ABOUT MEN WILL BE
|
|
|
- Horatio Hodges
- 5 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION Comparison of ations by Urologists and Oncologists for Treatment of Clinically Localized Prostate Cancer Floyd J. Fowler, Jr, PhD Mary McNaughton Collins, MD, MPH Peter C. Albertsen, MD, MS Anthony Zietman, MD Diana B. Elliott, BA Michael J. Barry, MD ABOUT 0 00 MEN WILL BE diagnosed as having prostate cancer in the United States this year, most with clinically localized disease. The majority of these men will choose among primary therapies: radical prostatectomy, external beam radiotherapy, or brachytherapy. The choice among these therapies is not easy. Because most prostate cancers are found in men in their 60s and 0s, and because these cancers generally grow slowly, many prostate cancer patients are destined to die of competing medical problems. 2 For others, especially men with poorly differentiated tumors or high prostate-specific antigen (PSA) levels, these therapies may not be curative. Moreover, while cohort studies following surgery and external beam radiotherapy patients for 0 to years have been done, patients receiving contemporary brachytherapy have not been followed up that long. Meanwhile, all of these therapies have the potential to create adverse effects or complications. For editorial comment see p 2. Context Multiple treatment options are available for men with prostate cancer, but therapeutic recommendations may differ depending on the type of specialist they consult. Objective To define and contrast the distribution of management recommendations by urologists and radiation oncologists for a spectrum of men with prostate cancer. Design, Setting, and Participants Mail survey sent in 99 to a random sample of physicians in the United States, who were listed as urologists (response rate 6%, n=0) and radiation oncologists (response rate 6%, n=9) in the American Medical Association Registry of Physicians and practicing at least 20 hours per week. Main Outcome Measure Questionnaire addressing beliefs and practices regarding prostate cancer management. Results Forty-three percent of radiation oncologists vs 6% of urologists would recommend routine prostate-specific antigen testing for men aged 0 years and older. For men with moderately differentiated, clinically localized cancers, and a more than 0-year life expectancy, 9% of urologists chose radical prostatectomy as the preferred treatment option, while 2% of radiation oncologists believed surgery and external beam radiotherapy were equivalent treatments. For most tumor grades and prostate-specific antigen levels, both specialty groups were significantly more likely to recommend the treatment in their specialty than the other treatment. Both groups reported giving patients similar estimates of the risks of complications due to surgery and radiation. Neither group favored watchful waiting in their treatment management except for a subset of men with life expectancies of less than 0 years and cancers with very favorable prognoses (Gleason score of or and prostate-specific antigen level ng/ml). Conclusions Based on this study, while urologists and radiation oncologists do agree on a variety of issues regarding detection and treatment of prostate cancer, specialists overwhelmingly recommend the therapy that they themselves deliver. JAMA. 2000;2: Author Affiliations: Center for Survey Research, University of Massachusetts, Boston (Dr Fowler and Ms Elliott); Medical Practices Evaluation Center (Drs McNaughton Collins and Barry) and the Department of Oncology (Dr Zietman), Massachusetts General Hospital, Boston; and the Division of The clinical judgment of the physicians who counsel patients can play a critical role in the treatments chosen. In a 9 survey, urologists and radiation oncologists were asked what they personally would do if they were diagnosed as having clinically localized prostate cancer. In that survey, 9% of US urologists said they would choose a radical prostatectomy, while 92% of radiation oncologists said they would choose external beam radiotherapy. Urology, University of Connecticut Health Center, Farmington (Dr Albertsen). Corresponding Author and Reprints: Michael J. Barry, MD, Medical Practices Evaluation Center, Massachusetts General Hospital, 0 Staniford St, 9th Floor, Boston, MA 02 ( mbarry@partners.org) American Medical Association. All rights reserved. (Reprinted) JAMA, June 2, 2000 Vol 2, No. 2 2 Downloaded From: on /0/20
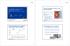
2 Table. Selected Respondent Characteristics Figure. ation of Routine Prostate-Specific Antigen (PSA) Testing for Men by Age % ing Routine PSA Testing Oncologists (n = 9) Urologists (n = 0) P = P<.00 P =.92 P< P< >0 Patient Age, y Obviously, depending on which physicians they consult, patients might well expect to get different counsel about optimal management. We were interested in extending our understanding of the differences between specialties beyond simply their preferences for treatment. We also P<.00 oncologists and urologists were asked: Do you recommend that primary care physicians include PSA testing as a part of the routine physical examination for men who are at average risk of prostate cancer, who are [each age group]? Oncologists, % (n = 9) Age, y Urologists, % (n = 0) P Value Sex Men 99 Women.00 Type of medical practice Solo 2 2 Single specialty group 0.00 Multispecialty group Average clinical time* Source of income Salaried 0 Mixture Fee-for-service Working at a hospital with a residency training program Yes 2 No 9 *Indicates the percentage of total professional time spent in clinical practice..0 wanted to see whether the different specialties continued to have such polar views regarding treatment 0 years later, well into the era of PSA testing. To these ends, in 99, we surveyed a nationwide random sample of practicing US urologists and radiation oncologists. METHODS A random sample of physicians who listed their specialty as either urology or radiation oncology were selected from the American Medical Association Master List of Physicians. Subsequently, the offices of the sampled physicians were contacted by telephone to verify the address and specialty, that they were not in residency training, and that they were in clinical practice for at least 20 hours weekly. Physicians then were sent a pretested questionnaire, a cover letter, and $0. A reminder postcard was sent to all sampled individuals; another survey instrument and cover letter were sent to nonrespondents after about weeks. Finally, for those physicians who had not responded to the questionnaire, follow-up telephone calls were made to the physicians offices to encourage response and to identify subjects who needed another questionnaire. The survey instrument for urologists contained questions about the diagnosis and treatment of benign prostatic hyperplasia and prostatitis, as well as prostate cancer. The instrument for radiation oncologists focused almost exclusively on prostate cancer. Whenever it made sense, comparable questions were asked of both specialties. RESULTS Questionnaires were returned by 6% of eligible radiation oncologists (n=9) and 6% of eligible urologists (n=0). TABLE compares the characteristics of the respondents in the 2 specialties. Responding urologists were older, more often male, more likely to be in solo practice, and less likely to be salaried. When respondents and nonrespondents were compared, using data from the file from which the sample was drawn, no significant differences were noted in terms of age or region of the country. Urologists who graduated from medical school less than 20 years previously were more likely to respond than earlier graduates. Physicians in multispecialty groups were also more likely to respond than physicians in solo practice in both specialties. FIGURE compares both groups of specialists answers to questions about their recommendations for routine PSA testing. For men up through age 0 years, members of the 2 specialties made similar recommendations. Urologists are slightly more aggressive about screening than radiation oncologists but significantly more aggressive when patients are men in their 0s. The clearer trend, however, is the much more aggressive stance of radiation oncologists regarding PSA testing for men 0 years and older, and particularly for men older than years. For example, while only 6% of urologists recommend routine PSA testing for men older than 0 years, % of the radiation oncologists do so. 2 JAMA, June 2, 2000 Vol 2, No. 2 (Reprinted) 2000 American Medical Association. All rights reserved. Downloaded From: on /0/20
3 FIGURE 2 presents these specialists beliefs about when aggressive treatments actually have a survival benefit. This figure presents the percentage of respondents saying that there is definitely or probably a survival benefit for each of the main therapies for men with clinically localized, moderately differentiated prostate cancer and less or more than a 0-year life expectancy, respectively. Although there are numerous statistically significant differences between the 2 groups given the large sample sizes, there is also considerable consistency in their answers. The majority of both groups of specialists think that all therapies have survival benefit for men with a 0-year or longer life expectancy; only a minority think there is benefit from any of the treatments for men with less than a 0-year life expectancy. More of both types of specialists, though, believe that radiation, either by external beam or brachytherapy, is more likely to offer a survival benefit for men with less than a 0-year life expectancy than a radical prostatectomy. Indeed, that perception is slightly but significantly more common among urologists than among radiation oncologists. Figure 2 also demonstrates that members of each specialty are generally somewhat more likely than those in the other specialty to believe in the efficacy of the treatments that they perform, and are also a little less positive about the survival benefits of the treatment offered by the other specialty group. TABLE 2 presents physicians responses to questions about head-tohead comparisons of the effectiveness of the major therapies. When comparing radical prostatectomy and external beam radiotherapy for patients with life expectancies of 0 years or longer, urologists are almost all convinced (9%) that radical prostatectomy is better. On the other hand, radiation oncologists perceptions (2%) are that surgery and radiotherapy are equivalent. Almost a third of urologists think neither treatment has survival value for men with less than a 0- year life expectancy, while only 9% of radiation oncologists agree. When deciding among treatment options, prostate cancer patients need to consider not only the effectiveness of the options at extending life, but also their adverse effects. Sexual dysfunction and incontinence are 2 potential adverse effects of aggressive therapy for prostate cancer. How are the likelihoods of these adverse effects presented to patients by urologists and radiation oncologists? TABLE presents the risks of these complications that the respondents said they quote to their patients. Table is most striking in how similarly the 2 groups estimate the probability of complications associated with surgery and radiation. Respondents were also asked to choose their preferred treatment for patients with tumors of varying Gleason scores and PSA levels. In FIGURE and FIGURE, the patient profiles are ordered based on the decreasing likelihood that such a cancer would be organconfined at surgical staging. 6 Subjects were given the options of expectant management (watchful waiting) and androgen deprivation (as primary therapy) in addition to the potentially curative therapies. For this analysis, both forms of radiotherapy were considered together. Both groups of specialists have some members (0%-20%) who are willing to consider watchful waiting for patients with cancers with Gleason scores Figure 2. Treatment Expectations for Clinically Organ-Confined, Moderate-Grade Prostate Cancers and Less or More Than 0-Year Life Expectancies Patients With Life Expectancy <0 y 6 9 Urologists (n = 0) Oncologists (n = 9) 22 Brachytherapy External Beam Radical Prostatectomy Patients With Life Expectancy 0 y % Who Say Treatments Have a Survival Benefit The left side of the figure shows the responses when asked: For a patient with clinically localized cancer (stage A or B, moderate grade), who has a life expectancy of less than 0 years, do you think that [name of treatment] as the primary therapy offers a survival benefit? The right side of the figure shows the responses when asked: For a patient with clinically localized cancer (stage A or B, moderate grade), whose life expectancy is clearly greater than 0 years, do you think [name of treatment] as the primary therapy offers a survival benefit? Table 2. Comparison of Treatments for Organ-Confined, Moderate-Grade Prostate Cancer* Comparison of Treatments (Patient Life Expectancy) Oncologists, % Urologists, % Radical prostatectomy vs external beam radiation ( 0 y) (n = 9) (n = 0) better 0 9 Both the same 6 0 Prostatectomy better 2 Neither offers survival benefit 9 2 Do not know 2 Radical prostatectomy vs external beam radiation ( 0 y) (n = 9) (n = 0) better 0 Both the same 2 6 Prostatectomy better 20 9 Neither offers survival benefit 0 Do not know 2 Brachytherapy vs external beam radiation ( 0 y) (n = ) (n = 9) Brachytherapy better 2 0 Both the same External beam radiation better Neither offers survival benefit 2 Do not know 20 *P.00 for all comparisons. Exact question wording: For a patient with clinically localized cancer (stage A or B, moderate grade), who has a life expectancy clearly [less or greater] than 0 years, how do you think [treatment and treatment 2] compare in terms of the survival benefit they offer? 2000 American Medical Association. All rights reserved. (Reprinted) JAMA, June 2, 2000 Vol 2, No Downloaded From: on /0/20
4 Table. Average Percentage Estimates of Chance for Loss of Sexual Function and Some Permanent Wetness for Various Prostate Cancer Treatment Options* Permanent Loss of Sexual Function, % Some Permanent Wetness, % Oncologists Urologists Oncologists Urologists Treatment (n = ) (n = 9) (n = 0) (n = ) External beam radiation Brachytherapy Non nerve-sparing prostatectomy Unilateral nerve-sparing prostatectomy Bilateral nerve-sparing prostatectomy *All differences between specialties were significant (P.0) with the exception of estimates for the permanent loss of sexual fuctioning for unilateral nerve-sparing prostatectomy (P =.99). The number of respondents differed slightly from question to question due to nonresponse. The numbers reflected are the maximum number of respondents to questions in this series. Exact question wording: A patient of yours with prostate cancer is 6 and has full sexual function and no sign of incontinence. What would you tell him his chances are of having loss of sexual functioning (permanent loss of the ability to have intercourse) and some incontinence (indefinitely experiencing leaking or wetness, enough to regularly wear a pad) for the following treatment options? Figure. ations of Androgen Deprivation and Watchful Waiting for Men With Clinically Localized Prostate Cancers 6 2 Urologists (n = 0) Oncologists (n = 9) 2 Gleason Score & PSA Level, ng/ml of or and PSA levels no higher than ng/ml. Beyond that low-risk subset, essentially no one in either group is willing to recommend watchful waiting (Figure ). As one would expect from the preceding data, the majority of both groups of specialists would recommend for most patients the therapy that they themselves deliver. However, there is a subset of radiation oncologists who indicated a preference for surgery for low-grade, low-psa tumors. There are very few urologists who prefer radiation for such tumors (Figure ). As Gleason scores reach or, both groups start to consider androgen deprivation as a primary therapy (Figure ). Urologists also begin to recommend radiation more often in relationship to surgery as Gleason scores and PSA levels increase (Figure ). As the probability of organ-confined disease decreases, urologists become divided about the value of surgery. For tumors with Gleason scores of or higher, or a Gleason score of with a high PSA level, they become as likely to recommend androgen deprivation or radiation as they do surgery. However, there is a substantial minority who continue to recommend surgery even when tumors are likely to be extracapsular. oncologists, on the other hand, continue to recommend radiation for higher-risk tumors. Finally, physicians were asked whether they believed that the main potentially curative prostate cancer therapies are overused or underused in the United States (TABLE ). A majority of radiation oncologists believe that radical prostatectomy is overused (2%), and about half think that radiation and brachytherapy are underused. In contrast, % of urologists think that radical prostatectomy is used at about the right rate and % think that external beam radiation is overused. Substantial percentages of both radiation oncologists and urologists believe that brachytherapy is both overused and underused, and a higher proportion express no opinion than for the other 2 primary therapies. COMMENT Although urologists and radiation oncologists differed in many of their beliefs regarding prostate cancer treatment, they also demonstrated agreement on a variety of issues. First, despite controversy over the value of PSA screening,, responding physicians in both these specialties are virtually unanimous in their recommendation that PSA testing be done routinely at least until around age years. For men older Androgen Deprivation Watchful Waiting The left side of the figure shows the responses recommending androgen deprivation treatment when asked: A prostate cancer patient of yours is 6, in good health, and has a negative digital rectal examination result and no evidence of extraprostatic spread. Which primary treatment would you be most likely to recommend for localized prostate cancer if this patient has the following biopsy results [list of Gleason/ PSA profiles]? The right side of the figure shows the responses recommending watchful waiting. than years, the 2 specialties differ, with radiation oncologists being considerably more positive about testing older men. This position is consistent with radiation oncologists perceptions that they have a therapy to offer that (according to nearly a majority) is beneficial to men even with less than a 0-year life expectancy. Second, despite the lack of published supporting evidence from randomized clinical trials, the vast majority of physicians in both specialties believe that all therapies offer a sur- 220 JAMA, June 2, 2000 Vol 2, No. 2 (Reprinted) 2000 American Medical Association. All rights reserved. Downloaded From: on /0/20
5 Figure. ations of Radical Prostatectomy and Therapy for Men With Clinically Localized Prostate Cancer Radical Prostatectomy Urologists (n = 0) Oncologists (n = 9) Gleason Score -6-6 & PSA Level, ng/ml External Beam The left side of the figure shows the responses recommending radical prostatectomy when asked: A prostate cancer patient of yours is 6, in good health, and has a negative digital rectal examination result and no evidence of extraprostatic spread. Which primary treatment would you be most likely to recommend for localized prostate cancer if this patient has the following biopsy results [list of Gleason/PSA profiles]? The right side of the figure shows the responses recommending external beam radiation. vival advantage for men with a 0- year or more life expectancy. Third, with respect to patients with less than a 0-year life expectancy, only a minority of members of either specialty thinks that any therapy offers a survival advantage. Within both groups, however, there are more physicians who think that radiation therapy offers a survival advantage than think that surgery does. Fourth, specialists generally agree on the probabilities of complications of all Table. Perceived Rates of Use of Treatments for Prostate Cancer* Treatment Oncologists Urologists Radical prostatectomy (n = 2) (n = 99) Overused 2 Underused 0 Used at about the right rate 6 No opinion 2 External beam (n = 2) (n = 99) radiation Overused Underused 0 Used at about the right rate No opinion 2 Brachytherapy (n = ) (n = 96) Overused 26 0 Underused 2 Used at about the right rate 20 2 No opinion 0 22 *P.00 for all comparisons. treatments. Both groups perceive surgery as being more likely to produce incontinence and sexual dysfunction than radiotherapy. Both urologists and radiation oncologists are generally convinced that nerve-sparing surgery substantially reduces the rate at which patients experience sexual dysfunction. Disagreements about probabilities of adverse effects, then, do not account for the differences in treatment recommendations noted between the specialties. Some recent studies actually suggest, however, that these estimated risks of complications for all treatments may be low, and particularly low for nerve-sparing radical prostatectomy. 9- Fifth, physicians from the 2 specialties are remarkably similar in the extent to which they would recommend either watchful waiting or androgen deprivation as primary therapies for particular subsets of men based on Gleason scores and PSA levels. Less than 2% of members of either specialty would recommend watchful waiting to men with a tumor with a Gleason score of, despite the fact that these patients appear to have an essentially normal life expectancy without aggressive treatment. Members of both specialties feel much more comfortable if patients with any degree of prostate cancer receive one of the major primary therapies. When the Gleason scores (-) and PSA levels ( 0 ng/ ml) are higher, increasing numbers in both specialties, eventually nearing half, would recommend androgen deprivation as the primary therapy. oncologists continue to recommend radiation for tumors with a higher likelihood of capsular penetration, while urologists appear more dubious about the value of surgery. This finding may reflect a difference in perspectives about when the 2 local therapies are likely to be still curative; that is, radiation oncologists may believe tumors with some degree of capsular penetration may still be effectively treated with radiation, while urologists may doubt that surgery will cure such tumors. Sixth, despite a relative shortage of long-term follow-up data, members of both specialties generally seem to accept brachytherapy as being at least as effective as external beam radiotherapy. Urologists seem to be slightly more positive about brachytherapy than about external beam radiation therapy. Of course, the most dramatic difference between these 2 groups of specialists is that members of each specialty tend to believe in the therapy that they themselves deliver. oncologists (2%) tend to believe that their therapy is just as good as radical prostatectomy for men with moderately differentiated, clinically localized cancer while urologists (9%) are overwhelmingly convinced that radical prostatectomy is better. This difference is critical in understanding what treatment recommendations patients are likely to hear. Presumably, the radiation therapists can justify their preference for recommending external beam radiotherapy on the basis that they believe it works just as well as surgery. In contrast, urologists believe that while men who have surgery do indeed have higher risks of sexual dysfunction and incontinence, cancer control is better with surgery, and thus radical prostatectomy is preferred American Medical Association. All rights reserved. (Reprinted) JAMA, June 2, 2000 Vol 2, No Downloaded From: on /0/20
6 While clinical trials have not proven that patient outcomes are improved by aggressive treatment with surgery or radiation, neither have they proven these treatments ineffective. Given our findings, it is also important to point out that the descriptions of the effectiveness of surgery and radiation therapy that patients receive from urologists and radiation oncologists would be expected to be quite different. Although some patients might find it confusing to hear quite different treatment recommendations from experienced physicians with access to the same medical literature, scheduling consultations with a member of each specialty may be the best approach to ensure that patients get a balanced picture regarding aggressive treatment options before making a decision. Neither group of specialists studied was supportive of expectant management for any but a limited subset of men; primary care physicians appear no more enthusiastic. Interestingly, however, when patients hear comprehensive presentations regarding the risks and benefits of all potential treatments, a substantial minority appears to choose expectant management. 6, Given that many more men are now being diagnosed as having prostate cancer than will ever die of it, expectant management would appear to be appropriate for some men. More research is needed to define those subgroups of men for whom an expectant approach is a reasonable, or even optimal, management strategy. An added challenge will be to ensure any such insights are effectively communicated to patients facing a treatment decision for prostate cancer. Funding/Support: This study was funded by grant HS 09 from the Agency for Healthcare Research and Quality (formerly the Agency for Health Care Policy and Research) to the Patient Outcomes Research Team. REFERENCES. Greenlee RT, Murray T, Bolden S, Wingo PA. Cancer statistics, CA Cancer J Clin. 2000;0:-. 2. Albertsen PC, Hanley JA, Gleason DF, Barry MJ. Competing risk analysis of men aged to years at diagnosis managed conservatively for clinically localized prostate cancer. JAMA. 99;20: Lu-Yao GL, Yao SL. Population-based study of longterm survival in patients with clinically localised prostate cancer. Lancet. 99;9: D Amico AV, Whittington R, Malkowicz B, et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA. 99;20: Moore MJ, O Sullivan BO, Tannock IF. How expert physicians would wish to be treated if they had genitourinary cancer. J Clin Oncol. 9;6: Partin AW, Kattan MW, Subong ENP, et al. Combination of prostate-specific antigen, clinical stage, and Gleason score to predict pathological stage of localized prostate cancer. JAMA. 99;2:-.. US Preventive Services Task Force. Screening for prostate cancer: commentary on the recommendations of the Canadian Task Force on the periodic health examination. Am J Prev Med. 99;0:- 9.. American College of Physicians. Screening for prostate cancer: Clinical Guideline, Part III. Ann Intern Med. 99;26: Fowler FJ, Barry MJ, Lu-Yao G, et al. Outcomes of external-beam radiation therapy for prostate cancer: a study of Medicare beneficiaries in three Surveillance, Epidemiology, and End Results areas. J Clin Oncol. 996;: Jonler M, Messing EM, Rhodes RP, et al. Sequelae of radical prostatectomy. Br J Urol. 99;: 2-.. Jonler M, Ritter MA, Brinkman R, et al. Sequelae of definitive radiation therapy for prostate cancer localized to the pelvis. Urology. 99;: Talcott JA, Rieker P, Propert KJ, et al. Patientreported impotence and incontinence after nervesparing radical prostatectomy. J Natl Cancer Inst. 99; 9:-2.. Stanford J, Feng Z, Hamilton A, et al. Urinary and sexual function after radical prostatectomy for clinically localized prostate cancer: The Prostate Cancer Outcomes Study. JAMA. 2000;2: Albertsen PC, Fryback DG, Storer BE, et al. Longterm survival among men with conservatively treated localized prostate cancer. JAMA. 99;2: Fowler FJ, Bin L, McNaughton Collins M, et al. Prostate cancer screening and beliefs about treatment efficacy: a national survey of primary care physicians and urologists. Am J Med. 99;0: Wilt TJ, Brawer MK. The Prostate cancer Intervention Versus Observation Trial (PIVOT). Oncology. 99;:-9.. Ontel E, Hamond C, Wasson JH, et al. Assessment of the feasibility and impact of shared decision making in prostate cancer. Urology. 99;: JAMA, June 2, 2000 Vol 2, No. 2 (Reprinted) 2000 American Medical Association. All rights reserved. Downloaded From: on /0/20
Outcomes With "Watchful Waiting" in Prostate Cancer in US Now So Good, Active Treatment May Not Be Better
 1 sur 5 19/09/2009 07:02 www.medscape.com From Medscape Medical News Outcomes With "Watchful Waiting" in Prostate Cancer in US Now So Good, Active Treatment May Not Be Better Zosia Chustecka September
1 sur 5 19/09/2009 07:02 www.medscape.com From Medscape Medical News Outcomes With "Watchful Waiting" in Prostate Cancer in US Now So Good, Active Treatment May Not Be Better Zosia Chustecka September
Information Content of Five Nomograms for Outcomes in Prostate Cancer
 Anatomic Pathology / NOMOGRAMS IN PROSTATE CANCER Information Content of Five Nomograms for Outcomes in Prostate Cancer Tarek A. Bismar, MD, 1 Peter Humphrey, MD, 2 and Robin T. Vollmer, MD 3 Key Words:
Anatomic Pathology / NOMOGRAMS IN PROSTATE CANCER Information Content of Five Nomograms for Outcomes in Prostate Cancer Tarek A. Bismar, MD, 1 Peter Humphrey, MD, 2 and Robin T. Vollmer, MD 3 Key Words:
TREATMENT OPTIONS FOR LOCALIZED PROSTATE CANCER: QUALITY-ADJUSTED LIFE YEARS AND THE EFFECTS OF LEAD-TIME
 ADULT UROLOGY TREATMENT OPTIONS FOR LOCALIZED PROSTATE CANCER: QUALITY-ADJUSTED LIFE YEARS AND THE EFFECTS OF LEAD-TIME VIBHA BHATNAGAR, SUSAN T. STEWART, WILLIAM W. BONNEY, AND ROBERT M. KAPLAN ABSTRACT
ADULT UROLOGY TREATMENT OPTIONS FOR LOCALIZED PROSTATE CANCER: QUALITY-ADJUSTED LIFE YEARS AND THE EFFECTS OF LEAD-TIME VIBHA BHATNAGAR, SUSAN T. STEWART, WILLIAM W. BONNEY, AND ROBERT M. KAPLAN ABSTRACT
Prostate Cancer Treatment for Economically Disadvantaged Men
 Prostate Cancer Treatment for Economically Disadvantaged Men A Comparison of County Hospitals and Private Providers J. Kellogg Parsons, MD, MHS 1,2 ; Lorna Kwan, MPH 3 ; Sarah E. Connor, MPH 4 ; David
Prostate Cancer Treatment for Economically Disadvantaged Men A Comparison of County Hospitals and Private Providers J. Kellogg Parsons, MD, MHS 1,2 ; Lorna Kwan, MPH 3 ; Sarah E. Connor, MPH 4 ; David
Helping you make better-informed decisions 1-5
 Helping you make better-informed decisions 1-5 The only test that provides an accurate assessment of prostate cancer aggressiveness A prognostic medicine product for prostate cancer. A common diagnosis
Helping you make better-informed decisions 1-5 The only test that provides an accurate assessment of prostate cancer aggressiveness A prognostic medicine product for prostate cancer. A common diagnosis
MORE THAN 140,000 men in the United States annually
 Time Course and Predictors of Symptoms After Primary Prostate Cancer Therapy By James A. Talcott, Judith Manola, Jack A. Clark, Irving Kaplan, Clair J. Beard, Sonya P. Mitchell, Ronald C. Chen, Michael
Time Course and Predictors of Symptoms After Primary Prostate Cancer Therapy By James A. Talcott, Judith Manola, Jack A. Clark, Irving Kaplan, Clair J. Beard, Sonya P. Mitchell, Ronald C. Chen, Michael
NICE BULLETIN Diagnosis & treatment of prostate cancer
 Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
Diagnosis & treatment of prostate cancer NICE provided the content for this booklet which is independent of any company or product advertised Diagnosis and treatment of prostate cancer Introduction In
Since the beginning of the prostate-specific antigen (PSA) era in the. Characteristics of Insignificant Clinical T1c Prostate Tumors
 2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
2001 Characteristics of Insignificant Clinical T1c Prostate Tumors A Contemporary Analysis Patrick J. Bastian, M.D. 1 Leslie A. Mangold, B.A., M.S. 1 Jonathan I. Epstein, M.D. 2 Alan W. Partin, M.D., Ph.D.
PSA testing in New Zealand general practice
 PSA testing in New Zealand general practice Ross Lawrenson, Charis Brown, Fraser Hodgson. On behalf of the Midland Prostate Cancer Study Group Academic Steering Goup: Zuzana Obertova, Helen Conaglen, John
PSA testing in New Zealand general practice Ross Lawrenson, Charis Brown, Fraser Hodgson. On behalf of the Midland Prostate Cancer Study Group Academic Steering Goup: Zuzana Obertova, Helen Conaglen, John
Prostate Cancer Screening. A Decision Guide
 Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Prostate Cancer Screening A Decision Guide This booklet was developed by the U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC). Is screening right for you?
Elevated PSA. Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017
 Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
Elevated PSA Dr.Nesaretnam Barr Kumarakulasinghe Associate Consultant Medical Oncology National University Cancer Institute, Singapore 9 th July 2017 Issues we will cover today.. The measurement of PSA,
BLADDER PROSTATE PENIS TESTICLES BE YO ND YO UR CA NC ER
 BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
BLADDER PROSTATE PENIS TESTICLES THE PROSTATE IS A SMALL, WALNUT-SIZED GLAND THAT IS PART OF THE MALE REPRODUCTIVE SYSTEM. IT RESTS BELOW THE BLADDER, IN FRONT OF THE RECTUM AND SURROUNDS PART OF THE URETHRA.
Mr PHIP No. 1 Prostate cancer: Should I be tested?
 Mr PHIP No. 1 cancer: Should I be tested? Having a large prostate doesn t increase your chances of having prostate cancer. No. 1 / 1 Key points cancer is the most common male cancer after skin cancer.
Mr PHIP No. 1 cancer: Should I be tested? Having a large prostate doesn t increase your chances of having prostate cancer. No. 1 / 1 Key points cancer is the most common male cancer after skin cancer.
A Competing Risk Analysis of Men Age Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer
 A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
A Competing Risk Analysis of Men Age 55-74 Years at Diagnosis Managed Conservatively for Clinically Localized Prostate Cancer Peter C. Albertsen, MD 1 James A. Hanley, PhD 2 Donald F.Gleason, MD, PhD 3
Prostate Cancer Incidence
 Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
Prostate Cancer: Prevention, Screening and Treatment Philip Kantoff MD Dana-Farber Cancer Institute Professor of fmedicine i Harvard Medical School Prostate Cancer Incidence # of patients 350,000 New Cases
The PSA debate. Question Answer Level of evidence and strength of recommendation
 THEME: Men s health forum The PSA debate Prostate cancer 1 Routine screening for prostate cancer with digital rectal examination (DRE), serum tumour markers or transabdominal ultrasound is not recommended
THEME: Men s health forum The PSA debate Prostate cancer 1 Routine screening for prostate cancer with digital rectal examination (DRE), serum tumour markers or transabdominal ultrasound is not recommended
ADVICE TO PATIENTS REQUESTING PSA MEASUREMENT FREQUENTLY-ASKED QUESTIONS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk ADVICE TO
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk ADVICE TO
Active surveillance for low-risk Prostate Cancer Compared with Immediate Treatment: A Canadian cost evaluation
 Active surveillance for low-risk Prostate Cancer Compared with Immediate Treatment: A Canadian cost evaluation Alice Dragomir, PhD Fabio Cury, MD Armen Aprikian, MD Introduction Clinical and economic burden
Active surveillance for low-risk Prostate Cancer Compared with Immediate Treatment: A Canadian cost evaluation Alice Dragomir, PhD Fabio Cury, MD Armen Aprikian, MD Introduction Clinical and economic burden
Advances and Challenges in Radiation Protection of Patients Modern Radiotherapy. Risk Acceptability
 Advances and Challenges in Radiation Protection of Patients Modern Radiotherapy Risk Acceptability Versailles, France December 2-4, 2009 Fred A. Mettler Jr. M.,D., M.P.H. New Mexico Federal Regional Medical
Advances and Challenges in Radiation Protection of Patients Modern Radiotherapy Risk Acceptability Versailles, France December 2-4, 2009 Fred A. Mettler Jr. M.,D., M.P.H. New Mexico Federal Regional Medical
ADVICE TO PATIENTS REQUESTING PSA MEASUREMENT
 Frequently-Asked Questions What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication of prostate cancer, is available to you if you want
Frequently-Asked Questions What is the aim of this leaflet? Prostate cancer is a serious condition. The PSA test, which can give an early indication of prostate cancer, is available to you if you want
Patient-Reported Impotence and Incontinence After Nerve-Sparing Radical Prostatectomy
 Patient-Reported Impotence and Incontinence After Nerve-Sparing Radical Prostatectomy James A. Talcott, Patricia Rieker, Kathleen J. Propert, Jack A. Clark, Kenneth I. Wishnow, Kevin R. Loughlin, Jerome
Patient-Reported Impotence and Incontinence After Nerve-Sparing Radical Prostatectomy James A. Talcott, Patricia Rieker, Kathleen J. Propert, Jack A. Clark, Kenneth I. Wishnow, Kevin R. Loughlin, Jerome
Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer
 Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Original Article Outcomes of Radical Prostatectomy in Thai Men with Prostate Cancer Sunai Leewansangtong, Suchai Soontrapa, Chaiyong Nualyong, Sittiporn Srinualnad, Tawatchai Taweemonkongsap and Teerapon
Quality of Life After Modern Treatment Options for Prostate Cancer Ronald Chen, MD, MPH
 Quality of Life After Modern Treatment Options I will be presenting some recently published data on the quality of life after modern treatment options for prostate cancer. My name is Dr. Ronald Chen. I'm
Quality of Life After Modern Treatment Options I will be presenting some recently published data on the quality of life after modern treatment options for prostate cancer. My name is Dr. Ronald Chen. I'm
An educational guide from Genomic Health
 Active Surveillance or Immediate Treatment? The Oncotype DX Prostate Cancer Assay helps you and your doctor choose with confidence. For more information, visit OncotypeDX.com. An educational guide from
Active Surveillance or Immediate Treatment? The Oncotype DX Prostate Cancer Assay helps you and your doctor choose with confidence. For more information, visit OncotypeDX.com. An educational guide from
Prostate Cancer: Is There Standard Treatment? Who has prostate cancer? In this article:
 Focus on CME at l Université de Montréal Prostate Cancer: Is There Standard Treatment? Pierre I. Karakiewicz, MD, FRCSC; Paul Perrotte, MD, FRCSC; Fred Saad, MD, FRCSC In this article: 1. Risk factors
Focus on CME at l Université de Montréal Prostate Cancer: Is There Standard Treatment? Pierre I. Karakiewicz, MD, FRCSC; Paul Perrotte, MD, FRCSC; Fred Saad, MD, FRCSC In this article: 1. Risk factors
THE UROLOGY GROUP
 THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
THE UROLOGY GROUP www.urologygroupvirginia.com 1860 Town Center Drive Suite 150/160 Reston, VA 20190 703-480-0220 19415 Deerfield Avenue Suite 112 Leesburg, VA 20176 703-724-1195 224-D Cornwall Street,
CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM
 RAPID COMMUNICATION CME ARTICLE CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM ALAN W. PARTIN, LESLIE A. MANGOLD, DANA M. LAMM, PATRICK C. WALSH, JONATHAN
RAPID COMMUNICATION CME ARTICLE CONTEMPORARY UPDATE OF PROSTATE CANCER STAGING NOMOGRAMS (PARTIN TABLES) FOR THE NEW MILLENNIUM ALAN W. PARTIN, LESLIE A. MANGOLD, DANA M. LAMM, PATRICK C. WALSH, JONATHAN
PCA MORTALITY VS TREATMENTS
 PCA MORTALITY VS TREATMENTS Terrence P McGarty White Paper No 145 July, 2017 In a recent NEJM paper the authors argue that there is no material difference between a prostatectomy and just "observation"
PCA MORTALITY VS TREATMENTS Terrence P McGarty White Paper No 145 July, 2017 In a recent NEJM paper the authors argue that there is no material difference between a prostatectomy and just "observation"
Mr PHIP No. 4 Life after treatment for localised prostate cancer
 Mr PHIP No. 4 Life after treatment for localised Mr Phip Mr Phip No. 4 / Key points PSA tests are used to monitor cancer control after treatment for. Your PSA drops more quickly after surgery than radiotherapy.
Mr PHIP No. 4 Life after treatment for localised Mr Phip Mr Phip No. 4 / Key points PSA tests are used to monitor cancer control after treatment for. Your PSA drops more quickly after surgery than radiotherapy.
Survival outcomes for men in rural and remote NSW. Trend in prostate cancer incidence and mortality rates in Australia. The prostate cancer conundrum
 7/8/20 7/8/20 Using PROMS to better understand prostate cancer outcomes: The NSW Prostate Cancer Care and Outcomes Study David Smith Research Fellow Cancer Research Division Monash Uni, 26 th June 20 Survival
7/8/20 7/8/20 Using PROMS to better understand prostate cancer outcomes: The NSW Prostate Cancer Care and Outcomes Study David Smith Research Fellow Cancer Research Division Monash Uni, 26 th June 20 Survival
Understanding the risk of recurrence after primary treatment for prostate cancer. Aditya Bagrodia, MD
 Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
Understanding the risk of recurrence after primary treatment for prostate cancer Aditya Bagrodia, MD Aditya.bagrodia@utsouthwestern.edu 423-967-5848 Outline and objectives Prostate cancer demographics
When to worry, when to test?
 Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Focus on CME at the University of Calgary Prostate Cancer: When to worry, when to test? Bryan J. Donnelly, MSc, MCh, FRCSI, FRCSC Presented at a Canadian College of Family Practitioner s conference (October
Consensus and Controversies in Cancer of Prostate BASIS FOR FURHTER STUDIES. Luis A. Linares MD FACRO Medical Director
 BASIS FOR FURHTER STUDIES Main controversies In prostate Cancer: 1-Screening 2-Management Observation Surgery Standard Laparoscopic Robotic Radiation: (no discussion on Cryosurgery-RF etc.) Standard SBRT
BASIS FOR FURHTER STUDIES Main controversies In prostate Cancer: 1-Screening 2-Management Observation Surgery Standard Laparoscopic Robotic Radiation: (no discussion on Cryosurgery-RF etc.) Standard SBRT
30-DAY FOLLOW-UP SURVEY (TELEPHONE TRANSCRIPT)
 30-DAY FOLLOW-UP SURVEY (TELEPHONE TRANSCRIPT) Hello, my name is . I m working with the doctors at the Jefferson Multidisciplinary Clinic. May I please speak to ? IF NOT THERE: Do you
30-DAY FOLLOW-UP SURVEY (TELEPHONE TRANSCRIPT) Hello, my name is . I m working with the doctors at the Jefferson Multidisciplinary Clinic. May I please speak to ? IF NOT THERE: Do you
PROSTATE CANCER SURVEILLANCE
 PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
PROSTATE CANCER SURVEILLANCE ESMO Preceptorship on Prostate Cancer Singapore, 15-16 November 2017 Rosa Nadal National Cancer Institute, NIH Bethesda, USA DISCLOSURE No conflicts of interest to declare
UCSF UC San Francisco Previously Published Works
 UCSF UC San Francisco Previously Published Works Title Patterns of practice in the United States: insights from CaPSURE on prostate cancer management. Permalink https://escholarship.org/uc/item/24j7405c
UCSF UC San Francisco Previously Published Works Title Patterns of practice in the United States: insights from CaPSURE on prostate cancer management. Permalink https://escholarship.org/uc/item/24j7405c
J Clin Oncol 28: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
VOLUME 28 NUMBER 1 JANUARY 1 2010 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Clinical Results of Long-Term Follow-Up of a Large, Active Surveillance Cohort With Localized Prostate Cancer
Prostate Cancer Case Study 1. Medical Student Case-Based Learning
 Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer Case Study 1 Medical Student Case-Based Learning The Case of Mr. Powers Prostatic Nodule The effervescent Mr. Powers is found by his primary care provider to have a prostatic nodule. You
Prostate Cancer: 2010 Guidelines Update
 Prostate Cancer: 2010 Guidelines Update James L. Mohler, MD Chair, NCCN Prostate Cancer Panel Associate Director for Translational Research, Professor and Chair, Department of Urology, Roswell Park Cancer
Prostate Cancer: 2010 Guidelines Update James L. Mohler, MD Chair, NCCN Prostate Cancer Panel Associate Director for Translational Research, Professor and Chair, Department of Urology, Roswell Park Cancer
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT
 MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
MODULE 8: PROSTATE CANCER: SCREENING & MANAGEMENT KEYWORDS: Prostate cancer, PSA, Screening, Radical Prostatectomy LEARNING OBJECTIVES At the end of this clerkship, the medical student will be able to:
Elsevier Editorial System(tm) for European Urology Manuscript Draft
 Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Elsevier Editorial System(tm) for European Urology Manuscript Draft Manuscript Number: EURUROL-D-13-00306 Title: Post-Prostatectomy Incontinence and Pelvic Floor Muscle Training: A Defining Problem Article
Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement
 Clinical Review & Education JAMA US Preventive Services Task Force RECOMMENDATION STATEMENT Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement US Preventive Services
Clinical Review & Education JAMA US Preventive Services Task Force RECOMMENDATION STATEMENT Screening for Prostate Cancer US Preventive Services Task Force Recommendation Statement US Preventive Services
The Royal Marsden. Prostate case study. Presented by Mr Alan Thompson Consultant Urological Surgeon
 Prostate case study Presented by Mr Alan Thompson Consultant Urological Surgeon 2 Part one Initial presentation A 62 year old male solicitor attends your GP surgery. He has rarely seen you over the last
Prostate case study Presented by Mr Alan Thompson Consultant Urological Surgeon 2 Part one Initial presentation A 62 year old male solicitor attends your GP surgery. He has rarely seen you over the last
Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer
 BRIEF COMMUNICATION Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer John L. Gore, Lorna Kwan, Steve P. Lee, Robert E. Reiter, Mark S.
BRIEF COMMUNICATION Survivorship Beyond Convalescence: 48-Month Quality-of-Life Outcomes After Treatment for Localized Prostate Cancer John L. Gore, Lorna Kwan, Steve P. Lee, Robert E. Reiter, Mark S.
Combined Reporting of Cancer Control and Functional Results of Radical Prostatectomy $
 European Urology European Urology 44 (2003) 656 660 Combined Reporting of Cancer Control and Functional Results of Radical Prostatectomy $ Laurent Salomon a,*, Fabien Saint a, Aristotelis G. Anastasiadis
European Urology European Urology 44 (2003) 656 660 Combined Reporting of Cancer Control and Functional Results of Radical Prostatectomy $ Laurent Salomon a,*, Fabien Saint a, Aristotelis G. Anastasiadis
INFORMED DECISION MAKING IN THE MANAGEMENT OF LOCALISED PROSTATE CANCER A POSITION STATEMENT ABOUT THIS POSITION STATEMENT DEVELOPMENT
 The Royal Australian and New Zealand College of Radiologists The Faculty of Radiation Oncology INFORMED DECISION MAKING IN THE MANAGEMENT OF LOCALISED PROSTATE CANCER A PATIENT-FOCUSED PERSPECTIVE A POSITION
The Royal Australian and New Zealand College of Radiologists The Faculty of Radiation Oncology INFORMED DECISION MAKING IN THE MANAGEMENT OF LOCALISED PROSTATE CANCER A PATIENT-FOCUSED PERSPECTIVE A POSITION
Chapter 2. Understanding My Diagnosis
 Chapter 2. Understanding My Diagnosis With contributions from Nancy L. Brown, Ph.D.,Palo Alto Medical Foundation Research Institute; and Patrick Swift, M.D., Alta Bates Comprehensive Cancer Program o Facts
Chapter 2. Understanding My Diagnosis With contributions from Nancy L. Brown, Ph.D.,Palo Alto Medical Foundation Research Institute; and Patrick Swift, M.D., Alta Bates Comprehensive Cancer Program o Facts
Management of Prostate Cancer
 Clinical Decisions Interactive at www.nejm.org Management of Prostate Cancer This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed by specific clinical
Clinical Decisions Interactive at www.nejm.org Management of Prostate Cancer This interactive feature addresses the diagnosis or management of a clinical case. A case vignette is followed by specific clinical
Prostate Cancer: from Beginning to End
 Prostate Cancer: from Beginning to End Matthew D. Katz, M.D. Assistant Professor Urologic Oncology Robotic and Laparoscopic Surgery University of Arkansas for Medical Sciences Winthrop P. Rockefeller Cancer
Prostate Cancer: from Beginning to End Matthew D. Katz, M.D. Assistant Professor Urologic Oncology Robotic and Laparoscopic Surgery University of Arkansas for Medical Sciences Winthrop P. Rockefeller Cancer
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION LESS IS MORE Risk Profiles and Treatment Patterns Among Men Diagnosed as Having Prostate Cancer and a Prostate-Specific Antigen Level Below 4. ng/ml Yu-Hsuan Shao, PhD; Peter C.
ORIGINAL INVESTIGATION LESS IS MORE Risk Profiles and Treatment Patterns Among Men Diagnosed as Having Prostate Cancer and a Prostate-Specific Antigen Level Below 4. ng/ml Yu-Hsuan Shao, PhD; Peter C.
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen).
 What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
What Is Prostate Cancer? Prostate cancer is the development of cancer cells in the prostate gland (a gland that produces fluid for semen). It is a very common cancer in men; some cancers grow very slowly,
Area offers new approach to detecting, diagnosing and treating prostate cancer. by ANDREA GABLE
 MAXIMIZING MEN S HEALTH Area offers new approach to detecting, diagnosing and treating prostate cancer by ANDREA GABLE From left, David Lowther, MD; Nayha Dixit; Leigh Collins; Erin Hutchinson; and Robert
MAXIMIZING MEN S HEALTH Area offers new approach to detecting, diagnosing and treating prostate cancer by ANDREA GABLE From left, David Lowther, MD; Nayha Dixit; Leigh Collins; Erin Hutchinson; and Robert
Measuring the value of healthcare activities. Susan Rollason, Director of Finance and Strategy
 Measuring the value of healthcare activities Susan Rollason, Director of Finance and Strategy Items covered What are we doing and why? What have we done so far? What challenges have we faced? What are
Measuring the value of healthcare activities Susan Rollason, Director of Finance and Strategy Items covered What are we doing and why? What have we done so far? What challenges have we faced? What are
Potency after unilateral nerve sparing surgery: a report on functional and oncological results of unilateral nerve sparing surgery
 Potency after unilateral nerve sparing surgery: a report on functional and oncological results of unilateral nerve sparing surgery F Van der Aa 1, S Joniau 1, D De Ridder 1 & H Van Poppel 1 * 1 Department
Potency after unilateral nerve sparing surgery: a report on functional and oncological results of unilateral nerve sparing surgery F Van der Aa 1, S Joniau 1, D De Ridder 1 & H Van Poppel 1 * 1 Department
PCSANM 2015 Seminar. Basic Knowledge: Test for Prostate Cancer. Jerry Cross. 15 item quiz, no grades given
 Basic Knowledge: Test for Prostate Cancer Jerry Cross 15 item quiz, no grades given Basic Knowledge: Test for Prostate Cancer From http://prostatesnatchers.blogspot.com/ January 27, 2015 BY MARK SCHOLZ,
Basic Knowledge: Test for Prostate Cancer Jerry Cross 15 item quiz, no grades given Basic Knowledge: Test for Prostate Cancer From http://prostatesnatchers.blogspot.com/ January 27, 2015 BY MARK SCHOLZ,
Preoperative Gleason score, percent of positive prostate biopsies and PSA in predicting biochemical recurrence after radical prostatectomy
 JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
JBUON 2013; 18(4): 954-960 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Gleason score, percent of positive prostate and PSA in predicting biochemical
FOR PATIENTS DIAGNOSED WITH EARLY-STAGE PROSTATE CANCER. Discover a test that can help you on your treatment journey
 FOR PATIENTS DIAGNOSED WITH EARLY-STAGE PROSTATE CANCER Discover a test that can help you on your treatment journey Jim G. Oncotype DX GPS patient navigating prostate cancer since 2014 Not all prostate
FOR PATIENTS DIAGNOSED WITH EARLY-STAGE PROSTATE CANCER Discover a test that can help you on your treatment journey Jim G. Oncotype DX GPS patient navigating prostate cancer since 2014 Not all prostate
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer
 Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
Factors Associated with Initial Treatment for Clinically Localized Prostate Cancer Preliminary Results from the National Program of Cancer Registries Patterns of Care Study (PoC1) NAACCR Annual Meeting
Prostate Cancer. Axiom. Overdetection Is A Small Issue. Reducing Morbidity and Mortality
 Overdetection Is A Small Issue (in the context of decreasing prostate cancer mortality rates and with appropriate, effective, and high-quality treatment) Prostate Cancer Arises silently Dwells in a curable
Overdetection Is A Small Issue (in the context of decreasing prostate cancer mortality rates and with appropriate, effective, and high-quality treatment) Prostate Cancer Arises silently Dwells in a curable
TOOKAD (padeliporfin) Patient Information Guide
 TOOKAD (padeliporfin) Patient Information Guide TOOKAD is used to treat low-risk localized prostate cancer This medicine is subject to additional monitoring. This will allow quick identification of new
TOOKAD (padeliporfin) Patient Information Guide TOOKAD is used to treat low-risk localized prostate cancer This medicine is subject to additional monitoring. This will allow quick identification of new
Causes of death in men with prostate cancer: an analysis of men from the Thames Cancer Registry
 Causes of death in men with prostate cancer: an analysis of 5 men from the Thames Cancer Registry Simon Chowdhury, David Robinson, Declan Cahill*, Alejo Rodriguez-Vida, Lars Holmberg and Henrik Møller
Causes of death in men with prostate cancer: an analysis of 5 men from the Thames Cancer Registry Simon Chowdhury, David Robinson, Declan Cahill*, Alejo Rodriguez-Vida, Lars Holmberg and Henrik Møller
Your Guide to Prostate Cancer
 Your Guide to Prostate Cancer If you face a diagnosis of prostate cancer, what s next? We can help. A prostate cancer diagnosis can be overwhelming. The good news is that while prostate cancer can be serious,
Your Guide to Prostate Cancer If you face a diagnosis of prostate cancer, what s next? We can help. A prostate cancer diagnosis can be overwhelming. The good news is that while prostate cancer can be serious,
The Selenium and Vitamin E Prevention Trial
 The largest-ever-prostate cancer prevention trial is now underway. The study will include a total of 32,400 men and is sponsored by the National Cancer Institute and a network of researchers known as the
The largest-ever-prostate cancer prevention trial is now underway. The study will include a total of 32,400 men and is sponsored by the National Cancer Institute and a network of researchers known as the
Prostate-Specific Antigen (PSA) Test
 Prostate-Specific Antigen (PSA) Test What is the PSA test? Prostate-specific antigen, or PSA, is a protein produced by normal, as well as malignant, cells of the prostate gland. The PSA test measures the
Prostate-Specific Antigen (PSA) Test What is the PSA test? Prostate-specific antigen, or PSA, is a protein produced by normal, as well as malignant, cells of the prostate gland. The PSA test measures the
The Prostate Cancer Surgery Tick List. Use these questions as starters for your first meeting with your prostate cancer surgeon.
 The Prostate Cancer Surgery Tick List Use these questions as starters for your first meeting with your prostate cancer surgeon. Print these out and had to your doctor at the start of your meeting. Tick
The Prostate Cancer Surgery Tick List Use these questions as starters for your first meeting with your prostate cancer surgeon. Print these out and had to your doctor at the start of your meeting. Tick
Radiation Therapy After Radical Prostatectomy
 Articles ISSN 1537-744X; DOI 10.1100/tsw.2004.93 Radiation Therapy After Radical Ali M. Ziada, M.D. and E. David Crawford, M.D. Division of Urology, University of Colorado, Denver, Colorado E-mails: aziada@mednet3.camed.eun.eg
Articles ISSN 1537-744X; DOI 10.1100/tsw.2004.93 Radiation Therapy After Radical Ali M. Ziada, M.D. and E. David Crawford, M.D. Division of Urology, University of Colorado, Denver, Colorado E-mails: aziada@mednet3.camed.eun.eg
IQSS 2019 QCDR and MIPS Measure Specifications
 IQSS1 Hypogonadism: Serum T, CBC, PSA, IPSS within 6 months of Rx Percentage of patients with a Effective Clinical Patients with documented new diagnosis of hypogonadism receiving androgen replacement
IQSS1 Hypogonadism: Serum T, CBC, PSA, IPSS within 6 months of Rx Percentage of patients with a Effective Clinical Patients with documented new diagnosis of hypogonadism receiving androgen replacement
BY PEGGY EASTMAN BETHESDA, MD A multidisciplinary panel of independent experts has concluded in a draft statement that
 Advertisement Wolters Kluwer Health Logo Login Register Subscribe etoc Help Enter Keywords Search Advanced Search Saved Searches HomePrevious IssuesBlogsCollectionsCEPodcastsInfo & Services Home > Blogs
Advertisement Wolters Kluwer Health Logo Login Register Subscribe etoc Help Enter Keywords Search Advanced Search Saved Searches HomePrevious IssuesBlogsCollectionsCEPodcastsInfo & Services Home > Blogs
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer
 Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
Guidelines for the Management of Prostate Cancer West Midlands Expert Advisory Group for Urological Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory Group
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options
 AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
AFTER DIAGNOSIS: PROSTATE CANCER Understanding Your Treatment Options INTRODUCTION This booklet describes how prostate cancer develops, how it affects the body and the current treatment methods. Although
PROSTATE CANCER: Meeting a Community Need
 outcomes REPORT 2017 PROSTATE CANCER: Meeting a Community Need 1 in 6 men will be diagnosed with prostate cancer in their lifetime. 1 southnassau.org/cancer outcomes REPORT 2017 Within the primary service
outcomes REPORT 2017 PROSTATE CANCER: Meeting a Community Need 1 in 6 men will be diagnosed with prostate cancer in their lifetime. 1 southnassau.org/cancer outcomes REPORT 2017 Within the primary service
PET imaging of cancer metabolism is commonly performed with F18
 PCRI Insights, August 2012, Vol. 15: No. 3 Carbon-11-Acetate PET/CT Imaging in Prostate Cancer Fabio Almeida, M.D. Medical Director, Arizona Molecular Imaging Center - Phoenix PET imaging of cancer metabolism
PCRI Insights, August 2012, Vol. 15: No. 3 Carbon-11-Acetate PET/CT Imaging in Prostate Cancer Fabio Almeida, M.D. Medical Director, Arizona Molecular Imaging Center - Phoenix PET imaging of cancer metabolism
NIH Public Access Author Manuscript World J Urol. Author manuscript; available in PMC 2012 February 1.
 NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
NIH Public Access Author Manuscript Published in final edited form as: World J Urol. 2011 February ; 29(1): 11 14. doi:10.1007/s00345-010-0625-4. Significance of preoperative PSA velocity in men with low
PSA Screening and Prostate Cancer. Rishi Modh, MD
 PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
PSA Screening and Prostate Cancer Rishi Modh, MD ABOUT ME From Tampa Bay Went to Berkeley Prep University of Miami for Undergraduate - 4 years University of Miami for Medical School - 4 Years University
HIGH MORTALITY AND POOR SURVIVAL OF MEN WITH PROSTATE CANCER IN RURAL AND REMOTE AUSTRALIA
 HIGH MORTALITY AND POOR SURVIVAL OF MEN WITH PROSTATE CANCER IN RURAL AND REMOTE AUSTRALIA The prostate is a small gland the size of a walnut which produces fluid to protect and lubricate the sperm It
HIGH MORTALITY AND POOR SURVIVAL OF MEN WITH PROSTATE CANCER IN RURAL AND REMOTE AUSTRALIA The prostate is a small gland the size of a walnut which produces fluid to protect and lubricate the sperm It
Detection & Risk Stratification for Early Stage Prostate Cancer
 Detection & Risk Stratification for Early Stage Prostate Cancer Andrew J. Stephenson, MD, FRCSC, FACS Chief, Urologic Oncology Glickman Urological and Kidney Institute Cleveland Clinic Risk Stratification:
Detection & Risk Stratification for Early Stage Prostate Cancer Andrew J. Stephenson, MD, FRCSC, FACS Chief, Urologic Oncology Glickman Urological and Kidney Institute Cleveland Clinic Risk Stratification:
Technology appraisal guidance Published: 21 November 2018 nice.org.uk/guidance/ta546
 Padeliporfin for untreated localised prostate cancer Technology appraisal guidance Published: 21 November 2018 nice.org.uk/guidance/ta546 NICE 2019. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Padeliporfin for untreated localised prostate cancer Technology appraisal guidance Published: 21 November 2018 nice.org.uk/guidance/ta546 NICE 2019. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Prostate Cancer Dashboard
 Process Risk Assessment Risk assessment: family history assessment of family history of prostate cancer Best Observed: 97 %1 ; Ideal Benchmark:100% measure P8 2 Process Appropriateness of Care Pre-treatment
Process Risk Assessment Risk assessment: family history assessment of family history of prostate cancer Best Observed: 97 %1 ; Ideal Benchmark:100% measure P8 2 Process Appropriateness of Care Pre-treatment
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #102 (NQF 0389): Prostate Cancer: Avoidance of Overuse of Bone Scan for Staging Low Risk Prostate Cancer Patients National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS
Quality ID #102 (NQF 0389): Prostate Cancer: Avoidance of Overuse of Bone Scan for Staging Low Risk Prostate Cancer Patients National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS
PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS
 ADULT UROLOGY PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS ABRAHAM MORGENTALER AND ERNANI LUIS RHODEN ABSTRACT Objectives. To determine
ADULT UROLOGY PREVALENCE OF PROSTATE CANCER AMONG HYPOGONADAL MEN WITH PROSTATE-SPECIFIC ANTIGEN LEVELS OF 4.0 ng/ml OR LESS ABRAHAM MORGENTALER AND ERNANI LUIS RHODEN ABSTRACT Objectives. To determine
EAU 2009: US Study Shows No Mortality Benefit From Prostate Cancer Screening, But European Study Suggests There May Be One
 From Medscape Medical News : www.medscape.com/viewarticle/589786 EAU 2009: US Study Shows No Mortality Benefit From Prostate Cancer Screening, But European Study Suggests There May Be One By Roxanne Nelson
From Medscape Medical News : www.medscape.com/viewarticle/589786 EAU 2009: US Study Shows No Mortality Benefit From Prostate Cancer Screening, But European Study Suggests There May Be One By Roxanne Nelson
Questions and Answers About the Prostate-Specific Antigen (PSA) Test
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Questions and Answers
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Questions and Answers
Division of Urologic Surgery and Duke Prostate Center (DPC), Duke University School of Medicine, Durham, NC
 LHRH AGONISTS: CONTEMPORARY ISSUES The Evolving Definition of Advanced Prostate Cancer Judd W. Moul, MD, FACS Division of Urologic Surgery and Duke Prostate Center (DPC), Duke University School of Medicine,
LHRH AGONISTS: CONTEMPORARY ISSUES The Evolving Definition of Advanced Prostate Cancer Judd W. Moul, MD, FACS Division of Urologic Surgery and Duke Prostate Center (DPC), Duke University School of Medicine,
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER?
 PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
PROSTATE CANCER 101 WHAT IS PROSTATE CANCER? Prostate cancer is cancer that begins in the prostate. The prostate is a walnut-shaped gland in the male reproductive system located below the bladder and in
Newer Aspects of Prostate Cancer Underwriting
 Newer Aspects of Prostate Cancer Underwriting Presented By: Jack Swanson, M.D. Keith Hoffman, NFP Moments Made Possible Objectives To review and discuss Conflicting messages about PSA testing Cautions
Newer Aspects of Prostate Cancer Underwriting Presented By: Jack Swanson, M.D. Keith Hoffman, NFP Moments Made Possible Objectives To review and discuss Conflicting messages about PSA testing Cautions
PROSTATE CANCER CONTENT CREATED BY. Learn more at
 PROSTATE CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Ask your doctor about screening and treatment options. WHAT IS PROSTATE CANCER? 4 WATCHFUL
PROSTATE CANCER CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Ask your doctor about screening and treatment options. WHAT IS PROSTATE CANCER? 4 WATCHFUL
Prostate Cancer UK Best Practice Pathway: ACTIVE SURVEILLANCE
 Prostate Cancer UK Best Practice Pathway: ACTIVE SURVEILLANCE Low risk localised PSA < 10 ng/ml and Gleason score 6, and clinical stage T1 - T2a Intermediate risk localised PSA 10-20 ng/ml, or Gleason
Prostate Cancer UK Best Practice Pathway: ACTIVE SURVEILLANCE Low risk localised PSA < 10 ng/ml and Gleason score 6, and clinical stage T1 - T2a Intermediate risk localised PSA 10-20 ng/ml, or Gleason
of Nebraska - Lincoln
 University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln U.S. Department of Veterans Affairs Staff Publications U.S. Department of Veterans Affairs 8-2000 Detection, Characterization,
University of Nebraska - Lincoln DigitalCommons@University of Nebraska - Lincoln U.S. Department of Veterans Affairs Staff Publications U.S. Department of Veterans Affairs 8-2000 Detection, Characterization,
A Decision Analysis Using Individual Patient Preferences to Determine Optimal Treatment for Localized Prostate Cancer
 This is a preprint of an article accepted for publication in CANCER Copyright (2007), American Cancer Society, Inc. A Decision Analysis Using Individual Patient Preferences to Determine Optimal Treatment
This is a preprint of an article accepted for publication in CANCER Copyright (2007), American Cancer Society, Inc. A Decision Analysis Using Individual Patient Preferences to Determine Optimal Treatment
QUESTIONS TO ASK A UROLOGIST
 QUESTIONS TO ASK A UROLOGIST For the patient: You should review these questions and determine if the answers would satisfy a better understanding of what to expect and ease your concerns. If there are
QUESTIONS TO ASK A UROLOGIST For the patient: You should review these questions and determine if the answers would satisfy a better understanding of what to expect and ease your concerns. If there are
MATERIALS AND METHODS
 Primary Triple Androgen Blockade (TAB) followed by Finasteride Maintenance (FM) for clinically localized prostate cancer (CL-PC): Long term follow-up and quality of life (QOL) SJ Tucker, JN Roundy, RL
Primary Triple Androgen Blockade (TAB) followed by Finasteride Maintenance (FM) for clinically localized prostate cancer (CL-PC): Long term follow-up and quality of life (QOL) SJ Tucker, JN Roundy, RL
Types of Prostate Radiation Data Points # 16
 Changes across time and geography in the use of prostate radiation technologies for newly diagnosed older cancer patients: 2006-2008 Types of Prostate Radiation Data Points # 16 Prostate cancer is the
Changes across time and geography in the use of prostate radiation technologies for newly diagnosed older cancer patients: 2006-2008 Types of Prostate Radiation Data Points # 16 Prostate cancer is the
Oncology member story: Barbara
 Oncology member story: Barbara The results from an initial mammogram concerned doctors enough that Barbara* was scheduled for a follow-up appointment for further investigation. A few months later, a sonogram
Oncology member story: Barbara The results from an initial mammogram concerned doctors enough that Barbara* was scheduled for a follow-up appointment for further investigation. A few months later, a sonogram
Percent Gleason pattern 4 in stratifying the prognosis of patients with intermediate-risk prostate cancer
 Review Article Percent Gleason pattern 4 in stratifying the prognosis of patients with intermediate-risk prostate cancer Meenal Sharma 1, Hiroshi Miyamoto 1,2,3 1 Department of Pathology and Laboratory
Review Article Percent Gleason pattern 4 in stratifying the prognosis of patients with intermediate-risk prostate cancer Meenal Sharma 1, Hiroshi Miyamoto 1,2,3 1 Department of Pathology and Laboratory
Treatment Failure After Primary and Salvage Therapy for Prostate Cancer
 307 Treatment Failure After Primary and Salvage Therapy for Prostate Cancer Likelihood, Patterns of Care, and Outcomes Piyush K. Agarwal, MD 1 Natalia Sadetsky, MD, MPH 2 Badrinath R. Konety, MD, MBA 2
307 Treatment Failure After Primary and Salvage Therapy for Prostate Cancer Likelihood, Patterns of Care, and Outcomes Piyush K. Agarwal, MD 1 Natalia Sadetsky, MD, MPH 2 Badrinath R. Konety, MD, MBA 2
PROSTATE CANCER Amit Gupta MD MPH
 PROSTATE CANCER Amit Gupta MD MPH Depts. of Urology and Epidemiology Amit-Gupta-1@uiowa.edu dramitgupta@gmail.com Tel: 319-384-5251 OUTLINE PSA screening controversy How to use PSA more effectively Treatment
PROSTATE CANCER Amit Gupta MD MPH Depts. of Urology and Epidemiology Amit-Gupta-1@uiowa.edu dramitgupta@gmail.com Tel: 319-384-5251 OUTLINE PSA screening controversy How to use PSA more effectively Treatment
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY
 BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
BIOCHEMICAL RECURRENCE POST RADICAL PROSTATECTOMY AZHAN BIN YUSOFF AZHAN BIN YUSOFF 2013 SCENARIO A 66 year old man underwent Robotic Radical Prostatectomy for a T1c Gleason 4+4, PSA 15 ng/ml prostate
Erectile Function Before and After Non-Nerve-Sparing Retropubic Radical Prostatectomy
 Archives of Urology ISSN: 2638-5228 Volume 1, Issue 2, 2018, PP: 5-9 Erectile Function Before and After Non-Nerve-Sparing Retropubic Radical Prostatectomy Jørgen Bjerggaard Jensen, MD 1, Jørgen K. Johansen,
Archives of Urology ISSN: 2638-5228 Volume 1, Issue 2, 2018, PP: 5-9 Erectile Function Before and After Non-Nerve-Sparing Retropubic Radical Prostatectomy Jørgen Bjerggaard Jensen, MD 1, Jørgen K. Johansen,
Treating Prostate Cancer
 Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Treating Prostate Cancer A Guide for Men With Localized Prostate Cancer Most men have time to learn about all the options for treating their prostate cancer. You have time to talk with your family and
Impact of PSA Screening on Prostate Cancer Incidence and Mortality in the US
 Impact of PSA Screening on Prostate Cancer Incidence and Mortality in the US Deaths per 100,000 Ruth Etzioni Fred Hutchinson Cancer Research Center JASP Symposium, Montreal 2006 Prostate Cancer Incidence
Impact of PSA Screening on Prostate Cancer Incidence and Mortality in the US Deaths per 100,000 Ruth Etzioni Fred Hutchinson Cancer Research Center JASP Symposium, Montreal 2006 Prostate Cancer Incidence
