Course of damage to the hallux over 5 years after forefoot resection arthroplasty in rheumatoid arthritis patients
|
|
|
- Gwen Porter
- 6 years ago
- Views:
Transcription
1 International Orthopaedics (SICOT) (2007) 31: DOI /s ORIGINAL PAPER Course of damage to the hallux over 5 years after forefoot resection arthroplasty in rheumatoid arthritis patients H. Hattori & J. Mibe & A. Nohara & K. Yamamoto Received: 19 May 2006 /Accepted: 12 June 2006 /Published online: 7 September 2006 # Springer-Verlag 2006 Abstract A retrospective study of 34 feet from 20 consecutive patients with rheumatoid arthritis was performed to investigate the development of damage to the hallux over 5 years after forefoot resection arthroplasty. Radiographically we analysed changes in two valgus angles and the interphalangeal joint (IP) damage of the hallux. These parameters were measured preoperatively, 12 months postoperatively, and at the latest follow-up. Although the average HVA (between the first metatarsal and the proximal phalanx) significantly decreased from 38.7 preoperatively to 8.66 postoperatively, the angle increased to 23.0 during the first 12 months following surgery. Further deterioration of the angle at the last follow-up was not detected (25.3 ; P=0.252). The average IPV (between the proximal phalanx and the distal phalanx) angle significantly increased from 6.65 preoperatively to months postoperatively and thereafter slightly increased to 13.3 at the latest follow-up. The average of the Sharp/van der Heijde score of the IP joint significantly increased from 5.71 preoperatively to months postoperatively and thereafter slightly increased to 9.65 at the latest follow-up. The deterioration and destruction process of the hallux after resection arthroplasty occurred soon after surgery, and the progression of the deformity was temporary. H. Hattori (*) : K. Yamamoto Department of Orthopedic Surgery, Tokyo Medical University, 6-7-1, Nishishinjuku, Shinjuku-ku, Tokyo , Japan hiroyuki.hattori@jcom.home.ne.jp J. Mibe : A. Nohara Department of Orthopedic Surgery, Tokyo Metropolitan OHTSUKA Hospital, Tokyo, Japan Résumé L étude rétrospective a porté sur 34 pieds chez 20 patients consécutifs présentant une arthrite rhumatoïde de façon à étudier l évolution de la déformation du gros orteil, 5 ans après une résection arthroplastique de l avant pied. Nous avons analysé de façon clinique et radiographique les angles des articulations du gros orteil. Ces paramètres ont été mesurés en préopératoire et en post-opératoire après 12 mois de suivi. L angle métatarso phalangien était significativement amélioré passant de 38.7 en préopératoire à 8.66 en post-opératoire avec une amélioration de 23 durant les 12 mois suivant l intervention chirurgicale. Il n y a pas eu d aggravation de cet angle au plus long recul. La moyenne de l angle inter phalangien a été significativement augmenté de 6.65 en préopératoire à 12.1 en postopératoire. Le score moyen de Sharp et Van Der Heijde relatif à l inter phalangienne a été significativement augmenté passant de 5.71 en préopératoire à 8.58 en post-opératoire. La destruction de l articulation du gros orteil après résection arthroplastique survient précocement après la chirurgie et la progression de la déformation est très temporaire. Introduction Rheumatoid arthritis (RA) frequently causes painful forefoot deformities that can interfere with standing and walking. The metatarsophalangeal (MTP) joints are the most common sites of this disease, which presents with an aggressive synovistis, capsular distention, and collateral ligament integrity. Continued walking with soft tissue instability, articular cartilage destruction, and subchondral bone resorption leads to common rheumatoid forefoot deformities, including hallux valgus, hammering of the lesser toes, and subluxation and dislocation of the lesser MTP. As the proximal phalanges are displaced dorsally, the
2 478 International Orthopaedics (SICOT) (2007) 31: plantar fat pad is drawn distally, leaving a relatively thin, insufficient soft tissue cushion beneath the metatarsal heads, where painful, thickened plantar callosities frequently develop and impair the ability of the affected individual to walk. Weight is shifted away from the painful part of the foot, which necessitates the use of custom-made shoes. In many cases, however, it is difficult to manage these deformities with conservative methods, and surgery is often required. Forefoot resection arthroplasty by various operative techniques has been widely recommended because most studies reported that a high percentage of the outcomes was satisfactory over the long term [1, 12, 14]. Some studies, however, reported a deterioration in the result over time, with a high recurrence rate for callosities and deformities, especially in the hallux [1, 9, 15]. Therefore, arthrodesis and implant arthroplasty of the first MTP joint have gained favour as alternatives to resection arthroplasty. Some of these authors reached their conclusions about the outcomes from forefoot resection arthroplasties on the basis of written questionnaires or telephone surveys [1, 9]. Most studies included only a comparison of preoperative and postoperative radiographs in the final assessment, even if radiographic measurements were analysed; detailed radiographic outcomes of the forefoot resection arthroplasties have not been well documented. The aim of this study was to assess the course of radiographic changes in the hallux over 5 years after resection arthroplasties in rheumatoid patients. Materials and methods Patients Medical records at our institution were reviewed to identify patients with RA who underwent a resection arthroplasty of the forefoot between 1995 and The inclusion criteria were the presence of RA, severe forefoot pain due to a deformity with subluxation of two or more MTP joints and plantar callosities, and bone destruction in two or more MTP joints. We identified 20 patients (all women with a total of 34 feet that had been operated on) that had undergone a resection arthroplasty for the first MTP joint, combined with resection of the metatarsal heads of the lesser toes through a plantar approach. Functional classification of these patients at the time of surgery was as follows: three women in class I, nine in class II, and eight in class III. The average age of the patients was 59.5 years (range: 36 to 76 years old), and the mean duration that they had been diagnosed with RA was 15.0 years (range: 7 to 38 years). The average follow-up period was 6.59 years (range: 5 to 8.83 years). Operative procedure The operative procedure was a combination of the Mayo procedure for the hallux and the Hoffman procedure for the lesser MTP joint, as has been described previously [8, 11]. The great toe was approached dorsomedially, with oval resection of the skin and bursa as needed. The capsular flap between the extensor and abductor tendons includes the short extensor tendon, which was incised off the proximal phalanx. After a synovectomy, the metatarsal head was resected as far as necessary to achieve soft tissue release. The dorsal flap was closed as far as possible, replacing the extensor tendon more medially and the abductor tendon more dorsally. The hallux was fixed with Kirschner wire. For the lesser MTP joints, we used a plantar transverse elliptic excision of skin calluses and bursae, which was convex, distally and waved proximally to adjust the lengths of both flaps. The perforated plantar capsules were split longitudinally underneath the metatarsal heads, which were resected such that their alignment and length corresponded with each other. The interphalangeal (IP) joints were corrected by manipulation, and Kirchner wires were used as needed to preserve the alignment for 3 weeks after the operation. If possible, patients were allowed to walk using a non-weight-bearing heel. The Kirschner wires were removed after 3 weeks, and then all the patients were allowed to walk in a full weight-bearing manner. Evaluation Radiographic deformities We measured three valgus angles of the hallux and second toe on plain anteroposterior (AP) radiographs (Fig. 1). The MTP valgus angles were formed by the intersections of the first metatarsal and the proximal phalanx (HVA), the second metatarsal and the proximal phalanx (MTP-2), and the first proximal phalanx and the distal phalanx (IPV). We also measured the intermetatarsal angle, which was defined as the intersection of the longitudinal axes of the first and the second metatarsals (M1/2). The HVA angle was measured before surgery, after the Kirschner wires were removed 3 weeks after operation, 12 months after surgery, and at the last follow-up examination. The IPV, MTP-2 and M1/M2 angles were measured before surgery, 12 months after surgery, and at the latest follow-up examination. Changes in the angles were then evaluated. Damage to the interphalangeal joint of the hallux Two methods were used to evaluate the AP radiographs for the extent of joint damage in the IP joint of the hallux. The first method was a modified Larsen score, which assessed
3 International Orthopaedics (SICOT) (2007) 31: follows: 0= normal; 1= focal or doubtful; 2= generalised, less than 50% of the original joint space; 3= generalised, more than 50% of the original joint space or subluxation; 4= bony ankylosis or complete luxation. Thus, the maximum score for a joint was 14. The grading and scoring were assessed before surgery, 12 months after the surgery and at the latest follow-up examination. Statistical analysis Paired t tests were used to assess the changes in the angles and scores that showed equal variance. When the data showed unequal variance, Wilcoxon signed-ranks tests were used. A P-value of less than 0.01 was considered to be statistically significant. Results Changes in the angles Fig. 1 HVA: valgus angle between the first metatarsal and the proximal phalanx. MTP-2: valgus angle between the second metatarsal and the proximal phalanx. IPV: valgus angle between the first proximal phalanx and the distal phalanx. M1/2: intermetatarsal angle between the first and second metatarsals the degree of joint destruction mainly determined using erosion changes [5]. The grading scale ranged from 0 to 5: 0= intact bony outlines and normal joint space; 1= erosion less than 1 mm in a diameter or joint space narrowing (JSN); 2= one or several small erosions (diameter more than 1 mm); 3= significant erosions; 4= severe erosions (usually no joint space left and the bony outlines were only partly preserved); 5= multiple changes (the original bony outlines were destroyed). The second method was a Sharp/ van der Heijde score (SHS), which assessed both joint erosion and JSN [13]. A score of one corresponded to discrete erosions, and the score rose to two, three, four, or five depending on the amount of surface area affected (complete collapse of the bone was scored as a five). JSN was combined with a score for subluxation and scored as Changes in the angles are shown in Table 1. Although the average HVA angle significantly decreased from a preoperative angle of 38.7 to a postoperative angle of 8.66 (P<0.01), the average HVA angle increased again to 23.0 during the first 12 months after the surgery (P<0.01). Significant deterioration of the angle from 12 months after the surgery to the last follow-up examination was not detected (25.3 at the last follow-up examination; P=0.252). There was still a significant difference between the preoperative angle and the angle at the last follow-up examination (P<0.01). The average MTP-2 angle was 17.6 (range: 40 to 70 ) before surgery, 16.3 (range: 0 to 30 ) 12 months after the Table 1 Average angles of measured at four times points Preoperative Postoperative Postoperative 12 mo Last follow-up HVA * 23.0** 25.3*## MTP * 18.2*## 2 IPV * 13.3*## M1/ # 13.4## HVA: valgus angle between the first metatarsal and the proximal phalanx MTP-2: valgus angle between the second metatarsal and the proximal phalanx IPV: valgus angle between the first proximal and the distal phalanx M1/2: intermetatarsal angle between the first and second metatarsals *P<0.01, significantly different from preoperative angle **P<0.01, significantly different from the postoperative angle # not significantly different from the preoperative angle ## not different from the postoperative angle measured 12 months after the surgery
4 480 International Orthopaedics (SICOT) (2007) 31: operation, and 18.2 (range: 15 to 55 ) at the last followup examination. We found that the postoperative changes in the MTP-2 angle, including improvement in the angle and deterioration over time, were not consistent for the different patients. The average IPV angle of the hallux significantly increased from a preoperative angle of 6.65 to months after the surgery (P<0.01). Thereafter, the angle slightly increased to 13.3 at the last follow-up examination, although the change was not significant (P=0.433). The average M1/2 angle decreased from 15.8 to months after the surgery, but the change was not significant (P=0.315). Deterioration of the angle from 12 months after the surgery to the last follow-up examination was not detected (13.4 at the last follow-up examination; P=0.373). There was no significant difference between the preoperative angle and the angle at the last follow-up examination (P=0.423). Damage to the interphalangeal joint of the hallux The changes in the scores for IP joint damage of the hallux are shown in Table 2. Before the surgery, small degenerative changes of the IP joint (grade 0, 1, or 2) were observed in 18 of the 34 feet (53%), whereas severe changes (grade 4 or 5) were found in less than 30% of the feet (7 of 34 feet). At the last follow-up examination, severe degenerative changes were observed in more than 50% of the feet (19 of 34 feet). The average SHS of the IP joint of the hallux significantly increased from a preoperative value of 5.71 to 8.58 during the first 12 months after the surgery (P<0.01). Thereafter, the SHS slightly increased to 9.65 at the last follow-up examination, although the change was not significant (P=0.0155); the highest scores from three of the feet were excluded. Table 2 Damage to the interphalangeal joint of the hallux Larsen grade Properative 12 months postoperative Last follow-up Grade Grade Grade Grade Grade Grade SHS score * 9.65# SHS score: Sharp/van der Heijde score *P<0.01, significantly different from preoperative ## not different from 12 months postoperatively Discussion In this study, we have shown that hallux deformities occurred soon after forefoot resection arthroplasties and that the radiographic progression of the deformities was most rapid during the first year following surgery. Moreover, the extent of the hallux deformity after surgery did not depend on the follow-up period. The prevalence of recurrent hallux valgus deformities after resection arthroplasties has been reported to be higher than 50%; the rate was 61% (109 of 179 feet) in the study by Vahvanen et al. [15] and was 68% (28 of 41 patients) in the study by van der Heijde et al. [12]. More recently, Fuhrmann and Anders found recurrent hallux valgus in 36.6% of the feet examined in their study (93 of 254 feet) [3]. Although in all of these studies, the hallux valgus deformities resulted in HVA angles of 20 or more, the mechanisms underlying the abnormal HVA angles in rheumatoid patients are not understood. In our study, none of the patients required a second operation because of recurrent hallux valgus, although 73.7% of the affected feet (28 of 38 feet) had an HVA angle of 20 or more. To our knowledge, there are no reports about the effects of the hallux on the IP joint after resection arthroplasty, although the changes in the IP joint after arthrodesis of the first MTP joint have been discussed. The prevalence of arthritis in the IP joint following arthrodesis of the first MTP joint in a rheumatoid foot has been reported to be relatively high [2, 6, 7]. We postulated that the effects on the IP joint of the hallux after resection arthroplasty should be less severe than those following arthrodesis of the first MTP joint, because the mobility of the first MTP joint after resection arthroplasty is preserved. It is known that the joint adjacent to the fused joint is often damaged. In this study, however, deformities and degenerative changes in the IP joint of the hallux after resection arthroplasty were unexpectedly severe and rapidly progressed during the early stages following surgery. Moreover, we could not predict the progression of the valgus deformity of the hallux IP joint after surgery. We predicted that a varus deformity of the IP joint would occur after the recurrence of a hallux valgus deformity due to direct contact between the hallux and the second toe. Moreover, the valgus deformity of the hallux IP joint did not relate to the course of a second valgus deformity in the MTP joint after surgery. We believe that these factors cause unnatural power to be applied to the IP joint of the hallux to support the instability of the forefoot and the decreased forefoot pain allows the great toe to contact the ground directly soon after surgery. Phillipson et al. used EMED F pressure to show that the total pressure and the pressuretime of the hallux significantly increased after forefoot resection arthroplasty, and the greatest area of change was
5 International Orthopaedics (SICOT) (2007) 31: the region of the first metatarsal head remnant [10]; these results support our hypothesis. This raises the possibility that deformity and degenerative changes of the IP joint of the hallux after surgery are affected not only by a mechanical factor, but also by rheumatoid arthritis. Deformity of the IP joint of the hallux, however, is relatively rare in rheumatoid patients. Kirkup et al. reported that in rheumatoid patients with hallux disorder, erosion changes in the IP joint were observed in 29% of the feet examined (57 of 194 feet), and IP valgus deformities were seen in only 6.7% of the affected feet (13 of 194 feet) [4]. Moreover, because the deformities and degenerative changes occur at an early postoperative stage, we believe that mechanical factors greatly contribute to the development of the deformities and degenerative changes in the IP joint of the hallux after the surgery. In conclusion, our study shows that the deterioration and destruction of the hallux after resection arthroplasty occur at a relatively early stage and that the progression of the deformity is a temporary process. Therefore, forefoot resection arthroplasty is a stable procedure for the patient with RA over the long term. References 1. Brattstrom H, Brasttstrom M (1970) Resection of the metatarsophangeal joints in rheumatoid arthritis. Acta Orthop Scand 41: Coughlin MJ (2000) Rheumatoid forefoot reconstruction. J Bone Jt Surg 82A: Fuhrmann RA, Anders JO (2001) The long-term results of resection arthroplasties of the first metarsophalangeal joint in rheumatoid arthritis. Int Orthop 25: Kirkup JR, Vidigal E, Jacoby RK (1977) The hallux and rheumatoid arthritis. Acta Orthop Scand 48: Larsen A (1995) How to apply Larsen score in evaluating radiographs of rheumatoid arthritis in long-term studies. J Rheumatol 22: Mann RA, Thompson FM (1984) Arthrodesis of the first metatarsophalangeal joint for hallux valgus in rheumatoid arthritis. J Bone Jt Surg 66A: Mann RA, Schakel ME (1995) Surgical correction of rheumatoid forefoot deformities. Foot Ankle Int 16: Mayo CG (1908) The surgical treatment of bunions. Ann Surg 48: Mc Garvey SR, Johnson KA (1988) Keller arthroplasty in combination with resection arthroplasty of lesser metatarsophalangeal joints in rheumatoid arthritis. Foot Ankle Int 9: Phillipson A, Dhar S, Linge K, Mc Cabe C, Klenerman L (1994) Forefoot arthroplasty and changes in plantar foot pressures. Foot Ankle Int 15: Tillmann K (1997) Surgery of the rheumatoid forefoot with special reference to plantar approach. Clin Orthop 340: van der Heijden KW, Rasker JJ, Jacob JW, Dey K (1992) Kates forefoot arthroplasty in rheumatoid arthritis. A 5-year follow-up study. J Rheumatol 19: van der Heijde DM, van Riel PL, Nuver-Zwart HH, Gribnau FW, van der Putte LB (1989) Effects of hydroxychloroquine and sulphasalazine on progression of joint damage in rheumatoid arthritis. Lancet i: van Loon PJ, Aries RP, Karthans RP, Steenaert BJ (1992) Metatarsal head resection in the deformed, symptomatic rheumatic foot. A comparison of two methods. Acta Orthop Belg 58: Vahvanen V, Piirainen H, Kettunen P (1980) Resection arthroplasty of metatarsophalangeal joints in rheumatoid arthritis. A follow-up study of 100 patients. Scand J Rheumatol 9:
Hallux Valgus Deformity: Preoperative Radiologic Assessment
 119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
119 Pictorial Essay H............ - Hallux Valgus Deformity: Preoperative Radiologic Assessment David Karasick1 and Keith L. Wapner An estimated 40% of the American adult population experiences foot problems,
Investigation performed at the Department of Orthopaedic and Trauma Surgery, Glasgow Royal Infirmary, Glasgow, United Kingdom
 748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
748 COPYRIGHT 2005 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Long-Term Results of the Modified Hoffman Procedure in the Rheumatoid Forefoot BY S. THOMAS, MBCHB, BSC, MRCS, A.W.G. KINNINMONTH,
Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot
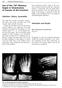 168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
168 Forefoot Reconstruction Use of the 20 Memory Staple in Osteotomies of Fusions of the Forefoot Definition, History, Generalities This staple first provides a permanent compression both in the prongs
Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy
 Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Journal of Orthopaedic Surgery 2005:13(3):245-252 Clinical results of modified Mitchell s osteotomy for hallux valgus augmented with oblique lesser metatarsal osteotomy K Yamamoto, A Imakiire, Y Katori,
Joint Preserving Surgery in Severe Forefoot Disorders
 Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Joint Preserving Surgery in Severe Forefoot Disorders J ORTHOP TRAUMA SURG REL RES 4 (12) 2008 Review article LOUIS S. BAROUK*, PIERRE BAROUK** * 39, Chemin de la Roche, 33370, Yvrac, France ** Clinique
Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity
 REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
REVIEW Proximal metatarsal osteotomy and distal soft tissue reconstruction as treatment for hallux valgus deformity Michael J. Coughlin and J. Speight Grimes Boise, Idaho, USA (Received for publication
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months.
 Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Case 57 What is the diagnosis? Insidious onset forefoot pain in a 50 year old female for last 3 months. Diagnosis: II MTP instability Demographics of MT instability Lesser MTP joint instability occurs
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus
 Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Comparison of Postoperative Outcomes between Modified Mann Procedure and Modified Lapidus Procedure for Hallux Valgus Yui Akiyama, Takaaki Hirano, Hiroyuki Mitsui Shingo Maeda, Hisateru Niki Department
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow.
 Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Medincenter GlavUpDK by the Ministry of Foreign Affairs of Russia, Moscow. Berezhnoy Sergey. Percutaneous First Metatarsocuneiform Joint Arthrodesis in a Treatment of Metatarsus Primus Varus: a Prospective
Lesser MPJ Hemi Implant
 Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Lesser MPJ Hemi Implant Surgical Technique Contents Product The BioPro Lesser MPJ Hemi Implant is a simple, durable, metallic hemiarthroplasty resurfacing prosthesis for the treatment of arthritis, Freiberg
Modified Proximal Scarf Osteotomy for Hallux Valgus
 Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Original Article Clinics in Orthopedic Surgery 2018;10:479-483 https://doi.org/10.4055/cios.2018.10.4.479 Modified Proximal Scarf Osteotomy for Hallux Valgus Ki Won Young, MD, Hong Seop Lee, MD, Seong
Resection Arthroplasty for Rheumatoid Forefoot Deformity
 Resection Arthroplasty for Rheumatoid Forefoot Deformity Jun-ichi Fukushi, M.D. Yasuharu Nakashima, M.D. Yukihide Iwamoto, M.D. Department of Orthopedic Surgery, Graduate School of Medical Sciences, Kyushu
Resection Arthroplasty for Rheumatoid Forefoot Deformity Jun-ichi Fukushi, M.D. Yasuharu Nakashima, M.D. Yukihide Iwamoto, M.D. Department of Orthopedic Surgery, Graduate School of Medical Sciences, Kyushu
Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2012.0400 Combination of First Metatarsophalangeal Joint Arthrodesis and Proximal Correction for Severe Hallux Valgus Deformity Pascal F. Rippstein, MD; Young-Uk
1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4
 1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4 Abstract 5 Background: To treat a patient with hallux
1 Relationship between degenerative change in the sesamoid-metatarsal joint and 2 displacement of the sesamoids in patients with hallux valgus 3 4 Abstract 5 Background: To treat a patient with hallux
SWANSON. Flexible Hinge Toe Implant SURGIC AL TECHNIQUE
 SWANSON Flexible Hinge Toe Implant SURGIC AL TECHNIQUE SWANSON flexible HINGE TOE IMPLANT with SWANSON Flexible Hinge Grommet surgical technique presented by ALFRED B. SWANSON, MD, FACS, GRAND RAPIDS,
SWANSON Flexible Hinge Toe Implant SURGIC AL TECHNIQUE SWANSON flexible HINGE TOE IMPLANT with SWANSON Flexible Hinge Grommet surgical technique presented by ALFRED B. SWANSON, MD, FACS, GRAND RAPIDS,
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD
 Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
Geoffrey Watson, MD Matthew McKean, MD Siddhant K. Mehta, MD Thom A. Tarquinio, MD University of Mississippi Medical Center Jackson, Mississippi American Orthopaedic Foot & Ankle Society ANNUAL MEETING
with regard to our presentation.
 Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Rotated Insertion Metatarsal Osteotomy with Distal Soft Tissue Procedure for Severe Hallux Valgus Deformity Novel Procedure of the 1 st metatarsal osteotomy Norihiro Samoto MD, Ph.D. Director of Department
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair
 Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Symptomatic Medial Exostosis of the Great Toe Distal Phalanx: A Complication Due to Over-correction Following Akin Osteotomy for Hallux Valgus Repair Carlos Villas, MD, PhD, 1 Javier Del Río, MD, 3 Andres
Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital review
 The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
The Foot and Ankle Online Journal Official publication of the International Foot & Ankle Foundation Complications associated with Mitchell s Osteotomy for Hallux Valgus Correction: A retrospective hospital
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus. Anand Vora, MD
 Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
Intermediate outcome of interpositional arthroplasty for the treatment of hallux rigidus Anand Vora, MD CONFLICT TO DISCLOSE Intermediate outcome of interpositional arthroplasty for the treatment of hallux
How to avoid complications of distraction osteogenesis for first brachymetatarsia
 220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
220 Acta Orthopaedica 2009; 80 (2): 220 225 How to avoid complications of distraction osteogenesis for first brachymetatarsia Keun-Bae Lee, Hyun-Kee Yang, Jae-Yoon Chung, Eun-Sun Moon, and Sung-Taek Jung
A New Incisional Approach to the Rheumatoid Foot
 A New Incisional Approach to the Rheumatoid Foot The authors introduce a new incisional approach to surgery of the rheumatoid foot. Advantages and disadvantages are presented. Historical comparisons are
A New Incisional Approach to the Rheumatoid Foot The authors introduce a new incisional approach to surgery of the rheumatoid foot. Advantages and disadvantages are presented. Historical comparisons are
High Rate of Recurrent Hallux Valgus Following Proximal Medial Opening Wedge Osteotomy for Correction of Moderate to Severe Deformity
 High Rate of Recurrent Hallux Valgus Following Proximal Medial Opening Wedge Osteotomy for Correction of Moderate to Severe Deformity Sravisht Iyer, MD 1 Constantine Demetracopoulos, MD Jeanne Yu, BS Sriniwasan
High Rate of Recurrent Hallux Valgus Following Proximal Medial Opening Wedge Osteotomy for Correction of Moderate to Severe Deformity Sravisht Iyer, MD 1 Constantine Demetracopoulos, MD Jeanne Yu, BS Sriniwasan
CURRENT METHODS OF TREATMENT
 ~ CURRENT METHODS OF TREATMENT Rheumatoid Deformity of the Foot* By LEONARD MARMOR T HE PATIENT with rheumatoid arthritis often develops severe, crippling deformities of his upper and lower limbs. The
~ CURRENT METHODS OF TREATMENT Rheumatoid Deformity of the Foot* By LEONARD MARMOR T HE PATIENT with rheumatoid arthritis often develops severe, crippling deformities of his upper and lower limbs. The
Merete PlantarMAX Lapidus Plate Surgical Technique. Description of Plate
 Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
Merete PlantarMAX Lapidus Plate Surgical Technique Description of Plate Merete Medical has designed the PlantarMax; a special Plantar/Medial Locking Lapidus plate which places the plate in the most biomechanically
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES
 FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
FREIBERG S INFRACTION TREATMENT WITH METATARSAL NECK DORSAL CLOSING WEDGE OSTEOTOMY: REPORT OF TWO CASES Sung-Yen Lin, 1 Yuh-Min Cheng, 1,2 and Peng-Ju Huang 1,2 1 Department of Orthopedics, Kaohsiung
19 Arthrodesis of the First Metatarsocuneiform Joint
 19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
19 Arthrodesis of the First Metatarsocuneiform Joint CHARLES GUDAS Abduction of the first metatarsal to correct metatarsus primus varus and hallux valgus was first described by Albrecht in 1911. 1 Lapidus
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS
 RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
RISK FACTORS FOR SUBOPTIMAL OUTCOMES IN HAMMERTOE SURGERY JACOB RANDICH BS RACHEL ALBRIGHT DPM, MOIZ HASSAN MS, ROBERT O KEEFE DPM, ERIN E. KLEIN DPM, MS, LOWELL WEIL JR. DPM, MBA, LOWELL WEIL SR. DPM,
JUVENILE AND ADOLESCENT HALLUX VALGUS. George E. Quill, Jr., M.D.
 JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
JUVENILE AND ADOLESCENT HALLUX VALGUS George E. Quill, Jr., M.D. The development of a hallux valgus deformity in children and adolescents is actually an uncommon entity. Most of these occurrences can be
Increased pressures at
 Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Surgical Off-loading of Plantar Hallux Ulcerations These approaches can be used to treat DFUs. By Adam R. Johnson, DPM Increased pressures at the plantar aspect of the hallux leading to chronic hyperkeratosis
Section 6: Preoperative Planning
 Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Clinical Relevance of the PedCat Study: In many ways the PedCat study confirmed radiographic findings. With the measuring tools embedded in the DICOM viewing software it was possible to gauge the thickness
Moderate to severe hallux valgus deformity: correction with proximal crescentic osteotomy and distal soft-tissue release
 Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Arch Orthop Trauma Surg (2000) 120 : 397 402 Springer-Verlag 2000 ORIGINAL ARTICLE R. Zettl H.-J. Trnka M. Easley M. Salzer P. Ritschl Moderate to severe hallux valgus deformity: correction with proximal
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint
 Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Medical Policy Partial or Total Replacement of First Metatarsophalangeal Joint Subject: Partial or Total Replacement of First Metatarsophalangeal (MTP) Joint Background: Underlying causes of disease or
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities
 Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Soft Tissue Rebalancing Procedures for the Treatment of Hallux Valgus Deformities NO DISCLOSURES Objectives The main objectives of any procedure in hallux abducto valgus surgery are to correct the deformity,
Bunions. A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus.
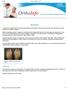 Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
Bunions A bunion is a painful bony bump that develops on the inside of the foot at the big toe joint. Bunions are often referred to as hallux valgus. Bunions develop slowly. Pressure on the big toe joint
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT. Miss Sue Kendall PhD FRCS (Orth&Trauma)
 THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
THE ROLE OF MINIMALLY INVASIVE SURGERY IN THE FOREFOOT Miss Sue Kendall PhD FRCS (Orth&Trauma) Is Minimally Invasive Surgery of the foot a good idea? Minimally invasive surgery, keyhole surgery entering
The Weil osteotomy. Lower limb A SEVEN-YEAR FOLLOW-UP. S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J.
 Lower limb The Weil osteotomy A SEVEN-YEAR FOLLOW-UP S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J. Trnka From Hospital Gersthof, Vienna, Austria We prospectively
Lower limb The Weil osteotomy A SEVEN-YEAR FOLLOW-UP S. G. Hofstaetter, J. G. Hofstaetter, J. A. Petroutsas, F. Gruber, P. Ritschl, H.-J. Trnka From Hospital Gersthof, Vienna, Austria We prospectively
Appendix H: Description of Foot Deformities
 Appendix H: Description of Foot Deformities The following table provides the description for several foot deformities: hammer toe, claw toe, hallux deformity, pes planus, pes cavus and charcot arthropathy.
Appendix H: Description of Foot Deformities The following table provides the description for several foot deformities: hammer toe, claw toe, hallux deformity, pes planus, pes cavus and charcot arthropathy.
THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery
 C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
C H A P T E R 1 4 THE FIBULAR SESAMOID ELEVATOR: A New Instrument to Aid the Lateral Release in Hallux Valgus Surgery Thomas F. Smith, DPM Lopa Dalmia, DPM INTRODUCTION Hallux valgus surgery is a complex
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant
 Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
Interphalangeal Arthrodesis of the Toe with a New Radiolucent Intramedullary Implant DIEBOLD P.-F., ROCHER H.,, DETERME P., CERMOLACCE C., GUILLO S., AVEROUS C., LEIBER WACKENHEIN F. Interphalangeal Arthrodesis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION. At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral)
 PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
PAINFUL SESAMOID OF THE GREAT TOE Dr Vasu Pai ANATOMICAL CONSIDERATION At the big toe MTP joint: Tibial sesamoid (medial) & fibular (lateral) They are contained within the tendons of Flexor Hallucis Brevis
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study
 Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Weil osteotomy and flexor to extensor transfer for irreparable plantar plate tear: prospective study Daniel Baumfeld, MD Fernando Raduan, MD Fernanda Catena, MD Tania Mann, MD Caio Nery, MD Disclosure
Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus
 Archives of Orthopedics and Rheumatology Volume 1, Issue 1, 2018, PP: 7-11 Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus Jorge de las Heras Romero 1 *, Ana María Lledó Alvarez
Archives of Orthopedics and Rheumatology Volume 1, Issue 1, 2018, PP: 7-11 Clinical Practice Guideline on the Diagnosis and Treatment of Hallux Valgus Jorge de las Heras Romero 1 *, Ana María Lledó Alvarez
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity
 Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
Re+Line Bunion Correction System for Correction of Hallux Abducto Valgus Deformity Amber M. Shane, DPM, FACFAS 1, Christopher L. Reeves, DPM, FACFAS 1 1. Orlando Foot & Ankle Clinic, Orlando, FL Abstract
University of Groningen. Forefoot disorders Schrier, Joost
 University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus
 FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
FOOT AND ANKLE Distal metatarsal osteotomy for hallux varus following surgery for hallux valgus K. J. Choi, H. S. Lee, Y. S. Yoon, S. S. Park, J. S. Kim, J. J. Jeong, Y. R. Choi From the Asan Medical Center,
RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS
 C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
C H A P T E R 1 7 RETROSPECTIVE ANALYSIS OF END-TO-END DIGITAL ARTHRODESIS Michelle L. Butterworth, DPM Michael S. Downey, DPM Digital deformities are one of the most common entities we face as foot and
Tomohiro Onodera 1*, Hiroaki Nakano 1, Kentaro Homan 1, Eiji Kondo 2 and Norimasa Iwasaki 1
 Onodera et al. BMC Musculoskeletal Disorders (2019) 20:87 https://doi.org/10.1186/s12891-019-2462-y RESEARCH ARTICLE Open Access Preoperative radiographic and clinical factors associated with postoperative
Onodera et al. BMC Musculoskeletal Disorders (2019) 20:87 https://doi.org/10.1186/s12891-019-2462-y RESEARCH ARTICLE Open Access Preoperative radiographic and clinical factors associated with postoperative
HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT
 C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
C H A P T E R 1 5 HEMI IMPLANT ARTHROPLASTY FOR THE SECOND METATARSOPHALANGEAL JOINT Joe T. Southerland, DPM Mickey D. Stapp, DPM INTRODUCTION Hemi-implant arthroplasty of the first metatarsophalangeal
A Patient s Guide to Claw Toes and Hammertoes
 A Patient s Guide to Claw Toes and Hammertoes 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Claw Toes and Hammertoes 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
Early Diagnosis. Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Progressive MTP joint subluxation
 Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Conflicts of interest Arthrex- consultant Arthrex- royalties Elsevier-book royalties Michael J Coughlin, M.D. Early
Instability of the lesser MTP joints (Crossover 2 nd toe deformity) -my 25 year journey- Conflicts of interest Arthrex- consultant Arthrex- royalties Elsevier-book royalties Michael J Coughlin, M.D. Early
Chevron Osteotomy With Lateral Soft Tissue Release
 5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
5(4):250 256, 2006 T E C H N I Q U E Chevron Osteotomy With Lateral Soft Tissue Release Hans-Jörg Trnka, MD, PhD and Stefan Gerhard Hofstaetter, MD Foot and Ankle Center Vienna Vienna, Austria Ó 2006 Lippincott
RECURRENT INTERMETATARSAL NEUROMA
 4 th Foot & Ankle Symposium RECURRENT INTERMETATARSAL NEUROMA Martin Berli, MD Department of Prosthetics and Orthotics Uniklinik Balgrist, Zurich martin.berli@balgrist.ch Recurrence: General Topics Pain
4 th Foot & Ankle Symposium RECURRENT INTERMETATARSAL NEUROMA Martin Berli, MD Department of Prosthetics and Orthotics Uniklinik Balgrist, Zurich martin.berli@balgrist.ch Recurrence: General Topics Pain
DuaFit. Proximal Interphal angeal Impl ant
 DuaFit Proximal Interphal angeal Impl ant DUAFIT - TABLE OF CONTENTS PRODUCT DESCRIPTION 3 INDICATIONS 6 SURGICAL TECHNIQUE #1 7 Without guide wire (DuaFit 0 10 17 ) SURGICAL TECHNIQUE #2 14 With guide
DuaFit Proximal Interphal angeal Impl ant DUAFIT - TABLE OF CONTENTS PRODUCT DESCRIPTION 3 INDICATIONS 6 SURGICAL TECHNIQUE #1 7 Without guide wire (DuaFit 0 10 17 ) SURGICAL TECHNIQUE #2 14 With guide
Investigation performed at Orthopaedic Hospital Gersthof, Vienna, Austria
 1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
1131 COPYRIGHT 2004 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED Salvage of a Failed Keller Resection Arthroplasty BY FELIX MACHACEK JR., MD, MARK E. EASLEY, MD, FLORIAN GRUBER, MD, PETER RITSCHL,
WHAT DO HALLUX VALGUS AND BUNION MEAN?
 Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
Mr Laurence James BSc MBBS MRCS(Eng) FRCS(Tr&Orth) Consultant Orthopaedic Surgeon Foot, Ankle and Sports Injuries WHAT DO HALLUX VALGUS AND BUNION MEAN? Hallux is Latin for great toe and Valgus is Latin
HemiEDGE. Patent No. 8,845,750. Surgical Technique
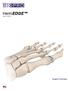 HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
HemiEDGE Patent No. 8,845,750 Surgical Technique Contents Product Based on the clinical success of our First MPJ Hemi Implant, the HemiEDGE, incorporates an overlapping edge extending around the medial,
A Patient s Guide to Claw Toes and Hammertoes
 A Patient s Guide to Claw Toes and Hammertoes Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information
A Patient s Guide to Claw Toes and Hammertoes Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information
Digital Surgery Complications
 Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
Annual Surgical Conference 2018 Digital Surgery Complications Zeeshan S. Husain, DPM, FACFAS, FASPS Great Lakes Foot and Ankle Institute September 21, 2018 None Disclosures Presentation Outline Differentials
PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE
 C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
C H A P T E R 5 PHALANGEAL BASE AUTOGRAFT FOR THE CORRECTION OF THE SUBLUXED HAMMERTOE Raymond G. Cavaliere, DPM INTRODUCTION Hammertoes can be classified as simple, moderate, and severe. The deformities
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES
 PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
PROstep Minimally Invasive Surgery HALLUX VALGUS CORRECTION USING PROSTEP MICA MINIMALLY INVASIVE FOOT SURGERY: TWO CASE STUDIES AS PRESENTED BY: JOEL VERNOIS M.D. 016798A Case Study 1 PROstep Minimally
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review
 Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Long Oblique Distal Osteotomy of the Fifth Metatarsal for Correction of Tailor s Bunion: A Retrospective Review Barry P. London, DPM, 1 Stephen F. Stern, DPM, 2 Mark A. Quist, DPM, 3 Robert K. Lee, DPM,
Foot and Ankle Surgeon (To the poor and ignomious)
 Foot and Ankle Surgeon (To the poor and ignomious) www.orthosports.com.au 47 49 Burwood Road, Concord 29 31 Dora Street, Hurstville 160 Belmore Road, Randwick Plantar plate repair A game changer John P.
Foot and Ankle Surgeon (To the poor and ignomious) www.orthosports.com.au 47 49 Burwood Road, Concord 29 31 Dora Street, Hurstville 160 Belmore Road, Randwick Plantar plate repair A game changer John P.
The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY
 60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
60 COPYRIGHT 2003 BY THE JOURNAL OF BONE AND JOINT SURGERY, INCORPORATED The Lapidus Procedure as Salvage After Failed Surgical Treatment of Hallux Valgus A PROSPECTIVE COHORT STUDY BY J. CHRIS COETZEE,
Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis
 FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
FOOT &ANKLE INTERNATIONAL DOI: 10.3113/FAI.2011.0704 Locked Versus Nonlocked Plate Fixation For Hallux MTP Arthrodesis Kenneth J. Hunt, MD; J. Kent Ellington, MD, MS; Robert B. Anderson, MD; Bruce E. Cohen,
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY
 SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
SEVERE VARUS AND VALGUS DEFORMITIES TREATED BY TOTAL KNEE ARTHROPLASTY Th. KARACHALIOS, P. P. SARANGI, J. H. NEWMAN From Winford Orthopaedic Hospital, Bristol, England We report a prospective case-controlled
Question: You trained as a general orthopaedic and trauma surgeon and became a Consultant in Newcastle in 1968.
 Question: You trained as a general orthopaedic and trauma surgeon and became a Consultant in Newcastle in 1968. How did you become so interested in conditions of the foot? As an Orthopaedic trainee in
Question: You trained as a general orthopaedic and trauma surgeon and became a Consultant in Newcastle in 1968. How did you become so interested in conditions of the foot? As an Orthopaedic trainee in
Forefoot Reconstruction Following Metatarsal Head Resection Arthroplasty With a Plantar Approach A 20-Year Follow-Up
 840814FAIXXX10.1177/1071100719840814Foot & Ankle InternationalSimon et al research-article2019 Article Forefoot Reconstruction Following Metatarsal Head Resection Arthroplasty With a Plantar Approach A
840814FAIXXX10.1177/1071100719840814Foot & Ankle InternationalSimon et al research-article2019 Article Forefoot Reconstruction Following Metatarsal Head Resection Arthroplasty With a Plantar Approach A
MiniRail System. Part B: Foot Applications. By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito
 Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Q U I C K R E F E R E N C E G U I D E 14 MiniRail System Part B: Foot Applications By Dr. B. Magnan, Dr. E. Rodriguez and Dr. G. Vito ORDERING INFORMATION MiniRail System Kit, M190C Contents: M 101 Standard
Clinical Policy Title: Hammer toe surgery
 Clinical Policy Title: Hammer toe surgery Clinical Policy Number: 18.03.04 Effective Date: July 1, 2016 Initial Review Date: July 15, 2016 Most Recent Review Date: May 1, 2018 Next Review Date: May 2019
Clinical Policy Title: Hammer toe surgery Clinical Policy Number: 18.03.04 Effective Date: July 1, 2016 Initial Review Date: July 15, 2016 Most Recent Review Date: May 1, 2018 Next Review Date: May 2019
Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position: radiological assessment
 Choi et al. Journal of Orthopaedic Surgery and Research (2018) 13:11 DOI 10.1186/s13018-017-0712-y RESEARCH ARTICLE Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position:
Choi et al. Journal of Orthopaedic Surgery and Research (2018) 13:11 DOI 10.1186/s13018-017-0712-y RESEARCH ARTICLE Effect of metatarsal osteotomy and open lateral soft tissue procedure on sesamoid position:
Implantable K-wire SURGIC A L T ECHNIQUE
 Implantable K-wire SURGIC A L T ECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description 4 Indications 4 Contraindications Chapter 2 5 Surgical Technique 5 Hammertoe Correction 6 MTP Joint
Implantable K-wire SURGIC A L T ECHNIQUE Contents Chapter 1 4 Product Information 4 Device Description 4 Indications 4 Contraindications Chapter 2 5 Surgical Technique 5 Hammertoe Correction 6 MTP Joint
Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus
 Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus Department of Orthopaedic Surgery, Faculty of Medicine, Fukuoka University Takefumi Nishino MD,
Efficacy of a Kirschner-Wire Guide in Distal Linear Metatarsal Osteotomy for Correction of Hallux Valgus Department of Orthopaedic Surgery, Faculty of Medicine, Fukuoka University Takefumi Nishino MD,
NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study
 Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
Scandinavian Journal of Surgery 91: 202 207, 2002 NON-CONSTRAINED TITANIUM-POLYETHYLENE TOTAL ENDOPROSTHESIS IN THE TREATMENT OF HALLUX RIGIDUS A prospective clinical 2-year follow-up study P. Ess, M.
REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY
 C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
C H A P T E R 2 1 REPAIR OF THE DISPLACED AUSTIN OSTEOTOMY John V. Vanore, DPM INTRODUCTION Bunion surgery is frequently performed by foot and ankle surgeons. Generally, bunion surgery is quite predictable,
Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy
 CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
CHAPTER 2 Minimally Invasive Bunionectomy: The Lam Modification of the Traditional Distal First Metatarsal Osteotomy Bunionectomy Kevin Lam, DPM Rikhil Patel, DPM Thomas Merrill, DPM Hallux abducto valgus
The Ludloff Osteotomy
 Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Techniques in Foot and Ankle Surgery 4(4):263 268, 2005 Ó 2005 Lippincott Williams & Wilkins, Philadelphia The Ludloff Osteotomy T E C H N I Q U E Hans-Jörg Trnka, MD, PhD and Stefan Hofstätter, MD Foot
Introduction Basics MIS Screw 2 System Characteristics 2 Indication 2
 Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
Clinical Advisor M. Walther. M.D., Ph.D. Professor of Orthopedic Surgery Head of Department Centre for Foot and Ankle Surgery Schön Klinik München Harlaching FIFA Medical Centre Table of Contents Introduction
EVALUATION OF THE INTERMETATARSAL ANGLE AFTER THE ARTHRODESIS OF THE FIRST METATARSOPHALANGEAL JOINT FOR TREATMENT OF THE HALLUX VALGUS
 ORIGINAL ARTICLE EVALUATION OF THE INTERMETATARSAL ANGLE AFTER THE ARTHRODESIS OF THE FIRST METATARSOPHALANGEAL Marco Túlio Costa 1, Douglas Lobato Lopes Neto 2, Fábio Henrique Kojima 2, Ricardo Cardenuto
ORIGINAL ARTICLE EVALUATION OF THE INTERMETATARSAL ANGLE AFTER THE ARTHRODESIS OF THE FIRST METATARSOPHALANGEAL Marco Túlio Costa 1, Douglas Lobato Lopes Neto 2, Fábio Henrique Kojima 2, Ricardo Cardenuto
MANAGEMENT OF NON-REDUCIBLE LESSER-TOE INTERPHALANGEAL DISLOCATION: AN UNUSUAL INJURY
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 MANAGEMENT OF NON-REDUCIBLE LESSER-TOE INTERPHALANGEAL DISLOCATION: AN UNUSUAL INJURY Interphalangeal joint (IPJ) dislocations
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 MANAGEMENT OF NON-REDUCIBLE LESSER-TOE INTERPHALANGEAL DISLOCATION: AN UNUSUAL INJURY Interphalangeal joint (IPJ) dislocations
Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion
 Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Surgical Technique Foot and Ankle Technique Guide Proximal Inter-Phalangeal (PIP) Fusion Prepared in consultation with: Phinit Phisitkul, MD Department of Orthopedics and Rehabilitation University of Iowa
Alberta Health Care Insurance Plan. Schedule Of Anaesthetic Rates Applicable To Podiatry. Procedure List. As Of. 01 April Government of Alberta
 Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Alberta Health Care Insurance Plan Procedure List As Of 01 April 2017 Alberta Health Care Insurance Plan Page i Generated 2017/03/14 TABLE OF CONTENTS As of 2017/04/01 II. OPERATIONS ON THE NERVOUS SYSTEM.......................
Lesser MTP joints Arthroscopy: Anatomical Description and Comparative Dissection
 Lesser MTP joints Arthroscopy: Anatomical Description and Comparative Dissection Caio Nery, MD Michael Coughlin, MD Daniel Baumfeld, MD Fernando Raduan, MD Carla Chertman, MD Disclosure Caio Nery, M.D.
Lesser MTP joints Arthroscopy: Anatomical Description and Comparative Dissection Caio Nery, MD Michael Coughlin, MD Daniel Baumfeld, MD Fernando Raduan, MD Carla Chertman, MD Disclosure Caio Nery, M.D.
University of Groningen. Forefoot disorders Schrier, Joost
 University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
University of Groningen Forefoot disorders Schrier, Joost IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document version
A Patient s Guide to Bunions. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Bunions Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
Bunions. Compliments of: Institute of Sports Medicine & Orthopaedics
 A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
A Patient s Guide to Bunions 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet is compiled
Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve. Lumbar radiculopathy Instability MTPJ joint or inflammatory MPJ
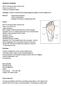 MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
MORTON S NEUROMA 80% III web space (next common is II). Never occurs in III or IV Common in females in fifties Aetiology: Pressure of Distal intermetatarsal ligament against common digital nerve Rule out
Foot and ankle update
 Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Foot and ankle update Mr Ian Garnham Consultant Foot and Ankle Surgeon Whipps Cross University Hospital Hallux Rigidus Symptoms first ray and 1st MTP pain and swelling worse with push off or forced dorsiflexion
Forefoot Procedures to Heal and Prevent Recurrence. Watermark. Diabetic Foot Update 2015 San Antonio, Texas
 Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Forefoot Procedures to Heal and Prevent Recurrence Diabetic Foot Update 2015 San Antonio, Texas J. Randolph Clements, DPM Assistant Professor of Orthopaedics Virginia Tech- Carilion School of Medicine
Arthrodesis of the first metatarsophalangeal joint using convex and concave drills A report on 50 cases
 Acta Orthop. Belg., 2005, 71, 76-82 ORIGINAL STUDY Arthrodesis of the first metatarsophalangeal joint using convex and concave drills A report on 50 cases Olivier JARDÉ, Zaccharie LAYA, Bruno OLORY, Gauthier
Acta Orthop. Belg., 2005, 71, 76-82 ORIGINAL STUDY Arthrodesis of the first metatarsophalangeal joint using convex and concave drills A report on 50 cases Olivier JARDÉ, Zaccharie LAYA, Bruno OLORY, Gauthier
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE. First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING.
 LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
LOWER EXTREMITIES SINGLE-USE INSTRUMENTATION SURGICAL IMPLANTATION TECHNIQUE First Metatarsal Phalangeal Joint FOOT THE DIFFERENCE IS MOVING. CARTIVA SYNTHETIC CARTILAGE IMPLANT SURGICAL IMPLANTATION TECHNIQUE
Fracture and Dislocation of the Carpus ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
3 section of the Foot
 TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
TERMINOLOGY 101 How many Bones 3 section of the Foot Bilateral Relating to both Plantar Relating to the bottom or sole Lateral Relating to the outside or farther from the median Medial Relating to the
AUTHOR(S): COUGHLIN, MICHAEL J., M.D., BOISE, IDAHO. An Instructional Course Lecture, The American Academy of Orthopaedic Surgeons
 JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
JBJA Journal of Bone and Joint Surgery - American 1996-1998 June 1996, Volume 78-A, Number 6 932 Instructional Course Lectures, The American Academy of Orthopaedic Surgeons - Hallux Valgus* Instructional
1. Orthoapedic Associates of Michigan, PC, Grand Rapids, MI 2. Michigan State University College of Human Medicine, Grand Rapids, MI
 Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Second Metatarsal Osteotomy Shortening with Tarsometatarsal Arthrodesis: Comparison of Outcomes Between MSP TM Metatarsal Shortening System and Plates and Screws Donald R. Bohay, MD, FACS 1 ; John G. Anderson,
Fracture and Dislocation of Metacarpal Bones, Metacarpophalangeal Joints, Phalanges, and Interphalangeal Joints ( 1-Jan-1985 )
 In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
In: Textbook of Small Animal Orthopaedics, C. D. Newton and D. M. Nunamaker (Eds.) Publisher: International Veterinary Information Service (www.ivis.org), Ithaca, New York, USA. Fracture and Dislocation
6/5/2018. Forefoot Disorders. Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) Hallux Rigidus
 Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Forefoot Disorders Mr Pinak Ray (MS, MCh(Orth), FRCS, FRCS(Tr&Orth)) Highgate Private Hospital (Royal Free London NHS Foundation Trust (Barnet & Chase Farm Hospitals) E: ray.secretary@uk-conslutants Our
Silicoplant. Well-being for your feet
 Silicoplant Well-being for your feet EMO designs, develops and manufactures using innovation as the way to offer advanced products and help the patients and users that need our products, solve their problems.
Silicoplant Well-being for your feet EMO designs, develops and manufactures using innovation as the way to offer advanced products and help the patients and users that need our products, solve their problems.
Osteotomy vs No Osteotomy Second Ray
 Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
Osteotomy vs No Osteotomy Second Ray Michael D. Dujela DPM, FACFAS Fellowship Trained Foot and Ankle Surgeon Washington Orthopaedic Center, Centralia, WA Chairman, Education and Scientific Affairs Committee
