NASS Diagnosis and Treatment of Low-Back Pain Guideline Draft Clinical Question Protocol
|
|
|
- Gerard Perkins
- 5 years ago
- Views:
Transcription
1 NASS Diagnosis and Treatment of Low-Back Pain Draft Clinical Questions Public Comment period: June 16-July 14, 2015 Comments should be sent to Background The North American Spine Society (NASS) is a multispecialty medical organization dedicated to fostering the highest quality, evidence-based, ethical spine care by promoting education, research and advocacy. NASS is comprised of more than 8,000 physician and non-physician members from several disciplines, including orthopedic surgery, neurosurgery, physiatry, pain management, neurology, radiology, anesthesiology, research, physical therapy and other spine care professionals. NASS will be conducting a systematic review of the literature to develop an evidence-based clinical practice guideline on low-back pain. The guideline panel is multi-stakeholder and composed of volunteer representatives from multiple specialties including: physical therapy, chiropractic care, research, psychology, family practice, neuroradiology, orthopedic surgery, neurosurgery, anesthesiology, pain medicine, physical medicine and rehabilitation, and physiatry. Author names will be released at time of publication. Notice of Public Comment Period The NASS Low-Back Pain Guideline Work Group recently drafted a list of clinical questions to be addressed in the guideline. The guideline will address 7 sections, including Diagnosis, Imaging, Medical & Psychological Treatment, Rehabilitation & Exercise, Interventional Treatment, Surgical Treatment and Cost-Effectiveness. The clinical question list is now available for public comment. Reviewers are requested to provide feedback on the proposed questions and suggest any additional questions that may be missing that are important to the low-back pain patient and their providers. The comment period closes on 11:59PM CST, Tuesday, July 14, 2015, and comments should be submitted to guidelines@spine.org. If applicable, please include your organizational affiliation in the response. All submissions received by the closing date will be reviewed and considered for potential inclusion in the clinical question protocol before conducting the systematic literature search and review. 1
2 Guideline Inclusion/Exclusion Criteria Definition Low-back pain is defined as pain of musculoskeletal origin extending from the lowest rib to the gluteal fold that may at times extend as somatic referred pain into the posterior thigh (above the knee). Inclusion Criteria Adult patients aged 18 and older Patients with low back pain limited to somatic referred pain/non-radicular pain limited to above the knee only Exclusion Criteria Patients less than 18 years of age Low back pain due to: o tumor o infection o Metabolic disease o Inflammatory arthritis o Fracture Patients with a diagnosed deformity, including spondylolisthesis, spondylolysis and scoliosis Pain experienced below the knee Extra-spinal conditions (ie, visceral, vascular, GU) Patients who have undergone prior lumbar surgery Presence of neurological deficit Back pain that is associated with widespread multi-site pain Literature Search Parameters Databases Searched: PubMed/Medline, EMBASE, Cochrane Library Date Range: all literature to current date Study Designs: Randomized Controlled Trials, Clinical Trials, Prospective/Retrospective Cohort and Comparative Studies, Observational Studies, Case-Control, Case-Series. Humans English only studies 2
3 Diagnosis Work Group Clinical Questions 1. In patients with acute or chronic low-back pain, are there specific history or physical examination findings that would indicate the structure causing pain and, therefore, guide treatment? a. Vertebral body b. Intervertebral disc c. Zygapophyseal joint d. Posterior elements e. Sacroiliac joint f. Muscle/tendon 2. In patients with acute or chronic low-back pain, are there history or physical examination findings that would serve as predictors for the recurrence of low-back pain? 3. In patients with acute low-back pain, are there history or physical examination findings that would predict that an episode will resolve within one month? 4. In patients with acute or chronic low-back pain, what history and/or physical examination findings are useful in determining if the cause is non-structural or non-mechanical in nature and, therefore, guide treatment? 5. In patients with acute or chronic low-back pain, what elements of the patient s history and findings from the physical examination would suggest the need for urgent or elective diagnostic laboratory studies? 6. In patients with acute or chronic low-back pain, are there specific findings on a pain diagram that help differentiate the structure which is causing pain? 7. What are the patient characteristics that increase or decrease the risk of developing chronic lowback pain after an acute episode? a. disability status b. substance abuse c. employment factors d. family support e. level of education f. coping strategies 8. Are there assessment tools or questionnaires that can help identify the cause of acute or chronic low back pain? 3
4 Imaging Work Group Clinical Questions 1. In patients with acute or chronic low-back pain, what elements of the patient s history and findings from the physical examination would suggest the need for urgent or elective diagnostic imaging studies? 2. What is the association between low-back pain and spondylosis on routine radiography? 3. Is there evidence to support the use of CT scans for the evaluation of low-back pain in the absence of radiographic abnormality? 4. In patients with low back pain, does duration of symptoms correlate with abnormal pathological findings on imaging? 5. What is the minimum CT or MR protocol that should be used in the setting of low-back pain? a. Are unique sequences considered preferential or optimal? b. What is the role of contrast enhanced imaging in patients with low-back pain? 6. In the absence of red flags, does imaging (X-ray, CT, MRI) in patients with acute or chronic low-back pain ultimately lead to different treatments? 7. Does the presence of a dorsal high intensity zone in a lumbar disc correlate to the presence of lowback pain? 4
5 Medical and Psychological Treatment Work Group Clinical Questions 1. Is smoking cessation effective in decreasing the frequency of low-back pain episodes? 2. In patients with acute or chronic low-back pain, is pharmacological treatment effective in improving duration of pain, intensity of pain, functional outcomes, anxiety, depression and return to work (RTW)? Vs: a. No treatment b. cognitive behavioral therapy (CBT) and/or psychosocial intervention alone c. patient education alone 3. In patients with acute or chronic low-back pain, is topical treatment (e.g. cream or gel) effective in improving duration of pain, intensity of pain, functional outcomes and RTW? 4. Following treatment for low-back pain, do patients with healthy sleep habits experience improved duration of pain, intensity of pain, functional outcomes and RTW compared to patients with poor sleeping habits? Commented [KR1]: Note: The lit search will include terms for: General pharmacological treatment search terms Analgesics NSAIDS Opioids Anxiolytics Antidepressants sleeping medications Commented [KR2]: Note: Sleep habits will include duration, quality, sleeping position, and mattress 5. In patients with acute or chronic low-back pain, is cognitive behavioral therapy (CBT) and/or psychosocial intervention effective in improving duration of pain, intensity of pain, functional outcomes, anxiety, depression and RTW? 6. In patients with acute or chronic low-pain pain, does the timing of cognitive behavioral therapy/psychosocial intervention affect duration of pain, intensity of pain, functional outcomes, anxiety, depression and RTW status? 7. In patients undergoing interventional or surgical treatment for low-back pain, does the addition of cognitive behavioral therapy (CBT) and/or psychosocial intervention add incremental benefit? 8. Does educating a patient about low-back pain improve treatment compliance and outcomes, including duration of pain, intensity of pain, functional outcomes, anxiety, depression and RTW? Commented [KR3]: Note: The lit search will include search terms for: cognitive behavior therapy psychosocial intervention coping skill straining biofeedback relaxation techniques psychotherapy 9. In patients undergoing treatment for low-back pain, what is the effectiveness of interventions that address fear avoidance behaviors? 10. Is active treatment (pharmacological or psychotherapeutic) of anxiety and depression effective in decreasing low-back pain? 11. What are the psychological factors influencing outcomes, including duration of pain, intensity of pain, functional outcomes and RTW status, of low-back pain treatment? 12. In patients with acute or chronic low-back pain, what psychosocial/cognitive/emotional or other assessments should be utilized to establish an accurate diagnosis? 5
6 Rehabilitation & Exercise Work Group Clinical Questions 1. In patients undergoing treatment for low-back pain, what is the effectiveness of the following in reducing the duration of pain, intensity of pain, functional outcomes and return to work (RTW), as compared with natural history plus or minus medication: a. Acute versus chronic i. Patient education and self-directed exercise program ii. Spinal manipulative therapy (SMT) iii. Physical agents (eg, heat, cold, ultrasound, electrical stimulation, laser, dry needling, traction, TENS) iv. Acupuncture v. Active stabilization exercise vi. McKenzie exercise (includes directional preference, centralization, and mechanical diagnosis and therapy (MDT) vii. Work hardening or conditioning viii. Bracing 2. Are there specific patient or treatment characteristics that predict improved duration of pain, intensity of pain, functional outcomes and RTW with SMT following an episode of low-back pain? 3. In patients undergoing treatment for low-back pain, what are outcomes, including duration of pain, intensity of pain, functional outcomes and RTW, for exercise therapy alone versus exercise with cognitive behavioral therapy (CBT)? Commented [KR4]: NOTE: SMT defined as spinal manipulative therapy, manual therapy, mobilization, high velocity thrusts 4. In patients undergoing treatment for low-back pain, what are outcomes, including duration of pain, intensity of pain, functional outcomes and RTW, for a lumbar stabilization program versus a general fitness program? 5. In patients undergoing treatment for low-back pain, what are outcomes, including duration of pain, intensity of pain, functional outcomes and RTW, for SMT versus SMT plus active exercise? 6. In patients undergoing treatment for low-back pain, what are the outcomes, including duration of pain, intensity of pain, functional outcomes and RTW, for bed rest versus active exercise/rehabilitation intervention? 7. In patients undergoing treatment for low-back pain, what is the appropriate timing, frequency and duration of treatment with a. Acute versus chronic i. Spinal manipulative therapy (SMT) ii. Physical agents (eg, heat, cold, ultrasound, electrical stimulation, laser, dry needling) iii. Acupuncture iv. Supervised exercise program v. Work hardening or conditioning vi. Yoga 6
7 8. In patients with low-back pain, does a regular exercise program (or pre-surgical intervention with exercise, PT, education) prior to lumbar surgery improve duration of pain, intensity of pain, functional outcomes and RTW compared to those who don t exercise? 9. In patients with low-back pain, does exercise treatment after epidural steroid injections/spinal interventions improve duration of pain, intensity of pain, functional outcomes and RTW compared to injections alone? 10. Following surgery for low-back pain, are outcomes, including duration of pain, intensity of pain, functional outcomes and RTW status, improved with a formal exercise/rehabilitation program versus home instruction plus or minus self-directed exercise program alone? 11. Can a clinical prediction rule determine appropriate indications and predict outcomes, including duration of pain, intensity of pain, functional outcomes and RTW status, for exercise for low-back pain? 7
8 Interventional Treatment Section Clinical Questions 1. In patients with acute or chronic low-back pain, does fluoroscopically guided epidural steroid injections improve duration of pain, intensity of pain, functional outcomes and return to work (RTW)? a. Does the effectiveness vary according to the characteristics of the injectate? b. Does the effectiveness vary with route of administration? 2. In patients with acute or chronic low-back pain, does fluoroscopically guided intra-articular lumbar facet joint injections improve duration of pain, intensity of pain, functional outcomes and RTW? a. Does the effectiveness vary according to the characteristics of the injectate? b. Do the indications for therapeutic facet joint injections vary with the duration of back pain/facet arthropathy? 3. In patients with acute or chronic low-back pain, do medial branch blocks have a role in defining treatment for low-back pain? a. Does duration of pain, intensity of pain, functional outcomes and RTW status vary when candidates for RFN are determined by single vs comparative medial branch blocks? b. Is there a threshold for the magnitude of relief from Dx facet nerve blocks that predict outcomes to RFN? c. Does duration of pain, intensity of pain, functional outcomes and RTW status vary when candidates for RFN are determined by Dx facet nerve blocks vs. intra-articular facet joint injections? 4. In patients with acute or chronic low-back pain due to lumbar facet joint arthropathy, does fluoroscopically guided radiofrequency neurotomy improve duration of pain, intensity of pain, functional outcomes and RTW? 5. In patients with acute or chronic low-back pain, do fluoroscopically guided sacroiliac joint injections improve duration of pain, intensity of pain, functional outcomes and RTW? a. When used therapeutically, does the effectiveness of SIJI vary according to the characteristics of the injectate? b. Does duration of pain, intensity of pain, functional outcomes and RTW status vary when candidates for RFN are determined by single vs. comparative SIJI? c. Is there a benefit to performing lateral branch blocks as compared with interarticular diagnostic injections as a predictor to response to lateral branch RFN? d. Is there a threshold for the magnitude of relief from Dx SIJI that predict improvement in duration of pain, intensity of pain, functional outcomes and RTW from SIJ RFN? 6. In patients with acute or chronic low-back pain emanating from the sacroiliac joint or posterior SIJ complex, does sacroiliac joint radiofrequency neurotomy improve duration of pain, intensity of pain, functional outcomes and RTW? 7. In patients with acute or chronic low-back pain, does spinal cord stimulation improve duration of pain, intensity of pain, functional outcomes and RTW? 8
9 8. In patients with acute or chronic low-back pain, does continuous delivery of intrathecal opioids improve duration of pain, intensity of pain, functional outcomes and RTW? 9. In patients with low back pain, is provocative lumbar discography more accurate than other diagnostic modalities in identifying the disc as the source of pain? 10. In patients with low back pain, is anesthetic lumbar discography more accurate than other diagnostic modalities in identifying the disc as the source of pain? 11. In patients with acute or chronic low-back pain, does intradiscal injection improve duration of pain, intensity of pain, functional outcomes and RTW? 12. In patients with acute or chronic low-back pain, does intradiscal electrothermal therapy improve duration of pain, intensity of pain, functional outcomes and RTW? 13. In patients with acute or chronic low-back pain, do trigger point injections improve duration of pain, intensity of pain, functional outcomes and RTW? Commented [KR5]: Note for literature search: including following search terms- platelet-rich-plasma, stem cell transplantation therapy, oxygen/ozone, methylene blue, corticosteroid, fibrin sealant Commented [KR6]: Note for literature search: include laser therapy 9
10 Surgical Treatment Work Group Clinical Questions 1. In patients with low-back pain, does surgical treatment vs. medical/interventional treatment alone yield better duration of pain, intensity of pain, functional outcomes and return to work (RTW)? 2. In patients with low-back pain, are there predictive factors which determine the benefit of initial treatment with surgical intervention versus initial medical/interventional treatment? Commented [KR7]: The term medical/interventional is meant to encompass pharmacological treatment, physical therapy, exercise therapy, manipulative therapy, modalities, various types of external stimulators and injections. 3. In patients undergoing fusion surgery for low-back pain, which fusion technique results in most improvement in duration of pain, intensity of pain, functional outcomes and RTW? a. Posterolateral fusion without internal fixation vs. b. Posterolateral transverse fusion with internal fixation vs. c. Stand-alone (anterior) interbody fusion vs. d. Transforaminal lumbar interbody fusion (TLIF) or posterior lumbar interbody fusion (PLIF) vs. e. Circumferential fusion (anterior interbody, lateral techniques) 4. In patients undergoing fusion surgery for low-back pain, are clinical outcomes, including duration of pain, intensity of pain, functional outcomes and RTW status, different for multi-level fusions vs. single level fusions? 5. In patients undergoing fusion surgery for low-back pain, does radiographic evidence of fusion correlate with improved duration of pain, intensity of pain, functional outcomes and RTW status? 6. In patients undergoing fusion surgery for low-back pain, does the use of bone growth stimulators (vs. fusion alone) improve duration of pain, intensity of pain, functional outcomes and RTW? 7. In patients undergoing fusion surgery for low back pain, does the use of BMP (vs. fusion alone) improve duration of pain, intensity of pain, functional outcomes and RTW? 8. In patients undergoing fusion surgery for low-back pain, does the use of minimally invasive techniques improve duration of pain, intensity of pain, functional outcomes and RTW compared to open fusion techniques? 9. In patients undergoing surgery for low-back pain, do motion preserving systems (disc prosthesis and dynamic stabilization systems) improve duration of pain, intensity of pain, functional outcomes and RTW compared to fusion surgery? 10. In patients undergoing surgery for low-back pain, do motion preserving systems (disc prosthesis and dynamic stabilization systems) result in lower incidence of symptomatic adjacent segment disease? 11. In patients with low-back pain, does fusion improve duration of pain, intensity of pain, functional outcomes and RTW compared to treatment with: a. Discectomy b. Discectomy plus rhizotomy c. Decompression alone 10
11 Cost-Effectiveness Work Group Clinical Questions Cost Effectiveness of Diagnosis/Screening/General Management Questions 1. What is the most cost-effective spinal care provider for evaluating patients with low back pain: a. Non-physician vs. b. General physician vs. c. Non-surgical spine specialist vs. d. Surgical spine specialist 2. What is the cost-effectiveness of diagnostic imaging studies/workup in the evaluation of low-back pain (acute, subacute, and chronic), in terms of influencing/altering treatment or in terms of leading to successful pain relief? a. X-rays (lumbar standing, lumbar flexion-extension, entire spine) b. CT scan / CT myelogram c. MRI (conventional vs. dynamic/upright/weight bearing) Cost Effectiveness of Medical/Interventional Treatments Questions 3. Are epidural steroid injections (including interlaminar, transforaminal, and caudal injections and selective nerve root blocks) more cost effective in the management of patients with chronic low back pain than other medical/interventional treatments? 4. Is spinal cord stimulation more cost effective in the management of patients with chronic low back pain than other medical/interventional treatments? Commented [KR8]: The term medical/interventional is meant to encompass pharmacological treatment, physical therapy, exercise therapy, manipulative therapy, modalities, various types of external stimulators and injections. 5. Is cognitive or psychological based therapy in the management of patients with chronic low back pain more cost effective than other medical/interventional treatments? 6. Is physical therapy in the management of patients with chronic low back pain more cost effective than other medical/interventional treatments? 7. Is pharmacological management (OTC + prescription medications) for patients with low back pain more or less cost-effective than interventional treatments including physical therapy and injection therapies? 8. Is manipulation in the management of patients with chronic low back pain more cost-effective than other medical/interventional treatments? 9. Is acupuncture based therapy in the management of patients with chronic low back pain more cost effective than other medical/interventional treatments? 10. Are OTC medications only without other medical interventions a more cost effective in the management of patients with chronic low back pain than other medical/interventional treatments 11. With chronic LBP > 6 weeks, is a symptom guided treatment approach using directional preference/centralization matched exercise more cost effective than usual care (Home Care vs. Medication vs Non Specific PT exercise vs Non Specific PT Modalities) long term at 12 months, 36 months? 11
12 Cost Effectiveness of Medical/Interventional Treatment vs. Surgical Treatment Questions 12. Is the surgical management (including fusion and lumbar disc replacement and spinal cord stimulators) of patients with chronic low back pain more cost effective than medical/interventional treatments? 13. Is cognitive or psychological based therapy in the management of patients with chronic low back pain more cost effective than surgical therapies? Cost Effectiveness of Surgical Treatment Questions 14. Are minimally invasive surgical procedures more cost effective in the management of patients with chronic low back pain than conventional open surgical procedures? 15. Is instrumented lumbar fusion more cost-effective compared to non-instrumented fusion for the treatment of patients with low back pain? 12
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Treatments for Common Pain Disorders. Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017
 Treatments for Common Pain Disorders Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017 Acute Disc Herniation Conservative Approach (Four to Six Weeks) Physical Therapy, exercise and gentle
Treatments for Common Pain Disorders Matthew R. Kohler, MD Hudson Spine and Pain Medicine 03/01/2017 Acute Disc Herniation Conservative Approach (Four to Six Weeks) Physical Therapy, exercise and gentle
Discussion Points 10/17/16. Spine Pain is Ubiquitous. Interventional Pain Management
 Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Interventional Pain Management Blake Christensen, D.O. Fellowship Trained Interventional Pain Management Board Eligible in Anesthesiology and Interventional Pain Management Oklahoma Interventional Pain
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Nonsurgical Interventional Treatments for Spinal Pain Management
 Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
Nonsurgical Interventional Treatments for Spinal Pain Management I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Spinal and Trigger Point Injections
 Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
Spinal and Trigger Point Injections I. Policy University Health Alliance (UHA) will reimburse for nonsurgical interventional treatment for subacute and chronic spinal pain when determined to be medically
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice
 The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
Table of Contents: Part 1 General principles. Section 1: Introduction. 1. Past, present and future of interventional physiatry 2.
 Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
Table of Contents: Part 1 General principles Section 1: Introduction 1. Past, present and future of interventional physiatry 2. Epidemiology Section 2: Spinal pain 3. Inflammatory basis of spinal pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Interventional Pain Management. Dr C Hearty 2016
 Interventional Pain Management Dr C Hearty 2016 Introduction Multiple Stakeholders GP Physiotherapy Surgery Radiology Oncology First described in 1899 Von Gaza (procain) Grew out of necessity Heretofore
Interventional Pain Management Dr C Hearty 2016 Introduction Multiple Stakeholders GP Physiotherapy Surgery Radiology Oncology First described in 1899 Von Gaza (procain) Grew out of necessity Heretofore
Chronic Low Back Pain Seminar Patient Engagement. NHS North West London CCGs 6 th February 2017
 Chronic Low Back Pain Seminar Patient Engagement NHS North West London CCGs 6 th February 2017 Aims and Objectives Welcome and introductions Why are we here? To hear patient views as CCGs plan to adopt
Chronic Low Back Pain Seminar Patient Engagement NHS North West London CCGs 6 th February 2017 Aims and Objectives Welcome and introductions Why are we here? To hear patient views as CCGs plan to adopt
PERCUTANEOUS FACET JOINT DENERVATION
 Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Surgery Policy Number: IV-95 Effective Date: 10/22/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Interventional Pain Management
 Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Origination: 5/21/08 Revised: 10/02/17 Annual Review: 11/02/17 Purpose: To provide interventional pain management clinical coordination criteria for the Medical Department staff to reference when making
Facet syndrome in the cervical (upper) spine
 Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Guideline Number: NIA_CG_301 Last Revised Date: March 2018 Responsible Department: Clinical Operations
 Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Magellan Healthcare Clinical guidelines PARAVERTEBRAL FACET JOINT INJECTIONS OR BLOCKS (no U/S) CPT Codes: Cervical Thoracic Region: 64490 (+ 64491, +64492) Lumbar Sacral Region: 64493 (+64494, +64495)
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain: Sacroiliac and Coccydynia Treatments PUM 250-0024-1706 Medical Policy Committee Approval 06/15/18 Effective Date 10/01/18 Prior Authorization Needed Yes Disclaimer:
Medical Affairs Policy Service: Back Pain: Sacroiliac and Coccydynia Treatments PUM 250-0024-1706 Medical Policy Committee Approval 06/15/18 Effective Date 10/01/18 Prior Authorization Needed Yes Disclaimer:
2/5/2019. Facet Joint Pain. Biomechanics
 Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Facet Arthropathy as a Pain Source Evaluation and Management Shelby Spine Jan 31 st Feb 2 nd, 2019 Kushagra Verma MD, MS Adult and Pediatric Scoliosis And Spine Deformity Beach Orthopaedics Specialty Institute
Management of Neuropathic pain
 Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Management of Neuropathic pain Ravi Parekodi Consultant in Anaesthetics and Pain Management 08/04/2014 Ref: BJA July2013, Map of Medicine2013, Pain Physician 2007, IASP 2012, Nice guideline 2013 Aims Highlight
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group. Policies for the Commissioning of Healthcare
 Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Blackburn with Darwen Clinical Commissioning Group and East Lancashire Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for Managing Back Pain Spinal /Facet Joint and Epidural
Orthopedic Coding Changes for 2012
 Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Orthopedic Coding Changes for Lynn M. Anderanin, CPC,CPC-I, COSC Vertebroplasty 22520- Percutaneous vertebroplasty, 1 vertebral body, unilateral or bilateral injection; thoracic 22520- Percutaneous vertebroplasty,
Regional Pain Syndromes: Neck and Low Back
 Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Regional Pain Syndromes: Neck and Low Back Srinivas Nalamachu, MD Disclosures Consultant/Independent Contractor/Honoraria: Ferring 1 Learning Objectives Identify the most common painful conditions in the
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Cover page DRAFT PROCEDURAL PAIN MANAGEMENT
 Cover page DRAFT PROCEDURAL PAIN MANAGEMENT 3 April 2018 Please find attached the DRAFT privileges for PROCEDURAL (INTERVENTIONAL) PAIN MANAGEMENT. THE PANEL: This draft was developed by a provincial panel
Cover page DRAFT PROCEDURAL PAIN MANAGEMENT 3 April 2018 Please find attached the DRAFT privileges for PROCEDURAL (INTERVENTIONAL) PAIN MANAGEMENT. THE PANEL: This draft was developed by a provincial panel
22110 vertebral segment; cervical vertebral segment; thoracic vertebral segment; lumbar
 The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
The following codes are authorized by Palladian Health for applicable product lines. Visit palladianhealth.com to request authorization and to access guidelines. Palladian Musculoskeletal Program Codes
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
This evidence-informed guideline is for non-specific, non-malignant low back pain in adults only
 A Summary of the Guideline for the Evidence-Informed Primary Care Management of Low Back Pain This evidence-informed guideline is for non-specific, non-malignant low back pain in adults only Red Flags
A Summary of the Guideline for the Evidence-Informed Primary Care Management of Low Back Pain This evidence-informed guideline is for non-specific, non-malignant low back pain in adults only Red Flags
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Outline. Introduction / Epidemiology. Anatomy / Pain generators. Diagnosis. Treatment. Most Important lecture!!
 Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
Acute Low Back Pain Outline Introduction / Epidemiology. Most Important lecture!! Anatomy / Pain generators Diagnosis Treatment Course Objectives Know the RED FLAGS in history taking. Know the Pain Generators
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Non-Operative Management of Low Back Pain in the Elderly
 www.4-no-pain.com Non-Operative Management of Low Back Pain in the Elderly Brian Kahan, D.O., FAAPMR Low Back Pain Outline Etiologies Initial Assessment Physical examination and Diagnostic work-up Clinical
www.4-no-pain.com Non-Operative Management of Low Back Pain in the Elderly Brian Kahan, D.O., FAAPMR Low Back Pain Outline Etiologies Initial Assessment Physical examination and Diagnostic work-up Clinical
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN
 EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN UnitedHealthcare Oxford Clinical Policy Policy Number: PAIN 019.21 T2 Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
EPIDURAL STEROID AND FACET INJECTIONS FOR SPINAL PAIN UnitedHealthcare Oxford Clinical Policy Policy Number: PAIN 019.21 T2 Effective Date: October 1, 2017 Table of Contents Page INSTRUCTIONS FOR USE...
Facet Joint Syndrome / Arthritis
 Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Facet Joint Syndrome / Arthritis Overview Facet joint syndrome is an arthritis-like condition of the spine that can be a significant source of back and neck pain. It is caused by degenerative changes to
Study Design: Prospective observational study of cervical transforaminal epidural steroid injections in patients with cervical radicular pain
 Study Design: Prospective observational study of cervical transforaminal epidural steroid injections in patients with cervical radicular pain Background and Significance To be completed by the project
Study Design: Prospective observational study of cervical transforaminal epidural steroid injections in patients with cervical radicular pain Background and Significance To be completed by the project
Karachi Spine - Pain and Minimally Invasive Spine Surgery Workshop. Lumbar Injections For Diagnosis and Treatment. Pain Management
 Lumbar Injections For Diagnosis and Treatment Pain Management Ovidiu Nicolae Palea Centrul de Diagnostic si Tratament ProVita Anesthesiology and Intensive Care 2009 decided to focus on Pain Management
Lumbar Injections For Diagnosis and Treatment Pain Management Ovidiu Nicolae Palea Centrul de Diagnostic si Tratament ProVita Anesthesiology and Intensive Care 2009 decided to focus on Pain Management
Interventional Pain. Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care
 Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
Interventional Pain Judith Dunipace MD Board certified in Anesthesiology, Pain Management and Hospice and Palliative Care IASP Definition of Pain Pain is an unpleasant sensory or emotional experience associated
2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves
 2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves Joseph S. Cheng, M.D., M.S. Associate Professor of Neurological Surgery, Orthopedic Surgery, and Rehabilitation
2012 CPT Coding Update AANS/CNS Joint Section on Disorders of the Spine and Peripheral Nerves Joseph S. Cheng, M.D., M.S. Associate Professor of Neurological Surgery, Orthopedic Surgery, and Rehabilitation
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
Basic Standards for. Fellowship Training in. Acute and Chronic Pain Management. in Anesthesiology
 Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Basic Standards for Fellowship Training in Acute and Chronic Pain Management in Anesthesiology American Osteopathic Association and American Osteopathic College of Anesthesiologists BOT, 7/1995 BOT, 11/2002
Interventional Pain Management
 Spinal Injections Can be beneficial for both chronic and acute pain depending on pathology Contraindications: Patient refusal Active infection Platelets less than 75 or inability to stop anticoagulation
Spinal Injections Can be beneficial for both chronic and acute pain depending on pathology Contraindications: Patient refusal Active infection Platelets less than 75 or inability to stop anticoagulation
GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE. A Guide for Patients
 GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE A Guide for Patients Your Spine Deserves Special Care Your spine is at the center of a delicately balanced system that controls all of your body s movements.
GET BACK TO YOUR FUTURE WITH SPECIALIZED SPINE CARE A Guide for Patients Your Spine Deserves Special Care Your spine is at the center of a delicately balanced system that controls all of your body s movements.
Thoracolumbar Spine Conditions: Treatment and Return to Play
 Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Thoracolumbar Spine Conditions: Treatment and Return to Play C H R I S T O P H E R B U R K S, MD B I E N V I L L E O R T H O P A E D I C S P E C I A L I S T S O C E A N S P R I N G S, MS Thoracolumbar
Study Design: Prospective observational study of cervical interlaminar injection of steroid in patients with cervical radicular pain
 Study Design: Prospective observational study of cervical interlaminar injection of steroid in patients with cervical radicular pain Background and Significance To be completed by the project s Principal
Study Design: Prospective observational study of cervical interlaminar injection of steroid in patients with cervical radicular pain Background and Significance To be completed by the project s Principal
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acetaminophen, in neck pain, 505 506 Acupuncture, chi and, 524 for mechanical neck disorders, 525 in neck pain, 524 525 safety of, 525 Adson
Note: Page numbers of article titles are in boldface type. A Acetaminophen, in neck pain, 505 506 Acupuncture, chi and, 524 for mechanical neck disorders, 525 in neck pain, 524 525 safety of, 525 Adson
Kevin S. Ladin, M.D. Board Certified in Physical Medicine & Rehabilitation ABMS Subspecialty Board Certified in Pain Medicine
 Kevin S. Ladin, M.D. Board Certified in Physical Medicine & Rehabilitation ABMS Subspecialty Board Certified in Pain Medicine kslmd@cox.net EBM in Pain Medicine Evidence-based medicine (EBM) is a form
Kevin S. Ladin, M.D. Board Certified in Physical Medicine & Rehabilitation ABMS Subspecialty Board Certified in Pain Medicine kslmd@cox.net EBM in Pain Medicine Evidence-based medicine (EBM) is a form
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Regions Hospital Delineation of Privileges Pain Medicine
 Regions Hospital Delineation of s Pain Medicine Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Regions Hospital Delineation of s Pain Medicine Applicant s Name: Last First M. Instructions: Place a check-mark where indicated for each core group you are requesting. Review education and basic formal
Evidence-based Clinical Practice Guidelines on Management of Pain in Older People Aza Abdulla, Margaret Bone, Nicola Adams, Alison M.
 Evidence-based Clinical Practice Guidelines on Management of Pain in Older People Aza Abdulla, Margaret Bone, Nicola Adams, Alison M. Elliott, Derek Jones, Roger Knaggs, Denis Martin, Elizabeth L. Sampson,
Evidence-based Clinical Practice Guidelines on Management of Pain in Older People Aza Abdulla, Margaret Bone, Nicola Adams, Alison M. Elliott, Derek Jones, Roger Knaggs, Denis Martin, Elizabeth L. Sampson,
Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center
 Oh My Aching Back! Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center Epidemiology 90% of episodes of LBP resolves
Oh My Aching Back! Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center Epidemiology 90% of episodes of LBP resolves
Are you getting the best treatment for your low back pain?
 Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
Are you getting the best treatment for your low back pain? Dr.Rahimian Orthopedic surgon Spine fellowship resident Why are we here? To update you on the best evidence for the treatments available To give
SpineFAQs. Neck Pain Diagnosis and Treatment
 SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
SpineFAQs Neck Pain Diagnosis and Treatment Neck pain is a common reason people visit their doctor. Neck pain typically doesn't start from a single injury. Instead, the problem usually develops over time
Placename CCG. Policies for the Commissioning of Healthcare. Policy for Managing Back Pain- Spinal Injections
 Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
Placename CCG Policies for the Commissioning of Healthcare Policy for Managing Back Pain- Spinal Injections 1 Introduction 1.1 This document is part of a suite of policies that the CCG uses to drive its
North American Spine Society Public Education Series
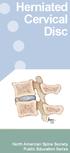 Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
Herniated Cervical Disc North American Spine Society Public Education Series What Is a Herniated Disc? The backbone, or spine, is composed of a series of connected bones called vertebrae. The vertebrae
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Roger Chou, MD John Loeser, MD Rick Rosenquist, MD Steve Stanos, DO (moderator)
 Evidence-based Medicine for Evaluation and Management of Low Back Pain: Update on Guidelines from the American Pain Society Richard W. Rosenquist, MD For the American Pain Society Low Back Pain Guidelines
Evidence-based Medicine for Evaluation and Management of Low Back Pain: Update on Guidelines from the American Pain Society Richard W. Rosenquist, MD For the American Pain Society Low Back Pain Guidelines
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Clinical Reference Guide
 Clinical Reference Guide Table of Clinical References PREVALENCE Bernard, 1987 Cohen, 2005 Weksler, 2007 Sembrano, 2009 POST LUMBAR FUSION Maigne, 2005 Ha, 2008 Ivanov, 2009 Liliang, 2011 DePalma, 2011
Clinical Reference Guide Table of Clinical References PREVALENCE Bernard, 1987 Cohen, 2005 Weksler, 2007 Sembrano, 2009 POST LUMBAR FUSION Maigne, 2005 Ha, 2008 Ivanov, 2009 Liliang, 2011 DePalma, 2011
PRECISE DIAGNOSIS AND TREATMENT OF NECK AND BACK PAIN
 PRECISE DIAGNOSIS AND TREATMENT OF NECK AND BACK PAIN MEDICAL DIRECTOR Elgin, Itasca, Lake Barrington, McHenry, Libertyville, Huntley, Elmhurst John V. Prunskis M.D. FIPP JOHN V. PRUNSKIS Illinois M.D.
PRECISE DIAGNOSIS AND TREATMENT OF NECK AND BACK PAIN MEDICAL DIRECTOR Elgin, Itasca, Lake Barrington, McHenry, Libertyville, Huntley, Elmhurst John V. Prunskis M.D. FIPP JOHN V. PRUNSKIS Illinois M.D.
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: facet_joint_denervation 6/2009 4/2017 4/2018 4/2017 Description of Procedure or Service Facet joint denervation
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: facet_joint_denervation 6/2009 4/2017 4/2018 4/2017 Description of Procedure or Service Facet joint denervation
UCSD DEPARTMENT OF ANESTHESIOLOGY
 UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
UCSD DEPARTMENT OF ANESTHESIOLOGY LEARNING OBJECTIVES FOR ADVANCED PAIN MEDICINE ROTATION, UCSD MEDICAL CENTER Competencies Objective Learning Environment Instructional Method Assessment Tool Patient Care:
Chapter 4 describes the results of systematic literature review of the diagnostic validity
 Summary The main aim of this thesis was to contribute to the diagnostics of SI joint pain. We performed anatomical and clinical research next to a systematic literature review regarding diagnostic criteria
Summary The main aim of this thesis was to contribute to the diagnostics of SI joint pain. We performed anatomical and clinical research next to a systematic literature review regarding diagnostic criteria
Adult Isthmic Spondylolisthesis
 Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Adult Isthmic Spondylolisthesis North American Spine Society Public Education Series What Is Adult Isthmic Spondylolisthesis? The spine is made up of a series of connected bones called vertebrae. In about
Medical Affairs Policy
 Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Medical Affairs Policy Service: Back Pain Procedures-Epidural Injection (Caudal Epidural, Selective Nerve Root Block, Interlaminar, Transforaminal, Translaminar Epidural Injection) PUM 250-0015-1706 Medical
Acute Low Back Pain. North American Spine Society Public Education Series
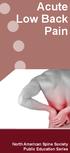 Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Acute Low Back Pain North American Spine Society Public Education Series What Is Acute Low Back Pain? Acute low back pain (LBP) is defined as low back pain present for up to six weeks. It may be experienced
Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers
 In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia
 Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Disclosure & Acknowledgment Getting at the CORE of Low-back pain Treatment Dr. John Flannery Dr. Carlo Ammendolia Disclosures - None Acknowledgements Dr. Andrea Furlan Dr. Julia Alleyne Dr. Hamilton Hall
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
10/8/2015. Consultant for Boston Scientific-no conflicts with this presentation
 Consultant for Boston Scientific-no conflicts with this presentation Mehul Sekhadia, DO Medical Director Advocate Lutheran General Hospital Park Ridge, IL Identify when to consider interventional pain
Consultant for Boston Scientific-no conflicts with this presentation Mehul Sekhadia, DO Medical Director Advocate Lutheran General Hospital Park Ridge, IL Identify when to consider interventional pain
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA Mailstop: CA
 To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
To: Manuel Suarez, M.D. Medical Director Neighborhood Health Plan Management Department 5757 Plaza Dr. Cyprus, CA 30630 Mailstop: CA124-01290 Subject: Denial of Cervical Spinal Injection Procedures Dear
Spinal Interventional Pain Management and Lumbar Spine Surgery
 Spinal Interventional Pain Management and Lumbar Spine Surgery Policy Number: Original Effective Date: MM.06.024 01/01/2014 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 08/22/2014
Spinal Interventional Pain Management and Lumbar Spine Surgery Policy Number: Original Effective Date: MM.06.024 01/01/2014 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 08/22/2014
2016 OPAM Mid-Year Educational Conference, sponsored by AOCOPM Thursday, March 10, 2016 C-1
 Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
Long-term Outcomes of Lumbar Fusion Among Workers Compensation Subjects : An Historical Cohort Study Trang Nguyen M.D., Ph.D. David C. Randolph M.D, M.P.H. James Talmage MD Paul Succop PhD Russell Travis
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Cox Technic Case Report #126 published at (sent December 2013 ) 1
 Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Cox Technic Case Report #126 published at www.coxtechnic.com (sent December 2013 ) 1 Cox Technic Decompression Spinal Manipulation Resolves Symptoms Associated with Disc Protrusion and S1 Radiculopathy,
Management of Spinal Pain
 Management of Spinal Pain Frequently Asked Questions For GPs and Clinicians Planned Procedures with a Threshold Policy Implementation V4 June 2018 1 FAQ Low Back Pain Policy Implementation_V4_June2018
Management of Spinal Pain Frequently Asked Questions For GPs and Clinicians Planned Procedures with a Threshold Policy Implementation V4 June 2018 1 FAQ Low Back Pain Policy Implementation_V4_June2018
Multidisciplinary Approach to Spine Care. Roland Kent, MD Axis Spine Center Post Falls, Idaho
 Multidisciplinary Approach to Spine Care Roland Kent, MD Axis Spine Center Post Falls, Idaho Objectives Epidemiology of chronic pain Pain as a disease What is multidisciplinary pain management (MDPM) Discuss
Multidisciplinary Approach to Spine Care Roland Kent, MD Axis Spine Center Post Falls, Idaho Objectives Epidemiology of chronic pain Pain as a disease What is multidisciplinary pain management (MDPM) Discuss
Back and Neck Injuries: Surgical Advances and Treatment
 Back and Neck Injuries: Surgical Advances and Treatment Ara Deukmedjian, MD Board Certified Neurosurgeon June 8, 2017 1 2 Spinal Joints: Anatomy Two types of Spinal Joints: Spinal (intervertebral) disc
Back and Neck Injuries: Surgical Advances and Treatment Ara Deukmedjian, MD Board Certified Neurosurgeon June 8, 2017 1 2 Spinal Joints: Anatomy Two types of Spinal Joints: Spinal (intervertebral) disc
Low back pain in a Nutshell Paul Manjaly. Paul Manjaly
 Low back pain in a Nutshell Paul Manjaly Paul Manjaly Pain: An unpleasant sensory and emotional experience which follows actual or potential tissue damage or is described in terms of such damage Unpleasant
Low back pain in a Nutshell Paul Manjaly Paul Manjaly Pain: An unpleasant sensory and emotional experience which follows actual or potential tissue damage or is described in terms of such damage Unpleasant
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18
 Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: MED Policy No: 391 Medical Policy Committee Approved Date: 6/17; 12/18 1/1/2019 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management.
 River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
River North Pain Management Consultants, S.C., Axel Vargas, M.D., Regional Anesthesiology and Interventional Pain Management. Chicago, Illinois, 60611 Phone: (888) 951-6471 Fax: (888) 961-6471 Clinical
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
DRAFT as posted for public comment 11/8/2016 to 8 a.m. 12/9/2016. HERC Coverage Guidance
 HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
HEALTH EVIDENCE REVIEW COMMISSION (HERC) COVERAGE GUIDANCE: LOW BACK PAIN - CORTICOSTEROID INJECTIONS HERC Coverage Guidance Corticosteroid injections (including epidural, facet joint, medial branch, and
MEDICAL POLICY EFFECTIVE DATE: 08/15/13 REVISED DATE: 07/17/14 SUBJECT: SPINAL INJECTIONS (EPIDURAL AND FACET INJECTIONS) FOR PAIN MANAGEMENT
 MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY SUBJECT: SPINAL INJECTIONS (EPIDURAL AND PAGE: 1 OF: 7 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Examination of the lumbosacral spine. Dr Lucy Holtzhausen Rotorua GP CME June 2015
 Examination of the lumbosacral spine Dr Lucy Holtzhausen Rotorua GP CME June 2015 Diagnostic Algorithm Presenting symptoms Diagnostic decisions Diagnostic triage LOW BACK PAIN Mechanical NON-SPECIFIC LBP
Examination of the lumbosacral spine Dr Lucy Holtzhausen Rotorua GP CME June 2015 Diagnostic Algorithm Presenting symptoms Diagnostic decisions Diagnostic triage LOW BACK PAIN Mechanical NON-SPECIFIC LBP
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Adhesiolysis Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Adhesiolysis Please check the indication (reason)
American Board of Anesthesiology Pain Medicine Content Outline January 2010
 American Board of Anesthesiology Pain Medicine Content Outline January 2010 Table of Contents 01 General... 2 02 Assessment and Psychology of Pain... 3 03 Treatment of Pain A Pharmacokinetics, pharmacodynamics,
American Board of Anesthesiology Pain Medicine Content Outline January 2010 Table of Contents 01 General... 2 02 Assessment and Psychology of Pain... 3 03 Treatment of Pain A Pharmacokinetics, pharmacodynamics,
Vijay Singh, M.D Roosevelt Rd., Niagara, WI 54151
 Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
Publications and Book Chapters Vijay Singh, M.D. 1601 Roosevelt Rd., Niagara, WI 54151 PUBLICATIONS Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 Jul-Aug 2012 July 2012 July 2012 May-Jun 2012 May-Jun
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
