Acta Dermatovenerol Croat 2008;16(2):60-64 CLINICAL ARTICLE
|
|
|
- Randolph Byrd
- 6 years ago
- Views:
Transcription
1 2008;16(2):60-64 CLINICAL ARTICLE Clinical Efficacy of Intramuscular Meglumine Antimoniate Alone and in Combination with Intralesional Meglumine Antimoniate in the Treatment of Old World Cutaneous Leishmaniasis Abrar Munir 1, Shahbaz A. Janjua 2, Ijaz Hussain 3 1 Combined Military Hospital, Kharian Cantt.; 2 Ayza Skin & Research Center, Lalamusa; 3 Department of Dermatology, Lahore General Hospital, Lahore, Pakistan Corresponding author: Shahbaz A. Janjua, MD Ayza Skin & Research Center Lalamusa, Pakistan shahbaz.janjua@gmail.com Received: November 9, 2007 Accepted: March 12, 2008 SUMMARY Treatment of cutaneous leishmaniasis is often difficult. Even though most cutaneous lesions will heal spontaneously, their duration cannot be predicted in an individual case. In general, only large, multiple or diffuse lesions of the face, head and neck need to be considered for therapeutic intervention. Pentavalent antimonials (sodium stibogluconate and meglumine antimoniate) administered intralesionally or parenterally (IM or IV) are the mainstays of systemic therapy despite the toxicity associated with their use. The objective of this study was to compare the clinical efficacy of intramuscular pentavalent antimonial compound meglumine antimoniate alone and in combination with intralesional therapy in the treatment of Old World cutaneous leishmaniasis. Study was conducted as a case controlled interventional prospective study. On the basis of demonstration of Leishmania tropica (LT) bodies in the skin slit smears/skin biopsies, 60 patients with cutaneous leishmaniasis were included in the study. The patients were randomly allocated to three groups of 20 patients each: group 1 treated with intramuscular injection of meglumine antimoniate (20 mg Sb/kg/day, maximum 850 mg) for 21 days; group 2 treated with intralesional injection of meglumine antimoniate (0.5 ml, 42.5 mg of Sb) into each lesion along with intramuscular injection of meglumine antimoniate (20 mg Sb/kg/day, maximum 850 mg) for 21 days; and group 3 as a control group. The patients were followed-up for therapeutic safety and efficacy at 10, 20 and 90 days. The rate of complete cure was 55% in group 1, 75% in group 2 and 10% of spontaneous cure cases in group 3. The conclusions derived from this study are limited by the relatively small number of patients. The combination of intramuscular meglumine antimoniate along with intralesional administration of the agent is superior therapy to intralesional administration of meglumine antimoniate alone. KEY WORDS: meglumine antimoniate, intramuscular administration, intralesional administration, cutaneous leishmaniasis Introduction Leishmaniases represent a spectrum of several vector-borne parasitic diseases of variable severity, ranging from self-healing cutaneous papular or ulcerated lesions to life-threatening visceral disease, each caused by one of the species of the genus Leishmania. Leishmaniasis is endemic in 60
2 88 countries throughout Asia, Africa, Europe and North and South America, and the population at risk is more than 350 million (1). The parasite is transmitted to humans by the bites of infected female sandflies (Phlebotomus in the Old World countries and Lutzomyia in the New World). Leishmaniases are classified into three forms: cutaneous (oriental sore), mucocutaneous (espundia) and visceral (kala azar). The World Health Organization estimates that at least 1.5 million cases of cutaneous leishmaniasis and 500,000 cases of visceral leishmaniasis occur each year (1). Individuals at high risk of cutaneous leishmaniasis include military personnel and those who travel to or live in areas of the tropics, subtropics and southern Europe where the disease is endemic (1,2). Approximately 90% of all cases of cutaneous leishmaniasis occur in Afghanistan, Brazil, Iran, Peru, Saudi Arabia and Syria. Cutaneous leishmaniasis is endemic along the northern areas of Baluchistan, Sindh, tribal area (refugees from Afghanistan), and western border of Pakistan. Sporadic cases have been reported from southern Punjab, Azad Kashmir, northern areas and Islamabad (3,4). The pentavalent antimony compounds sodium stibogluconate and meglumine antimoniate have been the mainstays of antileishmanial therapy for both visceral and cutaneous leishmaniasis (5,6). Rifampicin, ketoconazole, allopurinol, itraconazole, liposomal amphotericin B, topical paromomycin and dapsone were used in various studies, however, with conflicting results (7-11). The aim of the study was to monitor and compare clinical response to intramuscular meglumine antimoniate (MA) alone and in combination with intralesional meglumine antimoniate in cutaneous leishmaniasis. Patients and methods This case controlled interventional prospective study evaluated 60 patients admitted to Department of Medicine, Scouts Hospital Wana from January 2003 to December There were no sex differences. All patients were adults, their age ranging from 14 to 55 years and the number of lesions 2-5 per patient (Figures 1-10). The inclusion criteria were demonstration of Leishmania tropica (LT) bodies in skin slit smears/skin biopsies and Figure 2. Close-up view of Figure 1. lesions of less than 8-week duration to standardize the trial. The patients who had lesions more than 8 weeks old, those who had already been treated, patients with known hypersensitivity to antimonial compounds, those with cardiovascular, renal, hepatic or hematologic disorders and pregnant women were excluded from the study. Selected patients were explained the study purpose and gave their consent for inclusion. They were randomly divided into three groups of 20 patients each: group 1 received 20 mg of Sb/kg/day by intramuscular injection daily for 21 days; group 2 received 20 mg of Sb/kg/day by intramuscular Figure 1. Excoriated crusted plaques with erythematous indurated borders on the lower back. Figure 3. Erythematous indurated plaque on the back of left elbow. 61
3 Table 1. Clinical data No. of patients Mean age (yrs) Duration (weeks) Number of lesions Group (12-45) 6 (1-8) 4 (2-6) Group (18-50) 5 (1-8) 2 (2-6) Group (20-55) 5 (1-8) 3 (2-6) injection along with 0.5 ml (42.5 mg of meglumine antimoniate) into each lesion, upper and mid-dermis daily; and group 3 consisting of patients unwilling to receive treatment, thus serving as a control group. The patients were evaluated at 10, 20 and 90 days. The absence of exudation, erythema, induration and LT bodies in skin slit smears/biopsies was considered as a parameter of cure. Adverse effects were also recorded during treatment. Results were analyzed using x 2 method to calculate percentage, and p value was obtained according to appropriate degree of freedom. Adverse effects recorded in study patients are presented in Table 3. Myalgia, arthralgia, headache, nausea, urticaria and cardiomyopathy were common in group 2 (combination therapy), while cellulitis and pain at the injection site were common in group 1. Cardiomyopathy was observed in only one group 2 patient, with tachycardia and nonspecific ECG changes at 3 weeks of treatment, however, these changes reverted to normal upon therapy discontinuation. Figure 5. A crusted ulcer with indurated borders on the left forearm, and an indurated erythematous plaque on the left arm. Figure 4. Close-up view of Figure 3. Results Data on 60 study patients, mean age 27 years and a mean of 3 lesions, are shown in Table 1. Complete cure was ascertained by clinical and laboratory parameters already discussed. The patients on combination therapy with intramuscular and intralesional meglumine antimoniate showed better response (Table 2). At the end of follow up, complete cure was achieved in 11 of 20 (55%) patients in group 1 (p-0.001), 15 of 20 (75%) patients in group 2 (p ) and only two of 20 (10%) patients in group 3 as a control group. Discussion The treatment of cutaneous leishmaniasis is still controversial despite the fact that a wide variety of oral, parenteral, topical, surgical, combination and cryotherapy had been tried in the past with conflicting results in various studies. Pentavalent antimonial compounds, sodium stibogluconate and meglumine antimoniate, are still the drugs of first choice. The two compounds have almost similar efficacy and toxicity. Parenteral administration of meglumine antimoniate showed variable efficacy from 65% to 95% in various studies (12-16). In our study, group 1 administered only intramuscular therapy showed 55% cure rate that Table 2. Response to intramuscular meglumine antimoniate alone and in combination with intralesional therapy 10 days 20 days 90 days Group 1 7/20 (35%) 10/20 (50%) 11/20 (55%) Group 2 9/20 (45%) 10/20 (50%) 15/20 (75%) Group 3 1/20 (5%) 3/20(15%) 2/20 (10%) 62
4 Table 3. Adverse effects of treatment Adverse effect Group 1 Group 2 Group 3 Arthralgia 1 (5%) 3 (15%) - Myalgia 1 (5%) 3 (15%) - Headache - 2 (10%) - Urticaria - 1 (5%) - Cardiomyopathy - 1 (5%) - Cellulitis 2 (10%) 1 (5%) - Pain at injection site 4 (20%) 1 (5%) - Renal toxicity Hepatic toxicity Drug fever increased to 75% when intramuscular treatment was added to intralesional therapy which was in conformity to previous studies (12). A minor difference may have been due to different or resistant parasite strain or technique of intralesional treatment; however, in group 2 the efficacy was enhanced and the cost of few adverse effects (Table 3) as compared with group 1. Therapeutic Figure 6. Close-up view of Figure 5. decision depends on the site of lesion, e.g., face, which is too sensitive to be treated by intralesional route. Single lesions, especially on the extremities, may be treated exclusively by intralesional Figure 8. Close-up view of Figure 7. therapy, whereas for multiple and extensive lesions intramuscular therapy combined with intralesional therapy will be more effective than either therapy alone. In group 3, three (15%) patients showed spontaneous healing, one of them developing relapse at six months; the overall cure of 10% indicates that most patients require therapy, especially if the lesions are multiple, extensive, disfiguring, disseminating, and located at cosmetically unacceptable sites and joints. Figure 7. An erythematous indurated plaque with crusted ulcer. Figure 9. An ulcerated lesion with indurated borders on the left foot and a similar lesion on the right lower leg. 63
5 Figure 10. An ulcerated plaque with yellowish base on the left lower leg. Adverse effects commonly reported were mylagias, arthralgias, headache, urticaria, cellulitis and pain at injection sites. These were transient and disappeared upon treatment discontinuation, however, regular follow up for cardiac, hepatic, renal and hematologic toxicity was performed; only one patient developed early cardiotoxicity at the end of the 3 rd week of treatment that normalized upon treatment discontinuation. Conclusion Treatment of cutaneous leishmaniasis with combination therapy consisting of intramuscular and intralesional meglumine antimoniate showed high efficacy at the cost of few side effects. However, intralesional therapy should only be administered in case of multiple, extensive and disseminating lesions. References 1. The leishmaniases and Leishmania/HIV co-inf ections. WHO fact sheet ( mediacentre/ factsheets/fs116/en/) accessed January 23, Akilove OE, Khachemoune A, Hasan T. Clinical manifestations and classification of Old World cutaneous leishmaniasis. Int J Dermatol 2007;46: Rab MA, Azmi FA, Iqbal J, Hamid J, Ghafoor A, Burney MI, et al. Cutaneous leishmaniasis in Baluchistan: reservoir host and sandfly vector in Uthal, Lasbella. J Pak Med Assoc 1986;36: Mujtaba G, Khalid M. Cutaneous leishmaniasis in Multan, Pakistan. Int J Dermatol 1998:37; Khatami A, Firooz A, Gorouhi F, Dowlati Y. Treatment of acute Old World cutaneous leishmaniasis: a systematic review of the randomized controlled trials. J Am Acad Dermatol 2007 Mar 6; [Epub ahead of print]. 6. Bari AU, Rahman SB. A therapeutic update on cutaneous leishmaniasis. J Coll Physicians Surg Pak 2003;13: Urcuyo FG, Zaias N. Oral ketoconazole in the treatment of leishmaniasis. Int J Dermatol 1982;21: Moosavi Z, Nakhli A, Rassaii S. Comparing the efficiency of topical paromomycin with intralesional meglumine antimoniate for cutaneous leishmaniasis. Int J Dermatol 2005; 44: Dogra J. A double-blind study on the efficacy of oral dapsone in cutaneous leishmaniasis. Trans R Soc Trop Med Hyg 1991;85: Berman JD. Editorial response: U.S. Food and Drug Administration approval of AmBisome (liposomal amphotericin B) for treatment of visceral leishmaniasis. Clin Infect Dis 1999;28: El-Safi SH, Murph AG, Bryceson ADM, Neal RA. A double blind clinical trial of the treatment of cutaneous leishmaniasis with paromomycin ointment. Trans R Soc Trop Med Hyg 1990;84: Salman Pour R, Razmavar MR, Abtahi N. Comparison of intralesional meglumine antimoniate, cryotherapy and their combination in the treatment of cutaneous leishmaniasis. Int J Dermatol 2006;45: Alkhawajah AM, Larbi E, el-gindan Y, Abahussein A, Jain S. Treatment of cutaneous leishmaniasis with antimony: intramuscular versus intralesional administration. Ann Trop Med Parasitol 1997;91: Marsden PD, Sampaio RN, Carvalho EM, Veiga JP, Costa JL, Llanos-Cuentas EA. High continuous antimony therapy in two patients with unresponsive mucosal leishmaniasis. Am J Trop Med Hyg 1985;34: Oster CN, Chulay JD, Hendricks LD, Pamplin CL 3rd, Ballou WR, Berman JD, et al. American cutaneous leishmaniasis: a comparison of three sodium stibogluconate treatment schedules. Am J Trop Med Hyg 1985;34: Bogenreider T, Lehn N, Landthaler M, Stolz W. Treatment of Old World cutaneous leishmaniasis with intralesionally injected meglumine antimoniate using a Dermojet device. Dermatology 2003;206:
Original Article Chloroquine in cutaneous leishmaniasis
 Original Article Chloroquine in cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin, Iqbal Sidiqui Department of Dermatology, Pakistan Institute of Medical Sciences, Islamabad Abstract Background Chloroquine
Original Article Chloroquine in cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin, Iqbal Sidiqui Department of Dermatology, Pakistan Institute of Medical Sciences, Islamabad Abstract Background Chloroquine
Laboratory investigation of Cutaneous Leishmaniasis in Karachi
 Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Laboratory investigation of Cutaneous Leishmaniasis in Karachi Pages with reference to book, From 248 To 250 G.M. Rajpar, M.A. Khan, A. Hafiz ( Department of Microbiology, Jinnah Postgraduate Medical Centre,
Treatment of Cutaneous Leishmaniasis with Allopurinol and Stibogluconate
 165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
165 Treatment of Cutaneous Leishmaniasis with Allopurinol and S. Martinez, M. Gonzalez, and M. E. Vernaza From the Department of Internal Medicine, University of Cauca, Popayan, and the University Hospital
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin
 Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
Original Article Comparison of fine needle aspiration with biopsy in the diagnosis of cutaneous leishmaniasis Ikramullah Khan, Rifat Yasmin Department of Dermatology, Pakistan Institute of Medical Sciences,
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan
 Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Sodium Stibogluconate treatment for cutaneous leishmaniasis: A clinical study of 43 cases from the north of Jordan Mamoun Mohammad Al-Athamneh Hiathem Qasem Abu Al-haija Ra ed Smadi Ayman S. Qaqaa Heba
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar
 Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
Welcome to the Jungle! Dr Aileen Oon, 2017 Microbiology Registrar AA 55M presented with sores on left olecranon and umbilical area Umbilical sores present for 3 weeks Left olecranon lesions for 1 week
HAEMOFLAGELLATES. Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine
 HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
HAEMOFLAGELLATES Dr. Anuluck Junkum Department of Parasitology Faculty of Medicine Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of Leishmania spp. and Trypanosoma
World Health Organization Department of Communicable Disease Surveillance and Response
 WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
WHO Report on Global Surveillance of Epidemic-prone Infectious Diseases World Health Organization Department of Communicable Disease Surveillance and Response This document has been downloaded from the
Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A Case Report
 J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
J HEALTH POPUL NUTR 2014 Jun;32(2):372-376 ISSN 1606-0997 $ 5.00+0.20 INTERNATIONAL CENTRE FOR DIARRHOEAL DISEASE RESEARCH, BANGLADESH CASE STUDY Cutaneous Leishmaniasis in an Immigrant Saudi Worker: A
Table of Contents GUIDELINES FOR THE TREATMENT AND PREVENTION OF CUTANEOUS LEISHMANIASIS IN PAKISTAN
 GUIDELINES FOR THE TREATMENT AND PREVENTION OF CUTANEOUS LEISHMANIASIS IN PAKISTAN Table of Contents Acknowledgements 2 Introduction 3 1. Leishmaniasis 4 1.1. Disease incidence 5 1.2. Leishmaniasis in
GUIDELINES FOR THE TREATMENT AND PREVENTION OF CUTANEOUS LEISHMANIASIS IN PAKISTAN Table of Contents Acknowledgements 2 Introduction 3 1. Leishmaniasis 4 1.1. Disease incidence 5 1.2. Leishmaniasis in
Departments of Dermatology, Venereology and Leprosy and *Microbiology, Indira Gandhi Medical College, Shimla, India.
 Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
Net Study Comparative efþ cacy of intralesional sodium stibogluconate (SSG) alone and its combination with intramuscular SSG to treat localized cutaneous leishmaniasis: Results of a pilot study Ajeet K.
Control of leishmaniasis
 SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
SIXTIETH WORLD HEALTH ASSEMBLY A60/10 Provisional agenda item 12.3 22 March 2007 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
Leishmaniasis: A forgotten disease among neglected people
 ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
ISPUB.COM The Internet Journal of Health Volume 11 Number 2 Leishmaniasis: A forgotten disease among neglected people Y Homsi, G Makdisi Citation Y Homsi, G Makdisi. Leishmaniasis: A forgotten disease
The Most Common Parasitic Infections In Yemen. Medical Parasitology
 The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
The Most Common Parasitic Infections In Yemen Medical Parasitology ﻓﺎﯾز اﻟﺧوﻻﻧﻲ / د 2 : is a vector-borne disease that transmitted by sandflies and caused by obligate intracellular protozoa of the genus
Leishmaniasis. CDR R.L. Gutierrez Oct 2014
 Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
Leishmaniasis CDR R.L. Gutierrez Oct 2014 Overview Protozoan parasite(s) of tissue and WBCs Many species / Many Syndromes (Cutaneous / Visceral) Pathogen: Location - Old World vs. New World Host: Immune
ISPUB.COM. Cutaneous Leishmaniasis in Iran. C Yazdi, M Narmani, B Sadri INTRODUCTION CASE 1 CASE 2
 ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
ISPUB.COM The Internet Journal of Infectious Diseases Volume 3 Number 1 Cutaneous Leishmaniasis in Iran C Yazdi, M Narmani, B Sadri Citation C Yazdi, M Narmani, B Sadri. Cutaneous Leishmaniasis in Iran.
Leishmaniasis. By Joseph Knight, PA-C. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India.
 Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how
Leishmaniasis By Joseph Knight, PA-C Objectives 1. Identify the two types of leishmaniasis. 2. Explain the differences in the reasons leishmaniasis is spreading in Afghanistan and India. 3. Discuss how
Therapeutic Options for Visceral Leishmaniasis
 Drugs (2013) 73:1863 1888 DOI 10.1007/s40265-013-0133-0 REVIEW ARTICLE Therapeutic Options for Visceral Leishmaniasis Begoña Monge-Maillo Rogelio López-Vélez Published online: 30 October 2013 Ó The Author(s)
Drugs (2013) 73:1863 1888 DOI 10.1007/s40265-013-0133-0 REVIEW ARTICLE Therapeutic Options for Visceral Leishmaniasis Begoña Monge-Maillo Rogelio López-Vélez Published online: 30 October 2013 Ó The Author(s)
Leishmaniasis, Kala Azar(The Black Fever)
 Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
Leishmaniasis, Kala Azar(The Black Fever) By Lawrence Hall Etiologic agent Protist obligate intracellular parasite, Transmission Vectors Phylum: Euglenozoa (genus Leishmania) Over 21 species that infect
CUTANEOUS LEISHMANIASIS
 CUTANEOUS LEISHMANIASIS Why are you neglecting me? A WHO initiative to control Cutaneous Leishmaniasis in selected Old World areas This document has been produced as the result of a WHO Informal Consultative
CUTANEOUS LEISHMANIASIS Why are you neglecting me? A WHO initiative to control Cutaneous Leishmaniasis in selected Old World areas This document has been produced as the result of a WHO Informal Consultative
Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil
 Hong Kong J. Dermatol. Venereol. (2013) 21, 79-83 Case Report Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil JTHT Yu and SY Wong A 60-year-old man presented with ulcerated
Hong Kong J. Dermatol. Venereol. (2013) 21, 79-83 Case Report Cutaneous Leishmaniasis in a Chinese man returning from the Amazon forest in Brazil JTHT Yu and SY Wong A 60-year-old man presented with ulcerated
BIO Parasitology Spring 2009
 BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
BIO 475 - Parasitology Spring 2009 Stephen M. Shuster Northern Arizona University http://www4.nau.edu/isopod Lecture 5 Discovery of the Disease In 1924 the Kala-Azar Commission noted that the distribution
Authors Chappuis, François; Alirol, Emilie; Worku, Dagemlidet T; Mueller, Yolanda; Ritmeijer, Koert
 MSF Field Research High mortality among older patients treated with pentavalent antimonials for visceral leishmaniasis in East Africa and rationale for switch to liposomal amphotericin B Item type Article
MSF Field Research High mortality among older patients treated with pentavalent antimonials for visceral leishmaniasis in East Africa and rationale for switch to liposomal amphotericin B Item type Article
Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course
 Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course UNCLASSIFIED Acknowledgments LTC James E. Moon, MD Chief, Sleep Trials Branch Walter Reed Army Institute of Research CDR Ramiro
Leishmaniasis WRAIR- GEIS 'Operational Clinical Infectious Disease' Course UNCLASSIFIED Acknowledgments LTC James E. Moon, MD Chief, Sleep Trials Branch Walter Reed Army Institute of Research CDR Ramiro
Control of leishmaniasis
 EXECUTIVE BOARD EB118/4 118th Session 11 May 2006 Provisional agenda item 5.1 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
EXECUTIVE BOARD EB118/4 118th Session 11 May 2006 Provisional agenda item 5.1 Control of leishmaniasis Report by the Secretariat BACKGROUND 1. Leishmaniasis is endemic in 88 countries in the world and
Leishmaniasis. MAJ Kris Paolino September 2014
 Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
Leishmaniasis MAJ Kris Paolino September 2014 Thanks to COL (Ret) Kent Kester MAJ Leyi Lin http://www.niaid.nih.gov/topics/leishmaniasis History Sir William Boog Leishman (1865-1926) Matriculated at the
WMLN Case Study. Necrotizing Palate Biopsy Specimen. Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP)
 WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
WMLN Case Study Necrotizing Palate Biopsy Specimen Youngmi Kim Sr. Microbiologist TB Lab & Parasitology Lab MS, M(ASCP) 44 year old male from Honduras Immigrated to US 12 years ago to WI 4 years ago Seen
Human Cutaneous Leishmaniasis in Three Districts of Sindh in Pakistan
 Journal of Basic & Applied Sciences, 2017, 13, 611-615 611 Human Cutaneous Leishmaniasis in Three Districts of Sindh in Pakistan Farah Sharif 1,*, Imtiaz Ahmad 2 and Rafia Rehana Ghazi 3 1 Department of
Journal of Basic & Applied Sciences, 2017, 13, 611-615 611 Human Cutaneous Leishmaniasis in Three Districts of Sindh in Pakistan Farah Sharif 1,*, Imtiaz Ahmad 2 and Rafia Rehana Ghazi 3 1 Department of
SUMMARY. Cutaneous leishmaniasis with only skin involvement: single to multiple skin ulcers, satellite lesions and nodular lymphangitis.
 SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
SUMMARY Leishmaniasis is a disease affecting predominantly people in the developing countries; 350 million people worldwide are at risk and yearly more than 2 million new cases occur. Leishmaniasis is
Efficacy of pentavalent antimoniate intralesional infiltration therapy for cutaneous leishmaniasis: A systematic review
 COLLECTION REVIEW Efficacy of pentavalent antimoniate intralesional infiltration therapy for cutaneous leishmaniasis: A systematic review Nayara Castelano Brito, Ana Rabello, Gláucia Fernandes Cota* Pesquisas
COLLECTION REVIEW Efficacy of pentavalent antimoniate intralesional infiltration therapy for cutaneous leishmaniasis: A systematic review Nayara Castelano Brito, Ana Rabello, Gláucia Fernandes Cota* Pesquisas
ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY MAY 2012 ISBN X VOL 13(2)
 ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY MAY 2012 ISBN 1595-689X VOL 13(2) AJCEM/201179/21203 -http://www.ajol.info/journals/ajcem COPYRIGHT 2012 AFR. J. CLN. EXPER. MICROBIOL
ORIGINAL ARTICLE AFRICAN JOURNAL OF CLINICAL AND EXPERIMENTAL MICROBIOLOGY MAY 2012 ISBN 1595-689X VOL 13(2) AJCEM/201179/21203 -http://www.ajol.info/journals/ajcem COPYRIGHT 2012 AFR. J. CLN. EXPER. MICROBIOL
Cutaneous leishmaniasis in an overseas Filipino worker who responded favorably to oral itraconazole
 CSE REPORT Cutaneous leishmaniasis in an overseas Filipino worker who responded favorably to oral itraconazole udi, MD 1, ilza ellamy R. Limcangco, MD, FPDS 2, Johannes F, Dayrit, MD, FPDS 2,3 Introduction:
CSE REPORT Cutaneous leishmaniasis in an overseas Filipino worker who responded favorably to oral itraconazole udi, MD 1, ilza ellamy R. Limcangco, MD, FPDS 2, Johannes F, Dayrit, MD, FPDS 2,3 Introduction:
Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis
 ISRN Parasitology, Article ID 548010, 4 pages http://dx.doi.org/10.1155/2014/548010 Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis Shyam Sundar,
ISRN Parasitology, Article ID 548010, 4 pages http://dx.doi.org/10.1155/2014/548010 Research Article Efficacy and Safety of Paromomycin in Treatment of Post-Kala-Azar Dermal Leishmaniasis Shyam Sundar,
Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics
 Clinical dermatology Review article CED Clinical and Experimental Dermatology Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics M. Ameen Royal Free Hospital, Royal
Clinical dermatology Review article CED Clinical and Experimental Dermatology Cutaneous leishmaniasis: advances in disease pathogenesis, diagnostics and therapeutics M. Ameen Royal Free Hospital, Royal
Kala-Azar- Treatment Update
 JOURNAL OF ADVANCES IN MEDICINE (JAM) DOI: 10.5958/2319-4324.2016.00002.X REVIEW PAPER Kala-Azar- Treatment Update Anup Singh Associate Professor, Department of Medicine, Institute of Medical Sciences,
JOURNAL OF ADVANCES IN MEDICINE (JAM) DOI: 10.5958/2319-4324.2016.00002.X REVIEW PAPER Kala-Azar- Treatment Update Anup Singh Associate Professor, Department of Medicine, Institute of Medical Sciences,
KYAMC Journal Vol. 3, No.-1, June Evaluation of Adverse Effects of Sodium Stibogluconate in the Treatment of Visceral Leishmaniasis
 Original Article Evaluation of Adverse Effects of Sodium Stibogluconate in the Treatment of Visceral Leishmaniasis Dr. Md. Abdus Sattar Miah 1, Dr. Md. Abdus Salam 2, Dr. Md. Azizul Haque 3, Dr. Md. Azizul
Original Article Evaluation of Adverse Effects of Sodium Stibogluconate in the Treatment of Visceral Leishmaniasis Dr. Md. Abdus Sattar Miah 1, Dr. Md. Abdus Salam 2, Dr. Md. Azizul Haque 3, Dr. Md. Azizul
Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study
 MAJOR ARTICLE Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study S. Sundar, 1 T. K. Jha, 2 C. P. Thakur, 3 M. Mishra, 4 V. P. Singh, 1 and R.
MAJOR ARTICLE Single-Dose Liposomal Amphotericin B in the Treatment of Visceral Leishmaniasis in India: A Multicenter Study S. Sundar, 1 T. K. Jha, 2 C. P. Thakur, 3 M. Mishra, 4 V. P. Singh, 1 and R.
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças Red Room 17: 00h
 CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
CONTROLE DAS LEISHMANIOSES O QUE FALTA FAZER? Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000 deaths (6.7%) 310 million at
Treatment of Disseminated Leishmaniasis With Liposomal Amphotericin B
 MAJOR ARTICLE Treatment of Disseminated Leishmaniasis With Liposomal Amphotericin B Paulo R. L. Machado, 1,2 Maria Elisa A. Rosa, 1 Luís H. Guimarães, 1,2 Fernanda V. O. Prates, 1 Adriano Queiroz, 1,2
MAJOR ARTICLE Treatment of Disseminated Leishmaniasis With Liposomal Amphotericin B Paulo R. L. Machado, 1,2 Maria Elisa A. Rosa, 1 Luís H. Guimarães, 1,2 Fernanda V. O. Prates, 1 Adriano Queiroz, 1,2
Iranian J Parasitol: Vol. 8, No.3, July -Sep 2013, pp Iranian J Parasitol. Open access Journal at ijpa.tums.ac.ir
 Iranian J Parasitol: Vol. 8, No.3, July -Sep 2013, pp.396-401 Iranian J Parasitol Tehran University of Medical Sciences Publication http:// tums.ac.ir Open access Journal at http:// ijpa.tums.ac.ir Iranian
Iranian J Parasitol: Vol. 8, No.3, July -Sep 2013, pp.396-401 Iranian J Parasitol Tehran University of Medical Sciences Publication http:// tums.ac.ir Open access Journal at http:// ijpa.tums.ac.ir Iranian
Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis. Shyam Sundar Banaras Hindu University Varanasi, India
 Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis Shyam Sundar Banaras Hindu University Varanasi, India History of the Current Epidemic in India & Antimony Resistance 6 Official
Antimonial Resistance & Combination therapy in Indian Visceral Leishmaniasis Shyam Sundar Banaras Hindu University Varanasi, India History of the Current Epidemic in India & Antimony Resistance 6 Official
by author Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018
 Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018 Dr. Monique Wasunna, Director, DNDi Africa Regional Office Presentation Outline 1 2 4 5 Introduction leishmaniasis
Drug Therapy in African Visceral Leishmaniasis 28th ECCMID Conference, Madrid, Spain 21 April 2018 Dr. Monique Wasunna, Director, DNDi Africa Regional Office Presentation Outline 1 2 4 5 Introduction leishmaniasis
Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial
 Tropical Medicine and International Health doi:10.1111/tmi.12015 volume 18 no 1 pp 96 100 january 2013 Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial Shyam Sundar 1,
Tropical Medicine and International Health doi:10.1111/tmi.12015 volume 18 no 1 pp 96 100 january 2013 Oral miltefosine for Indian post-kala-azar dermal leishmaniasis: a randomised trial Shyam Sundar 1,
VISERAL LEISHMANIASI S (KALA-AZAR)
 VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
VISERAL LEISHMANIASI S (KALA-AZAR) :OUTLINES DEFINITION. EPIDEMIOLOGY. PARASITE & VECTOR. PATHOLOGY CLINICAL & LIFE CYCLE. PICTURE. COMPLICATIONS. DIAGNOSIS. INVESTIGATIONS. MANAGEMENT TREATMENT S CONTROL.
Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial
 MILITARY MEDICINE, 177, 3:345, 2012 Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial Najibullah Safi, MD*; COL Gary D. Davis,
MILITARY MEDICINE, 177, 3:345, 2012 Evaluation of Thermotherapy for the Treatment of Cutaneous Leishmaniasis in Kabul, Afghanistan: A Randomized Controlled Trial Najibullah Safi, MD*; COL Gary D. Davis,
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies. Centro de Convenções de Reboças Red Room 17: 00h
 Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Recommendations for Coping with Leishmaniasis: A Review of Control Strategies Centro de Convenções de Reboças 08.04.2014 Red Room 17: 00h Leishmaniasis - a Global Problem Visceral 2012 300 000 cases 20,000
Correlation of clinical, histopathological, and microbiological findings in 60 cases of cutaneous leishmaniasis
 Original Article Correlation of clinical, histopathological, and microbiological findings in 60 cases of cutaneous leishmaniasis Arfan ul Bari, Simeen ber Rahman* Combined Military Hospital, Muzaffarabad,
Original Article Correlation of clinical, histopathological, and microbiological findings in 60 cases of cutaneous leishmaniasis Arfan ul Bari, Simeen ber Rahman* Combined Military Hospital, Muzaffarabad,
Visceral childhood leishmaniasis in southern Turkey: experience of twenty years
 The Turkish Journal of Pediatrics 2009; 51: 1-5 Original Visceral childhood leishmaniasis in southern Turkey: experience of twenty years Oğuz Dursun 1, Seyhan Erişir 2, Akif Yeşilipek 3 Divisions of 1
The Turkish Journal of Pediatrics 2009; 51: 1-5 Original Visceral childhood leishmaniasis in southern Turkey: experience of twenty years Oğuz Dursun 1, Seyhan Erişir 2, Akif Yeşilipek 3 Divisions of 1
References for Application for inclusion of paromomycin in the WHO Model List of Essential Medicines
 6 (a) Visceral leishmaniasis disease burden. Desjeux P. Leishmaniasis: current situation and new perspectives. Comp Immunol Microbiol Infect Dis 2004:27:305-18. Sundar S, Murray HW. Availability of miltefosine
6 (a) Visceral leishmaniasis disease burden. Desjeux P. Leishmaniasis: current situation and new perspectives. Comp Immunol Microbiol Infect Dis 2004:27:305-18. Sundar S, Murray HW. Availability of miltefosine
Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment
 MAJOR ARTICLE Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment Shyam Sundar, Neha Agrawal, Rakesh Arora, Dipti Agarwal, Madhukar Rai, and Jaya Chakravarty
MAJOR ARTICLE Short-Course Paromomycin Treatment of Visceral Leishmaniasis in India: 14-Day vs 21-Day Treatment Shyam Sundar, Neha Agrawal, Rakesh Arora, Dipti Agarwal, Madhukar Rai, and Jaya Chakravarty
CUTANEOUS LEISHMANIASIS IN BALUCHISTAN : RESERVOIR HOST AND SANDFLY VECTOR IN UThAL, LASBELLA.
 CUTANEOUS LEISHMANIASIS IN BALUCHISTAN : RESERVOIR HOST AND SANDFLY VECTOR IN UThAL, LASBELLA. Pages with reference to book, From 134 To 138 M. A. Rab, F.A. Azmi, J. Iqbal, J. Hamid, A. Ghafoor, M.I. Burney
CUTANEOUS LEISHMANIASIS IN BALUCHISTAN : RESERVOIR HOST AND SANDFLY VECTOR IN UThAL, LASBELLA. Pages with reference to book, From 134 To 138 M. A. Rab, F.A. Azmi, J. Iqbal, J. Hamid, A. Ghafoor, M.I. Burney
Tropical medicine rounds
 Oxford, IJD International 0011-9059 Blackwell 41 UK Science, Journal Ltd 2002 of Dermatology Tropical medicine rounds Cutaneous André Báfica, Leishmaniasis Fabiano Oliveira, Luiz A. R. Freitas, Eliane
Oxford, IJD International 0011-9059 Blackwell 41 UK Science, Journal Ltd 2002 of Dermatology Tropical medicine rounds Cutaneous André Báfica, Leishmaniasis Fabiano Oliveira, Luiz A. R. Freitas, Eliane
Cutaneous Leishmania
 DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Cutaneous Leishmania Ibrahim Khalifeh, MD I do not have any relevant relationships with industry. Cutaneous Leishmania: Is it a Legend? Ibrahim Khalifeh,
DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Cutaneous Leishmania Ibrahim Khalifeh, MD I do not have any relevant relationships with industry. Cutaneous Leishmania: Is it a Legend? Ibrahim Khalifeh,
Cutaneous Leishmaniasis with Unusual Clinical and Histological Presentation: Report of Four Cases
 CASE REPORT Cutaneous Leishmaniasis with Unusual Clinical and Histological Presentation: Report of Four Cases Hamideh Moravvej 1, Mohammadreza Barzegar 1, Soheila Nasiri 1, Ehsan Abolhasani 1, and Mehdi
CASE REPORT Cutaneous Leishmaniasis with Unusual Clinical and Histological Presentation: Report of Four Cases Hamideh Moravvej 1, Mohammadreza Barzegar 1, Soheila Nasiri 1, Ehsan Abolhasani 1, and Mehdi
Elimination of VL in the Indian subcontinent is it achievable?
 Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
Elimination of VL in the Indian subcontinent is it achievable? P Das Rajendra Memorial Research Institute, Patna Jorge Alvar DNDi, Geneva Bhawna Sharma DNDi, India Leishmaniasis 350 million at risk worldwide
THE LEISHMANIA TEST IN EXPERIMENTAL LEISHMANIASIS (ORIENTAL SORE) IN HUMAN SUBJECTS
 THE IN EXPERIMENTAL SIS (ORIENTAL SORE) IN HUMAN SUBJECTS A. DOSTROVSKY, M.D. The reaction of the skin to the intracutaneous injection of leishmania vaccine has been studied and established as a diagnostic
THE IN EXPERIMENTAL SIS (ORIENTAL SORE) IN HUMAN SUBJECTS A. DOSTROVSKY, M.D. The reaction of the skin to the intracutaneous injection of leishmania vaccine has been studied and established as a diagnostic
Epidemiological Study of Cutaneous Leishmaniasis in Tuz
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 6 Number 1 (2017) pp. 477-483 Journal homepage: http://www.ijcmas.com Original Research Article http://dx.doi.org/10.20546/ijcmas.2017.601.056
Current therapeutics for visceral leischmaniasis. F.Amri
 Current therapeutics for visceral leischmaniasis F.Amri Department of pediatrics Kairouan Intoduction The visceral leischmaniasis is an anthropozoonose caused by a protozoar, the Leishmania infantum The
Current therapeutics for visceral leischmaniasis F.Amri Department of pediatrics Kairouan Intoduction The visceral leischmaniasis is an anthropozoonose caused by a protozoar, the Leishmania infantum The
WRAIR- GEIS 'OPERATIONAL CLINICAL INFECTIOUS DISEASE' COURSE
 Leishmaniasis WRAIR- GEIS 'OPERATIONAL CLINICAL INFECTIOUS DISEASE' COURSE The opinions or assertions contained herein are the private views of the author, and are not to be construed as official, or as
Leishmaniasis WRAIR- GEIS 'OPERATIONAL CLINICAL INFECTIOUS DISEASE' COURSE The opinions or assertions contained herein are the private views of the author, and are not to be construed as official, or as
JMSCR Vol 06 Issue 08 Page August 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i8.12 Original Research Article Lip
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i8.12 Original Research Article Lip
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT 2 QUALITATIVE AND QUANTITATIVE COMPOSITION
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Pentostam Injection. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Sodium Stibogluconate equivalent to 100 mg pentavalent antimony in each
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Pentostam Injection. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Sodium Stibogluconate equivalent to 100 mg pentavalent antimony in each
New insights on leishmaniasis in immunosuppressive conditions
 New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
New insights on leishmaniasis in immunosuppressive conditions Javier Moreno Immunoparasitology Unit WHO Collaborative Center for Leishmaniasis Centro Nacional de Microbiología INSTITUTO DE SALUD CARLOS
Cutaneous Leishmaniasis : Global overview
 Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Cutaneous Leishmaniasis : Global overview Meeting of stakeholders for selected Health R&D Demostration Projects, 7-10 May 2014, WHO, Geneva Dr. Daniel Argaw Dagne, NTD/WHO CSR - DDC AFRO Leishmaniasis
Drug resistance in Indian visceral leishmaniasis
 Tropical Medicine and International Health volume6no11pp849±854november2001 Drug resistance in Indian visceral leishmaniasis Shyam Sundar Kala-azar Medical Research Centre, Banaras Hindu University, Varanasi,
Tropical Medicine and International Health volume6no11pp849±854november2001 Drug resistance in Indian visceral leishmaniasis Shyam Sundar Kala-azar Medical Research Centre, Banaras Hindu University, Varanasi,
Lupoid Cutaneous Leishmaniasis: a Case Report
 Dermatol Ther (2011) 1(2):36-41. DOI 10.1007/s13555-011-0008-9 CASE REPORT Lupoid Cutaneous Leishmaniasis: a Case Report Aida Khaled Samia Goucha Sonia Trabelsi Rachida Zermani Bécima Fazaa To view enhanced
Dermatol Ther (2011) 1(2):36-41. DOI 10.1007/s13555-011-0008-9 CASE REPORT Lupoid Cutaneous Leishmaniasis: a Case Report Aida Khaled Samia Goucha Sonia Trabelsi Rachida Zermani Bécima Fazaa To view enhanced
Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar)
 SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
SEA-CD-274 Frequently Asked Questions on Visceral Leishmaniasis (Kala-azar) World Health Organization 2013 All rights reserved. Requests for publications, or for permission to reproduce or translate WHO
Children with Visceral Leishmaniasis Presented to Omdurman Emergency Hospital for Children
 Original Article Children with Visceral Leishmaniasis Presented to Omdurman Emergency Hospital for Children Elfakey Walyeldinl, Ahmed Muawial, Mohamed Abdurrahman2 and Suwar M 03 Department of Paediatrics
Original Article Children with Visceral Leishmaniasis Presented to Omdurman Emergency Hospital for Children Elfakey Walyeldinl, Ahmed Muawial, Mohamed Abdurrahman2 and Suwar M 03 Department of Paediatrics
Framework for action on cutaneous leishmaniasis in the Eastern Mediterranean Region
 Framework for action on cutaneous leishmaniasis in the Eastern Mediterranean Region 2014 2018 Framework for action on cutaneous leishmaniasis in the Eastern Mediterranean Region 2014 2018 WHO Library Cataloguing
Framework for action on cutaneous leishmaniasis in the Eastern Mediterranean Region 2014 2018 Framework for action on cutaneous leishmaniasis in the Eastern Mediterranean Region 2014 2018 WHO Library Cataloguing
The New England Journal of Medicine
 The New England Journal of Medicine Copyright 22 by the Massachusetts Medical Society VOLUME 347 N OVEMBER 28, 22 NUMBER 22 ORAL MILTEFOSINE FOR INDIAN VISCERAL LEISHMANIASIS SHYAM SUNDAR, M.D., T.K. JHA,
The New England Journal of Medicine Copyright 22 by the Massachusetts Medical Society VOLUME 347 N OVEMBER 28, 22 NUMBER 22 ORAL MILTEFOSINE FOR INDIAN VISCERAL LEISHMANIASIS SHYAM SUNDAR, M.D., T.K. JHA,
POST KALA-AZAR DERMAL LEISHMANIASIS WITH ULCERATION ON FOOT: AN ATYPICAL CASE PRESENTATION SUCCESSFULLY TREATED WITH MILTEFOSINE
 American Journal of Infectious Diseases 10 (2): 50-55, 2014 ISSN: 1553-6203 2014 Science Publication doi:10.3844/ajidsp.2014.50.55 Published Online 10 (2) 2014 (http://www.thescipub.com/ajid.toc) POST
American Journal of Infectious Diseases 10 (2): 50-55, 2014 ISSN: 1553-6203 2014 Science Publication doi:10.3844/ajidsp.2014.50.55 Published Online 10 (2) 2014 (http://www.thescipub.com/ajid.toc) POST
Interleukin-10 and Interferon-γ Levels in Patients with Cutaneous Leishmaniasis Treated with Cryotherapy
 IJMS Vol 42, No 5, September 2017 Brief Report Interleukin-10 and Interferon-γ Levels in Patients with Cutaneous Leishmaniasis Treated with Cryotherapy Farhad Handjani 1,2, MD; Saeed Reza Yousef 1,2, MD;
IJMS Vol 42, No 5, September 2017 Brief Report Interleukin-10 and Interferon-γ Levels in Patients with Cutaneous Leishmaniasis Treated with Cryotherapy Farhad Handjani 1,2, MD; Saeed Reza Yousef 1,2, MD;
SUDAN BASIC COUNTRY DATA
 SUDAN BASIC COUNTRY DATA Total Population: 43,551,941 Population 0-14 years: 40% Rural population: 55% Population living under USD 1.25 a day: no data Population living under the national poverty line:
SUDAN BASIC COUNTRY DATA Total Population: 43,551,941 Population 0-14 years: 40% Rural population: 55% Population living under USD 1.25 a day: no data Population living under the national poverty line:
~Trichinella Spiralis:
 Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
Musculoskeletal System **Today we are going to talk about the parasites that affect the musculoskeletal system ~Trichinella Spiralis: It s a small nematode that measures to about 2-3mm in length. In general
Asian Pacific Journal of Tropical Disease
 Asian Pac J Trop Dis 2016; 6(2): 1-19 1 Contents lists available at ScienceDirect Asian Pacific Journal of Tropical Disease journal homepage: www.elsevier.com/locate/apjtd Epidemiological investigation
Asian Pac J Trop Dis 2016; 6(2): 1-19 1 Contents lists available at ScienceDirect Asian Pacific Journal of Tropical Disease journal homepage: www.elsevier.com/locate/apjtd Epidemiological investigation
Transactions of the Royal Society of Tropical Medicine and Hygiene
 Transactions of the Royal Society of Tropical Medicine and Hygiene 104 (2010) 225 229 Contents lists available at ScienceDirect Transactions of the Royal Society of Tropical Medicine and Hygiene journal
Transactions of the Royal Society of Tropical Medicine and Hygiene 104 (2010) 225 229 Contents lists available at ScienceDirect Transactions of the Royal Society of Tropical Medicine and Hygiene journal
CLINCOPATHOLOGICAL CASE
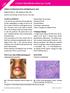 CLINCOPATHOLOGICAL CASE Solitary erythematous firm noduloplaque on nose Hassab El-Naby H., MD, Mosbeh Al Sadat, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt. CLINICAL FINDINGS A 36-year-old
CLINCOPATHOLOGICAL CASE Solitary erythematous firm noduloplaque on nose Hassab El-Naby H., MD, Mosbeh Al Sadat, MD Department of Dermatology, Al-Azhar University, Cairo, Egypt. CLINICAL FINDINGS A 36-year-old
Treatment of cutaneous leishmaniasis among travellers
 Journal of Antimicrobial Chemotherapy (2004) 53, 158 166 DOI: 10.1093/jac/dkh058 Advance Access publication 16 January 2004 Treatment of cutaneous leishmaniasis among travellers J. Blum 1 *, P. Desjeux
Journal of Antimicrobial Chemotherapy (2004) 53, 158 166 DOI: 10.1093/jac/dkh058 Advance Access publication 16 January 2004 Treatment of cutaneous leishmaniasis among travellers J. Blum 1 *, P. Desjeux
LeishMan Recommendations for Treatment of Cutaneous and Mucosal Leishmaniasis in Travelers, 2014
 I S T M 116 REVIEW LeishMan Recommendations for Treatment of Cutaneous and Mucosal Leishmaniasis in Travelers, 2014 Johannes Blum, MD, Pierre Buffet, MD, Leo Visser, MD, # Gundel Harms, MD, Mark S. Bailey,
I S T M 116 REVIEW LeishMan Recommendations for Treatment of Cutaneous and Mucosal Leishmaniasis in Travelers, 2014 Johannes Blum, MD, Pierre Buffet, MD, Leo Visser, MD, # Gundel Harms, MD, Mark S. Bailey,
Mucosal leishmaniasis: the experience of a Brazilian referral center
 Rev Soc Bras Med Trop 5(3):38-33, May-June, 08 doi: 0.590/0037-88-0478-07 Major Article Mucosal leishmaniasis: the experience of a Brazilian referral center Mariana Junqueira Pedras [],[], Janaína de Pina
Rev Soc Bras Med Trop 5(3):38-33, May-June, 08 doi: 0.590/0037-88-0478-07 Major Article Mucosal leishmaniasis: the experience of a Brazilian referral center Mariana Junqueira Pedras [],[], Janaína de Pina
Miltefosine for New World Cutaneous Leishmaniasis
 MAJOR ARTICLE for New World Cutaneous sis J. Soto, 1 B. A. Arana, 4 J. Toledo, 1 N. Rizzo, 4 J. C. Vega, 2 A. Diaz, 4 M. Luz, 1 P. Gutierrez, 1 M. Arboleda, 3 J. D. Berman, 6,a K. Junge, 5 J. Engel, 5
MAJOR ARTICLE for New World Cutaneous sis J. Soto, 1 B. A. Arana, 4 J. Toledo, 1 N. Rizzo, 4 J. C. Vega, 2 A. Diaz, 4 M. Luz, 1 P. Gutierrez, 1 M. Arboleda, 3 J. D. Berman, 6,a K. Junge, 5 J. Engel, 5
CASE OF CUTANEOUS LEISHMANIASIS OF THE LID*
 Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Brit. J. Ophthal. (1965) 49, 542 CASE OF CUTANEOUS LEISHMANIASIS OF THE LID* BY GWYN MORGAN Department ofpathology, Institute of Ophthalmology, University of London THE lid is involved only in about 2
Review Article Clinical Manifestations and Distribution of Cutaneous Leishmaniasis in Pakistan
 Tropical Medicine Volume 2011, Article ID 359145, 8 pages doi:10.1155/2011/359145 Review Article Clinical Manifestations and Distribution of Cutaneous Leishmaniasis in Pakistan Abaseen Khan Afghan, Masoom
Tropical Medicine Volume 2011, Article ID 359145, 8 pages doi:10.1155/2011/359145 Review Article Clinical Manifestations and Distribution of Cutaneous Leishmaniasis in Pakistan Abaseen Khan Afghan, Masoom
What is Kala-azar? What are Signs & Symptoms of Kala-Azar?
 What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
What is Kala-azar? Kala-azar is a slow progressing indigenous disease caused by a protozoan parasite of genus Leishmania In India Leishmania donovani is the only parasite causing this disease The parasite
Leishmaniaand Leishmaniasis
 Leishmaniaand Leishmaniasis Methodenseminar SS2014 IRMA SCHABUSSOVA, PhD Institute of Specific Prophylaxis and Tropical Medicine; Medical University Vienna Kinderspitalgasse 15, A-1090 Vienna, Austria
Leishmaniaand Leishmaniasis Methodenseminar SS2014 IRMA SCHABUSSOVA, PhD Institute of Specific Prophylaxis and Tropical Medicine; Medical University Vienna Kinderspitalgasse 15, A-1090 Vienna, Austria
Flagellates. Dr. Anuluck Junkum PARA
 Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
Flagellates Dr. Anuluck Junkum PARA 317242 Objective Can describe the morphology, life cycle, pathology, diagnosis and prevention of pathogenic flagellates Classification of Protozoa Based on locomotive
Case Report Development of Cutaneous Leishmaniasis after Leishmania Skin Test
 Case Reports in Medicine Volume 2011, Article ID 631079, 4 pages doi:10.1155/2011/631079 Case Report Development of Cutaneous Leishmaniasis after Leishmania Skin Test Paulo R. Machado, 1, 2 Augusto M.
Case Reports in Medicine Volume 2011, Article ID 631079, 4 pages doi:10.1155/2011/631079 Case Report Development of Cutaneous Leishmaniasis after Leishmania Skin Test Paulo R. Machado, 1, 2 Augusto M.
Egyptian Dermatology Online Journal Vol. 6 No 1: 14, June 2010
 Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
Wells Syndrome H. Gammaz, H. Amer, A. Adly and S. Mahmoud Egyptian Dermatology Online Journal 6 (1): 14 Al-Haud Al-Marsoud Hospital, Cairo, Egypt e-mail: hananderma@hotmail.com Submitted: April 15, 2010
A Novel Noninvasive Method for Diagnosis of Visceral Leishmaniasis by. rk39 Test in Sputum Samples
 JCM Accepts, published online ahead of print on 0 June 00 J. Clin. Microbiol. doi:0./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on 0 June 00 J. Clin. Microbiol. doi:0./jcm.00-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
Leishmaniasis impact and treatment access
 REVIEW 10.1111/j.1469-0691.2011.03635.x Leishmaniasis impact and treatment access M. den Boer, D. Argaw, J. Jannin and J. Alvar Leishmaniasis Control Programme, WHO/IDM. Av. Appia, Geneva, Switzerland
REVIEW 10.1111/j.1469-0691.2011.03635.x Leishmaniasis impact and treatment access M. den Boer, D. Argaw, J. Jannin and J. Alvar Leishmaniasis Control Programme, WHO/IDM. Av. Appia, Geneva, Switzerland
Epidemiological, clinical & pharmacological study of antimonyresistant visceral leishmaniasis in Bihar, India
 Indian J Med Res 120, September 2004, pp 166-172 Epidemiological, clinical & pharmacological study of antimonyresistant visceral leishmaniasis in Bihar, India C.P. Thakur, S. Narayan* & A. Ranjan* Balaji
Indian J Med Res 120, September 2004, pp 166-172 Epidemiological, clinical & pharmacological study of antimonyresistant visceral leishmaniasis in Bihar, India C.P. Thakur, S. Narayan* & A. Ranjan* Balaji
Case Report Localised Leishmaniasis of Oral Mucosa: Report of an Unusual Clinicopathological Entity
 Case Reports in Dentistry, Article ID 753149, 5 pages http://dx.doi.org/10.1155/2014/753149 Case Report Localised Leishmaniasis of Oral Mucosa: Report of an Unusual Clinicopathological Entity Deepak Passi,
Case Reports in Dentistry, Article ID 753149, 5 pages http://dx.doi.org/10.1155/2014/753149 Case Report Localised Leishmaniasis of Oral Mucosa: Report of an Unusual Clinicopathological Entity Deepak Passi,
Research Methods and Analysis
 Research Methods and Analysis Lecture 9 Analytic Experimental Studies Randomized Study Design Dr. Sayed Bahawaddin Hashemi, MD, MPH, ASCP Experimental Randomized Quasi Randomized Controlled Trial A study
Research Methods and Analysis Lecture 9 Analytic Experimental Studies Randomized Study Design Dr. Sayed Bahawaddin Hashemi, MD, MPH, ASCP Experimental Randomized Quasi Randomized Controlled Trial A study
Nanosilver in the treatment of localized cutaneous leishmaniasis caused by Leishmania major (MRHO/IR/75/ER): an in vitro and in vivo study
 DARU Vol. 17, No. 4 2009 285 Nanosilver in the treatment of localized cutaneous leishmaniasis caused by Leishmania major (MRHO/IR/75/ER): an in vitro and in vivo study *1 Mohebali M., 2 Rezayat M.M., 3
DARU Vol. 17, No. 4 2009 285 Nanosilver in the treatment of localized cutaneous leishmaniasis caused by Leishmania major (MRHO/IR/75/ER): an in vitro and in vivo study *1 Mohebali M., 2 Rezayat M.M., 3
Visceral leishmaniasis: an endemic disease with global impact
 Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Visceral leishmaniasis: an endemic disease with global impact Professor Olivier Lortholary, MD, PhD Department of Infectious and Tropical diseases Hôpital Necker-Enfants Malades Université Paris Descartes
Intralesional meglumine antimoniate for the treatment of localised cutaneous leishmaniasis: a retrospective review of a Brazilian referral centre
 512 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 111(8): 512-516, August 2016 Intralesional meglumine antimoniate for the treatment of localised cutaneous leishmaniasis: a retrospective review of a Brazilian
512 Mem Inst Oswaldo Cruz, Rio de Janeiro, Vol. 111(8): 512-516, August 2016 Intralesional meglumine antimoniate for the treatment of localised cutaneous leishmaniasis: a retrospective review of a Brazilian
Clinical pharmacology in leishmaniasis: treatment optimization of a neglected disease Dorlo, T.P.C.
 UvA-DARE (Digital Academic Repository) Clinical pharmacology in leishmaniasis: treatment optimization of a neglected disease Dorlo, T.P.C. Link to publication Citation for published version (APA): Dorlo,
UvA-DARE (Digital Academic Repository) Clinical pharmacology in leishmaniasis: treatment optimization of a neglected disease Dorlo, T.P.C. Link to publication Citation for published version (APA): Dorlo,
Development of Mathematical models predicting the density of vectors: Case of sandflies vectors of leishmaniasis
 Development of Mathematical models predicting the density of vectors: Case of sandflies vectors of leishmaniasis HABIBA MEJHED Département Génie Informatique, Ecole Nationale des sciences appliquées Université
Development of Mathematical models predicting the density of vectors: Case of sandflies vectors of leishmaniasis HABIBA MEJHED Département Génie Informatique, Ecole Nationale des sciences appliquées Université
2.Trichomonas vaginalis
 2.Trichomonas vaginalis 1. Pathogenic to human &causes vaginitis (trichomoniasis). 2. troph. Is round or pear like in shape, contains 4-6 flagella, all originating from anterior end & only one extend posteriorly.
2.Trichomonas vaginalis 1. Pathogenic to human &causes vaginitis (trichomoniasis). 2. troph. Is round or pear like in shape, contains 4-6 flagella, all originating from anterior end & only one extend posteriorly.
SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA. Lin Li, MD August, 2012
 SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA Lin Li, MD August, 2012 Case 1 32 year old male working in Arizona; on leave back in Singapore Presented to hospital A for fever x (7-10)
SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA Lin Li, MD August, 2012 Case 1 32 year old male working in Arizona; on leave back in Singapore Presented to hospital A for fever x (7-10)
