We have heard a great deal about "overactive" bladder recently. But what
|
|
|
- Lizbeth Oliver
- 5 years ago
- Views:
Transcription
1 BLADDER DYSFUNCTION Differential Diagnosis and Treatment of Impaired Bladder Emptying Naoki Yoshimura, MD, PhD, Michael B. Chancellor, MD Department of Urology, University of Pittsburgh School of Medicine, Pittsburgh, PA Although much attention is paid to urinary incontinence, the condition of incomplete bladder emptying is becoming more common with the aging of the US population and the widespread use of anticholinergic drugs to treat overactive bladder. This disorder can often be silent until end-stage presentation of overflow incontinence. In this article, we review the pathophysiologic conditions of the bladder and urethra that can cause impaired bladder emptying and discuss how to evaluate and screen the patient with a bladder that does not empty. In addition, we provide an overview of treatment options available for impaired bladder emptying and consider the research that is under way to find the best therapies for the failing bladder. [Rev Urol. 24;6(suppl 1):S24-S31] 24 MedReviews, LLC Key words: Bladder Urethra Urinary retention Ultrasound Bethanechol We have heard a great deal about "overactive" bladder recently. But what if your patients have the opposite problem a bladder that "won t go"? How do you evaluate the patient whose bladder does not empty? What are the most common and effective forms of therapy for impaired bladder emptying? S24 VOL. 6 SUPPL REVIEWS IN UROLOGY
2 Impaired Bladder Emptying Urinary retention and incomplete bladder emptying can be caused by an inadequately contractile bladder, urethral sphincter obstruction, or both. Because prostate enlargement has been addressed in a previous article in this supplement (see Lepor, p. S8), this article focuses on bladder dysfunction. The one unique case of urethral obstruction that is discussed is function retention due to non-neurogenic detrusor-sphincter dyssynergia, also referred to as shy bladder syndrome. Micturition Reflexes Normal micturition is completely dependent on neural pathways in the central nervous system. These pathways perform 3 major functions: amplification, coordination, and timing. 1 The nervous control of the lower urinary tract must be able to amplify weak smooth-muscle activity to provide sustained increases in intravesical pressures sufficient to empty the bladder. The bladder and urethral sphincter function must be coordinated to allow the sphincter to open during micturition but remain closed at all other times. Timing represents the voluntary control of voiding in the normal adult and the ability to initiate voiding over a wide range of bladder volumes. In this regard, the bladder is a unique visceral organ that exhibits predominantly voluntary rather than involuntary (autonomic) neural regulation. A number of important reflex mechanisms contribute to the storage and elimination of urine and modulate the voluntary control of micturition. Guarding Reflexes Against Stress Urinary Incontinence There is an important bladder-tourethra reflex that is mediated by sympathetic efferent pathways to the urethra. This is an excitatory reflex that contracts the urethral smooth muscle and, thus, is called a guarding reflex. The positive reflex is not activated during micturition but activates when bladder pressure is increased, such as during a cough or exercise. A second guarding reflex is triggered by activation of sacral motoneurons that, in turn, activate urethral external sphincter efferent neurons, which send axons into the pudendal nerves and the nerves innervating the pelvic floor. 2 This somatic guarding reflex is activated by bladder afferents and/or directly by stress such as sneezing. 3 The activation of somatic urethral and pelvic floor efferent pathways contracts the external urinary sphincter and the pelvic floor muscle, thus preventing stress urinary incontinence. The brain inhibits the guarding reflexes during micturition. Causes of Incomplete Bladder Emptying Urinary retention and incomplete emptying can result from a number of causes (Table 1). In some cases, the flow of urine is blocked, for example, in men with benign prostatic hyperplasia. This causes obstruction. Another form of impaired emptying is nonobstructive, that is, there is no problem with the urethra but the bladder muscle is less able to adequately contract. When the bladder cannot contract properly, some or all of the urine remains in the bladder. If left untreated, this condition can lead to urinary tract infection and damage to the kidneys. 4 Urethral Obstruction Functional obstruction at the pelvic floor external sphincter, sometimes called shy bladder syndrome, can cause just as much distress as prostatic mechanical obstruction of the urethra. At the University of Pittsburgh, we have seen a number of patients in end-stage renal failure resulting from the inability to relax the external sphincter over decades. The condition is believed to be an abnormal, learned, and upregulated guarding reflex. Before these patients are put on the transplant list, they are taught intermittent self-catheterization. Bladder Dysfunction Detrusor areflexia is defined as acontractility due to an abnormality of nervous control. In detrusor areflexia, Detrusor areflexia can develop from various conditions in which the neurologic pathways innervating the bladder are damaged. the bladder cannot be demonstrated to contract during urodynamic studies. Detrusor areflexia can develop from various conditions in which the neurologic pathways innervating the bladder are damaged. However, the contribution of myogenic factors should not be ignored. Common Neurologic Causes of Impaired Bladder Emptying Spinal cord injury. Any injury to the spinal cord, including blunt, degenerative, developmental, vascular, infectious, traumatic, and idiopathic injury, can cause voiding dysfunction. Injury to the cauda equina and peripheral sacral nerves can have devastating effects on bladder and urethral sphincter function. The true incidence of lower urinary tract dysfunction as a result of cauda equina and pelvic plexus injury is unknown, mainly because of the lack of prospective studies with preoperative and postoperative neurourologic evaluation of patients. Pelvic surgery. The incidence of VOL. 6 SUPPL REVIEWS IN UROLOGY S25
3 Impaired Bladder Emptying continued Table 1 Diagnosis, Evaluation, and Treatment of Impaired Bladder Emptying Causes Urethral obstruction Mechanical: benign prostatic hyperplasia and urethral stricture Functional obstruction at the pelvic floor external sphincter: shy bladder syndrome Bladder: detrusor muscle areflexia or impaired centricity Motor: neurologic diseases damaging the nerves that innervate the bladder, detrusor muscle damage, and anticholinergic drugs used to treat overactive bladder can induce high residual urine and impaired bladder emptying Sensory: the bladder gradually expands to large capacity due to sensory deficit seen commonly in patients with diabetic neuropathy Evaluation Urinalysis: rule out infection Residual urine screening: noninvasive ultrasonographic assessment of residual urine volume (preferred over catheterization for residual urine) Uroflow: noninvasive private test to screen for diminished flow rate that may predict impaired contractility, bladder outlet obstruction, or both Urodynamics: catheter-based test that can measure bladder sensation and contractility power Treatment Catheterization: indwelling urethral or suprapubic catheters or clean intermittent catheterization Biofeedback to teach the patient to relax his or her spastic sphincter muscle Drug: bethanechol chloride, 25 mg tid/qid, is the only drug approved for urinary retention Urethral sphincter botulinum toxin injection Neuromodulation with sacral nerve stimulation Basic research Muscle cell transplantation to reengineer the failing bladder Gene therapy to repair the damaged nerve to the bladder vesicourethral dysfunction has been reported to be 2% to 68% after abdominal perineal resection, 16% to 8% after radical hysterectomy, 1% to 2% after proctocolectomy, and 2% to 25% after anterior resection. 5 Pelvic and sacral fractures. Pelvic trauma can result in cauda equina and pelvic plexus injury. The frequency of neurologic injury after pelvic fracture is estimated to be between.75% and 11%. 5 The injury most closely correlated with neurologic damage is transverse sacral fracture. Approximately two thirds of these patients will have neurogenic bladder. 5 Because most of the injuries are incomplete, the majority of patients with neurourologic injury after pelvic and sacral fractures will improve over time. Herniated disc. Some reports indicate that the incidence of voiding dysfunction in patients with disc prolapse may approach 2%. Data have demonstrated that, once patients show evidence of bladder dysfunction following lumbar disc prolapse, detrusor recovery with treatment is uncommon. 5 Therefore, cauda equina syndrome from lumbar disc herniation should be considered a surgical emergency. Infectious neurologic processes. There are a number of infectious causes of incomplete emptying of the bladder: Acquired immune deficiency syndrome (AIDS): Neurologic complications, involving both the central and peripheral nervous systems, occur in as many as 4% of patients with AIDS. 5 Urinary retention is the most common presenting symptom. Neurosyphilis (tabes dorsalis): Neurosyphilis has long been recognized as a cause of central and peripheral nerve abnormalities. Voiding dysfunction related to neurosyphilis was common in the era before penicillin use. Herpes zoster and herpes simplex: Herpes zoster is an acute, painful mononeuropathy associated with a vesicular eruption in the distribution of the affected nerve. The viral activity is predominantly located in the dorsal root ganglia of the cranial nerves. However, sacral nerve involvement may be associated with loss of bladder and anal sphincter control. Lyme disease: Caused by the spirochete Borrelia burgdorferi, Lyme disease is associated with a variety of neurologic sequelae. Urologic manifestations of Lyme disease can be primary or late manifestations of disease and affect both sexes and persons of all ages. Urinary urgency, nocturia, and urge incontinence are the most common urologic symptoms. 6 Myogenic Failure Degeneration of or damage to bladder smooth muscle can also induce detru- S26 VOL. 6 SUPPL REVIEWS IN UROLOGY
4 Impaired Bladder Emptying Table 2 Symptoms of Impaired Bladder Emptying Fullness in the bladder area Straining to urinate Difficulty in starting the stream Inability to maintain a steady stream Sensation of incomplete emptying at end of micturition Discomfort in the lower abdomen Feeling of "having to go now" without being able to Constant dribbling Recurrent urinary tract infections sor hyporeflexia or areflexia. Chronic overdistension can result in detrusor myogenic failure, even if the neurologic disease is treated or reversed. Bladder management to avoid overdistension, such as institution of intermittent catheterization after spinal cord injury, may protect the bladder from permanent myogenic damage. Overactive Bladder Link to Impaired Bladder Emptying Anticholinergic drugs are now widely used to treat overactive bladder. A potential side effect of all anticholinergic agents is high residual urine volume and impaired bladder emptying. This can occur soon after initiation of therapy and is especially worrisome in the frail elderly and men with concomitant prostate hypertrophy. 7 A simple ultrasound check of residual urine after initiation of anticholinergic therapy can rule out potential problems. Sensory Uropathy It is widely accepted that diabetes results in sensory and autonomic polyneuropathy. When sensory and/or autonomic neurons innervating the bladder are damaged, bladder dysfunction, characterized by impaired sensation of bladder fullness, increased bladder capacity, reduced bladder contractility, and increased residual urine volume, can be observed. 8 The prevalence of diabetic cystopathy is related to the duration of diabetes and not to the sex and age of the patient. It has also been reported that diabetic cystopathy can occur silently and early in the course of diabetes. 8 In such cases, the bladder dysfunction is often detected only after careful questioning and/or urodynamic 1 Pves (cm H 2 O) 1 Pabd (cm H 2 O) 1 Pdet (cm H 2 O) EMG 1 2 testing. Thus, urodynamic testing in patients with diabetes is often key to the early diagnosis of bladder dysfunction. Diagnosis Table 2 lists some of the general symptoms of impaired bladder emptying. Patients with known or suspected neurologic damage due to pelvic or sacral injury should have a careful physical examination. The integrity of the sacral dermatomes is tested by assessing perianal sensation, anal sphincter tone, and control of the bulbocavernosus reflex. Many patients complain of straining to urinate, incontinence, and a sensation of incomplete bladder emptying. The urinary stream may be diminished and interrupted, since many of these patients rely on abdominal straining to urinate. On occasion, symptoms of voiding dysfunction may be the only initial clinical manifestation of a cauda equina lesion. 9 The varied and Figure 1. Detrusor areflexia without any voluntary or involuntary detrusor contraction to 5 ml volume on urodynamic study in a 61-year-old insulin-dependent diabetic woman. The patient is receiving intermittent catheterization approximately 4 times per 24 hours. Pves, intravesical pressure; Pabd, abdominal pressure; Pdet, detrusor pressure; EMG, electromyography. Volume (ml) VOL. 6 SUPPL REVIEWS IN UROLOGY S27
5 Impaired Bladder Emptying continued Volume (ml) mixed symptomatologies emphasize the need for a complete neurourologic evaluation. The physical examination may reveal a distended bladder, but the most characteristic features are elicited by a careful neurologic examination. Sensory loss in the perineum or perianal area is associated with the S2 through S4 dermatomes. The extent of perineal anesthesia can be a useful predictor in patients with lumbar disc prolapse. If saddle" anesthesia of the S2 through S4 dermatomes continues after surgical laminectomy and decompression, the urinary bladder rarely recovers. A unilateral or mild sensory disturbance indicates a better prognosis. Deep tendon reflexes in the lower extremities, clonus, and plantar responses, as well as the bulbocavernosus reflex, should be routinely evaluated. Urodynamic Findings The typical cystometrogram finding of cauda equina injury is detrusor areflexia (Figure 1). On the uroflowmetry, an abdominal straining, sawtooth pattern is generally seen (Figure 2). Urodynamic abnormalities may be the only aberration documented, with Q max = 29.1 ml/s Q mean = 11.5 ml/s Volume = 38 ml Time (s) Figure 2. Straining uroflowmetry of the diabetic woman in Figure 1. The patient complained of the sensation of incomplete emptying post-micturition, occasional incontinence, and straining to urinate. Although her maximum flow rate is normal (29.1 ml/s), the voiding pattern is classic for Valsalva voiding without true detrusor contractility. no other overt neurologic manifestations, in some patients with cauda equina injury. In cases of herniated disc not induced by trauma or acute conditions, the protrusion is usually slow and progressive and may result in nerve irritation and, consequently, detrusor hyperreflexia. 1 The integrity of the sacral reflex in men may be further studied with evaluation of the latency time of the sacral evoked potentials by stimulating the penile skin and recording the response with a needle electrode in the bulbocavernosus muscle. 11 In patients with complete cauda equina lesions, the sacral evoked response is either absent or significantly prolonged; this represents a more sensitive indicator of neuropathy than the classic electromyographic changes. In conclusion, the major urodynamic features in patients with cauda equina injury are an absent or diminished bulbocavernosus reflex, detrusor areflexia, neuropathic changes on perineal floor electromyography, and absent evoked electromyographic responses. Risks of Catheterization When evaluating impaired bladder emptying, it is important to avoid catheterizing a patient who has a large residual urine volume. Even with a sterile technique, it is difficult to avoid introducing bacteria into the bladder with catheterization. This is of little concern in the normal patient; however, in a patient with high residual urine, just a few bacteria can quickly multiply in the warm and wet environment of the bladder and can overgrow and become stagnant. Therefore, not only does an ultrasonographic residual urine check avoid the pain and irritation of urethral catheterization, it is medically safer. Use of the portable bladder When evaluating impaired bladder emptying, it is important to avoid catheterizing a patient who has a large residual urine volume. ultrasound machine, rather than catheterization, is recommended for routine residual urine check (Figure 3). Treatment Catheterization Indwelling urethral or suprapubic catheters and clean intermittent Figure 3. Checking residual urine volume is quicker, less irritating, and safer with a bladder scanner. S28 VOL. 6 SUPPL REVIEWS IN UROLOGY
6 Impaired Bladder Emptying Smooth muscle External sphincter Bladder catheterization are the options available when the bladder must be drained. Both urethral and suprapubic catheterization achieve this end; however, if long-term catheterization is required, most patients prefer a minor surgical procedure to place a suprapubic catheter. Suprapubic catheterization is more comfortable than urethral catheterization, allows the patient to have sexual intercourse, and is easier to change. Long-term urethral catheterization should especially be avoided in women, because of risk of chronic catheter pressure causing erosion damage and fistula formation to the vagina. Without question, if the patient can perform clean intermittent self-catheterization, it is almost always preferred over indwelling catheterization. Biofeedback Bladder retraining and biofeedback can help the patient with a spastic pelvic floor and external urinary sphincter to relearn how to relax during micturition. This technique is typically performed with perineal electromyographic electrodes connected to an electronic biofeedback Bladder afferent Sympathetic Somatic ( ) ( ) Brain SNS Figure 4. In cases of neurologic disease, the brain cannot turn off the guarding reflex and retention can occur. Sacral nerve stimulation (SNS) restores voluntary micturition in cases of voiding dysfunction and urinary retention by inhibiting the guarding reflex. machine. Over several sessions, patients get visual and auditory signals of what it feels like when they contract the pelvic floor muscles. Positive and negative feedback then can be used to teach the patient to relax specific muscles. Drug Treatment Bethanechol chloride, 25 mg tid/qid, is the only drug available for the treatment of urinary retention. Bethanechol is an agonist for the parasympathetic nerve mediated, acetylcholine-mediated detrusor muscle contraction. 12,13 It helps to increase bladder muscle tone and contractility. Bethanechol works within an hour after the pill is administered. Therefore, it takes only a few days to determine whether the medication is effective for a particular patient. Because of absorption issues, bethanechol generally should be taken on an empty stomach. Adverse effects include upset stomach, vomiting, dizziness, wheezing, sweating, and flushing. Urethral Botulinum Toxin Injection Another method of treating refractory sphincter spasticity is injection of botulinum toxin into the spastic pelvic floor. Although this technique may sound highly unusual, we have had great success with it at our institution. Botulinum toxin is a powerful site-specific muscle relaxant. We have employed the injection of botulinum toxin A in the lower urinary tract, as an FDA off-label use, in more than 125 patients since This therapy should not be used as firstline treatment; however, it can avoid the need for lifelong catheterization in patients who are refractory to therapy. 14 The technique is simple to perform and has been described in a previous issue of Reviews in Urology. 15 Sacral Nerve Stimulation Why would sacral nerve neuromodulation promote voiding in patients with voiding dysfunction? To understand this, it should be recognized that, in adults, functioning of brain pathways is necessary to turn off sphincter and urethral guarding reflexes and allow efficient bladder emptying. Spinal cord injury produces bladder sphincter dyssynergia and inefficient bladder emptying by interfering with these brain mechanisms (Figure 4). This may also occur with more subtle neurologic lesions in patients with idiopathic urinary retention; for example, after a bout of prostatitis or a urinary tract infection. It has been demonstrated in animals that, before the development of brain control of micturition, stimulation of somatic afferent pathways passing through the pudendal nerve to the perineum can initiate efficient voiding by activating bladder efferent pathways and turning off the excitatory pathways to the urethral outlet. 1 Tactile stimulation of the perineum in the cat also inhibits the bladder sympathetic reflex component of the guarding reflex mechanism. Sacral nerve stimulation can elicit similar VOL. 6 SUPPL REVIEWS IN UROLOGY S29
7 Impaired Bladder Emptying continued HSV-NGF injection Bladder C-fiber afferent responses in patients with urinary retention, turning off excitatory outflow to the urethral outlet and promoting bladder emptying. 16 Because sphincter activity can generate afferent input to the spinal cord that can, in turn, inhibit reflex bladder activity, an indirect benefit of suppressing sphincter reflexes would be a facilitation of bladder contraction. Efferent output Spinal cord L6-S1 spinal cord Figure 5. Herpes vector neurotrophic factor gene therapy: the herpes vector for nerve growth factor (HSV-NGF) is injected into the bladder and taken up by the sensory C-fiber afferent nerves. Research Muscle Cell Transplantation The aim of stem cell tissue engineering is to replace, repair, or enhance the biologic function of damaged tissue or organs. The process involves harvesting cells from patients or donors, isolating stem cells from the sample, expanding the cell number through cell culture techniques, and subsequently injecting or implanting the cells into the patient. One particular advantage of muscle stem cell transplantation is that it may augment impaired detrusor muscle function. It has been demonstrated that skeletal muscle stem cells, when injected into the failing bladder, can improve detrusor contractility and may be able to differentiate into bladder smooth muscle. 17 This treatment offers the only hope for patients with detrusor myogenic failure. Gene Therapy What can you do when the impaired bladder emptying is caused by damage to the nerve that innervates the bladder? We are studying the feasibility of gene therapy using a replication-deficient herpes simplex viral vector encoding neurotrophic factors that is injected into the bladder wall. 18 The herpes vector would hone in on the nerves that innervate the bladder. It is hoped that the payload it delivers, the transcription of neurotrophic factor proteins, will help improve nerve function. Thus, in the future, neurotrophic factors or other growth factors combined with targeted gene therapy techniques may be beneficial for patients with diabetic cystopathy or other forms of urologic nerve damage (Figure 5). Conclusion Impaired bladder emptying is a common and underdiagnosed condition. Main Points Urinary retention and incomplete bladder emptying can result from urethral obstruction (such as in men with benign prostatic hyperplasia), shy bladder syndrome, or detrusor areflexia (acontractility of the bladder due to an abnormality of nervous control). Incomplete bladder emptying is often neurologic in nature, as in patients who have had spinal cord injury, pelvic surgery or trauma, or herniated disc; it can also result from an infectious cause, presenting as a neurologic sequela of AIDS, Lyme disease, herpes zoster, or neurosyphilis. Patients with incomplete bladder emptying should undergo a careful physical and neurologic examination to assess for distended bladder, sensory loss in the perianal and perineal areas, deep tendon reflexes in the lower extremities, clonus, plantar responses, and bulbocavernosus reflex. Catheterization to evaluate impaired bladder emptying is not recommended in patients with a large residual urine volume because of the risk of bacteriuria. Ultrasonographic residual urine check, which is safer and more comfortable for the patient, should be employed in this population. Treatment options for patients with urinary retention include biofeedback to teach muscle relaxation, drug therapy with bethanechol chloride, and sacral nerve neuromodulation. In addition, injection of botulinum toxin to suppress pelvic floor spasticity has shown success in patients refractory to first-line therapy. Stem cell transplantation and gene therapy for impaired bladder emptying are also being investigated. S3 VOL. 6 SUPPL REVIEWS IN UROLOGY
8 Impaired Bladder Emptying With overactive bladder being treated more often, physicians should especially be on the lookout for impaired bladder emptying. Screening is simple and safe with portable bladder ultrasound scanners. Treatment ranges from bethanechol for stimulation of detrusor contraction to clean intermittent self-catheterization. Injection of botulinum toxin and acupuncture, like sacral nerve neuromodulation, can help a number of patients with refractory impaired bladder emptying. Exciting research on muscle stem cell transplantation and neurotrophic gene therapy is under way. References 1. Yoshimura N, de Groat WC. Neural control of the lower urinary tract. Int J Urol. 1997;4: de Groat WC. Inhibitory mechanisms in the sacral reflex pathways to the urinary bladder. In: Ryall RW, Kelly JS, eds. Iontophoresis and Transmitter Mechanisms in the Mammalian Central Nervous System. Holland: Elsevier; 1978: Kamo I, Torimoto K, Chancellor MB, et al. Urethral closure mechanisms under sneezeinduced stress condition in rats: a new animal model for evaluation of stress urinary incontinence. Am J Physiol Regul Integr Comp Physiol. 23;285:R356-R Chancellor MB, Yoshimura N. Physiology and pharmacology of the bladder and urethra. In: Walsh PC, Retik AB, Vaughan ED Jr, Wein AJ, eds. Campbell s Urology. Vol 2. 8th ed. Philadelphia: WB Saunders; 22: Chancellor MB, Blaivas JG, eds. Practical Neurourology: Genitourinary Complications in Neurologic Disease. Stoneham, Mass: Butterworth-Heinemann; Chancellor MB, McGinnis DE, Shenot PJ, et al. Lyme cystitis and neurogenic bladder dysfunction. Lancet. 1992;339: Yoshimura N, Chancellor MB. Current and future pharmacological therapy of the overactive bladder. J Urol. 22;168: Ueda T, Yoshimura N, Yoshida O. Diabetic cystopathy: relationship to autonomic neuropathy detected by sympathetic skin response. J Urol. 1997;157: Blaivas JG, Scott MR, Labib KB. Urodynamic evaluation as neurologic test for sacral cord function. Urology. 1979;8: Jones DL, Moore T. The types of neuropathic bladder dysfunction associated with prolapsed lumbar intervertebral discs. Br J Urol. 1973; 45: Krane RJ, Siroky MB. Studies on sacral-evoked potentials. J Urol. 198;124: Riedl CR, Stephen RL, Daha LK, et al. Electromotive administration of intravesical bethanechol and the clinical impact on acontractile detrusor management: introduction of a new test. J Urol. 2;164: Awad SA. Clinical use of bethanechol. J Urol. 1985;134: Phelan MW, Franks M, Somogyi GT, et al. Botulinum toxin urethral sphincter injection to restore bladder emptying in men and women with voiding dysfunction. J Urol. 21; 165: Smith CP, Somogyi GT, Chancellor MB. Botulinum toxin: poisoning the spastic bladder and urethra. Rev Urol. 22;4: Tanagho EA, Schmidt RA. Electrical stimulation in the clinical management of the neurogenic bladder. J Urol. 1988;14: Huard J, Yokoyama T, Pruchnic R, et al. Musclederived cell-mediated ex vivo gene therapy for urological dysfunction. Gene Ther. 22;9: Chancellor MB, Yoshimura N, Pruchnic R, Huard J. Gene therapy strategies for urological dysfunction. Trends Mol Med. 21;7: VOL. 6 SUPPL REVIEWS IN UROLOGY S31
TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TREATMENT METHODS FOR DISORDERS OF SMALL ANIMAL BLADDER FUNCTION Author : SIMONA T RADAELLI Categories : Vets Date : July
The Neurogenic Bladder
 The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
The Neurogenic Bladder Outline Brandon Haynes, MD Resident Physician Department of Urology Jelena Svircev, MD Assistant Professor Department of Rehabilitation Medicine Anatomy and Bladder Physiology Bladder
Neurogenic bladder. Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder.
 Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Definition: Neurogenic bladder Neurogenic bladder is a type of dysfunction of the bladder due to neurological disorder. Types: Nervous system diseases: Congenital: like myelodysplasia like meningocele.
Neuropathic Bladder. Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014
 Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
Neuropathic Bladder Magda Kujawa Consultant Urologist Stockport NHS Foundation Trust 12/03/2014 Plan Physiology- bladder and sphincter behaviour in neurological disease Clinical consequences of Symptoms
NEUROMODULATION FOR UROGYNAECOLOGISTS
 NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROMODULATION FOR UROGYNAECOLOGISTS Introduction The pelvic floor is highly complex structure made up of skeletal and striated muscle, support and suspensory ligaments, fascial coverings and an intricate
NEUROGENIC BLADDER. Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph
 NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
NEUROGENIC BLADDER Dr Harriet Grubb Dr Alison Seymour Dr Alexander Joseph OUTLINE Definition Anatomy and physiology of bladder function Types of neurogenic bladder Assessment and management Complications
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS
 Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Pelvic Floor Therapy for the Neurologic Client Carina Siracusa, PT, DPT, WCS OhioHealth, Columbus Ohio Disclosures I have nothing to disclose Objectives Describe the role of a pelvic floor therapist in
Spinal Cord Injury. R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH
 Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Spinal Cord Injury R Hamid Consultant Neuro-Urologist London Spinal Injuries Unit, Stanmore & National Hospital for Neurology & Neurosurgery, UCLH SCI 800 1000 new cases per year in UK Car accidents 35%
Summary. Neuro-urodynamics. The bladder cycle. and voiding. 14/12/2015. Neural control of the LUT Initial assessment Urodynamics
 Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
Neuro-urodynamics Summary Neural control of the LUT Initial assessment Urodynamics Marcus Drake, Bristol Urological Institute SAFETY FIRST; renal failure, dysreflexia, latex allergy SYMPTOMS SECOND; storage,
THE ACONTRACTILE BLADDER - FACT OR FICTION?
 THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
THE ACONTRACTILE BLADDER - FACT OR FICTION? Jacob Golomb Department of Urology Chaim Sheba Medical Center Tel Hashomer NEUROGENIC UNDERACTIVE DETRUSOR Central (complete/incomplete): Spinal cord injury-
Urodynamics in Neurological Lower Urinary Tract Dysfunction. Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne
 Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Urodynamics in Neurological Lower Urinary Tract Dysfunction Mr Chris Harding Consultant Urologist Freeman Hospital Newcastle-upon-Tyne Learning Objectives Review functional neurology relevant to lower
Neural control of the lower urinary tract in health and disease
 Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Neural control of the lower urinary tract in health and disease Jalesh N. Panicker MD, DM, FRCP Consultant Neurologist and Clinical lead in Uro-Neurology The National Hospital for Neurology and Neurosurgery
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
Guidelines on Neurogenic Lower Urinary Tract Dysfunction
 Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Guidelines on Neurogenic Lower Urinary Tract Dysfunction (Text update March 2009) M. Stöhrer (chairman), B. Blok, D. Castro-Diaz, E. Chartier- Kastler, P. Denys, G. Kramer, J. Pannek, G. del Popolo, P.
Overactive Bladder: Diagnosis and Approaches to Treatment
 Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Overactive Bladder: Diagnosis and Approaches to Treatment A Hidden Condition* Many Many patients self-manage by voiding frequently, reducing fluid intake, and wearing pads Nearly Nearly two-thirds thirds
Neural Control of Lower Urinary Tract Function. William C. de Groat University of Pittsburgh Medical School
 Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Neural Control of Lower Urinary Tract Function William C. de Groat University of Pittsburgh Medical School Disclosures Current funding: NIH Grants, DK093424, DK-091253, DK-094905, DK-090006. Other financial
Incontinence. When I was given this topic in urology to discuss with you today I
 Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
Incontinence When I was given this topic in urology to discuss with you today I was slightly disappointed. I personally see mostly men for problems such as stones, benign prostatic hyperplasia, prostate
Regulation of the Urinary Bladder Chapter 26
 Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Regulation of the Urinary Bladder Chapter 26 Anatomy 1. The urinary bladder is smooth muscle lined internally by transitional epithelium and externally by the parietal peritoneum. Contraction of the smooth
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
ATLAS OF URODYNAMICS. Bladder. Pure. Pves. Pabd. Pdet EMG. Bladder. volume. Cough Strain IDC. Filling. Pure. Pves. Pabd. Pdet EMG
 2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
2 Normal Micturition The micturition cycle (urine storage and voiding) is a nearly subconscious process that is under complete voluntary control. Bladder filling is accomplished without sensation and without
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist
 Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
Lower Urinary Tract Symptoms K Kuruvilla Zachariah Associate Specialist Lower Urinary Tract Symptoms Storage Symptoms Frequency, urgency, incontinence, Nocturia Voiding Symptoms Hesitancy, poor flow, intermittency,
NEUROPATHIC BLADDER DISORDERS
 NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
NEUROPATHIC BLADDER DISORDERS ANATOMY & PHYSIOLOGY The Bladder Unit The functional features of the bladder include (1) a normal capacity of 400 500 ml, (2) a sensation of fullness, (3) the ability to accommodate
Practical urodynamics What PA s need to know. Gary E. Lemack, MD Professor of Urology and Neurology
 Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Practical urodynamics What PA s need to know Gary E. Lemack, MD Professor of Urology and Neurology Urodynamics essential elements Urethral catheter Fill rate Catheter size Intravesical pressure measurements
Urodynamic and electrophysiological investigations in neuro-urology
 Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Urodynamic and electrophysiological investigations in neuro-urology Pr. Gerard Amarenco Neuro-Urology and Pelvic-Floor Investigations Department Tenon Hospital, Assistance Publique Hôpitaux de Paris, Er6,
Chapter 23. Micturition and Renal Insufficiency
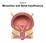 Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Chapter 23 Micturition and Renal Insufficiency Voiding Urine Between acts of urination, the bladder is filling. detrusor muscle relaxes urethral sphincters are tightly closed accomplished by sympathetic
Dr. Aso Urinary Symptoms
 Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Haematuria The presence of blood in the urine (haematuria) is always abnormal and may be the only indication of pathology in the urinary tract. False positive stick tests and the discolored urine caused
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Elimination Patterns: Bladder
 Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Elimination Patterns: Bladder CRRN Review Material Christa Carter, RN, BSN, CRRN Objectives Identify different types of neurogenic bladder Identify different types of incontinence Identify at least three
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests. Amelyn R.
 Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Renal Physiology: Filling of the Urinary Bladder, Micturition, Physiologic Basis of some Renal Function Tests Amelyn R. Rafael, MD 1 Functions of the Urinary Bladder 1. storage of urine 150 cc 1 st urge
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline
 Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Adult Urodynamics: American Urological Association (AUA)/Society of Urodynamics, Female Pelvic Medicine & Urogenital Reconstruction (SUFU) Guideline TARGET POPULATION Eligibility Decidable (Y or N) Inclusion
Physiologic Anatomy and Nervous Connections of the Bladder
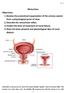 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Technologies and architectures" Stimulator, electrodes, system flexibility, reliability, security, etc."
 March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
March 2011 Introduction" Basic principle (Depolarization, hyper polarization, etc.." Stimulation types (Magnetic and electrical)" Main stimulation parameters (Current, voltage, etc )" Characteristics (Muscular
Mr. GIT KAH ANN. Pakar Klinikal Urologi Hospital Kuala Lumpur.
 Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
Mr. GIT KAH ANN Pakar Klinikal Urologi Hospital Kuala Lumpur drgitka@yahoo.com 25 Jan 2007 HIGHLIGHTS Introduction ICS Definition Making a Diagnosis Voiding Chart Investigation Urodynamics Ancillary Investigations
THE vesical dysfunction which follows injury or disease of the spinal cord
 VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
VESICAL NECK RESECTION FOR NEUROGENIC BLADDER WILLIAM J. ENGEL, M.D. Department of Urology THE vesical dysfunction which follows injury or disease of the spinal cord or cauda equina has always presented
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain
 Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Neuroanatomy, Neurophysiology and Clinical Presentation of Visceral Urological Pain Prof Dr K. Everaert Functional urology Department of Urology Ghent University Hospital Gent, Belgium Chronic pelvic pain
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Voiding Dysfunction Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU.
 Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Voiding Dysfunction 2009 Block lecture, 5 th year student. Choosak Pripatnanont, Department of Surgery, PSU. Objectives Understand and explain physiologic function and dysfunction of lower urinary tract.
Definitions of IC: U.S. perspective. Edward Stanford MD MS FACOG FACS Western Colorado
 Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Definitions of IC: U.S. perspective Edward Stanford MD MS FACOG FACS Western Colorado PURPOSE OF A DEFINITION? Identifies with specificity those patients who are most likely to have the disease. Identifies
Updates in the nonpharmacological. treatment on overactive bladder
 Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
Updates in the nonpharmacological treatment on overactive bladder Overactive Bladder Also known as urgency-frequency syndrome Symptoms Urgency Daytime frequency Nocturia Urge urinary incontinence Sudden
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER
 SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
SUPRAPUBIC PUNCTURE IN THE TREATMENT OF NEUROGENIC BLADDER CHARLES C. HIGGINS, M.D. W. JAMES GARDNER, M.D. WM. A. NOSIK, M.D. The treatment of "cord bladder", a disturbance of bladder function from disease
Neural control of the lower urinary tract
 Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
Neural control of the lower urinary tract Jalesh N. Panicker Consultant Neurologist and Honorary Senior Lecturer The National Hospital for Neurology and Neurosurgery and UCL Institute of Neurology Queen
NEUROUROLOGY BACKGROUND
 NEUROUROLOGY BACKGROUND Lower urinary tract dysfunction is common among patients with underlying neurologic conditions. Also known as neurogenic bladder, this occurs as a result of the disruption of the
NEUROUROLOGY BACKGROUND Lower urinary tract dysfunction is common among patients with underlying neurologic conditions. Also known as neurogenic bladder, this occurs as a result of the disruption of the
Normal micturition involves complex
 NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
NEW TARGET FOR INTERVENTION: THE NEUROUROLOGY CONNECTION * Donald R. Ostergard, MD, FACOG ABSTRACT Urine storage and release are under the control of the parasympathetic, sympathetic, and somatic nervous
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Tools for Evaluation. Urodynamics Case Studies. Case 1. Evaluation. Case 1. Bladder Diary SUI 19/01/2018
 Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
Urodynamics Case Studies Christopher K. Payne, MD Vista Urology & Pelvic Pain Partners Emeritus Professor of Urology, Stanford University Tools for Evaluation Ears, Eyes, and Brain Bladder diary Stress
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION
 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E. Chartier-Kastler, G. Kramer, A. Mattiasson, J-J. Wyndaele Introduction NLUTD (neurogenic lower urinary
Physiology & Neurophysiology of lower U.T.
 Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Physiology & Neurophysiology of lower U.T. Classification of voiding dysfunction Evaluation of a child with voiding dysfunction Management Storage Ø Adequate volume of urine Ø At LOW pressure Ø With NO
Ben Herbert Alex Wojtowicz
 Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
Ben Herbert Alex Wojtowicz 54 year old female presenting with: Dragging sensation Urinary incontinence Some faecal incontinence HPC Since May 14 had noticed a mass protruding from the vagina when going
This Special Report supplement
 ...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
...INTRODUCTION... Overactive Bladder: Defining the Disease Alan J. Wein, MD This Special Report supplement to The American Journal of Managed Care features proceedings from the workshop, Overactive Bladder:
The new International Continence Society
 ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
ROLE OF CYSTOMETRY IN EVALUATING PATIENTS WITH OVERACTIVE BLADDER ADAM J. FLISSER AND JERRY G. BLAIVAS ABSTRACT Overactive bladder (OAB) can be caused by a variety of conditions. We believe that cystometrography
URINARY INCONTINENCE. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
URINARY INCONTINENCE Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara Definition The involuntary loss of urine May denote a symptom, a sign or a condition Symptom the
Dysfunctional voiding
 Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
Dysfunctional voiding The importance of assessment, diagnosis and treatment of dysfunctional voiding and its role in recurrent UTI Dr Dean Wallace Consultant Paediatric Nephrologist RMCH Objectives Development
김준철 가톨릭대학교의과대학비뇨기과학교실
 비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
비뇨기계자율신경병증의치료 김준철 가톨릭대학교의과대학비뇨기과학교실 Introduction Urologic complications have increasingly become a concern in those affected by DM Genitourinary problems are included among these complications, related
How to manage a patient with bladder dysfunction
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Teaching Course 13 How to manage a patient with autonomic dysfunction - Level 2 How to manage a patient with
The Management of Female Urinary Incontinence. Part 1: Aetiology and Investigations
 The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
The Management of Female Urinary Incontinence Part 1: Aetiology and Investigations Dr Oseka Onuma Gynaecologist and Pelvic Reconstructive Surgeon 4 Robe Terrace Medindie SA 5081 Urinary incontinence has
Recommandations de prise en charge des vessies neurogènes EAU 2006
 Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
Annexe 4-1 Recommandations de prise en charge des vessies neurogènes EAU 2006 (Version courte) 685 686 GUIDELINES ON NEUROGENIC LOWER URINARY TRACT DYSFUNCTION M. Stöhrer (chairman), D. Castro-Diaz, E.
What neurologists need to understa
 98 PRACTICAL NEUROLOGY INTRODUCTION Urodynamics has been used in the investigation of bladder dysfunction since the 1950s, although the first report describing bladder pressure measurement dates from 1882
98 PRACTICAL NEUROLOGY INTRODUCTION Urodynamics has been used in the investigation of bladder dysfunction since the 1950s, although the first report describing bladder pressure measurement dates from 1882
Perineal Electrophysiologic Tests
 Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Perineal disorders and emg! Perineal Electrophysiologic Tests Voiding dysfunction Stress Urinary Incontinence urgency OAB Urge Incontinence nocturia Pr. Gerard Amarenco Mixed Incontinence frequency Service
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
What should we consider before surgery? BPH with bladder dysfunction. Inje University Sanggye Paik Hospital Sung Luck Hee
 What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
What should we consider before surgery? BPH with bladder dysfunction Inje University Sanggye Paik Hospital Sung Luck Hee Diagnostic tests in three categories Recommendation: there is evidence to support
EAU GUIDELINES ON NEURO-UROLOGY
 EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2016) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler. Guidelines Associates:
EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2016) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler. Guidelines Associates:
Electrostimulation Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
GBM8320 Dispositifs Médicaux Intelligents. Electrostimulation. Part 3: Bladder dysfunctions
 GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GBM8320 Dispositifs Médicaux Intelligents Electrostimulation Part 3: Bladder dysfunctions Mohamad Sawan et al Laboratoire de neurotechnologies Polystim!!! http://www.cours.polymtl.ca/gbm8320/! mohamad.sawan@polymtl.ca!
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
GUIDELINES ON NEURO-UROLOGY (Text update pril 2014) J. Pannek (co-chair), B. Blok (co-chair), D. Castro-Diaz, G. del Popolo, J. Groen, G. Karsenty, T.M. Kessler, G. Kramer, M. Stöhrer Eur Urol 2009 Jul;56(1):81-8
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH
 MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
MANAGING BENIGN PROSTATIC HYPERTROPHY IN PRIMARY CARE DR GEORGE G MATHEW CONSULTANT FAMILY PHYSICIAN FELLOW IN SEXUAL & REPRODUCTIVE HEALTH INTRODUCTION (1) Part of male sexual reproductive organ Size
CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1
 1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
1 CASES FOR TRAINING OF THE INTERNATIONAL SPINAL CORD INJURY LOWER URINARY TRACT FUNCTION BASIC DATA SET CASE 1 35 years old man, who previously has been completely healthy, was shot twice in the neck
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
Original Article Ann Rehabil Med 2014;38(3):342-346 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.342 Annals of Rehabilitation Medicine Phasic Changes in Bladder Compliance
EAU GUIDELINES ON NEURO-UROLOGY
 EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2017) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler Guidelines Associates:
EAU GUIDELINES ON NEURO-UROLOGY (Limited text update March 2017) B. Blok (Co-chair), J. Pannek (Co-chair) D. Castro-Diaz, G. del Popolo, J. Groen, R. Hamid, G. Karsenty, T.M. Kessler Guidelines Associates:
Neurourology, especially the video urodynamic
 NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
NEUROUROLOGIC FINDINGS WITH APPLICABILITY TO INCONTINENCE AND URETHRAL FUNCTION * Edward J. McGuire, MD ABSTRACT Neurourology is applicable to urinary incontinence and obstructive uropathy in the general
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction?
 London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
London, 2016 What is the role for neurophysiology in the evaluation of patients with uro-genito-anal dysfunction? David B. Vodušek Medical Faculty, University of Ljubljana, Slovenia vodusek.david.b@gmail.com
Guidelines on Urinary Incontinence
 Guidelines on Urinary Incontinence J. Thüroff (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck European Association of Urology 2006 TABLE OF CONTENTS
Guidelines on Urinary Incontinence J. Thüroff (chairman), P. Abrams, K.E. Andersson, W. Artibani, E. Chartier-Kastler, C. Hampel, Ph. van Kerrebroeck European Association of Urology 2006 TABLE OF CONTENTS
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN
 Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
Diane K. Newman DNP, ANP-BC, PCB-PMD, FAAN Diane K. Newman, DNP is a Biofeedback Certified Continence Specialist. With over 35-years experience, she is an expert in the assessment and management of pelvic-floor
The Enlarged Prostate Symptoms, Diagnosis and Treatment
 The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
The Enlarged Prostate Symptoms, Diagnosis and Treatment MAC00031-01 Rev G Financial support for this seminar has been provided by NeoTract, Inc., the manufacturer of the UroLift System. 1 Today s Agenda
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction
 Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
Annual Scientific Update in Urogynaecology- Joint RCOG/BSUG Meeting Neurogenic bladder dysfunction Clare J.Fowler National Hospital for Neurology and Neurosurgery & Institute of Neurology, UCL Aims Background
URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW Author : Ian Battersby Categories : Vets Date : August 3, 2009
Vet Times The website for the veterinary profession https://www.vettimes.co.uk URINARY TRACT NERVOUS SYSTEM DISORDERS: DRUG THERAPY REVIEW Author : Ian Battersby Categories : Vets Date : August 3, 2009
Sacral neuromodulation (SNM), using permanent foramen S3 electrode, Early versus late treatment of voiding dysfunction with pelvic neuromodulation
 ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
ORIGINAL RESEARCH Early versus late treatment of voiding dysfunction with pelvic neuromodulation Magdy M. Hassouna, MD, PhD; Mohamed S. Elkelini, MD See related article on page 111 Abstract Introduction:
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies. Dr. Boris Friedman May 2, 2012 OBJECTIVES
 Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Urinary Aspects of Multiple Sclerosis chronic condition with innovative treatment strategies Dr. Boris Friedman May 2, 2012 OBJECTIVES 1) Definition and classification of MS 2) Interventional radiology
Sacral neuromodulation for lower urinary tract dysfunction
 World J Urol (2012) 30:445 450 DOI 10.1007/s00345-011-0780-2 TOPIC PAPER Sacral neuromodulation for lower urinary tract dysfunction Philip E. V. Van Kerrebroeck Tom A. T. Marcelissen Received: 22 August
World J Urol (2012) 30:445 450 DOI 10.1007/s00345-011-0780-2 TOPIC PAPER Sacral neuromodulation for lower urinary tract dysfunction Philip E. V. Van Kerrebroeck Tom A. T. Marcelissen Received: 22 August
Male LUTS. Dr. Brian Ho. Division of Urology Department of Surgery Queen Mary Hospital
 Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Male LUTS Dr. Brian Ho Division of Urology Department of Surgery Queen Mary Hospital Mr. Siu M/78 Known to have HT & DM since 2008 on follow up with General ut-patient Clinic (GPC) Noticed to have worsening
Objectives. Key Outlines:
 Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Objectives! Iden8fy and describe the Func8onal Anatomy of Urinary Bladder! Describe the mechanism of filling and emptying of the urinary bladder! Cystometrogram! Appreciate neurogenic control of the mechanism
Neurological control of the bladder in health and disease
 Section 1 Chapter 1 Neurological control of pelvic organ functions Neurological control of the bladder in health and disease Derek J. Griffiths and Apostolos Apostolidis Peripheral control of micturition
Section 1 Chapter 1 Neurological control of pelvic organ functions Neurological control of the bladder in health and disease Derek J. Griffiths and Apostolos Apostolidis Peripheral control of micturition
Incontinence: Risks, Causes and Care
 Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
Welcome To Incontinence: Risks, Causes and Care Presented by Kamal Masaki, MD Professor and Chair Department of Geriatric Medicine John A. Burns School of Medicine, UH Manoa September 5, 2018 10:00 11:00
URGE MOTOR INCONTINENCE
 URGE MOTOR INCONTINENCE URGE INCONTINENCE COMMONEST TYPE IN ELDERLY WOMEN Causes: 1 - Defects in CNS regulation Stroke Parkinson s disease Dementia (Alzheimer s and other types) Normopressure hydrocephalus
URGE MOTOR INCONTINENCE URGE INCONTINENCE COMMONEST TYPE IN ELDERLY WOMEN Causes: 1 - Defects in CNS regulation Stroke Parkinson s disease Dementia (Alzheimer s and other types) Normopressure hydrocephalus
University of Alberta Reconstructive Urology Fellowship
 FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
FACULTY OF MEDICINE AND DENTISTRY DEPARTMENT OF SURGERY DIVISION OF UROLOGY Keith Rourke, MD, FRCSC Reconstructive Urology Professor Chair of Academic Urology Reconstructive Urology Fellowship Director
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics. Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital
 Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Lower Urinary Tract Symptoms (LUTS) and Nurse-Led Clinics Sean Diver Urology Advanced Nurse Practitioner candidate Letterkenny University Hospital 01/02/2018 Lower Urinary Tract Symptoms LUTS - one of
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Neurogenic Bladder: What You Should Know. A Guide for People with Spinal Cord Injury
 Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Neurogenic Bladder: What You Should Know A Guide for People with Spinal Cord Injury Why Is This Information Important? Before SCI, you didn t have to think about managing your bladder After SCI, you may
Urinary incontinence. Urology Department. Patient Information Leaflet
 Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Urinary incontinence Urology Department Patient Information Leaflet Introduction This leaflet is for people who have been diagnosed with urinary incontinence. It contains information about the bladder,
Diagnostic approach to LUTS in men. Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center
 Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
Diagnostic approach to LUTS in men Prof Dato Dr. Zulkifli Md Zainuddin Consultant Urologist / Head Of Urology Unit UKM Medical Center Classification of LUTS Storage symptoms Voiding symptoms Post micturition
GUIDELINES ON NEURO-UROLOGY
 GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
GUIDELINES ON NEURO-UROLOGY (Limited text update March 2015) B. Blok (Co-chair), J. Pannek (Co-chair), D. Castro Diaz, G. del Popolo, J. Groen, T. Gross (Guidelines ssociate), R. Hamid, G. Karsenty, T.M.
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME?
 URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
URODYNAMICS IN MALE LUTS: NECESSARY OR WASTE OF TIME? Andrea Tubaro, MD, FEBU Chairman Department of Urology Sant Andrea Hospital Sapienza University of Rome, Italy Disclosures Consultant, paid speaker,
Successful Therapy of Overactive Bladder Syndrome with Percutaneous Tibial Nerve Stimulation: A Case Report
 December, 2017 2017; Vol1; Issue11 http://iamresearcher.online Successful Therapy of Overactive Bladder Syndrome with Percutaneous Tibial Nerve Stimulation: A Case Report Nicole Keller, Seraina Schmid,
December, 2017 2017; Vol1; Issue11 http://iamresearcher.online Successful Therapy of Overactive Bladder Syndrome with Percutaneous Tibial Nerve Stimulation: A Case Report Nicole Keller, Seraina Schmid,
Urine a Mess: Micturition Disorders Joe Bartges, DVM, PhD, DACVIM, DACVN Cornell University Veterinary Specialists Stamford, CT
 Urine a Mess: Micturition Disorders Joe Bartges, DVM, PhD, DACVIM, DACVN Cornell University Veterinary Specialists Stamford, CT 1. Micturition refers to the process of storing and periodically voiding
Urine a Mess: Micturition Disorders Joe Bartges, DVM, PhD, DACVIM, DACVN Cornell University Veterinary Specialists Stamford, CT 1. Micturition refers to the process of storing and periodically voiding
1 Olsson CA, Willscher MK, Austen G Jr, Siroky MB and Krane RJ. Management of prostatic fistulas. Urol Surv 1976;25:135.
 Michael B. Siroky, MD FACS 720 Harrison Avenue Suite 606 Boston, Ma 02118 TEL: 617 638-8555 FAX: 617 638-8487 CHAPTERS, MONOGRAPHS, REVIEWS (Peer reviewed journals in bold) 1 Olsson CA, Willscher MK, Austen
Michael B. Siroky, MD FACS 720 Harrison Avenue Suite 606 Boston, Ma 02118 TEL: 617 638-8555 FAX: 617 638-8487 CHAPTERS, MONOGRAPHS, REVIEWS (Peer reviewed journals in bold) 1 Olsson CA, Willscher MK, Austen
