Downloaded from:
|
|
|
- Bertina Ferguson
- 5 years ago
- Views:
Transcription
1 Hanifa, Y; Fielding, KL; Charalambous, S; Variava, E; Luke, B; Churchyard, GJ; Grant, AD (2012) Tuberculosis among adults starting antiretroviral therapy in South Africa: the need for routine case finding. The international journal of tuberculosis and lung disease, 16 (9). pp ISSN DOI: Downloaded from: DOI: /ijtld Usage Guidelines Please refer to usage guidelines at or alternatively contact Available under license: Copyright the publishers
2 Tuberculosis among adults starting antiretroviral therapy in South Africa: the need for routine case finding Authors: Yasmeen Hanifa, MBBS MSc, 1 Katherine L Fielding, PhD, 2 Salome Charalambous, MBBCh MSc, 1 Ebrahim Variava, MBBCh, 3,4 Binu Luke, MBBS MD, 3,4 Gavin J Churchyard, MBBS PhD, 1,2,5 Alison D. Grant, MBBS PhD 2 Institutions: 1 Aurum Institute, Johannesburg, South Africa 2 London School of Hygiene & Tropical Medicine, London, UK 3 Tshepong Hospital Health Services, Klerksdorp, South Africa 4 University of Witwatersrand, Johannesburg, South Africa 5 CAPRISA, University of KwaZulu-Natal, Durban, South Africa Name and address of author for correspondence and reprints: Yasmeen Hanifa C/o Department of Clinical Research, London School of Hygiene & Tropical Medicine, Keppel Street, London WC1E 7HT, UK. Telephone: +44 (0) Fax: +44 (0) yhanifa@hotmail.com Sources of support in form of grants, gifts, equipment, and/or drugs: Partial costs of staff provided by PEPFAR. EV and BL received TB/HIV research training funded by the Fogarty International Center (twin grants RTW007370/3). Running head: High prevalence of TB prior to ART Word count: text 3249, abstract 203 Number of references: 35 Number of tables: 5 Number of figures: 1 Key words: tuberculosis, HIV infection, diagnosis, South Africa, screening. Burden of TB prior to ART Page 1 of 21
3 ABSTRACT Background: We investigated the prevalence of, and evaluated screening modalities for, undiagnosed tuberculosis in ART-eligible adults in South Africa. Methods: Individuals were screened for tuberculosis using symptoms, chest radiograph and two sputum specimens for microscopy and culture, then followed for <6 months to determine tuberculosis diagnoses. Results: Among 361 participants (67% female, median age 38, median CD4 count 120 cells/mm 3 ), 64/361 (18%) participants were sputum culture positive. 114 (32%) fulfilled any tuberculosis case definition (culture and/or smear positive; or improvement on specific treatment). A symptom screen comprising any of: cough or appetite loss or night sweats >2 weeks had sensitivity and specificity of 74.5% and 50.8% respectively. Sensitivity was increased by chest radiography (to 96.1%) but not by sputum microscopy. The WHO symptom screen had sensitivity and specificity of 96.1% and 5.2% respectively in our study population; addition of chest radiography increased sensitivity to 100%. Median time to TB treatment was 8 days for diagnoses based on chest radiograph (N=72), vs. 37 days for diagnoses based only on sputum culture (N=14). Conclusions: The very high prevalence of undiagnosed tuberculosis among patients presenting for ART mandates their routine investigation. Chest radiography improved sensitivity substantially, allowed rapid treatment initiation and should be routine, where available, pending better point-of-care diagnostics. Burden of TB prior to ART Page 2 of 21
4 INTRODUCTION Tuberculosis remains a key cause of death among people with HIV 1 in sub-saharan Africa despite wider use of antiretroviral therapy (ART). 2-4 Diagnosis is complicated by the high proportion who are smear-negative, 5,6 and atypical chest radiograph findings. 7 Intensified tuberculosis case finding (ICF) is recommended by the World Health Organization (WHO) 8 but is poorly implemented. 9 Screening prior to ART is particularly important because risk of tuberculosis and death is high for immunosuppressed individuals. 4,10 Individuals diagnosed with tuberculosis after, rather than before, ART initiation are more likely to die while on tuberculosis treatment, emphasising the need for prompt diagnosis and treatment initiation. 3 High tuberculosis incidence within the first few months of ART initiation suggests that cases are either missed at screening or subclinical disease is unmasked by immunological recovery The aim of our study was to determine the prevalence of previously undiagnosed active tuberculosis amongst ART-eligible adults at enrolment to a public sector HIV clinic in South Africa, and to evaluate the performance of combinations of symptoms and standard investigations in the diagnosis of tuberculosis. METHODS Study design and population Between August 2007 and January 2008, we recruited ART-eligible (WHO stage 4 or CD4<200 cells/mm 3 ) 13 adults (>17 years) to a prospective cohort study. Patients taking tuberculosis treatment currently or within the previous three months were excluded. Patients were referred to this clinic for ART initiation. South African guidelines 13 at the time of this study did not specify systematic screening for tuberculosis prior to ART. Clinic policy was for routine chest radiography at enrolment, but systematic tuberculosis screening was not routine; patients were assessed by clinicians for ART eligibility and investigated as deemed appropriate. All patients with CD4<200 Burden of TB prior to ART Page 3 of 21
5 cells/mm 3, or CD4<350 cells/mm 3 and WHO stage 2, 3 or 4 received cotrimoxazole; isoniazid preventive therapy was not given. Patients on tuberculosis treatment started ART after two weeks if CD4 count<50 cells/mm 3 or other serious HIV-related illness, or two months if CD4 count between 50 and 200 cells/mm 3 or WHO stage 4. Study procedures Trained nurses administered a symptom questionnaire and collected two spot sputum specimens for smear and mycobacterial culture from all participants. Chest radiographs were read by a consultant physician blinded to clinical details, using a standardised form adapted from a validated tool, 14 assigning radiographic diagnoses according to overall impression. We reviewed patients 3-6 months post enrolment, performing repeat symptom questionnaire and record review, and investigated symptomatic patients with chest radiography and two further sputum specimens. Symptomatic patients were those with any of: cough, night sweats, fever, appetite loss, tiredness for >2 weeks; or haemoptysis, chest pain, difficulty breathing, observed weight loss >1.5kg in previous month; or self-reported weight loss over the preceding 6 months. Patient records were used to ascertain CD4 and full blood counts, WHO clinical stage, tuberculosis diagnoses made outside of study visits, and evidence of clinical improvement at two months amongst those on tuberculosis treatment. Tuberculosis diagnosed at recruitment was not used to assign WHO stage. Laboratory methods Sputum specimens were examined at the National Health Laboratory Services by fluorochrome staining for acid-fast bacilli (AFB), and cultured using the BACTEC TM MGIT 960 TM system (Becton Dickinson Microbiology Systems, Sparks, MD, USA). Scanty positive smears were considered positive. All positive cultures were identified using a nucleic amplification technique (AccuProbe, Gen-Probe, San Diego, CA, USA). Burden of TB prior to ART Page 4 of 21
6 Case definition for tuberculosis Patients were classified as having pulmonary tuberculosis (PTB) if they had compatible clinical or radiological features and: sputum culture-positive for M. tuberculosis (definite PTB); sputum smear-positive, culture-negative (probable PTB); or no other cause of disease found and clinical improvement after two months of tuberculosis treatment, or lost to follow-up or died before two months (possible PTB). Patients were classified as having extrapulmonary tuberculosis (EPTB) if they had compatible clinical features and either had: M. tuberculosis cultured from a relevant site (definite EPTB); other diagnostic evidence of EPTB and improved after two months of tuberculosis treatment (probable EPTB); or no other cause of disease was found and the patient improved after two months of tuberculosis treatment or was lost to follow-up or died before two months (possible EPTB). Tuberculosis episodes were considered to start on the date tuberculosis treatment was started. Prevalent tuberculosis was defined as any tuberculosis episode fulfilling case definitions within three months of enrolment. Only study screening tests performed on the day of enrolment were used to calculate sensitivity, specificity, negative and positive predictive values for screening methods. Information from all available sources was used to assign tuberculosis case definitions. Statistical analysis Data were analysed using Intercooled Stata 10.0 (Stata Corporation, Texas, USA). We used logistic regression to calculate unadjusted and adjusted odds ratios for risk factors for prevalent tuberculosis and to assess the performance of symptoms for a screening tool using a gold standard of culture-positive tuberculosis. Risk factor analyses were restricted to "definite" (culture-positive) cases, as a robust case definition, comparable with other studies, 15,16 and probable and possible cases were excluded from these analyses. A priori, the multivariable model for the risk factor analysis included CD4 count and age category as established risk factors for tuberculosis, and other factors for which the P value in the univariable analysis was 0.2. From the multivariable model, we chose as screening criteria the three Burden of TB prior to ART Page 5 of 21
7 symptoms with the highest adjusted odds ratios. We also evaluated the new WHO ICF screening tool of any of current cough, fever, weight loss or night sweats. 17 To estimate mortality rates pre-art, person-time was calculated from date of recruitment to the study until the earliest of death; ART initiation; two weeks after last visit date (as all patients attend monthly to collect medication), or end of study (1 st July 2008). For mortality after ART start, person-time was calculated from date of ART initiation until the earliest of death; two weeks after last visit date, or end of study. Ethical approval The study received ethical approval from the Research Ethics Committee of the University of KwaZulu-Natal and the London School of Hygiene & Tropical Medicine. Written informed consent, or witnessed verbal consent for participants unable to read or write, was obtained for all participants. RESULTS Participation and demographics Figure 1 summarises study inclusions and exclusions, losses to follow-up, and tuberculosis case definitions. Among 381 participants recruited, 12 were treated for tuberculosis without fulfilling our case definitions, and a further 8 were culturepositive for non-tuberculous mycobacteria only. Amongst 361 participants analysed, 99% were Black African, 67% were female, median age was 38 (IQR 32-46) years, median CD4 was 120 (IQR ) cells/mm 3 and 171/305 (56%) were WHO stage 3 or (28%) reported a previous episode of tuberculosis, of whom 51% were treated 3 years ago. Prevalence of tuberculosis and basis of diagnosis 114/361 participants fulfilled our case definition for tuberculosis (definite, probable or possible) giving a prevalence of undiagnosed tuberculosis of 32% (95% confidence interval [CI] %). "Possible" cases, vs. "definite", were more likely to have Burden of TB prior to ART Page 6 of 21
8 more advanced WHO stage and EPTB only, but other markers of disease severity and radiographic patterns did not differ (see supplementary appendix table 1). 99/114 (87%) had PTB, 5 (4%) had EPTB, and 10 (9%) had both. Overall 64 (56%), 6 (5%), and 44 (39%) were classified as definite, probable and possible tuberculosis respectively. The prevalence of culture-proven tuberculosis was 17.7% (64/361; 95% CI %). Amongst 360 patients with complete data, 110/113 (97%) of tuberculosis patients and 236/247 (96%) of patients without tuberculosis had at least one of the following symptoms: cough, fever, drenching night sweats, self-reported weight loss, haemoptysis, dyspnoea, chest pain, loss of appetite or fatigue. Amongst 99 pulmonary tuberculosis cases (definite, probable and possible combined) the bases for diagnosis were: clinical, radiological, and microbiological (culture and/or smear) features for 39%; clinical and radiological features for 37%; clinical and microbiological features for 17%; and radiological and microbiological features for 2%. Sputum microscopy and culture results Amongst 350 individuals with sputum results available, 24 (7%) and 326 (90%) produced one or two adequate sputum specimens respectively. 9/350 (3%) were smear-positive and 64/350 (18%) were culture-positive for M. tuberculosis, of whom one was culture-negative at enrolment but culture-positive subsequently. 7/350 (2%) were both smear- and culture-positive. Amongst 300 patients with a negative or inadequate first sputum specimen, 14 (5%) had a culture-positive second specimen. 57/64 (89%) of culture-positive patients were smear-negative. Time from screening to start of treatment Amongst 86 patients with definite, probable or possible tuberculosis, and for whom the basis of starting treatment was clear, the median time to starting treatment was 13 (IQR 1, 35) days. 72/86 (84%) initiated treatment based on chest radiograph findings at median 8 (IQR 0, 24) days; of these 31/72 (43%) were initiated on the same or next day by the clinic doctor, and the remainder started treatment at a median of 20 (IQR 11, 36) days after enrolment, following further review of chest radiograph by consultant physician. 14/86 (16%) patients started treatment based on Burden of TB prior to ART Page 7 of 21
9 sputum culture result at a median of 37 (IQR 20, 49) days and two (2%) patients started treatment based on sputum smear result after median 9 (IQR 4, 13) days post enrolment. Amongst 45 culture-confirmed tuberculosis cases, 29/45 (64%) started treatment based on chest radiograph findings at median 1 (IQR 0, 8) day vs. 35 (IQR 20, 44) days for 14/45 (31%) patients started based on sputum culture result. Eight individuals had no evidence of active tuberculosis at the time of screening (and were included in the analysis as such) but at the time of final review were observed to have started tuberculosis treatment more than three months after screening (Figure 1). Demographic and clinical risk factors for undiagnosed prevalent tuberculosis Risk factor analyses were restricted to 300 individuals (6 probable and 44 possible tuberculosis cases, and 11 individuals without sputum results were excluded). In the univariable analysis (see supplementary appendix table 2), prevalent tuberculosis was associated with male sex, greater than six household members, ever having smoked, and no previous history of tuberculosis treatment. In the multivariable analysis only previous tuberculosis treatment, which was protective, (adjusted OR 0.29, 95% CI ) remained associated. Sensitivity, specificity and predictive values of markers for undiagnosed prevalent tuberculosis Using culture-positive tuberculosis as our gold standard we found that the presence of individual symptoms irrespective of duration was sensitive, but generally had low specificity, except for haemoptysis which had low prevalence (table 1). Addition of duration >2 weeks to individual symptoms reduced sensitivity, but improved specificity. Haemoglobin <10g/dl had a similar sensitivity to CD4 count<100 cells/mm 3 (38% vs. 35%), but had better specificity (80% vs. 62%). Sputum microscopy was very insensitive particularly when compared to chest radiographic features of active tuberculosis (11% vs. 77%), and overall only 7/300 (2%) patients were smear positive. In a sensitivity analysis including all tuberculosis cases (definite, probable and possible), there was little change in sensitivity and specificity values Burden of TB prior to ART Page 8 of 21
10 (data not shown) compared to those for only culture-positive tuberculosis cases. For example, sensitivity of radiographic features of active tuberculosis was 77.4% vs. 80.4% for culture-positive vs. all tuberculosis cases. The symptom, sign, and investigation with best performance in terms of sensitivity and negative predictive value were, respectively: self-reported weight loss, BMI <18.5kg/m 2, and any abnormality on chest radiograph (table 1). In terms of specificity and positive predictive value the best symptom, sign and investigation were fever >2 weeks, observed fever (although only two participants were febrile), and sputum microscopy respectively. Combinations of screening criteria The three symptoms with the highest adjusted odds ratios in multivariable analysis were cough>2 weeks, loss of appetite >2 weeks and night sweats >2 weeks (for details, see supplementary appendix table 3). Amongst 244 individuals with complete data the performance of these in combination was tested (table 2). A combination of any of: cough or appetite loss or night sweats for greater than two weeks (henceforth known as the symptom complex) had sensitivity, specificity, positive and negative predictive values of 75%, 51%, 29% and 88% respectively. Adding BMI <18.5kg/m 2 to our symptom complex made little difference to sensitivity and negative predictive values, in contrast to WHO clinical stage 3 or 4 which increased sensitivity and negative predictive values to 90% but halved specificity. Addition of haemoglobin <10g/dl improved the sensitivity and negative predictive value of the symptom complex to 82% and 90% respectively, and combining this with WHO stage 3 or 4 and BMI <18.5 further increased sensitivity to 90% but halved specificity. Sputum microscopy did not change the performance of the symptom complex, in contrast to chest radiography which increased sensitivity to 92% for features compatible with active tuberculosis, and 96% for any radiographic abnormality. A combination of symptom complex or any radiographic abnormality had sensitivity and negative predictive values of 96%, which was further improved by addition of CD4<100 which missed only 2% of tuberculosis cases and was our most sensitive combination (98%). Burden of TB prior to ART Page 9 of 21
11 The WHO symptom screen 17 had sensitivity, specificity, positive and negative predictive values of 96%, 5%, 21% and 83% respectively in our patients. Addition of chest radiography increased sensitivity and negative predictive value to 100% for both features compatible with active tuberculosis and any radiographic abnormality. Time to ART start and mortality 266/361 (74%) patients initiated ART by 1 st July 2008, at median of 70 days from recruitment (IQR 42, 105). Among 266 patients who started ART within the study period, the median time from enrolment to ART start was shorter for those without tuberculosis (median 64 days, N=190) vs. those with tuberculosis (median 94 days, N=76). In total 26/361 patients (7.2%) died, of whom 20/26 (77%) did not initiate ART. The pre-art mortality rate was 25.3/100 person-years (95% CI , vs. 6.8/100 person-years (95% CI ) after starting ART. Documented causes of death pre-art (N=20) were tuberculosis (4); acute renal failure (2); 1 each of septicaemia, gastroenteritis, cryptococcal meningitis, cardiomyopathy, and pneumonia; and unknown (9; of whom three fulfilled case definitions for tuberculosis but did not start tuberculosis treatment). Documented causes of on-art mortality (N=6) were one each of tuberculosis; cryptococcal meningitis; pneumonia and septicaemia; and unknown (3). Among 44 patients who did not meet TB case definitions based on investigations at enrolment but were not seen at the follow-up visit, 15 were known to have died (figure 1). DISCUSSION One-third of our patients referred to start ART had undiagnosed tuberculosis, a major burden of morbidity with life-threatening potential; 10,11 highlighting the need to investigate all of these patients, most of whom were highly symptomatic, for tuberculosis. Our prevalence is similar to recent data from Western Cape (32%), 12 but higher than generally reported among ART-eligible adults in Africa (3%- Burden of TB prior to ART Page 10 of 21
12 19%). 10,11,16,18-20 This reflects systematic screening of our patients using multiple modalities, and a broad case definition allowing diagnosis based on radiological and clinical features highlighting the real life burden, and recognising that sputum culture misses some cases of disseminated tuberculosis. 21 Our 18% prevalence of cultureconfirmed pulmonary tuberculosis accords with studies from Cambodia (17%), 22 KwaZulu-Natal (19%), 16 and Western Cape (17%). 15 We found demographic and clinical data unhelpful in identifying subgroups at higher risk of undiagnosed tuberculosis. Individuals with advanced HIV disease often reach HIV care due to symptoms of tuberculosis, underscoring the need for systematic case finding. Screening for this group requires high sensitivity to avoid missing cases, but in a resource-constrained setting, this must be balanced against the high costs resulting from a test combination with poor specificity. We found sputum microscopy had very poor sensitivity, consistent with other studies, 16,19,23-25 yet this remains a key component of National Tuberculosis control programmes in resource limited settings. The WHO symptom screen 17,26 had high sensitivity (96%) in our study population. It aims primarily to rule out tuberculosis among apparently healthy individuals prior to starting isoniazid preventive therapy, requiring a high sensitivity and negative predictive value; however this is at the cost of low specificity. If all individuals identified as tuberculosis suspects, based on a symptom combination with relatively low specificity, are investigated with new rapid molecular diagnostics, such as Xpert MTB/RIF 27 at US$17 per cartridge, 28 the cost to health services may be substantial, and the cost-effectiveness of a range of algorithms for different settings needs to be investigated. 90% of our culture-proven tuberculosis cases were smearnegative, and Xpert MTB/RIF has reported sensitivities from 43%-73% for smearnegative culture-positive tuberculosis from a single sputum sample. 15, 27 An algorithm requiring Xpert-negative tuberculosis suspects to undergo further evaluation using sputum culture, trial of antibiotic and chest radiograph has potential to delay tuberculosis treatment. Chest radiography improved sensitivity of our symptom screening complex substantially, consistent with our earlier data from South African gold miners with less advanced HIV disease. 23 Use of chest radiography to augment the WHO symptom screen in high tuberculosis prevalence settings is supported by a recent meta- Burden of TB prior to ART Page 11 of 21
13 analysis 26 and WHO guidance, 17 and in our study population increased sensitivity and negative predictive value to 100%. Our data show that chest radiography facilitates prompt tuberculosis treatment initiation. Although implementation of chest radiography can be challenging, 29,30 we suggest it should be done where possible. In high prevalence settings systematic sputum culture for all patients prior to ART has also been suggested, but presents the same challenges of access. 12,16 In our study, most culture-positive patients started tuberculosis treatment based on clinical and radiological features prior to availability of culture results; even with liquid culture, the median time to tuberculosis treatment start based on a positive culture was 37 days. Chest radiography provides a basis for rapid initiation of tuberculosis treatment both to reduce individual risk of death and also reduce risk of onward transmission in both clinic and community, and procedures must be in place to ensure follow-up of tuberculosis suspects. 30 The cost per chest radiograph has been estimated at only US$2. 30 The reported sensitivity of Xpert MTB/RIF among smear-negative tuberculosis cases (most ART-eligible patients will be smear-negative) is lower than chest radiography in this study, but it has much higher specificity. 27 Implementation of Xpert MTB/RIF should similarly reduce time to tuberculosis treatment start, but cost is likely to limit its wide use at peripheral health facilities, and effective low-cost point-ofcare diagnostic tools remain a pressing need. A low haemoglobin level is an independent predictor for mortality amongst patients commencing antiretroviral therapy and may reflect undiagnosed tuberculosis. Adding anaemia to our symptom complex increased sensitivity, and supports the clinical practice of investigating all anaemic patients for tuberculosis prior to initiation of ART. A major strength of our study was our longitudinal follow-up period, which is lacking from many screening studies, 19 minimising the number of tuberculosis cases missed and ensuring a robust case definition for possible tuberculosis. One-third of participants without a review visit are known to have died, underscoring how ill individuals were at enrolment. Tuberculosis cannot be excluded as cause of death amongst all; hence we may have underestimated the true tuberculosis prevalence. The study setting in a large public sector clinic is relatively typical of antiretroviral roll out sites, although better resourced than many in sub-saharan Africa. We had Burden of TB prior to ART Page 12 of 21
14 access to routine radiographs, read by an experienced physician, and mycobacterial cultures, and good patient retention in the study. Our screening procedure was straightforward to operationalise and did not appear to delay initiation of ART; the typical time from first visit to ART initiation in this clinic was days (personal communication, E Variaiva). In conclusion we found a very high prevalence of undiagnosed tuberculosis among patients presenting for ART to a public sector HIV clinic. These patients need routine systematic investigation for tuberculosis. Until accurate point-of-care diagnostic tests are available, our results suggest that chest radiography is a useful addition to routine screening which allows rapid initiation of tuberculosis treatment. Given the high mortality of patients awaiting investigation results, 2,4,34 presumptive tuberculosis treatment for high-risk individuals also needs to be evaluated. 35 Burden of TB prior to ART Page 13 of 21
15 Acknowledgements: We thank the study participants; the nursing and medical staff of Tshepong Hospital Health Services, South Africa; the staff of National Health Laboratory Services, Tshepong hospital, South Africa; and the staff of Aurum Institute for their essential contributions to this study. This work was supported by the Aurum Institute. Subjects in this study were enrolled in treatment programs supported by the U.S. President's Emergency Plan for AIDS Relief and by Cooperative Agreement Number PS from the Department of Health and Human Services/Centers for Disease Control and Prevention (CDC), National Center for HIV, Viral Hepatitis, STD, and TB Prevention (NCHHSTP), Global AIDS Program (GAP). The content of this manuscript are solely the responsibility of the authors and do not necessarily represent the official views of CDC. Professor Grant was supported by a UK Department of Health Public Health Career Scientist award. Burden of TB prior to ART Page 14 of 21
16 REFERENCES 1. Lucas SB, Hounnou A, Peacock C, et al. The mortality and pathology of HIV infection in a west African city. AIDS 1993;7: Etard JF, Ndiaye I, Thierry-Mieg M, et al. Mortality and causes of death in adults receiving highly active antiretroviral therapy in Senegal: a 7-year cohort study. AIDS 2006;20: Koenig SP, Riviere C, Leger P, et al. High mortality among patients with AIDS who received a diagnosis of tuberculosis in the first 3 months of antiretroviral therapy. Clin Infect Dis 2009;48: Lawn SD, Myer L, Orrell C, Bekker LG, Wood R. Early mortality among adults accessing a community-based antiretroviral service in South Africa: implications for programme design. AIDS 2005;19: Johnson JL, Vjecha MJ, Okwera A, et al. Impact of human immunodeficiency virus type-1 infection on the initial bacteriologic and radiographic manifestations of pulmonary tuberculosis in Uganda. Makerere University-Case Western Reserve University Research Collaboration. Int J Tuberc Lung Dis 1998;2: Samb B, Sow PS, Kony S, et al. Risk factors for negative sputum acid-fast bacilli smears in pulmonary tuberculosis: results from Dakar, Senegal, a city with low HIV seroprevalence. Int J Tuberc Lung Dis 1999;3: Perlman DC, el-sadr WM, Nelson ET, et al. Variation of chest radiographic patterns in pulmonary tuberculosis by degree of human immunodeficiency virus-related immunosuppression. The Terry Beirn Community Programs for Clinical Research on AIDS (CPCRA). The AIDS Clinical Trials Group (ACTG). Clin Infect Dis 1997;25: World Health Organization. WHO Three I s Meeting. Intensified Case Finding (ICF), Isoniazid Preventive Therapy (IPT) and TB Infection Control (IC) for people living with HIV. Report of a Joint World Health Organization HIV/AIDS and TB Department Meeting. 2-4 April, 2008, Geneva, Switzerland (Accessed 06/10/2008, at 9. World Health Organization. Global Tuberculosis Control: WHO Report (Accessed 12 December 2011, at Lawn SD, Myer L, Bekker LG, Wood R. Burden of tuberculosis in an antiretroviral treatment programme in sub-saharan Africa: impact on treatment outcomes and implications for tuberculosis control. AIDS 2006;20: Moore D, Liechty C, Ekwaru P, et al. Prevalence, incidence and mortality associated with tuberculosis in HIV-infected patients initiating antiretroviral therapy in rural Uganda. AIDS 2007;21: Lawn SD, Kranzer K, Edwards DJ, McNally M, Bekker LG, Wood R. Tuberculosis during the first year of antiretroviral therapy in a South African cohort using an intensive pretreatment screening strategy. AIDS 2010;24: National Department of Health South Africa. National Antiretroviral Treatment Guidelines. Jacana, (Accessed 24/09/2009, at Den Boon S, Bateman ED, Enarson DA, et al. Development and evaluation of a new chest radiograph reading and recording system for epidemiological surveys of tuberculosis and lung disease. Int J Tuberc Lung Dis 2005;9: Lawn SD, Brooks SV, Kranzer K, et al. Screening for HIV-Associated Tuberculosis and Rifampicin Resistance before Antiretroviral Therapy Using the Xpert MTB/RIF Assay: A Prospective Study. PLoS Med 2011;8:e Burden of TB prior to ART Page 15 of 21
17 16. Bassett IV, Wang B, Chetty S, et al. Intensive tuberculosis screening for HIV-infected patients starting antiretroviral therapy in Durban, South Africa. Clin Infect Dis 2010;51: World Health Organization. Guidelines for intensified tuberculosis case-finding and isoniazid preventive therapy for people living with HIV in resource-constrained settings. World Health Organization, (Accessed 5th September 2011, at Fairall LR, Bachmann MO, Louwagie GM, et al. Effectiveness of antiretroviral treatment in a South African program: a cohort study. Arch Intern Med 2008;168: Shah S, Demissie M, Lambert L, et al. Intensified tuberculosis case finding among HIV- Infected persons from a voluntary counseling and testing center in Addis Ababa, Ethiopia. J Acquir Immune Defic Syndr 2009;50: Were W, Moore D, Ekwaru P, et al. A simple screening tool for active tuberculosis in HIV-infected adults receiving antiretroviral treatment in Uganda. Int J Tuberc Lung Dis 2009;13: Shah M, Martinson NA, Chaisson RE, Martin DJ, Variava E, Dorman SE. Quantitative analysis of a urine-based assay for detection of lipoarabinomannan in patients with tuberculosis. J Clin Microbiol 2010;48: Tamhane A, Chheng P, Dobbs T, Mak S, Sar B, Kimerling ME. Predictors of smearnegative pulmonary tuberculosis in HIV-infected patients, Battambang, Cambodia. Int J Tuberc Lung Dis 2009;13: Day JH, Charalambous S, Fielding KL, Hayes RJ, Churchyard GJ, Grant AD. Screening for tuberculosis prior to isoniazid preventive therapy among HIV-infected gold miners in South Africa. Int J Tuberc Lung Dis 2006;10: Lawn S, Edwardsa D, Kranzer K, Vogta M, Bekker LG, Wood R. Urine lipoarabinomannan assay for tuberculosis screening before antiretroviral therapy diagnostic yield and association with immune reconstitution disease. AIDS 2009;23: Matee M, Mtei L, Lounasvaara T, et al. Sputum microscopy for the diagnosis of HIVassociated pulmonary tuberculosis in Tanzania. BMC Public Health 2008;8: Getahun H, Kittikraisak W, Heilig CM, et al. Development of a standardized screening rule for tuberculosis in people living with HIV in resource-constrained settings: individual participant data meta-analysis of observational studies. PLoS Med 2011;8:e Boehme CC, Nabeta P, Hillemann D, et al. Rapid molecular detection of tuberculosis and rifampin resistance. N Engl J Med 2010;363: Foundation for Innovative New Diagnostics. FIND negotiated prices for Xpert MTB/RIF and Country List (Accessed 5th September, 2011, at ) 29. Mosimaneotsile B, Talbot EA, Moeti TL, et al. Value of chest radiography in a tuberculosis prevention programme for HIV-infected people, Botswana. Lancet 2003;362: Shah NS, Anh MH, Thuy TT, et al. Population-based chest X-ray screening for pulmonary tuberculosis in people living with HIV/AIDS, An Giang, Vietnam. Int J Tuberc Lung Dis 2008;12: Johannessen A, Naman E, Ngowi BJ, et al. Predictors of mortality in HIV-infected patients starting antiretroviral therapy in a rural hospital in Tanzania. BMC Infect Dis 2008;8: Stringer JS, Zulu I, Levy J, et al. Rapid scale-up of antiretroviral therapy at primary care sites in Zambia: feasibility and early outcomes. JAMA 2006;296: Burden of TB prior to ART Page 16 of 21
18 33. Toure S, Kouadio B, Seyler C, et al. Rapid scaling-up of antiretroviral therapy in 10,000 adults in Cote d'ivoire: 2-year outcomes and determinants. AIDS 2008;22: Zachariah R, Fitzgerald M, Massaquoi M, et al. Risk factors for high early mortality in patients on antiretroviral treatment in a rural district of Malawi. AIDS 2006;20: Lawn SD, Wood R, Wilkinson RJ. Changing concepts of "latent tuberculosis infection" in patients living with HIV infection. Clin Dev Immunol pii: Burden of TB prior to ART Page 17 of 21
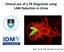
19 FIGURE LEGEND Figure 1 Study inclusions, exclusions, case definitions and basis for diagnosis Burden of TB prior to ART Page 18 of 21
20 Figure 1: Study inclusions, exclusions, case definitions and basis for diagnosis Recruited n = 381 Treated for TB but not fulfilling case definitions n = 12/381 (3.1%) NTM isolated n = 2 NTM only isolated n = 8 Definite TB n = 64/114 (56.1%) TB case definition not met: n = 247/361 (68.4%) TB case definition met: n = 114/361 (31.6%) Probable TB n = 6/114 (5.3%) Possible TB n = 44/114 (38.6%) No evidence of TB at review visit n = 195/247 (78.9%) Not seen for review visit n = 44/247 (17.8%) Started TB treatment >3months after screening n = 8/247 (3.2%) 21 defaulted 15 known dead 5 no information 3 transferred out TB = tuberculosis; NTM = non-tuberculous mycobacteria Burden of TB prior to ART Page 19 of 21
21 Table 1: Performance of symptoms, signs, investigations and WHO stage as markers for undiagnosed prevalent tuberculosis* Marker Prevalence of marker (N=300) % (n) Sensitivity (N=64) % (n) Specificity (N=236) % (n) SYMPTOMS Reported weight loss 90.0 (269/299) 90.5 (57/63) 10.2 (24) Any tiredness 69.3 (208) 81.3 (52) 33.9 (80) Tiredness > 2 weeks 47.0 (141) 70.3 (45) 59.3 (140) Any cough 44.0 (132) 68.8 (44) 62.7 (148) Cough > 2 weeks 24.3 (73) 43.8 (28) 80.9 (191) Cough > 3 weeks 22.3 (67) 42.2 (27) 83.1 (196) Any loss of appetite 50.0 (150) 62.5 (40) 53.4 (126) Loss of appetite > 2 weeks 32.0 (96) 51.6 (33) 73.3 (173) Any night sweats 40.7 (122) 59.4 (38) 64.4 (152) Night sweats > 2 weeks 28.7 (86) 45.3 (29) 75.9 (179) Any chest pain 46.3 (139) 53.1 (34) 55.5 (131) Chest pain > 2 weeks 27.3 (82) 37.5 (24) 75.4 (178) Any fever 27.0 (81) 35.9 (23) 75.4 (178) Fever > 2 weeks 12.7 (38) 25.0 (16) 90.7 (214) Any haemoptysis 7.7 (23) 9.4 (6) 92.8 (219) Any symptom 96.3 (288/299) 96.8 (61/63) 3.8 (9) SIGNS: Body Mass Index <18.5 kg/m (79/298) 37.5 (24) 76.5 (179/234) Temperature >37.4 C 0.7 (2) 3.1 (2) 100 (236) INVESTIGATIONS: Haemoglobin <8 g/dl 4.0 (12/297) 6.3 (4) 96.6(225/233) Haemoglobin <10 g/dl 23.6 (70/297) 37.5 (24) 80.3(187/233) Total lymphocyte count (10^9/l) < (66/295) 28.1 (18) 79.2(183/231) CD4 cell count <100 cells/mm (111/298) 34.9 (22/63) 62.1(146/235) Sputum AFB Positive 2.3 (7/300) 10.9 (7) 100 (236) Abnormal CXR 58.9 (175/297) 85.5 (53/62) 48.1(113/235) CXR compatible with active TB 45.1 (134/297) 77.4 (48/62) 63.4(149/235) Clinical classification WHO clinical stage 3 or (136/253) 55.6 (30/54) 46.7 (93/199) * Tuberculosis case defined as patients diagnosed within three months of recruitment who were culture-positive for tuberculosis; denominator =300 unless otherwise indicated (all participants with probable [n=6] or possible [n=44] tuberculosis, and those without sputum culture results [n=11] have been excluded); any of the following irrespective of duration: cough, sputum production, night sweats, self-reported weight loss, fever, haemoptysis, dyspnoea, chest pain, loss of appetite or fatigue; CXR = Chest radiograph; PPV= positive predictive value; NPV=negative predictive value; AFB = Acid-fast bacilli; HIV = human immunodeficiency virus; MTB = M. tuberculosis; WHO = World Health Organization PPV % NPV % Burden of TB prior to ART Page 20 of 21
22 Table 2: Combinations of tuberculosis* screening criteria from this study and performance of WHO algorithm 17 in our study population (N=244) Screening criteria: at least one of Present overall n=244 (%) Sensitivity % n=51 (95% CI) Specificity % n=193 (95% CI) PPV % (95% CI) NPV % (95% CI) Symptoms only C>2w, A>2w, S>2w 133 (54.5) 74.5 (69.0, 80.0) 50.8 (44.5, 57.1) 28.6 (22.9, 34.2) 88.3 (84.3, 92.3) Addition of clinical features C>2w, A>2w, S>2w, WHO 3/4 190 (77.9) 90.2 (86.5, 93.9) 25.4 (19.9,30.9) 24.2 (18.8, 29.6) 90.7 (87.1, 94.4) C>2w, A>2w, S>2w, BMI< (61.9) 78.4 (73.3, 83.6) 42.5 (36.3, 48.7) 26.5 (21.0,32.0) 88.2 (84.1,92.2) C>2w, A>2w, S>2w, WHO 3/4, BMI< (81.6) 90.2 (86.5, 93.9) 20.7 (15.6, 25.8) 23.1 (17.8, 28.4) 88.9 (85.0, 92.8) Addition of basic laboratory tests C>2w, A>2w, S>2w, Hb < (61.9) 82.4 (77.6, 87.1) 43.5 (37.3, 49.7) 27.8 (22.2, 33.4) 90.3 (86.6, 94.0) C>2w, A>2w, S>2w, Hb<10, BMI< (68.0) 84.3 (79.8, 88.9) 36.3 (30.2, 42.3) 25.9 (20.4, 31.4) 89.7 (85.9, 93.6) C>2w, A>2w, S>2w,WHO 3/4, Hb<10, 204 (83.6) 90.2 (86.5, 93.9) 18.1 (13.3, 23.0) 22.6 (17.3, 27.8) 87.5 (83.4, 91.7) BMI<18.5 Addition of sputum microscopy C>2w, A>2w, S>2w, Sputum AFB-positive 135 (55.3) 78.4 (73.3, 83.6) 50.8 (44.5, 57.1) 29.6 (23.9, 35.4) 89.9 (86.1, 93.7) Addition of CXR C>2w, A>2w, S>2w,any CXR abnormality 195 (79.9) 96.1 (93.6, 98.5) 24.4 (19.0, 29.7) 25.1 (19.7,30.6) 95.9 (93.4, 98.4) C>2w, A>2w, S>2w,CXR compatible with 179 (73.4) 92.2 (88.8, 95.5) 31.6 (25.8, 37.4) 26.3 (20.7, 31.8) 93.9 (90.8, 96.9) active TB Addition of CD4 count C>2w, A>2w, S>2w,CD4< (70.8) 82.4 (77.6, 87.1) 33.2 (27.3, 39.1) 24.6 (19.2, 30.0) 87.7 (83.6, 91.8) Addition of CXR and CD4 C>2w, A>2w, S>2w,any CXR abnormality, 211 (86.5) 98.0 (96.3, 99.8) 16.6 (11.9, 21.3) 23.7 (18.4, 29.0) 97.0 (94.8, 99.1) CD4<100 C>2w, A>2w, S>2w,CXR compatible with active TB, CD4< (81.6) 94.1 (91.2, 97.1) 21.8 (16.6, 26.9) 24.1 (18.8, 29.5) 93.3 (90.2, 96.5) WHO screening algorithm 17 C, F, W, S 232 (95.1) 96.1 (93.6, 98.5) 5.2 (2.4, 8.0) 21.1 (16.0, 26.2) 83.3 (78.7, 88.0) C, F, W, S, any CXR abnormality 240 (98.3) 100 (100,100) 2.1 (0.3, 3.9) 21.3 (16.1, 26.4) 100 (100, 100) *Tuberculosis case defined as patients diagnosed within three months of recruitment who were culture-positive for tuberculosis. All participants with probable [n=6] or possible tuberculosis [n=44] and those without sputum culture results [n=11] have been excluded. Participants with missing data have also been excluded: WHO clinical stage [n=47], haemoglobin [n=3], chest radiograph [n=3], BMI [n=2], and reported weight loss [n=1]. A, appetite loss; C, cough; F, fever; S, night sweats; W, weight loss PPV= positive predictive value; NPV=negative predictive value; 2w=2 weeks; WHO = World Health Organization clinical stage; BMI=Body mass index (kg/m 2 ); Hb=Haemoglobin g/dl; AFB = Acid-fast bacilli; CXR = Chest radiograph; CD4 = CD4 cell count (cells/mm 3 ); TB=tuberculosis Burden of TB prior to ART Page 21 of 21
Serial Clinical Screening for Active Tuberculosis among HIV-infected Kenyan Adults
 British Journal of Medicine & Medical Research 4(29): 4791-4801, 2014 SCIENCEDOMAIN international www.sciencedomain.org Serial Clinical Screening for Active Tuberculosis among HIV-infected Kenyan Adults
British Journal of Medicine & Medical Research 4(29): 4791-4801, 2014 SCIENCEDOMAIN international www.sciencedomain.org Serial Clinical Screening for Active Tuberculosis among HIV-infected Kenyan Adults
The New WHO guidelines on intensified TB case finding and Isoniazid preventive therapy and operational considerations
 Workshop to accelerate the implementation of the Three Is for HIV/TB and earlier initiation of ART in Southern Africa, March 14-18, 2011, Johannesburg, South Africa. The New WHO guidelines on intensified
Workshop to accelerate the implementation of the Three Is for HIV/TB and earlier initiation of ART in Southern Africa, March 14-18, 2011, Johannesburg, South Africa. The New WHO guidelines on intensified
MAJOR ARTICLE. Stephen D. Lawn, 1,4 Andrew D. Kerkhoff, 1,5 Monica Vogt, 1 Yonas Ghebrekristos, 3 Andrew Whitelaw, 2,3 and Robin Wood 1
 MAJOR ARTICLE Characteristics and Early Outcomes of Patients With Xpert MTB/RIF-Negative Pulmonary Tuberculosis Diagnosed During Screening Before Antiretroviral Therapy Stephen D. Lawn, 1,4 Andrew D. Kerkhoff,
MAJOR ARTICLE Characteristics and Early Outcomes of Patients With Xpert MTB/RIF-Negative Pulmonary Tuberculosis Diagnosed During Screening Before Antiretroviral Therapy Stephen D. Lawn, 1,4 Andrew D. Kerkhoff,
Diagnosis of HIV-Associated Tuberculosis
 Diagnosis of HIV-Associated Tuberculosis Stephen D. Lawn Desmond Tutu HIV Centre Institute of Infectious Disease and Molecular Medicine University of Cape Town Dept. Of Clinical Research, Faculty of Infectious
Diagnosis of HIV-Associated Tuberculosis Stephen D. Lawn Desmond Tutu HIV Centre Institute of Infectious Disease and Molecular Medicine University of Cape Town Dept. Of Clinical Research, Faculty of Infectious
The clinical utility of the urine based lateral flow lipoarabinomannan (LF-LAM) assay in HIV infected adults in Myanmar.
 The clinical utility of the urine based lateral flow lipoarabinomannan (LF-LAM) assay in HIV infected adults in Myanmar Josh Hanson Background Tuberculosis is the commonest cause of death in HIV infected
The clinical utility of the urine based lateral flow lipoarabinomannan (LF-LAM) assay in HIV infected adults in Myanmar Josh Hanson Background Tuberculosis is the commonest cause of death in HIV infected
Intensified TB Case Finding among HIV-infected Persons in Resource-limited Settings
 Intensified TB Case Finding among HIV-infected Persons in Resource-limited Settings Kevin Cain, MD Jay Varma, MD Division of Tuberculosis Elimination Centers for Disease Control and Prevention Need for
Intensified TB Case Finding among HIV-infected Persons in Resource-limited Settings Kevin Cain, MD Jay Varma, MD Division of Tuberculosis Elimination Centers for Disease Control and Prevention Need for
Intensified TB case finding among PLHIV and vulnerable population Identifying contacts Gunta Kirvelaite
 Intensified TB case finding among PLHIV and vulnerable population Identifying contacts Gunta Kirvelaite Riga East Clinical hospital, Centre for tuberculosis and lung diseases. Head of outpatient department.
Intensified TB case finding among PLHIV and vulnerable population Identifying contacts Gunta Kirvelaite Riga East Clinical hospital, Centre for tuberculosis and lung diseases. Head of outpatient department.
Clinical use of a TB Diagnostic using LAM Detection in Urine. Robin Wood, IDM, University of Cape Town
 Clinical use of a TB Diagnostic using LAM Detection in Urine Robin Wood, IDM, University of Cape Town Declaration of Interests Statement Robin Wood, FCP (SA), D.Sc.(Med), FRS (SA). Emeritus Professor of
Clinical use of a TB Diagnostic using LAM Detection in Urine Robin Wood, IDM, University of Cape Town Declaration of Interests Statement Robin Wood, FCP (SA), D.Sc.(Med), FRS (SA). Emeritus Professor of
Clinical Study Performance of Clinical Algorithms for Smear-Negative Tuberculosis in HIV-Infected PersonsinHoChiMinhCity,Vietnam
 Tuberculosis Research and Treatment Volume 2012, Article ID 360852, 6 pages doi:10.1155/2012/360852 Clinical Study Performance of Clinical Algorithms for Smear-Negative Tuberculosis in HIV-Infected PersonsinHoChiMinhCity,Vietnam
Tuberculosis Research and Treatment Volume 2012, Article ID 360852, 6 pages doi:10.1155/2012/360852 Clinical Study Performance of Clinical Algorithms for Smear-Negative Tuberculosis in HIV-Infected PersonsinHoChiMinhCity,Vietnam
Studies on the prevention and control of human immune deficiency virus associated tuberculosis Chakezha, Tendesayi
 UvA-DARE (Digital Academic Repository) Studies on the prevention and control of human immune deficiency virus associated tuberculosis Chakezha, Tendesayi Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Studies on the prevention and control of human immune deficiency virus associated tuberculosis Chakezha, Tendesayi Link to publication Citation for published version
Treating HIV and TB: New evidence, Challenges & Prospects
 Treating HIV and TB: New evidence, Challenges & Prospects Pre-IAS International consultative meeting on Transforming the HIV/TB response: defining the next 10 years July 21 st, 2012 Moses R. Kamya Professor
Treating HIV and TB: New evidence, Challenges & Prospects Pre-IAS International consultative meeting on Transforming the HIV/TB response: defining the next 10 years July 21 st, 2012 Moses R. Kamya Professor
Int.J.Curr.Microbiol.App.Sci (2015) 4(9):
 ISSN: 2319-7706 Volume 4 Number 9 (2015) pp. 744-748 http://www.ijcmas.com Original Research Article Prevalence of HIV-TB Co-Infection and Study of its Epidemiological Variant among Patient s Attending
ISSN: 2319-7706 Volume 4 Number 9 (2015) pp. 744-748 http://www.ijcmas.com Original Research Article Prevalence of HIV-TB Co-Infection and Study of its Epidemiological Variant among Patient s Attending
Intensive Tuberculosis Screening for HIV-Infected Patients Starting Antiretroviral Therapy in Durban, South Africa
 MAJOR ARTICLE HIV/AIDS Intensive Tuberculosis Screening for HIV-Infected Patients Starting Antiretroviral Therapy in Durban, South Africa Ingrid V. Bassett, 1,2 Bingxia Wang, 2,3 Senica Chetty, 7 Janet
MAJOR ARTICLE HIV/AIDS Intensive Tuberculosis Screening for HIV-Infected Patients Starting Antiretroviral Therapy in Durban, South Africa Ingrid V. Bassett, 1,2 Bingxia Wang, 2,3 Senica Chetty, 7 Janet
Modeling the diagnosis of HIVassociated
 Modeling the diagnosis of HIVassociated TB: key research questions and data gaps Patrick GT Cudahy, MD Clinical Instructor Yale School of Medicine S L I D E 0 Diagnosis of TB in people living with HIV
Modeling the diagnosis of HIVassociated TB: key research questions and data gaps Patrick GT Cudahy, MD Clinical Instructor Yale School of Medicine S L I D E 0 Diagnosis of TB in people living with HIV
Clinical and Public Health Impact of Nucleic Acid Amplification Tests (NAATs) for Tuberculosis
 Clinical and Public Health Impact of Nucleic Acid Amplification Tests (NAATs) for Tuberculosis Amit S. Chitnis, MD, MPH; Pennan M. Barry, MD, MPH; Jennifer M. Flood, MD, MPH. California Tuberculosis Controllers
Clinical and Public Health Impact of Nucleic Acid Amplification Tests (NAATs) for Tuberculosis Amit S. Chitnis, MD, MPH; Pennan M. Barry, MD, MPH; Jennifer M. Flood, MD, MPH. California Tuberculosis Controllers
Profile of Tuberculosis Infection among Current HIV+ Patients at the Philippine General Hospital
 Profile of Tuberculosis Infection among Current HIV+ Patients at the Albert B. Albay Jr., MD Jemylyn Garcia, MD Joel Santiaguel, MD UP- TB in the Philippines 6 th leading cause of morbidity and mortality
Profile of Tuberculosis Infection among Current HIV+ Patients at the Albert B. Albay Jr., MD Jemylyn Garcia, MD Joel Santiaguel, MD UP- TB in the Philippines 6 th leading cause of morbidity and mortality
CORRELATES OF DELAYED PULMONARY TUBERCULOSIS DIAGNOSIS AMONG HIV-INFECTED PULMONARY TUBERCULOSIS SUSPECTS IN A. Respicious L Boniface
 CORRELATES OF DELAYED PULMONARY TUBERCULOSIS DIAGNOSIS AMONG HIV-INFECTED PULMONARY TUBERCULOSIS SUSPECTS IN A RURAL HIV CLINIC, SOUTH AFRICA Respicious L Boniface A Research Report submitted to the Faculty
CORRELATES OF DELAYED PULMONARY TUBERCULOSIS DIAGNOSIS AMONG HIV-INFECTED PULMONARY TUBERCULOSIS SUSPECTS IN A RURAL HIV CLINIC, SOUTH AFRICA Respicious L Boniface A Research Report submitted to the Faculty
Risk factors for active tuberculosis following antiretroviral treatment initiation in Abidjan
 Risk factors for active tuberculosis following antiretroviral treatment initiation in Abidjan Catherine Seyler, Siaka Toure, Eugène Messou, Dominique Bonard, Delphine Gabillard, Xavier Anglaret Online
Risk factors for active tuberculosis following antiretroviral treatment initiation in Abidjan Catherine Seyler, Siaka Toure, Eugène Messou, Dominique Bonard, Delphine Gabillard, Xavier Anglaret Online
Open Forum Infectious Diseases MAJOR ARTICLE
 Open Forum Infectious Diseases MAJOR ARTICLE Clinic-Based Urinary Lipoarabinomannan as a Biomarker of Clinical Disease Severity and Mortality Among Antiretroviral Therapy-Naive Human Immunodeficiency Virus-Infected
Open Forum Infectious Diseases MAJOR ARTICLE Clinic-Based Urinary Lipoarabinomannan as a Biomarker of Clinical Disease Severity and Mortality Among Antiretroviral Therapy-Naive Human Immunodeficiency Virus-Infected
HIV Clinicians Society Conference TB/HIV Treatment Cascade
 HIV Clinicians Society Conference-2012 TB/HIV Treatment Cascade Dr Judith Mwansa-Kambafwile Wits Reproductive Health & HIV Institute University of Witwatersrand TB/HIV Treatment Cascade Overview TB stats
HIV Clinicians Society Conference-2012 TB/HIV Treatment Cascade Dr Judith Mwansa-Kambafwile Wits Reproductive Health & HIV Institute University of Witwatersrand TB/HIV Treatment Cascade Overview TB stats
Dr Clare van Halsema
 19 th Annual Conference of the British HIV Association (BHIVA) Dr Clare van Halsema North Manchester General Hospital 16-19 April 2013, Manchester Central Convention Complex The effect of antiretroviral
19 th Annual Conference of the British HIV Association (BHIVA) Dr Clare van Halsema North Manchester General Hospital 16-19 April 2013, Manchester Central Convention Complex The effect of antiretroviral
The need for new TB diagnostics in children and the way forward
 The need for new TB diagnostics in children and the way forward Steve Graham Centre for International Child Health University of Melbourne Department of Paediatrics Royal Children s Hospital Melbourne
The need for new TB diagnostics in children and the way forward Steve Graham Centre for International Child Health University of Melbourne Department of Paediatrics Royal Children s Hospital Melbourne
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Churchyard GJ, Stevens WS, Mametja LD, et al.
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Churchyard GJ, Stevens WS, Mametja LD, et al.
Xpert MTB/RIF use for TB diagnosis in TB suspects with no significant risk of drug resistance or HIV infection. Results of Group Work
 Xpert MTB/RIF use for TB diagnosis in TB suspects with no significant risk of drug resistance or HIV infection Results of Group Work DOTS expansion and enhancement Objective This group deals with the majority
Xpert MTB/RIF use for TB diagnosis in TB suspects with no significant risk of drug resistance or HIV infection Results of Group Work DOTS expansion and enhancement Objective This group deals with the majority
Urinary TB diagnostics in HIV
 Urinary TB diagnostics in HIV SAMRC UCT Eastern Cape collaborative research symposium 20 th October 2017 David Stead Prospective PM study in Zambian tertiary hospital - All medical deaths over 1 year -
Urinary TB diagnostics in HIV SAMRC UCT Eastern Cape collaborative research symposium 20 th October 2017 David Stead Prospective PM study in Zambian tertiary hospital - All medical deaths over 1 year -
TB & HIV CO-INFECTION IN CHILDREN. Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012
 TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
Let s Talk TB A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year
 A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Madhukar Pai, MD, PhD Author and Series Editor Camilla Rodrigues, MD co-author Abstract Most individuals who get exposed
A Series on Tuberculosis, A Disease That Affects Over 2 Million Indians Every Year Madhukar Pai, MD, PhD Author and Series Editor Camilla Rodrigues, MD co-author Abstract Most individuals who get exposed
Rapid PCR TB Testing Results in 68.5% Reduction in Unnecessary Isolation Days in Smear Positive Patients.
 Rapid PCR TB Testing Results in 68.5% Reduction in Unnecessary Isolation Days in Smear Positive Patients. Item Type Thesis Authors Patel, Ravikumar Publisher The University of Arizona. Rights Copyright
Rapid PCR TB Testing Results in 68.5% Reduction in Unnecessary Isolation Days in Smear Positive Patients. Item Type Thesis Authors Patel, Ravikumar Publisher The University of Arizona. Rights Copyright
Authors Nicholas, S; Sabapathy, K; Ferreyra, C; Varaine, F; Pujades-Rodríguez, M /QAI.0b013e318218a713
 MSF Field Research Incidence of Tuberculosis in HIV-Infected Patients Before and After Starting Combined Antiretroviral Therapy in 8 Sub- Saharan African HIV Programs. Authors Nicholas, S; Sabapathy, K;
MSF Field Research Incidence of Tuberculosis in HIV-Infected Patients Before and After Starting Combined Antiretroviral Therapy in 8 Sub- Saharan African HIV Programs. Authors Nicholas, S; Sabapathy, K;
Twelve-monthly versus six-monthly radiological screening for active case-finding of tuberculosis: a randomised controlled trial
 1 Aurum Institute for Health Research, Johannesburg, South Africa 2 Department of Infectious Disease Epidemiology, London School of Hygiene and Tropical Medicine, London, UK 3 Department of Clinical Research,
1 Aurum Institute for Health Research, Johannesburg, South Africa 2 Department of Infectious Disease Epidemiology, London School of Hygiene and Tropical Medicine, London, UK 3 Department of Clinical Research,
Comparative performance of emerging rapid diagnostics in HIV-infected individuals
 Comparative performance of emerging rapid diagnostics in HIV-infected individuals Maunank Shah M.D. Johns Hopkins University Clinical Diagnostics Research Consortium Background Emerging diagnostics may
Comparative performance of emerging rapid diagnostics in HIV-infected individuals Maunank Shah M.D. Johns Hopkins University Clinical Diagnostics Research Consortium Background Emerging diagnostics may
Principle of Tuberculosis Control. CHIANG Chen-Yuan MD, MPH, DrPhilos
 Principle of Tuberculosis Control CHIANG Chen-Yuan MD, MPH, DrPhilos Estimated global tuberculosis burden 2015 an estimated 10.4 million incident cases of TB (range, 8.7 million 12.2 million) 142 cases
Principle of Tuberculosis Control CHIANG Chen-Yuan MD, MPH, DrPhilos Estimated global tuberculosis burden 2015 an estimated 10.4 million incident cases of TB (range, 8.7 million 12.2 million) 142 cases
INTENSIFIED TB CASE FINDING
 INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
TOG The Way Forward
 TOG 2016- The Way Forward Main Changes in Diagnostic algorithm Definition (Type, Classification, Outcome) Registration at the time of Diagnosis (PHI level Notification Register) Long term follow up (till
TOG 2016- The Way Forward Main Changes in Diagnostic algorithm Definition (Type, Classification, Outcome) Registration at the time of Diagnosis (PHI level Notification Register) Long term follow up (till
Overview Treatment of latent TB infection Meta-analysis 36 months of IPT Screening for TB Adverse events INH Resistance IPT & ART TST Conclusions
 202/03/28 Isoniazid preventive therapy: evidence for safety and efficacy Clinician s course Gavin Churchyard/ Liesl Page-Shipp 6 March 202 Overview Treatment of latent TB infection Meta-analysis 36 months
202/03/28 Isoniazid preventive therapy: evidence for safety and efficacy Clinician s course Gavin Churchyard/ Liesl Page-Shipp 6 March 202 Overview Treatment of latent TB infection Meta-analysis 36 months
Downloaded from:
 Kerkhoff, AD; Barr, DA; Schutz, C; Burton, R; Nicol, MP; Lawn, SD; Meintjes, G (2017) Disseminated tuberculosis among hospitalised HIV patients in South Africa: a common condition that can be rapidly diagnosed
Kerkhoff, AD; Barr, DA; Schutz, C; Burton, R; Nicol, MP; Lawn, SD; Meintjes, G (2017) Disseminated tuberculosis among hospitalised HIV patients in South Africa: a common condition that can be rapidly diagnosed
Diagnosing Xpert MTB/RIF negative TB suspects: Impact and cost of an alternative algorithm
 Diagnosing Xpert MTB/RIF negative TB suspects: Impact and cost of an alternative algorithm Kathryn Schnippel 1, Gesine Meyer-Rath 1,2, Lawrence Long 1, Wendy Stevens 3,4, Ian Sanne 1,2, and Sydney Rosen
Diagnosing Xpert MTB/RIF negative TB suspects: Impact and cost of an alternative algorithm Kathryn Schnippel 1, Gesine Meyer-Rath 1,2, Lawrence Long 1, Wendy Stevens 3,4, Ian Sanne 1,2, and Sydney Rosen
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Cain KP, McCarthy KD, Heilig CM, et al. An algorithm for tuberculosis
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Cain KP, McCarthy KD, Heilig CM, et al. An algorithm for tuberculosis
Impact of HIV on the TB Epidemic in Africa
 Impact of HIV on the TB Epidemic in Africa Anthony David Harries Senior Advisor International Union against TB and Lung Disease The captain of all these men of death 1 Robert Koch 1882: Described the tubercle
Impact of HIV on the TB Epidemic in Africa Anthony David Harries Senior Advisor International Union against TB and Lung Disease The captain of all these men of death 1 Robert Koch 1882: Described the tubercle
Tuberculosis and HIV: key issues in diagnosis and management
 Tuberculosis and HIV: key issues in diagnosis and management Julian Elliott Infectious Diseases Unit, Alfred Hospital Centre for Population Health, Burnet Institute julian.elliott@alfred.org.au Outline
Tuberculosis and HIV: key issues in diagnosis and management Julian Elliott Infectious Diseases Unit, Alfred Hospital Centre for Population Health, Burnet Institute julian.elliott@alfred.org.au Outline
What Is New in Combination TB Prevention? Lisa J. Nelson Treatment and Care (TAC) Team HIV Department WHO HQ
 What Is New in Combination TB Prevention? Lisa J. Nelson Treatment and Care (TAC) Team HIV Department WHO HQ Outline Combination prevention for HIV Approaches to TB prevention Individual Household/key
What Is New in Combination TB Prevention? Lisa J. Nelson Treatment and Care (TAC) Team HIV Department WHO HQ Outline Combination prevention for HIV Approaches to TB prevention Individual Household/key
WHO Guidelines for IPT and ICF
 WHO Guidelines for IPT and ICF Reuben Granich HIV/AIDS Department World Health Organization Haileyesus Getahun STOP TB Department World Health Organization Outline Background Evidence Recommendations Adults
WHO Guidelines for IPT and ICF Reuben Granich HIV/AIDS Department World Health Organization Haileyesus Getahun STOP TB Department World Health Organization Outline Background Evidence Recommendations Adults
Interventions to improve screening for latent TB: effectiveness and outcomes
 Interventions to improve screening for latent TB: effectiveness and outcomes Fotinie Ntziora, Thushan DeSilva, Natasha Baker, Debbie Talbot, Louise Byrne, Karen Sherry, Sandra Booth, Janice Hobson, Karen
Interventions to improve screening for latent TB: effectiveness and outcomes Fotinie Ntziora, Thushan DeSilva, Natasha Baker, Debbie Talbot, Louise Byrne, Karen Sherry, Sandra Booth, Janice Hobson, Karen
Ken Jost, BA, has the following disclosures to make:
 Diagnosis of TB Disease: Laboratory Ken Jost, BA May 10, 2017 TB Intensive May 9-12, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Ken Jost, BA, has the following disclosures to make: No conflict
Diagnosis of TB Disease: Laboratory Ken Jost, BA May 10, 2017 TB Intensive May 9-12, 2017 San Antonio, TX EXCELLENCE EXPERTISE INNOVATION Ken Jost, BA, has the following disclosures to make: No conflict
Controlling TB in the era of HIV
 Controlling TB in the era of HIV Christy Hanson, PhD, MPH TB Research Advisor Amy Bloom, MD TB/HIV Advisor TB Incidence rates highest in Africa Estimated new TB cases (all forms) per 100 000 population
Controlling TB in the era of HIV Christy Hanson, PhD, MPH TB Research Advisor Amy Bloom, MD TB/HIV Advisor TB Incidence rates highest in Africa Estimated new TB cases (all forms) per 100 000 population
World Journal of Pharmaceutical and Life Sciences WJPLS
 wjpls, 2019, Vol. 5, Issue 2, 01-06 Research Article ISSN 2454-2229 WJPLS www.wjpls.org SJIF Impact Factor: 5.008 COMPARATIVE STUDY BETWEEN GENEXPERT MTB/RIF ASSAY AND DIRECT SMEAR MICROSCOPY(DSM) FOR
wjpls, 2019, Vol. 5, Issue 2, 01-06 Research Article ISSN 2454-2229 WJPLS www.wjpls.org SJIF Impact Factor: 5.008 COMPARATIVE STUDY BETWEEN GENEXPERT MTB/RIF ASSAY AND DIRECT SMEAR MICROSCOPY(DSM) FOR
Latent tuberculosis infection
 EXECUTIVE SUMMARY Latent tuberculosis infection Updated and consolidated guidelines for programmatic management Executive summary Latent tuberculosis infection (LTBI) is defined as a state of persistent
EXECUTIVE SUMMARY Latent tuberculosis infection Updated and consolidated guidelines for programmatic management Executive summary Latent tuberculosis infection (LTBI) is defined as a state of persistent
Algorithmic Approaches to Child TB Management in Resource-limited Settings
 Algorithmic Approaches to Child TB Management in Resource-limited Settings Steve Graham Centre for International Child Health University of Melbourne Department of Paediatrics Royal Children s Hospital
Algorithmic Approaches to Child TB Management in Resource-limited Settings Steve Graham Centre for International Child Health University of Melbourne Department of Paediatrics Royal Children s Hospital
Immune Reconstitution Inflammatory Syndrome. Dr. Lesego Mawela
 Immune Reconstitution Inflammatory Syndrome Dr. Lesego Mawela TOPICS FOR DISCUSSION IRIS Case Epidermiology Pathogenesis of IRIS Risk factors for IRIS Epidemiology of IRIS Health system burden of IRIS
Immune Reconstitution Inflammatory Syndrome Dr. Lesego Mawela TOPICS FOR DISCUSSION IRIS Case Epidermiology Pathogenesis of IRIS Risk factors for IRIS Epidemiology of IRIS Health system burden of IRIS
Downloaded from:
 van Halsema, CL; Fielding, KL; Chihota, VN; Lewis, JJ; Churchyard, GJ; Grant, AD (2012) Trends in drug-resistant tuberculosis in a gold-mining workforce in South Africa, 2002-2008. The international journal
van Halsema, CL; Fielding, KL; Chihota, VN; Lewis, JJ; Churchyard, GJ; Grant, AD (2012) Trends in drug-resistant tuberculosis in a gold-mining workforce in South Africa, 2002-2008. The international journal
IPT IMPLEMENTATION- SWAZILAND EXPERIENCE
 IPT IMPLEMENTATION- SWAZILAND EXPERIENCE Gugu Mchunu-National TB/HIV coordinator Programmatic Management of Latent TB infection consultation meeting Seoul, Republic of Korea,27-28 APRIL,2016 TB Epidemiology
IPT IMPLEMENTATION- SWAZILAND EXPERIENCE Gugu Mchunu-National TB/HIV coordinator Programmatic Management of Latent TB infection consultation meeting Seoul, Republic of Korea,27-28 APRIL,2016 TB Epidemiology
Factors associated with unsuppressed viral load in HIV-1 infected patients on 1 st line antiretroviral therapy in South Africa
 Factors associated with unsuppressed viral load in HIV-1 infected patients on 1 st line antiretroviral therapy in South Africa Dvora Joseph Davey 1, 2, PhD, Zulfa Abrahams 2, PhD 1 BroadReach, South Africa
Factors associated with unsuppressed viral load in HIV-1 infected patients on 1 st line antiretroviral therapy in South Africa Dvora Joseph Davey 1, 2, PhD, Zulfa Abrahams 2, PhD 1 BroadReach, South Africa
Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016
 Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016 Randy Culpepper, MD, MPH Deputy Heath Officer/Medical Director Frederick County Health Department March 16, 2016 2 No
Latent Tuberculosis Infections Controversies in Diagnosis and Management Update 2016 Randy Culpepper, MD, MPH Deputy Heath Officer/Medical Director Frederick County Health Department March 16, 2016 2 No
Tuberculosis active case finding: uptake and diagnostic yield among minibus drivers in urban South Africa
 Mabuto et al. BMC Public Health (2015) 15:242 DOI 10.1186/s12889-015-1592-x RESEARCH ARTICLE Open Access Tuberculosis active case finding: uptake and diagnostic yield among minibus drivers in urban South
Mabuto et al. BMC Public Health (2015) 15:242 DOI 10.1186/s12889-015-1592-x RESEARCH ARTICLE Open Access Tuberculosis active case finding: uptake and diagnostic yield among minibus drivers in urban South
Predictors of drug sensitive tuberculosis treatment outcomes among hospitalised
 Predictors of drug sensitive tuberculosis treatment outcomes among hospitalised patients in South Africa: a multinomial logit model Abiola O. Olaleye 1,* and Andy K. Beke 1 1 School of Health Systems and
Predictors of drug sensitive tuberculosis treatment outcomes among hospitalised patients in South Africa: a multinomial logit model Abiola O. Olaleye 1,* and Andy K. Beke 1 1 School of Health Systems and
Diagnostic challenges of active childhood TB in Tanzania. Michala Vaaben Rose, MD, Ph.D Department of Infectious Diseases, Hvidovre
 Diagnostic challenges of active childhood TB in Tanzania Michala Vaaben Rose, MD, Ph.D Department of Infectious Diseases, Hvidovre 1 Diagnosis of Childhood Tuberculosis Muheza hospital, TZ Hilleroedhospital.dk
Diagnostic challenges of active childhood TB in Tanzania Michala Vaaben Rose, MD, Ph.D Department of Infectious Diseases, Hvidovre 1 Diagnosis of Childhood Tuberculosis Muheza hospital, TZ Hilleroedhospital.dk
Epidemiology and diagnosis of MDR-TB in children H Simon Schaaf
 Epidemiology and diagnosis of MDR-TB in children H Simon Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health, Stellenbosch University, and Tygerberg Children s Hospital (TCH) Definitions
Epidemiology and diagnosis of MDR-TB in children H Simon Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health, Stellenbosch University, and Tygerberg Children s Hospital (TCH) Definitions
Ongoing Research on LTBI and Research priorities in India
 Ongoing Research on LTBI and Research priorities in India Dr. C.Padmapriyadarsini, MD, MS ICMR-National Institute for Research in Tuberculosis Chennai, India Technical Consultation Meeting on Programmatic
Ongoing Research on LTBI and Research priorities in India Dr. C.Padmapriyadarsini, MD, MS ICMR-National Institute for Research in Tuberculosis Chennai, India Technical Consultation Meeting on Programmatic
Title: Role of Interferon-gamma Release Assays in the Diagnosis of Pulmonary Tuberculosis in Patients with Advanced HIV infection
 Author's response to reviews Title: Role of Interferon-gamma Release Assays in the Diagnosis of Pulmonary Tuberculosis in Patients with Advanced HIV infection Authors: Adithya Cattamanchi (acattamanchi@medsfgh.ucsf.edu)
Author's response to reviews Title: Role of Interferon-gamma Release Assays in the Diagnosis of Pulmonary Tuberculosis in Patients with Advanced HIV infection Authors: Adithya Cattamanchi (acattamanchi@medsfgh.ucsf.edu)
Implementation and scale-up of the Xpert MTB/RIF system for rapid diagnosis of TB and MDR-TB. Global Consultation
 Implementation and scale-up of the Xpert MTB/RIF system for rapid diagnosis of TB and MDR-TB Global Consultation Geneva, 30 November 2010 Mario C. Raviglione, M.D. Director, Stop TB Department WHO, Geneva,
Implementation and scale-up of the Xpert MTB/RIF system for rapid diagnosis of TB and MDR-TB Global Consultation Geneva, 30 November 2010 Mario C. Raviglione, M.D. Director, Stop TB Department WHO, Geneva,
HIV antiretroviral therapy in Ethiopia. Paper IV. Degu Jerene Dare
 80 HIV antiretroviral therapy in Ethiopia Paper IV Degu Jerene Dare Acceptability of HIV counselling and testing among tuberculosis patients in south Ethiopia Degu Jerene 1, 2*, Aschalew Endale 2, Bernt
80 HIV antiretroviral therapy in Ethiopia Paper IV Degu Jerene Dare Acceptability of HIV counselling and testing among tuberculosis patients in south Ethiopia Degu Jerene 1, 2*, Aschalew Endale 2, Bernt
Isoniazid preventive therapy for HIV+:
 Isoniazid preventive therapy for HIV+: Controversial topics Gary Maartens Division of Clinical Pharmacology UNIVERSITY OF CAPE TOWN IYUNIVESITHI YASEKAPA UNIVERSITEIT VAN KAAPSTAD Risk of TB disease after
Isoniazid preventive therapy for HIV+: Controversial topics Gary Maartens Division of Clinical Pharmacology UNIVERSITY OF CAPE TOWN IYUNIVESITHI YASEKAPA UNIVERSITEIT VAN KAAPSTAD Risk of TB disease after
Tuberculosis in children: gaps and opportunities
 Tuberculosis in children: gaps and opportunities Mark Nicol Division of Medical Microbiology and Institute for Infectious Diseases and Molecular Medicine, University of Cape Town and National Health Laboratory
Tuberculosis in children: gaps and opportunities Mark Nicol Division of Medical Microbiology and Institute for Infectious Diseases and Molecular Medicine, University of Cape Town and National Health Laboratory
Isoniazid Preventive Therapy (IPT) in HIV-Infected and Uninfected Children. Réghana Taliep
 Isoniazid Preventive Therapy (IPT) in HIV-Infected and Uninfected Children Réghana Taliep Background Tuberculosis (TB) is a common complication and leading cause of death in HIV infection HIV is the strongest
Isoniazid Preventive Therapy (IPT) in HIV-Infected and Uninfected Children Réghana Taliep Background Tuberculosis (TB) is a common complication and leading cause of death in HIV infection HIV is the strongest
Abstract. PLoS Medicine 1 January 2011 Volume 8 Issue 1 e
 Development of a Standardized Screening Rule for Tuberculosis in People Living with HIV in Resource- Constrained Settings: Individual Participant Data Metaanalysis of Observational Studies Haileyesus Getahun
Development of a Standardized Screening Rule for Tuberculosis in People Living with HIV in Resource- Constrained Settings: Individual Participant Data Metaanalysis of Observational Studies Haileyesus Getahun
Pilot Summary Report Revisiting the cost-effectiveness of Xpert MTB/RIF: lessons learned from South Africa
 Pilot Summary Report Revisiting the cost-effectiveness of Xpert MTB/RIF: lessons learned from South Africa Background In 2014, 1.5 million people died from tuberculosis (TB), 25% of whom had HIV, and 13%
Pilot Summary Report Revisiting the cost-effectiveness of Xpert MTB/RIF: lessons learned from South Africa Background In 2014, 1.5 million people died from tuberculosis (TB), 25% of whom had HIV, and 13%
TB and HIV co-infection including IRIS
 TB and HIV co-infection including IRIS Richard Lessells SAHCS Conference 2018 Clinical scenario 1 36-year-old male Presents with cough, fever & weight loss HIV test positive (new diagnosis) Sputum Xpert
TB and HIV co-infection including IRIS Richard Lessells SAHCS Conference 2018 Clinical scenario 1 36-year-old male Presents with cough, fever & weight loss HIV test positive (new diagnosis) Sputum Xpert
Response to Treatment in Sputum Smear Positive Pulmonary Tuberculosis Patients In relation to Human Immunodeficiency Virus in Kano, Nigeria.
 Response to Treatment in Sputum Smear Positive Pulmonary Tuberculosis Patients In relation to Human Immunodeficiency Virus in Kano, Nigeria. Yusuf Mohammed, Mukhtar Dauda, Ifeanyi Oyeyi TB/HIV Unit, International
Response to Treatment in Sputum Smear Positive Pulmonary Tuberculosis Patients In relation to Human Immunodeficiency Virus in Kano, Nigeria. Yusuf Mohammed, Mukhtar Dauda, Ifeanyi Oyeyi TB/HIV Unit, International
Cost-effectiveness of ART and the Three I s for HIV/TB to prevent tuberculosis
 Cost-effectiveness of ART and the Three I s for HIV/TB to prevent tuberculosis among people living with HIV Somya Gupta, Taiwo Abimbola, Anand Date, Amitabh B. Suthar, Rod Bennett, Nalinee Sangrujee, Reuben
Cost-effectiveness of ART and the Three I s for HIV/TB to prevent tuberculosis among people living with HIV Somya Gupta, Taiwo Abimbola, Anand Date, Amitabh B. Suthar, Rod Bennett, Nalinee Sangrujee, Reuben
CRP as a potential TB triage or screening test: considerations for modelers
 CRP as a potential TB triage or screening test: considerations for modelers TB MAC Diagnostics Meeting September 14, 2018 Christina Yoon, MD, MAS, MPH Assistant Professor, UCSF Triage vs. Screening tests
CRP as a potential TB triage or screening test: considerations for modelers TB MAC Diagnostics Meeting September 14, 2018 Christina Yoon, MD, MAS, MPH Assistant Professor, UCSF Triage vs. Screening tests
DELAYS IN INITIATION OF ANTIRETROVIRAL THERAPY AMONG HIV-INFECTED CHILDREN IN RURAL ZAMBIA 9 th Interest Comference Francis H.
 DELAYS IN INITIATION OF ANTIRETROVIRAL THERAPY AMONG HIV-INFECTED CHILDREN IN RURAL ZAMBIA 9 th Interest Comference Francis H. Hamangaba Macha Research Trust Zambia Background Care and treatment are available
DELAYS IN INITIATION OF ANTIRETROVIRAL THERAPY AMONG HIV-INFECTED CHILDREN IN RURAL ZAMBIA 9 th Interest Comference Francis H. Hamangaba Macha Research Trust Zambia Background Care and treatment are available
Original Article Evaluation of Xpert MTB/RIF in detection of pulmonary and extrapulmonary tuberculosis cases in China
 Int J Clin Exp Pathol 2017;10(4):4847-4851 www.ijcep.com /ISSN:1936-2625/IJCEP0045802 Original Article Evaluation of Xpert MTB/RIF in detection of pulmonary and extrapulmonary tuberculosis cases in China
Int J Clin Exp Pathol 2017;10(4):4847-4851 www.ijcep.com /ISSN:1936-2625/IJCEP0045802 Original Article Evaluation of Xpert MTB/RIF in detection of pulmonary and extrapulmonary tuberculosis cases in China
Developing strategies for TB screening among HIV-infected and HIV-uninfected pregnant and postpartum women in Swaziland
 Developing strategies for TB screening among HIV-infected and HIV-uninfected pregnant and postpartum women in Swaziland Marianne Calnan Deputy Director www.urc-chs.com Background Recent research suggests
Developing strategies for TB screening among HIV-infected and HIV-uninfected pregnant and postpartum women in Swaziland Marianne Calnan Deputy Director www.urc-chs.com Background Recent research suggests
Evolving Realities of HIV Treatment in Resource-limited Settings
 Evolving Realities of HIV Treatment in Resource-limited Settings Papa Salif Sow MD, MSc Department of Infectious Diseases University of Dakar, Senegal Introduction: ARV access in RLS Scale-up of ART has
Evolving Realities of HIV Treatment in Resource-limited Settings Papa Salif Sow MD, MSc Department of Infectious Diseases University of Dakar, Senegal Introduction: ARV access in RLS Scale-up of ART has
Isoniazid Prevention Therapy for HIV Positive Patients
 Isoniazid Prevention Therapy for HIV Positive Patients Increasing Tuberculosis Prevention for HIV-Patients in Ethiopia QuickTime and a decompressor are needed to see this picture. Ashok Reddy, MD University
Isoniazid Prevention Therapy for HIV Positive Patients Increasing Tuberculosis Prevention for HIV-Patients in Ethiopia QuickTime and a decompressor are needed to see this picture. Ashok Reddy, MD University
UvA-DARE (Digital Academic Repository) Tuberculosis case finding in South Africa Claassens, M.M. Link to publication
 UvA-DARE (Digital Academic Repository) Tuberculosis case finding in South Africa Claassens, M.M. Link to publication Citation for published version (APA): Claassens, M. M. (2013). Tuberculosis case finding
UvA-DARE (Digital Academic Repository) Tuberculosis case finding in South Africa Claassens, M.M. Link to publication Citation for published version (APA): Claassens, M. M. (2013). Tuberculosis case finding
IPT BOTSWANA EXPERIENCE
 IPT BOTSWANA EXPERIENCE Oaitse I Motsamai RN, MW, B Ed, MPH Ministry of Health Botswana 11 th November 2008 Addis Ababa, Ethiopia OUTLINE Botswana context Rationale for IPT in Botswana Pilot Current Programme
IPT BOTSWANA EXPERIENCE Oaitse I Motsamai RN, MW, B Ed, MPH Ministry of Health Botswana 11 th November 2008 Addis Ababa, Ethiopia OUTLINE Botswana context Rationale for IPT in Botswana Pilot Current Programme
TB: A Supplement to GP CLINICS
 TB: A Supplement to GP CLINICS Chapter 10: Childhood Tuberculosis: Q&A For Primary Care Physicians Author: Madhukar Pai, MD, PhD Author and Series Editor What is Childhood TB and who is at risk? India
TB: A Supplement to GP CLINICS Chapter 10: Childhood Tuberculosis: Q&A For Primary Care Physicians Author: Madhukar Pai, MD, PhD Author and Series Editor What is Childhood TB and who is at risk? India
Multidrug-Resistant TB
 Multidrug-Resistant TB Diagnosis Treatment Linking Diagnosis and Treatment Charles L. Daley, M.D. National Jewish Health University of Colorado Denver Disclosures Chair, Data Monitoring Committee for delamanid
Multidrug-Resistant TB Diagnosis Treatment Linking Diagnosis and Treatment Charles L. Daley, M.D. National Jewish Health University of Colorado Denver Disclosures Chair, Data Monitoring Committee for delamanid
Downloaded from:
 Churchyard, GJ; Stevens, WS; Mametja, LD; McCarthy, KM; Chihota, V; Nicol, MP; Erasmus, LK; Ndjeka, NO; Mvusi, L; Vassall, A; Sinanovic, E; Cox, HS; Dye, C; Grant, AD; Fielding, KL (2015) Xpert MTB/RIF
Churchyard, GJ; Stevens, WS; Mametja, LD; McCarthy, KM; Chihota, V; Nicol, MP; Erasmus, LK; Ndjeka, NO; Mvusi, L; Vassall, A; Sinanovic, E; Cox, HS; Dye, C; Grant, AD; Fielding, KL (2015) Xpert MTB/RIF
Diagnosis and Treatment of Tuberculosis, 2011
 Diagnosis of TB Diagnosis and Treatment of Tuberculosis, 2011 Alfred Lardizabal, MD NJMS Global Tuberculosis Institute Diagnosis of TB, 2011 Diagnosis follows Suspicion When should we Think TB? Who is
Diagnosis of TB Diagnosis and Treatment of Tuberculosis, 2011 Alfred Lardizabal, MD NJMS Global Tuberculosis Institute Diagnosis of TB, 2011 Diagnosis follows Suspicion When should we Think TB? Who is
Recognizing MDR-TB in Children. Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention February 2016
 Recognizing MDR-TB in Children Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention 17-18 February 2016 Objectives Review the definitions and categorization of drugresistant tuberculosis Understand the
Recognizing MDR-TB in Children Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention 17-18 February 2016 Objectives Review the definitions and categorization of drugresistant tuberculosis Understand the
Lawn et al. BMC Medicine (2015) 13:192 DOI /s
 Lawn et al. BMC Medicine (2015) 13:192 DOI 10.1186/s12916-015-0432-2 RESEARCH ARTICLE Open Access Rapid microbiological screening for tuberculosis in HIV-positive patients on the first day of acute hospital
Lawn et al. BMC Medicine (2015) 13:192 DOI 10.1186/s12916-015-0432-2 RESEARCH ARTICLE Open Access Rapid microbiological screening for tuberculosis in HIV-positive patients on the first day of acute hospital
Abstract. n engl j med 370;4 nejm.org january 23,
 The new england journal of medicine established in 1812 january 23, 2014 vol. 370 no. 4 A Trial of Mass Isoniazid Preventive Therapy for Tuberculosis Control Gavin J. Churchyard, M.B., B.Ch., Ph.D., Katherine
The new england journal of medicine established in 1812 january 23, 2014 vol. 370 no. 4 A Trial of Mass Isoniazid Preventive Therapy for Tuberculosis Control Gavin J. Churchyard, M.B., B.Ch., Ph.D., Katherine
Subclinical tuberculosis among adults with HIV: clinical features and outcomes in a South African cohort
 Bajema et al. BMC Infectious Diseases (2019) 19:14 https://doi.org/10.1186/s12879-018-3614-7 RESEARCH ARTICLE Subclinical tuberculosis among adults with HIV: clinical features and outcomes in a South African
Bajema et al. BMC Infectious Diseases (2019) 19:14 https://doi.org/10.1186/s12879-018-3614-7 RESEARCH ARTICLE Subclinical tuberculosis among adults with HIV: clinical features and outcomes in a South African
Research Methods for TB Diagnostics. Kathy DeRiemer, PhD, MPH University of California, Davis Shanghai, China: May 8, 2012
 Research Methods for TB Diagnostics Kathy DeRiemer, PhD, MPH University of California, Davis Shanghai, China: May 8, 2012 Overview Why do we need good TB diagnostics? What works? What doesn t work? How
Research Methods for TB Diagnostics Kathy DeRiemer, PhD, MPH University of California, Davis Shanghai, China: May 8, 2012 Overview Why do we need good TB diagnostics? What works? What doesn t work? How
The relationship between adherence to clinic appointments and year-one mortality for HIV infected patients at a Referral Hospital in Western Kenya
 The relationship between adherence to clinic appointments and year-one mortality for HIV infected patients at a Referral Hospital in Western Kenya Muthusi, K; Burmen, B 8th International Workshop on HIV
The relationship between adherence to clinic appointments and year-one mortality for HIV infected patients at a Referral Hospital in Western Kenya Muthusi, K; Burmen, B 8th International Workshop on HIV
An Algorithm for Tuberculosis Screening and Diagnosis in People with HIV
 The new england journal of medicine original article An Algorithm for Tuberculosis Screening and Diagnosis in People with HIV Kevin P. Cain, M.D., Kimberly D. McCarthy, M.M., Charles M. Heilig, Ph.D.,
The new england journal of medicine original article An Algorithm for Tuberculosis Screening and Diagnosis in People with HIV Kevin P. Cain, M.D., Kimberly D. McCarthy, M.M., Charles M. Heilig, Ph.D.,
in South Africa. Authors Coetzee, D; Hilderbrand, K; Goemaere, E; Matthys, F; Boelaert, M /j x
 MSF Field Research Integrating tuberculosis and HIV care in the primary care setting in South Africa. Authors Coetzee, D; Hilderbrand, K; Goemaere, E; Matthys, F; Boelaert, M Citation DOI Journal Rights
MSF Field Research Integrating tuberculosis and HIV care in the primary care setting in South Africa. Authors Coetzee, D; Hilderbrand, K; Goemaere, E; Matthys, F; Boelaert, M Citation DOI Journal Rights
NATIONAL TUBERCULOSIS PREVALENCE SURVEY 2016
 NATIONAL TUBERCULOSIS PREVALENCE SURVEY 2016 Department of Health/National TB Control Program Philippine Council for Health Research and Development Foundation for the Advancement of Clinical Epidemiology,
NATIONAL TUBERCULOSIS PREVALENCE SURVEY 2016 Department of Health/National TB Control Program Philippine Council for Health Research and Development Foundation for the Advancement of Clinical Epidemiology,
Errors in Dx and Rx of TB
 Errors in Dx and Rx of TB David Schlossberg, MD, FACP Professor of Medicine Temple University School of Medicine Medical Director, TB Control Program Philadelphia Department of Public Health TB Still a
Errors in Dx and Rx of TB David Schlossberg, MD, FACP Professor of Medicine Temple University School of Medicine Medical Director, TB Control Program Philadelphia Department of Public Health TB Still a
Incremental cost-effectiveness of the second Xpert MTB/RIF assay to detect Mycobacterium tuberculosis
 Original Article Incremental cost-effectiveness of the second Xpert MTB/RIF assay to detect Mycobacterium tuberculosis Guirong Wang, Shuqi Wang, Guanglu Jiang, Yuhong Fu, Yuanyuan Shang, Hairong Huang
Original Article Incremental cost-effectiveness of the second Xpert MTB/RIF assay to detect Mycobacterium tuberculosis Guirong Wang, Shuqi Wang, Guanglu Jiang, Yuhong Fu, Yuanyuan Shang, Hairong Huang
Time to implement: WHO guidelines on TB Preventive Treatment
 Time to implement: WHO guidelines on TB Preventive Treatment WHO End TB Strategy TARGETS: 90% reduction of deaths and 80% reduction in incidence by 2030 Early diagnosis Integrated, of TB including universal
Time to implement: WHO guidelines on TB Preventive Treatment WHO End TB Strategy TARGETS: 90% reduction of deaths and 80% reduction in incidence by 2030 Early diagnosis Integrated, of TB including universal
Diagnosis of Extra Pulmonary Tuberculosis By Using Xpert MTB/RIF Assay (CBNAAT) And MGIT Liquid Culture.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 9 Ver. 10 (September. 2018), PP 65-70 www.iosrjournals.org Diagnosis of Extra Pulmonary Tuberculosis
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 9 Ver. 10 (September. 2018), PP 65-70 www.iosrjournals.org Diagnosis of Extra Pulmonary Tuberculosis
ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM
 ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM The form and content of the explanatory note is to: Inform those responsible for completing the DMR 164 Reporting Form - as to
ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM The form and content of the explanatory note is to: Inform those responsible for completing the DMR 164 Reporting Form - as to
Current status of implementation and monitoring and evaluation of collaborative TB/HIV activities. Avinash Kanchar
 Current status of implementation and monitoring and evaluation of collaborative TB/HIV activities Avinash Kanchar Outline WHO guide to M&E of collaborative TB/HIV activities: 2015 Reporting status on Global
Current status of implementation and monitoring and evaluation of collaborative TB/HIV activities Avinash Kanchar Outline WHO guide to M&E of collaborative TB/HIV activities: 2015 Reporting status on Global
