Techniques for Performing Tracheostomy
|
|
|
- Clyde Cannon
- 6 years ago
- Views:
Transcription
1 Techniques for Performing Tracheostomy Charles G Durbin Jr MD FAARC Introduction History of Tracheostomy Percutaneous Tracheostomy Techniques of Performing an Open or Surgical Tracheostomy Percutaneous Dilational Tracheostomy Choosing a Technique Summary One of the most commonly performed procedures in the critically ill, tracheostomy has been described and used for lifesaving treatment of upper-airway obstruction for at least 3,500 years. The procedure can be performed surgically in the operating room or at the bedside in the intensive care unit. Recently, percutaneous techniques performed by a variety of specialists have become popular alternatives to open surgical tracheostomy. Various devices have been developed to minimize identified risk and improve the simplicity of the procedure. These techniques and devices are described in this paper. Key words: tracheostomy, percutaneous, intensive care unit, surgical technique, medical devices. [Respir Care 2005;50(4): Daedalus Enterprises] History of Tracheostomy Introduction Besides being one of the most frequently performed procedures today, tracheostomy is one of the oldest described surgical procedures. It has been performed for over 3,500 years. Although it is not known when the first tracheostomy was actually placed, the procedure was probably performed by the ancient Egyptians. Possibly the earliest written descriptions are of tracheotomies performed in sheep, reported in the Babylonian Talmud and a similar Charles G Durbin Jr MD FAARC is affiliated with the Department of Anesthesiology, University of Virginia Health Science Center, Charlottesville, Virginia. Charles G Durbin Jr MD FAARC presented a version of this paper at the 20th Annual New Horizons Symposium at the 50th International Respiratory Congress, held December 4 7, 2004, in New Orleans, Louisiana. Correspondence: Charles G Durbin Jr MD FAARC, Department of Anesthesiology, University of Virginia Health Science Center, PO Box , Charlottesville VA cgd8v@virginia.edu. account in the Rig Veda, the sacred Hindu book. The eminent Greek physician Galen credited Asclepiades with originating tracheostomy for the treatment of upper-airway obstruction due to pharyngeal inflammation in the 2nd century BC. Later physicians also performed the procedure, including Antyllus in the 2nd century AD. Successes were uncommon, and the procedure seems to have been abandoned in humans until the 1500s, when Brasavola (1546) reported a survivor. This patient was almost dead, suffering from an abscess of the windpipe; the operation was performed with a vertical incision and a tube was inserted. 1 A major interest in tracheostomy developed during the 19th century, after Napoleon Bonaparte s nephew died of diphtheria in Research into the technique occurred, with resurrection of some of the old instruments, and use of tracheostomy for treatment of airway obstruction for diphtheria became accepted. Bretonneau and Trousseau demonstrated and popularized the technique. At this time mortality from the procedure was considered acceptable if 25% of the patients survived. 1 Chevalier Jackson standardized the indications for tracheostomy, the technique itself, and the instruments used, 488 RESPIRATORY CARE APRIL 2005 VOL 50 NO 4
2 around the turn of the 20th century. He developed anatomically correct tracheostomy tubes, recommended a high tracheostomy location (ring 2 or 3), and condemned cricothyroidotomy because of its high complication rate. 2 He is considered the father of the surgical specialty of ear, nose, and throat surgery, which has recently been reborn as otorhinolaryngology/head-and-neck surgery. Percutaneous Tracheostomy Placement of a tracheostomy percutaneously is not a new idea; pictures of devices that appear to have been developed for this purpose date back to the middle ages. A modern percutaneous tracheostomy device was developed by Toye and Weinstein in 1969, and its use in 100 trauma patients was reported in ,4 The wire-guided percutaneous technique for percutaneous tracheostomy was developed and reported in the same year by the American surgeon, Ciaglia, who combined the Seldinger wire nephrostomy tube multiple-dilator placement technique with a special, low-profile tracheostomy tube. 5 Several variants on the percutaneous tracheostomy technique have been developed, including a wire-guided sharp forceps (Griggs technique), 6 performance of the procedure under bronchoscopic control, using a single, tapered dilator (Blue Rhino), 7 passing the dilator from inside the trachea to the outside (Fantoni s technique), 8 and using a screw-like device to open the trachea wall (PercTwist). 9 Each of these variations came about as an attempt to improve some aspect of another technique. The classical surgical approach and percutaneous techniques will be described in this paper. Techniques of Performing an Open or Surgical Tracheostomy Surgical tracheostomy (ST) is usually performed in the operating room on a patient under general anesthesia, but it may be performed at the bedside in the intensive care unit. Usually the airway has been secured by a cuffed endotracheal tube; however, patients with partially obstructing pharyngeal or laryngeal tumors may undergo tracheostomy with light (or no) sedation and local anesthesia. The patient s shoulders are elevated with head extension (unless cervical disease or injury is present), elevating the larynx and exposing more of the upper trachea. Prophylactic antibiotics specific for skin pathogens should be administered min prior to skin incision. The skin from the chin to below the clavicles is sterilely prepared. If excessive hair is present, it should be removed with electric clippers immediately prior to skin preparation. Sterile drapes are placed, creating an opening from the top of the larynx to the suprasternal notch. Fig. 1. Creating a surgical tracheostomy. After incising the skin and dividing the strap muscles of the neck, the thyroid isthmus is mobilized with a hemostat. Local anesthesia with a vasoconstrictor is usually infiltrated into the skin and deeper tissues to reduce the amount of bleeding during the procedure. The skin of the neck over the 2nd tracheal ring is identified, and a vertical incision about 2 3 cm in length is created. Care to avoid cutting deeper than the subcutaneous tissues must be exercised to avoid lacerating the thyroid isthmus or a large neck vein. Sharp dissection following the skin incision is used to cut across the platysma muscle, with bleeding controlled by hemostats and ties or electocautery. Blunt dissection parallel to the long axis of the trachea is then used to spread the submuscular tissues until the thyroid isthmus is identified (Fig. 1). If the gland lies superior to the 3rd tracheal ring, it can be bluntly undermined and retracted superiorly to gain access to the trachea. If the isthmus overlies the 2nd and 3rd ring of the trachea, it must be mobilized and either a small incision made to clear a space for the tracheostomy (Fig. 2) or complete RESPIRATORY CARE APRIL 2005 VOL 50 NO 4 489
3 Fig. 2. Creating a surgical tracheostomy. If the thyroid cannot be retracted either superiorly or inferiorly to reveal the 2nd and 3rd tracheal rings, a small incision in the gland may be created to allow access to the trachea. Fig. 4. Creating the tracheal portal. There are 2 basic approaches to tracheal entry. As illustrated here, the 2nd tracheal ring is divided laterally and the anterior portion removed. Lateral sutures are used to provide counter traction during tracheostomy-tube insertion. These are left uncut to provide assistance should the tube be accidentally dislodged later. Fig. 3. Creating a surgical tracheostomy. If the thyroid isthmus remains in the way of the site of the tracheostomy, it may be completely divided, carefully ensuring there is no bleeding. This is the most common approach and gives the greatest access to the trachea. Fig. 5. Creating the tracheal portal. Instead of resecting and removing the tracheal ring, it can be used to create a flap, which can be attached to the skin. This method, described by Björk, 10 creates a stable tract for tube reinsertion. transection of the isthmus must be accomplished (Fig. 3). Blunt dissection is continued longitudinally through the pretracheal fascia, and the desired ring (usually the 2nd ring) is identified. One of 2 types of tracheal entry is usually used for ST. These are: complete removal of the anterior part of one of the tracheal rings to create the stoma, and creation of a flap with the severed part of the ring. In the ring-removal approach, the ring is lifted with a tracheal hook and 2 circumferential sutures are placed around the ring laterally. The portion of ring between the secured sutures is then cut and removed, leaving a hole in the anterior tracheal wall for the tracheostomy tube. The sutures are left in place and used to provide counter traction on the trachea as the tube is forced into the lumen. This is illustrated in Figure 4. The ring sutures are cut long and left out of the wound or used to secure the tracheostomy tube. These sutures can be used to identify the trachea and reinsert an inadvertently dislodged tracheostomy tube. After placement of an ST, the 490 RESPIRATORY CARE APRIL 2005 VOL 50 NO 4
4 Fig. 7. Fiberopic bronchoscopy is used to help place the guide wire correctly for PDT. Here the wire is seen in the anterior part or the trachea, passing between the 2nd and 3rd tracheal rings. Fig. 6. Using the Ciaglia method, a series of tapered dilators are sequentially inserted over the guide wire to create the stoma for placement of the tracheotomy tube. fistula tract is not stable for at least 4 5 days, and a tube dislodged soon after placement often cannot be reinserted through the fistula into the trachea. The ring sutures may help if this situation occurs. A second method for entry into the trachea involves creating a tracheal wall flap sutured to the skin. This is done by incising the fascia over the superior ring and entering the trachea along its inferior margin. This becomes the outer lip of the flap. Lateral cuts through the lower ring complete the sharp dissection. The flap thus created is reflected downward and attached with several sutures to the skin of the neck. This is shown in Figure This fistula is truly a stoma, with tracheal mucosa approximated to the skin. The stability of this tract is believed to be superior to the ring resection-removal technique; however, no study has convincingly demonstrated this. Percutaneous Dilational Tracheostomy Fig. 8. Here is the bronchoscopic view of the tip of a dilator entering the trachea over the guide wire during placement of a percutaneous dilational tracheostomy. As mentioned, an alterative to ST is percutaneous dilational tracheostomy (PDT), which has become a very common method of placing a tracheostomy in critically ill patients in the intensive care unit. It is rapid, simple, easy to learn, and cost-effective. While it seems superior to ST in some respects, some studies suggest a higher incidence of short-term but important problems. Long-term problems such as scar development, tracheal cutaneous fistula, and tracheal stenosis may be less with PDT, but more data will be needed to fully assess these risks. There are several different methods of performing PDT, the most common is that of Ciaglia, 5 in which a guide wire is placed between the first and second or second and third tracheal rings, and a series of stiff plastic dilators are sequentially forced into the tracheal wall over the guide wire RESPIRATORY CARE APRIL 2005 VOL 50 NO 4 491
5 Fig. 9. Important injuries to the vocal cords are often visualized during bronchoscopy through a laryngeal mask airway. Fig. 11. The guide wire is threaded through the catheter to act as a guide for the dilating forceps. (From Reference 6, with permission.) Fig. 10. An alternative to the sequential dilator technique was developed by Griggs. The trachea is entered between the appropriate tracheal rings with an intravenous catheter, with aspiration of air to confirm correct location. The needle is withdrawn and the catheter left in place as a conduit for the guide wire. (From Reference 6, with permission.) until a stoma of sufficient size to accommodate the desired tracheostomy tube is created (Fig. 6). As with placement of an ST, a PDT is usually performed in an anesthetized patient, can be done in the intensive care unit or operating room, and requires neck extension and a sterile field. Whether prophylactic antibiotics are useful for PDT is not yet known; however, one report suggests that they should be used and be tailored to the known flora of the tracheobronchial tree. 11,12 Fig. 12. This drawing depicts the sharp-tipped dilating forceps, with a channel for the guide wire developed by Griggs. (From Reference 6, with permission.) While some clinicians continue to perform PDT blindly, most have adopted a technique of observing and directing the needle and wire placement, using fiberoptic bronchoscopy. 13 This may help prevent inadvertent injury of the membranous tracheal (posterior) wall or too lateral a location of the tracheostomy. 14 In order to visualize the upper rings of the trachea with the bronchoscope, the endotracheal tube must be withdrawn until the tip is just in the larynx. This creates a substantial gas leak, as the cuff is no longer in the trachea. Patients experiencing severe hypoxic respiratory failure may deteriorate during this time and 492 RESPIRATORY CARE APRIL 2005 VOL 50 NO 4
6 Fig. 13. Griggs forceps are passed over the guide wire and spread in the skin and soft tissues of the neck (A) and into the trachea and spread again (B), to create a route though which the tracheostomy tube is inserted. (From Reference 6, with permission.) may benefit from conversion to ST rather than persistence with PDT. Patients requiring a tracheostomy only for airway access or protection often can have a laryngeal mask airway replace the endotracheal tube to provide the route for bronchoscopic visualization. The view of the larynx is unhampered when performed this way, making accurate identification of the tracheal rings easy. The bronchoscopic view of the wire being placed, seen in Figure 7, was obtained this way. In Figure 8 the dilator can be seen being passed over the wire. In addition to facilitating PDT, bronchoscopy through a laryngeal mask airway often reveals important pathology of the vocal cords (Fig. 9). An alternative to the sequential dilator technique was developed by Griggs et al. 6 Using a tracheal spreader modified to thread over the wire, this technique involves forceps dilation to create the skin path and tracheal stoma. As with the Ciaglia technique, the trachea is entered between Fig. 14. The Blue Rhino is a single dilator that can be used instead of the sequential dilators of the Ciaglia method. The outer surface of the dilator is very slippery, making insertion very easy. The size of the stoma must be carefully controlled by limiting the depth of insertion of the dilator. RESPIRATORY CARE APRIL 2005 VOL 50 NO 4 493
7 Fig. 15. Fantoni s translaryngeal placement of percutaneous dilational tracheostomy consists of a special tapered, flexible tracheostomy tube, the tip of which is cut off after placement, with the pilot balloon port secreted inside. (From Reference 8, with permission.) Fig. 17. The special tube is pulled from the inside through the trachea and dilates its own path. Digital counter-pressure provides tracheal stability. During placement, a small-diameter cuffed endotracheal tube can be used to support gas exchange while dilation is being performed. After placement, the dilating tip is removed, the upper part of the tube reversed in the trachea and the cuff inflated. (From Reference 8, with permission.) Fig. 16. After the guide wire is placed, a fiberoptic scope is used to direct the retrieval of the wire and bring it out of the endotracheal tube in Fantoni s technique. (From Reference 8, with permission.) the appropriate tracheal rings with an intravenous catheter (Fig. 10). Aspiration of air confirms tracheal entry. Bronchoscopy can also be used to prevent incorrect placement. The guide wire is threaded through the catheter (Fig. 11). The sharp-tipped dilating forceps (Fig. 12) are passed over the wire and spread in the skin and soft tissues of the neck (Fig. 13A) and into the trachea and spread again (see Fig. 13B). A tracheostomy tube is placed over the guide wire and through the passage created. Tracheal injury may be higher with this technique (especially if performed without bronchoscopy) than the other PDT techniques. The Blue Rhino dilator is a single, tapered dilator that is used instead of the sequential dilators of Ciaglia (Fig. 14). 15 It has a slippery coating that makes insertion very easy. It is softer and therefore (probably) less likely to damage the membranous tracheal wall. Since there is only a single dilator to pass, insertion is more rapid. 16 A substantial amount of force is needed to insert the dilators and tracheostomy tube, which often collapses the trachea and fractures a tracheal ring. The importance of ring fracture is not known. In an attempt to prevent membranous tracheal (posterior) wall injury and protect the anterior rings from fracture, Fantoni devised a special dilating tube that is placed translaryngeally through the trachea and pulled out rather than forced in. The technique, illustrated in Figures 15 17, is complicated and there are mixed reports regarding its success at protecting the trachea. Another attempt to solve the excessive-force problem with PDT is the PercTwist, a screw-action dilator that was designed to allow dilation with twisting while lifting the trachea rather than pushing down (Fig. 18). Reports with this method are preliminary and few. 17 Choosing a Technique The determining factors in deciding whether to use an ST or PDT in a particular situation include available resources (are there experienced clinicians available for either technique?) and patient factors. While there are no hard rules, some reasonable guidelines might include: 494 RESPIRATORY CARE APRIL 2005 VOL 50 NO 4
8 Fig. 18. The PercTwist is a screw-like dilating device, created to limit the amount of posterior force on the trachea during dilation. Here the device is shown, and what would be observed with a bronchoscope during the procedure. (From Reference 16, with permission.) 1. Coagulation abnormalities favor ST over PDT, since bleeding vessels are more easily controlled under direct vision. Limits on how abnormal should be in line with those set for other invasive procedures. 2. High levels of support need for oxygenation would favor ST over PDT (ie, fraction of inspired oxygen 0.7 and positive end-expiratory pressure 10 mm Hg have been suggested). 3. Patients with unstable or fragile cervical spines would favor ST over PDT. 4. Patients having recent surgical repair of neck injuries may benefit from PDT because of its lower wound-infection rate. 5. Patients with unfavorable neck anatomy would favor ST over PDT (ie, previous surgery, neck masses, poor neck mobility, or obesity may be more complicated for PDT). Summary ST has been performed for thousands of years to relieve upper airway obstruction; however, only in the past 200 years has survival of the operation been adequate to recommend its use. Currently, tracheostomy is performed in many situations and in critically ill patients with low morbidity. New percutaneous techniques offer advantages over standard open ST. However, operator experience and individual patient issues should control which technique is employed. PDT techniques are evolving and improving with time. ACKNOWLEDGMENT The author wishes to thank Brandy Durbin for her rendering of Figures 1 5. REFERENCES 1. Borman J, Davidson JT. A history of tracheostomy: Si Spiritum Ducit Vivit (Cicero). Br J Anaesth 1963;35: Jackson C. Tracheotomy. Laryngoscope 1909;19: Toy[sic] FJ, Weinstein JD. A percutaneous tracheostomy device. Surgery 1969;65(2): Toye FJ, Weinstein JD. Clinical experience with percutaneous tracheostomy and cricothyroidotomy in 100 trauma patients. J Trauma 1986;26(11): Ciaglia P, Firsching R, Syniec C. Elective percutaneous dilatational tracheostomy: a new simple bedside procedure; preliminary report. Chest 1985;87(6): Griggs WM, Worthley LI, Gilligan JE, Thomas PD, Myburg JA. A simple percutaneous tracheostomy technique. Surg Gynecol Obstet 1990;170(6): Ambesh SP, Pandey CK, Srivastava S, Agarwal A, Singh DK. Percutaneous tracheostomy with single dilatation technique: a prospective, randomized comparison of Ciaglia Blue Rhino versus Griggs guidewire dilating forceps. Anesth Analg 2002;95(6): Fantoni A, Ripamonti D. A non-derivative, non-surgical tracheostomy: the translaryngeal method. Intensive Care Med 1997;23(4): Westphal K, Maeser D, Scheifler G, Lischke V, Byhahn C. PercuTwist: a new single-dilator technique for percutaneous tracheostomy. Anesth Analg 2003;96(1): Björk VO. Partial resection of the only remaining lung with the aid of respirator treatment. J Thorac Cardiovasc Surg 1960;39: Jacobs S, Al Rasheed AM, Abdulsamat W, Al Barrak A, Al Omer NF, Tjan D, et al. Effects of a simple protocol on infective complications in intensive care unit patients undergoing percutaneous dilatational tracheostomy. Respir Care 2003;48(1): Durbin CG Jr. Bacteremia, infection, and antibiotic choices. Respir Care 2003;48(1): Oberwalder M, Weis H, Nehoda H, Kafka-Ritsch R, Bonatti H, Prommegger R, et al. Videobronchoscopic guidance makes percutaneous dilational tracheostomy safer. Surg Endosc 2004;18(5): Fernandez L, Norwood S, Roettger R, Gass D, Wilkins H 3rd. Bedside percutaneous tracheostomy with bronchoscopic guidance in critically ill patients. Arch Surg 1996;131(2): RESPIRATORY CARE APRIL 2005 VOL 50 NO 4 495
9 15. Bewsher MS, Adams AM, Clarke CW, McConachie I, Kelly DR. Evaluation of a new percutaneous dilatational tracheostomy set apparatus. Anaesthesia 2001;56(9): Byhahn C, Wilke HJ, Halbig S, Lischke V, Westphal K. Percutaneous tracheostomy: Ciaglia Blue Rhino versus the basic Ciaglia technique of percutaneous dilational tracheostomy. Anesth Analg 2000; 91(4): Frova G, Quintel M. A new simple method for percutaneous tracheostomy: controlled rotating dilation: a preliminary report. Intensive Care Med 2002;28(3): RESPIRATORY CARE APRIL 2005 VOL 50 NO 4
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Translaryngeal Tracheostomy - TLT Fantoni Method
 Translaryngeal Tracheostomy - TLT Fantoni Method Fantoni A., Ripamonti D., Lesmo A. About the Authors Fantoni Antonio Chief Emeritus of Department of Anaesthesia and Intensive Care - San Carlo Borromeo
Translaryngeal Tracheostomy - TLT Fantoni Method Fantoni A., Ripamonti D., Lesmo A. About the Authors Fantoni Antonio Chief Emeritus of Department of Anaesthesia and Intensive Care - San Carlo Borromeo
Comparison of Complications in Percutaneous Dilatational Tracheostomy versus Surgical Tracheostomy
 Global Journal of Health Science; Vol. 6, No. 4; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Comparison of Complications in Percutaneous Dilatational Tracheostomy
Global Journal of Health Science; Vol. 6, No. 4; 2014 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Comparison of Complications in Percutaneous Dilatational Tracheostomy
Indications for and Management of Tracheostomy
 Chapter 40 Indications for and Management of Tracheostomy Judi Anne B. Ramiscal, Michael S. Hayashi, and Mihae Yu Introduction A translaryngeal endotracheal tube (ETT) is the primary method of securing
Chapter 40 Indications for and Management of Tracheostomy Judi Anne B. Ramiscal, Michael S. Hayashi, and Mihae Yu Introduction A translaryngeal endotracheal tube (ETT) is the primary method of securing
Audit on Tracheostomies Performed at the General Intensive Care Unitt Kuala Lumpur Hospital
 ORIGINAL ARTICLE Audit on Tracheostomies Performed at the General Intensive Care Unitt Kuala Lumpur Hospital A S Rao, FANZCA, L Mansor, FRCA, K Inbasegaran, FANZCA Department of Anaesthesia and Intensive
ORIGINAL ARTICLE Audit on Tracheostomies Performed at the General Intensive Care Unitt Kuala Lumpur Hospital A S Rao, FANZCA, L Mansor, FRCA, K Inbasegaran, FANZCA Department of Anaesthesia and Intensive
Airway Management in the ICU
 Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
PRODUCTS FOR THE DIFFICULT AIRWAY. Courtesy of Cook Critical Care
 PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
PRODUCTS FOR THE DIFFICULT AIRWAY Courtesy of Cook Critical Care EMERGENCY CRICOTHYROTOMY Thyroid Cartilage Access Site Cricoid Cartilage Identify the cricothyroid membrane between the cricoid and thyroid
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
TRACHEOSTOMY 186 INTENSIVE CARE
 186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
186 INTENSIVE CARE Table 7.4 Indications for tracheostomy Upper-airway obstruction Prolonged mechanical ventilation To facilitate bronchopulmonary toilet To maintain and protect the airway use of oral
APPROACH TO THE EMERGENCY AIRWAY. Scott B. Davidson MD, FACS Trauma Surgery Service Bronson Methodist Hospital
 APPROACH TO THE EMERGENCY AIRWAY Scott B. Davidson MD, FACS Trauma Surgery Service Bronson Methodist Hospital Objectives History Initial recognition Get your act together Surgical options Complications
APPROACH TO THE EMERGENCY AIRWAY Scott B. Davidson MD, FACS Trauma Surgery Service Bronson Methodist Hospital Objectives History Initial recognition Get your act together Surgical options Complications
Trauma operating room
 Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Parma tracheostomy technique: a hybrid approach to tracheostomy between classical surgical and percutaneous tracheostomies
 Original Article Parma tracheostomy technique: a hybrid approach to tracheostomy between classical surgical and percutaneous tracheostomies Alberto Molardi 1, Filippo Benassi 1, Tullio Manca 2, Andrea
Original Article Parma tracheostomy technique: a hybrid approach to tracheostomy between classical surgical and percutaneous tracheostomies Alberto Molardi 1, Filippo Benassi 1, Tullio Manca 2, Andrea
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Is Percutaneous Tracheostomy Safe in Critically Ill Patients: A Retrospective Analysis
 ISSN: 2250-0359 Is Percutaneous Tracheostomy Safe in Critically Ill Patients: A Retrospective Analysis Ebru Tarıkçı Kılıç 1*, Mehmet Salim Akdemir 1, Ali İhsan Sert 2 1 Department of Anesthesiology and
ISSN: 2250-0359 Is Percutaneous Tracheostomy Safe in Critically Ill Patients: A Retrospective Analysis Ebru Tarıkçı Kılıç 1*, Mehmet Salim Akdemir 1, Ali İhsan Sert 2 1 Department of Anesthesiology and
External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other
 Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Etiology External trauma (MVA, surf board, assault, etc.) Internal trauma (Endotracheal intubation, tracheostomy) Other Systemic diseases (vasculitis, etc.) Chemo/XRT Idiopathic Trans nasal Esophagoscope
Subglottic stenosis, with involvement of the lower larynx
 Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Laryngotracheal Resection and Reconstruction John D. Mitchell, MD n, Subglottic stenosis is being recognized with increasing frequency in adults, and may be the most frequent indication for airway intervention
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
British Journal of Anaesthesia 104 (6): (2010) doi: /bja/aeq087 Advance Access publication April 21, 2010
 CRITICAL CARE Comparison between single-step and balloon dilatational tracheostomy in intensive care unit: a single-centre, randomized controlled study G. Cianchi 1, G. Zagli 1 *, M. Bonizzoli 1, S. Batacchi
CRITICAL CARE Comparison between single-step and balloon dilatational tracheostomy in intensive care unit: a single-centre, randomized controlled study G. Cianchi 1, G. Zagli 1 *, M. Bonizzoli 1, S. Batacchi
-Discussed in the Ebers Papyrus and the Rig Veda BC
 Tracheotomy History -Discussed in the Ebers Papyrus and the Rig Veda -1500 BC History -Treatment obstructive diseases (Antyllus, 2 nd century AD) -Discussed in the writings of Braassarolo (1546) -Considered
Tracheotomy History -Discussed in the Ebers Papyrus and the Rig Veda -1500 BC History -Treatment obstructive diseases (Antyllus, 2 nd century AD) -Discussed in the writings of Braassarolo (1546) -Considered
How to use the Control-Cric to perform a surgical cricothyrotomy
 TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
TRAININGGROUNDS How to use the Control-Cric to perform a surgical cricothyrotomy Product Description The Control-Cric is a System which verifies tracheal location during a surgical airway procedure, without
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Original Article Percutaneous dilational tracheostomy: An initial experience in community based teaching hospital
 Kathmandu University Medical Journal (2006), Vol. 4, No. 3, Issue 15, 275-280 Original Article Percutaneous dilational tracheostomy: An initial experience in community based teaching hospital Joshi S 1,
Kathmandu University Medical Journal (2006), Vol. 4, No. 3, Issue 15, 275-280 Original Article Percutaneous dilational tracheostomy: An initial experience in community based teaching hospital Joshi S 1,
Early Complications of Tracheostomy
 Early Complications of Tracheostomy Charles G Durbin Jr MD FAARC Introduction Definition of Risks Controlled, Randomized, Prospective Comparisons Anecdotal Reports of Complications Safety of Percutaneous
Early Complications of Tracheostomy Charles G Durbin Jr MD FAARC Introduction Definition of Risks Controlled, Randomized, Prospective Comparisons Anecdotal Reports of Complications Safety of Percutaneous
Policies and Procedures. I.D. Number: 1154
 Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
Policies and Procedures Title: TRACHEOSTOMY TUBE CHANGE - PEDIATRIC I.D. Number: 1154 Authorization: [X ] SHR Nursing Practice Committee Source: Nursing Date Effective: October 2008 Date Revised: March
PANELISTS. Controversial Issues In Common Interventions In ORL 4/10/2014
 Controversial Issues In Common Interventions In ORL Mohamed Hesham,MD Alexandria Faculty of Medicine PANELISTS Prof. Ahmed Eldaly Prof. Hamdy EL-Hakim Prof. Hossam Thabet Prof. Maged El-Shenawy Prof. Prince
Controversial Issues In Common Interventions In ORL Mohamed Hesham,MD Alexandria Faculty of Medicine PANELISTS Prof. Ahmed Eldaly Prof. Hamdy EL-Hakim Prof. Hossam Thabet Prof. Maged El-Shenawy Prof. Prince
Jay B. Brodsky, M.D. Professor Department of Anesthesia tel: (650) Stanford University School of Medicine fax: (650)
 Jay B. Brodsky, M.D. Professor Department of Anesthesia tel: (650) 725-5869 Stanford University School of Medicine fax: (650) 725-8544 Stanford, CA, 94305, USA e-mail: jbrodsky@stanford.edu RELIABLE SEPARATION
Jay B. Brodsky, M.D. Professor Department of Anesthesia tel: (650) 725-5869 Stanford University School of Medicine fax: (650) 725-8544 Stanford, CA, 94305, USA e-mail: jbrodsky@stanford.edu RELIABLE SEPARATION
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
Author's Accepted Manuscript
 Author's Accepted Manuscript One-lung ventilation via tracheostomy and left endobronchial microlaryngeal tube Stephen Howell MD, Monica Ata MD, Matthew Ellison MD, Colin Wilson MD www.elsevier.com/locate/buildenv
Author's Accepted Manuscript One-lung ventilation via tracheostomy and left endobronchial microlaryngeal tube Stephen Howell MD, Monica Ata MD, Matthew Ellison MD, Colin Wilson MD www.elsevier.com/locate/buildenv
Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis
 Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Use of the Silicone T-tube to Treat Tracheal Stenosis or Tracheal Injury
 Use of the Silicone T-tube to Treat Stenosis or Injury Chang-Jer Huang MD Backgound: stenosis or tracheal is a troublesome disease. Traditional temporary tracheostomy and reconstruction can resolve some
Use of the Silicone T-tube to Treat Stenosis or Injury Chang-Jer Huang MD Backgound: stenosis or tracheal is a troublesome disease. Traditional temporary tracheostomy and reconstruction can resolve some
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
Early Versus Late Tracheotomy in Patients with Severe Head Injury
 ORIGINAL ARTICLE Early Versus Late Tracheotomy in Patients with Severe Head Injury YASER UDDIN HOTI, MUHAMMAD IRFAN, AMIR AZIZ, AAMER UDDIN HOTI Khurram Ishaque and Tariq Salah Uddin Department of Neurosurgery
ORIGINAL ARTICLE Early Versus Late Tracheotomy in Patients with Severe Head Injury YASER UDDIN HOTI, MUHAMMAD IRFAN, AMIR AZIZ, AAMER UDDIN HOTI Khurram Ishaque and Tariq Salah Uddin Department of Neurosurgery
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Summary Report for Individual Task Perform a Surgical Cricothyroidotomy Status: Approved
 Report Date: 12 Jul 2011 Summary Report for Individual Task 081-833-3005 Perform a Surgical Cricothyroidotomy Status: Approved DISTRIBUTION RESTRICTION: Approved for public release; distribution is unlimited.
Report Date: 12 Jul 2011 Summary Report for Individual Task 081-833-3005 Perform a Surgical Cricothyroidotomy Status: Approved DISTRIBUTION RESTRICTION: Approved for public release; distribution is unlimited.
PERCUTANEOUS DILATIONAL TRACHEOSTOMY: A CONCISE CLINICAL REVIEW
 95 REVIEW ARTICLE PERCUTANEOUS DILATIONAL TRACHEOSTOMY: A CONCISE CLINICAL REVIEW Fares G. Mouchantaf, MD *, Carla R. Lamb, MD ** ABSTRACT Percutaneous dilational tracheostomy (PDT) is a commonly performed
95 REVIEW ARTICLE PERCUTANEOUS DILATIONAL TRACHEOSTOMY: A CONCISE CLINICAL REVIEW Fares G. Mouchantaf, MD *, Carla R. Lamb, MD ** ABSTRACT Percutaneous dilational tracheostomy (PDT) is a commonly performed
Nicolette Mosinski MPAS, PA-C
 Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Management of Pediatric Tracheostomy
 Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Management of Pediatric Tracheostomy Deepak Mehta Associate Professor Of Otolaryngology Director Pediatric Aerodigestive Center Definitions Tracheotomy: The making of an incision in the trachea The name
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Bronchoscopy SICU Protocol
 Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Bronchoscopy SICU Protocol Updated January 2013 Outline Clinical indications Considerations Preparation Bronchoscopy technique Bronchoalveolar Lavage (BAL) Post-procedure Purpose Bronchoscopy is a procedure
Educational Session: Evaluation and Management of the Difficult Airway
 Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Ponsky * PEG Safety System - "Pull" Bard * PEG Safety System - "Guidewire" Information for Use
 Ponsky * PEG Safety System - "Pull" Bard * PEG Safety System - "Guidewire" Information for Use Rx only Single patient use DEHP-Free This product and package do not contain natural rubber latex STERILE
Ponsky * PEG Safety System - "Pull" Bard * PEG Safety System - "Guidewire" Information for Use Rx only Single patient use DEHP-Free This product and package do not contain natural rubber latex STERILE
LESSON ASSIGNMENT. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
LESSON ASSIGNMENT LESSON 3 Cricothyroidotomy LESSON ASSIGNMENT Paragraphs 3-1 through 3-7. LESSON OBJECTIVES After completing this lesson, you should be able to: 3-1. Define cricothyroidotomy. 3-2. Identify
Department of Anesthesiology and Critical Care Medicine, Sanjay Gandhi Postgraduate Institute of Medical Sciences, Lucknow, India
 CRITICAL CARE AND TRAUMA SECTION EDITOR JUKKA TAKALA Percutaneous Tracheostomy with Single Dilatation Technique: A Prospective, Randomized Comparison of Ciaglia Blue Rhino Versus Griggs Guidewire Dilating
CRITICAL CARE AND TRAUMA SECTION EDITOR JUKKA TAKALA Percutaneous Tracheostomy with Single Dilatation Technique: A Prospective, Randomized Comparison of Ciaglia Blue Rhino Versus Griggs Guidewire Dilating
Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff
 2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
Percutaneous tracheostomy
 Bisanth Batuwitage MBBCh MRCS FRCA Stephen Webber MBChB FRCA FFICM Alastair Glossop BMed Sci BM BS MRCP FRCA DICM FFICM 1C02,2A01,2CO2 Key points Percutaneous tracheostomy is a safe and widely performed
Bisanth Batuwitage MBBCh MRCS FRCA Stephen Webber MBChB FRCA FFICM Alastair Glossop BMed Sci BM BS MRCP FRCA DICM FFICM 1C02,2A01,2CO2 Key points Percutaneous tracheostomy is a safe and widely performed
Management of pediatric cannot intubate, cannot oxygenate
 Acute Medicine & Surgery 2017; 4: 462 466 doi: 10.1002/ams2.305 Case Report Management of pediatric cannot intubate, cannot oxygenate Yohei Okada, 1 Wataru Ishii, 1 Norio Sato, 2 Hirokazu Kotani, 3 and
Acute Medicine & Surgery 2017; 4: 462 466 doi: 10.1002/ams2.305 Case Report Management of pediatric cannot intubate, cannot oxygenate Yohei Okada, 1 Wataru Ishii, 1 Norio Sato, 2 Hirokazu Kotani, 3 and
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS. - Our Perspective.
 ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY
 OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PAEDIATRIC TRACHEOSTOMY The open tracheostomy technique in the paediatric patient differs from that undertaken in the adult. In the paediatric
OPEN ACCESS ATLAS OF OTOLARYNGOLOGY, HEAD & NECK OPERATIVE SURGERY PAEDIATRIC TRACHEOSTOMY The open tracheostomy technique in the paediatric patient differs from that undertaken in the adult. In the paediatric
DIFFICULT AIRWAY MANAGMENT. Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr)
 DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
Peel-Apart Percutaneous Introducer Kits for
 Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Bard Access Systems Peel-Apart Percutaneous Introducer Kits for Table of Contents Contents Page Bard Implanted Ports Hickman*, Leonard*, Broviac*, Tenckhoff*, and Groshong* Catheters Introduction....................................
Which Percutaneous Tracheostomy Method Is Better? A Systematic Review
 Which Percutaneous Tracheostomy Method Is Better? A Systematic Review Alvaro Sanabria MD MSc PhD BACKGROUND: The aim of this study was to assess the different methods of percutaneous tracheostomy in terms
Which Percutaneous Tracheostomy Method Is Better? A Systematic Review Alvaro Sanabria MD MSc PhD BACKGROUND: The aim of this study was to assess the different methods of percutaneous tracheostomy in terms
Emergency Airway Management. Richard P. Dutton, M.D., M.B.A. Chief Quality Officer US Anesthesia Partners
 Emergency Airway Management Richard P. Dutton, M.D., M.B.A. Chief Quality Officer US Anesthesia Partners Disclosures I have studied a lot of airway gizmos over the years. I have no financial interest in
Emergency Airway Management Richard P. Dutton, M.D., M.B.A. Chief Quality Officer US Anesthesia Partners Disclosures I have studied a lot of airway gizmos over the years. I have no financial interest in
Feasibility of Percutaneous Dilatational Tracheostomy with a Light Source in the Surgical Intensive Care Unit
 Acute and Critical Care 2018 May 33(2):89-94 / ISSN 2586-6052 (Print) ㆍ ISSN 2586-6060 (Online) Original Article Feasibility of Percutaneous Dilatational Tracheostomy with a Light Source in the Surgical
Acute and Critical Care 2018 May 33(2):89-94 / ISSN 2586-6052 (Print) ㆍ ISSN 2586-6060 (Online) Original Article Feasibility of Percutaneous Dilatational Tracheostomy with a Light Source in the Surgical
Surgical Repair of Iatrogenic Cervical Tracheal Stenosis
 Surgical Repair of Iatrogenic Cervical Tracheal Stenosis Nirmal K. Veeramachaneni, MD, and Bryan F. Meyers, MD, MPH he advent of intensive care unit management has increased the potential opportunities
Surgical Repair of Iatrogenic Cervical Tracheal Stenosis Nirmal K. Veeramachaneni, MD, and Bryan F. Meyers, MD, MPH he advent of intensive care unit management has increased the potential opportunities
Surgical Technique. Proximal Humerus Locking Plate
 Surgical Technique Proximal Humerus Locking Plate PERI-LOC Upper Extremity Locked Plating System 3.5mm & 4.5mm Proximal Humerus Locking PlatesCatalog Infor Table of Contents Introduction.........................................................2
Surgical Technique Proximal Humerus Locking Plate PERI-LOC Upper Extremity Locked Plating System 3.5mm & 4.5mm Proximal Humerus Locking PlatesCatalog Infor Table of Contents Introduction.........................................................2
Airway management problem during anaesthesia. Airway management problem in ICU / HDU. Airway management problem occurring in the Emergency Department
 4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
4th National Audit Project of the Royal College of Anaesthetists: Major Complications of Airway Management in the UK Please select one form from the list below Airway management problem during anaesthesia
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator
 Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Airway Management in a Patient with Klippel-Feil Syndrome Using Extracorporeal Membrane Oxygenator Beckerman Z*, Cohen O, Adler Z, Segal D, Mishali D and Bolotin G Department of Cardiac Surgery, Rambam
Operative tracheotomy
 Operative Techniques in Otolaryngology (2007) 18, 85-89 Operative tracheotomy W. Cooper Scurry, Jr, MD, Johnathan D. McGinn, MD From the Department of Surgery, Division of Otolaryngology Head and Neck
Operative Techniques in Otolaryngology (2007) 18, 85-89 Operative tracheotomy W. Cooper Scurry, Jr, MD, Johnathan D. McGinn, MD From the Department of Surgery, Division of Otolaryngology Head and Neck
TRACHEOSTOMY. 28 August J Reddy CONTENTS
 28 August 2009 CONTENTS TRACHEOSTOMY J Reddy Commentator: L Pillay Moderator: D Muckart INTRODUCTION... 3 HISTORY OF TRACHEOSTOMY... 3 ANATOMY... 3 PHYSIOLOGY... 6 INDICATIONS FOR TRACHEOSTOMY... 9 CONTRAINDICATIONS...
28 August 2009 CONTENTS TRACHEOSTOMY J Reddy Commentator: L Pillay Moderator: D Muckart INTRODUCTION... 3 HISTORY OF TRACHEOSTOMY... 3 ANATOMY... 3 PHYSIOLOGY... 6 INDICATIONS FOR TRACHEOSTOMY... 9 CONTRAINDICATIONS...
Difficult Airway. Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital
 Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
Difficult Airway Victor M. Gomez, M.D. Pulmonary Critical Care Medicine Medical City Dallas Hospital Difficult Airway Definition Predicting a difficult airway Preparing for a difficult airway Extubation
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
The Impact of Obesity on Adult Tracheostomy Complication Rate
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS The Impact of Obesity on Adult Tracheostomy Complication Rate Susan
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS The Impact of Obesity on Adult Tracheostomy Complication Rate Susan
Case Review: Airway Trauma Case 1: Tracheal Transection Pre-hospital:
 (Prepared by: A. Bacevice, MD) The following two cases were submitted for the case competition in 2016. They are presented to illustrate the theme of airway trauma. Case Review: Airway Trauma Case 1: Tracheal
(Prepared by: A. Bacevice, MD) The following two cases were submitted for the case competition in 2016. They are presented to illustrate the theme of airway trauma. Case Review: Airway Trauma Case 1: Tracheal
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC
 Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Changing tracheostomy tubes
 Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Changing tracheostomy tubes Changing the tracheostomy tube should be a multidisciplinary decision. The first change should always be performed or supervised by a suitably trained member of the medical
Review of Posttracheostomy And Postintubation Tracheal Stenosis With Special Regard to Etiology and Treatment
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 6 Number 1 Review of Posttracheostomy And Postintubation Tracheal Stenosis With Special Regard to Etiology and A Sarper, A Ayten,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 6 Number 1 Review of Posttracheostomy And Postintubation Tracheal Stenosis With Special Regard to Etiology and A Sarper, A Ayten,
How do you use a bougie as an airway adjunct for endotracheal intubation?
 Ruth Bird, MBBCh -Specialist Registrar: Anaesthesia & Paediatric Trauma Fellow Daniel Nevin, MBBCh -Consultant in Anaesthesia & Pre-Hospital Care The Royal London Hospital London s Air Ambulance (HEMS)
Ruth Bird, MBBCh -Specialist Registrar: Anaesthesia & Paediatric Trauma Fellow Daniel Nevin, MBBCh -Consultant in Anaesthesia & Pre-Hospital Care The Royal London Hospital London s Air Ambulance (HEMS)
Flexible Fiberoptic Exam
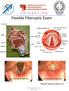 Flexible Fiberoptic Exam True Vocal Cords abducted True Vocal Cords adducted *Fiberoptic endoscopy, image is true. Cerumen Removal Position Patient -Explain Procedure Visualize Canal/Landmarks Determine
Flexible Fiberoptic Exam True Vocal Cords abducted True Vocal Cords adducted *Fiberoptic endoscopy, image is true. Cerumen Removal Position Patient -Explain Procedure Visualize Canal/Landmarks Determine
Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia
 DIFFICULT AIRWAY CANNOT VENTILATE, CANNOT INTUBATE. Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia Difficult airway According to AMERICAN SOCIETY OF ANAESTHESIOLOGISTS Difficult Airway is defined
DIFFICULT AIRWAY CANNOT VENTILATE, CANNOT INTUBATE. Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia Difficult airway According to AMERICAN SOCIETY OF ANAESTHESIOLOGISTS Difficult Airway is defined
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Policy x.xxx. Issued: Artificial Airways and Airway Care. ABC Home Medical Company Policy & Procedure Manual. A. Tracheostomy Tubes ( trach tubes)
 A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Surgical Management of Subglottic Stenosis
 Surgical Management of Subglottic Stenosis Cameron D. Wright, MD ubglottic stenosis is usually due to either endotracheal S tube ischemic necrosis or idiopathic larygotracheal stenosis. The ischemic area
Surgical Management of Subglottic Stenosis Cameron D. Wright, MD ubglottic stenosis is usually due to either endotracheal S tube ischemic necrosis or idiopathic larygotracheal stenosis. The ischemic area
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Imbibe Bone marrow aspiration needle. Operative technique
 Imbibe Bone marrow aspiration needle Operative technique Imbibe Bone Marrow Aspiration Needle Imbibe Bone marrow aspiration needle Contents 1. Smart design... 3 2. Operative technique... 4 Posterior iliac
Imbibe Bone marrow aspiration needle Operative technique Imbibe Bone Marrow Aspiration Needle Imbibe Bone marrow aspiration needle Contents 1. Smart design... 3 2. Operative technique... 4 Posterior iliac
Corkscrew stenosis : Defining and preventing a complication of percutaneous dilatational tracheostomy
 Corkscrew stenosis : Defining and preventing a complication of percutaneous dilatational tracheostomy Jordan V. Jacobs, MD, a David A. Hill, MD, a Scott R. Petersen, MD, a Ross M. Bremner, MD, PhD, b Richard
Corkscrew stenosis : Defining and preventing a complication of percutaneous dilatational tracheostomy Jordan V. Jacobs, MD, a David A. Hill, MD, a Scott R. Petersen, MD, a Ross M. Bremner, MD, PhD, b Richard
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of translaryngeal tracheostomy Tracheostomy using a breathing tube inserted from
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of translaryngeal tracheostomy Tracheostomy using a breathing tube inserted from
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Steroid Therapy for Tracheal Stenosis in Children
 Steroid Therapy for Tracheal Stenosis in Children Clinical Experience in 4 Children with Severe Strictures H. Biemann Othersen, Jr., M.D. ABSTRACT Recently a refinement in the treatment of tracheal stenosis
Steroid Therapy for Tracheal Stenosis in Children Clinical Experience in 4 Children with Severe Strictures H. Biemann Othersen, Jr., M.D. ABSTRACT Recently a refinement in the treatment of tracheal stenosis
Proceedings of the World Small Animal Veterinary Association Mexico City, Mexico 2005
 Close this window to return to IVIS Proceedings of the World Small Animal Veterinary Association Mexico City, Mexico 2005 Hosted by: Reprinted in the IVIS website with the permission of the WSAVA Surgery
Close this window to return to IVIS Proceedings of the World Small Animal Veterinary Association Mexico City, Mexico 2005 Hosted by: Reprinted in the IVIS website with the permission of the WSAVA Surgery
Adult Patients Going Home with a Tracheostomy
 Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Physiotherapy Department Adult Patients Going Home with a Tracheostomy Darent Valley Hospital Darenth Wood Road Dartford Kent DA2 8DA www.dvh.nhs.uk In case of emergencies you will need to dial 999 If
Airway Management. Teeradej Kuptanon, MD
 Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Tracheal Stenosis Following Cuffed Tube Tracheostomy
 Tracheal Stenosis Following Cuffed Tube Tracheostomy Anatomical Variation and Selected Treatment Armand A. Lefemine, M.D., Kenneth MacDonnell, M.D., and Hyung S. Moon, M.D. ABSTRACT Tracheal stenosis resulting
Tracheal Stenosis Following Cuffed Tube Tracheostomy Anatomical Variation and Selected Treatment Armand A. Lefemine, M.D., Kenneth MacDonnell, M.D., and Hyung S. Moon, M.D. ABSTRACT Tracheal stenosis resulting
Rotator Cuff Repair using JuggerKnot Soft Anchor 2.9mm Surgical Technique
 Rotator Cuff Repair using JuggerKnot Soft Anchor 2.9mm Surgical Technique It s small. It s strong. And it's all suture. The JuggerKnot Soft Anchor represents the next generation of suture anchor technology.
Rotator Cuff Repair using JuggerKnot Soft Anchor 2.9mm Surgical Technique It s small. It s strong. And it's all suture. The JuggerKnot Soft Anchor represents the next generation of suture anchor technology.
