Treatment of male idiopathic infertility with recombinant human follicle-stimulating hormone: a prospective, controlled, randomized clinical study
|
|
|
- Loren Welch
- 6 years ago
- Views:
Transcription
1 Treatment of male idiopathic infertility with recombinant human follicle-stimulating hormone: a prospective, controlled, randomized clinical study Carlo Foresta, M.D., Ph.D., a Andrea Bettella, M.D., Ph.D., a Andrea Garolla, M.D., Ph.D., a Guido Ambrosini, M.D., Ph.D., b and Alberto Ferlin, M.D., Ph.D. a a Centre for Male Gamete Cryopreservation, Department of Histology, Microbiology, and Medical Biotechnologies, and b Department of Gynecological and Human Reproduction Sciences, University of Padova, Padova, Italy Objective: To evaluate the effects of treatment with FSH on seminal parameters and spontaneous pregnancy in male infertility. Design: Prospective, controlled, randomized clinical study. Setting: Infertility center at a university hospital. Patient(s): One hundred twelve men affected by idiopathic oligozoospermia. Intervention(s): Patients were randomized into two groups: 62 subjects were treated with 100 IU of recombinant human FSH on alternate days for 3 months, and 50 patients did not receive any treatment. Semen analysis was performed in all subjects at the end of this period of treatment and after the following 3 months. Subjects who had not reached spontaneous pregnancy underwent assisted reproductive techniques. Main Outcome Measure(s): Seminal parameters, testicular cytologic analysis, FSH, LH, T, and inhibin B concentrations. Result(s): The treatment group considered as a whole did not show modifications in sperm parameters. However, a subgroup of these (30, 48.4%) had a significant increase of sperm count (responder group). In the period including 3 months after the withdrawal of FSH therapy, we observed a significantly higher spontaneous pregnancy rate in the responder group (5 of 30 [16.7%]) with respect to nonresponder and nontreated groups (1 of 32 [3.1%] and 2 of 50 [4.0%], respectively). Furthermore, the improvement of seminal parameters in the responder group allowed these patients to undergo less frequent IVF-ET/intracytoplasmic sperm injection. Conclusion(s): Results from this controlled, randomized clinical trial show that FSH therapy does not improve sperm concentration or pregnancy rate when infertile male patients are chosen solely by the clinical criteria of idiopathic oligospermia and normal FSH concentration. Subgroup analysis, however, does indicate that patients without maturation arrest in addition to the clinical scenario do benefit from medical therapy. (Fertil Steril 2005; 84: by American Society for Reproductive Medicine.) Key Words: Male infertility, FSH therapy, idiopathic oligozoospermia Follicle-stimulating hormone plays a crucial role in spermatogenesis (1, 2), and several experimental and clinical studies have demonstrated the importance of this hormone in regulating a normal quantitative spermatogenic process in animals and humans (3 7). Because of this physiologic role of FSH in spermatogenesis, various attempts have been made to treat idiopathic oligozoospermic subjects with this hormone. However, the results obtained so far are still controversial. In particular, several uncontrolled studies have shown an improvement of seminal parameters and/or an increase of pregnancy rates in infertile men treated with different doses of FSH (8 12). Nevertheless, these results have not been confirmed in randomized controlled studies. Only two randomized controlled clinical studies have been performed using both highly purified FSH and recombinant human FSH Received September 28, 2004; revised and accepted March 15, Reprint requests: Carlo Foresta, University of Padova, Department of Histology, Microbiology, and Medical Biotechnologies, Centre for Male Gamete Cryopreservation, Via Gabelli, 63, Padova 35121, Italy (FAX: ; carlo.foresta@unipd.it). (hfsh), and they did not show any improvement of seminal parameters or a significant increase in pregnancy rates in infertile men receiving the treatment compared with those receiving no treatment or placebo (13, 14). Controlled trials are crucial to evaluate the effectiveness of a novel therapeutic protocol, but this evaluation is extremely difficult in the setting of male infertility. In fact, fertility of a man should actually be considered in the setting of the fertility of the couple, and it is not always evident only from the man s semen analysis, with the exception of azoospermia or severe oligozoospermia. Furthermore, a reduction of sperm number in the ejaculate might be caused by different etiologies and might be related to different kinds of tubular disease, such as hypospermatogenesis or maturation arrest at different levels of spermatogenesis. These considerations should be kept in mind when recruiting infertile or oligozoospermic men as a whole to study the effectiveness of a therapeutic protocol. Recently, we demonstrated that FSH (highly purified FSH and recombinant hfsh) could be an appropriate and valid 654 Fertility and Sterility Vol. 84, No. 3, September /05/$30.00 Copyright 2005 American Society for Reproductive Medicine, Published by Elsevier Inc. doi: /j.fertnstert
2 treatment of oligozoospermic patients only when FSH and inhibin B plasma levels are in the normal range and the testicular tubular structure is characterized by hypospermatogenesis without germ cell maturation disturbances (15 18). No efficacy of FSH treatment is seen either when FSH plasma concentrations are higher than normal or when spermatogenic arrest is present. These preliminary studies were conducted primarily to verify the effectiveness of this therapy in male infertility and with particular attention to the criteria able to select appropriate clinical conditions predicting a seminal response to this specific hormonal treatment. Here, we better clarified the effectiveness of FSH therapy on sperm count and pregnancy rate by means of a prospective, controlled, randomized clinical study in a selected group of patients affected by idiopathic oligozoospermia. MATERIALS AND METHODS Our study was approved by the ethics committee of the University of Padova, and informed consent was obtained from each subject. All phases of the study were performed at the Infertility Centre of the University of Padova. All men were informed about the protocol of treatment and in particular about the different phases of the design of the study and about the possibility of undergoing assisted reproductive techniques (ARTs) during this period. Inclusion criteria were [1] a history of infertility for at least 2 years, [2] sperm count /ml on at least three separate occasions, according to World Health Organization guidelines (19), [3] idiopathic infertility with exclusion of common conditions, such as history of cryptorchidism, postmumps orchitis, testicular torsion or trauma, varicocele, seminal tract infections, antisperm antibodies and Y chromosome microdeletions, karyotypic abnormalities, and CFTR gene mutations, [4] normal plasma levels of FSH (range, 1 7 IU/L), LH (range, 2 6 IU/L), PRL (range, ng/ml), T (range 3 9 ng/ml), and inhibin B ( 150 pg/ml), and [5] exclusion of clear female factors, such as ovulatory disorders, tubal factor, and endocrine abnormalities as evaluated by endocrine evaluation, pelvic ultrasound examination, and hysterosalpingography. A total of 128 patients fulfilled the inclusion criteria and were enrolled in the study. Patients were randomly allocated to treatment or nontreatment groups in a blinded fashion by third-party true randomization in a 1:1 ratio with a random number generator. Sixty-five men were allocated to the treatment group and 63 to the nontreatment group. Of these, 6 couples (2 from the treatment group and 4 from the nontreatment group) were subsequently excluded from the study because of concurrent illnesses. Ten subjects (1 from the treatment group and 9 from the nontreatment group) dropped out before completing the study: 2 in the nontreatment group were lost, 7 in the nontreatment group dropped out by the patient s request, and 1 in the treatment group discontinued intervention. Therefore, 112 men affected by idiopathic oligozoospermia completed the study (62 in the treatment group and 50 in the nontreatment group), were analyzed, and are described here. There were no significant differences between the groups in the clinical characteristics that we assessed. The testicular structure was analyzed in all patients by means of bilateral fine needle aspiration cytology (FNAC) (20 22), to evaluate the tubular status related to the oligozoospermia. The methods of aspiration and cytologic analysis have been described previously in detail (20 22). Briefly, testicular aspiration is a simple procedure performed with a 23-gauge (0.6-mm) butterfly needle attached to a 20-mL syringe. The retrieved material is placed on two or more microscope slides for each testis, stained with May- Grünwald and Giemsa stains, and examined under a light microscope at magnifications of 125, 400, and 1,250, counting at least 200 spermatogenic cells (spermatogonia, primary and secondary spermatocytes, early and late spermatids, and spermatozoa) per smear and the interposed Sertoli cells. The cell number is expressed as a percentage. All patients underwent ultrasound scanning of the testis to evaluate testicular size and morphology before undergoing testicular aspiration. Semen evaluations were performed in a blinded fashion with regard to treatment and by the same operator. Plasma concentrations of FSH, LH, and T were measured by RIA with standard methods. Inhibin B plasma concentrations were measured by a solid-phase sandwich ELISA specific for the dimeric inhibin-b form (Serotec, Oxford, United Kingdom), as previously described (23, 24). Forty age-matched fertile and normozoospermic subjects were considered as controls for seminal and hormonal parameters. Design of the Study Improvement of seminal parameters is not always associated with an improvement in pregnancy rates. Therefore, to clarify the effectiveness of FSH therapy, subjects were studied in three consecutive phases, with primary outcomes being represented by both sperm parameters and pregnancy rate: [1] a period of treatment with recombinant hfsh for 3 months (therapy period), [2] the following 3-month period after the withdrawal of therapy, during which all subjects were monitored for semen parameters and spontaneous pregnancies (follow-up period), and [3] the following 3-month period, during which all subjects who had not reached pregnancy during the two previous periods underwent ART (ART period) (Fig. 1). Therapy Period After the initial assessment (basal hormonal parameters, three semen analyses, history and physical examination, ultrasound scanning of the testes, and FNAC), the patients were prospectively randomized into two groups: 62 subjects Fertility and Sterility 655
3 FIGURE 1 Study description. FIVET in vitro fertilization embryo transfer. PATIENTS STUDIED (112) Treated group (62) (r-hfsh 100 IU on alternate days) Infertile-control group (50) (no therapy) THERAPY PERIOD 3 months Responder group (30) Non-responder group (32) (50) FOLLOW UP PERIOD 3 months 16.7% 5/30 3.1% 1/32 4.0% 2/50 Spontaneous No (25) No (31) No (48) ART PERIOD 3 months IUI 20.0% 3/15 IUI n.s. IUI n.s. after ART IVF FIVET 30.0% 3/10 ICSI - IVF FIVET 18.2% 2/11 ICSI 20.0% 4/20 IVF FIVET 22.2% 4/18 ICSI 20.0% 6/30 n.s.: not suitable Foresta. FSH therapy in male idiopathic infertility. Fertil Steril received recombinant hfsh (100 IU IM on alternate days for 3 months) (treated group), and 50 patients did not receive any treatment (infertile control group). The two groups were comparable in terms of age ( years vs years), duration of infertility ( years vs years), and semen, hormonal, and cytologic parameters, as discussed below. At the end of this 3-month period, semen analysis was performed in all subjects (treated and controls) by the same operator. Pretreatment and posttreatment semen evaluations were performed in a blinded fashion with regard to treatment. All spontaneous pregnancies occurring during this period were recorded and eventually confirmed by measurement of hcg plasma levels. Follow-Up Period To evaluate the effectiveness of FSH treatment, we continued to study these 112 male-factor infertile couples during an additional 3-month period. All subjects were encouraged to have a special coitus frequency, at least two to three times per week, particularly at midcycle. All spontaneous pregnancies occurring during these 3 months were recorded and confirmed by measurement of hcg plasma levels. 656 Foresta et al. FSH therapy in male idiopathic infertility Vol. 84, No. 3, September 2005
4 TABLE 1 Clinical and hormonal features of oligozoospermic patients compared with controls (fertile subjects). Treated group (n 62) Infertile control group (n 50) Control group (n 40) Demographic data Age of patients (y) Age of partner (y) Infertility duration (y) Seminal parameters Sperm concentrations ( 10 6 /ml) a a Total no. of spermatozoa ( 10 6 ) a a Forward motility (%) b b Normal morphology (%) Hormone levels FSH (IU/L) LH (IU/L) T (ng/ml) Inhibin B (pg/ml) Testicular volume (ml) b b Note: Data are presented as mean SD. The treatment group received recombinant hfsh (100 IU on alternate days); the infertile control group received no treatment. a P.001 vs. control group. b P.05 vs. control group. Foresta. FSH therapy in male idiopathic infertility. Fertil Steril At the end of the follow-up period, all patients were reevaluated for semen analysis. ART Period Within 3 months after the follow-up period, all patients who had not reached spontaneous pregnancy underwent ARTs. Patients with a total number of motile postwash spermatozoa were randomly enrolled either to IUI for three cycles or IVF for 1 cycle (25, 26). If the number of total motile spermatozoa was not suitable for IUI ( ), couples were enrolled only in IVF programs, either IVF-ET or intracytoplasmic sperm injection (ICSI) (1 cycle), considering the specific indications. After this period, the new pregnancies were recorded. For IUI, ovarian stimulation started on day 3 of a spontaneous menstrual cycle with 100 mg of clomiphene citrate for 5 days. Ovarian monitoring was carried out by vaginal ultrasound, starting on day 10 of the menstrual cycle. Ovulation was induced with hcg (5,000 IU IM) when at least one follicle with a diameter 18 mm was observed. Two inseminations per cycle were performed, 24 hours and 48 hours after the administration of hcg. For IVF, the ovulation induction protocol used was the same for all the female partners and included down-regulation with a GnRH agonist and ovarian stimulation with recombinant hfsh. Follicular growth was monitored according to E 2 plasma levels and ultrasound measurements. Follicular aspiration was performed under transvaginal ultrasound guidance hours after hcg administration. The following steps, as regarding sperm preparation, insemination of oocytes, fertilization, embryo culture, and ET were performed according to European Society of Human Reproduction and Embryology indications (27). Statistical Analysis The results are expressed as mean SD. Comparisons between groups were performed with unpaired Student s t-tests. Comparisons of pretreatment and posttreatment data were performed with paired Student s t-tests. Comparisons of proportion were performed with a one-sided nonparametric resampling test. Probability (P) values of.05 were considered statistically significant. RESULTS Therapy Period The baseline clinical and hormonal data of the treated, infertile control, and normal control (fertile subjects) groups are summarized in Table 1. The treatment was well tolerated in all subjects, and no significant side effects were reported. In the treatment group considered as a whole, no modifications in sperm parameters were observed during the 3 Fertility and Sterility 657
5 TABLE 2 Sperm parameters observed during the different periods of the study in responder and nonresponder groups (treated subjects) and in the infertile control group (no treatment). Responder group (n 30) Non-responder group (n 32) Infertile control group (n 50) Sperm count ( 10 6 /ml) Total spermatozoa ( 10 6 ) Sperm count ( 10 6 /ml) Total spermatozoa ( 10 6 ) Sperm count ( 10 6 /ml) Total spermatozoa ( 10 6 ) Basal End of therapy period a a End of follow-up period b b End of ART period Note: Data are presented as mean SD. Therapy period: treatment with recombinant hfsh (100 IU IM) on alternate days for 3 months; follow-up period: an observation period of 3 months after the withdrawal of therapy; ART period: 3 months of ART. a P.01 vs. pretreatment. b P.05 vs. pretreatment. Foresta. FSH therapy in male idiopathic infertility. Fertil Steril months of therapy (sperm concentration /ml basal and /ml at the end of therapy). However, individual analysis of sperm parameters allowed us to identify two subgroups after the 3-month period of recombinant hfsh treatment: the responder group (30 of 62 subjects, 48.4%), who increased their sperm count after therapy, with a doubling of sperm concentration with respect to baseline; and the nonresponder group (32 of 62 subjects, 51.6%), who showed no increase in seminal parameters after FSH treatment. No significant variations were observed in other seminal parameters, such as forward motility and normal morphology, at the end of treatment in both groups (data not shown). In the infertile control group, no significant variations of sperm parameters were observed during this first period of observation. Table 2 summarizes the seminal parameters observed before and after recombinant hfsh therapy in the responder and nonresponder groups and in the infertile control group. Confirming previous studies, pretreatment testicular cytologic analysis of the patients in the responder group was characterized by isolated hypospermatogenesis (reduction in the number of germ cells without maturative disturbances); nonresponder patients had a cytologic picture of hypospermatogenesis, with maturative disturbances at different levels of the spermatogenetic process (spermatogonial spermatocytes or spermatidic arrest). During this first period, we did not observe spontaneous pregnancies in either the treated or the infertile control groups. Follow-Up Period Three months after the withdrawal of recombinant hfsh therapy, another sperm analysis was performed in all subjects. We did not observe any significant differences in seminal parameters in the treated group considered as a whole or in the nonresponder and infertile control groups. The responder group showed a significantly higher sperm concentration with respect to pretreatment sperm count. The mean sperm concentration in this group was not different from that observed after the 3-month period of FSH treatment (Table 2). During the follow-up period, the responder group showed significantly higher pregnancy rates. In fact, 5 patients achieved spontaneous pregnancies in the responder group (5 of 30, 16.7%), whereas one patient in the nonresponder group (1 of 32, 3.1%) and 2 in the infertile control group (2 of 50, 4.0%) achieved pregnancy (Fig. 1, Table 3). ART Period Six months after the withdrawal of recombinant hfsh therapy, another sperm analysis was performed in all subjects. No significant differences in seminal parameters were observed in the treated group considered as a whole or in the nonresponder and infertile control groups with respect to previous examinations. In the responder group, we observed a reduction of sperm concentration that was not, however, statistically different with respect to previous analyses. During this period, the patients who did not achieve pregnancy in the previous periods underwent ARTs. Because all patients in the responder group had a number of total motile postwash spermatozoa , they were randomly en- 658 Foresta et al. FSH therapy in male idiopathic infertility Vol. 84, No. 3, September 2005
6 TABLE 3 Pregnancy rates during the follow-up and ART periods in responder and nonresponder groups (treated subjects) and in infertile control group (no treatment). Follow-up period (spontaneous) ART period IUI IVF-ET ICSI Cumulative Treated subjects (n 62) 9.7 (6/62) 20.0 (3/15) 23.8 (5/21) 20.0 (4/20) 29.0 (18/62) Responder group (n 30) 16.7 (5/30) a 20.0 (3/15) 30.0 (3/10) 36.7 (11/30) Nonresponder group (n 32) 3.1 (1/32) Nonsuitable 18.2 (2/11) 20.0 (4/20) 21.9 (7/32) Infertile control group (n 50) 4.0 (2/50) Nonsuitable 22.2 (4/18) 20.0 (6/30) 24.0 (12/50) Note: Data are expressed as percentage (number). a P.05 vs. nonresponder and infertile control groups. Foresta. FSH therapy in male idiopathic infertility. Fertil Steril rolled in two ART programs: 15 subjects to IUI (three cycles) and 10 subjects to IVF-ET (one cycle). There were three pregnancies achieved in the patients assigned to IUI (3 of 15, 20.0%) and three pregnancies in the patients assigned to IVF-ET (3 of 10, 30.0%). The cumulative pregnancy rate in this group after ART was therefore 24.0% (6 of 25). In the other two groups, the number of total motile spermatozoa was not sufficient for an IUI program, so they were enrolled only for IVF (one cycle). Cumulative pregnancy rates in these groups after ART were 19.3% (6 of 31) and 20.8% (10 of 48) in the nonresponder and infertile control groups, respectively (Fig. 1, Table 3). In summary, during the follow-up and ART periods (i.e., during the 6-month period after the withdrawal of recombinant hfsh therapy), the cumulative pregnancy rate was 29.0% (18 of 62) in treated subjects. For the treatment subgroups, the pregnancy rates were 36.7% (11 of 30) in the responder group and 21.9% (7 of 32) in the nonresponder group. In the infertile control group, the pregnancy rate was 24.0% (12 of 50) (Table 3). DISCUSSION A male factor is the cause of infertility in approximately 25% 30% of infertile couples, and in an additional 30%, detectable abnormalities can be found in both partners (28, 29). Many aspects of male infertility are poorly understood, and medical therapy for these patients is mainly empiric and largely unsuccessful. Therefore, the management of male infertility often does not consider a pharmacologic treatment, and couples are directly treated with assisted reproduction. However, we think that medical therapy with FSH might be a valid method for improving spermatogenesis, although this treatment is effective only in selected cases. This is the first prospective, controlled, randomized clinical study showing that treatment with recombinant hfsh can improve seminal parameters and also spontaneous pregnancies in a selected group of idiopathic oligozoospermic patients. To evaluate the effectiveness of FSH therapy, we randomized infertile patients into two groups, treated or untreated. We did not observe any significant variation in seminal parameters in infertile control subjects and in the treatment group considered as a whole. However, in treated patients, a significant increase of sperm concentration was observed in approximately half the subjects (responder group). These subjects were affected by isolated hypospermatogenesis without spermatogenic arrest, as evaluated by FNAC before treatment. These data expand and confirm previous preliminary studies and strengthen the evidence that FSH treatment could be effective only in oligozoospermic subjects with normal FSH and inhibin B plasma concentrations and a testicular structure of moderate hypospermatogenesis without maturation defect. In such cases the spermatogenetic process can be efficaciously stimulated, thereby obtaining an increased sperm number in the ejaculate. The second aim of the present study was to evaluate the effectiveness of FSH therapy in terms of pregnancy rate. This is an important issue when evaluating the effect of a treatment for male infertility, because the improvement of seminal parameters often is not associated with an improvement of pregnancy rate, and conversely, spontaneous pregnancies can be achieved in infertile couples outside the treatment period. An improved pregnancy rate is also the primary endpoint for infertile couples, thus this parameter should be evaluated as a main outcome measurement of the effectiveness of a pharmacologic treatment in male infertility. Only two randomized, controlled clinical studies of FSH therapy in male infertility have been performed, and neither showed a significant increase in sperm concentrations or in pregnancy rates (13, 14). However, the selection criteria for infertile men recruited in these studies were not strict enough to derive conclusive information. Matorras et al. (13) evaluated 148 consecutive men undergoing IUI because of infertility, but they included men with a wide variation of sperm parameters. In fact, the mean sperm concentration in the FSH-treated group was /ml, with only Fertility and Sterility 659
7 18.2% of men presenting oligozoospermia. Kamischke et al. (14) studied a group of patients with different degrees of testicular alteration; in fact, selection criteria for treatment were limited to abnormal semen parameters and basal FSH concentrations 12 IU/L. In contrast to these studies, we detected a significant increase in spontaneous pregnancies in the responder group compared with both nonresponder and infertile control groups during the 3-month period after the withdrawal of recombinant hfsh therapy (16.7% vs. 3.1% and 4.0%, respectively, P.05). If we also add the pregnancies obtained with IUI during the following 3 months, pregnancy rates were 26.7% (8 of 30) in responder subjects, 3.1% (1 of 32) in nonresponder subjects, and 4.0% (2 of 50) in infertile control subjects. These data are very important because they highlight that FSH therapy, when performed in appropriate subjects, allows infertile couples to conceive spontaneously or by IUI in approximately one fourth of cases. In other words, these subjects benefitted from FSH therapy mainly because they could avoid more complex ART, such as IVF-ET or ICSI. Although the cumulative pregnancy rate, including with IVF-ET and ICSI cycles, seemed to be higher at the end of the study in responder subjects, it does not statistically differ with respect to the nonresponder and infertile control groups (36.7% vs. 21.9% and 24.0%, respectively), but a statistical analysis is difficult because of the dispersion of data. However, it is important to stress that the improvement of seminal parameters in the responder group after recombinant hfsh therapy and during the 6 months of follow-up allowed these patients to perform a less invasive method, whereas this was not possible for the other two patient groups. Intrauterine insemination is considered the most cost-effective and least-invasive treatment for male factor infertility when at least motile postwash spermatozoa are present in the ejaculate (25, 26, 30). Conversely, ICSI involves several risks in the female partners (multiple pregnancies, hyperstimulation syndrome, increase in abortion rate) and in the offspring (premature birth, low birthweight, chromosome abnormalities). In conclusion, this controlled, randomized clinical trial shows that FSH treatment is not effective in unselected oligozoospermic men. However, this is the first demonstration that such treatment can induce a significance increase in sperm count and an improvement in pregnancy rate in a subgroup of oligozoospermic patients (those with normal FSH plasma levels and absence of maturation arrest). These results underline the importance of strict criteria for the selection of patients to be treated with FSH. In our opinion, a deep understanding of the pathophysiologic conditions in male infertility has an important impact on the choice of medical treatment and on the perspectives of success. Indeed, the age of the female partner is an important aspect in decisions to treat the male for a long period. The results of this study suggest that a rational treatment of male infertility is possible. Therefore, in male infertility initial efforts should be directed to the study of infertile male patients and to improve sperm quality, whenever possible. Intracytoplasmic sperm injection should be applied only in the presence of severe male factor infertility or in the absence of a significant improvement of semen parameters after medical treatment. REFERENCES 1. Matsumoto AM. Hormonal control of human spermatogenesis. In: Burger H, de Kretser D, eds. The testis. New York: Raven Press, 1989: Sharpe RM. Follicle-stimulating hormone and spermatogenesis in adult male. J Endocrinol 1989;57: Matsumoto AM, Karpas AE, Bremmer WJ. Chronic human chorionic gonadotropin administration in normal men: evidence that follicle stimulating hormone is necessary for the maintenance of quantitative normal spermatogenesis in men. J Clin Endocrinol Metab 1986; 62: McLachlan RI, Wreford NG, de Kretser DM, Robertson DM. The effects of recombinant follicle-stimulating hormone on restoration of spermatogenesis in gonadotropin-releasing hormone-immunized adult rat. Endocrinology 1995;136: Marshall GR, Zorub DS, Plant TM. Follicle-stimulating hormone amplifies the population of differentiated spermatogonial in the hypophysectomized testosterone-replaced adult rhesus monkey (Macaca mulatta). Endocrinology 1995;136: Moudgal NR, Murthy GS, Prasanna KM, Martin F, Suresh R, Medhamurthy R, et al. Responsiveness of human male volunteers to immunization with ovine follicle stimulating hormone vaccine: results of a pilot study. Hum Reprod 1997;12: Tapanainen JS, Aittomaki K, Min J, Vaskivuo T, Huhtaniemi IT. Men homozygous for an inactivating mutation of the follicle-stimulating hormone (FSH) receptor gene present variable suppression of spermatogenesis and fertility. Nat Genet 1997;15: Acosta AA, Khalifa E, Oehninger S. Pure human follicle stimulating hormone has a role in the treatment of severe male infertility by assisted reproduction: Norfolk s total experience. Hum Reprod 1992;7: Bartoov B, Eltes F, Lunenfeld E. Sperm quality of subfertile males before and after treatment with human follicle-stimulating hormone. Fertil Steril 1994;61: Strehler E, Sterzik K, De Santo M, Abt M, Wiedemann R, Bellati U, et al. The effect of follicle-stimulating hormone therapy on sperm quality: an ultrastructural mathematical evaluation. J Androl 1997;18: Ashkenazi J, Bar-Hava I, Farhi J, Levy T, Feldberg D, Orvieto R, et al. The role of purified follicle stimulating hormone therapy in the male partner before intracytoplasmic sperm injection. Fertil Steril 1999;72: Ben-Rafael Z, Farhi J, Feldberg D, Bartoov B, Kovo M, Eltes F, et al. Follicle-stimulating hormone treatment for men with idiopathic oligoteratoasthenozoospermia before in vitro fertilization: the impact on sperm microstructure and fertilization potential. Fertil Steril 2000;73: Matorras R, Perez C, Corcostegui B, Pijoan JI, Ramon O, Delgado P, et al. Treatment of the male with follicle-stimulating hormone in intrauterine insemination with husband s spermatozoa: a randomized study. Hum Reprod 1997;12: Kamischke A, Behre HM, Bergmann M, Simoni M, Schafer T, Nieschlag E. Recombinant human follicle stimulating hormone for treatment of male idiopathic infertility: a randomized, double-blind, placebo-controlled, clinical trial. Hum Reprod 1998;13: Foresta C, Bettella A, Ferlin A, Garolla A, Rossato M. Evidence for a stimulatory role of follicle-stimulating hormone on the spermatogonial population in adult males. Fertil Steril 1998;69: Foresta C, Bettella A, Rossato M, La Sala G, De Paoli M, Plebani M. Inhibin B plasma concentrations in oligozoospermic subjects before 660 Foresta et al. FSH therapy in male idiopathic infertility Vol. 84, No. 3, September 2005
8 and after therapy with follicle stimulating hormone. Hum Reprod 1999;14: Foresta C, Bettella A, Merico M, Garolla A, Plebani M, Ferlin A, et al. FSH in the treatment of oligozoospermia. Mol Cell Endocrinol 2000; 161: Foresta C, Bettella A, Merico M, Garolla A, Ferlin A, Rossato M. Use of recombinant human follicle-stimulating hormone in the treatment of male factor infertility. Fertil Steril 2002;77: World Health Organization. Laboratory manual for the examination of human semen and sperm-cervical mucus interaction. 4th ed. Cambridge, United Kingdom: Cambridge University Press, Foresta C, Varotto A, Scandellari C. Assessment of testicular cytology by fine needle aspiration as a diagnostic parameter in the evaluation of the azoospermic subject. Fertil Steril 1992;57: Foresta C, Varotto A. Assessment of testicular cytology by fine needle aspiration as a diagnostic parameter in the evaluation of the oligospermic subject. Fertil Steril 1992;58: Foresta C, Ferlin A, Bettella A, Rossato M, Varotto A. Diagnostic and clinical features in azoospermia. Clin Endocrinol 1995;43: Groome NP, Illingworth PJ, O Brien M, Pai R, Rodger FE, Mather JP, et al. Measurement of dimeric inhibin B throughout the human menstrual cycle. J Clin Endocrinol Metab 1996;81: Illingworth PJ, Groome NP, Byrd W, Rainey WE, Mcneilly AS, Mather JP, et al. Inhibin-B: a likely candidate for the physiologically important form of inhibin in men. J Clin Endocrinol Metab 1996; 81: Oehninger S. Clinical and laboratory management of male infertility: an opinion on its current status. J Androl 2000;6: Khalil MR, Rasmussen PE, Erb K, Laursen SB, Rex S, Westergaard LG. Homologous intrauterine insemination. An evaluation of prognostic factors based on a review of 2473 cycles. Acta Obstet Gynecol Scand 2001;80: Gianaroli L, Plachot M, van Kooij R, Al-Hasani S, Dawson K, DeVos A, et al. ESHRE guidelines for good practice in IVF laboratories. Hum Reprod 2000;15: World Health Organization. Towards more objectivity in diagnosis and management of male infertility. Results of a World Health Organization multicenter study. Int J Androl 1987;10(Suppl 7): Bhasin S, de Krestser DM, Baker HWG. Pathophysiology and natural history of male infertility. J Clin Endocrinol Metab 1994;79: Comhaire F, Zalata A, Mahmoud A. Critical evaluation of the effectiveness of different modes of treatment of male infertility. Andrologia 1996;28(Suppl 1):31 5. Fertility and Sterility 661
Inhibin B plasma concentrations in infertile patients with DAZ gene deletions treated with FSH
 European Journal of Endocrinology (2002) 146 801 806 ISSN 0804-4643 CLINICAL STUDY Inhibin B plasma concentrations in infertile patients with DAZ gene deletions treated with FSH Carlo Foresta, Andrea Bettella,
European Journal of Endocrinology (2002) 146 801 806 ISSN 0804-4643 CLINICAL STUDY Inhibin B plasma concentrations in infertile patients with DAZ gene deletions treated with FSH Carlo Foresta, Andrea Bettella,
Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone
 Human Reproduction vol.14 no.4 pp.906 912, 1999 Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone Carlo Foresta 1,4, Andrea Bettella
Human Reproduction vol.14 no.4 pp.906 912, 1999 Inhibin B plasma concentrations in oligozoospermic subjects before and after therapy with follicle stimulating hormone Carlo Foresta 1,4, Andrea Bettella
Testicular fine needle aspiration as a diagnostic tool in nonobstructive
 Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
Asian J Androl 2005; 7 (3): 289 294 DOI: 10.1111/j.1745-7262.2005.00043.x. Original Article. Testicular fine needle aspiration as a diagnostic tool in nonobstructive azoospermia A. Bettella 1, A. Ferlin
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007
 ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
ESHRE Andrology Campus Course Reproductive Andrology Brussels 8-10 November 2007 To treat the man or his sperm? When to treat the man? Conventional non-surgical treatment of male infertility Axel Kamischke
Infertility treatment
 In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
In the name of God Infertility treatment Treatment options The optimal treatment is one that provide an acceptable success rate, has minimal risk and is costeffective. The treatment options are: 1- Ovulation
Functional and cytologic features of the contralateral testis in cryptorchidism
 FERTILITY AND STERILITY@ Copyright Ci') 1996 American Society for Reproductive Medicine Printed on acid-free paper in U. S. A. Functional and cytologic features of the contralateral testis in cryptorchidism
FERTILITY AND STERILITY@ Copyright Ci') 1996 American Society for Reproductive Medicine Printed on acid-free paper in U. S. A. Functional and cytologic features of the contralateral testis in cryptorchidism
Infertility. Review and Update Clifford C. Hayslip MD Intrauterine Inseminations
 Infertility Review and Update Clifford C. Hayslip MD Intrauterine Inseminations Beneficial effects of IUI not consistently documented in studies No deleterious effects on fertility 3-4 cycles of IUI should
Infertility Review and Update Clifford C. Hayslip MD Intrauterine Inseminations Beneficial effects of IUI not consistently documented in studies No deleterious effects on fertility 3-4 cycles of IUI should
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia
 Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Time to improvement in semen parameters after microsurgical varicocelectomy in men with severe oligospermia Thomas A. Masterson; Aubrey B. Greer; Ranjith Ramasamy University of Miami, Miami, FL, United
Assisted Reproduction. By Dr. Afraa Mahjoob Al-Naddawi
 Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Assisted Reproduction By Dr. Afraa Mahjoob Al-Naddawi Learning Objectives: By the end of this lecture, you will be able to: 1) Define assisted reproductive techniques (ART). 2) List indications for various
Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary
 Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Subfertility Infertility: failure to conceive within one year of unprotected regular sexual intercourse. Primary secondary Infertility affects about 15 % of couples. age of the female. Other factors that
Understanding Infertility, Evaluations, and Treatment Options
 Understanding Infertility, Evaluations, and Treatment Options Arlene J. Morales, M.D., F.A.C.O.G. Fertility Specialists Medical Group, Inc. What We Will Cover Introduction What is infertility? Briefly
Understanding Infertility, Evaluations, and Treatment Options Arlene J. Morales, M.D., F.A.C.O.G. Fertility Specialists Medical Group, Inc. What We Will Cover Introduction What is infertility? Briefly
Information Booklet. Exploring the causes of infertility and treatment options.
 Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
Information Booklet Exploring the causes of infertility and treatment options www.ptafertility.co.za info@ptafertility.co.za +27 12 998 8854 Faith is taking the first step even if you don t see the whole
NICE fertility guidelines. Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic
 NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
NICE fertility guidelines Hemlata Thackare MPhil MSc MRCOG Deputy Medical Director London Women s Clinic About the LWC 4 centres around the UK London Cardiff Swansea Darlington The largest sperm bank in
Introduction. Randomized controlled trial Recombinant human follicle stimulating hormone
 https://doi.org/10.1007/s40618-018-0843-y CONSENSUS STATEMENT The use of follicle stimulating hormone (FSH) for the treatment of the infertile man: position statement from the Italian Society of Andrology
https://doi.org/10.1007/s40618-018-0843-y CONSENSUS STATEMENT The use of follicle stimulating hormone (FSH) for the treatment of the infertile man: position statement from the Italian Society of Andrology
Evaluation and Treatment of the Subfertile Male. Karen Baker, MD Associate Professor Duke University, Division of Urology
 Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Evaluation and Treatment of the Subfertile Male Karen Baker, MD Associate Professor Duke University, Division of Urology Disclosures: None Off label uses: There are no oral medications approved by the
Neil Goodman, MD, FACE
 Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Initial Workup of Infertile Couple: Female Neil Goodman, MD, FACE Professor of Medicine Voluntary Faculty University of Miami Miller School of Medicine Scope of Infertility in the United States Affects
Chapter 1. Chapter 2. Chapter 3
 Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
Summary To perform IUI some conditions are required. This includes 1) a certain amount of progressively motile spermatozoa, 2) the presence of ovulation, 3) the presence of functional fallopian tubes,
A Therapeutic Scheme For Oligospermia Based On Serum Levels Of FSH And Estradiol
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 8 Number 1 A Therapeutic Scheme For Oligospermia Based On Serum Levels Of FSH And Estradiol P Sah Citation P Sah. A Therapeutic Scheme
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 8 Number 1 A Therapeutic Scheme For Oligospermia Based On Serum Levels Of FSH And Estradiol P Sah Citation P Sah. A Therapeutic Scheme
Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility
 Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
Article ID: WMC001510 ISSN 2046-1690 Role Of Serum Hormone Indices Including Inhibin B And Scrotal Ultrasound In Evaluation Of Non Obstructive Male Factor Infertility Author(s):Dr. Geetika, Dr. Sunita
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE. Anatomy : Male and Female genital tract
 POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
POST - DOCTORAL FELLOWSHIP PROGRAMME IN REPRODUCTIVE MEDICINE DURATION OF THE COURSE : TWO YEARS Detailed syllabus: Part 1 Basic Sciences: Anatomy : Male and Female genital tract Physiology Endocrinology
Complete failure of fertilization in couples with unexplained infertility: implications for subsequent in vitro fertilization cycles
 r FERTILITY AND STERILITY Copyright ~ 1993 The American Fertility Society Printed on acid-free paper in U.S.A. Complete failure of fertilization in couples with unexplained infertility: implications for
r FERTILITY AND STERILITY Copyright ~ 1993 The American Fertility Society Printed on acid-free paper in U.S.A. Complete failure of fertilization in couples with unexplained infertility: implications for
Clinical Policy Committee
 Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Northern, Eastern and Western Devon Clinical Commissioning Group South Devon and Torbay Clinical Commissioning Group Clinical Policy Committee Commissioning policy: Assisted Conception Fertility treatments
Comparison of single versus double intra uterine insemination
 International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pathak B. Int J Reprod Contracept Obstet Gynecol. 2017 Dec;6(12):5277-5281 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20175091
International Journal of Reproduction, Contraception, Obstetrics and Gynecology Pathak B. Int J Reprod Contracept Obstet Gynecol. 2017 Dec;6(12):5277-5281 www.ijrcog.org DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20175091
Fertility 101. About SCRC. A Primary Care Approach to Diagnosing and Treating Infertility. Definition of Infertility. Dr.
 Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Dr. Shahin Ghadir A Primary Care Approach to Diagnosing and Treating Infertility St. Charles Bend Grand Rounds November 30, 2018 I have no conflicts of interest to disclose. + About SCRC State-of-the-art
Infertility. Thomas Lloyd and Samera Dean
 Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Infertility Thomas Lloyd and Samera Dean Infertility Definition Causes Referral criteria Assisted reproductive techniques Complications Ethics What is infertility? Woman Reproductive age Has not conceived
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients
 Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Cytological findings of testicular fine needle aspiration in a sample of azoospermic Iraqi patients Basim Sh. Ahmed F.I.C.M.S Department of Pathology, College of Medicine, Al-Mustansiriya University, Baghdad,
Does previous response to clomifene citrate influence the selection of gonadotropin dosage given in subsequent superovulation treatment cycles?
 J Assist Reprod Genet (26) 23:427 431 DOI 1.17/s1815-6-965-x ASSISTED REPRODUCTION Does previous response to clomifene citrate influence the selection of gonadotropin dosage given in subsequent superovulation
J Assist Reprod Genet (26) 23:427 431 DOI 1.17/s1815-6-965-x ASSISTED REPRODUCTION Does previous response to clomifene citrate influence the selection of gonadotropin dosage given in subsequent superovulation
Controlled trial of high spermatic vein ligation for varicocele infertile men* Avraham Karasik, M.D.:j: Benad Goldwasser, M.D.t
 Urology-andrology FERTILITY AND STERILITY Copyright 1995 American Society for Reproductive Medicine Vol. 63, No. I, January 1995 Printed on acid-free paper in U. S. A. Controlled trial of high spermatic
Urology-andrology FERTILITY AND STERILITY Copyright 1995 American Society for Reproductive Medicine Vol. 63, No. I, January 1995 Printed on acid-free paper in U. S. A. Controlled trial of high spermatic
Testosterone Therapy-Male Infertility
 Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
Testosterone Therapy-Male Infertility Testosterone Therapy-Male Infertility Many men are prescribed testosterone for a variety of reasons. Low testosterone levels (Low T) with no symptoms, general symptoms
WHY INVESTIGATE FOR INFERTILITY
 WHY INVESTIGATE FOR INFERTILITY Intrauterine Insemination 1 About this booklet This series of booklets has been developed and written with the support of leading fertility clinics across Australia, and
WHY INVESTIGATE FOR INFERTILITY Intrauterine Insemination 1 About this booklet This series of booklets has been developed and written with the support of leading fertility clinics across Australia, and
I. ART PROCEDURES. A. In Vitro Fertilization (IVF)
 DFW Fertility Associates ASSISTED REPRODUCTIVE TECHNOLOGY (ART) Welcome to DFW Fertility Associates/ Presbyterian-Harris Methodist Hospital ARTS program. This document provides an overview of treatment
DFW Fertility Associates ASSISTED REPRODUCTIVE TECHNOLOGY (ART) Welcome to DFW Fertility Associates/ Presbyterian-Harris Methodist Hospital ARTS program. This document provides an overview of treatment
Subfertility B Y A L I S O N, B E N A N D J O H N
 Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
What You Need to Know
 UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
UW MEDICINE PATIENT EDUCATION What You Need to Know Facts about male infertility This handout explains what causes male infertility, how it is diagnosed, and possible treatments. Infertility is defined
Treatment of the male with follicle-stimulating hormone in intrauterine insemination with husband s spermatozoa: a randomized study
 hrep$$1251 Human Reproduction vol.12 no.1 pp.24 28, 1997 Treatment of the male with follicle-stimulating hormone in intrauterine insemination with husband s spermatozoa: a randomized study R.Matorras 1,3,
hrep$$1251 Human Reproduction vol.12 no.1 pp.24 28, 1997 Treatment of the male with follicle-stimulating hormone in intrauterine insemination with husband s spermatozoa: a randomized study R.Matorras 1,3,
The assessment and investigation of the infertile couple
 The assessment and investigation of the infertile couple BIRUTE ZILAITIENE, MD, PHD, PROF., FECSM DEPARTMENT OF ENDOCRINOLOGY AND INSTITUTE OF ENDOCRINOLOGY, LITHUANIAN UNIVERSITY OF HEALTH SCIENCES, KAUNAS,
The assessment and investigation of the infertile couple BIRUTE ZILAITIENE, MD, PHD, PROF., FECSM DEPARTMENT OF ENDOCRINOLOGY AND INSTITUTE OF ENDOCRINOLOGY, LITHUANIAN UNIVERSITY OF HEALTH SCIENCES, KAUNAS,
Clinical Policy Committee
 Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Clinical Policy Committee Commissioning policy: Assisted Conception Fertility assessment and investigations are commissioned where: A woman is of reproductive age and has not conceived after one (1) year
Recent Developments in Infertility Treatment
 Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Recent Developments in Infertility Treatment John T. Queenan Jr., MD Professor, Dept. Of Ob/Gyn University of Rochester Medical Center Rochester, NY Disclosures I don t have financial interest or other
Assisted Reproduction. Rajeevi Madankumar, 1,2 James Tsang, 1 Martin L. Lesser, 1 Daniel Kenigsberg, 1 and Steven Brenner 1 INTRODUCTION
 ( C 2005) DOI: 10.1007/s10815-005-4912-8 Assisted Reproduction Clomiphene citrate induced ovulation and intrauterine insemination: effect of timing of human chorionic gonadotropin injection in relation
( C 2005) DOI: 10.1007/s10815-005-4912-8 Assisted Reproduction Clomiphene citrate induced ovulation and intrauterine insemination: effect of timing of human chorionic gonadotropin injection in relation
Male Infertility Research
 Male Infertility Research Quantitative evaluation of spermatozoa ultrastructure after acupuncture treatment for idiopathic male infertility. Effect of Acupuncture on Sperm Parameters of Males Suffering
Male Infertility Research Quantitative evaluation of spermatozoa ultrastructure after acupuncture treatment for idiopathic male infertility. Effect of Acupuncture on Sperm Parameters of Males Suffering
Clinical evaluation of infertility
 Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Clinical evaluation of infertility DR. FARIBA KHANIPOUYANI OBSTETRICIAN & GYNECOLOGIST PRENATOLOGIST Definition: inability to achieve conception despite one year of frequent unprotected intercourse. Male
Cigna Drug and Biologic Coverage Policy
 Cigna Drug and Biologic Coverage Policy Subject Infertility Injectables Table of Contents Coverage Policy... 1 General Background...16 Coding/Billing Information...20 References...20 Effective Date...
Cigna Drug and Biologic Coverage Policy Subject Infertility Injectables Table of Contents Coverage Policy... 1 General Background...16 Coding/Billing Information...20 References...20 Effective Date...
Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia
 Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Urology Journal UNRC/IUA Vol. 3, No. 2, 92-96 Spring 2006 Printed in IRAN Prediction of Successful Sperm Retrieval in Patients with Nonobstructive Azoospermia Seyed Amirmohsen Ziaee, 1 * Mohammadreza Ezzatnegad,
Is the fallopian tube better than the uterus? Evidence on intrauterine insemination versus fallopian sperm perfusion
 F, V & V IN OBGYN, 2010, MONOGRAPH: 36-41 Artificial insemination Is the fallopian tube better than the uterus? Evidence on intrauterine insemination versus fallopian sperm perfusion Arne SUNDE 1, Jarl
F, V & V IN OBGYN, 2010, MONOGRAPH: 36-41 Artificial insemination Is the fallopian tube better than the uterus? Evidence on intrauterine insemination versus fallopian sperm perfusion Arne SUNDE 1, Jarl
In Vitro Fertilization in Clomiphene-Resistant Women with Polycystic Ovary Syndrome
 Original Article Effect of Laparoscopic Ovarian Drilling on Outcomes of In Vitro Fertilization in Clomiphene-Resistant Women with Polycystic Ovary Syndrome Maryam Eftekhar, M.D. 1, Razieh Deghani Firoozabadi,
Original Article Effect of Laparoscopic Ovarian Drilling on Outcomes of In Vitro Fertilization in Clomiphene-Resistant Women with Polycystic Ovary Syndrome Maryam Eftekhar, M.D. 1, Razieh Deghani Firoozabadi,
INDICATIONS OF IVF/ICSI
 PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
PROCESS OF IVF/ICSI INDICATIONS OF IVF/ICSI IVF is most clearly indicated when infertility results from one or more causes having no other effective treatment; Tubal disease. In women with blocked fallopian
Type of intervention Treatment. Economic study type Cost-effectiveness analysis.
 Recombinant versus urinary follicle-stimulating hormone in intrauterine insemination cycles: a prospective, randomized analysis of cost effectiveness Gerli S, Casini M L, Unfer V, Costabile L, Bini V,
Recombinant versus urinary follicle-stimulating hormone in intrauterine insemination cycles: a prospective, randomized analysis of cost effectiveness Gerli S, Casini M L, Unfer V, Costabile L, Bini V,
Male Factor Infertility
 Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Male Factor Infertility Simplified Evaluaon and Treatment* ^ * In 20 minutes or less In 20 slides ^ 5 minute office visit ALWAYS EVALUATE THE MALE & THE FEMALE Why 1. To help the coupleachieve a pregnancy
Interpreting follicular Progesterone: Late follicular Progesterone to Estradiol ratio is not influenced by protocols or gonadotropins used
 Interpreting follicular Progesterone: Late follicular Progesterone to Estradiol ratio is not influenced by protocols or gonadotropins used Ellenbogen A., M.D., Shalom-Paz E., M.D, Asalih N., M.D, Samara
Interpreting follicular Progesterone: Late follicular Progesterone to Estradiol ratio is not influenced by protocols or gonadotropins used Ellenbogen A., M.D., Shalom-Paz E., M.D, Asalih N., M.D, Samara
Low Dose hmg As a First choice for Ovarian Stimulation in IUI cycles
 Low Dose hmg As a First choice for Ovarian Stimulation in IUI cycles aslan, M.D Department of Obstetrics & Gynecology, Cairo University Abstract Objective: to compare pregnancy rates following low dose
Low Dose hmg As a First choice for Ovarian Stimulation in IUI cycles aslan, M.D Department of Obstetrics & Gynecology, Cairo University Abstract Objective: to compare pregnancy rates following low dose
INFERTILITY: DIAGNOSIS, WORKUP AND MANAGEMENT FOR THE COMMUNITY PHYSICIAN
 INFERTILITY: DIAGNOSIS, WORKUP AND MANAGEMENT FOR THE COMMUNITY PHYSICIAN Caitlin Dunne, MD, FRCSC Clinical Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics
INFERTILITY: DIAGNOSIS, WORKUP AND MANAGEMENT FOR THE COMMUNITY PHYSICIAN Caitlin Dunne, MD, FRCSC Clinical Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics
Understanding eggs, sperm and embryos. Marta Jansa Perez Wolfson Fertility Centre
 Understanding eggs, sperm and embryos Marta Jansa Perez Wolfson Fertility Centre What does embryology involve? Aims of the embryology laboratory Creation of a large number of embryos and supporting their
Understanding eggs, sperm and embryos Marta Jansa Perez Wolfson Fertility Centre What does embryology involve? Aims of the embryology laboratory Creation of a large number of embryos and supporting their
GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY
 GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G. Dohle (chairman), A. Jungwirth and W. Weidner. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 1. Introduction Infertility is
GUIDELINES ON THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G. Dohle (chairman), A. Jungwirth and W. Weidner. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 1. Introduction Infertility is
Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa
 andrologia 35, 220 226 (2003) Accepted: April 25, 2003 Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa J. U. Schwarzer, K. Fiedler, I.
andrologia 35, 220 226 (2003) Accepted: April 25, 2003 Male factors determining the outcome of intracytoplasmic sperm injection with epididymal and testicular spermatozoa J. U. Schwarzer, K. Fiedler, I.
Acupuncture Treatment For Infertile Women Undergoing Intracytoplasmic Sperm injection
 Acupuncture Treatment For Infertile Women Undergoing Intracytoplasmic Sperm injection Sandra L. Emmons, MD Phillip Patton, MD Source: Medical Acupuncture, A Journal For Physicians By Physicians Spring
Acupuncture Treatment For Infertile Women Undergoing Intracytoplasmic Sperm injection Sandra L. Emmons, MD Phillip Patton, MD Source: Medical Acupuncture, A Journal For Physicians By Physicians Spring
IVF (,, ) : (HP-hMG) - (IVF- ET) : GnRH, HP-hMG (HP-hMG )57, (rfsh )140, (Gn)
 34 11 Vol.34 No.11 2014 11 Nov. 2014 Reproduction & Contraception doi: 10.7669/j.issn.0253-3X.2014.11.0892 E-mail: randc_journal@163.com IVF ( 710003) : (H-hMG) - (IVF- ET) : GnRH H-hMG (H-hMG ) (rfsh
34 11 Vol.34 No.11 2014 11 Nov. 2014 Reproduction & Contraception doi: 10.7669/j.issn.0253-3X.2014.11.0892 E-mail: randc_journal@163.com IVF ( 710003) : (H-hMG) - (IVF- ET) : GnRH H-hMG (H-hMG ) (rfsh
Biology of fertility control. Higher Human Biology
 Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
Biology of fertility control Higher Human Biology Learning Intention Compare fertile periods in females and males What is infertility? Infertility is the inability of a sexually active, non-contracepting
2017 United HealthCare Services, Inc.
 UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
UnitedHealthcare Pharmacy Clinical Pharmacy Programs Program Number 2017 P 1143-4 Program Prior Authorization/Notification Medication Menopur (menotropins) * P&T Approval Date 8/2014, 5/2015, 5/2016, 5/2017
Original Article. Fauzia HaqNawaz 1*, Saadia Virk 2, Tasleem Qadir 3, Saadia Imam 3, Javed Rizvi 2
 Original Article Comparison of Letrozole and Clomiphene Citrate Efficacy along with Gonadotrophins in Controlled Ovarian Hyperstimulation for Intrauterine Insemination Cycles Fauzia HaqNawaz 1*, Saadia
Original Article Comparison of Letrozole and Clomiphene Citrate Efficacy along with Gonadotrophins in Controlled Ovarian Hyperstimulation for Intrauterine Insemination Cycles Fauzia HaqNawaz 1*, Saadia
Lars G.Westergaard 1, Karin Erb, Steen Laursen, Per E.Rasmussen and Sven Rex
 Human Reproduction vol.11 no.6 pp. 1209-1213, 19% The effect of human menopausal gonadotrophin and highly purified, urine-derived follicle stimulating hormone on the outcome of in-vitro fertuization in
Human Reproduction vol.11 no.6 pp. 1209-1213, 19% The effect of human menopausal gonadotrophin and highly purified, urine-derived follicle stimulating hormone on the outcome of in-vitro fertuization in
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Results and Discussion
 The AMH and Inhibin B in serum and follicular fluid was a very good predictive marker for assessment of oocyte quantity but did not correlate with the maturity of the oocyte or fertilization or reproductive
The AMH and Inhibin B in serum and follicular fluid was a very good predictive marker for assessment of oocyte quantity but did not correlate with the maturity of the oocyte or fertilization or reproductive
Rafael A. Cabrera, M.D., Laurel Stadtmauer, M.D., Ph.D., Jacob F. Mayer, Ph.D., William E. Gibbons, M.D., and Sergio Oehninger, M.D., Ph.D.
 Follicular phase serum levels of luteinizing hormone do not influence delivery rates in in vitro fertilization cycles down-regulated with a gonadotropin-releasing hormone agonist and stimulated with recombinant
Follicular phase serum levels of luteinizing hormone do not influence delivery rates in in vitro fertilization cycles down-regulated with a gonadotropin-releasing hormone agonist and stimulated with recombinant
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Infertility INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY To download lecture deck Reference Comprehensive Gynecology 7 th edition, 2017 (Lobo
Adoption and Foster Care
 GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GLOSSARY Family building via Adoption and Foster Care October 2018 www.familyequality.org/resources A Anonymous Donor: A person who donated sperm or eggs with the intention of never meeting resulting children.
GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY
 GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G.R. Dohle, Z. Kopa, A. Jungwirth, T.B. Hargreave. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 Definition Infertility is the
GUIDELINES FOR THE INVESTIGATION AND TREATMENT OF MALE INFERTILITY G.R. Dohle, Z. Kopa, A. Jungwirth, T.B. Hargreave. Eur Urol 2002;42(4):313-322 Eur Urol 2004;46(5):555-558 Definition Infertility is the
Brighton & Hove CCG PLS CONFERENCE Dr Carole Gilling-Smith Medical Director
 Brighton & Hove CCG PLS CONFERENCE 2016 Dr Carole Gilling-Smith Medical Director FERTILITY CHALLENGES IN THE NHS A TERTIARY CARE PERSPECTIVE LEARNING OBJECTIVES Understand the pathways through assisted
Brighton & Hove CCG PLS CONFERENCE 2016 Dr Carole Gilling-Smith Medical Director FERTILITY CHALLENGES IN THE NHS A TERTIARY CARE PERSPECTIVE LEARNING OBJECTIVES Understand the pathways through assisted
The predictive value of idiopathic failure to fertilize on the first in vitro fertilization attempt*
 FERTILITY AND STERILITY Copyright 1991 The American Fertility Society Printed on acid-free paper in U.S.A. The predictive value of idiopathic failure to fertilize on the first in vitro fertilization
FERTILITY AND STERILITY Copyright 1991 The American Fertility Society Printed on acid-free paper in U.S.A. The predictive value of idiopathic failure to fertilize on the first in vitro fertilization
ART Drugs. Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.02 Subject: ART Drugs Page: 1 of 7 Last Review Date: September 15, 2017 ART Drugs Description Bravelle
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.02 Subject: ART Drugs Page: 1 of 7 Last Review Date: September 15, 2017 ART Drugs Description Bravelle
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Low dose of cyproterone acetate and testosterone enanthate for contraception in men
 Human Reproduction vol.13 no.5 pp.1225 1229, 1998 Low dose of cyproterone acetate and testosterone enanthate for contraception in men M.Cristina Meriggiola 1,3, William J.Bremner 2, Antonietta Costantino
Human Reproduction vol.13 no.5 pp.1225 1229, 1998 Low dose of cyproterone acetate and testosterone enanthate for contraception in men M.Cristina Meriggiola 1,3, William J.Bremner 2, Antonietta Costantino
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 22 September 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 22 September 2010 100 µg/0.5 ml, solution for injection B/1 prefilled syringe + 1 needle (CIP code: 374 590-1) 150
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 22 September 2010 100 µg/0.5 ml, solution for injection B/1 prefilled syringe + 1 needle (CIP code: 374 590-1) 150
in vitro fertilization
 FERTILITY AND STERILITY VOL 69, NO. 6, JUNE 1998 Copyright (#1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Elevated levels of basal
FERTILITY AND STERILITY VOL 69, NO. 6, JUNE 1998 Copyright (#1998 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in U.S.A. Elevated levels of basal
JMSCR Vol 06 Issue 09 Page September 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i9.53 Role of Anti-Mullerian Hormone
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i9.53 Role of Anti-Mullerian Hormone
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Medical Benefit Effective: 8/15/18 Pharmacy- Formulary 1 x Next Review: 6/18 Pharmacy- Formulary 2 x Date of Origin: 7/00 Injectable Fertility Medications: Bravelle,
Drug Therapy Guidelines Applicable Medical Benefit Effective: 8/15/18 Pharmacy- Formulary 1 x Next Review: 6/18 Pharmacy- Formulary 2 x Date of Origin: 7/00 Injectable Fertility Medications: Bravelle,
Does triggering ovulation by 5000 IU of uhcg affect ICSI outcome? *
 Middle East Fertility Society Journal Vol. 11, No. 2, 2006 Copyright Middle East Fertility Society Does triggering ovulation by 5000 IU of uhcg affect ICSI outcome? * Amany A.M. Shaltout, M.D. Mohamed
Middle East Fertility Society Journal Vol. 11, No. 2, 2006 Copyright Middle East Fertility Society Does triggering ovulation by 5000 IU of uhcg affect ICSI outcome? * Amany A.M. Shaltout, M.D. Mohamed
Journal of Paramedical Sciences (JPS) Spring 2011 Vol.2, No.2 ISSN
 Rare association of multiple etiologies in a severe oligoasthenospermic male Vineeth V.S. 1, Mohsen Najafi 1, Sreenivasa G. 1, Sharath Kumar C. 2, Suttur S. Malini 1,* 1 Department of Studies in Zoology,
Rare association of multiple etiologies in a severe oligoasthenospermic male Vineeth V.S. 1, Mohsen Najafi 1, Sreenivasa G. 1, Sharath Kumar C. 2, Suttur S. Malini 1,* 1 Department of Studies in Zoology,
(BMI)=18.0~24.9 kg/m 2 ;
 33 10 Vol.33 No.10 2013 10 Oct. 2013 Reproduction & Contraception doi: 10.7669/j.issn.0253-357X.2013.10.0672 E-mail: randc_journal@163.com - ( 400013) : () GnRH-a - () : IVF- ET 233 A (I~II 102 ) B (III~IV
33 10 Vol.33 No.10 2013 10 Oct. 2013 Reproduction & Contraception doi: 10.7669/j.issn.0253-357X.2013.10.0672 E-mail: randc_journal@163.com - ( 400013) : () GnRH-a - () : IVF- ET 233 A (I~II 102 ) B (III~IV
Article Gonadotrophin therapy in combination with ICSI in men with hypogonadotrophic hypogonadism
 RBMOnline - Vol 15. No 2. 2007 156-160 Reproductive BioMedicine Online; www.rbmonline.com/article/2798 on web 14 June 2007 Article Gonadotrophin therapy in combination with ICSI in men with hypogonadotrophic
RBMOnline - Vol 15. No 2. 2007 156-160 Reproductive BioMedicine Online; www.rbmonline.com/article/2798 on web 14 June 2007 Article Gonadotrophin therapy in combination with ICSI in men with hypogonadotrophic
The prognostic factors for pregnancy after gonadotropin-induced controlled ovarian stimulation therapy with intrauterine insemination cycles
 Available online at www.medicinescience.org ORIGINAL RESEARCH Medicine Science International Medical Journal Medicine Science 2018; ( ): The prognostic factors for pregnancy after gonadotropin-induced
Available online at www.medicinescience.org ORIGINAL RESEARCH Medicine Science International Medical Journal Medicine Science 2018; ( ): The prognostic factors for pregnancy after gonadotropin-induced
Aromatase Inhibitors in Male Infertility:
 Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Aromatase Inhibitors in Male Infertility: The hype of hypogonadism? BEATRIZ UGALDE, PHARM.D. H-E-B/UNIVERSITY OF TEXAS COMMUNITY PHARMACY PGY1 03 NOVEMBER 2017 PHARMACOTHERAPY ROUNDS Disclosures No conflicts
Male factors can be identified as the cause of infertility in 30~40% of couples and a
 Focused Issue of This Month Causes and Diagnosis of Male Infertility Nam Cheol Park, MD Department of Urology, Pusan National University College of Medicine Email : pnc@pusan.ac.kr J Korean Med Assoc 2007;
Focused Issue of This Month Causes and Diagnosis of Male Infertility Nam Cheol Park, MD Department of Urology, Pusan National University College of Medicine Email : pnc@pusan.ac.kr J Korean Med Assoc 2007;
Indian Journal of Basic and Applied Medical Research; September 2015: Vol.-4, Issue- 4, P
 Original article: To study post intrauterine insemination conception rate among infertile women with polyp and women with normal uterine endometrium cavity 1Dr. Archana Meena, 2 Dr. Renu Meena, 3 Dr. Kusum
Original article: To study post intrauterine insemination conception rate among infertile women with polyp and women with normal uterine endometrium cavity 1Dr. Archana Meena, 2 Dr. Renu Meena, 3 Dr. Kusum
Evaluation of hormonal and physical factors responsible for male infertility in Sagamu South Western Nigeria
 Available online at wwwscholarsresearchlibrarycom Scholars Research Library Der Pharmacia Lettre, 2012, 4 (5):1475-1479 (http://scholarsresearchlibrarycom/archivehtml) ISSN 0975-5071 USA CODEN: DPLEB4
Available online at wwwscholarsresearchlibrarycom Scholars Research Library Der Pharmacia Lettre, 2012, 4 (5):1475-1479 (http://scholarsresearchlibrarycom/archivehtml) ISSN 0975-5071 USA CODEN: DPLEB4
The serum estradiol/oocyte ratio in patients with breast cancer undergoing ovarian stimulation with letrozole and gonadotropins
 Original Article Obstet Gynecol Sci 2018;61(2):242-246 https://doi.org/10.5468/ogs.2018.61.2.242 pissn 2287-8572 eissn 2287-8580 The serum estradiol/oocyte ratio in patients with breast cancer undergoing
Original Article Obstet Gynecol Sci 2018;61(2):242-246 https://doi.org/10.5468/ogs.2018.61.2.242 pissn 2287-8572 eissn 2287-8580 The serum estradiol/oocyte ratio in patients with breast cancer undergoing
Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection
 Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok
Variability in testis biopsy interpretation: implications for male infertility care in the era of intracytoplasmic sperm injection Matthew R. Cooperberg, M.D., a Thomas Chi, B.A., a Amir Jad, M.D., a Imok
Independent Review of Assisted Reproductive Technologies
 Assisted Reproductive Technologies Review Committee Report of the Independent Review of Assisted Reproductive Technologies APPENDICES Assisted Reproductive Technologies Review Committee APPENDIX A February
Assisted Reproductive Technologies Review Committee Report of the Independent Review of Assisted Reproductive Technologies APPENDICES Assisted Reproductive Technologies Review Committee APPENDIX A February
Clinical guideline Published: 20 February 2013 nice.org.uk/guidance/cg156
 Fertility problems: assessment and treatment Clinical guideline Published: 20 February 2013 nice.org.uk/guidance/cg156 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Fertility problems: assessment and treatment Clinical guideline Published: 20 February 2013 nice.org.uk/guidance/cg156 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Drug Therapy Guidelines
 Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
Drug Therapy Guidelines Applicable Injectable Fertility Medications: Bravelle, Cetrotide, Follistim AQ, Ganirelix, Gonal-F, human chorionic gonadotropin, leuprolide, Menopur, Novarel, Ovidrel, Pregnyl,
BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE
 Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
Authoriser: Moya O Doherty Page 1 of 7 BIOCHEMICAL TESTS FOR THE INVESTIGATION OF COMMON ENDOCRINE PROBLEMS IN THE MALE The purpose of this protocol is to describe common tests used for the investigation
IOF POI. hypergonadotropic hypogonadism primary ovarian insufficiency POI /premature ovarian failure POF. Van Kasteren. Coulam POI FSH E.
 hypergonadotropic hypogonadism primary ovarian insufficiency POI /premature ovarian failure POF Coulam POI Turner Fragile X premutation FSHR NOBOX FOXL etc POI FSH miu/ml AMH AMH AMH FSH / Knauff POI IOF
hypergonadotropic hypogonadism primary ovarian insufficiency POI /premature ovarian failure POF Coulam POI Turner Fragile X premutation FSHR NOBOX FOXL etc POI FSH miu/ml AMH AMH AMH FSH / Knauff POI IOF
MALE INFERTILITY & SEMEN ANALYSIS
 MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
MALE INFERTILITY & SEMEN ANALYSIS DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none Steps taken to review and mitigate potential
With advances in assisted reproduction techniques,
 Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Journal of Andrology, Vol. 26, No. 6, November/December 2005 Copyright American Society of Andrology Clomiphene Administration for Cases of Nonobstructive Azoospermia: A Multicenter Study ALAYMAN HUSSEIN,*
Puerto Rico Fertility Center
 Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
Puerto Rico Fertility Center General Information of the In-Vitro Fertilization Program Dr. Pedro J. Beauchamp First test-tube baby IN PUERTO RICO Dr. Pedro Beauchamp with Adlin Román in his arms. Paseo
IVM in PCOS patients. Introduction (1) Introduction (2) Michael Grynberg René Frydman
 IVM in PCOS patients Michael Grynberg René Frydman Department of Obstetrics and Gynecology A. Beclere Hospital, Clamart, France Maribor, Slovenia, 27-28 February 2009 Introduction (1) IVM could be a major
IVM in PCOS patients Michael Grynberg René Frydman Department of Obstetrics and Gynecology A. Beclere Hospital, Clamart, France Maribor, Slovenia, 27-28 February 2009 Introduction (1) IVM could be a major
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
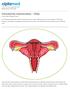 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Corrective measures and pregnancy outcome in in vitro fertilization in patients with severe sperm morphology abnormalities
 FERTILITY AND STERILITY Copyright e 1988 The American Fertility Society Printed in U.S.A. Corrective measures and pregnancy outcome in in vitro fertilization in patients with severe sperm morphology abnormalities
FERTILITY AND STERILITY Copyright e 1988 The American Fertility Society Printed in U.S.A. Corrective measures and pregnancy outcome in in vitro fertilization in patients with severe sperm morphology abnormalities
Utility of in vitro fertilization at diagnostic laparoscopy*
 FERTILITY AND STERILITY Copyright" 1994 The American Fertility Society Printed on acid-free paper in U. S. A. Utility of in vitro fertilization at diagnostic laparoscopy* Paul R. Gindoff, M.D.t Jerry L.
FERTILITY AND STERILITY Copyright" 1994 The American Fertility Society Printed on acid-free paper in U. S. A. Utility of in vitro fertilization at diagnostic laparoscopy* Paul R. Gindoff, M.D.t Jerry L.
Fertility assessment and assisted conception
 Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Fertility assessment and assisted conception Dr Geetha Venkat MD FRCOG Director Pulse Learning Women s health 14 September 2016 Disclosure statement Dr Venkat is a director of Harley Street Fertility Clinic.
Article Letrozole versus human menopausal gonadotrophin in women undergoing intrauterine insemination
 RBMOnline - Vol 13. No 2. 2006 208-212 Reproductive BioMedicine Online; www.rbmonline.com/article/2334 on web 30 May 2006 Article Letrozole versus human menopausal gonadotrophin in women undergoing intrauterine
RBMOnline - Vol 13. No 2. 2006 208-212 Reproductive BioMedicine Online; www.rbmonline.com/article/2334 on web 30 May 2006 Article Letrozole versus human menopausal gonadotrophin in women undergoing intrauterine
Comparison of the effectiveness of single intrauterine insemination (IUI) versus double IUI per cycle in infertile patients
 FERTILITY AND STERILITY VOL. 80, NO. 3, SEPTEMBER 2003 Copyright 2003 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Comparison of the effectiveness
FERTILITY AND STERILITY VOL. 80, NO. 3, SEPTEMBER 2003 Copyright 2003 American Society for Reproductive Medicine Published by Elsevier Inc. Printed on acid-free paper in U.S.A. Comparison of the effectiveness
