ONCOLOGY LETTERS 13: , 2017
|
|
|
- Karen James
- 6 years ago
- Views:
Transcription
1 ONCOLOGY LETTERS 13: , 2017 Integration of Child Pugh score with future liver remnant yields improved prediction of liver dysfunction risk for HBV related hepatocellular carcinoma following hepatic resection HENG ZOU, YIMING TAO and ZHI MING WANG Department of Hepatobiliary Surgery, Xiangya Hospital, Central South University, Changsha, Hunan , P.R. China Received March 20, 2016; Accepted January 31, 2017 DOI: /ol Abstract. Assessment of hepatic functional reserve is important to enable the selection of appropriate treatment methods and safe hepatic resection in hepatitis B virus (HBV) related hepatocellular carcinoma (HCC). In the present study, an evaluation was made of the clinical value of combining the Child Pugh score (CPS) with the standardized future liver remnant (sflr) measurement to predict postoperative liver dysfunction (PLD). A total of 61 HBV related HCC patients undergoing liver volumetry prior to hepatectomy were enrolled in the study. The sflr was calculated as the ratio of FLR volume to standardized liver volume. PLD was defined as a prothrombin time of >18 sec or a peak serum bilirubin level of >51.3 µmol/l for 7 days after surgery. Univariate analysis and multivariate logistic regression analysis were performed to identify risk factors associated with PLD. The correlation between PLD and the combination of sflr and CPS was analyzed. In total, 18 out of 61 patients developed PLD (29.5%), with a significantly higher PLD incidence for a CPS of 6 than a CPS of 5 (P<0.05). Multivariate logistic regression analysis revealed that a prothrombin time of <13.3 sec and an sflr of <0.55 were independent risk factors for PLD. Receiver operating characteristic (ROC) curve analysis revealed that the cut off values of sflr and sflr/cps for predicting PLD were 54.5% and , respectively, with areas under the ROC curve of and 0.860, respectively. The combination of CPS and sflr appears to yield improved prediction of the occurrence of PLD compared with either CPS or sflr alone. Introduction Liver cancer, primarily hepatocellular carcinoma (HCC), is the third most common cause of mortality from cancer Correspondence to: Dr Zhi Ming Wang, Department of Hepatobiliary Surgery, Xiangya Hospital, Central South University, 87 Xiangya Road, Changsha, Hunan , P.R. China E mail: wzmxycsu@hotmail.com Key words: hepatocellular carcinoma, Child Pugh score, future liver remnant, hepatectomy, postoperative liver dysfunction worldwide. Diagnostic and treatment strategies for liver cancer have improved, with hepatic resection being the preferred first line treatment (1,2). Patients' safety is paramount when performing hepatic surgery, although postoperative mortality occasionally occurs. Therefore, accurate assessment of hepatic functional reserve is important, particularly for hepatitis B virus (HBV) related HCC patients, since they often possess impaired livers. Hepatic functional reserve is determined by the quality and quantity of liver cells. The Child Pugh score (CPS) is widely used to assess the quality of the liver, and hepatic surgeons frequently use it to select HCC patients for resection. The CPS is calculated by five parameters: Presence or absence of encephalopathy, degree of ascites, total serum bilirubin, albumin concentration and prothrombin time. According to the total point score, CPS can be divided into grade A (5 6 points), B (7 9 points) or C (10 15 points) (3). In clinical practice, the majority of HCC patients who are eligible for resection are Child Pugh classification A patients (2,4). However, postoperative liver dysfunction (PLD) and postoperative mortality occasionally occur in Child Pugh A patients. It appears that the Child Pugh classification alone may be unreliable for predicting postoperative outcomes. To overcome the possible limitations of Child Pugh classification for predicting postoperative outcomes, liver computed tomography (CT) volumetry has been used to assist in the assessment of hepatic functional reserve in recent years, particularly when selecting HCC patients for major hepatic resection (5). Future liver remnant (FLR) volume measured preoperatively by three dimensional CT reconstruction can accurately reflect the size of the remnant liver (6,7). Patients with a smaller FLR are at a higher risk of developing PLD or postoperative liver failure (8 10). The main limitation of CT volumetry is the fact that volumetric assessment of the remnant liver does not take into account the quality of the liver parenchyma, and therefore is not reliable in predicting PLD in patients with impaired livers. The safe limit of FLR ranges from 35 to 50% in patients with chronic liver diseases (2,9,11). To improve the prediction of postoperative outcomes, CT volumetry should be complemented with a method that assesses hepatic function. In the present study, the CPS was used to assess the quality of the remnant liver, and the standardized FLR (sflr) measurement was used to evaluate the size of the remnant liver.
2 3632 ZOU et al: ROLE OF CPS AND FUTURE LIVER REMNANT IN HEPATIC RESECTION FOR LIVER CANCER In addition, risk factors were investigated in relation to PLD in patients with HBV related HCC. The CPS was combined with the sflr measurement in an attempt to predict PLD more accurately. Patients and methods Patients. Between March 2014 and February 2015, 70 patients with HCC underwent three dimensional CT reconstruction for the preoperative measurement of remnant liver volume prior to hepatectomy at the Department of Hepatobiliary Surgery, Xiangya Hospital, Central South University (Changsha, Hunan, China). Of these 70 patients, 1 patient who had undergone hepatectomy for HCC within 1 year of the present study and 8 patients who were negative for hepatitis B surface antigen were excluded. Ultimately, 61 patients with chronic hepatitis B were included. None of these patients had biliary obstruction prior to surgery or evidence of hepatitis C virus (HCV) specific antibodies or alcoholic cirrhosis. All surgery was performed through open hepatectomy by a single team of surgeons. Informed consent for the clinical study was obtained from all patients, and the present study was approved by the Institutional Review Board of Central South University. Postoperative liver dysfunction was defined as a prothrombin time of >18 sec (normal range, sec) or a peak serum bilirubin level of >51.3 µmol/l (normal range, µmol/l) (12,13) for 7 days after surgery. Liver volumetry and calculation of the FLR. Prior to surgery, all patients underwent a contrast enhanced CT angiography scan with a slice thickness of 0.8 mm. Automated volumetry was performed for three dimensional reconstruction of the liver using medical image analysis software (Myrian ; Intrasense S.A.S., Montpellier, France) and the results were modified by manual contour tracing of the hepatic contour following automated reconstruction. The gall bladder, hepatic inferior vena cava and main branches of the intrahepatic vascular structures were excluded from the reconstructional volume calculation, but the biliary structures were included. Preoperative virtual hepatic resection was performed according to the size and location of the tumors, which were evaluated by two experienced hepatic surgeons. The liver reconstruction and virtual hepatic resection are shown in Fig. 1. The total liver volume and FLR volume were calculated using image analysis software. The percentage of FLR was calculated as the sflr using the following equation: sflr=flr/standardized liver volume (SLV). The SLV was calculated using the following equation: SLV (cm 3 )=706.2 x body surface area (BSA; m 2 )+2.4 (14). The BSA was calculated using an equation that includes bodyweight and height: BSA (m 2 )= x height (cm) x weight (kg) for men; and BSA (m 2 )= x height (cm) x weight (kg) for women. The sflr/cps was calculated as a combinatorial measure of sflr and CPS. Statistical analysis. Continuous variables are expressed as medians (range) and were compared using the Mann Whitney U test. Discrete variables were compared using the χ 2 test or Fisher's exact test. Univariate analysis and multivariate logistic regression analysis were performed to identify risk factors associated with PLD. Correlation analyses were performed using Pearson's correlation coefficient. The cut off values for the occurrence of PLD were determined by receiver operating characteristic (ROC) curve analysis. Statistical analyses were performed using SPSS 17.0 (SPSS, Chicago, IL, USA). P<0.05 was considered to indicate a statistically significant difference. Results Clinicopathological characteristics and modalities of hepatic resection. A total of 61 patients were enrolled in the present study, comprising 52 men and 9 women, with a median age of 51 years (range, years). The surgical modalities were as follows: 18 patients underwent hemihepatectomy (right hemihepatectomy in 14 and left hemihepatectomy in 4), 17 patients underwent bisectionectomy (right anterior sectionectomy in 4, right posterior sectionectomy in 6 and left lateral sectionectomy in 7) and 26 patients underwent partial resection. None of the patients were allergic to anesthesia or experienced cardiac arrest during surgery. Postoperative pathological examinations revealed that 42 patients (68.9%) had liver cirrhosis. Postoperative liver dysfunction and complications. In total, 18 of the 61 patients (29.5%) developed PLD. Only 1 patient (1.6%) succumbed to intra abdominal bleeding 15 days after surgery. Of the 61 patients, 19 (31.1%) developed one or more complications after surgery and 11 (18.0%) developed postoperative infection, which was the most common complication. The following additional complications were observed: Pleural effusions in 5 patients (8.2%), bile leakage in 3 patients (4.9%), postoperative hemorrhage in 2 patients (3.3%) and temporary atrial fibrillation in 1 patient (1.6%). Child Pugh classification and postoperative liver dysfunction. According to the Child Pugh classification criteria, 58 patients were of Child Pugh grade A (with a CPS of 5 in 42 patients and a CPS of 6 in 16 patients) and 3 patients were of Child Pugh grade B (with a CPS of 7 in 2 patients and a CPS of 8 in 1 patient). A total of 16 of the 58 (27.6%) Child Pugh A patients developed PLD, and 2 of the 3 Child Pugh B patients developed PLD. Of the 58 Child Pugh A patients, 8 of the 42 (19.0%) patients with a CPS of 5 developed PLD and 8 of the 16 (50.0%) patients with a CPS of 6 developed PLD. This difference was significant (Fisher's exact test, P=0.026), indicating that the incidence of PLD for patients with a CPS of 6 was higher than that for patients with a CPS of 5. Prothrombin time and sflr are independent risk factors for postoperative liver dysfunction. The univariate analysis revealed no differences between the two groups in terms of age, body mass index, surgical duration, albumin, total bilirubin, alanine aminotransferase, aspartate aminotransferase, blood sugar, cholesterol, platelet count, presence of inflow occlusion, presence of blood transfusion, presence of hepatitis B e antigen, presence of HBV DNA or presence of liver cirrhosis (P>0.05; Table I). However, tumor diameter (P=0.043), blood loss (P=0.015), prothrombin time (PT) (P=0.007), CPS (P=0.007) and sflr (P<0.001) were significantly different between the two groups (Table I).
3 ONCOLOGY LETTERS 13: , Table I. Univariate analysis of risk factors of postoperative liver dysfunction. Postoperative liver dysfunction Variables Yes (n=18) No (n=43) P value Age, years 49.0 (26 65) 51.0 (21 70) BMI, kg/m 2a 22.1 ( ) 21.1 ( ) Tumor diameter, cm 8.0 ( ) 4.4 ( ) Operating time, min (90 280) (70 260) Blood loss, ml ( ) ( ) ALB, g/l 40.8 ( ) 40.8 ( ) Total bilirubin, µmol/l 14.2 ( ) 11.8 ( ) ALT, U/l 45.8 ( ) 36.7 ( ) AST, U/l 46.9 ( ) 37.0 ( ) Blood sugar, mmol/l 5.2 ( ) 5.0 ( ) Cholesterol, mmol/l 4.2 ( ) 4.2 ( ) PT, sec 13.9 ( ) 13.2 ( ) Platelet count, x10 9 /l (32 247) (48 437) Child Pugh score 6.0 (5 8) 5.0 (5 7) sflr ( ) ( ) <0.001 Inflow occlusion b Yes No 8 28 Blood transfusion Yes 4 5 No HBeAg Positive 3 4 Negative HBV DNA Positive (>500/copies) Negative (<500/copies) 5 18 Liver cirrhosis Yes No 6 13 a BMI, body mass index, BMI (kg/m 2 )=weight (kg)/height (m 2 ); b Patients received inflow occlusion during surgeries via the Pringle maneuver; c Pearson χ 2 ; d Fisher's exact test. ALB, albumin; ALT, alanine aminotransferase; AST, aspartate aminotransferase; PT, prothrombin time; sflr, standardized future liver remnant; HBeAg, hepatitis B e antigen; HBV DNA, hepatitis B virus DNA c d d c c A multivariate logistic regression analysis was performed to identify risk factors for PLD. Age, body mass index, operating time, albumin, total bilirubin, alanine aminotransferase, blood sugar, cholesterol, platelet count, inflow occlusion, positive HBeAg, liver cirrhosis, PT, blood loss, tumor diameter and sflr were entered into the multivariate logistic regression model to avoid collinearity (Table II). A prolonged PT and small sflr were identified as significant independent predictors of PLD (Table II). sflr and sflr/cps correlate with postoperative peak bilirubin levels and postoperative peak prothrombin time. Pearson's correlation analysis revealed that the postoperative peak bilirubin level had a stronger negative correlation with sflr/cps (P<0.0001, r= 0.547) than with sflr (P<0.0001, r= 0.488) (Fig. 2). The postoperative peak PT had a stronger negative correlation with sflr/cps (P<0.0001, r= 0.541) than with sflr (P<0.0001, r= 0.517) (Fig. 2). sflr and sflr/cps are predictors of postoperative liver dysfunction. ROC curve analysis revealed that the cut off value of sflr for predicting PLD was 54.5%, with 81.4% sensitivity and 77.8% specificity (Fig. 3). In total, 14 of the 22 (63.6%) patients with an sflr <54.5% developed PLD, compared with 4 of the 39 (10.3%) patients with a larger sflr. This difference was statistically significant (χ 2 =19.268, P<0.001). The cut off value of sflr/cps for predicting PLD was , with 86.0% sensitivity and 77.8% specificity (Fig. 3). Of the 20 patients with an sflr/cps of <0.0916, 14 (70.0%) developed PLD compared with 4 of 41 (9.8%)
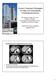
4 3634 ZOU et al: ROLE OF CPS AND FUTURE LIVER REMNANT IN HEPATIC RESECTION FOR LIVER CANCER Table II. Multivariate logistic regression analysis for risk factors of postoperative liver dysfunction. Variables Odds ratio 95% confidence interval P-value Age >60 years BMI >25 kg/m 2a Tumor diameter >5 cm Operating time >150 min Blood loss >400 ml ALB <40 g/l Total bilirubin >17.1 µmol/l ALT >40 U/l Blood sugar >6.1 mmol/l Cholesterol >4.2 mmol/l PT >13.3 sec Platelet count <100x10 9 /l sflr< Inflow occlusion Positive HBeAg Liver cirrhosis a BMI, body mass index, BMI (kg/m 2 )=weight (kg)/height (m 2 ); ALB, albumin; ALT, alanine aminotransferase; PT, prothrombin time; sflr, standardized future liver remnant; HBeAg, hepatitis B e antigen. Figure 1. Three dimensional reconstruction and virtual hepatic resection. Red, hepatic artery; pink, tumor; green, hepatic vein; blue, portal vein; light brown, hepatic parenchyma. (A) Computed tomography scan of the right hepatocellular carcinoma. (B) Volume of the reconstructional liver. (C) Virtual hepatic resection prior to surgery. (D) Remnant liver volume after virtual hepatic resection. patients with a higher sflr/cps, and this difference was statistically significant (χ 2 =23.455, P<0.001). This result indicates that sflr/cps was a more useful predictor of PLD in HBV related HCC patients following hepatic resection compared with sflr alone. sflr and CPS are linked to postoperative liver dysfunction. The distribution of PLD in patients with different CPSs and different sflrs is demonstrated in Fig. 4. According to the distribution of PLD, the majority of patients with a CPS of 5 who developed PLD had an sflr of <43%, and the majority
5 ONCOLOGY LETTERS 13: , Figure 2. Graphs showing strong negative correlations between (A) sflr and postoperative peak bilirubin levels, (B) sflr/cps and postoperative peak bilirubin levels, (C) sflr and postoperative peak PT, and (D) sflr/cps and postoperative peak PT. sflr, standardized future liver remnant; CPS, Child Pugh score; PT, prothrombin time. Figure 3. Receiver operating characteristic curve analysis of sflr and sflr/cps to predict postoperative liver dysfunction. A 54.5% cut off value for sflr was identified (area under the curve, 0.820; P<0.001; 95% confidence interval, ). A cut off value for sflr/cps was identified (area under the curve, 0.860; P<0.001; 95% confidence interval, ). sflr, standardized future liver remnant; CPS, Child Pugh score. of the patients with a CPS of 6 who developed PLD had an sflr of <54%. Discussion In the present study, the incidence of PLD among Child Pugh A patients was revealed to be significantly Figure 4. Distribution of PLD in patients with different Child Pugh scores and different sflrs. PLD, postoperative liver dysfunction; sflr, standardized future liver remnant. higher in patients with a CPS of 6 than in those patients with a CPS of 5 (P<0.05), indicating that hepatic function may not be the same for all HCC patients with Child Pugh A. For a number of years, the selection of HCC patients for hepatic resection has been based on the Child Pugh classification (15); however, flaws in this classification system have been described recently (16 18). First, a number of the variables included in the Child Pugh classification are interrelated (e.g., ascites and serum albumin levels). Second, the grading of ascites and encephalopathy is subjective. Third,
6 3636 ZOU et al: ROLE OF CPS AND FUTURE LIVER REMNANT IN HEPATIC RESECTION FOR LIVER CANCER the cut off value for each variable is selected empirically. Finally, the Child Pugh classification system does not offer a wide degree of discrimination for HCC patients undergoing hepatic resection, the majority of whom have Child Pugh A disease. Certain studies have reported the unreliability of the Child Pugh classification system for predicting postoperative outcomes (17,19 21). The data from the present study revealed that heterogeneity may exist in Child Pugh A patients. There is a requirement to identify good risk and poor risk Child Pugh A patients. Furthermore, even for multiple patients with a given CPS, different postoperative outcomes were observed in the present study, possibly since the remnant liver volume varied for these patients. More recently, with the advancement of three dimensional imaging technologies, the importance of preoperative volumetric analysis for major hepatic resection has been increasingly emphasized (5,22). Previous studies have demonstrated that a small FLR is associated with worse postoperative hepatic function (23,24). As in previous studies, the findings from the present study suggested that sflr is an independent risk factor for PLD. However, there were patients in the present study who had a small FLR but did not develop PLD, indicating that FLR may not be the only factor that affects postoperative outcomes. There is little doubt that hepatic function also plays an important role in predicting postoperative outcomes (25,26). Theoretically, with a higher CPS, a larger FLR is required to avoid PLD. Judging from the distribution of PLD (Fig. 4), data from the present study revealed that to avoid PLD in HBV related HCC patients following hepatic resection, an sflr of 43% is relatively safe when the CPS is 5, and an sflr of 54% is relatively safe when the CPS is 6. It is predicted that a higher sflr is required when the CPS is 7 or 8. These results require testing and verifying with more cases in clinical practice, in particular with more patients with a CPS of 7 or 8. In addition, by using sflr/cps as a combinatorial measure of sflr and CPS, it was revealed that sflr/cps showed a stronger negative correlation with postoperative peak bilirubin levels and postoperative peak PT than sflr, and ROC curve analysis revealed that the cut off value of sflr/cps could predict PLD more accurately than sflr. This indicates that sflr/cps is a more accurate predictor of postoperative hepatic function than sflr. The present study has a number of limitations. First, the time span of the study was short, and all the subjects were enrolled from a single study center. In addition, the study focused on HCC patients infected with HBV. It is possible that the results do not apply to HCC patients in other countries where HCV infection or alcoholic cirrhosis may be the most common cause of HCC. Therefore, these study results require validation in Western and Asia Pacific patient populations. Finally, no evaluation was performed of the correlations between the preoperative liver volumetry and the weight of the resected specimen. In conclusion, the combination of sflr and CPS was identified as aiding a more accurate assessment of hepatic functional reserve and improving prevention of the occurrence of postoperative liver dysfunction compared with either CPS or sflr alone. Acknowledgements The authors would like to thank Dr Saidan Zhang (Institute of Medical Science, Xiangya Hospital, Central South University, Changsha, China) for providing assistance with the statistical analysis. The present study was supported by the National Nature Science Foundation of China (grant nos and ). References 1. Cauchy F, Soubrane O and Belghiti J: Liver resection for HCC: Patient's selection and controversial scenarios. Best Pract Res Clin Gastroenterol 28: , Fonseca AL and Cha CH: Hepatocellular carcinoma: A comprehensive overview of surgical therapy. J Surg Oncol 110: , Pugh RN, Murray Lyon IM, Dawson JL, Pietroni MC and Williams R: Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 60: , Garcea G, Ong SL and Maddern GJ: Predicting liver failure following major hepatectomy. Dig Liver Dis 41: , Lim MC, Tan CH, Cai J, Zheng J and Kow AW: CT volumetry of the liver: Where does it stand in clinical practice? Clin Radiol 69: , Wigmore SJ, Redhead DN, Yan XJ, Casey J, Madhavan K, Dejong CH, Currie EJ and Garden OJ: Virtual hepatic resection using three dimensional reconstruction of helical computed tomography angioportograms. Ann Surg 233: , Simpson AL, Geller DA, Hemming AW, Jarnagin WR, Clements LW, D'Angelica MI, Dumpuri P, Gonen M, Zendejas I, Miga MI and Stefansic JD: Liver planning software accurately predicts postoperative liver volume and measures early regeneration. J Am Coll Surg 219: , Schindl MJ, Redhead DN, Fearon KC, Garden OJ and Wigmore SJ: The value of residual liver volume as a predictor of hepatic dysfunction and infection after major liver resection. Gut 54: , Clavien PA, Petrowsky H, DeOliveira ML and Graf R: Strategies for safer liver surgery and partial liver transplantation. N Engl J Med 356: , Ribero D, Amisamo M, Bertuzzo F, Langella S, Lo Tesoriere R, Ferrero A, Regge D and Capussotti L: Measured versus estimated total liver volume to preoperatively assess the adequacy of the future liver remnant: Which method should we use? Ann Surg 258: , Wagener G: Assessment of hepatic function, operative candidacy, and medical management after liver resection in the patient with underlying liver disease. Semin Liver Dis 33: , 2013 (In Danish, English). 12. Ribero D, Abdalla EK, Madoff DC, Donadon M, Loyer EM and Vauthey JN: Portal vein embolization before major hepatectomy and its effects on regeneration, resectability and outcome. Br J Surg 94: , Facciuto M, Contreras Saldivar A, Singh MK, Rocca JP, Taouli B, Oyfe I, LaPointe Rudow D, Gondolesi GE, Schiano TD, Kim Schluger L, et al: Right hepatectomy for living donation: Role of remnant liver volume in predicting hepatic dysfunction and complications. Surgery 153: , Urata K, Kawasaki S, Matsunami H, Hashikura Y, Ikegami T, Ishizone S, Momose Y, Komiyama A and Makuuchi M: Calculation of child and adult standard liver volume for liver transplantation. Hepatology 21: , Pugh RN, Murray Lyon IM, Dawson JL, Pietroni MC and Williams R: Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 60: , Durand F and Valla D: Assessment of prognosis of cirrhosis. Semin Liver Dis 28: , Johnson PJ, Berhane S, Kagebayashi C, Satomura S, Teng M, Reeves HL, O'Beirne J, Fox R, Skowronska A, Palmer D, et al: Assessment of liver function in patients with hepatocellular carcinoma: A new evidence based approach the ALBI grade. J Clin Oncol 33: , Kaplan DE, Dai F, Aytaman A, Baytarian M, Fox R, Hunt K, Knott A, Pedrosa M, Pocha C, Mehta R, et al: Development and performance of an algorithm to estimate the Child Turcotte Pugh Score from a national electronic healthcare database. Clin Gastroenterol Hepatol 13: e1 e6, 2015.
7 ONCOLOGY LETTERS 13: , Schneider PD: Preoperative assessment of liver function. Surg Clin North Am 84: , Hoekstra LT, de Graaf W, Nibourg GA, Heger M, Bennink RJ, Stieger B and van Gulik TM: Physiological and biochemical basis of clinical liver function tests: A review. Ann Surg 257: 27 36, Forner A, Llovet JM and Bruix J: Hepatocellular carcinoma. Lancet 379: , Cieslak KP, Runge JH, Heger M, Stoker J, Bennink RJ and van Gulik TM: New perspectives in the assessment of future remnant liver. Dig Surg 31: , Hirashita T, Ohta M, Iwashita Y, Iwaki K, Uchida H, Yada K, Matsumoto T and Kitano S: Risk factors of liver failure after right sided hepatectomy. Am J Surg 206: , Truant S, Boleslawski E, Sergent G, Leteurtre E, Duhamel A, Hebbar M and Pruvot FR: Liver function following extended hepatectomy can be accurately predicted using remnant liver volume to body weight ratio. World J Surg 39: , Stockmann M, Lock JF, Riecke B, Heyne K, Martus P, Fricke M, Lehmann S, Niehues SM, Schwabe M, Lemke AJ and Neuhaus P: Prediction of postoperative outcome after hepatectomy with a new beside test for maximal liver function capacity. Ann Surg 250: , Okabe H, Beppu T, Chikamoto A, Hayashi H, Yoshida M, Masuda T, Imai K, Mima K, Nakagawa S, Kuroki H, et al: Remnant liver volume based predictors of postoperative liver dysfunction after hepatectomy: Analysis of 625 consecutive patients from a single institution. Int J Clin Oncol 19: , 2014.
Combining albumin- bilirubin score with future liver remnant predicts post- hepatectomy liver failure in HBV- associated HCC patients
 Received: 7 April 2017 Accepted: 3 July 2017 DOI: 10.1111/liv.13514 ORIGINAL ARTICLE Combining albumin- bilirubin score with future liver remnant predicts post- hepatectomy liver failure in HBV- associated
Received: 7 April 2017 Accepted: 3 July 2017 DOI: 10.1111/liv.13514 ORIGINAL ARTICLE Combining albumin- bilirubin score with future liver remnant predicts post- hepatectomy liver failure in HBV- associated
ORIGINAL ARTICLE. Jun Zheng 1, Rong-chun Xing 1, Wei-hong Zheng 2, Wei Liu 1, Ru-cheng Yao 1, Xiao-song Li 1, Jian-ping Du 1, Lin Li 1.
 JBUON 2017; 22(3): 709-713 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE A comparative study on postoperative mortality prediction of SFLI scoring
JBUON 2017; 22(3): 709-713 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE A comparative study on postoperative mortality prediction of SFLI scoring
Prognostic nutritional index predicts short-term outcomes after liver resection for hepatocellular carcinoma within the Milan criteria
 /, 2016, Vol. 7, (No. 49), pp: 81611-81620 Prognostic nutritional index predicts short-term outcomes after liver resection for hepatocellular carcinoma within the Milan criteria Mengyun Ke 1,*, Tao Xu
/, 2016, Vol. 7, (No. 49), pp: 81611-81620 Prognostic nutritional index predicts short-term outcomes after liver resection for hepatocellular carcinoma within the Milan criteria Mengyun Ke 1,*, Tao Xu
Use of hepatic blood inflow occlusion and hemihepatic artery retention in liver resection for hepatocellular carcinoma
 Original Article Use of hepatic blood inflow occlusion and hemihepatic artery retention in liver resection for hepatocellular carcinoma Changjun Jia, Chaoliu Dai, Xingyu Zhao, Xianmin Bu, Feng Xu, Songlin
Original Article Use of hepatic blood inflow occlusion and hemihepatic artery retention in liver resection for hepatocellular carcinoma Changjun Jia, Chaoliu Dai, Xingyu Zhao, Xianmin Bu, Feng Xu, Songlin
University Medical Center, Kyungpook National University School of Medicine, Daegu, Korea
 Ann Hepatobiliary Pancreat Surg 2016;20:159-166 https://doi.org/10.14701/ahbps.2016.20.4.159 Original Article Impact of clinically significant portal hypertension on surgical outcomes for hepatocellular
Ann Hepatobiliary Pancreat Surg 2016;20:159-166 https://doi.org/10.14701/ahbps.2016.20.4.159 Original Article Impact of clinically significant portal hypertension on surgical outcomes for hepatocellular
Surgical resection for hepatocellular carcinoma (HCC)
 Surgical resection for hepatocellular carcinoma (HCC) Wojciech G Polak, MD, PhD, FEBS Department of Surgery, Division of HPB and Transplant Surgery, Erasmus MC, University Medical Center Rotterdam the
Surgical resection for hepatocellular carcinoma (HCC) Wojciech G Polak, MD, PhD, FEBS Department of Surgery, Division of HPB and Transplant Surgery, Erasmus MC, University Medical Center Rotterdam the
Clinical Study Clinical Characteristics and Surgical Prognosis of Hepatocellular Carcinoma with Bile Duct Invasion
 Gastroenterology Research and Practice, Article ID 604971, 7 pages http://dx.doi.org/10.1155/2014/604971 Clinical Study Clinical Characteristics and Surgical Prognosis of Hepatocellular Carcinoma with
Gastroenterology Research and Practice, Article ID 604971, 7 pages http://dx.doi.org/10.1155/2014/604971 Clinical Study Clinical Characteristics and Surgical Prognosis of Hepatocellular Carcinoma with
Albumin-to-bilirubin score for assessing the in-hospital death in cirrhosis
 Original Article Albumin-to-bilirubin score for assessing the in-hospital death in cirrhosis Lichun Shao 1 *, Bing Han 1 *, Shu An 2, Jiaxin Ma 1, Xiaozhong Guo 3, Fernando Gomes Romeiro 4, Andrea Mancuso
Original Article Albumin-to-bilirubin score for assessing the in-hospital death in cirrhosis Lichun Shao 1 *, Bing Han 1 *, Shu An 2, Jiaxin Ma 1, Xiaozhong Guo 3, Fernando Gomes Romeiro 4, Andrea Mancuso
Management of HepatoCellular Carcinoma
 9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
9th Symposium GIC St Louis - 2010 Management of HepatoCellular Carcinoma Overview Pierre A. Clavien, MD, PhD Department of Surgery University Hospital Zurich Zurich, Switzerland Hepatocellular carcinoma
Virtual Liver Resection and Volumetric Analysis of the Future Liver Remnant using Open Source Image Processing Software
 World J Surg (2010) 34:2426 2433 DOI 10.1007/s00268-010-0663-5 Virtual Liver Resection and Volumetric Analysis of the Future Liver Remnant using Open Source Image Processing Software Joost R. van der Vorst
World J Surg (2010) 34:2426 2433 DOI 10.1007/s00268-010-0663-5 Virtual Liver Resection and Volumetric Analysis of the Future Liver Remnant using Open Source Image Processing Software Joost R. van der Vorst
UvA-DARE (Digital Academic Repository) Towards safer liver resections Hoekstra, L.T. Link to publication
 UvA-DARE (Digital Academic Repository) Towards safer liver resections Hoekstra, L.T. Link to publication Citation for published version (APA): Hoekstra, L. T. (2012). Towards safer liver resections General
UvA-DARE (Digital Academic Repository) Towards safer liver resections Hoekstra, L.T. Link to publication Citation for published version (APA): Hoekstra, L. T. (2012). Towards safer liver resections General
Update in abdominal Surgery in cirrhotic patients
 Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
Update in abdominal Surgery in cirrhotic patients Safi Dokmak HBP department and liver transplantation Beaujon Hospital, Clichy, France Cairo, 5 April 2016 Cirrhosis Prevalence in France (1%)* Patients
CIRROSI E IPERTENSIONE PORTALE NELLA DONNA
 Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Treatment of HCC in real life-chinese perspective
 Treatment of HCC in real life-chinese perspective George Lau MBBS (HK), MRCP(UK), FHKCP, FHKAM (GI), MD(HK), FRCP (Edin, Lond), FAASLD (US) Chairman Humanity and Health Medical Group, Hong Kong SAR, CHINA
Treatment of HCC in real life-chinese perspective George Lau MBBS (HK), MRCP(UK), FHKCP, FHKAM (GI), MD(HK), FRCP (Edin, Lond), FAASLD (US) Chairman Humanity and Health Medical Group, Hong Kong SAR, CHINA
LiverGroup.org. Case Report Form (CRF) for STAGED procedures
 Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Ability of the ALBI grade to predict posthepatectomy liver failure and longterm survival after liver resection for different BCLC stages of HCC
 Zhang et al. World Journal of Surgical Oncology (2018) 16:208 https://doi.org/10.1186/s12957-018-1500-9 RESEARCH Open Access Ability of the ALBI grade to predict posthepatectomy liver failure and longterm
Zhang et al. World Journal of Surgical Oncology (2018) 16:208 https://doi.org/10.1186/s12957-018-1500-9 RESEARCH Open Access Ability of the ALBI grade to predict posthepatectomy liver failure and longterm
Impact of Three-Dimensional Reconstruction Technique in the Operation Planning of Centrally Located Hepatocellular Carcinoma
 Impact of Three-Dimensional Reconstruction Technique in the Operation Planning of Centrally Located Hepatocellular Carcinoma Chi-hua Fang, MD, Hai-su Tao, MM, Jian Yang, MD, Zhao-shan Fang, MM, Wei Cai,
Impact of Three-Dimensional Reconstruction Technique in the Operation Planning of Centrally Located Hepatocellular Carcinoma Chi-hua Fang, MD, Hai-su Tao, MM, Jian Yang, MD, Zhao-shan Fang, MM, Wei Cai,
RESEARCH ARTICLE. Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment
 DOI:10.22034/APJCP.2017.18.6.1697 RESEARCH ARTICLE Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment Alan Chuncharunee 1,
DOI:10.22034/APJCP.2017.18.6.1697 RESEARCH ARTICLE Validation of The Hong Kong Liver Cancer Staging System in Patients with Hepatocellular Carcinoma after Curative Intent Treatment Alan Chuncharunee 1,
Module 1 Introduction of hepatitis
 Module 1 Introduction of hepatitis 1 Training Objectives At the end of the module, trainees will be able to ; Demonstrate improved knowledge of the global epidemiology of the viral hepatitis Understand
Module 1 Introduction of hepatitis 1 Training Objectives At the end of the module, trainees will be able to ; Demonstrate improved knowledge of the global epidemiology of the viral hepatitis Understand
Negative impact of low body mass index on liver cirrhosis patients with hepatocellular carcinoma
 Li et al. World Journal of Surgical Oncology (2015) 13:294 DOI 10.1186/s12957-015-0713-4 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Negative impact of low body mass index on liver cirrhosis
Li et al. World Journal of Surgical Oncology (2015) 13:294 DOI 10.1186/s12957-015-0713-4 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Negative impact of low body mass index on liver cirrhosis
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance
 Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Preoperative Albumin-Bilirubin Score for Postoperative Solitary Hepatocellular Carcinoma within the Milan Criteria and Child-Pugh A Cirrhosis
 3862 Ivyspring International Publisher Research Paper Journal of Cancer 2017; 8(18): 3862-3867. doi: 10.7150/jca.21313 Preoperative Albumin-Bilirubin Score for Postoperative Solitary Hepatocellular Carcinoma
3862 Ivyspring International Publisher Research Paper Journal of Cancer 2017; 8(18): 3862-3867. doi: 10.7150/jca.21313 Preoperative Albumin-Bilirubin Score for Postoperative Solitary Hepatocellular Carcinoma
Role of Hepatitis B Virus Genotypes in Chronic Hepatitis B Exacerbation
 BRIEF REPORT Role of Hepatitis B Virus Genotypes in Chronic Hepatitis B Exacerbation Man-Fung Yuen, 1 Erwin Sablon, 2 Danny Ka-Ho Wong, 1 He-Jun Yuan, 1 Benjamin Chun-Yu Wong, 1 Annie On-On Chan, 1 and
BRIEF REPORT Role of Hepatitis B Virus Genotypes in Chronic Hepatitis B Exacerbation Man-Fung Yuen, 1 Erwin Sablon, 2 Danny Ka-Ho Wong, 1 He-Jun Yuan, 1 Benjamin Chun-Yu Wong, 1 Annie On-On Chan, 1 and
Upper abdominal shape as a risk factor of extended operation time and severe postoperative complications in HCC hepatectomy through subcostal incision
 Hou et al. World Journal of Surgical Oncology (2015) 13:298 DOI 10.1186/s12957-015-0702-7 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Upper abdominal shape as a risk factor of extended operation
Hou et al. World Journal of Surgical Oncology (2015) 13:298 DOI 10.1186/s12957-015-0702-7 WORLD JOURNAL OF SURGICAL ONCOLOGY RESEARCH Open Access Upper abdominal shape as a risk factor of extended operation
A novel scoring system to predict ascites development post hepatectomy for BCLC stage B hepatocellular carcinoma
 Original Article A novel scoring system to predict ascites development post hepatectomy for BCLC stage B hepatocellular carcinoma Hong-Gang Qian 1, Li-Ying Wu 2, Cheng-Peng Li 1, Ang Lv 1, Jian-Hui Wu
Original Article A novel scoring system to predict ascites development post hepatectomy for BCLC stage B hepatocellular carcinoma Hong-Gang Qian 1, Li-Ying Wu 2, Cheng-Peng Li 1, Ang Lv 1, Jian-Hui Wu
DISCLOSURES. This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea
 DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
DISCLOSURES This activity is jointly provided by Northwest Portland Area Indian Health Board and Cardea Cardea Services is approved as a provider of continuing nursing education by Montana Nurses Association,
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting?
 Rajani Sharma, PGY1 Geriatrics CRC Project, 12/19/13 Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting? A. Study Purpose and Rationale Hepatocellular carcinoma
Rajani Sharma, PGY1 Geriatrics CRC Project, 12/19/13 Are we adequately screening at-risk patients for hepatocellular carcinoma in the outpatient setting? A. Study Purpose and Rationale Hepatocellular carcinoma
King Abdul-Aziz University Hospital (KAUH) is a tertiary
 Modelling Factors Causing Mortality in Oesophageal Varices Patients in King Abdul Aziz University Hospital Sami Bahlas Abstract Objectives: The objective of this study is to reach a model defining factors
Modelling Factors Causing Mortality in Oesophageal Varices Patients in King Abdul Aziz University Hospital Sami Bahlas Abstract Objectives: The objective of this study is to reach a model defining factors
Posthepatectomy Liver Failure. C. Jeske
 Posthepatectomy Liver Failure C. Jeske Introduction Major source of morbidity and mortality after liver resection Devastating complication Little treatment Incidence: 4-19% Recently < 10% Mortality following
Posthepatectomy Liver Failure C. Jeske Introduction Major source of morbidity and mortality after liver resection Devastating complication Little treatment Incidence: 4-19% Recently < 10% Mortality following
MULTI-DISCIPLINARY MANAGEMENT OF INTERMEDIATE STAGE HCC
 Dr Apoorva Gogna MBBS FRCR FAMS Consultant Interventional Radiology Center Department of Diagnostic Radiology SingaporeGeneral Hospital MULTI-DISCIPLINARY MANAGEMENT OF INTERMEDIATE STAGE HCC CASE HISTORY
Dr Apoorva Gogna MBBS FRCR FAMS Consultant Interventional Radiology Center Department of Diagnostic Radiology SingaporeGeneral Hospital MULTI-DISCIPLINARY MANAGEMENT OF INTERMEDIATE STAGE HCC CASE HISTORY
Prognosis of untreated Primary Sclerosing Cholangitis (PSC) Erik Christensen Copenhagen, Denmark
 Prognosis of untreated Primary Sclerosing Cholangitis (PSC) Erik Christensen Copenhagen, Denmark Study of Prognosis of PSC Difficulties: Disease is rare The duration of the course of disease may be very
Prognosis of untreated Primary Sclerosing Cholangitis (PSC) Erik Christensen Copenhagen, Denmark Study of Prognosis of PSC Difficulties: Disease is rare The duration of the course of disease may be very
Laparoscopic Liver Resection for Hepatocellular Carcinoma
 Original Article Laparoscopic Liver Resection for Hepatocellular Carcinoma Carmen D. Chung, Lydia L. Lau, Kwan Lung Ko, Andrew C. Wong, Shezam Wong, Albert C. Chan, Ronnie T. Poon, Chung Mau Lo and Sheung
Original Article Laparoscopic Liver Resection for Hepatocellular Carcinoma Carmen D. Chung, Lydia L. Lau, Kwan Lung Ko, Andrew C. Wong, Shezam Wong, Albert C. Chan, Ronnie T. Poon, Chung Mau Lo and Sheung
Liver resection for HCC
 8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
8 th LIVER INTEREST GROUP Annual Meeting Cape Town 2017 Liver resection for HCC Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre The liver is almost unique in that treatment of the
Liver related complications in unresectable disease after portal vein embolization
 Original Article Liver related complications in unresectable disease after portal vein embolization Floor Huisman 1, Kasia P. Cieslak 1, Krijn P. van Lienden 2, Roelof J. Bennink 3, Thomas M. van Gulik
Original Article Liver related complications in unresectable disease after portal vein embolization Floor Huisman 1, Kasia P. Cieslak 1, Krijn P. van Lienden 2, Roelof J. Bennink 3, Thomas M. van Gulik
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary)
 Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
Hepatocellular Carcinoma HCC Updated November 2015 by: Dr. Mohammed Alghamdi (Medical Oncology Fellow, University of Calgary) Staff Reviewers: Dr. Yoo Joung Ko (Medical Oncologist, Sunnybrook Odette Cancer
IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS?
 IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS? Dr. Sammy Saab David Geffen School of Medicine, Los Angeles, USA April 2018 DISCLAIMER Please note: The views
IS THERE A DIFFERENCE IN LIVER CANCER RATES IN PATIENTS WHO RECEIVE TREATMENT FOR HEPATITIS? Dr. Sammy Saab David Geffen School of Medicine, Los Angeles, USA April 2018 DISCLAIMER Please note: The views
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Treatment of Colorectal Liver Metastases State of the Art
 Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Surveillance for Hepatocellular Carcinoma
 Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
Surveillance for Hepatocellular Carcinoma Marion G. Peters, MD John V. Carbone, MD, Endowed Chair Professor of Medicine Chief of Hepatology Research University of California San Francisco Recorded on April
(Received for Publication: March 24, 2015) Key words portal venous pressure, major hepatectomy, liver
 55 Original Article J. St. Marianna Univ. Vol. 6, pp. 55 61, 2015 Usefulness of Intraoperative Measurement of Portal Venous Pressure for Confirming the Most Appropriate Hepatectomy in Patients with Borderline
55 Original Article J. St. Marianna Univ. Vol. 6, pp. 55 61, 2015 Usefulness of Intraoperative Measurement of Portal Venous Pressure for Confirming the Most Appropriate Hepatectomy in Patients with Borderline
Functional assessment of the rapidly growing liver
 Functional assessment of the rapidly growing liver Erik Schadde Assistant Professor of Surgery Dept. of Surgery Liver Transplanation and Liver Surgery Rush University Medical Center Chicago Illinois Cantonal
Functional assessment of the rapidly growing liver Erik Schadde Assistant Professor of Surgery Dept. of Surgery Liver Transplanation and Liver Surgery Rush University Medical Center Chicago Illinois Cantonal
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis?
 Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Trans-arterial radioembolisation (TARE) of unresectable HCC using Y-90 microspheres: is it dangerous in case of portal vein thrombosis? Poster No.: C-1634 Congress: ECR 2014 Type: Authors: Keywords: DOI:
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma
 Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
Current Treatment Strategies for Hilar and Intrahepatic Cholangiocarcinoma Jean-Nicolas Vauthey, MD, FACS Professor of Surgery Chief Hepato-Pancreato-Biliary Section Department of Surgical Oncology Crescent
An investigation of pancreatic volume by disease using pancreatic volumetry
 Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Xiao-Ling Chi, Mei-Jie Shi, Huan-Ming Xiao, Yu-Bao Xie, and Gao-Shu Cai. Correspondence should be addressed to Xiao-Ling Chi;
 Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 3743427, 6 pages http://dx.doi.org/10.1155/2016/3743427 Research Article The Score Model Containing Chinese Medicine Syndrome
Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 3743427, 6 pages http://dx.doi.org/10.1155/2016/3743427 Research Article The Score Model Containing Chinese Medicine Syndrome
Cisplatin plus Gemcitabine versus Gemcitabine for Biliary Tract Cancer. Valle J et al. N Engl J Med 2010;362(14):
 Cisplatin plus Gemcitabine versus Gemcitabine for Biliary Tract Cancer Valle J et al. N Engl J Med 2010;362(14):1273-81. Introduction > Biliary tract cancers (BTC: cholangiocarcinoma, gall bladder cancer,
Cisplatin plus Gemcitabine versus Gemcitabine for Biliary Tract Cancer Valle J et al. N Engl J Med 2010;362(14):1273-81. Introduction > Biliary tract cancers (BTC: cholangiocarcinoma, gall bladder cancer,
Advances in percutaneous ablation for hepatocellular carcinoma
 Advances in percutaneous ablation for hepatocellular carcinoma P. Nahon1,2,3 1 Hepatology, Jean Verdier Hospital, APHP, Bondy, France 2 Paris 13 university, Sorbonne Paris Cité, UFRSMBH, Bobigny, France
Advances in percutaneous ablation for hepatocellular carcinoma P. Nahon1,2,3 1 Hepatology, Jean Verdier Hospital, APHP, Bondy, France 2 Paris 13 university, Sorbonne Paris Cité, UFRSMBH, Bobigny, France
Patterns of abnormal LFTs and their differential diagnosis
 Patterns of abnormal LFTs and their differential diagnosis Professor Matthew Cramp South West Liver Unit and Peninsula Schools of Medicine and Dentistry, Plymouth Outline liver function / liver function
Patterns of abnormal LFTs and their differential diagnosis Professor Matthew Cramp South West Liver Unit and Peninsula Schools of Medicine and Dentistry, Plymouth Outline liver function / liver function
Comparison of percutaneous cryosurgery and surgical resection for the treatment of small hepatocellular carcinoma
 ONCOLOGY LETTERS 6: 239-245, 2013 Comparison of percutaneous cryosurgery and surgical resection for the treatment of small hepatocellular carcinoma ZHIWEI LI 1, CHUNHUI ZHANG 1, CHANGJIE LOU 1, FEIHU YAN
ONCOLOGY LETTERS 6: 239-245, 2013 Comparison of percutaneous cryosurgery and surgical resection for the treatment of small hepatocellular carcinoma ZHIWEI LI 1, CHUNHUI ZHANG 1, CHANGJIE LOU 1, FEIHU YAN
An assessment of different scoring systems in cirrhotic patients undergoing nontransplant surgery
 The American Journal of Surgery (2012) 203, 589 593 North Pacific Surgical Association An assessment of different scoring systems in cirrhotic patients undergoing nontransplant surgery Marlin Wayne Causey,
The American Journal of Surgery (2012) 203, 589 593 North Pacific Surgical Association An assessment of different scoring systems in cirrhotic patients undergoing nontransplant surgery Marlin Wayne Causey,
UvA-DARE (Digital Academic Repository) Enhancement of liver regeneration and liver surgery Olthof, P.B. Link to publication
 UvA-DARE (Digital Academic Repository) Enhancement of liver regeneration and liver surgery Olthof, P.B. Link to publication Citation for published version (APA): Olthof, P. B. (2017). Enhancement of liver
UvA-DARE (Digital Academic Repository) Enhancement of liver regeneration and liver surgery Olthof, P.B. Link to publication Citation for published version (APA): Olthof, P. B. (2017). Enhancement of liver
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
MANAGEMENT OF COLORECTAL METASTASES. Robert Warren, MD. The Postgraduate Course in General Surgery March 22, /22/2011
 MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association
 CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
CIRRHOSIS AND PORTAL HYPERTENSION Cirrhosis and Portal Hypertension Gastroenterology Teaching Project American Gastroenterological Association WHAT IS CIRRHOSIS? What is Cirrhosis? DEFINITION OF CIRRHOSIS
Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D.
 Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D. Department of Surgery Grand Rounds University of Kentucky January 15, 2014 Metastatic Colorectal Cancer (CRC)
Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D. Department of Surgery Grand Rounds University of Kentucky January 15, 2014 Metastatic Colorectal Cancer (CRC)
Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy
 LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
Hepatocellular Carcinoma. Markus Heim Basel
 Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Hepatocellular Carcinoma Markus Heim Basel Outline 1. Epidemiology 2. Surveillance 3. (Diagnosis) 4. Staging 5. Treatment Epidemiology of HCC Worldwide, liver cancer is the sixth most common cancer (749
Surgical management of HCC. Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London
 Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Surgical management of HCC Evangelos Prassas Hepatobiliary and Pancreatic Surgery / Liver Transplantation Kings College Hospital / London Global distribution of HCC and staging systems WEST 1. Italy (Milan,
Does Viral Cure Prevent HCC Development
 Does Viral Cure Prevent HCC Development Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute of Digestive Disease Director, Center for Liver Health Assistant Dean,
Does Viral Cure Prevent HCC Development Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute of Digestive Disease Director, Center for Liver Health Assistant Dean,
Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis
 Original Article Page 1 of 9 Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis Rui Sun*, Xingshun Qi* #, Deli Zou, Xiaodong Shao, Hongyu Li, Xiaozhong
Original Article Page 1 of 9 Risk factors for 5-day bleeding after endoscopic treatments for gastroesophageal varices in liver cirrhosis Rui Sun*, Xingshun Qi* #, Deli Zou, Xiaodong Shao, Hongyu Li, Xiaozhong
Risk factors of postoperative ascites on hepatic resection for hepatocellular carcinoma
 Ann Hepatobiliary Pancreat Surg 2016;20:153-158 https://doi.org/10.14701/ahbps.2016.20.4.153 Original Article Risk factors of postoperative ascites on hepatic resection for hepatocellular carcinoma Seong
Ann Hepatobiliary Pancreat Surg 2016;20:153-158 https://doi.org/10.14701/ahbps.2016.20.4.153 Original Article Risk factors of postoperative ascites on hepatic resection for hepatocellular carcinoma Seong
Effect of hepatitis B virus DNA replication level and anti-hbv therapy on microvascular invasion of hepatocellular carcinoma
 Qu et al. Infectious Agents and Cancer (2019) 14:2 https://doi.org/10.1186/s13027-019-0219-8 RESEARCH ARTICLE Open Access Effect of hepatitis B virus DNA replication level and anti-hbv therapy on microvascular
Qu et al. Infectious Agents and Cancer (2019) 14:2 https://doi.org/10.1186/s13027-019-0219-8 RESEARCH ARTICLE Open Access Effect of hepatitis B virus DNA replication level and anti-hbv therapy on microvascular
Title:Identification of a novel microrna signature associated with intrahepatic cholangiocarcinoma (ICC) patient prognosis
 Author's response to reviews Title:Identification of a novel microrna signature associated with intrahepatic cholangiocarcinoma (ICC) patient prognosis Authors: Mei-Yin Zhang (zhangmy@sysucc.org.cn) Shu-Hong
Author's response to reviews Title:Identification of a novel microrna signature associated with intrahepatic cholangiocarcinoma (ICC) patient prognosis Authors: Mei-Yin Zhang (zhangmy@sysucc.org.cn) Shu-Hong
Arterial blood supply of hepatocellular carcinoma is associated with efficacy of sorafenib therapy
 Original Article Page 1 of 5 Arterial blood supply of hepatocellular carcinoma is associated with efficacy of sorafenib therapy Qian Zhu 1 *, Xianghua Zhang 2 *, Jing Li 2, Liang Huang 2, Jianjun Yan 2,
Original Article Page 1 of 5 Arterial blood supply of hepatocellular carcinoma is associated with efficacy of sorafenib therapy Qian Zhu 1 *, Xianghua Zhang 2 *, Jing Li 2, Liang Huang 2, Jianjun Yan 2,
Patterns of abnormal LFTs and their differential diagnosis
 Patterns of abnormal LFTs and their differential diagnosis Professor Matthew Cramp South West Liver Unit and Peninsula Schools of Medicine and Dentistry, Plymouth Outline liver function tests / tests of
Patterns of abnormal LFTs and their differential diagnosis Professor Matthew Cramp South West Liver Unit and Peninsula Schools of Medicine and Dentistry, Plymouth Outline liver function tests / tests of
Workup of a Solid Liver Lesion
 Workup of a Solid Liver Lesion Joseph B. Cofer MD FACS Chief Quality Officer Erlanger Health System Affiliate Professor of Surgery UTHSC-Chattanooga I have no financial or other relationships with any
Workup of a Solid Liver Lesion Joseph B. Cofer MD FACS Chief Quality Officer Erlanger Health System Affiliate Professor of Surgery UTHSC-Chattanooga I have no financial or other relationships with any
of bile leakage after liver resecti
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
Predictors of Mortality in Long-Term Follow-Up of Patients with Terminal Alcoholic Cirrhosis: Is It Time to Accept Remodeled Scores?
 Original Paper Received: March 8, 2015 Accepted: September 27, 2016 Published online: September 27, 2016 Predictors of Mortality in Long-Term Follow-Up of Patients with Terminal Alcoholic Cirrhosis: Is
Original Paper Received: March 8, 2015 Accepted: September 27, 2016 Published online: September 27, 2016 Predictors of Mortality in Long-Term Follow-Up of Patients with Terminal Alcoholic Cirrhosis: Is
Hepatocellular Carcinoma: Diagnosis and Management
 Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular Carcinoma: Diagnosis and Management Nizar A. Mukhtar, MD Co-director, SMC Liver Tumor Board April 30, 2016 1 Objectives Review screening/surveillance guidelines Discuss diagnostic algorithm
Hepatocellular carcinoma (HCC) is the most
 Original Article / Biliary Hepatobiliary & Pancreatic Diseases International Prognosis of hepatocellular carcinoma with bile duct tumor thrombus after R0 resection: a matched study Ding-Ding Wang, Li-Qun
Original Article / Biliary Hepatobiliary & Pancreatic Diseases International Prognosis of hepatocellular carcinoma with bile duct tumor thrombus after R0 resection: a matched study Ding-Ding Wang, Li-Qun
Evaluation of Serum Total Bile Acids in the Diagnosis of Hepatocellular Carcinoma
 Journal of the Egyptian Nat. Cancer Inst., Vol. 12, No. 4, December: 7-313, 2000 Evaluation of Serum Total Bile Acids in the Diagnosis of Hepatocellular Carcinoma MOTAWA E. EL-HOUSEINI, Ph.D.**; MAHMOUD
Journal of the Egyptian Nat. Cancer Inst., Vol. 12, No. 4, December: 7-313, 2000 Evaluation of Serum Total Bile Acids in the Diagnosis of Hepatocellular Carcinoma MOTAWA E. EL-HOUSEINI, Ph.D.**; MAHMOUD
Is surgical Apgar score an effective assessment tool for the prediction of postoperative complications in patients undergoing oesophagectomy?
 Interactive CardioVascular and Thoracic Surgery 27 (2018) 686 691 doi:10.1093/icvts/ivy148 Advance Access publication 9 May 2018 BEST EVIDENCE TOPIC Cite this article as: Li S, Zhou K, Li P, Che G. Is
Interactive CardioVascular and Thoracic Surgery 27 (2018) 686 691 doi:10.1093/icvts/ivy148 Advance Access publication 9 May 2018 BEST EVIDENCE TOPIC Cite this article as: Li S, Zhou K, Li P, Che G. Is
Ammonia level at admission predicts in-hospital mortality for patients with alcoholic hepatitis
 Gastroenterology Report, 5(3), 2017, 232 236 doi: 10.1093/gastro/gow010 Advance Access Publication Date: 1 May 2016 Original article ORIGINAL ARTICLE Ammonia level at admission predicts in-hospital mortality
Gastroenterology Report, 5(3), 2017, 232 236 doi: 10.1093/gastro/gow010 Advance Access Publication Date: 1 May 2016 Original article ORIGINAL ARTICLE Ammonia level at admission predicts in-hospital mortality
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
Analysis of short and long term therapeutic effects of radiofrequency hyperthermia combined with conformal radiotherapy in hepatocellular carcinoma
 JBUON 2016; 21(2): 407-411 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Analysis of short and long term therapeutic effects of radiofrequency
JBUON 2016; 21(2): 407-411 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Analysis of short and long term therapeutic effects of radiofrequency
Original Article Selective portal vein ligation promotes liver regeneration in rats with incomplete obstructive jaundice
 Int J Clin Exp Pathol 2017;10(2):1675-1682 www.ijcep.com /ISSN:1936-2625/IJCEP0040866 Original Article Selective portal vein ligation promotes liver regeneration in rats with incomplete obstructive jaundice
Int J Clin Exp Pathol 2017;10(2):1675-1682 www.ijcep.com /ISSN:1936-2625/IJCEP0040866 Original Article Selective portal vein ligation promotes liver regeneration in rats with incomplete obstructive jaundice
Healthy Liver Cirrhosis
 Gioacchino Angarano Clinica delle Malattie Infettive Università degli Studi di Foggia Healthy Liver Cirrhosis Storia naturale dell epatite HCVcorrelata in assenza di terapia Paestum 13-15 Maggio 24 The
Gioacchino Angarano Clinica delle Malattie Infettive Università degli Studi di Foggia Healthy Liver Cirrhosis Storia naturale dell epatite HCVcorrelata in assenza di terapia Paestum 13-15 Maggio 24 The
Hepatocellular carcinoma in Sri Lanka - where do we stand?
 SCIENTIFIC ARTICLE Hepatocellular carcinoma in Sri Lanka - where do we stand? R.C. Siriwardana 1, C.A.H. Liyanage 1, M.B. Gunethileke 2 1. Specialist Gastrointestinal and Hepatobilliary Surgeon, Senior
SCIENTIFIC ARTICLE Hepatocellular carcinoma in Sri Lanka - where do we stand? R.C. Siriwardana 1, C.A.H. Liyanage 1, M.B. Gunethileke 2 1. Specialist Gastrointestinal and Hepatobilliary Surgeon, Senior
Actual 10-year survival following hepatectomy for hepatocellular carcinoma
 DOI:10.1111/hpb.12206 HPB ORIGINAL ARTICLE Actual 10-year survival following hepatectomy for hepatocellular carcinoma Bernardo Franssen, Ghalib Jibara, Parissa Tabrizian, Myron E. Schwartz & Sasan Roayaie
DOI:10.1111/hpb.12206 HPB ORIGINAL ARTICLE Actual 10-year survival following hepatectomy for hepatocellular carcinoma Bernardo Franssen, Ghalib Jibara, Parissa Tabrizian, Myron E. Schwartz & Sasan Roayaie
Primary sclerosing cholangitis (PSC) is a chronic
 Predicting Clinical and Economic Outcomes After Liver Transplantation Using the Mayo Primary Sclerosing Cholangitis Model and Child-Pugh Score Jayant A. Talwalkar, * Eric Seaberg, W. Ray Kim, * and Russell
Predicting Clinical and Economic Outcomes After Liver Transplantation Using the Mayo Primary Sclerosing Cholangitis Model and Child-Pugh Score Jayant A. Talwalkar, * Eric Seaberg, W. Ray Kim, * and Russell
HPB ORIGINAL ARTICLE. Abstract. Correspondence. Introduction. Keith J. Roberts, Kishore G.S. Bharathy & J. Peter A. Lodge
 DOI:10.1111/j.1477-2574.2012.00593.x HPB ORIGINAL ARTICLE Kinetics of liver function tests after a hepatectomy for colorectal liver metastases predict post-operative liver failure as defined by the International
DOI:10.1111/j.1477-2574.2012.00593.x HPB ORIGINAL ARTICLE Kinetics of liver function tests after a hepatectomy for colorectal liver metastases predict post-operative liver failure as defined by the International
Hepatocellular carcinoma: Intra-arterial treatments
 Hepatocellular carcinoma: Intra-arterial treatments Irene Bargellini U.O. Radiologia Interventistica Azienda Ospedaliero Universitaria Pisana IRENE BARGELLINI,MD UO RADIOLOGIA INTERVENTISTICA, AZIENDA
Hepatocellular carcinoma: Intra-arterial treatments Irene Bargellini U.O. Radiologia Interventistica Azienda Ospedaliero Universitaria Pisana IRENE BARGELLINI,MD UO RADIOLOGIA INTERVENTISTICA, AZIENDA
Percutaneous Microwave Coagulation Therapy for Hepatocellular Carcinoma
 Hiroshima J. Med. Sci. Vol. 47, No.4, 151~155, December, 1998 HIJM47-2 151 Percutaneous Microwave Coagulation Therapy for Hepatocellular Carcinoma Toshimasa ASAHARA1l, Hideki NAKAHARA1l, Toshikatsu FUKUDA1l,
Hiroshima J. Med. Sci. Vol. 47, No.4, 151~155, December, 1998 HIJM47-2 151 Percutaneous Microwave Coagulation Therapy for Hepatocellular Carcinoma Toshimasa ASAHARA1l, Hideki NAKAHARA1l, Toshikatsu FUKUDA1l,
Hepatocellular Carcinoma in Qatar
 Hepatocellular Carcinoma in Qatar K. I. Rasul 1, S. H. Al-Azawi 1, P. Chandra 2 1 NCCCR, 2 Medical Research Centre, Hamad Medical Corporation, Doha, Qatar Abstract Objective The main aim of this study
Hepatocellular Carcinoma in Qatar K. I. Rasul 1, S. H. Al-Azawi 1, P. Chandra 2 1 NCCCR, 2 Medical Research Centre, Hamad Medical Corporation, Doha, Qatar Abstract Objective The main aim of this study
SIRTEX Lunch Symposium, Cebu, 23 Nov Dr. Stephen L. Chan Department of Clinical Oncology The Chinese University of Hong Kong
 SIRTEX Lunch Symposium, Cebu, 23 Nov 2013 Dr. Stephen L. Chan Department of Clinical Oncology The Chinese University of Hong Kong I will not talk on Mechanism of SIRT Data on efficacy of SIRT Epidemiology
SIRTEX Lunch Symposium, Cebu, 23 Nov 2013 Dr. Stephen L. Chan Department of Clinical Oncology The Chinese University of Hong Kong I will not talk on Mechanism of SIRT Data on efficacy of SIRT Epidemiology
Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis
 The Turkish Journal of Pediatrics 2015; 57: 492-497 Original Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis Aysel Ünlüsoy-Aksu 1,
The Turkish Journal of Pediatrics 2015; 57: 492-497 Original Aspartate aminotransferase-to-platelet ratio index in children with cholestatic liver diseases to assess liver fibrosis Aysel Ünlüsoy-Aksu 1,
SEQUENCING OF HCC TREATMENT. Dr. Amit G. Singal Medical Director, UT Southwestern Medical Center, USA
 SEQUENCING OF HCC TREATMENT Dr. Amit G. Singal Medical Director, UT Southwestern Medical Center, USA February 2018 DISCLAIMER Please note: The views expressed within this presentation are the personal
SEQUENCING OF HCC TREATMENT Dr. Amit G. Singal Medical Director, UT Southwestern Medical Center, USA February 2018 DISCLAIMER Please note: The views expressed within this presentation are the personal
Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis
 Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and
Korean J Hepatobiliary Pancreat Surg 212;16:15-19 Original Article Laparoscopic left hepatectomy in patients with intrahepatic duct stones and recurrent pyogenic cholangitis Sunjong Han, Insang Song, and
HEPATOCELLULAR CARCINOMA: AN OVERVIEW
 HEPATOCELLULAR CARCINOMA: AN OVERVIEW John K. Olynyk Head, Department of Gastroenterology & Hepatology Fiona Stanley Fremantle Hospital Group Dean of Research, Edith Cowan University RISING MORTALITY OF
HEPATOCELLULAR CARCINOMA: AN OVERVIEW John K. Olynyk Head, Department of Gastroenterology & Hepatology Fiona Stanley Fremantle Hospital Group Dean of Research, Edith Cowan University RISING MORTALITY OF
Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy: A Report of Two Cases
 Case Reports in Surgery Volume 2013, Article ID 238675, 4 pages http://dx.doi.org/10.1155/2013/238675 Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy:
Case Reports in Surgery Volume 2013, Article ID 238675, 4 pages http://dx.doi.org/10.1155/2013/238675 Case Report In Situ Split of the Liver When Portal Venous Embolization Fails to Induce Hypertrophy:
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days
 100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days TheraSphere [US package insert]. Surrey, UK: Biocompatibles UK Ltd,
100% pure beta emitter Decays to zirconium-90 Physical half-life of 64.1 hours (2.67 days) 94% of radiation delivered within 11 days TheraSphere [US package insert]. Surrey, UK: Biocompatibles UK Ltd,
Hepatic resection provided long-term survival for patients with intermediate and advanced-stage resectable hepatocellular carcinoma
 Liu et al. World Journal of Surgical Oncology (2016) 14:62 DOI 10.1186/s12957-016-0811-y RESEARCH Open Access Hepatic resection provided long-term survival for patients with intermediate and advanced-stage
Liu et al. World Journal of Surgical Oncology (2016) 14:62 DOI 10.1186/s12957-016-0811-y RESEARCH Open Access Hepatic resection provided long-term survival for patients with intermediate and advanced-stage
Anaesthetic considerations and peri-operative risks in patients with liver disease
 Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Anaesthetic considerations and peri-operative risks in patients with liver disease Dr. C. K. Pandey Professor & Head Department of Anaesthesiology & Critical Care Medicine Institute of Liver and Biliary
Management of hepatocellular carcinoma should consider both tumor factors and background liver factors
 Hepatocellular Carcinoma Column: Editorial Management of hepatocellular carcinoma should consider both tumor factors and background liver factors Shuji Nomoto, Mitsuhiro Hishida, Yoshikuni Inokawa, Hiroyuki
Hepatocellular Carcinoma Column: Editorial Management of hepatocellular carcinoma should consider both tumor factors and background liver factors Shuji Nomoto, Mitsuhiro Hishida, Yoshikuni Inokawa, Hiroyuki
간암의다양한병기분류법 : 현재사용중인병기분류를중심으로. Kim, Beom Kyung
 간암의다양한병기분류법 : 현재사용중인병기분류를중심으로 Kim, Beom Kyung Importance of staging system 환자의예후예측 적절한치료방법적용 ( 수술, 방사선, 항암..) 의료진간의 tumor burden 에대한적절한의사소통 향후연구및 clinical trial 시연구집단의성격에대한객관적기준제시 Requisites for good staging
간암의다양한병기분류법 : 현재사용중인병기분류를중심으로 Kim, Beom Kyung Importance of staging system 환자의예후예측 적절한치료방법적용 ( 수술, 방사선, 항암..) 의료진간의 tumor burden 에대한적절한의사소통 향후연구및 clinical trial 시연구집단의성격에대한객관적기준제시 Requisites for good staging
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Unmet needs in intermediate HCC. Korea University Guro Hospital Ji Hoon Kim
 Unmet needs in intermediate HCC Korea University Guro Hospital Ji Hoon Kim BCLC HCC Stage 0 PST 0, Child Pugh A Stage A C PST 0 2, Child Pugh A B Stage D PST > 2, Child Pugh C Very early stage (0) 1 HCC
Unmet needs in intermediate HCC Korea University Guro Hospital Ji Hoon Kim BCLC HCC Stage 0 PST 0, Child Pugh A Stage A C PST 0 2, Child Pugh A B Stage D PST > 2, Child Pugh C Very early stage (0) 1 HCC
