In 2007, an estimated 22,430 women in the United States
|
|
|
- Primrose Gibson
- 5 years ago
- Views:
Transcription
1 This material is protected by U.S. copyright law. Unauthorized reproduction is prohibited. To purchase quantity reprints, please or to request permission to reproduce multiple copies, please FEATURE ARTICLE Downloaded on Single-user license only. Copyright 2019 by the Oncology Nursing Society. For permission to post online, reprint, adapt, or reuse, please Evidence-Based Research for Intraperitoneal Chemotherapy in Epithelial Ovarian Cancer Lois Almadrones, RN, MS, FNP, MPA Intraperitoneal (IP) therapy is the administration of chemotherapy or biologic agents directly into the peritoneal cavity. A recent Gynecologic Oncology Group trial showed a survival advantage for women with advanced ovarian cancer and small residual disease after initial surgical staging and debulking who received IP therapy when compared to the standard IV regimen. The results prompted a National Cancer Institute announcement recommending the use of IP therapy in women who meet the criteria. This article describes the rationale for and underlying principles of IP therapy and summarizes the results of the three main clinical trials that led to the recommendation for incorporation of IP therapy into initial treatment of epithelial ovarian cancer. In 2007, an estimated 22,430 women in the United States will be diagnosed with epithelial ovarian cancer and 15,280 will die of the disease (Jemal et al., 2007). Ovarian cancer is the leading cause of death in women with gynecologic malignancies. Since 1996 (McGuire et al.), the standard treatment for advanced-stage ovarian cancer has been surgical debulking, followed by six cycles of IV paclitaxel and carboplatin administered every 21 days. Despite the aggressive treatment and some improvement in five-year survival, the median survival for patients with the disease remains about 40 months. Because of the less-than-optimal results, treatments using novel drug combinations or high-intensity chemotherapy have been researched, but neither has produced evidence of clinical benefit or improved survival. Hence, when the results of a Gynecologic Oncology Group trial using intraperitoneal (IP) and IV chemotherapy agents known to be active in ovarian cancer confirmed a definite survival advantage in the IP arm when compared to the IV standard, the National Cancer Institute issued a clinical announcement that strongly suggested a change in standard practice for the initial chemotherapy regimen for the disease. Although IP therapy is not a new method of drug delivery, it has been done principally as part of investigational research trials in cooperative groups participating institutions or comprehensive cancer centers. Therefore, many clinicians and nurses outside of the research clinical trial setting are not familiar with IP therapy rationale and basic principles and guidelines for its administration in patients with ovarian cancer. This article will review the rationale, principles, and evidence-based research for the use of IP therapy in this population. At a Glance Intraperitoneal (IP) therapy is the delivery of chemotherapy or biologic agents directly into the peritoneal cavity through a port and catheter. Results of a series of cooperative group clinical trials demonstrated improved survival for women who received IP therapy versus those who received only IV therapy. Basic principles of IP therapy must be adhered to for patient outcomes to be successful. Use of Intraperitoneal Chemotherapy Rationale IP therapy is the delivery of chemotherapy or biologic agents directly into the peritoneal cavity. It has been studied in investigational research trials in tumors confined to the peritoneal cavity since the late 1970s. The therapeutic advantage is thought to be the ability to deliver a higher concentration of drug and a longer exposure of active drug that, over time, penetrates directly into small tumor tissue in the peritoneal cavity. In addition, the active Lois Almadrones, RN, MS, FNP, MPA, is a clinical nurse specialist in the gynecology service at Memorial Sloan-Kettering Cancer Center in New York, NY. No fi nancial relationships to disclose. (Submitted March Accepted for publication June 4, 2006.) Digital Object Identifi er: /07.CJON Clinical Journal of Oncology Nursing Volume 11, Number 2 Evidence-Based Research for Intraperitoneal Chemotherapy 211
2 chemotherapy, after first-pass metabolism in the liver, has a systemic cytotoxic effect through capillary flow into the tumor bed. Dedrick, Myers, Bungay, and DeVita (1978) described the pharmacokinetic rationale of IP therapy using a mathematical model that suggests evidence about how chemicals move across the peritoneal membrane and are cleared from the systemic plasma. Dedrick et al. s model demonstrated that, on average, the concentration of methotrexate or cytosine arabinoside (ara- C) in the peritoneal cavity was one to three logs greater than its concentration in the blood. Since that initial research, many other chemotherapeutic agents have demonstrated a peritonealplasma ratio that exceeds a 20-fold concentration difference. In particular, Howell et al. (1982) demonstrated that cisplatin peritoneal concentrations were times greater than in the plasma; subsequently, Markman et al. (1992) reported a 1,000-fold difference in paclitaxel peritoneal-plasma concentrations. Many other chemotherapeutic and biologic agents also have been studied, and many show a similar pharmacokinetic advantage when administered through the IP route (Markman et al., 1989). The peritoneal cavity can be thought of as a compartment that has dynamic properties of permeability and absorption of the body s naturally occurring electrolytes, chemicals, proteins, and fluids. Compartment, or local, drug therapy is not a new concept. It is the basic underlying rationale for intrathecal therapy that is used successfully in leukemia. Intrathecal therapy also takes advantage of the restricted transfer of drugs from cerebrospinal fluid (CSF) and has shown a twofold higher difference in CSF compared to plasma concentrations (Bleyer & Dedrick, 1977; Shapiro, Young, & Mehta, 1975). Applying the same rationale for the use of IP therapy also will exploit the peritoneal-plasma ratio to benefit tumor types such as ovarian cancer that remain principally confined to the peritoneum for their natural lives in the majority of women with cancer. Principles The basic principles of IP therapy are listed in Figure 1 and must be adhered to for successful outcomes to occur (e.g., response, increased survival). Principle 1: The IP agent must have slow peritoneal clearance to maximize its direct exposure to the tumor. In contrast, when the agent reaches the systemic circulation, rapid clearance is necessary to minimize the toxicity of high-dose therapy (Dedrick, 1985; Dedrick et al., 1978; Markman et al., 1989; Markman & Walker, 2006). In the peritoneal cavity and the systemic circulation, the agent must maintain its anticancer properties. 1. The agent should have slow peritoneal clearance and rapid systemic clearance and should demonstrate activity against the tumor type. 2. The agent should have rapid and extensive hepatic metabolism into nontoxic metabolites during first pass through the liver. 3. Intraperitoneal tumors should be small, preferably less than 0.5 cm in greatest dimension. 4. Large treatment volumes are needed to ensure direct exposure of the agent to all peritoneal surfaces. 5. Administration of intraperitoneal therapy should be done through a port connected to a catheter that floats freely in the peritoneal cavity. Figure 1. Principles of Intraperitoneal Therapy Note. Based on information from Dedrick et al., 1978; Markman et al., Principle 2: The agent administered preferably is metabolized during the first pass through the liver into nontoxic metabolites. Most metabolism of peritoneal agents enters systemic circulation through the portal circulation (Kraft, Tompkins, & Jesseh, 1968). To minimize systemic toxicity, nontoxic metabolites need to enter the circulation. Similarly, drugs that compete for hepatic or renal clearance with the anticancer agents should not be coadministered to lessen the potential for more severe systemic toxicity (Dedrick et al., 1978). Women with severely compromised renal or hepatic function may have more severe toxicity, and adequate preventive measures need to be employed prior to IP therapy. Principle 3: The individual tumor size must be small (Alberts et al., 1996; Dedrick et al., 1978; Howell et al., 1982). The IP agent is limited and dependent on direct tumor diffusion in the peritoneal cavity and blood perfusion through capillary flow once the agent enters the systemic circulation. If the tumor size is larger than a few millimeters in greatest dimension, the diffusibilty of the agent is limited and a less-than-desirable response can be anticipated. A recent debulking laparotomy, preferably performed by a gynecologic oncologist, leaving either no gross residual or visible tumor greater than 0.5 cm in dimension prior to IP therapy, offers the best opportunity for an optimal response. However, the current IP standard is based on the Armstrong et al. (2006) trial, where eligibility was no tumor greater than 1 cm in dimension prior to IP. Principle 4: Sufficient volume of distillate with the antitumor agent must be instilled to ensure exposure of the agent and optimize the drug distribution to the entire peritoneal cavity (Alberts et al., 1996; Armstrong et al., 2006; Dedrick et al., 1978; Markman et al., 1989, 1992, 2001). All clinical trials that have demonstrated better response with IP versus IV therapy have used a volume of 2 L of normal saline solution in the peritoneal cavity. Although the principle is probably responsible for most of the toxicities related to IP therapy (i.e., abdominal bloating, pain, and temporary shortness of breath), it is important and cannot be modified without the possibility of compromising maximum tumor response. Principle 5: IP therapy should be administered through a port connected to a catheter that floats freely in the peritoneal cavity. The access system has evolved over time from a single-use percutaneous catheter placed and removed at each treatment to a transcutaneous, semipermanent catheter system and, finally, to the current subcutaneously placed, semipermanent port and catheter system. More research is needed to determine which type of catheter provides the best delivery and fewest catheter-related problems. Currently, studies recommend either a single-lumen polyurethane IV catheter or a fenestrated semipermanent catheter. Additional research may determine whether one of the catheters is superior. Complications related to the catheter and access system will be discussed in the article on pp Evidence-Based Research Data from phase I and II trials in the literature during the 1980s and early 1990s describe the potential response benefit of IP therapy when administered to women who meet the criteria for optimum response (e.g., small-volume disease confined to the peritoneal cavity with the potential for good peritoneal distribution of the anticancer agent) and have not demonstrated resistance to the particular chemotherapeutic agent. However, cooperative groups enlisted patients in phase III clinical trials that studied 212 April 2007 Volume 11, Number 2 Clinical Journal of Oncology Nursing
3 other experimental IV regimens that incorporated either highdose chemotherapy or multiple sequential agents using the known standard active agents. Results of intergroup trials (Southwest Oncology Group, Eastern Cooperative Oncology Group, and Gynecologic Oncology Group) by Alberts et al. in 1996 and Markman et al. in 2001, however, generated provocative results that initiated a third trial in the Gynecologic Oncology Group alone, recently published by Armstrong et al. (2006). Following are brief summaries of each of the major phase III IP trials. IV Cisplatin and Cyclophosphamide Versus IP Cisplatin and IV Cyclophosphamide Conducted from June 1986 July 1992, this trial enrolled 654 women (546 eligible for evaluation) with pathologically confirmed stage III epithelial ovarian cancer who, after surgical debulking, had no tumor nodules greater than 2 cm in dimension (see Figure 2). Each woman was stratified by size of the largest tumor after debulking surgery (< 0.5 cm versus > cm) and then randomized to receive either standard IV cisplatin and cyclophosphamide or the investigational arm of IP cisplatin and IV cyclophosphamide. Each regimen was given at three-week intervals. Results confirmed a modest survival advantage in the IP group (41 versus 47 months, respectively; p = 0.02). Covariates that determined survival included absence of gross disease at enrollment (p < 0.001), younger age (p < 0.001), tumor type other than clear cell or mucinous carcinoma (p < 0.001), and enrollment after surgery (p < 0.001) (Alberts et al., 1996). Conclusions of this trial demonstrated that a modest overall survival advantage was achieved in the IP group. However, another Gynecologic Oncology Group trial done during the same time period as the IP trial compared standard IV cisplatin and cyclophosphamide versus IV paclitaxel and cisplatin. Results of that trial suggested a significant survival time in the IV paclitaxel and cisplatin arm (McGuire et al., 1996). IV cisplatin 100 mg/m 2 and IV cyclophosphamide 600 mg/m 2 every 21 days IP intraperitoneal Ovarian Cancer Stage III Stratification by < 0.5 cm versus > cm Randomization Second-look laparotomy IP cisplatin 100 mg/m 2 and IV cyclophosphamide 600 mg/m 2 every 21 days Figure 2. Gynecologic Oncology Group Trial 104 and Southwestern Oncology Group Trial 8501 Note. Based on information from Alberts et al., IV cisplatin 75 mg/m 2 and IV cyclophosphamide 750 mg/m 2 every 21 days for six cycles Ovarian Cancer Stage III < 1.0 cm Randomization IV cisplatin 75 mg/m 2 and IV paclitaxel 135 mg/m 2 every 21 days Second-look laparotomy AUC area under the curve; IP intraperitoneal IV carboplatin AUC = 9 x 2 then IP cisplatin 100 mg/m 2 and IV paclitaxel 135 mg/m 2 every 21 days for six cycles Figure 3. Gynecologic Oncology Group Trial 114 Note. Based on information from Markman et al., Therefore, the IV regimen became the new gold standard, and the researchers advised that IP therapy needed further study. IV Paclitaxel and Cisplatin Versus Moderately High- Dose Carboplatin and IV Paclitaxel and IP Cisplatin Conducted from August 1992 April 1995, this trial enrolled 523 women (462 eligible for evaluation) with pathologically confirmed stage III epithelial ovarian cancer and largest residual tumor < 1 cm in diameter after surgical debulking (see Figure 3). The original trial had three arms. One arm included standard cisplatin and cyclophosphamide, but after the results of the paclitaxel and cisplatin trial became known, the arm was discontinued. The other two arms included the new standard IV paclitaxel and cisplatin versus IV carboplatin for two cycles followed by IP cisplatin and IV paclitaxel. Results showed modest improvement in progression-free (p = 0.01, one-tailed) and overall (p = 0.05, one-tailed) survival in the experimental group, but the improvement likely was explained by the two extra cycles given to women in the experimental arm of the trial rather than the IP route administration (Markman et al., 2001). However, further exploration with IP therapy was initiated by the Gynecologic Oncology Group. 24-Hour IV Paclitaxel and Cisplatin on Day 2 Versus 24-Hour IV Paclitaxel and IP Cisplatin on Day 2 and IP Paclitaxel on Day 8 Conducted from March 1998 January 2001, this Gynecologic Oncology Group trial enrolled 429 women (415 eligible for evaluation) with pathologically confirmed epithelial ovarian or primary peritoneal cancer with no residual disease mass greater than 1 cm after surgical debulking (see Figure 4). The trial randomized one group to the standard IV paclitaxel and cisplatin Clinical Journal of Oncology Nursing Volume 11, Number 2 Evidence-Based Research for Intraperitoneal Chemotherapy 213
4 IV paclitaxel 135 mg/ m 2 for 24 hours and IV cisplatin 75 mg/m 2 every 21 days IP intraperitoneal and a second group to IV paclitaxel and IP cisplatin and then IP paclitaxel on day eight of the 21-day regimen for each arm for six cycles. Results showed that the experimental arm had a progression-free survival advantage of 18.3 versus 23.8 months (p = 0.05 by the log-rank test) and an overall survival advantage of 49.5 months versus 66.9 months (p = 0.03 by the log-rank test). The trial reported the longest survival in women with advanced ovarian cancer, and the advantage was in women in the IP arm of the trial (Armstrong et al., 2006). Although the trial s results support further use of IP therapy in advanced ovarian cancer, the toxicity profile for this mode of therapy was higher than in the standard arm, and quality-of-life during treatment also was reduced. IP catheter complications were the major reason for discontinuation of therapy. Conclusion Ovarian Cancer Optimal (< 1 cm) Stage III Stratification by gross residual and planned second look Randomization Second-look laparotomy (if chosen) BRCA analysis DNA banking IV paclitaxel 135 mg/m 2 for 24 hours and IP cisplatin 100 mg/m 2 day 2 and IP paclitaxel 60 mg/m 2 day 8 every 21 days Figure 4. Gynecologic Oncology Group Trial 172 Note. Based on information from Armstrong et al., With the introduction of any new treatment regimen or mode of administration such as IP therapy, a learning curve is expected for all health professionals involved in the care of patients receiving such therapy. Understanding the rationale and principles that underlie the basic premises of IP therapy is the first step needed in the educational process to ensure successful treatment and avoid, or at least lessen, the complications that are associated with IP therapy. As nurses become more familiar with how to access the IP port and the correct way to administer therapy directly into the peritoneal cavity, the same or better survival benefit may be observed without increasing toxicity or having to sacrifice quality of life during treatment. The articles on pp and pp review the recommended nursing performance competency checklist for IP therapy and related patient education. See Appendix for a patient guide to IP therapy. Author Contact: Lois Almadrones, RN, MS, FNP, MPA, can be reached at almadrol@mskcc.org, with copy to editor at CJONEditor@ons.org. References Alberts, D.S., Liu, P.Y., Hannigan, E.V., O Toole, R., Williams, S., Young, J.A., et al. (1996). Intraperitoneal cisplatin plus intravenous cyclophosphamide versus cisplatin plus intravenous cyclophosphamide for stage III ovarian cancer. New England Journal of Medicine, 335, Armstrong, D.K., Bundy, B., Wenzel, L., Huang, H.Q., Baergan, R., Lele, S., et al. (2006). Intraperitoneal cisplatin and paclitaxel in ovarian cancer. New England Journal of Medicine, 354, Bleyer, W.A., & Dedrick, R.L. (1977). Clinical pharmacology of intrathecal methotrexate. I. Pharmacokinetics in nontoxic patients after lumbar injection. Cancer Treatment Reports, 61, Dedrick, R.L. (1985). Theoretical and experimental bases of intraperitoneal chemotherapy. Seminars in Oncology, 12(3, Suppl. 4), 1 6. Dedrick, R.L., Myers, C.E., Bungay, P.M., & DeVita, V.T., Jr. (1978). Pharmacokinetic rationale for peritoneal drug administration in the treatment of ovarian cancer. Cancer Treatment Reports, 62, 1 9. Howell, S.B., Pfeifle, C.L., Wung, W.E., Olshen, R.A., Lucas, W.E., Yon, J.L., et al. (1982). Intraperitoneal cisplatin with systemic thiosulfate protection. Annals of Internal Medicine, 97, Jemal, A., Siegel, R., Ward, E., Murray, T., Xu, J., & Thun, M. (2007). Cancer statistics, CA: A Cancer Journal for Clinicians, 57, Kraft, A.R., Tompkins, R.K., & Jesseh, J.E. (1968). Peritoneal electrolyte absorption: Analysis of portal, systemic venous and lymphatic transport. Surgery, 13, Markman, M., Bundy, B.N., Alberts, D.S., Fowler, J.M., Clark-Pearson, D.L., Carson, L.F., et al. (2001). Phase III trial of standard-dose intravenous cisplatin plus paclitaxel versus moderately high-dose carboplatin followed by intravenous paclitaxel and intraperitoneal cisplatin in small-volume stage II ovarian carcinoma: An intergroup study of the Gynecologic Oncology Group, Southwestern Oncology Group, and Eastern Cooperative Oncology Group. Journal of Clinical Oncology, 19, Markman, M., Hakes, T., Reichman, B., Hoskins, W., Rubin, S., Jones, W., et al. (1989). Intraperitoneal therapy in the management of ovarian carcinoma. Yale Journal of Biology and Medicine, 62, Markman, M., Rowinsky, E., Hakes, T., Reichman, B., Jones, W., Lewis, J.L., Jr., et al. (1992). Phase I trial of intraperitoneal Taxol: A Gynecologic Oncology Group study. Journal of Clinical Oncology, 10, Markman, M., & Walker, J.L. (2006). Intraperitoneal chemotherapy of ovarian cancer: A review, with a focus on practical aspects of treatment. Journal of Clinical Oncology, 24, McGuire, W.P., Hoskins, W.J., Brady, M.F., Kucera, P.R., Partridge, E.E., Look, K.Y., et al. (1996). Cyclophosphamide and cisplatin compared with paclitaxel and cisplatin in patients with stage III ovarian cancer. New England Journal of Medicine, 334, 1 6. Shapiro, W.R., Young, D.F., & Mehta, B.M. (1975). Methotrexate: Distribution in cerebrospinal fluid after intravenous, ventricular and lumbar injections. New England Journal of Medicine, 293, Receive continuing nursing education credit for reading this article and taking a brief quiz. See the Continuing Nursing Education in this issue for more information. 214 April 2007 Volume 11, Number 2 Clinical Journal of Oncology Nursing
5 Appendix. Your Guide to Intraperitoneal Therapy Lois Almadrones, RN, MPA, FNP, Anne Marie Flaherty, RN, MS, and Catherine Hydzik, RN, MS, AOCN Introduction This booklet is designed to provide you with information about intraperitoneal therapy and prepare you to participate in activities which will assist you during the time you receive this therapy. Peritoneal access port Catheter Peritoneal space What Intraperitoneal Therapy Is Intraperitoneal therapy is the Figure 1 delivery of anti-cancer drugs directly into the peritoneal space (abdominal cavity). This space lies Septum (disc) between the abdominal muscles and abdominal organs. The anti-cancer Side arm drug is mixed in a large volume of fluid and instilled into the peritoneal space Catheter through a port and catheter. Your surgeon will insert a peritoneal access port into Figure 2 a pocket beneath the skin near your rib cage. (See Figure 1.) The port consists of a raised chamber. Imbedded into the top of the chamber is a self-sealing silicone rubber septum (disc). The chamber also has a side arm for attaching the flexible catheter, which is placed in your peritoneal space. (See Figure 2.) Your surgeon usually inserts the port and catheter at the time of your surgery. Intraperitoneal therapy allows direct contact of the cancer-fighting drug with the cancer within your peritoneal space. The drug is left in the peritoneal space to bathe the cancer. This method of delivering it directly into the cavity where the cancer is located allows a higher concentration of the drug to be given. Where Your Intraperitoneal Therapy Will Be Administered Intraperitoneal therapy may be given in the inpatient or outpatient setting. Where you receive your intraperitoneal therapy, how many treatments you receive, and the duration of therapy depend on your condition and the particular anti-cancer drug your doctor has recommended. During the actual treatment you will be asked to remain in your bed. Who Will Administer Your Intraperitoneal Therapy Your intraperitoneal therapy will be administered by a registered nurse. Your nurse will review with you information explained in this booklet as well as review the Chemotherapy Fact Card about your anti-cancer drug. The Chemotherapy Fact Cards contain the important information you need to know about the drugs you will receive. How Your Intraperitoneal Therapy Will Be Administered Before and during the intraperitoneal treatment, intravenous fluid may be administered through a vein. The purpose of this fluid is to maintain your fluid level and to allow the administration of antinausea medicine if it is necessary during your treatment. To begin your intraperitoneal therapy, the nurse will place a special needle though your skin and into the self-sealing septum in the port chamber. This will feel similar to a small pin prick. The needle will be taped securely and covered with a small dressing. A fluid administration set, which contains the anti-cancer drug, will be attached to the needle. The volume of fluid your medication is mixed in is determined by the treatment you are receiving. This amount is given to allow the drug to reach and bathe all parts of the peritoneal space. The solution will be allowed to flow into your peritoneal space by gravity. The actual intraperitoneal therapy treatment time varies, but it is usually no more than 1 1/2 to 2 hours. More solution may be ordered after the treatment to improve the bathing of the peritoneal space. After the solution has flowed into your intraperitoneal space, the special needle will be removed and a bandage will be placed on the site. This bandage can be removed after about 30 minutes. Your nurse will ask you to move from side to side in bed a few times. This will help to distribute the anti-cancer drug solution evenly throughout your peritoneal space. Your intraperitoneal therapy will then be complete and you may be out of bed as desired. The solution in your peritoneal space will be absorbed by your body over the next few days. During this time, your abdomen may be bloated and you may feel some abdominal pressure. What to Do at Home to Prepare for Your Intraperitoneal Treatment Wear expandable or loose-fitting clothing to the hospital. Eat a light dinner the night before and a light breakfast the morning of the treatment. If you wish, bring a cassette or CD player or ipod and your favorite music to listen to during treatment. A television is provided in the room where you receive your treatment. It may be helpful to have a relative or friend accompany you home as some medicine may make you feel drowsy. Possible Side Effects of Intraperitoneal Therapy and Comfort Measures to Minimize These Effects You may not experience any side effects from your intraperitoneal therapy. The following are some effects that some patients have reported, and the comfort measures they have found helpful. POSSIBLE SIDE EFFECTS Abdominal pressure and bloating (caused by the large volume of fluid injected into the peritoneal space) Frequent urination/ bladder fullness (a desired side effect caused by the intravenous fluids) Breathing faster and more frequently (caused by the large volume of fluid injected into the peritoneal space) Nausea, vomiting, or both (caused by anti-cancer drugs) Decrease in appetite (caused by large volume of fluid injected into the peritoneal space and anticancer drugs) COMFORT MEASURES Walk around after the treatment is completed. Wear comfortable clothing with an expandable waistline, especially for the first few days after treatment. Empty your bladder just before beginning treatment. You will be allowed to use the bathroom, if needed, during the treatment. Elevate the head of your bed during treatment. Walk around after the treatment. Sit in an upright chair after the treatment. Antinausea medicine may be given to you before, during the therapy, or both. Your doctor will prescribe antinausea medicine for you to take at home if needed. Eat smaller meals more frequently. Drink high nutrition liquid supplements. Some of the drug you receive is absorbed and carried throughout your body. The effects you feel may be caused by the drug(s) given to you. Clinical Journal of Oncology Nursing Volume 11, Number 2 Evidence-Based Research for Intraperitoneal Chemotherapy 215
6 What You Need to Know About Home Care of the Peritoneal Port Since the peritoneal access port is located under your skin, no covering or bandage is required. You may bathe or shower. Having a port and catheter in place should not restrict your activities. Reasonable exercise is allowed after the incision is healed and your recovery from other surgery is complete. Ask your doctor or nurse about resuming your normal activities. Inspect the skin around your port daily. If this area becomes reddened, swollen, or tender to the touch, you should report this to your doctor or nurse. The port and catheter do not affect your dietary habits. You may continue on the diet which you normally eat. Questions for Your Doctor or Nurse The following section is where you may write any questions or comments you have about intraperitoneal therapy. We encourage you to discuss your therapy and any additional questions you have with your doctor or nurse. When You Should Notify Your Doctor Call your doctor if you: Experience unusual abdominal pain. Have a fever of 101 F (38.3 C) or higher. Develop redness, swelling, or tenderness around the port site. Have severe nausea, vomiting, diarrhea, or constipation that lasts more than 24 hours. Are unable to eat or drink for more than 24 hours. Have any unexpected or unexplained problems. Note. From Your Guide to Intraperitoneal Therapy (3rd ed.) [Booklet], by L. Almadrones, A.M. Flaherty, and C. Hydzik, Copyright 1988 by Memorial Sloan-Kettering Cancer Center. Reprinted with permission. 216 April 2007 Volume 11, Number 2 Clinical Journal of Oncology Nursing
Randomized Phase III Trials of Intravenous vs. Intraperitoneal Therapy in Optimal Ovarian Cancer
 Randomized Phase III Trials of Intravenous vs. Intraperitoneal Therapy in Optimal Ovarian Cancer Deborah K. Armstrong, M.D. Associate Professor of Oncology, Gynecology and Obstetrics Development of Intraperitoneal
Randomized Phase III Trials of Intravenous vs. Intraperitoneal Therapy in Optimal Ovarian Cancer Deborah K. Armstrong, M.D. Associate Professor of Oncology, Gynecology and Obstetrics Development of Intraperitoneal
Intraperitoneal Chemotherapy
 Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
Intraperitoneal Chemotherapy What is Intraperitoneal (IP) Chemotherapy? Intraperitoneal (IP) chemotherapy is a way to put some of your chemotherapy into your abdomen (also called the peritoneal cavity)
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
AHFS Final. IV and intraperitoneal regimen for. Criteria Used in. Strength. Strength. Use: Based on. taxane (either IV. following
 AHFS Final Determination of Medical Acceptance: Off-label Use of Sequential IV Paclitaxel, Intraperitoneal Cisplatin, and Intraperitoneal Paclitaxel for Initial Adjuvan nt Treatment of Optimally Debulked
AHFS Final Determination of Medical Acceptance: Off-label Use of Sequential IV Paclitaxel, Intraperitoneal Cisplatin, and Intraperitoneal Paclitaxel for Initial Adjuvan nt Treatment of Optimally Debulked
Intraperitoneal Cisplatin and Paclitaxel in Ovarian Cancer
 The new england journal of medicine original article Intraperitoneal Cisplatin and Paclitaxel in Ovarian Cancer Deborah K. Armstrong, M.D., Brian Bundy, Ph.D., Lari Wenzel, Ph.D., Helen Q. Huang, M.S.,
The new england journal of medicine original article Intraperitoneal Cisplatin and Paclitaxel in Ovarian Cancer Deborah K. Armstrong, M.D., Brian Bundy, Ph.D., Lari Wenzel, Ph.D., Helen Q. Huang, M.S.,
Epithelial ovarian carcinoma is the leading cause of death from gynecologic malignancies
 NCI Clinical Announcement Intraperitoneal chemotherapy for ovarian cancer Background Epithelial ovarian carcinoma is the leading cause of death from gynecologic malignancies in the developed world. In
NCI Clinical Announcement Intraperitoneal chemotherapy for ovarian cancer Background Epithelial ovarian carcinoma is the leading cause of death from gynecologic malignancies in the developed world. In
Current state of upfront treatment for newly diagnosed advanced ovarian cancer
 Current state of upfront treatment for newly diagnosed advanced ovarian cancer Ursula Matulonis, M.D. Associate Professor of Medicine, HMS Program Leader, Medical Gyn Oncology Dana-Farber Cancer Institute
Current state of upfront treatment for newly diagnosed advanced ovarian cancer Ursula Matulonis, M.D. Associate Professor of Medicine, HMS Program Leader, Medical Gyn Oncology Dana-Farber Cancer Institute
Why is an outpatient transplant best for you?
 Outpatient Autologous Transplant Why is an outpatient transplant best for you? An outpatient transplant allows you to: stay in the comfort of your own home sleep in your own bed eat your usual foods be
Outpatient Autologous Transplant Why is an outpatient transplant best for you? An outpatient transplant allows you to: stay in the comfort of your own home sleep in your own bed eat your usual foods be
Vaxcel Implantable Ports Valved and Non-Valved. A Patient s Guide
 Vaxcel Implantable Ports Valved and Non-Valved A Patient s Guide Vaxcel Implantable Port This pamphlet provides some answers to questions you may have about your implantable port and how to care for it
Vaxcel Implantable Ports Valved and Non-Valved A Patient s Guide Vaxcel Implantable Port This pamphlet provides some answers to questions you may have about your implantable port and how to care for it
Diagnostic Laparoscopy
 PATIENT & CAREGIVER EDUCATION Diagnostic Laparoscopy This information describes your diag nostic laparoscopy. About Your Diagnostic Laparoscopy A diag nostic laparoscopy is a minimally invasive procedure.
PATIENT & CAREGIVER EDUCATION Diagnostic Laparoscopy This information describes your diag nostic laparoscopy. About Your Diagnostic Laparoscopy A diag nostic laparoscopy is a minimally invasive procedure.
The New England Journal of Medicine
 CISPLATIN PLUS CYCLOPHOSPHAMIDE VERSUS CISPLATIN PLUS CYCLOPHOSPHAMIDE FOR STAGE III OVARIAN CANCER DAVID S. ALBERTS, M.D., P.Y. LIU, PH.D., EDWARD V. HANNIGAN, M.D., ROBERT O TOOLE, M.D., STEPHEN D. WILLIAMS,
CISPLATIN PLUS CYCLOPHOSPHAMIDE VERSUS CISPLATIN PLUS CYCLOPHOSPHAMIDE FOR STAGE III OVARIAN CANCER DAVID S. ALBERTS, M.D., P.Y. LIU, PH.D., EDWARD V. HANNIGAN, M.D., ROBERT O TOOLE, M.D., STEPHEN D. WILLIAMS,
Insertion of a totally implantable vascular access device (TIVAD)
 Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Insertion of a totally implantable vascular access device (TIVAD) What is a TIVAD? A TIVAD is a long hollow tube that is inserted into one of the large veins in your body. One end of the tube sits in a
Co-Chairs Helen J MacKay and Diane Provencher On behalf of the OV21/PETROC Investigators CCTG, NCRI (UK), GEICO and SWOG
 OV21/PETROC: A Randomized Gynecologic Cancer Intergroup (GCIG) Phase II Study of Intraperitoneal (IP) vs. Intravenous (IV) Chemotherapy Following Neoadjuvant Chemotherapy and Optimal Debulking Surgery
OV21/PETROC: A Randomized Gynecologic Cancer Intergroup (GCIG) Phase II Study of Intraperitoneal (IP) vs. Intravenous (IV) Chemotherapy Following Neoadjuvant Chemotherapy and Optimal Debulking Surgery
Winship Cancer Institute of Emory University Optimizing First Line Treatment of Advanced Ovarian Cancer
 Winship Cancer Institute of Emory University Optimizing First Line Treatment of Advanced Ovarian Cancer Ira R. Horowitz, MD, SM, FACOG, FACS John D. Thompson Professor and Chairman Department of Gynecology
Winship Cancer Institute of Emory University Optimizing First Line Treatment of Advanced Ovarian Cancer Ira R. Horowitz, MD, SM, FACOG, FACS John D. Thompson Professor and Chairman Department of Gynecology
Intraperitoneal chemotherapy: where are we going? A. Gadducci Pisa
 Intraperitoneal chemotherapy: where are we going? A. Gadducci Pisa Intraperitoneal Chemotherapy (IP) in advanced ovarian cancer (EOC): Rationale The spread of disease is often limited to the peritoneal
Intraperitoneal chemotherapy: where are we going? A. Gadducci Pisa Intraperitoneal Chemotherapy (IP) in advanced ovarian cancer (EOC): Rationale The spread of disease is often limited to the peritoneal
DATE: 22 May 2013 CONTEXT AND POLICY ISSUES
 TITLE: Intraperitoneal versus Intravenous Chemotherapy for the Treatment of Ovarian Cancer: A Review of the Comparative Clinical Evidence, Safety, Cost- Effectiveness, and Guidelines DATE: 22 May 2013
TITLE: Intraperitoneal versus Intravenous Chemotherapy for the Treatment of Ovarian Cancer: A Review of the Comparative Clinical Evidence, Safety, Cost- Effectiveness, and Guidelines DATE: 22 May 2013
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Prof A Pourazar Immunohematologist
 Prof A Pourazar Immunohematologist What is plasma? Plasma is part of blood. It is the liquid that supports the circulation of red blood cells, white blood cells and platelets. Plasma is mainly water and
Prof A Pourazar Immunohematologist What is plasma? Plasma is part of blood. It is the liquid that supports the circulation of red blood cells, white blood cells and platelets. Plasma is mainly water and
Appendicitis. Diagnosis and Surgery
 Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Intraperitoneal antineoplastic drug delivery: rationale and results. Cavity
 Intraperitoneal antineoplastic drug delivery: rationale and results Maurie Markman The use of intraperitoneal drug delivery in the treatment of malignant disease confined to the peritoneal cavity is based
Intraperitoneal antineoplastic drug delivery: rationale and results Maurie Markman The use of intraperitoneal drug delivery in the treatment of malignant disease confined to the peritoneal cavity is based
Esophagectomy Surgery
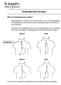 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Side Effects. PFS (months) Study Regimen No. patients. OS (months)
 Study Regimen No. patients PFS (months) OS (months) Side Effects Phase II PR ov ca 1 Phase II GOG PR+PS ov ca 1 Bev (15 mg/kg) q3wks Bev (15 mg/kg) q3wks 44 4.4 10.7 HTN, Proteinuria, GI perf (11%) stopped
Study Regimen No. patients PFS (months) OS (months) Side Effects Phase II PR ov ca 1 Phase II GOG PR+PS ov ca 1 Bev (15 mg/kg) q3wks Bev (15 mg/kg) q3wks 44 4.4 10.7 HTN, Proteinuria, GI perf (11%) stopped
ACRIN Gynecologic Committee
 ACRIN Gynecologic Committee Fall Meeting 2010 ACRIN Abdominal Committee Biomarkers & Endpoints in Ovarian Cancer Trials Robert L. Coleman, MD Professor and Vice Chair, Clinical Research Department of Gynecologic
ACRIN Gynecologic Committee Fall Meeting 2010 ACRIN Abdominal Committee Biomarkers & Endpoints in Ovarian Cancer Trials Robert L. Coleman, MD Professor and Vice Chair, Clinical Research Department of Gynecologic
Take control of your pain therapy. Getting started with Algovita SCS.
 Take control of your pain therapy. Getting started with Algovita SCS. The two-step approach to spinal cord stimulation therapy. You ve talked with your doctor. You ve discussed it with your family. You
Take control of your pain therapy. Getting started with Algovita SCS. The two-step approach to spinal cord stimulation therapy. You ve talked with your doctor. You ve discussed it with your family. You
Original Research. Background
 Original Research 849 in Carboplatin and Dose-Dense Paclitaxel Chemotherapy for Ovarian Malignancies: A Survey of NCCN Member Institutions Marina Stasenko, MD a ; R. Kevin Reynolds, MD a ; Carolyn Johnston,
Original Research 849 in Carboplatin and Dose-Dense Paclitaxel Chemotherapy for Ovarian Malignancies: A Survey of NCCN Member Institutions Marina Stasenko, MD a ; R. Kevin Reynolds, MD a ; Carolyn Johnston,
Heated Intraperitoneal Chemotherapy (HIPEC) for Advanced Abdominal Cancers
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/heated-intraperitonealchemotherapy-hipec-for-advanced-abdominal-cancers/7091/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/medical-breakthroughs-from-penn-medicine/heated-intraperitonealchemotherapy-hipec-for-advanced-abdominal-cancers/7091/
Patient & Family Guide. Bowel Surgery.
 Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Patient & Family Guide 2016 Bowel Surgery www.nshealth.ca Bowel Surgery This pamphlet will answer some of your questions about your stay in hospital and care at home. We hope this information will help
Transarterial Chemoembolization (TACE)
 Transarterial Chemoembolization (TACE) Princess Margaret Know what to expect Read this booklet to learn: What TACE is...1 How TACE works...2 The benefits of TACE...3 The risks and side effects of TACE...3
Transarterial Chemoembolization (TACE) Princess Margaret Know what to expect Read this booklet to learn: What TACE is...1 How TACE works...2 The benefits of TACE...3 The risks and side effects of TACE...3
Laparoscopic Gastric Bypass Information
 1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
1441 Constitution Boulevard, Salinas, CA 93906 (831) 783-2556 www.natividad.com/weight-loss (Roux-en-Y Gastric Bypass) What is gastric bypass surgery? Gastric bypass surgery, a type of bariatric surgery
Eligibility Form. 1. Patient Profile. (This form must be completed before the first dose is dispensed.) Request prior approval for enrolment
 Bevacizumab in combination with Paclitaxel and Carboplatin - Frontline Treatment (Previously Untreated) Ovarian, Fallopian Tube, and Primary Peritoneal Cancer (This form must be completed before the first
Bevacizumab in combination with Paclitaxel and Carboplatin - Frontline Treatment (Previously Untreated) Ovarian, Fallopian Tube, and Primary Peritoneal Cancer (This form must be completed before the first
UWMC Clinic Care After Discharge
 Patient Education UWMC Clinic Care After Discharge For a kidney/pancreas transplant Once you are discharged from the hospital, you will enter the next phase of transplant care, outpatient follow-up. You
Patient Education UWMC Clinic Care After Discharge For a kidney/pancreas transplant Once you are discharged from the hospital, you will enter the next phase of transplant care, outpatient follow-up. You
Interstitial Breast Brachytherapy
 Patient Education Questions? Your questions are important. Call your doctor or health care provider if you have questions or concerns. UWMC clinic staff are also available to help at any time. During normal
Patient Education Questions? Your questions are important. Call your doctor or health care provider if you have questions or concerns. UWMC clinic staff are also available to help at any time. During normal
Portacath Insertion. Patient Information Leaflet
 Portacath Insertion Patient Information Leaflet What is a Portacath? A Portacath (also referred to as Port, Chemoport or Power Port) is an implanted central venous access device (CVAD) recommended for
Portacath Insertion Patient Information Leaflet What is a Portacath? A Portacath (also referred to as Port, Chemoport or Power Port) is an implanted central venous access device (CVAD) recommended for
THERAPY Baclofen Pump Program at Boston Children s Hospital
 BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
BACLOFEN PUMP THERAPY Baclofen Pump Program at Boston Children s Hospital PAGER: 617-355-6369 and ask to page #7867 (PUMP) 1 Contents What is spasticity?... 3 What is baclofen?... 3 The evaluation for
Laparoscopic Inguinal Hernia Repair
 1 Laparoscopic Inguinal Hernia Repair Hernia is a medical condition where a part of the intestine bulges out of the weak abdominal muscles. Inguinal hernia is a type of hernia which occurs in the groin
1 Laparoscopic Inguinal Hernia Repair Hernia is a medical condition where a part of the intestine bulges out of the weak abdominal muscles. Inguinal hernia is a type of hernia which occurs in the groin
LAPAROSCOPIC APPENDICECTOMY
 LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
LAPAROSCOPIC APPENDICECTOMY WHAT IS THE APPENDIX? The appendix is a small, fingerlike pouch of the intestinal tract located where the small and large join. It has no known use. It is postulated that the
Debulking Surgery and HIPC to Treat Ovarian Cancer
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/debulking-surgery-and-hipc-to-treat-ovariancancer/3690/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/debulking-surgery-and-hipc-to-treat-ovariancancer/3690/
Renal Self Learning Package INTRODUCTION TO PERITONEAL DIALYSIS
 Renal Self Learning Package INTRODUCTION TO PERITONEAL DIALYSIS St George Hospital Renal Department, reviewed 2017 St George Hospital Renal Department RENAL SELF LEARNING PACKAGE INTRODUCTION TO PERITONEAL
Renal Self Learning Package INTRODUCTION TO PERITONEAL DIALYSIS St George Hospital Renal Department, reviewed 2017 St George Hospital Renal Department RENAL SELF LEARNING PACKAGE INTRODUCTION TO PERITONEAL
Review Heated Intraperitoneal Chemotherapy in the Management of Ovarian Cancer
 Review Heated Intraperitoneal Chemotherapy in the Management of Ovarian Cancer Andrea Jewell 1, Megan McMahon 1 and Dineo Khabele 1 1 Division of Gynecologic Oncology, Department of Obstetrics and Gynecology,
Review Heated Intraperitoneal Chemotherapy in the Management of Ovarian Cancer Andrea Jewell 1, Megan McMahon 1 and Dineo Khabele 1 1 Division of Gynecologic Oncology, Department of Obstetrics and Gynecology,
Ureteral Stenting and Nephrostomy
 Scan for mobile link. Ureteral Stenting and Nephrostomy Ureteral stenting and nephrostomy help restore urine flow through blocked ureters and return the kidney to normal function. Ureters are long, narrow
Scan for mobile link. Ureteral Stenting and Nephrostomy Ureteral stenting and nephrostomy help restore urine flow through blocked ureters and return the kidney to normal function. Ureters are long, narrow
Standard Operational Procedure. Drainage of Malignant Ascites (Abdominal Paracentesis)
 Standard Operational Procedure Drainage of Malignant Ascites (Abdominal Paracentesis) Background Cancers that involve the peritoneum can cause fluid to build up within the abdominal cavity. This is most
Standard Operational Procedure Drainage of Malignant Ascites (Abdominal Paracentesis) Background Cancers that involve the peritoneum can cause fluid to build up within the abdominal cavity. This is most
Caring for myself after Laparoscopic Appendectomy
 Caring for myself after Laparoscopic Appendectomy What is Laparoscopy Appendectomy? Laparoscopy appendectomy is a surgery to treat appendicitis infection of the appendix. During laparoscopic surgery, surgeons
Caring for myself after Laparoscopic Appendectomy What is Laparoscopy Appendectomy? Laparoscopy appendectomy is a surgery to treat appendicitis infection of the appendix. During laparoscopic surgery, surgeons
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
Lymphedema. Kelly Reichart, DNP, RN. About 246,660 women
 ADVANCED PRACTICE ASSOCIATE EDITOR DEBORAH "HUTCH" ALLEN, PhD, RN, CNS, FNP-BC, AOCNP Downloaded on 11 28 2018. Single-user license only. Copyright 2018 by the Oncology Nursing Society. For permission
ADVANCED PRACTICE ASSOCIATE EDITOR DEBORAH "HUTCH" ALLEN, PhD, RN, CNS, FNP-BC, AOCNP Downloaded on 11 28 2018. Single-user license only. Copyright 2018 by the Oncology Nursing Society. For permission
Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture
 Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture Patient name: Hospital Number: Consultant: Surgery
Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Instructions for Patients Following Vitreoretinal Surgery Who Need to Posture Patient name: Hospital Number: Consultant: Surgery
Rationale for the treatment. Peritoneal Surface Malignancy
 Rationale for the treatment of Peritoneal Surface Malignancy K. Van der Speeten 05/10/12 A full circle :acknowledgements Rationale for the treatment of Peritoneal Surface Malignancy K. Van der Speeten
Rationale for the treatment of Peritoneal Surface Malignancy K. Van der Speeten 05/10/12 A full circle :acknowledgements Rationale for the treatment of Peritoneal Surface Malignancy K. Van der Speeten
LAPAROSCOPIC HERNIA REPAIR
 LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
LAPAROSCOPIC HERNIA REPAIR Treating Your Hernia with Laparoscopy When You Have a Hernia Anyone can have a hernia. This is a weakness or tear in the wall of the abdomen. It often results from years of wear
Post Operative Instructions
 Mary A. Stanley, MD, FACS Breast Surgery Activity: Post Operative Instructions Gradually increase your activity the following day. You may drive as long as you are not taking narcotic pain medicine. It
Mary A. Stanley, MD, FACS Breast Surgery Activity: Post Operative Instructions Gradually increase your activity the following day. You may drive as long as you are not taking narcotic pain medicine. It
Patient Urinary Catheter Passport
 Useful contact details Name Contact Number Produced by Adapted from Worth by Michelle Pickering, Continence Specialist Practitioner Hambleton and Richmondshire Locality Continence Advisory Service and
Useful contact details Name Contact Number Produced by Adapted from Worth by Michelle Pickering, Continence Specialist Practitioner Hambleton and Richmondshire Locality Continence Advisory Service and
Renal Patient s Information Leaflet
 Renal (Haemodialysis) Unit Patient Information Renal Patient s Information Leaflet Opening hours: If you need this information in large print, easy read, on audiotape or in another language please call
Renal (Haemodialysis) Unit Patient Information Renal Patient s Information Leaflet Opening hours: If you need this information in large print, easy read, on audiotape or in another language please call
Peripherally Inserted Central Catheter (PICC) Booklet
 Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Aintree University Hospital FT PICC Booklet: a real world example This local booklet is an example used in the NICE medical technology guidance adoption support resource for SecurAcath for securing percutaneous
Radical Cystectomy A Patient s Guide
 Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
Radical Cystectomy A Patient s Guide Introduction The urinary system, which includes the bladder, urethra, ureters, and kidneys, helps maintain stable chemical conditions in the body, stores, and eliminates
PROGNOSTIC FACTORS AND FIRST LINE CHEMOTHERAPY IN AOC
 PROGNOSTIC FACTORS AND FIRST LINE CHEMOTHERAPY IN AOC Giorgia Mangili RUF ginecologia oncologica medica IRCCS San Raffaele Milano mangili.giorgia@hsr.it STANDARD CHEMOTHERAPY The standard chemotherapy
PROGNOSTIC FACTORS AND FIRST LINE CHEMOTHERAPY IN AOC Giorgia Mangili RUF ginecologia oncologica medica IRCCS San Raffaele Milano mangili.giorgia@hsr.it STANDARD CHEMOTHERAPY The standard chemotherapy
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
GOOVIPPC. Protocol Code: Gynecology. Tumour Group: Paul Hoskins. Contact Physician: James Conklin. Contact Pharmacist:
 BCCA Protocol Summary for Primary Treatment of Stage III less than or equal to 1 cm Visible Residual Invasive Epithelial Ovarian Cancer or Stage I Grade 3 or Stage II Grade 3 Papillary Serous Ovarian Cancer
BCCA Protocol Summary for Primary Treatment of Stage III less than or equal to 1 cm Visible Residual Invasive Epithelial Ovarian Cancer or Stage I Grade 3 or Stage II Grade 3 Papillary Serous Ovarian Cancer
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Kaiser Oakland Urology
 Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Kaiser Oakland Urology What is Laparoscopy? Minimally invasive surgical alternative to standard surgery How is Laparoscopy Performed? A laparoscope and video camera are used to visualize internal organs
Pain Relief Options for Labor. Providing you with quality care, information and support
 Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
My Urinary Catheter Passport Looking after my urinary catheter
 Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
Feedback We welcome your comments. If you have any ideas about how we could do something better or feedback about positive aspects of the service please let us know. If you have a complaint please let
STANDARDIZED PROCEDURE REPROGRAMMING AND REFILLING INTRATHECAL BACLOFEN PUMPS and ACCESSING THE CATHETER ACCESS PORT (Adult,Peds)
 I. Definition The purpose of this procedure is to allow the Advanced Health Practitioner (AHP) to reprogram and refill intrathecal Baclofen pumps, as well as access the catheter access port for those AHPs
I. Definition The purpose of this procedure is to allow the Advanced Health Practitioner (AHP) to reprogram and refill intrathecal Baclofen pumps, as well as access the catheter access port for those AHPs
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Select the dialysis treatment option that is best for you and your family.
 PEP CONNECT PEP Talk Outline P a t i e n t E d u c a t i o n P r o g r a m Your Treatment Options Part 1 Peritoneal Dialysis Select the dialysis treatment option that is best for you and your family. This
PEP CONNECT PEP Talk Outline P a t i e n t E d u c a t i o n P r o g r a m Your Treatment Options Part 1 Peritoneal Dialysis Select the dialysis treatment option that is best for you and your family. This
THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery
 THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery Clearance: Prior to surgery you will need surgical clearance from your Primary Care Physician and/ or Cardiologist, if recommended.
THORACIC SURGERY CHECKLIST Please review this checklist prior to surgery Clearance: Prior to surgery you will need surgical clearance from your Primary Care Physician and/ or Cardiologist, if recommended.
ABOUT THIS MEDICATION What are these drugs used for? Docetaxel is an anticancer drug used to treat cancers in the area of the neck and throat.
 For the Patient: HNAVDOC Treatment of Recurrent or Metastatic Squamous Cell Cancer of the Head and Neck with docetaxel HN=Head and Neck AV=Advanced DOC=Docetaxel ABOUT THIS MEDICATION What are these drugs
For the Patient: HNAVDOC Treatment of Recurrent or Metastatic Squamous Cell Cancer of the Head and Neck with docetaxel HN=Head and Neck AV=Advanced DOC=Docetaxel ABOUT THIS MEDICATION What are these drugs
Frequently Asked Questions About Photopheresis
 PATIENT & CAREGIVER EDUCATION Frequently Asked Questions About Photopheresis This information explains photopheresis, including how to prepare for the procedure and what to expect afterward. What is photopheresis?
PATIENT & CAREGIVER EDUCATION Frequently Asked Questions About Photopheresis This information explains photopheresis, including how to prepare for the procedure and what to expect afterward. What is photopheresis?
BMJ Case Reports Press Release
 2 November 2016 BMJ Case Reports Press Release Man develops acute hepatitis from consuming too many energy drinks A 50-year-old man was admitted to the emergency department with acute hepatitis, most likely
2 November 2016 BMJ Case Reports Press Release Man develops acute hepatitis from consuming too many energy drinks A 50-year-old man was admitted to the emergency department with acute hepatitis, most likely
Patient & Family Guide. Appendectomy. Aussi disponible en français : Appendicectomie (FF )
 Patient & Family Guide 2018 Appendectomy Aussi disponible en français : Appendicectomie (FF85-1895) www.nshealth.ca Appendectomy Your surgeon has arranged for you to have your appendix removed (appendectomy).
Patient & Family Guide 2018 Appendectomy Aussi disponible en français : Appendicectomie (FF85-1895) www.nshealth.ca Appendectomy Your surgeon has arranged for you to have your appendix removed (appendectomy).
Lower Anterior Resection (LAR) with Ileostomy
 Lower Anterior Resection (LAR) with Ileostomy Information for patients and families UHN Read this information to learn: what an LAR with ileostomy is how to care for yourself when you get home what problems
Lower Anterior Resection (LAR) with Ileostomy Information for patients and families UHN Read this information to learn: what an LAR with ileostomy is how to care for yourself when you get home what problems
About Implanted Ports
 PATIENT & CAREGIVER EDUCATION About Your Implanted Port This information will teach you about the placement and care of your implanted port. An implanted port is a type of central venous catheter (CVC).
PATIENT & CAREGIVER EDUCATION About Your Implanted Port This information will teach you about the placement and care of your implanted port. An implanted port is a type of central venous catheter (CVC).
If viewing a printed copy of this policy, please note it could be expired. Got to to view current policies.
 If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5555 Entity: Fairview Pharmacy Services
If viewing a printed copy of this policy, please note it could be expired. Got to www.fairview.org/fhipolicies to view current policies. Department Policy Code: D: PC-5555 Entity: Fairview Pharmacy Services
What is ureteral reimplantation?
 What is ureteral reimplantation? Ureteral reimplantation is surgery to disconnect the ureter from the bladder and reattach it in a better position. One or both ureters may need to be reimplanted. To understand
What is ureteral reimplantation? Ureteral reimplantation is surgery to disconnect the ureter from the bladder and reattach it in a better position. One or both ureters may need to be reimplanted. To understand
Clinical Trials. Ovarian Cancer
 1.0 0.8 0.6 0.4 0.2 0.0 < 65 years old 65 years old Events Censored Total 128 56 184 73 35 108 0 12 24 36 48 60 72 84 27-10-2012 Ovarian Cancer Stuart M. Lichtman, MD Attending Physician 65+ Clinical Geriatric
1.0 0.8 0.6 0.4 0.2 0.0 < 65 years old 65 years old Events Censored Total 128 56 184 73 35 108 0 12 24 36 48 60 72 84 27-10-2012 Ovarian Cancer Stuart M. Lichtman, MD Attending Physician 65+ Clinical Geriatric
Having MR Small Bowel (MR Enterography)
 Having MR Small Bowel (MR Enterography) Information for Patients In this leaflet: Introduction 2 What is an MR Small Bowel?..2 What do I need to do to before my scan?....2 Where do I go when I arrive at
Having MR Small Bowel (MR Enterography) Information for Patients In this leaflet: Introduction 2 What is an MR Small Bowel?..2 What do I need to do to before my scan?....2 Where do I go when I arrive at
For the Patient: Paclitaxel Other names: TAXOL
 For the Patient: Paclitaxel Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your doctor if
For the Patient: Paclitaxel Other names: TAXOL Paclitaxel (pak'' li tax' el) is a drug that is used to treat many types of cancer. It is a clear liquid that is injected into a vein. Tell your doctor if
UW MEDICINE PATIENT EDUCATION. Peritoneal Dialysis. A treatment option for kidney disease. There are 2 types of PD: continuous ambulatory
 UW MEDICINE PATIENT EDUCATION Peritoneal Dialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and basic principles of continuous ambulatory peritoneal dialysis (CAPD). 2.
UW MEDICINE PATIENT EDUCATION Peritoneal Dialysis A treatment option for kidney disease Class Goals 1. Understand the purpose and basic principles of continuous ambulatory peritoneal dialysis (CAPD). 2.
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Diagnostic Laparoscopy patient information from your surgeon & SAGES
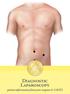 Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Diagnostic Laparoscopy patient information from your surgeon & SAGES Diagnostic Laparoscopy 1 Diagnostic Laparoscopy About conventional colon surgery: Patients may be referred to surgeons because of an
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~
 Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Orthotopic Bladder Reconstruction Surgery ~ Neobladder Surgery ~ Here are some words and pictures to help you understand this surgery: Kidney Ureter Bladder Urethra Small bowel An organ in the body that
Intrathecal chemotherapy
 Intrathecal chemotherapy Chemotherapy A guide for patients and carers Contents What is intrathecal chemotherapy?... 1 Why do I need intrathecal chemotherapy?... 1 What will happen before the procedure?...
Intrathecal chemotherapy Chemotherapy A guide for patients and carers Contents What is intrathecal chemotherapy?... 1 Why do I need intrathecal chemotherapy?... 1 What will happen before the procedure?...
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Robotic-Assisted Laparoscopic Pyeloplasty
 Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
Robotic-Assisted Laparoscopic Pyeloplasty What is a? Robotic-assisted pyeloplasty is a procedure to remove a blockage in the urinary tract that occurs where the kidney meets the ureter the Ureteropelvic
Sequential Dose-Dense Adjuvant Therapy With Doxorubicin, Paclitaxel, and Cyclophosphamide
 Sequential Dose-Dense Adjuvant Therapy With Doxorubicin, Paclitaxel, and Cyclophosphamide Review Article [1] April 01, 1997 By Clifford A. Hudis, MD [2] The recognition of paclitaxel's (Taxol's) activity
Sequential Dose-Dense Adjuvant Therapy With Doxorubicin, Paclitaxel, and Cyclophosphamide Review Article [1] April 01, 1997 By Clifford A. Hudis, MD [2] The recognition of paclitaxel's (Taxol's) activity
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
Robot Assisted Radical Prostatectomy
 For Patients Recovering from Robot Assisted Radical Prostatectomy This is a guide on what to expect before, during, and after your surgery and hospital stay. These are general guidelines that apply to
For Patients Recovering from Robot Assisted Radical Prostatectomy This is a guide on what to expect before, during, and after your surgery and hospital stay. These are general guidelines that apply to
Drafting a Coverage Authorization Request Letter
 Drafting a Coverage Authorization Request Letter The following information is presented for informational purposes only and is not intended to provide reimbursement or legal advice. Laws, regulations,
Drafting a Coverage Authorization Request Letter The following information is presented for informational purposes only and is not intended to provide reimbursement or legal advice. Laws, regulations,
Patient Urinary Catheter Passport
 Useful contact details: Continence Service (Community) 01724 298325 Continence Service (Goole) 01482 336951 Continence Service (SGH) 01724 282282 Ext 2823 Continence Service (DPOW) 01472 874111 Infection
Useful contact details: Continence Service (Community) 01724 298325 Continence Service (Goole) 01482 336951 Continence Service (SGH) 01724 282282 Ext 2823 Continence Service (DPOW) 01472 874111 Infection
After Shoulder Arthroscopic Surgery
 After Shoulder Arthroscopic Surgery Discharge Instructions Including: Examination of Joint Debridement of Joint Removal of Loose Bodies Arthroscope Important Points in Treatment Bleeding There may be some
After Shoulder Arthroscopic Surgery Discharge Instructions Including: Examination of Joint Debridement of Joint Removal of Loose Bodies Arthroscope Important Points in Treatment Bleeding There may be some
Wound care Keep your wound clean and dry. You do not need to have a dressing over it unless you are told otherwise by your hospital staff.
 After thoracic or lumbar spinal surgery We ve given you this factsheet because you have recently had thoracic or lumbar spinal surgery at Wessex Spinal Unit. It contains useful information and advice that
After thoracic or lumbar spinal surgery We ve given you this factsheet because you have recently had thoracic or lumbar spinal surgery at Wessex Spinal Unit. It contains useful information and advice that
Enhanced Recovery Patient Diary
 Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
How to Care for Yourself after Transcatheter Aortic Valve Replacement (TAVR)
 How to Care for Yourself after Transcatheter Aortic Valve Replacement (TAVR) When do I need to seek emergency care? Call 9-1-1 immediately if you develop: Sudden onset of chest pain Shortness of breath
How to Care for Yourself after Transcatheter Aortic Valve Replacement (TAVR) When do I need to seek emergency care? Call 9-1-1 immediately if you develop: Sudden onset of chest pain Shortness of breath
Going home after breast surgery without drains
 Going home after breast surgery without drains Princess Margaret Information for patients and families Read this resource to learn: How to care for yourself when you go home What activities you can do
Going home after breast surgery without drains Princess Margaret Information for patients and families Read this resource to learn: How to care for yourself when you go home What activities you can do
Laparoscopic Bowel Surgery
 Patient & Family Guide Laparoscopic Bowel Surgery 2016 www.nshealth.ca Laparoscopic Bowel Surgery Your surgeon has chosen for you to have laparoscopic bowel surgery instead of open bowel surgery. This
Patient & Family Guide Laparoscopic Bowel Surgery 2016 www.nshealth.ca Laparoscopic Bowel Surgery Your surgeon has chosen for you to have laparoscopic bowel surgery instead of open bowel surgery. This
Children's (Pediatric) PICC Line Placement
 Scan for mobile link. Children's (Pediatric) PICC Line Placement A peripherally inserted central catheter (PICC line) is most often used to deliver medication over a long period. The doctor or nurse inserts
Scan for mobile link. Children's (Pediatric) PICC Line Placement A peripherally inserted central catheter (PICC line) is most often used to deliver medication over a long period. The doctor or nurse inserts
Appendectomy. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Appendectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
Appendectomy Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information in this
patient decision aid advanced lung cancer
 patient decision aid advanced lung cancer Introduction This aid is meant to supplement conversations with your care team. Patients who have used a decision aid like this said it helped them make care choices
patient decision aid advanced lung cancer Introduction This aid is meant to supplement conversations with your care team. Patients who have used a decision aid like this said it helped them make care choices
Grey Bruce Health Network EVIDENCE-BASED CARE PROGRAM PATIENT EDUCATION BOOKLET TURP (TRANS URETHRAL RESECTION OF THE PROSTATE) PATHWAY
 Grey Bruce Health Network EVIDENCE-BASED CARE PROGRAM PATIENT EDUCATION BOOKLET TURP (TRANS URETHRAL RESECTION OF THE PROSTATE) PATHWAY Introduction: Prostate or bladder surgery requires special care.
Grey Bruce Health Network EVIDENCE-BASED CARE PROGRAM PATIENT EDUCATION BOOKLET TURP (TRANS URETHRAL RESECTION OF THE PROSTATE) PATHWAY Introduction: Prostate or bladder surgery requires special care.
For the Patient: GOOVCATM
 For the Patient: GOOVCATM Other Names: Treatment of No Visible Residual (Moderate- High Risk) Invasive Epithelial Ovarian, Fallopian Tube and Primary Peritoneal Cancer Using Carboplatin and Paclitaxel
For the Patient: GOOVCATM Other Names: Treatment of No Visible Residual (Moderate- High Risk) Invasive Epithelial Ovarian, Fallopian Tube and Primary Peritoneal Cancer Using Carboplatin and Paclitaxel
Transplant Surgery. Patient Education Guide to Your Kidney/Pancreas Transplant Page 9-1. For a kidney/pancreas transplant. Before Your Surgery
 Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Patient Education Page 9-1 Transplant Surgery For a kidney/pancreas transplant By the time you have your transplant surgery, you may have been waiting for some time. Reading this chapter before surgery
Daniel Calva, M.D. PHONE: (305) FAX: (305) Post Operative Instructions Breast Augmentation Surgery
 PHONE: (305) 203-3938 FAX: (305) 602-5956 Post Operative Instructions Breast Augmentation Surgery The goal is to make your surgical experience and recovery as comfortable as possible. Please call us with
PHONE: (305) 203-3938 FAX: (305) 602-5956 Post Operative Instructions Breast Augmentation Surgery The goal is to make your surgical experience and recovery as comfortable as possible. Please call us with
