Non-commercial use only
|
|
|
- Edith Claire Parks
- 6 years ago
- Views:
Transcription
1 Italian Journal of Medicine 2014; volume 8: Use of ursodeoxycholic acid in patients with hypertransaminasemia Claudio Puoti, 1 Maria Giuseppa Elmo 2 1 Department of Internal Medicine and Hepato-Gastroenterology, Marino General Hospital, Marino (RM); 2 Rome-A Health District, Rome, Italy ABSTRACT Ursodeoxycholic acid (UDCA) is a hydrophilic bile acid deriving from 7β epimerization of primary bile compound chenodeoxycholic acid. It may have antioxidant, immunomodulatory, antifibrotic and cytoprotective effects, therefore it has been extensively used in the treatment of cholestatic chronic liver diseases (primary biliary cirrhosis, primary sclerosing cholangitis, cholestasis of pregnancy, etc.). Due to the effectiveness of UDCA in decreasing serum liver enzyme levels also in non-cholestatic patients with chronic liver damage of various etiologies, this bile acid is now extensively used in clinical practice in combination with standard therapies, or as alternative treatment. In this paper, after a review of the biochemistry and physiology of UDCA, we have analyzed available data from the international literature on the efficacy and safety of UDCA in patients with hypertransaminasemia due to non-cholestatic chronic liver diseases, such as chronic viral hepatitis B and C and liver steatosis, the three main causes of aminotransferase elevation in western countries. Biosynthesis and functions of bile acids Correspondence: Claudio Puoti, Department of Internal Medicine and Hepato-Gastroenterology, Marino General Hospital, viale XXIV Maggio, Marino (RM), Italy. Mobile: Fax: puoti@epatologia.org Key words: aminotransferases, bile acids, chronic viral hepatitis, steatosis, ursodeoxycholic acid. Conflict of interests: the authors declare no potential conflict of interests. Received for publication: 17 August Revision received: 9 September Accepted for publication: 21 September This work is licensed under a Creative Commons Attribution NonCommercial 3.0 License (CC BY-NC 3.0). Copyright C. Puoti and M.G. Elmo, 2014 Licensee PAGEPress, Italy Italian Journal of Medicine 2014; 8: doi: /itjm Bile acids (BAs), the major constituents of bile, are synthesized in the liver from cholesterol. 1 Due to their biochemical characteristics, BAs allow the absorption and transport of dietary lipids and fat-soluble vitamins. 2 They may be classified into primary BAs, which are synthesized in the liver, such as the cholic acid (CA) and the chenodeoxycholic acid (CDCA), and secondary bile acids, such as deoxycholic acid and lithocholic acid (LA), which are formed in the intestine through 7α-dehydroxylation of primary bile acids by intestinal bacteria. 3 More in details, BAs synthesis starts from cholesterol, 4 following a classic or an alternative pathway. The former, which accounts for 90% of BAs synthesis, leads through a cascade of several enzymatic steps to the synthesis of CA (3α,7α,12α-trihydroxy-5β-cholanoic acid) and of CDCA (3α,7α-dihydroxy-5β-cholanoic acid), while the latter pathway leads to the formation of CDCA only. Under normal conditions, 70% of the human pool of BAs is composed by CA and its metabolites, while 30% is represented by CDCA. 1 After their synthesis, BAs are conjugated with glycine and taurine, improving their solubility. These conjugated BAs (glyco- and tauro-conjugated BAs) are present as anionic salts under physiological ph conditions and are therefore called bile salts. 5 After glyco- or tauro-conjugation, primary BAs are excreted in the intestine, where they are de-conjugated and converted by 7α-dehydroxylase in intestinal bacterial flora to the secondary BAs, deoxycholic acid (3α,12α-dihydroxy-5β-cholestanoic acid) and lithocholic acid (3α-hydroxy-5β-cholestanoic acid). 6 The intestinal conservation mechanism of bile salts is highly efficient. From g of bile salts excreted daily into the bile, only 0.5 g are lost through fecal excretion and have to be replaced by de novo BA synthesis. This conservation is achieved through the enterohepatic circulation of bile salts, which depends on the action of several transporter proteins expressed at the basolateral and apical membrane of liver, biliary and small intestinal epithelial cells. 6 In addition to their function of absorption and transport of dietary lipids and fat-soluble vitamins, BAs play an important role in decreasing cholesterol supersaturation human bile. 7 It is well-known that the relative concentrations of bile salts, phospholipids, and cholesterol are the major determinants of gallstone [page 141] [Italian Journal of Medicine 2014; 8:426] [page 141]
2 Review formation. 7 This separation was the result of an increase in the quantity of cholesterol relative to the amounts of bile salts and lecithin contained in the bile from patients with cholesterol gallstones. In other words, BAs and lecithin fully solubilize cholesterol through the formation of the so-called mixed micelles. Forty-five years ago, William Admirand and Donald Small 8 plotted these three constituents simultaneously on triangular coordinates (the so-called triangle of Admirand-Small), thus achieving a complete separation of the normal and abnormal bile. This separation was the result of an increase in the quantity of cholesterol relative to the amounts of bile salts and lecithin contained in the bile from patients with cholesterol gallstones (supersaturated bile). The enrichment of the BA pool by cholic acid did not desaturate the bile, 7 on the contrary, the other primary BA (CDCA) seemed to be able to reduce cholesterol biliary supersaturation, 9 although in several patients it induces an increase in serum aminotransferase levels. An outstanding progress in the treatment of gallstone disease came from Japanese studies, 10 showing that ursodeoxycholic acid (UDCA), another BA, might be more effective than CDCA in dissolving gallstones with no relevant side effects. This paved the way to the use of UDCA for gallstone dissolution, which is nowadays very widely used for this purpose. Ursodeoxycholic acid for the treatment of chronic liver diseases: a fascinating history UDCA is a BAs derived from CDCA and a highly hydrophilic dihydroxy (3α,7β-dihydroxy-5 β-cholanoic acid) bile acid. 2,11 In humans, UDCA accounts for up to 4-5% of the BA pool. It is not synthesized in the liver, but it probably originates in the colon from bacterial 7β epimerization of CDCA. 12 After its formation, UDCA is passively absorbed by the colonic mucosa, thus entering the portal circulation and subsequently it enriches the pool of BAs. BAs have both hydrophobic and hydrophilic properties that enable them to function as detergents. However, the different BAs have variable degrees of hydrophobicity and hydrophilicity, which are determined by their biochemical and physiochemical properties. LA acid is the least water soluble, whereas UDCA is much more hydrophilic. CA and CDCA acid have intermediate degrees of hydrophilicity. 2 The orientation (α or β) of the hydroxyl groups relative to each other determines the bile acid hydrophilicity in these planar molecules. Due to its high hydrophilic properties, its ability to reduce supersaturation of human bile and the lack of the hepatotoxicity of other endogenous BAs, UDCA was rapidly marketed globally for the non-surgical treatment of gallstones. Thus, millions of persons in the western countries were treated with the new drug. After a few years, however, it was clear that UDCA did perform some other therapeutic actions, beyond its biliary litholytic properties. In 1987, Poupon et al. suggested that long-term use of UDCA was safe and effective in patients suffering from primary biliary cirrhosis (PBC). 13 These preliminary results were confirmed 4 years later by a multicenter, prospective, placebo-controlled study in patients with PBC, 14 showing that UDCA therapy for 2-years has led to a reduction in clinically overt disease, improvement of liver blood tests and of Mayo risk score, a decrease in serum levels of immunoglobulin M class anti-mitochondial autoantibodies, and of the mean histologic score in the treated group compared with placebo. Subsequent studies have shown that UDCA delays the progression rate of PBC resulting in a decreased need for liver transplantation. 15 Lindor et al. reported a lower mortality or need for liver transplantation in the UDCA treatment group compared with patients receiving placebo. 16 These beneficial effects of UDCA were attributed to several other actions of this bile acid, such as expansion of hydrophilic pool of BAs with displacement of endogenous and more toxic BAs at hepatocyte level, competitive inhibition of the absorption of endogenous BAs at the terminal ileus, 2 choleretic effects, immunomodulatory properties, cytoprotection and stabilization of liver cell structures, anti-apoptotic effects, anti-inflammatory properties. 17 Several other studies did confirm the efficacy of UDCA in PBC, which is now widely used in clinical practice for the treatment of this and of other cholestatic diseases, such as primary sclerosing cholangitis and cholestatic disease of pregnancy. 7 However, in 1999, a meta-analysis 18 failed to show some efficacy of UDCA in patients with PBC. More recently, a Cochrane review 19 did conclude that UDCA does not demonstrate any significant benefits on mortality or liver transplantation, pruritus, or fatigue in patients with PBC. UDCA simply seemed to have a beneficial effect on serum liver enzyme levels and on histological progression compared with the control group. Anyway, due to the apparent beneficial effects of UDCA in cholestatic liver diseases, over the past 20 years, several studies have investigated the safety and efficacy of this BA also in non-cholestatic chronic liver diseases, such as chronic viral hepatitis [hepatitis B virus (HBV)- and hepatitis C virus (HCV)-related], non-alcoholic fatty liver disease (NAFLD) and non-alcoholic steatohepatitis (NASH), etc., mainly characterized by cytolysis and an increase of serum aminotransferase levels, rather than by cholestasis. [page 142] [Italian Journal of Medicine 2014; 8:426]
3 Use of ursodeoxycholic acid in patients with hypertransaminasemia Ursodeoxycholic acid and hypertransaminasemia: myth or fact? In their everyday clinical practice, physicians frequently must deal with patients showing increased aminotransferase levels, often found by chance in biochemical tests. Several causes for these enzyme alterations should be investigated, such as chronic hepatitis B or C (CHB, CHC), liver steatosis (NAFLD, NASH), autoimmune hepatitis, alcohol abuse, hemochromatosis, drugs, etc. To achieve a correct diagnosis, several parameters should be evaluated, such as the clinical history and age of the patient, lifestyle, body mass index, risk factors, magnitude of enzymatic elevations, duration, alanine transaminase (AST)/aspartate transaminase (ALT) ratio, presence of other biochemical alterations (e.g., gamma-glutamyl transpepidase (GGT), alkaline phosphatase, bilirubin, platelet count, etc.). 20 Studies on the general population in Italy have shown that approximately 17% of apparently healthy individuals have chronically elevated aminotransferase levels, often only slightly increased. In the majority of these patients the main cause is the steatosis of the liver, followed by CHC and CHB. 21 Due to the effectiveness of UDCA in decreasing serum liver enzyme levels in patients with chronic liver damage of various etiologies, this BA is now extensively used in clinical practice in combination with standard therapies or as an alternative treatment. We intend to examine here available data on the efficacy and safety of UDCA in the 3 main causes of aminotransferase elevation in our country: CHC, CHB and liver steatosis. Ursodeoxycholic acid and hepatitis C virus related chronic hepatitis Since the discovery of HCV in 1989, given the lack of optimal treatment and the severe side effects of the former available therapy with recombinant interferon (IFN) plus ribavirin, 22 several investigators began to evaluate the usefulness of UDCA in patients suffering from HCV-related CHC, non-candidates or non-responders to standard antiviral therapy. 23 These studies were aimed at evaluating whether UDCA might reduce serum aminotransferase and GGT levels, decrease viral load (serum HCV RNA amounts), improve liver histology, and finally favorably modify the natural history of the disease and the progression to more severe liver damage, such as cirrhosis and hepatocellular carcinoma (HCC). 24 Some trials compared UDCA versus placebo or no intervention for CHC. The dose of UDCA ranged from 400 to 800 mg/day, and the duration of treatment ranged from 3 to 12 months. 24 Two other trials compared tauro-conjugated UDCA (TUDCA) versus placebo 28 or no treatment. 29 Other trials compared UDCA combined with IFN versus IFN monotherapy in patients with CHC for chronic hepatitis C. 30 All these investigations reported a significant reduction in serum aminotransferase and GGT levels during the study ( 14% to 40%), and in several cases liver enzymes actually return within the normal range. However this biochemical normalization was lost at follow up, often returning to pre-treatment levels shortly after treatment. 23 Furthermore, it should be underlined that this transient beneficial effects on serum liver enzymes were not seen in all patients treated with UDCA, as at least 30-40% did not show any significant biochemical improvement. 26 The mechanisms of these biochemical remissions during UDCA treatment are not clearly understood. As mentioned above, it is possible that UDCA might exert some direct cytoprotective effects on the hepatocyte membrane, by replacing more toxic endogenous BAs at this level, or by modifying the hydrophobic/hydrophilic BA ratio It still remains unclear why UDCA treatment is effective on liver biochemistry in some patients with CHC, but ineffective in others. Some authors showed that a CDCA reduction in the hepatocytes is an important factor or cytoprotection, suggesting that UDCA exerts its cytoprotective action as a consequence of the stimulation of the efflux of cytotoxic BAs, such as CDCA from hepatocytes. 31 Nojiri et al. 32 reported that in patients with CHC responding to UDCA treatment the percentage of this BA in the serum and the percentage of CDCA in biliary bile were significantly higher than in the non-responders. This might indicate that, when effective, UDCA favors a decrease of CDCA in hepatocytes, thus contributing to hepatoprotection. Another important issue is that UDCA treatment fails to eradicate HCV infection, and does not decrease the amount of circulating genomes, as detected by HCV RNA serum levels. These disappointing results have been reported both in studies using only UDCA and in trials of a combined treatment with UDCA and IFN. 24 It is noteworthy that even in the latter, when comparing the efficacy of antiviral therapy with IFN plus UDCA versus IFN alone, the decrease of HCV RNA levels and the rate of responders (i.e., HCV RNA negative patients at the end of follow up) did not differ between the two groups. This means that, despite biochemical improvement, UDCA is not able to induce an enhanced clearance of HCV RNA from serum. 29 The third important question to be answered is whether UDCA treatment can improve liver histology in patients with CHC. Only a few studies actually address this issue, probably due to the difficulties to perform a second liver biopsy shortly after the pre-treatment one. In the study of Attili et al pa- [page 143] [Italian Journal of Medicine 2014; 8:426] [page 143]
4 Review tients with CHC were treated with UDCA 600 mg/day for 12 months, while 18 others did received placebo. A percutaneous liver biopsy was performed before and after 1 year of treatment. Histological analysis showed an improvement in the biliary features of the liver damage, although no significant modifications of the necroinflammatory scores were reported. 33 Similar unsatisfactory results were reported in studies comparing the effects of IFN plus UDCA treatment versus IFN alone on the portal and periportal inflammation scores or on the Knodell score. 24 Although no data exists on the ability of UDCA to modify the natural history of CHC, the lack of efficacy on viral replication and the failure to improve liver histology have led to conclude that UDCA treatment per se is not able to slowdown or prevent the progression of chronic hepatitis into liver cirrhosis and HCC. 24 At present, paramount advances in antiviral therapy introduce a new era of treatment for hepatitis C based on directly acting antiviral agents (oral protease inhibitors boceprevir and telaprevir), which are associated with a significant improvement in viral eradication rates in combination with pegylated IFN plus ribavirin. 34 Further antiviral drugs, even more potent and effective, are under study. Therefore the chance to eradicate HCV infection is strikingly increased with respect to past decades, thus decreasing the need for an alternative therapy with BAs. 34 Anyway, several patients with CHC are not candidates to new therapies, because of major contraindications, while others show non-response or relapses. In these cases, UDCA treatment might be taken into account with the aim to maintain low ALT levels, although it is not clear whether ALT normalization might modify the natural history of the disease. 26 Ursodeoxycholic acid and hepatitis B virus related chronic hepatitis Antiviral treatment of CHB is more effective than that of CHC, therefore treatment with UDCA has been less used in this setting. 35 The goal of antiviral therapy for CHB is to improve survival by preventing progression of the disease into cirrhosis and HCC. This goal can be achieved, if HBV replication can be suppressed in a sustained manner. 36 Two different types of drugs can be administered to patients with CHB, IFN and nucleoside/nucleotide analogues (NAs). IFN is a cytokine with antiviral, antiproliferative, and immunomodulatory effects. It has shown to be effective in suppressing HBV replication and in inducing remission of liver disease. 35,36 NAs act as inhibitors of the HBV polymerase activity. The more recent NAs (entecavir and tenofovir) show high potency, high genetic barrier, minimal side effects, low risk of viral resistance, oral administration, although they should be administered indefinitely. 36 For these reasons, trials examining the use of UDCA in CHB are few and less recent than those in CHC. Available data confirms that UDCA decreases aminotransferase levels in patients with CHB, similarly to CHC, although it is not be able to modify liver histology or decrease serum HBV DNA levels. 24 No data exists on the ability of UDCA treatment to modify clinical outcome and to prevent progression to more severe liver damage. 24 Ursodeoxycholic acid and steatosis of the liver In western countries, liver steatosis is the main cause of an apparently unexplained increase of aminotransferases in the general population with a preva- lence accounting for around 20-30%. 21 Liver fat derives from dietary free fatty acids (FFA), from liver FFA inflow, and from hepatic de novo lipogenesis. 37 Steatosis might be distinguished in 2 different forms, alcoholic and non-alcoholic. The latter may be secondary to a variety of causes, such as overweight/ obesity, insulin resistance (IR), HCV, drugs, diabetes mellitus, disorders of lipid metabolism, rapid and severe weight loss, etc. 37 NAFLD represents a spectrum of disorders characterized predominantly by macrovesicular steatosis occurring in individuals in the absence of significant alcohol consumption. 38 It is possible to distinguish a condition of simple fatty liver, where the only histologic finding is the presence of steatosis, from a state of NASH, a potentially progressive hepatic disorder leading to end-stage liver disease, characterized by hepatocellular injury/inflammation with or without fibrosis. 37 NAFLD is considered the hepatic manifestation of IR, and is therefore strongly associated with other clinical expressions of IR, such as metabolic syndrome and its features: obesity, type 2 diabetes, dyslipidemia and hypertension. 38 Although NAFLD is a rather benign condition, a fraction of these patients (20-30%) with non-alcoholic fatty liver disease might develop more severe liver damage and liver cirrhosis. 39 At present most hepatologists attempt to manage NASH using lifestyle changes to reverse the consequences of metabolic disease, such as weight reduction with or without exercise, as well as standard therapeutic interventions to control concomitant associated diseases, hyperlipidaemia, hypertension and type 2 diabetes. 39 Pharmacological treatment of steatosis is still an unmet medical need. Due to the lack of specific and effective agents, several drugs have been studied: insulin-sensitizing agents, antioxidant therapy, vitamin E, betaine, pentoxifilline, probucol, omega-3 polyunsaturated fatty acids, sartans and lastly UDCA. 40 [page 144] [Italian Journal of Medicine 2014; 8:426]
5 Use of ursodeoxycholic acid in patients with hypertransaminasemia In patients with fatty liver UDCA might prevent steatosis by protecting against mitochondrial injury, by inducing a plasma membrane stabilizing effect, and decreasing lipid peroxidation. Moreover, taurine-conjugated bile acids could inhibit the activity of some microsomal enzymes, which are induced by FFAs. UDCA inhibits the activation of Kupffer cells caused by toxic bile salts, thus acting as an antioxidant agent. 41 Furthermore, UDCA increases hepatocyte levels of glutathione and thio-containing protein, therefore protecting hepatocytes against oxidative injury. 42 UDCA may also reduce the expression of class II HLA inhibitors, the production of interleukin and interferon, thus acting as an immunomodulator. In addition, UDCA seems to reduce reactive oxygen species. 43 Both UDCA and TUDCA have been tested, alone or in combination with other drugs, versus no intervention or in randomized controlled trials versus placebo. 40 Biochemical response was assessed by serum activities of AST, ALT, alkaline phosphatase (ALP), GGT, and serum total bilirubin levels. UDCA or TUDCA treatments actually induce a decrease of AST and ALT serum levels, but there were no significant differences between patients treated with BAs and the control (placebo) group. Similarly, no significant decrease in GGT, ALP and bilirubin were seen. 40 Conflicting results were reported as to ultrasound (US) response. The majority of trials did not show significant improvement of US features of steatosis after UDCA treatment, 40 only one study reported a slight decrease in the US steatosis score. 44 Therefore, available data allow to exclude any radiological benefit of UDCA versus placebo/no intervention in patients with fatty liver. The major clinical outcome of such treatment should be the possible improvement of histological liver damage. Only a few studies have addressed this issue, failing to show significant modifications of degree of steatosis, inflammation, or fibrosis among treated patients. Lindor et al. 43 studied the efficacy of UDCA in 166 patients with biopsy-proven NASH. End-points included changes in liver test results and liver histology at 2 years of therapy. Unfortunately, also this study failed to show any biochemical or histological benefit of UDCA in patients with NASH. More recently, Ratziu et al. 41 investigated the efficacy and safety of high-dose UDCA (HD-UDCA, mg/kg per day) in a 12-month, randomized, double-blind, placebo-controlled multicenter trial enrolling 126 patients with biopsy-proven NASH and elevated ALT levels. The primary study end-point was a reduction in ALT levels from baseline in patients treated with HD-UDCA compared with placebo. Secondary study end-points were the proportion of patients with ALT normalization, a relative reduction in the scores of serum markers of fibrosis and hepatic inflammation, and safety and tolerability. In this study, HD-UDCA significantly reduced mean ALT levels ( 28.3% from baseline after 12 months compared with 1.6% with placebo, P<0.001). At the end of the trial, ALT levels normalized in 24.5% of patients treated with HD-UDCA and in 4.8% of patients who received placebo (P=0.003). Both results were not accounted for by changes in weight during the trial. HD-UDCA significantly reduced the serum fibrosis marker compared with placebo. Furthermore, this BA also significantly improved markers of glycemic control and insulin resistance. 41 The results of this study indicate that probably UDCA should be administered in a dosage higher than that reported in previous trials. Conclusions Although UDCA is extensively prescribed in clinical practice for the treatment of patients with hypertransaminasemia of various origins, its use is hampered by the fact that it is not clear whether biochemical remission seen during UDCA treatment might be associated with histological improvement and a favorable modification of the disease progression. Moreover, it should be underlined that in our country UDCA treatment for non-cholestatic chronic liver disease is considered off-label and therefore it is not refunded by our National Health System. On the other side, absence of evidence does not always mean absence of effect. 40 Furthermore, it should be considered that UDCA is a rather safe and relatively inexpensive drug. 26 The decrease of liver biochemistry during treatment often reduces patient anxiety, thus improving quality of life and mental health status (Elmo MG, unpublished data, 2012). Lastly, although it is not clear whether ALT levels actually correlate with the severity of liver damage and disease progression, particularly in CHC, 45 we cannot rule out the possibility that persistent ALT improvement or even normalization might favorably modify the clinical outcome and the long-term history of chronic liver diseases. In conclusion, further prospective studies using higher doses of UDCA and/or longer treatment periods are needed. Patients with CH should be clearly informed that this therapy might merely have cosmetic effects on the liver biochemistry. References 1. Hofmann AL. Bile acids: trying to understand their chemistry and biology with the hope of helping patients. Hepatology 2009;49: Lazaridis KN, Gores GJ, Lindor KD. Ursodeoxycholic [page 145] [Italian Journal of Medicine 2014; 8:426] [page 145]
6 Review acid. Mechanisms of action and clinical use in hepatobiliary disorders. J Hepatol 2001;35: Pauli-Magnus C, Stieger B, Meier Y, et al. Enterohepatic transport of bile acids and genetics of cholestasis. J Hepatol 2005;43: Chiang JYL. Regulation of bile acid synthesis: pathways, nuclear receptors, and mechanisms. J Hepatol 2004;40: Russel DW. The enzymes, regulation and genetics of bile acid synthesis. Ann Rev Biochem 2003;72: Meier PG, Stieger B. Bile salt transporters. News Physiol Sci 2000;15: Hofmann AL. Gallstone disease: physicochemical research sheds new light on an old disease and points the way to medical therapy (commentary). J Hepatol 2004;41: Admirand WH, Small DM. The physicochemical basis of cholesterol gallstones formation in man. J Clin Invest 1968;47: Danzinger RG, Hofmann AF, Schoenfield LJ, Thistle JL. Dissolution of cholesterol gallstones by chenodeoxycholic acid. N Engl J Med 1972;286: Nakagawa S, Makino I, Ishazaki T, Dohi I. Dissolution of cholesterol gallstones by ursodeoxycholic acid. Lancet 1977;2: Hofmann AF. Pharmacology of ursodeoxycholic acid, an enterohepatic drug. Scand J Gastroenterol 1994;29: Bachrach WH, Hofmann AF. Ursodeoxycholic acid in the treatment of cholesterol cholelithiasis. Dig Dis Sci 1982;27: Poupon R, Chretien Y, Poupon RE, et al. Is ursodeoxycholic acid an effective treatment for primary biliary cirrhosis? Lancet 1987;1: Poupon RE, Balkau B, Eschwege E, et al. A multicenter, controlled trial of ursodiol for the treatment of primary biliary cirrhosis. N Engl J Med 1991;324: Poupon RE, Poupon R, Balkau B, for the UDCA-PBC study group. Ursodiol for the long-term treatment of primary biliary cirrhosis. N Engl J Med 1994;330: Lindor KD, Therneau TM, Jorgensen RA, et al. Effects of ursodeoxycholic acid on survival in patients with primary biliary cirrhosis. Gastroenterology 1996;110: Kowdley KV. Ursodeoxycholic acid therapy in hepatobiliary disease. Am J Med 2000;108: Goulis J, Leandro G, Burroughs AK. Randomised controlled trials of ursodeoxycholic acid therapy for primary biliary cirrhosis: a meta-analysis. Lancet 1999;354: Rudic JS, Poropat G, Krstic MN, et al. Ursodeoxycholic acid for primary biliary cirrhosis. Cochrane Database Syst Rev 2012;12:CD Green RM, Flamm S. AGA technical review on the evaluation of liver chemistry tests. Gastroenterology 2002;123: Bellentan S, Tiribelli C. The spectrum of liver disease in the general population. Lessons from the Dyonisos study. J Hepatol 2001;35: Poynard T, Yuen MF, Ratziu V, Lai CL. Viral hepatitis C: review. Lancet 2003;362: Puoti C, Pannullo A, Annovazzi G, et al. Ursodeoxycholic acid and chronic hepatitis C infection. Lancet 1993;341: Chen W, Liu JP, Gluud C. Bile acids for viral hepatitis. Cochrane Database Syst Rev 2007;(4):CD Takano S, Nakamura K, Yokosuka O, et al. A multicenter randomized controlled dose study of ursodeoxycholic acid for chronic hepatitis C. Hepatology 1994; 20: Puoti C, Magrini A, Filippi T, et al. Effects of ursodeoxycholic acid on serum liver enzymes in patients with hepatitis C virus-related chronic liver disease. Eur J Gastroenterol Hepatol 1995;7: Scotto G. The ursodeoxycholic acid for the treatment of HCV infections. Inf Med 1997;3: Crosignani A, Battezzati PM, Cestari C, et al..tauroursodeoxycholic acid for the treatment of chronic hepatitis: a multicentre dose-response study. Hepatol Res 1998;13: Belloni G, Ferrari L, Balduzzi C, et al. Effect of tauroursodeoxycholic acid on ALT, GGT and viral load in patients with hepatitis C virus-related chronic hepatitis with reference to the genotype. Ital J Gastroenterol Hepatol 1999;31: Angelico M, Gandin C, Pescarmona E, et al. Recombinant interferon alpha and ursodeoxycholic acid versus interferon alpha alone in the treatment of chronic hepatitis C: a randomized clinical trial with long-term follow-up. Am J Gastroenterol 1995;90: Ohiwa T, Katagiri K, Hoshino M, et al. Tauroursodeoxycholate and tauro-beta-muricholate exert cytoprotection by reducing intrahepatocyte taurochenodeoxycholate content. Hepatology 1993;17: Nojiri S, Nakao H, Sugauchi F, et al. Effect of ursodeoxycholic acid on serum liver enzymes and bile acid metabolism in chronic active hepatitis C virus infection. Hepatol Res 2009;39: Attili AF, Rusticali A, Varriale M, et al. The effect of ursodeoxycholic acid on serum enzymes and liver histology in patients with chronic active hepatitis. A 12-month double-blind, placebo-controlled trial. J Hepatol 1994;20: Asselah T. A revolution in HCV treatment with directacting antivirals: From non-response to eradication. J Hepatol 2012;57: Puoti C. How to manage HBeAg-negative chronic HBV infection with normal alanine aminotransferase levels in clinical practice? Eur J Intern Med 2013;24: European Association for the Study of the Liver (EASL). EASL clinical practice guidelines: management of chronic hepatitis B virus infection. J Hepatol 2012;57: Sanyal AJ. AGA Technical review on non-alcoholic fatty liver disease. Gastroenterology 2002;123: Vuppalanchi R, Chalasani N. Non-alcoholic fatty liver disease and non-alcoholic steatohepatitis: selected practical issues in their evaluation and management. Hepatology 2009;49: Comar KM, Sterling RK. Drug therapy for non-alcoholic fatty liver disease. Aliment Pharmacol Ther 2006;23: Orlando R, Azzalini L, Orando S, Lirussi F. Bile acids for non-alcoholic fatty liver disease and/or steatohepatitis. Cochrane Database Syst Rev 2007;(1):CD Ratziu V, de Ledinghen V, Fréderic Oberti F, et al. A randomized controlled trial of high-dose ursodesoxycholic [page 146] [Italian Journal of Medicine 2014; 8:426]
7 Use of ursodeoxycholic acid in patients with hypertransaminasemia acid for non-alcoholic steatohepatitis. J Hepatol 2011; 54: Bellentani S, Chao YC, Ferretti I, et al. Chronic administration of ursodeoxycholic and tauroursodeoxycholic acid changes microsomal membrane lipid content and fatty acid compositions in rats. Biochem Biophys Res Commun 1996;220: Lindor KD, Kowdley KV, Heathcote EJ, et al. Ursodeoxycholic acid for treatment of non-alcoholic steatohepatitis: results of a randomized trial. Hepatology 2004;39: Mèndez-Sanchez N, Gonzalez V, Chavez-Tapia N, et al. Weight reduction and ursodeoxycholic acid in subjects with non-alcoholic fatty liver disease. A double-blind, placebo controlled trial. Ann Hepatol 2004;3: Puoti C. HCV carriers with persistently normal aminotransferase levels: normal does not always mean healthy. J Hepatol 2003;38: [page 147] [Italian Journal of Medicine 2014; 8:426] [page 147]
Ocaliva (obeticholic acid tablets)
 Ocaliva (obeticholic acid tablets) Policy Number: 5.01.619 Last Review: 11/2018 Origination: 11/2016 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
Ocaliva (obeticholic acid tablets) Policy Number: 5.01.619 Last Review: 11/2018 Origination: 11/2016 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage
EVALUATION OF ABNORMAL LIVER TESTS
 EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
THBA Platform - Bile acid imbalance
 - Bile acid imbalance Bile acids play an important role in maintaining human health by means of signaling molecules in the regulation of bile formation, liver function and metabolism. The detergent effect
- Bile acid imbalance Bile acids play an important role in maintaining human health by means of signaling molecules in the regulation of bile formation, liver function and metabolism. The detergent effect
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and
 Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Diagnosis and Management of PBC
 Diagnosis and Management of PBC Cynthia Levy, MD, FAASLD University of Miami Miller School of Medicine Miami, Florida 1 Primary Biliary Cholangitis (PBC) Chronic cholestatic liver disease Autoimmune in
Diagnosis and Management of PBC Cynthia Levy, MD, FAASLD University of Miami Miller School of Medicine Miami, Florida 1 Primary Biliary Cholangitis (PBC) Chronic cholestatic liver disease Autoimmune in
NONALCOHOLIC FATTY LIVER DISEASE. Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD. April 13, 2012
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
Bile acid metabolism. doc. Ing. Zenóbia Chavková, CSc.
 Bile acid metabolism doc. Ing. Zenóbia Chavková, CSc. Bile acid metabolism Importance: Availability for fat & cholesterol absorption Regulates total body pool of cholesterol Factors that synthesis promote
Bile acid metabolism doc. Ing. Zenóbia Chavková, CSc. Bile acid metabolism Importance: Availability for fat & cholesterol absorption Regulates total body pool of cholesterol Factors that synthesis promote
Fatty liver disease: What do we know?
 Fatty liver disease: What do we know? Prof. Dr. Claus Niederau Katholische Kliniken Oberhausen ggmbh St. Josef-Hospital Academic Teaching Hospital University of Duisburg-Essen NAFLD Non-Alcoholic Fatty
Fatty liver disease: What do we know? Prof. Dr. Claus Niederau Katholische Kliniken Oberhausen ggmbh St. Josef-Hospital Academic Teaching Hospital University of Duisburg-Essen NAFLD Non-Alcoholic Fatty
Hepatic Transporter Proteins involved in Bile Formation
 Bile salt synthesis Hepatic Transporter Proteins involved in Bile Formation Basolateral membrane transporter proteins fx: NTCP uptake of bile salts OATP bulky organic anions Canalicular membrane transporter
Bile salt synthesis Hepatic Transporter Proteins involved in Bile Formation Basolateral membrane transporter proteins fx: NTCP uptake of bile salts OATP bulky organic anions Canalicular membrane transporter
ABNORMAL LIVER FUNCTION TESTS. Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust
 ABNORMAL LIVER FUNCTION TESTS Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust INTRODUCTION Liver function tests Cases Non invasive fibrosis measurement Questions UK MORTALITY RATE
ABNORMAL LIVER FUNCTION TESTS Dr Uthayanan Chelvaratnam Hepatology Consultant North Bristol NHS Trust INTRODUCTION Liver function tests Cases Non invasive fibrosis measurement Questions UK MORTALITY RATE
Hepatocytes produce. Proteins Clotting factors Hormones. Bile Flow
 R.J.Bailey MD Hepatocytes produce Proteins Clotting factors Hormones Bile Flow Trouble.. for the liver! Trouble for the Liver Liver Gall Bladder Common Alcohol Hep C Fatty Liver Cancer Drugs Viruses Uncommon
R.J.Bailey MD Hepatocytes produce Proteins Clotting factors Hormones Bile Flow Trouble.. for the liver! Trouble for the Liver Liver Gall Bladder Common Alcohol Hep C Fatty Liver Cancer Drugs Viruses Uncommon
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy
 Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
TREATMENT OF PRIMARY BILIARY CIRRHOSIS (PBC)
 TREATMENT OF PRIMARY BILIARY CIRRHOSIS (PBC) URSO not indicated Therapy for PBC Difficulties Etiology is uncertain Therapies are based on ideas regarding pathogenesis Present medical therapies have a limited
TREATMENT OF PRIMARY BILIARY CIRRHOSIS (PBC) URSO not indicated Therapy for PBC Difficulties Etiology is uncertain Therapies are based on ideas regarding pathogenesis Present medical therapies have a limited
Update on Non-Alcoholic Fatty Liver Disease. Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI
 Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Ocaliva (obeticholic acid) Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Ocaliva (obeticholic acid) Prime Therapeutics will review Prior Authorization
Ocaliva (obeticholic acid) Page 1 of 6 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Ocaliva (obeticholic acid) Prime Therapeutics will review Prior Authorization
End Stage Liver Disease & Disease Specific Indications for Liver Transplant. Susan Kang, RN, MSN, ANP-BC
 End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP-BC Introduction (https://www.srtr.org) What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP-BC Introduction (https://www.srtr.org) What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC
 End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC Introduction (https://www.srtr.org) 1 What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
End Stage Liver Disease & Disease Specific Indications for Liver Transplant Susan Kang, RN, MSN, ANP BC Introduction (https://www.srtr.org) 1 What does the liver do? STORAGE METABOLIC DETOXIFICATION SYNTHETIC
Hangzhou, 15 March Ulrich Beuers Department of Gastroenterology and Hepatology Academic Medical Center University of Amsterdam
 Clinical Aspects of Primary Biliary Cirrhosis Hangzhou, 15 March 2008 Ulrich Beuers Department of Gastroenterology and Hepatology Academic Medical Center University of Amsterdam Epidemiology of Primary
Clinical Aspects of Primary Biliary Cirrhosis Hangzhou, 15 March 2008 Ulrich Beuers Department of Gastroenterology and Hepatology Academic Medical Center University of Amsterdam Epidemiology of Primary
Viral Hepatitis The Preventive Potential of Antiviral Therapy. Thomas Berg
 Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Liver function and clinical chemistry of liver
 INTRODUCTION Liver function and clinical chemistry of liver The liver plays a major role in carbohydrate, lipid and protein metabolism with the processes of glycolysis, the Krebs cycle,,homeostasis synthesis
INTRODUCTION Liver function and clinical chemistry of liver The liver plays a major role in carbohydrate, lipid and protein metabolism with the processes of glycolysis, the Krebs cycle,,homeostasis synthesis
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Cornerstones of Hepatitis B: Past, Present and Future
 Cornerstones of Hepatitis B: Past, Present and Future Professor Man-Fung Yuen Queen Mary Hospital The University of Hong Kong Hong Kong 1 Outline Past Natural history studies Development of HBV-related
Cornerstones of Hepatitis B: Past, Present and Future Professor Man-Fung Yuen Queen Mary Hospital The University of Hong Kong Hong Kong 1 Outline Past Natural history studies Development of HBV-related
Interpreting Liver Function Tests
 PSH Clinical Guidelines Statement 2017 Interpreting Liver Function Tests Dr. Asad A Chaudhry Consultant Hepatologist, Chaudhry Hospital, Gujranwala, Pakistan. Liver function tests (LFTs) generally refer
PSH Clinical Guidelines Statement 2017 Interpreting Liver Function Tests Dr. Asad A Chaudhry Consultant Hepatologist, Chaudhry Hospital, Gujranwala, Pakistan. Liver function tests (LFTs) generally refer
GI Workshop Case Studies
 GI Workshop Case Studies Cliff Titcomb MD Hannover Re AAIM Annual Meeting San Diego, October, 2012 5 Tests Commonly Known as Liver Function Tests Alanine Aminotransferase (ALT, SGPT) Aspartate Aminotransferase
GI Workshop Case Studies Cliff Titcomb MD Hannover Re AAIM Annual Meeting San Diego, October, 2012 5 Tests Commonly Known as Liver Function Tests Alanine Aminotransferase (ALT, SGPT) Aspartate Aminotransferase
Hepatitis C Management and Treatment
 Hepatitis C Management and Treatment Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology 1 Discovery of Hepatitis C Key facts Hepatitis C: the virus can cause
Hepatitis C Management and Treatment Kaya Süer Near East University Faculty of Medicine Infectious Diseases and Clinical Microbiology 1 Discovery of Hepatitis C Key facts Hepatitis C: the virus can cause
Improving the Lives of Patients with Liver Diseases
 Improving the Lives of Patients with Liver Diseases Corporate Presentation March 2019 Safe Harbor Statement This presentation contains "forward-looking" statements that involve risks, uncertainties and
Improving the Lives of Patients with Liver Diseases Corporate Presentation March 2019 Safe Harbor Statement This presentation contains "forward-looking" statements that involve risks, uncertainties and
Non-Alcoholic Fatty Liver Disease
 Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
NONALCOHOLIC FATTY LIVER DISEASE
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
NON-ALCOHOLIC FATTY LIVER DISEASE:
 NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health
 CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
Chronic Hepatitis B: management update.
 Chronic Hepatitis B: management update. E.O.Ogutu Department of clinical medicine & therapeutics, University of Nairobi. Physicians meeting,kisumu 2011. Background epidemiology Chronic hepatitis B (CHB)
Chronic Hepatitis B: management update. E.O.Ogutu Department of clinical medicine & therapeutics, University of Nairobi. Physicians meeting,kisumu 2011. Background epidemiology Chronic hepatitis B (CHB)
2. Liver blood tests and what they mean p2 Acute and chronic liver screen
 Hepatology referral pathways for GP 1 Scope For use within hepatology Contents 2. Liver blood tests and what they mean p2 Acute and chronic liver screen p2 Common reasons for hepatology referral 3. Raised
Hepatology referral pathways for GP 1 Scope For use within hepatology Contents 2. Liver blood tests and what they mean p2 Acute and chronic liver screen p2 Common reasons for hepatology referral 3. Raised
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
What is NAFLD?.NASH? Presenter Disclosure Information. Learning Objectives. Case 1: Rob. Questions Pertinent to Rob
 Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
-Liver function tests -
 -Liver function tests - Biochimestry teamwork Osamah Al-Jarallah Abdulaziz Al-Shamlan Abdullah Al-Mazyad Turki Al-Otaibi Khalid Al-Khamis Saud Al-awad KhaledAlmohaimede Meshal Al-Otaibi Al-Anood Asiri
-Liver function tests - Biochimestry teamwork Osamah Al-Jarallah Abdulaziz Al-Shamlan Abdullah Al-Mazyad Turki Al-Otaibi Khalid Al-Khamis Saud Al-awad KhaledAlmohaimede Meshal Al-Otaibi Al-Anood Asiri
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Bile acids, the major constituents of bile, are synthesized
 REVIEWS Ursodeoxycholic Acid Therapy in Hepatobiliary Disease Kris V. Kowdley, MD Ursodeoxycholic acid is a hydrophilic bile acid that under normal circumstances represents a small fraction of the bile
REVIEWS Ursodeoxycholic Acid Therapy in Hepatobiliary Disease Kris V. Kowdley, MD Ursodeoxycholic acid is a hydrophilic bile acid that under normal circumstances represents a small fraction of the bile
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016.
 Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
NUCs for Chronic Hepatitis B. Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona.
 NUCs for Chronic Hepatitis B Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona. Spain Disclosures Advisory board of, and/or, received speaker fee from
NUCs for Chronic Hepatitis B Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona. Spain Disclosures Advisory board of, and/or, received speaker fee from
Non-Alcoholic Fatty Liver Disease (NAFLD)
 HEPATO-PANCREATO-BILIARY STOMACH CANCER PROGRAM Non-Alcoholic Fatty Liver Disease (NAFLD) Steatosis and Non-Alcoholic Steatohepatitis (NASH) Management Recommendations UCSF Fresno Department of Surgery
HEPATO-PANCREATO-BILIARY STOMACH CANCER PROGRAM Non-Alcoholic Fatty Liver Disease (NAFLD) Steatosis and Non-Alcoholic Steatohepatitis (NASH) Management Recommendations UCSF Fresno Department of Surgery
Prolonged Follow-Up of Patients in the U.S. Multicenter Trial of Ursodeoxycholic Acid for Primary Biliary Cirrhosis
 American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j1572-0241.2004.04047.x Published by Blackwell Publishing Prolonged Follow-Up of Patients in the
American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j1572-0241.2004.04047.x Published by Blackwell Publishing Prolonged Follow-Up of Patients in the
Intron A Hepatitis B. Intron A (interferon alfa-2b) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES
 NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
Obeticholic Acid for the treatment of Primary Biliary Cholangitis: Effectiveness, Value, and Value-Based Price Benchmarks
 Obeticholic Acid for the treatment of Primary Biliary Cholangitis: Effectiveness, Value, and Value-Based Price Benchmarks Draft Background and Scope Background: April 21, 2016 Primary biliary cholangitis
Obeticholic Acid for the treatment of Primary Biliary Cholangitis: Effectiveness, Value, and Value-Based Price Benchmarks Draft Background and Scope Background: April 21, 2016 Primary biliary cholangitis
PBC treatment: the present and future. Maggie Bassendine Professor of Hepatology
 PBC treatment: the present and future Maggie Bassendine Professor of Hepatology Primary biliary cirrhosis 20-25yrs OLT/ Death Symptoms: Fatigue, itching, jaundice Autoimmune disease: Focal small bile duct
PBC treatment: the present and future Maggie Bassendine Professor of Hepatology Primary biliary cirrhosis 20-25yrs OLT/ Death Symptoms: Fatigue, itching, jaundice Autoimmune disease: Focal small bile duct
Steatosi epatica ed HCV
 Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
DATA SHEET URSOFALK. Ursodeoxycholic Acid
 URSOFALK - New Zealand Page 1 of 7 NAME OF DRUG DATA SHEET URSOFALK Ursodeoxycholic Acid DESCRIPTION Ursodeoxycholic acid (UDCA) is a white or almost white powder. It is practically insoluble in water,
URSOFALK - New Zealand Page 1 of 7 NAME OF DRUG DATA SHEET URSOFALK Ursodeoxycholic Acid DESCRIPTION Ursodeoxycholic acid (UDCA) is a white or almost white powder. It is practically insoluble in water,
I have no disclosures relevant to this presentation LIVER TESTS: WHAT IS INCLUDED? LIVER TESTS: HOW TO UTILIZE THEM OBJECTIVES
 LIVER TESTS: HOW TO UTILIZE THEM I have no disclosures relevant to this presentation José Franco, MD Professor of Medicine, Surgery and Pediatrics Medical College of Wisconsin OBJECTIVES Differentiate
LIVER TESTS: HOW TO UTILIZE THEM I have no disclosures relevant to this presentation José Franco, MD Professor of Medicine, Surgery and Pediatrics Medical College of Wisconsin OBJECTIVES Differentiate
Who to Treat? Consider biopsy Treat. > 2 ULN Treat Treat Treat Treat CIRRHOTIC PATIENTS Compensated Treat HBV DNA detectable treat
 Who to Treat? Parameter AASLD US Algorithm EASL APASL HBV DNA CRITERIA HBeAg+ >, IU/mL > 2, IU/mL > 2, IU/mL >, IU/mL HBeAg- > 2, IU/mL > 2, IU/mL > 2, IU/mL > 2, IU/mL ALT CRITERIA PNALT 1-2 ULN Monitor
Who to Treat? Parameter AASLD US Algorithm EASL APASL HBV DNA CRITERIA HBeAg+ >, IU/mL > 2, IU/mL > 2, IU/mL >, IU/mL HBeAg- > 2, IU/mL > 2, IU/mL > 2, IU/mL > 2, IU/mL ALT CRITERIA PNALT 1-2 ULN Monitor
AAIM: GI Workshop Follow Up to Case Studies. Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease
 AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
The Impact of HBV Therapy on Fibrosis and Cirrhosis
 The Impact of HBV Therapy on Fibrosis and Cirrhosis Jordan J. Feld, MD, MPH Associate Professor of Medicine University of Toronto Hepatologist Toronto Centre for Liver Disease Sandra Rotman Centre for
The Impact of HBV Therapy on Fibrosis and Cirrhosis Jordan J. Feld, MD, MPH Associate Professor of Medicine University of Toronto Hepatologist Toronto Centre for Liver Disease Sandra Rotman Centre for
Investigating and Referring Incidental Findings of Abnormal Liver Tests
 Investigating and Referring Incidental Findings of Abnormal Liver Tests Note on Referral Guidelines: these revised guidelines are presented as a tool to aid appropriate referral and management of common
Investigating and Referring Incidental Findings of Abnormal Liver Tests Note on Referral Guidelines: these revised guidelines are presented as a tool to aid appropriate referral and management of common
NAFLD/NASH. Definitions. Pathology NASH. Vicki Shah PA-C, MMS Rush University Hepatology
 NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
Hepatobiliary lipids איך טיפול נולד... from bench to bedside. Fred M Konikoff, MD, MSc, FAASLD
 Hepatobiliary lipids איך טיפול נולד... from bench to bedside Fred M Konikoff, MD, MSc, FAASLD Institute of Gastroenterology and Hepatology, Meir Medical Center, Kfar Saba, and Research Laboratory of Cholesterol
Hepatobiliary lipids איך טיפול נולד... from bench to bedside Fred M Konikoff, MD, MSc, FAASLD Institute of Gastroenterology and Hepatology, Meir Medical Center, Kfar Saba, and Research Laboratory of Cholesterol
Pathophysiology of Bile Secretion
 Pathophysiology of Bile Secretion Martin C. Carey, D.Sc., M.D. Division of Gastroenterology, Brigham and Women s Hospital and Department of Medicine, Harvard Medical School Boston, MA, U.S.A. Functions
Pathophysiology of Bile Secretion Martin C. Carey, D.Sc., M.D. Division of Gastroenterology, Brigham and Women s Hospital and Department of Medicine, Harvard Medical School Boston, MA, U.S.A. Functions
HEPATOPROTECTORS PLACE IN THERAPY OF CHRONIC VIRAL HEPATITIS. professor D.Gusev
 HEPATOPROTECTORS PLACE IN THERAPY OF CHRONIC VIRAL HEPATITIS professor D.Gusev St. Petersburg 2012 Hepatoprotectors and chronic viral hepatitis Do patients with chronic viral hepatitis need hepatoprotectors?
HEPATOPROTECTORS PLACE IN THERAPY OF CHRONIC VIRAL HEPATITIS professor D.Gusev St. Petersburg 2012 Hepatoprotectors and chronic viral hepatitis Do patients with chronic viral hepatitis need hepatoprotectors?
Current Concepts in the Management and Treatment of PBC & PSC
 Current Concepts in the Management and Treatment of PBC & PSC Michael A Heneghan, MD, MMedSc, FRCPI. Institute of Liver Studies, King s College Hospital, London A family affair? Central vein Hepatocytes
Current Concepts in the Management and Treatment of PBC & PSC Michael A Heneghan, MD, MMedSc, FRCPI. Institute of Liver Studies, King s College Hospital, London A family affair? Central vein Hepatocytes
Liver transplant: what is left after the viruses
 Riunione Monotematica A.I.S.F. 2016 The Future of Liver Disease: Beyond HCV is there a Role for Hepatologist? Milan 15 th 2016 Liver transplant: what is left after the viruses Stefano Ginanni Corradini
Riunione Monotematica A.I.S.F. 2016 The Future of Liver Disease: Beyond HCV is there a Role for Hepatologist? Milan 15 th 2016 Liver transplant: what is left after the viruses Stefano Ginanni Corradini
Hepatitis B Virus. Taylor Page PharmD Candidate 2019 February 1, 2019
 Hepatitis B Virus Taylor Page PharmD Candidate 2019 February 1, 2019 Epidemiology 3218 cases of acute HBV reported in 2016 847,000 non-institutionalized persons living with chronic HBV in 2011-2012 Viral
Hepatitis B Virus Taylor Page PharmD Candidate 2019 February 1, 2019 Epidemiology 3218 cases of acute HBV reported in 2016 847,000 non-institutionalized persons living with chronic HBV in 2011-2012 Viral
Screening for HCCwho,
 Screening for HCCwho, how and how often? Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital HCC Global Epidemiology
Screening for HCCwho, how and how often? Catherine Stedman Associate Professor of Medicine, University of Otago, Christchurch Gastroenterology Department, Christchurch Hospital HCC Global Epidemiology
New insights in pathogenesis and therapy of primary biliary cholangitis. Keith D. Lindor Dean Professor of Medicine
 New insights in pathogenesis and therapy of primary biliary cholangitis Keith D. Lindor Dean Professor of Medicine OUTLINE PBC Epidemiology Diagnosis Treatment Incidence of PBC and PSC Trends Boonstra
New insights in pathogenesis and therapy of primary biliary cholangitis Keith D. Lindor Dean Professor of Medicine OUTLINE PBC Epidemiology Diagnosis Treatment Incidence of PBC and PSC Trends Boonstra
Chronic Hepatitis B Infection
 Chronic Hepatitis B Infection Mohssen Nassiri Toosi, MD Imam Khomeinin Hospital Tehran University of Medical Sciences Chronic Hepatitis B Infection Virus : HBs Ag Positive Host Liver Health Chronic Hepatitis
Chronic Hepatitis B Infection Mohssen Nassiri Toosi, MD Imam Khomeinin Hospital Tehran University of Medical Sciences Chronic Hepatitis B Infection Virus : HBs Ag Positive Host Liver Health Chronic Hepatitis
29th Viral Hepatitis Prevention Board Meeting
 29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis B José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HBV INFECTION
29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis B José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HBV INFECTION
ACG Clinical Guideline: Primary Sclerosing Cholangitis
 ACG Clinical Guideline: Primary Sclerosing Cholangitis Keith D. Lindor, MD, FACG 1, Kris V. Kowdley, MD, FACG 2, and M. Edwyn Harrison, MD 3 1 College of Health Solutions, Arizona State University, Phoenix,
ACG Clinical Guideline: Primary Sclerosing Cholangitis Keith D. Lindor, MD, FACG 1, Kris V. Kowdley, MD, FACG 2, and M. Edwyn Harrison, MD 3 1 College of Health Solutions, Arizona State University, Phoenix,
Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition
 Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition Anna S. Lok, MD, DSc Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research
Consensus AASLD-EASL HBV Treatment Endpoint and HBV Cure Definition Anna S. Lok, MD, DSc Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research
NAFLD & NASH: Russian perspective
 NAFLD & NASH: Russian perspective Vasily Isakov, MD, PhD Professor, Chief, Department Gastroenterology & Hepatology, Federal Research Center of nutrition, biotechnology and food safety Disclosures Received
NAFLD & NASH: Russian perspective Vasily Isakov, MD, PhD Professor, Chief, Department Gastroenterology & Hepatology, Federal Research Center of nutrition, biotechnology and food safety Disclosures Received
Should Elderly CHC Patients (>70 years old) be Treated?
 Should Elderly CHC Patients (>70 years old) be Treated? Deepak Amarapurkar Consultant Gastroenterologist & Hepatologist Bombay Hospital & Medical Research Center, Mumbai & Jagjivanram Western Railway Hospital,
Should Elderly CHC Patients (>70 years old) be Treated? Deepak Amarapurkar Consultant Gastroenterologist & Hepatologist Bombay Hospital & Medical Research Center, Mumbai & Jagjivanram Western Railway Hospital,
HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM
 EVALUATION OF LIVER FUNCTION R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM METABOLIC FUNCTION
EVALUATION OF LIVER FUNCTION R. Mohammadi Biochemist (Ph.D.) Faculty member of Medical Faculty HEPETIC SYSTEMS BIOCHEMICAL HEPATOCYTIC SYSTEM HEPATOBILIARY SYSTEM RETICULOENDOTHELIAL SYSTEM METABOLIC FUNCTION
WHAT CAN YOU USE IN YOUR CLINIC TODAY FOR THE TREATMENT OF NASH?
 WHAT CAN YOU USE IN YOUR CLINIC TODAY FOR THE TREATMENT OF NASH? Helena Cortez-Pinto Laboratório de Nutrição, FML, Serviço de Gastrenterologia, Hospital St Maria, Lisboa, Portugal EASL Governing Board:
WHAT CAN YOU USE IN YOUR CLINIC TODAY FOR THE TREATMENT OF NASH? Helena Cortez-Pinto Laboratório de Nutrição, FML, Serviço de Gastrenterologia, Hospital St Maria, Lisboa, Portugal EASL Governing Board:
Management of Chronic Hepatitis B in Asian Americans
 Management of Chronic Hepatitis B in Asian Americans Myron J Tong; UCLA, CA Calvin Q. Pan; Mount Sinai, NY Hie-Won Hann; Thomas Jefferson, PA Kris V. Kowdley; Virginia Mason, WA Steven Huy B Han; UCLA,
Management of Chronic Hepatitis B in Asian Americans Myron J Tong; UCLA, CA Calvin Q. Pan; Mount Sinai, NY Hie-Won Hann; Thomas Jefferson, PA Kris V. Kowdley; Virginia Mason, WA Steven Huy B Han; UCLA,
CHRONIC HCV TREATMENT: In Special Populations.
 CHRONIC HCV TREATMENT: In Special Populations. By Taher EL-ZANATY Prof. of Internal Medicine CAIRO UNIVERSITY Introduction: HCV is the major cause of chronic hepatitis in Egypt. Its end stage is liver
CHRONIC HCV TREATMENT: In Special Populations. By Taher EL-ZANATY Prof. of Internal Medicine CAIRO UNIVERSITY Introduction: HCV is the major cause of chronic hepatitis in Egypt. Its end stage is liver
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids. Cholestasis
 Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
Noncalculous Biliary Disease Dean Abramson, M.D. Gastroenterologists, P.C. Cedar Rapids Cholestasis Biochemical hallmark Impaired bile flow from liver to small intestine Alkaline phosphatase is primary
BILE FORMATION, ENTEROHEPATIC CIRCULATION & BILE SALTS
 1 BILE FORMATION, ENTEROHEPATIC CIRCULATION & BILE SALTS Color index Important Further explanation 2 Mind map...3 Functions of bile & stages of bile secretion... 4 Characteristics & composition of bile...5
1 BILE FORMATION, ENTEROHEPATIC CIRCULATION & BILE SALTS Color index Important Further explanation 2 Mind map...3 Functions of bile & stages of bile secretion... 4 Characteristics & composition of bile...5
PREVALENCE OF NAFLD & NASH
 - - PREVALENCE OF & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology 2011; 140:124-31) Dallas Heart Study Prevalence Numbers (Browning et al., Hepatology 2004;40:1387-95)
- - PREVALENCE OF & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology 2011; 140:124-31) Dallas Heart Study Prevalence Numbers (Browning et al., Hepatology 2004;40:1387-95)
Key Points: Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective. Jenny Heathcote, MD. University of Toronto
 Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
Autoimmune Liver Disease: Update for Pathologists from the Hepatologist s Perspective Jenny Heathcote, MD University of Toronto Key Points: AILD comprise autoimmune hepatitis, primary biliary cirrhosis
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE
 PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
Assessment of Liver Stiffness by Transient Elastography in Diabetics with Fatty Liver A Single Center Cross Sectional observational Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
Risk Factors and Preventive Measures for Hepatocellular carcinoma (HCC) 울산의대울산대병원소화기내과박능화
 Risk Factors and Preventive Measures for Hepatocellular carcinoma (HCC) 울산의대울산대병원소화기내과박능화 Risk factors for HCC development (I) Environmental factors Infectious HBV HCV HDV Alimentary Alcohol Diet High
Risk Factors and Preventive Measures for Hepatocellular carcinoma (HCC) 울산의대울산대병원소화기내과박능화 Risk factors for HCC development (I) Environmental factors Infectious HBV HCV HDV Alimentary Alcohol Diet High
Chronic Cholestatic Liver Diseases
 Chronic Cholestatic Liver Diseases - EASL Clinical Practice Guidelines - Rome, 8 October 2010 Ulrich Beuers Department of Gastroenterology and Hepatology Tytgat Institute of Liver and Intestinal Research
Chronic Cholestatic Liver Diseases - EASL Clinical Practice Guidelines - Rome, 8 October 2010 Ulrich Beuers Department of Gastroenterology and Hepatology Tytgat Institute of Liver and Intestinal Research
MANAGEMENT OF HBV & HCV INFECTION---SIMILARITIES & DISSIMILARITIES---PAST AND PRESENT. Professor Salimur Rahman
 MANAGEMENT OF HBV & HCV INFECTION---SIMILARITIES & DISSIMILARITIES---PAST AND PRESENT Professor Salimur Rahman Department of Hepatology, BSMMU President, Association for the study of the liver, Dhaka,
MANAGEMENT OF HBV & HCV INFECTION---SIMILARITIES & DISSIMILARITIES---PAST AND PRESENT Professor Salimur Rahman Department of Hepatology, BSMMU President, Association for the study of the liver, Dhaka,
Bile Acids: Developments New and Very Old. William C. Duane, M.D. Department of Medicine, Veterans Affairs Medical Center and University of Minnesota,
 Bile Acids: Developments New and Very Old William C. Duane, M.D. Department of Medicine, Veterans Affairs Medical Center and University of Minnesota, Minneapolis, Minnesota 55417 Address for correspondence
Bile Acids: Developments New and Very Old William C. Duane, M.D. Department of Medicine, Veterans Affairs Medical Center and University of Minnesota, Minneapolis, Minnesota 55417 Address for correspondence
AASLD Immune tolerant phase HBV NAFLD diagnostic HCC
 AASLD 2016 Immune tolerant phase HBV NAFLD diagnostic HCC Immune tolerant 3 Modified from Chan HLY and Wong VWS. Hepatitis B. In Zakim and Boyers s Hepatology 2012 2015 AMERICAN ASSOCIATION FOR THE S1T6UDY
AASLD 2016 Immune tolerant phase HBV NAFLD diagnostic HCC Immune tolerant 3 Modified from Chan HLY and Wong VWS. Hepatitis B. In Zakim and Boyers s Hepatology 2012 2015 AMERICAN ASSOCIATION FOR THE S1T6UDY
Antiviral agents in HCV
 Antiviral agents in HCV : Upcoming Therapeutic Options Su Jong Yu, M.D., Ph.D. Department of Internal Medicine, Liver Research Institute, Seoul National University College of Medicine Estimated 170 Million
Antiviral agents in HCV : Upcoming Therapeutic Options Su Jong Yu, M.D., Ph.D. Department of Internal Medicine, Liver Research Institute, Seoul National University College of Medicine Estimated 170 Million
High dose UDCA in the Treatment of Primary Sclerosing Cholangitis. Falk Meeting,Freiberg2006 Dr RW Chapman John Radcliffe Hospital Oxford,UK
 High dose UDCA in the Treatment of Primary Sclerosing Cholangitis Falk Meeting,Freiberg2006 Dr RW Chapman John Radcliffe Hospital Oxford,UK Specific Medical Therapy for PSC Immunosuppressants -prednisolone
High dose UDCA in the Treatment of Primary Sclerosing Cholangitis Falk Meeting,Freiberg2006 Dr RW Chapman John Radcliffe Hospital Oxford,UK Specific Medical Therapy for PSC Immunosuppressants -prednisolone
Primary Sclerosing Cholangitis and Cholestatic liver diseases. Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants
 Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
Primary Sclerosing Cholangitis and Cholestatic liver diseases Ahsan M Bhatti MD, FACP Bhatti Gastroenterology Consultants I have nothing to disclose Educational Objectives What is PSC? Understand the cholestatic
[Sem Liver Disease 21(1):81-88, Thieme Medical Publishers, Inc.]
![[Sem Liver Disease 21(1):81-88, Thieme Medical Publishers, Inc.] [Sem Liver Disease 21(1):81-88, Thieme Medical Publishers, Inc.]](/thumbs/72/66425194.jpg) Treatment of Nonalcoholic Fatty Liver: Present and Emerging Therapies [Sem Liver Disease 21(1):81-88, 2001. 2001 Thieme Medical Publishers, Inc.] Paul Angulo, M.D., and Keith D. Lindor, M.D., Division
Treatment of Nonalcoholic Fatty Liver: Present and Emerging Therapies [Sem Liver Disease 21(1):81-88, 2001. 2001 Thieme Medical Publishers, Inc.] Paul Angulo, M.D., and Keith D. Lindor, M.D., Division
APO-URSODEOXYCHOLIC ACID CAPSULES
 APO-URSODEOXYCHOLIC ACID CAPSULES NAME OF THE MEDICINE Ursodeoxycholic Acid (UDCA) Chemical Name: 3α, 7ß-Dihydroxy-5ß-cholan-24-oic acid Structural Formula: Molecular Formula: Molecular Weight: C24H40O4
APO-URSODEOXYCHOLIC ACID CAPSULES NAME OF THE MEDICINE Ursodeoxycholic Acid (UDCA) Chemical Name: 3α, 7ß-Dihydroxy-5ß-cholan-24-oic acid Structural Formula: Molecular Formula: Molecular Weight: C24H40O4
Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia
 Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute
Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute
Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP
 Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP Autoimmune hepatobiliary diseases The liver is an important target for immunemediated injury. Three disease phenotypes are recognized:
Autoimmune Hepatobiliary Diseases PROF. DR. SABEHA ALBAYATI CABM,FRCP Autoimmune hepatobiliary diseases The liver is an important target for immunemediated injury. Three disease phenotypes are recognized:
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse
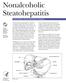 Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But
 HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But Hospital Universitario Valle Hebron and Ciberehd del Insttuto Carlos III. Barcelona. Spain Disclosures Advisory board of,
HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But Hospital Universitario Valle Hebron and Ciberehd del Insttuto Carlos III. Barcelona. Spain Disclosures Advisory board of,
METABOLIC SYNDROME AND HCV: FROM HCV
 METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
Title: Hepatocellular carcinoma in patients without advanced fibrosis after eradication of HCV with antiviral treatment
 Title: Hepatocellular carcinoma in patients without advanced fibrosis after eradication of HCV with antiviral treatment Authors: Yolanda Sánchez-Torrijos, Jara Eloísa Ternero Vega, Carmen Cepeda Franco
Title: Hepatocellular carcinoma in patients without advanced fibrosis after eradication of HCV with antiviral treatment Authors: Yolanda Sánchez-Torrijos, Jara Eloísa Ternero Vega, Carmen Cepeda Franco
Relationship between Serum Iron Indices and Hepatic Iron Quantitation in Patients with Fatty Liver Disease
 International Journal of Business, Humanities and Technology Vol. 2 No. 5; August 2012 Relationship between Serum Iron Indices and Hepatic Iron Quantitation in Patients with Fatty Liver Disease Dr. Mariana
International Journal of Business, Humanities and Technology Vol. 2 No. 5; August 2012 Relationship between Serum Iron Indices and Hepatic Iron Quantitation in Patients with Fatty Liver Disease Dr. Mariana
The impact of the treatment of HCV in developing Hepatocellular Carcinoma
 The impact of the treatment of HCV in developing Hepatocellular Carcinoma Paul Y Kwo, MD Professor of Medicine Medical Director, Liver Transplantation Gastroenterology/Hepatology Division Indiana University
The impact of the treatment of HCV in developing Hepatocellular Carcinoma Paul Y Kwo, MD Professor of Medicine Medical Director, Liver Transplantation Gastroenterology/Hepatology Division Indiana University
CIRROSI E IPERTENSIONE PORTALE NELLA DONNA
 Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar
 Original Research Article Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar Naresh Kumar 1, Jyoti Kumar Dinkar 2*, Chandrakishore
Original Research Article Prevalence of non-alcoholic fatty liver disease in type 2 diabetes mellitus patients in a tertiary care hospital of Bihar Naresh Kumar 1, Jyoti Kumar Dinkar 2*, Chandrakishore
Hepatitis C wi w t i h Ju J dy y W y W a y t a t t
 Hepatitis C with Judy Wyatt Hepatitis C and the histopathologist Pre-2006 biopsy based treatment of moderate-severe chronic hepatitis Now biopsy for: Watchful waiting, to confirm mild disease? Cirrhosis
Hepatitis C with Judy Wyatt Hepatitis C and the histopathologist Pre-2006 biopsy based treatment of moderate-severe chronic hepatitis Now biopsy for: Watchful waiting, to confirm mild disease? Cirrhosis
A Review of Liver Function Tests. James Gray Gastroenterology Vancouver
 A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
A Review of Liver Function Tests James Gray Gastroenterology Vancouver Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
A Young Man with Non-alcoholic Steatohepatitis and Serum Anti-mitochondrial Antibody Positivity: A Case Report
 doi: 10.2169/internalmedicine.0405-17 Intern Med Advance Publication http://internmed.jp CASE REPORT A Young Man with Non-alcoholic Steatohepatitis and Serum Anti-mitochondrial Antibody Positivity: A Case
doi: 10.2169/internalmedicine.0405-17 Intern Med Advance Publication http://internmed.jp CASE REPORT A Young Man with Non-alcoholic Steatohepatitis and Serum Anti-mitochondrial Antibody Positivity: A Case
