Endoscopic ultrasound-guided drainage of postoperative intra-abdominal abscesses
|
|
|
- Emily McCarthy
- 6 years ago
- Views:
Transcription
1 Submit a Manuscript: Help Desk: DOI: /wjg.v21.i World J Gastroenterol 2015 March 21; 21(11): ISSN (print) ISSN (online) 2015 Baishideng Publishing Group Inc. All rights reserved. CASE REPORT Endoscopic ultrasound-guided drainage of postoperative intra-abdominal abscesses Koichiro Mandai, Koji Uno, Kenjiro Yasuda Koichiro Mandai, Koji Uno, Kenjiro Yasuda, Department of Gastroenterology, Kyoto Second Red Cross Hospital, Kamigyoku, Kyoto , Japan Author contributions: Mandai K collected the data and wrote the paper; Uno K and Yasuda K revised the paper. Ethics approval: The study was reviewed and approved by the Kyoto Second Red Cross Hospital Institutional Review Board. Informed consent: All study participants provided informed consent prior to study enrollment. Conflict-of-interest: There are no conflicts of interest to declare. Open-Access: This article is an open-access article which was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: licenses/by-nc/4.0/ Correspondence to: Koichiro Mandai, MD, Department of Gastroenterology, Kyoto Second Red Cross Hospital, Haruobi-cho, Kamigyo-ku, Kyoto , Japan. mandai@gmail.com Telephone: Fax: Received: October 4, 2014 Peer-review started: October 6, 2014 First decision: October 29, 2014 Revised: November 12, 2014 Accepted: January 8, 2015 Article in press: January 8, 2015 Published online: March 21, 2015 Abstract Although endoscopic ultrasound (EUS)-guided drainage has become the standard procedure for pancreatic pseudocysts in recent years and is generally regarded as a safe and effective method, there have been few reports of EUS-guided drainage of postoperative intra-abdominal abscesses. Here we report our experience with 4 cases of postoperative intraabdominal abscesses for which EUS-guided drainage was performed between May 2011 and May Distal pancreatectomy had been performed in 3 cases, whereas low anterior resection for rectal cancer was performed in the remaining case. All patients underwent transgastric naso-cystic drainage, which resulted in clinical improvement without complications, even when performed within 4 wk after surgery. On average, the naso-cystic drain was removed 10 d after placement, with no abscess recurrence. Based on these findings, we believe that EUS-guided drainage of postoperative intraabdominal abscesses is a safe and effective method, although further large-scale investigations are required to confirm our findings. Key words: Postoperative intra-abdominal abscess; Endoscopic ultrasonography; endoscopic ultrasoundguided drainage; Transgastric drainage; Naso-cystic drainage The Author(s) Published by Baishideng Publishing Group Inc. All rights reserved. Core tip: There have been few reports of endoscopic ultrasound (EUS)-guided drainage of postoperative intra-abdominal abscesses, although EUS-guided drainage has become the standard procedure for pancreatic pseudocysts in recent years. Here we report our experience with 4 cases. Transgastric naso-cystic drainage was performed for all patients and resulted in clinical improvement without complications, even when performed within 4 wk after surgery. On average, the naso-cystic drain was removed 10 d after placement, with no abscess recurrence. We believe that EUSguided drainage of postoperative intra-abdominal abscesses is a safe and effective method, although further large-scale investigations are required to confirm our findings. Mandai K, Uno K, Yasuda K. Endoscopic ultrasound-guided 3402 March 21, 2015 Volume 21 Issue 11
2 drainage of postoperative intra-abdominal abscesses. World J Gastroenterol 2015; 21(11): Available from: URL: DOI: INTRODUCTION Traditionally, postoperative intra-abdominal abscesses have been managed by percutaneous or surgical drainage. Image-guided percutaneous drainage is reported to be a minimally invasive and effective method [1]. Although endoscopic ultrasound (EUS)-guided drainage for pancreatic pseudocysts is regarded as a safe and effective standard method [2-7], there have been few reports of EUS-guided drainage of postoperative intra-abdominal abscesses [8,9]. Herein, we examined 4 cases of EUS-guided drainage of postoperative intra-abdominal abscesses performed at our institution to evaluate the safety and efficacy of this procedure. CASE REPORT Between May 2011 and May 2014, we experienced 4 cases of postoperative intra-abdominal abscesses for which EUS-guided drainage was performed. The indication of EUS-guided drainage was limited to cases in which adhesion of the abscess and digestive wall was highly suspected on computed tomography (CT). All procedures were performed using a convextype echoendoscope (GE-UC2000P or GF-UCT260; Olympus Medical Systems, Tokyo, Japan). A 19-gauge needle (EchoTip; Cook Medical, Winston-Salem, NC, United States or Expect; Boston Scientific Japan, Tokyo, Japan, or SonoTip; Medi-Globe, Rosenheim, Germany) was used to puncture the abscess. The fluid content was aspirated, and a sample of the aspirate was sent for Gram staining and culture. Subsequently, a small dose of contrast agent was injected, and a inch guidewire (VisiGlide; Olympus Medical Systems) was introduced through the needle and coiled into the abscess under fluoroscopic guidance. In cases of only naso-cystic drainage, the fistula was dilated using a 7-Fr dilation catheter (Soehendra Biliary Dilation Catheter; Cook Medical), and a 6-Fr pigtail nasal biliary catheter (nasal biliary drainage set; Cook Medical) was subsequently placed. In cases of both naso-cystic and internal drainage, the fistula was dilated using a 7-Fr dilation catheter (Soehendra Biliary Dilation Catheter; Cook Medical) and a balloon catheter (Maxforce TTS biliary balloon dilator, 6 mm; Boston Scientific Japan). Next, two inch guidewires (VisiGlide; Olympus Medical Systems) were placed in the abscess using a double lumen catheter (Uneven Double Lumen Catheter; PIOLAX, Kanagawa, Japan), and a 6-Fr pigtail nasal biliary catheter (nasal biliary drainage set; Cook Medical) and 7-Fr double pigtail biliary stent (Zimmon Biliary Stent; Cook Medical) were subsequently placed. The naso-cystic drainage catheter was irrigated once daily with ml of sterile saline in all patients. Characteristics of the 4 cases are summarized in Table 1. Case 1 A 60-year-old woman underwent laparoscopic low anterior resection for rectal cancer. She developed a high fever after surgery, and CT revealed fluid collection around the anastomotic intestine and in the subdiaphragmatic area. We diagnosed this fluid collection as an abscess, and surgical drainage was consequently performed on postoperative day 17. Although the drain was removed and the patient was discharged on postoperative day 44, she was readmitted for high fever on postoperative day 64. CT revealed an encapsulated fluid collection (maximum axis, 61 mm) in the left subdiaphragmatic area close to the fornix of the stomach (Figure 1A). We again diagnosed this fluid collection as an abscess; and, as antibiotic administration did not improve the patient s condition, EUS-guided transgastric drainage was performed, and a 6-Fr pigtail nasal biliary catheter was placed on postoperative day 69 (Figure 1B, C). Gram staining and culture of a sample of the aspirate confirmed extended-spectrum beta lactamase (ESBL)-producing Escherichia coli, Enterococcus, and anaerobic bacteria. Antibiotics were administered until postoperative day 74, and CT on postoperative day 75 showed that the abscess had decreased in size (Figure 1D). The nasal biliary catheter was removed on postoperative day 80. The patient was discharged on postoperative day 99. At the latest follow-up (3 years after discharge), no abscess recurrence was noted. Case 2 A 46-year-old woman underwent distal pancreatectomy for a mucinous cystic neoplasm of the pancreas. She developed high fever on postoperative day 24, and CT revealed irregular fluid collection (maximum axis, 54 mm) around the resection stump of the pancreas close to the gastric wall (Figure 2A). The fluid collection was diagnosed as an abscess; and, accordingly, EUSguided transgastric drainage was performed and a 6-Fr pigtail nasal biliary catheter was placed on postoperative day 26 (Figure 2B-D). Gram staining and culture of a sample of the aspirate confirmed methicillin-resistant Staphylococcus aureus (MRSA). CT on postoperative day 37 showed that the abscess had decreased in size (Figure 2E), and the nasal biliary catheter was removed on the same day. Antibiotics were administered until postoperative day 38. The patient was discharged on postoperative day 40. At the latest follow-up (2 years after discharge), no abscess 3403 March 21, 2015 Volume 21 Issue 11
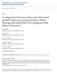
3 Table 1 Patient characteristics Case Age (yr)/ sex Primary disease Surgical procedure Abscess size (mm) Primary treatment for abscess EUS-D route Time to EUS-D (d) EUS-D modality Drainage length (d) Complications/ abscess recurrence 1 60/F Rectal cancer Low anterior rectal resection 2 46/F MCN Distal pancreatectomy 3 74/M PDAC Distal pancreatectomy 4 69/M IPMN Distal pancreatectomy Surgical TG 69 p.o. 6-Fr NB 11 None drainage None TG 26 p.o. 6-Fr NB 11 None None TG 10 p.o. 7-Fr stent 20 None None TG 21 p.o. 6-Fr NB 8 None Percutaneous drainage TG 18 p.o. 7-Fr stent, 6-Fr NB 7-Fr stent: no removal 6-Fr NB: 10 per-cutaneous: 24 None EUS-D: Endoscopic ultrasound-guided drainage; TG: Transgastric; p.o.: Postoperative day; MCN: Mucinous cystic neoplasm; NB: Nasal biliary catheter; PDAC: Pancreatic ductal adenocarcinoma; IPMN: Intraductal papillary mucinous neoplasm. A B C D Figure 1 Case 1. A: Computed tomography (CT) reveals an encapsulated fluid collection in the left subdiaphragmatic area close to the fornix of the stomach; B and C: Fluoroscopy image showing the guidewire inserted into the fluid collection under endoscopic ultrasound (EUS)-guidance and placement of a 6-Fr nasal biliary catheter; D: Six days after EUS-guided drainage, CT reveals that the drain was placed and that the fluid collection decreased. recurrence was observed. Case 3 A 74-year-old man underwent distal pancreatectomy for pancreatic ductal adenocarcinoma. He developed high fever on postoperative day 9, and CT revealed fluid collection (maximum axis, 62 mm) around the resection stump of the pancreas close to the gastric wall (Figure 3A). We diagnosed this fluid collection as an abscess, and EUS-guided transgastric drainage was performed and a 7-Fr double pigtail stent was placed on postoperative day 10 (Figure 3B). Gram staining and culture of a sample of the aspirate confirmed methicillin-susceptible Staphylococcus aureus (MSSA), and antibiotics were administered until postoperative day 15. However, the patient developed high fever after drainage, and CT on postoperative day 17 revealed another fluid collection (maximum axis, 66 mm) at the left side of the previously drained abscess (Figure 3C). EUS-guided transgastric drainage was performed again, and a 6-Fr pigtail nasal biliary catheter was placed on postoperative day 21 (Figure 3D, E). Gram staining and culture of a sample of the aspirate again 3404 March 21, 2015 Volume 21 Issue 11
4 A B C D E Figure 2 Case 2. A: Computed tomography (CT) reveals irregular fluid collection around the resection stump of the pancreas at the dorsal side of the stomach; B: Endoscopic ultrasound (EUS) reveals an irregular and cloudy fluid collection close to the gastric wall; C and D: Fluoroscopy image showing the dilation catheter inserted over the guidewire and placement of a 6-Fr nasal biliary catheter; E: Eleven days after EUS-guided drainage, CT reveals that the fluid collection decreased. confirmed MSSA, and antibiotics were administered until postoperative day 24. CT on postoperative day 28 showed that the abscess had decreased in size (Figure 3F), and the nasal biliary catheter and the 7-Fr double pigtail stent were removed on postoperative days 29 and 30, respectively. The patient was discharged on postoperative day 32. At the latest follow-up (1 year after discharge), no abscess recurrence was observed. Case 4 A 69-year-old man underwent distal pancreatectomy for intraductal papillary mucinous neoplasm of the pancreas. He developed high fever on postoperative day 9, and CT revealed a fluid collection (maximum axis, 70 mm) at the dorsal side of the fornix close to the gastric wall (Figure 4A). We diagnosed this fluid collection as an abscess, and conventional ultrasound- guided percutaneous drainage was performed on the same day. However, the high fever persisted after drainage, and EUS-guided transgastric drainage was consequently performed together with placement of a 7-Fr double pigtail stent and a 6-Fr pigtail nasal biliary catheter on postoperative day 18 (Figure 4B-D). Gram staining and culture of a sample of the aspirate revealed Enterococcus, and antibiotics were administered until postoperative day 21. CT on postoperative day 28 showed that the abscess had decreased in size (Figure 4E), and the nasal biliary catheter and the percutaneous drain were removed on postoperative days 28 and 33, respectively. The 7-Fr double pigtail stent was not removed, and the patient was discharged on postoperative day 36. At the latest follow-up (6 mo after discharge), no abscess recurrence was noted March 21, 2015 Volume 21 Issue 11
5 Mandai K et al. EUS drainage of postoperative abdominal abscesses A B C D E F Figure 3 Case 3. A: Computed tomography (CT) reveals fluid collection around the resection stump of the pancreas; B: Fluoroscopy image showing the dilation catheter inserted over the guidewire; C: Seven days after endoscopic ultrasound (EUS)-guided internal drainage, CT reveals another fluid collection on the left side of the previously drained abscess; D and E: Fluoroscopy image showing the placement of the 7-Fr double pigtail stent and insertion of the dilation catheter into the new abscess. Moreover, a 6-Fr nasal biliary catheter was placed; F: Seven days after EUS-guided naso-cystic drainage, CT reveals that the fluid collection decreased. A B C D E Figure 4 Case 4. A: Computed tomography (CT) reveals fluid collection at the dorsal side of the fornix close to the gastric wall; B: Endoscopic ultrasound (EUS) showing the fluid collection, which was punctured by a 19-gauge needle; C and D: Fluoroscopy image showing placement of the percutaneous drain and insertion of the 6-mm balloon catheter over the guidewire. Both a 7-Fr double pigtail stent and a 6-Fr nasal biliary catheter are placed; E: Ten days after EUS-guided drainage, CT reveals that the fluid collection decreased March 21, 2015 Volume 21 Issue 11
6 DISCUSSION Image-guided percutaneous drainage has been performed for postoperative intra-abdominal abscesses as a minimally invasive method. Azeem et al [10] reported that endoscopic drainage with or without EUS was as effective as percutaneous drainage in patients with pancreatic fluid collection after distal pancreatectomy, and that primary endoscopic drainage may be associated with a shorter hospital stay. Although their report suggested the importance of endoscopic drainage of pancreatic fluid collection after pancreatic resection, to our knowledge, there have been no reports comparing the outcomes of EUS-guided drainage and image-guided percutaneous drainage for the treatment of postoperative intraabdominal abscesses. In this study, EUS-guided transgastric drainage for postoperative intra-abdominal abscesses was performed in all 4 patients and resulted in clinical improvement in all cases. Furthermore, naso-cystic drainage was performed within 4 wk of surgery in 3 of the 4 patients, with no complications in any patient, suggesting that early EUS-guided drainage after surgery is safe. Similarly, Tilara et al [8] also reported that early drainage (within 30 d after surgery) of postoperative pancreatic fluid collections was not associated with an increased risk of complications. In all 4 of our cases, naso-cystic drainage was performed. The naso-cystic drain was removed on day 11 after placement in cases 1 and 2, day 8 in Case 3, and day 10 in Case 4 (mean, day 10 after nasocystic drainage), and there was no recurrence of the abscess after naso-cystic drain removal in any case. Taken together, these outcomes suggest the efficacy of naso-cystic drainage, but further investigations are required to confirm these results and to determine whether naso-cystic drainage alone is effective, as internal drainage and percutaneous drainage were also performed before naso-cystic drainage in Cases 3 and 4, respectively. Furthermore, the necessity of internal drainage stent removal and the appropriate time of stent removal should be investigated in cases of both naso-cystic and internal drainage. Several recent studies of EUS-guided drainage of pancreatic pseudocysts recommend both internal and naso-cystic drain placement by first using the double guidewire technique, followed by naso-cystic drain removal after improvement of infection [3,6] ; however, there is no consensus regarding the optimal drainage method and time for drain removal. Thus, based on our present cases, we believe that EUS-guided drainage of postoperative intra-abdominal abscesses is a safe and effective method; however, further large-scale investigations are required to confirm our findings. COMMENTS Case characteristics The 4 patients (2 male, 2 female) developed high fever after abdominal surgery (pancreatectomy or low anterior resection for rectal cancer). Clinical diagnosis In addition to high fever, all patients had general fatigue. Differential diagnosis Postoperative intra-abdominal fluid collection was performed to diagnose infection. Laboratory diagnosis Gram staining and culture of samples of collected fluid confirmed extendedspectrum beta lactamase-producing Escherichia coli, Enterococcus, and anaerobic bacteria in the first patient, methicillin-resistant Staphylococcus aureus in the second patient, methicillin-susceptible Staphylococcus aureus in the third patient, and Enterococcus in the fourth patient. Imaging diagnosis Computed tomography revealed fluid collection close to the gastric wall in all 4 patients. Pathological diagnosis Pathological examination of the fluid collection was not performed in any of the patients. Treatment All 4 patients underwent endoscopic ultrasound (EUS)-guided transgastric naso-cystic drainage, and in 2 of the 4 patients, internal drainage was also performed. Related reports Earlier reports state that EUS-guided drainage of postoperative peripancreatic fluid collections is safe and effective, and we believe that this case report adds our findings that early EUS-guided transgastric drainage within 4 wk of surgery is also safe and effective. Term explanation Naso-cystic drainage describes a method of external drainage via the nose. Experiences and lessons This case report presents data showing that early EUS-guided drainage within 4 wk of surgery for postoperative intra-abdominal abscesses is safe and effective. Peer-review This is a well-written case report of a novel application of therapeutic EUS. Although 3 of 4 cases death with post-pancreatic surgery fluid collections, the 4th case is the first to report drainage of an abscess by EUS after colorectal surgery. REFERENCES 1 Kassi F, Dohan A, Soyer P, Vicaut E, Boudiaf M, Valleur P, Pocard M. Predictive factors for failure of percutaneous drainage of postoperative abscess after abdominal surgery. Am J Surg 2014; 207: [PMID: DOI: /j.amjsurg ] 2 Lopes CV, Pesenti C, Bories E, Caillol F, Giovannini M. Endoscopic-ultrasound-guided endoscopic transmural drainage of pancreatic pseudocysts and abscesses. Scand J Gastroenterol 2007; 42: [PMID: DOI: / ] 3 Itoi T, Itokawa F, Tsuchiya T, Kawai T, Moriyasu F. EUS-guided pancreatic pseudocyst drainage: simultaneous placement of stents and nasocystic catheter using double-guidewire technique. Dig Endosc 2009; 21 Suppl 1: S53-S56 [PMID: DOI: / j x] 4 Seewald S, Ang TL, Richter H, Teng KY, Zhong Y, Groth S, Omar S, Soehendra N. Long-term results after endoscopic drainage and necrosectomy of symptomatic pancreatic fluid collections. Dig Endosc 2012; 24: [PMID: DOI: / j x] 5 Sadik R, Kalaitzakis E, Thune A, Hansen J, Jönson C. EUS-guided drainage is more successful in pancreatic pseudocysts compared 3407 March 21, 2015 Volume 21 Issue 11
7 with abscesses. World J Gastroenterol 2011; 17: [PMID: DOI: /wjg.v17.i4.499] 6 Kato S, Katanuma A, Maguchi H, Takahashi K, Osanai M, Yane K, Kim T, Kaneko M, Takaki R, Matsumoto K, Matsumori T, Gon K, Tomonari A. Efficacy, Safety, and Long-Term Follow-Up Results of EUS-Guided Transmural Drainage for Pancreatic Pseudocyst. Diagn Ther Endosc 2013; 2013: [PMID: DOI: /2013/924291] 7 Lin H, Zhan XB, Sun SY, Yang XJ, Jin ZD, Zou DW, Li ZS. Stent selection for endoscopic ultrasound-guided drainage of pancreatic fluid collections: a multicenter study in china. Gastroenterol Res Pract 2014; 2014: [PMID: DOI: /2014/193562] 8 Tilara A, Gerdes H, Allen P, Jarnagin W, Kingham P, Fong Y, DeMatteo R, D Angelica M, Schattner M. Endoscopic ultrasoundguided transmural drainage of postoperative pancreatic collections. J Am Coll Surg 2014; 218: [PMID: DOI: / j.jamcollsurg ] 9 Varadarajulu S, Wilcox CM, Christein JD. EUS-guided therapy for management of peripancreatic fluid collections after distal pancreatectomy in 20 consecutive patients. Gastrointest Endosc 2011; 74: [PMID: DOI: / j.gie ] 10 Azeem N, Baron TH, Topazian MD, Zhong N, Fleming CJ, Kendrick ML. Outcomes of endoscopic and percutaneous drainage of pancreatic fluid collections arising after pancreatic tail resection. J Am Coll Surg 2012; 215: [PMID: DOI: / j.jamcollsurg ] P- Reviewer: Chisthi MM, Teshima CW, Yoshida H S- Editor: Ma YJ L- Editor: A E- Editor: Wang CH 3408 March 21, 2015 Volume 21 Issue 11
8 Published by Baishideng Publishing Group Inc 8226 Regency Drive, Pleasanton, CA 94588, USA Telephone: Fax: Help Desk: I S S N Baishideng Publishing Group Inc. All rights reserved.
Tomonari, Akiko; Katanuma, Akio; Ma Author(s)
 Resected tumor seeding in stomach w Titleultrasonography-guided fine needle adenocarcinoma Tomonari, Akiko; Katanuma, Akio; Ma Author(s) Yamazaki, Hajime; Sano, Itsuki; Min Manabu; Ikarashi, Satoshi; Kin,
Resected tumor seeding in stomach w Titleultrasonography-guided fine needle adenocarcinoma Tomonari, Akiko; Katanuma, Akio; Ma Author(s) Yamazaki, Hajime; Sano, Itsuki; Min Manabu; Ikarashi, Satoshi; Kin,
EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice
 CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
CASE REPORT EUS-Guided Transduodenal Biliary Drainage in Unresectable Pancreatic Cancer with Obstructive Jaundice Tiing Leong Ang, Eng Kiong Teo, Kwong Ming Fock Division of Gastroenterology, Department
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
Original Article INTRODUCTION
 Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Original Article A retrospective study evaluating endoscopic ultrasound guided drainage of pancreatic fluid collections using a novel lumen apposing metal stent on an electrocautery enhanced delivery system
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Endoscopic pancreatic necrosectomy in 2017
 Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Endoscopic pancreatic necrosectomy in 2017 Mouen Khashab, MD Associate Professor of Medicine Director of Therapeutic Endoscopy The Johns Hopkins Hospital Revised Atlanta Classification Entity Acute fluid
Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance for Extraluminal Complicated Cysts
 Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
Gastroenterology Research and Practice Volume 2016, Article ID 1249064, 8 pages http://dx.doi.org/10.1155/2016/1249064 Clinical Study Endoscopic Ultrasound-Guided Drainage without Fluoroscopic Guidance
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies. Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels
 PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
PANCREATIC PSEUDOCYSTS: Optimal therapeutic strategies Jacques DEVIERE, MD, PhD Erasme University Hospital Brussels 1. Diagnosis. 2. Multidisciplinary approach. 3. Therapeutic planning. 4. How? 5. Follow-up
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection
 Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Original Article Clinical evaluation of endoscopic ultrasonography-guided drainage using a novel flared-type biflanged metal stent for pancreatic fluid collection Shuntaro Mukai, Takao Itoi, Atsushi Sofuni,
Therapeutic EUS: today & tomorrow Pietro Fusaroli
 Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Therapeutic EUS: today & tomorrow Pietro Fusaroli Gastroenterologia Università di Bologna AUSL di Imola, Castel S. Pietro Terme (BO) Direttore Prof. G. Caletti EUS FNA: CONVEX ARRAY Olympus, Pentax, Toshiba
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica
 Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Title: The endoscopic ultrasound-assisted Rendez-Vous technique for treatment of recurrent pancreatitis due to pancreas divisum and ansa pancreatica Authors: Sergio López-Durán, Celia Zaera, Juan Ángel
Endoscopic Ultrasound-Guided Pancreatic Duct Intervention
 FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
FOCUSED REVIEW SERIES: EUS-Guided Therapeutic Interventions Clin Endosc 2017;50:112-116 https://doi.org/10.5946/ce.2017.046 Print ISSN 2234-2400 On-line ISSN 2234-2443 Open Access Endoscopic Ultrasound-Guided
Performance of novel tissue harmonic echo imaging using endoscopic ultrasound for pancreatic diseases
 E Performance of novel tissue harmonic echo imaging using endoscopic ultrasound for pancreatic diseases Authors Kazuyuki Matsumoto, *, Akio Katanuma, *, Hiroyuki Maguchi, Kuniyuki Takahashi, Manabu Osanai,
E Performance of novel tissue harmonic echo imaging using endoscopic ultrasound for pancreatic diseases Authors Kazuyuki Matsumoto, *, Akio Katanuma, *, Hiroyuki Maguchi, Kuniyuki Takahashi, Manabu Osanai,
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY
 A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
A LEADER IN ADVANCED ENDOSCOPY AND HEPATOBILIARY SURGERY St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center Welcome The St. Peter s Hospital Advanced Endoscopy & Hepatobiliary Center is a leader
PANCREATIC PSEUDOCYSTS. Madhuri Rao MD PGY-5 Kings County Hospital Center
 PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
PANCREATIC PSEUDOCYSTS Madhuri Rao MD PGY-5 Kings County Hospital Center 34 yo M Case Presentation PMH: Chronic pancreatitis (ETOH related) PSH: Nil Meds: Nil NKDA www.downstatesurgery.org Symptoms o Chronic
Endoscopic Management of Acute Pancreatitis. Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018
 Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
Endoscopic Management of Acute Pancreatitis Theo Doukides, MD Gastroenterology and Therapeutic Endoscopy February 13, 2018 Objectives Assessment of acute pancreatitis Early management Who needs an ERCP
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 1-6 Endoscopic ultrasound-guided placement of AXIOS stent for drainage of pancreatic fluid collections Rashmee Patil a, Mel A. Ona b, Charilaos Papafragkakis
Successful Endoscopic Treatment of Severe Pancreaticojejunostomy Strictures by Puncturing the Anastomotic Site with an EUS-guided Guidewire
 doi: 10.2169/internalmedicine.9133-17 http://internmed.jp CASE REPORT Successful Endoscopic Treatment of Severe Pancreaticojejunostomy Strictures by Puncturing the Anastomotic Site with an EUS-guided Guidewire
doi: 10.2169/internalmedicine.9133-17 http://internmed.jp CASE REPORT Successful Endoscopic Treatment of Severe Pancreaticojejunostomy Strictures by Puncturing the Anastomotic Site with an EUS-guided Guidewire
Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage
 Shimane J. Med. Sci., Vol.34 pp.73-80, 2017 73 Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage Ahmed SELIM 1,2), Nobuhiko FUKUBA 1), Ichiro MORIYAMA 3), Hiroki
Shimane J. Med. Sci., Vol.34 pp.73-80, 2017 73 Recurrence of Pancreatic Pseudocyst following Endoscopic Ultrasonography-Guided Drainage Ahmed SELIM 1,2), Nobuhiko FUKUBA 1), Ichiro MORIYAMA 3), Hiroki
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE. PRESENTED BY: Susan DePasquale, CGRN, MSN
 PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
PANCREATIC PSEUDOCYST DRAINAGE: ENDOSCOPIC APPROACHES & THE NURSING ROLE PRESENTED BY: Susan DePasquale, CGRN, MSN Pancreatic Fluid Collection (PFC) A result of pancreatic duct (PD) and side branch disruption,
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Endoscopic ultrasound guided gastrojejunostomy
 Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
Review Article Endoscopic ultrasound guided gastrojejunostomy Enad Dawod 1, Jose M. Nieto 2 1 Weill Cornell Medicine, Department of Gastroenterology and Hepatology, New York, NY, USA; 2 Borland Groover
The Risk Factors for Acute Pancreatitis after Endoscopic Ultrasound Guided Biopsy
 Korean J Gastroenterol Vol. 72 No. 3, 135-140 https://doi.org/10.4166/kjg.2018.72.3.135 pissn 1598-9992 eissn 2233-6869 ORIGINAL ARTICLE The Risk Factors for Acute Pancreatitis after Endoscopic Ultrasound
Korean J Gastroenterol Vol. 72 No. 3, 135-140 https://doi.org/10.4166/kjg.2018.72.3.135 pissn 1598-9992 eissn 2233-6869 ORIGINAL ARTICLE The Risk Factors for Acute Pancreatitis after Endoscopic Ultrasound
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
CASE REPORT. Masakuni Fujii 1*, Masao Yoshioka 1, Takefumi Niguma 2, Hiroaki Saito 1,ToruKojima 2, Soichiro Nose 3 and Junji Shiode 1
 Fujii et al. Journal of Medical Case Reports 2014, 8:243 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A solid pseudopapillary neoplasm without cysts that occurred in a patient diagnosed by endoscopic
Fujii et al. Journal of Medical Case Reports 2014, 8:243 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A solid pseudopapillary neoplasm without cysts that occurred in a patient diagnosed by endoscopic
Title. CitationSurgical Endoscopy, 26(6): Issue Date Doc URL. Rights. Type. File Information. surgery
 Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
Title Endoscopic ultrasound-guided transmural drainage for surgery Onodera, Manabu; Kawakami, Hiroshi; Kuwatani, Masaki Author(s) Eto, Kazunori; Nasu, Yuya; Tanaka, Eiichi; Hirano, S CitationSurgical Endoscopy,
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal Extension
 Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Gut and Liver, Vol. 4, No. 1, March 2010, pp. 140-145 Case report EUS-Guided Multitransgastric Endoscopic Necrosectomy for Infected Pancreatic Necrosis with Noncontagious Retroperitoneal and Peritoneal
Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas
 ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
ACG CASE REPORTS JOURNAL CASE REPORT ENDOSCOPY Endoscopic Ultrasound-Guided Treatment of Pancreaticocutaneous Fistulas Abdul Haseeb, MD, Barham K. Abu Dayyeh, MD, Michael J. Levy, MD, Larissa L. Fujii,
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study
 609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
609285TAG0010.1177/1756283X15609285Therapeutic Advances in GastroenterologyW Takagi, T Ogura research-article2015 Therapeutic Advances in Gastroenterology Original Research EUS-guided cholecystoduodenostomy
Original article. Introduction!
 382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
of EUS-guided transesophageal, transgastric, and transcolonic drainage of intra-abdominal fluid collections and abscesses
 CASE STUDIES EUS-guided transesophageal, transgastric, and transcolonic drainage of intra-abdominal fluid collections and abscesses Cyrus Piraka, MD, Raj J. Shah, MD, Norio Fukami, MD, Krishnavel V. Chathadi,
CASE STUDIES EUS-guided transesophageal, transgastric, and transcolonic drainage of intra-abdominal fluid collections and abscesses Cyrus Piraka, MD, Raj J. Shah, MD, Norio Fukami, MD, Krishnavel V. Chathadi,
Electrocautery vs non-electrocautery dilation catheters in endoscopic ultrasonography-guided pancreatic fluid collection drainage
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v8.i13.458 World J Gastrointest Endosc 2016 July 10; 8(13): 458-465 ISSN 1948-5190
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4253/wjge.v8.i13.458 World J Gastrointest Endosc 2016 July 10; 8(13): 458-465 ISSN 1948-5190
Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis
 ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 162-166 Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis Surinder
ORIGINAL ARTICLE Annals of Gastroenterology (2014) 27, 162-166 Comparative evaluation of structural and functional changes in pancreas after endoscopic and surgical management of pancreatic necrosis Surinder
Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report
 CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
CASE REPORT Endoscopic Resolution of Pseudocyst Infection and Necrosis as a Complication of Endoscopic Pseudocyst Drainage. A Case Report Rodrigo Azevedo Rodrigues, Lucianna Pereira da Motta Pires Correia,
Endosonography guided management of pancreatic fluid collections
 Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i41.11842 World J Gastroenterol 2015 November 7; 21(41): 11842-11853 ISSN 1007-9327
Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.3748/wjg.v21.i41.11842 World J Gastroenterol 2015 November 7; 21(41): 11842-11853 ISSN 1007-9327
ACUTE CHOLANGITIS AS a result of an occluded
 Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Digestive Endoscopy 2017; 29 (Suppl. 2): 88 93 doi: 10.1111/den.12836 Current status of biliary drainage strategy for acute cholangitis Endoscopic treatment for acute cholangitis with common bile duct
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Diagnostic performance of endoscopic ultrasound-guided fine-needle aspiration in pancreatic lesions
 European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
Follow this and additional works at:
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2016 A comparison between endoscopic ultrasoundguided rendezvous and percutaneous biliary drainage after failed
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction
 Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
Double endoscopic bypass for gastric outlet obstruction and biliary obstruction Authors Olaya I. Brewer Gutierrez 1,JoseNieto 2, Shayan Irani 3, Theodore James 4,RenataPierattiBueno 1, Yen-I Chen 1, Majidah
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction
 A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
A tale of two LAMS: a report of benign tissue ingrowth resulting in recurrent gastric outlet obstruction Authors Parth J. Parekh, Mohammad H. Shakhatreh, Paul Yeaton Institution Department of Internal
Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas
 CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
CASE REPORT Management of the Mucin Filled Bile Duct. A Complication of Intraductal Papillary Mucinous Tumor of the Pancreas Anand Patel, Louis Lambiase, Antonio Decarli, Ali Fazel Division of Gastroenterology
Key words: gastric cancer, postoperative complication, total gastrectomy
 Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
VIDEO ASSISTED RETROPERITONEAL DEBRIDEMENT IN HUGE INFECTED PANCREATIC PSEUDOCYST
 Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Types of IPMN. Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy. Cysts: Early Neoplasia. Mucinous Cystic Lesions. EUS-guided FNA EUS
 Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Does it matter what we drain?
 Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Endoscopic Management of Pancreatic Fluid Collections Shyam Varadarajulu, MD Medical Director Center for Interventional Endoscopy Florida Hospital, Orlando Does it matter what we drain? Makes all the difference!
Effectiveness and safety of metallic stent for ileocecal obstructive colon cancer: a report of 4 cases
 Effectiveness and safety of metallic stent for ileocecal obstructive colon cancer: a report of 4 cases Authors Tatsuya Ishii 1,KosukeMinaga 2, Satoshi Ogawa 3, Maiko Ikenouchi 1, Tomoe Yoshikawa 1,TakujiAkamatsu
Effectiveness and safety of metallic stent for ileocecal obstructive colon cancer: a report of 4 cases Authors Tatsuya Ishii 1,KosukeMinaga 2, Satoshi Ogawa 3, Maiko Ikenouchi 1, Tomoe Yoshikawa 1,TakujiAkamatsu
Safety and Efficacy of Endoscopic Ultrasound-Guided Drainage of Pancreatic Fluid Collections With Lumen-Apposing Covered Self-Expanding Metal Stents
 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line. Studies cannot be publicized as accepted manuscripts
All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line. Studies cannot be publicized as accepted manuscripts
An Intraductal Papillary Neoplasm of the Bile Duct at the Duodenal Papilla
 Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Published online: July 2, 2014 1662 6575/14/0072 0417$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial 3.0 Unported license (CC BY-NC)
Fine-Needle Aspiration Biopsy of Solid Pancreatic Masses: Comparison of CT and Endoscopic Sonography Guidance
 Comparison of Guidance Techniques for Pancreatic Mass Biopsy Abdominal Imaging Original Research A C D E M N E U T R Y L I A M C A I G O F I N G Sukru Mehmet Erturk 1 Koenraad J. Mortelé 1 Kemal Tuncali
Comparison of Guidance Techniques for Pancreatic Mass Biopsy Abdominal Imaging Original Research A C D E M N E U T R Y L I A M C A I G O F I N G Sukru Mehmet Erturk 1 Koenraad J. Mortelé 1 Kemal Tuncali
Naoyuki Toyota, Tadahiro Takada, Hodaka Amano, Masahiro Yoshida, Fumihiko Miura, and Keita Wada
 J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
J Hepatobiliary Pancreat Surg (2006) 13:80 85 DOI 10.1007/s00534-005-1062-4 Endoscopic naso-gallbladder drainage in the treatment of acute cholecystitis: alleviates inflammation and fixes operator s aim
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage?
 EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
EUS- Gallbladder Drainage: is it time to replace percutaneous drainage? Jessica Widmer, DO 1, Juveria Abdullah 1, Michel Kahaleh, MD. 1 Division of Gastroenterology and Hepatology, Department of Medicine,
Making ERCP Easy: Tips From A Master
 Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
Making ERCP Easy: Tips From A Master Raj J. Shah, M.D., FASGE Associate Professor of Medicine University of Colorado School of Medicine Co-Director, Endoscopy Director, Pancreaticobiliary Endoscopy Services
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT
 O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
O r i g i n a l a r t i c l e Endoscopic ultrasonography in suspected pancreatic malignancy and indecisive CT O.L.M. Meijer 1, R.K. Weersma 1, E.J. van der Jagt 2, H.M. van Dullemen 1 * Departments of
An investigation of pancreatic volume by disease using pancreatic volumetry
 Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Keywords. Abstract. Introduction
 The Safety of Endoscopic Ultrasonography-Guided Drainage of Pancreatic Fluid Collections Without Fluoroscopic Control: a Single Tertiary Center Experience Andrada Seicean 1, Roxana Stan-Iuga 1, Radu Badea
The Safety of Endoscopic Ultrasonography-Guided Drainage of Pancreatic Fluid Collections Without Fluoroscopic Control: a Single Tertiary Center Experience Andrada Seicean 1, Roxana Stan-Iuga 1, Radu Badea
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Paolo Giorgio Arcidiacono MD FASGE
 LOCAL ABLATIVE TREATMENT OF PANCREATIC SOLID LESIONS. WHERE ARE WE NOW? Paolo Giorgio Arcidiacono MD FASGE Pancreato-Biliary Endoscopy & Endosonography Division Pancreas Translational & Clinical Research
LOCAL ABLATIVE TREATMENT OF PANCREATIC SOLID LESIONS. WHERE ARE WE NOW? Paolo Giorgio Arcidiacono MD FASGE Pancreato-Biliary Endoscopy & Endosonography Division Pancreas Translational & Clinical Research
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Gallbladder drainage guided by endoscopic ultrasound
 Online Submissions: http://www.wjgnet.com/1948-5190office wjge@wjgnet.com doi:10.4253/wjge.v2.i6.203 World J Gastrointest Endosc 2010 June 16; 2(6): 203-209 ISSN 1948-5190 (online) 2010 Baishideng. All
Online Submissions: http://www.wjgnet.com/1948-5190office wjge@wjgnet.com doi:10.4253/wjge.v2.i6.203 World J Gastrointest Endosc 2010 June 16; 2(6): 203-209 ISSN 1948-5190 (online) 2010 Baishideng. All
Endoscopic Management of the Iatrogenic CBD Injury
 The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
The Liver Week 2014, Jeju, Korea Endoscopic Management of the Iatrogenic CBD Injury Jong Ho Moon, MD, PhD Department of Internal Medicine Soon Chun Hyang University School of Medicine Bucheon/Seoul, KOREA
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
BILIARY CANNULATION FOR the treatment of biliary
 Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Digestive Endoscopy 2016; 28 (Suppl. 1): 96 101 doi: 10.1111/den.12611 Current situation of cannulation and salvage for difficult cases Endoscopic ultrasonography-guided rendezvous technique Takayoshi
Prognostic influence of endoscopic ultrasound-guided fine needle aspiration in IPMN-derived invasive adenocarcinoma
 Suzuki et al. BMC Cancer (2018) 18:974 https://doi.org/10.1186/s12885-018-4896-2 RESEARCH ARTICLE Open Access Prognostic influence of endoscopic ultrasound-guided fine needle aspiration in IPMN-derived
Suzuki et al. BMC Cancer (2018) 18:974 https://doi.org/10.1186/s12885-018-4896-2 RESEARCH ARTICLE Open Access Prognostic influence of endoscopic ultrasound-guided fine needle aspiration in IPMN-derived
Clinical Study Bedside Endoscopic Ultrasound in Critically Ill patients
 Diagnostic and Therapeutic Endoscopy Volume 2011, Article ID 529791, 4 pages doi:10.1155/2011/529791 Clinical Study Bedside Endoscopic Ultrasound in Critically Ill patients Mehdi Mohamadnejad, 1, 2 Julia
Diagnostic and Therapeutic Endoscopy Volume 2011, Article ID 529791, 4 pages doi:10.1155/2011/529791 Clinical Study Bedside Endoscopic Ultrasound in Critically Ill patients Mehdi Mohamadnejad, 1, 2 Julia
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm
 Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
Intra-channel stent release technique for fluoroless endoscopic ultrasound-guided lumen-apposing metal stent placement: changing the paradigm Authors Andrea Anderloni 1,FabiaAttili 2, Silvia Carrara 1,
EUS Guided Pancreatic Duct Drainage: When? How?
 PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
PBS-IV Beyond the Horizon of Interventional EUS EUS Guided Pancreatic Duct Drainage: When? How? Uzma D. Siddiqui, M.D. Center for Endoscopic Research and Therapeutics (CERT), University of Chicago Medicine,
CURRICULUM VITAE
 CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
CURRICULUM VITAE Name Date of Birth Nationality Marital Status Permanent Address Sang Soo Lee, M. D. August 6, 1968 Korean Married, one child 217-704 Hanshin APT 137-949 Jamwon dong, Seocho-gu, Seoul,
Safety and utility of endoscopic ultrasound-guided fine-needle aspiration of focal splenic lesions: a retrospective analysis
 ORIGINAL ARTICLE Annals of Gastroenterology (2017) 30, 1-5 Safety and utility of endoscopic ultrasound-guided fine-needle aspiration of focal splenic lesions: a retrospective analysis Surinder S. Rana
ORIGINAL ARTICLE Annals of Gastroenterology (2017) 30, 1-5 Safety and utility of endoscopic ultrasound-guided fine-needle aspiration of focal splenic lesions: a retrospective analysis Surinder S. Rana
WallFlex Stents Technique Spotlights
 WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
WallFlex Stents Technique Spotlights OPEN TO THE POSSIBILITIES SEAN E. McGarr, do Kennebec Gastrointestinal Associates Maine General Medical Center, Augusta, ME 04330, United States Director of Gastrointestinal
Gastrointestinal Intervention
 Gastrointest Interv 2013; 2:24 29 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Self-expandable metal stents
Gastrointest Interv 2013; 2:24 29 Contents lists available at SciVerse ScienceDirect Gastrointestinal Intervention journal homepage: www.gi-intervention.org Review Article Self-expandable metal stents
Pancreatic Cystic Neoplasms: Guidelines and beyond
 Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 8 Case Report: Paraspinal Abscess Complicating Crohn s Disease Joseph J. Kim Adrian Greenstein Marissa Jaffe Alexander J. Greenstein The
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 8 Case Report: Paraspinal Abscess Complicating Crohn s Disease Joseph J. Kim Adrian Greenstein Marissa Jaffe Alexander J. Greenstein The
Complicated surgical infections
 Complicated surgical infections JASLYN DOSHI ID ADVANCED TRAINEE, WESTMEAD HOPC 46 F admitted 13 th March 2017 Epigastric pain Vomiting Diarrhoea Background Gastric banding 2009 Vomiting since last year
Complicated surgical infections JASLYN DOSHI ID ADVANCED TRAINEE, WESTMEAD HOPC 46 F admitted 13 th March 2017 Epigastric pain Vomiting Diarrhoea Background Gastric banding 2009 Vomiting since last year
Endoscopic Ultrasound-Guided Fine Needle Aspiration Used for the Diagnosis of a Retroperitoneal Abscess. A Case Report
 EUS guided fine needle aspiration of a retroperitoneal abscess CASE REPORTS Endoscopic Ultrasound-Guided Fine Needle Aspiration Used for the Diagnosis of a Retroperitoneal Abscess. A Case Report Adrian
EUS guided fine needle aspiration of a retroperitoneal abscess CASE REPORTS Endoscopic Ultrasound-Guided Fine Needle Aspiration Used for the Diagnosis of a Retroperitoneal Abscess. A Case Report Adrian
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Review Article Endoscopic Ultrasound-Guided Radiofrequency Ablation of the Pancreatic Tumors: A Promising Tool in Management of Pancreatic Tumors
 Hindawi Publishing Corporation Canadian Journal of Gastroenterology and Hepatology Volume 2016, Article ID 4189358, 5 pages http://dx.doi.org/10.1155/2016/4189358 Review Article Endoscopic Ultrasound-Guided
Hindawi Publishing Corporation Canadian Journal of Gastroenterology and Hepatology Volume 2016, Article ID 4189358, 5 pages http://dx.doi.org/10.1155/2016/4189358 Review Article Endoscopic Ultrasound-Guided
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Title: EUS-GUIDED FNA: HOW DO I INCREASE THE YIELD? Session No.: 7
 Title: EUS-GUIDED FNA: HOW DO I INCREASE THE YIELD? Session No.: 7 Name: Tomas Hucl Institution: Department of Gastroenterology and Hepatology Institute of Clinical and Experimental Medicine Country: Czech
Title: EUS-GUIDED FNA: HOW DO I INCREASE THE YIELD? Session No.: 7 Name: Tomas Hucl Institution: Department of Gastroenterology and Hepatology Institute of Clinical and Experimental Medicine Country: Czech
Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct
 CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
Percutaneous cholecystostomy for the treatment of acute cholecystitis in the critically ill and elderly
 ORIGINAL ARTICLE Key words: Cholecystectomy; Cholecystostomy!!"#!" JCM Li DWH Lee CW Lai ACN Li DW Chu ACW Chan Hong Kong Med J 2004;10:389-93 North District Hospital, New Territories East Cluster, 9 Po
ORIGINAL ARTICLE Key words: Cholecystectomy; Cholecystostomy!!"#!" JCM Li DWH Lee CW Lai ACN Li DW Chu ACW Chan Hong Kong Med J 2004;10:389-93 North District Hospital, New Territories East Cluster, 9 Po
Evaluation of a new stent for EUS-guided pancreatic duct drainage: long-term follow-up outcome
 Evaluation of a new stent for EUS-guided pancreatic duct drainage: long-term follow-up outcome Authors Yukitoshi Matsunami 1,TakaoItoi 1, Atsushi Sofuni 1, Takayoshi Tsuchiya 1,KentaroKamada 1, Reina Tanaka
Evaluation of a new stent for EUS-guided pancreatic duct drainage: long-term follow-up outcome Authors Yukitoshi Matsunami 1,TakaoItoi 1, Atsushi Sofuni 1, Takayoshi Tsuchiya 1,KentaroKamada 1, Reina Tanaka
Imaging Guided Biopsy. Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer
 Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
NYU School of Medicine Department of Radiology Rotation-Specific House Staff Evaluation
 Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Vascular & Interventional Radiology Rotation 1 Core competency in vascular and interventional radiology during the first resident rotation consists of clinical objectives, technical objectives and image
Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis
 MULTIMEDIA ARTICLE - Videoclips Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis Rakesh Kalapala 1, Lingareddy Sunitha 2, Reddy D Nageshwar 1, Guduru V Rao 1,
MULTIMEDIA ARTICLE - Videoclips Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis Rakesh Kalapala 1, Lingareddy Sunitha 2, Reddy D Nageshwar 1, Guduru V Rao 1,
AXIOS Stent and Electrocautery Enhanced Delivery System. Quick Reference Guide
 AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
AXIOS Stent and Electrocautery Enhanced Delivery System Quick Reference Guide AXIOS Stent (front and side views) UPN Codes Flange Diameter (mm) Lumen Diamter (mm) Saddle Length (mm) Catheter OD (Fr) Catheter
Review Article EUS-Guided Biliary Drainage
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2012, Article ID 348719, 5 pages doi:10.1155/2012/348719 Review Article EUS-Guided Biliary Drainage Marc Giovannini and Erwan
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis. William H. Nealon M.D.
 The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
The Influence of Pancreatic Ductal Anatomy on the Complications of Pancreatitis William H. Nealon M.D. Students and Trainees: Guide to Creativity, Productivity and Innovation in a Clinical Career Choose
Diagnosis of tumor extension in biliary carcinoma has. Differential Diagnosis and Treatment of Biliary Strictures
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:S79 S83 Differential Diagnosis and Treatment of Biliary Strictures KAZUO INUI, JUNJI YOSHINO, and HIRONAO MIYOSHI Department of Internal Medicine, Second
