Outcomes of Moderate-to-Severe Pneumocystis Pneumonia Treated with Adjunctive Steroid in Non-HIV-Infected Patients
|
|
|
- Hector Shelton
- 5 years ago
- Views:
Transcription
1 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 2011, p Vol. 55, No /11/$12.00 doi: /aac Copyright 2011, American Society for Microbiology. All Rights Reserved. Outcomes of Moderate-to-Severe Pneumocystis Pneumonia Treated with Adjunctive Steroid in Non-HIV-Infected Patients Song Mi Moon, 1 Tark Kim, 1 Heungsup Sung, 2 Mi-Na Kim, 2 Sung-Han Kim, 1 Sang-Ho Choi, 1 Jin-Yong Jeong, 1 Jun Hee Woo, 1 Yang Soo Kim, 1 and Sang-Oh Lee 1 * Departments of Infectious Diseases 1 and Laboratory Medicine, 2 Asan Medical Center, University of Ulsan College of Medicine, Seoul, Republic of Korea Received 16 May 2011/Returned for modification 4 July 2011/Accepted 16 July 2011 While it is well-known that adjunctive corticosteroid use improves the outcome of moderate-to-severe Pneumocystis jirovecii pneumonia (PcP) in patients with human immunodeficiency virus (HIV), there are limited data on its efficacy in non-hiv-infected patients with PcP. Patients undergoing fiber-optic bronchoscopy with bronchoalveolar lavage for suspected PcP from January 2007 through December 2010 were reviewed retrospectively. We compared demographics, clinical characteristics, and outcomes in 88 non-hiv-infected patients with moderate-to-severe PcP with (n 59) and without (n 29) adjunctive corticosteroid use. Outcomes of PcP were assessed by respiratory failure and 30-day and 90-day all-cause mortality. Survival curves were analyzed by the Kaplan-Meier method and estimated by the log rank test. All-cause mortality of moderate-to-severe PcP at 90 days was lower in the solid-organ transplant recipients than in all other patients (6/26 [23%] versus 34/62 [55%], respectively; P 0.006), and mortality at 30 days was lower in patients with hematologic malignancies than in all other patients (4/26 [15%] versus 24/62 [39%], respectively; P 0.03). The outcomes of PcP were not significantly different in moderate-to-severe PcP patients with and without adjunctive corticosteroid use, regardless of recent corticosteroid use. Survival analysis of PcP patients with and without corticosteroid use by the Kaplan-Meier method also did not reveal any difference (log rank test; P 0.81). There again was no difference within the subgroup of PcP patients with solid-organ transplants. Adjunctive corticosteroid use may not improve the outcome of moderate-to-severe PcP in non-hiv-infected patients. Pneumocystis jirovecii pneumonia (PcP) remains an important opportunistic infection in the context of human immunodeficiency virus (HIV) infection as well as in other immunocompromised conditions (4, 14). Several important advances have greatly influenced the treatment of PcP in HIV-infected patients, notably the introduction of adjunctive corticosteroids (4, 14). In HIV-infected patients with PcP, further deterioration of oxygenation is often observed during the first 3 to 5 days of specific PcP therapy. Why therapy provokes a decline in pulmonary function is unclear, but one hypothesis is that the drug-induced death of microorganisms exacerbates pulmonary inflammation (1). Accordingly, early in the HIV epidemic, randomized trials evaluated the efficacy of adjunctive corticosteroid therapy in reducing morbidity and mortality in HIVinfected patients with moderate-to-severe PcP (3, 7, 11, 12). These trials demonstrated a survival benefit of corticosteroid administration. Because of this, corticosteroid should be given within 72 h of initiating antimicrobial therapy in an HIVinfected patient with PcP if the partial pressure of arterial oxygen (PaO 2 )is 70 mmhg or the alveolar-arterial oxygen difference (AaDO 2 )is 35 (9). * Corresponding author. Mailing address: Department of Infectious Diseases, Asan Medical Center, University of Ulsan College of Medicine, Pungnap-2dong, Songpa-gu, Seoul , Republic of Korea. Phone: Fax: Supplemental material for this article may be found at Published ahead of print on 25 July The clinical characteristics and outcomes of PcP differ in HIV-infected and non-hiv-infected patients (6, 10). However, there are very limited data on the efficacy of adjunctive corticosteroid in non-hiv-infected patients with PcP (5, 13), and no randomized studies have been conducted. In contrast to the data for HIV-infected patients, the data for non-hiv-infected PcP patients suggest that adjunctive corticosteroid might not improve outcomes (5, 13). The problems encountered in analyzing and interpreting these data are that the non-hiv-immunocompromised hosts were a nonhomogeneous group of patients and that most of them had been on corticosteroids at the time they developed PcP. Therefore, we evaluated the effects of adjunctive corticosteroid treatment on the outcomes of non-hiv-infected patients with moderate-to-severe PcP, using adjustments for recent use of corticosteroid and underlying disease. MATERIALS AND METHODS Study population. This study was performed at the Asan Medical Center, a 2,700-bed tertiary care teaching hospital in Seoul, Republic of Korea. Patients undergoing fiber-optic bronchoscopy with bronchoalveolar lavage for suspected PcP from January 2007 through December 2010 were identified by examining bronchoscopy logs and laboratory databases. Only the first bronchoscopy in patients undergoing multiple bronchoscopies during a single clinical episode was analyzed. Patients under 16 years of age and HIV-infected patients were excluded from the analysis. Microbiological methods. Bronchoalveolar lavage was performed through a fiber-optic bronchoscope using standard techniques (2). Diagnosis of PcP was based on a positive result in the direct immunofluorescence assay for P. jirovecii (Light Diagnostics Pneumocystis carinii DFA kit; Millipore, Billerica, MA). Additional microbiological investigations performed on bronchoalveolar lavage 4613
2 4614 MOON ET AL. ANTIMICROB. AGENTS CHEMOTHER. TABLE 1. Outcomes of moderate-to-severe P. jirovecii pneumonia according to underlying disease a Underlying disease Respiratory failure 30-day all-cause mortality 90-day all-cause mortality Solid-organ transplant recipient (n 26) 15 (57.7) 5 (19.2) 6 (23.1) b Hematologic malignancy (n 26) 17 (65.4) 4 (15.4) b 10 (38.5) Non-hematologic malignancy (n 12) 6 (50.0) 5 (41.7) 8 (66.7) Interstitial lung disease (n 9) 6 (66.7) 5 (55.6) 7 (77.8) Connective tissue disease (n 7) 6 (85.7) 4 (57.1) 4 (57.1) Others (n 8) 4 (50.0) 5 (62.5) 5 (62.5) Total (n 88) 54 (61.4) 28 (31.8) 40 (45.5) a Data are numbers (%) of patients. b s of 0.05 between patients with a given underlying disease and all other underlying diseases. specimens included culture for conventional bacteria, mycobacteria, fungi, and viruses. Quantitative culture of bronchoalveolar lavage specimens was used to assay conventional bacteria, and the threshold value was 10 4 CFU/ml (8). Cytomegalovirus (CMV) was cultured by standard techniques; samples were inoculated into shell vial cultures of human fetal lung fibroblasts (Diagnostic Hybrids, Athens, OH), and growth was examined on days 1 and 7 by direct immunofluorescence staining. Viruses other than CMV, including respiratory syncytial virus, influenza virus, parainfluenza virus, and adenovirus, were detected by means of a direct immunofluorescence assay employing a respiratory virus screening and identification kit (Diagnostic Hybrids). TABLE 2. Demographics, clinical characteristics, and outcomes of moderate-to-severe P. jirovecii pneumonia with and without adjunctive steroid therapy in non-hiv-infected patients a Characteristic therapy (n 59) No adjunctive steroid therapy (n 29) Demographics Age, median years (IQR) b 59 (45 69) 54 (39 60) 0.01 Male gender 38 (64.4) 18 (62.1) 0.83 Underlying disease Solid-organ transplant recipient 12 (20.3) 14 (48.3) Hematologic malignancy 21 (35.6) 5 (17.2) 0.08 Hematopoietic stem cell transplant recipient 4 (6.8) 1 (3.4) 0.99 Nonhematologic malignancy 9 (15.3) 3 (10.3) 0.74 Interstitial lung disease 6 (10.2) 3 (10.3) 0.99 Connective tissue disease 6 (10.2) 1 (3.4) 0.42 Others 5 (8.5) 3 (10.3) 0.99 Immunosuppressive agents use, previous month Steroid 23 (39.0) 11 (37.9) 0.92 T-cell immunosuppressant 16 (27.1) 15 (51.7) 0.02 Anticancer agent 27 (45.8) 10 (34.5) 0.31 Time to BAL after admission, median days (IQR) c 2 (1 5) 6 (1 16) 0.13 Pulmonary coinfection Bacteria 0 (0) 1 (3.4) 0.33 Cytomegalovirus 14 (23.7) 9 (31.0) 0.46 Virus other than cytomegalovirus 0 (0) 1 (3.4) 0.33 Treatment duration, median days (IQR) 18 (14 24) 16 (13 23) 0.59 Initial treatment regimen Trimethoprim-sulfamethoxazole 59 (100) 28 (96.6) 0.33 Change to second-line regimen 24 (40.7) 7 (24.1) 0.13 Due to treatment failure 19 (32.2) 6 (20.7) 0.26 Due to adverse reaction 5 (8.5) 1 (3.4) 0.66 Respiratory failure 37 (62.7) 17 (58.6) day all-cause mortality 18 (30.5) 10 (34.5) day all-cause mortality 28 (47.5) 12 (41.4) 0.59 a Data are numbers (%) of patients, unless otherwise indicated. b IQR, interquartile range. c BAL, bronchoalveolar lavage.
3 VOL. 55, 2011 PcP WITH ADJUNCTIVE STEROID IN NON-HIV PATIENTS 4615 Clinical data. All medical records were reviewed retrospectively. Based on the PaO 2 while breathing room air, or the AaDO 2, prior to the first bronchoscopy, patients were classified into those with mild (PaO2 70 mmhg or AaDO2 35), moderate (PaO2 70 mmhg or AaDO2 35), or severe (PaO2 60 mmhg or AaDO2 45) PcP (14). We compared demographics, clinical characteristics, and outcomes in the moderate-to-severe PcP patients with and without the use of adjunctive corticosteroid. Use of adjunctive corticosteroid was defined as use started within 72 h of initiating specific PcP therapy and consisting of at least 40 mg prednisone twice daily for 5 days, regardless of the subsequent tapering schedule, and of use of corticosteroid prior to the onset of PcP (17). The outcome of PcP was assessed by respiratory failure and 30-day and 90-day all-cause mortality. Respiratory failure was defined as use of mechanical ventilation for more than 48 h. The reason for the choice of 48 h was to avoid analyzing instances of temporary use of mechanical ventilation for bronchoscopic examination. To adjust for recent use of corticosteroid, we performed the same comparisons between moderate-to-severe PcP patients with and without the use of adjunctive corticosteroid after subdivision into those with and without recent corticosteroid use. Recent corticosteroid use was defined as use of more than 0.3 mg/kg body weight/day for over 3 weeks in the month preceding the onset of PcP. To adjust for underlying disease, the outcomes of the PcP patients with and without adjunctive corticosteroid use were compared within groups with a given underlying disease. Clinical decisions concerning treatment regimens for PcP were made by the physicians. Failure of initial treatment regimen was defined as clinical deterioration during the first 5 days of treatment or lack of improvement after 7 or more days of treatment (16). Statistical analysis. All statistics were calculated using SPSS version 12.0 (SPSS, Chicago, IL). Categorical variables were compared using the chi-square test or Fisher s exact test. Continuous variables were analyzed by the Mann- Whitney U test. Time-to-event analysis was performed using Kaplan-Meier estimates and the log rank test. All tests were two tailed, and differences were considered significant at s of RESULTS FIG. 1. Kaplan-Meier survival curves in patients with moderate-tosevere Pneumocystis jirovecii pneumonia (PcP) with or without adjunctive steroid therapy. During the study period, 135 patients with PcP were identified. Among these, the following 24 patients were excluded: pediatric patients (n 7) and HIV-infected patients (n 17). Of the remaining 111 patients, 23 (20.7%) had mild PcP, 8 (7.2%) had moderate PcP, and 80 (72.1%) had severe PcP. Therefore, a total of 88 patients with moderate-to-severe PcP were included in the study. Of these, 26 (29.5%) were solidorgan transplant recipients (14 kidneys, 8 livers, 2 hearts, 2 pancreases), 26 (29.5%) had hematologic malignancies, including 5 (5.7%) hematopoietic stem cell transplant recipients, 12 (13.7%) had nonhematologic malignancies (7 had lung cancer, 3 colon cancer, 1 gastric cancer, 1 prostatic cancer), 9 (10.2%) had interstitial lung disease, and 7 (8.0%) had connective tissue disease. The majority of patients were treated with trimethoprim-sulfamethoxazole (98.9%). In the organ transplant recipients, the median interval from transplantation to the onset of PcP was 12 months (interquartile range, 9 to 16 months). Outcome of moderate-to-severe PcP according to underlying disease. Table 1 shows the outcomes of moderate-to-severe PcP according to the underlying disease. All-cause mortality at 90 days was lower in the solid-organ transplant recipients than in all others (6/26 [23.1%] versus 34/62 [54.8%], respectively; P 0.006), and mortality at 30 days was lower in patients with hematologic malignancies than in all others (4/26 [15.4%] versus 24/62 [38.7%], respectively; P 0.03). However, there was no significant difference in the incidence of respiratory failure according to the underlying disease. Comparison of moderate-to-severe PcP patients with and without adjunctive corticosteroid use. Table 2 presents the demographics, clinical characteristics, and outcomes in the patients with and without adjunctive corticosteroid use. Of the 88 patients, 59 (67%) received adjunctive corticosteroid therapy, and 29 (33%) did not. The PcP patients with adjunctive corticosteroid use were older than those without (59 versus 29 years old; P 0.01). Those with adjunctive corticosteroid use also included fewer solid-organ transplant recipients (20.3% versus 48.3%, respectively; P 0.007) and patients who received T-cell immunosuppressants (27.1% versus 51.7%, respectively; P 0.02) compared to those without adjunctive corticosteroid. There were no significant differences in rates of pulmonary coinfection with bacteria, cytomegalovirus, and other viruses or in the rate of respiratory failure and 30-day and 90-day all-cause mortality between the two groups. Survival analysis by the Kaplan-Meier method also did not reveal a significant difference between the groups (log rank test, P 0.81) (Fig. 1). Using the median age (56 years old) of all the moderate-tosevere PcP patients as a reference point, we divided the patients into younger and older groups and compared the outcomes between patients with and without adjunctive corticosteroid according to age. Again there was no significant difference of outcomes (see Table S1 in the supplemental material), and the same was true when we first divided the patients into those receiving T-cell immunosuppressants and those not receiving them (see Table S2 in the supplemental material). Again, when we first divided the patients into those with and without recent corticosteroid use and compared the outcomes between patients with and without adjunctive corticosteroid (Table 3), the outcomes in terms of respiratory failure rate and 30-day and 90-day mortality did not differ significantly, and this proved also to be the case when we adjusted for underlying disease by comparing the outcomes in moderate-to-severe PcP
4 4616 MOON ET AL. ANTIMICROB. AGENTS CHEMOTHER. TABLE 3. Demographics, clinical characteristics, and outcomes of moderate-to-severe P. jirovecii pneumonia with and without adjunctive steroid therapy in non-hiv-infected patients with or without recent steroid use a Recent steroid use No recent steroid use Characteristic therapy (n 23) No adjunctive steroid therapy (n 11) therapy (n 36) No adjunctive steroid therapy (n 18) Demographics Age, median years (IQR) b 57 (40 70) 55 (38 64) (45 69) 54 (37 59) 0.02 Male gender 15 (65.2) 6 (54.5) (63.9) 12 (66.7) 0.84 Underlying disease Solid-organ transplant recipient 2 (8.7) 1 (9.1) (27.8) 13 (72.2) Hematologic malignancy 3 (13.0) 3 (27.3) (50.0) 2 (11.1) Hematopoietic stem cell transplant recipient 1 (4.3) 1 (9.1) (8.3) 0 (0) 0.54 Nonhematologic malignancy 3 (13.0) 1 (9.1) (16.7) 2 (11.1) 0.70 Interstitial lung disease 6 (26.1) 3 (27.3) (0) 0 (0) Connective tissue disease 5 (21.7) 1 (9.1) (2.8) 0 (0) 0.99 Others 4 (17.4) 2 (18.2) (2.8) 1 (5.6) 0.99 Immunosuppressive agents use, previous month T-cell immunosuppressant 5 (21.7) 2 (18.2) (30.6) 13 (72.2) Anticancer agent 7 (30.4) 5 (45.5) (55.6) 5 (27.8) Time to BAL after admission, median days (IQR) c 2 (1 6) 6 (1 14) (1 5) 6 (1 23) 0.24 Pulmonary coinfection Bacteria 0 (0) 1 (9.1) (0) 0 (0) Cytomegalovirus 9 (39.1) 3 (27.3) (13.9) 6 (33.3) 0.15 Virus other than cytomegalovirus 0 (0) 1 (9.1) (0) 0 (0) Treatment duration, median days (IQR) 20 (14 23) 14 (9 22) (13 24) 19 (14 25) 0.67 Initial treatment regimen Trimethoprim-sulfamethoxazole 23 (100) 10 (90.9) (100) 18 (100) Change to second-line regimen 12 (52.2) 3 (27.3) (33.3) 4 (22.2) 0.40 Due to treatment failure 9 (39.1) 3 (27.3) (27.8) 3 (16.7) 0.51 Due to adverse reaction 3 (13.0) 0 (0) (5.6) 1 (5.6) 0.99 Respiratory failure 15 (65.2) 6 (54.5) (61.1) 11 (61.1) day all-cause mortality 11 (47.8) 4 (36.4) (19.4) 6 (33.3) day all-cause mortality 12 (52.2) 6 (54.5) (44.4) 6 (33.3) 0.43 a Data are numbers (%) of patients, unless otherwise indicated. b IQR, interquartile range. c BAL, bronchoalveolar lavage. patients receiving solid-organ transplantation with (n 12) and without (n 14) adjunctive corticosteroid use (Table 4). Patients with other underlying diseases were not analyzed because of the small sample sizes. TABLE 4. Outcomes of moderate-to-severe P. jirovecii pneumonia with and without adjunctive steroid therapy in solid-organ transplant recipients a Outcome therapy (n 12) No adjunctive steroid therapy (n 14) Respiratory failure 6 (50.0) 9 (64.3) day all-cause mortality 3 (25.0) 2 (14.3) day all-cause mortality 4 (33.3) 2 (14.3) 0.37 a Data are numbers (%) of patients. DISCUSSION There have been many advances in the treatment of PcP in HIV-infected patients (4, 14). One is the use of adjunctive corticosteroid. Many studies have shown that adjunctive corticosteroid use prevents early deterioration after PcP treatment (3, 11) and decreases the rates of respiratory failure and mortality of HIVinfected moderate-to-severe PcP patients (1, 3, 7, 12, 17). Based on these results, adjunctive corticosteroid use within 72 h of initiating antimicrobial therapy is recommended in HIV-infected patients with PcP, if PaO 2 is 70 mmhg or AaDO 2 is 35 (9). Many clinicians have used adjunctive corticosteroid in this way in HIV-infected patients with PcP. However, there have been very few studies of the efficacy of adjunctive corticosteroid use in non-hiv-infected patients with PcP, but a number of retrospective studies have failed to show significant differences in morbidity and mortality in non-hiv-infected PcP
5 VOL. 55, 2011 PcP WITH ADJUNCTIVE STEROID IN NON-HIV PATIENTS 4617 patients with and without adjunctive corticosteroid use (5, 13, 15). In a previous study of non-hiv-infected PcP patients with a variety of underlying diseases, mortality of PcP patients with low-dose steroid use was not significantly different from that of PcP patients with high-dose steroid use (5/14 [36%] versus 7/16 [44%], respectively; P 0.65) (13). Another study showed that the need for mechanical ventilation (10/23 [43%] versus 4/8 [50%]; P 0.75) and the mortality rate (9/23 [39%] versus 4/8 [50%]; P 0.59) were similar in the two groups (5). In a third study, of PcP patients with hematologic malignancies, there was even a trend toward increased mortality in the PcP patients with adjunctive corticosteroid compared to those without (15/35 [42.9%] versus 5/25 [20%], respectively; P 0.06) (15). To the best of our knowledge, ours is the largest retrospective study aimed at determining the efficacy of adjunctive corticosteroid therapy in non-hiv-infected PcP patients. Our results support the previous smaller-sized reports indicating that adjunctive corticosteroid use may not improve the outcome of PcP in non-hiv-infected patients. During the study period from January 2007 to December 2010, 135 PcP patients were identified. Among these, 7 pediatric patients were excluded. Of the remaining 128 patients, 111 (86%) patients were non-hiv-infected patients, and 17 (14%) were HIV-infected patients. It should be pointed out that the incidence of PcP in non-hiv-infected versus HIVinfected patients may not reflect the general population in Republic of Korea. During the study period, 2,353 cases of solid-organ transplantations (22% of nationwide cases) and 806 cases of hematologic stem cell transplantations were treated at the Asan Medical Center. On the other hand, only 291 HIV-infected patients were treated in our hospital. It is well-known that the clinical characteristics and outcomes of PcP in HIV-infected patients are different from those in non-hiv-infected patients (6, 10). In addition, non-hivinfected patients with PcP suffer from different underlying diseases, and these may affect the clinical outcomes of PcP. That is one of the reasons why there have been limited studies of the efficacy of adjunctive corticosteroid use in non-hiv-infected patients with PcP. To adjust for underlying diseases, we compared the outcomes of moderate-to-severe PcP in patients with and without adjunctive corticosteroid use according to underlying disease and found no significant difference between PcP patients receiving solid-organ transplantation with and without adjunctive corticosteroid use (Table 4). Unfortunately, we could not analyze PcP patients with other underlying diseases, such as hematologic malignancies, nonhematologic malignancies, interstitial lung disease, and connective tissues disease, due to the small sample sizes. Another reason why it is difficult to analyze and interpret the efficacy of adjunctive corticosteroid use in non-hiv-infected PcP patients is that a considerable proportion of the patients have received corticosteroids previously for various reasons. In our study, 39% of the patients had received corticosteroid at a dose of more than 0.3 mg/kg/day for more than 3 weeks in the month prior to the onset of PcP. For this reason, we divided patients into two groups according to recent steroid use and found no significant difference of outcome (Table 3). The current study showed a 6% difference (P 0.59) in 90-day all-cause mortality between the group receiving adjunctive steroid therapy and the group not receiving adjunctive steroid therapy. It had 80% power to detect a 30% difference in 90-day all-cause mortality at a 5% significance level. It is possible that our sample size was too small to achieve statistical significance. Due to the limitation of statistical power, subgroup analysis by age, underlying disease analysis, and recent medication history have been conducted. The consistent results from the subgroup analysis support our result. We divided the patients into younger and older groups and compared the outcomes between patients with and without adjunctive corticosteroid separately for the ages, and there again was no significant difference of outcomes between those with and without adjunctive corticosteroid (see Table S1 in the supplemental material). There was also no significant difference of outcomes between PcP patients with and without adjunctive corticosteroid, regardless of the use/nonuse of T-cell immunosuppressants (see Table S2 in the supplemental material). In conclusion, adjunctive corticosteroid use may not improve the outcome of moderate-to-severe PcP in non-hiv-infected patients, regardless of recent corticosteroid use. The current practice of using adjunctive corticosteroid in non-hiv-infected PcP patients as is done with HIV-infected PcP patients should be reconsidered. Well-designed prospective studies should be undertaken to reach a more reliable conclusion. ACKNOWLEDGMENT We have no potential conflicts of interest, and there is no financial support to report. REFERENCES 1. Anonymous Consensus statement on the use of corticosteroids as adjunctive therapy for pneumocystis pneumonia in the acquired immunodeficiency syndrome. The National Institutes of Health University of California Expert Panel for Corticosteroids as Adjunctive Therapy for Pneumocystis Pneumonia. N. Engl. J. Med. 323: Anonymous Technical recommendations and guidelines for bronchoalveolar lavage (BAL). Report of the European Society of Pneumology Task Group. Eur. Respir. J. 2: Bozzette, S. A., et al A controlled trial of early adjunctive treatment with corticosteroids for Pneumocystis carinii pneumonia in the AIDS. California Collaborative Treatment Group. N. Engl. J. Med. 323: Catherinot, E., et al Pneumocystis jirovecii Pneumonia. Infect. Dis. Clin. North Am. 24: Delclaux, C., et al Corticosteroids as adjunctive therapy for severe Pneumocystis carinii pneumonia in non-human immunodeficiency virus-infected patients: retrospective study of 31 patients. Clin. Infect. Dis. 29: Ewig, S., et al Clinical characteristics and outcome of Pneumocystis carinii pneumonia in HIV-infected and otherwise immunosuppressed patients. Eur. Respir. J. 8: Gagnon, S., et al Corticosteroids as adjunctive therapy for severe Pneumocystis carinii pneumonia in the AIDS. A double-blind, placebocontrolled trial. N. Engl. J. Med. 323: Horan, T. C., M. Andrus, and M. A. Dudeck CDC/NHSN surveillance definition of health care-associated infection and criteria for specific types of infections in the acute care setting. Am. J. Infect. Control 36: Kaplan, J. E., et al Guidelines for prevention and treatment of opportunistic infections in HIV-infected adults and adolescents: recommendations from CDC, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. MMWR Recommend. Rep. 58(RR-4): (Quiz, CE1 CE4.) 10. Mansharamani, N. G., R. Garland, D. Delaney, and H. Koziel Management and outcome patterns for adult Pneumocystis carinii pneumonia, 1985 to 1995: comparison of HIV-associated cases to other immunocompromised states. Chest 118: Montaner, J. S., et al Corticosteroids prevent early deterioration in patients with moderately severe Pneumocystis carinii pneumonia and the AIDS. Ann. Intern. Med. 113: Nielsen, T. L., et al Adjunctive corticosteroid therapy for Pneumocystis carinii pneumonia in AIDS: a randomized European multicenter open label study. J. Acquir. Immune Defic. Syndr. 5: Pareja, J. G., R. Garland, and H. Koziel Use of adjunctive cortico-
6 4618 MOON ET AL. ANTIMICROB. AGENTS CHEMOTHER. steroids in severe adult non-hiv Pneumocystis carinii pneumonia. Chest 113: Pfaller, M. A., and E. J. Anaissie Pneumocystis, p In E. J. Anaissie, M. R. McGinnis, and M. A. Pfaller (ed.), Clinical mycology, 2nd ed. Churchill Livingstone, Oxford, United Kingdom. 15. Roblot, F., et al Pneumocystis carinii pneumonia in patients with hematologic malignancies: a descriptive study. J. Infect. 47: Smego, R. A., Jr., S. Nagar, B. Maloba, and M. Popara A metaanalysis of salvage therapy for Pneumocystis carinii pneumonia. Arch. Intern. Med. 161: Walmsley, S., et al A multicenter randomized double-blind placebocontrolled trial of adjunctive corticosteroids in the treatment of Pneumocystis carinii pneumonia complicating the AIDS. J. Acquir. Immune Defic. Syndr. Hum. Retrovirol. 8:
Cellular Profiles of Bronchoalveolar Lavage Fluid and Their Prognostic. Significance in Non-HIV-Infected Patients with Pneumocystis jirovecii
 JCM Accepted Manuscript Posted Online 11 February 2015 J. Clin. Microbiol. doi:10.1128/jcm.03494-14 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 3 Cellular Profiles of Bronchoalveolar
JCM Accepted Manuscript Posted Online 11 February 2015 J. Clin. Microbiol. doi:10.1128/jcm.03494-14 Copyright 2015, American Society for Microbiology. All Rights Reserved. 1 2 3 Cellular Profiles of Bronchoalveolar
Original Article. Noparat Oniem, M.D., Somnuek Sungkanuparph, M.D.
 Original Article Vol. 29 No. 1 Primary prophylaxis for cryptococcosis with fluconazole:- Oniem N & Sungkanuparph S. 5 Primary prophylaxis for cryptococcosis with fluconazole among HIV-infected patients
Original Article Vol. 29 No. 1 Primary prophylaxis for cryptococcosis with fluconazole:- Oniem N & Sungkanuparph S. 5 Primary prophylaxis for cryptococcosis with fluconazole among HIV-infected patients
Value of Bronchoalveolar Lavage Fluid Cytology in the Diagnosis of Pneumocystis jirovecii Pneumonia: A Review of 30 Cases
 http://dx.doi.org/10.4046/trd.2011.71.5.322 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2011;71:322-327 CopyrightC2011. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2011.71.5.322 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2011;71:322-327 CopyrightC2011. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Adjunctive steroid in HIV-negative patients with severe Pneumocystis pneumonia
 Lemiale et al. Respiratory Research 2013, 14:87 RESEARCH Open Access Adjunctive steroid in HIV-negative patients with severe Pneumocystis pneumonia Virginie Lemiale 1*, Alexandre Debrumetz 1, Alexandra
Lemiale et al. Respiratory Research 2013, 14:87 RESEARCH Open Access Adjunctive steroid in HIV-negative patients with severe Pneumocystis pneumonia Virginie Lemiale 1*, Alexandre Debrumetz 1, Alexandra
Supplementary Online Content
 Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
Supplementary Online Content Torres A, Sibila O, Ferrer M, et al. Effect of corticosteroids on treatment failure among hospitalized patients with severe community-acquired pneumonia and high inflammatory
11/19/2012. The spectrum of pulmonary diseases in HIV-infected persons is broad.
 The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
The spectrum of pulmonary diseases in HIV-infected persons is broad. HIV-associated Opportunistic infections Neoplasms Miscellaneous conditions Non HIV-associated Antiretroviral therapy (ART)-associated
Predictors of high flow nasal cannula failure in immunocompromised patients with acute respiratory failure due to non-hiv pneumocystis pneumonia
 Original Article Predictors of high flow nasal cannula failure in immunocompromised patients with acute respiratory failure due to non-hiv pneumocystis pneumonia Won-Young Kim 1,2, Heungsup Sung 3, Sang-Bum
Original Article Predictors of high flow nasal cannula failure in immunocompromised patients with acute respiratory failure due to non-hiv pneumocystis pneumonia Won-Young Kim 1,2, Heungsup Sung 3, Sang-Bum
Pneumocystis. Pneumocystis BIOL Summer Introduction. Mycology. Introduction (cont.) Introduction (cont.)
 Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Introduction Pneumocystis Disclaimer: This lecture slide presentation is intended solely for educational purposes. Many of the images contained herein are the property of the original owner, as indicated
Cytomegalovirus (CMV) Viral Load in Bronchoalveolar Lavage Fluid (BALF) and Plasma to Diagnose Lung Transplant Associated CMV Pneumonia
 Cytomegalovirus (CMV) Viral Load in Bronchoalveolar Lavage Fluid (BALF) and Plasma to Diagnose Lung Transplant Associated CMV Pneumonia I.P. Lodding 1,2, H.H. Schultz 3, J.U. Jensen 1,5, C. Andersen 4,
Cytomegalovirus (CMV) Viral Load in Bronchoalveolar Lavage Fluid (BALF) and Plasma to Diagnose Lung Transplant Associated CMV Pneumonia I.P. Lodding 1,2, H.H. Schultz 3, J.U. Jensen 1,5, C. Andersen 4,
Open Forum Infectious Diseases Advance Access published February 11, 2016
 Open Forum Infectious Diseases Advance Access published February 11, 2016 1 A Critical Reappraisal of Prolonged Neutropenia as a Risk Factor for Invasive Pulmonary Aspergillosis Michael S. Abers 1,2, Musie
Open Forum Infectious Diseases Advance Access published February 11, 2016 1 A Critical Reappraisal of Prolonged Neutropenia as a Risk Factor for Invasive Pulmonary Aspergillosis Michael S. Abers 1,2, Musie
Adjunctive Options for Severe PCP. Dr Erica Shaddock Division of Pulmonology and Critical Care Charlotte Maxeke Johannesburg Academic Hospital
 Adjunctive Options for Severe PCP Dr Erica Shaddock Division of Pulmonology and Critical Care Charlotte Maxeke Johannesburg Academic Hospital Is this topic still relevant? Is this topic still relevant?
Adjunctive Options for Severe PCP Dr Erica Shaddock Division of Pulmonology and Critical Care Charlotte Maxeke Johannesburg Academic Hospital Is this topic still relevant? Is this topic still relevant?
Pneumocystis carinii Pneumonia in Critically Ill Patients with Malignancy: A Descriptive Study
 MAJOR ARTICLE Pneumocystis carinii Pneumonia in Critically Ill Patients with Malignancy: A Descriptive Study J. R. Zahar, 1,a M. Robin, 1 E. Azoulay, 2 F. Fieux, 2 G. Nitenberg, 1 and B. Schlemmer 2 1
MAJOR ARTICLE Pneumocystis carinii Pneumonia in Critically Ill Patients with Malignancy: A Descriptive Study J. R. Zahar, 1,a M. Robin, 1 E. Azoulay, 2 F. Fieux, 2 G. Nitenberg, 1 and B. Schlemmer 2 1
ESCMID Online Lecture Library. by author
 Up to date management of Pneumocystis pneumonia ECCMID April 30th 2013 Mark G.J. de Boer MD PhD Leiden University Medical Ctr Disclosures: none Leiden University Medical Ctr Leiden, The Netherlands Introduction
Up to date management of Pneumocystis pneumonia ECCMID April 30th 2013 Mark G.J. de Boer MD PhD Leiden University Medical Ctr Disclosures: none Leiden University Medical Ctr Leiden, The Netherlands Introduction
Eastern Mediterranean Health Journal, Vol. 14, No. 5,
 Eastern Mediterranean Health Journal, Vol. 14, No. 5, 2008 1217 Case report Inappropriate use of steroid and Pneumocystis jiroveci pneumonia: report of two cases P. Tabarsi, 1 M. Mirsaeidi, 1 M. Amiri,
Eastern Mediterranean Health Journal, Vol. 14, No. 5, 2008 1217 Case report Inappropriate use of steroid and Pneumocystis jiroveci pneumonia: report of two cases P. Tabarsi, 1 M. Mirsaeidi, 1 M. Amiri,
Late diagnosis of influenza in adult patients during a seasonal outbreak
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:391-396 Late diagnosis of influenza in adult patients during a seasonal outbreak Seong-Ho Choi 1, Jin-Won Chung 1, Tark Kim 2, Ki-Ho Park 3, Mi Suk Lee 3, and
ORIGINAL ARTICLE Korean J Intern Med 2018;33:391-396 Late diagnosis of influenza in adult patients during a seasonal outbreak Seong-Ho Choi 1, Jin-Won Chung 1, Tark Kim 2, Ki-Ho Park 3, Mi Suk Lee 3, and
CLINICAL GUIDELINES. Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P.
 CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
Viral Threat on Respiratory Failure
 Viral Threat on Respiratory Failure Younsuck Koh, MD, PhD, FCCM Department of Pulmonary and Critical Care Medicine Asan Medical Center University of Ulsan College of Medicine Seoul, Korea No Conflict of
Viral Threat on Respiratory Failure Younsuck Koh, MD, PhD, FCCM Department of Pulmonary and Critical Care Medicine Asan Medical Center University of Ulsan College of Medicine Seoul, Korea No Conflict of
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Invasive Pulmonary Aspergillosis in
 Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
Infection & Sepsis Symposium Porto, April 1-3, 2009 Invasive Pulmonary Aspergillosis in Non-Immunocompromised Patients Stijn BLOT, PhD General Internal Medicine & Infectious Diseases Ghent University Hospital,
PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES
 PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES DEFINITIONS AND BACKGROUND Uncomplicated influenza illness is characterized by the abrupt onset of constitutional and respiratory signs and symptoms. Signs
PEDIATRIC INFLUENZA CLINICAL PRACTICE GUIDELINES DEFINITIONS AND BACKGROUND Uncomplicated influenza illness is characterized by the abrupt onset of constitutional and respiratory signs and symptoms. Signs
Polmoniti: Steroidi sì, no, quando. Alfredo Chetta Clinica Pneumologica Università degli Studi di Parma
 Polmoniti: Steroidi sì, no, quando Alfredo Chetta Clinica Pneumologica Università degli Studi di Parma Number of patients Epidemiology and outcome of severe pneumococcal pneumonia admitted to intensive
Polmoniti: Steroidi sì, no, quando Alfredo Chetta Clinica Pneumologica Università degli Studi di Parma Number of patients Epidemiology and outcome of severe pneumococcal pneumonia admitted to intensive
Prognostic Value of Bronchoalveolar Lavage in Patients with Non-HIV Pneumocystis Pneumonia
 ORIGINAL ARTICLE Prognostic Value of Bronchoalveolar Lavage in Patients with Non-HIV Pneumocystis Pneumonia Koji Tamai, Ryo Tachikawa, Keisuke Tomii, Kazuma Nagata, Kojiro Otsuka, Atsushi Nakagawa, Kyoko
ORIGINAL ARTICLE Prognostic Value of Bronchoalveolar Lavage in Patients with Non-HIV Pneumocystis Pneumonia Koji Tamai, Ryo Tachikawa, Keisuke Tomii, Kazuma Nagata, Kojiro Otsuka, Atsushi Nakagawa, Kyoko
Adjunctive corticosteroids for the treatment of Pneumocystis jiroveci pneumonia in patients with HIV: A meta analysis
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 11: 683-687, 2016 Adjunctive corticosteroids for the treatment of Pneumocystis jiroveci pneumonia in patients with HIV: A meta analysis LI WANG 1, HAO LIANG 1,2, LI
EXPERIMENTAL AND THERAPEUTIC MEDICINE 11: 683-687, 2016 Adjunctive corticosteroids for the treatment of Pneumocystis jiroveci pneumonia in patients with HIV: A meta analysis LI WANG 1, HAO LIANG 1,2, LI
New respiratory symptoms and lung imaging findings in a woman with polymyositis
 Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Maria Bolaki 1, Konstantinos Karagiannis 1, George Bertsias 2, Ioanna Mitrouska 1, Nikolaos Tzanakis 1, Katerina M. Antoniou 1 kantoniou@uoc.gr 1 Dept of Thoracic Medicine, Heraklion University Hospital,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Jain S, Kamimoto L, Bramley AM, et al. Hospitalized patients
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Jain S, Kamimoto L, Bramley AM, et al. Hospitalized patients
EMERGING FUNGAL INFECTIONS IN IMMUNOCOMPROMISED PATIENTS
 EMERGING FUNGAL INFECTIONS IN IMMUNOCOMPROMISED PATIENTS DR LOW CHIAN YONG MBBS, MRCP(UK), MMed(Int Med), FAMS Consultant, Dept of Infectious Diseases, SGH Introduction The incidence of invasive fungal
EMERGING FUNGAL INFECTIONS IN IMMUNOCOMPROMISED PATIENTS DR LOW CHIAN YONG MBBS, MRCP(UK), MMed(Int Med), FAMS Consultant, Dept of Infectious Diseases, SGH Introduction The incidence of invasive fungal
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
BRINCIDOFOVIR WAS USED TO SUCCESSFULLY TREAT ADENOVIRUS INFECTIONS IN SOLID ORGAN TRANSPLANT RECIPIENTS AND OTHER IMMUNOCOMPROMISED PATIENTS
 BRINCIDOFOVIR WAS USED TO SUCCESSFULLY TREAT ADENOVIRUS INFECTIONS IN SOLID ORGAN TRANSPLANT RECIPIENTS AND OTHER IMMUNOCOMPROMISED PATIENTS Diana F. Florescu, MD 1, Michael S. Grimley, MD 2, Genovefa
BRINCIDOFOVIR WAS USED TO SUCCESSFULLY TREAT ADENOVIRUS INFECTIONS IN SOLID ORGAN TRANSPLANT RECIPIENTS AND OTHER IMMUNOCOMPROMISED PATIENTS Diana F. Florescu, MD 1, Michael S. Grimley, MD 2, Genovefa
The Utility of Surgical Lung Biopsy in Immunocompromised Children
 The Utility of Surgical Lung Biopsy in Immunocompromised Children Jessica A. Naiditch, MD, Katherine A. Barsness, MD, and David H. Rothstein, MD Objective To determine the utility of lung biopsy in immunocompromised
The Utility of Surgical Lung Biopsy in Immunocompromised Children Jessica A. Naiditch, MD, Katherine A. Barsness, MD, and David H. Rothstein, MD Objective To determine the utility of lung biopsy in immunocompromised
by author ESCMID Online Lecture Library Steroids in acute bacterial meningitis
 Steroids in acute bacterial meningitis Javier Garau, MD, PhD University of Barcelona Spain ESCMID Summer School, Porto, July 2009 Dexamethasone treatment in childhood bacterial meningitis in Malawi: a
Steroids in acute bacterial meningitis Javier Garau, MD, PhD University of Barcelona Spain ESCMID Summer School, Porto, July 2009 Dexamethasone treatment in childhood bacterial meningitis in Malawi: a
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Acute kidney injury and outcomes in acute decompensated heart failure in Korea
 Acute kidney injury and outcomes in acute decompensated heart failure in Korea Mi-Seung Shin 1, Seong Woo Han 2, Dong-Ju Choi 3, Eun Seok Jeon 4, Jae-Joong Kim 5, Myeong-Chan Cho 6, Shung Chull Chae 7,
Acute kidney injury and outcomes in acute decompensated heart failure in Korea Mi-Seung Shin 1, Seong Woo Han 2, Dong-Ju Choi 3, Eun Seok Jeon 4, Jae-Joong Kim 5, Myeong-Chan Cho 6, Shung Chull Chae 7,
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance
 Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
Long-term Clinical Outcomes and Risk of Hepatocellular Carcinoma in Chronic Hepatitis B Patients with HBsAg Seroclearance Gi-Ae Kim, Han Chu Lee *, Danbi Lee, Ju Hyun Shim, Kang Mo Kim, Young-Suk Lim,
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Clinical syndromes: experience from the bedside. Professor Rob Miller University College Hospital, London
 Clinical syndromes: experience from the bedside Professor Rob Miller University College Hospital, London Presented at ECCMID Berlin April 30 th 2013 Pneumocystis jirovecii pneumonia http://commons.wikimedia.org/wiki/file
Clinical syndromes: experience from the bedside Professor Rob Miller University College Hospital, London Presented at ECCMID Berlin April 30 th 2013 Pneumocystis jirovecii pneumonia http://commons.wikimedia.org/wiki/file
ARDS during Neutropenia. D Mokart DAR IPC GRRRRROH 2010
 ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
ARDS during Neutropenia D Mokart DAR IPC GRRRRROH 2010 Definitions Neutropenia is a decrease in circulating neutrophil white cells in the peripheral blood. neutrophil count of 1,000 1,500 cells/ml = mild
Appendix E1. Epidemiology
 Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Test Requested Specimen Ordering Recommendations
 Microbiology Essentials Culture and Sensitivity (C&S) Urine C&S Catheter Surgical (excluding kidney aspirates) Voided Requisition requirements o Specific method of collection MUST be indicated o Indicate
Microbiology Essentials Culture and Sensitivity (C&S) Urine C&S Catheter Surgical (excluding kidney aspirates) Voided Requisition requirements o Specific method of collection MUST be indicated o Indicate
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia)
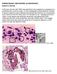 PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
PARASITOLOGY CASE HISTORY 10 (HISTOLOGY) (Lynne S. Garcia) A 46-year-old man with AIDS was admitted to the hospital for complaints of a persisting fever and dry cough. A chest radiograph showed bilateral
The Younger Patients Have More Better Prognosis in Limited Disease Small Cell Lung Cancer
 ORIGINAL ARTICLE http://dx.doi.org/10.4046/trd.2016.79.4.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:274-281 The Younger Patients Have More Better Prognosis in Limited Disease
ORIGINAL ARTICLE http://dx.doi.org/10.4046/trd.2016.79.4.274 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:274-281 The Younger Patients Have More Better Prognosis in Limited Disease
ECMM Excellence Centers Quality Audit
 ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
ECMM Excellence Centers Quality Audit Person in charge: Department: Head of Department: Laboratory is accredited according to ISO 15189 (Medical Laboratories Requirements for quality and competence) Inspected
Immunizing the Immunocompromised. Leilani T. Sanchez, MD, DPPS, DPIDSP Crowne Plaza Galleria Manila, 21 February 2013
 Immunizing the Immunocompromised Leilani T. Sanchez, MD, DPPS, DPIDSP Crowne Plaza Galleria Manila, 21 February 2013 WHO World Health Statistics 2012 2 Immunizing the Immunocompromised Leilani T. Sanchez
Immunizing the Immunocompromised Leilani T. Sanchez, MD, DPPS, DPIDSP Crowne Plaza Galleria Manila, 21 February 2013 WHO World Health Statistics 2012 2 Immunizing the Immunocompromised Leilani T. Sanchez
HIV-HBV coinfection in HIV population horizontally infected in early childhood between
 UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE HIV-HBV coinfection in HIV population horizontally infected in early childhood between 1987-1990 Supervising professor: Prof. Cupşa Augustin
UNIVERSITY OF MEDICINE AND PHARMACY OF CRAIOVA FACULTY OF MEDICINE HIV-HBV coinfection in HIV population horizontally infected in early childhood between 1987-1990 Supervising professor: Prof. Cupşa Augustin
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS*
 clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
clinical investigations in critical care The Role of Open-Lung Biopsy in ARDS* Sanjay R. Patel, MD; Dimitri Karmpaliotis, MD; Najib T. Ayas, MD; Eugene J. Mark, MD; John Wain, MD, FCCP; B. Taylor Thompson,
Incidence and Predictors of Stent Thrombosis after Percutaneous Coronary Intervention in Acute Myocardial Infarction
 Incidence and Predictors of Stent Thrombosis after Percutaneous Coronary Intervention in Acute Myocardial Infarction Sungmin Lim, Yoon Seok Koh, Hee Yeol Kim, Ik Jun Choi, Eun Ho Choo, Jin Jin Kim, Mineok
Incidence and Predictors of Stent Thrombosis after Percutaneous Coronary Intervention in Acute Myocardial Infarction Sungmin Lim, Yoon Seok Koh, Hee Yeol Kim, Ik Jun Choi, Eun Ho Choo, Jin Jin Kim, Mineok
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
EGIS BILIARY STENT. 1. Features & Benefits 2. Ordering information 3. References
 EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
EGIS BILIARY STENT 1. Features & Benefits 2. Ordering information 3. References 1. Features & Benefits (1) Features Superior flexibility & conformability 4 Types Single bare, Single cover, Double bare,
P neumocystis jirovecii pneumonia (PCP) continues to be a
 716 RESPIRATORY INFECTION Improved survival for HIV infected patients with severe Pneumocystis jirovecii pneumonia is independent of highly active antiretroviral therapy R F Miller, E Allen, A Copas, M
716 RESPIRATORY INFECTION Improved survival for HIV infected patients with severe Pneumocystis jirovecii pneumonia is independent of highly active antiretroviral therapy R F Miller, E Allen, A Copas, M
Pneumocystis jirovecii (Pj) quantitative PCR to differentiate Pj pneumonia from Pj colonization in immunocompromised patients
 DOI 10.1007/s10096-013-1960-3 ARTICLE Pneumocystis jirovecii (Pj) quantitative PCR to differentiate Pj pneumonia from Pj colonization in immunocompromised patients M. Maillet & D. Maubon & J. P. Brion
DOI 10.1007/s10096-013-1960-3 ARTICLE Pneumocystis jirovecii (Pj) quantitative PCR to differentiate Pj pneumonia from Pj colonization in immunocompromised patients M. Maillet & D. Maubon & J. P. Brion
Influenza Backgrounder
 Influenza Backgrounder Influenza Overview Influenza causes an average of 36,000 deaths and 200,000 hospitalizations in the U.S. every year. 1,2 Combined with pneumonia, influenza is the seventh leading
Influenza Backgrounder Influenza Overview Influenza causes an average of 36,000 deaths and 200,000 hospitalizations in the U.S. every year. 1,2 Combined with pneumonia, influenza is the seventh leading
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer
 Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
Indeterminate Pulmonary Nodules in Patients with Colorectal Cancer Jai Sule 1, Kah Wai Cheong 2, Stella Bee 2, Bettina Lieske 2,3 1 Dept of Cardiothoracic and Vascular Surgery, University Surgical Cluster,
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage)
 NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
NONGYNECOLOGICAL CYTOLOGY PULMONARY SPECIMENS (Sputum, Post-Bronchoscopy Sputum, Bronchial Brushings, Bronchial Washings, Bronchoalveolar Lavage) I. Purpose The adequacy of a sputum specimen is determined
ORIGINAL ARTICLE INTRODUCTION
 ORIGINAL ARTICLE Korean J Intern Med 2017;32:478-485 Clinical significance of positive Pneumocystis jirovecii polymerase chain reaction in non-human immunodeficiency virus immunocompromised patients in
ORIGINAL ARTICLE Korean J Intern Med 2017;32:478-485 Clinical significance of positive Pneumocystis jirovecii polymerase chain reaction in non-human immunodeficiency virus immunocompromised patients in
Chapter 22. Pulmonary Infections
 Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Chapter 22 Pulmonary Infections Objectives State the incidence of pneumonia in the United States and its economic impact. Discuss the current classification scheme for pneumonia and be able to define hospital-acquired
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Diagnosis and management of influenza: Information for medical staff and ANPs
 Diagnosis and management of influenza: Information for medical staff and ANPs Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications
Diagnosis and management of influenza: Information for medical staff and ANPs Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications
Clinical Policy: Pyrimethamine (Daraprim) Reference Number: ERX.NPA.44 Effective Date:
 Clinical Policy: (Daraprim) Reference Number: ERX.NPA.44 Effective Date: 12.01.15 Last Review Date: 08.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Daraprim) Reference Number: ERX.NPA.44 Effective Date: 12.01.15 Last Review Date: 08.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Supplementary Online Content
 Supplementary Online Content Uranga A, España, Bilbao A, et al. Duration of antibiotic treatment in communityacquired pneumonia: a multicenter randomized clinical trial. JAMA Intern Med. ublished online
Supplementary Online Content Uranga A, España, Bilbao A, et al. Duration of antibiotic treatment in communityacquired pneumonia: a multicenter randomized clinical trial. JAMA Intern Med. ublished online
SYNOPSIS. Clinical Study Report IM Double-blind Period
 Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier SYNOPSIS (For National Authority
Name of Sponsor/Company: Bristol-Myers Squibb Name of Finished Product: Abatacept () Name of Active Ingredient: Abatacept () Individual Study Table Referring to the Dossier SYNOPSIS (For National Authority
Ischemic Stroke in Critically Ill Patients with Malignancy
 Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
Care Guideline DRAFT for review cycle 08/02/17 CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: All MHS employed providers within Primary Care, Urgent Care, and In-Hospital Care. The secondary audience
PNEUMONIA IN CHILDREN. IAP UG Teaching slides
 PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
PNEUMONIA IN CHILDREN 1 INTRODUCTION 156 million new episodes / yr. worldwide 151 million episodes developing world 95% in developing countries 19% of all deaths in children
Potential etiologies of infection in these patients are diverse, including common and uncommon opportunistic infections.
 In the name of God Principles of post Tx infections 1: Potential etiologies of infection in these patients are diverse, including common and uncommon opportunistic infections. Infection processes can progress
In the name of God Principles of post Tx infections 1: Potential etiologies of infection in these patients are diverse, including common and uncommon opportunistic infections. Infection processes can progress
Viral infections Cytomegalovirus pneumonia in adult autologous blood and marrow transplant recipients
 (2001) 27, 877 881 2001 Nature Publishing Group All rights reserved 0268 3369/01 $15.00 www.nature.com/bmt Viral infections Cytomegalovirus pneumonia in adult autologous blood and marrow transplant recipients
(2001) 27, 877 881 2001 Nature Publishing Group All rights reserved 0268 3369/01 $15.00 www.nature.com/bmt Viral infections Cytomegalovirus pneumonia in adult autologous blood and marrow transplant recipients
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Infections in immunocompromised host
 Infections in immunocompromised host Immunodeficiencies Primary immunodeficiencies Neutrophil defect Humoral: B cell defect Humoral: Complement Cellular: T cells Combined severe immunodeficiency Secondary
Infections in immunocompromised host Immunodeficiencies Primary immunodeficiencies Neutrophil defect Humoral: B cell defect Humoral: Complement Cellular: T cells Combined severe immunodeficiency Secondary
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Research & Reviews of. Pneumonia
 Chapter Clinical Presentation and Diagnosis of VAP in Adult ICU Patients Priyam Batra * ; Purva Mathur Research & Reviews of Department of Laboratory Medicine, AIIMS, Trauma Centre, New Delhi, India. *
Chapter Clinical Presentation and Diagnosis of VAP in Adult ICU Patients Priyam Batra * ; Purva Mathur Research & Reviews of Department of Laboratory Medicine, AIIMS, Trauma Centre, New Delhi, India. *
Research Article Eosinophil as a Protective Cell in S. aureus Ventilator-Associated Pneumonia
 Hindawi Publishing Corporation Mediators of Inflammation Volume 2013, Article ID 152943, 5 pages http://dx.doi.org/10.1155/2013/152943 Research Article Eosinophil as a Protective Cell in S. aureus Ventilator-Associated
Hindawi Publishing Corporation Mediators of Inflammation Volume 2013, Article ID 152943, 5 pages http://dx.doi.org/10.1155/2013/152943 Research Article Eosinophil as a Protective Cell in S. aureus Ventilator-Associated
Quality of End-of-Life Care in Patients with Hematologic Malignancies: A Retrospective Cohort Study
 Quality of End-of-Life Care in Patients with Hematologic Malignancies: A Retrospective Cohort Study David Hui, Neha Didwaniya, Marieberta Vidal, Seong Hoon Shin, Gary Chisholm, Joyce Roquemore, Eduardo
Quality of End-of-Life Care in Patients with Hematologic Malignancies: A Retrospective Cohort Study David Hui, Neha Didwaniya, Marieberta Vidal, Seong Hoon Shin, Gary Chisholm, Joyce Roquemore, Eduardo
The 1-year survival rate approaches 80% for patients
 Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
UPDATE IN HOSPITAL MEDICINE
 UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
UPDATE IN HOSPITAL MEDICINE FLORIDA CHAPTER ACP MEETING 2016 Himangi Kaushal, M.D., F.A.C.P. Program Director Memorial Healthcare System Internal Medicine Residency DISCLOSURES None OBJECTIVES Review some
Clinical Infectious Diseases Advance Access published April 11, What is the real role of respiratory viruses in severe community-acquired
 Clinical Infectious Diseases Advance Access published April 11, 2014 1 What is the real role of respiratory viruses in severe community-acquired pneumonia? Olli Ruuskanen 1 and Asko Järvinen 2 1 Department
Clinical Infectious Diseases Advance Access published April 11, 2014 1 What is the real role of respiratory viruses in severe community-acquired pneumonia? Olli Ruuskanen 1 and Asko Järvinen 2 1 Department
MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
 MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSP There are no translations available. MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSP There are no translations available. MANAGEMENT OF FEVER IN PEDIATRIC PATIENTS FOLLOWING HEMATOPOIETIC STEM CELL TRANSPLANTATION
A Randomized Clinical Trial Comparing 6 EH vs 36H for TB Prevention in HIV-infected Adults in south India: Impact on Mortality
 A Randomized Clinical Trial Comparing 6 EH vs 36H for TB Prevention in HIV-infected Adults in south India: Impact on Mortality Soumya Swaminathan,, PA Menon,, P Venkatesan et al Indian Council of Medical
A Randomized Clinical Trial Comparing 6 EH vs 36H for TB Prevention in HIV-infected Adults in south India: Impact on Mortality Soumya Swaminathan,, PA Menon,, P Venkatesan et al Indian Council of Medical
Pneumocystis Pneumonia. Dr. Pradeep kumar II yr Pulmonary Medicine
 Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Pneumocystis Pneumonia Dr. Pradeep kumar II yr Pulmonary Medicine PNEUMOCYSTIS CARINII PNEUMONIA Pneumocystis carinii pneumonia (PCP), is commonly termed Pneumocystis jiroveci pneumonia, is the 2 nd most
Tarrant County Influenza Surveillance Weekly Report CDC Week 11: Mar 10-16, 2019
 Tarrant County Public Health Division of Epidemiology and Health Information Tarrant County Influenza Surveillance Weekly Report 11: Mar 10-16, 2019 Influenza Activity Code: County and State Levels Tarrant
Tarrant County Public Health Division of Epidemiology and Health Information Tarrant County Influenza Surveillance Weekly Report 11: Mar 10-16, 2019 Influenza Activity Code: County and State Levels Tarrant
Critically Ill Patients with Pandemic Influenza A/H1N at a Medical Center in Korea
 DOI: 10.4046/trd.2011.70.1.28 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2011;70:28-35 CopyrightC2011. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights reserved.
DOI: 10.4046/trd.2011.70.1.28 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2011;70:28-35 CopyrightC2011. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights reserved.
Haemophilus influenzae
 Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
Haemophilus influenzae type b Severe bacterial infection, particularly among infants During late 19th century believed to cause influenza Immunology and microbiology clarified in 1930s Haemophilus influenzae
pneumonia 2015;6:48 56
 pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
pneumonia 2015 Aug 21;6:48 56 pneumonia Brief Report Anne B Chang a,b, Heidi Smith-Vaughan a,c, Theo P Sloots f, Patricia C Valery a, David Whiley f, Jemima Beissbarth a, Paul J Torzillo d,e a Menzies
Clinical Outcomes of Lung Transplantation: Experience at Asan Medical Center
 Korean J Thorac Cardiovasc Surg 2018;51:22-28 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.1.22 Clinical Outcomes of Lung Transplantation: Experience
Korean J Thorac Cardiovasc Surg 2018;51:22-28 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) CLINICAL RESEARCH https://doi.org/10.5090/kjtcs.2018.51.1.22 Clinical Outcomes of Lung Transplantation: Experience
The Burden of Viruses in Pneumonia Associated With Acute Respiratory Failure An Underappreciated Issue
 [ Original Research ] The Burden of Viruses in Pneumonia Associated With Acute Respiratory Failure An Underappreciated Issue Andrew F. Shorr, MD, MPH; Kristen Fisher, MD; Scott T. Micek, PharmD; and Marin
[ Original Research ] The Burden of Viruses in Pneumonia Associated With Acute Respiratory Failure An Underappreciated Issue Andrew F. Shorr, MD, MPH; Kristen Fisher, MD; Scott T. Micek, PharmD; and Marin
2. Clinical Manifestations (Pediatric HIV Infection)
 Page 1 of 6 HOUSTON ROMANIA SOUTHERN AFRICA MEXICO HOME CONTACT Friday, July 25, 2003 Pediatric HIV Infection by Mark W. Kline, M.D. 1. Introduction 2. Clinical Manifestations 3. Diagnosis 2. Clinical
Page 1 of 6 HOUSTON ROMANIA SOUTHERN AFRICA MEXICO HOME CONTACT Friday, July 25, 2003 Pediatric HIV Infection by Mark W. Kline, M.D. 1. Introduction 2. Clinical Manifestations 3. Diagnosis 2. Clinical
The pages that follow contain information critical to protecting the health of your patients and the citizens of Colorado.
 Health Alert Network Tri-County Health Department Serving Adams, Arapahoe and Douglas Counties Phone 303/220-9200 Fax 303/741-4173 www.tchd.org Follow us on Twitter @TCHDHealth and @TCHDEmergency John
Health Alert Network Tri-County Health Department Serving Adams, Arapahoe and Douglas Counties Phone 303/220-9200 Fax 303/741-4173 www.tchd.org Follow us on Twitter @TCHDHealth and @TCHDEmergency John
Outpatient treatment in women with acute pyelonephritis after visiting emergency department
 LETTER TO THE EDITOR Korean J Intern Med 2017;32:369-373 Outpatient treatment in women with acute pyelonephritis after visiting emergency department Hee Kyoung Choi 1,*, Jin-Won Chung 2, Won Sup Oh 3,
LETTER TO THE EDITOR Korean J Intern Med 2017;32:369-373 Outpatient treatment in women with acute pyelonephritis after visiting emergency department Hee Kyoung Choi 1,*, Jin-Won Chung 2, Won Sup Oh 3,
2009 (Pandemic) H1N1 Influenza Virus
 2009 (Pandemic) H1N1 Influenza Virus September 15, 2009 Olympia, Washington Anthony A Marfin Washington State Department of Health Goals Understand current situation & pattern of transmission of 2009 H1N1
2009 (Pandemic) H1N1 Influenza Virus September 15, 2009 Olympia, Washington Anthony A Marfin Washington State Department of Health Goals Understand current situation & pattern of transmission of 2009 H1N1
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: The National Heart, Lung, and Blood Institute Acute Respiratory
CARE OF THE ADULT PNEUMONIA PATIENT
 Care Guideline CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: The target audience for this Care Guideline is all MultiCare providers and staff, including those associated with our clinically integrated
Care Guideline CARE OF THE ADULT PNEUMONIA PATIENT Target Audience: The target audience for this Care Guideline is all MultiCare providers and staff, including those associated with our clinically integrated
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Daraprim) Reference Number: CP.PMN.44 Effective Date: 11.01.15 Last Review Date: 08.18 Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this
Clinical Policy: (Daraprim) Reference Number: CP.PMN.44 Effective Date: 11.01.15 Last Review Date: 08.18 Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this
Corticosteroids in Severe CAP. Mervyn Mer Department of Medicine & ICU Johannesburg Hospital University of the Witwatersrand
 Corticosteroids in Severe CAP Mervyn Mer Department of Medicine & ICU Johannesburg Hospital University of the Witwatersrand Introduction Much controversy and debate regarding the use of corticosteroids
Corticosteroids in Severe CAP Mervyn Mer Department of Medicine & ICU Johannesburg Hospital University of the Witwatersrand Introduction Much controversy and debate regarding the use of corticosteroids
HAEMOPHILUS INFLUENZAE INVASIVE DISEASE
 23 Annual Morbidity Report HAEMOPHILUS INFLUENZAE INVASIVE DISEASE CRUDE DATA 35 Annual Incidence a LA County.37 California b. United States c.2 Age at Diagnosis Mean 4. years Median 36. years Range Birth
23 Annual Morbidity Report HAEMOPHILUS INFLUENZAE INVASIVE DISEASE CRUDE DATA 35 Annual Incidence a LA County.37 California b. United States c.2 Age at Diagnosis Mean 4. years Median 36. years Range Birth
Pneumocystis Pneumonia -- Los Angeles
 Pneumocystis Pneumonia -- Los Angeles As part of its commemoration of CDC's 50th anniversary, MMWR is reprinting selected MMWR articles of historical interest to public health, accompanied by a current
Pneumocystis Pneumonia -- Los Angeles As part of its commemoration of CDC's 50th anniversary, MMWR is reprinting selected MMWR articles of historical interest to public health, accompanied by a current
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids
 Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Treatment of Coccidioidomycosis-associated Eosinophilic Pneumonia with Corticosteroids Joshua Malo, MD Yuval Raz, MD Linda Snyder, MD Kenneth Knox, MD University of Arizona Medical Center Department of
Streptococcus pneumoniae CDC
 Streptococcus pneumoniae CDC Pneumococcal Disease Infection caused by the bacteria, Streptococcus pneumoniae» otitis media 20 million office visits (28-55% Strep)» pneumonia 175,000 cases annually» meningitis
Streptococcus pneumoniae CDC Pneumococcal Disease Infection caused by the bacteria, Streptococcus pneumoniae» otitis media 20 million office visits (28-55% Strep)» pneumonia 175,000 cases annually» meningitis
Methods ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE
 ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
ROLE OF OPEN LUNG BIOPSY IN PATIENTS WITH DIFFUSE LUNG INFILTRATES AND ACUTE RESPIRATORY FAILURE Li-Hui Soh, Chih-Feng Chian, Wen-Lin Su, Horng-Chin Yan, Wann-Cherng Perng, and Chin-Pyng Wu Background
