Lymphedema In Ovarian Cancer Survivors: Assessing Diagnostic Methods And Risk Factors
|
|
|
- Laura Stephens
- 6 years ago
- Views:
Transcription
1 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Public Health Theses School of Public Health January 2013 Lymphedema In Ovarian Cancer Survivors: Assessing Diagnostic Methods And Risk Factors Neel Subramanian Iyer Yale University, neelsiyer@gmail.com Follow this and additional works at: Recommended Citation Iyer, Neel Subramanian, "Lymphedema In Ovarian Cancer Survivors: Assessing Diagnostic Methods And Risk Factors" (2013). Public Health Theses This Open Access Thesis is brought to you for free and open access by the School of Public Health at EliScholar A Digital Platform for Scholarly Publishing at Yale. It has been accepted for inclusion in Public Health Theses by an authorized administrator of EliScholar A Digital Platform for Scholarly Publishing at Yale. For more information, please contact elischolar@yale.edu.
2 Lymphedema in Ovarian Cancer Survivors: Assessing Diagnostic Methods and Risk Factors By Neel Subramanian Iyer A Thesis Presented to The Faculty of the Yale School of Public Health Yale University In Candidacy for the Degree of Masters of Public Health 2013
3 Abstract Purpose: Lymphedema is a poorly understood but significant side effect of treatment for gynecologic cancer. We sought to determine the prevalence of lower limb lymphedema (LLL) in a sample of ovarian cancer survivors via three different diagnostic methods while also evaluating the agreement between each method and assessing potential risk factors for LLL. Methods: LLL was measured via self-report questionnaire, optoelectric perometry, and evaluation by a certified lymphedema specialist in women (n = 48) who had completed treatment for their ovarian cancer and were physically inactive. Results: LLL prevalence ranged from 19-42% depending on the diagnostic method, with the self-report questionnaire and the lymphedema specialist evaluation having the highest agreement (κ = 0.646). No risk factors were significantly associated with LLL, although there was a trend towards higher total body fat and BMI among those with LLL versus lower body fat and BMI among those without LLL. Conclusion: There is a strong need for further research, given that the prevalence of LLL could be as high as 42 percent among women treated for ovarian cancer. 2
4 Acknowledgements Firstly, I would like to thank Dr. Melinda Irwin, PhD, MPH, and Dr. Brenda Cartmel, PhD, for their constant support, insight, and guidance throughout the thesis process. I gratefully acknowledge the support of Louis Friedman, PT CLT-LANA, our lymphedema specialist, for his involvement in the study and his availability throughout the process. We are appreciative of the help provided by the Yale Cancer Center, specifically Rajni Mehta, MPH, of the Rapid Case Ascertainment team. The cooperation of 23 Connecticut hospitals, including Stanford Hospital, in allowing patient access, is gratefully acknowledged. This study was approved by the State of Connecticut Department of Public Health Human Investigation Committee. Certain data used in this study were obtained from the Connecticut Tumor Registry located in the Connecticut Department of Public Health. The authors assume full responsibility for analyses and interpretation of these data. Finally, we gratefully acknowledge the cooperation of our study participants. 3
5 Table of Contents List of Tables... 5 Introduction... 6 Methods... 8 Study Population... 8 Baseline Measures... 9 Defining Lymphedema Statistical Analysis Results Participant Characteristics Prevalence of Lower Limb Lymphedema Diagnostic Method Agreement Analysis of Potential Risk Factors Discussion Conclusion References
6 List of Tables Table 1. WALC Study Eligibility Criteria Table 2. Baseline Characteristics of Study Participants (n=48) Table 3. Prevalence of Lower Limb Lymphedema (n=48) Table 4. Agreement of the Self-Report Questionnaire and Optoelectric Perometer with the Lymphedema Specialist Evaluation Table 5. Comparison of Means (Diagnosis by Any Method) Table 6. Comparison of Means (Diagnosis via Lymphedema Specialist Evaluation) Table 7. Comparison of Means (Diagnosis via Self-Report Questionnaire) Table 8. Comparison of Means (Diagnosis via Optoelectric Perometer) Table 9. Comparison of Means (Diagnosis via Lymphedema Specialist Evaluation -or- Self-Report Questionnaire) Table 10. Comparison of Means (Diagnosis via Lymphedema Specialist Evaluation -or- Optoelectric Perometer)
7 Introduction Ovarian cancer represents a significant number of gynecological cancers in the United States, accounting for more than 20,000 cases per year. 1 It is the fourth most frequent cause of cancer death in women, after lung, breast, and colorectal cancer. 2 It is difficult to treat, as patients frequently present late in the course of the disease, which may be asymptomatic until advanced stages. The five year survival for stage I ovarian cancer is over 90 percent, but is only 25 percent for women with stage IV ovarian cancer. 1 Unfortunately more than 60 percent of ovarian cancers are diagnosed at stage IV, which portends a poor prognosis and represents the majority of the estimated 15,000 deaths in ,2 The current standard treatment of ovarian cancer is to optimally remove the tumor surgically and follow with adjuvant chemotherapy. Standard initial therapy most often is five to six courses of systematic chemotherapy with a platinum and taxane regimen. This treatment approach results in a complete clinical response to therapy in percent of patients with advanced stage disease. 3 Despite the often seen dramatic clinical response to treatment, the disease will recur in percent of patients diagnosed with advanced disease. 1 Unfortunately, no proven curative therapy exists for this group of patients, and the optimal treatment approach for those who relapse after initial treatment remains unknown. However, a growing number of new chemotherapeutic agents for recurrent advanced ovarian cancer have been successful at stabilization of disease and thus are increasing length of survival of women with recurrent ovarian cancer. In turn, the goals of treatment for women with ovarian cancer are to maximize survival and disease-free intervals and to improve quality of life. Each year, thousands of ovarian cancer patients and survivors will develop and endure the side effects of their cancer, which negatively affect their quality of life. One such side effect, lymphedema, is a debilitating, chronic condition that causes localized swelling when lymph vessels 6
8 become blocked, occurring after surgery and treatment for various cancers. 4 Given that the surgical treatment of ovarian cancer often involves removal of the lymph beds in the pelvic sidewalls and para-aortic area, the risk of lower limb lymphedema (LLL) is high. 7 However, few women diagnosed with ovarian cancer know that they are at risk for LLL, and few gynecological oncologists discuss this potential side effect with their patients when discussing treatment for their cancer. 12 Therefore, currently, most women are only referred to a lymphedema specialist when they complain of swelling and pain, signs that LLL may already be occurring. To date, the majority of research on lymphedema has occurred primarily in patients treated for breast cancer. 5 Existing research on LLL in ovarian cancer patients is extremely limited, with only three published studies. Of the three studies that have examined LLL in women diagnosed with ovarian cancer, all have been retrospective chart reviews examining prevalence of LLL based on a singular diagnostic method These retrospective chart reviews have reported LLL prevalence rates ranging from 7-38 percent. The variation in these reported prevalence rates are the result of different measurement techniques used in each of the studies. Beyond these retrospective chart reviews, no current estimate exists on the prevalence of LLL based on a prospective method, using objective and valid measures that clinicians can use to help guide them to identify those most at risk for developing LLL. The current gold standard for measuring lymphedema is evaluation by a trained lymphedema specialist, although most recently diagnosis via optoelectric perometry has become increasingly common. 13 Previously, a self-report questionnaire has been developed to assess lymphedema in breast cancer patients, 14 providing a quick, low cost method to collect information on a large sample of patients. However, the validity of this questionnaire has not been assessed in ovarian cancer patients. Due to the limited number of studies, data on the prevalence of LLL in ovarian cancer patients is inadequate as is data on effective treatment of LLL in this population. Improving our 7
9 knowledge would help guide clinicians in diagnosing and treating LLL. The purpose of this study was to determine the prevalence of LLL via perometry, self-report questionnaire and an evaluation by a certified lymphedema specialist in a sample of ovarian cancer survivors and to determine risk factors for LLL. A second purpose of our study was to determine the validity of a LLL self-report questionnaire and optoelectric perometry against the lymphedema specialist evaluation. Methods Study Participants Women diagnosed with ovarian cancer (stage I-IV) were recruited as part of an NCI-funded (CA R ) study entitled, The Women s Activity and Lifestyle Study in Connecticut (WALC). The WALC study is a randomized controlled trial in physically inactive ovarian cancer survivors examining the impact of a moderate-intensity aerobic exercise intervention (vs. attention control) on overall quality of life, body composition, and serum hormones possibly associated with physical activity and ovarian cancer prognosis. Women diagnosed with ovarian cancer between the years of 2007 and 2013, were identified from the Rapid Case Ascertainment (RCA) Shared Resource of the Yale Cancer Center, a field arm of the Connecticut Tumor Registry. After Connecticut Department of Public Health and hospital IRB approvals, RCA identified women diagnosed with ovarian cancer at 23 Connecticut hospitals. After study staff initially contacted the women s physician for consent to contact the patient, potential participants were contacted individually and invited to participate in the WALC study, once eligibility was established (see Table 1). Women who contacted study staff without having received a letter of invitation were invited to participate once eligibility had been verified and upon written approval by their physician allowing them to participate in a moderate-intensity exercise program. All women were under the age of 75, had completed adjuvant treatment at least one month prior to 8
10 randomization, and were diagnosed within the past four years. They each exhibited a sedentary physical activity pattern (< 90 min/week of moderate-intensity exercise). Baseline Measures Baseline visits were scheduled with all new participants, either at their home or in the WALC research center, at which point baseline characteristics, including treatment characteristics were collected via interview-administered questionnaires by WALC research staff. Within one week of completing the initial baseline visit, study participants visited the Smilow Cancer Hospital at Yale- New Haven to receive a physical exam to collect physical characteristics (height, weight, BMI), receive a full-body dual-energy X-ray absorptiometry (DEXA) scan to measure total and percent body fat, and where the initial lymphedema evaluation was completed. Lower limb lymphedema was assessed using the Norman Lymphedema Survey, a selfadministered questionnaire. The Norman Lymphedema Survey is a multi-section survey created to evaluate lymphedema that has been validated in breast cancer survivors. 14 The sections focused on lower limb lymphedema, asked women if they had observed differences in their feet, lower (ankle to knee) legs, upper (knee to hip) legs, and abdomen following treatment for ovarian cancer. The questionnaire also asked about the frequency of these differences, and whether medical evaluation and treatment had been sought when differences were seen. Importantly, the questionnaire also asked women if they had ever been informed about lymphedema previously. During the baseline visit, an optoelectric perometer test measuring leg volume conducted by a trained lymphedema specialist was also used to assess LLL. The perometer (1000M Perometer: Juzo, Cuyahoga Falls, OH) measures circumference transections every 3mm and sums these to a volume using a computer. It has been evaluated extensively for validity and reliability, with one recent study finding both high intra-rater reliability (ICC = 0.989, 95% CI: ) and inter-rater 9
11 reliability (ICC = 0.993, 95% CI: ) when compared to other volumetric assessments for lymphedema. 13,15 With the participant standing, leg volume was measured once for each leg. Prior to the assessment, women removed all clothing and jewelry from the area. Following the perometer measurement, the specialist conducted his own lymphedema assessment. Women were asked if they had any history of swelling in their legs prior to surgery, and any perceived changes in leg swelling following surgery. They were also asked if swelling occurred with physical activity and if any changes in leg appearance were seen in the morning compared to later in the day. Palpations assessing for pitting or induration were performed on both legs and compared. The specialist also conducted a visual assessment of both legs, notably looking for differences at the dorsum of the foot, toes, and ankles. Defining Lymphedema Using the results of the self-report questionnaire, lymphedema was defined as seeing any regular difference in limb/abdomen appearance, compared to the other leg/side of abdomen and/or to appearance prior to treatment for ovarian cancer. This was based on the four main questions in the survey asking about differences in the women s feet, lower and upper legs, and abdomen. Using the optoelectric perometer assessment, lymphedema was defined as having five percent or more inter-limb volume discrepancy. This was based on standard definitions set forth by the International Society of Lymphology, defining mild lymphedema as five percent or more limb volume difference, moderate lymphedema as percent discrepancy, and severe lymphedema as more than 30 percent discrepancy. 16 The lymphedema specialist categorized lymphedema as either lymphedema occurrence or no lymphedema occurrence. Using his visual inspection and palpations, the specialist defined no lymphedema as: no pitting, no palpable induration, no patient-reported history of swelling (with and 10
12 without physical activity), no patient-reported appearance change between pre- and post-treatment, and no visual differences in appearance at assessment. Statistical Analysis We performed descriptive statistics to describe the characteristics of our study population. To assess agreement between the three diagnostic methods simple kappa (κ) statistics were calculated. A simple kappa statistic was used to measure the level of agreement, and the degree of disagreement, with a maximum value of 1 (perfect agreement) and values great than 0.75 suggest strong agreement. 14 Optoelectric perometer and self-report questionnaire results were compared to results of the lymphedema specialist evaluation, as the gold-standard diagnosis method. Because of the small sample size, logistic regression models could not be used to identify risk factors for LLL. Instead we conducted an analysis of the means of all continuous variables, using a Student s t-test to compare those diagnosed with lymphedema to those without lymphedema, for the various diagnostic methods. A continuous variable, total number of surgical procedures was created, to account for the various surgical procedures that the women could have received as part of their ovarian cancer treatments. These surgical procedures included total abdominal hysterectomy, bilateral salpingo oophorectomy, omenectomy, lymph node removal, tumor debulking, bowel resection, and colon resection, as well as any other surgery that they might have undergone as part of their treatment. Fisher s exact tests were run to evaluate differences among the categorical variables. P-values were two-sided and p < 0.05 was used as the threshold for statistical significance. All statistical analyses were conducted using SAS 9.3 (Cary, North Carolina). 11
13 Results Participant Characteristics A total of 83 women completed the baseline evaluations as part of the WALC study. Fortyeight women (57.8%) received all three of the lymphedema diagnostic evaluations (self-report questionnaire, optoelectric perometer, lymphedema specialist evaluation), limiting our analyses to these women. Demographic and clinical characteristics of the study participants are depicted in Table 2. The age of participants ranged from years, with a mean of 56.1 years (SD: 7.2). The majority of participants were non-hispanic white (95.8%) and had at least a high school diploma (95.8%). The body mass index (BMI) of study participants ranged from kg/m 2, with an average of 30 kg/m 2 (SD: 7.9). Fifty percent of study participants reported having heard of the condition of lymphedema before participating in the study. The time since diagnosis ranged from 7 months to 48 months, with an average of 17.6 months since diagnosis. The majority of women had been diagnosed with stage III (41.7%) ovarian cancer or later. Forty-six percent of women in the study were diagnosed with localized (stage I or II) ovarian cancer, much higher than the national average of 15 percent. 1 Nearly all of the women had received chemotherapy as part of their cancer treatment (91.7%), and a small minority of the women (16.7%) had experienced recurrence of their ovarian cancer. In terms of surgical treatments for their ovarian cancer treatment, nearly every woman had a total-abdominal hysterectomy (95.8%), a bilateral salpingo oophorectomy (95.8%), an omenectomy (95.8%), and a local lymph node dissection (91.7%). Of the 33 percent of women who reported having other surgery (n=15) related to their ovarian cancer treatment, 60 percent of surgeries were appendectomies. 12
14 Prevalence of Lower Limb Lymphedema Lower limb lymphedema diagnosis ranged from 19 percent to 23 percent across the various diagnostic methods individually. Twenty-three percent of women (n=11) in our study were diagnosed with LLL via the trained lymphedema specialist evaluation. Among the 23 percent of women (n=11) who were diagnosed via the self-report questionnaire, six women saw lymphedemalike symptoms in their feet, seven saw symptoms in their lower legs, one saw symptoms in her upper leg, and four saw symptoms in their abdomen area. Four women reported lymphedema-like symptoms in multiple regions of their lower limbs. Nineteen percent of women (n=9) were diagnosed via the optoelectric perometer. Of these women, the inter-limb difference ranged from five to nine percent, with an average inter-limb difference of 6.1 percent, indicating that all women would be classified as having mild lymphedema. Forty-two percent of women (n=20) had LLL diagnosis by at least one of the three diagnostic methods, while zero study participants had diagnosis by all three methods. Prevalence results are summarized in Table 3. Diagnostic Method Agreement The self-report questionnaire showed stronger agreement (κ = 0.646) with the lymphedema specialist evaluation diagnosis compared to the agreement of the optoelectric perometer with the lymphedema specialist evaluation (κ = 0.011). Hence, neither method met the kappa statistic threshold for strong agreement with the gold standard, the lymphedema specialist evaluation. The comparison of the self-report questionnaire and the optoelectric perometer produced a negative kappa statistics (κ = ), indicating no agreement between the two methods. Eight of the 11 women (72.7%) diagnosed by the lymphedema specialist were also diagnosed by the self-report questionnaire. Comparatively only two of the 11 women diagnosed by the lymphedema specialist (18.2%) were also diagnosed by the optoelectric perometer. Only one woman was diagnosed with 13
15 LLL by both the self-report questionnaire and the optoelectric perometer (out of the 19 women who were diagnosed by either method). Analysis of Potential Risk Factors Tables 5-10 summarize the differences in age, BMI, total body fat, percent body fat, time since diagnosis, and number of surgical procedures between those diagnosed with LLL and those not diagnosed with LLL, based on the various diagnostic methods. No statistically significant differences were observed between the two groups among any of the potential risk factors independent of diagnostic method. However, those without LLL were consistently found to have a longer time since diagnosis in every comparison, across all diagnostic methods. Total body fat was found to be higher among those with LLL in five of the six comparisons. Similarly, age, BMI, and percent body fat were found to be higher among those with LLL in four of the six comparisons. No statistically significant differences in stage at diagnosis, chemotherapy as part of treatment, and ovarian cancer recurrence were detected between the two groups. Discussion We found that the prevalence of lower limb lymphedema in ovarian cancer survivors ranged from 19 to 42 percent depending on the diagnostic method used. Individually, the three diagnostic methods evaluated, self-report questionnaire, optoelectric perometer, and lymphedema specialist evaluation, each found a prevalence of LLL of about 20 percent, but when used collectively found a prevalence of 42 percent. The self-report questionnaire had a much higher agreement with the gold standard evaluation by a trained lymphedema specialist than the agreement between the optoelectric perometer and the evaluation by a trained lymphedema specialist, although neither achieved strong agreement (defined as a kappa statistic of 0.75 or higher). Those with LLL were consistently found 14
16 to have a shorter time since diagnosis across all diagnostic measures compared to women without LLL, although this trend was not statistically significant. Also of interest was the fact that only 50 percent of our study population had heard about lymphedema, and only 60 percent of those diagnosed with lymphedema via any diagnostic method had previous knowledge about the condition prior to study participation. The prevalence differences observed from using the different diagnostic methods indicate the limitations of each method, even the gold standard method, evaluation by a lymphedema specialist. While the self-report questionnaire is easy and quick to administer, it remains a subjective evaluation of LLL that has not been validated before for LLL or in gynecologic cancer survivors. Our findings represent initial validation for the questionnaire in this population, and indicate that it may be a preferable diagnostic method when compared to the perometer. Unlike the questionnaire, the perometer does provide an objective measurement of limb volume on which to base LLL diagnosis. Furthermore, it can detect even very small differences in limb volume that are symptomatic of lymphedema, which may be overlooked by even the lymphedema specialist. However, it is severely limited by the fact that it is unable to diagnose lymphedema in women who are experiencing LLL in both legs. For these women who would be experiencing swelling in both legs, the perometer would fail to identify a meaningful inter-limb volume difference needed to diagnose LLL. Additionally, the perometer would fail to identify LLL that may be occurring in a woman s abdomen because it is limited to the measurement of limb volume. This may be why the optoelectric perometer had such a low agreement with both of the other diagnostic methods. The lymphedema specialist evaluation remains the likely gold standard because it takes both subjective factors, like patient-reported history of swelling, and objective factors, like induration and pitting, into consideration in diagnosing LLL, but the evaluation is a time-intensive process. The reasonably 15
17 high agreement of the self-report questionnaire with the lymphedema specialist indicates that with further validation the self-report questionnaire could be a useful tool in diagnosing LLL. Previous literature on LLL has found a prevalence of LLL of 7-38 percent in women following treatment for ovarian cancer. All of these studies evaluated LLL through retrospective chart reviews of clinically diagnosed lymphedema via different singular diagnostic methods, a limitation of their findings. These previous results are similar to those seen in the study reported here, a LLL prevalence ranging from percent. One previous study found that elevated BMI, at levels consistent with being overweight (BMI of 25-30) or obese (BMI greater than 30), was a strong risk factor for LLL among gynecologic cancer survivors. 12 While our results were not statistically significant, the trend towards higher BMI, percent body fat and total body fat among those with LLL in our study supports this finding. These findings are consistent with literature published about upper limb lymphedema following treatment for breast cancer which has been shown to be strongly associated with greater body weight and higher BMI. 17,18 Previous research has also shown an association between lymph node dissection and LLL, as well as post-operative radiation and LLL. 10 Unfortunately because more than 90 percent of the women in our study received a lymph node dissection as part of their treatment, we had very limited power to detect an association between lymph node removal and LLL in our study. Interestingly, previous research has also shown a general lack of knowledge among patients about lymphedema related to gynecologic cancer treatment, 12 supporting our finding that only 50 percent of our study population had been informed about the condition previously. This represents a deficiency in the current standard of care, particularly if LLL prevalence could be as high as 40 percent. The finding of an association between lymph node dissection as part of cancer treatment and LLL in previous literature provides insight into the mechanism behind lymphedema occurrence. While no specific literature has been published on the mechanism for LLL related to gynecologic 16
18 cancer, previous research has illustrated the mechanism for lymphedema following treatment for breast cancer. When lymph node dissection is performed it can disrupt the flow of lymph through the lymphatic system. This can cause lymph vessels to become congested and dilated, resulting in lymph accumulation in the limbs. 19 Steady accumulation of the lymph fluid, and the failure of reparative and compensatory mechanisms in the body, like lymphatic regeneration, is consistent with lymphedema. 19 Because similar lymph node dissections in the pelvic area are required for treatment of ovarian and other gynecologic cancers, it is probable that LLL follows a similar mechanism. Furthermore, whereas most breast cancers are diagnosed at stage I, before they have metastasized to local lymph nodes, most ovarian cancers are diagnosed at stage III and IV, once the cancer has already spread to local lymph nodes. 1 Thus lymph node dissection is more likely to be required as part of treatment for ovarian cancer, illustrated by the fact that more than 90 percent of the women in our study received lymph node dissection, increasing the risk for lymphedema occurrence. Our study was the first study to look at LLL prevalence in ovarian cancer survivors utilizing multiple diagnostic methods. While previous studies calculated LLL prevalence via retrospective chart reviews, which was diagnosed by various singular methods, ours used the latest diagnostic standards to assess LLL in ovarian cancer survivors, as they were experiencing symptoms, likely a better measure of LLL prevalence. Furthermore, because each participant was evaluated using all three diagnostic measures, our prevalence findings may be more accurate, because they overcome many of the limitations associated with each diagnostic method individually, such as the failure of the optoelectric perometer to diagnose LLL when it is occurring in both legs. These findings indicate that diagnosis via multiple methods may be the most accurate way of diagnosing LLL, as this may be the best way to detect lymphedema symptoms in the entire leg from abdomen to feet and even in the mildest forms. 17
19 However, limitations of our study need to be considered when interpreting our results. While the cross-sectional design was sufficient to assess LLL prevalence, causality between our hypothesized risk factors and LLL was not possible to infer. This was furthered by our small sample size, which limited our ability to detect significant differences between those with and without LLL. Future studies should focus on looking at lymphedema incidence, to better quantify the risk of LLL among ovarian cancer survivors. Furthermore, a prospective cohort design, rather than a crosssectional design, should be utilized comparing limb appearance and volume pre-and post-treatment for ovarian cancer in order to more accurately measure LLL occurrence, and allow for a better evaluation of potential risk factors. Conclusion Among ovarian cancer survivors the prevalence of LLL ranged from percent. The fairly high diagnostic agreement between the self-report questionnaire and the lymphedema specialist evaluation indicates the usefulness of the self-report questionnaire in diagnosing LLL. Similarly the low agreement of both of those methods with the optoelectric perometer, illustrates the major limitation of the perometer, that it cannot diagnose LLL when it is occurring in both legs simultaneously or in the abdomen. While our study did not identify any significant risk factors associated with LLL, the trends towards higher BMI and body fat in those with LLL are consistent with previous literature and warrant further study. Despite the fairly high prevalence of LLL that we found, only about half of the women in our study had heard of lymphedema prior to participation indicating a large information gap. The lack of significant literature on the subject on LLL in ovarian cancer survivors, and related to gynecologic cancers in general, indicates a strong need for further research, particularly if the prevalence of LLL could be as high as 42 percent among women treated for these cancers. 18
20 References 1. Howlader N, Noone AM, Krapcho M, Neyman N, Aminou R, Altekruse SF, Kosary CL, Ruhl J, Tatalovich Z, Cho H, Mariotto A, Eisner MP, Lewis DR, Chen HS, Feuer EJ, Cronin KA (eds). SEER Cancer Statistics Review, (Vintage 2009 Populations), National Cancer Institute. Bethesda, MD, based on November 2011 SEER data submission, posted to the SEER web site, American Cancer Society. Cancer facts and figures Atlanta, GA: American Cancer Society, Piccart MJ, Bertelsen K, James K, et al. Randomized intergroup trial of cisplatin-paclitaxel versus cisplatin-cyclophosphamide in women with advanced epithelial ovarian cancer: Three-year results. JNCI 2000; 92: Daroczy J. Pathology of lymphedema. Clin Dermatol 1995; 13: Ahmed R, Prizment A, Lazovich D, Schmitz K, Folsom A. Lymphedema and quality of life in breast cancer survivors. J Clin Oncol 2008; 26(35): Velanovich V, Szymanski, W. Quality of life of breast cancer patients with lymphedema. American Journal of Surgery 1999; 177(3): Levenback CF, van der Zee AG, Rob L, et al. Sentinel lymph node biopsy in patients with gynecological cancers. Expert panel statement from the International Sentinel Node Society Mtg, Feb 21, Gynecol Oncol 2009; 114: Abu-Rustum N, Alektiar K, Iasonos A, et al. The incidence of symptomatic lower-extremity lymphedema following treatment of uterine corpus malignancies: a 12-year experience at Memorial Sloan-Kettering Cancer Center. Gynecol Oncol 2006; 103: Todo Y, Yamamoto R, Minobe S, et al. Risk factors for postoperative lower-extremity lymphedema in endometrial cancer survivors who had treatment including lymphadenectomy. Gynecol Oncol 2010; 119: Tada H, Teramukai S, Fukushima M, et al. Risk factors for lower limb lymphedema after lymph node dissection in patients with ovarian and endometrial carcinoma. BMC Cancer 2009; 9: 47: Ryan M, Stainton M, Slaytor E, et al. Aetiology and prevalence of lower limb lymphedema following treatment for gynaecological cancer. Aust NZ J Obstet Gynaecol 2003; 43: Beesley V, Janda M, Eakin E, et al. Lymphedema after gynecological cancer treatment. Cancer 2007; 109: Stanton AW, Northfield JW, Holroyd B, et al. Validation of an optoelectronic limb volumeter (perometer). Lymphology 1997; 39(2): Norman SA, Miller LT, Erikson HB, et al. Development and validation of a telephone questionnaire to characterize lymphedema in women treated for breast cancer. Phys Ther. 2001; 81: Lee MJ, Boland RA, Czerniec S, Kilbreath SL. Reliability and concurrent validity of the perometer for measuring hand volume in women with and without lymphedema. Lymphatic Research and Biology 2011; 9(1): The diagnosis and treatment of peripheral lymphedema. Consensus Document of the International Society of Lymphology. Lymphology 2003; 36: McLaughlin SA, Wright MJ, et al. Prevalence of lymphedema in woman with breast cancer 5 years after sentinel lymph node biopsy or axillary dissection: objective measurements. Journal of Clinical Oncology 2008; 26 (32): Meeske KA, Sullivan-Halley J, et al. Risk factors for arm lymphedema following breast cancer diagnosis in Black women and White women. Breast Cancer Research and Treatment 2009; 113 (2):
21 19. Sakorafas GH, Peros G, et al. Lymphedema following axillary lymph node dissection for breast cancer. Surgical Oncology 2006; 15 (3):
22 Table 1. WALC Study Eligibility Criteria Ages at the time of initial contact AJCC Stage I-IV invasive epithelial ovarian cancer Completed adjuvant therapy (i.e. chemotherapy and/or radiation therapy) at least one month prior to enrollment Diagnosed within the past four years Physically able to exercise and physician consent given to start an exercise program Sedentary activity pattern (< 90 min/week of moderate-to-vigorous recreational physical activity) Agreed to be randomly assigned to either the exercise or health education groups Able to travel to New Haven for a baseline and a six-month visit Accessible by phone English speaking No recent (within the past 6 months) history of stroke or myocardial infarction 21
23 Table 2. Baseline Characteristics of Study Participants a Total Patient Population (n=48) b Characteristic Age (years) 56.1±7.2 BMI (kg/m 2 ) 30.0±7.9 Total Body Fat (kg) 31.2±12.1 Percent Body Fat (%) 39.9±5.1 Race/ethnicity Non-Hispanic White Black Hispanic 46 (95.8) 0 2 (4.2) Time since diagnosis (months) 17.6±9.8 Stage at diagnosis Stage I Stage II Stage III Stage IV Education Some high school High school graduate Some college College graduate Graduate school Surgical procedure Total abdominal hysterectomy Bilateral salpingo-oophorectomy Omenectomy Lymph node removal Tumor debulking Bowel resection Colon resection Other surgical procedure 10 (20.8) 12 (25.0) 20 (41.7) 6 (12.5) 2 (4.2) 6 (12.5) 12 (25.0) 13 (27.1) 15 (31.3) 46 (95.8) 46 (95.8) 46 (95.8) 44 (91.7) 20 (41.7) 6 (12.8) 4 (8.3) 15 (32.6) Total number of surgical procedures c 4.7±1.2 Chemotherapy 44 (91.7) Ovarian cancer recurrence 8 (16.7) a Table values are mean ± SD for continuous variables and n (column %) for categorical variables. For surgical procedure, values are the number of subjects who received that procedure (% of subjects). b Numbers may not sum to total due to missing data, and percentages may not sum to 100% due to rounding c Total number of surgical procedures is defined as total number of surgical procedures received related to ovarian cancer diagnosis 22
24 Table 3. Prevalence of Lower Limb Lymphedema a (n=48) Optoelectric Perometer Lymphedema Specialist Self-report Questionnaire 9 (18.8) 11 (22.9) 11 (22.9) Diagnosis via perometer -or- lymphedema specialist: 18 (37.5) Diagnosis via self-report questionnaire -or- lymphedema specialist: 14 (29.2) Any diagnosis of lymphedema: 20 (41.7) a Table values are the number of subjects diagnosed with lymphedema by that method (% of subjects) 23
25 Table 4. Agreement of the Self-Report Questionnaire and Optoelectric Perometer with the Lymphedema Specialist Evaluation Self-Report Questionnaire Optoelectric Perometer κ = [0.387,0.905] κ = [-0.278, 0.300] Self-report questionnaire vs. optoelectric perometer κ = [-0.354,0.113] 24
26 Table 5. Comparison of Means (Diagnosis via Any Method) a Characteristic LLL (n=20) Non-LLL (n=28) p b Age (years) 56.7± ± BMI (kg/m 2 ) 31.4± ± Total body fat 33.8± ± Percent body fat 40.5± ± Time since diagnosis (months) 15.6± ± Number of surgical procedures 4.6± ± a Table values are mean ± SD b p-value is for t-test comparing statistical difference between the two groups 25
27 Table 6. Comparison of Means (Diagnosis via Lymphedema Specialist Evaluation) a Characteristic LLL (n=11) Non-LLL (n=37) p b Age (years) 57.5± ± BMI (kg/m 2 ) 30.1± ± Total body fat (kg) 32.7± ± Percent body fat 40.0± ± Time since diagnosis (months) 15.3± ± Number of surgical procedures 4.8± ± a Table values are mean ± SD b p-value is for t-test comparing statistical difference between the two groups 26
28 Table 7. Comparison of Means (Diagnosis via Self-Report Questionnaire) a Characteristic LLL (n=11) Non-LLL (n=37) p b Age (years) 58.6± ± BMI (kg/m 2 ) 28.5± ± Total body fat (kg) 30.8± ± Percent body fat (%) 38.9± ± Time since diagnosis (months) 14.9± ± Number of surgical procedures 4.8± ± a Table values are mean ± SD b p-value is for t-test comparing statistical difference between the two groups 27
29 Table 8. Comparison of Means (Diagnosis via Optoelectric Perometer) a Characteristic LLL (n=9) Non-LLL (n=39) p b Age (years) 53.2± ± BMI (kg/m 2 ) 34.5± ± Total body fat (kg) 35.5± ± Percent body fat (%) 41.4± ± Time since diagnosis (months) 16.5± ± Number of surgical procedures 4.4± ± a Table values are mean ± SD b p-value is for t-test comparing statistical difference between the two groups 28
30 Table 9. Comparison of Means (Diagnosis via Lymphedema Specialist Evaluation -or- Self- Report Questionnaire) a Characteristic LLL (n=14) Non-LLL (n=34) p b Age (years) 57.4± ± BMI (kg/m 2 ) 29.9± ± Total body fat (kg) 31.9± ± Percent body fat 39.6± ± Time since diagnosis (months) 14.4± ± Number of surgical procedures 4.7± ± a Table values are mean ± SD b p-value is for t-test comparing statistical difference between the two groups 29
31 Table 10. Comparison of Means (Diagnosis via Lymphedema Specialist Evaluation -or- Optoelectric Perometer) a Characteristic LLL (n=18) Non-LLL (n=30) p b Age (years) 56.0± ± BMI (kg/m 2 ) 31.5± ± Total body fat (kg) 34.2± ± Percent body fat 40.7± ± Time since diagnosis (months) 15.9± ± Number of surgical procedures 4.6± ± a Table values are mean ± SD b p-value is for t-test comparing statistical difference between the two groups 30
Colorectal Cancer Statistics in Virginia - Maps. July
 July 2011 5 July 2011 6 July 2011 7 July 2011 8 Colorectal Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health Statistics);
July 2011 5 July 2011 6 July 2011 7 July 2011 8 Colorectal Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health Statistics);
Lung and Bronchus Cancer Statistics in Virginia - Maps. July
 July 2011 4 July 2011 5 July 2011 6 July 2011 7 Lung and Bronchus Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health
July 2011 4 July 2011 5 July 2011 6 July 2011 7 Lung and Bronchus Cancer Statistics in Virginia - Notes Sources: Incidence and percent local staging (VA Cancer Registry); mortality (VDH Division of Health
Mercy s 2013 Cancer Program Annual Report
 Mercy s 2013 Cancer Program Annual Report Mercy Hospital & Medical Center is accredited by the Commission on Cancer as an Academic Comprehensive Cancer Program. This study directed by the Mercy s Cancer
Mercy s 2013 Cancer Program Annual Report Mercy Hospital & Medical Center is accredited by the Commission on Cancer as an Academic Comprehensive Cancer Program. This study directed by the Mercy s Cancer
Cancer of the Breast (Female) - Cancer Stat Facts
 Page 1 of 9 Home Statistical Summaries Cancer Stat Facts Cancer of the Breast (Female) Cancer Stat Facts: Female Breast Cancer Statistics at a Glance At a Glance Estimated New Cases in 2016 % of All New
Page 1 of 9 Home Statistical Summaries Cancer Stat Facts Cancer of the Breast (Female) Cancer Stat Facts: Female Breast Cancer Statistics at a Glance At a Glance Estimated New Cases in 2016 % of All New
Percent Surviving 5 Years 89.4%
 Page 1 of 8 Surveillance, Epidemiology, and End Results Program Turning Cancer Data Into Discovery Home Statistical Summaries Cancer Stat Fact Sheets Cancer of the Breast SEER Stat Fact Sheets: Breast
Page 1 of 8 Surveillance, Epidemiology, and End Results Program Turning Cancer Data Into Discovery Home Statistical Summaries Cancer Stat Fact Sheets Cancer of the Breast SEER Stat Fact Sheets: Breast
Overview of All SEER-Medicare Publications
 Overview of All SEER-Medicare Publications Outcomes Insights, Inc. Mark D. Danese, MHS, PhD Claire Cangialose February 22, 2017 Overview Information was extracted from the National Cancer Institute (NCI)
Overview of All SEER-Medicare Publications Outcomes Insights, Inc. Mark D. Danese, MHS, PhD Claire Cangialose February 22, 2017 Overview Information was extracted from the National Cancer Institute (NCI)
Breast Cancer Survivorship: Physical Activity
 WORKING EVERYDAY TO PROVIDE THE HIGHEST QUALITY OF LIFE FOR PEOPLE WITH CANCER Breast Cancer Survivorship: What is the Role of Diet and Physical Activity WENDY DEMARK-WAHNEFRIED, PHD, RD PROFESSOR AND
WORKING EVERYDAY TO PROVIDE THE HIGHEST QUALITY OF LIFE FOR PEOPLE WITH CANCER Breast Cancer Survivorship: What is the Role of Diet and Physical Activity WENDY DEMARK-WAHNEFRIED, PHD, RD PROFESSOR AND
Diet, Physical Activity, Weight & Cancer Survivorship: Perspectives from the NCI
 Diet, Physical Activity, Weight & Cancer Survivorship: Perspectives from the NCI American Institute for Cancer Research Meeting October 21, 2010 Catherine M. Alfano, Ph.D. Program Director & Behavioral
Diet, Physical Activity, Weight & Cancer Survivorship: Perspectives from the NCI American Institute for Cancer Research Meeting October 21, 2010 Catherine M. Alfano, Ph.D. Program Director & Behavioral
Healthcare Reform and Cancer Survivorship: Implications for Care & Research
 Healthcare Reform and Cancer Survivorship: Implications for Care & Research Julia H. Rowland, Ph.D., Director Office of Cancer Survivorship National Cancer Institute National Institutes of Health DHHS
Healthcare Reform and Cancer Survivorship: Implications for Care & Research Julia H. Rowland, Ph.D., Director Office of Cancer Survivorship National Cancer Institute National Institutes of Health DHHS
Early Detection: Screening Guidelines
 Early Detection: Screening Guidelines National Cancer Statistics 2015 National Cancer Statistics 1. 6 Million Cases Expected 589,430 Cancer Deaths expected 2015 Virginia Cancer Statistics: Projected cases:
Early Detection: Screening Guidelines National Cancer Statistics 2015 National Cancer Statistics 1. 6 Million Cases Expected 589,430 Cancer Deaths expected 2015 Virginia Cancer Statistics: Projected cases:
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type)
 Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer
 THIS DOCUMENT North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer Based on WOSCAN CMG with further extensive consultation within NOSCAN UNCONTROLLED WHEN PRINTED DOCUMENT
THIS DOCUMENT North of Scotland Cancer Network Clinical Management Guideline for Endometrial Cancer Based on WOSCAN CMG with further extensive consultation within NOSCAN UNCONTROLLED WHEN PRINTED DOCUMENT
Impact of Surgery Extent on Survival and Recurrence Rate of Stage ⅠEndometrial Adenocarcinoma
 Hou et al. / Cancer Cell Research 3 (2014) 65-69 Cancer Cell Research Available at http:// http://www.cancercellresearch.org/ ISSN 2161-2609 Impact of Surgery Extent on Survival and Recurrence Rate of
Hou et al. / Cancer Cell Research 3 (2014) 65-69 Cancer Cell Research Available at http:// http://www.cancercellresearch.org/ ISSN 2161-2609 Impact of Surgery Extent on Survival and Recurrence Rate of
Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer
 HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
HEALTH SERVICES RESEARCH FUND Risk factors for the initiation and aggravation of lymphoedema after axillary lymph node dissection for breast cancer Key Messages 1. Previous inflammation or infection of
Factors predictive of myoinvasion in cases of Complex Atypical Hyperplasia diagnosed on endometrial biopsy or curettage
 Factors predictive of myoinvasion in cases of Complex Atypical Hyperplasia diagnosed on endometrial biopsy or curettage Jessica Johns, MD Jeffrey Killeen, MD Robert Kim, MD Hyeong Jun Ahn, PhD None Disclosures
Factors predictive of myoinvasion in cases of Complex Atypical Hyperplasia diagnosed on endometrial biopsy or curettage Jessica Johns, MD Jeffrey Killeen, MD Robert Kim, MD Hyeong Jun Ahn, PhD None Disclosures
1 Oregon Health & Science University, Portland, OR 2 Stritch School of Medicine, Loyola University Chicago, Chicago, IL
 Current treatment practices for limited-stage small cell lung cancer: A survey of US radiation oncologists on the timing of thoracic radiotherapy with chemotherapy Matthew J. Farrell 1, Jehan Yahya 1,
Current treatment practices for limited-stage small cell lung cancer: A survey of US radiation oncologists on the timing of thoracic radiotherapy with chemotherapy Matthew J. Farrell 1, Jehan Yahya 1,
Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy
 Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy Stephanie Yap, M.D. University Gynecologic Oncology Northside Cancer Institute Our Learning Objectives Review survival rates,
Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy Stephanie Yap, M.D. University Gynecologic Oncology Northside Cancer Institute Our Learning Objectives Review survival rates,
2016 Uterine Cancer Annual Report
 2016 Uterine Cancer Annual Report Overview At Carolinas HealthCare System s Levine Cancer Institute, we offer comprehensive care focused on using the latest technology and innovative techniques in the
2016 Uterine Cancer Annual Report Overview At Carolinas HealthCare System s Levine Cancer Institute, we offer comprehensive care focused on using the latest technology and innovative techniques in the
receive adjuvant chemotherapy
 Women with high h risk early stage endometrial cancer should receive adjuvant chemotherapy Michael Friedlander The Prince of Wales Cancer Centre and Royal Hospital for Women The Prince of Wales Cancer
Women with high h risk early stage endometrial cancer should receive adjuvant chemotherapy Michael Friedlander The Prince of Wales Cancer Centre and Royal Hospital for Women The Prince of Wales Cancer
Estimated Minnesota Cancer Prevalence, January 1, MCSS Epidemiology Report 04:2. April 2004
 MCSS Epidemiology Report 04:2 Suggested citation Perkins C, Bushhouse S.. Minnesota Cancer Surveillance System. Minneapolis, MN, http://www.health.state.mn.us/divs/hpcd/ cdee/mcss),. 1 Background Cancer
MCSS Epidemiology Report 04:2 Suggested citation Perkins C, Bushhouse S.. Minnesota Cancer Surveillance System. Minneapolis, MN, http://www.health.state.mn.us/divs/hpcd/ cdee/mcss),. 1 Background Cancer
Impact of BIS Technology
 Skilled nursing leaders know that the number of women surviving breast cancer is rising. While this is good news, survivorship care has grown more complex and challenging for clinicians in skilled nursing
Skilled nursing leaders know that the number of women surviving breast cancer is rising. While this is good news, survivorship care has grown more complex and challenging for clinicians in skilled nursing
One Breast Cancer Annual Report
 One 2015 Breast Cancer Annual Report One OVERVIEW The Breast Program at Carolinas HealthCare System s Levine Cancer Institute, offers comprehensive care. Patients with benign and malignant disease of the
One 2015 Breast Cancer Annual Report One OVERVIEW The Breast Program at Carolinas HealthCare System s Levine Cancer Institute, offers comprehensive care. Patients with benign and malignant disease of the
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact
 Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
Update on Sentinel Node Biopsy in Endometrial Cancer: Feasibility, Technique, Impact Bjørn Hagen, MD, PhD St Olavs Hospital Trondheim University Hospital Trondheim, Norway Endometrial Cancer (EC) The most
North of Scotland Cancer Network Clinical Management Guideline for Carcinoma of the Uterine Cervix
 THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
THIS DOCUMENT North of Scotland Cancer Network Carcinoma of the Uterine Cervix UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Prepared by A Kennedy/AG Macdonald/Others Approved by NOT APPROVED Issue date April
Submitted by: Date of request: 28 th October 2015
 Submitted by: Frank Vicini, MD, FACR Chief Medical Officer ImpediMed, Inc. 5900 Pasteur Court Suite 125 Carlsbad, CA 92008 Phone: 760 585 2100 Email: fvicini@impedimed.com Date of request: 28 th October
Submitted by: Frank Vicini, MD, FACR Chief Medical Officer ImpediMed, Inc. 5900 Pasteur Court Suite 125 Carlsbad, CA 92008 Phone: 760 585 2100 Email: fvicini@impedimed.com Date of request: 28 th October
Predictors of Palliative Therapy Receipt in Stage IV Colorectal Cancer
 Predictors of Palliative Therapy Receipt in Stage IV Colorectal Cancer Osayande Osagiede, MBBS, MPH 1,2, Aaron C. Spaulding, PhD 2, Ryan D. Frank, MS 3, Amit Merchea, MD 1, Dorin Colibaseanu, MD 1 ACS
Predictors of Palliative Therapy Receipt in Stage IV Colorectal Cancer Osayande Osagiede, MBBS, MPH 1,2, Aaron C. Spaulding, PhD 2, Ryan D. Frank, MS 3, Amit Merchea, MD 1, Dorin Colibaseanu, MD 1 ACS
What Is Small Cell Lung Cancer?
 About Small Cell Lung Cancer Overview If you have been diagnosed with small cell lung cancer or are worried about it, you likely have a lot of questions. Learning some basics is a good place to start.
About Small Cell Lung Cancer Overview If you have been diagnosed with small cell lung cancer or are worried about it, you likely have a lot of questions. Learning some basics is a good place to start.
GYNECOLOGIC MALIGNANCIES: Ovarian Cancer
 GYNECOLOGIC MALIGNANCIES: Ovarian Cancer KRISTEN STARBUCK, MD ROSWELL PARK CANCER INSTITUTE DEPARTMENT OF SURGERY DIVISION OF GYNECOLOGIC ONCOLOGY APRIL 19 TH, 2018 Objectives Basic Cancer Statistics Discuss
GYNECOLOGIC MALIGNANCIES: Ovarian Cancer KRISTEN STARBUCK, MD ROSWELL PARK CANCER INSTITUTE DEPARTMENT OF SURGERY DIVISION OF GYNECOLOGIC ONCOLOGY APRIL 19 TH, 2018 Objectives Basic Cancer Statistics Discuss
Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122
 Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Lymphoedema following treatment for breast cancer: a new approach to an old problem
 Lymphoedema following treatment for breast cancer: a new approach to an old problem Screening breast cancer patients for lymphoedema makes it possible to identify problems early and take action to halt
Lymphoedema following treatment for breast cancer: a new approach to an old problem Screening breast cancer patients for lymphoedema makes it possible to identify problems early and take action to halt
Gynecologic Cancer InterGroup Cervix Cancer Research Network. Management of Cervical Cancer in Resource Limited Settings.
 Management of Cervical Cancer in Resource Limited Settings Linus Chuang MD Conflict of Interests None Cervical cancer is the fourth most common malignancy in women worldwide 530,000 new cases per year
Management of Cervical Cancer in Resource Limited Settings Linus Chuang MD Conflict of Interests None Cervical cancer is the fourth most common malignancy in women worldwide 530,000 new cases per year
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO)
 North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
North of Scotland Cancer Network Clinical Management Guideline for Metastatic Malignancy of Undefined Primary Origin (MUO) UNCONTROLLED WHEN PRINTED DOCUMENT CONTROL Original Prepared by NMcL April 2016
What You Need to Know About Ovarian Cancer
 What You Need to Know About Ovarian Cancer About Us The Rhode Island Ovarian Cancer Alliance (RIOCA) was formed in honor and memory of Jessica Morris. Jessica was diagnosed with Stage IIIC Ovarian Cancer
What You Need to Know About Ovarian Cancer About Us The Rhode Island Ovarian Cancer Alliance (RIOCA) was formed in honor and memory of Jessica Morris. Jessica was diagnosed with Stage IIIC Ovarian Cancer
Wellness Coaching for People with Prediabetes
 Wellness Coaching for People with Prediabetes PUBLIC HEALTH RESEARCH, PRACTICE, AND POLICY Volume 12, E207 NOVEMBER 2015 ORIGINAL RESEARCH Wellness Coaching for People With Prediabetes: A Randomized Encouragement
Wellness Coaching for People with Prediabetes PUBLIC HEALTH RESEARCH, PRACTICE, AND POLICY Volume 12, E207 NOVEMBER 2015 ORIGINAL RESEARCH Wellness Coaching for People With Prediabetes: A Randomized Encouragement
Identifying Risk Factors for Occult Lower Extremity Lymphedema using Computed
 Identifying Risk Factors for Occult Lower Extremity Lymphedema using Computed Tomography in Patients undergoing Lymphadenectomy for Gynecologic Cancers Miseon Kim a*, Dong Hoon Suh a*, Eun Joo Yang b,
Identifying Risk Factors for Occult Lower Extremity Lymphedema using Computed Tomography in Patients undergoing Lymphadenectomy for Gynecologic Cancers Miseon Kim a*, Dong Hoon Suh a*, Eun Joo Yang b,
Early detection and prevention of lymphoedema
 Early detection and prevention of lymphoedema Katie Riches Senior Research Nurse Derby Hospitals NHSF Trust Background: Derby Lymphoedema Service Three lymphoedema services based in Acute Hospitals at
Early detection and prevention of lymphoedema Katie Riches Senior Research Nurse Derby Hospitals NHSF Trust Background: Derby Lymphoedema Service Three lymphoedema services based in Acute Hospitals at
Chapter 13 Cancer of the Female Breast
 Lynn A. Gloeckler Ries and Milton P. Eisner INTRODUCTION This study presents survival analyses for female breast cancer based on 302,763 adult cases from the Surveillance, Epidemiology, and End Results
Lynn A. Gloeckler Ries and Milton P. Eisner INTRODUCTION This study presents survival analyses for female breast cancer based on 302,763 adult cases from the Surveillance, Epidemiology, and End Results
Study Title The SACS trial - Phase II Study of Adjuvant Therapy in CarcinoSarcoma of the Uterus
 Study Title The SACS trial - Phase II Study of Adjuvant Therapy in CarcinoSarcoma of the Uterus Investigators Dr Bronwyn King, Peter MacCallum Cancer Centre Dr Linda Mileshkin, Peter MacCallum Cancer Centre
Study Title The SACS trial - Phase II Study of Adjuvant Therapy in CarcinoSarcoma of the Uterus Investigators Dr Bronwyn King, Peter MacCallum Cancer Centre Dr Linda Mileshkin, Peter MacCallum Cancer Centre
One of the commonest gynecological cancers,especially in white Americans.
 Gynaecology Dr. Rozhan Lecture 6 CARCINOMA OF THE ENDOMETRIUM One of the commonest gynecological cancers,especially in white Americans. It is a disease of postmenopausal women with a peak incidence in
Gynaecology Dr. Rozhan Lecture 6 CARCINOMA OF THE ENDOMETRIUM One of the commonest gynecological cancers,especially in white Americans. It is a disease of postmenopausal women with a peak incidence in
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER CERVIX Site Group: Gynecology Cervix Author: Dr. Stephane Laframboise 1. INTRODUCTION 3 2. PREVENTION 3 3. SCREENING AND
Chemotherapy or Observation in Stage I-II Intermediate or High Risk Endometrial Cancer
 Find Studies About Studies Submit Studies Resources About Site Chemotherapy or Observation in Stage I-II Intermediate or High Risk Endometrial Cancer The safety and scientific validity of this study is
Find Studies About Studies Submit Studies Resources About Site Chemotherapy or Observation in Stage I-II Intermediate or High Risk Endometrial Cancer The safety and scientific validity of this study is
SLN Mapping in Cervical Cancer. Memorial Sloan Kettering Cancer Center New York, USA
 Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Lead Grou p Log SLN Mapping in Cervical Cancer Nadeem R. Abu-Rustum, M.D. Memorial Sloan Kettering Cancer Center New York, USA Conflict of Interest Disclosure Nadeem R. Abu-Rustum, M.D. I have no financial
Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
Adjuvant Therapies in Endometrial Cancer. Emma Hudson
 Adjuvant Therapies in Endometrial Cancer Emma Hudson Endometrial Cancer Most common gynaecological cancer Incidence increasing in Western world 1-2% cancer deaths 75% patients postmenopausal 97% epithelial
Adjuvant Therapies in Endometrial Cancer Emma Hudson Endometrial Cancer Most common gynaecological cancer Incidence increasing in Western world 1-2% cancer deaths 75% patients postmenopausal 97% epithelial
The Study of Tamoxifen and Raloxifene (STAR): Questions and Answers. Key Points
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s The Study of Tamoxifen
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s The Study of Tamoxifen
Trends in Oncology Care. Challenges and Obstacles. Lawrence N. Shulman, MD Dana-Farber Cancer Institute Brigham and Women s Hospital
 Trends in Oncology Care Challenges and Obstacles Lawrence N. Shulman, MD Dana-Farber Cancer Institute Brigham and Women s Hospital Navigation Through The Continuum of Cancer Care Education Screening Early
Trends in Oncology Care Challenges and Obstacles Lawrence N. Shulman, MD Dana-Farber Cancer Institute Brigham and Women s Hospital Navigation Through The Continuum of Cancer Care Education Screening Early
Relapse Patterns and Outcomes Following Recurrence of Endometrial Cancer in Northern Thai Women
 DOI:http://dx.doi.org/10.7314/APJCP.2015.16.9.3861 Relapse Patterns and Outcomes Following Recurrence of Endometrial Cancer in Northern Thai Women RESEARCH ARTICLE Relapse Patterns and Outcomes Following
DOI:http://dx.doi.org/10.7314/APJCP.2015.16.9.3861 Relapse Patterns and Outcomes Following Recurrence of Endometrial Cancer in Northern Thai Women RESEARCH ARTICLE Relapse Patterns and Outcomes Following
Bringing the Fight to Cancer Annual Report
 Bringing the Fight to Cancer. 216 Annual Report Quality Study Adherence to Adjuvant System Therapy Following Primary Surgery in Stage II Breast Cancer Patients: Baylor Scott & White Medical Center Irving
Bringing the Fight to Cancer. 216 Annual Report Quality Study Adherence to Adjuvant System Therapy Following Primary Surgery in Stage II Breast Cancer Patients: Baylor Scott & White Medical Center Irving
Prof. Dr. Aydın ÖZSARAN
 Prof. Dr. Aydın ÖZSARAN Adenocarcinomas of the endometrium Most common gynecologic malignancy in developed countries Second most common in developing countries. Adenocarcinomas, grade 1 and 2 endometrioid
Prof. Dr. Aydın ÖZSARAN Adenocarcinomas of the endometrium Most common gynecologic malignancy in developed countries Second most common in developing countries. Adenocarcinomas, grade 1 and 2 endometrioid
Research. Breast cancer represents a major
 Research GENERAL GYNECOLOGY Gynecologic conditions in participants in the NSABP breast cancer prevention study of tamoxifen and raloxifene (STAR) Carolyn D. Runowicz, MD; Joseph P. Costantino, DrPH; D.
Research GENERAL GYNECOLOGY Gynecologic conditions in participants in the NSABP breast cancer prevention study of tamoxifen and raloxifene (STAR) Carolyn D. Runowicz, MD; Joseph P. Costantino, DrPH; D.
Carcinosarcoma Trial rial in s a in rare malign rare mali ancy
 Carcinosarcoma Trials in a rare malignancy BACKGROUND Rare and highly aggressive epithelial malignancies Biphasic tumors with epithelial and mesenchymal components Uterine carcinomas (UCS) uncommon with
Carcinosarcoma Trials in a rare malignancy BACKGROUND Rare and highly aggressive epithelial malignancies Biphasic tumors with epithelial and mesenchymal components Uterine carcinomas (UCS) uncommon with
Lifestyle Factors and Cancer Survivorship: Observational Findings of Weight, Physical Activity, and Diet on Survival
 Lifestyle Factors and Cancer Survivorship: Observational Findings of Weight, Physical Activity, and Diet on Survival Melinda L. Irwin, PhD, MPH Associate Professor of Epidemiology Yale School of Medicine
Lifestyle Factors and Cancer Survivorship: Observational Findings of Weight, Physical Activity, and Diet on Survival Melinda L. Irwin, PhD, MPH Associate Professor of Epidemiology Yale School of Medicine
Breast Cancer in Childhood Cancer Survivors: The Impact of Screening on Morbidity
 Breast Cancer in Childhood Cancer Survivors: The Impact of Screening on Morbidity WORKING GROUP: This report will be written within the Cancer Control Working Group with oversight from the Second Malignant
Breast Cancer in Childhood Cancer Survivors: The Impact of Screening on Morbidity WORKING GROUP: This report will be written within the Cancer Control Working Group with oversight from the Second Malignant
Bringing the Fight to Cancer Annual Report
 Bringing the Fight to Cancer. 21 Annual Report Quality Study Adherence to Adjuvant Systemic Therapy Following Primary Surgery in Stage II Breast Cancer Patients: Baylor Scott & White Medical Center Grapevine
Bringing the Fight to Cancer. 21 Annual Report Quality Study Adherence to Adjuvant Systemic Therapy Following Primary Surgery in Stage II Breast Cancer Patients: Baylor Scott & White Medical Center Grapevine
Endometrial Cancer. Saudi Gynecology Oncology Group (SGOG) Gynecological Cancer Treatment Guidelines
 Saudi Gynecology Oncology Group (SGOG) Gynecological Cancer Treatment Guidelines Endometrial Cancer Emad R. Sagr, MBBS, FRCSC Consultant Gynecology Oncology Security forces Hospital, Riyadh Epidemiology
Saudi Gynecology Oncology Group (SGOG) Gynecological Cancer Treatment Guidelines Endometrial Cancer Emad R. Sagr, MBBS, FRCSC Consultant Gynecology Oncology Security forces Hospital, Riyadh Epidemiology
Bringing the Fight to Cancer Annual Report
 Bringing the Fight to Cancer. 1 Annual Report Quality Study Adherence to Adjuvant Systemic Therapy Following Primary Surgery in Stage II Breast Cancer Patients: Baylor Scott & White Medical Center McKinney
Bringing the Fight to Cancer. 1 Annual Report Quality Study Adherence to Adjuvant Systemic Therapy Following Primary Surgery in Stage II Breast Cancer Patients: Baylor Scott & White Medical Center McKinney
It is a malignancy originating from breast tissue
 59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
59 Breast cancer 1 It is a malignancy originating from breast tissue including both early stages which are potentially curable, and metastatic breast cancer (MBC) which is usually incurable. Most breast
PET/CT in Gynaecological Cancers. Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp
 PET/CT in Gynaecological Cancers Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp Cervix cancer Outline of this talk Initial staging Treatment monitoring/guidance
PET/CT in Gynaecological Cancers Stroobants Sigrid, MD, PhD Departement of Nuclear Medicine University Hospital,Antwerp Cervix cancer Outline of this talk Initial staging Treatment monitoring/guidance
Lymphedema. Kelly Reichart, DNP, RN. About 246,660 women
 ADVANCED PRACTICE ASSOCIATE EDITOR DEBORAH "HUTCH" ALLEN, PhD, RN, CNS, FNP-BC, AOCNP Downloaded on 11 28 2018. Single-user license only. Copyright 2018 by the Oncology Nursing Society. For permission
ADVANCED PRACTICE ASSOCIATE EDITOR DEBORAH "HUTCH" ALLEN, PhD, RN, CNS, FNP-BC, AOCNP Downloaded on 11 28 2018. Single-user license only. Copyright 2018 by the Oncology Nursing Society. For permission
ENDOMETRIAL CANCER. Endometrial cancer is a great concern in UPDATE. For personal use only. Copyright Dowden Health Media
 For mass reproduction, content licensing and permissions contact Dowden Health Media. UPDATE ENDOMETRIAL CANCER Are lymphadenectomy and external-beam radiotherapy valuable in women who have an endometrial
For mass reproduction, content licensing and permissions contact Dowden Health Media. UPDATE ENDOMETRIAL CANCER Are lymphadenectomy and external-beam radiotherapy valuable in women who have an endometrial
Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care
 Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: The percentage
Measure #264: Sentinel Lymph Node Biopsy for Invasive Breast Cancer National Quality Strategy Domain: Effective Clinical Care 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION: The percentage
Surveillance Guidelines Section 1. Surveillance Imaging Section 2. Lymphedema Section 3. Fatigue / Dyspnea Section 4. Weight Gain Section 5
 Surveillance Guidelines Section 1 Surveillance Imaging Section 2 Lymphedema Section 3 Fatigue / Dyspnea Section 4 Weight Gain Section 5 Menopausal Symptoms Section 6 Peripheral Neuropathy / Arthralgia
Surveillance Guidelines Section 1 Surveillance Imaging Section 2 Lymphedema Section 3 Fatigue / Dyspnea Section 4 Weight Gain Section 5 Menopausal Symptoms Section 6 Peripheral Neuropathy / Arthralgia
Chapter 8 Adenocarcinoma
 Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
Page 80 Chapter 8 Adenocarcinoma Overview In Japan, the proportion of squamous cell carcinoma among all cervical cancers has been declining every year. In a recent survey, non-squamous cell carcinoma accounted
After primary tumor treatment, 30% of patients with malignant
 ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
ESTS METASTASECTOMY SUPPLEMENT Alberto Oliaro, MD, Pier L. Filosso, MD, Maria C. Bruna, MD, Claudio Mossetti, MD, and Enrico Ruffini, MD Abstract: After primary tumor treatment, 30% of patients with malignant
Debate Axillary dissection - con. Prof. Dr. Rodica Anghel Institute of Oncology Bucharest
 Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Improving Representation of Diverse Patients in Clinical Trials
 Improving Representation of Diverse Patients in Clinical Trials Coleman Obasaju, MD, PhD, Senior Medical Director US Medical Division, Oncology, Eli Lilly and Company Lilly s commitment to clinical diversity
Improving Representation of Diverse Patients in Clinical Trials Coleman Obasaju, MD, PhD, Senior Medical Director US Medical Division, Oncology, Eli Lilly and Company Lilly s commitment to clinical diversity
A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY. Helen Mari Parsons
 A Culture of Quality? Lymph Node Evaluation for Colon Cancer Care A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Helen Mari Parsons IN PARTIAL FULFILLMENT
A Culture of Quality? Lymph Node Evaluation for Colon Cancer Care A DISSERTATION SUBMITTED TO THE FACULTY OF THE GRADUATE SCHOOL OF THE UNIVERSITY OF MINNESOTA BY Helen Mari Parsons IN PARTIAL FULFILLMENT
Staging and Treatment Update for Gynecologic Malignancies
 Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Staging and Treatment Update for Gynecologic Malignancies Bunja Rungruang, MD Medical College of Georgia No disclosures 4 th most common new cases of cancer in women 5 th and 6 th leading cancer deaths
Squamous cell carcinoma arising in a dermoid cyst of the ovary: a case series
 DOI: 10.1111/j.1471-0528.2007.01478.x www.blackwellpublishing.com/bjog Gynaecological oncology Squamous cell carcinoma arising in a dermoid cyst of the ovary: a case series JL Hurwitz, a A Fenton, a WG
DOI: 10.1111/j.1471-0528.2007.01478.x www.blackwellpublishing.com/bjog Gynaecological oncology Squamous cell carcinoma arising in a dermoid cyst of the ovary: a case series JL Hurwitz, a A Fenton, a WG
Ovarian cancer: clinical practice the Arabic perspective
 Lead Group Log Ovarian cancer: clinical practice the Arabic perspective Experience of Hôtel-Dieu de France University Hospital (Beirut, LEBANON) in supraradical surgery for ovarian cancer David ATALLAH
Lead Group Log Ovarian cancer: clinical practice the Arabic perspective Experience of Hôtel-Dieu de France University Hospital (Beirut, LEBANON) in supraradical surgery for ovarian cancer David ATALLAH
Cancer Services 2018 Quality Report
 Cancer Services 2018 Quality Report MAURY REGIONAL CANCER CENTER Clinical Excellence The Maury Regional Cancer Center is a comprehensive treatment center committed to medical excellence. We combine stringent
Cancer Services 2018 Quality Report MAURY REGIONAL CANCER CENTER Clinical Excellence The Maury Regional Cancer Center is a comprehensive treatment center committed to medical excellence. We combine stringent
Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer
 Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer Gabriela M. Vargas, MD Kristin M. Sheffield, PhD, Abhishek Parmar, MD, Yimei Han, MS, Kimberly M. Brown,
Physician Follow-Up and Guideline Adherence in Post- Treatment Surveillance of Colorectal Cancer Gabriela M. Vargas, MD Kristin M. Sheffield, PhD, Abhishek Parmar, MD, Yimei Han, MS, Kimberly M. Brown,
5/8/2014. AJCC Stage Introduction and General Rules. Acknowledgements* Introduction. Melissa Pearson, CTR North Carolina Central Cancer Registry
 AJCC Stage Introduction and General Rules Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
AJCC Stage Introduction and General Rules Linda Mulvihill Public Health Advisor NCRA Annual Meeting May 2014 National Center for Chronic Disease Prevention and Health Promotion Division of Cancer Prevention
Prognostic factors in adult granulosa cell tumors of the ovary: a retrospective analysis of 80 cases
 J Gynecol Oncol Vol. 20, No. 3:158-163, September 2009 DOI:10.3802/jgo.2009.20.3.158 Original Article Prognostic factors in adult granulosa cell tumors of the ovary: a retrospective analysis of 80 cases
J Gynecol Oncol Vol. 20, No. 3:158-163, September 2009 DOI:10.3802/jgo.2009.20.3.158 Original Article Prognostic factors in adult granulosa cell tumors of the ovary: a retrospective analysis of 80 cases
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008
 A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
A phase II study of weekly paclitaxel and cisplatin followed by radical hysterectomy in stages IB2 and IIA2 cervical cancer AGOG14-001/TGOG1008 NCT02432365 Chyong-Huey Lai, MD On behalf of Principal investigator
Updates on the Conflict of Postoperative Radiotherapy Impact on Survival of Young Women with Cancer Breast: A Retrospective Cohort Study
 International Journal of Medical Research & Health Sciences Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2017, 6(7): 14-18 I J M R
International Journal of Medical Research & Health Sciences Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2017, 6(7): 14-18 I J M R
Influence of Weight Management and Exercise on Other Outcomes
 Influence of Weight Management and Exercise on Other Outcomes Melinda L. Irwin, PhD, MPH Professor of Epidemiology, Yale School of Public Health Associate Director for Population Sciences, Yale Cancer
Influence of Weight Management and Exercise on Other Outcomes Melinda L. Irwin, PhD, MPH Professor of Epidemiology, Yale School of Public Health Associate Director for Population Sciences, Yale Cancer
Presented by: Lillian Erdahl, MD
 Presented by: Lillian Erdahl, MD Learning Objectives What is Breast Cancer Types of Breast Cancer Risk Factors Warning Signs Diagnosis Treatment Options Prognosis What is Breast Cancer? A disease that
Presented by: Lillian Erdahl, MD Learning Objectives What is Breast Cancer Types of Breast Cancer Risk Factors Warning Signs Diagnosis Treatment Options Prognosis What is Breast Cancer? A disease that
4:00 into mp3 file Huang_342831_5_v1.mp3
 Support for Yale Cancer Answers comes from AstraZeneca, providing important treatment options for women living with advanced ovarian cancer. Learn more at astrazeneca-us.com. Welcome to Yale Cancer Answers
Support for Yale Cancer Answers comes from AstraZeneca, providing important treatment options for women living with advanced ovarian cancer. Learn more at astrazeneca-us.com. Welcome to Yale Cancer Answers
The ACA and Breast Cancer: Danger for Disparities Still Exists, Despite Law s Intentions
 The ACA and Breast Cancer: Danger for Disparities Still Exists, Despite Law s Intentions Join the conversation on Twitter: #BreakingDownWalls Thursday, September 25, 2014 Presenters September 25, 2014
The ACA and Breast Cancer: Danger for Disparities Still Exists, Despite Law s Intentions Join the conversation on Twitter: #BreakingDownWalls Thursday, September 25, 2014 Presenters September 25, 2014
Case Scenario 1. Pathology report Specimen from mediastinoscopy Final Diagnosis : Metastatic small cell carcinoma with residual lymphatic tissue
 Case Scenario 1 Oncology Consult: Patient is a 51-year-old male with history of T4N3 squamous cell carcinoma of tonsil status post concurrent chemoradiation finished in October two years ago. He was hospitalized
Case Scenario 1 Oncology Consult: Patient is a 51-year-old male with history of T4N3 squamous cell carcinoma of tonsil status post concurrent chemoradiation finished in October two years ago. He was hospitalized
Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical trial for low-risk patients?
 bs_bs_banner doi:10.1111/jog.12281 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 322 326, February 2014 Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical
bs_bs_banner doi:10.1111/jog.12281 J. Obstet. Gynaecol. Res. Vol. 40, No. 2: 322 326, February 2014 Risk assessment of lymph node metastasis before surgery in endometrial cancer: Do we need a clinical
is time consuming and expensive. An intra-operative assessment is not going to be helpful if there is no more tissue that can be taken to improve the
 My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
My name is Barry Feig. I am a Professor of Surgical Oncology at The University of Texas MD Anderson Cancer Center in Houston, Texas. I am going to talk to you today about the role for surgery in the treatment
Radiation Oncology MOC Study Guide
 Radiation Oncology MOC Study Guide The following study guide is intended to give a general overview of the type of material that will be covered on the Radiation Oncology Maintenance of Certification (MOC)
Radiation Oncology MOC Study Guide The following study guide is intended to give a general overview of the type of material that will be covered on the Radiation Oncology Maintenance of Certification (MOC)
Original Research. Background
 Original Research 849 in Carboplatin and Dose-Dense Paclitaxel Chemotherapy for Ovarian Malignancies: A Survey of NCCN Member Institutions Marina Stasenko, MD a ; R. Kevin Reynolds, MD a ; Carolyn Johnston,
Original Research 849 in Carboplatin and Dose-Dense Paclitaxel Chemotherapy for Ovarian Malignancies: A Survey of NCCN Member Institutions Marina Stasenko, MD a ; R. Kevin Reynolds, MD a ; Carolyn Johnston,
The Effect of Changing Hysterectomy Prevalence on Trends in Endometrial Cancer, SEER
 The Effect of Changing Hysterectomy Prevalence on Trends in Endometrial Cancer, SEER 1992-2008 Annie Noone noonea@mail.nih.gov Missy Jamison, Lynn Ries, Brenda Edwards NAACCR 2012 Portland, OR Outline
The Effect of Changing Hysterectomy Prevalence on Trends in Endometrial Cancer, SEER 1992-2008 Annie Noone noonea@mail.nih.gov Missy Jamison, Lynn Ries, Brenda Edwards NAACCR 2012 Portland, OR Outline
1. Study Title. Exercise and Late Mortality in 5-Year Survivors of Childhood Cancer: a Report from the Childhood Cancer Survivor Study.
 CCSS Analysis Concept Proposal Exercise, Mortality, & Childhood Cancer 1 1. Study Title. Exercise and Late Mortality in 5-Year Survivors of Childhood Cancer: a Report from the Childhood Cancer Survivor
CCSS Analysis Concept Proposal Exercise, Mortality, & Childhood Cancer 1 1. Study Title. Exercise and Late Mortality in 5-Year Survivors of Childhood Cancer: a Report from the Childhood Cancer Survivor
TMIST: Frequently Asked Questions
 TMIST: Frequently Asked Questions Key Topics for Site Investigators and Staff This document answers frequently asked questions about the Tomosynthesis Mammographic Imaging Screening Trial (TMIST/EA1151);
TMIST: Frequently Asked Questions Key Topics for Site Investigators and Staff This document answers frequently asked questions about the Tomosynthesis Mammographic Imaging Screening Trial (TMIST/EA1151);
Eligibility Form. 1. Patient Profile. (This form must be completed before the first dose is dispensed.) Request prior approval for enrolment
 Bevacizumab in combination with Paclitaxel and Carboplatin - Frontline Treatment (Previously Untreated) Ovarian, Fallopian Tube, and Primary Peritoneal Cancer (This form must be completed before the first
Bevacizumab in combination with Paclitaxel and Carboplatin - Frontline Treatment (Previously Untreated) Ovarian, Fallopian Tube, and Primary Peritoneal Cancer (This form must be completed before the first
Index. B Bilateral salpingo-oophorectomy (BSO), 69
 A Advanced stage endometrial cancer diagnosis, 92 lymph node metastasis, 92 multivariate analysis, 92 myometrial invasion, 92 prognostic factors FIGO stage, 94 histological grade, 94, 95 histologic cell
A Advanced stage endometrial cancer diagnosis, 92 lymph node metastasis, 92 multivariate analysis, 92 myometrial invasion, 92 prognostic factors FIGO stage, 94 histological grade, 94, 95 histologic cell
Measuring Performance Of Physicians In The Diagnosis Of Endometriosis Using An Expectation-Maximization Algorithm
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Public Health Theses School of Public Health January 2014 Measuring Performance Of Physicians In The Diagnosis Of Endometriosis
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Public Health Theses School of Public Health January 2014 Measuring Performance Of Physicians In The Diagnosis Of Endometriosis
Menopause and Cancer risk; What to do overcome the risks? Fatih DURMUŞOĞLU,M.D
 Menopause and Cancer risk; What to do overcome the risks? Fatih DURMUŞOĞLU,M.D Menopause and Cancer How does menopause affect a woman s cancer risk? Ø Menopause does not cause cancer.but risk of developing
Menopause and Cancer risk; What to do overcome the risks? Fatih DURMUŞOĞLU,M.D Menopause and Cancer How does menopause affect a woman s cancer risk? Ø Menopause does not cause cancer.but risk of developing
X-Plain Ovarian Cancer Reference Summary
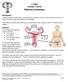 X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
X-Plain Ovarian Cancer Reference Summary Introduction Ovarian cancer is fairly rare. Ovarian cancer usually occurs in women who are over 50 years old and it may sometimes be hereditary. This reference
UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER
 UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER Susan Davidson, MD Professor Department of Obstetrics and Gynecology Division of Gynecologic Oncology University of Colorado- Denver Anatomy Review
UPDATE IN THE MANAGEMENT OF INVASIVE CERVICAL CANCER Susan Davidson, MD Professor Department of Obstetrics and Gynecology Division of Gynecologic Oncology University of Colorado- Denver Anatomy Review
Vagina. 1. Introduction. 1.1 General Information and Aetiology
 Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Vagina 1. Introduction 1.1 General Information and Aetiology The vagina is part of internal female reproductive system. It is an elastic, muscular tube that connects the outside of the body to the cervix.
Cancer Endorsement Maintenance 2011-Maintenance Measures
 Measure Number Title Description Measure Steward 0210 Proportion receiving chemotherapy in the last 14 days of life 0211 Proportion with more than one emergency room visit in the last days of life 0212
Measure Number Title Description Measure Steward 0210 Proportion receiving chemotherapy in the last 14 days of life 0211 Proportion with more than one emergency room visit in the last days of life 0212
I ing therapy, the most commonly used index
 WHEN MAY ENDOMETRIAL CANCER BE CONSIDERED CURED? RICHARD R. MONSON, MD,* BRIAN MACMAHON, &ID,* AND JAMES H. AUSTIN, MD+ To assess when a woman may be considered cured following treatment for endometrial
WHEN MAY ENDOMETRIAL CANCER BE CONSIDERED CURED? RICHARD R. MONSON, MD,* BRIAN MACMAHON, &ID,* AND JAMES H. AUSTIN, MD+ To assess when a woman may be considered cured following treatment for endometrial
What is ovarian cancer?
 What is ovarian cancer? Ovarian cancer is a type of cancer that forms in tissues of the ovary. Most ovarian cancers are either ovarian epithelial cancers (cancer that begins in the cells on the surface
What is ovarian cancer? Ovarian cancer is a type of cancer that forms in tissues of the ovary. Most ovarian cancers are either ovarian epithelial cancers (cancer that begins in the cells on the surface
7. Cytoreductive surgery in endometrial cancer and uterine sarcomas
 Transworld Research Network 37/661 (2), Fort P.O. Trivandrum-695 023 Kerala, India Cytoreductive Surgery in Gynecologic Oncology: A Multidisciplinary Approach, 2010: 123-151 ISBN: 978-81-7895-484-4 Editor:
Transworld Research Network 37/661 (2), Fort P.O. Trivandrum-695 023 Kerala, India Cytoreductive Surgery in Gynecologic Oncology: A Multidisciplinary Approach, 2010: 123-151 ISBN: 978-81-7895-484-4 Editor:
