Biliary Atresia. A Guide. An explanation of the symptoms and diagnosis of Biliary Atresia
|
|
|
- Imogen McDowell
- 5 years ago
- Views:
Transcription
1 A Guide An explanation of the symptoms and diagnosis of Biliary Atresia
2 Introduction... 5 What is biliary atresia?... 5 What causes biliary atresia?... 6 What are the signs of biliary atresia?... 6 How is biliary atresia diagnosed?... 7 Is there more than one type of biliary atresia?... 8 How can biliary atresia be treated?... 9 What happens before the operation?... 9 What happens during the operation? How long will the operation last? Are there any other complications of biliary atresia? What happens immediately after the Kasai operation? When will my baby be able to leave hospital and what happens next? What options are there for feeding my baby after the operation? What should I do when I am back at home with my baby?
3 What medicines may my baby need and why are they given? How is it possible to tell if the operation has been successful? What happens if the biliary atresia is not treated or treatment is unsuccessful? What other problems might occur? What will happen in the future?
4 This information has primarily been written for: Parents/carers of children and young people with biliary atresia Others may also find this information useful: Young people with biliary atresia Healthcare professionals who would like to find out more about the condition It provides information on: The symptoms of biliary atresia Diagnosis Treatment Possible complications You may find it helpful to also read the following CLDF leaflets: An Introduction to Liver Disease Nutrition Leaflet 4
5 Introduction An important function of the liver is to make a substance called bile. Bile is a liquid which passes into the gut through small tubes called bile ducts and is stored in the gall bladder. Bile contains waste products and other products needed to digest food. What is biliary atresia? Biliary atresia is a medical condition. It can occur either: Before birth due to the bile ducts developing abnormally Shortly after birth due to the bile ducts becoming inflamed or obstructed In most babies with biliary atresia bile ducts on the inside and outside of the liver are affected eventually leading to a complete blockage of bile flow from the liver. This in turn causes scarring (fibrosis) in the liver. Liver Liver Intrahepatic ducts (partially blocked & abnormal) Bile Duct Bile Duct (maybe blocked or missing) Gallbladder Duodenum Pancreas Gallbladder (often shrunken) Duodenum Pancreas Diagram One Showing the normal liver, gall bladder, bile ducts and upper intestine in a healthy child Diagram Two Showing the liver, gall bladder, bile ducts and upper intestine of a child with biliary atresia 5
6 What causes biliary atresia? The cause of biliary atresia is unknown. Research is being carried out but it hasn t provided any definite answers yet. Parents often feel guilty that they may have, in some way, contributed to their child having the condition. These feelings are understandable but there is no evidence to suggest that biliary atresia is hereditary (can be passed on to children by their parents) or due to anything parents might have done or taken. Children with biliary atresia will not pass the condition on to their own children. What are the signs of biliary atresia? In the first weeks of life babies with biliary atresia often seem well apart from being jaundiced (yellow discolouration of the skin and of the whites of the eyes) and in some cases feeding more often. There are two types of jaundice in babies: 1) Physiological Jaundice The first is very common and in most babies it clears within the first two weeks of life. The Children s Liver Disease Foundation has a booklet explaining baby jaundice which is available online. 2) Pathological Jaundice This is caused by a problem with the liver. This type of jaundice does not fade and babies who are jaundiced after two weeks (three weeks if pre-term) should have a split bilirubin blood test performed to find out which type of jaundice it is. 6
7 The other important signs of pathological jaundice are: Urine colour Normally the urine of a newborn baby is colourless. If a baby s urine is persistently yellow or dark in colour this can be an indication of liver disease. Pale Stools Normally the stools of a baby are green or yellow. If the stools of a baby are grey, white, fawn or pale then this can be an indication of liver disease. CLDF have a stool chart which includes the colours of healthy and potentially unhealthy stools. You can use this to examine your baby s stool. You can download a stool chart or order a hard copy on CLDF s website: How is biliary atresia diagnosed? If a baby has the signs and symptoms above then they may be admitted to hospital for further investigation. A number of investigations will need to be carried out in order to make a diagnosis. These may include: Blood tests Urine test An ultrasound Liver excretion test Some children will need a liver biopsy and/or a small operation to confirm or rule out a diagnosis. These investigations are completed over the course of a few days. To find out more about routine liver investigations please see our leaflet: An Introduction to Liver Disease. 7
8 Is there more than one type of biliary atresia? Yes, there are three types of biliary atresia. In all three types the bile ducts in the liver are affected. In type one and two some of the bile ducts near the liver may stay open. In type three all of the ducts outside the liver are blocked. Type three is the most common type of biliary atresia. The treatment for all three types is the same but the results are slightly better if your baby has a type one or type two biliary atresia. Type 1 (~5%) Type 2 (~2%) Gallbladder contains bile Often cystic Common bile duct Common hepatic duct Visible patent ducts at porta Type 3 (>90%) Gallbladder solid or mucocele Solid porta hepatis microscopic ductules only 8
9 How can biliary atresia be treated? If the tests show that there is a strong indication that your baby has biliary atresia, he/she will require surgery. This will involve carrying out an investigation called an operative cholangiogram under a general anaesthetic to confirm the diagnosis. If biliary atresia is confirmed then this will be followed by a Kasai procedure, usually done under the same general anaesthetic at the same time. This procedure was named after the Japanese surgeon who first performed the operation in The aim of the operation is to help bile drain from the liver into the gut. What happens before the operation? Blood tests will be performed and will include checking your baby s blood group in case there is a need to give blood to your baby before, during or after surgery. Your baby may be given special medicines to prepare the gut for surgery. Your baby will not be fed milk for a number of hours before the operation. This will differ depending on which liver unit your baby is having the operation at. The team caring for your baby will explain what this involves. If you are breast feeding, speak to your nurse regarding expression and storage of milk. You will be allowed to go down to the operating theatre with your baby and stay until just before your baby is asleep. 9
10 What happens during the operation? The aim of the operation is to make a drainage tube to allow bile to drain from the liver. During the operation the surgeon will look at the liver and see if there are abnormalities. The surgeon will also remove a tiny piece of the liver to send to the laboratory for further tests (a liver biopsy). The surgeon will carry out the operation called the Kasai operation (Kasai portoenterostomy). Normal Anatomy Liver Normal bile ducts Gallbladder Pancreas Duodenum Jejunum 10
11 Diagram of Surgery Loop of bowel (called a Roux Loop) joined to the underside of the liver During the operation the gallbladder and all the abnormal bile ducts outside the liver are removed. At the highest point, along the surface of the liver, there are usually enough very small bile ducts which will allow some bile flow to be re-established. The surgeon will join a loop of intestine to the under surface of the liver. How long will the operation last? The operation will last a whole morning or afternoon. Putting your baby to sleep, inserting lines (tubes) so that your child can have fluids through their vein, giving your child pain management and then waiting for your baby to wake up will take longer. The doctor responsible for putting your child to sleep (the anaesthetist) can explain the kind of lines they will insert to monitor your child and to give them medications or blood products after the operation. 11
12 Are there any other complications of biliary atresia? Between babies out of 100 with biliary atresia may have additional problems found during surgery. These may include the following: Some children with biliary atresia can have multiple small spleens (polysplenia) or the spleen can be absent (asplenia). The spleen is an organ which sits under the left lower ribs next to the stomach and helps to fight against infection. It also removes blood cells, especially platelets at the end of their life. It is normally a solid single organ. It is believed that multiple small spleens do not function normally and do not protect the baby against infection the way a normal spleen does. The intestine may not have properly curled up into the abdomen during development (intestinal malrotation). This will need to be corrected at the time the surgeon operates for biliary atresia. Some abnormalities of the veins in the abdomen Heart defects If some or all of these complications occur it is a condition known as biliary atresia splenic malformation syndrome (BASM). This group of children with biliary atresia may be less likely to clear their jaundice after the operation. They also need additional tests such as a heart scan to check for problems. It may also be necessary for them to take daily antibiotics to reduce their risk of infection. 12
13 What happens immediately after the Kasai operation? You will be able to collect your child from the operation recovery area. There will be a tube running through your baby s nose down into the stomach. This is called a naso-gastric tube. This usually drains into a clear bag and keeps the stomach empty which helps to prevent sickness. It is important to keep your baby s stomach empty for hours until the feeds are commenced. You will not be able to feed your baby for a couple of days. This is because the surgeon operates on the bowel which stops it from working for a short time. There is a danger of leakage from the point where the bile ducts have been joined to the bowel if the feeds are started too early. The bowel recovers within a couple of days and feeding can resume. Until then your baby will be fed through an intravenous drip. Intravenous Drips A central line will be placed into one of the bigger blood vessels in the neck at the time of the surgery. It will be used to provide fluids, medication including pain relief, antibiotics and blood products. It will be taken out when these are no longer needed. Fluids are given in order to keep the sugar, salt and water levels at the right level in the body. Blood tests will be carried out to check these levels so that they can be changed if needed. All fluids required by your baby will be given through the drip until feeding is re-started. 13
14 Pain relieving drugs These are often given nonstop via the central line or a cannula (a tube inserted into a vein). A special pump controls the rate and amount of the drug given. Sometimes pain relief is given through a small tube inserted into a baby s back at the time of the operation. This is similar to those used for women in labour. This is called an epidural catheter. Pain relief will be discussed with you. Antibiotics Your baby will receive antibiotics through a vein (intravenously) for three to five days after surgery. Urinary catheter Your child will have a urinary catheter which will drain urine from the bladder. This is to ensure their urine output is measured accurately to check how well the kidneys are working. Abdominal drain An abdominal drain will be placed during surgery to drain excess blood and fluid from around the liver. This will be removed as the drainage decreases. A dressing may cover the wound on your baby s tummy for the first few days. The dressing will be changed as needed. The stitches do not need to be removed as they will dissolve after the wound has healed. It will be possible for you to hold your baby the day following the surgery, the nurse will help you. 14
15 When will my baby be able to leave hospital and what happens next? If there are no problems after the surgery then your baby will be allowed to go home, usually around seven to ten days after the operation, once you and the medical team are happy with your baby s condition. Before going home the clinical staff will make sure that the wound is healing and there is no suggestion of infection anywhere in the body. You will be given or sent an outpatient appointment. Before your baby leaves the hospital you will be given an initial supply of medicines and feeds. More will be arranged through your GP. It is quite common for the hospital staff to advise your health visitor, GP and local hospital about your child s condition and any special care which is needed so that they can offer you useful support when you are at home. Your Clinical Nurse Specialist (CNS) will stay in touch with you and you will be able to ring them whenever necessary so you are not alone. Once your child can leave the hospital they will require longterm follow-up by the doctors, specialist nurses and dieticians. It is often helpful for your baby to be weighed on a weekly basis to monitor weight gain. It is important that your child receives their immunisations and to discuss timing and additional immunisations with their medical team. 15
16 What options are there for feeding my baby after the operation? If your baby was being breast fed before you found out they had biliary atresia it may be possible to start breast feeding again, normally alongside other formula feeds. It is important that your milk has been maintained by expressing milk while your baby is unable to feed. The nursing staff will help and advise you with this. Most babies with biliary atresia are unable to gain enough weight on breast milk alone. Your baby might need special milk formula. There are a number of special milks for babies suffering from liver disease. These milks have fats which are more easily digested by babies with liver disease. Powders can be added to the formula to increase the number of calories given to your child. This will make sure your child can gain weight. If this is needed a dietician will tell you how to combine breast and bottle-feeding. The doctor will prescribe extra vitamins for your baby. This is because babies with prolonged jaundice also have problems absorbing certain vitamins. CLDF s Nutrition leaflet has more detailed information on this. 16
17 What should I do when I am back at home with my baby? When you get home you should try and treat your baby as normally as possible. Obviously you will be worried at times and this is quite normal. Babies with biliary atresia get common illnesses just like any other baby. Symptoms for which you should seek advice from your GP or hospital are: A raised temperature of 37.8ºC or more, or non-specific illness with a raised temperature More jaundice with paler stools and darker urine The child is generally unwell If you have any queries regarding your child, please do not hesitate to contact your Clinical Nurse Specialist at the liver unit treating your child. Children s Liver Disease Foundation provides family support and is on hand to provide help and information whenever you need it. The contact details can be found at the back of this leaflet. 17
18 What medicines may my baby need and why are they given? The medicines required will depend upon your child s condition and progress as well as the liver unit you are at. The medical team will help you to understand which medicines your baby will need to take and when. It is important to note that some medicines are not available straight away at pharmacies. You may need to order them from the pharmacy two to three days in advance. Some commonly used medicines are: Antibiotics After the operation antibiotics are given by a drip at first and then by mouth. They are used to reduce the risk of infection in the bile ducts (cholangitis). Further antibiotics may be given as needed. Vitamins Additional vitamins are necessary because poor bile flow can reduce the absorption of vitamins. Phenobarbital This may be given to increase the flow of bile. As it may make your baby sleepy at first, it is usually given as a single dose, in the evening. 18
19 URSO (Ursodeoxycholic acid) This drug is given after restarting feeding after the Kasai operation. It aims to promote the flow of bile. Colestyramine This comes in the form of a powder in individual sachets. Each sachet is mixed with water and given in liquid form. This may be given to improve liver function and remove substances which may otherwise cause the skin to itch. A side effect of colestyramine is that it can affect the absorption of some drugs, especially vitamins and ursodeoxycholic acid. Therefore, with babies it is best to give some at each feed time except when vitamins are given. As your baby becomes older and manages larger volumes, the daily dose of colestyramine can be given all at once or split into two. For a toddler or older child needing colestyramine it is best given in one or two doses away from the main meal times and vitamins. Always leave at least two hours between giving colestyramine and vitamins. Ranitidine It is common to find stomach irritation after any type of abdominal operation and this drug may be given to help lessen this problem. Steroids Steroids are also given to reduce inflammation. 19
20 Occasionally the medical team will need to use the following medicines: Spironolactone This may need to be given to help your baby get rid of extra fluid which otherwise collects in the abdomen and is called ascites. It is not needed in all cases. If your child needs medicine to reduce a high temperature please use paracetamol (panadol/calpol etc.). Remember aspirin, ibuprofen and other drugs containing aspirin and ibuprofen (calprofen/nurofen) must not be given. Please make sure all medicines are stored correctly and in a safe place. Your child s medication and dosage will be reviewed at clinic appointments. 20
21 How is it possible to tell if the operation has been successful? At the time of the operation the surgeon will not be able to tell if the Kasai operation has been successful. The first stools after the operation are usually very dark and will then become paler. If the operation is a success and bile drainage does occur the stools gradually change to a yellow/green/brown colour and later the urine becomes paler. The colour of the stools will be checked whilst your baby is in hospital. It is not unusual for there to be difference in the colour of the stools and every baby is different. If bile drainage is established the jaundice gradually fades. Blood tests will show that bilirubin levels, which cause jaundice, drop towards a normal level. Most babies who clear jaundice after a Kasai procedure do so in two to three months after surgery. It is not unusual for liver function tests to remain abnormal even if the jaundice completely clears. Even if the jaundice clears after a Kasai operation some children will develop complications due to liver damage. Therefore, all children should continue to be seen for regular check ups. Of those babies who clear their jaundice some will achieve completely normal liver function and may never experience any further problems. Children who clear their jaundice but have persistently abnormal liver function tests may develop treatable problems such as portal hypertension or deteriorating liver function eventually. These can lead to liver transplantation. Many children who undergo a successful Kasai will be well with their own liver ten years later. 21
22 What happens if the biliary atresia is not treated or treatment is unsuccessful? If a baby has not had a Kasai procedure in the first two to three months of life the success rate the operation is very low. If biliary atresia is not treated or the treatment isn t successful the bile produced in the liver builds up causing damage to the cells of the liver eventually resulting in severe scarring (cirrhosis). If this continues liver function deteriorates, complications occur and general health suffers. Liver transplantation is often the accepted form of treatment. Transplant is a huge step and is only considered when other treatments are ineffective. Liver transplantation became available for children in the 1980 s. The results of liver transplantation are encouraging and are steadily improving. UK liver transplant centres are reporting an overall 90% 10-year survival rate for liver transplantation. Liver transplantation is now possible in children of any age. If liver transplantation is an option for your child this will be discussed with you by your child s medical team. The aim of liver transplantation is to restore your child to good health. 22
23 What other problems might occur? In any baby who undergoes a Kasai procedure, even if they clear their jaundice completely, a number of problems may occur. Cholangitis Cholangitis is an infection of the bile ducts in the liver resulting in inflammation. This may cause a fever, worsening or recurrent jaundice, or both. It requires urgent treatment with intravenous antibiotics which can only be given at your local hospital or the liver unit treating your child. If the treatment is given locally, please ask the doctors to contact the liver unit treating your child. If cholangitis is left untreated it can cause further damage to the liver. That is why prompt investigation of any high temperature (over 37.8ºC) or a non-specific illness is necessary in babies who have undergone a Kasai procedure. Although cholangitis most commonly occurs in the first year or two after a Kasai procedure it can occur at any time. Ascites Ascites is an abnormal collection of fluid in the abdomen. A small amount of ascites can be present for up to six weeks after the operation but should then disappear. If it recurs at any time this is usually a sign that the disease has affected the ability of the liver to make a protein called albumin. When the albumin level is too low, water from the child s blood leaks out of the blood vessels and collects in the abdomen. In severe cases it may also collect in other parts of the body. 23
24 The first sign of this problem is often when clothes and nappies do not fit so well over the tummy. This usually occurs gradually but may be started or made worse by infection. If your child s tummy becomes noticeably bigger, or your child has rapid weight gain that is not consistent with normal growth rates you should contact your liver team. Treatment for ascites may be started by your GP or local paediatrician in consultation with the liver unit and does not necessarily need admission to hospital. Treatment can include medicines and altering the child s diet. The aim is to make sure there is a high amount of energy in the food given (calorie intake) but less fluid and salt. In more serious cases it may be necessary to admit your child to hospital and give albumin intravenously through a drip. You should never attempt to alter your child s diet and, in particular, the fluid intake without medical advice. Portal Hypertension Portal Hypertension is high blood pressure in the portal vein which is the main vein carrying blood from the gut to the liver. It may occur due to scarring in the liver which causes back pressure in the portal vein. This may cause veins, like varicose veins, to develop in the lining of the gullet, stomach or gut. These are called varices. These veins become fragile and may bleed. It is uncommon for this to occur before the child is two years old. Bleeding can cause black stools, paleness or vomiting of blood. If bleeding does occur you will need to ring for an ambulance which will take you to your local hospital. 24
25 Itching (Pruritus) Some children with reduced bile flow experience itching of the skin. This can develop at any time and may be upsetting for your child. If you think your child may be affected talk to your GP or liver unit. The itching may not be because of the liver dysfunction. Additional medicine may be required. CLDF has a leaflet explaining ascites, portal hypertension and pruritus in more detail. 25
26 What will happen in the future? Your baby/child s growth and development will be followed up by periodic visits to the hospital. How often you will need to go to the hospital will vary for each child. Blood tests will be done to measure your child s bilirubin level and liver function. Periodically an ultrasound will be performed to assess the size of the liver and other structures in the abdomen (e.g. the spleen). CLDF is in touch with a large number of families who have children with biliary atresia. These children can live happy, fulfilling lives and achieve a huge amount. Biliary atresia doesn t have to hold a child back from living a relatively normal life. CLDF is here to support you throughout your child s development. Further details can be found at the back of this leaflet. 26
27 CLDF produces a wide variety of information resources for children and young people up to the age of 25 with liver disease, their families and the healthcare professionals who look after them. This information can be downloaded or ordered from CLDF s website For further enquiries regarding CLDF s information please contact the Health and Research Information Manager by at hrim@ childliverdisease.org or call Thanks The booklet has been written, edited and reviewed with the help of staff at each of the specialist paediatric liver centres: Birmingham Children s Hospital, King s College Hospital and Leeds Children s Hospital. Thank you to all of the staff involved who have made the production of this leaflet possible. Disclaimer This leaflet provides general information but does not replace medical advice. It is important to contact your/your child s medical team if you have any worries or concerns. Feedback and Information Sources Information within this leaflet has been produced with input from the three specialist paediatric liver centres in the UK. To provide feedback on this leaflet, for more information on the content of this leaflet including references and how it was developed contact Children s Liver Disease Foundation: info@ childliverdisease.org This leaflet has been reviewed in September It is due to be reviewed by September
28 What is Children s Liver Disease Foundation (CLDF)? CLDF is the UK s leading organisation dedicated to fighting all childhood liver diseases. CLDF provides information and support services to young people up to the age of 25 with liver conditions and their families, is the voice of children, young people and young adults with a childhood liver disease and their families and funds vital medical research into childhood liver disease. Are you a young person up to the age of 25 with a liver condition or a family member? CLDF s Families and Young People s teams are here for you, whether you want to talk about issues affecting you, meet and share with others, or just belong to a group which cares, knows what it s like and is fighting to make a difference. You are not alone. If you are a parent/carer or family member then get in touch with CLDF s Families Team: Phone: families@childliverdisease.org If you are a young person and want to find out more about CLDF s services you can contact CLDF s Young People s Team: Phone: youngpeople@childliverdisease.org CLDF have a dedicated website for young people called Focus as well as a social media platform called HIVE for year olds with a liver disease/transplant to make new friends, connect and share stories Would you like to help us support the fight against childhood liver disease? All of CLDF s work is funded entirely through voluntary donations and fundraising. Please help us to continue to support young people, families and adults diagnosed in childhood now and in the future. To find out more about fundraising and how you can join the fight against childhood liver disease you can visit Alternatively you can contact the Fundraising Team by fundraising@childliverdisease.org or call Children s Liver Disease Foundation, 36 Great Charles Street, Birmingham, B3 3JY info@childliverdisease.org CLDF September 2016 Main site: childliverdisease.org Registered Charity Number: Young people s site: cldf-focus.org Charity registered in Scotland: SC044387
Acute Liver Failure. A Guide. An explanation of what Acute Liver Failure is, symptoms, diagnosis and treatment
 A Guide An explanation of what is, symptoms, diagnosis and treatment Introduction... 4 What is ALF?... 4 What can cause ALF?... 4 What are the signs and symptoms of ALF?... 5 Why does my child need to
A Guide An explanation of what is, symptoms, diagnosis and treatment Introduction... 4 What is ALF?... 4 What can cause ALF?... 4 What are the signs and symptoms of ALF?... 5 Why does my child need to
Autoimmune Liver Disease
 Autoimmune Liver Disease A Guide An explanation of what autoimmune liver diseases are including autoimmune hepatitis and autoimmune sclerosis cholangitis What are autoimmune diseases?... 4 What is autoimmune
Autoimmune Liver Disease A Guide An explanation of what autoimmune liver diseases are including autoimmune hepatitis and autoimmune sclerosis cholangitis What are autoimmune diseases?... 4 What is autoimmune
Liver Transplantation
 An Overview General information on liver transplantation in children and young people What is a liver transplant?... 4 When does a child or young person need a liver transplant?... 4 What is a transplant
An Overview General information on liver transplantation in children and young people What is a liver transplant?... 4 When does a child or young person need a liver transplant?... 4 What is a transplant
Nutrition. A Guide. A guide to the nutrition of babies and children with liver disease
 A Guide A guide to the nutrition of babies and children with liver disease Why is nutrition so important?... 4 What is a nutritional assessment?... 5 Why do some children with liver disease have poor nutrition?...
A Guide A guide to the nutrition of babies and children with liver disease Why is nutrition so important?... 4 What is a nutritional assessment?... 5 Why do some children with liver disease have poor nutrition?...
Wilson's Disease. A Guide. An explanation of what Wilson's disease is, symptoms, diagnosis and treatment
 A Guide An explanation of what Wilson's disease is, symptoms, diagnosis and treatment What is Wilson's disease?... 4 Why does the body contain copper?... 4 What causes Wilson s disease?... 5 Are males
A Guide An explanation of what Wilson's disease is, symptoms, diagnosis and treatment What is Wilson's disease?... 4 Why does the body contain copper?... 4 What causes Wilson s disease?... 5 Are males
Pruritus. A Guide. A guide to pruritus in children and young people
 A Guide A guide to pruritus in children and young people What is pruritus and what causes it?... 3 How can pruritus affect a child or young person?... 3 What treatment is available for pruritus?... 4 This
A Guide A guide to pruritus in children and young people What is pruritus and what causes it?... 3 How can pruritus affect a child or young person?... 3 What treatment is available for pruritus?... 4 This
BILIARY ATRESIA. What is biliary atresia?
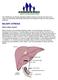 The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. BILIARY ATRESIA What is
The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. BILIARY ATRESIA What is
Cystic Fibrosis and Liver Disease a guide
 fighting childhood liver disease Cystic Fibrosis and Liver Disease a guide Medical Information Series Cystic Fibrosis and Liver Disease a guide 1 Welcome This leaflet has been written for: Parents/carers
fighting childhood liver disease Cystic Fibrosis and Liver Disease a guide Medical Information Series Cystic Fibrosis and Liver Disease a guide 1 Welcome This leaflet has been written for: Parents/carers
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
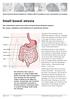 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
LAPAROSCOPIC GALLBLADDER SURGERY
 LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
LAPAROSCOPIC GALLBLADDER SURGERY Treating Gallbladder Problems with Laparoscopy A Common Problem If you ve had an attack of painful gallbladder symptoms, you re not alone. Gallbladder disease is very common.
Chronic Pancreatitis (1 of 4) i
 Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
Chronic Pancreatitis (1 of 4) i If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk.
YOUR OPERATION EXPLAINED
 RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
RIGHT HEMICOLECTOMY This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer Research
Gallstones Information Leaflet THE DIGESTIVE SYSTEM. Gutscharity.org.uk
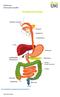 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about gallstones Gall is an old-fashioned word for bile, a liquid made in the liver and stored in the gall bladder
Information leaflet for parents/carers. Fundoplication
 Information leaflet for parents/carers Fundoplication Introduction Your child has gastro oesophageal reflux disease (GORD), which is where acid from the stomach leaks up into the oesophagus (gullet). It
Information leaflet for parents/carers Fundoplication Introduction Your child has gastro oesophageal reflux disease (GORD), which is where acid from the stomach leaks up into the oesophagus (gullet). It
Biliary Atresia. Who is at risk for biliary atresia?
 Biliary Atresia Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic
Biliary Atresia Biliary atresia is a life-threatening condition in infants in which the bile ducts inside or outside the liver do not have normal openings. Bile ducts in the liver, also called hepatic
Portal Hypertension and Varices a guide
 fighting childhood liver disease Portal Hypertension and Varices a guide Medical Information Series 4 Welcome This leaflet has been written specifically for: Parents/carers of a child with portal hypertension
fighting childhood liver disease Portal Hypertension and Varices a guide Medical Information Series 4 Welcome This leaflet has been written specifically for: Parents/carers of a child with portal hypertension
Laparotomy for large retroperitoneal mass:
 Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparotomy for large retroperitoneal mass: procedure-specific information UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Laparoscopic (keyhole) colorectal (bowel) resection
 Laparoscopic (keyhole) colorectal (bowel) resection Your operation explained Information for patients Colorectal Surgery Introduction This leaflet should be read together with a booklet which explains
Laparoscopic (keyhole) colorectal (bowel) resection Your operation explained Information for patients Colorectal Surgery Introduction This leaflet should be read together with a booklet which explains
DRAFT. Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect. What is a transjugular intrahepatic portosystemic shunt?
 UW MEDICINE PATIENT EDUCATION Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect This handout explains a transjugular intrahepatic portosystemic shunt and what to expect when
UW MEDICINE PATIENT EDUCATION Angiography: Transjugular Intrahepatic Portosystemic Shunt (TIPS) What to expect This handout explains a transjugular intrahepatic portosystemic shunt and what to expect when
Your Bowel Operation Hartmanns Procedure
 Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Your Bowel Operation Hartmanns Procedure Introduction You are having an operation called Hartmanns Procedure and this booklet aims to help you to understand your condition and this operation. The nurses
Acute pancreatitis. Information for patients Hepatobiliary
 Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Acute pancreatitis Information for patients Hepatobiliary What is acute pancreatitis? Acute pancreatitis is an inflammation of the pancreas gland. The main symptoms are: severe abdominal pain severe back
Having an operation on the pancreas
 Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Having an operation on the pancreas Let us assume you (the reader) are going to have a pancreatic resection. The following section attempts to answer some of the questions you may have in mind, and the
Mr Sanjeev Sarin MS FRCS. Aortic Aneurysms Patient Information Sheet
 Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Aortic Aneurysms Patient Information Sheet The aim of this information sheet is to ensure that you understand the nature of the treatment you wish to undertake. Please read it carefully and discuss any
Treating your abdominal aortic aneurysm by open repair (surgery)
 Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Patient information Abdominal aortic aneurysm open surgery Treating your abdominal aortic aneurysm by open repair (surgery) Introduction This leaflet tells you about open repair of abdominal aortic aneurysm,
Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure
 Patient Education Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure This handout explains what a transjugular intrahepatic portosystemic shunt is and what to expect when you have
Patient Education Transjugular Intrahepatic Portosystemic Shunt (TIPS) About your procedure This handout explains what a transjugular intrahepatic portosystemic shunt is and what to expect when you have
Making the most of an appointment
 Making the most of an appointment fighting childhood liver disease Support Series JOB 11565 PROOF 04 14/03/2006 Welcome This leaflet has been written for: Parents/carers of a child/young person diagnosed
Making the most of an appointment fighting childhood liver disease Support Series JOB 11565 PROOF 04 14/03/2006 Welcome This leaflet has been written for: Parents/carers of a child/young person diagnosed
PROGRESSIVE FAMILIAL INTRAHEPATIC CHOLESTASIS (PFIC)
 The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. PROGRESSIVE FAMILIAL INTRAHEPATIC
The Childhood Liver Disease Research Network strives to provide information and support to individuals and families affected by liver disease through its many research programs. PROGRESSIVE FAMILIAL INTRAHEPATIC
Bereavement. A Guide. Information on coping with the loss of a child
 A Guide Information on coping with the loss of a child Coping with grief... 3 Seeking peace, comfort and hope: Religious and spiritual care... 4 Advice for parents regarding how to deal with siblings and
A Guide Information on coping with the loss of a child Coping with grief... 3 Seeking peace, comfort and hope: Religious and spiritual care... 4 Advice for parents regarding how to deal with siblings and
Having a pancreas transplant alone (PTA)
 Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
Having a pancreas transplant alone (PTA) This leaflet explains more about having a pancreas transplant alone (PTA), including the benefits, risks, alternatives, and what you can expect at the time of the
The Children s Hospital Intussusception and its treatment Information for parents
 The Children s Hospital Intussusception and its treatment Information for parents What is intussusception? Intussusception occurs when one part of the bowel slides into another part of bowel, like a telescope,
The Children s Hospital Intussusception and its treatment Information for parents What is intussusception? Intussusception occurs when one part of the bowel slides into another part of bowel, like a telescope,
ABDOMINAL PERINEAL RESECTION
 ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
ABDOMINAL PERINEAL RESECTION This leaflet is produced by the Department of Colorectal Surgery at Beaumont Hospital supported by an unrestricted grant to better Beaumont from the Beaumont Hospital Cancer
Transjugular intrahepatic portosystemic shunt (TIPS) Information for patients Sheffield Vascular Institute
 Transjugular intrahepatic portosystemic shunt (TIPS) Information for patients Sheffield Vascular Institute You have been given this leaflet because you need a procedure called a transjugular intrahepatic
Transjugular intrahepatic portosystemic shunt (TIPS) Information for patients Sheffield Vascular Institute You have been given this leaflet because you need a procedure called a transjugular intrahepatic
Subtotal and Total Gastrectomy
 DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
DR ADEEB MAJID MBBS, MS, FRACS, ANZHPBA FELLOWSHIP GENERAL, HEPATOBILIARY AND PANCREATIC SURGEON CALVARY MATER HOSPITAL NEWCASTLE Information for patients and carers Subtotal and Total Gastrectomy Introduction
Surgery. In this fact sheet. Surgery: English
 Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Surgery: English Surgery This information is about surgery (having an operation). Any words that are underlined are explained in the glossary at the end. Many people with cancer will have surgery as part
Acute kidney injury. Information for patients Sheffield Teaching Hospitals
 Acute kidney injury Information for patients Sheffield Teaching Hospitals page 2 of 12 Acute kidney injury You have been given this leaflet because you have had an episode of acute kidney injury (AKI).
Acute kidney injury Information for patients Sheffield Teaching Hospitals page 2 of 12 Acute kidney injury You have been given this leaflet because you have had an episode of acute kidney injury (AKI).
Laparoscopic Ventral Mesh Rectopexy
 Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
Laparoscopic Ventral Mesh Rectopexy (LVMR) Information for patients General Surgery What is a LVMR? A laparoscopic ventral mesh rectopexy (LVMR) is an operation in which the rectum (last part of the bowel)
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer.
 What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
What is a TURBT? Removal of an abnormal area within the bladder which may, or may not, prove to be cancer. What are the benefits of this operation? Removal of an abnormality which is sent for analysis
ABDOMINAL PERINEAL RESECTION. Patient information Leaflet
 ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
ABDOMINAL PERINEAL RESECTION Patient information Leaflet April 2017 WHAT IS AN ABDOMINAL PERINEAL RESECTION? This is an operation which involves removing the lower end of your large bowel along with the
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Laparoscopic cholecystectomyy
 Laparoscopic cholecystectomyy What is the gall bladder? The gallbladder is a small pear sized organ that stores bile. Bile is necessary for the digestion of fatty food. The bile duct is a tube that carries
Laparoscopic cholecystectomyy What is the gall bladder? The gallbladder is a small pear sized organ that stores bile. Bile is necessary for the digestion of fatty food. The bile duct is a tube that carries
HARTMANNS PROCEDURE. Patient information Leaflet
 HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
HARTMANNS PROCEDURE Patient information Leaflet April 2017 WHAT IS A HARTMANNS PROCEDURE? This operation is necessary to remove the area of bowel that is diseased. The operation removes a piece of your
Inguinal hernias may be present from birth but may not become evident until later in life. They are usually more common in men.
 This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
This booklet is designed to give you information about inguinal hernia repair done under general anaesthesia. We hope it will answer some of the questions that you or those who care for you may have at
The peritoneal dialysis catheter
 The peritoneal dialysis catheter Department of Renal Medicine Patient Information Leaflet Introduction The information contained in this booklet is for: Patients who have renal failure and need a peritoneal
The peritoneal dialysis catheter Department of Renal Medicine Patient Information Leaflet Introduction The information contained in this booklet is for: Patients who have renal failure and need a peritoneal
Gallstones and Cholecystectomy Information Sheet
 Gallstones and Cholecystectomy Information Sheet Gallstones & Cholecystectomy This information sheet desrcibes what they are, the treatment options, and what to expect following a operation. The following
Gallstones and Cholecystectomy Information Sheet Gallstones & Cholecystectomy This information sheet desrcibes what they are, the treatment options, and what to expect following a operation. The following
What Is Cirrhosis? CIRRHOSIS. Cirrhosis occurs when the liver is. by chronic conditions and diseases. permanently scarred or injured
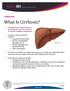 What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
What Is Cirrhosis? Cirrhosis occurs when the liver is permanently scarred or injured by chronic conditions and diseases. Common causes of cirrhosis include: Long-term alcohol abuse. Chronic viral hepatitis
Malrotation and volvulus
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Malrotation and volvulus This leaflet explains about malrotation and volvulus, how they can be treated, and what
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Malrotation and volvulus This leaflet explains about malrotation and volvulus, how they can be treated, and what
Pain relief after major surgery
 Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Page 1 of 6 Pain relief after major surgery Introduction The aim of this leaflet is to tell you about the main pain relief options available after major surgery. You will probably only need this for the
Package leaflet: Information for the user. Ursodeoxycholic Acid Capsules 250mg (Ursodeoxycholic acid)
 Package leaflet: Information for the user Ursodeoxycholic Acid Capsules 250mg (Ursodeoxycholic acid) Read all of this leaflet carefully before you start taking this medicine because it contains important
Package leaflet: Information for the user Ursodeoxycholic Acid Capsules 250mg (Ursodeoxycholic acid) Read all of this leaflet carefully before you start taking this medicine because it contains important
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients
 Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Retroperitoneal Lymph Node Dissection (RPLND) Department of Urology Information for patients i What is a retroperitoneal lymph node dissection (RPLND)? You have probably already undergone surgery and treatment
Pyloric Stenosis Advice for Parents & Carers
 Pyloric Stenosis Advice for Parents & Carers Children s Services The aim of this leaflet is to provide you as carers or parents all the relevant information regarding Pyloric Stenosis and answer some common
Pyloric Stenosis Advice for Parents & Carers Children s Services The aim of this leaflet is to provide you as carers or parents all the relevant information regarding Pyloric Stenosis and answer some common
X-Plain Pancreatic Cancer Reference Summary
 X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
X-Plain Pancreatic Cancer Reference Summary Introduction Pancreatic cancer is the 4th leading cause of cancer deaths in the U.S. About 37,000 new cases of pancreatic cancer are diagnosed each year in the
What can you expect after your ERCP?
 ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
ERCP Explained and respond to bed rest, pain relief and fasting to rest the gut with the patient needing to stay in hospital for only a few days. Some patients develop severe pancreatitis and may require
Urology Department Percutaneous Nephrolithotomy (PCNL)
 Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Urology Department Percutaneous Nephrolithotomy (PCNL) Your consultant has diagnosed that you have a problem with kidney stones and has recommended that you have an operation called a percutaneous nephrolithotomy
Varicose Veins Operation. Patient Information Leaflet
 Varicose Veins Operation Patient Information Leaflet April 2017 1 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the leaky
Varicose Veins Operation Patient Information Leaflet April 2017 1 WHAT IS VARICOSE VEIN SURGERY (HIGH LIGATION AND MULTIPLE AVULSIONS) The operation varies from case to case, depending on where the leaky
Laparoscopic partial removal of the kidney
 Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
Laparoscopic partial removal of the kidney Department of Urology 2 Patient Information What evidence is this information based on? This booklet includes advice from consensus panels, the British Association
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
Pancreatic Cancer (1 of 5)
 i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
i If you need your information in another language or medium (audio, large print, etc) please contact Customer Care on 0800 374 208 or send an email to: customercare@ salisbury.nhs.uk You are entitled
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon
 Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Having a nephrostomy tube inserted
 Having a nephrostomy tube inserted Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been advised to have a nephrostomy tube inserted. It includes information
Having a nephrostomy tube inserted Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been advised to have a nephrostomy tube inserted. It includes information
Laser Trans Urethral Resection of Prostate (TURP)
 Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laser Trans Urethral Resection of Prostate (TURP) Department of Urology Information for patients i Introduction The prostate is a small gland, which is found only in men. It is found at the base of the
Laparoscopic Cholecystectomy
 Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Treatment Centre Laparoscopic Cholecystectomy What is a laparoscopic cholecystectomy? You need this operation because stones have collected in your gallbladder (the area where a small amount of bile is
Percutaneous transhepatic cholangiogram (PTC) and biliary drainage. An information guide
 TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Percutaneous transhepatic cholangiogram (PTC) and biliary drainage An information guide Percutaneous transhepatic cholangiogram (PTC) and
TO PROVIDE THE VERY BEST CARE FOR EACH PATIENT ON EVERY OCCASION Percutaneous transhepatic cholangiogram (PTC) and biliary drainage An information guide Percutaneous transhepatic cholangiogram (PTC) and
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER
 INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
INFORMATION ON PANCREATIC HEAD AND PERIAMPULLARY CANCER What is Pancreas? The pancreas is a gland located in the back of your abdomen behind the stomach. pancreas is divided into four parts: the head,
Reproduced with the kind permission of Health Press Ltd, Oxford
 Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Trans Urethral Resection of the Prostate (TURP) Department of Urology Where is the Prostate Gland? The prostate gland sits below the bladder which lies behind the pubic bone see diagram below. The urethra
Caring for a Nephrostomy and what is Ureteric Stenting
 Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Useful contacts: Macmillan Cancer Support Tel: 0808 808 00 00 www.macmillan.org.uk Buckinghamshire Healthcare NHS Trust Cancer Education, Information & Support Service Tel: 01296 316954 How can I help
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet
 Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Crossover Bypass Graft Surgery Vascular Surgery Patient Information Leaflet Originator: Mr Jayatunga, Consultant Vascular surgeon. Joy Lewis, Vascular Nurse Specialist Date: October 2011 Version: 1 Date
Hydrocele repair. Information for parents and carers
 Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
Hydrocele repair Information for parents and carers A hydrocele is a swelling in the scrotum or groin caused by a collection of fluid surrounding the testicle. The testes start developing inside a baby
LAPAROSCOPIC RADICAL REMOVAL OF THE KIDNEY INFORMATION FOR PATIENTS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk LAPAROSCOPIC
Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile)
 Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
Patient information - Radiology Unit Tel 0118 322 7991 Inserting a percutaneous biliary drain and biliary stent (a tube to drain bile) Introduction This leaflet tells you about the procedures known as
EVALUATION & LISTING. Your Child s Liver Transplant Evaluation. What is the Liver?
 EVALUATION & LISTING Your Child s Liver Transplant Evaluation The University of Michigan is a national leader in liver transplantation, as well as the surgical and medical management of patients with liver
EVALUATION & LISTING Your Child s Liver Transplant Evaluation The University of Michigan is a national leader in liver transplantation, as well as the surgical and medical management of patients with liver
Northumbria Healthcare NHS Foundation Trust. Laparoscopic Cholecystectomy. Issued by the Department of Upper Gastrointestinal Surgery
 Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
Northumbria Healthcare NHS Foundation Trust Laparoscopic Cholecystectomy Issued by the Department of Upper Gastrointestinal Surgery Laparoscopic Cholecystectomy This leaflet explains why you have been
Acute Kidney Injury. Patient Information Leaflet
 Acute Kidney Injury Patient Information Leaflet What is Acute Kidney Injury (AKI)? Acute Kidney injury is a rapid fall in kidney function in a person who has become unwell. It can happen over hours or
Acute Kidney Injury Patient Information Leaflet What is Acute Kidney Injury (AKI)? Acute Kidney injury is a rapid fall in kidney function in a person who has become unwell. It can happen over hours or
Treatment for cancer of the gall bladder
 Treatment for cancer of the gall bladder Hepatobiliary Services Information for Patients Liver i Stomach Pancreas Gall bladder Introduction The aim of this booklet is to help you understand more about
Treatment for cancer of the gall bladder Hepatobiliary Services Information for Patients Liver i Stomach Pancreas Gall bladder Introduction The aim of this booklet is to help you understand more about
Kelly procedure. How does the urinary system work? What is a Kelly procedure and why does my child need one?
 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Kelly procedure This information sheet from Great Ormond Street Hospital (GOSH) explains the Kelly procedure used
Parent/Carer Information Leaflet
 Hydrocele repair Children s Ward Parent/Carer Information Leaflet Introduction Your doctor has recommended that your son has a hydrocele repair. This leaflet is for parents who are considering this operation
Hydrocele repair Children s Ward Parent/Carer Information Leaflet Introduction Your doctor has recommended that your son has a hydrocele repair. This leaflet is for parents who are considering this operation
Patient Information Leaflet Liver Transplantation Assessment
 Patient Information Leaflet Liver Transplantation Assessment South West Liver Unit Derriford Hospital Plymouth PL6 8DH Tel: 01752 431320 Information about Liver Transplantation: Your specialist may recommend
Patient Information Leaflet Liver Transplantation Assessment South West Liver Unit Derriford Hospital Plymouth PL6 8DH Tel: 01752 431320 Information about Liver Transplantation: Your specialist may recommend
PERCUTANEOUS BILIARY DRAINAGE
 PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
PERCUTANEOUS BILIARY DRAINAGE MEDICAL IMAGING INFORMATION FOR PATIENTS Introduction This booklet tells you about the procedure known as percutaneous biliary drainage, explains what is involved and what
PERCUTANEOUS NEPHROLITHOTOMY
 PERCUTANEOUS NEPHROLITHOTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport Tel: 0161 419 5698 Website: www.stockport.nhs.uk Tameside Tel: 0161 922 6696/6698 Website: www.tameside.nhs.uk
PERCUTANEOUS NEPHROLITHOTOMY AN INFORMATION LEAFLET Written by: Department of Urology May 2011 Stockport Tel: 0161 419 5698 Website: www.stockport.nhs.uk Tameside Tel: 0161 922 6696/6698 Website: www.tameside.nhs.uk
Jaundice Protocol. Early identification and referral of liver disease in infants. fighting childhood liver disease. fighting childhood liver disease
 fighting childhood liver disease Jaundice Protocol Early identification and referral of liver disease in infants fighting childhood liver disease 36 Great Charles Street Birmingham B3 3JY Telephone: 0121
fighting childhood liver disease Jaundice Protocol Early identification and referral of liver disease in infants fighting childhood liver disease 36 Great Charles Street Birmingham B3 3JY Telephone: 0121
The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS)
 n The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS) Information for patients Your liver doctor has recommended that you have a Transjugular Intrahepatic Portosystemic
n The Leeds Teaching Hospitals NHS Trust Transjugular Intrahepatic Portosystemic Shunt (TIPS) Information for patients Your liver doctor has recommended that you have a Transjugular Intrahepatic Portosystemic
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon
 Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Dr Candice Silverman MBBS (HONS) FRACS General & Laparoscopic Surgeon Core Specialist Group Suite 5G, John Flynn Medical Centre 42 Inland Drive TUGUN QLD 4224 Tel: 07 5598 0955 Write questions or notes
Gynaecology Department Patient Information Leaflet
 Laparoscopy Gynaecology Department Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called a laparoscopy. It explains what the operation involves, why it is
Laparoscopy Gynaecology Department Patient Information Leaflet Introduction This leaflet is for people who are having a procedure called a laparoscopy. It explains what the operation involves, why it is
Acute Pancreatitis. What is the Pancreas? What does it do? What is acute pancreatitis? What causes acute pancreatitis? What symptoms do you get?
 In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Acute Pancreatitis www.corecharity.org.uk What is the Pancreas? What does it do? What is acute pancreatitis? What causes
In association with: Primary Care Society for Gastroenterology INFORMATION ABOUT Acute Pancreatitis www.corecharity.org.uk What is the Pancreas? What does it do? What is acute pancreatitis? What causes
Laparoscopic Nephrectomy
 Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Laparoscopic Nephrectomy Department of Urology Patient Information What What is Laparoscopic is Laparoscopic Nephrectomy? Nephrectomy? Laparoscopic Nephrectomy is a minimal invasive procedure or key-hole
Laparoscopy. What you need to know. 139 Dumaresq Street Campbelltown Phone Fax
 Laparoscopy What you need to know 139 Dumaresq Street Campbelltown Phone 4628 5292 Fax 4628 0349 www.nureva.com.au September 2015 Laparoscopy is a procedure where I insert a telescope through your navel,
Laparoscopy What you need to know 139 Dumaresq Street Campbelltown Phone 4628 5292 Fax 4628 0349 www.nureva.com.au September 2015 Laparoscopy is a procedure where I insert a telescope through your navel,
The organs and tissues of the body are made up of tiny building blocks called cells. Cancer is a disease of these cells.
 Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Surgery: English Surgery This fact sheet is about surgery for cancer. This is when someone has an operation to remove part of the body where the cancer is growing. It is also used to help diagnose cancer.
Primary Liver Cancer or Hepatocellular Carcinoma (HCC)
 Primary Liver Cancer or Hepatocellular Carcinoma (HCC) Patient Information Booklet UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Primary Liver Cancer or Hepatocellular Carcinoma (HCC) Patient Information Booklet UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Appendicitis. Diagnosis and Surgery
 Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Appendicitis Diagnosis and Surgery What Is Appendicitis? Your side may hurt so much that you called your doctor. Or maybe you went straight to the hospital emergency room. If the symptoms came on quickly,
Steroid Joint Injections under General Anaesthetic. Information for young people
 Steroid Joint Injections under General Anaesthetic Information for young people What is a Joint Injection? A joint injection is a treatment that is used for Juvenile Idiopathic Arthritis (J.I.A). It means
Steroid Joint Injections under General Anaesthetic Information for young people What is a Joint Injection? A joint injection is a treatment that is used for Juvenile Idiopathic Arthritis (J.I.A). It means
Having an ERCP (endoscopic retrograde cholangio pancreatogram)
 Having an ERCP (endoscopic retrograde cholangio pancreatogram) The aim of this information sheet is to help answer some of the questions you may have about having an ERCP. It explains what it is, why it
Having an ERCP (endoscopic retrograde cholangio pancreatogram) The aim of this information sheet is to help answer some of the questions you may have about having an ERCP. It explains what it is, why it
Cholangiocarcinoma (Bile Duct Cancer)
 Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
Cholangiocarcinoma (Bile Duct Cancer) The Bile Duct System (Biliary Tract) A network of bile ducts (tubes) connects the liver and the gallbladder to the small intestine. This network begins in the liver
University Hospitals Bristol NHS Foundation Trust NHS. Catheterisation using a Mitrofanoff
 University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
University Hospitals Bristol NHS Foundation Trust NHS Tel: 0117 342 8840 DEPARTMENT OF PAEDIATRIC UROLOGY Fax 0117 342 8845 Bristol Royal Hospital for Children Paul O Gorman Building Family information
Roboticassisted. laparoscopic nephrectomy
 Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
Roboticassisted laparoscopic nephrectomy This leaflet is designed to give you information on why this procedure may be suitable for you, and what you can expect from it. It outlines the advantages and
My Passport. Name: Date of birth:
 My Passport Name: Date of birth: This passport has been developed to help you keep track of important information related to your liver condition. You can use this passport to record important details
My Passport Name: Date of birth: This passport has been developed to help you keep track of important information related to your liver condition. You can use this passport to record important details
CATHETER PASSPORT. Looking after your Urinary Catheter. The Catheter Passport should be given to all patients with a urinary catheter.
 CATHETER PASSPORT Looking after your Urinary Catheter The Catheter Passport should be given to all patients with a urinary catheter. Health care staff should ensure that page 10 is completed. This document
CATHETER PASSPORT Looking after your Urinary Catheter The Catheter Passport should be given to all patients with a urinary catheter. Health care staff should ensure that page 10 is completed. This document
Femoropopliteal/distal. bypass grafts. Vascular Surgery Patient Information Leaflet
 Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
Femoropopliteal/distal bypass grafts Vascular Surgery Patient Information Leaflet Femoro-popliteal/distal bypass grafts This leaflet tells you about the operation known as a femoropopliteal bypass graft.
ERCP. Patient Information
 ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
Treatment for early pancreatic cancer
 13 11 20 Information and support Treatment for pancreatic cancer Contents Treatment for early pancreatic cancer Surgery What to expect after surgery Neoadjuvant and adjuvant therapies Treatment for advanced
13 11 20 Information and support Treatment for pancreatic cancer Contents Treatment for early pancreatic cancer Surgery What to expect after surgery Neoadjuvant and adjuvant therapies Treatment for advanced
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
