Rehabilitation Guidelines for UCL Repair
|
|
|
- Jennifer Gilbert
- 5 years ago
- Views:
Transcription
1 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for UCL Repair The elbow is a complex system of three joints formed from three bones; the humerus (the upper arm bone), the ulna (the larger bone of the forearm, on the small finger side) and the radius (the smaller bone of the forearm, on the thumb side). This complex system allows a hinging action (bending and straightening) and a rotation action. The stability of the elbow joint is maintained by the bony congruency, the muscular attachments and the ligaments. There are several important ligaments in the elbow. Ligaments are soft tissue that connect bones to bones. The ligaments around a joint usually combine together to form a joint capsule. A joint capsule is a watertight sac that surrounds a joint and contains lubricating fluid called synovial fluid. In the elbow, two of the most important ligaments are the ulnar collateral ligament (UCL) and the lateral collateral ligament (LCL). The UCL is also known as the medial collateral ligament. The UCL is on the medial (the side of the elbow that s next to the body when your arms are at your side with your palms up or facing out in front of you) side of the elbow and LCL is on the outside of your elbow. The ulnar collateral ligament is a thick band of tissue that forms a triangular shape along the inside of the elbow. It has an anterior bundle, posterior bundle and a thinner, transverse ligament. These ligaments can be torn when there is an injury or dislocation of the elbow. If the injury to the ligament(s) affects the stability of the joint, it is possible that the function of the elbow will be compromised. Injury to the UCL in overhead athletes has been widely reported. Normal activities of daily living rarely place enough stress on the UCL to create instability but throwing sports place high stresses on the elbow supporting structures. Over time, the high repetitive stresses associated with throwing and overhead activity may create overload to the supporting ligamentous support, resulting in a UCL tear. Athletes with UCL injury report a history of repetitive throwing with complaints of pain at the medial (inside) aspect of the elbow during or after their activity. Onset occurs from either one traumatic incident or can develop throughout a long period of time due to repetitive elbow stress. Eventually the athlete loses their velocity and accuracy of throwing. More than 40% of athletes with UCL injury also report symptoms of ulnar nerve irritation from friction or snapping of the nerve during activity. The overhead thrower often experiences pain with the arm fully cocked (shoulder in full external rotation or the arm rotated all the way back) and as it accelerates through the throw and release of the ball. While throwing, the elbow can straighten at speeds of over 2300 degrees per second and may have a valgus (side) force that exceeds the ultimate strength of the normal uninjured UCL. Proper mechanics and optimal strength and endurance of the muscles of the upper extremity are needed to assist with injury prevention. Trauma or injury to the UCL results in significant functional limitations including medial elbow pain, loss of velocity and accuracy with throwing, instability, neurologic (nerve) symptoms and decreased muscular strength. The consequences of this injury usually leave the athlete who has a torn UCL with two options: rehabilitation with activity modification (i.e. avoidance of pitching and performance throwing) or surgical correction with postoperative rehabilitation prior to return to pitching and performance throwing. The two types of surgical correction are UCL reconstruction and UCL repair. A reconstruction involves replacing the torn UCL with a different tendon, where as a repair involves suturing the torn UCL back to its original location. UCL reconstruction surgery is performed through an incision on the medial (inside) side of the elbow joint. The damaged ulnar collateral ligament is replaced with a tendon taken from somewhere else in the body. The tendon graft can come from the patient s own forearm, The world class health care team for the UW Badgers and proud sponsor of UW Athletics UWSPORTSMEDICINE.ORG
2 hamstring, knee or foot. This is called an autograft. This tendon is weaved through drill holes in the humerus and ulna to re-create the triangular shape of the UCL. If the ulnar collateral ligament is pulled off the bone (avulsed) at the time of injury (as opposed to being torn in the middle of the ligament) AND the ligament itself looks strong and healthy then an option for surgical correction is a UCL repair. In this procedure suture anchors are drilled in to the bone at the ligament s original attachment site. Then fiber tape sutures are put through the avulsed ligament and pulled back to the bone and tied off securely. Rehabilitation following surgical repair of the UCL begins with range of motion and initial protection of the repair, along with resistive exercises to keep the shoulder and core strong. This is followed by progressions for resistive exercise that attempt to fully restore strength and muscular endurance to allow for a safe return to throwing and overhead functional activities. These guidelines also include aerobic training throughout the rehabilitation process and, for many, a later stage an interval throwing program. This multi-faceted rehabilitation approach often includes biomechanical video analysis to ensure proper throwing mechanics before an athlete returns to their sport. The early phases of post-operative care for UCL repair involve specific time frames, restrictions and precautions to protect healing tissues and the surgical fixation/ reconstruction. The later phases of rehabilitation are presented in a criterion based progression, where advancement to subsequent levels is based on strength and control. Return to competitive throwing will take 6-9 months. Not all athletes will be able to return to competitive throwing. The athlete should ice the elbow for minutes after their rehabilitation program to help decrease pain and swelling. 2 UWSPORTSMEDICINE.ORG
3 PHASE I (surgery to 3 weeks after surgery) Suggested therapeutic exercise Rehbilitation appointments begin days after surgery, after the first physician visit and continue 1 time per week Protect healing tissues Decrease pain and inflammation Prevent muscular atrophy Initiate elbow range of motion (ROM) Week 1 = immobilized at 90 of elbow flexion in hard brace Week 2 = functional hinged brace with ROM from Week 3 = functional hinged brace with a ROM of Gentle active and active assistive ROM for the elbow and wrist Gentle and gradual overpressure to meet ROM guidelines Note: be sure to avoid valgus force or positioning during ROM exercises Begin week 2 with sub-maximal isometrics for shoulder internal rotation (IR), shoulder abduction, biceps, wrist flexors and extensors Hand gripping Cervical spine and scapular active ROM Walking, stationery bike-brace on No treadmill Avoid running and jumping due to the distractive and compressive forces that can occur at landing PHASE II (begin after meeting Phase 1 criteria, usually 4-8 weeks after surgery) Rehabilitation appointments are 1 time per week Gradual increase in elbow ROM to near full ROM by week 9-10 Protect reconstruction during continued healing Improve muscular strength of the arm, shoulder and trunk Week 4 = functional hinged brace with ROM from Week 5 = functional hinged brace with ROM from Week 6 = functional hinged brace with ROM from Discontinue brace at 6-8 weeks except in unsafe environments (this time frame may vary from patient to patient per physician recommendation) Avoid all valgus positions and minimize valgus stress to the elbow during all rehab exercises Gentle active and active assistive ROM for elbow and wrist Passive range of motion (PROM) should be initiated in a very controlled and gentle fashion 3 UWSPORTSMEDICINE.ORG
4 Suggested Therapeutic Exercise Isotonics with light resistance for shoulder IR/external rotation (ER), shoulder abduction, elbow flexion/extension, pronation/supination, wrist flexion/extension (all in a protective elbow position-hand staying on the medial side of the elbow for all shoulder rotation exercises) Walking, stationery bike-brace on No treadmill Avoid running and jumping due to the distractive and compressive forces that can occur at landing PHASE III (begin after meeting Phase II criteria, usually 9-12 weeks after surgery) Rehabilitation appointments are once every 1-2 weeks Increase overall strength and endurance Achieve and maintain full elbow ROM Transition to entry level plyometrics There should be no pain while doing the strengthening exercises Post-exercise soreness; should be less than 4/10 and return to baseline within hours ROM should be full at post-operative week 10. If not, please consult with the physician prior to week 12 appointment Suggested Therapeutic Exercises Progressive isotonics for shoulder and elbow strengthening with the arm <45 abduction positions, controlling speed of the movement and valgus force at the elbow Initiate eccentric elbow flexion strengthening Assess shoulder mobility and address any imbalances (such as posterior capsular tightness (which may prevent optimal throwing biomechanics in the next phase Manual resistance diagonal patterns Hip, lower extremity and core strengthening Scapular strengthening and stabilization Walking, stationery bike-brace off Continue to avoid running and jumping 4 UWSPORTSMEDICINE.ORG
5 PHASE IV (begin after meeting Phase III criteria, usually weeks after surgery) Suggested Therapeutic Exercises Rehabilitation appointments are once every 1-2 weeks Maximize rotator cuff and scapular strength in throwing positions and postures Initiate education on throwing mechanics Transition to higher level plyometrics There should be no pain while doing the strengthening exercises Post-exercise soreness; should be less than 4/10 and return to baseline within hours ROM should be full at this point. If not, please consult with the physician Shoulder and elbow strengthening with the arm in > 45 abducted position, controlling speed of the movement and valgus force at the elbow Initiate rhythmic stabilization drills for the elbow and shoulder in protected positions (at athlete s side) Initiate plyometrics-2 hand drills only Begin throwing mechanics education-including slow motion air throws, posture and position check points Hip, lower extremity and core strengthening Scapular strengthening and stabilization Week 16; athlete may be running and sprinting at 75% speed, monitoring the environment to minimize the risk of falls 5 UWSPORTSMEDICINE.ORG
6 PHASE V (begin after meeting Phase IV criteria, usually weeks after surgery) Suggested Therapeutic Exercises Rehabilitation appointments are once every 2-3 weeks Maximize dynamic neuromuscular control with shoulder and elbow stabilization Develop biomechanically sound throwing mechanics Maximize muscular endurance and strength of the muscles involved in throwing, including core, upper and lower extremity There should be no pain while throwing or doing sport specific drills Post-throwing soreness or post-sport specific drill soreness; should be less than 4/10 and return to baseline within hours ROM should be full at this point. If not, please consult with the physician Multi-joint, multi-planar strengthening program Shoulder and elbow stabilization and proprioceptive drills Plyometric progressions (over several weeks); transition from 2 arms in the sagittal plane, progressing to 1 arm sagittal plane to 2 arm rotational movements to 1 arm rotational movement Initiate interval throwing program, progressing to a position specific throwing program around week 28 if the athlete has no pain or problems with the baseline throwing program Initiate sport specific return program for golf, tennis, basketball or volleyball Hip, lower extremity and core strengthening Training should be targeted toward sport specific energy systems These rehabilitation guidelines were developed collaboratively between UW Health Sports Rehabilitation and the UW Health Sports Medicine physician group. Updated 11/2018 REFERENCES 1. Ulnar Collateral Ligament Reconstuction in High School Baseball Players: Clinical Results and Injury Risk Factors. AJSM 32(5), pp , Current Concepts in the Rehabilitation of the Overhead Throwing Athlete. AJSM 30, pp , Cain EL, Dugas JR, Wolf RS, Andrews JR. Elbow injuries in throwing athletes: a current concepts review. Am J Sports Med. 2003; 31(4): Conway JE, Jobe FW, Glousman RE, Pink M. Medial instability of the elbow in throwing athletes: surgical treatment by ulnar collateral ligament repair or reconstruction. J Bone Joint Surg Am. 1992; 74: Ellenbecker TS, Wilk KE, Altchek DW, Andrews JR. Current concepts in rehabilitation following ulnar collateral ligament reconstruction. Sports Health. 2009; 1(4): Flesig GS, Andrews JR, Dillman CJ, Escamilla RF. Kinetics of baseball pitching with implications about injury mechanisms. Am J Sports Med. 1995; 23: Vitale MA, Ahmad CS. The outcome of elbow ulnar collateral ligament reconstruction in overhead athletes: a systematic review. Am J Sports Med. 2008; 36: At UW Health, patients may have advanced diagnostic and /or treatment options, or may receive educational materials that vary from this information. Please be aware that this information is not intended to replace the care or advice given by your physician or health care provider. It is neither intended nor implied to be a substitute for professional advice. Call your health provider immediately if you think you may have a medical emergency. Always seek the advice of your physician or other qualified health provider prior to starting any new treatment or with any question you may have regarding a medical condition. Copyright 2018 UW Health Sports Medicine 6 UWSPORTSMEDICINE.ORG SM
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Open Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared
Ulnar Collateral Ligament Reconstruction
 Ulnar Collateral Ligament Reconstruction 1. Defined a. The ulnar collateral ligament is critical for valgus stability of the elbow. It serves as the primary elbow stabilizer and as such, serves a very
Ulnar Collateral Ligament Reconstruction 1. Defined a. The ulnar collateral ligament is critical for valgus stability of the elbow. It serves as the primary elbow stabilizer and as such, serves a very
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
Rehabilitation Guidelines for Large Rotator Cuff Repair
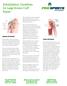 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Arthroscopic Capsular Shift
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Arthroscopic Capsular Shift The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a golf ball on a tee.
Introduction. Anatomy
 Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Introduction The doctors call it a UCLR ulnar collateral ligament reconstruction. Baseball players and fans call it Tommy John surgery -- named after the pitcher (Los Angeles Dodgers) who was the first
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Rehabilitation Guidelines for Shoulder Arthroscopy
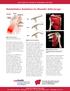 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Shoulder Arthroscopy Front View Acromion Supraspinatus Back View Supraspinatus Long head of bicep Type I Infraspinatus Short head of bicep
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR
 REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ANTERIOR SHOULDER RECONSTRUCTION WITH BANKART REPAIR The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
PHASE I (Begin PT 3-5 days post-op) DOS:
 REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR POSTERIOR SHOULDER RECONSTRUCTION +/- LABRAL REPAIRS The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Patellar Tendon and Quadriceps Tendon Repair The knee consists of four bones that form three joints. The femur is the large bone in the thigh
POST-OPERATIVE REHABILITATION PROTOCOL FOLLOWING ULNAR COLLATERAL LIGAMENT RECONSTRUCTION USING AUTOGENOUS GRACILIS GRAFT
 Therapist POST-OPERATIVE REHABILITATION PROTOCOL FOLLOWING ULNAR COLLATERAL LIGAMENT RECONSTRUCTION USING AUTOGENOUS GRACILIS GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (0-3 weeks) Protect healing tissue
Therapist POST-OPERATIVE REHABILITATION PROTOCOL FOLLOWING ULNAR COLLATERAL LIGAMENT RECONSTRUCTION USING AUTOGENOUS GRACILIS GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (0-3 weeks) Protect healing tissue
ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete)
 ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete) This rehabilitation program's goal is to return the patient/athlete to their activity/sport as quickly and safely as
ANTERIOR OPEN CAPSULAR SHIFT REHABILITATION PROTOCOL (Accelerated - Overhead Athlete) This rehabilitation program's goal is to return the patient/athlete to their activity/sport as quickly and safely as
A Patient s Guide to. Ulnar Collateral Ligament Reconstruction (Tommy John Surgery)
 A Patient s Guide to Ulnar Collateral Ligament Reconstruction (Tommy John Surgery) 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER:
A Patient s Guide to Ulnar Collateral Ligament Reconstruction (Tommy John Surgery) 228 West Main St., Suite D Missoula, MT 59802-4345 Phone: 406-721-3072 Fax: 406-721-2619 info@eorthopod.com DISCLAIMER:
Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Latarjet Anterior Shoulder Stabilization The anatomic configuration of the shoulder joint (glenohumeral joint) is often compared to a
A Patient s Guide to Ulnar Collateral Ligament Injuries
 A Patient s Guide to Ulnar Collateral Ligament Injuries 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
A Patient s Guide to Ulnar Collateral Ligament Injuries 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE II TEARS (MASSIVE)(+/- SUBACROMIAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
ULNAR COLLATERAL LIGAMENT (UCL) RECONSTRUCTION REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION)
 REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
REHABILITATION GUIDELINES FOR ROTATOR CUFF REPAIR FOR TYPE I TEARS (+/- SUBACROMINAL DECOMPRESSION) The rehabilitation guidelines are presented in a criterion based progression. General time frames are
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 1 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
Rehabilitation Guidelines for Meniscal Repair
 Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Meniscal Repair The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
UHealth Sports Medicine
 UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
UHealth Sports Medicine Rehabilitation Guidelines for Arthroscopic Rotator Cuff Repair Type 2 Repairs (+/- subacromial decompression) The rehabilitation guidelines are presented in a criterion based progression.
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson
 REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
REHABILITATION GUIDELINES FOR SUBSCAPULARIS (+/- SUBACROMIAL DECOMPRESSION) Dr. Carson The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction
 Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Rehabilitation Guidelines for Anterior Cruciate Ligament (ACL) Reconstruction The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
Rehabilitation Guidelines for Biceps Tenodesis with Hardware Fixation
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Biceps Tenodesis with Hardware Fixation The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Biceps Tenodesis with Hardware Fixation The shoulder has two primary joints. One part of the shoulder blade, called the glenoid fossa forms
Superior Labrum Repair Protocol - SLAP
 Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Superior Labrum Repair Protocol - SLAP Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Patient Education Ulnar Collateral Ligament Reconstruction
 Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Explanation of Procedure and/or Diagnosis Overview is commonly referred to as Tommy John Surgery. Tommy John was a baseball pitcher who played for the Los Angeles Dodgers. He was the first person to have
Rehabilitation Guidelines for Meniscal Repair
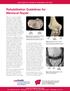 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Meniscal Repair There are two types of cartilage in the knee, articular cartilage and cartilage. Articular cartilage is made up of collagen,
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline
 Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Arthroscopic SLAP Lesion Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol
 Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol The following document is an evidence-based protocol for arthroscopic rotator cuff repair rehabilitation. The protocol is both chronologically
Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol The following document is an evidence-based protocol for arthroscopic rotator cuff repair rehabilitation. The protocol is both chronologically
Rehabilitation Guidelines for Knee Arthroscopy
 Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Rehabilitation Guidelines for Knee Arthroscopy The knee is the body's largest joint, and the place where the femur, tibia, and patella meet to form a hinge-like joint. These bones are supported by a large
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Rehabilitation following Arthroscopic Rotator Cuff Repair: Medium Tears Phase I: Immediate Postsurgical Phase (Days 10-14) Precautions: No lifting of objects; No excessive arm motions; No excessive external
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) BENJAMIN J. DAVIS, MD
 I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative effects of immobilization Promote dynamic stability Diminish pain and inflammation
I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative effects of immobilization Promote dynamic stability Diminish pain and inflammation
Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft
 Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
Day of Surgery Post-Operative Instructions Glenoid Reconstruction using Fresh Distal Tibial Allograft A. Relax. Diet as tolerated. B. Icing is important for the first 5-7 days post-op. While the post-op
ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE
 ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative
ARTHROSCOPIC SLAP LESION REPAIR (TYPE II) WITH THERMAL CAPSULAR SHRINKAGE I. Phase I Immediate Postoperative Phase Restrictive Motion (Day 1 to Week 6) Goals: Protect the anatomic repair Prevent negative
Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Medial Patellofemoral Ligament Repair and Reconstruction The knee consists of four bones that form three joints. The femur is the large bone
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm)
 Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
Type Three Rotator Cuff Repair Arthroscopic Assisted with SAD Large to Massive Tears (Greater than 4 cm) Therapist Phone I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity
ROTATOR CUFF REPAIR REHAB PROTOCOL
 Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Overview a. Begin passive shoulder ROM after surgery (beginning week 1) b. Active assist ROM beginning week 7 after surgery (weeks 7-8) c. Active ROM beginning week 9 after
Rotator Cuff Repair Protocol Overview a. Begin passive shoulder ROM after surgery (beginning week 1) b. Active assist ROM beginning week 7 after surgery (weeks 7-8) c. Active ROM beginning week 9 after
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate
 Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
Bicep Tenodesis D. WATTS, M.D. Progression to the next phase based on Clinic Criteria and or Time Frames as Appropriate PHASE I PASSIVE RANG OF MOTION PHASE (STARTS APPROXIMATELY POST OP WEEKS 1-2) Minimize
THERMAL - ASSISTED CAPSULORRAPHY With or without SLAP Repair
 THERMAL - ASSISTED CAPSULORRAPHY With or without SLAP Repair **It is important for the clinician to determine the capsular response to the heat probe. Patients that have excessive ROM early in the rehab
THERMAL - ASSISTED CAPSULORRAPHY With or without SLAP Repair **It is important for the clinician to determine the capsular response to the heat probe. Patients that have excessive ROM early in the rehab
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Arthroscopic Anterior Stabilization Rehab
 Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
Arthroscopic Anterior Stabilization Rehab Phase I (0-3weeks) Sling immobilization-md directed Codmans/Pendulum exercises Wrist/Elbow ROM Gripping exercises FF-AAROM (supine)-limit to 90 o ER to 0 o Sub
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL BENJAMIN J. DAVIS, MD Type Two Rotator Cuff Repair
 I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
I. Phase I - Immediate Post-Surgical Phase (Day 1-10) Goals: Maintain Integrity of the Repair Gradually Increase Passive Range of Motion Diminish Pain and Inflammation Prevent Muscular Inhibition Passive
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Pectoralis Major Tendon Repair The pectoralis major is a thick, fan-shaped
Mark Adickes, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-6016 Fax: 713-986-5411 Pectoralis Major Tendon Repair The pectoralis major is a thick, fan-shaped
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Elbow Dislocation 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
Sterile gauze used at incision site. Check brace for rubbing or irritation. Compression garment at elbow to be used with physician s authorization
 ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
ULNAR COLLATERAL LIGAMENT RECONSTRUCTION GUIDELINE Functional Outcome Measure KJOC (Appendix 1) should be completed at initial evaluation and at all identified times through guideline, Phase 1 Immediate
Small Rotator Cuff Repair
 Small Rotator Cuff Repair 1. Defined a. Surgical repair of the rotator cuff (most commonly supraspinatus muscle) utilizing sutures b. May be done arthroscopically or open. c. May be done in conjunction
Small Rotator Cuff Repair 1. Defined a. Surgical repair of the rotator cuff (most commonly supraspinatus muscle) utilizing sutures b. May be done arthroscopically or open. c. May be done in conjunction
Rotator Cuff Repair Protocol
 Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
AC reconstruction Protocol: Dr. Rolf
 AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
AC reconstruction Protocol: Dr. Rolf The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient that has undergone a AC reconstruction
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Rehabilitation of Overhead Shoulder Injuries
 Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
MUCL REPAIR. Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA
 MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
MUCL REPAIR Felix H. Savoie III, MD Ray J. Haddad Professor & Chairman Department of Orthopaedic Surgery Tulane University New Orleans, LA MUCL INJURY EPIDEMIC Frequency increasing despite major efforts
Pectorlais Major Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Pectorlais Major Tendon Repair The pectoralis major muscle
(PROTOCOL #18) REVERSE TOTAL SHOULDER ARTHROPLASTY PROTOCOL
 The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
The following is a set of general guidelines. It is important to remember that each patient is different. The progression of the patient depends on many factors including age and medical health of the
Rehabilitation Following Arthroscopic Anterior Shoulder Plication in the Overhead Athlete
 Rehabilitation Following Arthroscopic Anterior Shoulder Plication in the Overhead Athlete PHASE I IMMEDIATE GUARDED MOTION PHASE (Weeks 0-6) Reduce postoperative pain and inflammation Promote capsular
Rehabilitation Following Arthroscopic Anterior Shoulder Plication in the Overhead Athlete PHASE I IMMEDIATE GUARDED MOTION PHASE (Weeks 0-6) Reduce postoperative pain and inflammation Promote capsular
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE
 ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
ANTERIOR SHOULDER STABILIZATION CLINICAL PRACTICE GUIDELINE Background Ohio State s Anterior Shoulder Stabilization Rehabilitation Guideline is to be utilized following open or arthroscopic anterior shoulder
A Patient s Guide to Elbow Anatomy
 A Patient s Guide to Elbow Anatomy Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can better understand and
A Patient s Guide to Elbow Anatomy Iain is a specialist in musculoskeletal imaging and the diagnosis of musculoskeletal pain. This information is provided with the hope that you can better understand and
Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Elbow Injuries in the Throwing Athlete
 Elbow Injuries in the Throwing Athlete Overhand throwing places extremely high stresses on the elbow. In baseball pitchers and other throwing athletes, these high stresses are repeated many times and can
Elbow Injuries in the Throwing Athlete Overhand throwing places extremely high stresses on the elbow. In baseball pitchers and other throwing athletes, these high stresses are repeated many times and can
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Disclosures. Throwing is NOT Normal MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS. Joshua S. Dines, MD. Sports Medicine and Shoulder Service
 MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS Joshua S. Dines, MD Sports Medicine and Shoulder Service Disclosures Consultant: Arthrex, Conmed Linvatec, Ossur IP/Royalties: Conmed Linvatec Editorial
MCL RECONSTRUCTION: INDICATIONS, TECHNIQUE, RESULTS Joshua S. Dines, MD Sports Medicine and Shoulder Service Disclosures Consultant: Arthrex, Conmed Linvatec, Ossur IP/Royalties: Conmed Linvatec Editorial
Upper Extremity Injuries in Youth Baseball: Causes and Prevention
 Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
Upper Extremity Injuries in Youth Baseball: Causes and Prevention Biomechanics Throwing a baseball is an unnatural movement Excessively high forces are generated at the elbow and shoulder Throwing requires
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
Large/Massive Rotator Cuff Repair
 Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Large/Massive Rotator Cuff Repair 1. Defined a. Suturing of tears within the rotator cuff (most commonly supraspinatus muscle). Massive RCR usually involve more than the supraspinatus. b. May be done arthroscopically
Recurrent and Chronic Elbow Instability
 Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Recurrent and Chronic Elbow Instability Elbow instability is a looseness in the elbow joint that may cause the joint to catch, pop, or slide out of place during certain arm movements. It most often occurs
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) Arthroscopic Posterior Labral Repair
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Arthroscopic
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Arthroscopic
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas Phone: Fax:
 Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 DISTAL BICEPS TENDON REPAIR PROTOCOL This rehabilitation protocol
Theodore B. Shybut, M.D. Orthopedics and Sports Medicine 7200 Cambridge St. #10A Houston, Texas 77030 Phone: 713-986-5590 Fax: 713-986-5521 DISTAL BICEPS TENDON REPAIR PROTOCOL This rehabilitation protocol
Slide 1. Slide 2. Slide 3. The Thrower s Elbow: When to Operate. Medial Elbow Pain in the Athlete. Goal of This Talk
 Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Slide 1 The Thrower s Elbow: When to Operate Luke S. Oh, MD Massachusetts General Hospital Team Physician, Boston Red Sox Team Physician, New England Revolution Consultant, Harvard University Athletics
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
Index Note: Page numbers of article titles are in boldface type. A Achilles tendonitis, criteria for full competition in, 164 165 description of, 164 patient education in, 165 prophylactic support in,
Rehabilitation Guidelines for Knee Arthroscopy
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Knee Arthroscopy Arthroscopy is a common surgical procedure in which a joint is viewed using a small camera. This technique allows the surgeon
