David M. Miller 1,2*, Ryan M. Trowbridge 3, Anupam Desai 1 and Reed E. Drews 1
|
|
|
- Barbra Cooper
- 5 years ago
- Views:
Transcription
1 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 CASE REPORT Kaposi s varicelliform eruption in a patient with metastatic melanoma and primary cutaneous anaplastic large cell lymphoma treated with talimogene laherparepvec and nivolumab David M. Miller 1,2*, Ryan M. Trowbridge 3, Anupam Desai 1 and Reed E. Drews 1 Open Access Abstract Background: Immune-directed therapies have become front-line therapy for melanoma and are transforming the management of advanced disease. In refractory cases, multi-modal immunoncology (IO) approaches are being utilized, including combining immune checkpoint blockade (ICB) with oncolytic herpes viruses. Talimogene laherparepvec (T-VEC) is the first genetically modified oncolytic viral therapy (OVT) approved for the treatment of recurrent and unresectable melanoma. The use of IO in patients with concomitant malignancies and/or compromised immune systems is limited due to systematic exclusion from clinical trials. For example, a single case report of a solid organ transplant patient successfully treated with T-VEC for metastatic melanoma has been reported. Furthermore, the use of ICB in T-cell malignancies is limited and paradoxical worsening has been described. To our knowledge, this is the first report of dual ICB/T-VEC being administered to a patient with concurrent primary cutaneous anaplastic large cell lymphoma (pcalcl) and melanoma. Case presentation: Here we present the case of a patient with concomitant primary cutaneous ALCL and metastatic melanoma, progressing on anti-programmed death (PD)-1 therapy, who developed Kaposi s varicelliform eruption after receiving the first dose of Talimogene laherparepvec. Conclusion: This case highlights the complexities of care of patients with coexistent cancers, demonstrates rapid progression of primary cutaneous ALCL on nivolumab and introduces a novel adverse effect of Talimogene laherparepvec. Keywords: Talimogene laherparepvec, Melanoma, Anaplastic large cell lymphoma, Kaposi varicelliform eruption, eczema TVECium, Immunocompromised Background Immune-directed therapies have become front-line for the vast majority of advanced melanoma cases. ICB with anti-pd-1 antibodies are routinely used as first-line options for patients with high-risk resected or metastatic disease. For patients with unresectable disease, oncolytic * Correspondence: dmmiller12345@gmail.com 1 Division of Hematology/Oncology, Beth Israel Deaconess Medical Center, Boston, MA, USA 2 Department of Dermatology, Massachusetts General Hospital, 50 Staniford Street, Boston, MA 02114, USA Full list of author information is available at the end of the article virus therapy with talimogene laherparepvec (T-VEC, or Imlygic, BioVex Inc., a subsidiary of Amgen Inc., based in Thousand Oaks, California) has become an option [1]. In refractory cases, ICB is being combined with OVT [2, 3], with off-target or abscopal responses occurring in up to 20% of patients 3. Although many patients are actualizing the benefits of IO therapies, adverse effects (AEs) of these approaches affect the majority of those treated and new AEs are still emerging. For example, the rapid progression of adult T-cell leukemia-lymphoma (ATLL) following PD-1 inhibitor The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 Page 2 of 7 therapy was recently described [4]. Furthermore, the delivery of IO therapies is complicated by the fact that many of the patients treated in routine clinical practice are excluded from clinical trials due to comorbidities; thus, the efficacy and risks are not effectively attributed to all patients. In particular, the risks and benefits of OVT in patients with concomitant malignancies and/or compromised immune systems are almost completely unknown. Due to concerns for disseminated viral infection, OVT is not recommended in patients with compromised immune systems or with malignancies such as leukemia or lymphoma, though there is little published clinical experience highlighting the risks and benefits of OVT in this population. Currently, the successful administration of T-VEC in a patient on immunosuppressive therapy for an allogeneic heart transplantation 5 is the only case we are aware of that details OVT delivery to a patient for which it is contraindicated. To date, there have been no reports of the use of dual ICB/OVT in patients with coexistent primary cutaneous ALCL (pcalcl) and metastatic melanoma. In addition, there have been no publications demonstrating Kaposi s varicelliform eruption after receiving a cycle of T-VEC. Case presentation Herein, we describe an 81-year-old male with concomitant metastatic melanoma and pcalcl whose disease progressed on nivolumab and who then developed Kaposi s varicelliform eruption following one cycle of T-VEC. The patient had a complicated past medical history including coronary artery disease, treated with a coronary artery bypass graft, cerebral vascular accident following a left knee arthroplasty with residual partial aphasia, and a low-grade CD5+ B-cell lymphoproliferative disease, presenting as a large pleural effusion, which was put in a complete remission following 6 cycles of bendamustine and rituximab (R-Benda) (Figure 1). Nearly two and a half years following completion of R-Benda, the patient developed ulcerative plaques on his chin, scalp, lip, right inner canthus and penile foreskin (Figure 2A-C). A skin biopsy was obtained and was consistent with an anaplastic lymphoma kinase (ALK)-negative, CD4 + CD30 +, PD-1, primary cutaneous anaplastic large cell lymphoma (ALCL). In addition to highlighting the cutaneous plaques of ALCL, a staging positron emission tomography-computed tomography (PET-CT) scan demonstrated a cm fludeoxyglucose (FDG) avid right axillary lymph node. A core needle biopsy of the lymph node demonstrated melanoma. Five of 10 lymph nodes were positive for melanoma upon a right axillary lymphadenectomy. A subsequent dermatological evaluation revealed a new 1 cm red/bluish nodule on the right forearm. Surgical excision of the lesion confirmed a 4.7 mm thick, nodular, BRAF wild-type melanoma. Concurrent with the diagnostic work up for his melanoma, the patient underwent targeted radiotherapy to the cutaneous ALCL lesions with excellent response. Following excisions of the right forearm and right axillary melanoma, a re-staging PET-CT demonstrated no additional areas concerning for metastatic melanoma. The patient was then started on nivolumab for his resected, but high-risk, melanoma. At the time of Fig. 1 Timeline of the patient s clinical course. A time reference has been included, with Day 0 referring to the day of the diagnosis of pcalcl. C1D1, cycle 1 day 1; c/f, concerning for; Dx:, diagnosis; Gy, gray; Hosp adm, hospital admission; KVE, kaposi s varicelliform eruption; pcalcl, primary cutaneous anaplastic large cell lymphoma; R-Benda, rituximab-bendamustine; T-VEC, Talimogene laherparepvec; WBC, white blood cell count; WLE, wide-local excision; XRT, radiotherapy
3 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 Page 3 of 7 Fig. 2 Progression of the patient s primary cutaneous anaplastic large cell lymphoma. The patient s lesions prior to nivolumab treatment (a-c); on treatment (d-h), with corresponding cycle days denoted in the white box on the bottom of each insert nivolumab initiation, the patient had pink ulcerative, but improving, plaques of ALCL on his right tragus, chin, left preauricular skin and penile foreskin. He also had faint scaly plaques, without ulceration of the bilateral peri-ocular skin. On cycle 2 day 8 of nivolumab he developed new ulcerative plaques on his upper lip, left upper arm and left pre-auricular skin (Figure 2E) and worsening scale and erythema of his face that were consistent with progressing ALCL. Two new lesions consistent with melanoma recurrence were also noted on the right wrist at the site of the previous melanoma excision. Due to apparent worsening of his ALCL on nivolumab, the decision was made to treat concurrently with radiotherapy and brentuximab. Given the early time point, the appearance of new melanoma nodules were not considered to be a nivolumab failure, and he was continued on therapy. On cycle 3 day 1 of nivolumab, the patient was given an initial dose of brentuximab vedotin. He also received external beam radiotherapy to his upper lip, left ear and left upper arm. On cycle 3 day 11, the patient was admitted for clostridium difficile-toxin positive colitis, which improved with oral vancomycin. A restaging PET-CT during cycle 3 demonstrated multiple new pulmonary nodules concerning for metastatic melanoma. On cycle 3 day 20, the patient was admitted again secondary to
4 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 Page 4 of 7 worsening fatigue and a concern for cellulitis surrounding a radiotherapy-treated ALCL lesion of his left upper arm. The patient was treated with antibiotics and improved. During this admission, new ulcerative plaques were noted on the scalp concerning for progression of the ALCL and cutaneous lesions of metastatic melanoma were identified on the right arm and right chest. Due to worsening disease and declining performance status, the patient s treatment options were limited. Ipilimumab was deemed inappropriate due to the recent clostridium difficile infection and worsening fatigue. There was also concern that his pcalcl was being exacerbated by ICB and that treatment with brentuximab may have accelerated the melanoma. Thus, after discussing the risks and benefits, the decision was made to discontinue brentuximab and treat the in-transit lesions of melanoma with talimogene laherparepvec concurrently with nivolumab. On cycle 4 day 1 of nivolumab, the patient was treated with 1.7 ml of 1 million plaque-forming-units/ml to three melanoma lesions on the right forearm and two on the right chest. At that visit, the patient was noted to have worsening erythema and scale of his upper extremities, upper chest and face. This was thought to be multifactorial, with asteatosis cutis a prominent feature, as well as either an ICB-related dermatitis or worsening pcalcl. On cycle 4 day 3, the patient presented to clinic febrile (temperature F), fatigued and was noted to have a leukocytosis (21,200 white blood cells per microliter). He was subsequently hospitalized for 4 days and the presentation was attributed to an AE of T-VEC. During the admission, the patient had a skin biopsy of the worsening erythema and scale on his face (Figure 2F), which demonstrated features consistent with pcalcl. In anticipation of a second cycle of T-VEC, the patient returned to clinic on cycle 4 day 22. On examination, a diffuse eruption of eroded papules was noted on his bilateral upper extremities, chest, flank and back (Figure 3A-C). A few intact vesicles were visible on the right forearm. The lesions were notably asymmetrical in distribution, with the highest density occurring on the right upper arm and right chest. The patient was afebrile and reported mild pruritus of the eruption, which he reported began a few days previously. A Tzanck smear was performed from one of the intact vesicles. Multinucleated giant cells with cytopathic changes were noted (Figure 4). Due to concern for Kaposi s varicelliform eruption (KVE), the patient was started on intravenous (IV) acyclovir. A direct fluorescence antibody test performed on a vesicle confirmed HSV1 infection. A skin biopsy demonstrated epidermal ulceration with acute inflammation and viral cytopathic effects. HSV I/II-specific immunoperoxidase stain was positive, while a specific immunostain for VZV was negative. HSV viremia was not detected by polymerase chain reaction. He was given 48 hours of IV acyclovir Fig. 3 Kaposi s varicelliform eruption. Scattered 2 3 mm eroded and crusted papules on the bilateral upper arms and trunk. Lesions are concentrated on the right upper arm and trunk and when the vesicles had completely crusted over, he was discharged on a 14-day course of oral valacyclovir. He experienced a complete resolution of his KVE; however, due to his progressing melanoma, ALCL and declining performance status, the patient was transitioned to hospice care. Discussion and concluding remarks There are several unique aspects to this case. To our knowledge, this is the first reported use of ICB in a patient with both metastatic melanoma and pcalcl. It is also the first report of a patient receiving OVT in the setting of lymphoma. And finally, this is the first
5 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 Fig. 4 Tzanck smear from a vesicle on the right arm. Under medium power, multinucleated giant cells with viral cytopathic effects, including nuclear molding, are seen publication of Kaposi s varicelliform eruption developing in the setting of T-VEC. This case highlights the challenges of treating two concurrent malignancies in the context of immunotherapy. Although the benefits of ICB for melanoma [5 7] and B-cell lymphoma [8, 9] have been well documented, the data for ICB in T-cell lymphomas are more limited, and conflicting results have been reported. Previously, Lesokhin et al. reported 4 of 23 patients with various forms of T-cell lymphoma exhibited responses to nivolumab [10]. In addition, two complete responses have been published in nivolumab-treated patients with ALK-positive systemic ALCL [11, 12]. However recently, Ratner et al. reported rapid progression of ATLL following PD-1 inhibitor therapy [4]. The effects of anti-pd-1 therapy on ALK-negative pcalcl have not been described. Our patient s ALK-negative pcalcl significantly worsened after the first cycle of nivolumab, and continued to rapidly progress with subsequent doses (Figure 2 D-H). Previously, it was hypothesized that PD-1 may act as a tumor suppressor for T-cell lymphomas, possibly accounting for the rapid progression seen in nivolumab-treated ATLL patients [4]. Our patient s pcalcl biopsy was negative for PD-1 by immunohistochemistry prior to treatment, making this mechanism less likely to explain the rapid progression of our patient s ALCL. Whether the patient s worsening pcalcl contributed to the development of a hitherto unreported adverse effect of OVT is unclear. AEs are experienced by nearly all patients treated with T-VEC, with chills, pyrexia and Page 5 of 7 injection-site pain being the most common [1]. Additional cutaneous AEs that have been described include injection-site erythema, cellulitis and chronic granulomatous dermatitis [13]. KVE has not previously been reported. Kaposi s varicelliform eruption was first described by Moritz Kaposi in 1887 [14]. KVE is the presentation of widespread cutaneous infection of viral pathogens, most commonly herpes simplex virus. KVE has, however, also been reported in the context of other viral infections such as vaccinia, varicella zoster, and coxsackie virus [15]. Although classically seen in patients with atopic dermatitis, in which the eruption is also called eczema herpeticum, KVE can also occur in patients with impaired skin barrier function due to a wide variety of conditions. These include: thermal trauma, ichthyosis vulgaris, pemphigus foliaceus, Darier disease, Hailey Hailey disease, mycosis fungoides, and Sézary syndrome [16]. KVE most commonly presents as small 2 3 mm, discrete, punched-out erosions with hemorrhagic crusts, rather than intact vesicles, similar to what was observed in our patient. Prior to the use of anti-viral therapy, KVE had an approximate mortality rate of 10 50% [17]. Causes of death include viral pneumonia, adrenal hemorrhage, encephalitis, meningitis and bacterial super-infection. Additional causes of morbidity include viral keratitis. Management of KVE typically involves assessment of systemic involvement, ophthalmologic evaluation for keratitis, systemic antiviral therapy and treatment of bacterial superinfection, as necessary. There is very little data regarding the use of OVT in patients with compromised immunity. As most patients with additional primary malignancies or immunocompromise are excluded from clinical trials, there is little data to guide clinical care in these complex scenarios. T-VEC use in immunosuppressed patients or those with leukemia/lymphoma is not recommend by the product label given the posited risk of disseminated viral infection. However, in certain clinical contexts, when treatment options are limited, the unknown risks of postulated AEs must be weighed heavily with the potential of clinical benefit. Recently, T-VEC was shown to be safe and effective in an allogeneic heart-transplant recipient on cyclosporine [18]. Thus, case reports can provide real-world examples outside of clinical trials or in scenarios cautioned on product labels. Furthermore, it is particularly relevant given that T-VEC is being investigated in clinical trials for patients with refractory cutaneous T-cell lymphoma (e.g. NCT ). We suspect that our patient s impaired skin barrier secondary to a combination of asteatosis cutis, ICB-mediated
6 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 Page 6 of 7 dermatitis and worsening cutaneous lymphoma contributed to epidermal spread of the engineered herpes virus, analogous to what is seen in eczema herpeticum, eczema vaccinatum or eczema coxsackium. Epidermal spread, rather than hematological transmission, is supported by a negative HSV1 PCR from the blood and the fact that the highest density of herpetic lesions were concentrated around the sites previously injected with T-VEC: the right arm and right chest. Thus, caution should be used in employing OVT in areas of compromised skin integrity to prevent the development of an eczema herpeticum-like eruption termed eczema TVECium or lymphoma tvecium. This case also highlights that although engineering efforts were made to attenuate off-target AEs and induce preferential replication within tumors cells-e.g. by deleting the HSV1 virulence genes ICP34.5 and ICP47 [19] T-VEC retains the potential to replicate in non-neoplastic keratinocytes. Fortunately, our patient had no evidence of keratitis or systemic organ involvement, and his KVE resolved without sequelae. Thus, despite the eruption being widespread, our patient s KVE was effectively managed with antiviral therapy and the overall clinical impact was limited. Unfortunately, neither ICB nor OVT were effective in controlling the patient s malignancies and the decision was made to transition to symptom-directed therapy. In summary, we present a case of a patient with melanoma and pcalcl who was treated with ICB and oncolytic viral therapy and developed a novel adverse effect: eczema TVECium. Abbreviations AE: Adverse effect; ALK: Anaplastic lymphoma kinase; ATLLL: Adult T-cell leukemialymphoma; c/f: Concerning for; C1D1: Cycle 1 day 1; DFA: Direct fluorescence antibody; Dx: Diagnosis; FDG: Fludeoxyglucose; Gy: Gray; Hosp adm: Hospital admission; HSV: Herpes simplex virus; ICB: Immune checkpoint blockade; IO: Immunoncology; IV: Intravenous; KVE: Kaposi s varicelliform eruption; OVT: Oncolytic viral therapy; pcalcl: Primary cutaneous anaplastic large cell lymphoma; PD-1: Programmed-death 1; PET-CT: Positron emission tomographycomputed tomography; R-Benda: Rituximab-bendamustine; T-VEC: Talimogene laherparepvec; WBC: White blood cell count; XRT: Radiotherapy Acknowledgements The authors acknowledge the patient and his family who agreed to share his experience. We also acknowldge Dr. Paul Vanderlaan for his expert analysis of the Tzanck smear. Funding This work was not supported by funding. Availability of data and materials Not applicable. Disclosures Dr. Miller has received honoraria for serving as a healthcare consultant for Pzifer, Inc. Authors contributions All authors contributed to the care of the patient. All authors read and approved the final manuscript. Ethics approval and consent to participate Patient described in this case signed a case report informed consent form, which is available for review. Consent for publication Patient consented to publication of the case report. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Division of Hematology/Oncology, Beth Israel Deaconess Medical Center, Boston, MA, USA. 2 Department of Dermatology, Massachusetts General Hospital, 50 Staniford Street, Boston, MA 02114, USA. 3 Department of Dermatology, University of Nebraska Medical Center, Omaha, NE, USA. Received: 13 August 2018 Accepted: 28 October 2018 References 1. Andtbacka RH, Kaufman HL, Collichio F, et al. Talimogene Laherparepvec improves durable response rate in patients with advanced melanoma. J Clin Oncol. 2015;33(25): Puzanov I, Milhem MM, Minor D, et al. Talimogene Laherparepvec in combination with Ipilimumab in previously untreated, Unresectable stage IIIB-IV melanoma. J Clin Oncol. 2016;34(22): Sun L, Funchain P, Song JM, et al. Talimogene Laherparepvec combined with anti-pd-1 based immunotherapy for unresectable stage III-IV melanoma: a case series. J Immunother Cancer. 2018;6(1): Ratner L, Waldmann TA, Janakiram M, Brammer JE. Rapid progression of adult T-cell leukemia-lymphoma after PD-1 inhibitor therapy. N Engl J Med. 2018;378(20): Weber J, Mandala M, Del Vecchio M, et al. Adjuvant Nivolumab versus Ipilimumab in resected stage III or IV melanoma. N Engl J Med Hodi FS, O'Day SJ, McDermott DF, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010;363(8): Robert C, Long GV, Brady B, et al. Nivolumab in previously untreated melanoma without BRAF mutation. N Engl J Med. 2015;372(4): Ansell SM, Lesokhin AM, Borrello I, et al. PD-1 blockade with nivolumab in relapsed or refractory Hodgkin's lymphoma. N Engl J Med. 2015; 372(4): Chen R, Zinzani PL, Fanale MA, et al. Phase II study of the efficacy and safety of Pembrolizumab for relapsed/refractory classic Hodgkin lymphoma. J Clin Oncol. 2017;35(19): Lesokhin AM, Ansell SM, Armand P, et al. Nivolumab in patients with relapsed or refractory hematologic malignancy: preliminary results of a phase Ib study. J Clin Oncol. 2016;34(23): Hebart H, Lang P, Woessmann W. Nivolumab for refractory anaplastic large cell lymphoma: a case report. Ann Intern Med. 2016;165(8): Rigaud C, Abbou S, Minard-Colin V, et al. Efficacy of nivolumab in a patient with systemic refractory ALK+ anaplastic large cell lymphoma. Pediatr Blood Cancer. 2018;65(4). 13. Everett AS, Pavlidakey PG, Contreras CM, et al. Chronic granulomatous dermatitis induced by talimogene laherparepvec therapy of melanoma metastases. J Cutan Pathol. 2018;45(1): Kaposi M. Pathologie und Therapie der Hautkrankheiten. Vorlesungen für praktische Aerzte und Studirende. Vol 3. Vienna: Urban und Schwarzenberg; Mathes EF, Oza V, Frieden IJ, et al. Eczema coxsackium and unusual cutaneous findings in an enterovirus outbreak. Pediatrics. 2013;132(1): e Wollenberg A, Wetzel S, Burgdorf WH, Haas J. Viral infections in atopic dermatitis: pathogenic aspects and clinical management. J Allergy Clin Immunol. 2003;112(4):
7 Miller et al. Journal for ImmunoTherapy of Cancer (2018) 6:122 Page 7 of Wheeler CE Jr, Abele DC. Eczema herpeticum, primary and recurrent. Arch Dermatol. 1966;93(2): Schvartsman G, Perez K, Flynn JE, Myers JN, Tawbi H. Safe and effective administration of T-VEC in a patient with heart transplantation and recurrent locally advanced melanoma. J Immunother Cancer. 2017;5: Rehman H, Silk AW, Kane MP, Kaufman HL. Into the clinic: Talimogene laherparepvec (T-VEC), a first-in-class intratumoral oncolytic viral therapy. J Immunother Cancer. 2016;4:53.
Limitations of Use: Imlygic has not been shown to improve overall survival or have an effect on visceral metastases (1).
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.66 Subject: Imlygic Page: 1 of 5 Last Review Date: June 22, 2017 Imlygic Description Imlygic (talimogene
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.66 Subject: Imlygic Page: 1 of 5 Last Review Date: June 22, 2017 Imlygic Description Imlygic (talimogene
What's New in Oncodermatopathology: Immunotherapy Reactions
 What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
What's New in Oncodermatopathology: Immunotherapy Reactions Emily Y. Chu, M.D., Ph.D. Assistant Professor of Dermatology & Pathology and Laboratory Medicine Hospital of the University of Pennsylvania March
Talimogene Laherparepvec (T-VEC) at the SCCA: an update
 Talimogene Laherparepvec (T-VEC) at the SCCA: an update Jennifer M. Gardner, MD Assistant Professor, Division of Dermatology University of Washington jen1110@uw.edu Northwest Melanoma Symposium: Science
Talimogene Laherparepvec (T-VEC) at the SCCA: an update Jennifer M. Gardner, MD Assistant Professor, Division of Dermatology University of Washington jen1110@uw.edu Northwest Melanoma Symposium: Science
NCCN Guidelines for Cutaneous Melanoma V Meeting on 06/20/18
 ME-1, ME-3, ME-B Submission from Castle Biosciences, Inc (05/30/18) to consider inclusion of the DecisionDx-Melanoma test in the guidelines as a prognostic test that provides stratification according to
ME-1, ME-3, ME-B Submission from Castle Biosciences, Inc (05/30/18) to consider inclusion of the DecisionDx-Melanoma test in the guidelines as a prognostic test that provides stratification according to
Kamakshi V Rao, PharmD, BCOP, FASHP University of North Carolina Medical Center UPDATE IN REFRACTORY HODGKIN LYMPHOMA
 Kamakshi V Rao, PharmD, BCOP, FASHP University of North Carolina Medical Center UPDATE IN REFRACTORY HODGKIN LYMPHOMA Objectives Describe the current standard approach for patients with relapsed/refractory
Kamakshi V Rao, PharmD, BCOP, FASHP University of North Carolina Medical Center UPDATE IN REFRACTORY HODGKIN LYMPHOMA Objectives Describe the current standard approach for patients with relapsed/refractory
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Metastatic Melanoma. Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds
 Metastatic Melanoma Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds Case Presentation 77 year old male with previous history of scalp melanoma and thyroid
Metastatic Melanoma Cynthia Kwong February 16, 2017 SUNY Downstate Medical Center Department of Surgery Grand Rounds Case Presentation 77 year old male with previous history of scalp melanoma and thyroid
Immune checkpoint inhibitors in Hodgkin and non-hodgkin Lymphoma: How do they work? Where will we use them? Stephen M. Ansell, MD, PhD Mayo Clinic
 Immune checkpoint inhibitors in Hodgkin and non-hodgkin Lymphoma: How do they work? Where will we use them? Stephen M. Ansell, MD, PhD Mayo Clinic Conflicts of Interest Research Funding from Bristol Myers
Immune checkpoint inhibitors in Hodgkin and non-hodgkin Lymphoma: How do they work? Where will we use them? Stephen M. Ansell, MD, PhD Mayo Clinic Conflicts of Interest Research Funding from Bristol Myers
Locally Advanced and Metastatic Melanoma. Relevant disclosures 6/23/2018. What is the median survival of metastatic melanoma? Abel D.
 Locally Advanced and Metastatic Melanoma Abel D. Jarell, MD, FAAD Adjunct Dartmouth School of Medicine, Hanover, NH Northeast Dermatology Associates, Portsmouth, NH Relevant disclosures What is the median
Locally Advanced and Metastatic Melanoma Abel D. Jarell, MD, FAAD Adjunct Dartmouth School of Medicine, Hanover, NH Northeast Dermatology Associates, Portsmouth, NH Relevant disclosures What is the median
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Malignant melanoma: assessment and management of malignant melanoma 1.1 Short title Malignant Melanoma 2 The remit The Department
Two roads for oncolytic immunotherapy development
 Kaufman and Bommareddy Journal for ImmunoTherapy of Cancer (2019) 7:26 https://doi.org/10.1186/s40425-019-0515-2 COMMENTARY Two roads for oncolytic immunotherapy development Howard L. Kaufman 1,2* and
Kaufman and Bommareddy Journal for ImmunoTherapy of Cancer (2019) 7:26 https://doi.org/10.1186/s40425-019-0515-2 COMMENTARY Two roads for oncolytic immunotherapy development Howard L. Kaufman 1,2* and
Melanoma: Therapeutic Progress and the Improvements Continue
 Melanoma: Therapeutic Progress and the Improvements Continue David W. Ollila, MD Professor of Surgery Jesse and James Millis Professor of Melanoma Research May 20, 2016 Disclosures: NONE Outline 2016 Therapeutic
Melanoma: Therapeutic Progress and the Improvements Continue David W. Ollila, MD Professor of Surgery Jesse and James Millis Professor of Melanoma Research May 20, 2016 Disclosures: NONE Outline 2016 Therapeutic
Evolving Treatment Strategies in the Management of Metastatic Melanoma: Novel Therapies for Improved Patient Outcomes. Disclosures
 Evolving Treatment Strategies in the Management of Metastatic Melanoma: Novel Therapies for Improved Patient Outcomes Fall Managed Care Forum November 11, 2016 Matthew Taylor, M.D. Disclosures Consulting/Advisory
Evolving Treatment Strategies in the Management of Metastatic Melanoma: Novel Therapies for Improved Patient Outcomes Fall Managed Care Forum November 11, 2016 Matthew Taylor, M.D. Disclosures Consulting/Advisory
Current Trends in Melanoma Theresa Medina, MD UCD Cutaneous Oncology
 Current Trends in Melanoma Theresa Medina, MD UCD Cutaneous Oncology Overview Melanoma incidence and prevention Approach to surgical management of early melanoma Landscape of Advanced Melanoma Therapy
Current Trends in Melanoma Theresa Medina, MD UCD Cutaneous Oncology Overview Melanoma incidence and prevention Approach to surgical management of early melanoma Landscape of Advanced Melanoma Therapy
Opdivo. Opdivo (nivolumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.53 Subsection: Antineoplastic Agents Original Policy Date: January 16, 2015 Subject: Opdivo Page:
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.53 Subsection: Antineoplastic Agents Original Policy Date: January 16, 2015 Subject: Opdivo Page:
Subject Index. Dry desquamation, see Skin reactions, radiotherapy
 Subject Index Actinic keratosis disseminated disease 42 surgical excision 42 AIDS, see Kaposi s sarcoma Amifostine, skin reaction prophylaxis 111 Basal cell carcinoma, superficial X-ray therapy Bowen s
Subject Index Actinic keratosis disseminated disease 42 surgical excision 42 AIDS, see Kaposi s sarcoma Amifostine, skin reaction prophylaxis 111 Basal cell carcinoma, superficial X-ray therapy Bowen s
Tumor control with PD-1 inhibition in a patient with concurrent metastatic melanoma and renal cell carcinoma
 Marmarelis et al. Journal for ImmunoTherapy of Cancer (2016) 4:26 DOI 10.1186/s40425-016-0129-x CASE REPORT Tumor control with PD-1 inhibition in a patient with concurrent metastatic melanoma and renal
Marmarelis et al. Journal for ImmunoTherapy of Cancer (2016) 4:26 DOI 10.1186/s40425-016-0129-x CASE REPORT Tumor control with PD-1 inhibition in a patient with concurrent metastatic melanoma and renal
Index. Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, Anorectal melanoma RT for, 1035
 Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Index Note: Page numbers of article titles are in boldface type. A Age as factor in melanoma, 947 948 Anorectal melanoma RT for, 1035 B Bacille Calmette-Guerin (BCG) in melanoma, 1008 BCG. See Bacille
Product: Talimogene Laherparepvec Clinical Study Report: Date: 31 October 2018 Page 1
 Date: 31 October 2018 Page 1 2. SYNOPSIS Name of Sponsor: Amgen Inc., Thousand Oaks, CA, USA Name of Finished Product: Imlygic Name of Active Ingredient: Talimogene laherparepvec Title of Study: A Phase
Date: 31 October 2018 Page 1 2. SYNOPSIS Name of Sponsor: Amgen Inc., Thousand Oaks, CA, USA Name of Finished Product: Imlygic Name of Active Ingredient: Talimogene laherparepvec Title of Study: A Phase
Immunotherapy for the Treatment of Melanoma. Marlana Orloff, MD Thomas Jefferson University Hospital
 Immunotherapy for the Treatment of Melanoma Marlana Orloff, MD Thomas Jefferson University Hospital Disclosures Immunocore and Castle Biosciences, Consulting Fees I will be discussing non-fda approved
Immunotherapy for the Treatment of Melanoma Marlana Orloff, MD Thomas Jefferson University Hospital Disclosures Immunocore and Castle Biosciences, Consulting Fees I will be discussing non-fda approved
ISPUB.COM. Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose Methotrexate. S Parker INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
Recommendations for VZV management in. Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman
 Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Recommendations for VZV management in patients Cas cliniques with leukemia Dan Engelhard, Pierre Reusser, Rafael de la Camara, Hermann Einsele, Jan Styczynski, Kate Ward, Per Ljungman Introduction Acute
Concept of oncolytic virotherapyclinical
 Concept of oncolytic virotherapyclinical implementation Simona Donina A. Kirchenstein Institute of Microbiology and Virology, Riga Stradiņš University Riga East University Hospital 4.04.2014. Timeline
Concept of oncolytic virotherapyclinical implementation Simona Donina A. Kirchenstein Institute of Microbiology and Virology, Riga Stradiņš University Riga East University Hospital 4.04.2014. Timeline
Surgical Oncology Perspective of Melanoma
 Surgical Oncology Perspective of Melanoma Hans F. Schoellhammer, MD, FACS Assistant Clinical Professor Division of Surgical Oncology September 20, 2018 Nothing to disclose DISCLOSURE Discussion Objectives
Surgical Oncology Perspective of Melanoma Hans F. Schoellhammer, MD, FACS Assistant Clinical Professor Division of Surgical Oncology September 20, 2018 Nothing to disclose DISCLOSURE Discussion Objectives
Dr Rosalie Stephens. Mr Richard Martin. Medical Oncologist Auckland City Hospital Auckland
 Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Dr Rosalie Stephens Medical Oncologist Auckland City Hospital Auckland Mr Richard Martin General Surgeon Melanoma Unit Team Waitemata District Health Board Auckland 8:30-9:25 WS #99: Interactive Case Studies
Summary of the risk management plan (RMP) for Imlygic (talimogene laherparepvec)
 EMA/713818/2015 Summary of the risk management plan (RMP) for Imlygic ( laherparepvec) This is a summary of the risk management plan (RMP) for Imlygic, which details the measures to be taken in order to
EMA/713818/2015 Summary of the risk management plan (RMP) for Imlygic ( laherparepvec) This is a summary of the risk management plan (RMP) for Imlygic, which details the measures to be taken in order to
A. Viral infections whose main symptom is blistering
 Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Viral Infections A virus is a particle of DNA or RNA enclosed by structural proteins. Viruses infect cells and proliferate to
Go Back to the Top To Order, Visit the Purchasing Page for Details Chapter Viral Infections A virus is a particle of DNA or RNA enclosed by structural proteins. Viruses infect cells and proliferate to
OPTIMAL MANAGEMENT OF IMMUNE- RELATED ADVERSE EVENTS ASSOCIATED WITH CHECKPOINT INHIBITORS
 OPTIMAL MANAGEMENT OF IMMUNE- RELATED ADVERSE EVENTS ASSOCIATED WITH CHECKPOINT INHIBITORS Alberto Fusi Charité Comprehensive Cancer Centre Berlin, Germany 1 Immune check point blockade with CTLA-4, anti-pd-1
OPTIMAL MANAGEMENT OF IMMUNE- RELATED ADVERSE EVENTS ASSOCIATED WITH CHECKPOINT INHIBITORS Alberto Fusi Charité Comprehensive Cancer Centre Berlin, Germany 1 Immune check point blockade with CTLA-4, anti-pd-1
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Tumor Immunology: A Primer
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Case Scenario 1 Worksheet. Primary Site C44.4 Morphology 8743/3 Laterality 0 Stage/ Prognostic Factors
 CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
CASE SCENARIO 1 9/10/13 HISTORY: Patient is a 67-year-old white male and presents with lesion located 4-5cm above his right ear. The lesion has been present for years. No lymphadenopathy. 9/10/13 anterior
6/7/16. Melanoma. Updates on immune checkpoint therapies. Molecularly targeted therapies. FDA approval for talimogene laherparepvec (T- VEC)
 Melanoma John A Thompson MD July 17, 2016 Featuring: Updates on immune checkpoint therapies Molecularly targeted therapies FDA approval for talimogene laherparepvec (T- VEC) 1 Mechanism of ac-on of Ipilimumab
Melanoma John A Thompson MD July 17, 2016 Featuring: Updates on immune checkpoint therapies Molecularly targeted therapies FDA approval for talimogene laherparepvec (T- VEC) 1 Mechanism of ac-on of Ipilimumab
Approaches To Treating Advanced Melanoma
 Approaches To Treating Advanced Melanoma Suraj Venna, MD Medical Director, Melanoma and Cutaneous Oncology Inova Schar Cancer Institute Associate Professor, VCU Fairfax VA Disclosures No relevant disclosures
Approaches To Treating Advanced Melanoma Suraj Venna, MD Medical Director, Melanoma and Cutaneous Oncology Inova Schar Cancer Institute Associate Professor, VCU Fairfax VA Disclosures No relevant disclosures
Yervoy. Yervoy (ipilimumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.13 Subject: Yervoy Page: 1 of 5 Last Review Date: September 15, 2017 Yervoy Description Yervoy (ipilimumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.13 Subject: Yervoy Page: 1 of 5 Last Review Date: September 15, 2017 Yervoy Description Yervoy (ipilimumab)
Adverse effects of Immunotherapy. Asha Nayak M.D
 Adverse effects of Immunotherapy Asha Nayak M.D None Financial Disclosures Objectives Understand intensity of the AEs. Understanding unique side-effects. Develop effective monitoring and management guidelines.
Adverse effects of Immunotherapy Asha Nayak M.D None Financial Disclosures Objectives Understand intensity of the AEs. Understanding unique side-effects. Develop effective monitoring and management guidelines.
REQUEST FOR PROJECT TEAM MEMBER APPLICATION FOR CONDUCTING CLINICAL TRIALS USING TALIMOGENE LAHERPAREPVEC
 REQUEST FOR PROJECT TEAM MEMBER APPLICATION FOR CONDUCTING CLINICAL TRIALS USING TALIMOGENE LAHERPAREPVEC The Cancer Therapy Evaluation Program (CTEP) is accepting Project Team Member Applications (PTMAs)
REQUEST FOR PROJECT TEAM MEMBER APPLICATION FOR CONDUCTING CLINICAL TRIALS USING TALIMOGENE LAHERPAREPVEC The Cancer Therapy Evaluation Program (CTEP) is accepting Project Team Member Applications (PTMAs)
Exploring Immunotherapies: Beyond Checkpoint Inhibitors
 Exploring Immunotherapies: Beyond Checkpoint Inhibitors Authored by: Jennifer Dolan Fox, PhD VirtualScopics (Now part of BioTelemetry Research) jennifer_fox@virtualscopics.com +1 585 249 6231 Introduction
Exploring Immunotherapies: Beyond Checkpoint Inhibitors Authored by: Jennifer Dolan Fox, PhD VirtualScopics (Now part of BioTelemetry Research) jennifer_fox@virtualscopics.com +1 585 249 6231 Introduction
Current State of Immunotherapy for Metastatic Melanoma
 Current State of Immunotherapy for Metastatic Melanoma Background: The Duval County Medical Society (DCMS) is proud to provide its members with free continuing medical education (CME) opportunities in
Current State of Immunotherapy for Metastatic Melanoma Background: The Duval County Medical Society (DCMS) is proud to provide its members with free continuing medical education (CME) opportunities in
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Single Technology Appraisal (STA) Nivolumab for adjuvant treatment of resected stage III and IV melanoma
 Single Technology Appraisal (STA) Nivolumab for adjuvant treatment of resected stage III and IV Response to consultee and commentator comments on the draft remit and draft scope (pre-referral) Comment:
Single Technology Appraisal (STA) Nivolumab for adjuvant treatment of resected stage III and IV Response to consultee and commentator comments on the draft remit and draft scope (pre-referral) Comment:
ESCMID Online Lecture Library. by author. CASE PRESENTATION ECCMID clinical grand round May Anat Stern, MD Rambam medical center Haifa, Israel
 CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
CASE PRESENTATION ECCMID clinical grand round May 2014 Anat Stern, MD Rambam medical center Haifa, Israel An 18 years old Female, from Ukraine, diagnosed with acute lymphoblastic leukemia (ALL) in 2003.
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia
 Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
Immunotherapy for the Treatment of Brain Metastases
 Society for Immunotherapy of Cancer (SITC) Immunotherapy for the Treatment of Brain Metastases Lawrence G. Lum, MD, DSc Karmanos Cancer Institute and Wayne State University Advances in Cancer Immunotherapy
Society for Immunotherapy of Cancer (SITC) Immunotherapy for the Treatment of Brain Metastases Lawrence G. Lum, MD, DSc Karmanos Cancer Institute and Wayne State University Advances in Cancer Immunotherapy
Immune-Related Adverse Events (IRAEs) due to Cancer Immunotherapy
 Immune-Related Adverse Events (IRAEs) due to Cancer Immunotherapy Philip Mease MD Director, Rheumatology Clinical Research, Swedish- Providence St. Joseph Health Clinical Professor, University of Washington
Immune-Related Adverse Events (IRAEs) due to Cancer Immunotherapy Philip Mease MD Director, Rheumatology Clinical Research, Swedish- Providence St. Joseph Health Clinical Professor, University of Washington
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Dr Sneha Shah Tata Memorial Hospital, Mumbai.
 Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
Dr Sneha Shah Tata Memorial Hospital, Mumbai. Topics covered Lymphomas including Burkitts Pediatric solid tumors (non CNS) Musculoskeletal Ewings & osteosarcoma. Neuroblastomas Nasopharyngeal carcinomas
A case report of using nivolumab for a malignant melanoma patient with rheumatoid arthritis
 Int Canc Conf J (6) 5:9 96 DOI.7/s369-6-56-8 CASE REPORT A case report of using nivolumab for a malignant melanoma patient with rheumatoid arthritis Shun-Ichiro Kageyama Shigeo Yamaguchi Shin Ito Yoshiyuki
Int Canc Conf J (6) 5:9 96 DOI.7/s369-6-56-8 CASE REPORT A case report of using nivolumab for a malignant melanoma patient with rheumatoid arthritis Shun-Ichiro Kageyama Shigeo Yamaguchi Shin Ito Yoshiyuki
CLINICAL MEDICATION POLICY
 CLINICAL MEDICATION POLICY Policy Name: Opdivo (nivolumab) injection Policy Number: Approved By: Medical Management, Clinical Pharmacy Products: Highmark Health Options Application: All participating hospitals
CLINICAL MEDICATION POLICY Policy Name: Opdivo (nivolumab) injection Policy Number: Approved By: Medical Management, Clinical Pharmacy Products: Highmark Health Options Application: All participating hospitals
IMMUNE CHECKPOINT THERAPY FOR GENITOURINARY CANCERS: KIDNEY CANCER AND TRANSITIONAL CELL CARCINOMA
 IMMUNE CHECKPOINT THERAPY FOR GENITOURINARY CANCERS: KIDNEY CANCER AND TRANSITIONAL CELL CARCINOMA Kathleen Mahoney, M.D., Ph.D. Instructor of Medicine, Harvard Medical School Attending, Beth Israel Deaconess
IMMUNE CHECKPOINT THERAPY FOR GENITOURINARY CANCERS: KIDNEY CANCER AND TRANSITIONAL CELL CARCINOMA Kathleen Mahoney, M.D., Ph.D. Instructor of Medicine, Harvard Medical School Attending, Beth Israel Deaconess
Immune checkpoint inhibitors in lymphoma. Catherine Hildyard Haematology Senior Registrar Oxford University Hospitals NHS Foundation Trust
 Immune checkpoint inhibitors in lymphoma Catherine Hildyard Haematology Senior Registrar Oxford University Hospitals NHS Foundation Trust Aims How immune checkpoint inhibitors work Success of immune checkpoint
Immune checkpoint inhibitors in lymphoma Catherine Hildyard Haematology Senior Registrar Oxford University Hospitals NHS Foundation Trust Aims How immune checkpoint inhibitors work Success of immune checkpoint
Immunotherapy Case Studies Weighing risks and benefits when risks are difficult to predict
 Immunotherapy Case Studies Weighing risks and benefits when risks are difficult to predict Ari VanderWalde, MD, MPH Director of Clinical Research West Cancer Center Assistant Professor Hematology/Oncology
Immunotherapy Case Studies Weighing risks and benefits when risks are difficult to predict Ari VanderWalde, MD, MPH Director of Clinical Research West Cancer Center Assistant Professor Hematology/Oncology
Cancer Immunotherapy Survey
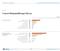 CHAPTER 8: Cancer Immunotherapy Survey All (N=100) Please classify your organization. Academic lab or center Small biopharmaceutical company Top 20 Pharma Mid-size pharma Diagnostics company Other (please
CHAPTER 8: Cancer Immunotherapy Survey All (N=100) Please classify your organization. Academic lab or center Small biopharmaceutical company Top 20 Pharma Mid-size pharma Diagnostics company Other (please
Immunotherapy Overview, Rationale, and Role in Clinical Practice
 Immunotherapy Overview, Rationale, and Role in Clinical Practice Financial Disclosure Bradi L. Frei, PharmD, BCOP, BCPS has no relevant financial relationships with commercial interests to disclose. OBJECTIVES
Immunotherapy Overview, Rationale, and Role in Clinical Practice Financial Disclosure Bradi L. Frei, PharmD, BCOP, BCPS has no relevant financial relationships with commercial interests to disclose. OBJECTIVES
Subunit adjuvanted zoster vaccine: why the fuss?
 Subunit adjuvanted zoster vaccine: why the fuss? Soren Gantt, MD PhD MPH Pediatric Infectious Diseases Vaccine Evaluation Center BC Children s Hospital University of British Columbia Disclosures Research
Subunit adjuvanted zoster vaccine: why the fuss? Soren Gantt, MD PhD MPH Pediatric Infectious Diseases Vaccine Evaluation Center BC Children s Hospital University of British Columbia Disclosures Research
Re-emergence of old viruses
 Re-emergence of old viruses Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco American Academy of Dermatology Annual Meeting, February 2018 Disclosures
Re-emergence of old viruses Erin Mathes, MD Associate Professor of Dermatology and Pediatrics University of California, San Francisco American Academy of Dermatology Annual Meeting, February 2018 Disclosures
Relapsed/Refractory Hodgkin Lymphoma
 Relapsed/Refractory Hodgkin Lymphoma Anas Younes, MD Chief, Lymphoma Service Memorial Sloan-Kettering Cancer Center New York, New York, United States Case Study 32-year-old woman was diagnosed with stage
Relapsed/Refractory Hodgkin Lymphoma Anas Younes, MD Chief, Lymphoma Service Memorial Sloan-Kettering Cancer Center New York, New York, United States Case Study 32-year-old woman was diagnosed with stage
Oncologic Dermatology and Surgery. Dra. Elena de las Heras
 Oncologic Dermatology and Surgery Dra. Elena de las Heras Review and Updates: Clinical oncology: Lymphomas PROspective Cutaneous Lymphoma International Prognostic Index (PROCLIPI) study Launched in 2015
Oncologic Dermatology and Surgery Dra. Elena de las Heras Review and Updates: Clinical oncology: Lymphomas PROspective Cutaneous Lymphoma International Prognostic Index (PROCLIPI) study Launched in 2015
PART VI: SUMMARY OF THE RISK MANAGEMENT PLAN BY PRODUCT
 PAGE 175 PART VI: SUMMARY OF THE RISK MANAGEMENT PLAN BY PRODUCT Summary of risk management plan for pembrolizumab This is a summary of the risk management plan (RMP) for pembrolizumab. The RMP details
PAGE 175 PART VI: SUMMARY OF THE RISK MANAGEMENT PLAN BY PRODUCT Summary of risk management plan for pembrolizumab This is a summary of the risk management plan (RMP) for pembrolizumab. The RMP details
Clinical Policy: Nivolumab (Opdivo) Reference Number: CP.PHAR.121 Effective Date: Last Review Date: Line of Business: Medicaid
 Clinical Policy: (Opdivo) Reference Number: CP.PHAR.121 Effective Date: 07.15 Last Review Date: 01.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Opdivo) Reference Number: CP.PHAR.121 Effective Date: 07.15 Last Review Date: 01.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: Nivolumab (Opdivo) Reference Number: CP.PHAR.121
 Clinical Policy: (Opdivo) Reference Number: CP.PHAR.121 Effective Date: 07/15 Last Review Date: 04/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Clinical Policy: (Opdivo) Reference Number: CP.PHAR.121 Effective Date: 07/15 Last Review Date: 04/17 Coding Implications Revision Log See Important Reminder at the end of this policy for important regulatory
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Clinical Policy: Nivolumab (Opdivo) Reference Number: ERX.SPA.302 Effective Date:
 Clinical Policy: (Opdivo) Reference Number: ERX.SPA.302 Effective Date: 03.01.19 Last Review Date: 02.19 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Opdivo) Reference Number: ERX.SPA.302 Effective Date: 03.01.19 Last Review Date: 02.19 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
HSV1716 Dose levels and Cohort size Dose level No of Patients HSV1716 Dosage 1* 3 to 6 1 ml of 1 x 10 5 infectious units HSV1716 per ml 2
 Abstract and Schema: Description and Rationale: Pediatric high grade gliomas have a progressive initial course and high risk of relapse/ progression; making the 5-year overall survival rate 15-35% with
Abstract and Schema: Description and Rationale: Pediatric high grade gliomas have a progressive initial course and high risk of relapse/ progression; making the 5-year overall survival rate 15-35% with
Opdivo. Opdivo (nivolumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.53 Subsection: Antineoplastic nts Original Policy Date: January 16, 2015 Subject: Opdivo Page: 1 of
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.53 Subsection: Antineoplastic nts Original Policy Date: January 16, 2015 Subject: Opdivo Page: 1 of
Vaccination to protect against shingles
 Vaccination to protect against shingles - An update for registered healthcare practitioners The programme from September 2018 and contraindications and precautions Revised July 2018 NES and HPS accept
Vaccination to protect against shingles - An update for registered healthcare practitioners The programme from September 2018 and contraindications and precautions Revised July 2018 NES and HPS accept
Relapse After Transplant: Next Steps for Patients with Hodgkin Lymphoma
 Hi! My name is Alison Moskowitz. I am an attending at Memorial Sloan Kettering Cancer Center within the Lymphoma Department. I am speaking on behalf of ManagingHodgkinLymphoma.com. I will be discussing
Hi! My name is Alison Moskowitz. I am an attending at Memorial Sloan Kettering Cancer Center within the Lymphoma Department. I am speaking on behalf of ManagingHodgkinLymphoma.com. I will be discussing
VARICELLA. Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara
 VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
Alexander Fosså, M.D. PhD.
 Alexander Fosså, M.D. PhD. Current position: Senior Consultant, Department of Medical Oncology Oslo University Hospital Focus of work: - Malignant lymphoma - Chemotherapy, immunotherapy, radiotherapy -
Alexander Fosså, M.D. PhD. Current position: Senior Consultant, Department of Medical Oncology Oslo University Hospital Focus of work: - Malignant lymphoma - Chemotherapy, immunotherapy, radiotherapy -
Navigating Treatment Pathways in Relapsed/Refractory Hodgkin Lymphoma
 Welcome to Managing Hodgkin Lymphoma. I am Dr. John Sweetenham from Huntsman Cancer Institute at the University of Utah. In today s presentation, I will be discussing navigating treatment pathways in relapsed
Welcome to Managing Hodgkin Lymphoma. I am Dr. John Sweetenham from Huntsman Cancer Institute at the University of Utah. In today s presentation, I will be discussing navigating treatment pathways in relapsed
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Efficacy and toxicity of rechallenge with combination immune checkpoint blockade in metastatic melanoma: a case series
 Efficacy and toxicity of rechallenge with combination immune checkpoint blockade in metastatic melanoma: a case series Lavinia Spain, 1 Gerard Walls, 1 Christina Messiou, 2 Samra Turajlic, 1,3 Martin Gore,
Efficacy and toxicity of rechallenge with combination immune checkpoint blockade in metastatic melanoma: a case series Lavinia Spain, 1 Gerard Walls, 1 Christina Messiou, 2 Samra Turajlic, 1,3 Martin Gore,
Bendamustine for Hodgkin lymphoma. Alison Moskowitz, MD Assistant Attending Memorial Sloan Kettering, Lymphoma Service
 Bendamustine for Hodgkin lymphoma Alison Moskowitz, MD Assistant Attending Memorial Sloan Kettering, Lymphoma Service Bendamustine in Hodgkin lymphoma Bifunctional molecule Nitrogen mustard component (meclorethamine)
Bendamustine for Hodgkin lymphoma Alison Moskowitz, MD Assistant Attending Memorial Sloan Kettering, Lymphoma Service Bendamustine in Hodgkin lymphoma Bifunctional molecule Nitrogen mustard component (meclorethamine)
Checkpoint Blockade in Hematology and Stem Cell Transplantation
 Checkpoint Blockade in Hematology and Stem Cell Transplantation Saad S. Kenderian, MD Assistant Professor of Medicine and Oncology Mayo Clinic College of Medicine October 14, 2016 2015 MFMER slide-1 Disclosures
Checkpoint Blockade in Hematology and Stem Cell Transplantation Saad S. Kenderian, MD Assistant Professor of Medicine and Oncology Mayo Clinic College of Medicine October 14, 2016 2015 MFMER slide-1 Disclosures
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d oncologie et d hématologie pédiatrique des provinces de l Atlantique
 Atlantic Provinces Pediatric Hematology Oncology Network Réseau d oncologie et d hématologie pédiatrique des provinces de l Atlantique Reviewed and approved by specialists at the IWK Health Centre, Halifax,
Atlantic Provinces Pediatric Hematology Oncology Network Réseau d oncologie et d hématologie pédiatrique des provinces de l Atlantique Reviewed and approved by specialists at the IWK Health Centre, Halifax,
Priming the Immune System to Kill Cancer and Reverse Tolerance. Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics
 Priming the Immune System to Kill Cancer and Reverse Tolerance Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics Learning Objectives Describe the role of the immune system in cancer
Priming the Immune System to Kill Cancer and Reverse Tolerance Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics Learning Objectives Describe the role of the immune system in cancer
Pembrolizumab 200mg Monotherapy
 Pembrolizumab 200mg This regimen supercedes NCCP Regimen 00347 Pembrolizumab 2mg/kg as of September 2018 due to a change in the licensed dosing posology. INDICATIONS FOR USE: INDICATION ICD10 Regimen Code
Pembrolizumab 200mg This regimen supercedes NCCP Regimen 00347 Pembrolizumab 2mg/kg as of September 2018 due to a change in the licensed dosing posology. INDICATIONS FOR USE: INDICATION ICD10 Regimen Code
Cutaneous Malignancies: A Primer COPYRIGHT. Marissa Heller, M.D.
 Cutaneous Malignancies: A Primer Marissa Heller, M.D. Associate Director of Dermatologic Surgery Department of Dermatology Beth Israel Deaconess Medical Center December 10, 2016 Skin Cancer Non-melanoma
Cutaneous Malignancies: A Primer Marissa Heller, M.D. Associate Director of Dermatologic Surgery Department of Dermatology Beth Israel Deaconess Medical Center December 10, 2016 Skin Cancer Non-melanoma
UC Davis Dermatology Online Journal
 UC Davis Dermatology Online Journal Title Disseminated varicella-zoster virus in an immunocompetent adult Permalink https://escholarship.org/uc/item/3cz2x99b Journal Dermatology Online Journal, 21(3) Authors
UC Davis Dermatology Online Journal Title Disseminated varicella-zoster virus in an immunocompetent adult Permalink https://escholarship.org/uc/item/3cz2x99b Journal Dermatology Online Journal, 21(3) Authors
COMMON VIRAL INFECTIONS. Dr D. Tenea Department of Dermatology University of Pretoria
 COMMON VIRAL INFECTIONS Dr D. Tenea Department of Dermatology University of Pretoria GENERAL Viral infections of the skin important in immunocompromised Pts. Infection: direct inoculation ( warts ) or
COMMON VIRAL INFECTIONS Dr D. Tenea Department of Dermatology University of Pretoria GENERAL Viral infections of the skin important in immunocompromised Pts. Infection: direct inoculation ( warts ) or
A Phase I Dose Escalation Study of Intratumoral Herpes Simplex Virus 1 Mutant rrp450 in Patients with Refractory Sarcoma or Neuroblastoma
 A Phase I Dose Escalation Study of Intratumoral Herpes Simplex Virus 1 Mutant rrp450 in Patients with Refractory Sarcoma or Neuroblastoma Timothy P. Cripe, M.D., Ph.D. Associate Professor Division of Hematology/Oncology
A Phase I Dose Escalation Study of Intratumoral Herpes Simplex Virus 1 Mutant rrp450 in Patients with Refractory Sarcoma or Neuroblastoma Timothy P. Cripe, M.D., Ph.D. Associate Professor Division of Hematology/Oncology
POSITRON EMISSION TOMOGRAPHY (PET)
 Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
Status Active Medical and Behavioral Health Policy Section: Radiology Policy Number: V-27 Effective Date: 08/27/2014 Blue Cross and Blue Shield of Minnesota medical policies do not imply that members should
CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series
 Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
Malalagama et al. Cancer Imaging (2017) 17:17 DOI 10.1186/s40644-017-0119-3 CASE SERIES CT findings in patients with Cabazitaxel induced pelvic pain and haematuria: a case series Geethal N. Malalagama
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Viewpoint from a health care professional
 Viewpoint from a health care professional Christoph Hoeller Skin Cancer Center at the Department of Dermatology Medical University of Vienna Austria Certified Skin Tumor Center The fifth annual regulatory
Viewpoint from a health care professional Christoph Hoeller Skin Cancer Center at the Department of Dermatology Medical University of Vienna Austria Certified Skin Tumor Center The fifth annual regulatory
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Medicine Type of Article: Case Report Title:
Human Herpes Virus-6 Limbic Encephalitis
 Case Studies [1] March 19, 2013 Case history: A 32-year-old Caucasian female with newly diagnosed acute myeloid leukemia (AML) was treated with induction chemotherapy and attained complete remission. She
Case Studies [1] March 19, 2013 Case history: A 32-year-old Caucasian female with newly diagnosed acute myeloid leukemia (AML) was treated with induction chemotherapy and attained complete remission. She
General Information, efficacy and safety data
 Horizon Scanning in Oncology Horizon Scanning in Oncology 23 rd Prioritization 2 nd quarter 2015 General Information, efficacy and safety data Eleen Rothschedl Anna Nachtnebel Priorisierung XXIII HSS Onkologie
Horizon Scanning in Oncology Horizon Scanning in Oncology 23 rd Prioritization 2 nd quarter 2015 General Information, efficacy and safety data Eleen Rothschedl Anna Nachtnebel Priorisierung XXIII HSS Onkologie
حسام أبو عوض. 1 P a g e
 2 حسام أبو عوض - - 1 P a g e For the remaining of the MSS (microbiology) we will be discussing types of lesions and microorganisms and diseases related to them. Vesicles A vesicle may have begun as a macule/papule
2 حسام أبو عوض - - 1 P a g e For the remaining of the MSS (microbiology) we will be discussing types of lesions and microorganisms and diseases related to them. Vesicles A vesicle may have begun as a macule/papule
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Treatment and management of advanced melanoma: Paul B. Chapman, MD Melanoma Clinical Director, Melanoma and Immunotherapeutics Service MSKCC
 Treatment and management of advanced melanoma: 2018 Paul B. Chapman, MD Melanoma Clinical Director, Melanoma and Immunotherapeutics Service MSKCC Disclosure Paul B. Chapman, MD Nothing to disclose. Off
Treatment and management of advanced melanoma: 2018 Paul B. Chapman, MD Melanoma Clinical Director, Melanoma and Immunotherapeutics Service MSKCC Disclosure Paul B. Chapman, MD Nothing to disclose. Off
NK/T cell lymphoma Recent advances. Y.L Kwong University Department of Medicine Queen Mary Hospital
 NK/T cell lymphoma Recent advances Y.L Kwong University Department of Medicine Queen Mary Hospital Natural killer cell lymphomas NK cell lymphomas are mainly extranodal lymphomas Clinical classification
NK/T cell lymphoma Recent advances Y.L Kwong University Department of Medicine Queen Mary Hospital Natural killer cell lymphomas NK cell lymphomas are mainly extranodal lymphomas Clinical classification
0BCore Safety Profile. Pharmaceutical form(s)/strength: Cream 1% DK/H/PSUR/0009/005 Date of FAR:
 0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
0BCore Safety Profile Active substance: Pimecrolimus Pharmaceutical form(s)/strength: Cream 1% P-RMS: DK/H/PSUR/0009/005 Date of FAR: 06.06.2013 4.3 Contraindications Hypersensitivity to pimecrolimus,
Mantle-Cell Leukemia: Lessons in Life and Death
 Mantle-Cell Leukemia: Lessons in Life and Death James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation 60 y.o.
Mantle-Cell Leukemia: Lessons in Life and Death James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation 60 y.o.
Delayed onset of neurosarcoidosis after concurrent ipilimumab/nivolumab therapy
 Tan et al. Journal for ImmunoTherapy of Cancer (2018) 6:77 https://doi.org/10.1186/s40425-018-0390-2 CASE REPORT Open Access Delayed onset of neurosarcoidosis after concurrent ipilimumab/nivolumab therapy
Tan et al. Journal for ImmunoTherapy of Cancer (2018) 6:77 https://doi.org/10.1186/s40425-018-0390-2 CASE REPORT Open Access Delayed onset of neurosarcoidosis after concurrent ipilimumab/nivolumab therapy
Keytruda. Keytruda (pembrolizumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.50 Subject: Keytruda Page: 1 of 6 Last Review Date: September 15, 2017 Keytruda Description Keytruda
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.50 Subject: Keytruda Page: 1 of 6 Last Review Date: September 15, 2017 Keytruda Description Keytruda
For more information about how to cite these materials visit
 Author(s): David Miller, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): David Miller, M.D., Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Varicella (Chickenpox) and Varicella Vaccines
 Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Varicella (Chickenpox) and Varicella Vaccines September 2018 Photographs and images included in this
Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Varicella (Chickenpox) and Varicella Vaccines September 2018 Photographs and images included in this
