PAPER. High Morbidity of Enterostomy and Its Closure in Premature Infants With Necrotizing Enterocolitis
|
|
|
- Delilah Jordan
- 5 years ago
- Views:
Transcription
1 High Morbidity of Enterostomy and Its Closure in Premature Infants With Necrotizing Enterocolitis Ann O Connor, MD; Robert S. Sawin, MD PAPER Objective: To review the morbidity and mortality among 68 premature infants treated with enterostomy for necrotizing enterocolitis. Design: Data were collected retrospectively from hospital medical records to include the period between January 1, 1987, and September 30, Setting: Tertiary care children s hospital. Patients: A group of 68 infants aged 2 to 35 days (mean age, 12.5 days), weighing 1500 g or less, with necrotizing enterocolitis necessitating surgical enterostomy for treatment. Interventions: Creation of any enterostomy during exploratory laparotomy for necrotizing enterocolitis and subsequent closure. Main Outcome Measures: Morbidity and mortality associated with infant enterostomy and its closure. Results: Thirty-nine infants underwent ileostomy with mucous fistula, 16 underwent ileostomy with a Hartmann pouch, 7 had jejunostomy with mucous fistula, 2 had colostomy with mucous fistula, and 4 had colostomy with a Hartmann pouch. Eighteen (26%) of the 68 infants died in the postoperative period of sepsis (n = 10), continuing necrotizing enterocolitis (n = 5), or respiratory distress (n = 3). Of the remaining 50 infants, complications developed in 34 (68%). These complications included strictures requiring further resection at the time of enterostomy closure in 20 infants; stricture of the enterostomy requiring surgical revision in 6; incisional hernia in 3; parastomal hernia in 4; enterostomal prolapse or intussusception in 6 and 1, respectively; wound dehiscence in 4; wound infection in 8; small-bowel obstruction requiring laparotomy in 2; and anastomotic complications in 2. Only 16 enterostomies were closed uneventfully, with 3 of these infants subsequently dying of sudden infant death syndrome between 6 and 8 months after the operation. Of the surviving infants, 3 (6%) continue to require home hyperalimentation. Conclusions: Although enterostomy in infants with low birth weight with necrotizing enterocolitis may be lifesaving, it is also a major cause of morbidity. These data suggest the feasibility of a prospective study comparing resection and primary anastomosis with resection and enterostomy. Arch Surg. 1998;133: From the Department of Surgery, Children s Hospital and Regional Medical Center, University of Washington School of Medicine, Seattle. PREMATURE NEONATES undergoing surgical intervention for necrotizing enterocolitis (NEC) are undoubtedly among the most critically ill infants treated by pediatric surgeons. The resection of necrotic intestine with the creation of an enterostomy has been the accepted surgical therapy for NEC for many years. 1-3 Although most authors agree that an enterostomy in patients with NEC can be lifesaving, others have suggested the use of primary anastomosis, 4,5 drainage without resection, 6 or even enterostomy without resection 7 as superior methods. Few studies have reviewed the morbidity and mortality of enterostomy among premature infants with NEC. To determine the standard against which alternative surgical treatment of NEC can be compared, we retrospectively reviewed our surgical experience with enterostomy and its closure in premature infants with NEC during 10 years 10 months. RESULTS Seventy infants weighing 1500 g or less underwent exploratory laparotomy for NEC during the nearly 11-year review period. Two infants (3%) did not undergo resection due to NEC totalis. Of the remaining 68 infants, 18 (26%) died in the immediate postoperative period (day 0-30). Deaths were attributed to sepsis with multiple organ failure and disseminated intra- 875
2 PATIENTS AND METHODS From January 1, 1987, to September 30, 1997, 148 infants required laparotomy for the treatment of NEC. Twenty of these infants underwent resection with primary anastomosis, and the remaining 128 infants had resection with enterostomy. Sixty-eight (53.1%) of these 128 infants weighed 1500 g or less (mean, 1097 g) and were the population studied. A retrospective review of all available medical records was performed to obtain as much follow-up information as possible. The patients undergoing enterostomy were evaluated for a number of complications, shown in the following table. Complication Patients, No. Postoperative death 18 SIDS 3 Ileostomy stricture 6 Distal stricture 20 Anastomotic stricture 1 Anastomotic leak 1 Parastoma hernia (ileostomy) 4 Incisional hernia 3 Ileostomy prolapse 6 Wound infection 8 Wound dehiscence 4 Ileostomy intussusception 1 Small-bowel obstruction 2 (SIDS indicates sudden infant death syndrome.) Infants ranged in age from 2 to 35 days (mean, 12.5 days) at the time of the initial resection. All infants were of less than 36 weeks gestation, with 9 (13%) being of 32 to 36 weeks gestation, 34 (50%) being of 28 to 31 weeks gestation, and 25 (37%) being of 24 to 27 weeks gestation. There was an equal distribution of male to female infants (31:37). Fifteen infants (22%) had concomitant anomalies, including patent ductus arteriosus, aortic coarctation, pulmonary atresia, tetralogy of Fallot, endocardial septal defects, duodenal atresia, and trisomy 21. Thirtyeight infants (56%) were also products of high-risk pregnancies, including young age ( 16 years old), women without prenatal care, women requiring urgent delivery (placental abruption, placenta previa, and eclampsia), and women addicted to narcotics or alcohol. Thirty-four infants (50%) had substantial infant respiratory tract disease requiring prolonged ventilation therapy (defined as 7 days), with 1 infant requiring home ventilator therapy before and after enterostomy closure. Serum albumin levels before resection and enterostomy were measured in 58 infants (85%) to estimate their nutritional status and ranged from 4 to 30 g/l (mean, 18 g/l), with reference levels in our institution ranging from 29 to 55 g/l. Seventy-two infants underwent enterostomy at various levels based on the distribution of disease. Enterostomy Level Patients, No. Ileostomy with mucous fistula 39 Ileostomy with Hartmann pouch 16 Jejunostomy with mucous fistula 9* Colostomy with mucous fistula 2 Colostomy with Hartmann pouch 4 No resection 2 (Asterisk indicates that 2 infants required multiple simultaneous enterostomies.) Forty-five infants (66%) had evidence of perforation at the time of the initial resection. Most functional enterostomies were exteriorized at a point separate from the laparotomy incision, whereas most mucous fistulas were exteriorized through the edge of the laparotomy incision. The decision to create either a distal mucous fistula or a Hartmann pouch was made based on the ability to create the mucous fistula without sacrificing additional bowel length. Fifty infants survived until the time of enterostomy closure and ranged in age from 1.5 to 20 months (mean, 5 months). Albumin levels were measured in only 19 (38%) infants at the time of enterostomy closure and ranged from 10 to 48 g/l (mean, 31 g/l). In general, albumin levels at the time of enterostomy closure were measured only in infants who either continued to require hyperalimentation (n = 8) or were still in the hospital (n = 11). The average weight gain for the 50 infants who survived to enterostomy closure was 2.4 kg. The enterostomies were closed when the infants were medically stable or when the respiratory status was maximized. In 6 infants, enterostomies were closed early because of problems of high stomal output or poor weight gain. Closure was always preceded by a contrast study to ensure distal bowel patency and was usually accomplished by a single-layer, end-to-end anastomosis with a small, nonabsorbable suture. vascular coagulation (n = 10), continued NEC with total remaining bowel necrosis (n = 5), or infant respiratory distress primarily due to prematurity (n = 3). Three infants (4%) died of SIDS between 6 and 8 months following enterostomy closure, making the overall mortality of 31% for the entire group of patients. There were no deaths as a direct result of enterostomy or its closure. Eight infants continued to require hyperalimentation (mean of 41 days) at the time of enterostomy closure. Three infants were successfully weaned off home hyperalimentation following enterostomy closure, with only 3 requiring home hyperalimentation due to shortgut syndrome. Of the 3 infants who died of SIDS following enterostomy closure, 2 had been receiving home hyperalimentation at the time of their death. After intestinal continuity was restored and bowel function had resumed, enteral feedings were begun between 3 and 11 days (mean, 4 days). At the time of the initial resection, the distribution of disease was recorded (Figure 1), as was the distribution of perforations. Disease was frequently distributed in more than 1 region. Forty-five patients (66%) had evidence of perforation at the time of the initial exploration, most of whom had gross peritoneal contamination. Perforations were frequently multiple and predominantly in the ileum and the ascending colon (Figure 2). Of the 18 patients who died in the postoperative period, 11 (61%) had multiple free perforations in several locations at the time of resection (as did all 3 infants who died of SIDS). Despite having similar disease distribution and severity, none of the infants who underwent un- 876
3 Table 1. Enterostomal Complications by Level Jejunum Ileum 15% 83% 63% Figure 1. Distribution of disease at the time of resection. 3% 46% 28% 23% Complication by Level (Total No. Created) No. of Events Ileostomy (55) Stricture with repair 6 Prolapse 6 Intussusception 1 Wound infection 2 Wound dehiscence 2 Small bowel obstruction 1 Distal stricture 16 Incisional hernia 2 Parastomal hernia 4 Total, No. (%) 40 (73) Colostomy (6) Wound infection 4 Distal stricture 1 Total, No. (%) 5 (83) Jejunostomy (9) Distal stricture 3 Incisional hernia 1 Wound infection 2 Wound dehiscence 2 Small bowel obstruction 1 Total, No. (%) 9 (100) Ileum Jejunum 58% 53% 9% Figure 2. Distribution of perforations at the time of resection. 36% 24% eventful enterostomy and closure had perforated NEC at the time of the initial resection. Only 16 infants (24%) underwent uneventful enterostomy and closure, with complications developing in 34 (68%) of the 50 infants who had survived until the time of enterostomy closure (Table 1). Many infants had more than 1 complication. Distal stricture developed in 20 infants (29%), predominantly (80%) among infants who required an ileostomy (Table 2). These strictures were always in the colon and were discovered by contrast studies before the enterostomy closure. Of the 55 ileostomies created, 6 (11%) developed a subsequent stomal stricture that required operative repair, usually following several failed attempts to dilate the ileostomy. Ten ileostomies (18%) required dilatation but no operative repair. No enterostomal strictures developed in those created at the jejunal or colonic level. Parastomal hernias requiring repair developed in 4 patients (6%). All of these hernias were among infants with ileostomies and occurred at the enterostomy only, regardless of whether a mucous fistula was created. All 6 (9%) of the prolapsed enterostomies and the single intussuscepted enterostomy were also limited to infants with ileostomies, and all of these patients had concomitant distal mucous fistulae (Table 2). None of the distal mucous fistulae underwent retraction. Complications with the laparotomy incision developed in 15 infants (22%). In 3 infants, incisional hernias developed that were repaired at the time of the ileostomy closure. Eight infants had wound infections that were treated with dressing changes and antibiotics. Four of the wound infections developed in infants who had a colostomy and a distal mucous fistula, 2 in patients with a jejunostomy and mucous fistula and 2 in patients with ileostomies (1 with a mucous fistula and 1 without). Wound dehiscence requiring operative repair developed in 4 infants, all of whom later died of multiple organ failure and sepsis. The incidence of wound dehiscence was evenly distributed among infants with an ileostomy and those with a jejunostomy. Small-bowel obstruction developed in only 2 patients, 11 and 18 months, respectively, after the enterostomy closure. Both patients had previously had multiple enterostomies at the jejunal level with distal mucous fistulae for the treatment of NEC. Both patients required adhesiolysis without further bowel resection and have remained well. Anastomotic complications developed in 2 infants after enterostomy closure. One infant required reoperation 10 days after the initial operation due to stricture formation, and another was reexplored 3 days postoperatively 877
4 Table 2. Enterostomal Complications by Location in 68 Premature Infants With Necrotizing Enterocolitis Complications, No. (%) Enterostomy Stomal Stricture Distal Stricture Hernia Prolapse Intussusception Ileostomy with mucous fistula 4 (67) 10 (50) 2 (50) 6 (100) 1 (100) Ileostomy with Hartmann pouch 27 (33) 6 (30) 2 (50) 0 (0) 0 (0) Jejunostomy with mucous fistula 0 (0) 3 (15) 0 (0) 0 (0) 0 (0) Colostomy with mucous fistula 0 (0) 0 (0) 0 (0) 0 (0) 0 (0) Colostomy with Hartmann pouch 0 (0) 1 (5) 0 (0) 0 (0) 0 (0) due to disruption of the anastomosis. This latter infant had been receiving parenteral steroid therapy because of his poor respiratory status at the time of the anastomosis but did well after the disruption was repaired. The percentage of complications as a function of disease distribution at the time of resection demonstrates that most infants who died in the immediate postoperative period had ileal (95% [n = 17]), ascending colon (67% [n = 12]), and transverse colon (57% [n = 10]) disease, with disease distributed less frequently in the jejunum and distal colon. The same pattern of disease distribution applies to nearly all the other complications listed, with the exception of wound infections, which appeared more frequently associated with colonic NEC. COMMENT ThestandardsurgicaltherapyforprematureinfantswithNEC has long been the resection of necrotic intestine with enterostomy for both decompression and diversion. 1-3,8-11 Debate continues in the literature 4,5,8,12 regarding the technique of resection and primary anastomosis for infants with NEC, although primary anastomosis remains inherently attractive. Objections to resection and primary anastomosis are multiple 6,11 and include the fear of increased anastomotic complications, the resection of more bowel than necessary, and the concept of enterostomal decompression until an optimal weight has been maintained before intestinal continuity is restored. Our series of premature infants with NEC treated with resection and enterostomy demonstrates that although enterostomal decompression may be lifesaving, it is not without significant morbidity and mortality. This series shows a mortality of 26% in the immediate postoperative period, which is similar to rates described by other authors. 1,4,5,7,8,11 Most infants had disease distributed predominantly in the ileum and ascending colon, which is also consistent with other reports. Accordingly, perforations were most common in the ileum and ascending colon. The observed mortality of 24% among infants with intestinal perforation did not differ significantly from that for infants without perforation (26%). None of the infants who underwent treatment without complication had perforation at the time of the initial resection, implying that whereas the mortality is not different, perforation may be a prediction of increased morbidity. Most striking in this series is the high complication rate observed among infants treated with enterostomy. Our seriesconfirmsmanyauthors 1-3,7,9,10 observationthat the most common complication of enterostomy is distal bowel stricture. Our observed distal stricture rate of 40% is similar to the published stricture rate of 38% 12 among infants evaluated with contrast studies following nonoperative treatment of NEC. Half of the strictures found in the medically treated patients with NEC were asymptomatic and not treated. 12 In our series, all distal strictures were resected at the time of anastomosis, and therefore, the prospective use of contrast studiesinfluencedthesurgicalmanagementofthesepatients. Perhaps strictures are less likely to resolve among infants with more severe NEC treated with enterostomy. Distal strictures were found predominantly among infants who were treated with an ileostomy. The percentage of distal strictures in these infants did not differ significantly between those who had a distal mucous fistula (50% [n = 10]) and those who did not (30% [n = 6]). The strictures were located in the descending and rectosigmoid colon almost exclusively, implying that NEC may cause continued damage in those areas of intestine that are deemed grossly free of disease at the time of resection. It is also possible that the blood supply to the remaining distal bowel is tenuous, resulting in ischemia and subsequent stricture formation. Perhaps the early restoration of intestinal continuity provides intrinsic dilatation due to fecal boluses or encourages the trophic effects of feedings and succus entericus. The timing of enterostomy closure among infants with NEC is debated, 3 and our data support the need to investigate further the role of early restoration of continuity with regard to the rate of distal stricture. The creation of an ileostomy, either with or without a distal mucous fistula, proved to be a morbid procedure. Ileostomy complications have been reported, 9,10 but our series reports a markedly higher rate. Of the 55 ileostomies, 6 (11%) developed stricture and required revision after failed attempts at dilation. Half of these infants underwent anastomosis at that time, which was generally considered sooner than planned. Prolapse occurred in 6 (11%) of the 55 ileostomies, all of which were repaired at the time of anastomosis. The only intussuscepted ileostomy (which was a case of prolapse severe enough to result in complete obstruction) required urgent exploration and the resection of approximately 5 cm of distal ileum in addition to an anastomosis. Four parastomal hernias occurred in this group, with all of them repaired electively at the time of anastomosis. When wound infection (n = 2), wound dehiscence (n = 2), small-bowel obstruction (n = 1), incisional hernia (n = 2), and distal stricture (n = 16) are included with the aforementioned complications, the total percentage of ileostomies with complications is 73%. If distal stricture is excluded from the list of complications, the percentage of ileostomy complications decreases to 44%, which is closer to the rate reported by others. 9,10 878
5 Although only 9 infants underwent jejunostomy with mucous fistula, there were a total of 9 complications. In addition to the infants who suffered wound dehiscence and died, small-bowel obstruction later developed in 2 infants. Both infants had multiple ileal and jejunal enterostomies for the initial treatment of NEC. Both infants had dense adhesions but needed no further bowel resection at the time of exploration for small-bowel obstruction. Again, if distal bowel stricture is not included in the list of complications, the percentage of complications decreases to 67%, which approaches the rate reported by other authors. 10 Most complications associated with colostomy in these infants (67%) were wound infections. Only 1 infant had a distal stricture develop after colostomy with a Hartmann pouch. Of the 50 infants who underwent ileostomy closure, only 2 had anastomotic complications, and 3 later died of SIDS. Our rate of anastomotic complications is lower than that reported by some authors. 10 Differences between the postclosure group complication rate (10%) vs the preclosure group complication rate (68%) may be ascribed to factors other than the technical creation of the enterostomy. Most of these premature infants exhibited some degree of malnutrition (mean albumin level, 18 g/l) at the time of enterostomy and resection, but not at the time of stomal closure (mean albumin level, 31 g/l). In addition, all infants who suffered wound dehiscence after both ileostomy and jejunostomy were malnourished (albumin levels, 4-18 g/l) and subsequently died of continued sepsis. Also, many infants received mechanical ventilation for prolonged periods following resection and enterostomy. Many infants were taking broad-spectrum antibiotic therapy and hyperalimentation for prolonged periods following enterostomy creation. It is also possible that to save as much intestine as possible, enterostomies were created using bowel that had tenuous viability. These factors imply that the high complication rate among infants with an enterostomy in this series may be due to poor nutritional status, ongoing sepsis, respiratory distress, and continued NEC. Because the operative management of NEC is so complex,someauthors 6,7 haveadoptedalternativesurgicalstrategies. Few of the patients in our series were treated with preoperative peritoneal drainage, and none were treated with patch,drain,andwait 6 orenterostomy withoutresection. 7 The claim for both techniques is that they maximize intestinal salvage while providing adequate decompression and a short operation for infants who are premature and critically ill. The usefulness of these approaches has not been universally accepted, perhaps because philosophically and technically, treatment of these premature infants has changed from the need to perform the shortest operation to the ability to perform the most inclusive operation. During our review period, 20 infants underwent resection with primary anastomosis for NEC. Of these 20 infants, 10 (50%) weighed 1500 g or less. Complications developed in only 2 (20%) of these 10 infants and included 1 death from overwhelming sepsis with multiple organ failure and 1 wound infection treated with dressing changes and antibiotics. In none of the infants did distal strictures or anastomotic complications develop (data not shown). The possibility remains that these patients with primary anastomosis were a selected group of infants who were less critically ill than the infants who underwent enterostomy, but the results of this limited review suggest that resection with primary anastomosis may be a safe alternative to enterostomy. CONCLUSIONS Necrotizing enterocolitis remains a difficult management issue for pediatric surgeons. Our data show that enterostomy in premature infants is a seriously morbid procedure, which supports the need to prospectively compare resection and primary anastomosis with resection and enterostomy. Presented at the 69th Annual Session of the Pacific Coast Surgical Association, Maui, Hawaii, February 18, Reprints: Robert S. Sawin, MD, Department of Surgery, Children s Hospital and Regional Medical Center, University of Washington School of Medicine, 4800 Sand Point Way NE, Mailstop CH-78, Seattle, WA REFERENCES 1. Ricketts RR, Jerles ML. Neonatal necrotizing enterocolitis: experience with 100 consecutive surgical patients. World J Surg. 1990;14: Rescorla FJ. Surgical management of pediatric necrotizing enterocolitis. Curr Opin Pediatr. 1995;7: Musemeche CA, Kosloske AM, Ricketts RR. Enterostomy in necrotizing enterocolitis: an analysis of techniques and timing of closure. J Pediatr Surg. 1987;22: Ade-Ajayi N, Kiely E, Drake D, Wheeler R, Spitz L. Resection and primary anastomosis in necrotizing enterocolitis. J R Soc Med. 1996;89: Harberg FJ, McGill CW, Saleem MM, Halbert R, Anastassiou P. Resection with primary anastomosis for necrotizing enterocolitis. J Pediatr Surg. 1983;18: Moore TC. The management of necrotizing enterocolitis by patch, drain, and wait. Pediatr Surg Int. 1989;4: Luzzatto C, Previtera C, Boscolo R, Katende M, Orzali A, Guglielmi M. Necrotizing enterocolitis: late surgical results after enterostomy without resection. Eur J Pediatr Surg. 1996;6: Fasching G, Hollwarth ME, Schmidt B, Mayr J. Surgical strategies in very-low birthweight neonates with necrotizing enterocolitis. Acta Paediatr Suppl. 1994;396: Haberlik A, Hollwarth ME, Windhager U, Schober PH. Problems of ileostomy in necrotizing enterocolitis. Acta Paediatr Suppl. 1994;396: Weber TR, Tracy TF, Silen ML, Powell MA. Enterostomy and its closure in newborns. Arch Surg. 1995;130: Cooper A, Ross AJ, O Neill JA, Schnaufer L. Resection with primary anastomosis for necrotizing enterocolitis: a contrasting view. J Pediatr Surg. 1988;23: Born M, Holgersen LO, Shahrivar F, Stanley-Brown E, Hilfer C. Routine contrast enemas for diagnosing and managing strictures following non-operative treatment of necrotizing enterocolitis. J Pediatr Surg. 1985;20: DISCUSSION Harry Applebaum, MD, Los Angeles, Calif: Drs O Connor and Sawin have compiled an excellent analysis that can greatly help pediatric surgeons deal with one of their more common and most frustrating problems what to do in the middle of the night when confronted with gangrenous bowel in a very sick and very small premature infant. As they note, the choice for an initial operation in NEC usually combines a conservative resection of compromised bowel with proximal diversion. Unfortunately, this seemingly safe surgical approach is too often the prelude to a whole chain of adverse events that are often related to the stoma. And, as might be anticipated, the sicker an infant at the outset, the greater the number of complications that can be expected. They, therefore, suggest that primary resection and anastomosis might supplant the staged approach, theorizing that if there are no stomas, they cannot cause problems. Although this concept was first introduced by Harberg more than 15 years ago, it has failed to gain wide acceptance. Most still find it suitable only for selected good-risk patients of the type that successfully un- 879
6 derwent a 1-stage procedure in this nonrandomized study. Primary anastomosis requires the excision of any questionably viable bowel, thus increasing the risk of the short-gut syndrome, and would be difficult to apply to the large number of patients with skip areas of involvement. And, most important, the stomarelated complications that are reported pale in comparison with those that would accompany any potential anastomotic disruptions. It is also not likely that a primary anastomotic approach would have benefited the 26% of patients in this series who died of sepsis and the progression of disease in the immediate postoperative period. The authors conclude that a prospective trial comparing resection and enterostomy with resection and primary anastomosis is warranted. With the preceding concepts in mind, I would be interested in hearing their thoughts on which patients should be specifically included or excluded from a randomized trial that compares these 2 alternatives. Second, in my experience, the incidence of stomal complications is directly related to the length of time that the stoma is left in place. Although most pediatric surgeons continue to use stomas, the trend has been toward more rapid closure, with a perceived decreased incidence not only of stoma-related problems but also of short-gut symptoms and total parenteral nutrition induced cholestatic jaundice. In this series, the average age for closure was 5 months. Would earlier stomal closure safely lead to fewer complications, and how should we currently determine its optimal timing? Last, some stricture-related issues: The postoperative stricture rate is comparable to that observed in other series of less severely affected patients who could be managed nonoperatively. This would suggest that strictures are a consequence of the disease rather than of stomas and fecal diversion. Also, perhaps 50% of radiographically diagnosed strictures in nonoperative patients never become clinically significant. When discovered in surgically treated patients before stomal closure, could some strictures be balloon dilated or even ignored, rather than routinely resected? John German, MD, Orange, Calif: The invited discussant hit all of the right points that were asked by this paper. Dr Paul W. Johnson and I have wondered exactly the issue Dr Applebaum brought up. Is definitive surgical intervention for these patients delayed beyond what we consider a window of opportunity? In the management of these patients, once you get them as stable as you possibly can, it doesn t get any better than that. The reasonwerecommendthatiswestartseeingthecomplicationsoutlined in this paper in those patients whom we have lost control of. Those patients were transferred to our neonatal unit, operated on, stabilized, and returned to their home unit, and they bounce back to us because they were not closed during the initial admission. We, therefore, feelthatadefinitiveprocedureshouldbedonewhen youhaveawindowofopportunitytogivethepatientthebestchance for overall lowest morbidity during the first admission. A final point is, I hope that in your prospective study, you evaluate abdominal drainage alone in the management of NEC. Claude H. Organ, Jr, MD, Oakland, Calif: Among the options listed in the surgical management of these patients, you did not mention the Santulli chimney. Is this operation of historic interest only? Is there a place for it in the management of this difficult disease? Richard A. Crass, MD, Portland, Ore: As an adult surgeon, I am reluctant to comment on a pediatric paper, but it seems you can t do much worse than the wound infection rate in the colostomy group. I wonder if you are considering other strategies such as leaving the skin open in these patients. David Tapper, MD, Seattle, Wash: When you reviewed the data, was there a group of neonates who had a primary anastomosis? Were there any major complications associated with that procedure? In this group of low-birth-weight infants, 50 of them survived, which is impressive, and so I would like to ask you to speculate as to why you think neonates with a distal stoma do so poorly. Is it because you are waiting too long to do your reanastomosis, or is it the distance from the colon? I noticed that the higher the diversion, the greater the incidence of stricture. How significant is a distal stricture? I assume that before closure, you are evaluating the distal intestine to make sure that you don t do your anastomosis proximal to a stricture, so just how significant is it? Do you think it was associated with the incidence of short intestine? Did you have to resect the stricture, or was that something that in your careful study you looked at? John A. Ryan, Jr, MD, Seattle: Congratulations for having two thirds of these low-weight premature children survive. If you propose resection and primary anastomosis, will the high incidence of distal strictures predispose to anastomotic dehiscence? Tell us more of the pathogenesis of distal strictures. Dr Sawin: Dr Ryan asked about the distal stricture and how this might affect the primary anastomosis. This touches on some of the other questions as well. There is a theory that something about the small-bowel succus entericus is preventing these distal strictures. Some people have theorized that if you do a proximal diversion, perhaps you should feed the distal bowel, and then you will prevent that distal stricture from developing. Our experience reported here would support that in the infants who had colostomies, distal strictures never developed only those who had proximal small-bowel diversion. Interestingly, almost all of the strictures were in the rectosigmoid. I can t really explain that. That leads to Dr Tapper s question about why children with distal strictures do so poorly. I really don t have a good explanation for that, unless it can be attributed to what Dr German alluded to, and that is that perhaps had we closed them earlier, this distal stricture would not have developed. Perhaps what we are seeing is that stricture is a marker of having waited too long. DrOrganaskedabouttheSantullioperation. Itstillhasaplace in pediatric surgery, but I don t think it does in patients with NEC. It s probably something that we use more frequently in some of the complicated intestinal atresias. It is an interesting idea, but I have never seen it used in the treatment of these patients with NEC. Dr Crass asked about wound infection, particularly in the patients with a colostomy. I would concur that it is a high enough rate that I have changed the way I close those incisions. Typically, ratherthanclosingtheminanairtightmanner, Iputjustafewloose interrupted sutures in and maybe even put some wicks in between. Despite that, we still see a high incidence of wound infection. Dr Applebaum asked about the severity of the complications. Were we to do more primary anastomoses, would we be trading offstomalcomplicationsformuchworse? IthinkthatTomMoore s revolutionary concept of the patch, drain, and wait and the other peoplewhoadvocateprimarybedsidedrainagewouldindicatethat maybe the most important part of this operation is doing the laparotomy and irrigating out everything that is going on in there. How we handle the bowel may be less important because, even if you did a primary anastomosis and had an anastomotic leak down the road, perhaps that wouldn t be as big a problem 2, 3, or 4 days after you have resuscitated them with this laparotomy. Regarding balloon dilatation and whether all of these distal strictures need to be treated, we have had little success with balloon dilatation of these post-nec strictures. I don t know why that is. I have seen 1 child in particular who initially had a balloon dilatation, then a stricturoplasty, and then ultimately a resection. The histopathological examination showed an intense fibrosis, and I just think it s not amenable to dilatation. Perhaps the most important question is the one that Dr Applebaum raised. If we were to do a prospective trial, how could we possibly do it without having apples and oranges? It would have to be a pretty homogeneous population, and, in fact, in our series, about 60% had fairly homogeneous disease, ie, distal ileal and cecal disease. If we chose a specified population like that, perhaps we could get enough pediatric surgeons to agree to a randomized trial. 880
Colostomy & Ileostomy
 Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Colostomy & Ileostomy Indications, problems and preference By Waleed Omar Professor of Colorectal surgery, Mansoura University. Disclosure I have no disclosures. Presentation outline Stoma: Definition
Index. Note: Page numbers of article title are in boldface type.
 Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
Index Note: Page numbers of article title are in boldface type. A Abscess(es) in Crohn s disease, 168 169 IPAA and, 110 114 as unexpected finding in colorectal surgery, 46 Adhesion(s) trocars-related laparoscopy
NEC. cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine
 NEC cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine Necrotizing enterocolitis (NEC) the most common and most lethal disease
NEC cathy e. shin childrens hospital los angeles department of surgery university of southern california keck school of medicine Necrotizing enterocolitis (NEC) the most common and most lethal disease
INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC
 INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC Pages with reference to book, From 14 To 16 S. Amjad Hussain, Chinda Suriyapa, Karl Grubaugh ( Depts. of Surger and
INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC Pages with reference to book, From 14 To 16 S. Amjad Hussain, Chinda Suriyapa, Karl Grubaugh ( Depts. of Surger and
Complications of laparoscopic protective loop ileostomy in patients with colorectal cancer
 ISPUB.COM The Internet Journal of Surgery Volume 19 Number 2 Complications of laparoscopic protective loop ileostomy in patients with colorectal cancer F Puccio, M Solazzo, G Pandolfo, P Marcianò Citation
ISPUB.COM The Internet Journal of Surgery Volume 19 Number 2 Complications of laparoscopic protective loop ileostomy in patients with colorectal cancer F Puccio, M Solazzo, G Pandolfo, P Marcianò Citation
Product Adaptations in Pediatric Ostomy Care
 Product Adaptations in Pediatric Ostomy Care Teri Robinson, RN, BSN, CWON-Arnold Palmer Hospital for Children, Orlando, FL Bonita Yarjau RN, BN, ET-Health Sciences Centre, Winnipeg, MB, Canada Bev Biller,
Product Adaptations in Pediatric Ostomy Care Teri Robinson, RN, BSN, CWON-Arnold Palmer Hospital for Children, Orlando, FL Bonita Yarjau RN, BN, ET-Health Sciences Centre, Winnipeg, MB, Canada Bev Biller,
Neonatal Perforated Gut: Etiology and Risk Factors
 Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Mostafa Kotb 1 * and Marwa Beyaly 2 1 Pediatric Surgery Department, Alexandria Faculty of Medicine, Egypt. 2 Human Genetics Department, Medical Research
Cronicon OPEN ACCESS EC PAEDIATRICS Research Article Mostafa Kotb 1 * and Marwa Beyaly 2 1 Pediatric Surgery Department, Alexandria Faculty of Medicine, Egypt. 2 Human Genetics Department, Medical Research
Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates
 Annals of Pediatric Surgery Vol 5, No 1, January 2009, PP 31-35 Original Article Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates Almoutaz A. Eltayeb Pediatric
Annals of Pediatric Surgery Vol 5, No 1, January 2009, PP 31-35 Original Article Different Surgical Techniques in Management of Small Intestinal Atresia in High Risk Neonates Almoutaz A. Eltayeb Pediatric
Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts Correspondence to
 East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
East and Central African Journal of Surgery http://www.bioline.org.br/js 9 Outcomes of Colostomy Reversal Procedures in Two Teaching Hospitals in Addis Ababa, Ethiopia A. Bekele, B. Kotisso, H. Biluts
Case Report The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in a Newborn
 Case Reports in Pediatrics Volume 2015, Article ID 129098, 4 pages http://dx.doi.org/10.1155/2015/129098 Case Report The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in a Newborn
Case Reports in Pediatrics Volume 2015, Article ID 129098, 4 pages http://dx.doi.org/10.1155/2015/129098 Case Report The Combination of Gastroschisis, Jejunal Atresia, and Colonic Atresia in a Newborn
A Multi center Randomized Trial of Laparotomy vs. Drainage
 A Multi center Randomized Trial of Laparotomy vs. Drainage as the Initial Surgical Therapy for ELBW Infants with Necrotizing Enterocolitis (NEC) or Isolated Intestinal Perforation (IP): Outcomes at 18
A Multi center Randomized Trial of Laparotomy vs. Drainage as the Initial Surgical Therapy for ELBW Infants with Necrotizing Enterocolitis (NEC) or Isolated Intestinal Perforation (IP): Outcomes at 18
SWISS SOCIETY OF NEONATOLOGY. Neonatal gastric perforation
 SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
SWISS SOCIETY OF NEONATOLOGY Neonatal gastric perforation September 2002 2 Zankl A, Stähelin J, Roth K, Boudny P and Zeilinger G, Children s Hospital of Aarau (ZA, SJ, RK, ZG) and Institute of Pathology
Acute Care Surgery: Diverticulitis
 Acute Care Surgery: Diverticulitis Madhulika G. Varma, MD Associate Professor and Chief Section of Colorectal Surgery University of California, San Francisco Modern Treatment of Diverticular Disease Increasing
Acute Care Surgery: Diverticulitis Madhulika G. Varma, MD Associate Professor and Chief Section of Colorectal Surgery University of California, San Francisco Modern Treatment of Diverticular Disease Increasing
Vacuum-Assisted Closure: A Novel Method of Managing Surgical Necrotizing Enterocolitis
 Original Article 41 Vacuum-Assisted Closure: A Novel Method of Managing Surgical Necrotizing Enterocolitis Stephanie Sea 1 Teerin Meckmongkol 1 Matthew L. Moront 1 Shaheen Timmapuri 1 Rajeev Prasad 1 Marshall
Original Article 41 Vacuum-Assisted Closure: A Novel Method of Managing Surgical Necrotizing Enterocolitis Stephanie Sea 1 Teerin Meckmongkol 1 Matthew L. Moront 1 Shaheen Timmapuri 1 Rajeev Prasad 1 Marshall
GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM
 GASTROENTEROLOGY 64: 1071-1076, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.6 Printed in U.S.A. GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM JAMES A. NELSON,
GASTROENTEROLOGY 64: 1071-1076, 1973 Copyright 1973 by The Williams & Wilkins Co. Vol. 64, No.6 Printed in U.S.A. GRANULOMATOUS COLITIS: SIGNIFICANCE OF INVOLVEMENT OF THE TERMINAL ILEUM JAMES A. NELSON,
Ileo-rectal anastomosis for Crohn's disease of
 Ileo-rectal anastomosis for Crohn's disease of the colon W. N. W. BAKER From the Research Department, St Mark's Hospital, London Gut, 1971, 12, 427-431 SUMMARY Twenty-six cases of Crohn's disease of the
Ileo-rectal anastomosis for Crohn's disease of the colon W. N. W. BAKER From the Research Department, St Mark's Hospital, London Gut, 1971, 12, 427-431 SUMMARY Twenty-six cases of Crohn's disease of the
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
DIGESTIVE SYSTEM SURGICAL PROCEDURES December 22, 2015 (effective March 1, 2016) INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
December 22, 2015 (effective March 1, 201) INTESTINES (EXCEPT RECTUM) Z513 Hydrostatic - Pneumatic dilatation of colon stricture(s) through colonoscope... 10.50 Z50 Fulguration of first polyp through colonoscope...
Perforated Necrotizing Enterocolitis: What Is The Rational Approach? Peritoneal Drainage or Laparotomy?
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 17, Issue 5 Ver. 12(May. 218), PP 19-23 www.iosrjournals.org Perforated Necrotizing Enterocolitis: What
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-853, p-issn: 2279-861.Volume 17, Issue 5 Ver. 12(May. 218), PP 19-23 www.iosrjournals.org Perforated Necrotizing Enterocolitis: What
Advanced Necrotizing Enterocolitis Part 1: Mortality
 8 Original Article Advanced Necrotizing Enterocolitis Part 1: Mortality M. Thyoka 1 P. de Coppi 1 S. Eaton 1 K. Khoo 1 N.J. Hall 1 J. Curry 1 E. Kiely 1 D. Drake 1 K. Cross 1 A. Pierro 1 1 Department of
8 Original Article Advanced Necrotizing Enterocolitis Part 1: Mortality M. Thyoka 1 P. de Coppi 1 S. Eaton 1 K. Khoo 1 N.J. Hall 1 J. Curry 1 E. Kiely 1 D. Drake 1 K. Cross 1 A. Pierro 1 1 Department of
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT
 STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
STOMA SITING & PARASTOMAL HERNIA MANAGEMENT Professor Hany S. Tawfik Head of the Department of Surgery & Chairman of Colorectal Surgery Unit Benha University Disclosure No financial affiliation to disclose
University of Groningen. Colorectal Anastomoses Bakker, Ilsalien
 University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
University of Groningen Colorectal Anastomoses Bakker, Ilsalien IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it. Please check the document
The Hierarchy of Evidence
 The Hierarchy of Evidence The Hierarchy of evidence is based on summaries from the National Health and Medical Research Council (2009), the Oxford Centre for Evidencebased Medicine Levels of Evidence (2011)
The Hierarchy of Evidence The Hierarchy of evidence is based on summaries from the National Health and Medical Research Council (2009), the Oxford Centre for Evidencebased Medicine Levels of Evidence (2011)
Small bowel atresia. Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families
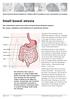 Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Great Ormond Street Hospital for Children NHS Foundation Trust: Information for Families Small bowel atresia This information sheet from Great Ormond Street Hospital explains the causes, symptoms and treatment
Abdominal Wall Modification for the Difficult Ostomy
 Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Abdominal Wall Modification for the Difficult Ostomy David E. Beck, M.D. 1 ABSTRACT A select group of patients with major stomal problems may benefit from operative modification of the abdominal wall.
Comparison of Loop Ileostomy and Loop Colostomy as Defunctioning Stoma in Low Rectal Cancer Surgery NCI Experience
 Kasr El Aini Journal of Surgery VOL., 12, NO 1 January 2011 75 Comparison of Loop Ileostomy and Loop Colostomy as Defunctioning Stoma in Low Rectal Cancer Surgery NCI Experience Ahmed Abbas, MD MRCS General
Kasr El Aini Journal of Surgery VOL., 12, NO 1 January 2011 75 Comparison of Loop Ileostomy and Loop Colostomy as Defunctioning Stoma in Low Rectal Cancer Surgery NCI Experience Ahmed Abbas, MD MRCS General
AN EXPERIMENTAL TUBE PEDICLE LINED WITH SMALL BOWEL. By J. H. GOLDIN, F.R.C.S.(Edin.) Plastic Surgery Unit, St Thomas' Hospital, London
 British Journal of Plastic Surgery (I972), 25, 388-39z AN EXPERIMENTAL TUBE PEDICLE LINED WITH SMALL BOWEL By J. H. GOLDIN, F.R.C.S.(Edin.) Plastic Surgery Unit, St Thomas' Hospital, London ONE of the
British Journal of Plastic Surgery (I972), 25, 388-39z AN EXPERIMENTAL TUBE PEDICLE LINED WITH SMALL BOWEL By J. H. GOLDIN, F.R.C.S.(Edin.) Plastic Surgery Unit, St Thomas' Hospital, London ONE of the
11/13/11. Biologics for CD and CUC: The Impact on Surgical Outcomes. Principles of Successful Intestinal Surgery
 Biologics for CD and CUC: The Impact on Surgical Outcomes Robert R. Cima, M.D., M.A. Associate Professor of Surgery Division of Colon and Rectal Surgery Overview Antibody based medications (biologics)
Biologics for CD and CUC: The Impact on Surgical Outcomes Robert R. Cima, M.D., M.A. Associate Professor of Surgery Division of Colon and Rectal Surgery Overview Antibody based medications (biologics)
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 9 ISSUE 1 Perforation Of The Caecum Owing To Benign Rectal Obstruction: A Paradigm Of Damage Control In Emergency Colorectal Surgery DIMITRIOS
World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 9 ISSUE 1 Perforation Of The Caecum Owing To Benign Rectal Obstruction: A Paradigm Of Damage Control In Emergency Colorectal Surgery DIMITRIOS
DIVERTICULAR DISEASE. Dr. Irina Murray Casanova PGY IV
 DIVERTICULAR DISEASE Dr. Irina Murray Casanova PGY IV Diverticular Disease Colonoscopy Abdpelvic CT Scan Surgical Indications Overall, approximately 20% of patients with diverticulitis require surgical
DIVERTICULAR DISEASE Dr. Irina Murray Casanova PGY IV Diverticular Disease Colonoscopy Abdpelvic CT Scan Surgical Indications Overall, approximately 20% of patients with diverticulitis require surgical
Inflammatory Bowel Disease and Surgery: What You Should Know
 Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
Inflammatory Bowel Disease and Surgery: What You Should Know Ask the Experts March 9, 2019 Kristen Blaker, MD Colon and Rectal Surgery MetroHealth Medical Center Disclosures None Outline Who undergoes
ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM
 ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM DATA COLLECTION FORM Most Australian hospitals contribute data
ANZ Emergency Laparotomy Audit Quality Improvement (ANZELA-QI) Pilot Collaboration between RACS, ANZCA, GSA, NZAGS, ASA, NZSA, ACEM, CICM DATA COLLECTION FORM Most Australian hospitals contribute data
Colostomy in anorectal malformations: a procedure with serious but preventable complications
 Journal of Pediatric Surgery (2006) 41, 748 756 www.elsevier.com/locate/jpedsurg Colostomy in anorectal malformations: a procedure with serious but preventable complications Alberto Pena a, *, Melissa
Journal of Pediatric Surgery (2006) 41, 748 756 www.elsevier.com/locate/jpedsurg Colostomy in anorectal malformations: a procedure with serious but preventable complications Alberto Pena a, *, Melissa
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN)
 An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
An 8-year experience of esophageal atresia repair in Sarvar children hospital (Mashhad- IRAN) Mehran Hiradfar* Ahmad Bazrafshan* Marjan Judi** Mohammad Gharavi*** - Reza Shojaeian**** * Associate professor
MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION
 Basrah Journal Of Surgery MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION Haithem Hussein Ali Almoamin MB, ChB, FIBMS Pediatric Surgery, Lecturer, Department of Surgery, College of Medicine,
Basrah Journal Of Surgery MORTALITY RISK FACTORS FOR NEONATAL INTESTINAL OBSTRUCTION Haithem Hussein Ali Almoamin MB, ChB, FIBMS Pediatric Surgery, Lecturer, Department of Surgery, College of Medicine,
1 p-issn: ,e-issn: Original Article. Neonatal Intestinal Obstruction-Four Year Experience. BJKines-NJBAS Volume-7(1), June
 Neonatal Intestinal Obstruction-Four Year Experience D. Rathore 1, J. Ramji 2*, R. Joshi 3, A. Shah 4, T. Dihare 5, M. Bachani 6 1 Pediatric Surgeon, 2 Associate Professor, 3 Professor & Head, 4,5 Resident,
Neonatal Intestinal Obstruction-Four Year Experience D. Rathore 1, J. Ramji 2*, R. Joshi 3, A. Shah 4, T. Dihare 5, M. Bachani 6 1 Pediatric Surgeon, 2 Associate Professor, 3 Professor & Head, 4,5 Resident,
Unusual presentations of late onset diaphragmatic hernia: a six year study
 International Surgery Journal Aggarwal S et al. Int Surg J. 2017 Apr;4(4):1180-1184 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170895
International Surgery Journal Aggarwal S et al. Int Surg J. 2017 Apr;4(4):1180-1184 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170895
Homayoon Akbari, MD, PhD
 Recent Advances in IBD Surgery Homayoon M. Akbari, MD, PhD, FRCS(C), FACS Associate Professor of Surgery Virginia Commonwealth University Crohn s disease first described as a surgical condition, with the
Recent Advances in IBD Surgery Homayoon M. Akbari, MD, PhD, FRCS(C), FACS Associate Professor of Surgery Virginia Commonwealth University Crohn s disease first described as a surgical condition, with the
Surgery for Inflammatory Bowel Disease
 Surgery for Inflammatory Bowel Disease Emily Steinhagen, MD Assistant Professor Department of Surgery, Division of Colorectal Surgery University Hospitals Cleveland Medical Center Common Questions Why
Surgery for Inflammatory Bowel Disease Emily Steinhagen, MD Assistant Professor Department of Surgery, Division of Colorectal Surgery University Hospitals Cleveland Medical Center Common Questions Why
Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of Conservative Treatment
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 645104, 4 pages doi:10.5402/2011/645104 Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 645104, 4 pages doi:10.5402/2011/645104 Clinical Study Adhesive Intestinal Obstruction in Infants and Children: The Place of
Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery
 SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
SCIENTIFIC PAPER Inadvertent Enterotomy in Minimally Invasive Abdominal Surgery Steven J. Binenbaum, MD, Michael A. Goldfarb, MD ABSTRACT Background: Inadvertent enterotomy (IE) in laparoscopic abdominal
JMSCR Vol 05 Issue 04 Page April 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i4.206 Acute Presentations of Abdominal Tuberculosis
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i4.206 Acute Presentations of Abdominal Tuberculosis
The jury is still out: changes in gastroschisis management over the last decade are associated with both benefits and shortcomings
 Journal of Pediatric Surgery (2012) 47, 119 124 www.elsevier.com/locate/jpedsurg The jury is still out: changes in gastroschisis management over the last decade are associated with both benefits and shortcomings
Journal of Pediatric Surgery (2012) 47, 119 124 www.elsevier.com/locate/jpedsurg The jury is still out: changes in gastroschisis management over the last decade are associated with both benefits and shortcomings
Surgery and Crohn s. Crohn s Disease 70 % Why Operate? Complications of Disease. The Gastrointestinal Tract. Surgery for Inflammatory Bowel Disease
 The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
The Gastrointestinal Tract Surgery for Inflammatory Bowel Disease Jonathan Chun, MD The regon Clinic Gastrointestinal and Minimally Invasive Surgery Crohn s Disease Can affect anywhere in the GI tract,
ORIGINAL ARTICLE. Surgery for Ulcerative Colitis in Elderly Persons. Changes in Indications for Surgery and Outcome Over Time
 ORIGINAL ARTICLE Surgery for Ulcerative Colitis in Elderly Persons Changes in Indications for Surgery and Outcome Over Time Gidon Almogy, MD; David B. Sachar, MD; Carol A. Bodian, DrPH; Adrian J. Greenstein,
ORIGINAL ARTICLE Surgery for Ulcerative Colitis in Elderly Persons Changes in Indications for Surgery and Outcome Over Time Gidon Almogy, MD; David B. Sachar, MD; Carol A. Bodian, DrPH; Adrian J. Greenstein,
Difficult Abdominal Closure. Mark A. Carlson, MD
 Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Difficult Abdominal Closure Mark A. Carlson, MD Illustrative case 14 yo boy with delayed diagnosis of appendicitis POD9 Appendectomy 2 wk after onset of symptoms POD4: return to OR for midline laparotomy
Management of Perforated Colon Cancers
 Management of Perforated Colon Cancers Introduction Colon and rectal cancers are the most common gastrointestinal cancers. They are 3 rd most common and 2 nd most common causes of cancer deaths among men
Management of Perforated Colon Cancers Introduction Colon and rectal cancers are the most common gastrointestinal cancers. They are 3 rd most common and 2 nd most common causes of cancer deaths among men
AMERICAN ACADEMY OF PEDIATRICS 993 THE NATURAL HISTORY OF CERTAIN CONGENITAL CARDIOVASCULAR MALFORMATIONS. Alexander S. Nadas, M.D.
 AMERICAN ACADEMY OF PEDIATRICS 993 tnicular overload is the major problem and left ventricular failure occurs. Since for many years the importance of hepatomegaly in the diagnosis of cardiac failure has
AMERICAN ACADEMY OF PEDIATRICS 993 tnicular overload is the major problem and left ventricular failure occurs. Since for many years the importance of hepatomegaly in the diagnosis of cardiac failure has
Surgical Management of IBD in the Age of Biologics
 Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
Surgical Management of IBD in the Age of Biologics Lisa S. Poritz, M.D Associate Professor of Surgery Division of Colon and Rectal Surgery Objectives Discuss surgical management of IBD When to operate
FECAL DIVERSION is often required
 Temporary Transverse Colostomy vs Loop Ileostomy in Diversion A Case-Matched Study ORIGINAL ARTICLE Yasuo Sakai, MD, PhD; Heidi Nelson, MD; Dirk Larson; Laurie Maidl, RN; Tonia Young-Fadok, MD, MS; Duane
Temporary Transverse Colostomy vs Loop Ileostomy in Diversion A Case-Matched Study ORIGINAL ARTICLE Yasuo Sakai, MD, PhD; Heidi Nelson, MD; Dirk Larson; Laurie Maidl, RN; Tonia Young-Fadok, MD, MS; Duane
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications
 Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Peutz Jegher's Syndrome (Gastro-intestinal Polyposis) and Its Complications Pages with reference to book, From 154 To 155 Zakiuddin G. Oonwala, Sina Aziz ( Department of Surgery, Dow Medical College and
Colorectal non-inflammatory emergencies
 Colorectal non-inflammatory emergencies Prof. Hesham Amer Professor of general surgery, Kasr Alainy hospital, Cairo university Dr. Doaa Mansour Dr. Ahmed Nabil Dr. Ahmed Abdel-Salam Lecturers of general
Colorectal non-inflammatory emergencies Prof. Hesham Amer Professor of general surgery, Kasr Alainy hospital, Cairo university Dr. Doaa Mansour Dr. Ahmed Nabil Dr. Ahmed Abdel-Salam Lecturers of general
Kyoko Mochizuki *, Masato Shinkai, Norihiko Kitagawa, Hiroshi Take, Hidehito Usui, Takashi Hosokawa and Kaori Yamoto
 Mochizuki et al. Surgical Case Reports (2017) 3:42 DOI 10.1186/s40792-017-0318-y CASE REPORT Open Access Continuous transanal decompression for infants with long- and total-type Hirschsprung s diseases
Mochizuki et al. Surgical Case Reports (2017) 3:42 DOI 10.1186/s40792-017-0318-y CASE REPORT Open Access Continuous transanal decompression for infants with long- and total-type Hirschsprung s diseases
Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic Surgery for Colorectal Disease
 ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
ORIGINAL ARTICLE pissn 2234-778X eissn 2234-5248 J Minim Invasive Surg 2018;21(1):38-42 Journal of Minimally Invasive Surgery Repeat Single Incision Laparoscopic Surgery after Primary Single Incision Laparoscopic
Case discussion. Anastomotic leakage. intern superviser
 Case discussion Anastomotic leakage intern superviser Basic data Name : XX ID: M101881671 Age:51 Y Gender: male Past history: Hospitalized for acute diverticulitis on 2004/7/17, 2005/5/28 controlled by
Case discussion Anastomotic leakage intern superviser Basic data Name : XX ID: M101881671 Age:51 Y Gender: male Past history: Hospitalized for acute diverticulitis on 2004/7/17, 2005/5/28 controlled by
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
A novel and simple method using a transanal intestinal long tube for protecting intestinal anastomosis and decompressing the small bowel
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.93.3.137 Annals of Surgical Treatment and Research A novel and simple method using a transanal intestinal long tube for
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 https://doi.org/10.4174/astr.2017.93.3.137 Annals of Surgical Treatment and Research A novel and simple method using a transanal intestinal long tube for
E n t e r o c u t a n e o u s F i s t u l a : Outcome in a Tertiary Center in Nigeria
 E n t e r o c u t a n e o u s F i s t u l a : Aetiology and Management Outcome in a Tertiary Center in Nigeria 2 2 Okoli C, Oparocha D, Onyemkpa J ABSTRACT Background: Enterocutaneous fistula is a major
E n t e r o c u t a n e o u s F i s t u l a : Aetiology and Management Outcome in a Tertiary Center in Nigeria 2 2 Okoli C, Oparocha D, Onyemkpa J ABSTRACT Background: Enterocutaneous fistula is a major
Citation for published version (APA): Bartels, S. A. L. (2013). Laparoscopic colorectal surgery: beyond the short-term effects
 UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
UvA-DARE (Digital Academic Repository) Laparoscopic colorectal surgery: beyond the short-term effects Bartels, S.A.L. Link to publication Citation for published version (APA): Bartels, S. A. L. (2013).
Pediatric SCR Discussion of Complex Clinical Scenarios NSQIP Annual Meeting July 26, 2015
 Pediatric SCR Discussion of Complex Clinical Scenarios NSQIP Annual Meeting July 26, 2015 Scenario 1: Postoperative SSI A 16 year-old patient Principal Operative Procedure: Incision and Drainage for monoarticular
Pediatric SCR Discussion of Complex Clinical Scenarios NSQIP Annual Meeting July 26, 2015 Scenario 1: Postoperative SSI A 16 year-old patient Principal Operative Procedure: Incision and Drainage for monoarticular
Safety of short stay Hospitalization in Reversal of Loop Ileostomy
 Original Article Safety of short stay Hospitalization in Reversal of Loop Ileostomy Tayyab Abbas, Abid Nazir, Muhammad Lateef, Faisal Rauf, Zafar Ali Choudhary Abstract Study Design: Prospective, randomized
Original Article Safety of short stay Hospitalization in Reversal of Loop Ileostomy Tayyab Abbas, Abid Nazir, Muhammad Lateef, Faisal Rauf, Zafar Ali Choudhary Abstract Study Design: Prospective, randomized
Early Reoperations after Primary Repair of Jejunoileal Atresia in Newborns
 Journal of Neonatal Surgery 2016; 5(4):42 Doi:10.21699/jns.v5i4.444 ORIGINAL ARTICLE Early Reoperations after Primary Repair of Jejunoileal Atresia in Newborns Fanny Yeung, Yuk Him Tam,* Yuen Shan Wong,
Journal of Neonatal Surgery 2016; 5(4):42 Doi:10.21699/jns.v5i4.444 ORIGINAL ARTICLE Early Reoperations after Primary Repair of Jejunoileal Atresia in Newborns Fanny Yeung, Yuk Him Tam,* Yuen Shan Wong,
Anorectal malformations include a wide spectrum of
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 20, Number 1, 2010 ª Mary Ann Liebert, Inc. DOI: 10.1089=lap.2008.0343 Laparoscopic-Assisted Pull-Through for Congenital Rectal Stenosis
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience
 Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
Journal of Neonatal Surgery 2013;2(4):39 ORIGINAL ARTICLE Single Stage Transanal Pull-Through for Hirschsprung s Disease in Neonates: Our Early Experience Pradeep Bhatia,* Rakesh S Joshi, Jaishri Ramji,
SWISS SOCIETY OF NEONATOLOGY. Congenital omphalo-mesenteric fistula in a newborn
 SWISS SOCIETY OF NEONATOLOGY Congenital omphalo-mesenteric fistula in a newborn NOVEMBER 2011 2 Dommange SJ, Lhermitte B, de Buys Roessingh A, Cachat F, Panchard MA, Department of Pediatrics (DSJ, CF,
SWISS SOCIETY OF NEONATOLOGY Congenital omphalo-mesenteric fistula in a newborn NOVEMBER 2011 2 Dommange SJ, Lhermitte B, de Buys Roessingh A, Cachat F, Panchard MA, Department of Pediatrics (DSJ, CF,
SOUTHERN WEST MIDLANDS NEWBORN NETWORK
 SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title : Person Responsible for Review : Management of Gastro-Intestinal Stomata In Neonates R. Wragg & G.Jawaheer
SOUTHERN WEST MIDLANDS NEWBORN NETWORK Hereford, Worcester, Birmingham, Sandwell & Solihull Title : Person Responsible for Review : Management of Gastro-Intestinal Stomata In Neonates R. Wragg & G.Jawaheer
LONG TERM FOLLOW-UP OF HIRSCHSPRUNG'S DISEASE: REVIEW OF EARLY AND LATE COMPLICATIONS. S. Agarwala, V. Bhatnagar and D.K. Mitra
 Original Articles LONG TERM FOLLOW-UP OF HIRSCHSPRUNG'S DISEASE: REVIEW OF EARLY AND LATE COMPLICATIONS S. Agarwala, V. Bhatnagar and D.K. Mitra From the Department of Pediatric Surgery, All India Institute
Original Articles LONG TERM FOLLOW-UP OF HIRSCHSPRUNG'S DISEASE: REVIEW OF EARLY AND LATE COMPLICATIONS S. Agarwala, V. Bhatnagar and D.K. Mitra From the Department of Pediatric Surgery, All India Institute
Current Surgical Management of Enterocutaneous Fistulas
 LONDON NORTH WEST HOSPITALS Current Surgical Management of Enterocutaneous Fistulas THIS TALK Surgical prevention of ECF formation Preparing the patient for surgery The surgery to the bowel The surgery
LONDON NORTH WEST HOSPITALS Current Surgical Management of Enterocutaneous Fistulas THIS TALK Surgical prevention of ECF formation Preparing the patient for surgery The surgery to the bowel The surgery
Prevention and Surgical management of Parastomal hernias; When to treat?
 Prevention and Surgical management of Parastomal hernias; When to treat? Sabry A. Mahmoud (MD) Prof of General & Colorectal Surgery Mansoura University It is an incisional hernia that develops at the site
Prevention and Surgical management of Parastomal hernias; When to treat? Sabry A. Mahmoud (MD) Prof of General & Colorectal Surgery Mansoura University It is an incisional hernia that develops at the site
Resuscitating neonatal and infant organs and preserving function. GI Tract and Kidneys
 Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Resuscitating neonatal and infant organs and preserving function GI Tract and Kidneys Australian and New Zealand Resuscitation Council Joint Guidelines Outline Emphasis on the infant - PICU Kidney Gastrointestinal
Gastroschisis Sequelae and Management
 Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
Gastroschisis Sequelae and Management Mary Finn Gillian Lieberman, MD Primary Care Radiology Beth Israel Deaconess Medical Center Harvard Medical School April 2014 Outline I. Definition and Epidemiology
Necrotizing Enterocolitis: the role of ultrasound in the assessment of bowel viability
 Necrotizing Enterocolitis: the role of ultrasound in the assessment of bowel viability Ricardo Faingold, MD. Department of Medical Imaging The Montreal Children s Hospital McGill University SPR Vancouver
Necrotizing Enterocolitis: the role of ultrasound in the assessment of bowel viability Ricardo Faingold, MD. Department of Medical Imaging The Montreal Children s Hospital McGill University SPR Vancouver
ARE TEMPORARY STOMAS HELPFUL TO MANAGE COMPLEX WOUNDS? Rosine van den Bulck BRUSSELS
 ARE TEMPORARY STOMAS HELPFUL TO MANAGE COMPLEX WOUNDS? Rosine van den Bulck BRUSSELS WHY TEMPORARY STOMAS? Patient AGE AGING POPULATION CO MORBIDITIES OVERALL CONDITION MULTIPLE SURGICAL PROCEDURES POOR
ARE TEMPORARY STOMAS HELPFUL TO MANAGE COMPLEX WOUNDS? Rosine van den Bulck BRUSSELS WHY TEMPORARY STOMAS? Patient AGE AGING POPULATION CO MORBIDITIES OVERALL CONDITION MULTIPLE SURGICAL PROCEDURES POOR
Adult Intussusception
 Bahrain Medical Bulletin, Vol. 27, No. 3, September 2005 Adult Intussusception Suhair Alsaad, MBCHB, CABS, FRCSI* Mariam Al-Muftah, MBCHB** Objectives: Adult intussusception is a rare entity. We present
Bahrain Medical Bulletin, Vol. 27, No. 3, September 2005 Adult Intussusception Suhair Alsaad, MBCHB, CABS, FRCSI* Mariam Al-Muftah, MBCHB** Objectives: Adult intussusception is a rare entity. We present
Rectal Cancer. About the Colon and Rectum. Symptoms. Colorectal Cancer Screening
 Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Patient information regarding care and surgery associated with RECTAL CANCER by Robert K. Cleary, M.D., John C. Eggenberger, M.D., Amalia J. Stefanou., M.D. location: Michigan Heart and Vascular Institute,
Abstract Introduction We present the experiences from two European centers performing the
 Original Article 3 The Foker Technique (FT) and Kimura Advancement (KA) for the Treatment of Children with Long-Gap Esophageal Atresia (LGEA): Lessons Learned at Two European Centers Mariusz Sroka 1 Robin
Original Article 3 The Foker Technique (FT) and Kimura Advancement (KA) for the Treatment of Children with Long-Gap Esophageal Atresia (LGEA): Lessons Learned at Two European Centers Mariusz Sroka 1 Robin
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 6 Case report: Intussusception of the colon through a colostomy: A rare presentation of colonic intussusception. Dr. Nora Trabulsi Dr.
World Journal of Colorectal Surgery Volume 3, Issue 4 2013 Article 6 Case report: Intussusception of the colon through a colostomy: A rare presentation of colonic intussusception. Dr. Nora Trabulsi Dr.
Management of colorectal anastomotic leakage: differences between salvage and anastomotic takedown
 The American Journal of Surgery (2012) 204, 671 676 Clinical Science Management of colorectal anastomotic leakage: differences between salvage and anastomotic takedown Domenico Fraccalvieri, M.D., Sebastiano
The American Journal of Surgery (2012) 204, 671 676 Clinical Science Management of colorectal anastomotic leakage: differences between salvage and anastomotic takedown Domenico Fraccalvieri, M.D., Sebastiano
National Emergency Laparotomy Audit. Help Box Text
 National Emergency Laparotomy Audit Help Box Text Version Control Version 1.1 06/12/13 1.2 13/12/13 1.3 20/12/13 1.4 20/01/14 1.5 30/01/14 1.6 13/03/14 1.7 07/04/14 1.8 01/12/14 1.9 05/05/15 1.10 02/07/15
National Emergency Laparotomy Audit Help Box Text Version Control Version 1.1 06/12/13 1.2 13/12/13 1.3 20/12/13 1.4 20/01/14 1.5 30/01/14 1.6 13/03/14 1.7 07/04/14 1.8 01/12/14 1.9 05/05/15 1.10 02/07/15
Proximal Loop Ileostomy-A Life Saving Approach in ComplicatedEnterocutaneous Fistulas
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 8 Ver. III (Aug. 2014), PP 58-67 Proximal Loop Ileostomy-A Life Saving Approach in ComplicatedEnterocutaneous
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 8 Ver. III (Aug. 2014), PP 58-67 Proximal Loop Ileostomy-A Life Saving Approach in ComplicatedEnterocutaneous
DIGESTIVE SYSTEM SURGICAL PROCEDURES May 1, 2015 INTESTINES (EXCEPT RECTUM) Asst Surg Anae
 ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
ENDOSCOPY Z50 Duodenoscopy (not to be claimed if Z399 and/or Z00 performed on same patient within 3 months)... 92.10 Z9 Subsequent procedure (within three months following previous endoscopic procedure)...
Open abdomen in trauma. Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland
 Open abdomen in trauma Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland Frequency and causes of open abdomen - in 23% (344/1531) after trauma laparotomies - damage control
Open abdomen in trauma Ari Leppäniemi Abdominal Center Meilahti hospital University of Helsinki Finland Frequency and causes of open abdomen - in 23% (344/1531) after trauma laparotomies - damage control
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of reinforcement of a permanent stoma with mesh to prevent a parastomal hernia A
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of reinforcement of a permanent stoma with mesh to prevent a parastomal hernia A
Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai
 Original Research Article Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai S. Vijayalakshmi 1, Sriramchristopher M 2* 1 Associate
Original Research Article Retrospective study analyzing the data on non-traumatic abdominal emergency surgeries done tertiary care hospital, Chennai S. Vijayalakshmi 1, Sriramchristopher M 2* 1 Associate
Atypical use of button gastrostomy tube for children with complex colorectal malformations (ileostomy, vesicostomy, vaginostomy)
 Atypical use of button gastrostomy tube for children with complex colorectal malformations (ileostomy, vesicostomy, vaginostomy) Christian PIOLAT, Yohann Robert, Pierre-Yves Rabattu, Youssef Teklali, Catherine
Atypical use of button gastrostomy tube for children with complex colorectal malformations (ileostomy, vesicostomy, vaginostomy) Christian PIOLAT, Yohann Robert, Pierre-Yves Rabattu, Youssef Teklali, Catherine
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children
 Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Ileal Pouch Anal Anastomosis: The Preferred Method of Reconstruction after Proctocolectomy in Children Stephanie Jones, D.O. Surgical Fellow March 21, 2011 Ulcerative Colitis Spectrum of inflammatory bowel
Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help. Print this Page Add to my Bookmarks Page 3 of 10
 Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Welcome Kristin Ingstrup [ Logout ] SEARCH Home FAQ Archives ABP Topics NeoReviews.org My Bookmarks CME Information Help Overview Editorial Board My Learning Plan January February March May June July August
Screening for Critical Congenital Heart Disease
 Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Screening for Critical Congenital Heart Disease Caroline K. Lee, MD Pediatric Cardiology Disclosures I have no relevant financial relationships or conflicts of interest 1 Most Common Birth Defect Most
Perforated duodenal ulcer in Reading from 1950 to 1959
 Gut, 1969, 1, 454-459 Perforated duodenal ulcer in Reading from 195 to 1959 PAUL CASSELL From the Royal Berkshire Hospital, Reading During the last 15 years there has been an evolution in the management
Gut, 1969, 1, 454-459 Perforated duodenal ulcer in Reading from 195 to 1959 PAUL CASSELL From the Royal Berkshire Hospital, Reading During the last 15 years there has been an evolution in the management
NEC- What Lies Under the Big Umbrella?
 NEC- What Lies Under the Big Umbrella? Instructor in Surgery Associate Surgical Director, Center for Advanced Intestinal Rehabilitation Department of Surgery, Boston Children's Hospital Harvard Medical
NEC- What Lies Under the Big Umbrella? Instructor in Surgery Associate Surgical Director, Center for Advanced Intestinal Rehabilitation Department of Surgery, Boston Children's Hospital Harvard Medical
Necrotizing Enterocolitis
 CHAPTER 1 CHAPTER Necrotizing Enterocolitis Fawn C. Lewis and Daniel A. Bambini Incidence The incidence of necrotizing enterocolitis (NEC) in the United States is 1-3 cases per thousand live births, or
CHAPTER 1 CHAPTER Necrotizing Enterocolitis Fawn C. Lewis and Daniel A. Bambini Incidence The incidence of necrotizing enterocolitis (NEC) in the United States is 1-3 cases per thousand live births, or
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.142 Clinical Factors Affecting Outcome
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.142 Clinical Factors Affecting Outcome
SUSTAIN BASELINE DATA COLLECTION FORM. Revised 2/4/2014 (both pediatric and adult data elements) 1. Gestational age at birth ( weeks gestation)
 SUSTAIN BASELINE DATA COLLECTION FORM Patient Demographics Revised 2/4/2014 (both pediatric and adult data elements) Did the patient begin Home PN over 90 days ago? Yes No Date began Home PN Patient Number
SUSTAIN BASELINE DATA COLLECTION FORM Patient Demographics Revised 2/4/2014 (both pediatric and adult data elements) Did the patient begin Home PN over 90 days ago? Yes No Date began Home PN Patient Number
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE
 PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations
 Original paper Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations Paweł Nachulewicz 1, Kamila Zaborowska 1, Błażej Rogowski 1, Anita Kalińska 1, Marzena
Original paper Thoracoscopic repair of esophageal atresia with a distal fistula lessons from the first 10 operations Paweł Nachulewicz 1, Kamila Zaborowska 1, Błażej Rogowski 1, Anita Kalińska 1, Marzena
The Emergency Hernia or The call you don t want at 2:00 a.m.*
 or The call you don t want at 2:00 a.m.* *Or even at 8:00 a.m. Michael G. Sarr, MD Professor of Surgery Mayo Clinic South Canada WEST CANADA EAST CANADA Clinical talk Hernias Inguinal Umbilical Incisional
or The call you don t want at 2:00 a.m.* *Or even at 8:00 a.m. Michael G. Sarr, MD Professor of Surgery Mayo Clinic South Canada WEST CANADA EAST CANADA Clinical talk Hernias Inguinal Umbilical Incisional
THE BEST OF TISSUE REGENERATION FOCUSED ON PATIENTS NEEDS
 THE BEST OF TISSUE REGENERATION FOCUSED ON PATIENTS NEEDS Tissue regeneration is a natural process by which the body forms a functional neo-tissue to repair a wound. This process requires the patient s
THE BEST OF TISSUE REGENERATION FOCUSED ON PATIENTS NEEDS Tissue regeneration is a natural process by which the body forms a functional neo-tissue to repair a wound. This process requires the patient s
Surgical Approach to Crohn s Colitis Segmental or Total Colectomy? Can We Avoid the Stoma?
 17 th Panhellenic IBD Congress Thessaloniki May 2018 Surgical Approach to Crohn s Colitis Segmental or Total Colectomy? Can We Avoid the Stoma? Janindra Warusavitarne Consultant Colorectal Surgeon, St
17 th Panhellenic IBD Congress Thessaloniki May 2018 Surgical Approach to Crohn s Colitis Segmental or Total Colectomy? Can We Avoid the Stoma? Janindra Warusavitarne Consultant Colorectal Surgeon, St
Colorectal procedure guide
 Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
Colorectal procedure guide Illustrations by Lisa Clark Biodesign ADVANCED TISSUE REPAIR cookmedical.com 2 INDEX Anal fistula repair Using the Biodesign plug with no button.... 4 Anal fistula repair Using
