Clinical Study Ultrasound Guided Core Biopsy versus Fine Needle Aspiration for Evaluation of Axillary Lymphadenopathy in Patients with Breast Cancer
|
|
|
- Marylou Elliott
- 5 years ago
- Views:
Transcription
1 ISRN Oncology, Article ID , 9 pages Clinical Study Ultrasound Guided Core Biopsy versus Fine Needle Aspiration for Evaluation of Axillary Lymphadenopathy in Patients with Breast Cancer Marie A. Ganott, 1 Margarita L. Zuley, 1 Gordon S. Abrams, 1 Amy H. Lu, 1 Amy E. Kelly, 1 Jules H. Sumkin, 1 Mamatha Chivukula, 2 Gloria Carter, 3 R. Marshall Austin, 3 and Andriy I. Bandos 4 1 Department of Radiology at Magee-Womens Hospital of the University of Pittsburgh Medical Center, 300 Halket Street, Pittsburgh, PA 15213, USA 2 Department of Pathology, Mills-Peninsula Hospital of Sutter Health Affiliate, 383 East Grand Avenue suite A, South San Francisco, CA 94080, USA 3 Department of Pathology at Magee-Womens Hospital of the University of Pittsburgh Medical Center, 300 Halket Street, Pittsburgh, PA 15213, USA 4 Department of Biostatistics, University of Pittsburgh, Graduate School of Public Health, A414 Crabtree Hall, 130 DeSoto Street, Pittsburgh, PA 15213, USA Correspondence should be addressed to Marie A. Ganott; mganott@mail.magee.edu Received 23 September 2013; Accepted 24 November 2013; Published 4 February 2014 Academic Editors: K. H. Tkaczuk and T. Yokoe Copyright 2014 Marie A. Ganott et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Rationale and Objectives. To compare the sensitivities of ultrasound guided core biopsy and fine needle aspiration (FNA) for detection of axillary lymph node metastases in patients with a current diagnosis of ipsilateral breast cancer. Materials and Methods. From December 2008 to December 2010, 105 patients with breast cancer and abnormal appearing lymph nodes in the ipsilateral axilla consented to undergo FNA of an axillary node immediately followed by core biopsy of the same node, both with ultrasound guidance. Experienced pathologists evaluated the aspirate cytology without knowledge of the core histology. Cytology and core biopsy results were compared to sentinel node excision or axillary dissection pathology. Sensitivities were compared using McNemar s test. Results. Of 70 patients with axillary node metastases, FNA was positive in 55/70 (78.6%) and core was positive in 61/70 (87.1%) (P = 0.18). The FNA and core results were discordant in 14/70 (20%) patients. Ten cases were FNA negative/core positive. Four cases were FNA positive/core negative. Conclusion. Core biopsy detected six (8.6%) more cases of metastatic lymphadenopathy than FNA but the difference in sensitivities was not statistically significant. Core biopsy should be considered if the node is clearly imaged and readily accessible. FNA is a good alternative when a smaller needle is desired due to node location or other patient factors. This trial is registered with NCT Introduction The prognosis of the newly diagnosed breast cancer patient depends on a number of factors, among the most important of which is the extent of spread of disease to the axillary lymph nodes [1, 2]. Because treatment is influenced by the presence and number of axillary lymph nodes involved, evaluation of the axillary nodes has been performed in every patient that could tolerate it after a diagnosis of invasive carcinoma [3].Inthepast,acompletesurgicaldissectionoftheaxilla was performed, resulting in significant morbidity, including a 30% incidence of lymphedema [4]. The development of sentinel node mapping resulted in a notable reduction in morbidity; however, if a sentinel node was positive, often not discovered until final pathologic processing done postoperatively, complete axillary dissection would be performed at a later date to assess the total number of lymph nodes involved, thus requiring a second surgical procedure and anesthesia
2 2 ISRN Oncology [5 7]. A preoperative diagnosis of axillary metastasis by ultrasound guided node biopsy would streamline patient care and reduce operating room time and expense by allowing definitive breast surgery and complete axillary dissection in the same operative setting, eliminating an unnecessary sentinel node procedure. While the need for preoperative node sampling in patients with nonpalpable nodes and T1 and T2 cancers has been challenged by the ACOSOG Z 11 study [8], there are subgroups of women for whom initial ultrasound guided node sampling is desirable, including those planning mastectomy or neoadjuvant chemotherapy. Using current high frequency transducers, the axillary lymph nodes are usually well visualized sonographically. Studies have been performed attempting to identify malignant lymph nodes by their morphology but there is overlap both in the appearance of benign and malignant lymphadenopathy and in the appearance of normal and abnormal lymph nodes, with benign causes of axillary adenopathy being relatively common [9 11]. Therefore, tissue diagnosis of axillary node status remains important when it will affect patient management. Tissue sampling of suspicious axillary lymph nodes with ultrasound guidance has been performed for many years with a fine needle to obtain aspirates for cytologic evaluation. Reports in the literature have shown that FNA is useful for evaluation of metastatic disease, with sensitivities ranging from 44 to 100%, the variability being likely due at least in part to patient selection [12 18]. Studies comparing FNA to large needle core biopsy of breast masses haveshowncorebiopsytobemoreaccurateandeasierto interpret than FNA [19], leading breast care specialists to wonder if that is the case for sampling of axillary lymph nodes. While it is reasonable to expect the use of a core biopsy device to obtain a larger and architecturally intact piece of tissue to increase diagnostic accuracy as compared to obtaining an aspirate of cells with a fine needle, if the only question to be answered in sampling the axillary node is whether or not metastatic carcinoma cells are present along with lymphocytes, a larger architecturally intact piece of tissue may not be required. Although core biopsy is more invasive than FNA due to the larger needle size, reports have shown that core biopsy of axillary nodes is a safe and effective procedure [20, 21]. Retrospective comparisons of FNA and core accuracy in the axilla have been performed [22, 23], but to our knowledge, only one other prospective study [24] has been published directly comparing fine needle aspiration to core biopsy of an axillary lymph node for the diagnosis of metastatic breast cancer. The purpose of this study was to determine if there is a difference between ultrasound guided core biopsy and FNA in their ability to detect metastatic disease in the axillary lymph nodes of patients with a current diagnosis of ipsilateral breast cancer. 2. Materials and Methods 2.1. Study Design. From December 2008 through December 2010, women with suspected or recently diagnosed breast carcinoma and at least one lymph node in the ipsilateral axilla judged to be abnormal in sonographic appearance were approached for participation in this IRB-approved, HIPIAA-compliant prospective study. 105 women gave written informed consent to undergo ultrasound guided FNA, immediately followed by core biopsy of the same node, followed by clip placement. Patients unable to consent due to language or comprehension difficulties and patients deemed emotionallytoofragiletodiscussthesubjectofmetastatic disease required in the consent form were excluded. Other patients excluded themselves, not wishing to undergo a second needle procedure for research purposes. One patient was excluded due to difficulty accessing the node with a core biopsy due to its location. The outcome of percutaneous node sampling was correlated with surgical pathology from sentinel node excision or axillary dissection. Priortonodesampling,thecorticalthickness,presenceor absence of a hilus, presence or absence of cortical flow, node shape, and number of nodes thought to be abnormal were recorded. A Phillips iu22 ultrasound unit (Phillips Healthcare, Andover, MA) with 12 or 17 MHz transducers was used for imaging. Criteria used in determining appropriateness for node sampling were loss of the normal hilus, abnormal shape including focal bulging of the cortex, presence of cortical flow, and cortical thickening. A strict threshold for cortical thickness was not used; a node with a cortex between 2 and 3 mm was considered suspicious if the other nodes had cortices less than 2 mm. The patients were asked to rate their pain during each procedure on a scale of 1 to 10 and were informed of which procedure was being performed. The degree of bleeding (minimal or moderate) or hematoma formation, if any, was documented Study Population. Of the 105 patients, 7 patients percutaneous breast biopsies were unexpectedly negative for malignancy (their node biopsies were all negative also). Of the remaining 98 with breast malignancy, 3 patients with both FNA and core negative nodes were excluded due to lack of histopathologic axillary surgical correlation. Thus, 95 patients constitute the cohort for assessing percutaneous node biopsy sensitivity. We included 4 patients who did not have axillary surgery but were assumed to be true positives as they were both core and FNA positive. Time between biopsy and surgery ranged from 9 days to 10 months. However, 47 of the patients had neoadjuvant chemotherapy prior to surgery. Tumorsizerangedfrom6mmto10.7cm,with12patients having tumor size greater than 5 cm. Cortical thickness of the sampled noderangedfrom2mm to over 6mm. Table 1 shows features of the study population Tissue Sampling Procedures. To mimic the actual range of clinical practice, variability in sampling devices was allowed. FNA was performed using a 21 or 25 g, 2-inch needle, with one (90 cases), 2 (11 cases), or 3 (4 cases) needle entries of multiple needle excursions through the cortex of the node. The number of excursions was not recorded, but radiologists preferring more than one entry typically made fewer excursions per entry, estimated at 10 versus 20 to 30. The aspirated material was placed both on slides in 95%
3 ISRN Oncology 3 Table 1: Features of population of 95 patients in study cohort. Number of patients Node positive Number of patients Node negative Number of patients Neoadjuvant therapy Number of patients No chemotherapy Other Number of patients Tumor size by imaging 5 mm 1 cm 4 (6) 6 (24) 3 (6) 7 (16) 0(0) >1cm-2cm 19 (27) 7 (28) 12 (26) 13 (30) 1(25) >2 cm 5 cm 36 (51) 11 (44) 25 (53) 20 (45) 2(50) >5cm 11 (16) 1 (4) 7 (15) 4 (9) 1(25) Hilus present 51 (73) 22 (88) 34 (72) 36 (82) 3(75) Hilus absent 19(27) 3(12) 13(28) 8(18) 1(25) Cortex 2mm 1(1) 0(0) 1(2) 0(0) 0(0) mm 13 (19) 18 (72) 9 (19) 22 (50) 0(0) mm 20(29) 3(12) 13(28) 9(20) 1(25) >6mm 36 (51) 4 (16) 24 (51) 13 (30) 3(75) Shape Normal 21 (30) 9 (36) 13 (28) 17 (39) 0(0) Focal bulge 20 (29) 12 (48) 14 (30) 10 (23) 3(75) Round 23(33) 4(16) 16(34) 15(34) 1(25) Ill-defined 6 (9) 0 (0) 4 (8) 2 (4) 0(0) Number of suspicious nodes 1 31 (44) 14 (56) 18 (38) 24 (55) 3(75) 2 16 (23) 3 (12) 11 (23) 10 (23) 0(0) 3 10 (14) 5 (16) 7 (15) 5 (11) 1(25) 4ormore 13 (19) 3 (12) 11 (24) 5 (11) 0(0) Note. Numbers in parentheses are percentages. Percentages are rounded. Other: 4 patients were both core and FNA positive but did not have axillary surgery. Number of cases Case distribution by radiologist Radiologist identification number Core positive FNA positive Number of positive cases Figure 1: The graph illustrates the number of cases positive for malignancy for each radiologist and the number testing positive by core biopsy and FNA. (The 12th radiologist was not included, with only negative cases.) alcohol and in buffered Formalin for cell block preparation; a pathologist was not present at the time of the procedure to evaluate the adequacy of the samples. Core biopsy was performed immediately following the FNA with either a 14 g (86 cases), 12 g (16 cases), or 18 g (3 cases) biopsy device. The 12 g device used was Celero (Hologic, Bedford, MA). The 14 g devices were Bard Monopty, Bard Maxcore, Finesse (Bard, Tempe, AZ), and Achieve (Cardinal Health, Dublin, OH), and the 18 g devices were Achieve. One to four cores were obtained (one core in 23 cases, 2 cores in 54 cases, 3 cores in 20 cases, and 4 cores in 8 cases). With 14 g devices, only one core was obtained in 11 of 86 cases. With 12 g devices, one core only was obtained in 12 of 16 cases. With 18 g devices, 2, 3, or 4 cores were obtained. The procedures were performed by 12 different academic radiologists experienced (range 3 21 years, with over half performed by those with over 16 years of experience) in breast imaging and biopsy (Figure 1). However, for a given patient, the same radiologist performed both the FNA and the core biopsy. The cytologic material obtained was evaluated by one of three pathologists experienced in breast pathology and cytology, without the knowledge of the core biopsy result. No immunostains were used. The FNA result was categorized as negative if reported as containing suspicious cells but not actually stating
4 4 ISRN Oncology (a) (b) (c) Figure 2: Ultrasound images of the right axilla of a 65-year-old woman with infiltrating lobular carcinoma show (a) a round lymph node (arrows) with a 5 mm cortex, (b) a 25 g FNA needle (arrows) traversing the cortex of the node, and (c) the open trough (arrows) of a 12 g core biopsy needle in the node. The FNA was single entry. The core was 1 pass. The FNA cytology was negative but the core biopsy was positive formalignancy;7of18lymphnodeswerepositiveataxillarydissectionperformedlessthan2monthsafterthebiopsy. that metastatic cancer cells were present. The core biopsy samples were evaluated separately by different pathologists. Suboptimal specimens were categorized as negative for both core and FNA, because the course of action in our institution in most cases would be to proceed with sentinel node biopsy rather than to repeat the percutaneous biopsy. Figure 2 shows images from an axillary node sampling procedure Statistical Analysis. Statistical analysis was performed using SAS v.9.2. The sensitivities of the FNA and core biopsy procedures were compared using McNemar s exact test for correlated proportions. The trends in sensitivities with changing numbers of passes, entries, or needle sizes were assessed with the exact Cochran-Armitage test. Patients subjective perception of pain levels was compared using the exact Wilcoxon sign test. 3. Results Of the 95 patients in the study cohort, 70 patients (74%) had metastatic adenopathy. This group included 5 patients that were both core and FNA positive at percutaneous biopsy but were node negative after chemotherapy, 2 discordant (FNA negative, core positive or FNA positive, core negative) cases with complete pathologic response to chemotherapy resulting in negative nodes at surgery, and 4 core and FNA positive patients without axillary surgical correlation. (59 patients had positive nodes at axillary surgery.) We assumed no results were false positive. Figure 3 is a flow chart of the procedures and results. FNAwaspositivein55/70(78.6%)andcorewaspositive in 61/70 (87.1%) (P = 0.18 (95% CI )). 65 of the 70 (92.9%) patients had a positive axillary node by tissue sampling:51bybothfnaandcore,4onlybyfna,and10
5 ISRN Oncology 5 US guided lymph node biopsy in patients with breast CA (n = 95) FNA negative Core negative (n = 30) FNA negative FNA positive FNA positive Core positive Core negative Core positive (n = 10) (n = 4) (n = 51) Surgery Neoadjuvant Surgery Neoadjuvant Surgery Neoadjuvant Surgery Neoadjuvant (n = 23) (n = 7) (n = 4) (n = 6) (n = 1) (n = 3) (n = 16) (n = 31) Total surgeries Total neoadjuvant (n = 44) (n = 47) No metastasis Metastasis No metastasis Metastasis (n = 18) (n = 26) (n = 7) (n = 40) FNA positive 17/26 Core positive 20/26 FNA positive 34/40 Core positive 37/40 FNA positive 55/70 Core positive 61/70 No axillary surgery (n = 4) Figure 3: Flowchart of patients undergoing lymph node biopsy. Total surgeries = number of patients without chemotherapy before surgery. Total neoadjuvant = number of patients having chemotherapy before surgery. only by core biopsy. Thus, in this group of 70, there were 14 cases (20%) where FNA and core results were discordant (K = 0.3 (95% CI 0.03 to 0.58)). The sensitivity for single pass core biopsy was 78.6% (11/14) and for multipass cores was 89.3% (50/56), which was not a statistically significant difference (P = 0.37). The sensitivity for the 12 g device was 89.9% (8/9), for 14 g devices was 86.7% (52/60), and for 18 g devices was 1/1; the differences in sensitivity using the 12 g vacuum assisted device versus other devices together were not statistically significant (P > 0.99). The sensitivity for 21 g single entry FNA was 76.1% (35/46) not different from 25 g single entry FNA at 78.6% (11/14) (P = 0.85). The sensitivity for single entry FNA was 76.7% (46/60) not statistically significantly different from multientry FNA at 90% (9/10) (P > 0.41)(Table 2). The sensitivities of FNA and core biopsy were compared in Table 2 for numbers of suspicious nodes, for node hilus, cortex, and shape, and also for tumor size. FNA was the least sensitive in normal shaped nodes. FNA sensitivity was inferior to core sensitivity (P = 0.04) when the node hilus was visible but improved with hilar absence. Both FNA and core sensitivities improved with cortical thickness increasing beyond 2 mm, and when 3 or more abnormal appearing nodes were noted. Ofthe10FNAnegative/corepositivepatients,allbutone had positive nodes at surgery; that patient had a complete pathologic response to chemotherapy and 20 negative nodes. One cytology specimen was reported as less than optimal, and 2 mentioned suspicious cells but were not diagnostic for malignancy. Of the 4 FNA positive/core negative cases, each performed by a different radiologist, all of the core specimens were reported as suboptimal, 2 with scant lymphoid tissue, and two with absent lymphoid tissue. In 2 of the 4 (one scant and one absent lymphoid tissue), only one core was obtained. Three of the 4 had positive nodes at surgery, and one patient had negative nodes but had a complete pathologic response to chemotherapy with neoadjuvant related changes in the axilla. Of the 5 core and FNA negative patients with positive nodes at surgery, the clip was noted to be in a negative node in 2 cases indicating that the wrong node was chosen for sampling. The presence of a clip or evidence of biopsy was commented on in 59% (54/91) axillary surgical reports. There was no difference in bleeding between the 2 procedures, which was minimal for all but one case that
6 6 ISRN Oncology Table 2: Sensitivity of core biopsy versus FNA for detection of 70 patients with Axillary node metastases. Factor N Core detected FNA detected Difference in N (%) N (%) sensitivities (core-fna) Discordant P value Overall (87.1) 55 (78.6) 8.6% Number of core passes 1pass (78.6) > (89.3) Core needle size 12 g 9 8 (88.9) 1corepass 8 7(87.5) >1corepass 1 1(100) 14 g or 18 g (86.9) 1corepass 6 4 (66.7) >1corepass (89.1) Number of FNA entries 1entry (76.7) >1 10 9(90) FNA needle size 21g (77.4) 1FNAentry (76.1) >1FNAentry 7 6(85.7) 25g (82.4) 1FNAentry (78.6) >1FNAentry 3 3(100) Hilus Present (86.3) 36 (70.6) 15.7% 12 Absent (89.5) 19 (100) 10.5% 2 Cortex 2mm 1 1 (100) 0 (0) 100.0% mm 13 8 (61.5) 7 (53.8) 7.7% mm (90) 15 (75) 15.0% 5 >6mm (94.4) 33 (91.7) 2.8% 5 Shape Normal (76.2) 11 (52.4) 23.8% 5 Focal bulge (95) 16 (80) 15.0% 5 Round (95.7) 22 (95.7) 0.0% 2 Ill-defined 6 4 (66.7) 6 (100) 33.3% 2 Number of suspicious nodes (83.9) 23 (74.2) 9.7% (81.3) 11 (68.8) 12.5% (100) 9 (90) 10.0% 1 4ormore (92.3) 12 (92.3) 0.0% 2 Tumor size by imaging 5 mm 1 cm 4 4 (100) 2 (50) 50.0% 2 >1cm-2cm (84.2) 14 (73.7) 10.5% 4 >2 cm 5 cm (86.1) 31 (86.1) 2.8% 5 >5cm 11 9 (81.8) 8 (72.7) 9.1% 3 Chemotherapy status No chemotherapy (76.9) 17 (65.4) 11.5% 5 Neoadjuvant (92.5) 34 (85.0) 7.5% 9 Other 4 4 (100) 4 (100) 0.0% 0 Other: 4 patients were both core and FNA positive but did not have axillary surgery. wasmoderateforbothfnaandcore.themeanpainscore for FNA was 2.0 and for core was 2.4 while the range was from 1 to 8 for FNA and from 1 to 10 for core. Reported pain levels were similar during FNA and core in 63 patients (60%), greater with core in 31 patients (29.5%), and greater with FNA in 11 patients (10.5%). The higher pain level was reported significantly more frequently for core than for FNA (P < 0.01). 4. Discussion Our results show that although core biopsy had greater sensitivity than FNA in detecting metastasis, it did not approach statistical significance, probably primarily due to the small number of patients. These results are in agreement with the meta-analysis by Houssami et al. [22]whoreported a sensitivity for FNA (24 studies) of 72.2% and sensitivity for
7 ISRN Oncology 7 core biopsy (4 studies) of 83.3%, which were not statistically significantlydifferent.theonlyotherprospectivecomparison study [24] reportedasignificantlygreatersensitivityforcore biopsy (88.2%) than for FNA (72.5%) but had a small sample size of 51 patients undergoing percutaneous node biopsy with axillary metastasis. Our study included several experienced radiologists and allowed a variety of sampling devices to simulate actual clinical practice. While axillary node FNA is technically easy to perform for one experienced in image-guided procedures, the radiologist must obtain an aspirate that is both sufficient in the amount of material and at the same time not overly bloody, to enable an optimal interpretation. It is not clear why there were fewer false negative results when multiple FNA entries were performed, as the total number of needle excursions likely did not differ greatly. Perhaps the chance of obtaining a better sample was increased by using different entry sites or obtaining less blood mixed with cells from the node. The number of slides used, actual number of excursions, and length of procedure were not recorded, which could have affected the results. In some institutions, a pathologist is present when cytologic samples are obtained and can request additional sampling if the specimen is deemed suboptimal; the presence of a pathologist at the time of sampling could have improved the yield from FNA. In our institution, immunostains may be used to aid in interpretation when FNA alone is performed. Our pathologists have extensive experience in cytopathology but in this study therewerenoimmunostainsusedinthecytologicevaluation; because the pathologists knew that additional tissue would be examined by core biopsy, a factor that may have decreased the sensitivity of FNA. As demonstrated by the core negative/fna positive cases, care must be taken to be certain that the core specimen is being taken from the node; the node may be more difficult to visualize due to its depth and is frequently very mobile, making the core biopsy procedure quite challenging. Obtaining more than one core sample should insure a greater chance of obtaining an adequate specimen, as shown by the trend (albeit statistically not significant) for increased sensitivity with a greater number of core passes. Obtaining one core with a 14 g device was the least sensitive technique in this study and would not be recommended. If it is not certain that adequate cores were obtained, the radiologist should perform FNA of the node or take additional cores. In either case, samples should be taken from the node s cortex, where the metastatic cells would lodge, avoiding the hilus where the vascular supply to the node is located. Both FNA and core biopsy (excluding the insufficient cores of ill-defined nodes) were least sensitive when the node appearance was least abnormal. This can be due to difficulty in choosing the appropriate node for sampling or due to smaller metastatic deposits in the sampled node. In 4 of the 5 cases that were both core and FNA negative, the nodes had a normal shape, visible hilus, and cortical thickness of 2.1 to 4 mm. In our study core biopsy had no more morbidity than FNA, even with the largest gauge device. Use of a biopsy device with a nonthrow option should diminish the chance of vascular injury. However, patients whose suspect node was immediately adjacent to a vessel or very deep and difficult to access were not asked to participate in the study and hence were not subjected to core biopsy. Despite the statistically significant difference we observed in the number of patients reporting pain being greater during core than FNA, the majority of patients tolerated the pain equally well during both procedures, and we do not believe this should be a factor in deciding which procedure to perform. Limitations of our study included its small size, in particular, the small size of subgroups of needle types and number of samples obtained. Although there may have been some selection bias due to excluding patients with nodes not suited to core biopsy, the aim of the study was to compare the two methods when both were possible. In all cases,thecorebiopsywasperformedafterthefna,with additional lidocaine, which may have minimized the pain associated with core biopsy. FNA was always performed first because of concern that core biopsy might cause sufficient bleeding to have to abort the second sampling procedure, but bleeding was not a significant problem. A large fraction of patients underwent neoadjuvant chemotherapy, which was not predicted at the time of initiation of the study. This could have rendered some patients node negative that were initially node positive, but there were only 7 that were node negative after chemotherapy and node negative by both core and FNA. If FNA and core were both falsely negative, there would be a similar reduction in sensitivity for each method. Unsuccessful neoadjuvant chemotherapy could result in nodes initially negative becoming positive. However, the 5 patients which were both FNA and core negative and with positive nodes at surgery did not have neoadjuvant chemotherapy. Table 2 shows the sensitivities of core biopsy and FNA in patients chosen to receive chemotherapy to be better than in those going directly to surgery, which is likely a reflection of the fact that the neoadjuvant group had more abnormal appearing nodes with thicker cortices. Our study began before the ACOSOG Z0011 trial [8] that reported in 2010 no statistically significant differences in local or regional recurrence after median follow-up of 6.3 years between those randomized to sentinel node dissection alone versus completion axillary dissection in patients with clinically negative axillae and T1 or T2 invasive breast cancers treated with lumpectomy and radiation and 1 or 2 positive sentinel nodes. As a result of this trial, surgeons indicated that they would perform sentinel node biopsy even after a positive percutaneous node biopsy to determine if only one or two nodes were positive rather than perform axillary dissectioninpatientswithtumorslessthan5cm.consequently some surgeons have requested that radiologists not biopsy suspicious nodes in these patients. However, the Z0011 patient population had a low tumor burden with median tumor sizes of 1.6 and 1.8 cm, and a high percentage of micrometastases and solitary positive nodes, suggesting that their outcome may be different than those with positive percutaneous node biopsies. Although the Z0011 trial results have called into question the value of preoperative tissue sampling of axillary nodes in a selected population, the preoperative detection of metastatic adenopathy at the time of breast cancer diagnosis
8 8 ISRN Oncology will continue to be helpful in management of patients with a larger tumor burden and allow many women to have axillary dissection at the time of definitive breast surgery, sparing them an unnecessary sentinel node procedure. For patients who will undergo neoadjuvant chemotherapy, the Z0011 results do not apply; percutaneous axillary node sampling will aidinproperstagingpriortotreatment. The decision to perform core biopsy versus FNA should be based on the pathologist s experience in interpreting cytology and the accessibility of the lymph node. Core biopsy should be considered if the node is clearly imaged and readily accessible. Fine needle aspiration is a good alternative to core biopsy when a smaller needle is desired due to node location orotherpatientrelatedfactors.careshouldbetakentoobtain sufficient material for cytologic or histopathologic evaluation. Conflict of Interests The authors declare that there is no conflict of interests regarding the publication of this paper. Funding Partial funding from Magee-Womens Foundation and Suros Surgical, Inc. (now Hologic, Inc.). Acknowledgments The authors would like to acknowledge the assistance of Linda Lovy, Michele Gruss, and Erica Brown. References [1] B. Fisher, M. Bauer, D. L. Wickerham et al., Relation of number of positive axillary nodes to the prognosis of patients with primary breast cancer. An NSABP update, Cancer,vol.52,no. 9, pp , [2]S.Masood, Prognosticfactorsinbreastcancer, The Breast Journal,vol.3,no.5,pp ,1997. [3] Z. U. Rahman, A. U. Buzdar, E. Singletary et al., Selection of systemic therapy: is axillary lymph node status important? Seminars in Breast Disease,vol.1,no.3,pp ,1998. [4] D. Brenin and M. Morrow, Conventional axillary dissection: extent, local control, and morbidity, Seminars in Breast Disease, vol. 1, no. 3, pp , [5] J.J.Albertini,G.H.Lyman,C.Coxetal., Lymphaticmapping and sentinel node biopsy in the patient with breast cancer, JournaloftheAmericanMedicalAssociation,vol.276,no.22, pp ,1996. [6] N. M. Hansen, Historical review of sentinel node biopsy for breast cancer, Seminars in Breast Disease,vol.5,no.1,pp.2 9, [7] B. J. Grube and A. E. Giuliano, Implications of sentinel lymphadenectomy and management options of the axilla after sentinel node biopsy: sentinel node negative and sentinel node positive, Seminars in Breast Disease, vol.5,no.2,pp.61 75, [8] A. E. Giuliano, L. McCall, P. Beitsch et al., Locoregional recurrence after sentinel lymph node dissection with or without axillary dissection in patients with sentinel lymph node metastases: the American college of surgeons oncology group z0011 randomized trial, Annals of Surgery, vol.252,no.3,pp , [9]R.Welsh,P.J.Kornguth,M.S.Soo,R.Bentley,andD.M. DeLong, Axillary lymph nodes: mammographic, pathologic, and clinical correlation, American Journal of Roentgenology, vol. 168, no. 1, pp , [10] P.Vassallo,K.Wernecke,N.Roos,andP.E.Peters, Differentiation of benign from malignant superficial lymphadenopathy: the role of high-resolution US, Radiology, vol. 183, no. 1, pp , [11] E. E. Deurloo, P. J. Tanis, K. G. A. Gilhuijs et al., Reduction in the number of sentinel lymph node procedures by preoperative ultrasonography of the axilla in breast cancer, European Journal of Cancer,vol.39,no.8,pp ,2003. [12] V. Kuenen-Boumeester, M. Menke-Pluymers, A. Y. de Kanter, I.-M. A. Obdeijn, D. Urich, and T. H. van der Kwast, Ultrasound-guided fine needle aspiration cytology of axillary lymph nodes in breast cancer patients. A preoperative staging procedure, European Journal of Cancer, vol.39,no.2,pp , [13] S.Sahoo,M.A.Sanders,L.Roland,N.Pile,andA.B.Chagpar, Astrategicapproachtotheevaluationofaxillarylymphnodes in breast cancer patients: analysis of 168 patients at a single institution, American Journal of Surgery,vol.194,no.4,pp , [14] S. Krishnamurthy, N. Sneige, D. G. Bedi et al., Role of ultrasound-guided fine-needle aspiration of indeterminate and suspicious axillary lymph nodes in the initial staging of breast carcinoma, Cancer, vol. 95, no. 5, pp , [15] J.U.N.Oruwari,M.A.Chung,S.Koelliker,M.M.Steinhoff,and B. Cady, Axillary staging using ultrasound-guided fine needle aspiration biopsy in locally advanced breast cancer, American Journal of Surgery,vol.184,no.4,pp ,2002. [16] A. Sapino, P. Cassoni, E. Zanon et al., Ultrasonographicallyguided fine-needle aspiration of axillary lymph nodes: role in breast cancer management, British Journal of Cancer, vol. 88, no.5,pp ,2003. [17] B.Brancato,M.Zappa,D.Bricoloetal., Roleofultrasoundguided fine needle cytology of axillary lymph nodes in breast carcinoma staging, Radiologia Medica,vol.108,no.4,pp , [18] S. L. Koelliker, M. A. Chung, M. B. Mainiero, M. M. Steinhoff, and B. Cady, Axillary lymph nodes: US guided fine-needle aspiration for initial staging of breast cancer Correlation with primary tumor size, Radiology, vol. 246, no. 1, pp , [19] W. A. Berg, Image-guided breast biopsy and management of high-risk lesions, Radiologic Clinics of North America, vol. 42, no.5,pp ,2004. [20] U. Topal, Ş. Punar, I. Taşdelen, and S. B. Adim, Role of ultrasound-guided core needle biopsy of axillary lymph nodes in the initial staging of breast carcinoma, European Journal of Radiology,vol.56,no.3,pp ,2005. [21] H. Abe, R. A. Schmidt, C. A. Sennett, A. Shimauchi, and G. M. Newstead, US-guided core needle biopsy of axillary lymph nodes in patients with breast cancer: why and how to do it, Radiographics,vol.27,pp.S91 S99,2007. [22]N.Houssami,S.Ciatto,R.M.Turner,H.S.Cody,andP. MacAskill, Preoperative ultrasound-guided needle biopsy of axillary nodes in invasive breast cancer: meta-analysis of its
9 ISRN Oncology 9 accuracy and utility in staging the axilla, Annals of Surgery,vol. 254, no. 2, pp , [23]R.Rao,L.Lilley,V.Andrews,L.Radford,andM.Ulissey, Axillary staging by percutaneous biopsy: sensitivity of fineneedle aspiration versus core needle biopsy, Annals of Surgical Oncology,vol.16,no.5,pp ,2009. [24] S. Rautianen, A. Masarwah, M. Sudah et al., Axillary iymph node biopsy in newly diagnosed breast cancer: comparative accuracy of fine-needle aspiration biopsy versus core needle biopsy, Radiology, vol. 269, pp.54 60, 2013.
10 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Women s Imaging Original Research
 Women s Imaging Original Research Mainiero et al. Ultrasound-Guided FN in Breast Cancer Patients Women s Imaging Original Research WOMEN S IMGING Martha B. Mainiero 1 Christina M. Cinelli 2 Susan L. Koelliker
Women s Imaging Original Research Mainiero et al. Ultrasound-Guided FN in Breast Cancer Patients Women s Imaging Original Research WOMEN S IMGING Martha B. Mainiero 1 Christina M. Cinelli 2 Susan L. Koelliker
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Study on Efficacy of Preoperative Ultrasonography for Axillary Lymph Node Involvement In Breast Carcinoma
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 4 Ver. II. (Apr. 2014), PP 01-05 Study on Efficacy of Preoperative Ultrasonography for Axillary
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 4 Ver. II. (Apr. 2014), PP 01-05 Study on Efficacy of Preoperative Ultrasonography for Axillary
Donna Plecha, MD 1, Shiyu Bai, BS 2, Helen Patterson 3, Cheryl Thompson, PhD 4, and Robert Shenk, MD 5
 Ann Surg Oncol DOI 10.1245/s10434-015-4527-y ORIGINAL ARTICLE BREAST ONCOLOGY Improving the Accuracy of Axillary Lymph Node Surgery in Breast Cancer with Ultrasound-Guided Wire Localization of Biopsy Proven
Ann Surg Oncol DOI 10.1245/s10434-015-4527-y ORIGINAL ARTICLE BREAST ONCOLOGY Improving the Accuracy of Axillary Lymph Node Surgery in Breast Cancer with Ultrasound-Guided Wire Localization of Biopsy Proven
The Safety and Efficiency of the Ultrasound-guided Large Needle Core Biopsy of Axilla Lymph Nodes
 Yonsei Med J 49(2):249-254, 2008 DOI 10.3349/ymj.2008.49.2.249 The Safety and Efficiency of the Ultrasound-guided Large Needle Core Biopsy of Axilla Lymph Nodes Ki Hong Kim, 1 Eun Ju Son, 1 Eun-Kyung Kim,
Yonsei Med J 49(2):249-254, 2008 DOI 10.3349/ymj.2008.49.2.249 The Safety and Efficiency of the Ultrasound-guided Large Needle Core Biopsy of Axilla Lymph Nodes Ki Hong Kim, 1 Eun Ju Son, 1 Eun-Kyung Kim,
Utility of Preoperative Ultrasound for Predicting pn2 or Higher Stage Axillary Lymph Node Involvement in Patients With Newly Diagnosed Breast Cancer
 Women s Imaging Original Research Abe et al. Preoperative Ultrasound to Predict Axillary Lymph Node Involvement Women s Imaging Original Research Hiroyuki Abe 1 David Schacht Charlene A. Sennett Gillian
Women s Imaging Original Research Abe et al. Preoperative Ultrasound to Predict Axillary Lymph Node Involvement Women s Imaging Original Research Hiroyuki Abe 1 David Schacht Charlene A. Sennett Gillian
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
Mandana Moosavi 1 and Stuart Kreisman Background
 Case Reports in Endocrinology Volume 2016, Article ID 6471081, 4 pages http://dx.doi.org/10.1155/2016/6471081 Case Report A Case Report of Dramatically Increased Thyroglobulin after Lymph Node Biopsy in
Case Reports in Endocrinology Volume 2016, Article ID 6471081, 4 pages http://dx.doi.org/10.1155/2016/6471081 Case Report A Case Report of Dramatically Increased Thyroglobulin after Lymph Node Biopsy in
EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY
 EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY AXILLARY LYMPH NODE METASTASIS Axillary lymph node metastasis is one of the most
EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY AXILLARY LYMPH NODE METASTASIS Axillary lymph node metastasis is one of the most
Original Article. J Fac Med Baghdad 193. Introduction:
 Original Article The value of Gray scale, color doppler and ultrasound guided- FNA in detection metastasis to the axillary lymph node in patient with primary breast cancer. * Qusay A. Fahad* Enam A.Al
Original Article The value of Gray scale, color doppler and ultrasound guided- FNA in detection metastasis to the axillary lymph node in patient with primary breast cancer. * Qusay A. Fahad* Enam A.Al
Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer
 - Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
- Official Statement - Position Statement on Management of the Axilla in Patients with Invasive Breast Cancer Sentinel lymph node (SLN) biopsy has replaced axillary lymph node dissection (ALND) for the
Evaluation of the Axilla Post Z-0011 Trial New Paradigm
 Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
The American Society of Breast Surgeons
 The American Journal of Surgery (2008) 196, 477 482 The American Society of Breast Surgeons Scientific Presentation Award: The combination of axillary ultrasound and ultrasound-guided biopsy is an accurate
The American Journal of Surgery (2008) 196, 477 482 The American Society of Breast Surgeons Scientific Presentation Award: The combination of axillary ultrasound and ultrasound-guided biopsy is an accurate
Axillary ultrasound in patients with breast cancer: which lymph nodes should be targeted for fine needle aspiration?
 Axillary ultrasound in patients with breast cancer: which lymph nodes should be targeted for fine needle aspiration? Poster No.: C-0289 Congress: ECR 2011 Type: Scientific Paper Authors: M. J. Diaz-Ruiz,
Axillary ultrasound in patients with breast cancer: which lymph nodes should be targeted for fine needle aspiration? Poster No.: C-0289 Congress: ECR 2011 Type: Scientific Paper Authors: M. J. Diaz-Ruiz,
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Targeting Surgery for Known Axillary Disease. Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center
 Targeting Surgery for Known Axillary Disease Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center Nodal Ultrasound at Diagnosis Whole breast and draining lymphatic
Targeting Surgery for Known Axillary Disease Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center Nodal Ultrasound at Diagnosis Whole breast and draining lymphatic
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES
 RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
RUTGERS CANCER INSTITUTE OF NEW JERSEY - ROBERT WOOD JOHNSON MEDICAL SCHOOL INTERDISCIPLINARY BREAST SURGERY FELLOWSHIP CORE EDUCATIONAL OBJECTIVES At the completion of Breast Fellowship training, the
Correspondence should be addressed to Taha Numan Yıkılmaz;
 Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
Advances in Medicine Volume 2016, Article ID 8639041, 5 pages http://dx.doi.org/10.1155/2016/8639041 Research Article External Validation of the Cancer of the Prostate Risk Assessment Postsurgical Score
The Clinical Value of Axillary Ultrasonography for Detection of Axillary Lymph Node Metastasis in Cases with Breast Cancer
 Original Article Middle East Journal of Cancer; October 2014; 5(4): 215-220 The Clinical Value of Axillary Ultrasonography for Detection of Axillary Lymph Node Metastasis in Cases with Breast Cancer Sedigheh
Original Article Middle East Journal of Cancer; October 2014; 5(4): 215-220 The Clinical Value of Axillary Ultrasonography for Detection of Axillary Lymph Node Metastasis in Cases with Breast Cancer Sedigheh
Ultrasound or FNA for Predicting Node Positive in Breast Cancer
 Ultrasound or FNA for Predicting Node Positive in Breast Cancer Chiun Sheng Huang, MD, PhD, MPH Professor and Chairman Department of Surgery Director of Breast Care Center National Taiwan University Hospital
Ultrasound or FNA for Predicting Node Positive in Breast Cancer Chiun Sheng Huang, MD, PhD, MPH Professor and Chairman Department of Surgery Director of Breast Care Center National Taiwan University Hospital
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions
 Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
Consensus Guideline on Image-Guided Percutaneous Biopsy of Palpable and Nonpalpable Breast Lesions Purpose: To outline the use of minimally invasive biopsy techniques (MIBT) for palpable and nonpalpable
Research Article A Structured Assessment to Decrease the Amount of Inconclusive Endometrial Biopsies in Women with Postmenopausal Bleeding
 International Surgical Oncology Volume 2016, Article ID 3039261, 5 pages http://dx.doi.org/10.1155/2016/3039261 Research Article A Structured Assessment to Decrease the Amount of Inconclusive Endometrial
International Surgical Oncology Volume 2016, Article ID 3039261, 5 pages http://dx.doi.org/10.1155/2016/3039261 Research Article A Structured Assessment to Decrease the Amount of Inconclusive Endometrial
Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma of Thyroid
 Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Research Article Papillary Thyroid Cancer, Macrofollicular Variant: The Follow-Up and Analysis of Prognosis of 5 Patients
 yroid Research, Article ID 818134, 4 pages http://dx.doi.org/10.1155/2014/818134 Research Article Papillary Thyroid Cancer, Macrofollicular Variant: The Follow-Up and Analysis of Prognosis of 5 Patients
yroid Research, Article ID 818134, 4 pages http://dx.doi.org/10.1155/2014/818134 Research Article Papillary Thyroid Cancer, Macrofollicular Variant: The Follow-Up and Analysis of Prognosis of 5 Patients
Updates on management of the axilla in breast cancer the surgical point of view
 Updates on management of the axilla in breast cancer the surgical point of view Edwige Bourstyn Centre des maladies du sein Hôpital Saint Louis Paris Sentinel lymph node biopsy (SLNB) is the standard of
Updates on management of the axilla in breast cancer the surgical point of view Edwige Bourstyn Centre des maladies du sein Hôpital Saint Louis Paris Sentinel lymph node biopsy (SLNB) is the standard of
Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule
 Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
 Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Case Reports in Otolaryngology Volume 2016, Article ID 5393404, 4 pages http://dx.doi.org/10.1155/2016/5393404 Case Report Metastatic Malignant Melanoma of Parotid Gland with a Regressed Primary Tumor
Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication for Repeat Metastasectomy
 Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Axillary ultrasound is frequently used to assess axillary nodes at
 ORIGINAL ARTICLE Identification and Resection of Clipped Node Decreases the False-negative Rate of Sentinel Lymph Node Surgery in Patients Presenting With Node-positive Breast Cancer (T0 T4, N1 N2) Who
ORIGINAL ARTICLE Identification and Resection of Clipped Node Decreases the False-negative Rate of Sentinel Lymph Node Surgery in Patients Presenting With Node-positive Breast Cancer (T0 T4, N1 N2) Who
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
R. F. Falkenstern-Ge, 1 S. Bode-Erdmann, 2 G. Ott, 2 M. Wohlleber, 1 and M. Kohlhäufl Introduction. 2. Histology
 Case Reports in Oncological Medicine Volume 2013, Article ID 167585, 4 pages http://dx.doi.org/10.1155/2013/167585 Case Report Late Lung Metastasis of a Primary Eccrine Sweat Gland Carcinoma 10 Years after
Case Reports in Oncological Medicine Volume 2013, Article ID 167585, 4 pages http://dx.doi.org/10.1155/2013/167585 Case Report Late Lung Metastasis of a Primary Eccrine Sweat Gland Carcinoma 10 Years after
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach
 Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Research Article A Clinicopathological Analysis of Soft Tissue Sarcoma with Telangiectatic Changes
 Sarcoma Volume 2015, Article ID 740571, 5 pages http://dx.doi.org/10.1155/2015/740571 Research Article A Clinicopathological Analysis of Soft Tissue Sarcoma with Telangiectatic Changes Hiroshi Kobayashi,
Sarcoma Volume 2015, Article ID 740571, 5 pages http://dx.doi.org/10.1155/2015/740571 Research Article A Clinicopathological Analysis of Soft Tissue Sarcoma with Telangiectatic Changes Hiroshi Kobayashi,
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Research Article Comparison of Colour Duplex Ultrasound with Computed Tomography to Measure the Maximum Abdominal Aortic Aneurysmal Diameter
 International Vascular Medicine, Article ID 574762, 4 pages http://dx.doi.org/10.1155/2014/574762 Research Article Comparison of Colour Duplex Ultrasound with Computed Tomography to Measure the Maximum
International Vascular Medicine, Article ID 574762, 4 pages http://dx.doi.org/10.1155/2014/574762 Research Article Comparison of Colour Duplex Ultrasound with Computed Tomography to Measure the Maximum
Correspondence should be addressed to Alicia McMaster;
 Cancer Research Volume 2013, Article ID 308236, 5 pages http://dx.doi.org/10.1155/2013/308236 Research Article Taxpas: Epidemiological and Survival Data in Breast Cancer Patients Treated with a Docetaxel-Based
Cancer Research Volume 2013, Article ID 308236, 5 pages http://dx.doi.org/10.1155/2013/308236 Research Article Taxpas: Epidemiological and Survival Data in Breast Cancer Patients Treated with a Docetaxel-Based
Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Quality ID #263: Preoperative Diagnosis of Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION:
Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus Irinotecan and Radiotherapy
 Case Reports in Otolaryngology Volume 2013, Article ID 893638, 4 pages http://dx.doi.org/10.1155/2013/893638 Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus
Case Reports in Otolaryngology Volume 2013, Article ID 893638, 4 pages http://dx.doi.org/10.1155/2013/893638 Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus
Breast Cancer: Management of the Axilla in Greg McKinnon MD FRCSC SON Vancouver Oct 2016
 Breast Cancer: Management of the Axilla in 2016 Greg McKinnon MD FRCSC SON Vancouver Oct 2016 No Disclosures Principle #1 There is no point talking about surgical therapy in isolation. From a patient
Breast Cancer: Management of the Axilla in 2016 Greg McKinnon MD FRCSC SON Vancouver Oct 2016 No Disclosures Principle #1 There is no point talking about surgical therapy in isolation. From a patient
Savitri Krishnamurthy, MD 1
 EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
EVOLVING TRENDS IN PATHOLOGIC EVALUATION OF AXILLARY LYMPH NODES IN BREAST CANCER Savitri Krishnamurthy, M.D. Professor Department of Pathology University of Texas M. D. Anderson Cancer Center AXILLARY
The Value of Ultrasonographic Detection for Metastatic Axillary Lymph Nodes in Breast Cancer 1
 The Value of Ultrasonographic Detection for Metastatic Axillary Lymph Nodes in Breast Cancer 1 Jung Hee Shin, M.D., Asiry Hwang, M.D., Hye-Young Choi, M.D., Seung Yon Baek, M.D. Purpose: We evaluated the
The Value of Ultrasonographic Detection for Metastatic Axillary Lymph Nodes in Breast Cancer 1 Jung Hee Shin, M.D., Asiry Hwang, M.D., Hye-Young Choi, M.D., Seung Yon Baek, M.D. Purpose: We evaluated the
NICE diagnostics guidance on intraoperative tests (RD 100i OSNA system and Metasin test) for detecting sentinel lymph node metastases in breast cancer
 NICE diagnostics guidance on intraoperative tests (RD 100i OSNA system and Metasin test) for detecting sentinel lymph node metastases in breast cancer NICE provided the content for this booklet which is
NICE diagnostics guidance on intraoperative tests (RD 100i OSNA system and Metasin test) for detecting sentinel lymph node metastases in breast cancer NICE provided the content for this booklet which is
Recent Update in Surgery for the Management of Breast Cancer
 Recent Update in Surgery for the Management of Breast Cancer Wonshik Han, MD, PhD Professor, Department of Surgery, Seoul National University College of Medicine Chief of Breast Care Center, Seoul National
Recent Update in Surgery for the Management of Breast Cancer Wonshik Han, MD, PhD Professor, Department of Surgery, Seoul National University College of Medicine Chief of Breast Care Center, Seoul National
Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control Study
 Advances in Endocrinology, Article ID 954194, 4 pages http://dx.doi.org/10.1155/2014/954194 Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control
Advances in Endocrinology, Article ID 954194, 4 pages http://dx.doi.org/10.1155/2014/954194 Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control
Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study
 [ABS-0078] GBCC 2018 Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study Eun Young Kim 1, Kwan Ho Lee 1, Yong
[ABS-0078] GBCC 2018 Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study Eun Young Kim 1, Kwan Ho Lee 1, Yong
Correspondence should be addressed to Donald R. Lannin;
 Hindawi Surgery Research and Practice Volume 2017, Article ID 5924802, 5 pages https://doi.org/10.1155/2017/5924802 Research Article Intraoperative Injection of Technetium-99m Sulfur Colloid for Sentinel
Hindawi Surgery Research and Practice Volume 2017, Article ID 5924802, 5 pages https://doi.org/10.1155/2017/5924802 Research Article Intraoperative Injection of Technetium-99m Sulfur Colloid for Sentinel
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Guideline for the Diagnosis of Breast Cancer
 Guideline for the Diagnosis of Breast Cancer Version History Version Date Brief Summary of Change Issued 2.0 May 2007 Approved by the Governance Committee 2.0 25.11.08 Discussed at the NSSG 2.1 5.12.08
Guideline for the Diagnosis of Breast Cancer Version History Version Date Brief Summary of Change Issued 2.0 May 2007 Approved by the Governance Committee 2.0 25.11.08 Discussed at the NSSG 2.1 5.12.08
Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report of Neoadjuvant Use Enabling Complete Surgical Resection
 Case Reports in Oncological Medicine Volume 2013, Article ID 496351, 4 pages http://dx.doi.org/10.1155/2013/496351 Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report
Case Reports in Oncological Medicine Volume 2013, Article ID 496351, 4 pages http://dx.doi.org/10.1155/2013/496351 Case Report Denosumab Chemotherapy for Recurrent Giant-Cell Tumor of Bone: A Case Report
Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder in an Elderly Patient
 Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Research Article Predictions of the Length of Lumbar Puncture Needles
 Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Clinical Study Accuracy of Individual Descriptors and Grading of Nodal Involvement by Axillary Ultrasound in Patients of Breast Cancer
 International Breast Cancer Volume 2013, Article ID 930596, 6 pages http://dx.doi.org/10.1155/2013/930596 Clinical Study Accuracy of Individual Descriptors and Grading of Nodal Involvement by Axillary
International Breast Cancer Volume 2013, Article ID 930596, 6 pages http://dx.doi.org/10.1155/2013/930596 Clinical Study Accuracy of Individual Descriptors and Grading of Nodal Involvement by Axillary
Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma
 Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Case Reports in Otolaryngology Volume 2013, Article ID 384238, 4 pages http://dx.doi.org/10.1155/2013/384238 Case Report A Case of Primary Submandibular Gland Oncocytic Carcinoma Kunihiko Tokashiki, Kiyoaki
Abstract. Introduction. Salah Abobaker Ali
 Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
Case Report Tubular Carcinoma of the Breast: Advantages and Limitations of Breast Tomosynthesis
 Case Reports in Radiology Volume 2016, Article ID 3906195, 4 pages http://dx.doi.org/10.1155/2016/3906195 Case Report Tubular Carcinoma of the Breast: Advantages and Limitations of Breast Tomosynthesis
Case Reports in Radiology Volume 2016, Article ID 3906195, 4 pages http://dx.doi.org/10.1155/2016/3906195 Case Report Tubular Carcinoma of the Breast: Advantages and Limitations of Breast Tomosynthesis
Research Article Can Breast Self-Examination Continue to Be Touted Justifiably as an Optional Practice?
 International Surgical Oncology Volume 2011, Article ID 965464, 5 pages doi:10.1155/2011/965464 Research Article Can Breast Self-Examination Continue to Be Touted Justifiably as an Optional Practice? T.T.Fancher,J.A.Palesty,J.J.Paszkowiak,R.P.Kiran,A.D.Malkan,andS.J.Dudrick
International Surgical Oncology Volume 2011, Article ID 965464, 5 pages doi:10.1155/2011/965464 Research Article Can Breast Self-Examination Continue to Be Touted Justifiably as an Optional Practice? T.T.Fancher,J.A.Palesty,J.J.Paszkowiak,R.P.Kiran,A.D.Malkan,andS.J.Dudrick
Prediction of Postoperative Tumor Size in Breast Cancer Patients by Clinical Assessment, Mammography and Ultrasonography
 Prediction of Postoperative Tumor Size in Breast Cancer Patients by Clinical Assessment, Mammography and Ultrasonography Eyad Fawzi AlSaeed 1 and Mutahir A. Tunio 2* 1 Consultant Radiation Oncology, Chairman
Prediction of Postoperative Tumor Size in Breast Cancer Patients by Clinical Assessment, Mammography and Ultrasonography Eyad Fawzi AlSaeed 1 and Mutahir A. Tunio 2* 1 Consultant Radiation Oncology, Chairman
Journal of Breast Cancer
 Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2012 June; 15(2): 211-217 Efficiency of Ultrasound and Ultrasound-Guided Fine Needle Aspiration Cytology in Preoperative Assessment of Axillary
Journal of Breast Cancer ORIGINAL ARTICLE J Breast Cancer 2012 June; 15(2): 211-217 Efficiency of Ultrasound and Ultrasound-Guided Fine Needle Aspiration Cytology in Preoperative Assessment of Axillary
J.N., PRADHAN A.K., KUSTA M.K. ABSTRACT
 Axillary Ultrasound Examination in the Selection of Carcinoma of Breast Patients for Sentinel Node Biopsy - A Prospective Study MISRA J.N., PRADHAN A.K., KUSTA M.K. ABSTRACT Background: Axillary lymph
Axillary Ultrasound Examination in the Selection of Carcinoma of Breast Patients for Sentinel Node Biopsy - A Prospective Study MISRA J.N., PRADHAN A.K., KUSTA M.K. ABSTRACT Background: Axillary lymph
Effective Health Care Program
 Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
Comparative Effectiveness Review Number 19 Effective Health Care Program Comparative Effectiveness of Core-Needle and Open Surgical Biopsy for the Diagnosis of Breast Lesions Executive Summary Background
Minimizing Errors in Diagnostic Pathology
 Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine-Jacksonville Medical Director, Shands Jacksonville Breast Health Center
Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine-Jacksonville Medical Director, Shands Jacksonville Breast Health Center
Research Article Stromal Expression of CD10 in Invasive Breast Carcinoma and Its Correlation with ER, PR, HER2-neu, and Ki67
 SAGE-Hindawi Access to Research International Breast Cancer Volume 20, Article ID 47957, 4 pages doi:0.406/20/47957 Research Article Stromal Expression of CD0 in Invasive Breast Carcinoma and Its Correlation
SAGE-Hindawi Access to Research International Breast Cancer Volume 20, Article ID 47957, 4 pages doi:0.406/20/47957 Research Article Stromal Expression of CD0 in Invasive Breast Carcinoma and Its Correlation
Why Do Axillary Dissection? Nodal Treatment and Survival NSABP B04. Revisiting Axillary Dissection for SN Positive Patients
 Memorial Sloan-Kettering Cancer Center 1275 York Avenue, New York, NY 10065 10th International Congress on the Future of Breast Cancer Coronado, CA Why Do Axillary Dissection? 6 August 2011 Implications
Memorial Sloan-Kettering Cancer Center 1275 York Avenue, New York, NY 10065 10th International Congress on the Future of Breast Cancer Coronado, CA Why Do Axillary Dissection? 6 August 2011 Implications
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Debate Axillary dissection - con. Prof. Dr. Rodica Anghel Institute of Oncology Bucharest
 Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Implications of ACOSOG Z11 for Clinical Practice: Surgical Perspective
 :$;7)#*8'-87*4BCD'E7)F'31$4.$&'G$H'E7)F&'GE'>??ID >?,"'@4,$)4*,#74*8'!74/)$++'74',"$'A.,.)$'7%'()$*+,'!*42$)!7)74*67&'!3 6 August 2011 Implications of ACOSOG Z11 for Clinical
:$;7)#*8'-87*4BCD'E7)F'31$4.$&'G$H'E7)F&'GE'>??ID >?,"'@4,$)4*,#74*8'!74/)$++'74',"$'A.,.)$'7%'()$*+,'!*42$)!7)74*67&'!3 6 August 2011 Implications of ACOSOG Z11 for Clinical
Solitary Contralateral Adrenal Metastases after Nephrectomy for Renal Cell Carcinoma
 Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Original Report ISSN 1537-744X; DOI 10.1100/tsw.2004.39 Solitary Contralateral Adrenal after Nephrectomy for Renal Cell Carcinoma Nikolaos Antoniou, M.D. and Demetrios Karanastasis, M.D. General Hospital
Cervical Lymph Nodes
 Cervical Lymph Nodes Diana Gaitini, MD Unit of Ultrasound, Department of Medical Imaging Rambam Medical Center and Faculty of Medicine Technion, Israel Institute of Technology Haifa, Israel Learning Targets
Cervical Lymph Nodes Diana Gaitini, MD Unit of Ultrasound, Department of Medical Imaging Rambam Medical Center and Faculty of Medicine Technion, Israel Institute of Technology Haifa, Israel Learning Targets
Preoperative axillary lymph node staging by ultrasound-guided cytology using a four-level sonographic score
 De Coninck et al. BMC Medical Imaging (2016) 16:13 DOI 10.1186/s12880-016-0116-1 RESEARCH ARTICLE Open Access Preoperative axillary lymph node staging by ultrasound-guided cytology using a four-level sonographic
De Coninck et al. BMC Medical Imaging (2016) 16:13 DOI 10.1186/s12880-016-0116-1 RESEARCH ARTICLE Open Access Preoperative axillary lymph node staging by ultrasound-guided cytology using a four-level sonographic
Implications of ACOSOG Z11 for Clinical Practice: Surgical Perspective
 Memorial Sloan-Kettering Cancer Center 1275 York Avenue, New York, NY 10065 10th International Congress on the Future of Breast Cancer Coronado, CA 6 August 2011 Implications of ACOSOG Z11 for Clinical
Memorial Sloan-Kettering Cancer Center 1275 York Avenue, New York, NY 10065 10th International Congress on the Future of Breast Cancer Coronado, CA 6 August 2011 Implications of ACOSOG Z11 for Clinical
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy
 Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Atypical Ductal Hyperplasia and Papillomas: A Comparison of Ultrasound Guided Breast Biopsy and Stereotactic Guided Breast Biopsy Breast Cancer is the most common cancer diagnosed in women in the United
Ultrasound-guided fine needle aspiration cytology in staging clinically node-negative invasive breast cancer
 Gynecol Surg (2012) 9:185 191 DOI 10.1007/s10397-011-0712-6 ORIGINAL ARTICLE Ultrasound-guided fine needle aspiration cytology in staging clinically node-negative invasive breast cancer Daniela Huber &
Gynecol Surg (2012) 9:185 191 DOI 10.1007/s10397-011-0712-6 ORIGINAL ARTICLE Ultrasound-guided fine needle aspiration cytology in staging clinically node-negative invasive breast cancer Daniela Huber &
Case Report Tortuous Common Carotid Artery: A Report of Four Cases Observed in Cadaveric Dissections
 Case Reports in Otolaryngology Volume 2016, Article ID 2028402, 4 pages http://dx.doi.org/10.1155/2016/2028402 Case Report Tortuous Common Carotid Artery: A Report of Four Cases Observed in Cadaveric Dissections
Case Reports in Otolaryngology Volume 2016, Article ID 2028402, 4 pages http://dx.doi.org/10.1155/2016/2028402 Case Report Tortuous Common Carotid Artery: A Report of Four Cases Observed in Cadaveric Dissections
Page 1. AHN-JHU Breast Cancer Symposium. Novel Local Regional Clinical Trials. Background. Neoadjuvant Chemotherapy Benefit.
 AHN-JHU Breast Cancer Symposium Novel Local Regional Clinical Trials March 22, 2019 Thomas B. Julian, MD, FACS Associate Medical Director, Cancer Program Development, ANH Cancer Institute Background In
AHN-JHU Breast Cancer Symposium Novel Local Regional Clinical Trials March 22, 2019 Thomas B. Julian, MD, FACS Associate Medical Director, Cancer Program Development, ANH Cancer Institute Background In
Fine needle aspiration cytology guided by ultrasound of suspicious axillary lymph nodes in breast cancer patients
 Hematology & Medical Oncology Research Article ISSN: 2398-8495 Fine needle aspiration cytology guided by ultrasound of suspicious axillary lymph nodes in breast cancer patients Waldeir de Almeida Júnior
Hematology & Medical Oncology Research Article ISSN: 2398-8495 Fine needle aspiration cytology guided by ultrasound of suspicious axillary lymph nodes in breast cancer patients Waldeir de Almeida Júnior
STEREOTACTIC BREAST BIOPSY: CORRELATION WITH HISTOLOGY
 3-rd Baltic Congress of Radiology, October 8-9, 2010 Riga Rūta Briedienė, Rūta Grigienė, Raimundas Meškauskas Institute of Oncology Vilnius University, National Centre of Pathology STEREOTACTIC BREAST
3-rd Baltic Congress of Radiology, October 8-9, 2010 Riga Rūta Briedienė, Rūta Grigienė, Raimundas Meškauskas Institute of Oncology Vilnius University, National Centre of Pathology STEREOTACTIC BREAST
The Efficacy of Axillary Ultrasound in the Detection of Nodal Metastasis in Breast Cancer
 Women s Imaging Original Research Lee et al. Ultrasound Detection of Nodal Metastasis Women s Imaging Original Research Belinda Lee 1 Adrian K. Lim 2 Jonathan Krell 1 Keshthra Satchithananda 2 R. Charles
Women s Imaging Original Research Lee et al. Ultrasound Detection of Nodal Metastasis Women s Imaging Original Research Belinda Lee 1 Adrian K. Lim 2 Jonathan Krell 1 Keshthra Satchithananda 2 R. Charles
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report 005 Produced by: BreastScreen Victoria Coordination Unit Level, Pelham Street, Carlton South Victoria 05 PH 0 9660 6888 FX 0 966 88 EM info@breastscreen.org.au
BreastScreen Victoria Annual Statistical Report 005 Produced by: BreastScreen Victoria Coordination Unit Level, Pelham Street, Carlton South Victoria 05 PH 0 9660 6888 FX 0 966 88 EM info@breastscreen.org.au
Evaluation of the effect of neoadjuvant chemotherapy on tumor and axillary lymph nodes in locally advanced breast cancer: a study of 50 patients
 Chinese-German J Clin Oncol DOI 10.1007/s10330-014-0005-4 Evaluation of the effect of neoadjuvant chemotherapy on tumor and axillary lymph nodes in locally advanced breast cancer: a study of 50 patients
Chinese-German J Clin Oncol DOI 10.1007/s10330-014-0005-4 Evaluation of the effect of neoadjuvant chemotherapy on tumor and axillary lymph nodes in locally advanced breast cancer: a study of 50 patients
Research Article Prognostic Implication of Predominant Histologic Subtypes of Lymph Node Metastases in Surgically Resected Lung Adenocarcinoma
 BioMed Research International, Article ID 64568, 6 pages http://dx.doi.org/.55/24/64568 Research Article Prognostic Implication of Predominant Histologic Subtypes of Lymph Node Metastases in Surgically
BioMed Research International, Article ID 64568, 6 pages http://dx.doi.org/.55/24/64568 Research Article Prognostic Implication of Predominant Histologic Subtypes of Lymph Node Metastases in Surgically
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy
 Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
ROLE OF MRI IN SCREENING, DIAGNOSIS AND MANAGEMENT OF BREAST CANCER. B.Zandi Professor of Radiology
 ROLE OF MRI IN SCREENING, DIAGNOSIS AND MANAGEMENT OF BREAST CANCER B.Zandi Professor of Radiology Introduction In the USA, Breast Cancer is : The Most Common Non-Skin Cancer The Second Leading cause of
ROLE OF MRI IN SCREENING, DIAGNOSIS AND MANAGEMENT OF BREAST CANCER B.Zandi Professor of Radiology Introduction In the USA, Breast Cancer is : The Most Common Non-Skin Cancer The Second Leading cause of
Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
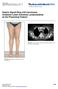 Clinical Image TheScientificWorldJOURNAL (2007) 7, 1189 1192 ISSN 1537-744X; DOI 10.1100/tsw.2007.199 Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
Clinical Image TheScientificWorldJOURNAL (2007) 7, 1189 1192 ISSN 1537-744X; DOI 10.1100/tsw.2007.199 Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY
 EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
EARLY DETECTION: MAMMOGRAPHY AND SONOGRAPHY Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School Breast Cancer Screening Early detection of
Breast Surgery When Less is More and More is Less. E MacIntosh, MD June 6, 2015
 Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Relevance. Axillary Node Recurrence. Purpose. Case Presentation: Is axillary staging required? Two trends have emerged:
 Axillary Node Recurrence N.L. Davis Associate Professor of Surgery, UBC Head of Surgical Oncology, BCCA Relevance In an attempt to minimize long term complications and to maximize cancer control, the management
Axillary Node Recurrence N.L. Davis Associate Professor of Surgery, UBC Head of Surgical Oncology, BCCA Relevance In an attempt to minimize long term complications and to maximize cancer control, the management
Research Article Does Tumor Size Influence the Diagnostic Accuracy of Ultrasound-Guided Fine-Needle Aspiration Cytology for Thyroid Nodules?
 International Endocrinology Volume 2016, Article ID 3803647, 6 pages http://dx.doi.org/10.1155/2016/3803647 Research Article Does Tumor Size Influence the Diagnostic Accuracy of Ultrasound-Guided Fine-Needle
International Endocrinology Volume 2016, Article ID 3803647, 6 pages http://dx.doi.org/10.1155/2016/3803647 Research Article Does Tumor Size Influence the Diagnostic Accuracy of Ultrasound-Guided Fine-Needle
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation
 Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Surgical Therapy: Sentinel Node Biopsy and Breast Conservation Stephen B. Edge, MD Professor of Surgery and Oncology Roswell Park Cancer Institute University at Buffalo Dr. Roswell Park: Tradition in Cancer
Case Report Liver Metastases of Unknown Primary: Malignant Melanoma
 Case Reports in Hepatology, Article ID 131708, 4 pages http://dx.doi.org/10.1155/2014/131708 Case Report Liver Metastases of Unknown Primary: Malignant Melanoma Ozgur Bostanci, Kinyas Kartal, and Muharrem
Case Reports in Hepatology, Article ID 131708, 4 pages http://dx.doi.org/10.1155/2014/131708 Case Report Liver Metastases of Unknown Primary: Malignant Melanoma Ozgur Bostanci, Kinyas Kartal, and Muharrem
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection
 The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
Breast Imaging: Multidisciplinary Approach. Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina
 Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Breast Imaging: Multidisciplinary Approach Madelene Lewis, MD Assistant Professor Associate Program Director Medical University of South Carolina No Disclosures Objectives Discuss a multidisciplinary breast
Pre- operative staging of the axilla
 Pre- operative staging of the axilla Anthony J Maxwell University Hospital of South Manchester Outline Why stage the axilla? Optimising conventional US & needle sampling Other imaging and needle sampling
Pre- operative staging of the axilla Anthony J Maxwell University Hospital of South Manchester Outline Why stage the axilla? Optimising conventional US & needle sampling Other imaging and needle sampling
Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome to Cutaneous Melanoma
 ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
ISRN Dermatology Volume 2013, Article ID 586915, 5 pages http://dx.doi.org/10.1155/2013/586915 Clinical Study Mucosal Melanoma in the Head and Neck Region: Different Clinical Features and Same Outcome
Case Report Multiple Giant Cell Tumors of Tendon Sheath Found within a Single Digit of a 9-Year-Old
 Case Reports in Orthopedics Volume 2016, Article ID 1834740, 4 pages http://dx.doi.org/10.1155/2016/1834740 Case Report Multiple Giant Cell Tumors of Tendon Sheath Found within a Single Digit of a 9-Year-Old
Case Reports in Orthopedics Volume 2016, Article ID 1834740, 4 pages http://dx.doi.org/10.1155/2016/1834740 Case Report Multiple Giant Cell Tumors of Tendon Sheath Found within a Single Digit of a 9-Year-Old
