Does inhalational nitrous oxide affect induction dose of propofol and haemodynamic?
|
|
|
- Augustus Webb
- 5 years ago
- Views:
Transcription
1 Journal of Anesthesiology 2014; 2(5): Published online November 17, 2014 ( doi: /j.ja Does inhalational nitrous oxide affect induction dose of propofol and haemodynamic? 1, 2, 3 Sanjeev Singh 1 Department of Anaesthesia and Intensive care, School of Medical Sciences, College of Health Sciences, Kwame Nkrumah University of Science and Technology, Kumasi, Ghana, West Africa 2 Department of Anaesthesia and Intensive care, Satyabhama Academy Of Medical Sciences & Research Institute, Lucknow, India 3 Department of Cardiac Anaesthesia, Artemis Health Institute, Gurgaon, India address: drsanjeev73@rediffmail.com To cite this article: Sanjeev Singh. Does Inhalational Nitrous Oxide Affect Induction Dose of Propofol and Haemodynamic? Journal of Anesthesiology. Vol. 2, No. 5, 2014, pp doi: /j.ja Abstract: Background: Propofol is a commonly used induction agent. Propofol does not possess any strong analgesic effect, when used alone for induction of anaesthesia. In dose of more than 2 mg/kg bolus known to cause hypotension even requiring vasopressors. Nitrous oxide (N 2 O) has been in use for more than 150 years. Although N 2 O reduces the requirement of propofol for induction and maintenance, the effects of both the drugs on overall haemodynamic remain controversial. The aim of this study was to evaluate the efficacy and safety of induction dose of propofol when N 2 O was concurrently administered and haemodynamic alteration with addition of N 2 O to therapeutic dose of propofol. Materials and Methods: This was a prospective, randomized and double blinded comparison study that was conducted after obtaining institutional ethical approval. The study population consisted of eighty patients aged between 18 to 60 years from either sex and classified as American Society of Anaesthesiologists (ASA) physical status I or II which were scheduled for various elective surgical procedures under general anaesthesias. Participants were randomly allocated into two groups comprising 40 subjects each. received breathed 67% N 2 O (4 L/min) + 33% O2 (2L/min) and propofol. : breathed 100 % O 2 (6L/min) and propofol. Changes in heart rate (HR), systolic blood pressure (SBP), mean arterial pressure (MAP) and Oxygen saturation (SpO 2 ) were measured Preoperatively (baseline T0), After 3minutes of premedication (T1), After 1minute of inhalation of 100% O 2 before induction of anesthesia (T2), After induction (T3), At 2, 5 and 10 minutes after induction (T4), (T5), and (T6). Results: Induction time and dose of propofol in PN group were significantly less. As 42.5% of the patients were induced in less than 100 sec, 57.5% in less than 200 sec and none of the patients required more than 200 sec for induction as compare to group PO where 77.5% required more than 200 sec, 22.5% in less than 200 sec and none of the patients were induced in less than 100 sec. The mean ± SD of induction time in groups PN and PO were ±35.93 and ±59.43 seconds respectively with p < In group PN, 57.5% required mg/kg, 40% required less than 0.5mg/kg unlike group PO where 77.5% required 1-2mg/kg. The mean ± SD induction dose required for induction of anesthesia were 0.58±0.19 mg/kg and 1.43±0.40 mg/kg with and without 67% N 2 O in O 2. Increase in HR in groups PN and PO 16.38% and 6.42% respectively. Conclusions: Co-administration of N 2 O during induction of anaesthesia achieves significant reduction in induction dose as well as induction time of propofol. It provides significant stability in SBP, and MAP, without affecting arterial oxygen saturation. N 2 O causes significant increase in HR. Keywords: Blood Pressure, Heart Rate, Nitrous Oxide, Propofol (Source: Mesh, NLM) 1. Introduction Propofol an intravenous ( IV) anaesthetic agent, is widely used for induction of anaesthesia due to rapid onset, recovery and low degree of excitatory activity.[1] However, as propofol alone possesses no strong analgesic effect, it is often administered in combination with additional analgesics. Addition of analgesics and volatile anaesthetic agents augments induction characteristics and reduces the dose of propofol.[2] Propofol commonly produces decrease in systemic vascular resistance (SVR %), Stroke volume (SV- 20%), cardiac Index (CI-15%), left ventricular stroke work index (30%), myocardial contractility as well as It causes transient apnea mostly in a dose and rate dependent
2 33 Sanjeev Singh: Does Inhalational Nitrous Oxide Affect Induction Dose of Propofol and Haemodynamic manner.[3] At higher doses it causes significant decrease in arterial blood pressure and heart rate by 37% and 24%, respectively [4], which is particularly undesirable in elderly, and high risk group of patients as may cause hypotension. N 2 O has been a cornerstone of anaesthetic practice since its first use because of its analgesic, anxiolytic and anaesthetic properties. It is good analgesic but a weak anaesthetic agent. It is used commonly as an adjunct to balanced general anaesthesia (GA) and a gaseous vehicle for the administration of more potent volatile anaesthetics. When used as an adjunct, the resulting minimum alveolar concentration (MAC) reduction for the other volatile anaesthetic agent. Potential side effects like acute and chronic pain, neurological, cardiovascular outcomes, and wound infection remain controversial. Certain characteristics of nitrous oxide as its propensity to postoperative nausea and vomiting, expansion of gas-filled cavities, the second-gas effect, and diffusion hypoxia are very well known.[5] It remains incumbent upon the practitioner to utilize the patient history and data to evaluate the risk benefit profile for the use of nitrous oxide. Many authors have studied the reduction in effective concentration (EC 50 ), plasma concentration (CP 50 ) for noxious stimulus, CP 50 LOR (loss of response) of propofol with N 2 O.[6, 7] Although N 2 O reduces the requirement of propofol for induction and maintenance, the effects of both drugs on overall haemodynamic remain controversial.[7] However use of N 2 O as an inhaled additional drug for the induction of propofol anaesthesia has not been studied extensively.[8] The present study was designed primarily to determine the efficacy and safety of minimum induction dose of propofol, when N 2 O was concurrently administered and haemodynamic variations Material and Methods This study was undertaken after an institutional approval by the Committee on Human Research Publications and Ethics was obtained. The study was conducted at Satyabhama Academy Of Medical Sciences & Research Institute in Informed consent was obtained from 80 patients. The study population consisted of ASA physical status I (normal healthy patients) or II (patients with mild systemic disease), male and female adults between the ages of years scheduled for various elective surgical procedures Study Design This study was a prospective, randomized, and double blinded clinical comparison study. The Sample size for the study was 80 generated using a sample size calculator. The study participants were randomly divided into two groups by a computer generated randomization table. A study nurse (Person A) who was not involved in the randomization process of N 2 O to enhance blinding. Person B monitored the heart rate (HR), systolic blood pressure (SBP), mean arterial pressure (MAP) and oxygen saturation (SpO 2 ) with respect to time, whilst Person C was responsible for intubation of the patients. Person A and C were kept constant throughout the study. Person B, C, and the patient were kept unaware of the N 2 O to enable double blinding. Inclusion criteria: for the study were ASA class I or II, age range 18 60, oropharyngeal anatomy of Mallampati class I and any operation other than cardiac surgery performed under general anesthesia with endotracheal intubation. Exclusion criteria: for the study included patients who were pregnant, morbidly obese, with risk of aspiration of gastric contents, cardiovascular disease, heart rate <60 beats per minute (bpm), basal SBP < 100 mm Hg, and other conditions such as bronchial asthma, diabetes mellitus, drug allergies. Duration of laryngoscopy was noted and in case where duration exceeded 15 sec was excluded from this study. Patients with relative contraindication to the use of halothane as well as N 2 O during induction of anesthesia such as intestinal obstruction, middle ear disease, pneumothorax, air embolism, sinus or middle ear surgery. 2. Pre-Surgical Protocol Prior to surgery all patients underwent pre-anaesthetic evaluation for systemic diseases and routine laboratory investigations such as haemoglobin (Hb), total lymphocyte count, differential lymphocyte count, urine analysis and other investigations were done as necessary. Information collected also included weight, nutritional status, airway assessment by the Mallampatti scoring system, a detailed examination of the respiratory, cardiovascular, central nervous system. Patients looked for hypotension (basal SBP < 100 mm Hg, or a decrease in the initial systolic arterial pressure of 20% from baseline, or both),[9] and hypoxemia (SpO 2 < 90 that correlates with a PaO 2 of < 60 mmhg).[10] The procedure of general anaesthesia was explained to the patient. Patients were explained about the purpose and procedure. Informed consent was obtained. All patients were kept fasting overnight. Premedication included tablet alprazolam 0.25 mg and tablet ranitidine 150 mg orally, night prior and on the morning of the surgery Anaesthetic Technique On arrival to the operation theatre (OT), patients were identified, a short preoperative history was taken, clinical examination and routine investigations were rechecked in all patients. Monitors were attached to patient and baseline HR, MAP, SBP and SpO 2 were recorded. The procedure was again explained to the patients. An intravenous (IV) line was established and all patients were premedicated with IV glycopyrrolate 0.2 mg, IV ondansetron 4 mg and IV fentanyl 1 mcg/kg. After 3 minutes of pre-oxygenation patients were made to breathe respective gases (67% N 2 O +33% O 2 in group PN and 100% O 2 in group PO) via a tight fitting face mask using a closed circuit breathing system with CO 2 absorber for 1 minute. Lidocaine 10 mg was given followed by IV propofol at a rate of 20 mg/min to maintain uniformity in all patients
3 Journal of Anesthesiology 2014; 2(5): (as titrated doses of 10 mg every 30 seconds). Propofol was stopped when there was loss of response to verbal command (ie, to open eyes). Onset of anaesthesia was confirmed with disappearance of the eyelash reflex. The induction time was taken as time from the start of propofol to loss of response and induction dose as the amount of propofol administered in that time. The study drug N 2 O was randomly allocated to patients in a double blinded manner. Patients were ventilated with oxygen and 1% halothane using IPPV. About 2 min after IV vecuronium, laryngoscopy was performed with a Macintosh laryngoscope blade and trachea intubated with an appropriate size cuffed endotracheal tube. After confirmation of correct placement of ET tube, anaesthesia was then maintained with O 2 and halothane. During the study HR, MAP, SBP and SpO 2 were monitored at preoperatively (baseline T0), After 3 minutes of premedication (T1), After 1 minute of inhalation of 100% O 2 before induction of anaesthesia (T2), After induction (T3), At 2, 5 and 10 minutes after induction (T4), (T5), and (T6) respectively. Any complications like hypoxia, respiratory depression, allergic reactions etc were noted. 3. Parameters and Statistical Analysis Summary statistics of patient gender, age, and weight for all three groups were reported as means±standard deviation (SD). HR, SBP, MAP, Sp0 2 were recorded using Infinity Delta XL Drager, Draeger Medical Systems, Inc. Telford, PA 18969, USA. Patients were also observed for complications like hypotension, hypertension, arrhythmias, and hypoxaemia. Statistical analysis was done by student t test, Chi-square/ Fisher Exact test has been used to find the significance of study parameters on categorical scale between two or more groups and P values were calculated. Levenes test has been performed to assess the homogeneity of variance. Haemodynamic variables were represented by mean±sd. In all analyses, p<0.05 was considered statistically significant. The Statistical software package SAS 9.2, SPSS 15.0, Stata 10.1, MedCalc 9.0.1, Systat 12.0 and R environment ver were used for the analysis of the data. 4. Results Table 1. Age distribution of patients. Age in years Total Mean ± SD 37.05± ±11.35 Samples are age matched with p=0.731 All the demographic profiles in the PN and PO groups were comparable [Table 1]. The age range was years for both PN and PO group. The mean values of the age with standard deviations are 37.05±10.70 and for PN and PO groups respectively. There was no significant difference between the two groups (p>0.05). In groups PN and PO 45% patients were males and 55% were females respectively. No significant difference was observed in sex wise distribution of the cases between the two groups (p>0.05) [Table 2] The Male: Female ratio is maintained in both the groups of the study. Gender Table 2. Gender distribution of patients. Male Female Total M: F Ratio 1:1.2 1:1.2 Samples are gender matched with p=1.000 Weight (kg) Table 3. Weight (kg) distribution of patients Total Mean ± SD 60.22± ±11.41 Samples are weight matched with p=0.507 As shown above (Table 3), the weights of the patients were between kgs with a mean and standard deviation of 60.22±9.28 and 58.67±11.41 for PN and PO groups respectively. No significant difference was observed in the weight distribution in the two groups (p>0.05). In majority of the patients of both the groups, the body weight range between kg. The mean body weight is comparable in both the study groups. Table 4. ASA Physical status distribution of patients. ASA ASA I ASA II Total Distribution ASA is statistically similar in two groups with p=0.633 Table 5. Operative procedure of the patients. Operative procedures (n=40) (n=40) General surgery procedures ENT procedures Urological procedures Gynaecological procedures Neurosurgical procedures Others
4 35 Sanjeev Singh: Does Inhalational Nitrous Oxide Affect Induction Dose of Propofol and Haemodynamic Table 6. Distribution of Induction time (sec) in patients. Induction (n=40) (n=40) time (sec) < > Mean ± SD ± ±59.43 Induction time (sec) is significantly less in Inference ( ±35.93sec) when compared to (258.00sec±59.43) with p<0.001** In group PN, 42.5% patients were induced in less than 100 sec and 57.5% required less than 200 sec for induction of anaesthesia. None of the patients required more than 200 sec. Where as in group PO, (77.5%) required more than 200 sec for induction of anaesthesia. None of the patients were induced in less than 100 sec as compared to 42.5% in group PN. The mean induction time was significantly less in group PN ( ) as compared to group PO ( ) (p < 0.001) Table 7. Distribution of Induction dose (mg/kg) in patients. Induction (n=40) (n=40) dose (mg/kg) < > Mean ± SD 0.58± ±0.40 Induction dose is significantly less s in Inference (0.58±0.19 mg/kg) when compared to (1.43±0.40 mg/kg) with p<0.001** * In group PN, about 40% patients required induction dose less than 0.5 mg/kg and 57.5% patients were induced with mg/kg. None of the patients required more than 2mg/kg for the induction of anaesthesia. In group PO, 77.5% of the patients were induced d with 1 2 mg/kg induction dose. But none of the patients were induced with less than 0.5 mg/kg as compared to 40% in group PN. The induction dose was significantly less in group PN ( ), as compared to group PO ( ) with p< Table 8. Comparison of heart rate (bpm) in the two study groups of patients. HR (bpm) (n=40) T ±12.45 T ±13.55 T ±15.01 T ±11.27 T ±10.59 T ±8.82 T ±10.60 (n=40) p value 82.50± ± ± ± * 87.70±13.36 <0.001** 86.25±12.17 <0.001** 91.20± * The baseline mean heart rate and standard deviation were and in groups PN and PO respectively, which were statistically comparable (p= 0.446). In group PN, there was significant increase in mean heart rate after induction of anaesthesia ( ). There was continuous increase in heart rate till 10 mins after induction. Heart rates were 98.25±10.59, 99.35±8.82 and 97.15±10.60 at 2, 5 and 10 min respectively. In group PO, no significant change in mean heart rate was observed immediately after induction of anaesthesia (87.80±12.61). The mean heart rate was stable at 2 and 5min 87.70±13.36 and 86.25±12.17 respectively. The inter group PN had statistically significant increase in heart rate as compared to group PO (p<0.001). Fig 1. Line diagram changes in heart rate in each group.
5 Journal of Anesthesiology 2014; 2(5): Fig 2. Changes in mean arterial pressure in each group. In group PN, the baseline mean arterial pressure and standard deviation were 97.40± Immediately after induction there was reduction in mean arterial pressure 77.80±8.53 and mean arterial pressure returns to baseline value at about 10 min after induction of anaesthesia 85.93± Whereas, in group PO, the baseline mean arterial pressure and standard deviation were 95.50±17.65, immediately after induction of anaesthesia there was statistically significant reduction in mean arterial pressure to 70.28±16.65 and the reduction were observed even at 5 min after induction (72.33±15.25). The inter group analysis shows that the reduction in mean arterial pressure in group PO was highly significant when compared to group PN (p<0.001). Table 9. Comparison of mean arterial pressure in the two study groups of patients. MAP (mm Hg) P value (n=40) (n=40) T ± ± T ± ± T ± ± T ± ± * T ± ± ** T ± ± ** T ± ± The baseline systolic blood pressure and standard deviation were ±17.95 and ±22.42 in groups PN and group PO respectively, which were comparable in both the groups. In group PO there was fall in systolic blood pressure immediately after induction of anaesthesia to 94.78± The fall in systolic blood pressure was observed even at 10 min after induction (103.88±16.22). In group PN the systolic blood pressure immediately after induction was ±9.9, but it remained stable thereafter ±12.00, ±12.86, and ±10.46 at 2, 5, and 10 min respectively. Inter group analysis shows group PN had stable systolic blood pressure after induction of anaesthesia as compared to group PO. Table 10. Comparison of systolic blood pressure in the two study groups of patients. SBP (mm Hg) (n=40) T ±17.95 T ±17.37 T ±11.00 T ±9.99 T ±12.00 T ±12.86 T ±10.46 p value (n=40) ± ± ± ±15.74 <0.001** 94.78±15.81 <0.001** 95.55±14.78 <0.001** ± **
6 37 Sanjeev Singh: Does Inhalational Nitrous Oxide Affect Induction Dose of Propofol and Haemodynamic Fig 3. Changes in systolic blood pressure in each group. Fig 4. Changes in arterial oxygen saturation in each group. Table 11. Comparison of Oxygen saturation (SpO 2) in the two study groups. S PO 2% (n=40) (n=40) p value T ± ± T ± ± T ± ± T ± ± T ± ± * T ± ± T ± ± The baseline arterial oxygen saturation and standard deviation were 99.38±0.59 and 99.13±0.53 in groups PN and PO respectively. In group PN reduction in arterial oxygen saturation was observed at 2 min 98.80±0.61. However it is statistically significant but did not resulted in hypoxia clinically. In group PO, there was no statistically significant reduction in arterial oxygen saturation 99.03±0.16, after induction 99.00±0.00 and thereafter. None of the patients in PN and PO group had any complications during the study period.
7 Journal of Anesthesiology 2014; 2(5): Discussion Propofol is a commonly used induction agent, often used in combination with benzodiazepinesand opioids.[11] If not used carefully may cause hypotension and require vassopressors. Since last 150 years N 2 O has been a cornerstone of anaesthetic practice and often used with intravenous anaesthetic induction agents. In our study propofol was administered in titrated doses. With a slower infusion rate of 10mg/30 sec, we found that the induction time prolonged as in study by Ju in control group, however co-administration of 67% N 2 O in O 2 shortened the induction time.[12] In our study the induction time and dose of propofol in PN group were significantly less as compared to control group. In PN group 42.5% of the patients were induced in less than 100 sec, whereas in group PO 77.5 % required more than 200 sec for induction. The mean ± SD induction time was significantly less in group PN (113.38±35.93sec) as compared to group PO (258.00±59.43sec) with p < 0.001, which is highly significant. We studied the induction dose of propofol with and without N 2 O. Our analysis showed that in group PN, 57.5% required mg/kg, and 40% required less than 0.5mg/kg, where as in group PO 77.5% required 1-2mg/kg. The mean ± SD for induction of anaesthesia was 0.58±0.19 mg/kg and 1.43±0.40 mg/kg with and without N 2 O. Our findings were similar to Ju that the induction dose of propofol was reduced by almost 40% with concurrent use of N 2 O.[12] In our study where induction time with N 2 O was ±35.93 sec as compared to 141.8±46.7 sec in the study by Ju. This may be was due to all our patients received fentanyl but in Ju study patients received N 2 O were not given fentanyl.[12] Infusion rates of propofol ranging from mg/ min were compared in several studies. Reduction in total dose of propofol used with slower infusion rates with an increase in the induction time.[13] In the study by Kumar mean induction dose of propofol was 2mg/kg in control group. In study group propofol priming with 20% calculated dose 30 seconds before remaining dose of propofol until loss of eyelash reflex reduced requirement of propofol by 27.48%. In our study with addition of nitrous oxide 97.5% patients induction with 50% reduced dose of propofol of 5-1mg/kg. In his study in control and study groups 8% and 1% of patients had complications like hypotension which were not visible in our study.[14] It shows that cardiovascular changes occurring in response to the amount of drug administered and not the rate of administration.[15] Target controlled infusion (TCI) is a recently developed system that aids rapid recovery from propofol anaesthesia. When the target concentration of propofol required to prevent movements in 50% (CP 50 ) and 95% (CP 95 ) of patients were studied with and without 50% N 2 O, it was concluded that CP 50 value was significantly higher in those who did not receive N 2 O than in those who did. [16] Studies have shown reduction of CP 50, CP 95 of propofol by 25-28% with 67% N 2 O, 43% reduction of CP 50 LOR of propofol with 67% N 2 O. [6, 7] Our study results are similar to these studies which showed that co-administration of N 2 O not only achieves more acceptable induction time with slow propofol infusion, but also results in a reduction in the total dose of propofol required.[12-14] Reports on the effect of nitrous oxide in combination with volatile anaesthetic agents on heart rate have been inconsistent.[13 15] In contrast to McKinney study, we observed an increase in HR to statistically significant value immediately after induction, at 2 min, and 5 min in group PN.[16] The circulatory effects of N 2 O can be explained by its tendency to stimulate sympathetic nervous system (SNS). Though it directly depresses myocardial contractility but arterial blood pressure, CO and HR are essentially unchanged or slightly elevated because of its stimulation of catecholamines or SNS activation.[17,18] 40-70% N 2 O causes modest increases in HR in healthy patients, however, decline in HR can occur with N 2 O in patients with coronary artery disease (CAD).[18] In McKinney study average age was about 70 years as compare to our 37 years. This decrease in heart rate attributed to the limited responsiveness of the aged cardiovascular system to sympathomimetic effects, may explain the absence of an increase in heart rate in his study. An increase in HR to significant value with nitrous oxide compensate well with decrease in systolic blood pressure with propofol. As RPP (rate pressure product) was calculated by multiplying heart rate with systolic blood pressure. RPP is a good estimate of myocardial oxygen requirement.[19] The RPP levels close to 20,000 are normally associated with angina and myocardial ischemia, which is not noticed in our patients. 6. Conclusions The present data suggests that Co-administration of N 2 O during induction of anaesthesia achieves significant reduction in induction dose as well as induction time of propofol. It provides significant stability in SBP, and MAP, without affecting arterial oxygen saturation with increase in heart rate. Comments We accept the fact that there were few limitations to our study. We used end point for induction of anaesthesia as loss of verbal response and disappearance of eyelash reflex, which had its own limitations. End tidal N 2 O monitoring would have been a better indicator of effective administration of N 2 O than inspired N 2 O used in our study. Further studies needs to be done in high-risk patients with BIS and end tidal N 2 O monitoring. References [1] Perouansky M, Hemmings HC Jr. Intravenous anesthetic agents. In: HC Hemmings Jr, PM Hopkins, eds. Foundations of Anesthesia: Basic Science and Clinical Practice. 2nd ed. London: Mosby Elsevier; 2006:
8 39 Sanjeev Singh: Does Inhalational Nitrous Oxide Affect Induction Dose of Propofol and Haemodynamic [2] Krzych LJ,Szurlej D, Bochenek A. Rationale for propofol use in cardiac surgery. Journal of Cardiothoracic and Vascular Anesthesia. 2009;23: [3] Rasooli S, Parish M, Mahmoodpoor A, Moslemi F, Sanaie S, Faghfuri S. The effect of intramuscular ephedrine in prevention of hypotension due to propofol. Pak J Med Sci. 2007;23: [4] Hashiba E, Hirota K, Suzuki K, Matsuki A. Effects of propofol on bronchoconstriction and bradycardia induced by vagal nerve stimulation. Acta Anaesthesiologica Scandinavica. 2003; 47: [5] Vasconcellos KD, Sneyd JR. Nitrous oxide: are we still in equipoise? A qualitative review of current controversies. BJA. 2013;111: [6] Davidson JAH, Macleod AD, Howie JC, White M, Kenny GNC. Effective concentration 50 for propofol with and without 67% nitrous oxide. Acta Anesthesiol Scand 1993; 37: [7] Stuart PC, Stott SM, Millar A, Kenny GNC, Russell D. CP50 of propofol with and without nitrous oxide 67%. Br J Anaesth 2000; 84: [8] Shiga T, Wajima Z, Inoue T, Ogawa R. Nitrous oxide produces minimal hemodynamic changes in patients receiving a propofol-based anesthetic: an esophageal Doppler ultrasound study. Can J Anaesth. 2003; 50 : [9] Annamalai A, Singh S, Singh A, Mahrous DE. Can Intravenous Dexmedetomidine Prolong Bupivacaine Intrathecal Spinal Anesthesia? J Anesth Clin Res. 2013; 12: 1-5. [10] Ehrenfeld JM, Funk LM, Schalkwyk JV, Merry AF, Sandberg WS, Gawande A. The incidence of hypoxemia during surgery: evidence from two institutions. Can J Anaesth. 2010; 57: [11] Tanaka M, Nishikawa T. Propofol requirement for insertion of cuffed oropharyngeal airway versus laryngeal mask airway with and without fentanyl: a dose finding study. Br J Anaesth 2003; 90: [12] Ju-Mei Ng and Nian-Chih Hwang. Inhaling nitrous oxide reduces the induction dose requirements of propofol. Anesth Analg 2000; 90: [13] Uzun S, Ozkaya BA, Yilbaş SO, Ayhan B, Sahin A, Aypar U. Effects of different propofol injection speeds on blood pressure, dose, and time of induction. Turk J Med Sci 2011; 41: [14] Kumar AA, Sanikop CS, Kotur PF. Clinical investigation effect of priming principle on the induction dose requirements of propofol - a randomized clinical trial. Indian J. Anaesth. 2006; 50: [15] Peacock JE, Lewis RP, Reilly CS, Nimmo WS. Effect of different rates of propofol for induction of anaesthesia in elderly patients. Br J Anaesth. 1990; 65: [16] McKinney MS, Fee JPH. Cardiovascular effects of 50% nitrous oxide in older adult patients anaesthetized with isoflurane or halothane.bja. 1998; 80: [17] Robert K. Stoelting. Inhaled Anesthetics. In: Pharmacology and Physiology in Anesthetic Practice. Stoelting RK, Hiller SC, 4 th Edition. Philadelphia: Lippincott Williams and Wilkins; 2006: p [18] Edmond I. Eger II. Inhaled Anesthetics: Uptake and Distribution. In: Miller s Anaesthesia. Miller RD. 7 th Edition. Philadelphia: Churchill Livingstone; 2010: p [19] Singh S, Laing EF, Owiredu WKBA, Singh A. Comparison of esmolol and lidocaine for attenuation of cardiovascular stress response to laryngoscopy and endotracheal intubation in a Ghanaian population. Anesthesia: Essays and Researches. 2013; 7:
Veena Mathur, Deepak Garg, Neena Jain, Vivek Singhal, Arvind Khare, Surendra K. Sethi*
 International Journal of Research in Medical Sciences Mathur V et al. Int J Res Med Sci. 2016 Aug;4(8):3421-3426 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162305
International Journal of Research in Medical Sciences Mathur V et al. Int J Res Med Sci. 2016 Aug;4(8):3421-3426 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162305
Comparison of the Hemodynamic Responses with. with LMA vs Endotracheal Intubation
 Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Original article Comparison of the Hemodynamic Responses 10.5005/jp-journals-10045-0060 with LMA vs Endotracheal Intubation Comparison of the Hemodynamic Responses with Laryngeal Mask Airway vs Endotracheal
Comparison of Ease of Insertion and Hemodynamic Response to Lma with Propofol and Thiopentone.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 14, Issue 12 Ver. IV (Dec. 2015), PP 22-30 www.iosrjournals.org Comparison of Ease of Insertion and Hemodynamic
Pharmacokinetics. Inhalational Agents. Uptake and Distribution
 Pharmacokinetics Inhalational Agents The pharmacokinetics of inhalational agents is divided into four phases Absorption Distribution (to the CNS Metabolism (minimal Excretion (minimal The ultimate goal
Pharmacokinetics Inhalational Agents The pharmacokinetics of inhalational agents is divided into four phases Absorption Distribution (to the CNS Metabolism (minimal Excretion (minimal The ultimate goal
P V Praveen Kumar 1*, P. Archana 2. Original Research Article. Abstract
 Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Original Research Article Comparative clinical study of attenuation of cardiovascular responses to laryngoscopy intubation diltiazem, lignocaine and combination of diltiazem and lignocaine P V Praveen
Evaluation of Dexmedetomidine 0.5 µg/kg and 1 µg/kg in Blunting the Responses to Laryngoscopy and Intubation
 Original Article DOI: 10.17354/ijss/2016/74 Evaluation of Dexmedetomidine 0.5 µg/kg and 1 µg/kg in Blunting the Responses to Laryngoscopy and Intubation Bansal Rachit 1, H S Nanda 2, Kashyap Mahesh 3 1
Original Article DOI: 10.17354/ijss/2016/74 Evaluation of Dexmedetomidine 0.5 µg/kg and 1 µg/kg in Blunting the Responses to Laryngoscopy and Intubation Bansal Rachit 1, H S Nanda 2, Kashyap Mahesh 3 1
General anesthesia. No single drug capable of achieving these effects both safely and effectively.
 General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
General anesthesia General anesthesia is essential to surgical practice, because it renders patients analgesic, amnesia, and unconscious reflexes, while causing muscle relaxation and suppression of undesirable
Journal of Anesthesia & Clinical
 Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Journal of Anesthesia & Clinical Research ISSN: 2155-6148 Journal of Anesthesia & Clinical Research Balasubramanian and Menaha, J Anesth Clin Res 2017, 8:12 DOI: 10.4172/2155-6148.1000791 Research Article
Research Article. Shital S. Ahire 1 *, Shweta Mhambrey 1, Sambharana Nayak 2. Received: 22 July 2016 Accepted: 08 August 2016
 International Journal of Research in Medical Sciences Ahire SS et al. Int J Res Med Sci. 2016 Sep;4(9):3838-3844 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162824
International Journal of Research in Medical Sciences Ahire SS et al. Int J Res Med Sci. 2016 Sep;4(9):3838-3844 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162824
ISSN X (Print) Research Article. *Corresponding author Dr. Souvik Saha
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(6B):2238-2243 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(6B):2238-2243 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Study Of Effects Of Varying Durations Of Pre-Oxygenation. J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh
 ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh Citation J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh.. The Internet
ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 1 J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh Citation J Khandrani, A Modak, B Pachpande, G Walsinge, A Ghosh.. The Internet
JMSCR Vol 04 Issue 01 Page January 2016
 www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i1.04 Haemodynamic Effects during Induction in
www.jmscr.igmpublication.org Impact Factor 3.79 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i1.04 Haemodynamic Effects during Induction in
Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study
 Original article Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study Shishir Ramachandra Sonkusale 1, RajulSubhash
Original article Evaluation of Postoperative Complications Occurring in Patients after Desflurane or Sevoflurane in Outpatient Anaesthesia: A Comparative Study Shishir Ramachandra Sonkusale 1, RajulSubhash
Low dose fentanyl attenuates hypertension but not tachycardia during laryngoscopy and tracheal intubation in a three arm study
 Original Research Article Low dose fentanyl attenuates hypertension but not tachycardia during laryngoscopy and tracheal intubation in a three arm study Valluri Anil Kumar 1*, Vaddineni Jagadish 1, Netra
Original Research Article Low dose fentanyl attenuates hypertension but not tachycardia during laryngoscopy and tracheal intubation in a three arm study Valluri Anil Kumar 1*, Vaddineni Jagadish 1, Netra
Propofol or etomidate: Does it genuinely matter for induction in cardiac surgical procedures?
 Original Research Article DOI: 10.18231/2394-4994.2016.0012 Propofol or etomidate: Does it genuinely matter for induction in cardiac surgical procedures? Manjunath Ratnakara Kamath 1,*, Suchitha Kamath
Original Research Article DOI: 10.18231/2394-4994.2016.0012 Propofol or etomidate: Does it genuinely matter for induction in cardiac surgical procedures? Manjunath Ratnakara Kamath 1,*, Suchitha Kamath
Type of intervention Anaesthesia. Economic study type Cost-effectiveness analysis.
 Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
Comparison of the costs and recovery profiles of three anesthetic techniques for ambulatory anorectal surgery Li S T, Coloma M, White P F, Watcha M F, Chiu J W, Li H, Huber P J Record Status This is a
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
S.No. 1. COMPARATIVE STUDY OF CENTRAL VENOUS CANNULATION USING ULTRASOUND GUIDANCE VERSUS LANDMARK TECHNIQUE IN PAEDIATRIC CARDIAC PATIENT. 2. TO EVALUATE THE ABILITY OF SVV OBTAINED BY VIGILEO-FLO TRAC
Effect of Vecuronium in different age group
 Original Research Article Effect of Vecuronium in different age group Bharti Rajani 1, Hitesh Brahmbhatt 2, Hemlata Chaudhry 2, Hiren Parmar 3* 1 Associate Professor, Department of Anesthesiology, GMERS
Original Research Article Effect of Vecuronium in different age group Bharti Rajani 1, Hitesh Brahmbhatt 2, Hemlata Chaudhry 2, Hiren Parmar 3* 1 Associate Professor, Department of Anesthesiology, GMERS
Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy
 Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy Amir Murad Khudad* Hoshyar Najeeb Karem** ABSTRACT Background and Objectives: The cardiovascular response
Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy Amir Murad Khudad* Hoshyar Najeeb Karem** ABSTRACT Background and Objectives: The cardiovascular response
Journal of Anesthesiology
 Journal of Anesthesiology 213; 1(1): 1-8 Published online June 3, 213 (http://www.sciencepublishinggroup.com/j/ja) doi: 1.11648/j.ja.21311.11 A study of the efficacy of cardiac antidysrhythmic drugs in
Journal of Anesthesiology 213; 1(1): 1-8 Published online June 3, 213 (http://www.sciencepublishinggroup.com/j/ja) doi: 1.11648/j.ja.21311.11 A study of the efficacy of cardiac antidysrhythmic drugs in
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS)
 Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Optimal sedation and management of anxiety in patients undergoing endobronchial ultrasound (EBUS) Georgios Dadoudis Anesthesiologist ICU DIRECTOR INTERBALKAN MEDICAL CENTER Optimal performance requires:
Keywords: Dexmedetomidine, fentanyl, tympanoplasty, monitored anaesthesia care. INTRODUCTION:
 13 Original article A COMPARATIVE OBSERVATIONAL STUDY BETWEEN DEXMEDETOMIDINE V/S COMBINATION OF MIDAZOLAM- FENTANYL FOR TYMPANOPLASTY SURGERY UNDER MONITORED ANESTHESIA CARE Dr. Parul Pachotiya (Professor
13 Original article A COMPARATIVE OBSERVATIONAL STUDY BETWEEN DEXMEDETOMIDINE V/S COMBINATION OF MIDAZOLAM- FENTANYL FOR TYMPANOPLASTY SURGERY UNDER MONITORED ANESTHESIA CARE Dr. Parul Pachotiya (Professor
General Anesthesia. Mohamed A. Yaseen
 General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
General Anesthesia Mohamed A. Yaseen M.S,c Surgery Before Anesthesia General Anesthesia ( GA ) Drug induced absence of perception of all sensation allowing surgery or other painful procedure to be carried
Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant
 Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Original Article Tracheal intubation in children after induction of anesthesia with propofol and remifentanil without a muscle relaxant Mirmohammad Taghi Mortazavi, 1 Masood Parish, 1 Naghi Abedini, 2
Bispectral index (Bis) guided comparison of control of haemodynamic responses by fentanyl and butorphanol during tracheal intubation in neurosurgical
 Page 1 of 5 Pharmacology Bispectral index (Bis) guided comparison of control of haemodynamic responses by fentanyl and butorphanol during tracheal intubation in neurosurgical S Kumar 1, A Singh 3*, LD
Page 1 of 5 Pharmacology Bispectral index (Bis) guided comparison of control of haemodynamic responses by fentanyl and butorphanol during tracheal intubation in neurosurgical S Kumar 1, A Singh 3*, LD
Setting The setting was a hospital (tertiary care). The economic study was carried out in Ankara, Turkey.
 Inhalation versus total intravenous anesthesia for lumbar disc herniation: comparison of hemodynamic effects, recovery characteristics, and cost Ozkose Z, Ercan B, Unal Y, Yardim S, Kaymaz M, Dogulu F,
Inhalation versus total intravenous anesthesia for lumbar disc herniation: comparison of hemodynamic effects, recovery characteristics, and cost Ozkose Z, Ercan B, Unal Y, Yardim S, Kaymaz M, Dogulu F,
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Pharmacology: Inhalation Anesthetics
 Pharmacology: Inhalation Anesthetics This is an edited and abridged version of: Pharmacology: Inhalation Anesthetics by Jch Ko, DVM, MS, DACVA Oklahoma State University - Veterinary Medicine, February
Pharmacology: Inhalation Anesthetics This is an edited and abridged version of: Pharmacology: Inhalation Anesthetics by Jch Ko, DVM, MS, DACVA Oklahoma State University - Veterinary Medicine, February
As laparoscopic surgeries are gaining popularity, Original Article. Maharjan SK 1, Shrestha S 2 1. Introduction
 , Vol. 1, No. 1, Issue 1, Jul.-Sep., 2012 Original Article Maharjan SK 1, Shrestha S 2 1 Associate Professor, 2 Assistant Professor, Department of Anaesthesiology and Intensive Care Kathmandu Medical College,
, Vol. 1, No. 1, Issue 1, Jul.-Sep., 2012 Original Article Maharjan SK 1, Shrestha S 2 1 Associate Professor, 2 Assistant Professor, Department of Anaesthesiology and Intensive Care Kathmandu Medical College,
GENERAL ANAESTHESIA AND FAILED INTUBATION
 GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
GENERAL ANAESTHESIA AND FAILED INTUBATION INTRODUCTION The majority of caesarean sections in the UK are performed under regional anaesthesia. However, there are situations where general anaesthesia (GA)
ANESTHESIA EXAM (four week rotation)
 SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
SPARROW HEALTH SYSTEM ANESTHESIA SERVICES ANESTHESIA EXAM (four week rotation) Circle the best answer 1. During spontaneous breathing, volatile anesthetics A. Increase tidal volume and decrease respiratory
Efficacy Of Ropivacaine - Fentanyl In Comparison To Bupivacaine - Fentanyl In Epidural Anaesthesia
 ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 Efficacy Of Ropivacaine - Fentanyl In Comparison To Bupivacaine - Fentanyl In Epidural Anaesthesia S Gautam, S Singh, R Verma, S Kumar,
ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 Efficacy Of Ropivacaine - Fentanyl In Comparison To Bupivacaine - Fentanyl In Epidural Anaesthesia S Gautam, S Singh, R Verma, S Kumar,
Induction position for spinal anaesthesia: Sitting versus lateral position
 11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
11 ORIGINAL ARTICLE Induction position for spinal anaesthesia: Sitting versus lateral position Khurrum Shahzad, Gauhar Afshan Abstract Objective: To compare the effect of induction position on block characteristics
ORIGINAL RESEARCH Attenuation Of Rise In Blood Pressure And Heart Rate During Direct Laryngoscopy And Intubation
 IJCMR 428 ORIGINAL RESEARCH Attenuation Of Rise In Blood Pressure And Heart Rate During Direct Laryngoscopy And Intubation Kailash Chandra Sharma 1, Subodh Kumar 2, Sujata Singh 3 ABSTRACT Introduction:
IJCMR 428 ORIGINAL RESEARCH Attenuation Of Rise In Blood Pressure And Heart Rate During Direct Laryngoscopy And Intubation Kailash Chandra Sharma 1, Subodh Kumar 2, Sujata Singh 3 ABSTRACT Introduction:
Rocuronium versus Vecuronium for laparoscopic cholecystectomy
 Original Article, Vol. 2, No. 4, Issue 6, Oct.-Dec., 2013 Rocuronium versus Vecuronium for laparoscopic cholecystectomy Tabdar S 1, Kadariya ER 2 1 Sushila Tabdar, Assistant Professor, Department of Anaesthesiology
Original Article, Vol. 2, No. 4, Issue 6, Oct.-Dec., 2013 Rocuronium versus Vecuronium for laparoscopic cholecystectomy Tabdar S 1, Kadariya ER 2 1 Sushila Tabdar, Assistant Professor, Department of Anaesthesiology
MD (Anaesthesiology) Title (Plan of Thesis) (Session )
 S.No. 1. Comparative Assessment of Sequential organ failure Assessment (SOFA) score and Multiple Organ Dysfunction Score (Mode) in Outcome Prediction among ICU Patients. 2. Comparison of Backpain after
S.No. 1. Comparative Assessment of Sequential organ failure Assessment (SOFA) score and Multiple Organ Dysfunction Score (Mode) in Outcome Prediction among ICU Patients. 2. Comparison of Backpain after
Regional Anaesthesia for Caesarean Section
 Regional Anaesthesia for Caesarean Section "The Best Recipe" Warwick D. Ngan Kee Dept of Anaesthesia & Intensive Care The Chinese University of Hong Kong What I will not do. Magic recipes One shoe to fit
Regional Anaesthesia for Caesarean Section "The Best Recipe" Warwick D. Ngan Kee Dept of Anaesthesia & Intensive Care The Chinese University of Hong Kong What I will not do. Magic recipes One shoe to fit
General anesthetics. Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine
 General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
General anesthetics Dr. Shamil AL-Noaimy Lecturer of Pharmacology Dept. of Pharmacology College of Medicine Rationale General anesthesia is essential to surgical practice, because it renders patients analgesic,
Original Article INTRODUCTION. Abstract. hypothermia. Shivering obscures intraoperative monitoring like electrocardiogram, SPO 2
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/431 Compare the Efficacy of Dexmedetomidine and Tramadol in Preventing Intraoperative Shivering in Patients Undergoing
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/431 Compare the Efficacy of Dexmedetomidine and Tramadol in Preventing Intraoperative Shivering in Patients Undergoing
Preparation for Premedication
 Preparation for Premedication Recommendations for Premedication in Rapid Sequence Intubation David J. Roy, PharmD, BCPS PGY2 Emergency Medicine Pharmacy Resident Pharmacy Grand Rounds January 17 th, 2017
Preparation for Premedication Recommendations for Premedication in Rapid Sequence Intubation David J. Roy, PharmD, BCPS PGY2 Emergency Medicine Pharmacy Resident Pharmacy Grand Rounds January 17 th, 2017
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 3/ Issue 74/Dec 29, 2014 Page 15535
 RANDOMISED CLINICAL TRIAL TO COMPARE THE EFFECT OF PRETREATMENT OF KETAMINE AND LIGNOCAINE ON PROPOFOL INJECTION PAIN Hanumanthappa V. Airani 1, Bhagyashree Amingad 2, Chandra Kumar B. M 3 HOW TO CITE
RANDOMISED CLINICAL TRIAL TO COMPARE THE EFFECT OF PRETREATMENT OF KETAMINE AND LIGNOCAINE ON PROPOFOL INJECTION PAIN Hanumanthappa V. Airani 1, Bhagyashree Amingad 2, Chandra Kumar B. M 3 HOW TO CITE
Remifentanil. Addressing the challenges of ambulatory orthopedic procedures 1-3
 Remifentanil Addressing the challenges of ambulatory orthopedic procedures 1-3 INDICATIONS AND IMPORTANT RISK INFORMATION INDICATIONS ULTIVA (remifentanil HCl) for Injection is indicated for intravenous
Remifentanil Addressing the challenges of ambulatory orthopedic procedures 1-3 INDICATIONS AND IMPORTANT RISK INFORMATION INDICATIONS ULTIVA (remifentanil HCl) for Injection is indicated for intravenous
PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older)
 Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Name Score PHYSICIAN COMPETENCY FOR ADULT DEEP SEDATION (Ages 14 and older) 1. Pre-procedure evaluation for moderate sedation should involve all of the following EXCEPT: a) Airway Exam b) Anesthetic history
Chapter 25. General Anesthetics
 Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Chapter 25 1. Introduction General anesthetics: 1. Analgesia 2. Amnesia 3. Loss of consciousness 4. Inhibition of sensory and autonomic reflexes 5. Skeletal muscle relaxation An ideal anesthetic: 1. A
Inhalational Agents in Bariatric Procedures
 Inhalational Agents in Bariatric Procedures Overweight The term overweight signifies an excess body weight when compared to established standards. This weight may derive from muscle, bone, fat, and/or
Inhalational Agents in Bariatric Procedures Overweight The term overweight signifies an excess body weight when compared to established standards. This weight may derive from muscle, bone, fat, and/or
Crresponding Author: * Gurpreet Singh
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. V (Sep. 2017), PP 28-35 www.iosrjournals.org A Comparative Evaluation of Fixed High
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 9 Ver. V (Sep. 2017), PP 28-35 www.iosrjournals.org A Comparative Evaluation of Fixed High
Beta Blockers for ENT Surgery
 Beta Blockers for ENT Surgery Dr. Giuliano Michelagnoli U.O. Anestesia e Rianimazione Nuovo Ospedale di Prato Perioperative Beta-Blockade 1. Reduction of perioperative cardiovascular risk 2. Multimodal
Beta Blockers for ENT Surgery Dr. Giuliano Michelagnoli U.O. Anestesia e Rianimazione Nuovo Ospedale di Prato Perioperative Beta-Blockade 1. Reduction of perioperative cardiovascular risk 2. Multimodal
Anesthesia Final Exam
 Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Antiemetic Effect Of Propofol Administered At The End Of Surgery
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 11 Ver. III (November. 2016), PP 54-58 www.iosrjournals.org Antiemetic Effect Of Propofol Administered
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 11 Ver. III (November. 2016), PP 54-58 www.iosrjournals.org Antiemetic Effect Of Propofol Administered
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Comparison of intracuff dexamethasone, lignocaine and normal saline on post extubation response - A prospective study
 Original Research Article Comparison of intracuff dexamethasone, lignocaine and normal saline on post extubation response - A prospective study Soumya M V 1, Sanjeev G M 2* 1 Senior Resident, 2 Associate
Original Research Article Comparison of intracuff dexamethasone, lignocaine and normal saline on post extubation response - A prospective study Soumya M V 1, Sanjeev G M 2* 1 Senior Resident, 2 Associate
ABSTRACT. Alexandria Journal of Anaesthesia and Intensive Care INTRODUCTION. AJAIC-Vol. (9) No. 1 Marsh 2006
 1 COMPARISON BETWEEN THE INDUCTION OF ANESTHESIA USING SEVOFLURANE-NITROUS OXIDE, PROPOFOL OR COMBINATION OF PROPOFOL AND SEVOFLURANE-NITROUS OXIDE USING LARYNGEAL MASK AIRWAY(LMA) IN HYPERTENSIVE PATIENTS
1 COMPARISON BETWEEN THE INDUCTION OF ANESTHESIA USING SEVOFLURANE-NITROUS OXIDE, PROPOFOL OR COMBINATION OF PROPOFOL AND SEVOFLURANE-NITROUS OXIDE USING LARYNGEAL MASK AIRWAY(LMA) IN HYPERTENSIVE PATIENTS
SEEING KETAMINE IN A NEW LIGHT
 SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SEEING KETAMINE IN A NEW LIGHT BobbieJean Sweitzer, M.D., FACP Professor of Anesthesiology Director of Perioperative Medicine Northwestern University Bobbie.Sweitzer@northwestern.edu LEARNING OBJECTIVES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION
 SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
SECTION 1: INCLUSION, EXCLUSION & RANDOMISATION INFORMATION DEMOGRAPHIC INFORMATION Given name Family name Date of birth Consent date Gender Female Male Date of surgery INCLUSION & EXCLUSION CRITERIA YES
Internet Journal of Medical Update
 Internet Journal of Medical Update 2011 July;6(2):20-24. Internet Journal of Medical Update Journal home page: http://www.akspublication.com/ijmu Original Work Circulatory responses to propofol-ketamine
Internet Journal of Medical Update 2011 July;6(2):20-24. Internet Journal of Medical Update Journal home page: http://www.akspublication.com/ijmu Original Work Circulatory responses to propofol-ketamine
Attenuation of the Hemodynamic Responses to Endotracheal Intubation with Gabapentin Versus Fentanyl: A Randomized Double Blind Controlled Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 18, Issue 2 Ser. 1 (February. 2019), PP 83-88 www.iosrjournals.org Attenuation of the Hemodynamic Responses
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 18, Issue 2 Ser. 1 (February. 2019), PP 83-88 www.iosrjournals.org Attenuation of the Hemodynamic Responses
COMPARISON OF INDUCTION WITH SEVOFLURANE-FENTANYL AND PROPOFOL-FENTANYL ON POSTOPERATIVE NAUSEA AND VOMITING AFTER LAPAROSCOPIC SURGERY
 RESEARCH ARTICLE COMPARISON OF INDUCTION WITH SEVOFLURANE-FENTANYL AND PROPOFOL-FENTANYL ON POSTOPERATIVE NAUSEA AND VOMITING AFTER LAPAROSCOPIC SURGERY ABSTRACT Ghanta.V. Nalini Kumari 1,*, Sushma Ladi
RESEARCH ARTICLE COMPARISON OF INDUCTION WITH SEVOFLURANE-FENTANYL AND PROPOFOL-FENTANYL ON POSTOPERATIVE NAUSEA AND VOMITING AFTER LAPAROSCOPIC SURGERY ABSTRACT Ghanta.V. Nalini Kumari 1,*, Sushma Ladi
THE EFFECT OF INTRAMUSCULAR EPHEDRINE IN PREVENTION OF HYPOTENSION DUE TO PROPOFOL
 Original Article THE EFFECT OF INTRAMUSCULAR EPHEDRINE IN PREVENTION OF HYPOTENSION DUE TO PROPOFOL Susan Rasooli 1, Masoud Parish 2, Ata Mahmoodpoor 3, Farnaz Moslemi 4, Sarvin Sanaie 5, Sara Faghfuri
Original Article THE EFFECT OF INTRAMUSCULAR EPHEDRINE IN PREVENTION OF HYPOTENSION DUE TO PROPOFOL Susan Rasooli 1, Masoud Parish 2, Ata Mahmoodpoor 3, Farnaz Moslemi 4, Sarvin Sanaie 5, Sara Faghfuri
JMSCR Vol 06 Issue 11 Page November 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i11.98 IV Nalbuphine vs IV Fentanyl
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i11.98 IV Nalbuphine vs IV Fentanyl
International Journal of Medical and Health Sciences
 International Journal of Medical and Health Sciences Journal Home Page: http://www.ijmhs.net ISSN:2277-4505 Original article A Comparative Study Of Etomidate And Midazolam Induction In Patients Undergoing
International Journal of Medical and Health Sciences Journal Home Page: http://www.ijmhs.net ISSN:2277-4505 Original article A Comparative Study Of Etomidate And Midazolam Induction In Patients Undergoing
J M e d A l l i e d S c i ; 7 ( 1 ) : w w w. j m a s. i n. P r i n t I S S N : O n l i n e I S S N : X
 J M e d A l l i e d S c i 2 0 1 7 ; 7 ( 1 ) : 09-13 w w w. j m a s. i n P r i n t I S S N : 2 2 3 1 1 6 9 6 O n l i n e I S S N : 2 2 3 1 1 7 0 X Journal of M e d i cal & Allied Sciences Original article
J M e d A l l i e d S c i 2 0 1 7 ; 7 ( 1 ) : 09-13 w w w. j m a s. i n P r i n t I S S N : 2 2 3 1 1 6 9 6 O n l i n e I S S N : 2 2 3 1 1 7 0 X Journal of M e d i cal & Allied Sciences Original article
Original contribution. Department of Anesthesiology, Sapporo Medical University, School of Medicine, Sapporo, Hokkaido, Japan
 Journal of Clinical Anesthesia (2007) 19, 25 29 Original contribution A comparison of spinal anesthesia with small-dose lidocaine and general anesthesia with fentanyl and propofol for ambulatory prostate
Journal of Clinical Anesthesia (2007) 19, 25 29 Original contribution A comparison of spinal anesthesia with small-dose lidocaine and general anesthesia with fentanyl and propofol for ambulatory prostate
May 2013 Anesthetics SLOs Page 1 of 5
 May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
May 2013 Anesthetics SLOs Page 1 of 5 1. A client is having a scalp laceration sutured and is to be given Lidocaine that contains Epinephrine. The nurse knows that this combination is desgined to: A. Cause
S. K. Gvalani 1 *, Sushant Mane 2
 International Journal of Research in Medical Sciences Gvalani SK et al. Int J Res Med Sci. 2016 Sep;4(9):3858-3864 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162848
International Journal of Research in Medical Sciences Gvalani SK et al. Int J Res Med Sci. 2016 Sep;4(9):3858-3864 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20162848
Comparison of tramadol and pethidine for control of shivering in regional anesthesia
 International Journal of Research in Medical Sciences Paul C et al. Int J Res Med Sci. 2017 Jul;5(7):2890-2894 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20172621
International Journal of Research in Medical Sciences Paul C et al. Int J Res Med Sci. 2017 Jul;5(7):2890-2894 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20172621
Controlled Trial of Wound Infiltration with Bupivacaine for Post Operative Pain Relief after Caesarean Section
 Bahrain Medical Bulletin, Vol.23, No.2, June 2001 Controlled Trial of Wound Infiltration with Bupivacaine for Post Operative Pain Relief after Caesarean Section Omar Momani, MD, MBBS, JBA* Objective: The
Bahrain Medical Bulletin, Vol.23, No.2, June 2001 Controlled Trial of Wound Infiltration with Bupivacaine for Post Operative Pain Relief after Caesarean Section Omar Momani, MD, MBBS, JBA* Objective: The
Labor Epidural: Local Anesthetics and Beyond
 Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Goals: Labor Epidural: Local Anesthetics and Beyond Pedram Aleshi MD The Changing Practice of Anesthesia September 2012 Review Concept of MLAC Local anesthetic efficacy Local anesthetic sparing effects:
Regional Anaesthesia for Children
 Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Regional Anaesthesia for Children Indispensable! but also safe? PD Dr. med. Jacqueline Mauch Outline Significance of regional anaesthesia in paediatric surgery Risks and complications of regional anaesthesia
Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol and sevoflurane
 Clinical Research Article Korean J Anesthesiol 2011 January 60(1): 36-40 DOI: 10.4097/kjae.2011.60.1.36 Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol
Clinical Research Article Korean J Anesthesiol 2011 January 60(1): 36-40 DOI: 10.4097/kjae.2011.60.1.36 Post-operative nausea and vomiting after gynecologic laparoscopic surgery: comparison between propofol
COMPARATIVE STUDY OF PROPOFOL-NITROUS OXIDE(N 2 O) WITH CONVENTIONAL BALANCED ANAESTHETIC TECHNIQUE FOR DAY CARE LAPAROSCOPIC SURGERY.
 COMPARATIVE STUDY OF PROPOFOL-NITROUS OXIDE(N 2 O) WITH CONVENTIONAL BALANCED ANAESTHETIC TECHNIQUE FOR DAY CARE LAPAROSCOPIC SURGERY. Alka Kewalramani. 1*,Dr.Gaurav Chhabra 2,Dr.Vaishali Shelgoankar 3
COMPARATIVE STUDY OF PROPOFOL-NITROUS OXIDE(N 2 O) WITH CONVENTIONAL BALANCED ANAESTHETIC TECHNIQUE FOR DAY CARE LAPAROSCOPIC SURGERY. Alka Kewalramani. 1*,Dr.Gaurav Chhabra 2,Dr.Vaishali Shelgoankar 3
Paediatric neuraxial anaesthesia asleep or awake, what is the best for safety?
 ISPUB.COM The Internet Journal of Anesthesiology Volume 21 Number 1 Paediatric neuraxial anaesthesia asleep or awake, what is the best for safety? A Shabana, A Shorrab Citation A Shabana, A Shorrab. Paediatric
ISPUB.COM The Internet Journal of Anesthesiology Volume 21 Number 1 Paediatric neuraxial anaesthesia asleep or awake, what is the best for safety? A Shabana, A Shorrab Citation A Shabana, A Shorrab. Paediatric
Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries and Perineal Surgeries
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/229 Comparative Study of Equal Doses of Intrathecal Isobaric Bupivacaine and Isobaric Ropivacaine for Lower Limb Surgeries
Sleep Apnea and ifficulty in Extubation. Jean Louis BOURGAIN May 15, 2016
 Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
Sleep Apnea and ifficulty in Extubation Jean Louis BOURGAIN May 15, 2016 Introduction Repetitive collapse of the upper airway > sleep fragmentation, > hypoxemia, hypercapnia, > marked variations in intrathoracic
*Author for Correspondence
 COMPARATIVE EVALUATION OF ONSET TIME INTUBATING CONDITION JUDGED BY CLINICAL CRITERIA AND HAEMODYNAMIC RESPONSE AFTER THE INTUBATING DOSE OF ROCURONIUM AND VECURONIUM *Namita Gupta 1, Mamta Sharma 2, Pusplata
COMPARATIVE EVALUATION OF ONSET TIME INTUBATING CONDITION JUDGED BY CLINICAL CRITERIA AND HAEMODYNAMIC RESPONSE AFTER THE INTUBATING DOSE OF ROCURONIUM AND VECURONIUM *Namita Gupta 1, Mamta Sharma 2, Pusplata
SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE
 Br. J. Anaesth. (987), 59, 24-28 SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE J. M. LAMBERTY AND I. H. WILSON Two studies have demonstrated that the induction of anaesthesia using a single breath
Br. J. Anaesth. (987), 59, 24-28 SINGLE BREATH INDUCTION OF ANAESTHESIA WITH ISOFLURANE J. M. LAMBERTY AND I. H. WILSON Two studies have demonstrated that the induction of anaesthesia using a single breath
ABHINAV NATIONAL MONTHLY REFEREED JOURNAL OF RESEARCH IN SCIENCE & TECHNOLOGY
 A COMPARATIVE STUDY OF BUTORPHANOL AND NALBUPHINE USING PROPOFOL AND ISOFLURANE IN PATIENTS UNDERGOING ELECTIVE CRANIOTOMY UNDER GENERAL ANAESTHESIA Dr. S.C. Dulara 1 and Dr. Sushil Chhabra 2 1 Professor,
A COMPARATIVE STUDY OF BUTORPHANOL AND NALBUPHINE USING PROPOFOL AND ISOFLURANE IN PATIENTS UNDERGOING ELECTIVE CRANIOTOMY UNDER GENERAL ANAESTHESIA Dr. S.C. Dulara 1 and Dr. Sushil Chhabra 2 1 Professor,
Pressor Response to Laryngeal Mask Airway Insertion versus Endotracheal Intubation in Standard Anesthetic Practice
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/239 Pressor Response to Laryngeal Mask Airway Insertion versus Endotracheal Intubation in Standard Anesthetic Practice
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2018/239 Pressor Response to Laryngeal Mask Airway Insertion versus Endotracheal Intubation in Standard Anesthetic Practice
Haemodynamic response to endotrachial intubation: direct versus video laryngoscopy
 International Journal of Research in Medical Sciences Kamewad AK et al. Int J Res Med Sci. 2016 Dec;4(12):5196-5200 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164040
International Journal of Research in Medical Sciences Kamewad AK et al. Int J Res Med Sci. 2016 Dec;4(12):5196-5200 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Original Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20164040
Multi-center (5 centers); United States and Canada. September 10, 1992 to April 9, 1993
 vi STUDY SYNOPSIS Study Number: Title: Investigator: GHBA-534 A Phase III, Randomized, Open-Label Study To Compare The Safety, Tolerability And Recovery Characteristics of Sevoflurane Versus Halothane
vi STUDY SYNOPSIS Study Number: Title: Investigator: GHBA-534 A Phase III, Randomized, Open-Label Study To Compare The Safety, Tolerability And Recovery Characteristics of Sevoflurane Versus Halothane
Table showing induction time (seconds) among studied groups Induction time (Seconds)
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. IV(Aug. 2017), PP 73-77 www.iosrjournals.org Comparison of Intraoperative Haemodynamic
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 8 Ver. IV(Aug. 2017), PP 73-77 www.iosrjournals.org Comparison of Intraoperative Haemodynamic
Use of the Intubating Laryngeal Mask Airway
 340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Surgical Care at the District Hospital 1 14 Practical Anesthesia Key Points 2 14.1 General Anesthesia Have a clear plan before starting anesthesia Never use an unfamiliar anesthetic technique in an emergency
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair. Krista Madden, MSNA. Westminster College
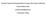 Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent Option For Day Care Surgeries
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 2 Ver. III. (Feb. 2014), PP 09-13 Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 13, Issue 2 Ver. III. (Feb. 2014), PP 09-13 Hyperbaric 2% Lignocaine In Spinal Anaesthesia An Excellent
Suggested items to be included in obstetric anaesthesia records
 Suggested items to be included in obstetric anaesthesia records This list is intended as a guide to what fields could be included in an anaesthesia record used in obstetric practice. It is merely a suggested
Suggested items to be included in obstetric anaesthesia records This list is intended as a guide to what fields could be included in an anaesthesia record used in obstetric practice. It is merely a suggested
Neostigmine as an adjunct to Bupivacaine, for caudal block in burned children, undergoing skin grafting of the lower extremities
 Neostigmine as an adjunct to Bupivacaine, for caudal block in burned children, undergoing skin grafting of the lower extremities Dr. Pramod Gupta, Dr Amy Grace MD Department of Anaesthesiology and Critical
Neostigmine as an adjunct to Bupivacaine, for caudal block in burned children, undergoing skin grafting of the lower extremities Dr. Pramod Gupta, Dr Amy Grace MD Department of Anaesthesiology and Critical
Anesthesia Monitoring. D. J. McMahon rev cewood
 Anesthesia Monitoring D. J. McMahon 150114 rev cewood 2018-01-19 Key Points Anesthesia Monitoring: - Understand the difference between guidelines & standards - ASA monitoring Standard I states that an
Anesthesia Monitoring D. J. McMahon 150114 rev cewood 2018-01-19 Key Points Anesthesia Monitoring: - Understand the difference between guidelines & standards - ASA monitoring Standard I states that an
Downloaded from armaghanj.yums.ac.ir at 21: on Thursday November 29th 2018
 : :.. :. II I ) II ( ) I. (.. SPSS. ) I : ) (. ( ) ( ) II ( ) ( ( ) I.(p=/) II. /±.. * * ** *** * ** *** //: //: : Khosro_kolahdozan@yahoo.com : :. : ..().()...()...()..( )...( ). ( ) /.. / : I / /) :
: :.. :. II I ) II ( ) I. (.. SPSS. ) I : ) (. ( ) ( ) II ( ) ( ( ) I.(p=/) II. /±.. * * ** *** * ** *** //: //: : Khosro_kolahdozan@yahoo.com : :. : ..().()...()...()..( )...( ). ( ) /.. / : I / /) :
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Indian Journal of Basic and Applied Medical Research; June 2015: Vol.-4, Issue- 3, P
 Original article: A randomised controlled study of tracheal extubation response following nitroglycerine (NTG) sublingual spray in normotensive and hypertensive patients Dr. sunil tuljapure, Dr. Vaishali
Original article: A randomised controlled study of tracheal extubation response following nitroglycerine (NTG) sublingual spray in normotensive and hypertensive patients Dr. sunil tuljapure, Dr. Vaishali
Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery
 Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Article ID: WMC002013 2046-1690 Dexamethasone Compared with Metoclopramide in Prevention of Postoperative Nausea and Vomiting in Orthognathic Surgery Corresponding Author: Dr. Agreta Gashi, Anesthesiologist,
Study of effectiveness of Dexmedetomidine and Fentanyl in attenuating the pressor responses associated with laryngoscopy and endotracheal intubation
 Original article: Study of effectiveness of Dexmedetomidine and Fentanyl in attenuating the pressor responses associated with laryngoscopy and endotracheal intubation Dr. G. Anjana Purnima 1, Dr. Pravin
Original article: Study of effectiveness of Dexmedetomidine and Fentanyl in attenuating the pressor responses associated with laryngoscopy and endotracheal intubation Dr. G. Anjana Purnima 1, Dr. Pravin
PROPHYLACTIC ORAL EPHEDRINE IN PREVENTION OF HYPOTENSION FOLLOWING SPINAL ANAESTHESIA R. Vasanthageethan 1, S. Ramesh Kumar 2, Ilango Ganesan 3
 PROPHYLACTIC ORAL EPHEDRINE IN PREVENTION OF HYPOTENSION FOLLOWING SPINAL ANAESTHESIA R. Vasanthageethan 1, S. Ramesh Kumar 2, Ilango Ganesan 3 HOW TO CITE THIS ARTICLE: R. Vasanthageethan, S. Ramesh Kumar,
PROPHYLACTIC ORAL EPHEDRINE IN PREVENTION OF HYPOTENSION FOLLOWING SPINAL ANAESTHESIA R. Vasanthageethan 1, S. Ramesh Kumar 2, Ilango Ganesan 3 HOW TO CITE THIS ARTICLE: R. Vasanthageethan, S. Ramesh Kumar,
Manual versus target-controlled infusions of propofol
 Manual versus target-controlled s of propofol D. S. Breslin, 1 R. K. Mirakhur, 2 J. E. Reid 3 and A. Kyle 4 1 Research Fellow, 2 Professor, 3 SpR, 4 Research Nurse, Department of Anaesthetics and Intensive
Manual versus target-controlled s of propofol D. S. Breslin, 1 R. K. Mirakhur, 2 J. E. Reid 3 and A. Kyle 4 1 Research Fellow, 2 Professor, 3 SpR, 4 Research Nurse, Department of Anaesthetics and Intensive
Pain & Sedation Management in PICU. Marut Chantra, M.D.
 Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Pain & Sedation Management in PICU Marut Chantra, M.D. Pain Diseases Trauma Procedures Rogers Textbook of Pediatric Intensive Care, 5 th ed, 2015 Emotional Distress Separation from parents Unfamiliar
Comparative study of effective-site target controlled infusion with standard bolus induction of propofol for laryngeal mask airway insertion
 Asian Biomedicine Vol. 4 No. 1 February 2010; 177-182 Brief communication (Original) Comparative study of effective-site target controlled infusion with standard bolus induction of propofol for laryngeal
Asian Biomedicine Vol. 4 No. 1 February 2010; 177-182 Brief communication (Original) Comparative study of effective-site target controlled infusion with standard bolus induction of propofol for laryngeal
EFFECT OF PROPOFOL TITRATION V/S BOLUS DURING INDUCTION OF ANESTHESIA ON HEMODYNAMICS AND BISPECTRAL INDEX
 EFFECT OF PROPOFOL TITRATION V/S BOLUS DURING INDUCTION OF ANESTHESIA ON HEMODYNAMICS AND BISPECTRAL INDEX EFFECT OF PROPOFOL TITRATION V/S BOLUS DURING INDUCTION OF ANESTHESIA ON HEMODYNAMICS AND BISPECTRAL
EFFECT OF PROPOFOL TITRATION V/S BOLUS DURING INDUCTION OF ANESTHESIA ON HEMODYNAMICS AND BISPECTRAL INDEX EFFECT OF PROPOFOL TITRATION V/S BOLUS DURING INDUCTION OF ANESTHESIA ON HEMODYNAMICS AND BISPECTRAL
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
