Disturbance of uterine bleeding patterns, often anecdotally
|
|
|
- Janel Collins
- 6 years ago
- Views:
Transcription
1 Management of Initial Bleeding or Spotting After Levonorgestrel-Releasing Intrauterine System Placement A Randomized Controlled Trial Terje Sørdal, MD, Pirjo Inki, MD, PhD, John Draeby, MD, Mary O Flynn, MB, and Thomas Schmelter, PhD OBJECTIVE: To assess the efficacy of tranexamic acid or mefenamic acid in the management of the initial nuisance bleeding or spotting in the period immediately after placement of the levonorgestrel-releasing intrauterine system. METHODS: Women were randomized after levonorgestrelreleasing intrauterine system placement to oral tranexamic acid (500 mg), mefenamic acid (500 mg), or placebo three times daily during bleeding or spotting episodes over a 90-day treatment period. Treatment was initiated from onset of a bleeding or spotting episode and continued until the first day after bleeding or spotting stopped and restarted with a new bleeding or spotting episode. The primary efficacy variable was reduction in the number of bleeding or spotting days. Tranexamic acid and mefenamic acid were compared with placebo using a one-sided See related editorial on page 919. From the Medicus AS, Trondheim, Norway; Global Medical Affairs Women s HealthCare and Global Clinical Statistics, Bayer Healthcare, Berlin, Germany; Gynecology, Skt Anne Plads, Odense, Denmark; and Town Centre Medical Practice, Cork, Ireland. Funded by Bayer Healthcare, Berlin, Germany. The authors thank Karin Burock (BIOP, Basel, Switzerland) for additional statistical support and Luana Atherly-Henderson and Richard Glover of in- Science Communications, Springer Healthcare, for medical writing support, funded by Bayer Healthcare. Corresponding author: Terje Sørdal, MD, Medicus AS, Sverres gate 15 E, Trondheim, 7012 Norway; terje@medicus.no. Financial Disclosure Dr. Sørdal is an employee of Medicus AS, who received financial support from Bayer HealthCare to conduct this clinical trial. Dr. Draeby and Ms. O Flynn received financial support from Bayer HealthCare to conduct this clinical trial. Drs. Inki and Schmelter are employees of Bayer Healthcare by The American College of Obstetricians and Gynecologists. Published by Lippincott Williams & Wilkins. ISSN: /13 Wilcoxon rank-sum test. Bonferroni-Holm adjustment was used to account for multiple testing. RESULTS: A total of 204 women were screened; 187 were randomized to tranexamic acid (n563), mefenamic acid (n563), or placebo (n561). The median number of bleeding or spotting days experienced during treatment was 25, 29, and 33 days in the three groups, respectively. The median number of bleeding or spotting days was reduced by 6 days (95% confidence interval [CI] 14.0 to 1.0, P5.049) with tranexamic acid and by 3 days (95% CI 11.0 to 5.0, P5.229) with mefenamic acid compared with placebo. The relative risk of bleeding or spotting compared with placebo with tranexamic acid and mefenamic acid was 0.82 (95% CI ) and 0.89 (95% CI ), respectively. Most women (85% or more) were satisfied with the levonorgestrel-releasing intrauterine system across the groups. CONCLUSIONS: Tranexamic acid and mefenamic acid during the first 90 days after levonorgestrel-releasing intrauterine system placement do not alleviate nuisance bleeding or spotting. CLINICAL TRIAL REGISTRATION: ClinicalTrials.gov, www. clinicaltrials.gov, NCT (Obstet Gynecol 2013;121:934 41) DOI: /AOG.0b013e31828c65d8 LEVEL OF EVIDENCE: I Disturbance of uterine bleeding patterns, often anecdotally referred to as nuisance bleeding, is common during the first few months after placement of the levonorgestrel-releasing intrauterine system. During the first 3 months of use, prolonged bleeding has been reported by 22% and irregular bleeding by 67% of women after postmenstrual placement of the levonorgestrel-releasing intrauterine system, which declined to 3% and 19%, respectively, by the end of the first 934 VOL. 121, NO. 5, MAY 2013 OBSTETRICS & GYNECOLOGY
2 year. 1 To avoid unnecessary removals as a result of initial bleeding-related issues, women wishing to use the levonorgestrel-releasing intrauterine system need to be counseled regarding the expected bleeding pattern. The limited data on the medical management of uterine bleeding disturbances after levonorgestrelreleasing intrauterine system placement suggest an inconclusive benefit with mifepristone or a progesterone receptor modulator. 2,3 Tranexamic acid, which reduces menstrual blood loss by 28 58% in women with heavy menstrual blood loss, 4 may be an effective treatment for irregular bleeding associated with depot medroxyprogesterone acetate 5 or the subdermal levonorgestrelreleasing implant. 6 Nonsteroidal anti-inflammatory drugs (NSAIDs) are superior to placebo for the treatment of heavy menstrual blood loss (reduce menstrual blood loss by 20 49% 4 ) and dysmenorrhea, 7,8 and in the management of bleeding or spotting, or dysmenorrhea associated with copper intrauterine device (IUD) use. 8 Naproxen was shown to achieve a 10% reduction in bleeding and spotting days compared with placebo in recent study. 9 We undertook this study to investigate whether counseling plus tranexamic acid or the NSAID, mefenamic acid, was superior to counseling plus placebo in the management of initial bleeding or spotting after levonorgestrel-releasing intrauterine system placement. MATERIALS AND METHODS This prospective, double-blind, three-arm, randomized placebo-controlled, phase IV study was conducted between March and December 2011 in 12 study centers in Denmark, Ireland, and Norway. The protocol and all protocol amendments were reviewed and approved by each study site s institutional review board before the start of the study and before implementation of the amendment, respectively. The study was conducted according to the principles of Declaration of Helsinki of 1975, which was revised in All participants provided written, informed consent before entry into the study. Healthy women aged years requesting contraception and who had a history of regular, cyclic menstrual cycles (cycle length days) without use of hormonal contraceptives, normal or clinically insignificant cervical smear not requiring further follow-up, were recruited to the study. Ultrasonographic examination was not part of the trial procedures because routine vaginal ultrasound in these women was not standard practice before IUD placement in the participating countries. Women were excluded if they were pregnant or breastfeeding, had not had at least two complete menstrual cycles after removal of a previous levonorgestrelreleasing intrauterine system, had a vaginal or cesarean delivery or abortion within 6 weeks of initial screening, hadaninfectedabortionorpostpartumendometritis within 90 days of screening, had been indicated for treatment of idiopathic heavy menstrual bleeding or had a history of abnormal bleeding, had any pelvic, genital, or gynecologic abnormalities, had any malignancy or severe hypertension, or had used long-acting contraceptive methods within 90 days of screening. Women who had daily or frequent NSAID use for any condition or those unwilling to use non-nsaids (eg, paracetamol) for pain management were also excluded. Use of medications known to affect vaginal bleeding patterns (eg, gonadotropin-releasing hormone analogs, danazol, or anticoagulants as well as oral, vaginal, injectable, or transdermal hormonal contraception, copper IUDs, and implants) or other NSAIDs was prohibited during the study. Women enrolled to the study received standardized structured preplacement counseling on the bleeding or spotting associated with levonorgestrel-releasing intrauterine system use. The women undertook a pregnancy test to exclude the possibility of pregnancy. The levonorgestrel-releasing intrauterine system was then placed within 7 days of the onset of menstruation or withdrawal bleeding. Women with successful levonorgestrel-releasing intrauterine system placement were randomized 1:1:1 to treatment with encapsulated (all study drug capsules were identical in appearance to maintain blinding) oral tranexamic acid (500 mg), mefenamic acid (500 mg), or placebo (lactose and magnesium stearate, encapsulated to appear identical to study treatments) three times daily during bleeding or spotting episodes. Randomization was performed in a sequential manner in blocks of six using a SAS-generated randomization list prepared by the study sponsor. Oral study treatment was scheduled to start on the first day of a bleeding or spotting episode (however, if the bleeding or spotting episode started in the afternoon or evening, the women were instructed to start study drug treatment the morning of the next day) until bleeding or spotting stopped (ie, first bleeding-free or spotting-free day) without restriction to treatment length. The first treatment was to be started on the day after levonorgestrel-releasing intrauterine system placement and continued as described and was to be restarted on occurrence of all bleeding or spotting episodes during the 90 days of study assessment followed by a 30-day follow-up period without oral study treatment. The women were also instructed to take a full day s dose of study drug (ie, one capsule three times per day). VOL. 121, NO. 5, MAY 2013 Sørdal et al Bleeding Management After IUD Placement 935
3 All women were given diary cards to record on a daily basis vaginal bleeding, study drug intake, and use of pain medication for dysmenorrhea. Occurrence of dysmenorrhea was also recorded at the end of study treatment and at the end of study. The intensity of vaginal bleeding was recorded according to bleeding intensity based on the woman s subjective experience as follows: none, no vaginal bleeding; spotting, less than associated with normal menstruation relative to the woman s experience with no need for sanitary protection (except for panty liners); light, less than associated with normal menstruation relative to the woman s experience with need for sanitary protection; normal, like normal menstruation relative to the woman s experience; and heavy, more than normal menstruation relative to the woman s experience. Compliance to treatment was assessed through diary card recordings of the number of capsules taken, along with all used study drug packaging and any remaining unused study drug. Bleeding and spotting days and episodes were assessed for the full analysis set (all randomized women with at least one clinical observation) using the terminology proposed by the World Health Organization. 10 In our study, bleeding intensity rated as light, normal, or heavy was classified as bleeding to be consistent with the World Health Organization definitions. A one-sided, nonparametric Wilcoxon rank-sum test was used to compare the cumulative number of bleeding or spotting days during the 90-day treatment period observed in the placebo group pairwise with the two active study drug treatment groups. The Bonferroni-Holm procedure was used to adjust the a level to take into account multiplicity testing to keep the overall significance level of a55%. The Hodges-Lehmann estimates for the differences in the number of bleeding or spotting days between the treatment groups with active oral study drug and the placebo treatment group were accompanied by corresponding unadjusted exact 95% confidence intervals. The Hodges-Lehmann estimator is a robust estimator for the shift in the distribution of two groups. A direct comparison between tranexamic acid and mefenamic acid was also performed using a two-sided Wilcoxon rank-sum test providing the P value, Hodges-Lehmann estimate, and corresponding 95% confidence interval. No a adjustments were performed between active treatments comparison because this analysis was considered to be secondary. The number of bleeding or spotting days was compared using univariable and multivariable Poisson regression models to estimate the relative risk (RR) between treatment groups along with 95% confidence intervals and to explore the effects of the following baseline characteristics: age (in years) or age category (younger than 35 years compared with 35 years or older); current smoker (yes or no); body mass index (as continuous variable, calculated as weight (kg)/ [height (m)] 2 ); and parity status (number of births, zero compared with one or more). The sample size (calculated using nquery Advisor 6.01) was based on experience from a previous study with the levonorgestrel-releasing intrauterine system. 11 Assuming a mean reduction in the number of bleeding or spotting days during the 90-day treatment period of at least 25% (consider the convention margin for superiority, corresponding to a reduction by 12.5 bleeding or spotting days) with active study drug treatment compared with placebo and a common standard deviation of 20 bleeding or spotting days, then 62 women per treatment group (assuming a 20% dropout rate) would be needed for a one-sided Wilcoxon rank sum test at a 5% a level to achieve a 90% power for a single comparison. Based on a Bonferroni adjustment, ie, a significance level of 2.5% per one-sided test, a power of more than 83% could be achieved for a single test based on the aforementioned assumptions. RESULTS The flow of participants through the study is shown in Figure 1. A total of 204 women were screened, of whom 187 were randomized after successful placement of the levonorgestrel-releasing intrauterine system to receive oral tranexamic acid (n563), mefenamic acid (n563), or placebo (n561). Demographic and baseline characteristics of the women enrolled to the study are summarized in Table 1. There were no statistically significant differences between the treatment groups. There were 41 (22.3%) nulliparous women included in the study. Compliance to 80% or more of planned days (ie, the percentage of days with bleeding or spotting where study medication was taken) of oral study drug intake was recorded in 83.9%, 87.1%, and 90.0% of participants in the tranexamic acid, mefenamic acid, and placebo groups, respectively. Total average cumulative numbers of capsules taken were , , and in the three groups, respectively. Figure 2 shows the box whisker plot of the number of bleeding or spotting days during the 90-day treatment period. The median number of bleeding or spotting days was lowest in the tranexamic acid group followed by the mefenamic acid and placebo groups, respectively. The median reduction in the number of bleeding or spotting days was estimated 936 Sørdal et al Bleeding Management After IUD Placement OBSTETRICS & GYNECOLOGY
4 Potential participants screened n=204 Denmark: 93 Ireland: 34 Norway: 77 Participants randomized 87 Screening failures: 7 Denmark: 4 Ireland: 6 Norway: 7 Tranexamic acid n=63 Mefenamic acid n=63 Placebo n=61 Excluded from full analysis set because of no observation after randomization Excluded from full analysis set because of no observation after randomization Excluded from full analysis set because of no observation after randomization Full analysis set n=62 Full analysis set n=62 Full analysis set n=60 Did not complete treatment phase: n=5 Adverse event: 3 Withdrawal of consent: 1 Lost to follow-up: 1 Did not complete treatment phase: n=6 Adverse event: 4 Lost to follow-up: 2 Did not complete treatment phase: n=3 Withdrawal of consent: 2 Lost to follow-up: 1 treatment phase n=57 treatment phase n=56 treatment phase n=57 Did not complete follow-up period; adverse event Did not complete follow-up period; adverse event Did not complete follow-up period; withdrawal of consent follow-up period n=56 Fig. 1. Flow of participants through the study. follow-up period n=55 Sørdal. Bleeding Management After IUD Placement. Obstet Gynecol follow-up period n=56 to be 6 days (95% confidence interval [CI] 14.0 to 1.0, P5.049) for tranexamic acid and 3 days (95% CI 11.0 to 5.0, P5.229) for mefenamic acid compared with placebo. These reductions were not statistically significant at an overall significance level a55% after using the Bonferroni-Holm procedure to adjust for multiplicity. Thus, both active study drugs were not superior to placebo because they did not reduce by at least 25% the number of bleeding or spotting days during the first 90 days after levonorgestrel-releasing intrauterine system placement. Table 2 summarizes the data for the additional bleeding or spotting parameters assessed. The number of bleeding-only days and the length of the bleeding or spotting episodes tended to be lower with tranexamic acid compared with mefenamic acid or placebo. The number of spotting-only days and number of bleeding or spotting episodes were similar between the groups. The change in the number of bleeding or spotting days between the last 30 days on study drug treatment and the 30-day follow-up period was also evaluated to determine whether the treatments assessed were only postponing the initial nuisance bleeding or spotting. There was no increase observed in the number of bleeding or spotting days in any of the treatment groups, suggesting that study treatments do not postpone the initial nuisance bleeding or spotting (Table 2). VOL. 121, NO. 5, MAY 2013 Sørdal et al Bleeding Management After IUD Placement 937
5 Table 1. Demographic and Baseline Characteristics of Women (Full Analysis set) Enrolled After Successful Placement of the Levonorgestrel-Releasing Intrauterine System Characteristic Tranexamic Acid (n562) Mefenamic Acid (n562) Placebo (n560) Age (y) Ethnicity White 61 (98.4) 61 (98.4) 58 (96.7) Asian 0 1 (1.6) 2 (3.3) Not reported 1 (1.6) 0 0 Weight (kg) BMI (kg/m 2 ) Cigarette smoker Never 42 (67.7) 46 (74.2) 45 (75.0) Former 7 (11.3) 5 (8.1) 5 (8.3) Current 13 (21.0) 11 (17.7) 10 (16.7) Parity Length of menstrual cycle (d) Duration of menstrual or withdrawal bleeding (d) Intensity of menstrual or withdrawal bleeding Spotting (1.7) Light 8 (12.9) 9 (14.5) 7 (11.7) Normal 40 (64.5) 46 (74.2) 43 (71.7) Heavy 14 (22.6) 7 (11.3) 9 (15.0) BMI, body mass index. Data are mean6standard deviation or n (%). There were no statistically significant differences in any of the characteristics between the three treatment groups (P values not shown). Outcomes of univariable and multivariable analyses of the number of bleeding or spotting days during the 90-day treatment period using Poisson regression models are summarized in Table 3. There was no Total bleeding or spotting days Tranexamic acid Mefenamic acid Placebo Fig. 2. Box whisker plot of the number of bleeding or spotting days during the 90-day treatment period by treatment group (full analysis set). The lower and upper ends of the box indicate the first to third quartile, respectively; the horizontal line indicates the median and the cross indicates the mean. Vertical lines (whiskers) indicate the minimum to maximum. Sørdal. Bleeding Management After IUD Placement. Obstet Gynecol significant difference in the RR of bleeding or spotting with tranexamic acid compared with placebo. Variables such as age, body mass index, or smoking status did not have a marked influence on bleeding or spotting compared with placebo. The proportion of women who reported being satisfied with the study drug (ie, when specifically questioned about satisfaction with study drug) used to manage initial bleeding or spotting ranged between 63.8% and 66.4% across the three study groups (Fig. 3). In addition, there were no marked differences in participant satisfaction with the levonorgestrelreleasing intrauterine system (ie, when specifically questioned about satisfaction with the levonorgestrelreleasing intrauterine system) between the treatment groups with 85% or more women reporting being satisfied across the groups. This indicates that satisfaction with the study drug does not influence overall satisfaction with the levonorgestrel-releasing intrauterine system. Continuation rates after 16 weeks were 96.7%, 96.6%, and 98.3% in the tranexamic acid, mefenamic acid, and placebo groups, respectively, indicating no influence of study drug on early discontinuation among the treatment groups. The proportion of women with dysmenorrhea decreased from 40% at baseline to approximately 20% in all three groups at the end of treatment and at the end of the study (data not shown). Only one woman 938 Sørdal et al Bleeding Management After IUD Placement OBSTETRICS & GYNECOLOGY
6 Table 2. Bleeding or Spotting Parameters During the 90-Day Treatment Phase (Full Analysis Set) Parameter Tranexamic Acid (n555) Mefenamic Acid (n557) Placebo (n556) No. of bleeding or spotting days 25.0 (13.0, 40.0) 29.0 (15.0, 44.0) 33.0 (15.0, 53.5) No. of bleeding-only days 8.0 (4.0, 16.0) 10.0 (5.0, 18.0) 11.5 (6.0, 19.5) No. of spotting-only days 15.0 (7.0, 22.0) 16.0 (8.0, 25.0) 16.0 (7.0, 27.0) No. of bleeding or spotting episodes 5.0 (3.0, 6.0) 4.0 (3.0, 5.0) 4.0 (3.0, 5.0) Length of bleeding or spotting episodes (d) 5.2 (3.5, 7.0) 7.0 (4.7, 9.6) 7.0 (4.0, 12.0) Change in the no. of bleeding or spotting days* 0 ( 1.0, 3.0) 1.0 ( 1.0, 4.0) 0 ( 4.0, 3.0) Data are median (quartile 1, quartile 3). * Change in the number of bleeding or spotting days from the last 30 days of oral blinded treatment to the first 30 days without blinded treatment. reported severe dysmenorrhea at the end of treatment and none at the end of the study compared with nine women (approximately 5%) at baseline. Inversely, the proportion of women free of dysmenorrhea increased from approximately 60% at screening to approximately 80% at the end of the study, showing the effect of the levonorgestrel-releasing intrauterine system in the alleviation of dysmenorrhea. The median number of days of pain medication use to alleviate dysmenorrhea during the treatment period was zero in all groups. The treatment-emergent adverse events are summarized in Table 4. Adverse events related to the gastrointestinal tract tended to be higher in the tranexamic acid group compared with the other two groups, and occurrence of headache tended to be lower in the mefenamic acid group compared with the other groups; however, there was no statistically significant difference in the occurrence of any single adverse event nor in the occurrence of different adverse events belonging to the same organ class between the treatment groups. Two women receiving tranexamic acid experienced a serious adverse event. One had a previously inserted, asymptomatic intraabdominal copper IUD that was assumed spontaneously expelled (it was not removed according to investigator clinical judgment). Another had endometritis resulting in hospitalization, which resolved completely after antibiotic treatment and removal of the levonorgestrel-releasing intrauterine system. DISCUSSION Tranexamic acid and mefenamic acid during the first 90 days after levonorgestrel-releasing intrauterine system placement do not alleviate the initial nuisance bleeding or spotting associated with the intrauterine system to a clinically meaningful degree. We do not believe that there were any relevant placebo effects to confound our results because the mean number of bleeding or spotting days observed in the placebo group in this study was consistent with those reported in a similar group of patients in another study that assessed the contraceptive effectiveness of the levonorgestrel-releasing intrauterine system (35 days compared with 36 days). 11 The strengths of our study include the randomized, blinded, placebo-controlled design, use of standardized structured levonorgestrel-releasing intrauterine system preplacement counseling, and the careful monitoring of compliance with study drug treatment. Potential weaknesses included patient selection, more than 95% of the women recruited were white, and it is possible that our results may not be generally applicable to other ethnic groups. In addition, a greater reduction in bleeding or Table 3. Univariable and Multivariable Poisson Regression Analyses of the Number of Bleeding or Spotting Days During the 90-Day Treatment Period (Full Analysis Set) Independent Variables Univariable (n5168) Multivariable (n5168) Tranexamic acid vs placebo 0.81 ( ) 0.82 ( ) Mefenamic acid vs placebo 0.90 ( ) 0.89 ( ) Tranexamic acid vs mefenamic acid 0.90 ( ) 0.92 ( ) Age (y) 1.00 ( ) 1.00 ( ) BMI at baseline (kg/m 2 ) 0.98 ( ) 0.98 ( ) Current smoker (yes vs. no) 0.89 ( ) 0.91 ( ) BMI, body mass index. Data are relative risk (95% confidence interval). VOL. 121, NO. 5, MAY 2013 Sørdal et al Bleeding Management After IUD Placement 939
7 Proportion of women (%) Very dissatisfied Dissatisfied Satisfied Very satisfied Neither satisfied nor dissatisfied Tranexamic acid Mefenamic acid Placebo Treatment Fig. 3. Satisfaction with the levonorgestrel-releasing intrauterine system (full analysis set). There was no statistically significant difference in women who were very satisfied or satisfied compared with those who were very dissatisfied or dissatisfied among the three treatment-groups (P values not shown). Sørdal. Bleeding Management After IUD Placement. Obstet Gynecol spotting days may have been easier to show in women using the levonorgestrel-releasing intrauterine system for treatment of heavy menstrual blood loss. However, this would have resulted in a highly selected patient population, preventing extrapolation of our results to the general population of women using the levonorgestrelreleasing intrauterine system for contraception. Alternatively, we could have selected only women with a high number of bleeding or spotting days during the first month after levonorgestrel-releasing intrauterine system placement or women with a subjective complaint of irregular bleeding or spotting (two overlapping but not identical groups). However, this may have increased the screening phase to at least 30 days, after which the condition may have resolved without intervention; most nuisance bleeding or spotting occurs during the first month followed by a rapid reduction in these events. 1 Treatment of bleeding or spotting with tranexamic acid tended to be associated with fewer bleeding or spotting days, shorter bleeding or spotting episodes, compared with mefenamic acid or placebo. It may be argued that the dose of tranexamic acid (1.5 g/d) used in this study was too low and that a higher dose may have resulted in a higher treatment effect. However, 1 g tranexamic acid per day has been previously shown to be more effective than Table 4. Treatment-Emergent Adverse Events Reported for 2% or More of Participants by Primary System Organ Class and Preferred Term (Full Analysis Set) Primary System Organ Class Preferred Term Tranexamic Acid (n562) Mefenamic Acid (n562) Placebo (n560) Total (N5184) Participants with any adverse event 29 (46.8) 29 (46.8) 26 (43.3) 84 (45.7) Gastrointestinal disorders 12 (19.4) 4 (6.5) 6 (10.0) 22 (12.0) Abdominal distension 3 (4.8) 1 (1.6) 0 4 (2.2) Abdominal pain 1 (1.6) 2 (3.2) 3 (5.0) 6 (3.3) Abdominal pain lower 3 (4.8) 0 2 (3.3) 5 (2.7) Nausea 2 (3.2) 0 3 (5.0) 5 (2.7) General disorders and administration site 2 (3.2) 1 (1.6) 2 (3.3) 5 (2.7) conditions* Infections and infestations 7 (11.3) 7 (11.3) 6 (10.0) 20 (10.9) Influenza 1 (1.6) 3 (4.8) 0 4 (2.2) Musculoskeletal and connective tissue disorders 4 (6.5) 0 2 (3.3) 6 (3.3) Nervous system disorders 5 (8.1) 2 (3.2) 7 (11.7) 14 (7.6) Headache 5 (8.1) 2 (3.2) 7 (11.7) 14 (7.6) Psychiatric disorders 3 (4.8) 2 (3.2) 1 (1.7) 6 (3.3) Reproductive system and breast disorders 13 (21.0) 15 (24.2) 15 (25.0) 43 (23.4) Breast tenderness 1 (1.6) 1 (1.6) 2 (3.3) 4 (2.2) Dysmenorrhea 8 (12.9) 10 (16.1) 10 (16.7) 28 (15.2) Pelvic pain 3 (4.8) 3 (4.8) 2 (3.3) 8 (4.3) Skin and subcutaneous tissue disorders 0 2 (3.2) 4 (6.7) 6 (3.3) Data are n (%). * The general disorders and administration site conditions were: expulsion (n52), previously inserted copper intrauterine device diagnosed as intraabdominal (n51), and fatigue (n52). 940 Sørdal et al Bleeding Management After IUD Placement OBSTETRICS & GYNECOLOGY
8 placebo in stopping bleeding episodes in women using subdermal contraceptive implants and depot medroxyprogesterone acetate. 5,6 Moreover, in our study, treatment with a higher tranexamic acid dose may have resulted in lower compliance and more frequent adverse events as a result of the increased pill burden. A recently published, placebo-controlled study with naproxen showed a nonsignificant reduction in bleeding or spotting of 4.5 days during the first 90 days after levonorgestrel-releasing intrauterine system placement. 9 In that study, women received 500 mg naproxen or placebo twice daily for 5 days every 4 weeks during three 4-week periods. As such, the drug intake could have occurred at a time without any bleeding (expected menstrual bleeding or irregular bleeding or spotting). The relative risk of bleeding or spotting for naproxen compared with placebo was 0.90 (95% CI ). Despite the difference in treatment regimen, the RR reported by Madden et al is similar to that observed for mefenamic acid (0.89, 95% CI ) in our study, although our CI was wider despite the larger sample size and similar distribution of bleeding or spotting days. The narrower 95% CI reported by Madden et al suggests that they used a Poisson regression analysis without accounting for overdispersion. We believe that a statistical model of these data accounting for overdispersion would not have resulted in a significant effect for NSAIDs in reducing the initial bleeding or spotting associated with the levonorgestrel-releasing intrauterine system in the first few months after placement. None of our comparisons resulted in statistically significant differences, because we accounted for the additional variability in the bleeding or spotting days in our Poisson regression analysis. Had we not done so, the 95% CI for the RR would have excluded 1 as well and would have indicated a significant effect. In conclusion, considering the overall risk benefit, we cannot recommend either tranexamic acid or mefenamic acid for prophylactic use in the management of initial nuisance bleeding or spotting with the levonorgestrel-releasing intrauterine system, because both drugs did not result in at least 25% reduction in the number of bleeding or spotting days during the first 3 months of levonorgestrel-releasing intrauterine system use. Future trials are needed to confirm whether tranexamic acid or other drugs can be used for the management of bleeding or spotting among levonorgestrel-releasing intrauterine system users with a subjective complaint of bleeding or spotting. REFERENCES 1. Suvisaari J, Lähteenmäki P. Detailed analysis of menstrual bleeding patterns after postmenstrual and postabortal insertion of a copper IUD or a levonorgestrel-releasing intrauterine system. Contraception 1996;54: Warner P, Guttinger A, Glasier AF, Lee RJ, Nickerson S, Brenner RM, et al. Randomized placebo-controlled trial of CDB-2914 in new users of a levonorgestrel-releasing intrauterine system shows only short-lived amelioration of unscheduled bleeding. Hum Reprod 2010;25: Lal S, Kriplani A, Kulshrestha V, Sharma M, Agarwal N. Efficacy of mifepristone in reducing intermenstrual vaginal bleeding in users of the levonorgestrel intrauterine system. Int J Gynaecol Obstet 2010;109: National Institute for Health and Clinical Excellence. Heavy menstrual bleeding (NICE clinical guideline 44). London (UK): National Institute for Health and Clinical Excellence; Senthong AJ, Taneepanichskul S. The effect of tranexamic acid for treatment irregular uterine bleeding secondary to DMPA use. J Med Assoc Thai 2009;92: Phupong V, Sophonsritsuk A, Taneepanichskul S. The effect of tranexamic acid for treatment of irregular uterine bleeding secondary to Norplant use. Contraception 2006;73: Lethaby A, Augood C, Duckitt K, Farquhar C. Nonsteroidal anti-inflammatory drugs for heavy menstrual bleeding. The Cochrane Database of Systematic Reviews 2007, Issue 4. Art. No: CD DOI: / CD pub2. 8. Grimes DA, Hubacher D, Lopez LM, Schulz KF. Non-steroidal anti-inflammatory drugs for heavy bleeding or pain associated with intrauterine-device use. The Cochrane Database of Systematic Reviews 2011, Issue 10. Art. No.: CD DOI: / CD pub2. 9. Madden T, Proehl S, Allsworth JE, Secura GM, Peipert JF. Naproxen or estradiol for bleeding and spotting with the levonorgestrel intrauterine system: a randomized controlled trial. Am J Obstet Gynecol 2012;206:129.e Belsey EM, Machin D, d Arcangues C. The analysis of vaginal bleeding patterns induced by fertility regulating methods. World Health Organization Special Programme of Research, Development and Research Training in Human Reproduction. Contraception 1986;34: Gemzell-Danielsson K, Schellschmidt I, Apter D. A randomized, phase II study describing the efficacy, bleeding profile, and safety of two low-dose levonorgestrel-releasing intrauterine contraceptive systems and Mirena. Fertil Steril 2012;97: e1 3. VOL. 121, NO. 5, MAY 2013 Sørdal et al Bleeding Management After IUD Placement 941
Instruction for the patient
 WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage:
 Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
What s New in Adolescent Contraception?
 What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
Lindsey Tingen, MD Department of Obstetrics and Gynecology, Greenville Health System Greenville, SC
 Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
Postpartum IUD Insertion: Continued Usage at Six Months Based on Expulsion and Removal Rates at Greenville Memorial Hospital in the First Year After Adoption of the Practice Lindsey Tingen, MD Department
Product Information. Confidence that lasts
 Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
LONG-ACTING REVERSIBLE CONTRACEPTION. Summary Tables
 LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
BRIEF REPORTS. Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH
 Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH BACKGROUND AND OBJECTIVES: Providing long-acting reversible contraception
Providing Long-Acting Reversible Contraception in an Academic Family Medicine Center Jennifer Amico, MD, MPH; Justine Wu, MD, MPH BACKGROUND AND OBJECTIVES: Providing long-acting reversible contraception
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer
 levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
LEARNING OBJECTIVES. Beyond the Pill: Long Acting Contraception. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy is Common
 4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
2
 1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
Unintended Pregnancy is Common LEARNING OBJECTIVES. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy And Contraceptive Use
 3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines
 Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines 1. Summary statement of the proposal for inclusion LNG-IUS is an effective contraceptive;
Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines 1. Summary statement of the proposal for inclusion LNG-IUS is an effective contraceptive;
LARC: Disclosures. Long Acting Reversible Contraception. Objectives 10/23/2013. I have no relevant financial disclosures
 LARC: Long Acting Reversible Contraception Disclosures I have no relevant financial disclosures Jennifer Kerns, MD, MPH Assistant Professor, UCSF Obstetrics, Gynecology and Reproductive Sciences San Francisco
LARC: Long Acting Reversible Contraception Disclosures I have no relevant financial disclosures Jennifer Kerns, MD, MPH Assistant Professor, UCSF Obstetrics, Gynecology and Reproductive Sciences San Francisco
1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7:
 1 2 1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7: 777 85. 3 1. Wu JP et al. Extended use of the intrauterine device: a
1 2 1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7: 777 85. 3 1. Wu JP et al. Extended use of the intrauterine device: a
Simplifying Vide Contraception. University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok
 Simplifying Vide Contraception University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok Background Objectives At the conclusion of this presentation participants will be able
Simplifying Vide Contraception University of Utah Department of Ob/Gyn Post Grad Course February 13, 2017 David Turok Background Objectives At the conclusion of this presentation participants will be able
1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7:
 1 2 1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7: 777 85. 3 1. Wu JP et al. Extended use of the intrauterine device: a
1 2 1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7: 777 85. 3 1. Wu JP et al. Extended use of the intrauterine device: a
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Women spend about 5 years of their
 CONTRACEPTION Why we have not yet reduced the unintended pregnancy rate Melody Y. Hou, MD, MPH Dr. Hou is Assistant Professor of Obstetrics and Gynecology at the University of California, Davis, in Sacramento.
CONTRACEPTION Why we have not yet reduced the unintended pregnancy rate Melody Y. Hou, MD, MPH Dr. Hou is Assistant Professor of Obstetrics and Gynecology at the University of California, Davis, in Sacramento.
1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S.
 1 2 1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S. The contraceptive action of all IUDs is mainly in the uterine cavity. The major effect
1 2 1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S. The contraceptive action of all IUDs is mainly in the uterine cavity. The major effect
Contraception and gynecological pathologies
 1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
BLEEDING PATTERNS AND CONTRACEPTIVE DISCONTINUATION FG MHLANGA MTN ANNUAL MEETING 20 MARCH 2018
 BLEEDING PATTERNS AND CONTRACEPTIVE DISCONTINUATION FG MHLANGA MTN ANNUAL MEETING 20 MARCH 2018 Introduction Bleeding with contraception may lead to discontinuation and possible unintended pregnancy What
BLEEDING PATTERNS AND CONTRACEPTIVE DISCONTINUATION FG MHLANGA MTN ANNUAL MEETING 20 MARCH 2018 Introduction Bleeding with contraception may lead to discontinuation and possible unintended pregnancy What
Levosert levonorgestrel 20mcg/24hour intrauterine device
 Levosert levonorgestrel 20mcg/24hour intrauterine device Verdict: Formulary inclusion: Formulary category: Restrictions: Reason for inclusion: Link to formulary: Link to medicine review summary: Levosert
Levosert levonorgestrel 20mcg/24hour intrauterine device Verdict: Formulary inclusion: Formulary category: Restrictions: Reason for inclusion: Link to formulary: Link to medicine review summary: Levosert
Welcome to Mirena. The Mirena Handbook: A Personal Guide to Your New Mirena. mirena.com. Mirena is the #1 prescribed IUD * in the U.S.
 Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
The number of women using long-acting reversible
 Long-acting reversible contraception: Who, what, when, and how This review provides practical tips and dispels some common misconceptions about these devices, which have higher rates of patient satisfaction
Long-acting reversible contraception: Who, what, when, and how This review provides practical tips and dispels some common misconceptions about these devices, which have higher rates of patient satisfaction
Contraception: Common Problems Faced in Office Practice. Jane S. Sillman, MD Brigham and Women s Hospital
 Contraception: Common Problems Faced in Office Practice Jane S. Sillman, MD Brigham and Women s Hospital Disclosures I have no conflicts of interest Contraception: Common Problems How to discuss contraception
Contraception: Common Problems Faced in Office Practice Jane S. Sillman, MD Brigham and Women s Hospital Disclosures I have no conflicts of interest Contraception: Common Problems How to discuss contraception
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system)
 FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
Reproductive health research at WHO
 Reproductive health research at WHO Paul F.A. Van Look, MD PhD Department of Reproductive Health and Research World Health Organization Geneva, 11 March 2004 PVL_GE_StudCourse_MAR04/1 Health is a state
Reproductive health research at WHO Paul F.A. Van Look, MD PhD Department of Reproductive Health and Research World Health Organization Geneva, 11 March 2004 PVL_GE_StudCourse_MAR04/1 Health is a state
Gayatrri Anipindi *, Vani I. Original Research Article. Abstract
 Original Research Article Role of levonorgestrel releasing intrauterine device in management of heavy menstrual bleeding: A safe and effective option for all PALM COEIN variants Gayatrri Anipindi *, Vani
Original Research Article Role of levonorgestrel releasing intrauterine device in management of heavy menstrual bleeding: A safe and effective option for all PALM COEIN variants Gayatrri Anipindi *, Vani
Coding for the Contraceptive Implant and IUDs
 LARC Quick Coding Guide 2018 UPDATE Coding for the Contraceptive Implant and IUDs CORRECT CODING can result in more appropriate compensation for services and devices. To help practices receive appropriate
LARC Quick Coding Guide 2018 UPDATE Coding for the Contraceptive Implant and IUDs CORRECT CODING can result in more appropriate compensation for services and devices. To help practices receive appropriate
Picking the Perfect Pill How to Effectively Choose an Oral Contraceptive
 Focus on CME at Queen s University Picking the Perfect Pill How to Effectively Choose an Oral Contraceptive By Susan Chamberlain, MD, FRCSC There are over 20 oral contraceptive (OC) preparations on the
Focus on CME at Queen s University Picking the Perfect Pill How to Effectively Choose an Oral Contraceptive By Susan Chamberlain, MD, FRCSC There are over 20 oral contraceptive (OC) preparations on the
prevalence was 13.8% among females
 1 2 3 1. Woldeamanuel YW et al. Migraine affects 1 in 10 people worldwide featuring recent rise: a systematic review and meta-analysis of communitybased studies involving 6 million participants. J Neurol
1 2 3 1. Woldeamanuel YW et al. Migraine affects 1 in 10 people worldwide featuring recent rise: a systematic review and meta-analysis of communitybased studies involving 6 million participants. J Neurol
Original Article ABSTRACT
 Original Article Effectiveness and safety of Levonorgestrel Releasing Intrauterine System in treatment of menorrhagia secondary to oral anticoagulations and chronic liver disease Abeera Choudry, Ayesha
Original Article Effectiveness and safety of Levonorgestrel Releasing Intrauterine System in treatment of menorrhagia secondary to oral anticoagulations and chronic liver disease Abeera Choudry, Ayesha
Contraceptive Updates and Recommendations
 Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations
 Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Medical Eligibility for Contraception Use
 Medical Eligibility for Contraception Use DIVISION OF REPRODUCTIVE HEALTH CENTERS FOR DISEASE CONTROL AND PREVENTION 2016 US Medical Eligibility Criteria for Contraceptive Use (US MEC) Purpose To assist
Medical Eligibility for Contraception Use DIVISION OF REPRODUCTIVE HEALTH CENTERS FOR DISEASE CONTROL AND PREVENTION 2016 US Medical Eligibility Criteria for Contraceptive Use (US MEC) Purpose To assist
The use of long-acting reversible contraceptive
 Overcoming LARC complications: 7 case challenges The strings to your patient s intrauterine device (IUD) are missing. Clinical experience and ACOG direction guide the management plans for this and more
Overcoming LARC complications: 7 case challenges The strings to your patient s intrauterine device (IUD) are missing. Clinical experience and ACOG direction guide the management plans for this and more
Research. Reported weight gain is one of the
 Research www.ajog.org GENERAL GYNECOLOGY Validity of perceived weight gain in women using long-acting reversible contraception and depot medroxyprogesterone acetate Ashley M. Nault, BS; Jeffrey F. Peipert,
Research www.ajog.org GENERAL GYNECOLOGY Validity of perceived weight gain in women using long-acting reversible contraception and depot medroxyprogesterone acetate Ashley M. Nault, BS; Jeffrey F. Peipert,
Expanding Access to Birth Control: Will Women Get the Care They Need?
 Expanding Access to Birth Control: Will Women Get the Care They Need? Target Audience: Pharmacists ACPE#: 0202-0000-18-045-L01-P Activity Type: Application-based Target Audience: ACPE#: Activity Type:
Expanding Access to Birth Control: Will Women Get the Care They Need? Target Audience: Pharmacists ACPE#: 0202-0000-18-045-L01-P Activity Type: Application-based Target Audience: ACPE#: Activity Type:
An Overview of Long Acting Reversible Contraception Methods
 An Overview of Long Acting Reversible Contraception Methods Unintended Pregnancy All pregnancies should be intended; that is, they should be consciously and clearly desired at the time of conception. -
An Overview of Long Acting Reversible Contraception Methods Unintended Pregnancy All pregnancies should be intended; that is, they should be consciously and clearly desired at the time of conception. -
Uterine-Sparing Treatment Options for Symptomatic Uterine Fibroids
 Uterine-Sparing Treatment Options for Symptomatic Uterine Fibroids Developed in collaboration Learning Objective Upon completion, participants should be able to: Review uterine-sparing fibroid therapies
Uterine-Sparing Treatment Options for Symptomatic Uterine Fibroids Developed in collaboration Learning Objective Upon completion, participants should be able to: Review uterine-sparing fibroid therapies
Dr. Nancy Van Eyk Associate Professor, Dalhousie University Chief of Gynaecology, IWK Health Centre
 Dr. Nancy Van Eyk Associate Professor, Dalhousie University Chief of Gynaecology, IWK Health Centre AUB Outline Terminology Classification/Etiology Assessment Treatment Referral to Gynaecology U c pt 4
Dr. Nancy Van Eyk Associate Professor, Dalhousie University Chief of Gynaecology, IWK Health Centre AUB Outline Terminology Classification/Etiology Assessment Treatment Referral to Gynaecology U c pt 4
2. Studies of Cancer in Humans
 346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
346 IARC MONOGRAPHS VOLUME 72 2. Studies of Cancer in Humans 2.1 Breast cancer 2.1.1 Results of published studies Eight studies have been published on the relationship between the incidence of breast cancer
2/4/2011. What is your specialty? A. Family practice B. Internal medicine and subs C. OB/GYN D. Peds E. Surgery and subs
 Steve P. Buchanan D.O. FACOOG(Dist.) TOMA Mid Winter February 11, 2011 Dallas,TX Associate Professor OB/GYN UNTHSC/TCOM 1987- present Executive Vice President, American College of Osteopathic Obstetricians
Steve P. Buchanan D.O. FACOOG(Dist.) TOMA Mid Winter February 11, 2011 Dallas,TX Associate Professor OB/GYN UNTHSC/TCOM 1987- present Executive Vice President, American College of Osteopathic Obstetricians
New Zealand Datasheet
 New Zealand Datasheet 1 PRODUCT NAME POSTINOR-1 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Levonorgestrel 1.5 mg 3 PHARMACEUTICAL FORM Each round white tablet contains 1.5 mg of levonorgestrel. The tablet
New Zealand Datasheet 1 PRODUCT NAME POSTINOR-1 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Levonorgestrel 1.5 mg 3 PHARMACEUTICAL FORM Each round white tablet contains 1.5 mg of levonorgestrel. The tablet
Intrauterine contraceptive devices (IUDs) are becoming
 Malpositioned Intrauterine Contraceptive Devices Risk Factors, Outcomes, and Future Pregnancies Kari P. Braaten, MD, MPH, Carol B. Benson, MD, Rie Maurer, MA, and Alisa B. Goldberg, MD, MPH OBJECTIVE:
Malpositioned Intrauterine Contraceptive Devices Risk Factors, Outcomes, and Future Pregnancies Kari P. Braaten, MD, MPH, Carol B. Benson, MD, Rie Maurer, MA, and Alisa B. Goldberg, MD, MPH OBJECTIVE:
Review of IUCD Complications: Lessons from CAT. Dr FG Mhlanga CAT Meeting 24 September 2016
 Review of IUCD Complications: Lessons from CAT Dr FG Mhlanga CAT Meeting 24 September 2016 INTRODUCTION The intrauterine device (IUD) is a reliable long term reversible, cost-effective,easy to use and
Review of IUCD Complications: Lessons from CAT Dr FG Mhlanga CAT Meeting 24 September 2016 INTRODUCTION The intrauterine device (IUD) is a reliable long term reversible, cost-effective,easy to use and
Differences in Women Who Choose Subdermal Implants Versus Intrauterine Devices
 The Journal of Reproductive Medicine Differences in Women Who Choose Subdermal Implants Versus Intrauterine Devices Vien C. Lam, M.D., Emily E. Hadley, M.D., Abbey B. Berenson, M.D., Ph.D., Jacqueline
The Journal of Reproductive Medicine Differences in Women Who Choose Subdermal Implants Versus Intrauterine Devices Vien C. Lam, M.D., Emily E. Hadley, M.D., Abbey B. Berenson, M.D., Ph.D., Jacqueline
Contraception. Objectives. Unintended Pregnancy. Unintended Pregnancy in the US. What s the Impact? 10/7/2014
 Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Fertility control: what do women want?
 FIAPAC 2018 Fertility control: what do women want? Dr. Raymond H.W. Li MBBS, MMedSC, FRCOG, FHKAM (O&G) Cert RCOG/HKCOG (Reprod Med) Department of O&G, The University of Hong Kong The Family Planning Association
FIAPAC 2018 Fertility control: what do women want? Dr. Raymond H.W. Li MBBS, MMedSC, FRCOG, FHKAM (O&G) Cert RCOG/HKCOG (Reprod Med) Department of O&G, The University of Hong Kong The Family Planning Association
4. Timing of post-abortion contraception
 Web annexes: Medical management of abortion: evidence summary* 4. Timing of post-abortion contraception * This publication forms part of the WHO guideline entitled Medical Management of Abortion. The full
Web annexes: Medical management of abortion: evidence summary* 4. Timing of post-abortion contraception * This publication forms part of the WHO guideline entitled Medical Management of Abortion. The full
Family Planning UNMET NEED. The Nurse Mildred Radio Talk Shows
 Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
The most commonly chosen methods of contraception
 Original Research Effects of Age, Parity, and Device Type on Complications and Discontinuation of Intrauterine Devices Joelle Aoun, MD, Virginia A. Dines, BS, Dale W. Stovall, MD, Mihriye Mete, PhD, Casey
Original Research Effects of Age, Parity, and Device Type on Complications and Discontinuation of Intrauterine Devices Joelle Aoun, MD, Virginia A. Dines, BS, Dale W. Stovall, MD, Mihriye Mete, PhD, Casey
A Comparative Study between the Side Effects of Copper Intrauterine Device in Women with Non-scarred and Scarred Uterus
 Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 161-659 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ A Comparative Study between the Side Effects of Copper Intrauterine
Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 161-659 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ A Comparative Study between the Side Effects of Copper Intrauterine
Hormonal Contraception: Asian View. Hormonal Contraception: Asian View: focused on Chinese View. Prof.Dr.Xiangyan Ruan, MD.PhD
 Asian View Prof.Dr.Xiangyan Ruan, MD.PhD Beijing Obstetrics & Gynecology Hospital, Capital Medical University (China) WHO Collaborative Centre - Director of Dept. of Gynecological Endocrinology & & - Fertility
Asian View Prof.Dr.Xiangyan Ruan, MD.PhD Beijing Obstetrics & Gynecology Hospital, Capital Medical University (China) WHO Collaborative Centre - Director of Dept. of Gynecological Endocrinology & & - Fertility
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Table I. Examples of Hormone and Tapering Regimens
 Table I. Examples of Hormone and Tapering Regimens Severe AUB Heavy bleeding (soaking through 2 maxi pads an hour, 2 hours in a row) History of heavy menses Hemodynamically un (tachycardia, hypotensive,
Table I. Examples of Hormone and Tapering Regimens Severe AUB Heavy bleeding (soaking through 2 maxi pads an hour, 2 hours in a row) History of heavy menses Hemodynamically un (tachycardia, hypotensive,
Maximizing LARC Availability: Bringing the Lessons of the CHOICE Project to Your Community
 Maximizing LARC Availability: Bringing the Lessons of the CHOICE Project to Your Community Reproductive Health 2012 September 21, 2012 David Turok, MD/MPH Objectives Communicate to colleagues the reduction
Maximizing LARC Availability: Bringing the Lessons of the CHOICE Project to Your Community Reproductive Health 2012 September 21, 2012 David Turok, MD/MPH Objectives Communicate to colleagues the reduction
Ardhanu Kusumanto Oktober Contraception methods for gyne cancer survivors
 Ardhanu Kusumanto Oktober 2017 Contraception methods for gyne cancer survivors Background cancer treatment Care of gyn cancer survivor Promotion of sexual, cardiovascular, bone, and brain health management
Ardhanu Kusumanto Oktober 2017 Contraception methods for gyne cancer survivors Background cancer treatment Care of gyn cancer survivor Promotion of sexual, cardiovascular, bone, and brain health management
INTRAUTERINE DEVICES AND INFECTIONS. Tips for Evaluation and Management
 INTRAUTERINE DEVICES AND INFECTIONS Tips for Evaluation and Management Objectives At the end of this presentation, the participant should be able to: 1. Diagnose infection after IUD placement 2. Provide
INTRAUTERINE DEVICES AND INFECTIONS Tips for Evaluation and Management Objectives At the end of this presentation, the participant should be able to: 1. Diagnose infection after IUD placement 2. Provide
INTERVENTIONAL PROCEDURES PROGRAMME
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of microwave endometrial ablation Introduction This overview has been prepared to assist
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of microwave endometrial ablation Introduction This overview has been prepared to assist
Information for Informed Consent for Insertion of a Mirena IUD
 Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
World Health Organization Medical Eligibility for Contraceptive Use. Connie Kraus, PharmD, BCACP Professor (CHS) Director Office of Global Health
 World Health Organization Medical Eligibility for Contraceptive Use Connie Kraus, PharmD, BCACP Professor (CHS) Director Office of Global Health Objectives After this session, learners should be able to:
World Health Organization Medical Eligibility for Contraceptive Use Connie Kraus, PharmD, BCACP Professor (CHS) Director Office of Global Health Objectives After this session, learners should be able to:
PALM-COEIN: Your AUB Counseling Guide
 PALM-COEIN: Your AUB Counseling Guide 10 million+ Treat the cause, not the symptom In the U.S, more than 10 million women between the ages of 35 and 49 are affected by AUB 1 Diagnosis Cause Structural
PALM-COEIN: Your AUB Counseling Guide 10 million+ Treat the cause, not the symptom In the U.S, more than 10 million women between the ages of 35 and 49 are affected by AUB 1 Diagnosis Cause Structural
2
 1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
REPRODUCTIVE ENDOCRINOLOGY
 REPRODUCTIVE ENDOCRINOLOGY FERTILITY AND STERILITY VOL. 76, NO. 2, AUGUST 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in
REPRODUCTIVE ENDOCRINOLOGY FERTILITY AND STERILITY VOL. 76, NO. 2, AUGUST 2001 Copyright 2001 American Society for Reproductive Medicine Published by Elsevier Science Inc. Printed on acid-free paper in
Please fill out the following information and have it returned to our office prior to your consultation.
 Please fill out the following information and have it returned to our office prior to your consultation. Patient s Name Partner s Name Address: City: State: Zip: Phone (day#): ( ) (eve#) ( ) (cell) ( )
Please fill out the following information and have it returned to our office prior to your consultation. Patient s Name Partner s Name Address: City: State: Zip: Phone (day#): ( ) (eve#) ( ) (cell) ( )
Management of Emergency Contraception (EC)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Management of Emergency Contraception (EC) The risks and benefits of an IUD or oral EC should be discussed and documented (see appendix). Reasonable measures
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Management of Emergency Contraception (EC) The risks and benefits of an IUD or oral EC should be discussed and documented (see appendix). Reasonable measures
الحمد هلل رب العالمين والصالة والسالم علي محمد الصادق الوعد األمين اللهم أخرجنا من ظلمات الجهل والوهم إلى نور المعرفة والعلم..
 الحمد هلل رب العالمين والصالة والسالم علي محمد الصادق الوعد األمين اللهم أخرجنا من ظلمات الجهل والوهم إلى نور المعرفة والعلم.. سيدنا 11/6/2013 1 Goals of Family Planning services : 1- Enable women and
الحمد هلل رب العالمين والصالة والسالم علي محمد الصادق الوعد األمين اللهم أخرجنا من ظلمات الجهل والوهم إلى نور المعرفة والعلم.. سيدنا 11/6/2013 1 Goals of Family Planning services : 1- Enable women and
ClincialTrials.gov Identifier: sanofi-aventis. Sponsor/company:
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClincialTrials.gov
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription Sponsor/company: sanofi-aventis ClincialTrials.gov
Emergency Contraception THE FACTS
 Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
CURRENT HORMONAL CONTRACEPTION - LIMITATIONS
 CURRENT HORMONAL CONTRACEPTION - LIMITATIONS Oral Contraceptives - Features MERITS Up to 99.9% efficacy if used correctly and consistently Reversible method rapid return of fertility Offer non-contraceptive
CURRENT HORMONAL CONTRACEPTION - LIMITATIONS Oral Contraceptives - Features MERITS Up to 99.9% efficacy if used correctly and consistently Reversible method rapid return of fertility Offer non-contraceptive
Intrauterine Devices (IUDs): Access for Women in the U.S.
 November 2016 Fact Sheet Intrauterine Devices (IUDs): Access for Women in the U.S. Intrauterine devices (IUDs) are one of the most effective forms of reversible contraception. IUDs, along with implants,
November 2016 Fact Sheet Intrauterine Devices (IUDs): Access for Women in the U.S. Intrauterine devices (IUDs) are one of the most effective forms of reversible contraception. IUDs, along with implants,
 Non-contraceptive Uses of the Levonorgestrel Intrauterine Device Elena Gates, MD http://www.mirena-us.com/pvs1/pri/whatisframe.html Progestin levels with LNG- IUS Lower plasma levels Mirena 150-200 pg/ml
Non-contraceptive Uses of the Levonorgestrel Intrauterine Device Elena Gates, MD http://www.mirena-us.com/pvs1/pri/whatisframe.html Progestin levels with LNG- IUS Lower plasma levels Mirena 150-200 pg/ml
WHAT ARE CONTRACEPTIVES?
 CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
Orals,Transdermals, and Other Estrogens in the Perimenopause
 Orals,Transdermals, and Other Estrogens in the Perimenopause Cases Denise Black, MD, FRCSC Assistant Professor, Obstetrics, Gynecology and Reproductive Sciences University of Manitoba 6/4/18 197 Faculty/Presenter
Orals,Transdermals, and Other Estrogens in the Perimenopause Cases Denise Black, MD, FRCSC Assistant Professor, Obstetrics, Gynecology and Reproductive Sciences University of Manitoba 6/4/18 197 Faculty/Presenter
the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD your guide to
 your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
PFIZER INC. THERAPEUTIC AREA AND FDA APPROVED INDICATIONS: See USPI.
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
Unintended Pregnancy in U.S. The Importance of LARC: What have We Learned? Long-acting Reversible Contraception (LARC)
 Unintended Pregnancy in U.S. The Importance of LARC: What have We Learned? Colleen McNicholas, DO, MSCI Department of Obstetrics & Gynecology Washington University in St. Louis School of Medicine Over
Unintended Pregnancy in U.S. The Importance of LARC: What have We Learned? Colleen McNicholas, DO, MSCI Department of Obstetrics & Gynecology Washington University in St. Louis School of Medicine Over
UKMEC SUMMARY TABLE HORMONAL AND INTRAUTERINE CONTRACEPTION
 SUMMARY TABLE SUMMARY TABLE HORMONAL AND INTRAUTERINE CONTRACEPTION Cu-IUD = Copper-bearing intrauterine device; LNG-IUS = Levonorgestrel-releasing intrauterine system; IMP = Progestogen-only implant;
SUMMARY TABLE SUMMARY TABLE HORMONAL AND INTRAUTERINE CONTRACEPTION Cu-IUD = Copper-bearing intrauterine device; LNG-IUS = Levonorgestrel-releasing intrauterine system; IMP = Progestogen-only implant;
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial
 The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial A Multi-Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot Medroxyprogesterone
The Evidence for Contraceptive Options and HIV Outcomes (ECHO) Trial A Multi-Center, Open-Label, Randomised Clinical Trial Comparing HIV Incidence and Contraceptive Benefits in Women using Depot Medroxyprogesterone
CODING GUIDELINES FOR CONTRACEPTIVES. Effective June 1, 2017 Version 1.40
 CODING GUIDELINES FOR CONTRACEPTIVES Effective June 1, 2017 Version 1.40 TABLE OF CONTENTS ICD-10 CM Diagnosis Codes: Encounter for Contraception page 2 Coding for IUD Insertion and Removal Procedures
CODING GUIDELINES FOR CONTRACEPTIVES Effective June 1, 2017 Version 1.40 TABLE OF CONTENTS ICD-10 CM Diagnosis Codes: Encounter for Contraception page 2 Coding for IUD Insertion and Removal Procedures
Jadelle Contraceptive Implants up to 5 years Insertion and Removal
 Contraceptive Implants up to 5 years Bayer AG Global HealthCare Programs Family Planning 13342 Berlin, Germany www.bayer.com September 2017 Global HealthCare Programs Family Planning Contraceptive Independence»»
Contraceptive Implants up to 5 years Bayer AG Global HealthCare Programs Family Planning 13342 Berlin, Germany www.bayer.com September 2017 Global HealthCare Programs Family Planning Contraceptive Independence»»
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Partial and complete expulsion of the Multiload 375 IUD and the levonorgestrel-releasing
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Partial and complete expulsion of the Multiload 375 IUD and the levonorgestrel-releasing
Long-Acting Reversible Contraception: The Contraceptive CHOICE Project
 Long-Acting Reversible Contraception: The Contraceptive CHOICE Project Jeffrey F. Peipert, M.D., Ph.D. Vice Chair of Clinical Research Robert J. Terry Professor Department of Obstetrics & Gynecology Washington
Long-Acting Reversible Contraception: The Contraceptive CHOICE Project Jeffrey F. Peipert, M.D., Ph.D. Vice Chair of Clinical Research Robert J. Terry Professor Department of Obstetrics & Gynecology Washington
Primary Care Gynaecology Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
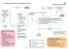 Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
The modern intrauterine device (IUD) is highly reliable and
 Intrauterine Device Knowledge and Practices: A National Survey of Obstetrics and Gynecology Residents Jennifer Tang, MD, MSCR, Rie Maurer, MA, and Deborah Bartz, MD, MPH Objectives: The primary objective
Intrauterine Device Knowledge and Practices: A National Survey of Obstetrics and Gynecology Residents Jennifer Tang, MD, MSCR, Rie Maurer, MA, and Deborah Bartz, MD, MPH Objectives: The primary objective
Contraception for Obese Women RENEE E. MESTAD, MD, MSCI ACOG DISTRICT II UPSTATE MEETING APRIL 29, 2016
 Contraception for Obese Women RENEE E. MESTAD, MD, MSCI ACOG DISTRICT II UPSTATE MEETING APRIL 29, 2016 Disclosure I am a Nexplanon trainer for Merck. Objectives Understand how obesity may affect pharmacokinetics
Contraception for Obese Women RENEE E. MESTAD, MD, MSCI ACOG DISTRICT II UPSTATE MEETING APRIL 29, 2016 Disclosure I am a Nexplanon trainer for Merck. Objectives Understand how obesity may affect pharmacokinetics
Patient or Clinician: Duration of Use of Intrauterine Devices Based on Who Initiated Discussion of Placement
 ORIGINAL RESEARCH Patient or Clinician: Duration of Use of Intrauterine Devices Based on Who Initiated Discussion of Placement Tammy Chang, MD, MPH, MS, Michelle H. Moniz, MD, MSc, Melissa A. Plegue, MA,
ORIGINAL RESEARCH Patient or Clinician: Duration of Use of Intrauterine Devices Based on Who Initiated Discussion of Placement Tammy Chang, MD, MPH, MS, Michelle H. Moniz, MD, MSc, Melissa A. Plegue, MA,
Reproductive and Sexual Health Subcommittee of PTAC. Meeting held 10 April (minutes for web publishing)
 Reproductive and Sexual Health Subcommittee of PTAC Meeting held 10 April 2017 (minutes for web publishing) Reproductive and Sexual Health Subcommittee minutes are published in accordance with the Terms
Reproductive and Sexual Health Subcommittee of PTAC Meeting held 10 April 2017 (minutes for web publishing) Reproductive and Sexual Health Subcommittee minutes are published in accordance with the Terms
Removing Unnecessary Barriers to Contraceptive Services
 Title X Grantee Meeting July 31, 2013 Seattle, WA Removing Unnecessary Barriers to Contraceptive Services Michael Policar, MD, MPH Professor of Ob, Gyn, and Repro Sciences UCSF School of Medicine policarm@obgyn.ucsf.edu
Title X Grantee Meeting July 31, 2013 Seattle, WA Removing Unnecessary Barriers to Contraceptive Services Michael Policar, MD, MPH Professor of Ob, Gyn, and Repro Sciences UCSF School of Medicine policarm@obgyn.ucsf.edu
CHINA STUDY. Friendly Collaboration And Fruitful Achievement. Introduction
 CHINA STUDY Friendly Collaboration And Fruitful Achievement Some Experiences and Understandings of the Research Work on the Billings Ovulation Method used in Shanghai, China by: Dr. Zhang De-wei, Advisor-
CHINA STUDY Friendly Collaboration And Fruitful Achievement Some Experiences and Understandings of the Research Work on the Billings Ovulation Method used in Shanghai, China by: Dr. Zhang De-wei, Advisor-
Immediate Postpartum Long-Term Reversible Contraception (LARC) Bethany Berry, CNM, MSN and Alyssa Givens, MSN, RN
 Immediate Postpartum Long-Term Reversible Contraception (LARC) Bethany Berry, CNM, MSN and Alyssa Givens, MSN, RN Disclosures O Bethany Berry CNM is a Nexplanon trainer with Merck O Alyssa Givens, RN has
Immediate Postpartum Long-Term Reversible Contraception (LARC) Bethany Berry, CNM, MSN and Alyssa Givens, MSN, RN Disclosures O Bethany Berry CNM is a Nexplanon trainer with Merck O Alyssa Givens, RN has
The 45-year-old woman with monthly headaches. Anne MacGregor Barts and the London School of Medicine and Dentistry
 The 45-year-old woman with monthly headaches Anne MacGregor Barts and the London School of Medicine and Dentistry Learning Objectives Use of diary cards for establishing patterns of attacks Importance
The 45-year-old woman with monthly headaches Anne MacGregor Barts and the London School of Medicine and Dentistry Learning Objectives Use of diary cards for establishing patterns of attacks Importance
Dr Mary Birdsall. Fertility Associates Auckland
 Dr Mary Birdsall Fertility Associates Auckland Period Problems Mary Birdsall Medical Director Fertility Associates Auckland Period Problems Basic Physiology No Periods Irregular Periods Heavy Periods
Dr Mary Birdsall Fertility Associates Auckland Period Problems Mary Birdsall Medical Director Fertility Associates Auckland Period Problems Basic Physiology No Periods Irregular Periods Heavy Periods
PFIZER INC. What is the difference in incidence of fracture in women who ever or never used DMPA for contraception?
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
MDHHS: Coding and Billing for Contraceptive Services
 1 The correct answer is B. A separate preventive E/M service was provided and a 25 modifier is necessary. The correct code is 99385 based on Lisa being new to the practice and being between 18 and 39 years
1 The correct answer is B. A separate preventive E/M service was provided and a 25 modifier is necessary. The correct code is 99385 based on Lisa being new to the practice and being between 18 and 39 years
Contraception for Adolescents: What s New?
 Contraception for Adolescents: What s New? US Medical Eligibility Criteria for Contraceptive Use Kathryn M. Curtis, PhD Division of Reproductive Health, CDC Expanding Our Experience and Expertise: Implementing
Contraception for Adolescents: What s New? US Medical Eligibility Criteria for Contraceptive Use Kathryn M. Curtis, PhD Division of Reproductive Health, CDC Expanding Our Experience and Expertise: Implementing
CLEAR COVERAGE HYSTERECTOMY CHECKLISTS
 CLEAR COVERAGE HYSTERECTOMY CHECKLISTS Click on the link below to access the checklist sheet. Abnormal Uterine Bleeding Adenomyosis Chronic Abdominal or Pelvic Pain Endometriosis Fibroids General Guidelines
CLEAR COVERAGE HYSTERECTOMY CHECKLISTS Click on the link below to access the checklist sheet. Abnormal Uterine Bleeding Adenomyosis Chronic Abdominal or Pelvic Pain Endometriosis Fibroids General Guidelines
Long Acting Reversible Contraception: First Line Care for Adolescents. David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG
 Long Acting Reversible Contraception: First Line Care for Adolescents David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG Disclosures Melissa Kottke is a Nexplanon trainer for Merck Objectives Describe
Long Acting Reversible Contraception: First Line Care for Adolescents David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG Disclosures Melissa Kottke is a Nexplanon trainer for Merck Objectives Describe
