PROLONGED EXPOSURE THERAPY, A
|
|
|
- Easter White
- 5 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION Integrated Exposure-Based Therapy for Co-occurring Posttraumatic Stress Disorder and Substance Dependence A Randomized Controlled Trial Katherine L. Mills, PhD Maree Teesson, PhD Sudie E. Back, PhD Kathleen T. Brady, MD, PhD Amanda L. Baker, PhD Sally Hopwood, MPsych (Clin) Claudia Sannibale, PhD Emma L. Barrett, PhD Sabine Merz, PhD Julia Rosenfeld, MPsych (Clin) Philippa L. Ewer, BPsych (Hons) PROLONGED EXPOSURE THERAPY, A cognitive-behavioral therapy (CBT) involving exposure to memories and reminders of past trauma, has long been regarded as a gold standard treatment for posttraumatic stress disorder (PTSD). Although there are other evidence-based treatments for PTSD, such as eye movement desensitization and reprocessing therapy, there is more empirical evidence for the efficacy of prolonged exposure than for any other treatment. 1 Indeed, the International Consensus Group on Depression and Anxiety recommends prolonged exposure as the most appropriate form of psychotherapy for PTSD, 2 and it was the only treatment for PTSD endorsed in a US Institute of Medicine study as evidence based. 3 The efficacy of prolonged exposure in reducing PTSD symptom severity has been demonstrated among persons from a number of populations who have been exposed to a wide variety of trauma types. 4 There is, however, a notable absence of research examining the See also p 714 and Patient Page. Context There is concern that exposure therapy, an evidence-based cognitivebehavioral treatment for posttraumatic stress disorder (PTSD), may be inappropriate because of risk of relapse for patients with co-occurring substance dependence. Objective To determine whether an integrated treatment for PTSD and substance dependence, Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE), can achieve greater reductions in PTSD and substance dependence symptom severity compared with usual treatment for substance dependence. Design, Setting, and Participants Randomized controlled trial enrolling 103 participants who met DSM-IV-TR criteria for both PTSD and substance dependence. Participants were recruited from in Sydney, Australia; outcomes were assessed at 9 months postbaseline, with interim measures collected at 6 weeks and 3 months postbaseline. Interventions Participants were randomized to receive COPE plus usual treatment (n=55) or usual treatment alone (control) (n=48). COPE consists of 13 individual 90- minute sessions (ie, 19.5 hours) with a clinical psychologist. Main Outcome Measures Change in PTSD symptom severity as measured by the Clinician-Administered PTSD Scale (CAPS; scale range, 0-240) and change in severity of substance dependence as measured by the number of dependence criteria met according to the Composite International Diagnostic Interview version 3.0 (CIDI; range, 0-7), from baseline to 9-month follow-up. A change of 15 points on the CAPS scale and 1 dependence criterion on the CIDI were considered clinically significant. Results From baseline to 9-month follow-up, significant reductions in PTSD symptom severity were found for both the treatment group (mean difference, [95% CI, to 28.54]) and the control group (mean difference, [95% CI, to 13.95]); however,thetreatmentgroupdemonstratedasignificantlygreaterreductioninptsdsymptom severity(meandifference, 16.09[95% CI, 29.00to 3.19]). Nosignificantbetween-group difference was found in relation to improvement in severity of substance dependence (0.43 vs 0.52; incidence rate ratio, 0.85 [95% CI, 0.60 to 1.21), nor were there any significant between-group differences in relation to changes in substance use, depression, or anxiety. Conclusion Among patients with PTSD and substance dependence, the combined use of COPE plus usual treatment, compared with usual treatment alone, resulted in improvement in PTSD symptom severity without an increase in severity of substance dependence. Trial Registration isrctn.org Identifier: ISRCTN JAMA. 2012;308(7): efficacy of prolonged exposure among individuals with co-occurring PTSD and substance dependence. Epidemiologicandclinicalresearchhas demonstrated that trauma exposure amongindividualswithsubstancedependence is almost universal, and up to 62% experience comorbid PTSD. 5,6 Similarly, up to 65% of patients with PTSD have been found to have a comorbid substance use disorder. 7,8 Although PTSD is perva- Author Affiliations are listed at the end of this article. Corresponding Author: Katherine L. Mills, PhD, National Drug and Alcohol Research Centre, University of New South Wales, Sydney, New South Wales, Australia 2052 (k.mills@unsw.edu.au). 690 JAMA, August 15, 2012 Vol 308, No American Medical Association. All rights reserved.
2 sive across all drug classes, there is some evidence to suggest that individuals with opiate, sedative, and stimulant use disorders are at greatest risk. 5 Thus, there is a clear need for PTSD treatment in this population. Until recently, however, many experts and clinicians considered the use of prolonged exposure therapy amongindividualswithsubstancedependencetobeinappropriateunlessalengthy periodofabstinencehadbeenachieved. 9,10 Based on early case reports, it was widely believed that the intense emotions elicited during prolonged exposure therapy could place individuals at increased risk for relapse. 9 There is, however, an absence of evidence to support or refute this recommendation, because most trials of PTSD treatment have excludedindividualswithsubstancedependence. 11 Although a small number of pilot studies have examined the efficacy of integratedtreatmentprograms(whichaddress both PTSD and substance dependence at the same time) that incorporate prolongedexposure, thesetreatments havenotyetbeenexaminedinalargerandomized controlled trial. The aim of the present study was to address this gap in the literature by conducting what is to our knowledge the first randomized controlled trial of an integrated treatment for PTSD and substance dependence that incorporates prolonged exposure therapy. METHODS Design Participants were randomly assigned to 1 of 2 conditions. The treatment condition consisted of an integrated treatment for PTSD and substance dependence, calledconcurrenttreatmentofptsdand SubstanceUseDisordersUsingProlonged Exposure (COPE), plus usual treatment for substance dependence. The control conditionconsistedofusualtreatmentfor substance dependence only. Block randomization was conducted in groups of 10, stratified according to sex, by a person independent of the research. It was hypothesized that participants randomized to the treatment group would demonstrate greater reductions in PTSD and substance dependence symptom severity compared with those randomized to the control group. Participants were interviewed on entry to the study, and primary outcome measures were assessed at 9monthspostbaseline. Twointerimmeasures of outcome were also obtained at 6 weeksand3monthspostbaselinetomonitor participants status and increase the likelihood of retention at 9 months. Ethical approval was granted by the human ethics review committees of the University of New South Wales and the Northern Sydney Central Coast Area Health Service. Written informed consent was obtained from all participants prior to participation. Recruitment Participants were recruited between April 2007 and June 2009 from substance use treatment services, media advertisements, and practitioner referrals within the greater Sydney region, Australia. Inclusion criteria were past-month Diagnostic and Statistical Manual of Mental Disorders (Fourth Edition, Text Revision) (DSM-IV-TR) diagnoses of PTSD and substance dependence, age 18 years or older, and fluency in English. Individuals were excluded from participating if they were currently suicidal (expressed suicidal ideation accompanied by a plan and intent), had a recent history of self-harm (past 6 months), had current active symptoms of psychosis, or experienced cognitive impairment severe enough to impede treatment. Structured Interviews All participants were administered a structured, face-to-face interview at baseline. The primary outcomes, severity of PTSD and severity of substance dependence (as indicated by the number of dependence criteria met), were assessed using the Clinician-Administered PTSD Scale (CAPS) (range, 0-240; higher scores indicate more severe PTSD) 15 and the Composite International Diagnostic Interview version 3.0 (CIDI) (range, 0-7 dependence criteria; higher scores indicate more severe substance dependence), 16 respectively. The interview also assessed demographic characteristics; lifetime and current use of heroin, other opiates, amphetamines, cocaine, hallucinogens, benzodiazepines, alcohol, cannabis, and inhalants using the Opiate Treatment Index 17 ; DSM-IV-TR diagnoses of current substance dependence for main drug of concern (using the CIDI 16 ) ; trauma history using the CIDI version ; DSM- IV-TR diagnoses of PTSD in the past month using the CAPS 15 ; depression using the Beck Depression Inventory II (range, 0-63; higher scores indicate more severe depression) 19 ; state and trait anxiety using the State-Trait Anxiety Inventory (range, 20-80; higher scores indicate more severe anxiety) 20 ; the possible presence of borderline personality disorder using the International Personality Disorder Examination Questionnaire 21 ; and history of attempted suicide. To assess history of treatment for substance dependence, participants were asked whether they had commenced any of the following forms of treatment for their substance use: substitution pharmacotherapies (including methadone, buprenorphine, buprenorphine plus naloxone, and naltrexone maintenance); outpatient or inpatient detoxification; residential rehabilitation; and outpatient counseling. To assess PTSD treatment history, participants were asked whether they had ever commenced any of the following forms of treatment for their PTSD: inpatient hospitalization; outpatient counseling or psychotherapy; and medication (such as antidepressants). The sections of the assessment pertaining to current drug use, substance dependence, PTSD, depression, and anxiety were readministered at each follow-up interview. Participants were also asked whether they had been exposed to any further traumatic events, had experienced any suicidal ideation or attempted suicide, or had undergone any treatment over the follow-up period. Participants were paid A$30 (US $30.75) for completing each interview. Interviews were administered by 2 trained research officers blinded to group allocation. Interventions COPE Treatment. COPE is a modified version of Concurrent Treatment of 2012 American Medical Association. All rights reserved. JAMA, August 15, 2012 Vol 308, No
3 PTSD and Cocaine Dependence. 22 The version of COPE used in the present study represents an integration of existing evidence-based manualized CBT interventions for PTSD and substance dependence The intervention consists of 13 individual 90-minute sessions (ie, 19.5 hours) delivered by a clinical psychologist. Although designed to be delivered weekly, flexibility is permitted. Treatment components include motivational enhancement and CBT for substance use (sessions 1-4 and throughout); psychoeducation relating to both disorders and their interaction (sessions 1-4); in vivo exposure (sessions 5-12); imaginal exposure (sessions 6-12); and cognitive therapy for PTSD (sessions 8-12). The final session (session 13) is dedicated to providing a review of the treatment, devising an after-care plan, and termination of therapy. COPE was delivered by 2 clinical psychologists employed on the project who received fortnightly supervision for the duration of the study. All treatment sessions were recorded. Ten percent of participants were randomly selected to have their sessions rated for treatment fidelity (ie, compliance with the treatment manual) by an independent assessor. Fidelity was rated for 53 of a total of 323 sessions (16.4%) conducted as part of the study. Average fidelity ratings were high, with a mean score of 4.13 (SD, 0.95) of a possible score of 5 indicating strong adherence to the treatment manual. Usual Treatment. Both the treatment and the control group were able to engage in usual treatment for substance dependence. As such, participants could access any type of substance use treatment currently available in the community, including outpatient counseling, inpatient or outpatient detoxification, residential rehabilitation, and pharmacotherapies (eg, methadone, buprenorphine, buprenorphine plus naloxone, naltrexone). Sample Size Calculations Power analysis on the primary outcome variables (ie, change in CAPS score and number of dependence criteria met) was conducted using RMASS2 (Phar Lap Software Inc). The target sample size (n=150) was conservatively designed to have 90% power to detect a time-averaged difference between groups of 5 points on the CAPS scale and 0.5 points in severity of substance dependence, at =.05. The final sample size was 103 because of a lower-than-expected recruitment rate. The final sample size had 80% power to detect a difference between groups of 10 points on the CAPS scale at 9-month follow-up but only 60% power to detect a 1-point difference in the number of dependence criteria met at 9-month follow-up, at =.05. A difference of 15 points on the CAPS scale is considered clinically significant. 26 With regard to severity of substance dependence, we considered a 1-unit change in the number of DSM-IV-TR criteria met to be clinically significant, because research has demonstrated a 1-unit change to be associated with level of impairment, mental health, and risk of attempted suicide. 27,28 Missing Data Analysis of missing data revealed 18.7% missing data across the follow-up period. According to the results of the Little missing completely at random test, the data could be considered to be missing completely at random ( 2 36=14.28, P.99). To satisfy the intention-to-treat (ITT) requirement that analyses be undertaken on all participants, missing data were imputed using multiple imputation, which allows for the uncertainty about the missingdatabycreatingseveraldifferentplausible imputed data sets and appropriately combiningresultsobtainedfromeach. 29,30 Multiple imputation is recommended over single-imputation techniques because the missing values for each participant are predicted from his or her own observed values, and the estimates produced take into account the uncertainty of the imputation process. 29 Because the pattern of missing data was nonmonotone, the Markov chain Monte Carlo method of multiple imputation was used. 30 As suggested by Schafer and Graham, 29 5 imputations were used. Imputations were constrained to plausible values for the scales used. Statistical Analyses Two-sided analyses were conducted with IBM SPSS Statistics 20 using a predetermined level of P.05. Baseline differences between groups were examined using t tests for normally distributed measures, Mann-Whitney U-tests for nonnormally distributed data, and 2 test for categorical variables. 2 and linear regression analyses were undertaken to ascertain whether there were any between-group differences in exposure to usual treatment for substance dependence over the follow-up period. Intention-to-treat analyses were conducted for all outcomes. Primary unadjusted analyses were undertaken comparing the treatment and control groups. Secondary analyses were undertaken adjusting for covariates found to be unbalanced between groups (ie, history of childhood trauma, history of childhood sexual abuse, percentage of time spent in usual treatment during the study). Outcomes were examined using a series of binomial logistic, linear, and Poisson-distributed generalized estimatingequationsforcategorical, continuous, and count data, respectively. Analyses were undertaken using an exchangeable correlation matrix. Linear and Poisson models used data from all points (baseline and each follow-up). These models testedwhetherthescoresobtainedateach point differed significantly between the 2 groups, the change in scores from baseline to 9 months differed for each group, and the degree of change between baseline and 9 months differed between the 2groups.Binomialmodelsdidnotinclude baseline data for the dependent variables, because these values were constant and hence the models could not converge. Thus, the binomial models examined whether the scores obtained at each point differed significantly between the 2 groups. Results are reported as the unstandardized mean difference with 95% CIs for linear models, odds ratios (ORs) with 95% CIs for binomial logistic models, and incidence rate ratios (IRRs) with 95% CIs for Poisson models. 692 JAMA, August 15, 2012 Vol 308, No American Medical Association. All rights reserved.
4 Figure. Study Flow 55 Randomized to receive COPE + usual treatment 45 Received intervention as randomized 10 Did not receive intervention as randomized (did not attend any sessions) Follow-up 6 Weeks 37 Assessed 16 Could not be contacted 2 Refused 3 Months 41 Assessed 10 Could not be contacted 4 Refused 9 Months 39 Assessed 11 Could not be contacted 4 Refused 1 Died RESULTS Sample Recruitment and Retention Ofthe334individualsassessed, morethan one-third (103 [37.1%]) were eligible to participate (FIGURE). The primary reasons for exclusion were not meeting criteria for a diagnosis of PTSD (111 [52.9%]) or no substance use in the preceding month(82[39.0%]); 14 individuals(6.7%) were currently suicidal or selfharming, 2 (1.0%) exhibited cognitive impairment severe enough to impede treatment, and 1 (0.5%) was younger than 18 years. The majority of eligible individuals agreed to participate (103 [83.1%]). A total of 74, 82, and 77 participants were reinterviewed at 6 weeks, 3 months, and 9 months postbaseline, respectively, representing 71.8%, 79.6%, and 74.8% of participants enrolled in the study at baseline (Figure). Ninety-three participants (90.3%) completed at least 1 of the 3 follow-up interviews; 57 (55.3%) completed all 3 follow-up interviews. Detail regardingthepatternoffollow-updatacollected is provided in the efigure available at Study retention was not related to randomization. There were no significant differences between the treatment and control groups in the likelihood of completing interviews at 6 weeks (37 [67.3%] vs 37 [77.1%], respectively; OR, 0.61 [95% CI, 0.25 to 1.47]), 3 months (41 [74.5%] vs 41 [85.4%]; OR, 0.50 [95% CI, 0.18 to 1.37]), or 9 months (39 [70.9%] vs 38 [79.2%]; OR, 0.64 [95% CI, 0.26 to 1.59]) or in the number of follow-up interviews completed (median, 3.0 vs 3.0; U=1142.5; P=.19). Patternsofstudyretentionwerelargely unrelated to current substance use, severity of substance dependence, types of trauma exposure, age of first trauma exposure, or severity of PTSD (etable 1). However, participants who completed the 6-week follow-up, compared with those who did not, were more likely to have experienced sexual molestation (54 [73.0%] vs 14 [48.3%], respectively; OR, 2.89 [95% CI, 1.19 to 7.05]). Participants who completed the 3-month follow-up, compared with those who did not, were more likely to have experienced rape (60 [73.2%] vs 10 [47.6%]; OR, 3.00 [95% CI, 1.12 to 8.04]) and less likely to have used inhalants in the month prior to baseline (3 [3.7%] vs 4 [19.0%]; OR, 0.16 [95% CI, 0.03 to 0.79]). Participants who completed the 9-month follow-up, compared with those who did not, were also more likely to have experienced rape (57 [74.0%] vs 13 [50.0%]; OR, 2.85 [95% CI, 1.13 to 7.17]). None of the substance use, trauma, or PTSD variables examined were related to the number of follow-up interviews completed (etable 1). Baseline Sample Characteristics There were no significant differences between the treatment and control groups in demographic characteristics, lifetime or current substance use, severity of substance dependence, or history of treatment for substance use (TABLE 1 and TABLE 2). Polysubstance use was the norm, with participants using a median 334 Participants assessed for eligibility 103 Randomized 231 Excluded 210 Did not meet inclusion criteria 14 Declined to participate 7 Other 48 Randomized to receive usual treatment only 42 Received intervention as randomized 6 Did not receive intervention as randomized (not currently in or did not enter usual treatment for substance use at study entry) Follow-up 6 Weeks 37 Assessed 9 Could not be contacted 2 Refused 3 Months 41 Assessed 5 Could not be contacted 2 Refused 9 Months 38 Assessed 7 Could not be contacted 3 Refused 55 Included in primary analysis 48 Included in primary analysis COPE indicates Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure. of 4.0 different drug classes in the preceding month, most commonly benzodiazepines, cannabis, and alcohol, followed by heroin, amphetamines, other opiates, cocaine, hallucinogens, and inhalants. The most commonly reported main drug of concern was heroin (22 [21.4%]), followed by cannabis (20 [19.4%]), amphetamines (18 [17.5%]), benzodiazepines (16 [15.5%]), alcohol (12 [11.7%]), cocaine (7 [6.8%]), other opiates (5 [4.9%]), and hallucinogens (1 [1.0%]). The distribution of main drug of concern did not differ according to group ( 2 8=8.03, P=.43). The treatment and control groups were similar in terms of trauma history (Table 1); however, participants randomized to the control group were more likely to have experienced childhood sexual abuse compared with participants randomized to the treatment group. All participants had experienced multiple traumas and met crite American Medical Association. All rights reserved. JAMA, August 15, 2012 Vol 308, No
5 ria for current PTSD. There were no significant differences between groups in PTSD, depression, or anxiety symptomology (Table 2). Treatment Exposure COPE Treatment. Forty-five participants (81.8%) randomized to the treatment group attended at least 1 session. Among those randomized to receive COPE, the median number of sessions attended was 5 (range, 0-13). Thirty participants (54.5%) attended sessions in which imaginal or in vivo exposure were covered (22 [40.0%] imaginal, 28 [50.9%] in vivo). Participants attended a median of 0 sessions covering imaginal exposure (range, 0-7) and 1 covering in vivo exposure (range, 0-8). Ten participants (18.2%) attended all 13 sessions. Although the 13-session intervention was designed to be delivered weekly, appointment scheduling and treatment retention was made difficult by the chaotic lifestyle associated with substance dependence and comorbidity. There was, Table 1. Baseline Characteristics According to Group No. (%) Characteristic Treatment (n = 55) Control (n = 48) Total (n = 103) OR (95% CI) Demographic Age, mean (SD), y a 33.4 (7.4) 33.5 (8.6) 33.7 (7.9) Women 33 (60.0) 31 (64.6) 64 (62.1) 0.82 (0.37 to 1.83) Australian born 47 (85.5) 40 (83.3) 87 (84.5) 1.18 (0.40 to 3.42) Aboriginal or Torres Strait Islander 2 (3.6) 4 (8.3) 6 (5.8) 0.42 (0.07 to 2.37) School completed, median (range), y b 10 (7-12) 10 (7-12) 10 (7-12) Completed tertiary education 40 (72.7) 36 (75.0) 76 (73.8) 0.89 (0.37 to 2.15) Unemployed 42 (76.4) 39 (81.3) 81 (78.6) 0.75 (0.29 to 1.94) Prison history 17 (30.9) 19 (39.6) 36 (35.0) 0.68 (0.30 to 1.54) Substance use Age of first intoxication, median (range) c 13 (7-29) 13 (6-27) 13 (6-29) History of injection drug use 43 (78.2) 39 (81.2) 82 (79.6) 0.83 (0.31 to 2.18) Prior substance use treatment 50 (90.9) 46 (95.8) 96 (93.2) 0.44 (0.08 to 2.35) Trauma exposure Type Physical assault 52 (94.5) 44 (91.7) 96 (93.2) 1.58 (0.34 to 7.42) Threatened or held captive 50 (90.9) 42 (87.5) 92 (89.3) 1.43 (0.41 to 5.02) Witnessed injury or death 46 (83.6) 35 (72.9) 81 (78.6) 1.90 (0.73 to 4.94) Sexual assault d 42 (76.4) 38 (79.2) 80 (77.7) 0.85 (0.33 to 2.16) Accident or disaster 40 (72.7) 28 (58.3) 68 (66.0) 1.90 (0.83 to 4.35) Torture 15 (27.3) 10 (20.8) 25 (24.3) 1.43 (0.57 to 3.56) Combat experience 1 (1.8) 1 (2.1) 2 (1.9) 0.87 (0.05 to 14.30) Other 39 (70.9) 31 (64.6) 70 (68.0) 1.34 (0.58 to 3.06) No. of trauma types experienced, median (range) e 6.0 (2-9) 5.5 (2-10) 6.0 (2-10) Age at first trauma, median (range) f 10 (1-44) 7 (2-28) 8 (1-44) Experienced trauma during childhood 38 (69.1) 41 (85.4) 79 (76.7) 0.38 (0.14 to 1.02) Experienced sexual abuse during childhood 25 (45.5) 32 (66.7) 57 (55.3) 0.42 (0.19 to 0.93) g PTSD Delayed onset h 14 (25.5) 11 (22.9) 25 (24.3) 1.15 (0.46 to 2.84) Duration of trauma symptoms, median (range), y i 9 ( ) 12 ( ) 10 ( ) Prior PTSD treatment 17 (30.9) 19 (39.6) 36 (35.0) 0.68 (0.30 to 1.54) Other mental health history Screened positive for BPD 38 (69.1) 37 (77.1) 75 (72.8) 0.67 (0.28 to 1.61) Attempted suicide Lifetime 32 (58.2) 22 (45.8) 54 (52.4) 1.64 (0.75 to 3.59) Past year 6 (10.9) 4 (8.3) 10 (9.7) 1.35 (0.36 to 5.09) Abbreviations: BPD, borderline personality disorder; OR, odd ratio; PTSD, posttraumatic stress disorder. a t=0.17 (df=101), P=.87 for between-group comparisons. b U=1316.0, P=.98 for between-group comparisons. c U=1286.0, P=.82 for between-group comparisons. d Includes rape and sexual molestation. e U=1100.5, P=.14 for between-group comparisons. f U=1087.0, P=.12 for between-group comparisons. g P=.03. h Symptoms had their onset more than 6 months following trauma exposure. i U=1085.5, P=.12 for between-group comparisons. 694 JAMA, August 15, 2012 Vol 308, No American Medical Association. All rights reserved.
6 therefore, considerable variability in the time taken to deliver the COPE treatment, ranging from 0 to 271 days (median, 71 days). Twenty-two participants (40.0%) randomized to receive COPE treatment were still receiving COPE after 3 months. Usual Treatment. The majority of both the treatment and the control group were enrolled in usual treatment for substance dependence at study entry (44 [80.0%] vs 42 [87.5%], respectively; OR, 0.57 [95% CI, 0.19 to 1.68]). The type of usual treatment enrolled in at baseline did not differ significantly between the 2 groups ( 2 4=7.00, P=.14). The most common treatment enrolled in for the treatment group was detoxification (28 [50.0%]), followed by maintenance therapies (12 [21.8%]) and residential rehabilitation (4 [7.3%]). The most common treatment enrolled in for the control group was detoxification (29 [60.4%]), followed by maintenance therapies (7 [14.6%]), residential rehabilitation (3 [6.5%]), and outpatient counseling (3 [6.3%]). Percentage of time spent in treatment over the follow-up period was analyzed instead of days in treatment to control for differences in time to follow-up. As shown in TABLE 3, the treatment group spent significantly less time in usual treatment compared with the control group over the entire 9-month follow-up period; however, there were no differences between groups in the percentage of time spent in treatment between follow-up points. Primary Treatment Outcome Analysis PTSD. There was a significant group time interaction in relation to PTSD symptom severity ( 2 1=5.38, P=.02). From baseline to 9-month follow-up, significant reductions in PTSD symptom severity were found for both the treatment group (mean difference, Table 2. Unadjusted Comparisons Between the Treatment and Control Groups on Continuous Measures of Outcome Mean (95% CI) a Outcome Measure Baseline 6 wk 3 mo 9 mo No. of drug classes used COPE usual care (n = 55) (3.32 to 4.10) (1.57 to 2.51) (1.62 to 2.52) (1.68 to 2.58) Usual care only (n = 48) 3.81 (3.40 to 4.22) Between-group difference at each interview, IRR (95% CI) c 0.97 (0.84 to 1.13) No. of dependence criteria met COPE usual care (n = 55) 5.33 (5.09 to 5.57) Usual care only (n = 48) 5.58 (5.36 to 5.80) Between-group difference at each interview, IRR (95% CI) c 0.95 (0.90 to 1.01) CAPS COPE usual care (n = 55) (87.03 to 95.23) Usual care only (n = 48) (84.70 to 94.06) Mean between-group difference at each interview (95% CI) c 1.75 ( 4.41 to 7.92) BDI-II COPE usual care (n = 55) (33.17 to 38.97) Usual care only (n = 48) (28.08 to 35.30) Mean between-group difference at each interview (95% CI) c 4.38 ( 0.20 to 8.97) STAI COPE usual care (n = 55) (51.16 to 58.22) Usual care only (n = 48) (46.89 to 53.95) Mean between-group difference at each interview (95% CI) c 4.27 ( 0.66 to 9.21) 2.26 (1.67 to 2.85) 0.90 (0.65 to 1.26) 2.62 (1.68 to 3.56) 2.96 (2.22 to 3.70) 0.88 (0.57 to 1.37) (60.15 to 77.71) (69.03 to 82.83) 7.00 ( to 4.96) (22.55 to 32.85) (21.82 to 28.96) 2.31 ( 3.86 to 8.48) (43.85 to 54.63) (43.29 to 51.41) 1.89 ( 4.03 to 7.81) 2.31 (1.80 to 2.82) 0.89 (0.65 to 1.22) 2.49 (1.75 to 3.23) 3.41 (2.70 to 4.12) 0.73 (0.50 to 1.05) (59.93 to 75.77) (66.79 to 79.97) 5.53 ( to 4.05) (25.74 to 33.74) (21.71 to 30.17) 3.80 ( 1.81 to 9.40) (45.83 to 53.95) (44.19 to 53.09) 1.25 ( 4.65 to 7.15) 2.28 (1.71 to 2.85) 0.94 (0.67 to 1.30) 2.27 (1.58 to 2.96) 2.98 (2.27 to 3.69) 0.76 (0.51 to 1.14) (43.72 to 62.06) (59.21 to 75.25) ( to 1.75) d (19.29 to 29.59) (20.15 to 29.41) 0.35 ( 7.72 to 7.03) (42.09 to 50.79) (43.15 to 51.85) 1.06 ( 7.55 to 5.43) Within-Group Difference Between Baseline and 9-mo Follow-up IRR (95% CI) Between-Group Difference Between Baseline and 9-mo Follow-up 0.57 (0.46 to 0.72) b 0.96 (0.69 to 1.34) 0.60 (0.47 to 0.76) b 1 [Reference] 0.43 (0.31 to 0.58) b 0.85 (0.60 to 1.21) 0.52 (0.41 to 0.66) b 1 [Reference] Mean Difference (95% CI) Mean Difference (95% CI) ( to 28.54) b ( to 3.19) d ( to 13.95) b 1 [Reference] ( to 6.19) b 4.73 ( to 2.29) 6.90 ( to 2.97) b 1 [Reference] 8.25 ( to 2.86) b 5.34 ( to 1.80) 2.91 ( 7.16 to 1.34) 1 [Reference] Abbreviations: BDI-II, Beck Depression Inventory II; CAPS, Clinician-Administered PTSD Scale; COPE, Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure; IRR, incidence rate ratio; STAI, State-Trait Anxiety Inventory. a Group time interaction effect not significant at P.05, except for CAPS, for which group time interaction effect was significant at P=.02. b P.001. c Reference category is the control group. d P= American Medical Association. All rights reserved. JAMA, August 15, 2012 Vol 308, No
7 Table 3. Comparisons Between the Treatment and Control Groups of Percentage of Time Spent in Usual Treatment for Substance Dependence Over the Follow-up Period Time in Treatment Treatment (n = 55) Mean % (95% CI) Control (n = 48) Total (n = 103) Difference Between Treatment and Control Groups, Mean % (95% CI) Cumulative (since baseline) 6 wk (40.50 to 60.46) (49.54 to 70.32) (47.69 to 62.07) 9.45 ( to 5.01) 3 mo (46.64 to 67.38) (56.47 to 76.55) (54.19 to 68.69) 9.49 ( to 5.07) 9 mo (43.85 to 65.49) (59.50 to 79.34) (53.84 to 69.24) ( to 0.33) a Since last interview 6 wk (40.50 to 60.46) (49.54 to 70.32) (47.69 to 62.07) 9.45 ( to 5.01) 3 mo (39.54 to 61.84) (49.83 to 72.91) (47.63 to 63.71) ( to 5.48) 9 mo (41.29 to 64.53) (56.36 to 79.06) (51.42 to 68.20) ( to 1.25) a P= ; [95% CI, to 28.54]) and the control group (mean difference, [95% CI, to 13.95]); however, the treatment group demonstrated a significantly greater reduction in PTSD symptom severity compared with the control group (mean difference, [95% CI, to 3.19]) (Table 3). At 9-month follow-up, PTSD symptom severity was significantly lower in the treatment group compared with the control group (52.89 vs 67.23; mean difference, [95% CI, to 1.75). Although the prevalence of PTSD diagnosis at 9-month follow-up appears to be significantly lower in the treatment group compared with the control group (31 [56.4%] vs 38 [79.2%]; OR, 0.32 [95% CI, ]) (TABLE 4), the group time interaction in relation to PTSD diagnosis was not significant ( 2 1=0.30, P=.58). Substance Use and Dependence. The group time interactions in relation to rates of substance use ( 2 1=0.00, P.99) and the number of drug classes used ( 2 1=0.10, P=.76) were not significant, indicating that the prevalence of abstinence and number of drug classes used over the follow-up period did not differ between the treatment and control groups. Although the majority of participants in both the treatment and the control group continued to use substances at 9-month follow-up (45 [81.8%] vs 35 [72.9%]) (Table 4), both the treatment and the control group demonstrated significant reductions in the number of drug classes used from baseline to 9-month follow-up (Table 2). The degree of improvement in number of drug classes used did not differ significantly between groups (0.57 vs 0.60; IRR, 0.96 [95% CI, ]). The group time interactions in relation to rates of substance dependence ( 2 1=0.00, P.99) and severity of substancedependence( 2 1=2.09,P=.15)were not significant, indicating that the prevalenceofsubstancedependenceanddegree of change in severity of substance dependence over the follow-up period did not differ between the treatment and control groups. By the 9-month follow-up, rates of substance dependence had decreased to 45.4% (n=25) in the treatment group and 56.2% (n=27) in the control group; however, the difference between groups was not significant (OR, 0.64 [95% CI, 0.28 to 1.48]) (Table 4). Both the treatment and the control group also demonstrated significant reductions in severity of dependence from baseline to 9-month follow-up (Table 2); however, the degree of change did not differ significantly between groups (0.43 vs 0.52; IRR, 0.85 [95% CI, 0.60 to 1.21]). Depression and Anxiety. The group time interactions in relation to severity of depression ( 2 1=1.31, P=.26) and anxiety ( 2 1=2.69, P=.10) were not significant, indicating that severity of depression and anxiety did not differ between the treatment and control groups over the follow-up period. Both the treatment and the control group demonstrated significant reductions in severity of depression from baseline to 9-month follow-up (Table 2); however, the degree of change did not differ significantly between groups ( vs 6.90; mean difference, 4.73 [95% CI, to 2.29). There was also no significant difference between the treatment and control groups in the degree of change in severity of anxiety from baseline to 9-month follow-up ( 8.25 vs 2.91; mean difference, 5.34 [95% CI, to 1.80]) (Table 2). Secondary Treatment Outcome Analysis Secondary analyses were undertaken adjusting for covariates found to be unbalancedbetweengroups(ie, historyofchildhood trauma, history of childhood sexual abuse, percentage of time spent in usual treatment during the study). The results of these analyses (etable 2 and etable 3) were consistent with those of the unadjusted analyses. Serious Adverse Events Two participants from the treatment group (3.6%) and 5 participants from the control group (10.4%) attempted suicide during the study (OR, 0.32 [95% CI, ]). Although it is possible that these attempts were related to participation in the study, all 7 individuals reported that this was not the case and elected to remain involved with the study. Additionally, 1 participant from the treatment group (1.8%) died as a result of a preexisting medical condition. COMMENT Findings from the present study provide support for the efficacy of integrated exposure-basedtherapiesforthetreatment 696 JAMA, August 15, 2012 Vol 308, No American Medical Association. All rights reserved.
8 Table 4. Unadjusted Comparisons Between the Treatment and Control Groups on Categorical Measures of Outcome No. (%) Outcome Measure Baseline 6 wk 3 mo 9 mo Abstinent, % a COPE usual treatment (n = 55) 0 12 (21.8) 10 (18.2) 10 (18.2) Usual treatment only (n = 48) 0 15 (31.3) 12 (25.0) 13 (27.1) Between-group difference at each interview, OR (95% CI) b NA 0.59 (0.24 to 1.46) 0.70 (0.24 to 1.99) 0.59 (0.21 to 1.65) Diagnosis of substance dependence, % a COPE usual treatment (n = 55) 55 (100) 26 (47.3) 26 (47.3) 25 (45.4) Usual treatment only (n = 48) 48 (100) 28 (58.3) 28 (58.3) 27 (56.2) Between-group difference at each interview, OR (95% CI) b NA 0.64 (0.25 to 1.63) 0.62 (0.25 to 1.54) 0.64 (0.28 to 1.48) Diagnosis of PTSD, % a COPE usual treatment (n = 55) 55 (100) 48 (87.3) 47 (85.4) 31 (56.4) Usual treatment only (n = 48) 48 (100) 45 (93.8) 43 (89.6) 38 (79.2) Between-group difference at each interview, OR (95% CI) b NA 0.41 (0.06 to 2.63) 0.68 (0.19 to 2.44) 0.32 (0.13 to 0.81) c Abbreviations: COPE, Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure; NA, not applicable; OR, odds ratio; PTSD, posttraumatic stress disorder. a Group time interaction effect not significant at P.05. b Reference category is the control group. c P=.02. of PTSD among patients with substance dependence. Consistentwithourhypothesis, participants randomized to receive COPEplususualtreatmentdemonstrated significantly greater reductions in PTSD symptom severity compared with participants randomized to receive usual treatment alone (mean difference, 16.09). Thisalsorepresentsaclinicallysignificant difference. 26 It is important to note that most participants randomized to receive COPE plus usual treatment continued to use substances throughout the study. These findings challenge the widely held view that patients need to be abstinent beforeanytraumawork, letaloneprolonged exposure therapy, is commenced. 10 Although we agree that patients need to show some improvement in their substance use and an ability to use alternativecopingstrategiesbeforeprolongedexposure therapy is initiated, findings from the present study demonstrate that abstinence is not required. Our second hypothesis, that individuals randomized to receive COPE plus usual care would demonstrate significantly greater reductions in severity of substance dependence, was not confirmed. Both groups demonstrated significant reductions in severity of substance dependence, but the difference between groups was not significant. This may be attributable to a lack of statistical power, because the final sample size had only 60% power to detect a 1-point difference in the number of dependence criteria met across the 9-month follow-up period. Comparable reductions in severity of depression and anxiety were also observed between groups. Further research with larger samples sufficiently powered to detect differences in these domains is needed. It is important to note, however, that studies examining the temporal sequencing of changes in PTSD and substance dependence symptoms have shown that improvements in PTSD symptoms are associated with subsequent improvements in substance dependence, but the reciprocal relationship is not observed. 31,32 These findings highlight the importance of treating PTSD to improve substance dependence outcomes for individuals with this comorbidity. The improvements in PTSD, substance dependence, and depression observed in the present study are consistent with the findings of a pilot study by Brady et al 13 of an earlier version of the COPE treatment. Brady et al did not use a control group; however, similar withingroup pretreatment to posttreatment effects were observed in both studies. These similarities are encouraging, given that Brady et al examined outcomes for treatment completers only (ie, patients who completed 10 of 16 sessions), and the baseline severity of PTSD symptoms in their study was considerably lower than that of participants randomized to receive COPE plus usual treatment in the present study (mean CAPS scores, 45.2 vs 91.1, respectively). The present findings add to those of Brady et al by demonstrating the efficacy of COPE using a more conservative ITT approach in a sample of substantially more disabled individuals. It should be noted however, that although those randomized to receive COPE plus usual treatment demonstrated significantly greater improvements in PTSD, at the end of the study 56.4% continued to meet diagnostic criteria for PTSD. Further analysis of these data will examine the characteristics of this group and the importance of particular treatment components to inform further development of the intervention. The overall lack of between-group differences found in the present study is similar to the findings of a study by Triffleman et al 12 of Substance Dependency Post-Traumatic Stress Disorder Therapy, an integrated 40-session therapy for PTSD and substance dependence that includes in vivo (but not imaginal) exposure. Substance Dependency Post-Traumatic Stress Disorder Therapy was compared with Twelve-Step Facilitation Therapy, an evidence-based treatment for substance dependence that does not address trauma, in a sample of American Medical Association. All rights reserved. JAMA, August 15, 2012 Vol 308, No
9 methadone-maintained patients. As in the present study, both groups demonstrated significant improvements in PTSD and substance dependence symptoms; however, no between-group differences were found in relation to PTSD or substance dependence outcomes. Like the findings of the present study, the lack of differences observed by Triffleman et al 12 may also be attributable to insufficient power. Aside from measures of treatment outcome, treatment retention is an important indicator of a treatment s acceptability and utility. Consistent with the findings of Brady et al, 13 the present study demonstrated high treatment dropout rates, with participants attending a median of 5 of the 13 sessions offered. Although higher retention rates would be optimal, it is important to note that low attendance in addiction treatment has been identified as a pervasive clinical challenge, particularly in cases in which there is comorbidity. 33,34 High dropout rates and attrition have been observed across treatment settings, interventions, and substances of abuse. Indeed, treatment retention in the present study is comparable with that in studies of integrated PTSD treatments for patients with substance dependence that are not trauma-focused, studies of treatments for substance dependence alone, and studies of treatments for other mental health disorders. 32,35 For example, in a study by Hien et al 32 of Seeking Safety (a non trauma-focused integrated treatment for substance dependence and PTSD), 82% of participants attended at least 1 session, with a mean of 6 (of a possible total of 12 sessions) completed. Only 12% of the sample completed all 12 sessions. The corresponding values for the present study were 82% attendance, for a median of 5 sessions, with 18% completing all 13 sessions. Given that the treatment aims to address 2 disorders characterized by extreme avoidance among individuals with severe and chronic symptomology (in addition to many other current life stressors that make it difficult for them to engage in treatment), it is imperative that future research incorporate and examine methods to improve retention in treatment. Based on observations made in the present study, it appears that the provision of ancillary support services that provide concurrent case management may be useful. The characteristics of the sample lend support to the generalizability of the findings. Participants had experienced a wide range of traumas, were using a variety of substances, and experienced significant comorbidity, including likely borderline personality disorder features typical of patients with PTSD and substance dependence. 5,36 However, the findings cannot be generalized to individuals younger than 18 years; those not fluent in English; those currently suicidal, self-harming, or psychotic; or those with severe cognitive impairment, because these individuals were excluded from study participation. A number of other limitations should also be noted. First, the study relied on measures of self-report alone. There is much controversy regarding the reliability and validity of self-reported drug use; however, an extensive literature documents its reliability and validity. 37 Overall, agreement between self-report and biomarkers is high; indeed, when there are discrepancies, this tends to be when respondents report drug use that has failed to be detected by the biological measures. 37 Sherman and Bigelow 38 suggested that drug use information reported by persons seeking treatment is likely to be highly valid, given that they are seeking treatment for that drug use and have no need to conceal their use. Two studies examining self-reported substance use among patients with PTSD found participants responses to be highly valid, with less than 10% of participants not reporting substance use detected by urine screens. 39,40 Second, although the effects observed remained after controlling for between-group differences in exposure to usual treatment and in the prevalence of childhood sexual abuse and childhood trauma, the outcomes observed may have been influenced by confounding factors not measured by the present study. It could also be argued that the differences observed may be attributed to more general therapist effects (ie, the treatment group received up to 13 sessions with a therapist that the control group did not). Thus, although the present study provides evidence in support of COPE, it does not speak to its efficacy in comparison with other treatments. Further research examining the efficacy of COPE relative to other active treatments of equivalent duration is necessary. With regard to the analyses, it should also be noted that to satisfy the ITT requirement that outcome data be analyzed for all participants, missing data were imputed. Although the methods used in the present study are considered optimal and take into account the uncertainty surrounding the imputation process, the actual values for missing participants remain unknown. The analyses were also based on a predetermined level of P.05, and adjustments were not made to take into account multiple comparisons. The present study provides evidence in support of integrated treatment for PTSD and substance dependence using prolonged exposure. The COPE treatment was found to be efficacious in reducing PTSD symptom severity when combined with usual treatment; however, no other between-group differences were observed in relation to severity of substance dependence, substance use, depression, or anxiety. Contrary to popular belief, participants randomized to receive the exposurebased intervention did not demonstrate poorer substance use outcomes relative to those randomized to receive usual treatment only. The complex trauma, substance use, and psychiatric presentations commonly found among individuals with PTSD and substance dependence should not be a deterrent to providing trauma-focused treatment. Author Affiliations: National Drug and Alcohol Research Centre (Drs Mills, Teesson, Sannibale, Barrett, and Merz and Mss Rosenfeld and Ewer) and Traumatic Stress Clinic (Ms Hopwood), University of New South Wales, Sydney, New South Wales, Australia; Medical University of South Carolina and the Ralph H. Johnston Veterans Affairs Medical Center, Charleston (Drs Back and Brady); and Centre for Brain and 698 JAMA, August 15, 2012 Vol 308, No American Medical Association. All rights reserved.
10 Mental Health Research, University of Newcastle, Newcastle, New South Wales, Australia (Dr Baker). Author Contributions: Dr Mills had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Study concept and design: Mills, Teesson, Back, Brady, Baker, Hopwood, Sannibale. Acquisition of data: Teesson, Baker, Barrett, Merz, Rosenfeld, Ewer. Analysis and interpretation of data: Mills, Teesson, Back, Brady, Baker. Drafting of the manuscript: Mills, Teesson, Baker. Critical revision of the manuscript for important intellectual content: Teesson, Back, Brady, Baker, Hopwood, Sannibale, Barrett, Merz, Rosenfeld, Ewer. Statistical analysis: Mills, Teesson, Barrett, Rosenfeld, Ewer. Obtained funding: Mills, Teesson, Back, Baker, Hopwood, Sannibale. Administrative, technical, or material support: Teesson, Brady, Hopwood, Barrett, Merz, Rosenfeld, Ewer. Study supervision: Mills, Teesson, Brady, Baker. Conflict of Interest Disclosures: All authors have completed and submitted the ICMJE Form for Disclosure of Potential Conflicts of Interest. Dr Mills reported that her institution receives funding for her salary from the National Health and Medical Research Council and reported receiving payment for providing lectures for the Richmond Fellowship of New South Wales; receiving payment for the development of educational presentations for the University of New South Wales, the Alcohol Tobacco and Other Drug Association ACT, and the New South Wales Institute of Psychiatry; receiving funding from the Alcohol, Tobacco and Other Drugs Council of Tasmania to present at a symposium; and receiving payment from the Cancer Council of New South Wales to conduct an ethics review. Dr Back reported that her institution received funding from the Australian-American Fulbright Commission to support travel to meetings for this study and other purposes and reported serving as a consultant for California State University and receiving payment for lectures and travel expenses from the National Institute on Drug Abuse. Dr Barrett reported receiving funding from the University of New South Wales for the development of educational presentations and travel expenses. No other authors reported disclosures. Funding/Support: This study was funded by Australian National Health and Medical Research Council (NHMRC) project grant Role of the Sponsor: The NHMRC had no role in the design and conduct of the study; the collection, management, analysis, and interpretation of the data; or the preparation, review, or approval of the manuscript. Online-Only Material: etables 1-3 and the efigure are available at Additional Contributions: We thank Kim Felmingham, PhD, and Catherine Cahill, PhD (Trauma Stress Clinic, University of New South Wales, Sydney, New South Wales, Australia), for providing clinical supervision. Drs Felmingham and Cahill were remunerated for their contributions. REFERENCES 1. Foa EB, Keane TM, Friedman MJ, Cohen JA. Effective Treatments for PTSD: Practice Guidelines From the International Society for Traumatic Stress Studies. 2nd ed. New York, NY: Guilford Press; Ballenger JC, Davidson JRT, Lecrubier Y, et al. Consensus statement on posttraumatic stress disorder from the International Consensus Group on Depression and Anxiety. J Clin Psychiatry. 2000;61(suppl 5): Institute of Medicine. Treatment of Posttraumatic Stress Disorder: An Assessment of the Evidence. Washington, DC: National Academies Press; Cahill SP, Rothbaum BO, Resick PA, Follette VM. Cognitive-Behavioral Therapy for Adults: Effective Treatments for PTSD: Practice Guidelines From the International Society for Traumatic Stress Studies. 2nd ed. New York, NY: Guilford Press; 2009: Mills KL, Teesson M, Ross J, Peters L. Trauma, PTSD, and substance use disorders: findings from the Australian National Survey of Mental Health and Well-Being. Am J Psychiatry. 2006;163(4): Dore G, Mills K, Murray R, Teesson M, Farrugia P. Post-traumatic stress disorder, depression and suicidality in inpatients with substance use disorders. Drug Alcohol Rev. 2012;31(3): Krystal JH, Rosenheck RA, Cramer JA, et al; Veterans Affairs Cooperative Study No. 504 Group. Adjunctive risperidone treatment for antidepressantresistant symptoms of chronic military service related PTSD: a randomized trial. JAMA. 2011;306(5): Pietrzak RH, Goldstein RB, Southwick SM, Grant BF. Prevalence and axis I comorbidity of full and partial posttraumatic stress disorder in the United States: results from wave 2 of the National Epidemiologic Survey on Alcohol and Related Conditions. J Anxiety Disord. 2011;25(3): Pitman RK, Altman B, Greenwald E, et al. Psychiatric complications during flooding therapy for posttraumatic stress disorder. J Clin Psychiatry. 1991; 52(1): Becker CB, Zayfert C, Anderson E. A survey of psychologists attitudes towards and utilization of exposure therapy for PTSD. Behav Res Ther. 2004; 42(3): Bradley R, Greene J, Russ E, Dutra L, Westen D. A multidimensional meta-analysis of psychotherapy for PTSD. Am J Psychiatry. 2005;162(2): Triffleman E. Gender differences in a controlled pilot study of psychosocial treatments in substance dependent patients with post-traumatic stress disorder: design considerations and outcomes. Alcohol Treat Q. 2000;18(3): Brady KT, Dansky BS, Back SE, Foa EB, Carroll KM. Exposure therapy in the treatment of PTSD among cocaine-dependent individuals: preliminary findings. J Subst Abuse Treat. 2001;21(1): Najavits LM, Schmitz M, Gotthardt S, Weiss RD. Seeking Safety plus Exposure Therapy: an outcome study on dual-diagnosis men. J Psychoactive Drugs. 2005;37(4): Blake DD, Weathers FW, Nagy LM, et al. The development of a Clinician-Administered PTSD Scale. J Trauma Stress. 1995;8(1): Kessler RC, Ustün TB. The World Mental Health (WMH) Survey Initiative Version of the World Health Organization (WHO) Composite International Diagnostic Interview (CIDI). Int J Methods Psychiatr Res. 2004;13(2): Darke S, Hall W, Wodak A, Heather N, Ward J. Development and validation of a multi-dimensional instrument for assessing outcome of treatment among opiate users: the Opiate Treatment Index. Br J Addict. 1992;87(5): World Health Organisation. Composite International Diagnostic Interview (CIDI) Core Version 2.1, 12 Month Version. Geneva, Switzerland: World Health Organisation; Beck AT, Steer RA, Brown GK. Manual for the Beck Depression Inventory-II. San Antonio, TX: Psychological Corp; Spielberger CD. Manual for the State-Trait Anxiety Inventory. Palo Alto, CA: Consulting Psychologists Press; Loranger AW, Janca A, Sartorius N. Assessment and Diagnosis of Personality Disorders. Cambridge, United Kingdom: Cambridge University Press; Back SE, Dansky BS, Carroll KM, Foa EB, Brady KT. Exposure therapy in the treatment of PTSD among cocaine-dependent individuals: description of procedures. J Subst Abuse Treat. 2001;21(1): Carroll KM. A Cognitive-Behavioral Approach: Treating Cocaine Addiction. Rockville, MD: US Dept of Health and Human Services, National Institute on Drug Abuse; Foa EB, Rothbaum BO. Treating the Trauma of Rape: Cognitive-Behavioral Therapy for PTSD. New York, NY: Guilford Press; Baker A, Kay-Lambkin F, Lee NK, Claire M, Jenner L. A Brief Cognitive Behavioural Intervention for Regular Amphetamine Users. Canberra: Australian Government Department of Health and Ageing; Weathers FW, Keane TM, Davidson JRT. Clinicianadministered PTSD scale: a review of the first ten years of research. Depress Anxiety. 2001;13(3): McBride O, Adamson G, Bunting BP, McCann S. Assessing the general health of diagnostic orphans using the Short Form Health Survey (SF-12v2): a latent variable modelling approach. Alcohol Alcohol. 2009;44(1): Preuss UW, Schuckit MA, Smith TL, et al. Predictors and correlates of suicide attempts over 5 years in 1,237 alcohol-dependent men and women. Am J Psychiatry. 2003;160(1): Schafer JL, Graham JW. Missing data: our view of the state of the art. Psychol Methods. 2002; 7(2): Zhang P. Multiple imputation: theory and method. Int Stat Rev. 2003;71(3): Back SE, Brady KT, Sonne SC, Verduin ML. Symptom improvement in co-occurring PTSD and alcohol dependence. J Nerv Ment Dis. 2006;194(9): Hien DA, Jiang H, Campbell ANC, et al. Do treatment improvements in PTSD severity affect substance use outcomes? a secondary analysis from a randomized clinical trial in NIDA s Clinical Trials Network. Am J Psychiatry. 2010;167(1): Beynon CM, Bellis MA, McVeigh J. Trends in drop out, drug free discharge and rates of re-presentation: a retrospective cohort study of drug treatment clients in the North West of England. BMC Public Health. 2006;6: Tate SR, Mrnak-Meyer J, Shriver CL, Atkinson JH, Robinson SK, Brown SA. Predictors of treatment retention for substance-dependent adults with cooccurring depression. Am J Addict. 2011;20(4): Craske MG, Stein MB, Sullivan G, et al. Disorderspecific impact of coordinated anxiety learning and management treatment for anxiety disorders in primary care. Arch Gen Psychiatry. 2011;68(4): Mills KL, Lynskey M, Teesson M, Ross J, Darke S. Post-traumatic stress disorder among people with heroin dependence in the Australian Treatment Outcome Study (ATOS): prevalence and correlates. Drug Alcohol Depend. 2005;77(3): Darke S. Self-report among injecting drug users: a review. Drug Alcohol Depend. 1998;51(3): Sherman MF, Bigelow GE. Validity of patients selfreported drug use as a function of treatment status. Drug Alcohol Depend. 1992;30(1): Calhoun PS, Sampson WS, Bosworth HB, et al. Drug use and validity of substance use self-reports in veterans seeking help for posttraumatic stress disorder. J Consult Clin Psychol. 2000;68(5): Weiss RD, Najavits LM, Greenfield SF, Soto JA, Shaw SR, Wyner D. Validity of substance use selfreports in dually diagnosed outpatients. Am J Psychiatry. 1998;155(1): American Medical Association. All rights reserved. JAMA, August 15, 2012 Vol 308, No
Therapeutic approaches to the treatment of post traumatic stress disorder and substance use in adults and adolescents
 Therapeutic approaches to the treatment of post traumatic stress disorder and substance use in adults and adolescents Natalie Peach 1, Katherine Mills 1, Emma Barrett 1, Vanessa Cobham 2, Joanne Ross 1,
Therapeutic approaches to the treatment of post traumatic stress disorder and substance use in adults and adolescents Natalie Peach 1, Katherine Mills 1, Emma Barrett 1, Vanessa Cobham 2, Joanne Ross 1,
Katherine Mills, Michael Lynskey, Maree Teesson, Joanne Ross & Shane Darke
 Katherine Mills, Michael Lynskey, Maree Teesson, Joanne Ross & Shane Darke Prevalence and correlates of Post Traumatic Stress Disorder (PTSD) among people with heroin dependence: Findings from the Australian
Katherine Mills, Michael Lynskey, Maree Teesson, Joanne Ross & Shane Darke Prevalence and correlates of Post Traumatic Stress Disorder (PTSD) among people with heroin dependence: Findings from the Australian
PTSD, Addictions and Veterans
 PTSD, Addictions and Veterans Malcolm Battersby Head, Discipline of Psychiatry Centre for Anxiety and Related Disorders Master of Mental Health Sciences Post Traumatic Stress Disorder and comorbidities
PTSD, Addictions and Veterans Malcolm Battersby Head, Discipline of Psychiatry Centre for Anxiety and Related Disorders Master of Mental Health Sciences Post Traumatic Stress Disorder and comorbidities
The influence of depression on treatment for methamphetamine use
 SUPPLEMENT The influence of depression on treatment for methamphetamine use Frances J Kay-Lambkin, Amanda L Baker, Nicole M Lee, Linda Jenner and Terry J Lewin Methamphetamine use is common internationally,
SUPPLEMENT The influence of depression on treatment for methamphetamine use Frances J Kay-Lambkin, Amanda L Baker, Nicole M Lee, Linda Jenner and Terry J Lewin Methamphetamine use is common internationally,
Secondary traumatic stress among alcohol and other drug workers. Philippa Ewer, Katherine Mills, Claudia Sannibale, Maree Teesson, Ann Roche
 Secondary traumatic stress among alcohol and other drug workers Philippa Ewer, Katherine Mills, Claudia Sannibale, Maree Teesson, Ann Roche Trauma and PTSD among clients AOD clients Dore et al. (2012).
Secondary traumatic stress among alcohol and other drug workers Philippa Ewer, Katherine Mills, Claudia Sannibale, Maree Teesson, Ann Roche Trauma and PTSD among clients AOD clients Dore et al. (2012).
Comorbidity With Substance Abuse P a g e 1
 Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients. Centerstone Research Institute
 American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients Centerstone Research Institute 2018 1 AAC Outcomes Study: Long-Term Outcomes Executive Summary
American Addiction Centers Outcomes Study Long-Term Outcomes Among Residential Addiction Treatment Clients Centerstone Research Institute 2018 1 AAC Outcomes Study: Long-Term Outcomes Executive Summary
IDDT Fidelity Action Planning Guidelines
 1a. Multidisciplinary Team IDDT Fidelity Action Planning Guidelines Definition: All clients targeted for IDDT receive care from a multidisciplinary team. A multi-disciplinary team consists of, in addition
1a. Multidisciplinary Team IDDT Fidelity Action Planning Guidelines Definition: All clients targeted for IDDT receive care from a multidisciplinary team. A multi-disciplinary team consists of, in addition
Centerstone Research Institute
 American Addiction Centers Outcomes Study 12 month post discharge outcomes among a randomly selected sample of residential addiction treatment clients Centerstone Research Institute 2018 1 AAC Outcomes
American Addiction Centers Outcomes Study 12 month post discharge outcomes among a randomly selected sample of residential addiction treatment clients Centerstone Research Institute 2018 1 AAC Outcomes
Acute Stabilization In A Trauma Program: A Pilot Study. Colin A. Ross, MD. Sean Burns, MA, LLP
 In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
We acknowledge the traditional custodians of the land on which we meet today and pay respect to Elders past, present and emerging.
 We acknowledge the traditional custodians of the land on which we meet today and pay respect to Elders past, present and emerging. We also extend that respect to other Aboriginal and/or Torres Strait Islanders
We acknowledge the traditional custodians of the land on which we meet today and pay respect to Elders past, present and emerging. We also extend that respect to other Aboriginal and/or Torres Strait Islanders
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
CO-OCCURRING SUBSTANCE USE AND PSYCHIATRIC DISORDERS INTEGRATING COMBINED THERAPIES (ICT) FOR CO-OCCURRING SUBSTANCE USE AND PSYCHIATRIC DISORDERS
 INTEGRATING COMBINED THERAPIES (ICT) FOR CO-OCCURRING SUBSTANCE USE AND PSYCHIATRIC DISORDERS 2009 MARRCH CONFERENCE 22 October 2009 CO-OCCURRING SUBSTANCE USE AND PSYCHIATRIC DISORDERS 1. Common in the
INTEGRATING COMBINED THERAPIES (ICT) FOR CO-OCCURRING SUBSTANCE USE AND PSYCHIATRIC DISORDERS 2009 MARRCH CONFERENCE 22 October 2009 CO-OCCURRING SUBSTANCE USE AND PSYCHIATRIC DISORDERS 1. Common in the
BEST in MH clinical question-answering service
 1 BEST.awp.nhs.uk Best Evidence Summaries of Topics in Mental Healthcare BEST in MH clinical question-answering service Question In adults who have suffered an injury/accident, which group interventions
1 BEST.awp.nhs.uk Best Evidence Summaries of Topics in Mental Healthcare BEST in MH clinical question-answering service Question In adults who have suffered an injury/accident, which group interventions
Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence
 Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
To Reduce or Abstain? Substance Use Goals in the Treatment of Veterans With Substance Use Disorders and Comorbid PTSD
 The American Journal on Addictions, 24: 578 581, 2015 Copyright American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/ajad.12263 To Reduce or Abstain? Substance
The American Journal on Addictions, 24: 578 581, 2015 Copyright American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/ajad.12263 To Reduce or Abstain? Substance
Description of intervention
 Helping to Overcome PTSD through Empowerment (HOPE) Johnson, D., Zlotnick, C. and Perez, S. (2011) Johnson, D. M., Johnson, N. L., Perez, S. K., Palmieri, P. A., & Zlotnick, C. (2016) Description of Helping
Helping to Overcome PTSD through Empowerment (HOPE) Johnson, D., Zlotnick, C. and Perez, S. (2011) Johnson, D. M., Johnson, N. L., Perez, S. K., Palmieri, P. A., & Zlotnick, C. (2016) Description of Helping
ADVANCED BEHAVIORAL HEALTH, INC. Clinical Level of Care Guidelines
 The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
The Clinical Level of Care Guidelines contained on the following pages have been developed as a guide to assist care managers, physicians and providers in making medical necessity decisions about the least
Models of good practice in drug treatment in Europe. Project group
 Models of good practice in drug treatment in Europe ( moretreat 2006329 ) Project group Hamburg, London, Rome, Stockholm, Vienna, Warsaw, Zurich Project duration: 17 months from April 2006 August 2008
Models of good practice in drug treatment in Europe ( moretreat 2006329 ) Project group Hamburg, London, Rome, Stockholm, Vienna, Warsaw, Zurich Project duration: 17 months from April 2006 August 2008
TITLE: Naltrexone for the Treatment of Alcohol Dependence in Individuals with Co- Dependencies: A Review of the Clinical Effectiveness
 TITLE: Naltrexone for the Treatment of Alcohol Dependence in Individuals with Co- Dependencies: A Review of the Clinical Effectiveness DATE: 08 October 2009 CONTEXT AND POLICY ISSUES: Poly-drug abuse is
TITLE: Naltrexone for the Treatment of Alcohol Dependence in Individuals with Co- Dependencies: A Review of the Clinical Effectiveness DATE: 08 October 2009 CONTEXT AND POLICY ISSUES: Poly-drug abuse is
Referral to Treatment: Utilizing the ASAM Criteria
 Referral to Treatment: Utilizing the ASAM Criteria AOAAM Essentials in Addiction Medicine October 22, 2016 East Lansing, MI Stephen A. Wyatt, DO Medical Director, Addiction Medicine Behavioral Health Service
Referral to Treatment: Utilizing the ASAM Criteria AOAAM Essentials in Addiction Medicine October 22, 2016 East Lansing, MI Stephen A. Wyatt, DO Medical Director, Addiction Medicine Behavioral Health Service
Evidence table for systematic reviews
 Evidence table for systematic reviews Topic: CB use and dependence Reviewer: CMF Abbreviations: y- years Reference Research Parameters Population Outcomes Funding Additional comments Bibliographic reference
Evidence table for systematic reviews Topic: CB use and dependence Reviewer: CMF Abbreviations: y- years Reference Research Parameters Population Outcomes Funding Additional comments Bibliographic reference
The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders
 AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
Kim L. Gratz Department of Psychiatry and Human Behavior University of Mississippi Medical Center (UMMC)
 Efficacy of an Acceptance-based Emotion Regulation Group Therapy for Deliberate Self-Harm among Women with Borderline Personality Pathology: Randomized Controlled Trial and 9-month Follow-up Kim L. Gratz
Efficacy of an Acceptance-based Emotion Regulation Group Therapy for Deliberate Self-Harm among Women with Borderline Personality Pathology: Randomized Controlled Trial and 9-month Follow-up Kim L. Gratz
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION In military veterans, what is the effect of virtual reality exposure therapy (VRE) on posttraumatic stress disorder (PTSD) and depressive symptoms, as
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION In military veterans, what is the effect of virtual reality exposure therapy (VRE) on posttraumatic stress disorder (PTSD) and depressive symptoms, as
FRN Research Report April 2012: Treatment Outcomes for Women at The Canyon
 FRN Research Report April 2012: Treatment Outcomes for Women at The Canyon Background The Canyon Treatment Center treats substance abuse disorders along with mental health issues in Malibu, Calif. The
FRN Research Report April 2012: Treatment Outcomes for Women at The Canyon Background The Canyon Treatment Center treats substance abuse disorders along with mental health issues in Malibu, Calif. The
The Intersection of Post-Traumatic Stress and Substance Use Disorders. Implications for an emerging integrated treatment approach
 The Intersection of Post-Traumatic Stress and Substance Use Disorders Implications for an emerging integrated treatment approach Christal L. Badour, PhD Assistant Professor Department of Psychology Overview
The Intersection of Post-Traumatic Stress and Substance Use Disorders Implications for an emerging integrated treatment approach Christal L. Badour, PhD Assistant Professor Department of Psychology Overview
Mental health among clients of the Sydney Medically Supervised Injecting Centre (MSIC)
 Goodhew et al. Harm Reduction Journal (2016) 13:29 DOI 10.1186/s12954-016-0117-y BRIEF REPORT Mental health among clients of the Sydney Medically Supervised Injecting Centre (MSIC) Mark Goodhew 1*, Allison
Goodhew et al. Harm Reduction Journal (2016) 13:29 DOI 10.1186/s12954-016-0117-y BRIEF REPORT Mental health among clients of the Sydney Medically Supervised Injecting Centre (MSIC) Mark Goodhew 1*, Allison
We also Know INTEGRATED GROUP COGNITIVE BEHAVIORAL THERAPY FOR PATIENTS WITH CONCURRENT DEPRESSIVE AND SUBSTANCE USE DISORDERS
 INTEGRATED GROUP COGNITIVE BEHAVIORAL THERAPY FOR PATIENTS WITH CONCURRENT DEPRESSIVE AND SUBSTANCE USE DISORDERS May 13, 2010 Kasia Galperyn, Ph.D., R. Psych. Kelly Rose, B.A. David Crockford, MD, FRCPC
INTEGRATED GROUP COGNITIVE BEHAVIORAL THERAPY FOR PATIENTS WITH CONCURRENT DEPRESSIVE AND SUBSTANCE USE DISORDERS May 13, 2010 Kasia Galperyn, Ph.D., R. Psych. Kelly Rose, B.A. David Crockford, MD, FRCPC
Workshop I. Dialectical Behaviour Therapy Workshop Saturday March 12 th, About Dialectical Behaviour Therapy
 Workshop I Dialectical Behaviour Therapy Workshop Saturday March 12 th, 2014 About Dialectical Behaviour Therapy Dialectical Behaviour Therapy, or DBT, is an innovative and comprehensive psycho-educational
Workshop I Dialectical Behaviour Therapy Workshop Saturday March 12 th, 2014 About Dialectical Behaviour Therapy Dialectical Behaviour Therapy, or DBT, is an innovative and comprehensive psycho-educational
The Importance of Psychological Treatment and Behavioral Support
 The Importance of Psychological Treatment and Behavioral Support Michael W. Otto, PhD Department of Psychological and Brain Science Boston University Conflicts and Acknowledgements No industry funding
The Importance of Psychological Treatment and Behavioral Support Michael W. Otto, PhD Department of Psychological and Brain Science Boston University Conflicts and Acknowledgements No industry funding
Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE): A Pilot Study in Alcohol-dependent Women
 ORIGINAL RESEARCH Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE): A Pilot Study in Alcohol-dependent Women Anna Persson, MSc, Sudie E. Back, PhD, Therese K. Killeen,
ORIGINAL RESEARCH Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE): A Pilot Study in Alcohol-dependent Women Anna Persson, MSc, Sudie E. Back, PhD, Therese K. Killeen,
MI and CBT to reduce substance use problems and improve mental health and well-being Amanda Baker PhD
 MI and CBT to reduce substance use problems and improve mental health and well-being Amanda Baker PhD Acknowledgments Clinical Psychology /PhD Peter Wilson (Syd Uni) Nick Heather (UNSW) Alex Wodak (UNSW)
MI and CBT to reduce substance use problems and improve mental health and well-being Amanda Baker PhD Acknowledgments Clinical Psychology /PhD Peter Wilson (Syd Uni) Nick Heather (UNSW) Alex Wodak (UNSW)
Healing after Rape Edna B. Foa. Department of Psychiatry University of Pennsylvania
 Healing after Rape Edna B. Foa Department of Psychiatry University of Pennsylvania Outline of Lecture What is a trauma? What are common reactions to trauma? Why some people do not recover? How can we help
Healing after Rape Edna B. Foa Department of Psychiatry University of Pennsylvania Outline of Lecture What is a trauma? What are common reactions to trauma? Why some people do not recover? How can we help
Alberta Alcohol and Drug Abuse Commission. POSITION ON ADDICTION AND MENTAL HEALTH February 2007
 Alberta Alcohol and Drug Abuse Commission POSITION ON ADDICTION AND MENTAL HEALTH POSITION The Alberta Alcohol and Drug Abuse Commission (AADAC) recognizes that among clients with addiction problems, there
Alberta Alcohol and Drug Abuse Commission POSITION ON ADDICTION AND MENTAL HEALTH POSITION The Alberta Alcohol and Drug Abuse Commission (AADAC) recognizes that among clients with addiction problems, there
Intro to Concurrent Disorders
 CSAM-SCAM Fundamentals Intro to Concurrent Disorders Presentation provided by Jennifer Brasch, MD, FRCPC Psychiatrist, Concurrent Disorders Program, St. Joseph s Healthcare There are all kinds of addicts,
CSAM-SCAM Fundamentals Intro to Concurrent Disorders Presentation provided by Jennifer Brasch, MD, FRCPC Psychiatrist, Concurrent Disorders Program, St. Joseph s Healthcare There are all kinds of addicts,
Clinical Guidelines and Procedures for the Use of Naltrexone in the Management of Opioid Dependence Abbreviated Version
 Clinical Guidelines and Procedures for the Use of Naltrexone in the Management of Opioid Dependence Abbreviated Version Clinical Guidelines and Procedures for the Use of Naltrexone in the Management of
Clinical Guidelines and Procedures for the Use of Naltrexone in the Management of Opioid Dependence Abbreviated Version Clinical Guidelines and Procedures for the Use of Naltrexone in the Management of
TITLE: Practice parameters for the assessment and treatment of children and adolescents with posttraumatic stress disorder.
 Brief Summary TITLE: Practice parameters for the assessment and treatment of children and adolescents with posttraumatic stress disorder. SOURCE(S): Practice parameters for the assessment and treatment
Brief Summary TITLE: Practice parameters for the assessment and treatment of children and adolescents with posttraumatic stress disorder. SOURCE(S): Practice parameters for the assessment and treatment
PTSD and Other Invisible Wounds affecting our Service Members and Veterans. Alan Peterson, PhD, ABPP
 PTSD and Other Invisible Wounds affecting our Service Members and Veterans Alan Peterson, PhD, ABPP 1 Alan Peterson, PhD, ABPP Retired USAF Lt Col Clinical Health Psychologist Former Chair, Department
PTSD and Other Invisible Wounds affecting our Service Members and Veterans Alan Peterson, PhD, ABPP 1 Alan Peterson, PhD, ABPP Retired USAF Lt Col Clinical Health Psychologist Former Chair, Department
A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer
 A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer CARLOS BLANCO, M.D., Ph.D.* JOHN C. MARKOWITZ, M.D.* DAWN L. HERSHMAN, M.D., M.S.# JON A. LEVENSON, M.D.* SHUAI WANG,
A Pilot Study of Interpersonal Psychotherapy for Depressed Women with Breast Cancer CARLOS BLANCO, M.D., Ph.D.* JOHN C. MARKOWITZ, M.D.* DAWN L. HERSHMAN, M.D., M.S.# JON A. LEVENSON, M.D.* SHUAI WANG,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE. Personality Disorder: the clinical management of borderline personality disorder
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Personality Disorder: the clinical management of borderline personality disorder 1.1 Short title Borderline personality disorder
Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes
 MILITARY MEDICINE, 178, 12:1328, 2013 Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes Meaghan O Donnell, PhD*; Tracey Varker, PhD*; Desmond Perry,
MILITARY MEDICINE, 178, 12:1328, 2013 Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes Meaghan O Donnell, PhD*; Tracey Varker, PhD*; Desmond Perry,
The Role of Social Identity and Support in Recovery from Alcohol and Drug Dependence Dr Genevieve Dingle and Claire Stark School of Psychology,
 The Role of Social Identity and Support in Recovery from Alcohol and Drug Dependence Dr Genevieve Dingle and Claire Stark School of Psychology, University of QLD A therapeutic community is a treatment
The Role of Social Identity and Support in Recovery from Alcohol and Drug Dependence Dr Genevieve Dingle and Claire Stark School of Psychology, University of QLD A therapeutic community is a treatment
CHAPTER 9.1. Summary
 CHAPTER 9.1 Summary 174 TRAUMA-FOCUSED TREATMENT IN PSYCHOSIS Treating PTSD in psychosis The main objective of this thesis was to test the effectiveness and safety of evidence-based trauma-focused treatments
CHAPTER 9.1 Summary 174 TRAUMA-FOCUSED TREATMENT IN PSYCHOSIS Treating PTSD in psychosis The main objective of this thesis was to test the effectiveness and safety of evidence-based trauma-focused treatments
Calculating clinically significant change: Applications of the Clinical Global Impressions (CGI) Scale to evaluate client outcomes in private practice
 University of Wollongong Research Online Faculty of Health and Behavioural Sciences - Papers (Archive) Faculty of Science, Medicine and Health 2010 Calculating clinically significant change: Applications
University of Wollongong Research Online Faculty of Health and Behavioural Sciences - Papers (Archive) Faculty of Science, Medicine and Health 2010 Calculating clinically significant change: Applications
CHARACTERISTICS OF ADMISSIONS TO RESIDENTIAL DRUG TREATMENT AGENCIES IN NEW SOUTH WALES, : ALCOHOL PROBLEMS
 CHARACTERISTICS OF ADMISSIONS TO RESIDENTIAL DRUG TREATMENT AGENCIES IN NEW SOUTH WALES, 1988-1992: ALCOHOL PROBLEMS Shane Darke 1, Margaret Kelahar 1, Wayne Hall 1 & Bruce Flaherty 2 1 National Drug and
CHARACTERISTICS OF ADMISSIONS TO RESIDENTIAL DRUG TREATMENT AGENCIES IN NEW SOUTH WALES, 1988-1992: ALCOHOL PROBLEMS Shane Darke 1, Margaret Kelahar 1, Wayne Hall 1 & Bruce Flaherty 2 1 National Drug and
Setting The setting was secondary care. The economic study was carried out in the UK.
 The cost-effectiveness of cognitive behavior therapy for borderline personality disorder: results from the BOSCOT trial Palmer S, Davidson K, Tyrer P, Gumley A, Tata P, Norrie J, Murray H, Seivewright
The cost-effectiveness of cognitive behavior therapy for borderline personality disorder: results from the BOSCOT trial Palmer S, Davidson K, Tyrer P, Gumley A, Tata P, Norrie J, Murray H, Seivewright
In 2008, an estimated 282,000 persons
 National Survey of Substance Abuse Treatment Services The N-SSATS Report January 28, 2010 Similarities and Differences in Opioid Treatment Programs that Provide Methadone Maintenance or Buprenorphine Maintenance
National Survey of Substance Abuse Treatment Services The N-SSATS Report January 28, 2010 Similarities and Differences in Opioid Treatment Programs that Provide Methadone Maintenance or Buprenorphine Maintenance
SUBSTANCE USE DISORDER IN ADOLESCENT POPULATION
 Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences SUBSTANCE USE DISORDER IN ADOLESCENT POPULATION ANNABELLE SIMPSON, MD UNIVERSITY OF WASHINGTON GENERAL DISCLOSURES
Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences SUBSTANCE USE DISORDER IN ADOLESCENT POPULATION ANNABELLE SIMPSON, MD UNIVERSITY OF WASHINGTON GENERAL DISCLOSURES
Dynamic Deconstructive Psychotherapy
 This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
This program description was created for SAMHSA s National Registry for Evidence-based Programs and Practices (NREPP). Please note that SAMHSA has discontinued the NREPP program and these program descriptions
RECOMMENDATIONS FOR HEALTH CARE PROVIDERS
 Ending Addiction Changes Everything RECOMMENDATIONS FOR HEALTH CARE PROVIDERS CRITICAL ADDICTION PREVENTION, TREATMENT AND MANAGEMENT SERVICES TO INCLUDE IN ROUTINE HEALTH CARE PRACTICE JULY 2013 In the
Ending Addiction Changes Everything RECOMMENDATIONS FOR HEALTH CARE PROVIDERS CRITICAL ADDICTION PREVENTION, TREATMENT AND MANAGEMENT SERVICES TO INCLUDE IN ROUTINE HEALTH CARE PRACTICE JULY 2013 In the
Dialectical Behaviour Therapy in an Outpatient Drug and Alcohol Setting
 Dialectical Behaviour Therapy in an Outpatient Drug and Alcohol Setting Distinguishing features of DBT Implementing DBT within Drug Health Services RPAH Case Study Background to DBT Developed in early
Dialectical Behaviour Therapy in an Outpatient Drug and Alcohol Setting Distinguishing features of DBT Implementing DBT within Drug Health Services RPAH Case Study Background to DBT Developed in early
Exploring the connection between early trauma and later negative life events among Cork Simon service users.
 Adverse Childhood Experiences ACEs at Cork Simon: Exploring the connection between early trauma and later negative life events among Cork Simon service users. Extracted and elaborated information from
Adverse Childhood Experiences ACEs at Cork Simon: Exploring the connection between early trauma and later negative life events among Cork Simon service users. Extracted and elaborated information from
Manual Supplement. Posttraumatic Stress Disorder Checklist (PCL)
 Manual Supplement V OLUME 1, I SSUE 1 N OVEMBER 18, 2014 Posttraumatic Stress Disorder Checklist (PCL) The Posttraumatic Stress Disorder Checklist (PCL) is one of the most frequently used standardized
Manual Supplement V OLUME 1, I SSUE 1 N OVEMBER 18, 2014 Posttraumatic Stress Disorder Checklist (PCL) The Posttraumatic Stress Disorder Checklist (PCL) is one of the most frequently used standardized
Implementing Dialectical Behaviour Therapy (DBT) Skills training on a male low secure ward
 Implementing Dialectical Behaviour Therapy (DBT) Skills training on a male low secure ward Dr Louise Roberts (Lead Clinical Psychologist) Viktoria Nagy (Assistant Psychologist) Robin Pinto Unit 12.06.2018
Implementing Dialectical Behaviour Therapy (DBT) Skills training on a male low secure ward Dr Louise Roberts (Lead Clinical Psychologist) Viktoria Nagy (Assistant Psychologist) Robin Pinto Unit 12.06.2018
Early Life Trauma and Sensitivity to Current Life Stressors in Individuals With and Without Cocaine Dependence
 The American Journal of Drug and Alcohol Abuse, 34: 389 396, 2008 Copyright Informa Healthcare USA, Inc. ISSN: 0095-2990 print / 1097-9891 online DOI: 10.1080/00952990802122614 Early Life Trauma and Sensitivity
The American Journal of Drug and Alcohol Abuse, 34: 389 396, 2008 Copyright Informa Healthcare USA, Inc. ISSN: 0095-2990 print / 1097-9891 online DOI: 10.1080/00952990802122614 Early Life Trauma and Sensitivity
PRIMUM NON NOCERE (FIRST DO NO HARM): SYMPTOM WORSENING AND IMPROVEMENT IN FEMALE ASSAULT VICTIMS AFTER PROLONGED EXPOSURE FOR PTSD
 Research Article DEPRESSION AND ANXIETY 31:412 419 (2014) PRIMUM NON NOCERE (FIRST DO NO HARM): SYMPTOM WORSENING AND IMPROVEMENT IN FEMALE ASSAULT VICTIMS AFTER PROLONGED EXPOSURE FOR PTSD Nuwan Jayawickreme,
Research Article DEPRESSION AND ANXIETY 31:412 419 (2014) PRIMUM NON NOCERE (FIRST DO NO HARM): SYMPTOM WORSENING AND IMPROVEMENT IN FEMALE ASSAULT VICTIMS AFTER PROLONGED EXPOSURE FOR PTSD Nuwan Jayawickreme,
The traditional approach to. Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans
 Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans John A. Schinka, Ph.D. Roger J. Casey, Ph.D., M.S.W. Wesley Kasprow, Ph.D., M.P.H. Robert
Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans John A. Schinka, Ph.D. Roger J. Casey, Ph.D., M.S.W. Wesley Kasprow, Ph.D., M.P.H. Robert
Evidence-Based Practice: Psychosocial Interventions
 Evidence-Based Practice: Psychosocial Interventions Maxine Stitzer, Ph.D. Johns Hopkins Univ SOM NIDA Blending Conference June 3, 2008 Cincinnati, Ohio Talk Outline What is an evidence-based practice?
Evidence-Based Practice: Psychosocial Interventions Maxine Stitzer, Ph.D. Johns Hopkins Univ SOM NIDA Blending Conference June 3, 2008 Cincinnati, Ohio Talk Outline What is an evidence-based practice?
MEDICAL POLICY EFFECTIVE DATE: 04/28/11 REVISED DATE: 04/26/12, 04/25/13, 04/24/14, 06/25/15, 06/22/16, 06/22/17
 MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
MEDICAL POLICY SUBJECT: STANDARD DIALECTICAL BEHAVIOR A nonprofit independent licensee of the BlueCross BlueShield Association PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered,
Cognitive Processing Therapy: Moving Towards Effectiveness Research
 Cognitive Processing Therapy: Moving Towards Effectiveness Research Courtney Chappuis, M.A., Chelsea Gloth, M.A., & Tara Galovski, Ph.D. University of Missouri-St. Louis Overview Brief review of trauma
Cognitive Processing Therapy: Moving Towards Effectiveness Research Courtney Chappuis, M.A., Chelsea Gloth, M.A., & Tara Galovski, Ph.D. University of Missouri-St. Louis Overview Brief review of trauma
Addressing Mental Health in HIV Prevention and Treatment Research Kathleen J. Sikkema, Ph.D.
 Addressing Mental Health in HIV Prevention and Treatment Research Kathleen J. Sikkema, Ph.D. Professor of Psychology and Neuroscience, Global Health, and Psychiatry and Behavioral Sciences Director, Social
Addressing Mental Health in HIV Prevention and Treatment Research Kathleen J. Sikkema, Ph.D. Professor of Psychology and Neuroscience, Global Health, and Psychiatry and Behavioral Sciences Director, Social
Professional Doctorate in Counselling Psychology
 Professional Doctorate in Counselling Psychology Institute of Sport and Human Science Location Study mode Duration Start date Wolverhampton City Campus Full-time 3 year(s) 24/09/2018 Employability Counselling
Professional Doctorate in Counselling Psychology Institute of Sport and Human Science Location Study mode Duration Start date Wolverhampton City Campus Full-time 3 year(s) 24/09/2018 Employability Counselling
Improving Outcomes in Methadone Treatment
 Improving Outcomes in Methadone Treatment Cognitive/Behavioral Treatment Contingency Management Michael J. McCann, MA Matrix Institute on Addictions COMP Symposium September 11, 2007 Overview of Presentation
Improving Outcomes in Methadone Treatment Cognitive/Behavioral Treatment Contingency Management Michael J. McCann, MA Matrix Institute on Addictions COMP Symposium September 11, 2007 Overview of Presentation
Advances in Clinical Research for Prescription Opioid Dependence
 Advances in Clinical Research for Prescription Opioid Dependence Scott E. Provost, M.M., M.S.W. Jennifer Sharpe Potter, Ph.D., M.P.H. Roger D. Weiss, M.D. Objectives To learn about: 1. the prevalence of
Advances in Clinical Research for Prescription Opioid Dependence Scott E. Provost, M.M., M.S.W. Jennifer Sharpe Potter, Ph.D., M.P.H. Roger D. Weiss, M.D. Objectives To learn about: 1. the prevalence of
Behavioral Therapies for Methamphetamine Use
 Behavioral Therapies for Methamphetamine Use Will M. Aklin, PhD National Institute on Drug Abuse Division of Therapeutics and Medical Consequences June 27, 2017 1 Behavioral Therapy Development Program
Behavioral Therapies for Methamphetamine Use Will M. Aklin, PhD National Institute on Drug Abuse Division of Therapeutics and Medical Consequences June 27, 2017 1 Behavioral Therapy Development Program
Why the need for comorbidity guidelines?
 National comorbidity guidelines: Guidelines on the management of co-occurring alcohol and other drug and mental health conditions in alcohol and other drug treatment settings Dr Christina Marel Why the
National comorbidity guidelines: Guidelines on the management of co-occurring alcohol and other drug and mental health conditions in alcohol and other drug treatment settings Dr Christina Marel Why the
Case Series Utilizing Exposure, Relaxation, and Rescripting Therapy: Impact on Nightmares, Sleep Quality, and Psychological Distress
 BEHAVIORAL SLEEP MEDICINE, 3(3), 151 157 Copyright 2005, Lawrence Erlbaum Associates, Inc. Case Series Utilizing Exposure, Relaxation, and Rescripting Therapy: Impact on Nightmares, Sleep Quality, and
BEHAVIORAL SLEEP MEDICINE, 3(3), 151 157 Copyright 2005, Lawrence Erlbaum Associates, Inc. Case Series Utilizing Exposure, Relaxation, and Rescripting Therapy: Impact on Nightmares, Sleep Quality, and
CADTH HEALTH TECHNOLOGY ASSESSMENT Cognitive Processing Therapy for Post-traumatic Stress Disorder: A Systematic Review and Meta-analysis
 CADTH HEALTH TECHNOLOGY ASSESSMENT Cognitive Processing Therapy for Post-traumatic Stress Disorder: A Systematic Review and Meta-analysis Product Line: Health Technology Assessment Issue Number: 141 Publication
CADTH HEALTH TECHNOLOGY ASSESSMENT Cognitive Processing Therapy for Post-traumatic Stress Disorder: A Systematic Review and Meta-analysis Product Line: Health Technology Assessment Issue Number: 141 Publication
Everything You Always Wanted to Know about PTSD and Substance Abuse, But Were Afraid to Ask: Now You Can!
 Everything You Always Wanted to Know about PTSD and Substance Abuse, But Were Afraid to Ask: Now You Can! Brian L. Meyer, Ph.D. Interim Associate Chief, Mental Health Clinical Services McGuire VA Medical
Everything You Always Wanted to Know about PTSD and Substance Abuse, But Were Afraid to Ask: Now You Can! Brian L. Meyer, Ph.D. Interim Associate Chief, Mental Health Clinical Services McGuire VA Medical
Medication Assisted Treatment. Karen Drexler, MD National Mental Health Program Director-Substance Use Disorders Department of Veterans Affairs
 Medication Assisted Treatment Karen Drexler, MD National Mental Health Program Director-Substance Use Disorders Department of Veterans Affairs Disclosures Employed by the Department of Veterans Affairs
Medication Assisted Treatment Karen Drexler, MD National Mental Health Program Director-Substance Use Disorders Department of Veterans Affairs Disclosures Employed by the Department of Veterans Affairs
A healthy lifestyles approach to co-existing mental health and substance use problems Amanda Baker PhD
 A healthy lifestyles approach to co-existing mental health and substance use problems Amanda Baker PhD Outline 2 Context Early studies addressing co-existing problems Depression and AOD use Smoking in
A healthy lifestyles approach to co-existing mental health and substance use problems Amanda Baker PhD Outline 2 Context Early studies addressing co-existing problems Depression and AOD use Smoking in
POLYSUBSTANCE USE IN THE TREATMENT OF OPIOID USE DISORDER WITH BUPRENORPHINE
 Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences POLYSUBSTANCE USE IN THE TREATMENT OF OPIOID USE DISORDER WITH BUPRENORPHINE MARK DUNCAN, MD November 8, 2018 SPEAKER
Psychiatry and Addictions Case Conference UW Medicine Psychiatry and Behavioral Sciences POLYSUBSTANCE USE IN THE TREATMENT OF OPIOID USE DISORDER WITH BUPRENORPHINE MARK DUNCAN, MD November 8, 2018 SPEAKER
The age of feeling in-between : Factors that influence emerging adult outcomes during and after residential substance use disorder treatment
 The age of feeling in-between : Factors that influence emerging adult outcomes during and after residential substance use disorder treatment Brandon G. Bergman, PhD Associate Director & Research Scientist,
The age of feeling in-between : Factors that influence emerging adult outcomes during and after residential substance use disorder treatment Brandon G. Bergman, PhD Associate Director & Research Scientist,
Metacognitive therapy for generalized anxiety disorder: An open trial
 Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Journal of Behavior Therapy and Experimental Psychiatry 37 (2006) 206 212 www.elsevier.com/locate/jbtep Metacognitive therapy for generalized anxiety disorder: An open trial Adrian Wells a,, Paul King
Supplementary Online Content
 Supplementary Online Content Saitz R, Palfai TPA, Cheng DM, et al. Screening and brief intervention for drug use in primary care: the ASPIRE randomized clinical trial. JAMA. doi:10.1001/jama.2012.9630.
Supplementary Online Content Saitz R, Palfai TPA, Cheng DM, et al. Screening and brief intervention for drug use in primary care: the ASPIRE randomized clinical trial. JAMA. doi:10.1001/jama.2012.9630.
CANDIS. A Marijuana Treatment Program for Youth and Adults SCOPE AND SEQUENCE. An Evidence-Based Program from
 A Marijuana Treatment Program for Youth and Adults SCOPE AND SEQUENCE An Evidence-Based Program from For more information about this program, visit hazelden.org/bookstore or call 800-328-9000. Introduction
A Marijuana Treatment Program for Youth and Adults SCOPE AND SEQUENCE An Evidence-Based Program from For more information about this program, visit hazelden.org/bookstore or call 800-328-9000. Introduction
East-West Research. Samples of Journal Abstracts
 East-West Research Samples of Journal Abstracts # 1 Sapir-Weise, R., Berglund, M., Frank, A., and Kristenson, H. (1999) Acupuncture in Alcoholism Treatment: A Randomized Out-Patient Study. Alcohol & Alcoholism
East-West Research Samples of Journal Abstracts # 1 Sapir-Weise, R., Berglund, M., Frank, A., and Kristenson, H. (1999) Acupuncture in Alcoholism Treatment: A Randomized Out-Patient Study. Alcohol & Alcoholism
Difference Between Men and Women in Drug Use Disorders
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550056 Volume 3, Issue 1 Research Article Difference Between Men and Women in Drug Use Disorders Clairmont Griffith, Bernice La France*
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550056 Volume 3, Issue 1 Research Article Difference Between Men and Women in Drug Use Disorders Clairmont Griffith, Bernice La France*
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care
 Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Obsessive-Compulsive Disorder Clinical Practice Guideline Summary for Primary Care CLINICAL ASSESSMENT AND DIAGNOSIS (ADULTS) Obsessive-Compulsive Disorder (OCD) is categorized by recurrent obsessions,
Primary Health Networks
 Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Primary Health Networks Drug and Alcohol Treatment Activity Work Plan 2016-17 to 2018-19 Hunter New England & Central Coast Please note: This Activity Work Plan was developed in response to the HNECC PHN
Trigger. Myths About the Use of Medication in Recovery BUPRENORPHINE TREATMENT: A TRAINING FOR MULTIDISCIPLINARY ADDICTION PROFESSIONALS
 BUPRENORPHINE TREATMENT: A TRAINING FOR MULTIDISCIPLINARY ADDICTION PROFESSIONALS Module VI Counseling Buprenorphine Patients Myths About the Use of Medication in Recovery! Patients are still addicted!
BUPRENORPHINE TREATMENT: A TRAINING FOR MULTIDISCIPLINARY ADDICTION PROFESSIONALS Module VI Counseling Buprenorphine Patients Myths About the Use of Medication in Recovery! Patients are still addicted!
10 INDEX Acknowledgements, i
 INDEX 10 INDEX Acknowledgements, i Acute Care, Admissions to, 3.83 Discharge Planning, 3.86 Involuntary Admission Criteria, 3.84 List of Designated Provincial and Regional Mental Health Facilities, 3.83
INDEX 10 INDEX Acknowledgements, i Acute Care, Admissions to, 3.83 Discharge Planning, 3.86 Involuntary Admission Criteria, 3.84 List of Designated Provincial and Regional Mental Health Facilities, 3.83
Abnormal Respiratory Physiology and Capnometry Guided Respiratory Intervention for Anxiety, Panic, and PTSD
 Abnormal Respiratory Physiology and Capnometry Guided Respiratory Intervention for Anxiety, Panic, and PTSD Saturday, April 7: 3:30 PM - 5:00 PM 336R Symposium Credits: 1.5 Anxiety disorder, panic disorder
Abnormal Respiratory Physiology and Capnometry Guided Respiratory Intervention for Anxiety, Panic, and PTSD Saturday, April 7: 3:30 PM - 5:00 PM 336R Symposium Credits: 1.5 Anxiety disorder, panic disorder
HA Corporate Scholarship Program:
 HA Corporate Scholarship Program: Substance Abuse Service in Psychiatry Ronnie Pao 02-10-10 The Maudsley Hospital Marina House Community Drug & Alcohol Team London Borough of Southwark Provides a Tier
HA Corporate Scholarship Program: Substance Abuse Service in Psychiatry Ronnie Pao 02-10-10 The Maudsley Hospital Marina House Community Drug & Alcohol Team London Borough of Southwark Provides a Tier
The Practitioner Scholar: Journal of Counseling and Professional Psychology 1 Volume 5, 2016
 The Practitioner Scholar: Journal of Counseling and Professional Psychology 1 Assessing the Effectiveness of EMDR in the Treatment of Sexual Trauma Shanika Paylor North Carolina Central University and
The Practitioner Scholar: Journal of Counseling and Professional Psychology 1 Assessing the Effectiveness of EMDR in the Treatment of Sexual Trauma Shanika Paylor North Carolina Central University and
General Principles for the Use of Pharmacological Agents for Co- Occurring Disorders
 General Principles for the Use of Pharmacological Agents for Co- Occurring Disorders Individuals with co-occurring mental and substance use disorders (COD) are common in behavioral and primary health settings
General Principles for the Use of Pharmacological Agents for Co- Occurring Disorders Individuals with co-occurring mental and substance use disorders (COD) are common in behavioral and primary health settings
Behavioral Self-management in an Inpatient Headache Treatment Unit: Increasing Adherence and Relationship to Changes in Affective Distress
 Behavioral Self-management in an Inpatient Headache Treatment Unit: Increasing Adherence and Relationship to Changes in Affective Distress F. Hoodin, PhD; B.J. Brines, PhD; A.E. Lake III, PhD; J. Wilson,
Behavioral Self-management in an Inpatient Headache Treatment Unit: Increasing Adherence and Relationship to Changes in Affective Distress F. Hoodin, PhD; B.J. Brines, PhD; A.E. Lake III, PhD; J. Wilson,
Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study
 Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
Cognitive Behaviour Therapy Vol 39, No 1, pp. 24 27, 2010 Cognitive Behavioral Therapy Plus Motivational Interviewing Improves Outcome for Pediatric Obsessive Compulsive Disorder: A Preliminary Study Lisa
Philadelphia College of Osteopathic Medicine. ReAnna Gibbs Philadelphia College of Osteopathic Medicine,
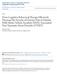 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Cognitive Behavioral Therapy Effectively
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Cognitive Behavioral Therapy Effectively
An event where a person is exposed to: death threatened death actual or threatened serious injury actual or threatened sexual violence
 By Jo Lunn An event where a person is exposed to: death threatened death actual or threatened serious injury actual or threatened sexual violence Characterized by symptoms of: } Intrusion/re experiencing
By Jo Lunn An event where a person is exposed to: death threatened death actual or threatened serious injury actual or threatened sexual violence Characterized by symptoms of: } Intrusion/re experiencing
IMPACT OF INCLUSION/ EXCLUSION CRITERIA ON ENROLLMENT
 2014 CTN Web Seminar Series IMPACT OF INCLUSION/ EXCLUSION CRITERIA ON ENROLLMENT Presented by: Robert Lindblad, MD & Gaurav Sharma, PhD NIDA Clinical Coordinating & Data and Statistics Centers The EMMES
2014 CTN Web Seminar Series IMPACT OF INCLUSION/ EXCLUSION CRITERIA ON ENROLLMENT Presented by: Robert Lindblad, MD & Gaurav Sharma, PhD NIDA Clinical Coordinating & Data and Statistics Centers The EMMES
Tammy Filby ( address: 4 th year undergraduate occupational therapy student, University of Western Sydney
 There is evidence from one RCT that an energy conservation course run by an occupational therapist decreased the impact of fatigue by 7% in persons with multiple sclerosis Prepared by; Tammy Filby (email
There is evidence from one RCT that an energy conservation course run by an occupational therapist decreased the impact of fatigue by 7% in persons with multiple sclerosis Prepared by; Tammy Filby (email
Cannabis Use Disorders: Using Evidenced Based Interventions to Engage Students in Reducing Harmful Cannabis Use or Enter Recovery
 Cannabis Use Disorders: Using Evidenced Based Interventions to Engage Students in Reducing Harmful Cannabis Use or Enter Recovery Lisa Laitman MSEd, LCADC Rutgers, The State University of New Jersey National
Cannabis Use Disorders: Using Evidenced Based Interventions to Engage Students in Reducing Harmful Cannabis Use or Enter Recovery Lisa Laitman MSEd, LCADC Rutgers, The State University of New Jersey National
2/19/18. Today s talk. Today s talk. The Role of Behavioral Interventions in Buprenorphine Treatment of Opioid Use Disorders
 The Role of Behavioral Interventions in Buprenorphine Treatment of Opioid Use Disorders Roger D. Weiss, MD Chief, Division of Alcohol and Drug Abuse, McLean Hospital, Belmont, MA Professor of Psychiatry,
The Role of Behavioral Interventions in Buprenorphine Treatment of Opioid Use Disorders Roger D. Weiss, MD Chief, Division of Alcohol and Drug Abuse, McLean Hospital, Belmont, MA Professor of Psychiatry,
ADHD and Substance Use Disorders: An Intoxicating Combination
 ADHD and Substance Use Disorders: An Intoxicating Combination Timothy E. Wilens, MD Chief, Division of Child & Adolescent Psychiatry Director, Center for Addiction Medicine Massachusetts General Hospital
ADHD and Substance Use Disorders: An Intoxicating Combination Timothy E. Wilens, MD Chief, Division of Child & Adolescent Psychiatry Director, Center for Addiction Medicine Massachusetts General Hospital
Perceived Stigma and Barriers to Mental Health Care Utilization Among OEF-OIF Veterans
 Brief Reports Perceived Stigma and Barriers to Mental Health Care Utilization Among OEF-OIF Veterans Robert H. Pietrzak, Ph.D., M.P.H. Douglas C. Johnson, Ph.D. Marc B. Goldstein, Ph.D. James C. Malley,
Brief Reports Perceived Stigma and Barriers to Mental Health Care Utilization Among OEF-OIF Veterans Robert H. Pietrzak, Ph.D., M.P.H. Douglas C. Johnson, Ph.D. Marc B. Goldstein, Ph.D. James C. Malley,
Referral to the Women s Alcohol and Drug Service (WADS) Procedure
 Procedure Referral to the Women s Alcohol and Drug Service (WADS) Procedure. Purpose The following document describes criteria for the referral to Women s Alcohol and Drug Service (WADS) and how a referral
Procedure Referral to the Women s Alcohol and Drug Service (WADS) Procedure. Purpose The following document describes criteria for the referral to Women s Alcohol and Drug Service (WADS) and how a referral
Developing a new treatment approach to binge eating and weight management. Clinical Psychology Forum, Number 244, April 2013.
 Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Lecture Outline Signs and symptoms in psychiatry Adjustment Disorders Other conditions that may be a focus of clinical attention
 V Codes & Adjustment Disorders Cornelia Pinnell, Ph.D. Argosy University/Phoenix Lecture Outline Signs and symptoms in psychiatry Adjustment Disorders Other conditions that may be a focus of clinical attention
V Codes & Adjustment Disorders Cornelia Pinnell, Ph.D. Argosy University/Phoenix Lecture Outline Signs and symptoms in psychiatry Adjustment Disorders Other conditions that may be a focus of clinical attention
