Subject: Infertility DESCRIPTION: Original Effective Date: 11/15/00. Reviewed: 09/27/18. Revised: 10/15/18
|
|
|
- Lydia Underwood
- 5 years ago
- Views:
Transcription
1 Original Effective Date: 11/15/00 Reviewed: 09/27/18 Revised: 10/15/18 Subject: Infertility THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION, CERTIFICATION, EXPLANATION OF BENEFITS, OR A GUARANTEE OF PAYMENT, NOR DOES IT SUBSTITUTE FOR OR CONSTITUTE MEDICAL ADVICE. ALL MEDICAL DECISIONS ARE SOLELY THE RESPONSIBILITY OF THE PATIENT AND PHYSICIAN. BENEFITS ARE DETERMINED BY THE GROUP CONTRACT, MEMBER BENEFIT BOOKLET, AND/OR INDIVIDUAL SUBSCRIBER CERTIFICATE IN EFFECT AT THE TIME SERVICES WERE RENDERED. THIS MEDICAL COVERAGE GUIDELINE APPLIES TO ALL LINES OF BUSINESS UNLESS OTHERWISE NOTED IN THE PROGRAM EXCEPTIONS SECTION. Position Statement Billing/Coding Reimbursement Program Exceptions Definitions Related Guidelines Other References Updates DESCRIPTION: Infertility diagnosis, treatment, assisted reproductive technologies (e.g., IVF, ZIFT, GIFT) and artificial and intrauterine insemination (AI) vary by member s benefits. Infertility is defined as inability to conceive a child despite trying for one year, or the inability of the woman to carry a pregnancy that results in live birth. Some causes of infertility include the following: Abnormalities in the semen (male factor infertility) Ovulatory disorders (ovulatory factor) Tubal injury, blockage, paratubal adhesions, or endometriosis (tubal/peritoneal factor) Abnormalities in cervical mucus-sperm interaction (cervical factor) Rarer conditions such as uterine abnormalities, immunologic aberrations, and infections. In some cases, no specific cause of infertility is detected despite an extensive and complete evaluation. Assisted reproductive technologies (ART) refer to several interventions designed to establish a viable pregnancy for individuals who have been diagnosed with infertility; due either to female factors (e.g., pelvic adhesions, ovarian dysfunction, endometriosis, prior tubal ligation), male factors (e.g., abnormalities in sperm; production, function, transport, or prior vasectomy), a combination of both male and female factors, or unknown causes.
2 Assisted reproductive technologies include: in vitro fertilization (IVF), gamete intrafallopian transfer (GIFT), zygote intra-fallopian transfer (ZIFT), donor oocytes, and cryopreserved embryo transfers (CET). ART incorporates some type of in vitro fertilization (IVF) procedure in which oocytes harvested from the female are inseminated in vitro with sperm harvested from the male. Following the fertilization procedure, the zygote is cultured and ultimately transferred back into the female s uterus or fallopian tubes (zygote intrafallopian transfer [ZIFT]). In some instances, the oocyte and sperm are collected, but no in vitro fertilization takes place, and the gametes are reintroduced into the fallopian tubes (gamete intrafallopian transfer [GIFT]). Artificial Insemination (AI) encompasses a variety of procedures (e.g., intracervical, intrauterine (IUI)) involving placement of whole semen or processed sperm into the female reproductive tract, which permits sperm-oocyte interaction in the absence of intercourse. AI uses processed sperm from the male partner or a donor. Relatively new ART techniques include: intracytoplasmic sperm injection (ICSI), assisted hatching, coculture of embryos, and cryopreservation of reproductive tissue (e.g., ovarian, oocytes, testicular). Intracytoplasmic Sperm Injection (ICSI) is performed in cases of male factor infertility when either insufficient numbers of sperm, abnormal morphology, or poor motility preclude unassisted in vitro fertilization. Assisted Hatching one key component of a successful attempt at in vitro fertilization is implantation of the embryo in the uterus. It is hypothesized that during the in vitro component of the IVF, the zona pellucid becomes hardened, thus impairing the hatching process. Alternatively, some embryos may have some inherent inability to induce thinning of the zona pellucida before hatching. Mechanical disruption of the zona pellucida (e.g., assisted hatching) has been proposed as a mechanism to improve implantation rates. There is no evidence that assisted hatching improves the live birth rate compared with standard of care. Embryo Co-Culture a variety of co-culture techniques have been investigated, involving the use of feeder cell layers derived from a range of tissues, including the use of human reproductive tissues (e.g., oviducts) to non-human cells (e.g., fetal bovine uterine or oviduct cells) to established cell lines (e.g., Vero cells or bovine kidney cells). No standardized method of co-culture has emerged and no controlled trials have evaluated an improved implantation or pregnancy rate associated with co-culture. Cryopreservation of Ovarian tissue with subsequent auto or heterotopic transplant has been investigated as a technique to sustain the reproductive function of women or children who are faced with sterilizing procedures, such as chemotherapy, radiation therapy, surgery, or due to malignant diseases. Cryopreservation of ovarian tissue techniques is not standardized, and the overall success of the procedure cannot be determined from individual case reports. Cryopreservation of Oocytes is less commonly performed in the setting of malignancy due to the time constraints inherent in ovarian stimulation. Oocyte cryopreservation has been primarily investigated as an alternative to embryo cryopreservation due to ethical or religious reasons. The technique for
3 cryopreservation and thawing of oocytes has not been established and there is a lack of long-term experience with this technique. Cryopreservation of Testicular Tissue/Testicular sperm extraction (TESE) refers to the collection of sperm from testicular tissue in men with azoospermia. TESE may be performed at the time of a diagnostic biopsy, or performed as a subsequent procedure, specifically for the collection of spermatozoa. The spermatozoa may be isolated immediately and a portion used for an ICSI procedure at the time of oocyte retrieval from the partner, with the remainder cryopreserved. Alternatively, the entire tissue sample can be cryopreserved with portion thawed and sperm isolation performed at subsequent ICSI cycles. This technique appears to be a well-established component of the overall ICSI procedure; cryopreservation of either the isolated sperm of the tissue sample eliminates the need for multiple biopsies to obtain fresh tissue in the event of a failed initial ICSI cycle. Cryopreservation of Testicular Tissue in prepubertal boys may be considered in those undergoing chemotherapy for cancer. The goal of cryopreservation in prepubertal boys undergoing chemotherapy is maintenance of fertility potential by auto-transplanting the testicular tissue when chemotherapy has been completed. While cryopreservation of testicular tissue in prepubertal boys have been explored in animals, there are inadequate human studies. Blastocyst Transfer refers to the extended culture of oocytes/embryos, i.e., for greater than 4 days. The development of commercially available sequential media designed to reproduce the changes in nutrient requirements as the embryo develops has permitted the extended culture of embryos to the blastocyst stage, at which point the embryos are transferred. The rationale behind blastocyst transfer is that embryos progressing to the blastocyst stage have a much greater chance of implanting successfully in the uterus and resulting in an ongoing pregnancy. Blastocyst culture allows one to select the best quality embryo with the highest implantation potential. POSITION STATEMENT: NOTE: Coverage for infertility is subject to the member s benefit terms, limitations and maximums. Refer to contract language regarding infertility. If the benefit for coverage for infertility treatment is available and there is documentation of infertility for at least one year s duration, the following indications meet the definition of medical necessity: Diagnostic test or procedures to determine female infertility and or male infertility Artificial or intrauterine insemination (AI). NOTE: For AI, during one ovulatory cycle, sperm may be inseminated twice (once before human chorionic gonadotropin (hcg) and once after hcg. This is considered to be two attempts during one cycle) Assisted Reproductive Technologies (ARTs): IVF, ZIFT, GIFT Four (4) cycles for any Assisted Reproductive Technologies (ARTs): IVF, ZIFT, GIFT, AI A cycle (ovulatory) of infertility treatment may include ovulation monitoring, egg retrieval, sperm retrieval, embryo transfer, egg fertilization. NOTE: If medical circumstances warrant consideration of more than four (4) cycles, additional cycles will be reviewed for medical appropriateness (e.g., a new cause of infertility is discovered and treated during covered therapy)
4 Services associated with the diagnosis and treatment of infertility. For fertility drug coverage, refer to member s contract benefits. For diagnostic testing coverage for infertility, refer to member s contract benefits. NOTE: Family balancing is not eligible for coverage. Family balancing is a measured approach to a nonmedically indicated use of preconception gender selection. Family balancing provides couples having at least one child the opportunity to use MicroSort to increase the chance of having another child of the less represented sex in the family. The following assisted reproductive techniques meet the definition of medically necessity: Cryopreservation of testicular tissue/sperm in adult men with azoospermia as part of an intracytoplasmic sperm injection (ICSI) procedure Intracytoplasmic sperm injection (ICSI) for male factor infertility Blastocyst transfer The following assisted reproductive techniques are considered experimental or investigational. Assisted hatching is considered experimental or investigational, as there is insufficient clinical evidence to support the use of assisted hatching. The evidence is insufficient to determine the effects of assisted hatching on health outcomes. Embryo co-culture of oocyte(s)/embryos is considered experimental or investigational as there is insufficient clinical evidence to support the use of embryo co-culture of oocyte/embryo to improve the culture media for embryos, in order for a greater proportion of embryos to remain viable until implantation. Embryo co-culture techniques are not standardized embryos and a higher clinical pregnancy rate. The evidence is insufficient to determine the effects of embryo co-culture of oocyte(s)/embryos on health outcomes. Cryopreservation of ovarian tissue, including storage and thawing of ovarian tissue is considered experimental or investigational, as there is insufficient clinical evidence to support the use of cryopreservation of ovarian tissue, including storage and thawing of ovarian tissue. Cryopreservation of ovarian tissue is not standardized. The evidence is insufficient to determine the effects of cryopreservation of ovarian tissue on health outcomes. Cryopreservation of ovarian tissue with subsequent auto-or heterotopic transplant has been investigated as a technique to sustain the reproductive function of women or children who are faced with sterilizing procedures, such as chemotherapy, radiation therapy, or surgery (frequently due to
5 malignant diseases). Cryopreservation of ovarian tissue with subsequent auto-or heterotopic transplant is considered experimental or investigational. The evidence is insufficient to determine the effects of cryopreservation of ovarian tissue with subsequent auto-or heterotopic transplant on health outcomes. Cryopreservation of oocyte(s), including storage and thawing of oocytes, is considered experimental or investigational, as there is insufficient clinical evidence to support the use of cryopreservation of oocytes. The evidence is insufficient to determine the effects of cryopreservation of oocyte(s) on health outcomes. Cryopreservation of testicular tissue, including storage and thawing of testicular tissue in prepubertal boys is considered experimental or investigational, as there is insufficient clinical evidence to support the use of cryopreservation of testicular tissue in prepubertal boys. Cryopreservation of testicular tissue in prepubertal boys has been explored in animals; there are inadequate human studies for cryopreservation of testicular tissue in prepubertal boys. The evidence is insufficient to determine the effects of cryopreservation of testicular tissue on health outcomes. Intracytoplasmic sperm injection in the absence of male factor infertility is considered experimental or investigational. The evidence is insufficient to determine the effects of intracytoplasmic sperm injection in the absence of male factor infertility on health outcomes. BILLING/CODING INFORMATION: The following are some of the codes that may be used to report services that may be associated with infertility and diagnostic testing for infertility. NOTE: Coverage for infertility is subject to the member s benefit terms, limitations and maximums. Refer to contract language regarding infertility. NOTE: Coverage for diagnostic testing for infertility is subject to the member s benefit terms, limitations and maximums. Refer to contract language regarding diagnostic testing for infertility. CPT Coding: Fine needle aspiration; without imaging guidance Fine needle aspiration; with imaging guidance Biopsy of the testis, needle
6 54800 Biopsy of epididymis, needle Vasovasostomy, vas vasorrhaphy Electroejaculation (may be used in patients who are unable to produce a normal ejaculate due to spinal cord or other nervous system disorder i.e., diabetic neuropathy) Artificial insemination; intra-cervical Artificial insemination; intra-uterine Sperm washing for artificial insemination Transcervical introduction of fallopian tube catheter for diagnosis and/or re-establishing patency (any method), with or without hysterosalpingography Follicle puncture for oocyte retrieval, any method Embryo transfer, intrauterine Gamete, zygote or embryo intrafallopian transfer, any method Culture of oocyte(s)/embryo(s), less than 4 days Culture of oocyte(s)/embryo(s), less than 4 days; with co-culture of oocyte(s)/embryos (investigational) Assisted embryo hatching, micro techniques (any method) Oocyte identification from follicular fluid Preparation of embryo for transfer (any method) Sperm identification from aspirate (other than seminal fluid) Cryopreservation; embryo(s) Cryopreservation sperm Sperm isolation; simple prep (e. g., sperm wash and swim-up) for insemination or
7 diagnosis with semen analysis Sperm isolation; complex prep (e. g., Percoll gradient, albumin gradient) for insemination or diagnosis with semen analysis Sperm identification from testis tissue, fresh or cryopreserved Insemination of oocytes Extended culture oocyte(s)/embryo(s), 4 7 days Assisted oocyte fertilization, micro technique; less than or equal to 10 oocytes Assisted oocyte fertilization, micro technique; greater than 10 oocytes Biopsy, oocyte polar body or embryo blastomere, micro technique (for pre-implantation genetic diagnosis); less than or equal to 5 embryos Biopsy, oocyte polar body or embryo blastomere, micro technique (for pre-implantation genetic diagnosis); greater than 5 embryos (non-covered) Semen analysis; presence and/or motility of sperm including Huhner test (post coital) Semen analysis; motility and count (not including Huhner test) Semen analysis; volume, count, motility, and differential Semen analysis; sperm presence and motility of sperm, if performed Semen analysis; volume, count, motility, and differential using strict morphologic criteria (e.g., Kruger) Sperm antibodies Sperm evaluation; hamster penetration test Sperm evaluation; cervical mucus penetration test, with or without spinnbarkeit test Sperm evaluation, for retrograde ejaculation, urine (sperm concentration, motility, and morphology, as indicated)
8 89335 Cryopreservation, reproductive tissue, testicular Cryopreservation, mature oocyte(s) (investigational) Storage, (per year); embryo(s) Storage, (per year); sperm/semen Storage, (per year); reproductive tissue, testicular/ovarian (investigational) Storage, (per year); oocyte (investigational) Thawing of cryopreserved; embryo(s) Thawing of cryopreserved; sperm/semen, each aliquot Thawing of cryopreserved; reproductive tissue, testicular/ovarian (investigational) Thawing of cryopreserved; oocytes, each aliquot (investigational) 0058T 0357T Cryopreservation; reproductive tissue, ovarian (investigational) Cryopreservation; immature oocyte(s) (investigational) HCPCS Coding: S3655 S4011 S4013 S4014 S4015 S4016 Antisperm antibodies test (immunobead) In vitro fertilization; including but not limited to identification and incubation of mature oocytes, fertilization with sperm, incubation of embryo(s), and subsequent visualization for determination of development Complete cycle, gamete intrafallopian transfer (GIFT), case rate Complete cycle, zygote intrafallopian transfer (ZIFT), case rate Complete in vitro fertilization cycle, not other wise specified case rate Frozen in vitro fertilization cycle, case rate
9 S4017 S4018 S4020 S4021 S4022 S4023 S4025 S4026 S4027 S4028 S4030 S4031 S4035 S4037 S4040 S4042 Incomplete cycle, treatment canceled prior to stimulation, case rate Frozen embryo transfer procedure canceled before transfer, case rate In vitro fertilization procedure cancelled before aspiration, case rate In vitro fertilization procedure cancelled after aspiration, case rate Assisted oocyte fertilization, case rate Donor egg cycle, incomplete, case rate Donor services for in vitro fertilization (sperm or embryo), case rate Procurement of donor sperm from sperm bank Storage of previously frozen embryos Microsurgical epididymal sperm aspiration (MESA) Sperm procurement and cryopreservation services; initial visit Sperm procurement and cryopreservation services; subsequent visit Stimulated intrauterine insemination (IUI), case rate Cryopreserved embryo transfer, case rate Monitoring and storage of cryopreserved embryos, per 30 days Management of ovulation induction (interpretation of diagnostic tests and studies, nonface-to-face medical management of the patient), per cycle REIMBURSEMENT INFORMATION: Refer to section entitled POSITION STATEMENT and BILLING/CODING INFORMATION. PROGRAM EXCEPTIONS: Federal Employee Program (FEP): Follow FEP guidelines.
10 State Account Organization (SAO): Follow SAO guidelines. Medicare Advantage products: The following National Coverage Determination was reviewed on the last guideline reviewed date: Medicare Benefit Policy Manual Chapter 15-Covered Medical and Other Health Services-20.1 Physician Expense for Surgery, Childbirth and Treatment for Infertility. The following Local Coverage Determination (LCD) was reviewed on the last guideline reviewed date: Noncovered Services, (L33777) located at fcso.com. DEFINITIONS: ART: Assisted Reproductive Technologies. Artificial insemination (AI): placement of semen into the uterus with a syringe. Azoospermia: lack of live spermatozoa in the semen. Cryopreservation: special freezing process. Cryopreserved embryo transfer (CET): once embryos have been fertilized in the lab, they are frozen (reserved) and later transferred to the uterus. Direct intra-peritoneal insemination (DIPI): process-attempting fertilization inside the body by placing a needle into the abdomen. Donor egg (DE): an egg donated from a woman other than the patient. Electroejaculation: this procedure assists men who are unable to ejaculate; electricity is sent through the pelvic area to assist in ejaculation. Embryo: an egg fertilized with sperm. Fallopian tubes: tubes connecting the uterus to the area around the ovaries. Eggs travel through the tubes to reach the uterus. Fertilization: egg penetrated by sperm to form an embryo. Gamete intrafallopian transfer (GIFT): a form of IVF; eggs are harvested from the ovary, loaded into a tube with sperm, and immediately placed into the fallopian tube with special scope for fertilization inside the body. Gamete: a mature male or female reproductive cell (sperm or ovum). Hysterosalpingography: x-ray test where dye is injected into the uterus and fallopian tubes, to see their structure.
11 In vitro fertilization (IVF): the egg is fertilized with sperm in a dish in a laboratory, rather than inside a woman s body. The resulting embryo is placed into the uterus later. One cycle of IVF includes using medicines to stimulate the ovaries to ovulate, harvesting the eggs with an instrument, attempting to fertilize the eggs with sperm in the lab, and placing any embryos into the uterus. Intra-cytoplasmic sperm injection (ICSI sperm): ICSI can be used to treat male infertility disorders, such as low sperm count, low sperm motility, abnormally shaped sperm, or azoospermia (complete absence of sperm in the man s ejaculate). In a dish in the lab, sperm is injected into the egg to fertilize it, rather than letting it penetrate the egg naturally. Embryos are transferred to the uterus. Intrauterine: inside the uterus. IUI: intrauterine insemination. A procedure, which involves placing sperm inside a women s uterus to facilitate fertilization. Laparoscopy: a small cut is made in the skin, and a scope with a light on the end is placed inside the abdomen. Microfertilization (egg drilling or tweaking): this technique creates a cut in the egg, so that sperm can get in more easily. A subzonal microinjection places the sperm between the egg and it s outer covering, and a partial zonal dissection cuts the egg before it is incubated with sperm. In either case, embryos are transferred from the lab dish into the uterus. Microsurgical epididymal sperm aspiration (MESA): in men who were born without a vas deferens, there is no way for sperm to reach the penis. This procedure places a needle into the testicle area to aspirate sperm for fertilization. Natural oocyte retrieval (NORIVF): harvesting eggs from the ovary, when the egg has ovulated naturally. Obstruction: blockage. Oocyte: egg. Ovulation: the monthly process of eggs released from the ovaries. Sperm penetration assay: lab test designed to check the ability of sperm to enter eggs. Other terms for this test are the heterologous ovum penetration test, and hamster ovum test. A hamster egg (ovum) is used as the target, and sperm are placed in a dish with these eggs for several hours. The number of eggs with sperm penetration is counted, and the semen sample is rated as fertile or non-fertile. Spermatozoa: a mature male germ cell, the specific output of the testes. It is the generative element of the semen, which serves to fertilize the ovum, and contains the genetic information to be transmitted to the zygote by the male.
12 Vas deferens: tube connecting the testicles to the penis. Sperm travels along this path during ejaculation. Voluntary sterilization: choosing to undergo a process that makes a person unable to reproduce (e.g., tubal ligation (tubes tied) in women or vasectomy in males. Zygote intra-fallopian transfer (ZIFT): a form of IVF. Eggs are harvested and fertilized in a dish in the laboratory. The fertilized egg is placed inside the fallopian tube. Zygote: a fertilized egg that has not yet divided. RELATED GUIDELINES: None applicable. OTHER: Coverage for office visits, and infertility diagnostic services (e.g., diagnostic procedures to determine the cause of infertility (diagnosis), and laboratory procedures) are covered services if the member has a benefit to cover these services. Other names used to report infertility: Assisted Oocyte Fertilization (AOF), formerly known as ICSI Assisted Hatching Assisted Oocyte Fertilization Assisted Reproductive Technologies (ART) Blastocyst Transfer Cryopreserved Embryo Transfer (CET) Electroejaculation Gamete Intrafallopian Transfer (GIFT) Intracytoplasmic Sperm Injection (ICSI) In Vitro Fertilization (IVF) Natural Oocyte Retrieval (NORIVF) Zygote Intrafallopian Transfer (ZIFT). REFERENCES: 1. American College of Obstetricians and Gynecologists Committee Opinion No. 584: oocyte cryopreservation. Obstetrics & Gynecology 2014 Jan;123(1):221-2, Reaffirmed American Society for Reproductive Medicine, Report on Management of Obstructive Azoospermia, American Urological Association (AUA), Inc.-Infertility Report on Evaluation of the Azoospermic Male (An AUA Best Practice Policy and American Society of Reproductive Medicine (ASRM) Practice committee Report), Bahadur G, Chatterjee R, Ralph D. Testicular Tissue Cryopreservation in Boys. Ethical and Legal Issues: Case Report. Human Reproduction 2000; 15: Blue Cross Blue Shield Association Medical Policy Reference Manual Assisted Reproductive Technologies, 08/18.
13 6. D Angelo A, Amso N, Embryo Freezing for Preventing Ovarian Hyperstimulation Syndrome, 02/27/ Donnez J, Dolmans MM, Dennylle D et al. Live birth After Orthotopic Transplantation of Cryopreserved Ovarian Tissue. Lancet 2004; 364(9443): Glujovsky D. Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology. Cochrane Database Syst Rev Goodwin PJ, Oktay KH, Lobo RA. Options for Preservation of Fertility in Women. New England Journal of Medicine 2005; (Correspondence). 10. Kaur P, Swarankar ML, Maheshwari M et al. A comparative study between cleavage stage embryo transfer at day 3 and blastocyst stage transfer at day 5 in in-vitro fertilization/intra-cytoplasmic sperm injection on clinical pregnancy rates. Journal of Human Reproductive Sciences 2014 Jul;7(3): Lee SJ, Schover LR, Patridge AH. American Society of Clinical Oncology Recommendations on Fertility Preservation in Cancer Patients. Journal of Clinical Oncology 2006; 24(18): Lobo RA. Current Concepts: Potential Options for Preservation of Fertility in Women. New England Journal of Medicine 2005; Meirow D, Levron J, Eldar-Geva T et al. Pregnancy After Transplantation of Cryopreserved Ovarian Tissue in a Patient with Ovarian Failure After Chemotherapy. New England Journal of Medicine 2005; (Correspondence). 14. Myers ER, McCrory DC, Mills AA, Price TM, Swamy GK, Tantibhedhyangkul J, Wu JM, Matchar DB. Effectiveness of Assisted Reproductive Technology. Evidence Report/Technology Assessment No. 167 (Prepared by the Duke University Evidence-based Practice Center under Contract No ) AHRQ Publication No. 08-E012. Rockville, MD: Agency for Healthcare Research and Quality. May Oatway C, Gunby J Daya S. Day Three Versus Day Two Embryo Transfer Following In Vitro Fertilization or Intracytoplasmic Sperm Injection. Cochrane Database of Systematic Reviews 2004, Issue Oktay K, Buyuk E, Veeck L et al. Embryo Development After Heterotopic Transplantation of Cryopreserved Ovarian Tissue. Lancet 2004; 363: Palermo G, Joris H, Devroey P. Pregnancies After Intracytoplasmic Injection of Single Spermatozoon Into an Oocyte. The Lancet 1992; 340: Pandian Z, Bhattacharya S, Vale L, Templeton A. In Vitro Fertilization for Unexplained Subfertility. Cochrane Database of Systematic Reviews 2005, Issue Porcu E, Fabbri R, Damiano G et al. Clinical Experience and Applications of Oocyte Cryopreservation. Molecular and Cellular Endocrinology 2000; 169: Practice Committee of the American Society for Reproductive Medicine and Practice Committee of the Society for Assisted Reproductive Technology. Blastocyst culture and transfer in clinical-assisted reproduction. Fertility and Sterility 2008; 90:S Practice Committee of the American Society for Reproductive Medicine and Practice Committee of the Society for Assisted Reproductive Technology. Intracytoplasmic sperm injection (ICSI). Fertility and Sterility 2008; 90: S Practice Committee of the American Society for Reproductive Medicine and the Practice Committee of the Society for Assisted Reproductive Technology. Ovarian tissue and oocyte cryopreservation. Fertility and Sterility 2008; 90: S241-S Practice Committee of the American Society of Reproductive Medicine and Practice Committee of the Society for Assisted Reproductive Technology.The role of assisted hatching in in vitro fertilization: a review of the literature. a committee opinion. Fertility and Sterility 2008; 90: S196-S198.
14 24. Practice Committee of the American Society for Reproductive Medicine and Practice Committee of the Society for Assisted Reproductive Technology. Role of assisted hatching in in vitro fertilization: a guideline. Fertility and Sterility. Aug 2014;102(2): Seif MMW, Edi-Osagie ECO, Farquhar C, Hooper L, Blake D, McGinlay P. Assisted Hatching on Assisted Conception (IVF & ICSI). Cochrane Database of Systematic Reviews 2006, Issue The Ethics committee of the American Society for Reproductive Medicine-Fertility Preservation and Reproduction in Cancer Patients. Fertility and Sterility 2005; 83(6): The National Women s Health Information Center U.S. Department of Health & Human Services- Infertility, 05/ Toledo AA, Wright G, Jones AE et al. Blastocyst Transfer: A Useful Tool for Reduction of High-Order Multiple Gestations in a Human Assisted Reproduction Program. American Journal of Obstetrics and Gynecology 2000; 183(2): COMMITTEE APPROVAL: This Medical Coverage Guideline (MCG) was approved by the BCBSF Medical Policy & Coverage Committee on 09/27/18. GUIDELINE UPDATE INFORMATION: 11/15/00 Medical Coverage Guideline Revised. 01/01/02 Annual HCPCS coding update. 04/01/02 HCPCS changes. 08/15/02 Added CPT codes (89254, 89320, 89321, 89325, 89329, 89330). 01/01/03 Annual review and annual HCPCS coding update. 01/01/04 Annual HCPCS coding update: revise descriptors for the following: 89250, 89251, and Deleted the following: and Added the following: 89268, 89272, 89280, 89281, 89290, 89291, 89335, 89342, 89343, 89344, 89346, 89352, 89353, 89354, and Changed from non-covered to investigational (per BCBSA medical policy). Added 0058T and 0059T (considered investigational). Revised program exception for Medicare & More. 12/15/04 Added code and descriptor under billing/coding information-in vitro laboratory procedures. Deleted code and replace with Deleted covered codes for Medicare & More under program exceptions (Medicare Policy retired). Added code (non-covered) for Medicare & More under program exceptions. Deleted coverage statement for State group and Tropicana & Fowler White.
15 01/01/05 Annual HCPCS coding update: revised code descriptor. Added S /15/05 Deleted ICD-9 diagnoses that support medical necessity. 09/15/05 Added S /15/06 Updated DESCRIPTION section to include information regarding: intracytoplasmic sperm injection (ICSI), assisted hatching, embryo co-culture, cryopreservation of ovarian and testicular tissue and oocytes. Added coverage statement (investigational) regarding storage and thawing of ovarian tissue and oocytes and cryopreservation of testicular tissue to the WHEN SERVICES ARE NOT COVERED section. Revised CPT BILLING/CODING INFORMATION section. Deleted code (invalid code) and (unlisted procedure, male genital system). Added code to list of procedures not covered by Medicare. Added azoospermia and spermatozoa to the DEFINITIONS section. Updated references. 01/01/07 Annual HCPCS coding update: deleted S /15/07 Annual review, coverage statements maintained, guideline reformatted, references updated. 01/01/08 Annual HCPCS coding update: revised and descriptor. Added and /01/09 Annual HCPCS coding update: deleted 0058T and 0059T. Updated references. 12/15/09 Annual review; no change in position statement. Updated references. 01/01/11 Annual HCPCS coding update; added 0058T and 0059T. 12/15/11 Annual review; revised description, member s benefit statement, added information regarding blastocyst transfer to description, updated position statement (added assisting hatching and blastocyst transfer) and updated billing/coding and references. 12/15/12 Annual review; added cryopreservation of testicular tissue in adult men with azoospermia as part of an intracytoplasmic sperm injection procedure, intracytoplasmic sperm injection, blastocyst transfer and updated references. 05/11/14 Revision: Program Exceptions section updated.
16 07/01/14 Quarterly HCPCS update; added 0357T. 01/01/15 Annual HCPCS code update. Deleted 0059T. Added /15/16 Revision: Updated description section. Added statement for diagnostic testing for infertility to position statement section. Added note for infertility and diagnostic testing for infertility to the billing/coding information section. Added for male factor infertility to intracytoplasmic sperm injection. Added including storage and thawing to cryopreservation of testicular tissue experimental or investigational statement. Updated references. 1015/18 Review; Added intracytoplasmic sperm injection in the absence of male factor infertility to experimental or investigational statement. Added sperm to cryopreservation of testicular tissue statement. Revised position statements. Updated references.
Medical Coverage Policy Infertility Services EFFECTIVE DATE:03/01/2017 POLICY LAST UPDATED: 03/06/2018
 Medical Coverage Policy Infertility Services EFFECTIVE DATE:03/01/2017 POLICY LAST UPDATED: 03/06/2018 OVERVIEW The policy addresses medical necessity criteria and coverage guidelines related to the treatment
Medical Coverage Policy Infertility Services EFFECTIVE DATE:03/01/2017 POLICY LAST UPDATED: 03/06/2018 OVERVIEW The policy addresses medical necessity criteria and coverage guidelines related to the treatment
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
INFERTILITY SERVICES
 INFERTILITY SERVICES Protocol: OBG036 Effective Date: August 1, 2018 Table of Contents Page COMMERCIAL COVERAGE RATIONALE... 1 DEFINITIONS... 4 MEDICARE AND MEDICAID COVERAGE RATIONALE... 5 REFERENCES...
INFERTILITY SERVICES Protocol: OBG036 Effective Date: August 1, 2018 Table of Contents Page COMMERCIAL COVERAGE RATIONALE... 1 DEFINITIONS... 4 MEDICARE AND MEDICAID COVERAGE RATIONALE... 5 REFERENCES...
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: PA.018.MH Last Review Date: 08/04/2016 Effective Date: 01/01/2017
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.018.MH Infertility- Treatment This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
Reproductive Techniques
 Reproductive Techniques Policy Number: 4.02.04 Last Review: 12/2018 Origination: 10/1988 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for assisted
Reproductive Techniques Policy Number: 4.02.04 Last Review: 12/2018 Origination: 10/1988 Next Review: 12/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for assisted
Reproductive Techniques
 Reproductive Techniques Policy Number: 4.02.04 Last Review: 12/2017 Origination: 10/1988 Next Review: 12/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for assisted
Reproductive Techniques Policy Number: 4.02.04 Last Review: 12/2017 Origination: 10/1988 Next Review: 12/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for assisted
MEDICAL POLICY No R8 INFERTILITY DIAGNOSIS AND TREATMENT/ ASSISTED REPRODUCTION/ARTIFICIAL CONCEPTION
 INFERTILITY DIAGNOSIS AND TREATMENT/ ASSISTED REPRODUCTION/ARTIFICIAL CONCEPTION Effective Date: June 4, 2015 Review Dates: 1/93, 12/99, 12/01, 11/02, 11/03, 11/04, 10/05, 10/06, 7/07, 6/08, 6/09, 6/10,
INFERTILITY DIAGNOSIS AND TREATMENT/ ASSISTED REPRODUCTION/ARTIFICIAL CONCEPTION Effective Date: June 4, 2015 Review Dates: 1/93, 12/99, 12/01, 11/02, 11/03, 11/04, 10/05, 10/06, 7/07, 6/08, 6/09, 6/10,
Treating Infertility
 Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
Treating Infertility WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 About 10% of couples in the United States are infertile. Infertility is a condition in which a woman has not been able
LISI CARRIERS INFERTILITY COMPARISON
 AETNA Diagnostic services for the diagnosis and treatment of the underlying medical condition, and: Infertility Treatment - AI/OI Advanced Reproductive Technology including but not limited to GIFT, ZIFT,
AETNA Diagnostic services for the diagnosis and treatment of the underlying medical condition, and: Infertility Treatment - AI/OI Advanced Reproductive Technology including but not limited to GIFT, ZIFT,
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Fertility treatment and referral criteria for tertiary level assisted conception Version Number Name of Originator/Author Cross Reference V2 East of England Consortium Commissioning Policy for Fertility
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: PA.017.MH Last Review Date: 08/04/2016 Effective Date: 01/01/2016
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.017.MH Infertility- Diagnosis This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL PA.017.MH Infertility- Diagnosis This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP (Not Covered) MedStar
East and North Hertfordshire CCG. Fertility treatment and referral criteria for tertiary level assisted conception
 East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
East and North Hertfordshire CCG Fertility treatment and referral criteria for tertiary level assisted conception December 2015 1 1. Introduction This policy sets out the entitlement and service that will
ASSISTED REPRODUCTIVE TECHNOLOGIES (ART)
 ASSISTED REPRODUCTIVE TECHNOLOGIES (ART) Dr. Herve Lucas, MD, PhD, Biologist, Andrologist Dr. Taher Elbarbary, MD Gynecologist-Obstetrician Geneva Foundation for Medical Education and research Definitions
ASSISTED REPRODUCTIVE TECHNOLOGIES (ART) Dr. Herve Lucas, MD, PhD, Biologist, Andrologist Dr. Taher Elbarbary, MD Gynecologist-Obstetrician Geneva Foundation for Medical Education and research Definitions
Advanced Assisted Reproductive Technologies
 Advanced Assisted Reproductive Technologies 體外受孕中心 IVF Centre IVF CENTRE at Hong Kong Sanatorium & Hospital The IVF Centre at Hong Kong Sanatorium & Hospital has been offering excellent patient care and
Advanced Assisted Reproductive Technologies 體外受孕中心 IVF Centre IVF CENTRE at Hong Kong Sanatorium & Hospital The IVF Centre at Hong Kong Sanatorium & Hospital has been offering excellent patient care and
Assisted Reproduction. By Dr. Afraa Mahjoob Al-Naddawi
 Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
What to do about infertility?
 What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
What to do about infertility? Dr. M.A. Fischer Section Head, Division of Urology, Department of Surgery Assistant Clinical Professor, Department of Obstetrics and Gynecology Hamilton Health Sciences, Hamilton,
Clinical Policy: Fertility Preservation Reference Number: CP.MP.130
 Clinical Policy: Reference Number: CP.MP.130 Effective Date: 9/16 Last Review Date: 11/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Clinical Policy: Reference Number: CP.MP.130 Effective Date: 9/16 Last Review Date: 11/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and
Reproductive Endocrinology & Infertility Glossary
 Reproductive Endocrinology & Infertility Glossary The following is a glossary of terms you may hear during your association with the University of Mississippi Health Care's reproductive endocrinology and
Reproductive Endocrinology & Infertility Glossary The following is a glossary of terms you may hear during your association with the University of Mississippi Health Care's reproductive endocrinology and
Fertility Services Commissioning Policy
 Fertility Services Commissioning Policy Author: Commissioning Team Version No: Two Policy Effective From: 29 September 2016 Review Date: September 2017 Policy Amendment: 02 August 2017 Document Reader
Fertility Services Commissioning Policy Author: Commissioning Team Version No: Two Policy Effective From: 29 September 2016 Review Date: September 2017 Policy Amendment: 02 August 2017 Document Reader
Puerto Rico Fertility Center
 Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Male Fertility: Your Questions Answered
 Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Male Fertility: Your Questions Answered Michael S. Neal Scientific Director, ONE Fertility, 3210 Harvester Rd. Burlington, Ontario www.onefertility.com mneal@onefertility.com Outline Assisted Conception
Intrauterine (IUI) and Donor Insemination (DI) Policy (excluding In vitro fertilisation (IVF) & Intracytoplasmic sperm injection (ICSI) treatment)
 Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Leicester City Clinical Commissioning Group West Leicestershire Clinical Commissioning Group East Leicestershire and Rutland Clinical Commissioning Group POLICY DOCUMENT Intrauterine (IUI) and Donor Insemination
Fertility 101. About SCRC. A Primary Care Approach to Diagnosing and Treating Infertility. Definition of Infertility. Dr.
 Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Fertility Assisted Conception Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives
 NHS Dorset Clinical Commissioning Group Fertility Assisted Conception Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives POLICY TRAIL AND VERSION CONTROL SHEET: Policy Reference:
NHS Dorset Clinical Commissioning Group Fertility Assisted Conception Criteria Based Access Protocol Supporting people in Dorset to lead healthier lives POLICY TRAIL AND VERSION CONTROL SHEET: Policy Reference:
Chris Davies & Greg Handley
 Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
Chris Davies & Greg Handley Contents Definition Epidemiology Aetiology Conditions for pregnancy Female Infertility Male Infertility Shared infertility Treatment Definition Failure of a couple to conceive
LCCG Fertility Services Commissioning Policy
 LCCG Fertility Services Commissioning Policy Author: Emma Dwyer & Dr Fiona Sim Version No: V.4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces all previous versions.
LCCG Fertility Services Commissioning Policy Author: Emma Dwyer & Dr Fiona Sim Version No: V.4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces all previous versions.
PROCEDURES LAPAROSCOPY
 PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
PROCEDURES - Further infertility work-up if indicated (ultrasound examination / semen decontamination etc.) - Office Hysteroscopy where indicated - Laparoscopic and /or hysteroscopic surgery where indicated
Infertility. F r e q u e n t l y A s k e d Q u e s t i o n s. Q: What causes infertility in men? A: Infertility in men is most often caused by:
 Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Infertility Q: What is infertility? A: Infertility means not being able to get pregnant after one year of trying. Or, six months, if a woman is 35 or older. Women who can get pregnant but are unable to
Fertility treatment and referral criteria for tertiary level assisted conception
 Fertility treatment and referral criteria for tertiary level assisted conception Version Number 2.0 Ratified by HVCCG Exec Team Date Ratified 9 th November 2017 Name of Originator/Author Dr Raj Nagaraj
Fertility treatment and referral criteria for tertiary level assisted conception Version Number 2.0 Ratified by HVCCG Exec Team Date Ratified 9 th November 2017 Name of Originator/Author Dr Raj Nagaraj
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: infertility_diagnosis_and_treatment 1/2000 9/2017 9/2018 9/2017 Description of Procedure or Service Infertility
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: infertility_diagnosis_and_treatment 1/2000 9/2017 9/2018 9/2017 Description of Procedure or Service Infertility
Getting Help for Obstructive Azoospermia A BASIC GUIDE TO MALE. A doctor s guide for patients developed by the American Urological Association, Inc.
 A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
A BASIC GUIDE TO MALE Getting Help for Obstructive Azoospermia A doctor s guide for patients developed by the American Urological Association, Inc. Based on the AUA Best Practice Policy and ASRM Practice
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
Infertility. Thomas Lloyd and Samera Dean
 Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Information Booklet. Exploring the causes of infertility and treatment options.
 Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
COMMISSIONING POLICY. Tertiary treatment for assisted conception services
 Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Final Version COMMISSIONING POLICY Tertiary treatment for assisted conception services Designated providers for patients registered with a Worcestershire GP BMI The Priory Hospital, Birmingham - 1 - Commissioning
Clinical Policy: Assisted Reproductive Technology
 Clinical Policy: Reference Number: CP.MP.55 Last Review Date: 03/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Clinical Policy: Reference Number: CP.MP.55 Last Review Date: 03/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Independent Review of Assisted Reproductive Technologies
 Assisted Reproductive Technologies Review Committee Report of the Independent Review of Assisted Reproductive Technologies APPENDICES Assisted Reproductive Technologies Review Committee APPENDIX A February
Assisted Reproductive Technologies Review Committee Report of the Independent Review of Assisted Reproductive Technologies APPENDICES Assisted Reproductive Technologies Review Committee APPENDIX A February
NHS FUNDED TREATMENT FOR SUBFERTILITY. ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs
 NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA POLICY GUIDANCE/OPTIONS FOR CCGs CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO
INFERTILITY. Services - Part 2
 INFERTILITY Services - Part 2 1 Imprint Published in January, 2013 By Victory A.R.T. Laboratory Phils, Inc. These articles were compiled by in hopes of helping bring into light infertility questions and
INFERTILITY Services - Part 2 1 Imprint Published in January, 2013 By Victory A.R.T. Laboratory Phils, Inc. These articles were compiled by in hopes of helping bring into light infertility questions and
Wiltshire CCG Fertility Policy
 Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
Wiltshire CCG Fertility Policy Introduction This policy sets out the limits within which WCCG will fund treatment with either Intrauterine Insemination [IUI], ovulation induction medication or donor insemination
Policy statement. Commissioning of Fertility treatments
 Policy statement Commissioning of Fertility treatments NB: The policy relating to commissioning of fertility treatments is unchanged from the version approved by the CCG in March 2017. The clinical thresholds
Policy statement Commissioning of Fertility treatments NB: The policy relating to commissioning of fertility treatments is unchanged from the version approved by the CCG in March 2017. The clinical thresholds
Blackpool CCG. Policies for the Commissioning of Healthcare. Assisted Conception
 1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
1 Introduction Blackpool CCG Policies for the Commissioning of Healthcare Assisted Conception 1.1 This policy describes circumstances in which NHS Blackpool Clinical Commissioning Group (CCG) will fund
NHS WEST ESSEX CLINICAL COMMISSIONING GROUP. Fertility Services Commissioning Policy Policy No. WECCG89. This policy replaces all previous versions.
 NHS WEST ESSEX CLINICAL COMMISSIONING GROUP Fertility Services Commissioning Policy Policy No. WECCG89 Description This policy replaces all previous versions. This policy sets out the entitlement and service
NHS WEST ESSEX CLINICAL COMMISSIONING GROUP Fertility Services Commissioning Policy Policy No. WECCG89 Description This policy replaces all previous versions. This policy sets out the entitlement and service
HALTON CLINICAL COMMISSIONING GROUP NHS FUNDED TREATMENT FOR SUBFERTILITY. CONTENTS Page
 HALTON CLINICAL COMMISSIONING GROUP NHS FUNDED TREATMENT FOR SUBFERTILITY CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO TREATMENT 3 4. DEFINITION
HALTON CLINICAL COMMISSIONING GROUP NHS FUNDED TREATMENT FOR SUBFERTILITY CONTENTS Page 1. INTRODUCTION 2 2. GENERAL PRINCIPLES 2 3. DEFINITION OF SUBFERTILITY AND TIMING OF ACCESS TO TREATMENT 3 4. DEFINITION
Infertility. Review and Update Clifford C. Hayslip MD Intrauterine Inseminations
 Infertility Review and Update Clifford C. Hayslip MD Intrauterine Inseminations Beneficial effects of IUI not consistently documented in studies No deleterious effects on fertility 3-4 cycles of IUI should
Infertility Review and Update Clifford C. Hayslip MD Intrauterine Inseminations Beneficial effects of IUI not consistently documented in studies No deleterious effects on fertility 3-4 cycles of IUI should
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE
 ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
ASSISTED CONCEPTION NHS FUNDED TREATMENT FOR SUBFERTILITY ELIGIBILITY CRITERIA & POLICY GUIDANCE Version 1.0 Page 1 of 11 MARCH 2014 POLICY DOCUMENT VERSION CONTROL CERTIFICATE TITLE Title: Assisted Conception
St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16
 St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16 1 Standard Operating Procedure St Helens CCG NHS Funded Treatment for Sub Fertility Policy Version 1 Implementation Date May 2015 Review
St Helens CCG NHS Funded Treatment for Subfertility Policy 2015/16 1 Standard Operating Procedure St Helens CCG NHS Funded Treatment for Sub Fertility Policy Version 1 Implementation Date May 2015 Review
Reversible Conditions Organising More Information semen analysis Male Infertility at Melbourne IVF Fertility Preservation
 Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
Male Infertility Understanding fertility in men Conceiving a baby depends on a number of factors, including healthy sperm. After a woman s age, this can be the biggest issue. Reproduction, although simple
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES
 COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES Version number V2.3 Responsible individual Author(s) Barry Weaver Trish
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES Version number V2.3 Responsible individual Author(s) Barry Weaver Trish
Contents Overview... 2 Coverage Guidelines... 2 MassHealth, and Certain Custom Plans... 2 Covered Services/Procedures... 2
 Medical Policy Infertility Services Document Number: 002 *Commercial MassHealth and Qualified Health Plans Authorization required X Notification within 24 hours or the next business day No notification
Medical Policy Infertility Services Document Number: 002 *Commercial MassHealth and Qualified Health Plans Authorization required X Notification within 24 hours or the next business day No notification
Medical Policy Infertility Services
 Medical Policy Infertility Services Document Number: 002 *Commercial and Qualified Health Plans MassHealth Authorization required X No notification or authorization Not covered X *Not all commercial plans
Medical Policy Infertility Services Document Number: 002 *Commercial and Qualified Health Plans MassHealth Authorization required X No notification or authorization Not covered X *Not all commercial plans
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.
 COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.3 2017 Agreed at Cannock Chase CCG Signature: Designation: Chair of
COMMISSIONING POLICY FOR IN VITRO FERTILISATION (IVF)/ INTRACYTOPLASMIC SPERM INJECTION (ICSI) WITHIN TERTIARY INFERTILITY SERVICES V2.3 2017 Agreed at Cannock Chase CCG Signature: Designation: Chair of
WHAT IS A PATIENT CARE ADVOCATE?
 WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
WHAT IS A PATIENT CARE ADVOCATE? Fertility treatments can be overwhelming. As a member, you have unlimited access to a dedicated Patient Care Advocate (PCA), who acts as your expert resource for discussing
Assisted Conception Policy
 Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
Assisted Conception Policy NHS Eligibility Criteria for assisted conception services (excluding In vitro fertilisation (IVF) Intracytoplasmic sperm injection (ICSI) treatment) for people with infertility
MEDICAL POLICY Infertility and Reproductive Services
 POLICY: PG0098 ORIGINAL EFFECTIVE: 01/01/09 LAST REVIEW: 02/13/18 MEDICAL POLICY Infertility and Reproductive Services GUIDELINES This policy does not certify benefits or authorization of benefits, which
POLICY: PG0098 ORIGINAL EFFECTIVE: 01/01/09 LAST REVIEW: 02/13/18 MEDICAL POLICY Infertility and Reproductive Services GUIDELINES This policy does not certify benefits or authorization of benefits, which
Bringing Life to the Living
 Bringing Life to the Living ReGenesis Where Life Begins Centre for Assisted Reproduction, Endoscopy and Fetal Medicine Traditionally, infertility is defined as the inability to conceive for more than two
Bringing Life to the Living ReGenesis Where Life Begins Centre for Assisted Reproduction, Endoscopy and Fetal Medicine Traditionally, infertility is defined as the inability to conceive for more than two
INDICATIONS OF IVF/ICSI
 PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
Possibilities Plan. Access to the care you need.
 Possibilities Plan If you do not have insurance or have insurance but lack coverage for infertility services and are concerned about the cost of infertility services, The Center for Advanced Reproductive
Possibilities Plan If you do not have insurance or have insurance but lack coverage for infertility services and are concerned about the cost of infertility services, The Center for Advanced Reproductive
MEDICAL POLICY SUBJECT: ASSISTED REPRODUCTIVE TECHNOLOGIES FOR INFERTILITY
 MEDICAL POLICY Retrospective effective date: 01/01/16 PAGE: 1 OF: 13 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
MEDICAL POLICY Retrospective effective date: 01/01/16 PAGE: 1 OF: 13 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
Health Service System City & County of San Francisco
 Health Service System City & County of San Francisco Health Service Board Meeting Infertility Coverage January 12, 2017 Prepared by: Infertility Infertility is defined as not being able to get pregnant
Health Service System City & County of San Francisco Health Service Board Meeting Infertility Coverage January 12, 2017 Prepared by: Infertility Infertility is defined as not being able to get pregnant
DESTINATION :FAMILY. Reproductive Services TABLE OF CONTENTS
 DESTINATION :FAMILY Reproductive Services TABLE OF CONTENTS Which doctor should I choose? What resources are available to help me? What is covered? How will I afford treatment? What can I do to help prepare
DESTINATION :FAMILY Reproductive Services TABLE OF CONTENTS Which doctor should I choose? What resources are available to help me? What is covered? How will I afford treatment? What can I do to help prepare
OUR CENTER HISTORY THE FERTIVITRO
 OUR CENTER - HISTORY THE FERTIVITRO The Center for Human Reproduction FERTIVITRO that was founded in March, 2001 has the goal to increase the number of success cases in the area of infertility treatments.
OUR CENTER - HISTORY THE FERTIVITRO The Center for Human Reproduction FERTIVITRO that was founded in March, 2001 has the goal to increase the number of success cases in the area of infertility treatments.
Recent Developments in Infertility Treatment
 Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Clinical Policy: Fertility Preservation
 Clinical Policy: Reference Number: CP.MP.130 Last Review Date: 09/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Clinical Policy: Reference Number: CP.MP.130 Last Review Date: 09/18 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description
Reproductive Technology, Genetic Testing, and Gene Therapy
 Michael Cummings Chapter 16 Reproductive Technology, Genetic Testing, and Gene Therapy David Reisman University of South Carolina 16.1 Infertility Is a Common Problem In the US, about 13% of all couples
Michael Cummings Chapter 16 Reproductive Technology, Genetic Testing, and Gene Therapy David Reisman University of South Carolina 16.1 Infertility Is a Common Problem In the US, about 13% of all couples
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
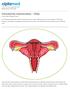 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
IVF. NHS North West London CCGs
 IVF NHS North West London CCGs Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services Adopted by NWL CCGs to be effective from
IVF NHS North West London CCGs Commissioning Policy for In Vitro Fertilisation (IVF)/ Intracytoplasmic Sperm Injection (ICSI) within tertiary Infertility Services Adopted by NWL CCGs to be effective from
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition
 Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
Consent for In Vitro Fertilization (IVF), Intracytoplasmic Sperm Injection (ICSI), and Embryo Cryopreservation/Disposition Patient Name (please print) Patient DOB (MM/DD/YYYY) Patient eivf number Partner
Section III Consent Forms
 Section III Consent Forms Please read the consents prior to your IVF consultation appointment. Most people have questions regarding the consent forms. Your questions will be addressed during the appointment.
Section III Consent Forms Please read the consents prior to your IVF consultation appointment. Most people have questions regarding the consent forms. Your questions will be addressed during the appointment.
Always placing innovation and excellence at the heart of our strategy, clinique ovo aims to meet your expectations and support your family project.
 Always placing innovation and excellence at the heart of our strategy, clinique ovo aims to meet your expectations and support your family project. Since 2003, ovo fertility offers comprehensive assisted
Always placing innovation and excellence at the heart of our strategy, clinique ovo aims to meet your expectations and support your family project. Since 2003, ovo fertility offers comprehensive assisted
Assisted Reproductive Technologies
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Assisted Reproductive Technologies A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Assisted Reproductive Technologies A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction
Androgens Hormones that are produced by the testes of the male and in small amounts by the ovaries and adrenal glands of the female.
 http://www.myfertility.ca/glossary.xhtml (February 27, 2015) Glossary Acrosome This is a membrane-bound cap-like structure found at the head of the sperm. It contains enzymes that are thought to help the
http://www.myfertility.ca/glossary.xhtml (February 27, 2015) Glossary Acrosome This is a membrane-bound cap-like structure found at the head of the sperm. It contains enzymes that are thought to help the
INSEMINATION IUI. Engelsk Info IUI ~ 1 ~
 Engelsk Info IUI ~ 1 ~ INSEMINATION IUI Engelsk Info IUI ~ 2 ~ In cases of unexplained infertility, irregular periods, ovulatory dysfunction or poor sperm quality, insemination of sperm cells directly
Engelsk Info IUI ~ 1 ~ INSEMINATION IUI Engelsk Info IUI ~ 2 ~ In cases of unexplained infertility, irregular periods, ovulatory dysfunction or poor sperm quality, insemination of sperm cells directly
Reproductive Medicine Module 4a: Subfertility and Assisted Conception 4a: General Subfertility
 Reproductive Medicine Module 4a: Subfertility and Assisted Conception 4a: General Subfertility = Not required Pathology/Immunology/Anatomy Uterus, tubes, ovaries Adrenal/thyroid Pituitary Testis Investigation
Reproductive Medicine Module 4a: Subfertility and Assisted Conception 4a: General Subfertility = Not required Pathology/Immunology/Anatomy Uterus, tubes, ovaries Adrenal/thyroid Pituitary Testis Investigation
Assisted Reproductive Technologies
 Assisted Reproductive Technologies Textbook pages 224 231 Section 6.3 Summary Before You Read What do you think the phrase test-tube baby refers to? Write your ideas on the lines below. Mark the Text Check
Assisted Reproductive Technologies Textbook pages 224 231 Section 6.3 Summary Before You Read What do you think the phrase test-tube baby refers to? Write your ideas on the lines below. Mark the Text Check
Chapter 7 Infertility, Contraception, and Abortion
 Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
FACT SHEET. Failure of Ovulation Blocked or Damaged Fallopian TubesHostile Cervical Mucus Endometriosis Fibroids
 FACT SHEET Overview of infertility If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the Lithuania are infertile. Infertility is defined
FACT SHEET Overview of infertility If getting pregnant has been a challenge for you and your partner, you're not alone. Ten to 15 percent of couples in the Lithuania are infertile. Infertility is defined
Fertility Services Commissioning Policy
 Fertility Services Commissioning Policy NEE CCG Policy Reference: Where patients have commenced treatment in any cycle prior to this version becoming effective, they are subject to the eligibility criteria
Fertility Services Commissioning Policy NEE CCG Policy Reference: Where patients have commenced treatment in any cycle prior to this version becoming effective, they are subject to the eligibility criteria
Lecture 14: Conception, Fertility, Early Fetal Loss. provera. Depo-provera. Early Fetal Loss. Implanon. Norplant. Nuva Ring.
 Lecture 14: Conception, Fertility, Early Fetal Loss Birth Control (cont.) Conception What Influences Probability of Conception? Early Fetal Loss Infertility Fertility Enhancement Depo-provera provera Injectable
Lecture 14: Conception, Fertility, Early Fetal Loss Birth Control (cont.) Conception What Influences Probability of Conception? Early Fetal Loss Infertility Fertility Enhancement Depo-provera provera Injectable
Fertility Policy. December Introduction
 Fertility Policy December 2015 Introduction Camden Clinical Commissioning Group (CCG) is responsible for commissioning a range of health services including hospital, mental health and community services
Fertility Policy December 2015 Introduction Camden Clinical Commissioning Group (CCG) is responsible for commissioning a range of health services including hospital, mental health and community services
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 Cryopreservation to preserve e fertility in people diagnosed with cancer bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They
Cryopreservation to preserve e fertility in people diagnosed with cancer bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They
College of Physicians and Surgeons of Saskatchewan STANDARDS. Assisted Reproductive Technology PREAMBLE
 College of Physicians and Surgeons of Saskatchewan STANDARDS Assisted Reproductive Technology STATUS: UNDER REVIEW Approved by Council: September 2012 Amended: November 2015 To be reviewed: November 2020
College of Physicians and Surgeons of Saskatchewan STANDARDS Assisted Reproductive Technology STATUS: UNDER REVIEW Approved by Council: September 2012 Amended: November 2015 To be reviewed: November 2020
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
I would be happy to discuss all of these options for fertility after vasectomy with you at the time of our consultation or over the phone.
 F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
F Sperm Aspiration We perform and, in fact, are pioneers in sperm aspiration here at The New York Presbyterian Hospital-Cornell Medical Center. Sperm aspiration involves extraction of sperm from either
Appendix 1: Specialist Fertility Services Commissioning Policy
 Appendix 1: Specialist Fertility Services Commissioning Policy Author: EoE CCG Fertility Consortium Version No: 4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces
Appendix 1: Specialist Fertility Services Commissioning Policy Author: EoE CCG Fertility Consortium Version No: 4 Policy Effective from: 1 st December 2014 Review Date: December 2015 This policy replaces
Fertility Services Commissioning Policy (Level 3)
 Fertility Services Commissioning Policy (Level 3) Author: Karin Bryant (Norwich CCG) has coordinated the refresh of policy Version No: V54 Policy Effective from: TBC Review Date: TBC This policy replaces
Fertility Services Commissioning Policy (Level 3) Author: Karin Bryant (Norwich CCG) has coordinated the refresh of policy Version No: V54 Policy Effective from: TBC Review Date: TBC This policy replaces
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE. Anatomy : Male and Female genital tract
 POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Haringey CCG Fertility Policy April 2014
 Haringey CCG Fertility Policy April 2014 1 SUMMARY This policy describes the clinical pathways and entry criteria for Haringey patients wishing to access NHS funded fertility treatment. 2 RESPONSIBLE PERSON:
Haringey CCG Fertility Policy April 2014 1 SUMMARY This policy describes the clinical pathways and entry criteria for Haringey patients wishing to access NHS funded fertility treatment. 2 RESPONSIBLE PERSON:
Realizing dreams booklet.indd 1 5/20/ :26:52 AM
 Realizing dreams. 18891booklet.indd 1 5/20/2010 11:26:52 AM The Journey To Parenthood The first Gator Baby was born in 1988 through the in vitro fertilization program at the University of Florida. Since
Realizing dreams. 18891booklet.indd 1 5/20/2010 11:26:52 AM The Journey To Parenthood The first Gator Baby was born in 1988 through the in vitro fertilization program at the University of Florida. Since
DRAFT Policy for the Provision of NHS funded Gamete Retrieval and Cryopreservation for the Preservation of Fertility
 NHS Birmingham and Solihull Clinical Commissioning Group NHS Sandwell and West Birmingham Clinical Commissioning Group DRAFT Policy for the Provision of NHS funded Gamete Retrieval and Cryopreservation
NHS Birmingham and Solihull Clinical Commissioning Group NHS Sandwell and West Birmingham Clinical Commissioning Group DRAFT Policy for the Provision of NHS funded Gamete Retrieval and Cryopreservation
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Fertility Services Commissioning Policy
 Fertility Services Policy Author: EOE CCGs Fertility Consortia Version No: Policy Effective from: 01 December 2014 Review Date: 01 December 2016 This policy replaces all versions. Where patients have commenced
Fertility Services Policy Author: EOE CCGs Fertility Consortia Version No: Policy Effective from: 01 December 2014 Review Date: 01 December 2016 This policy replaces all versions. Where patients have commenced
OVERVIEW AND FACTS: CRYOPRESERVATION
 OVERVIEW AND FACTS: CRYOPRESERVATION Imprint Published in August, 2013 By Victory A.R.T. Laboratory Phils, Inc. This ebook was created by http://www.ivfvictoryphilippines.com/ in hopes of helping bring
OVERVIEW AND FACTS: CRYOPRESERVATION Imprint Published in August, 2013 By Victory A.R.T. Laboratory Phils, Inc. This ebook was created by http://www.ivfvictoryphilippines.com/ in hopes of helping bring
