JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY VOL. 65, NO. 9, 2015 ª 2015 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN /$36.
|
|
|
- Rolf Harper
- 5 years ago
- Views:
Transcription
1 JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY VOL. 65, NO. 9, 2015 ª 2015 BY THE AMERICAN COLLEGE OF CARDIOLOGY FOUNDATION ISSN /$36.00 PUBLISHED BY ELSEVIER INC. Implantable Cardioverter-Defibrillator TherapyinBrugadaSyndrome A 20-Year Single-Center Experience Giulio Conte, MD,* Juan Sieira, MD,* Giuseppe Ciconte, MD,* Carlo de Asmundis, MD,* Gian-Battista Chierchia, MD,* Giannis Baltogiannis, MD,* Giacomo Di Giovanni, MD,* Mark La Meir, MD,y Francis Wellens, MD,y Jens Czapla, MD,y Kristel Wauters, MD,* Moises Levinstein, MD,* Yukio Saitoh, MD,* Ghazala Irfan, MD,* Justo Julià, MD,* Gudrun Pappaert, RN,* Pedro Brugada, MD* ABSTRACT BACKGROUND Patients with Brugada syndrome and aborted sudden cardiac death or syncope have higher risks for ventricular arrhythmias (VAs) and should undergo implantable cardioverter-defibrillator (ICD) placement. Device-based management of asymptomatic patients is controversial. ICD therapy is associated with high rates of inappropriate shocks and device-related complications. OBJECTIVES The objective of this study was to investigate clinical features, management, and long-term follow-up of ICD therapy in patients with Brugada syndrome. METHODS Patients presenting with spontaneous or drug-induced Brugada type 1 electrocardiographic findings, who underwent ICD implantation and continuous follow-up at a single institution, were eligible for this study. RESULTS A total of 176 consecutive patients were included. During a mean follow-up period of months, spontaneous sustained VAs occurred in 30 patients (17%). Eight patients (4.5%) died. Appropriate ICD shocks occurred in 28 patients (15.9%), and 33 patients (18.7%) had inappropriate shocks. Electrical storm occurred in 4 subjects (2.3%). Twenty-eight patients (15.9%) experienced device-related complications. In multivariate Cox regression analysis, aborted sudden cardiac death and VA inducibility on electrophysiologic studies were independent predictors of appropriate shock occurrence. CONCLUSIONS ICD therapy was an effective strategy in Brugada syndrome, treating potentially lethal arrhythmias in 17% of patients during long-term follow-up. Appropriate shocks were significantly associated with the presence of aborted sudden cardiac death but also occurred in 13% of asymptomatic patients. Risk stratification by electrophysiologic study may identify asymptomatic patients at risk for arrhythmic events and could be helpful in investigating syncope not related to VAs. ICD placement is frequently associated with device-related complications, and rates of inappropriate shocks remain high regardless of careful device programming. (J Am Coll Cardiol 2015;65:879 88) 2015 by the American College of Cardiology Foundation. Brugada syndrome (BS) is an inheritable syndrome characterized by coved-type STsegment elevation in the right precordial leads (V 1 to V 3 ) and increased risk for sudden cardiac death (SCD) in the absence of structural heart disease (1). Today, the placement of an implantable cardioverter-defibrillator (ICD) remains the only therapy with proven efficacy for the management of ventricular arrhythmias (VAs) in patients with BS (2). Patients experiencing syncope or aborted SCD, who are considered to be the patients with BS at higher From the *Heart Rhythm Management Centre UZ Brussel-VUB, Brussels, Belgium; and the ycardiac Surgery Department, UZ Brussel-VUB, Brussels, Belgium. Dr. Brugada has received research grants from Biotronik, Medtronic, St. Jude Medical, and Sorin. All other authors have reported that they have no relationships relevant to the contents of this paper to disclose. Drs. Conte and Sieira contributed equally to this work. Manuscript received June 3, 2014; revised manuscript received December 7, 2014, accepted December 12, 2014.
2 880 Conte et al. JACC VOL. 65, NO. 9, 2015 ICD Therapy in Brugada Syndrome MARCH 10, 2015: ABBREVIATIONS AND ACRONYMS risk for recurrent arrhythmic events during follow-up, are the best candidates to undergo ICD therapy (3,4). However, although appropriate AF = atrial fibrillation BS = Brugada syndrome CI = confidence interval ECG = electrocardiographic EPS = electrophysiologic study HR = hazard ratio ICD = implantable cardioverter-defibrillator SCD = sudden cardiac death SND = sinus node dysfunction VA = ventricular arrhythmia VF = ventricular fibrillation VT = ventricular tachycardia ICD therapies are more prevalent in symptomatic patients, they are not insignificant in asymptomatic ones (5). Todate,risk assessment of patients with asymptomatic BS has not been well established, and devicebased management in this setting remains controversial. Data on long-term follow-up (>6 years)of patients with BS with ICDs are sparse. In our previous study, 15% of 47 patients who underwent primary prophylactic ICD therapy experienced appropriate interventions during a 4-year follow-up period (6). But ICD implantation was not without problems, including high rates of inappropriate shocks and device-related complications. SEE PAGE 889 The purpose of this study was to analyze our single-center experience with ICD therapy in patients with BS over the past 20 years, since the first description of the syndrome. Particularly, we aimed to assess the clinical features and the long-term follow-up of patients with BS who underwent ICD placement and the evolution of device-based management over the past 2 decades. METHODS STUDY POPULATION. Since 1992, all consecutive patients diagnosed with BS have been included in a registry and followed in a prospective fashion. The ethics committee of UZ Brussel-VUB approved the study protocol. A total of 524 patients with BS were included in the registry from 1992 to Among them, 181 patients (34.5%) received ICD therapy. Study inclusion criteria consisted of 1) spontaneous or drug-induced Brugada type 1 electrocardiographic (ECG) pattern, (2) ICD implantation, and (3) continuous follow-up at our institution. One-hundred seventy-six patients (97.2%) fulfilled the inclusion criteria. Five patients (2.8%) were not included because of a follow-up time of <6 months.medical history, physical examination, and baseline electrocardiography were performed, and underlying structural cardiac abnormalities were excluded in all patients. All patients with syncope before receiving ICDs underwent careful diagnostic work-up for arrhythmic origins of the events. The work-up included a careful examination of the patient s history, 12-lead electrocardiography, transthoracic echocardiography, and Holter monitoring. Electrophysiologic study (EPS) was performed in patients with syncope potentially related to supraventricular arrhythmias. Arrhythmic syncope was suspected in the absence of prodromes and specific triggering circumstances and in the presence of brief loss of consciousness and rapid return to consciousness or severe trauma. A tilt-table test was performed in patients with suspected vasovagal syncope. ECG patterns were classified as Brugada coved type (type 1) or saddleback (type 2) or normal. An electrocardiogram was considered diagnostic of BS if a coved-type STsegment elevation of $2 mmwasdocumentedin$1 lead from V 1 to V 3 in the presence or absence of a sodium-channelblocker.abnormalfragmentationof the QRS complex was defined as the presence of multiple spikes within the QRS complex ($4 spikesin 1leador$8 spikes in leads V 1,V 2,andV 3 ) (7). All baseline and drug-induced 12-lead electrocardiograms were recorded at a paper speed of 25 mm/s and amplitude of 10 mm/mv, with the right precordial leads positioned at the sternal margin of the third and fourth intercostal space. Two independent experienced electrophysiologists analyzed all electrocardiograms;incasesofdisagreement,athirdphysician wasconsulted.patientswereconsideredsymptomatic if they presented with syncope and/or aborted SCD. EPS was performed at the investigators preference to assess risk stratification. Programmed ventricular stimulation consisted of a maximum of 3 ventricular extrastimuli with a minimal coupling interval of 200 ms delivered from 1 ventricular site unless ventricular fibrillation (VF) or sustained ventricular tachycardia (VT) lasting at least 30 s, accompanied with syncope or requiring intervention for termination was induced. Genetic testing with sequence analysis of SCN5A was recommendedforallpatientswithdiagnosesofbs. AJMALINE CHALLENGE. Ajmaline (1 mg/kg) was administered intravenously over a 5-min period to unmask the diagnostic ECG pattern of BS in case of a nondiagnostic baseline electrocardiogram. The test was considered positive for BS only if coved-type ECG pattern was documented in $1 right precordial lead (V 1 to V 3 ). Ajmaline infusion was discontinued before reaching the target dose if QRS prolongation exceeded 30% compared with the baseline interval, when frequent premature ventricular beats or Brugada type 1 ECG pattern occurred or in case of development of high-degree atrioventricular block. Ajmaline-induced VAs were defined as the occurrence of sustained episodes of VF or VT. ICD IMPLANTATION. Beginning in 2005, the indications for ICD therapy were determined using the
3 JACC VOL. 65, NO. 9, 2015 MARCH 10, 2015: Conte et al. ICD Therapy in Brugada Syndrome 881 recommendations of the second Brugada consensus conference (4). The decision to perform epicardial or endocardial lead implantation or to place the device in a thoracic or subcostal pocket was made according to the patient s age, anthropometric characteristics, and level of physical activity. The choice between single- and dual-chamber devices was driven by the presence of previous episodes of supraventricular arrhythmias or evidence of sinus node dysfunction (SND). ICD programming at thetimeofimplantation changed over time. After our initial experience, the VF detection rate was increased from 180 to more than 200 beats/min for primary prevention implantations, and a monitor zone was added (6,8). In accordance with more recently published data, apart from setting a high cutoff rate, long detection intervals (30 of 40 intervals) were adopted to avoid unnecessary therapies (9 11). Conversely, in patients undergoing ICD therapy for secondary prevention, a monitor zone (>150 beats/min) and a fast VT zone (180 to 200 beats/min) with antitachycardia pacing and shocks were programmed in all cases, and supraventricular tachycardia discriminators were activated if available. These settings were adjusted during follow-up on the basis of individual clinical history and to avoid recurrences of inappropriate interventions. FOLLOW-UP. Clinical follow-up of patients consisted of physical examinations and electrocardiography at least every 6 months. Follow-up of the device was performed at 1 and 3 months after implantation and thereafter every 6 months. Clinical data were regularly collected. From 2006, home monitoring devices were implanted either de novo or at battery change, in case of prior implantation, in all patients younger than 12 years and in 30% of older patients. Arrhythmic events receiving ICD therapies were pre-defined according to the cycle lengths of the arrhythmias. All available electrograms of appropriate and inappropriate shocks were analyzed by at least 2 investigators independently. Electrograms were derived from various bipolar configurations involving the tip and ring electrodes or shocking coils on the pacing or defibrillating lead or a wide bipolar recording between one of the ventricular electrodes and the ICD casing. For primary prevention implantations, the VF detection rate was usually higher than 180 to 200 beats/min (according to the year of implantation). For these patients, an attempt to discriminaterapidpolymorphicvtandvfwasmade when possible on the basis of the electrographic configuration derived from multiple ICD channels. Monomorphic VTs were defined as arrhythmias with constant electrographic configuration and a stable rate within a few beats. Polymorphic VTs had a changing rate and demonstrated varying configurations and rate between 180 and 200 beats/min. Conversely, an arrhythmia was characterized as VF if the cycle length was irregular and had a rate higher than 200 beats/min and/or occurred in the presence of electrograms of continuously varying configuration. Appropriate therapies were defined as shocks or antitachycardia pacing delivered for VT or VF, and inappropriate therapies were defined as those delivered in the absence of VAs. Electrical storm was defined by 3 or more sustained episodes of VT, VF, or appropriate ICD shocks within 24 h. STATISTICAL ANALYSIS. Data are presented as mean SD or as absolute values and percents as appropriate. Comparisons between continuous variables were performed using the unpaired Student t test or analysis of variance as appropriate. The chisquare test was used to compare categorical variables. Event-free survival was estimated by the Kaplan-Meier method and compared by the log-rank test. Hazard ratios (HRs) were calculated using Cox proportional hazards regression models. Cox regression analysis was used for the predictor model. Variables were selected on the basis of univariate significance and/or if they were known predictors in published research. The final model was selected by stepwise regression on the basis of likelihood ratios. A pvalueof<0.05 was considered to indicate statistical significance. Statistical analyses were conducted using SPSS version 22 (SPSS, Inc., Chicago, Illinois). RESULTS BASELINE CHARACTERISTICS. A total of 176 consecutive patients (118 male [67%]; mean age years; range: 2 to 77 years) received ICDs at our institution from 1992 to 2012 and met the inclusion criteria for this study. Baseline clinical and procedural characteristics of the study population are shown in Table 1. Patients belonged to 92 different families. At the time of implantation, 19 patients (10.8%) were younger than 18 years. Family histories of SCD were present in 90 patients (51%). Twenty-five subjects (14.2%) presented with aborted SCD before ICD placement. One-hundred five patients (59.7%) had at least 1 episode of syncope, and 46 (25.1%) were completely asymptomatic before receiving ICDs. Twenty-four patients (13.6%) had documented episodes of sustained atrial arrhythmias (atrial fibrillation [AF] or atrial flutter). Moreover, 9 patients (5.1%) presented with SND. Spontaneous Brugada type 1 ECG pattern was documented in 37 patients (21%).
4 882 Conte et al. JACC VOL. 65, NO. 9, 2015 ICD Therapy in Brugada Syndrome MARCH 10, 2015: TABLE 1 Baseline Clinical and Procedural Characteristics of the Study Population According to Year of Implantation Overall (n ¼ 176) Group I (n ¼ 82) Group II (n ¼ 94) p Value Age, yrs Male 118 (67.0) 62 (75.6) 56 (59.6) 0.02 Spontaneous type 1 ECG pattern 37 (21.0) 28 (34.1) 9 (9.6) <0.01 Aborted SCD 25 (14.2) 15 (18.3) 10 (10.6) 0.15 Syncope 105 (59.7) 39 (47.6) 66 (70.2) <0.01 Asymptomatic 46 (26.1) 28 (34.1) 18 (19.1) 0.01 Family history of SCD 90 (51.1) 47 (57.3) 43 (45.7) 0.13 Previous atrial arrhythmias 24 (13.6) 14 (17.1) 10 (10.6) 0.22 Previous SND 9 (5.1) 6 (7.3) 3 (3.2) 0.31 Inducible on EPS* 72 (43.6) 58 (75.3) 14 (15.9) <0.01 SCN5A mutation* 23 (21.9) 13 (21.7) 10 (22.2) 0.95 Abdominal implantation 19 (10.8) 6 (7.3) 13 (13.8) 0.19 Epicardial lead placement 8 (4.5) 3 (3.7) 5 (5.3) 0.73 Values are mean SD or n (%). Group I included patients who underwent ICD placement before 2005, and group II included patients who underwent ICD placement during or after *Percents refer to patients who underwent EPS and genetic testing. ECG ¼ electrocardiographic; EPS ¼ electrophysiologic study; ICD ¼ implantable cardioverter-defibrillator; SCD ¼ sudden cardiac death; SND ¼ sinus node dysfunction. The diagnosis was induced by ajmaline challenge in the remaining 139 patients (79%). Among them, 9 patients (6.5%) experienced drug-induced sustained VAs. EPS was performed in 165 patients (93.7%). Sustained VAs were induced during programmed ventricular stimulation in 72 patients (43.6%). A total of 105 genetic tests (59.7%) were performed; 23 of them (21.9%) were positive for mutations in the SCN5A gene. The clinical profile of the patients who received ICDs during the 20-year study period changed over time (Table 1). In particular, the rate of asymptomatic patients significantly decreased after 2005 (from 34.1% before 2005 to 19.1% during or after 2005; p ¼ 0.01). Similarly, there was a significant reduction in the number of patients with inducible arrhythmias during EPS (from 75.3% before 2005 to 15.9% during or after 2005; p < 0.01). Conversely, the rate of patients with syncope increased (from 47.6% before 2005 to 70.2% during or after 2005; p < 0.01). No significant temporal difference was found in the number of patients presenting with aborted SCD or in those with family histories of SCD in whom ICDs were placed before or after Moreover, the number of patients with spontaneous Brugada type 1 ECG pattern undergoing ICD placement decreased over time (from 34.1% before 2005 vs. 9.6% during or after 2005; p < 0.01). SYMPTOM STATUS. A total of 130 patients (73.8%) presented with syncope and/or aborted SCD before ICD implantation. The remaining 46 patients were asymptomatic. Clinical characteristics of patients according to their symptom status are shown in Table 2. No significant difference was found in the clinical features among patients presenting with syncope and aborted SCD and asymptomatic patients. Aborted SCD. Twenty-five patients (14.2%) presented with previous episodes of aborted SCD due to spontaneous sustained VAs. Sixteen (64%) were male, and 10 (40%) had family histories of SCD. Spontaneous Brugada type 1 ECG pattern was documented in 7 patients (28%). The mean age at the time of SCD was years, ranging from 6 days to 61 years. One infant and 1 child experienced multiple episodes of aborted SCD before reaching 2 years of age. Aborted SCD was the first clinical manifestation of the syndrome in 20 patients (11.3%). SCD was preceded by episodes of syncope and by palpitations in 4 patients and 1 patient, respectively. Sudden death occurred at rest in 16 patients, during exercise in 5, during sleep in 3, and during a febrile episode in 1. Syncope. Syncope was the clinical manifestation of the syndrome in 105 patients (59.7%). Sixty-six (62.8%) were male, and 53 (50.4%) had family histories of SCD. Forty-eight patients (45.7%) were family members of patients with BS. Spontaneous Brugada type 1 ECG pattern was documented in 19 patients (18.1%). The mean age at the time of first syncope was years. The mean number of episodes of syncope per patient was Syncope occurred at rest in 72 patients (68.6%) and during exercise in 27 subjects (25.7%). Syncope was associated exclusively with fever in 6 patients (5.7%). Asymptomatic patients. Forty-six patients (26.1%) did not report any symptoms before receiving ICDs. Twenty-seven (58.7%) were family members of BS patients. Indications for ICD therapy in these patients were: 1) the presence of spontaneous Brugada type 1 ECG pattern and family history of SCD in 2 patients (4.3%); 2) spontaneous Brugada type 1 ECG pattern and sustained VA induced during EPS in 9 patients (19.6%); and 3) sustained VA during ajmaline challenge in 5 patients (10.9%). The remaining 30 patients (65.2%) received ICDs because of ajmaline-induced Brugada type 1 ECG pattern with sustained VA induced during EPS (n ¼ 17) or family histories of SCD (n ¼ 13). PROCEDURAL CHARACTERISTICS. One-hundred nine patients (62%) received single-chamber transvenous devices, and 59 (33.5%) underwent dual-chamber transvenous ICD implantation. Single and dual epicardial leads were implanted in 6 and 2 patients (4.5%), respectively. No patient received a totally subcutaneous system. Nineteen subjects (10.8%)
5 JACC VOL. 65, NO. 9, 2015 MARCH 10, 2015: Conte et al. ICD Therapy in Brugada Syndrome 883 underwent abdominal pulse generator placement. Mean R-wave amplitude at implantation was mv. After ICD implantation, 4 patients (2.3%) experienced device-related early complications: 2 pneumothoraxes, 1 episode of pericarditis that occurred 1 month after epicardial lead placement, and a dislocation of the abdominal generator that led to the revision of the device 1 week after implantation. LONG-TERM FOLLOW-UP. After a mean follow-up period of months, spontaneous sustained VAs were documented in 30 patients (17%). Sustained VA was terminated by ICD shocks in 28 patients (15.9%) and by antitachycardia pacing in 2 patients (1.1%). Thirty-three patients (18.7%) experienced inappropriate shocks. Electrical storm occurred in 4 subjects (2.3%). Nonsustained VAs were documented in 10 patients (5.7%). Of note, 30 patients (21.6%) with drug-induced BS presented with spontaneous Brugada type 1 ECG pattern during follow-up. Spontaneous Brugada type 1 ECG pattern could be documented on at least 1 occasion during the followup period in 67 patients (38.1%). After ICD placement, 21 patients (11.9%) experienced episodes of syncope. Of them, 5 patients had neurally mediated syncope. In 8 patients with recurrent syncope after ICD implantation, the rate of ventricular pacing was <1%, and no VAs were detected. Among initially asymptomatic patients, 3 (6.5%) experienced syncope during follow-up. Thirty-two patients (18.2%) developed paroxysmal AF: 6 in the asymptomatic group, 21 (20%) in the syncope group, and 5 (20%) in the aborted SCD group (p ¼ 0.58). Six patients (3.4%) with ICDs and drug-resistant AF underwent pulmonary vein isolation by means of radiofrequency energy source (n ¼ 5) or cryoballoon ablation (1 patient). At last follow-up, a total of 19 patients (10.8%) with documented atrial arrhythmias were under pharmacological treatment with sotalol or beta-blockers. Fifty-two patients (29.5%) underwent generator replacement. The mean number of battery changes during the follow-up was per patient. MORTALITY. Eight patients (4.5%) died during follow-up. The mean age at death was years. The mean time from BS diagnosis to death was years. Cardiac death occurred in 3 patients. One subject died in the hospital because of cardiogenic shock complicating an acute anterolateral wall myocardial infarction that presented with persistent ST-segment elevation. Another patient experienced septic shock with fatal consequences shortly after device revision. A third patient died as consequence of an arrhythmic event (Central Illustration). He was the first patient ever diagnosed TABLE 2 Clinical Characteristics and Outcomes of Patients According to ICD Indication Overall (n ¼ 176) Aborted SCD (n ¼ 25) Syncope (n ¼ 105) with BS. He had presented at 3 years of age with syncope and recurrent aborted SCDs and had concomitant SND and AF and atrial flutter. He first received a pacemaker and pharmacologic therapy with amiodarone, beta-blockers, digoxin, and diphenylhydantoin but had 2 further episodes of syncope. Subsequently, he was asymptomatic for 13 years, at which point the family agreed to undergo ICD implantation. After the implantation, antiarrhythmic therapy was discontinued. The patient died suddenly 11 months after ICD implantation, at 18 years of age, becauseofvfrefractorytobothinternalandexternal defibrillations. In the remaining 5 cases, death was due to noncardiac causes. None of the asymptomatic patients died. APPROPRIATE SHOCKS. Twenty-eight patients (15.9%) experienced at least 1 appropriate shock during the follow-up period (Central Illustration). Twenty-four (85.7%) were male, and 22 (78.6%) were symptomatic. Six patients (21.4%) had neither aborted SCD nor previous syncope. Of note, appropriate shocks occurred in 13% of asymptomatic patients. However, therateofappropriateshockswassignificantly higher in patients presenting with aborted SCD compared with the other patients (p < 0.01) (Table 2). Sixteen of these patients (53.6%) presented with spontaneous Asymptomatic (n ¼ 46) p Value Clinical features Age, yrs Male 118 (67.0) 16 (64.0) 66 (62.9) 36 (78.3) 0.17 Proband 92 (52.3) 16 (64.0) 57 (54.3) 19 (41.3) 0.15 Spontaneous type 1 ECG 37 (21.0) 7 (28.0) 19 (18.1) 11 (23.9) 0.47 pattern Family history of SCD 90 (51.1) 10 (40.0) 53 (50.5) 27 (58.7) 0.32 Previous atrial 24 (13.6) 3 (12.0) 14 (13.3) 7 (15.2) 0.92 arrhythmias Previous SND 9 (5.1) 1 (4.0) 5 (4.8) 3 (6.5) 0.87 Inducible on EPS* 72 (43.6) 5 (26.3) 39 (37.9) 28 (65.1) <0.01 SCN5A mutations* 23 (21.9) 6 (26.1) 9 (15.8) 8 (32) 0.23 Outcomes Appropriate shocks 28 (15.9) 11 (44.0) 11 (10.5) 6 (13.0) <0.01 Time to first therapy, months Shock rate per year Inappropriate shocks 33 (18.8) 8 (32.0) 18 (17.1) 7 (15.2) 0.54 Time to first therapy (months) Shock rate per year Deaths 8 (4.5) 3 (12.0) 5 (4.8) 0 (0) 0.10 Values are mean SD or n (%). *Percents refer to patients who underwent EPS and genetic testing. Abbreviations as in Table 1.
6 884 Conte et al. JACC VOL. 65, NO. 9, 2015 ICD Therapy in Brugada Syndrome MARCH 10, 2015: CENTRAL ILLUSTRATION ICD Therapy in Brugada Syndrome 5 (17.9%) received 3 or more shocks. Twenty-two patients received ICD shocks for VF and 3 for polymorphic VT. ICD therapy was delivered for monomorphic VT in the remaining 3 patients. All VF and VT episodes had ventricular rates higher than 200 and 180 beats/min, respectively. On univariate analysis, male sex (HR: 2.95; 95% confidence interval [CI]: 1.02 to 8.53; p ¼ 0.04), spontaneous Brugada type 1 ECG pattern (HR: 2.50; 95% CI: 1.16 to 5.39; p ¼ 0.02), aborted SCD (HR: 4.53; 95% CI: 1.57 to 13.0; p < 0.01), and VA inducibility on EPS (HR: 2.44; 95% CI: 1.18 to 6.02; p ¼ 0.04) were shown to confer a higher risk for experiencing an appropriate shock during follow-up. Implantation after 2005 was shown to be a protective factor (HR: 0.31; 95% CI: 0.12 to 0.77; p ¼ 0.01) (Table 3). Aborted SCD (HR: 5.13; 95% CI: 2.03 to 12.96; p < 0.01) and VA inducibility on EPS (HR: 3.38; 95% CI: 1.33 to 8.59; p ¼ 0.01) remained the only significant predictors of appropriate shocks on multivariate analysis. Kaplan-Meier curve analyzing freedom from appropriate shocks according to implantable cardioverter-defibrillator (ICD) indication. SD ¼ sudden cardiac death. Brugada type 1 ECG pattern. The median time to first therapy was 11.6 months (interquartile range: 5.3 to 33.0 months). The mean number of shocks delivered per patient was Seventeen patients (60.7%) had 1 shock, 6 (21.4%) experienced 2 shocks, and TABLE 3 Univariate Cox Regression Analysis Among Patients Experiencing Appropriate Shocks b Coefficient HR (95% CI) p Value Age ( ) 0.12 Male ( ) 0.04 Proband ( ) 0.38 Spontaneous type 1 ECG pattern ( ) 0.02 Symptoms ( ) <0.01 Syncope ( ) 0.89 Aborted SCD ( ) <0.01 Family history of SCD ( ) 0.29 Previous AF ( ) 0.61 Previous SND ( ) 0.44 EPS inducibility ( ) 0.04 SCN5A mutation ( ) 0.74 Implantation during or after ( ) 0.01 The HR for age considers every year increase. AF ¼ atrial fibrillation; CI ¼ confidence interval; HR ¼ hazard ratio; other abbreviations as in Table 1. ELECTRICAL STORM. Four patients (2.3%) presented with electrical storm during the follow-up period (Table 4, Figure 1).Threeweremale(75%).Themean age at the time of electrical storm was years. Electrical storm occurred years after ICD implantation. Aborted SCD was the indication for ICD therapy in all patients. Two patients had experienced episodes of appropriate shocks 3 and 5 years before the occurrence of electrical storm. After the electrical storm, 2 patients were treated with quinidine with no further arrhythmic recurrences, and 1 patient underwent VF ablation with no subsequent episodes of electrical storm. The remaining patient who experienced another episode of electrical storm underwent heart transplantation. INAPPROPRIATE SHOCKS. Thirty-three patients (18.7%) had inappropriate shocks a median of 36.9 months (interquartile range: 9.4 to 75.4 months) after ICD implantation. The mean number of inappropriate shocks delivered per patient was Eighteen patients (54%) experienced 1 shock, and 15 had 2 or more episodes of inappropriate shocks (46%). Inappropriate shocks were due to sinus tachycardia in 5 patients, noise on the ventricular channel after lead fracture in 7 patients, and T-wave oversensing in 6 patients. The remaining 15 subjects experienced inappropriate shocks because of episodes of AF with fast ventricular rate. Among these patients, 3 underwent pulmonary vein isolation because of drugresistant paroxysmal AF. At follow-up, the remaining 12 patients were under pharmacological treatment with sotalol (n ¼ 10) or beta-blockers and sotalol (n ¼ 2). Conversely, none of the patients who
7 JACC VOL. 65, NO. 9, 2015 MARCH 10, 2015: Conte et al. ICD Therapy in Brugada Syndrome 885 experienced inappropriate shocks because of sinus tachycardia were treated pharmacologically. Of note, the incidence of inappropriate shocks did not differ depending on patients previous symptom status (Table 2). DEVICE-RELATED COMPLICATIONS. During followup, 28 patients (15.9%) experienced device-related complications. Twenty-one (75%) were younger than 40 years at the time of implantation. Complications consisted of fracture of the ventricular electrode and subsequent extraction and replacement in 14 patients, lead dislocation in 7 patients, and pulse generator migration in 2 patients, leading to revision of the device in all patients. The other 5 patients had device infections, which led to replacement of the devices. TABLE 4 DISCUSSION Clinical Characteristics of Patients Experiencing Electrical Storm Patient # Sex Age (yrs) Proband Family History of SCD Spontaneous Type 1 ECG Pattern ICD Indication f-qrs 1 Male 34 No Yes Yes Aborted SCD No 2 Male 24 No Yes Yes Aborted SCD No 3 Male 53 Yes No No Aborted SCD Yes 4 Female 41 No No No Aborted SCD No f-qrs ¼ fragmentation of QRS complex; other abbreviations as in Table 1. CLINICAL PROFILE OF PATIENTS WITH BS WHO RECEIVE ICDs. Patients presenting with either symptomatic or asymptomatic BS are usually in their FIGURE 1 Baseline Electrocardiograms of Patients With Electrical Storm Fragmentation of the terminal portion of the QRS complex can be appreciated in all leads of the baseline electrocardiogram of Patient #3. *Electrocardiogram after ajmaline challenge. Pt ¼ patient.
8 886 Conte et al. JACC VOL. 65, NO. 9, 2015 ICD Therapy in Brugada Syndrome MARCH 10, 2015: fourth or fifth decade of life (3), andinourstudy,patients with BS receiving ICDs presented with a mean age of 40 years. Most were male, and 74% were symptomatic, presenting with aborted SCD or syncope before ICD placement. Interestingly, the clinical profile of patients undergoing ICD therapy changed during the 20-year study period, particularly after the second Brugada consensus conference recommendations (4). The rate of asymptomatic patients significantly decreased after 2005 (from 34.1% to 19.1%), and there was a significant reduction in the number of patients with inducible arrhythmias during EPS (from 75.3% to 15.9%). Conversely, the rate of patients with syncope increased (from 47.6% to 70.2%). No significant temporal difference was found in the number of patients presenting with aborted SCD or in those with family histories of SCD. Although it has a psychological impact for patients and their families, family history of SCD has not been shown to be predictive of future arrhythmic events in patients with BS, and it does not appear to be of prognostic value in patients with ICDs (12). Thus, asymptomatic patients with family histories of SCD do not have an indication for ICD placement on that basis alone. Clinical followup with electrocardiography should be performed every 6 months in these patients, and EPS should be considered for risk stratification purposes. Of note, therateofpatientswithspontaneousbrugadatype1 ECG pattern undergoing ICD placement decreased over time (from 34.1% to 9.6%). This could be explained by a more proactive attitude developed after 2005 in the diagnosis of the syndrome in patients with syncope and in asymptomatic family members. APPROPRIATE SHOCKS. An important finding of the present study concerns the considerable risk for SCD during long-term follow-up, affecting patients with BS with ICDs for primary or secondary prevention. In our study, 17% of patients experienced documented life-threatening arrhythmias during a mean follow-up period of 7 years. Moreover, 1 patient died because of an arrhythmic event. The rate of appropriate shocks was 16%. The discharge rate was comparable to the rate reported in our previous follow-up study (14.9%) conducted in patients undergoing ICD implantation for prophylactic purposes only (6). This previous study was not able to identify any independent predictors of future arrhythmic events, possibly because of the relatively low event rate in a small patient population. In the present study, including a larger number of patients, aborted SCD (HR: 5.13) and VA inducibility on EPS (HR: 3.38) were found to be the only independent predictors of appropriate shocks in multivariate analysis. Moreover, in univariate analysis, apart from aborted SCD and VA inducibility on EPS, male sex and spontaneous Brugada type 1 ECG pattern were shown to confer a higher risk for experiencing an appropriate shock during follow-up. Although the device-based therapeutic management of BS in asymptomatic patients is challenging, the decision to implant an ICD after an episode of aborted SCD is straightforward. In our study, the appropriate device therapy rate at 7 years was 44% in patients in whom the ICD therapy indication was aborted SCD. Previously, Sacher et al. (5) reported a similar rate of appropriate shocks after ICD therapy for secondary prevention. Although low, the rate of sustained VA in asymptomatic patients with ICD has been reported as 0.81% per year (5). Ofnote,inourstudy,itwasnotas low as previously thought, affecting 13% of previously asymptomatic patients. In patients without histories of VT or VF, the identification of potential predictors of arrhythmic events during follow-up has been assessed in different studies, with controversial results, and the role of EPS has been considered questionable. Data from the PRELUDE (Programmed Electrical Stimulation Predictive Value) study identified the presence of spontaneous Brugada type 1 ECG pattern and history of syncope as the only significant predictors of arrhythmias (13). Conversely, the presence of VT or VF inducibility on EPS failed to identify patients at risk for developing arrhythmic events during follow-up (13). In our study, VA inducibility during EPS appeared to confer a significantly higher risk for experiencing appropriate shocks during follow-up. Therefore, risk assessment on the basis of clinicalfeatures,suchasmalesex,baselineelectrocardiography, or the results of EPS, should be always taken into account when considering ICD therapy. Moreover, EPS might be valuable in the clinical evaluation of patients with syncope to rule out the presence of SND or supraventricular arrhythmias as potential causes of the event. Interestingly, in the present study, syncope was not found to be an independent predictor of future VAs, and freedom over time from appropriate shocks did not differ between asymptomatic patients and those with syncope (Figure 1). Despite performing a proper diagnostic work-up, in some cases, it remains difficult to determine whether syncope is truly due to VA. All large registries of patients with BS and syncope report that 6% to 19% of patients experience arrhythmic events during follow-up of 24 to 39 months (5,6,8). In our study, 11% of patients with syncope received appropriate shocks. Currently, ICD therapy is considered in order to prevent SCD in patients presenting with episodes of syncope if no
9 JACC VOL. 65, NO. 9, 2015 MARCH 10, 2015: Conte et al. ICD Therapy in Brugada Syndrome 887 other cause of syncope is found (4). The decision to perform ICD implantation in this setting must be taken after a careful evaluation of the episode, as in this category of patients, it is not always easy to differentiate its origin. In our study, 8% of patients with syncope experienced further episodes of syncope during follow-up, but no VA was detected by the device. Moreover, 18% of patients developed paroxysmal AF. It has been shown that approximately 20% of patients with BS can develop supraventricular arrhythmias that can be a potential cause of syncope (14). Similarly, a prolonged sinus node recovery time and sinoatrial conduction time as well as slowed atrial conduction and atrial standstill have been reported in association with the syndrome and can lead to syncope (15). Thus, in any case of syncope suspected to be attributable to arrhythmic causes other than VAs, an EPS should be always performed to clarify the diagnosis before ICD implantation. Interestingly, 2% of our study population presented with electrical storm during follow-up, requiring drug therapy initiation, ablation, or cardiac transplantation. Electrical storm occurrence is always a tragic event, even more so when the patient is young. Pharmacologic therapy aimed at rebalancing the currents active during the early phases of the epicardial right ventricular action potentials can be useful to abort electrical storms. In particular, drugs such as quinidine inhibit the transient outward current, acting to diminish the action potential notch and thus suppress the substrate and trigger for VAs (16). ADVERSE EFFECTS OF ICD THERAPY. Inappropriate shocksareamongthemostimportantadverseeffects of ICD therapy. In our study, 18.7% of patients experienced inappropriate shocks due to supraventricular arrhythmias, lead fracture, and T-wave oversensing. The frequency of inappropriate shocks in our study is consistent with the data previously reported by other groups. Steven et al. (17) reported a 15% rate of inappropriate shocks in series of 33 patients at 8-year follow-up. Similarly, Sacher et al. (5) reported inappropriate shocks in 24% of patients during 6-year follow-up. On the basis of the results of our previous study (6), in 2006 we started to program a single VF zone with a lower detection rate (>200 beats/min) in patients younger than 50 years and to adjust these settings on the basis of the individual clinical history. However, in this study, no significant temporal difference was found in terms of the rate of inappropriate shocks between patients implanted before or after 2005 (implantation after 2005: HR: 1.1; 95% CI: 0.43 to 2.78; p ¼ 0.83). Young age, an active profile, and the predisposition of these patients to atrial arrhythmias likely increase the risk for inappropriate shocks. Moreover, the incidence of atrial arrhythmias has been reported to be higher in patients with ICDs (27%) compared with those without indications for ICD (13%), suggesting a more advanced disease process in patients with spontaneous atrial arrhythmias (18). Apartfromsettinghigh rate cutoffs, a strategy to reduce unnecessary therapies might be the insertion of a high VT zone with supraventricular tachycardia discriminators and a prolongeddelayintherapydeliverybyincreasingthe number of intervals to detect (11,19,20). Patients with BS with ICDs have already been demonstrated to be more difficult to manage, not only because of the high incidence of inappropriate therapies but also because of their long life expectancy compared with the conventional ICD patient population, in which lead failure rates have been reported to range from 15% to 40% after 5 and 8 years, respectively (21). In this study, the rate of devicerelated complications was 16% at 7-year follow-up, and 75% of patients were younger than 40 years. It is well established that ICD placement in patients with BS is not without potential problems (5,6). Of note, in a previous study from our group, complications affected up to 33% of children with ICDs (22). In this particularly active category of patients, lead fracture can more frequently occur. Moreover, their long life expectancy leads to multiple generator change procedures, with a potential increased rate of device-related complications. Finally, lead-related problems can give rise to inappropriate therapies, with a significant impact on the quality of life of patients and relatives. STUDY LIMITATIONS. Our study was a single-center experience conducted in a population of patients with heterogeneous clinical characteristics. The nature of this analysis, conducted on ICD implantations performed over 20 years, was retrospective. Thus, the ICD programming evolution over this period of time and the lack of consistent or pre-specified settings might be limitations of the study. EPS with programmed ventricular stimulation and genetic testing were not performed in all patients. Furthermore, in patients with lifelong risk for arrhythmias, a mean follow-up period of 7 years might be too short. CONCLUSIONS ICDtherapywasaneffectivestrategyinpatientswith BS, treating potentially lethal arrhythmias in 17% of patients during long-term follow-up. Appropriate shocks were significantly associated with the
10 888 Conte et al. JACC VOL. 65, NO. 9, 2015 ICD Therapy in Brugada Syndrome MARCH 10, 2015: presence of aborted SCD, but they also occurred in 13% of asymptomatic patients. On the basis of our findings, risk stratification by means of EPS might identify asymptomatic patients at risk for arrhythmic events and could be helpful in investigating syncope potentially not related to VA. ICD placement is frequently associated with device-related complications, affecting 16% of patients. Moreover, inappropriate shock rates remain high regardless of careful device programming. REPRINT REQUSTS AND CORRESPONDENCE: Dr. Giulio Conte, Heart Rhythm Management Centre, UZ Brussel-VUB, Laarbeeklaan 101, 1090 Brussels, Belgium. PERSPECTIVES COMPETENCY IN INTERPERSONAL AND COMMUNICATION SKILLS: Before the implantation of ICDs, physicians should explain to patients with BS the potential benefits and risks of devicerelated complications. TRANSLATIONAL OUTLOOK: Longer term followup studies are needed to better identify patients with BS prone to developing life-threatening arrhythmias and to clarify the value of diagnostic electrophysiologic testing. REFERENCES 1. Brugada P, Brugada J. Right bundle branch block, persistent ST segment elevation and sudden cardiac death: a distinct clinical and electrocardiographic syndrome. A multicenter report. J Am Coll Cardiol 1992;20: Brugada J, Brugada R, Brugada P. Pharmacological and device approach to therapy of inherited cardiac diseases associated with cardiac arrhythmias and sudden death. J Electrocardiol 2000;33 Suppl: Priori SG, Napolitano C, Gasparini M, et al. Natural history of Brugada syndrome: insights for risk stratification and management. Circulation 2002;105: Antzelevitch C, Brugada P, Borggrefe M, et al. Brugada syndrome: report of the second consensus conference: endorsed by the Heart Rhythm Society and the European Heart Rhythm Association. Circulation 2005;111: Sacher F, Probst V, Maury P, et al. Outcome after implantation of a cardioverter-defibrillator in patients with Brugada syndrome: a multicenter study-part 2. Circulation 2013;128: Sarkozy A, Boussy T, Kourgiannides G, et al. Long-term follow-up of primary prophylactic implantable cardioverter-defibrillator therapy in Brugada syndrome. Eur Heart J 2007;28: Morita H, Kusano KF, Miura D, et al. Fragmented QRS as a marker of conduction abnormality and a predictor of prognosis of Brugada syndrome. Circulation 2008;118: Sarkozy A, Brugada P, Mont L, Brugada J. Optimizing the clinical use of implantable defibrillators in patients with Brugada syndrome. Eur Heart J 2007;9 Suppl I:I Wilkoff BL, Williamson BD, Stern RS, et al. Strategic programming of detection and therapy parameters in implantablecardioverter-defibrillators reduces shocks in primary prevention patients: results from the PREPARE (Primary Prevention Parameters Evaluation) study. J Am Coll Cardiol 2008;52: Gasparini M, Menozzi C, Proclemer A, et al. A simplified biventricular defibrillator with fixed long detection intervals reduces implantable cardioverter defibrillator (ICD) interventions and heart failure hospitalizations in patients with non-ischaemic cardiomyopathy implanted for primary prevention: the RELEVANT [Role of Long Detection Window Programming in Patients With Left Ventricular Dysfunction, Non-Ischemic Etiology in Primary Prevention Treated With a Biventricular ICD] study. Eur Heart J 2009;30: Moss AJ, Schuger C, Beck CA, et al. Reduction in inappropriate therapy and mortality through ICD programming. N Engl J Med 2012;367: Sarkozy A, Sorgente A, Boussy T, et al. The value of a family history of sudden death in patients with diagnostic type I Brugada ECG pattern. Eur Heart J 2011;32: Priori SG, Gasparini M, Napolitano C, et al. Risk stratification in Brugada syndrome: results of the PRELUDE (Programmed Electrical Stimulation Predictive Value) registry. J Am Coll Cardiol 2012; 59: Morita H, Kusano-Fukushima K, Nagase S, et al. Atrial fibrillation and atrial vulnerability in patients with Brugada syndrome. J Am Coll Cardiol 2002;40: Morita H, Fukushima-Kusano K, Nagase S, et al. Sinus node function in patients with Brugada-type ECG. Circ J 2004;68: Hermida JS, Denjoy I, Clerc J, et al. Hydroquinidine therapy in Brugada syndrome. J Am Coll Cardiol 2004;43: Steven D, Roberts-Thomson KC, Inada K, et al. Long-term follow-up in patients with presumptive Brugada syndrome treated with implanted defibrillators. J Cardiovasc Electrophysiol 2011;22: Bordachar P, Reuter S, Garrigue S, Caï X, et al. Incidence, clinical implications and prognosis of atrial arrhythmias in Brugada syndrome. Eur Heart J 2004;25: Gasparini M, Proclemer A, Klersy C. Effect of long-detection interval vs standard-detection interval for implantable cardioverter-defibrillators on antitachycardia pacing and shock delivery: the ADVANCE III randomized clinical trial. JAMA 2013; 309: Saeed M, Hanna I, Robotis D, et al. Programming implantable cardioverter-defibrillators in patients with primary prevention indication to prolong time to first shock: results from the PROVIDE study. J Cardiovasc Electrophysiol 2014;25: Kleemann T, Becker T, Doenges K, et al. Annual rate of transvenous defibrillation lead defects in implantable cardioverter-defibrillators over a period of >10 years. Circulation 2007;115: Conte G, Dewals W, Sieira J, et al. Drug-induced Brugada syndrome in children: clinical features, device-based management and long-term followup. J Am Coll Cardiol 2014;63: KEY WORDS Brugada syndrome, implantable cardioverter-defibrillator, sudden cardiac death, ventricular arrhythmias
Ripolarizzazione precoce. Torino, 24th October Non così innocente come si pensava
 Asymptomatic inherited arrhythmia syndromes: Drug induced Brugada Syndrome: when a prophylactic ICD is indicated? how high (or low) is QT the risk? Asymptomatic short Ripolarizzazione precoce. Torino,
Asymptomatic inherited arrhythmia syndromes: Drug induced Brugada Syndrome: when a prophylactic ICD is indicated? how high (or low) is QT the risk? Asymptomatic short Ripolarizzazione precoce. Torino,
Are there low risk patients in Brugada syndrome?
 Are there low risk patients in Brugada syndrome? Pedro Brugada MD, PhD Andrea Sarkozy MD Risk stratification in Brugada syndrome In the last years risk stratification in Brugada syndrome has become the
Are there low risk patients in Brugada syndrome? Pedro Brugada MD, PhD Andrea Sarkozy MD Risk stratification in Brugada syndrome In the last years risk stratification in Brugada syndrome has become the
Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation
 J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
J Arrhythmia Vol 25 No 1 2009 Original Article Clinical and Electrocardiographic Characteristics of Patients with Brugada Syndrome: Report of Five Cases of Documented Ventricular Fibrillation Seiji Takashio
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
The Therapeutic Role of the Implantable Cardioverter Defibrillator in Arrhythmogenic Right Ventricular Dysplasia
 The Therapeutic Role of the Implantable Cardioverter Defibrillator in Arrhythmogenic Right Ventricular Dysplasia By Sandeep Joshi, MD and Jonathan S. Steinberg, MD Arrhythmia Service, Division of Cardiology
The Therapeutic Role of the Implantable Cardioverter Defibrillator in Arrhythmogenic Right Ventricular Dysplasia By Sandeep Joshi, MD and Jonathan S. Steinberg, MD Arrhythmia Service, Division of Cardiology
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm
 Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Syncope in patients with inherited arrhythmogenic syndromes. Is it enough to justify ICD implantation?
 Innovations in Interventional Cardiology and Electrophysiology Thessaloniki 2014 Syncope in patients with inherited arrhythmogenic syndromes. Is it enough to justify ICD implantation? K. Letsas, MD, FESC
Innovations in Interventional Cardiology and Electrophysiology Thessaloniki 2014 Syncope in patients with inherited arrhythmogenic syndromes. Is it enough to justify ICD implantation? K. Letsas, MD, FESC
Journal of the American College of Cardiology Vol. 37, No. 2, by the American College of Cardiology ISSN /01/$20.
 Journal of the American College of Cardiology Vol. 37, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)01133-5 Coronary
Journal of the American College of Cardiology Vol. 37, No. 2, 2001 2001 by the American College of Cardiology ISSN 0735-1097/01/$20.00 Published by Elsevier Science Inc. PII S0735-1097(00)01133-5 Coronary
When the rhythm of life is disturbed
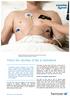 Brugada Syndrome has the capacity to cause abnormal heart rhythms originating in the upper chambers of the heart When the rhythm of life is disturbed Cardiovascular disease continues to be a leading cause
Brugada Syndrome has the capacity to cause abnormal heart rhythms originating in the upper chambers of the heart When the rhythm of life is disturbed Cardiovascular disease continues to be a leading cause
Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks
 Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks Alireza Ghorbani Sharif, MD Interventional Electrophysiologist Tehran Arrhythmia Clinic January 2016 Recurrent ICD shocks are associated
Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks Alireza Ghorbani Sharif, MD Interventional Electrophysiologist Tehran Arrhythmia Clinic January 2016 Recurrent ICD shocks are associated
Tachycardia Devices Indications and Basic Trouble Shooting
 Tachycardia Devices Indications and Basic Trouble Shooting Peter A. Brady, MD., FRCP Cardiology Review Course London, March 6 th, 2014 2011 MFMER 3134946-1 Tachycardia Devices ICD Indications Primary and
Tachycardia Devices Indications and Basic Trouble Shooting Peter A. Brady, MD., FRCP Cardiology Review Course London, March 6 th, 2014 2011 MFMER 3134946-1 Tachycardia Devices ICD Indications Primary and
Optimal management of Brugada syndrome
 Optimal management of Brugada syndrome Cristian Stătescu 1,2, Teodor Vasilcu 1,2, Ioana Mădălina Chiorescu*,1,2, Grigore Tinică 1,2, Cătălina Arsenescu-Georgescu 1,2, Radu Sascău 1,2 1 "Grigore T. Popa"
Optimal management of Brugada syndrome Cristian Stătescu 1,2, Teodor Vasilcu 1,2, Ioana Mădălina Chiorescu*,1,2, Grigore Tinică 1,2, Cătălina Arsenescu-Georgescu 1,2, Radu Sascău 1,2 1 "Grigore T. Popa"
Brugada syndrome (BS) is an inheritable syndrome characterized
 Original Article Prognostic Value of Programmed Electrical Stimulation in Brugada Syndrome 20 Years Experience Juan Sieira, MD; Giulio Conte, MD; Giuseppe Ciconte, MD; Carlo de Asmundis, MD; Gian-Battista
Original Article Prognostic Value of Programmed Electrical Stimulation in Brugada Syndrome 20 Years Experience Juan Sieira, MD; Giulio Conte, MD; Giuseppe Ciconte, MD; Carlo de Asmundis, MD; Gian-Battista
2017 AHA/ACC/HRS Ventricular Arrhythmias and Sudden Cardiac Death Guideline. Top Ten Messages. Eleftherios M Kallergis, MD, PhD, FESC
 2017 AHA/ACC/HRS Ventricular Arrhythmias and Sudden Cardiac Death Guideline Top Ten Messages Eleftherios M Kallergis, MD, PhD, FESC Cadiology Department - Heraklion University Hospital No actual or potential
2017 AHA/ACC/HRS Ventricular Arrhythmias and Sudden Cardiac Death Guideline Top Ten Messages Eleftherios M Kallergis, MD, PhD, FESC Cadiology Department - Heraklion University Hospital No actual or potential
that number is extremely high. It s 16 episodes, or in other words, it s 14, one-four, ICD shocks per patient per day.
 Doctor Karlsner, Doctor Schumosky, ladies and gentlemen. It s my real pleasure to participate in this session on controversial issues in the management of ventricular tachycardia and I m sure that will
Doctor Karlsner, Doctor Schumosky, ladies and gentlemen. It s my real pleasure to participate in this session on controversial issues in the management of ventricular tachycardia and I m sure that will
Ripolarizzazione precoce.
 Controversia: impianto di defibrillatore in prevenzione primaria Caso clinico: Ripolarizzazione precoce. Sindrome di Brugada Non così innocente come si pensava Torino, 31 marzo 2017 Carla Giustetto Carla
Controversia: impianto di defibrillatore in prevenzione primaria Caso clinico: Ripolarizzazione precoce. Sindrome di Brugada Non così innocente come si pensava Torino, 31 marzo 2017 Carla Giustetto Carla
Διαχείρηση Ασυμπτωματικού ασθενούς με ΗΚΓ τύπου Brugada
 Διαχείρηση Ασυμπτωματικού ασθενούς με ΗΚΓ τύπου Brugada Άννα Κωστοπούλου Επιμελήτρια Α Ωνάσειο Καρδιοχειρουργικό Κέντρο Τμήμα Ηλεκτροφυσιολογίας και Βηματοδότησης BrS: Diagnosis 5:10000 First described
Διαχείρηση Ασυμπτωματικού ασθενούς με ΗΚΓ τύπου Brugada Άννα Κωστοπούλου Επιμελήτρια Α Ωνάσειο Καρδιοχειρουργικό Κέντρο Τμήμα Ηλεκτροφυσιολογίας και Βηματοδότησης BrS: Diagnosis 5:10000 First described
Invasive Risk Stratification: When is it needed?
 Inherited Cardiomyopathies and Channelopathies: Who is at risk for Sudden Cardiac Death? Invasive Risk Stratification: When is it needed? Hung-Fat Tse, MD, PhD Department of Medicine The University of
Inherited Cardiomyopathies and Channelopathies: Who is at risk for Sudden Cardiac Death? Invasive Risk Stratification: When is it needed? Hung-Fat Tse, MD, PhD Department of Medicine The University of
Shock Reduction Strategies Michael Geist E. Wolfson MC
 Shock Reduction Strategies Michael Geist E. Wolfson MC Shock Therapy Thanks, I needed that! Why Do We Need To Reduce Shocks Long-term outcome after ICD and CRT implantation and influence of remote device
Shock Reduction Strategies Michael Geist E. Wolfson MC Shock Therapy Thanks, I needed that! Why Do We Need To Reduce Shocks Long-term outcome after ICD and CRT implantation and influence of remote device
CME Article Brugada pattern masking anterior myocardial infarction
 Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Summary, conclusions and future perspectives
 Summary, conclusions and future perspectives Summary The general introduction (Chapter 1) of this thesis describes aspects of sudden cardiac death (SCD), ventricular arrhythmias, substrates for ventricular
Summary, conclusions and future perspectives Summary The general introduction (Chapter 1) of this thesis describes aspects of sudden cardiac death (SCD), ventricular arrhythmias, substrates for ventricular
Brugada syndrome is a cardiac disease caused by an
 Efficacy of Quinidine in High-Risk Patients With Brugada Syndrome Bernard Belhassen, MD; Aharon Glick, MD; Sami Viskin, MD Background Automatic implantable cardioverter-defibrillator therapy is considered
Efficacy of Quinidine in High-Risk Patients With Brugada Syndrome Bernard Belhassen, MD; Aharon Glick, MD; Sami Viskin, MD Background Automatic implantable cardioverter-defibrillator therapy is considered
ICD in a young patient with syncope
 ICD in a young patient with syncope Konstantinos P. Letsas, MD, FESC Second Department of Cardiology Evangelismos General Hospital of Athens Athens, Greece Case presentation A 17-year-old apparently healthy
ICD in a young patient with syncope Konstantinos P. Letsas, MD, FESC Second Department of Cardiology Evangelismos General Hospital of Athens Athens, Greece Case presentation A 17-year-old apparently healthy
Εκθορηίζεις απινιδωηή και θνηηόηηηα: μέθοδοι μείωζης ηων θεραπειών απινίδωζης
 Εκθορηίζεις απινιδωηή και θνηηόηηηα: μέθοδοι μείωζης ηων θεραπειών απινίδωζης Εμμ. Μ. Κανοσπάκης Καρδιολογική Κλινική Πανεπιζηημίοσ Κρήηης Lessons from large trials Conditioning Rhythm and Electrical Therapy
Εκθορηίζεις απινιδωηή και θνηηόηηηα: μέθοδοι μείωζης ηων θεραπειών απινίδωζης Εμμ. Μ. Κανοσπάκης Καρδιολογική Κλινική Πανεπιζηημίοσ Κρήηης Lessons from large trials Conditioning Rhythm and Electrical Therapy
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
How to manage a patient with short QT syndrome?
 How to manage a patient with short QT syndrome? Torino, 27 ottobre2012 Carla Giustetto Division of Cardiology University of Torino QT 280 ms QTc 260 ms Narrow, tall and peaked T waves High incidence of
How to manage a patient with short QT syndrome? Torino, 27 ottobre2012 Carla Giustetto Division of Cardiology University of Torino QT 280 ms QTc 260 ms Narrow, tall and peaked T waves High incidence of
Brugada Syndrome: Age is just a number
 Brugada Syndrome: Age is just a number 1 Deepthi Kagolanu, MD, 2 Cynthia Pacas, 1 Usman Jilani, DO, 1 Ebisa Bekele, MD, 3 Christopher Henessey, 4 Kent Stephenson MD 1 Nassau University Medical Center,
Brugada Syndrome: Age is just a number 1 Deepthi Kagolanu, MD, 2 Cynthia Pacas, 1 Usman Jilani, DO, 1 Ebisa Bekele, MD, 3 Christopher Henessey, 4 Kent Stephenson MD 1 Nassau University Medical Center,
Subcutaneous implantable cardioverter defibrillator insertion for preventing sudden cardiac death
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Subcutaneous implantable cardioverter defibrillator insertion for preventing sudden cardiac death A subcutaneous
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Subcutaneous implantable cardioverter defibrillator insertion for preventing sudden cardiac death A subcutaneous
Abbreviation List: 2017 by the American Heart Association, Inc. and the American College of Cardiology Foundation. 1
 2017 AHA/ACC/HRS Systematic Review for the Guideline for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death Data Supplement Table of Contents Part 1. For Asymptomatic
2017 AHA/ACC/HRS Systematic Review for the Guideline for Management of Patients With Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death Data Supplement Table of Contents Part 1. For Asymptomatic
Inappropriate electrical shocks: Tackling the beast
 ESC Paris 2011 Inappropriate electrical shocks: Tackling the beast Gerhard Hindricks University of Leipzig Heart Center Dept. of Electrophysiology ESC Paris 2011 Inappropriate electrical shocks: Tackling
ESC Paris 2011 Inappropriate electrical shocks: Tackling the beast Gerhard Hindricks University of Leipzig Heart Center Dept. of Electrophysiology ESC Paris 2011 Inappropriate electrical shocks: Tackling
State of the Art: Brugada Syndrome Novel diagnostic approaches and risk stratification
 State of the Art: Brugada Syndrome Novel diagnostic approaches and risk stratification Lars Eckardt Division Electrophysiology Department of Cardiovascular Medicine University of Münster, Germany I have
State of the Art: Brugada Syndrome Novel diagnostic approaches and risk stratification Lars Eckardt Division Electrophysiology Department of Cardiovascular Medicine University of Münster, Germany I have
Continuous ECG telemonitoring with implantable devices: the expected clinical benefits
 Continuous ECG telemonitoring with implantable devices: the expected clinical benefits C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany Carsten.Israel@evkb.de Declaration of
Continuous ECG telemonitoring with implantable devices: the expected clinical benefits C. W. Israel, M.D. Dept. of Cardiology Evangelical Hospital Bielefeld Germany Carsten.Israel@evkb.de Declaration of
ICD THERAPIES: are they harmful or just high risk markers?
 ICD THERAPIES: are they harmful or just high risk markers? Konstantinos P. Letsas, MD, PhD, FESC LAB OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL ATHENS ICD therapies are common In a meta-analysis
ICD THERAPIES: are they harmful or just high risk markers? Konstantinos P. Letsas, MD, PhD, FESC LAB OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL ATHENS ICD therapies are common In a meta-analysis
Subcutaneous Implantable Cardioverter Defibrillator (S-ICD)
 Subcutaneous Implantable Cardioverter Defibrillator (S-ICD) D. D. MANOLATOS, MD, PhD, FESC Electrophysiology and Device Lab General Hospital Evangelismos, Athens The Problem: 300,000 people die each year
Subcutaneous Implantable Cardioverter Defibrillator (S-ICD) D. D. MANOLATOS, MD, PhD, FESC Electrophysiology and Device Lab General Hospital Evangelismos, Athens The Problem: 300,000 people die each year
Ripolarizzazione precoce. Non così innocente come si pensava
 La sincope nel paziente con ECG Brugada-like Stresa, 9 giugno 2017 Ripolarizzazione precoce. Non così innocente come si pensava Carla Giustetto Carla Giustetto Divisione di Cardiologia Divisione Università
La sincope nel paziente con ECG Brugada-like Stresa, 9 giugno 2017 Ripolarizzazione precoce. Non così innocente come si pensava Carla Giustetto Carla Giustetto Divisione di Cardiologia Divisione Università
Tailored treatment in Brugada syndrome
 Tailored treatment in Brugada syndrome Lars Eckardt Department of Cardiology and Angiology Division of Experimental and Clinical Electrophysiology University of Münster, Germany 45 yr old male preoperative
Tailored treatment in Brugada syndrome Lars Eckardt Department of Cardiology and Angiology Division of Experimental and Clinical Electrophysiology University of Münster, Germany 45 yr old male preoperative
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs
 EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
EHRA Accreditation Exam - Sample MCQs Cardiac Pacing and ICDs Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important step for
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
Atrial Fibrillation: Rate vs. Rhythm. Michael Curley, MD Cardiac Electrophysiology
 Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Prevention of Sudden Death in ARVC
 ESC Munich, August 29, 2012 Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC): Prevention of Sudden Death in ARVC Thomas Wichter, MD, FESC Professor of Medicine - Cardiology Marienhospital Osnabrück
ESC Munich, August 29, 2012 Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC): Prevention of Sudden Death in ARVC Thomas Wichter, MD, FESC Professor of Medicine - Cardiology Marienhospital Osnabrück
Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators
 22 March 2002 Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators F. HINTRINGER, O. PACHINGER Division of Cardiology, Department for Internal Medicine, University
22 March 2002 Interactive Simulator for Evaluating the Detection Algorithms of Implantable Defibrillators F. HINTRINGER, O. PACHINGER Division of Cardiology, Department for Internal Medicine, University
Original Article. Introduction. Korean Circulation Journal
 Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Tachyarrhythmia Cycle Length in Appropriate versus Inappropriate Defibrillator Shocks in Brugada Syndrome, Early
Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Tachyarrhythmia Cycle Length in Appropriate versus Inappropriate Defibrillator Shocks in Brugada Syndrome, Early
Subcutaneous ICD Emerging Role of Sudden Cardiac Death Prevention
 Subcutaneous ICD Emerging Role of Sudden Cardiac Death Prevention Dr Ngai-Yin Chan, MBBS, FRCP(Lond), FRCP(Edin), FRCP(Glasg), FACC, FHRS, Consultant Physician, Department of Medicine & Geriatrics, Princess
Subcutaneous ICD Emerging Role of Sudden Cardiac Death Prevention Dr Ngai-Yin Chan, MBBS, FRCP(Lond), FRCP(Edin), FRCP(Glasg), FACC, FHRS, Consultant Physician, Department of Medicine & Geriatrics, Princess
Prophylactic ablation
 Ventricular tachycardia in ischaemic heart disease. Update on electrical therapy 29 august 2010 Prophylactic ablation Pasquale Notarstefano Cardiovacular Department S. Donato Hospital, Arezzo (IT) Prophylactic
Ventricular tachycardia in ischaemic heart disease. Update on electrical therapy 29 august 2010 Prophylactic ablation Pasquale Notarstefano Cardiovacular Department S. Donato Hospital, Arezzo (IT) Prophylactic
Atrial Fibrillation and Brugada Syndrome
 Journal of the American College of Cardiology Vol. 51, No. 12, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.10.062
Journal of the American College of Cardiology Vol. 51, No. 12, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.10.062
Low Prevalence of Risk Markers in Cases of Sudden Death Due to Brugada Syndrome
 Journal of the American College of Cardiology Vol. 57, No. 23, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2010.11.067
Journal of the American College of Cardiology Vol. 57, No. 23, 2011 2011 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2010.11.067
P. Brugada 1, R. Brugada 2 and J. Brugada 3. Introduction. U.S.A.; 3 Unitat d Arritmias, Hospital Clinic, Barcelona, Spain
 European Heart Journal (2000) 21, 321 326 Article No. euhj.1999.1751, available online at http://www.idealibrary.com on Sudden death in patients and relatives with the syndrome of right bundle branch block,
European Heart Journal (2000) 21, 321 326 Article No. euhj.1999.1751, available online at http://www.idealibrary.com on Sudden death in patients and relatives with the syndrome of right bundle branch block,
Case Presentation. Asaad Khan University College Hospital Galway Rep of Ireland
 Case Presentation Asaad Khan University College Hospital Galway Rep of Ireland Case History 32 male Married Working as a chartered accountant P/C:Admitted to a Regional hospital to be investigated for
Case Presentation Asaad Khan University College Hospital Galway Rep of Ireland Case History 32 male Married Working as a chartered accountant P/C:Admitted to a Regional hospital to be investigated for
Evaluation of Sum Absolute QRST Integral as a Clinical Marker for Ventricular Arrhythmias. Markus Kowalsky Group 11
 Evaluation of Sum Absolute QRST Integral as a Clinical Marker for Ventricular Arrhythmias Markus Kowalsky Group 11 Selected Paper Ventricular arrhythmia is predicted by sum absolute QRST integral but not
Evaluation of Sum Absolute QRST Integral as a Clinical Marker for Ventricular Arrhythmias Markus Kowalsky Group 11 Selected Paper Ventricular arrhythmia is predicted by sum absolute QRST integral but not
Silvia G Priori MD PhD
 The approach to the cardiac arrest survivor Silvia G Priori MD PhD Molecular Cardiology, IRCCS Fondazione Salvatore Maugeri Pavia, Italy AND Leon Charney Division of Cardiology, Cardiovascular Genetics
The approach to the cardiac arrest survivor Silvia G Priori MD PhD Molecular Cardiology, IRCCS Fondazione Salvatore Maugeri Pavia, Italy AND Leon Charney Division of Cardiology, Cardiovascular Genetics
Ripolarizzazione precoce. Non così innocente come si pensava
 Brugada syndrome: tests and diagnosis. Torino, 27 ottobre 2017 Ripolarizzazione precoce. Non così innocente come si pensava Carla Giustetto Carla Giustetto Divisione di Cardiologia Divisione Università
Brugada syndrome: tests and diagnosis. Torino, 27 ottobre 2017 Ripolarizzazione precoce. Non così innocente come si pensava Carla Giustetto Carla Giustetto Divisione di Cardiologia Divisione Università
ICD: Basics, Programming and Trouble-shooting
 ICD: Basics, Programming and Trouble-shooting Amir AbdelWahab, MD Electrophysiology and Pacing Service Cardiology Department Cairo University Feb 2013 Evolution of ICD Technology ICD Evolution Indications
ICD: Basics, Programming and Trouble-shooting Amir AbdelWahab, MD Electrophysiology and Pacing Service Cardiology Department Cairo University Feb 2013 Evolution of ICD Technology ICD Evolution Indications
Different indications for pacemaker implantation are the following:
 Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Patient Resources: ICD/Pacemaker Overview ICD/Pacemaker Overview What is a pacemaker? A pacemaker is a device that uses low energy electrical pulses to prompt the heart to beat whenever a pause in the
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Pearls of the ESC/ERS Guidelines 2015 Channelopathies
 Pearls of the ESC/ERS Guidelines 2015 Channelopathies Carina Blomstrom Lundqvist Dept Cardiology, Uppsala, Sweden Content 2015 ESC Guidelines for the Management of Patients with Ventricular Arrhythmias
Pearls of the ESC/ERS Guidelines 2015 Channelopathies Carina Blomstrom Lundqvist Dept Cardiology, Uppsala, Sweden Content 2015 ESC Guidelines for the Management of Patients with Ventricular Arrhythmias
Long QT Syndrome in Children in the Era of Implantable Defibrillators
 Journal of the American College of Cardiology Vol. 50, No. 14, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.05.042
Journal of the American College of Cardiology Vol. 50, No. 14, 2007 2007 by the American College of Cardiology Foundation ISSN 0735-1097/07/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2007.05.042
How agressively should we treat asymptomatic patients with Brugada syndrome. Josep Brugada Medical Director Hospital Clínic, University of Barcelona
 How agressively should we treat asymptomatic patients with Brugada syndrome Josep Brugada Medical Director Hospital Clínic, University of Barcelona The ECG in Brugada syndrome - Prolonged PR - RBBB - ST
How agressively should we treat asymptomatic patients with Brugada syndrome Josep Brugada Medical Director Hospital Clínic, University of Barcelona The ECG in Brugada syndrome - Prolonged PR - RBBB - ST
FANS Paediatric Pathway for Inherited Arrhythmias*
 FANS Paediatric Pathway for Inherited Arrhythmias* The pathway is based on the HRS/EHRA/APHRS Expert Consensus Statement on the Diagnosis and Management of Patients with Inherited Primary Arrhythmia Syndromes
FANS Paediatric Pathway for Inherited Arrhythmias* The pathway is based on the HRS/EHRA/APHRS Expert Consensus Statement on the Diagnosis and Management of Patients with Inherited Primary Arrhythmia Syndromes
Arrhythmias Focused Review. Who Needs An ICD?
 Who Needs An ICD? Cesar Alberte, MD, Douglas P. Zipes, MD, Krannert Institute of Cardiology, Indiana University School of Medicine, Indianapolis, IN Sudden cardiac arrest is one of the most common causes
Who Needs An ICD? Cesar Alberte, MD, Douglas P. Zipes, MD, Krannert Institute of Cardiology, Indiana University School of Medicine, Indianapolis, IN Sudden cardiac arrest is one of the most common causes
Device Interrogation- Pacemakers, ICD and Loop Recorders. Dulce Obias-Manno, RN, MHSA, CCDS,CEPS, FHRS Device Clinic Coordinator, MHVI
 Device Interrogation- Pacemakers, ICD and Loop Recorders Dulce Obias-Manno, RN, MHSA, CCDS,CEPS, FHRS Device Clinic Coordinator, MHVI Disclosures Consultant: Medtronic Speaker s Bureau: St. Jude Medical
Device Interrogation- Pacemakers, ICD and Loop Recorders Dulce Obias-Manno, RN, MHSA, CCDS,CEPS, FHRS Device Clinic Coordinator, MHVI Disclosures Consultant: Medtronic Speaker s Bureau: St. Jude Medical
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013
 Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm
 April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
April 2000 107 Clinical Results with the Dual-Chamber Cardioverter Defibrillator Phylax AV - Efficacy of the SMART I Discrimination Algorithm B. MERKELY Semmelweis University, Dept. of Cardiovascular Surgery,
A Prospective Study Comparing the Sensed R Wave in Bipolar and Extended Bipolar Configurations: The PropR Study
 A Prospective Study Comparing the Sensed R Wave in Bipolar and Extended Bipolar Configurations: The PropR Study ANEESH V. TOLAT, M.D.,* MELISSA WOICIECHOWSKI, M.S.N.,* ROSEMARIE KAHR, R.C.I.S.,* JOSEPH
A Prospective Study Comparing the Sensed R Wave in Bipolar and Extended Bipolar Configurations: The PropR Study ANEESH V. TOLAT, M.D.,* MELISSA WOICIECHOWSKI, M.S.N.,* ROSEMARIE KAHR, R.C.I.S.,* JOSEPH
The impact of clinical and genetic findings on the management of young Brugada Syndrome patients
 12 ème Congrès Médico-Chirugical de la FCPC 21 au 24 novembre 2015 Schoelcher, Martinique The impact of clinical and genetic findings on the management of young Brugada Syndrome patients Institut du Thorax,
12 ème Congrès Médico-Chirugical de la FCPC 21 au 24 novembre 2015 Schoelcher, Martinique The impact of clinical and genetic findings on the management of young Brugada Syndrome patients Institut du Thorax,
file://c:\documents and Settings\admin\My Documents\CV\92.htm
 Page 1 of 5 Amir Farjam Fazelifar, M.D. Assistant Professor of Cardiac Electrophysiology Academic Address: Shaheed Rajaei Cardiovascular, Medical & Research Center, Vali- Asr Avenue Tehran- Iran Tel /
Page 1 of 5 Amir Farjam Fazelifar, M.D. Assistant Professor of Cardiac Electrophysiology Academic Address: Shaheed Rajaei Cardiovascular, Medical & Research Center, Vali- Asr Avenue Tehran- Iran Tel /
Original Article Fragmented QRS as a Predictor of Appropriate Implantable Cardioverter-defibrillator Therapy
 4 Original Article Fragmented QRS as a Predictor of Appropriate Implantable Cardioverter-defibrillator Therapy Sirin Apiyasawat, Dujdao Sahasthas, Tachapong Ngarmukos, Pakorn Chandanamattha, Khanchit Likittanasombat
4 Original Article Fragmented QRS as a Predictor of Appropriate Implantable Cardioverter-defibrillator Therapy Sirin Apiyasawat, Dujdao Sahasthas, Tachapong Ngarmukos, Pakorn Chandanamattha, Khanchit Likittanasombat
Defibrillation threshold testing should no longer be performed: contra
 Defibrillation threshold testing should no longer be performed: contra Andreas Goette St. Vincenz-Hospital Paderborn Dept. of Cardiology and Intensive Care Medicine Germany No conflict of interest to disclose
Defibrillation threshold testing should no longer be performed: contra Andreas Goette St. Vincenz-Hospital Paderborn Dept. of Cardiology and Intensive Care Medicine Germany No conflict of interest to disclose
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Synopsis of Management on Ventricular arrhythmias. M. Soni MD Interventional Cardiologist
 Synopsis of Management on Ventricular arrhythmias M. Soni MD Interventional Cardiologist No financial disclosure Premature Ventricular Contraction (PVC) Ventricular Bigeminy Ventricular Trigeminy Multifocal
Synopsis of Management on Ventricular arrhythmias M. Soni MD Interventional Cardiologist No financial disclosure Premature Ventricular Contraction (PVC) Ventricular Bigeminy Ventricular Trigeminy Multifocal
What s new in my specialty?
 What s new in my specialty? Jon Melman, MD Heart Rhythm Specialists McKay-Dee Hospital some would say some would say my specialty 1 some would say my specialty First pacemaker 1958 some would say my specialty
What s new in my specialty? Jon Melman, MD Heart Rhythm Specialists McKay-Dee Hospital some would say some would say my specialty 1 some would say my specialty First pacemaker 1958 some would say my specialty
Exercise guidelines in athletes with isolated repolarisation abnormalities and structurally normal heart.
 Exercise guidelines in athletes with isolated repolarisation abnormalities and structurally normal heart. Hanne Rasmusen Consultant cardiologist, PhD Dept. of Cardiology Bispebjerg University Hospital
Exercise guidelines in athletes with isolated repolarisation abnormalities and structurally normal heart. Hanne Rasmusen Consultant cardiologist, PhD Dept. of Cardiology Bispebjerg University Hospital
AF and arrhythmia management. Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire
 AF and arrhythmia management Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire Atrial fibrillation Paroxysmal AF recurrent AF (>2 episodes) that
AF and arrhythmia management Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire Atrial fibrillation Paroxysmal AF recurrent AF (>2 episodes) that
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh
 Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT JANUARY 24, 2012
 IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
Antony French Consultant Cardiologist & Electrophysiologist
 Antony French Consultant Cardiologist & Electrophysiologist Palpitations Unpleasant awareness of rapid or forceful heart beat Not all tachycardias cause palpitations, and not all palpitations are due to
Antony French Consultant Cardiologist & Electrophysiologist Palpitations Unpleasant awareness of rapid or forceful heart beat Not all tachycardias cause palpitations, and not all palpitations are due to
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS
 NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
NEIL CISPER TECHNICAL FIELD ENGINEER ICD/CRTD BASICS OBJECTIVES Discuss history of ICDs Review the indications for ICD and CRT therapy Describe basic lead and device technology Discuss different therapies
Electrophysiologic investigation in Brugada syndrome
 European Heart Journal (2002) 23, 1394 1401 doi:10.1053/euhj.2002.3256, available online at http://www.idealibrary.com on Electrophysiologic investigation in Brugada syndrome Yield of programmed ventricular
European Heart Journal (2002) 23, 1394 1401 doi:10.1053/euhj.2002.3256, available online at http://www.idealibrary.com on Electrophysiologic investigation in Brugada syndrome Yield of programmed ventricular
Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life
 Chapter 3 Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life Guido H. van Welsenes, MS, Johannes B. van Rees, MD, Joep Thijssen, MD, Serge
Chapter 3 Primary prevention ICD recipients: the need for defibrillator back-up after an event-free first battery service-life Guido H. van Welsenes, MS, Johannes B. van Rees, MD, Joep Thijssen, MD, Serge
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
ΔΠΔΜΒΑΣΙΚΗ ΘΔΡΑΠΔΙΑ ΚΟΙΛΙΑΚΩΝ ΑΡΡΤΘΜΙΩΝ
 ΔΠΔΜΒΑΣΙΚΗ ΘΔΡΑΠΔΙΑ ΚΟΙΛΙΑΚΩΝ ΑΡΡΤΘΜΙΩΝ ΣΔΛΙΟ ΠΑΡΑΚΔΤΑÏΓΗ ΓΙΔΤΘΤΝΣΗ ΔΤ Α Καρδιολογική Κλινική ΑΠΘ, Νοζοκομείο ΑΧΕΠΑ, Θεζζαλονίκη NO CONFLICT OF INTEREST INTRODUCTION Sustained VT is an important cause
ΔΠΔΜΒΑΣΙΚΗ ΘΔΡΑΠΔΙΑ ΚΟΙΛΙΑΚΩΝ ΑΡΡΤΘΜΙΩΝ ΣΔΛΙΟ ΠΑΡΑΚΔΤΑÏΓΗ ΓΙΔΤΘΤΝΣΗ ΔΤ Α Καρδιολογική Κλινική ΑΠΘ, Νοζοκομείο ΑΧΕΠΑ, Θεζζαλονίκη NO CONFLICT OF INTEREST INTRODUCTION Sustained VT is an important cause
SVT Discriminators. Definition of SVT Discrimination. Identify which patient populations might benefit from these features
 Definition of SVT Discrimination Identify which patient populations might benefit from these features Understand the 4 types of SVT discriminators used by St Jude Medical Be aware of programmable parameters
Definition of SVT Discrimination Identify which patient populations might benefit from these features Understand the 4 types of SVT discriminators used by St Jude Medical Be aware of programmable parameters
Ventricular arrhythmia during ajmaline challenge for the Brugada syndrome
 Europace (2016) 18, 1501 1506 doi:10.1093/europace/euw008 REVIEW Ventricular arrhythmia during ajmaline challenge for the Brugada syndrome Bieke Dobbels 1 *, Dieter De Cleen 2,3, and Joris Ector 4,5 1
Europace (2016) 18, 1501 1506 doi:10.1093/europace/euw008 REVIEW Ventricular arrhythmia during ajmaline challenge for the Brugada syndrome Bieke Dobbels 1 *, Dieter De Cleen 2,3, and Joris Ector 4,5 1
Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification. Carlo Pappone, MD, PhD, FACC
 Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification Carlo Pappone, MD, PhD, FACC The Wolff-Parkinson-White Syndrome Demographics Δ waves detectable on
Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification Carlo Pappone, MD, PhD, FACC The Wolff-Parkinson-White Syndrome Demographics Δ waves detectable on
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
J Wave Syndromes. Osama Diab Lecturer of Cardiology Ain Shams University
 J Wave Syndromes Osama Diab Lecturer of Cardiology Ain Shams University J Wave Syndromes Group of electric disorders characterized by > 1 mm elevation of the J point or prominent J wave with or without
J Wave Syndromes Osama Diab Lecturer of Cardiology Ain Shams University J Wave Syndromes Group of electric disorders characterized by > 1 mm elevation of the J point or prominent J wave with or without
Management strategies for atrial fibrillation Thursday, 20 October :27
 ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists
 PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
PERMANENT PACEMAKERS AND IMPLANTABLE DEFIBRILLATORS Considerations for intensivists Craig A. McPherson, MD, FACC Associate Professor of Medicine Constantine Manthous, MD, FACP, FCCP Associate Clinical
Automatic External Defibrillators
 Last Review Date: April 21, 2017 Number: MG.MM.DM.10dC3v4 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: April 21, 2017 Number: MG.MM.DM.10dC3v4 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Short QT Syndrome: Pharmacological Treatment
 Journal of the American College of Cardiology Vol. 43, No. 8, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.02.034
Journal of the American College of Cardiology Vol. 43, No. 8, 2004 2004 by the American College of Cardiology Foundation ISSN 0735-1097/04/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2004.02.034
Brugada Syndrome: An Update
 Brugada Syndrome: An Update Osama Diab Associate professor of Cardiology Ain Shams university, Cairo, Egypt Updates Mechanism and Genetics Risk stratification Treatment 1 Brugada syndrome causes 4 12%
Brugada Syndrome: An Update Osama Diab Associate professor of Cardiology Ain Shams university, Cairo, Egypt Updates Mechanism and Genetics Risk stratification Treatment 1 Brugada syndrome causes 4 12%
Implantable cardioverter defibrillator, Inappropriate shock, Lead failure
 Inappropriate Discharges of Intravenous Implantable Cardioverter Defibrillators Owing to Lead Failure Takashi WASHIZUKA, 1 MD, Masaomi CHINUSHI, 1 MD, Ryu KAZAMA, 1 MD, Takashi HIRONO, 1 MD, Hiroshi WATANABE,
Inappropriate Discharges of Intravenous Implantable Cardioverter Defibrillators Owing to Lead Failure Takashi WASHIZUKA, 1 MD, Masaomi CHINUSHI, 1 MD, Ryu KAZAMA, 1 MD, Takashi HIRONO, 1 MD, Hiroshi WATANABE,
MADIT-RIT: Simple programming change averts most inappropriate ICD therapy
 Print MADIT-RIT: Simple programming change averts most inappropriate ICD therapy NOV 6, 2012 Steve Stiles Los Angeles, CA - A large randomized trial has identified specific programming criteria for implantable
Print MADIT-RIT: Simple programming change averts most inappropriate ICD therapy NOV 6, 2012 Steve Stiles Los Angeles, CA - A large randomized trial has identified specific programming criteria for implantable
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Electrical Storm in Coronary Artery Disease. Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic July 2016
 Electrical Storm in Coronary Artery Disease Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic July 2016 48 yrs. Old diabetic with ACS 48 yrs. Old diabetic with ACS
Electrical Storm in Coronary Artery Disease Saeed Oraii MD, Cardiologist Interventional Electrophysiologist Tehran Arrhythmia Clinic July 2016 48 yrs. Old diabetic with ACS 48 yrs. Old diabetic with ACS
Primary Therapy for High Risk LQT Patients Should Be an ICD
 Primary Therapy for High Risk LQT Patients Should Be an ICD Raul Weiss MD, FAHA, FACC, FHRS, CCDS Director, Electrophysiology Fellowship Program Associate Professor of Medicine The Ohio State University
Primary Therapy for High Risk LQT Patients Should Be an ICD Raul Weiss MD, FAHA, FACC, FHRS, CCDS Director, Electrophysiology Fellowship Program Associate Professor of Medicine The Ohio State University
PARAD/PARAD+ : P and R Based Arrhythmia Detection
 Tech Corner PARAD/PARAD+ : P and R Based Arrhythmia Detection NOTE: PLEASE NOTE THAT THE FOLLOWING INFORMATION IS A GENERAL DESCRIPTION OF THE FUNCTION. DETAILS AND PARTICULAR CASES ARE NOT DESCRIBED IN
Tech Corner PARAD/PARAD+ : P and R Based Arrhythmia Detection NOTE: PLEASE NOTE THAT THE FOLLOWING INFORMATION IS A GENERAL DESCRIPTION OF THE FUNCTION. DETAILS AND PARTICULAR CASES ARE NOT DESCRIBED IN
Risk Stratification in Patients With Brugada Syndrome Without Previous Cardiac Arrest
 310 OKAMURA H et al. Circulation Journal ORIGINAL ARTICLE Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp Arrhythmia/Electrophysiology Risk Stratification in Patients With
310 OKAMURA H et al. Circulation Journal ORIGINAL ARTICLE Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp Arrhythmia/Electrophysiology Risk Stratification in Patients With
Remote Monitoring & the Smart Home of the 21 Century
 Cardiostim EHRA Europace 2016, Nice - June 8-11, 2016 Remote Monitoring & the Smart Home of the 21 Century Antonio Raviele, MD, FESC, FHRS President ALFA -Alliance to Fight Atrial fibrillation- Venezia
Cardiostim EHRA Europace 2016, Nice - June 8-11, 2016 Remote Monitoring & the Smart Home of the 21 Century Antonio Raviele, MD, FESC, FHRS President ALFA -Alliance to Fight Atrial fibrillation- Venezia
