HEDIS Guidelines for Health Care Providers
|
|
|
- Beverly Atkins
- 5 years ago
- Views:
Transcription
1 75 Vanderbilt Ave Staten Island NY CPHL-CARES HEDIS Guidelines for Health Care Providers Adult BMI Assessment (ABA) Members years of age who had an outpatient visit and whose body mass index (BMI) was documented during the measurement year or the year prior to the measurement year Medical record documentation must include: For members 21 years and older on the date of service, include documentation of weight and BMI value. For members younger than 21 years on the date of service, include height, weight, and BMI percentile. Tips for Success: Height and weight are usually documented but calculation of the BMI is often missing. Work with your EMR vendor to update your system with the calculation. Code appropriately. Members who have a diagnosis of pregnancy during the measurement year or the year prior to the measurement year can be excluded from the measure. ABA Codes BMI:ICD-10: Z68.1, Z68.20, Z68.21, Z68.22, Z68.23, Z68.24, Z68.25, Z68.2,Z68.2, Z68.28, Z68.2, Z68.30, Z68.31, Z68.32, Z68.33, Z68.34, Z68.35,Z68.36, Z68.37, Z68.38, Z68.39, Z68.41, Z68.42, Z68.43, Z68.44, Z68.45 BMI Percentile: ICD-10: Z68.51, Z68.52, Z68.53, Z68.54
2 Controlling High Blood Pressure (CBP) Members years of age with diagnosis of Hypertension (HTN) prior to June 30 of the measurement year and whose B P was adequately controlled during the measurement year based on the following criteria: Members years of age whose BP was <140/90 mm Hg. Members years of age with a diagnosis of diabetes whose BP was <140/90 mm Hg. Members years of age without a diagnosis of diabetes whose BP was <150/mm Hg. Medical record documentation must include: The most recent BP reading (date and result) in the measurement year AFTER the diagnosis of HTN is made. Tips for Success: when the member s BP is elevated at the visit, be sure to repeat the measurement AND document the new result. The repeat BP is often lower! CBP Codes Essential Hypertension: ICD-10: I10 Exclusions: Members with evident ESRD; Diagnosis of pregnancy during the year prior to the measurement year; Members who had an admission to a non-acute inpatient setting in the year prior to the measurement year;
3 Comprehensive Diabetes Care (CDC) Members with diabetes (Type I and Type 2) who had each of the following: Hemoglobin A1c testing o HbA1c control (<8.0%) o HbA1c poor control (>9.0%) Eye exam (retinal) Medical attention for nephropathy BP control <140/90 mm Hg Medical record documentation must include: Most recent blood pressure readings. Most recent lab test for HbA1c with date of test and result. A nephropathy screening or monitoring test (urine protein) during the measurement year or evidence of nephropathy during the measurement year. A retinal or dilated eye exam by an eye care professional (optometrist or ophthalmologist) in the measurement year or a negative retinal or dilated eye exam (negative for retinopathy) by an eye care professional in the year prior to the measurement year. Tips for Success: Labs indicating poor control should be repeated again later in the calendar year. Bring the member back in for testing! The intent of the eye exam indicator is to ensure that members with evidence of any type of retinopathy have an eye exam annually. Communicate the importance of this exam and help coordinate the scheduling if Indicated: Hemoglobin A1c (HbA1c) testing. Eye exam (retinal) performed. Medical attention for nephropathy. BP control (<140/90 mm Hg).
4 CDC Codes Exclusions: Gestational diabetes, steroid induced diabetes Diabetic Retinal Screening: CPT: 67028, 67030, 67031, 67036, 67039, 67040, 67041, 67042, 67043,67101, 67105, 67107, 67108, 67110, 67112, 67113, 67121, 67141, 67145, 67208, 67210, 67218, 67220, 67221, 67227, 67228, 92002,92004, 92012, 92014, 92018, 92019, 92134, 92225,92226, 92227,92228, 92230, 92235, 92240, 92250, HCPCS: S0620, S0621, S3000 Diabetic Retinal Screening Negative: 3072F Diabetic Retinal Screening with Eye Care Professional CPT II: 2022F, 2024F, 2026F, S0625 HbA1c HbA1c Test: CPT: 83036, HbA1c Level Less the 7.0: CPT II: 3044F HbA1c Level : CPT II: 3045F HbA1c Level Greater Than 9.0: CPT II 3046F
5 Blood Pressure Diastolic 80-89: CPT II: 3079F Diastolic Greater than/equal to 90: CPT II: 3080F Diastolic Less than 80: CPT II: 3078F Systolic Greater than/equal to 140: CPT II: 3077F Systolic Less than 140: CPT II: 3074F, 3075F Nephropathy Nephropathy Treatment: CPT II: 3066F, 4010F Urine Protein Tests: CPT: 81000, 81001, 81002, 81003, 81005, 82042, 82043, 82044, CPT II: 3060F, 3061F, 3062F Dialysis HCPCS: G0257, S2065, S9339
6 Colorectal Cancer Screening (COL) Members years of age who had appropriate screening for colorectal cancer. Medical record documentation must include evidence of one of the following: Colonoscopy (within last 10 years). FOBT (gfobt or ifobt in the measurement year). Flexible Sigmoidoscopy (within last 5 years). FIT-DNA test during the measurement year or the two years prior to the measurement year. CT Colonography during the measurement year or the four years prior to the measurement year. Tips for Success: Providers should review/confirm all preventive health screenings at each visit. Dates and results need to be consistently documented. When colorectal screening is reported, obtain report from specialist to ensure medical record is complete. COL Codes Colonoscopy CPT: 44388, 44389, 44390, 44391, 44392, 44393, 44394,44397, , 45355,45378,45379, 45380, 45381, 45382, 45383, 45384,45385, 45386,45387, 45391, HCPCS: G0105, G0121, G0213, G0214, G0215 FOBT CPT: 82270, HCPCS: G0328 Flexible Sigmoidoscopy CPT: , , , HCPCS: G0104 CT Colonography CPT:
7 FIT DNA CPT: 81528, HCPCS: G0464 Medication Reconciliation Post-Discharge (MRP) Members 18 years and older with discharges (acute and non-acute inpatient) from January,1 to December,1 of the measurement year, for whom medications were reconciled the date of discharge through 30 days after discharge (31 days total) Medical record documentation must include: Evidence of medication reconciliation AND the date when it was performed. Must be conducted by a prescribing practitioner, clinical pharmacist, or RN. Only documentation in the outpatient chart meets the intent of the measure, but an outpatient visit is not required. Tips for Successful Hybrid Chart Review: Any of the following meet criteria: Documentation that the provider reconciled the current and discharge medications. Documentation of the current medication with a notation that references the Discharge medications. Documentation of the member s current medications with a notation that the discharge medications were reviewed. Documentation of a current medication list, a discharge medication list, and notation that both lists were reviewed on the same date of service. Notation that no medications were prescribed or ordered upon discharge. Medication Reconciliation (MRP) Codes CPT: 99495, CPT II: 1111F, 1159F, 1160F
8 Transitions of Care (TRC) Members 18 years of age and older with discharges (acute and non-acute inpatient) who had documentation by the Provider of each of the following during the measurement year. 1. Notification of Inpatient Admission Documentation of receipt of notification of inpatient admission on the day of admission or the following day. Documentation in your outpatient record of any tests and treatments ordered during the member s inpatient stay. Documentation that the admission was elective and you had performed a preadmission exam or were notified of pre-admission testing results. 2. Receipt of Discharge Information Documentation of receipt of discharge information on the day of discharge or the following day. 3. Patient Engagement after Inpatient Discharge Documentation of patient engagement (e.g., office visits, visits to the home, telehealth) provided within 30 days after discharge (does not include the date of discharge). Codes CPT: , , , , , , , , , 99429, HCPCS: T1015, G0402, G0438, G0439, G Medication Reconciliation Post-Discharge Documentation of medication reconciliation on the date of discharge through 30 days after discharge (31 total days). (See MRP measure)
9 Care of Older Adults (COA) The percentage of adults 66+ years old who had each of the following during the measurement year: 1. Advance care planning Includes a discussion about preferences for resuscitation, life sustaining treatment and end of life care. Examples include: Advance Directives Actionable Medical Orders Living Will Codes: CPT: CPT II: 1123F, 1124F, 1157F, 1158F HCPCS: S Medication review Includes at least one medication review conducted by a prescribing practitioner or clinical pharmacist in the measurement year and the presence of a medication list or includes notation that the member is not taking any medication and the date when it was noted. Codes: Medication review Codes: CPT: 90863, 99605, CPT II: 1160F Medication list Codes: CPT II: 1159F HCPCS: G8427 Transitional care management services Codes: CPT: 99495, 99496
10 3. Functional status assessment Includes evidence of at least one functional status assessment and the date it was performed as documented by: Instrumental Activity of Daily Living (IADL) or - Activities of Daily Living (ADL) or - Results of a standardized functional status assessment tool or Notation that at least 3 of the 4 following were assessed: notation of functional independence, sensory ability, cognitive status, and ambulatory status Functional status assessment Codes: CPT II:1170F 4. Pain assessment Includes evidence of a pain assessment using a standardized pain assessment tool and the date it was performed Pain assessment Codes: CPT II: 1125F,1126F How to Improve your HEDIS Rates Timely submission of all claims and encounter data Complete and accurate coding of all services performed Document all services and care provided in the medical record Schedule patients for their annual screenings and check- ups Continually monitor patients with chronic conditions Continually monitor patients on persistent medications Understand the HEDIS measure criteria and the standard practice guidelines
Clinical HEDIS Medicare Stars Quick Reference Guide
 Clinical HEDIS Medicare Stars Quick Reference Guide MEASURE Adult BMI Assessment (ABA) Breast Cancer Screening (BCS) SPECIFICATIONS The percentage of members 18 74 years of age who had an outpatient visit
Clinical HEDIS Medicare Stars Quick Reference Guide MEASURE Adult BMI Assessment (ABA) Breast Cancer Screening (BCS) SPECIFICATIONS The percentage of members 18 74 years of age who had an outpatient visit
Adult-Peds Quality Measure Information Sheet 2018
 Prevention and Screening Adolescent Preventive Care Measures (ADL) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Prevention and Screening Adolescent Preventive Care Measures (ADL) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Michigan Complete Health strives to provide
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Michigan Complete Health strives to provide
2017 Medicare STARs Provider Quality Indicators Guide
 2017 Medicare STARs Provider Quality Indicators Guide Medicare STARs Rating Centers for Medicare & Medicaid Services (CMS) created a Five-Star Quality Rating System to help measure the quality in care
2017 Medicare STARs Provider Quality Indicators Guide Medicare STARs Rating Centers for Medicare & Medicaid Services (CMS) created a Five-Star Quality Rating System to help measure the quality in care
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Healthcare Effectiveness Data and Information Set Quality Assurance Reporting Requirements
 HEDIS/QARR Healthcare Effectiveness Data and Information Set Quality Assurance Reporting Requirements 2015 Quick Reference Guide ADULTS Avoidance of Antibiotic Treatment in Adults with Acute Bronchitis
HEDIS/QARR Healthcare Effectiveness Data and Information Set Quality Assurance Reporting Requirements 2015 Quick Reference Guide ADULTS Avoidance of Antibiotic Treatment in Adults with Acute Bronchitis
This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings.
 2019 HEDIS AT-A-GLANCE GUIDE STAR MEASURES This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. At WellCare, we value everything
2019 HEDIS AT-A-GLANCE GUIDE STAR MEASURES This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. At WellCare, we value everything
STRIDE SM Quality Program 2017 Program Overview
 STRIDE SM Quality Program 2017 Program Overview Health Services 2017 Program 1 Quality Program Program Overview The Plan will support the efforts of the LCU and LCU Participating Providers in managing
STRIDE SM Quality Program 2017 Program Overview Health Services 2017 Program 1 Quality Program Program Overview The Plan will support the efforts of the LCU and LCU Participating Providers in managing
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service. Updated January 20, 2016
 Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
Provider STAR Ratings Quick Reference Guide 2016 Dates of Service Updated January 20, 2016 Adult BMI (Body Mass Index) Assessment (ABA) EXCLUSIONS: Members who have a diagnosis of pregnancy during the
PROVIDER GUIDE Required information on targeted HEDIS and Part D measures
 PROVIDER GUIDE Required information on targeted HEDIS and Part D measures Visit www.atriohp.com/star-ratings-program for full measure descriptions. Contact QI@atriohp.com with any questions. Adult Body
PROVIDER GUIDE Required information on targeted HEDIS and Part D measures Visit www.atriohp.com/star-ratings-program for full measure descriptions. Contact QI@atriohp.com with any questions. Adult Body
Medicare STRIDE SM Physician Quality Program 2019 Program Overview
 Medicare STRIDE SM Quality Program 2019 Program Overview Health Services- Managed by Network Medical Management 2019 Program 1 Medicare Advantage Quality Program Program Overview The Plan will support
Medicare STRIDE SM Quality Program 2019 Program Overview Health Services- Managed by Network Medical Management 2019 Program 1 Medicare Advantage Quality Program Program Overview The Plan will support
Blue Cross and Blue Shield of Louisiana 2016 Healthcare Effectiveness Data and Information Set (HEDIS) Coding and Documentation Guide
 Blue Cross and Blue Shield of Louisiana 2016 Healthcare Effectiveness Data and Information Set (HEDIS) Coding and Documentation Guide Measure Measure Description Protocol or Documentation Required Coding
Blue Cross and Blue Shield of Louisiana 2016 Healthcare Effectiveness Data and Information Set (HEDIS) Coding and Documentation Guide Measure Measure Description Protocol or Documentation Required Coding
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS QUICK REFERENCE GUIDE: DOCUMENTATION TIPS FOR ADULT MEASURES
 HEDIS QUICK REFERENCE GUIDE: DOCUMENTATION TIPS FOR ADULT MEASURES For Health Care Providers January 2018 Helping you improve your scores, as you improve the health of your patients. Healthcare Effectiveness
HEDIS QUICK REFERENCE GUIDE: DOCUMENTATION TIPS FOR ADULT MEASURES For Health Care Providers January 2018 Helping you improve your scores, as you improve the health of your patients. Healthcare Effectiveness
HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS )
 STARS MEASURES 2015 HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS ) Developed by the National Committee for Quality Assurance (NCQA), HEDIS is the most widely used set of performance measures
STARS MEASURES 2015 HEALTHCARE EFFECTIVENESS DATA AND INFORMATION SET (HEDIS ) Developed by the National Committee for Quality Assurance (NCQA), HEDIS is the most widely used set of performance measures
HEDIS Quality Measure Descriptions
 HEDIS Quality Measure Descriptions Updated January 18, Highlighted areas indicate change from prior version. Adolescent well care (AWC) Patients ages 12 to 21 who has at least one comprehensive well child
HEDIS Quality Measure Descriptions Updated January 18, Highlighted areas indicate change from prior version. Adolescent well care (AWC) Patients ages 12 to 21 who has at least one comprehensive well child
December 2018 CTC/OHIC Measure Specifications
 Overarching Principles and Definitions Active Patients: Patients seen by a primary care clinician of the PCMH anytime within the last 24 months Definition of primary care clinician includes the following:
Overarching Principles and Definitions Active Patients: Patients seen by a primary care clinician of the PCMH anytime within the last 24 months Definition of primary care clinician includes the following:
April Thank you for attending today s Webinar. We will begin shortly Aetna Inc.
 April 2018 Thank you for attending today s Webinar. We will begin shortly. April 2018 1 Brian Clark Jacob Stipe Debbie Barkley Diana Charlton Welcome Illinois, New Jersey, Florida, Louisiana, Ohio, Pennsylvania,
April 2018 Thank you for attending today s Webinar. We will begin shortly. April 2018 1 Brian Clark Jacob Stipe Debbie Barkley Diana Charlton Welcome Illinois, New Jersey, Florida, Louisiana, Ohio, Pennsylvania,
Multi-Specialty Quality Measure Information Sheet 2017
 Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2017 Technical Specifications Michigan Complete Health Medicare-Medicaid Plan
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2017 Technical Specifications Michigan Complete Health Medicare-Medicaid Plan
HEDIS Measure 2018 Physician Documentation Guidelines and Administrative Codes
 Each HEDIS measure identified below has criteria that is required for your patient s chart or claims review to be considered valid towards HEDIS measurement. To make the most of your office visits towards
Each HEDIS measure identified below has criteria that is required for your patient s chart or claims review to be considered valid towards HEDIS measurement. To make the most of your office visits towards
2017 PCP INCENTIVE AWARD PROGRAM MEASURES & TIPS
 Childhood Immunization Status (CIS) Combo 10 Immunizations for Adolescents (IMA) Combo 1 Lead Screening in Children (LSC) Immunizations completed prior to a child turning 2 years of age in 2017 as follows:
Childhood Immunization Status (CIS) Combo 10 Immunizations for Adolescents (IMA) Combo 1 Lead Screening in Children (LSC) Immunizations completed prior to a child turning 2 years of age in 2017 as follows:
2017 MSSP Clinical Quality Measures
 *The information contained in this document relies heavily on information supplied by CMS. GPRO CARE-1 (NQF 0097): Medication Reconciliation Post-Discharge DESCRIPTION: Percentage of discharges from any
*The information contained in this document relies heavily on information supplied by CMS. GPRO CARE-1 (NQF 0097): Medication Reconciliation Post-Discharge DESCRIPTION: Percentage of discharges from any
HEDIS Documentation and Coding Adult Guidelines 2017
 HEDIS Documentation and Coding Adult Guidelines 2017 Reproduced with permission from HEDIS 2017, Volume 2: Technical Specifications for Health Plans by the National Committee for Quality Assurance (NCQA).
HEDIS Documentation and Coding Adult Guidelines 2017 Reproduced with permission from HEDIS 2017, Volume 2: Technical Specifications for Health Plans by the National Committee for Quality Assurance (NCQA).
QBPC Claims Based Provider Quick Reference Guide
 QBPC Claims Based Provider Quick Reference Guide Category: Diabetes Chronic Suite ICD-10-CM diagnosis HbA1c Test Codes LOINC Evidence of Treatment for Nephropathy Codes E10; E11; E13 83036-37 17856-6,
QBPC Claims Based Provider Quick Reference Guide Category: Diabetes Chronic Suite ICD-10-CM diagnosis HbA1c Test Codes LOINC Evidence of Treatment for Nephropathy Codes E10; E11; E13 83036-37 17856-6,
2017 BlueCare Plus (HMO SNP) SM Stars Quality Attestation Form
 2017 BlueCare Plus (HMO SNP) SM Stars Quality Attestation Form Provider Name Contract Entity/Group Name Patient Preventive Screenings Breast Cancer Screening Colorectal Cancer Screening The Breast Cancer
2017 BlueCare Plus (HMO SNP) SM Stars Quality Attestation Form Provider Name Contract Entity/Group Name Patient Preventive Screenings Breast Cancer Screening Colorectal Cancer Screening The Breast Cancer
Quick Reference Guide
 Breast Cancer Screening (BCS) STAR RATING: Percentage of members ages 50-74 who had a mammogram screening in last 27 reported months. Test performed between: Oct. 1 two years prior to the measurement year
Breast Cancer Screening (BCS) STAR RATING: Percentage of members ages 50-74 who had a mammogram screening in last 27 reported months. Test performed between: Oct. 1 two years prior to the measurement year
Quality Indicator Physician Medicare HEDIS, HOS, CAHPS and Part D Safety Measures Guide for 2017
 Quality Indicator Physician Medicare HEDIS, HOS, CAHPS and Part D Safety s Guide for 2017 Note: HEDIS codes can change from year to year. The codes in this document are from the HEDIS 2017 specifications.
Quality Indicator Physician Medicare HEDIS, HOS, CAHPS and Part D Safety s Guide for 2017 Note: HEDIS codes can change from year to year. The codes in this document are from the HEDIS 2017 specifications.
HEDIS Adult. Documentation and Coding Guidelines Medical record documentation required. Measure description. Coding ICD-10: Z68.1 Z68.45, Z68.
 HEDIS Adult Documentation and Guidelines 2017 description Adult BMI Assessment (ABI) Members 18 74 years of age who had an outpatient visit and whose body mass index (BMI) was documented during the measurement
HEDIS Adult Documentation and Guidelines 2017 description Adult BMI Assessment (ABI) Members 18 74 years of age who had an outpatient visit and whose body mass index (BMI) was documented during the measurement
PENNSYLVANIA MEDICAID AND MEDICARE Explanation of HEDIS Measures
 Each year, NCQA (National Committee for Quality Assurance) publishes HEDIS (Healthcare Effectiveness Data and Information Set), a set of standardized performance measures used in the managed care industry
Each year, NCQA (National Committee for Quality Assurance) publishes HEDIS (Healthcare Effectiveness Data and Information Set), a set of standardized performance measures used in the managed care industry
Adult HEDIS & STARs Measures
 HEDIS AND MEDICARE STAR DOCUMENTATION & CODING GUIDE Adult HEDIS & STARs Measures Adult BMI Assessment (ABA) 18 74-year-old Antidepressant Medication Management (AMM) Breast Cancer Screening (BCS) Cervical
HEDIS AND MEDICARE STAR DOCUMENTATION & CODING GUIDE Adult HEDIS & STARs Measures Adult BMI Assessment (ABA) 18 74-year-old Antidepressant Medication Management (AMM) Breast Cancer Screening (BCS) Cervical
HEDIS Documentation & Coding Guidelines 2015
 Effectiveness of Care: Prevention & Screening Members 18 74 years of age who had an outpatient visit and BMI ICD-9: V85.0 - V85.45 whose body mass index (BMI) was documented during the measurement year
Effectiveness of Care: Prevention & Screening Members 18 74 years of age who had an outpatient visit and BMI ICD-9: V85.0 - V85.45 whose body mass index (BMI) was documented during the measurement year
HEDIS/QARR 2018 Quick Reference Guide ALL MEASURES
 2018 HEDIS Codes HEDIS/QARR 2018 Quick Reference Guide ALL MEASURES Code Age Band Denominator Event Numerator Requirement ADL AAB AAP ABA ADV Adolescent Preventive Care Avoidance of Antibiotic in Adults
2018 HEDIS Codes HEDIS/QARR 2018 Quick Reference Guide ALL MEASURES Code Age Band Denominator Event Numerator Requirement ADL AAB AAP ABA ADV Adolescent Preventive Care Avoidance of Antibiotic in Adults
2017 HEDIS Measures. PREVENTIVE SCREENING 2017 Measure Quality Indicator
 PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
2017 CMS Web Interface Reporting
 2017 CMS Web Interface Reporting Measure Specification Review May 18, 2017 Sherry Grund, Telligen Mary Schrader, Telligen Medicare Shared Savings Program and Next Generation ACO Model DISCLAIMER This presentation
2017 CMS Web Interface Reporting Measure Specification Review May 18, 2017 Sherry Grund, Telligen Mary Schrader, Telligen Medicare Shared Savings Program and Next Generation ACO Model DISCLAIMER This presentation
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
GlobalHealth has improved ratings in the following HEDIS measures: Antidepressant Medication Management Continuation Phase
 August 2013, Dear GlobalHealth Network Practitioners and Providers: Each year, GlobalHealth selects and examines a sample of medical records to ensure quality care is being provided to our members. These
August 2013, Dear GlobalHealth Network Practitioners and Providers: Each year, GlobalHealth selects and examines a sample of medical records to ensure quality care is being provided to our members. These
COMMUNITY HEALTH GROUP HEDIS MEASURES (CY 2012) MEDICARE QUICK REFERENCE GUIDE FOR BILLING DEPARTMENT
 HEDIS MEASURES (CY ) MEDICARE QUICK REFERENCE GUIDE FOR BILLING DEPARTMENT Care for Older Adults Colorectal Cancer Screening Annual Monitoring for Patients on Persistent Medications COA COL MPM Age Description
HEDIS MEASURES (CY ) MEDICARE QUICK REFERENCE GUIDE FOR BILLING DEPARTMENT Care for Older Adults Colorectal Cancer Screening Annual Monitoring for Patients on Persistent Medications COA COL MPM Age Description
Changes for Physician Measurement 2018
 Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
2019 HEDIS 1 Measures Healthcare Effectiveness Data and Information Set
 209 HEDIS s Healthcare Effectiveness Data and Information Set *s collected with medical record review. Red= new/addition to measures Blue= Medicare only Prevention and Screening Adult Immunization Status
209 HEDIS s Healthcare Effectiveness Data and Information Set *s collected with medical record review. Red= new/addition to measures Blue= Medicare only Prevention and Screening Adult Immunization Status
May 2016 CTC/OHIC Measure Specifications
 Active Patients: Overarching Principles and Definitions Out patients seen by a primary care clinician of the PCMH anytime within the last 24 months. Definition of primary care clinician includes the following:
Active Patients: Overarching Principles and Definitions Out patients seen by a primary care clinician of the PCMH anytime within the last 24 months. Definition of primary care clinician includes the following:
Key Behavioral Measures (17 Years and Younger)
 2018 HEDIS At-A-Glance Key Behavioral Measures (17 Years and Younger) At WellCare/Harmony, we value everything you do to deliver quality care for our members your patients to make sure they have a positive
2018 HEDIS At-A-Glance Key Behavioral Measures (17 Years and Younger) At WellCare/Harmony, we value everything you do to deliver quality care for our members your patients to make sure they have a positive
IHA P4P Measure Manual Measure Year Reporting Year 2018
 ADULT PREVENTIVE CARE IHA P4P Measure Manual Measure Year 2017 - Reporting Year 2018 *If line of business not labeled, measure is Commercial only Adult BMI (Medicare) 18-74 Medicare members ages 18-74
ADULT PREVENTIVE CARE IHA P4P Measure Manual Measure Year 2017 - Reporting Year 2018 *If line of business not labeled, measure is Commercial only Adult BMI (Medicare) 18-74 Medicare members ages 18-74
Quality Program Measures
 QUALITY+ Quality Program Measures BLUEADVANTAGE (PPO) SM BLUECARE PLUS (HMO SNP) SM We value your partnership and participation in the 2018 Medicare Advantage Quality+ Partnership Program, and hope you
QUALITY+ Quality Program Measures BLUEADVANTAGE (PPO) SM BLUECARE PLUS (HMO SNP) SM We value your partnership and participation in the 2018 Medicare Advantage Quality+ Partnership Program, and hope you
HEDIS Stars Measures Reference Guide for 2018
 HEDIS Stars Measures Reference Guide for 2018 Here s a handy guide to help you check criteria, codes and exceptions of HEDIS Stars measures. For questions about HEDIS measures, contact us at carole.wright@floridablue.com.
HEDIS Stars Measures Reference Guide for 2018 Here s a handy guide to help you check criteria, codes and exceptions of HEDIS Stars measures. For questions about HEDIS measures, contact us at carole.wright@floridablue.com.
PQRS in TRAKnet 2015 GUIDE TO SUBMIT TING AND REPORTING PQRS IN 2015 THROUGH TRAKNET
 PQRS in TRAKnet 2015 GUIDE TO SUBMITTING AND REPORTING PQRS IN 2015 THROUGH TRAKNET What is PQRS? PQRS is a quality reporting program that uses negative payment adjustments to promote reporting of quality
PQRS in TRAKnet 2015 GUIDE TO SUBMITTING AND REPORTING PQRS IN 2015 THROUGH TRAKNET What is PQRS? PQRS is a quality reporting program that uses negative payment adjustments to promote reporting of quality
Total Health Quality Indicators For Providers 2018
 Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2018 Adult- Preventive Z00.00 Report ALL components of an annual visit
Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2018 Adult- Preventive Z00.00 Report ALL components of an annual visit
KEY BEHAVIORAL MEASURES
 2019 HEDIS AT-A-GLANCE: KEY BEHAVIORAL MEASURES (17 Years and Younger) At WellCare, we value everything you do to deliver quality care for our members your patients to make sure they have a positive healthcare
2019 HEDIS AT-A-GLANCE: KEY BEHAVIORAL MEASURES (17 Years and Younger) At WellCare, we value everything you do to deliver quality care for our members your patients to make sure they have a positive healthcare
2017 Top Ten Quality Metrics Quick Reference Guide POWER OUR
 2017 Top Ten Quality Metrics Quick Reference Guide POWER OUR Population Health Strategy Population Health Services Organization (PHSO) an optimized, physician-partnered operations entity that powers a
2017 Top Ten Quality Metrics Quick Reference Guide POWER OUR Population Health Strategy Population Health Services Organization (PHSO) an optimized, physician-partnered operations entity that powers a
HEDIS PLUS PROVIDER TRAINING
 HEDIS PLUS PROVIDER TRAINING With a focus on: 2018 LDH Incentive Based or Monitoring Measures, 2018 NCQA Accreditation Measures, and 2018 AmeriHealth Caritas Louisiana Quality Enhancement Program Measures
HEDIS PLUS PROVIDER TRAINING With a focus on: 2018 LDH Incentive Based or Monitoring Measures, 2018 NCQA Accreditation Measures, and 2018 AmeriHealth Caritas Louisiana Quality Enhancement Program Measures
5 x 7 spiral bound - prints front and back sheets - 1/1 - black MEASURE DESCRIPTION
 Requirements for Meeting Clinical Goals - Last Updated 11-1-2016 TABLE OF CONTENTS MEASURE ABBREVIATION AAB ABA ADD AMM AMR ART BCS CBP CCS CDC CDC CDC CDC CHL CWP CIS COL FUH IMA IET LBP MPM MEASURE DESCRIPTION
Requirements for Meeting Clinical Goals - Last Updated 11-1-2016 TABLE OF CONTENTS MEASURE ABBREVIATION AAB ABA ADD AMM AMR ART BCS CBP CCS CDC CDC CDC CDC CHL CWP CIS COL FUH IMA IET LBP MPM MEASURE DESCRIPTION
Quality Measures Guide. Medicare Star Rating and HEDIS measures
 Quality Measures Guide Medicare Star Rating and HEDIS measures February 2018 About the Quality Measures Guide A key component of our Quality Program is Healthcare Effectiveness Data and Information Set
Quality Measures Guide Medicare Star Rating and HEDIS measures February 2018 About the Quality Measures Guide A key component of our Quality Program is Healthcare Effectiveness Data and Information Set
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications MHS Health Wisconsin strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications MHS Health Wisconsin strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
Key Behavioral Health Measures (18 Years and Older)
 At WellCare, we value everything you do to deliver quality care for our members your patients to make sure they have a positive health care experience. That s why we ve created this easy-to-use, informative
At WellCare, we value everything you do to deliver quality care for our members your patients to make sure they have a positive health care experience. That s why we ve created this easy-to-use, informative
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO
 The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
Frequently Asked Questions (FAQ) IHA Align. Measure. Perform. (AMP) Programs January Audit Audit Roadmap Posted 1/23/19
 Frequently Asked Questions (FAQ) IHA Align. Measure. Perform. (AMP) Programs January 2019 Audit Audit Roadmap Question: For the AMP MY 2018 Roadmap, is the last part of question 5.2W in Section 5, Describe
Frequently Asked Questions (FAQ) IHA Align. Measure. Perform. (AMP) Programs January 2019 Audit Audit Roadmap Question: For the AMP MY 2018 Roadmap, is the last part of question 5.2W in Section 5, Describe
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Humana Practitioner Assessment Form
 Humana Practitioner Assessment Form Please fill in the information requested in this box only. Your physician will complete the remaining sections of this assessment. Patient name: Date of service: Humana
Humana Practitioner Assessment Form Please fill in the information requested in this box only. Your physician will complete the remaining sections of this assessment. Patient name: Date of service: Humana
INTERNAL MEDICINE PRACTICES
 2018 Primary Care Provider Quality Improvement Program (PCP QIP) Measurement Specifications INTERNAL MEDICINE PRACTICES Developed by: The QIP Team QIP@partnershiphp.org Published: November 28, 2017 Updated:
2018 Primary Care Provider Quality Improvement Program (PCP QIP) Measurement Specifications INTERNAL MEDICINE PRACTICES Developed by: The QIP Team QIP@partnershiphp.org Published: November 28, 2017 Updated:
2018 Blue Cross NC. Provider Quality Pocket Guide
 2018 Blue Cross NC Provider Quality Pocket Guide 5 x 7 spiral bound - prints front and back sheets - 1/1 - black Requirements for Meeting Clinical Goals - Last Updated October 2017 TABLE OF CONTENTS MEASURE
2018 Blue Cross NC Provider Quality Pocket Guide 5 x 7 spiral bound - prints front and back sheets - 1/1 - black Requirements for Meeting Clinical Goals - Last Updated October 2017 TABLE OF CONTENTS MEASURE
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Ambetter from Arkansas Health & Wellness strives
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Ambetter from Arkansas Health & Wellness strives
RECOMMENDED SCREENINGS & IMMUNIZATIONS TO KEEP YOU HEALTHY
 RECOMMENDED SCREENINGS RECOMMENDED SCREENINGS & IMMUNIZATIONS TO KEEP YOU HEALTHY AGE 18+ 30 40 50 60 70 80+ Breast Cancer (for women) Cervical Cancer (for women) Colorectal Cancer Have a Pap test every
RECOMMENDED SCREENINGS RECOMMENDED SCREENINGS & IMMUNIZATIONS TO KEEP YOU HEALTHY AGE 18+ 30 40 50 60 70 80+ Breast Cancer (for women) Cervical Cancer (for women) Colorectal Cancer Have a Pap test every
Reference Guide for Adult Health PATH HEDIS, CMS Part D, CAHPS and HOS Measures
 Reference Guide for Adult Health 2018 HEDIS, CMS Part D, CAHPS and HOS Measures HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Information contained in this guide
Reference Guide for Adult Health 2018 HEDIS, CMS Part D, CAHPS and HOS Measures HEDIS is a registered trademark of the National Committee for Quality Assurance (NCQA). Information contained in this guide
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications IlliniCare Health strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications IlliniCare Health strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Nebraska Total Care strives to provide quality
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Nebraska Total Care strives to provide quality
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
Practitioner Assessment Form (PAF)
 Practitioner Assessment Form (PAF) What is the PAF? The practitioner assessment form is a health assessment designed to assist the physician in collecting specific information on Medicare Advantage patients.
Practitioner Assessment Form (PAF) What is the PAF? The practitioner assessment form is a health assessment designed to assist the physician in collecting specific information on Medicare Advantage patients.
SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES
 Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
HEDIS 2018 MEASURES. Performance Ratings Operations Department
 HEDIS 2018 MEASURES Performance Ratings Operations Department ABA Adult BMI Assessment Members ages 18 74 years of age What makes them compliant? Documentation in the medical record must reflect office
HEDIS 2018 MEASURES Performance Ratings Operations Department ABA Adult BMI Assessment Members ages 18 74 years of age What makes them compliant? Documentation in the medical record must reflect office
Trending Determinations by Measure
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Parties FROM: Cindy Ottone, Director, Policy DATE: March 2019 RE: HEDIS 1 2019 Measure
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Parties FROM: Cindy Ottone, Director, Policy DATE: March 2019 RE: HEDIS 1 2019 Measure
KEY BEHAVIORAL MEASURES
 2019 HEDIS AT-A-GLANCE: KEY BEHAVIORAL MEASURES (18 Years and Older) At WellCare, we value everything you do to deliver quality care for our members your patients to make sure they have a positive healthcare
2019 HEDIS AT-A-GLANCE: KEY BEHAVIORAL MEASURES (18 Years and Older) At WellCare, we value everything you do to deliver quality care for our members your patients to make sure they have a positive healthcare
HEDIS. Quick Reference Guide. For more information, visit
 HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2019 Technical Specifications SilverSummit Healthplan strives to provide quality
HEDIS Quick Reference Guide For more information, visit www.ncqa.org HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2019 Technical Specifications SilverSummit Healthplan strives to provide quality
HEDIS Quick Reference Guide
 SHP_20174053 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Superior HealthPlan strives to provide quality health care to our membership as measured through Healthcare
SHP_20174053 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2018 Technical Specifications Superior HealthPlan strives to provide quality health care to our membership as measured through Healthcare
2018 P4P Overview 0518.PR.P.PP.1 6/18
 2018 P4P Overview Agenda MHS Pay For Performance (P4P) Ambetter P4P Program Secure Web Reporting Question and Answer What You Will Learn 1. Measure Overviews & Specifications 2. Documentation Requirements
2018 P4P Overview Agenda MHS Pay For Performance (P4P) Ambetter P4P Program Secure Web Reporting Question and Answer What You Will Learn 1. Measure Overviews & Specifications 2. Documentation Requirements
Wisconsin Chronic Disease Quality Improvement Project. HEDIS 2017 Summary Data
 Wisconsin Chronic Disease Quality Improvement Project HEDIS 2017 Summary Data CDQIP Results: HEDIS 2017 Data Year 19 of data collection for CDQIP Plans voluntarily submit HEDIS data for selected measures
Wisconsin Chronic Disease Quality Improvement Project HEDIS 2017 Summary Data CDQIP Results: HEDIS 2017 Data Year 19 of data collection for CDQIP Plans voluntarily submit HEDIS data for selected measures
AETNA BETTER HEALTH Brian Clark
 AETNA BETTER HEALTH Brian Clark Diana Charlton The webinar will begin shortly. 2017 Erin Goodard Aetna Inc. March 20181 The teenage years up to age 21 HEDIS measures, and a focus on maximizing administrative
AETNA BETTER HEALTH Brian Clark Diana Charlton The webinar will begin shortly. 2017 Erin Goodard Aetna Inc. March 20181 The teenage years up to age 21 HEDIS measures, and a focus on maximizing administrative
BlueAdvantage (PPO) SM. and BlueChoice (HMO) SM. BlueCare Plus (HMO SNP) SM
 We value your partnership and participation in the 2017 Quality Rewards Program, and hope you will find this guide helpful. It will provide information and tips to assist you in maximizing your STAR rating
We value your partnership and participation in the 2017 Quality Rewards Program, and hope you will find this guide helpful. It will provide information and tips to assist you in maximizing your STAR rating
Medicare & Dual Options Annual Comprehensive Exam FAX COMPLETED FORM TO: Patient Personal Information
 FAX COMPLETED FM TO: 877-682-2216 All fields marked with an * are required to be completed in order to receive payment for the ACE Form, unless indicated otherwise. Please refer to the document titled
FAX COMPLETED FM TO: 877-682-2216 All fields marked with an * are required to be completed in order to receive payment for the ACE Form, unless indicated otherwise. Please refer to the document titled
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015
 Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
Medicare Advantage Measurement Period Handbook for Enhanced Personal Health Care Measurement Period beginning January 1, 2015 Amerivantage is an HMO plan with a contract with the New Mexico Medicare program.
2017 Performance Recognition Program PROVIDER INCENTIVE PROGRAM FOR: BCN HMO SM Commercial BCN Advantage SM Blue Cross Medicare Plus Blue SM PPO
 Confidence comes with every card. 2017 Performance Recognition Program PROVIDER INCENTIVE PROGRAM FOR: BCN HMO SM Commercial BCN Advantage SM Blue Cross Medicare Plus Blue SM PPO Revised October 2017 CONTENTS
Confidence comes with every card. 2017 Performance Recognition Program PROVIDER INCENTIVE PROGRAM FOR: BCN HMO SM Commercial BCN Advantage SM Blue Cross Medicare Plus Blue SM PPO Revised October 2017 CONTENTS
HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING
 HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING ATTENTION-DEFICIT/HYPERACTIVITY DISORDER 1. Follow-up Care for Children Prescribed ADHD Medication (ADD) Percent children newly
HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING ATTENTION-DEFICIT/HYPERACTIVITY DISORDER 1. Follow-up Care for Children Prescribed ADHD Medication (ADD) Percent children newly
FAMILY MEDICINE PRACTICES
 2018 Primary Care Provider Quality Improvement Program (PCP QIP) Measurement Specifications FAMILY MEDICINE PRACTICES Developed by: The QIP Team QIP@partnershiphp.org Published: November 28, 2017 Updated:
2018 Primary Care Provider Quality Improvement Program (PCP QIP) Measurement Specifications FAMILY MEDICINE PRACTICES Developed by: The QIP Team QIP@partnershiphp.org Published: November 28, 2017 Updated:
HEDIS Adult Resource Guide
 HEDIS Adult Resource Guide What s Inside Adult Resource Guide Adult and Behavioral Health Measures 1 What is HEDIS? 2 HEDIS Reference Guide for Adults 16 How to Be a Quality Star 17 Medicare STAR Measures
HEDIS Adult Resource Guide What s Inside Adult Resource Guide Adult and Behavioral Health Measures 1 What is HEDIS? 2 HEDIS Reference Guide for Adults 16 How to Be a Quality Star 17 Medicare STAR Measures
Quality measures a for measurement year 2016
 Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
2016 PQRS Diabetes Measures Group
 Measures #1 : Hemoglobin A1c Poor Control #110 Preventive Care and Screening: Influenza Immunization #117 : Eye Exam #119 : Medical Attention for Nephropathy #126 Mellitus: Diabetic Foot and Ankle Care,
Measures #1 : Hemoglobin A1c Poor Control #110 Preventive Care and Screening: Influenza Immunization #117 : Eye Exam #119 : Medical Attention for Nephropathy #126 Mellitus: Diabetic Foot and Ankle Care,
QUALITY IMPROVEMENT Section 9
 Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Provider Toolkit. Y0067_PR_Tlkt_0316 IA 03/09/2016
 Provider Toolkit 2016 2017 Y0067_PR_Tlkt_0316 IA 03/09/2016 PFFS/PPO/TOHMO TABLE OF CONTENTS Sample Letter from Physician to Patient...4 HEDIS Quick Reference Guide...5 Fax Cover Sheet...10 Preventive
Provider Toolkit 2016 2017 Y0067_PR_Tlkt_0316 IA 03/09/2016 PFFS/PPO/TOHMO TABLE OF CONTENTS Sample Letter from Physician to Patient...4 HEDIS Quick Reference Guide...5 Fax Cover Sheet...10 Preventive
Hedis Behavioral Health Measures
 Hedis Behavioral Health Measures Generating better health outcomes and improving HEDIS scores is a positive outcome for everyone. Magellan Complete Care is offering support by providing the details of
Hedis Behavioral Health Measures Generating better health outcomes and improving HEDIS scores is a positive outcome for everyone. Magellan Complete Care is offering support by providing the details of
Medicare Advantage and BlueCare Plus
 Medicare Advantage and BlueCare Plus QUALITY CARE REWARDS PROGRAM MEASURES 2017 We value your partnership and participation in the 2017 Quality Rewards Program, and hope you will find this guide helpful.
Medicare Advantage and BlueCare Plus QUALITY CARE REWARDS PROGRAM MEASURES 2017 We value your partnership and participation in the 2017 Quality Rewards Program, and hope you will find this guide helpful.
2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW
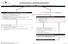 2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW REMEMBER! Abstract only those cases belonging to your ACO and use only MiShare (https://mishare.med.umich.edu/) when communicating PHI! STEP 1:
2017 CMS Quality Reporting - ABSTRACTION PROCESS OVERVIEW REMEMBER! Abstract only those cases belonging to your ACO and use only MiShare (https://mishare.med.umich.edu/) when communicating PHI! STEP 1:
Consensus Core Set: ACO and PCMH / Primary Care Measures Version 1.0
 Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Validating and Reporting the 2017 ACO Clinical Measures (Version 1)
 Validating and Reporting the 2017 ACO Clinical Measures Author: Ben Fouts, Informatics Redwood Community Health Coalition 1310 Redwood Way Petaluma, California 94954 support@rchc.net Document Last Updated:
Validating and Reporting the 2017 ACO Clinical Measures Author: Ben Fouts, Informatics Redwood Community Health Coalition 1310 Redwood Way Petaluma, California 94954 support@rchc.net Document Last Updated:
A Partnership in Quality Reporting. Effectiveness of Care: Prevention and Screening
 A Partnership in Quality Reporting Effectiveness of Care: Prevention and Screening Codes to Identify Well-Child Visits Completed during First 15 Months of Life ICD-9-CM Diagnosis Codes 99381, 99382, 99391,
A Partnership in Quality Reporting Effectiveness of Care: Prevention and Screening Codes to Identify Well-Child Visits Completed during First 15 Months of Life ICD-9-CM Diagnosis Codes 99381, 99382, 99391,
Quality Care Plus 2015 Primary Care Physician Incentive Program. Now includes Medicare patients!
 Quality Care Plus 2015 Primary Care Physician Incentive Program Now includes Medicare patients! Health Partners Plans (HPP) would like to express our appreciation for the invaluable role our primary care
Quality Care Plus 2015 Primary Care Physician Incentive Program Now includes Medicare patients! Health Partners Plans (HPP) would like to express our appreciation for the invaluable role our primary care
ABCBS PCMH Specifications. ARKANSAS BLUE CROSS and BLUE SHIELD An Independent Licensee of the Blue Cross and Blue Shield Association
 ABCBS PCMH 2016 Specifications An Independent Licensee of the Blue Cross and Blue Shield Association Table of Contents I. Terminology 3 II. Transformation Activities 2016 List of Activities 4 3 month 5-9
ABCBS PCMH 2016 Specifications An Independent Licensee of the Blue Cross and Blue Shield Association Table of Contents I. Terminology 3 II. Transformation Activities 2016 List of Activities 4 3 month 5-9
HEDIS/QARR 2017 Quick Reference Guide ALL MEASURES
 2017 HEDIS s HEDIS/QARR 2017 Quick Reference Guide ALL MEASURES Measure Age Band Denominator Event Numerator Requirement Line of Business AAB Avoidance of Antibiotic Treatment in Adults with Acute Bronchitis
2017 HEDIS s HEDIS/QARR 2017 Quick Reference Guide ALL MEASURES Measure Age Band Denominator Event Numerator Requirement Line of Business AAB Avoidance of Antibiotic Treatment in Adults with Acute Bronchitis
