PERCUTANEOUS DILATIONAL TRACHEOSTOMY: A CONCISE CLINICAL REVIEW
|
|
|
- Madlyn Singleton
- 5 years ago
- Views:
Transcription
1 95 REVIEW ARTICLE PERCUTANEOUS DILATIONAL TRACHEOSTOMY: A CONCISE CLINICAL REVIEW Fares G. Mouchantaf, MD *, Carla R. Lamb, MD ** ABSTRACT Percutaneous dilational tracheostomy (PDT) is a commonly performed procedure in any intensive care unit. We hope to provide a concise review of the basic anatomy, technique, indications, contraindications, and complications of PDT. PDT is now a long established procedure for most physicians caring for intensive care unit patients. Not all clinicians will be able to perform the procedure but everyone caring for these patients should be familiar with the technique, indications, and potential adverse effects. BACKGROUND Tracheostomy is a long established tool for physicians treating patients with respiratory failure. It is one of the oldest surgical procedures. Chevalier Jackson published his techniques of surgical tracheostomy in Prior to Jackson s technique, mortality from the procedure was considered acceptable if 25% of patients survived 2. Open surgical tracheostomy (OST) was the dominant mode of tracheostomy in the 20 th century till Ciaglia described the initial percutaneous technique in Percutaneous dilatational tracheostomy (PDT) provides a means for a less invasive technique to access the patient s trachea. While the debate over timing to tracheostomy, patient selection, and technique continues, few will argue that a designated team of nurses, well trained physicians, and support staff are needed for a successful, safe, and efficient procedure to occur. Anatomy It is essential for all physicians performing tracheostomy to understand the basic anatomy of the neck. As the proceduralist approaches the patient s neck the important anatomic features include the thyroid cartilage, cricoid cartilage, cricothyroid membrane, manubrium, sternal notch, internal carotid artery, and internal jugular vein, see Figure I. The tracheal length is approximately 10 to 13 cm with an anterior-posterior diameter of 1.8 cm. It begins approximately 1.5 cm below the vocal cords. However, variation in anatomy is common and several factors may alter the usual landmarks. For example, goiter, tracheal deviation, kyphoscoliosis, or obesity can alter the procedural approach. External visual cues and bronchoscopic recognition of important landmarks must be understood by both the proceduralist and bronchoscopist. As the bronchoscopist enters the endotracheal tube with the bronchoscope the carina, anterior trachea, subglottic shelf, cricoid cartilage should be identified. A coordinated step by step approach should be taken by both proceduralist and bronchoscopist in order to confirm proper positioning of the tracheostomy tube, avoid damage to equipment, and loss of control of the patient s airway. Patient Selection, Indications, and Timing Patient selection criteria are similar for both approaches, PDT or OST. Patients with large goiter or tumor may be better served with a surgical tracheostomy given the difficulty identifying palpable landmarks. Several different techniques have been developed using the percutaneous approach 4,5,6. A recent meta-analysis by Cabrini et. Al 7 compared different techniques for PDT. They evaluated whether multiple dilators, rotational dilation, retrograde tracheostomy, single step dilatation, or balloon dilation techniques was superior to one another. In their review the single step dilatation technique seemed to have fewer failures and mild complications compared to rotational dilatation, balloon dilatation, and guide wire dilating forceps. * Interventional Pulmonary Fellow, Lahey Clinic Medical Center, Burlington, MA, USA ** Director of Interventional Pulmonary, Lahey Clinic Medical Center, Burlington, MA, USA
2 96 General indications for tracheostomy include the need for prolonged ventilator weaning, management of respiratory secretions, failed extubation, enhanced patient comfort to facilitate weaning, and upper airway obstruction. Indications and contraindications are indicated in Table I and II. Contraindications can be divided into relative and absolute categories. Kornblith et. al recently reported a single center experience with bedside percutaneous tracheostomy. They retrospectively reviewed 1000 percutaneous tracheostomy within their surgical intensive care unit and found an average complication rate of 1.2% percent in normal risk patients and 1.7% in high risk patients. Their most common reported complication was misplacement of the tracheal tube and bleeding. Their study reported no deaths attributed to percutaneous tracheostomy 8. They concluded that PDT should be the new gold standard of care for patients being considered for tracheostomy. Timing of tracheostomy has been a highly debated topic within the medical literature. Tracheostomy should be performed when endotracheal intubation is projected to be prolonged. A recent trial in the U.K. and U.S. (TracMan, 9 attempted to answer if there are any differences in patients receiving early or late tracheostomy. Patients were screened at 72 hours of intubation and if the clinician believed they would require mechanical ventilation beyond 14 days they were asked to participate in the study. Patients were randomized to an early vs. late tracheostomy group, with approximately 900 patients were enrolled in the study. The early group received a tracheostomy immediately, whereas the late group were delayed for at least 10 days. They found patient demographics to be similar in both groups. They concluded that the early tracheotomy group had fewer days of sedation, however, over half of the patients in the late tracheotomy group were either weaned and successfully extubated or died prior to 14 days. A major inadvertent finding of the study is that clinicians are poor predictors of who will require prolonged ventilation and intubation. A recent randomized controlled trial conducted in Italy compared two groups of ICU (intensive care unit) patients. They enrolled 600 adult ICU patients without lung infection after 24 hours of ventilation. Patients who had worsening respiratory condition, unchanged sequential organ failure assessment score, and no pneumonia at 48 hours were randomized into early (between 6 to 8 days of laryngeal intubation) and late (between 13 to 15 days of laryngeal intubation). Ventilator associated pneumonia and survival was no different between both groups 10. This study has led many clinicians to acknowledge that early tracheotomy likely will not lead to reduced ventilator associated pneumonia, shorter hospital stay, or lower mortality. Therefore, based on these two large randomized controlled trials our practice has been to only consider tracheostomy in medical ICU patients likely to fail extubation after at least 10 days of laryngeal intubation. At this time early tracheostomy can only be advocated for trauma patients based on class II data and recent guidelines published by the Eastern Association for the Surgery of Trauma. This Level II recommendation states that fewer days of mechanical ventilation will be needed and ICU stay will be shorter with early tracheostomy (within 5 days of injury) 11. Technique of PDT Tracheostomy can be done with several different techniques. We will only discuss the percutaneous single dilator technique, which is the most common and widely accepted technique. A pre-procedure checklist with a trained procedural team is ideal as indicated in Table III. After informed consent is obtained and the procedure team is assembled, the patient is positioned with a towel roll between the scapula. The head and neck should be maintained in a midline position throughout the procedure to prevent inadvertent malposition of the tracheostomy. In the United States, standard universal protocol is mandatory to assure all necessary staff and personnel are present and agree. In most of these patients the technique assumes mechanical ventilation with a preexisting endotracheal tube. A laryngeal mask airway can be safely used in selected patients (i.e. patients with progressive neuromuscular disease requiring long term airway management). The patient should be evaluated for coagulation disorders and presence of uremia. If uremia is present we typically give a dose of intravenous 1-desamino-8-arginine vasopressin at 0.3 µg/kg one hour prior to start of procedure. PDT can be performed if the prothrombin time/international normalized ratio (INR) is <1.6 times control and the platelet count is >50,000. The proceduralist identifies the appropriate landmarks. The patient is prepped and draped in sterile fashion. Topical anesthetic with 1% lidocaine with epinephrine is given within the subcutaneous tissue and pretracheal fascia. The
3 97 patient is premedicated with an intravenous narcotic and benzodiazepine or propofol. A paralytic agent may be given to prevent coughing, unless otherwise contraindicated. The patient is preoxygenated with 100% oxygen and the ventilator is placed on a set rate using either pressure or volume mode. Bronchoscopy is used for optimal placement of the guide wire and immediate confirmation of tracheostomy placement into the airway. Recently, ultrasound has been used as a possible means for guidance of PDT. Rajajee et. Al 12 recently conducted a feasibility study on 13 neurosurgical patients using ultrasound guidance as means for successful guide wire placement. They subsequently confirmed guidewire placement using bronchoscopy and found ultrasound feasible, safely avoids vital vascular structure with no cases of tube misplacement, pneumothorax, posterior wall injury, or significant bleeding. Optimal position of the tracheostomy should be between 10 o clock and 2 o clock between the 1 st and 2 nd or 2 nd and 3 rd tracheal ring as indicated in Figure II. Bronchoscopy should be limited to confirm placement of guide wire and tracheostomy, since bronchoscopy is thought to cause progressive hypercapnea and hypoxemia due to transient obstruction of the endotracheal tube. Bronchoscopy is best utilized during the initial entry, for confirming that the direction of the guidewire is distal in the trachea, and there is no inadvertent false tract entry. Lastly, it allows suctioning of any peri-procedural bleeding or clots, and confirms final position of tracheostomy. The most widely used technique is the single dilator method, which is described below. After proper patient positioning, sterile prep and drape, topical anesthetic, intravenous sedation with analgesia, and a muscle relaxant, a cm incision is made guided by identified landmarks. The incision can be made horizontally or vertically at the level between the 1 st and 4 th tracheal cartilaginous rings. A blunt dissection clamp can be used to gently spread the pretracheal planes and palpate the tracheal rings. This clamp can also be used to apply pressure to the anterior tracheal wall to confirm anticipated point of entry. First, the introducer needle is passed through the incision and between the tracheal rings. The needle is attached to a saline or lidocaine filled syringe so that air bubbles can be aspirated once inside the trachea. The bronchoscopist then confirms the point of entry. A guide wire is passed into the trachea via the introducer needle. The introducer needle is then removed. A punch dilator is passed over the guidewire creating the initial tract. A small catheter is then placed over the guidewire to prevent kinking of the guidewire as the large dilator is inserted into the trachea. The tracheostomy tube is then preloaded onto a dilator/loader and passed over the guidewire and catheter into the newly established tract 13. The endotracheal tube is then removed followed by bronchoscopic intubation of the tracheostomy for final confirmation of positioning within the trachea. COMPLICATIONS OF PDT The complications of PDT are similar to those of ST. We will highlight those complications, which are specific to PDT. Complications most commonly reported are bleeding, infection, malposition, and stenosis. Death is rare from tracheostomy and has been reported in 0 to 1.6% of cases 8, 14, 16. Complications should be categorized as early or late. Often early is defined as within 48 hours of procedure, whereas late and long term complications are seen within weeks of the procedure. Many early complications are self limited and require little or no intervention. Well established surgical back up is important for any non-surgical proceduralist to insure patient safety and timely intervention. Complications of PDT are highlighted in Table IV. CONCLUSION PDT is a safe and efficient procedure when performed by an adequately trained team of physicians, nurses, respiratory therapist, and necessary assistants. Published guidelines from the American College of Chest Physicians and the American Thoracic Society/European Respiratory Society have recommended a minimum of 20 supervised procedures to be performed 17, 18. The timing of tracheostomy will remain a challenge until we can better define particular characteristics of those ICU patients who will require prolonged mechanical ventilation at the onset of their initial respiratory failure. Conflict of Interest: none for both authors Funding: none for both authors
4 98 REFERENCES 1. Jackson C. Tracheotomy. Laryngoscope ;19: Borman J, Davidson JT. A history of tracheostomy: si spiritum ducit vivit (Cicero). Br J Anaesth Jun;35: Ciaglia P, Firsching R, Syniec C. Elective percutaneous dilatational tracheostomy. A new simple bedside procedure; preliminary report. Chest Jun;87(6): Delaney A, Bagshaw SM, Nalos M. Percutaneous dilatational tracheostomy versus surgical tracheostomy in critically ill patients: a systematic review and meta-analysis. Crit Care. 2006;10(2):R Durbin CG, Jr. Techniques for performing tracheostomy. Respir Care Apr;50(4): Rana S, Pendem S, Pogodzinski MS, Hubmayr RD, Gajic O. Tracheostomy in critically ill patients. Mayo Clin Proc Dec;80(12): Cabrini L, Monti G, Landoni G, Biondi-Zoccai G, Boroli F, Mamo D, et al. Percutaneous tracheostomy, a systematic review. Acta Anaesthesiol Scand Dec Kornblith LZ, Burlew CC, Moore EE, Haenel JB, Kashuk JL, Biffl WL, et al. One thousand bedside percutaneous tracheostomies in the surgical intensive care unit: time to change the gold standard. J Am Coll Surg Feb;212(2): Young D. The Tracheostomy Managment in Critical Care 10. Terragni PP, Antonelli M, Fumagalli R, Faggiano C, Berardino M, Pallavicini FB, et al. Early vs late tracheotomy for prevention of pneumonia in mechanically ventilated adult ICU patients: a randomized controlled trial. JAMA Apr 21;303(15): Holevar M, Dunham JC, Brautigan R, Clancy TV, Como JJ, Ebert JB, et al. Practice management guidelines for timing of tracheostomy: the EAST Practice Management Guidelines Work Group. J Trauma Oct;67(4): Rajajee V, Fletcher JJ, Rochlen LR, Jacobs TL. Real-time ultrasound-guided percutaneous dilatational tracheostomy: a feasibility study. Crit Care. 2011;15(1):R Beamis JF, Mathur PN, Mehta AC, editors. Interventional pulmonary medicine. 2nd ed. New York: Informa Healthcare; Beiderlinden M, Karl Walz M, Sander A, Groeben H, Peters J. Complications of bronchoscopically guided percutaneous dilational tracheostomy: beyond the learning curve. Intensive Care Med Jan;28(1): Pandit RA, Jacques TC. Audit of over 500 percutaneous dilational tracheostomies. Crit Care Resusc Jun;8(2): Walz MK, Peitgen K, Thurauf N, Trost HA, Wolfhard U, Sander A, et al. Percutaneous dilatational tracheostomy--early results and long-term outcome of 326 critically ill patients. Intensive Care Med Jul;24(7): Ernst A, Silvestri GA, Johnstone D. Interventional pulmonary procedures: Guidelines from the American College of Chest Physicians. Chest May;123(5): Bolliger CT, Mathur PN, Beamis JF, Becker HD, Cavaliere S, Colt H, et al. ERS/ATS statement on interventional pulmonology. European Respiratory Society/American Thoracic Society. Eur Respir J Feb;19(2):
5 99 Table I. INDICATIONS FOR PDT Prolonged mechanical ventilation: anticipated > 10 days Improved management of respiratory secretions Upper airway obstruction Enhance patient comfort and allow for weaning with reduction of sedation Failed extubation Reduction of extubation risk in a known difficult airway Table II. CONTRAINDICATIONS FOR PDT Relative Contraindications Unstable cervical spine Prior neck surgery or radiation Extensive burns to the neck Morbid obesity (BMI > 40) FIO2 >60 PEEP > 15 Surgical wounds near planned site Large thyroid goiter or local malignancy at planned site Anatomic variations (severe tracheal deviation and superficial vasculature at planned site Severe trachomalacia Absolute Contraindications Infants Clinical instability Uncorrectable coagulopathy Significant infection at anticipated site Emergency airway access Patient unlikely to survive > 48 hours Unable to define and/or palpate tracheal anatomy after proper patient positioning Absence of informed consent Lack of operator training Table III. PROCEDURE TEAM AND PRE-PROCEDURE CHECKLIST TEAM MEMBERS Proceduralist: Guides steps of procedure and assures safety of patient Bronchoscopist: Inspects airway, maintains control of airway, and familiar of necessary bronchoscopic landmarks Bronchoscopy technician: Provides all necessary bronchoscopic equipment Bronchoscopy nurse: assists bronchoscopist in management of endotracheal tube repositioning Respiratory Therapist: confirms patient ventilator settings and oxygenation ICU Nurse: provides continuous assessment of patient and provides necessary sedation, analgesia, and paralytics as needed PREPROCEDURE CHECKLIST Consent signed Labs reviewed and medications reviewed Coagulopathies corrected Patient positioning Anticipates difficult airway Verifies ventilator settings
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Is Percutaneous Tracheostomy Safe in Critically Ill Patients: A Retrospective Analysis
 ISSN: 2250-0359 Is Percutaneous Tracheostomy Safe in Critically Ill Patients: A Retrospective Analysis Ebru Tarıkçı Kılıç 1*, Mehmet Salim Akdemir 1, Ali İhsan Sert 2 1 Department of Anesthesiology and
ISSN: 2250-0359 Is Percutaneous Tracheostomy Safe in Critically Ill Patients: A Retrospective Analysis Ebru Tarıkçı Kılıç 1*, Mehmet Salim Akdemir 1, Ali İhsan Sert 2 1 Department of Anesthesiology and
Airway Management in the ICU
 Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Indications for and Management of Tracheostomy
 Chapter 40 Indications for and Management of Tracheostomy Judi Anne B. Ramiscal, Michael S. Hayashi, and Mihae Yu Introduction A translaryngeal endotracheal tube (ETT) is the primary method of securing
Chapter 40 Indications for and Management of Tracheostomy Judi Anne B. Ramiscal, Michael S. Hayashi, and Mihae Yu Introduction A translaryngeal endotracheal tube (ETT) is the primary method of securing
PRODUCTS FOR THE DIFFICULT AIRWAY. Courtesy of Cook Critical Care
 PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
Feasibility of Percutaneous Dilatational Tracheostomy with a Light Source in the Surgical Intensive Care Unit
 Acute and Critical Care 2018 May 33(2):89-94 / ISSN 2586-6052 (Print) ㆍ ISSN 2586-6060 (Online) Original Article Feasibility of Percutaneous Dilatational Tracheostomy with a Light Source in the Surgical
Acute and Critical Care 2018 May 33(2):89-94 / ISSN 2586-6052 (Print) ㆍ ISSN 2586-6060 (Online) Original Article Feasibility of Percutaneous Dilatational Tracheostomy with a Light Source in the Surgical
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Bronchoscopy SICU Protocol
 Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Tracheostomy practice in adults with acute respiratory failure
 本檔僅供內部教學使用檔案內所使用之照片之版權仍屬於原期刊公開使用時, 須獲得原期刊之同意授權 Tracheostomy practice in adults with acute respiratory failure Bradley D. Freeman, MD, FACS; Peter E. Morris, MD, FCCP Crit Care Med 2012 Vol. 40, No. 10
本檔僅供內部教學使用檔案內所使用之照片之版權仍屬於原期刊公開使用時, 須獲得原期刊之同意授權 Tracheostomy practice in adults with acute respiratory failure Bradley D. Freeman, MD, FACS; Peter E. Morris, MD, FCCP Crit Care Med 2012 Vol. 40, No. 10
Trauma operating room
 Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Audit on Tracheostomies Performed at the General Intensive Care Unitt Kuala Lumpur Hospital
 ORIGINAL ARTICLE Audit on Tracheostomies Performed at the General Intensive Care Unitt Kuala Lumpur Hospital A S Rao, FANZCA, L Mansor, FRCA, K Inbasegaran, FANZCA Department of Anaesthesia and Intensive
ORIGINAL ARTICLE Audit on Tracheostomies Performed at the General Intensive Care Unitt Kuala Lumpur Hospital A S Rao, FANZCA, L Mansor, FRCA, K Inbasegaran, FANZCA Department of Anaesthesia and Intensive
Original Article Percutaneous dilational tracheostomy: An initial experience in community based teaching hospital
 Kathmandu University Medical Journal (2006), Vol. 4, No. 3, Issue 15, 275-280 Original Article Percutaneous dilational tracheostomy: An initial experience in community based teaching hospital Joshi S 1,
Kathmandu University Medical Journal (2006), Vol. 4, No. 3, Issue 15, 275-280 Original Article Percutaneous dilational tracheostomy: An initial experience in community based teaching hospital Joshi S 1,
Percutaneous tracheostomy
 Bisanth Batuwitage MBBCh MRCS FRCA Stephen Webber MBChB FRCA FFICM Alastair Glossop BMed Sci BM BS MRCP FRCA DICM FFICM 1C02,2A01,2CO2 Key points Percutaneous tracheostomy is a safe and widely performed
Bisanth Batuwitage MBBCh MRCS FRCA Stephen Webber MBChB FRCA FFICM Alastair Glossop BMed Sci BM BS MRCP FRCA DICM FFICM 1C02,2A01,2CO2 Key points Percutaneous tracheostomy is a safe and widely performed
Kingdom; 2 University of Cambridge, Cambridge, United Kingdom
 P-111 TIMING OF TRACHEOSTOMY AND ASSOCIATED COMPLICATIONS IN CARDIOTHORACIC INTENSIVE CARE PATIENTS Zochios, Vasileios 1 ; Casey, Jessica 2 ; Vuylsteke, Alain 1 1 Cardiac Critical Care Unit, Papworth Hospital
P-111 TIMING OF TRACHEOSTOMY AND ASSOCIATED COMPLICATIONS IN CARDIOTHORACIC INTENSIVE CARE PATIENTS Zochios, Vasileios 1 ; Casey, Jessica 2 ; Vuylsteke, Alain 1 1 Cardiac Critical Care Unit, Papworth Hospital
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
British Journal of Anaesthesia 104 (6): (2010) doi: /bja/aeq087 Advance Access publication April 21, 2010
 CRITICAL CARE Comparison between single-step and balloon dilatational tracheostomy in intensive care unit: a single-centre, randomized controlled study G. Cianchi 1, G. Zagli 1 *, M. Bonizzoli 1, S. Batacchi
CRITICAL CARE Comparison between single-step and balloon dilatational tracheostomy in intensive care unit: a single-centre, randomized controlled study G. Cianchi 1, G. Zagli 1 *, M. Bonizzoli 1, S. Batacchi
Comparison of Complications in Percutaneous Dilatational Tracheostomy versus Surgical Tracheostomy
 Global Journal of Health Science; Vol. 6, No. 4; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Comparison of Complications in Percutaneous Dilatational Tracheostomy
Global Journal of Health Science; Vol. 6, No. 4; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Comparison of Complications in Percutaneous Dilatational Tracheostomy
APPROACH TO THE EMERGENCY AIRWAY. Scott B. Davidson MD, FACS Trauma Surgery Service Bronson Methodist Hospital
 APPROACH TO THE EMERGENCY AIRWAY Scott B. Davidson MD, FACS Trauma Surgery Service Bronson Methodist Hospital Objectives History Initial recognition Get your act together Surgical options Complications
APPROACH TO THE EMERGENCY AIRWAY Scott B. Davidson MD, FACS Trauma Surgery Service Bronson Methodist Hospital Objectives History Initial recognition Get your act together Surgical options Complications
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Translaryngeal Tracheostomy - TLT Fantoni Method
 Translaryngeal Tracheostomy - TLT Fantoni Method Fantoni A., Ripamonti D., Lesmo A. About the Authors Fantoni Antonio Chief Emeritus of Department of Anaesthesia and Intensive Care - San Carlo Borromeo
Translaryngeal Tracheostomy - TLT Fantoni Method Fantoni A., Ripamonti D., Lesmo A. About the Authors Fantoni Antonio Chief Emeritus of Department of Anaesthesia and Intensive Care - San Carlo Borromeo
Percutaneous Dilatational Tracheostomy. Consensus Statement
 Percutaneous Dilatational Tracheostomy Consensus Statement Australian New Zealand intensive Care Society (ANZICS) 2010 Suggested Citation: ANZICS, Percutaneous Dilatational Tracheostomy Consensus Statement,
Percutaneous Dilatational Tracheostomy Consensus Statement Australian New Zealand intensive Care Society (ANZICS) 2010 Suggested Citation: ANZICS, Percutaneous Dilatational Tracheostomy Consensus Statement,
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Techniques for Performing Tracheostomy
 Techniques for Performing Tracheostomy Charles G Durbin Jr MD FAARC Introduction History of Tracheostomy Percutaneous Tracheostomy Techniques of Performing an Open or Surgical Tracheostomy Percutaneous
Techniques for Performing Tracheostomy Charles G Durbin Jr MD FAARC Introduction History of Tracheostomy Percutaneous Tracheostomy Techniques of Performing an Open or Surgical Tracheostomy Percutaneous
TRACHEOSTOMY 186 INTENSIVE CARE
 186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
ENDOBRONCHIAL ABLATIVE THERAPIES. Christopher Cortes, MD, FPCCP
 ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
ENDOBRONCHIAL ABLATIVE THERAPIES Christopher Cortes, MD, FPCCP Choice of Ablative Therapy Size of the lesion Location of the lesion Characteristics of the lesion Availability of the different therapies
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
How to use the Control-Cric to perform a surgical cricothyrotomy
 TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
Corkscrew stenosis : Defining and preventing a complication of percutaneous dilatational tracheostomy
 Corkscrew stenosis : Defining and preventing a complication of percutaneous dilatational tracheostomy Jordan V. Jacobs, MD, a David A. Hill, MD, a Scott R. Petersen, MD, a Ross M. Bremner, MD, PhD, b Richard
Corkscrew stenosis : Defining and preventing a complication of percutaneous dilatational tracheostomy Jordan V. Jacobs, MD, a David A. Hill, MD, a Scott R. Petersen, MD, a Ross M. Bremner, MD, PhD, b Richard
The Ventilator Liberation Process: Update on Technique, Timing, and Termination of Tracheostomy
 The Ventilator Liberation Process: Update on Technique, Timing, and Termination of Tracheostomy Edward A Bittner MD PhD and Ulrich H Schmidt MD PhD Introduction Indications for Tracheostomy and Patient
The Ventilator Liberation Process: Update on Technique, Timing, and Termination of Tracheostomy Edward A Bittner MD PhD and Ulrich H Schmidt MD PhD Introduction Indications for Tracheostomy and Patient
Advocate Christ Medical Center CVC Placement Certification Course
 Advocate Christ Medical Center CVC Placement Certification Course July 12th, 2012 Hannah Watts, MD Medical Simulation Director Modified August 10, 2017 Taajwar Khan, MD Chief Resident of Internal Medicine
Advocate Christ Medical Center CVC Placement Certification Course July 12th, 2012 Hannah Watts, MD Medical Simulation Director Modified August 10, 2017 Taajwar Khan, MD Chief Resident of Internal Medicine
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation
 I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
I. Subject: Therapeutic Bronchoscopy and Bronchoscope Assisted Intubation II. Policy: Therapeutic flexible fiberoptic bronchoscopy procedures and bronchoscope assisted intubations will be performed by
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
How do you use a bougie as an airway adjunct for endotracheal intubation?
 Ruth Bird, MBBCh -Specialist Registrar: Anaesthesia & Paediatric Trauma Fellow Daniel Nevin, MBBCh -Consultant in Anaesthesia & Pre-Hospital Care The Royal London Hospital London s Air Ambulance (HEMS)
Ruth Bird, MBBCh -Specialist Registrar: Anaesthesia & Paediatric Trauma Fellow Daniel Nevin, MBBCh -Consultant in Anaesthesia & Pre-Hospital Care The Royal London Hospital London s Air Ambulance (HEMS)
Emergency Cricothyrotomy
 Emergency Cricothyrotomy SWORBHP Live Paramedic Rounds June 15, 2012 Sameer Mal PGY4 Emergency Medicine Dwayne Cottel Regional Paramedic Educator Overview BVM Ventilation Intro to Cricothyrotomy Relevant
Emergency Cricothyrotomy SWORBHP Live Paramedic Rounds June 15, 2012 Sameer Mal PGY4 Emergency Medicine Dwayne Cottel Regional Paramedic Educator Overview BVM Ventilation Intro to Cricothyrotomy Relevant
General OR Rotations GOALS & OBJECTIVES
 General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
General OR Rotations GOALS & OBJECTIVES Goals At the end of the CA 1 year General OR rotations, the resident should competently manage uncomplicated ambulatory, orthopedic, maxillo-facial, ENT, gynecologic,
Airway management problem during anaesthesia. Airway management problem in ICU / HDU. Airway management problem occurring in the Emergency Department
 4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital,
 H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital, Montreal General Hospital, McGill University Health Center
H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital, Montreal General Hospital, McGill University Health Center
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Adult Intubation Skill Sheet
 Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Adult Intubation 2. Opens the airway manually and inserts an oral airway *** 3. Ventilates the patient with BVM attached to oxygen at 15 lpm *** 4. Directs assistant to oxygenate the patient 5. Selects
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
신경계중환자실에서시행한경피적확장기관절개술의안정성과타당성
 Original article J Neurocrit Care 2018;11(1):32-38 eissn 2508-1349 신경계중환자실에서시행한경피적확장기관절개술의안정성과타당성 이동현 1,2 정진헌 1,3 동아대학교의과대학동아대학교병원 1 중환자의학과, 2 호흡기내과, 3 신경과 Safety and Feasibility of Percutaneous Dilatational
Original article J Neurocrit Care 2018;11(1):32-38 eissn 2508-1349 신경계중환자실에서시행한경피적확장기관절개술의안정성과타당성 이동현 1,2 정진헌 1,3 동아대학교의과대학동아대학교병원 1 중환자의학과, 2 호흡기내과, 3 신경과 Safety and Feasibility of Percutaneous Dilatational
Difficult Airway. Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital
 Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
Airway Management. Teeradej Kuptanon, MD
 Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Central Venous Line Insertion
 Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Central Venous Line Insertion Understand the indications and risks of CVC insertion Understand and troubleshoot the seldinger technique Understand available sites and select the appropriate site for clinical
Intubation sedation intubation
 Intubation sedation Mar 29, 2017. When a paralytic agent is used for intubation without sedation, the patient may be fully aware of his or. Oct 11, 2016. This post will review sedation and analgesia regimens
Intubation sedation Mar 29, 2017. When a paralytic agent is used for intubation without sedation, the patient may be fully aware of his or. Oct 11, 2016. This post will review sedation and analgesia regimens
Summary Report for Individual Task Perform a Surgical Cricothyroidotomy Status: Approved
 Report Date: 12 Jul 2011 Summary Report for Individual Task 081-833-3005 Perform a Surgical Cricothyroidotomy Status: Approved DISTRIBUTION RESTRICTION: Approved for public release; distribution is unlimited.
Report Date: 12 Jul 2011 Summary Report for Individual Task 081-833-3005 Perform a Surgical Cricothyroidotomy Status: Approved DISTRIBUTION RESTRICTION: Approved for public release; distribution is unlimited.
Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
CASE PRIMERS. Pediatric Anesthesia Fellowship Program. Laryngotracheal Reconstruction (LTR) Tufts Medical Center
 CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
CASE PRIMERS Pediatric Anesthesia Fellowship Program Tufts Medical Center Department of Anesthesiology and Perioperative Medicine Division of Pediatric Anesthesia 800 Washington Street, Box 298 Boston,
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
ADVANCED AIRWAY MANAGEMENT
 The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
The Advanced Airway Management protocol should be used on all patients requiring advanced airway management procedures. This protocol is divided into three sections the Crash Airway Algorithm, the Rapid
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
ENDOTRACHEAL INTUBATION POLICY
 POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
POLICY Indications: Ineffective ventilation with mask and t-piece, or mask and bag technique Inability to maintain a patent airway Need or anticipation of need for prolonged ventilation Need for endotracheal
Since central airway stenosis is often a lifethreatening. Double Y-stenting for tracheobronchial stenosis. Masahide Oki and Hideo Saka
 Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Eur Respir J 2012; 40: 1483 1488 DOI: 10.1183/09031936.00015012 CopyrightßERS 2012 Double Y-stenting for tracheobronchial stenosis Masahide Oki and Hideo Saka ABSTRACT: The purpose of the present study
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
General Medical Procedure. Emergency Airway Techniques (General Airway Protocol)
 General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
Effectiveness of Fiberoptic Intubation in Anticipated Difficult Airway
 Original Article Effectiveness of Fiberoptic Intubation in Anticipated Difficult Airway Khawaja Kamal Nasir, Faraz Mansoor From Department of Anesthesia, Pakistan Institute of Medical Sciences, Islamabad.
Original Article Effectiveness of Fiberoptic Intubation in Anticipated Difficult Airway Khawaja Kamal Nasir, Faraz Mansoor From Department of Anesthesia, Pakistan Institute of Medical Sciences, Islamabad.
PERCUTANEOUS DILATATIONAL TRACHEOSTOMY: A PROSPECTIVE ANALYSIS ABOUT THE SAFETY OF PROCEDURE AMONG ICU PATIENTS ABSTRACT
 ORIGINAL ARTICLE PERCUTANEOUS DILATATIONAL TRACHEOSTOMY: A PROSPECTIVE ANALYSIS ABOUT THE SAFETY OF PROCEDURE AMONG ICU PATIENTS Syed Mazhar Ali Naqvi 1, Muhammad Javed Bashir 2, Muhammad Hussain 3, Hamna
ORIGINAL ARTICLE PERCUTANEOUS DILATATIONAL TRACHEOSTOMY: A PROSPECTIVE ANALYSIS ABOUT THE SAFETY OF PROCEDURE AMONG ICU PATIENTS Syed Mazhar Ali Naqvi 1, Muhammad Javed Bashir 2, Muhammad Hussain 3, Hamna
TRACHEOSTOMY. 28 August J Reddy CONTENTS
 28 August 2009 CONTENTS TRACHEOSTOMY J Reddy Commentator: L Pillay Moderator: D Muckart INTRODUCTION... 3 HISTORY OF TRACHEOSTOMY... 3 ANATOMY... 3 PHYSIOLOGY... 6 INDICATIONS FOR TRACHEOSTOMY... 9 CONTRAINDICATIONS...
28 August 2009 CONTENTS TRACHEOSTOMY J Reddy Commentator: L Pillay Moderator: D Muckart INTRODUCTION... 3 HISTORY OF TRACHEOSTOMY... 3 ANATOMY... 3 PHYSIOLOGY... 6 INDICATIONS FOR TRACHEOSTOMY... 9 CONTRAINDICATIONS...
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
The Use of Fiberoptic Bronchoscopy During Percutaneous Dilatational Tracheostomy with Laryngeal Mask
 Diagnostic and Therapeutic Endoscopy, Vol. 4, pp. 13-18 Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 4, pp. 13-18 Reprints available directly from the publisher Photocopying permitted by license only (C) 1997 OPA (Overseas Publishers Association) Amsterdam B.V.
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Airway complications on the general medical unit after prolonged ICU admission
 Airway complications on the general medical unit after prolonged ICU admission Palash Kar Discipline of Acute Care Medicine, University of Adelaide Intensive Care Unit, Royal Adelaide Hospital, Adelaide,
Airway complications on the general medical unit after prolonged ICU admission Palash Kar Discipline of Acute Care Medicine, University of Adelaide Intensive Care Unit, Royal Adelaide Hospital, Adelaide,
Equipment: NRP algorithm, MRSOPA table, medication chart, SpO 2 table Warm
 NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
NRP Skills Stations Performance Skills Station OR Integrated Skills Station STATION: Assisting with and insertion of endotracheal tube (ETT) Equipment: NRP algorithm, MRSOPA table, medication chart, SpO
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other
 Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Joint Theater Trauma System Clinical Practice Guideline
 Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Page 1 of 7 Joint Theater Trauma System Clinical Practice Guideline TRAUMA AIRWAY MANAGEMENT Original Release/Approval 18 Dec 2004 Note: This CPG requires an annual review. Reviewed: May 2012 Approved:
Overview. Chapter 37. Advanced Airway Techniques. Sellick Maneuver 9/11/2012
 Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
Chapter 37 Advanced Airway Techniques Slide 1 Sellick Maneuver Purpose Anatomic Location Technique Special Considerations Overview Advanced Airway Management of Adults Esophageal Tracheal Combitubes Tracheal
Mobilizing the Patient in the Intensive Care Unit: The Role of Early Tracheotomy
 Crit Care Clin 23 (2007) 71 79 Mobilizing the Patient in the Intensive Care Unit: The Role of Early Tracheotomy Stephen R. Clum, MD, PhD, Mark J. Rumbak, MD, FCCP* Department of Internal Medicine, Division
Crit Care Clin 23 (2007) 71 79 Mobilizing the Patient in the Intensive Care Unit: The Role of Early Tracheotomy Stephen R. Clum, MD, PhD, Mark J. Rumbak, MD, FCCP* Department of Internal Medicine, Division
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Jefferson Tower Task Trainer List
 Jefferson Tower Task Trainer List Table of Contents Blue Phantom Ultrasound Central Line Training Model 2 Blue Phantom Femoral Vascular Access Training Model 3 Blue Phantom Thoracentesis Ultrasound Training
Jefferson Tower Task Trainer List Table of Contents Blue Phantom Ultrasound Central Line Training Model 2 Blue Phantom Femoral Vascular Access Training Model 3 Blue Phantom Thoracentesis Ultrasound Training
Trust Guidelines. Title: Guidelines for chest drain insertion
 Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Trust Guidelines Title: Guidelines for chest drain insertion Authors: Dr JCT Pepperell; Dr J Tipping; J Hansford Ratified by: Planned Care and Emergency & Urgent Care Divisional Governance Committees Active
Interfacility Protocol Protocol Title:
 Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interfacility Protocol Protocol Title: Mechanical Ventilator Monitoring & Management Original Adoption Date: 05/2009 Past Protocol Updates 05/2009, 12/2013 Date of Most Recent Update: March 23, 2015 Medical
Interesting Case Series. Pulmonary Injury Secondary to Feeding Tube Misplacement
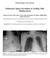 Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Tracheostomy/ Laryngectomy PRODUCT CATALOG
 1 Tracheostomy/ Laryngectomy PRODUCT CATALOG 2 3 is a highly experienced manufacturer of medical devices for tracheostomized and laryngectomized patients. For many years we have been supplying our customers
1 Tracheostomy/ Laryngectomy PRODUCT CATALOG 2 3 is a highly experienced manufacturer of medical devices for tracheostomized and laryngectomized patients. For many years we have been supplying our customers
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
Airway Workshop Lecture. University of Ottawa
 Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Management of pediatric cannot intubate, cannot oxygenate
 Acute Medicine & Surgery 2017; 4: 462 466 doi: 10.1002/ams2.305 Case Report Management of pediatric cannot intubate, cannot oxygenate Yohei Okada, 1 Wataru Ishii, 1 Norio Sato, 2 Hirokazu Kotani, 3 and
Acute Medicine & Surgery 2017; 4: 462 466 doi: 10.1002/ams2.305 Case Report Management of pediatric cannot intubate, cannot oxygenate Yohei Okada, 1 Wataru Ishii, 1 Norio Sato, 2 Hirokazu Kotani, 3 and
Subglottic stenosis, with involvement of the lower larynx
 Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Emergency Airway Management. Richard P. Dutton, M.D., M.B.A. Chief Quality Officer US Anesthesia Partners
 Emergency Airway Management Richard P. Dutton, M.D., M.B.A. Chief Quality Officer US Anesthesia Partners Disclosures I have studied a lot of airway gizmos over the years. I have no financial interest in
Emergency Airway Management Richard P. Dutton, M.D., M.B.A. Chief Quality Officer US Anesthesia Partners Disclosures I have studied a lot of airway gizmos over the years. I have no financial interest in
Review July Page 1 of 36. Title of Guideline. Contact Names and Job Title (authors) Directorate & Speciality
 Title of Guideline Contact Names and Job Title (authors) Directorate & Speciality Date of submission 06/07/2017 Date on which guideline must be reviewed Explicit definition of patient group to which it
Title of Guideline Contact Names and Job Title (authors) Directorate & Speciality Date of submission 06/07/2017 Date on which guideline must be reviewed Explicit definition of patient group to which it
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
PANELISTS. Controversial Issues In Common Interventions In ORL 4/10/2014
 Controversial Issues In Common Interventions In ORL Mohamed Hesham,MD Alexandria Faculty of Medicine PANELISTS Prof. Ahmed Eldaly Prof. Hamdy EL-Hakim Prof. Hossam Thabet Prof. Maged El-Shenawy Prof. Prince
Controversial Issues In Common Interventions In ORL Mohamed Hesham,MD Alexandria Faculty of Medicine PANELISTS Prof. Ahmed Eldaly Prof. Hamdy EL-Hakim Prof. Hossam Thabet Prof. Maged El-Shenawy Prof. Prince
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Educational Session: Evaluation and Management of the Difficult Airway
 Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Tracheostomy in pediatric. Tran Quoc Huy, MD ENT department
 Tracheostomy in pediatric Tran Quoc Huy, MD ENT department 1. History 2. Indication 3. Tracheostomy vs Tracheal intubation 4. A systematic review 5. Decannulation 6. Swallowing 7. Communication concerns
Tracheostomy in pediatric Tran Quoc Huy, MD ENT department 1. History 2. Indication 3. Tracheostomy vs Tracheal intubation 4. A systematic review 5. Decannulation 6. Swallowing 7. Communication concerns
Difficult Airway. Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.)
 Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Changing tracheostomy tubes
 Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
