Year 1 Peer Based Learning 2018 Respiratory System
|
|
|
- Elmer Reeves
- 5 years ago
- Views:
Transcription
1 Please note this learning resource has been produced by the GUMS Academic Team. It is possible that there are some minor errors in the questions/answers, and other possible answers that are not included below. Make sure to check with other resources. Scenario 1: Stem 1: Toby Acco is a 70 year old male. He has a 20 pack year history of smoking. His flow volume loop is shown below; normal is shown for reference. Question 1: Define pack year Number of packs of cigarettes smoked per day by the number of years the person has smoked Question 2: What is the difference between a lung capacity and volume A capacity = 2 or more lung volumes totaled together Question 3: Define the lung volumes/capacity shown on the graph at the right VC = vital capacity = maximum volume of gas that can be expired after a maximal inspiration RV = residual volume = air remaining in lung after a maximal expiration TLC = sum of all volumes - volume of gas in lung after a maximal inspiration (IRV + TV + ERV + RV)
2 Question 4: State the pattern of lung disease Toby has and how RV and TLC from question 3 have changed. State the underlying mechanism for this. Obstructive disease. RV and TLC have both increased (RV goes from 0 to about 4 now; TLC goes from 0 to 8). The mechanism for this is air trapping Question 5: Summarise the main spirometry/lung volume/capacity findings in obstructive disease and restrictive disease by completing the below table: Obstructive Disease Restrictive Disease RV increased Decreased TLC Increased Decreased FRC Increased Decreased FEV1:FVC Decreased Normal or increased (discuss how this ratio is changed with the students: in obstructive FEV1 drops more than FVC > decreases ratio; in restrictive there is low FEV1 and low to very low FVC > normal or increased ratio)
3 Question 6: What is the most likely diagnosis? Define this disease COPD - broad term for chronic bronchitis and emphysema. Explain that even though these are two different diseases, because the major risk factor for both is smoking, they commonly occur together - this is why the blanket term COPD is given Question 7: Contrast the pathophysiology mechanism of obstruction in chronic bronchitis and emphysema Both are caused by smoking (which acts as an irritant). Chronic bronchitis. It results mainly from hypertrophy and hyperplasia of bronchial mucinous glands (mainly) and also goblet cells. This leads to increased mucous production leading to mucous plugging this is an obstruction. Smoking also causes shortened and immotile cilia, which further decreases ability to clear mucus. Emphysema. Smoking causes inflammation in the airways, leading to production of proteases via inflammatory cells such as macrophages and neutrophils. These proteases (eg, collagenases, elastases) cause destruction of elastin and collagen, which are responsible for elastic recoil of the lung. Normally, when air leaves the lungs, there is negative pressure which acts to collapse the airways, however the elastic recoil of the lungs prevents this from occurring. In emphysema, the loss of elastin leads to: Collapsing airway walls on expiration (due to negative pressure) leading to air-trapping More compliant (stretchy) alveoli on inspiration, increasing lung volumes There is also degradation of fibrous septa in the lungs, leading to alveoli collapsing into larger alveoli, decreasing the surface area for gas exchange to occur. Question 8: for the following signs/symptoms, state which is more characteristic of chronic bronchitis vs emphysema and explain why: - cyanosis - chronic bronchitis: mucus plugging causes a low V/Q ratio (decreased ventilation across the entire lungs) à hypercapnia and hypoxaemia. This is not as much of an issue in emphysema, because the V/Q ratio is more normal or even high (increased ventilation due to increased lung compliance, and decreased blood flow due to reduced surface area with the alveoli) - prolonged expiration with pursed lips - emphysema: breathing with pursed lips forces a back pressure into the airways > ensures smaller airways remain patent - productive cough - chronic bronchitis: huge mucus production results in coughing; no where near as much mucus in emphysema (it does occur, just not as much) - wheezing - chronic bronchitis: this is the sound of air ossicilating within narrowed airways - the intense mucus plugging causes this. also ask students: name another disease where wheezing is seen and state the mechanism for this: answer = asthma; mechanism = bronchoconstriction AND mucus plugging
4 Year 1 Peer Based Learning 2018 Question 9: What if a patient also presented with liver cirrhosis? Which one of the diseases (chronic bronchitis or emphysema) is more likely to also occur concurrently? State what protein is defective and the mechanism for developing the disease it causes Alpha-1-antitrypsin deficiency. Causes emphysema. Alpha-1-antitrypsin is an anti-protease. Explain that emphysema is caused by an imbalance of proteases and anti-proteases. In smoking, there is increased inflammation > more proteases released > number of antiproteases cannot counteract this. In alpha-1-antitrypsin deficiency, even if the person doesn t smoke, the fact that there are no anti-proteases can t counteract the inflammation that will naturally occur as life goes on > emphysema Question 10: Which disease is more likely to have the following x-ray? Explain increased AP diameter = barrel chest = emphysema, for expansion of the thorax, it is a battle between the chest wall and lung tissue. lung recoil has a tendency to collapse inwards, and the chest wall has a tendency to pull the thorax outwards. because of loss of elastic recoil, the chest wall wins this war > barrel chest Ask what other features might be seen on X-ray: increased lung field lucency and flattened diaphragm both due to hyperinflation
5 Q11. Which disease is more likely to cause infection as a complication? Explain Infection is more likely in chronic bronchitis. a general principle in pathology is that if there is an obstruction, you get infection down-stream e.g. give a faecolith causing appendicitis as an example Question 12: What is the effect of hypoxia on the pulmonary vasculature? Explain in ONE sentence the impact of long-term COPD on the heart and name this condition Hypoxia causes vasoconstriction. Give the example of an upper lobar bronchus obstruction. Here, it is advantageous to constrict the pulmonary vasculature, because you divert the blood to the other lobes of the lung and can still get sufficiency gas exchange. Now, nowhere is getting enough oxygen in COPD, so everywhere constricts. One sentence: hypoxic vasoconstriction > increases afterload > RVH and heart failure - cor pulmonale Question 13: You administer ipratropium. State the MOA muscarinic antagonist > bronchodilation Question 14: Would you administer supplemental oxygen? Discuss It may lead to hypercapnic respiratory failure (Type II respiratory failure) in some COPD patients. This is because, in COPD, patients are able to optimise their gas exchange by hypoxic vasoconstriction. By administering excessive oxygen, this overcomes the hypoxic vasoconstriction, increasing blood supply to areas which are poorly ventilated, creating a V/Q mismatch (low V and high Q). Stem 2: 10 years later, he presents with distended neck veins, ipsilateral partial ptosis, miosis and anhidrosis. Question 15: What disease (don t need to be specific) has he most likely developed now? What lobe of the lung is most likely affected? What other structures could also be compressed here and what should you look for? lung cancer. upper lobe = pancoast tumour = compresses sympathetic chain (e.g. stellate ganglion) and SVC or brachiocephalic veins. also should check for: - recurrent laryngeal nerve (hoarseness of voice) - thoracic outlet syndrome: compression of lower trunk or T1 of brachial plexus plus subclavian vessels - intrinsic hand muscle wasting (e.g. thenar, hypothenar wasting - get a picture from google images and show them), ischaemia, pain and oedema in lower limb from vessel compression Stem 3: The patient complains of altered mental state.
6 Question 16: If these were caused by his lung cancer, elucidate TWO possible mechanisms for this prompt students with: think about paraneoplastic syndromes small cell lung cancer > releases ADH, causing SIADH > hyponatraemia > altered mental state squamous cell clung cancer > releases PTHrP (Parathyroid hormone-related protein), causing hypercalcaemia > altered mental state Question 17: complete the following table, comparing the main features of lung cancers: also explain that small cell lung cancer is its own category - the others (squamous cell, adenocarcinoma etc.) are all types of non-small cell lung cancer. small cell treated by chemo/radiotherapy; non-small treated by surgery give them the following mnemonic to help them remember: squamous cell and small cell lung cancer are s entral, caused by smoking, have paraneoplastic syndromes and are more common in males. the one thing that is different is treatment. then, adenocarcinoma, is mostly the opposite! location in lung risk factors paraneoplastic syndromes histological features treatment small cell lung cancer central male smoke SIADH, Lambert-Eaton syndrome, ACTH neuroendocrine tumour, poorly differentiated chemotherapy adenocarcinom a peripheral non-smokers and female smokers nil back to back glands, mucin surgery squamous cell central male smokers hypercalcaemia keratin pearls, intercellular bridges surgery
7 Stem 4: The patient goes onto develop a fever and the following x-ray whilst in hospital: Question 18: State the diagnosis. What predisposed him to this infection? What is the most common causative organism? What is the treatment for this? What is this patient s prognosis? Lobar pneumonia COPD (esp. chronic bronchitis) S. pneumoniae Penicillin (State strep has no resistance to penicllins) Poor (state pneumonia is a common cause of death of the elderly in the hospital Wrap up: state other important topics for them to study: pleural effusion, pneumothorax other types of pneumonia etc.
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
The role of lung function testing in the assessment of and treatment of: AIRWAYS DISEASE
 The role of lung function testing in the assessment of and treatment of: AIRWAYS DISEASE RHYS JEFFERIES ARTP education Learning Objectives Examine the clinical features of airways disease to distinguish
The role of lung function testing in the assessment of and treatment of: AIRWAYS DISEASE RHYS JEFFERIES ARTP education Learning Objectives Examine the clinical features of airways disease to distinguish
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Respiratory Medicine
 Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
Lab 4: Respiratory Physiology and Pathophysiology
 Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
Lab 4: Respiratory Physiology and Pathophysiology This exercise is completed as an in class activity and including the time for the PhysioEx 9.0 demonstration this activity requires ~ 1 hour to complete
COPD. Information is arranged in a way to make it easy to understand.
 COPD The sheet is divided into : 1- Some types of COPD 2- Tests for diagnosis of COPD Information is arranged in a way to make it easy to understand. First part: COPDs The term means Chronic Obstructive
COPD The sheet is divided into : 1- Some types of COPD 2- Tests for diagnosis of COPD Information is arranged in a way to make it easy to understand. First part: COPDs The term means Chronic Obstructive
How does COPD really work?
 How does COPD really work? by Alex Goodell View online Where does COPD fit in the mix of respiratory diseases? I ve made a map of the major pathologies outlined in Robbins and First Aid (obviously these
How does COPD really work? by Alex Goodell View online Where does COPD fit in the mix of respiratory diseases? I ve made a map of the major pathologies outlined in Robbins and First Aid (obviously these
Chronic Obstructive Pulmonary Disease
 136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
136 PHYSIOLOGY CASES AND PROBLEMS Case 24 Chronic Obstructive Pulmonary Disease Bernice Betweiler is a 73-year-old retired seamstress who has never been married. She worked in the alterations department
The Aging Lung. Sidney S. Braman MD FACP FCCP Professor of Medicine Brown University Providence RI
 The Aging Lung Sidney S. Braman MD FACP FCCP Professor of Medicine Brown University Providence RI Is the respiratory system of the elderly different when compared to younger age groups? Respiratory Changes
The Aging Lung Sidney S. Braman MD FACP FCCP Professor of Medicine Brown University Providence RI Is the respiratory system of the elderly different when compared to younger age groups? Respiratory Changes
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
PULMONARY FUNCTION. VOLUMES AND CAPACITIES
 PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
PULMONARY FUNCTION. VOLUMES AND CAPACITIES The volume of air a person inhales (inspires) and exhales (expires) can be measured with a spirometer (spiro = breath, meter = to measure). A bell spirometer
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Lecture Notes. Chapter 4: Chronic Obstructive Pulmonary Disease (COPD)
 Lecture Notes Chapter 4: Chronic Obstructive Pulmonary Disease (COPD) Objectives Define COPD Estimate incidence of COPD in the US Define factors associated with onset of COPD Describe the clinical features
Lecture Notes Chapter 4: Chronic Obstructive Pulmonary Disease (COPD) Objectives Define COPD Estimate incidence of COPD in the US Define factors associated with onset of COPD Describe the clinical features
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
What do pulmonary function tests tell you?
 Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
Pulmonary Function Testing Michael Wert, MD Assistant Professor Clinical Department of Internal Medicine Division of Pulmonary, Critical Care, and Sleep Medicine The Ohio State University Wexner Medical
COPD: Change in Definition. COPD Pathology with 3D Interactive. COPD: Definitions of 21st Century 1. COPD Includes Chronic Bronchitis 2
 COPD: Change in Definition COPD Pathology with 3D Interactive by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org COPD used to include 5 disease processes 1 1 Chronic Bronchitis 2 Emphysema
COPD: Change in Definition COPD Pathology with 3D Interactive by Scott Cerreta, BS, RRT Director of Education www.copdfoundation.org COPD used to include 5 disease processes 1 1 Chronic Bronchitis 2 Emphysema
Physiology lab (RS) First : Spirometry. ** Objectives :-
 Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Physiology lab (RS) ** Objectives :- 1. Spirometry in general. 2. Spirogram (volumes and capacities). 3. The importance of vital capacity in diagnosis. 4. Flow volume loop. 5. Miss Arwa s part (the practical
Chapter 10. Respiratory System and Gas Exchange. Copyright 2005 Pearson Education, Inc. publishing as Benjamin Cummings
 Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Your Lungs and COPD. Patient Education Pulmonary Rehabilitation. A guide to how your lungs work and how COPD affects your lungs
 Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
Patient Education Your Lungs and COPD A guide to how your lungs work and how COPD affects your lungs Your lungs are organs that process every breath you take. They provide oxygen (O 2 ) to the blood and
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chronic Obstructive Pulmonary Disease (COPD)
 Chronic Obstructive Pulmonary Disease (COPD) Definition of COPD Airflow obstruction that is: o Not fully reversible o Progressive o Does not change markedly over several months Combination of airway and
Chronic Obstructive Pulmonary Disease (COPD) Definition of COPD Airflow obstruction that is: o Not fully reversible o Progressive o Does not change markedly over several months Combination of airway and
Pathophysiology of COPD 건국대학교의학전문대학원
 Pathophysiology of COPD 건국대학교의학전문대학원 내과학교실 유광하 Rate per 100 0,000 population 550 500 450 400 350 300 250 200 150 100 50 0 Heart disease Cancer Stroke 1970 1974 1978 1982 1986 1990 1994 1998 2002 Year of
Pathophysiology of COPD 건국대학교의학전문대학원 내과학교실 유광하 Rate per 100 0,000 population 550 500 450 400 350 300 250 200 150 100 50 0 Heart disease Cancer Stroke 1970 1974 1978 1982 1986 1990 1994 1998 2002 Year of
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
6- Lung Volumes and Pulmonary Function Tests
 6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
6- Lung Volumes and Pulmonary Function Tests s (PFTs) are noninvasive diagnostic tests that provide measurable feedback about the function of the lungs. By assessing lung volumes, capacities, rates of
Unit 9. Respiratory System 16-1
 Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
Unit 9 Respiratory System 16-1 Works together with the circulatory system Exchange of gases between atmosphere, blood, and cells If respiratory system and/or circulatory system fails, death will occur
بسم هللا الرحمن الرحيم
 بسم هللا الرحمن الرحيم Yesterday we spoke of the increased airway resistance and its two examples: 1) emphysema, where we have destruction of the alveolar wall and thus reducing the area available for
بسم هللا الرحمن الرحيم Yesterday we spoke of the increased airway resistance and its two examples: 1) emphysema, where we have destruction of the alveolar wall and thus reducing the area available for
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
Slide 120, Lobar Pneumonia. Slide 120, Lobar Pneumonia. Slide 172, Interstitial Pneumonia. Slide 172, Interstitial Pneumonia. 53 Year-Old Smoker
 Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
Respiratory System Mechanics
 M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
M56_MARI0000_00_SE_EX07.qxd 8/22/11 3:02 PM Page 389 7 E X E R C I S E Respiratory System Mechanics Advance Preparation/Comments 1. Demonstrate the mechanics of the lungs during respiration if a bell jar
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS
 DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS INTRDUCTION In the last lecture we discussed the difference between restrictive and obstructive lung
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 3: CHRONIC BRNCHITIS AND BRONCHIECTASIS INTRDUCTION In the last lecture we discussed the difference between restrictive and obstructive lung
Respiratory Physiology In-Lab Guide
 Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Physiology In-Lab Guide Read Me Study Guide Check Your Knowledge, before the Practical: 1. Understand the relationship between volume and pressure. Understand the three respiratory pressures
Respiratory Pathophysiology
 Respiratory Pathophysiology Objectives: Respiratory infections and lung cancer. Pleural effusion & edema, pleuritis, pneumothorax and atelectasis. Obstructive airway disease and chronic interstitial lung
Respiratory Pathophysiology Objectives: Respiratory infections and lung cancer. Pleural effusion & edema, pleuritis, pneumothorax and atelectasis. Obstructive airway disease and chronic interstitial lung
Notes to complete gas exchange in mammals
 Notes to complete gas exchange in mammals Mass flow of air to respiratory surface this is achieved through the mechanics of ventilation (breathing). This ensures a regular supply of air into and out of
Notes to complete gas exchange in mammals Mass flow of air to respiratory surface this is achieved through the mechanics of ventilation (breathing). This ensures a regular supply of air into and out of
Diseases of the Lung and Respiratory Tract, Part I. William Bligh-Glover M.D. Department of Anatomy, CWRU
 Diseases of the Lung and Respiratory Tract, Part I William Bligh-Glover M.D. Department of Anatomy, CWRU Educational objectives: Distinguish the types of atelectasis and their etiologies Distinguish the
Diseases of the Lung and Respiratory Tract, Part I William Bligh-Glover M.D. Department of Anatomy, CWRU Educational objectives: Distinguish the types of atelectasis and their etiologies Distinguish the
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA
 DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA INTRODUCTION In this lecture we will discuss atelectasis which is a complication of several medical and surgical
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA INTRODUCTION In this lecture we will discuss atelectasis which is a complication of several medical and surgical
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Clinical Pathological Correlation of Chronic Obstructive Pulmonary Disease (COPD)*
 Clinical Pathological Correlation of Chronic Obstructive Pulmonary Disease (COPD)* ORHAN MUREN, M.D. Associate Professor of Medicine and Anesthesiology, Medical College of Virginia, Health Sciences Division
Clinical Pathological Correlation of Chronic Obstructive Pulmonary Disease (COPD)* ORHAN MUREN, M.D. Associate Professor of Medicine and Anesthesiology, Medical College of Virginia, Health Sciences Division
PFT Interpretation and Reference Values
 PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
PFT Interpretation and Reference Values September 21, 2018 Eric Wong Objectives Understand the components of PFT Interpretation of PFT Clinical Patterns How to choose Reference Values 3 Components Spirometry
COPD/ Asthma. Dr Heather Lewis Honorary Clinical Lecturer
 COPD/ Asthma Dr Heather Lewis Honorary Clinical Lecturer Objectives To understand the pathogenesis of asthma/ COPD To recognise the clinical features of asthma/ COPD To know how to diagnose asthma/ COPD
COPD/ Asthma Dr Heather Lewis Honorary Clinical Lecturer Objectives To understand the pathogenesis of asthma/ COPD To recognise the clinical features of asthma/ COPD To know how to diagnose asthma/ COPD
Respiration Lesson 3. Respiration Lesson 3
 Respiration Lesson 3 and Airway Resistance (key factors affecting air flow) 1) What is the arterial blood pressure in a healthy 18 year old male? 2) What would his venous blood pressure be? 3) What is
Respiration Lesson 3 and Airway Resistance (key factors affecting air flow) 1) What is the arterial blood pressure in a healthy 18 year old male? 2) What would his venous blood pressure be? 3) What is
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
PATHOPHYSIOLOGY OF RESPIRATION 2
 PATHOPHYSIOLOGY OF RESPIRATION 2 Obstructive disorders R. Benacka Department of Pathophysiology, Medical faculty, P.J. Safarik University Košice Respiratory diseases Obstructive diseases (OPD) - restricted
PATHOPHYSIOLOGY OF RESPIRATION 2 Obstructive disorders R. Benacka Department of Pathophysiology, Medical faculty, P.J. Safarik University Košice Respiratory diseases Obstructive diseases (OPD) - restricted
Objectives. Pulmonary Assessment 12/13/2017
 Pulmonary Assessment Reid Blackwelder, MD, FAAFP Professor and Chair, Family Medicine Quillen Colege of Medicine, ETSU Objectives Understand anatomy and physiology of pulmonary assessment techniques Remember
Pulmonary Assessment Reid Blackwelder, MD, FAAFP Professor and Chair, Family Medicine Quillen Colege of Medicine, ETSU Objectives Understand anatomy and physiology of pulmonary assessment techniques Remember
Overview of Obstructive Diseases of the Lung, Lung Physiology and Imaging Modalities
 Overview of Obstructive Diseases of the Lung, Lung Physiology and Imaging Modalities Jann Mortensen Final Phil meeting, 29 april 2004 Obstructive disease Definition Epidemiologi Mechanisms Natural history
Overview of Obstructive Diseases of the Lung, Lung Physiology and Imaging Modalities Jann Mortensen Final Phil meeting, 29 april 2004 Obstructive disease Definition Epidemiologi Mechanisms Natural history
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Respiratory Pathophysiology Cases Linda Costanzo Ph.D.
 Respiratory Pathophysiology Cases Linda Costanzo Ph.D. I. Case of Pulmonary Fibrosis Susan was diagnosed 3 years ago with diffuse interstitial pulmonary fibrosis. She tries to continue normal activities,
Respiratory Pathophysiology Cases Linda Costanzo Ph.D. I. Case of Pulmonary Fibrosis Susan was diagnosed 3 years ago with diffuse interstitial pulmonary fibrosis. She tries to continue normal activities,
PULMONARY FUNCTION TESTING. Purposes of Pulmonary Tests. General Categories of Lung Diseases. Types of PF Tests
 PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
Ch 16 A and P Lecture Notes.notebook May 03, 2017
 Table of Contents # Date Title Page # 1. 01/30/17 Ch 8: Muscular System 1 2. 3. 4. 5. 6. 7. 02/14/17 Ch 9: Nervous System 12 03/13/17 Ch 10: Somatic and Special Senses 53 03/27/17 Ch 11: Endocrine System
Table of Contents # Date Title Page # 1. 01/30/17 Ch 8: Muscular System 1 2. 3. 4. 5. 6. 7. 02/14/17 Ch 9: Nervous System 12 03/13/17 Ch 10: Somatic and Special Senses 53 03/27/17 Ch 11: Endocrine System
The development of chronic obstructive pulmonary
 THE PATHOGENESIS AND PATHOLOGY OF COPD: IDENTIFYING RISK FACTORS AND IMPROVING MORBIDITY AND MORTALITY * Paul D. Scanlon, MD ABSTRACT Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory
THE PATHOGENESIS AND PATHOLOGY OF COPD: IDENTIFYING RISK FACTORS AND IMPROVING MORBIDITY AND MORTALITY * Paul D. Scanlon, MD ABSTRACT Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory
5/5/2013. The Respiratory System. Chapter 16 Notes. The Respiratory System. Nasal Cavity. Sinuses
 The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
The Respiratory System Chapter 16 Notes The Respiratory System Objectives List the general functions of the respiratory system. Identify the organs of the respiratory system. Describe the functions of
Chapter Effects of Smoke on the Respiratory System Part 2 pages
 Chapter 18.1 Effects of Smoke on the Respiratory System Part 2 pages 417-419 Hemoglobin has 4 separate protein chains. Each protein chain has a single iron atom (Fe 3+ ). Each iron atom can bind to a single
Chapter 18.1 Effects of Smoke on the Respiratory System Part 2 pages 417-419 Hemoglobin has 4 separate protein chains. Each protein chain has a single iron atom (Fe 3+ ). Each iron atom can bind to a single
Lesson 9.1: Learning the Key Terms
 131 Lesson 9.1: Learning the Key Terms Directions: Place the letter of the best definition next to each key term. 1. alveolar capillary membrane 2. alveoli 3. bronchioles 4. cardiopulmonary system 5. conchae
131 Lesson 9.1: Learning the Key Terms Directions: Place the letter of the best definition next to each key term. 1. alveolar capillary membrane 2. alveoli 3. bronchioles 4. cardiopulmonary system 5. conchae
Spirometry. Obstruction. By Helen Grim M.S. RRT. loop will have concave appearance. Flows decreased consistent with degree of obstruction.
 1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
1 2 Spirometry By Helen Grim M.S. RRT 3 4 Obstruction loop will have concave appearance. Flows decreased consistent with degree of obstruction. Volumes may be normal, but can decrease with severity of
WHAT ARE THE PHYSIOLOGICAL DETERMINANTS OF EXPIRATORY FLOW?
 Lung Volume the physiology of breathing: OBSTRUCTIVE LUNG DISORDERS Dr. Andrew Fon MBBS FRACP Respiratory and Sleep Medicine Physician PhD Research Fellow Dept. of Thoracic Medicine, ROYAL ADELAIDE HOSPITAL
Lung Volume the physiology of breathing: OBSTRUCTIVE LUNG DISORDERS Dr. Andrew Fon MBBS FRACP Respiratory and Sleep Medicine Physician PhD Research Fellow Dept. of Thoracic Medicine, ROYAL ADELAIDE HOSPITAL
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air
 Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Medicine Dr. Kawa Lecture 1 Asthma Obstructive & Restrictive Pulmonary Diseases Obstructive Pulmonary Disease Indicate obstruction to flow of air through the airways. As asthma, COPD ( chronic bronchitis
Known Allergies: Shellfish. Symptoms: abdominal pain, nausea, diarrhea, or vomiting. congestion, trouble breathing, or wheezing.
 CSTAR CASE STUDIES: BLOCK B Asthma or COPD? Setting: Walk in clinic. Dan: I havi g that cough thi g agai HPI: Dan is a 49-year-old male teacher who reports having had episodes of cough with mucus production
CSTAR CASE STUDIES: BLOCK B Asthma or COPD? Setting: Walk in clinic. Dan: I havi g that cough thi g agai HPI: Dan is a 49-year-old male teacher who reports having had episodes of cough with mucus production
People with asthma who smoke. The combination of asthma, a chronic airway disease, and smoking increases the risk of COPD even more.
 COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
COPD Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, sputum (phlegm) production
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Basic approach to PFT interpretation. Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic
 Basic approach to PFT interpretation Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic Disclosures Received honorarium from Astra Zeneca for education presentations Tasked Asked
Basic approach to PFT interpretation Dr. Giulio Dominelli BSc, MD, FRCPC Kelowna Respiratory and Allergy Clinic Disclosures Received honorarium from Astra Zeneca for education presentations Tasked Asked
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
COPD. Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS
 IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
B Unit III Notes 6, 7 and 8
 The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
The Respiratory System Why do we breathe? B. 2201 Unit III Notes 6, 7 and 8 Respiratory System We know that our cells respire to produce ATP (energy). All organisms need energy to live, so that s why we
COPD COPD. C - Chronic O - Obstructive P - Pulmonary D - Disease OBJECTIVES
 COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
Chapter 16. The Respiratory System. Mosby items and derived items 2010, 2006, 2002, 1997, 1992 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 16 The Respiratory System Objectives Discuss the generalized functions of the respiratory system List the major organs of the respiratory system and describe the function of each Compare, contrast,
Chapter 16 The Respiratory System Objectives Discuss the generalized functions of the respiratory system List the major organs of the respiratory system and describe the function of each Compare, contrast,
#8 - Respiratory System
 Page1 #8 - Objectives: Study the parts of the respiratory system Observe slides of the lung and trachea Equipment: Remember to bring photographic atlas. Figure 1. Structures of the respiratory system.
Page1 #8 - Objectives: Study the parts of the respiratory system Observe slides of the lung and trachea Equipment: Remember to bring photographic atlas. Figure 1. Structures of the respiratory system.
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
COPD Management in LTC: Presented By: Jessica Denney RRT
 COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
COPD Management in LTC: Presented By: Jessica Denney RRT Sponsored by Z & D Medical Services, Diamond Sponsor Seizing Opportunities to Provide Individualized Treatment and Device Selection for your COPD
Biochemistry of Lungs. Lecture # 35 Lecturer: Alexander Koval
 Biochemistry of Lungs Lecture # 35 Lecturer: Alexander Koval Introduction Biochemistry of lungs Overview of substances produced (surfactant, mucus, collagen), inactivated (ROS, kinins, serotonin, catecholamines)
Biochemistry of Lungs Lecture # 35 Lecturer: Alexander Koval Introduction Biochemistry of lungs Overview of substances produced (surfactant, mucus, collagen), inactivated (ROS, kinins, serotonin, catecholamines)
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Anyone who smokes and/or has shortness of breath and sputum production could have COPD
 COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
COPD DIAGNOSIS AND MANAGEMENT CHECKLIST Anyone who smokes and/or has shortness of breath and sputum production could have COPD Confirm Diagnosis Presence and history of symptoms: Shortness of breath Cough
CHAPTER 22 RESPIRATORY
 pulmonary ventilation move air external respiration exchange gases transportation of gases internal respiration exchange gases CHAPTER 22 RESPIRATORY in / out lungs air - blood blood - cells cell respiration
pulmonary ventilation move air external respiration exchange gases transportation of gases internal respiration exchange gases CHAPTER 22 RESPIRATORY in / out lungs air - blood blood - cells cell respiration
Lung Cancer. Definition of lung cancer Malignancy arising from lung tissue
 Lung Cancer Definition of lung cancer Malignancy arising from lung tissue Epidemiology of lung cancer Commonest malignancy in western world Commonest cause of death in men and women in the UK Approximately
Lung Cancer Definition of lung cancer Malignancy arising from lung tissue Epidemiology of lung cancer Commonest malignancy in western world Commonest cause of death in men and women in the UK Approximately
Wash your hands, introduce yourself, obtain consent.
 Introduction At the start: Wash your hands, introduce yourself, obtain consent. Patient position: Sitting upright (45 o ) & adequately exposed (undress to waist). NB: if you have a female patient, the
Introduction At the start: Wash your hands, introduce yourself, obtain consent. Patient position: Sitting upright (45 o ) & adequately exposed (undress to waist). NB: if you have a female patient, the
THE AUSTRALIAN JOURNAL OF PHYSIOTHERAPY
 THE AUSTRALIAN JOURNAL OF PHYSIOTHERAPY VOLUME XVIV DECEMBER, 1973 NUMBER 4 ASPECTS OF APPLIED PHYSIOLOGY IN CHRONIC BRONCHITIS AND EMPHYSEMA 1 G* B. FIELD, M.D., F.R.A.C.P.? B.SC. (MED.) The terms chronic
THE AUSTRALIAN JOURNAL OF PHYSIOTHERAPY VOLUME XVIV DECEMBER, 1973 NUMBER 4 ASPECTS OF APPLIED PHYSIOLOGY IN CHRONIC BRONCHITIS AND EMPHYSEMA 1 G* B. FIELD, M.D., F.R.A.C.P.? B.SC. (MED.) The terms chronic
Altered Ventilation and Diffusion
 Respiratory Structures Altered Ventilation and Diffusion Alveolar type 1: provide structure and air exchange Alveolar type 2: lubricant that coats the inner portion of the alveolus, promotes easy expansion,
Respiratory Structures Altered Ventilation and Diffusion Alveolar type 1: provide structure and air exchange Alveolar type 2: lubricant that coats the inner portion of the alveolus, promotes easy expansion,
Chapter 10 Lecture Outline
 Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
Chapter 10 Lecture Outline See separate PowerPoint slides for all figures and tables preinserted into PowerPoint without notes. Copyright 2016 McGraw-Hill Education. Permission required for reproduction
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Respiratory System. December 20, 2011
 Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Respiratory System December 20, 2011 Nasal Cavity: Contains cilia (hair cells) to prevent particles from entering the respiratory tract Mucus does the same, in addition to warming and moistening the air
Emphysema. Lungs The lungs help us breathe in oxygen and breathe out carbon dioxide. Everyone is born with 2 lungs: a right lung and a left lung.
 Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects millions of people worldwide. Emphysema involves damage to the air sacs in the lungs. This makes
Emphysema Introduction Emphysema is a type of chronic obstructive pulmonary disease, or COPD. COPD affects millions of people worldwide. Emphysema involves damage to the air sacs in the lungs. This makes
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Internal medicine. Lec #: 4 Date: COPD-Definition
 Internal medicine Topic: COPD Dr: mousa malkawy Lec #: 4 Date: 26-10-2009 COPD-Definition A disease state characterized by airflow limitation that is not fully reversible and usually it is progressive
Internal medicine Topic: COPD Dr: mousa malkawy Lec #: 4 Date: 26-10-2009 COPD-Definition A disease state characterized by airflow limitation that is not fully reversible and usually it is progressive
The Respiratory System
 The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
The Respiratory System Respiratory Anatomy Upper respiratory tract Nose Nasal passages Pharynx Larynx Respiratory Anatomy Functions of the upper respiratory tract: Provide entry for inhaled air Respiratory
Respiratory Pathology. Kristine Krafts, M.D.
 Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
Respiratory Pathology Kristine Krafts, M.D. Normal lung: alveolar spaces Respiratory Pathology Outline Acute respiratory distress syndrome Obstructive lung diseases Restrictive lung diseases Vascular
THE RESPIRATORY SYSTEM. Pages and
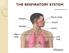 THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
The Respiratory System
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 14 The Respiratory System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
Chronic Obstructive Pulmonary Disease (COPD) Clinical Guideline
 Chronic Obstructive Pulmonary Disease (COPD) Clinical These clinical guidelines are designed to assist clinicians by providing an analytical framework for the evaluation and treatment of patients. They
Chronic Obstructive Pulmonary Disease (COPD) Clinical These clinical guidelines are designed to assist clinicians by providing an analytical framework for the evaluation and treatment of patients. They
BELLWORK page 343. Apnea Dyspnea Hypoxia pneumo pulmonary Remember the structures of the respiratory system 1
 BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
Why do you breathe? What is oxygen used for? Where does CO2 come from?
 RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
RESPIRATORY SYSTEM How You Breathe Why do you breathe? What is oxygen used for? Where does CO2 come from? Respiration: exchange of gases between air & your body cells 1. Outside air (O2) lungs metabolism
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Lab Activity 27. Anatomy of the Respiratory System. Portland Community College BI 233
 Lab Activity 27 Anatomy of the Respiratory System Portland Community College BI 233 1 Terminology Pulmonary Ventilation: aka breathing, is the movement of air into and out of the lungs External Respiration:
Lab Activity 27 Anatomy of the Respiratory System Portland Community College BI 233 1 Terminology Pulmonary Ventilation: aka breathing, is the movement of air into and out of the lungs External Respiration:
