Original article RHEUMATOLOGY
|
|
|
- Tyler Dominic Parks
- 5 years ago
- Views:
Transcription
1 RHEUMATOLOGY Rheumatology 2015;54: doi: /rheumatology/kev249 Advance Access publication 21 July 2015 Original article Final 10-year effectiveness and safety results from study DE020: adalimumab treatment in patients with rheumatoid arthritis and an inadequate response to standard therapy Daniel E. Furst 1, Arthur Kavanaugh 2, Stefan Florentinus 3, Hartmut Kupper 4, Mahinda Karunaratne 5 and Charles A. Birbara 6 CLINICAL SCIENCE Abstract Objective. To evaluate the long-term effectiveness and safety of 10 years of adalimumab (ADA) treatment in DMARD-refractory RA patients and to analyse efficacy based on RF status and baseline disease duration. Methods. DE020 was a multicentre, phase 3, open-label continuation study. Adult RA patients who received s.c. ADA (40 mg every other week or monthly) in one of four early assessment studies could receive ADA for 410 years in DE020. Assessments included the 28-joint DAS with CRP (DAS28-CRP), Simplified Disease Activity Index (SDAI), HAQ Disability Index (HAQ-DI) and safety as events per 100 patient-years. Results. Of 846 enrolled patients, mean age at baseline was 55.6 years, 78.1% were women, mean disease duration was 11.7 years and 27.0% were RF. Among 286 (33.8%) patients who completed 10 years of ADA, 168/236 (71.2%) achieved DAS28-CRP 43.2, 101/238 (42.4%) achieved HAQ-DI <0.5 and 90/241 (37.3%) achieved DAS28-CRP 43.2 plus HAQ-DI <0.5. DAS28-CRP- or SDAI-based remission was observed in 135/236 (57.2%) and 70/236 (29.7%) patients, respectively. Effectiveness outcomes were similar regardless of RF status. Higher proportions of patients with shorter vs longer baseline disease duration (42 vs >2 years) achieved HAQ-DI <0.5 (60.6% vs 39.5%; P = 0.023) and DAS28-CRP 43.2 plus HAQ-DI <0.5 (58.1% vs 32.5%; P = 0.006). Adverse events (317.2 events per 100 patient-years) during ADA exposure were consistent with the expected safety profile for TNF inhibitors. Conclusion. ADA led to sustained clinical and functional responses in the 33.8% of treatment-refractory RA patients who completed 10 years of treatment. Patients with shorter disease duration achieved better outcomes, highlighting the need for early treatment. No unexpected safety findings were observed. Trial registration: ClinicalTrials.gov, NCT Key words: adalimumab, long-term therapy, rheumatoid arthritis. Rheumatology key messages. Ten year adalimumab treatment led to clinical and functional improvements in patients with DMARD-refractory RA.. Safety findings from 5224 patient-years of adalimumab exposure in RA were as expected.. RA patients with shorter disease duration (i.e. earlier treatment) achieved better long-term outcomes with adalimumab. 1 Department of Medicine, David Geffen School of Medicine, University of California Los Angeles, Los Angeles, 2 Department of Medicine, University of California San Diego School of Medicine, San Diego, CA, USA, 3 Global Medical Affairs, AbbVie, Rungis, France, 4 Pharmaceutical Development, AbbVie Deutschland, Ludwigshafen, Germany, 5 Data and Statistical Sciences, AbbVie, North Chicago, IL and 6 Department of Medicine, University of Massachusetts School of Medicine, Worcester, MA, USA Submitted 30 April 2014; revised version accepted 1 June 2015 Correspondence to: Daniel E. Furst, UCLA Medical School, Rheumatology Division, 1000 Veteran Avenue, Rehab Center Room 32-59, Los Angeles, CA , USA. defurst@mednet.ucla.edu! The Author Published by Oxford University Press on behalf of the British Society for Rheumatology. All rights reserved. For Permissions, please journals.permissions@oup.com
2 Long-term adalimumab treatment for RA Introduction RA is a chronic inflammatory disorder of the joints, with a reported prevalence of 0.5 1% worldwide [1]. RA is associated with substantial morbidity and mortality. Recommendations formulated by the EULAR and ACR for the management of RA are aimed at achieving remission or low disease activity (LDA) [2, 3]. First-line treatment includes conventional synthetic DMARDs; in particular, MTX. If disease control or a target is not achieved within the first 6 months of treatment, recommendations suggest treatment with a second DMARD or the addition of a biologic DMARD if poor prognostic factors are present. Because RA is a chronic disease, patients may require continued, long-term therapy with biologic DMARDs in order to suppress disease activity, prevent structural progression and maintain physical function. Considering the likelihood of lifelong therapy, studies reporting long-term effectiveness and safety observations with biologic DMARDs are warranted. Disease characteristics, such as the presence of autoantibodies, high disease activity and early joint damage, have been shown to impact effective management of RA [3]. In addition, therapeutic response may be influenced by disease duration at the time of treatment initiation. For example, there appears to be a window of opportunity for adding a TNF inhibitor to standard therapy; a delay of >2 years has been shown to result in a suboptimal clinical response [4, 5]. Thus a better understanding of the impact of disease duration on clinical outcomes is needed, particularly in patients who have failed several DMARD therapies. The TNF inhibitor adalimumab (ADA), either as monotherapy or in combination with MTX, has demonstrated efficacy and safety in patients with RA in multiple studies [4 9]. This study (DE020) was a long-term extension of four studies (DE005/DE005X, DE009/DE009X, DE031 and DE037) that were conducted in the early development programme of ADA [8, 10 12]. All four studies enrolled patients with active RA and an inadequate response to MTX and/or other DMARDs. We report the final 10 year results from DE020 on the long-term effectiveness and safety of adalimumab exposure in patients with RA and previous DMARD failure. Further objectives of this post hoc analysis were to assess the long-term effectiveness of ADA in patients with RA on the basis of RF status and baseline disease duration. Methods Study design and patients DE020 was a 10 year, multicentre, phase 3, open-label continuation study (NCT ) evaluating the longterm effectiveness, safety and tolerability of ADA in patients with RA. Adults with RA who completed one of four ADA studies conducted in the USA or Canada (DE005/ DE005X, DE009/DE009X, DE031 or DE037) were eligible for enrolment in this rollover study. Patients with known HIV infection, a history of tuberculosis (TB) or listeriosis, any ongoing chronic or active infection, chronic use of oral antibiotics or any major episode of infection requiring hospitalization or treatment with i.v. antibiotics within 30 days of study entry were excluded. Patients received s.c. injections of ADA 40 mg every other week (eow) for up to 10 years. Patients who had received monthly dosing in their initial study continued monthly dosing in DE020. In addition, any patients who received ADA eow in the current study and maintained a 50% improvement in ACR criteria (ACR50) for two consecutive visits could change to monthly dosing. In contrast, patient dosing frequency could be increased to ADA 40 mg/week in response to any increase in disease activity. Concomitant DMARD therapy was allowed at the discretion of the investigator. The study was approved by 21 institutional review boards and was conducted in accordance with the International Conference on Harmonisation Good Clinical Practice Guideline, US Food and Drug Administration regulations governing clinical study conduct and principles that have their origin in the Declaration of Helsinki. All patients provided written informed consent prior to study initiation. Effectiveness assessments Clinical and functional responses to ADA treatment were assessed at year 10. Clinical effectiveness was assessed by the ACR20, ACR50 and ACR70 criteria [13], the 28-joint DAS based on CRP (DAS28-CRP) [14, 15], the Simplified Disease Activity Index (SDAI) [16] and CRP concentration. The proportions of patients with clinical responses were compared based on achieving the ACR criteria, DAS28- CRP LDA or remission (score 43.2 or <2.6, respectively), SDAI remission (score 43.3) and CRP concentration 41.0 mg/dl. Physical function was assessed using the HAQ Disability Index (HAQ-DI) [17]. Normal physical function was defined as HAQ-DI <0.5. Combined clinical and functional response was assessed as the percentage of patients achieving simultaneous LDA and normal function (DAS28-CRP43.2 and HAQ-DI <0.5). Safety assessments All patients who received one or more doses of study drug were included in the safety analysis. Safety was assessed in terms of adverse event (AE) incidence and events per 100 patient-years (E/100-PYs). Treatment-emergent AEs (TEAEs) were defined as AEs occurring from the date of the first dose of ADA in DE020 until 70 days after the last dose of ADA. TEAEs were coded according to the Medical Dictionary for Regulatory Activities, version 14.0, and analysed by severity and relationship to the study drug. A serious AE was defined as hospitalization, significant disability/incapacity, congenital anomaly, new diagnosis of cancer, life-threatening event or death. Statistical analyses Results of this post hoc analysis are reported through 10 years of ADA treatment. All patients who had one or more effectiveness measurement after the first dose of study drug in DE020 were included in the intent-to-treat (ITT) population. Baseline and demographic data and numbers
3 Daniel E. Furst et al. of patients achieving effectiveness endpoints were summarized descriptively. Nonresponder imputation was used as a sensitivity analysis to account for discontinuations during the 10 year study for the ITT population. For analyses using observed data, only patients with nonmissing values were included. The impact of several baseline variables, including sex, age, body weight, CS use, RF status (positive or negative) and disease duration (42 or >2 years) on 10 year effectiveness outcomes was also assessed. Differences in effectiveness outcomes between disease duration and RF status subgroups were analysed using the Pearson chi-square test or Fisher s exact test. Results Patients Of the 846 patients in the ITT population of DE020, 321 (37.9%) completed the study and 286 (33.8%) received a full 10 years of ADA treatment (Fig. 1A). Overall, there was an increase in discontinuation 6 months after the study began, followed by a fairly linear rate of withdrawal afterwards of approximately 410% annually; the rate of discontinuation was statistically similar regardless of baseline disease duration (Fig. 1B). Baseline demographics and disease characteristics in the initial studies were typical for patients with chronic RA (Table 1). Most patients were women (78.1%); the mean baseline age of patients was 55.0 years in the initial studies and 55.6 years in the current study. The majority of patients (95.9%) had been treated with DMARDs prior to participation in the initial studies; 73.0% of patients were seropositive for RF. Before participation in the initial studies, the majority of patients (86.0%) had a disease duration of >2 years. Patients had more severe disease activity at baseline in the initial studies compared with the current study (Table 1). Most patients began the study with 40 mg eow dosing of ADA [n = 829 (98.0%)], 17 (2.0%) patients were on monthly ADA and 31 patients (3.7%) switched from eow to monthly dosing during the course of the study. Concomitant use of a nonbiologic DMARD for RA or an NSAID or CS for any reason occurred in 89.2%, 85.6% and 80.1% of patients, respectively, at some point during this 10 year study. The reasons for discontinuation were AE development [n = 194 (22.9%)], lack of efficacy/disease progression [n = 99 (11.7%)], administrative reason [n = 83 (9.8%)], withdrawal of consent [n =67 (7.9%)], loss to follow-up [n = 44 (5.2%)], death [n = 23 (2.7%)] and protocol violation [n = 15 (1.8%)]. Among the 194 patients who withdrew from the study due to AEs, 185 stopped study treatment permanently. Effectiveness outcomes Clinical and functional improvements in ACR responses, DAS28-CRP, HAQ-DI, SDAI and serum CRP levels persisted over the course of the study with ADA treatment, based on observed data at each time point (Fig, 2; solid symbols). Based on observed data at year 10, ACR20, ACR50 and ACR70 responses were achieved by 78.6%, 55.5%, and 32.8% of treatment completers, respectively (Fig. 2A; solid symbols). Remission, defined as DAS28- CRP <2.6 or SDAI 43.3, was observed for 57.2% and 29.7% of treatment completers, respectively, at year 10 (Fig. 2B; solid circle and square). LDA, defined as DAS28- CRP 43.2, was achieved by 71.2% of treatment completers at year 10 (Fig. 2C; solid circle); the only statistically significant baseline and week 24 predictors of LDA at 10 years, based on logistic regression, were male sex [odds ratio (OR) (95% CI 1.096, 8.340), P = 0.033] and DAS28 at week 24 [OR (95% CI 0.194, 0.928), P = 0.032]. At year 10, 42.4% of treatment completers had normal physical function (HAQ-DI <0.5) and 37.3% exhibited both LDA and normal function (Fig. 2C; solid square and triangle). Suppression of CRP concentration to 41.0 mg/dl was achieved by 92.9% of patients after completing 10 years of treatment (Fig. 2D; solid circle). Based on non-responder imputation, the response rate for each effectiveness outcome gradually decreased over the course of the study, corresponding to the steady rate of treatment discontinuation (Fig. 2; open symbols). The observed effectiveness outcome response rates at the final visit generally remained high (Fig. 2; bars within inset plots). Among the ITT patients who completed 10 years of ADA treatment, those with normal physical function at year 10 had consistently lower DAS28-CRP scores over the course of the study compared with those without normal function at year 10 (Fig. 3). Among 836 ITT patients with observed HAQ-DI and DAS28-CRP data, time-averaged physical function [area under the time curve (AUC) for HAQ-DI] was most favourable among patients who achieved remission (DAS28-CRP <2.6; n = 266; mean AUC of HAQ-DI 154.6). Time-averaged physical function was comparable among patients who achieved LDA (DAS28-CRP ; n = 178; mean AUC of HAQ-DI 283.4) or neither remission nor LDA (DAS28-CRP >3.2; n = 392; mean AUC of HAQ-DI 307.4). Effects of RF status Based on RF status assessed at baseline of their initial study, identical proportions of RF and RF + ITT patients completed 10 years of ADA treatment (33.8% each; Table 2). Clinical and functional responses were generally similar among patients regardless of RF status (Table 2). Larger proportions of RF than RF + patients achieved an ACR50 response (63.2% vs 52.4%) or remission according to DAS28-CRP (63.6% vs 54.7%), although these differences were not statistically significant. No differences were observed between RF and RF + patients when the normal physical function criterion was combined with LDA. Effects of baseline disease duration Similar proportions of ITT patients with baseline disease duration 42 or >2 years completed 10 years of ADA treatment (32.2% vs 34.1%, respectively; Table 2). A significantly greater proportion of patients with baseline disease duration >2 vs 42 years were receiving concomitant DMARDs at the start of DE020 (86.2% vs 75.4%;
4 Long-term adalimumab treatment for RA FIG. 1Patient (A) disposition and (B) discontinuation over the course of the 10-year study A ITT Analysis Set N=846 Ini al Studies DE005/005X (n=39) DE009/009X (n=217) DE031 (n=554) DE037 (n=36) Discon nued Study, N=525 (62.1%) Reasons for discon nua on: B Percentage of Patients Completed DE020, N=321 (37.9%) Completed 10 Years of Treatment in DE020, N=286 (33.8%) Adverse event, n=194 (22.9%) a Lack of efficacy/progression of disease, n=99 (11.7%) Administra ve reasons, n=83 (9.8%) Withdrawal of consent, n=67 (7.9%) Lost to follow-up, n=44 (5.2%) Death, n=23 (2.7%) Protocol viola on, n=15 (1.8%) Study Year All patients 2 years disease duration <2 years disease duration a Nine patients withdrew from the study due to adverse events but did not permanently discontinue treatment. P = 0.004); there were no significant differences in systemic CS use. At initial study entry, patients with longer disease duration were significantly more likely to be RF + than patients with shorter disease duration (74.6% vs 64.4%; P = 0.021) and were significantly older on average at initial study entry (mean age 55.5 vs 51.8 years; P = 0.002) and at the start of DE020 (mean age 56.2 vs 52.4 years; P = 0.002). Response rates for effectiveness outcomes were consistently numerically higher among patients with shorter baseline disease duration (Table 2). Of note, the proportion of patients achieving an ACR50 response at 10 years was statistically greater among patients with baseline disease duration 42 years compared with >2 years (71.9% vs 52.9%, respectively; P = 0.045); a trend was also observed for ACR70 response (46.9% vs 30.6%, respectively; P = 0.068). A statistically significant difference was observed in the proportion of patients who achieved normal function with a disease duration
5 Daniel E. Furst et al. TABLE 1 Demographics and baseline characteristics Initial study 42 years compared with >2 years at baseline (60.6% vs 39.5%, respectively; P = 0.023). The percentage of patients achieving simultaneous LDA and normal function was also statistically greater among patients with baseline disease duration 42 years compared with >2 years (58.1% vs 32.5%; P = 0.006). Long-term ACR20 non-responders Current study Women, n (%) 661 (78.1) 661 (78.1) Age at first dose, years 55.0 (12.2) 55.6 (12.2) Race, n (%) White 734 (86.8) 734 (86.8) Black 41 (4.8) 41 (4.8) Hispanic 43 (5.1) 43 (5.1) Other 28 (3.3) 28 (3.3) Duration of RA, years 11.1 (9.5) a 11.7 (9.6) a 42 years, n (%) 118 (14.0) a 90 (10.7) a >2 years, n (%) 727 (86.0) a 755 (89.3) a Prior DMARD use for 811 (95.9) NA RA, n (%) MTX 709 (83.8) NA HCQ 433 (51.2) NA SSZ 239 (28.3) NA Gold 154 (18.2) NA LEF 120 (14.2) NA Prior CS use for any 476 (56.3) NA reason, n (%) Prior NSAID use for 681 (80.5) NA any reason, n (%) Presence of morning stiffness Yes, n/n b (%) 556/590 (94.2) 573/842 (68.1) TJC, 68 joints 27.9 (13.2) 13.3 (14.3) SJC, 66 joints 20.1 (10.4) 10.5 (10.9) TJC, 28 joints 15.1 (6.6) 6.8 (7.3) SJC, 28 joints 13.5 (5.8) 7.2 (6.6) PtGA pain, 54.4 (22.2) 33.4 (25.3) 100 mm VAS PtGA disease activity, 53.5 (22.8) 32.2 (24.6) 100 mm VAS PGA, 100 mm VAS 59.2 (16.5) 29.6 (22.3) CRP, mg/l 18.0 (21.4) 10.0 (15.3) RF status 228 (27.0) NA negative, c n (%) HAQ-DI 1.4 (0.6) 0.9 (0.7) DAS28-CRP 5.7 (0.9) d 3.9 (1.5) Data are mean (S.D.) unless otherwise indicated. a n = 845. b n indicates the number of patients without missing values. c Not assessed before the first dose of open-label adalimumab in the current study. d n = 844. DAS28-CRP: 28-joint DAS with CRP; HAQ-DI: HAQ Disability Index; NA: not available; PGA: physician s global assessment of disease activity; PtGA: patient s global assessment of disease activity; SJC: swollen joint count; TJC: tender joint count; VAS: visual analogue scale. Nine patients never achieved an ACR20 response and yet continued in the study for at least 5 years. The degree of improvement in individual components of the ACR response criteria for these patients is presented in supplementary Table S1, available at Rheumatology Online. Each patient showed some level of improvement in at least one of the individual component measures. The majority of these patients experienced 520% improvements in patient-reported measures of disease activity and/or pain. Safety All 846 patients enrolled in the study received one or more injections of ADA. The mean duration of ADA exposure was 6.2 years (median 7.1 years), which totalled 5224 patient-years of exposure. The majority of patients (95.5%) reported one or more TEAEs during the 10 year study (Table 3). Approximately half of patients experienced a severe TEAE (51.2%; 22.8 E/100-PYs) or a serious TEAE (51.1%; 18.2 E/100-PYs). A TEAE considered at least possibly related to the study drug was experienced by 69.0% of patients (52.7 E/100-PYs). TEAEs led to permanent study drug discontinuation in 22.3% of patients and a dose reduction in 1.3% of patients. Four of the 189 patients who permanently discontinued study treatment due to TEAEs withdrew from the study for other reasons (two deaths and two withdrawals of consent). The majority of TEAEs that occurred in 510% of patients (supplementary Table S2, available at Rheumatology Online) are consistent with the safety profile for ADA, are associated with RA or are common in a middle-aged population. Upper respiratory tract infection (46.3%), RA disease flare (34.0%) and sinusitis (25.1%) were the most frequently reported TEAEs. Over the course of the 10 year study, 125 patients had serious infections (3.1 E/100-PYs; Table 3). Serious infections reported by 52% of patients were cellulitis (2.4%) and pneumonia (4.3%). Opportunistic infections occurred in eight patients (0.9%) and included oesophageal candidiasis (n = 3), coccidioidomycosis (n = 2), Mycobacterium avium complex infection (n = 1), nocardiosis (n = 1) and systemic Candida (n = 1). Over the 10 year period, two cases of TB were reported (0.1 E/100-PYs); both were serious and one was severe. One case of TB occurred in a 41-year-old woman 1286 days after the first dose of ADA in the current study; another case occurred in a 68- year-old woman 388 days after the first dose of ADA in the current study. Both cases were considered probably related to the study drug and led to study discontinuation. Treatment-emergent malignancies were reported in 14.8% of patients; 6 patients reported leukaemia (0.7%; 0.1 E/100-PYs), 9 patients reported lymphoma (1.1%; 0.2 E/100-PYs) and 10 patients reported melanoma (1.2%; 0.2 E/100-PYs). A total of 56 patients reported a treatment-emergent non-melanoma skin cancer (NMSC) event (6.6%; 1.5 E/100-PYs). Most malignancies were considered by the investigator as unrelated or unlikely to be related to the study drug. The standardized incidence ratio (SIR) for all malignancies was 1.14 [66 observed/ expected (95% CI 0.88, 1.46)]. The SIR was 2.69 [6 observed/2.23 expected (95% CI 0.98, 5.86)] for
6 Long-term adalimumab treatment for RA FIG. 2Clinical and functional responses through year 10 (NRI, obs) and the final visit (obs) (A) ACR20, ACR50 and ACR70. (B) DAS28-CRP remission (<2.6); SDAI remission (43.3). (C) DAS28-CRP LDA (43.2); normal function (HAQ-DI <0.5); simultaneous DAS28-CRP LDA (43.2) and normal function (HAQ-DI <0.5). (D) CRP 41.0 mg/dl. ACR20, 50, 70: 20, 50 or 70% improvement, respectively, in ACR criteria; DAS28-CRP: 28-joint DAS with CRP; HAQ-DI: HAQ Disability Index; LDA: low disease activity; NRI: non-responder imputation; obs: observed; SDAI: Simplified Disease Activity Index. FIG. 3Mean DAS28-CRP scores over time for patients with HAQ-DI 50.5 or <0.5 at year 10 Mean DAS28(CRP) Score HAQ-DI 0.5 at Year 10 HAQ-DI <0.5 at Year Study Year Baseline N obs*= N obs*= DAS28-CRP: 28-joint DAS with CRP; HAQ-DI: HAQ Disability Index. melanoma and 2.12 [65 observed/30.60 expected (95% CI 1.64, 2.71)] for NMSC. The incidence rates of myocardial infarction, cerebrovascular accident and congestive heart failure were 0.4, 0.8 and 0.6 E/100-PYs, respectively, during this study A total of 35 patients died over the course of the study, and 25 deaths occurred during or within 70 days of ADA treatment. Most treatment-emergent deaths were considered unrelated or likely unrelated to treatment with ADA (supplementary Table S3, available at Rheumatology Online). Five patient deaths were deemed possibly related to the study drug, including one patient each with acute myeloid leukaemia, breast cancer, nonsmall cell lung cancer, metastases to the liver and sepsis. Overall, the standardized mortality ratio (SMR) was 0.76 (95% CI 0.53, 1.05). Using the 25 treatment-emergent deaths, the SMR was 0.54 (95% CI 0.35, 0.80). These SMRs indicate that long-term exposure to ADA was not associated with increased mortality in this patient population. Discussion The DE020 study was conceived with the goal of longterm follow-up, with effectiveness and safety data over 10 years in patients with DMARD-refractory RA; a strength of this final report is that it includes 5224 patient-years of prospective follow-up. As expected, long-term treatment with ADA reduced disease activity and improved physical function in patients who continued in the study. At year 10, the majority of patients exhibited LDA, and over half of the
7 Daniel E. Furst et al. TABLE 2 Proportion of patients achieving clinical and functional response at year 10 by RF status and baseline disease duration RF status (n = 846), n/n obs a (%) Baseline disease duration (n = 845), n/n obs a (%) RF RF + 42 years >2 years Completed 10 years 77/228 (33.8) 209/618 (33.8) 38/118 (32.2) 248/727 (34.1) ACR20 53/68 (77.9) 134/170 (78.8) 26/32 (81.3) 161/206 (78.2) ACR50 43/68 (63.2) 89/170 (52.4) 23/32 (71.9) 109/206 (52.9)* ACR70 23/68 (33.8) 55/170 (32.4) 15/32 (46.9) 63/206 (30.6) LDA, DAS28-CRP /66 (74.2) 119/170 (70.0) 26/31 (83.9) 142/205 (69.3) DAS28-CRP remission (<2.6) 42/66 (63.6) 93/170 (54.7) 21/31 (67.7) 114/205 (55.6) Normal function, HAQ-DI <0.5 30/66 (45.5) 71/172 (41.3) 20/33 (60.6) 81/205 (39.5)** DAS28-CRP HAQ-DI <0.5 25/64 (39.1) 59/170 (34.7) 18/31 (58.1) 66/203 (32.5)*** SDAI remission (43.3) 22/66 (33.3) 48/170 (28.2) 13/31 (41.9) 57/205 (27.8) CRP 41.0, mg/dl 62/67 (92.5) 160/172 (93.0) 32/34 (94.1) 190/205 (92.7) Bold values showed a statistically significant difference when compared between patients with 42 vs >2 years of baseline disease duration. a N obs indicates the number of patients with non-missing values. *P = for the difference between subgroups; **P = for the difference between subgroups; ***P = for difference between subgroups (Pearson chisquare test or Fisher exact test). ACR20, 50, 70: 20, 50 or 70% improvement, respectively, in ACR criteria; DAS28-CRP: 28-joint DAS with CRP; HAQ-DI: HAQ Disability Index; LDA: low disease activity; SDAI: Simplified Disease Activity Index. TABLE 3 Overview of treatment-emergent adverse events Incidence (n = 846), n (%) E/100-PYs (ADA exposure = 5224 PYs), n (%) Any AE 808 (95.5) (317.2) At least possibly drug-related AE 584 (69.0) 2753 (52.7) Severe or life-threatening AE 433 (51.2) 1193 (22.8) Serious AE 432 (51.1) 953 (18.2) Fatal treatment-emergent AE 25 (3.0) 25 (0.5) Deaths, including non-treatment emergent deaths 35 (4.1) 35 (0.7) AE leading to permanent discontinuation of study drug 189 (22.3) a 239 (4.6) AE leading to study drug dose reduction 11 (1.3) 12 (0.2) Infections 678 (80.1) 4485 (85.9) Serious infections 125 (14.8) 162 (3.1) Opportunistic infections excluding TB and oral candidiasis 8 (0.9) 10 (0.2) Serious opportunistic infections excluding TB and oral candidiasis 3 (0.4) 3 (0.1) Active TB 2 (0.2) 3 (0.1) Parasitic infections other than opportunistic infection 4 (0.5) 4 (0.1) Malignancies 125 (14.8) 160 (3.1) Lymphoma 9 (1.1) 10 (0.2) NMSC 56 (6.6) 79 (1.5) Malignancies other than lymphoma and NMSC 67 (7.9) 71 (1.4) Malignancies other than NMSC 75 (8.9) 81 (1.6) HSTCL 0 0 Leukaemia 6 (0.7) 6 (0.1) Melanoma 10 (1.2) 10 (0.2) Demyelinating disorder 5 (0.6) 5 (0.1) Cerebrovascular accident 33 (3.9) 44 (0.8) Congestive heart failure 27 (3.2) 33 (0.6) Myocardial infarction 20 (2.4) 22 (0.4) Injection-site reaction 116 (13.7) 210 (4.0) Hepatic event 20 (2.4) 24 (0.5) Elevated ALT levels 86 (10.2) 173 (3.3) a One patient was found to have permanently discontinued from the study due to melanoma in situ after the database lock and is not reflected in the n (%) or E/100-PYs for permanent discontinuation of the study. ADA: adalimumab; AE: adverse event; ALT: alanine transaminase; E/100-PYs: events per 100 patient-years; HSTCL: hepatosplenic T cell lymphoma; NMSC: non-melanoma skin cancer; PY: patient-years; TB: tuberculosis
8 Long-term adalimumab treatment for RA patients were in remission according to DAS28-CRP. When using SDAI-based criteria, the number of patients in remission was lower, but still clinically relevant. Despite long-standing disease, normal physical function was observed for >40% of patients, and more than one-third of patients attained simultaneous normal function and LDA. The safety profile of ADA, observed using combined data from 10 years of treatment in the current study, demonstrated no new findings compared with earlier reports [18, 19]. As is usual in long-term studies of biologics [20 25] and non-biologic DMARDs [26, 27], TEAEs were common. Approximately 80% of patients experienced treatmentemergent infections, with a rate of 85.9 E/100-PYs. Serious infections in ADA-treated patients occurred at a rate of 3.1 E/100-PYs, which is slightly lower than rates observed in published trials of TNF inhibitors ( E/ 100-PYs) [19, 21, 28], but is consistent with other reports in the literature [29]. Of interest, two patients developed active TB and eight patients had other opportunistic infections over the 10 year period of DE020. Although patients were screened before study entry, they were not routinely rescreened on an ongoing basis for TB or other opportunistic infections; these infrequent events reflect the low rates of mycobacterial TB and other opportunistic infections in the USA, even among those using TNF inhibitors. Approximately 15% of patients experienced a treatment-emergent malignancy. In the current study, the SIR for overall malignancies was 1.14, with 95% CIs that encompassed 1, compared with the Surveillance, Epidemiology, and End Results (SEER) data for individuals without RA. Similarly the SIR for overall malignancies (excluding NMSC) was not elevated [0.64 (95% CI 0.53, 0.76)] in a 5 year observational study of 3435 patients with RA treated with ADA [30]. In contrast, the SIR was 1.28 (95% CI 1.10, 1.48) for malignancies observed in a cohort of 3771 patients with RA who were naive to biologic DMARDs compared with the general population in the UK [31]. The elevated SIRs for melanoma and NMSC in DE020 may reflect a more careful medical surveillance of patients in the study than is typical for individuals in the SEER database. However, the longitudinal data may militate against such an association, as the incidence of melanoma and NMSC did not increase with increasing ADA exposure (data not shown). SMRs indicate that long-term treatment with ADA was not associated with increased mortality in this patient population. The low incidences of myocardial infarction, cerebrovascular accident and congestive heart failure observed in this pre-selected population do not indicate an increased risk of these events with ADA use and are consistent with cardiovascular event rates reported in the Consortium of Rheumatology Researchers of North America database [32]. Similar percentages of patients with RF + and RF status completed 10 years of treatment with ADA. Clinical and functional response rates were generally similar between RF and RF + patients, although a greater proportion of RF patients achieved remission at year 10. These similarities support previous observations that RF status is not a conclusive predictor of response to anti-tnf therapy [33] or to MTX [34]. In the current study, patients with early disease, defined by convention as 42 years of disease duration, achieved better clinical and functional responses. Normal function was reported to a greater extent among patients who began ADA treatment within 2 years of disease onset. Better outcomes for patients with shorter disease duration were not due to concomitant treatments, as patients with shorter disease duration had lower rates of DMARD use and similar rates of CS use. These results support the earlier initiation of effective therapy, including ADA, with the goal of improving long-term outcomes and limiting functional loss that seemingly cannot be recovered in patients with long-standing disease. Ten year results from the PREMIER trial led to similar conclusions [4]. This study had limitations that are characteristic of any open-label design; there also was bias towards responders, as only the patients who continued in the study were followed. Only 34% of the original cohort completed 10 years of ADA treatment and were included in the 10 year analysis, although similar completion rates were observed in patients with early RA (disease duration 42 years; 32.2%) and established RA (disease duration >2 years; 34.1%), which may be expected due to these patients receiving the same long-term treatment. The overall 10 year treatment completion rate is comparable to the completion rates seen in the DE019 (44%) [7] and PREMIER (50%) [4] studies for patients who entered the open-label periods. Lack of effectiveness led 12% of patients to discontinue study treatment. In addition, there are no radiographic data available; however, physical function was assessed. In conclusion, 10 year treatment with ADA led to clinical and functional improvements in the 286 of 846 patients (34%) with DMARD-refractory RA who continued therapy throughout the entire study period. Safety findings from the 5224 patient-years of exposure are reassuring for infections, malignancies and cardiovascular outcomes; no new signals were found. RF status did not influence outcomes in this population, while those with shorter disease duration typically achieved better outcomes, underscoring the benefit of early treatment. Acknowledgements The authors are grateful to the investigators of the DE020 study for their efforts in collecting patient data. Medical writing support was provided by Amanda Sheldon, PhD, and Jennifer Han, MS, of Complete Publication Solutions; this support was funded by AbbVie. The authors thank Su Chen, PhD, of AbbVie for statistical support. Funding: This work was supported by AbbVie Inc., who sponsored the study, contributed to its design and participated in the collection, analysis and interpretation of the data and in the writing, reviewing and approval of the final version
9 Daniel E. Furst et al. Disclosure statement: A.K. has conducted clinical studies sponsored by AbbVie, Amgen, Bristol-Myers Squibb, Janssen, Pfizer and UCB. M.K. is an employee of and own stocks in AbbVie. D.E.F. has received grant/research support from AbbVie, Actelion, Amgen, BMS, Gilead, GSK, the National Institutes of Health (NIH), Novartis, Pfizer, Roche/Genentech and UCB; is a consultant for AbbVie, Actelion, Amgen, BMS, Cytori, Janssen, Gilead, GSK, NIH, Novartis, Pfizer, Roche/Genentech and UCB; and has served on the speaker s bureau (continuing medical education only) for AbbVie, Actelion and UCB. S.F. is a full-time employee of AbbVie and holds AbbVie shares and stock options. C.A.B. has performed clinical studies for AbbVie, Bristol-Myers Squibb, Genentech, Amgen, Celgene and Janssen. H.K. is a full-time employee of AbbVie and holds AbbVie shares and stock options. Supplementary data Supplementary data are available at Rheumatology Online. References 1 Sangha O. Epidemiology of rheumatic diseases. Rheumatology 2000;39: Singh JA, Furst DE, Bharat A et al update of the 2008 American College of Rheumatology recommendations for the use of disease-modifying antirheumatic drugs and biologic agents in the treatment of rheumatoid arthritis. Arthritis Care Res 2012;64: Smolen JS, Landewe R, Breedveld FC et al. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2013 update. Ann Rheum Dis 2014;73: Keystone EC, Breedveld FC, van der Heijde D et al. Longterm effect of delaying combination therapy with tumor necrosis factor inhibitor in patients with aggressive early rheumatoid arthritis: 10-year efficacy and safety of adalimumab from the randomized controlled PREMIER trial with open-label extension. J Rheumatol 2014;41: van der Heijde D, Breedveld FC, Kavanaugh A et al. Disease activity, physical function, and radiographic progression after longterm therapy with adalimumab plus methotrexate: 5-year results of PREMIER. J Rheumatol 2010;37: Keystone EC, Kavanaugh AF, Sharp JT et al. Radiographic, clinical, and functional outcomes of treatment with adalimumab (a human anti-tumor necrosis factor monoclonal antibody) in patients with active rheumatoid arthritis receiving concomitant methotrexate therapy: a randomized, placebo-controlled, 52-week trial. Arthritis Rheum 2004;50: Keystone EC, van der Heijde D, Kavanaugh A et al. Clinical, functional, and radiographic benefits of longterm adalimumab plus methotrexate: final 10-year data in longstanding rheumatoid arthritis. J Rheumatol 2013;40: Weinblatt ME, Keystone EC, Furst DE et al. Adalimumab, a fully human anti-tumor necrosis factor alpha monoclonal antibody, for the treatment of rheumatoid arthritis in patients taking concomitant methotrexate: the ARMADA trial. Arthritis Rheum 2003;48: Smolen JS, Emery P, Fleischmann R et al. Adjustment of therapy in rheumatoid arthritis on the basis of achievement of stable low disease activity with adalimumab plus methotrexate or methotrexate alone: the randomised controlled OPTIMA trial. Lancet 2014;383: Weisman MH, Moreland LW, Furst DE et al. Efficacy, pharmacokinetic, and safety assessment of adalimumab, a fully human anti-tumor necrosis factor-alpha monoclonal antibody, in adults with rheumatoid arthritis receiving concomitant methotrexate: a pilot study. Clin Ther 2003;25: Furst DE, Schiff MH, Fleischmann RM et al. Adalimumab, a fully human anti tumor necrosis factor-alpha monoclonal antibody, and concomitant standard antirheumatic therapy for the treatment of rheumatoid arthritis: results of STAR (Safety Trial of Adalimumab in Rheumatoid Arthritis). J Rheumatol 2003;30: Weinblatt ME, Keystone EC, Furst DE et al. Change over time in the safety, efficacy, and remission profiles of patients with rheumatoid arthritis receiving adalimumab for up to 7 years [abstract]. Arthritis Rheum 2007;56(Suppl):S Felson DT, Anderson JJ, Boers M et al. The American College of Rheumatology preliminary core set of disease activity measures for rheumatoid arthritis clinical trials. The Committee on Outcome Measures in Rheumatoid Arthritis Clinical Trials. Arthritis Rheum 1993;36: Prevoo ML, van t Hof MA, Kuper HH et al. Modified disease activity scores that include twenty-eight-joint counts. Development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum 1995;38: Inoue E, Yamanaka H, Hara M, Tomatsu T, Kamatani N. Comparison of Disease Activity Score (DAS)28- erythrocyte sedimentation rate and DAS28- C-reactive protein threshold values. Ann Rheum Dis 2007;66: Smolen JS, Breedveld FC, Schiff MH et al. A simplified disease activity index for rheumatoid arthritis for use in clinical practice. Rheumatology 2003;42: Fries JF, Spitz P, Kraines RG, Holman HR. Measurement of patient outcome in arthritis. Arthritis Rheum 1980;23: Schiff MH, Burmester GR, Kent JD et al. Safety analyses of adalimumab (HUMIRA) in global clinical trials and US postmarketing surveillance of patients with rheumatoid arthritis. Ann Rheum Dis 2006;65: Burmester GR, Panaccione R, Gordon KB, McIlraith MJ, Lacerda AP. Adalimumab: long-term safety in patients from global clinical trials in rheumatoid arthritis, juvenile idiopathic arthritis, ankylosing spondylitis, psoriatic arthritis, psoriasis and Crohn s disease. Ann Rheum Dis 2013;72: Smolen JS, Emery P. Infliximab: 12 years of experience. Arthritis Res Ther 2011;13(Suppl 1):S2. 21 Klareskog L, Gaubitz M, Rodriguez-Valverde V et al. Assessment of long-term safety and efficacy of etanercept
10 Long-term adalimumab treatment for RA in a 5-year extension study in patients with rheumatoid arthritis. Clin Exp Rheumatol 2011;29: van Vollenhoven RF, Emery P, Bingham CO 3rd et al. Long-term safety of rituximab in rheumatoid arthritis: 9.5-year follow-up of the global clinical trial programme with a focus on adverse events of interest in RA patients. Ann Rheum Dis 2013;72: Genovese MC, Rubbert-Roth A, Smolen JS et al. Longterm safety and efficacy of tocilizumab in patients with rheumatoid arthritis: a cumulative analysis of up to 4.6 years of exposure. J Rheumatol 2013;40: Kremer JM, Russell AS, Emery P et al. Long-term safety, efficacy and inhibition of radiographic progression with abatacept treatment in patients with rheumatoid arthritis and an inadequate response to methotrexate: 3-year results from the AIM trial. Ann Rheum Dis 2011;70: Fleischmann RM, Tesser J, Schiff MH et al. Safety of extended treatment with anakinra in patients with rheumatoid arthritis. Ann Rheum Dis 2006;65: Salliot C, van der Heijde D. Long-term safety of methotrexate monotherapy in patients with rheumatoid arthritis: a systematic literature research. Ann Rheum Dis 2009;68: Kalden JR, Schattenkirchner M, Sorensen H et al. The efficacy and safety of leflunomide in patients with active rheumatoid arthritis: a five-year followup study. Arthritis Rheum 2003;48: Moreland LW, Weinblatt ME, Keystone EC et al. Etanercept treatment in adults with established rheumatoid arthritis: 7 years of clinical experience. J Rheumatol 2006;33: Curtis JR, Jain A, Askling J et al. A comparison of patient characteristics and outcomes in selected European and U.S. rheumatoid arthritis registries. Semin Arthritis Rheum 2010;40:2 14 e1. 30 Burmester GR, Matucci-Cerinic M, Mariette X et al. Safety and effectiveness of adalimumab in patients with rheumatoid arthritis over 5 years of therapy in a phase 3b and subsequent postmarketing observational study. Arthritis Res Ther 2014;16:R Mercer LK, Davies R, Galloway JB et al. Risk of cancer in patients receiving non-biologic disease-modifying therapy for rheumatoid arthritis compared with the UK general population. Rheumatology 2013;52: Greenberg JD, Kremer JM, Curtis JR et al. Tumour necrosis factor antagonist use and associated risk reduction of cardiovascular events among patients with rheumatoid arthritis. Ann Rheum Dis 2011;70: Marotte H, Miossec P. Biomarkers for prediction of TNFa blockers response in rheumatoid arthritis. Joint Bone Spine 2010;77: Drouin J, Haraoui B, 3e Initiative Group. Predictors of clinical response and radiographic progression in patients with rheumatoid arthritis treated with methotrexate monotherapy. J Rheumatol 2010;37:
New Evidence reports on presentations given at EULAR Safety and Efficacy of Tocilizumab as Monotherapy and in Combination with Methotrexate
 New Evidence reports on presentations given at EULAR 2009 Safety and Efficacy of Tocilizumab as Monotherapy and in Combination with Methotrexate Report on EULAR 2009 presentations Tocilizumab inhibits
New Evidence reports on presentations given at EULAR 2009 Safety and Efficacy of Tocilizumab as Monotherapy and in Combination with Methotrexate Report on EULAR 2009 presentations Tocilizumab inhibits
Annual Rheumatology & Therapeutics Review for Organizations & Societies
 Annual Rheumatology & Therapeutics Review for Organizations & Societies Comparative Effectiveness Studies of Biologics Learning Objectives Understand the motivation for comparative effectiveness research
Annual Rheumatology & Therapeutics Review for Organizations & Societies Comparative Effectiveness Studies of Biologics Learning Objectives Understand the motivation for comparative effectiveness research
New Evidence reports on presentations given at ACR Improving Radiographic, Clinical, and Patient-Reported Outcomes with Rituximab
 New Evidence reports on presentations given at ACR 2009 Improving Radiographic, Clinical, and Patient-Reported Outcomes with Rituximab From ACR 2009: Rituximab Rituximab in combination with methotrexate
New Evidence reports on presentations given at ACR 2009 Improving Radiographic, Clinical, and Patient-Reported Outcomes with Rituximab From ACR 2009: Rituximab Rituximab in combination with methotrexate
2.0 Synopsis. Adalimumab (HUMIRA ) W Clinical Study Report R&D/15/0629. Individual Study Table Referring to Part of Dossier: Volume:
 2.0 Synopsis AbbVie Inc. Name of Study Drug: Adalimumab / HUMIRA Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only)
2.0 Synopsis AbbVie Inc. Name of Study Drug: Adalimumab / HUMIRA Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only)
New Evidence reports on presentations given at EULAR Tocilizumab for the Treatment of Rheumatoid Arthritis and Juvenile Idiopathic Arthritis
 New Evidence reports on presentations given at EULAR 2011 Tocilizumab for the Treatment of Rheumatoid Arthritis and Juvenile Idiopathic Arthritis Report on EULAR 2011 presentations Benefit of continuing
New Evidence reports on presentations given at EULAR 2011 Tocilizumab for the Treatment of Rheumatoid Arthritis and Juvenile Idiopathic Arthritis Report on EULAR 2011 presentations Benefit of continuing
Efficacy and Safety of Tocilizumab in the Treatment of Rheumatoid Arthritis and Juvenile Idiopathic Arthritis
 New Evidence reports on presentations given at EULAR 2010 Efficacy and Safety of Tocilizumab in the Treatment of Rheumatoid Arthritis and Juvenile Idiopathic Arthritis Report on EULAR 2010 presentations
New Evidence reports on presentations given at EULAR 2010 Efficacy and Safety of Tocilizumab in the Treatment of Rheumatoid Arthritis and Juvenile Idiopathic Arthritis Report on EULAR 2010 presentations
Supplemental Table 1. Key Inclusion Criteria Inclusion Criterion OPTIMA PREMIER 18 years old with RA (per 1987 revised American College of General
 Supplemental Table 1. Key Inclusion Criteria Inclusion Criterion OPTIMA PREMIER 18 years old with RA (per 1987 revised American College of General Rheumatology classification criteria) 34 ; erythrocyte
Supplemental Table 1. Key Inclusion Criteria Inclusion Criterion OPTIMA PREMIER 18 years old with RA (per 1987 revised American College of General Rheumatology classification criteria) 34 ; erythrocyte
Abatacept (Orencia) for active rheumatoid arthritis. August 2009
 Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC
 Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Update on the Treatment of Rheumatoid Arthritis Sabrina Fallavollita MDCM McGill University Canadian Society of Internal Medicine
Canadian Society of Internal Medicine Annual Meeting 2016 Montreal, QC Update on the Treatment of Rheumatoid Arthritis Sabrina Fallavollita MDCM McGill University Canadian Society of Internal Medicine
New Evidence reports on presentations given at EULAR Tocilizumab for the Treatment of Rheumatoid Arthritis
 New Evidence reports on presentations given at EULAR 2012 Tocilizumab for the Treatment of Rheumatoid Arthritis Report on EULAR 2012 presentations Tocilizumab monotherapy is superior to adalimumab monotherapy
New Evidence reports on presentations given at EULAR 2012 Tocilizumab for the Treatment of Rheumatoid Arthritis Report on EULAR 2012 presentations Tocilizumab monotherapy is superior to adalimumab monotherapy
Criteria Inclusion criteria Exclusion criteria. despite treatment with csdmards, NSAIDs, and/or previous anti-tnf therapy and/or
 Supplementary Material Table S1 Eligibility criteria (PICOS) for the SLR Criteria Inclusion criteria Exclusion criteria Population Adults (aged 18 years) with active PsA despite treatment with csdmards,
Supplementary Material Table S1 Eligibility criteria (PICOS) for the SLR Criteria Inclusion criteria Exclusion criteria Population Adults (aged 18 years) with active PsA despite treatment with csdmards,
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,700 108,500 1.7 M Open access books available International authors and editors Downloads Our
University of California, San Diego, School of Medicine, La Jolla, CA, USA; 2
 2194 Long-term (104-Week) Efficacy and Safety Profile of Apremilast, an Oral Phosphodiesterase 4 Inhibitor, in Patients With Psoriatic Arthritis: Results From a Phase III, Randomized, Controlled Trial
2194 Long-term (104-Week) Efficacy and Safety Profile of Apremilast, an Oral Phosphodiesterase 4 Inhibitor, in Patients With Psoriatic Arthritis: Results From a Phase III, Randomized, Controlled Trial
Bringing the clinical experience with anakinra to the patient
 Rheumatology 2003;42(Suppl. 2):ii36 ii40 doi:10.1093/rheumatology/keg331, available online at www.rheumatology.oupjournals.org Bringing the clinical experience with anakinra to the patient S. B. Cohen
Rheumatology 2003;42(Suppl. 2):ii36 ii40 doi:10.1093/rheumatology/keg331, available online at www.rheumatology.oupjournals.org Bringing the clinical experience with anakinra to the patient S. B. Cohen
Scottish Medicines Consortium
 Scottish Medicines Consortium abatacept, 250mg powder for concentrate for solution (Orencia ) No. (400/07) Bristol Myers Squibb Pharmaceuticals Ltd 10 August 2007 The Scottish Medicines Consortium has
Scottish Medicines Consortium abatacept, 250mg powder for concentrate for solution (Orencia ) No. (400/07) Bristol Myers Squibb Pharmaceuticals Ltd 10 August 2007 The Scottish Medicines Consortium has
Charité - University Hospital, Free University and Humboldt University of Berlin, Berlin, Germany; 2 Sanofi Genzyme, Bridgewater, NJ, USA; 3
 Efficacy and Safety of Sarilumab Versus Adalimumab in a Phase 3, Randomized, Double-blind, Monotherapy Study in Patients With Active Rheumatoid Arthritis With Intolerance or Inadequate Response to Methotrexate
Efficacy and Safety of Sarilumab Versus Adalimumab in a Phase 3, Randomized, Double-blind, Monotherapy Study in Patients With Active Rheumatoid Arthritis With Intolerance or Inadequate Response to Methotrexate
Comparison of long-term clinical outcome with etanercept and adalimumab treatment of rheumatoid arthritis with respect to immunogenicity
 7 Comparison of long-term clinical outcome with etanercept and adalimumab treatment of rheumatoid arthritis with respect to immunogenicity Charlotte Krieckaert* Anna Jamnitski* Mike Nurmohamed Piet Kostense
7 Comparison of long-term clinical outcome with etanercept and adalimumab treatment of rheumatoid arthritis with respect to immunogenicity Charlotte Krieckaert* Anna Jamnitski* Mike Nurmohamed Piet Kostense
METHODS In the context of an indirect comparison metaanalysis between tocilizumab and other biological
 c Additional data are published online only at http://ard.bmj. com/content/vol69/issue1 Correspondence to: Professor M Boers, Department of Epidemiology and Biostatistics, VU University Medical Centre,
c Additional data are published online only at http://ard.bmj. com/content/vol69/issue1 Correspondence to: Professor M Boers, Department of Epidemiology and Biostatistics, VU University Medical Centre,
Treat to a Target The New Paradigm in the Management of RA. Boulos Haraoui, MD FRCPC Université de Montréal Institut de rhumatologie de Montréal
 Treat to a Target The New Paradigm in the Management of RA Boulos Haraoui, MD FRCPC Université de Montréal Institut de rhumatologie de Montréal Disclosure Dr Boulos Haraoui Advisor/Research Grants/Speakers
Treat to a Target The New Paradigm in the Management of RA Boulos Haraoui, MD FRCPC Université de Montréal Institut de rhumatologie de Montréal Disclosure Dr Boulos Haraoui Advisor/Research Grants/Speakers
10/28/2013. Disclosures. Objectives. Background. Study Design. Key Inclusion Criteria
 Randomization (1:1:1:1) /28/13 Tocilizumab in Combination Therapy and Monotherapy Versus Methotrexate in Methotrexate-Naive Patients With Early Rheumatoid Arthritis: Clinical and Radiographic Outcomes
Randomization (1:1:1:1) /28/13 Tocilizumab in Combination Therapy and Monotherapy Versus Methotrexate in Methotrexate-Naive Patients With Early Rheumatoid Arthritis: Clinical and Radiographic Outcomes
Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis
 New Evidence reports on presentations given at ACR/ARHP 2010 Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis Report on ACR/ARHP 2010 presentations
New Evidence reports on presentations given at ACR/ARHP 2010 Efficacy and Safety of Rituximab in the Treatment of Rheumatoid Arthritis and ANCA-associated Vasculitis Report on ACR/ARHP 2010 presentations
2.0 Synopsis. Adalimumab DE019 OLE (5-year) Clinical Study Report Amendment 1 R&D/06/095. (For National Authority Use Only)
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Humira Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only) Title
2.0 Synopsis Abbott Laboratories Name of Study Drug: Humira Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only) Title
What I Have Learned Over the Years - Keystone s Top 10 -
 What I Have Learned Over the Years - Keystone s Top 10 - Edward Keystone, MD FRCP(C) Professor of Medicine University of Toronto, CANADA Ontario Rheumatology Association Meeting Muskoka, Canada Sunday,
What I Have Learned Over the Years - Keystone s Top 10 - Edward Keystone, MD FRCP(C) Professor of Medicine University of Toronto, CANADA Ontario Rheumatology Association Meeting Muskoka, Canada Sunday,
Primary Results Citation 2
 Table S1. Adalimumab clinical trials 1 ClinicalTrials.gov Rheumatoid Arthritis 3 NCT00195663 Breedveld FC, Weisman MH, Kavanaugh AF, et al. The PREMIER study. A multicenter, randomized, double-blind clinical
Table S1. Adalimumab clinical trials 1 ClinicalTrials.gov Rheumatoid Arthritis 3 NCT00195663 Breedveld FC, Weisman MH, Kavanaugh AF, et al. The PREMIER study. A multicenter, randomized, double-blind clinical
Practical RA Treatment: James R. O Dell, M.D. University of Nebraska Medical Center May 24, 2014
 Practical RA Treatment: 2014 James R. O Dell, M.D. University of Nebraska Medical Center May 24, 2014 Disclosures James R. O Dell PI of Multinational RA trial supported by VA and NIH (NIAMS) that receives
Practical RA Treatment: 2014 James R. O Dell, M.D. University of Nebraska Medical Center May 24, 2014 Disclosures James R. O Dell PI of Multinational RA trial supported by VA and NIH (NIAMS) that receives
Received: 27 May 2003 Revisions requested: 26 Jun 2003 Revisions received: 14 Aug 2003 Accepted: 19 Aug 2003 Published: 1 Oct 2003
 Research article Etanercept versus etanercept plus methotrexate: a registrybased study suggesting that the combination is clinically more efficacious Ronald F van Vollenhoven 1, Sofia Ernestam 2, Anders
Research article Etanercept versus etanercept plus methotrexate: a registrybased study suggesting that the combination is clinically more efficacious Ronald F van Vollenhoven 1, Sofia Ernestam 2, Anders
Introduction ORIGINAL ARTICLE
 Mod Rheumatol (2007) 17:28 32 Japan College of Rheumatology 2007 DOI 10.1007/s10165-006-0532-0 ORIGINAL ARTICLE Hisashi Yamanaka Yoshiya Tanaka Naoya Sekiguchi Eisuke Inoue Kazuyoshi Saito Hideto Kameda
Mod Rheumatol (2007) 17:28 32 Japan College of Rheumatology 2007 DOI 10.1007/s10165-006-0532-0 ORIGINAL ARTICLE Hisashi Yamanaka Yoshiya Tanaka Naoya Sekiguchi Eisuke Inoue Kazuyoshi Saito Hideto Kameda
The Journal of Rheumatology Volume 41, no. 2
 The Volume 41, no. 2 Clinical, Functional, and Radiographic Implications of Time to Treatment Response in Patients With Early Rheumatoid Arthritis: a Posthoc Analysis of the PREMIER Study Edward C. Keystone,
The Volume 41, no. 2 Clinical, Functional, and Radiographic Implications of Time to Treatment Response in Patients With Early Rheumatoid Arthritis: a Posthoc Analysis of the PREMIER Study Edward C. Keystone,
Appendix 2 (as provided by the authors): List of studies in the reviews included for analyses in the overview. Trial duration in months
 Appendix 2 (as provided by the authors): List of studies in the reviews included for analyses in the overview Study Name Year Reference ABATACEPT (n=7) Moreland 2002 Moreland LW, Alten R, Van den Bosch
Appendix 2 (as provided by the authors): List of studies in the reviews included for analyses in the overview Study Name Year Reference ABATACEPT (n=7) Moreland 2002 Moreland LW, Alten R, Van den Bosch
Research Article. Efficacy and safety of abatacept therapy for rheumatoid arthritis in routine clinical practice
 Research Article Efficacy and safety of abatacept therapy for rheumatoid arthritis in routine clinical practice Aim: To evaluate treatment of rheumatoid arthritis with abatacept in the real-life clinic
Research Article Efficacy and safety of abatacept therapy for rheumatoid arthritis in routine clinical practice Aim: To evaluate treatment of rheumatoid arthritis with abatacept in the real-life clinic
ABSTRACT. DMARD- and biologic-naïve Japanese patients
 DOI 10.1007/s40744-017-0059-1 ORIGINAL RESEARCH Adalimumab with Methotrexate in Treatment-Naïve Japanese Patients with Rheumatoid Arthritis at Risk of Progressive Structural Joint Damage: A Postmarketing
DOI 10.1007/s40744-017-0059-1 ORIGINAL RESEARCH Adalimumab with Methotrexate in Treatment-Naïve Japanese Patients with Rheumatoid Arthritis at Risk of Progressive Structural Joint Damage: A Postmarketing
Orencia (abatacept) for Rheumatoid Arthritis. Media backgrounder
 Orencia (abatacept) for Rheumatoid Arthritis Media backgrounder What is Orencia (abatacept)? Orencia (abatacept) is the first biologic agent to be available in both an intravenous (IV) and a self-injectable,
Orencia (abatacept) for Rheumatoid Arthritis Media backgrounder What is Orencia (abatacept)? Orencia (abatacept) is the first biologic agent to be available in both an intravenous (IV) and a self-injectable,
M. Schoels 1, F. Alasti 2, J. S. Smolen 1,2 and D. Aletaha 2*
 Schoels et al. Arthritis Research & Therapy (2017) 19:155 DOI 10.1186/s13075-017-1346-5 RESEARCH ARTICLE Evaluation of newly proposed remission cut-points for disease activity score in 28 joints (DAS28)
Schoels et al. Arthritis Research & Therapy (2017) 19:155 DOI 10.1186/s13075-017-1346-5 RESEARCH ARTICLE Evaluation of newly proposed remission cut-points for disease activity score in 28 joints (DAS28)
New Evidence reports on presentations given at EULAR Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis
 New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
New Evidence reports on presentations given at EULAR 2011 Rituximab for the Treatment of Rheumatoid Arthritis and Vasculitis Report on EULAR 2011 presentations Anti-TNF failure and response to rituximab
Safety and effectiveness of biologic Disease-Modifying Antirheumatic Drugs in elderly patients with rheumatoid arthritis
 1. Title: Safety and effectiveness of biologic Disease-Modifying Antirheumatic Drugs in elderly patients with rheumatoid arthritis 2. Background: The population of older individuals with rheumatoid arthritis
1. Title: Safety and effectiveness of biologic Disease-Modifying Antirheumatic Drugs in elderly patients with rheumatoid arthritis 2. Background: The population of older individuals with rheumatoid arthritis
2.0 Synopsis. Adalimumab M Clinical Study Report Final R&D/15/1093. (For National Authority Use Only)
 2.0 Synopsis AbbVie Inc. Name of Study Drug: Adalimumab Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only) Title
2.0 Synopsis AbbVie Inc. Name of Study Drug: Adalimumab Name of Active Ingredient: Adalimumab Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority Use Only) Title
James R. O Dell, M.D. University of Nebraska Medical Center
 Not everyone in the world needs a biologic: Lessons from TEAR and RACAT James R. O Dell, M.D. University of Nebraska Medical Center Disclosure Declaration James O Dell, MD Advisory Board for Crescendo,
Not everyone in the world needs a biologic: Lessons from TEAR and RACAT James R. O Dell, M.D. University of Nebraska Medical Center Disclosure Declaration James O Dell, MD Advisory Board for Crescendo,
Individual Study Table Referring to Part of Dossier: Use Only) Name of Study Drug:
 2.0 Synopsis AbbVie Inc. Individual Study Table Referring to Part of Dossier: (For National Authority Use Only) Name of Study Drug: Volume: Adalimumab (Humira ) Page: Name of Active Ingredient: Adalimumab
2.0 Synopsis AbbVie Inc. Individual Study Table Referring to Part of Dossier: (For National Authority Use Only) Name of Study Drug: Volume: Adalimumab (Humira ) Page: Name of Active Ingredient: Adalimumab
Efficacy of tofacitinib monotherapy in methotrexate-naive patients with early or established rheumatoid arthritis
 To cite: Fleischmann RM, Huizinga TWJ, Kavanaugh AF, et al. Efficacy of tofacitinib monotherapy in methotrexate-naive patients with early or established rheumatoid arthritis. RMD Open 2016;2:e000262. doi:10.1136/rmdopen-2016-000262
To cite: Fleischmann RM, Huizinga TWJ, Kavanaugh AF, et al. Efficacy of tofacitinib monotherapy in methotrexate-naive patients with early or established rheumatoid arthritis. RMD Open 2016;2:e000262. doi:10.1136/rmdopen-2016-000262
6 ADRs, 2 LOE. 2 ADRs, 4 LOE. Ineffectiveness 24 ADRs 7, 1 pt for convenience. 48% had antibodies against Infliximab at baseline
 Summary of Published Switch data Table 1. Information Patients Switch from (n) Reason for switch Switch to: (n) Results Numbers Presse Med. 2002 (1) 14 Infliximab (8) (6) 6 ADRs, 2 LOE 2 ADRs, 4 LOE (8)
Summary of Published Switch data Table 1. Information Patients Switch from (n) Reason for switch Switch to: (n) Results Numbers Presse Med. 2002 (1) 14 Infliximab (8) (6) 6 ADRs, 2 LOE 2 ADRs, 4 LOE (8)
London, 1 June 2006 Product name: REMICADE Procedure number: Remicade-H-240-II-73-AR SCIENTIFIC DISCUSSION 1/8
 London, 1 June 2006 Product name: REMICADE Procedure number: Remicade-H-240-II-73-AR SCIENTIFIC DISCUSSION 1/8 1. Introduction Infliximab is a chimeric human-murine IgG1κ monoclonal antibody, which binds
London, 1 June 2006 Product name: REMICADE Procedure number: Remicade-H-240-II-73-AR SCIENTIFIC DISCUSSION 1/8 1. Introduction Infliximab is a chimeric human-murine IgG1κ monoclonal antibody, which binds
Efficacy and safety of ascending methotrexate dose in combination with adalimumab: the randomised CONCERTO trial
 Downloaded from http://ard.bmj.com/ on May 2, 216 - Published by group.bmj.com Clinical and epidemiological research EXTENDED REPORT Efficacy and safety of ascending methotrexate dose in combination with
Downloaded from http://ard.bmj.com/ on May 2, 216 - Published by group.bmj.com Clinical and epidemiological research EXTENDED REPORT Efficacy and safety of ascending methotrexate dose in combination with
G Wells, 1 J-C Becker, 2 J Teng, 2 M Dougados, 3 M Schiff, 4 J Smolen, 5 D Aletaha, 6 P L C M van Riel 7. Extended report
 1 Department of Epidemiology and Community Medicine, University of Ottawa, Ottawa, Canada; 2 Bristol-Myers Squibb, Princeton, New Jersey, USA; 3 Paris-Descartes University, Medicine Faculty and UPRES-EA
1 Department of Epidemiology and Community Medicine, University of Ottawa, Ottawa, Canada; 2 Bristol-Myers Squibb, Princeton, New Jersey, USA; 3 Paris-Descartes University, Medicine Faculty and UPRES-EA
ORIGINAL ARTICLE R. F. VAN VOLLENHOVEN, 1 D. FELSON, 2 V. STRAND, 3 M. E. WEINBLATT, 4 K. LUIJTENS, 5 AND E. C. KEYSTONE 6 INTRODUCTION
 Arthritis Care & Research Vol. 63, No. 1, January 2011, pp 128 134 DOI 10.1002/acr.20331 2011, American College of Rheumatology ORIGINAL ARTICLE American College of Rheumatology Hybrid Analysis of Certolizumab
Arthritis Care & Research Vol. 63, No. 1, January 2011, pp 128 134 DOI 10.1002/acr.20331 2011, American College of Rheumatology ORIGINAL ARTICLE American College of Rheumatology Hybrid Analysis of Certolizumab
Rheumatoid arthritis 2010: Treatment and monitoring
 October 12, 2010 By Yusuf Yazici, MD [1] The significant changes in the way rheumatoid arthritis has been managed include earlier, more aggressive treatment with combination therapy. Significant changes
October 12, 2010 By Yusuf Yazici, MD [1] The significant changes in the way rheumatoid arthritis has been managed include earlier, more aggressive treatment with combination therapy. Significant changes
ORENCIA (abatacept) Demonstrates Comparable Efficacy to Humira ( adalimumab
 ORENCIA (abatacept) Demonstrates Comparable Efficacy to Humira (adalimumab) in Patients with Moderate to Severe Rheumatoid Arthritis in First Head-to-Head Study of These Agents ORENCIA demonstrated comparable
ORENCIA (abatacept) Demonstrates Comparable Efficacy to Humira (adalimumab) in Patients with Moderate to Severe Rheumatoid Arthritis in First Head-to-Head Study of These Agents ORENCIA demonstrated comparable
Characteristics Associated with Biologic Monotherapy Use in Biologic-Naive Patients with Rheumatoid Arthritis in a US Registry Population
 Rheumatol Ther (2015) 2:85 96 DOI 10.1007/s40744-015-0008-9 ORIGINAL RESEARCH Characteristics Associated with Biologic Monotherapy Use in Biologic-Naive Patients with Rheumatoid Arthritis in a US Registry
Rheumatol Ther (2015) 2:85 96 DOI 10.1007/s40744-015-0008-9 ORIGINAL RESEARCH Characteristics Associated with Biologic Monotherapy Use in Biologic-Naive Patients with Rheumatoid Arthritis in a US Registry
Inflammatory arthritis, such as rheumatoid arthritis (RA), is
 O r i g i n a l A r t i c l e Using Biologics in Inflammatory Arthritis: Assessing the Risks and Benefits Gina Rohekar MD FRCPC MSc (Clin Epi) About the Author Gina Rohekar is an assistant professor at
O r i g i n a l A r t i c l e Using Biologics in Inflammatory Arthritis: Assessing the Risks and Benefits Gina Rohekar MD FRCPC MSc (Clin Epi) About the Author Gina Rohekar is an assistant professor at
M Schiff, 1 C Pritchard, 2 J E Huffstutter, 3 V Rodriguez-Valverde, 4 P Durez, 5 X Zhou, 6 T Li, 6 K Bahrt, 6 S Kelly, 6 M Le Bars, 7 M C Genovese 8
 The 6-month safety and efficacy of abatacept in patients with rheumatoid arthritis who underwent a washout after anti-tumour necrosis factor therapy or were directly switched to abatacept: the ARRIVE trial
The 6-month safety and efficacy of abatacept in patients with rheumatoid arthritis who underwent a washout after anti-tumour necrosis factor therapy or were directly switched to abatacept: the ARRIVE trial
M Schiff, 1 C Pritchard, 2 J E Huffstutter, 3 V Rodriguez-Valverde, 4 P Durez, 5 X Zhou, 6 T Li, 6 K Bahrt, 6 S Kelly, 6 M Le Bars, 7 M C Genovese 8
 1 University of Colorado, Denver, Colorado, USA; 2 Rheumatology Specialty Center, Willow Grove, Pennsylvania, USA; 3 Arthritis Associates, Hixson, Tennessee, USA; 4 Hospital Universitario Marques De Valdecilla,
1 University of Colorado, Denver, Colorado, USA; 2 Rheumatology Specialty Center, Willow Grove, Pennsylvania, USA; 3 Arthritis Associates, Hixson, Tennessee, USA; 4 Hospital Universitario Marques De Valdecilla,
Golimumab: In Combination with Methotrexate as Once Monthly Treatment for Moderate to Severe Rheumatoid Arthritis
 Clinical Medicine Reviews in Therapeutics Review Golimumab: In Combination with Methotrexate as Once Monthly Treatment for Moderate to Severe Rheumatoid Arthritis Lauren Keyser McCluggage 1 and Kelly Michelle
Clinical Medicine Reviews in Therapeutics Review Golimumab: In Combination with Methotrexate as Once Monthly Treatment for Moderate to Severe Rheumatoid Arthritis Lauren Keyser McCluggage 1 and Kelly Michelle
ABSTRACT. Keywords: Africa; Efficacy; Etanercept; Maintenance therapy; Middle East; Rheumatoid arthritis ORIGINAL RESEARCH
 Rheumatol Ther (2018) 5:149 158 https://doi.org/10.1007/s40744-018-0094-6 ORIGINAL RESEARCH Maintenance of Remission with Etanercept DMARD Combination Therapy Compared with DMARDs Alone in African and
Rheumatol Ther (2018) 5:149 158 https://doi.org/10.1007/s40744-018-0094-6 ORIGINAL RESEARCH Maintenance of Remission with Etanercept DMARD Combination Therapy Compared with DMARDs Alone in African and
Rheumatology journal club October 20, 2017 Presented by: Matthew Stoll MD,PhD,PSCS
 Efficacy and safety of abatacept, a T-cell modulator, in a randomised, double-blind, placebo-controlled, phase III study in psoriatic arthritis (Mease et al., 2017) Rheumatology journal club October 20,
Efficacy and safety of abatacept, a T-cell modulator, in a randomised, double-blind, placebo-controlled, phase III study in psoriatic arthritis (Mease et al., 2017) Rheumatology journal club October 20,
What prescribers need to know
 HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
HUMIRA Citrate-free presentations in an Electronic Medical Record (EMR) What prescribers need to know 2 / This is your guide to identifying HUMIRA Citrate-free presentations in your Electronic Medical
Tanaka et al. Arthritis Research & Therapy (2017) 19:56 DOI /s
 Tanaka et al. Arthritis Research & Therapy (217) 19:6 DOI 1.1186/s137-17-1264-6 RESEARCH ARTICLE Open Access Low disease activity for up to 3 years after adalimumab discontinuation in patients with early
Tanaka et al. Arthritis Research & Therapy (217) 19:6 DOI 1.1186/s137-17-1264-6 RESEARCH ARTICLE Open Access Low disease activity for up to 3 years after adalimumab discontinuation in patients with early
Pros and Cons of Combination MTX+ Biologics vs Monotherapy with Biologics: the place of immunogenicity
 Pros and Cons of Combination MTX+ Biologics vs Monotherapy with Biologics: the place of immunogenicity Daniel E Furst MD University of California in Los Angeles University of Washington University of Florence
Pros and Cons of Combination MTX+ Biologics vs Monotherapy with Biologics: the place of immunogenicity Daniel E Furst MD University of California in Los Angeles University of Washington University of Florence
Pharmacy Medical Necessity Guidelines: Orencia (abatacept)
 Pharmacy Medical Necessity Guidelines: Effective: October 23, 2017 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review SQ: RXUM/ RX / Pharmacy (RX) or
Pharmacy Medical Necessity Guidelines: Effective: October 23, 2017 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review SQ: RXUM/ RX / Pharmacy (RX) or
intolerance to tumour necrosis
 To cite: Nash P, Behrens F, Orbai A-M, et al. Ixekizumab is efficacious when used alone or when added to conventional synthetic diseasemodifying antirheumatic drugs (cdmards) in patients with active psoriatic
To cite: Nash P, Behrens F, Orbai A-M, et al. Ixekizumab is efficacious when used alone or when added to conventional synthetic diseasemodifying antirheumatic drugs (cdmards) in patients with active psoriatic
SYNOPSIS. Issue Date: 17 Jan 2013
 STELARA (ustekinumab) Clinical Study Report CNTO1275PSA3002 24-Week CSR SYNOPSIS Issue Date: 17 Jan 2013 Name of Sponsor/Company Name of Finished Product Name of Active Ingredient(s) Janssen Research &
STELARA (ustekinumab) Clinical Study Report CNTO1275PSA3002 24-Week CSR SYNOPSIS Issue Date: 17 Jan 2013 Name of Sponsor/Company Name of Finished Product Name of Active Ingredient(s) Janssen Research &
Horizon Scanning Centre November Secukinumab for active and progressive psoriatic arthritis. SUMMARY NIHR HSC ID: 5330
 Horizon Scanning Centre November 2012 Secukinumab for active and progressive psoriatic arthritis. SUMMARY NIHR HSC ID: 5330 Secukinumab is a high-affinity fully human monoclonal antibody that antagonises
Horizon Scanning Centre November 2012 Secukinumab for active and progressive psoriatic arthritis. SUMMARY NIHR HSC ID: 5330 Secukinumab is a high-affinity fully human monoclonal antibody that antagonises
Division of Rheumatology, Department of Internal Medicine and Gerontology, Jagiellonian University Medical College, Kraków, Poland 4
 Original papers Efficacy and safety of golimumab as add-on therapy to standard disease-modifying antirheumatic drugs: Results of the GO-MORE study in the Polish population Sławomir Jeka 1,A,B,D F, Bogdan
Original papers Efficacy and safety of golimumab as add-on therapy to standard disease-modifying antirheumatic drugs: Results of the GO-MORE study in the Polish population Sławomir Jeka 1,A,B,D F, Bogdan
Abatacept: first T cell co-stimulation modulator for severe active RA
 Abatacept: first T cell co-stimulation modulator for severe active RA Steve Chaplin MSc, MRPharmS and Andrew Ostor FRACP PRODUCT PROFILE Proprietary name: Orencia Constituents: abatacept Dosage and method
Abatacept: first T cell co-stimulation modulator for severe active RA Steve Chaplin MSc, MRPharmS and Andrew Ostor FRACP PRODUCT PROFILE Proprietary name: Orencia Constituents: abatacept Dosage and method
Head-to-head comparison of subcutaneous abatacept versus adalimumab for rheumatoid arthritis: two-year efficacy and safety findings from AMPLE trial
 Handling editor Tore K Kvien For numbered affiliations see end of article. Correspondence to Dr Michael Schiff, University of Colorado, School of Medicine, 5400 South Monaco Street, Greenwood Village,
Handling editor Tore K Kvien For numbered affiliations see end of article. Correspondence to Dr Michael Schiff, University of Colorado, School of Medicine, 5400 South Monaco Street, Greenwood Village,
Principal Investigator. General Information. Conflict of Interest. Certification Published on The YODA Project (
 Principal Investigator First Name: Liana Last Name: Fraenkel Degree: MD, MPH Primary Affiliation: Yale University School of Medicine E-mail: christine.ramsey@gmail.com Phone number: 610-613-6745 Address:
Principal Investigator First Name: Liana Last Name: Fraenkel Degree: MD, MPH Primary Affiliation: Yale University School of Medicine E-mail: christine.ramsey@gmail.com Phone number: 610-613-6745 Address:
ORIGINAL ARTICLE. Rheumatoid arthritis
 To cite: Tanaka Y, Yamanaka H, Ishiguro N, et al. Adalimumab discontinuation in patients with early rheumatoid arthritis who were initially treated with methotrexate alone or in combination with adalimumab:
To cite: Tanaka Y, Yamanaka H, Ishiguro N, et al. Adalimumab discontinuation in patients with early rheumatoid arthritis who were initially treated with methotrexate alone or in combination with adalimumab:
Physical function continues to improve when clinical remission is sustained in rheumatoid arthritis patients
 Radner et al. Arthritis Research & Therapy (2015) 17:203 DOI 10.1186/s13075-015-0719-x RESEARCH ARTICLE Open Access Physical function continues to improve when clinical remission is sustained in rheumatoid
Radner et al. Arthritis Research & Therapy (2015) 17:203 DOI 10.1186/s13075-015-0719-x RESEARCH ARTICLE Open Access Physical function continues to improve when clinical remission is sustained in rheumatoid
1.0 Abstract. Title. Keywords. Adalimumab, Rheumatoid Arthritis, Effectiveness, Safety. Rationale and Background
 1.0 Abstract Title Assessment of the safety of adalimumab in rheumatoid arthritis (RA) patients showing rapid progression of structural damage of the joints, who have no prior history of treatment with
1.0 Abstract Title Assessment of the safety of adalimumab in rheumatoid arthritis (RA) patients showing rapid progression of structural damage of the joints, who have no prior history of treatment with
Treatment of Rheumatoid Arthritis: The Past, the Present and the Future
 Treatment of Rheumatoid Arthritis: The Past, the Present and the Future Lai-Ling Winchow FCP(SA) Cert Rheum(SA) Chris Hani Baragwanath Academic Hospital University of the Witwatersrand Outline of presentation
Treatment of Rheumatoid Arthritis: The Past, the Present and the Future Lai-Ling Winchow FCP(SA) Cert Rheum(SA) Chris Hani Baragwanath Academic Hospital University of the Witwatersrand Outline of presentation
PsA. SIMPONI (golimumab) Rheumatoid arthritis. Psoriatic arthritis. Ankylosing spondylitis EFFICACY EFFICACY EFFICACY. QoL. QoL.
 RA Rheumatoid arthritis PsA Psoriatic arthritis AS Ankylosing spondylitis EFFICACY EFFICACY EFFICACY QoL QoL QoL SAFETY SAFETY SAFETY EXPERIENCE EXPERIENCE EXPERIENCE SUMMARY SUMMARY SUMMARY Copyright
RA Rheumatoid arthritis PsA Psoriatic arthritis AS Ankylosing spondylitis EFFICACY EFFICACY EFFICACY QoL QoL QoL SAFETY SAFETY SAFETY EXPERIENCE EXPERIENCE EXPERIENCE SUMMARY SUMMARY SUMMARY Copyright
Recommendations for RA management: what has changed?
 The 2016 Update of the EULAR Recommendations for RA management: what has changed? Baltics Rheumatology Conference Vilnius, September 21-22 Prof. Diego Kyburz University Hospital of Basel Switzerland Multiple
The 2016 Update of the EULAR Recommendations for RA management: what has changed? Baltics Rheumatology Conference Vilnius, September 21-22 Prof. Diego Kyburz University Hospital of Basel Switzerland Multiple
Non-commercial use only
 Reumatismo, 2016; 68 (2): 90-96 Real-world experiences of folic acid supplementation (5 versus 30 mg/week) with methotrexate in rheumatoid arthritis patients: a comparison study K.T. Koh 1, C.L. Teh 2,
Reumatismo, 2016; 68 (2): 90-96 Real-world experiences of folic acid supplementation (5 versus 30 mg/week) with methotrexate in rheumatoid arthritis patients: a comparison study K.T. Koh 1, C.L. Teh 2,
Optimizing outcomes in rheumatoid arthritis patients with inadequate responses to disease-modifying anti-rheumatic drugs
 RHEUMATOLOGY Rheumatology 2012;51:v12 v21 doi:10.1093/rheumatology/kes111 Optimizing outcomes in rheumatoid arthritis patients with inadequate responses to disease-modifying anti-rheumatic drugs Karel
RHEUMATOLOGY Rheumatology 2012;51:v12 v21 doi:10.1093/rheumatology/kes111 Optimizing outcomes in rheumatoid arthritis patients with inadequate responses to disease-modifying anti-rheumatic drugs Karel
Certolizumab pegol (Cimzia) for psoriatic arthritis second line
 Certolizumab pegol (Cimzia) for psoriatic arthritis second line This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Certolizumab pegol (Cimzia) for psoriatic arthritis second line This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Pharmacy Medical Necessity Guidelines: Actemra (tocilizumab)
 Pharmacy Medical Necessity Guidelines: Effective: July 11, 2017 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review SQ: RXUM/ RX / Pharmacy (RX) or Medical
Pharmacy Medical Necessity Guidelines: Effective: July 11, 2017 Prior Authorization Required Type of Review Care Management Not Covered Type of Review Clinical Review SQ: RXUM/ RX / Pharmacy (RX) or Medical
Tofacitinib Therapy for Rheumatoid Arthritis: A Direct Comparison Study between Biologic-naïve and Experienced Patients
 doi: 10.2169/internalmedicine.9341-17 Intern Med Advance Publication http://internmed.jp ORIGINAL ARTICLE Tofacitinib Therapy for Rheumatoid Arthritis: A Direct Comparison Study between Biologic-naïve
doi: 10.2169/internalmedicine.9341-17 Intern Med Advance Publication http://internmed.jp ORIGINAL ARTICLE Tofacitinib Therapy for Rheumatoid Arthritis: A Direct Comparison Study between Biologic-naïve
Key Words: Rheumatoid Arthritis, etanercept, post-marketing study, comparative study
 CLINICAL DATA GAP BETWEEN PHASE III CLINICAL TRIALS (PRE-MARKETING) AND PHASE IV (POST-MARKETING) STUDIES: EVALUATION OF ETANERCEPT IN RHEUMATOID ARTHRITIS Pendar Farahani 1,3, Mitchell Levine 1,2, Kathryn
CLINICAL DATA GAP BETWEEN PHASE III CLINICAL TRIALS (PRE-MARKETING) AND PHASE IV (POST-MARKETING) STUDIES: EVALUATION OF ETANERCEPT IN RHEUMATOID ARTHRITIS Pendar Farahani 1,3, Mitchell Levine 1,2, Kathryn
Citation for final published version:
 This is an Open Access document downloaded from ORCA, Cardiff University's institutional repository: http://orca.cf.ac.uk/97756/ This is the author s version of a work that was submitted to / accepted
This is an Open Access document downloaded from ORCA, Cardiff University's institutional repository: http://orca.cf.ac.uk/97756/ This is the author s version of a work that was submitted to / accepted
K., "Insights into the efficacy of golimumab plus methotrexate in patients with active rheumatoid arthritis who discontinued prior antitumour
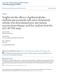 University of Massachusetts Medical School escholarship@umms Rheumatology Publications and Presentations Rheumatology 10-2014 Insights into the efficacy of golimumab plus methotrexate in patients with
University of Massachusetts Medical School escholarship@umms Rheumatology Publications and Presentations Rheumatology 10-2014 Insights into the efficacy of golimumab plus methotrexate in patients with
N Nishimoto, 1 N Miyasaka, 2 K Yamamoto, 3 S Kawai, 4 T Takeuchi, 5 J Azuma 1. Extended report
 1 Osaka University, Osaka, Japan; 2 Tokyo Medical and Dental University, Tokyo, Japan; 3 University of Tokyo, Tokyo, Japan; 4 Toho University Omori Medical Center, Tokyo, Japan; 5 Saitama Medical Center/
1 Osaka University, Osaka, Japan; 2 Tokyo Medical and Dental University, Tokyo, Japan; 3 University of Tokyo, Tokyo, Japan; 4 Toho University Omori Medical Center, Tokyo, Japan; 5 Saitama Medical Center/
GSK 165: anti-gm-csf antibody
 GSK 165: anti-gm-csf antibody A novel mechanism with potentially differentiated impact on pain in the treatment of Rheumatoid Arthritis 23 October 2018 Cautionary statement regarding forward-looking statements
GSK 165: anti-gm-csf antibody A novel mechanism with potentially differentiated impact on pain in the treatment of Rheumatoid Arthritis 23 October 2018 Cautionary statement regarding forward-looking statements
SCIENTIFIC DISCUSSION. London, 27 April 2006 Product name: HUMIRA/TRUDEXA Procedure number: EMEA/H/C/ /II/26
 SCIENTIFIC DISCUSSION London, 27 April 2006 Product name: HUMIRA/TRUDEXA Procedure number: EMEA/H/C/481-482/II/26 3.1. Introduction Adalimumab is a recombinant human immunoglobulin (IgG 1 ) monoclonal
SCIENTIFIC DISCUSSION London, 27 April 2006 Product name: HUMIRA/TRUDEXA Procedure number: EMEA/H/C/481-482/II/26 3.1. Introduction Adalimumab is a recombinant human immunoglobulin (IgG 1 ) monoclonal
Ustekinumab (Stelara) for psoriatic arthritis second line after disease modifying anti rheumatic drugs (DMARDs)
 Ustekinumab (Stelara) for psoriatic arthritis second line after disease modifying anti rheumatic drugs (DMARDs) January 2010 This technology summary is based on information available at the time of research
Ustekinumab (Stelara) for psoriatic arthritis second line after disease modifying anti rheumatic drugs (DMARDs) January 2010 This technology summary is based on information available at the time of research
(tofacitinib) are met.
 Xeljanz (tofacitinib) Policy Number: 5.01. 560 Origination: 3/2014 Last Review: 3/2014 Next Review: 3/2015 Policy BCBSKC will provide coverage for Xeljanz (tofacitinib) when it is determined to be medically
Xeljanz (tofacitinib) Policy Number: 5.01. 560 Origination: 3/2014 Last Review: 3/2014 Next Review: 3/2015 Policy BCBSKC will provide coverage for Xeljanz (tofacitinib) when it is determined to be medically
PRODUCT INFORMATION HUMIRA
 NAME OF THE MEDICINE Adalimumab (rch) DESCRIPTION PRODUCT INFORMATION HUMIRA (adalimumab) is a recombinant human immunoglobulin (IgG1) monoclonal antibody containing only human peptide sequences. was created
NAME OF THE MEDICINE Adalimumab (rch) DESCRIPTION PRODUCT INFORMATION HUMIRA (adalimumab) is a recombinant human immunoglobulin (IgG1) monoclonal antibody containing only human peptide sequences. was created
Horizon Scanning Technology Summary. Adalimumab (Humira) for juvenile idiopathic arthritis. National Horizon Scanning Centre.
 Horizon Scanning Technology Summary National Horizon Scanning Centre Adalimumab (Humira) for juvenile idiopathic arthritis June 2007 This technology summary is based on information available at the time
Horizon Scanning Technology Summary National Horizon Scanning Centre Adalimumab (Humira) for juvenile idiopathic arthritis June 2007 This technology summary is based on information available at the time
Biologics and Psoriasis: The Beat Goes On
 Biologics and Psoriasis: The Beat Goes On Mark Lebwohl, MD Waldman Professor And Chairman Kimberly and Eric J. Waldman Department of Dermatology Icahn School of Medicine at Mount Sinai Mark Lebwohl is
Biologics and Psoriasis: The Beat Goes On Mark Lebwohl, MD Waldman Professor And Chairman Kimberly and Eric J. Waldman Department of Dermatology Icahn School of Medicine at Mount Sinai Mark Lebwohl is
The Effects of Golimumab on Radiographic Progression in Rheumatoid Arthritis
 ARTHRITIS & RHEUMATISM Vol. 63, No. 5, May 2011, pp 1200 1210 DOI 10.1002/art.30263 2011, American College of Rheumatology The Effects of Golimumab on Radiographic Progression in Rheumatoid Arthritis Results
ARTHRITIS & RHEUMATISM Vol. 63, No. 5, May 2011, pp 1200 1210 DOI 10.1002/art.30263 2011, American College of Rheumatology The Effects of Golimumab on Radiographic Progression in Rheumatoid Arthritis Results
CADTH Therapeutic Review Panel
 Therapeutic Review Panel Final Recommendations Biological Response Modifier Agents for Adults with Rheumatoid Arthritis July 2010 RECOMMENDATIONS The Therapeutic Review Panel (TRP) recommends that in adult
Therapeutic Review Panel Final Recommendations Biological Response Modifier Agents for Adults with Rheumatoid Arthritis July 2010 RECOMMENDATIONS The Therapeutic Review Panel (TRP) recommends that in adult
ABSTRACT ORIGINAL RESEARCH
 Rheumatol Ther (2018) 5:203 214 https://doi.org/10.1007/s40744-018-0093-7 ORIGINAL RESEARCH Effect of Discontinuation or Initiation of Methotrexate or Glucocorticoids on Tofacitinib Efficacy in Patients
Rheumatol Ther (2018) 5:203 214 https://doi.org/10.1007/s40744-018-0093-7 ORIGINAL RESEARCH Effect of Discontinuation or Initiation of Methotrexate or Glucocorticoids on Tofacitinib Efficacy in Patients
Cimzia (certolizumab pegol) Data Showed Broad and Rapid Relief From Burden of Symptoms In Rheumatoid Arthritis Patients
 Cimzia (certolizumab pegol) Data Showed Broad and Rapid Relief From Burden of Symptoms In Rheumatoid Arthritis Patients Rapid, sustained and clinically meaningful improvement in wideranging patient-reported
Cimzia (certolizumab pegol) Data Showed Broad and Rapid Relief From Burden of Symptoms In Rheumatoid Arthritis Patients Rapid, sustained and clinically meaningful improvement in wideranging patient-reported
Summary of Risk Minimization Measures
 Table 6.1.4-1: Summary of Risk Minimization Measures Safety Concern Vaccination Hepatic and renal impairment Combination therapy Elderly Routine Risk Minimization Measures Specific subsection on vaccination
Table 6.1.4-1: Summary of Risk Minimization Measures Safety Concern Vaccination Hepatic and renal impairment Combination therapy Elderly Routine Risk Minimization Measures Specific subsection on vaccination
Golimumab: a novel anti-tumor necrosis factor
 Golimumab: a novel anti-tumor necrosis factor Rossini M, De Vita S, Ferri C, et al. Biol Ther. 2013. This slide deck represents the opinions of the authors, and not necessarily the opinions of the publisher
Golimumab: a novel anti-tumor necrosis factor Rossini M, De Vita S, Ferri C, et al. Biol Ther. 2013. This slide deck represents the opinions of the authors, and not necessarily the opinions of the publisher
Clinical Policy: Certolizumab (Cimzia) Reference Number: PA.CP.PHAR.247 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid
 Clinical Policy: (Cimzia) Reference Number: PA.CP.PHAR.247 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid Coding Implications Revision Log Description (Cimzia ) is a tumor necrosis
Clinical Policy: (Cimzia) Reference Number: PA.CP.PHAR.247 Effective Date: 01/18 Last Review Date: 08/17 Line of Business: Medicaid Coding Implications Revision Log Description (Cimzia ) is a tumor necrosis
Smolen et al. Arthritis Research & Therapy (2015) 17:157 DOI /s
 Smolen et al. Arthritis Research & Therapy (215) 17:157 DOI 1.1186/s1375-15-671-9 RESEARCH ARTICLE Open Access Attainment and characteristics of clinical remission according to the new ACR-EULAR criteria
Smolen et al. Arthritis Research & Therapy (215) 17:157 DOI 1.1186/s1375-15-671-9 RESEARCH ARTICLE Open Access Attainment and characteristics of clinical remission according to the new ACR-EULAR criteria
Gerd R Burmester 1*, Marco Matucci-Cerinic 2, Xavier Mariette 3, Francisco Navarro-Blasco 4, Sonja Kary 5, Kristina Unnebrink 5 and Hartmut Kupper 5
 Burmester et al. Arthritis Research & Therapy 2014, 16:R24 RESEARCH ARTICLE Open Access Safety and effectiveness of adalimumab in patients with rheumatoid arthritis over 5 years of therapy in a phase 3b
Burmester et al. Arthritis Research & Therapy 2014, 16:R24 RESEARCH ARTICLE Open Access Safety and effectiveness of adalimumab in patients with rheumatoid arthritis over 5 years of therapy in a phase 3b
Comprehensive disease control (CDC): what does achieving CDC mean for patients with rheumatoid arthritis?
 Handling editor Tore K Kvien 1 Leeds Institute of Rheumatic & Musculoskeletal Medicine, University of Leeds, Chapel Allerton Hospital and NIHR Leeds Musculoskeletal Biomedical Research Unit, Leeds Teaching
Handling editor Tore K Kvien 1 Leeds Institute of Rheumatic & Musculoskeletal Medicine, University of Leeds, Chapel Allerton Hospital and NIHR Leeds Musculoskeletal Biomedical Research Unit, Leeds Teaching
Received: 28 November 2007 / Revised: 11 February 2008 / Accepted: 12 February 2008 / Published online: 19 March 2008 # The Author(s) 2008
 Clin Rheumatol (08) 27:1021 1028 DOI 10.1007/s10067-008-0866-4 ORIGINAL ARTICLE An open-label pilot study of the effectiveness of adalimumab in patients with rheumatoid arthritis and previous infliximab
Clin Rheumatol (08) 27:1021 1028 DOI 10.1007/s10067-008-0866-4 ORIGINAL ARTICLE An open-label pilot study of the effectiveness of adalimumab in patients with rheumatoid arthritis and previous infliximab
CLINICAL BRIEFS. Tumor Necrosis Factor Inhibitors In the Treatment of Chronic Inflammatory Diseases
 CLINICAL BRIEFS Tumor Necrosis Factor Inhibitors In the Treatment of Chronic Inflammatory Diseases A review of immunogenicity and potential implications By Joseph Flood, MD, FACR President, Musculoskeletal
CLINICAL BRIEFS Tumor Necrosis Factor Inhibitors In the Treatment of Chronic Inflammatory Diseases A review of immunogenicity and potential implications By Joseph Flood, MD, FACR President, Musculoskeletal
