Inpatient Psychiatric Length of Stay. And Readmission Rates. Katrina A. Drager
|
|
|
- Samantha Young
- 5 years ago
- Views:
Transcription
1 Inpatient Psychiatric Length of Stay And Readmission Rates by Katrina A. Drager A ResearchPaper Submitted in Partial Fulfillment of the Requirements for the MasterofScienceDegree in Applied Psychology Mitdadl SIIcrma., PIt.D. / L: The Graduate School University of Wisconsin-Stout December, 2007
2 ii The Graduate School University of Wisconsin-Stout Menomonie, WI Author: Katrina A. Drager Title: Inpatient Psychiatric Length ofstay and Readmission Rates Graduate Degree/ Major: MS Applied Psychology Research Adviser: Mitchell Sherman, Ph.D. MonthlYear: December, 2007 Number of Pages: 70 Style Manual Used: American Psychological Association, 5 th edition ABSTRACT Average length of inpatient hospital stays are a concern of many stakeholders within the mental health care community, mental health providers, clinics, hospitals, and insurance companies. An analysis was conducted to determine whether average length of stay is significantly related to readmission rates at industry standard levels of 7 day readmission and 30 day readmission. The results showed that the shortest stay group of 2-3 days and the longest stay group of 8+ days had significantly higher rates of readmission both at 7 day and 30 day readmissions. Further research is necessary to determine both the reliability of these results, and causal explanations.
3 iii The Graduate School University of Wisconsin Stout Menomonie, WI Acknowledgments I would like to thank my Husband Michael D. Drager Jr. and my son Ayden D. Drager for allowing me the time to complete this work. I also would like to thank my parents, Dean & MaryAnn Cranston for always believing in my talents. In addition, I would like to thank my Mother-In-Law Sandra Drager for all the babysitting and help around the house while I worked on my degree.
4 iv TABLE OF CONTENTS...Page Abstract List of Tables Chapter I: Introduction Statement ofthe Problem Purpose ofthe Study Assumptions ofthe Study Definition ofterms Methodology Chapter II: Literature Review Chapter III: Methodology Participant Selection and Description ii vi Instrumentation Data Collection Procedures Limitations Summary Chapter IV: Results Cohort July 1,2003 -June 30,2005 Cohort January 1, December 31, 2006 Combined Cohorts Chapter V: Discussion Limitations Conclusions
5 v Recommendations References Appendix A: Diagnostic Codes for Eating Disorders Appendix B Diagnostic Codes for Complex Cases Appendix C: Diagnostic Codes for Substance Abuse and Detoxification
6 VI List of Tables Table 1: Cumulative Percent of Days Paid for All Claims 16 Table 2: Comparison of the Number of Claims for Each Subpopulation Based on Claim Time Period 20 Table 3: One-Way ANOVA for Days Paid Groups and Readmission Rate at 7 Days for July 1,2003 to June 30, Table 4: HSD Comparisons Days Paid Groups and Readmission Rate at 7 Days for July, 2003 to June 30, Table 5: One-Way ANOVA for Days Paid Groups and Readmission Rate at 30 Days for July 1,2003 to June 30, Table 6: HSD Comparisons Days Paid Groups and Readmission Rate at 30 Days for July, 2003 to June 30, Table 7: One-Way ANOVA for Days Paid Groups and Readmission Rate at 7 Days for January 1,2005 to December 31, Table 8: HSD Comparisons Days Paid Groups and Readmission Rate at 7 Days for January 1,2005 to December 31, Table 9: One-Way ANOVA for Days Paid Groups and Readmission Rate at 30 Days for January 1,2005 to December 31, 2006, 26 Table 10: HSD Comparisons Days Paid Groups and Readmission Rate at 30 Days for January 1,2005 to December 31, Table 11: One-Way ANOVA for Adult General Mental Health Days Paid Groups and Readmission Rate at 7 Days 28 Table 12: HSD Comparisons Adult General Mental Health Days Paid Groups and Readmission Rate at 7 Days 28 Table 13: One-Way ANOVA for Adult General Mental Health Days Paid Groups and Readmission Rate at 30 Days 29 Table 14: HSD Comparisons Adult General Mental Health Days Paid Groups and Readmission Rate at 30 Days Table 15: One-Way ANOVA for Complex Case Population Days Paid Groups and Readmission Rate at 7 Days Table 16: HSD Comparisons Complex Case Population Days Paid Groups and Readmission Rate at 7 Days
7 vii Table 17: One-Way ANOVA for Complex Case Population Days Paid Groups and Readmission Rate at 30 Days 32 Table 18: One-Way ANOVA for Child General Mental Health Days Paid Groups and Readmission Rate at 7 Days 32 Table 19: HSD Comparisons Child General Mental Health Days Paid Groups and Readmission Rate at 7 Days 33 Table 20: One-Way ANOVA for Child General Mental Health Days Paid Groups and Readmission Rate at 30 Days 34 Table 21: HSD Comparisons Child General Mental Health Days Paid Groups and Readmission Rate at 30 Days 34 Table 22: One-Way ANOVA for Substance Abuse and Detoxification Population Days Paid Groups and Readmission Rate at 7 Days 35 Table 23: HSD Comparisons Substance Abuse and Detoxification Populations Days Paid Groups and Readmission Rate at 7 Days 35 Table 24: One-Way ANOVA for Substance Abuse and Detoxification Populations Days Paid Groups and Readmission Rate at 30 Days 36 Table 25: One-Way ANOVA for Eating Disorders Population Days Paid Groups and Readmission Rate at 7 Days 37 Table 26: One-Way ANOVA for Eating Disorders Population Days Paid Groups and Readmission Rate at 30 Days 38 Table 27: HSD Eating Disorders Population Days Paid Groups and Readmission Rate at 30 Days 38
8 1 Chapter I: Introduction Average length of stay and readmission rates are a common concern of healthcare providers, mental healthcare providers, and insurance companies alike. The length of an inpatient's hospital stay may predict whether they will consequently return to a normal life or be readmitted to another inpatient stay. The length of an inpatient hospital stay is expensive for everyone involved, but it is also a critical variable in the effective treatment of many psychiatric illnesses. Therefore, it may partially determine the likelihood of readmission of the patient into inpatient care at a later time. The determination of how long a patient should be in the hospital for psychiatric treatment is not an easy decision for anyone involved. There are many factors which affect the length of stay ranging from diagnosis, co-morbidity of medical illnesses, and age of the patient. Additional contributing factors include previous success of the particular inpatient program related to the particular case at hand, availability of effective outpatient treatment options, availability of effective partial hospitalization options, and so forth. The intention of the present research is the initiation of a series of studies to delineate and thoroughly describe length of stay, readmission, and its implications to the field. Statement ofthe Problem Differing lengths of hospital stay are differentially effective at reducing the readmission rate. The intent ofthis research is to examine what length of stay serves the psychiatric patient best in regards to avoidance of readmission to inpatient care.
9 2 Purpose ofthe Study The purpose of this study was to examine variances between different groupings of average length of stay and readmission rates at 7 days and 30 days. Readmission rates at 7 days and 30 days post discharge are considered a facility standard for quality care. Assumptions ofthe Study It is assumed that the membership ofthe mental health insurance company is similar to the overall mental health patient population. Industry standard of care related to readmission rates at 7 days and 30 days are assumed to be valid measures for quality of care. Definition ofterms Average length of stay is defined as the length of stay that is typical for an inpatient hospital stay. Readmission is defined as the re-admittance of an inpatient mental health patient to another inpatient mental health stay. Readmission at 7 days is defined as re-admittance within 7 days of discharge from an inpatient mental health stay. Readmission at 30 days is defined as re-admittance within 30 days of discharge from an inpatient mental health stay, not including those counted as re-admitted within 7 days of discharge. Days paid is assumed equivalent to length of stay, as the length of stay and the days paid are essentially the same. Partial hospitalization is defined as a patient commuting to the hospital up to 7 days a week for treatment but residing at home.
10 3 Methodology The population consisted of all members of the mental health insurance company who had claims paid between July 1,2003 to June 30, 2005 and January 1,2005 to December 31, 2006, including children, adolescents, adults, geriatric, eating disorders, complex cases, and substance abuse and detoxification inpatients. No claims were excluded from the analysis. Diagnostic population types for Eating Disorders, Complex Cases, and Alcohol & Substance Abuse were separated based upon the primary and secondary diagnosis code on the claim. If the claim did not fit into one of those three diagnostic populations, then the claim was assigned to Adult General Mental Health Diagnostic Population if the age of the patient was 18 years or older, and Child General Mental Health Diagnostic Population if the age of the patient was under 18 years. A thorough literature review was conducted before data analysis was begun in order to ensure a comprehensive understanding of the problem. After the literature review was complete the data set was formatted and analyzed using SAS Version 9.1.
11 4 Chapter II: Literature Review According to Lieberman, Wiitala, Elliott, McCormick, & Goyette (1998), The past decade has seen dramatic changes in the role played by psychiatric hospitals in the care of patients. Patients who would have remained hospitalized for weeks, months, or even years are now treated mostly or entirely in outpatient settings. Lengths of stay are measured in days. Goals of admission have also changed greatly, from furthering development and building psychological "structure" to stabilizing symptoms, adjusting medication, and facilitating connections to outpatient care. (p.905) Lieberman, et ai., (1998) conducted a study at Dartmouth-Hitchcock Medical Center in New Hampshire while the program went through a change from longer lengths of stay in 1988 to shorter lengths of stay up to approximately The study consisted of three cohorts during this time frame. They were grouped as follows: cohort 1, ; cohort 2, ; and cohort 3, It was discovered that the final cohort 3, consisting of patients with the shortest hospital stay, showed no significant difference in levels of functioning between those in earlier cohort 1 who were solely hospitalized versus those in cohort 2 who were hospitalized and then followed up with partial hospitalization. This finding could be due to the differences in overall level of illness between the two subgroups, further investigation is needed. Another finding was that the length of stay for those not experiencing a partial hospitalization was approximately 9.6 days, in contrast to those experiencing a partial hospitalization, whose length of stay averaged 6.7 days, followed by weeks ofpartial
12 5 hospitalization. Additionally, readmission rates from cohort 1,N=12 (17.6%) to cohort 2, N=2 (6.3%) decreased, but they increased from cohort 2, N=2 (6.3%) to cohort 3, N=12 (17.1%). Although, there seemed to be no change in readmission rates in relation to the reduction in the average length of stay, there did appear to be adverse affects suffered by the patient population as shown through the study. These adverse affects are indicated by Liberman, et al., (1998) as he concluded "patients are now more depressed and more globally impaired when they leave the hospital." (p.908) According to the work of Liberman, et al., (1998),... as clinical experience suggests, depressed patients are now discharged more depressed than they previously were, and with lower scores on the Global Assessment of Functioning Scale. One month after discharge, although readmission rates were equal, global and work functioning remained lower among the short-stay group. (p.908) The findings of Liberman, et al., (1998) should not only be of concern to researchers and clinicians, but to patients, counselors, and insurance companies. This seems to be a time when we are all considering the rising levels of stress within our culture and the rising cost of healthcare. An individual deserves the care that best treats their illness so that they can return to their lives and their work functioning at levels that are as high as possible. Outpatient care may appear to be cheaper, but the length ofthe care may be more costly and more stressful than inpatient care. In this study this seems to be the case as indicated by longer rather than shorter hospital stays or partial hospitalization.
13 6 An analysis completed by Case, Olfson, Marcus, and Siegel (2007) on children and adolescents in community based hospitals indicated by ICD-9-CM codes 290 to 319 showed no significant changes in discharge rates in the decade of 1990 to In addition, "The proportion of discharges diagnosed with principal bipolar disorders rose dramatically from 2.9% to 15.21%. Increases were also observed in the proportion diagnosed with psychotic disorders" (p.92). Despite the decrease in length of stay and the increase in severity of illness in this particular population, it appears that clinicians are doing more in a shorter amount of time. "Inpatient clinicians who on average evaluated, treated, and discharged mentally ill children over the course of 12 days in 1990 routinely accomplished these tasks in 4 1/2 days by 2000" (Case, et ai., 2007, p.94). It is important to note that alarmingly, the quartile with the longest length of stay had the greatest reduction in length ofstay"... while the 75 th percentile fell significantly from 27.2 to 7.7 days, a decline of 72%" (Case, et ai., 2007, p.94). Case, et ai., (2007) follows with, Declines in average length of stay over the period were generally greatest for diagnoses and other characteristics associated with the longest average length of stay in Rather than a targeted reduction of average length of stay for treatment of patients with less severe illnesses and, presumably, less complex clinical needs, this trend in average length of stay suggests the emergence of a more uniform standard of inpatient treatment duration irrespective of patient need. (p.94) This leads to another fact of concern, "Inpatient mental health professionals routinely evaluate, treat, and discharge depressed children and adolescents in 4 days, well before the onset of response to selective serotonin reuptake inhibitor pharmacotherapy or the emergence of adverse effects" (Case, et ai., 2007, p.95). This not only leads to a potential
14 7 health risk but an issue of follow-up care. Accounting for the effects of anti-depressant medication and the increase in suicidal ideation at the beginning of anti-depressant treatment in children and adolescents, discharging them within days of beginning this medication is alarming without intensive follow-up to insure the safety ofthe patient. In addition, research by Case, et al. (2007) indicates that transfers to other inpatient facilities and subsequent treatment are on the decline, with the majority of discharges being to home. Considering the severity of the majority ofthe illnesses at admission this fact is disconcerting. Additionally, this particular study did not address readmission, as the patients were not identified as to allow such analysis, lending to an uncertainty about the effectiveness of the initial admission. Several possible conclusions could be garnered from this information. To name a few, first, in order to provide the care the patient needs"...under scrutiny ofmanaged care review, inpatient providers may be indicating more serious diagnoses to justify admission or secure greater reimbursement, a process termed "diagnostic upcoding"" (Case, et al., 2007, p.95). Second, there is a disproportionate case mix found at community hospitals. Third, private hospitals and programs are not accounted for within this study. According to work done by Horvitz-Lennon, Normand, Gaccione, and Frank (2001), "Rising mental health spending has triggered cost-containment efforts primarily aimed at decreasing inpatient utilization" (p. 676). They discovered that, "Regardless of study design, the most frequent exclusion criterion was, by far, "too severely ill" (i.e., dangerousness to self or others; disruptive behavior). Other frequent exclusion criteria were cognitive impairment and antisocial behavior" (Horvitz-Lennon et al., 2001, p.680).
15 8 The determination made at the end ofthe study was that there was no difference in effect between partial hospitalization and inpatient treatments. It is important to note that this result cannot be generalized beyond the applicable population of this research, due to the large amount of exclusions and transference of care from partial to inpatient. In addition, Horvitz-Lennon et al., (2001) also assert"...61% to approximately 80% of partial care patients will eventually be transferred and fully hospitalized. Conversely, approximately 21% to 39% of acutely ill patients may be solely treated with partial hospitalization" (p.682). The average length of a hospital stay for a psychiatric patient can also be complicated by co-morbidity of medical illness. Work done by Lyketsos, Dunn, Kaminsky, and Breakey (2002) details the issues of comorbidity in psychiatric inpatient cases. According to Lyketsos, et al., (2002), "A wide range of comorbidity has been described, with chronic medical illnesses such as hypertension, heart disease, pulmonary disease, and diabetes, being the most common" (p.24). This is a concern considering these medical illnesses are chronic and require monitoring and in many cases medications in order to control. According to Lyketsos, et al., (2002) this can have effects on psychiatric outcomes, average length of stay, and overall patient functioning. The concern is that "Psychiatric medications also have health effects, such as impaired glucose tolerances, effects on renal function, effects on liver function, and many others" (Lyketsos, et al., 2002, p.24), leading to further medical complications in treatment and effects. In addition, Lyketsos, et al., (2002) state, "Medications used to treat medical illness often have psychiatric effects" (p.24), which leads also to the concern that medications used to treat medical illnesses are contributing to the outcomes of psychiatric
16 9 diagnosis and treatments, a viscous circle ofmedicating to counter the effects ofthe medications. Additionally, Lyketsos, et al. (2002) believe that, "another link is that psychiatric patients are less motivated to seek care for medical illness. They are often neglectful of their health and self-care" (p.24), which leads to the possibility that psychiatric patients are at greater risk for medication non-compliance, greater levels of morbidity, and mortality related to medical illness due to their psychiatric illness. A serious concern for doctors, mental health professionals, and insurance companies alike is the statement by Lyketsos, et al., (2002) that, "... psychiatric patients are less likely to receive necessary medical care and have higher rates ofmorbidity and mortality from medical illnesses when compared with control populations" (p.25). Psychiatric patients need more attention and care in order to avoid the higher rates of morbidity and mortality rates. In addition, Lyketsos, et al. (2002) state that"... medically ill psychiatric patients might have more severe psychiatric symptoms, might have greater functional impairment, and might have longer lengths of stay when hospitalized on psychiatric units" (p.25), due to the greater need for more specialized and intensive care brought on by the combination of psychiatric illness, side effects of a medical nature due to psychiatric medications, medical illness, and psychiatric side effects of medically needed medications. "The presence of a physical diagnosis in depressed inpatients was associated with a stay on the psychiatric unit of a general hospital that was on average 4 days longer" (Lyketsos, et al., 2002, p.25), assumed to be due to the intensity of care required for complicated cases. Despite the longer hospital stay required by cases of a co-morbid nature at discharge these patients are more impaired in their functioning. According to Lyketsos, et
17 10 al., (2002), "... average length of stay was significantly longer by an average of 5.4 days" (p.27). This is concern considering that the stay was longer yet the functioning more impaired upon discharge, most likely leading to another inpatient admission or further outpatient care upon discharge. Work completed by Pavkov, Boerge, and Czapkowicz (1997) address the concern of average length of stay related to youth hospitalizations in Illinois. The findings showed that, "those diagnosed with attention deficit, psychotic, and conduct disorder experienced longer hospitalizations, in contrast youths diagnosed with depressive disorders, drug and alcohol disorders, and adjustment disorders had shorter hospitalizations" (Pavkov, et al., 1997, p.221). In their work, Pavkov, et al., (1997) point out that, "Some investigators have speculated that the length of hospitalization is dependent upon the type and array of community-based services available in different geographic locations" (p.222). Interestingly, the work by Grinshpoon, Shershevsky, Levinson, and Ponozovsky (2003) in Israel on a population of long term stay patients, of whom 70% were schizophrenic with an ICD-I0 diagnosis, supports the notion that residential treatment does in fact save inpatient hospitalization time. "...(1) only one out of three residents was rehospitalized, (2) and whenever hospitalization was needed, the inpatient stay was substantially shorter" (Grinshpoon, et al., 2003, p.272). Unfortunately, the study did not assess the levels of functioning attained or not attained by the patients who were transferred from inpatient to residential care. The primary goal of treatment should be the improvement of patient functioning using the most effective means available, regardless of whether the means which achieve the goal are inpatient hospitalization, outpatient treatment options, or a combination. The study provides evidence that the
18 11 "...rehospitalized residents tended to be younger at first-in-life hospitalization... than their nonhospitalized counterparts... " (p.272). A note ofcaution was included by Grinshpoon, et al. (2003). "However, we are aware that the overall cost of community care is higher than the cost of running the residences, because services that were provided within the hospital are now only available outside ofthe hospitals... a more rigorous design comparing direct and indirect expenditures in hospital and community is required to answer this question" (p.272). This indication that there is a lack of overall cost benefit analysis between residential, community, and inpatient costs is a concern. Work would need to be completed first to determine which methods of treatments are most effective in terms of different diagnoses. Second, the costs of different methods oftreatment would have to be determined. Third, the cost and benefit of each treatment would have to be laid out and analyzed in order to give a more definitive answer to the question, Should long term hospitalized patients remain hospitalized or should they be moved to residential or community treatment options? This particular research doesn't truly answer this question. It tells us that residential and community treatment options save inpatient hospital days. The real question is, at what cost does the saving of inpatient days come? Research completed by Kunik, Edwards, Molinari, Hale, and Orengo (2001) on geriatric patients specifically suffering from dementia show support for decreasing length ofstay. Although the length of stay considered in this particular study could be construed as a long length of stay in general, "a length of stay beyond 20 days rather than beyond 30 days, as previously required' (Kunik, et al., 2001, p.376) requires reporting to their chief. This reduction in average length of stay by 10 days did"... indicate that the
19 12 cognitive and emotional status ofpatients discharged since that time are equivalent to those of patients discharged after longer hospital stays" (Kunik, et ai., 2001, p.376), suggesting that this reduction did not have any effect on patient outcomes. Although there was a possible change in outpatient services due to, "shortened lengths of stay, geropsychiatry outpatient services were enhanced - for example, a geropychologist was added to the outpatient treatment plan" (Kunik, et ai., 2001, p.377). This leaves unanswered the question, did outpatient services increase and at what cost? Was there an increase in readmissions? It would be valuable to know whether the outpatient treatment had to be extended, since it appears that patient outcome remained the same regardless of the change in average length of stay.
20 13 Chapter III: Methodology This section is a review of the methods used to complete this study. The problem this research addresses is whether average length of stay is at all indicative of readmission rate. In other words does average length ofhospital inpatient stay explain any variance in the rate of inpatient readmission, defined as an industry standard of readmission within 7 days of discharge or readmission within 30 days of discharge? The following section discusses the participant selection and description, instrumentation, data collection procedures, data analysis, and limitations ofthis study. Participant Selection and Description The population consists of all members ofthe mental health insurance company, and may be representative of all mental health patients throughout the country. The sample consisted of all claims paid by the mental health insurance company between July 1,2003 through June 30, 2005 and between January 1,2005 through December 31,2006. In the first two experiments all population subgroups were combined in the final experiment the population subgroups were separated. In order to determine population subgroups first, the claim was assessed by determining if there was a diagnosis for eating disorders, as seen in Appendix A. Ifthe claim did not have a diagnosis for eating disorders, it was examined for diagnosis codes for complex cases, as seen in Appendix B. Ifthe claim was not related to an eating disorder or complex case diagnosis, it was then tested for substance abuse and detoxification diagnosis codes, as seen in Appendix C. If the claim did belong to one of those classifications the claim was then classified as adult general mental health or child
21 14 general mental health based upon the age of the patient. The dates selected were based upon convenience as those were the dates which data was readily available to analyze. Instrumentation SAS for Windows, version service pack 4, was used to complete the data analysis. Data Collection Procedures The sample consisted of all claims paid by the mental health insurance company between July 1,2003 through June 30, 2005 and between January 1, 2005 through December 31, This data is contained in the data warehouse within the mental health insurance company, the data used is based on claims paid. The data were pooled after a minimum of 90 days from the date of service related to the claim to ensure that a limited number of claims would be lost in adjudication. The data sets are limited to those members with an inpatient mental health stay. Access to this data is limited to authorized personnel working within the company which this research was completed. Limitations This study is limited to claims data alone, meaning that any inpatient admissions or readmissions which were not paid by the mental health insurance company were not included in the research. This is considered a serious limitation considering the lack of generalizability of the research to all inpatient stays. Readmissions which were not covered by the mental health insurance company are not included in the study. Those people who do not have access to mental health insurance from the mental health insurance company are not included in the study as we do not have any information beyond those claims which the mental health insurance company has paid. It could be
22 15 assumed that people who do not have access to mental health insurance will be a population ofdifferent demographics and socio-economical status therefore these results in no way should be generalized to a population ofnon-mental health insured individuals. Another limitation is the short time frame, limiting the variety of claims. Additionally, this study only assesses industry standard 7 day readmissions and 30 day readmissions, but long term affects of inpatient stays in terms of readmission would be of interest. Finally, this research was conducted within a single mental health insurance company. Summary The data was divided into length of stay groupings for analysis as described above. The groupings were based on approximate quartiles of the data. The analyses will consisted of fourteen, one-way ANOVAs, comparing the different length of stay groupings to readmission rates at 7 and 30 days. Keeping in mind the limitation that this research was conducted within a single mental health insurance company, the results should be interpreted with caution with regard to generalizability.
23 16 Chapter IV: Results The analysis began with frequencies for days paid to determine groupings for average length of stay. Days paid indicated that stays in length of 2 to 3 days accounted for 30.69% of claims and were assigned Group 1; stays in length of 4 to 5 days accounted for 29.02% of claims and were assigned Group 2; stays in length of 6 to 7 days accounted for 18.4% of claims and were assigned Group 3; and last, stays in length of 8+ days accounted for 21.89% of claims and were assigned to Group 4; as shown in table 1. The data were quartile to allow for more meaningful analysis, exact quartering was not possible so, approximate quartiles were used. Table 1 Cumulative Percent ofdays Paidfor All Claims Days Paid Frequency Cumulative Percent 2 12, % 3 16, % 4 15, % 5 12, % 6 9, % 7 7, % 8 4, % 9 3, % 10 2, % 11 1, %
24 17 Days Paid Frequency Cumulative Percent 12 1, , , % 93.51% 94.76% 95.54% 96.16% 96.69% 97.20% 97.55% 97.88% 98.19% 98.37% 98.55% 98.71% 98.84% 98.95% 99.07% 99.18% 99.29% 99.43% 99.49% 99.53% 99.56%
25 18 Days Paid Frequency Cumulative Percent % 99.64% 99.69% 99.70% 99.73% 99.74% 99.77% 99.79% 99.81% 99.83% 99.84% 99.92% 99.92% 99.92% 99.93% 99.94% 99.95% 99.96% 99.96% 99.97% 99.97% 99.97%
26 19 Days Paid Frequency Cumulative Percent % % % % % % % % % % % % % Frequency distribution information for claims data from July 1,2003 through June 30, 2005 revealed that 30,782 claims were for adult general mental health, 4,391 claims were for complex cases, 10,109 claims were for child general mental health, 10,973 claims were for substance abuse & detoxification, and 364 claims were for eating disorders, as indicated in table 2. Frequency distribution information for claims data from January 1,2005 through December 31,2006 revealed that 20,841 claims were for adult general mental health, 3,084 claims were for complex cases, 6,550 claims were for child
27 20 general mental health, 7,662 claims were for substance abuse & detoxification, and 287 claims were for eating disorders, also indicated in table 2. Table 2 Comparison ofthe Number ofclaims for Each Subpopulation Based on Claim Time Period Time Period Eating Complex Substance Adult Child Disorders Cases Abuse & General General Detoxification Mental Mental Health Health July 1, 2003 through 364 4,391 10,973 30,782 10,109 June 30, 2005 January 1,2005 through 287 3,084 7,662 20,841 6,550 December 31, 2006 Total Claims 651 7,475 18,635 51,623 16,659 Fourteen One-Way Analyses of Variance (ANOYA) were completed. They included two on the claims from July 1,2003 through June 30, 2005, two on claims from January 1, 2005 through December 31, 2006, and ten on the combined claims of July 1, 2003 through June, and January 1,2005 through December 31, 2006 which were separated by diagnosis code into population subgroups, to determine if different population subgroups have different needs regarding length of stay in relation to readmission rates.
28 21 The following are the results ofthree sets of one-way ANOVA on the inpatient hospital stay claims data collected at CIGNA Behavioral Health. The first two one-way ANOVA are completed on claims data July 1, 2003 to June 30, 2005, the second two one-way ANOVA are completed on claims data January 1, 2005 to December 31, 2006 in order to show repeatability ofthe results ofthe first two ANOVA. The third set of ANOVA is on the combined claims data found in the first two sets of ANOVA, separated out by population. This separation by population is an attempt to ascertain the effects of the days paid groupings on different populations. The goal of all three sets of analyses is to ascertain the effects of the length of inpatient stay on readmission rates at 7 days and 30 days. Cohort July 1, June 30, 2005 The first set of one-way ANOVA was completed on data ranging July 1,2003 to June 30, As stated earlier, the groupings of days paid were used in the analyses to compare shorter lengths ofstay to longer lengths of stay, to determine whether there was an effect on readmission rates at 7 and 30 days. The data set included 56,619 observations. The results for readmission rates at 7 days indicate F (3, 56615) = 14.34, P <.01, as indicated in Table 3. Group 1 had 17,690 observations (M =.089), Group 2 had 16,280 observations (M =.082), Group 3 had 10,199 observations (M =.086), and Group 4 had 12,450 observations (M =.104). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 1, Group 4 to Group 3, Group 4 to Group 2, and Group 1 to Group 3, as indicated in Table 4.
29 22 Table 3 One-Way ANOVAfor Days Paid Groups and Readmission Rate at 7 Days July 1,2003 to June 30, 2005 Source Df SS MS F p Days Paid Grouped <.0001 ** Error 56,615 4, Corrected Total 56,618 4, * p <.05 ** p <.01 Table 4 HSD Comparisons Days Paid Groups and Readmission Rate at 7 Daysfor July 1, 2003 to June 30, 2005 Days Paid Group Comparison Difference Between Means Simultaneous 95% Confidence Limits Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 1 - Group * Group 1 - Group Group 3 - Group * p <.05 ** p <.01 The results for readmission rates at 30 days indicate F (3, 56615) = 31.72, p <.01, as indicated in Table 5. Group 1 had 17,690 observations (M=.136), Group 2 had 16,280 observations (M=.135), Group 3 had 10,199 observations (M=.148), and Group
30 23 4 had 12,450 observations (M=.171). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 1, Group 4 to Group 2, Group 3 to Group 1, and Group 2 to Group 3, as indicated in Table 6. Table 5 One-Way ANOVAfor Days Paid Groups and Readmission Rate at 30 Days for July 1, 2003 to June 30, 2005 Source Df SS MS F P Days Paid Grouped <.0001 ** Error 56,615 7, Corrected Total 56,618 7, * p <.05 ** p <.01 Table 6 HSD Comparisons Days Paid Groups and Readmission Rate at 30 Daysfor July 1,2003 to June 30,2005 Days Paid Group Comparison Difference Between Means Simultaneous 95%.Confidence Limits Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 3 - Group * Group 3 - Group *
31 24 Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 3 - Group * Group 1 - Group * p <.05 ** P <.01 Cohort January 1,2005 to December 31,2006 The second set of one-way ANOVA was completed on data ranging January 1, 2005 to December 31, The groupings of days paid as stated previously in the methods section were used in analysis to compare shorter lengths of stay to longer lengths of stay to determine ifthere was an effect on readmission rates at 7 and 30 days. The data set included 38,424 observations. The results for readmission rates at 7 days indicate F (3,38420) = 10.67,p <.01, as indicated in Table 7. Group 1 had 11,482 observations (M=.093), Group 2 had 11,299 observations (M=.087), Group 3 had 7,290 observations (M=.097), and Group 4 had 8,353 observations (M=.110). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 1, and Group 4 to Group 2, as indicated in Table 8.
32 25 Table 7 One-Way ANOVAfor Days Paid Groups and Readmission Rate at 7 Days for January 1, 2005 to December 31, 2006 Source Df SS MS F p Days Paid Grouped <.0001 ** Error 38,420 3, Corrected Total 38,423 3, * p <.05 ** P <.01 Table 8 HSD Comparisons Days Paid Groups and Readmission Rate at 7 Days January 1, 2005 to December 31, 2006 Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 3 - Group Group 3 - Group Group 1 - Group *P <.05 ** P <.01 The results for readmission rates at 30 days indicate F (3, 38420) = 26.28, P<.01, as indicated in Table 9. Group 1 had 11,482 observations (M =.139), Group 2 had 11,299 (M=.146), Group 3 had 7,290 observations (M=.097), and Group 4 had 8,353
33 26 observations (M=.110). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 2, Group 4 to Group 1, Group 3 to Group 2, Group 3 to Group 1, and Group 1 to Group 3, as indicated in Table 10. Table 9 One-Way ANOVAfor Days Paid Groups and Readmission Rate at 30 Days for January 1, 2005 to December 31, 2006 Source Df SS MS F p Days Paid Grouped <.0001 ** Error 38,420 5, Corrected Total 38,423 5, *P <.05 ** P <.01 Table 10 HSD Comparisons Days Paid Groups and Readmission Rate at 30 Days January 1,2005 to December 31, 2006 Days Paid Group Comparison Difference Between Means Simultaneous 95% Confidence Limits Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 3 - Group * Group 3 - Group * Group 2 - Group *p <.05 ** P <.01
34 27 Combined Cohorts The third set ofone-way ANOVA was completed on the combined cohorts of data ranging July 1, 2003 to June 30, 2005 and January 1,2005 to December 31, The groupings of days paid as stated previously in the methods section were used in analysis to compare shorter lengths of stay to longer lengths of stay to determine if there was an effect on readmission rates at 7 and 30 days. The analysis was conducted by populations and they were divided out by Adult General Mental Health, Child General Mental Health, Eating Disorders, Complex Cases, and Substance Abuse & Detoxification. Adult General Mental Health The data set Adult General Mental Health included 51,622 observations. The results for readmission rates at 7 days indicate F (3,51619) = 18.83,p <.01, as indicated in Table 11. Group 1 had 15,587 observations (M=.087), Group 2 had 13,575 observations (M=.087), Group 3 had 9,519 observations (M=.091), and Group 4 had 12,942 (M =.110). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 1, and Group 4 to Group 2, as indicated in Table 12.
35 28 Table 11 One-Way ANOVAfor Adult General Mental Health Population Days Paid Groups and. Readmission Rate at 7 Days Source Df SS MS F p Days Paid Grouped <.0001 ** Error 51,619 4, Corrected Total 51,622 4, * p <.05 ** p <.01 Table 12 HSD Comparisons Adult General Mental Health Population Days Paid Groups and Readmission Rate at 7 Days Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 3 - Group Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 3 - Group Group 1 - Group * p <.05 ** p <.01
36 29 The results for readmission rates at 30 days indicate F (3,51619) = 48.69,p<.01, as indicated in Table 13. Group 1 had 15,587 observations (M=.133), Group 2 had 13,575 observations (M=.148), Group 3 had 9,519 observations (M=.160), and Group 4 had 12,942 observations (M=.184). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 2, Group 4 to Group 1, Group 3 to. Group 1, and Group 2 to Group 1, as indicated in Table 14. Table 13 One-Way ANOVAfor Adult General Mental Health Population Days Paid Groups and Readmission Rate at 30 Days Source Df SS MS F P Days Paid Grouped <.0001 * Error 51,619 6, Corrected Total 51,622 6, * p <.05 ** p <.01 Table 14 HSD Comparisons Adult General Mental Health Population Days Paid Groups and Readmission Rate at 30 Days Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group *
37 30 Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 3 - Group Group 3 - Group * Group 2 - Group * * p <.05 ** P <.01 Complex Cases The data set Complex Cases included 7,475 observations. The results for readmission rates at 7 days indicate F (3, 7471) = 3.04, P =.03, as indicated in Table 15. Group 1 had 1,615 observations (M=.099), Group 2 had 1,722 observations (M=.070), Group 3 had 1,366 observations (M=.089), and Group 4 had 2,772 observations (M=.090). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. The only significant pair was between Group 1 to Group 2, as indicated in Table 16. Table 15 One-Way ANOVAfor Complex Cases Population Days Paid Groups and Readmission Rate at 7 Days Source Df SS MS F' p Days Paid Grouped * Error 7, Corrected Total 7, * p <.05 ** p <.01
38 31 Table 16 HSD Comparisons Complex Case Population Days Paid Groups and Readmission Rate at 7 Days Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 1 - Group Group 1 -Group Group 1 - Group * Group 4 - Group Group 4 - Group Group 3 - Group * P <.05 ** p <.01 The results for readmission rates at 30 days indicate F (3, 7471) = 1.22, p =.30, as indicated in Table 17. Group 1 had 1,615 observations (M=.143), Group 2 had 1,722 observations (M=.124), Group 3 had 1,366 observations (M=.089), and Group 4 had 2,772 observations (M=.142). Tukey's Studentized Range (HSD) was not completed for this population as the results ofthe one-way ANOVA are not significant.
39 32 Table 17 One-Way ANOVAfor Complex Cases Population Days Paid Groups and Readmission Rate at 30 Days Source Pi ss MS F p Days Paid Grouped Error 7, Corrected Total 7, * p <.05 **p <.01 Child General Mental Health The data set Child General Mental Health included 16,659 observations. The results for readmission rates at 7 days indicate F (3, 16655) = 15.25,p <.01, as indicated in Table 18. Group 1 had 4,189 observations (M=.073), Group 2 had 4,891 observations (M=.072), Group 3 had 3,798 observations (M=.086), and Group 4 had 3,781 observations (M=.109). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 1, and Group 4 to Group 2, as indicated in Table 19. Table 18 One-Way ANOVAfor Child General Mental Health Population Days Paid Groups and Readmission Rate at 7 Days Source Df SS MS F p Days Paid Grouped <.0001 * Error 16, Corrected Total 16, * p <.05 ** p <.01
40 33 Table 19 HSD Comparisons Child General Mental Health Population Days Paid Groups and Readmission Rate at 7 Days Days Paid Group Comparison Difference Between Means Simultaneous 95% Confidence Limits Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 3 - Group Group 3 - Group Group 1 - Group * p <.05 ** p <.01 The results for readmission rates at 30 days indicate F (3, 16655) = 36.46, P<.01, as indicated in Table 20. Group 1 had 4,189 observations (M=.118), Group 2 had 4,891 observations (M=-.116), Group 3 had 3,798 observations (M=.147), Group 4 had 3,781 observations (M=.186). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. Significant results included; Group 4 to Group 3, Group 4 to Group 1, Group 4 to Group 2, Group 3 to Group 1, and Group 3 to Group 2, as indicated in Table 21.
41 34 Table 20 One-Way ANOVAfor Child General Mental Health Population Days Paid Groups and Readmission Rate at 30 Days Source Df SS MS F P Days Paid Grouped <.0001 * Error 16,655 1, Corrected Total 16,658 2, * p <.05 ** p <.01 Table 21 HSD Comparisons Child General Mental Health Population Days Paid Groups and Readmission Rate at 30 Days Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 4 - Group * Group 4 - Group * Group 4 - Group * Group 3 - Group * Group 3 - Group 2.03] * Group 1 - Group * p <.05 ** P <.01 Substance Abuse and Detoxification The data set Substance Abuse and Detoxification included 18,635 observations. The results for readmission rates at 7 days indicate F (3, 18631) = 3.27,p <.05, as
42 35 indicated in Table 22. Group 1 had 7,675 observations (M=.103), Group 2 had 7,283 observations (M =.088), Group 3 had 2,690 observations (M=.095), and Group 4 had 987 observations (M =.087). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. The only significant result was between Group 1 to Group 2, as indicated in Table 23. Table 22 One-Way ANOVAfor Substance Abuse and Detoxification Population Days Paid Groups and Readmission Rate at 7 Days Source Df SS MS F p Days Paid Grouped * Error 18,631 1, Corrected Total 18,634 1, *p <.05 ** p <.01 Table 23 HSD Comparisons Substance Abuse and Detoxification Population Days Paid Groups and Readmission Rate at 7 Days Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 1 - Group Group 1 - Group * Group 1 - Group Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound
43 36 Days Paid Group Difference Simultaneous 95% Confidence Limits Comparison Between Means Lower Bound Upper Bound Group 3 - Group Group 3 - Group Group 2 - Group, * p <.05 ** p <.01 The results for readmission rates at 30 days indicate F (3, 18631) = 2.61,p =.05, as indicated in Table 24. Group 1 had 7,675 observations (M=.153), Group 2 had 7,283 observations (M=.144), Group 3 had 2,690 observations (M=.153), and Group 4 had 987 observations (M=.124). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. No significant results were found between any ofthe groups indicating there is no real significant difference. Table 24 One-Way ANOVAfor Substance Abuse and Detoxification Population Days Paid Groups and Readmission Rate at 30 Days Source Df SS MS F p Days Paid Grouped * Error 18,631 2, Corrected Total 18,634 2, * p <.05 ** p <.01
44 37 Eating Disorders The data set Eating Disorders included 651 observations. The results for readmission rates at 7 days indicate F (3, 647) =.54,p =.65, as indicated in Table 25. Group 1 had 106 observations (M =.160), Group 2 had 108 observations (M=.166), Group 3 had 116 observations (M=.137), and Group 4 had 321 observations and (M=.124). Tukey's Studentized Range (HSD) was not completed as the results were not significant. Table 25 One-Way ANOVAfor Eating Disorders Population Days Paid Groups and Readmission Rate at 7 Days Source Df SS MS F p Days Paid Grouped Error Corrected Total *p <.05 **p <.01 The results for readmission rates at 30 days indicate F (3, 647) = 2.59, p =.05, as indicated in Table 26. Group 1 had 106 observations (M =.179), Group 2 had 108 observations (M=.222), Group 3 had 116 observations (M=.275), and Group 4 had 321 observations (M=.161). Tukey's Studentized Range (HSD) was then completed to determine significance within specific comparisons. The only significant result was between Group 3 to Group 4, as indicated in Table 27.
Hospital Length of Stay and Readmission for Individuals Diagnosed With Schizophrenia: Are They Related?
 April 17, 2008 Hospital Length of Stay and Readmission for Individuals Diagnosed With Schizophrenia: Are They Related? Summary Pan-Canadian data show relatively high rates of readmission and declining
April 17, 2008 Hospital Length of Stay and Readmission for Individuals Diagnosed With Schizophrenia: Are They Related? Summary Pan-Canadian data show relatively high rates of readmission and declining
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
Value of Hospice Benefit to Medicaid Programs
 One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
One Pennsylvania Plaza, 38 th Floor New York, NY 10119 Tel 212-279-7166 Fax 212-629-5657 www.milliman.com Value of Hospice Benefit May 2, 2003 Milliman USA, Inc. New York, NY Kate Fitch, RN, MEd, MA Bruce
RISK FACTORS FOR PSYCHIATRIC HOSPITALIZATION AMONG ADOLESCENTS
 SILBERMAN S C H O O L of S O C I A L W O R K RISK FACTORS FOR PSYCHIATRIC HOSPITALIZATION AMONG ADOLESCENTS Jonathan D. Prince, Ph.D Marina Lalayants, Ph.D. Child Welfare in the U.S. and Russia May 30
SILBERMAN S C H O O L of S O C I A L W O R K RISK FACTORS FOR PSYCHIATRIC HOSPITALIZATION AMONG ADOLESCENTS Jonathan D. Prince, Ph.D Marina Lalayants, Ph.D. Child Welfare in the U.S. and Russia May 30
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
ADVANCED BEHAVIORAL HEALTH, INC. Clinical Level of Care Guidelines
 The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
Suicide Risk Assessment Self-Test
 Suicide Risk Assessment Self-Test The 30 item true or false self-test is designed to enhance clinician suicide risk assessment by incorporating evidence-based risk and protective factors. This self-test
Suicide Risk Assessment Self-Test The 30 item true or false self-test is designed to enhance clinician suicide risk assessment by incorporating evidence-based risk and protective factors. This self-test
SPARRA Mental Disorder: Scottish Patients at Risk of Readmission and Admission (to psychiatric hospitals or units)
 SPARRA Mental Disorder: Scottish Patients at Risk of Readmission and Admission (to psychiatric hospitals or units) A report on the work to identify patients at greatest risk of readmission and admission
SPARRA Mental Disorder: Scottish Patients at Risk of Readmission and Admission (to psychiatric hospitals or units) A report on the work to identify patients at greatest risk of readmission and admission
Medical Necessity Criteria
 SECTION 3: MEDICAL NECESSITY CRITERIA 3.0 Definition of Medical Necessity Medical necessity is the principal criteria by which the Fresno County Mental Health Plan (FCMHP) decides to accept and approve
SECTION 3: MEDICAL NECESSITY CRITERIA 3.0 Definition of Medical Necessity Medical necessity is the principal criteria by which the Fresno County Mental Health Plan (FCMHP) decides to accept and approve
Behavioral Health Hospital and Emergency Department Health Services Utilization
 Behavioral Health Hospital and Emergency Department Health Services Utilization Rhode Island Fee-For-Service Medicaid Recipients Calendar Year 2000 Prepared for: Prepared by: Medicaid Research and Evaluation
Behavioral Health Hospital and Emergency Department Health Services Utilization Rhode Island Fee-For-Service Medicaid Recipients Calendar Year 2000 Prepared for: Prepared by: Medicaid Research and Evaluation
Cost-Motivated Treatment Changes in Commercial Claims:
 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non- Medical Switching August 2017 THE MORAN COMPANY 1 Cost-Motivated Treatment Changes in Commercial Claims: Implications for Non-Medical
Heart Attack Readmissions in Virginia
 Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
Heart Attack Readmissions in Virginia Schroeder Center Statistical Brief Research by Mitchell Cole, William & Mary Public Policy, MPP Class of 2017 Highlights: In 2014, almost 11.2 percent of patients
The Value of Engagement in Substance Use Disorder (SUD) Treatment
 The Value of Engagement in Substance Use Disorder (SUD) Treatment A Report from Allegheny HealthChoices, Inc. June 2016 Introduction When considering substance use disorder (SUD) treatment, the length
The Value of Engagement in Substance Use Disorder (SUD) Treatment A Report from Allegheny HealthChoices, Inc. June 2016 Introduction When considering substance use disorder (SUD) treatment, the length
Alberta Alcohol and Drug Abuse Commission. POSITION ON ADDICTION AND MENTAL HEALTH February 2007
 Alberta Alcohol and Drug Abuse Commission POSITION ON ADDICTION AND MENTAL HEALTH POSITION The Alberta Alcohol and Drug Abuse Commission (AADAC) recognizes that among clients with addiction problems, there
Alberta Alcohol and Drug Abuse Commission POSITION ON ADDICTION AND MENTAL HEALTH POSITION The Alberta Alcohol and Drug Abuse Commission (AADAC) recognizes that among clients with addiction problems, there
National Council on Ageing and Older People
 National Council on Ageing and Older People LONG-STAY CARE Ageing In Ireland Fact File No. 7 While the future development of the Irish health services is in the direction of community-based care, there
National Council on Ageing and Older People LONG-STAY CARE Ageing In Ireland Fact File No. 7 While the future development of the Irish health services is in the direction of community-based care, there
Guidelines for the Utilization of Psychotropic Medications for Children in Foster Care. Illinois Department of Children and Family Services
 Guidelines for the Utilization of Psychotropic Medications for Children in Foster Care Illinois Department of Children and Family Services Introduction With few exceptions, children and adolescents in
Guidelines for the Utilization of Psychotropic Medications for Children in Foster Care Illinois Department of Children and Family Services Introduction With few exceptions, children and adolescents in
Texas Council Endorsed Measurement Strategy
 Texas Council Endorsed Measurement Strategy During 2013, the Data Work Group of the Texas Council of Community Centers met to identify a set of clinical quality measures that can be used across the entire
Texas Council Endorsed Measurement Strategy During 2013, the Data Work Group of the Texas Council of Community Centers met to identify a set of clinical quality measures that can be used across the entire
Mentors on Discharge
 Mentors on Discharge Repeated psychiatric hospitalizations are costly, impede recovery and are demoralizing to individuals, families, and clinicians. Between 40 to 50 percent of patients with a history
Mentors on Discharge Repeated psychiatric hospitalizations are costly, impede recovery and are demoralizing to individuals, families, and clinicians. Between 40 to 50 percent of patients with a history
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 2 Episodes Acute COPD exacerbation (COPD); Screening and surveillance colonoscopy (COL); and Outpatient and non-acute
Chapter 5: Acute Kidney Injury
 Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
Chapter 5: Acute Kidney Injury Introduction In recent years, acute kidney injury (AKI) has gained increasing recognition as a major risk factor for the development of chronic kidney disease (CKD). The
New York Medicaid Beneficiaries with Mental Health and Substance Abuse Conditions
 Medicaid institute at united Hospital Fund New York Medicaid Beneficiaries with Mental Health and Substance Abuse Conditions About the Medicaid Institute at United Hospital Fund Established in 2005, the
Medicaid institute at united Hospital Fund New York Medicaid Beneficiaries with Mental Health and Substance Abuse Conditions About the Medicaid Institute at United Hospital Fund Established in 2005, the
ADDICTION AND CO-OCCURRING DISORDERS
 ADDICTION AND CO-OCCURRING DISORDERS Exceptional Care in an Exceptional Setting Silver Hill Hospital is an academic affiliate of Yale University School of Medicine, Department of Psychiatry. SILVER HILL
ADDICTION AND CO-OCCURRING DISORDERS Exceptional Care in an Exceptional Setting Silver Hill Hospital is an academic affiliate of Yale University School of Medicine, Department of Psychiatry. SILVER HILL
MENTAL HEALTH INDICATORS: WITHIN 30-DAY HOSPITAL RE-ADMISSION
 MENTAL HEALTH INDICATORS: WITHIN 30-DAY HOSPITAL RE-ADMISSION OECD HCQI Expert Meeting Rie Fujisawa November 16 th 2012 Within 30-day hospital re-admission Data are collected in two different ways: The
MENTAL HEALTH INDICATORS: WITHIN 30-DAY HOSPITAL RE-ADMISSION OECD HCQI Expert Meeting Rie Fujisawa November 16 th 2012 Within 30-day hospital re-admission Data are collected in two different ways: The
Residential Treatment (RTC)
 An Independent Licensee of the Blue Cross and Blue Shield Association Residential Treatment (RTC) BEACON HEALTH STRATEGIES, LLC ORIGINAL EFFECTIVE DATE HAWAII LEVEL OF CARE CRITERIA 2013 CURRENT EFFECTIVE
An Independent Licensee of the Blue Cross and Blue Shield Association Residential Treatment (RTC) BEACON HEALTH STRATEGIES, LLC ORIGINAL EFFECTIVE DATE HAWAII LEVEL OF CARE CRITERIA 2013 CURRENT EFFECTIVE
ANNOTATIONS. Beds Observation Unit A 82 Observation Unit B 76
 BE ANNOTATIONS M M ENTAL ILLNESS IN L O N D O N 1 h i s publication represents a substantial contribution of mental hospital statistics, a useful commentary on some Tof the methodological problems, and
BE ANNOTATIONS M M ENTAL ILLNESS IN L O N D O N 1 h i s publication represents a substantial contribution of mental hospital statistics, a useful commentary on some Tof the methodological problems, and
MEDICAL POLICY EFFECTIVE DATE: 04/28/11 REVISED DATE: 04/26/12, 04/25/13, 04/24/14, 06/25/15, 06/22/16, 06/22/17
 MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care
 Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care New Futures mission is to advocate, educate, and collaborate to reduce alcohol and other drug problems in New Hampshire. Expanding
Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care New Futures mission is to advocate, educate, and collaborate to reduce alcohol and other drug problems in New Hampshire. Expanding
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Chapter 3: Morbidity and Mortality in Patients with CKD
 Chapter 3: Morbidity and Mortality in Patients with CKD In this 2017 Annual Data Report (ADR) we introduce analysis of a new dataset. To provide a more comprehensive examination of morbidity patterns,
Chapter 3: Morbidity and Mortality in Patients with CKD In this 2017 Annual Data Report (ADR) we introduce analysis of a new dataset. To provide a more comprehensive examination of morbidity patterns,
CALIFORNIA COUNTIES TREATMENT RECORD REQUIREMENTS
 CALIFORNIA COUNTIES TREATMENT RECORD REQUIREMENTS Every service provided is subject to Beacon Health Options, State of California and federal audits. All treatment records must include documentation of
CALIFORNIA COUNTIES TREATMENT RECORD REQUIREMENTS Every service provided is subject to Beacon Health Options, State of California and federal audits. All treatment records must include documentation of
MYTH BUSTERS. Market Intelligence Reveals New Insights to Old Growth Measures. Excel Health TM. Myth vs. Reality
 Excel Health TM MYTH BUSTERS Market Intelligence Reveals New Insights to Old Growth Measures By looking deeply into the CMS Chronic Conditions Data Warehouse, Excel Health challenges the hospice industry
Excel Health TM MYTH BUSTERS Market Intelligence Reveals New Insights to Old Growth Measures By looking deeply into the CMS Chronic Conditions Data Warehouse, Excel Health challenges the hospice industry
Mental Illness and Substance Use Hospitalizations in New Hampshire,
 Mental Illness and Substance Use Hospitalizations in New Hampshire, 1997-2006 May, 2008 Part of the Access New Hampshire: Living with Disability in the Granite State Project To learn more about the Access
Mental Illness and Substance Use Hospitalizations in New Hampshire, 1997-2006 May, 2008 Part of the Access New Hampshire: Living with Disability in the Granite State Project To learn more about the Access
Cambia Palliative Care Metrics: Where are we and where are we going?
 Cambia Palliative Care Metrics: Where are we and where are we going? J. Randall Curtis, MD, MPH Director, Cambia Palliative Care Center of Excellence www.uwpalliativecarecenter.com Overview of System-Wide
Cambia Palliative Care Metrics: Where are we and where are we going? J. Randall Curtis, MD, MPH Director, Cambia Palliative Care Center of Excellence www.uwpalliativecarecenter.com Overview of System-Wide
Connecticut Medicaid Emerging Adults
 Connecticut Medicaid Emerging Adults Child/Adolescent Quality, Access & Policy Committee April 18, 2018 Christopher Bory, PsyD, Beacon Health Options Agenda 1. National Context a. Gap in understanding
Connecticut Medicaid Emerging Adults Child/Adolescent Quality, Access & Policy Committee April 18, 2018 Christopher Bory, PsyD, Beacon Health Options Agenda 1. National Context a. Gap in understanding
Drug Overdose Morbidity and Mortality in Kentucky,
 Drug Overdose Morbidity and Mortality in Kentucky, 2000-2010 An examination of statewide data, including the rising impact of prescription drug overdose on fatality rates, and the parallel rise in associated
Drug Overdose Morbidity and Mortality in Kentucky, 2000-2010 An examination of statewide data, including the rising impact of prescription drug overdose on fatality rates, and the parallel rise in associated
Study Links Use of Intraoperative Neuromonitoring during Spine Surgery to Improved Outcomes, Lower Opioid Use
 SpecialtyCare Insight Study Links Use of Intraoperative Neuromonitoring during Spine Surgery to Improved Outcomes, Lower Opioid Use INSIGHT Spine surgery is a commonly performed procedure today, but even
SpecialtyCare Insight Study Links Use of Intraoperative Neuromonitoring during Spine Surgery to Improved Outcomes, Lower Opioid Use INSIGHT Spine surgery is a commonly performed procedure today, but even
Combination therapy compared to monotherapy for moderate to severe Alzheimer's Disease. Summary
 Combination therapy compared to monotherapy for moderate to severe Alzheimer's Disease Summary Mai 17 th 2017 Background Alzheimer s disease is a serious neurocognitive disorder which is characterized
Combination therapy compared to monotherapy for moderate to severe Alzheimer's Disease Summary Mai 17 th 2017 Background Alzheimer s disease is a serious neurocognitive disorder which is characterized
Centerstone Research Institute
 American Addiction Centers Outcomes Study 12 month post discharge outcomes among a randomly selected sample of residential addiction treatment clients Centerstone Research Institute 2018 1 AAC Outcomes
American Addiction Centers Outcomes Study 12 month post discharge outcomes among a randomly selected sample of residential addiction treatment clients Centerstone Research Institute 2018 1 AAC Outcomes
Suicide Risk Screening, Assessment and Management
 Approved by: Vice President & Chief Medical Officer, and Vice President & Chief Operating Officer Suicide Risk Screening, Assessment and Management Corporate Policy & Procedures Manual Number: VII-B-200
Approved by: Vice President & Chief Medical Officer, and Vice President & Chief Operating Officer Suicide Risk Screening, Assessment and Management Corporate Policy & Procedures Manual Number: VII-B-200
Setting Non-profit psychiatric hospital. The economic analysis was carried out in the USA.
 Inpatient alcohol treatment in a private healthcare setting: which patients benefit and at what cost? Pettinati H M, Meyers K, Evans B D, Ruetsch C R, Kaplan F N, Jensen J M, Hadley T R Record Status This
Inpatient alcohol treatment in a private healthcare setting: which patients benefit and at what cost? Pettinati H M, Meyers K, Evans B D, Ruetsch C R, Kaplan F N, Jensen J M, Hadley T R Record Status This
FAMILY FUNCTIONAL THERAPY (FFT) - Youth. Program Description
 Clinical FAMILY FUNCTIONAL THERAPY (FFT) - Youth Program Description Family Functional Therapy (FFT) is a family-focused, community-based treatment for youth who are either at risk for, or who manifest,
Clinical FAMILY FUNCTIONAL THERAPY (FFT) - Youth Program Description Family Functional Therapy (FFT) is a family-focused, community-based treatment for youth who are either at risk for, or who manifest,
Legal 2000 and the Mental Health Crisis in Clark County. Lesley R. Dickson, M.D. Executive Director, Nevada Psychiatric Association
 Legal 2000 and the Mental Health Crisis in Clark County Lesley R. Dickson, M.D. Executive Director, Nevada Psychiatric Association Civil action: Civil Commitment Definition a legal action to recover money
Legal 2000 and the Mental Health Crisis in Clark County Lesley R. Dickson, M.D. Executive Director, Nevada Psychiatric Association Civil action: Civil Commitment Definition a legal action to recover money
Functional Outcomes among the Medically Complex Population
 Functional Outcomes among the Medically Complex Population Paulette Niewczyk, PhD, MPH Director of Research Uniform Data System for Medical Rehabilitation 2015 Uniform Data System for Medical Rehabilitation,
Functional Outcomes among the Medically Complex Population Paulette Niewczyk, PhD, MPH Director of Research Uniform Data System for Medical Rehabilitation 2015 Uniform Data System for Medical Rehabilitation,
Defining High Users in Acute Care: An Examination of Different Approaches. Better data. Better decisions. Healthier Canadians.
 Defining High Users in Acute Care: An Examination of Different Approaches July 2015 Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the development and maintenance of
Defining High Users in Acute Care: An Examination of Different Approaches July 2015 Our Vision Better data. Better decisions. Healthier Canadians. Our Mandate To lead the development and maintenance of
Emergency Department Boarding of Psychiatric Patients in Oregon
 College of Public Health and Human Sciences Emergency Department Boarding of Psychiatric Patients in Oregon Jangho Yoon, PhD, Jeff Luck, PhD April 25, 2017 Scope Quantify the extent of psychiatric emergency
College of Public Health and Human Sciences Emergency Department Boarding of Psychiatric Patients in Oregon Jangho Yoon, PhD, Jeff Luck, PhD April 25, 2017 Scope Quantify the extent of psychiatric emergency
The dramatic growth of managed. Use of Psychiatrists, Psychologists, and Master s-level Therapists in Managed Behavioral Health Care Carve-Out Plans
 Use of Psychiatrists, Psychologists, and Master s-level Therapists in Managed Behavioral Health Care Carve-Out Plans Roland Sturm, Ph.D. Ruth Klap, Ph.D. Objective: Outpatient claims data from a managed
Use of Psychiatrists, Psychologists, and Master s-level Therapists in Managed Behavioral Health Care Carve-Out Plans Roland Sturm, Ph.D. Ruth Klap, Ph.D. Objective: Outpatient claims data from a managed
USRDS UNITED STATES RENAL DATA SYSTEM
 USRDS UNITED STATES RENAL DATA SYSTEM Chapter 6: Medicare Expenditures for Persons With CKD Medicare spending for patients with CKD aged 65 and older exceeded $50 billion in 2013, representing 20% of all
USRDS UNITED STATES RENAL DATA SYSTEM Chapter 6: Medicare Expenditures for Persons With CKD Medicare spending for patients with CKD aged 65 and older exceeded $50 billion in 2013, representing 20% of all
City of Lawrence 2010 Alcohol Tax Funds Request for Proposals Calendar Year 2010 ( January December) Cover Page
 City of Lawrence 2010 Alcohol Tax Funds Request for Proposals Calendar Year 2010 ( January December) Cover Page Agency Name: Program Name: Contact Person: DCCCA, Inc First Step at Lake View Lisa Carter,
City of Lawrence 2010 Alcohol Tax Funds Request for Proposals Calendar Year 2010 ( January December) Cover Page Agency Name: Program Name: Contact Person: DCCCA, Inc First Step at Lake View Lisa Carter,
Studies that have evaluated the relationship between length of stay and rate of readmission have reported contradictory results.
 Use of Claims Data to Examine the Impact of Length of Inpatient Psychiatric Stay on Readmission Rate Roberto Figueroa, M.D., M.P.P.M. Jeffrey Harman, Ph.D. John Engberg, Ph.D. Objective: This study analyzed
Use of Claims Data to Examine the Impact of Length of Inpatient Psychiatric Stay on Readmission Rate Roberto Figueroa, M.D., M.P.P.M. Jeffrey Harman, Ph.D. John Engberg, Ph.D. Objective: This study analyzed
Report on Medicaid Data Analyses For
 Report on Medicaid Data Analyses For King, Pierce, Spokane, Thurston, Skagit and Kitsap Counties NW HIDTA/DASA Drug Court Evaluation Alcohol and Drug Abuse Institute University of Washington April 25,
Report on Medicaid Data Analyses For King, Pierce, Spokane, Thurston, Skagit and Kitsap Counties NW HIDTA/DASA Drug Court Evaluation Alcohol and Drug Abuse Institute University of Washington April 25,
Huangdao People's Hospital
 Table of contents 1. Background... 3 2. Integrated care pathway implementation... 6 (1) Workload indicators... 6 A. In eligible for care pathway... 6 B. Care pathway implementation... 7 (2) Outcome indicators...
Table of contents 1. Background... 3 2. Integrated care pathway implementation... 6 (1) Workload indicators... 6 A. In eligible for care pathway... 6 B. Care pathway implementation... 7 (2) Outcome indicators...
May 16, Division of Dockets Management (HFA-305) Food and Drug Administration 5630 Fishers Lane, Room 1061 Rockville, MD 20852
 701 Pennsylvania Avenue, NW Suite 800 Washington, D.C. 20004 2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org May 16, 2014 Division of Dockets Management (HFA-305) Food and Drug Administration
701 Pennsylvania Avenue, NW Suite 800 Washington, D.C. 20004 2654 Tel: 202 783 8700 Fax: 202 783 8750 www.advamed.org May 16, 2014 Division of Dockets Management (HFA-305) Food and Drug Administration
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psychosis and schizophrenia in children and young people: recognition and management 1.1 Short title Psychosis and schizophrenia
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psychosis and schizophrenia in children and young people: recognition and management 1.1 Short title Psychosis and schizophrenia
INTERQUAL BEHAVIORAL HEALTH CRITERIA ADOLESCENT PSYCHIATRY REVIEW PROCESS
 INTERQUAL BEHAVIORAL HEALTH CRITERIA ADOLESCENT PSYCHIATRY REVIEW PROCESS RP-1 RP-2 AGE PARAMETERS Adolescent Psychiatry Behavioral Health Criteria are for the review of patients who are ages 13 to 17
INTERQUAL BEHAVIORAL HEALTH CRITERIA ADOLESCENT PSYCHIATRY REVIEW PROCESS RP-1 RP-2 AGE PARAMETERS Adolescent Psychiatry Behavioral Health Criteria are for the review of patients who are ages 13 to 17
Florida s Mental Health Act
 Florida s Mental Health Act By Rene Jackson, RN, BSN, MS, LHRM At the completion of this course, the learner will be able to: 1. Define mental illness according to Florida s Mental Health Act 2. Identify
Florida s Mental Health Act By Rene Jackson, RN, BSN, MS, LHRM At the completion of this course, the learner will be able to: 1. Define mental illness according to Florida s Mental Health Act 2. Identify
Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia
 Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia I. Key Points a. Schizophrenia is a chronic illness affecting all aspects of person s life i. Treatment Planning Goals 1.
Condensed Clinical Practice Guideline Treatment Of Patients With Schizophrenia I. Key Points a. Schizophrenia is a chronic illness affecting all aspects of person s life i. Treatment Planning Goals 1.
Medicare Severity-adjusted Diagnosis Related Groups (MS-DRGs) Coding Adjustment
 American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
American Hospital association December 2012 TrendWatch Are Medicare Patients Getting Sicker? Today, Medicare covers more than 48 million people, and that number is growing rapidly baby boomers are reaching
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Personality Disorder: the clinical management of borderline personality disorder
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
FULTON COUNTY GOVERNMENT RYAN WHITE PART A PROGRAM. Atlanta Eligible Metropolitan Area HIV/AIDS Unmet Need Estimate
 FULTON COUNTY GOVERNMENT RYAN WHITE PART A PROGRAM Atlanta Eligible Metropolitan Area HIV/AIDS Unmet Need Estimate Southeast AIDS Training and Education Center Department of Family and Preventative Medicine
FULTON COUNTY GOVERNMENT RYAN WHITE PART A PROGRAM Atlanta Eligible Metropolitan Area HIV/AIDS Unmet Need Estimate Southeast AIDS Training and Education Center Department of Family and Preventative Medicine
PHPG. Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions
 PHPG The Pacific Health Policy Group Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions Prepared for: State of Oklahoma Oklahoma Health Care Authority April
PHPG The Pacific Health Policy Group Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions Prepared for: State of Oklahoma Oklahoma Health Care Authority April
ACUTE INPATIENT TREATMENT
 I. Definition of Service: ACUTE INPATIENT TREATMENT Acute inpatient hospitalization represents the most intensive level of psychiatric care. Multidisciplinary assessments and multimodal interventions are
I. Definition of Service: ACUTE INPATIENT TREATMENT Acute inpatient hospitalization represents the most intensive level of psychiatric care. Multidisciplinary assessments and multimodal interventions are
Maryland s Behavioral Health Crisis. The Hospital Perspective
 Maryland s Behavioral Health Crisis The Hospital Perspective Topics to Cover The National Experience Maryland s Experience Hospital Data 2 The National Experience 3 Behavioral and Physical Health are Linked
Maryland s Behavioral Health Crisis The Hospital Perspective Topics to Cover The National Experience Maryland s Experience Hospital Data 2 The National Experience 3 Behavioral and Physical Health are Linked
Depression Disease Navigation
 Depression Disease Navigation The depression disease navigation program is designed to reach out to members who have been diagnosed with major depression disorder. This is accomplished by promoting treatment
Depression Disease Navigation The depression disease navigation program is designed to reach out to members who have been diagnosed with major depression disorder. This is accomplished by promoting treatment
2016 Collier County Florida Health Assessment Executive Summary
 2016 Florida Health Assessment Executive Summary Prepared by: The Health Planning Council of Southwest Florida, Inc. www.hpcswf.com Executive Summary To access the report in its entirety, visit http://www.hpcswf.com/health-planning/health-planningprojects/.
2016 Florida Health Assessment Executive Summary Prepared by: The Health Planning Council of Southwest Florida, Inc. www.hpcswf.com Executive Summary To access the report in its entirety, visit http://www.hpcswf.com/health-planning/health-planningprojects/.
Standard emergency department care vs. admission to an observation unit for low-risk chest pain patients. A two-phase prospective cohort study
 Standard emergency department care vs. admission to an observation unit for low-risk chest pain patients A. STUDY PURPOSE AND RATIONALE Rationale: A two-phase prospective cohort study IRB Proposal Sara
Standard emergency department care vs. admission to an observation unit for low-risk chest pain patients A. STUDY PURPOSE AND RATIONALE Rationale: A two-phase prospective cohort study IRB Proposal Sara
JC Sunnybrook HEALTH SCIENCES CENTRE
 Dear Referring Provider: Thank you for referring your patient to the Frederick W. Thompson Anxiety Disorders Centre at Sunnybrook Health Sciences Centre. The attached form will assist us in determining
Dear Referring Provider: Thank you for referring your patient to the Frederick W. Thompson Anxiety Disorders Centre at Sunnybrook Health Sciences Centre. The attached form will assist us in determining
Oklahoma Department of Mental Health And Substance Abuse Services. Regional Performance Management Report. Report for Third Quarter of FY2003
 Oklahoma Department of Mental Health And Substance Abuse Services al Performance Management Report Report for Third Quarter of FY23 Reported September 23 By ODMHSAS Decision Support Services Table of Contents
Oklahoma Department of Mental Health And Substance Abuse Services al Performance Management Report Report for Third Quarter of FY23 Reported September 23 By ODMHSAS Decision Support Services Table of Contents
Eating disorders. Introduction SUMMARY
 8 Eating disorders SUMMARY The eating disorders included in this chapter are relatively uncommon and in many cases are not treated. The numbers of people with these eating disorders is likely to increase
8 Eating disorders SUMMARY The eating disorders included in this chapter are relatively uncommon and in many cases are not treated. The numbers of people with these eating disorders is likely to increase
Performance Analysis:
 Performance Analysis: Healthcare Utilization of CCNC- Population 2007-2010 Prepared by Treo Solutions JUNE 2012 Table of Contents SECTION ONE: EXECUTIVE SUMMARY 4-5 SECTION TWO: REPORT DETAILS 6 Inpatient
Performance Analysis: Healthcare Utilization of CCNC- Population 2007-2010 Prepared by Treo Solutions JUNE 2012 Table of Contents SECTION ONE: EXECUTIVE SUMMARY 4-5 SECTION TWO: REPORT DETAILS 6 Inpatient
Psychotropic Medication
 FOM 802-1 1 of 10 OVERVIEW The use of psychotropic medication as part of a child s comprehensive mental health treatment plan may be beneficial and should include consideration of all alternative interventions.
FOM 802-1 1 of 10 OVERVIEW The use of psychotropic medication as part of a child s comprehensive mental health treatment plan may be beneficial and should include consideration of all alternative interventions.
Epidemiology of adolescent and young adult hospital utilization for alcohol and drug use, poisoning, and suicide attempts in the United States
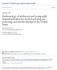 Journal of Adolescent and Family Health Volume 6 Issue 2 Article 4 November 2014 Epidemiology of adolescent and young adult hospital utilization for alcohol and drug use, poisoning, and suicide attempts
Journal of Adolescent and Family Health Volume 6 Issue 2 Article 4 November 2014 Epidemiology of adolescent and young adult hospital utilization for alcohol and drug use, poisoning, and suicide attempts
Chapter 5: Cost of Chiropractic Compared to Family Physician
 ICA Best Practices & Practice Guidelines 47 Chapter 5: Cost of Chiropractic Compared to Family Physician Introduction Here we explore the cost of chiropractic care versus the cost of care provided by medical
ICA Best Practices & Practice Guidelines 47 Chapter 5: Cost of Chiropractic Compared to Family Physician Introduction Here we explore the cost of chiropractic care versus the cost of care provided by medical
Voluntary Mental Health Treatment Laws for Minors & Length of Inpatient Stay. Tori Lallemont MPH Thesis: Maternal & Child Health June 6, 2007
 Voluntary Mental Health Treatment Laws for Minors & Length of Inpatient Stay Tori Lallemont MPH Thesis: Maternal & Child Health June 6, 2007 Introduction 1997: Nearly 300,000 children were admitted to
Voluntary Mental Health Treatment Laws for Minors & Length of Inpatient Stay Tori Lallemont MPH Thesis: Maternal & Child Health June 6, 2007 Introduction 1997: Nearly 300,000 children were admitted to
Creating Better Health
 Creating Better Health With the Diabetes Prevention Program (DPP) [date] Presented by: [Presenter name/logo] Agenda Introductions Diabetes and prediabetes facts Health and financial cost of diabetes How
Creating Better Health With the Diabetes Prevention Program (DPP) [date] Presented by: [Presenter name/logo] Agenda Introductions Diabetes and prediabetes facts Health and financial cost of diabetes How
Chapter 3: Morbidity and Mortality
 Chapter 3: Morbidity and Mortality Introduction In this chapter we evaluate the morbidity and mortality of chronic kidney disease (CKD) patients continuously enrolled in Medicare. Each year s analysis
Chapter 3: Morbidity and Mortality Introduction In this chapter we evaluate the morbidity and mortality of chronic kidney disease (CKD) patients continuously enrolled in Medicare. Each year s analysis
and Independence PROVIDING RESIDENTIAL AND OUTPATIENT TREATMENT FOR ADOLESCENTS WITH BEHAVIORAL, EMOTIONAL AND SUBSTANCE ABUSE PROBLEMS
 The Center for Success and Independence PROVIDING RESIDENTIAL AND OUTPATIENT TREATMENT FOR ADOLESCENTS WITH BEHAVIORAL, EMOTIONAL AND SUBSTANCE ABUSE PROBLEMS THE CENTER FOR SUCCESS AND INDEPENDENCE 3722
The Center for Success and Independence PROVIDING RESIDENTIAL AND OUTPATIENT TREATMENT FOR ADOLESCENTS WITH BEHAVIORAL, EMOTIONAL AND SUBSTANCE ABUSE PROBLEMS THE CENTER FOR SUCCESS AND INDEPENDENCE 3722
A Community Wide Approach to Innovating Outreach, Crisis Intervention, and Community Education for Youth affected by Mental Health Challenges
 Waukesha County Health and Human Services A Community Wide Approach to Innovating Outreach, Crisis Intervention, and Community Education for Youth affected by Mental Health Challenges Quick Review of the
Waukesha County Health and Human Services A Community Wide Approach to Innovating Outreach, Crisis Intervention, and Community Education for Youth affected by Mental Health Challenges Quick Review of the
Making the Business Case for Long-Acting Injectables
 Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Making the Business Case for Long-Acting Injectables David R. Swann, MA, LCAS, CCS, LPC, NCC Senior Healthcare Integration Consultant MTM Services Chief Clinical Officer Partners Behavioral Health Management
Executive Summary. Context. Guideline Origins
 Executive Summary Context In America today, tobacco stands out as the agent most responsible for avoidable illness and death. Millions of Americans consume this toxin on a daily basis. Its use brings premature
Executive Summary Context In America today, tobacco stands out as the agent most responsible for avoidable illness and death. Millions of Americans consume this toxin on a daily basis. Its use brings premature
CIGNA STANDARDS AND GUIDELINES/MEDICAL NECESSITY CRITERIA
 CIGNA STANDARDS AND GUIDELINES/MEDICAL NECESSITY CRITERIA For Treatment of Mental Health and Substance Use Disorders Revised Edition: October 15, 2017 0 Table of Contents Foreword... 3 Core Principles...
CIGNA STANDARDS AND GUIDELINES/MEDICAL NECESSITY CRITERIA For Treatment of Mental Health and Substance Use Disorders Revised Edition: October 15, 2017 0 Table of Contents Foreword... 3 Core Principles...
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/22306 holds various files of this Leiden University dissertation. Author: Vochteloo, Anne Jochem Hendrik Title: Determinants of outcome in hip fracture
Cover Page The handle http://hdl.handle.net/1887/22306 holds various files of this Leiden University dissertation. Author: Vochteloo, Anne Jochem Hendrik Title: Determinants of outcome in hip fracture
Mental Health Statistics, to
 , 1982-83 to 1993-94 Jean Randhawa and Rod Riley* Since the early 1980s, in relation to the size of the population, general and psychiatric hospitals have seen a drop in separations for mental disorders.
, 1982-83 to 1993-94 Jean Randhawa and Rod Riley* Since the early 1980s, in relation to the size of the population, general and psychiatric hospitals have seen a drop in separations for mental disorders.
Appendix A AUTIM SPECTRUM DISORDER FEASIBILITY STUDY
 Appendix A AUTIM SPECTRUM DISORDER FEASIBILITY STUDY Description: Representatives from the Departments of Social Services (DSS), Mental Health and Addiction Services (DMHAS), Children and Families (DCF),
Appendix A AUTIM SPECTRUM DISORDER FEASIBILITY STUDY Description: Representatives from the Departments of Social Services (DSS), Mental Health and Addiction Services (DMHAS), Children and Families (DCF),
Cost of Mental Health Care
 Section 4 Cost of Mental Health Care Per capita mental health spending for Americans with a mental health diagnosis has increased among children, peaking in. For adults, the spending has been more stable.
Section 4 Cost of Mental Health Care Per capita mental health spending for Americans with a mental health diagnosis has increased among children, peaking in. For adults, the spending has been more stable.
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010
 Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Health Services Utilization and Medical Costs Among Medicare Atrial Fibrillation Patients / September 2010 AF Stat is sponsored by sanofi-aventis, U.S. LLC, which provided funding for this report. Avalere
Cost-effectiveness of Hepatitis A and Hepatitis B Vaccination for Jail Inmates
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2007 Cost-effectiveness of Hepatitis A and Hepatitis B Vaccination
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2007 Cost-effectiveness of Hepatitis A and Hepatitis B Vaccination
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report. User s Guide Sixth Edition. Prepared by
 Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Partial Hospitalization Program Program for Evaluating Payment Patterns Electronic Report User s Guide Sixth Edition Prepared by Partial Hospitalization Program Program for Evaluating Payment Patterns
Palliative Care and End of Life Care
 Palliative Care and End of Life Care Relevant Data and References Victorian Population 1 Total Victorian Population as at June 2016 was 6.1 million (6,179,249) Victorian 60 plus population as at June 2016
Palliative Care and End of Life Care Relevant Data and References Victorian Population 1 Total Victorian Population as at June 2016 was 6.1 million (6,179,249) Victorian 60 plus population as at June 2016
The Allegheny County HealthChoices Program, 2008: The Year in Review
 The Allegheny County HealthChoices Program, : The Year in Review A publication of Allegheny HealthChoices, Inc. August 2009 Overview and Highlights HealthChoices is Pennsylvania s managed care program
The Allegheny County HealthChoices Program, : The Year in Review A publication of Allegheny HealthChoices, Inc. August 2009 Overview and Highlights HealthChoices is Pennsylvania s managed care program
Inpatient psychiatric care in Medicare: Trends and issues
 C h a p t e r6 Inpatient psychiatric care in Medicare: Trends and issues C H A P T E R 6 Inpatient psychiatric care in Medicare: Trends and issues Chapter summary In this chapter Medicare beneficiaries
C h a p t e r6 Inpatient psychiatric care in Medicare: Trends and issues C H A P T E R 6 Inpatient psychiatric care in Medicare: Trends and issues Chapter summary In this chapter Medicare beneficiaries
Inpatient Psychiatric Facilities
 Payment Integrity Compass Inpatient Psychiatric Facilities Understanding IPF Calculations Updated 12/05/12 2 Questions from the Group Please use GoToMeeting to Ask a Question Use the Raise Hand function
Payment Integrity Compass Inpatient Psychiatric Facilities Understanding IPF Calculations Updated 12/05/12 2 Questions from the Group Please use GoToMeeting to Ask a Question Use the Raise Hand function
Chapter six Outcomes: hospitalization & mortality. There is an element of death in life, and I am astonished
 INTRODUCTION 1 OVERALL HOSPITALIZATION & MORTALITY 1 hospital admissions & days, by primary diagnosis & patient vintage five-year survival mortality rates, by patient vintage expected remaining lifetimes
INTRODUCTION 1 OVERALL HOSPITALIZATION & MORTALITY 1 hospital admissions & days, by primary diagnosis & patient vintage five-year survival mortality rates, by patient vintage expected remaining lifetimes
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
In each hospital-year, we calculated a 30-day unplanned. readmission rate among patients who survived at least 30 days
 Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Romley JA, Goldman DP, Sood N. US hospitals experienced substantial productivity growth during 2002 11. Health Aff (Millwood). 2015;34(3). Published online February 11, 2015. Appendix Adjusting hospital
Heroin Use in Illinois: A Ten-Year Multiple Indicator Analysis, 1998 to 2008
 Heroin Use in Illinois: A Ten-Year Multiple Indicator Analysis, 1998 to 2008 EXECUTIVE SUMMARY AND FINDINGS Co-authored by: Stephanie Schmitz Kathleen Kane-Willis Research Support: Laura Reichel, Elizabeth
Heroin Use in Illinois: A Ten-Year Multiple Indicator Analysis, 1998 to 2008 EXECUTIVE SUMMARY AND FINDINGS Co-authored by: Stephanie Schmitz Kathleen Kane-Willis Research Support: Laura Reichel, Elizabeth
Integrated Payment & Reporting System (IPRS) Target Population Details FY Child Substance Abuse Assessment Only (CSAO)
 Assessment Only (CSAO) Client Eligibility Criteria Children, starting on the third birthday until the 18 th birthday, who: are seeking or needing services for a current substance abuse problem or symptom,
Assessment Only (CSAO) Client Eligibility Criteria Children, starting on the third birthday until the 18 th birthday, who: are seeking or needing services for a current substance abuse problem or symptom,
Supplementary Online Content
 Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Supplementary Online Content Lee JS, Nsa W, Hausmann LRM, et al. Quality of care for elderly patients hospitalized for pneumonia in the United States, 2006 to 2010. JAMA Intern Med. Published online September
Care of Adults With Mental Health. U.S. Community Hospitals, 2004
 t t 4 t t 10 t t Care of Adults With Mental Health t and Substance Abuse Disorders in t t U.S. Community Hospitals, 2004 t t t t t t t t t t t t t t t t t t t Care of Adults With Mental Health and Substance
t t 4 t t 10 t t Care of Adults With Mental Health t and Substance Abuse Disorders in t t U.S. Community Hospitals, 2004 t t t t t t t t t t t t t t t t t t t Care of Adults With Mental Health and Substance
Child and Adolescent Residential Services Referral Packet
 Patient Name: Date of Birth: Child and Adolescent Residential Services Referral Packet Please do not reply. See attached questions. We require that you directly answer all questions in this referral packet.
Patient Name: Date of Birth: Child and Adolescent Residential Services Referral Packet Please do not reply. See attached questions. We require that you directly answer all questions in this referral packet.
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
