CERVICAL SCREENING. a pocket guide. Cancer Screening Programmes
|
|
|
- Flora Nicholson
- 5 years ago
- Views:
Transcription
1 CERVICAL SCREENING a pocket guide Cancer Screening Programmes
2 CERVICAL SCREENING a pocket guide This booklet is a simple guide to cervical screening. We hope you find it useful whether you work for or take a professional interest in the NHS Cervical Screening Programme. Your comments about the pocket guide are welcome and should be sent to: Julietta Patnick Director NHS Cervical Screening Programme The Manor House 260 Ecclesall Road South Sheffield S11 9PS Further copies of this guide are available from: Department of Health publications orderline Telephone: Fax: orders: doh@prolog.uk.com Cancer Screening Programmes
3 CONTENTS The NHS Cervical Screening Programme Cervical cancer incidence, mortality and risk factors Cervical screening results and treatment Future developments in cervical screening Informed choice CERVICAL SCREENING What happens in the NHS Cervical Screening Programme 22 Directory 24 1
4 The NHS Cervical Screening Programme What is cervical screening? Cervical screening is not a test for cancer. It is a method of preventing cancer by detecting and treating early abnormalities which, if left untreated, could lead to cancer in a woman s cervix (the neck of the womb). Early detection and treatment can prevent around 75 per cent of cancers developing but like other screening tests, it is not perfect. It may not always detect early cell changes that could lead to cancer. The first stage in cervical screening is either a smear test or a liquid based cytology (LBC) test. Most women consider these procedures to be only mildly uncomfortable. What is a smear test? A sample of cells is taken from the cervix for analysis. A doctor or nurse inserts an instrument (a speculum) to open the woman s vagina and uses a spatula to sweep around the cervix. The sample of cells is smeared on to a slide which is sent to a laboratory for examination under a microscope. What is LBC? LBC is a new way of preparing cervical samples for examination in the laboratory. A sample of cells is taken using a spatula which brushes cells from the cervix. Rather than smearing the sample onto a microscope slide as happens with the conventional smear, the head of the spatula, where the cells are lodged, is broken off into a small glass vial containing preservative fluid or rinsed directly into the preservative fluid. 2
5 The sample is sent to the laboratory where it is spun and treated to remove obscuring material, for example mucus or pus, and a random sample of the remaining cells is taken. A thin layer of the cells is deposited onto a slide. The slide is examined in the usual way under a microscope by a cytologist. LBC is currently being introduced. Due to retraining of laboratory staff and sample takers, roll-out is expected to take place over the next five years. LBC will: Reduce the number of inadequate cervical tests (for example, the introduction of LBC at the pilot sites reduced the reported rate of inadequate tests from 9 per cent to 1-2 per cent). Reduce the pressure on a skilled workforce (fewer inadequate tests and clearer to read samples). Nationally, the workload would be reduced from 4.2 million slides per annum to 3.9 million slides. Reduce levels of anxiety in women who accept their invitation for cervical screening due to quicker reporting time and a reduction in the number of women recalled. CERVICAL SCREENING What does the NHS Cervical Screening Programme do? The programme aims to reduce the number of women who develop invasive cervical cancer (incidence) and the number of women who die from it (mortality). It does this by regularly screening all women at risk so that conditions which might otherwise develop into invasive cancer can be identified and treated. 3
6 Who is eligible for screening? Cancer Research UK (CRUK) evaluated the interval for cervical screening. The findings indicate that a more effective and targeted programme can be provided by changing the frequency of screening according to a woman s age. 1 The Advisory Committee on Cervical Screening has accepted recommendations made by CRUK scientists. National recommendations have been changed as follows: Age Group (Years) Frequency of Screening 25 First invitation yearly yearly The change is recommended to take place after a woman s next cervical test. The NHS call and recall system invites women who are registered with a GP. This also keeps track of any follow-up investigation and, if all is well, recalls the woman for screening in three or five years time. It is therefore important that all women ensure their GP has their correct name and address. Women who have not had a recent cervical test may be offered one when they attend their GP or family planning clinic on another matter. Why are women under 25 and women over 65 not invited? Invasive cancer is rare in women under 25 but changes in the cervix are common. This means that younger women may get an abnormal result when there is nothing wrong. 1 P Sasieni, J Adams and J Cuzick, Benefits of cervical screening at different ages: evidence from the UK audit of screening histories, British Journal of Cancer, July
7 Cervical cancer is very rare in women under 25. Evidence suggests that screening women under the age of 25 may do more harm than good by resulting in unnecessary investigations after false positive results suggest that they appear to have cervical abnormalities when in fact they do not. Screening women from the age of 25 will help reduce anxiety as well as the number of unnecessary investigations and treatments in younger women. Any woman under 25 who is concerned about her risk of developing cervical cancer, or her sexual health generally, should contact her GP or Genito-Urinary Medicine (GUM) clinic. Women aged 65 and over who have had three consecutive negative cervical tests in the preceding ten years are taken out of the recall system. The natural history and progression of cervical cancer means it is highly unlikely that such women will go on to develop the disease. Women aged 65 and over who have never had a cervical test are entitled to one. What about women who are not sexually active? CERVICAL SCREENING The NHS Cervical Screening Programme invites all women between the ages of 25 and 64 for cervical screening. If a woman has never been sexually active with a man, research evidence shows that her chance of developing cervical cancer is very low. In these circumstances, a woman might choose to decline the invitation for cervical screening on this occasion. 5
8 When was the NHS Cervical Screening Programme set up? Cervical screening began in Britain in the mid-1960s. Although many women were having regular smear tests by the mid-1980s, there was concern that those at greatest risk were not being tested and that those who had positive results were not being followed up and treated effectively. The NHS Cervical Screening Programme was set up in 1988 when the Department of Health instructed all health authorities to introduce computerised call-recall systems and to meet certain quality standards. How many women are screened? The programme screens almost four million women in England each year. Of the 3.6 million women in the target age group screened in , 2.7 million were tested following an invitation and about 0.9 million were screened opportunistically at the suggestion of the sample taker or of the woman herself. 2 For clinical reasons some women have more than one cervical test during the course of a year and an estimated 4.1 million tests were examined by pathology laboratories during Of the 13.8 million women aged eligible for cervical screening in , 81.2 per cent had been screened within the previous five years. 2 How is the programme organised? More than 100,000 people are involved in cervical screening. They include the doctors and nurses who take the tests in GP surgeries and community clinics, the laboratory staff who review the slides and the people who run the computer systems. 2 Department of Health Statistical Bulletin, Cervical Screening Programme, England
9 The National Coordination Office, based in Sheffield, is responsible for improving the overall performance of the programme. Set up in 1994, its priorities are to: Develop systems and guidelines which will assure a high quality of cervical screening throughout the country. Improve communications within the programme and to women. Identify important policy issues and help resolve them. Every Primary Care Trust has a nominated person responsible for its cervical screening programme. Regional Directors of Public Health are responsible for the quality assurance network in their region. How much does the programme cost and how is it funded? Cervical screening, including the cost of treating pre-cancerous lesions, has been estimated to cost around 150 million a year in England. The cost per woman screened equates to Primary Care Trusts commission cervical screening from the overall allocation they receive from the Department of Health. The new General Medical Services (GMS) Contract for GPs came into effect on 1st April Under the new contract, target payments no longer exist. Instead, GPs are being funded to provide a cervical screening service to national guidelines. Cervical screening is funded through the global sum paid to each GP practice monthly in advance. In addition, further funding is available for delivering a quality service. For example, half of the available extra funding is rewarded on a sliding scale for screening between 25 per cent and 80 per cent of eligible women who have had an adequate cervical screening test performed in the last three to five years. CERVICAL SCREENING 7
10 Cervical cancer incidence, mortality and risk factors What is the incidence of cervical cancer? There were an estimated 2,400 new cases of invasive cervical cancer in England in Cervical cancer incidence fell by 42 per cent between 1988 and 1997 (England and Wales). This fall is directly related to the cervical screening programme. 4 There was a 25 per cent decrease in the incidence rate of cervical cancer for women under the age of 70 from 1990 to This has been attributed to the rapid increase in coverage of the cervical screening programme which occurred from 1989 onwards. 5 In 1995 there were 10.4 newly diagnosed cases of cervical cancer per 100,000 women. 6 By 1999 this had fallen to 9.3 per 100,000 women. 7 Cervical screening now saves approximately 1,300 lives per year. 8 In ,617 women in England were found to have the most severe type of Cervical Intraepithelial Neoplasia 3 (CIN3). 7 This can only be detected by screening and is treated to prevent invasive cancer developing. UK incidence rates are slightly below the European Union average while the mortality rates are slightly above. 9 An estimated 471,000 new cases of cervical cancer are diagnosed each year in the world with 80 per cent of these occurring in the less developed world. 9 3 National Statistics, Cancer Registrations, England National Statistics, Health Statistics Quarterly 07, Autumn Cancer Incidence and Mortality in England and Wales: trends and risk factors. Swerdlow, Silva and Doll OUP National Statistics MB1 No 28 Cancer statistics. Registrations National Statistics MB1 No 30 Registrations of cancer diagnosed in Sasieni P, Adams J, BMJ 1999; 318: Cancer Stats, Cervical Cancer UK, January 2003, Cancer Research UK, London 8
11 How many women die from cervical cancer? For the first time ever death rates from cervical cancer have fallen below 1,000 in England. In 2002, 927 deaths from cervical cancer were registered. 10 Mortality rates generally increase with age. Less than 5 per cent of cervical cancer deaths occur in women under Mortality rates in 2000 were 60 per cent lower (3.3 per 100,000 women) than they were 30 years earlier (8.3 per 100,000 in 1971). 11 Cervical cancer is the eleventh most common cause of cancer deaths in women in the UK, compared with third world countries where it is one of the most common killers. It accounts for around 2 per cent of all female cancers in the UK. 11 The latest relative survival figures for England show that an average of 84 per cent of women diagnosed with cervical cancer between 1993 and 1995 were alive one year later and 66 per cent were alive five years later. 11 CERVICAL SCREENING 10 Health Statistics Quarterly, Summer 2003, National Statistics 11 Cancer Stats, Cervical Cancer UK, January 2003, Cancer Research UK, London 9
12 Death from cancer of the cervix in England and Wales, Year of death Introduction of national call-recall system All ages (rate per 100,000 women) 10
13 What are the risk factors for cervical cancer? The exact cause of cervical cancer is not known. However, it is known that certain types of human papilloma virus (HPV) are linked with around 95 per cent of all cases of cervical cancer. Women with many sexual partners, or whose partners have had many partners, are more at risk. Using a condom gives some protection while long term use of oral contraceptives increases the risk. The benefits of taking oral contraceptives far outweigh the risks for the majority of women. Women who smoke are about twice as likely to develop cervical cancer as non-smokers. Women with a late first pregnancy have a lower risk than those with an early pregnancy; the risk rises with the number of pregnancies. Women in manual social classes are at higher risk than those in non-manual social classes. Women who have had a total hysterectomy for other non-malignant reasons cannot get cervical cancer and no longer need cervical screening. Women who take immunosuppressant drugs (for example, after an organ transplant) are at increased risk of developing cervical cancer. Despite the risk factors, cervical screening can prevent around 75 per cent of cancer cases in women who attend regularly. Screening is one of the best defences against cervical cancer. Many of those who develop it have never been screened. The biggest risk factor therefore is non-attendance. CERVICAL SCREENING 11
14 Cervical screening results and treatment Under national quality assurance guidelines, 80 per cent of women should receive the result of their cervical test in writing within four weeks and all women should be informed within six weeks. 12 Cytology, the study of cells, enables cervical tests to be grouped into different grades. This helps the doctors decide what action needs to be taken. GRADE EXPLANATION ACTION NEGATIVE No abnormalities detected Routine recall after three to five years ABNORMAL Cellular appearances which Refer for colposcopy after cannot be described as one borderline change or normal three abnormal tests at any grade in a ten year period Borderline changes Endocervical cell changes Refer for colposcopy after one test is reported as borderline Squamous cell changes Refer for colposcopy after three tests in a series are reported as borderline Mild dyskaryosis Cellular appearances Ideally refer for colposcopy consistent with CIN* 1 but it remains acceptable to recommend a repeat test after one test reported as mild dyskaryosis. If two tests are reported as mild dyskaryosis refer for colposcopy Moderate Cellular appearances Refer for colposcopy dyskaryosis consistent with CIN 2 Severe dyskaryosis Cellular appearances Refer for colposcopy consistent with CIN 3 Suspected Possibility of invasive cancer Refer for colposcopy. Women invasive cancer should be seen urgently within two weeks of referral INADEQUATE The test cannot be interpreted. Repeat the test. Refer for It may be too thick or colopscopy after three too thin, obscured by consecutive inadequate inflammatory cells, blood, samples incorrectly labelled or does not contain the right type of cells NHSCSP Publication No.20: Colposcopy and Programme Management Guidelines for the NHS Cervical Screening Programmes *The abnormal changes, or lesions, on the skin of the cervix are known as cervical intraepithelial neoplasia (CIN). The appearance that is noted when cells are scraped from the surface of CIN lesions onto a slide in a cervical test is called dyskaryosis. 12 Quality assurance guidelines for the cervical screening programme, NHSCSP publication no. 3, January
15 What is colposcopy? Colposcopy is performed by specially trained clinicians at an outpatient appointment. A colposcope, a low-powered microscope, is used to examine the woman s cervix to assess the extent and severity of any problem and to determine appropriate treatment. Colposcopy further examines noninvasive conditions (CIN 1-3) so that a sample of tissue can be taken from the cervix for diagnosis and/or treatment as required. When should the cervix be treated? Not all grades of abnormality are referred for immediate treatment. Some abnormalities may disappear on their own without treatment. The Colposcopy and Programme Management Guidelines for the NHS Cervical Screening Programme 13 set out a clear protocol which aims to ensure that women at a very low risk of developing cervical cancer are not referred unnecessarily. Following referral to colposcopy a rapid return to community based cytology is also recommended for women at low risk, whereas those at high risk will be maintained on follow-up for up to ten years following treatment. At colposcopy samples can be taken from the cervix. If histological diagnosis indicates CIN 2 or 3 the affected part of the cervix can be removed or destroyed. Women with CIN 1 may be treated or kept under surveillance with repeat cervical tests. CIN 1 often disappears without treatment. CERVICAL SCREENING 13 NHSCSP Publication No.20: Colposcopy and Programme Management Guidelines for the NHS Cervical Screening Programmes 13
16 What kind of treatment is available? There are two main methods of treatment. The abnormal cells in the cervix may be destroyed using laser ablation or cold coagulation treatments or the abnormality may be cut away using loop diathermy or laser excision. Loop diathermy, where a thin wire loop cuts through and removes the abnormal area, is the most common treatment, used by 71 per cent of clinics. Hysterectomy is not usually necessary for CIN. Treatment aims to preserve a woman s fertility and ability to have children wherever possible. Surgery is the main form of treatment for localised cases for the few women who have cancer, while radiotherapy and chemotherapy may be used for more extensive disease. 14
17 Future developments in cervical screening Human Papilloma Virus (HPV) Human papilloma viruses are a group of more than 80 viruses, some of which are associated with an increased risk of cervical cancer. Most women are infected with the virus at some point, but it is not yet possible to tell which of these will go on to develop CIN, abnormalities of the cervix, nor which of them will naturally expel the virus by the normal functioning of their immune system. Most HPV infections disappear without treatment and even those women who contract high risk HPVs rarely go on to develop cervical cancer. Carrying out an HPV test at the same time as a woman has a cervical test may help to decide how to manage the woman if her test shows minor abnormalities, and could avoid referral to colposcopy with its associated anxiety. The LBC pilot also looked at using HPV testing as triage. The evaluation results from the HPV pilot should be available by the end of 2004 as the women need to be followed up. CERVICAL SCREENING ARTISTIC trial Professor Henry Kitchener is leading a trial investigating HPV as a primary screening test. The trial, entitled ARTISTIC (A Randomised Trial of HPV Testing in Primary Cervical Screening), is taking place in Manchester, Stockport, Wigan & Leigh and Salford & Trafford, and began in June It will last for six years. The trial should: Provide clear evidence on the costs, medical effects and psychosocial impact of adding HPV testing to cervical cytology. 15
18 Provide an estimate of the effectiveness and costs of HPV as a stand-alone test. Determine the contribution of HPV detection to the cervical screening programme, particularly to sensitivity, specificity and inadequate smears. Address methodological issues in HPV testing. The study population comprises 25,000 women aged who are attending general practices for routine cervical screening and who consent to having a HPV test. TOMBOLA study The Trial of Management of Borderline and other Low grade Abnormal smears (TOMBOLA) was established to understand the most appropriate way to deal with HPV positive results and associated psychological issues. Funded by the Medical Research Council, the study started recruiting women in December It is a seven year multi-centre trial and is being run from Dundee, Aberdeen and Nottingham. Our answers to questions asked about HPV infection Questions from women Is there any treatment? There is no reliable treatment to get rid of the virus, but since it disappears spontaneously over time in most women, a wait and see policy is the usual management. 16
19 Should women and/or their partner practise safe sex or use barrier methods of contraception? Correct and consistent use of male or female condoms would appear to be a sensible precaution. The virus might, however, have been present for some time before its detection and thereby passed on before condoms were used and so it is difficult to give specific advice on this. Some people come across the virus and never show its presence, developing a kind of immunity. Others harbour it for short or long periods of time without its presence being detected. There are no clinical trials to prove the efficacy or otherwise of barrier methods in this respect. The presence of HPV is not a contraindication to attempting to become pregnant. How long might she have had the infection? This is an impossible question to answer since the virus can remain in your body without harm for considerable periods of time or be quickly dealt with by the immune system. Questions from men Should they see a doctor or attend a GUM clinic? If men are worried about their partners having HPV found in screening, they might wish to visit their GP or GUM clinic for a further explanation and/or examination. Can he be tested to see if he has HPV? At present there is no reliable test to demonstrate the presence of the virus in men. Can he be treated? This is unnecessary (just as it is in women) unless the virus develops into clinical warts (growths), which project above the surrounding skin. CERVICAL SCREENING 17
20 How long might he have had the infection? This is an impossible question to answer since the virus can remain in your body without harm for considerable periods of time or be quickly dealt with by the immune system. New ways of working Since December 2001 the NHS Cervical Screening Programme has been instrumental in the development of new ways of working with professional scientists in the programme. A new grade of Advanced Biomedical Scientist Practitioner has been introduced which brings additional reporting skills to the service. These practitioners undergo substantial extra training and study culminating in a qualification by examination run jointly by the Royal College of Pathologists and the Institute of Biomedical Science. 18
21 Informed choice Every woman registered with a GP will receive her first invitation for a cervical test at 25 years old. Every effort is made to minimise women s anxiety at all stages of screening. Invitations and recall letters are carefully worded and include a contact number for those who have questions. To help them make an informed choice about whether or not to come for cervical screening, all eligible women receive a leaflet Cervical Screening THE FACTS with their invitation. The leaflet explains the benefits and limitations of cervical screening. This initiative is part of the NHS Cancer Plan and follows efforts to make the limitations of screening better understood in the wake of the Bristol Inquiry and Alder Hey. The leaflet also addresses the need to inform patients about the use of personal information for audit, as advised in General Medical Council guidance as well as tying in with the Data Protection Act, the Human Rights Act and Disability Discrimination Act. The leaflet has been produced in Braille and on tape in English and has been translated into 17 languages: Arabic, Bengali, Cantonese, Farsi, French, Greek, Gujarati, Hindi, Italian, Polish, Punjabi, Somali, Spanish, Turkish, Ukrainian, Urdu and Vietnamese. CERVICAL SCREENING 19
22 What happens to samples once they have been looked at? Samples are kept for 10 years by the laboratory so that they can compare a patient s most recent cervical test with their screening history. The laboratory may review all screening records as part of the programme s aim to offer a quality service and help increase the expertise of staff. When a review shows that a woman should have been cared for differently, she will be contacted and offered information about the reviewed case. Coverage of the target population The effectiveness of the programme can also be judged by coverage. This is the percentage of women in the target age group (25 to 64) who have been screened in the last five years. If overall coverage of 80 per cent can be achieved, the evidence suggests that a reduction in death rates of 65 to 70 per cent is possible in the long term. In 2002/03 the coverage of eligible women was 81.2 per cent. 14 Coverage of the target age group by the NHS Cervical Screening Programme has almost doubled from 45 per cent in 1988/89 to around 81 per cent in 2002/03. Coverage (less than five years since last adequate test) of the target age group (25-64) Coverage (%) /6 1996/7 1997/8 1998/9 1999/ /1 2001/2 2002/3 Year 14 Department of Health Statistical Bulletin, Cervical Screening Programme, England, 2002 /
23 Coverage (%) Coverage by NHS region: Percentage of women who had a smear test in the last five years on 31 March N England Yo Humber North East East of England Yorkshire & Humber London South Eas South es Results of screening in 2002/2003 In 2002/03, 3.6 million women were screened in England. About one in 10 cervical tests examined were inadequate specimens where no result could be determined. Of the adequate tests 92.4 per cent were negative. The test results for adequate cervical tests are shown below. 15 East 84.6 West M North Wes South East South West East Midlands West Midlands North West CERVICAL SCREENING Negative cervical tests 92.4% Borderline changes 3.9% Mild dyskaryosis 2.2% Abnormal cervical tests 7.5% Moderate dyskaryosis 0.8% Severe dyskaryosis 0.6 % 15 Department of Health Statistical Bulletin, Cervical Screening Programme, England, 2002 /
24 The NHS Call and Recall system: Holds a list of all patients registered with a GP in the area it covers. Sends the list of women due for screening to each GP to check the records (for correct name and address and in case it is not appropriate for them to be invited). Sends the invitation letters and reminder letters. Sends the results letters. What happens in the NHS Cervical Screening programme? The sample takers: A woman can choose to be screened at her GP surgery, by the GP practice nurse or at a community clinic, such as a family planning or well-woman clinic. Sample takers: Take the samples in line with quality standards and using the most up-to-date methods. Check that the results are returned to the GP surgery and to the woman. Arrange for repeat screening if necessary. The laboratory: Interprets the tests. All slides are screened by a bio-medical scientist or a cytology screener. Tests which are thought to be abnormal are screened again by senior laboratory staff and are given a result code which depends on the degree of abnormality seen. Follows strict quality assurance procedures, including rapid review by a senior member of staff of all tests originally classed as negative. Sends the results to the Primary Care Trust, the GP and the sample taker (if not the GP). 22
25 Runs a failsafe system for checking that all abnormal tests are followed up. Reports on biopsies (samples of tissue taken at colposcopy) and provides a histological diagnosis. Tests are screened in the hospital s pathology department. A consultant pathologist has overall responsibility. The colposcopy service: Accepts referrals from GPs. Takes samples from the cervix (a biopsy) to obtain a histological diagnosis. Diagnoses conditions from colposcopic examination. Treats the condition. Follows up treatment with further investigation if necessary. Discharges the patient back to the call-recall system. Runs a failsafe system for checking the follow-up of all patients treated. This service is provided in the gynaecology and genitourinary medicine departments of the general hospital. CERVICAL SCREENING The primary care team: This includes the woman s GP and all practice staff. Encourages women to be screened when they are due and keeps women informed about the different stages of the screening programme. Answers questions and concerns that women may have regarding test results, follow-up and treatment. The GP refers women for further treatment if necessary, regardless of whether he or she was the sample taker. Incidental findings of infections are not part of the NHS Cervical Screening Programme but may be reported and acted upon according to local protocols. 23
26 Directory The NHS Cervical Screening Programme National coordination office: Julietta Patnick Director NHS Cancer Screening Programmes The Manor House 260 Ecclesall Road South Sheffield S11 9PS Telephone: /1 Fax: Public relations and press enquiries: NHS Cancer Screening Programmes press office 3 London Wall Buildings London Wall London EC2M 5SY Telephone: Fax: screening@westminster.com NHS Direct Telephone:
27 Cancer Charities CancerBACUP 3 Bath Place Rivington Street London EC2A 3JR Telephone: (freephone) Macmillan Cancer Relief 89 Albert Embankment London SE1 7UQ Telephone: (Macmillan Cancer Line) Marie Curie Cancer Care 89 Albert Embankment London SE1 7TP Telephone: CERVICAL SCREENING Cancer Research UK P.O. Box 123 Lincoln s Inn Fields London WC2A 3PX Telephone: Cancerkin Royal Free Hospital Hampstead London NW3 2QG Telephone: NHS Cervical Screening Programme, January All information is correct at time of going to press.
28 NHSCSP January 2004 Cancer Screening Programmes
Human Papilloma Virus (HPV) A patient s guide
 Patient advice and liaison service (PALS) If you have a question, compliment, comment or concern please contact our PALS team on 020 7288 5551 or whh-tr.whitthealthpals@nhs.net If you need a large print,
Patient advice and liaison service (PALS) If you have a question, compliment, comment or concern please contact our PALS team on 020 7288 5551 or whh-tr.whitthealthpals@nhs.net If you need a large print,
Cervical Screening - The Facts Sgrinio Serfigol - Y Ffeithiau AWARDED FOR EXCELLENCE
 Cervical Screening - The Facts Sgrinio Serfigol - Y Ffeithiau AWARDED FOR EXCELLENCE This leaflet tells you about cervical screening. Cervical Screening Wales (CSW) invites all eligible women who live
Cervical Screening - The Facts Sgrinio Serfigol - Y Ffeithiau AWARDED FOR EXCELLENCE This leaflet tells you about cervical screening. Cervical Screening Wales (CSW) invites all eligible women who live
Northern Ireland Cervical Screening Programme
 Northern Ireland Cervical Screening Programme ANNUAL REPORT & STATISTICAL BULLETIN 2010-2011 1 Report produced by : Quality Assurance Reference Centre, PHA Date of Publication: September 2012 2 Contents
Northern Ireland Cervical Screening Programme ANNUAL REPORT & STATISTICAL BULLETIN 2010-2011 1 Report produced by : Quality Assurance Reference Centre, PHA Date of Publication: September 2012 2 Contents
NHS cervical screening
 NHS cervical screening Cervical screening the facts This leaflet tells you about cervical screening. It aims to help you choose whether or not to take part in the NHS Cervical Screening Programme. What
NHS cervical screening Cervical screening the facts This leaflet tells you about cervical screening. It aims to help you choose whether or not to take part in the NHS Cervical Screening Programme. What
Scottish Cervical Screening Programme. Colposcopy and Programme Management
 Scottish Cervical Screening Programme Colposcopy and Programme Management Addendum to NHSCSP Publication No 20 Second Edition Exceptions Applicable in NHS Scotland April 2013 (Final Version 2.8 to incorporate
Scottish Cervical Screening Programme Colposcopy and Programme Management Addendum to NHSCSP Publication No 20 Second Edition Exceptions Applicable in NHS Scotland April 2013 (Final Version 2.8 to incorporate
NHS cervical screening Helping you decide
 NHS cervical screening Helping you decide What is cervical cancer? 2 What causes cervical cancer? 2 What is cervical screening? 3 Cervical screening results 6 What is a colposcopy? 8 Making a choice the
NHS cervical screening Helping you decide What is cervical cancer? 2 What causes cervical cancer? 2 What is cervical screening? 3 Cervical screening results 6 What is a colposcopy? 8 Making a choice the
TO TEST, OR NOT TO TEST? THAT IS THE QUESTION. Cervical screening guide for lesbian and bisexual women in Norfolk and Waveney.
 TO TEST, OR NOT TO THAT IS THE QUESTION. Cervical screening guide for lesbian and bisexual women in Norfolk and Waveney. TEST? Every effort has been made to ensure that the information provided is accurate.
TO TEST, OR NOT TO THAT IS THE QUESTION. Cervical screening guide for lesbian and bisexual women in Norfolk and Waveney. TEST? Every effort has been made to ensure that the information provided is accurate.
Cancer Screening Programmes CERVICAL SCREENING. The Facts
 Cancer Screening Programmes CERVICAL SCREENING The Facts What is cervical screening? Cervical screening is not a test for diagnosing cervical cancer. It is a test to check the health of the cervix, which
Cancer Screening Programmes CERVICAL SCREENING The Facts What is cervical screening? Cervical screening is not a test for diagnosing cervical cancer. It is a test to check the health of the cervix, which
About your cervical screening (smear test) Going for screening could save your life.
 About your cervical screening (smear test) Going for screening could save your life. STOP Cancer, before it starts This leaflet is available in Easy Read, BSL, audio and large print. www.cervicalscreeningwales.wales.nhs.uk
About your cervical screening (smear test) Going for screening could save your life. STOP Cancer, before it starts This leaflet is available in Easy Read, BSL, audio and large print. www.cervicalscreeningwales.wales.nhs.uk
Information on: Cervical. screening. (smear test) jostrust.org.uk
 Information on: Cervical screening (smear test) jostrust.org.uk Cervical screening This booklet covers: What is cervical screening? Who is eligible for screening? What happens when I have a screening sample
Information on: Cervical screening (smear test) jostrust.org.uk Cervical screening This booklet covers: What is cervical screening? Who is eligible for screening? What happens when I have a screening sample
You have been asked to come for a Colposcopy examination because your cervical screening test (smear) has shown evidence of abnormal cells.
 Colposcopy Examination One Stops Patient Information Sheet Why do I need a Colposcopy examination at the one stop clinic? You have been asked to come for a Colposcopy examination because your cervical
Colposcopy Examination One Stops Patient Information Sheet Why do I need a Colposcopy examination at the one stop clinic? You have been asked to come for a Colposcopy examination because your cervical
Information on: Cervical. screening. (smear test) jostrust.org.uk
 Information on: Cervical screening (smear test) jostrust.org.uk Cervical screening This booklet covers: What is cervical screening? Who is eligible for screening? What happens when I have a screening sample
Information on: Cervical screening (smear test) jostrust.org.uk Cervical screening This booklet covers: What is cervical screening? Who is eligible for screening? What happens when I have a screening sample
STOP Cancer, before it starts*
 About your cervical screening (smear test) Going for screening could save your life. STOP Cancer, before it starts* This leaflet is available in Easy Read, BSL, audio and large print. www.cervicalscreeningwales.wales.nhs.uk
About your cervical screening (smear test) Going for screening could save your life. STOP Cancer, before it starts* This leaflet is available in Easy Read, BSL, audio and large print. www.cervicalscreeningwales.wales.nhs.uk
CERVICAL SCREENING WALES CERVICAL SCREENING PROGRAMME, WALES: 2001/02
 CERVICAL SCREENING WALES INFORMATION TEAM STATISTICAL REPORT CERVICAL SCREENING PROGRAMME, WALES: 2001/02 For more information about this report contact: Helen Beer, Information Analyst / Manager, Screening
CERVICAL SCREENING WALES INFORMATION TEAM STATISTICAL REPORT CERVICAL SCREENING PROGRAMME, WALES: 2001/02 For more information about this report contact: Helen Beer, Information Analyst / Manager, Screening
A Guide To Understanding Your Cervical Screening Test Results
 A Guide To Understanding Your Cervical Screening Test Results INTRODUCTION This booklet provides you with information to help you better understand your Cervical Screening Test results. Your healthcare
A Guide To Understanding Your Cervical Screening Test Results INTRODUCTION This booklet provides you with information to help you better understand your Cervical Screening Test results. Your healthcare
NHS Cervical Screening Programme in Kingston and Richmond ANNUAL REPORT
 Kingston Borough Team Richmond and Twickenham Borough Team 1. Introduction NHS Cervical Screening Programme in Kingston and Richmond ANNUAL REPORT 2010-12 All women between the ages of 25 and 64 are eligible
Kingston Borough Team Richmond and Twickenham Borough Team 1. Introduction NHS Cervical Screening Programme in Kingston and Richmond ANNUAL REPORT 2010-12 All women between the ages of 25 and 64 are eligible
Breast Screening. a pocket guide. Breast Screening Programme NHS_BSP_booklet_AW.indd 1 8/4/08 12:17:46
 Breast Screening a pocket guide Breast Screening Programme 11345 NHS_BSP_booklet_AW.indd 1 8/4/08 12:17:46 Breast Screening a pocket guide This booklet is a simple guide to breast screening. We hope you
Breast Screening a pocket guide Breast Screening Programme 11345 NHS_BSP_booklet_AW.indd 1 8/4/08 12:17:46 Breast Screening a pocket guide This booklet is a simple guide to breast screening. We hope you
Pap test results FOR WOMEN WITH AN ABNORMAL PAP TEST
 Pap test results FOR WOMEN WITH AN ABNORMAL PAP TEST Introduction This booklet provides women with information about abnormal Pap test results. Many women feel anxious or worried when they are told their
Pap test results FOR WOMEN WITH AN ABNORMAL PAP TEST Introduction This booklet provides women with information about abnormal Pap test results. Many women feel anxious or worried when they are told their
Abnormal Smear (Cytology) Results What do they mean?
 Abnormal Smear (Cytology) Results What do they mean? Obstetrics & Gynaecology Women & Children s Services This leaflet has been designed to give you important information about your condition / procedure,
Abnormal Smear (Cytology) Results What do they mean? Obstetrics & Gynaecology Women & Children s Services This leaflet has been designed to give you important information about your condition / procedure,
Northern Ireland cervical screening programme. Information for primary care and smear takers
 Northern Ireland cervical screening programme Information for primary care and smear takers From January 2011, the Northern Ireland cervical screening programme will no longer invite women aged under 25
Northern Ireland cervical screening programme Information for primary care and smear takers From January 2011, the Northern Ireland cervical screening programme will no longer invite women aged under 25
Cervical Screening. What Pacific women need to know
 Cervical Screening What Pacific women need to know To avoid cervical cancer and to stay well, Pacific women aged from 20 until they turn 70 need to have smear tests every three years. The smear tests look
Cervical Screening What Pacific women need to know To avoid cervical cancer and to stay well, Pacific women aged from 20 until they turn 70 need to have smear tests every three years. The smear tests look
POLICY FOR CLINICAL AUDIT OF NEW CASES OF INVASIVE CERVICAL CANCER AND DISCLOSURE OF RESULTS
 POLICY FOR CLINICAL AUDIT OF NEW CASES OF INVASIVE CERVICAL CANCER AND DISCLOSURE OF RESULTS Reference Number Version: Status Author: Alison Cropper CL-CP/2009/010 V3 Final Job Title: Hospital Based Programme
POLICY FOR CLINICAL AUDIT OF NEW CASES OF INVASIVE CERVICAL CANCER AND DISCLOSURE OF RESULTS Reference Number Version: Status Author: Alison Cropper CL-CP/2009/010 V3 Final Job Title: Hospital Based Programme
NATIONAL CERVICAL CANCER SCREENING PROGRAMME Monitor 2017
 a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a NATIONAL CERVICAL CANCER SCREENING PROGRAMME Monitor
a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a a NATIONAL CERVICAL CANCER SCREENING PROGRAMME Monitor
Information on: HPV testing. jostrust.org.uk
 Information on: HPV testing jostrust.org.uk HPV testing This booklet covers: What is HPV? How do you get HPV? HPV testing Results of HPV testing Jo s Cervical Cancer Trust 2 What is HPV testing? Human
Information on: HPV testing jostrust.org.uk HPV testing This booklet covers: What is HPV? How do you get HPV? HPV testing Results of HPV testing Jo s Cervical Cancer Trust 2 What is HPV testing? Human
GYNAECOLOGICAL CYTOLOGY
 The laboratory runs a tour of the department for Practice Nurses on request, as part of their training, explaining the procedures and requirements for Gynae LBC. RECOMMENDED PROTOCOL FOR SMEAR TAKERS Only
The laboratory runs a tour of the department for Practice Nurses on request, as part of their training, explaining the procedures and requirements for Gynae LBC. RECOMMENDED PROTOCOL FOR SMEAR TAKERS Only
For all women aged Cervical Screening. Frequently Asked Questions. States of Guernsey Public Health Services
 For all women aged 25-65 Cervical Screening Frequently Asked Questions States of Guernsey Public Health Services What is cervical screening? The Cervical Screening Programme now uses human papillomavirus
For all women aged 25-65 Cervical Screening Frequently Asked Questions States of Guernsey Public Health Services What is cervical screening? The Cervical Screening Programme now uses human papillomavirus
CELLULAR PATHOLOGY DEPARTMENT STANDARD OPERATING PROCEDURE INSTRUCTIONS FOR CERVICAL CYTOLOGY SAMPLE TAKERS
 Implementation date: October 2006 Page 1 of 7 CELLULAR PATHOLOGY DEPARTMENT STANDARD OPERATING PROCEDURE INSTRUCTIONS FOR CERVICAL CYTOLOGY SAMPLE TAKERS Purpose: This procedure has been written to provide
Implementation date: October 2006 Page 1 of 7 CELLULAR PATHOLOGY DEPARTMENT STANDARD OPERATING PROCEDURE INSTRUCTIONS FOR CERVICAL CYTOLOGY SAMPLE TAKERS Purpose: This procedure has been written to provide
WIRRAL UNIVERSITY TEACHING HOSPITAL CYTOLOGY NHS CERVICAL SCREENING PROGRAMME INFORMATION PACK FOR SAMPLE TAKERS
 Author J. Evans BMS 3 Authoriser A. Bamber Page 1 of 16 WIRRAL UNIVERSITY TEACHING HOSPITAL CYTOLOGY NHS CERVICAL SCREENING PROGRAMME INFORMATION PACK FOR SAMPLE TAKERS Author J. Evans BMS 3 Authoriser
Author J. Evans BMS 3 Authoriser A. Bamber Page 1 of 16 WIRRAL UNIVERSITY TEACHING HOSPITAL CYTOLOGY NHS CERVICAL SCREENING PROGRAMME INFORMATION PACK FOR SAMPLE TAKERS Author J. Evans BMS 3 Authoriser
Cervical Skills. Dr Margaret Laing Queen Elizabeth University Hospital
 Cervical Skills Dr Margaret Laing Queen Elizabeth University Hospital What is screening? Screening is a test offered to an apparently well person with the possibility of detecting a serious disease before
Cervical Skills Dr Margaret Laing Queen Elizabeth University Hospital What is screening? Screening is a test offered to an apparently well person with the possibility of detecting a serious disease before
Cervical screening: it s best to take the test. Updated guidance
 Cervical screening: it s best to take the test Updated guidance This leaflet gives information about cervical screening in Northern Ireland. It will help you to understand why it is important to be screened.
Cervical screening: it s best to take the test Updated guidance This leaflet gives information about cervical screening in Northern Ireland. It will help you to understand why it is important to be screened.
CERVICAL SCREENING WALES
 CERVICAL SCREENING WALES Cervical Screening Wales Audit of Cervical Cancer (CSWACC) National Report 1999-2009 For more information about this report contact: Dr Rose Fox Director Cervical Screening Wales
CERVICAL SCREENING WALES Cervical Screening Wales Audit of Cervical Cancer (CSWACC) National Report 1999-2009 For more information about this report contact: Dr Rose Fox Director Cervical Screening Wales
The introduction of HPV testing to cervical screening in Scotland
 The introduction of HPV testing to cervical screening in Scotland Frequently asked questions for professionals Key messages From early 2020, cervical cytology (looking at cells under a microscope) will
The introduction of HPV testing to cervical screening in Scotland Frequently asked questions for professionals Key messages From early 2020, cervical cytology (looking at cells under a microscope) will
CERVICAL CANCER FACTSHEET. What is cervical cancer?
 CERVICAL CANCER FACTSHEET What is cervical cancer? ENGAGe is releasing a series of factsheets to raise awareness of gynaecological cancers and to support its network to work at a grassroots level. Take-up
CERVICAL CANCER FACTSHEET What is cervical cancer? ENGAGe is releasing a series of factsheets to raise awareness of gynaecological cancers and to support its network to work at a grassroots level. Take-up
Cervical Screening A guide for women in New Zealand
 Cervical Screening 4/15/08 1:48 PM Page 1 Cervical Screening A guide for women in New Zealand Taku hauora, taku tinana, taku tūmanako My health, my body, my future Cervical Screening 4/15/08 1:48 PM Page
Cervical Screening 4/15/08 1:48 PM Page 1 Cervical Screening A guide for women in New Zealand Taku hauora, taku tinana, taku tūmanako My health, my body, my future Cervical Screening 4/15/08 1:48 PM Page
Cervical cancer is almost always linked to HPV, which is spread through genital-skin to genital-skin contact during sexual activity.
 Image description. Better Health Channel logo End of image description. Pap tests Ima ge des crip The Pap test is a quick and simple test that checks for particular changes to the cells of a woman s cervix
Image description. Better Health Channel logo End of image description. Pap tests Ima ge des crip The Pap test is a quick and simple test that checks for particular changes to the cells of a woman s cervix
The Renewed National Cervical Screening Program:
 The Renewed National Cervical Screening Program: Key information for Health Professionals Contents: Overview: National Cervical Screening Program... 2 Background: HPV and cervical cancer... 3 HPV testing
The Renewed National Cervical Screening Program: Key information for Health Professionals Contents: Overview: National Cervical Screening Program... 2 Background: HPV and cervical cancer... 3 HPV testing
Your Colposcopy Visit
 Introduction Welcome to the colposcopy clinic. This booklet tells you about. The colposcopy examination.. Tests that are done in the colposcopy clinic.. What these tests look for Take a few minutes to
Introduction Welcome to the colposcopy clinic. This booklet tells you about. The colposcopy examination.. Tests that are done in the colposcopy clinic.. What these tests look for Take a few minutes to
NHSCSP proposals for cervical screening intervals. Comments and recommendations of Council of the British Society for Clinical Cytology
 NHSCSP proposals for cervical screening intervals Comments and recommendations of Council of the British Society for Clinical Cytology The following paper is written on behalf of BSCC Council to express
NHSCSP proposals for cervical screening intervals Comments and recommendations of Council of the British Society for Clinical Cytology The following paper is written on behalf of BSCC Council to express
The Pap Smear Test. The Lebanese Society of Obstetrics and Gynecology. Women s health promotion series
 The Lebanese Society of Obstetrics and Gynecology Women s health promotion series The Pap Smear Test Since the Pap smear test started to be used the number of cases of cervical cancer was greatly reduced.
The Lebanese Society of Obstetrics and Gynecology Women s health promotion series The Pap Smear Test Since the Pap smear test started to be used the number of cases of cervical cancer was greatly reduced.
Primary High Risk HPV Testing with Cytology Triage
 Primary High Risk HPV Testing with Cytology Triage NHS Cervical Screening Programme Public Health England leads the NHS Screening Programmes Human papillomavirus (HPV) High risk (HR) HPV is associated
Primary High Risk HPV Testing with Cytology Triage NHS Cervical Screening Programme Public Health England leads the NHS Screening Programmes Human papillomavirus (HPV) High risk (HR) HPV is associated
The new Cervical Screening Test for Australian women: Louise Farrell
 The new Cervical Screening Test for Australian women: Louise Farrell Outline and explain the changes to the National Cervical Screening Program due to commence in Dec 2017 LEARNING OBJECTIVES FOR TODAY
The new Cervical Screening Test for Australian women: Louise Farrell Outline and explain the changes to the National Cervical Screening Program due to commence in Dec 2017 LEARNING OBJECTIVES FOR TODAY
HPV testing For women with high-grade abnormal Pap tests. p 1
 HPV testing For women with high-grade abnormal Pap tests p 1 It is common for abnormal changes in the cells of the cervix to be found when you have a Pap test. In most cases, these changes are caused by
HPV testing For women with high-grade abnormal Pap tests p 1 It is common for abnormal changes in the cells of the cervix to be found when you have a Pap test. In most cases, these changes are caused by
Cytology Update M Laing QEUH
 Cytology Update M Laing QEUH Age change to 25 to 65 Age 25 to 50 Three yearly smear invitation Age 50 to 65 Five yearly smear invitation Women on non routine screening will be invited up to age 70 OUTCOME
Cytology Update M Laing QEUH Age change to 25 to 65 Age 25 to 50 Three yearly smear invitation Age 50 to 65 Five yearly smear invitation Women on non routine screening will be invited up to age 70 OUTCOME
KC53/61/65 Statistical Report Adroddiad Ystadegol 2012/13 Prepared by Cervical Screening Wales
 KC53/61/65 Statistical Report Adroddiad Ystadegol 2012/13 Prepared by Cervical Screening Wales CERVICAL SCREENING WALES STATISTICAL REPORT CERVICAL SCREENING PROGRAMME, WALES: 2012/2013 For more information
KC53/61/65 Statistical Report Adroddiad Ystadegol 2012/13 Prepared by Cervical Screening Wales CERVICAL SCREENING WALES STATISTICAL REPORT CERVICAL SCREENING PROGRAMME, WALES: 2012/2013 For more information
Information for trans people
 NHS Screening Programmes Public Health England leads the NHS Screening Programmes About this leaflet This leaflet is for trans (transgender) and non-binary people in England. It tells you about the adult
NHS Screening Programmes Public Health England leads the NHS Screening Programmes About this leaflet This leaflet is for trans (transgender) and non-binary people in England. It tells you about the adult
How invasive cervical cancer audit affects clinical practice
 How invasive cervical cancer audit affects clinical practice Referring to NHSCSP and EU guidelines and audits in Southampton and London Amanda Herbert Guy s & St Thomas Foundation NHS Trust How invasive
How invasive cervical cancer audit affects clinical practice Referring to NHSCSP and EU guidelines and audits in Southampton and London Amanda Herbert Guy s & St Thomas Foundation NHS Trust How invasive
Colposcopy. Information for women. Taku hauora, taku tinana, taku tūmanako My health, my body, my future.
 Colposcopy Information for women Taku hauora, taku tinana, taku tūmanako My health, my body, my future. www.timetoscreen.nz Kia ora and welcome This information is for women referred to colposcopy (kol-poss-kapee).
Colposcopy Information for women Taku hauora, taku tinana, taku tūmanako My health, my body, my future. www.timetoscreen.nz Kia ora and welcome This information is for women referred to colposcopy (kol-poss-kapee).
National Screening Programmes (Adult Population) Annual Report
 National Screening Programmes (Adult Population) Annual Report 2011-12 1 This report details the range of national screening programmes for the adult population offered by NHS Shetland and reports the
National Screening Programmes (Adult Population) Annual Report 2011-12 1 This report details the range of national screening programmes for the adult population offered by NHS Shetland and reports the
GUIDELINES FOR CERVICAL CYTOLOGY SPECIMENS CA1066 (V8) Approved by Guidelines Assessment Panel
 NORFOLK & WAVENEY CELLULAR PATHOLOGY SERVICE GUIDELINES FOR CERVICAL CYTOLOGY SPECIMENS CA1066 (V8) DEPT. SOP NO.:C.SC.I.806b EDITION: 8 AUTHORISED BY: See table below AUTHOR: VIKI FREW DATE OF ISSUE:
NORFOLK & WAVENEY CELLULAR PATHOLOGY SERVICE GUIDELINES FOR CERVICAL CYTOLOGY SPECIMENS CA1066 (V8) DEPT. SOP NO.:C.SC.I.806b EDITION: 8 AUTHORISED BY: See table below AUTHOR: VIKI FREW DATE OF ISSUE:
Cervical screening update What you need to know about HPV primary testing
 even if you ve had the HPV vaccine whether you re sexually active or not and whatever your sexual orientation And speak to your GP if you haven t GPN Insight January 2019 Cervical screening update What
even if you ve had the HPV vaccine whether you re sexually active or not and whatever your sexual orientation And speak to your GP if you haven t GPN Insight January 2019 Cervical screening update What
NHS breast screening Helping you decide
 NHS breast screening Helping you decide 1 What is breast cancer? 2 What is breast screening? 3 Breast screening results 6 Making a choice the possible benefits 9 and risks of breast screening What are
NHS breast screening Helping you decide 1 What is breast cancer? 2 What is breast screening? 3 Breast screening results 6 Making a choice the possible benefits 9 and risks of breast screening What are
ZedScan delivers improvements in clinical performance and more efficient patient management at Sheffield Teaching Hospitals NHS Foundation Trust
 ZedScan Case Study NHS Hospital, UK. ZedScan delivers improvements in clinical performance and more efficient patient management at Sheffield Teaching Hospitals NHS Foundation Trust Increased detection
ZedScan Case Study NHS Hospital, UK. ZedScan delivers improvements in clinical performance and more efficient patient management at Sheffield Teaching Hospitals NHS Foundation Trust Increased detection
Awareness of cervical cancer and prevention among women eligible for cervical screening in Scotland
 Awareness of cervical cancer and prevention among women eligible for cervical screening in Scotland A project funded by the Scottish Government Screening Inequalities Fund Contents 1. Background... 2 2.
Awareness of cervical cancer and prevention among women eligible for cervical screening in Scotland A project funded by the Scottish Government Screening Inequalities Fund Contents 1. Background... 2 2.
Treating cancer of the endometrium. Information for patients Gynaecology
 Treating cancer of the endometrium Information for patients Gynaecology We have written this leaflet to provide you with information following your diagnosis of cancer of the endometrium. We understand
Treating cancer of the endometrium Information for patients Gynaecology We have written this leaflet to provide you with information following your diagnosis of cancer of the endometrium. We understand
Hysteroscopy Clinic. Patient Information. Women and Children - Gynaecology
 8 Hysteroscopy Clinic Patient Information Women and Children - Gynaecology When a woman is first told that she has a gynaecological condition that requires further investigation at a specialised hospital
8 Hysteroscopy Clinic Patient Information Women and Children - Gynaecology When a woman is first told that she has a gynaecological condition that requires further investigation at a specialised hospital
Information about. Cervical screening. (smear test) jostrust.org.uk
 Information about Cervical screening Cervical screening (smear test) jostrust.org.uk About this booklet This booklet is for anyone who has been invited for cervical screening (a smear test) or is interested
Information about Cervical screening Cervical screening (smear test) jostrust.org.uk About this booklet This booklet is for anyone who has been invited for cervical screening (a smear test) or is interested
2. CANCER AND CANCER SCREENING
 2. CANCER AND CANCER SCREENING INTRODUCTION The incidence of cancer and premature mortality from cancer are higher in Islington compared to the rest of England. Although death rates are reducing, this
2. CANCER AND CANCER SCREENING INTRODUCTION The incidence of cancer and premature mortality from cancer are higher in Islington compared to the rest of England. Although death rates are reducing, this
Human Papillomavirus (HPV) vaccination to protect against cervical cancer
 Community Immunisation Service IMPORTANT INFORMATION Human Papillomavirus (HPV) vaccination to protect against cervical cancer School year 8 GIRLS ONLY COMMUNITY IMMUNISATION TEAM IN SCHOOL TUESDAY, 13
Community Immunisation Service IMPORTANT INFORMATION Human Papillomavirus (HPV) vaccination to protect against cervical cancer School year 8 GIRLS ONLY COMMUNITY IMMUNISATION TEAM IN SCHOOL TUESDAY, 13
The Future of Cervical Screening. Jenny Ross
 The Future of Cervical Screening Jenny Ross Introduction Cervical cancer and the Pap smear History of cervical screening in Australia New knowledge about HPV and cervical cancer HPV Vaccination Program
The Future of Cervical Screening Jenny Ross Introduction Cervical cancer and the Pap smear History of cervical screening in Australia New knowledge about HPV and cervical cancer HPV Vaccination Program
TARGETS To reduce the age-standardised mortality rate from cervical cancer in all New Zealand women to 3.5 per or less by the year 2005.
 Cervical Cancer Key points Annually, around 85 women die from, and 230 women are registered with, cervical cancer. The decline in both incidence and mortality rates for cervical cancer has accelerated
Cervical Cancer Key points Annually, around 85 women die from, and 230 women are registered with, cervical cancer. The decline in both incidence and mortality rates for cervical cancer has accelerated
NHSCSP AUDIT OF INVASIVE CERVICAL CANCER: NATIONAL REPORT
 NHSCSP AUDIT OF INVASIVE CERVICAL CANCER: NATIONAL REPORT 2009-2012 NHSCSP audit of invasive cervical cancer: national report 2009-2012 i Lead Authors Professor Peter Sasieni Professor of Biostatistics
NHSCSP AUDIT OF INVASIVE CERVICAL CANCER: NATIONAL REPORT 2009-2012 NHSCSP audit of invasive cervical cancer: national report 2009-2012 i Lead Authors Professor Peter Sasieni Professor of Biostatistics
Cuid d Fheidhmeannacht na Seirbhíse Sláinte. Part of the Health Service Executive. CS/PR/PM-20 Rev 2 ISBN Programme Report 2014/2015
 Programme Report 2014/2015 Contents Summary points 2 Introduction to the statistics 2014/2015 3 Part 1 Cervical screening activity 3 Programme coverage 4 Laboratory turnaround time 7 Notification of results
Programme Report 2014/2015 Contents Summary points 2 Introduction to the statistics 2014/2015 3 Part 1 Cervical screening activity 3 Programme coverage 4 Laboratory turnaround time 7 Notification of results
The Northern Ireland breast screening programme
 The Northern Ireland breast screening programme Guide for health professionals The HSC offers breast screening to reduce the number of women who die from breast cancer. Breast cancer is the second most
The Northern Ireland breast screening programme Guide for health professionals The HSC offers breast screening to reduce the number of women who die from breast cancer. Breast cancer is the second most
Cervical screening: your results explained. Updated guidance
 Cervical screening: your results explained Updated guidance This leaflet will explain the results of your cervical screening test which is designed to pick up any changes in cells on the cervix (lower
Cervical screening: your results explained Updated guidance This leaflet will explain the results of your cervical screening test which is designed to pick up any changes in cells on the cervix (lower
NHS breast screening Helping you decide
 NHS breast screening Helping you decide What is breast cancer?... 3 What is breast screening?... 4 Breast screening results... 7 Making a choice the possible benefits and risks of breast screening... 11
NHS breast screening Helping you decide What is breast cancer?... 3 What is breast screening?... 4 Breast screening results... 7 Making a choice the possible benefits and risks of breast screening... 11
NHS breast screening Helping you decide
 NHS breast screening Helping you decide What is breast cancer?... 3 What is breast screening?... 3 Breast screening results... 5 Making a choice the possible benefits and risks of breast screening... 8
NHS breast screening Helping you decide What is breast cancer?... 3 What is breast screening?... 3 Breast screening results... 5 Making a choice the possible benefits and risks of breast screening... 8
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines
 Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Appropriate Use of Cytology and HPV Testing in the New Cervical Cancer Screening Guidelines Tim Kremer, MD Ralph Anderson, MD 1 Objectives Describe the natural history of HPV particularly as it relates
Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two
 Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two Seshu P. Sarma, MD, FAAP Emory University Regional Training Center Atlanta, Georgia Produced by the Alabama Department of Public Health
Faculty Pap Smear Guidelines: Family Planning Update 2008 Part Two Seshu P. Sarma, MD, FAAP Emory University Regional Training Center Atlanta, Georgia Produced by the Alabama Department of Public Health
Preventing Cervical Cancer 2018 WHAT THIS WILL MEAN FOR PRIMARY CARE
 Preventing Cervical Cancer 2018 WHAT THIS WILL MEAN FOR PRIMARY CARE DR GARY FENTIMAN, CLINICAL LEADER COLPOSCOPY, N C S P TAKE-HOME LESSONS Vaccination is Primary Prevention for Cervical Cancer Women
Preventing Cervical Cancer 2018 WHAT THIS WILL MEAN FOR PRIMARY CARE DR GARY FENTIMAN, CLINICAL LEADER COLPOSCOPY, N C S P TAKE-HOME LESSONS Vaccination is Primary Prevention for Cervical Cancer Women
Estimated New Cancers Cases 2003
 Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz Estimated New Cancers Cases 2003 Images removed due to copyright reasons.
Harvard-MIT Division of Health Sciences and Technology HST.071: Human Reproductive Biology Course Director: Professor Henry Klapholz Estimated New Cancers Cases 2003 Images removed due to copyright reasons.
PAP SMEAR and BD SurePath TM Tests
 PAP SMEAR and BD SurePath TM Tests What is a Pap smear? A Pap smear is a simple procedure in which cells are removed from the lower end of the womb (cervix) during an internal examination of the vagina.
PAP SMEAR and BD SurePath TM Tests What is a Pap smear? A Pap smear is a simple procedure in which cells are removed from the lower end of the womb (cervix) during an internal examination of the vagina.
European Union survey on organization and quality control of cervical cancer screening and HPV vaccination programs
 European Union survey on organization and quality control of cervical cancer screening and HPV vaccination programs Introduction to the Survey The purpose of this project is to collect information regarding
European Union survey on organization and quality control of cervical cancer screening and HPV vaccination programs Introduction to the Survey The purpose of this project is to collect information regarding
ANNEX 07 - LATVIA MEDIA GUIDE on CERVICAL CANCER IN LATVIA
 European Commission Directorate C Public Health and Risk Assessment Health & Consumer Protection Directorate general GRANT AGREEMENT n 2007121 EUROCHIP-III European Cancer Health Indicator Project-III
European Commission Directorate C Public Health and Risk Assessment Health & Consumer Protection Directorate general GRANT AGREEMENT n 2007121 EUROCHIP-III European Cancer Health Indicator Project-III
Objectives. I have no financial interests in any product I will discuss today. Cervical Cancer Screening Guidelines: Updates and Controversies
 Cervical Cancer Screening Guidelines: Updates and Controversies I have no financial interests in any product I will discuss today. Jody Steinauer, MD, MAS University of California, San Francisco Objectives
Cervical Cancer Screening Guidelines: Updates and Controversies I have no financial interests in any product I will discuss today. Jody Steinauer, MD, MAS University of California, San Francisco Objectives
BREAST CANCER & CERVICAL CANCER SCREENING
 BREAST CANCER & CERVICAL CANCER 1 BREAST Cancer WHAT IS BREAST CANCER? Breast cancer starts when cells in the breast begin to grow in an uncontrolled way and build up to form a lump (also known as a tumour).
BREAST CANCER & CERVICAL CANCER 1 BREAST Cancer WHAT IS BREAST CANCER? Breast cancer starts when cells in the breast begin to grow in an uncontrolled way and build up to form a lump (also known as a tumour).
What is HPV and why is it so important?
 Understanding HPV For many years, Pap smears have been the most effective way to tell if a woman is at risk of developing cervical cancer. The Pap smear may also identify a common viral infection called
Understanding HPV For many years, Pap smears have been the most effective way to tell if a woman is at risk of developing cervical cancer. The Pap smear may also identify a common viral infection called
07 August Dear Colleague,
 07 August 2018 Dear Colleague, Further to our letter dated 9 May 2018, we are writing today to all healthcare professionals registered with CervicalCheck with updated advice and information regarding CervicalCheck.
07 August 2018 Dear Colleague, Further to our letter dated 9 May 2018, we are writing today to all healthcare professionals registered with CervicalCheck with updated advice and information regarding CervicalCheck.
Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families
 Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast and Ovarian Cancer is a genetic condition which
Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast and Ovarian Cancer is a genetic condition which
Translation and Interpretation Policy
 Translation and Interpretation Policy Version 1 Ratified By NHS West Cheshire Clinical Commissioning Group Governing Body Date Ratified 16 th November 2017 Author(s) Jonathan Taylor Responsible Committee
Translation and Interpretation Policy Version 1 Ratified By NHS West Cheshire Clinical Commissioning Group Governing Body Date Ratified 16 th November 2017 Author(s) Jonathan Taylor Responsible Committee
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs. Gynaecological sarcomas Version 1
 Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Gynaecological sarcomas Version 1 Background This guidance is to provide direction for the management of patients with sarcomas
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Gynaecological sarcomas Version 1 Background This guidance is to provide direction for the management of patients with sarcomas
Northern Ireland breast screening. Helping you decide
 Northern Ireland breast screening Helping you decide What is breast cancer? 4 What is breast screening? 5 Breast screening results 8 Making a choice the possible benefits 11 and risks of breast screening
Northern Ireland breast screening Helping you decide What is breast cancer? 4 What is breast screening? 5 Breast screening results 8 Making a choice the possible benefits 11 and risks of breast screening
Northern Ireland breast screening. Helping you decide
 Northern Ireland breast screening Helping you decide 1 What is breast cancer? 4 What is breast screening? 5 Breast screening results 9 Making a choice the possible benefits and risks of breast screening
Northern Ireland breast screening Helping you decide 1 What is breast cancer? 4 What is breast screening? 5 Breast screening results 9 Making a choice the possible benefits and risks of breast screening
Barrett s Oesophagus
 PATIENT INFORMATION Barrett s Oesophagus Radiofrequency Ablation of Barrett s Columnar Lined Oesophagus and Squamous Dysplasia MulticentreTrial with Long Term Follow Up Using a Central Database Project
PATIENT INFORMATION Barrett s Oesophagus Radiofrequency Ablation of Barrett s Columnar Lined Oesophagus and Squamous Dysplasia MulticentreTrial with Long Term Follow Up Using a Central Database Project
UK National Screening Committee HPV as primary screen for cervical cancer - an evidence review. Consultation comments pro-forma.
 UK National Screening Committee HPV as primary screen for cervical cancer - an evidence review Consultation comments pro-forma Name: Sarah May Email address: sarahmay@ibms.org Organisation (if appropriate):
UK National Screening Committee HPV as primary screen for cervical cancer - an evidence review Consultation comments pro-forma Name: Sarah May Email address: sarahmay@ibms.org Organisation (if appropriate):
Cervical cancer screening in Norway
 Cervical cancer screening in Norway «The future of cancer screening in Estonia: health benefits and best practices» 17 November 2016, Tartu Stefan Lönnberg Cancer Registry of Norway Screening governance
Cervical cancer screening in Norway «The future of cancer screening in Estonia: health benefits and best practices» 17 November 2016, Tartu Stefan Lönnberg Cancer Registry of Norway Screening governance
News. Laboratory NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING TIMOTHY UPHOFF, PHD, DABMG, MLS (ASCP) CM
 Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Laboratory News Inside This Issue NEW GUIDELINES DEMONSTRATE GREATER ROLE FOR HPV TESTING IN CERVICAL CANCER SCREENING...1 NEW HPV TEST METHODOLOGY PROVIDES BETTER SPECIFICITY FOR CERVICAL CANCER...4 BEYOND
Manchester Cytology Centre APRIL 2012
 Directorate of Laboratory Medicine Manchester Cytology Centre NHS Cervical Screening Programme INFORMATION PACK FOR SAMPLE TAKERS APRIL 2012 April 2012 [CYT GEN 029 Version 004] 1 SUMMARY OF CHANGES Page
Directorate of Laboratory Medicine Manchester Cytology Centre NHS Cervical Screening Programme INFORMATION PACK FOR SAMPLE TAKERS APRIL 2012 April 2012 [CYT GEN 029 Version 004] 1 SUMMARY OF CHANGES Page
APPENDIX A SERVICE SPECIFICATION
 Service Specification No. Service Authority Lead Provider Lead 2013/14 APPENDIX A SERVICE SPECIFICATION Participation in the Ruclear chlamydia and gonorrhoea screening programme (General practices) Period
Service Specification No. Service Authority Lead Provider Lead 2013/14 APPENDIX A SERVICE SPECIFICATION Participation in the Ruclear chlamydia and gonorrhoea screening programme (General practices) Period
Cervical Screening. Bexley Bromley and Greenwich (BBG) Annual Report 2009/10. Dr Angela Bhan Screening Commissioner
 Cervical Screening Bexley Bromley and Greenwich (BBG) Annual Report 2009/10 Dr Angela Bhan Screening Commissioner 1 Contents EXECUTIVE SUMMARY 3 1. NHS Cervical Screening Programme 1.1 Local programme
Cervical Screening Bexley Bromley and Greenwich (BBG) Annual Report 2009/10 Dr Angela Bhan Screening Commissioner 1 Contents EXECUTIVE SUMMARY 3 1. NHS Cervical Screening Programme 1.1 Local programme
Keywords Cytology-screening, statistics-epidemiological surveys.
 DOI: 10.1111/j.1471-0528.2007.01467.x www.blackwellpublishing.com/bjog Epidemiology An examination of the role of opportunistic smear taking in the NHS cervical screening programme using data from the
DOI: 10.1111/j.1471-0528.2007.01467.x www.blackwellpublishing.com/bjog Epidemiology An examination of the role of opportunistic smear taking in the NHS cervical screening programme using data from the
Helping you decide 2014 edition Easy Read
 Breast Screening Helping you decide 2014 edition Easy Read We have made this leaflet as accessible as possible. There are still some difficult ideas in it. You might need to ask a friend, family member,
Breast Screening Helping you decide 2014 edition Easy Read We have made this leaflet as accessible as possible. There are still some difficult ideas in it. You might need to ask a friend, family member,
cle Modern management of abnormal cervical smear Tint Tint Wai and Dilip Patil BJMP 2008:1(2) 18-22
 BJMP 2008:1(2) 18-22 Review Articl cle Modern management of abnormal cervical smear Tint Tint Wai and Dilip Patil Abbreviations BSCCP British Society of Colposcopy and Cervical Pathology CIN Cervical intraepithelial
BJMP 2008:1(2) 18-22 Review Articl cle Modern management of abnormal cervical smear Tint Tint Wai and Dilip Patil Abbreviations BSCCP British Society of Colposcopy and Cervical Pathology CIN Cervical intraepithelial
ADVICE TO PATIENTS REQUESTING PSA MEASUREMENT FREQUENTLY-ASKED QUESTIONS
 The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk ADVICE TO
The British Association of Urological Surgeons 35-43 Lincoln s Inn Fields London WC2A 3PE Phone: Fax: Website: E-mail: +44 (0)20 7869 6950 +44 (0)20 7404 5048 www.baus.org.uk admin@baus.org.uk ADVICE TO
Northern Ireland Abdominal Aortic Aneurysm (AAA) Screening Programme
 Northern Ireland Abdominal Aortic Aneurysm (AAA) Screening Programme Frequently asked questions The condition What is an abdominal aortic aneurysm (AAA)? The aorta is the main blood vessel that supplies
Northern Ireland Abdominal Aortic Aneurysm (AAA) Screening Programme Frequently asked questions The condition What is an abdominal aortic aneurysm (AAA)? The aorta is the main blood vessel that supplies
abcdefghijklmnopqrstu
 Chief Medical Officer Directorate Chief Medical Officer and Secretariat Division abcdefghijklmnopqrstu T: 0131-244 2399 F: 0131-244 2989 E: sandra.falconer@scotland.gsi.gov.uk NHS Board Medical and Nursing
Chief Medical Officer Directorate Chief Medical Officer and Secretariat Division abcdefghijklmnopqrstu T: 0131-244 2399 F: 0131-244 2989 E: sandra.falconer@scotland.gsi.gov.uk NHS Board Medical and Nursing
Cervical Cancer : Pap smear
 Taking a PAP SMEAR Cervical Cancer : Pap smear George N Papanicolaou introduced cervical cytology in clinical practice in 1940 In 1945, PAP smear was endorsed by American cancer society as an effective
Taking a PAP SMEAR Cervical Cancer : Pap smear George N Papanicolaou introduced cervical cytology in clinical practice in 1940 In 1945, PAP smear was endorsed by American cancer society as an effective
Questions and answers paper
 Questions and answers paper From Monday, June 6 th 2016*, the age range for cervical screening will change from ages 20 60 years, to ages 25 64 years plus 364 days. The frequency of cervical screening
Questions and answers paper From Monday, June 6 th 2016*, the age range for cervical screening will change from ages 20 60 years, to ages 25 64 years plus 364 days. The frequency of cervical screening
PATIENT INFORMATION. about CERVICAL CANCER
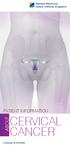 PATIENT INFORMATION about CERVICAL CANCER What is Cervical Cancer? The cervix is the lower part of the uterus (womb) connecting the body of the uterus to the vagina (birth canal). Cancer of the cervix
PATIENT INFORMATION about CERVICAL CANCER What is Cervical Cancer? The cervix is the lower part of the uterus (womb) connecting the body of the uterus to the vagina (birth canal). Cancer of the cervix
ZedScan delivers improvements in clinical performance and more efficient patient management at Sheffield Teaching Hospitals NHS Foundation Trust
 ZedScan Case Study NHS Hospital, UK. ZedScan delivers improvements in clinical performance and more efficient patient management at Sheffield Teaching Hospitals NHS Foundation Trust Increased detection
ZedScan Case Study NHS Hospital, UK. ZedScan delivers improvements in clinical performance and more efficient patient management at Sheffield Teaching Hospitals NHS Foundation Trust Increased detection
Department of Health Standard for the Cervical Cancer Screening Program. Approval Date: 08 May 2018 Effective Date: 13 May 2018
 Document Title: Department of Health Standard for the Cervical Cancer Screening Program Document Ref. Number: DOH/CCSC/SD/1.0 Version: 1.0 Approval Date: 08 May 2018 Effective Date: 13 May 2018 Last Reviewed:
Document Title: Department of Health Standard for the Cervical Cancer Screening Program Document Ref. Number: DOH/CCSC/SD/1.0 Version: 1.0 Approval Date: 08 May 2018 Effective Date: 13 May 2018 Last Reviewed:
