Extramammary Paget s Disease in an Asian Population: A Single Centre s Experience
|
|
|
- Ada Nash
- 6 years ago
- Views:
Transcription
1 Extramammary Paget s Disease in an Asian Population: A Single Centre s Experience Lee Chee Meng; MBBS, MRCS, Cheong Kai Xiong, Kesavan S; MBBS, FRCPA, MBA, Melissa Teo Ching Ching; MBBS, MMed, FRCSEd, FAMS, MPH. National Cancer Centre Singapore. Abstract Aims: Extramammary Paget s Disease (EMPD) is a rare intra-epithelial neoplasm affecting the skin of areas such as the scrotum, vulva and perineal region. This study examines the patient demographics, presenting symptoms, disease characteristics, and recurrence rates after surgical treatment, and overall prognosis of the condition. Methods: This retrospective analysis examined all patients (n=11) who were treated at the National Cancer Centre Singapore from 2003 to Information regarding the patients demographics, disease characteristics, treatment modalities and outcomes were collected. Key Words: Extramammary Paget s Disease; Apocrine gland tumors; Lymphadenopathy; Invasiveness; Prognosis; Management Results: The median age was 68 years, and patients were predominantly Chinese males who presented with skin rash. No concomitant malignancy was picked up amongst all the patients. All patients underwent wide excision, while groin dissection was performed in 2 patients with clinical lymphadenopathy. 5 patients had microscopically invasive disease while 6 had intraepidermal EMPD. Patients with intraepidermal EMPD had a significantly longer mean overall survival period of 35.5 months (range: 5-104) compared to 29 months (range: 3-59) for those with invasive disease. (p=0.0855). Mortality rate was 40% in those with microinvasive disease, at time of follow up. The 2 patients who eventually passed away were noted to have lymphadenopathy at diagnosis. Corresponding author: Dr. Melissa Teo, National Cancer Centre Singapore, Department of Surgical Oncology, 11 Hospital Drive, Singapore Tel: , Fax: , Address: melissa.teo.c.c@nccs.com.sg 21
2 Lee Chee Meng Conclusions: Physicians should consider EMPD as a differential in the evaluation of persistent skin rash, especially for that in the genital region. The best chance of cure remains surgical resection, with adequate margins. Computed Tomography should be used as an adjunct to look for concomitant malignancy and to assess nodal disease. Patients who presented with metastatic disease had poor outcomes even with surgery, and should be considered for palliative management. INTRODUCTION Extramammary Paget s Disease (EMPD) is a rare form of intra-epithelial neoplasm of apocrine glands of the skin, characterised by the presence of Paget cells on histology. The common sites of EMPD include the vulva, scrotum, perineum, and perianal region, with rarer manifestations in sites such as the axilla, thigh, umbilicus and nose. The first cases of penoscrotal, perianal, and vulva EMPD were reported by Crocker, 1 Darier and Couillaud, 2 and Dubreuilh 3 respectively. It predominantly affects patients between 50 years to 80 years of age, with a peak at 65 years. It has a higher prevalence in Caucasians and in females. 4 However, various Asian studies 5-6 have reported more males being affected. Major symptoms and signs of EMPD include rash, pruritus, plaque, pigmentary changes, erythema, ulceration, and erosion. 7 As EMPD often presents very non-specifically, the diagnosis is often delayed, and is reached only after prolonged treatment failure. The median delay before the correct diagnosis is made is reported to be 2 years. 8 EMPD can occasionally be associated with internal malignancies such as colorectal, gastric, renal, bladder, urethral, prostate, and endocervical carcinomas, 9-14 and some authors have advocated screening for these cancers. Localised EMPD has a good prognosis because the tumour cells tend to spread only intraepidermally. However, invasive EMPD is frequently associated with lymph node metastasis, with reported rates of close to 26% and thus has a poorer prognosis. 8-9 Surgery represents the mainstay of treatment, especially for localised EMPD. Non-surgical modalities, in the form of various forms of phototherapy, laser therapy, radiotherapy, and chemotherapy have also been developed to reduce the morbidity and mortality associated with surgery The recurrence rates post-surgical resection is also reported to be fairly high, i.e. from 8% to 44%, 8,18 which is likely due to the tendency of EMPD to be multifocal and to have ill-defined margins. 19 Recurrences occurring up to 12 years after initial treatment have been reported. 20 The rarity of this condition has caused difficulty in its characterisation. To date, there exist only a small number of retrospective studies which attempt to characterize EMPD. 8,21-26 Hence, the aim of this paper is to describe our experience with EMPD at the National Cancer Centre Singapore (NCCS) and suggest a management strategy for this rare disease. METHODS Study Population All patients who were evaluated and treated for EMPD at the Singapore NCC from January 2003 to December 2011 were included in this study. A retrospective crosssectional study of the eligible patients was conducted. The study population was identified from a prospectively maintained database at the NCC, and clinical charts were reviewed. Ethical approval was obtained from the Centralised Institutional Review Board in Singapore. Data Collection Information regarding the patients demographics, age at diagnosis, presenting symptoms, disease sites and presence of synchronous lesions, evaluations, definitive treatments, post-operative adjuvant therapies, follow-up periods, survival periods, complications, recurrences, and deaths were collected. Data Analysis The data were reviewed and analysed using the computer software IBM SPSS Statistics for Windows, Version 19.0 (IBM, Chicago, IL). Descriptive analysis was performed. The means, standard deviations, ranges, and medians were reported for categorical variables where appropriate, and the numbers and individual percentages were reported for categorical variables. The overall survival period was defined as the length of time from the date of diagnosis to the point of death or time of analysis, whichever earlier. The disease-free 22
3 Extramammary Paget s Disease survival period was defined as the length of time from the date of surgery to the point of recurrence, or death, or time of analysis, whichever was the earliest, and was calculated for the patients who underwent resection for all known disease. RESULTS Demographics A total of 11 patients presented to the NCC for EMPD from January 2003 to December 2011 and were included in this study. The patients were of 53 to 85 years of age at diagnosis, with the median age of 68 years. 8 patients were male, and the remaining 3 patients were female. All the patients in this study were of Chinese in ethnicity, except for 1 patient who was Malay (Table 1). Table 1. Summary of Demographics, Presentation, Disease Characteristics, Evaluation, Management, and Outcomes Characteristics Gender Male 8 (72.7%) Female 3 (27.3%) Age at Diagnosis (Years) 69.8 ± 11.2 (Range: ) Ethnic Group Chinese 10 (90.9%) Malay 1 (9.1%) Primary Site Scrotum +/- Penile Shaft 8 (72.7%) Vulva 2 (18.2%) Perianal Region +/- Anal canal 1 (9.1%) Common Symptoms for First Presentation Rash 11 (100.0%) Plaque 6 (54.5%) Pruritus 4 (36.4%) Duration of Symptoms Prior to Diagnosis (Years) 1.72 ± 0.94 (Range: ; Median: 1.50) Surgico-Pathological Characteristics Intraepidermal 6 (54.5%) Invasive Carcinoma 5 (45.5%) Primary Treatment Wide local excision 5 (45.5%) Wide local excision with skin grafts/ 4 (36.3%) flaps Wide local excision with lymph node 2 (18.2%) dissection Post-Operative Complications Yes 5 (45.5%) No 6 (54.5%) Recurrence Yes 1 (9.1%) No 10 (90.9%) Death Yes 2 (18.2%) No 9 (81.8%) Overall Survival Period (Months) Disease-Free Survival Period (Months) Presentation 31.2 (Range: 3-104) 29.8 (Range: 3-89) The means, standard deviations, ranges, and medians were reported as appropriate for continuous variables The most common presenting symptoms were that of rash, plaque, followed by pruritus. Rash was a common complaint amongst all of the patients. In addition, 6 patients presented with plaques, 4 with pruritus, and 3 with skin discolouration. 2 patients had palpable inguinal lymph nodes on examination. Prior to referral to NCC for management, patients had experienced symptoms for a mean duration of 1.65 years during which they either did not seek help or were conservatively managed by their primary healthcare provider. 7 of the 8 male patients had scrotal EMPD. This was unilateral (left) in 5 of them, and bilateral in 2 others. 2 of the 3 female patients had vulva EMPD, with unilateral labial involvement in 1, and bilateral labial involvement in the other. The last male patient had perineal EMPD, similarly observed in the last female patient (Table 2). 23
4 Lee Chee Meng Table 2. Presentation and Disease Characteristics at Diagnosis Patient Number Presenting Symptoms Duration Prior to Diagnosis (Years) Synchronous Skin Lesions Lymphadenopathy on Computed Tomography Extranodal Metastasis 1 Rash, Discolouration 0.54 No No No 2 Rash, Plaque, Pruritus, Ulceration/ Erosion 1.0 No No No 3 Rash, Discolouration 1.0 No No No 4 Rash 3.0 No No No 5 Rash, Plaque 2.0 No No No 6 Rash, Plaque, Lymphadenopathy, Discharge 2.0 No Yes Bone 7 Rash 1.5 No No No 8 Rash, Pruritus 1.0 No No No 9 Rash, Plaque, Pruritus, Lymphadenopathy 3.0 No Yes No 10 Rash, Plaque, Pruritus 3.0 No No No 10 Rash, Pruritus, Discolouration 1.0 No No No 11 Rash, Plaque 0.83 No No No Patient experienced recurrence. Investigation Modalities All 11 patients were diagnosed with EMPD after incisional biopsies were performed. Subsequently, Computed Tomography (CT) scans and a Fluorodeoxyglucose- Positron Emission Tomography (FDG-PET) with contrast-enhanced CT scan were performed in 10 and one patients respectively, to exclude the presence of nodal and distant metastases. It confirmed the presence of lymphadenopathy in 2 male patients in whom palpable lymph nodes were noted on physical examination. At diagnosis, one of these 2 patients already had extra-nodal metastasis to the bone, noted on the CT scan. Underlying Malignancy Only 1 patient had a background of malignancy. She was previously diagnosed with left breast ductal carcinoma in situ (DCIS), underwent a simple mastectomy with axillary clearance (in February 2007), and subsequently presented to us for EMPD in Her first malignancy was not thought to be associated with the diagnosis of EMPD. 10 of the 11 patients had a CT Abdomen and Pelvis while 7 of the 11 patients underwent colonoscopies, which picked up benign colonic polyps in 3 patients. No one was found to have underlying malignancy after CT scans and colonoscopies. Management The main treatment modality was surgery. 5 patients underwent wide local excisions, while 4 patients underwent wide local excisions with skin grafts or regional flaps. The 2 patients with clinical lymphadenopathy, confirmed to be metastatic on fine needle aspiration cytology, underwent a concomitant modified inguinal lymphadenectomy, with dissection of the superficial and deep inguinal lymph node groups. The depth of the excision is down to Scarpa s fascia with a superior limit at the inguinal ligament, medial limit at the border of the adductor longus, lateral limit at the lateral border of the femoral artery and inferior limit at the apex of the femoral triangle. 24
5 Extramammary Paget s Disease Intra-operative frozen section analyses of the margins were performed for all the 11 patients. Frozen section margins were clear for 9 patients while the remaining 2 patients with positive margins underwent wider excision. However, the wider margins remain persistently positive up to the perianal and peri-urethral region. Decision was made to withhold further surgery for these 2 patients as further resection would result in the involvement of the anal canal and urethra respectively. Both patients were then counseled on wider resections that would entail an abdomino-perineal resection in one, and a urethral resection with an ileal conduit in the other. Both patients declined the respective surgeries and the former patient underwent 10 cycles of radiotherapy (RT), whilst the latter had a further resection up to the level of urethra and closure with vertical rectus abdominis myocutaneous (VRAM) flap cover. 2 of the 9 patients who were thought to have clear resection margins after frozen section were subsequently found to have involved resection margins after the full histology was reviewed. These 2 patients underwent wider excision of involved margins with flap covers within a month of the initial surgery, attaining clear margins in the second surgery. Post-operatively, both patients with nodal disease were offered chemotherapy. The patient who had nodal and bone metastases died before he could receive palliative chemotherapy, while the patient with isolated nodal involvement declined adjuvant chemotherapy. Histological Results 5 patients were found to have invasive carcinomas microscopically, and the remaining 6 patients were found to have intraepithelial lesions. The choice of immunohistochemical markers for surgico-pathological evaluation was not standardised for all of the patients. Markers which were used included the CK5, CK6, CK7 and CK20. CK 7 was tested in 7 of the 11 patients and it was positive in all of them, while CK 20 was negative in all 6 patients who were tested for it. Outcomes A total of 3 patients suffered from wound infections post-operatively. 2 of these patients had undergone groin dissection, of whom 1 subsequently required vacuum assisted closure. All 3 patients were treated with a course of oral antibiotics, and the infections resolved subsequently after 1 week. One of the patients who had undergone lymph node dissection for nodal involvement had persistent post-operative secondary lymphedema. No other post-operative complications were noted for other patients. 1 patient had metastatic disease on initial diagnosis. Of the remaining 10 patients, 1 had local recurrence, which occurred at 89 months. He had bilateral scrotal EMPD, for which he underwent wide local excision initially, and frozen sections revealed negative margins. Post-operatively, full histology revealed intraepidermal EMPD, but the surgical margins were involved, and he thus underwent a wider excision with a split skin graft cover, attaining clear margins. At the 7 th year of follow up, he was noted to have recurrence of a scrotal rash at the previous operative site, and an incisional biopsy was performed, which confirmed the recurrence of Paget s disease. A wider excision with split skin graft cover was subsequently performed. He has remained disease-free 14 months after the last surgery. The mean overall survival period was 31.2 months (range: 3-104) while the mean disease-free survival period was 29.8 months (range: 3-89). Both patients with nodal involvement at presentation were deceased at time of evaluation. The patient with bone metastases died 3 months after surgery. The other patient was noted to develop cervical lymph node metastasis at 29 months post-operatively and eventually died at 51 months postoperatively (Table 3). Differences in Characteristics between Intraepidermal and Invasive EMPD Although patients with intra-epithelial disease only appeared to present at an earlier time than those who had invasive disease, with duration of symptoms experienced for a median of 1.00 and 1.75 years respectively, there was no significant difference (p=0.514; Mann-Whitney s U test). Patients with intraepidermal EMPD had a mean overall survival period of 35.5 months (range: 5-104), compared to 29 months (range: 3-59) for those with invasive disease and this was found to be significant (p=0.0855; Mann- Whitney s U test). 25
6 Lee Chee Meng Table 3. Management and Outcomes Patient No. Primary Treatment Lymph Node Dissection Adjuvant Therapy Surgico-Pathological Characteristics Sequelae and Complications Recurrence Death Survival Period (Months) 1 Wide local excision No No Invasive malignancy No No No 6 (adenocarcinoma) 2 Wide local excision No No Invasive maligancy No No No 59 (adenocarcinoma) 3 Wide local excision No No Intraepidermal No No No 56 with skin grafts/flaps 4 Wide local excision No No Intraepidermal No No No 9 5 Wide local excision No No Intraepidermal Surgical site infection No No 5 6 Wide local excision Yes Offered chemotherapy, but died before receiving it Invasive malignancy (adenocarcinoma) Surgical site infection Synchronous metastasis No Yes 3 7 Wide local excision No No Intraepidermal No No No 16 with skin grafts/flaps 8 Wide local excision No No Invasive malignancy (adenocarcinoma) No No No 26 9 Wide local excision Yes Offered chemotherapy, but declined 10 Wide local excision with skin grafts/flaps 10 Wide local excision with skin grafts/flaps Invasive malignancy (adenocarcinoma) Surgical site infection, and secondary lymphedema in left lower limb Metachronous metastasis to supraclavicular LN No Yes 51 No No Intraepidermal No Local recurrence No 104 (at 89 months) No No Intraepidermal No No No Wide local excision No Underwent radiotherapy Intraepidermal No No No 8 Patient experienced recurrence DISCUSSION EMPD is a rare condition, and there is very little information available regarding the disease patterns and outcomes in an Asian population. To the best of our knowledge, this cohort of 11 patients over 8 years represents the largest number of cases treated at a single centre in Singapore. Our aim was to analyze the epidemiology, presenting symptoms, disease characteristics, management strategies, and the long-term outcomes of patients who are treated at a large tertiary referral centre. In doing so, we hope to determine the prognostic factors and develop a better management strategy for patients with this rare disease. Patients experienced symptoms of EMPD for a mean period of 1.65 years prior to presentation at our centre. As all of the patients complained of skin rash, the delay in diagnosis can be attributed to the fact that rash is a common and non-specific skin condition. Many patients could have downplayed its significance, and not sought medical attention until further symptoms arose. Although EMPD is rare, clinicians should consider this differential diagnosis in a patient who presents with a persistent and suspicious-looking rash, especially that in the genitalia region. Although Chanda et al., in a review of 197 cases, 10 had reported that EMPD may be associated with underlying malignancies, Asian studies had demonstrated lower incidences, particularly in men with penoscrotal EMPD. The results of our study are consistent with the Asian studies, i.e. none of the patients were found to have internal malignancies after colonoscopies and CT scans. CT or PET scans can assess for nodal involvement, metastatic disease or other concurrent malignancies. In our study, no one was noted to have concurrent 26
7 Extramammary Paget s Disease malignancy. CT revealed sizeable lymphadenopathy, both in the superficial and deep inguinal chains, in the 2 patients with clinically palpable lymph nodes, proving to be a useful adjunct to determine the extent of groin dissection. In one of the 2 patients with lymphadenopathy, CT also revealed the presence of synchronous bone metastases. PET CT did not provide us with any additional information during staging and this concurred with a systematic review of 17 primary studies, where PET- CT was found not to have any patient-relevant benefit 27 over conventional CT in detecting lymphadenopathy during the staging of malignant melanoma. groin dissection should be carried out in addition to wide excision. If FNAC is negative, an excision biopsy of the lymph node should be carried out during wide excision of EMPD. The lymph node would be sent for frozen section, with a groin dissection performed if positive for metastasis. In some situations, a CT may be useful in detecting enlarged lymph nodes that are not clinically palpable. If these can be biopsied under radiological image guidance, this should be performed to confirm the presence of metastatic nodal disease that can be managed with a concomitant nodal dissection. If access for biopsy There is currently no internationally recognised consensus regarding the standard work up for the detection of concomitant internal malignancies after EMPD has been diagnosed. A thorough history and physical examination remain imperative in guiding the initial clinical evaluation, as with any other disease. Specific investigations like gastroscopies, colonoscopies, PAP smears, colposcopies, cystoscopies, mammograms, abdomino-pelvic ultrasounds, serum CEA and PSA may then be carried out, especially if there are organ-specific symptoms and signs. The choice of specific investigations may also be guided by the site of the lesion, for instance, colonoscopy for perianal lesions, cystoscopy for genitourinary lesions, since Chanda et al. has reported a strong association between the anatomical site of EMPD and that of internal malignancies. However, this was not noted in our study. Patients with lymph node disease have poorer outcomes. As such, we propose a workflow for the management of such patients (Figure 1). Patients diagnosed with EMPD should be carefully examined for the presence of nodal involvement or distant metastases. In patients with clinically palpable nodes, a fine needle aspiration cytology should be performed. If FNAC is positive, a 27
8 Lee Chee Meng is an issue, and the nodes are suspicious for metastasis by size criteria or are significantly FDG-avid on the PET scan, the patient can be offered a nodal dissection. In cases where there is no lymphadenopathy detected on clinical examination and CT scan, a wide excision should be performed. It is our practice to perform a CT or PET scan upon diagnosis, in order that surgical management can be confined to a single episode, although patients with intra-epidermal EMPD (non evidence of invasion) may possibly avoid the need for imaging. Post-operatively, clinicians should base their next management step on whether there is microscopically invasive disease on final histology. As expected, patients with microscopically invasive disease fared poorly compared to those with intraepithelial disease. At time of follow up, there was a 40% mortality rate in the former group, and 2 of these 5 patients had lymph node metastases from the onset. Studies have reported the high sensitivity of sentinel lymph node biopsy in cutaneous malignancies, with Hatta 28 et al reporting a 100% detection rate in 23 patients with EMPD, and a 0% false negative rate. If there is micro-invasion and no clinical evidence of lmyphadenopathy, it might be worthwhile to consider offering an elective sentinel lymph node biopsy, keeping in view groin dissection in cases with positive nodes. Otherwise, regular follow up with careful clinical examination for lymphadenopathy, coupled with surveillance CT will be useful in this group of patients as it is difficult to predict if they will eventually develop nodal spread. Frozen section analyses of resection margins were performed in all patients treated at our centre. In 9 patients, frozen sections reported clear margins, yet final histologies revealed false negative results in 2 of them (22.2%). This inherent risk was also reported in other studies with rates approaching 40%, 19,30 but this had little effect on disease outcomes. 17,31-32 In our series, outcomes were unchanged as the 2 mentioned patients were subjected to a second surgery allowing them to achieve negative margins. Studies on immuno-histochemical analysis have shown that certain markers have a relationship in the manifestation of EMPD. CK 7, CEA and GCDFP-15 are known to be positive for all forms of EMPD, while those patients with an underlying malignancy usually test positive for CK Amongst the mucinous markers, MUC 1 and MUC 2 are occasionally expressed in EMPD but MUC 5 has the highest prognostic potential 36 as they are expressed more frequently in microinvasive EMPD. One of the limitations in our study was that immunohistochemical analysis was not uniform. In our series, all patients who were tested with CK 7 all ended with positive results whereas CK 20 was negative amongst those tested, correlating with the absence of underlying malignancy. Apart from validating our results with known disease patterns associated with CK 7 and CK 20, we were unable to further derive any other meaningful results regarding immuno-histochemical evaluation of EMPD. We recommend that histological reports for future patients adopt a standardised set of markers for testing, namely CK 7, CK 20, CEA, GCDFP-15, MUC 1, MUC 2 and MUC 5 as this may allow researchers to find a link between the presence and absence of markers with prognosis. Besides chemotherapy, radiotherapy has been used as alternative form of treatment, particularly in patients who are at a high risk for surgery or in those with large lesions, where further wide excision may cause compromise to vital structures such as the anus or urethra. In such cases, radiotherapy may be more acceptable to patients than an abdominal perineal resection or the creation of an uretero-ileal conduit. Although radiotherapy is useful in some patients recurrences has also been reported in these studies. Furthermore, there are no studies that have recommended any fixed dose or duration of radiotherapy, and its use has to be carefully considered on a case-by-case basis as there are acute and chronic toxicity effects. The only patient who underwent radiotherapy for persistently positive margins at the perianal region remains disease-free to date, at 8 months of follow up. EMPD is known to have high local recurrence rates despite adequate surgical resection. 30 In our study, there was only 1 patient who had locoregional recurrence. This was the first EMPD patient managed by our center, with recurrence at 89 months after disease clearance. After the original surgery, full histology showed that margins were involved and he subsequently went for wider excision 1 month later. The margins were cleared after the second surgery and full histology revealed intraepithelial disease. Apart from him, there were 4 other patients who similarly did not have clear margins after the first operations and 2 of them underwent further surgeries, and the final margins were clear of EMPD. Till date, these patients have not developed evidence of recurrence. Our next longest follow up was only up to 54 months. A review of patient outcomes after a longer duration post-operatively may provide us with greater clarity on 28
9 Extramammary Paget s Disease disease patterns in the local population. We recommend that patients have long term follow ups, and clinicians should have low thresholds for suspecting recurrence upon detecting new skin lesions on follow ups. CONCLUSION In summary, this study represents a retrospective analysis of EMPD. It has contributed to the small corpus of knowledge of EMPD, which has remained largely controversial. Our results reflected similarities with those in overseas centers apart from the findings of male predominance of the disease, low incidence of internal malignancy, and low recurrence rates. Although EMPD is rare, it remains an important differential for non-resolving skin rash. With early diagnosis and adequate surgical resection, it remains treatable with a fairly good prognosis. Poor prognostic factors include those with nodal metastases on presentation and microscopically invasive disease on final histology; and the role of adjuvant chemotherapy in such patients should be further explored. Patients need to be placed on long term follow up to look for recurrence and scans should be considered, particularly in those with microscopically invasive disease. We propose a workflow for the treatment of future patients in our center, and this can be validated with a prospective study. ACKNOWLEDGEMENTS No funding has been sought in this research. The authors hereby thank all physicians who have been involved in the care of the patients described in this paper. REFERENCES 1. Crocker HR: Paget s disease affecting the scrotum and the penis. Trans Pathol Soc Lond 1889; 40: Darier J, Couillaud P: Sur un cas de maladie de Paget de la region perinea-annale et scrotale. Ann Dermatol Syphiligr 1893; 4: Dubreuilh W: Paget s disease of the vulva. Br J Dermatol 1901; 13: Shepherd V, Davidson EJ, Davies-Humphreys J: Extramammary Paget s disease. BJOG 2005; 112:273e9. 5. Kanitakis J: Mammary and extramammary Paget s disease. J Eur Acad Dermatol Venereol 2007; 21(5): 581e Curtin JP, Rubin SC, Jones WB, et al.: Paget s disease of the vulva. Gynecol Oncol 1990; 39:374e7. 7. Chiba H, Kazama T, Takenouchi T, et al.: Two cases of vulval pigmented extramammary Paget s disease: Histochemical and immunohistochemical studies. Br J Dermatol 2000; 142:1190e4. 8. Hatta N, Yamada M, Hirano T, et al.: Extramammary Paget s disease: Treatment, prognostic factors and outcome in 76 patients. Br J Dermatol Feb; 158(2): Tsutsumida A, Yamamoto Y, Minakawa H, et al. Indications for lymph node dissection in the treatment of extramammary Paget s disease. Dermatol Surg. 2003;29: Chanda JJ: Extramammary Paget s disease: Prognosis and relationship to internal malignancy. J Am Acad Dermatol 1985; 13: Ojeda VJ, Heenan PJ and Watson SH: Paget s disease of the groin associated with adenocarcinoma of the urinary bladder. J Cutan Pathol 1987; 14: Koh KBH and Nazarina AR: Paget s disease of the scrotum: Report of a case with underlying carcinoma of the prostate. Br J Dermatol 1995; 133: Hoffman MS, Cavanagh D: Malignancies of the vulva. In: Rock JA, Thompson JD, (eds). The Linde s operative gynecology. 8th ed. Philadelphia: Lippincott-Raven; p Allan SJR, McLaren K and Aldridge RD: Paget s disease of the scrotum: A case exhibiting positive prostate-specific antigen staining and associated with prostatic adenocarcinoma. Br J Dermatol 1998; 138: Im M, Kye KC, Kim JM et al.: Extramammary Paget s disease of the scrotum with adenocarcinoma of the stomach. J Am Acad Dermatol 2007; 57: S Petkovic S, Jeremic K, Vidakovic S, et al.: Paget s disease of the vulva review of our experience. Eur J Gynaecol Oncol 2006; 27(6):611e Louis-Sylvestre C, Haddad B, Paniel BJ: Paget s disease of the vulva: Results of different conservative treatments. Eur J Obstet Gynecol Reprod Biol 2001; 99:253e Pierie JP, Choudry U, Muzikansky A, et al.: Prognosis and management of extramammary Paget s disease and the association with secondary malignancies. J Am Coll Surg 2003; 196:45e Gunn RA, Gallager HS: Vulvar Paget s disease: A topographic study. Cancer 1980; 46:590e Goldblum JR, Hart WR: Perianal Paget s disease: A histologic and immunohistochemical study of 11 cases with and without associated rectal adenocarcinoma. Am J Surg Pathol 1998; 22(2):170e Hegarty PK, Suh J, Fisher MB, et al.: Penoscrotal extramammary Paget s disease: The University of Texas M. D. Anderson Cancer Center contemporary experience. J Urol Jul; 186(1): Zhang N, Gong K, Zhang X, et al.: Extramammary Paget s disease of scrotum--report of 25 cases and literature review. Urol Oncol Jan-Feb; 28(1): Jones IS, Crandon A, Sanday K: Paget s disease of the vulva: Diagnosis and follow-up key to management; a retrospective study of 50 cases from Queensland. Gynecol Oncol Jul; 122(1): Lee SJ, Choe YS, Jung HD, et al.: A multicenter study on extramammary Paget s disease in Korea. Int J Dermatol May; 50(5): Chiu TW, Wong PSY, Ahmed K, et al.: Extramammary Paget s disease in Chinese males: A 21-year experience. World J Surg 2007; 31: Chang YT, Liu HN, Wong CK: Extramammary Paget s disease: A report of 22 cases in Chinese males. J Dermatol May; 23(5): Morton DL, Wen DR, Wong JH, et al.: Technical details of intraoperative lymphatic mapping for early stage melanoma. Arch Surg 1992; 127(4):392e Hatta N, Morita R, Yamada M, et al.: Sentinel lymph node biopsy in patients with extramammary Paget s disease. Dermatol Surg 29
10 Lee Chee Meng 2004; 30(10):1329e Longo MI, Lázaro P, Bueno C, et al.: Fluorodeoxyglucose-positron emission tomography imaging versus sentinel node biopsy in the primary staging of melanoma patients. Dermatol Surg Mar;29(3): Fishman DA, Chambers SK, Schwartz PE, et al.: Extramammary Paget s disease of the vulva. Gynecol Oncol 1995; 56:266e Zollo JD, Zeitouni NC: The Roswell Park Cancer Institute experience with extramammary Paget s disease. Br J Dermatol 2000 Jan; 142(1): Preti M, Micheletti B, Ghiringhello B, et al.: La malattia di Paget vulvare. Minerva Ginecol 2000; 52:203e Goldblum JR, Hart WR: Vulvar Paget s disease: A clinicopathologic and immunohistochemical study of 19 cases. Am J Surg Pathol Oct; 21(10): Nowak MA, Guerriere-Kovach P, Pathan A, et al.: Perianal Paget s disease distinguishing primary and secondary lesions using immunohistochemical studies including gross cystic disease fluid protein-15 and cytokeratin 20 expression. Arch Pathol Lab Med 1998; 12: Prieto VG, Ivan D: The use of immunohistochemistry in the differential diagnosis of primary cutaneous adnexal neoplasms and metastatic adenocarcinomas to the skin. Diagnostic Histopathology Sep; 16(9): Hata H, Abe R, Hoshina D, et al.: MUC5AC expression correlates with invasiveness and progression of extramammary Paget s disease. J Eur Acad Dermatol Venereol. doi: /jdv Luk NM, Yu KH, Yeung WK, et al.: Extramammary Paget s disease: outcome of radiotherapy with curative intent. Clin Exp Dermatol Jul; 28(4): Hata M, Koike I, Wada H, et al.: Definitive radiation therapy for extramammary Paget s disease. Anticancer Res Aug;32(8):
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Proposed All Wales Vulval Cancer Guidelines. Dr Amanda Tristram
 Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Proposed All Wales Vulval Cancer Guidelines Dr Amanda Tristram Previous FIGO staging FIGO Stage Features TNM Ia Lesion confined to vulva with
Guideline for the Management of Vulval Cancer
 Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
Version History Guideline for the Management of Vulval Cancer Version Date Brief Summary of Change Issued 2.0 20.02.08 Endorsed by the Governance Committee 2.1 19.11.10 Circulated at NSSG meeting 2.2 13.04.11
BAP-oma & BEYOND MICHAEL A NOWAK, MD
 BAP-oma & BEYOND MICHAEL A NOWAK, MD CONFLICTS No conflicts with the content of this lecture BAP-oma Wiesner 2011: Families with multiple tan dome-shaped papules of head, neck, trunk, and extremities.
BAP-oma & BEYOND MICHAEL A NOWAK, MD CONFLICTS No conflicts with the content of this lecture BAP-oma Wiesner 2011: Families with multiple tan dome-shaped papules of head, neck, trunk, and extremities.
Clinical Pathological Conference. Malignant Melanoma of the Vulva
 Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Clinical Pathological Conference Malignant Melanoma of the Vulva History F/48 Chinese Married Para 1 Presented in September 2004 Vulval mass for 2 months Associated with watery and blood stained discharge
Management of Neck Metastasis from Unknown Primary
 Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
COLORECTAL CARCINOMA
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
Pruritus Ani in an Elderly Man
 Pruritus Ani in an Elderly Man Pedro Redondo, MD; Michel Idoate, MD; Agustín España, MD; Emilio Quintanilla, MD; University of Navarra, Pamplona, Spain REPORT OF A CASE A 78-year-old man presented with
Pruritus Ani in an Elderly Man Pedro Redondo, MD; Michel Idoate, MD; Agustín España, MD; Emilio Quintanilla, MD; University of Navarra, Pamplona, Spain REPORT OF A CASE A 78-year-old man presented with
Case history: Figure 1. H&E, 5x. Figure 2. H&E, 20x.
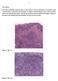 1 Case history: A 49 year-old female presented with a 5 year history of chronic anal fissure. The patient s past medical history is otherwise unremarkable. On digital rectal examination there was a very
1 Case history: A 49 year-old female presented with a 5 year history of chronic anal fissure. The patient s past medical history is otherwise unremarkable. On digital rectal examination there was a very
World Articles of Ear, Nose and Throat Page 1
 World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
World Articles of Ear, Nose and Throat ---------------------Page 1 Primary Malignant Melanoma of the Tongue: A Case Report Authors: Nanayakkara PR*, Arudchelvam JD** Ariyaratne JC*, Mendis K*, Jayasekera
Table of contents. Page 2 of 40
 Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
Metachronic solitary breast metastasis from renal cell carcinoma: case report
 Metachronic solitary breast metastasis from renal cell carcinoma: case report Abstract We describe the case of a patient with solitary and metachronic breast metastasis, 3 years after nephrectomy for renal
Metachronic solitary breast metastasis from renal cell carcinoma: case report Abstract We describe the case of a patient with solitary and metachronic breast metastasis, 3 years after nephrectomy for renal
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Vagina. 1. Introduction. 1.1 General Information and Aetiology
 Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter.
 Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Skin Cancer follow up guidelines If NEW serious diagnosis given: 1. Written information to patient /GP: fax ASAP to GP & offer copy of consultation letter. 2. Free prescription information details. 3.
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Staging and Treatment Update for Gynecologic Malignancies
 Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Koebner Phenomenon in Radiation Associated Angiosarcoma of the Breast: Linear Metastasis in Split Skin Graft Donor Site
 ISPUB.COM The Internet Journal of Surgery Volume 9 Number 2 Koebner Phenomenon in Radiation Associated Angiosarcoma of the Breast: Linear Metastasis in Split Skin Graft Donor Site A Chhabra, A Goyal, R
ISPUB.COM The Internet Journal of Surgery Volume 9 Number 2 Koebner Phenomenon in Radiation Associated Angiosarcoma of the Breast: Linear Metastasis in Split Skin Graft Donor Site A Chhabra, A Goyal, R
The Effectiveness of Mapping Biopsy in Patients with Extramammary Paget s Disease
 The Effectiveness of Mapping Biopsy in Patients with Extramammary Paget s Disease Byung Jun Kim, Shin Ki Park, Hak Chang Department of Plastic and Reconstructive Surgery, Seoul National University Hospital,
The Effectiveness of Mapping Biopsy in Patients with Extramammary Paget s Disease Byung Jun Kim, Shin Ki Park, Hak Chang Department of Plastic and Reconstructive Surgery, Seoul National University Hospital,
Vaginal intraepithelial neoplasia
 Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Vaginal intraepithelial neoplasia The terminology and pathology of VAIN are analogous to those of CIN (VAIN I-III). The main difference is that vaginal epithelium does not normally have crypts, so the
Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva Malignant melanoma sho
 Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Carcinoma Vulva & Vagina Subdivisi Onkologi Ginekologi Bagian Obgin FK USU Vulvar Carcinoma. Definition: Cases should be classified as carsinoma of the vulva when the primary site growth is in the vulva
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Metastatic mechanism of spermatic cord tumor from stomach cancer
 Int Canc Conf J (2013) 2:191 195 DOI 10.1007/s13691-013-0-9 CANCER BOARD CONFERENCE Metastatic mechanism of spermatic cord tumor from stomach cancer Masahiro Seike Yoshikazu Kanazawa Ryuji Ohashi Tadashi
Int Canc Conf J (2013) 2:191 195 DOI 10.1007/s13691-013-0-9 CANCER BOARD CONFERENCE Metastatic mechanism of spermatic cord tumor from stomach cancer Masahiro Seike Yoshikazu Kanazawa Ryuji Ohashi Tadashi
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy
 Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Paget's Disease of the Breast: Clinical Analysis of 45 Patients
 236 Paget's Disease of the Breast: Clinical Analysis of 45 Patients Mingfian Yang Hao Long Jiehua He Xi Wang Zeming Xie Department of Thoracic Oncology, Cancer Center of Sun Yat-sen University, Guangzhou
236 Paget's Disease of the Breast: Clinical Analysis of 45 Patients Mingfian Yang Hao Long Jiehua He Xi Wang Zeming Xie Department of Thoracic Oncology, Cancer Center of Sun Yat-sen University, Guangzhou
Melanoma Quality Reporting
 Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Melanoma Quality Reporting September 1, 2013 December 31, 2016 Laurence McCahill, MD Surgical Oncologist Metro Health Surgical Oncology Metro Health Professional Building 2122 Health Drive SW Wyoming,
Invasive Papillary Breast Carcinoma
 410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
410 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), E. Compérat, S. Minhas, A. Necchi, C. Protzel, N. Watkin Guidelines Associate: R. Robinson Introduction and epidemiology
A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study
 ORIGINAL ARTICLE A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study Joon-Hyop Lee, MD, Yoo Seung Chung, MD, PhD,* Young Don Lee, MD, PhD
ORIGINAL ARTICLE A variation in recurrence patterns of papillary thyroid cancer with disease progression: A long-term follow-up study Joon-Hyop Lee, MD, Yoo Seung Chung, MD, PhD,* Young Don Lee, MD, PhD
Ines Buccimazza 16 TH UP CONTROVERSIES AND PROBLEMS IN SURGERY SYMPOSIUM
 BILATERAL MASTECTOMY IS NOT ROUTINELY JUSTIFIED IN PATIENTS WITH BILATERAL AXILLARY LYMPHADENOPATHY AND ONLY ONE DETECTABLE PRIMARY BREAST CANCER LESION SURGERY SYMPOSIUM Ines Buccimazza Breast Unit Department
BILATERAL MASTECTOMY IS NOT ROUTINELY JUSTIFIED IN PATIENTS WITH BILATERAL AXILLARY LYMPHADENOPATHY AND ONLY ONE DETECTABLE PRIMARY BREAST CANCER LESION SURGERY SYMPOSIUM Ines Buccimazza Breast Unit Department
Metachronous anterior urethral metastasis of prostatic ductal adenocarcinoma
 http://dx.doi.org/10.7180/kmj.2016.31.1.66 KMJ Case Report Metachronous anterior urethral metastasis of prostatic ductal adenocarcinoma Jeong Hyun Oh 1, Taek Sang Kim 1, Hyun Yul Rhew 1, Bong Kwon Chun
http://dx.doi.org/10.7180/kmj.2016.31.1.66 KMJ Case Report Metachronous anterior urethral metastasis of prostatic ductal adenocarcinoma Jeong Hyun Oh 1, Taek Sang Kim 1, Hyun Yul Rhew 1, Bong Kwon Chun
Primary invasive carcinoma associated with penoscrotal extramammary Paget's disease: a clinicopathological analysis of 56 cases
 Sexual Medicine Primary invasive carcinoma associated with penoscrotal extramammary Paget's disease: a clinicopathological analysis of 56 cases Bo Dai*, Yun-Yi Kong, Kun Chang*, Yuan-Yuan Qu*, Ding-Wei
Sexual Medicine Primary invasive carcinoma associated with penoscrotal extramammary Paget's disease: a clinicopathological analysis of 56 cases Bo Dai*, Yun-Yi Kong, Kun Chang*, Yuan-Yuan Qu*, Ding-Wei
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER
 MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
MUSCLE-INVASIVE AND METASTATIC BLADDER CANCER (Text update March 2008) A. Stenzl (chairman), N.C. Cowan, M. De Santis, G. Jakse, M. Kuczyk, A.S. Merseburger, M.J. Ribal, A. Sherif, J.A. Witjes Introduction
Guidelines for Management of Penile Cancer
 Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Guidelines for Management of Penile Cancer Date Approved by Network Governance July 2012 Date for Review July 2015 Changes Between Versions 2 and 3 Sections 3, 5, 6 and 16 updated. Page 1 of 10 1. Scope
Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer
 - Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
- Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
SCAN Gynaecological Group. Clinical Management Protocols vulval cancer
 SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer 2009 www.scan.scot.nhs.uk August 2001 updated annually, most recently INTRODUCTION The South East Scotland
SE Scotland Cancer Network SCAN Gynaecological Group Clinical Management Protocols vulval cancer 2009 www.scan.scot.nhs.uk August 2001 updated annually, most recently INTRODUCTION The South East Scotland
Acantholytic Anaplastic Extramammary Paget s Disease: A Case Report and Review of the Literature
 Ann Dermatol Vol. 23, Suppl. 2, 2011 http://dx.doi.org/10.5021/ad.2011.23.s2.s226 CASE REPORT Acantholytic Anaplastic Extramammary Paget s Disease: A Case Report and Review of the Literature Yu-Jin Oh,
Ann Dermatol Vol. 23, Suppl. 2, 2011 http://dx.doi.org/10.5021/ad.2011.23.s2.s226 CASE REPORT Acantholytic Anaplastic Extramammary Paget s Disease: A Case Report and Review of the Literature Yu-Jin Oh,
Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ).
 SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
SOLID TUMORS WORKSHOP Cases for review Prostate Cancer Case #1: 75 y/o Male (treated and followed by prostate cancer oncology specialist ). January 2009 PSA 4.4, 20% free; August 2009 PSA 5.2; Sept 2009
Canadian Scientific Journal. Intraoperative color detection of lymph nodes metastases in thyroid cancer
 Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
Canadian Scientific Journal 2 (2014) Contents lists available at Canadian Scientific Journal Canadian Scientific Journal journal homepage: Intraoperative color detection of lymph nodes metastases in thyroid
EAU GUIDELINES ON PENILE CANCER
 EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
EAU GUIDELINES ON PENILE CANCER (Text update April 2014) O.W. Hakenberg (Chair), N. Watkin, E. Compérat, S. Minhas, A. Necchi, C. Protzel Introduction and epidemiology The incidence of penile cancer increases
Extramammary Paget Disease of External Genitalia: Surgical Excision and Follow-up Experiences With 19 Patients
 www.kjurology.org http://dx.doi.org/10.4111/kju.013.54.1.834 Urological Oncology Extramammary Paget Disease of External Genitalia: Surgical Excision and Follow-up Experiences With 19 Patients Jae Hyun
www.kjurology.org http://dx.doi.org/10.4111/kju.013.54.1.834 Urological Oncology Extramammary Paget Disease of External Genitalia: Surgical Excision and Follow-up Experiences With 19 Patients Jae Hyun
Cervical Cancer: 2018 FIGO Staging
 Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Cervical Cancer: 2018 FIGO Staging Jonathan S. Berek, MD, MMS Laurie Kraus Lacob Professor Stanford University School of Medicine Director, Stanford Women s Cancer Center Senior Scientific Advisor, Stanford
Glossary of Terms Primary Urethral Cancer
 Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Patient Information English Glossary of Terms Primary Urethral Cancer Advanced cancer A tumour that grows into deeper layers of tissue, adjacent organs, or surrounding muscles. Anaesthesia (general, spinal,
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
8. The polyp in the illustration can be described as (circle all that apply) a. Exophytic b. Pedunculated c. Sessile d. Frank
 Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
GUIDELINES ON PENILE CANCER (Text updated March 2005) G. Pizzocaro (chairman), F. Algaba, S. Horenblas, H. van der Poel, E. Solsona, S. Tana, N. Watkin 58 Penile Cancer Eur Urol 2004;46(1);1-8 Introduction
BLADDER CANCER: PATIENT INFORMATION
 BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
BLADDER CANCER: PATIENT INFORMATION The bladder is the balloon like organ located in the pelvis that stores and empties urine. Urine is produced by the kidneys, is conducted to the bladder by the ureters,
SEER Summary Stage Still Here!
 SEER Summary Stage Still Here! CCRA NORTHERN REGION STAGING SYMPOSIUM SEPTEMBER 20, 2017 SEER Summary Stage Timeframe: includes all information available through completion of surgery(ies) in the first
SEER Summary Stage Still Here! CCRA NORTHERN REGION STAGING SYMPOSIUM SEPTEMBER 20, 2017 SEER Summary Stage Timeframe: includes all information available through completion of surgery(ies) in the first
When to Integrate Surgery for Metatstatic Urothelial Cancers
 When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
Case Report Management of Adenocarcinoma in the Setting of Recently Operated Perianal Paget s Disease
 Case Reports in Surgery Volume 2013, Article ID 510813, 5 pages http://dx.doi.org/10.1155/2013/510813 Case Report Management of Adenocarcinoma in the Setting of Recently Operated Perianal Paget s Disease
Case Reports in Surgery Volume 2013, Article ID 510813, 5 pages http://dx.doi.org/10.1155/2013/510813 Case Report Management of Adenocarcinoma in the Setting of Recently Operated Perianal Paget s Disease
Extramammary Paget s disease: a report of 2 cases and a review of the literature
 Malaysian J Pathol 2003; 25(1) : 73 78 EXTRAMAMMARY PAGET S DISEASE CASE REPORT Extramammary Paget s disease: a report of 2 cases and a review of the literature Joon Joon KHOO, MBBS, MPath, and Siew Eng
Malaysian J Pathol 2003; 25(1) : 73 78 EXTRAMAMMARY PAGET S DISEASE CASE REPORT Extramammary Paget s disease: a report of 2 cases and a review of the literature Joon Joon KHOO, MBBS, MPath, and Siew Eng
BreastScreen Aotearoa Annual Report 2015
 BreastScreen Aotearoa Annual Report 2015 EARLY AND LOCALLY ADVANCED BREAST CANCER PATIENTS DIAGNOSED IN NEW ZEALAND IN 2015 Prepared for Ministry of Health, New Zealand Version 1.0 Date November 2017 Prepared
BreastScreen Aotearoa Annual Report 2015 EARLY AND LOCALLY ADVANCED BREAST CANCER PATIENTS DIAGNOSED IN NEW ZEALAND IN 2015 Prepared for Ministry of Health, New Zealand Version 1.0 Date November 2017 Prepared
Rare Case of Metastatic Colorectal Cancer to Uretral Meatus with Rapid Progression and Fatal Outcomes
 Rare Case of Metastatic Colorectal Cancer to Uretral Meatus with Rapid Progression and Fatal Outcomes Marwane Andaloussi Benatiya Department of Urology, Hassan 2 Hospital, Agadir, Morocco Zakaria El Asri
Rare Case of Metastatic Colorectal Cancer to Uretral Meatus with Rapid Progression and Fatal Outcomes Marwane Andaloussi Benatiya Department of Urology, Hassan 2 Hospital, Agadir, Morocco Zakaria El Asri
Rebecca Vogel, PGY-4 March 5, 2012
 Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
Rebecca Vogel, PGY-4 March 5, 2012 Historical Perspective Changes In The Staging System Studies That Started The Talk Where We Go From Here Cutaneous melanoma has become an increasingly growing problem,
American Journals of Cancer Case Reports. A Rare Case of Rectal Metastasis from Sarcomatoid Variant of Urothelial Carcinoma: A Case Report
 American Journals of Cancer Case Reports Lin JYJ et al. American Journals of Cancer Case Reports 2014, 3:1-5 http://ivyunion.org/index.php/ajccr Page 1 of 5 Vol 3 Article ID 20140539, 5 pages Case Report
American Journals of Cancer Case Reports Lin JYJ et al. American Journals of Cancer Case Reports 2014, 3:1-5 http://ivyunion.org/index.php/ajccr Page 1 of 5 Vol 3 Article ID 20140539, 5 pages Case Report
Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy
 Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy Stephanie Yap, M.D. University Gynecologic Oncology Northside Cancer Institute Our Learning Objectives Review survival rates,
Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy Stephanie Yap, M.D. University Gynecologic Oncology Northside Cancer Institute Our Learning Objectives Review survival rates,
Cancer of Unknown Primary (CUP)
 Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
GUIDELINES ON PENILE CANCER
 GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
GUIDELINES ON PENILE CANCER (Text update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin 78 Penile Cancer Eur Urol 2010 Jun;57(6):1002-12 Introduction
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact
 Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
So, we already talked about that recognition is the key to optimal treatment and outcome.
 Hi, I m Dr. Anthony Lucci from the University of Texas MD Anderson Cancer Center in Houston. And today, I d like to talk to you about the role of surgery in inflammatory breast cancer patients. So, there
Hi, I m Dr. Anthony Lucci from the University of Texas MD Anderson Cancer Center in Houston. And today, I d like to talk to you about the role of surgery in inflammatory breast cancer patients. So, there
Diagnosis and staging of breast cancer and multidisciplinary team working
 1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Cancer of Unknown Primary Network Site Specific Group. Clinical Guidelines
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Chapter 8 Adenocarcinoma
 Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Multidisciplinary management of retroperitoneal sarcomas
 Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Take Home Quiz 1 Please complete the quiz below prior to the session. Use the Multiple Primary and Histology Rules
 Take Home Quiz 1 Please complete the quiz below prior to the session. Use the Multiple Primary and Histology Rules Case 1 72 year old white female presents with a nodular thyroid. This was biopsied in
Take Home Quiz 1 Please complete the quiz below prior to the session. Use the Multiple Primary and Histology Rules Case 1 72 year old white female presents with a nodular thyroid. This was biopsied in
PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT
 PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT Author: Dr Sally Ann Hales On behalf of the Breast and pathology CNGs Written: March 2005 Reviewed by CNG: June 2009 &
PROTOCOL SENTINEL NODE BIOPSY (NON OPERATIVE) BREAST CANCER - PATHOLOGY ASSESSMENT Author: Dr Sally Ann Hales On behalf of the Breast and pathology CNGs Written: March 2005 Reviewed by CNG: June 2009 &
FDG-PET/CT in Gynaecologic Cancers
 Friday, August 31, 2012 Session 6, 9:00-9:30 FDG-PET/CT in Gynaecologic Cancers (Uterine) cervical cancer Endometrial cancer & Uterine sarcomas Ovarian cancer Little mermaid (Edvard Eriksen 1913) honoring
Friday, August 31, 2012 Session 6, 9:00-9:30 FDG-PET/CT in Gynaecologic Cancers (Uterine) cervical cancer Endometrial cancer & Uterine sarcomas Ovarian cancer Little mermaid (Edvard Eriksen 1913) honoring
ACOS Inquiry and Response Selected Inquires CS Tumor Size/Extension Evaluation, CS Lymph Nodes Evaluation, CS Metastasis at Diagnosis Evaluation *
 ACOS Inquiry and Response Selected Inquires CS Tumor Size/Extension Evaluation, CS Lymph Nodes Evaluation, CS Metastasis at Diagnosis Evaluation * CS Tumor Size/Extension Evaluation 24842 12/11/2007: Q:
ACOS Inquiry and Response Selected Inquires CS Tumor Size/Extension Evaluation, CS Lymph Nodes Evaluation, CS Metastasis at Diagnosis Evaluation * CS Tumor Size/Extension Evaluation 24842 12/11/2007: Q:
Clinical indications for positron emission tomography
 Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Clinical indications for positron emission tomography Oncology applications Brain and spinal cord Parotid Suspected tumour recurrence when anatomical imaging is difficult or equivocal and management will
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Da Costa was the first to coin the term. Marjolin s Ulcer: A Case Report and Literature Review. Case Report. Introduction
 E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO)
 North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
North of Scotland Cancer Network Clinical Management Guideline for Malignant Melanoma
 Nth of Scotland Cancer Netwk Clinical Management Guideline f Malignant Melanoma Based on WOSCAN CMG with further consultation within NOSCAN UNCONTROLLED WHEN PRINTED Prepared by Approved by Issue date
Nth of Scotland Cancer Netwk Clinical Management Guideline f Malignant Melanoma Based on WOSCAN CMG with further consultation within NOSCAN UNCONTROLLED WHEN PRINTED Prepared by Approved by Issue date
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES
 RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
Dr Rosalie Stephens. Mr Richard Martin. Medical Oncologist Auckland City Hospital Auckland
 Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Management of recurrent phyllodes with full thickness chest wall resection
 ORIGINAL ARTICLES Management of recurrent phyllodes with full thickness chest wall resection R Awwal a, SA Shashi b, MS Khondokar c, SH Khundkar d Abstract: Phyllodes tumours are biphasic fibroepithelial
ORIGINAL ARTICLES Management of recurrent phyllodes with full thickness chest wall resection R Awwal a, SA Shashi b, MS Khondokar c, SH Khundkar d Abstract: Phyllodes tumours are biphasic fibroepithelial
Skin lesions suspicious for melanoma: New Zealand excision margin guidelines in practice
 Skin lesions suspicious for melanoma: excision margin guidelines in practice Tess Brian MBBS; 1 Michael B. Jameson MBChB, FRACP, FRCP, PhD 2,3 1 Department of Plastic and Reconstructive Surgery, Waikato
Skin lesions suspicious for melanoma: excision margin guidelines in practice Tess Brian MBBS; 1 Michael B. Jameson MBChB, FRACP, FRCP, PhD 2,3 1 Department of Plastic and Reconstructive Surgery, Waikato
IMAGING GUIDELINES - COLORECTAL CANCER
 IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
IMAGING GUIDELINES - COLORECTAL CANCER DIAGNOSIS The majority of colorectal cancers are diagnosed on colonoscopy, with some being diagnosed on Ba enema, ultrasound or CT. STAGING CT chest, abdomen and
GUIDELINEs ON PENILE CANCER
 GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
GUIDELINEs ON PENILE CANCER (update April 2010) G. Pizzocaro, F. Algaba, S. Horenblas, E. Solsona, S. Tana, H. Van Der Poel, N. Watkin Eur Urol 2010, doi:10.1016/j.eururo.2010.01.039 Introduction Over
Quiz. b. 4 High grade c. 9 Unknown
 Quiz 1. 10/11/12 CT scan abdomen/pelvis: Metastatic liver disease with probable primary colon malignancy. 10/17/12 Colonoscopy with polypectomy: Adenocarcinoma of sigmoid colon measuring at least 6 mm
Quiz 1. 10/11/12 CT scan abdomen/pelvis: Metastatic liver disease with probable primary colon malignancy. 10/17/12 Colonoscopy with polypectomy: Adenocarcinoma of sigmoid colon measuring at least 6 mm
Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate surgical options
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Breast cancer reconstruction surgery (immediate and delayed) across Ontario: Patient indications and appropriate
Case 18. M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is:
 Case 18 M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is: A. Pilomatrical carcinoma B. Adnexal carcinoma NOS C. Metastatic squamous cell carcinoma D.Primary squamous cell carcinoma
Case 18 M75. Excision of mass on scalp. Clinically SCC. The best diagnosis is: A. Pilomatrical carcinoma B. Adnexal carcinoma NOS C. Metastatic squamous cell carcinoma D.Primary squamous cell carcinoma
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
Prognostic factors in squamous cell anal cancers
 Prognostic factors in squamous cell anal cancers Zainul Abedin Kapacee Year 4-5 Intercalating Medical Student, University of Manchester Dr. Shabbir Susnerwala, Mr. Nigel Scott Dr. Falalu Danwata, Dr. Marcus
Prognostic factors in squamous cell anal cancers Zainul Abedin Kapacee Year 4-5 Intercalating Medical Student, University of Manchester Dr. Shabbir Susnerwala, Mr. Nigel Scott Dr. Falalu Danwata, Dr. Marcus
Primary Malignant Melanoma of the Vagina: Report of Two Cases and Review of the Literature
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.9655007 Volume 1, Issue 2 Case Report Primary Malignant Melanoma of the Vagina: Report of Two Cases and Review of the Literature Guler
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.9655007 Volume 1, Issue 2 Case Report Primary Malignant Melanoma of the Vagina: Report of Two Cases and Review of the Literature Guler
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy
 Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Desmoplastic Melanoma: Surgical Management and Adjuvant Therapy Dale Han, MD Assistant Professor Department of Surgery Section of Surgical Oncology No disclosures Background Desmoplastic melanoma (DM)
Cervical Cancer 3/25/2019. Abnormal vaginal bleeding
 Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Cervical Cancer Abnormal vaginal bleeding Postcoital, intermenstrual or postmenopausal Vaginal discharge Pelvic pain or pressure Asymptomatic In most patients who are not sexually active due to symptoms
Penis Cancer. What is penis cancer? Symptoms. Patient Information. Pagina 1 / 9. Patient Information - Penis Cancer
 Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Patient Information English 31 Penis Cancer The underlined terms are listed in the glossary. What is penis cancer? Cancer is abnormal cell growth in the skin or organ tissue. When this cell growth starts
Oncology General Principles L A U R I E S I M A R D B R E A S T S U R G I C A L O N C O L O G Y F E L L O W D E C E M B E R
 Oncology General Principles L A U R I E S I M A R D B R E A S T S U R G I C A L O N C O L O G Y F E L L O W D E C E M B E R 2 0 1 2 Objectives Discuss Diagnostic and staging strategies in oncology Know
Oncology General Principles L A U R I E S I M A R D B R E A S T S U R G I C A L O N C O L O G Y F E L L O W D E C E M B E R 2 0 1 2 Objectives Discuss Diagnostic and staging strategies in oncology Know
A superficial radiotherapy B single pass curettage C excision with 2 mm margins D excision with 5 mm margins E Mohs micrographic surgery.
 1- A 63-year-old woman presents with a non-healing lesion on her right temple that has been present for over two years. On examination there is a 6 mm well defined lesion with central ulceration, telangiectasia
1- A 63-year-old woman presents with a non-healing lesion on her right temple that has been present for over two years. On examination there is a 6 mm well defined lesion with central ulceration, telangiectasia
