Title: Navigating through Mutations in Acute Myeloid Leukemia. What Do We Know and What Do We Do with It?
|
|
|
- Brenda Black
- 5 years ago
- Views:
Transcription
1 DOI: /etd Manuscript Type: Invited Review Title: Navigating through Mutations in Acute Myeloid Leukemia. What Do We Know and What Do We Do with It? Running Head: Mutations in AML Author: Deniz Peker Institution: The University of Alabama at Birmingham, Comprehensive Cancer Center, US Address for Correspondence: Deniz Peker Phone: Cite this article as: Peker D. Navigating through Mutations in Acute Myeloid Leukemia. What Do We Know and What Do We Do with
2 Abstract Acute myeloid leukemia (AML) is a clonal hematopoietic disease characterized by abnormal proliferation of early precursors of myeloid cells and blasts. AML represents a heterogeneous disease group with a significantly complex biology and pathophysiology. Various translocations, chromosome copy number changes and mutations have been described in AML, some of which help define the diagnosis, prognosis and management. The optimal treatment in most cases remains cytarabine and anthracycline-based combination regimens followed by the allogeneic stem cell transplant. However, older age and decreased tolerance to conventional therapies pose a major challenge for the conventional therapies which has lead to the development of effective and less toxic therapy modalities as reviewed in this manuscript. Keywords: AML, mutations, cytogenetics, targeted therapies INTRODUCTION Acute myeloid leukemia (AML) represents a group of diseases characterized by clonal expansion of myeloid blasts in peripheral blood, bone marrow, other organs and cavities. The worldwide incidence of AML is cases per 100,000 population annually and reportedly most common in the Western World (1). A diagnosis of AML can be made based on 1) 20% blasts of myeloid and/or monocytic or megakaryocytic lineages and 2) presence of recurrent cytogenetic abnormalities including t(8;21) (q22;q22.1), inv16 (p13.1q22) or t(16;16) (p13.1:q22) and PML-RARA fusion (1). AML can arise de novo or evolve from myelodysplastic syndromes (MDS) and/or myeloproliferative neoplasms (MPN). The
3 current risk stratification for AML is primarily based on cytogenetics and molecular genetic abnormalities (Table 1) according to the European Leukemia Net (2). Recent developments in the molecular biology of this clinically, morphologically and phenotypically heterogeneous disease lead us to a more comprehensive diagnostic approach, including conventional karyotyping, fluorescence in situ hybridization (FISH), polymerase chain reaction (PCR) and next generation DNA sequencing (NGS), enable us to predict prognosis in these patients and develop of more effective targeted treatments. NGS is a fairly novel technology that massively parallels or deep sequences the DNA, allowing us to sequence the entire human genome within a day (3). Detection of somatic mutations by NGS in AML cases using large multi-gene panels provides important information that can be used in diagnosis, prognostic risk stratification, evaluation for targeted treatments, and monitoring for minimal residual disease (MRD). Mutations in AML and Clinical Consequences In AML, the transcription-factor fusions [e.g. t (8;21), inv(16) and t(15;17)] are the first identified genomic alteration and have been linked to disease initiation (4, 5). A recent whole genome sequencing study on 200 adult de novo AML patients published by The Cancer Genome Atlas (TCGA) Research Network classified AML associated mutations in functional categories (Table 2) according to the results of this comprehensive analysis (6). This data suggests that one mutation in any of these pathways is sufficient for pathogenesis of AML and certain mutations that are common in AML (e.g., in DNMT3A, NPM1, CEPBA, IDH1/2, and RUNX1) to play a role in the initiation of AML similar to the fusion genes. In addition to the role in the pathogenesis of AML, these mutations appear to have clinical utility in prognostication, determining the therapy options and detecting MRD. Recently approved and under investigation agents targeting these mutations are summarized in Table 3.
4 FLT3 mutation: Mutations involving FLT3 gene, a member of the class II tyrosine kinase receptor, has been extensively studied and shown to play a crucial role in AML promoting expansion of hematopoietic precursors (7). FLT3 is not uncommonly expressed in AML blasts and is associated with poor prognosis. FLT3 internal tandem duplication (FLT3-ITD) mutations result in increased tyrosine kinase activity and are the first mutations reported that have a prognostic impact in AML (8). Subsequent large cohort studies as well as sporadic case reports demonstrate the association between FLT3-ITD mutations and an increased relapse rate as well as decreased overall survival (9-11). Point mutations occurring in the FLT3 gene in the constitutive activation of the kinase domain are known as FLT3-TKD mutations. Both FLT3-ITD and FLT3-TKD mutations occur in AML with normal karyotype (~35% and 10%, respectively) as well as AML with recurrent cytogenetics (12). FLT3 mutation analysis was historically performed for prognostication in AML; however, with the advances in FLT3-inhibitors, it now clear that it has prognostic and predictive value. NPM1 mutation: Nucleaophosmin (NPM) is a protein that is important in a wide-spectrum of cell processes including cell proliferation, DNA repair and genome stability (13). Frameshift mutations of the NPM1 gene are observed in one third of adult patients with de novo AML; WHO classifies AML with NPM1 mutation as a separate entity (13). NPM1 mutations are associated with a favorable prognosis in AML with normal karyotype without other mutations. AML with mutated NPM1 commonly harbors other mutations involving the FLT3 gene (in 40-50% of patients), DNMT3A, TET2, IDH1, and, IDH2 (14). A recent large retrospective study performed by Ostronoff et al., showed that AML patients ages 55 to 65 years and NPM1+/FLT3-ITD+ have an improved survival when compared to the group without this phenotype (15). Mason et al. studied 133 cases with NPM1 mutated AML; 40% of these cases demonstrated an APL-like phenotype with lack of CD34 and HLA-DR expression (14) suggesting a
5 maturation arrest of myeloid differentiation, closer to the promyelocytic stage. Furthermore, these APLlike cases also showed TET2, IDH1, or IDH2 mutations with a superior outcome and lower frequency of DNMT3A mutations. The results of this study were interesting and indicated a potential use of ATRA and ATO in the cases of AML with mutated NPM1 and APL-like phenotype. CEBPA mutation: CEBPA, a transcription factor in hematopoietic stem cells, is responsible for the differentiation to the myeloid progenitors and functions as promoter for myeloid and monocytic differentiation (16). CEBPA is expressed in granulocytes, monocytes and eosinophils. CEBPA mutations occur in approximately 10% of AML cases and double mutations confer a favorable diagnosis (16, 17). However, when single mutation of CEBPA occurs, other concurrent mutations, including NPM1 and FLT3-ITD affect the outcome in these cases (18). Other mutations not uncommonly detected in AML include DNMT3A, IDH1 and IDH2, RUNX1, ASXL1, TP53, KIT, and TET2. DNMT3A mutation: DNMT genes play a role in methylation of CpG islands and reduce the expression of downstream genes resulting in genome instability and cancer (19). DNMT3A mutations occur in 18%- 22% of AML cases and one third of AML cases with normal cytogenetics (20-23). Studies showed that DNMT3A mutations are often accompanied by other mutations including FLT3, NPM1, and IDH1 and IDH2 mutations (24) and confer an unfavorable prognosis in both younger and older patients (17). Treatment with high dose daunorubicin (25) and hematopoietic stem cell transplant (19) have been shown to increase the overall survival in AML patients with DNMT3A mutation. IDH1 and IDH2 mutation: IDH is an essential enzyme in cell metabolism and gain of function mutations in IDH lead to DNA methylation and impaired myeloid differentiation (26). Approximately 20% of all AML
6 and 30% of AML with normal karyotype cases harbor IDH1 or IDH2 mutations (27). IDH1 mutations have been shown to confer an overall unfavorable prognosis in AML with shorter OS and event-free survival, while the impact of mutations of IDH2 mutation differs based on type of mutation: IDH2 R140 are associated with a better prognosis in younger AML patients whereas IDH2 R172 is associated with a poorer outcome (28, 29). IDH1/IDH2 small inhibitor molecules are available in treatment of AML. RUNX1 mutation: AML with RUNX1 is a relatively infrequent provisional AML entity. RUNX1 mutation frequency increased with age: 5%-10% in patients <60 years and 10-20% 60 years. It is more frequent in men than women and is often associated with secondary AML evolving from MDS, failure of induction therapy and inferior OS (30). ASXL1 mutation: ASXL1 mutations are detected in approximately 10% of all de novo AML cases and frequency increases significantly with age, particularly in patients more than 60 years old. ASXL1 mutation in AML constitutes an inferior outcome with low complete remission rates. TP53 mutation: p53 is a tumor suppressor transcription factor that is actively involved in hematopoietic stem cell quiescence and self-renewal preventing leukomogenesis (31). TP53 mutations in AML have recently been the focus of investigations. TP53 mutations occur in 8% of de novo AML and are early leukomogenic initiating driver mutations resulting in an aggressive disease course, therapy-resistance and poor outcome even after allogeneic HSCT (32). MDM2 inhibitors appear to be promising in targeting mutant p53 in AML treatment, although the therapeutic progress is still inadequate. KIT mutation: KIT mutation is found in 13%-46% of core-binding protein factor (CBF) AML including t(8;21)(q22;q22) and inv(16)(p13;q22) (33). While CBF-AML is generally considered to be in the
7 favorable risk group, co-existence of KIT mutation is associated with unfavorable prognosis. Targeted tyrosine kinase inhibition of KIT is still in development. TET2 mutation: Somatic methylcytosine dioxygenase ten eleven translocation 2 (TET2) mutations occur in approximately 23% of AML (34). TET2 mutation is a common finding among the elderly population with clonal hematopoiesis. TET2 is often associated with AML with normal karyotype and NPM1 mutation (30). CONCLUSION AML is the most common acute leukemia in the adult population with a complex biology and significant heterogeneity. Over the last few decades, many balanced and unbalanced chromosomal abnormalities and mutation have been described that are used to diagnose and also prognosticate the disease. Despite the advances in molecular pathogenesis and targeted drug discoveries, the overall long-term survival in the majority of the patients remains poor. The advanced age of onset and exclusion of optimal cytotoxic treatments in the elderly patient group due to increased complications and decreased tolerance makes the treatment of AML using conventional therapies challenging. Several targeted therapies, i.e. FLT3-inhibitors, have been introduced for AML. However, the molecular heterogeneity of the disease and co-existing mutations and translocations makes single-targeted-therapy option less likely to succeed. Further understanding of the complex biology of AML and identification of the optimal targeted treatments will benefit particularly patients of older age as well as patients with complex karyotype and refractory disease.
8 REFERENCES 1. Swerdlow SH, World Health Organization, International Agency for Research on Cancer. WHO classification of tumours of haematopoietic and lymphoid tissues. Revised 4th edition. ed. Lyon: International Agency for Research on Cancer; pages p. 2. Dohner H, Estey EH, Amadori S, Appelbaum FR, Buchner T, Burnett AK, et al. Diagnosis and management of acute myeloid leukemia in adults: recommendations from an international expert panel, on behalf of the European LeukemiaNet. Blood. 2010;115(3): Behjati S, Tarpey PS. What is next generation sequencing? Arch Dis Child Educ Pract Ed. 2013;98(6): Rowley JD. Chromosomal translocations: revisited yet again. Blood. 2008;112(6): Mrozek K, Heerema NA, Bloomfield CD. Cytogenetics in acute leukemia. Blood Rev. 2004;18(2): Cancer Genome Atlas Research N, Ley TJ, Miller C, Ding L, Raphael BJ, Mungall AJ, et al. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N Engl J Med. 2013;368(22): Lyman SD, Jacobsen SE. c-kit ligand and Flt3 ligand: stem/progenitor cell factors with overlapping yet distinct activities. Blood. 1998;91(4): Kiyoi H, Naoe T, Nakano Y, Yokota S, Minami S, Miyawaki S, et al. Prognostic implication of FLT3 and N-RAS gene mutations in acute myeloid leukemia. Blood. 1999;93(9): Kottaridis PD, Gale RE, Langabeer SE, Frew ME, Bowen DT, Linch DC. Studies of FLT3 mutations in paired presentation and relapse samples from patients with acute myeloid leukemia: implications for the role of FLT3 mutations in leukemogenesis, minimal residual disease detection, and possible therapy with FLT3 inhibitors. Blood. 2002;100(7):
9 10. Frohling S, Schlenk RF, Breitruck J, Benner A, Kreitmeier S, Tobis K, et al. Prognostic significance of activating FLT3 mutations in younger adults (16 to 60 years) with acute myeloid leukemia and normal cytogenetics: a study of the AML Study Group Ulm. Blood. 2002;100(13): Pratz KW, Levis M. How I treat FLT3-mutated AML. Blood. 2017;129(5): Patnaik MM. The importance of FLT3 mutational analysis in acute myeloid leukemia. Leuk Lymphoma. 2017: Handschuh L, Wojciechowski P, Kazmierczak M, Marcinkowska-Swojak M, Luczak M, Lewandowski K, et al. NPM1 alternative transcripts are upregulated in acute myeloid and lymphoblastic leukemia and their expression level affects patient outcome. J Transl Med. 2018;16(1): Mason EF, Kuo FC, Hasserjian RP, Seegmiller AC, Pozdnyakova O. A distinct immunophenotype identifies a subset of NPM1-mutated AML with TET2 or IDH1/2 mutations and improved outcome. Am J Hematol. 2018;93(4): Ostronoff F, Othus M, Lazenby M, Estey E, Appelbaum FR, Evans A, et al. Prognostic significance of NPM1 mutations in the absence of FLT3-internal tandem duplication in older patients with acute myeloid leukemia: a SWOG and UK National Cancer Research Institute/Medical Research Council report. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2015;33(10): Song G, Wang L, Bi K, Jiang G. Regulation of the C/EBPalpha signaling pathway in acute myeloid leukemia (Review). Oncol Rep. 2015;33(5): Dohner K, Paschka P. Intermediate-risk acute myeloid leukemia therapy: current and future. Hematology Am Soc Hematol Educ Program. 2014;2014(1):34-43.
10 18. Taskesen E, Bullinger L, Corbacioglu A, Sanders MA, Erpelinck CA, Wouters BJ, et al. Prognostic impact, concurrent genetic mutations, and gene expression features of AML with CEBPA mutations in a cohort of 1182 cytogenetically normal AML patients: further evidence for CEBPA double mutant AML as a distinctive disease entity. Blood. 2011;117(8): Yang X, Shi J, Zhang X, Zhang G, Zhang J, Yang S, et al. Biological and clinical influences of NPM1 in acute myeloid leukemia patients with DNMT3A mutations. Cancer Manag Res. 2018;10: Ley TJ, Ding L, Walter MJ, McLellan MD, Lamprecht T, Larson DE, et al. DNMT3A mutations in acute myeloid leukemia. The New England journal of medicine. 2010;363(25): Thol F, Damm F, Ludeking A, Winschel C, Wagner K, Morgan M, et al. Incidence and prognostic influence of DNMT3A mutations in acute myeloid leukemia. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2011;29(21): Gaidzik VI, Schlenk RF, Paschka P, Stolzle A, Spath D, Kuendgen A, et al. Clinical impact of DNMT3A mutations in younger adult patients with acute myeloid leukemia: results of the AML Study Group (AMLSG). Blood. 2013;121(23): Marcucci G, Metzeler KH, Schwind S, Becker H, Maharry K, Mrozek K, et al. Age-related prognostic impact of different types of DNMT3A mutations in adults with primary cytogenetically normal acute myeloid leukemia. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2012;30(7): Yohe S. Molecular Genetic Markers in Acute Myeloid Leukemia. J Clin Med. 2015;4(3): Patel JP, Gonen M, Figueroa ME, Fernandez H, Sun Z, Racevskis J, et al. Prognostic relevance of integrated genetic profiling in acute myeloid leukemia. The New England journal of medicine. 2012;366(12):
11 26. Zhang X, Shi J, Zhang J, Yang X, Zhang G, Yang S, et al. Clinical and biological implications of IDH1/2 in acute myeloid leukemia with DNMT3A(mut). Cancer Manag Res. 2018;10: Marcucci G, Haferlach T, Dohner H. Molecular genetics of adult acute myeloid leukemia: prognostic and therapeutic implications. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2011;29(5): Rakheja D, Konoplev S, Medeiros LJ, Chen W. IDH mutations in acute myeloid leukemia. Hum Pathol. 2012;43(10): Xu Q, Li Y, Lv N, Jing Y, Xu Y, Li Y, et al. Correlation Between Isocitrate Dehydrogenase Gene Aberrations and Prognosis of Patients with Acute Myeloid Leukemia: A Systematic Review and Meta- Analysis. Clin Cancer Res. 2017;23(15): Bullinger L, Dohner K, Dohner H. Genomics of Acute Myeloid Leukemia Diagnosis and Pathways. Journal of clinical oncology : official journal of the American Society of Clinical Oncology. 2017;35(9): Pant V, Quintas-Cardama A, Lozano G. The p53 pathway in hematopoiesis: lessons from mouse models, implications for humans. Blood. 2012;120(26): Prokocimer M, Molchadsky A, Rotter V. Dysfunctional diversity of p53 proteins in adult acute myeloid leukemia: projections on diagnostic workup and therapy. Blood. 2017;130(6): Ayatollahi H, Shajiei A, Sadeghian MH, Sheikhi M, Yazdandoust E, Ghazanfarpour M, et al. Prognostic Importance of C-KIT Mutations in Core Binding Factor Acute Myeloid Leukemia: A Systematic Review. Hematol Oncol Stem Cell Ther. 2017;10(1): Shih AH, Abdel-Wahab O, Patel JP, Levine RL. The role of mutations in epigenetic regulators in myeloid malignancies. Nat Rev Cancer. 2012;12(9):
12 Table 1. Risk stratification for AML according to the European LeukemiaNet (2) Genetic Group Favorable Subsets t(8;21)(q22;q22); RUNX1-RUNX1T1 inv(16)(p13.1q22) or t(16;16)(p13.1;q22); CBFB- MYH11 Mutated NPM1 without FLT3-ITD (normal karyotype) Mutated CEBPA (normal karyotype) Intermediate-I Mutated NPM1 and FLT3-ITD (normal karyotype) Wild-type NPM1 and FLT3-ITD (normal karyotype) Wild-type NPM1 without FLT3-ITD (normal karyotype) Intermediate-II t(9;11)(p22;q23); MLLT3-MLL Cytogenetic abnormalities not classified as favorable or adverse Adverse inv(3)(q21q26.2) or t(3;3)(q21;q26.2); RPN1-EVI1 t(6;9)(p23;q34); DEK-NUP214 t(v;11)(v;q23); MLL rearranged -5 or del(5q); -7; abnl(17p); complex karyotype*
13 * Complex karyotype is defined by three or more chromosome abnormalities in the absence of designated recurrent translocations or inversions by the WHO. Table 2. Functional gene groups in AML according to the The Cancer Genome Atlas Research Network (6) Functional gene group Spliceosome Genes in the group CSTF2T, DDX1, DDX23, DHX32, HNRNPK, METTL3, PLRG1, PRPF3, PRPF8, RBMX, F3B1, SNRNP200, SRRM2, SRSF6, SUPT5H, TRA2B, U2AF1, U2AF1L4, U2AF2 Cohesin complex MLL-X fusions RAS protein Other epigenetic modifiers SMC1A, SMC3, SMC5, STAG2, RAD21 MLL-ELL, MLL-MLLT4, MLL-MLLT3, MLLT10-MLL KRAS, NRAS ARID4B, ASXL2, ASXL3, BRPF1, CBX5, CBX7, EED, HDAC2, HDAC3, JMJD1C, KAT6B, KDM2B, KDM3B, MLL2, MLL3, MTA2, PRDM9, PRDM16, RBBP4, SAP130, SCML2, SUDS3, SUZ12, ZBTB33, ZBTB7B, EBBPKAT6A, RPN1-MECOM, RUNX1-MECOM
14 Other Tyrosine Kinase ABL1, DYRK4, EPHA2, EPHA3, JAK3, MST1R, OBSCN, PDGFRB, WEE1 Serine/Threonine Kinase ACVR2B, ADRBK1, AKAP13, BUB1, CPNE3, DCLK1, MAPK1, YLK2, MYO3A, NRK, PRKCG, RPS6KA6, SMG1, STK32A, STK33, STK36, TRIO, TTBK1, WNK3, WNK4 Protein tyrosine phosphatase Other myeloid transcription factors PTPN11, PTPRT, PTPN14 GATA2, CBFB, ETV6, ETV3, GLI1, IKZF1, MYB, MYC, MLLT10-CEP164
15 Table 3. Targeted treatments for AML, FDA-approved and under investigation agents Target Drug(s) Approval status* Indication FLT3 Crenolanib Gilteritinib Midastaurin Quizartinib Sorafenib Approved New dx AML with FLT3 mutation IDH2 Enasidenib Approved Adults with relapsed or refractory AML associated with IDH2 mutations. IDH1 Ivosidenib Approved Adults with relapsed or refractory AML associated with IDH1 mutation FT-2102 and others Investigational BCL2 Venetoclax Investigational TET2 Vitamin C and hypomethylating agents Approved* AML with low blast count* CD33 gemtuzumab ozogamicin Approved Newly diagnosed CD33-positive AML MDM2 idasanutlin Investigational *US Food and Drug Administration (FDA) approval status # Hypomethylating agent (Azacitidine) approved for low blast count AML in the US.
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017
 Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia
 Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia Hartmut Döhner Medical Director, Department of Internal Medicine III Director, Comprehensive Cancer Center Ulm Ulm University,
Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia Hartmut Döhner Medical Director, Department of Internal Medicine III Director, Comprehensive Cancer Center Ulm Ulm University,
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Treatments and Current Research in Leukemia. Richard A. Larson, MD University of Chicago
 Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
AML: WHO classification, biology and prognosis. Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen
 AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
SUPPLEMENTARY INFORMATION
 Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Update on the WHO Classification of Acute Myeloid Leukemia. Kaaren K. Reichard, MD Mayo Clinic Rochester
 Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota
 Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia
 Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schlenk RF, Döhner K, Krauter J, et al. Mutations and treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schlenk RF, Döhner K, Krauter J, et al. Mutations and treatment
Corporate Medical Policy. Policy Effective February 23, 2018
 Corporate Medical Policy Genetic Testing for FLT3, NPM1 and CEBPA Mutations in Acute File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_flt3_npm1_and_cebpa_mutations_in_acute_myeloid_leukemia
Corporate Medical Policy Genetic Testing for FLT3, NPM1 and CEBPA Mutations in Acute File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_flt3_npm1_and_cebpa_mutations_in_acute_myeloid_leukemia
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1
 Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
ESTABLISHED AND EMERGING THERAPIES FOR ACUTE MYELOID LEUKAEMIA. Dr Rob Sellar UCL Cancer Institute, London, UK
 ESTABLISHED AND EMERGING THERAPIES FOR ACUTE MYELOID LEUKAEMIA Dr Rob Sellar UCL Cancer Institute, London, UK OVERVIEW Main focus on patients fit for intensive treatment Biological and Clinical Heterogeneity
ESTABLISHED AND EMERGING THERAPIES FOR ACUTE MYELOID LEUKAEMIA Dr Rob Sellar UCL Cancer Institute, London, UK OVERVIEW Main focus on patients fit for intensive treatment Biological and Clinical Heterogeneity
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH )
 Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Molecularly Targeted Therapies - Strategies of the AMLSG
 Molecularly Targeted Therapies - Strategies of the AMLSG Richard Schlenk Department of Internal Medicine III Ulm University, Germany Genotype-adapted Leukemia Program NAPOLEON GIMEMA/AMLSG/SAL APL [t(15;17)]
Molecularly Targeted Therapies - Strategies of the AMLSG Richard Schlenk Department of Internal Medicine III Ulm University, Germany Genotype-adapted Leukemia Program NAPOLEON GIMEMA/AMLSG/SAL APL [t(15;17)]
Acute Myeloid Leukemia
 Acute Myeloid Leukemia Guido Marcucci, M.D. Director, Gehr Family Center for Leukemia Research Hematologic Malignancies and Stem Cell Transplantation Institute City of Hope Acute Myeloid Leukemia Gene
Acute Myeloid Leukemia Guido Marcucci, M.D. Director, Gehr Family Center for Leukemia Research Hematologic Malignancies and Stem Cell Transplantation Institute City of Hope Acute Myeloid Leukemia Gene
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
Classification and risk assessment in AML: integrating cytogenetics and molecular profiling
 ACUTE MYELOID LEUKEMIA: HOW CAN WE IMPROVE UPON STANDARD THERAPY? Classification and risk assessment in AML: integrating cytogenetics and molecular profiling Matahi Moarii and Elli Papaemmanuil Department
ACUTE MYELOID LEUKEMIA: HOW CAN WE IMPROVE UPON STANDARD THERAPY? Classification and risk assessment in AML: integrating cytogenetics and molecular profiling Matahi Moarii and Elli Papaemmanuil Department
N Engl J Med Volume 373(12): September 17, 2015
 Review Article Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. N Engl J Med Volume 373(12):1136-1152 September 17, 2015 Acute Myeloid Leukemia Most
Review Article Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. N Engl J Med Volume 373(12):1136-1152 September 17, 2015 Acute Myeloid Leukemia Most
Evolving Targeted Management of Acute Myeloid Leukemia
 Evolving Targeted Management of Acute Myeloid Leukemia Jessica Altman, MD Robert H. Lurie Comprehensive Cancer Center of Northwestern University Learning Objectives Identify which mutations should be assessed
Evolving Targeted Management of Acute Myeloid Leukemia Jessica Altman, MD Robert H. Lurie Comprehensive Cancer Center of Northwestern University Learning Objectives Identify which mutations should be assessed
Acute myeloid leukemia: a comprehensive review and 2016 update
 OPEN Citation: (2016) 6, e441; doi:10.1038/bcj.2016.50 www.nature.com/bcj REVIEW Acute myeloid leukemia: a comprehensive review and 2016 update I De Kouchkovsky 1 and M Abdul-Hay 1,2 Acute myeloid leukemia
OPEN Citation: (2016) 6, e441; doi:10.1038/bcj.2016.50 www.nature.com/bcj REVIEW Acute myeloid leukemia: a comprehensive review and 2016 update I De Kouchkovsky 1 and M Abdul-Hay 1,2 Acute myeloid leukemia
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
New drugs in Acute Leukemia. Cristina Papayannidis, MD, PhD University of Bologna
 New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
Measure Specifications Measure Description
 CMS ID/CMS QCDR ID: CAP 17 Title: FMS-like Tyrosine 3-Internal Tandem Duplication (FLT3-ITD) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Acute Myeloid Leukemia
CMS ID/CMS QCDR ID: CAP 17 Title: FMS-like Tyrosine 3-Internal Tandem Duplication (FLT3-ITD) Biomarker Testing to Inform Clinical Management and Treatment Decisions in Patients with Acute Myeloid Leukemia
The Past, Present, and Future of Acute Myeloid Leukemia
 The Past, Present, and Future of Acute Myeloid Leukemia Carter T. Davis, MD Hematology-Oncology Fellow Duke University Health System September 10, 2016 Overview Overview of Acute Myeloid Leukemia Review
The Past, Present, and Future of Acute Myeloid Leukemia Carter T. Davis, MD Hematology-Oncology Fellow Duke University Health System September 10, 2016 Overview Overview of Acute Myeloid Leukemia Review
«Adverse Prognosis» Acute Myeloid Leukemia
 23. Fortbildungskurs Lausanne, 11.11.2017 «Adverse Prognosis» Acute Myeloid Leukemia Markus G. Manz Zentrum für Hämatologie und Onkologie UniversitätsSpital Zürich Content AML Update on current definition
23. Fortbildungskurs Lausanne, 11.11.2017 «Adverse Prognosis» Acute Myeloid Leukemia Markus G. Manz Zentrum für Hämatologie und Onkologie UniversitätsSpital Zürich Content AML Update on current definition
Acute leukemia and myelodysplastic syndromes
 11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
Acute Myeloid Leukemia with RUNX1 and Several Co-mutations
 Case SH2017-0281 Acute Myeloid Leukemia with RUNX1 and Several Co-mutations James Bauer, MD, PhD David Yang, MD Erik Ranheim, MD, PhD Catherine Leith, MB, Bchir Clinical History Chief Complaint: 72 year
Case SH2017-0281 Acute Myeloid Leukemia with RUNX1 and Several Co-mutations James Bauer, MD, PhD David Yang, MD Erik Ranheim, MD, PhD Catherine Leith, MB, Bchir Clinical History Chief Complaint: 72 year
New concepts in the management of elderly patients with AML
 New concepts in the management of elderly patients with AML Martha L. Arellano, MD Associate Professor of Hematology/Oncology Director, Hematology & Medical Oncology Fellowship Program Winship Cancer Institute
New concepts in the management of elderly patients with AML Martha L. Arellano, MD Associate Professor of Hematology/Oncology Director, Hematology & Medical Oncology Fellowship Program Winship Cancer Institute
Kevin Kelly, MD, Phd Acute Myeloid and Lymphoid Leukemias
 Kevin Kelly, MD, Phd Acute Myeloid and Lymphoid Leukemias Relevant financial relationships in the past twelve months by presenter or spouse/partner. Speakers bureau: Novartis, Janssen, Gilead, Bayer The
Kevin Kelly, MD, Phd Acute Myeloid and Lymphoid Leukemias Relevant financial relationships in the past twelve months by presenter or spouse/partner. Speakers bureau: Novartis, Janssen, Gilead, Bayer The
Available online at
 Annals of Clinical & Laboratory Science, vol. 45, no. 5, 2015 Available online at www.annclinlabsci.org Bioinformatics Analysis to Determine Prognostic Mutations of 72 de novo Acute Myeloid Leukemia Cases
Annals of Clinical & Laboratory Science, vol. 45, no. 5, 2015 Available online at www.annclinlabsci.org Bioinformatics Analysis to Determine Prognostic Mutations of 72 de novo Acute Myeloid Leukemia Cases
Cytogenetics and FLT3 ITD mutation predict clinical outcomes in non transplant patients with acute myeloid leukemia
 https://doi.org/10.1186/s40164-019-0127-z Experimental Hematology & Oncology RESEARCH Open Access Cytogenetics and FLT3 ITD mutation predict clinical outcomes in non transplant patients with acute myeloid
https://doi.org/10.1186/s40164-019-0127-z Experimental Hematology & Oncology RESEARCH Open Access Cytogenetics and FLT3 ITD mutation predict clinical outcomes in non transplant patients with acute myeloid
All patients with FLT3 mutant AML should receive midostaurin-based induction therapy. Not so fast!
 All patients with FLT3 mutant AML should receive midostaurin-based induction therapy Not so fast! Harry P. Erba, M.D., Ph.D. Professor, Internal Medicine Director, Hematologic Malignancy Program University
All patients with FLT3 mutant AML should receive midostaurin-based induction therapy Not so fast! Harry P. Erba, M.D., Ph.D. Professor, Internal Medicine Director, Hematologic Malignancy Program University
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD
 Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD What is it? clonal expansion of myeloid precursor cells with reduced capacity to differentiate as opposed to ALL/CLL, it is limited to the myeloid cell
Meeting VAKB 8 februari 2011 Nancy Boeckx, MD, PhD What is it? clonal expansion of myeloid precursor cells with reduced capacity to differentiate as opposed to ALL/CLL, it is limited to the myeloid cell
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Acute Leukemia. Sebastian Giebel. Geneva 03/04/
 Acute Leukemia (including ALL) Sebastian Giebel Geneva 03/04/2012 www.ebmt.org Acute leukemias: EBMT survey 2 AML: EBMT survey Gratwohl A, et al. Bone Marrow Transplant 2009 3 Acute leukemias: INCIDENCE
Acute Leukemia (including ALL) Sebastian Giebel Geneva 03/04/2012 www.ebmt.org Acute leukemias: EBMT survey 2 AML: EBMT survey Gratwohl A, et al. Bone Marrow Transplant 2009 3 Acute leukemias: INCIDENCE
Personalized Therapy for Acute Myeloid Leukemia. Patrick Stiff MD Loyola University Medical Center
 Personalized Therapy for Acute Myeloid Leukemia Patrick Stiff MD Loyola University Medical Center 708-327-3216 Major groups of Mutations in AML Targets for AML: Is this Achievable? Chronic Myeloid Leukemia:
Personalized Therapy for Acute Myeloid Leukemia Patrick Stiff MD Loyola University Medical Center 708-327-3216 Major groups of Mutations in AML Targets for AML: Is this Achievable? Chronic Myeloid Leukemia:
Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome
 Molecular profiling of early MDS Hematopathology - March 2016 Article Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome Maya Thangavelu 1,*, Ryan Olson 2, Li Li 2, Wanlong
Molecular profiling of early MDS Hematopathology - March 2016 Article Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome Maya Thangavelu 1,*, Ryan Olson 2, Li Li 2, Wanlong
Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia
 Acute Myeloid Leukemia Articles Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia Bruno C. Medeiros, 1 Megan Othus, 2,3 Min Fang, 3,4 Frederick R. Appelbaum,
Acute Myeloid Leukemia Articles Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia Bruno C. Medeiros, 1 Megan Othus, 2,3 Min Fang, 3,4 Frederick R. Appelbaum,
Case 1. Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX
 Case 1 Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX Disclosure of Relevant Financial Relationships The USCAP requires that anyone in a position to influence or control the content of all CME
Case 1 Sa A.Wang, MD UT MD Anderson Cancer Center Houston, TX Disclosure of Relevant Financial Relationships The USCAP requires that anyone in a position to influence or control the content of all CME
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
REVIEW. Prognostic Value of RUNX1 Mutations in AML: A Meta-Analysis
 DOI:10.22034/APJCP.2018.19.2.325 REVIEW Editorial Process: Submission:10/03/2017 Acceptance:12/16/2017 Prognostic Value of RUNX1 Mutations in AML: A Meta-Analysis Mahdi Jalili 1,2, Marjan Yaghmaie 1, Mohammad
DOI:10.22034/APJCP.2018.19.2.325 REVIEW Editorial Process: Submission:10/03/2017 Acceptance:12/16/2017 Prognostic Value of RUNX1 Mutations in AML: A Meta-Analysis Mahdi Jalili 1,2, Marjan Yaghmaie 1, Mohammad
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Initial Diagnostic Workup of Acute Leukemia
 Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Krishna Reddy CH and Ashwin Dalal. Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad
 Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Next Generation Sequencing in Haematological Malignancy: A European Perspective. Wolfgang Kern, Munich Leukemia Laboratory
 Next Generation Sequencing in Haematological Malignancy: A European Perspective Wolfgang Kern, Munich Leukemia Laboratory Diagnostic Methods Cytomorphology Cytogenetics Immunophenotype Histology FISH Molecular
Next Generation Sequencing in Haematological Malignancy: A European Perspective Wolfgang Kern, Munich Leukemia Laboratory Diagnostic Methods Cytomorphology Cytogenetics Immunophenotype Histology FISH Molecular
Case Report Blasts-more than meets the eye: evaluation of post-induction day 21 bone marrow in CBFB rearranged acute leukemia
 Int J Clin Exp Pathol 2014;7(7):4498-4502 www.ijcep.com /ISSN:1936-2625/IJCEP0000851 Case Report Blasts-more than meets the eye: evaluation of post-induction day 21 bone marrow in CBFB rearranged acute
Int J Clin Exp Pathol 2014;7(7):4498-4502 www.ijcep.com /ISSN:1936-2625/IJCEP0000851 Case Report Blasts-more than meets the eye: evaluation of post-induction day 21 bone marrow in CBFB rearranged acute
GENETICS OF HEMATOLOGICAL MALIGNANCIES
 de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
How do novel molecular genetic markers influence treatment decisions in acute myeloid leukemia?
 ACUTE MYELOID LEUKEMIA: NEWLY DISCOVERED GENES, SCREENS (FOR MINIMAL RESIDUAL DISEASE), AND THERAPEUTIC MEANS How do novel molecular genetic markers influence treatment decisions in acute myeloid leukemia?
ACUTE MYELOID LEUKEMIA: NEWLY DISCOVERED GENES, SCREENS (FOR MINIMAL RESIDUAL DISEASE), AND THERAPEUTIC MEANS How do novel molecular genetic markers influence treatment decisions in acute myeloid leukemia?
RUNX1 and FPD/AML Translational Research. The Leukemia and Lymphoma Society / Babich Family Foundation Partnership. September 2016
 www.lls.org www.runx1.com RUNX1 and FPD/AML Translational Research The Leukemia and Lymphoma Society / Babich Family Foundation Partnership September 2016 Prepared by L. Greenberger, PhD Chief Scientific
www.lls.org www.runx1.com RUNX1 and FPD/AML Translational Research The Leukemia and Lymphoma Society / Babich Family Foundation Partnership September 2016 Prepared by L. Greenberger, PhD Chief Scientific
Changing AML Outcomes via Personalized Medicine: Transforming Cancer Management with Genetic Insight
 Changing AML Outcomes via Personalized Medicine: Transforming Cancer Management with Genetic Insight Co-Moderators: Rick Winneker, PhD, Senior Vice President, Research, Leukemia & Lymphoma Society Mike
Changing AML Outcomes via Personalized Medicine: Transforming Cancer Management with Genetic Insight Co-Moderators: Rick Winneker, PhD, Senior Vice President, Research, Leukemia & Lymphoma Society Mike
Acute Myeloid Leukemia
 The new england journal of medicine Review Article Dan L. Longo, M.D., Editor Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. From the Department of
The new england journal of medicine Review Article Dan L. Longo, M.D., Editor Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. From the Department of
New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke
 University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
Acute myeloid leukemia: prognosis and treatment. Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg
 Acute myeloid leukemia: prognosis and treatment Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg Patient Female, 39 years History: hypothyroidism Present:
Acute myeloid leukemia: prognosis and treatment Dimitri A. Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Campus Stuivenberg Patient Female, 39 years History: hypothyroidism Present:
Supplemental Material. The new provisional WHO entity RUNX1 mutated AML shows specific genetics without prognostic influence of dysplasia
 Supplemental Material The new provisional WHO entity RUNX1 mutated AML shows specific genetics without prognostic influence of dysplasia Torsten Haferlach, 1 Anna Stengel, 1 Sandra Eckstein, 1 Karolína
Supplemental Material The new provisional WHO entity RUNX1 mutated AML shows specific genetics without prognostic influence of dysplasia Torsten Haferlach, 1 Anna Stengel, 1 Sandra Eckstein, 1 Karolína
Out-Patient Billing CPT Codes
 Out-Patient Billing CPT Codes Updated Date: August 3, 08 Client Billed Molecular Tests HPV DNA Tissue Testing 8764 No Medicare Billed - Molecular Tests NeoARRAY NeoARRAY SNP/Cytogenetic No 89 NeoLAB NeoLAB
Out-Patient Billing CPT Codes Updated Date: August 3, 08 Client Billed Molecular Tests HPV DNA Tissue Testing 8764 No Medicare Billed - Molecular Tests NeoARRAY NeoARRAY SNP/Cytogenetic No 89 NeoLAB NeoLAB
* University of Pennsylvania +Kaiser Permanente, California
 SH2017-0144: Differential response to FLT3 inhibition (using quizartinib/ac220) in acute myeloid leukemia is affected by baseline molecular genetics and cytogenetics Siddharth Bhattacharyya, MD*, Grant
SH2017-0144: Differential response to FLT3 inhibition (using quizartinib/ac220) in acute myeloid leukemia is affected by baseline molecular genetics and cytogenetics Siddharth Bhattacharyya, MD*, Grant
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Patel JP, Gönen M, Figueroa ME, et al. Prognostic relevance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Patel JP, Gönen M, Figueroa ME, et al. Prognostic relevance
Management of Myelodysplastic Syndromes
 Management of Myelodysplastic Syndromes Peter L. Greenberg, MD Stanford Cancer Institute Myelodysplastic Syndromes: Clinical & Molecular Advances for Disease Classification and Prognostication MDSs: A
Management of Myelodysplastic Syndromes Peter L. Greenberg, MD Stanford Cancer Institute Myelodysplastic Syndromes: Clinical & Molecular Advances for Disease Classification and Prognostication MDSs: A
Neue zielgerichtete Behandlungsoptionen der neu diagnostizierten FLT3-positiven Akuten Myeloischen Leukämie (AML)
 Neue zielgerichtete Behandlungsoptionen der neu diagnostizierten FLT3-positiven Akuten Myeloischen Leukämie (AML) Prof. Hartmut Döhner Klinik für Innere Medizin III, Universitätsklinikum Ulm Midostaurin
Neue zielgerichtete Behandlungsoptionen der neu diagnostizierten FLT3-positiven Akuten Myeloischen Leukämie (AML) Prof. Hartmut Döhner Klinik für Innere Medizin III, Universitätsklinikum Ulm Midostaurin
Acute Myeloid Leukemia Progress at last
 Acute Myeloid Leukemia Progress at last Bruno C. Medeiros, MD September 9, 217 Introduction Mechanisms of leukemogenesis Emerging therapies in AML Previously untreated AML Relapsed and refractory patients
Acute Myeloid Leukemia Progress at last Bruno C. Medeiros, MD September 9, 217 Introduction Mechanisms of leukemogenesis Emerging therapies in AML Previously untreated AML Relapsed and refractory patients
Clinical Overview on Measurable Residual Disease (MRD) in Acute Myeloid Leukemia(AML)
 Clinical Overview on Measurable Residual Disease (MRD) in Acute Myeloid Leukemia(AML) Konstanze Döhner Department of Internal Medicine III, University Hospital of Ulm, Ulm Germany DISCLOSURES OF COMMERCIAL
Clinical Overview on Measurable Residual Disease (MRD) in Acute Myeloid Leukemia(AML) Konstanze Döhner Department of Internal Medicine III, University Hospital of Ulm, Ulm Germany DISCLOSURES OF COMMERCIAL
Minimal residual disease (MRD) in AML; coming of age. Dr. Mehmet Yılmaz Gaziantep University Medical School Sahinbey Education and Research hospital
 Minimal residual disease (MRD) in AML; coming of age Dr. Mehmet Yılmaz Gaziantep University Medical School Sahinbey Education and Research hospital 1. The logistics of MRD assessment in AML 2. The clinical
Minimal residual disease (MRD) in AML; coming of age Dr. Mehmet Yılmaz Gaziantep University Medical School Sahinbey Education and Research hospital 1. The logistics of MRD assessment in AML 2. The clinical
Molecularly targeted therapies for acute myeloid leukemia
 Molecularly targeted therapies for acute myeloid leukemia Eytan M. Stein 1 TREATMENT OF ACUTE MYELOID LEUKEMIA:MOVING BEYOND 3 7 1 Leukemia Service, Memorial Sloan Kettering Cancer Center, New York, NY
Molecularly targeted therapies for acute myeloid leukemia Eytan M. Stein 1 TREATMENT OF ACUTE MYELOID LEUKEMIA:MOVING BEYOND 3 7 1 Leukemia Service, Memorial Sloan Kettering Cancer Center, New York, NY
Cost-Effective Strategies in the Workup of Hematologic Neoplasm. Karl S. Theil, Claudiu V. Cotta Cleveland Clinic
 Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
How the Treatment of Acute Myeloid Leukemia is Changing in 2019
 How the Treatment of Acute Myeloid Leukemia is Changing in 2019 Guido Marcucci, M.D. Director, Gehr Family Center for Leukemia Research Chair, Dept. Hematologic Malignancies Translational Science City
How the Treatment of Acute Myeloid Leukemia is Changing in 2019 Guido Marcucci, M.D. Director, Gehr Family Center for Leukemia Research Chair, Dept. Hematologic Malignancies Translational Science City
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities
 Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Page: 1 of 12. Genetic Testing for FLT3, NPM1, and CEBPA Mutations in Acute Myeloid Leukemia
 Page: 1 of 12 Last Review Status/Date: September 2015 Genetic Testing for FLT3, NPM1, and CEBPA Mutations in Acute Myeloid Description Treatment of acute myeloid leukemia (AML) is based upon risk stratification,
Page: 1 of 12 Last Review Status/Date: September 2015 Genetic Testing for FLT3, NPM1, and CEBPA Mutations in Acute Myeloid Description Treatment of acute myeloid leukemia (AML) is based upon risk stratification,
Trapianto allogenico convenzionale
 Il trapianto nella leucemia acuta mieloide a rischio intermedio Trapianto allogenico convenzionale Trapianto allogenico nelle Leucemie Acute Mieloidi in I RC D. Pastore Ematologia con Trapianto-Bari Domenico
Il trapianto nella leucemia acuta mieloide a rischio intermedio Trapianto allogenico convenzionale Trapianto allogenico nelle Leucemie Acute Mieloidi in I RC D. Pastore Ematologia con Trapianto-Bari Domenico
Cytogenetic and molecular abnormalities in AML. Dr Elizabeth Tegg Director of haematology Pathology West
 Cytogenetic and molecular abnormalities in AML Dr Elizabeth Tegg Director of haematology Pathology West Outline Classification of AML Types of genetic changes Next generation sequencing in HM Outline Classification
Cytogenetic and molecular abnormalities in AML Dr Elizabeth Tegg Director of haematology Pathology West Outline Classification of AML Types of genetic changes Next generation sequencing in HM Outline Classification
FLT-3 inhibitors in AML
 FLT-3 inhibitors in AML Jorge Sierra Hospital de la Santa Creu i Sant Pau Autonomous University of Barcelona Rome, September 24, 2017 Disclosures Advisory board: Pfizer, NovarHs, Jazz, Celgene, SeaIle
FLT-3 inhibitors in AML Jorge Sierra Hospital de la Santa Creu i Sant Pau Autonomous University of Barcelona Rome, September 24, 2017 Disclosures Advisory board: Pfizer, NovarHs, Jazz, Celgene, SeaIle
Disclosure: Objectives/Outline. Leukemia: Genealogy of Pathology Practice: Old Diseases New Expectations. Nothing to disclose.
 RC1 Leukemia: Genealogy of Pathology Practice: Old Diseases New Expectations RC2 Disclosure: Nothing to disclose Henry Moon Lecture: UCSF Annual Conference Kathryn Foucar, MD kfoucar@salud.unm.edu May
RC1 Leukemia: Genealogy of Pathology Practice: Old Diseases New Expectations RC2 Disclosure: Nothing to disclose Henry Moon Lecture: UCSF Annual Conference Kathryn Foucar, MD kfoucar@salud.unm.edu May
Review Article The Epigenetic Landscape of Acute Myeloid Leukemia
 Advances in Hematology, Article ID 103175, 15 pages http://dx.doi.org/10.1155/2014/103175 Review Article The Epigenetic Landscape of Acute Myeloid Leukemia Emma Conway O Brien, Steven Prideaux, and Timothy
Advances in Hematology, Article ID 103175, 15 pages http://dx.doi.org/10.1155/2014/103175 Review Article The Epigenetic Landscape of Acute Myeloid Leukemia Emma Conway O Brien, Steven Prideaux, and Timothy
Enhancing Assessment of Myeloid Disorders in the Era of Precision Medicine
 Enhancing Assessment of Myeloid Disorders in the Era of Precision Medicine Michelle Afkhami, M.D. Medical Director, Clinical Molecular Diagnostic Laboratory City of Hope National Medical Center Objectives
Enhancing Assessment of Myeloid Disorders in the Era of Precision Medicine Michelle Afkhami, M.D. Medical Director, Clinical Molecular Diagnostic Laboratory City of Hope National Medical Center Objectives
Molecular. Oncology & Pathology. Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine. Liquid Biopsy.
 Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
Cytogenetic heterogeneity negatively impacts outcomes in patients with acute myeloid leukemia
 Published Ahead of Print on December 19, 2014, as doi:10.3324/haematol.2014.117267. Copyright 2014 Ferrata Storti Foundation. Cytogenetic heterogeneity negatively impacts outcomes in patients with acute
Published Ahead of Print on December 19, 2014, as doi:10.3324/haematol.2014.117267. Copyright 2014 Ferrata Storti Foundation. Cytogenetic heterogeneity negatively impacts outcomes in patients with acute
Therapy-related MDS/AML with KMT2A (MLL) Rearrangement Following Therapy for APL Case 0328
 Therapy-related MDS/AML with KMT2A (MLL) Rearrangement Following Therapy for APL Case 0328 Kenneth N. Holder, Leslie J. Greebon, Gopalrao Velagaleti, Hongxin Fan, Russell A. Higgins Initial Case: Clinical
Therapy-related MDS/AML with KMT2A (MLL) Rearrangement Following Therapy for APL Case 0328 Kenneth N. Holder, Leslie J. Greebon, Gopalrao Velagaleti, Hongxin Fan, Russell A. Higgins Initial Case: Clinical
Remission induction in acute myeloid leukemia
 Int J Hematol (2012) 96:164 170 DOI 10.1007/s12185-012-1121-y PROGRESS IN HEMATOLOGY How to improve the outcome of adult acute myeloid leukemia? Remission induction in acute myeloid leukemia Eytan M. Stein
Int J Hematol (2012) 96:164 170 DOI 10.1007/s12185-012-1121-y PROGRESS IN HEMATOLOGY How to improve the outcome of adult acute myeloid leukemia? Remission induction in acute myeloid leukemia Eytan M. Stein
Leukaemia - New Therapeutic Approaches. Professor Paresh Vyas
 Leukaemia - New Therapeutic Approaches Professor Paresh Vyas Oxford Center for Haematology & MRC Molecular Unit University of Oxford and University of Oxford Hospitals Foundation NHS Trust Outline of Presentation
Leukaemia - New Therapeutic Approaches Professor Paresh Vyas Oxford Center for Haematology & MRC Molecular Unit University of Oxford and University of Oxford Hospitals Foundation NHS Trust Outline of Presentation
Post-remission therapy for acute myeloid leukemia
 Review Articles Post-remission therapy for acute myeloid leukemia Richard F. Schlenk Department of Internal Medicine III, University Hospital Ulm, Germany ABSTRACT Induction followed by post-remission
Review Articles Post-remission therapy for acute myeloid leukemia Richard F. Schlenk Department of Internal Medicine III, University Hospital Ulm, Germany ABSTRACT Induction followed by post-remission
GENETIC TESTING FOR FLT3, NPM1 AND CEBPA VARIANTS IN CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA
 CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
A pediatric patient with acute leukemia of ambiguous lineage with a NUP98-NSD1 rearrangement SH
 A pediatric patient with acute leukemia of ambiguous lineage with a NUP98NSD1 rearrangement SH20170203 Rebecca LeemanNeill, Ronald Rice, Anita Malek, Patricia Raciti, Susan Hsiao, Mahesh Mansukhani, Bachir
A pediatric patient with acute leukemia of ambiguous lineage with a NUP98NSD1 rearrangement SH20170203 Rebecca LeemanNeill, Ronald Rice, Anita Malek, Patricia Raciti, Susan Hsiao, Mahesh Mansukhani, Bachir
AML Emerging Treatment Strategies
 Welcome and Introduction Clare Karten, MS Senior Director, Mission Education The Leukemia & Lymphoma Society AML Emerging Treatment Strategies Wendy Stock, MD Professor of Medicine, Section of Hematology/Oncology
Welcome and Introduction Clare Karten, MS Senior Director, Mission Education The Leukemia & Lymphoma Society AML Emerging Treatment Strategies Wendy Stock, MD Professor of Medicine, Section of Hematology/Oncology
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Molecular Advances in Hematopathology
 Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
Molecular Advances in Hematopathology HOW MOLECULAR METHODS HAVE CHANGED MY PRACTICE Objectives Understand the importance of cytogenetic/molecular studies in hematolymphoid diseases Know some of the important
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 5.21.93 Rydapt (midostaurin) Genetic Testing for FLT3, NPM1, and CEBPA Variants in Description Treatment of acute myeloid leukemia
FEP Medical Policy Manual Effective Date: April 15, 2018 Related Policies: 5.21.93 Rydapt (midostaurin) Genetic Testing for FLT3, NPM1, and CEBPA Variants in Description Treatment of acute myeloid leukemia
TEST MENU TEST CPT CODES TAT. Chromosome Analysis Bone Marrow x 2, 88264, x 3, Days
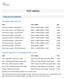 TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party. The European Group for Blood and Marrow Transplantation
 36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
Keywords: Acute Myeloid Leukemia, FLT3-ITD Mutation, FAB Subgroups, Cytogenetic Risk Groups
 Original Articleeee fms Like Tyrosine kinase3- Internal Tandem Duplication (FLT3-ITD) in Acute Myeloid Leukemia, Mutation Frequency and its Relation with Complete Remission, 2007-2008 Emami AH, 1 Shekarriz
Original Articleeee fms Like Tyrosine kinase3- Internal Tandem Duplication (FLT3-ITD) in Acute Myeloid Leukemia, Mutation Frequency and its Relation with Complete Remission, 2007-2008 Emami AH, 1 Shekarriz
Minimal Residual Disease as a Surrogate Endpoint in Acute Myeloid Leukemia Clinical Trials
 Minimal Residual Disease as a Surrogate Endpoint in Acute Myeloid Leukemia Clinical Trials Fda.gov Adriano Venditti Hematology, University Tor Vergata, Rome, Italy Minimal Residual Disease 10 12 Relapse
Minimal Residual Disease as a Surrogate Endpoint in Acute Myeloid Leukemia Clinical Trials Fda.gov Adriano Venditti Hematology, University Tor Vergata, Rome, Italy Minimal Residual Disease 10 12 Relapse
Acute Leukemia Diagnosis
 Acute Leukemia Diagnosis Elizabeth A. Griffiths, MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine 3 841,390 843,820 Blood cancers are normal blood cells
Acute Leukemia Diagnosis Elizabeth A. Griffiths, MD Leukemia Service, Department of Medicine Roswell Park Cancer Institute SUNY-UB School of Medicine 3 841,390 843,820 Blood cancers are normal blood cells
Mixed Phenotype Acute Leukemias
 Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Myelodysplastic syndromes
 Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
Myelodysplastic syndromes Robert P Hasserjian Massachusetts General Hospital, Boston, MA Disclosure of Relevant Financial Relationships Dr. Hasserjian declares he has no conflict(s) of interest to disclose.
BCR-ABL1 positive Myeloid Sarcoma Nicola Austin
 BCR-ABL1 positive Myeloid Sarcoma Nicola Austin Cytocell UK & Ireland User Group Meeting Jesus College, Cambridge 4 th - 5 th April 2017 Myeloid Sarcoma WHO Classification Tumours of Haematopoietic and
BCR-ABL1 positive Myeloid Sarcoma Nicola Austin Cytocell UK & Ireland User Group Meeting Jesus College, Cambridge 4 th - 5 th April 2017 Myeloid Sarcoma WHO Classification Tumours of Haematopoietic and
Test Name Results Units Bio. Ref. Interval. Positive
 Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
