Emergency and Critical Care Pharmacology: Commonly Used Drugs
|
|
|
- Georgiana Cole
- 6 years ago
- Views:
Transcription
1 Emergency and Critical Care Pharmacology: Commonly Used Drugs HAROLD DAVIS, BA, RVT, VTS (ECC) (ANESTH/ANALGESIA ) General Nursing Considerations Indications Medication dilution Constant rate infusions (CRI) Medication compatibility The Kings Guide to Parenteral Admixtures ( Handbook of Injectable Drugs Knowledge of potential side effects or adverse reactions Plumb s Veterinary Drug Handbook Kings Guide to Parenteral Admixtures 1
2 Constant Rate Infusions (CRI) Used in drugs that have rapid onset and short duration of action Reduces amount of drug used over time Avoids peaks and valleys Quick CRI Formula #1 45 kg patient to receive 5 µg/kg/min dopamine CRI BW kg x Dose (µg/kg/min) = mg drug qs to 250 ml of NaCl Administer at 15 ml/hr 45 x 5 = 225 mg 5.6 ml of 40 mg/ml dopamine is placed in 244 ml NaCl and given at 15 ml/hr CRI Formula # 2 (Mg Drug to Add to a Solution) 45 kg patient to receive 5 µg/kg/min dopamine CRI M = (D) (W) (V) / (R) (16.67) M = (5) (45) (250) / (15) (16.67) M = 56,250 / 250 M = 225 mg M = milligrams of drug to add to base solution D = dosage of drug in mcg per kg per min D adjusted = new dose rate of drug W = body weight in kg V = volume in ml of base solution R = fluid rate in ml/hr = conversion factor 2
3 CRI Formula # 2 (Change in Rate) 45 kg patient to receive 10 µg/kg/min dopamine CRI R = (D adjusted) (W) (V) / (M) (16.67) R = (10) (45) (250) / (225) (16.67) R = 112,500 / 3, R = 30 ml/hr M = milligrams of drug to add to base solution D = dosage of drug in mcg per kg per min D adjusted = new dose rate of drug W = body weight in kg V = volume in ml of base solution R = fluid rate in ml/hr = conversion factor Oxygen Therapy Indications Hypoxemia PaO 2 < 80 mmhg SpO 2 < 95% Respiratory distress Objective Correct hypoxemia using the lowest possible FIO 2 techniques Pros Cons Oxygen Therapy 3
4 Oxygen Therapy Oxygen Therapy Contraindications Potential complications Diminished or lost the hypercapnic respiratory stimulus to breath Oxygen toxicity FIO 2 100% hrs FIO 2 > 60 % not more than hrs. Airway inflammation, increased tissue permeability resulting in pulmonary edema, and finally interstitial fibrosis and permanent lung damage Crystalloids Composition Sodium, chloride, potassium, magnesium or calcium, buffer Sodium distribution Sodium major solute in extracellular space, majority extracellular space is extravascular, therefore sodium will reside outside the vascular space Classification Extracellular fluid (ECF) replacement (Isotonic) Maintenance (Hypotonic) Hypertonic 4
5 Electrolyte Composition of Fluids Solution Na + K + Cl - Ca 2+ Mg 2+ HCO 3 Osmolarity (meq/l) (meq/l) (meq/l) Like anion (mosm/l) (meq/l) ECF (Plasma) Lactated Ringers Lactate 274 Hartmann s Lactate 278 Normosol R Acetate Gluconate Plasmalyte Acetate 23 Gluconate % NaCl % NaCl Normosol M in5% Dextrose Acetate 364 Plasmalyte Acetate % Dextrose in ½ strength Lactated Ringers Lactate 263 Colloids Large molecular weight solutions Colloid fluids contain a suspension of particles that exert an oncotic pressure that attracts water Better blood volume expanders than isotonic crystalloids, 50-80% of the infused volume remains in the intravascular space Colloid types Naturally occurring Synthetic Colloid Indications Crystalloids not effectively improving or maintaining blood volume restoration Administered when the total protein or albumin are decreased below 3.5 g/dl (35 g/l) or 1.5 g/dl (15 g/l) respectively To support colloid oncotic pressure when the COP is measured in the low teens If edema develops prior to adequate blood volume restoration Capillary permeability problems or capillary leak syndrome. Clotting factor replacement (Plasma) 5
6 Physical Properties of Isotonic Crystalloids and HES Isotonic crystalloids Hetastarch6% Average MW - kd Number Av MW-kD 0 69 Osmolality-mOsm/L COP - mmhg 0 33 Maximum volume expansion -% Duration of volume expansion - hrs Plasma half-life - hrs General Concerns Calculation of fluid volume are based on subjective data, potential inaccuracies occur. Necessary to reassess the patient often. The patient may require more or less of the original calculated fluid volume. You are looking for a resolution in the signs that indicated that the patient needed fluids. It is necessary to reassess the patient s condition frequently (i.e. about every minutes) during large or rapid volume fluid administration. Colloids and crystalloids can negatively affect coagulation factors HES solutions impairs coagulation Decreasing von Willebrand factor and factor VIII up to 80% Platelet function is also inhibited Anticholinergics - Atropine & Glycopyrrolate Parasympatholytic Blocks muscarinic stimulatory effects Salivation, lacrimation, vomiting diarrhea, miosis and bradycardia Indications Treat vagally mediated bradycardia Treat organophosphate carbamate toxicity Pre-anesthetic medication Atropine vs Glycopyrrolate Longer duration of action Does not cross theplacental or blood-brain barrier. Administration IM, IV 6
7 Sympathomimetics Indications When patient is unresponsive to vigorous fluid therapy When arterial blood pressure (BP), vasomotor tone, and tissue perfusion have not returned to acceptable levels Support myocardial contractility Examples: Dopamine Dobutamine Epinephrine Norepinephrine Components of O 2 Delivery Preload Map SVR SV Contractility CO Afterload DO 2 HR Hgb O 2 Content PaO 2 Dopamine Dose dependent effects Dopaminergic Beta 1 Alpha Given as CRI dilute D5W or 0.9% NaCl Starting in midrange dose, titrate (0.5-1µ/kg/min) to effect 7
8 Dobutamine Primarily beta 1 Increase contractility Reduce systemic vascular resistance Given as CRI dilute D5W or 0.9% NaCl Titrate to effect Epinephrine Alpha 1 Vasoconstriction Beta 1 Increase heart rate Beta 2 Dilates bronchioles Bolus or CRI Bolus in CPR Norepinephrine Alpha 1 Beta 1 Given as CRI dilute D5W or 0.9% NaCl Titrate to effect 8
9 Smooth Muscle Vasoconstrictor - Vasopressin Vasopressin acts as a direct peripheral smooth muscle vasoconstrictor Uses CPR alternative to epinephrine Septic shock Vasodilators Venodilators Expands vascular capacity by dilating veins, which, reduces preload and venous pressure. Reduce congestion but not improve cardiac output Example: Nitroglycerin Arterial vasodilators Decrease systemic vascular resistance, which reduces afterload and improves cardiac output Decreases the work of the heart Example: Clevidipine Venodilator - Nitroglycerin Applied transdermally, usually on the pinna of the ear or some other hairless spot Dose measured in inches by application of a strip of ointment to a measuring paper Gloves should be worn when applying the ointment Should not be touch application site with bare hands Application site should be rotated. 9
10 Arterial Vasodilator - Clevidipine Dihydropyridine calcium channel blocker and is a smooth muscle vasodilator Uses Goal reduce blood pressure Treat fulminant heart failure Severe hypertension Aseptic technique used when handling this medication Not diluted Dedicated IV line Should be used within 12 hours Arterial Vasodilator - Clevidipine Titrated to effect by doubling the dose every 90 seconds. As the blood pressure approaches goal, the infusion rate should be increased in smaller increments and titrated less frequently Primary concern is hypotension Heart rate and blood pressure should be measured continually Assess perfusion parameters until the patient is stable If hypotension, the drug is reduced or turned off; effects will dissipate within a few minutes. General Concerns - Vasoactive Drugs Most if not all drugs are titrated to effect Monitor Direct BP monitoring is desirable but indirect methods are also acceptable Regardless, it is recommended that BP is monitored Perfusion parameters Mentation, mucus membrane color, capillary refill time, heart rate, and pulse quality Sympathomimetics should not be a substitute for adequate volume restoration 10
11 Antiarrhythmic Lidocaine (Class 1B) Sodium channel blocker, binds to and block fast sodium channels responsible for rapid depolarization Indications Used to treat premature ventricular contractions or ventricular tachycardia if cardiovascularly unstable Initial bolus (undiluted), ifresponsive then CRI CRI Diluted in either D 5W or 0.9% NaCl compatible with LRS CRI is titrated to effect Titrated in 5 µg/kg/min increments every 10 to 15 min until: Desired effect is seen Maximum dose has been reached Adverse signs are seen Antiarrthymic Lidocaine (Class 1B) Potential adverse effect: Nausea Vomiting Tremors Seizures Hypotension Bradycardia General Cats more sensitive than dogs Used in much lower doses May exhibit central nervous system signs Weaning Slow or stop infusion, notify clinician Diuretic - Furosemide Loop diuretic, meaning it acts primarily in the ascending Loop of Henle Natriuretic Renal vasodilator Anuria / Oliguria Used in high doses for anuria If no effect another diuretic or combination of diuretics Used in low doses for oliguria Given as a IV bolus or CRI 11
12 Diuretic - Furosemide In heart failure decreases blood volumeand reduces capillary pressure Heart Failure IV bolus, IM, CRI As frequently as every hour until decrease in respiratory rate and /or effort improves CRI loading dose first Potential adverse effects Excessive diuresis and dehydration, Hypovolemia Hypotension Hypokalemia, hyponatremia, metabolic alkalosis Vomiting and diarrhea Potential for potentiating nephrotoxic effects of certain drugs Mannitol s Osmotic diuretic Free radical scavenger Rheologic properties Indications Increased intracranial pressure, cerebral edema Cushing s triad Deterioration level of consciousness Posturing Changes in resting pupil size and/or loss of pupillary light response Acute kidney injury Anuria / oliguria Mannitol May be given as an intermittent bolus or as a CRI. 20% and 25% mannitol Dilute 1:1 with D 5W for peripheral vein Use a 18 micron Hemo-Nate filter General Response may be seen within 10 minutes, maximal effects are noted at minutes. Mannitol may be contraindicated in patients with volume overload and intracranial hemorrhage Can be piggybacked with other crystalloids May crystalize when exposed to low temperatures; solutions less than 15% are less likely to crystalize 12
13 Regular Crystalline Insulin Promotes entry of glucose and potassium into the cell Inhibits the release of glucagon (prevents gluconeogenesis / glycogenolysis) Inhibit ketone production Indications Treatment of hyperglycemia secondary to DKA Treatment option for hyperkalemia Regular Crystalline Insulin - DKA Insulin Administration Intramuscular technique Insulin is administered every 2 hours based upon the blood glucose level while adjusting the dose up or down depending on the rate of declining glucose levels As blood glucose approaches 250 mg/dl the q 2 hour IM insulin dose can be changed to the subcutaneous route and administered everyfour to six hours. When the patient is eating and drinking, no longer ketotic and is not vomiting the regular insulin may be switched to a long acting form. Regular Crystalline Insulin - DKA Insulin Administration CRI technique With the regular insulin CRI, the regular insulin dose is diluted in 250 ml of 0.9 % saline. Insulin binds to glass and plastic, so, the first 50 ml of the infusion should be discarded. Insulin infusion is piggybacked on to the primary fluid line and administered with a fluid infusion pump Insulin rate is adjusted according to a dosing table The goal is essentially the same as the IM technique. 13
14 Regular Crystalline Insulin - Hyperkalemia Insulin Administration Insulin is given with dextrose to minimize the risk of the patient becoming hypoglycemic General Concerns Regular insulin is considered a fast acting insulin with a duration of 1 4 hours Blood glucose is monitored at the appropriate frequency Potential for adverse effects Signs seen related to overdose, at risk for hypoglycemia Weakness Ataxia Seizures Cerebral edema secondary to rapid glucose reduction (> 75 mg/dl/hr) Regular Crystalline Insulin General Concerns Regular insulin is considered a fast acting insulin with a duration of 1 4 hours Blood glucose is monitored at the appropriate frequency Potential for adverse effects: Signs seen related to overdose, at risk for hypoglycemia Weakness Ataxia Seizures Cerebral edema secondary to rapid glucose reduction (> 75 mg/dl/hr) Prokinetic - Metoclopramide Antiemetic action due to its antagonist activity at Dopamine D 2 receptors in the chemoreceptor trigger zone Mixed serotonin 5-HT3 receptor antagonist/5-ht4 receptor agonist Indication Enhance gastrointestinal motility and promote gastric emptying Can be given IV, subcutaneously, and orally CRI Dilute the drug to a concentration of 1 mg/ml in 0.9% NaCl Dose is divided over 24 hrs 14
15 Prokinetic - Metoclopramide Contraindications Contraindicated in cases of gastric outflow or gastrointestinal obstruction due to foreign body or intussusception Potential adverse effects Increase in seizure activity in epileptics Sedation Hyperactivity Changes in behavior Constipation Diarrhea Abdominal pain Serotonin 5HT 3 Antagonist - Ondansetron Indications Antiemetic and nausea Administered intravenously over 2 to 5 mins but no less than 30 seconds Compatibilities Plasmalyte A, 0.9 % NaCl, D 5W Incompatibilities Ampicillin, Timentin, Furosemide, and Enrofloxacin Potential adverse effect (Rare People) Hypotension, tachycardia, rash, neurologic signs and hypokalemia Protein pump inhibitor - Pantoprazole Indication Acid reducer GI protectant Standard dilution Administered over 3 5 minutes Dilution for CRI - diluted to 0.4 mg/ml in 0.9% NaCl Over 30 minutes Compatibilities Lactated Ringer s solution and D 5W Incompatibilities Midazolam, magnesium sulfate and zinc containing solutions Plasmalyte Adverse effects reported in people headache, diarrhea, constipation and abdominal pain 15
16 Summary Medication administration is not a benign procedure. Medication administration requires Forethought Attention to detail Vigilance 16
GENERAL NURSING CONSIDERATIONS
 Emergency and Critical Care Pharmacology: Commonly Used Drugs Harold Davis, BA, RVT, VTS (ECC) (Anesth/Analgesia) William R. Pritchard Veterinary Medical Teaching Hospital, University of California Davis,
Emergency and Critical Care Pharmacology: Commonly Used Drugs Harold Davis, BA, RVT, VTS (ECC) (Anesth/Analgesia) William R. Pritchard Veterinary Medical Teaching Hospital, University of California Davis,
HYPOVOLEMIA AND HEMORRHAGE UPDATE ON VOLUME RESUSCITATION HEMORRHAGE AND HYPOVOLEMIA DISTRIBUTION OF BODY FLUIDS 11/7/2015
 UPDATE ON VOLUME RESUSCITATION HYPOVOLEMIA AND HEMORRHAGE HUMAN CIRCULATORY SYSTEM OPERATES WITH A SMALL VOLUME AND A VERY EFFICIENT VOLUME RESPONSIVE PUMP. HOWEVER THIS PUMP FAILS QUICKLY WITH VOLUME
UPDATE ON VOLUME RESUSCITATION HYPOVOLEMIA AND HEMORRHAGE HUMAN CIRCULATORY SYSTEM OPERATES WITH A SMALL VOLUME AND A VERY EFFICIENT VOLUME RESPONSIVE PUMP. HOWEVER THIS PUMP FAILS QUICKLY WITH VOLUME
Vasoactive Medications. Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis
 Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Fundamentals of Pharmacology for Veterinary Technicians Chapter 19
 Figure 19-1 Figure 19-2A Figure 19-2B Figure 19-3 Figure 19-4A1 Figure 19-4A2 Figure 19-4B Figure 19-4C Figure 19-4D Figure 19-5 Figure 19-6A Figure 19-6B A Figure 19-7A B Figure 19-7B C Figure 19-7C D
Figure 19-1 Figure 19-2A Figure 19-2B Figure 19-3 Figure 19-4A1 Figure 19-4A2 Figure 19-4B Figure 19-4C Figure 19-4D Figure 19-5 Figure 19-6A Figure 19-6B A Figure 19-7A B Figure 19-7B C Figure 19-7C D
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES
 Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
KASHVET VETERINARIAN RESOURCES FLUID THERAPY AND SELECTION OF FLUIDS
 KASHVET VETERINARIAN RESOURCES FLUID THERAPY AND SELECTION OF FLUIDS INTRODUCTION Formulating a fluid therapy plan for the critical small animal patient requires careful determination of the current volume
KASHVET VETERINARIAN RESOURCES FLUID THERAPY AND SELECTION OF FLUIDS INTRODUCTION Formulating a fluid therapy plan for the critical small animal patient requires careful determination of the current volume
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
FLUID THERAPY: IT S MORE THAN JUST LACTATED RINGERS
 FLUID THERAPY: IT S MORE THAN JUST LACTATED RINGERS Elisa M. Mazzaferro, MS, DVM, PhD, DACVECC Cornell University Veterinary Specialists, Stamford, CT, USA Total body water constitutes approximately 60%
FLUID THERAPY: IT S MORE THAN JUST LACTATED RINGERS Elisa M. Mazzaferro, MS, DVM, PhD, DACVECC Cornell University Veterinary Specialists, Stamford, CT, USA Total body water constitutes approximately 60%
Taking the shock factor out of shock
 Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
INTRAVENOUS FLUIDS. Ahmad AL-zu bi
 INTRAVENOUS FLUIDS Ahmad AL-zu bi Types of IV fluids Crystalloids colloids Crystalloids Crystalloids are aqueous solutions of low molecular weight ions,with or without glucose. Isotonic, Hypotonic, & Hypertonic
INTRAVENOUS FLUIDS Ahmad AL-zu bi Types of IV fluids Crystalloids colloids Crystalloids Crystalloids are aqueous solutions of low molecular weight ions,with or without glucose. Isotonic, Hypotonic, & Hypertonic
Body fluid compartments Fluid Pharmacology Phases of fluid therapy. Fluid therapy during anesthesia Subcutaneous fluids
 Edward Cooper, VMD, MS, DACVECC Professor, Emergency and Critical Care The Ohio State University Body fluid compartments Fluid Pharmacology Phases of fluid therapy Resuscitation Replacement Maintenance
Edward Cooper, VMD, MS, DACVECC Professor, Emergency and Critical Care The Ohio State University Body fluid compartments Fluid Pharmacology Phases of fluid therapy Resuscitation Replacement Maintenance
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua
 Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients. Keliana O Mara, PharmD August 4, 2018
 The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments
 ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
Principles of Infusion Therapy: Fluids
 Principles of Infusion Therapy: Fluids Christie Heinzman, MSN, APRN-CNP Acute Care Pediatric Nurse Practitioner Cincinnati Children s Hospital Medical Center May 22, 2018 Conflict of Interest Disclosure
Principles of Infusion Therapy: Fluids Christie Heinzman, MSN, APRN-CNP Acute Care Pediatric Nurse Practitioner Cincinnati Children s Hospital Medical Center May 22, 2018 Conflict of Interest Disclosure
Proceeding of the LAVC Latin American Veterinary Conference Oct , 2011 Lima, Peru
 Close this window to return to IVIS www.ivis.org Proceeding of the LAVC Latin American Veterinary Conference Oct. 24-26, 2011 Lima, Peru Next LAVC Conference: Apr. 24-26, 2012 Lima, Peru Reprinted in the
Close this window to return to IVIS www.ivis.org Proceeding of the LAVC Latin American Veterinary Conference Oct. 24-26, 2011 Lima, Peru Next LAVC Conference: Apr. 24-26, 2012 Lima, Peru Reprinted in the
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Principles of Fluid Balance
 Principles of Fluid Balance I. The Cellular Environment: Fluids and Electrolytes A. Water 1. Total body water (TBW) = 60% of total body weight 2. Fluid Compartments in the Body a. Intracellular Compartment
Principles of Fluid Balance I. The Cellular Environment: Fluids and Electrolytes A. Water 1. Total body water (TBW) = 60% of total body weight 2. Fluid Compartments in the Body a. Intracellular Compartment
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE
 Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
How Normal Body Processes Are Altered By Disease and Injury
 1 Chapter 4, GENERAL PRINCIPLES OF PATHOPHYSIOLOGY. Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
1 Chapter 4, GENERAL PRINCIPLES OF PATHOPHYSIOLOGY. Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
9/13/2015. Laboratory. HPI and PE
 Critical Care HPI and PE 74 yo male confused SBP 90/20 MAP50, P 122, RR 34 Ox1 w/o nuchal rigidity S1S2 wo m RLL reduced breath sounds Skin warm dry Laboratory» WBC 15,600 Hgb 8.4 HCt 23%, Plts 95000,
Critical Care HPI and PE 74 yo male confused SBP 90/20 MAP50, P 122, RR 34 Ox1 w/o nuchal rigidity S1S2 wo m RLL reduced breath sounds Skin warm dry Laboratory» WBC 15,600 Hgb 8.4 HCt 23%, Plts 95000,
SHOCK. Pathophysiology
 SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
What would be the response of the sympathetic system to this patient s decrease in arterial pressure?
 CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Contra Costa County Emergency Medical Services Drug Reference. Indication Dosing Cautions Comments
 Drug Adenosine Albuterol Indication Dosing Cautions Comments Narrow complex tachycardia Bronchospasm Crush injury - hyperkalemia Initial 6mg rapid IV Repeat 12mg rapid IV Follow each dose with 20ml NS
Drug Adenosine Albuterol Indication Dosing Cautions Comments Narrow complex tachycardia Bronchospasm Crush injury - hyperkalemia Initial 6mg rapid IV Repeat 12mg rapid IV Follow each dose with 20ml NS
9/11/2012. Chapter 11. Learning Objectives. Learning Objectives. Endocrine Emergencies. Differentiate type 1 and type 2 diabetes
 Chapter 11 Endocrine Emergencies Learning Objectives Differentiate type 1 and type 2 diabetes Explain roles of glucagon, glycogen, and glucose in hypoglycemia Learning Objectives Discuss following medications
Chapter 11 Endocrine Emergencies Learning Objectives Differentiate type 1 and type 2 diabetes Explain roles of glucagon, glycogen, and glucose in hypoglycemia Learning Objectives Discuss following medications
Intravenous Infusions
 Intravenous Infusions 1) An IV insulin infusion can be used for patients: a) with out of control diabetes b) with DKA (Diabetic Ketoacidosis) c) after a heart attack 2) Hyperglycemia is an adaptive response
Intravenous Infusions 1) An IV insulin infusion can be used for patients: a) with out of control diabetes b) with DKA (Diabetic Ketoacidosis) c) after a heart attack 2) Hyperglycemia is an adaptive response
6 th Floor and 7 East Nurses Guide Intravenous Drip List Approved for RN Administration University of Kentucky Chandler Medical Center
 RATE Abciximab (Reopro) Alteplase (tpa, Activase) All units 6S and 6W ONLY Platelet aggregation inhibitor Thrombolytic agent Bolus: 0.25 mg/kg IV over 5 min Infusion: 0.125 0.9 mg/kg (max 90 mg); 10% of
RATE Abciximab (Reopro) Alteplase (tpa, Activase) All units 6S and 6W ONLY Platelet aggregation inhibitor Thrombolytic agent Bolus: 0.25 mg/kg IV over 5 min Infusion: 0.125 0.9 mg/kg (max 90 mg); 10% of
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Drug Max dose approved for IVP Dilution Rate Monitoring Parameters. Dilution not necessary (Available in prefilled syringe)
 Drug Max dose approved for IVP Dilution Rate Monitoring Parameters Acetazolamide 500 mg Reconstitute with at least 5ml sterile water (max concentration should not exceed 100mg/ml) 100-500 mg/min Hypotension
Drug Max dose approved for IVP Dilution Rate Monitoring Parameters Acetazolamide 500 mg Reconstitute with at least 5ml sterile water (max concentration should not exceed 100mg/ml) 100-500 mg/min Hypotension
How Normal Body Processes Are Altered By Disease and Injury
 1 Chapter 4, General Principles of Pathophysiology Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
1 Chapter 4, General Principles of Pathophysiology Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
How and why I give IV fluid Disclosures SCA Fluids and public health 4/1/15. Andrew Shaw MB FRCA FCCM FFICM
 How and why I give IV fluid Andrew Shaw MB FRCA FCCM FFICM Professor and Chief Cardiothoracic Anesthesiology Vanderbilt University Medical Center 2015 Disclosures Consultant for Grifols manufacturer of
How and why I give IV fluid Andrew Shaw MB FRCA FCCM FFICM Professor and Chief Cardiothoracic Anesthesiology Vanderbilt University Medical Center 2015 Disclosures Consultant for Grifols manufacturer of
PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker
 PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Human Albumin 200 g/l Baxter is a solution containing 200 g/l of total protein of which at least 95% is human albumin.
 1. NAME OF THE MEDICINAL PRODUCT Human Albumin 200 g/l Baxter Solution for Infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Human Albumin 200 g/l Baxter is a solution containing 200 g/l of total protein
1. NAME OF THE MEDICINAL PRODUCT Human Albumin 200 g/l Baxter Solution for Infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Human Albumin 200 g/l Baxter is a solution containing 200 g/l of total protein
SHOCK. May 12, 2011 Body and Disease
 SHOCK May 12, 2011 Body and Disease Shock Definition of shock Pathophysiology Types of shock Management of shock Shock Definition? Shock What the Duke Community would have experienced if Gordon Hayward
SHOCK May 12, 2011 Body and Disease Shock Definition of shock Pathophysiology Types of shock Management of shock Shock Definition? Shock What the Duke Community would have experienced if Gordon Hayward
Nursing Process Focus: Patients Receiving Dextran 40 (Gentran 40)
 Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT 2 QUALITATIVE AND QUANTITATIVE COMPOSITION
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Albunorm 20%, 200 g/l, solution for infusion 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Albunorm 20% is a solution containing 200 g/l
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Albunorm 20%, 200 g/l, solution for infusion 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Albunorm 20% is a solution containing 200 g/l
Dr. Nai Shun Tsoi Department of Paediatric and Adolescent Medicine Queen Mary Hospital Hong Kong SAR
 Dr. Nai Shun Tsoi Department of Paediatric and Adolescent Medicine Queen Mary Hospital Hong Kong SAR A very important aspect in paediatric intensive care and deserve more attention Basic principle is to
Dr. Nai Shun Tsoi Department of Paediatric and Adolescent Medicine Queen Mary Hospital Hong Kong SAR A very important aspect in paediatric intensive care and deserve more attention Basic principle is to
Diabetic Ketoacidosis
 Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Diabetic Ketoacidosis Definition: Diabetic Ketoacidosis is one of the most serious acute complications of diabetes. It s more common in young patients with type 1 diabetes mellitus. It s usually characterized
Change in Practice PCP Autonomous IV OBHG Education Subcommittee
 Change in Practice PCP Autonomous IV Intravenous and Fluid Therapy Medical Directive Auxiliary Ability to initiate IV access and Ability to administer fluid and fluid boluses in general IV Therapy Actual
Change in Practice PCP Autonomous IV Intravenous and Fluid Therapy Medical Directive Auxiliary Ability to initiate IV access and Ability to administer fluid and fluid boluses in general IV Therapy Actual
Nitroglycerin and Heparin Drip Interfacility Protocols
 Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Nitroglycerin and Heparin Drip Interfacility Protocols EMS Protocol This protocol applies to nitroglycerin and Heparin drips that are initiated at the transferring facility prior to transport and are not
Neonatal Fluid Therapy Not my mother s physiology!!
 Neonatal Fluid Therapy Not my mother s physiology!! Physiologic Approach to Neonatal Fluid Therapy General principles of fluid balance Fetal physiology of fluid balance Neonatal physiology of fluid balance
Neonatal Fluid Therapy Not my mother s physiology!! Physiologic Approach to Neonatal Fluid Therapy General principles of fluid balance Fetal physiology of fluid balance Neonatal physiology of fluid balance
Division 1 Introduction to Advanced Prehospital Care
 Division 1 Introduction to Advanced Prehospital Care Topics Fluids & fluid imbalances IV Therapy Hypoperfusion Shock Fluids and Fluid Imbalances 1 Water is the most abundant substance in the human body.
Division 1 Introduction to Advanced Prehospital Care Topics Fluids & fluid imbalances IV Therapy Hypoperfusion Shock Fluids and Fluid Imbalances 1 Water is the most abundant substance in the human body.
7/21/2017. Learning Objectives. Current Cardiovascular Pharmacology. Epinephrine. Cardiotonic Agents. Epinephrine. Epinephrine. Arthur Jones, EdD, RRT
 Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
(human albumin solution) POM SUMMARY OF PRODUCT CHARACTERISTICS
 albunorm TM 20% (human albumin solution) POM SUMMARY OF PRODUCT CHARACTERISTICS UK IRELAND and Ireland Octapharma Limited The Zenith Building, 26 Spring Gardens Manchester M2 1AB United Kingdom 1. Name
albunorm TM 20% (human albumin solution) POM SUMMARY OF PRODUCT CHARACTERISTICS UK IRELAND and Ireland Octapharma Limited The Zenith Building, 26 Spring Gardens Manchester M2 1AB United Kingdom 1. Name
3. PHARMACEUTICAL FORM Solution for infusion. A clear, slightly viscous liquid; it is almost colourless, yellow, amber or green.
 1. NAME OF THE MEDICINAL PRODUCT Albutein 250 g/l, solution for infusion. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Human albumin Albutein 250 g/l is a solution containing 250 g/l of total protein of
1. NAME OF THE MEDICINAL PRODUCT Albutein 250 g/l, solution for infusion. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Human albumin Albutein 250 g/l is a solution containing 250 g/l of total protein of
2 QUALITATIVE AND QUANTITATIVE COMPOSITION
 SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Albunorm 5%, 50 g/l, solution for infusion 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Albunorm 5% is a solution containing 50 g/l of total
SUMMARY OF PRODUCT CHARACTERISTICS 1 NAME OF THE MEDICINAL PRODUCT Albunorm 5%, 50 g/l, solution for infusion 2 QUALITATIVE AND QUANTITATIVE COMPOSITION Albunorm 5% is a solution containing 50 g/l of total
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Understanding the pediatric patient and basics of pediatric emergencies. Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS
 Understanding the pediatric patient and basics of pediatric emergencies Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS Stages of development Neonatal period - from birth till 3 rd -4 th week Weaning period
Understanding the pediatric patient and basics of pediatric emergencies Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS Stages of development Neonatal period - from birth till 3 rd -4 th week Weaning period
SUMMARY OF PRODUCT CHARACTERISTICS. Flexbumin 200 g/l is a solution containing 200 g/l (20%) of total protein of which at least 95% is human albumin.
 SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Flexbumin 200g/l solution for infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Flexbumin 200 g/l is a solution containing 200 g/l
SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT Flexbumin 200g/l solution for infusion 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Flexbumin 200 g/l is a solution containing 200 g/l
Standard Operating Procedure (SOP) Management of intervention group patients SOP 001
 ` Standard Operating Procedure (SOP) Management of intervention group patients SOP 001 Authors: Mark Edwards & Rupert Pearse Authorisation: Rupert Pearse (Chief Investigator) Scope To provide guidance
` Standard Operating Procedure (SOP) Management of intervention group patients SOP 001 Authors: Mark Edwards & Rupert Pearse Authorisation: Rupert Pearse (Chief Investigator) Scope To provide guidance
Medical Treatment for acute Decompensated Heart Failure. Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011
 Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Medical Treatment for acute Decompensated Heart Failure Vlasis Ninios Cardiologist St. Luke s s Hospital Thessaloniki 2011 2010 HFSA guidelines for ADHF 2009 focused update of the 2005 American College
Presented by: Indah Dwi Pratiwi
 Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Presented by: Indah Dwi Pratiwi Normal Fluid Requirements Resuscitation Fluids Goals of Resuscitation Maintain normal body temperature In most cases, elevate the feet and legs above the level of the heart
Failure of the circulation to maintain Tissue cellular. Tissue hypoperfusion Cellular hypoxia SHOCK. Perfusion
 Shock SHOCK Failure of the circulation to maintain Tissue cellular Perfusion Organs Syndrome RR
Shock SHOCK Failure of the circulation to maintain Tissue cellular Perfusion Organs Syndrome RR
COMPANY CORE PACKAGE INSERT CCPI (PI/CORE/ENGLISH)
 COMPANY CORE PACKAGE INSERT CCPI (PI/CORE/ENGLISH) HUMAN ALBUMIN 20 % BEHRING Rev.: 05-MAR-2008 / PEI approval 26.02.08 Supersedes previous versions Rev.: 28-NOV-2007 / Adaptation to Core SPC Rev.: 02-JAN-2007
COMPANY CORE PACKAGE INSERT CCPI (PI/CORE/ENGLISH) HUMAN ALBUMIN 20 % BEHRING Rev.: 05-MAR-2008 / PEI approval 26.02.08 Supersedes previous versions Rev.: 28-NOV-2007 / Adaptation to Core SPC Rev.: 02-JAN-2007
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers HOW
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers HOW
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
DRUG GUIDELINE. HYDRALAZINE (Intravenous severe hypertension in pregnancy)
 DRUG GUIDELINE HYDRALAZINE (Intravenous severe hypertension SCOPE (Area): FOR USE IN: Labour Ward, HDU, Theatre and ED EXCLUSIONS: Paediatrics (seek Paediatrician advice) and other general wards. SCOPE
DRUG GUIDELINE HYDRALAZINE (Intravenous severe hypertension SCOPE (Area): FOR USE IN: Labour Ward, HDU, Theatre and ED EXCLUSIONS: Paediatrics (seek Paediatrician advice) and other general wards. SCOPE
Pare. Blalock. Shires. shock caused by circulating toxins treatment with phlebotomy. shock caused by hypovolemia treatment with plasma replacement
 Pare shock caused by circulating toxins treatment with phlebotomy Blalock shock caused by hypovolemia treatment with plasma replacement Shires deficit in functional extracellular volume treatment with
Pare shock caused by circulating toxins treatment with phlebotomy Blalock shock caused by hypovolemia treatment with plasma replacement Shires deficit in functional extracellular volume treatment with
The Mentally Altered Diabetic Diagnosis and Management of Hyperosmolar Hyperglycemic Syndrome Christy Michael, BVMS, MBA
 The Mentally Altered Diabetic Diagnosis and Management of Hyperosmolar Hyperglycemic Syndrome Christy Michael, BVMS, MBA Introduction When a mentally altered patient arrives on the scene at any veterinary
The Mentally Altered Diabetic Diagnosis and Management of Hyperosmolar Hyperglycemic Syndrome Christy Michael, BVMS, MBA Introduction When a mentally altered patient arrives on the scene at any veterinary
MOVING IN AND PREVENTING THE KILL Elke Rudloff, DVM, DACVECC
 RESUSCITATION FROM HYPOVOLEMIC SHOCK: MOVING IN AND PREVENTING THE KILL Elke Rudloff, DVM, DACVECC EMERGENCY AND CRITICAL CARE Shock is a phenomenon manifesting as inadequate tissue perfusion resulting
RESUSCITATION FROM HYPOVOLEMIC SHOCK: MOVING IN AND PREVENTING THE KILL Elke Rudloff, DVM, DACVECC EMERGENCY AND CRITICAL CARE Shock is a phenomenon manifesting as inadequate tissue perfusion resulting
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
Medical Management of Acutely Decompensated Heart Failure. William T. Abraham, MD Director, Division of Cardiovascular Medicine
 Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
Medical Management of Acutely Decompensated Heart Failure William T. Abraham, MD Director, Division of Cardiovascular Medicine Orlando, Florida October 7-9, 2011 Goals of Acute Heart Failure Therapy Alleviate
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
ALS MODULE 7 Pharmacology
 ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
Acute Liver Failure: Supporting Other Organs
 Acute Liver Failure: Supporting Other Organs Michael A. Gropper, MD, PhD Professor of Anesthesia and Physiology Director, Critical Care Medicine University of California San Francisco Acute Liver Failure
Acute Liver Failure: Supporting Other Organs Michael A. Gropper, MD, PhD Professor of Anesthesia and Physiology Director, Critical Care Medicine University of California San Francisco Acute Liver Failure
Electrolytes Solution
 Electrolytes Solution Substances that are not dissociated in solution are called nonelectrolytes, and those with varying degrees of dissociation are called electrolytes. Urea and dextrose are examples
Electrolytes Solution Substances that are not dissociated in solution are called nonelectrolytes, and those with varying degrees of dissociation are called electrolytes. Urea and dextrose are examples
Dr. Rezzan Khan Consultant Nutritionist Shifa International Hospital
 Dr. Rezzan Khan Consultant Nutritionist Shifa International Hospital Concept of Fluid & Electrolyte Balance Body fluid and electrolyte homeostasis Differentiate between hypovolemic, euvolemic, and hypervolemic
Dr. Rezzan Khan Consultant Nutritionist Shifa International Hospital Concept of Fluid & Electrolyte Balance Body fluid and electrolyte homeostasis Differentiate between hypovolemic, euvolemic, and hypervolemic
Organ Donor Management Recommended Guidelines ADULT Brain Death (NDD)
 Date: Time: = Always applicable = Check if applicable ADMISSION INSTRUCTIONS Neurological Determination of Death (NDD) has been performed by at least 2 licensed physicians Contact initiated with BC Transplant
Date: Time: = Always applicable = Check if applicable ADMISSION INSTRUCTIONS Neurological Determination of Death (NDD) has been performed by at least 2 licensed physicians Contact initiated with BC Transplant
Sodium Bicarbonate Injection, USP
 Sodium Bicarbonate Injection, USP FOR THE CORRECTION OF METABOLIC ACIDOSIS AND OTHER CONDITIONS REQUIRING SYSTEMIC ALKALINIZATION. Plastic Ansyr II Syringe R x only DESCRIPTION Sodium Bicarbonate Injection,
Sodium Bicarbonate Injection, USP FOR THE CORRECTION OF METABOLIC ACIDOSIS AND OTHER CONDITIONS REQUIRING SYSTEMIC ALKALINIZATION. Plastic Ansyr II Syringe R x only DESCRIPTION Sodium Bicarbonate Injection,
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Blanchard Valley Hospital Pharmacy Code Blue Overview
 Blanchard Valley Hospital Pharmacy Code Blue Overview Adapted from Gary Spanik, RPh Edited by Kate Reeves, Pharm D, RPh Jon Manocchio, Pharm D, RPh Pharmacist Responsibilities Be aware of basic ACLS tenets
Blanchard Valley Hospital Pharmacy Code Blue Overview Adapted from Gary Spanik, RPh Edited by Kate Reeves, Pharm D, RPh Jon Manocchio, Pharm D, RPh Pharmacist Responsibilities Be aware of basic ACLS tenets
Categories & Complications
 Shock, Fluid & Therapy Arthur Jones, EdD, RRT Learning Objectives: Explain the etiologies, manifestations and management of shock. Describe specific agents used to maintain blood pressure, fluid balance
Shock, Fluid & Therapy Arthur Jones, EdD, RRT Learning Objectives: Explain the etiologies, manifestations and management of shock. Describe specific agents used to maintain blood pressure, fluid balance
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION
 DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
DBL MAGNESIUM SULFATE CONCENTRATED INJECTION NAME OF MEDICINE Magnesium Sulfate BP DESCRIPTION DBL Magnesium Sulfate Concentrated Injection is a clear, colourless, sterile solution. Each ampoule contains
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
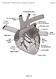 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Unit 11. Objectives. Indications for IV Therapy. Intravenous Access Devices & Common IV Fluids. 3 categories. Maintenance Replacement Restoration
 Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
Unit 11 Fluids, Electrolytes and Acid Base Imbalances Intravenous Access Devices & Common IV Fluids Objectives Review the purpose and types of intravenous (IV) therapy. Recall the nursing care related
*Sections or subsections omitted from the full prescribing information are not listed.
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use GIAPREZA TM safely and effectively. See full prescribing information for GIAPREZA. GIAPREZA (angiotensin
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use GIAPREZA TM safely and effectively. See full prescribing information for GIAPREZA. GIAPREZA (angiotensin
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
CCRN Review - Renal. CCRN Review - Renal 10/16/2014. CCRN Review Renal. Sodium Critical Value < 120 meq/l > 160 meq/l
 CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
CCRN Review Renal Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Sodium 136-145 Critical Value < 120 meq/l > 160 meq/l Sodium Etiology
2
 1 2 3 4 5 6 7 8 Please check regional policy on Tetracaine and Morgan Lens this may be optional in your region. *Ketamine and Fentanyl must be added to your controlled substance license if required by
1 2 3 4 5 6 7 8 Please check regional policy on Tetracaine and Morgan Lens this may be optional in your region. *Ketamine and Fentanyl must be added to your controlled substance license if required by
VENTRICULAR FIBRILLATION. 1. Safe scene, standard precautions. 2. Establish unresponsiveness, apnea, and pulselessness. 3. Quick look (monitor)
 LUCAS COUNTY EMS SUMMARY PAGES VENTRICULAR FIBRILLATION 2. Establish unresponsiveness, apnea, and pulselessness 3. Quick look (monitor) 4. Identify rhythm 5. Provide 2 minutes CPR if unwitnessed by EMS
LUCAS COUNTY EMS SUMMARY PAGES VENTRICULAR FIBRILLATION 2. Establish unresponsiveness, apnea, and pulselessness 3. Quick look (monitor) 4. Identify rhythm 5. Provide 2 minutes CPR if unwitnessed by EMS
Hypertensives Emergency and Urgency
 Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Hypertensives Emergency and Urgency Budi Yuli Setianto Cardiology Divisision Department of Internal Medicine Faculty of Medicine UGM Sardjito Hospital Yogyakarta Background USA: Hypertension is 30% of
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
For The Management Of. Diabetic Ketoacidosis
 Guidelines For The Management Of Diabetic Ketoacidosis By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council
Guidelines For The Management Of Diabetic Ketoacidosis By Dr. Sinan Butrus F.I.C.M.S Clinical Standards & Guidelines Dr.Layla Al-Shahrabani F.R.C.P (UK) Director of Clinical Affairs Kurdistan Higher Council
Chapter 21. Diuretic Agents. Mosby items and derived items 2008, 2002 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Chapter 21 Diuretic Agents Renal Structure and Function Kidneys at level of umbilicus Each weighs 160 to 175 g and is 10 to 12 cm long Most blood flow per gram of weight in body 22% of cardiac output (CO)
Calcium (Ca 2+ ) mg/dl
 Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
