Reduced telaprevir dosing in combination therapy for patients with chronic hepatitis C
|
|
|
- James Daniels
- 5 years ago
- Views:
Transcription
1 Original Contribution Kitasato Med J 2017; 47: 1-9 Reduced telaprevir dosing in combination therapy for patients with chronic hepatitis C Wataru Ando, 1 Yumi Fukunaga, 1 Hiroaki Yokomori, 2 Takako Komiyama 1 1 Department of Clinical Pharmacy, Center for Clinical Pharmacy and Sciences, School of Pharmacy, Kitasato University, Tokyo 2 Department of General Medicine, Kitasato University Medical Center, Saitama Background: Telaprevir (TVR) is used for chronic hepatitis C (CHC) treatment and is reported to be effective in maintaining higher rates of sustained virological response (SVR) than conventional therapy (CT) using peginterferon alpha-2b (PEG-IFN) and ribavirin (RBV). However, TVR has serious side effects. Therefore, we proposed the use of a moderate TVR dose and evaluated treatment completion and SVR. Methods: CHC patients were divided into a PEG-IFN and RBV group (the CT group, n = 82) and a PEG-IFN, RBV and TVR group (the TVR group, n = 28). The TVR group was comprised of a lowdose group (1,000 mg/day) and a moderate-dose group (1,500 mg/day). The safety and efficacy were compared among these groups. Results: The treatment completion rate was 78.6% (22/28) in the TVR group and 59.8% (49/82) in the CT group (odds ratio [OR]: 2.47, 95% confidence interval [CI]: , P = 0.108). The SVR rate was 60.7% (17/28) in the TVR group and 27% (22/82) in the CT group (OR: 4.15, 95% CI: , P = 0.002). The SVR rate was 80.0% (12/15) in the moderate-dose group and 38.4% (5/13) in the low-dose group (OR: 6.40, 95% CI: , P = 0.031). Conclusion: Moderate TVR doses improved the treatment completion rates and led to a high SVR. Key words: Hepatitis C, peginterferon, ribavirin, telaprevir, anemia Background hronic Hepatitis C (CHC) causes a variety of liver C damage, leading to the development of liver cirrhosis and hepatocellular carcinoma. 1 CHC treatment should be considered from the interrelation of patients' reaction to hepatitis C virus (HCV) therapy and HCV genotype. Telaprevir (TVR) is an inhibitor of HCV NS3/ 4A serine protease 2 and is administered with peginterferon alpha-2b (PEG-IFN) and ribavirin (RBV). High sustained viral response (SVR) has been reported with TVR use 3,4 ; however, side effects, such as rash (38% 39%) and hemoglobin level (Hb) decrease (91.3% 100%), are observed with a high frequency. 3,4 Simeprevir (SMV), a NS3/4A protease inhibitor, is a next generation of TVR and is currently used worldwide. However, although response rates are similar between combination therapy of PEG-IFN, RBV, and SMV and combination therapy of PEG-IFN, RBV, and TVR, side effects are less frequent with SMV use than those with TVR. 5 Recently, we had an opportunity to treat CHC patients with TVR and conventional therapy of PEG-IFN and RBV. Therefore, we proposed the use of a moderate TVR dose to decrease side effects, increase treatment completion rates, and improve SVR rates. This study aimed to evaluate the efficacy and safety of moderate TVR doses in combination therapy for CHC patients. Materials and Methods Study design This interventional study was conducted at Kitasato University Medical Center (Kitamoto, Saitama, Japan). The study protocol was approved by Ethical Committee Received 6 July 2016, accepted 2 September 2016 Correspondence to: Wataru Ando, Department of Clinical Pharmacy, Center for Clinical Pharmacy and Sciences, School of Pharmacy, Kitasato University Shirokane, Minato-ku, Tokyo , Japan andow@pharm.kitasato-u.ac.jp 1
2 Ando W. et al. of Kitasato University Medical Center before initiation. The study adheres to the Declaration of Helsinki. The following genetic analyses were conducted in patients in the TVR group following the receipt of written informed consent: IL-28B (rs , rs , and rs ) and ITPA (94C>A, rs ). All of the patients who started PEG-IFN and RBV between April 1, 2000 and March 31, 2011, or PEG-IFN, RBV, and TVR between June 1, 2012 and December 31, 2012 were enrolled in this study. The enrolled CHC patients were divided into two groups: patients treated with two conventional drugs, PEG-IFN and RBV (CT group) and patients treated with three dugs, PEG-IFN, RBV, and TVR (TVR group). Patients in the CT group were treated with a standard regimen comprised of PEG-IFN and RBV for 48 weeks. Patients in the TVR group were treated with a triple regimen, PEG-IFN, RBV, and TVR for the first 12 weeks followed by PEG-IFN and RBV for the next 12 weeks. Both groups received weekly doses of 1.5μg/kg PEG- IFN and 600, 800, and 1,000 mg/day RBV for patients with body weights of <60 kg, kg, and >80 kg, respectively. In this study, a reduced dose of TVR was administered, although the Guideline or the Treatment of CHC issued by the Japan Society of Hepatology 6 recommended a TVR dose of 2,250 mg/day. The TVR group was further divided into a low-tvr dose group (Low-TVR group; 1,000 mg/day TVR) and a moderate- TVR dose group (Mod-TVR group; 1,500 mg/day TVR). The Low-TVR group included only female patients, and the physician determined that the patients would not tolerate with adverse effects induced Mod-TVR dose. Mod-TVR dose was used for the other patients. Treatment stop was set when severe adverse event appeared, the will of the patient, or the physician's decision. The safety and efficacy of treatment regimens were compared between groups. Antiviral effects were evaluated at enrollment, after 12 weeks treatment, at end of treatment, 12 weeks after end of treatment. SVR to treatment was evaluated 24 weeks after end of treatment. The exclusion criteria included infection of hepatitis B virus or human immunodeficiency virus, hepatocellular carcinoma, determined unsuitable for treatment by physician. Relapse was defined as one instance of undetectable HCV virus levels following treatment with PEG-IFN and/or RBV prior to relapse within 6 months of treatment completion. Non-response was defined as persistently detectable HCV virus levels by PCR even if levels had decreased following treatment with PEG-IFN and/or RBV. Table 1. Baseline patients' characteristics in the TVR and CT groups CT group TVR group n = 82 n = 28 P value Sex (men/women) 34/48 9/ Age (years) 63 (30 75) 63 (24 74) 0.11 Weight (kg) 57 (48 84) 54 (44 84) 0.16 WBC (cells/mm 3 ) 4,300 (2,200 9,300) 4,800 (2,500 8,400) 0.75 Plt (10 4 /mm 3 ) 14.9 ( ) 13.7 ( ) 0.32 Hb (g/dl) 13.6 ( ) 13.0 ( ) 0.06 AST (IU/l) 44 (17 414) 41 (22 138) 0.96 ALT (IU/l) 46 (13 629) 45 (17 133) 0.50 γgtp (IU/l) 33 (10 284) 30 (14 69) 0.16 HCV genotype (1/2) 62/20 28/0 HCV RNA (log10 IU/ml) 6.5 ( ) 6.6 ( ) 0.08 IL28B rs (TT/TG/GG/UK) 16/10/0/2 IL28B rs (CC/CT/TT/UK) 15/11/0/2 IL28B rs (CC/CA/AA/UK) 15/11/0/2 ITPA rs (CC/CC+AA/AA) 59/23/0 21/6/ PEG-IFN dose (μg/week) 70 (50 100) 60 (30 100) <0.01 RBV dose (mg/day) 600 ( ) 400 ( ) 0.03 ALT, alanine aminotransferase; AST, aspartate transaminase; γgtp, g-glutamyltransferase; Hb, hemoglobin level; HCV, hepatitis virus C; IL-28B, interlukin 28B; ITPA, inosine triphosphatase; PEG- IFN, pegylated interferon; Plt, platelets; RBV, ribavirin; Std, standard TVR dose; UK, unknown; WBC, white blood cells. Age, weight, WBC, Plt, Hb, AST, ALT, γgtp, HCV RNA, PEG-IFN dose, RBV dose; median (range) 2
3 Reduced telaprevir for chronic hepatitis C Patients The CT and TVR groups comprised 82 patients (34 men, and 48 women, mean age 63 [range 30 75] years) and 28 patients (9 men, 19 women, median age 63 [range 24 74] years), respectively (Table 1). Of the 82 patients in the CT group, 9 had previously relapsed, 7 were previous non-responders, and 57 were treatment-naïve, whereas the remaining 9 had interrupted previous treatments. Of the 28 patients in the TVR group, 14 had previously relapsed, 13 were previous non-responders, and 1 was treatment-naive. The Low TVR groups comprised 13 patients (no men, and 13 women, median age 60 [range 24 71] years) and the Mod TVR group was 15 patients (9 men, 6 women, median age 64 [range 27 74] years). The median PEG-IFN dose in the TVR group was less than in the CT group (60μg/week vs. 70μg/week, P < 0.01). The median RBV dose in the TVR group was less than in the CT group (400 mg/day vs. 600 mg/day, P = 0.03). Laboratory data No difference in WBC or platelet counts was observed between the groups. However, there was a trend toward lower Hb in the TVR group compared with the CT group (13.0 mg/dl vs mg/dl, P = 0.06). No significant difference in Hb was observed between the Mod TVR group and the Low TVR group (Table 2). No significant difference in serum AST, ALT, and γgtp levels were observed between the CT and TVR groups (Table 2). Serum creatinine levels were significantly higher in the Mod TVR group than in the Low TVR group, most likely because of the substantially higher proportion of women in the Low TVR group (Table 2). Analysis of gene polymorphisms contribute to the antiviral effect and side effects IL-28B is an immune response gene involved in antiviral effect during HCV therapy. 7 Major alleles of IL-28B are reported to be associated with greater antiviral effect Table 2. Baseline characteristics in groups according to Mod or Low TVR dose TVR group Mod Low n = 15 n = 13 P value Sex (men/women) 9/6 0/13 <0.01 Age (years) 64 (27 74) 60 (24 71) 0.36 Weight (kg) 59 (53 84) 51 (44 60) 0.03 WBC (cells/mm 3 ) 4,900 (2,700 6,900) 4,500 (2,500 8,400) 0.62 Hb (g/dl) 13.1 ( ) 12.7 ( ) 0.47 Plt (10 4 /mm 3 ) 13.5 ( ) 13.9 ( ) 0.93 ALT (IU/l) 50.5 (24 92) 36 (17 133) 0.79 γgtp (IU/l) 34 (23 69) 29 (14 43) 0.41 Creatinine (g/dl) 0.78 ( ) 0.57 ( ) <0.01 egfr (ml/min) 69.9 (53 109) 76.5 ( ) 0.39 HCV RNA (log10 IU/ml) 6.7 ( ) 6.5 ( ) 0.83 IL28B rs (TT/TG/GG/UK) 6/7/0/2 10/3/0/ IL28B rs (CC/CT/TT/UK) 6/7/0/2 9/4/0/ IL28B rs (CC/CA/AA/UK) 6/7/0/2 9/4/0/ ITPA rs (CC/CC+AA/AA) 10/4/1 11/2/ PEG-IFN dose (μg/week) 70 (35 100) 60 (30 80) <0.01 RBV dose (mg/day) 600 ( ) 400 ( ) <0.01 History of IFN-based therapy (n) Initial therapy Retreatment Previous virological response Non-response Relapse ALT, alanine aminotransferase; AST, aspartate transaminase; egfr, estimated glomerular filtration rate; γgtp, g-glutamyltransferase; Hb, hemoglobin level; IL-28B, interleukin 28B; IFN, interferon; ITPA, inosine triphosphatase; Mod, moderate; PEG, pegylated; Plt, platelets; RBV, ribavirin; UK, unknown; WBC, white blood cells Age, weight, WBC, Hb, Plt, ALT, γgtp, creatinine, egfr, HCV RNA, PEG-IFN dose, RBV dose; median (range) 3
4 Ando W. et al. during HCV therapy than hetero or minor alleles. Polymorphisms of the ITPA gene are reportedly associated with decreased Hb in response to RBV 8 with ITPA CC genotype (wild type) found to be associated with greater decreases in Hb than CA genotype (heterotype). In patients of the CT group, only the ITPA genotype was examined; IL-28B was not examined. IL- 28B genotypes were determined using a DNA direct sequencing method (LSI Medience Co., Tokyo). ITPA genotypes were determined using a StepOne TM Real Time PCR system (Applied Biosystems, CA, USA) and Taqman SNP Genotyping Assays (Applied Biosystems). Experimental procedures were conducted according to industry protocols. Statistical analyses Statistical analyses were conducted using SPSS statistics 19 (IBM SPSS Inc., Chicago, IL, USA). Baseline continuous data are expressed as median (first-third quartiles) or mean (±standard deviation); categorical variables are reported as frequencies and percentages. Contentious variables between groups were compared by student's t-test, Mann-Whitney U-test, or Odds ratio, confidence limits by Fisher's exact test. P-values <0.05 were considered statistically significant in all analyses. Results Treatment completion and discontinuation between TVRreduced and PEG-IFN plus RBV group The treatment completion rate was 82.1% (23/28) in the TVR group and 59.8% (49/82) in the CT group (odds ratio [OR]: 3.10, 95% CI: , P = 0.039). In the CT group, 73.7% (42/57) of treatment naïve, 28.0% (7/ 25) of re-treated, and 55.6% (5/9) of relapsed patients completed therapy. The treatment completion rate of treatment-naïve patients was higher than re-treated patients (OR: 2.63, 95% CI: , P < 0.001). No previous non-responders completed therapy. Treatment completion rates in the Mod TVR and Low TVR groups were 87.5% (14/15) and 68.2% (9/13), respectively (OR: 6.22, 95% CI: , P = 0.153). All 9 relapsed patients in the Mod TVR group completed therapy and 83% (5/6) of relapsed patients in the Low TVR group completed therapy. Treatment completion rates among non-responders in the Mod TVR and Low TVR groups were 83% (5/6) and 50% (3/6), respectively (OR: 5.00, 95% CI: , P = 0.4). The rate of treatment completion trended to be higher in relapsed patients and non-responders in the Mod TVR group than those in the Low TVR group. Treatment discontinuation was defined to interrupt the medication of TVR and/or PEG-IFN plus RBV because of adverse events. Treatment discontinuation occurred in 40% (33/82) and 18% (5/28) patients in the CT and TVR groups. Treatment discontinuations in CT group were due to non-response (no decrease in HCV RNA levels during the treatment period, n = 6), liver cancer (n = 3), retinal bleeding (n = 2), breakthrough (increased HCV RNA levels following initially reduced levels, n = 2), thyroid dysfunction (n = 2), anemia (n = 1), reported visual disturbance (n = 1), facial nerve paralysis (n = 1), depression (n = 1), loss of consciousness (n = 1), gait disturbance (n = 1), otitis media (n = 1), ascites (n = Table 3. Efficacy of antiviral effect in relapsed and non-responsive patients between the TVR and CT groups CT group TVR group Treatment or Response Mod Low Relapsed Non-Responder Relapsed Non-Responder Initial n (%) n = 82 n = 9 n = 6 n = 6 n = 6 n = 1 Completed treatment 49 (60) 9 (100) 5 (83) 5 (83) 3 (50) 1 Discontinuation of treatment 33 (40) 0 (0) 1 (17) 1 (17) 3 (50) 0 RVR 12 (15) 9 (100) 3 (50) 5 (83) 5 (83) 1 ETR 37 (45) 9 (100) 5 (83) 5 (83) 5 (83) 1 SVR 22 (27) 9 (100) 3 (50) 2 (33) 2 (33) 1 Relapse 26 (32) 0 (0) 1 (17) 1 (17) 3 (50) 0 Non-response 16 (20) 0 (0) 0 (0) 0 (0) 0 (0) 0 VBT 1 (1) 0 (0) 1 (17) 1 (17) 0 (0) 0 RVR, rapid virological response; ETR, end of therapy response; SVR, sustained virological response; VBT, virological breakthrough 4
5 Reduced telaprevir for chronic hepatitis C 1), left subdural hematoma (1), and unknown (n = 5). In the TVR group, treatment discontinuations were due to retinal bleeding (n = 2), severe skin rash (n = 1), psychiatric symptoms (n = 1), and unknown infection disease (n = 1). Comparison of virological response among the groups The SVR rate of the TVR group (60.7%, 17/28) was higher than that in the CT group (27%, 22/82) (OR: 4.15, 95% CI: , P = 0.002). The SVR rate in treatment-naive patients in the CT group was 36.8% (21/ 57) and no relapsed patients or non-responders in the CT group completed therapy. The SVR rate was 80.0% (12/15) and 38.4% (5/13) in the Mod TVR and the Low TVR groups, respectively (OR: 6.40, 95% CI: , P = 0.031) (Table 3). The SVR rate was 73% (11/15) and 42% (5/12) among all relapsed patients and non-responders, respectively (OR: 3.85, 95% CI: , P = 0.13). Among relapsed patients, SVR was observed 100% (9/9) and 33% (2/3) in the Mod TVR and the Low TVR groups, respectively (OR: 1.5, 95% CI: , P = 0.25). Among non-responders, SVR was observed 50% (3/6) and 33% (2/6) in the Mod TVR and the Low TVR groups, respectively (OR: 2.0, 95% CI: , P = 1). The TVR group acquired a higher SVR rate than did the CT group. The Mod TVR group acquired a higher SVR rate than did the Low TVR group. Moreover, the relapsed patients had a higher SVR rate than did the nonresponders in each TVR dose group. No significant difference in SVR rates was observed between patients homozygous for the major IL-28B allele (12/16; 75.0%) and heterozygous (4/10; 40.0%) in the TVR group (OR: 4.5, 95% CI: , P = 0.19). In the Mod TVR group, SVR rates were 100% (6/6) in patients with major IL-28B alleles, and 57.1% (4/7) in heterozygous patients (OR: 5.6, 95% CI: , P = 0.29). In the Low TVR group, the SVR rate in patients homozygous for IL-28B major alleles was 60.0% (6/10); no patients with heterozygous genotypes had a SVR (OR: 9.4, 95% CI: , P = 0.29). There was a trend towards higher SVR rates in relapsed patients homozygous for IL-28B than in relapsed patients heterozygous for IL-28B alleles in both the Mod TVR and the Low TVR groups. Hemoglobin levels in the TVR-reduced and PEG-IFN plus RBV groups in relation to ITPA genotypes Adverse events are shown in Table 4. The most frequent adverse event was anemia. Anemia was observed 14/15 (93.3%) in the Mod TVR group and 13/13 (100%) in the Low TVR group. The baseline of Hb in the TVR group was 13.0 ± 1.3 g/dl and that in the CT group was 13.5 ± 1.2 g/dl. Hb levels after 12 weeks of treatment in the TVR group were significantly lower than those in the CT group (9.9 ± 1.9 g/dl vs ± 1.0 g/dl, P = 0.02). Table 4. Adverse events in CT and TVR groups CT group TVR group Mod Low Total (Mod and Low) n (%) n = 82 n = 15 n = 13 n = 28 Anemia 81 (98.6) 14 (93.3) 13 (100.0) 27 (96.4) Injection site erythema 58 (71.1) 11 (73.3) 12 (92.3) 23 (82.1) Decreased platelet count 52 (63.4) 9 (60.0) 9 (69.2) 18 (64.3) Increased serum uric acid N/A 14 (93.3) 9 (69.2) 23 (82.1) Pruritus 29 (35.4) 6 (40.0) 9 (69.2) 15 (53.6) Rash 9 (11.0) 7 (46.7) 2 (15.4) 9 (32.1) Decreased WBC count 54 (65.9) 7 (46.7) 7 (53.8) 14 (50.0) Fatigue or malaise 31 (37.8) 6 (40.0) 6 (46.2) 12 (42.9) Fever 7 (5.1) 13 (86.7) 5 (38.5) 18 (64.3) Increased serum creatine 13 (15.9) 12 (80.0) 5 (38.5) 17 (60.7) Headache 26 (31.7) 1 (6.7) 5 (38.5) 6 (21.4) Anorexia 38 (27.1) 9 (60.0) 2 (15.4) 11 (39.3) Nausea 19 (13.6) 4 (26.7) 4 (30.8) 8 (28.6) Alopecia 18 (22.0) 3 (20.0) 1 (7.7) 4 (14.3) Dysgeusia 7 (5.1) 1 (6.7) 4 (30.8) 5 (17.9) Nasopharyngitis 5 (6.1) 1 (6.7) 2 (15.4) 3 (10.7) Vomiting 10 (6.8) 1 (6.7) 2 (15.4) 3 (10.7) 5
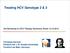
6 Ando W. et al. Figure 1. Comparison of hemoglobin levels according to hemoglobin level at initiation and ITPA genotype between the TVR and the CT groups (A) Hb 13 g/dl, (B) <13 g/dl at initiation of therapy, (C) TVR group and (D) CT group. Hb in patients with wild-type ITPA were significantly decreased compared to patients with mutant ITPA genotypes. Similar results were observed in both TVR and CT groups. (E) ITPA wild type and (F) ITPA mutant type showed Hb decline levels in the Low and the Mod TVR group. Hb levels were calculated by subtracting values at each point (2, 4, 6, 8, 12 weeks, end of treatment (EOT), and 12 weeks after EOT) from values at treatment initiation. Statistical analyses were performed for each point. Symbols and bars represent mean values ± standard deviations, respectively. Hb, hemoglobin level; ITPA, inosine triphosphate. *P < 0.05, **P <
7 Reduced telaprevir for chronic hepatitis C When patients were divided into 2 groups according to Hb at the initiation of therapy of greater or less than 13 g/ dl, a significantly higher incidence of decreased Hb was observed in patients in the TVR group with Hb of <13 g/ dl at treatment initiation (Figures 1A, 1B). Decreased Hb in the TVR group were clearly observed from the second week of treatment to the 12th week, whereas decreases in the CT group were maintained until treatment completion. In both the TVR and the CT groups, Hb levels in patients with wild-type ITPA genotypes were significantly lower than those in patients with mutant ITPA genotypes (Figures 1C, 1D). Despite no difference in RBV doses between patients with wild-type and mutant ITPA genotypes, Hb levels were significantly lower in patients with the wild-type genotypes during the early stage of treatment. In patients with wild-type ITPA genotypes, Hb levels were lower in the TVR group than those in the CT group. The Mod TVR group acquired a greater Hb decline than did the Low TVR group regardless of whether the ITPA genotype was the wild or the mutant type (Figures 1E, 1F). Discussion TVR efficacy that has been demonstrated in numerous clinical trials and clinical studies and suggest reduced TVR doses may be effective (Table 5). The moderate TVR dose in the present study and the standard TVR dose in those reference were almost the same rates of SVR. A SVR rate of 36.8% in treatment-naïve patients treated with PEG-IFN and RBV was used as the baseline treatment response in the present study. The addition of TVR to treatment regimens was found to increase SVR rates in previously relapsed and non-responsive HCV patients in the Mod TVR group (80%). The result of previous treatment using PEG-IFN and RBV affected SVR rates in each TVR group. The relapsed patients were expected to achieve higher SVR rates than the nonresponders. Moreover, in this study, IL-28B polymorphisms were found to influence SVR in the TVR group. The Low TVR dose selected for the patients who would not tolerate adverse effects induced Mod TVR dose, as a result, all Low TVR group patients were women with a relatively low body weight. And patients who achieved SVR in the Low TVR group had a tendency of IL-28B major alleles. Therefore, when selecting the TVR dose, it was important to lead a good SVR by considering patients gender, body weight, IL-28B polymorphism, past history of interferon therapy, and tolerance to adverse effects. IL-28B is a cytokine that belongs to the IFNλ family. When IFNλ bound to a complex of IFNλ receptor 1 (R1) and the IL10 receptor 2 (R2), IFNλ activates the STAT1/STAT2 through the Janus kinase (JAK) 1 and tyrosine kinase (TYK) 2, finally by promoting the expression of Interferon-simulated gene, it is considered to induce anti-viral activity. 9 Besides IL- 28B gene polymorphisms, an as yet undiscovered critical mechanism underlying host virus elimination capacity is expected to be present. 10 Treatment completion rates in the CT and the TVR groups were 59.8% and 82.1%, respectively. Thus, the addition of TVR demonstrated efficacy improving the treatment success rates. This effect may have been because of the shortened treatment duration. 11 Hayashi et al. 12 reported the results of Phase III clinical trial in Japan evaluating the use of a PEG-IFN, RBV, and the standard dose of TVR (2,250 mg/day) regimen for the re-treatment of Japanese HCV-infected patients. This reference showed the SVR rate in relapse patients was 88% (96/109) and that in non-responders was 34% (11/ 32). Treatment discontinuation due to side effects in the Table 5. Summary of treatment completion and SVR rates following PEG-IFN, RBV, and TVR treatment in patients with HCV genotype 1b in Japan TVR dose Number of Treatment Author Year Sex (M/F) Age (years) SVR (%) (mg) patients completion (%) Kumada H, et al , / (20 65) 79% 73% Furusyo N, et al , / (61 73)* (25 60)* 2 86% 80% Sezaki H, et al , /30 60 (53 63) 92% 83% 1, /30 62 (56 64) 98% 93% Oze T, et al , / ± % 85% 1, / ± % 85% * 1 Patient aged over 60 years, * 2 patient aged less than 59 years 7
8 Ando W. et al. clinical trial were anemia (9.9%, 14/141), severe skin rash (2.8%, 4/141), and death possibly related to pulmonary embolism (0.7%, 1/141), among others (2.8%, 4/141). Treatment discontinuation due to side effects was less frequent in the Mod TVR and the Low TVR groups than in the clinical trial. The side effects including anemia (90.8%) and rash (39%) were a similar rate between reduced dose of TVR and the clinical trial. It was considered that the SVR rates of the Mod group and those of the standard TVR regimen were not significantly different. However, the baselines of patients, dose protocol and discontinuation criteria of this clinical trial were not significant in the present study. As described above, SVR rates with SMV therapy are typically higher in relapsed patients than those in previous non-responders. Protease inhibitors were hoped to represent an efficacious treatment option in patients infected with difficult-to-treat HCV genotypes, particularly given the predominance of HCV genotype 1b in Japanese patients. Protease inhibitors should be considered in previously non-responsive patients with genotype 1b and expectations for antiviral efficacy on re-treatment. A high incidence of RBV-induced anemia has been reported during PEG-IFN and RBV-based therapies. Modification of RBV dosing according to the patient's body weight is important for the prevention of anemia. The next approach to prevent anemia is to examine ITPA genotype because the wild type is known to be associated with anemia during RBV administration. 7 Although the TVR group had greater decreases in Hb than in the CT group, Hb recovered to comparable levels after 12 weeks treatment. Since the duration of TVR administration was 12 weeks, it was suggested that TVR had enhanced the RBV-induced Hb decrease. However, we demonstrated that the discontinuation of TVR group was only one patient because TVR dose was moderate or low. Such low rate of discontinuation has not been reported. TVR is currently applicable only for the re-treatment of genotype 2 HCV as Japanese guidelines; however, trade in this will continue, although it may soon disappear from Japanese market in the future. Because TVR is still available in Japan and some other countries, the results of this study has the potential to be useful for the new combination anti-viral therapy in future and for patients unable to receive the latest treatment for various reasons such as drug allergy, TVR can be selected for treatment. It has to clarify the relationship between dose adjustment and safety. Conclusion Moderate TVR dose contributed to improve the achievement of treatment by reducing the incidence of adverse side effects and to lead to a high SVR. Author contributions WA contributed to the conception and design of this study, data analysis, drafting of this manuscript, and critically revising it for important intellectual content. YF contributed to data collection and data analysis. HY recruited patients for this study, data analysis, and critically reviewed this manuscript. TK was responsible for this research idea and contributed to the conception and design of this study. All authors reviewed the article and approved the final manuscript for submission. Acknowledgments We thank Akiko Izumisawa, and Yuna Mitsuki at Kitasato University School of Pharmacy for analysis of ITPA gene polymorphisms. References 1. Di Bisceglie AM. Hepatitis C and hepatocellular carcinoma. Hepatology 1997; 26 (3 Suppl 1): 34s- 8s. 2. McHutchison JG, Everson GT, Gordon SC, et al. Telaprevir with peginterferon and ribavirin for chronic HCV genotype 1 infection. N Engl J Med 2009; 360: Reddy KR, Zeuzem S, Zoulim F, et al. Simeprevir versus telaprevir with peginterferon and ribavirin in previous null or partial responders with chronic hepatitis C virus genotype 1 infection (ATTAIN): a randomised, double-blind, non-inferiority phase 3 trial. Lancet Infect Dis 2015; 15: Thomas DL, Thio CL, Martin MP, et al. Genetic variation in IL28B and spontaneous clearance of hepatitis C virus. Nature 2009; 461: Fellay J, Thompson AJ, Ge D, et al. ITPA gene variants protect against anaemia in patients treated for chronic hepatitis C. Nature 2010; 464: Asahina Y, Izumi N, Oketani M, et al. Treatment Guidelines of Hepatitis C. Kanzo 2012; 53: Ge D, Fellay J, Thompson AJ, et al. Genetic variation in IL28B predicts hepatitis C treatment-induced viral. Nature 2009; 461:
9 Reduced telaprevir for chronic hepatitis C 8. Muir AJ, Poordad FF, McHutchison JG, et al. Retreatment with telaprevir combination therapy in hepatitis C patients with. Hepatology 2011; 54: Ahlenstiel G, Booth DR, George J. IL28B in hepatitis C virus infection: translating pharmacogenomics into clinical practice. J Gastroenterol 2010; 45: Hayashi N, Okanoue T, Tsubouchi H, et al. Efficacy and safety of telaprevir, a new protease inhibitor, for difficult-to-treat patients with genotype 1 chronic hepatitis C. J Viral Hepat 2012; 19: e Kumada H, Toyota J, Okanoue T, et al. Telaprevir with peginterferon and ribavirin for treatment-naive patients. J Hepatol 2012; 56: Furusyo N, Ogawa E, Nakamuta M, et al. Telaprevir can be successfully and safely used to treat older patients with genotype 1b chronic hepatitis C. J Hepatol 2013; 59: Sezaki H, Suzuki F, Hosaka T, et al. Effectiveness and safety of reduced-dose telaprevir-based triple therapy in chronic hepatitis C patients. Hepatol Res 2014; 44: E Oze T, Hiramatsu N, Yakushijin T, et al. The prospective randomized study on telaprevir at 1500 or 2250 mg with pegylated interferon plus ribavirin in Japanese patients with HCV genotype 1. J Gastroenterol 2015; 50:
doi: /jvh.12162
 Journal of Viral Hepatitis, 214, 21, 341 347 doi:1.1111/jvh.12162 Telaprevir impairs renal function and increases blood ribavirin concentration during telaprevir/pegylated interferon/ribavirin therapy
Journal of Viral Hepatitis, 214, 21, 341 347 doi:1.1111/jvh.12162 Telaprevir impairs renal function and increases blood ribavirin concentration during telaprevir/pegylated interferon/ribavirin therapy
The role of triple therapy with protease inhibitors in hepatitis C virus genotype 1na «ve patients
 The role of triple therapy with protease inhibitors in hepatitis C virus genotype 1na «ve patients David R. Nelson Clinical and Translational Science Institute, University of Florida, FL, USA Liver International
The role of triple therapy with protease inhibitors in hepatitis C virus genotype 1na «ve patients David R. Nelson Clinical and Translational Science Institute, University of Florida, FL, USA Liver International
Simeprevir + PEG + RBV in Treatment-Naïve Genotype 1 QUEST-1 Trial
 Phase 3 Treatment Naïve Simeprevir + in Treatment-Naïve Genotype 1 QUEST-1 Trial Jacobson IM, et al. Lancet. 2014;384:403-13. Simeprevir + PEG + Ribavirin for Treatment-Naïve HCV GT1 QUEST-1 Trial QUEST-1
Phase 3 Treatment Naïve Simeprevir + in Treatment-Naïve Genotype 1 QUEST-1 Trial Jacobson IM, et al. Lancet. 2014;384:403-13. Simeprevir + PEG + Ribavirin for Treatment-Naïve HCV GT1 QUEST-1 Trial QUEST-1
SYNOPSIS Final Clinical Study Report for Study AI444031
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Name of Active Ingredient: () Individual Study Table Referring to the Dossier (For National Authority Use Only) SYNOPSIS for Study
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Name of Active Ingredient: () Individual Study Table Referring to the Dossier (For National Authority Use Only) SYNOPSIS for Study
Efficacy and safety of telaprevir, a new protease inhibitor, for difficult-to-treat patients with genotype 1 chronic hepatitis C
 Journal of Viral Hepatitis, 2012, 19, e134 e142 doi:10.1111/j.1365-2893.2011.01528.x Efficacy and safety of telaprevir, a new protease inhibitor, for difficult-to-treat patients with genotype 1 chronic
Journal of Viral Hepatitis, 2012, 19, e134 e142 doi:10.1111/j.1365-2893.2011.01528.x Efficacy and safety of telaprevir, a new protease inhibitor, for difficult-to-treat patients with genotype 1 chronic
Clinical Cases Hepatitis C Naïve Patients. Rafael Esteban Liver Unit. Hospital General Universitari Vall Hebron. Barcelona.
 Clinical Cases Hepatitis C Naïve Patients Rafael Esteban Liver Unit. Hospital General Universitari Vall Hebron. Barcelona. Case study 1 27 year old woman, Diagnosed with Chronic Hepatitis C 3 years ago
Clinical Cases Hepatitis C Naïve Patients Rafael Esteban Liver Unit. Hospital General Universitari Vall Hebron. Barcelona. Case study 1 27 year old woman, Diagnosed with Chronic Hepatitis C 3 years ago
Oral combination therapy: future hepatitis C virus treatment? "Lancet Oct 30;376(9751): Oral combination therapy with a nucleoside
 Author manuscript, published in "Journal of Hepatology 2011;55(4):933-5" DOI : 10.1016/j.jhep.2011.04.018 Oral combination therapy: future hepatitis C virus treatment? Commentary article on the following
Author manuscript, published in "Journal of Hepatology 2011;55(4):933-5" DOI : 10.1016/j.jhep.2011.04.018 Oral combination therapy: future hepatitis C virus treatment? Commentary article on the following
ةي : لآا ةرقبلا ةروس
 سورة البقرة: اآلية HCV RELAPSERS AND NONRESPONDERS: How to deal with them? BY Prof. Mohamed Sharaf-Eldin Prof. of Hepatology and Gastroenterology Tanta University Achieving SVR The ability to achieve a
سورة البقرة: اآلية HCV RELAPSERS AND NONRESPONDERS: How to deal with them? BY Prof. Mohamed Sharaf-Eldin Prof. of Hepatology and Gastroenterology Tanta University Achieving SVR The ability to achieve a
Hepatitis C: Management of Previous Non-responders with First Line Protease Inhibitors
 Hepatitis C: Management of Previous Non-responders with First Line Protease Inhibitors Fred Poordad, MD The Texas Liver Institute Clinical Professor of Medicine University of Texas Health Science Center
Hepatitis C: Management of Previous Non-responders with First Line Protease Inhibitors Fred Poordad, MD The Texas Liver Institute Clinical Professor of Medicine University of Texas Health Science Center
Pegylated Interferon Alfa-2b (Peg-Intron) Plus Ribavirin (Rebetol)in the Treatment of Chronic Hepatitis C: A Local Experience
 Pegylated Interferon Alfa-2b (Peg-Intron) Plus Ribavirin (Rebetol)in the Treatment of Chronic Hepatitis C: A Local Experience E L Seow, PH Robert Ding Island Hospital, Penang, Malaysia. Introduction Hepatitis
Pegylated Interferon Alfa-2b (Peg-Intron) Plus Ribavirin (Rebetol)in the Treatment of Chronic Hepatitis C: A Local Experience E L Seow, PH Robert Ding Island Hospital, Penang, Malaysia. Introduction Hepatitis
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA DOCTORAL SCHOOL DOCTORAL THESIS
 UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA DOCTORAL SCHOOL DOCTORAL THESIS PHARMACOGENETICS AND THE APPLICATION OF SINGLE NUCLEOTIDE POLYMORPHISMS IN RESPONSE TO PEGYLATED INTERFERON AND RIBAVIRIN
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA DOCTORAL SCHOOL DOCTORAL THESIS PHARMACOGENETICS AND THE APPLICATION OF SINGLE NUCLEOTIDE POLYMORPHISMS IN RESPONSE TO PEGYLATED INTERFERON AND RIBAVIRIN
Bacterial Infection as an Adverse Effect of Telaprevir-based Triple Therapy for Chronic Hepatitis C Infection
 ORIGINAL ARTICLE Bacterial Infection as an Adverse Effect of Telaprevir-based Triple Therapy for Chronic Hepatitis C Infection Akira Kawano 1, Eiichi Ogawa 2, Norihiro Furusyo 2, Makoto Nakamuta 3, Eiji
ORIGINAL ARTICLE Bacterial Infection as an Adverse Effect of Telaprevir-based Triple Therapy for Chronic Hepatitis C Infection Akira Kawano 1, Eiichi Ogawa 2, Norihiro Furusyo 2, Makoto Nakamuta 3, Eiji
Emerging Therapies for HCV: Highlights from AASLD 2012 (Part 2)
 Emerging Therapies for HCV: Highlights from AASLD 2012 (Part 2) Goals for Hepatitis C Therapy Compared to PegIFN α/rbv, new treatment regimens for chronic hepatitis C should offer: Improved efficacy Efficacy
Emerging Therapies for HCV: Highlights from AASLD 2012 (Part 2) Goals for Hepatitis C Therapy Compared to PegIFN α/rbv, new treatment regimens for chronic hepatitis C should offer: Improved efficacy Efficacy
Ritsuzo Kozuka, Hoang Hai, Yuga Teranishi, Hiroyuki Motoyama, Etsushi Kawamura, Atsushi Hagihara, Sawako Uchida
 Correlation between polymorphism in the inosine triphosphatase and the reductions in hemoglobin concentration and ribavirin dose during sofosbuvir and ribavirin therapy Ritsuzo Kozuka, Hoang Hai, Yuga
Correlation between polymorphism in the inosine triphosphatase and the reductions in hemoglobin concentration and ribavirin dose during sofosbuvir and ribavirin therapy Ritsuzo Kozuka, Hoang Hai, Yuga
CASE STUDY. Adverse Events in treatment chronic hepatitis C patients with PegInterferon and Ribavirin What would your management decision be?
 Adverse Events in treatment chronic hepatitis C patients with PegInterferon and Ribavirin What would your management decision be? CASE STUDY Pham Thi Thu Thuy MD, PhD Ho Chi Minh City Vietnam Serious Adverse
Adverse Events in treatment chronic hepatitis C patients with PegInterferon and Ribavirin What would your management decision be? CASE STUDY Pham Thi Thu Thuy MD, PhD Ho Chi Minh City Vietnam Serious Adverse
CURRENT TREATMENTS. Mitchell L Shiffman, MD Director Liver Institute of Virginia. Richmond and Newport News, VA, USA
 CURRENT TREATMENTS FOR HCV Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, VA, USA Liver Institute of Virginia Education, Research and
CURRENT TREATMENTS FOR HCV Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, VA, USA Liver Institute of Virginia Education, Research and
Antiviral agents in HCV
 Antiviral agents in HCV : Upcoming Therapeutic Options Su Jong Yu, M.D., Ph.D. Department of Internal Medicine, Liver Research Institute, Seoul National University College of Medicine Estimated 170 Million
Antiviral agents in HCV : Upcoming Therapeutic Options Su Jong Yu, M.D., Ph.D. Department of Internal Medicine, Liver Research Institute, Seoul National University College of Medicine Estimated 170 Million
EASL 2013 Interferon Free, All Oral Regimens for Hepatitis C. Maria Buti Hospital Universitario Valle Hebron Barcelona Spain
 EASL 2013 Interferon Free, All Oral Regimens for Hepatitis C Maria Buti Hospital Universitario Valle Hebron Barcelona Spain The first Results with Oral therapy: a Protease Inhibitor and NS5A inhibitor
EASL 2013 Interferon Free, All Oral Regimens for Hepatitis C Maria Buti Hospital Universitario Valle Hebron Barcelona Spain The first Results with Oral therapy: a Protease Inhibitor and NS5A inhibitor
Triple therapy with telaprevir or boceprevir: management of side effects
 Triple therapy with telaprevir or boceprevir: management of side effects Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber
Triple therapy with telaprevir or boceprevir: management of side effects Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber
Tratamiento de la Hepatitis C Rafael Esteban Hospital General Universitario Valle de Hebrón Barcelona
 Tratamiento de la Hepatitis C Rafael Esteban Hospital General Universitario Valle de Hebrón Barcelona rrent HCV Therapy 8% % sustained response 6% 4% 2% % 54-61% 41% 34% 25% 16% 6% IFN 24w IFN 48w Peg
Tratamiento de la Hepatitis C Rafael Esteban Hospital General Universitario Valle de Hebrón Barcelona rrent HCV Therapy 8% % sustained response 6% 4% 2% % 54-61% 41% 34% 25% 16% 6% IFN 24w IFN 48w Peg
Phase 3. Treatment Experienced. Ledipasvir-Sofosbuvir +/- Ribavirin in HCV Genotype 1 ION-2. Afdhal N, et al. N Engl J Med. 2014;370:
 Phase 3 Treatment Experienced Ledipasvir-Sofosbuvir +/- Ribavirin in HCV Genotype 1 ION-2 Afdhal N, et al. N Engl J Med. 2014;370:1483-93. Ledipasvir-Sofosbuvir +/- Ribavirin in Treatment-Experienced HCV
Phase 3 Treatment Experienced Ledipasvir-Sofosbuvir +/- Ribavirin in HCV Genotype 1 ION-2 Afdhal N, et al. N Engl J Med. 2014;370:1483-93. Ledipasvir-Sofosbuvir +/- Ribavirin in Treatment-Experienced HCV
Hepatitis C: Management of Treatment Naïve Patients with First Line Protease Inhibitors
 Hepatitis C: Management of Treatment Naïve Patients with First Line Protease Inhibitors Eric Lawitz, MD, AGAF, CPI The Texas Liver Institute Clinical Professor of Medicine University of Texas Health Science
Hepatitis C: Management of Treatment Naïve Patients with First Line Protease Inhibitors Eric Lawitz, MD, AGAF, CPI The Texas Liver Institute Clinical Professor of Medicine University of Texas Health Science
How to optimize current therapy for GT1 patients Shortened therapy with IFNa-based therapy
 How to optimize current therapy for GT1 patients Shortened therapy with IFNa-based therapy Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber- und Studienzentrum
How to optimize current therapy for GT1 patients Shortened therapy with IFNa-based therapy Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber- und Studienzentrum
5/12/2016. Learning Objectives. Management of Hepatitis C Virus Genotype 2 or 3 Infected Treatment-Naive or Experienced Patients
 5/12/216 Management of Hepatitis C Virus Genotype 2 or 3 Infected Treatment-Naive or Experienced Patients Alexander Monto, MD Professor of Clinical Medicine University of California San Francisco San Francisco,
5/12/216 Management of Hepatitis C Virus Genotype 2 or 3 Infected Treatment-Naive or Experienced Patients Alexander Monto, MD Professor of Clinical Medicine University of California San Francisco San Francisco,
Effects on anemia of drug adjustment in patients with chronic hepatitis C during telaprevir-combined therapy
 ORIGINAL ARTICLE January-February, Vol. 14 No. 1, 2015: 28-35 Effects on anemia of drug adjustment in patients with chronic hepatitis C during telaprevir-combined therapy Akihiro Tamori,* Kiyohide Kioka,**
ORIGINAL ARTICLE January-February, Vol. 14 No. 1, 2015: 28-35 Effects on anemia of drug adjustment in patients with chronic hepatitis C during telaprevir-combined therapy Akihiro Tamori,* Kiyohide Kioka,**
Should Elderly CHC Patients (>70 years old) be Treated?
 Should Elderly CHC Patients (>70 years old) be Treated? Deepak Amarapurkar Consultant Gastroenterologist & Hepatologist Bombay Hospital & Medical Research Center, Mumbai & Jagjivanram Western Railway Hospital,
Should Elderly CHC Patients (>70 years old) be Treated? Deepak Amarapurkar Consultant Gastroenterologist & Hepatologist Bombay Hospital & Medical Research Center, Mumbai & Jagjivanram Western Railway Hospital,
The Real-World Safety and Efficacy of Daclatasvir and Asunaprevir for Elderly Patients
 Gut and Liver, Published online August 14, 2017 ORiginal Article The Real-World Safety and Efficacy of Daclatasvir and Asunaprevir for Elderly Patients Shinya Taki 1, Hideyuki Tamai 1, Yoshiyuki Ida 1,
Gut and Liver, Published online August 14, 2017 ORiginal Article The Real-World Safety and Efficacy of Daclatasvir and Asunaprevir for Elderly Patients Shinya Taki 1, Hideyuki Tamai 1, Yoshiyuki Ida 1,
Detection and significance of PD-1.3 SNP (rs ) and IL28B SNP (rs ) in patients with current or past hepatitis B virus (HBV) infection
 Detection and significance of PD-1.3 SNP (rs11568821) and IL28B SNP (rs12979860) in patients with current or past hepatitis B virus (HBV) infection Asterios Saitis 1, Nikolaos K. Gatselis 1, Kalliopi Azariadi
Detection and significance of PD-1.3 SNP (rs11568821) and IL28B SNP (rs12979860) in patients with current or past hepatitis B virus (HBV) infection Asterios Saitis 1, Nikolaos K. Gatselis 1, Kalliopi Azariadi
1.0 Abstract. Title. Keywords
 1.0 Abstract Title Real World Evidence of the Effectiveness of Paritaprevir/r Ombitasvir, ± Dasabuvir, ± Ribavirin in Patients with Chronic Hepatitis C - An Observational Study in Austria (REAL) Keywords
1.0 Abstract Title Real World Evidence of the Effectiveness of Paritaprevir/r Ombitasvir, ± Dasabuvir, ± Ribavirin in Patients with Chronic Hepatitis C - An Observational Study in Austria (REAL) Keywords
Program Disclosure. Provider is approved by the California Board of Registered Nursing, Provider #13664, for 1.5 contact hours.
 Program Disclosure This activity has been planned and implemented in accordance with the Essential Areas and policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint-sponsorship
Program Disclosure This activity has been planned and implemented in accordance with the Essential Areas and policies of the Accreditation Council for Continuing Medical Education (ACCME) through the joint-sponsorship
RECENTLY, THE MANAGEMENT of chronic hepatitis
 bs_bs_banner Hepatology Research 214; 44 (Suppl. 1): 59 7 doi: 1.1111/hepr.12272 Special Report JSH Guidelines for the Management of Hepatitis C Virus Infection: A 214 Update for Genotype 1 Drafting Committee
bs_bs_banner Hepatology Research 214; 44 (Suppl. 1): 59 7 doi: 1.1111/hepr.12272 Special Report JSH Guidelines for the Management of Hepatitis C Virus Infection: A 214 Update for Genotype 1 Drafting Committee
PEARL-I. Ombitasvir + Paritaprevir + Ritonavir +/- Ribavirin in HCV GT4. Treatment Naïve and Treatment Experienced
 Phase 2b Treatment Naïve and Treatment Experienced Ombitasvir + Paritaprevir + Ritonavir +/- Ribavirin in HCV GT4 PEARL-I Hézode C, et al. Lancet. 2015 March 30. [Epub ahead of print] PEARL-I: Study Design
Phase 2b Treatment Naïve and Treatment Experienced Ombitasvir + Paritaprevir + Ritonavir +/- Ribavirin in HCV GT4 PEARL-I Hézode C, et al. Lancet. 2015 March 30. [Epub ahead of print] PEARL-I: Study Design
Treatement Experienced patients without cirrhosis. Rafael Esteban Hospital Universitario Valle Hebron Barcelona
 Treatement Experienced patients without cirrhosis Rafael Esteban Hospital Universitario Valle Hebron Barcelona Agenda With IFN PegIFN+ Ribavirin + Simeprevir PegIFN+ Ribavirin+ Sofosbuvir Without IFN Sofosbuvir
Treatement Experienced patients without cirrhosis Rafael Esteban Hospital Universitario Valle Hebron Barcelona Agenda With IFN PegIFN+ Ribavirin + Simeprevir PegIFN+ Ribavirin+ Sofosbuvir Without IFN Sofosbuvir
Protease inhibitor based triple therapy in treatment experienced patients
 Protease inhibitor based triple therapy in treatment experienced patients Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber
Protease inhibitor based triple therapy in treatment experienced patients Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber
Management of CHC G1 patients who are relapsers or non-responders to Peg IFN and RBV therapy: Wait or Triple Therapy?
 Management of CHC G1 patients who are relapsers or non-responders to Peg IFN and RBV therapy: Wait or Triple Therapy? Prof. Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of
Management of CHC G1 patients who are relapsers or non-responders to Peg IFN and RBV therapy: Wait or Triple Therapy? Prof. Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Thompson AJV; Expert panel representing the Gastroenterological
Appendix This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Appendix to: Thompson AJV; Expert panel representing the Gastroenterological
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 14 December 2011
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 14 December 2011 INCIVO 375 mg, film-coated tablet B/4 bottles of 42 tablets (CIP code: 217 378-5) B/1 bottle of 42
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 14 December 2011 INCIVO 375 mg, film-coated tablet B/4 bottles of 42 tablets (CIP code: 217 378-5) B/1 bottle of 42
2.0 Synopsis. ABT-450/r, ABT-267 M Clinical Study Report R&D/17/0539. (For National Authority Use Only)
 2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-450, ritonavir, ABT-267, ribavirin, pegylated interferon Name of Active Ingredient: ABT-450, Ritonavir, ABT-267, Ribavirin, Pegylated interferon Individual
2.0 Synopsis AbbVie Inc. Name of Study Drug: ABT-450, ritonavir, ABT-267, ribavirin, pegylated interferon Name of Active Ingredient: ABT-450, Ritonavir, ABT-267, Ribavirin, Pegylated interferon Individual
Strategies towards cure of HCV infection: a personalized approach. Heiner Wedemeyer Hannover Medical School Hannover, Germany
 Strategies towards cure of HCV infection: a personalized approach Heiner Wedemeyer Hannover Medical School Hannover, Germany 1 Disclosures Honoraria for consulting or speaking (last 5 years): Abbott, Biolex,
Strategies towards cure of HCV infection: a personalized approach Heiner Wedemeyer Hannover Medical School Hannover, Germany 1 Disclosures Honoraria for consulting or speaking (last 5 years): Abbott, Biolex,
Evolution of Therapy in HCV
 Hepatitis C: Update on New Therapies and AASLD 13 David Bernstein, MD, FACP, AGAF, FACP Professor of Medicine Hofstra North Shore-LIJ School of Medicine Evolution of Therapy in HCV 199 1999 1 13 (%) SVR
Hepatitis C: Update on New Therapies and AASLD 13 David Bernstein, MD, FACP, AGAF, FACP Professor of Medicine Hofstra North Shore-LIJ School of Medicine Evolution of Therapy in HCV 199 1999 1 13 (%) SVR
Hepatitis C Treatment 2014
 Hepatitis C Treatment 214 Brendan M. McGuire, MD UAB Liver Center Outline Epidemiology/National History Terminology for Treatment Treatment Considerations Current Treatment Options Genotype 1 (GT 1) Genotype
Hepatitis C Treatment 214 Brendan M. McGuire, MD UAB Liver Center Outline Epidemiology/National History Terminology for Treatment Treatment Considerations Current Treatment Options Genotype 1 (GT 1) Genotype
MEDIC CENTER. Case 2
 Case 2 Case history 57 year old Vietnamese man He lives in HCM city and works as a engineer The patient presented in July 2012 with fatigue Diagnosed with HCV in 2004 Negative for both HBV and HIV antibodies
Case 2 Case history 57 year old Vietnamese man He lives in HCM city and works as a engineer The patient presented in July 2012 with fatigue Diagnosed with HCV in 2004 Negative for both HBV and HIV antibodies
Bristol-Myers Squibb. HCV Full Development Portfolio Overview. Richard Bertz Int Workshop CP HIV Meeting Amsterdam, Netherlands 24 April 2013
 Bristol-Myers Squibb HCV Full Development Portfolio Overview Richard Bertz Int Workshop CP HIV Meeting Amsterdam, Netherlands 24 April 2013 1 BMS Agents in Clinical Development: DAAs and INF Lambda Lambda
Bristol-Myers Squibb HCV Full Development Portfolio Overview Richard Bertz Int Workshop CP HIV Meeting Amsterdam, Netherlands 24 April 2013 1 BMS Agents in Clinical Development: DAAs and INF Lambda Lambda
Introduction. The ELECTRON Trial
 63rd AASLD November 9-13, 12 Boston, Massachusetts Faculty Douglas T. Dieterich, MD Professor of Medicine and Director of CME Department of Medicine Director of Outpatient Hepatology Division of Liver
63rd AASLD November 9-13, 12 Boston, Massachusetts Faculty Douglas T. Dieterich, MD Professor of Medicine and Director of CME Department of Medicine Director of Outpatient Hepatology Division of Liver
Original article Ledipasvir and sofosbuvir for HCV infection in patients coinfected with HBV
 Antiviral Therapy 2016; 21:605 609 (doi: 10.3851/IMP3066) Original article Ledipasvir and sofosbuvir for HCV infection in patients coinfected with HBV Edward J Gane 1,2 *, Robert H Hyland 3, Di An 3, Evguenia
Antiviral Therapy 2016; 21:605 609 (doi: 10.3851/IMP3066) Original article Ledipasvir and sofosbuvir for HCV infection in patients coinfected with HBV Edward J Gane 1,2 *, Robert H Hyland 3, Di An 3, Evguenia
ROLE OF IL28B AND ITPA POLYMORPHISMS IN DIFFERENT GENOTYPES OF HCV
 ROLE OF IL28B AND ITPA POLYMORPHISMS IN DIFFERENT GENOTYPES OF HCV (Especially HCV-6) WK Seto Clinical Assistant Professor Department of Medicine Queen Mary Hospital The University of Hong Kong HCV GENOTYPES:
ROLE OF IL28B AND ITPA POLYMORPHISMS IN DIFFERENT GENOTYPES OF HCV (Especially HCV-6) WK Seto Clinical Assistant Professor Department of Medicine Queen Mary Hospital The University of Hong Kong HCV GENOTYPES:
Clinical Сase A previously relapse to PEG IFN + RBV in HCV G3a patient. Konstantin Zhdanov
 Clinical Сase A previously relapse to PEG IFN + RBV in HCV G3a patient Konstantin Zhdanov Genotype 3 in Europe Canada Norway Germany Sweden Czech Republic Poland Approximately 1/3 of HCV-infected patients
Clinical Сase A previously relapse to PEG IFN + RBV in HCV G3a patient Konstantin Zhdanov Genotype 3 in Europe Canada Norway Germany Sweden Czech Republic Poland Approximately 1/3 of HCV-infected patients
Clinical Management: Treatment of HCV Mono-infection
 Clinical Management: Treatment of HCV Mono-infection Curtis Cooper, MD, FRCPC Associate Professor-University of Ottawa The Ottawa Hospital- Infections Diseases Viral Hepatitis Program- Director Industry
Clinical Management: Treatment of HCV Mono-infection Curtis Cooper, MD, FRCPC Associate Professor-University of Ottawa The Ottawa Hospital- Infections Diseases Viral Hepatitis Program- Director Industry
Case 4: A 61-year-old man with HCV genotype 3 with cirrhosis. Ira M. Jacobson, M.D. Weill Cornell Medical College New York, New York USA
 Case 4: A 61-year-old man with HCV genotype 3 with cirrhosis Ira M. Jacobson, M.D. Weill Cornell Medical College New York, New York USA 1 Genotype 3 case 61-year-old man with HCV genotype 3 Cirrhosis on
Case 4: A 61-year-old man with HCV genotype 3 with cirrhosis Ira M. Jacobson, M.D. Weill Cornell Medical College New York, New York USA 1 Genotype 3 case 61-year-old man with HCV genotype 3 Cirrhosis on
29th Viral Hepatitis Prevention Board Meeting
 29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis C José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HEPATITIS C
29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis C José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HEPATITIS C
Saeed Hamid, MD Alex Thompson, MD, PhD
 Saeed Hamid, MD Alex Thompson, MD, PhD 1 We will review some top line data from EASL Majority of the time discussing how the data affects daily practice 2 Grazoprevir (GZR; MK-5172) + Elbasvir (EBR; MK-
Saeed Hamid, MD Alex Thompson, MD, PhD 1 We will review some top line data from EASL Majority of the time discussing how the data affects daily practice 2 Grazoprevir (GZR; MK-5172) + Elbasvir (EBR; MK-
Emerging Therapies for HCV: Highlights from AASLD 2012 (Part 2)
 Emerging Therapies for HCV: Highlights from AASLD 2012 (Part 2) PegIFN and RBV remain vital components of HCV therapy-- selected presentations from: Program Disclosure This activity has been planned and
Emerging Therapies for HCV: Highlights from AASLD 2012 (Part 2) PegIFN and RBV remain vital components of HCV therapy-- selected presentations from: Program Disclosure This activity has been planned and
Efficacy and safety of protease inhibitors for sever hepatitis C recurrence after liver transplantation: a first multicentric experience
 Efficacy and safety of protease inhibitors for sever hepatitis C recurrence after liver transplantation: a first multicentric experience A. Coilly, B. Roche, J. Dumortier, D. Botta-Fridlund, V. Leroy,
Efficacy and safety of protease inhibitors for sever hepatitis C recurrence after liver transplantation: a first multicentric experience A. Coilly, B. Roche, J. Dumortier, D. Botta-Fridlund, V. Leroy,
ASSAYS UTILZIED TO MONITOR HCV AND ITS TREATMENT
 ASSAYS UTILZIED TO MONITOR HCV AND ITS TREATMENT Mitchell L Shiffman, MD Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, VA Liver Institute of Virginia Education, Research
ASSAYS UTILZIED TO MONITOR HCV AND ITS TREATMENT Mitchell L Shiffman, MD Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, VA Liver Institute of Virginia Education, Research
HEPATITIS WEB STUDY. Treatment of Hepatitis C following Liver Transplantation
 HEPATITIS WEB STUDY Treatment of Hepatitis C following Liver Transplantation Terry D. Box, MD Associate Professor of Medicine Division of Gastroenterology/Hepatology University of Utah Health Sciences
HEPATITIS WEB STUDY Treatment of Hepatitis C following Liver Transplantation Terry D. Box, MD Associate Professor of Medicine Division of Gastroenterology/Hepatology University of Utah Health Sciences
IFN-free for Genotype 1 HCV: the current landscape. Prof. Graham R Foster
 IFN-free for Genotype 1 HCV: the current landscape Prof. Graham R Foster Wonderful new drugs are coming Poordad F, et al. New Engl J Med 2014; online DOI: 10.1056/NEJMoa1402869. 2 The New Drugs Two treatment
IFN-free for Genotype 1 HCV: the current landscape Prof. Graham R Foster Wonderful new drugs are coming Poordad F, et al. New Engl J Med 2014; online DOI: 10.1056/NEJMoa1402869. 2 The New Drugs Two treatment
Safety of Treatment in Cirrhotics in the Era of New Antiviral Therapies for Hepatitis C Virus
 Safety of Treatment in Cirrhotics in the Era of New Antiviral Therapies for Hepatitis C Virus JEFFREY NADELSON MD, ALAN EPSTEIN MD, THOMAS SEPE MD BOSTON UNIVERSITY SCHOOL OF MEDICINE ROGER WILLIAMS MEDICAL
Safety of Treatment in Cirrhotics in the Era of New Antiviral Therapies for Hepatitis C Virus JEFFREY NADELSON MD, ALAN EPSTEIN MD, THOMAS SEPE MD BOSTON UNIVERSITY SCHOOL OF MEDICINE ROGER WILLIAMS MEDICAL
Topic: Sovaldi, sofosbuvir Date of Origin: March 14, Committee Approval Date: August 15, 2014 Next Review Date: March 2015
 Medication Policy Manual Policy No: dru332 Topic: Sovaldi, sofosbuvir Date of Origin: March 14, 2014 Committee Approval Date: August 15, 2014 Next Review Date: March 2015 Effective Date: October 1, 2014
Medication Policy Manual Policy No: dru332 Topic: Sovaldi, sofosbuvir Date of Origin: March 14, 2014 Committee Approval Date: August 15, 2014 Next Review Date: March 2015 Effective Date: October 1, 2014
Pharmacological management of viruses in obese patients
 Cubist Pharmaceuticals The Shape of Cures to Come Pharmacological management of viruses in obese patients Dr. Dimitar Tonev, Medical Director UKINORD 1 Disclosures } The author is a pharmaceutical physician
Cubist Pharmaceuticals The Shape of Cures to Come Pharmacological management of viruses in obese patients Dr. Dimitar Tonev, Medical Director UKINORD 1 Disclosures } The author is a pharmaceutical physician
Glecaprevir-Pibrentasvir in Cirrhotic Genotype 1, 2, 4, 5, and 6 EXPEDITION-1
 Phase 3 Treatment-Naïve and Treatment-Experienced Glecaprevir-Pibrentasvir in Cirrhotic Genotype 1, 2, 4, 5, and 6 EXPEDITION-1 EXPEDITION-1: Study Features EXPEDITION-1 Trial Design: Open-label, single-arm,
Phase 3 Treatment-Naïve and Treatment-Experienced Glecaprevir-Pibrentasvir in Cirrhotic Genotype 1, 2, 4, 5, and 6 EXPEDITION-1 EXPEDITION-1: Study Features EXPEDITION-1 Trial Design: Open-label, single-arm,
SOLAR-1 (Cohorts A and B)
 Phase 2 Treatment Naïve and Treatment Experienced Ledipasvir-Sofosbuvir + RBV in HCV GT 1,4 and Advanced Liver Disease SOLAR-1 (Cohorts A and B) Charlton M, al. Gastroenterology. 2015; 149:649-59. Ledipasvir-Sofosbuvir
Phase 2 Treatment Naïve and Treatment Experienced Ledipasvir-Sofosbuvir + RBV in HCV GT 1,4 and Advanced Liver Disease SOLAR-1 (Cohorts A and B) Charlton M, al. Gastroenterology. 2015; 149:649-59. Ledipasvir-Sofosbuvir
ABCs of Hepatitis C: What s New. The Long-Awaited New Era: Protease Inhibitors for HCV Genotype 1
 ABCs of Hepatitis C: What s New ACG Postgraduate Course Washington, DC October 30, 2011 Ira M. Jacobson, M.D. Vincent Astor Professor of Medicine Chief, Division of Gastronterology and Hepatology Medical
ABCs of Hepatitis C: What s New ACG Postgraduate Course Washington, DC October 30, 2011 Ira M. Jacobson, M.D. Vincent Astor Professor of Medicine Chief, Division of Gastronterology and Hepatology Medical
Interferon-based and interferon-free new treatment options
 Interferon-based and interferon-free new treatment options White Nights of Hepatology St. Petersburg, 7. June 2013 Christoph Sarrazin Klinikum der J. W. Goethe-Universität Medizinische Klinik I Frankfurt
Interferon-based and interferon-free new treatment options White Nights of Hepatology St. Petersburg, 7. June 2013 Christoph Sarrazin Klinikum der J. W. Goethe-Universität Medizinische Klinik I Frankfurt
TITLE: Re-treatment with Direct Acting Antivirals for Chronic Hepatitis C Genotype 1: Emerging Evidence of Clinical Effectiveness and Safety An Update
 TITLE: Re-treatment with Direct Acting Antivirals for Chronic Hepatitis C Genotype 1: Emerging Evidence of Clinical Effectiveness and Safety An Update DATE: 02 January 2015 RESEARCH QUESTION What is the
TITLE: Re-treatment with Direct Acting Antivirals for Chronic Hepatitis C Genotype 1: Emerging Evidence of Clinical Effectiveness and Safety An Update DATE: 02 January 2015 RESEARCH QUESTION What is the
Treating HCV Genotype 2 & 3
 Treating HCV Genotype 2 & 3 3rd Workshop on HCV Therapy Advances, Rome 14.12.2013 Christoph Sarrazin Klinikum der J. W. Goethe-Universität Frankfurt am Main, Germany HCV Genotypes 2 & 3 Laurel and Hardy
Treating HCV Genotype 2 & 3 3rd Workshop on HCV Therapy Advances, Rome 14.12.2013 Christoph Sarrazin Klinikum der J. W. Goethe-Universität Frankfurt am Main, Germany HCV Genotypes 2 & 3 Laurel and Hardy
Treatment strategies for recurrent hepatitis C after living donor liver transplantation (from Kyushu University experience)
 Korean Association of HBP Surgery President: Dong Wook Choi, MD, PhD, Samsung Medical Center Session : 09:50-10:50, 2 nd /3, Apr 27, 2013 Venue: Lotte Hotel, Jeju Island, Korea Session: Prevention of original
Korean Association of HBP Surgery President: Dong Wook Choi, MD, PhD, Samsung Medical Center Session : 09:50-10:50, 2 nd /3, Apr 27, 2013 Venue: Lotte Hotel, Jeju Island, Korea Session: Prevention of original
Treatment with the New Direct Acting Antivirals for Hepatitis C
 Treatment with the New Direct Acting Antivirals for Hepatitis C Mary Olson, DNP, ANP-BC Clinical Trials Program Director Weill Cornell Medical College The Center for the Study of Hepatitis C Objectives
Treatment with the New Direct Acting Antivirals for Hepatitis C Mary Olson, DNP, ANP-BC Clinical Trials Program Director Weill Cornell Medical College The Center for the Study of Hepatitis C Objectives
EPIDEMIOLOGY, CLINICAL FEATURES AND OUTCOME OF ACUTE HEPATITIS C IN HIV-POSITIVE PATIENTS: PRESENTATION OF OUR EXPERIENCE
 EPIDEMIOLOGY, CLINICAL FEATURES AND OUTCOME OF ACUTE HEPATITIS C IN HIV-POSITIVE PATIENTS: PRESENTATION OF OUR EXPERIENCE E. Angeli, A. Mainini, C. Atzori, G. Gubertini and G. Rizzardini II Dept. Infectious
EPIDEMIOLOGY, CLINICAL FEATURES AND OUTCOME OF ACUTE HEPATITIS C IN HIV-POSITIVE PATIENTS: PRESENTATION OF OUR EXPERIENCE E. Angeli, A. Mainini, C. Atzori, G. Gubertini and G. Rizzardini II Dept. Infectious
Expert Perspectives: Best of HCV from EASL 2015
 Best of HCV from EASL 2015 Expert Perspectives: Best of HCV from EASL 2015 Saeed Hamid, MD Alex Thompson, MD, PhD This activity is supported by educational grants from AbbVie, Bristol-Myers Squibb, and
Best of HCV from EASL 2015 Expert Perspectives: Best of HCV from EASL 2015 Saeed Hamid, MD Alex Thompson, MD, PhD This activity is supported by educational grants from AbbVie, Bristol-Myers Squibb, and
Disclosures 29/09/2014. Genetic determinants of. HCV treatment outcome. IDEAL: IL28B-type is the strongest pre-treatment predictor of SVR
 29/9/214 Genetic determinants of ᴧ HCV treatment outcome Disclosures Advisory board member - Gilead, Abbvie, Bristol-Myers Squibb (BMS), Janssen, Merck, and oche Speaker - Gilead, Janssen, Merck, BMS,
29/9/214 Genetic determinants of ᴧ HCV treatment outcome Disclosures Advisory board member - Gilead, Abbvie, Bristol-Myers Squibb (BMS), Janssen, Merck, and oche Speaker - Gilead, Janssen, Merck, BMS,
Hepatitis C Medications Prior Authorization Criteria
 Hepatitis C Medications Authorization Criteria Epclusa (/velpatasvir), Harvoni (ledipasvir/), Sovaldi (), Daklinza (daclatasvir), Zepatier (elbasvir/grazoprevir), Olysio (simeprevir), Viekira Pak (ombitasvir/paritaprevir/ritonavir;
Hepatitis C Medications Authorization Criteria Epclusa (/velpatasvir), Harvoni (ledipasvir/), Sovaldi (), Daklinza (daclatasvir), Zepatier (elbasvir/grazoprevir), Olysio (simeprevir), Viekira Pak (ombitasvir/paritaprevir/ritonavir;
Division of Gastroenterology and Hepatology, Kawasaki Municipal Tama Hospital, Kawasaki, Japan 3
 Turk J Gastroenterol 2016; 27: 165-72 Can the Abbott RealTime hepatitis C virus assay be used to predict therapeutic outcomes in hepatitis C virus-infected patients undergoing triple therapy? LIVER Hiroki
Turk J Gastroenterol 2016; 27: 165-72 Can the Abbott RealTime hepatitis C virus assay be used to predict therapeutic outcomes in hepatitis C virus-infected patients undergoing triple therapy? LIVER Hiroki
Gane et al. BMC Infectious Diseases (2017) 17:389 DOI /s
 Gane et al. BMC Infectious Diseases (2017) 17:389 DOI 10.1186/s12879-017-2444-3 RESEARCH ARTICLE Simeprevir with peginterferon α-2a/ribavirin for chronic hepatitis C virus genotype 1 infection in treatment-experienced
Gane et al. BMC Infectious Diseases (2017) 17:389 DOI 10.1186/s12879-017-2444-3 RESEARCH ARTICLE Simeprevir with peginterferon α-2a/ribavirin for chronic hepatitis C virus genotype 1 infection in treatment-experienced
Genetic Determinants in HCV
 Genetic Determinants in HCV Lynn E. Taylor, MD Assistant Professor of Medicine Warren Alpert Medical School of Brown University The Miriam Hospital Providence, RI April 27, 2011 Disclosure My presentation
Genetic Determinants in HCV Lynn E. Taylor, MD Assistant Professor of Medicine Warren Alpert Medical School of Brown University The Miriam Hospital Providence, RI April 27, 2011 Disclosure My presentation
New Therapies on the Horizon in Hepatitis C Patients Paul Y. Kwo, MD
 Viral Targets for HCV New Therapies on the Horizon in Hepatitis C Patients Paul Y. Kwo, MD Sites for development of inhibitors Metalloproteinase Serine protease (trans) Core E E2 NS2 NS3 NS4a/NS4b NS5a/NS5b
Viral Targets for HCV New Therapies on the Horizon in Hepatitis C Patients Paul Y. Kwo, MD Sites for development of inhibitors Metalloproteinase Serine protease (trans) Core E E2 NS2 NS3 NS4a/NS4b NS5a/NS5b
Future strategies with new DAAs
 Future strategies with new DAAs Ola Weiland professor New direct antiviral drugs Case no 1 male with genotype 2b Male with gt 2b chronic HCV Male with gt 2b relapse afer peg-ifn + RBV during 24 weeks
Future strategies with new DAAs Ola Weiland professor New direct antiviral drugs Case no 1 male with genotype 2b Male with gt 2b chronic HCV Male with gt 2b relapse afer peg-ifn + RBV during 24 weeks
Express Scripts, Inc. monograph dated 5/25/2011; selected revision 6/1/2011
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Coverage Criteria: Approval Period: Victrelis (boceprevir capsules)
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Coverage Criteria: Approval Period: Victrelis (boceprevir capsules)
Antiviral Therapy 2015; 20: (doi: /IMP2805)
 Antiviral Therapy 2015; 20:185 192 (doi: 10.3851/IMP2805) Original article Non-invasive fibrosis assessment predicts sustained virological response to telaprevir with pegylated interferon and ribavirin
Antiviral Therapy 2015; 20:185 192 (doi: 10.3851/IMP2805) Original article Non-invasive fibrosis assessment predicts sustained virological response to telaprevir with pegylated interferon and ribavirin
Treatment Options in HCV Relapsers and Nonresponders. Raymond T. Chung, M.D.
 Session IV Treatment Options in HCV Relapsers and Nonresponders Raymond T. Chung, M.D. Director of Hepatology, Massachusetts General Hospital, Associate Professor of Medicine, Harvard Medical School, Boston,
Session IV Treatment Options in HCV Relapsers and Nonresponders Raymond T. Chung, M.D. Director of Hepatology, Massachusetts General Hospital, Associate Professor of Medicine, Harvard Medical School, Boston,
Intravenous drug use is currently the main transmission
 A Prospective Controlled Study of Interferon-Based Therapy of Chronic Hepatitis C in Patients on Methadone Maintenance Stefan Mauss, 1 Florian Berger, 1 Joerg Goelz, 2 Bernhard Jacob, 3 and Günther Schmutz
A Prospective Controlled Study of Interferon-Based Therapy of Chronic Hepatitis C in Patients on Methadone Maintenance Stefan Mauss, 1 Florian Berger, 1 Joerg Goelz, 2 Bernhard Jacob, 3 and Günther Schmutz
Glecaprevir-Pibrentasvir in Non-Cirrhotic Genotype 2 ENDURANCE-2
 Phase 3 Treatment Naïve or Experienced Glecaprevir-Pibrentasvir in Non-Cirrhotic Genotype 2 ENDURANCE-2 *ENDURANCE-2: Study Features ENDURANCE-2 Trial Design: Randomized, double-blind, placebo-controlled
Phase 3 Treatment Naïve or Experienced Glecaprevir-Pibrentasvir in Non-Cirrhotic Genotype 2 ENDURANCE-2 *ENDURANCE-2: Study Features ENDURANCE-2 Trial Design: Randomized, double-blind, placebo-controlled
Hepatitis C Therapy Falk Symposium September 20, 2008
 Hepatitis C Therapy Falk Symposium September 20, 2008 Ira M. Jacobson, MD Vincent Astor Professor of Clinical Medicine Chief, Division of Gastroenterology and Hepatology Medical Director, Center for the
Hepatitis C Therapy Falk Symposium September 20, 2008 Ira M. Jacobson, MD Vincent Astor Professor of Clinical Medicine Chief, Division of Gastroenterology and Hepatology Medical Director, Center for the
Original article Daclatasvir combined with peginterferon alfa-2a and ribavirin in Japanese patients infected with hepatitis C genotype 1
 Antiviral Therapy 2014; 19:501 510 (doi: 10.3851/IMP2731) Original article Daclatasvir combined with peginterferon alfa-2a and ribavirin in Japanese patients infected with hepatitis C genotype 1 Namiki
Antiviral Therapy 2014; 19:501 510 (doi: 10.3851/IMP2731) Original article Daclatasvir combined with peginterferon alfa-2a and ribavirin in Japanese patients infected with hepatitis C genotype 1 Namiki
Emerging Approaches for the Treatment of Hepatitis C Virus
 Emerging Approaches for the Treatment of Hepatitis C Virus Gap Analysis 1 Physicians may not be sufficiently familiar with the latest guidelines for chronic HCV treatment, including the initiation and
Emerging Approaches for the Treatment of Hepatitis C Virus Gap Analysis 1 Physicians may not be sufficiently familiar with the latest guidelines for chronic HCV treatment, including the initiation and
Glecaprevir-Pibrentasvir in HCV GT 1 or 4 & Prior DAA Treatment MAGELLAN-1 (Part 2)
 Phase 3 Treatment-Experienced in HCV GT 1 or 4 & Prior DAA Treatment MAGELLAN-1 (Part 2) in HCV GT 1 or 4 & Prior DAA Treatment MAGELLAN-1 (Part 2): Study Features MAGELLAN-1 (Part 2) Trial Design: Randomized,
Phase 3 Treatment-Experienced in HCV GT 1 or 4 & Prior DAA Treatment MAGELLAN-1 (Part 2) in HCV GT 1 or 4 & Prior DAA Treatment MAGELLAN-1 (Part 2): Study Features MAGELLAN-1 (Part 2) Trial Design: Randomized,
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Long-term Pegylated Interferon Monotherapy Following 72 Weeks of Pegylated Interferon and Ribavirin in Hepatitis C Virus Genotype-1-infected Slow Responders Shinya Watanabe 1, Yoshimasa
ORIGINAL ARTICLE Long-term Pegylated Interferon Monotherapy Following 72 Weeks of Pegylated Interferon and Ribavirin in Hepatitis C Virus Genotype-1-infected Slow Responders Shinya Watanabe 1, Yoshimasa
Antiviral treatment in HCV cirrhotic patients on waiting list
 Antiviral treatment in HCV cirrhotic patients on waiting list Krzysztof Tomasiewicz Department of Hepatology and Infectious Diseases Medical University of Lublin, Poland Disclosures Consultancy/Advisory
Antiviral treatment in HCV cirrhotic patients on waiting list Krzysztof Tomasiewicz Department of Hepatology and Infectious Diseases Medical University of Lublin, Poland Disclosures Consultancy/Advisory
New developments in HCV research and their implications for front-line practice
 New developments in HCV research and their implications for front-line practice Dr. Curtis Cooper Associate Professor, University of Ottawa Director, Ottawa Hospital Viral Hepatitis Program June 17, 2013
New developments in HCV research and their implications for front-line practice Dr. Curtis Cooper Associate Professor, University of Ottawa Director, Ottawa Hospital Viral Hepatitis Program June 17, 2013
Stick or twist management options in hepatitis C
 Stick or twist management options in hepatitis C Dr. Chris Durojaiye & Dr. Matthijs Backx SpR Microbiology and Infectious Diseases University Hospital of Wales, Cardiff Patient history 63 year old female
Stick or twist management options in hepatitis C Dr. Chris Durojaiye & Dr. Matthijs Backx SpR Microbiology and Infectious Diseases University Hospital of Wales, Cardiff Patient history 63 year old female
Ombitasvir-Paritaprevir-Ritonavir + Dasabuvir (Viekira Pak)
 HEPATITIS WEB STUDY HEPATITIS C ONLINE Ombitasvir-Paritaprevir-Ritonavir + Dasabuvir (Viekira Pak) Prepared by: Sophie Woolston, MD and David H. Spach, MD Last Updated: December 29, 2014 OMBITASVIR-PARITAPREVIR-RITONAVIR
HEPATITIS WEB STUDY HEPATITIS C ONLINE Ombitasvir-Paritaprevir-Ritonavir + Dasabuvir (Viekira Pak) Prepared by: Sophie Woolston, MD and David H. Spach, MD Last Updated: December 29, 2014 OMBITASVIR-PARITAPREVIR-RITONAVIR
TRANSPARENCY COMMITTEE
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 10 December 2008 REBETOL 200 mg capsules Pack of 84 (CIP code: 351 971.9) Pack of 112 (CIP code: 373 277.8) Pack of
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 10 December 2008 REBETOL 200 mg capsules Pack of 84 (CIP code: 351 971.9) Pack of 112 (CIP code: 373 277.8) Pack of
Assessment of the Efficacy of Reducing Peginterferon Alfa-2a and Ribavirin Dose on Virologic Response in Koreans with Chronic Hepatitis C
 ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.3.203 Assessment of the Efficacy of Reducing Peginterferon Alfa-2a and Ribavirin Dose on Virologic Response in Koreans with Chronic Hepatitis C Jung Hyun Kwon
ORIGINAL ARTICLE DOI: 10.3904/kjim.2009.24.3.203 Assessment of the Efficacy of Reducing Peginterferon Alfa-2a and Ribavirin Dose on Virologic Response in Koreans with Chronic Hepatitis C Jung Hyun Kwon
Global Hepatitis Programme. Guideline development for Hepatitis C virus Screening, Care and Treatment in low- and middle-income countries
 WHO/HIV/2014.26 World Health Organization 2014 Global Hepatitis Programme Guideline development for Hepatitis C virus Screening, Care and Treatment in low- and middle-income countries WHO TECHNICAL REPORT
WHO/HIV/2014.26 World Health Organization 2014 Global Hepatitis Programme Guideline development for Hepatitis C virus Screening, Care and Treatment in low- and middle-income countries WHO TECHNICAL REPORT
Hepatitis C: How sick can we treat? Robert S. Brown, Jr., MD, MPH Vice Chair, Transitions of Care Interim Chief, Division of
 Hepatitis C: How sick can we treat? Robert S. Brown, Jr., MD, MPH Vice Chair, Transitions of Care Interim Chief, Division of Gastroenterology & Hepatology www.livermd.org HCV in advanced disease In principle
Hepatitis C: How sick can we treat? Robert S. Brown, Jr., MD, MPH Vice Chair, Transitions of Care Interim Chief, Division of Gastroenterology & Hepatology www.livermd.org HCV in advanced disease In principle
Prior Authorization Guideline
 Prior Authorization Guideline Guideline Name Olysio (simeprevir) Formulary UnitedHealthcare Community & State Formulary Note Approval Date 2/19/2014 Revision Date 7/9/2014 1. Indications Drug Name: Olysio
Prior Authorization Guideline Guideline Name Olysio (simeprevir) Formulary UnitedHealthcare Community & State Formulary Note Approval Date 2/19/2014 Revision Date 7/9/2014 1. Indications Drug Name: Olysio
Hepatitis C Treatment
 Hepatitis C Treatment Standard of care & Managing advrse events Mohssen Nassiri Toosi, MD A s s o c i a t e P ro f e s s o r Of Internal M e d i c i n e Te h r a n U n i v e r s i t y O f M e d i c a l
Hepatitis C Treatment Standard of care & Managing advrse events Mohssen Nassiri Toosi, MD A s s o c i a t e P ro f e s s o r Of Internal M e d i c i n e Te h r a n U n i v e r s i t y O f M e d i c a l
V.G. Bain, P. Marotta, K. Kaita, E. Yoshida, M. Swain, R. Bailey, A. Neumann, P. Cronin, J. McHutchison, E. Pulkstenis, M.
 COMPARABLE ANTIVIRAL RESPONSE RATES WITH ALBINTERFERON ALFA-2B DOSED AT Q2W OR Q4W INTERVALS IN NAIVE SUBJECTS WITH GENOTYPE 2 OR 3 CHRONIC HEPATITIS C V.G. Bain, P. Marotta, K. Kaita, E. Yoshida, M. Swain,
COMPARABLE ANTIVIRAL RESPONSE RATES WITH ALBINTERFERON ALFA-2B DOSED AT Q2W OR Q4W INTERVALS IN NAIVE SUBJECTS WITH GENOTYPE 2 OR 3 CHRONIC HEPATITIS C V.G. Bain, P. Marotta, K. Kaita, E. Yoshida, M. Swain,
Treatment of Hepatitis C in HIV-Coinfected Patients. Vincent Soriano Department of Infectious Diseases Hospital Carlos III Madrid, Spain
 Treatment of Hepatitis C in HIV-Coinfected Patients Vincent Soriano Department of Infectious Diseases Hospital Carlos III Madrid, Spain Estimated no. of persons infected with HIV and hepatitis viruses
Treatment of Hepatitis C in HIV-Coinfected Patients Vincent Soriano Department of Infectious Diseases Hospital Carlos III Madrid, Spain Estimated no. of persons infected with HIV and hepatitis viruses
SECTION 1: OLYSIO with (PEGASYS) AND RIBAVIRIN SECTION 2: OLYSIO with (PEGINTRON) AND RIBAVIRIN RATIONALE FOR INCLUSION IN PA PROGRAM
 SECTION 1: OLYSIO with (PEGASYS) AND RIBAVIRIN SECTION 2: OLYSIO with (PEGINTRON) AND RIBAVIRIN RATIONALE FOR INCLUSION IN PA PROGRAM SECTION 1: OLYSIO with (PEGASYS) AND RIBAVIRIN Background Hepatitis
SECTION 1: OLYSIO with (PEGASYS) AND RIBAVIRIN SECTION 2: OLYSIO with (PEGINTRON) AND RIBAVIRIN RATIONALE FOR INCLUSION IN PA PROGRAM SECTION 1: OLYSIO with (PEGASYS) AND RIBAVIRIN Background Hepatitis
Direct acting anti-virals: the near future
 Direct acting anti-virals: the near future Heiner Wedemeyer Hannover Medical School Germany Will IFN-free treatment be possible in the near future? Interferon-free regimens to treat hepatitis C What should
Direct acting anti-virals: the near future Heiner Wedemeyer Hannover Medical School Germany Will IFN-free treatment be possible in the near future? Interferon-free regimens to treat hepatitis C What should
