Survival of Liver Transplant Recipients With Hemochromatosis in the United States
|
|
|
- Lambert Elliott
- 5 years ago
- Views:
Transcription
1 GASTROENTEROLOGY 2007;133: Survival of Liver Transplant Recipients With Hemochromatosis in the United States LEI YU*, and GEORGE N. IOANNOU*, *Division of Gastroenterology, Department of Medicine Veterans Affairs Puget Sound Health Care System and University of Washington, Seattle Washington; Research Enhancement Award Program Veterans Affairs Puget Sound Health Care System Background & Aims: Earlier studies have suggested that patients with have poor posttransplantation. We aimed to compare patients with to those with other causes of liver disease with regard to post-transplantation. Methods: We compared the posttransplant of patients with and without using data provided by the United Network for Organ Sharing on 50,306 adult, cadaveric liver transplantations performed in the United States between January 1, 1990, and July 18, Results: During , the post-transplantation of patients with (n 177) at 1 year (79.1%), 3 years (71.8%), and 5 years (64.6%) was lower than the average 1-year (86.4%), 3-year (79.5%), and 5-year (73.8%) of all other transplant recipients (hazard ratio for death, 1.38; 95% confidence interval [CI], ). In contrast, during , patients with (n 217) had excellent 1-year (86.1%), 3-year (80.8%), and 5-year (77.3%) post-transplantation, which was not different from the 1-year (88.4%), 3-year (80.3%), and 5-year (74.0%) post-transplantation of all other transplant recipients (hazard ratio for death, 0.89; 95% CI, ). Adjustment for donor and recipient characteristics did not substantially change these results. Compared with recipients without, those with were more likely to die of cardiovascular diseases and less likely to die as a result of graft failure. Conclusions: The post-transplantation of patients with, which was previously reported to be poor, has been excellent in the United States during the past 10 years. It has been suggested that patients who undergo liver transplantation for cirrhosis related to have a higher than average post-transplantation mortality. Kilpe et al 1 reported that 1-year after liver transplantation for between 1982 and 1991 in 37 US centers was 54% (30/56), whereas the 1-year post-transplantation of all patients was 80% (4092/5180). Kowdley et al 2 reported that among 37 patients with -related cirrhosis who underwent liver transplantation in 5 US centers between 1988 and 1993, 1-year post-transplantation was 58%. More recently, Kowdley et al 3 reported that the 1-year post-transplantation of 25 patients with HFE-related who underwent liver transplantation at 1 of 12 US centers before 1996 was 64% which was lower than the 1-year post-transplantation (84%) of all liver transplant recipients in these 12 centers before Those studies may not accurately reflect the current post-transplantation of patients with for a number of reasons. All those studies analyzed liver transplantations performed before 1996, and in patients with may have improved since then (for instance, as a result of more aggressive iron depletion before and after transplantation or more careful patient selection). 4 6 Those studies included a relatively small number of patients because is a rare indication for liver transplantation. As a result, none of the previous studies adequately adjusted for other predictors of post-transplantation, such as donor age, cold ischemia time, recipient age, and causes of liver disease, 7 or directly compared the post-transplantation of patients with -related cirrhosis with the posttransplantation of patients with other causes of cirrhosis such as viral hepatitis, alcoholic liver disease, or primary biliary cirrhosis. Finally, it is possible that those studies included patients with -related cirrhosis with worse than the average post-transplantation of all patients with related cirrhosis in the United States. To resolve these issues, we compared the post-transplantation of patients with to the post-transplantation of patients with other causes of liver disease with and without adjusting for predictors of post-transplantation using data reported to the United Network for Organ Sharing Abbreviations used in this paper: BMI, body mass index; CI, confidence interval; HCV, hepatitis C virus; NASH, nonalcoholic steatohepatitis; UNOS, United Network for Organ Sharing by the AGA Institute /07/$32.00 doi: /j.gastro
2 490 YU AND IOANNOU GASTROENTEROLOGY Vol. 133, No. 2 (UNOS) for all liver transplantations performed in the United States from January 1, 1990, until July18, Materials and Methods Data Collection Transplantation centers and organ procurement organizations in the United States are required to submit to UNOS 8 standardized data collection forms, including the Transplant Candidate Registration Form, which contains patient information at the time of listing for liver transplantation; the Deceased Donor Registration Form, which contains information on all consented recovered and nonrecovered donors; the Transplant Recipient Registration Form, which includes the patient status at discharge, clinical information before and after transplantation, as well as treatment data; and the Transplant Recipient Follow-up Form, which is generated 6 months after transplantation and on each subsequent transplantation anniversary and includes patient status and clinical and treatment information. These forms are currently submitted to UNOS electronically, and the information is entered into a single Standard Transplant Analysis and Research file that includes one record per transplantation event and the most recent follow-up information on patient status as of the date the file was created. The Standard Transplant Analysis and Research file created by UNOS on July 18, 2006, was kindly provided to the authors for this study. Study Population Of 63,679 liver transplantations involving recipients 18 years of age which were performed in the United States between January 1, 1990, and July 18, 2006, we excluded patients who had donors 10 or 75 years of age (n 1472), living donors (n 2040), split-liver donors (n 763), and non heart-beating donors (n 916). We also excluded patients with multiple simultaneous organ transplantations (n 2278) or previous liver transplantation (n 5904), leaving 50,306 participants in univariate analyses. We divided these patients into 2 time periods, (n 16,286) and (n 34,020) for more direct comparison with previous studies performed before 1996 and to look for any changes in the post-transplantation of patients with in more recent years for which no data are currently available. We additionally wanted to explore whether any difference in post-transplantation between patients with and without could be explained by differences in donor or recipient characteristics. For these multivariate analyses, we excluded patients with missing information in donor characteristics, including cold ischemia time (n 5206), and race (n 353), and recipient characteristics, including age (n 1), body mass index (BMI; calculated as the weight in kilograms divided by the square of height in meters [kg/m 2 ]; n 1375), race (n 281), serum albumin (n 1509), bilirubin (n 368), and creatinine (n 67). Finally, we excluded 943 patients with very abnormal values of cold ischemia time, BMI, serum bilirubin, creatinine, and albumin, (because they might have been recorded erroneously) and 183 with implausible values for these variables (almost certainly recorded erroneously), leaving 40,020 patients in multivariate analyses, including 13,342 who received transplants in and 26,678 in ( Very abnormal values were defined as follows: cold ischemia time, 0.5 to 1 hour or 24 to 48 hours; BMI, or 55 65; serum creatinine, 0 to 0.1 or 15 to 20 mg/dl; serum total bilirubin, 0 to 0.1 or mg/dl; and serum albumin, 0 to 0.5 or 6 to 10 g/dl. Implausible were values even more extreme than the abnormal values). Definition of Hemochromatosis and Comparable Liver Diseases The recipient s primary diagnosis leading to liver transplantation was identified by using the UNOS variable diag. This variable describes the recipient s primary diagnosis that was derived from information at discharge from the hospital after the transplantation, that is, after the explanted liver was also available for analysis. If the recipient s primary diagnosis at the time of discharge was not recorded, then the diagnosis at transplantation was used, and, if that was not available, the diagnosis at listing. By using this variable, we divided liver transplant recipients into the following categories:, hepatitis C virus (HCV; including HCV and alcoholic liver disease or hepatitis B virus), hepatitis B virus, alcoholic liver disease, primary biliary cirrhosis, primary sclerosing cholangitis, cryptogenic cirrhosis and fatty liver or nonalcoholic steatohepatitis (NASH), hepatocellular carcinoma, acute hepatic necrosis (excluding acute viral hepatitis B and C and acute alcoholic hepatitis), and others. We attempted to identify if any of the patients with a diagnosis of also had a diagnosis of hepatocellular carcinoma by looking at secondary diagnoses, which have been reported to UNOS only since April 1, In addition, since the introduction of the model for end-stage liver disease allocation system on February 27, 2002, an exception has been recorded for patients with hepatocellular carcinoma who receive a high priority score, and this was also used to identify patients with who also had hepatocellular carcinoma. Predictors of Post-Transplantation Survival We wanted to investigate whether any observed difference in post-transplantation between patients with and without was due to differences in the following donor and recipient characteristics that are predictors of post-transplantation sur-
3 August 2007 HEMOCHROMATOSIS AND LIVER TRANSPLANTATION 491 vival: donor age, cold ischemia time, race, and sex; recipient age, race, sex, BMI, serum albumin, bilirubin, and creatinine. 7 All variables were modeled as continuous variables except for race and sex. All these characteristics were ascertained at the time of transplantation. We did not consider diabetes as a potential confounder because causes diabetes; hence, diabetes may be one of the mechanisms by which could lead to worse post-transplantation. Causes of Death We categorized causes of recipient death, recorded by UNOS variable cod, into cardiovascular, graft failure, infection, malignancy, multiple organ system failure, and others. Statistical Analysis The Kaplan Meier method was used to calculate patient at 1, 3, and 5 years after transplantation. Cox proportional-hazards regression was used to compare patients with to patients with other liver diseases with regard to patient and graft after liver transplantation with and without adjusting for the predictors of post-transplantation listed earlier. 9 For the analysis of post-transplantation, patients were censored at the time when they were last traced alive. Graft failure was defined as liver failure (with or without retransplantation) or patient death from any cause. Time was measured from the date of liver transplantation to the date of liver failure, death, or last follow-up. Patients who remained alive without liver failure were censored at the time they were last traced alive. Results The proportion of transplant recipients with was 1.1% (177/16,286) in and 0.6% (217/34,020) in Compared with transplant recipients without, those with were older and more likely to be male and white in both time periods (Table 1). The presence of diabetes was routinely reported after 1997, and it was more common in recipients with. BMI and serum levels of bilirubin, creatinine, and albumin were similar in recipients with and without. Also, recipients with were similar to patients without with respect to donor characteristics in both time periods (Table 1). During , the post-transplantation of recipients with at 1 year (79.1%), 3 years (71.8%), and 5 years (64.6%) was lower than the post-transplantation of recipients without at 1 year (86.4%), 3 years (79.5%), and 5 years (73.8%) (Table 2). Compared with recipients without, those with were more likely to die (hazard ratio, 1.38; 95% confidence interval [CI], ) or to develop graft failure (hazard ratio, 1.27; 95% CI, ). Adjustment for all the Table 1. Donor and Recipient Characteristics of Liver Transplantations for Patients With and Without Hemochromatosis Patients with (N 177) Patients without (N 16,109) Patients with (N 217) Patients without (N 33,803) Donor characteristics Age (y), mean SD Cold ischemia time (h), mean SD Race or ethnicity White, % Black and African American, % Hispanic, % Others (mostly Asian), % Male, % Recipient characteristics Body mass index (kg/m 2 ), mean SD Age (y), mean SD Male, % Race or ethnicity White, % Black and African American, % Hispanic, % Other (mostly Asian) Diabetes, % NA NA Albumin (g/dl), mean SD Total bilirubin (mg/dl), mean SD Serum creatinine (mg/dl), mean SD
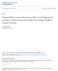
4 492 YU AND IOANNOU GASTROENTEROLOGY Vol. 133, No. 2 Table 2. Comparison of Liver Transplant Recipients With and Without Hemochromatosis With Regard to Patient and Graft Survival After Transplantation in the United States for Periods and Patients (n) Patientyears (n) Patient deaths (n) Mortality per 100 patientyears Hazard ratio (95% CI) for patient Hazard ratio (95% CI) for graft 1-Year patient (%) 3-Year patient (%) 5-Year patient (%) Time period No 16, ,928 6, Hemochromatosis ( ) 1.27 ( ) Time period No 33,803 96, Hemochromatosis ( ) 0.96 ( ) donor and recipient characteristics shown in Table 1 had little effect on these hazard ratios (adjusted hazard ratio for patient death, 1.30; 95% CI, ; adjusted hazard ratio for graft failure, 1.24; 95% CI, ). During the period , recipients with had the worst post-transplantation of any other recipient group defined by cause of liver disease other than hepatocellular carcinoma (Table 3; Figure 1A). In contrast, during , recipients with had similar post-transplantation at 1 year (86.1%), 3 years (80.8%), and 5 years (77.3%) to recipients without (88.4%, 80.3%, and 74.0% at 1, 3, and 5 years, respectively). Adjusted (hazard ratio for patient death, 0.78; 95% CI, ; and for graft failure, 0.88; 95% CI, ) and unadjusted (Table 2) hazard ratios comparing recipients with and without did not show any significant difference. During , recipients with had 5-year post-transplantation that was superior to not only recipients with hepatocellular carcinoma but also those with HCV infection, NASH-induced or cryptogenic cirrhosis, alcoholic liver disease, or acute Table 3. Patient Survival After Transplantation for Selected Causes of Liver Disease for Periods and Year 3-Year 5-Year Hepatocellular carcinoma Hemochromatosis Cryptogenic-NASH Hepatitis B virus Alcohol Hepatitis C virus Acute hepatic failure Autoimmune hepatitis PSC PBC Hepatocellular carcinoma Hepatitis C virus Cryptogenic-NASH Alcohol Acute hepatic failure Hemochromatosis Hepatitis B virus Autoimmune hepatitis PBC PSC NOTE. Causes of liver disease are arranged in order of increasing 5-year. NASH, nonalcoholic steatohepatitis; PSC, primary sclerosing cholangitis; PBC, primary biliary cirrhosis. Figure 1. Kaplan Meier curves of patient after liver transplantation for recipients with and selected causes of liver disease during (A) and (B).
5 August 2007 HEMOCHROMATOSIS AND LIVER TRANSPLANTATION 493 Table 4. Causes of Post-Transplantation Death Among Recipients With and Without Hemochromatosis During the Periods , , and Combined Cause of death Hemochromatosis, No, Hemochromatosis, No, Hemochromatosis, No, P value a Cardiovascular 23 (27) 922 (15) 6 (15) 864 (13) 29 (23) 1786 (14).002 Graft failure 4 (5) 843 (13) 3 (8) 981 (15) 7 (6) 1824 (14).07 Infection 18 (21) 1213 (19) 11 (28) 1142 (17) 29 (23) 2355 (18).1 Malignancy 11 (13) 886 (14) 3 (8) 777 (12) 14 (11) 1663 (13).6 Multiple organ 5 (6) 424 (7) 2 (5) 663 (10) 7 (6) 1087 (8).3 system failure Other 25 (29) 2,023 (32) 14 (36) 2299 (34) 39 (31) 4322 (33).6 Total 86 (100) 6311 (100) 39 (100) 6726 (100) 125 (100) 13,037 (100) a The P value refers to the comparison of patients with to patients without with respect to the proportion with each cause of death for the entire study period ( ). hepatic failure (Table 3; Figure 1B). Compared with recipients without, those with were more likely to die of cardiovascular diseases and less likely to die as a result of graft failure (Table 4). In the period we could only identify 3 patients (of 177) with who were recorded to have a secondary diagnosis of hepatocellular carcinoma (of which one was identified in the explanted liver after transplantation). In , 30 of 217 patients with were identified as also having hepatocellular carcinoma, of which 25 were listed as exceptions for priority score after February 27, Removing these 30 patients did not change 1-, 3-, and 5-year of patients with appreciably. Discussion The most important finding of this study is that in recent years ( ) the 1-year (86.1%), 3-year (80.8%), and 5-year (77.3%) post-transplantation of patients with in the United States was excellent. Post-transplantation in patients with during was almost identical to the average of all liver transplant recipients and was better than the of recipients with hepatocellular carcinoma, HCV infection, NASHinduced or cryptogenic cirrhosis, alcoholic liver disease, or acute hepatic failure. In contrast, during , 1-year (79.3%), 3-year (71.8%), and 5-year (64.6%) post-transplantation in patients with in the United States was worse than average. In fact, during that time period, patients with had the worst post-transplantation of any major group of patients defined by cause of liver disease, with the exception of patients with hepatocellular carcinoma. From to , 5-year post-transplantation improved by 13% (from 64.6% to 77.3%) in patients with, whereas it remained almost unchanged in all other patients without (73.8% to 74%). We can only speculate as to the causes of the difference in post-transplantation of patients with between periods and In theory, this could be due to better patient selection that may have been prompted by previous studies that reported recipients with to have significantly higher proportion of cardiac disease related mortality than recipients with other liver diseases. 2,10,11 In more recent years, transplantation centers may have been more rigorous at identifying cardiac disease in patients with and excluding them from transplantation. This is suggested by our finding that cardiovascular deaths were more common in patients with than other patients in the period but not in Second, although prior studies failed to show an association between the presence of hepatocellular carcinoma and poor after transplantation among recipients with, 2,11 we suspect hepatocellular carcinoma was another important reason for the low post-transplantation during , particularly if patients had large tumors such that they would not have received transplants in more recent years. 12 For example, in the study by Crawford et al, 12 6 of 22 recipients with had hepatocellular carcinoma, including 4 patients with tumors 7, 9, 10, and 12 cm in diameter. All 4 patients died of recurrent hepatocellular cancer. 12 We cannot tell for sure in our study exactly what proportion of patients with also had hepatocellular carcinoma. However, since 1997 hepatocellular carcinoma within the Milan criteria 13 has been recognized as an indication for transplantation in the United States, and patients have been listed as status 2B for the period or with a high priority score under the model for end-stage liver disease allocation period (2002 to now). This suggests that any patients with hepatocellular carcinoma among those with in the period would likely be within the Milan cri-
6 494 YU AND IOANNOU GASTROENTEROLOGY Vol. 133, No. 2 teria, for which post-transplantation is generally good. In contrast, it is likely that many of the patients with during the period had large tumors (as was consistently shown by earlier studies) which are associated with high post-transplantation mortality. Therefore, we speculate that one of the reasons for the improvement in post-transplantation that we observed in patients with may be that patients with concurrent large hepatocellular carcinomas have been excluded from transplantation since It is also theoretically possible that better care before and after transplantation may have improved post-transplantation in patients with. Two small studies reported that a total of 8 patients with who underwent adequate iron depletion before transplantation had good post-transplantation. 14,15 Whether iron depletion before transplantation really improves post-transplantation and whether it has been widely adopted since 1997 is unclear. In addition, previous reports highlighted excess infectious complications in liver transplant recipients with, 16 which may have led to greater awareness and early treatment of such infections. Our study is limited by the fact that the diagnosis of was based on the diagnosis reported to UNOS by the transplantation centers. We do not have data on hepatic iron concentration or related end-organ damage to confirm the diagnosis. However, these diagnoses were all made by experienced hepatologists at transplantation centers with knowledge of the explant liver pathology who recorded as the cause of liver disease requiring liver transplantation. We doubt that the diagnosis of made under these circumstances would be wrong in more than an insignificant minority of cases. The proportion of transplant recipients with in this study (1.1% for period and 0.6% for period ) is similar to the proportion reported in earlier studies in which patients with were individually identified and the diagnosis confirmed. 3,12,16 Another limitation of our study is that we cannot determine accurately what proportion of patients with also had hepatocellular carcinoma, which precluded us from analyzing its association with the observed change in post-transplantation in recipients. We attempted to determine the presence of hepatocellular carcinoma in patients with a diagnosis of hepatocellular carcinoma by seeing whether it was reported as a secondary diagnosis (reported only after 1994) or as an exception with high priority score for liver transplantation (reported after 2002). These techniques probably did not identify all patients with who also had hepatocellular carcinoma even in the period However, the post-transplantation of patients with in was excellent despite the fact that this group included a proportion of recipients with concurrent hepatocellular carcinoma, and the would be expected to be even better among those who did not have hepatocellular carcinoma, if we could accurately identify them. Finally, our study is limited by the lack of information on the HFE genotype of patients with a diagnosis of. In 5 previous studies, the cumulative proportion of patients with HFE- (C282Y homozygotes or C282Y/H63D compound heterozygotes) among patients who underwent liver transplantation for was 46/84 or 55% (2/4, 17 4/7, 18 3/5, 16 17/22, 12 and 20/46 3 ). Four of those studies analyzed patients transplanted before the discovery of the HFE gene in1996, and one study analyzed patients transplanted between 1982 and It is possible that among patients with, those with homozygosity for the C282Y mutation or compound heterozygosity for the C282Y/H63D mutation may have worse post-transplantation than patients without these mutations in the HFE gene. This was suggested by a recent study, 3 which is not directly analogous to ours because the majority (82%) of patients in that study were included on the basis of having elevated hepatic iron concentration or hepatic iron index in the explanted liver irrespective of any additional liver diseases, such as viral hepatitis, which may have caused or contributed to the cirrhosis (ie, was not the primary cause for liver transplantation). This study analyzed patients transplanted before 1996, and the impact of HFE genotype should probably be reassessed in more recent populations of liver transplant recipients, given our finding of a significant change in post-transplantation among patients with in It is also possible that since the discovery of the HFE gene in 1996, the proportion of patients with HFE- among those transplanted for has increased. However, if this were true and if patients with HFE- have worse post-transplantation than patients with non HFE- or iron overload as suggested by Kowdley et al, 3 then this would have led to a decrease in post-transplantation of patients with in compared with (not an increase, as we report here). In conclusion, our study shows that liver transplant recipients with a diagnosis of in the United States in had excellent that was comparable to all other transplant recipients. This reflects a significant improvement in post-transplantation among recipients with who before 1997 had one of the worst post-transplantation s compared with recipients with other liver disease causes. Our findings are important for patients
7 August 2007 HEMOCHROMATOSIS AND LIVER TRANSPLANTATION 495 with -related cirrhosis who are contemplating liver transplantation and for liver transplantation centers evaluating such patients because they suggest that a diagnosis of alone does not necessarily predict poor post-transplantation. Although we speculate that more careful patient selection with regard to cardiac diseases and hepatocellular carcinoma and improved care before and after transplantation are potential reasons for this observed change in, future research should attempt to confirm these hypotheses by analyzing recent cohorts of recipients with with more complete clinical data before and after transplantation. References 1. Kilpe VE, Krakauer H, Wren RE. An analysis of liver transplant experience from 37 transplant centers as reported to Medicare. Transplantation 1993;56: Kowdley KV, Hassanein T, Kaur S, Farrell FJ, Van Thiel DH, Keeffe EB, Sorrell MF, Bacon BR, Weber FL Jr, Tavill AS. Primary liver cancer and in patients undergoing liver transplantation for. Liver Transpl Surg 1995;1: Kowdley KV, Brandhagen DJ, Gish RG, Bass NM, Weinstein J, Schilsky ML, Fontana RJ, McCashland T, Cotler SJ, Bacon BR, Keeffe EB, Gordon F, Polissar N. Survival after liver transplantation in patients with hepatic iron overload: the national transplant registry. Gastroenterology 2005;129: Niederau C, Fischer R, Purschel A, Stremmel W, Haussinger D, Strohmeyer G. Long-term in patients with hereditary. Gastroenterology 1996;110: Niederau C, Fischer R, Sonnenberg A, Stremmel W, Trampisch HJ, Strohmeyer G. Survival and causes of death in cirrhotic and in noncirrhotic patients with primary. N Engl J Med 1985;313: Powell LW. Hemochromatosis: the impact of early diagnosis and therapy. Gastroenterology 1996;110: Ioannou GN. Development and validation of a model predicting graft after liver transplantation. Liver Transpl 2006;12: United Network for Organ Sharing. Accessed February 2, Cox DR. Regression models and life tables. J Royal Stat Soc Ser B 1972;34: Farrell FJ, Nguyen M, Woodley S, Imperial JC, Garcia-Kennedy R, Man K, Esquivel CO, Keeffe EB. Outcome of liver transplantation in patients with. Hepatology 1994;20: Tung BY, Farrell FJ, McCashland TM, Gish RG, Bacon BR, Keeffe EB, Kowdley KV. Long-term follow-up after liver transplantation in patients with hepatic iron overload. Liver Transpl Surg 1999;5: Crawford DH, Fletcher LM, Hubscher SG, Stuart KA, Gane E, Angus PW, Jeffrey GP, McCaughan GW, Kerlin P, Powell LW, Elias EE. Patient and graft after liver transplantation for hereditary : implications for pathogenesis. Hepatology 2004;39: Mazzaferro V, Regalia E, Doci R, Andreola S, Pulvirenti A, Bozzetti F, Montalto F, Ammatuna M, Morabito A, Gennari L. Liver transplantation for the treatment of small hepatocellular carcinomas in patients with cirrhosis. N Engl J Med 1996;334: Pillay P, Tzoracoleftherakis E, Tzakis AG, Kakizoe S, Van Thiel DH, Starzl TE. Orthotopic liver transplantation for. Transplant Proc 1991;23: Poulos JE, Bacon BR. Liver transplantation for hereditary. Dig Dis 1996;14: Brandhagen DJ, Alvarez W, Therneau TM, Kruckeberg KE, Thibodeau SN, Ludwig J, Porayko MK. Iron overload in cirrhosis-hfe genotypes and outcome after liver transplantation. Hepatology 2000;31: Fiel MI, Schiano TD, Bodenheimer HC, Thung SN, King TW, Varma CR, Miller CM, Brunt EM, Starnes S, Prass C, Wolff RK, Bacon BR. Hereditary in liver transplantation. Liver Transpl Surg 1999;5: Stuart KA, Fletcher LM, Clouston AD, Lynch SV, Purdie DM, Kerlin P, Crawford DH. Increased hepatic iron and cirrhosis: no evidence for an adverse effect on patient outcome following liver transplantation. Hepatology 2000;32: Received March 1, Accepted May 10, Address requests for reprints to: George Ioannou, MD, MS, Veterans Affairs Puget Sound Health Care System, Gastroenterology, S-111- Gastro, 1660 S. Columbian Way, Seattle, Washington georgei@medicine.washington.edu; fax: (206) Supported by American Liver Foundation and American Association for the Study of Liver Diseases Jan Albrecht Award (to G.N.I.), Research Enhancement Award Program, Veterans Affairs Puget Sound Health Care System (to L.Y.). All authors declare that they have no conflict of interest to disclose.
Survival After Orthotopic Liver Transplantation: The Impact of Antibody Against Hepatitis B Core Antigen in the Donor
 LIVER TRANSPLANTATION 15:1343-1350, 2009 ORIGINAL ARTICLE Survival After Orthotopic Liver Transplantation: The Impact of Antibody Against Hepatitis B Core Antigen in the Donor Lei Yu, 1-3 Thomas Koepsell,
LIVER TRANSPLANTATION 15:1343-1350, 2009 ORIGINAL ARTICLE Survival After Orthotopic Liver Transplantation: The Impact of Antibody Against Hepatitis B Core Antigen in the Donor Lei Yu, 1-3 Thomas Koepsell,
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995
 Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Frequency and Outcomes of Liver Transplantation for Nonalcoholic Steatohepatitis in the United States
 GASTROENTEROLOGY 2011;141:1249 1253 Frequency and Outcomes of Liver Transplantation for Nonalcoholic Steatohepatitis in the United States MICHAEL R. CHARLTON,* JUSTIN M. BURNS, RACHEL A. PEDERSEN, KYMBERLY
GASTROENTEROLOGY 2011;141:1249 1253 Frequency and Outcomes of Liver Transplantation for Nonalcoholic Steatohepatitis in the United States MICHAEL R. CHARLTON,* JUSTIN M. BURNS, RACHEL A. PEDERSEN, KYMBERLY
ORIGINAL ARTICLE. Eric F. Martin, 1 Jonathan Huang, 3 Qun Xiang, 2 John P. Klein, 2 Jasmohan Bajaj, 4 and Kia Saeian 1
 LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
LIVER TRANSPLANTATION 18:914 929, 2012 ORIGINAL ARTICLE Recipient Survival and Graft Survival are Not Diminished by Simultaneous Liver-Kidney Transplantation: An Analysis of the United Network for Organ
Minimal But Significant Improvement in Survival for Non Hepatitis C Related Adult Liver Transplant Patients Beyond the One-Year Posttransplant Mark
 LIVER TRANSPLANTATION 16:130-137, 2010 ORIGINAL ARTICLE Minimal But Significant Improvement in Survival for Non Hepatitis C Related Adult Liver Transplant Patients Beyond the One-Year Posttransplant Mark
LIVER TRANSPLANTATION 16:130-137, 2010 ORIGINAL ARTICLE Minimal But Significant Improvement in Survival for Non Hepatitis C Related Adult Liver Transplant Patients Beyond the One-Year Posttransplant Mark
Survival Outcomes Following Liver Transplantation (SOFT) Score: A Novel Method to Predict Patient Survival Following Liver Transplantation
 American Journal of Transplantation 2008; 8: 2537 2546 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2537 2546 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
What Is the Real Gain After Liver Transplantation?
 LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
Hwm YI Yoo, * Ernest0 Molmenti, ' and PuulJ Tbuluvutb"
 The Effect of Donor Body Mass Index on Primary Nonfunction, Retransplantation Rate, and Early and Patient Survival After Liver Transplantation Hwm YI Yoo, * Ernest0 Molmenti, ' and PuulJ Tbuluvutb" Previous
The Effect of Donor Body Mass Index on Primary Nonfunction, Retransplantation Rate, and Early and Patient Survival After Liver Transplantation Hwm YI Yoo, * Ernest0 Molmenti, ' and PuulJ Tbuluvutb" Previous
Research Article New Onset Diabetes Mellitus in Living Donor versus Deceased Donor Liver Transplant Recipients: Analysis of the UNOS/OPTN Database
 Transplantation Volume 2013, Article ID 269096, 7 pages http://dx.doi.org/10.1155/2013/269096 Research Article New Onset Diabetes Mellitus in Living Donor versus Deceased Donor Liver Transplant Recipients:
Transplantation Volume 2013, Article ID 269096, 7 pages http://dx.doi.org/10.1155/2013/269096 Research Article New Onset Diabetes Mellitus in Living Donor versus Deceased Donor Liver Transplant Recipients:
Obesity is perhaps the most significant public health problem
 Obesity and Its Effect on Survival in Patients Undergoing Orthotopic Liver Transplantation in the United States Satheesh Nair, 1 Sumita Verma, 2 and Paul J. Thuluvath 2 Studies assessing morbidity and
Obesity and Its Effect on Survival in Patients Undergoing Orthotopic Liver Transplantation in the United States Satheesh Nair, 1 Sumita Verma, 2 and Paul J. Thuluvath 2 Studies assessing morbidity and
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Liver Cancer: Epidemiology and Health Disparities. Andrea Goldstein NP, MS, MPH Scientific Director Onyx Pharmaceuticals
 Liver Cancer: Epidemiology and Health Disparities Andrea Goldstein NP, MS, MPH Scientific Director Onyx Pharmaceuticals 1. Bosch FX, et al. Gastroenterology. 2004;127(5 suppl 1):S5-S16. 2. American Cancer
Liver Cancer: Epidemiology and Health Disparities Andrea Goldstein NP, MS, MPH Scientific Director Onyx Pharmaceuticals 1. Bosch FX, et al. Gastroenterology. 2004;127(5 suppl 1):S5-S16. 2. American Cancer
Genetic Testing for Hereditary Hemochromatosis
 Medical Policy Manual Genetic Testing, Policy No. 48 Genetic Testing for Hereditary Hemochromatosis Next Review: December 2018 Last Review: December 2017 Effective: February 1, 2018 IMPORTANT REMINDER
Medical Policy Manual Genetic Testing, Policy No. 48 Genetic Testing for Hereditary Hemochromatosis Next Review: December 2018 Last Review: December 2017 Effective: February 1, 2018 IMPORTANT REMINDER
The Effect of Donor Race on the Survival of Black Americans Undergoing Liver Transplantation for Chronic Hepatitis C
 LIVER TRANSPLANTATION 15:1126-1132, 2009 ORIGINAL ARTICLE The Effect of Donor Race on the Survival of Black Americans Undergoing Liver Transplantation for Chronic Hepatitis C Phillip S. Pang, 1,2 * Ahmad
LIVER TRANSPLANTATION 15:1126-1132, 2009 ORIGINAL ARTICLE The Effect of Donor Race on the Survival of Black Americans Undergoing Liver Transplantation for Chronic Hepatitis C Phillip S. Pang, 1,2 * Ahmad
Liver transplantation is the only hope for patients with terminal. Indication and Prognosis of Liver Transplantation. Abstract
 Indication and Prognosis of Liver Transplantation Jae Won Joh, M.D. Department of General Surgery Sungkyunkwan University School of Medicine Samsung Medical Center E mail: jwjoh@smc.samsung.co.kr Abstract
Indication and Prognosis of Liver Transplantation Jae Won Joh, M.D. Department of General Surgery Sungkyunkwan University School of Medicine Samsung Medical Center E mail: jwjoh@smc.samsung.co.kr Abstract
Liver grafts for transplantation from donors with diabetes: an analysis of the Scientific Registry of Transplant Recipients database
 Title Liver grafts for transplantation from donors with diabetes: an analysis of the Scientific Registry of Transplant Recipients database Author(s) Zheng, J; Xiang, J; Zhou, J; Li, Z; Hu, Z; Lo, CM; Wang,
Title Liver grafts for transplantation from donors with diabetes: an analysis of the Scientific Registry of Transplant Recipients database Author(s) Zheng, J; Xiang, J; Zhou, J; Li, Z; Hu, Z; Lo, CM; Wang,
Transplant Hepatology
 Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
PAPER. Liver Transplant for Hepatitis C Virus. Effect of Using Older Donor Grafts on Short- and Medium-Term Survival
 PAPER Liver Transplant for Hepatitis C Virus Effect of Using Older Donor Grafts on Short- and Medium-Term Survival M. B. Majella Doyle, MD; Christopher D. Anderson, MD; Neeta Vachharajani, MD; Jeffrey
PAPER Liver Transplant for Hepatitis C Virus Effect of Using Older Donor Grafts on Short- and Medium-Term Survival M. B. Majella Doyle, MD; Christopher D. Anderson, MD; Neeta Vachharajani, MD; Jeffrey
Waitlist Priority for Hepatocellular Carcinoma Beyond Milan Criteria: A Potentially Appropriate Decision Without a Structured Approach
 American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
American Journal of Transplantation 2014; 14: 79 87 Wiley Periodicals Inc. C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/ajt.12530
PATIENTS AND METHODS. Data Source
 LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
LIVER TRANSPLANTATION 20:1045 1056, 2014 ORIGINAL ARTICLE Waiting Time Predicts Survival After Liver Transplantation for Hepatocellular Carcinoma: A Cohort Study Using the United Network for Organ Sharing
In the United States, the Model for End-Stage Liver. Re-weighting the Model for End-Stage Liver Disease Score Components
 GASTROENTEROLOGY 2008;135:1575 1581 Re-weighting the Model for End-Stage Liver Disease Score Components PRATIMA SHARMA,* DOUGLAS E. SCHAUBEL,, CAMELIA S. SIMA,, ROBERT M. MERION,, and ANNA S. F. LOK* *Division
GASTROENTEROLOGY 2008;135:1575 1581 Re-weighting the Model for End-Stage Liver Disease Score Components PRATIMA SHARMA,* DOUGLAS E. SCHAUBEL,, CAMELIA S. SIMA,, ROBERT M. MERION,, and ANNA S. F. LOK* *Division
The pediatric end-stage liver disease (PELD) score
 Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Selection of Pediatric Candidates Under the PELD System Sue V. McDiarmid, 1 Robert M. Merion, 2 Dawn M. Dykstra, 2 and Ann M. Harper 3 Key Points 1. The PELD score accurately predicts the 3 month probability
Organ allocation for liver transplantation: Is MELD the answer? North American experience
 Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
Organ allocation for liver transplantation: Is MELD the answer? North American experience Douglas M. Heuman, MD Virginia Commonwealth University Richmond, VA, USA March 1998: US Department of Health and
During the past 2 decades, an increase in the ageadjusted
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:104 110 Racial Differences in Survival of Hepatocellular Carcinoma in the United States: A Population-Based Study JESSICA A. DAVILA* and HASHEM B. EL SERAG*,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:104 110 Racial Differences in Survival of Hepatocellular Carcinoma in the United States: A Population-Based Study JESSICA A. DAVILA* and HASHEM B. EL SERAG*,
H common genetic disease in Caucasians, with a
 Primary liver Cancer and Survival in Patients Undergoing Liver Transplantation for Hemochromatosis Kvis V. Kowdley, * Taveh Hassanein, # Sumanjit Kaur, # Fvanh]. Fawell, 3 David H. Van Thiel,# Emmet B.
Primary liver Cancer and Survival in Patients Undergoing Liver Transplantation for Hemochromatosis Kvis V. Kowdley, * Taveh Hassanein, # Sumanjit Kaur, # Fvanh]. Fawell, 3 David H. Van Thiel,# Emmet B.
Experience with Liver Transplantation in patients over 65 years of Age at the Hospital Pablo Tobón Uribe in Medellin, Colombia from 2004 to 2010
 Original articles Experience with Liver Transplantation in patients over 65 years of Age at the Hospital Pablo Tobón Uribe in Medellin, Colombia from 2004 to 2010 Octavio Muñoz, MD, 1 Laura Ovadía, MD,
Original articles Experience with Liver Transplantation in patients over 65 years of Age at the Hospital Pablo Tobón Uribe in Medellin, Colombia from 2004 to 2010 Octavio Muñoz, MD, 1 Laura Ovadía, MD,
Liver transplant: what is left after the viruses
 Riunione Monotematica A.I.S.F. 2016 The Future of Liver Disease: Beyond HCV is there a Role for Hepatologist? Milan 15 th 2016 Liver transplant: what is left after the viruses Stefano Ginanni Corradini
Riunione Monotematica A.I.S.F. 2016 The Future of Liver Disease: Beyond HCV is there a Role for Hepatologist? Milan 15 th 2016 Liver transplant: what is left after the viruses Stefano Ginanni Corradini
For the past two decades, the number of patients
 When Shouldn t We Retransplant? Michael A. Zimmerman and R. Mark Ghobrial Key Points 1. In the setting of early graft failure after primary transplantation, orthotopic liver retransplantation (re-olt)
When Shouldn t We Retransplant? Michael A. Zimmerman and R. Mark Ghobrial Key Points 1. In the setting of early graft failure after primary transplantation, orthotopic liver retransplantation (re-olt)
Association of Hepatic Iron Overload With Invasive Fungal Infection in Liver Transplant Recipients
 LIVER TRANSPLANTATION 12:1799-1804, 2006 ORIGINAL ARTICLE Association of Hepatic Iron Overload With Invasive Fungal Infection in Liver Transplant Recipients Jacob Alexander, 1 Ajit P. Limaye, 2 Cynthia
LIVER TRANSPLANTATION 12:1799-1804, 2006 ORIGINAL ARTICLE Association of Hepatic Iron Overload With Invasive Fungal Infection in Liver Transplant Recipients Jacob Alexander, 1 Ajit P. Limaye, 2 Cynthia
IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS?
 IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS? Dr. Sammy Saab David Geffen School of Medicine, Los Angeles, USA April 2018 DISCLAIMER Please note: The views
IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS? Dr. Sammy Saab David Geffen School of Medicine, Los Angeles, USA April 2018 DISCLAIMER Please note: The views
Corporate Medical Policy Genetic Testing for Hereditary Hemochromatosis
 Corporate Medical Policy Genetic Testing for Hereditary Hemochromatosis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_hemochromatosis 5/2012 3/2018 3/2019 3/2018
Corporate Medical Policy Genetic Testing for Hereditary Hemochromatosis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_hemochromatosis 5/2012 3/2018 3/2019 3/2018
Geographic Differences in Event Rates by Model for End-Stage Liver Disease Score
 American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2006; 6: 2470 2475 Blackwell Munksgaard C 2006 The Authors Journal compilation C 2006 The American Society of Transplantation and the American Society of Transplant
Role of Liver Biopsy. Role of Liver Biopsy 9/3/2009. Liver Biopsies in Viral Hepatitis: Beyond Grading and Staging
 Liver Biopsies in Viral Hepatitis: Beyond Grading and Staging for further reference: Liver biopsy assessment in chronic viral hepatitis: a personal, practical approach Neil Theise, MD. Depts of Pathology
Liver Biopsies in Viral Hepatitis: Beyond Grading and Staging for further reference: Liver biopsy assessment in chronic viral hepatitis: a personal, practical approach Neil Theise, MD. Depts of Pathology
UK Liver Transplant Audit
 November 2012 UK Liver Transplant Audit In patients who received a Liver Transplant between 1 st March 1994 and 31 st March 2012 ANNUAL REPORT Advisory Group for National Specialised Services Prepared
November 2012 UK Liver Transplant Audit In patients who received a Liver Transplant between 1 st March 1994 and 31 st March 2012 ANNUAL REPORT Advisory Group for National Specialised Services Prepared
The Effect of HLA Class I (A and B) and Class II (DR) Compatibility on Liver Transplantation Outcomes: An Analysis of the OPTN Database
 LIVER TRANSPLANTATION 12:652-658, 2006 ORIGINAL ARTICLE The Effect of HLA Class I (A and B) and Class II (DR) Compatibility on Liver Transplantation Outcomes: An Analysis of the OPTN Database Victor Navarro,
LIVER TRANSPLANTATION 12:652-658, 2006 ORIGINAL ARTICLE The Effect of HLA Class I (A and B) and Class II (DR) Compatibility on Liver Transplantation Outcomes: An Analysis of the OPTN Database Victor Navarro,
Hepatocellular Carcinoma: Epidemiology and Screening
 Hepatocellular Carcinoma: Epidemiology and Screening W. Ray Kim, MD Professor and Chief Gastroenterology and Hepatology Stanford University School of Medicine Case A 67 year old Filipino-American woman
Hepatocellular Carcinoma: Epidemiology and Screening W. Ray Kim, MD Professor and Chief Gastroenterology and Hepatology Stanford University School of Medicine Case A 67 year old Filipino-American woman
Autoimmune Hepatitis: Defining the need for Liver Transplantation
 Autoimmune Hepatitis: Defining the need for Liver Transplantation Michael A Heneghan, MD, MMedSc, FRCPI. Institute of Liver Studies, King s College Hospital, London Outline Autoimmune Hepatitis Background
Autoimmune Hepatitis: Defining the need for Liver Transplantation Michael A Heneghan, MD, MMedSc, FRCPI. Institute of Liver Studies, King s College Hospital, London Outline Autoimmune Hepatitis Background
ORIGINAL ARTICLE. Received April 30, 2007; accepted June
 LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
Liver and intestine transplantation: summary analysis,
 American Journal of Transplantation 25; 5 (Part 2): 916 933 Blackwell Munksgaard Blackwell Munksgaard 25 Liver and intestine transplantation: summary analysis, 1994 23 Douglas W. Hanto a,, Thomas M. Fishbein
American Journal of Transplantation 25; 5 (Part 2): 916 933 Blackwell Munksgaard Blackwell Munksgaard 25 Liver and intestine transplantation: summary analysis, 1994 23 Douglas W. Hanto a,, Thomas M. Fishbein
Diabetes, Hypertension and Hyperlipidemia: Prevalence Over Time and Impact on Long-Term Survival After Liver Transplantation
 American Journal of Transplantation 2012; 12: 2181 2187 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/j.1600-6143.2012.04077.x
American Journal of Transplantation 2012; 12: 2181 2187 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons doi: 10.1111/j.1600-6143.2012.04077.x
Hepatitis C: Difficult-to-treat Patients 11th Paris Hepatology Conference 16th January 2018 Stefan Zeuzem, MD University Hospital, Frankfurt, Germany
 Hepatitis C: Difficult-to-treat Patients 11th Paris Hepatology Conference 16th January 2018 Stefan Zeuzem, MD University Hospital, Frankfurt, Germany PHC 2018 - www.aphc.info Disclosures Advisory boards:
Hepatitis C: Difficult-to-treat Patients 11th Paris Hepatology Conference 16th January 2018 Stefan Zeuzem, MD University Hospital, Frankfurt, Germany PHC 2018 - www.aphc.info Disclosures Advisory boards:
Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors?
 Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance
 Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
OHSU Digital Commons. Oregon Health & Science University. Barry Schlansky. Scholar Archive. July 2013
 Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Oregon Health & Science University OHSU Digital Commons Scholar Archive July 2013 Waitlist time predicts survival after liver transplantation for hepatocellular carcinoma : a cohort study in the United
Long-term Outcomes After Third Liver Transplant
 ArtıcLe Long-term Outcomes After Third Liver Transplant C. Burcin Taner, 1 Deniz Balci, 1 Darrin L. Willingham, 1 Andrew P. Keaveny, 1 Barry G. Rosser, 1 Juan M. Canabal, 1 Timothy S. J. Shine, 2 Denise
ArtıcLe Long-term Outcomes After Third Liver Transplant C. Burcin Taner, 1 Deniz Balci, 1 Darrin L. Willingham, 1 Andrew P. Keaveny, 1 Barry G. Rosser, 1 Juan M. Canabal, 1 Timothy S. J. Shine, 2 Denise
There are approximately 1 million new cases of primary hepatocellular
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:800 806 Liver Transplantation in Patients With Nonalcoholic Steatohepatitis-Related Hepatocellular Carcinoma SHAHID M. MALIK,* PARIJAT A. GUPTE,* MICHAEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:800 806 Liver Transplantation in Patients With Nonalcoholic Steatohepatitis-Related Hepatocellular Carcinoma SHAHID M. MALIK,* PARIJAT A. GUPTE,* MICHAEL
CLINICAL UPDATE Haemochromatosis 3rd Edition 2007 Digestive Health Foundation 2007
 CLINICAL UPDATE Haemochromatosis 3rd Edition 2007 Digestive Health Foundation 2007 Table of Contents 2 Definition Iron Studies Genetics of Hereditary Haemochromatosis 4 Clinical Manifestations Diagnosis
CLINICAL UPDATE Haemochromatosis 3rd Edition 2007 Digestive Health Foundation 2007 Table of Contents 2 Definition Iron Studies Genetics of Hereditary Haemochromatosis 4 Clinical Manifestations Diagnosis
Liver Cancer: Diagnosis and Treatment Options
 Liver Cancer: Diagnosis and Treatment Options Fred Poordad, MD Chief, Hepatology University Transplant Center Professor of Medicine UT Health, San Antonio VP, Academic and Clinical Affairs, Texas Liver
Liver Cancer: Diagnosis and Treatment Options Fred Poordad, MD Chief, Hepatology University Transplant Center Professor of Medicine UT Health, San Antonio VP, Academic and Clinical Affairs, Texas Liver
POST TRANSPLANT OUTCOMES IN PSC
 POST TRANSPLANT OUTCOMES IN PSC Kidist K. Yimam, MD Medical Director, Autoimmune Liver Disease Program Division of Hepatology and Liver Transplantation California Pacific Medical Center (CPMC) PSC Partners
POST TRANSPLANT OUTCOMES IN PSC Kidist K. Yimam, MD Medical Director, Autoimmune Liver Disease Program Division of Hepatology and Liver Transplantation California Pacific Medical Center (CPMC) PSC Partners
Hepatocellular carcinoma
 Hepatocellular carcinoma Mary Ann Y. Huang, M.D., M.S., FAASLD Transplant hepatologist Peak Gastroenterology Associates Porter Adventist Hospital Denver, Colorado Background - Worldwide Hepatocellular
Hepatocellular carcinoma Mary Ann Y. Huang, M.D., M.S., FAASLD Transplant hepatologist Peak Gastroenterology Associates Porter Adventist Hospital Denver, Colorado Background - Worldwide Hepatocellular
4/26/2017. Liver Transplant and Palliative Care: Teaming up to improve care
 Liver Transplant and Palliative Care: Teaming up to improve care Jody C. Olson, M.D., FACP Assistant Professor of Medicine and Surgery Hepatology and Critical Care Medicine All patients with end-stage
Liver Transplant and Palliative Care: Teaming up to improve care Jody C. Olson, M.D., FACP Assistant Professor of Medicine and Surgery Hepatology and Critical Care Medicine All patients with end-stage
Despite recent advances in the care of patients with
 Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Liver Transplantation for Hepatocellular Carcinoma: Lessons from the First Year Under the Model of End- Stage Liver Disease (MELD) Organ Allocation Policy Francis Y. Yao, 1,2 Nathan M. Bass, 1 Nancy L.
Transient elastography in chronic liver diseases of other etiologies
 4 Post Meeting A.I.S.F. Unmet Clinical Needs in Hepatology: New and upcoming diagnostic tools" Transient elastography in chronic liver diseases of other etiologies Dr. Vincenza Calvaruso Gastroenterologia
4 Post Meeting A.I.S.F. Unmet Clinical Needs in Hepatology: New and upcoming diagnostic tools" Transient elastography in chronic liver diseases of other etiologies Dr. Vincenza Calvaruso Gastroenterologia
Peri-operative challenges and long-term outcomes in liver transplantation for polycystic liver disease
 DOI:10.1111/j.1477-2574.2012.00579.x HPB ORIGINAL ARTICLE Peri-operative challenges and long-term outcomes in liver transplantation for polycystic liver disease Roberto Gedaly, Paige Guidry, Daniel Davenport,
DOI:10.1111/j.1477-2574.2012.00579.x HPB ORIGINAL ARTICLE Peri-operative challenges and long-term outcomes in liver transplantation for polycystic liver disease Roberto Gedaly, Paige Guidry, Daniel Davenport,
ORIGINAL ARTICLE Gastroenterology & Hepatology INTRODUCTION
 ORIGINAL ARTICLE Gastroenterology & Hepatology http://dx.doi.org/10.3346/jkms.2013.28.8.1207 J Korean Med Sci 2013; 28: 1207-1212 The Model for End-Stage Liver Disease Score-Based System Predicts Short
ORIGINAL ARTICLE Gastroenterology & Hepatology http://dx.doi.org/10.3346/jkms.2013.28.8.1207 J Korean Med Sci 2013; 28: 1207-1212 The Model for End-Stage Liver Disease Score-Based System Predicts Short
Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients
 Accepted Manuscript Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients George Cholankeril, MD, Andrew A. Li, MD, Brittany B. Dennis, PhD, Alice E. Toll, MS, Donghee
Accepted Manuscript Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients George Cholankeril, MD, Andrew A. Li, MD, Brittany B. Dennis, PhD, Alice E. Toll, MS, Donghee
Supplementary Digital Content
 Geissler et al: Sirolimus and Hepatocellular Carcinoma in Liver Transplantation Page 1 of 10 Supplementary Digital Content Supplementary Table 1. Surgical procedures used Total Transplant technique Piggy
Geissler et al: Sirolimus and Hepatocellular Carcinoma in Liver Transplantation Page 1 of 10 Supplementary Digital Content Supplementary Table 1. Surgical procedures used Total Transplant technique Piggy
I have no disclosures relevant to this presentation LIVER TESTS: WHAT IS INCLUDED? LIVER TESTS: HOW TO UTILIZE THEM OBJECTIVES
 LIVER TESTS: HOW TO UTILIZE THEM I have no disclosures relevant to this presentation José Franco, MD Professor of Medicine, Surgery and Pediatrics Medical College of Wisconsin OBJECTIVES Differentiate
LIVER TESTS: HOW TO UTILIZE THEM I have no disclosures relevant to this presentation José Franco, MD Professor of Medicine, Surgery and Pediatrics Medical College of Wisconsin OBJECTIVES Differentiate
Access and Outcomes Among Minority Transplant Patients, , with a Focus on Determinants of Kidney Graft Survival
 American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
American Journal of Transplantation 2010; 10 (Part 2): 1090 1107 Wiley Periodicals Inc. Special Feature No claim to original US government works Journal compilation C 2010 The American Society of Transplantation
Death in patients waiting for liver transplantation. Liver Transplant Recipient Selection: MELD vs. Clinical Judgment
 ORIGINAL ARTICLES Liver Transplant Recipient Selection: MELD vs. Clinical Judgment Michael A. Fink, 1,2 Peter W. Angus, 1 Paul J. Gow, 1 S. Roger Berry, 1,2 Bao-Zhong Wang, 1,2 Vijayaragavan Muralidharan,
ORIGINAL ARTICLES Liver Transplant Recipient Selection: MELD vs. Clinical Judgment Michael A. Fink, 1,2 Peter W. Angus, 1 Paul J. Gow, 1 S. Roger Berry, 1,2 Bao-Zhong Wang, 1,2 Vijayaragavan Muralidharan,
Screening for HCCwho,
 Screening for HCCwho, how and how often? Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital HCC Global Epidemiology
Screening for HCCwho, how and how often? Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital HCC Global Epidemiology
Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison
 ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 722-727 Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison Georgios
ORIGINAL ARTICLE Annals of Gastroenterology (2018) 31, 722-727 Liver transplantation for hepatocellular carcinoma with live donors or extended criteria donors: a propensity score-matched comparison Georgios
The New Kidney Allocation System: What You Need to Know. Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health
 The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation
 Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
The future of liver transplantation for viral hepatitis
 The future of liver transplantation for viral hepatitis François Durand Hepatology & Liver Intensive Care Hospital Beaujon, Clichy University Paris Diderot France Liver transplantation in France 2013:
The future of liver transplantation for viral hepatitis François Durand Hepatology & Liver Intensive Care Hospital Beaujon, Clichy University Paris Diderot France Liver transplantation in France 2013:
Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation
 8 Original Article Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation Neema Kaseje 1 Samuel Lüthold 2 Gilles Mentha 3 Christian Toso 3 Dominique Belli 2 Valérie McLin 2 Barbara
8 Original Article Donor Hypernatremia Influences Outcomes Following Pediatric Liver Transplantation Neema Kaseje 1 Samuel Lüthold 2 Gilles Mentha 3 Christian Toso 3 Dominique Belli 2 Valérie McLin 2 Barbara
LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES
 LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES No conflict of interest Objectives Introduction Methods Results Conclusions Objectives Introduction Methods Results Conclusions
LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES No conflict of interest Objectives Introduction Methods Results Conclusions Objectives Introduction Methods Results Conclusions
Primary sclerosing cholangitis (PSC) is a chronic
 Predicting Clinical and Economic Outcomes After Liver Transplantation Using the Mayo Primary Sclerosing Cholangitis Model and Child-Pugh Score Jayant A. Talwalkar, * Eric Seaberg, W. Ray Kim, * and Russell
Predicting Clinical and Economic Outcomes After Liver Transplantation Using the Mayo Primary Sclerosing Cholangitis Model and Child-Pugh Score Jayant A. Talwalkar, * Eric Seaberg, W. Ray Kim, * and Russell
Liver Pathology in the 0bese
 Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Effect of Body Mass Index on the Survival Benefit of Liver Transplantation
 LIVER TRANSPLANTATION 13:1678-1683, 2007 ORIGINAL ARTICLE Effect of Body Mass Index on the Survival Benefit of Liver Transplantation Shawn J. Pelletier, 1 Douglas E. Schaubel, 2,3 Guanghui Wei, 2 Michael
LIVER TRANSPLANTATION 13:1678-1683, 2007 ORIGINAL ARTICLE Effect of Body Mass Index on the Survival Benefit of Liver Transplantation Shawn J. Pelletier, 1 Douglas E. Schaubel, 2,3 Guanghui Wei, 2 Michael
Hereditary hemochromatosis, which results predominantly. Prognostic factors and survival in patients with hereditary hemochromatosis and cirrhosis
 ORIGINAL ARTICLE Prognostic factors and survival in patients with hereditary hemochromatosis and cirrhosis Melanie D Beaton MD, Paul C Adams MD MD Beaton, PC Adams. Prognostic factors and survival in patients
ORIGINAL ARTICLE Prognostic factors and survival in patients with hereditary hemochromatosis and cirrhosis Melanie D Beaton MD, Paul C Adams MD MD Beaton, PC Adams. Prognostic factors and survival in patients
Journal of the American College of Cardiology Vol. 60, No. 1, by the American College of Cardiology Foundation ISSN /$36.
 Journal of the American College of Cardiology Vol. 60, No. 1, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.02.031
Journal of the American College of Cardiology Vol. 60, No. 1, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2012.02.031
Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting?
 Rajani Sharma, PGY1 Geriatrics CRC Project, 12/19/13 Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting? A. Study Purpose and Rationale Hepatocellular carcinoma
Rajani Sharma, PGY1 Geriatrics CRC Project, 12/19/13 Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting? A. Study Purpose and Rationale Hepatocellular carcinoma
Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from Oregon Health & Science University
 Portland State University PDXScholar University Honors Theses University Honors College 2016 Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from
Portland State University PDXScholar University Honors Theses University Honors College 2016 Hepatocellular Carcinoma Recurrence After Liver Transplantation: an Analysis of Risk Factors and Incidence from
Portal Vein Thrombosis and Outcomes for Pediatric Liver Transplant Candidates and Recipients in the United States
 LIVER TRANSPLANTATION 17:1066-1072, 2011 ORIGINAL ARTICLE Portal Vein Thrombosis and Outcomes for Pediatric Liver Transplant Candidates and Recipients in the United States Seth A. Waits, 1 Brandon M. Wojcik,
LIVER TRANSPLANTATION 17:1066-1072, 2011 ORIGINAL ARTICLE Portal Vein Thrombosis and Outcomes for Pediatric Liver Transplant Candidates and Recipients in the United States Seth A. Waits, 1 Brandon M. Wojcik,
Inverse relationship between cirrhosis and massive tumours in hepatocellular carcinoma
 DOI:10.1111/j.1477-2574.2012.00507.x HPB ORIGINAL ARTICLE Inverse relationship between cirrhosis and massive tumours in hepatocellular carcinoma Umut Sarpel 1, Diego Ayo 2, Iryna Lobach 3, Ruliang Xu 4
DOI:10.1111/j.1477-2574.2012.00507.x HPB ORIGINAL ARTICLE Inverse relationship between cirrhosis and massive tumours in hepatocellular carcinoma Umut Sarpel 1, Diego Ayo 2, Iryna Lobach 3, Ruliang Xu 4
Overall Goals and Objectives for Transplant Hepatology EPAs:
 Overall Goals and Objectives for Transplant Hepatology EPAs: 1. DIAGNOSTIC LIST During the one-year Advanced Pediatric Transplant Hepatology Program, fellows are expected to develop comprehensive skills
Overall Goals and Objectives for Transplant Hepatology EPAs: 1. DIAGNOSTIC LIST During the one-year Advanced Pediatric Transplant Hepatology Program, fellows are expected to develop comprehensive skills
Kidney Transplant in the Elderly. Robert Santella, M.D., F.A.C.P.
 Kidney Transplant in the Elderly! Robert Santella, M.D., F.A.C.P. Incident Rate of ESRD by Age Age 75+ 65-74 From US Renal Data System, 2012 Should there be an age limit? Various guidelines: Canadian,
Kidney Transplant in the Elderly! Robert Santella, M.D., F.A.C.P. Incident Rate of ESRD by Age Age 75+ 65-74 From US Renal Data System, 2012 Should there be an age limit? Various guidelines: Canadian,
The Effect of Liver Transplantation on Autonomic Dysfunction in Patients with End-Stage Liver Disease
 LIVER TRANSPLANTATION 14:235-239, 2008 ORIGINAL ARTICLE The Effect of Liver Transplantation on Autonomic Dysfunction in Patients with End-Stage Liver Disease Elizabeth J. Carey, Manjushree Gautam, 3 Timothy
LIVER TRANSPLANTATION 14:235-239, 2008 ORIGINAL ARTICLE The Effect of Liver Transplantation on Autonomic Dysfunction in Patients with End-Stage Liver Disease Elizabeth J. Carey, Manjushree Gautam, 3 Timothy
Developing a Kidney Waiting List Calculator
 Developing a Kidney Waiting List Calculator Jon J. Snyder, PhD* Nicholas Salkowski, PhD, Jiannong Liu, PhD, Kenneth Lamb, PhD, Bryn Thompson, MPH, Ajay Israni, MD, MS, and Bertram Kasiske, MD, FACP *Presenter
Developing a Kidney Waiting List Calculator Jon J. Snyder, PhD* Nicholas Salkowski, PhD, Jiannong Liu, PhD, Kenneth Lamb, PhD, Bryn Thompson, MPH, Ajay Israni, MD, MS, and Bertram Kasiske, MD, FACP *Presenter
Hepatitis After Liver Transplantation: The Role of the Known and Unknown Viruses
 Hepatitis After Liver Transplantation: The Role of the Known and Unknown Viruses Mario G. Pessoa,*00 Norah A. Terrault,*00 Linda D. Ferrell, Jill Detmer, Janice Kolberg, Mark L. Collins, Maurene Viele,
Hepatitis After Liver Transplantation: The Role of the Known and Unknown Viruses Mario G. Pessoa,*00 Norah A. Terrault,*00 Linda D. Ferrell, Jill Detmer, Janice Kolberg, Mark L. Collins, Maurene Viele,
THE MODEL FOR END-STAGE
 ORIGINAL CONTRIBUTION Disparities in Liver Transplantation Before and After Introduction of the MELD Score Cynthia A. Moylan, MD Carla W. Brady, MD, MHS Jeffrey L. Johnson, MS Alastair D. Smith, MB, ChB
ORIGINAL CONTRIBUTION Disparities in Liver Transplantation Before and After Introduction of the MELD Score Cynthia A. Moylan, MD Carla W. Brady, MD, MHS Jeffrey L. Johnson, MS Alastair D. Smith, MB, ChB
Chronic liver failure Assessment for liver transplantation
 Chronic liver failure Assessment for liver transplantation Liver Transplantation Dealing with the organ shortage Timing of listing must reflect length on waiting list Ethical issues Justice, equity, utility
Chronic liver failure Assessment for liver transplantation Liver Transplantation Dealing with the organ shortage Timing of listing must reflect length on waiting list Ethical issues Justice, equity, utility
Type of intervention Other: transplantation. Economic study type Cost-utility analysis.
 Midterm cost-effectiveness of the liver transplantation program of England and Wales for three disease groups Longworth L, Young T, Buxton M J, Ratcliffe J, Neuberger J, Burroughs A, Bryan S Record Status
Midterm cost-effectiveness of the liver transplantation program of England and Wales for three disease groups Longworth L, Young T, Buxton M J, Ratcliffe J, Neuberger J, Burroughs A, Bryan S Record Status
Evaluation Process for Liver Transplant Candidates
 Evaluation Process for Liver Transplant Candidates 2 Objectives Identify components of the liver transplant referral to evaluation Describe the role of the liver transplant coordinator Describe selection
Evaluation Process for Liver Transplant Candidates 2 Objectives Identify components of the liver transplant referral to evaluation Describe the role of the liver transplant coordinator Describe selection
HPB ORIGINAL ARTICLE. Abstract. Correspondence. Introduction
 http://dx.doi.org/10.1016/j.hpb.2015.10.001 HPB ORIGINAL ARTICLE Long-term outcome of patients undergoing liver transplantation for mixed hepatocellular carcinoma and cholangiocarcinoma: an analysis of
http://dx.doi.org/10.1016/j.hpb.2015.10.001 HPB ORIGINAL ARTICLE Long-term outcome of patients undergoing liver transplantation for mixed hepatocellular carcinoma and cholangiocarcinoma: an analysis of
Peritransplant Pancreatitis: A Marker of High Mortality and Graft Failure in Liver Transplant Patients
 ORIGINAL ARTICLE RUSSELL ET AL. Peritransplant Pancreatitis: A Marker of High Mortality and Graft Failure in Liver Transplant Patients Tara A. Russell, 1 Sarah Park, 2 Vatche G. Agopian, 3 Ali Zarrinpar,
ORIGINAL ARTICLE RUSSELL ET AL. Peritransplant Pancreatitis: A Marker of High Mortality and Graft Failure in Liver Transplant Patients Tara A. Russell, 1 Sarah Park, 2 Vatche G. Agopian, 3 Ali Zarrinpar,
Recurrence of hepatitis C virus (HCV) after orthotopic. Poor Survival After Liver Retransplantation: Is Hepatitis C to Blame?
 RAPID COMMUNICATION Poor Survival After Liver Retransplantation: Is Hepatitis C to Blame? Kymberly D.S. Watt, Elizabeth R. Lyden, and Timothy M. McCashland Data from 1990 to 1996 suggest that the prevalence
RAPID COMMUNICATION Poor Survival After Liver Retransplantation: Is Hepatitis C to Blame? Kymberly D.S. Watt, Elizabeth R. Lyden, and Timothy M. McCashland Data from 1990 to 1996 suggest that the prevalence
Readmission to the hospital after discharge is an important
 Defining Readmission Risk Factors for Liver Transplantation Recipients Neil Shankar, Paul Marotta, MD, William Wall, MD, Mamoun AlBasheer, MD, Roberto Hernandez-Alejandro, MD, and Natasha Chandok, MD,
Defining Readmission Risk Factors for Liver Transplantation Recipients Neil Shankar, Paul Marotta, MD, William Wall, MD, Mamoun AlBasheer, MD, Roberto Hernandez-Alejandro, MD, and Natasha Chandok, MD,
Ammonia level at admission predicts in-hospital mortality for patients with alcoholic hepatitis
 Gastroenterology Report, 5(3), 2017, 232 236 doi: 10.1093/gastro/gow010 Advance Access Publication Date: 1 May 2016 Original article ORIGINAL ARTICLE Ammonia level at admission predicts in-hospital mortality
Gastroenterology Report, 5(3), 2017, 232 236 doi: 10.1093/gastro/gow010 Advance Access Publication Date: 1 May 2016 Original article ORIGINAL ARTICLE Ammonia level at admission predicts in-hospital mortality
The transplant benefit score and the national liver offering scheme
 The transplant benefit score and the national liver offering scheme New national offering scheme The development of a national set of rules to offer livers to named adult patients on the elective liver
The transplant benefit score and the national liver offering scheme New national offering scheme The development of a national set of rules to offer livers to named adult patients on the elective liver
Professor Norbert Bräu
 Sixth Annual BHIVA Conference for the Management of HIV/Hepatitis Co-Infection in collaboration with BASL and BVHG Professor Norbert Bräu James J Peters VA Medical Center, New York, USA COMPETING INTEREST
Sixth Annual BHIVA Conference for the Management of HIV/Hepatitis Co-Infection in collaboration with BASL and BVHG Professor Norbert Bräu James J Peters VA Medical Center, New York, USA COMPETING INTEREST
CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease
 CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease Maria Isabel Fiel, M.D. The Mount Sinai Medical Center New York, New York Case A 57 yo man, 7 months
CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease Maria Isabel Fiel, M.D. The Mount Sinai Medical Center New York, New York Case A 57 yo man, 7 months
Liver Transplantation: The End of the Road in Chronic Hepatitis C Infection
 University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2012 UMass Center for Clinical and Translational Science Research Retreat
University of Massachusetts Medical School escholarship@umms UMass Center for Clinical and Translational Science Research Retreat 2012 UMass Center for Clinical and Translational Science Research Retreat
Related Policies: None
 Medical Policy MP 7.03.06 Original Policy Date: December 1995 Last Review: 09/28/2017 Effective Date: 11/15/2017 Section: Surgery End Date: Related Policies: None Disclaimer Our medical policies are designed
Medical Policy MP 7.03.06 Original Policy Date: December 1995 Last Review: 09/28/2017 Effective Date: 11/15/2017 Section: Surgery End Date: Related Policies: None Disclaimer Our medical policies are designed
Understanding Liver Disease
 Visit us on the Web at: clevelandclinic.org/liver To make an appointment call: 888.410.1775, option 1 International patients call: 001.216.444.8184 WOULD YOU LIKE A SECOND OPINION? If you would like a
Visit us on the Web at: clevelandclinic.org/liver To make an appointment call: 888.410.1775, option 1 International patients call: 001.216.444.8184 WOULD YOU LIKE A SECOND OPINION? If you would like a
ORIGINAL ARTICLE. Hung-Tien Kuo, 1,2 Erik Lum, 1 Paul Martin, 3 and Suphamai Bunnapradist ORIGINAL ARTICLE
 ORIGINAL ARTICLE Effect of Diabetes and Acute Rejection on Liver Transplant Outcomes: An Analysis of the Organ rocurement and Transplantation Network/United Network for Organ Sharing Database Hung-Tien
ORIGINAL ARTICLE Effect of Diabetes and Acute Rejection on Liver Transplant Outcomes: An Analysis of the Organ rocurement and Transplantation Network/United Network for Organ Sharing Database Hung-Tien
Retransplantation for Recurrent Hepatitis C in the MELD Era: Maximizing Utility
 Retransplantation for Recurrent Hepatitis C in the MELD Era: Maximizing Utility James R. Burton, Jr., 1,2 Amnon Sonnenberg, 1,2 and Hugo R. Rosen 1,2 Key Points 1. Retransplantation (re-lt) for hepatitis
Retransplantation for Recurrent Hepatitis C in the MELD Era: Maximizing Utility James R. Burton, Jr., 1,2 Amnon Sonnenberg, 1,2 and Hugo R. Rosen 1,2 Key Points 1. Retransplantation (re-lt) for hepatitis
Liver Transplant: Alcoholic liver disease as first indication
 Monotematica AISF The future of liver disease: beyond HCV there is a role for hepatologist? Milano, 13-15 Ottobre 2016 Liver Transplant: Alcoholic liver disease as first indication Giacomo Germani Multivisceral
Monotematica AISF The future of liver disease: beyond HCV there is a role for hepatologist? Milano, 13-15 Ottobre 2016 Liver Transplant: Alcoholic liver disease as first indication Giacomo Germani Multivisceral
NONALCOHOLIC FATTY LIVER DISEASE. Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD. April 13, 2012
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
