Aalborg Universitet. Published in: Acta Oncologica. DOI (link to publication from Publisher): / X
|
|
|
- Garry Morton
- 5 years ago
- Views:
Transcription
1 Aalborg Universitet A five-factor biomarker profile obtained week 4-12 of treatment for improved prognostication in metastatic renal cell carcinoma Soerensen, Anne V; Geertsen, Poul F; Christensen, Ib J; Hermann, Gregers G; Jensen, Niels V; Fode, Kirsten; Petersen, Astrid Christine; Sandin, Rickard; Donskov, Frede Published in: Acta Oncologica DOI (link to publication from Publisher): / X Creative Commons License CC BY-NC-ND 3.0 Publication date: 2016 Document Version Publisher's PDF, also known as Version of record Link to publication from Aalborg University Citation for published version (APA): Soerensen, A. V., Geertsen, P. F., Christensen, I. J., Hermann, G. G., Jensen, N. V., Fode, K.,... Donskov, F. (2016). A five-factor biomarker profile obtained week 4-12 of treatment for improved prognostication in metastatic renal cell carcinoma: Results from DARENCA study 2. Acta Oncologica, 55(3), DOI: / X General rights Copyright and moral rights for the publications made accessible in the public portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognise and abide by the legal requirements associated with these rights.? Users may download and print one copy of any publication from the public portal for the purpose of private study or research.? You may not further distribute the material or use it for any profit-making activity or commercial gain? You may freely distribute the URL identifying the publication in the public portal? Take down policy If you believe that this document breaches copyright please contact us at vbn@aub.aau.dk providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from vbn.aau.dk on: september 18, 2018
2 Acta Oncologica ISSN: X (Print) X (Online) Journal homepage: A five-factor biomarker profile obtained week 4 12 of treatment for improved prognostication in metastatic renal cell carcinoma: Results from DARENCA study 2 Anne V. Soerensen, Poul F. Geertsen, Ib J. Christensen, Gregers G. Hermann, Niels V. Jensen, Kirsten Fode, Astrid Petersen, Rickard Sandin & Frede Donskov To cite this article: Anne V. Soerensen, Poul F. Geertsen, Ib J. Christensen, Gregers G. Hermann, Niels V. Jensen, Kirsten Fode, Astrid Petersen, Rickard Sandin & Frede Donskov (2016) A fivefactor biomarker profile obtained week 4 12 of treatment for improved prognostication in metastatic renal cell carcinoma: Results from DARENCA study 2, Acta Oncologica, 55:3, , DOI: / X To link to this article: Taylor & Francis View supplementary material Published online: 08 Oct Submit your article to this journal Article views: 530 View related articles View Crossmark data Citing articles: 5 View citing articles Full Terms & Conditions of access and use can be found at
3 ACTA ONCOLOGICA, 2016 VOL. 55, NO. 3, ORIGINAL ARTICLE A five-factor biomarker profile obtained week 4 12 of treatment for improved prognostication in metastatic renal cell carcinoma: Results from DARENCA study 2 ANNE V. SOERENSEN 1, POUL F. GEERTSEN 1, IB J. CHRISTENSEN 2, GREGERS G. HERMANN 3, NIELS V. JENSEN 4, KIRSTEN FODE 5, ASTRID PETERSEN 6, RICKARD SANDIN 7 & FREDE DONSKOV 5 1 Department of Oncology, Herlev Hospital, University of Copenhagen, Herlev, Denmark, 2 The Finsen Laboratory, Rigshospitalet and Biotech Research and Innovation Centre (BRIC), University of Copenhagen, Copenhagen, Denmark, 3 Department of Urology, Rigshospitalet, University of Copenhagen, Copenhagen, Denmark, 4 Department of Oncology, Odense University Hospital, Odense, Denmark, 5 Department of Oncology, Aarhus University Hospital, Aarhus, Denmark, 6 Department of Pathology, Aalborg University Hospital, Aalborg, Denmark, and 7 Pfizer Oncology, Sollentuna, Sweden ABSTRACT Background: Several biomarkers of treatment efficacy have been associated with a better prognosis in patients with metastatic renal cell carcinoma (mrcc). The prognostic significance of biomarkers in the early treatment phase is unclear. Material and methods: In a complete national cohort of mrcc patients receiving first-line tyrosine kinase inhibitors (TKI) or interleukin-2 based immunotherapy (IT) from 2006 to 2010, overall survival (OS) was analysed for baseline International mrcc Database Consortium (IMDC) classification factors and on-treatment time-dependent biomarkers obtained day 1 each cycle week 4 12 after treatment initiation with multivariate analysis and bootstrap validation. Results: A total of 735 patients received first-line TKI (59%) or IT (41%). Median OS was overall 14.0 months and 33.4, 18.5, and 5.8 months for baseline IMDC favourable, intermediate, and poor risk groups, respectively (p ). Systolic blood pressure 140 mmhg, neutrophils5lower level of normal (LLN), platelets5lln, sodium LLN, and LDH 1.5 times upper level of normal after treatment initiation were significantly associated with favourable OS independent of baseline IMDC risk group in multivariate analyses stratified for TKI and IT (p 0.04). Concordance (C)-index for IMDC classification alone was (95% CI ) and combined with the five-factor biomarker profile (95% CI ). For patients with good (3 5 factors) and poor (0 2 factors) biomarker profile median OS were 23.5 and 9.6 months, respectively (p ). Adding the fivefactor biomarker profile significantly improved prognostication in IMDC intermediate (25.7 vs months, p ) and poor (12.8 vs. 6.4 months, p ) risk groups. A trend was seen in IMDC favourable risk group (38.9 vs months, p ¼ 0.112). Conclusion: On-treatment hypertension, neutropenia, thrombocytopenia, LDH below 1.5 times upper level of normal, and normal sodium, obtained week 4 12 of treatment, are independent biomarkers of favourable outcome in mrcc, independent of treatment type. HISTORY Received 19 May 2015 Revised 27 August 2015 Accepted 2 September 2015 Published online 7 October 2015 The introduction of tyrosine kinase inhibitors (TKI) has resulted in a major change in the treatment of patients with metastatic renal cell carcinoma (mrcc). Overall survival (OS) has been improved and a higher number of patients are now able to receive treatment compared with the cytokine era [1]. However, mrcc is a heterogeneous disease where patients vary with regard to their disease course and many real-life patients still have a poor outcome. An early identification of patients with a higher probability to benefit from treatment would aid the clinical decision whether to keep these patients on treatment or consider alternative treatment options. Biomarkers to improve prognostication or to predict responsiveness to a particular treatment are therefore highly needed. For patients treated with TKI, the development of hypertension [2 4], hypothyroidism [5], or thrombocytopenia [4] during treatment have independently been associated with improved OS. The development of neutropenia [4] during treatment or normal baseline sodium [6 8] have independently been associated with favourable outcome both for patients treated with TKI or immunotherapy. However, adding these biomarkers to established prognostic models [9 13] have not been attempted and the clinical implication of the biomarkers restricted to the early treatment phase is unknown. The aim of this study was to assess paraclinical data obtained week 4 12 after treatment initiation in a complete national cohort of mrcc patients and to integrate Correspondence: A. V. Soerensen, Department of Oncology, Herlev University Hospital, Herlev Ringvej 75, 2730 Herlev, Denmark. Tel: Fax: Anne.Vest.Soerensen@regionh.dk ß 2015 Taylor & Francis. This is an open-access article distributed under the terms of the CC-BY-NC-ND 3.0 License which permits users to download and share the article for non-commercial purposes, so long as the article is reproduced in the whole without changes, and provided the original source is credited. ß 2015 Taylor & Francis
4 342 A. V. SOERENSEN ET AL. independent biomarkers in an established prognostic model in order to improve prognostication. Patients and methods This population-based analysis comprised a complete national cohort of Danish patients who received TKI (sorafenib and sunitinib) or interleukin-2 (IL2)-based immunotherapy (subcutaneous low-dose IL2 mainly administered as a two-week on/two-week off schedule and interferon-alpha given four weeks on) as first-line treatment from 1 January 2006 to 31 December The clinical results have previously been published [1]. A central pathology review confirmed mrcc. Baseline patient characteristics, outcome data, and paraclinical data were collected retrospectively with uniform data collection templates. Blood pressure (BP) and blood samples (BS) were measured on day 1 in each cycle for the first 12-week on treatment (week 4 12). BS were standardised to upper (ULN) and lower level of normal (LLN) for the treating hospital. If neutrophils or platelets were measured below LLN, haemoglobin or sodium at or above LLN, calcium at or below ULN, LDH at or below 1.5 ULN, and thyroid-stimulating hormone (TSH) above ULN at any time after baseline but within or equal to 12 week (week 4 12) after treatment initiation the patient would remain in the category despite subsequent reversal of values. Hypertension was defined as systolic BP (SBP) above or equal to 140 mmhg or diastolic BP (DBP) above or equal to 90 mmhg. Statistical analysis OS was defined from start of first-line treatment to death of any cause. Patients alive were censored at time of last follow-up. Data were right-censored. Patients who emigrated (n ¼ 4) were censored at time of last contact. OS was calculated with Kaplan-Meier method and median follow-up with the reverse Kaplan-Meier method. All analyses were complete cases. BS and BP within 12 weeks (week 4 12) after treatment initiation were analysed as binary time-dependent covariates along with baseline IMDC risk groups in a univariate Cox proportional hazard model. A multivariable time-dependent Cox regression analysis with time-dependent covariates and baseline IMDC risk groups including covariates with a univariate p 0.1 was performed. The model was then reduced retaining covariates with two-sided p The model was stratified for TKI and IL2-based therapies after prior test for interaction between drug and time-dependent covariates and analysed separately for TKI and IL2-based therapy. A prognostic index was constructed based on all significant time-dependent covariates from the stratified multivariate model. A forest plot was created to demonstrate the effect of adding covariates to the index by assigning all significant timedependent variables 1 point each except LDH and then scored by the sum. The multivariate model was validated internally with bootstrap analysis with 300 random samples. Concordance (C)- index was used to evaluate both the original and the bootstrap models predictive accuracy where a value of 0.5 represents no predictive accuracy and 1 represents complete accuracy that is patients predicted to survive will actually survive [14]. Database management and statistical calculations were performed using SAS (v9.3, SAS Institute, Cary, NC, USA) and R [R Core Team (2013)]. Ethics The study was approved by the Danish Health Authorities, the Danish Research Ethics Committee and the Danish Data Protection Agency. The study was registered with ClinicalTrials.gov NCT Results Patients Patient characteristics are summarised in Table I. A total of 735 patients started first-line treatment; 431 patients received TKI (sunitinib, n ¼ 364; sorafenib, n ¼ 67) and 304 patients received IL2-based immunotherapy. A flowchart is shown in Figure 1. In total 596 (81%) of the 735 patients received at least a second cycle and were evaluable for time-dependent analyses. After initiation but within 12-week (week 4 12) treatment 451 (82%), 88 (16%), and 153 (28%) patients had sodium LLN, platelets5lln, and neutrophils5lln, respectively. A total of 224 (56%) patients had SBP 140 mmhg (Table II) of which 50 patients were treated with IL2-based immunotherapy. Median OS for all patients was 14.0 months [95% confidence interval (CI) ] and 33.4, 18.5, and 5.8 months for IMDC favourable, intermediate, and poor risk group (p ), respectively, with a median follow-up of 50.2 months (range ). Median OS was 2.5 months (95% CI ) for the 139 patients who did not start a second cycle of treatment. Univariate analyses Univariate analyses were stratified for TKI and IL2-based immunotherapy. The time-dependent variables obtained within 12 weeks (week 4 12) after treatment initiation that were significantly associated with longer OS are given in Table II. SBP 140 mmhg and DBP 90 mmhg were both significantly associated with favourable OS but these were highly correlated (data not shown). SBP was therefore included in the multivariate analyses as the association with OS was the strongest. Patients with SBP 140 mmhg within 12 weeks (week 4 12) treatment had a median OS of 18.4 (95% CI ) versus 15.1 (95% CI ) months for patients with SBP5 140 mmhg (p ¼ ). Patients treated with IL2-based immunotherapy and SBP 140 mmhg had a median OS of 34.5 (95% CI ) versus 22.7 (95% CI 24.0 NA) months for patients with SBP5140 mmhg (p ¼ ). Patients with sodium LLN had a median OS of 19.8 (95% CI ) versus 8.3 (95% CI ) months for sodium5lln (p ). Few patients had complete data to examine changes from baseline to on-treatment, however, OS for 53 patients with normalisation of sodium (LLN) from baseline5lln was 11.5 (95% CI ) compared to 6.5 months (95% CI ) for 56 patients with unchanged sodium5lln (p ¼ ). Only 41 of 72 patients with baseline LDH41.5 times ULN
5 ACTA ONCOLOGICA 343 Table I. Baseline characteristics of patients receiving first-line TKI and IL2-based immunotherapy for metastatic renal cell carcinoma. Variable TKI a + IL2-based immunotherapy TKI a IL2-based immunotherapy Total number of patients (%) 735 (100) 431 (100) 304 (100) Emigrated (%) 4 (1) 4 (1) 0 (0) Median age (IQR) 63 (57 69) 66 (60-73) 60 (53 64) Male sex (%) 507 (69) 298 (69) 209 (69) PS 0 (%) 292 (40) 120 (28) 172 (57) 1 (%) 286 (39) 176 (41) 110 (36) 2 (%) 126 (17) 116 (27) 10 (3) 3 (%) 10 (1) 10 (2) 0 (0) NA (%) 21 (3) 9 (2) 12 (4) IMDC Favourable (%) 78 (11) 38 (9) 40 (13) Intermediate (%) 364 (50) 190 (44) 174 (57) Poor (%) 285 (39) 201 (47) 84 (28) NA (%) 8 (1) 2 (51) 6 (2) Known hypothyroidism (%) 24 (3) 14 (3) 10 (3) NA (%) 2 (51) 1 (51) 1 (51) TSH4ULN (%) 37 (6) 25 (8) 12 (5) NA (%) 150 (20) 111 (26) 39 (13) Known hypertension (%) 332 (45) 197 (46) 135 (44) NA (%) 1 (51) 1 (51) 0 (0) Systolic BP 140 mmhg (%) 252 (51) 189 (51) 63 (49) NA (%) 239 (33) 63 (15) 176 (58) Diastolic BP 90 mmhg (%) 183 (37) 130 (35) 53 (41) NA (%) 237 (32) 62 (14) 175 (58) Sodium5LLN (%) 182 (25) 133 (31) 49 (16) NA (%) 4 (1) 2 (51) 2 (1) Hemoglobin5LLN (%) 362 (49) 233 (54) 129 (43) NA (%) 2 (51) 0 (0) 2 (1) LDH41.5 times ULN (%) 72 (10) 55 (13) 17 (6) NA (%) 15 (2) 11 (3) 4 (1) Platelets4ULN (%) 207 (28) 131 (30) 76 (25) NA (%) 3 (51) 1 (51) 2 (1) Neutrophils4ULN (%) 222 (30) 166 (39) 56 (19) NA (%) 7 (1) 5 (1) 2 (1) Ca 2+ 4ULN (%) 159 (22) 94 (22) 65 (22) NA (%) 15 (2) 8 (2) 7 (2) Nephrectomy performed (%) 451 (61) 239 (55) 212 (70) Histology Clearcell (%) 606 (82) 342 (79) 264 (87) Non-clearcell (%) 118 (16) 83 (19) 35 (12) NA (%) 11 (1) 6 (1) 5 (2) Less than 1 year from diagnose (%) 548 (75) 329 (76) 219 (72) CNS metastases present (%) 52 (7) 47 (11) 5 (2) Liver metastases present (%) 156 (21) 105 (24) 51 (17) Metastatic sites 1 2 (%) 365 (50) 199 (46) 166 (55) More than 2 (%) 370 (50) 232 (54) 138 (45) a Sunitinib and sorafenib. BP, blood pressure; IL2, interleukin-2; IMDC, international mrcc Database Consortium; IQR, interquartile range; LDH, lactate dehydrogenase; LLN, lower level of normal; NA, not applicable; PS, performance status; TKI, tyrosine kinase inhibitor; TSH, thyroidea stimulating hormone; ULN, upper level of normal. Blood samples and blood pressures below or above levels are given as a proportion of the available samples. started a second cycle of first-line treatment. Twelve patients obtained LDH 1.5 times ULN within 12 weeks (week 4 12) of treatment resulting in almost doubling OS to 7.7 (95% CI 6.5 NA) compared to 4.1 (95% CI ) months for 20 patients with unchanged LDH levels41.5 times ULN (p ¼ ). Multivariate analysis There was an interaction between haemoglobin and treatment type; demonstrating an OS benefit for patients treated with IL2-based immunotherapy with normal haemoglobin values during therapy while there was no effect for TKI-treated patients. No other interactions between type of treatment and time-dependent covariates in the multivariate analyses were found (data not shown). Removal of haemoglobin from the multivariate analysis enabled stratification for TKI and IL2- based immunotherapy (Table III). Eight patients were excluded due to missing values. In multivariate analysis, LDH 1.5 times ULN within 12 weeks (week 4 12) after treatment initiation was the strongest predictor of OS among the five significant time-dependent covariates with a hazard ratio (HR) of 0.45 (95% CI , p ). Sodium LLN was independently associated with improved OS with HR of 0.63 (95% CI , p ¼ ). Similar significant HRs for OS were observed for SBP 140 mmhg, and neutrophils or platelets5lln. These time-dependent covariates were significantly associated with OS independent of baseline IMDC risk group status. Comparable results were seen if DBP was used instead of SBP (data not shown). The C-index for baseline IMDC risk group
6 344 A. V. SOERENSEN ET AL. 9 patients received first-line treatment with mtor-inhibitors or dendritic cell vaccination 139 patients discontinued first-line treatment before the second cycle 129 patients had one or more (on treatment) missing value(s) of the variables in the index 5 patients had missing IMDC classification 744 patients with confirmed diagnose received first-line treatment for mrcc in Denmark patients were treated with firstline TKI or IL2-based immunotherapy 596 patients received at least a second cycle of first-line TKI or IL2-based immunotherapy 467 patients had complete data for the index analysis 462 patients had complete data for the index analysis and baseline IMDC classification Table II. Univariate analyses of time-dependent covariates after the first cycle but within the first 12 weeks (week 4 12) on first-line treatment of patients with mrcc stratified by TKI and IL2-based immunotherapy. N (%) HR 95% CI p-value Age 596 (100) Sex (male) 416 (70) Baseline PS 0 vs (46) NA 17 (3) Baseline IMDC risk group Favourable 71 (12) 1.00 Intermediate 322 (54) Poor 197 (33) NA 6 (1) Sodium LLN 451 (82) NA 44 (7) LDH 1.5 times ULN 466 (92) NA 92 (15) Platelets5LLN 88 (16) NA 38 (6) Neutrophils5LLN 153 (28) NA 42 (7) Systolic BP 140 mmhg 224 (56) NA 196 (33) Diastolic BP 90 mmhg 187 (47) NA 197 (33) TSH4ULN 70 (20) NA 250 (42) Hemoglobin LLN 276 (50) NA 40 (7) Ca 2+ ULN 441 (92) NA 118 (20) BP, blood pressure; CI, confidence interval; HR, hazard ratio; IL2, interleukin-2; IMDC, International mrcc Database Consortium; LDH, lactate dehydrogenase; mrcc, metastatic renal cell carcinoma; N, number; NA, not applicable; PS, performance status; TKI, tyrosine kinase inhibitor; TSH, thyroid stimulating hormone; ULN, upper Level of normal. Blood samples and blood pressure below or above levels are given as a proportion of the available samples. Figure 1. Flowchart of first-line patients with mrcc treated with TKI or IL2-based immunotherapy. IL2, interleukin-2; IMDC, International mrcc Database Consortium; mrcc, metastatic renal cell carcinoma; mtor, mammalian target of rapamycin; TKI, tyrosine kinase inhibitor. alone in this heterogeneous cohort was (CI ) and increased to (CI ) when baseline IMDC risk group was combined with the five time-dependent covariates. HRs were almost similar when multivariate analyses were restricted to patients treated with TKI and IL2-based therapy separately, but did not reach similar significance levels for all variables probably due to low patient numbers in subgroups (Supplementary Table I, available online at More extreme values within the first 12-weeks of treatment (week 4 12), such as neutropenia grade 2 ( /L) or higher levels of sodium than LLN were associated with even longer OS [HR 0.60 (95% CI , p ¼ using cut-off for neutrophils of /L]. Cut-offs with LLN and ULN were chosen because they are practical and easy-to-use in the routine clinic. It also illustrates that less extreme values are sufficient to predict outcome. Bootstrap validation The multivariate analysis was internally validated with 300 random bootstrap samples (Table III). The mean HRs were similar to the original model. The C-index from the bootstrap analysis with combined five covariates and IMDC risk groups was Biomarker index All significant time-dependent variables were assigned 1 point each: LDH 1.5 times ULN, SBP 140 mmhg, sodium LLN, neutrophils or platelets5lln. Any combinations of 1 5 biomarkers in a constructed biomarker index gradually reduced the HR for death with the lowest HR seen in the index comprising all five biomarkers (Figure 2A). LDH had higher weight than the other covariates (black bars in Figure 2B) but was still assigned 1 point to create a feasible and easy-to-use tool. Of 596 patients that received at least two cycles of treatment, 467 patients had complete data available. Patients were assigned a biomarker profile based on numbers of favourable features; good biomarker profile (3 5 biomarkers) and poor biomarker profile (0 2 biomarkers) with median OS from baseline of 23.5 (95% CI ) and 9.6 (95% CI ) months (p ), respectively (Table IV, Figure 3A). For the 462 patients with complete baseline and biomarker data, OS for IMDC favourable, intermediate, and poor risk group was 33.4 (95% CI ), 19.8 (95% CI ), and 9.0 (95% CI ) months, respectively. OS for patients with good versus poor biomarker profile in IMDC poor prognostic group was 12.8 (95% CI ) and 6.4 (95% CI ) months, respectively, and for patients in IMDC intermediate risk group 25.7 (95% CI ) and 12.0 (95% CI )
7 ACTA ONCOLOGICA 345 Table III. Multivariate analyses with bootstrap analysis of time-dependent covariates after the first cycle but within the first 12 weeks (week 4 12) on first-line treatment of patients with mrcc stratified by TKI and IL2-based immunotherapy. N ¼ 588. Multivariate analysis a Bootstrap analysis b HR 95% CI p-value Mean HR 95% CI p-value Baseline IMDC risk group Favourable versus poor Intermediate versus poor Biomarkers within 12 weeks Sodium LLN LDH 1.5 times ULN Platelets5LLN Neutrophils5LLN Systolic BP 140 mmhg a Time-dependent Cox proportional hazard model; b 300 samples. BP, blood pressure; CI, confidence interval; HR, hazard ratio; IL2, interleukin-2; IMDC, International mrcc Database Consortium; LDH, lactate dehydrogenase; LLN, lower level of normal; mrcc, metastatic renal cell carcinoma; TKI, tyrosine kinase inhibitor; ULN, upper level of normal. Figure 2. Forest plot of hazard ratio s (HR) for survival from combining biomarkers stratified for first-line treatment with tyrosine kinase inhibitors and interleukin-2 based immunotherapy. (A) HR for adding a favourable biomarker to the index adjusted for Heng risk group status. Combining all 5 favourable biomarkers resulted in the lowest HR compared to an index consisting of only two, three or four favourable biomarkers. 1. Any biomarker. 2. Any two biomarkers. 3. Any three biomarkers. 4. Any four biomarkers. 5. All five biomarkers. (B) HR of adding a biomarker to the index with (black bars) or without (red bars) LDH to assess the impact of LDH on the index. 1. Any biomarker not containing LDH. 2. LDH alone. 3. Any two biomarkers not containing LDH. 4. LDH and any biomarker. 5. Any three biomarkers not containing LDH. 6. LDH and any two biomarkers. 7. All four biomarkers not containing LDH. 8. LDH and any three biomarkers. months (both p ), respectively (Table V and Figure 3B, C and D). A separation of OS per biomarker profile was observed for patients in IMDC favourable risk group [38.9 (95% CI 29.7 NA) and 28.7 (95% CI 23.4 NA) months, p ¼ 0.112], though not significant probably due to the low number of patients (n ¼ 57). Discussion This study is to our knowledge the first to demonstrate that systolic hypertension, neutropenia, thrombocytopenia, LDH 1.5 times ULN, and normal sodium assessed week 4 12 after treatment initiation are independent prognostic biomarkers associated with improved OS for patients with mrcc. These five biomarkers were able to predict OS independent of baseline IMDC variables and irrespectively of treatment type and may therefore be considered as true prognostic factors. Adjusted for baseline IMDC classification the biomarker index provided additional significant prognostic information for patients in IMDC intermediate and poor prognostic groups and also provided prognostic information in IMDC favourable group, albeit not statistically significant, probably due to the
8 346 A. V. SOERENSEN ET AL. low number of patients. Our findings may reflect treatmentinduced tumour biology alterations suggesting that prognostic risk features are dynamic variables instead of static that need readjustment during treatment. Along with the detection of new biomarkers [15] inclusion of biomarkers in established prognostic models [9 13] is needed for improved prognostication and individualised therapies for patients [16]. Our biomarker index is readily available, easily obtained, and routinely measured during clinical visit. Importantly, the biomarker index provide clinically meaningful information by adjusting prognosis and early counselling especially for poor and intermediate risk patients before the first computed tomography assessment routinely obtained at a three-month time point on top of baseline IMDC prognostic stratification. Low sodium at baseline has been shown to predict poor OS for both targeted therapy and immunotherapy [6 8] but the Table IV. Biomarker index. On-treatment biomarkers a Observation Points Sodium LLN 1 5LLN 0 LDH 1.5 times ULN times ULN 0 Platelets 5LLN 1 LLN 0 Neutrophils 5LLN 1 LLN 0 Systolic blood pressure 140 mmhg mmhg 0 a Measured after treatment start and within 12 weeks of treatment. LDH, lactate dehydrogenase; LLN, lower level of normal; ULN, upper level of normal. Good biomarker profile: 3 5 points. Poor biomarker profile: 0 2 points. significance of reversal to normal sodium during treatment has until now been unknown. The mechanism behind hyponatraemia is not clearly understood but a relation to chronic inflammation caused by elevated interleukin-6 has been suggested [7,17]. Hyponatraemia could also be caused by renal impairment though both Jeppesen et al. [6] and Kawashima et al. [7] could not find a correlation between hyponatraemia and estimated glomerular filtration rate, adrenal metastases, or nephrectomy. Similarly, Marfarlane et al. [18] found that impaired renal function did not impact objective response or OS for patients treated with vascular endothelial growth factor (VEGF)-targeted therapy. Other factors, such as co-morbidity or diuretics [19,20] could influence the development of hyponatraemia and this area needs further research. Elevated LDH at baseline has been shown to predict poor OS in patients with mrcc [9,11,12,16] but the significance of LDH below 1.5 times ULN during treatment has not been analysed previously. In our analysis LDH had higher weight with HR of 0.45 compared to other biomarkers. However, to establish a simple and easy-to-use tool all variables were assigned 1 point each in the biomarker index. Elevated TSH has been associated with improved outcome by others [3,5,21,22] but was not associated with OS in our study. Many of our patients did not have TSH measured prior to each treatment cycle which resulted in a high amount of missing values and this may have influenced our results. Several studies have shown that adverse events, such as hypertension, thrombocytopenia and neutropenia are biomarkers of efficacy in patients treated with targeted therapy [2 5]. We validated these findings and also extended the findings to be evident during the early treatment phase independent of type of therapy. However, it is counterintuitive that hypertension is a biomarker of efficacy in IL2-based Figure 3. Kaplan-Meier estimates of median overall survival (OS) per biomarker profile and combined with baseline International Metastatic renal cell carcinoma Database Consortium (IMDC) risk group status. A good biomarker profile comprised 3 5 biomarkers within 12-weeks after treatment initiation and a poor profile 0 2 biomarkers. (A) OS for patients with a good versus poor biomarker profile. (B) OS for patients in IMDC favourable risk group with a good versus poor biomarker profile. (C) OS for patients in IMDC intermediate risk group with a good versus poor biomarker profile. (D) OS for patients in IMDC poor risk group with a good versus poor biomarker profile.
9 ACTA ONCOLOGICA 347 Table V. Overall survival per biomarker profile per IMDC risk group for patients with mrcc stratified by TKI and IL2-based immunotherapy. IMDC risk group Biomarker profile N % Alive OS 95% CI p-value Favourable Good NA Poor NA Intermediate Good Poor Poor Good Poor CI, confidence interval; IL2, interleukin-2; IMDC, International mrcc Database Consortium; mrcc, metastatic renal cell carcinoma; N, number; NA, not applicable; OS, overall survival; TKI, tyrosine kinase inhibitors. immunotherapy as it often results in hypotension when administered. Both activation of the endothelin-1 axis [23] and inhibition of vascular relaxation due to decreased production of nitric oxide have been mentioned to lead to hypertension which is a group effect of VEGF inhibitors [24]. Whether hypertension between IL-2 courses is due to the same mechanism is unclear. BP values were obtained at every cycle initiation after a two-week treatment break from IL2 which may explain our findings as it could be related to baseline hypertension [2]. Multivariate analyses looking at changes from baseline to on-treatment values were not possible due to a high amount of missing values. We have recently shown that implementation of targeted therapy did not lead to an increase in total health care costs per patient per treatment year compared with a pre-tki era [25]. However, we have also previously shown that patients in IMDC poor prognostic group had limited OS benefit from treatment [1]. The implication of our present study is that baseline adverse prognostic features established by Motzer and IMDC [9,10] can be supplemented with early on-treatment biomarkers for improved prognostication thereby better identifying patients that will benefit from treatment. Adding the prognostic index to IMDC poor risk group adjusted prognostication as patients with a good biomarker profile during early treatment had doubled OS compared to patients with a poor biomarker profile. Similar separation was observed for IMDC intermediate prognostic group and a trend was seen in the favourable group. Thus, the biomarker index identifies a subgroup of IMDC patients that achieve clear survival benefit from treatment. This tool may therefore aid clinicians with supplementary prognostic information to guide treatment counselling with the patient. However, our index needs validation in another cohort and further testing of the relation to outcome in patients treated with mammalian target of rapamycin (mtor)-inhibitors is needed as well as prospective testing. Limitations are the retrospective design, missing data and low number of patients in IMDC favourable risk. Not all available published baseline prognostic factors were included in the multivariate model. However, we controlled for IMDC status as no other prognostic models have shown improved accuracy [13]. Also, the effect of the biomarkers may have been underestimated as they were measured day 1 each cycle after a treatment break for sunitinib and IL-2. Conclusion On-treatment hypertension, neutropenia, thrombocytopenia, LDH below 1.5 times upper level of normal, and normal sodium, obtained week 4 12 of treatment, are independent biomarkers of favourable outcome in mrcc, independent of treatment type. Acknowledgements This work was supported by Pfizer; Axel Muusfeldts fund; Christian Larsen and judge Ellen Larsens fund; Else and Mogens Wedell-Wedellsborgs Fund; Timber merchant Johannes Fogs Fund; Svend H.A. Schroeder and wife Ketty K. Larsen Fund; Novartis grant and the Department of Oncology and Research Fund at Herlev University Hospital. Results of this study were presented at the 2014 ESMO conference September 26 30, 2014, Madrid, Spain (poster presentation). Declaration of interest: A.V. Soerensen has received travel grants to conferences and research grants from Pfizer and Novartis. F. Donskov has received research grants from the research fund of central Denmark Region, Novartis and GSK. R. Sandin is an employee at Pfizer and has stockownership in Pfizer. All remaining authors have no conflict of interest. References 1. Soerensen AV, Donskov F, Hermann GG, Jensen NV, Petersen A, Spliid H, et al. Improved overall survival after implementation of targeted therapy for patients with metastatic renal cell carcinoma: Results from the Danish Renal Cancer group (DARENCA) study-2. Eur J Cancer 2014;50: Rini BI, Cohen DP, Lu DR, Chen I, Hariharan S, Gore ME, et al. Hypertension as a biomarker of efficacy in patients with metastatic renal cell carcinoma treated with sunitinib. J Natl Cancer Inst 2011;103: Bono P, Rautiola J, Utriainen T, Joensuu H. Hypertension as a predictor of sunitinib treatment outcome in metastatic renal cell carcinoma. Acta Oncol 2011;50: Rautiola J, Donskov F, Peltola K, Joensuu H, Bono P. Sunitinib-induced hypertension, neutropenia and thrombocytopenia as predictors of good prognosis in metastatic renal cell carcinoma patients. BJU Int Epub 2014 Sep Schmidinger M, Vogl UM, Bojic M, Lamm W, Heinzl H, Haitel A, et al. Hypothyroidism in patients with renal cell carcinoma: Blessing or curse? Cancer 2011;117: Jeppesen AN, Jensen HK, Donskov F, Marcussen N, von der Maase H. Hyponatremia as a prognostic and predictive factor in metastatic renal cell carcinoma. Br J Cancer 2010;102: Kawashima A, Tsujimura A, Takayama H, Arai Y, Nin M, Tanigawa G, et al. Impact of hyponatremia on survival of patients with metastatic renal cell carcinoma treated with molecular targeted therapy. Int J Urol 2012;19: Schutz FA, Xie W, Donskov F, Sircar M, McDermott DF, Rini BI, et al. The impact of low serum sodium on treatment outcome of targeted therapy in metastatic renal cell carcinoma: Results from the International Metastatic Renal Cell Cancer Database Consortium. Eur Urol 2014;65: Motzer RJ, Mazumdar M, Bacik J, Berg W, Amsterdam A, Ferrara J. Survival and prognostic stratification of 670 patients with advanced renal cell carcinoma. J Clin Oncol 1999;17:
10 348 A. V. SOERENSEN ET AL. 10. Heng DY, Xie W, Regan MM, Warren MA, Golshayan AR, Sahi C, et al. Prognostic factors for overall survival in patients with metastatic renal cell carcinoma treated with vascular endothelial growth factortargeted agents: Results from a large, multicenter study. J Clin Oncol 2009;27: Motzer RJ, Bacik J, Murphy BA, Russo P, Mazumdar M. Interferon-alfa as a comparative treatment for clinical trials of new therapies against advanced renal cell carcinoma. J Clin Oncol 2002;20: Manola J, Royston P, Elson P, McCormack JB, Mazumdar M, Négrier S, et al. Prognostic model for survival in patients with metastatic renal cell carcinoma: Results from the international kidney cancer working group. Clin Cancer Res 2011;17: Heng DY, Xie W, Regan MM, Harshman LC, Bjarnason GA, Vaishampayan UN, et al. External validation and comparison with other models of the International Metastatic Renal-Cell Carcinoma Database Consortium prognostic model: A population-based study. Lancet Oncol 2013;14: Harrell FE, Lee KL, Mark DB. Multivariate prognostic models: Issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat Med 1996;15: Tran HT, Liu Y, Zurita AJ, Lin Y, Baker-Neblett KL, Martin AM, et al. Prognostic or predictive plasma cytokines and angiogenic factors for patients treated with pazopanib for metastatic renal-cell cancer: A retrospective analysis of phase 2 and phase 3 trials. Lancet Oncol 2012;13: Donskov F, von der Maase H. Impact of immune parameters on longterm survival in metastatic renal cell carcinomas. J Clin Oncol 2006; 24: Hashizume M, Higuchi Y, Uchiyama Y, Mihara M. IL-6 plays an essential role in neutrophilia under inflammation. Cytokine 2011;54: Marfarlane R, Heng DY, Xie W, Knox JJ, McDermott DF, Rini BI, et al. The impact of kidney function on the outcome of metastatic renal cell carcinoma treated with vascular endothelial growth factor-targeted therapy. Cancer 2012;118: Spital A. Diuretic-induced hyponatremia. Am J Nephrol 1999;19: Gankam-Kengne F, Ayers C, Khera A, de Lemos J, Maalouf NM. Mild hyponatremia is associated with increased risk of death in an ambulatory setting. Kidney Int 2013;83: Riesenbeck LM, Bierer S, Hoffmeister I, Köpke T, Papavassilis P, Hertle L, et al. Hypothyroidism correlates with a better prognosis in metastatic renal cell cancer patients treated with sorafenib and sunitinib. World J Urol 2011;29: Franzke A, Peest D, Probst-Kepper M, Buer J, Kirchner GI, Brabant G, et al. Autoimmunity resulting from cytokine treatment predicts long-term survival in patients with metastatic renal cell cancer. J Clin Oncol 1999;17: Erratum in J Clin Oncol 1999;17: Lankhorst S, Kappers MH, van Esch JH, Danser AH, van der Meiracker AH. Hypertension during vascular endothelial growth factor inhibition: Focus on nitric oxide, endothelin-1, and oxidative stress. Antioxid Redox Signal 2014;20: Klümpen HJ, Samer CF, Mathijssen RH, Schellens JH, Gurney H. Moving towards dose individualization of tyrosine kinase inhibitors. Cancer Treat Rev 2011;37: Soerensen AV, Donskov F, Kjellberg J, Ibsen R, Hermann GG, Jensen NV, et al. Health economic changes as a result of implementation of targeted therapy for metastatic renal cell carcinoma: National results from Darenca study 2. Eur Urol 2014; 68: Supplementary Material available online. Supplementary Table I
Toxicity as a Biomarker
 Toxicity as a Biomarker Frede Donskov, M.D., PhD Chair, Danish Renal Cancer Group, DARENCA Aarhus University Hospital Denmark Thirteenth International COI Research funding from Novartis, GSK, Pfizer and
Toxicity as a Biomarker Frede Donskov, M.D., PhD Chair, Danish Renal Cancer Group, DARENCA Aarhus University Hospital Denmark Thirteenth International COI Research funding from Novartis, GSK, Pfizer and
Metastatic renal cancer (mrcc): Evidence-based treatment
 Metastatic renal cancer (mrcc): Evidence-based treatment José M. Ruiz Morales, M.D. Hospital Médica Sur April 18th, 2018 4th ESO-ESMO Latin American Masterclass in Clinical Oncology Disclosures Consulting:
Metastatic renal cancer (mrcc): Evidence-based treatment José M. Ruiz Morales, M.D. Hospital Médica Sur April 18th, 2018 4th ESO-ESMO Latin American Masterclass in Clinical Oncology Disclosures Consulting:
Characterization of Patients with Poor-
 Characterization of Patients with Poor- Risk Metastatic Renal Cell Carcinoma Hamieh L 1 *, McKay RR 1 *, Lin X 2, Simantov R 2, Choueiri TK 1 *Equal contributions 1 Dana-Farber Cancer Institute, Boston,
Characterization of Patients with Poor- Risk Metastatic Renal Cell Carcinoma Hamieh L 1 *, McKay RR 1 *, Lin X 2, Simantov R 2, Choueiri TK 1 *Equal contributions 1 Dana-Farber Cancer Institute, Boston,
Prognostic Factors for mrcc: Relevance in Clinical Practice
 Prognostic Factors for mrcc: Relevance in Clinical Practice Daniel Heng MD MPH FRCPC Chair, GU Tumor Group Tom Baker Cancer Center University of Calgary Prognostic Factors Patient Factors Performance Status
Prognostic Factors for mrcc: Relevance in Clinical Practice Daniel Heng MD MPH FRCPC Chair, GU Tumor Group Tom Baker Cancer Center University of Calgary Prognostic Factors Patient Factors Performance Status
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense?
 Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Surgical Management of Metastatic and Locally Recurrent Kidney Cancer: Does it Make Sense? Philippe E. Spiess, MD, FACS Associate Member Department of GU Oncology Department of Tumor Biology Moffitt Cancer
Prognostic Factors: Does It Really Matter if New Drugs for Targeted Therapy Will Be Used?
 european urology supplements 8 (2009) 478 482 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prognostic Factors: Does It Really Matter if New Drugs for Targeted Therapy Will
european urology supplements 8 (2009) 478 482 available at www.sciencedirect.com journal homepage: www.europeanurology.com Prognostic Factors: Does It Really Matter if New Drugs for Targeted Therapy Will
David N. Robinson, MD
 David N. Robinson, MD Background and Treatment of mrcc Background ~ 64,770 new cases of kidney/renal pelvis cancers will be diagnosed in the US in 2012 with an estimated 13,570 deaths [1] ~ 75% are clear-cell
David N. Robinson, MD Background and Treatment of mrcc Background ~ 64,770 new cases of kidney/renal pelvis cancers will be diagnosed in the US in 2012 with an estimated 13,570 deaths [1] ~ 75% are clear-cell
CANCER UROLOGY VOL. 12. P. S. Borisov 1, M. I. Shkol nik 2, R. V. Orlova 3, P. A. Karlov 1 DOI: /
 CANCER UROLOGY 3 6 VOL. The use of targeted therapies and selection of the optimal treatment sequence in heterogeneous population of patients with metastatic kidney cancer. Results of retrospective study
CANCER UROLOGY 3 6 VOL. The use of targeted therapies and selection of the optimal treatment sequence in heterogeneous population of patients with metastatic kidney cancer. Results of retrospective study
Introduction. Pawel Chrom, MD Rafal Stec, MD, PhD Lubomir Bodnar, MD, PhD Cezary Szczylik, MD, PhD. pissn , eissn
 pissn 1598-2998, eissn 25-9256 Original Article https://doi.org/1.414/crt.217. Open Access Incorporating Neutrophil-to-Lymphocyte Ratio and Platelet-to-Lymphocyte Ratio in Place of Neutrophil Count and
pissn 1598-2998, eissn 25-9256 Original Article https://doi.org/1.414/crt.217. Open Access Incorporating Neutrophil-to-Lymphocyte Ratio and Platelet-to-Lymphocyte Ratio in Place of Neutrophil Count and
pan-canadian Oncology Drug Review Stakeholder Feedback on a pcodr Request for Advice Axitinib (Inlyta) for Metastatic Renal Cell Carcinoma
 pan-canadian Oncology Drug Review Stakeholder Feedback on a pcodr Request for Advice Axitinib (Inlyta) for Metastatic Renal Cell Carcinoma Pfizer Canada Inc. June 29, 2017 3 Stakeholder Feedback on a pcodr
pan-canadian Oncology Drug Review Stakeholder Feedback on a pcodr Request for Advice Axitinib (Inlyta) for Metastatic Renal Cell Carcinoma Pfizer Canada Inc. June 29, 2017 3 Stakeholder Feedback on a pcodr
Management of High Risk Renal Cell Carcinoma
 Management of High Risk Renal Cell Carcinoma Peter E. Clark, MD Professor and Chair, Department of Urology Carolinas HealthCare System Chair, Urologic Oncology Levine Cancer Institute October 14, 2017
Management of High Risk Renal Cell Carcinoma Peter E. Clark, MD Professor and Chair, Department of Urology Carolinas HealthCare System Chair, Urologic Oncology Levine Cancer Institute October 14, 2017
Sustained Response to Temsirolimus in Chromophobe variant of Metastatic Renal Cell Carcinoma
 JOURNAL OF CASE REPORTS 2015;5(1):280-284 Sustained Response to Temsirolimus in Chromophobe variant of Metastatic Renal Cell Carcinoma Chanchal Goswami, Aditi Mandal B. P. Poddar Hospital & Medical Research
JOURNAL OF CASE REPORTS 2015;5(1):280-284 Sustained Response to Temsirolimus in Chromophobe variant of Metastatic Renal Cell Carcinoma Chanchal Goswami, Aditi Mandal B. P. Poddar Hospital & Medical Research
Timing of targeted therapy in patients with low volume mrcc. Eli Rosenbaum Davidoff Cancer Center Beilinson Hospital
 1 Timing of targeted therapy in patients with low volume mrcc Eli Rosenbaum Davidoff Cancer Center Beilinson Hospital 2 Wont be discussing: Symptomatic patients High volume disease Rapidly growing metastases
1 Timing of targeted therapy in patients with low volume mrcc Eli Rosenbaum Davidoff Cancer Center Beilinson Hospital 2 Wont be discussing: Symptomatic patients High volume disease Rapidly growing metastases
Dose individualization of sunitinib in mrcc: Toxicity-adjusted dose or Therapeutic drug monitoring
 Dose individualization of sunitinib in mrcc: Toxicity-adjusted dose or Therapeutic drug monitoring Alison Zhang 1, Peter Fox 1, Sally Coulter 4, Val Gebski 5, Bavanthi Balakrishnar 1, Christopher Liddle
Dose individualization of sunitinib in mrcc: Toxicity-adjusted dose or Therapeutic drug monitoring Alison Zhang 1, Peter Fox 1, Sally Coulter 4, Val Gebski 5, Bavanthi Balakrishnar 1, Christopher Liddle
Sergio Bracarda MD. Head, Medical Oncology Department of Oncology AUSL-8 Istituto Toscano Tumori (ITT) San Donato Hospital Arezzo, Italy
 Sergio Bracarda MD Head, Medical Oncology Department of Oncology AUSL-8 Istituto Toscano Tumori (ITT) San Donato Hospital Arezzo, Italy Ninth European International Kidney Cancer Symposium Dublin 25-26
Sergio Bracarda MD Head, Medical Oncology Department of Oncology AUSL-8 Istituto Toscano Tumori (ITT) San Donato Hospital Arezzo, Italy Ninth European International Kidney Cancer Symposium Dublin 25-26
Clinical Biomarker in Kidney Cancer. Maria Nirvana Formiga, M.D., Ph.D.
 Clinical Biomarker in Kidney Cancer Maria Nirvana Formiga, M.D., Ph.D. Disclosures I am on the Speaker s Bureau with Pfizer and Bayer Clinical trials of BMS and Pfizer Kidney Cancer 70% new cases in developed
Clinical Biomarker in Kidney Cancer Maria Nirvana Formiga, M.D., Ph.D. Disclosures I am on the Speaker s Bureau with Pfizer and Bayer Clinical trials of BMS and Pfizer Kidney Cancer 70% new cases in developed
Metastatic Renal Cancer Medical Treatment
 Metastatic Renal Cancer Medical Treatment Bohuslav Melichar, M.D., Ph.D. Professor and Head Department of Oncology Palacký University Medical School and Teaching Hospital Olomouc, Czech Republic Peculiarities
Metastatic Renal Cancer Medical Treatment Bohuslav Melichar, M.D., Ph.D. Professor and Head Department of Oncology Palacký University Medical School and Teaching Hospital Olomouc, Czech Republic Peculiarities
Have Results of Recent Randomized Trials Changed the Role of mtor Inhibitors?
 Have Results of Recent Randomized Trials Changed the Role of mtor Inhibitors? Bernard Escudier Institut Gustave Roussy Villejuif, France EIKCS Lyon April 2015 What is the current role of mtor inhibitors?
Have Results of Recent Randomized Trials Changed the Role of mtor Inhibitors? Bernard Escudier Institut Gustave Roussy Villejuif, France EIKCS Lyon April 2015 What is the current role of mtor inhibitors?
Linee guida terapeutiche oncologiche. Francesco Massari U.O.C. di Oncologia Medica d.u. Azienda Ospedaliera Universitaria Integrata Verona
 Linee guida terapeutiche oncologiche Francesco Massari U.O.C. di Oncologia Medica d.u. Azienda Ospedaliera Universitaria Integrata Verona 1 YOUNG SPECIALIST RENAL CARE Verona, 07-08 Marzo 2014 Clinical
Linee guida terapeutiche oncologiche Francesco Massari U.O.C. di Oncologia Medica d.u. Azienda Ospedaliera Universitaria Integrata Verona 1 YOUNG SPECIALIST RENAL CARE Verona, 07-08 Marzo 2014 Clinical
Efficacy and safety of advanced renal cell carcinoma patients treated with sorafenib: roles of cytokine pretreatment
 Efficacy and safety of advanced renal cell carcinoma patients treated with sorafenib: roles of cytokine pretreatment Hisanori Suzuki 1),2), Toshiro Suzuki 1),2), Osamu Ishizuka 1),2), Osamu Nishizawa 1),2),
Efficacy and safety of advanced renal cell carcinoma patients treated with sorafenib: roles of cytokine pretreatment Hisanori Suzuki 1),2), Toshiro Suzuki 1),2), Osamu Ishizuka 1),2), Osamu Nishizawa 1),2),
Sequencing of therapies in mrcc. Ari Hakimi MD Assistant Professor Urology Service, Department of Surgery MSKCC
 Sequencing of therapies in mrcc Ari Hakimi MD Assistant Professor Urology Service, Department of Surgery MSKCC Old Paradigm Sequencing approved agents VEGF TKI Sunitinib Pazopanib Axitinib TKI TKI MTORi
Sequencing of therapies in mrcc Ari Hakimi MD Assistant Professor Urology Service, Department of Surgery MSKCC Old Paradigm Sequencing approved agents VEGF TKI Sunitinib Pazopanib Axitinib TKI TKI MTORi
Medical Management of Renal Cell Carcinoma
 Medical Management of Renal Cell Carcinoma Lin Mei, MD Hematology-Oncology Fellow Hematology, Oncology and Palliative Care Virginia Commonwealth University Educational Objectives Background of RCC (epidemiology,
Medical Management of Renal Cell Carcinoma Lin Mei, MD Hematology-Oncology Fellow Hematology, Oncology and Palliative Care Virginia Commonwealth University Educational Objectives Background of RCC (epidemiology,
I Kid(ney) You Not: Updates on Renal Cell Carcinoma
 Disclosures I Kid(ney) You Not: Updates on Renal Cell Carcinoma Nothing to disclose Renee McAlister, PharmD, BCOP Clinical Pharmacist, GU/Melanoma Vanderbilt Ingram Cancer Center September 29, 2018 Objectives
Disclosures I Kid(ney) You Not: Updates on Renal Cell Carcinoma Nothing to disclose Renee McAlister, PharmD, BCOP Clinical Pharmacist, GU/Melanoma Vanderbilt Ingram Cancer Center September 29, 2018 Objectives
UPDATE FROM ASCO GU FEBRUARY 2018, SAN FRANCISCO, USA. Prof. David Pfister University Hospital of Cologne Germany RENAL CELL CARCINOMA
 UPDATE FROM ASCO GU FEBRUARY 2018, SAN FRANCISCO, USA Prof. David Pfister University Hospital of Cologne Germany RENAL CELL CARCINOMA DISCLAIMER Please note: The views expressed within this presentation
UPDATE FROM ASCO GU FEBRUARY 2018, SAN FRANCISCO, USA Prof. David Pfister University Hospital of Cologne Germany RENAL CELL CARCINOMA DISCLAIMER Please note: The views expressed within this presentation
Scottish Medicines Consortium
 Scottish Medicines Consortium sorafenib 200mg tablets (Nexavar ) (No. 321/06) Bayer Plc 6 October 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
Scottish Medicines Consortium sorafenib 200mg tablets (Nexavar ) (No. 321/06) Bayer Plc 6 October 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
The Therapeutic Landscape in Advanced Renal Cell Carcinoma
 The Therapeutic Landscape in Advanced Renal Cell Carcinoma Cora Sternberg, MD, FACP Chairman, Department of Medical Oncology San Camillo-Forlanini Hospital Rome, Italy What best describes the change in
The Therapeutic Landscape in Advanced Renal Cell Carcinoma Cora Sternberg, MD, FACP Chairman, Department of Medical Oncology San Camillo-Forlanini Hospital Rome, Italy What best describes the change in
Immunotherapy versus targeted treatments in metastatic renal cell carcinoma: The return game?
 Immunotherapy versus targeted treatments in metastatic renal cell carcinoma: The return game? Sylvie NEGRIER MD, PhD Centre Léon Bérard, Lyon Université Lyon I IMMUNOTHERAPY: A LONG AND WIDING ROAD! WHERE
Immunotherapy versus targeted treatments in metastatic renal cell carcinoma: The return game? Sylvie NEGRIER MD, PhD Centre Léon Bérard, Lyon Université Lyon I IMMUNOTHERAPY: A LONG AND WIDING ROAD! WHERE
Evidenze cliniche nel trattamento del RCC
 Criteri di scelta nel trattamento sistemico del carcinoma renale Evidenze cliniche nel trattamento del RCC Alessandro Morabito Unità Sperimentazioni Cliniche Istituto Nazionale Tumori di Napoli Napoli,
Criteri di scelta nel trattamento sistemico del carcinoma renale Evidenze cliniche nel trattamento del RCC Alessandro Morabito Unità Sperimentazioni Cliniche Istituto Nazionale Tumori di Napoli Napoli,
PROGNOSTIC FACTORS FOR SURVIVAL IN PATIENTS WITH METASTATIC RENAL CELL CARCINOMA TREATED WITH CHEMOTHERAPY
 Journal of IMAB ISSN: 1312-773X http://www.journal-imab-bg.org http://dx.doi.org/10.5272/jimab.2016221.1045 Journal of IMAB - Annual Proceeding (Scientific Papers) 2016, vol. 22, issue 1 PROGNOSTIC FACTORS
Journal of IMAB ISSN: 1312-773X http://www.journal-imab-bg.org http://dx.doi.org/10.5272/jimab.2016221.1045 Journal of IMAB - Annual Proceeding (Scientific Papers) 2016, vol. 22, issue 1 PROGNOSTIC FACTORS
Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients
 Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients Bradley Carthon, MD, PhD Assistant Professor, Genitourinary Medical Oncology Winship
Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients Bradley Carthon, MD, PhD Assistant Professor, Genitourinary Medical Oncology Winship
Negative Trials in RCC: Where Did We Go Wrong? Can We Do Better?
 Negative Trials in RCC: Where Did We Go Wrong? Can We Do Better? 9 th European Kidney Cancer Symposium, Dublin, April 2014 Tim Eisen Tim Eisen - Disclosures Company Research Support Advisory Board Trial
Negative Trials in RCC: Where Did We Go Wrong? Can We Do Better? 9 th European Kidney Cancer Symposium, Dublin, April 2014 Tim Eisen Tim Eisen - Disclosures Company Research Support Advisory Board Trial
Aalborg Universitet. Statistical analysis plan Riis, Allan; Karran, E. L. ; Jørgensen, Anette; Holst, S.; Rolving, N. Publication date: 2017
 Aalborg Universitet Statistical analysis plan Riis, Allan; Karran, E. L. ; Jørgensen, Anette; Holst, S.; Rolving, N. Publication date: 2017 Document Version Publisher's PDF, also known as Version of record
Aalborg Universitet Statistical analysis plan Riis, Allan; Karran, E. L. ; Jørgensen, Anette; Holst, S.; Rolving, N. Publication date: 2017 Document Version Publisher's PDF, also known as Version of record
CLINICAL INVESTIGATION of new agents and combination
 Interferon-Alfa as a Comparative Treatment for Clinical Trials of New Therapies Against Advanced Renal Cell Carcinoma By Robert J. Motzer, Jennifer Bacik, Barbara A. Murphy, Paul Russo, and Madhu Mazumdar
Interferon-Alfa as a Comparative Treatment for Clinical Trials of New Therapies Against Advanced Renal Cell Carcinoma By Robert J. Motzer, Jennifer Bacik, Barbara A. Murphy, Paul Russo, and Madhu Mazumdar
Plasma fibrinogen as prognostic predictor in patients with metastatic renal cell carcinoma receiving target therapy
 Original Article Plasma fibrinogen as prognostic predictor in patients with metastatic renal cell carcinoma receiving target therapy Lihe Wang 1#, Wen Cai 2#, Wen Kong 2, Jin Zhang 2, Yonghui Chen 2, Jiwei
Original Article Plasma fibrinogen as prognostic predictor in patients with metastatic renal cell carcinoma receiving target therapy Lihe Wang 1#, Wen Cai 2#, Wen Kong 2, Jin Zhang 2, Yonghui Chen 2, Jiwei
Medical treatment of metastatic renal cell carcinoma (mrcc) in the elderly ( 65y): Position of a SIOG Taskforce
 Medical treatment of metastatic renal cell carcinoma (mrcc) in the elderly ( 65y): Position of a SIOG Taskforce Medical treatment of metastatic RCC in the elderly ( 65y): Members of the SIOG Taskforce
Medical treatment of metastatic renal cell carcinoma (mrcc) in the elderly ( 65y): Position of a SIOG Taskforce Medical treatment of metastatic RCC in the elderly ( 65y): Members of the SIOG Taskforce
The Scandinavian Sarcoma Group skeletal metastasis register: Survival after surgery for bone metastases in the pelvis and extremities
 The Scandinavian Sarcoma Group skeletal metastasis register: Survival after surgery for bone metastases in the pelvis and extremities Hansen, B. H.; Keller, J.; Laitinen, M.; Berg, P.; Skjeldal, S.; Trovik,
The Scandinavian Sarcoma Group skeletal metastasis register: Survival after surgery for bone metastases in the pelvis and extremities Hansen, B. H.; Keller, J.; Laitinen, M.; Berg, P.; Skjeldal, S.; Trovik,
EVIDENCE IN BRIEF OVERALL CLINICAL BENEFIT
 ipilimumab aligned with patient values. Although few patients had direct experience using this combination agent, patients indicated that side effects associated with nivolumab plus ipilimumab were few
ipilimumab aligned with patient values. Although few patients had direct experience using this combination agent, patients indicated that side effects associated with nivolumab plus ipilimumab were few
Emerging Biomarkers of VEGF and mtor Inhibitors in 2015
 Emerging Biomarkers of VEGF and mtor Inhibitors in 2015 Laurence Albiges Institut Gustave Roussy, France Fourteenth International Kidney Cancer Symposium Miami, Florida, USA November 6-7, 2015 www.kidneycancersymposium.com
Emerging Biomarkers of VEGF and mtor Inhibitors in 2015 Laurence Albiges Institut Gustave Roussy, France Fourteenth International Kidney Cancer Symposium Miami, Florida, USA November 6-7, 2015 www.kidneycancersymposium.com
Treatment of everolimus-resistant metastatic renal cell carcinoma with VEGF-targeted therapies
 British Journal of Cancer (2011) 105, 1635 1639 All rights reserved 0007 0920/11 www.bjcancer.com Short Communication Treatment of everolimus-resistant metastatic renal cell carcinoma with VEGF-targeted
British Journal of Cancer (2011) 105, 1635 1639 All rights reserved 0007 0920/11 www.bjcancer.com Short Communication Treatment of everolimus-resistant metastatic renal cell carcinoma with VEGF-targeted
Chinese Journal of Cancer. Open Access ORIGINAL ARTICLE
 DOI 10.1186/s40880-017-0230-7 Chinese Journal of Cancer ORIGINAL ARTICLE Open Access Comparison of efficacy, safety, and quality of life between sorafenib and sunitinib as first line therapy for Chinese
DOI 10.1186/s40880-017-0230-7 Chinese Journal of Cancer ORIGINAL ARTICLE Open Access Comparison of efficacy, safety, and quality of life between sorafenib and sunitinib as first line therapy for Chinese
Renal Cell Cancer: Present and Future. Bernard Escudier, Gustave Roussy
 Renal Cell Cancer: Present and Future Bernard Escudier, Gustave Roussy [HKIOF May 2017] Sponsored by Bristol- Myers Squibb OPDIVO Hong Kong prescribing information is available upon request Disclosures
Renal Cell Cancer: Present and Future Bernard Escudier, Gustave Roussy [HKIOF May 2017] Sponsored by Bristol- Myers Squibb OPDIVO Hong Kong prescribing information is available upon request Disclosures
Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute
 Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 23 March 2012, Sao Paulo, Brazil Surgery of RCC Locally confined (small) renal tumours Locally advanced disease Metastatic
Surgery of Renal Cell Carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 23 March 2012, Sao Paulo, Brazil Surgery of RCC Locally confined (small) renal tumours Locally advanced disease Metastatic
CLINICAL CHALLENGES IN METASTATIC RENAL CELL CARCINOMA: THE RIGHT THERAPY FOR THE RIGHT PATIENT
 Daniel Heng, MD, MPH, FRCPC @DrDanielHeng Chair GU Tumour Group, Tom Baker Cancer Centre Clinical Professor, University of Calgary CLINICAL CHALLENGES IN METASTATIC RENAL CELL CARCINOMA: THE RIGHT THERAPY
Daniel Heng, MD, MPH, FRCPC @DrDanielHeng Chair GU Tumour Group, Tom Baker Cancer Centre Clinical Professor, University of Calgary CLINICAL CHALLENGES IN METASTATIC RENAL CELL CARCINOMA: THE RIGHT THERAPY
Treatment of Renal Cell Carcinoma (RCC) in the Era of Targeted Agents
 Conflict of Interest Treatment of Renal Cell Carcinoma (RCC) in the Era of Targeted Agents None Patrick Medina, PharmD, BCOP Associate Professor University of Oklahoma OKC, OK Learning Objectives Epidemiology
Conflict of Interest Treatment of Renal Cell Carcinoma (RCC) in the Era of Targeted Agents None Patrick Medina, PharmD, BCOP Associate Professor University of Oklahoma OKC, OK Learning Objectives Epidemiology
A Korean multi-center, real-world, retrospective study of first-line pazopanib in unselected patients with metastatic renal clear-cell carcinoma
 Kim et al. BMC Urology (2016) 16:46 DOI 10.1186/s12894-016-0163-5 RESEARCH ARTICLE Open Access A Korean multi-center, real-world, retrospective study of first-line pazopanib in unselected patients with
Kim et al. BMC Urology (2016) 16:46 DOI 10.1186/s12894-016-0163-5 RESEARCH ARTICLE Open Access A Korean multi-center, real-world, retrospective study of first-line pazopanib in unselected patients with
Sequential Therapy in Renal Cell Carcinoma*
 Sequential Therapy in Renal Cell Carcinoma* Bernard Escudier, MD, Marine Gross Goupil, MD, Christophe Massard, MD, and Karim Fizazi, MD, PhD Because of the recent approval of several drugs for the treatment
Sequential Therapy in Renal Cell Carcinoma* Bernard Escudier, MD, Marine Gross Goupil, MD, Christophe Massard, MD, and Karim Fizazi, MD, PhD Because of the recent approval of several drugs for the treatment
Cytoreductive Nephrectomy
 Cytoreductive Nephrectomy Stephen H. Culp, M.D., Ph.D. Assistant Professor, Department of Urology Outline The Historics of CN The current status of CN The importance of patient selection Cytoreductive
Cytoreductive Nephrectomy Stephen H. Culp, M.D., Ph.D. Assistant Professor, Department of Urology Outline The Historics of CN The current status of CN The importance of patient selection Cytoreductive
Efficacy and Toxicity of Sunitinib in Metastatic Renal Cell Carcinoma Patients in Egypt
 DOI:http://dx.doi.org/10.7314/APJCP.2015.16.5.1971 Efficacy and Toxicity of Sunitinib in Egyptian Patients with Metastatic Renal Cell Carcinoma RESEARCH ARTICLE Efficacy and Toxicity of Sunitinib in Metastatic
DOI:http://dx.doi.org/10.7314/APJCP.2015.16.5.1971 Efficacy and Toxicity of Sunitinib in Egyptian Patients with Metastatic Renal Cell Carcinoma RESEARCH ARTICLE Efficacy and Toxicity of Sunitinib in Metastatic
Lymphadenectomy in RCC: Yes, No, Clinical Trial?
 Lymphadenectomy in RCC: Yes, No, Clinical Trial? Viraj Master MD PhD FACS Professor Associate Chair for Clinical Affairs and Quality Director of Clinical Research Unit Department of Urology Emory University
Lymphadenectomy in RCC: Yes, No, Clinical Trial? Viraj Master MD PhD FACS Professor Associate Chair for Clinical Affairs and Quality Director of Clinical Research Unit Department of Urology Emory University
New strategies and future of target therapy in advanced kidney cancer
 New strategies and future of target therapy in advanced kidney cancer VHL Gene Inactivation VHL Complex Disrupted VHL Protein HIF1-a, HIF2-a Accumulation VEGF PDGF TGF-α, CXCR4 Angiogenesis Endothelial
New strategies and future of target therapy in advanced kidney cancer VHL Gene Inactivation VHL Complex Disrupted VHL Protein HIF1-a, HIF2-a Accumulation VEGF PDGF TGF-α, CXCR4 Angiogenesis Endothelial
Multidisciplinary approach for renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute
 Multidisciplinary approach for renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 20 April, Antalya, Turkey RCC European Union 60.000 new diagnoses/year 26.000 Cancer related deaths
Multidisciplinary approach for renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute 20 April, Antalya, Turkey RCC European Union 60.000 new diagnoses/year 26.000 Cancer related deaths
Key Words. Metastatic kidney cancer Prognosis Body mass index BMI Body surface area BSA Visceral fat Subcutaneous fat Obesity Overweight
 The Oncologist Genitourinary Cancer: Renal, Bladder, and Testicular Does Obesity Influence the Prognosis of Metastatic Renal Cell Carcinoma in Patients Treated with Vascular Endothelial Growth Factor Targeted
The Oncologist Genitourinary Cancer: Renal, Bladder, and Testicular Does Obesity Influence the Prognosis of Metastatic Renal Cell Carcinoma in Patients Treated with Vascular Endothelial Growth Factor Targeted
Revisione Oral Abstracts
 Revisione Oral Abstracts Francesco Massari Oncologia Medica Azienda Ospedaliero Universitaria di Bologna Policlinico S. Orsola-Malpighi UPDATES and NEWS from the Genitourinary Cancers Symposium - Milano,
Revisione Oral Abstracts Francesco Massari Oncologia Medica Azienda Ospedaliero Universitaria di Bologna Policlinico S. Orsola-Malpighi UPDATES and NEWS from the Genitourinary Cancers Symposium - Milano,
Innovaciones en el tratamiento del ca ncer renal. Enrique Grande
 Innovaciones en el tratamiento del ca ncer renal Enrique Grande The enriched inflammatory environment of RCC Chen Z, et al. Nat Rev Cancer 2014 Available agents are expanding across the three eras of arcc
Innovaciones en el tratamiento del ca ncer renal Enrique Grande The enriched inflammatory environment of RCC Chen Z, et al. Nat Rev Cancer 2014 Available agents are expanding across the three eras of arcc
Treatment with sorafenib and sunitinib in renal cell cancer: a Swedish register-based study
 Med Oncol (2013) 30:331 DOI 10.1007/s12032-012-0331-8 ORIGINAL PAPER Treatment with sorafenib and sunitinib in renal cell cancer: a Swedish register-based study Anneli Ambring Ingela Björholt Eva Lesén
Med Oncol (2013) 30:331 DOI 10.1007/s12032-012-0331-8 ORIGINAL PAPER Treatment with sorafenib and sunitinib in renal cell cancer: a Swedish register-based study Anneli Ambring Ingela Björholt Eva Lesén
Local survival outcomes in metastatic renal cell carcinoma
 Local survival outcomes in metastatic renal cell carcinoma Gerald Busuttil, Joseph Attard, David Farrugia, John Sciberras, Stephen Mattocks, Karl German, Patrick Zammit Abstract A quarter of patients who
Local survival outcomes in metastatic renal cell carcinoma Gerald Busuttil, Joseph Attard, David Farrugia, John Sciberras, Stephen Mattocks, Karl German, Patrick Zammit Abstract A quarter of patients who
Horizon Scanning Technology Briefing. Sutent (Sunitinib) for first-line and adjuvant treatment of renal cell carcinoma
 Horizon Scanning Technology Briefing National Horizon Scanning Centre Sutent (Sunitinib) for first-line and adjuvant treatment of renal cell carcinoma August 2006: Updated October 2006 This technology
Horizon Scanning Technology Briefing National Horizon Scanning Centre Sutent (Sunitinib) for first-line and adjuvant treatment of renal cell carcinoma August 2006: Updated October 2006 This technology
The role of cytoreductive. nephrectomy in elderly patients. with metastatic renal cell. carcinoma in an era of targeted. therapy
 The role of cytoreductive nephrectomy in elderly patients with metastatic renal cell carcinoma in an era of targeted therapy Dipesh Uprety, MD Amir Bista, MD Yazhini Vallatharasu, MD Angela Smith, MA David
The role of cytoreductive nephrectomy in elderly patients with metastatic renal cell carcinoma in an era of targeted therapy Dipesh Uprety, MD Amir Bista, MD Yazhini Vallatharasu, MD Angela Smith, MA David
Sequential Use of the Tyrosine Kinase Inhibitors Sorafenib and Sunitinib in Metastatic Renal Cell Carcinoma: A Retrospective Outcome Analysis
 available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Sequential Use of the Tyrosine Kinase Inhibitors Sorafenib and Sunitinib in Metastatic Renal Cell Carcinoma: A
available at www.sciencedirect.com journal homepage: www.europeanurology.com Kidney Cancer Sequential Use of the Tyrosine Kinase Inhibitors Sorafenib and Sunitinib in Metastatic Renal Cell Carcinoma: A
Treatment Algorithm and Therapy Management in mrcc. Manuela Schmidinger Medical University of Vienna Austria
 Treatment Algorithm and Therapy Management in mrcc Manuela Schmidinger Medical University of Vienna Austria A Paradigm Shift in the Treatment of mrcc 1. Sunitinib 2. Sorafenib 3. Bevacizumab+IFN-alpha
Treatment Algorithm and Therapy Management in mrcc Manuela Schmidinger Medical University of Vienna Austria A Paradigm Shift in the Treatment of mrcc 1. Sunitinib 2. Sorafenib 3. Bevacizumab+IFN-alpha
Introduction. pissn , eissn Cancer Res Treat. 2014;46(4):
 pissn 1598-2998, eissn 2005-9256 Original Article http://dx.doi.org/10.4143/crt.2013.154 Open Access Efficacy and Safety of Everolimus in Korean Patients with Metastatic Renal Cell Carcinoma Following
pissn 1598-2998, eissn 2005-9256 Original Article http://dx.doi.org/10.4143/crt.2013.154 Open Access Efficacy and Safety of Everolimus in Korean Patients with Metastatic Renal Cell Carcinoma Following
NEXT GENERATION DRUGS IN KIDNEY CANCER. Dr Aine O Reilly Karolinska Institutet Stockholm, Sweden
 NEXT GENERATION DRUGS IN KIDNEY CANCER Dr Aine O Reilly Karolinska Institutet Stockholm, Sweden KIDNEY CANCER SUBTYPES Papillary Type 1 and 2 Medullary Collecting duct Chromophobe Translocation Clear cell
NEXT GENERATION DRUGS IN KIDNEY CANCER Dr Aine O Reilly Karolinska Institutet Stockholm, Sweden KIDNEY CANCER SUBTYPES Papillary Type 1 and 2 Medullary Collecting duct Chromophobe Translocation Clear cell
CLINICAL POLICY Department: Medical Management Document Name: Inlyta Reference Number: NH.PHAR.100 Effective Date: 05/12
 Page: 1 of 5 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Page: 1 of 5 IMPORTANT REMINDER This Clinical Policy has been developed by appropriately experienced and licensed health care professionals based on a thorough review and consideration of generally accepted
Targeted and immunotherapy in RCC
 Targeted and immunotherapy in RCC Treatment options Surgery (radical VS partial nephrectomy) Thermal ablation therapy Surveillance Immunotherapy Molecular targeted therapy Molecular targeted therapy Targeted
Targeted and immunotherapy in RCC Treatment options Surgery (radical VS partial nephrectomy) Thermal ablation therapy Surveillance Immunotherapy Molecular targeted therapy Molecular targeted therapy Targeted
Cytoreductive nephrectomy and its role in the present-day period of targeted therapy
 585501TAU0010.1177/1756287215585501Therapeutic Advances in UrologySH Culp review-article2015 Therapeutic Advances in Urology Review Cytoreductive nephrectomy and its role in the present-day period of targeted
585501TAU0010.1177/1756287215585501Therapeutic Advances in UrologySH Culp review-article2015 Therapeutic Advances in Urology Review Cytoreductive nephrectomy and its role in the present-day period of targeted
Axitinib in renal cell carcinoma: now what do we do?
 Renal Cell Carcinoma Axitinib in renal cell carcinoma: now what do we do? Ian D. Davis Monash University Eastern Health Clinical School, Level 2, Box Hill, Victoria 3128, Australia Correspondence to: Ian
Renal Cell Carcinoma Axitinib in renal cell carcinoma: now what do we do? Ian D. Davis Monash University Eastern Health Clinical School, Level 2, Box Hill, Victoria 3128, Australia Correspondence to: Ian
pan-canadian Oncology Drug Review Final Clinical Guidance Report Axitinib (Inlyta) for metastatic Renal Cell Carcinoma March 7, 2013
 pan-canadian Oncology Drug Review Final Clinical Guidance Report Axitinib (Inlyta) for metastatic Renal Cell Carcinoma March 7, 2013 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
pan-canadian Oncology Drug Review Final Clinical Guidance Report Axitinib (Inlyta) for metastatic Renal Cell Carcinoma March 7, 2013 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
Pazopanib as a second-line treatment for non-cytokine-treated metastatic renal cell carcinoma: a meta-analysis of the effect of treatment
 Kok and Kuo BMC Urology (2016) 16:34 DOI 10.1186/s12894-016-0156-4 RESEARCH ARTICLE Pazopanib as a second-line treatment for non-cytokine-treated metastatic renal cell carcinoma: a meta-analysis of the
Kok and Kuo BMC Urology (2016) 16:34 DOI 10.1186/s12894-016-0156-4 RESEARCH ARTICLE Pazopanib as a second-line treatment for non-cytokine-treated metastatic renal cell carcinoma: a meta-analysis of the
EVIDENCE IN BRIEF OVERALL CLINICAL BENEFIT
 into consideration the concerns of the patient. Upon reconsideration of the perc Initial Recommendation,the Committee discussed feedback from the patient advocacy group reporting concerns that the definition
into consideration the concerns of the patient. Upon reconsideration of the perc Initial Recommendation,the Committee discussed feedback from the patient advocacy group reporting concerns that the definition
Research Report. ISSN /17/$ IOS Press and the authors. All rights reserved
 Kidney Cancer 1 (2017) 41 47 DOI 10.3233/KCA-160002 IOS Press Research Report 41 Outcomes of Metastatic Chromophobe Renal Cell Carcinoma (chrrcc) in the Targeted Therapy Era: Results from the International
Kidney Cancer 1 (2017) 41 47 DOI 10.3233/KCA-160002 IOS Press Research Report 41 Outcomes of Metastatic Chromophobe Renal Cell Carcinoma (chrrcc) in the Targeted Therapy Era: Results from the International
Association of post treatment hypoalbuminemia and survival in Chinese patients with metastatic renal cell carcinoma
 DOI 10.1186/s40880-017-0214-7 Chinese Journal of Cancer ORIGINAL ARTICLE Open Access Association of post treatment hypoalbuminemia and survival in Chinese patients with metastatic renal cell carcinoma
DOI 10.1186/s40880-017-0214-7 Chinese Journal of Cancer ORIGINAL ARTICLE Open Access Association of post treatment hypoalbuminemia and survival in Chinese patients with metastatic renal cell carcinoma
Syddansk Universitet. Stem cell divisions per se do not cause cancer. Wensink, Maarten Jan; Vaupel, James W. ; Christensen, Kaare
 Syddansk Universitet Stem cell divisions per se do not cause cancer Wensink, Maarten Jan; Vaupel, James W. ; Christensen, Kaare Published in: Epidemiology DOI: 10.1097/EDE.0000000000000612 Publication
Syddansk Universitet Stem cell divisions per se do not cause cancer Wensink, Maarten Jan; Vaupel, James W. ; Christensen, Kaare Published in: Epidemiology DOI: 10.1097/EDE.0000000000000612 Publication
Ito et al. BMC Cancer 2012, 12:337
 Ito et al. BMC Cancer 212, 12:337 RESEARCH ARTICLE Open Access C-reactive protein in patients with advanced metastatic renal cell carcinoma: Usefulness in identifying patients most likely to benefit from
Ito et al. BMC Cancer 212, 12:337 RESEARCH ARTICLE Open Access C-reactive protein in patients with advanced metastatic renal cell carcinoma: Usefulness in identifying patients most likely to benefit from
Current experience in immunotherapy for metastatic renal cell carcinoma
 Current experience in immunotherapy for metastatic renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute FOIU, Tel Aviv, 3 July 2018 Financial and Other Disclosures Off-label use of drugs,
Current experience in immunotherapy for metastatic renal cell carcinoma Axel Bex, MD, PhD The Netherlands Cancer Institute FOIU, Tel Aviv, 3 July 2018 Financial and Other Disclosures Off-label use of drugs,
Title. CitationCancer science, 106(5): Issue Date Doc URL. Rights(URL)
 Title Prognosis of Japanese patients with previously untre therapy Shinohara, Nobuo; Obara, Wataru; Tatsugami, Katsunor Author(s) Sachiyo; Abe, Takashige; Oba, Koji; Naito, Seiji CitationCancer science,
Title Prognosis of Japanese patients with previously untre therapy Shinohara, Nobuo; Obara, Wataru; Tatsugami, Katsunor Author(s) Sachiyo; Abe, Takashige; Oba, Koji; Naito, Seiji CitationCancer science,
The incidence and mortality rates of renal cell carcinoma (RCC) have been rising steadily worldwide at a rate of 2% to
 Pretreatment Assessment of Tumor Enhancement on Contrast-Enhanced Computed Tomography as a Potential Predictor of Treatment Outcome in Metastatic Renal Cell Carcinoma Patients Receiving Antiangiogenic
Pretreatment Assessment of Tumor Enhancement on Contrast-Enhanced Computed Tomography as a Potential Predictor of Treatment Outcome in Metastatic Renal Cell Carcinoma Patients Receiving Antiangiogenic
Novel ceramic membranes for water purification and food industry Boffa, Vittorio
 Aalborg Universitet Novel ceramic membranes for water purification and food industry Boffa, Vittorio Published in: PPM 2013 abstracts Publication date: 2013 Document Version Early version, also known as
Aalborg Universitet Novel ceramic membranes for water purification and food industry Boffa, Vittorio Published in: PPM 2013 abstracts Publication date: 2013 Document Version Early version, also known as
Kidney Cancer Session
 New Frontiers in Urologic Oncology September 12 th, 2015 Kidney Cancer Session Moderator: Philippe E. Spiess, M.D. Invited Faculty Members: Wade J. Sexton, MD Jeremiah J. Morrissey, PhD Agenda for Session
New Frontiers in Urologic Oncology September 12 th, 2015 Kidney Cancer Session Moderator: Philippe E. Spiess, M.D. Invited Faculty Members: Wade J. Sexton, MD Jeremiah J. Morrissey, PhD Agenda for Session
Immunotherapy for Renal Cell Carcinoma. James Larkin
 Immunotherapy for Renal Cell Carcinoma James Larkin Disclosures Institutional research support: BMS, MSD, Novartis, Pfizer Consultancy (all non-remunerated): Eisai, BMS, MSD, GSK, Pfizer, Novartis, Roche/Genentech
Immunotherapy for Renal Cell Carcinoma James Larkin Disclosures Institutional research support: BMS, MSD, Novartis, Pfizer Consultancy (all non-remunerated): Eisai, BMS, MSD, GSK, Pfizer, Novartis, Roche/Genentech
symposium article introduction symposium article
 Annals of Oncology 17 (Supplement 5): v118 v122, 2006 doi:10.1093/annonc/mdj965 Long-term survival results of a randomized trial comparing gemcitabine/cisplatin and methotrexate/ vinblastine/doxorubicin/cisplatin
Annals of Oncology 17 (Supplement 5): v118 v122, 2006 doi:10.1093/annonc/mdj965 Long-term survival results of a randomized trial comparing gemcitabine/cisplatin and methotrexate/ vinblastine/doxorubicin/cisplatin
Does organic food intervention in the Danish schools lead to change dietary patterns? He, Chen; Mikkelsen, Bent Egberg
 Aalborg Universitet Does organic food intervention in the Danish schools lead to change dietary patterns? He, Chen; Mikkelsen, Bent Egberg Published in: Like what you get? Is it good for you? Organic food,
Aalborg Universitet Does organic food intervention in the Danish schools lead to change dietary patterns? He, Chen; Mikkelsen, Bent Egberg Published in: Like what you get? Is it good for you? Organic food,
The Use of Inhibitors of Angiogenesis in Patients with Inoperable Locally Advanced or Metastatic Renal Cell Cancer: Guideline Recommendations
 Evidence-Based Series #3-8-4: Section 1 The Use of Inhibitors of Angiogenesis in Patients with Inoperable Locally Advanced or Metastatic Renal Cell Cancer: Guideline Recommendations S. Hotte, T. Waldron,
Evidence-Based Series #3-8-4: Section 1 The Use of Inhibitors of Angiogenesis in Patients with Inoperable Locally Advanced or Metastatic Renal Cell Cancer: Guideline Recommendations S. Hotte, T. Waldron,
Complete Remission is a Reachable Goal in mrcc L. Albiges Institut Gustave Roussy
 Complete Remission is a Reachable Goal in mrcc L. Albiges Institut Gustave Roussy Is complete remission an achievable goal in mrcc? Lessons from observation Lessons from immunotherapy Current status in
Complete Remission is a Reachable Goal in mrcc L. Albiges Institut Gustave Roussy Is complete remission an achievable goal in mrcc? Lessons from observation Lessons from immunotherapy Current status in
Oncology A Phase II Study of Presurgical Sunitinib in Patients with Metastatic Clear-cell Renal Carcinoma and the Primary Tumor In Situ
 Oncology A Phase II Study of Presurgical Sunitinib in Patients with Metastatic Clear-cell Renal Carcinoma and the Primary Tumor In Situ Axel Bex, Christian Blank, Wim Meinhardt, Harm van Tinteren, Simon
Oncology A Phase II Study of Presurgical Sunitinib in Patients with Metastatic Clear-cell Renal Carcinoma and the Primary Tumor In Situ Axel Bex, Christian Blank, Wim Meinhardt, Harm van Tinteren, Simon
Supplementary Online Content
 Supplementary Online Content Mezquita L, Auclin E, Ferrara R, et al. Association of the Lung Immune Prognostic Index with immune checkpoint inhibitor outcomes in patients with advanced non small cell lung
Supplementary Online Content Mezquita L, Auclin E, Ferrara R, et al. Association of the Lung Immune Prognostic Index with immune checkpoint inhibitor outcomes in patients with advanced non small cell lung
Reference No: Author(s) Approval date: June Committee. Operational Date: July Review:
 Reference No: Title: Author(s) Systemic anti-cancer therapy (SACT) guidelines for renal cell cancer Dr Alison Clayton Consultant Medical Oncologist & Dr Jane Hurwitz Consultant Medical Oncologist, Cancer
Reference No: Title: Author(s) Systemic anti-cancer therapy (SACT) guidelines for renal cell cancer Dr Alison Clayton Consultant Medical Oncologist & Dr Jane Hurwitz Consultant Medical Oncologist, Cancer
John Fitzpatrick Memorial Lecture. John Fitzpatrick Memorial lecture
 John Fitzpatrick Memorial Lecture John Fitzpatrick Memorial Lecture John M Fitzpatrick, 1948 2014 Head of Research at the Irish Cancer Society Professor of Surgery and Consultant Urologist at the Mater
John Fitzpatrick Memorial Lecture John Fitzpatrick Memorial Lecture John M Fitzpatrick, 1948 2014 Head of Research at the Irish Cancer Society Professor of Surgery and Consultant Urologist at the Mater
Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target?
 Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target? New Frontiers in Urologic Oncology Juan Chipollini, MD Clinical Fellow Department of Genitourinary Oncology Moffitt Cancer
Androgen Receptor Expression in Renal Cell Carcinoma: A New Actionable Target? New Frontiers in Urologic Oncology Juan Chipollini, MD Clinical Fellow Department of Genitourinary Oncology Moffitt Cancer
Tyrosine Kinase Inhibitors in Clinical Practice: Case Reports
 european urology supplements 7 (2008) 610 614 available at www.sciencedirect.com journal homepage: www.europeanurology.com Tyrosine Kinase Inhibitors in Clinical Practice: Case Reports Vincenzo Ficarra
european urology supplements 7 (2008) 610 614 available at www.sciencedirect.com journal homepage: www.europeanurology.com Tyrosine Kinase Inhibitors in Clinical Practice: Case Reports Vincenzo Ficarra
Opinion 26 June 2013
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 26 June 2013 VOTRIENT 200 mg, film-coated tablets B/30 (CIP: 491 313 4) VOTRIENT 400 mg, film-coated tablets B/30
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 26 June 2013 VOTRIENT 200 mg, film-coated tablets B/30 (CIP: 491 313 4) VOTRIENT 400 mg, film-coated tablets B/30
Validation of preoperative variables and stratification of patients to help predict benefit of cytoreductive nephrectomy in the targeted therapy ERA
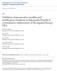 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Validation of preoperative variables and stratification of patients to help predict benefit of cytoreductive
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Validation of preoperative variables and stratification of patients to help predict benefit of cytoreductive
ANTICANCER RESEARCH 35: (2015)
 No Significant Correlation of Clinical Outcomes Between First- and Second-line Tyrosine Kinase Inhibitors in Patients with Metastatic Renal Cell Carcinoma AKIRA MIYAZAKI, HIDEAKI MIYAKE, KEN-ICHI HARADA
No Significant Correlation of Clinical Outcomes Between First- and Second-line Tyrosine Kinase Inhibitors in Patients with Metastatic Renal Cell Carcinoma AKIRA MIYAZAKI, HIDEAKI MIYAKE, KEN-ICHI HARADA
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva
 Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Locoregional treatment Session Oral Abstract Presentation Saulo Brito Silva Background Post-operative radiotherapy (PORT) improves disease free and overall suvivallin selected patients with breast cancer
Patients with metastatic renal cell carcinoma who benefit from axitinib dose titration: analysis from a randomised, double-blind phase II study
 Tomita et al. BMC Cancer (219) 19:17 https://doi.org/1.1186/s12885-18-5224-6 RESEARCH ARTICLE Open Access Patients with metastatic renal cell carcinoma who benefit from axitinib dose titration: analysis
Tomita et al. BMC Cancer (219) 19:17 https://doi.org/1.1186/s12885-18-5224-6 RESEARCH ARTICLE Open Access Patients with metastatic renal cell carcinoma who benefit from axitinib dose titration: analysis
Case(s): How to Deal with Mixed Response Giuseppe Procopio
 Case(s): How to Deal with Mixed Response Giuseppe Procopio Fondazione IRCCS Istituto Nazionale dei Tumori, Milano Disclosures Advisory: Astellas, Bayer, GSK Consultant: Pfizer, Novartis Background Mixed
Case(s): How to Deal with Mixed Response Giuseppe Procopio Fondazione IRCCS Istituto Nazionale dei Tumori, Milano Disclosures Advisory: Astellas, Bayer, GSK Consultant: Pfizer, Novartis Background Mixed
CheckMate 025, as patients may derive a benefit, based on the opinion of the CGP and the mechanism of action of nivolumab.
 CheckMate 025, as patients may derive a benefit, based on the opinion of the CGP and the mechanism of action of nivolumab. perc noted that patients with brain metastases were excluded from the CheckMate
CheckMate 025, as patients may derive a benefit, based on the opinion of the CGP and the mechanism of action of nivolumab. perc noted that patients with brain metastases were excluded from the CheckMate
Summary BREAST CANCER - Early Stage Breast Cancer... 3
 ESMO 2016 Congress 7-11 October, 2016 Copenhagen, Denmark Table of Contents Summary... 2 BREAST CANCER - Early Stage Breast Cancer... 3 Large data analysis reveals similar survival outcomes with sequential
ESMO 2016 Congress 7-11 October, 2016 Copenhagen, Denmark Table of Contents Summary... 2 BREAST CANCER - Early Stage Breast Cancer... 3 Large data analysis reveals similar survival outcomes with sequential
The plan. Overview of clinical trials Current clinical trials in renal cancer Future treatment of renal cancer
 Relevant disclosure Bayer - consultancy GSK research funding, consultancy, speaker honoraria Novartis research funding Pfizer research funding, consultancy Roche / Genentech research funding, consultancy
Relevant disclosure Bayer - consultancy GSK research funding, consultancy, speaker honoraria Novartis research funding Pfizer research funding, consultancy Roche / Genentech research funding, consultancy
Response Assessment Classification in Patients with Advanced Renal Cell Carcinoma Treated on Clinical Trials
 1611 Response Assessment Classification in Patients with Advanced Renal Cell Carcinoma Treated on Clinical Trials Effect of Measurement Criteria and Other Parameters Lawrence H. Schwartz, M.D. 1,2 Madhu
1611 Response Assessment Classification in Patients with Advanced Renal Cell Carcinoma Treated on Clinical Trials Effect of Measurement Criteria and Other Parameters Lawrence H. Schwartz, M.D. 1,2 Madhu
Hyponatremia in small cell lung cancer is associated with a poorer prognosis
 Original Article Hyponatremia in small cell lung cancer is associated with a poorer prognosis Wenxian Wang 1, Zhengbo Song 1,2, Yiping Zhang 1,2 1 Department of Chemotherapy, Zhejiang Cancer Hospital,
Original Article Hyponatremia in small cell lung cancer is associated with a poorer prognosis Wenxian Wang 1, Zhengbo Song 1,2, Yiping Zhang 1,2 1 Department of Chemotherapy, Zhejiang Cancer Hospital,
