A practical clinical approach to liver fibrosis
|
|
|
- Joel Weaver
- 5 years ago
- Views:
Transcription
1 Singapore Med J 2018; 59(12): CMEArticle A practical clinical approach to liver fibrosis Rahul Kumar 1, MBBS, MRCP, Eng Kiong Teo 1, MBBS MRCP, How Choon How 2,3, MMed, FCFP, Teck Yee Wong 4, MMed, MHPEd, Tiing Leong Ang 1, FRCPEd, FAMS Ms Chew, a 35-year-old executive, was found to have fatty liver on her recent pre-employment health checkup. She visited your clinic and showed you her test results. Her liver biochemistry assessment was normal. Ultrasonography of the liver was normal except for mild fatty infiltration of the liver. Her body mass index was 24, and she was generally well. Ms Chew was concerned about her liver health and whether she had liver hardening or fibrosis. WHAT IS LIVER FIBROSIS? Liver fibrosis, regardless of the underlying aetiology, is a consequence of the accumulation of extracellular matrix protein, including collagen, in the liver. It is a dynamic process that reflects imbalanced extracellular matrix turnover. This process is caused by persistent liver damage and consequent wound healing reaction. It can progress to cirrhosis, portal hypertension and hepatocellular carcinoma, leading to increased morbidity and mortality. (1,2) Common causes of liver fibrosis that also lead to chronic liver disease (CLD) are listed in Box 1. Liver fibrosis has an insidious onset, slowly progressing over many years and typically taking over 20 years to develop into liver cirrhosis. Rapid progression over a few years to liver cirrhosis can also occur in some cases. Genetic as well as environmental factors influence the natural history of liver fibrosis. Genetic variations in candidate genes may influence the rate of fibrosis progression, (3) which may explain the broad spectrum of clinical phenotypes with the same aetiological agents. Effectively treating and controlling the aetiology and risk factors of fibrosis progression can potentially reverse fibrosis. HOW COMMON IS THIS IN MY PRACTICE? Liver fibrosis results from persistent liver damage and consequent wound healing reaction due to CLD. In Singapore, chronic hepatitis B (CHB), non-alcoholic fatty liver disease (NAFLD) and alcoholic liver disease are common causes of CLD. Chronic hepatitis C (CHC) is more prevalent among intravenous drug users. Other aetiological factors that can give rise to CLD are primary biliary cirrhosis, autoimmune hepatitis and haemochromatosis. The prevalence of CLD and consequent liver fibrosis is challenging to assess. Recently, epidemiological data from an Italian general practitioner database revealed that 37.2% of patients had either overt or occult CLD based on liver function and imaging modalities. (4) CLD is typically diagnosed on health screening or incidentally, after the investigation of an abnormal liver panel. This is because CLD, or even liver cirrhosis, is often asymptomatic until complications appear. Hence, a high index of suspicion is necessary. The stages of liver fibrosis in CLD, such as NAFLD, define the patient s overall morbidity and mortality; the higher the stage of fibrosis, the worse the prognosis (Fig. 1). (5) The amount of liver fibrosis is correlated with the risk of developing liver cirrhosis and liver-related complications in viral and non-viral CLD. (6,7) The assessment of liver fibrosis is thus crucial in making therapeutic decisions and predicting outcomes. WHAT CAN I DO IN MY PRACTICE? After establishing the presence of CLD and determining the aetiology, the next step would be to determine whether a patient needs specialised care, including follow-up and treatment. Patients who have CHB with persistently elevated transaminases Box 1. Common causes of liver fibrosis: Chronic viral hepatitis B and C Non alcoholic fatty liver disease Alcoholic liver disease Autoimmune liver diseases Iron and copper overload Mortality rate (per 1,000 PYF) F0 F1 F2 F3 F4 Fibrosis stage Fig. 1 Fibrosis stage-specific liver-related mortality rate in non-alcoholic fatty liver disease (adapted from Dulai et al). (5) PYF: patient-years of follow-up 1 Department of Gastroenterology and Hepatology, 2 Care and Health Integration, Changi General Hospital, 3 Family Medicine Academic Clinical Programme, SingHealth Duke-NUS Academic Medical Centre, 4 Department of Continuing and Community Care, Tan Tock Seng Hospital, Singapore Correspondence: Dr Rahul Kumar, Associate Consultant, Department of Gastroenterology and Hepatology, Changi General Hospital, 2 Simei Street 3, Singapore rahul_kumar@cgh.com.sg 628
2 (> 2 upper limit of normal), patients of any aetiology with advanced fibrosis, and those with unknown aetiology should be referred for specialist care. The fibrosis assessment of patients should divide them into the advanced fibrosis or not-advanced fibrosis groups. (8,9) Noninvasive tests, especially serology-based composite scores, can be used to determine whether patients with mild abnormalities in liver chemical values need referrals to liver specialists. With NAFLD on the rise due to the epidemic of diabetes mellitus and obesity, this becomes even more relevant. (10) Depending on the aetiology, composite scores such as the NAFLD fibrosis score (NFS) and Fibrosis-4 (FIB-4) index for NAFLD; FIB-4 for CHB; and aspartate aminotransferase to platelet ratio index (APRI) score for the hepatitis C virus (HCV) provide cost-effective and efficient risk stratification when performed in the primary care clinic, identifying patients who have advanced fibrosis or indeterminate scores warranting referral to a specialist. (11,12) Most patients having NAFLD with low risk on the composite scoring systems can be followed up at the primary care clinic. Patients with intermediate risk should be reassessed with another composite scoring system and referred to liver specialists if their risk level remains unchanged. Those with high risk should be referred to specialist care. For example, NAFLD patients with NFS < or FIB-4 index < 1.3 have a 93% negative predictive value for advanced fibrosis and cirrhosis. They can hence be safely managed in the primary care clinic. The physician should provide advice on weight loss, and encourage the patient to adopt a hypocaloric diet rich in antioxidants and fibre, as well as regular exercise. Weight loss of at least 3% 5% of body weight improves steatosis, and up to 10% weight loss improves necroinflammation in patients with NAFLD or non-alcoholic steatohepatitis (NASH). (13) Aggressive control of hypertension, hyperlipidaemia and diabetes mellitus should be considered in these patients. Patients with CHB in the absence of necroinflammation defined as raised alanine aminotransferase (ALT) and aspartate aminotransferase (AST) and with low composite scores can similarly be managed in the primary care setting with six-monthly hepatocellular carcinoma surveillance ultrasonography and blood tests when indicated. (14,15) Periodic monitoring of fibrosis assessment based on composite scores should be carried out. CHB patients with necroinflammation (raised ALT and AST) should be referred for specialist care, as they may benefit from treatment of CHB. Table I summarises the risk stratification for common causes of CLD in Singapore based on noninvasive composite scoring systems. HOW DO I DIAGNOSE SIGNIFICANT FIBROSIS? Liver biopsy is the gold standard for diagnosis and staging of liver fibrosis. Other well-validated methods, known as noninvasive markers of liver fibrosis, are composite scores, direct serum biomarkers and liver imaging-based techniques (Fig. 2). These methods can be used to assess liver fibrosis in an outpatient, office setting as an alternative to liver biopsy, (16,17,18) but come with limitations. Table I. Noninvasive risk stratification for various liver diseases (adapted from Tapper EB and Lok AS). (10) Test Cut-off for AF AF probability* after ve vs. +ve test (%) Hepatitis B FIB 4 < vs. 77 NAFLD > vs. 95 FIB 4 < vs. 72 > vs. 94 NFS < vs. 73 Hepatitis C > vs. 91 FIB 4 < vs. 80 > vs. 68 APRI > vs. 63 > vs. 79 *Advanced fibrosis (AF) is defined as F3/F4 stage. ve: negative; +ve: positive; APRI: aspartate aminotransferase to platelet ratio index; FIB 4: Fibrosis 4 index; NAFLD: non alcoholic fatty liver disease; NFS: NAFLD fibrosis score Composite scores Fibrosis-4 index AST to platelet ratio index NAFLD fibrosis score Liver biopsy Staging of fibrosis Liver imaging VCTE ARFI imaging MR imaging SWE Direct biomarkers Leptin Laminin Procollagen Fibronectin Fig. 2 Diagram shows modes of staging for liver fibrosis (black arrows: invasive; white arrows: minimally invasive or noninvasive). ARFI: acoustic radiation force impulse; AST: aspartate aminotransferase; MR: magnetic resonance; NAFLD: non-alcoholic fatty liver disease; SWE: shear wave elastography; VCTE: vibration-controlled transient elastography Indirect serum markers and composite scores Various serum markers have been shown to correlate well with the presence or absence of liver fibrosis. These serum markers can be divided into two groups: indirect serum biomarkers with composite scores (based on simple laboratory tests and scoring systems); and direct serum biomarkers. Direct serum biomarkers reflect extracellular matrix turnover, whereas indirect markers reflect alterations in hepatic function rather than the metabolism of the hepatic extracellular matrix. Indirect serum markers of fibrosis and composite scores include scoring systems based on patients age, body mass index, platelet count, coagulation studies, and levels of serum albumin, AST and ALT. The most validated aetiology-specific scoring systems include FIB-4 index, APRI and NFS. These composite scoring systems are well validated in the prediction of fibrosis due to many aetiological agents (i.e. NAFLD, CHB and HCV), and have sufficient diagnostic accuracy in determining both minimal and advanced fibrosis. These simple scoring systems can assess 629
3 the severity of liver fibrosis based on readily available laboratory parameters. As invasive reassessments may carry significant risks for patients, composite scores provide an excellent method for reassessing fibrosis over time. Composite scoring systems are, however, not without disadvantages and limitations. While they can predict advanced and minimal fibrosis with reasonable certainty, they often fail to predict the exact grade of fibrosis. None of the composite scores are liver-specific, and the results can be influenced by comorbid conditions. For example, APRI can be falsely elevated in acute hepatitis. In addition, composite scoring systems require critical interpretation in terms of aetiology one size does not fit all. For example, NFS can only be applied for NAFLD and is not validated for other aetiologies. While calculating composite scores, one should also keep in mind that the same test has a different cut-off depending on the aetiology. Overall, these scores are excellent screening tests, especially to exclude advance fibrosis, with good negative predictive value. The following is a summary of these composite scoring systems and how they can be applied. Many non-patented free online calculators and websites can be used to calculate FIB-4, APRI and NFS, and provide instantaneous results once the data input fields have been filled in. Fibrosis-4 index The FIB-4 index is based on age, and AST, ALT and platelet levels. Although it was initially developed for fibrosis assessment in patients with HCV and HIV coinfected patients, (19) it has been subsequently validated for use in HCV mono-infection, CHB infection (20) and NAFLD/NASH. (21) FIB-4 scores < 1.45 have a negative predictive value of 90% for advanced fibrosis (meaning minimal amount of scarring) with 81% sensitivity. FIB-4 scores > 3.25 have a positive predictive value of 65% for advanced fibrosis with 97% specificity. Patients with low fibrosis scores (< 1.45) can safely be followed up in the primary care clinic with yearly assessment of fibrosis scores. Any patient with an FIB-4 score > 1.45 should undergo further evaluation to assess the stage of liver fibrosis. Table II. Interpretation of the NAFLD fibrosis score (adapted from Angulo et al). (24) NAFLD fibrosis score < F0 F2 Correlated fibrosis severity to Indeterminate score/fibrosis > F3 F4 NAFLD: non alcoholic fatty liver disease who have been diagnosed with NAFLD should have the first assessment of liver fibrosis based on NAFLD scores. Patients with an NFS < can safely be followed up in primary care clinics. Their fibrosis score trends should be tracked over time to evaluate for progression or stabilisation. Table II outlines the interpretation of NFS. Direct serum biomarkers Direct serum biomarkers such as leptin, laminin, hyaluronic acid, procollagen III N-terminal peptide, tissue inhibitor of metalloproteinase-1 and fibronectin are extensively studied for prediction of liver fibrosis. Hyaluronic acid seems to be most closely associated with fibrosis severity. (26) Outside of clinical research and trial settings, these biomarkers are not available for routine use, as commercial kits are not readily available. Available commercial kits include enhanced liver function panel and FibroTest, which are increasingly being used to determine the extent of fibrosis. Imaging-based methods Imaging-based methods, including vibration-controlled transient elastography (or FibroScan ), magnetic resonance imaging, acoustic radiation force impulse imaging and shear wave elastography, typically use the principle of shaking the liver with an external probe. This is based on the theory that as the liver becomes increasingly stiff, the velocity of the shear wave increases. However, these methods require specialised equipment and training, and are costly to set up, limiting their use in the primary care setting. AST to platelet ratio APRI scores have been demonstrated to correlate well with fibrosis in many CLDs. (22,23) However, apart from HCV infection, APRI values generally do not predict minimal or advanced fibrosis as well as the other scores, such as FIB-4 or NFS. Most experts recommend using APRI scores in conjunction with other noninvasive scores, especially with intermediate values for greater accuracy. An APRI score > 1 is approximately 77% sensitive and 75% specific in predicting advanced fibrosis and cirrhosis (> F3) in patients with HCV infection. NAFLD fibrosis score NFS was derived by Angulo et al in a multicentre study. (24) Its utility in excluding advanced fibrosis was validated in a separate study comparing multiple noninvasive models for fibrosis. (25) NFS reliably predicts (with 90% accuracy) which patients are unlikely to have advanced fibrosis on liver biopsy. Patients Liver biopsy Liver biopsy is the gold standard test to measure liver fibrosis. (27) However, it is an invasive procedure and not only has minor complications such as pain (20%), but also major complications such as haemobilia, intraperitoneal bleeding (0.5%), (28) and even death (0.009% 0.12%). (29,30) Other major drawbacks of liver biopsy include sampling errors: an adequate liver biopsy specimen can only assess a tiny fraction (1/50000) of the liver; (31) and inter- and intraobserver variability in reporting limits its use in clinical practice. (32) In a sentinel study involving 51 patients with NAFLD in whom two biopsy samples were obtained on the same day, 35% of the patients who had F3 fibrosis in one sample had F0 or F1 fibrosis in the other sample. (33) WHEN SHOULD I REFER TO A SPECIALIST? A vast majority of CLD patients can be managed in the outpatient primary care setting. Referral to specialists should be made for 630
4 Suspicion of CLD Laboratory tests to confirm CLD No CLD Extrahepatic disease Unknown aetiology CHB (> 2 ALT/AST) Cirrhosis HCC Partial hypertension CLD confirmed Assessment of liver fibrosis + US Use noninvasive composite scores Fibrosis-4 index NAFLD fibrosis score APRI High risk Medium risk Low risk Refer to specialist urgently Refer to specialist, non-urgent Reassess in 12 mth Fig. 3 Flowchart shows the noninvasive approach to clinical staging of chronic liver disease (CLD) based on composite scores. ALT: alanine aminotransferase; APRI: AST to platelet ratio index; AST: aspartate aminotransferase; CHB: chronic hepatitis B; FIB-4: Fibrosis-4 index; HCC: hepatocellular carcinoma; NAFLD: non-alcoholic fatty liver disease; US: ultrasonography patients with signs of advanced liver disease or persistently elevated ALT and AST levels, and those without a confirmed aetiology. Any clinical evidence of cirrhosis (i.e. ascites, jaundice, spider naevi, palmar erythema, gynaecomastia) should prompt a referral to liver specialists for further evaluation and management, as these signs are consistent with decompensated liver disease. Any radiological evidence of liver cirrhosis and portal hypertension also warrants review by liver specialists. If other causes of thrombocytopenia are ruled out, a low platelet count (typically < /ul) is often the first biochemical marker of liver cirrhosis; any patient with persistently low platelet values should be referred for further evaluation. Patients with noninvasive composite scores (i.e. FIB-4, NFS, APRI) suggestive of advanced fibrosis ( F3), or those with CHB infection and persistently raised ALT levels (an indication for antiviral therapy) should be referred for further management. Fig. 3 shows the noninvasive approach to clinical staging of CLD using composite scores. TAKE HOME MESSAGES 1. CLD is becoming more prevalent as NAFLD increases rapidly due to the obesity and diabetes mellitus epidemic. 2. A high index of suspicion is essential for CLD, as most patients are asymptomatic and incidentally diagnosed. 3. Easy-to-use composite scoring systems for fibrosis assessment can identify patients who are at risk for minimal or advanced fibrosis, and should be an integral part of the decision on whether to refer to specialist care. 4. NAFLD patients with minimal or no fibrosis based on composite scores can be safely managed in primary care clinics. 5. Patients with high likelihood of advanced fibrosis based on composite scores, CHB with necroinflammation (raised ALT and AST) or deranged liver function tests of uncertain aetiology should be referred to a liver specialist. ABSTRACT Liver fibrosis is a slow, insidious process involving accumulation of extracellular matrix protein in the liver. The stage of liver fibrosis in chronic liver disease (CLD) determines overall morbidity and mortality; the higher the stage, the worse the prognosis. Noninvasive composite scores can be used to determine whether patients with CLD have significant or advanced fibrosis. Patients with low composite scores can be safely followed up in primary care with periodic reassessment. Those with higher scores should be referred to a specialist. As the epidemic of diabetes mellitus, obesity and non-alcoholic fatty liver diseases is rising, CLD is becoming more prevalent. Easy-to-use fibrosis assessment composite scores can identify patients with minimal or advanced fibrosis, and should be an integral part of decision-making. Patients with cirrhosis, high composite scores, chronic hepatitis B with elevated alanine aminotransferase and aspartate aminotransferase, or deranged liver panel of uncertain aetiology should be referred to a specialist. Keywords: chronic liver disease, fibrosis assessment, noninvasive composite scores REFERENCES 1. Friedman SL. Evolving challenges in hepatic fibrosis. Nat Rev Gastroenterol Hepatol 2010; 7: Kawada N. Evolution of hepatic fibrosis research. Hepatol Res 2011; 41: Bataller R, North KE, Brenner DA. Genetic polymorphisms and the progression 631
5 of liver fibrosis: a critical appraisal. Hepatology 2003; 37: Martini A, Ceranto E, Gatta A, Angeli P, Pontisso P. Occult liver disease burden: analysis from a large general practitioners database. United European Gastroenterol J 2017; 5: Dulai PS, Singh S, Patel J, et al. Increased risk of mortality by fibrosis stage in nonalcoholic fatty liver disease: systematic review and metaanalysis. Hepatology 2017; 65: Yano M, Kumada H, Kage M, et al. The long-term pathological evolution of chronic hepatitis C. Hepatology 1996; 23: Younossi ZM, Stepanova M, Rafiq N, et al. Pathologic criteria for nonalcoholic steatohepatitis: interprotocol agreement and ability to predict liver-related mortality. Hepatology 2011; 53: Angulo P, Kleiner DE, Dam-Larsen S, et al. Liver fibrosis, but no other histologic features, is associated with long-term outcomes of patients with nonalcoholic fatty liver disease. Gastroenterology 2015; 149: e Ekstedt M, Hagström H, Nasr P, et al. Fibrosis stage is the strongest predictor for disease-specific mortality in NAFLD after up to 33 years of follow-up. Hepatology 2015; 61: Tapper EB, Lok AS. Use of liver imaging and biopsy in clinical practice. N Engl J Med 2017; 377: Tapper EB, Hunink MG, Afdhal NH, Lai M, Sengupta N. Cost-effectiveness analysis: risk stratification of nonalcoholic fatty liver disease (NAFLD) by the primary care physician using the NAFLD fibrosis score. PLoS One 2016; 11:e Tapper EB, Sengupta N, Hunink MG, Afdhal NH, Lai M. Cost-effective evaluation of nonalcoholic fatty liver disease with NAFLD fibrosis score and vibration controlled transient elastography. Am J Gastroenterol 2015; 110: Yamamoto M, Iwasa M, Iwata K, et al. Restriction of dietary calories, fat and iron improves non-alcoholic fatty liver disease. J Gastroenterol Hepatol 2007; 22: Terrault NA, Bzowej NH, Chang KM, et al; American Association for the Study of Liver Diseases. AASLD guidelines for treatment of chronic hepatitis B. Hepatology 2016; 63: European Association for the Study of the Liver. EASL 2017 clinical practice guidelines on the management of hepatitis B virus infection. J Hepatol 2017; 67: Pinzani M, Vizzutti F, Arena U, Marra F. Technology insight: noninvasive assessment of liver fibrosis by biochemical scores and elastography. Nat Clin Pract Gastroenterol Hepatol 2008; 5: Martínez SM, Crespo G, Navasa M, Forns X. Noninvasive assessment of liver fibrosis. Hepatology 2011; 53: Castera L. Noninvasive methods to assess liver disease in patients with hepatitis B or C. Gastroenterology 2012; 142: e Sterling RK, Lissen E, Clumeck N, et al; APRICOT Clinical Investigators. Development of a simple noninvasive index to predict significant fibrosis in patients with HIV/HCV coinfection. Hepatology 2006; 43: Kim BK, Kim DY, Park JY, et al. Validation of FIB-4 and comparison with other simple noninvasive indices for predicting liver fibrosis and cirrhosis in hepatitis B virus-infected patients. Liver Int 2010; 30: Shah AG, Lydecker A, Murray K, et al; Nash Clinical Research Network. Comparison of noninvasive markers of fibrosis in patients with nonalcoholic fatty liver disease. Clin Gastroenterol Hepatol 2009; 7: Lin ZH, Xin YN, Dong QJ, et al. Performance of the aspartate aminotransferaseto-platelet ratio index for the staging of hepatitis C-related fibrosis: an updated meta-analysis. Hepatology 2011; 53: Sirli R, Sporea I. Aspartate aminotransferase to platelet ratio index for the assessment of liver fibrosis severity in patients with chronic hepatitis. Hepat Mon 2011; 11: Angulo P, Hui JM, Marchesini G, et al. The NAFLD fibrosis score: a noninvasive system that identifies liver fibrosis in patients with NAFLD. Hepatology 2007; 45: McPherson S, Stewart SF, Henderson E, Burt AD, Day CP. Simple non-invasive fibrosis scoring systems can reliably exclude advanced fibrosis in patients with non-alcoholic fatty liver disease. Gut 2010; 59: Lydatakis H, Hager IP, Kostadelou E, et al. Non-invasive markers to predict the liver fibrosis in non-alcoholic fatty liver disease. Liver Int 2006; 26: Afdhal NH, Nunes D. Evaluation of liver fibrosis: a concise review. Am J Gastroenterol 2004; 99: Cadranel JF, Rufat P, Degos F. Practices of liver biopsy in France: results of a prospective nationwide survey. For the Group of Epidemiology of the French Association for the Study of the Liver (AFEF). Hepatology 2000; 32: West J, Card TR. Reduced mortality rates following elective percutaneous liver biopsies. Gastroenterology 2010; 139: Terjung B, Lemnitzer I, Dumoulin FL, et al. Bleeding complications after percutaneous liver biopsy. An analysis of risk factors. Digestion 2003; 67: Bedossa P, Dargère D, Paradis V. Sampling variability of liver fibrosis in chronic hepatitis C. Hepatology 2003; 38: Ter Borg F, ten K, Cuypers H, et al. A survey of liver pathology in needle biopsies from HBsAg and anti-hbe positive individuals. J Clin Pathol 2000; 53: Ratziu V, Charlotte F, Heurtier A, et al; LIDO Study Group. Sampling variability of liver biopsy in nonalcoholic fatty liver disease. Gastroenterology 2005; 128:
6 SINGAPORE MEDICAL COUNCIL CATEGORY 3B CME PROGRAMME (Code SMJ A) 1. Liver fibrosis, regardless of the underlying aetiology, is a consequence of the accumulation of extracellular matrix protein, including collagen, in the liver. 2. Environmental and not genetic factors influence the natural history of liver fibrosis. 3. The stages of liver fibrosis in chronic liver disease (CLD) define the patient s overall morbidity and mortality. 4. Noninvasive tests, especially serology-based composite score, cannot be used to determine whether patients with mild abnormalities in liver chemical values need referrals to liver specialists. 5. In patients with CLD, the assessment of liver fibrosis is not required for making therapeutic decisions and predicting outcomes. 6. The Fibrosis-4 (FIB-4) index is based on age and aspartate aminotransferase, alanine aminotransferase and platelet levels. 7. Imaging-based methods of measuring liver fibrosis are based on the theory that the stiffer the liver is, the higher the velocity of the shear wave. 8. Liver biopsy is not the gold standard test for liver fibrosis. 9. Patients with advanced fibrosis should be referred to specialist care. 10. The most common cause of liver fibrosis in Singapore is autoimmune liver disease. 11. Chronic hepatitis C is more prevalent among intravenous drug users. 12. Leptin, laminin, hyaluronic acid and procollagen III N-terminal peptide are examples of direct serum biomarkers for liver fibrosis. 13. A high index of suspicion is essential for diagnosis of CLD, as most patients are asymptomatic and diagnosed incidentally. 14. Liver fibrosis generally has an insidious onset, slowly progressing over many years, and typically takes over 20 years to develop into liver cirrhosis. 15. Liver fibrosis can be staged using composite scoring systems, liver imaging techniques, direct serum biomarkers or liver biopsy. 16. No online calculators and websites offer free calculation of FIB-4 index, APRI (aspartate aminotransferase to platelet ratio index) and NFS (non-alcoholic fatty liver disease fibrosis score). 17. Liver biopsy has complications such as bleeding, pain and even death. 18. Patients with clinical evidence of cirrhosis should be referred to liver specialists for further evaluation and management. 19. Patients with minimal or no fibrosis based on composite scores can be safely managed in primary care clinics. 20. Easy-to-use composite scoring systems for fibrosis assessment can identify patients who are at high risk for minimal or advanced fibrosis. True False Doctor s particulars: Name in full: MCR no.: Specialty: SUBMISSION INSTRUCTIONS: Visit the SMJ website: and select the appropriate quiz. You will be redirected to the SMA login page. For SMA member: (1) Log in with your username and password (if you do not know your password, please click on Forgot your password? ). (2) Select your answers for each quiz and click Submit. For non-sma member: (1) Create an SMJ CME account, or login with your SMJ CME username and password (for returning users). (2) Make payment of SGD (inclusive of 7% GST) via PayPal to access this month s quizzes. (3) Select your answers for each quiz and click Submit. RESULTS: (1) Answers will be published online in the SMJ February 2019 issue. (2) The MCR numbers of successful candidates will be posted online at the SMJ website by 1 February (3) Passing mark is 60%. No mark will be deducted for incorrect answers. (4) The SMJ editorial office will submit the list of successful candidates to the Singapore Medical Council. (5) One CME point is awarded for successful candidates. (6) SMC credits CME points according to the month of publication of the CME article (i.e. points awarded for a quiz published in the December 2017 issue will be credited for the month of December 2017, even if the deadline is in January 2018). Deadline for submission (December 2018 SMJ 3B CME programme): 12 noon, 25 January
The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis
 The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis Objectives: Liver biopsy is the gold standard for diagnosing the extent of fibrosis in NAFLD/NASH;
The role of non-invasivemethods in evaluating liver fibrosis of patients with non-alcoholic steatohepatitis Objectives: Liver biopsy is the gold standard for diagnosing the extent of fibrosis in NAFLD/NASH;
Non-Invasive Testing for Liver Fibrosis
 NORTHWEST AIDS EDUCATION AND TRAINING CENTER Non-Invasive Testing for Liver Fibrosis John Scott, MD, MSc Associate Professor, University of Washington Associate Clinic Director, Hep/Liver Clinic, Harborview
NORTHWEST AIDS EDUCATION AND TRAINING CENTER Non-Invasive Testing for Liver Fibrosis John Scott, MD, MSc Associate Professor, University of Washington Associate Clinic Director, Hep/Liver Clinic, Harborview
Pretreatment Evaluation
 Pretreatment Evaluation Disclosures Research supported by Gilead Sciences Inc.: Site investigator for HIV/HCV SWITCH Registry Study Key personnel for FOCUS HCV Screening Program through Vanderbilt University
Pretreatment Evaluation Disclosures Research supported by Gilead Sciences Inc.: Site investigator for HIV/HCV SWITCH Registry Study Key personnel for FOCUS HCV Screening Program through Vanderbilt University
National Horizon Scanning Centre. Enhanced Liver Fibrosis Test (ELF) for evaluating liver fibrosis. June 2008
 Enhanced Liver Fibrosis Test (ELF) for evaluating liver fibrosis June 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
Enhanced Liver Fibrosis Test (ELF) for evaluating liver fibrosis June 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not intended
In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease
 REVIEW In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease Ting-Ting Chan, M.R.C.P., and Vincent Wai-Sun Wong, M.D. Nonalcoholic fatty liver disease (NAFLD) affects 15% to 40% of the general
REVIEW In Search of New Biomarkers for Nonalcoholic Fatty Liver Disease Ting-Ting Chan, M.R.C.P., and Vincent Wai-Sun Wong, M.D. Nonalcoholic fatty liver disease (NAFLD) affects 15% to 40% of the general
HEP DART 2017, Kona, Hawaii
 HEP DART 2017, Kona, Hawaii Rong Yu 1, Ke Xu 1, Jing Li 1, Tong Sun 1, Shengjiang Zhang 2, Jinhua Shao 2, Jin Sun 2, Qiong He 3, Jianwen Luo 3, Cheng Wang 4, Yudong Wang 4, Jing Chen 4, Vanessa Wu 4, George
HEP DART 2017, Kona, Hawaii Rong Yu 1, Ke Xu 1, Jing Li 1, Tong Sun 1, Shengjiang Zhang 2, Jinhua Shao 2, Jin Sun 2, Qiong He 3, Jianwen Luo 3, Cheng Wang 4, Yudong Wang 4, Jing Chen 4, Vanessa Wu 4, George
Update on Non-Alcoholic Fatty Liver Disease. Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI
 Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Transient elastography the state of the art
 Transient elastography the state of the art Laurent CASTERA, MD PhD Department of Hepatology, Hôpital Beaujon, Clichy Université Paris-7, France White Nights of Hepatology, St Petersburg, Russia, june
Transient elastography the state of the art Laurent CASTERA, MD PhD Department of Hepatology, Hôpital Beaujon, Clichy Université Paris-7, France White Nights of Hepatology, St Petersburg, Russia, june
Medical Policy Non-invasive Tests for Hepatic Fibrosis
 Medical Policy Non-invasive Tests for Hepatic Fibrosis Subject: Non-invasive Tests for Hepatic Fibrosis Background: Accurately diagnosing liver fibrosis and inflammatory activity are the most important
Medical Policy Non-invasive Tests for Hepatic Fibrosis Subject: Non-invasive Tests for Hepatic Fibrosis Background: Accurately diagnosing liver fibrosis and inflammatory activity are the most important
/ FIB4 Index , simple steatosis. FIB4 Index. FIB4 Index. FIB4 Index FIB4 Index. Sterling FIB4 Index. FIB4 Index AST AST ALT
 原 著 29 34-41, 2014 FIB4 Index 1 1 1 1 2 1 1 FIB4 Index FIB4 Index cut off 2.67 2.67 12,059 FIB4 IndexFIB4 Index 2.67 / FIB4 Index AST ALT FIB4 Index 2.67 161 1.3% FIB4 Index 5 FIB4 Index 1.1 5 1.6 FIB4
原 著 29 34-41, 2014 FIB4 Index 1 1 1 1 2 1 1 FIB4 Index FIB4 Index cut off 2.67 2.67 12,059 FIB4 IndexFIB4 Index 2.67 / FIB4 Index AST ALT FIB4 Index 2.67 161 1.3% FIB4 Index 5 FIB4 Index 1.1 5 1.6 FIB4
Pretreatment Evaluation
 Pretreatment Evaluation Disclosures Research supported by Gilead Sciences Inc.: Site investigator for HIV/HCV SWITCH Registry Study Key personnel for FOCUS HCV Screening Program through Vanderbilt University
Pretreatment Evaluation Disclosures Research supported by Gilead Sciences Inc.: Site investigator for HIV/HCV SWITCH Registry Study Key personnel for FOCUS HCV Screening Program through Vanderbilt University
WHEN HCV TREATMENT IS DEFERRED WV HEPC ECHO PROJECT
 WHEN HCV TREATMENT IS DEFERRED WV HEPC ECHO PROJECT October 13, 2016 Reminder - treatment is recommended for all patients with chronic HCV infection Except short life expectancies that cannot be remediated
WHEN HCV TREATMENT IS DEFERRED WV HEPC ECHO PROJECT October 13, 2016 Reminder - treatment is recommended for all patients with chronic HCV infection Except short life expectancies that cannot be remediated
NAFLD and NASH: The Not-So-New Kids on the Block
 NAFLD and NASH: The Not-So-New Kids on the Block Mary E. Rinella, MD Associate Professor of Medicine Feinberg School of Medicine Northwestern University Chicago, Illinois This program is supported by an
NAFLD and NASH: The Not-So-New Kids on the Block Mary E. Rinella, MD Associate Professor of Medicine Feinberg School of Medicine Northwestern University Chicago, Illinois This program is supported by an
Non-Invasive Assessment of Liver Fibrosis. Patricia Slev, PhD University of Utah Department of Pathology
 Non-Invasive Assessment of Liver Fibrosis Patricia Slev, PhD University of Utah Department of Pathology Disclosure Patricia Slev has no relevant financial relationships to disclose. 2 Chronic Liver Disease
Non-Invasive Assessment of Liver Fibrosis Patricia Slev, PhD University of Utah Department of Pathology Disclosure Patricia Slev has no relevant financial relationships to disclose. 2 Chronic Liver Disease
Noninvasive Diagnosis and Staging of Liver Disease. Naveen Gara, MD
 Noninvasive Diagnosis and Staging of Liver Disease Naveen Gara, MD Outline Brief overview of the anatomy of liver Liver-related lab tests Chronic liver disease progression Estimation of liver fibrosis
Noninvasive Diagnosis and Staging of Liver Disease Naveen Gara, MD Outline Brief overview of the anatomy of liver Liver-related lab tests Chronic liver disease progression Estimation of liver fibrosis
The role of ARFI and APRI in diagnosis of liver fibrosis on patients with common chronic liver diseases
 RESEARCH ARTICLE The role of ARFI and APRI in diagnosis of liver fibrosis on patients with common chronic liver diseases Objective: This study aimed to investigate the value of liver fibrosis assessment
RESEARCH ARTICLE The role of ARFI and APRI in diagnosis of liver fibrosis on patients with common chronic liver diseases Objective: This study aimed to investigate the value of liver fibrosis assessment
Invasive. Sampling error. Interobserver variability. Nondynamic evaluation of
 How to assess liver fibrosis Serum markers or FibroScan vs. liver biopsy? Laurent CASTERA & Pierre BEDOSSA Hôpital Beaujon, AP-HP, Clichy Université Paris-VII France 4 th Paris Hepatitis Conference, Paris,
How to assess liver fibrosis Serum markers or FibroScan vs. liver biopsy? Laurent CASTERA & Pierre BEDOSSA Hôpital Beaujon, AP-HP, Clichy Université Paris-VII France 4 th Paris Hepatitis Conference, Paris,
INHSU th International Symposium on Hepatitis Care In Substance Users
 INHSU 2015 4 th International Symposium on Hepatitis Care In Substance Users Sydney, 7 October 2015 Non-invasive liver fibrosis assessment: Opportunities for enhanced liver disease assessment and treatment
INHSU 2015 4 th International Symposium on Hepatitis Care In Substance Users Sydney, 7 October 2015 Non-invasive liver fibrosis assessment: Opportunities for enhanced liver disease assessment and treatment
National Horizon Scanning Centre. Transient elastography (FibroScan) for evaluating liver fibrosis. April 2008
 Transient elastography (FibroScan) for evaluating liver fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Transient elastography (FibroScan) for evaluating liver fibrosis April 2008 This technology summary is based on information available at the time of research and a limited literature search. It is not
Practical Diagnosis and Staging of Nonalcoholic Fatty Liver Disease: A Narrative Review
 Practical Diagnosis and Staging of Nonalcoholic Fatty Liver Disease: A Narrative Review Authors: Jennifer Gallacher, 1 *Stuart McPherson 1,2 1. Liver Unit, Newcastle Upon Tyne Hospitals NHS Trust, Freeman
Practical Diagnosis and Staging of Nonalcoholic Fatty Liver Disease: A Narrative Review Authors: Jennifer Gallacher, 1 *Stuart McPherson 1,2 1. Liver Unit, Newcastle Upon Tyne Hospitals NHS Trust, Freeman
Pretreatment Evaluation
 Pretreatment Evaluation Objective At the end of this lecture, the learner will be able to: Outline the appropriate evaluation of a person infected with HCV in order to assess the benefits and risks of
Pretreatment Evaluation Objective At the end of this lecture, the learner will be able to: Outline the appropriate evaluation of a person infected with HCV in order to assess the benefits and risks of
Liver 102: Injury and Healing
 Liver 102: Injury and Healing Dawn Pease, MSN, RN, ANP-BC Brackenridge Specialty Clinics University Medical Center Brackenridge Austin, TX Seton Healthcare Family Liver 102 Outline Biochemical patterns
Liver 102: Injury and Healing Dawn Pease, MSN, RN, ANP-BC Brackenridge Specialty Clinics University Medical Center Brackenridge Austin, TX Seton Healthcare Family Liver 102 Outline Biochemical patterns
Screening cardiac patients for advanced liver disease
 HKASLD 30 th ASM and International Symposium on Hepatology 2017 Screening cardiac patients for advanced liver disease 5 Nov 2017 Dr. Lau Yue Leung Joulen Pamela Youde Nethersole Eastern Hospital NAFLD
HKASLD 30 th ASM and International Symposium on Hepatology 2017 Screening cardiac patients for advanced liver disease 5 Nov 2017 Dr. Lau Yue Leung Joulen Pamela Youde Nethersole Eastern Hospital NAFLD
Evaluating Obese Persons With Abnormal Liver Chemistries
 Mary E. Rinella, MD, FAASLD Evaluating Obese Persons With Abnormal Liver Chemistries Postgraduate Course: Challenges in Management of Common Liver Diseases 275 1 25 year old obese Hispanic man with obesity,
Mary E. Rinella, MD, FAASLD Evaluating Obese Persons With Abnormal Liver Chemistries Postgraduate Course: Challenges in Management of Common Liver Diseases 275 1 25 year old obese Hispanic man with obesity,
AASLD Immune tolerant phase HBV NAFLD diagnostic HCC
 AASLD 2016 Immune tolerant phase HBV NAFLD diagnostic HCC Immune tolerant 3 Modified from Chan HLY and Wong VWS. Hepatitis B. In Zakim and Boyers s Hepatology 2012 2015 AMERICAN ASSOCIATION FOR THE S1T6UDY
AASLD 2016 Immune tolerant phase HBV NAFLD diagnostic HCC Immune tolerant 3 Modified from Chan HLY and Wong VWS. Hepatitis B. In Zakim and Boyers s Hepatology 2012 2015 AMERICAN ASSOCIATION FOR THE S1T6UDY
Hepatology For The Nonhepatologist
 Hepatology For The Nonhepatologist Andrew Aronsohn, MD Associate Professor of Medicine University of Chicago Chicago, Illinois Learning Objectives After attending this presentation, learners will be able
Hepatology For The Nonhepatologist Andrew Aronsohn, MD Associate Professor of Medicine University of Chicago Chicago, Illinois Learning Objectives After attending this presentation, learners will be able
Transient elastography in chronic liver diseases of other etiologies
 4 Post Meeting A.I.S.F. Unmet Clinical Needs in Hepatology: New and upcoming diagnostic tools" Transient elastography in chronic liver diseases of other etiologies Dr. Vincenza Calvaruso Gastroenterologia
4 Post Meeting A.I.S.F. Unmet Clinical Needs in Hepatology: New and upcoming diagnostic tools" Transient elastography in chronic liver diseases of other etiologies Dr. Vincenza Calvaruso Gastroenterologia
ABNORMAL LIVER FUNCTION TESTS. Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust
 ABNORMAL LIVER FUNCTION TESTS Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust INTRODUCTION Liver function tests Cases Non invasive fibrosis measurement Questions UK MORTALITY RATE
ABNORMAL LIVER FUNCTION TESTS Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust INTRODUCTION Liver function tests Cases Non invasive fibrosis measurement Questions UK MORTALITY RATE
NON INVASIVE EVALUATION OF DISEASE PROGRESSION IN CHRONIC LIVER DISEASES
 Best of EASL -, Ethiopia 29 Sep to 01 Oct, 2016 Inaugural meeting of the Sub Saharan GI-Hepatology Working Group Incorporating Best of AGA and Best of EASL NON INVASIVE EVALUATION OF DISEASE PROGRESSION
Best of EASL -, Ethiopia 29 Sep to 01 Oct, 2016 Inaugural meeting of the Sub Saharan GI-Hepatology Working Group Incorporating Best of AGA and Best of EASL NON INVASIVE EVALUATION OF DISEASE PROGRESSION
Assessment of Liver Stiffness by Transient Elastography in Diabetics with Fatty Liver A Single Center Cross Sectional observational Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
NHSScotland is required to consider the Scottish Health Technologies Group (SHTG) advice.
 Advice Statement 010-18 July 2018 Advice Statement What is the most accurate and cost-effective direct test (ELF test, hyaluronic acid, P3NP, Fibroscan or ARFI elastography) for detecting and staging liver
Advice Statement 010-18 July 2018 Advice Statement What is the most accurate and cost-effective direct test (ELF test, hyaluronic acid, P3NP, Fibroscan or ARFI elastography) for detecting and staging liver
Hepatology for the Nonhepatologist
 Hepatology for the Nonhepatologist Kenneth E. Sherman, MD, PhD Gould Professor of Medicine Director, Division of Digestive Diseases University of Cincinnati College of Medicine Cincinnati, Ohio Learning
Hepatology for the Nonhepatologist Kenneth E. Sherman, MD, PhD Gould Professor of Medicine Director, Division of Digestive Diseases University of Cincinnati College of Medicine Cincinnati, Ohio Learning
Transient elastography in chronic viral liver diseases
 4 th AISF POST-MEETING COURSE Roma, 26 Febbraio 2011 Transient elastography in chronic viral liver diseases CRISTINA RIGAMONTI, M.D., Ph.D. Transient elastography (TE): a rapid, non-invasive technique
4 th AISF POST-MEETING COURSE Roma, 26 Febbraio 2011 Transient elastography in chronic viral liver diseases CRISTINA RIGAMONTI, M.D., Ph.D. Transient elastography (TE): a rapid, non-invasive technique
At Least 1 in 5 Patients in Your Practice Have Fatty Liver
 At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
New Tools for Assessing Disease Sererity, progression and regression in HBV and HCV
 New Tools for Assessing Disease Sererity, progression and regression in HBV and HCV Jidong Jia, MD, PhD Beijing Friendship Hospital, Capital Medical University 2016-3-14 Disclosure Consultation for Abbvie
New Tools for Assessing Disease Sererity, progression and regression in HBV and HCV Jidong Jia, MD, PhD Beijing Friendship Hospital, Capital Medical University 2016-3-14 Disclosure Consultation for Abbvie
DISCLOSURES. This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea
 DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
Bio Predictive. FibroTest/FibroSure Scientific Publications. Houot 2015 FibroTest, TE, FIB-4, APRI Meta-analysis
 AASLD 2015 /FibroSure Scientific Publications Section 1 - compared to APRI, FIB-4 and transient elastography Houot 2015, TE, FIB-4, APRI Meta-analysis is superior to TE by Fibroscan, APRI and Fib-4 using
AASLD 2015 /FibroSure Scientific Publications Section 1 - compared to APRI, FIB-4 and transient elastography Houot 2015, TE, FIB-4, APRI Meta-analysis is superior to TE by Fibroscan, APRI and Fib-4 using
SMJ Singapore Medical Journal
 SMJ Singapore Medical Journal ONLINE FIRST PUBLICATION Online first papers have undergone full scientific review and copyediting, but have not been typeset or proofread. To cite this article, use the DOIs
SMJ Singapore Medical Journal ONLINE FIRST PUBLICATION Online first papers have undergone full scientific review and copyediting, but have not been typeset or proofread. To cite this article, use the DOIs
In response to an enquiry from the Scottish Clinical Biochemistry Managed Diagnostic Network
 Evidence Note Number 82 July 2018 In response to an enquiry from the Scottish Clinical Biochemistry Managed Diagnostic Network What is the most accurate and cost-effective direct test (ELF test, hyaluronic
Evidence Note Number 82 July 2018 In response to an enquiry from the Scottish Clinical Biochemistry Managed Diagnostic Network What is the most accurate and cost-effective direct test (ELF test, hyaluronic
NON-ALCOHOLIC FATTY LIVER DISEASE:
 NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
Clinical Policy Title: Liver elastography
 Clinical Policy Title: Liver elastography Clinical Policy Number: CCP.1118 Effective Date: October 1, 2014 Initial Review Date: June 18, 2014 Most Recent Review Date: August 7, 2018 Next Review Date: August
Clinical Policy Title: Liver elastography Clinical Policy Number: CCP.1118 Effective Date: October 1, 2014 Initial Review Date: June 18, 2014 Most Recent Review Date: August 7, 2018 Next Review Date: August
The New World of HCV Therapy
 HCV: Assessing the Patient Prior to Treatment: Diagnostic Testing and Strategy JORGE L. HERRERA, MD, MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE, MOBILE, AL The New World of HCV Therapy Interferon-free
HCV: Assessing the Patient Prior to Treatment: Diagnostic Testing and Strategy JORGE L. HERRERA, MD, MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE, MOBILE, AL The New World of HCV Therapy Interferon-free
American Gastroenterological Association Institute Guideline on the Role of Elastography in the Evaluation of Liver Fibrosis
 American Gastroenterological Association Institute Guideline on the Role of Elastography in the Evaluation of Liver Fibrosis Joseph K. Lim, 1 Steven L. Flamm, 2 Siddharth Singh, 3 Yngve T. Falck-Ytter,
American Gastroenterological Association Institute Guideline on the Role of Elastography in the Evaluation of Liver Fibrosis Joseph K. Lim, 1 Steven L. Flamm, 2 Siddharth Singh, 3 Yngve T. Falck-Ytter,
Simple Tests to Predict Hepatic Fibrosis in Nonalcoholic Chronic Liver Diseases
 Gut and Liver, Vol. 1, No. 2, December 2007, pp. 145-150 original article Simple Tests to Predict Hepatic Fibrosis in Nonalcoholic Chronic Liver Diseases Woon Geon Shin*, Sang Hoon Park*, Sun-Young Jun,
Gut and Liver, Vol. 1, No. 2, December 2007, pp. 145-150 original article Simple Tests to Predict Hepatic Fibrosis in Nonalcoholic Chronic Liver Diseases Woon Geon Shin*, Sang Hoon Park*, Sun-Young Jun,
Bio Predictive. FibroTest Scientific Publications. Ratziu 2016 FibroMax NASH. Friedman 2016 FibroTest NASH EASL Key Publications for 2017
 EASL 2017 Scientific Publications Ratziu 2016 NASH Friedman 2016 NASH SteatoTest and sensitive markers of improvement in NASH trial using Elafibranor Elafibranor, an agonist of the peroxisome proliferator
EASL 2017 Scientific Publications Ratziu 2016 NASH Friedman 2016 NASH SteatoTest and sensitive markers of improvement in NASH trial using Elafibranor Elafibranor, an agonist of the peroxisome proliferator
The Liver for the Nonhepatologist
 The Liver for the Nonhepatologist Michael R. Charlton, MBBS, FRCP Hepatology Director and Medical Director of Liver Transplantation Intermountain Medical Center Salt Lake City, Utah FORMATTED: 05-14-15
The Liver for the Nonhepatologist Michael R. Charlton, MBBS, FRCP Hepatology Director and Medical Director of Liver Transplantation Intermountain Medical Center Salt Lake City, Utah FORMATTED: 05-14-15
NASH : Diagnosis and investigation. VII Workshop international, Curitiba, Brazil 29/08/2014
 NASH : Diagnosis and investigation VII Workshop international, Curitiba, Brazil 29/08/2014 Vlad Ratziu, Université Pierre et Marie Curie, Hôpital Pitié Salpêtrière, Paris, France Usual diagnostic circumstances
NASH : Diagnosis and investigation VII Workshop international, Curitiba, Brazil 29/08/2014 Vlad Ratziu, Université Pierre et Marie Curie, Hôpital Pitié Salpêtrière, Paris, France Usual diagnostic circumstances
Liver biopsy as the gold standard for diagnosis. Pierre BEDOSSA
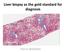 Liver biopsy as the gold standard for diagnosis Pierre BEDOSSA 1 PATHOLOGY OF NAFLD CONFLICTS OF INTEREST Grants and funding from Genfit, Intercept, Allergan, Inventiva, OWL, Echosens CEO and funding of
Liver biopsy as the gold standard for diagnosis Pierre BEDOSSA 1 PATHOLOGY OF NAFLD CONFLICTS OF INTEREST Grants and funding from Genfit, Intercept, Allergan, Inventiva, OWL, Echosens CEO and funding of
NAFLD: evidence-based management. Curso de residentes AEEH Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain
 NAFLD: evidence-based management Curso de residentes AEEH 2017 Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain Clinical case - 55 yo female - Sent for incidental steatosis at abdominal
NAFLD: evidence-based management Curso de residentes AEEH 2017 Salvador Augustin, MD Liver Unit Vall d Hebron Hospital Barcelona, Spain Clinical case - 55 yo female - Sent for incidental steatosis at abdominal
Management of Hepatitis C in Primary Care BABAFEMI ONABANJO, MD & BEN ALFRED, FNP UMASS FAMILY HEALTH CENTER WORCESTER
 Management of Hepatitis C in Primary Care BABAFEMI ONABANJO, MD & BEN ALFRED, FNP UMASS FAMILY HEALTH CENTER WORCESTER Objective Epidemiology Screening criteria Appropriate work up Treatment Guidelines
Management of Hepatitis C in Primary Care BABAFEMI ONABANJO, MD & BEN ALFRED, FNP UMASS FAMILY HEALTH CENTER WORCESTER Objective Epidemiology Screening criteria Appropriate work up Treatment Guidelines
Simple non-invasive fibrosis scoring systems can reliably exclude advanced fibrosis in patients with non-alcoholic fatty liver disease
 1 Liver Unit, Newcastle Upon Tyne Hospitals NHS Trust, Freeman Hospital, Newcastle upon Tyne, UK 2 Institute of Cellular Medicine, Faculty of Medical Sciences, Newcastle University, Newcastle Upon Tyne,
1 Liver Unit, Newcastle Upon Tyne Hospitals NHS Trust, Freeman Hospital, Newcastle upon Tyne, UK 2 Institute of Cellular Medicine, Faculty of Medical Sciences, Newcastle University, Newcastle Upon Tyne,
Initial Evaluation for HCV Therapy. Hope McGratty PA-C, MPH
 Initial Evaluation for HCV Therapy Hope McGratty PA-C, MPH Conflict of Interest Disclosure Statement None Who are we talking about today? Treatment naïve Chronic infection This patient seems complicated
Initial Evaluation for HCV Therapy Hope McGratty PA-C, MPH Conflict of Interest Disclosure Statement None Who are we talking about today? Treatment naïve Chronic infection This patient seems complicated
DISCLOSURES. This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea
 DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease
 Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease Policy Number: 2.04.41 Last Review: 2/2018 Origination: 2/2017 Next Review: 2/2019 Policy Blue Cross and
Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease Policy Number: 2.04.41 Last Review: 2/2018 Origination: 2/2017 Next Review: 2/2019 Policy Blue Cross and
Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease
 Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease Policy Number: 2.04.41 Last Review: 2/2019 Origination: 2/2017 Next Review: 2/2020 Policy Blue Cross and
Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease Policy Number: 2.04.41 Last Review: 2/2019 Origination: 2/2017 Next Review: 2/2020 Policy Blue Cross and
Module 1 Introduction of hepatitis
 Module 1 Introduction of hepatitis 1 Training Objectives At the end of the module, trainees will be able to ; Demonstrate improved knowledge of the global epidemiology of the viral hepatitis Understand
Module 1 Introduction of hepatitis 1 Training Objectives At the end of the module, trainees will be able to ; Demonstrate improved knowledge of the global epidemiology of the viral hepatitis Understand
What to do about the high ALT picked up at the annual review. Dr Michael Yee Consultant in Diabetes and Endocrinology
 What to do about the high ALT picked up at the annual review Dr Michael Yee Consultant in Diabetes and Endocrinology Mrs DC HPC PMH Type 2 Diabetes (decades) Regular retinal screening No foot complications/neuropathy
What to do about the high ALT picked up at the annual review Dr Michael Yee Consultant in Diabetes and Endocrinology Mrs DC HPC PMH Type 2 Diabetes (decades) Regular retinal screening No foot complications/neuropathy
LFTs: an update A MacGilchrist PLIG meeting 31st January 2019
 LFTs: an update A MacGilchrist PLIG meeting 31 st January 2019 LFTs: what are we trying to achieve? (1) The case against investigation abnormal LFTs in up to 21% of the population only 1-2% develop significant
LFTs: an update A MacGilchrist PLIG meeting 31 st January 2019 LFTs: what are we trying to achieve? (1) The case against investigation abnormal LFTs in up to 21% of the population only 1-2% develop significant
Natural History of Chronic Hepatitis B
 Natural History of Chronic Hepatitis B Anna SF Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor,
Natural History of Chronic Hepatitis B Anna SF Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor,
What is NAFLD?.NASH? Presenter Disclosure Information. Learning Objectives. Case 1: Rob. Questions Pertinent to Rob
 Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES
 NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NONINVASIVE TECHNIQUES FOR EVALUATION AND MONITORING OF CHRONIC LIVER DISEASE
 LIVER DISEASE Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
LIVER DISEASE Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are
Journal of the Egyptian Society of Parasitology, Vol.46, No.1, April 2016 J. Egypt. Soc. Parasitol. (JESP), 46(1), 2016:
 Journal of the Egyptian Society of Parasitology, Vol.46, No.1, April 2016 J. Egypt. Soc. Parasitol. (JESP), 46(1), 2016: 125-130 SERUM MARKERS FOR ASSESSING LIVER FIBROSIS IN EGYPTIAN PA- TIENTS WITH CHRONIC
Journal of the Egyptian Society of Parasitology, Vol.46, No.1, April 2016 J. Egypt. Soc. Parasitol. (JESP), 46(1), 2016: 125-130 SERUM MARKERS FOR ASSESSING LIVER FIBROSIS IN EGYPTIAN PA- TIENTS WITH CHRONIC
Clinical Policy Title: Noninvasive assessment of hepatic fibrosis
 Clinical Policy Title: Noninvasive assessment of hepatic fibrosis Clinical Policy Number: 08.01.03 Effective Date: Oct. 1, 2014 Initial Review Date: June 18, 2014 Most Recent Review Date: August 17, 2017
Clinical Policy Title: Noninvasive assessment of hepatic fibrosis Clinical Policy Number: 08.01.03 Effective Date: Oct. 1, 2014 Initial Review Date: June 18, 2014 Most Recent Review Date: August 17, 2017
When to Treat: Staging Liver Disease David L. Thomas, MD, MPH
 When to Treat: Staging Liver Disease David L. Thomas, MD, MPH Professor of Medicine Johns Hopkins School of Medicine Disclosures Received royalties from UpToDate, Inc. Staging refers to the assessment
When to Treat: Staging Liver Disease David L. Thomas, MD, MPH Professor of Medicine Johns Hopkins School of Medicine Disclosures Received royalties from UpToDate, Inc. Staging refers to the assessment
EASL EASD EASO Clinical practice guidelines for the management of nonalcoholic fatty liver disease.
 Commentary. EASL EASD EASO Clinical practice guidelines for the management of nonalcoholic fatty liver disease. Christopher D. Byrne 1,2, Giovanni Targher 3 1 Nutrition and Metabolism, Faculty of Medicine,
Commentary. EASL EASD EASO Clinical practice guidelines for the management of nonalcoholic fatty liver disease. Christopher D. Byrne 1,2, Giovanni Targher 3 1 Nutrition and Metabolism, Faculty of Medicine,
Making the best use of liver biopsy: clinical perspective. Steve Ryder Wolfson Digestive Diseases Centre University of Nottingham
 Making the best use of liver biopsy: clinical perspective Steve Ryder Wolfson Digestive Diseases Centre University of Nottingham Trepanning most efficacious for the relief of maladies so diverse and troublesome
Making the best use of liver biopsy: clinical perspective Steve Ryder Wolfson Digestive Diseases Centre University of Nottingham Trepanning most efficacious for the relief of maladies so diverse and troublesome
PHC, Paris, 30th Jan 2017 PATHOLOGY OF NAFLD. Pierre Bedossa. Departement of Pathology Hôpital Beaujon University Paris-Diderot Paris - FRANCE
 PHC, Paris, 30th Jan 2017 PATHOLOGY OF NAFLD Pierre Bedossa Departement of Pathology Hôpital Beaujon University Paris-Diderot Paris - FRANCE 1 PATHOLOGY OF NAFLD NAFLD: a chronic liver disease with a wide
PHC, Paris, 30th Jan 2017 PATHOLOGY OF NAFLD Pierre Bedossa Departement of Pathology Hôpital Beaujon University Paris-Diderot Paris - FRANCE 1 PATHOLOGY OF NAFLD NAFLD: a chronic liver disease with a wide
Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease
 ORIGINAL ARTICLE Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease Takashi Wada and Mikio Zeniya Abstract Objective We investigated the distribution and characteristics of the
ORIGINAL ARTICLE Background of the FIB-4 Index in Japanese Non-Alcoholic Fatty Liver Disease Takashi Wada and Mikio Zeniya Abstract Objective We investigated the distribution and characteristics of the
Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting?
 Rajani Sharma, PGY1 Geriatrics CRC Project, 12/19/13 Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting? A. Study Purpose and Rationale Hepatocellular carcinoma
Rajani Sharma, PGY1 Geriatrics CRC Project, 12/19/13 Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting? A. Study Purpose and Rationale Hepatocellular carcinoma
NICE guideline Published: 6 July 2016 nice.org.uk/guidance/ng49
 Non-alcoholic fatty liver disease (NAFLD): assessment and management NICE guideline Published: 6 July 20 nice.org.uk/guidance/ng49 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Non-alcoholic fatty liver disease (NAFLD): assessment and management NICE guideline Published: 6 July 20 nice.org.uk/guidance/ng49 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Non-invasive diagnosis of hepatitis B virus-related cirrhosis
 Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v20.i2.445 World J Gastroenterol 2014 January 14; 20(2): 445-459 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2014
Online Submissions: http://www.wjgnet.com/esps/ bpgoffice@wjgnet.com doi:10.3748/wjg.v20.i2.445 World J Gastroenterol 2014 January 14; 20(2): 445-459 ISSN 1007-9327 (print) ISSN 2219-2840 (online) 2014
The Future is Here Now!
 HCV Treatment: Assessing the Patient Prior to Treatment. How Will This Change in the Future? JORGE L. HERRERA M.D., FACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE, MOBILE, AL The Future is Here Now!
HCV Treatment: Assessing the Patient Prior to Treatment. How Will This Change in the Future? JORGE L. HERRERA M.D., FACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE, MOBILE, AL The Future is Here Now!
M30 Apoptosense ELISA. A biomarker assay for detection and screening of NASH
 M30 Apoptosense ELISA A biomarker assay for detection and screening of NASH NASH A Global Disease In the Western countries, Non-Alcoholic Fatty Liver Disease (NAFLD) is the most common liver disease, strongly
M30 Apoptosense ELISA A biomarker assay for detection and screening of NASH NASH A Global Disease In the Western countries, Non-Alcoholic Fatty Liver Disease (NAFLD) is the most common liver disease, strongly
Screening for HCCwho,
 Screening for HCCwho, how and how often? Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital HCC Global Epidemiology
Screening for HCCwho, how and how often? Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital HCC Global Epidemiology
The New World of HCV Therapy
 HCV: Assessing the Patient Prior to Treatment: Diagnostic Testing and Strategy JORGE L. HERRERA M.D., MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE, MOBILE, AL The New World of HCV Therapy Interferon-free
HCV: Assessing the Patient Prior to Treatment: Diagnostic Testing and Strategy JORGE L. HERRERA M.D., MACG UNIVERSITY OF SOUTH ALABAMA COLLEGE OF MEDICINE, MOBILE, AL The New World of HCV Therapy Interferon-free
MR Elastography of Liver
 MR Elastography of Liver Sudhakar K. Venkatesh, MD, FRCR Professor of Radiology Mayo Clinic College of Medicine Consultant, Abdominal Division Radiology, Mayo Clinic Rochester, MN, USA 19 th May 2018 2018
MR Elastography of Liver Sudhakar K. Venkatesh, MD, FRCR Professor of Radiology Mayo Clinic College of Medicine Consultant, Abdominal Division Radiology, Mayo Clinic Rochester, MN, USA 19 th May 2018 2018
Surveillance for Hepatocellular Carcinoma
 Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
HEPATIC ELASTOGRAPHY AND FIB-4 SCORE VERSUS LIVER BIOPSY FOR ASSESSMENT OF LIVER FIBROSIS IN CHRONIC HCV PATIENTS
 HEPATIC ELASTOGRAPHY AND FIB-4 SCORE VERSUS LIVER BIOPSY FOR ASSESSMENT OF LIVER FIBROSIS IN CHRONIC HCV PATIENTS Essam A. Wahab*, Talaat Fathy** Sameh Saber*** and Hanan S. Ahmad**** Internal Medicine*,
HEPATIC ELASTOGRAPHY AND FIB-4 SCORE VERSUS LIVER BIOPSY FOR ASSESSMENT OF LIVER FIBROSIS IN CHRONIC HCV PATIENTS Essam A. Wahab*, Talaat Fathy** Sameh Saber*** and Hanan S. Ahmad**** Internal Medicine*,
Diagnostic Challenges of Nonalcoholic Fatty Liver Disease/ Nonalcoholic Steatohepatitis
 REVIEW Diagnostic Challenges of Nonalcoholic Fatty Liver Disease/ Nonalcoholic Steatohepatitis Erin Cleveland, M.D.,* Andrew Bandy, M.D., and Lisa B. VanWagner, M.D., M.Sc. *, Nonalcoholic fatty liver
REVIEW Diagnostic Challenges of Nonalcoholic Fatty Liver Disease/ Nonalcoholic Steatohepatitis Erin Cleveland, M.D.,* Andrew Bandy, M.D., and Lisa B. VanWagner, M.D., M.Sc. *, Nonalcoholic fatty liver
Hepatitis C Policy Discussion
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Learning Objectives. After attending this presentation, participants will be able to:
 Learning Objectives After attending this presentation, participants will be able to: Describe HCV in 2015 Describe how to diagnose advanced liver disease and cirrhosis Identify the clinical presentation
Learning Objectives After attending this presentation, participants will be able to: Describe HCV in 2015 Describe how to diagnose advanced liver disease and cirrhosis Identify the clinical presentation
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Follow-up of patients with SVR Lawrence Serfaty Service d Hépatologie, UMR_S 938 Hôpital Saint-Antoine Université Pierre&Marie Curie Paris, France
 9th Paris Hepatitis Conference, January 11-12, 2016 Follow-up of patients with SVR Lawrence Serfaty Service d Hépatologie, UMR_S 938 Hôpital Saint-Antoine Université Pierre&Marie Curie Paris, France Disclosures
9th Paris Hepatitis Conference, January 11-12, 2016 Follow-up of patients with SVR Lawrence Serfaty Service d Hépatologie, UMR_S 938 Hôpital Saint-Antoine Université Pierre&Marie Curie Paris, France Disclosures
New HCV reimbursement criteria Chronic hepatitis C regardless of fibrosis stage if:
 New HCV reimbursement criteria 01-2018 Chronic hepatitis C with F2 fibrosis stage Chronic hepatitis C regardless of fibrosis stage if: HIV-HCV coinfection HBV-HCV coinfection Listed for or post-solid organ
New HCV reimbursement criteria 01-2018 Chronic hepatitis C with F2 fibrosis stage Chronic hepatitis C regardless of fibrosis stage if: HIV-HCV coinfection HBV-HCV coinfection Listed for or post-solid organ
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Noninvasive Techniques for the Evaluation and Monitoring of Page 1 of 38 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Noninvasive Techniques for the Evaluation
Noninvasive Techniques for the Evaluation and Monitoring of Page 1 of 38 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Noninvasive Techniques for the Evaluation
Health Clinical Practice Guidelines:
 Clinical Practice Guidelines Singapore Med J 2010; 51(6) : 518 CME Article Health Promotion Board-Ministry of Health Clinical Practice Guidelines: Functional Screening for Older Adults in the Community
Clinical Practice Guidelines Singapore Med J 2010; 51(6) : 518 CME Article Health Promotion Board-Ministry of Health Clinical Practice Guidelines: Functional Screening for Older Adults in the Community
We don t need a liver biopsy. We have non-invasive tests
 We don t need a liver biopsy We have non-invasive tests Laurent CASTERA, MD PhD Department of Hepatology, Hôpital Beaujon, Clichy Université Paris Diderot, France PHC 2018 www.aphc.info Liver biopsy: an
We don t need a liver biopsy We have non-invasive tests Laurent CASTERA, MD PhD Department of Hepatology, Hôpital Beaujon, Clichy Université Paris Diderot, France PHC 2018 www.aphc.info Liver biopsy: an
New HCV reimbursement criteria Chronic hepatitis C regardless of fibrosis stage if:
 New HCV reimbursement criteria 01-2018 Chronic hepatitis C with F2 fibrosis stage Chronic hepatitis C regardless of fibrosis stage if: HIV-HCV coinfection HBV-HCV coinfection Listed for or post-solid organ
New HCV reimbursement criteria 01-2018 Chronic hepatitis C with F2 fibrosis stage Chronic hepatitis C regardless of fibrosis stage if: HIV-HCV coinfection HBV-HCV coinfection Listed for or post-solid organ
MP Noninvasive Techniques for the Evaluation and Monitoring of Patients With Chronic Liver Disease
 Medical Policy BCBSA Ref. Policy: 2.04.41 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our medical policies
Medical Policy BCBSA Ref. Policy: 2.04.41 Last Review: 11/15/2018 Effective Date: 11/15/2018 Section: Medicine Related Policies 9.01.502 Experimental / Investigational Services DISCLAIMER Our medical policies
Evaluation of liver and spleen stiffness using a ultrasound guided method: Accuracy of ARFI(R) measurements in liver disease patients
 Evaluation of liver and spleen stiffness using a ultrasound guided method: Accuracy of ARFI(R) measurements in liver disease patients Poster No.: C-3242 Congress: ECR 2010 Type: Topic: Authors: Keywords:
Evaluation of liver and spleen stiffness using a ultrasound guided method: Accuracy of ARFI(R) measurements in liver disease patients Poster No.: C-3242 Congress: ECR 2010 Type: Topic: Authors: Keywords:
Faculty Disclosure. Objectives. Cirrhosis Management for the Family Physician 18/11/2014
 Cirrhosis Management for the Family Physician Mang Ma, MD, FRCP Professor University of Alberta Faculty: Mang Ma Faculty Disclosure Relationships with commercial interests: Advisory Board: Merck, Gilead
Cirrhosis Management for the Family Physician Mang Ma, MD, FRCP Professor University of Alberta Faculty: Mang Ma Faculty Disclosure Relationships with commercial interests: Advisory Board: Merck, Gilead
Medical technologies guidance Published: 23 September 2015 nice.org.uk/guidance/mtg27
 Virtual Touch Quantification to diagnose and monitor liver fibrosis in chronic hepatitis B and C Medical technologies guidance Published: 23 September 2015 nice.org.uk/guidance/mtg27 NICE 2017. All rights
Virtual Touch Quantification to diagnose and monitor liver fibrosis in chronic hepatitis B and C Medical technologies guidance Published: 23 September 2015 nice.org.uk/guidance/mtg27 NICE 2017. All rights
Non invasive assessment of liver fi brosis ONLY. liver diseases liver biopsy liver fibrosis biomarkers fibrotest fibroscan
 Ann Transplant, 2008; 13(2): 5-11 Received: 2008.04.15 Accepted: 2008.04.29 Published: 2008.06.17 Key words Full-text PDF: Word count: 1979 Tables: 1 Figures: 2 References: 50 Author s address: Non invasive
Ann Transplant, 2008; 13(2): 5-11 Received: 2008.04.15 Accepted: 2008.04.29 Published: 2008.06.17 Key words Full-text PDF: Word count: 1979 Tables: 1 Figures: 2 References: 50 Author s address: Non invasive
Hepatitis B screening and surveillance in primary care
 Hepatitis B screening and surveillance in primary care Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital Disclosures
Hepatitis B screening and surveillance in primary care Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital Disclosures
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Noninvasive Techniques for the Evaluation and Page 1 of 34 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Noninvasive Techniques for the Evaluation and Professional
Noninvasive Techniques for the Evaluation and Page 1 of 34 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Noninvasive Techniques for the Evaluation and Professional
EVALUATION OF ABNORMAL LIVER TESTS
 EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
Management of Hepatitis B - Information for primary care providers
 Management of Hepatitis B - Information for primary care providers July 2018 Chronic hepatitis B (CHB) is often a lifelong condition. Not everyone infected needs anti-viral therapy. This document outlines
Management of Hepatitis B - Information for primary care providers July 2018 Chronic hepatitis B (CHB) is often a lifelong condition. Not everyone infected needs anti-viral therapy. This document outlines
