Mycobacterium abscessus Lung Disease in a Patient with Kartagener Syndrome
|
|
|
- Ruby Kelley
- 5 years ago
- Views:
Transcription
1 CASE REPORT ISSN: (Print)/ (Online) Tuberc Respir Dis 2014;77: Mycobacterium abscessus Lung Disease in a Patient with Kartagener Syndrome Jung Hoon Kim, M.D. 1, *, Won Jun Song, M.D. 1, *, Ji Eun Jun, M.D. 1, Duck Hyun Ryu, M.D. 1, Ji Eun Lee, M.D. 1, Ho Jung Jeong, M.D. 1, Suk Hyeon Jeong, M.D. 1, Hyung Koo Kang, M.D. 1, Jung Soo Kim, M.D. 1, Hyun Lee, M.D. 1, Hae Ri Chon, M.D. 1, Kyeongman Jeon, M.D. 1, Dohun Kim, M.D. 2,, Jhingook Kim, M.D. 2 and Won-Jung Koh, M.D. 1 1 Division of Pulmonary and Critical Care Medicine, Department of Medicine, 2 Department of Thoracic Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Primary ciliary dyskinesia (PCD) is characterized by the congenital impairment of mucociliary clearance. When accompanied by situs inversus, chronic sinusitis and bronchiectasis, PCD is known as Kartagener syndrome. The main consequence of impaired ciliary function is a reduced mucus clearance from the lungs, and susceptibility to chronic respiratory infections due to opportunistic pathogens, including nontuberculous mycobacteria (NTM). There has been no report of NTM lung disease combined with Kartagener syndrome in Korea. Here, we report an adult patient with Kartagener syndrome complicated with Mycobacterium abscessus lung disease. A 37-year-old female presented to our hospital with chronic cough and sputum. She was ultimately diagnosed with M. abscessus lung disease and Kartagener syndrome. M. abscessus was repeatedly isolated from sputum specimens collected from the patient, despite prolonged antibiotic treatment. The patient s condition improved and negative sputum culture conversion was achieved after sequential bilateral pulmonary resection. Keywords: Kartagener Syndrome; Primary Ciliary Dyskinesia; Bronchiectasis; Nontuberculous Mycobacteria; Mycobacterium Infections, Nontuberculous Introduction Address for correspondence: Won-Jung Koh, M.D. Division of Pulmonary and Critical Care Medicine, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, 81 Irwon-ro, Gangnam-gu, Seoul , Korea Phone: , Fax: wjkoh@skku.edu *Jung Hoon Kim and Won Jun Song contributed equally to this work. Present address: Department of Thoracic Surgery, Chungbuk National University Hospital, Cheongju, Korea Received: May 3, 2014 Revised: May 27, 2014 Accepted: Jun. 17, 2014 cc It is identical to the Creative Commons Attribution Non-Commercial License ( Copyright 2014 The Korean Academy of Tuberculosis and Respiratory Diseases. All rights reserved. Primary ciliary dyskinesia (PCD) is associated with abnormal ciliary structure and function, which results in the retention of mucus and bacteria in the respiratory tract, leading to chronic oto-sino-pulmonary disease, situs abnormalities and abnormal sperm motility 1. The initial recognition of this syndrome in 1933 was based on the triad of chronic sinusitis, bronchiectasis, and situs inversus, known as Kartagener syndrome 2. About 55% of PCD patients present with situs inversus 2. PCD causes abnormal and permanent dilatation of the bronchi, known as bronchiectasis, which is caused by inflammation and destruction of the structural components of the bronchial walls. Most experts accept that a vicious cycle of infection and inflammation is created by this basic defect in host airway defenses. This generates airway damage and further impairs airway clearance; eventually chronic microbial colonization/infection develops, leading to further infection and 136
2 M. abscessus lung disease and Kartagener syndrome inflammation with subsequent destruction of the conducting airways 1,2. Airway infections with Haemophilus influenzae, Staphylococcus aureus, and Streptococcus pneumoniae are common, infections with Pseudomonas aeruginosa have also been reported, usually in adults 1. Approximately 15% of adult patients with PCD have positive sputum cultures of nontuberculous mycobacteria (NTM); however, the prevalence in children with PCD is lower 3. To the best of our knowledge, there has been no report of NTM lung disease combined with Kartagener syndrome in Korea, although the number of patients with NTM lung disease has been increasing in recent years 4,5. Here, we report an adult case of Kartagener syndrome complicated with Mycobacterium abscessus lung disease who was successfully treated with bilateral pulmonary resection combined with antibiotic therapy. Case Report A 37-year-old female was referred to our hospital for further management of NTM lung disease. During the 4 months before the patient arrived at our hospital, she had a productive cough and hemoptysis. She was initially diagnosed as having smear-positive pulmonary tuberculosis, and received antituberculosis drugs. During treatment, her symptoms did not improve and NTM were repeatedly isolated from her sputum specimens. She was then referred to our hospital. The patient was a nonsmoker. Twenty years earlier, the patient had undergone surgery for chronic rhinosinusitis. Chest radiography showed dextrocardia and situs inversus and paranasal sinus radiography showed total opacification involving the bilateral ethmoid sinus and bilateral maxillary sinus (Figure 1A, B). Chest high-resolution computed tomography (HRCT) scans showed multiple cavitary lesions in both upper lobes, bronchiectasis, and multiple nodules in the left middle lobe and the lingular segment of the right upper lobe (Figure 2A, C, E, G). The patient s sputum was positive for acid-fast bacilli (AFB) stain, and M. abscessus (sensu stricto) was repeatedly isolated from sputum specimens collected from the patient. The identification of M. abscessus (sensu stricto) was performed using a polymerase chain reaction-restriction fragment length polymorphism analysis of rpob and sequence analysis of rpob and hsp65 6. Drug susceptibility test showed the isolate was susceptible amikacin (minimum inhibitory concentration [MIC], 16 μg/ml) and imipenem (MIC, 4 μg/ ml), intermediate to cefoxitin (MIC, 32 μg/ml), and resistant to ciprofloxacin (MIC, >16 μg/ml), moxifloxacin (MIC, 8 μg/ ml) and doxycycline (MIC, >32 μg/ml). The isolate had inducible resistance to clarithromycin, as it was susceptible (MIC, 0.5 μg/ml) to clarithromycin at day 3 but resistant to clarithromycin (MIC, >64 μg/ml) at day 14. The patient received oral clarithromycin and fluoroquinolone antibiotics (initially ciprofloxacin, later moxifloxacin), along with an initial 4-week course of intravenous amikacin and cefoxitin 7. Although the cavitary lesion in the right upper lobe improved after 20 months of antibiotic therapy, the size of the multiple cavities in the left upper lobe increased (Figure 2B, D, F, H). The patient s symptoms worsened and follow-up AFB staining of sputum and sputum cultures were persistently positive. Considering the patient s age, persistent symptoms, and aggravation of cavitary lesions in the left lung after antibiotic therapy, we decided to perform surgical resection. Preoperative pulmonary function test revealed that forced vital capacity was 2.82 L (95% predicted) and forced expiratory volume in one second was 1.46 L (63% predicted). The patient underwent a left upper bilobectomy (left upper lobectomy plus left middle lobectomy). She was discharged 8 days after surgery without postoperative complications. After surgery, Figure 1. (A) Chest radiography showed dextrocardia and situs inversus. Note the cavitary lesions in the right upper lobe and nodulostreaky opacity, suggesting bronchiectasis in the left middle lung zones. (B) Paranasal sinus radiography showed total opacification involving the bilateral ethmoid sinus and bilateral maxillary sinus
3 JH Kim et al. Figure 2. (A, C, E, G) Chest high-resolution computed tomography showed multiple cavities in both upper lobes. Note the severe bronchiectasis in the left middle lobe and the lingular segment of the right upper lobe. (B, D, F, H) Although the cavitary lesion in the right upper lobe improved after 20 months of antibiotic treatment, the size of the multiple cavities in the left upper lobe increased. her symptoms improved. However, cultures of the patient s sputum were persistently positive for M. abscessus, although AFB staining of sputum showed negative conversion. At 9 months after surgery, an AFB-positive sputum smear was obtained, and the cavitary lesion in the right upper lobe was aggravated (Figure 3A, C, E, G). Thus, a right upper lobectomy was performed and the patient was discharged 8 days after surgery without postoperative complications. Soon after the second operation, the patient s symptoms improved and negative sputum smears and culture conversion were achieved. The patient was maintained on oral antibiotic treatment with clarithromycin and moxifloxacin. Antibiotic therapy was successfully discontinued 24 months after the second operation. At 2 years since the second surgery, the patient is doing well: sputum AFB smears and cultures are consistently negative and follow-up chest HRCT scans indicate no new lesions (Figure 3B, D, F, H). Discussion PCD is a genetically heterogeneous recessive disorder of motile cilia that leads to oto-sino-pulmonary disease 1,2. Kartagener syndrome, which consists of situs inversus totalis, bronchiectasis and sinusitis, is a well-known but less common presentation of PCD. In patients with PCD, recurrent and chronic bacterial infections in the lower airways inevitably occur, and there is age-dependent development of bronchiectasis, which is a nearly universal complication of PCD in adults 3. Initially, sputum cultures are positive for H. influenzae, S. pneumoniae, and S. aureus. Once bronchiectasis is evident on chest HRCT, P. aeruginosa and other opportunistic pathogens may be present. NTM may also be isolated; a previous study from the United States reported that NTM infections are not uncommon, especially in older patients, and that NTM were present in 8 of 59 patients (14%) with PCD in whom sputum for microbiologic testing was obtained (Mycobacterium avium complex [n=3], M. abscessus [n=2], M. gordonae [n=2], and mixed M. avium complex/m. gordonae [n=1]) 3. The prevalence of lung diseases caused by NTM is increasing worldwide, affecting both immunocompetent and immunocompromised individuals 8. In Korea, M. abscessus complex is the second most common pathogen responsible for lung diseases caused by NTM, after M. avium complex 6,7, Tuberc Respir Dis 2014;77:
4 M. abscessus lung disease and Kartagener syndrome Figure 3. (A, C, E, G) At 9 months after the left-sided surgery, chest high-resolution computed tomography showed an aggravation of the cavitary lesion in the right upper lobe. (B, D, F, H) At 24 months of the right-sided surgery, follow-up chest high-resolution computed tomography scans indicate no new lesions. M. abscessus complex (M. abscessus sensu lato) are divided into three closely related subspecies: M. abscessus (sensu stricto), Mycobacterium massiliense, and Mycobacterium bolletii 6,10,11. Within the M. abscessus complex, M. abscessus (44 53%) and M. massiliense (45 55%) are equally distributed, while M. bolletii is a relatively rare pathogen (1 2%) in Korea 6,10,11. M. abscessus (sensu stricto) is resistant in vitro to many antibiotics and thus is very difficult to treat 6,7. Isolates are usually susceptible in vitro to some parenteral agents (e.g., amikacin, cefoxitin, and imipenem) and to macrolides (e.g., clarithromycin and azithromycin) 8. Combination therapy with intravenous amikacin and cefoxitin or imipenem and an oral macrolide has been recommended by the American Thoracic Society/Infectious Diseases Society of America and many other experts 8. However, treatment response rates are not satisfactory and optimal therapeutic regimens and treatment durations are not well established 6,7. Curative therapy for M. abscessus lung disease is more likely to be obtained with limited disease and a combination of surgical resection of the involved lung and chemotherapy 8. Patients with focal lung disease and symptoms that significantly impair their quality of life who can withstand lung resection should be treated surgically after an initial period on antimicrobials to lessen the microbial burden 8,12. Some patients who have bilateral disease could undergo staged sequential surgery The fact that sputum conversion was obtained only after the second pulmonary resection underscores the necessity of bilateral resection in this patient. In summary, this is the first reported case of NTM lung disease in a patient with Kartagener syndrome in Korea. AFB smear cannot differentiate between Mycobacterium tuberculosis and NTM. The recovery rate of NTM from respiratory specimens and the number of patients with NTM lung disease has been rapidly increasing in Korea. An early differential diagnosis of NTM lung disease from pulmonary tuberculosis is important, as the therapeutic regimen differs from that of pulmonary tuberculosis. This case also suggests that if medical treatment fails for NTM lung disease, resection of the diseased lobes should be considered, even in patients with bilateral lesions
5 JH Kim et al. Conflicts of Interest No potential conflict of interest relevant to this article was reported. Acknowledgements This study was supported by a grant of the Korean Health technology R&D Project, Ministry for Health & Welfare, Republic of Korea (A120647). References 1. Barbato A, Frischer T, Kuehni CE, Snijders D, Azevedo I, Baktai G, et al. Primary ciliary dyskinesia: a consensus statement on diagnostic and treatment approaches in children. Eur Respir J 2009;34: Knowles MR, Daniels LA, Davis SD, Zariwala MA, Leigh MW. Primary ciliary dyskinesia. Recent advances in diagnostics, genetics, and characterization of clinical disease. Am J Respir Crit Care Med 2013;188: Noone PG, Leigh MW, Sannuti A, Minnix SL, Carson JL, Hazucha M, et al. Primary ciliary dyskinesia: diagnostic and phenotypic features. Am J Respir Crit Care Med 2004;169: Yoo JW, Jo KW, Kim MN, Lee SD, Kim WS, Kim DS, et al. Increasing trend of isolation of non-tuberculous mycobacteria in a tertiary university hospital in South Korea. Tuberc Respir Dis 2012;72: Koh WJ, Chang B, Jeong BH, Jeon K, Kim SY, Lee NY, et al. Increasing recovery of nontuberculous mycobacteria from respiratory specimens over a 10-year period in a tertiary referral hospital in South Korea. Tuberc Respir Dis 2013;75: Koh WJ, Jeon K, Lee NY, Kim BJ, Kook YH, Lee SH, et al. Clinical significance of differentiation of Mycobacterium massiliense from Mycobacterium abscessus. Am J Respir Crit Care Med 2011;183: Jeon K, Kwon OJ, Lee NY, Kim BJ, Kook YH, Lee SH, et al. Antibiotic treatment of Mycobacterium abscessus lung disease: a retrospective analysis of 65 patients. Am J Respir Crit Care Med 2009;180: Griffith DE, Aksamit T, Brown-Elliott BA, Catanzaro A, Daley C, Gordin F, et al. An official ATS/IDSA statement: diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. Am J Respir Crit Care Med 2007;175: Koh WJ, Jeong BH, Jeon K, Lee NY, Lee KS, Woo SY, et al. Clinical significance of the differentiation between Mycobacterium avium and Mycobacterium intracellulare in M avium complex lung disease. Chest 2012;142: Koh WJ, Stout JE, Yew WW. Advances in the management of pulmonary disease due to Mycobacterium abscessus complex. Int J Tuberc Lung Dis 2014;18: Lee SH, Yoo HK, Kim SH, Koh WJ, Kim CK, Park YK, et al. The drug resistance profile of Mycobacterium abscessus group strains from Korea. Ann Lab Med 2014;34: Koh WJ, Kim YH, Kwon OJ, Choi YS, Kim K, Shim YM, et al. Surgical treatment of pulmonary diseases due to nontuberculous mycobacteria. J Korean Med Sci 2008;23: Mitchell JD, Bishop A, Cafaro A, Weyant MJ, Pomerantz M. Anatomic lung resection for nontuberculous mycobacterial disease. Ann Thorac Surg 2008;85: Yu JA, Pomerantz M, Bishop A, Weyant MJ, Mitchell JD. Lady Windermere revisited: treatment with thoracoscopic lobectomy/segmentectomy for right middle lobe and lingular bronchiectasis associated with non-tuberculous mycobacterial disease. Eur J Cardiothorac Surg 2011;40: Lee SH, Min JW, Um SW, Han SS, Han SK, Shim YS, et al. Sequential bilateral lung resection in a patient with Mycobacterium abscessus lung disease refractory to medical treatment. Yonsei Med J 2010;51: Tuberc Respir Dis 2014;77:
Diagnosis of Pulmonary Tuberculosis and Nontuberculous Mycobacterial Lung Disease in Korea
 REVIEW http://dx.doi.org/10.4046/trd.2014.77.1.1 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:1-5 Diagnosis of Pulmonary Tuberculosis and Nontuberculous Mycobacterial Lung Disease
REVIEW http://dx.doi.org/10.4046/trd.2014.77.1.1 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:1-5 Diagnosis of Pulmonary Tuberculosis and Nontuberculous Mycobacterial Lung Disease
Implication of species change of Nontuberculous Mycobacteria during or after treatment
 Lee et al. BMC Pulmonary Medicine (2017) 17:213 DOI 10.1186/s12890-017-0539-7 RESEARCH ARTICLE Open Access Implication of species change of Nontuberculous Mycobacteria during or after Jong Sik Lee 1, Jong
Lee et al. BMC Pulmonary Medicine (2017) 17:213 DOI 10.1186/s12890-017-0539-7 RESEARCH ARTICLE Open Access Implication of species change of Nontuberculous Mycobacteria during or after Jong Sik Lee 1, Jong
Antibiotic Treatment of Mycobacterium abscessus Lung Disease A Retrospective Analysis of 65 Patients
 Antibiotic Treatment of Mycobacterium abscessus Lung Disease A Retrospective Analysis of 65 Patients Kyeongman Jeon 1, O Jung Kwon 1, Nam Yong Lee 2, Bum-Joon Kim 3, Yoon-Hoh Kook 3, Seung-Heon Lee 4,
Antibiotic Treatment of Mycobacterium abscessus Lung Disease A Retrospective Analysis of 65 Patients Kyeongman Jeon 1, O Jung Kwon 1, Nam Yong Lee 2, Bum-Joon Kim 3, Yoon-Hoh Kook 3, Seung-Heon Lee 4,
Clarithromycin-resistant Mycobacterium Shinjukuense Lung Disease: Case Report and Literature Review
 Showa Univ J Med Sci 28 4, 373 377, December 2016 Case Report Clarithromycin-resistant Mycobacterium Shinjukuense Lung Disease: Case Report and Literature Review Makoto HAYASHI 1, Satoshi MATSUKURA 1,
Showa Univ J Med Sci 28 4, 373 377, December 2016 Case Report Clarithromycin-resistant Mycobacterium Shinjukuense Lung Disease: Case Report and Literature Review Makoto HAYASHI 1, Satoshi MATSUKURA 1,
Nontuberculous mycobacteria isolated during the treatment of pulmonary tuberculosis
 Respiratory Medicine (2009) 103, 1936e1940 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Nontuberculous mycobacteria isolated during the treatment of pulmonary tuberculosis
Respiratory Medicine (2009) 103, 1936e1940 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Nontuberculous mycobacteria isolated during the treatment of pulmonary tuberculosis
Pathologic Findings of Surgically Resected Nontuberculous Mycobacterial Pulmonary Infection
 The Korean Journal of Pathology 2010; 44: 56-62 DOI: 10.4132/KoreanJPathol.2010.44.1.56 Pathologic Findings of Surgically Resected Nontuberculous Mycobacterial Pulmonary Infection Hye-Jong Song Jung Suk
The Korean Journal of Pathology 2010; 44: 56-62 DOI: 10.4132/KoreanJPathol.2010.44.1.56 Pathologic Findings of Surgically Resected Nontuberculous Mycobacterial Pulmonary Infection Hye-Jong Song Jung Suk
Hyun Su Kim, MD Kyung Soo Lee, MD Won-Jung Koh, MD Kyeongman Jeon, MD Eun Ju Lee, MD Hee Kang, MD Joonghyun Ahn, PhD. Purpose: Materials and Methods:
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Original Research
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Original Research
Recent Advances in Tuberculosis and Nontuberculous Mycobacteria Lung Disease
 http://dx.doi.org/10.4046/trd.2013.74.6.251 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:251-255 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2013.74.6.251 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:251-255 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Treatment of Mycobacterium avium Complex Pulmonary Disease
 REVIEW https://doi.org/10.4046/trd.2018.0060 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2019;82:15-26 Treatment of Mycobacterium avium Complex Pulmonary Disease Yong-Soo Kwon, M.D. 1, Won-Jung
REVIEW https://doi.org/10.4046/trd.2018.0060 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2019;82:15-26 Treatment of Mycobacterium avium Complex Pulmonary Disease Yong-Soo Kwon, M.D. 1, Won-Jung
Increasing Trend of Isolation of Non-Tuberculous Mycobacteria in a Tertiary University Hospital in South Korea
 http://dx.doi.org/10.4046/trd.2012.72.5.409 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2012;72:409-415 CopyrightC2012. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2012.72.5.409 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2012;72:409-415 CopyrightC2012. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Diagnosis and Treatment of Nontuberculous Mycobacterial Lung Disease
 REVIEW Respiratory Diseases http://dx.doi.org/10.3346/jkms.2016.31.5.649 J Korean Med Sci 2016; 31: 649-659 Diagnosis and Treatment of Nontuberculous Mycobacterial Lung Disease Yong-Soo Kwon 1 and Won-Jung
REVIEW Respiratory Diseases http://dx.doi.org/10.3346/jkms.2016.31.5.649 J Korean Med Sci 2016; 31: 649-659 Diagnosis and Treatment of Nontuberculous Mycobacterial Lung Disease Yong-Soo Kwon 1 and Won-Jung
Consolidations in Nodular Bronchiectatic Mycobacterium Avium Complex Lung Disease: Mycobacterium Avium Complex or Other Infection?
 Original Article DOI 10.3349/ymj.2010.51.4.546 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):546-551, 2010 Consolidations in Nodular Bronchiectatic Mycobacterium Avium Complex Lung Disease: Mycobacterium
Original Article DOI 10.3349/ymj.2010.51.4.546 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 51(4):546-551, 2010 Consolidations in Nodular Bronchiectatic Mycobacterium Avium Complex Lung Disease: Mycobacterium
Slowly Growing Nontuberculous Mycobacterial Infections
 Slowly Growing Nontuberculous Mycobacterial Infections Charles L. Daley, MD National Jewish Health University of Colorado, Denver Disclosures Advisory Board Horizon, Johnson and Johnson, Otsuka and Spero
Slowly Growing Nontuberculous Mycobacterial Infections Charles L. Daley, MD National Jewish Health University of Colorado, Denver Disclosures Advisory Board Horizon, Johnson and Johnson, Otsuka and Spero
Nontuberculous Mycobacteria
 Nontuberculous Mycobacteria When antibiotics are not enough a surgical approach John D. Mitchell, M.D. Davis Endowed Chair in Thoracic Surgery Professor and Chief Section of General Thoracic Surgery University
Nontuberculous Mycobacteria When antibiotics are not enough a surgical approach John D. Mitchell, M.D. Davis Endowed Chair in Thoracic Surgery Professor and Chief Section of General Thoracic Surgery University
Is the Initial Size of Tuberculous Lymphadenopathy associated with Lymph Node Enlargement during Treatment?
 Brief Communication https://doi.org/10.3947/ic.2017.49.2.130 Infect Chemother 2017;49(2):130-134 ISSN 2093-2340 (Print) ISSN 2092-6448 (Online) Infection & Chemotherapy Is the Initial Size of Tuberculous
Brief Communication https://doi.org/10.3947/ic.2017.49.2.130 Infect Chemother 2017;49(2):130-134 ISSN 2093-2340 (Print) ISSN 2092-6448 (Online) Infection & Chemotherapy Is the Initial Size of Tuberculous
Nontuberculous Mycobacterial Lung Disease
 Non-TB Mycobacterial Disease Jeffrey P. Kanne, MD Nontuberculous Mycobacterial Lung Disease Jeffrey P. Kanne, M.D. Consultant Disclosures Perceptive Informatics Royalties (book author) Amirsys, Inc. Wolters
Non-TB Mycobacterial Disease Jeffrey P. Kanne, MD Nontuberculous Mycobacterial Lung Disease Jeffrey P. Kanne, M.D. Consultant Disclosures Perceptive Informatics Royalties (book author) Amirsys, Inc. Wolters
Shannon Kasperbauer, M.D. National Jewish Health University of Colorado Health Sciences Center. Property of Presenter. Not for Reproduction
 Shannon Kasperbauer, M.D. National Jewish Health University of Colorado Health Sciences Center Consultant: Johnson and Johnson Speaker/consultant: Insmed Examine characteristics of the RGM Define the main
Shannon Kasperbauer, M.D. National Jewish Health University of Colorado Health Sciences Center Consultant: Johnson and Johnson Speaker/consultant: Insmed Examine characteristics of the RGM Define the main
Diagnosis and Treatment of Nontuberculous Mycobacterial Pulmonary Diseases
 Diagnosis and Treatment of Nontuberculous Mycobacterial Pulmonary Diseases Jae Joon Yim, M.D. Sung Koo Han, M.D. Division of Pulmonary and Critical Care Medicine Department of Internal Medicine Seoul National
Diagnosis and Treatment of Nontuberculous Mycobacterial Pulmonary Diseases Jae Joon Yim, M.D. Sung Koo Han, M.D. Division of Pulmonary and Critical Care Medicine Department of Internal Medicine Seoul National
Nontuberculous Mycobacteria (NTM) in Patients with Cystic Fibrosis
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/cystic-fibrosis-in-focus/nontuberculous-mycobacteria-ntm-in-patientswith-cystic-fibrosis/8337/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/cystic-fibrosis-in-focus/nontuberculous-mycobacteria-ntm-in-patientswith-cystic-fibrosis/8337/
Title: Cefoxitin Continuous Infusion for Lung Infection Caused by M. abscessus group
 AAC Accepts, published online ahead of print on 14 April 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.02763-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 Title: Cefoxitin
AAC Accepts, published online ahead of print on 14 April 2014 Antimicrob. Agents Chemother. doi:10.1128/aac.02763-14 Copyright 2014, American Society for Microbiology. All Rights Reserved. 1 Title: Cefoxitin
How Do I Manage Nontuberculous Mycobacterial (NTM) Lung Disease Patients?
 How Do I Manage Nontuberculous Mycobacterial (NTM) Lung Disease Patients? David E. Griffith, M.D. Professor of Medicine University of Texas Health Science Center, Tyler Potential COI Statement I was a
How Do I Manage Nontuberculous Mycobacterial (NTM) Lung Disease Patients? David E. Griffith, M.D. Professor of Medicine University of Texas Health Science Center, Tyler Potential COI Statement I was a
Diagnostic Evaluation of NTM and Bronchiectasis
 Division of Pulmonary, Critical Care and Sleep Medicine Diagnostic Evaluation of NTM and Bronchiectasis Ashwin Basavaraj, MD, FCCP NTM patient education program November 9, 2016 Involves a combination
Division of Pulmonary, Critical Care and Sleep Medicine Diagnostic Evaluation of NTM and Bronchiectasis Ashwin Basavaraj, MD, FCCP NTM patient education program November 9, 2016 Involves a combination
A Vietnamese woman with a 2-week history of cough
 Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Delphine Natali 1, Hai Tran Pham 1, Hung Nguyen The 2 delphinenatali@gmail.com Case report A Vietnamese woman with a 2-week history of cough A 52-year-old nonsmoker Vietnamese woman without any past medical
Inhaled Amikacin for Treatment of Refractory Pulmonary Nontuberculous Mycobacterial Disease
 Inhaled Amikacin for Treatment of Refractory Pulmonary Nontuberculous Mycobacterial Disease Kenneth N. Olivier 1, Pamela A. Shaw 2, Tanya S. Glaser 1, Darshana Bhattacharyya 1, Michelle Fleshner 1, Carmen
Inhaled Amikacin for Treatment of Refractory Pulmonary Nontuberculous Mycobacterial Disease Kenneth N. Olivier 1, Pamela A. Shaw 2, Tanya S. Glaser 1, Darshana Bhattacharyya 1, Michelle Fleshner 1, Carmen
Mycobacterium intracellulare Pleurisy Identified on Liquid Cultures of the Pleural Fluid and Pleural Biopsy
 http://dx.doi.org/10.4046/trd.2013.74.3.124 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:124-128 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2013.74.3.124 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2013;74:124-128 CopyrightC2013. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Prevalence of Gastroesophageal Reflux Disease in Patients With Nontuberculous Mycobacterial Lung Disease*
 Original Research MYCOBACTERIAL DISEASE Prevalence of Gastroesophageal Reflux Disease in Patients With Nontuberculous Mycobacterial Lung Disease* Won-Jung Koh, MD; Jun Haeng Lee, MD; Yong Soo Kwon, MD;
Original Research MYCOBACTERIAL DISEASE Prevalence of Gastroesophageal Reflux Disease in Patients With Nontuberculous Mycobacterial Lung Disease* Won-Jung Koh, MD; Jun Haeng Lee, MD; Yong Soo Kwon, MD;
2018 Vindico Medical Education. Non-tuberculous Mycobacteria: Circumventing Difficulties in Diagnosis and Treatment
 Activity presentations are considered intellectual property. These slides may not be published or posted online without permission from Vindico Medical Education (cme@vindicocme.com). Please be respectful
Activity presentations are considered intellectual property. These slides may not be published or posted online without permission from Vindico Medical Education (cme@vindicocme.com). Please be respectful
Serial CT Findings of Nodular Bronchiectatic Mycobacterium avium Complex Pulmonary Disease With Antibiotic Treatment
 Cardiopulmonary Imaging Original Research Lee et al. Serial CT of MAC Pulmonary Disease Cardiopulmonary Imaging Original Research Geewon Lee 1 Hyun Su Kim 1 Kyung Soo Lee 1 Won-Jung Koh 2 Kyeongman Jeon
Cardiopulmonary Imaging Original Research Lee et al. Serial CT of MAC Pulmonary Disease Cardiopulmonary Imaging Original Research Geewon Lee 1 Hyun Su Kim 1 Kyung Soo Lee 1 Won-Jung Koh 2 Kyeongman Jeon
CASE REPORT. 1. Assistant Professor. Department of Paediatrics, Vinayaka Missions Medical College, Karaikal
 A CASE OF KARTAGENER SYNDROME Pagadpally Srinivas 1. Assistant Professor. Department of Paediatrics, Vinayaka Missions Medical College, Karaikal CORRESPONDING AUTHOR: Pagadpally Srinivas, 72, Vellai Pillaiyar
A CASE OF KARTAGENER SYNDROME Pagadpally Srinivas 1. Assistant Professor. Department of Paediatrics, Vinayaka Missions Medical College, Karaikal CORRESPONDING AUTHOR: Pagadpally Srinivas, 72, Vellai Pillaiyar
NTM Lecture Series. Challenging Cases: Part 1. Property of Presenter
 NTM Lecture Series Challenging Cases: Part 1 Dr. Wendi Kay Drummond DO, MPH Assistant Professor of Medicine Division of Mycobacterial and Infectious Diseases Department of Medicine September 27, 2018 Disclosures
NTM Lecture Series Challenging Cases: Part 1 Dr. Wendi Kay Drummond DO, MPH Assistant Professor of Medicine Division of Mycobacterial and Infectious Diseases Department of Medicine September 27, 2018 Disclosures
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Treatment outcomes and survival based on drug resistance patterns in multidrug-resistant
 Treatment outcomes and survival based on drug resistance patterns in multidrug-resistant tuberculosis Doh Hyung Kim, Hee Jin Kim, Seung-Kyu Park, Suck-Jun Kong, Young Sam Kim, Tae-Hyung Kim, Eun Kyung
Treatment outcomes and survival based on drug resistance patterns in multidrug-resistant tuberculosis Doh Hyung Kim, Hee Jin Kim, Seung-Kyu Park, Suck-Jun Kong, Young Sam Kim, Tae-Hyung Kim, Eun Kyung
Rapid Diagnosis of Tuberculosis and Multidrug Resistance Using a MGIT 960 System
 Original Article Clinical Microbiology Ann Lab Med 2012;32:264-269 ISSN 2234-3806 eissn 2234-3814 Rapid Diagnosis of Tuberculosis and Multidrug Resistance Using a MGIT 960 System Won-Jung Koh, M.D. 1,
Original Article Clinical Microbiology Ann Lab Med 2012;32:264-269 ISSN 2234-3806 eissn 2234-3814 Rapid Diagnosis of Tuberculosis and Multidrug Resistance Using a MGIT 960 System Won-Jung Koh, M.D. 1,
Bronchiectasis: An Imaging Approach
 Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Bronchiectasis: An Imaging Approach Travis S Henry, MD Associate Professor of Clinical Radiology Cardiac and Pulmonary Imaging Section University of California, San Francisco Large Middle Small 1 Bronchiectasis
Original Article Tree-in-bud pattern of chest CT images for diagnosis of Mycobacterium abscesses
 Int J Clin Exp Med 2015;8(10):18705-18712 www.ijcem.com /ISSN:1940-5901/IJCEM0013538 Original Article Tree-in-bud pattern of chest CT images for diagnosis of Mycobacterium Haiqing Chu 1, Bing Li 1, Lan
Int J Clin Exp Med 2015;8(10):18705-18712 www.ijcem.com /ISSN:1940-5901/IJCEM0013538 Original Article Tree-in-bud pattern of chest CT images for diagnosis of Mycobacterium Haiqing Chu 1, Bing Li 1, Lan
Prognostic factors for surgical resection in patients with multidrug-resistant tuberculosis
 Eur Respir J 2006; 28: 576 580 DOI: 10.1183/09031936.06.00023006 CopyrightßERS Journals Ltd 2006 Prognostic factors for surgical resection in patients with multidrug-resistant tuberculosis H.J. Kim*, C.H.
Eur Respir J 2006; 28: 576 580 DOI: 10.1183/09031936.06.00023006 CopyrightßERS Journals Ltd 2006 Prognostic factors for surgical resection in patients with multidrug-resistant tuberculosis H.J. Kim*, C.H.
Nontuberculous Mycobacteria (NTM)
 Nontuberculous Mycobacteria (NTM) Bacteria, like plants and animals, have been classified into similar groups. The groups are called "families." One such family of bacteria is known as the Mycobacteriaceae.
Nontuberculous Mycobacteria (NTM) Bacteria, like plants and animals, have been classified into similar groups. The groups are called "families." One such family of bacteria is known as the Mycobacteriaceae.
Non-CF bronchiectasis: Alexander Duarte, MD Pulmonary, Critical Care & Sleep Medicine University of Texas Medical Branch Galveston, TX
 Non-CF bronchiectasis: Alexander Duarte, MD Pulmonary, Critical Care & Sleep Medicine University of Texas Medical Branch Galveston, TX Pioneer of Respiratory Medicine 2016 marked 200th anniversary of his
Non-CF bronchiectasis: Alexander Duarte, MD Pulmonary, Critical Care & Sleep Medicine University of Texas Medical Branch Galveston, TX Pioneer of Respiratory Medicine 2016 marked 200th anniversary of his
CHAPTER 3: DEFINITION OF TERMS
 CHAPTER 3: DEFINITION OF TERMS NOTE: TB bacteria is used in place of Mycobacterium tuberculosis and Mycobacterium tuberculosis complex in most of the definitions presented here. 3.1 Acid-fast bacteria
CHAPTER 3: DEFINITION OF TERMS NOTE: TB bacteria is used in place of Mycobacterium tuberculosis and Mycobacterium tuberculosis complex in most of the definitions presented here. 3.1 Acid-fast bacteria
TB Intensive San Antonio, Texas August 7-10, 2012
 TB Intensive San Antonio, Texas August 7-10, 2012 Nontuberculosis Mycobacterial Lung Disease David Griffith, MD August 8, 2012 David Griffith, MD has the following disclosures to make: No conflict of interests
TB Intensive San Antonio, Texas August 7-10, 2012 Nontuberculosis Mycobacterial Lung Disease David Griffith, MD August 8, 2012 David Griffith, MD has the following disclosures to make: No conflict of interests
Bronchiectasis in Adults - Suspected
 Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Hypothesis on the Evolution of Cavitary Lesions in Nontuberculous Mycobacterial Pulmonary Infection: Thin-Section CT and Histopathologic Correlation
 CT of Nontuberculous Mycobacterial Pulmonary Infection Tae Sung Kim 1 Won-Jung Koh 2 Joungho Han 3 Myung Jin Chung 1 Ju Hyun Lee 1 Kyung Soo Lee 1 O Jung Kwon 2 Kim TS, Koh W-J, Han J, et al. Received
CT of Nontuberculous Mycobacterial Pulmonary Infection Tae Sung Kim 1 Won-Jung Koh 2 Joungho Han 3 Myung Jin Chung 1 Ju Hyun Lee 1 Kyung Soo Lee 1 O Jung Kwon 2 Kim TS, Koh W-J, Han J, et al. Received
Communicable Disease Control Manual Chapter 4: Tuberculosis
 Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Definitions Page 1 2.0 DEFINITIONS Many of the definitions that follow are taken from
Provincial TB Services 655 West 12th Avenue Vancouver, BC V5Z 4R4 www.bccdc.ca Communicable Disease Control Manual Definitions Page 1 2.0 DEFINITIONS Many of the definitions that follow are taken from
Mycobacterium Avium Complex Infection Presenting as an Endobronchial Mass in a Patient with Acquired Immune Deficiency Syndrome
 The Korean Journal of Internal Medicine : 22:215-219, 2007 Mycobacterium Avium Complex Infection Presenting as an Endobronchial Mass in a Patient with Acquired Immune Deficiency Syndrome Ho Cheol Kim,
The Korean Journal of Internal Medicine : 22:215-219, 2007 Mycobacterium Avium Complex Infection Presenting as an Endobronchial Mass in a Patient with Acquired Immune Deficiency Syndrome Ho Cheol Kim,
Bronchiectasis. Examples include: Viral infections (measles, adenovirus, influenza)
 Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
Bronchiectasis What is Bronchiectasis? Bronchiectasis (pronounced bron-kee-ek'-tas-is) is a condition of the airways in the lungs. These airways (bronchial tubes) are tubelike structures that branch from
Nontuberculous Mycobacteria
 Nontuberculous Mycobacteria Epidemiology and Clinical Management Kevin L. Winthrop, MD, MPH Associate Professor, Divisions of Infectious Diseases, Public Health and Preventive Medicine Oregon Health &
Nontuberculous Mycobacteria Epidemiology and Clinical Management Kevin L. Winthrop, MD, MPH Associate Professor, Divisions of Infectious Diseases, Public Health and Preventive Medicine Oregon Health &
Validity and Reliability of CAT and Dyspnea-12 in Bronchiectasis and Tuberculous Destroyed Lung
 http://dx.doi.org/10.4046/trd.2012.72.6.467 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2012;72:467-474 CopyrightC2012. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
http://dx.doi.org/10.4046/trd.2012.72.6.467 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2012;72:467-474 CopyrightC2012. The Korean Academy of Tuberculosis and Respiratory Diseases. All rights
Primary Ciliary Dyskinesia (PCD) Angelo Barbato Department of Pediatrics Padova University/General Hospital Padova-Italy
 Primary Ciliary Dyskinesia (PCD) Angelo Barbato Department of Pediatrics Padova University/General Hospital Padova-Italy barbato@pediatria.unipd.it PCD IS A RARE DISEASE THAT BEGINS IN CHILDHOOD AND CONTINUES
Primary Ciliary Dyskinesia (PCD) Angelo Barbato Department of Pediatrics Padova University/General Hospital Padova-Italy barbato@pediatria.unipd.it PCD IS A RARE DISEASE THAT BEGINS IN CHILDHOOD AND CONTINUES
Postgraduate Course ERS Glasgow 2004 Surgical approach to multiresistant cavitary mycobacteriosis
 REVIEW Postgraduate Course ERS Glasgow 2004 Surgical approach to multiresistant cavitary mycobacteriosis Educational aims To explain the present importance of surgery in TB management. To describe the
REVIEW Postgraduate Course ERS Glasgow 2004 Surgical approach to multiresistant cavitary mycobacteriosis Educational aims To explain the present importance of surgery in TB management. To describe the
Natural history of Mycobacterium avium complex lung disease in untreated patients with stable course
 ORIGINAL ARTICLE RESPIRATORY INFECTIONS Natural history of Mycobacterium avium complex lung disease in untreated patients with stable course Ji An Hwang 1,3, Sunyoung Kim 2,3, Kyung-Wook Jo 1 and Tae Sun
ORIGINAL ARTICLE RESPIRATORY INFECTIONS Natural history of Mycobacterium avium complex lung disease in untreated patients with stable course Ji An Hwang 1,3, Sunyoung Kim 2,3, Kyung-Wook Jo 1 and Tae Sun
Respiratory Review of 2014: Tuberculosis and Nontuberculous Mycobacterial Pulmonary Disease
 REVIEW http://dx.doi.org/10.4046/trd.2014.77.4.161 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:161-166 Respiratory Review of 2014: Tuberculosis and Nontuberculous Mycobacterial Pulmonary
REVIEW http://dx.doi.org/10.4046/trd.2014.77.4.161 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:161-166 Respiratory Review of 2014: Tuberculosis and Nontuberculous Mycobacterial Pulmonary
Characteristics associated with progression in patients with of nontuberculous mycobacterial lung disease : a prospective cohort study
 Kim et al. BMC Pulmonary Medicine (2017) 17:5 DOI 10.1186/s12890-016-0349-3 RESEARCH ARTICLE Open Access Characteristics associated with progression in patients with of nontuberculous mycobacterial lung
Kim et al. BMC Pulmonary Medicine (2017) 17:5 DOI 10.1186/s12890-016-0349-3 RESEARCH ARTICLE Open Access Characteristics associated with progression in patients with of nontuberculous mycobacterial lung
Carbapenem Susceptibility Patterns for Clinical Isolates of Mycobacterium abscessus by
 JCM Accepts, published online ahead of print on 16 December 2009 J. Clin. Microbiol. doi:10.1128/jcm.01930-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All
JCM Accepts, published online ahead of print on 16 December 2009 J. Clin. Microbiol. doi:10.1128/jcm.01930-09 Copyright 2009, American Society for Microbiology and/or the Listed Authors/Institutions. All
Cavitary Pulmonary Nontuberculous Mycobacterium Infection in an Adult Patient with Cyanotic Congenital Heart Disease
 PEDIATRIC CARDIOLOGY and CARDIAC SURGERY VOL. 25 NO. 1 (56 60) 1 1 1 2 2 3 4 1 2 3 4 Cavitary Pulmonary Nontuberculous Mycobacterium Infection in an Adult Patient with Cyanotic Congenital Heart Disease
PEDIATRIC CARDIOLOGY and CARDIAC SURGERY VOL. 25 NO. 1 (56 60) 1 1 1 2 2 3 4 1 2 3 4 Cavitary Pulmonary Nontuberculous Mycobacterium Infection in an Adult Patient with Cyanotic Congenital Heart Disease
High prevalence of Primary Ciliary Dyskinesia in a British Asian population
 High prevalence of Primary Ciliary Dyskinesia in a British Asian population Chris O Callaghan 1, Phil Chetcuti 2, Eduardo Moya 3 1. University of Leicester, Leicester, United Kingdom 2. Leeds General Infirmary,
High prevalence of Primary Ciliary Dyskinesia in a British Asian population Chris O Callaghan 1, Phil Chetcuti 2, Eduardo Moya 3 1. University of Leicester, Leicester, United Kingdom 2. Leeds General Infirmary,
RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION. Tilman Koelsch, MD National Jewish Health - Department of Radiology
 Pr N op ot e fo rty rr o f ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures None Goals Identify
Pr N op ot e fo rty rr o f ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures None Goals Identify
Kartagener s Syndrome STEFANIE CORRADINI - PMU SALZBURG (AUSTRIA) GILLIAN LIEBERMAN, MD
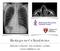 Kartagener s Syndrome STEFANIE CORRADINI - PMU SALZBURG (AUSTRIA) GILLIAN LIEBERMAN, MD let s meet our patient.. 75 y/o woman presents to the ED complaining of chest pain over the anterior right chest
Kartagener s Syndrome STEFANIE CORRADINI - PMU SALZBURG (AUSTRIA) GILLIAN LIEBERMAN, MD let s meet our patient.. 75 y/o woman presents to the ED complaining of chest pain over the anterior right chest
Bronchiectasis. Introduction. Key points
 15 Bronchiectasis Introduction i Key points Patients with bronchiectasis typically have chronic airway infection, punctuated by acute exacerbations and accompanied by progressive airflow obstruction. Bronchiectasis
15 Bronchiectasis Introduction i Key points Patients with bronchiectasis typically have chronic airway infection, punctuated by acute exacerbations and accompanied by progressive airflow obstruction. Bronchiectasis
Down-Regulation of Serum High- Mobility Group Box 1 Protein in Patients with Pulmonary Tuberculosis and Nontuberculous Mycobacterial Lung Disease
 ORIGINAL ARTICLE https://doi.org/10.4046/trd.2017.80.2.153 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2017;80:153-158 Down-Regulation of Serum High- Mobility Group Box 1 Protein in Patients
ORIGINAL ARTICLE https://doi.org/10.4046/trd.2017.80.2.153 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2017;80:153-158 Down-Regulation of Serum High- Mobility Group Box 1 Protein in Patients
Clinical Commissioning Policy: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages)
 Clinical Commissioning Policy: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages) Reference: NHS England: 16029/P NHS England INFORMATION READER BOX Directorate Medical Operations and
Clinical Commissioning Policy: Dornase alfa inhaled therapy for primary ciliary dyskinesia (all ages) Reference: NHS England: 16029/P NHS England INFORMATION READER BOX Directorate Medical Operations and
RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION. Tilman Koelsch, MD National Jewish Health - Department of Radiology
 Pr N op ot er fo ty r R of ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures No relevant financial
Pr N op ot er fo ty r R of ep Pr ro es du en ct te io r n RADIOLOGIC EVALUATION OF PULMONARY NTM INFECTION Tilman Koelsch, MD National Jewish Health - Department of Radiology Disclosures No relevant financial
Acute necrotizing pneumonia combined with parapneumonic effusion caused by Mycobacterium lentiflavum: a case report
 Lee et al. BMC Infectious Diseases (2015) 15:354 DOI 10.1186/s12879-015-1100-z CASE REPORT Open Access Acute necrotizing pneumonia combined with parapneumonic effusion caused by Mycobacterium lentiflavum:
Lee et al. BMC Infectious Diseases (2015) 15:354 DOI 10.1186/s12879-015-1100-z CASE REPORT Open Access Acute necrotizing pneumonia combined with parapneumonic effusion caused by Mycobacterium lentiflavum:
Primary Ciliary Dyskinesia (PCD) Angelo Barbato Department of Pediatrics Padova University/General Hospital Padova-Italy
 Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Thank you for viewing this presentation. We would like to remind you that this material is the property of the author. It is provided to you by the ERS for your personal use only, as submitted by the author.
Mycobacterium fortuitum,
 2009 177 Mycobacterium fortuitum 1 1) 2) 3) 1) 1) 4) 4) 5) 2) 1) 1) 2) 3) 4) 5) 21 3 16 21 7 1 Mycobacterium fortuitum 1 39 BHI 2 Ziehl Neelsen M. fortuitum MIC CPFX 0.2 mg/ml, MINO 0.78 mg/ml, CAM 100
2009 177 Mycobacterium fortuitum 1 1) 2) 3) 1) 1) 4) 4) 5) 2) 1) 1) 2) 3) 4) 5) 21 3 16 21 7 1 Mycobacterium fortuitum 1 39 BHI 2 Ziehl Neelsen M. fortuitum MIC CPFX 0.2 mg/ml, MINO 0.78 mg/ml, CAM 100
Nontuberculous Mycobacterial Pulmonary Diseases in Immunocompetent Patients
 Nontuberculous Mycobacterial Pulmonary Diseases in Immunocompetent Patients Won-Jung Koh, MD 1 O Jung Kwon, MD 1 Kyung Soo Lee, MD 2 Nontuberculous mycobacterial (NTM) infections are an increasingly recognized
Nontuberculous Mycobacterial Pulmonary Diseases in Immunocompetent Patients Won-Jung Koh, MD 1 O Jung Kwon, MD 1 Kyung Soo Lee, MD 2 Nontuberculous mycobacterial (NTM) infections are an increasingly recognized
TB Intensive Houston, Texas October 15-17, 2013
 TB Intensive Houston, Texas October 15-17, 2013 Nontuberculous Mycobacterial Lung Disease David Griffith, MD October 15, 2013 David Griffith, MD has the following disclosures to make: No conflict of interests
TB Intensive Houston, Texas October 15-17, 2013 Nontuberculous Mycobacterial Lung Disease David Griffith, MD October 15, 2013 David Griffith, MD has the following disclosures to make: No conflict of interests
Ryo Takahashi 1,2,3, Taiki Fujiwara 1,2, Hisami Yamakawa 1,2. Introduction
 Case Report Completion pneumonectomy after fenestration for empyema due to nontuberculous mycobacteriosis associated with destroyed lung as a result of cancer surgery Ryo Takahashi 1,2,3, Taiki Fujiwara
Case Report Completion pneumonectomy after fenestration for empyema due to nontuberculous mycobacteriosis associated with destroyed lung as a result of cancer surgery Ryo Takahashi 1,2,3, Taiki Fujiwara
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D.
 Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
Eun-Young Kang, M.D., Jae Wook Lee, M.D., Ji Yung Choo, M.D., Hwan Seok Yong, M.D., Ki Yeol Lee, M.D., Yu-Whan Oh, M.D. Department of Radiology, Korea University Guro Hospital, College of Medicine, Korea
C.S. HAWORTH 1, A. WANNER 2, J. FROEHLICH 3, T. O'NEAL 3, A. DAVIS 4, I. GONDA 3, A. O'DONNELL 5
 Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
Inhaled Liposomal Ciprofloxacin in Patients With Non-Cystic Fibrosis Bronchiectasis and Chronic Pseudomonas aeruginosa: Results From Two Parallel Phase III Trials (ORBIT-3 and -4) C.S. HAWORTH 1, A. WANNER
Infection With the Mycobacterium avium Complex in Patients Without Predisposing Conditons A Case Report and Literature Review
 BJID 2005; 9 (April) 173 Infection With the Mycobacterium avium Complex in Patients Without Predisposing Conditons A Case Report and Literature Review Andrea Barral Martins 1, Eliana Dias Matos 2,3 and
BJID 2005; 9 (April) 173 Infection With the Mycobacterium avium Complex in Patients Without Predisposing Conditons A Case Report and Literature Review Andrea Barral Martins 1, Eliana Dias Matos 2,3 and
Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino Jul-Aug; 21(4):423-7
 AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
AMINOGLYCOSIDES Dose-dependent effects of tobramycin in an animal model of Pseudomonas sinusitis Am J Rhino. 2007 Jul-Aug; 21(4):423-7 http://www.ncbi.nlm.nih.gov/pubmed/17882910 Evaluation of the in-vivo
Delayed Perforation Occurring after Endoscopic Submucosal Dissection for Early Gastric Cancer
 CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
CASE REPORT Clin Endosc 2015;48:251-255 Print ISSN 2234-2400 / On-line ISSN 2234-2443 http://dx.doi.org/10.5946/ce.2015.48.3.251 Open Access Delayed Perforation Occurring after Endoscopic Submucosal Dissection
Peritoneal dialysis associated peritonitis secondary to Mycobacterium fortuitum
 Case Reports Peritoneal dialysis associated peritonitis secondary to Mycobacterium fortuitum Paula McKenzie MD, David Sotello MD, Kunal Parekh MD, Kristen Fuhrmann PharmD, Richard Winn MD Abstract We report
Case Reports Peritoneal dialysis associated peritonitis secondary to Mycobacterium fortuitum Paula McKenzie MD, David Sotello MD, Kunal Parekh MD, Kristen Fuhrmann PharmD, Richard Winn MD Abstract We report
Comparison of CT Findings
 Newly Detected Pulmonary Nontuberculous Mycobacterial Infection and Peripheral Lung Cancers in Patients During Follow-Up of Idiopathic Interstitial Pneumonia Comparison of CT Findings Sang Young Oh, MD,
Newly Detected Pulmonary Nontuberculous Mycobacterial Infection and Peripheral Lung Cancers in Patients During Follow-Up of Idiopathic Interstitial Pneumonia Comparison of CT Findings Sang Young Oh, MD,
NON-CF BRONCHIECTASIS IN ADULTS
 Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
후인두농양의치료에대한고찰 정지성 이동욱 연제엽. Adequate Management of Retropharyngeal Abscess. Ji-Seong Jeong, MD, Dong Wook Lee, MD and Je-Yeob Yeon, MD
 KISEP Head and Neck Korean J Otolaryngol 004;4:899-90 후인두농양의치료에대한고찰 충북대학교의과대학이비인후과학교실 정지성 이동욱 연제엽 Adequate Management of Retropharyngeal Abscess Ji-Seong Jeong, MD, Dong Wook Lee, MD and Je-Yeob Yeon,
KISEP Head and Neck Korean J Otolaryngol 004;4:899-90 후인두농양의치료에대한고찰 충북대학교의과대학이비인후과학교실 정지성 이동욱 연제엽 Adequate Management of Retropharyngeal Abscess Ji-Seong Jeong, MD, Dong Wook Lee, MD and Je-Yeob Yeon,
Left middle lobectomy for bronchiectasis in a patient with Kartagener syndrome: a case report
 Lin et al. Journal of Cardiothoracic Surgery (2016) 11:37 DOI 10.1186/s13019-016-0426-y CASE REPORT Open Access Left middle lobectomy for bronchiectasis in a patient with Kartagener syndrome: a case report
Lin et al. Journal of Cardiothoracic Surgery (2016) 11:37 DOI 10.1186/s13019-016-0426-y CASE REPORT Open Access Left middle lobectomy for bronchiectasis in a patient with Kartagener syndrome: a case report
Six-month Therapy with Aerosolized Interferon-γfor Refractory Multidrug-Resistant Pulmonary Tuberculosis
 J Korean Med Sci 2004; 19: 167-71 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Six-month Therapy with Aerosolized Interferon-γfor Refractory Multidrug-Resistant Pulmonary Tuberculosis
J Korean Med Sci 2004; 19: 167-71 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Six-month Therapy with Aerosolized Interferon-γfor Refractory Multidrug-Resistant Pulmonary Tuberculosis
Kartagener s Syndrome: Presenting in Fourth Decade
 August, 2017 2017; Vol1; Issue7 http://iamresearcher.online Kartagener s Syndrome: Presenting in Fourth Decade Sejal Sejwani, Pramod Jha, Krunal Tamakuwala, Garvit Garg, Smit Shah SBKS & MIRC Vadodara,
August, 2017 2017; Vol1; Issue7 http://iamresearcher.online Kartagener s Syndrome: Presenting in Fourth Decade Sejal Sejwani, Pramod Jha, Krunal Tamakuwala, Garvit Garg, Smit Shah SBKS & MIRC Vadodara,
Diagnosis and Treatment of Latent Tuberculosis Infection in Healthcare Workers
 REVIEW http://dx.doi.org/10.4046/trd.2016.79.3.127 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:127-133 Diagnosis and Treatment of Latent Tuberculosis Infection in Healthcare Workers
REVIEW http://dx.doi.org/10.4046/trd.2016.79.3.127 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2016;79:127-133 Diagnosis and Treatment of Latent Tuberculosis Infection in Healthcare Workers
Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010
 Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Evaluation of Patients with Diffuse Bronchiectasis
 Evaluation of Patients with Diffuse Bronchiectasis Dr. Patricia Eshaghian, MD Assistant Clinical Professor of Medicine Director, UCLA Adult Cystic Fibrosis Affiliate Program UCLA Division of Pulmonary
Evaluation of Patients with Diffuse Bronchiectasis Dr. Patricia Eshaghian, MD Assistant Clinical Professor of Medicine Director, UCLA Adult Cystic Fibrosis Affiliate Program UCLA Division of Pulmonary
NTM AND BRONCHIECTASIS (BXSIS): THE CHICKEN AND THE EGG
 REMINGTON WINTER COURSE IN ID VAIL, CO FEBRUARY, 2010 NONTUBERCULOSIS MYCOBACTERIA AND BRONCHIECTASIS: Revised 1/28/10 10:31 AM- CQ MICHAEL D. ISEMAN, MD OR In some cases NTMs invade pre-existing BXSIS
REMINGTON WINTER COURSE IN ID VAIL, CO FEBRUARY, 2010 NONTUBERCULOSIS MYCOBACTERIA AND BRONCHIECTASIS: Revised 1/28/10 10:31 AM- CQ MICHAEL D. ISEMAN, MD OR In some cases NTMs invade pre-existing BXSIS
Management of Drug-resistant Tuberculosis (DR-TB)
 Management of Drug-resistant Tuberculosis (DR-TB) Nitipatana Chierakul Division of Respiratory Disease & Tuberculosis Department of Medicine Faculty of Medicine Siriraj Hospital October 14 th, 2008 Tropical
Management of Drug-resistant Tuberculosis (DR-TB) Nitipatana Chierakul Division of Respiratory Disease & Tuberculosis Department of Medicine Faculty of Medicine Siriraj Hospital October 14 th, 2008 Tropical
Chronic Mycobacterium abscessus infection and lung function decline in cystic fibrosis
 Journal of Cystic Fibrosis 9 (2010) 117 123 www.elsevier.com/locate/jcf Original article Chronic Mycobacterium abscessus infection and lung function decline in cystic fibrosis Charles R. Esther Jr., Denise
Journal of Cystic Fibrosis 9 (2010) 117 123 www.elsevier.com/locate/jcf Original article Chronic Mycobacterium abscessus infection and lung function decline in cystic fibrosis Charles R. Esther Jr., Denise
Mycobacterial diseases developed during anti-tumour necrosis factor-a therapy
 ORIGINAL ARTICLE PULMONARY INFECTIONS Mycobacterial diseases developed during anti-tumour necrosis factor-a therapy Jung-Wan Yoo 1, Kyung-Wook Jo 1, Bo-Hyung Kang 1, Mi Young Kim 2, Bin Yoo 3, Chang-Keun
ORIGINAL ARTICLE PULMONARY INFECTIONS Mycobacterial diseases developed during anti-tumour necrosis factor-a therapy Jung-Wan Yoo 1, Kyung-Wook Jo 1, Bo-Hyung Kang 1, Mi Young Kim 2, Bin Yoo 3, Chang-Keun
A Case of Delayed Diagnosis of Pulmonary Paragonimiasis due to Improvement after Anti-tuberculosis Therapy
 CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.4.178 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:178-183 A Case of Delayed Diagnosis of Pulmonary Paragonimiasis due to Improvement
CASE REPORT http://dx.doi.org/10.4046/trd.2014.77.4.178 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;77:178-183 A Case of Delayed Diagnosis of Pulmonary Paragonimiasis due to Improvement
Novel Therapies for NTM
 NTM Lecture Series for Providers Novel Therapies for NTM Kenneth N Olivier, MD, MPH Laboratory of Chronic Airway Infection Chief, Pulmonary Branch/DIR October 20, 2017 Disclosures Past: Cooperative Research
NTM Lecture Series for Providers Novel Therapies for NTM Kenneth N Olivier, MD, MPH Laboratory of Chronic Airway Infection Chief, Pulmonary Branch/DIR October 20, 2017 Disclosures Past: Cooperative Research
High dose amoxicillin for sinusitis
 High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
High dose amoxicillin for sinusitis Amoxil ( amoxicillin ) is a commonly used penicillin antibiotic. It is produced in tablets (500 mg 875 mg), capsules, chewable tablets and oral suspensions. 6-3-2018
NON-TUBERCULOUS MYCOBACTERIAL (NTM) INFECTIONS ISOLATED FROM BIRMINGHAM HEARTLANDS HOSPITAL: A CASE NOTES REVIEW.
 NON-TUBERCULOUS MYCOBACTERIAL (NTM) INFECTIONS ISOLATED FROM BIRMINGHAM HEARTLANDS HOSPITAL: A CASE NOTES REVIEW. K. Clay 1, K. Bhatt 1, D. Burns 1, J. Evans 2, S. Gardiner 2, EG. Smith 2, P. Hawkey 2,
NON-TUBERCULOUS MYCOBACTERIAL (NTM) INFECTIONS ISOLATED FROM BIRMINGHAM HEARTLANDS HOSPITAL: A CASE NOTES REVIEW. K. Clay 1, K. Bhatt 1, D. Burns 1, J. Evans 2, S. Gardiner 2, EG. Smith 2, P. Hawkey 2,
Jihoon Cha, MD 1 Ho Yun Lee, MD 1 Kyung Soo Lee, MD 1 Won-Jung Koh, MD 2 O Jung Kwon, MD 2 Chin A Yi, MD 1 Tae Sung Kim, MD 1 Myung Jin Chung, MD 1
 Radiological Findings of Extensively Drug-Resistant Pulmonary Tuberculosis in Non-AIDS Adults: Comparisons with Findings of Multidrug-Resistant and Drug-Sensitive Tuberculosis Jihoon Cha, MD 1 Ho Yun Lee,
Radiological Findings of Extensively Drug-Resistant Pulmonary Tuberculosis in Non-AIDS Adults: Comparisons with Findings of Multidrug-Resistant and Drug-Sensitive Tuberculosis Jihoon Cha, MD 1 Ho Yun Lee,
Surgery for MDR/XDR Tuberculosis
 Surgery for MDR/XDR Tuberculosis John D. Mitchell, M.D. Davis Endowed Chair in Thoracic Surgery Professor and Chief, General Thoracic Surgery Department of Surgery University of Colorado School of Medicine
Surgery for MDR/XDR Tuberculosis John D. Mitchell, M.D. Davis Endowed Chair in Thoracic Surgery Professor and Chief, General Thoracic Surgery Department of Surgery University of Colorado School of Medicine
PULMONARY EMERGENCIES
 EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
EMERGENCIES I. Pneumonia A. Bacterial Pneumonia (most common cause of a focal infiltrate) 1. Epidemiology a. Accounts for up to 10% of hospital admissions in the U.S. b. Most pneumonias are the result
Serodiagnosis of Mycobacterium avium complex pulmonary disease in the USA
 ORIGINAL ARTICLE PULMONARY INFECTIONS Serodiagnosis of Mycobacterium avium complex pulmonary disease in the USA Seigo Kitada 1, Adrah Levin 2, Melissa Hiserote 3, Ron J. Harbeck 3, Chris A. Czaja 2,4,
ORIGINAL ARTICLE PULMONARY INFECTIONS Serodiagnosis of Mycobacterium avium complex pulmonary disease in the USA Seigo Kitada 1, Adrah Levin 2, Melissa Hiserote 3, Ron J. Harbeck 3, Chris A. Czaja 2,4,
Dr Conroy Wong. Professor Richard Beasley. Dr Sarah Mooney. Professor Innes Asher
 Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
Professor Richard Beasley University of Otago Director Medical Research Institute of New Zealand Wellington Dr Sarah Mooney Physiotherapy Advanced Clinician Counties Manukau Health NZ Respiratory and Sleep
Mycobacterium avium complex disease: prognostic implication of high-resolution computed tomography findings
 Eur Respir J 2008; 32: 147 152 DOI: 10.1183/09031936.00074207 CopyrightßERS Journals Ltd 2008 Mycobacterium avium complex disease: prognostic implication of high-resolution computed tomography findings
Eur Respir J 2008; 32: 147 152 DOI: 10.1183/09031936.00074207 CopyrightßERS Journals Ltd 2008 Mycobacterium avium complex disease: prognostic implication of high-resolution computed tomography findings
Best Practices for Pulmonary Nontuberculous Mycobacteria
 Best Practices for Pulmonary Nontuberculous Mycobacteria June 2017 Public Health Ontario Public Health Ontario is a Crown corporation dedicated to protecting and promoting the health of all Ontarians and
Best Practices for Pulmonary Nontuberculous Mycobacteria June 2017 Public Health Ontario Public Health Ontario is a Crown corporation dedicated to protecting and promoting the health of all Ontarians and
DOWNLOAD OR READ : NONTUBERCULOUS MYCOBACTERIA NTM PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : NONTUBERCULOUS MYCOBACTERIA NTM PDF EBOOK EPUB MOBI Page 1 Page 2 nontuberculous mycobacteria ntm nontuberculous mycobacteria ntm pdf nontuberculous mycobacteria ntm patients and those
DOWNLOAD OR READ : NONTUBERCULOUS MYCOBACTERIA NTM PDF EBOOK EPUB MOBI Page 1 Page 2 nontuberculous mycobacteria ntm nontuberculous mycobacteria ntm pdf nontuberculous mycobacteria ntm patients and those
Comparison of CT findings between MDR-TB and XDR-TB
 Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
Comparison of CT findings between MDR-TB and XDR-TB Poster No.: C-0757 Congress: ECR 2017 Type: Authors: Keywords: DOI: Scientific Exhibit K. Yoon, H. Soohee; Changwon-si/KR Thorax, Lung, Respiratory system,
A survey of dental treatment under general anesthesia in a Korean university hospital pediatric dental clinic
 Original Article pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2016;16(3):203-208 http://dx.doi.org/10.17245/jdapm.2016.16.3.203 A survey of dental treatment under general anesthesia in a Korean
Original Article pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2016;16(3):203-208 http://dx.doi.org/10.17245/jdapm.2016.16.3.203 A survey of dental treatment under general anesthesia in a Korean
