FINAL CENSORED REPORT: Treatment for Chronic Hepatitis B. Systematic Review and Network Meta-Analysis. September 28 th, 2015
|
|
|
- Barry Watts
- 5 years ago
- Views:
Transcription
1 FINAL CENSORED REPORT: Treatment for Chronic Hepatitis B Systematic Review and Network Meta-Analysis William W. L. Wong, Petros Pechlivanoglou, Aysegul Erman, Yasmin Saeed, Mona Younis, Noha Zaki Rayad, Joanna Bielecki, Valeria Rac, Murray D. Krahn September 28 th, Bond Street, Toronto ON, M5B 1W8 info@odprn.ca
2 Table of Contents Executive Summary... 3 Results... 9 Efficacy Virologic response ALT normalization HBeAg Loss HBeAg Seroconversion HBsAg Loss Histological improvement Comparisons among the CHB therapies Safety Serious adverse events Any adverse events Withdrawal due to adverse events Observational Studies Discussion Key Messages Reference List Appendix A: Study selection Diagrams and Search terms Appendix B: Cochrane risk of bias tool results Appendix C: Included Randomized Controlled Trial List Appendix D: Characteristics of included RCTs Appendix E: Observational Study List Appendix F: Full NMA RESULTS (EFFICACY): ODDS RATIOS FOR RANDOM EFFECTS MODEL (SIGNIFICANT IN RED FONTS) Appendix G: Full NMA RESULTS (SAFETY): ODDS RATIOS FOR RANDOM EFFECTS MODEL (SIGNIFICANT IN RED FONTS)... 84
3 3 Executive Summary Objective The objective of this review is to identify the available evidence on Randomized Controlled Trial (RCT) and observational studies investigating the comparative effectiveness and safety between the available chronic hepatitis B (CHB) treatments (standard interferon (IFN), pegylated interferon-alfa (PEG), adefovir (ADV), lamivudine (LAM), entecavir (ETV), telbivudine (LDT), and tenofovir (TDF), and their combinations) through a systematic review and synthesize this evidence using network meta-analysis. Systematic Reviews Randomized Control trial (RCT) studies A total of 5,021 studies were identified from the published literature. Upon screening the titles and abstracts, 884 potentially relevant publications were retrieved for further screening. Of the 884 potentially relevant articles, a total of 62 studies were selected for inclusion. These 62 studies were focused on mono-infected patients (40 in HBeAg positive, 22 in HBeAg negative). The total number of participants in each study ranged from 10 to 657. The overall number of included participants was 13,697. Observational Studies A total of 4,530 studies were identified from the published literature and, upon screening the titles and abstracts, 452 potentially relevant publications were retrieved for further screening. Of the 452 potentially relevant reports, a total of 52 studies were selected for inclusion. Network Meta Analyses Network meta-analyses (NMA) were conducted to estimate pooled effectiveness and safety data from the RCT studies on the following outcomes: Efficacy for HBeAg positive patients: virologic response; alanine aminotransferase (ALT) normalization; HBeAg loss; HBeAg seroconversion; and HBsAg loss; Efficacy for HBeAg negative patients: virologic response and ALT normalization. Safety: Serious adverse events, any adverse events, and withdrawal due to adverse events Results In terms of efficacy for HBeAg positive patients: LDT, TDF and ETV were found to be significantly better than LAM, PEG or IFN in terms of virologic response; TDF was also found to be significantly better than ADV, LDT, ETV, PEG and IFN in terms of virologic response. In terms of normalization of ALT, LDT was also significantly better than LAM, PEG or IFN for the HBeAg positive patients. ETV was significantly better than LAM, PEG or IFN in terms of normalization of ALT. In addition, LDT and PEG were significantly better than LAM in terms of HBeAg loss and HBeAg seroconversion. PEG was also significantly better than ETV in terms of HBeAg loss and HBeAg seroconversion.
4 4 For HBeAg negative patients: LDT, ADV, TDF and ETV were found significantly better than LAM in terms of virologic response; TDF was also found to be significantly better than ADV, LDT, PEG and IFN in terms of virologic response. In terms of normalization of ALT, only ETV was significantly better than LAM. PEG was not significantly better than IFN in terms of efficacy for both HBeAg positive and HBeAg negative patients. In terms of safety, PEG was associated with a significantly higher number of serious adverse events than LAM, LDT, and ETV. The likelihood of any adverse event was also significantly higher in studies involving PEG than LAM, PLA, ADV, LDT, TDF and ETV. Withdrawal due to adverse events was significantly less frequent in ETV compared to LAM and PEG.Other than these, there was no significant difference was found between oral agents in terms of safety. Conclusion Our systematic review of RCT studies and network meta-analysis show that for HBeAg positive patients, tenofovir is the most effective treatment followed by entecavir, in terms of virologic response and ALT normalization. In terms of HBeAg loss and HBeAg seroconversion, pegylated interferon is the most effective treatment. In terms of HBsAg loss, pegylated interferon is the most effective treatment followed by tenofovir. For HBeAg negative patients, tenofovir is also the most effective treatment, followed by adefovir and entecavir, in terms of virologic response and ALT normalization. Findings of the observational studies show that the probability of achieving virologic response and ALT normalization in a real-world setting is high among the oral agents assessed, while the probability of achieving HBeAg loss, HBeAg seroconversion, and HBsAg loss was generally low. However, direct comparisons between the treatments with respect to their relative effectiveness could not be achieved through the observational studies. More research on the comparative effectiveness of the treatments in a real-world setting is needed.
5 5 Efficacy and Safety Systematic Review Literature Search Strategy The literature search was performed by an information specialist using a peer-reviewed search strategy (Appendix A). Published literature was identified by searching the following bibliographic databases: Ovid MEDLINE (1946 ), Ovid MEDLINE In-Process; Ovid Embase (1974 ); the Cochrane Central Register of Controlled Trials; and Web of Science: Science Citation Index Expanded (1900-) and Conference Proceedings Citation Index- Science (1990-). Our search started from the date of inception of each database until October 29, Search terms included controlled vocabulary (MeSH) and text-words in the following three concept areas: chronic hepatitis B (CHB), antiviral agents (standard interferon, pegylated interferon, lamivudine, adefovir, entecavir, telbivudine, tenofovir) and the following published and validated filters were applied consecutively: Randomized Control Trials (RCTs) 1 or Prognosis studies 2 or Causation (Etiology) studies 3 or Cohort and case-control studies 4. Selection Criteria and Methods The systematic review included RCTs and observational studies (i.e. case-control and cohort studies) that compared at least two CHB treatments or placebo/no treatment in adults patients diagnosed with HBeAg-positive and/or HBeAg-negative CHB. Studies were selected for inclusion in the systematic review based on the selection criteria presented in Table 1 and 2. The review included treatment options of standard and pegylated interferon-alfa, lamivudine, adefovir, entecavir, telbivudine, and tenofovir as monotherapy or combination therapy. Table 1: Inclusion and Exclusion Criteria for Randomized Controlled Trials Inclusion Criteria Population Adult patients diagnosed with HBeAg-positive and/or HBeAg-negative CHB Treatment of interest (TO) standard interferon (IFN) pegylated interferon (PEG) lamivudine (LAM) adefovir (ADV) entecavir (ETV) telbivudine (LDT) tenofovir (TDF) Comparators Treatment of interest (TO) can be monotherapy or combination therapy TO v. placebo TO v. TO (different TO)
6 6 Inclusion Criteria Outcomes (Efficacy) virologic response alanine aminotransferase (ALT) normalization HBeAg loss HBeAg seroconversion HBsAg loss histologic improvement Outcomes (Safety) serious adverse events any adverse events withdrawals due to adverse events Study design Published, randomized, controlled interventional studies Exclusion Criteria Studies that did not meet the aforementioned selection criteria; provided results of a qualitative study; or were follow-up, extension, or observational studies. Duplicate publications, narrative reviews, and editorials were also excluded. Additional criteria include: Studies not conducted in English Uncontrolled non-randomized studies Studies breaking randomization treatment duration shorter than 48 weeks treatment experienced population > 50% Table 2: Inclusion and Exclusion Criteria for Observational studies Inclusion Criteria Population Adults patients diagnosed with HBeAg-positive and/or HBeAg-negative CHB Interventions standard interferon (IFN) pegylated interferon (PEG) lamivudine (LAM) adefovir (ADV) entecavir (ETV) telbivudine (LDT) tenofovir (TDF)
7 7 Inclusion Criteria Comparators Treatment of interest (TO) can be monotherapy or combination therapy Outcomes (Efficacy) virologic response alanine aminotransferase (ALT) normalization HBeAg loss HBeAg seroconversion HBsAg loss histologic improvement Outcomes (Safety) serious adverse events withdrawals due to adverse events any adverse events Study design Published, randomize but not included in NMA, non-randomized, controlled or uncontrolled, prospective, retrospective interventional studies. Exclusion Criteria Studies that did not meet the aforementioned selection criteria; provided results of a qualitative study; Duplicate publications, narrative reviews, and editorials were also excluded. Additional criteria include: Studies not conducted in English Uncontrolled non-randomized studies Less than 50 patients in the study scientific abstract treatment duration shorter than 48 weeks treatment experienced population > 50% Study selection and screening process Two reviewers independently screened the titles and abstracts of the studies identified by the search strategy to determine if they met the inclusion criteria, using a hierarchical screening method adapted from Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 5. Subsequently, the full text of the eligible studies was assessed by the same reviewers independently to determine if they met the inclusion criteria. Disagreements between the two reviewers at any stage of the study selection process were resolved with discussion. Clinical experts were consulted and existing systematic reviews and meta-analysis were reviewed to identify any relevant studies that were not identified through the screening process.
8 8 Data Analysis Methods The characteristics of randomized identified studies were presented narratively while the patient characteristics of the identified studies were pooled separately for RCTs and observational studies to create descriptive summary estimates for the synthesized population. For patient characteristics that could not be pooled, the estimates from each study were narratively described. Risk of bias for each study and bias domain were accessed. Network meta-analysis (NMA) methods were used to synthesize the evidence from the RCTs identified on relative effectiveness and safety across the treatment options. Binomial NMA models were applied for all the outcomes. The NMA was conducted within a Bayesian framework using WinBUGS v (MRC Biostatistics Unit, Cambridge, England) 6. Under this framework the distribution of each parameter of interest (posterior distribution) was estimated through a Markov Chain Monte Carlo simulation method. Both fixed and random effect models were considered based on the data availability in the included studies. Mean or median estimates for the parameters of interest together with their 95% credible intervals were constructed from the posterior distributions of the MCMC simulations. An important assumption underlying network meta-analysis is that of consistency between the direct and indirect evidence of relative efficacy, safety and tolerability. Any presence of inconsistency in closed loops was visually assessed using coherence plots 7, which statistically compares the similarity of the pooled estimates from the direct evidence to those from indirect evidence. Sensitivity analyses were performed to assess the impact of assumptions related to the type of model (fixed vs random) and the prior distributions of the model (e.g. informative vs vague, type of distribution assumed etc.) on the estimates of relative efficacy and safety.
9 9 Results Selection of Randomized Control trials A total of 5,021 studies were identified from the original literature. Upon screening the titles and abstracts, 884 potentially relevant publications were retrieved for further screening. Of the 884 potentially relevant articles, a total of 62 studies, were selected for inclusion (See Appendix B for Risk of bias for each study, and Appendix C for the included study characteristics). These 62 studies were for mono-infected patients (40 in HBeAg positive 8-47, 22 in HBeAg negative 22,25,27,29,32,34,37,43,44, Table 3 summarizes the included studies by interventions according to the HBeAg status. Table 3: Summary of Interventions Evaluated Interventions Publications (n) DB RCT (n) Patients (n) Publication Years Included in the NMA HBeAg Positive Patients Lamivudine (LAM) Adefovir (ADV) Telbivudine (LDT) Tenofovir (TDF) Entecavir (ETV) pegylated interferon (PEG) Conventional interferon (IFN) Combination therapies TOTAL 40* 18* 10,071 HBeAg Negative Patients Lamivudine (LAM) Adefovir (ADV) Telbivudine (LDT) Tenofovir (TDF)
10 10 Interventions Publications (n) DB RCT (n) Patients (n) Publication Years Entecavir (ETV) pegylated interferon (PEG) Conventional interferon (IFN) Combination therapies TOTAL 22* 12* 3,616 *unique publication/study Abbreviations: DB RCT: Double Blind Randomized Controlled Trial The total number of participants in each study ranged from 10 to 657. The overall number of included participants was 13,697. See Appendix D for participant baseline characteristics.
11 11 Efficacy Network meta-analyses (NMA) were conducted for 5 efficacy outcomes in HBeAg positive patients: virologic response; alanine aminotransferase (ALT) normalization; HBeAg loss; HBeAg seroconversion; and HBsAg loss; and NMA were conducted for 2 efficacy outcomes in HBeAg negative patients: virologic response and ALT normalization. The choice of these outcomes for NMA was based on their importance and the sufficiency of the data available to derive robust and consistent network models. To illustrate, the evidence networks for virologic response (Figure 1a: HBeAg positive patients; Figure 1b: HBeAg negative patients) and ALT normalization (Figure 2a: HBeAg positive patients; Figure 2b: HBeAg negative patients) are provided in below. Figure 1a: Evidence network for virologic response for HBeAg positive patients Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; PEGPEG2: double duration of PEG; ADV2: additional dose of ADV;
12 12 Figure 1b: Evidence network for virologic response for HBeAg negative patients Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; PEGPEG2: double duration of PEG; ADV2: additional dose of ADV; Figure 2a: Evidence network for alt normalization for HBeAg positive patients Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; PEGPEG2: double duration of PEG; ADV2: additional dose of ADV;
13 13 Figure 2b: Evidence network for alt normalization for HBeAg negative patients Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; PEGPEG2: double duration of PEG; ADV2: additional dose of ADV; A variety of doses were found in the included studies. Treatment nodes in the network were assigned based on product brand name if available and by generic formulation if brand names were not available. Trial dosing strategies were collapsed for nodes except where specifically noted in this report. As the predicted probabilities of an outcome with a given treatment are more readily understood than the odd ratios (OR) comparing treatments, based on the NMA, we estimated these posterior probabilities. A summary of the efficacy results for the posterior probability of outcomes are provided in Figure 3 for HBeAg positive patients and in Figure 4 for HBeAg negative patients.
14 Figure 3: PREDICTED posterior probability of efficacy outcomes based on network meta-analysis for HBeAg positive patients Posterior probability of patients achieved virologic response for HBeAg+ patients LAM PLA ADV LDT TDF ETV PEG IFN Posterior probability of patients achieved ALT normalization for HBeAg+ patients LAM PLA ADV LDT TDF ETV PEG IFN Posterior probability of patients achieved HBeAg loss for HBeAg+ patients LAM PLA ADV LDT TDF ETV PEG IFN
15 15 Posterior probability of patients achieved HBeAg seroconversion for HBeAg+ patients LAM PLA ADV LDT TDF ETV PEG IFN Posterior probability of patients achieved HBsAg loss for HBeAg+ patients LAM PLA ADV LDT TDF ETV PEG IFN Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir;;
16 Figure 4: Predicted posterior probability of efficacy outcomes based on network meta-analysis for HBeAg negative patients Posterior probability of patients achieved virologic response for HBeAg- patients LAM PLA ADV LDT TDF ETV PEG IFN Posterior probability of patients achieved ALT normalization for HBeAg- patients LAM PLA ADV LDT TDF ETV PEG IFN Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; Exhibit 4: Serum testosterone level, quality of life, erectile dysfunction, libido, and depression: mean (SD) differences from Placebo based on network meta-analysis
17 17 Virologic response Virologic response was defined as attainment of undetectable levels of HBV DNA as determined by the PCR test for the particular study. Threshold values for undetectable DNA levels according to method of techniques used for measurement were documented, as they could be a source of heterogeneity. Only studies where the threshold of detection was 1,000 copies/milliliter were used in the analysis of undetectable HBV DNA levels. Thirty-six of the 40 included HBeAg positive studies reported 1,000 copies/milliliter at the end of treatment / fellow up, and were included in the NMA 8-15,17,19-25,27,28,30-33,35-47,61. In particular, LAM+ETV (0.952 ( )) and TDF (0.856 ( )), were associated with an over 70% virologic response rate at the end of treatment (Table 3). Twenty-one of the 22 included HBeAg negative studies reported 1,000 copies/milliliter at the end of treatment / follow up, and were included in the NMA 22,25,27,29,32,34,37,43,44, From the NMA, TDF (0.981 ( )), was associated with an over 70% virologic response rate at the end of treatment (Table 4). Some of the included studies used more than one scale to evaluate virologic response. Undetected scales were chosen over subscales if possible. ALT normalization ALT normalization was defined as normalization of alanine aminotransferase (ALT) levels to below the upper limit of normal for that study. Of the included HBeAg positive studies, 27 studies assessed the efficacy of CHB therapies on participants ALT normalization 9,10,13,14,19-28,30,31,33,34,36-42,44,47. From the NMA, LDT (0.722 ( )) and ETV (0.741 ( )), were associated with a higher chance of achieving normalization of ALT at the end of treatment/follow-up than the other treatment therapies. (Table 3). Of the included HBeAg negative studies, 19 studies assessed the efficacy of CHB therapy on participants ALT normalization 22,25,27,29,32,34,37,44,48-55,57,59,60. From the NMA, ETV (0.846 ( )), ETV+TDF (0.874 ( )) and IFN (0.863 ( )), were associated with a higher chance of achieving normalization of ALT at the end of treatment/follow-up than the other treatment therapies (Table 4). HBeAg Loss In HBeAg positive patients, HBeAg loss were defined as undetectable, using the threshold of detection used in each corresponding study. Twenty-four studies 11,13-15,19,20,22-25,27,28,30-32,34-36,38,41,42,44,47,61 assessed the efficacy of HBeAg loss for HBeAg positive patients. From the NMA, ADV+LDT (0.423 ( )) and PEG+ADV (0.499 ( )), were associated with a higher chance of achieving HBeAg loss at the end of treatment/follow-up than the other treatment therapies. (Table 3).
18 18 HBeAg Seroconversion In HBeAg positive patients, seroconversion was defined as undetectable HBeAg and presence of anti-hbeag. Thirty studies 8,10,12-16,18-28,30-32,34,36,37,41,42,45,47,61 assessed the efficacy of HBeAg seroconversion for HBeAg positive patient. From the NMA, LAM+ETV (0.578 ( )) was associated with a higher chance of achieving HBeAg seroconversion at the end of treatment/follow-up than the other treatment therapies. (Table 3). HBsAg Loss HBeAg loss was defined as undetectable, using the threshold of detection used in each corresponding study. For the HBeAg positive patients, seventeen studies 9,14,22,24-26,28,32-35,37,38,41,45,47 assessed the efficacy of CHB therapies on HBsAg loss. From the NMA, TDF (0.202 ( )), LAM+PEG (0.246 ( )) and PEG+ADV (0.262 ( )), were associated with a higher chance of achieving HBsAg loss at the end of treatment/follow-up than the other treatment therapies. (Table 3). For the HBeAg negative patients, HBsAg loss was a rare event, and only four studies 22,29,37,60 assessed the efficacy of CHB therapies on HBsAg loss. NMA cannot be conducted due to limitation of data. Other efficacy outcomes were considered, but the data on these outcomes were limited: Histological Improvement Histological improvement of the liver was defined as a two point improvement on the Knodell inflammation score without an increase in fibrosis. In the HBeAg positive group, only eight studies assessed histological improvement as an efficacy outcome 9,14,20,24,26,27,36,37. Only four studies 27,29,37,51 assessed for the HBeAg negative patients. As the network was unstable due to limitation of the data, NMA was not performed on histological improvement for both HBeAg positive and HBeAg negative patients. HCC Incidence None of the included studies investigated HCC incidence as an outcome. Comparisons among the CHB therapies Summaries of the NMA comparisons among the included doses of CHB therapies are presented in Appendix F, for both HBeAg positive and HBeAg negative patients. Table 5 summaries the NMA comparisons among the monotherapies. In general for monotherapies:
19 19 Most of the treatment therapies are significantly better than PLA in terms of virologic response, normalization of ALT, HBeAg loss and HBeAg seroconversion. LAM for HBeAg positive patients LDT, TDF and ETV are significantly better than LAM in terms of virologic response. LDT, ETV are significantly better than LAM in terms of normalization of ALT. However, LAM is significantly better than PEG. LDT and PEG are significantly better than LAM in terms of HBeAg loss. LDT and PEG are significantly better than LAM in terms of HBeAg seroconversion. LAM for HBeAg negative patients ADV, LDT, TDF and ETV are significantly better than LAM in terms of virologic response. ETV is significantly better than LAM in terms of normalization of ALT. ADV for HBeAg positive patients LDT, TDF and ETV are significantly better than ADV in terms of virologic response. LDT and PEG are significantly better than ADV in terms of HBeAg loss. LDT for HBeAg positive patients LDT is significantly better than PEG and IFN in terms of virologic response. However, TDF is significantly better than LDT. LDT is significantly better than PEG and IFN in terms of normalization of ALT. LDT is significantly better than ETV in terms of HBeAg loss and HBeAg seroconversion. TDF for HBeAg positive patients TDF is significantly better than ETV, PEG and IFN in terms of virologic response. TDF is significantly better than PEG and IFN in terms of normalization of ALT. TDF for HBeAg negative patients TDF is significantly better than LAM, ADV, LDT, PEG and IFN in terms of virologic response. ETV for HBeAg positive patients ETV is significantly better than PEG and IFN in terms of virologic response normalization of ALT. However, PEG is significantly better than ETV in terms of HBeAg loss and HBeAg seroconversion. IFN for HBeAg positive or HBeAg negative patients PEG is NOT significantly better than IFN in terms of virologic response, normalization of ALT, HBeAg loss, HBeAg seroconversion and HBsAg loss. Note that some of the comparison have a large confidence interval due to the limitation of the data.
20 20 Table 5: NMA Results (EFFICACY): Odds ratios for Random Effects Model (Significant in Red Fonts) Odds ratios (95 % confidence interval) Tx Outcomes PLA ADV LDT TDF ETV PEG IFN HBeAg Positive LAM HBV DNA 0.09 ( ) 0.8 ( ) 2.43 ( ) ( ) 3 ( ) 0.65 ( ) 0.35 ( ) ALT norm 0.15 ( ) 0.98 ( ) 1.5 ( ) 1.53 ( ) 1.66 ( ) 0.46 ( ) 0.42 ( ) HBeAg loss 0.29 ( ) 0.79 ( ) 1.44 ( ) (-) 0.87 ( ) 1.6 ( ) 1.29 ( ) HBeAg sero 0.33 ( ) 0.87 ( ) 1.41 ( ) 0.97 ( ) 0.8 ( ) 1.51 ( ) 1.06 ( ) HBsAg loss 0.37 ( ) 0.73 ( ) 0.99 ( ) 3.78 (0-3442) 0.83 ( ) 6.56 ( ) 2.22 ( ) PLA HBV DNA 9.17 ( ) ( ) ( ) ( ) 7.47 ( ) 4.04 ( ) ALT norm 6.56 ( ) ( ) ( ) ( ) 3.1 ( ) 2.79 ( ) HBeAg loss 2.67 ( ) 4.89 ( ) (-) 2.92 ( ) 5.41 ( ) 4.37 ( ) HBeAg sero 2.64 ( ) 4.3 ( ) 2.94 ( ) 2.42 ( ) 4.58 ( ) 3.23 ( ) HBsAg loss 2.14 ( ) 2.71 ( ) ( ) 2.28 ( ) ( ) 6 ( ) ADV HBV DNA 3.02 ( ) ( ) 3.74 ( ) 0.81 ( ) 0.44 ( ) ALT norm 1.53 ( ) 1.56 ( ) 1.69 ( ) 0.47 ( ) 0.42 ( ) HBeAg loss 1.83 ( ) (-) 1.1 ( ) 2.03 ( ) 1.64 ( ) HBeAg sero 1.62 ( ) 1.11 ( ) 0.91 ( ) 1.73 ( ) 1.21 ( ) HBsAg loss 1.36 ( ) 4.83 ( ) 1.11 ( ) 9.17 ( ) 2.86 ( ) LDT HBV DNA 4.13 ( ) 1.23 ( ) 0.27 ( ) 0.15 ( ) ALT norm 1.02 ( ) 1.11 ( ) 0.31 ( ) 0.28 ( ) HBeAg loss (-) 0.6 ( ) 1.11 ( ) 0.89 ( ) HBeAg sero 0.68 ( ) 0.57 ( ) 1.07 ( ) 0.75 ( ) HBsAg loss 3.73 ( ) 0.84 ( ) 6.63 ( ) 2.21 ( ) TDF HBV DNA 0.3 ( ) 0.07 ( ) 0.04 ( ) ALT norm 1.09 ( ) 0.3 ( ) 0.27 ( ) HBeAg loss (-) (-) (-) HBeAg sero 0.83 ( ) 1.56 ( ) 1.09 ( ) HBsAg loss 0.22 ( ) 1.86 ( ) 0.57 ( ) ETV HBV DNA 0.22 ( ) 0.12 ( ) ALT norm 0.28 ( ) 0.25 ( ) HBeAg loss 1.85 ( ) 1.5 ( ) HBeAg sero 1.89 ( ) 1.32 ( ) HBsAg loss 7.66 ( ) 2.68 ( ) PEG HBV DNA 0.54 ( ) ALT norm 0.9 ( ) HBeAg loss 0.81 ( ) HBeAg sero 0.7 ( )
21 21 Odds ratios (95 % confidence interval) Tx Outcomes PLA ADV LDT TDF ETV PEG IFN HBsAg loss 0.31 ( ) HBeAg Negative LAM HBV DNA 0.21 ( ) 20.4 ( ) 3.08 ( ) ( ) 5 ( ) 3.04 ( ) 3.31 ( ) ALT norm 0.39 ( ) 2.61 ( ) 1.03 ( ) 2.51 ( ) 3.06 ( ) 1.93 ( ) 4.8 ( ) PLA HBV DNA ( ) ( ) ( ) ( ) ( ) ( ) ALT norm 6.8 ( ) 2.66 ( ) 6.56 ( ) 7.92 ( ) 4.99 ( ) ( ) ADV HBV DNA 0.15 (0-3.1) 8.05 ( ) 0.24 (0-5.32) 0.14 (0-4.1) 0.16 (0-3.8) ALT norm 0.39 ( ) 0.96 ( ) 1.16 ( ) 0.75 ( ) 1.81 ( ) LDT HBV DNA 54.8 ( ) 1.61 ( ) 0.98 ( ) 1.07 ( ) ALT norm 2.45 ( ) 2.97 ( ) 1.89 ( ) 4.64 ( ) TDF HBV DNA 0.03 (0-1.04) 0.02 (0-0.78) 0.02 (0-0.77) ALT norm 1.2 ( ) 0.77 ( ) 1.9 ( ) ETV HBV DNA 0.61 ( ) 0.66 ( ) ALT norm 0.64 ( ) 1.56 ( ) PEG HBV DNA 1.09 ( ) ALT norm 2.5 ( ) Abbreviations: Tx: Treatment; PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; HBV DNA, undetectable HBV DNA levels; ALT norm, normalization of serum alanine aminotransferase levels; HBeAg sero, hepatitis B e antigen seroconversion; HBeAg loss, hepatitis B e antigen loss; HBsAg loss, hepatitis B surface antigen loss; Histo Improv, histological improvement of the liver
22 22 Safety NMA were conducted for 3 safety outcomes: serious adverse events, any adverse events and withdrawal due to adverse events. Serious adverse events Twenty trials 9,10,12,14,25,27,29-32,34,36,37,44,47,50,51,54,55,60 reported serious adverse events (SAE; as defined by the authors). Table 6 summarizes the posterior probability of the serious adverse events, Table 7 summarizes the head-to-head comparison among mono-therapies, and Appendix G summarizes the full head-to-head comparison. In terms of serious adverse events, PEG has significantly more serious adverse events than LAM, LDT, and ETV. Any adverse events Twenty trials 9,14,17,22,25-29,31,32,34,36,37,42,44,51,54,55 reported any adverse events (AE; as defined by the authors). Table 6 summarizes the posterior probability of the any adverse events, Table 7 summarizes the headto-head comparison among mono-therapies, and Appendix G summarizes the full head-to-head comparison. In terms of any adverse events, PEG has statistically significantly more any adverse events than LAM, PLA, ADV, LDT, TDF and ETV. Withdrawal due to adverse events Seventeen trials 9-11,14,15,25,29-31,34,36,37,42,44,47,55,60 reported withdrawal due to adverse events (as defined by the authors). Table 6 summarizes the posterior probability of the withdrawal due to adverse events, Table 7 summarizes the head-to-head comparison among mono-therapies, and Appendix G summarizes the full head-to-head comparison. In terms of the results, PEG has significantly more withdrawal due to adverse events than ETV. In addition, ETV has significantly fewer withdrawal due to adverse events than LAM.
23 23 Table 6: Posterior probability of safety outcomes based on network meta-analysis Posterior probability of an outcome Treatment Any AE Serious AE Withdrawal due to AE LAM ( ) ( ) 0.02 ( ) PLA ( ) ( ) ( ) ADV ( ) ( ) ( ) LDT ( ) 0.04 ( ) ( ) TDF ( ) ( ) ( ) ETV ( ) ( ) ( ) PEG 0.93 ( ) ( ) ( ) LAMPEG ( ) ( ) ( ) LAMLDT ( ) (-) (-) PEGADV (-) ( ) ( ) ETVTDF ( ) ( ) ( ) IFNLAM (-) (-) ( ) ADVLDT (-) (-) 0.08 (0-0.64) ADV2 (-) ( ) ( ) PEGPEG ( ) ( ) (-) Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir; PEGPEG2: double duration of PEG; ADV2: additional dose of ADV;
24 24 Table 7: NMA Results (SAFTY): Odds ratios for Random Effects Model (Significant in Red Fonts) Odds ratios (95 % confidence interval) Tx Outcomes PLA ADV LDT TDF ETV PEG LAM Any AE 0.92 ( ) 1.14 ( ) 1.19 ( ) 1.18 ( ) 1.09 ( ) 6.91 ( ) Serious AE 3.85 ( ) 3.9 ( ) 0.73 ( ) 3.91 ( ) 0.85 ( ) 2.19 ( ) Withdrawal due to AE 0.45 ( ) 0.71 ( ) 0.19 (0-2.83) 0.76 ( ) 0.25 ( ) 4.2 ( ) PLA Any AE 1.24 ( ) 1.3 ( ) 1.28 ( ) 1.18 ( ) 7.54 ( ) Serious AE 1.04 ( ) 0.19 ( ) 1.02 ( ) 0.23 ( ) 0.57 ( ) Withdrawal due to AE 1.56 ( ) 0.37 ( ) 1.58 ( ) 0.54 ( ) 9.07 ( ) ADV Any AE 1.05 ( ) 1.04 ( ) 0.96 ( ) 6.1 ( ) Serious AE 0.19 (0.01-2) 0.98 ( ) 0.22 ( ) 0.57 ( ) Withdrawal due to AE 0.23 ( ) 0.98 ( ) 0.35 ( ) 5.76 ( ) LDT Any AE 0.99 ( ) 0.92 ( ) 5.82 ( ) Serious AE 5.35 ( ) 1.16 ( ) 3.01 ( ) Withdrawal due to AE 4.06 ( ) 1.29 ( ) ( ) TDF Any AE 0.93 ( ) 5.84 ( ) Serious AE 0.22 ( ) 0.57 ( ) Withdrawal due to AE 0.34 (0-11.6) 5.59 ( ) ETV Any AE 6.35 ( ) Serious AE 2.57 ( ) Withdrawal due to AE 17.3 ( ) Abbreviations: AE: adverse event; PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir
25 25 Observational Studies Selection of Observational studies A total of 4,530 studies were identified from the original literature, and, upon screening the titles and abstracts, 452 potentially relevant publications were retrieved for further screening. Of the 452 potentially relevant reports, a total of 52 studies, were selected for inclusion (See Appendix D for selection detail). Note that these studies were for mono-infected treatment naïve patients only. A summary of the included studies can be found in Table 8. A detailed description of the included observational studies can be found in Appendix E. Table 8: Summary of observational studies Interventions Publications (n) Patients (n) Publication Years Lamivudine (LAM) Adefovir (ADV) Telbivudine (LDT) Tenofovir (TDF) Entecavir (ETV) pegylated interferon (PEG) Conventional interferon (IFN) Combination therapies TOTAL 52 11,256 Abbreviations: PLA, placebo; LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir Results of Observational studies A summary of the efficacy results based on meta-analysis for the observation studies are provided in Figure 5 for both HBeAg positive and negative patients in a forest plot in terms of virologic response and normalization of ALT.
26 26 Figure 5: Meta-analyses results from observational studies proportion of patients achieved virologic response for HBeAg positive patients LAM LDT TDF ETV PEG IFN proportion of patients achieved ALT normalization for HBeAg positive patients LAM LDT TDF ETV PEG IFN proportion of patients achieved virologic response for HBeAg negative patients LAM LDT TDF ETV PEG IFN proportion of patients achieved ALT normalization for HBeAg negative patients LAM LDT TDF ETV PEG IFN Abbreviations: LAM, lamivudine; IFN, conventional interferon; PEG, pegylated interferon; LdT, telbivudine; ETV, entecavir; ADV, adefovir; TDF, tenofovir;
27 27 A total of four studies reported outcomes for IFN treatment. Only one study 65 reported virologic response (34%) and ALT normalization (34%). Two studies 62,63 reported HBeAg loss (47.1%-70%). One study 64 reported HBeAg seroconversion (20.5%-36.8%) and HBsAg loss (3.2%-5.7%). A total of five studies reported outcomes for PEG treatment. One study 69 reported virologic response (28%) for HBeAg+ patients, and three studies 67,68,70 for HBeAg- patients (19.2%-61.1%); One study 70 reported ALT normalization (27%) for HBeAg+ patients and two studies 68,70 reported for HBeAgpatients (33.3%-47%). Three studies 66,69,70 reported HBeAg loss (25%-46.7%), and one reported 69 HBeAg seroconversion (35%). A total of four studies 66,68-70 reported HBsAg loss (6.7%-13% for HBeAg+ patients; 2.8%-14% for HBeAg- patients). A total of fifteen studies 62,68,71-83 reported outcomes for LAM treatment. Five studies 71,76,78,82,83 reported virologic response (38.1%-93.1%%) for HBeAg+ patients, and six studies 68,73,75-77,81 reported for HBeAgpatients (10%-91.6%). Four studies 71,78,82,83 reported ALT normalization for HBeAg+ patients (52.6%- 83.1%) while only three studies 68,77,81 reported for HBeAg- patients (24%-72.4%). Seven studies 62,71,74,76,78,82,83 reported HBeAg loss (4.1%-80.3%), and six reported 71,74,76,78,82,83 HBeAg seroconversion (6.7%-80.3%). A total of five studies 72,73,75,79,82 reported HBsAg loss (0%-2.1% for HBeAg+ patients; 4.8%-11.7% for HBeAg- patients). Five studies 74,84-87 reported outcomes for LDT treatment. Four studies reported virologic response (25.6%-85.7%) for HBeAg+ patients, and three studies 84,86,87 reported for HBeAg- patients (77.2%- 93.1%). Three studies reported ALT normalization for HBeAg+ patients (81.0%-100%) while only two studies 84,86 reported for HBeAg- patients (79.3%-82.8%). Two studies 74,84 reported HBeAg loss (13.3%- 51.9%), and three 74,84,86 reported HBeAg seroconversion (8.9%-57.1%). A total of two studies 84,86 reported HBsAg loss (0%-1.6% for HBeAg+ patients; 0% for HBeAg- patients). Only two studies 88,89 for TDF were included. The main reason for exclusion was co-infection. Among this two studies, virologic response was reported (71.4%-72% for HBeAg+ patients and 27.3%-91% for HBeAg- patients). ALT normalization (82% for HBeAg+ patients and 70% for HBeAg- patients) and HBeAg seroconversion (5.1%) were reported from one study 88. A total of seventeen studies 86,88, reported outcomes for ETV treatment. Thirteen studies 86,88,91-97,99,100,103,104 reported virologic response (39%-82.5%) for HBeAg+ patients, and eleven studies 86,88,91-95,97,98,100,104 reported for HBeAg- patients (61.7%-100%). Nine studies 86,88,93-97,99,103 reported ALT normalization for HBeAg+ patients (31.4%-98%) while only six studies 86,93-95,97,98 reported for HBeAgpatients (60.9%-95%). Seven studies reported 91,94-97,99 HBeAg loss (3.5%-48.9%), and six reported 88,90,93,97,99 HBeAg seroconversion (2.2%-68%). A total of three studies 86,93,98 reported HBsAg loss (0% for both HBeAg+ patients and HBeAg- patients). Only three observation studies 68,69,99 reported for outcomes for combination treatment. The combination included PEG+LAM and LAM+ADV.
28 28 Discussion In this study, we identified the available evidence on comparable benefits and harms of the available CHB treatments through systematic reviews and synthesized this evidence using network metaanalysis (NMA). We used NMA to evaluate the relative efficacy of all available treatments across 5 surrogate clinical outcomes and 3 safety outcomes. We consolidated the information of all RCTs that included the treatments of interest to provide the probability of an outcome. The framework of our analysis was largely based on our previous publication 105. We expanded our review to studies with a standard interferon arm as well as to scientific abstracts. The total number of the included RCT studies in the NMA was increased from 15 to 40 for HBeAg positive patients, and from 8 studies to 22 studies for HBeAg negative patients. With additional evidence serving as input to the NMA, our study was able to provide narrower confidence intervals than the previous study. However, the main conclusion on most of the results did not change. In terms of mono-therapies, TDF, ETV and LDT were still the most effective in terms of virologic response and ALT normalization for HBeAg positive patients; TDF, ETV and ADV were the most effective treatments in terms of the same outcomes for HBeAg negative patients. In the five years since our previous review, a number of combination therapies studies were conducted and reported. New combination therapies included ADV+LDT, ETV+LAM and ETV+TDF. Our study had limitations. Firstly, given that our review was limited to studies written in English, a number of useful studies that were written in other languages might have been ignored. For example, a number of clinical studies of CHB have been conducted and published in Chinese and Japanese. Other limitations include variation in outcome definition, especially in terms of virologic response viral load, duration of study treatment and follow up and patient characteristics. These variations may increase the risk of bias in the NMA estimates. In addition, the number of studies included for some pair-wise comparisons was small. This is particularly true for tenofovir, standard interferon and most of the combination therapies. Thus, it will create wide confidence intervals in the NMA for these therapies. Statistical significant inconsistency was not observed within the networks. However, some of the inconsistency estimates presented wide confidence intervals, indicating the likelihood of a type II error in some of the inconsistency tests. We were not able to test for heterogeneity and subgroup analysis due to time constraints. Finally, NMAs for some of the outcomes with rare events that were infrequently reported were characterized by large parameter uncertainty especially in indirect comparisons. The comparisons in these outcomes were also limited due to lack of connectivity in the study network for some of the treatments. In conclusion, our systematic review of RCT studies and network meta-analysis show that for HBeAg positive patients, tenofovir is the most effective treatment followed by entecavir, in terms of virologic response and ALT normalization. In terms of HBeAg loss and HBeAg seroconversion, pegylated interferon is the most effective treatment. In terms of HBsAg loss, pegylated interferon is the most effective treatment followed by tenofovir. For HBeAg negative patients, tenofovir is also the most
29 effective treatment, followed by adefovir and entecavir, in terms of virologic response and ALT normalization. Findings of the observational studies show that the probability of achieving virologic response and ALT normalization in a real-world setting is high among the oral agents assessed, while the probability of achieving HBeAg loss, HBeAg seroconversion, and HBsAg loss was generally low. However, direct comparisons between the treatments with respect to their relative effectiveness could not be achieved through the observation studies. More research on the comparative effectiveness of the treatments in a real-world setting is needed. 29 Key Messages PEG is not significantly better than IFN in both HBeAg positive and negative patients. When we compare with LAM for HBeAg positive patients, LDT, TDF and ETV are significantly better than LAM in terms of virologic response. LDT and ETV are significantly better than LAM in terms of normalization of ALT. However, LAM is significantly better than PEG in terms of normalization of ALT. LDT and PEG are significantly better than LAM in terms of HBeAg loss and HBeAg seroconversion. When we compare with LAM for HBeAg negative patients, ADV, LDT, TDF and ETV are significantly better than LAM in terms of virologic response. ETV is significantly better than LAM in terms of normalization of ALT. When we compare with TDF for HBeAg positive patients, TDF is significantly better than LAM, ADV, LDT, ETV, PEG and IFN in terms of virologic response. TDF is significantly better than PEG and IFN in terms of normalization of ALT. When we compare with TDF for HBeAg negative patients, TDF is significantly better than LAM, ADV, LDT, PEG and IFN in terms of virologic response. When we compare with PEG and IFN for HBeAg positive patients: LDT, TDF and ETV are significantly better than PEG and IFN in terms of virologic response. LDT and ETV are significantly better than PEG and IFN in terms of normalization of ALT. On the other hand, PEG is significantly better than ETV in terms of HBeAg loss and HBeAg seroconversion. In terms of safety, PEG has significantly more serious adverse events than LAM, LDT, and ETV. PEG also has statistically significantly more any adverse events than LAM, PLA,
30 ADV, LDT, TDF and ETV. PEG has significantly more withdrawal due to adverse events than ETV. LAM has significantly more withdrawal due to adverse events than ETV. Beside this, there are no significant different in terms of safety among all other oral agents. 30
31 31 Reference List 1. Higgins JPT, Green S. Cochrane Handbook for Systematic Reviews of Interventions Version ; 2. Wilczynski NL, Haynes RB, Hedges T. Developing optimal search strategies for detecting clinically sound prognostic studies in MEDLINE: an analytic survey. BMC medicine. 2004;2: Wilczynski NL, Haynes RB, Hedges T. Developing optimal search strategies for detecting clinically sound causation studies in MEDLINE. AMIA... Annual Symposium proceedings / AMIA Symposium. AMIA Symposium. 2003: Rao W, Wu X, Xiu D. Lamivudine or lamivudine combined with hepatitis B immunoglobulin in prophylaxis of hepatitis B recurrence after liver transplantation: a meta-analysis. Transplant international : official journal of the European Society for Organ Transplantation. 2009;22: Moher D, Liberati A, Tetzlaff J, Altman DG, Group P. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264-9, W Lunn DJ, Thomas A, Best N, Spiegelhalter D. WinBUGS-a Bayesian modelling framework concepts, structure, and extensibility. Statistics and computing. 2000;10: Salanti G, Higgins JP, Ades AE, Ioannidis JP. Evaluation of networks of randomized trials. Statistical methods in medical research. 2008;17: Ahn SH, Park JY, Lee HJ, et al. Prospective randomized trial of switching to entecavir in chronic hepatitis B patients with suboptimal virologic response to lamivudine: Interim analysis at 48 weeks. Hepatology International. 2010;4 (1): Akarca US, Ersoz G, Gunsar F, et al. Interferon-lamivudine combination is no better than lamivudine alone in anti-hbe-positive chronic hepatitis B. Antiviral Therapy. 2004;9: Ayaz C, Celen MK, Colak H, Hosoglu S, Geyik MF. Comparison of lamivudine and alpha-interferon combination with alpha-interferon alone in the treatment of HBeAg-positive chronic hepatitis B. Indian Journal of Gastroenterology. 2006;25: Bzowej N, Chan HLY, Lai CL, et al. A randomized trial of telbivudine (LDT) vs. adefovir for HBeAgpositive chronic hepatitis B: Final week 52 results. Hepatology. 2006;44:563A-A. 12. Cao ZH, Ma LN, Zhang HW, Liu YL, Chen XY. Extended treatment with peginterferon alpha-2a in combination with lamivudine or adefovir for 96 weeks yields high rates of HBeAg and HBsAg seroconversion. Journal of Digestive Diseases. 2013;14: Chan HL, Leung NW, Hui AY, et al. A randomized, controlled trial of combination therapy for chronic hepatitis B: comparing pegylated interferon-alpha2b and lamivudine with lamivudine alone. Ann Intern Med. 2005;142: Chang TT, Gish RG, de Man R, et al. A comparison of entecavir and lamivudine for HBeAg-positive chronic hepatitis B. N Engl J Med. 2006;354: Chen X. Effect of telbivudine and entecavir on HBeAg-positive chronic hepatitis B: A 4-year follow-up. Hepatology International. 2013;7:S195-S Chen XFP, Chen XFP, Huang J, et al. Extending peginterferon alfa-2a therapy in patients with HBeAgpositive chronic hepatitis B who did not achieve a response at week 48 can lead to HBeAg seroconversion and HBsAg clearance. Hepatology. 2009;50:499a. 17. Chen YC, Hsu CW, Chao YC, Lee CM, Chang TT, Liaw YF. A randomized, double-blind trial of telbivudine versus lamivudine in adults with compensated chronic hepatitis B week sub-study result in Taiwan. Hepatology International. 2009;3 (1): Cooksley G, Manns M, Lau GKK, et al. Effect of genotype and other baseline factors on response to peginterferon alpha-2a (40 kda) (PEGASYS (R)) in HBeAg-POSITIVE chronic hepatitis B: Results from a
32 large, randomised study. Journal of Hepatology. 2005;42: Cooksley WGE, Piratvisuth T, Lee SD, et al. Peginterferon alpha-2a (40 kda): an advance in the treatment of hepatitis B e antigen-positive chronic hepatitis B. Journal of Viral Hepatitis. 2003;10: Dienstag JL, Schiff ER, Wright TL, et al. Lamivudine as initial treatment for chronic hepatitis B in the United States. N Engl J Med. 1999;341: He F, FanXiao T, Xiernayi H. Randomized trial of telbivudine or lamivudine treatment in chinese patients with decompensated HBV cirrhosis. Hepatology International. 2011;5 (1): Hou J, Yin YK, Xu D, et al. Telbivudine versus lamivudine in Chinese patients with chronic hepatitis B: Results at 1 year of a randomized, double-blind trial. Hepatology. 2008;47: Huang J, Chen X. Predictors of HBeAg-seroconversion in HBeAg-positive chronic hepatitis B patients treated with telbivudine and entecavir. Hepatology International. 2014;1):S Janssen HL, van Zonneveld M, Senturk H, et al. Pegylated interferon alfa-2b alone or in combination with lamivudine for HBeAg-positive chronic hepatitis B: a randomised trial. Lancet. 2005;365: Jia JD, Hou JL, Yin YK, et al. Two-year results of a randomized, phase III comparative trial of telbivudine versus lamivudine in Chinese patients. Hepatology International. 2014;8: Lai CL, Chien RN, Leung NW, et al. A one-year trial of lamivudine for chronic hepatitis B. Asia Hepatitis Lamivudine Study Group. N Engl J Med. 1998;339: Lai CL, Gane E, Liaw YF, et al. Telbivudine versus lamivudine in patients with chronic hepatitis B. N Engl J Med. 2007;357: Lai CL, Leung N, Teo EK, et al. A 1-year trial of telbivudine, lamivudine, and the combination in patients with hepatitis B e antigen-positive chronic hepatitis B. Gastroenterology. 2005;129: Lai CL, Shouval D, Lok AS, et al. Entecavir versus lamivudine for patients with HBeAg-negative chronic hepatitis B. N Engl J Med. 2006;354: Lau GK, Piratvisuth T, Luo KX, et al. Peginterferon Alfa-2a, lamivudine, and the combination for HBeAg-positive chronic hepatitis B. N Engl J Med. 2005;352: Leung N, Peng CY, Hann HW, et al. Early hepatitis B virus DNA reduction in hepatitis B e antigenpositive patients with chronic hepatitis B: A randomized international study of entecavir versus adefovir. Hepatology. 2009;49: Liaw YF, Gane E, Leung N, et al. 2-Year GLOBE trial results: telbivudine Is superior to lamivudine in patients with chronic hepatitis B. Gastroenterology. 2009;136: Liu YH, Wu T, Sun N, et al. Combination therapy with pegylated interferon alpha-2b and adefovir dipivoxil in HBeAg-positive chronic hepatitis B versus interferon alone: a prospective, randomized study. Journal of Huazhong University of Science and Technology. Medical Sciences. 2014;34: Lok AS, Trinh H, Carosi G, et al. Efficacy of entecavir with or without tenofovir disoproxil fumarate for nucleos(t)ide-nave patients with chronic hepatitis B. Gastroenterology. 2012;143: e Ma H, Yang R, Wei L. On-treatment HBsAg and HBeAg levels as potential predictors of durable offtreatment HBeAg seroconversion for HBeAg-positive chb patients treated with peginterferon alfa2b not conventional interferon alfa-2b. Hepatology. 2009;50:527A. 36. Marcellin P, Chang TT, Lim SG, et al. Adefovir dipivoxil for the treatment of hepatitis B e antigenpositive chronic hepatitis B. N Engl J Med. 2003;348: Marcellin P, Heathcote EJ, Buti M, et al. Tenofovir Disoproxil Fumarate versus Adefovir Dipivoxil for Chronic Hepatitis B. N Engl J Med. 2008;359: Mazzella G, Saracco G, Festi D, et al. Long-term results with interferon therapy in chronic type B hepatitis: A prospective randomized trial. American Journal of Gastroenterology. 1999;94: Murray KF, Szenborn L, Wysocki J, et al. Tenofovir disoproxil fumarate treatment results in high rates of virologic suppression and ALT response in adolescents with chronic active hepatitis B regardless of 32
Hepatitis B Virus therapy. Maria Buti Hospital Universitario Valle Hebron Barcelona Spain
 Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Hepatitis B Virus therapy. Maria Buti Hospital Universitario Valle Hebron Barcelona Spain
 Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Hepatitis B Virus therapy Maria Buti Hospital Universitario Valle Hebron Barcelona Spain Disclosures Advisor: AbbVie, Boehringer Ingelheim, Bristol-Myers Squibb, Gilead Sciences, Janssen, Merck Sharp &
Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia
 Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute
Treatment as a form of liver cancer prevention The clinical efficacy and cost effectiveness of treatment across Asia Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute
An estimated 400 million people worldwide are chronically
 GASTROENTEROLOGY 2010;139:1218 1229 Tenofovir and Entecavir Are the Most Effective Antiviral Agents for Chronic Hepatitis B: A Systematic Review and Bayesian Meta-analyses GLORIA WOO,*, GEORGE TOMLINSON,*,,
GASTROENTEROLOGY 2010;139:1218 1229 Tenofovir and Entecavir Are the Most Effective Antiviral Agents for Chronic Hepatitis B: A Systematic Review and Bayesian Meta-analyses GLORIA WOO,*, GEORGE TOMLINSON,*,,
Who to Treat? Consider biopsy Treat. > 2 ULN Treat Treat Treat Treat CIRRHOTIC PATIENTS Compensated Treat HBV DNA detectable treat
 Who to Treat? Parameter AASLD US Algorithm EASL APASL HBV DNA CRITERIA HBeAg+ >, IU/mL > 2, IU/mL > 2, IU/mL >, IU/mL HBeAg- > 2, IU/mL > 2, IU/mL > 2, IU/mL > 2, IU/mL ALT CRITERIA PNALT 1-2 ULN Monitor
Who to Treat? Parameter AASLD US Algorithm EASL APASL HBV DNA CRITERIA HBeAg+ >, IU/mL > 2, IU/mL > 2, IU/mL >, IU/mL HBeAg- > 2, IU/mL > 2, IU/mL > 2, IU/mL > 2, IU/mL ALT CRITERIA PNALT 1-2 ULN Monitor
Does Viral Cure Prevent HCC Development
 Does Viral Cure Prevent HCC Development Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute of Digestive Disease Director, Center for Liver Health Assistant Dean,
Does Viral Cure Prevent HCC Development Prof. Henry LY Chan Head, Division of Gastroenterology and Hepatology Director, Institute of Digestive Disease Director, Center for Liver Health Assistant Dean,
HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But
 HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But Hospital Universitario Valle Hebron and Ciberehd del Insttuto Carlos III. Barcelona. Spain Disclosures Advisory board of,
HBeAg-positve chronic hepatts B: Why do I treat my patent with a NA? Maria But Hospital Universitario Valle Hebron and Ciberehd del Insttuto Carlos III. Barcelona. Spain Disclosures Advisory board of,
Novedades en el tratamiento de la hepatitis B: noticias desde la EASL. Maria Buti Hospital Universitario Valle Hebrón Barcelona
 Novedades en el tratamiento de la hepatitis B: noticias desde la EASL Maria Buti Hospital Universitario Valle Hebrón Barcelona Milestones in CHB treatment Conventional IFN 1991 Lamivudine (LAM) 1998 Adefovir
Novedades en el tratamiento de la hepatitis B: noticias desde la EASL Maria Buti Hospital Universitario Valle Hebrón Barcelona Milestones in CHB treatment Conventional IFN 1991 Lamivudine (LAM) 1998 Adefovir
Is there a need for combination therapy? No. Maria Buti Hospital General Universitario Valle Hebron Barcelona. Spain
 Is there a need for combination therapy? No Maria Buti Hospital General Universitario Valle Hebron Barcelona. Spain No, No and No EASL Update HBV Guidelines 2012 The most potent drugs with the optimal
Is there a need for combination therapy? No Maria Buti Hospital General Universitario Valle Hebron Barcelona. Spain No, No and No EASL Update HBV Guidelines 2012 The most potent drugs with the optimal
NUCs for Chronic Hepatitis B. Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona.
 NUCs for Chronic Hepatitis B Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona. Spain Disclosures Advisory board of, and/or, received speaker fee from
NUCs for Chronic Hepatitis B Rafael Esteban Hospital Universitario Valle Hebron and Ciberehd del Instituto Carlos III. Barcelona. Spain Disclosures Advisory board of, and/or, received speaker fee from
How to use pegylated Interferon for Chronic Hepatitis B in 2015
 How to use pegylated Interferon for Chronic Hepatitis B in 215 Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of Songkla University, Thailand ASIAN-PACIFIC CLINICAL PRACTICE
How to use pegylated Interferon for Chronic Hepatitis B in 215 Teerha Piratvisuth NKC Institute of Gastroenterology and Hepatology Prince of Songkla University, Thailand ASIAN-PACIFIC CLINICAL PRACTICE
29th Viral Hepatitis Prevention Board Meeting
 29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis B José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HBV INFECTION
29th Viral Hepatitis Prevention Board Meeting Madrid, November 2006 Treatment of chronic hepatitis B José M. Sánchez-Tapias Liver Unit Hospital Clínic University of Barcelona Spain CHRONIC HBV INFECTION
Research Article The Effectiveness of Antiviral Treatments for Patients with HBeAg-Positive Chronic Hepatitis B: A Bayesian Network Analysis
 Canadian Journal of Gastroenterology and Hepatology, Article ID 357665, 9 pages https://doi.org/0.55/08/357665 Research Article The Effectiveness of Antiviral Treatments for Patients with HBeAg-Positive
Canadian Journal of Gastroenterology and Hepatology, Article ID 357665, 9 pages https://doi.org/0.55/08/357665 Research Article The Effectiveness of Antiviral Treatments for Patients with HBeAg-Positive
Prediction of HBsAg Loss by Quantitative HBsAg Kinetics during Long-Term 2015
 THAI J 16 GASTROENTEROL Treatment with Nucleos(t)ide Original Analogues Article Prediction of HBsAg Loss by Quantitative HBsAg Kinetics during Long-Term Treatment with Nucleos(t)ide Analogues Sombutsook
THAI J 16 GASTROENTEROL Treatment with Nucleos(t)ide Original Analogues Article Prediction of HBsAg Loss by Quantitative HBsAg Kinetics during Long-Term Treatment with Nucleos(t)ide Analogues Sombutsook
Management of Decompensated Chronic Hepatitis B
 Management of Decompensated Chronic Hepatitis B Dr James YY Fung, FRACP, MD Department of Medicine The University of Hong Kong Liver Transplant Center Queen Mary Hospital State Key Laboratory for Liver
Management of Decompensated Chronic Hepatitis B Dr James YY Fung, FRACP, MD Department of Medicine The University of Hong Kong Liver Transplant Center Queen Mary Hospital State Key Laboratory for Liver
Management of chronic hepatitis B : recent advance in the treatment of antiviral resistance
 anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance / 김강모 연수강좌 anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance 김강모 울산대학교의과대학서울아산병원소화기내과
anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance / 김강모 연수강좌 anagement of chronic hepatitis B : recent advance in the treatment of antiviral resistance 김강모 울산대학교의과대학서울아산병원소화기내과
Our better understanding of the natural
 TREATMENT OF CHRONIC HEPATITIS B: MASTERING THE BASICS ON A COMPLEX TOPIC Ke-Qin Hu, MD* ABSTRACT The availability of newer antiviral agents, as well as comprehensive treatment recommendations, has equipped
TREATMENT OF CHRONIC HEPATITIS B: MASTERING THE BASICS ON A COMPLEX TOPIC Ke-Qin Hu, MD* ABSTRACT The availability of newer antiviral agents, as well as comprehensive treatment recommendations, has equipped
Response-guided antiviral therapy in chronic hepatitis B: nucleot(s)ide analogues vs. pegylated interferon
 Response-guided antiviral therapy in chronic hepatitis B: Sang Hoon Ahn, M.D., Ph.D. Department of Internal Medicine, Yonsei University College of Medicine, Institute of Gastroenterology, Liver Cirrhosis
Response-guided antiviral therapy in chronic hepatitis B: Sang Hoon Ahn, M.D., Ph.D. Department of Internal Medicine, Yonsei University College of Medicine, Institute of Gastroenterology, Liver Cirrhosis
The Impact of HBV Therapy on Fibrosis and Cirrhosis
 The Impact of HBV Therapy on Fibrosis and Cirrhosis Jordan J. Feld, MD, MPH Associate Professor of Medicine University of Toronto Hepatologist Toronto Centre for Liver Disease Sandra Rotman Centre for
The Impact of HBV Therapy on Fibrosis and Cirrhosis Jordan J. Feld, MD, MPH Associate Professor of Medicine University of Toronto Hepatologist Toronto Centre for Liver Disease Sandra Rotman Centre for
The role of entecavir in the treatment of chronic hepatitis B
 REVIEW The role of entecavir in the treatment of chronic hepatitis B Evangelini Dimou Vasilios Papadimitropoulos Stephanos J Hadziyannis Department of Medicine and Liver Unit, Henry Dunant Hospital, Athens,
REVIEW The role of entecavir in the treatment of chronic hepatitis B Evangelini Dimou Vasilios Papadimitropoulos Stephanos J Hadziyannis Department of Medicine and Liver Unit, Henry Dunant Hospital, Athens,
entecavir, 0.5mg and 1mg film-coated tablets and 0.05 mg/ml oral solution, Baraclude SMC No. (747/11) Bristol-Myers Squibb Pharmaceuticals Ltd
 entecavir, 0.5mg and 1mg film-coated tablets and 0.05 mg/ml oral solution, Baraclude SMC No. (747/11) Bristol-Myers Squibb Pharmaceuticals Ltd 09 December 2011 The Scottish Medicines Consortium (SMC) has
entecavir, 0.5mg and 1mg film-coated tablets and 0.05 mg/ml oral solution, Baraclude SMC No. (747/11) Bristol-Myers Squibb Pharmaceuticals Ltd 09 December 2011 The Scottish Medicines Consortium (SMC) has
Scottish Medicines Consortium
 Scottish Medicines Consortium pegylated Interferon alfa 2a, 180 mcg for subcutaneous injection (Pegasys ) No. (186/05) Roche New indication (chronic hepatitis B) 10 June 2005 The Scottish Medicines Consortium
Scottish Medicines Consortium pegylated Interferon alfa 2a, 180 mcg for subcutaneous injection (Pegasys ) No. (186/05) Roche New indication (chronic hepatitis B) 10 June 2005 The Scottish Medicines Consortium
Pros and Cons of Peginterferon Versus Nucleos(t)ide Analogues for Treatment of Chronic Hepatitis B
 Curr Hepatitis Rep (2010) 9:91 98 DOI 10.1007/s11901-010-0041-7 Pros and Cons of Peginterferon Versus Nucleos(t)ide Analogues for Treatment of Chronic Hepatitis B Milan J. Sonneveld & Harry L. A. Janssen
Curr Hepatitis Rep (2010) 9:91 98 DOI 10.1007/s11901-010-0041-7 Pros and Cons of Peginterferon Versus Nucleos(t)ide Analogues for Treatment of Chronic Hepatitis B Milan J. Sonneveld & Harry L. A. Janssen
Landmarks for Prevention and Treatment
 HBeAg-positive chronic hepatitis B Why do I treat my patient with a nucleos(t)ide analogue? Dr. Nancy Leung BSc(Lon) MSc(Lon) MBBS(Lon) MD(Lon), FRCP(Lon) FRCP(Edin) FHKCP FHKAM Consultant Physician, Alice
HBeAg-positive chronic hepatitis B Why do I treat my patient with a nucleos(t)ide analogue? Dr. Nancy Leung BSc(Lon) MSc(Lon) MBBS(Lon) MD(Lon), FRCP(Lon) FRCP(Edin) FHKCP FHKAM Consultant Physician, Alice
New therapeutic perspectives in HBV: when to stop NAs
 Liver International ISSN 1478-3223 REVIEW ARTICLE New therapeutic perspectives in HBV: when to stop NAs Cristina Perez-Cameo, Monica Pons and Rafael Esteban Liver Unit, Department of Internal Medicine,
Liver International ISSN 1478-3223 REVIEW ARTICLE New therapeutic perspectives in HBV: when to stop NAs Cristina Perez-Cameo, Monica Pons and Rafael Esteban Liver Unit, Department of Internal Medicine,
Chronic hepatitis B - New goals, new treatment. New England Journal Of Medicine, 2008, v. 359 n. 23, p
 Title Chronic hepatitis B - New goals, new treatment Author(s) Lai, CL; Yuen, MF Citation New England Journal Of Medicine, 2008, v. 359 n. 23, p. 2488-2491 Issued Date 2008 URL http://hdl.handle.net/10722/59270
Title Chronic hepatitis B - New goals, new treatment Author(s) Lai, CL; Yuen, MF Citation New England Journal Of Medicine, 2008, v. 359 n. 23, p. 2488-2491 Issued Date 2008 URL http://hdl.handle.net/10722/59270
Gish RG and AC Gadano. J Vir Hep
 Treatment in Hepatitis B and C There are options! Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Hepatitis B Virus Epidemiology and natural history 400
Treatment in Hepatitis B and C There are options! Karen F. Murray, MD Professor of Pediatrics Director, Hepatobiliary Program Seattle Children s Hepatitis B Virus Epidemiology and natural history 400
Hepatitis B: Future treatment developments
 Hepatitis B: Future treatment developments VIII International Update Workshop in Hepatology Curitiba, 27.08.2016 Christoph Sarrazin St. Josefs-Hospital Wiesbaden and Goethe-University, Frankfurt am Main
Hepatitis B: Future treatment developments VIII International Update Workshop in Hepatology Curitiba, 27.08.2016 Christoph Sarrazin St. Josefs-Hospital Wiesbaden and Goethe-University, Frankfurt am Main
Dual Therapy for Chronic Hepatitis B Virus
 Dual Therapy for Chronic Hepatitis B Virus Hussien Elsiesy, MD, and Douglas Dieterich, MD Corresponding author Douglas Dieterich, MD Division of Liver Diseases, Mount Sinai School of Medicine, One Gustave
Dual Therapy for Chronic Hepatitis B Virus Hussien Elsiesy, MD, and Douglas Dieterich, MD Corresponding author Douglas Dieterich, MD Division of Liver Diseases, Mount Sinai School of Medicine, One Gustave
CURRENT TREATMENT. Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, Virginia
 CURRENT TREATMENT OF HBV Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, Virginia CHRONIC HBV INFECTION DEMOGRAPHICS IN THE USA Estimated
CURRENT TREATMENT OF HBV Mitchell L Shiffman, MD Director Liver Institute of Virginia Bon Secours Health System Richmond and Newport News, Virginia CHRONIC HBV INFECTION DEMOGRAPHICS IN THE USA Estimated
Update on HBV Treatment
 Update on HBV Treatment Calvin Q. Pan MD, FAASLD, FACG, MACP Professor of Medicine Division of Gastroenterology and Hepatology Department of Medicine, NYU Langone Health New York University School of Medicine,
Update on HBV Treatment Calvin Q. Pan MD, FAASLD, FACG, MACP Professor of Medicine Division of Gastroenterology and Hepatology Department of Medicine, NYU Langone Health New York University School of Medicine,
HBV Therapy in Special Populations: Liver Cirrhosis
 HBV Therapy in Special Populations: Liver Cirrhosis Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber- und Studienzentrum
HBV Therapy in Special Populations: Liver Cirrhosis Universitätsklinikum Leipzig Thomas Berg Sektion Hepatologie Klinik und Poliklinik für Gastroenterologie und Rheumatologie Leber- und Studienzentrum
Cornerstones of Hepatitis B: Past, Present and Future
 Cornerstones of Hepatitis B: Past, Present and Future Professor Man-Fung Yuen Queen Mary Hospital The University of Hong Kong Hong Kong 1 Outline Past Natural history studies Development of HBV-related
Cornerstones of Hepatitis B: Past, Present and Future Professor Man-Fung Yuen Queen Mary Hospital The University of Hong Kong Hong Kong 1 Outline Past Natural history studies Development of HBV-related
Drug Class Monograph
 Drug Class Monograph Class: Chronic Hepatitis B Drug: Baraclude (entecavir), Epivir (lamivudine), Hepsera (adefovir), Intron A (interferon alfa- 2b), Pegasys (peginterferon alfa-2a), Tyzeka (telbivudine),
Drug Class Monograph Class: Chronic Hepatitis B Drug: Baraclude (entecavir), Epivir (lamivudine), Hepsera (adefovir), Intron A (interferon alfa- 2b), Pegasys (peginterferon alfa-2a), Tyzeka (telbivudine),
Clinical impact of the early alanine amininotransferase flare during tenofovir monotherapy in treatment-naïve patients with chronic hepatitis B
 pissn 2287-2728 eissn 2287-285X Original Article Clinical and Molecular Hepatology 217;23:154-159 Clinical impact of the early alanine amininotransferase flare during tenofovir monotherapy in treatment-naïve
pissn 2287-2728 eissn 2287-285X Original Article Clinical and Molecular Hepatology 217;23:154-159 Clinical impact of the early alanine amininotransferase flare during tenofovir monotherapy in treatment-naïve
Optimized HBV Treatment Through Baseline and on-treatment Predictor Oral Antiviral Therapy. Watcharasak Chotiyaputta
 Optimized HBV Treatment Through Baseline and on-treatment Predictor Oral Antiviral Therapy Watcharasak Chotiyaputta Progression of Liver Disease Goal of HBV Treatment: prevention the development of cirrhosis
Optimized HBV Treatment Through Baseline and on-treatment Predictor Oral Antiviral Therapy Watcharasak Chotiyaputta Progression of Liver Disease Goal of HBV Treatment: prevention the development of cirrhosis
Treatment of chronic hepatitis B 2013 update
 22 February 213 Treatment of chronic hepatitis B 213 update Pietro Lampertico 1st Gastroenterology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico Università di Milano EASL 212 Clinical
22 February 213 Treatment of chronic hepatitis B 213 update Pietro Lampertico 1st Gastroenterology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico Università di Milano EASL 212 Clinical
Hepatitis B Prior Authorization Policy
 Hepatitis B Prior Authorization Policy Line of Business: Medi-Cal P&T Approval Date: November 15, 2017 Effective Date: January 1, 2018 This policy has been developed through review of medical literature,
Hepatitis B Prior Authorization Policy Line of Business: Medi-Cal P&T Approval Date: November 15, 2017 Effective Date: January 1, 2018 This policy has been developed through review of medical literature,
Chronic hepatitis B virus (HBV) infection is an important. New and Emerging Treatment of Chronic Hepatitis B
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:285 294 New and Emerging Treatment of Chronic Hepatitis B EMMET B. KEEFFE* and PATRICK MARCELLIN *Division of Gastroenterology and Hepatology, Stanford University
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:285 294 New and Emerging Treatment of Chronic Hepatitis B EMMET B. KEEFFE* and PATRICK MARCELLIN *Division of Gastroenterology and Hepatology, Stanford University
Endpoints of hepatitis B treatment
 Journal of Viral Hepatitis, 2010, 17, 675 684 doi:10.1111/j.1365-2893.2010.01369.x REVIEW Endpoints of hepatitis B treatment W. Chotiyaputta and A. S. F. Lok Division of Gastroenterology, Department of
Journal of Viral Hepatitis, 2010, 17, 675 684 doi:10.1111/j.1365-2893.2010.01369.x REVIEW Endpoints of hepatitis B treatment W. Chotiyaputta and A. S. F. Lok Division of Gastroenterology, Department of
Scottish Medicines Consortium
 Scottish Medicines Consortium tenofovir disoproxil (as fumarate), 245 mg film-coated tablet (Viread ) No. (479/08) Gilead Sciences 06 June 2008 The Scottish Medicines Consortium has completed its assessment
Scottish Medicines Consortium tenofovir disoproxil (as fumarate), 245 mg film-coated tablet (Viread ) No. (479/08) Gilead Sciences 06 June 2008 The Scottish Medicines Consortium has completed its assessment
Entecavir for the treatment of chronic hepatitis B infection
 DOI: 10.3310/hta13suppl3/05 Health Technology Assessment 2009; Vol. 13: Suppl. 3 Entecavir for the treatment of chronic hepatitis B infection J Shepherd,* E Gospodarevskaya, G Frampton and K Cooper Southampton
DOI: 10.3310/hta13suppl3/05 Health Technology Assessment 2009; Vol. 13: Suppl. 3 Entecavir for the treatment of chronic hepatitis B infection J Shepherd,* E Gospodarevskaya, G Frampton and K Cooper Southampton
Perspective Hepatitis B Virus Infection: What Is Current and New
 Perspective Hepatitis B Virus Infection: What Is Current and New Hepatitis B virus (HBV) infection is a lifelong dynamic disease that can be controlled with treatment but cannot yet be cured. Risk of end-stage
Perspective Hepatitis B Virus Infection: What Is Current and New Hepatitis B virus (HBV) infection is a lifelong dynamic disease that can be controlled with treatment but cannot yet be cured. Risk of end-stage
HBeAg-negative chronic hepatitis B. with a nucleos(t)ide analogue?
 4 th PARIS HEPATITIS CONFERENCE HBeAg-negative chronic hepatitis B Why do I treat my chronic hepatitis B patients with a nucleos(t)ide analogue? George V. Papatheodoridis, MD 2nd Department of Internal
4 th PARIS HEPATITIS CONFERENCE HBeAg-negative chronic hepatitis B Why do I treat my chronic hepatitis B patients with a nucleos(t)ide analogue? George V. Papatheodoridis, MD 2nd Department of Internal
HBV (AASLD) CHB, HBV, CHB , ( < 5% ) 11 ( immune tolerant phase) : 21 ( immune clearance phase ) : 31 ( inactive phase) : HBeAg - HBe HBV DNA ALT
 2010262 125 R51216 + 2 C 1001-5256 (2010) 02-0125 - 06 2005 12 [ 1 ], (HBV ) (APASL) ( EASL ) (AASLD) (CHB) [ 2 4 ], ( ) ( ), CHB,, CHB CHB,, CHB,, 2 1 HBV hepatitis B virus CHB chronic hepatitis B HB
2010262 125 R51216 + 2 C 1001-5256 (2010) 02-0125 - 06 2005 12 [ 1 ], (HBV ) (APASL) ( EASL ) (AASLD) (CHB) [ 2 4 ], ( ) ( ), CHB,, CHB CHB,, CHB,, 2 1 HBV hepatitis B virus CHB chronic hepatitis B HB
Basics of hepatitis B diagnostics. Dr Emma Page MRCP MD(Res) Locum Consultant Sexual Health & Virology
 Basics of hepatitis B diagnostics Dr Emma Page MRCP MD(Res) Locum Consultant Sexual Health & Virology Basics of hepatitis B diagnostics Background Epidemiology Morphology Life-cycle Diagnostic markers
Basics of hepatitis B diagnostics Dr Emma Page MRCP MD(Res) Locum Consultant Sexual Health & Virology Basics of hepatitis B diagnostics Background Epidemiology Morphology Life-cycle Diagnostic markers
HBV Diagnosis and Treatment
 HBV Diagnosis and Treatment Anna S. F. Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor, MI, USA
HBV Diagnosis and Treatment Anna S. F. Lok, MD Alice Lohrman Andrews Professor in Hepatology Director of Clinical Hepatology Assistant Dean for Clinical Research University of Michigan Ann Arbor, MI, USA
February 8, World Journal of Gastroenterology. Re: ESPS Manuscript No Dear Dr. Qi:
 February 8, 2017 World Journal of Gastroenterology Re: ESPS Manuscript No. 32025 Dear Dr. Qi: My co-authors and I respectfully submit the accompanying revised manuscript, Early hepatitis B viral DNA clearance
February 8, 2017 World Journal of Gastroenterology Re: ESPS Manuscript No. 32025 Dear Dr. Qi: My co-authors and I respectfully submit the accompanying revised manuscript, Early hepatitis B viral DNA clearance
Chronic HBV Management in 2013
 Chronic HBV Management in 2013 Mohammad Hossein Somi MD Professor of Gastroentrology and hepatology Liver and Gastrointestinal Disease Research Center Tabriz University of Medical Sciences 1 HBV in 2013
Chronic HBV Management in 2013 Mohammad Hossein Somi MD Professor of Gastroentrology and hepatology Liver and Gastrointestinal Disease Research Center Tabriz University of Medical Sciences 1 HBV in 2013
Chronic Hepatitis B: management update.
 Chronic Hepatitis B: management update. E.O.Ogutu Department of clinical medicine & therapeutics, University of Nairobi. Physicians meeting,kisumu 2011. Background epidemiology Chronic hepatitis B (CHB)
Chronic Hepatitis B: management update. E.O.Ogutu Department of clinical medicine & therapeutics, University of Nairobi. Physicians meeting,kisumu 2011. Background epidemiology Chronic hepatitis B (CHB)
Pegasys Hepatitis B. Pegasys (peginterferon alfa-2a) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.03.02 Subject: Pegasys Hepatitis B Page: 1 of 5 Last Review Date: September 18, 2015 Pegasys Hepatitis
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.03.02 Subject: Pegasys Hepatitis B Page: 1 of 5 Last Review Date: September 18, 2015 Pegasys Hepatitis
Hepatocellular Carcinoma: Can We Slow the Rising Incidence?
 Hepatocellular Carcinoma: Can We Slow the Rising Incidence? K.Rajender Reddy M.D. Professor of Medicine Director of Hepatology Medical Director of Liver Transplantation University of Pennsylvania Outline
Hepatocellular Carcinoma: Can We Slow the Rising Incidence? K.Rajender Reddy M.D. Professor of Medicine Director of Hepatology Medical Director of Liver Transplantation University of Pennsylvania Outline
Viral Hepatitis The Preventive Potential of Antiviral Therapy. Thomas Berg
 Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Viral Hepatitis The Preventive Potential of Antiviral Therapy Thomas Berg Therapeutic and preventive strategies in patients with hepatitis virus infection Treatment of acute infection Treatment of chronic
Recent achievements in the treatment of hepatitis B by nucleosides and nucleotides. K. Zhdanov
 EASL endorsed conference White Nights of Hepatology 2012 Adverse events during antiviral therapy: how to predict, manage and monitor June 7-8 Saint-Petersburg Recent achievements in the treatment of hepatitis
EASL endorsed conference White Nights of Hepatology 2012 Adverse events during antiviral therapy: how to predict, manage and monitor June 7-8 Saint-Petersburg Recent achievements in the treatment of hepatitis
Need for long-term evaluation of therapy in Chronic Hepatitis B
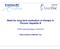 Need for long-term evaluation of therapy in Chronic Hepatitis B VHPB meeting Budapest 18/03/2010 Solko Schalm & Mehlika Toy Licensed Therapy Chronic hepatitis B Drug Date of Efficacy Disease Clinical Mortality
Need for long-term evaluation of therapy in Chronic Hepatitis B VHPB meeting Budapest 18/03/2010 Solko Schalm & Mehlika Toy Licensed Therapy Chronic hepatitis B Drug Date of Efficacy Disease Clinical Mortality
Choice of Oral Drug for Hepatitis B: Status Asokananda Konar
 Choice of Oral Drug for Hepatitis B: Status 2011 Asokananda Konar Chronic hepatitis B (CHB) is a global public health challenge with an estimated 350 to 400 million people with chronic HBV infection, despite
Choice of Oral Drug for Hepatitis B: Status 2011 Asokananda Konar Chronic hepatitis B (CHB) is a global public health challenge with an estimated 350 to 400 million people with chronic HBV infection, despite
tenofovir disoproxil (as fumarate), 245mg, film-coated tablet (Viread ) SMC No. (720/11) Gilead Sciences Ltd
 tenofovir disoproxil (as fumarate), 245mg, film-coated tablet (Viread ) SMC No. (720/11) Gilead Sciences Ltd 05 August 2011 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
tenofovir disoproxil (as fumarate), 245mg, film-coated tablet (Viread ) SMC No. (720/11) Gilead Sciences Ltd 05 August 2011 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
Individualizing Treatment in the Patient With Chronic HBV Infection: When to Start, What to Use, and When to Stop CME
 Individualizing Treatment in the Patient With Chronic HBV Infection: When to Start, What to Use, and When to Stop CME Chia C. Wang, MD, MS Anna S. F. Lok, MD Kris V. Kowdley, MD Supported by an independent
Individualizing Treatment in the Patient With Chronic HBV Infection: When to Start, What to Use, and When to Stop CME Chia C. Wang, MD, MS Anna S. F. Lok, MD Kris V. Kowdley, MD Supported by an independent
J.C. WANG, L.L. HE, Q. CHEN 1. Introduction. Abstract. BACKGROUND: Either combination. European Review for Medical and Pharmacological Sciences
 European Review for Medical and Pharmacological Sciences Comparison of re-treatment outcomes of lamivudine plus adefovir or entecavir in chronic hepatitis B patients with viral relapse after cessation
European Review for Medical and Pharmacological Sciences Comparison of re-treatment outcomes of lamivudine plus adefovir or entecavir in chronic hepatitis B patients with viral relapse after cessation
Tenofovir as a drug of choice for the chronic hepatitis B treatment
 EASL endorsed conference White Nights of Hepatology 2013 Symposium Perspectives of chronic viral hepatitis B and C treatment June 6-7 Saint-Petersburg Tenofovir as a drug of choice for the chronic hepatitis
EASL endorsed conference White Nights of Hepatology 2013 Symposium Perspectives of chronic viral hepatitis B and C treatment June 6-7 Saint-Petersburg Tenofovir as a drug of choice for the chronic hepatitis
Management of Chronic Hepatitis B in Asian Americans
 Management of Chronic Hepatitis B in Asian Americans Myron J Tong; UCLA, CA Calvin Q. Pan; Mount Sinai, NY Hie-Won Hann; Thomas Jefferson, PA Kris V. Kowdley; Virginia Mason, WA Steven Huy B Han; UCLA,
Management of Chronic Hepatitis B in Asian Americans Myron J Tong; UCLA, CA Calvin Q. Pan; Mount Sinai, NY Hie-Won Hann; Thomas Jefferson, PA Kris V. Kowdley; Virginia Mason, WA Steven Huy B Han; UCLA,
Medicine. Ka Zhang, MD a, Hong Cao, MD a, Jiayi Liang, MD b, Xin Shu, MD a, Haixia Sun, MD a, Gang Li, PhD a, Qihuan Xu, PhD a,
 Clinical Trial/Experimental Study Medicine CONSORT: Effects of adding adefovirdipivoxil to peginterferon alfa-2a at different time points on HBeAg-positivepatients A prospective, randomized study Ka Zhang,
Clinical Trial/Experimental Study Medicine CONSORT: Effects of adding adefovirdipivoxil to peginterferon alfa-2a at different time points on HBeAg-positivepatients A prospective, randomized study Ka Zhang,
The advent of sensitive assays for the detection of hepatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;-:1 10 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;-:1 10 All studies published in Clinical Gastroenterology and Hepatology are embargoed until 3PM ET of the day they are published as corrected proofs on-line.
Currently status of HBV therapy: efficacy and limitations
 9 November 2016 Currently status of HBV therapy: efficacy and limitations Pietro Lampertico Gastroenterology and Hepatology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico University of
9 November 2016 Currently status of HBV therapy: efficacy and limitations Pietro Lampertico Gastroenterology and Hepatology Unit Fondazione IRCCS Cà Granda - Ospedale Maggiore Policlinico University of
Horizon Scanning Technology Summary. Tenofovir disoproxil fumarate for hepatitis B. National Horizon Scanning Centre. April 2007
 Horizon Scanning Technology Summary National Horizon Scanning Centre Tenofovir disoproxil fumarate for hepatitis B April 2007 This technology summary is based on information available at the time of research
Horizon Scanning Technology Summary National Horizon Scanning Centre Tenofovir disoproxil fumarate for hepatitis B April 2007 This technology summary is based on information available at the time of research
How find a solution for alternative to indefinite nucleoside analogue therapy in patients chronic HBV infection?
 How find a solution for alternative to indefinite nucleoside analogue therapy in patients chronic HBV infection? Philippe Halfon, MD,PhD Associate Professor of Medicine Hôpital Europeen Marseille, France
How find a solution for alternative to indefinite nucleoside analogue therapy in patients chronic HBV infection? Philippe Halfon, MD,PhD Associate Professor of Medicine Hôpital Europeen Marseille, France
Hepatitis B virus infection (HBV) is global epidemic. Current Treatment Strategies for the Management of Chronic Hepatitis B CHRONIC HEPATITIS B
 CHRONIC HEPATITIS B Current Treatment Strategies for the Management of Chronic Hepatitis B Case Study and Commentary, Robert J. Wong, MD, and Walid S. Ayoub, MD ABSTRACT Objective: To review current treatment
CHRONIC HEPATITIS B Current Treatment Strategies for the Management of Chronic Hepatitis B Case Study and Commentary, Robert J. Wong, MD, and Walid S. Ayoub, MD ABSTRACT Objective: To review current treatment
Supplementary materials: Predictors of response to pegylated interferon in chronic hepatitis B: a
 Supplementary materials: Predictors of response to pegylated interferon in chronic hepatitis B: a real-world hospital-based analysis Yin-Chen Wang 1, Sien-Sing Yang 2*, Chien-Wei Su 1, Yuan-Jen Wang 3,
Supplementary materials: Predictors of response to pegylated interferon in chronic hepatitis B: a real-world hospital-based analysis Yin-Chen Wang 1, Sien-Sing Yang 2*, Chien-Wei Su 1, Yuan-Jen Wang 3,
Potential Efficacy of Pegylated Interferon-α and a Nucleos(t)ide Analogue as Combination Therapy for HBeAg-Positive Chronic Hepatitis B
 Gut and Liver, Vol. 10, No. 4, July 2016, pp. 611-616 ORiginal Article Potential Efficacy of Pegylated Interferon-α and a Nucleos(t)ide Analogue as Combination Therapy for HBeAg-Positive Chronic Hepatitis
Gut and Liver, Vol. 10, No. 4, July 2016, pp. 611-616 ORiginal Article Potential Efficacy of Pegylated Interferon-α and a Nucleos(t)ide Analogue as Combination Therapy for HBeAg-Positive Chronic Hepatitis
The effect of pegylated interferon-a on the treatment of lamivudine resistant chronic HBeAg positive hepatitis B virus infection *
 Journal of Hepatology 44 (2006) 507 511 www.elsevier.com/locate/jhep The effect of pegylated interferon-a on the treatment of lamivudine resistant chronic HBeAg positive hepatitis B virus infection * Wilhelmus
Journal of Hepatology 44 (2006) 507 511 www.elsevier.com/locate/jhep The effect of pegylated interferon-a on the treatment of lamivudine resistant chronic HBeAg positive hepatitis B virus infection * Wilhelmus
Antiviral Therapy 14:
 Antiviral Therapy 14:679 685 Original article Combination of baseline parameters and on-treatment hepatitis B virus DNA levels to start and continue patients with lamivudine therapy Man-Fung Yuen 1 *,
Antiviral Therapy 14:679 685 Original article Combination of baseline parameters and on-treatment hepatitis B virus DNA levels to start and continue patients with lamivudine therapy Man-Fung Yuen 1 *,
Disclaimer. Presenter Release are for reactive use by Medical Information only internal learning/educational use only
 Disclaimer Presenter Release are for reactive use by Medical Information only internal learning/educational use only Any unsolicited request from HCP must be forwarded to Medical Information Housekeeping
Disclaimer Presenter Release are for reactive use by Medical Information only internal learning/educational use only Any unsolicited request from HCP must be forwarded to Medical Information Housekeeping
Chronic Hepatitis B - Antiviral Resistance in Korea -
 Chronic Hepatitis B - Antiviral Resistance in Korea - Young-Suk Lim University of Ulsan College of Medicine Asan Medical Center Seoul, Korea HBV Genome partially double-stranded DNA genome about 3200 nucleotides
Chronic Hepatitis B - Antiviral Resistance in Korea - Young-Suk Lim University of Ulsan College of Medicine Asan Medical Center Seoul, Korea HBV Genome partially double-stranded DNA genome about 3200 nucleotides
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Hepatitis B (chronic): diagnosis and management of chronic hepatitis B in children, young
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Centre for Clinical Practice SCOPE Clinical guideline title: Hepatitis B (chronic): diagnosis and management of chronic hepatitis B in children, young
Terapia dell epatite cronica B: paradigmi attuali e possibili scenari futuri
 Terapia dell epatite cronica B: paradigmi attuali e possibili scenari futuri Nicola Coppola Dipartimento di Salute Mentale e Medicina Preventiva Seconda Università di Napoli Main goal of treatment of chronic
Terapia dell epatite cronica B: paradigmi attuali e possibili scenari futuri Nicola Coppola Dipartimento di Salute Mentale e Medicina Preventiva Seconda Università di Napoli Main goal of treatment of chronic
Yunhua Liu*, Weikun Li, Ting Jia, Dan Peng, Huimin Li, Xiaofei Li and Songqin Lv. Introduction
 Original Article Sustained Responses in Chronic Hepatitis B Patients with Nucleos(t)ide Analogue Drug-resistance after Peg-interferon Alfa-2a Add-on Treatment: A Long-term Cohort Study Yunhua Liu*, Weikun
Original Article Sustained Responses in Chronic Hepatitis B Patients with Nucleos(t)ide Analogue Drug-resistance after Peg-interferon Alfa-2a Add-on Treatment: A Long-term Cohort Study Yunhua Liu*, Weikun
High Rates of Viral Suppression After Long-term Entecavir Treatment of Asian Patients With Hepatitis B e Antigen Positive Chronic Hepatitis B
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1047 1050 BRIEF COMMUNICATIONS High Rates of Viral Suppression After Long-term Entecavir Treatment of Asian Patients With Hepatitis B e Antigen Positive
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1047 1050 BRIEF COMMUNICATIONS High Rates of Viral Suppression After Long-term Entecavir Treatment of Asian Patients With Hepatitis B e Antigen Positive
MedInform. HBsAg-guided extension of Peg-IFN therapy in HBeAg-negative responders. Original Article
 HBsAg-guided extension of Peg-IFN therapy in HBeAg-negative responders Nina Nikolova, Deian Jelev, Krassimir Antonov, Lyudmila Mateva, Zahariy Krastev. University Hospital St. Ivan Rilski Sofia, Clinic
HBsAg-guided extension of Peg-IFN therapy in HBeAg-negative responders Nina Nikolova, Deian Jelev, Krassimir Antonov, Lyudmila Mateva, Zahariy Krastev. University Hospital St. Ivan Rilski Sofia, Clinic
Off-Therapy Durability of Response to Entecavir Therapy in Hepatitis B e Antigen-Negative Chronic Hepatitis B Patients
 VIRAL HEPATITIS Off-Therapy Durability of Response to Entecavir Therapy in Hepatitis B e Antigen-Negative Chronic Hepatitis B Patients Wen-Juei Jeng, 1,2 I-Shyan Sheen, 1,2 Yi-Cheng Chen, 1,2 Chao-Wei
VIRAL HEPATITIS Off-Therapy Durability of Response to Entecavir Therapy in Hepatitis B e Antigen-Negative Chronic Hepatitis B Patients Wen-Juei Jeng, 1,2 I-Shyan Sheen, 1,2 Yi-Cheng Chen, 1,2 Chao-Wei
Hepatitis B Treatment Pearls. Agenda
 Hepatitis B Treatment Pearls Fredric D. Gordon, MD Vice Chair Dept. of Transplantation and Hepatobiliary Diseases Lahey Hospital & Medical Center Associate Professor of Medicine Tufts Medical School Boston,
Hepatitis B Treatment Pearls Fredric D. Gordon, MD Vice Chair Dept. of Transplantation and Hepatobiliary Diseases Lahey Hospital & Medical Center Associate Professor of Medicine Tufts Medical School Boston,
Chronic hepatitis B is one of the leading causes of hepatocellular. Surrogate End Points and Long-Term Outcome in Patients With Chronic Hepatitis B
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1113 1120 Surrogate End Points and Long-Term Outcome in Patients With Chronic Hepatitis B VINCENT WAI SUN WONG,*, GRACE LAI HUNG WONG,*, ANGEL MEI LING CHIM,*,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2009;7:1113 1120 Surrogate End Points and Long-Term Outcome in Patients With Chronic Hepatitis B VINCENT WAI SUN WONG,*, GRACE LAI HUNG WONG,*, ANGEL MEI LING CHIM,*,
Is there a need for combination treatment? Yes!
 18.0.2012 C Hep Meeting Berlin Is there a need for combination treatment? Yes! Florian van Bömmel University Hospital Leipzig Hepatology Section Germany Most patients respond to monotherapy with entecavir
18.0.2012 C Hep Meeting Berlin Is there a need for combination treatment? Yes! Florian van Bömmel University Hospital Leipzig Hepatology Section Germany Most patients respond to monotherapy with entecavir
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.02 An Open Label Prospective Study to Evaluate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.02 An Open Label Prospective Study to Evaluate
Title: Off therapy durability of response to Entecavir therapy in hepatitis B e
 Title: Off therapy durability of response to Entecavir therapy in hepatitis B e antigen negative chronic hepatitis B patients Wen-Juei Jeng, MD 1,3, I-Shyan Sheen, MD 1-3, Yi-Cheng Chen, MD 1,3, Chao-Wei
Title: Off therapy durability of response to Entecavir therapy in hepatitis B e antigen negative chronic hepatitis B patients Wen-Juei Jeng, MD 1,3, I-Shyan Sheen, MD 1-3, Yi-Cheng Chen, MD 1,3, Chao-Wei
ESCMID Online Lecture Library. by author
 Pro-Con: To stop or not to stop hepatitis B treatment? To Stop HBV Treatment Resat Ozaras, MD, Professor Istanbul University, Cerrahpasa Medical School, Infection Dept. HBV Therapy Nucleos(t)ide analogues
Pro-Con: To stop or not to stop hepatitis B treatment? To Stop HBV Treatment Resat Ozaras, MD, Professor Istanbul University, Cerrahpasa Medical School, Infection Dept. HBV Therapy Nucleos(t)ide analogues
Efficacy of Tenofovir Disoproxil Fumarate at 240 Weeks in Patients With Chronic Hepatitis B With High Baseline Viral Load
 Efficacy of Tenofovir Disoproxil Fumarate at 240 Weeks in Patients With Chronic Hepatitis B With High Baseline Viral Load Stuart C. Gordon, 1 Zahary Krastev, 2 Andrzej Horban, 3 J org Petersen, 4 Jan Sperl,
Efficacy of Tenofovir Disoproxil Fumarate at 240 Weeks in Patients With Chronic Hepatitis B With High Baseline Viral Load Stuart C. Gordon, 1 Zahary Krastev, 2 Andrzej Horban, 3 J org Petersen, 4 Jan Sperl,
New therapeutic strategies in HBV patients
 New therapeutic strategies in HBV patients Philippe HALFON MD, PhD Associate Professor of Medecine Internal Medecine and Infectious Diseases, Hopital Europeen, Marseille, France. NUC + PEG IFN, HBsAg Clearance
New therapeutic strategies in HBV patients Philippe HALFON MD, PhD Associate Professor of Medecine Internal Medecine and Infectious Diseases, Hopital Europeen, Marseille, France. NUC + PEG IFN, HBsAg Clearance
Acute Hepatitis B Virus Infection with Recovery
 Hepatitis B: Clear as Mud Melissa Osborn, MD, MSCR Assistant Professor Emory University School of Medicine Atlanta, GA 1 Objectives 1. Distinguish the various stages in the natural history of chronic hepatitis
Hepatitis B: Clear as Mud Melissa Osborn, MD, MSCR Assistant Professor Emory University School of Medicine Atlanta, GA 1 Objectives 1. Distinguish the various stages in the natural history of chronic hepatitis
Hepatitis B Update. Jorge L. Herrera, M.D. University of South Alabama Mobile, AL. Gastroenterology
 Hepatitis B Update Jorge L. Herrera, M.D. University of South Alabama Mobile, AL Deciding Who to Treat Is hepatitis B a viral disease or a liver disease? Importance of HBV-DNA Levels in the Natural History
Hepatitis B Update Jorge L. Herrera, M.D. University of South Alabama Mobile, AL Deciding Who to Treat Is hepatitis B a viral disease or a liver disease? Importance of HBV-DNA Levels in the Natural History
Tenofovir (Viread ) for the treatment of chronic hepatitis B SINGLE TECHNOLOGY APPRAISAL
 Tenofovir (Viread ) for the treatment of chronic hepatitis B SINGLE TECHNOLOGY APPRAISAL Submission to the National Institute for Health and Clinical Excellence December 2008 Amended version in response
Tenofovir (Viread ) for the treatment of chronic hepatitis B SINGLE TECHNOLOGY APPRAISAL Submission to the National Institute for Health and Clinical Excellence December 2008 Amended version in response
EASL Clinical Practice Guidelines: Management of chronic hepatitis B virus infection
 EASL Clinical Practice Guidelines: Management of chronic hepatitis B virus infection European Association for the Study of the Liver Introduction Our understanding of the natural history of hepatitis B
EASL Clinical Practice Guidelines: Management of chronic hepatitis B virus infection European Association for the Study of the Liver Introduction Our understanding of the natural history of hepatitis B
Journal of Antimicrobial Chemotherapy Advance Access published April 25, 2013
 Journal of Antimicrobial Chemotherapy Advance Access published April 25, 213 J Antimicrob Chemother doi:1.193/jac/dkt147 Virological response to entecavir reduces the risk of liver disease progression
Journal of Antimicrobial Chemotherapy Advance Access published April 25, 213 J Antimicrob Chemother doi:1.193/jac/dkt147 Virological response to entecavir reduces the risk of liver disease progression
Management of hepatitis B virus
 Journal of Antimicrobial Chemotherapy Advance Access published May 14, 2008 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkn188 Management of hepatitis B virus Nidhi A. Singh and Nancy Reau* Section
Journal of Antimicrobial Chemotherapy Advance Access published May 14, 2008 Journal of Antimicrobial Chemotherapy doi:10.1093/jac/dkn188 Management of hepatitis B virus Nidhi A. Singh and Nancy Reau* Section
Intron A Hepatitis B. Intron A (interferon alfa-2b) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Hepatitis B and D Update on clinical aspects
 Hepatitis B and D Update on clinical aspects B. Müllhaupt Gastroenterology and Hepatology Swiss Transplant and HPB-Center University Hospital Zurich beat.muellhaupt@usz.ch B.M. 11.11.17 Hepatitis Strategy
Hepatitis B and D Update on clinical aspects B. Müllhaupt Gastroenterology and Hepatology Swiss Transplant and HPB-Center University Hospital Zurich beat.muellhaupt@usz.ch B.M. 11.11.17 Hepatitis Strategy
Hepatitis B. Epidemiology and Natural History and Implications for Treatment
 Hepatitis B Epidemiology and Natural History and Implications for Treatment Norah Terrault, MD Professor of Medicine and Surgery Director, Viral Hepatitis Center University of California San Francisco
Hepatitis B Epidemiology and Natural History and Implications for Treatment Norah Terrault, MD Professor of Medicine and Surgery Director, Viral Hepatitis Center University of California San Francisco
MedInform. HBV DNA loss in Bulgarian patients on NUC therapy. Speed related factors. (NUC related speed of HBV DNA loss in Bulgaria) Original Article
 DOI: 10.18044/Medinform.201852.897 ISSUE 3, 2018 HBV DNA loss in Bulgarian patients on NUC therapy. Speed related factors. (NUC related speed of HBV DNA loss in Bulgaria) Donika Krasteva, Radosveta Tomova,
DOI: 10.18044/Medinform.201852.897 ISSUE 3, 2018 HBV DNA loss in Bulgarian patients on NUC therapy. Speed related factors. (NUC related speed of HBV DNA loss in Bulgaria) Donika Krasteva, Radosveta Tomova,
Beyond the Tip of the Iceberg: Strategies to Ensure Optimal HBV Screenin g, Diagnosis, and Initial Therapy
 : Strategies to Ensure Optimal HBV Screenin g, Diagnosis, and Initial Therapy Sunday, November 1, 2009 Back Bay Ballroom Sheraton Boston Hotel Boston, Massachusetts This program is supported by an educational
: Strategies to Ensure Optimal HBV Screenin g, Diagnosis, and Initial Therapy Sunday, November 1, 2009 Back Bay Ballroom Sheraton Boston Hotel Boston, Massachusetts This program is supported by an educational
Hepatitis B (chronic)
 National Clinical Guideline Centre. Hepatitis B (chronic) Appendices H - 0 Hepatitis B Guideline Appendices June 2013 Final Commissioned by the National Institute for Health and Care Excellence Final:
National Clinical Guideline Centre. Hepatitis B (chronic) Appendices H - 0 Hepatitis B Guideline Appendices June 2013 Final Commissioned by the National Institute for Health and Care Excellence Final:
Treatment of chronic hepatitis B: Evolution over two decades_
 doi:10.1111/j.1440-1746.2010.06545.x REVIEW Treatment of chronic hepatitis B: Evolution over two decades_6545 138..143 Man-Fung Yuen and Ching-Lung Lai Department of Medicine, the University of Hong Kong,
doi:10.1111/j.1440-1746.2010.06545.x REVIEW Treatment of chronic hepatitis B: Evolution over two decades_6545 138..143 Man-Fung Yuen and Ching-Lung Lai Department of Medicine, the University of Hong Kong,
