AFTER A STROKE, PEOPLE develop multiple impairments
|
|
|
- June Johnston
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Walking Recovery After an Acute Stroke: Assessment With a New Functional Classification and the Barthel Index Enrique Viosca, PhD, MD, Rubén Lafuente, PhD, José L. Martínez, MD, Pedro L. Almagro, MD, Antonio Gracia, MD, Carmen González, MD ABSTRACT. Viosca E, Lafuente R, Martínez JL, Almagro PL, Gracia A, González C. Walking recovery after an acute stroke: assessment with a new functional classification and the Barthel Index. Arch Phys Med Rehabil 2005;86: Objectives: To investigate walking recovery after an acute stroke by using both a new functional classification and the Barthel Index, and to identify factors associated with good recovery. Design: A 1-year inception cohort study. Setting: In- and outpatient setting in a district hospital. Participants: Twenty-six patients with a prognosis of intermediate walking recovery. Intervention: Conventional physical rehabilitation under professional supervision. Main Outcome Measures: Walking capacity was assessed with a new classification scale and the Barthel Index during 5 patient evolution stages (admission to the hospital, hospital and physiotherapy discharge, clinical review, end of study). We also assessed the severity of the paresis of the affected lower limb, the time lapse between the stroke until the recovery of the weight-bearing capacity of the affected leg, and finally the time until standing balance was regained. Results: We detected improvement in walking capacity throughout the follow-up process with our new classification scale, but not with the Barthel Index. Significant improvements were observed from the initial assessment, from 1 month onward, and from 3 to 12 months. The functional level of the final ambulation correlated negatively and significantly with the initial time to achieve weight-bearing capacity on the affected leg and also with the standing balance. There was also a significant correlation with the severity of lower-extremity paresis. Conclusions: Patients experienced an improvement in walking recovery throughout the first year after their stroke. The early weight-bearing capacity of the affected leg and standing balance were associated with higher walking levels 1 year after the stroke. Key Words: Cerebrovascular accident; Gait; Rehabilitation; Stroke; Walking by American Congress of Rehabilitation Medicine and the American Academy of Physical Medicine and Rehabilitation From the Departments of Physical Medicine and Rehabilitation (Viosca, Martínez, Almagro, Gracia) and Preventive Medicine (González), Hospital de Sagunt y C.E.; and the Instituto de Biomecánica de Valencia (Lafuente), Puerto de Sagunto, Valencia, Spain. Presented to the II Mediterranean Congress of Physical Medicine and Rehabilitation, May 20 23, 1998, Valencia, Spain. No commercial party having a direct financial interest in the results of the research supporting this article has or will confer a benefit upon the author(s) or upon any organization with which the author(s) is/are associated. Reprint requests to Enrique Viosca, PhD, MD, Hospital de Sagunt y C.E., Servicio de Rehabilitación, Av Ramón y Cajal s/n, 46520, Puerto de Sagunto, Valencia, Spain, eviosca@ibv.upv.es /05/ $30.00/0 doi: /j.apmr AFTER A STROKE, PEOPLE develop multiple impairments and disabilities (eg, motor deficits, difficulties in activities of daily living, sphincter muscle control, perceptive faculties, communication and cognitive capacities, mobility, walking problems), 1 all of which must be considered to adequately assess rehabilitation outcomes. Thus, clinicians tend to use an overall functional index that provides a comprehensive view of a patient s status. The Barthel Index and the FIM instrument are examples of such an index, although many more exist. 2,3 However, one of the most valued and important aspects for patients and relatives is the patient s recovery of walking function. This is probably because changes in walking function are among the most frequent causes for physical dependency in these patients. 4 Because no specific and commonly accepted walking assessment tool is available, many published studies of poststroke gait recovery are based on the Barthel Index score for walking, the FIM motor score, or other global functional scales. 5 There are other specific methods, such as the Functional Ambulation Classification (FAC), which includes 6 categories (4 for dependent walking, 2 for independent walking), or the protocol adopted in Gothenburg at the 1971 World Health Organization (WHO) meeting on Community Control of Stroke and Hypertension, which includes 3 grades. However, all these methods could be summarized into 3 categories for walking that are similar to those of Barthel Index score (no walking function, dependent walking, independent walking). 6-8 On the basis of the results obtained with these methods, it would appear that walking recovery only happens between 3 to 6 months after a stroke. 8,9 However, these data do not coincide with our clinical observations or with those of other authors Among the possible reasons for this discrepancy could be the short-term follow-up of the studies and/or the lack of sensitivity of the Barthel Index (and similar methods) to detect clinical changes in walking recovery. This is known as the ceiling effect and occurs particularly in the first 6 months after the stroke. 6,9 Our objective in this study was to investigate walking recovery in a group of postacute stroke subjects by using a new functional ambulation classification scale that we developed and validated. 13 The scale is both specific and sensitive in detecting clinical ambulation changes. We compared our results with those obtained by using the Barthel Index. This study included a 1-year follow-up. Furthermore, as a secondary goal, we also searched for factors associated with a good walking recovery prognosis, especially those reported in the literature, such as standing balance, the severity of lower-extremity paresis, and the capacity of weight bearing on the affected leg. 5-7 METHODS We conducted a prospective study with 41 consecutive hemiplegic patients who were referred to our rehabilitation unit after an acute stroke. Most were inpatients in the rehabilitation ward of a district hospital, and all were diagnosed by a neu-
2 1240 WALKING RECOVERY AFTER ACUTE STROKE, Viosca rologist according to the WHO definition of stroke. Computed tomography scans confirmed the diagnosis; we divided the patients into infarction or hemorrhage subgroups. All patients signed informed consent forms before participating in the study. Patients Selection Our inclusion criteria were the following. One, all patients were either hemiparetic or hemiplegic, unable to walk or had impaired walking capacity, and who were admitted to rehabilitation after their medical condition stabilized. Two, patients had to be conscious and oriented. They had to show an ability to follow simple instructions and had to take an active role in physiotherapy (PT). Finally, patients had to be able to maintain seating balance. This was assessed on their admission to the rehabilitation unit and was considered to be positive when the patient was able to sit on the side of the hospital bed for 5 seconds without needing any back support. However, patients were allowed to place their hands on their lap or on the bed. Patients were excluded if they had had a previous stroke (even if their recovery was complete), had a swift or complete walking recovery in the first week after the stroke, or had had an incomplete follow-up in clinical check-ups. Our intention was to select a middle band of stroke patients with an intermediate prognosis from a walking recovery point of view, who were most likely to derive maximum benefit from rehabilitation. We therefore discarded the data on those patients with the best and the worst walking recovery prognosis, according to our own experience and that of others A prospective cohort study of 41 patients was undertaken over a 9-month period. Three patients were excluded because of a previous stroke, and 2 were excluded because they were unable to maintain sitting balance. Another 4 were excluded because of their swift recovery of walking ability, and 6 were disqualified because of incomplete follow-up (2 were transferred to another hospital). The remaining 26 patients comprised our study sample and were followed for 1 year poststroke. From the total number of cases, 19 remained in the rehabilitation ward for 23 9 days (mean standard deviation [SD]) after being admitted to the neurology service, where they had remained for an average of days. Another 7 patients started the outpatient rehabilitation program. During follow-up, 1 suffered another stroke 10 months later and was then excluded from the study in later sessions. Procedures We performed 5 clinical study sessions for all patients throughout the 12-month follow-up to analyze the temporal evolution of different variables being studied. These reviews coincided with clinically relevant events, when clinical-therapeutic decisions were made (table 1). Thus, session 0 (S0) coincided with the time each patient was selected to be included in the study group, which, in most cases, coincided with admission to the rehabilitation ward. Session 1 (S1) corresponded to their hospital discharge. Session 2 (S2) took place during the first outpatient visit (this often occurred on completion of PT). Session 3 (S3) coincided with the second outpatient visit and involved a follow-up of the patient s progress. Finally, session 4 (S4) took place approximately 1 year poststroke, and it coincided with the final assessment and medical discharge. The Barthel Index (score for walking) was used to assess walking capacity for all patients as was our new functional classification scale, 13 which was modified based on the Hoffer Table 1: Average Times of Clinical Assessments Study Session Poststroke Time (d) Clinical Decision Taken S Admission to rehabilitation department S Hospital discharge S st assessment (PT discharge) S nd assessment (control) S End of study NOTE. Values are mean SD. classification. We call our scale Functional Ambulation Classification of the Hospital at Sagunto (FACHS). The levels of the scale are as follows: Level 0: Nonambulation. Level 1: Nonfunctional or dependent ambulation. Level 2: Household ambulation. Level 3: Surroundings of the house ambulation (neighborhood). Level 4: Community ambulation. Level 5: Normal ambulation. To assess the severity of the affected lower-extremity paresis, the number of joints involved during volitional movements were scored while the patient lay supine on the bed, whether there were associated movements or synergies, etc, or whether they seemed abnormal or uncoordinated. Patients were asked to move their affected leg into a global flexion and extension movement and then to move each joint separately. A score of 0 points was assigned when no joint movement was detected; a score of 1 point was given if there was only hip movement; 2 points were given hip and knee movement; 3 points were given for hip, knee, and ankle-foot movements; and 4 points were assigned when these movements were performed in the lower limb with strength against manual resistance. We also studied standing balance. Balance was considered to be positive when the patient could stand for 5 seconds with his/her eyes open, feet apart, and without any external assistance or body support. Finally, we qualitatively assessed the affected leg s weightbearing capacity (without any type of quantitative measurement). We considered only the presence or absence of body weight-bearing capacity while patients stood, attempted to stand on their affected leg, and took a step forward with the other leg while being firmly held by 2 examiners. Analysis A descriptive statistical analysis of the study sample was performed by analyzing the following variables: age, sex, type of stroke (ischemic or hemorrhagic), and anatomic stroke site (anterior cerebral artery [ACA], middle cerebral artery [MCA], posterior cerebral artery [PCA], or undetermined focus). Different time parameters were also considered, such as the time patients remained in rehabilitation and the amount of time required for PT. The functional ambulation level was registered with both the Barthel Index and our classification, as was the time from the stroke needed to reach this level. We used the nonparametric Friedman test for repeated measurements to compare the functional ambulation levels from among the 5 sessions. The Wilcoxon signed-rank test was used to perform pairwise multiple comparisons. We used the nonparametric Kruskal-Wallis test to compare the functional level
3 WALKING RECOVERY AFTER ACUTE STROKE, Viosca 1241 among independent groups, should there be more than 2 groups, and the Mann-Whitney U test if there were only 2 groups. The linear relation between the functional level and the different variables was measured by the Spearman correlation coefficient. The significance level was set at P less than.05 and was corrected by using the Bonferroni adjustment in multiple comparisons. We used the SPSS 8.0, a statistical package. RESULTS Table 2 shows the general characteristics of the study sample of 41 potential participants with postacute stroke gait disorders, along with the characteristics of the 26 patients who qualified for the study group. The average length of stay in the rehabilitation department was 23 9 days, whereas the average length of PT was days. The average time from stroke to when the weight-bearing capacity on the affected leg returned was days. Finally, the average time before standing balance was achieved was days. The mean times of clinical assessments for the study group are shown in table 1. Figure 1 shows the ambulation recovery of analyzed patients when our classification system was used. Each study session is also represented. Figure 2 shows the ambulation recovery assessed with the Barthel Index (score for walking). There were significant differences (Friedman test, P.001) when analyzing the functional level evolution of the entire sample in all the follow-up sessions. These differences were seen both with our classification system and with the Barthel Index. When pairwise multiple comparisons were made by using the Wilcoxon test and the Bonferroni adjustment was applied, significant differences were observed between the S0 session and the other sessions and between the S1 session and all the others (with both the FACHS and the Barthel Index). Nevertheless, there were significant differences only between sessions S2 and S4 sessions when we used our classification scale. There were no significant differences between the S2 and S3 results or between the S3 and S4 results. Table 3 shows the complete ambulation recovery data of the patients analyzed. S0 reports on the 26 patients who formed the study group. There were only 19 patients in S1 (hospital discharge) because 7 were outpatients and were treated after the selection visit. Improvement was seen at all functional ambulation levels in all but 7 patients (37%), all of whom Fig 1. Ambulation recovery of patients according to the FACHS system. remained at level 0. All 26 patients improved at S2. Everyone improved in S3 except for 1 patient who suffered another stroke. That patient left the study group, and another patient did not come for the check-up, leaving only 24 subjects at S3. At S4 (end of the study and final discharge), we assessed the 25 patients who finished the study, including the 1 who did not attend session 3. A close analysis of table 3 indicates that when our classification system was used, patients walking ability continued to improve beyond 6 months (S3). Seven of our patients improved from this session onward, although the majority improved substantially between sessions S1 and S2. This improvement persisted throughout the 1-year follow-up period. These results differ considerably when walking was scored with the Barthel Index (table 4). As for our secondary objective, we found no association between the functional ambulation level finally achieved and the left- or the right-sided hemiplegia (Mann-Whitney U test 69.0, P.65), the site of stroke (MCA, PCA, ACA, or Table 2: Description of the Study Sample Variable Selected Patients Excluded Patients Mean age SD (y) Sex, n (%) Male 15 (56.0) 8 (53.3) Female 11 (44.0) 7 (46.6) Side of hemiparesis, n (%) Right 12 (49.0) 9 (60.0) Left 14 (50.5) 6 (40.0) Stroke type, n (%) Ischemic 19 (74.0) 13 (86.6) Hemorrhagic 7 (26.0) 2 (13.3) Anatomic site, n (%) MCA 20 (77.0) 11 (73.3) Vertebro-basilar artery 3 (11.0) 0 (0.0) PCA 2 (8.0) 2 (13.3) ACA 1 (4.0) 2 (13.3) No. of patients Fig 2. Ambulation recovery of patients according to the Barthel Index.
4 1242 WALKING RECOVERY AFTER ACUTE STROKE, Viosca Table 3: Temporal Evolution of Gait Recovery in the Study Group as Measured With the FACHS Functional Level S0 (%) S1 (%) S2 (%) S3 (%) S4 (%) 5 2 (8) 5 (21) 4 (16) 4 7 (27) 5 (21) 8 (32) 3 5 (19) 6 (25) 8 (32) 2 2 (8) 6 (32) 7 (27) 6 (25) 3 (12) 1 4 (15) 6 (32) 5 (19) 2 (8) 2 (8) 0 20 (77) 7 (37) Total vertebro-basilar) (Kruskal-Wallis test 4.9, P.18), or the type of stroke (hemorrhagic or ischemic) (Mann-Whitney U test 43, P.24). There was a significant negative linear association between the final achieved functional ambulation level and the time from the resumption of the weight-bearing capacity on the affected lower limb (Spearman.522, P.007) or between the time from the resumption of the standing balance (Spearman.415, P.039). On the other hand, no significant linear correlation was found between the final functional level and the length of time in PT (Spearman.330, P.107). There was also a significant correlation between the time when the weight bearing returned on the affected inferior limb and the resumption of the standing balance (Spearman.42, P.032). The severity of the lower-extremity paresis correlated with the functional ambulation level found at all times throughout the study (Spearman.52, P.001). DISCUSSION There are 3 fundamental findings in this work. The first is the importance of using tools that are sensitive enough to assess walking recovery and the importance of extending the follow-up time. When this occurs, we obtain results different from published reports. Most reports have been based on the Barthel Index or on similar instruments that lack this required sensitivity. Our findings agree with results reported by Skilbeck, 9 Lindmark, 18 and Jorgensen 5 and colleagues, who showed that gait recovery occurs in the majority of patients mainly during the first 3 months after stroke. However, we disagree with their suggestion that the percentage of patients who recover their walking capacity is very small after this period. (Jorgensen 5 put it at 5%). In our study, there were 7 cases (37%) whose functional level improved after 8 months (S3). We cannot affirm any significant differences in the functional ambulation level improvement when comparing S2 and S3, or S3 and S4; however, we can affirm significant differences when a longer term is considered. This occurs between the S2 and S4 sessions. Therefore, we do not agree with those who indicate that gait recovery only occurs in the 6-month poststroke period. We observed that recovery occurs during the entire first year, and we cannot discount that it continues afterward. We have shown that this observation is because of the sensitivity of the method used. Although their samples were not comparable to our sample, results similar to ours were published by Dam 10 and Rodriguez 12 and colleagues who found walking improvement even beyond a 1-year poststroke period. The only explanation to these findings is the greater sensitivity and discrimination capacity of our classification and also the longer follow-up period time. Appendix 1 shows our classification in detail in comparison with the levels established by the Hoffer classification and the Barthel Index. We distinguish 6 functional levels, whereas the Barthel Index does so only with 3. It is precisely in independent walking that we define 4 functional levels (household, surroundings of the house, community, and normal ambulation). It is, therefore, more sensitive at detecting slight functional improvements. It is obvious that because the Barthel Index summarizes walking ability in just 3 categories, there is little chance of detecting further improvement, especially in the upper range of function. This has been reported as a ceiling effect, 9 as figure 2 clearly shows. Andrews et al 8 give a similar explanation for the scant percentage of walking improvement detected in a group of 135 patients (4%) after 6 months because they used a method similar to the Barthel Index. Because the Barthel Index only has 3 levels, the potential to move from 1 level to the next is smaller, if compared with other tests that include more levels. 8 Jorgensen 5 also pointed out that their measurements possibly had limited sensitivity because of the use of the Barthel Index score for walking, yet they used it because it is widely used, is valid, and offers the possibility to compare results with those of other authors. Our work shows that their conclusions are erroneous since they used insensitive methods. The second point to discuss is the great variability in the percentage of independent gait reported by authors, ranging from between 53.3% 19 to 84% 8 at 8 weeks after stroke. We believe that the greater variability results from the difference in the ambulation assessment methods, in both the conceptual and the sensitivity approaches. Another point to bear in mind is that the selection of cases is not always comparable in different studies. Global functional assessment methods, which are neither specific nor sensitive to the walking function, are used in most cases. Thus, Wade et al, 20 who had used the FAC (from the Massachusetts General Hospital), found that 60% of stroke survivors achieved independent walking after 3 months. In the Copenhagen study, Jorgensen affirmed that 64% of their subjects could walk independently at rehabilitation discharge, 14% needed assistance, and 22% could not walk. We are aware that our study has its limitations namely, that the sample size was small and therefore we cannot generalize our results or compare them with those of larger study groups because the designs differ. However, we defend our claim that a method that is specific to the walking function assessment, such as the ones we propose, ought to be used. Any assessment method with these requisites offers more complete information on this particular function. It would make more sense and would have more clinical significance than an assessment obtained with instruments that are summarized into 3 walking categories (nonwalking, dependent, Table 4: Temporal Evolution of Gait Recovery in the Study Group as Measured With the Barthel Index (score for walking) Barthel Index (score for walking) S0 (%) S1 (%) S2 (%) S3 (%) S4 (%) 2 2 (8) 6 (32) 21 (81) 22 (92) 23 (92) 1 4 (15) 6 (32) 5 (19) 2 (8) 2 (8) 0 20 (77) 7 (37) Total
5 WALKING RECOVERY AFTER ACUTE STROKE, Viosca 1243 independent). 5,20 Many aspects of walking development and performance can be determined with our assessment method. It distinguishes among 4 functional levels (from 2 to 5) and, in our work, we obtained independent walking in 92% of cases after 1 year poststroke with the Barthel Index (table 4). With our FACHS, we found that 12% of our subjects were independent in household ambulation, 32% were independent in surroundings of the house ambulation, 32% were independent in community ambulation, and 16% achieved normal ambulation (in appearance and development). Furthermore, although 8% of the patients walk with assistance as measured by the Barthel Index, we can be more precise with our instrument by pointing out that 8% of the patients could walk but with nonfunctional ambulation. Finally, the third point is concerned with factors associated with a prognosis that walking recovery will be good. Generally speaking, our findings coincide with those of other researchers. We found no link between walking recovery and the hemiplegic side, the site, or the type of stroke. 5,10,21 Nor was there any correlation with the length of time in PT. 5 As with other authors, we found a significant correlation between a good finally achieved functional level and the severity of the paresis of the affected lower limb. The same happened with the early (precocity) beginning of weight-bearing capacity on the same affected limb 22,23 and with an early resumption of the standing balance. 5,7,14,16,21,22 Furthermore, we found a significant association between these 2 variables; the sooner weight bearing began, the sooner the standing balance and the better the functional ambulation level were achieved. Therefore, although more thorough research is required, 2 factors linked to a good walking recovery prognosis appeared in our series: the early appearance of both the weight-bearing capacity on the affected limb and the standing balance. CONCLUSIONS By using a specific, valid, reliable, and sensitive assessment method, poststroke walking recovery was observed throughout the first year after a stroke. We cannot ignore the possibility that it may continue beyond that time. Although thorough research would be needed for confirmation purposes, we hypothesize that an early appearance of the weight-bearing capacity on the affected lower limb, as well as an early resumption of recovery of standing balance, could well be 2 factors that indicate a good prognosis for walking recovery. Acknowledgments: We thank the Foreign Language Co-ordination Office at the Polytechnic University of Valencia for its help in revising this article. APPENDIX 1: COMPARISON OF DIFFERENT DISCRIMINATION LEVELS OF WALKING AMONG THE BARTHEL INDEX, HOFFER CLASSIFICATION, AND THE FACHS BARTHEL INDEX HOFFER CLASSIFICATION The FACHS 5. Normal ambulation Community ambulation 4. Community ambulation 3. Surroundings of the house Independent walking Household ambulation 2. Household ambulation Walking with assistance Nonfunctional 1. Nonfunctional No walking function Nonambulation 0. Nonambulation References 1. Hajek VE, Gagnon S, Ruderman JE. Cognitive and functional assessment of stroke patients: an analysis of their relation. Arch Phys Med Rehabil 1997;78: Granger CV, Hamilton BB, Gresham GE. The stroke rehabilitation outcome study Part I: general description. Arch Phys Med Rehabil 1997;69: Linacre JM, Heinemann AW, Wright BD, Granger CV, Hamilton BB. The structure and stability of the Functional Independence Measure. Arch Phys Med Rehabil 1994;75: Scranton RN, Fogel ML, Erdman WJ. Evaluation of functional levels of patients during and following rehabilitation. Arch Phys Med Rehabil 1970;51: Jorgensen HS, Nakayama H, Raaschou HO, Olsen TS. Recovery of walking function in stroke patients: the Copenhagen Stroke Study. Arch Phys Med Rehabil 1995;76: Wade DT, Hewer RL. Functional abilities after stroke: measurement, natural history and prognosis. J Neurol Neurosurg Psychiatry 1987;50: Bohannon RW. Selected determinants of ambulatory capacity in patients with hemiplegia. Clin Rehabil 1989;3: Andrews K, Brocklehurst JC, Richards B, Laycock PJ. The rate of recovery from stroke and its measurements. Int Rehabil Med 1981;3: Skilbeck CE, Wade DT, Hewer RL, Wood VA. Recovery after stroke. J Neurol Neurosurg Psychiatry 1983;46: Dam M, Tonin P, Casson S, et al. The effects of long-term rehabilitation therapy on poststroke hemiplegic patients. Stroke 1993;24: Panturin E. Stroke patients and walking [letter]. Arch Phys Med Rehabil 1995;76: Rodriguez AA, Black PO, Kile KA, et al. Gait training efficacy using a home-based practice model in chronic hemiplegia. Arch Phys Med Rehabil 1996;77: Viosca E, Martínez JL, Almagro PL, Gracia A, González C. Proposal and validation of a new functional ambulation classification scale for clinical use. Arch Phys Med Rehabil 2005;86: Prescott RJ, Garraway WM, Akhtar AJ. Predicting functional outcome following acute stroke using a standard clinical examination. Stroke 1982;13: Sandin KJ, Smith BS. The measure of balance in sitting in stroke rehabilitation prognosis. Stroke 1990;21: Brun V, Dhoms G, Henrion G, Codine P, Founau H, Terraza M. L équilibre postural de l hémiplégique par accident vasculaire cérébral: méthodologie d évaluation et étude corrélative. Ann Réadaptation Méd Phys 1993;36:
6 1244 WALKING RECOVERY AFTER ACUTE STROKE, Viosca 17. Hoffer MM, Feiwell E, Perry R, Perry J, Bonnett C. Functional ambulation in patients with myelomeningocele. J Bone Joint Surg Am 1973;55: Lindmark B. Evaluation of functional capacity after stroke with special emphasis on motor function and activities of daily living. Scand J Rehabil Med Suppl 1988;21: Partridge CJ, Johnston M, Edwards S. Recovery from physical disability after stroke: normal patterns as a basis for evaluation. Lancet 1987;14: Wade DT, Wood VA, Heller A, Maggs J, Langston Hewer R. Walking after stroke. Measuring and recovery over the first 3 months. Scand J Rehabil Med 1987;19: Bohannon RW. Gait performance of hemiparetic stroke patients: selected variables. Arch Phys Med Rehabil 1987;68: Dettmann MA, Linder MT, Sepic SB. Relationships among walking performance, postural stability, and functional assessments of the hemiplegic patient. Am J Phys Med 1987;66: Nugent JA, Schurr KA, Adams RD. A dose-response relationship between amount of weight-bearing exercise and walking outcome following cerebrovascular accident. Arch Phys Med Rehabil 1994;75: Supplier a. SPSS Inc, 233 S Wacker Dr, 11th Fl, Chicago, IL
Predicting the outcome of acute stroke: prospective evaluation of five multivariate models
 Journal of Neurology, Neurosurgery, and Psychiatry 1992;55:347-351 Department of Health Care of the Elderly, University Hospital, Nottingham J R F Gladman Department of Medicine, Ipswich Hospital D M J
Journal of Neurology, Neurosurgery, and Psychiatry 1992;55:347-351 Department of Health Care of the Elderly, University Hospital, Nottingham J R F Gladman Department of Medicine, Ipswich Hospital D M J
Outcome and Time Course of Recovery in Stroke. Part II: Time Course of Recovery. The Copenhagen Stroke Study
 406 Outcome and Time Course of Recovery in Stroke. Part II: Time Course of Recovery. The Copenhagen Stroke Study Henrik S. JCrgensen, MD, Hirofumi Nakayama, MD, Hans O. Raaschou, MD, JCrgen Vive-Larsen,
406 Outcome and Time Course of Recovery in Stroke. Part II: Time Course of Recovery. The Copenhagen Stroke Study Henrik S. JCrgensen, MD, Hirofumi Nakayama, MD, Hans O. Raaschou, MD, JCrgen Vive-Larsen,
Short-Term Recovery of Limb Muscle Strength After Acute Stroke
 125 Short-Term Recovery of Limb Muscle Strength After Acute Stroke A. Williams Andrews, PT, MS, Richard W. Bohannon, PT, EdD ABSTRACT. Andrews AW, Bohannon RW. Short-term IN THE 1970s, CERTAIN AUTHORS
125 Short-Term Recovery of Limb Muscle Strength After Acute Stroke A. Williams Andrews, PT, MS, Richard W. Bohannon, PT, EdD ABSTRACT. Andrews AW, Bohannon RW. Short-term IN THE 1970s, CERTAIN AUTHORS
Stroke patients constitute an increasing challenge
 236 Outcome After Stroke in Patients Discharged to Independent Living Margareta Thorngren, MD, Britt Westling, MD, and Bo Norrving, MD In a prospective, population-based study, we evaluated rehabilitation
236 Outcome After Stroke in Patients Discharged to Independent Living Margareta Thorngren, MD, Britt Westling, MD, and Bo Norrving, MD In a prospective, population-based study, we evaluated rehabilitation
Sitting Balance: Its Relation to Function in Individuals With Hemiparesis
 865 Sitting Balance: Its Relation to Function in Individuals With Hemiparesis Deborah S. Nichols, Phi), PT, Laura Miller, MS, PT, Lynn A. Colby, MS, PT, William S. Pease, MD ABSTRACT. Nichols DS, Miller
865 Sitting Balance: Its Relation to Function in Individuals With Hemiparesis Deborah S. Nichols, Phi), PT, Laura Miller, MS, PT, Lynn A. Colby, MS, PT, William S. Pease, MD ABSTRACT. Nichols DS, Miller
SITTING, A PREREQUISITE FOR most functional activities, Sit-and-Reach Test Can Predict Mobility of Patients Recovering From Acute Stroke
 94 Sit-and-Reach Test Can Predict Mobility of Patients Recovering From Acute Stroke Yuk Lan Tsang, MSc, Margaret Kit Mak, PhD ABSTRACT. Tsang YL, Mak MK. Sit-and-reach test can predict mobility of patients
94 Sit-and-Reach Test Can Predict Mobility of Patients Recovering From Acute Stroke Yuk Lan Tsang, MSc, Margaret Kit Mak, PhD ABSTRACT. Tsang YL, Mak MK. Sit-and-reach test can predict mobility of patients
PEOPLE WITH STROKE often have difficulties changing
 2156 ORIGINAL ARTICLE The Four Square Step Test is a Feasible and Valid Clinical Test of Dynamic Standing Balance for Use in Ambulant People Poststroke Jannette M. Blennerhassett, PhD, Victoria M. Jayalath,
2156 ORIGINAL ARTICLE The Four Square Step Test is a Feasible and Valid Clinical Test of Dynamic Standing Balance for Use in Ambulant People Poststroke Jannette M. Blennerhassett, PhD, Victoria M. Jayalath,
Gait dysfunction is a particularly prevalent and important
 Modified Emory Functional Ambulation Profile An Outcome Measure for the Rehabilitation of Poststroke Gait Dysfunction Heather R. Baer, MD; Steven L. Wolf, PhD, PT, FAPTA Background and Purpose The modified
Modified Emory Functional Ambulation Profile An Outcome Measure for the Rehabilitation of Poststroke Gait Dysfunction Heather R. Baer, MD; Steven L. Wolf, PhD, PT, FAPTA Background and Purpose The modified
For the stroke patient and
 Prue Morgan The relationship between sitting balance and mobility outcome in stroke The purpose of this study was to identify the relationship between static sitting balance in the acute post stroke patient
Prue Morgan The relationship between sitting balance and mobility outcome in stroke The purpose of this study was to identify the relationship between static sitting balance in the acute post stroke patient
CHAPTER 6. Predicting improvement in gait after stroke: A longitudinal prospective study
 CHAPTER 6 Predicting improvement in gait after stroke: A longitudinal prospective study Boudewijn Kollen, Ingrid van de Port, Eline Lindeman, Jos Twisk and Gert Kwakkel Stroke 2005; 36: 2676-2680 79 Abstract
CHAPTER 6 Predicting improvement in gait after stroke: A longitudinal prospective study Boudewijn Kollen, Ingrid van de Port, Eline Lindeman, Jos Twisk and Gert Kwakkel Stroke 2005; 36: 2676-2680 79 Abstract
Localizing lesion locations to predict extent of aphasia recovery. Abstract
 Localizing lesion locations to predict extent of aphasia recovery Abstract Extensive research has related specific lesion locations to language impairment in aphasia. However, far less work has focused
Localizing lesion locations to predict extent of aphasia recovery Abstract Extensive research has related specific lesion locations to language impairment in aphasia. However, far less work has focused
To Study the Effects of Forced Used Training and Capsular Stretching To Improve the Movement of the Shoulder Joint in Chronic Stroke Patients
 International Journal of Science and Healthcare Research Vol.3; Issue: 4; Oct.-Dec. 2018 Website: www.ijshr.com Original Research Article ISSN: 2455-7587 To Study the Effects of Forced Used Training and
International Journal of Science and Healthcare Research Vol.3; Issue: 4; Oct.-Dec. 2018 Website: www.ijshr.com Original Research Article ISSN: 2455-7587 To Study the Effects of Forced Used Training and
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training.
 Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Akita J Med 44 : , (received 11 December 2017, accepted 18 December 2017)
 Akita J Med 44 : 111-116, 2017 (33) Takashi Mizutani 1), Toshiki Matsunaga 2), Kimio Saito 2), Takehiro Iwami 3), Satoru Kizawa 4), Toshihiko Anbo 3) and Yoichi Shimada 1) 1) Department of Orthopedic Surgery,
Akita J Med 44 : 111-116, 2017 (33) Takashi Mizutani 1), Toshiki Matsunaga 2), Kimio Saito 2), Takehiro Iwami 3), Satoru Kizawa 4), Toshihiko Anbo 3) and Yoichi Shimada 1) 1) Department of Orthopedic Surgery,
ALLOCATING REHABILITATION resources, planning
 865 ARTICLES Recovery of Ambulation After Traumatic Brain Injury Douglas I. Katz, MD, Daniel K. White, MSPT, Michael P. Alexander, MD, Reva B. Klein, MD ABSTRACT. Katz DI, White DK, Alexander MP, Klein
865 ARTICLES Recovery of Ambulation After Traumatic Brain Injury Douglas I. Katz, MD, Daniel K. White, MSPT, Michael P. Alexander, MD, Reva B. Klein, MD ABSTRACT. Katz DI, White DK, Alexander MP, Klein
Balance training is an important component of stroke
 Analysis and Comparison of the Psychometric Properties of Three Balance Measures for Stroke Patients Hui-Fen Mao, MS; I-Ping Hsueh, MA; Pei-Fang Tang, PhD; Ching-Fan Sheu, PhD; Ching-Lin Hsieh, PhD Background
Analysis and Comparison of the Psychometric Properties of Three Balance Measures for Stroke Patients Hui-Fen Mao, MS; I-Ping Hsueh, MA; Pei-Fang Tang, PhD; Ching-Fan Sheu, PhD; Ching-Lin Hsieh, PhD Background
DO STROKE REHABILITATION inpatients whose urinary. Urinary Incontinence and Stroke Outcomes. Jan C. Gross, PhD, RN, CS
 22 Urinary Incontinence and Stroke Outcomes Jan C. Gross, PhD, RN, CS ABSTRACT. Gross JC. Urinary incontinence and stroke outcomes. Arch Phys Med Rehabil 2000;81:22-7. Objective: To examine the relation
22 Urinary Incontinence and Stroke Outcomes Jan C. Gross, PhD, RN, CS ABSTRACT. Gross JC. Urinary incontinence and stroke outcomes. Arch Phys Med Rehabil 2000;81:22-7. Objective: To examine the relation
Efficiency, Effectiveness, and Duration of Stroke Rehabilitation
 241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
Activity of Daily Living and Motor Evoked Potentials in the Subacute Stroke Patients Kil Byung Lim, MD, Jeong-Ah Kim, MD
 Original Article Ann Rehabil Med 2013;37(1):82-87 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.1.82 Annals of Rehabilitation Medicine Activity of Daily Living and Motor Evoked
Original Article Ann Rehabil Med 2013;37(1):82-87 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.1.82 Annals of Rehabilitation Medicine Activity of Daily Living and Motor Evoked
The Stroke Impairment Assessment Set: Its Internal Consistency and Predictive Validity
 863 The Stroke Impairment Assessment Set: Its Internal Consistency and Predictive Validity Tetsuya Tsuji, MD, Meigen Liu, MD, DMSc, Shigeru Sonoda, MD, DMSc, Kazuhisa Domen, MD, DMSc, Naoichi Chino, MD,
863 The Stroke Impairment Assessment Set: Its Internal Consistency and Predictive Validity Tetsuya Tsuji, MD, Meigen Liu, MD, DMSc, Shigeru Sonoda, MD, DMSc, Kazuhisa Domen, MD, DMSc, Naoichi Chino, MD,
Predicting Improvement in Gait After Stroke A Longitudinal Prospective Study
 Predicting Improvement in Gait After Stroke A Longitudinal Prospective Study Boudewijn Kollen; Ingrid van de Port, MS; Eline Lindeman, MD, PhD; Jos Twisk, PhD; Gert Kwakkel, PhD Background and Purpose
Predicting Improvement in Gait After Stroke A Longitudinal Prospective Study Boudewijn Kollen; Ingrid van de Port, MS; Eline Lindeman, MD, PhD; Jos Twisk, PhD; Gert Kwakkel, PhD Background and Purpose
Clinical Problem Solving 1: Using the Short Form Berg Balance Scale to Detect Change in Post Acute Stroke Patients
 Clinical Problem Solving 1: Using the Short Form Berg Balance Scale to Detect Change in Post Acute Stroke Patients By Caroline Owen November 12, 2015 Purpose 1. To present the physical therapy evaluation
Clinical Problem Solving 1: Using the Short Form Berg Balance Scale to Detect Change in Post Acute Stroke Patients By Caroline Owen November 12, 2015 Purpose 1. To present the physical therapy evaluation
Research Report. Key Words: Functional status; Orthopedics, general; Treatment outcomes. Neva J Kirk-Sanchez. Kathryn E Roach
 Research Report Relationship Between Duration of Therapy Services in a Comprehensive Rehabilitation Program and Mobility at Discharge in Patients With Orthopedic Problems Background and Purpose. The purpose
Research Report Relationship Between Duration of Therapy Services in a Comprehensive Rehabilitation Program and Mobility at Discharge in Patients With Orthopedic Problems Background and Purpose. The purpose
CLINICAL OUTCOME VARIABLES SCALE: A RETROSPECTIVE
 J Rehabil Med 2010; 42: 609 613 ORIGINAL REPORT CLINICAL OUTCOME VARIABLES SCALE: A RETROSPECTIVE VALIDATION STUDY in patients after stroke Katherine Salter, BA 1, Jeffrey Jutai, PhD 1,2, Norine Foley,
J Rehabil Med 2010; 42: 609 613 ORIGINAL REPORT CLINICAL OUTCOME VARIABLES SCALE: A RETROSPECTIVE VALIDATION STUDY in patients after stroke Katherine Salter, BA 1, Jeffrey Jutai, PhD 1,2, Norine Foley,
Brunel balance assessment (BBA)
 Brunel balance assessment (BBA) Tyson, S Title Authors Type URL Brunel balance assessment (BBA) Tyson, S Published Date 2004 Monograph This version is available at: http://usir.salford.ac.uk/4886/ USIR
Brunel balance assessment (BBA) Tyson, S Title Authors Type URL Brunel balance assessment (BBA) Tyson, S Published Date 2004 Monograph This version is available at: http://usir.salford.ac.uk/4886/ USIR
THE WORLD HEALTH ORGANIZATION defines mobility
 9 Validity and Reliability Comparison of 4 Mobility Measures in Patients Presenting With Neurologic Impairment Philippe Rossier, MD, Derick T. Wade, MA, MD, FRCP ABSTRACT. Rossier P, Wade DT. Validity
9 Validity and Reliability Comparison of 4 Mobility Measures in Patients Presenting With Neurologic Impairment Philippe Rossier, MD, Derick T. Wade, MA, MD, FRCP ABSTRACT. Rossier P, Wade DT. Validity
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center
 Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
CORE MEASURE: CORE MEASURE: BERG BALANCE SCALE (BBS)
 OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
OVERVIEW NUMBER OF TEST ITEMS SCORING EQUIPMENT TIME (NEW CLINICIAN) TIME (EXPERIENCED CLINICIAN) COST o The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and
SEVERAL STUDIES ON spinal cord injury (SCI) recovery. Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study
 512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
The effects of repetitive task training combined with neuromuscular electrical stimulation on extremities for acute cerebral paralysis
 The effects of repetitive task training combined with neuromuscular electrical stimulation on extremities for acute cerebral paralysis Xingnan Liu 1,2 and Chunli Mei 1,a 1 Department of Nursing, Beihua
The effects of repetitive task training combined with neuromuscular electrical stimulation on extremities for acute cerebral paralysis Xingnan Liu 1,2 and Chunli Mei 1,a 1 Department of Nursing, Beihua
FES Standing: The Effect of Arm Support on Stability and Fatigue During Sit-to-Stand Manoeuvres in SCI Individuals
 FES Standing: The Effect of Arm Support on Stability and Fatigue During Sit-to-Stand Manoeuvres in SCI Individuals Musfirah Abd Aziz and Nur Azah Hamzaid Abstract Functional Electrical Stimulation (FES)
FES Standing: The Effect of Arm Support on Stability and Fatigue During Sit-to-Stand Manoeuvres in SCI Individuals Musfirah Abd Aziz and Nur Azah Hamzaid Abstract Functional Electrical Stimulation (FES)
A Study on the Validity and Reliability of 6-Metre Timed Walk in Stroke Patients. Sau Ping Helen Lam PT, HHH
 A Study on the Validity and Reliability of 6-Metre Timed Walk in Stroke Patients. Sau Ping Helen Lam PT, HHH INTRODUCTION Stroke is also known as cerebro-vascular accident (CVA). Survivors can experience
A Study on the Validity and Reliability of 6-Metre Timed Walk in Stroke Patients. Sau Ping Helen Lam PT, HHH INTRODUCTION Stroke is also known as cerebro-vascular accident (CVA). Survivors can experience
MEASUREMENT OF FUNCTIONAL ABILITIES is an. Recovery of Functional Status After Right Hemisphere Stroke: Relationship With Unilateral Neglect
 322 Recovery of Functional Status After Right Hemisphere Stroke: Relationship With Unilateral Neglect Leora R. Cherney, PhD, BC-NCD, Anita S. Halper, MA, BC-NCD, Christina M. Kwasnica, MD, Richard L. Harvey,
322 Recovery of Functional Status After Right Hemisphere Stroke: Relationship With Unilateral Neglect Leora R. Cherney, PhD, BC-NCD, Anita S. Halper, MA, BC-NCD, Christina M. Kwasnica, MD, Richard L. Harvey,
STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB
 STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB PRESENTED BY: Francine Carrier-Stevens, PT. Natasha Uens, PT. Chelsea Foster, RN. OVERVIEW Objectives Factors affecting mobility
STROKE POSITIONING, TRANSFERRING & SHOULDER MANAGEMENT IN ACUTE AND REHAB PRESENTED BY: Francine Carrier-Stevens, PT. Natasha Uens, PT. Chelsea Foster, RN. OVERVIEW Objectives Factors affecting mobility
Evaluating the Effectiveness of Stroke Rehabilitation: Choosing a Discriminative Measure
 92 Evaluating the Effectiveness of Stroke Rehabilitation: Choosing a Discriminative Measure Kim A. Brock, PhD, Patricia A. Goldie, PhD, Kenneth M. Greenwood, PhD ABSTRACT. Brock KA, Goldie PA, Greenwood
92 Evaluating the Effectiveness of Stroke Rehabilitation: Choosing a Discriminative Measure Kim A. Brock, PhD, Patricia A. Goldie, PhD, Kenneth M. Greenwood, PhD ABSTRACT. Brock KA, Goldie PA, Greenwood
Day Hospital Rehabilitation for the Elderly: A Retrospective Study
 468 Day Hospital Elderly Rehabilitation S F Wong et al Day Hospital Rehabilitation for the Elderly: A Retrospective Study S F Wong,*MBBS, MRCP, K B Yap,**FAMS, M Med (Int Med), MRCP, K M Chan,***FAMS,
468 Day Hospital Elderly Rehabilitation S F Wong et al Day Hospital Rehabilitation for the Elderly: A Retrospective Study S F Wong,*MBBS, MRCP, K B Yap,**FAMS, M Med (Int Med), MRCP, K M Chan,***FAMS,
Stroke Rehabilitation
 Stroke Rehabilitation Three Exercise Therapy Approaches RUTH DICKSTEIN, SHRAGA HOCHERMAN, THOMAS PILLAR, and RACHEL SHAHAM The purpose of this study was to compare the therapeutic efficacy of three exercise
Stroke Rehabilitation Three Exercise Therapy Approaches RUTH DICKSTEIN, SHRAGA HOCHERMAN, THOMAS PILLAR, and RACHEL SHAHAM The purpose of this study was to compare the therapeutic efficacy of three exercise
Reliability of the Modified Motor Assessment Scale and the Barthel Index
 Reliability of the Modified Motor Assessment Scale and the Barthel Index SANDY C. LOEWEN and BRIAN A. ANDERSON Many physical therapists use descriptive and functional assessments of motor recovery for
Reliability of the Modified Motor Assessment Scale and the Barthel Index SANDY C. LOEWEN and BRIAN A. ANDERSON Many physical therapists use descriptive and functional assessments of motor recovery for
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Selection of aphasic stroke patients for intensive speech therapy
 Journal of Neurology, Neurosurgery, and Psychiatry 1987;50:1488-1492 Selection of aphasic stroke patients for intensive speech therapy JULIA A LEGH-SMITH, ROSA DENIS, RICHARD LANGTON-HEWER PAMELA M ENDERBY,
Journal of Neurology, Neurosurgery, and Psychiatry 1987;50:1488-1492 Selection of aphasic stroke patients for intensive speech therapy JULIA A LEGH-SMITH, ROSA DENIS, RICHARD LANGTON-HEWER PAMELA M ENDERBY,
Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance.
 Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Core Measure: Berg Balance Scale (BBS) Overview The BBS is a widely-used, clinician-rated scale used to assess sitting and standing, static and dynamic balance. Number of Test Items The BBS consists of
Stroke & the Emergency Department. Dr. Barry Moynihan, March 2 nd, 2012
 Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Stroke & the Emergency Department Dr. Barry Moynihan, March 2 nd, 2012 Outline Primer Stroke anatomy & clinical syndromes Diagnosing stroke Anterior / Posterior Thrombolysis Haemorrhage The London model
Implementing a Structured Cognitive Orientation Program on an Inpatient Rehabilitation Unit: A Pilot Project Lauren Fletcher
 Implementing a Structured Cognitive Orientation Program on an Inpatient Rehabilitation Unit: A Pilot Project Lauren Fletcher The Royal Melbourne Hospital Royal Park Campus Inpatient Rehabilitation Unit
Implementing a Structured Cognitive Orientation Program on an Inpatient Rehabilitation Unit: A Pilot Project Lauren Fletcher The Royal Melbourne Hospital Royal Park Campus Inpatient Rehabilitation Unit
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Functional Ability Screening Tools for the Clinic
 Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
Functional Ability Screening Tools for the Clinic Shelley Hockensmith,, P.T., NCS Objectives Review screening tools for physical or functional ability including Five Times Sit to Stand, Walking Speed,
Using the AcuteFIM Instrument for Discharge Placement
 Using the AcuteFIM Instrument for Discharge Placement Paulette Niewczyk, MPH, PhD Manager of CFAR / Director of Research Center for Functional Assessment Research Uniform Data System for Medical Rehabilitation
Using the AcuteFIM Instrument for Discharge Placement Paulette Niewczyk, MPH, PhD Manager of CFAR / Director of Research Center for Functional Assessment Research Uniform Data System for Medical Rehabilitation
Measuring Outcomes in Acute Neurorehabilitation in General Hospital Setting Our Experience
 & Measuring Outcomes in Acute Neurorehabilitation in General Hospital Setting Our Experience Emela Mujić-Skikić¹*, Suad Trebinjac¹, Dijana Avdić², Amra Džumhur-Sarić³ 1. Physical Medicine & Rehabilitation
& Measuring Outcomes in Acute Neurorehabilitation in General Hospital Setting Our Experience Emela Mujić-Skikić¹*, Suad Trebinjac¹, Dijana Avdić², Amra Džumhur-Sarić³ 1. Physical Medicine & Rehabilitation
POSTURAL DISORDERS are frequent in victims of hemiplegia
 793 Rehabilitation of Postural Disturbances of Hemiplegic Patients by Using Trunk Control Retraining During Exploratory Exercises Marianne de Sèze, MD, Laurent Wiart, MD, Alain Bon-Saint-Côme, PT, Xavier
793 Rehabilitation of Postural Disturbances of Hemiplegic Patients by Using Trunk Control Retraining During Exploratory Exercises Marianne de Sèze, MD, Laurent Wiart, MD, Alain Bon-Saint-Côme, PT, Xavier
Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works
 Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works Emily R. Rosario, PhD Why is Casa Colina unique? Continuum of care offering medical and rehabilitation services
Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works Emily R. Rosario, PhD Why is Casa Colina unique? Continuum of care offering medical and rehabilitation services
INTRACEREBRAL HEMORRHAGE (ICH) is a major
 968 Functional Recovery Following Rehabilitation After Hemorrhagic and Ischemic Stroke Peter J. Kelly, MB, MRCPI, Karen L. Furie, MD, MPH, Saad Shafqat, MD, PhD, Nikoletta Rallis, BA, Yuchiao Chang, PhD,
968 Functional Recovery Following Rehabilitation After Hemorrhagic and Ischemic Stroke Peter J. Kelly, MB, MRCPI, Karen L. Furie, MD, MPH, Saad Shafqat, MD, PhD, Nikoletta Rallis, BA, Yuchiao Chang, PhD,
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Huseyinsinoglu, B. E., Ozdincler, A. R., & Krespi, Y. (2012). Bobath concept versus constraint-induced movement therapy to improve arm functional recovery in stroke patients:
CRITICALLY APPRAISED PAPER (CAP) Huseyinsinoglu, B. E., Ozdincler, A. R., & Krespi, Y. (2012). Bobath concept versus constraint-induced movement therapy to improve arm functional recovery in stroke patients:
Treadmill training with partial body weight support and physiotherapy in stroke patients: a preliminary comparison
 European Journal of Neurology 2002, 9: 639 644 Treadmill training with partial body weight support and physiotherapy in stroke patients: a preliminary comparison C. Werner a, A. Bardeleben a, K-H. Mauritz
European Journal of Neurology 2002, 9: 639 644 Treadmill training with partial body weight support and physiotherapy in stroke patients: a preliminary comparison C. Werner a, A. Bardeleben a, K-H. Mauritz
Berg Balance Scale. CVA, Parkinson Disease, Pediatrics
 CVA, Parkinson Disease, Pediatrics CVA Highly recommended for inpatient and outpatient rehabilitation Recommended for acute care Parkinson s Disease Recommended for H and Y stages 2 and 3 G code-changing
CVA, Parkinson Disease, Pediatrics CVA Highly recommended for inpatient and outpatient rehabilitation Recommended for acute care Parkinson s Disease Recommended for H and Y stages 2 and 3 G code-changing
The influence of age on corrected motor FIM effectiveness
 56 Japanese Journal of Comprehensive Rehabilitation Science (2014) Original Article The influence of age on corrected motor FIM effectiveness Makoto Tokunaga, MD, PhD, 1 Ryoji Nakanishi, MD, PhD, 1 Gihachiro
56 Japanese Journal of Comprehensive Rehabilitation Science (2014) Original Article The influence of age on corrected motor FIM effectiveness Makoto Tokunaga, MD, PhD, 1 Ryoji Nakanishi, MD, PhD, 1 Gihachiro
University of Salford
 University of Salford College of Health and Social Care A systematic review to examine the functional balance in individuals with stroke 2013 MSc Degree R. M. WAHBA Abstract Background: Treadmill training
University of Salford College of Health and Social Care A systematic review to examine the functional balance in individuals with stroke 2013 MSc Degree R. M. WAHBA Abstract Background: Treadmill training
ebavir, easy Balance Virtual Rehabilitation system: a study with patients
 ebavir, easy Balance Virtual Rehabilitation system: a study with patients M. González-Fernández 1, José-Antonio Gil-Gómez 1, M. Alcañiz 1, E. Noé 2, C. Colomer 2 1 Instituto Interuniversitario de Investigación
ebavir, easy Balance Virtual Rehabilitation system: a study with patients M. González-Fernández 1, José-Antonio Gil-Gómez 1, M. Alcañiz 1, E. Noé 2, C. Colomer 2 1 Instituto Interuniversitario de Investigación
TOTAL HIP REPLACEMENT is one of the most effective
 1652 ORIGINAL ARTICLE Effect of Multiple Physiotherapy Sessions on Functional Outcomes in the Initial Postoperative Period After Primary Total Hip Replacement: A Randomized Controlled Trial Kellie A. Stockton,
1652 ORIGINAL ARTICLE Effect of Multiple Physiotherapy Sessions on Functional Outcomes in the Initial Postoperative Period After Primary Total Hip Replacement: A Randomized Controlled Trial Kellie A. Stockton,
Expert Transfers in Rehabilitation: A Safety and Utilisation Review
 Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction
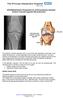 GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
GG10Rehabilitation Programme for Arthroscopically Assisted Anterior Cruciate Ligament Reconstruction Femur ACL Graft Fibula Tibia The Anterior Cruciate Ligament (ACL) is one of the main ligaments in the
University of South Australia, 2 Royal Adelaide Hospital Australia
 English et al: Shoulder pain after stroke Incidence and severity of shoulder pain does not increase with the use of circuit class therapy during inpatient stroke rehabilitation: a controlled trial Coralie
English et al: Shoulder pain after stroke Incidence and severity of shoulder pain does not increase with the use of circuit class therapy during inpatient stroke rehabilitation: a controlled trial Coralie
IN STROKE REHABILITATION, it is common practice for. Selecting Patients for Rehabilitation After Acute Stroke: Are There Variations in Practice?
 788 ORIGINAL ARTICLE Selecting Patients for Rehabilitation After Acute Stroke: Are There Variations in Practice? Paul A. Ilett, BAppSc (Physio), Kim A. Brock, PhD, Christine J. Graven, PostGradDip (Health
788 ORIGINAL ARTICLE Selecting Patients for Rehabilitation After Acute Stroke: Are There Variations in Practice? Paul A. Ilett, BAppSc (Physio), Kim A. Brock, PhD, Christine J. Graven, PostGradDip (Health
Quiz ACUTE STROKE UNIT ORIENTATION MODULE 7: MOBILITY, POSITIONING, AND TRANSFERS
 ACUTE STROKE UNIT ORIENTATION 2014 MODULE 7: MOBILITY, POSITIONING, AND TRANSFERS Name: Date: 1. Fill in the blanks (2 points) The goal of assisting the stroke survivor is to functional recovery and independence
ACUTE STROKE UNIT ORIENTATION 2014 MODULE 7: MOBILITY, POSITIONING, AND TRANSFERS Name: Date: 1. Fill in the blanks (2 points) The goal of assisting the stroke survivor is to functional recovery and independence
AQUATIC PHYSIOTHERAPY IN PERIPHERAL NEUROPATHIES: A REHABILITATIVE PROTOCOL
 AQUATIC PHYSIOTHERAPY IN PERIPHERAL NEUROPATHIES: A REHABILITATIVE PROTOCOL Ilaria Zivi, MD Department of Brain Injury and Parkinson Disease Rehabilitation Moriggia-Pelascini Hospital, Gravedona ed Uniti
AQUATIC PHYSIOTHERAPY IN PERIPHERAL NEUROPATHIES: A REHABILITATIVE PROTOCOL Ilaria Zivi, MD Department of Brain Injury and Parkinson Disease Rehabilitation Moriggia-Pelascini Hospital, Gravedona ed Uniti
University of Groningen
 University of Groningen Functional recovery of gait and joint kinematics after right hemispheric stroke Huitema, RB; Mulder, T; Brouwer, Wiebo; Dekker, Rienk; Postema, Klaas; Hof, At L. Published in: Archives
University of Groningen Functional recovery of gait and joint kinematics after right hemispheric stroke Huitema, RB; Mulder, T; Brouwer, Wiebo; Dekker, Rienk; Postema, Klaas; Hof, At L. Published in: Archives
Controlled randomised crossover trial of the evects of physiotherapy on mobility in chronic multiple sclerosis
 174 Department of Medicine (Neurology (C4)), University of Wales College of Medicine, CardiV CF14 4XN, Wales, UK C M Wiles T P Pickersgill Medical Computing and Statistics R G Newcombe Department of Physiotherapy,
174 Department of Medicine (Neurology (C4)), University of Wales College of Medicine, CardiV CF14 4XN, Wales, UK C M Wiles T P Pickersgill Medical Computing and Statistics R G Newcombe Department of Physiotherapy,
Manual of basic physiotherapeutic exercises for family and caregivers of stroke patients
 Neurology and Neuroscience Reports Research Article ISSN: 2631-4010 Manual of basic physiotherapeutic exercises for family and caregivers of stroke patients Dérrick Patrick Artioli 1 and Gladson Ricardo
Neurology and Neuroscience Reports Research Article ISSN: 2631-4010 Manual of basic physiotherapeutic exercises for family and caregivers of stroke patients Dérrick Patrick Artioli 1 and Gladson Ricardo
A ccurate prediction of outcome in the acute and
 401 PAPER Predicting functional outcome in acute stroke: comparison of a simple six variable model with other predictive systems and informal clinical prediction C Counsell, M Dennis, M McDowall... See
401 PAPER Predicting functional outcome in acute stroke: comparison of a simple six variable model with other predictive systems and informal clinical prediction C Counsell, M Dennis, M McDowall... See
The triage of stroke rehabilitation
 Journal of Epidemiology and Community Health, 1981, 35, 39-44 The triage of stroke rehabilitation W. M. GARRAWAY,' A. J. AKHTAR,2 D. L. SMITH,2 AND M. E. SMITH' From 'the Department of Community Medicine,
Journal of Epidemiology and Community Health, 1981, 35, 39-44 The triage of stroke rehabilitation W. M. GARRAWAY,' A. J. AKHTAR,2 D. L. SMITH,2 AND M. E. SMITH' From 'the Department of Community Medicine,
EFFECTS OF FUNCTIONAL ELECTRICAL STIMULATION IN REHABILITATION WITH HEMIPARESIS PATIENTS
 & EFFECTS OF FUNCTIONAL ELECTRICAL STIMULATION IN REHABILITATION WITH HEMIPARESIS PATIENTS Edina Tanović* Institute for Physiotherapy and Rehabilitation, University of Sarajevo Clinics Centre, Bolnička
& EFFECTS OF FUNCTIONAL ELECTRICAL STIMULATION IN REHABILITATION WITH HEMIPARESIS PATIENTS Edina Tanović* Institute for Physiotherapy and Rehabilitation, University of Sarajevo Clinics Centre, Bolnička
Physical Therapy Diagnosis and Documentation Tips
 1 This tool is designed to assist the Physical Therapist in consultation with the physician, in the selection of an appropriate according to Medicare coverage guidelines. The documentation tips will add
1 This tool is designed to assist the Physical Therapist in consultation with the physician, in the selection of an appropriate according to Medicare coverage guidelines. The documentation tips will add
Comprehensive Joint Replacement Therapeutic Approaches: Leading the Way as Clinicians, Care Managers, and Colleagues
 Comprehensive Joint Replacement Therapeutic Approaches: Leading the Way as Clinicians, Care Managers, and Colleagues Greg Young, PT, OCS Senior Director of Rehab Infinity Rehab My Background Joint replacement
Comprehensive Joint Replacement Therapeutic Approaches: Leading the Way as Clinicians, Care Managers, and Colleagues Greg Young, PT, OCS Senior Director of Rehab Infinity Rehab My Background Joint replacement
APPROXIMATELY 70% OF STROKE survivors have
 214 ORIGINAL ARTICLE Measuring Upper Limb Capacity in Poststroke Patients: Development, Fit of the Monotone Homogeneity Model, Unidimensionality, Fit of the Double Monotonicity Model, Differential Item
214 ORIGINAL ARTICLE Measuring Upper Limb Capacity in Poststroke Patients: Development, Fit of the Monotone Homogeneity Model, Unidimensionality, Fit of the Double Monotonicity Model, Differential Item
Visual Field Defects and the Prognosis of Stroke Patients
 Visual Field Defects and the Prognosis of Stroke Patients BY ARMIN F. HAERER, M.D. Abstract: Visual Field Defects and the Prognosis of Stroke Patients The prognosis of stroke patients is related to the
Visual Field Defects and the Prognosis of Stroke Patients BY ARMIN F. HAERER, M.D. Abstract: Visual Field Defects and the Prognosis of Stroke Patients The prognosis of stroke patients is related to the
AROC Outcome Targets Report Inpatient Pathway 3
 AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
What is Occupational Therapy?
 Introduction to Occupational Therapy Services What is Occupational Therapy? Alice Chan, OTI Tai Po Hospital a health profession that focuses on promoting health and well being through engagement in meaningful
Introduction to Occupational Therapy Services What is Occupational Therapy? Alice Chan, OTI Tai Po Hospital a health profession that focuses on promoting health and well being through engagement in meaningful
RECOVERY OF LINGUISTIC DEFICITS IN STROKE PATIENTS; A THREE- YEAR-FOLLOW UP STUDY.
 RECOVERY OF LINGUISTIC DEFICITS IN STROKE PATIENTS; A THREE- YEAR-FOLLOW UP STUDY. Introduction For the diagnosis of aphasia early after stroke, several screening tests are available to support clinical
RECOVERY OF LINGUISTIC DEFICITS IN STROKE PATIENTS; A THREE- YEAR-FOLLOW UP STUDY. Introduction For the diagnosis of aphasia early after stroke, several screening tests are available to support clinical
Many upper extremity motor function outcome measures do
 Assessing Wolf Motor Function Test as Outcome Measure for Research in Patients After Stroke Steven L. Wolf, PhD, PT; Pamela A. Catlin, EdD, PT; Michael Ellis, MPT; Audrey Link Archer, MPT; Bryn Morgan,
Assessing Wolf Motor Function Test as Outcome Measure for Research in Patients After Stroke Steven L. Wolf, PhD, PT; Pamela A. Catlin, EdD, PT; Michael Ellis, MPT; Audrey Link Archer, MPT; Bryn Morgan,
10/13/2017. The K2A Cycle. Focused Intensive Repetitive Step Training (FIRST)
 Walking the Walk: Translation of Scientific Findings into Clinical Practice September 14 and 15, 2017 State of the Science Chicago, IL T. George Hornby PT, PhD Jennifer Moore PT, DHSc, NCS The K2A Cycle
Walking the Walk: Translation of Scientific Findings into Clinical Practice September 14 and 15, 2017 State of the Science Chicago, IL T. George Hornby PT, PhD Jennifer Moore PT, DHSc, NCS The K2A Cycle
Trunk Control as an Early Predictor of Comprehensive Activities of Daily Living Function in Stroke Patients
 Trunk Control as an Early Predictor of Comprehensive Activities of Daily Living Function in Stroke Patients Ching-Lin Hsieh, PhD; Ching-Fan Sheu, PhD; I-Ping Hsueh, MA; Chun-Hou Wang, BS Background and
Trunk Control as an Early Predictor of Comprehensive Activities of Daily Living Function in Stroke Patients Ching-Lin Hsieh, PhD; Ching-Fan Sheu, PhD; I-Ping Hsueh, MA; Chun-Hou Wang, BS Background and
Original Article. Japanese Journal of Comprehensive Rehabilitation Science (2015) Kumamoto Kinoh Hospital, Kumamoto, Japan
 86 Japanese Journal of Comprehensive Rehabilitation Science (2015) Original Article The relationship between measured values and values predicted using multiple regression analysis for mean motor FIM at
86 Japanese Journal of Comprehensive Rehabilitation Science (2015) Original Article The relationship between measured values and values predicted using multiple regression analysis for mean motor FIM at
Arm function after stroke: measurement and recovery
 Journal of Neurology, Neurosurgery, and Psychiatry 1987;50:714-719 Arm function after stroke: measurement and recovery over the first three months ANDREW HELLER, DERICK T WADE, VICTORINE A WOOD, ALAN SUNDERLAND,
Journal of Neurology, Neurosurgery, and Psychiatry 1987;50:714-719 Arm function after stroke: measurement and recovery over the first three months ANDREW HELLER, DERICK T WADE, VICTORINE A WOOD, ALAN SUNDERLAND,
STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT
 STROKE HKJOT REHABILITATION 2004;14:3 11 STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT Fung Mei Ling Background: Stroke is the third leading cause of death in Hong
STROKE HKJOT REHABILITATION 2004;14:3 11 STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT Fung Mei Ling Background: Stroke is the third leading cause of death in Hong
Bryan Andresen MD Advances in Clinical Neuroscience Practice /2/11
 Bryan Andresen MD Advances in Clinical Neuroscience Practice 2011 5/2/11 Intro/History Definition Differential Diagnosis Clinical Characteristics Exam Findings Treatment Outcomes 46 yo female admitted
Bryan Andresen MD Advances in Clinical Neuroscience Practice 2011 5/2/11 Intro/History Definition Differential Diagnosis Clinical Characteristics Exam Findings Treatment Outcomes 46 yo female admitted
Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the patient
 () 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
() 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
Evaluation of the functional independence for stroke survivors in the community
 Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Evaluation of the Family - Rated Kinder Infant Development Scale (KIDS) for Disabled Children
 Jikeikai Med J 2012 ; 59 : 5-10 Evaluation of the Family - Rated Kinder Infant Development Scale (KIDS) for Disabled Children Keiji Hashimoto, Naoko Matsui, Hidemi Yakuwa, and Kohei Miyamura Division of
Jikeikai Med J 2012 ; 59 : 5-10 Evaluation of the Family - Rated Kinder Infant Development Scale (KIDS) for Disabled Children Keiji Hashimoto, Naoko Matsui, Hidemi Yakuwa, and Kohei Miyamura Division of
ii. Reduction of tone in upper limb Lycra arm splints improve movement fluency in children with cerebral palsy.
 Guidelines for the Provision of Dynamic Compression for people diagnosed with Multiple Sclerosis The use of Lycra garments in patients with the diagnosis of Multiple Sclerosis has been initiated with very
Guidelines for the Provision of Dynamic Compression for people diagnosed with Multiple Sclerosis The use of Lycra garments in patients with the diagnosis of Multiple Sclerosis has been initiated with very
Margaret Schenkman, PT, PhD, FAPTA University of Colorado, Denver Colorado
 Margaret Schenkman, PT, PhD, FAPTA University of Colorado, Denver Colorado Present a framework for clinical reasoning with emphasis on Patient centered care Application of enablement and disablement frameworks
Margaret Schenkman, PT, PhD, FAPTA University of Colorado, Denver Colorado Present a framework for clinical reasoning with emphasis on Patient centered care Application of enablement and disablement frameworks
Review of Selected Physical Therapy Interventions for School Age Children with Disabilities
 Review of Selected Physical Therapy Interventions for School Age Children with Disabilities Prepared for the Center on Personnel Studies in Special Education EXECUTIVE SUMMARY by Susan K. Effgen University.
Review of Selected Physical Therapy Interventions for School Age Children with Disabilities Prepared for the Center on Personnel Studies in Special Education EXECUTIVE SUMMARY by Susan K. Effgen University.
Effect of Mobility on Community Participation at 1 year Post-Injury in Individuals with Traumatic Brain Injury (TBI)
 Effect of Mobility on Community Participation at 1 year Post-Injury in Individuals with Traumatic Brain Injury (TBI) Irene Ward, PT, DPT, NCS Brain Injury Clinical Research Coordinator Kessler Institute
Effect of Mobility on Community Participation at 1 year Post-Injury in Individuals with Traumatic Brain Injury (TBI) Irene Ward, PT, DPT, NCS Brain Injury Clinical Research Coordinator Kessler Institute
Dr Nancy Low Choy, Bond University, Gold Coast. Paige Hooper, Physiotherapist, Bond University, Gold Coast
 Associations between vestibular system function, perceived confidence, falls efficacy, balance and mobility in older fallers undertaking home rehabilitation Dr Nancy Low Choy, Bond University, Gold Coast
Associations between vestibular system function, perceived confidence, falls efficacy, balance and mobility in older fallers undertaking home rehabilitation Dr Nancy Low Choy, Bond University, Gold Coast
Int J Physiother. Vol 1(5), , December (2014) ISSN:
 Int J Physiother. Vol (5), 4-47, December (04) ISSN: 48-86 B. Deekshita V. Srikumari K. Madhavi ABSTRACT Background: Stroke is an acute onset of neurological dysfunction resulting in the most common disability.
Int J Physiother. Vol (5), 4-47, December (04) ISSN: 48-86 B. Deekshita V. Srikumari K. Madhavi ABSTRACT Background: Stroke is an acute onset of neurological dysfunction resulting in the most common disability.
Using Individual Growth Curve Models to Predict Recovery and Activities of Daily Living After Spinal Cord Injury: An SCIRehab Project Study
 Archives of Physical Medicine and Rehabilitation journal homepage: Archives of Physical Medicine and Rehabilitation 2013;94(4 Suppl 2):S154-64 ORIGINAL ARTICLE Using Individual Growth Curve Models to Predict
Archives of Physical Medicine and Rehabilitation journal homepage: Archives of Physical Medicine and Rehabilitation 2013;94(4 Suppl 2):S154-64 ORIGINAL ARTICLE Using Individual Growth Curve Models to Predict
After a stroke, the ability to control balance in the sitting
 Validation of a Standardized Assessment of Postural Control in Stroke Patients The Postural Assessment Scale for Stroke Patients (PASS) Charles Benaim, MD; Dominique Alain Pérennou, MD, PhD; Jacqueline
Validation of a Standardized Assessment of Postural Control in Stroke Patients The Postural Assessment Scale for Stroke Patients (PASS) Charles Benaim, MD; Dominique Alain Pérennou, MD, PhD; Jacqueline
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents
 Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
Appendix E : Evidence table 9 Rehabilitation: Other Key Documents 1. Cameron et al. Geriatric rehabilitation following following fractures in older people: a systematic review. Health Technology Assessment
Enhanced physical therapy improves recovery of
 530 5Journal of Neurology, Neurosurgery, and Psychiatry 1992;55:530-535 The Stroke Research Unit, Frenchay Hospital, Bristol, UK A Sunderland D J Tinson E L Bradley D Fletcher R Langton Hewer Rivermead
530 5Journal of Neurology, Neurosurgery, and Psychiatry 1992;55:530-535 The Stroke Research Unit, Frenchay Hospital, Bristol, UK A Sunderland D J Tinson E L Bradley D Fletcher R Langton Hewer Rivermead
M ost people who suffer movement problems caused by
 PAPER Comparison of Bobath based and movement science based treatment for stroke: a randomised controlled trial P M van Vliet, N B Lincoln, A Foxall... See Editorial Commentary, p 465 See end of article
PAPER Comparison of Bobath based and movement science based treatment for stroke: a randomised controlled trial P M van Vliet, N B Lincoln, A Foxall... See Editorial Commentary, p 465 See end of article
Table 3.1: Canadian Stroke Best Practice Recommendations Screening and Assessment Tools for Acute Stroke Severity
 Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Cumulated Ambulation Score to evaluate mobility is feasible in geriatric patients and in patients with hip fracture
 Cumulated Ambulation Score to evaluate mobility is feasible in geriatric patients and in patients with hip fracture Morten Tange Kristensen 1, 2,Thomas Linding Jakobsen 3, 4, Jesper Westphal Nielsen 1,
Cumulated Ambulation Score to evaluate mobility is feasible in geriatric patients and in patients with hip fracture Morten Tange Kristensen 1, 2,Thomas Linding Jakobsen 3, 4, Jesper Westphal Nielsen 1,
Sensory Retraining of the Lower Limb After Acute Stroke: A Randomized Controlled Pilot Trial
 ORIGINAL ARTICLE Sensory Retraining of the Lower Limb After Acute Stroke: A Randomized Controlled Pilot Trial Elizabeth A. Lynch, BAppSc, Susan L. Hillier, PhD, Kathy Stiller, PhD, Rachel R. Campanella,
ORIGINAL ARTICLE Sensory Retraining of the Lower Limb After Acute Stroke: A Randomized Controlled Pilot Trial Elizabeth A. Lynch, BAppSc, Susan L. Hillier, PhD, Kathy Stiller, PhD, Rachel R. Campanella,
