Mortality rates are higher in anorexia nervosa than
|
|
|
- Joel Holland
- 6 years ago
- Views:
Transcription
1 Article A Longitudinal Investigation of Mortality in Anorexia Nervosa and Bulimia Nervosa Debra L. Franko, Ph.D. Aparna Keshaviah, Sc.M. Kamryn T. Eddy, Ph.D. Meera Krishna, B.A. Martha C. Davis, B.A. Pamela K. Keel, Ph.D. David B. Herzog, M.D. Objective: Although anorexia nervosa has a high mortality rate, our understanding of the timing and predictors of mortality in eating disorders is limited. The authors investigated mortality in a long-term study of patients with eating disorders. Method: Beginning in 1987, 246 treatmentseeking female patients with anorexia nervosa or bulimia nervosa were interviewed every 6 months for a median of 9.5 years to obtain weekly ratings of eating disorder symptoms, comorbidity, treatment participation, and psychosocial functioning. From January 2007 to December 2010 (median follow-up of 20 years), vital status was ascertained with a National Index search. Results: Sixteen deaths (6.5%) were recorded (lifetime anorexia N=14; bulimia nervosa with no history of anorexia N=2). The standardized mortality ratio was 4.37 (95% CI= ) for lifetime anorexia nervosa and 2.33 (95% CI= ) for bulimia nervosa with no history of anorexia nervosa. Risk of premature death among patients with lifetime anorexia nervosa peaked within the first 10 years of follow-up, resulting in a standardized mortality ratio of 7.7 (95% CI= ). The standardized mortality ratio varied by duration of illness and was 3.2 (95% CI= ) for patients with lifetime anorexia nervosa for 0 to 15 years (4/119 died), and 6.6 (95% CI= ) for those with lifetime anorexia nervosa for.15 to 30 years (10/67 died). Multivariate predictors of mortality included alcohol abuse, low body mass index, and poor social adjustment. Conclusions: These findings highlight the need for early identification and intervention and suggest that a long duration of illness, substance abuse, low weight, and poor psychosocial functioning raise the risk for mortality in anorexia nervosa. (Am J Psychiatry 2013; 170: ) Mortality rates are higher in anorexia nervosa than in other psychiatric disorders (1), but few studies have examined when death is more likely to occur in the course of this eating disorder. Most commonly, rates of premature death are described by the standardized mortality ratio, calculated as the number of observed deaths during a given period in a specific population of interest divided by the number of deaths expected in the general population, matched for age, race, and sex. A meta-analysis of 25 studies of patients with anorexia nervosa found a standardized mortality ratio of 5.9 in studies with a mean follow-up duration of 12.8 years (1). A similar standardized mortality ratio of 6.2 over 13.4 years of follow-up has also been reported (2). Although both are elevated, there was considerable variability in standardized mortality ratios across studies included in the meta-analysis (1), and these standardized mortality ratios are lower than those reported in studies with shorter follow-up periods (3, 4). Such variability across studies might be accounted for by ascertainment rates, sample size, severity of illness, and duration of follow-up, which may differ substantially from study to study. Thus, it would be instructive to examine the standardized mortality ratio in relation to the duration of follow-up as well as the duration of illness to understand whether there are high-risk periods for premature death in eating disorders. Six longitudinal studies, including three in adolescents (5 7) and three in adults (8 10), have examined mortality rates over time. All of these investigations assessed anorexia nervosa patients at inpatient admission and again at multiple varying time points, ranging from 2 to 20 years after admission. Four of these studies found that the number of deaths increased with increasing duration of follow-up, with greater consistency in the adult studies than in the adolescent studies. However, it is unclear whether risk of death remained constant during followup because at least three studies (5, 9, 10) detected a majority of recorded deaths earlier in the follow-up period. In the literature, it remains unknown at what point in the progression of the disorder death is more likely to occur and whether there are differences between patients with anorexia nervosa who die relatively early in the follow-up period (or early in the course of the disorder) and those who die later (after a more protracted or chronic course). These two variables, timing of follow-up assessment and duration of illness, are distinct; individuals with eating disorders do not necessarily seek treatment or enter a study at the exact point when they meet full diagnostic criteria. To This article is featured in this month s AJP Audio, is the subject of a CME course (p. 935), and is discussed in an Editorial by Dr. Crow (p. 824) Am J Psychiatry 170:8, August 2013 ajp.psychiatryonline.org 917
2 MORTALITY RATES IN EATING DISORDERS clarify this distinction, our first aim in this longitudinal study was to examine standardized mortality ratios at two time points as well as at varying years of duration of illness. Such data might be informative as to whether there is a peak period for death in eating disorders. Our second aim was to examine factors that might increase vulnerability to premature death. Studies have indicated that older age at hospital admission, longer duration of eating disorder, history of attempted suicide, use of diuretics, more severe eating disorder symptoms, desire for lower weight at admission, repeated admission, and psychiatric comorbidity predict mortality (2 4, 11). We address the question of which variables predict mortality whenexaminedatalaterfollowup point in this longitudinal study. Predictor variables included eating disorder symptoms, comorbidity, treatment, and psychosocial functioning assessed both at intake and through interviews conducted over the study period. Method Participants The sample consisted of females recruited for participation in the Massachusetts General Hospital Longitudinal Study of Anorexia and Bulimia Nervosa between 1987 and Most participants were seeking outpatient treatment for their eating disorder. Participants who met the following inclusion criteria were invited to participate: DSM-III-R diagnosis of anorexia nervosa or bulimia nervosa; female; age $12 years old; reside within 200 miles of Boston; English speaking; and no evidence of organic brain syndrome or terminal illness. Of the 294 individuals who met the study criteria, 250 (85%) agreed to participate; four dropped out after their intake interview, resulting in a sample size of 246. Participants were reclassified according to DSM-IV criteria, resulting in 51 with anorexia, 85 with anorexia, and 110 with bulimia nervosa. Of these, 186 (76%) were identified as having lifetime presence of anorexia which was defined as 1) being diagnosed at study intake with anorexia nervosa (N=136), 2) having a history of anorexia nervosa prior to study intake (N=26), or 3) developing anorexia nervosa over the course of the study (N=24). Given our previous observations that individuals with lifetime anorexia nervosa who die continue to be at risk even when not actively ill and our previous analyses suggesting that deaths observed among individuals with intake diagnoses of bulimia nervosa might be attributable to a lifetime diagnosis of anorexia nervosa (11), we chose to analyze mortality by lifetime presence (not just intake diagnosis) of anorexia nervosa. Procedure This study was approved by the institutional review board at Massachusetts General Hospital. After brief telephone screening, individuals were scheduled for a face-to-face interview to confirm eating disorder diagnoses, assess other psychiatric disorders and treatment history, and measure height and weight. Follow-up interviews were conducted every 6 to 12 months until Measures During intake interviews, participants lifetime axis I psychiatric history was assessed using the Schedule for Affective s and Schizophrenia Lifetime Version (12), modified to include DSM-III-R diagnostic criteria for anorexia nervosa and bulimia nervosa. The 1983 Metropolitan Insurance Company (13) height and weight norms were used to calculate percent ideal body weight. Over the course of the study, the Longitudinal Interval Follow- Up Evaluation, adapted for eating disorders (14), was used to assess eating pathology, treatment, and comorbid psychiatric disorders. Once a diagnosis was determined, the course of psychopathology was coded on a week-by-week basis using the Psychiatric Status Rating Scale (11), with scores ranging from 1 (no symptoms) to 6 (full diagnostic criteria). Major depressive disorder and substance use disorders were rated similarly. Psychosocial functioning was assessed longitudinally using semistructured interviews to examine interpersonal relationships and functioning at work, in household chores, and in recreational activities, as well as global life satisfaction and overall functioning (15, 16). Ratings were made on a 5-point scale ranging from 1, no impairment, to 5, severe impairment. We refer to the global score measuring overall psychosocial functioning as the social adjustment score. The Global Assessment of Functioning Scale was used to evaluate overall level of symptom severity and impairment, with higher scores indicating better functioning. Further study details have been presented elsewhere (17). Ascertainment of Vital Status Vital status was ascertained in 2010 by searching the National Index (18). This index represents a branch of the National Center for Health Statistics with a national death certificate database updated through December 31, 2008, at the time of this investigation (19). Cause of death was obtained from death certificates, and, whenever possible, interviews were conducted with the deceased participant s relatives to collect data concerning the participant immediately prior to her death. The median time from study intake to last study visit was 9 years (range, 13 weeks 12 years), and the median time from last study visit to ascertainment of vital status was 11 years (range, 9 weeks 11 years), resulting in a median total follow-up time of 20 years (range, 13 weeks 23 years). Statistical Data To summarize mortality, we calculated crude mortality ratios, annual mortality rates (deaths per person-years), and standardized mortality ratios quantifying the excess number of deaths in our study population compared with what would be expected after adjusting for age, sex, and duration of follow-up. The expected number of deaths for a general white female population, adjusted for age, was derived from U.S. decennial life tables for Massachusetts from 1989 to 1991 (20). Fisher s exact 95% confidence intervals around the standardized mortality ratios were calculated using chi-square centile cutoffs (21). We examined how risk of death changed over time by comparing the standardized mortality ratio by years of follow-up (0 10 years compared with years) and by total duration of eating disorder (0 15 years compared with years; from full-onset eating disorder through last study visit, excluding weeks with full eating disorder recovery). Formal comparison of the standardized mortality ratios by years of follow-up was not conducted because the ratios are not independent, and comparison by duration of illness is not recommended because our standardized mortality ratios were obtained by indirect standardization (because of the small number of deaths). Cox proportional hazards regression was used to identify predictors of mortality. The proportional hazards assumption and functional form of the continuous covariates were verified using the methods of Lin et al. (22). Because mortality status was ascertained for many participants after the last study measurement of the course variables, use of time-varying covariates was not possible. Instead, we summarized the variability in course variables using mean scores for continuous 918 ajp.psychiatryonline.org Am J Psychiatry 170:8, August 2013
3 FRANKO, KESHAVIAH, EDDY, ET AL. TABLE 1. Summary of Covariates Analyzed for Female Patients With Lifetime Anorexia Nervosa a Variable Alive (N=172) Died (N=14) b Mean SD Mean SD Intake covariate Age (years) at eating disorder onset Age (years) at study intake Years of eating disorder prior to study intake Body mass index (BMI) Percent ideal body weight N % N % disorder diagnosis Anorexia Anorexia Bulimia nervosa History of hospitalization for an eating disorder History of alcohol abuse History of drug use disorder History of bipolar disorder Any suicidal gestures or attempts Mean SD Mean SD Course covariate Years from study intake to last visit Years from last visit to last follow-up or death Total years of eating disorder Number of changes in eating disorder diagnosis Psychiatric Status Rating Scale Anorexia nervosa score, percent of weeks $ Anorexia nervosa score, last visit Weight loss, percent of weeks $21% 29% below ideal body weight BMI, percent of 13-week periods, Last visit covariate BMI, last visit Psychiatric Status Rating Scale Alcohol abuse score, percent of weeks $ Alcohol abuse score, last visit Major depressive disorder score, percent of weeks $ Major depressive disorder score, last visit Manic score, last visit Social adjustment rating c Average during study Last visit Global Assessment of Functioning Scale score Average during study Last visit a Other course variables analyzed included the percent of study weeks meeting the following criteria: bulimia psychiatric status rating score $5 (percent of weeks dichotomized as above compared with at or below the median); (including vomiting, laxative use, and diuretic use); other compensatory behavior (including diet pill use, fasting, and vigorous exercise); drug abuse psychiatric status rating score $3; hospitalized for an eating disorder; and suicidal gestures or attempts. Also analyzed were sessions of individual therapy received (mean over time) and marital status at last visit (single; married or living with a partner; or separated, divorced, or widowed). b A total of 16 patients died during the course of the study; two of the 16 had bulimia nervosa with no history of anorexia nervosa. c The ratings for social adjustment were as follows: 1=very good; 2=good; 3=fair; 4=poor; 5=very poor. covariates and percentage of weeks below or above a cutoff for ordinal or categorical covariates. All covariates analyzed are listed in Table 1. Univariate analyses were conducted first to ensure that relationships were not obscured by collinearity among the covariates; consistent with methods used previously (11), we conservatively applied a Bonferroni-corrected significance threshold of , adjusting for the 46 individual comparisons made. Significant covariates were then entered into multivariate models, and stepwise variable selection (with alpha=0.01 to enter and alpha=0.05 to remain) was used to identify a final model. To facilitate comparison with cross-sectional studies that examined only intake covariates, we performed automated selection separately on variables measured at intake, over the course of the study, and at last study visit. AllanalyseswereconductedusingSAS,version9.3(SASInstitute, Cary, N.C.). Am J Psychiatry 170:8, August 2013 ajp.psychiatryonline.org 919
4 MORTALITY RATES IN EATING DISORDERS TABLE 2. Clinical Characteristics of 16 Women With an Who Died During the Course of the Study Diagnosis Participant at Intake 1 Anorexia 2 Anorexia 3 Anorexia 4 Anorexia 5 Anorexia 6 Anorexia 7 Anorexia 8 Anorexia 9 Anorexia 10 Anorexia 11 Anorexia 12 Anorexia Lifetime Anorexia Nervosa Age at Intake (Years) Age at (Years) Years of at Intake Total Years of Number of Changes in Diagnosis Percent Below Ideal Body Weight at Last Visit Years From Intake to Years From Last Visit to Yes Suicide Cause of Yes Complications of resuscitated cardiac arrest; acute methadone, diazepam, and chloral hydrate intoxication Yes a Suicide Yes $ Respiratory failure due to amyotrophic lateral sclerosis Yes Suicide Yes Gastrointestinal hemorrhage, esophageal ulceration Yes Anoxic brain injury, septic shock Yes Fungal pneumonia Yes Cardiac arrhythmia, seizure disorder Yes Acute ethanol intoxication Yes a Cardiopulmonary arrest, cardiovascular disease, diabetes mellitus Yes $ Suicide continued 920 ajp.psychiatryonline.org Am J Psychiatry 170:8, August 2013
5 FRANKO, KESHAVIAH, EDDY, ET AL. TABLE 2. Clinical Characteristics of 16 Women With an Who Died During the Course of the Study (continued) Participant Diagnosis at Intake 13 Anorexia 14 Bulimia nervosa 15 Bulimia nervosa 16 Bulimia nervosa Lifetime Anorexia Nervosa Age at Intake (Years) Age at (Years) Years of at Intake Total Years of Number of Changes in Diagnosis Percent Below Ideal Body Weight at Last Visit Years From Intake to Years From Last Visit to Cause of Yes $ Cardiorespiratory failure, hepatic failure, cirrhosis Yes b Chronic ethanol abuse with early cirrhosis of liver No Acute bronchopneumonia; cerebral glioma No Mitral valve prolapse a Participant recovered from eating disorder during follow-up but subsequently relapsed. b Participant had recovered from eating disorder by the time of her last study visit. Results Overall, 16 deaths (6.5%) were observed among the 246 participants (Table 2). Among the 186 individuals with a lifetime history of anorexia 14 (7.5%) died, which translated to an annual mortality rate of 3.87 deaths per 1,000 person-years. After adjusting for age, sex, and race, the standardized mortality ratio for individuals with lifetime anorexia nervosa was 4.37 (95% exact confidence interval [CI]= ). Among the 60 participants with bulimia nervosa and no history of anorexia two (3.3%) died, which translates to an annual mortality rate of 1.63 deaths per 1,000 person-years and a standardized mortality ratio of 2.33 (95% CI= ). When standardized mortality ratios were calculated by intake diagnosis rather than presence of lifetime anorexia findings were consistent in that individuals with anorexia nervosa at intake had significantly elevated mortality (6.2 times the expected rate), while those with an intake diagnosis of bulimia nervosa did not (1.5 times the expected rate, with the confidence interval overlapping 1.0). Given the small number of deaths in the bulimia nervosa group, and the fact that the confidence interval for the standardized mortality ratio includes 1.0 (no elevated mortality), additional analyses focused primarily on participants with lifetime anorexia nervosa. Of the 16 deaths, four occurred by suicide (all four of these patients had anorexia nervosa). We previously reported the standardized mortality ratio for suicide in our sample to be 56.9 (11). With no new completed suicides in the sample, but an increased number of expected suicides in the demographically matched population since our last analysis, the standardized mortality ratio for suicide among individuals with lifetime anorexia in this sample is now substantially lower, calculated to be 25.2 [95% CI= ]. Risk of premature mortality appeared to decrease over time among individuals with lifetime anorexia nervosa. Within the first 10 years of follow-up, the annual mortality rate for this group was 5.49 deaths per 1,000 person-years, compared with 1.13 deaths per 1,000 person-years thereafter. The standardized mortality ratio also varied substantially by follow-up time. For the follow-up duration from 0 to 10 years (10/186 died), the standardized mortality ratio was 7.7 (95% CI= ), and for the follow-up duration.10 to 20 years (4/176 died), the ratio was 0.7 (95% CI= ). When we examined the standardized mortality ratio by illness duration, we again found considerable variation. The standardized mortality ratio for those with an eating disorder for 0 to 15 years (4/119 died) was 3.2 (95% CI= ), and for those with an eating disorder lasting.15 to 30 years (10/67 died), the ratio was 6.6 (95% CI= ). In other words, the standardized mortality ratio was higher within the first decade of the study compared with the second decade and for those with a longer duration of illness. Specifically, seven of the 10 patients with a longer duration of illness died in the first decade of the study (Table 2), although three of the four patients who died in the second decade also had a longer duration of illness. Thus, the 10 patients who died in the first decade were not the same 10 patients with.15 years of an eating disorder, suggesting that these covariates capture somewhat different information. The number of changes in eating disorder diagnosis over the course of the study is presented in Table 2. Our previous work indicated that over time, the majority of Am J Psychiatry 170:8, August 2013 ajp.psychiatryonline.org 921
6 MORTALITY RATES IN EATING DISORDERS FIGURE 1. Survival Curve Comparing Female Patients With and Without a Lifetime History of Anorexia Nervosa Survival Probability : Lifetime anorexia nervosa 2: No lifetime anorexia nervosa Censored Time (years) from study intake to last follow-up visit or death patients with an intake diagnosis of anorexia nervosa in the entire sample experienced crossover between the anorexia nervosa subs or from anorexia nervosa to bulimia nervosa; crossover was recurrent and bidirectional with the subs (23, 24). In contrast, crossover from bulimia nervosa to anorexia nervosa in individuals without a history of anorexia nervosa at intake was less common (23). It is noteworthy that two of the three individuals with an intake diagnosis of bulimia nervosa who died did not meet criteria for anorexia nervosa during the course of follow-up, nor did they have a history of anorexia nervosa at intake. It is possible that associations between mortality and eating disorder diagnoses depend on when in the course of illness diagnostic status is assessed. Importantly, however, an examination of diagnostic crossover in our predictor analyses indicated that it was not a significant predictor of mortality. Values of covariates ascertained at intake and course variables examined as predictors of mortality are summarized in Table 1. Although the mean age at eating disorder onset was similar between participants who were still alive at last follow-up and those who died prematurely, those who were still alive at last follow-up entered the study at a much earlier age than those who died prematurely, indicating that those who died had a longer duration of illness prior to study intake, which may reflect delays between disorder onset and seeking treatment. As shown in the survival curve (Figure 1), whereas individuals without lifetime anorexia nervosa were more likely to die later in the study, most deaths among those with lifetime anorexia nervosa occurred at varying times within the first 10 years of follow-up. Furthermore, while lifetime anorexia nervosa appeared to confer greater risk of mortality, the overall mortality rate was still low in both groups (survival at 20 years after study intake among individuals with and without lifetime anorexia nervosa was 92% and 97%, respectively). Significant univariate predictors (before and after Bonferroni correction) are presented in Table 3. After applying automated model selection separately to the significant intake, course, and last visit variables, duration of illness was the only significant intake variable to predict mortality. Among course variables, percent of weeks with alcohol abuse and percent of weeks with low body mass index (BMI) (,16) remained in the model. Among last visit covariates, alcohol abuse, BMI, and social adjustment score remained significant. To determine which of the intake, course, and last visit variables together best predicted mortality, we conducted one final automated stepwise selection, which resulted in three variables remaining significant: percent of weeks with alcohol abuse, BMI at last visit, and social adjustment score at last visit. Finally, to account for the fact that, by definition, the last study visit was closer to the time of death than to the time of 922 ajp.psychiatryonline.org Am J Psychiatry 170:8, August 2013
7 FRANKO, KESHAVIAH, EDDY, ET AL. TABLE 3. Significant Univariate Predictors of Mortality Among Female Patients With Lifetime Anorexia Nervosa Univariate Predictor Time Point Estimate Standard Error Hazard Ratio 95% CI p Age (years) Intake a ** disorder diagnosis Last visit 0.04* disorder diagnosis Last visit (bulimia nervosa * compared with anorexia ) disorder diagnosis, last visit Last visit (full eating disorder * recovery compared with anorexia ) Years of eating disorder Intake a ** Years of eating disorder Total a 0.03* Anorexia nervosa Percent of weeks $ b 0.002* Psychiatric Status Rating Scale score Anorexia nervosa Last visit * Psychiatric Status Rating Scale score Bulimia nervosa Percent of weeks $5 above b 0.04* Psychiatric Status Rating Scale score compared with at or below median (6.5%) Percent ideal body weight Intake b 0.009* Weight loss Percent of weeks $21% 29% b 0.003* below ideal body weight Weight loss Last visit 0.04* Weight loss Last visit; 6% 9% compared * with 21% 29% below ideal body weight BMI Intake * BMI Percent of 13-week b ** periods,16 BMI Last visit b,0.0001** Alcohol abuse Psychiatric Status Percent of weeks $ b,0.0001** Rating Scale score Alcohol abuse Psychiatric Status Last visit ,0.0001** Rating Scale score Major depressive disorder Psychiatric Percent of weeks $ b 0.01* Status Rating Scale score Major depressive disorder Psychiatric Last visit * Status Rating Scale score Social adjustment score Average during study ,0.0001** Social adjustment score Last visit ,0.0001** Global Assessment of Functioning Average during study b,0.0001** Scale score Global Assessment of Functioning Scale score Last visit b,0.0001** a The hazard ratio is calculated for a 5-year increase in the covariate. b The hazard ratio is calculated for a 10-unit increase in the covariate. * Indicates significance at an alpha level of 0.05; ** indicates significance at a Bonferroni-corrected alpha level of the last follow-up for those still alive, we forced age at intake into the final model to account for the passage of calendar time. Both the significance and the direction of effect of the covariates were maintained in the final model after adjusting for age. To understand the factors captured by the social adjustment score, we compared social adjustment components at last visit by mortality status. Women who died had moderate to severe impairment in employment (t= 4.92, df=160, p,0.0001), mild to moderate impairment in household functioning (t= 4.24, df=174, p,0.0001), and fair to poor interpersonal relationships with friends (t= 2.96, df=184, p=0.003) and siblings (t= 2.35, df=184, p=0.02) and were more likely to be single (Fisher s exact p=0.07). They also had fair to poor enjoyment of recreational activities (t= 3.00, df=184, p=0.003) and low global satisfaction (t= 2.88, df=184, p=0.004). There were no significant differences in interpersonal relationships with partners or with parents. Discussion Our analyses revealed that patients with lifetime anorexia nervosa had higher premature mortality rates than the general population and that risk of premature death was highest in the first 10 years of follow-up and among Am J Psychiatry 170:8, August 2013 ajp.psychiatryonline.org 923
8 MORTALITY RATES IN EATING DISORDERS individuals with the longest duration of illness. This finding may be explained by the fact that most of the women who died came into the study with a long duration of illness. With one exception, those who died reported an illness duration spanning 7 to 25 years before entry into the study. It may be that their deaths tended to come early in the study because they had already suffered a long period of time with an eating disorder. Thus, while mortality rates in anorexia nervosa varied based on when inthecourseofthislongitudinal study mortality was assessed as well as by the duration of the disorder, it seems likely that chronicity is a crucial factor in premature death. In some (25) but not all (26, 27) studies, the standardized mortality ratio for bulimia nervosa has been reported to be lower than that for anorexia nervosa. Interestingly, however, two of the three women with bulimia nervosa in our study who died had never been diagnosed with anorexia nervosa. Future research might investigate causes of death in bulimia as well as potential predictors, by combining data sets in order to achieve adequate sample sizes. The age and cause of death in this sample of patients with anorexia nervosa are noteworthy. All deaths occurred in middle adulthood, with all but three deaths occurring between ages 35 and 48 years, suggesting that for women with long-standing histories of eating disorders, middle adulthood is a particularly high-risk period for dying. Furthermore, the causes of death, with a few exceptions (e.g., amyotrophic lateral sclerosis), may have been related to eating disorder symptoms, although given the time lapse between the last interview and death, we are not able to address this issue definitively. In the case of the four suicides, the causes of death represent extreme methods with high lethality (28). Although a number of predictor variables were significant in univariate analyses, alcohol abuse over the course of the study and BMI and social adjustment at the last interview remained significant in multivariate analyses. Our earlier analyses at the 10-year follow-up found that longer duration of illness at intake and severity of alcohol use disorder during follow-up increased the risk of mortality (11). Over the longer follow-up period, the degree of low weight and the social adjustment score at the last visit also emerged as significant multivariate predictors of mortality. Social adjustment has been linked to mortality in depression and substance abuse (29, 30). While it is difficult to know in what ways poor social adjustment may be related to mortality (i.e., directly, in concert with comorbidity, or as a reflection of eating disorder severity), our findings indicate that assessing the quality of relationships, the capacity for work and play, and the degree of impairment in psychosocial functioning is vital when working with patients with anorexia nervosa. Recent efforts examining the care of individuals with long-term anorexia nervosa are important, given how little is known about how to treat patients with a chronic eating disorder (31, 32). Strengths of our study include the large well-maintained sample, the long duration of follow-up, and the careful assessment of diagnoses. Limitations include that the assessment of comorbidity was limited to substance abuse and depression and that no longitudinal data were available between the last study visit and the assessment of mortality, which constituted a lengthy period in some cases. Thus, it is possible that mortality was affected by unobserved life events that occurred between the last study visit and death. Furthermore, the National Index does not report deaths that occur outside the United States. In conclusion, anorexia nervosa continues to be a disorder with high mortality rates and one for which effective treatment remains elusive (33). Our findings highlight the need for early identification and intervention and suggest that among those with a long duration of illness, particularly when substance abuse, low weight, or poor psychosocial functioning are also present, the risk for mortality increases substantially. Presented in part at the 2012 International Conference on s, Austin, Tex., May 3 5, Received July 2, 2012; revisions received Oct. 24, Nov. 1, and Dec. 7, 2012; accepted Jan. 3, 2013 (doi: /appi.ajp ). From the Harris Center for Education and Advocacy in s and the Department of Psychiatry, Massachusetts General Hospital, Boston; Department of Counseling and Applied Educational Psychology, Northeastern University, Boston; and Department of Psychology, Florida State University, Tallahassee, Fla. Address correspondence to Dr. Franko (d.franko@neu.edu). The authors report no financial relationships with commercial interests. Supported by NIMH grants R01 MH (to Dr. Herzog) and R03 MH (to Drs. Eddy and Herzog). References 1. Arcelus J, Mitchell A, Wales J, Nielsen S: Is there an elevated mortality rate in anorexia nervosa and other eating disorders? a meta-analysis of 36 studies. Arch Gen Psychiatry 2011; 68: Papadopoulos FC, Ekbom A, Brandt L, Ekselius L: Excess mortality, causes of death and prognostic factors in anorexia nervosa. Br J Psychiatry 2009; 194: Button EJ, Chadalavada B, Palmer RL: Mortality and predictors of death in a cohort of patients presenting to an eating disorders service. Int J Eat Disord 2010; 43: Huas C, Caille A, Godart N, Foulon C, Pham-Scottez A, Divac S, Dechartres A, Lavoisy G, Guelfi JD, Rouillon F, Falissard B: Factors predictive of ten-year mortality in severe anorexia nervosa patients. Acta Psychiatr Scand 2011; 123: Steinhausen HC, Seidel R, Winkler Metzke C: Evaluation of treatment and intermediate and long-term outcome of adolescent eating disorders. Psychol Med 2000; 30: Herpertz-Dahlmann B, Müller B, Herpertz S, Heussen N, Hebebrand J, Remschmidt H: Prospective 10-year follow-up in adolescent anorexia nervosa: course, outcome, psychiatric comorbidity, and psychosocial adaptation. J Child Psychol Psychiatry 2001; 42: ajp.psychiatryonline.org Am J Psychiatry 170:8, August 2013
9 FRANKO, KESHAVIAH, EDDY, ET AL. 7. Strober M, Freeman R, Morrell W: The long-term course of severe anorexia nervosa in adolescents: survival analysis of recovery, relapse, and outcome predictors over years in a prospective study. Int J Eat Disord 1997; 22: Ratnasuriya RH, Eisler I, Szmukler GI, Russell GF: Anorexia nervosa: outcome and prognostic factors after 20 years. Br J Psychiatry 1991; 158: Löwe B, Zipfel S, Buchholz C, Dupont Y, Reas DL, Herzog W: Long-term outcome of anorexia nervosa in a prospective 21- year follow-up study. Psychol Med 2001; 31: Fichter MM, Quadflieg N, Hedlund S: Twelve-year course and outcome predictors of anorexia nervosa. Int J Eat Disord 2006; 39: Keel PK, Dorer DJ, Eddy KT, Franko D, Charatan DL, Herzog DB: Predictors of mortality in eating disorders. Arch Gen Psychiatry 2003; 60: Spitzer RL, Endicott J: Schedule for Affective s and Schizophrenia (SADS), 3rd ed. New York, New York State Psychiatric Institute, Biometrics Research, Metropolitan Life Insurance Company: 1983 metropolitan height and weight tables. Stat Bull Metrop Life Found 1983; 64: Keller MB, Lavori PW, Friedman B, Nielsen E, Endicott J, McDonald-Scott P, Andreasen NC: The Longitudinal Interval Follow-up Evaluation: a comprehensive method for assessing outcome in prospective longitudinal studies. Arch Gen Psychiatry 1987; 44: Leon AC, Solomon DA, Mueller TI, Turvey CL, Endicott J, Keller MB: The Range of Impaired Functioning Tool (LIFE-RIFT): a brief measure of functional impairment. Psychol Med 1999; 29: Leon AC, Solomon DA, Mueller TI, Endicott J, Posternak M, Judd LL, Schettler PJ, Akiskal HS, Keller MB: A brief assessment of psychosocial functioning of subjects with bipolar I disorder: the LIFE-RIFT. Longitudinal Interval Follow-up Evaluation- Range Impaired Functioning Tool. J Nerv Ment Dis 2000; 188: Herzog DB, Dorer DJ, Keel PK, Selwyn SE, Ekeblad ER, Flores AT, Greenwood DN, Burwell RA, Keller MB: Recovery and relapse in anorexia and bulimia nervosa: a 7.5-year follow-up study. J Am Acad Child Adolesc Psychiatry 1999; 38: Horm J: National Index User s Manual, Appendix A: Assignment of Probabilistic Scores to National Index Record Matches. Hyattsville, Md, National Center for Health Statistics, Calle EE, Terrell DD: Utility of the National Index for ascertainment of mortality among cancer prevention study II participants. Am J Epidemiol 1993; 137: National Center for Health Statistics: U.S. Decennial Life Tables for , vol 2, State Life Tables, No 22, Massachusetts. Hyattsville, Md, National Center for Health Statistics, Ulm K: A simple method to calculate the confidence interval of a standardized mortality ratio (SMR). Am J Epidemiol 1990; 131: Lin D, Wei LJ, Ying Z: Checking the cox model with cumulative sums of martingale-based residuals. Biometrika 1993; 80: Eddy KT, Dorer DJ, Franko DL, Tahilani K, Thompson-Brenner H, Herzog DB: Diagnostic crossover in anorexia nervosa and bulimia nervosa: implications for DSM-V. Am J Psychiatry 2008; 165: Eddy KT, Swanson SA, Crosby RD, Franko DL, Engel S, Herzog DB: How should DSM-V classify eating disorder not otherwise specified (EDNOS) presentations in women with lifetime anorexia or bulimia nervosa? Psychol Med 2010; 40: Smink FRE, van Hoeken D, Hoek HW: Epidemiology of eating disorders: incidence, prevalence and mortality rates. Curr Psychiatry Rep 2012; 14: Crow SJ, Peterson CB, Swanson SA, Raymond NC, Specker S, Eckert ED, Mitchell JE: Increased mortality in bulimia nervosa and other eating disorders. Am J Psychiatry 2009; 166: Crow SJ, Swanson SA, Peterson CB, Crosby RD, Wonderlich SA, Mitchell JE: Latent class analysis of eating disorders: relationship to mortality. J Abnorm Psychol 2012; 121: Holm-Denoma JM, Witte TK, Gordon KH, Herzog DB, Franko DL, Fichter M, Quadflieg N, Joiner TE Jr: s by suicide among individuals with anorexia as arbiters between competing explanations of the anorexia-suicide link. J Affect Disord 2008; 107: Feigelman W, Gorman BS: Prospective predictors of premature death: evidence from the National Longitudinal Study of Adolescent Health. J Psychoactive Drugs 2010; 42: Holwerda TJ, Beekman AT, Deeg DJ, Stek ML, van Tilburg TG, Visser PJ, Schmand B, Jonker C, Schoevers RA: Increased risk of mortality associated with social isolation in older men: only when feeling lonely? results from the Amsterdam Study of the Elderly (AMSTEL). Psychol Med 2012; 42: Bamford BH, Mountford VA: Cognitive behavioural therapy for individuals with longstanding anorexia nervosa: adaptations, clinician survival and system issues. Eur Eat Disord Rev 2012; 20: Wonderlich S, Mitchell JE, Crosby RD, Myers TC, Kadlec K, Lahaise K, Swan-Kremeier L, Dokken J, Lange M, Dinkel J, Jorgensen M, Schander L: Minimizing and treating chronicity in the eating disorders: a clinical overview. Int J Eat Disord 2012; 45: Keel PK, Brown TA: Update on course and outcome in eating disorders. Int J Eat Disord 2010; 43: Am J Psychiatry 170:8, August 2013 ajp.psychiatryonline.org 925
With the preparation for the fifth edition of the Diagnostic
 Article Diagnostic Crossover in Anorexia Nervosa and Bulimia Nervosa: Implications for DSM-V Kamryn T. Eddy, Ph.D. David J. Dorer, Ph.D. Debra L. Franko, Ph.D. Kavita Tahilani, B.S. Heather Thompson-Brenner,
Article Diagnostic Crossover in Anorexia Nervosa and Bulimia Nervosa: Implications for DSM-V Kamryn T. Eddy, Ph.D. David J. Dorer, Ph.D. Debra L. Franko, Ph.D. Kavita Tahilani, B.S. Heather Thompson-Brenner,
ORIGINAL ARTICLE. Predictors of Mortality in Eating Disorders
 ORIGINAL ARTICLE Predictors of Mortality in Eating Disorders Pamela K. Keel, PhD; David J. Dorer, PhD; Kamryn T. Eddy, BA; Debra Franko, PhD; Dana L. Charatan, BA; David B. Herzog, MD Background: Anorexia
ORIGINAL ARTICLE Predictors of Mortality in Eating Disorders Pamela K. Keel, PhD; David J. Dorer, PhD; Kamryn T. Eddy, BA; Debra Franko, PhD; Dana L. Charatan, BA; David B. Herzog, MD Background: Anorexia
Relapse is a significant problem for individuals with
 Article Postremission Predictors of Relapse in Women With Eating Disorders Pamela K. Keel, Ph.D. David J. Dorer, Ph.D. Debra L. Franko, Ph.D. Safia C. Jackson, B.S. David B. Herzog, M.D. Objective: The
Article Postremission Predictors of Relapse in Women With Eating Disorders Pamela K. Keel, Ph.D. David J. Dorer, Ph.D. Debra L. Franko, Ph.D. Safia C. Jackson, B.S. David B. Herzog, M.D. Objective: The
Eating Disorders Detection and Treatment. Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program
 Eating Disorders Detection and Treatment Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program Obesity Trends* Among U.S. Adults BRFSS, 1990, 1995, 2005
Eating Disorders Detection and Treatment Scott Crow, M.D. Professor of Psychiatry University of Minnesota Chief Research Officer The Emily Program Obesity Trends* Among U.S. Adults BRFSS, 1990, 1995, 2005
Comparison of DSM-IV Versus Proposed DSM-5 Diagnostic Criteria for Eating Disorders: Reduction of Eating Disorder Not Otherwise Specified and Validity
 CE ACTIVITY Comparison of DSM-IV Versus Proposed DSM-5 Diagnostic Criteria for Eating Disorders: Reduction of Eating Disorder Not Otherwise Specified and Validity Pamela K. Keel, PhD 1 * Tiffany A. Brown,
CE ACTIVITY Comparison of DSM-IV Versus Proposed DSM-5 Diagnostic Criteria for Eating Disorders: Reduction of Eating Disorder Not Otherwise Specified and Validity Pamela K. Keel, PhD 1 * Tiffany A. Brown,
Weight Suppression Predicts Time to Remission From Bulimia Nervosa
 Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 6, 772 776 0022-006X/11/$12.00 DOI: 10.1037/a0025714 Weight Suppression Predicts Time to Remission
Journal of Consulting and Clinical Psychology 2011 American Psychological Association 2011, Vol. 79, No. 6, 772 776 0022-006X/11/$12.00 DOI: 10.1037/a0025714 Weight Suppression Predicts Time to Remission
Short-term outcome of anorexia nervosa in adolescents after inpatient treatment: a prospective study
 Short-term outcome of anorexia nervosa in adolescents after inpatient treatment: a prospective study Harriet Salbach-Andrae, Nora Schneider, Katja Seifert, Ernst Pfeiffer, Klaus Lenz, Ulrike Lehmkuhl,
Short-term outcome of anorexia nervosa in adolescents after inpatient treatment: a prospective study Harriet Salbach-Andrae, Nora Schneider, Katja Seifert, Ernst Pfeiffer, Klaus Lenz, Ulrike Lehmkuhl,
NIH Public Access Author Manuscript Int J Eat Disord. Author manuscript; available in PMC 2014 December 01.
 NIH Public Access Author Manuscript Published in final edited form as: Int J Eat Disord. 2013 December ; 46(8): 849 854. doi:10.1002/eat.22163. Restrictive Eating Behaviors are a Non-Weight-Based Marker
NIH Public Access Author Manuscript Published in final edited form as: Int J Eat Disord. 2013 December ; 46(8): 849 854. doi:10.1002/eat.22163. Restrictive Eating Behaviors are a Non-Weight-Based Marker
AP-HP, Hôpital Sainte-Anne, Clinique des maladies mentales et de l Encéphale, Paris, France
 TITLE PAGE Factors predictive of ten-year mortality in severe anorexia nervosa patients Running head: mortality in severe anorexia nervosa patients Huas Caroline, MD 1,2,3, Caille Agnès, MD 1,2, Godart
TITLE PAGE Factors predictive of ten-year mortality in severe anorexia nervosa patients Running head: mortality in severe anorexia nervosa patients Huas Caroline, MD 1,2,3, Caille Agnès, MD 1,2, Godart
Comparison of Long-Term Outcomes in Adolescents With Anorexia Nervosa Treated With Family Therapy
 Comparison of Long-Term Outcomes in Adolescents With Anorexia Nervosa Treated With Family Therapy JAMES LOCK, M.D., PH.D., JENNIFER COUTURIER, M.D., AND W. STEWART AGRAS, M.D. ABSTRACT Objective: To describe
Comparison of Long-Term Outcomes in Adolescents With Anorexia Nervosa Treated With Family Therapy JAMES LOCK, M.D., PH.D., JENNIFER COUTURIER, M.D., AND W. STEWART AGRAS, M.D. ABSTRACT Objective: To describe
META-ANALYSIS. Mortality Rates in Patients With Anorexia Nervosa and Other Eating Disorders
 META-ANALYSIS Mortality Rates in Patients With Anorexia Nervosa and Other Eating Disorders A Meta-analysis of 36 Studies Jon Arcelus, LMS, MSc, FRCPsych, PhD; Alex J. Mitchell, MRCPsych; Jackie Wales,
META-ANALYSIS Mortality Rates in Patients With Anorexia Nervosa and Other Eating Disorders A Meta-analysis of 36 Studies Jon Arcelus, LMS, MSc, FRCPsych, PhD; Alex J. Mitchell, MRCPsych; Jackie Wales,
1. We ask the Secretary to replace the sizeable flexibility given to the states with national uniform standards for the EHB categories.
 1 January 31, 2012 The Honorable Kathleen Sebelius U.S. Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201 Re: Essential Health Benefits Bulletin Dear Secretary Sebelius:
1 January 31, 2012 The Honorable Kathleen Sebelius U.S. Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201 Re: Essential Health Benefits Bulletin Dear Secretary Sebelius:
Importance of Multiple Purging Methods in the Classification of Eating Disorder Subtypes
 REGULAR ARTICLE Importance of Multiple Purging Methods in the Classification of Eating Disorder Subtypes Alissa A. Haedt, BS 1 Crystal Edler, BS 1 Todd F. Heatherton, PhD 2 Pamela K. Keel, PhD 1 * ABSTRACT
REGULAR ARTICLE Importance of Multiple Purging Methods in the Classification of Eating Disorder Subtypes Alissa A. Haedt, BS 1 Crystal Edler, BS 1 Todd F. Heatherton, PhD 2 Pamela K. Keel, PhD 1 * ABSTRACT
Eating Disorders: Clinical Features, Comorbidity, and Treatment
 Eating Disorders: Clinical Features, Comorbidity, and Treatment Carol B. Peterson, PhD Associate Professor Eating Disorders Research Program Department of Psychiatry University of Minnesota peter161@umn.edu
Eating Disorders: Clinical Features, Comorbidity, and Treatment Carol B. Peterson, PhD Associate Professor Eating Disorders Research Program Department of Psychiatry University of Minnesota peter161@umn.edu
Prospective assessment of treatment use by patients with personality disorders
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
The Course of Illness Following Inpatient Treatment of Adults with Longstanding Eating Disorders: A 5-Year Follow-Up
 REGULAR ARTICLE The Course of Illness Following Inpatient Treatment of Adults with Longstanding Eating Disorders: A 5-Year Follow-Up KariAnne R. Vrabel, CandPsych 1 * Jan H. Rosenvinge, PhD 2 Asle Hoffart,
REGULAR ARTICLE The Course of Illness Following Inpatient Treatment of Adults with Longstanding Eating Disorders: A 5-Year Follow-Up KariAnne R. Vrabel, CandPsych 1 * Jan H. Rosenvinge, PhD 2 Asle Hoffart,
NIH Public Access Author Manuscript J Clin Psychiatry. Author manuscript; available in PMC 2008 August 31.
 NIH Public Access Author Manuscript Published in final edited form as: J Clin Psychiatry. 2007 May ; 68(5): 738 746. Natural Course of Bulimia Nervosa and of Eating Disorder Not Otherwise Specified: 5-Year
NIH Public Access Author Manuscript Published in final edited form as: J Clin Psychiatry. 2007 May ; 68(5): 738 746. Natural Course of Bulimia Nervosa and of Eating Disorder Not Otherwise Specified: 5-Year
Relapse in anorexia nervosa: a survival analysis
 Psychological Medicine, 2004, 34, 671 679. f 2004 Cambridge University Press DOI: 10.1017/S0033291703001168 Printed in the United Kingdom Relapse in anorexia nervosa: a survival analysis J. C. CARTER,
Psychological Medicine, 2004, 34, 671 679. f 2004 Cambridge University Press DOI: 10.1017/S0033291703001168 Printed in the United Kingdom Relapse in anorexia nervosa: a survival analysis J. C. CARTER,
Paper s Information. Eating Disorder Diagnoses. Paper Type: Essay. Word Count: 1700 words. Referencing Style: APA Style
 1 Paper s Information Topic: Eating Disorder Diagnoses Paper Type: Essay Word Count: 1700 words Pages: 7pages Referencing Style: APA Style Education Level: Under Graduate 2 Running Head: EATING DISORDER
1 Paper s Information Topic: Eating Disorder Diagnoses Paper Type: Essay Word Count: 1700 words Pages: 7pages Referencing Style: APA Style Education Level: Under Graduate 2 Running Head: EATING DISORDER
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI
 Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia Nervosa A. A refusal to maintain body weight
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia Nervosa A. A refusal to maintain body weight
DSM-5 Reduces the Proportion of EDNOS Cases: Evidence from Community Samples
 REGULAR ARTICLE DSM-5 Reduces the Proportion of EDNOS Cases: Evidence from Community Samples Paulo P.P. Machado, PhD 1 * Sónia Gonçalves, PhD 1 Hans W. Hoek, MD, PhD 2,3,4 ABSTRACT Objective: Eating Disorder
REGULAR ARTICLE DSM-5 Reduces the Proportion of EDNOS Cases: Evidence from Community Samples Paulo P.P. Machado, PhD 1 * Sónia Gonçalves, PhD 1 Hans W. Hoek, MD, PhD 2,3,4 ABSTRACT Objective: Eating Disorder
Final Outcomes Report. Sherry Van Blyderveen, M.A. Pediatric Eating Disorders Program McMaster Children s Hospital. April 30,
 Understanding Pediatric Eating Disorders and their Treatment: Evaluating an Outpatient Treatment Program for Children and Youth Struggling with Eating Disorders Final Outcomes Report Sherry Van Blyderveen,
Understanding Pediatric Eating Disorders and their Treatment: Evaluating an Outpatient Treatment Program for Children and Youth Struggling with Eating Disorders Final Outcomes Report Sherry Van Blyderveen,
8/10/2012. Education level and diabetes risk: The EPIC-InterAct study AIM. Background. Case-cohort design. Int J Epidemiol 2012 (in press)
 Education level and diabetes risk: The EPIC-InterAct study 50 authors from European countries Int J Epidemiol 2012 (in press) Background Type 2 diabetes mellitus (T2DM) is one of the most common chronic
Education level and diabetes risk: The EPIC-InterAct study 50 authors from European countries Int J Epidemiol 2012 (in press) Background Type 2 diabetes mellitus (T2DM) is one of the most common chronic
Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample
 Available online at www.sciencedirect.com Drug and Alcohol Dependence 96 (2008) 187 191 Short communication Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample Lara A.
Available online at www.sciencedirect.com Drug and Alcohol Dependence 96 (2008) 187 191 Short communication Diagnostic orphans for alcohol use disorders in a treatment-seeking psychiatric sample Lara A.
Anxiety disorders in mothers and their children: prospective longitudinal community study
 Anxiety disorders in mothers and their children: prospective longitudinal community study Andrea Schreier, Hans-Ulrich Wittchen, Michael Höfler and Roselind Lieb Summary The relationship between DSM IV
Anxiety disorders in mothers and their children: prospective longitudinal community study Andrea Schreier, Hans-Ulrich Wittchen, Michael Höfler and Roselind Lieb Summary The relationship between DSM IV
A Comparison of Quality of Life and. Psychosocial Functioning in Obsessive-Compulsive Disorder and Body Dysmorphic Disorder
 Annals of Clinical Psychiatry, 19[3]:181 186, 2007 Copyright American Academy of Clinical Psychiatrists ISSN: 1040-1237 print / 1547-3325 online DOI: 10.1080/10401230701468685 A Comparison of Quality of
Annals of Clinical Psychiatry, 19[3]:181 186, 2007 Copyright American Academy of Clinical Psychiatrists ISSN: 1040-1237 print / 1547-3325 online DOI: 10.1080/10401230701468685 A Comparison of Quality of
Maintenance Treatment for Anorexia Nervosa: A Comparison of Cognitive Behavior Therapy and Treatment as Usual
 REGULAR ARTICLE Maintenance Treatment for Anorexia Nervosa: A Comparison of Cognitive Behavior Therapy and Treatment as Usual Jacqueline C. Carter, PhD 1,2 * Traci L. McFarlane, PhD 1,2 Carmen Bewell,
REGULAR ARTICLE Maintenance Treatment for Anorexia Nervosa: A Comparison of Cognitive Behavior Therapy and Treatment as Usual Jacqueline C. Carter, PhD 1,2 * Traci L. McFarlane, PhD 1,2 Carmen Bewell,
OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL. Ng CG
 ORIGINAL PAPER OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL Ng CG Department of Psychological Medicine, Faculty of Medicine, University Malaya,
ORIGINAL PAPER OUTCOMES OF DICHOTOMIZING A CONTINUOUS VARIABLE IN THE PSYCHIATRIC EARLY READMISSION PREDICTION MODEL Ng CG Department of Psychological Medicine, Faculty of Medicine, University Malaya,
Online publication date: 24 February 2011 PLEASE SCROLL DOWN FOR ARTICLE
 This article was downloaded by: [Brewerton, Timothy D.] On: 24 February 2011 Access details: Access Details: [subscription number 933991272] Publisher Routledge Informa Ltd Registered in England and Wales
This article was downloaded by: [Brewerton, Timothy D.] On: 24 February 2011 Access details: Access Details: [subscription number 933991272] Publisher Routledge Informa Ltd Registered in England and Wales
Outcome of Anorexia Nervosa: results of a 5 year follow-up study
 Outcome of Anorexia Nervosa: results of a 5 year follow-up study Annemarie A. van Elburg, Jacquelien J.G. Hillebrand, Karlijn Kampman, Marinus J.C. Eijkemans, Martien J.H. Kas, Herman van Engeland, Hans
Outcome of Anorexia Nervosa: results of a 5 year follow-up study Annemarie A. van Elburg, Jacquelien J.G. Hillebrand, Karlijn Kampman, Marinus J.C. Eijkemans, Martien J.H. Kas, Herman van Engeland, Hans
Eating Disorders: recognition and treatment
 National Guideline Alliance Version 1.0 Eating Disorders: recognition and treatment Appendix O - HE evidence checklists NICE Guideline Methods, evidence and recommendations December 2016 Draft for Consultation
National Guideline Alliance Version 1.0 Eating Disorders: recognition and treatment Appendix O - HE evidence checklists NICE Guideline Methods, evidence and recommendations December 2016 Draft for Consultation
Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence
 Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa?
 Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa? Marisol Perez, 1 Thomas E. Joiner, Jr., 1 * and Peter M. Lewinsohn 2 1 Department of Psychology, Florida State University,
Is Major Depressive Disorder or Dysthymia More Strongly Associated with Bulimia Nervosa? Marisol Perez, 1 Thomas E. Joiner, Jr., 1 * and Peter M. Lewinsohn 2 1 Department of Psychology, Florida State University,
Eating Disorder Awareness: Assess, Diagnose, and Refer! Kristin Francis, MD Assistant Professor University of Utah Department of Psychiatry
 Eating Disorder Awareness: Assess, Diagnose, and Refer! Kristin Francis, MD Assistant Professor University of Utah Department of Psychiatry Goals of our time together WHY are eating disorders so important
Eating Disorder Awareness: Assess, Diagnose, and Refer! Kristin Francis, MD Assistant Professor University of Utah Department of Psychiatry Goals of our time together WHY are eating disorders so important
Hafizullah Azizi M.D.
 Hafizullah Azizi M.D. Eating disorders Feeding and Eating Disorders of Infancy and Early Childhood and Obesity Anorexia Nervosa Bulimia Nervosa EDNOS Binge Eating Disorder Purging Disorder Night Eating
Hafizullah Azizi M.D. Eating disorders Feeding and Eating Disorders of Infancy and Early Childhood and Obesity Anorexia Nervosa Bulimia Nervosa EDNOS Binge Eating Disorder Purging Disorder Night Eating
Abstract. Comprehensive Psychiatry 48 (2007)
 Comprehensive Psychiatry 48 (2007) 329 336 www.elsevier.com/locate/comppsych Psychosocial impairment and treatment utilization by patients with borderline personality disorder, other personality disorders,
Comprehensive Psychiatry 48 (2007) 329 336 www.elsevier.com/locate/comppsych Psychosocial impairment and treatment utilization by patients with borderline personality disorder, other personality disorders,
Mild, moderate, meaningful? Examining the psychological and functioning correlates of DSM-5 eating disorder severity specifiers
 Received: 9 August 2016 Revised: 14 April 2017 Accepted: 17 April 2017 DOI: 10.1002/eat.22728 ORIGINAL ARTICLE Mild, moderate, meaningful? Examining the psychological and functioning correlates of DSM-5
Received: 9 August 2016 Revised: 14 April 2017 Accepted: 17 April 2017 DOI: 10.1002/eat.22728 ORIGINAL ARTICLE Mild, moderate, meaningful? Examining the psychological and functioning correlates of DSM-5
The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders
 AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH
 Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Early-onset eating disorders
 Early-onset eating disorders Principal investigators Debra K. Katzman, MD, FRCPC, Division of Adolescent Medicine, Department of Paediatrics* Anne Morris, MB, BS, MPH, FRACP, Division of Adolescent Medicine,
Early-onset eating disorders Principal investigators Debra K. Katzman, MD, FRCPC, Division of Adolescent Medicine, Department of Paediatrics* Anne Morris, MB, BS, MPH, FRACP, Division of Adolescent Medicine,
Application of Cox Regression in Modeling Survival Rate of Drug Abuse
 American Journal of Theoretical and Applied Statistics 2018; 7(1): 1-7 http://www.sciencepublishinggroup.com/j/ajtas doi: 10.11648/j.ajtas.20180701.11 ISSN: 2326-8999 (Print); ISSN: 2326-9006 (Online)
American Journal of Theoretical and Applied Statistics 2018; 7(1): 1-7 http://www.sciencepublishinggroup.com/j/ajtas doi: 10.11648/j.ajtas.20180701.11 ISSN: 2326-8999 (Print); ISSN: 2326-9006 (Online)
Challenges to Recovery Following Early Psychosis: Implications of Recovery Rate and Timing
 Challenges to Recovery Following Early Psychosis: Implications of Recovery Rate and Timing Mental Health Exchange Group December 3, 2014 W Joy Maddigan, PhD RN Background One component [the quantitative
Challenges to Recovery Following Early Psychosis: Implications of Recovery Rate and Timing Mental Health Exchange Group December 3, 2014 W Joy Maddigan, PhD RN Background One component [the quantitative
INSTRUCTION MANUAL Instructions for Patient Health Questionnaire (PHQ) and GAD-7 Measures
 PHQ and GAD-7 Instructions P. 1/9 INSTRUCTION MANUAL Instructions for Patient Health Questionnaire (PHQ) and GAD-7 Measures TOPIC PAGES Background 1 Coding and Scoring 2, 4, 5 Versions 3 Use as Severity
PHQ and GAD-7 Instructions P. 1/9 INSTRUCTION MANUAL Instructions for Patient Health Questionnaire (PHQ) and GAD-7 Measures TOPIC PAGES Background 1 Coding and Scoring 2, 4, 5 Versions 3 Use as Severity
Clinical Trial Results Database Page 1
 Clinical Trial Results Database Page 1 Sponsor Novartis Pharmaceuticals Corporation Generic Drug Name Therapeutic Area of Trial Major Depressive Disorder (MDD) Approved Indication Treatment of major depressive
Clinical Trial Results Database Page 1 Sponsor Novartis Pharmaceuticals Corporation Generic Drug Name Therapeutic Area of Trial Major Depressive Disorder (MDD) Approved Indication Treatment of major depressive
Child and Adolescent Eating Disorders: Diagnoses and Treatment Innovations
 Child and Adolescent Eating Disorders: Diagnoses and Treatment Innovations Kamryn T. Eddy, Ph.D. Co-Director, Eating Disorders Clinical and Research Program, Massachusetts General Hospital Associate Professor
Child and Adolescent Eating Disorders: Diagnoses and Treatment Innovations Kamryn T. Eddy, Ph.D. Co-Director, Eating Disorders Clinical and Research Program, Massachusetts General Hospital Associate Professor
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Severe and enduring anorexia nervosa? Illness severity and duration are unrelated to outcomes from enhanced cognitive behaviour therapy. White Rose Research Online URL for
This is a repository copy of Severe and enduring anorexia nervosa? Illness severity and duration are unrelated to outcomes from enhanced cognitive behaviour therapy. White Rose Research Online URL for
Developing a new treatment approach to binge eating and weight management. Clinical Psychology Forum, Number 244, April 2013.
 Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
Developing a new treatment approach to binge eating and weight management Clinical Psychology Forum, Number 244, April 2013 Dr Marie Prince 1 Contents Service information Binge Eating Disorder Binge Eating
BRIEF REPORT FACTORS ASSOCIATED WITH UNTREATED REMISSIONS FROM ALCOHOL ABUSE OR DEPENDENCE
 Pergamon Addictive Behaviors, Vol. 25, No. 2, pp. 317 321, 2000 Copyright 2000 Elsevier Science Ltd. Printed in the USA. All rights reserved 0306-4603/00/$ see front matter PII S0306-4603(98)00130-0 BRIEF
Pergamon Addictive Behaviors, Vol. 25, No. 2, pp. 317 321, 2000 Copyright 2000 Elsevier Science Ltd. Printed in the USA. All rights reserved 0306-4603/00/$ see front matter PII S0306-4603(98)00130-0 BRIEF
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/45091 holds various files of this Leiden University dissertation. Author: Aardoom, J.J. Title: Just a click away... E-mental health for eating disorders
Cover Page The handle http://hdl.handle.net/1887/45091 holds various files of this Leiden University dissertation. Author: Aardoom, J.J. Title: Just a click away... E-mental health for eating disorders
Declaration. Overview Eating Disorders in Children and Adolescents
 Eating Disorders in Children and Adolescents Dr Pei-Yoong Lam FRACP Assistant Clinical Professor, Division of Adolescent Health and Medicine Declaration I have no commercial affiliations or conflicts of
Eating Disorders in Children and Adolescents Dr Pei-Yoong Lam FRACP Assistant Clinical Professor, Division of Adolescent Health and Medicine Declaration I have no commercial affiliations or conflicts of
METHODS RESULTS. Supported by funding from Ortho-McNeil Janssen Scientific Affairs, LLC
 PREDICTORS OF MEDICATION ADHERENCE AMONG PATIENTS WITH SCHIZOPHRENIC DISORDERS TREATED WITH TYPICAL AND ATYPICAL ANTIPSYCHOTICS IN A LARGE STATE MEDICAID PROGRAM S.P. Lee 1 ; K. Lang 2 ; J. Jackel 2 ;
PREDICTORS OF MEDICATION ADHERENCE AMONG PATIENTS WITH SCHIZOPHRENIC DISORDERS TREATED WITH TYPICAL AND ATYPICAL ANTIPSYCHOTICS IN A LARGE STATE MEDICAID PROGRAM S.P. Lee 1 ; K. Lang 2 ; J. Jackel 2 ;
Identifying Adult Mental Disorders with Existing Data Sources
 Identifying Adult Mental Disorders with Existing Data Sources Mark Olfson, M.D., M.P.H. New York State Psychiatric Institute Columbia University New York, New York Everything that can be counted does not
Identifying Adult Mental Disorders with Existing Data Sources Mark Olfson, M.D., M.P.H. New York State Psychiatric Institute Columbia University New York, New York Everything that can be counted does not
study of anorexia nervosa
 222 Original Article Singapore Med 1 2007, 48 (3) : The pursuit of thinness: an outcome study of anorexia nervosa Lim S L, Sinaram S, Ung E K, Kua E H ABSTRACT Introduction: Anorexia nervosa (AN) is a
222 Original Article Singapore Med 1 2007, 48 (3) : The pursuit of thinness: an outcome study of anorexia nervosa Lim S L, Sinaram S, Ung E K, Kua E H ABSTRACT Introduction: Anorexia nervosa (AN) is a
Posttraumatic Stress Disorder and Suicidal Behavior: Current Understanding and Future Directions
 Posttraumatic Stress Disorder and Suicidal Behavior: Current Understanding and Future Directions Jaimie L. Gradus, DSc, MPH Epidemiologist, National Center for PTSD, VA Boston Healthcare System Associate
Posttraumatic Stress Disorder and Suicidal Behavior: Current Understanding and Future Directions Jaimie L. Gradus, DSc, MPH Epidemiologist, National Center for PTSD, VA Boston Healthcare System Associate
Final Outcomes Report. Sherry Van Blyderveen, Ph.D. Pediatric Eating Disorders Program McMaster Children s Hospital. April 30,
 Understanding Pediatric Eating Disorders and their Treatment: Evaluating an Outpatient Treatment Program for Children and Youth Struggling with Eating Disorders Final Outcomes Report Sherry Van Blyderveen,
Understanding Pediatric Eating Disorders and their Treatment: Evaluating an Outpatient Treatment Program for Children and Youth Struggling with Eating Disorders Final Outcomes Report Sherry Van Blyderveen,
Substance Use Among Potential Kidney Transplant Candidates and its Impact on Access to Kidney Transplantation: A Canadian Cohort Study
 Substance Use Among Potential Kidney Transplant Candidates and its Impact on Access to Kidney Transplantation: A Canadian Cohort Study Evan Tang 1, Aarushi Bansal 1, Michelle Kwok 1, Olusegun Famure 1,
Substance Use Among Potential Kidney Transplant Candidates and its Impact on Access to Kidney Transplantation: A Canadian Cohort Study Evan Tang 1, Aarushi Bansal 1, Michelle Kwok 1, Olusegun Famure 1,
How can we predict & change the course and outcome of anorexia nervosa?
 Download slides bit.do/annakeski How can we predict & change the course and outcome of anorexia nervosa? Anna Keski-Rahkonen Associate Professor University of Helsinki, Finland How can we change the course
Download slides bit.do/annakeski How can we predict & change the course and outcome of anorexia nervosa? Anna Keski-Rahkonen Associate Professor University of Helsinki, Finland How can we change the course
Outcomes of Eating Disorders: A Systematic Review of the Literature
 SPECIAL SECTION ARTICLE Outcomes of Eating Disorders: A Systematic Review of the Literature Nancy D. Berkman, PhD 1 Kathleen N. Lohr, PhD 1 Cynthia M. Bulik, PhD 2,3 * ABSTRACT Objective: The RTI International-University
SPECIAL SECTION ARTICLE Outcomes of Eating Disorders: A Systematic Review of the Literature Nancy D. Berkman, PhD 1 Kathleen N. Lohr, PhD 1 Cynthia M. Bulik, PhD 2,3 * ABSTRACT Objective: The RTI International-University
ORIGINAL ARTICLE. Psychosocial Disability in the Course of Bipolar I and II Disorders
 ORIGINAL ARTICLE Psychosocial Disability in the Course of Bipolar I and II Disorders A Prospective, Comparative, Longitudinal Study Lewis L. Judd, MD; Hagop S. Akiskal, MD; Pamela J. Schettler, PhD; Jean
ORIGINAL ARTICLE Psychosocial Disability in the Course of Bipolar I and II Disorders A Prospective, Comparative, Longitudinal Study Lewis L. Judd, MD; Hagop S. Akiskal, MD; Pamela J. Schettler, PhD; Jean
Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna
 University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
University of Groningen Developing bipolar disorder. A study among children of patients with bipolar disorder Hillegers, Manon Hubertine Johanna IMPORTANT NOTE: You are advised to consult the publisher's
ARTICLE. The Economic Effect of Planet Health on Preventing Bulimia Nervosa
 ARTICLE The Economic Effect of Planet Health on Preventing Bulimia Nervosa Li Yan Wang, MBA, MA; Lauren P. Nichols, BA; S. Bryn Austin, ScD Objectives: To assess the economic effect of the schoolbased
ARTICLE The Economic Effect of Planet Health on Preventing Bulimia Nervosa Li Yan Wang, MBA, MA; Lauren P. Nichols, BA; S. Bryn Austin, ScD Objectives: To assess the economic effect of the schoolbased
Resolution of Vital Sign Instability: An Objective Measure of Medical Stability in Anorexia Nervosa
 JOURNAL OF ADOLESCENT HEALTH 2003;32:73 77 ORIGINAL ARTICLE Resolution of Vital Sign Instability: An Objective Measure of Medical Stability in Anorexia Nervosa TABASSUM SHAMIM, M.D., NEVILLE H. GOLDEN,
JOURNAL OF ADOLESCENT HEALTH 2003;32:73 77 ORIGINAL ARTICLE Resolution of Vital Sign Instability: An Objective Measure of Medical Stability in Anorexia Nervosa TABASSUM SHAMIM, M.D., NEVILLE H. GOLDEN,
Depression, anxiety, and obsessionality in long-term recovered patients with adolescent-onset anorexia nervosa
 Eur Child Adolesc Psychiatry (2005) 14:106 110 DOI 10.1007/s00787-005-0431-5 BRIEF REPORT K. Holtkamp B. Müller N. Heussen H. Remschmidt B. Herpertz-Dahlmann Depression, anxiety, and obsessionality in
Eur Child Adolesc Psychiatry (2005) 14:106 110 DOI 10.1007/s00787-005-0431-5 BRIEF REPORT K. Holtkamp B. Müller N. Heussen H. Remschmidt B. Herpertz-Dahlmann Depression, anxiety, and obsessionality in
BGS Falls Severe mental illness, poor bone health and falls: The potential role for physical activity
 Severe mental illness, poor bone health and falls: The potential role for physical activity Brendon Stubbs MCSP, PhD Head of Physiotherapy South London and Maudsley NHS Foundation Trust Post Doctoral Research
Severe mental illness, poor bone health and falls: The potential role for physical activity Brendon Stubbs MCSP, PhD Head of Physiotherapy South London and Maudsley NHS Foundation Trust Post Doctoral Research
ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS
 CHAPTER 5 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS J. AM. GERIATR. SOC. 2013;61(6):882 887 DOI: 10.1111/JGS.12261 61 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER,
CHAPTER 5 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS J. AM. GERIATR. SOC. 2013;61(6):882 887 DOI: 10.1111/JGS.12261 61 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER,
Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts Future Cardiovascular Events
 Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
* Manuscript. A comparison between the costs of Australian and. Mandometer treatment of eating disorders
 * Manuscript A comparison between the costs of Australian and Mandometer treatment of eating disorders 1 Abstract We have estimated the costs of the treatment of a group of patients with eating disorders
* Manuscript A comparison between the costs of Australian and Mandometer treatment of eating disorders 1 Abstract We have estimated the costs of the treatment of a group of patients with eating disorders
Eating Disorders Are we doing enough? Tracey Wade Professor, School of Psychology
 Eating Disorders Are we doing enough? Tracey Wade Professor, School of Psychology 25 June 2013 Myth 1 Anorexia nervosa is the most serious eating disorder Isabelle Caro 1982-2010 Fact 1 All eating disorders
Eating Disorders Are we doing enough? Tracey Wade Professor, School of Psychology 25 June 2013 Myth 1 Anorexia nervosa is the most serious eating disorder Isabelle Caro 1982-2010 Fact 1 All eating disorders
Defense mechanisms and symptom severity in panic disorder
 ACTA BIOMED 2010; 81: 30-34 Mattioli 1885 O R I G I N A L A R T I C L E Defense mechanisms and symptom severity in panic disorder Marco Fario, Sonja Aprile, Chiara Cabrino, Carlo Maggini, Carlo Marchesi
ACTA BIOMED 2010; 81: 30-34 Mattioli 1885 O R I G I N A L A R T I C L E Defense mechanisms and symptom severity in panic disorder Marco Fario, Sonja Aprile, Chiara Cabrino, Carlo Maggini, Carlo Marchesi
Personality traits predict current and future functioning comparably for individuals with major depressive and personality disorders
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. March, 2007 Personality traits predict current and future functioning comparably for individuals with major depressive and personality
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. March, 2007 Personality traits predict current and future functioning comparably for individuals with major depressive and personality
Hopelessness Predicts Suicide Ideation But Not Attempts: A 10-Year Longitudinal Study
 Suicide and Life-Threatening Behavior 1 2017 The American Association of Suicidology DOI: 10.1111/sltb.12328 Hopelessness Predicts Suicide Ideation But Not Attempts: A 10-Year Longitudinal Study TIANYOU
Suicide and Life-Threatening Behavior 1 2017 The American Association of Suicidology DOI: 10.1111/sltb.12328 Hopelessness Predicts Suicide Ideation But Not Attempts: A 10-Year Longitudinal Study TIANYOU
Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents
 BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
BadgerCare Plus Preferred Practice Guidelines Bipolar Disorder in Children and Adolescents These Guidelines are based in part on the following: American Academy of Child and Adolescent Psychiatry s Practice
Prevalence of psychosomatic and other medical illnesses in anorexic and bulimic patients 1
 Behavioural Neurology (1993),6, 123-127 Prevalence of psychosomatic and other medical illnesses in anorexic and bulimic patients 1 A.-M. Ghadirian, F. Engelsmann, P. Leichner and M. Marshall Department
Behavioural Neurology (1993),6, 123-127 Prevalence of psychosomatic and other medical illnesses in anorexic and bulimic patients 1 A.-M. Ghadirian, F. Engelsmann, P. Leichner and M. Marshall Department
In the last few years, evidence for the efficacy of psychotherapy
 Article Relapse Prevention in With Bipolar Disorder: Outcome After 2 Years Dominic H. Lam, Ph.D. Peter Hayward, Ph.D. Edward R. Watkins, Ph.D. Kim Wright, B.A. Pak Sham, Ph.D. Objective: In a previous
Article Relapse Prevention in With Bipolar Disorder: Outcome After 2 Years Dominic H. Lam, Ph.D. Peter Hayward, Ph.D. Edward R. Watkins, Ph.D. Kim Wright, B.A. Pak Sham, Ph.D. Objective: In a previous
Supplementary Methods
 Supplementary Materials for Suicidal Behavior During Lithium and Valproate Medication: A Withinindividual Eight Year Prospective Study of 50,000 Patients With Bipolar Disorder Supplementary Methods We
Supplementary Materials for Suicidal Behavior During Lithium and Valproate Medication: A Withinindividual Eight Year Prospective Study of 50,000 Patients With Bipolar Disorder Supplementary Methods We
Alberta Alcohol and Drug Abuse Commission. POSITION ON ADDICTION AND MENTAL HEALTH February 2007
 Alberta Alcohol and Drug Abuse Commission POSITION ON ADDICTION AND MENTAL HEALTH POSITION The Alberta Alcohol and Drug Abuse Commission (AADAC) recognizes that among clients with addiction problems, there
Alberta Alcohol and Drug Abuse Commission POSITION ON ADDICTION AND MENTAL HEALTH POSITION The Alberta Alcohol and Drug Abuse Commission (AADAC) recognizes that among clients with addiction problems, there
Eating Disorders in Youth
 Eating Disorders in Youth Evaluating and Treating in the Medical Home February 27, 2017 Rebecca Marshall, MD, MPH Outline Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Avoidant Restrictive Food
Eating Disorders in Youth Evaluating and Treating in the Medical Home February 27, 2017 Rebecca Marshall, MD, MPH Outline Anorexia Nervosa Bulimia Nervosa Binge Eating Disorder Avoidant Restrictive Food
Prevalence of anxiety and depressive symptoms in men with erectile dysfunction
 Prevalence of anxiety and depressive symptoms in men with erectile dysfunction K Pankhurst, MB ChB G Joubert, BA, MSc P J Pretorius, MB ChB, MMed (Psych) Departments of Psychiatry and Biostatistics, University
Prevalence of anxiety and depressive symptoms in men with erectile dysfunction K Pankhurst, MB ChB G Joubert, BA, MSc P J Pretorius, MB ChB, MMed (Psych) Departments of Psychiatry and Biostatistics, University
Familial Aggregation of Eating Disorders: Results from a Controlled Family Study of Bulimia Nervosa
 Familial Aggregation of Eating Disorders: Results from a Controlled Family Study of Bulimia Nervosa Daniel Stein, 1 Lisa R. Lilenfeld, 1 Katherine Plotnicov, 1 Christine Pollice, 1 Radhika Rao, 1 Michael
Familial Aggregation of Eating Disorders: Results from a Controlled Family Study of Bulimia Nervosa Daniel Stein, 1 Lisa R. Lilenfeld, 1 Katherine Plotnicov, 1 Christine Pollice, 1 Radhika Rao, 1 Michael
Factors Associated with Suicide Attempts in Women with Eating Disorders. Emily M. Pisetsky. Chapel Hill 2013
 Factors Associated with Suicide Attempts in Women with Eating Disorders Emily M. Pisetsky A dissertation submitted to the faculty of the University of North Carolina at Chapel Hill in partial fulfillment
Factors Associated with Suicide Attempts in Women with Eating Disorders Emily M. Pisetsky A dissertation submitted to the faculty of the University of North Carolina at Chapel Hill in partial fulfillment
Avoidant/restrictive food intake disorder: Introducing a new DSM-5 eating disorder
 Avoidant/restrictive food intake disorder: Introducing a new DSM-5 eating disorder Debra Katzman, MD FRCPC, The Hospital for Sick Children and University of Toronto Karizma Mawjee, BA MA, The Hospital
Avoidant/restrictive food intake disorder: Introducing a new DSM-5 eating disorder Debra Katzman, MD FRCPC, The Hospital for Sick Children and University of Toronto Karizma Mawjee, BA MA, The Hospital
Incidence and Risk of Alcohol Use Disorders by Age, Gender and Poverty Status: A Population-Based-10 Year Follow-Up Study
 Incidence and Risk of Alcohol Use Disorders by Age, Gender and Poverty Status: A Population-Based-10 Year Chun-Te Lee 1,2, Chiu-Yueh Hsiao 3, Yi-Chyan Chen 4,5, Oswald Ndi Nfor 6, Jing-Yang Huang 6, Lee
Incidence and Risk of Alcohol Use Disorders by Age, Gender and Poverty Status: A Population-Based-10 Year Chun-Te Lee 1,2, Chiu-Yueh Hsiao 3, Yi-Chyan Chen 4,5, Oswald Ndi Nfor 6, Jing-Yang Huang 6, Lee
Consecutive mental health patients of a family doctor in Shanghai 6 years experience
 Consecutive mental health patients of a family doctor in Shanghai 6 years experience Date: 13 th January 2015 Time: 12:15 Location: UFH Presenter: Lincoln Miyasaka Introduction: The prevalence of generalized
Consecutive mental health patients of a family doctor in Shanghai 6 years experience Date: 13 th January 2015 Time: 12:15 Location: UFH Presenter: Lincoln Miyasaka Introduction: The prevalence of generalized
Rates and patterns of participation in cardiac rehabilitation in Victoria
 Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Rates and patterns of participation in cardiac rehabilitation in Victoria Vijaya Sundararajan, MD, MPH, Stephen Begg, MS, Michael Ackland, MBBS, MPH, FAPHM, Ric Marshall, PhD Victorian Department of Human
Eating Disorders in Old Age
 Eating Disorders in Old Age Dr. William Rhys Jones Consultant Psychiatrist & Clinical Lead CONNECT: The West Yorkshire and Harrogate Adult Eating Disorders Service r.jones9@nhs.net 0113 855 6400 Eating
Eating Disorders in Old Age Dr. William Rhys Jones Consultant Psychiatrist & Clinical Lead CONNECT: The West Yorkshire and Harrogate Adult Eating Disorders Service r.jones9@nhs.net 0113 855 6400 Eating
DMRI Drug Misuse Research Initiative
 DMRI Drug Misuse Research Initiative Executive Summary Comorbidity in the national psychiatric morbidity surveys Research Report submitted to the Department of Health in February 2004 Report prepared by:
DMRI Drug Misuse Research Initiative Executive Summary Comorbidity in the national psychiatric morbidity surveys Research Report submitted to the Department of Health in February 2004 Report prepared by:
2010 EDRS PROGRAM AND SCHEDULE. 1:15 3:00 p.m. Symposium 1: Prevention of Eating Disorders and Obesity
 THURSDAY, OCTOBER 7, 2010: 1:00 1:15 p.m. Welcome from President 2010 EDRS PROGRAM AND SCHEDULE 1:15 3:00 p.m. Symposium 1: Prevention of Eating Disorders and Obesity Linking Eating Disorders and Overweight
THURSDAY, OCTOBER 7, 2010: 1:00 1:15 p.m. Welcome from President 2010 EDRS PROGRAM AND SCHEDULE 1:15 3:00 p.m. Symposium 1: Prevention of Eating Disorders and Obesity Linking Eating Disorders and Overweight
Clinical experience suggests. Ten-Year Use of Mental Health Services by Patients With Borderline Personality Disorder and With Other Axis II Disorders
 Ten-Year Use of Mental Health Services by Patients With Borderline Personality Disorder and With Other Axis II Disorders Susanne Hörz, Dipl.-Psych., Ph.D. Mary C. Zanarini, Ed.D. Frances R. Frankenburg,
Ten-Year Use of Mental Health Services by Patients With Borderline Personality Disorder and With Other Axis II Disorders Susanne Hörz, Dipl.-Psych., Ph.D. Mary C. Zanarini, Ed.D. Frances R. Frankenburg,
Change in Self-Rated Health and Mortality Among Community-Dwelling Disabled Older Women
 The Gerontologist Vol. 45, No. 2, 216 221 In the Public Domain Change in Self-Rated Health and Mortality Among Community-Dwelling Disabled Older Women Beth Han, PhD, MD, MPH, 1 Caroline Phillips, MS, 2
The Gerontologist Vol. 45, No. 2, 216 221 In the Public Domain Change in Self-Rated Health and Mortality Among Community-Dwelling Disabled Older Women Beth Han, PhD, MD, MPH, 1 Caroline Phillips, MS, 2
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI
 Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia A. A refusal to maintain body weight at or
Appendix Table 1. Operationalization in the CIDI of criteria for DSM-IV eating disorders and related entities Criteria* Operationalization from CIDI 1 Anorexia A. A refusal to maintain body weight at or
Long-term outcome of anorexia nervosa in a prospective 21-year follow-up study
 Psychological Medicine, 2001, 31, 881 890. 2001 Cambridge University Press Printed in the United Kingdom Long-term outcome of anorexia nervosa in a prospective 21-year follow-up study B. LO WE, S. ZIPFEL,
Psychological Medicine, 2001, 31, 881 890. 2001 Cambridge University Press Printed in the United Kingdom Long-term outcome of anorexia nervosa in a prospective 21-year follow-up study B. LO WE, S. ZIPFEL,
Eating Disorders. Sristi Nath, D.O. Early Identification and Proactive Treatment November 12, Disclosures
 Eating Disorders Sristi Nath, D.O. Early Identification and Proactive Treatment November 12, 2016 1 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation.
Eating Disorders Sristi Nath, D.O. Early Identification and Proactive Treatment November 12, 2016 1 Disclosures I have no actual or potential conflict of interest in relation to this program/presentation.
An Overview of Survival Statistics in SEER*Stat
 An Overview of Survival Statistics in SEER*Stat National Cancer Institute SEER Program SEER s mission is to provide information on cancer statistics in an effort to reduce the burden of cancer among the
An Overview of Survival Statistics in SEER*Stat National Cancer Institute SEER Program SEER s mission is to provide information on cancer statistics in an effort to reduce the burden of cancer among the
Date: Dear Mental Health Professional,
 Date: Dear Mental Health Professional, Attached is the Referral Form required to receive PRP services from Mosaic Community Services. The following is required to complete the application process: Completed
Date: Dear Mental Health Professional, Attached is the Referral Form required to receive PRP services from Mosaic Community Services. The following is required to complete the application process: Completed
The relationship between adolescent/young adult BMI and subsequent non-problem and problem alcohol use
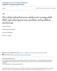 Washington University School of Medicine Digital Commons@Becker Posters 2007: Alcohol Use Across the Lifespan 2007 The relationship between adolescent/young adult BMI and subsequent non-problem and problem
Washington University School of Medicine Digital Commons@Becker Posters 2007: Alcohol Use Across the Lifespan 2007 The relationship between adolescent/young adult BMI and subsequent non-problem and problem
Exercise Behavior & Major Cardiac Events: CCSS 1 STUDY TITLE
 STUDY TITLE Exercise Behavior & Major Cardiac Events: CCSS 1 Association Between Exercise Behavior and Incidence of Major Cardiac Events in Adult Survivors of Childhood Cancer: A Report from the Childhood
STUDY TITLE Exercise Behavior & Major Cardiac Events: CCSS 1 Association Between Exercise Behavior and Incidence of Major Cardiac Events in Adult Survivors of Childhood Cancer: A Report from the Childhood
An estimated 18% of women and 3% of men
 Gender and Time Differences in the Associations Between Sexual Violence Victimization, Health Outcomes, and Risk Behaviors American Journal of Men s Health Volume 2 Number 3 September 2008 254-259 2008
Gender and Time Differences in the Associations Between Sexual Violence Victimization, Health Outcomes, and Risk Behaviors American Journal of Men s Health Volume 2 Number 3 September 2008 254-259 2008
University of Groningen. Children of bipolar parents Wals, Marjolein
 University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Children of bipolar parents Wals, Marjolein IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES
 APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
APPENDIX 11: CASE IDENTIFICATION STUDY CHARACTERISTICS AND RISK OF BIAS TABLES 1 Study characteristics table... 3 2 Methodology checklist: the QUADAS-2 tool for studies of diagnostic test accuracy... 4
Association between Bulimia Nervosa, Body Mass Index and Depression in Period of Puberty
 Association between Bulimia Nervosa, Body Mass Index and Depression in Period of Puberty Ahmeti Aferdita, PhD Faculty of Psychology, University AAB of Kosovo, Faculty of Arts, University of Pristina, Hasan
Association between Bulimia Nervosa, Body Mass Index and Depression in Period of Puberty Ahmeti Aferdita, PhD Faculty of Psychology, University AAB of Kosovo, Faculty of Arts, University of Pristina, Hasan
