AN ESTIMATED 500,000 to 1.5 million patients are admitted
|
|
|
- Annabella Adams
- 6 years ago
- Views:
Transcription
1 1441 The Relationship Between Therapy Intensity and Rehabilitative Outcomes After Traumatic Brain Injury: A Multicenter Analysis David X. Cifu, MD, Jeffrey S. Kreutzer, PhD, ABPP, Stephanie A. Kolakowsky-Hayner, MA, Jennifer H. Marwitz, MA, Jeffrey Englander, MD From the Department of Physical Medicine and Rehabilitation, Virginia Commonwealth University, Medical College of Virginia Campus, Richmond, VA (Cifu, Kreutzer, Kolakowsky-Hayner, Marwitz); and Rehabilitation Research Center for Traumatic Brain Injury and Spinal Cord Injury, Santa Clara Valley Medical Center, Santa Clara, CA (Englander). Supported in part by the National Institute on Disability and Rehabilitation Research, Office of Special Education and Rehabilitative Services, US Department of Education (grant nos. H133A980026, H133A70018). Data were contributed by the Santa Clara Valley Medical Center, TIRR, and Virginia Commonwealth University, Medical College of Virginia Campus. No commercial party having a direct financial interest in the results of the research supporting this article has or will confer a benefit upon the author(s) or upon any organization with which the author(s) is/are associated. Reprint requests to Jeffrey S. Kreutzer, PhD, ABPP, Dept of Physical Medicine and Rehabilitation, Virginia Commonwealth University, Medical College of Virginia Campus, 1200 E Broad St, Rm 3-102, Box , Richmond, VA , jskreutz@hsc.vcu.edu /03/ $30.00/0 doi: /s (03) ABSTRACT. Cifu DX, Kreutzer JS, Kolakowsky-Hayner SA, Marwitz JH, Englander J. The relationship between therapy intensity and rehabilitative outcomes after traumatic brain injury: a multicenter analysis. Arch Phys Med Rehabil 2003;84: Objectives: To identify factors relating to the intensity of rehabilitation services received and to ascertain the relation between injury outcomes, demographics, types of therapy, and the intensity of rehabilitation services provided. Design: A multicenter, prospective, nonrandomized study with inpatient rehabilitation data collected between 1989 and Setting: Three medical centers in the federally sponsored Traumatic Brain Injury Model Systems. In each setting, the continuum of care includes emergency medical services, intensive and acute medical care, and inpatient rehabilitation. Participants: A total of 491 consecutively enrolled patients with a mean age standard deviation of years recruited from 3 medical centers. To be included in the study, patients must have been at least 16 years of age, have presented to the emergency department within 24 hours of injury, and have received acute care and inpatient rehabilitation. Interventions: Patients received comprehensive medical care along with a combination of rehabilitative therapies, including physical, occupational, psychologic, and speech therapy. Main Outcome Measures: Therapy intensity; levels of functional independence, cognitive function, functional gain, and treatment efficiency, as indicated by the FIM instrument; rehabilitation length of stay (LOS); and charges. Results: Age predicted the intensity of both psychologic (P.001) and total therapy (P.01) services. Acute care LOS was also a significant predictor of psychologic services (P.01). Only admission motor FIM was relevant in predicting speech services intensity (P.01). Therapy intensity was predictive of motor functioning at discharge (P.001). However, therapy intensity did not predict cognitive gain (P.05). Conclusions: This study is among the first multicenter efforts to examine the potential benefits of individual therapy services. Findings support assertions that increased therapy intensity, particularly physical and psychologic therapies, enhances functional outcomes. Key Words: Brain injuries; Rehabilitation; Treatment outcome by the American Congress of Rehabilitation Medicine and the American Academy of Physical Medicine and Rehabilitation AN ESTIMATED 500,000 to 1.5 million patients are admitted to acute care hospitals with traumatic brain injury (TBI) annually. 1,2 A recent multicenter study 3 found that the average combined cost of acute care and inpatient rehabilitation was $154,152 per patient. The recent development of a continuum of care model of rehabilitation introduced the idea of cost shifting by varying the intensity and site of the rehabilitation services provided, depending on the stage of recovery after TBI and patient tolerance. Providing more intensive therapy on a daily basis has been suggested as a way to reduce costs by further shortening the rehabilitation length of stay (LOS) and improving short- and long-term outcomes. Unfortunately, there are limited data on the efficacy of varying therapy intensity within a continuum of rehabilitation services. Initial research into therapy intensity focused on patients with stroke; it yielded equivocal findings. More recent investigations 4-9 have found improved outcomes with increased therapy intensity and use of specialized therapy techniques. Other researchers have found no meaningful relation between therapy intensity and outcomes. A recent critical review 14 of the stroke literature attributed equivocal findings to differences in samples and variations in methodology. Few studies have investigated the relation between therapy intensity and outcomes in the TBI population. Several studies, however, have found a correlation between increased therapy and decreased LOS or improved functional outcomes. For example, Blackerby 15 studied the effect of increased therapy intensity on rehabilitation LOS in patients with TBI at 2 regional hospitals. At both hospitals, a new therapeutic model was introduced that increased the number of therapy hours. Patients admitted before and after the increase were similar in age, injury severity, and functional status. Analyses showed that patients in the greater therapy intensity group had stays that were significantly shorter than those of patients in the lesser therapy intensity group. Similarly, Aronow 16 found that patients who received more rehabilitation therapy overall had better outcomes as measured by self-care skills, mobility, and symptoms at 2 or more years after injury. More recently, investigators have focused on the type of therapy delivered, as well as its intensity. Spivack et al 17 were among the first to investigate the relation between therapy and
2 1442 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu specific outcomes. Their study included 95 patients with mild to severe injuries who were admitted to a comprehensive rehabilitation program. Measures of therapy intensity, including totals from various types of therapy (eg, physical, speech) and LOS, with division of participants into short-stay and long-stay groups, were designated as the independent variables. Retrospectively, participants were divided into high- and lowintensity groups, based on therapy totals for the entire LOS. The dependent measures consisted of measurement in 3 main areas: physical performance (eg, motor strength, bladder control); cognitively mediated physical skills (eg, visuoperceptual skills, swallowing ability); and higher-level cognitive skills (eg, memory, problem-solving). Analyses showed no effect of therapy intensity on outcomes in any of the 3 domains. However, although the high-intensity group had lower functional scores at the time of admission, their scores were at the same levels as those of the low-intensity group at discharge. The researchers concluded, therefore, that the higher intensity had beneficial effects. Heinemann et al 18 expanded on previous studies by investigating the effect of specific therapy intensities, including physical, occupational, speech, and psychology. Participants were 140 patients with TBI. The cognitive and motor scales of the FIM instrument were used as outcome measures. Achievement of potential was defined as the gain between admission and discharge divided by the potential gain (maximum possible score minus admission score). Efficiency scores were calculated by dividing the difference between admission and discharge scores by the LOS. After controlling for age, functional status at admission, and interruption of stay, greater intensity of psychology services was associated with better cognitive scores at discharge. Intensity of psychologic services was not related to motor outcome. The intensity of physical, occupational, or speech therapy was unrelated to motor or cognitive outcome. The intensity of all therapy types was positively correlated. Of note, physical and occupational therapy intensities were most closely related. Heinemann 18 recommended cross-validation of the findings with another sample. Our purpose in this study was to replicate and expand on Heinemann s therapy intensity study by using data from hospitals that participate in the Traumatic Brain Injury Model Systems (TBIMS). The primary goals were to determine the relation between intensity of therapy services and functional outcome, LOS, and hospital charges. The relative intensities of each therapy type were calculated, compared, and correlated. Statistical procedures were used to control for the effects of age, injury severity, and functional status at admission. A large, multicenter sample was studied to enhance generalization. The intensities of different therapy types were hypothesized to directly affect certain functional areas. Specifically, the intensity of physical and occupational therapy was expected to be most related to motor tasks, whereas speech and psychology services were expected to correlate with cognitive skills. Consistent with other research results, a relation between global outcome measures and therapy intensity was not anticipated. 18 METHODS Participants Participants were 491 patients who were enrolled in the TBIMS program, which is funded by the National Institute on Disability and Rehabilitation Research (NIDRR). 3,19 They were recruited from 3 participating medical centers, representing geographically diverse regions of the United States. To be included in the study, patients had to be at least 16 years old, had to have presented to the emergency department of a TBIMS trauma center within 24 hours of injury, and had to have received acute care and inpatient rehabilitation at a TBIMS center. The mean age standard deviation (SD) of patients was years. Most patients were male (72%) and white (63%). The sample also included African Americans (18%), Asian Americans (3%), Hispanics (11%), and other (5%). Regarding education, 41% of the sample had less than a high school education, 27% reported having completed high school, 20% had attended trade school or had some college background, and 12% had earned a higher education degree (eg, associate s, bachelor s). Glasgow Coma Scale scores at hospital admission showed a full range of injury severity, with most patients having severe or moderate injuries (mean, ). Patients mean interval between injury and admission to rehabilitation was days. Mean LOS in inpatient rehabilitation was days. Measures Therapy hours. As part of the TBIMS data collection protocol, information is collected on the total number of minutes spent in inpatient rehabilitation therapy. 3 Values reflect actual time in therapy and the time required for chart documentation. Typically, more than 90% of therapy hours is composed of hands-on intervention. Separate totals are also recorded for 4 therapy types: speech, occupational, physical, and psychologic. For each therapy type, the total number of minutes was divided by 60 to yield the number of therapy hours. Therapy intensity. To control for variations in LOS, an intensity score depicting daily therapy hours was computed for each of the 4 therapy types. For each patient, the total number of therapy hours was divided by LOS (days). No distinction was made between services provided on weekends and weekdays. Total therapy hours per day. For each patient, the sum of speech, occupational, psychologic, and physical therapy hours was calculated and divided by the LOS. Rehabilitation charges. Total rehabilitation charges for each patient were obtained from billing records. FIM instrument. The FIM was completed at both admission and discharge from the rehabilitation hospital. This instrument is an 18-item rating scale that assesses patients levels of independence. Each item is rated on a scale of 1 (total assistance) to 7 (complete independence). Scores range from a minimum of 18 to a maximum of 126. The FIM identifies levels of independence in self-care, mobility, bowel and bladder management, communication, cognition, and psychosocial adjustment The following scores were calculated from the FIM: (1) FIM motor score, derived from the subscale containing the 13 items relevant to mobility, daily living skills, and continence; (2) FIM cognitive score, derived from the subscale containing the 5 items relating to cognition, communication, and psychosocial functioning; (3) FIM change score, determined by subtracting admission scores from discharge scores; (4) cognitive and motor efficiency, determined by dividing FIM motor and cognitive subscale change scores by LOS; (5) functional potential gained, calculated by subtracting each patient s admission score from the maximum subscale score (motor 91; cognitive 35); and (6) functional potential achieved, calculated as the difference between admission and discharge scores, divided by the functional potential gained. As noted by Heinemann, 18 the score reflects the mathematical rather than the biologic potential of each patient.
3 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu 1443 Settings and Procedures Each of the 3 TBIMS centers provides a comprehensive array of services, including physiatry; nursing; physical, occupational, and speech therapy; social work; psychology; and therapeutic recreation. Treatment protocols are individualized to meet patients unique needs and levels of functioning. All centers have been accredited by the Commission on Accreditation of Rehabilitation Facilities (CARF). Admission and discharge decisions are based on CARF guidelines, patients capabilities to participate in acute rehabilitation programs, a viable discharge plan, patients needs, and funding availability. As part of the TBIMS protocol, comprehensive data are collected for each patient, including demographics, injury severity, medical treatment and complications, types of therapy received, LOS, and rehabilitation costs. Data are gathered and coded by experienced staff members through record reviews, patient and family interviews, and consultation with treatment professionals. The FIM is completed by 1 or more members of the rehabilitation team within 72 hours after rehabilitation admission and 72 hours before discharge. Statistical Analyses Means, SDs, and ranges were calculated for all variables. Linear multiple regression was used to determine whether therapy intensity was predicted by age and admission variables, including (1) FIM cognitive and motor subscale scores at admission; (2) the interval between injury and admission to rehabilitation; and (3) whether rehabilitation was continuous or interrupted. Histograms and skewness statistics showed that the distributions for onset-admission interval, LOS, and hospital charges were skewed. Logarithms for onset-admission interval, LOS, and hospital charges were used to correct for skewness. We did a 2-step multiple regression analysis to determine the relation between therapy intensity and functional outcomes. Step 1 contained nontherapy variables such as age, logarithm of onset-admission interval, logarithm of LOS, interruption in rehabilitation (dummy coded as 0 no, 1 yes), and FIM cognitive and motor subscale scores at discharge. Step 2 contained therapy intensity variables for physical, psychologic, occupational, and speech therapies. To distinguish the contribution of each variable set, the R 2 values were examined incrementally after each step. RESULTS Variance of Therapy Intensities Descriptive statistics for therapy intensities and total therapy hours were examined because of concerns about limited variance in intensities among patients (table 1). Evaluation of scatterplots and histograms shows relatively normal distributions for intensities of all 4 therapy types but suggests a restricted range of intensities. Most patients received occupational (95.5%), physical (95.9%), speech (94.7%), and psychologic (86.4%) therapies. On average, patients received the most occupational therapy per day, with a mean of 1.09 hours, or approximately 65 minutes, followed by physical therapy (mean,.90h, or 54min), speech therapy (mean,.58h, or 35min), and psychologic services (mean,.32h, or 19min). SDs ranged from.55 hours (33min) for occupational therapy to.27 hours (16min) for psychologic services. The mean number of total therapy hours per day was 2.91 (2h, 55min), with an SD of 1.09 hours (1h, 5min). The 95th percentile was 4.36 hours. Examination of the percentiles shows that few people received more than 2 hours a day of 1 type of therapy. The 95th percentile cutoff was 1.02 hours a day for speech therapy, 1.53 Table 1: Therapy Hours and Intensities Mean SD Minimum Maximum Total therapy hours PT OT Psychologic therapy Speech therapy Therapy intensity (h/d) PT OT Psychologic therapy Speech therapy Abbreviations: PT, physical therapy; OT, occupational therapy. hours a day for physical therapy, 1.78 hours a day for occupational therapy, and.86 hours a day of psychologic services. In our analysis, we did not examine differences between services provided on weekends and weekdays. Table 2 presents the amount of each type of therapy and total therapy hours received in the course of a day. These results indicate that variance is small for each type of therapy and for total therapy hours. Interpretation of regression analyses should consider the relatively small amount of variance for patients receiving each type of therapy. Cognitive and Motor Scores Patients mean FIM cognitive admission score was , and their mean FIM motor admission score was The mean cognitive discharge score was , and the mean motor discharge score was , yielding mean change scores of and , respectively. Predictions of Therapeutic Intensity Multiple regression analyses were used to determine whether age, functional status at admission, interruption in rehabilitation, LOS, or onset-admission interval predicted therapy intensity. Table 3 shows the results of regression analyses for each of the 4 therapeutic intensities and total number of therapy hours per day. R 2 values did not differ significantly from 0 for occupational or physical therapy intensities. Models for psychologic (R 2.130, F 5, , P.001), speech (R 2.063, F 5, , P.001), and total therapy hours per day (R 2.045, F 5, , P.01) differed significantly from 0. Lower age and shorter onset-admission interval were significant predictors of increased psychologic therapy intensity. FIM motor score at admission was a significant predictor of speech therapy. The higher the motor score, the more that speech therapy was provided. The number of total therapy hours per day was significantly predicted by age, with older patients receiving less therapy per day. Therapy Intensity and Cognitive Outcome Examination of cognitive outcomes indicates that therapeutic intensity did not contribute to gains in cognitive ability. Age and admission variables entered as set 1 predicted a significant amount of the variance for cognitive discharge scores (R 2.476, F 6,403 change , P.001), cognitive potential achieved (R 2.100, F 6,403 change 7.478, P.001), and cognitive efficiency (R 2.312, F 6,403 change , P.001). Beta weight and squared semipartial correlations for each cognitive outcome are provided in tables 4 through 6. In each case,
4 1444 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu Table 2: Hours of Therapy Per Day Occupational Psychologic Physical Speech n % Cum% n % Cum% n % Cum% n % Cum% 0h/d h/d h/d h/d h/d h/d Total N NOTE. Values may not equal 100% due to rounding. Abbreviation: Cum%, cumulative percentage. Total Hours Per Day n % Cum % 0h/d h/d h/d h/d h/d h/d h/d Total when therapeutic intensities were entered in set 2, they did not significantly add to the predictive model. Therapy Intensity and Motor Outcome Motor outcomes were also significantly predicted by set 1 age and admission variables. Beta weight and squared semipartial correlations for each motor outcome are provided in tables 4 through 6. After step 1, FIM motor discharge (R 2.405, F 6,402 change , P.001), motor potential achieved (R F 6,400 change , P.001), and motor efficiency (R 2.394, F 6,402 change , P.001) were significant. Onset-admission interval and FIM motor admission score were significant predictors in all models. FIM cognitive admission score was a significant predictor of motor potential achieved, but not of motor efficiency or FIM motor discharge score. Longer LOS in rehabilitation significantly predicted greater motor potential achieved and lower motor efficiency. Therapy intensity yielded a significant addition to the predicted variance for FIM motor discharge score (R 2 change.064, F 4,398 change , P.001), FIM motor potential achieved (R 2 change.099, F 4,396 change , P.001), and FIM motor efficiency (R 2 change.074, F 4,398 change , P.001). For all 3 models, speech and physical therapy were significant predictors, whereas psychologic and occupational therapies did not contribute significantly to motor outcome at discharge. Therapy Intensity and Rehabilitation LOS Age and admission status significantly predicted rehabilitation LOS (R 2.576, F 4,411 change , P.001). FIM motor admission score, FIM cognitive admission score, and onset-admission interval were significant predictors of rehabilitation LOS. Results of this analysis are presented in table 7. The addition of the therapy intensity variables to the model did not significantly increase prediction. Therapy Intensity and Rehabilitation Charges Sets that included the same variables used for models of functional status were also used in hierarchical regression to Table 3: Regression Analyses for 4 Therapeutic Intensities OT OT r 2 PT PT r 2 Psych Psych r 2 Speech Speech r 2 Total h/d Total r 2 Age Admission cognition Admission motor Interrupted rehab Onset-admission interval R F df P Abbreviations: Psych, psychologic; rehab, rehabilitation.
5 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu 1445 Table 4: FIM Outcome Scores Discharge Motor Discharge Cognitive Step 1 Step 2 Step 1 Step 2 r 2 r 2 r 2 r 2 Age and admission variables (step 1) Age Admission cognition Admission motor Onset-admission interval LOS Interrupted stay R 2 change (step 1) F change df 6,402 6,403 Therapy intensities (step 2) PT (h/d) OT (h/d) Speech therapy (h/d) Psychologic therapy (h/d) R 2 change F change df 4,398 4,399 R 2 total F df 10,309 10,399 evaluate the effect of therapeutic intensities on hospital charges (table 7). After age and admission variables were entered at step 1 (R 2.628, F 6,399 change , P.001), rehabilitation LOS was the primary significant predictor of rehabilitation charges (P.001). Rehabilitation LOS uniquely accounted for approximately 24% of the variance. The addition of therapy intensities significantly increased prediction, with an additional 1.3% of the variance accounted for (R 2.013, F 4,572 change 3.572, P.01). Physical therapy intensity was a significant predictor of increased rehabilitation charges. Table 5: FIM Potential Achieved Discharge Motor Potential Achieved Discharge Cognitive Potential Achieved Step 1 Step 2 Step 1 Step 2 r 2 r 2 r 2 r 2 Age and admission variables (step 1) Age Admission cognition Admission motor Onset-admission interval LOS Interrupted stay R 2 change (step 1) F change df 6,400 6,403 Therapy intensities (step 2) PT (h/d) OT (h/d) Speech therapy (h/d) Psych therapy (h/d) R 2 change F change df 4,396 4,399 R 2 total F df 10,396 10,399
6 1446 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu Table 6: FIM Efficiency Motor Efficiency Cognitive Efficiency Step 1 Step 2 Step 1 Step 2 r 2 r 2 r 2 r 2 Age and admission variables (step 1) Age Admission cognition Admission motor Onset-admission interval LOS Interrupted stay R 2 change (step 1) F change df 6,402 6,403 Therapy intensities (step 2) PT (h/d) OT (h/d) Speech therapy (h/d) Psych therapy (h/d) R 2 change F change df 4,398 4,399 R 2 Total F df 10,398 10,399 DISCUSSION For many years, rehabilitation clinicians have advocated for patients access to rehabilitation services. Their advocacy stems from a belief that higher intensities of medical, therapy, social work, psychologic, nursing, and other rehabilitative services yield improved outcomes. Unfortunately, research into the benefits of more intensive services has been limited. The overwhelming majority of studies have focused on speech, occupational, and physical therapies. Research findings suggest that there is a tenuous relation between the intensity of therapy services provided after TBI and the functional outcome. For example, early researchers 15,16 Table 7: LOS and Charges Rehabilitation LOS Rehabilitation Charges Step 1 Step 2 Step 1 Step 2 r 2 r 2 r 2 r 2 Age and admission variables (step 1) Age Admission cognition Admission motor Onset-admission interval Interrupted stay LOS R 2 change (step 1) F change df 5,411 6,399 Therapy intensities (step 2) PT (h/d) OT (h/d) Speech therapy (h/d) Psych therapy (h/d) R 2 change F change df 4,407 4,395 R 2 total F
7 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu 1447 found that patients who received more overall hours of therapy were more likely to have shorter LOSs, greater levels of independence in self-care, and improved mobility. Later researchers 17,18 reported equivocal findings. Many insurers dictate minimum amounts of therapy. Patient endurance, personnel, and financial allocation constraints control the upper limits of service delivery. Such boundaries have led to assertions that equivocal findings are attributable to limited variance in therapy services between patients. Our study provides information about variability in service delivery patterns for specific types of therapies. Substantial variation was noted. For example, occupational therapy was the most intensively provided service. Approximately 15% of the patients received 30 minutes or less a day, whereas 18% received more than 90 minutes. Similar patterns of variation were found for physical, psychologic, and speech therapy. As one might expect, more substantial variation was found in the total number of daily therapy hours. Approximately 17% of patients received 2 hours or less of daily therapy services, whereas another 8% received more than 4 hours. Weekend and weekday service delivery patterns were not examined, and future research separating the 2 may prove helpful. Heinemann et al 18 attributed variations in therapy intensity to differences in age, admission functional status, interruption in care, and acute care LOS. We used regression analysis to examine their assertion. Analyses indicated that age predicted the intensity of both psychologic and total therapy services. Perhaps because of ageism bias, greater functional reserve, and higher endurance, younger persons received a greater intensity of services. Acute care LOS was also a significant predictor of psychologic services. Shorter LOSs were associated with higher intensities of psychologic services. Only the admission motor FIM score was relevant in predicting speech services intensity, with higher motor scores being associated with higher intensity speech services. None of the variables was useful in predicting the intensity of occupational or physical therapy services. In summary, age, acute LOS, and admission motor FIM scores were the most useful predictor variables, and the intensity of cognitively based therapies was most predictable. Our results support Heinemann s assertions about salient predictors of therapy intensity. Research has provided little evidence of a relation between the intensity of therapy services and cognitive outcome at rehabilitation discharge. Spivack et al 17 reported that therapy intensity was not related to cognitively mediated physical skills. Similarly, Heinemann 18 found that the intensity of physical, occupational, and speech therapy services was unrelated to cognitive outcome. However, Heinemann also noted that the intensity of psychologic services was associated with improved cognitively based outcome at rehabilitation discharge. We found no relation between therapy intensity and cognitive functioning at rehabilitation discharge. Aronow 16 provided evidence that rehabilitation therapy services are effective. Our study has provided data that help to substantiate the efficacy of speech and physical therapy services. The intensity of these services predicted FIM motor discharge score, FIM motor potential achieved, and FIM motor efficiency. Similar to the findings reported by Spivack 17 and Heinemann, 18 psychologic and occupational therapy intensity did not predict functional motor outcomes. Some clinicians have asserted that increased therapy intensity is costly because of the additional personnel needed. Yet others have argued that added therapy costs are justified because increased service intensity improves efficiency by reducing LOS. For example, in 1990, Blackerby 15 indicated that increased overall therapy intensity was associated with decreased LOS. However, arguments have continued, because few investigators have examined the relation among intensity of services, LOS, and charges. Our study provides little evidence that LOS or charges are related to therapy intensity. The primary limitations of our study should be acknowledged. First, because of ethical considerations, the investigators did not randomly assign patients to treatment groups with varying treatment intensities. Second, we used ordinal-level data that were subjected to parametric analysis. Third, the use of multiple regression, a form of correlational analysis, raises questions about causation. Fourth, data were collected on a limited number of clinical services. For example, data regarding the intensity of nursing or therapeutic recreation services were not collected. Finally, data were collected solely at TBIMS rehabilitation centers, which can raise questions about generalization. Keith 23 described the challenges of evaluating therapy efficacy in a research context, arguing that equivocal findings may be attributable to variations in treatment and provider characteristics. We did not collect data about service types (eg, assessment vs treatment), provider credentials and experience, or the nature of treatment goals (eg, skill improvement vs education). Collecting more specific information in future studies will permit more careful analysis of therapy benefits and make possible more rigorous comparisons between studies. CONCLUSIONS Practitioners who manage patients with acute infectious processes have established evidence-based guidelines to help them in prescribing the specific type and intensity of services (ie, varying dosing of differing antibiotics). In contrast, physicians who prescribe inpatient rehabilitation for patients with acute disabilities after TBI have few empirically based guidelines. In most cases, these patients are offered a generic package of services that includes nursing care, physician monitoring, psychologic and social work intervention, speech therapy, and physical and occupational therapy services. In a few cases, patients with special needs (eg, non weight bearing, contact precautions) may receive more specialized and intensive services. However, the type and intensity of the services provided are invariably determined by minimal standards that have been established by insurers, and by the availability of staffing. Several single-center investigations have delineated the benefits of interdisciplinary inpatient TBI rehabilitation. 18,24 Our study is among the first multicenter efforts to examine the potential benefits of individual therapy services. Its results support assertions that increased therapy intensity potentially enhances outcomes. For example, increased physical and psychologic therapies appear to ameliorate FIM motor deficits. A multitude of additional treatment factors may be of benefit to outcomes, and additional research is needed to identify those factors. 25 Rehabilitation outcomes research should help guide the development of evidence-based guidelines for rehabilitation. Until then, clinical practice will be guided by experience, common sense, and professional standards of care. Acknowledgments: The contributions of the NIDRR-funded TBIMS centers are gratefully acknowledged. References 1. Kalsbeek WD, McLaurin RL, Harris BS, Miller JD. The national head injury and spinal cord injury survey: major findings. J Neurosurg 1980;53:
8 1448 THERAPY INTENSITY AFTER BRAIN INJURY, Cifu 2. Kraus JF, Black MA, Hessol N, et al. The incidence of acute brain injury and serious impairment in a defined population. Am J Epidemiol 1984;119: Harrison-Felix C, Newton CN, Hall KM, Kreutzer JS. Descriptive findings from the traumatic brain injury model systems national data base. J Head Trauma Rehabil 1996;11(5): Kramer AM, Steiner JF, Schlenker RE, et al. Outcomes and costs after hip fracture and stroke. A comparison of rehabilitation settings. JAMA 1997;277: Basmajian JV, Gowland CA, Finlayson MA, et al. Stroke treatment: comparison of integrated behavioral-physical therapy vs traditional physical therapy programs. Arch Phys Med Rehabil 1987;67(5 Pt 1): Carey L, Matyas T, Oke L. Sensory loss in stroke patients: effective training of tactile and proprioceptive discrimination. Arch Phys Med Rehabil 1993;74: Hesse SA, Jahnke MT, Bertelt CM, Schreiner C, Lucke D, Mauritz KH. Gait outcome in ambulatory hemiparetic patients after a 4-week comprehensive rehabilitation program and prognostic factors. Stroke 1994;25: Macdonell R. Functional electrical stimulation to the affected lower limb and recovery after cerebral infarction. J Stroke Cerebrovasc Dis 1994;4: Richards C, Malouin F, Wood-Dauphinee S, Williams JI, Bouchard JP, Brunet D. Task-specific physical therapy for optimization of gait recovery in acute stroke patients. Arch Phys Med Rehabil 1993;74: Lorenze EG, Cancro R. Dysfunction in visual perception with hemiplegia: its relation to activities of daily living. Arch Phys Med Rehabil 1962;43: Stern PH, McDowell F, Miller JM, Robinson M. Factors influencing stroke rehabilitation. Stroke 1971;2: Jongbloed L. Prediction of function after stroke: a critical review. Stroke 1986;17: Ottenbacher KJ, Jannell S. The results of clinical trials in stroke rehabilitation research. Arch Neurol 1993;50: Cifu DX, Stewart DG. Factors affecting functional outcome after stroke: a critical review of rehabilitation interventions. Arch Phys Med Rehabil 1999;80(5 Suppl 1):S Blackerby WF. Intensity of rehabilitation and length of stay. Brain Inj 1990;4: Aronow HU. Rehabilitation effectiveness with severe brain injury: translating research into policy. J Head Trauma Rehabil 1987; 2(3): Spivack G, Spettell CM, Ellis DW, Ross SE. Effect of intensity of treatment and length of stay on rehabilitation outcomes. Brain Inj 1992;6: Heinemann AW, Hamilton B, Linacre JM, Wright BD, Granger C. Functional status and therapeutic intensity during inpatient rehabilitation. Am J Phys Med Rehabil 1995;74: Dahmer ER, Schilling MA, Hamilton BB, et al. A model systems data base for traumatic brain injury. J Head Trauma Rehabil 1993;8(2): Hall KM, Johnston MV. Outcomes evaluation in TBI rehabilitation. Part II: measurement tools for a nationwide data system. Arch Phys Med Rehabil 1994;75(12 Spec. No):SC10-8; discussion SC Keith RA, Granger CV, Hamilton BB, Sherman FS. The functional independence measure: a new tool for rehabilitation, In: Eisenberg MG, Grzesiak RC, editors. Advances in clinical rehabilitation. Vol 2. New York: Springer; p Guide for Uniform Data System for Medical Rehabilitation (Adult FIM), version 4.0. Buffalo: State Univ New York; Keith RA. Treatment strength in rehabilitation. Arch Phys Med Rehabil 1997;78: Semlyen JK, Summers SJ, Barnes MP. Traumatic brain injury: efficacy of multidisciplinary rehabilitation. Arch Phys Med Rehabil 1998;79: NIH Consensus Development Panel on Rehabilitation of Persons with Traumatic Brain Injury. Rehabilitation of persons with traumatic brain injury. JAMA 1999;282:
Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1, Raisa Deber, PhD 3, Junlang Yin, MSc 1 and Hwan Kim, PhD candidate 1
 J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
Age as a Predictor of Functional Outcome in Anoxic Brain Injury
 Age as a Predictor of Functional Outcome in Anoxic Brain Injury Mrugeshkumar K. Shah, MD, MPH, MS Samir Al-Adawi, PhD David T. Burke, MD, MA Department of Physical Medicine and Rehabilitation, Spaulding
Age as a Predictor of Functional Outcome in Anoxic Brain Injury Mrugeshkumar K. Shah, MD, MPH, MS Samir Al-Adawi, PhD David T. Burke, MD, MA Department of Physical Medicine and Rehabilitation, Spaulding
Research Report. Key Words: Functional status; Orthopedics, general; Treatment outcomes. Neva J Kirk-Sanchez. Kathryn E Roach
 Research Report Relationship Between Duration of Therapy Services in a Comprehensive Rehabilitation Program and Mobility at Discharge in Patients With Orthopedic Problems Background and Purpose. The purpose
Research Report Relationship Between Duration of Therapy Services in a Comprehensive Rehabilitation Program and Mobility at Discharge in Patients With Orthopedic Problems Background and Purpose. The purpose
The need to understand what types and intensities of
 Original Contributions Relative Importance of Rehabilitation Therapy Characteristics on Functional Outcomes for Persons With Stroke Rita K. Bode, PhD; Allen W. Heinemann, PhD; Patrick Semik, BS; Trudy
Original Contributions Relative Importance of Rehabilitation Therapy Characteristics on Functional Outcomes for Persons With Stroke Rita K. Bode, PhD; Allen W. Heinemann, PhD; Patrick Semik, BS; Trudy
Pattern of Functional Change During Rehabilitation of Patients With Hip Fracture
 111 ORIGINAL ARTICLE Pattern of Functional Change During Rehabilitation of Patients With Hip Fracture Nancy K. Latham, PhD, PT, Diane U. Jette, DSc, PT, Reg L. Warren, PhD, Christopher Wirtalla, BA ABSTRACT.
111 ORIGINAL ARTICLE Pattern of Functional Change During Rehabilitation of Patients With Hip Fracture Nancy K. Latham, PhD, PT, Diane U. Jette, DSc, PT, Reg L. Warren, PhD, Christopher Wirtalla, BA ABSTRACT.
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center
 Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
Functional Independent Recovery among Stroke Patients at King Hussein Medical Center Ali Al-Hadeed MD*, Amjad Banihani MD**, Tareq Al-Marabha MD* ABSTRACT Objective: To describe the functional independent
COMMON GOALS OF REHABILITATION are to decrease
 373 The Relation Between Therapy Intensity and Outcomes of Rehabilitation in Skilled Nursing Facilities Diane U. Jette, PT, DSc, Reg L. Warren, PhD, Christopher Wirtalla, BA ABSTRACT. Jette DU, Warren
373 The Relation Between Therapy Intensity and Outcomes of Rehabilitation in Skilled Nursing Facilities Diane U. Jette, PT, DSc, Reg L. Warren, PhD, Christopher Wirtalla, BA ABSTRACT. Jette DU, Warren
Efficiency, Effectiveness, and Duration of Stroke Rehabilitation
 241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
241 Efficiency, Effectiveness, and Duration of Stroke Rehabilitation Surya Shah, MEd OTR/L, Frank Vanclay, MSocSci, and Betty Cooper, BAppSc This prospective multicenter study identifies the variables
The Uniform Data System for Medical Rehabilitation Report of Patients with Debility Discharged from Inpatient Rehabilitation Programs in 2000Y2010
 Authors: Rebecca V. Galloway, PT, MPT Carl V. Granger, MD Amol M. Karmarkar, PhD, OTR James E. Graham, PhD, DC Anne Deutsch, RN, PhD, CRRN Paulette Niewczyk, PhD, MPH Margaret A. DiVita, MS Kenneth J.
Authors: Rebecca V. Galloway, PT, MPT Carl V. Granger, MD Amol M. Karmarkar, PhD, OTR James E. Graham, PhD, DC Anne Deutsch, RN, PhD, CRRN Paulette Niewczyk, PhD, MPH Margaret A. DiVita, MS Kenneth J.
Canadian Stroke Best Practices Table 3.3A Screening and Assessment Tools for Acute Stroke
 Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Canadian Stroke Best Practices Table 3.3A Screening and s for Acute Stroke Neurological Status/Stroke Severity assess mentation (level of consciousness, orientation and speech) and motor function (face,
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project
 Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Low Tolerance Long Duration (LTLD) Stroke Demonstration Project Interim Summary Report October 25 Table of Contents 1. INTRODUCTION 3 1.1 Background.. 3 2. APPROACH 4 2.1 LTLD Stroke Demonstration Project
Table 3.1: Canadian Stroke Best Practice Recommendations Screening and Assessment Tools for Acute Stroke Severity
 Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Table 3.1: Assessment Tool Number and description of Items Neurological Status/Stroke Severity Canadian Neurological Scale (CNS)(1) Items assess mentation (level of consciousness, orientation and speech)
Spinal Cord Injury Fact Sheet
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Comprehensive Acute. Rehabilitation Unit
 Comprehensive Acute Rehabilitation Unit The Comprehensive Acute Rehabilitation Unit at Thomas Jefferson University Hospital has provided excellence in patient-focused acute rehabilitative care since 1963.
Comprehensive Acute Rehabilitation Unit The Comprehensive Acute Rehabilitation Unit at Thomas Jefferson University Hospital has provided excellence in patient-focused acute rehabilitative care since 1963.
MEASUREMENT OF FUNCTIONAL ABILITIES is an. Recovery of Functional Status After Right Hemisphere Stroke: Relationship With Unilateral Neglect
 322 Recovery of Functional Status After Right Hemisphere Stroke: Relationship With Unilateral Neglect Leora R. Cherney, PhD, BC-NCD, Anita S. Halper, MA, BC-NCD, Christina M. Kwasnica, MD, Richard L. Harvey,
322 Recovery of Functional Status After Right Hemisphere Stroke: Relationship With Unilateral Neglect Leora R. Cherney, PhD, BC-NCD, Anita S. Halper, MA, BC-NCD, Christina M. Kwasnica, MD, Richard L. Harvey,
The Veterans Health Administration TBI/Polytrauma Program
 The Veterans Health Administration TBI/Polytrauma Program Joel Scholten, MD Special Projects Director, Physical Medicine and Rehab Program Office September 10, 2012 Physical Medicine & Rehabilitation National
The Veterans Health Administration TBI/Polytrauma Program Joel Scholten, MD Special Projects Director, Physical Medicine and Rehab Program Office September 10, 2012 Physical Medicine & Rehabilitation National
BACKGROUND ON INPATIENT REHAB FACILITIES (IRF)
 BACKGROUND ON INPATIENT REHAB FACILITIES (IRF) There are 1,140 IRFs in the US 1,000 rehab units within hospitals 217 freestanding rehabilitation hospitals 68% for-profit; 30% nonprofit. Most with designated
BACKGROUND ON INPATIENT REHAB FACILITIES (IRF) There are 1,140 IRFs in the US 1,000 rehab units within hospitals 217 freestanding rehabilitation hospitals 68% for-profit; 30% nonprofit. Most with designated
Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works
 Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works Emily R. Rosario, PhD Why is Casa Colina unique? Continuum of care offering medical and rehabilitation services
Casa Colina Centers for Rehabilitation: A unique physician-directed model of care that works Emily R. Rosario, PhD Why is Casa Colina unique? Continuum of care offering medical and rehabilitation services
Using Individual Growth Curve Models to Predict Recovery and Activities of Daily Living After Spinal Cord Injury: An SCIRehab Project Study
 Archives of Physical Medicine and Rehabilitation journal homepage: Archives of Physical Medicine and Rehabilitation 2013;94(4 Suppl 2):S154-64 ORIGINAL ARTICLE Using Individual Growth Curve Models to Predict
Archives of Physical Medicine and Rehabilitation journal homepage: Archives of Physical Medicine and Rehabilitation 2013;94(4 Suppl 2):S154-64 ORIGINAL ARTICLE Using Individual Growth Curve Models to Predict
LIFE-CHANGING CARE INPATIENT CARE
 LIFE-CHANGING CARE INPATIENT CARE Helping Patients Get the Most out of Rehab When a stroke, accident or other traumatic incident turns a person s world upside down, there s a place in Indiana where he
LIFE-CHANGING CARE INPATIENT CARE Helping Patients Get the Most out of Rehab When a stroke, accident or other traumatic incident turns a person s world upside down, there s a place in Indiana where he
Functional Level During the First Year After Moderate and Severe Traumatic Brain Injury: Course and Predictors of Outcome
 Original Article Elmer ress Functional Level During the First Year After Moderate and Severe Traumatic Brain Injury: Course and Predictors of Outcome Maria Sandhaug a, b, e, Nada Andelic c, Svein A Berntsen
Original Article Elmer ress Functional Level During the First Year After Moderate and Severe Traumatic Brain Injury: Course and Predictors of Outcome Maria Sandhaug a, b, e, Nada Andelic c, Svein A Berntsen
Influence of Early Variables in Traumatic Brain Injury on Functional Independence Measure Scores and Rehabilitation Length of Stay and Charges
 797 Influence of Early Variables in Traumatic Brain Injury on Functional Independence Measure Scores and Rehabilitation Length of Stay and Charges Todd D. Cowen, MD, Jay M. Meythaler, MD, Michael J. DeVivo,
797 Influence of Early Variables in Traumatic Brain Injury on Functional Independence Measure Scores and Rehabilitation Length of Stay and Charges Todd D. Cowen, MD, Jay M. Meythaler, MD, Michael J. DeVivo,
National Stroke Association s Guide to Choosing Stroke. Rehabilitation Services
 National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
Evaluation of the functional independence for stroke survivors in the community
 Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Asian J Gerontol Geriatr 2009; 4: 24 9 Evaluation of the functional independence for stroke survivors in the community ORIGINAL ARTICLE CKC Chan Bsc, DWC Chan Msc, SKM Wong MBA, MAIS, BA, PDOT ABSTRACT
Original Article. Japanese Journal of Comprehensive Rehabilitation Science (2011)
 77 Japanese Journal of Comprehensive Rehabilitation Science (2011) Original Article Relationship between the intensity of stroke rehabilitation and outcome: A survey conducted by the Kaifukuki Rehabilitation
77 Japanese Journal of Comprehensive Rehabilitation Science (2011) Original Article Relationship between the intensity of stroke rehabilitation and outcome: A survey conducted by the Kaifukuki Rehabilitation
OUR BRAINS!!!!! Stroke Facts READY SET.
 HealthSouth Rehabilitation Hospital Huntington Dr. Timothy Saxe, Medical Director READY SET. OUR BRAINS!!!!! Stroke Facts 795,000 strokes each year- 600,000 new strokes 5.5 million stroke survivors Leading
HealthSouth Rehabilitation Hospital Huntington Dr. Timothy Saxe, Medical Director READY SET. OUR BRAINS!!!!! Stroke Facts 795,000 strokes each year- 600,000 new strokes 5.5 million stroke survivors Leading
DO STROKE REHABILITATION inpatients whose urinary. Urinary Incontinence and Stroke Outcomes. Jan C. Gross, PhD, RN, CS
 22 Urinary Incontinence and Stroke Outcomes Jan C. Gross, PhD, RN, CS ABSTRACT. Gross JC. Urinary incontinence and stroke outcomes. Arch Phys Med Rehabil 2000;81:22-7. Objective: To examine the relation
22 Urinary Incontinence and Stroke Outcomes Jan C. Gross, PhD, RN, CS ABSTRACT. Gross JC. Urinary incontinence and stroke outcomes. Arch Phys Med Rehabil 2000;81:22-7. Objective: To examine the relation
Effects of age on functional independence measure score gain in stroke patients in kaifukuki rehabilitation ward
 32 Japanese Journal of Comprehensive Rehabilitation Science (2012) Original Article Effects of age on functional independence measure score gain in stroke patients in kaifukuki rehabilitation ward Makoto
32 Japanese Journal of Comprehensive Rehabilitation Science (2012) Original Article Effects of age on functional independence measure score gain in stroke patients in kaifukuki rehabilitation ward Makoto
EVIDENCE OF THE BENEFITS of medical rehabilitation
 100 Course of Functional Improvement After Stroke, Spinal Cord Injury, and Traumatic Brain Injury Rita K. Bode, PhD, Allen W. Heinemann, PhD ABSTRACT. Bode RK, Heinemann AW. Course of functional improvement
100 Course of Functional Improvement After Stroke, Spinal Cord Injury, and Traumatic Brain Injury Rita K. Bode, PhD, Allen W. Heinemann, PhD ABSTRACT. Bode RK, Heinemann AW. Course of functional improvement
Surgery saved my life. Rehab is restoring my future.
 The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
APPROXIMATELY 500,000 MEDICARE patients are
 934 ORIGINAL ARTICLE A Comparative Evaluation of Inpatient Rehabilitation for Older Adults With Debility, Hip Fracture, and Myopathy Patrick Kortebein, MD, Carl V. Granger, MD, Dennis H. Sullivan, MD ABSTRACT.
934 ORIGINAL ARTICLE A Comparative Evaluation of Inpatient Rehabilitation for Older Adults With Debility, Hip Fracture, and Myopathy Patrick Kortebein, MD, Carl V. Granger, MD, Dennis H. Sullivan, MD ABSTRACT.
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit
 rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
2014 Report Card. 62 acute inpatient rehabilitation beds days
 Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Effect of Mobility on Community Participation at 1 year Post-Injury in Individuals with Traumatic Brain Injury (TBI)
 Effect of Mobility on Community Participation at 1 year Post-Injury in Individuals with Traumatic Brain Injury (TBI) Irene Ward, PT, DPT, NCS Brain Injury Clinical Research Coordinator Kessler Institute
Effect of Mobility on Community Participation at 1 year Post-Injury in Individuals with Traumatic Brain Injury (TBI) Irene Ward, PT, DPT, NCS Brain Injury Clinical Research Coordinator Kessler Institute
SINCE THE PROSPECTIVE payment system (PPS), based
 1514 Functional Gains and Therapy Intensity During Subacute Rehabilitation: A Study of 20 Facilities Christine C. Chen, ScD, OTR/L, Allen W. Heinemann, PhD, ABPP, Carl V. Granger, MD, Richard T. Linn,
1514 Functional Gains and Therapy Intensity During Subacute Rehabilitation: A Study of 20 Facilities Christine C. Chen, ScD, OTR/L, Allen W. Heinemann, PhD, ABPP, Carl V. Granger, MD, Richard T. Linn,
SEVERAL STUDIES ON spinal cord injury (SCI) recovery. Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study
 512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
Frequently Asked Questions: Riverview Rehabilitation Center
 Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities
 Predicting Potential for Positive Outcomes in a Slow-stream Rehabilitation Program Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities Ideas Fund Final Report
Predicting Potential for Positive Outcomes in a Slow-stream Rehabilitation Program Collaborative Research Grant Initiative: Mental Wellness in Seniors and Persons with Disabilities Ideas Fund Final Report
Functional Outcomes of Cancer Patients in an Inpatient Rehabilitation Setting
 Original Article 197 Functional Outcomes of Cancer Patients in an Inpatient Rehabilitation Setting San San Tay, 1 MBBS, MMed (Int Med), MRCP (UK), Yee Sien Ng, 1 MBBS, MRCP (UK), Peter AC Lim, 1 MBBS,
Original Article 197 Functional Outcomes of Cancer Patients in an Inpatient Rehabilitation Setting San San Tay, 1 MBBS, MMed (Int Med), MRCP (UK), Yee Sien Ng, 1 MBBS, MRCP (UK), Peter AC Lim, 1 MBBS,
STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT
 STROKE HKJOT REHABILITATION 2004;14:3 11 STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT Fung Mei Ling Background: Stroke is the third leading cause of death in Hong
STROKE HKJOT REHABILITATION 2004;14:3 11 STROKE REHABILITATION: PREDICTING INPATIENT LENGTH OF STAY AND DISCHARGE PLACEMENT Fung Mei Ling Background: Stroke is the third leading cause of death in Hong
10/13/2017. The K2A Cycle. Focused Intensive Repetitive Step Training (FIRST)
 Walking the Walk: Translation of Scientific Findings into Clinical Practice September 14 and 15, 2017 State of the Science Chicago, IL T. George Hornby PT, PhD Jennifer Moore PT, DHSc, NCS The K2A Cycle
Walking the Walk: Translation of Scientific Findings into Clinical Practice September 14 and 15, 2017 State of the Science Chicago, IL T. George Hornby PT, PhD Jennifer Moore PT, DHSc, NCS The K2A Cycle
Mai 2017 INDICATORS EXAMPLES
 Mai 2017 INDICATORS EXAMPLES SECTIONS INDICATORS A. Key Components of TBI Rehabilitation Proportion of individuals with TBI who required and received rehabilitation services within two working days of
Mai 2017 INDICATORS EXAMPLES SECTIONS INDICATORS A. Key Components of TBI Rehabilitation Proportion of individuals with TBI who required and received rehabilitation services within two working days of
Perceived pain and satisfaction with medical rehabilitation after hospital discharge
 Clinical Rehabilitation 2006; 20: 724730 Perceived pain and satisfaction with medical rehabilitation after hospital discharge Ivonne-Marie Bergés Sealy Center on Aging, University of Texas Medical Branch
Clinical Rehabilitation 2006; 20: 724730 Perceived pain and satisfaction with medical rehabilitation after hospital discharge Ivonne-Marie Bergés Sealy Center on Aging, University of Texas Medical Branch
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
Severe Penetrating Head Injury: A Study of Outcomes
 306 Severe Penetrating Head Injury: A Study of Outcomes Ross D. Zafonte, DO, Deborah L. Wood, MS, Cynthia L. Harrison-Felix, MS, Scott R. Millis, PhD, Nelson V. Valena, MD ABSTRACT. Zafonte RD, Wood DL,
306 Severe Penetrating Head Injury: A Study of Outcomes Ross D. Zafonte, DO, Deborah L. Wood, MS, Cynthia L. Harrison-Felix, MS, Scott R. Millis, PhD, Nelson V. Valena, MD ABSTRACT. Zafonte RD, Wood DL,
Central Cord Syndrome: Does early surgical intervention improve neurological outcome
 Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
WHO WAITS FOR INPATIENT REHABILITATION SERVICES IN CANADA
 J Rehabil Med 2010; 42: 773 779 ORIGINAL REPORT WHO WAITS FOR INPATIENT REHABILITATION SERVICES IN CANADA AFTER NEUROTRAUMA? A POPULATION-BASED STUDY Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark
J Rehabil Med 2010; 42: 773 779 ORIGINAL REPORT WHO WAITS FOR INPATIENT REHABILITATION SERVICES IN CANADA AFTER NEUROTRAUMA? A POPULATION-BASED STUDY Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark
The influence of age on corrected motor FIM effectiveness
 56 Japanese Journal of Comprehensive Rehabilitation Science (2014) Original Article The influence of age on corrected motor FIM effectiveness Makoto Tokunaga, MD, PhD, 1 Ryoji Nakanishi, MD, PhD, 1 Gihachiro
56 Japanese Journal of Comprehensive Rehabilitation Science (2014) Original Article The influence of age on corrected motor FIM effectiveness Makoto Tokunaga, MD, PhD, 1 Ryoji Nakanishi, MD, PhD, 1 Gihachiro
Evaluating inpatient public rehabilitation in Australia using a utilization review tool developed in North America
 University of Wollongong Research Online Graduate School of Medicine - Papers (Archive) Faculty of Science, Medicine and Health 2010 Evaluating inpatient public rehabilitation in Australia using a utilization
University of Wollongong Research Online Graduate School of Medicine - Papers (Archive) Faculty of Science, Medicine and Health 2010 Evaluating inpatient public rehabilitation in Australia using a utilization
Specialty Rehabilitation Fact Sheet
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Logan, D. E., Carpino, E. A., Chiang, G., Condon, M., Firn, E., Gaughan, V. J.,... Berde, C. B. (2012). A day-hospital approach to treatment of pediatric complex regional
CRITICALLY APPRAISED PAPER (CAP) Logan, D. E., Carpino, E. A., Chiang, G., Condon, M., Firn, E., Gaughan, V. J.,... Berde, C. B. (2012). A day-hospital approach to treatment of pediatric complex regional
Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab)
 Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab) TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted
Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab) TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted
OUTCOMES AND DATA 2016
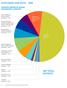 AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
2017 Report Card. 62 acute inpatient rehabilitation beds 13 DAYS
 Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Sentinel Stroke National Audit Programme (SSNAP)
 Sentinel Stroke National Audit Programme (SSNAP) Changes over Time: 4 years of data April 2013 March 2017 National results Based on stroke patients admitted to and/or discharged from hospital between April
Sentinel Stroke National Audit Programme (SSNAP) Changes over Time: 4 years of data April 2013 March 2017 National results Based on stroke patients admitted to and/or discharged from hospital between April
Recovery of function after stroke: principles of motor rehabilitation
 Recovery of function after stroke: principles of motor rehabilitation Horst Hummelsheim NRZ Neurologisches Rehabilitationszentrum Leipzig Universität Leipzig Berlin, 13.11.2009 1 Target symptoms in motor
Recovery of function after stroke: principles of motor rehabilitation Horst Hummelsheim NRZ Neurologisches Rehabilitationszentrum Leipzig Universität Leipzig Berlin, 13.11.2009 1 Target symptoms in motor
DIFFERENTIAL ITEM FUNCTIONING OF THE FUNCTIONAL INDEPENDENCE MEASURE IN HIGHER PERFORMING NEUROLOGICAL PATIENTS
 J Rehabil Med 5; 7: 6 5 DIFFERENTIAL ITEM FUNCTIONING OF THE FUNCTIONAL INDEPENDENCE MEASURE IN HIGHER PERFORMING NEUROLOGICAL PATIENTS Annet J. Dallmeijer,, Joost Dekker,, Leo D. Roorda,, Dirk L. Knol,,
J Rehabil Med 5; 7: 6 5 DIFFERENTIAL ITEM FUNCTIONING OF THE FUNCTIONAL INDEPENDENCE MEASURE IN HIGHER PERFORMING NEUROLOGICAL PATIENTS Annet J. Dallmeijer,, Joost Dekker,, Leo D. Roorda,, Dirk L. Knol,,
EARLY EXPOSURE TO comprehensive rehabilitation is. Impact of Transfer Delays to Rehabilitation in Patients With Severe Trauma
 184 Impact of Transfer Delays to Rehabilitation in Patients With Severe Trauma Marie-Josée Sirois, MSc, André Lavoie, PhD, Clermont E. Dionne, PhD From the Research Center, Laval University Affiliated
184 Impact of Transfer Delays to Rehabilitation in Patients With Severe Trauma Marie-Josée Sirois, MSc, André Lavoie, PhD, Clermont E. Dionne, PhD From the Research Center, Laval University Affiliated
CLINICIANS AND INVESTIGATORS have long recognized
 1788 ORIGINAL ARTICLE Co-Occurring Traumatic Brain Injury and Acute Spinal Cord Injury Rehabilitation Outcomes Stephen Macciocchi, hd, AB, Ronald T. Seel, hd, Adam Warshowsky, hd, Nicole Thompson, MH,
1788 ORIGINAL ARTICLE Co-Occurring Traumatic Brain Injury and Acute Spinal Cord Injury Rehabilitation Outcomes Stephen Macciocchi, hd, AB, Ronald T. Seel, hd, Adam Warshowsky, hd, Nicole Thompson, MH,
2016 Rehabilitation Services. Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital
 2016 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
2016 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
THE ESSENTIAL BRAIN INJURY GUIDE
 THE ESSENTIAL BRAIN INJURY GUIDE Outcomes Section 9 Measurements & Participation Presented by: Rene Carfi, LCSW, CBIST Senior Brain Injury Specialist Brain Injury Alliance of Connecticut Contributors Kimberly
THE ESSENTIAL BRAIN INJURY GUIDE Outcomes Section 9 Measurements & Participation Presented by: Rene Carfi, LCSW, CBIST Senior Brain Injury Specialist Brain Injury Alliance of Connecticut Contributors Kimberly
3/5/2014. Longitudinal Databases and Registries. The Spinal Cord Injury Model Systems of Care. Project Design. Project Design
 The Spinal Cord Injury Model Systems of Care Longitudinal Databases and Registries International SCI Conference: Toward Better Quality of Life Sultan Bin Abdulaziz Humanitarian City Riyadh, KSA Tamara
The Spinal Cord Injury Model Systems of Care Longitudinal Databases and Registries International SCI Conference: Toward Better Quality of Life Sultan Bin Abdulaziz Humanitarian City Riyadh, KSA Tamara
2017 Rehabilitation Services. Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital
 2017 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
2017 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
We Have a Great Story to Tell
 We Have a Great Story to Tell Inpatient Outpatient Day Neuro Baylor Scott & White Institute for Rehabilitation Frisco is dedicated to helping patients find their way back from all types of injuries, illnesses,
We Have a Great Story to Tell Inpatient Outpatient Day Neuro Baylor Scott & White Institute for Rehabilitation Frisco is dedicated to helping patients find their way back from all types of injuries, illnesses,
Poststroke Rehabilitation Outcomes and Reimbursement of Inpatient Rehabilitation Facilities and Subacute Rehabilitation Programs
 Poststroke Rehabilitation Outcomes and Reimbursement of Inpatient Rehabilitation Facilities and Subacute Rehabilitation Programs Anne Deutsch, PhD, RN, CRRN; Carl V. Granger, MD; Allen W. Heinemann, PhD,
Poststroke Rehabilitation Outcomes and Reimbursement of Inpatient Rehabilitation Facilities and Subacute Rehabilitation Programs Anne Deutsch, PhD, RN, CRRN; Carl V. Granger, MD; Allen W. Heinemann, PhD,
Inpatient Acute Rehabilitation
 Inpatient Acute Rehabilitation A massive stroke. A major illness. A debilitating injury. At first, you can t imagine how life will ever be the same. Affiliated with the renowned Dignity Health Neurological
Inpatient Acute Rehabilitation A massive stroke. A major illness. A debilitating injury. At first, you can t imagine how life will ever be the same. Affiliated with the renowned Dignity Health Neurological
Hip fracture rehabilitation: important program and outcome characteristics. Disclosure
 Hip fracture rehabilitation: important program and outcome characteristics Karl J. Sandin MD MPH Medical Director, Immanuel Rehabilitation Institute Assistant Professor of Surgery (trauma), Creighton University
Hip fracture rehabilitation: important program and outcome characteristics Karl J. Sandin MD MPH Medical Director, Immanuel Rehabilitation Institute Assistant Professor of Surgery (trauma), Creighton University
Original Article. Client-centred assessment and the identification of meaningful treatment goals for individuals with a spinal cord injury
 (2004) 42, 302 307 & 2004 International Society All rights reserved 1362-4393/04 $25.00 www.nature.com/sc Original Article Client-centred assessment and the identification of meaningful treatment goals
(2004) 42, 302 307 & 2004 International Society All rights reserved 1362-4393/04 $25.00 www.nature.com/sc Original Article Client-centred assessment and the identification of meaningful treatment goals
Stroke Special Project 640 and 740 Resource For Health Information Management Professionals
 Stroke Special Project 640 and 740 Resource For Health Information Management Professionals Linda Gould RPN Erin Kelleher, BA, CHIM Stefan Pagliuso PT, B.A. Kin(Hon.) Overview of this Resource Overview
Stroke Special Project 640 and 740 Resource For Health Information Management Professionals Linda Gould RPN Erin Kelleher, BA, CHIM Stefan Pagliuso PT, B.A. Kin(Hon.) Overview of this Resource Overview
restoring hope rebuilding lives
 Spinal Cord Injury Brain Injury Stroke Neurologic Diseases Orthopedic Conditions Amputation Cancer Cardiac Recovery The patient experience: 2015 in review restoring hope rebuilding lives Advancing care
Spinal Cord Injury Brain Injury Stroke Neurologic Diseases Orthopedic Conditions Amputation Cancer Cardiac Recovery The patient experience: 2015 in review restoring hope rebuilding lives Advancing care
For the stroke patient and
 Prue Morgan The relationship between sitting balance and mobility outcome in stroke The purpose of this study was to identify the relationship between static sitting balance in the acute post stroke patient
Prue Morgan The relationship between sitting balance and mobility outcome in stroke The purpose of this study was to identify the relationship between static sitting balance in the acute post stroke patient
Rick Hansen Spinal Cord Injury Registry: special report
 Rick Hansen Spinal Cord Injury Registry: special report 11 13 acknowledgements Thank you to the dedicated clinicians, researchers and coordinators who collect, analyze and input data into the Rick Hansen
Rick Hansen Spinal Cord Injury Registry: special report 11 13 acknowledgements Thank you to the dedicated clinicians, researchers and coordinators who collect, analyze and input data into the Rick Hansen
REHABILITATION UNIT ANNUAL OUTCOMES REPORT Prepared by
 REHABILITATION UNIT ANNUAL OUTCOMES Prepared by REPORT - 2014 Keir Ringquist, PT, PhD, GCS Rehabilitation Program Manager Director of Occupational and Physical Therapy DEMOGRAPHICS OF THE REHABILITATION
REHABILITATION UNIT ANNUAL OUTCOMES Prepared by REPORT - 2014 Keir Ringquist, PT, PhD, GCS Rehabilitation Program Manager Director of Occupational and Physical Therapy DEMOGRAPHICS OF THE REHABILITATION
Measuring Outcomes in Acute Neurorehabilitation in General Hospital Setting Our Experience
 & Measuring Outcomes in Acute Neurorehabilitation in General Hospital Setting Our Experience Emela Mujić-Skikić¹*, Suad Trebinjac¹, Dijana Avdić², Amra Džumhur-Sarić³ 1. Physical Medicine & Rehabilitation
& Measuring Outcomes in Acute Neurorehabilitation in General Hospital Setting Our Experience Emela Mujić-Skikić¹*, Suad Trebinjac¹, Dijana Avdić², Amra Džumhur-Sarić³ 1. Physical Medicine & Rehabilitation
General Medical Rehabilitation
 General Medical Rehabilitation Outcomes Report 20 Rehabilitation Hospital is part of the Rehabilitation system of care, a post-acute provider of neuro-rehabilitation for over 45 years. Our 160-bed acute,
General Medical Rehabilitation Outcomes Report 20 Rehabilitation Hospital is part of the Rehabilitation system of care, a post-acute provider of neuro-rehabilitation for over 45 years. Our 160-bed acute,
TOTAL HIP AND KNEE REPLACEMENTS. FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES
 TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
TOTAL HIP AND KNEE REPLACEMENTS FISCAL YEAR 2002 DATA July 1, 2001 through June 30, 2002 TECHNICAL NOTES The Pennsylvania Health Care Cost Containment Council April 2005 Preface This document serves as
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Tsang, M. H., Sze, K. H., & Fong, K. N. K. (2008). Occupational therapy treatment with right half-field eye-patching for patients with subacute stroke and unilateral neglect:
CRITICALLY APPRAISED PAPER (CAP) Tsang, M. H., Sze, K. H., & Fong, K. N. K. (2008). Occupational therapy treatment with right half-field eye-patching for patients with subacute stroke and unilateral neglect:
The Stroke Impairment Assessment Set: Its Internal Consistency and Predictive Validity
 863 The Stroke Impairment Assessment Set: Its Internal Consistency and Predictive Validity Tetsuya Tsuji, MD, Meigen Liu, MD, DMSc, Shigeru Sonoda, MD, DMSc, Kazuhisa Domen, MD, DMSc, Naoichi Chino, MD,
863 The Stroke Impairment Assessment Set: Its Internal Consistency and Predictive Validity Tetsuya Tsuji, MD, Meigen Liu, MD, DMSc, Shigeru Sonoda, MD, DMSc, Kazuhisa Domen, MD, DMSc, Naoichi Chino, MD,
Fall Risk Factors Fall Prevention is Everyone s Business
 Fall Risk Factors Fall Prevention is Everyone s Business Part 2 Prof (Col) Dr RN Basu Adviser, Quality & Academics Medica Superspecilalty Hospital & Executive Director Academy of Hospital Administration
Fall Risk Factors Fall Prevention is Everyone s Business Part 2 Prof (Col) Dr RN Basu Adviser, Quality & Academics Medica Superspecilalty Hospital & Executive Director Academy of Hospital Administration
Occupational Therapy (OC_THR)
 Occupational Therapy (OC_THR) 1 Occupational Therapy (OC_THR) OC_THR 1000: Introduction to Occupational Therapy Introductory course to provide students information about the occupational therapy profession.
Occupational Therapy (OC_THR) 1 Occupational Therapy (OC_THR) OC_THR 1000: Introduction to Occupational Therapy Introductory course to provide students information about the occupational therapy profession.
Reasons for Extending Length of Stay in Inpatient Spinal Cord Rehabilitation
 Reasons for Extending Length of Stay in Inpatient Spinal Cord Rehabilitation September 5, 2012 Heather Flett MSc, BScPT, BA Advanced Practice Leader- Spinal Cord Rehab Toronto Rehab UHN, University of
Reasons for Extending Length of Stay in Inpatient Spinal Cord Rehabilitation September 5, 2012 Heather Flett MSc, BScPT, BA Advanced Practice Leader- Spinal Cord Rehab Toronto Rehab UHN, University of
Department of Rehabilitation, Kumamoto Kinoh Hospital, Kumamoto, Japan 2. Department of Orthopedic Surgery, Kumamoto Kinoh Hospital, Kumamoto, Japan 3
 16 Japanese Journal of Comprehensive Rehabilitation Science (2017) Original Article Increasing the prediction accuracy of FIM gain by adding FIM improvement for one month from admission to the explanatory
16 Japanese Journal of Comprehensive Rehabilitation Science (2017) Original Article Increasing the prediction accuracy of FIM gain by adding FIM improvement for one month from admission to the explanatory
Parental Perception of Quality of Hospital Care for Children with Sickle Cell Disease
 Parental Perception of Quality of Hospital Care for Children with Sickle Cell Disease Jared Kam, BS; Julie A. Panepinto, MD, MSPH; Amanda M. Brandow, DO; David C. Brousseau, MD, MS Abstract Problem Considered:
Parental Perception of Quality of Hospital Care for Children with Sickle Cell Disease Jared Kam, BS; Julie A. Panepinto, MD, MSPH; Amanda M. Brandow, DO; David C. Brousseau, MD, MS Abstract Problem Considered:
Using the AcuteFIM Instrument for Discharge Placement
 Using the AcuteFIM Instrument for Discharge Placement Paulette Niewczyk, MPH, PhD Manager of CFAR / Director of Research Center for Functional Assessment Research Uniform Data System for Medical Rehabilitation
Using the AcuteFIM Instrument for Discharge Placement Paulette Niewczyk, MPH, PhD Manager of CFAR / Director of Research Center for Functional Assessment Research Uniform Data System for Medical Rehabilitation
More capacity for healing. More focus on you.
 REHABILITATION PROGRAM small means more. More capacity for healing. More focus on you. The Rehabilitation Center at Mt. Ascutney Hospital offering patient-centered rehabilitative care for your best possible
REHABILITATION PROGRAM small means more. More capacity for healing. More focus on you. The Rehabilitation Center at Mt. Ascutney Hospital offering patient-centered rehabilitative care for your best possible
Centerstone Research Institute
 American Addiction Centers Outcomes Study 12 month post discharge outcomes among a randomly selected sample of residential addiction treatment clients Centerstone Research Institute 2018 1 AAC Outcomes
American Addiction Centers Outcomes Study 12 month post discharge outcomes among a randomly selected sample of residential addiction treatment clients Centerstone Research Institute 2018 1 AAC Outcomes
Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the patient
 () 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
() 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
Occupational Therapy. Undergraduate. Graduate. Accreditation & Certification. Financial Aid from the Program. Faculty. Occupational Therapy 1
 Occupational Therapy 1 Occupational Therapy Department of Occupational Therapy School of Health Professions 801B Clark Hall Columbia, Missouri 65211 (573) 882-3988 Advising Contact MUOT@health.missouri.edu
Occupational Therapy 1 Occupational Therapy Department of Occupational Therapy School of Health Professions 801B Clark Hall Columbia, Missouri 65211 (573) 882-3988 Advising Contact MUOT@health.missouri.edu
Critical Thinking Assessment at MCC. How are we doing?
 Critical Thinking Assessment at MCC How are we doing? Prepared by Maura McCool, M.S. Office of Research, Evaluation and Assessment Metropolitan Community Colleges Fall 2003 1 General Education Assessment
Critical Thinking Assessment at MCC How are we doing? Prepared by Maura McCool, M.S. Office of Research, Evaluation and Assessment Metropolitan Community Colleges Fall 2003 1 General Education Assessment
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Comparing the CR-3 Injury Severity Categories (KABCO) to Injury Severity Metrics
 Comparing the CR-3 Injury Severity Categories (KABCO) to Injury Severity Metrics Texas EMS & Trauma Registries Injury Epidemiology & Surveillance Branch Environmental & Injury Epidemiology & Toxicology
Comparing the CR-3 Injury Severity Categories (KABCO) to Injury Severity Metrics Texas EMS & Trauma Registries Injury Epidemiology & Surveillance Branch Environmental & Injury Epidemiology & Toxicology
Nathan Schomburg PT, NCS 2535 Shellburne Dr. Wexford, PA (412)
 Nathan Schomburg PT, NCS 2535 Shellburne Dr. Wexford, PA 15090 (412) 310-6837 schomburgn@upmc.edu EDUCATION Duquesne University, Pittsburgh, PA Masters of Physical Therapy 1997-2002 2001 Recipient of John
Nathan Schomburg PT, NCS 2535 Shellburne Dr. Wexford, PA 15090 (412) 310-6837 schomburgn@upmc.edu EDUCATION Duquesne University, Pittsburgh, PA Masters of Physical Therapy 1997-2002 2001 Recipient of John
Hips & Knees Priority Action Team
 Hips & Knees Priority Action Team Current State Data Refresh September 5, 27 Overview Population Profile Health Status Utilization of Hip & Knee Total Joint Services 1 1 Population Profile 2 SouthWest
Hips & Knees Priority Action Team Current State Data Refresh September 5, 27 Overview Population Profile Health Status Utilization of Hip & Knee Total Joint Services 1 1 Population Profile 2 SouthWest
Oral Presentation to the H.E.L.P. Committee on February 14, 2012 Philip A. Pizzo, MD
 Oral Presentation to the H.E.L.P. Committee on February 14, 2012 Philip A. Pizzo, MD 1. I am Dr. Philip A Pizzo, Dean of the Stanford University School of Medicine as well as Professor of Pediatrics and
Oral Presentation to the H.E.L.P. Committee on February 14, 2012 Philip A. Pizzo, MD 1. I am Dr. Philip A Pizzo, Dean of the Stanford University School of Medicine as well as Professor of Pediatrics and
AVERT Trial Debate: Implications for Practice Have we AVERT ed the real message?
 AVERT Trial Debate: Implications for Practice Have we AVERT ed the real message? Jackie Bosch, PhD, OT Reg(Ont) School of Rehabilitation Science McMaster University Vince DePaul PT PhD School of Rehabilitation
AVERT Trial Debate: Implications for Practice Have we AVERT ed the real message? Jackie Bosch, PhD, OT Reg(Ont) School of Rehabilitation Science McMaster University Vince DePaul PT PhD School of Rehabilitation
Bryan Andresen MD Advances in Clinical Neuroscience Practice /2/11
 Bryan Andresen MD Advances in Clinical Neuroscience Practice 2011 5/2/11 Intro/History Definition Differential Diagnosis Clinical Characteristics Exam Findings Treatment Outcomes 46 yo female admitted
Bryan Andresen MD Advances in Clinical Neuroscience Practice 2011 5/2/11 Intro/History Definition Differential Diagnosis Clinical Characteristics Exam Findings Treatment Outcomes 46 yo female admitted
Relationship between motor FIM improvement (corrected motor FIM effectiveness) and age in proximal femoral fractures
 131 Japanese Journal of Comprehensive Rehabilitation Science (2014) Original Article Relationship between motor FIM improvement (corrected motor FIM effectiveness) and age in proximal femoral fractures
131 Japanese Journal of Comprehensive Rehabilitation Science (2014) Original Article Relationship between motor FIM improvement (corrected motor FIM effectiveness) and age in proximal femoral fractures
The Complex Rehab Technology Company. Focused on Providing Specialized Products and Related Services to People with Disabilities
 The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
