Citation for published version (APA): Lutke Holzik, M. F. (2007). Genetic predisposition to testicular cancer s.n.
|
|
|
- Dinah Green
- 5 years ago
- Views:
Transcription
1 University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version below. Document Version Publisher's PDF, also known as Version of record Publication date: 2007 Link to publication in University of Groningen/UMCG research database Citation for published version (APA): Lutke Holzik, M. F. (2007). Genetic predisposition to testicular cancer s.n. Copyright Other than for strictly personal use, it is not permitted to download or to forward/distribute the text or part of it without the consent of the author(s) and/or copyright holder(s), unless the work is under an open content license (like Creative Commons). Take-down policy If you believe that this document breaches copyright please contact us providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from the University of Groningen/UMCG research database (Pure): For technical reasons the number of authors shown on this cover page is limited to 0 maximum. Download date:
2 Chapter, aim and outline of the thesis
3 , aim and outline of the thesis Testicular tumours can be divided into germ cell tumours, stromal tumours and other tumours (e.g. malignant lymphomas). Tumours of paratesticular structures form a separate group. The research in this thesis focused solely on the testicular germ cell tumours (TGCT) seminoma and non-seminoma. TGCT are rare, but they are the most frequently occurring tumour in men aged between 5 and 40 years. In the Netherlands, 536 men were diagnosed with TGCT in 2003, while in 2004, 30 men died of this malignancy. Although the incidence of TGCT has increased sharply in recent years, survival of patients with TGCT has improved enormously. Five year survival in the nineteen seventies was about 65% compared to more than 90% at present (Figures and 2). () Improved survival can chiefly be attributed to the cisplatin-based polychemotherapy that was introduced in the nineteen eighties to treat patients with metastasized TGCT. In addition, new strategies have been developed in the surgical approach to metastasized/non-metastasized TGCT and alterations have been made to the radiotherapy technique and radiation dose for seminoma. (2;3) The progress in diagnosis, treatment and the subsequent treatment outcomes in patients with TGCT are the ultimate result of multidisciplinary team work. At the University Medical Center Groningen (UMCG), this multidisciplinary approach was started at the end of the nineteen seventies to provide every patient with tailored treatment. These accomplishments in the treatment of TGCT have led to the present goal of further optimising the treatment for TGCT, Figure : Incidence of TGCT 2 3
4 Figure 2: Survival of TGCT in which the research and treatment chiefly concentrate on reducing the toxic side-effects of chemotherapy and radiotherapy. In patients with prognostically favourable factors (Table 2) (4), the number of courses of chemotherapy can be reduced, whereas in patients with prognostically unfavourable factors, more intensive chemotherapy is necessary to improve the chances of survival. Nowadays the majority of TGCT patients can be cured by the multidisciplinary treatment. Therefore, the number of TGCT survivors will continue to increase. In principle, these TGCT survivors will be exposed to the long-term consequences of chemotherapy-related toxicity (side-effects) cq the long-term side-effects of radiotherapy. TGCT survivors are mostly young men who can be expected to have a long life ahead of them. This has meant that over the past few years, scientific research has centred on studying the long-term effects of treatment (5-8) and the quality of life of these TGCT survivors. (9) All this research has the ultimate aim of achieving further improvement in the treatment and follow-up of TGCT patients. The genetic background of TGCT Carcinoma in situ (CIS) (or intra-tubular germ cell neoplasia) is the precursor of TGCT and is found in nearly all TGCT together with an invasive component. CIS cells originate from primordial germ cells that escaped normal differentiation in utero. It is assumed that over the course of time, CIS develops into an invasive TGCT, but the precise transformation of premalignant CIS into a TGCT is not yet clear. It is suggested that the default pathway follows the development of CIS into seminoma and that non-seminoma requires activation of pluripotency (reprogramming) Figure and 2 from: Signaleringsrapport kanker: () of a CIS or seminoma cell. (0;) A theoretical model of TGCT development as part of testicular dysgenesis, taking into account a range of reported TGCT risk factors, has been developed by Skaekebaek et al (2) and is discussed in subsequent chapters. In recent years several studies have looked into chromosomal abnormalities and more recently at gene mutations and gene activity in TGCT to unravel the molecular pathways underlying these tumours. A detailed overview of (non-inherited) genomic aberrations in TGCT was recently published by Von Eyben. (3) Aneuploidy has been found in nearly all cases and triploidy is a common finding. Seminoma have a mean hypertriploid DNA index and non-seminoma have a mean hypotriploid DNA index (due to loss of chromosomal material during cancer progression). () When looking at individual chromosomal regions, an isochromosome of the short arm of chromosome 2, i(2p), (resulting in a duplication of the short arm of chromosome 2) is found in about 80% of TGCT. The remainder have excess 2p genetic material in derivative chromosomes. (4) The exact relation between these changes and TGCT is unclear but the absence of amplification of a section of 2p in intratubular germ cell neoplasia, suggests that this amplification may be related to progression of the disease rather than initiation. (5) A recent gene expression profile study on TGCT material identified differentiated expressed genes on 2p. Seventy-three genes on 2p were significantly overexpressed, indicating that the p arm of chromosome 2 may play an important role in TGCT tumorigenesis. (6) In addition to the genes located on 2p, a growing list of genes is implicated in the various stages of TGCT development. In particular, TGCT has been shown to be associated with a characteristic series of abnormalities in the retinoblastoma pathway including upregulation of cyclin D2 and p27 and downregulation of RB and the cyclin-dependent kinase inhibitors of p6, p8, p9 and p2. (3) A gain of activity of the KIT gene, a member of the tyrosine kinase family, appears to play a role in the progression of CIS towards seminomas. (7) Recently, the scope of genetic study of TGCT has been extended to include the role of naturally occurring micro RNAs (mirnas). Indeed, some of these mirnas (mirna-372 and 373) were shown to allow tumorigenic growth. As they have also been observed to be expressed in human seminomas and non-seminomas, but not in normal testicular tissue, it has been suggested that these mirna may represent a new class of oncogenes involved in TGCT. (8) Studies of hereditary genetic changes and TGCT are widely discussed in the subsequent chapters. Histology TGCT can be divided into two important histological subtypes: seminoma and non-seminoma. Pure seminoma occurs in about 50% of the cases and often (in 20%) contains trophoblastic giant cells that can produce beta-human chorionic gonadotrophin (ß-HCG). Non-seminoma chiefly comprises two or more cell types, for example embryonal carcinoma, choriocarcinoma (also contains trophoblastic giant cells), yolk sac tumour, teratoma, whether or not in combination with seminoma. Embryonal carcinoma and yolk sac tumour elements are associated with the production of alpha-fetoprotein (AFP). Clinically, there are three important tumour markers in the diagnosis and follow-up of TGCT: ß-HCG, alpha-fetoprotein (AFP) and lactate dehydrogenase (LDH). (2) 4 5
5 Clinical presentation and initial therapy Patients who present with a painless swelling of the testicle and increased levels of AFP, ß-HCG and/or LDH have a TGCT until proven otherwise. Clinical presentation varies widely. TGCT can also show extra-testicular clinical manifestation (without any testicular complaints). Retroperitoneal lymph node metastases can cause (lower) back pain, while haemoptysis can be the result of pulmonary metastases. Ultrasound examination of the testicle is useful to establish possible testicular abnormalities. Radical inguinal orchidectomy with high ligation of the spermatic cord, blood vessels and lymph vessels is the surgical treatment for patients who are suspected of having a TGCT. Originally, the testicles descend embryologically via the retroperitoneal route and inguinal canal into the scrotum. This often results in regional metastases from a TGCT that first arise in the retroperitoneal lymph nodes. A right-sided TGCT tends to metastasize to the inter-aorto-caval lymph nodes, whereas a left-sided TGCT tends to metastasize to the para-aortal lymph nodes. At a higher, supradiaphragmatic level, metastases can spread via the thoracic duct and result in mediastinal or supraclavicular metastases. Haematogenically, TGCT chiefly metastasize to the lungs, later to the liver, the skeleton and the cerebrum. (3;9) Staging When a patient has been diagnosed with a TGCT, the malignancy must be staged. This can be done by means of tumour markers (AFP and ß-HCG, LDH) and spiral CT (computed tomography) scanning of the lungs, the retroperitoneum and pelvis. On indication (anamnestic complaints of the cerebrum and/or sharply elevated ß-HCG), CT scanning of the cerebrum is conducted. Table : Royal Marsden staging classification of testicular germ cell tumours Stage Criteria Stage I No evidence of metastases Stage IM No clinical evidence of metastases, but persistent elevation of serum tumour markers AFP and/or hcg Stage II Infradiaphragmatic lymph node metastases IIA Metastases < 2 cm in diameter IIB Metastases 2-5 cm in diameter IIC Metastases > 5 cm in diameter Stage III Supradiaphragmatic lymph node metastases; Status A, B, C as for stage II Stage IV Extra lymphatic metastases L < - 3 Lung metastases L2 > 3 Lung metastases, all < - 2 cm in diameter L3 > 3 Lung metastases, one or more > 2 cm in diameter H+, Br+, Bo+ Liver, brain, or bone metastases The roles and/or additional value of magnetic resonance imaging (MRI) and positron emission tomography (PET) are currently under investigation. (20) At the UMCG, patients with TGCT are staged according to the Royal Marsden classification (Table ). Patients with stage I have no radiological or biochemical evidence of metastases. Patients with stages II to IV have metastasized disease. These patients are subsequently classified according to the prognostic factors formulated by the International Germ Cell Cancer Collaborative Group (IGCCCG) (Table 2) and a treatment plan is drawn up on the basis of the subgroup classification (good / intermediate / poor). (4) Table 2: IGCCCG prognostic classification for germ cell cancer (4) Non-seminoma Seminoma Good prognosis Testis / retroperitoneal primary Any primary site and No non-pulmonary and No non-pulmonary and AFP<000 ng/ml and and Normal AFP, any hcg, hcg<000 ng/ml and any LDH LDH<.5x N* Intermediate prognosis Testis / retroperitoneal primary Any primary site and No non-pulmonary and Non-pulmonary and and Normal AFP, any hcg, 000 < - AFP < ng/ml or any LDH 000 < - hcg < ng/ml or.5x N < - LDH < - 0x N Poor prognosis Mediastinal primary No patients classified as or Non-pulmonary visceral poor prognosis metastases or AFP>0.000 ng/ml or hcg>0.000 ng/ml or LDH>0xN * N=normal range Treatment Stage I disease (=non-metastasized disease) About half of the patients with a non-seminoma present with stage I disease. Presently, the treatment comprises radical orchidectomy with high ligation of the spermatic cord, blood vessels and lymph vessels, followed by regular outpatient visits (wait and see policy) or modified unilateral nerve-sparing retroperitoneal lymph node dissection. The UMCG has been applying the wait and see policy to patients with stage I disease since 982. (2) In the meantime, world- 6 7
6 wide consensus has been reached about the treatment for stage I non-seminoma patients in the low risk group (i.e. histological examination does not show any vascular invasion of the tumour). These patients have 5% risk of TGCT relapse, thus the wait and see policy is justified and comprises regular outpatient visits for 5 years after orchidectomy with physical examination, tumour marker analysis and frequent radiological investigation. There is a great deal of discussion about the current treatment policy for patients with stage I non-seminoma in the high risk group (i.e. histo-pathological investigation shows vascular invasion). Unilateral nervesparing retroperitoneal lymph node dissection (RPLND) or adjuvant chemotherapy leads to a considerable reduction in the risk of relapse of about 5%. However, the disadvantages of RPLND (loss of ejaculatory function) or chemotherapy (toxicity) must be taken into consideration. The UMCG applies still the wait and see policy to these high risk patients. In the UK and many other European countries, the preferred approach for high risk patients is often to administer two courses of adjuvant chemotherapy, whereas in the USA it is the trend to perform nerve-sparing unilateral RPLND. (2;3) Which treatment policy is the best for these so called high-risk patients is unknow. About 75% of the patients with seminoma have stage I disease. The standard treatment after orchidectomy is radiotherapy of the retroperitoneal para-aortal lymph nodes with a total dose of 20 Gy. In this way the relapse rate is reduced to -3%. (2) The advantage of para-aortal radiotherapy (while excluding the ipsilateral lymph nodes) is less gastrointestinal and gonadal toxicity. As an alternative for radiotherapy, adjuvant chemotherapy can be administered. The latter approach results in the same relapse rates. (22) A wait and see policy alone would lead to relapse rates of 5% to 20% and is less suitable, because there are no sensitive tumour markers for seminoma and the patient would therefore have to undergo frequent radiological investigation. (2;3) Metastasized disease Patients with stage IIa and IIb seminoma receive radiotherapy with a total dose of 30 Gy and 36 Gy, respectively. In contrast with stage I seminoma, the ipsilateral iliac lymph nodes are also included in the treatment volume (dog-leg field) in patients with stage II seminoma. This approach achieves 6-year relapse-free survival of 95% in stage IIa patients and 89% in stage IIb patients. Alternative treatments for radiotherapy can be considered in stage IIb patients, for example 3 courses of BEP (bleomycin, etoposide and cisplatin) or 4 courses of EP (etoposide and cisplatin). (2;3) Treatment for patients with stage IIc - IV metastasized seminoma and with stage II IV metastasized non-seminoma comprises chemotherapy in accordance with the prognostic factor classification. In the good prognosis group, patients with non-seminoma / seminoma receive chemotherapy in the form of 3 courses of BEP or 4 courses of EP. Patients in the intermediate and poor prognosis groups are treated with 4 courses of BEP. (2;23;24) Surgery after chemotherapy After completion of the chemotherapy, patients with a metastasized tumour (TGCT) at the UMCG undergo restaging with the aid of serum tumour marker analyses (as described above) and spiral CT scanning of the lungs and retroperitoneum. When radiological investigation shows residual disease after completion of the chemotherapy in patients with seminoma, surgical resection is not performed, but instead the abnormality is followed radiologically. Generally, a new indication will arise for chemotherapy or radiotherapy, which if necessary is combined with surgical resection of the residual tumour. Presently, positron emission tomography (PET) scanning can be applied to help identify viable cancer. (25) After patients with non-seminomatous TGCT have completed the chemotherapy, there is no indication for surgical resection when they do not show any residual disease, or the residual abnormality is smaller than cm, the tumour markers have normalised and mature teratoma is absent from the primary tumour. Follow-up is then conducted on the basis of tumour markers. However, when residual (abdominal / pulmonary) disease is identified, surgical resection must be performed on the residual retroperitoneal tumour mass (RRRTM), or local resection in the case of residual pulmonary tumour tissue. When residual tumour persists after completion of the chemotherapy and the tumour markers remain high, an individual treatment plan must be drawn up: salvage chemotherapy or salvage surgery. In patients with non-seminomatous TGCT, it is not possible to predict the histology of the residual tumour. After surgical resection, histological examination shows that the mass consists of necrosis in 45% of the cases, mature teratoma in 40%, viable tumour tissue in 0% and non-germ cell malignancies in the remaining 5%. (26) When the resected residual tumour only contains necrosis or mature teratoma, no further treatment is necessary and the patient has an excellent prognosis. However, when viable tumour tissue is present, the prognosis is less favourable and depending on factors such as the initial prognostic classification (Table 2), the volume (percentage) of residual viable cancer and the completeness of the resection, it may be necessary to administer adjuvant salvage chemotherapy. (27) The clinical significance of mature teratoma in the residual tumour is not yet completely clear and it is impossible to predict the course that can be expected from mature teratoma left in situ. In the literature, growing teratoma is a well-known phenomenon and it can lead to (very) late tumour recurrence. In addition, there is a risk that mature teratoma will de-differentiate into a non-germ cell malignancy (e.g. sarcoma). In such cases, the prognosis of the patient is far less favourable. Radical surgery is the only curative treatment option for these non-germ cell tumours. When the primary TGCT contains elements of mature teratoma, there is a greater chance that the residual tumour will also contain teratomatous elements. Therefore, at the UMCG, all patients with elements of teratoma in the primary tumour undergo laparotomy and partial retroperitoneal 8 9
7 dissection at the original tumour site after chemotherapy, even when there are no radiological signs of residual disease. (26) Aim and outline of this thesis Over the past few years, there has been growing interest in the genetic aspects of testicular cancer for a variety of reasons. In general terms, there is a scientific need to unravel the oncogenetic steps of all types of cancer in the hope that understanding the genetic changes will lead to better (early) diagnosis and treatment options. Some of these genetic changes have a hereditary nature, i.e. they can be passed on from one generation to the next and they must therefore be distinguished from the non-hereditary, somatic mutations that occur in the course of life. Studies on the hereditary predisposition of testicular cancer may lead to the identification of men with a strongly increased risk of developing testicular cancer who might benefit from preventive measures. Cure rates for testicular cancer are now high, so there is increasing interest in fertility aspects and the possible consequences of passing on the predisposition of testicular cancer to the offspring. Nowadays all patients with testicular cancer who undergo chemotherapy are in principle offered the opportunity to freeze their semen (cryopreservation). If a patient is less fertile or infertile after chemotherapy, it is possible to achieve pregnancy by means of artificial insemination. In this way, there is a risk of transmitting the hereditary predisposition. Another reason to study testicular cancer predisposition is that as a rule, finding hereditary cancer-predisposing mutations in genes leads to increased insight into the development of nonhereditary (so-called sporadic) tumours. In many cases, it has been found that genes involved in hereditary tumours also play a role in non-hereditary types of cancer. Now that the genomes of humans and other species are being systematically mapped and the scope of molecular and statistical analyses in genetic studies is expanding, there has been rapid progress in tumour genetic research. In contrast with studies on the hereditary aspects of breast cancer, colorectal cancer and a series of relatively rare tumour syndromes (such as multiple endocrine neoplasia (MEN and MEN2), Von Hippel Lindau, neuro-fibromatosis (NF and NF2) and Li-Fraumeni s syndrome), studies on the hereditary aspects of testicular cancer have been unable to identify any germline mutations in genes that could be associated with a high risk of developing testicular cancer. The research described in this thesis aimed to contribute to knowledge on hereditary predisposition to TGCT and focuses on the following aspects: The literature on the hereditary and syndromal aspects of TGCT Epidemiological aspects of TGCT The HLA and Xq27 regions on the genome that might harbour genes contributing to the development of TGCT Occurrence of constitutional deletions of the Yq region in men with TGCT Interest of men in genetic testing for TGCT 20 2
GUIDELINES ON TESTICULAR CANCER
 38 (Text updated March 2005) P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro Introduction Compared with other types of cancer
38 (Text updated March 2005) P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro Introduction Compared with other types of cancer
EAU GUIDELINES ON TESTICULAR CANCER
 EAU GUIDELINES ON TESTICULAR CANCER (Limited text update March 2018) P. Albers (Chair), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna (Vice-chair), N. Nicolai,
EAU GUIDELINES ON TESTICULAR CANCER (Limited text update March 2018) P. Albers (Chair), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna (Vice-chair), N. Nicolai,
EAU GUIDELINES ON TESTICULAR CANCER
 EU GUIDELINES ON TESTICULR CNCER (Limited text update March 2017) P. lbers (Chair), W. lbrecht, F. lgaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi,. Horwich, M.P. Laguna, N. Nicolai, J. Oldenburg Introduction
EU GUIDELINES ON TESTICULR CNCER (Limited text update March 2017) P. lbers (Chair), W. lbrecht, F. lgaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi,. Horwich, M.P. Laguna, N. Nicolai, J. Oldenburg Introduction
EAU GUIDELINES ON TESTICULAR CANCER
 EAU GUIDELINES ON TESTICULAR CANCER (Limited text update March 2015) P. Albers (Chair), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna, N. Nicolai, J. Oldenburg
EAU GUIDELINES ON TESTICULAR CANCER (Limited text update March 2015) P. Albers (Chair), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna, N. Nicolai, J. Oldenburg
NICaN Testicular Germ Cell Tumours SACT protocols
 Reference No: Title: Author(s) Ownership: Approval by: Systemic Anti-Cancer Therapy (SACT) Guidelines for Germ Cell Tumours Dr Audrey Fenton Consultant Medical Oncologist, Dr Vicky Coyle Consultant Medical
Reference No: Title: Author(s) Ownership: Approval by: Systemic Anti-Cancer Therapy (SACT) Guidelines for Germ Cell Tumours Dr Audrey Fenton Consultant Medical Oncologist, Dr Vicky Coyle Consultant Medical
ESMO Consensus Empfehlungen 2017
 ESMO Consensus Empfehlungen 2017 What s old, what s new, what s missing? Jörg Beyer, Klinik für Onkologie Offenlegung Interessenskonflikte 1. Anstellungsverhältnis oder Führungsposition Keine 2. Beratungs-
ESMO Consensus Empfehlungen 2017 What s old, what s new, what s missing? Jörg Beyer, Klinik für Onkologie Offenlegung Interessenskonflikte 1. Anstellungsverhältnis oder Führungsposition Keine 2. Beratungs-
STAGING AND FOLLOW-UP STRATEGIES
 ATHENS 4-6 October 2018 European Society of Urogenital Radiology STAGING AND FOLLOW-UP STRATEGIES Ahmet Tuncay Turgut, MD Professor of Radiology Hacettepe University, Faculty of Medicine Ankara 2nd ESUR
ATHENS 4-6 October 2018 European Society of Urogenital Radiology STAGING AND FOLLOW-UP STRATEGIES Ahmet Tuncay Turgut, MD Professor of Radiology Hacettepe University, Faculty of Medicine Ankara 2nd ESUR
Testicular Malignancies /8/15
 Collecting Cancer Data: Testis 2014-2015 NAACCR Webinar Series January 8, 2015 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Collecting Cancer Data: Testis 2014-2015 NAACCR Webinar Series January 8, 2015 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants watching
Cardiff MRCS OSCE Courses Testicular Cancer
 Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Testicular Cancer Scenario: A 40-year-old male presents to the surgical out-patient clinic with a 6-8 week history of a painless lump in his left scrotum. He however complains of a dull ache in the scrotum
Case Scenario 1 Discharge Summary Pathology Report Final Diagnosis: Oncology Consult
 Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Case Scenario 1 Discharge Summary Pathology Report Final Diagnosis: Oncology Consult
 Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Case Scenario 1 Discharge Summary A 31-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was
Doppler ultrasound of the abdomen and pelvis, and color Doppler
 - - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
- - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
-The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - include: I. Germ cell tumors : (95%); all are malignant. II. Sex cord-stromal tumors: from Sertoli or Leydig cells; usually
- In the 15- to 34-year-old age group, they are the most common tumors of men. - include: I. Germ cell tumors : (95%); all are malignant. II. Sex cord-stromal tumors: from Sertoli or Leydig cells; usually
Exercise. Discharge Summary
 Exercise Discharge Summary A 32-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was present
Exercise Discharge Summary A 32-year-old Brazilian male presented with a 6 month history of right-sided scrotal swelling. Backache was present for 2 months and a history of right epididymitis was present
Guidelines on Testicular Cancer
 Guidelines on Testicular Cancer P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna European Association of Urology 2009 TABLE OF CONTENTS
Guidelines on Testicular Cancer P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna European Association of Urology 2009 TABLE OF CONTENTS
GUIDELINES ON TESTICULAR CANCER
 European Association of Urology GUIDELINES ON TESTICULAR CANCER P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro UPDATE MARCH
European Association of Urology GUIDELINES ON TESTICULAR CANCER P. Albers (chairman), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, A. Horwich, O. Klepp, M.P. Laguna, G. Pizzocaro UPDATE MARCH
Testicular Cancer: Questions and Answers. Testicular cancer is a disease in which cells become malignant (cancerous) in one or both testicles.
 CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Testicular Cancer: Questions
CANCER FACTS N a t i o n a l C a n c e r I n s t i t u t e N a t i o n a l I n s t i t u t e s o f H e a l t h D e p a r t m e n t o f H e a l t h a n d H u m a n S e r v i c e s Testicular Cancer: Questions
Fellow GU Lecture Series, Testicular Cancer. Asit Paul, MD, PhD 02/06/2018
 Fellow GU Lecture Series, 2018 Testicular Cancer Asit Paul, MD, PhD 02/06/2018 Rare cancer worldwide, approximately 1% of all male cancers There is a large difference among ethnic/racial groups. Rates
Fellow GU Lecture Series, 2018 Testicular Cancer Asit Paul, MD, PhD 02/06/2018 Rare cancer worldwide, approximately 1% of all male cancers There is a large difference among ethnic/racial groups. Rates
Fellow GU Lecture Series, Testicular Cancer. Asit Paul, MD, PhD 02/06/2018
 Fellow GU Lecture Series, 2018 Testicular Cancer Asit Paul, MD, PhD 02/06/2018 Rare cancer worldwide, approximately 1% of all male cancers There is a large difference among ethnic/racial groups. Rates
Fellow GU Lecture Series, 2018 Testicular Cancer Asit Paul, MD, PhD 02/06/2018 Rare cancer worldwide, approximately 1% of all male cancers There is a large difference among ethnic/racial groups. Rates
Note: The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
- In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
Citation for published version (APA): Bleeker, W. A. (2001). Therapeutic considerations in Dukes C colon cancer s.n.
 University of Groningen Therapeutic considerations in Dukes C colon cancer Bleeker, Willem Aldert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Therapeutic considerations in Dukes C colon cancer Bleeker, Willem Aldert IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation in the Treatment of Germ File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_in_the_treatment_of_germ_cell_tumor
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation in the Treatment of Germ File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_in_the_treatment_of_germ_cell_tumor
Quiz 1. Assign Race 1, Race 2 and Spanish Hispanic Origin to the following scenarios.
 Quiz 1 Assign Race 1, Race 2 and Spanish Hispanic Origin to the following scenarios. 1. 62 year old Brazilian female Race 1 Race 2 Spanish/Hispanic Origin 2. 43 year old Asian male born in Japan Race 1
Quiz 1 Assign Race 1, Race 2 and Spanish Hispanic Origin to the following scenarios. 1. 62 year old Brazilian female Race 1 Race 2 Spanish/Hispanic Origin 2. 43 year old Asian male born in Japan Race 1
Testicular germ cell tumors
 Testicular germ cell tumors Introduction Most common solid tumor in young adult men with 3 6 new cases/100,000 men/year. They acc ount for 1.5% of male malignancies and 5% of urological tumors. Bilateral
Testicular germ cell tumors Introduction Most common solid tumor in young adult men with 3 6 new cases/100,000 men/year. They acc ount for 1.5% of male malignancies and 5% of urological tumors. Bilateral
ANZUP SURVEILLANCE RECOMMENDATIONS FOR METASTATIC TESTICULAR CANCER POST-CHEMOTHERAPY
 ANZUP SURVEILLANCE RECOMMENDATIONS FOR METASTATIC TESTICULAR CANCER POST-CHEMOTHERAPY Note: These surveillance recommendations are provided as recommendations only. Clinicians should take into account
ANZUP SURVEILLANCE RECOMMENDATIONS FOR METASTATIC TESTICULAR CANCER POST-CHEMOTHERAPY Note: These surveillance recommendations are provided as recommendations only. Clinicians should take into account
UK CAA Oncology Certification Charts
 UK CAA Oncology Certification Charts 1. Colorectal 2. Malignant Melanoma 3. Germ Cell Tumour of Testis 4. Renal Cell Carcinoma 5. Breast Carcinoma 6. Non-small Cell Lung Cancer Note: All Class 1 cases
UK CAA Oncology Certification Charts 1. Colorectal 2. Malignant Melanoma 3. Germ Cell Tumour of Testis 4. Renal Cell Carcinoma 5. Breast Carcinoma 6. Non-small Cell Lung Cancer Note: All Class 1 cases
Testis. Protocol applies to all malignant germ cell and malignant sex cord-stromal tumors of the testis, exclusive of paratesticular malignancies.
 Testis Protocol applies to all malignant germ cell and malignant sex cord-stromal tumors of the testis, exclusive of paratesticular malignancies. Protocol revision date: January 2005 Based on AJCC/UICC
Testis Protocol applies to all malignant germ cell and malignant sex cord-stromal tumors of the testis, exclusive of paratesticular malignancies. Protocol revision date: January 2005 Based on AJCC/UICC
Improving quality of care for patients with ovarian and endometrial cancer Eggink, Florine
 University of Groningen Improving quality of care for patients with ovarian and endometrial cancer Eggink, Florine IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Improving quality of care for patients with ovarian and endometrial cancer Eggink, Florine IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
What is Testicular cancer?
 Testicular Cancer What is Testicular cancer? Testicular cancer is a disease in which cancer cells form in the tissues of one or both testicles. The testicles are 2 egg-shaped glands located inside the
Testicular Cancer What is Testicular cancer? Testicular cancer is a disease in which cancer cells form in the tissues of one or both testicles. The testicles are 2 egg-shaped glands located inside the
Resection of retroperitoneal residual mass after chemotherapy in patients with nonseminomatous testicular cancer
 Turkish Journal of Cancer Vol.31/ No. 2/2001 Resection of retroperitoneal residual mass after chemotherapy in patients with nonseminomatous testicular cancer AHMET ÖZET 1, ALİ AYDIN YAVUZ 1, MURAT BEYZADEOĞLU
Turkish Journal of Cancer Vol.31/ No. 2/2001 Resection of retroperitoneal residual mass after chemotherapy in patients with nonseminomatous testicular cancer AHMET ÖZET 1, ALİ AYDIN YAVUZ 1, MURAT BEYZADEOĞLU
ASYMPTOMATIC COMPLEX TESTICULAR NEOPLASIA ASSOCIATED WITH ORCHIEPIDIDYMITIS. CASE REPORT
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 4 SURGERY CASE REPORTS ASYMPTOMATIC COMPLEX TESTICULAR NEOPLASIA ASSOCIATED WITH ORCHIEPIDIDYMITIS. CASE REPORT Ș. Iacob 1, R. Vrînceanu 2,3, B.
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2017 vol. 121, no. 4 SURGERY CASE REPORTS ASYMPTOMATIC COMPLEX TESTICULAR NEOPLASIA ASSOCIATED WITH ORCHIEPIDIDYMITIS. CASE REPORT Ș. Iacob 1, R. Vrînceanu 2,3, B.
Testicular Cancer. J. Richard Auman, MD. James J. Stark, MD. Jerry Singer, MD. September 19, 2008
 Testicular Cancer J. Richard Auman, MD James J. Stark, MD Jerry Singer, MD September 19, 2008 Testicular Cancer From mystery to far-advanced disease: a remarkable case Case Presentation. 23 y. o. male
Testicular Cancer J. Richard Auman, MD James J. Stark, MD Jerry Singer, MD September 19, 2008 Testicular Cancer From mystery to far-advanced disease: a remarkable case Case Presentation. 23 y. o. male
Collecting Cancer Data: Testis 2/3/11. Collecting Cancer Data: NAACCR Webinar Series 1. Agenda. Fabulous Prizes
 Collecting Cancer Data: Testis February 3, 2011 NAACCR 2010-2011 Webinar Series Agenda Coding moment Race/Hispanic origin Overview Collaborative Stage Treatment Exercises Fabulous Prizes NAACCR 2010-2011
Collecting Cancer Data: Testis February 3, 2011 NAACCR 2010-2011 Webinar Series Agenda Coding moment Race/Hispanic origin Overview Collaborative Stage Treatment Exercises Fabulous Prizes NAACCR 2010-2011
It is known, from comparisons of lymphography. with lymph-node histology, that 250 of clinical Stage I patients have
 Br. J. ('ancer (1982) 45, 167 PROGNOSTIC FACTORS IN CLINICAL STAGE I NON-SEMINOMATOUS GERM-CELL TUMOURS OF THE TESTIS D. RAGHAVAN*, M. J. PECKHAM, E. HEYDERMANt, J. S. TOBIAS AND D. E. AUSTIN From, the
Br. J. ('ancer (1982) 45, 167 PROGNOSTIC FACTORS IN CLINICAL STAGE I NON-SEMINOMATOUS GERM-CELL TUMOURS OF THE TESTIS D. RAGHAVAN*, M. J. PECKHAM, E. HEYDERMANt, J. S. TOBIAS AND D. E. AUSTIN From, the
Citation for published version (APA): Francken, A. B. (2007). Primary and metastatic melanoma: aspects of follow-up and staging s.n.
 University of Groningen Primary and metastatic melanoma Francken, Anne Brecht IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen Primary and metastatic melanoma Francken, Anne Brecht IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Citation for published version (APA): Lutke Holzik, M. F. (2007). Genetic predisposition to testicular cancer s.n.
 University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Testis tumors. Richard Epstein
 Testis tumors Richard Epstein TKCC/SVH, August 5 2016 Testis cancer - Remains virtually the only solid (nonhaematologic) metastatic tumour that is routinely curable by drug therapy. What we will discuss
Testis tumors Richard Epstein TKCC/SVH, August 5 2016 Testis cancer - Remains virtually the only solid (nonhaematologic) metastatic tumour that is routinely curable by drug therapy. What we will discuss
EAU Guidelines on Testicular Cancer
 EAU Guidelines on Testicular Cancer P. Albers (Chair), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna, N. Nicolai, J. Oldenburg Guidelines Associates: J.L.
EAU Guidelines on Testicular Cancer P. Albers (Chair), W. Albrecht, F. Algaba, C. Bokemeyer, G. Cohn-Cedermark, K. Fizazi, A. Horwich, M.P. Laguna, N. Nicolai, J. Oldenburg Guidelines Associates: J.L.
Prof. Dr. med. Beata BODE-LESNIEWSKA Institute of Pathology and Molecular Pathology University Hospital; Zurich
 Prof. Dr. med. Beata BODE-LESNIEWSKA Institute of Pathology and Molecular Pathology University Hospital; Zurich 32 year old man 2 months history of growing left supraclavicular lymph nodes Antibiotic treatment
Prof. Dr. med. Beata BODE-LESNIEWSKA Institute of Pathology and Molecular Pathology University Hospital; Zurich 32 year old man 2 months history of growing left supraclavicular lymph nodes Antibiotic treatment
TESTICULAR CANCER Updated March 2016 by Dr. Safiya Karim (PGY-5 Medical Oncology Resident, University of Toronto)
 TESTICULAR CANCER Updated March 2016 by Dr. Safiya Karim (PGY-5 Medical Oncology Resident, University of Toronto) Reviewed by Dr. Aaron Hansen (Staff Medical Oncologist, University of Toronto) DISCLAIMER:
TESTICULAR CANCER Updated March 2016 by Dr. Safiya Karim (PGY-5 Medical Oncology Resident, University of Toronto) Reviewed by Dr. Aaron Hansen (Staff Medical Oncologist, University of Toronto) DISCLAIMER:
Twelve Years of Experience in the Management of Testicular Germ Cell Tumors at a Referral Center in Portugal
 Elmer Press Original Article Twelve Years of Experience in the Management of Testicular Germ Cell Tumors at a Referral Center in Portugal Diana Valadares a, c, Filipe Nery a, Franklim Marques a, b Abstract
Elmer Press Original Article Twelve Years of Experience in the Management of Testicular Germ Cell Tumors at a Referral Center in Portugal Diana Valadares a, c, Filipe Nery a, Franklim Marques a, b Abstract
Testicular Cancer. Regional Follow-up Guidelines
 Urological Cancers Managed Clinical Network Testicular Cancer Regional Follow-up Guidelines Prepared by Drs J White/ A Waterston, J Salmond, J Wallace, Mr D Hendry, Approved by Urological Cancers MCN and
Urological Cancers Managed Clinical Network Testicular Cancer Regional Follow-up Guidelines Prepared by Drs J White/ A Waterston, J Salmond, J Wallace, Mr D Hendry, Approved by Urological Cancers MCN and
Tumour Markers. For these reasons, only a handful of tumour markers are commonly used by most doctors.
 Tumour Markers What are Tumour Markers? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer
Tumour Markers What are Tumour Markers? Tumour markers are substances that can be found in the body when cancer is present. They are usually found in the blood or urine. They can be products of cancer
Cover Page. Author: Willemse, Peter-Paul M. Title: Skeletal and metabolic complications of testicular germ cell tumours Issue Date:
 Cover Page The handle http://hdl.handle.net/1887/24412 holds various files of this Leiden University dissertation Author: Willemse, Peter-Paul M. Title: Skeletal and metabolic complications of testicular
Cover Page The handle http://hdl.handle.net/1887/24412 holds various files of this Leiden University dissertation Author: Willemse, Peter-Paul M. Title: Skeletal and metabolic complications of testicular
Teratocarcinoma In A Young Boy- An Unusual Presentation
 Human Journals Case Report November 2015 Vol.:2, Issue:1 All rights are reserved by Atia Zaka-ur-Rab et al. Teratocarcinoma In A Young Boy- An Unusual Presentation Keywords: Boy, Testicular Mass, Teratocarcinoma
Human Journals Case Report November 2015 Vol.:2, Issue:1 All rights are reserved by Atia Zaka-ur-Rab et al. Teratocarcinoma In A Young Boy- An Unusual Presentation Keywords: Boy, Testicular Mass, Teratocarcinoma
Citation for published version (APA): Weert, E. V. (2007). Cancer rehabilitation: effects and mechanisms s.n.
 University of Groningen Cancer rehabilitation Weert, Ellen van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Cancer rehabilitation Weert, Ellen van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Male Genital Cancers in the US in Frequency of Types
 Germ Cell Tumors of the Testis Pathology, Immunohistochemistry, and the Often Confusing Appearance of Their Metastases Charles Zaloudek, MD Department of Pathology UCSF Male Genital Cancers in the US in
Germ Cell Tumors of the Testis Pathology, Immunohistochemistry, and the Often Confusing Appearance of Their Metastases Charles Zaloudek, MD Department of Pathology UCSF Male Genital Cancers in the US in
Leukaemia 35% Lymphoma 14%
 Distribution ib ti of Cancers in Children under 15 years Leukaemia 35% Lymphoma 14% Neuroblastoma 9% Other 5% Liver 1% Retinoblastoma 3% Bone and STS 15% CNS 20% Wilms' 8% 30-40% Mortality Germ Cell Tumours
Distribution ib ti of Cancers in Children under 15 years Leukaemia 35% Lymphoma 14% Neuroblastoma 9% Other 5% Liver 1% Retinoblastoma 3% Bone and STS 15% CNS 20% Wilms' 8% 30-40% Mortality Germ Cell Tumours
BENIGN & MALIGNANT TESTIS DISEASES. Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES
 BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
BENIGN & MALIGNANT TESTIS DISEASES Gary J. Faerber, M.D. Associate Professor, Dept of Urology March 2009 OBJECTIVES 1. Become familiar with the scrotal contents and their anatomical relationship with each
Viable Germ Cell Tumor at Postchemotherapy Retroperitoneal Lymph Node Dissection. Can We Predict Patients at Risk of Disease Progression?
 2700 Viable Germ Cell Tumor at Postchemotherapy Retroperitoneal Lymph Node Dissection Can We Predict Patients at Risk of Disease Progression? Philippe E. Spiess, MD 1 Nizar M. Tannir, MD 2 Shi-Ming Tu,
2700 Viable Germ Cell Tumor at Postchemotherapy Retroperitoneal Lymph Node Dissection Can We Predict Patients at Risk of Disease Progression? Philippe E. Spiess, MD 1 Nizar M. Tannir, MD 2 Shi-Ming Tu,
Running Title: Utility of HCG Washout in Cervical LND FNA
 AACE Clinical Case Reports Rapid Electronic Articles in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited,
AACE Clinical Case Reports Rapid Electronic Articles in Press Rapid Electronic Articles in Press are preprinted manuscripts that have been reviewed and accepted for publication, but have yet to be edited,
Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy
 Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy Stephanie Yap, M.D. University Gynecologic Oncology Northside Cancer Institute Our Learning Objectives Review survival rates,
Gynecologic Cancer Surveillance and Survivorship: Informing Practice and Policy Stephanie Yap, M.D. University Gynecologic Oncology Northside Cancer Institute Our Learning Objectives Review survival rates,
Uncommon secondary tumour of the stomach
 Uncommon secondary tumour of the stomach B. Bancel, Hôpital CROIX ROUSSE LYON Bucharest Nov 2013 Case report 33-year old man Profound mental retardation and motor disturbances (sequelae of neonatal meningeal
Uncommon secondary tumour of the stomach B. Bancel, Hôpital CROIX ROUSSE LYON Bucharest Nov 2013 Case report 33-year old man Profound mental retardation and motor disturbances (sequelae of neonatal meningeal
Testicular Cancer. What is cancer?
 What is cancer? Testicular Cancer The body is made up of trillions of living cells. Normal body cells grow, divide, and die in an orderly fashion. During the early years of a person's life, normal cells
What is cancer? Testicular Cancer The body is made up of trillions of living cells. Normal body cells grow, divide, and die in an orderly fashion. During the early years of a person's life, normal cells
Cancer of Unknown Primary (CUP)
 Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Cancer of Unknown Primary (CUP) Pathways and Guidelines V1.0 London Cancer September 2013 The following pathways and guidelines document has been compiled by the London Cancer CUP technical subgroup and
Stage 3c breast cancer survival rate
 Stage 3c breast cancer survival rate There are five main subtypes of ovarian carcinoma, of which high-grade serous carcinoma is the most common. [3]. Testicular cancer is generally found in young men.
Stage 3c breast cancer survival rate There are five main subtypes of ovarian carcinoma, of which high-grade serous carcinoma is the most common. [3]. Testicular cancer is generally found in young men.
Mixed Germ Cell Testis Tumor Presenting with Massive Lung Metastasis
 International Archives of Medical Research Volume 10, No.1, pp.21-26, 2018. CASE REPORT RESEARCH Mixed Germ Cell Testis Tumor Presenting with Massive Lung Metastasis Zuhat Urakci 1, Senar Ebinc 1, Ogur
International Archives of Medical Research Volume 10, No.1, pp.21-26, 2018. CASE REPORT RESEARCH Mixed Germ Cell Testis Tumor Presenting with Massive Lung Metastasis Zuhat Urakci 1, Senar Ebinc 1, Ogur
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Cancer of Unknown Primary Network Site Specific Group. Clinical Guidelines
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Analysis of the prognosis of patients with testicular seminoma
 ONCOLOGY LETTERS 11: 1361-1366, 2016 Analysis of the prognosis of patients with testicular seminoma WEI DONG 1, WANG GANG 1, MIAOMIAO LIU 2 and HONGZHEN ZHANG 2 1 Department of Urology; 2 Department of
ONCOLOGY LETTERS 11: 1361-1366, 2016 Analysis of the prognosis of patients with testicular seminoma WEI DONG 1, WANG GANG 1, MIAOMIAO LIU 2 and HONGZHEN ZHANG 2 1 Department of Urology; 2 Department of
Testicular Germ Cell Tumors; A Simplistic Approach
 Testicular Germ Cell Tumors; A Simplistic Approach Merce Jorda, MD, PhD, MBA Professor and Vice Chair, Director of Anatomic Pathology Director of Genitourinary Pathology Service Interim Director of Cytopathology
Testicular Germ Cell Tumors; A Simplistic Approach Merce Jorda, MD, PhD, MBA Professor and Vice Chair, Director of Anatomic Pathology Director of Genitourinary Pathology Service Interim Director of Cytopathology
Testicular tumours are uncommon but constitute an
 09010:Layout 1 3/18/10 9:26 PM Page E19 CONSENSUS GUIDELINE Canadian consensus guidelines for the management of testicular germ cell cancer Lori Wood, MD; * Christian Kollmannsberger, MD, FRCSC; Michael
09010:Layout 1 3/18/10 9:26 PM Page E19 CONSENSUS GUIDELINE Canadian consensus guidelines for the management of testicular germ cell cancer Lori Wood, MD; * Christian Kollmannsberger, MD, FRCSC; Michael
MULTIDISCIPLINARY GENITOURINARY ONCOLOGY COURSE
 MULTIDISCIPLINARY GENITOURINARY ONCOLOGY COURSE Case 2 Testicular Cancer Nuno Sineiro Vau Medical Oncologist Champalimaud Foundation, Lisbon October 2017 Male, 36 year-old, sales manager. Past medical
MULTIDISCIPLINARY GENITOURINARY ONCOLOGY COURSE Case 2 Testicular Cancer Nuno Sineiro Vau Medical Oncologist Champalimaud Foundation, Lisbon October 2017 Male, 36 year-old, sales manager. Past medical
Testicular cancer and other germ cell tumours. London Cancer Jonathan Shamash
 Testicular cancer and other germ cell tumours London Cancer 2018 Jonathan Shamash Background Testicular germ cell tumours are the commonest cancers of young men Overall they are curable but long term side
Testicular cancer and other germ cell tumours London Cancer 2018 Jonathan Shamash Background Testicular germ cell tumours are the commonest cancers of young men Overall they are curable but long term side
GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCER
 GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCER Testicular Tumour Treatment Guidelines Authors: Professor Peter Clark Mr Mark Fordham Review Date: May 2017 CONTENTS Page 1. Introduction 4 2. Details
GUIDELINES FOR THE MANAGEMENT OF UROLOGICAL CANCER Testicular Tumour Treatment Guidelines Authors: Professor Peter Clark Mr Mark Fordham Review Date: May 2017 CONTENTS Page 1. Introduction 4 2. Details
Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122
 Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Chemotherapy for Urological Cancers
 Chemotherapy for Urologic Cancers Matthew Rettig, MD Associate Professor Department of Medicine Division of Hematology-Oncology Department of Urology Medical Director, Prostate Cancer Program Institute
Chemotherapy for Urologic Cancers Matthew Rettig, MD Associate Professor Department of Medicine Division of Hematology-Oncology Department of Urology Medical Director, Prostate Cancer Program Institute
Testicular Germ Cell Cancer Explained
 The Beatson West of Scotland Cancer Centre Pan Glasgow Urology / Oncology Patient Information Testicular Germ Cell Cancer Explained The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow
The Beatson West of Scotland Cancer Centre Pan Glasgow Urology / Oncology Patient Information Testicular Germ Cell Cancer Explained The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow
Surgery Illustrated Surgical Atlas Inguinal orchidectomy for testicular cancer
 Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
Surgery Illustrated Focus on Details SURGERY ILLUSTRATED SURGICAL ATLASPIZZOCARO and GUARNERI PIZZOCARO and GUARNERI BJUI BJU INTERNATIONAL Surgery Illustrated Surgical Atlas Inguinal orchidectomy for
Long-Term Outcome for Men With Teratoma Found at Postchemotherapy Retroperitoneal Lymph Node Dissection
 Original Article Long-Term Outcome for Men With Teratoma Found at Postchemotherapy Retroperitoneal Lymph Node Dissection Robert S. Svatek, MD 1, Philippe E. Spiess, MD 2, Debasish Sundi, BS 1, Shi-ming
Original Article Long-Term Outcome for Men With Teratoma Found at Postchemotherapy Retroperitoneal Lymph Node Dissection Robert S. Svatek, MD 1, Philippe E. Spiess, MD 2, Debasish Sundi, BS 1, Shi-ming
Slide 1. Slide 2. Slide 3. Investigation and management of lung cancer Robert Rintoul. Epidemiology. Risk factors/aetiology
 Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
Slide 1 Investigation and management of lung cancer Robert Rintoul Department of Thoracic Oncology Papworth Hospital Slide 2 Epidemiology Second most common cancer in the UK (after breast). 38 000 new
AMORE (Ablative surgery, MOulage technique brachytherapy and REconstruction) for childhood head and neck rhabdomyosarcoma Buwalda, J.
 UvA-DARE (Digital Academic Repository) AMORE (Ablative surgery, MOulage technique brachytherapy and REconstruction) for childhood head and neck rhabdomyosarcoma Buwalda, J. Link to publication Citation
UvA-DARE (Digital Academic Repository) AMORE (Ablative surgery, MOulage technique brachytherapy and REconstruction) for childhood head and neck rhabdomyosarcoma Buwalda, J. Link to publication Citation
Germ Cell Tumors. Karim Fizazi, MD, PhD Institut Gustave Roussy, France
 Germ Cell Tumors Karim Fizazi, MD, PhD Institut Gustave Roussy, France Surveillance for stage I GCT NSGCT A 26 year-old patient had a orchiectomy revealing embryonal carcinoma (40%), seminoma (40%) and
Germ Cell Tumors Karim Fizazi, MD, PhD Institut Gustave Roussy, France Surveillance for stage I GCT NSGCT A 26 year-old patient had a orchiectomy revealing embryonal carcinoma (40%), seminoma (40%) and
Management of Testicular Cancer
 Management of Testicular Cancer Christian Kollmannsberger MD FRCPC Clinical Professor Div. of Medical Oncology BC Cancer - Vancouver Cancer Centre Dept. of Medicine, University of British Columbia Associate
Management of Testicular Cancer Christian Kollmannsberger MD FRCPC Clinical Professor Div. of Medical Oncology BC Cancer - Vancouver Cancer Centre Dept. of Medicine, University of British Columbia Associate
Citation for published version (APA): Lutke Holzik, M. F. (2007). Genetic predisposition to testicular cancer s.n.
 University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Management preferences following radical inguinal orchidectomy for Stage I testicular seminoma in Australasia
 Radiation Oncology Australasian Radiology (2002) 46, 280 284 Management preferences following radical inguinal orchidectomy for Stage I testicular seminoma in Australasia G Hruby, 1 R Choo, 2 M Jackson,
Radiation Oncology Australasian Radiology (2002) 46, 280 284 Management preferences following radical inguinal orchidectomy for Stage I testicular seminoma in Australasia G Hruby, 1 R Choo, 2 M Jackson,
University of Groningen. BNP and NT-proBNP in heart failure Hogenhuis, Jochem
 University of Groningen BNP and NT-proBNP in heart failure Hogenhuis, Jochem IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
University of Groningen BNP and NT-proBNP in heart failure Hogenhuis, Jochem IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check
Testicular Cancer. NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Version December 8, NCCN.org.
 NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Version 2.2017 December 8, 2016 NCCN.org Continue Version 2.2017, 12/08/16 National Comprehensive Cancer Network, Inc. 2016, All rights
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines ) Version 2.2017 December 8, 2016 NCCN.org Continue Version 2.2017, 12/08/16 National Comprehensive Cancer Network, Inc. 2016, All rights
MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER
 10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
10 MUSCLE - INVASIVE AND METASTATIC BLADDER CANCER Recommendations from the EAU Working Party on Muscle Invasive and Metastatic Bladder Cancer G. Jakse (chairman), F. Algaba, S. Fossa, A. Stenzl, C. Sternberg
University of Groningen. Morbidity after neck dissection in head and neck cancer patients Wilgen, Cornelis Paul van
 University of Groningen Morbidity after neck dissection in head and neck cancer patients Wilgen, Cornelis Paul van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
University of Groningen Morbidity after neck dissection in head and neck cancer patients Wilgen, Cornelis Paul van IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if
Citation for published version (APA): van Kruchten, M. (2015). Molecular imaging of estrogen receptors [Groningen]: University of Groningen
![Citation for published version (APA): van Kruchten, M. (2015). Molecular imaging of estrogen receptors [Groningen]: University of Groningen Citation for published version (APA): van Kruchten, M. (2015). Molecular imaging of estrogen receptors [Groningen]: University of Groningen](/thumbs/89/99843822.jpg) University of Groningen Molecular imaging of estrogen receptors van Kruchten, Michel IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
University of Groningen Molecular imaging of estrogen receptors van Kruchten, Michel IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please
Regressed Testicular Seminoma with Extensive Metastases. S Andhavarapu, B Low, J Raj, S Skinner, J Armenta-Corona
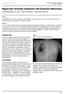 ISPUB.COM The Internet Journal of Oncology Volume 5 Number 1 S Andhavarapu, B Low, J Raj, S Skinner, J Armenta-Corona Citation S Andhavarapu, B Low, J Raj, S Skinner, J Armenta-Corona.. The Internet Journal
ISPUB.COM The Internet Journal of Oncology Volume 5 Number 1 S Andhavarapu, B Low, J Raj, S Skinner, J Armenta-Corona Citation S Andhavarapu, B Low, J Raj, S Skinner, J Armenta-Corona.. The Internet Journal
European consensus on diagnosis and treatment of germ cell cancer: a report of the European Germ Cell Cancer Consensus Group (EGCCCG)
 Original article Annals of Oncology 15: 1377 1399, 2004 doi:10.1093/annonc/mdh301 European consensus on diagnosis and treatment of germ cell cancer: a report of the European Germ Cell Cancer Consensus
Original article Annals of Oncology 15: 1377 1399, 2004 doi:10.1093/annonc/mdh301 European consensus on diagnosis and treatment of germ cell cancer: a report of the European Germ Cell Cancer Consensus
GERM-CELL TUMOURS. ESMO Preceptorship on Adolescents and Young Adults with cancer Lugano, May 2018
 ESMO Preceptorship on Adolescents and Young Adults with cancer Lugano, 11-12 May 2018 GERM-CELL TUMOURS Giannis Mountzios MSc, PhD Medical Oncology University of Athens School of Medicine Athens, Greece
ESMO Preceptorship on Adolescents and Young Adults with cancer Lugano, 11-12 May 2018 GERM-CELL TUMOURS Giannis Mountzios MSc, PhD Medical Oncology University of Athens School of Medicine Athens, Greece
Cancer: recent advances and implications for underwriting
 Cancer: recent advances and implications for underwriting Robert Rubens Select 74 Bristol 25 February 2010 Agenda Epidemiology - changing mortality Evidence-base for underwriting breast cancer ovarian
Cancer: recent advances and implications for underwriting Robert Rubens Select 74 Bristol 25 February 2010 Agenda Epidemiology - changing mortality Evidence-base for underwriting breast cancer ovarian
The Importance of One-Stage Median Stemotomy and Retroperitoneal Node Dissection in Disseminated Testicular Cancer
 The Importance of One-Stage Median Stemotomy and Retroperitoneal Node Dissection in Disseminated Testicular Cancer Isidore Mandelbaum, M.D., Peter B. Yaw, M.D., Lawrence H. Einhorn, M.D., Stephen D. Williams,
The Importance of One-Stage Median Stemotomy and Retroperitoneal Node Dissection in Disseminated Testicular Cancer Isidore Mandelbaum, M.D., Peter B. Yaw, M.D., Lawrence H. Einhorn, M.D., Stephen D. Williams,
Germ cell tumours UK SH. Ivo Leuschner. Kiel Pediatric Tumor Registry, Institute of Pathology University Hospital of Schleswig-Holstein Campus Kiel
 Germ cell tumours Ivo Leuschner Kiel Pediatric Tumor Registry, Institute of Pathology University Hospital of Schleswig-Holstein Campus Kiel UK SH Old histogenetic Concept of Germ cell tumours Pluripotent
Germ cell tumours Ivo Leuschner Kiel Pediatric Tumor Registry, Institute of Pathology University Hospital of Schleswig-Holstein Campus Kiel UK SH Old histogenetic Concept of Germ cell tumours Pluripotent
Populations Interventions Comparators Outcomes Individuals: With previously untreated germ cell tumors
 Hematopoietic Cell Transplantation in the Treatment of Germ Cell (80135) (Formerly Hematopoietic Stem Cell Transplantation in the Treatment of Germ Cell ) Medical Benefit Effective Date: 04/01/13 Next
Hematopoietic Cell Transplantation in the Treatment of Germ Cell (80135) (Formerly Hematopoietic Stem Cell Transplantation in the Treatment of Germ Cell ) Medical Benefit Effective Date: 04/01/13 Next
Clinical and genetic aspects of testicular germ cell tumours
 Hereditary Cancer in Clinical Practice 2008; 6(1) pp. 3-14 Clinical genetic aspects of testicular germ cell tumours Martijn F. Lutke Holzik 1,2, Rolf H. Sijmons 3, Josette E.H.M. Hoekstra-Weebers 4,5,
Hereditary Cancer in Clinical Practice 2008; 6(1) pp. 3-14 Clinical genetic aspects of testicular germ cell tumours Martijn F. Lutke Holzik 1,2, Rolf H. Sijmons 3, Josette E.H.M. Hoekstra-Weebers 4,5,
Germ cell tumours local perspectives on a curable cancer
 REVIEW Germ cell tumours local perspectives on a curable cancer ATC Chan, MMC Cheung, WH Lau, PJ Johnson Germ cell tumours are among the most curable solid cancers and have become a model for the multimodality
REVIEW Germ cell tumours local perspectives on a curable cancer ATC Chan, MMC Cheung, WH Lau, PJ Johnson Germ cell tumours are among the most curable solid cancers and have become a model for the multimodality
Germ cell tumors (GCT) are uncommon neoplasms
 ORIGINAL ARTICLES: GENERAL THORACIC Pulmonary Metastasectomy for Testicular Germ Cell Tumors: A 28-Year Experience David Liu, MD, Amir Abolhoda, MD, Michael E. Burt, MD, PhD, Nael Martini, MD, Manjit S.
ORIGINAL ARTICLES: GENERAL THORACIC Pulmonary Metastasectomy for Testicular Germ Cell Tumors: A 28-Year Experience David Liu, MD, Amir Abolhoda, MD, Michael E. Burt, MD, PhD, Nael Martini, MD, Manjit S.
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type)
 Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Chapter 2: Initial treatment for endometrial cancer (including histologic variant type) CQ01 Which surgical techniques for hysterectomy are recommended for patients considered to be stage I preoperatively?
Nerve-sparing retroperitoneal lymph node dissection for advanced testicular cancer after chemotherapy
 Blackwell Science, LtdOxford, UK IJU International Journal of Urology 0919-81722002 Blackwell Science Asia Pty Ltd 910October 2002 520 Postchemotherapy nerve-sparing RPLND N Nonomura et al. 10.1046/j.0919-8172.2002.00520.x
Blackwell Science, LtdOxford, UK IJU International Journal of Urology 0919-81722002 Blackwell Science Asia Pty Ltd 910October 2002 520 Postchemotherapy nerve-sparing RPLND N Nonomura et al. 10.1046/j.0919-8172.2002.00520.x
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM GERM CELL TUMOURS CNS Site Group Germ Cell Tumours Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM GERM CELL TUMOURS CNS Site Group Germ Cell Tumours Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Pharmacoeconomic analysis of proton pump inhibitor therapy and interventions to control Helicobacter pylori infection Klok, Rogier Martijn
 University of Groningen Pharmacoeconomic analysis of proton pump inhibitor therapy and interventions to control Helicobacter pylori infection Klok, Rogier Martijn IMPORTANT NOTE: You are advised to consult
University of Groningen Pharmacoeconomic analysis of proton pump inhibitor therapy and interventions to control Helicobacter pylori infection Klok, Rogier Martijn IMPORTANT NOTE: You are advised to consult
ISSN: X (Print) X (Online) Journal homepage:
 Acta Oncologica ISSN: 0284-186X (Print) 1651-226X (Online) Journal homepage: http://www.tandfonline.com/loi/ionc20 Testicular Cancer Michael Peckham To cite this article: Michael Peckham (1988) Testicular
Acta Oncologica ISSN: 0284-186X (Print) 1651-226X (Online) Journal homepage: http://www.tandfonline.com/loi/ionc20 Testicular Cancer Michael Peckham To cite this article: Michael Peckham (1988) Testicular
Ultrasound of malignant testicular lesions. Arne Hørlyck Department of Radiology Aarhus University Hospital, Skejby
 Ultrasound of malignant testicular lesions Arne Hørlyck Department of Radiology Aarhus University Hospital, Skejby Testis Ultrasound is fantastic!! Scrotum Extratesticular mass: Benign Intratesticular
Ultrasound of malignant testicular lesions Arne Hørlyck Department of Radiology Aarhus University Hospital, Skejby Testis Ultrasound is fantastic!! Scrotum Extratesticular mass: Benign Intratesticular
Acute: Symptoms that start and worsen quickly but do not last over a long period of time.
 Cancer Glossary Acute: Symptoms that start and worsen quickly but do not last over a long period of time. Adjuvant therapy: Treatment given after the main treatment. It usually refers to chemotherapy,
Cancer Glossary Acute: Symptoms that start and worsen quickly but do not last over a long period of time. Adjuvant therapy: Treatment given after the main treatment. It usually refers to chemotherapy,
University of Groningen. Colorectal Anastomoses Bakker, Ilsalien
 University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
Citation for published version (APA): Lutke Holzik, M. F. (2007). Genetic predisposition to testicular cancer s.n.
 University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Genetic predisposition to testicular cancer Lutke Holzik, Martijn Frederik IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
