PSYCHONEUROIMMUNOLOGIC ASPECTS OF SKIN DISEASES
|
|
|
- Susanna Harris
- 5 years ago
- Views:
Transcription
1 Acta Clin Croat 2013; 52: Review PSYCHONEUROIMMUNOLOGIC ASPECTS OF SKIN DISEASES Liborija Lugović-Mihić 1, Luka Ljubešić 1, Josip Mihić 2, Vlasta Vuković-Cvetković 3, Nina Troskot 1 and Mirna Šitum 1 1 Clinical Department of Dermatovenereology, Sestre milosrdnice University Hospital Center, Zagreb; 2 Division of Neurosurgery, Dr. Josip Benčević General Hospital, Slavonski Brod; 3 Clinical Department of Neurology, Sestre milosrdnice University Hospital Center, Zagreb, Croatia SUMMARY As mental and psychological issues are important in the development of many dermatologic diseases, these factors are of special interest in research. Psychoneuroimmunology is the study of interaction between psychological processes and the nervous and immune systems of the human body, and it was comprehensively described for the first time about 30 years ago. Communication between the mind and the skin involves the psycho-immuno-endocrine-cutaneous system, encompassing the activities of the brain, the immune system and the skin, with participation of different neuropeptides, interleukins, and immune system messengers. Many common dermatologic diseases have some form of psychomediated pathogenesis that partially accounts for the development of skin lesions. There is a link between emotional stressors (acute or chronic), psychiatric diseases, and dermatoses (e.g., psoriasis, atopic dermatitis, urticaria, viral warts, herpes simplex, vitiligo, acnes, alopecia, prurigo, etc.) and different cytokines and mediators produced in the skin and involved in their pathogenesis. A prominent role is played by those agents that belong to the hypothalamic-pituitary-adrenal axis. Key words: Psychoneuroimmunology; Skin; Skin diseases; Interleukins; Neuropeptides; Hormones Introduction Mental and psychological issues are important in the genesis and development of many diseases, including different dermatoses 1. Psychoneuroimmunology encompasses the interaction of the nervous system and immunity, being for the first time comprehensively described about 30 years ago, although the influence of mental status on the course and outcome of numerous diseases had been suspected long before 1-4. The primary route of communication between the mind and the body is the psycho-immuno-endocrine-cutaneous Correspondence to: Liborija Lugović-Mihić, MD, PhD, Clinical Department of Dermatovenereology, Sestre milosrdnice University Hospital Center, Vinogradska c. 29, HR Zagreb, Croatia liborija@gmail.com Received September 17, 2012, accepted May 10, 2013 system, connecting the activity of the brain, the immune system, and the skin. This communication involves different neuropeptides, interleukins, immune system messengers, hormones, etc. There is clinical and experimental evidence that the brain can start, affect, and halt biological skin events and that the skin, as a relevant part of the diffuse brain, can modify the quality of perceptions and feelings. Many common dermatologic diseases have some form of psychomediated pathogenesis that partially accounts for the development of lesions. Clinical observations support a link between emotional stressors (acute or chronic), psychiatric diseases, and many dermatoses and also report positive effects of psychopharmacology and psychotherapy in their treatment. Thus, different dermatoses can be associated with some psychomediated mechanism, e.g., psoriasis, atopic dermatitis (AD), urticaria, viral warts, herpes Acta Clin Croat, Vol. 52, No. 3,
2 simplex, vitiligo, acnes, hyperhidrosis, effluvium, alopecia, idiopathic itch, lichen simplex, rosacea, seborrheic dermatitis, etc. 1. The main neuroendocrine and nervous pathways of carrying out the physiological effect of psychological, biological, and social factors on the immunity and disease development are the hypothalamic-pituitaryadrenal axis (HPA axis) and the sympathetic, adrenomedullary, and parasympathetic systems 2. These systems react to stressogenic stimuli and can cause pathological occurrences in acute or chronic stress. It is significant that stress resistance can be enhanced by personal coping mechanisms, social support, and favorable psychosocial constellations. According to the biopsychosocial model, psychosocial factors interact with the person s biological characteristics (e.g., genetic or constitutional) engendering vulnerability to disease processes 5. Thus, genetic predisposition to disease development ( diathesis ) may remain latent until stress events, represented as an interaction between the biopsychosocial factors and the person s biology 2. Psychological and social factors are believed to influence disease processes via two main mechanisms: psychosocial processes (e.g., mental health and mood factors, personality characteristics, resources, social relationships) and health-oriented behaviors (e.g., hygiene, protective measures such as sun protection, exercise, nutrition, smoking) 2,6. Studies have shown the association between illness, behavior and psychological state (anxiety, depression, sleep loss, bereavement, etc.) and certain external stress factors (e.g., family illness, academic stress, unemployment), which seem to affect the immune system in some way 4,7. As data on personality and coping suggest, differences in perceptions and reactions to the same events can provoke different endocrine and immune responses. In fact, neuroendocrine mechanisms may mediate the associations between personality and coping styles and immune function 2,8. When talking about the skin, the neuroendocrine substances originate from nerve fibers that innervate it, or from skin cells that can produce and secrete humoral signal molecules (neurotransmitters, neuropeptides and hormones), which enter the HPA axis and are analogous to its own neurotransmitters, neuropeptides and hormones 2. Neuromediators in the skin also include classical neurotransmitters (catecholamines and acetylcholine), released from autonomous nerve fiber endings in the skin and skin cells. Skin proteinases also have a regulatory role in immune and inflammatory reactions, acting as enzymes or ligands of specific receptors (proteinase-activated receptor, PAR). It is important that there is also evidence that at the local level (in the skin) a neuroendocrine control mechanism exists, similar to the central one that acts at the level of the whole body. Cellular Elements of the Skin Immune System and Cytokine Secretion In the epidermis and dermis, there are various immune cells [keratinocytes, dermal dendritic cells (DCs), epidermal Langerhans cells (LSs), melanocytes, T cells and others], which reach the skin through recirculation 2. So, when stimulated, skin cells (primarily keratinocytes) produce various cytokines. Although keratinocytes of healthy skin do not express class II major histocompatibility complex (MHC-IL) or adhesion molecules ICAM-l (an important component for antigen presentation), it is possible in some skin diseases (acting as accessory cells that stimulate proliferation of antigen-stimulated T cells) 2. Keratinocytes synthesize various chemokines and cytokines that act through corresponding receptors on skin cells, having numerous effects on the migration of inflammatory cells, proliferation and differentiation of keratinocytes, synthesis of other cytokines, and on the immune system. After skin contact with the antigen, keratinocytes are activated and produce and secrete various cytokines and chemokines, through which they regulate inflammatory and immune reactions in the skin. Activated keratinocytes secrete proinflammatory cytokines (IL-1α, IL-6, IFN-γ), which enhance migratory activity of LCs leaving for regional lymph nodes, where they stimulate proliferation of specific T cells 9. Thus, keratinocytes can have a role of accessory cells for antigen presentation (under the influence of proinflammatory cytokine IFN-γ they express MHC-lI). Specific T cells enter the circulation and, attracted by chemokines, arrive in the skin where they remain due to increased expression of adhesion molecules on endothelial cells of dermal blood vessels. After initial stimulation of inflammatory and immune reactions, they are inhibited to preserve ho- 338 Acta Clin Croat, Vol. 52, No. 3, 2013
3 meostasis [keratinocytes participate by secreting antiinflammatory cytokines IL-10 and transforming growth factor-β (TGF-β)] 2,9. Keratinocytes produce IL-1 and IL-6 whose basal synthesis is enhanced by some allergens or superantigens. IL-1 is stored in the skin (predominantly as IL-1α) and probably waits to act immediately after an injury or bionoxa. So, IL-1α induces several genes in skin cells, including keratinocytes, fibroblasts (FBLs) and endothelial cells of blood vessels, e.g., genes for adhesion molecules, chemokines, cytokines, proteolytic enzymes and matrix proteins. Keratinocytes also produce IL-6, which stimulates keratinocyte proliferation and it is important in different pathologic conditions (e.g., psoriasis, lichen planus, wound healing), after exposure to UV radiation or after treatment with tumor necrosis factor (TNF-α) 2. Keratinocytes also produce immunomodulatory cytokines that have systemic effects, IL-10 and IL-12, and act antagonistically. After exposure to UV radiation, immunosuppression occurs for which keratinocyte IL-10 is responsible because it shifts the cytokine profile from T helper type 1 (Th1) to T helper type 2 (Th2) cell type (suppresses cellular immunoreaction). On the other hand, IL-12 has an important role in Th1 response induction. It was found that allergens stimulate keratinocytes to secrete IL-12, as in allergic contact dermatitis (as opposed to irritant contact dermatitis). Recently, it has been shown that keratinocytes secrete IL-18, a key mediator that induces Th1 response (e.g., in AD). It is significant that keratinocytes synthesize growth factor and chemokines (IL-8, TNF-α). Chemokines are small cytokines which, during inflammation, are involved in chemotaxis, cell migration and activation, especially of phagocytes and lymphocytes. Thereby, IL-8 is a chemotactic factor for neutrophils and is secreted after contact with various irritants and in autoimmune skin diseases, while TNF-α is released after UV radiation (when it induces keratinocyte apoptosis) and in some skin diseases (e.g., psoriasis and skin T- lymphomas) 2. The Role of Hypothalamic, Hypophyseal and Adrenocortical Hormones It has been determined that skin produces hypothalamic and hypophyseal signal peptides, which are secreted in the intercellular space. So, epidermal keratinocytes and dermal FBLs synthesize hypothalamic and hypophyseal signal peptides and express receptors for them 2. Thus, the skin synthesizes all peptide hormones that enter the HPA axis (the main mediator in stress response), hypothalamic corticotropin-releasing hormone (CRH) and urocortin (a peptide similar to CRH). CRH is a central component of the HPA axis and regulates the expression of pro-opiomelanocortin (POMC) and pituitary POMC-derived peptides [(ACTH, α-melanocyte-stimulating hormone (α-msh) and β-endorphin)] (from the anterior pituitary gland) 10. The skin is directly exposed to various environmental stressors (UV radiation, pathogens, thermal and chemical insults) and the skin cells have developed a number of defense mechanisms that are coordinated by messages from the local neuroendocrineimmune system. The predominant skin stressor from the environment is sun radiation (particularly the UV spectrum) that increases the expression of the gene for prostaglandin metabolism and the genes for IL- 1, IL-6, IL-8, IL-10, for some metalloproteinases, whilst decreasing the activity of the genes for growth factors (KGF, FGF). It has been found that UV radiation leads to increased expression of CRH receptor (CRH-R1). Recent studies have identified the existence of a peripheral skin stress response system (equivalent to the central HPA axis) It is well known that pituitary ACTH stimulates adrenal cortisol and glucocorticoid production. Stress influences cellular and humoral immune responses by releasing glucocorticoid, catecholamine, and CRH and POMC peptide secretion as well as by altering cytokine profiles 11,12. Accordingly, the skin would be a peripheral neuroendocrine organ, and local homeostasis is regulated through hormones, neurotransmitters, neuropeptides, cytokines and their receptors Also, the presence of CRH, urocortin, POMC-derived peptides and their receptors is proven in normal skin: in the epidermis, hair follicles, blood vessel walls, etc. Thus, HPA axis activation at the central, hypothalamic level is stimulated by hormones in the skin, which are a product of various cellular elements 2. POMC is a significant hypophyseal hormone (also found in the skin and other organs), a precur- Acta Clin Croat, Vol. 52, No. 3,
4 sor molecule by whose breakdown [by serine proteases PC1 and PC2 (prohormone-convertase)] active neuropeptides and neurohormones are created: MSH (α-msh, β-msh, γ-msh), ACTH, β-lipotropic hormone (β-lph)) and β-endorphin. These peptides are bound to melanocortin receptors on skin cells: MC-1R (binds α-msh and ACTH) and MC- 2R (selectively binds ACTH). Thus, POMC and its dissolution peptides participate in growth regulation and differentiation, immunomodulatory activities and melanogenesis stimulation, and is found in the skin in keratinocytes, melanocytes, DCs and FBLs. The level of POMC peptide is low in healthy skin and increased in various skin diseases (e.g., AD, melanoma, carcinoma). The expression of POMC is increased under the influence of proinflammatory cytokines (IL-l, IL-6, TNF-α) and UV radiation, and decreased under the influence of antiinflammatory cytokine TGF-β 2. α-msh is a neuropeptide (13-amino-acid polypeptide) derived from POMC and primarily a hypophyseal product (but also synthesized in the skin), whose immune-modulating activity seems to inhibit skin inflammation. Thus, α-msh modulates inflammatory and immune response (by anti-inflammatory action), and it increases the secretion of anti-inflammatory cytokines (IL-10), suppresses the secretion of proinflammatory cytokines (IL-l, IL-6, TNF-α) and limits antigen presentation (decreases expression of MHC-1 and co-stimulatory molecules on DCs). The skin can also release α-msh during the process of synthesis and release of POMC, its derivatives and a series of other substances [substance P (SP), calcitonin gene-related peptide, vasoactive intestinal peptide (VIP), neuropeptide Y (NPY), etc.] 1. Skin cells and Aδ and C nerve fibers release neuropeptides that link the nervous system and the skin itself. Furthermore, α-msh may regulate the expression of cell mediators on the surface of immune cells and decrease IFN-γ release from activated lymphocytes. α-msh also seems to interfere with leukocyte migration from blood to the sites of inflammation, modifying the expression of leukocyte and endothelial adhesion molecules and endothelial leukocyte and vascular cell adhesion molecules-1 (VCAM-1). Thus, α-msh and other neuropeptides may function as a potential therapeutic, anti-inflammatory agent in dermatology. The Role of Corticotropin-Releasing Hormone Stress activates several neural pathways, but the main stress response systems are the locus caeruleus, sympathetic-adrenal-medullary system, and HPA axis The stressors stimulate the paraventricular nuclei of the hypothalamus, whereas the corticotropin-releasing hormone (CRH) and arginine vasopressin (AVP) are synthesized. Thus, CRH stimulates the secretion of AVP (which has a synergistic effect with CRH), particularly under chronic stress, while pituitary ACTH stimulates adrenal cortisol and glucocorticoid production. It can be said that the skin is homologous to the HPA axis and corresponds in organization to the central hypothalamic-hypophyseal axis, CRH-POMC- ACT 13,14. Recently, it has been demonstrated that dermal FBLs respond to CRH by activating the gene for POMC, and subsequently by secreting ACTH 2. Thus, FBLs demonstrate a functional CRH-POMC- ACTH-corticosterone axis similar to the hypothalamus-hypophysis-adrenal gland axis (systemic response to stress), except that FBLs synthesize corticosterone (instead of cortisol). In contrast to FBLs, keratinocytes do not respond to ACTH by secreting corticosterone, although they express CRH R1 and the gene for POMC (they do not demonstrate a functional CRH-POMC axis). Normal skin expresses CRH, urocortin, POMCderived peptides and their receptors. Various skin cells can secrete CRH (including epidermal and hair follicle keratinocytes, sebocytes and mast cells), and melanocytes and FBLs response to local CRH stimulation, confirming the presence of a functional local HPA axis Local production of stress hormones of the HPA axis enables the skin to regulate local homeostasis under stress. CRH acts through CRH receptor (CRH-R), which belongs to the calcitonin/vip/growth hormone-releasing hormone subfamily of the G protein-coupled receptors. These include CRH-R1 (the major receptor in the epidermis and dermis) and CRH-R2 (the predominant type of receptor in adnexal structures) 17. CRH has a different skin effect, i.e. stimulates diverse signaling pathways (via CRH-R1 activation), which modulate proliferation, differentiation, apoptosis and pro- or anti-inflammatory activities of skin cells Acta Clin Croat, Vol. 52, No. 3, 2013
5 CRH activates various skin cells to release the proinflammatory cytokines (e.g., IL-6 release by keratinocytes and IL-1β release by monocytes). As skin mast cells function as sensors of environmental and emotional stress, their CRH-induced activation may be associated with exacerbation of skin diseases 12,19. CRH and urocortin activate skin mast cells (through activation of CRH-R1) and increase mast cell s selective release of vascular endothelial growth factor (VEGF) and IL-6 (vascular permeability) 19. Moreover, human mast cells can produce CRH and urocortin. It could also be mentioned that local concentration of neuropeptides and some chemokines is adjusted by peptidases on skin cell membranes. Some peptidases are expressed on mastocytes, e.g., the neutral peptidase (NEP; CD10), which regulates the concentration of several neuropeptides (substance P, VIP and bradykinin), and adjusts the concentration of opioid peptides Len-enkephalins and Met-enkephalins 2. Hence, CRH has anti-inflammatory activity and diminishes NF-kB activation in epidermal melanocytes and inhibits IL-18 expression [through the mitogen-activated protein kinase (MAPK) signaling pathway] in human HaCaT keratinocytes (cell type belonging to an immortal human keratinocyte line used in scientific research) 20. ACTH stimulates human keratinocytes to secrete IL-18 through melanocortin receptors (MC1R and MC2R), p38 and ERK MAPK pathways. Since CRH inhibits IL-18 expression in HaCaT cells, IL-18 may play an important role in the negative feedback loop of CRH regulation 21. The Influence of Psychosocial and Psychiatric Factors on Dermatologic Diseases Only a few clinical and experimental studies have investigated the association of psychoneuroimmunology and skin diseases (psoriasis, AD, urticaria, viral warts, herpes simplex, vitiligo, acnes, itch, etc.). However, the majority of observations are limited to comparison of clinical pictures of skin diseases and psychological states. It has been observed that psoriasis is worsened by stress, but there is no clear evidence defining the exact pathomechanisms 1. Many psoriatic patients believe that there is a causal relationship between stressors and their disease outcome. Earlier studies have suggested that exacerbation of psoriasis occurs a few weeks to months after a stressful event, which might be related to the alteration of the HPA axis and the release of neuropeptides 12,22. Thus, a recent prospective study demonstrated a positive significant correlation between preceding daily stressors and clinical pictures (Psoriasis Area and Severity Index) and itch (4 weeks later) 23. Earlier studies found a hyporesponsiveness of HPA axis function in psoriatic patients during exposure to an acute stressor, which might result in exaggerated clinical picture due to diminished suppressive effect of the low level of cortisol (indicating they are more vulnerable to the influence of stressors) 12. Recent data revealed associations between daily stressors and an increase in disease severity a month later, with a significant association between the highest levels of daily stressors and a lower cortisol level. Schmid-Ott et al. proved that after a psychosocial stress, psoriatic patients showed an increased number of activated T cells with a shift towards Th1-cytokines and an increased number of cutaneous lymphocyte-associated antigen-positive T cells and natural killer (NK) cells (relevant in aggravation of psoriatic plaques) 24. However, other studies demonstrated no alteration of the HPA axis function in psoriasis, indicating that the systemic HPA axis response could be normal in a Th1-dominant inflammatory condition 12,25. It is interesting to observe the role of β-endorphin (one of the POMC-related peptides) in psoriasis, which is produced by the HPA axis or secreted by immune cells. Psoriatic patients with actively spreading plaque lesions showed increased serum β-endorphin and high lesional β-endorphin, which might induce SP-mediated neurogenic inflammation and has an anti-nociceptive effect on peripheral sensory nerve function (possibly responsible for the absence of itching). It is supposed that β-endorphin may be produced by lesional inflammatory cells rather than by the activation of HPA axis in chronic stress 12. Many researchers focus on the proinflammatory role of CRH in psoriasis. So, CRH may activate mast cells (via CRH-R), leading to the release of histamine with increased vascular permeability. Simultaneously, mast cells secrete the proinflammatory cytokines IL- 1, IL-6 and TNF-α (up-regulated in psoriatic skin), which are potent stimulators of CRH and POMC Acta Clin Croat, Vol. 52, No. 3,
6 production in the skin. In psoriasis, increased serum CRH and decreased lesional CRH/CRH-R1 gene expression suggest that down-regulated lesional CRH/ CRH-R1 expression in psoriatic lesions may be the result of negative feedback of systemic CRH elevation. Thereby, CRH might have a protective function from developing psoriatic lesions 12. However, there are also some conflicting results of peripheral HPA axis expression in psoriatic lesions 12,18. The exposure to stressors (real life and experimental) showed dysregulated HPA activity, which might result in changes of immune responses and peripheral CRH levels. Inflammatory mediators released from psoriatic lesions interact with peripheral HPA axis and may influence the central HPA axis, which should be studied further 12,26. Concerning AD, a chronic allergic skin disease, psychological aspects of the disease must also be taken into account. Investigations have revealed that in AD patients psychological factors seemed to increase serum IFN-γ and IL-4, whereas NK activity was decreased mainly by anxiety (not by psychosomatic complaints) 1. The studies also suggest that psychological stress triggers and aggravates AD by involving the activation of the HPA axis and inducing a shift toward Th2 cell phenotype 12. After stress, AD patients showed blunted HPA axis responsiveness and increased reactivity of the sympathetic adrenomedullary system 27. Interestingly, neonates with a parental atopic history and elevated cord IgE had significantly increased HPA responsiveness to the stress of heel prick (possibly due to hormonal effect to maternal stress), which may increase the vulnerability to develop AD later in life. Additionally, adolescents with AD had an attenuated cortisol response to laboratory stress. However, Afsar et al. identified that AD children did not differ in basal cortisol levels or anxiety compared with normal children 28. There is also an influence of stress-induced CRH on the immune response and DCs which promote allergic responses by inducing Th2 cell differentiation. So, Lee et al. detected CRH-R1α, 1β, 2α mrna and CRH-R1, CRH-R2 protein in mononuclear cellderived DCs in AD patients and revealed that CRH significantly decreased the expression of IL-18 in DCs 29,30. In AD patients, stress-induced CRH may enhance Th2 immune responses by acting directly on DCs (via CRH-R) and may aggravate the disease 29,30. Additionally, patients with severe AD have increased serum levels of β-endorphin produced from lesional inflammatory cells (rather than by activation of central HPA axis in chronic stress). Thereby, stressrelated pruritus may be associated with a systemic pruritic effect of β-endorphin 29,31,32. It has been found that exercise-induced stress differently affects the AD symptoms and POMC-related hormone level, depending on the strength of exercise. As β-endorphin strengthens natural immunity, proper exercise might be helpful to control the AD symptoms by stimulating the HPA axis and inducing balanced Th1/Th2 immunity. Exacerbation of AD due to stress also manifests through mast cell activation 29. In the presence of stem cell factor (SCF) and IL-4, mast cells produce mostly Th2-cytokines and release neuropeptides (such as SP and nerve growth factor, NGF) 19. Experimental stress in AD patients also stimulates enhanced allergen-specific immune responses with elevated levels of plasma SP, VIP and NGF, and concomitant increase of Th2- cytokines 33. There are few studies about local stress hormone expression in AD lesions. The neuropeptides NGF and NPY are known to be associated with anxiety (anxiety score positively correlated with pruritus in AD patients) 33. According to study results, the epidermis of AD skin lesions showed significantly higher NGF and NPY expression, indicating that they participate in the activation of intraepidermal mast cells, contributing to stress-induced pruritus 34,35. AD patients also showed blunted HPA axis responses to stressors. In general, stress negatively affects the severity of AD by down-regulating cellular immunity and enhancing humoral immunity. Thus, CRH and POMC-related peptide hormones, as well as the neuropeptides SP, NGF and NPY modulate immune and inflammatory response under stress. However, psychological interventions have been shown to have positive effects on skin status, itch and scratching behavior in patients 36. Regarding urticaria, it has also been indicated that psychological factors may contribute to its occurrence, especially in chronic urticaria. Psychosocial and psychiatric factors may act in the pathogenesis of urti- 342 Acta Clin Croat, Vol. 52, No. 3, 2013
7 caria, mostly by increasing the release of neuro- and immune mediators, mainly from mast cells (e.g., IL-4, IL-5, IFN-γ, and TNF-α) and the release of vasoactive peptides (including histamine) 1. There is also evidence of the psychoneuroimmune mechanisms in the pathogenesis of vitiligo 37. Some investigators revealed a higher number of stressful life events in these patients compared to controls, as well as abnormal secretion of neuromediators (e.g., β-endorphin and metenkephalin) and higher immunoreactivity to NPY and VIP. Not all effects of neuropeptides on melanocytes are known, although nervous system seems to play a role in activating melanocytes 1. Alternatively, clinical and experimental evidence suggests a role of humoral and cellular autoimmunity in vitiligo pathogenesis. It is important to mention that some infective skin diseases are also under psychological influence (e.g., viral warts, herpes simplex) 38,39. There are also other dermatologic diseases for which there is evidence of psychological and psychiatric etiological factors. This indicates its importance in considering the possibility that those patients could benefit from cognitive behavioral and psychological therapy 1,40. As dermatologists and dermatologic patients have long acknowledged the effect of stress on the skin and its capability to initiate, maintain, or exacerbate several skin diseases, it is important to understand skin vulnerability to psychological stress It is significant that stress resistance can be enhanced by personal coping mechanisms, social support, and favorable psychosocial constellations. A multidisciplinary approach for treatment from both dermatologic and psychiatric viewpoints is suggested. Conclusion The link between emotional stressors (acute or chronic), psychiatric diseases, and dermatoses (e.g., psoriasis, AD, urticaria, viral warts, herpes simplex, vitiligo, acnes, alopecia, prurigo, etc.) has been evidenced. Thereby, different cytokines, mediators and hormones are produced in the skin and involved in the pathogenesis of these skin disorders. A prominent role is played by those agents that belong to the HPA axis and there is plenty of evidence that the skin includes a neuroendocrine control mechanism similar to the central one. This indicates its importance in considering the possibility that these patients could benefit from cognitive behavioral and psychological therapy or other therapeutic methods. However, the psychological and psychiatric genesis of a skin disease is still a topic of investigation. References 1. Urpe M, Buggiani G, Lotti T. Stress and psychoneuroimmunologic factors in dermatology. Dermatol Clin 2005;23(4): Gabrilovac J. Neuroendokrina regulacija imunosnog odgovara u koži. In: Boranić M et al., editors. Psihoneuroimunologija. Zagreb: Školska knjiga, 2008: (in Croatian) 3. Lugović L, Šitum M, Vurnek M, Buljan M. Influence of psychoneuroimmunologic factors on patients with malignant skin diseases. Acta Med Croatica 2007;61(4): Vidrih B, Karlović D, bošnjak Pašić M, Uremović M, KOVAK Mufić A, MatoŠić A. A review of the psychoneuroimmunologic concepts on the etiology of depressive disorders. Acta Clin Croat 2012;51(3): Engel GF. The need for a new medical model: a challenge for biomedicine. Science 1977;196: Kiecolt-Glaser JK, McGuire L, Robles TF. Emotions, morbidity, and mortality. New perspectives from psychoneuroimmunology. Annu Rev Psychol 2002;53: Moldofsky H, Lue FA, Davidson JR. Effect of sleep deprivation on human immune function. FASEB J 1989;3(8): Segerstrom SC. Personality and the immune system: models, methods, and mechanisms. Annu Rev Behav Med 2000;22(3): Bakula A, Lugović-Mihić L, Šitum M, Turčin J, Šinković A. Contact allergy in the mouth: diversity of clinical presentations and diagnosis of common allergens relevant to dental practice. Acta Clin Croat 2011;50(4): Chrousos GP. Stressors, stress, and neuroendocrine integration of the adaptive response. Ann N Y Acad Sci 1998;30(851): Elenkov IJ, Chrousos GP. Stress hormones, Th1/Th2 patterns, pro/anti-inflammatory cytokines and susceptibility to disease. Trends Endocrinol Metab 1999;10(9): Kim JE, Park HJ. Stress hormone and skin disease [homepage on the Internet]. Korea: Department of Dermatology, College of Medicine; 2012 [updated 17 May 2012; cited 30 May 2012]. Available from: com/pdfs/22589/intech-stress_hormone_and_skin_disease.pdf Acta Clin Croat, Vol. 52, No. 3,
8 13. Slominski A, Wortsman J, Luger T, Paus R, Solomon S. Corticotropin releasing hormone and proopiomelanocortin involvement in the cutaneous response to stress. Physiol Rev 2000;80(3): Slominski A, Zbytek B, Pisarchik A, Slominski RM, Zmijewski MA, Wortsman J. CRH functions as a growth factor/cytokine in the skin. J Cell Physiol 2006;206(3): Slominski A, Wortsman J, Tuckey RC, Paus R. Differential expression of HPA axis homolog in the skin. Mol Cell Endocrinol 2007; : Zhang X, Sliwowska JH, Weinberg J. Prenatal alcohol exposure and fetal programming: effects on neuroendocrine and immune function. Exp Biol Med (Maywood) 2005;230(6): Pisarchik A, Slominski A. Molecular and functional characterization of novel CRHR1 isoforms from the skin. Eur J Biochem 2004;271(13): O Kane M, Murphy EP, Kirby B. The role of corticotropin-releasing hormone in immune-mediated cutaneous inflammatory disease. Exp Dermatol 2006;15(3): Theoharides TC, Alysandratos KD, Angelidou A, et al. Mast cells and inflammation. Biochim Biophys Acta 2012;1822(1): Park HJ, Kim HJ, Lee JH, et al. Corticotropin-releasing hormone (CRH) downregulates interleukin-18 expression in human HaCaT keratinocytes by activation of p38 mitogenactivated protein kinase (MAPK) pathway. J Invest Dermatol 2005;124(4): Park HJ, Kim HJ, Lee JY, et al. Adrenocorticotropin hormone stimulates interleukin-18 expression in human HaCaT keratinocytes. J Invest Dermatol 2007;127(5): Gupta MA, Gupta AK, Kirkby S, et al. Pruritus in psoriasis. A prospective study of some psychiatric and dermatologic correlates. Arch Dermatol 1988;124(7): Verhoeven EW, Kraaimaat FW, Jong EM, et al. Effect of daily stressors on psoriasis: a prospective study. J Invest Dermatol 2009;129(8): Schmid-Ott G, Jaeger B, Boehm T, et al. Immunological effects of stress in psoriasis. Br J Dermatol 2009;160(4): Karanikas E, Harsoulis F, Giouzepas I, Griveas I, Chrisomallis F. Neuroendocrine stimulatory tests of hypothalamus-pituitary-adrenal axis in psoriasis and correlative implications with psychopathological and immune parameters. J Dermatol 2009;36(1): Leibovici V, Canetti L, Yahalomi S, et al. Well being, psychopathology and coping strategies in psoriasis compared with atopic dermatitis: a controlled study. J Eur Acad Dermatol Venereol 2010;24(8): Buske-Kirschbaum A, Ebrecht M, Hellhammer DH. Blunted HPA axis responsiveness to stress in atopic patients is associated with the acuity and severeness of allergic inflammation. Brain Behav Immun 2010;24(8): Afsar FS, Isleten F, Sonmez N. Children with atopic dermatitis do not have more anxiety or different cortisol levels compared with normal children. J Cutan Med Surg 2010;14(1): Lee CH., Chuang HY, Shih CC, et al. Transepidermal water loss, serum IgE and beta-endorphin as important and independent biological markers for development of itch intensity in atopic dermatitis. Br J Dermatol 2006;154(6): Lee HJ, Kwon YS, Park CO, et al. Corticotropin-releasing factor decreases IL-18 in the monocyte-derived dendritic cell. Exp Dermatol 2009;18(3): Glinski W, Brodecka H, Glinska-Ferenz M, Kowalski D. Increased concentration of beta-endorphin in the sera of patients with severe atopic dermatitis. Exp Dermatol 1995;75(1): Katsarou-Katsari A, Filippou A, Theoharides TC. Effect of stress and other psychological factors on the pathophysiology and treatment of dermatoses. Int J Immunopathol Pharmacol 1999;12(1): Kimata H. Enhancement of allergic skin wheal responses in patients with atopic eczema/dermatitis syndrome by playing video games or by a frequently ringing mobile phone. Eur J Clin Invest 2003;3(6): Oh SH, Bae BG, Park CO, et al. Association of stress with symptoms of atopic dermatitis. Acta Derm Venereol 2010;90(6): Dou YC, Hagströmer L, Emtestam L, Johansson O. Increased nerve growth factor and its receptors in atopic dermatitis: an immunohistochemical study. Arch Dermatol Res 2006;298(1): Schut C, Weik U, Tews N, Gieler U, Deinzer R, Kupfer J. Psychophysiological effects of stress management in patients with atopic dermatitis: a randomized controlled trial. Acta Derm Venereol 2013;93(1): Schwartz R, Sepúlveda JE, Quintana T. Possible role of psychological and environmental factors in the genesis of childhood vitiligo. Rev Med Chil 2009;137(1): Dhabhar FS. Psychological stress and immunoprotection versus immunopathology in the skin. Clin Dermatol 2013;31(1): Chida Y, Mao X. Does psychosocial stress predict symptomatic herpes simplex virus recurrence? A meta-analytic investigation on prospective studies. Brain Behav Immun 2009;23(7): Chung WL, Ng SS, Koh M, Peh LH, Liu TT. A review of patients managed at a combined psychodermatology clinic: a Singapore experience. Singapore Med J 2012;53(12): Acta Clin Croat, Vol. 52, No. 3, 2013
9 41. Orion E, Wolf R. Psychological stress and epidermal barrier function. Clin Dermatol 2012;30(3): Basavaraj KH, Navya MA, Rashmi R. Relevance of psychiatry in dermatology: present concepts. Indian J Psychiatry 2010;52(3): Sažetak PSIHONEUROIMUNOLOŠKI ASPEKTI KOŽNIH BOLESTI L. Lugović-Mihić, L. Ljubešić, J. Mihić, V. Vuković-Cvetković, N. Troskot i M. Šitum S obzirom na to da su mentalne i psihološke značajke važne u razvoju mnogih dermatoloških bolesti, ovi čimbenici su od posebnog interesa za istraživanja. Psihoneuroimunologija obuhvaća međudjelovanje psiholoških procesa, živčanog i imunog sustava te ljudskog tijela, a prvi put je jasno opisana prije oko 30 godina. Komunikacija između psihe i kože uključuje psihološki-imuni-endokrini-kožni sustav obuhvaćajući aktivnosti mozga, imunog sustava i kože, uza sudjelovanje različitih neuropeptida, interleukina i posrednika imunog sustava. Mnoge česte dermatološke bolesti imaju neki oblik psihološki uvjetovane patogeneze koja dijelom doprinosi razvoju kožnih promjena. Pritom postoji veza između emocionalnih stresora (akutnih ili kroničnih), psihijatrijskih bolesti i dermatoza (npr. psorijaza, atopijski dermatitis, urtikarija, akne, virusne bradavice, herpes simpleks, vitiligo, alopecia, prurigo itd.) te različitih citokina i medijatora stvorenih u koži koji su uključeni u njihovu patogenezu. Istaknutu ulogu imaju tvari koje pripadaju osi hipotalamus-hipofiza-nadbubrežna žlijezda. Ključne riječi: Psihoneuroimunologija; Koža; Kožne bolesti; Interleukini; Neuropeptidi; Hormoni Acta Clin Croat, Vol. 52, No. 3,
Cutaneous Immunology: Innate Immune Responses. Skin Biology Lecture Series
 Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
Cutaneous Immunology: Innate Immune Responses Skin Biology Lecture Series The Immune Response: Innate and Adaptive Components Source: Wolff, Goldsmith, Katz, Gilchrest, Paller, Leffell. Fitzpatrick s Dermatology
The Immune System: The Mind Body Connection. Presented by Margaret Kemeny, Ph.D. Department of Psychiatry, University of California, San Francisco
 The Immune System: The Mind Body Connection Presented by Margaret Kemeny, Ph.D. Department of Psychiatry, University of California, San Francisco Psychoneuroimmunology Investigation of the bidirectional
The Immune System: The Mind Body Connection Presented by Margaret Kemeny, Ph.D. Department of Psychiatry, University of California, San Francisco Psychoneuroimmunology Investigation of the bidirectional
Neuroimmunology. Innervation of lymphoid organs. Neurotransmitters. Neuroendocrine hormones. Cytokines. Autoimmunity
 Neuroimmunology Innervation of lymphoid organs Neurotransmitters Neuroendocrine hormones Cytokines Autoimmunity CNS has two ways of contacting and regulating structures in the periphery Autonomic
Neuroimmunology Innervation of lymphoid organs Neurotransmitters Neuroendocrine hormones Cytokines Autoimmunity CNS has two ways of contacting and regulating structures in the periphery Autonomic
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A
 HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
HYPERSENSITIVITY REACTIONS D R S H O AI B R AZ A HYPERSENSITIVITY REACTIONS Are exaggerated immune response upon antigenic stimulation Individuals who have been previously exposed to an antigen are said
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Stress and Disease. Chapter 8. Elsevier items and derived items 2008 by Mosby, Inc., an affiliate of Elsevier Inc.
 Stress and Disease Chapter 8 Stress A person experiences stress when a demand exceeds a person s coping abilities, resulting in reactions such as disturbances of cognition, emotion, and behavior that can
Stress and Disease Chapter 8 Stress A person experiences stress when a demand exceeds a person s coping abilities, resulting in reactions such as disturbances of cognition, emotion, and behavior that can
Basis of Immunology and
 Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Basis of Immunology and Immunophysiopathology of Infectious Diseases Jointly organized by Institut Pasteur in Ho Chi Minh City and Institut Pasteur with kind support from ANRS & Université Pierre et Marie
Neurobiology of Addiction
 Neurobiology of Addiction Domenic A. Ciraulo, MD Director of Alcohol Pharmacotherapy Research Center for Addiction Medicine Department of Psychiatry Massachusetts General Hospital Disclosure Neither I
Neurobiology of Addiction Domenic A. Ciraulo, MD Director of Alcohol Pharmacotherapy Research Center for Addiction Medicine Department of Psychiatry Massachusetts General Hospital Disclosure Neither I
IL-17 in health and disease. March 2014 PSO13-C051n
 IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
IL-17 in health and disease March 2014 PSO13-C051n Originally Researchers Suggested That IL-12 and IL-4 drove Th Cell Differentiation Naïve CD4 + T cell Question: Which of these cell types is responsible
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
Stress, Immunity and the HPA axis
 Stress, Immunity and the HPA axis The goal of these lectures is to discuss basic physiology associated with the control of stress and immunity. This lecture together with the previous one (biological rhythms)
Stress, Immunity and the HPA axis The goal of these lectures is to discuss basic physiology associated with the control of stress and immunity. This lecture together with the previous one (biological rhythms)
PASPCR June, 2006 Commentary
 Scientific journey: from Bomirski melanoma to a stress- response system in the skin Andrzej Slominski, MD, PhD Department of Pathology and Laboratory Medicine, University of Tennessee HSC 1. Introduction
Scientific journey: from Bomirski melanoma to a stress- response system in the skin Andrzej Slominski, MD, PhD Department of Pathology and Laboratory Medicine, University of Tennessee HSC 1. Introduction
Overview of the Lymphoid System
 Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
Overview of the Lymphoid System The Lymphoid System Protects us against disease Lymphoid system cells respond to Environmental pathogens Toxins Abnormal body cells, such as cancers Overview of the Lymphoid
NROSCI/BIOSC 1070 and MSNBIO 2070 September 11, 2017 Control Mechanisms 2: Endocrine Control
 NROSCI/BIOSC 1070 and MSNBIO 2070 September 11, 2017 Control Mechanisms 2: Endocrine Control Hormones are chemical messengers that are secreted into the blood by endocrine cells or specialized neurons.
NROSCI/BIOSC 1070 and MSNBIO 2070 September 11, 2017 Control Mechanisms 2: Endocrine Control Hormones are chemical messengers that are secreted into the blood by endocrine cells or specialized neurons.
Chapter 16: Endocrine System 1
 Ch 16 Endocrine System Bi 233 Endocrine system Endocrine System: Overview Body s second great controlling system Influences metabolic activities of cells by means of hormones Slow signaling Endocrine glands
Ch 16 Endocrine System Bi 233 Endocrine system Endocrine System: Overview Body s second great controlling system Influences metabolic activities of cells by means of hormones Slow signaling Endocrine glands
Fluid movement in capillaries. Not all fluid is reclaimed at the venous end of the capillaries; that is the job of the lymphatic system
 Capillary exchange Fluid movement in capillaries Not all fluid is reclaimed at the venous end of the capillaries; that is the job of the lymphatic system Lymphatic vessels Lymphatic capillaries permeate
Capillary exchange Fluid movement in capillaries Not all fluid is reclaimed at the venous end of the capillaries; that is the job of the lymphatic system Lymphatic vessels Lymphatic capillaries permeate
Allergic rhinitis (Hay fever) Asthma Anaphylaxis Urticaria Atopic dermatitis
 Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
Hypersensitivity Disorders Hypersensitivity Disorders Immune Response IgE Disease Example Ragweed hay fever IgG Cytotoxic Immune complex T Cell Hemolytic anemia Serum sickness Poison ivy IgE-mediated Diseases
ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES:
 ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES: -In a living organism there must be coordination of number of physiological activities taking place simultaneously such as: movement, respiration,
ENDOCRINOLOGY COORDINATION OF PHYSIOLOGICAL PROCESSES: -In a living organism there must be coordination of number of physiological activities taking place simultaneously such as: movement, respiration,
NTD Vaccine Design Toolkit and Training Workshop Providence, RI January 05, 2011 Cytokines Leslie P. Cousens, PhD EpiVax, Inc.
 NTD Vaccine Design Toolkit and Training Workshop Providence, RI January 05, 2011 Cytokines Leslie P. Cousens, PhD EpiVax, Inc. Cytokines Properties of Cytokines Cytokines are proteins with specific roles
NTD Vaccine Design Toolkit and Training Workshop Providence, RI January 05, 2011 Cytokines Leslie P. Cousens, PhD EpiVax, Inc. Cytokines Properties of Cytokines Cytokines are proteins with specific roles
Subject Index. hypothalamic-pituitary-adrenal axis 158. Atherosclerosis, ghrelin role AVP, see Arginine vasopressin.
 Subject Index Acromegaly, somatostatin analog therapy dopamine agonist combination therapy 132 efficacy 132, 133 overview 130, 131 receptor subtype response 131, 132 SOM30 studies 131, 132 ACTH, see Adrenocorticotropic
Subject Index Acromegaly, somatostatin analog therapy dopamine agonist combination therapy 132 efficacy 132, 133 overview 130, 131 receptor subtype response 131, 132 SOM30 studies 131, 132 ACTH, see Adrenocorticotropic
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
The Skinny of the Immune System
 The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
The Skinny of the Immune System Robert Hostoffer, DO, FACOP, FAAP Associate Professor of Pediatrics Case Western Reserve University, Cleveland, Ohio Overview 1. Immune system of the skin 2. Immune Players
Chapter 21: Innate and Adaptive Body Defenses
 Chapter 21: Innate and Adaptive Body Defenses I. 2 main types of body defenses A. Innate (nonspecific) defense: not to a specific microorganism or substance B. Adaptive (specific) defense: immunity to
Chapter 21: Innate and Adaptive Body Defenses I. 2 main types of body defenses A. Innate (nonspecific) defense: not to a specific microorganism or substance B. Adaptive (specific) defense: immunity to
Anatomy 36 Study Guide Unit 3
 Anatomy 36 Study Guide Unit 3 Chapter 11 Amine hormones Peptide hormones Steroid hormones 11 4 Hormones of the adrenal cortex 11 6 Hormones of the gonads Categories of hormones Table 11 2 Hormone receptors
Anatomy 36 Study Guide Unit 3 Chapter 11 Amine hormones Peptide hormones Steroid hormones 11 4 Hormones of the adrenal cortex 11 6 Hormones of the gonads Categories of hormones Table 11 2 Hormone receptors
Introduction to Immunopathology
 MICR2209 Introduction to Immunopathology Dr Allison Imrie 1 Allergy and Hypersensitivity Adaptive immune responses can sometimes be elicited by antigens not associated with infectious agents, and this
MICR2209 Introduction to Immunopathology Dr Allison Imrie 1 Allergy and Hypersensitivity Adaptive immune responses can sometimes be elicited by antigens not associated with infectious agents, and this
Immune System. Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka
 Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
Immune System Presented by Kazzandra Anton, Rhea Chung, Lea Sado, and Raymond Tanaka Content Standards 35.1 In innate immunity, recognition and response rely on traits common to groups of pathogens 35.2
The Adaptive Immune Responses
 The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
Mucosal Immune System
 Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Strategies to Gain Acceptance for Wellness/ Mind-Body Programs by Skeptical Residents and Clinical Faculty: Stress Physiology
 Strategies to Gain Acceptance for Wellness/ Mind-Body Programs by Skeptical Residents and Clinical Faculty: Stress Physiology Michael D. Lumpkin, PhD Professor of Integrative Physiology and Biochemistry
Strategies to Gain Acceptance for Wellness/ Mind-Body Programs by Skeptical Residents and Clinical Faculty: Stress Physiology Michael D. Lumpkin, PhD Professor of Integrative Physiology and Biochemistry
Skin Immune Mechanisms in Health and Disease
 Skin Immune Mechanisms in Health and Disease by Barbara S. Baker Published by Garner Press (http://www.garnerpress.com) Copyright 2006 Garner Press All rights reserved. This book, or parts thereof, may
Skin Immune Mechanisms in Health and Disease by Barbara S. Baker Published by Garner Press (http://www.garnerpress.com) Copyright 2006 Garner Press All rights reserved. This book, or parts thereof, may
Cytokines, adhesion molecules and apoptosis markers. A comprehensive product line for human and veterinary ELISAs
 Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
Cytokines, adhesion molecules and apoptosis markers A comprehensive product line for human and veterinary ELISAs IBL International s cytokine product line... is extremely comprehensive. The assays are
Autoimmune Diseases. Betsy Kirchner CNP The Cleveland Clinic
 Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
Autoimmune Diseases Betsy Kirchner CNP The Cleveland Clinic Disclosures (financial) No relevant disclosures Learning Objectives Explain the pathophysiology of autoimmune disease Discuss safe administration
The recruitment of leukocytes and plasma proteins from the blood to sites of infection and tissue injury is called inflammation
 The migration of a particular type of leukocyte into a restricted type of tissue, or a tissue with an ongoing infection or injury, is often called leukocyte homing, and the general process of leukocyte
The migration of a particular type of leukocyte into a restricted type of tissue, or a tissue with an ongoing infection or injury, is often called leukocyte homing, and the general process of leukocyte
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel:
 Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Cytokines (II) Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Understand the physiological
Chapter 9 The Endocrine System and Hormone Activity
 Chapter 9 The Endocrine System and Hormone Activity Overview Coordinates and directs the activity of cells. Interacts with the nervous system Uses chemical messengers called hormones released by organs
Chapter 9 The Endocrine System and Hormone Activity Overview Coordinates and directs the activity of cells. Interacts with the nervous system Uses chemical messengers called hormones released by organs
Stimulation of the hypothalamic-pituitary-adrenal axis with corticotropin releasing hormone in patients with psoriasis
 HORMONES 2007, 6(4):314-320 Research paper Stimulation of the hypothalamic-pituitary-adrenal axis with corticotropin releasing hormone in patients with psoriasis Evangelos Karanikas, Faidon Harsoulis,
HORMONES 2007, 6(4):314-320 Research paper Stimulation of the hypothalamic-pituitary-adrenal axis with corticotropin releasing hormone in patients with psoriasis Evangelos Karanikas, Faidon Harsoulis,
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep
 The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
Immunology lecture: 14. Cytokines: Main source: Fibroblast, but actually it can be produced by other types of cells
 Immunology lecture: 14 Cytokines: 1)Interferons"IFN" : 2 types Type 1 : IFN-Alpha : Main source: Macrophages IFN-Beta: Main source: Fibroblast, but actually it can be produced by other types of cells **There
Immunology lecture: 14 Cytokines: 1)Interferons"IFN" : 2 types Type 1 : IFN-Alpha : Main source: Macrophages IFN-Beta: Main source: Fibroblast, but actually it can be produced by other types of cells **There
Mast cells as targets of corticotropinreleasing factor and related peptides
 Opinion TRENDS in Pharmacological Sciences Vol.25 No.11 November 2004 Mast cells as targets of corticotropinreleasing factor and related peptides Theoharis C. Theoharides 1,2,3, Jill M. Donelan 1, Nikoletta
Opinion TRENDS in Pharmacological Sciences Vol.25 No.11 November 2004 Mast cells as targets of corticotropinreleasing factor and related peptides Theoharis C. Theoharides 1,2,3, Jill M. Donelan 1, Nikoletta
Immunology for the Rheumatologist
 Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
INFLAMMATION & REPAIR
 INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
INFLAMMATION & REPAIR Lecture 7 Chemical Mediators of Inflammation Winter 2013 Chelsea Martin Special thanks to Drs. Hanna and Forzan Course Outline i. Inflammation: Introduction and generalities (lecture
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline Consensus characteristics/incidence data Immune/inflammatory basis Etiology/Genetic basis Hygiene
PRURITOCEPTIVE AND PSYCHOGENIC PRURITUS IN LICHEN SIMPLEX CHRONICUS
 ORIGINAL ARTICLES PRURITOCEPTIVE AND PSYCHOGENIC PRURITUS IN LICHEN SIMPLEX CHRONICUS Department of Dermatology and Venerology, ABSTRACT Pruritus is a diagnostic hallmark for Lichen Simplex Chronicus (LSC).
ORIGINAL ARTICLES PRURITOCEPTIVE AND PSYCHOGENIC PRURITUS IN LICHEN SIMPLEX CHRONICUS Department of Dermatology and Venerology, ABSTRACT Pruritus is a diagnostic hallmark for Lichen Simplex Chronicus (LSC).
Chapter 6 Communication, Integration, and Homeostasis
 Chapter 6 Communication, Integration, and Homeostasis About This Chapter Cell-to-cell communication Signal pathways Novel signal molecules Modulation of signal pathways Homeostatic reflex pathways Cell-to-Cell
Chapter 6 Communication, Integration, and Homeostasis About This Chapter Cell-to-cell communication Signal pathways Novel signal molecules Modulation of signal pathways Homeostatic reflex pathways Cell-to-Cell
Cell-Derived Inflammatory Mediators
 Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
Cell-Derived Inflammatory Mediators Introduction about chemical mediators in inflammation Mediators may be Cellular mediators cell-produced or cell-secreted derived from circulating inactive precursors,
T Cell Effector Mechanisms I: B cell Help & DTH
 T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
T Cell Effector Mechanisms I: B cell Help & DTH Ned Braunstein, MD The Major T Cell Subsets p56 lck + T cells γ δ ε ζ ζ p56 lck CD8+ T cells γ δ ε ζ ζ Cα Cβ Vα Vβ CD3 CD8 Cα Cβ Vα Vβ CD3 MHC II peptide
Mechanisms of disease
 PP Mechanisms of disease Stress and disease Homeostasis - Responsible for maintaining a constant, safe internal environment - Controlled by feedback loops o Negative feedback loop: temperature, blood glucose
PP Mechanisms of disease Stress and disease Homeostasis - Responsible for maintaining a constant, safe internal environment - Controlled by feedback loops o Negative feedback loop: temperature, blood glucose
Chapter 13: Cytokines
 Chapter 13: Cytokines Definition: secreted, low-molecular-weight proteins that regulate the nature, intensity and duration of the immune response by exerting a variety of effects on lymphocytes and/or
Chapter 13: Cytokines Definition: secreted, low-molecular-weight proteins that regulate the nature, intensity and duration of the immune response by exerting a variety of effects on lymphocytes and/or
Stress and the aging brain
 Stress and the aging brain Stress and the aging brain: What are the issues? Aging makes us less able to adjust to change Reactions of elderly to change generate stress Stress response involves acute reactions
Stress and the aging brain Stress and the aging brain: What are the issues? Aging makes us less able to adjust to change Reactions of elderly to change generate stress Stress response involves acute reactions
Adrenal Steroid Hormones (Chapter 15) I. glucocorticoids cortisol corticosterone
 Adrenal Steroid Hormones (Chapter 15) I. glucocorticoids cortisol corticosterone II. mineralocorticoids i id aldosterone III. androgenic steroids dehydroepiandrosterone testosterone IV. estrogenic steroids
Adrenal Steroid Hormones (Chapter 15) I. glucocorticoids cortisol corticosterone II. mineralocorticoids i id aldosterone III. androgenic steroids dehydroepiandrosterone testosterone IV. estrogenic steroids
Immunology of Asthma. Kenneth J. Goodrum,Ph. Ph.D. Ohio University College of Osteopathic Medicine
 Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Immunology of Asthma Kenneth J. Goodrum,Ph Ph.D. Ohio University College of Osteopathic Medicine Outline! Consensus characteristics! Allergens:role in asthma! Immune/inflammatory basis! Genetic basis!
Basis and Clinical Applications of Interferon
 Interferon Therapy Basis and Clinical Applications of Interferon JMAJ 47(1): 7 12, 2004 Jiro IMANISHI Professor, Kyoto Prefectural University of Medicine Abstract: Interferon (IFN) is an antiviral substance
Interferon Therapy Basis and Clinical Applications of Interferon JMAJ 47(1): 7 12, 2004 Jiro IMANISHI Professor, Kyoto Prefectural University of Medicine Abstract: Interferon (IFN) is an antiviral substance
Stressed skin? a molecular psychosomatic update on stress-causes and effects in dermatologic diseases
 Submitted: 5.11.2015 Accepted: 30.12.2015 Conflict of interest None. DOI: 10.1111/ddg.12957 Stressed skin? a molecular psychosomatic update on stress-causes and effects in dermatologic diseases Eva M.J.
Submitted: 5.11.2015 Accepted: 30.12.2015 Conflict of interest None. DOI: 10.1111/ddg.12957 Stressed skin? a molecular psychosomatic update on stress-causes and effects in dermatologic diseases Eva M.J.
1. Specificity: specific activity for each type of pathogens. Immunity is directed against a particular pathogen or foreign substance.
 L13: Acquired or adaptive (specific) immunity The resistance, which absent at the time of first exposure to a pathogen, but develops after being exposed to the pathogen is called acquired immunity. It
L13: Acquired or adaptive (specific) immunity The resistance, which absent at the time of first exposure to a pathogen, but develops after being exposed to the pathogen is called acquired immunity. It
Cytokines. Luděk Šefc. Cytokines Protein regulators of cellular communication. Cytokines x hormones
 Cytokines Luděk Šefc Cytokines Protein regulators of cellular communication Cytokines x hormones Hormones Cytokines Production sites few many Cell targets few many Presence in blood yes rarely Biological
Cytokines Luděk Šefc Cytokines Protein regulators of cellular communication Cytokines x hormones Hormones Cytokines Production sites few many Cell targets few many Presence in blood yes rarely Biological
DNA vaccine, peripheral T-cell tolerance modulation 185
 Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Subject Index Airway hyperresponsiveness (AHR) animal models 41 43 asthma inhibition 45 overview 41 mast cell modulation of T-cells 62 64 respiratory tolerance 40, 41 Tregs inhibition role 44 respiratory
Everant.in/index.php/jmpr. Journal of Medical Practice and Review
 Everant.in/index.php/jmpr Journal of Medical Practice and Review Real world Efficacy and Tolerance of Bepotastine, a new 2 nd generation antihistamine, in Pruritis and other symptoms associated with cutaneous
Everant.in/index.php/jmpr Journal of Medical Practice and Review Real world Efficacy and Tolerance of Bepotastine, a new 2 nd generation antihistamine, in Pruritis and other symptoms associated with cutaneous
BIOLOGY - CLUTCH CH.45 - ENDOCRINE SYSTEM.
 !! www.clutchprep.com Chemical signals allow cells to communicate with each other Pheromones chemical signals released to the environment to communicate with other organisms Autocrine signaling self-signaling,
!! www.clutchprep.com Chemical signals allow cells to communicate with each other Pheromones chemical signals released to the environment to communicate with other organisms Autocrine signaling self-signaling,
Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals. Taniawati Supali. Department of Parasitology
 Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals Taniawati Supali Department of Parasitology 1 Defense mechanism in human Th17 (? ) Acute Chronic Th1 Th 2 Intracellular Treg
Immunological Aspects of Parasitic Diseases in Immunocompromised Individuals Taniawati Supali Department of Parasitology 1 Defense mechanism in human Th17 (? ) Acute Chronic Th1 Th 2 Intracellular Treg
Why do we itch and scratch? Radhika Bali 6 th Year Medical Student University of Cambridge
 Why do we itch and scratch? Radhika Bali 6 th Year Medical Student University of Cambridge Introduction Itch is an increasingly common symptom presenting in both dermatology and primary care, which may
Why do we itch and scratch? Radhika Bali 6 th Year Medical Student University of Cambridge Introduction Itch is an increasingly common symptom presenting in both dermatology and primary care, which may
Innate Immunity. Chapter 3. Connection Between Innate and Adaptive Immunity. Know Differences and Provide Examples. Antimicrobial peptide psoriasin
 Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Chapter Know Differences and Provide Examples Innate Immunity kin and Epithelial Barriers Antimicrobial peptide psoriasin -Activity against Gram (-) E. coli Connection Between Innate and Adaptive Immunity
Art labeling Activity: Figure 16.1
 ANP 1105D Winter 2013 Assignment 6 part I: The Endocrine Sy... Assignment 6 part I: The Endocrine System, Chapter 16 Due: 11:59pm on Monday, March 4, 2013 Note: To understand how points are awarded, read
ANP 1105D Winter 2013 Assignment 6 part I: The Endocrine Sy... Assignment 6 part I: The Endocrine System, Chapter 16 Due: 11:59pm on Monday, March 4, 2013 Note: To understand how points are awarded, read
Nonspecific External Barriers skin, mucous membranes
 Immune system Chapter 36 BI 103 Plant-Animal A&P Levels of Defense Against Disease Nonspecific External Barriers skin, mucous membranes Physical barriers? Brainstorm with a partner If these barriers are
Immune system Chapter 36 BI 103 Plant-Animal A&P Levels of Defense Against Disease Nonspecific External Barriers skin, mucous membranes Physical barriers? Brainstorm with a partner If these barriers are
TRAUMATIC BRAIN INJURY: FROM PHYSIOLOGY TO TREATMENT Presented by: Dr. J. Brandon Brock, DC, MSN, RN, NP-C, DAAIM, DACNB, BCIM, FICC
 TRAUMATIC BRAIN INJURY: FROM PHYSIOLOGY TO TREATMENT Presented by: Dr. J. Brandon Brock, DC, MSN, RN, NP-C, DAAIM, DACNB, BCIM, FICC https://www.facebook.com/drbrandonbrock/ The Problem!!! What are We
TRAUMATIC BRAIN INJURY: FROM PHYSIOLOGY TO TREATMENT Presented by: Dr. J. Brandon Brock, DC, MSN, RN, NP-C, DAAIM, DACNB, BCIM, FICC https://www.facebook.com/drbrandonbrock/ The Problem!!! What are We
INNATE IMMUNITY Non-Specific Immune Response. Physiology Unit 3
 INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
INNATE IMMUNITY Non-Specific Immune Response Physiology Unit 3 Protection Against Infection The body has several defenses to protect itself from getting an infection Skin Mucus membranes Serous membranes
Recent insights into atopic dermatitis and implications for management of infectious complications
 Mark Boguniewicz, MD Professor, Division of Allergy-Immunology Department of Pediatrics National Jewish Health and University of Colorado School of Medicine Denver, Colorado USA Recent insights into atopic
Mark Boguniewicz, MD Professor, Division of Allergy-Immunology Department of Pediatrics National Jewish Health and University of Colorado School of Medicine Denver, Colorado USA Recent insights into atopic
TCR, MHC and coreceptors
 Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cellular Immune response. Jianzhong Chen, Ph.D Institute of immunology, ZJU
 Cellular Immune response Jianzhong Chen, Ph.D Institute of immunology, ZJU Concept of adaptive immune response T cell-mediated adaptive immune response I. Concept of immune response A collective and coordinated
Cellular Immune response Jianzhong Chen, Ph.D Institute of immunology, ZJU Concept of adaptive immune response T cell-mediated adaptive immune response I. Concept of immune response A collective and coordinated
Hormonal regulation of. Physiology Department Medical School, University of Sumatera Utara
 Hormonal regulation of nutrient metabolism Physiology Department Medical School, University of Sumatera Utara Homeostasis & Controls Successful compensation Homeostasis reestablished Failure to compensate
Hormonal regulation of nutrient metabolism Physiology Department Medical School, University of Sumatera Utara Homeostasis & Controls Successful compensation Homeostasis reestablished Failure to compensate
Anatomy and Physiology I Student Outline The Integumentary System. Integumentary System. Page 1
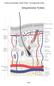 Anatomy and Physiology I Student Outline The Integumentary System Integumentary System Page 1 Have a very clear understanding of the each particular tissue and their unique functions in each layer of the
Anatomy and Physiology I Student Outline The Integumentary System Integumentary System Page 1 Have a very clear understanding of the each particular tissue and their unique functions in each layer of the
CELL BIOLOGY - CLUTCH CH THE IMMUNE SYSTEM.
 !! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
!! www.clutchprep.com CONCEPT: OVERVIEW OF HOST DEFENSES The human body contains three lines of against infectious agents (pathogens) 1. Mechanical and chemical boundaries (part of the innate immune system)
Crosstalk between Adiponectin and IGF-IR in breast cancer. Prof. Young Jin Suh Department of Surgery The Catholic University of Korea
 Crosstalk between Adiponectin and IGF-IR in breast cancer Prof. Young Jin Suh Department of Surgery The Catholic University of Korea Obesity Chronic, multifactorial disorder Hypertrophy and hyperplasia
Crosstalk between Adiponectin and IGF-IR in breast cancer Prof. Young Jin Suh Department of Surgery The Catholic University of Korea Obesity Chronic, multifactorial disorder Hypertrophy and hyperplasia
BIOL 2458 A&P II CHAPTER 18 SI Both the system and the endocrine system affect all body cells.
 BIOL 2458 A&P II CHAPTER 18 SI 1 1. Both the system and the endocrine system affect all body cells. 2. Affect on target cells by the system is slow. Affect on target cells by the system is fast. INTERCELLULAR
BIOL 2458 A&P II CHAPTER 18 SI 1 1. Both the system and the endocrine system affect all body cells. 2. Affect on target cells by the system is slow. Affect on target cells by the system is fast. INTERCELLULAR
Diseases-causing agents, pathogens, can produce infections within the body.
 BIO 212: ANATOMY & PHYSIOLOGY II 1 CHAPTER 16 Lecture: Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. LYMPHATIC and IMMUNE Systems Body Defenses Against
BIO 212: ANATOMY & PHYSIOLOGY II 1 CHAPTER 16 Lecture: Dr. Lawrence G. Altman www.lawrencegaltman.com Some illustrations are courtesy of McGraw-Hill. LYMPHATIC and IMMUNE Systems Body Defenses Against
DermaPep A530. Multifunctional anti-inflammatory peptide for irritated and sensitive skin. Experience The Magic of Science
 Experience The Magic of Science DermaPep A53 Multifunctional anti-inflammatory peptide for irritated and sensitive skin DermaP ep Experience the magic of science Anti-aging DermaPep A35 DermaPep A42 DermaPep
Experience The Magic of Science DermaPep A53 Multifunctional anti-inflammatory peptide for irritated and sensitive skin DermaP ep Experience the magic of science Anti-aging DermaPep A35 DermaPep A42 DermaPep
CYTOKINES. Marion C. Cohen, Ph.D. MSB C
 CYTOKINES Marion C. Cohen, Ph.D. MSB C538 973-972-5995 cohenma@umdnj.edu Last week s EMT group was at full strength, although they were now tossing around phrases like cytokines and pyruvic acid. A Few
CYTOKINES Marion C. Cohen, Ph.D. MSB C538 973-972-5995 cohenma@umdnj.edu Last week s EMT group was at full strength, although they were now tossing around phrases like cytokines and pyruvic acid. A Few
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
THE ADRENAL (SUPRARENAL) GLANDS
 THE ADRENAL (SUPRARENAL) GLANDS They are two glands, present above the kidneys. One adrenal gland is sufficient for human beings/mammals (example: we also have two kidneys but one is sufficient). The Adrenal
THE ADRENAL (SUPRARENAL) GLANDS They are two glands, present above the kidneys. One adrenal gland is sufficient for human beings/mammals (example: we also have two kidneys but one is sufficient). The Adrenal
Prevalence of pruritus in psoriatic skin lesions and its relations to different variables
 Original Article Prevalence of pruritus in psoriatic skin lesions and its relations to different variables Satyendra Kumar Singh Department of Dermatology & Venereology, Institute of Medical Sciences,
Original Article Prevalence of pruritus in psoriatic skin lesions and its relations to different variables Satyendra Kumar Singh Department of Dermatology & Venereology, Institute of Medical Sciences,
NIH Public Access Author Manuscript J Invest Dermatol. Author manuscript; available in PMC 2014 April 01.
 NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2013 October ; 133(10): 2311 2314. doi:10.1038/jid.2013.239. Mechanisms of contact sensitization offer insights
NIH Public Access Author Manuscript Published in final edited form as: J Invest Dermatol. 2013 October ; 133(10): 2311 2314. doi:10.1038/jid.2013.239. Mechanisms of contact sensitization offer insights
Ch45: Endocrine System
 Ch45: Endocrine System Endocrine System Homeostasis is the tendency to maintain a stable internal environment. Function = coordinate and control the body with hormones to maintain homeostasis Works with
Ch45: Endocrine System Endocrine System Homeostasis is the tendency to maintain a stable internal environment. Function = coordinate and control the body with hormones to maintain homeostasis Works with
Reactivity and Resistance
 Reactivity and Resistance 1. Resistance is: 1.The ability of the living system to respond precisely to irritants. 2. The ability of the living system not to respond to irritants. 3. The ability of the
Reactivity and Resistance 1. Resistance is: 1.The ability of the living system to respond precisely to irritants. 2. The ability of the living system not to respond to irritants. 3. The ability of the
Third line of Defense
 Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
Chapter 15 Specific Immunity and Immunization Topics -3 rd of Defense - B cells - T cells - Specific Immunities Third line of Defense Specific immunity is a complex interaction of immune cells (leukocytes)
LYMPHOCYTES & IMMUNOGLOBULINS. Dr Mere Kende, Lecturer SMHS
 LYMPHOCYTES & IMMUNOGLOBULINS Dr Mere Kende, Lecturer SMHS Immunity Immune- protection against dangers of non-self/invader eg organism 3 components of immune system 1 st line: skin/mucosa/cilia/hair/saliva/fatty
LYMPHOCYTES & IMMUNOGLOBULINS Dr Mere Kende, Lecturer SMHS Immunity Immune- protection against dangers of non-self/invader eg organism 3 components of immune system 1 st line: skin/mucosa/cilia/hair/saliva/fatty
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION
 CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
CYTOKINE RECEPTORS AND SIGNAL TRANSDUCTION What is Cytokine? Secreted popypeptide (protein) involved in cell-to-cell signaling. Acts in paracrine or autocrine fashion through specific cellular receptors.
Effects of biological response modifiers in psoriasis and psoriatic arthritis Goedkoop, A.Y.
 UvA-DARE (Digital Academic Repository) Effects of biological response modifiers in psoriasis and psoriatic arthritis Goedkoop, A.Y. Link to publication Citation for published version (APA): Goedkoop, A.
UvA-DARE (Digital Academic Repository) Effects of biological response modifiers in psoriasis and psoriatic arthritis Goedkoop, A.Y. Link to publication Citation for published version (APA): Goedkoop, A.
Rheumatology Advance Access published May 20, Immune responses to stress in rheumatoid arthritis and psoriasis
 Concise report Rheumatology Advance Access published May 20, 2014 RHEUMATOLOGY 53, 263 doi:10.1093/rheumatology/keu221 Immune responses to stress in rheumatoid arthritis and psoriasis Sabine J. M. de Brouwer
Concise report Rheumatology Advance Access published May 20, 2014 RHEUMATOLOGY 53, 263 doi:10.1093/rheumatology/keu221 Immune responses to stress in rheumatoid arthritis and psoriasis Sabine J. M. de Brouwer
1. The scavenger receptor, CD36, functions as a coreceptor for which TLR? a. TLR ½ b. TLR 3 c. TLR 4 d. TLR 2/6
 Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Allergy and Immunology Review Corner: Cellular and Molecular Immunology, 8th Edition By Abul K. Abbas, MBBS, Andrew H. H. Lichtman, MD, PhD and Shiv Pillai, MBBS, PhD. Chapter 4 (pages 62-74): Innate Immunity
Chapter 9. The Endocrine System. Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical College Pearson Education, Inc.
 Chapter 9 The Endocrine System Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical College Intro to the Endocrine System Chief Complaint:8-year-old girl with excessive thirst, frequent
Chapter 9 The Endocrine System Lecture Presentation by Patty Bostwick-Taylor Florence-Darlington Technical College Intro to the Endocrine System Chief Complaint:8-year-old girl with excessive thirst, frequent
Corticosteroids. Veterinary Pharmacology Endocrine System. University of Tehran Faculty of Veterinary Medicine Academic Year
 Veterinary Pharmacology Endocrine System Corticosteroids University of Tehran Faculty of Veterinary Medicine Academic Year 2008-9 Goudarz Sadeghi, DVM, PhD, DSc Associate Professor of Pharmacology Introduction
Veterinary Pharmacology Endocrine System Corticosteroids University of Tehran Faculty of Veterinary Medicine Academic Year 2008-9 Goudarz Sadeghi, DVM, PhD, DSc Associate Professor of Pharmacology Introduction
Lymphoid System: cells of the immune system. Answer Sheet
 Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
A New Era of Migraine Management: The Challenging Landscape in Prevention
 Provided by MediCom Worldwide, Inc. Supported by an educational grant from Teva Pharmaceuticals What is a Neuropeptide? Small chains of amino acids released by neural cells (neurons or glial cells) to
Provided by MediCom Worldwide, Inc. Supported by an educational grant from Teva Pharmaceuticals What is a Neuropeptide? Small chains of amino acids released by neural cells (neurons or glial cells) to
74. Hormone synthesis in the adrenal cortex. The glucocorticoids: biosynthesis, regulation, effects. Adrenal cortex is vital for life!
 74. Hormone synthesis in the adrenal cortex. The glucocorticoids: biosynthesis, regulation, effects. Adrenal cortex is vital for life! 5 g each Zona glomerulosa : Mineralocorticoids ALDOSTERON Zona fasciculata:
74. Hormone synthesis in the adrenal cortex. The glucocorticoids: biosynthesis, regulation, effects. Adrenal cortex is vital for life! 5 g each Zona glomerulosa : Mineralocorticoids ALDOSTERON Zona fasciculata:
Lecture 4. T lymphocytes
 Lecture 4 T lymphocytes Objectives Mention the types of T cells List the Types of T helper cell (CD4+) Discuss the Activation of T cells Define Interleukins Distinguish the Super Ag from ordinary Ag Show
Lecture 4 T lymphocytes Objectives Mention the types of T cells List the Types of T helper cell (CD4+) Discuss the Activation of T cells Define Interleukins Distinguish the Super Ag from ordinary Ag Show
Quality of Life of Saudi Patients with Dermatologic Disorders
 Clinical Medicine and Diagnostics 2018, 8(1): 1-6 DOI: 10.5923/j.cmd.20180801.01 Quality of Life of Saudi Patients with Dermatologic Disorders Bassam Ahmed Almutlaq 1, Fatemah Kadhem Aljishi 2, Rawan Ahmed
Clinical Medicine and Diagnostics 2018, 8(1): 1-6 DOI: 10.5923/j.cmd.20180801.01 Quality of Life of Saudi Patients with Dermatologic Disorders Bassam Ahmed Almutlaq 1, Fatemah Kadhem Aljishi 2, Rawan Ahmed
BIOLOGY 2402 Anatomy and Physiology Lecture. Chapter 18 ENDOCRINE GLANDS
 BIOLOGY 2402 Anatomy and Physiology Lecture Chapter 18 ENDOCRINE GLANDS 1 ENDOCRINE GLANDS Homeostasis depends on the precise regulation of the organs and organ systems of the body. Together the nervous
BIOLOGY 2402 Anatomy and Physiology Lecture Chapter 18 ENDOCRINE GLANDS 1 ENDOCRINE GLANDS Homeostasis depends on the precise regulation of the organs and organ systems of the body. Together the nervous
Physiological processes controlled by hormones?
 : the study of hormones, their receptors, the intracellular signaling pathways they invoke, and the diseases and conditions associated with them. What are hormones? Major endocrine glands? Fig 7-2 Physiological
: the study of hormones, their receptors, the intracellular signaling pathways they invoke, and the diseases and conditions associated with them. What are hormones? Major endocrine glands? Fig 7-2 Physiological
Ch 11: Endocrine System
 Ch 11: Endocrine System SLOs Describe the chemical nature of hormones and define the terms proand prepro-hormone. Explain mechanism of action of steroid and thyroid hormones Create chart to distinguish
Ch 11: Endocrine System SLOs Describe the chemical nature of hormones and define the terms proand prepro-hormone. Explain mechanism of action of steroid and thyroid hormones Create chart to distinguish
