! # % & & () & +,., / 0) %& 4 % 5 6! & ) 6,,7 + & % 1, + & 0 12 )& / 4..&89&7.&7! 0 % 45& & 2
|
|
|
- Juliet Anthony
- 6 years ago
- Views:
Transcription
1 # % & & () & +,., / 0) %& 4 % & ) 6,,7 + & % 1, + & 0 12 )& / 4..&89&7.&7 0 % 45& & 2 :
2 *Manuscript The global burden of drug-resistant tuberculosis in children: a mathematical model P.J. Dodd 1,*, PhD, C. Sismanidis 2, PhD, and J.A. Seddon 3, PhD 1. School of Health and Related Research, University of Sheffield, Sheffield, UK 2. Global TB Programme, World Health Organization, Geneva, Switzerland 3. Department of Paediatric Infectious Diseases, Imperial College London, London, UK * p.j.dodd@sheffield.ac.uk +44(0) Abstract Background: Following infection with M. tuberculosis, children are at increased risk of progression to tuberculosis disease; a condition that can be challenging to diagnose. New estimation approaches for children have highlighted the gap between incidence and notifications, and suggest there is much more isoniazid-resistant and multidrug-resistant (MDR) disease than is identified. No work has yet quantified the burden of drug-resistant infection, considered other types of drug-resistance, or accounted for sampling uncertainty. Methods: We combined a mathematical model of tuberculosis in children with an analysis of drug-resistance patterns to produce country-level, regional, and global estimates of drugresistant infection and disease. We estimated the proportions of tuberculosis cases at a country-level with: isoniazid-monoresistance (HMR), rifampicin mono-resistance, MDR, fluoroquinolone-resistant MDR, second-line injectable resistant MDR, and MDR with resistance to both a fluoroquinolone and a second-line injectable (XDR). Findings: We estimate 850,000 children developed tuberculosis in 2014; 58,000 with HMRtuberculosis, 25,000 with MDR-tuberculosis, and 1,200 with XDR-tuberculosis. We estimate 67 million children are infected with M. tuberculosis; 5 million with HMR, 2 million with MDR, and 100,000 with XDR. Africa and South-East Asia have the highest numbers of tuberculosis in children, but WHO EMR, EUR and WPR regions also contribute substantially to the burden of drug-resistant tuberculosis due to their much higher proportions of resistance. Interpretation: Far more drug-resistant tuberculosis occurs in children than is diagnosed, and there is a large pool of drug-resistant infection. This has implications for approaches to empiric treatment and preventive therapy in some regions. Funding: UNITAID
3 Introduction Tuberculosis in children is increasingly being recognised as a significant public health problem, and an important component of the total global burden of tuberculosis. 1 New methodological developments for estimating the burden of tuberculosis in children have been adopted in the estimation process used by the Global Tuberculosis Programme (GTB) at the World Health Organization (WHO). 2,3 The GTB estimated that in 2014, 1 million children developed tuberculosis disease. 4 Understanding the burden is central to resource allocation, estimation of market size for potential drug, diagnostic or vaccine development, a tool to evaluate programmes and for advocacy. Following infection with Mycobacterium tuberculosis (M. tuberculosis) young children are at particularly high risk of progressing to tuberculosis disease. They are also more likely to develop severe forms of disease such as tuberculous meningitis and disseminated tuberculosis. 5,6 WHO guidance suggests use of isoniazid preventive therapy (IPT) in children under five years who have been exposed to tuberculosis. 7 IPT has been shown to reduce the risk of progression from tuberculosis infection to tuberculosis disease by around 60% in HIVuninfected people (including children) 8, and comparable reductions have been seen in children with HIV infection. 9 Without treatment, tuberculosis disease carries a substantial risk of death in children, but if diagnosed and treated, outcomes are excellent. 10 Anti-tuberculosis drug resistance is frequently divided into drug-susceptible (DS)- tuberculosis and multidrug-resistant (MDR)-tuberculosis. DS-tuberculosis suggests that the organism is susceptible to the two most effective first-line medications (isoniazid and rifampicin), whereas MDR-tuberculosis is defined as disease caused by M. tuberculosis resistant to both of these drugs. This division has programmatic motivations, as patients with strains that are resistant to only isoniazid can largely be treated successfully with standard first-line therapy, whereas those with MDR-tuberculosis cannot. However, the importance of isoniazid-mono-resistant (HMR)-tuberculosis is increasingly recognised. First, MDR strains have normally acquired resistance to isoniazid first and then resistance to rifampicin, in effect making HMR-tuberculosis the usual gateway to MDR disease. Second, those with asymptomatic HMR-tuberculosis infection are unlikely to respond to IPT. In addition to the emerging recognition of the importance of HMR-tuberculosis, a more comprehensive approach to second-line drug (SLD) resistance is required. The most important drug classes for treating MDR-tuberculosis are the fluoroquinolones and the second-line injectable medications; resistance to these drugs can influence MDR-tuberculosis treatment outcomes. Children are increasingly being identified, diagnosed and started on treatment for drugresistant (DR)-tuberculosis either when DR-tuberculosis is confirmed in an isolate from the child or when a child develops clinical disease in conjunction with exposure to a source case that has DR-tuberculosis. 11 In addition, there is increasing recognition that to reduce the burden of tuberculosis it is necessary to identify and treat infected contacts before they become unwell. 12 Children with DR-tuberculosis infection are a reservoir from which future cases will develop and children exposed to DR-tuberculosis are at times treated with nonstandardised preventive therapy. 13 The treatment of DR-tuberculosis infection is usually directed against the drug susceptibility test (DST) pattern of the identified source case as child contacts demonstrate high concordance with the source case, if they do progress to disease. 14,15
4 We previously estimated the burden of childhood tuberculosis in the 22 high tuberculosis burden countries but did not estimate a global burden or evaluate drug resistance. Other estimates of paediatric tuberculosis incidence exist, based on upwardly adjusting paediatric notification rates. 3 These approaches do not, however, permit quantification of the burden of infection. Although previous estimates of isoniazid-resistant disease and MDR disease in children have been made, 3,16 no investigators have quantified the burden of DR-tuberculosis infection in children. In addition, there have been no comprehensive attempts to quantify the different types of DR-tuberculosis disease in children. Moreover, approaches to date have not accounted for sample uncertainty associated with numbers of cases with drug-susceptibility testing.
5 Methods We extended a previously published model of tuberculosis burden estimation in children to 180 countries for which the necessary input data were available, accounting for over 99% of the world population (see Appendix pages 3-5). 2 Briefly, this model uses the WHO estimates of adult tuberculosis prevalence and a revised Styblo rule to estimate the annual risk of infection for children. Data on underlying demography, BCG coverage, HIV prevalence, and the natural history of disease in children is then used to estimate incidence of disease at a country-level. Uncertainty in all data is included and propagated through to results. We used the following classification and notation for drug-resistance types: DS - susceptible to isoniazid and rifampicin; HMR - isoniazid mono-resistant; RMR - rifampicin monoresistant; MDR - multidrug-resistant (resistant to at least isoniazid and rifampicin); MDR# - only resistant to isoniazid and rifampicin; FQR MDR# with additional resistance to 1 fluoroquinolone but not any second line injectables; SLR MDR# with additional resistance to 1 second line injectable but not any fluoroquinolone; XDR MDR# with additional resistance to 1 fluoroquinolone and to 1 second line injectable. We did not consider resistance to other anti-tuberculosis drugs, such as ethambutol, pyrazinamide, streptomycin, nor any second-line drugs other than the fluoroquinolones and second-line injectable medications. This classification of resistance can thus be summarised as follows: all TB = DS + HMR + RMR + MDR; and MDR = MDR# + FQR + SLR + XDR (see Figure 1). Given the difficulties of bacteriological confirmation of tuberculosis in children, direct data on drug resistance types are rare. Systematic reviews suggest that the proportion of isoniazid resistance and MDR in treatment-naïve adults is a reasonable proxy for the proportion of the corresponding resistance in children 3,16. Analysis of surveillance data failed to find a difference between proportions of first-line drug resistance in children and adults regardless of treatment status. 17 For first-line resistance, we therefore based the proportions of children resistant to each compound on data in treatment-naïve adults. For second-line resistance, data were not available stratified by treatment history; we therefore directly applied the proportions of drug resistance in these data. Drug resistance was determined using data from the Global Project on Anti-tuberculosis Drug Resistance Surveillance at WHO. Data comprised counts of resistance by type from routine surveillance, and proportions (with confidence intervals) for each resistance type from surveys reported to WHO between 1988 and 2014, 4,17 following guidelines for drug resistance surveillance. 18 In most countries these data relate to patients with pulmonary tuberculosis, nearly all of whom are adults. Because of the potential for bias, data were not used from surveillance systems where less than 60% of treatment-naïve patients had a rifampicin-resistance result. 18 For surveys, 82 countries contributed 166 country-years with complete data on HMR, RMR and MDR. For surveillance data, 87 countries contributed 627 country-years with complete data on HMR, RMR and MDR, and there were a further 288 country-years with data on only MDR resistance. 90 countries reported data on second-line resistance among MDR-tuberclosis individuals (MDR#, FQR, SLR and XDR): 33 countryyears from surveys and 273 country-years from surveillance; 227 country-years with complete data, 40 country-years with only data on XDR and FQR resistance, 43 countryyears with only data on XDR resistance. We converted proportions from survey data into counts by multiplying by the survey sample size. Exploratory data analysis suggested no clear trends so we aggregated data over the years
6 To sample the uncertain proportions for each DR category in each country, we used the following algorithm: 1) if a country had data, we used a Bayesian approach assuming multinomial counts with a flat Dirichlet prior on proportions, allowing sampling from the closed-form posterior for proportions (approach to missing category counts described Appendix page 9); 2) if a country had no data but 2 or more of its 5 nearest neighbours did, for each sample we randomly chose a neighbouring country and sampled its proportions as in 1); 3) if a country had no data and fewer than 2 of its 5 nearest neighbours did, we randomly chose a country from the same epidemiological region and sampled its proportions as in 1); 4) if a country had no data and no countries in the same epidemiological region had data, we randomly chose a country with data globally and sampled its proportions as in 1). The nine epidemiological regions used for analysis were the those defined in the WHO report methodological appendix 19 for MDR analyses but the results are presented and discussed for the standard six WHO regions (see Appendix pages 8-9). 4 We combined 1,000 sampled proportions for each country using this algorithm with 10,000 sampled country estimates of tuberculosis disease incidence and M. tuberculosis infection prevalence from our model (resampling the proportions to generate 10,000 stratified incidences). Country estimates of tuberculosis disease incidence and M. tuberculosis infection prevalence by drug-resistance type were then aggregated by WHO region and globally. Reported aggregate proportions of drug-resistance type are among total tuberculosis incidence in children. Standard world maps and a Gastner-Newman cartogram 20 (which represents data by scaling areas) were used to visualize the geographic variation in median quantities. Role of the funding source The sponsor of the study had no role in study design, data collection, data analysis, data interpretation, or writing of the report. The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit for publication.
7 Results Proportions of DR-tuberculosis Overall we find that 6.9% (Inter-quartile range [IQR]: 6.6% 7.1%) of tuberculosis in children is HMR and 2.9% (IQR: 2.7% 3.1%) MDR (see Figure 2A and Appendix page 11). Of MDR-tuberculosis in children, we find that 4.7% (IQR: 4.3% 5.1%) is XDR (see Figure 2B and Appendix page 11). These patterns of drug resistance vary strongly both by region (see Figure 2 and Appendix page 11) and within region (see Appendix page 13-14). In the EUR region, in contrast to all the other regions, the proportion of cases that are MDR is now higher than HMR. While uncertain, the proportion of children with MDR who have second-line drug resistance seems lowest in the AFR and WPR regions. Global resampling was not reached for first- or second-line resistance estimates (see Appendix page 10). Incident DR-tuberculosis disease We estimate a total global paediatric incidence in 2014 of 847,000 (IQR: 558,000 1,280,000) of which 58,300 (IQR: 38,300 87,000) were HMR-tuberculosis, 24,800 (IQR: 16,100 37,400) MDR-tuberculosis and 1,160 (IQR: 757 1,770) XDR-tuberculosis. There is substantial variation regionally (see Table 1 for all drug resistance categories and also incidence in children under 5). The proportion of incident tuberculosis in children in 2014 with MDR-tuberculosis varies from very low percentages in the Americas and Western Europe (light red in Figure 3), through to over 30% in some of the former Soviet states in the WHO European (EUR) region (dark red, Figure 3). However, countries with low or moderate proportions of resistance in the SEA, AFR and WPR regions contribute to the majority of the incident MDR-tuberculosis in children, due to their high incidences and large child populations. Prevalent DR-tuberculosis infection We estimate that in 2014 the global paediatric burden of tuberculosis infection was 67.0 million (IQR: 52.3 million 85.7 million). Of these infections, 4.8 million (IQR: 3.8 million 6.2 million) were HMR, 2.0 million (IQR: 1.6 million 2.6 million) were MDR and 101,000 (IQR: 78, ,000) were XDR. There is substantial regional variation (see Table 2 for all drug resistance categories and Appendix pages 17-18).
8 All TB Resistant to second line MDR TB injectables DS SLR RMR MDR# XDR HMR FQR Rifampicin resistant TB Resistant to Isoniazid resistant TB fluoroquinolones Figure 1: Definitions of drug-resistance types used. DS - susceptible to isoniazid and rifampicin; HMR - isoniazid mono-resistant; RMR - rifampicin mono-resistant; MDR - multidrug-resistant (resistant to at least isoniazid and rifampicin); MDR# - only resistant to isoniazid and rifampicin; FQR MDR# with additional resistance to 1 fluoroquinolone but not any second line injectables; SLR MDR# with additional resistance to 1 second line injectable but not any fluoroquinolone; XDR MDR# with additional resistance to 1 fluoroquinolone and to 1 second line injectable. We did not consider resistance to other anti-tuberculosis drugs.
9 A B Proportion of incident tuberculosis in children (%) DR type DS HMR RMR MDR Proportion of incident MDR tuberculosis in children (%) MDR type MDR# FQR SLR XDR 0 0 AFR AMR EMR EUR SEA WPR GLOBAL WHO region AFR AMR EMR EUR SEA WPR GLOBAL WHO region Figure 2: Proportion of incident tuberculosis in children by drug-resistance status, DS=drug-susceptible, HMR=isoniazid mono-resistant, RMR=rifampicin mono-resistant, MDR=multidrug-resistant; MDR#=MDR only, FQR=MDR# + resistant to a fluoroquinolone, SLR=MDR# + resistant to a second-line injectable, XDR=extensively drug-resistant. WHO regions: AFR=African, AMR=Americas, EMR=Eastern Mediterranean, EUR=European, SEA=South-East Asia, WPR=Western Boxand-whiskers depict mean, inter-quartile range, and 95th percentiles.
10 MDR (%) Figure 3: Cartogram showing total incidence of MDR tuberculosis in children in 2014 by area (using the Gastner-Newman method 20 ) and the proportion of incident in children with MDR tuberculosis by colour (grey shading indicates no estimate)
11 Table 1: Estimates of incident tuberculosis in children by drug resistance type and WHO region, DS=drug-susceptible, HMR=isoniazid mono-resistant, RMR=rifampicin mono-resistant, MDR=multidrug-resistant; MDR#=MDR only, FQR=MDR# + resistant to a fluoroquinolone, SLR=MDR# + resistant to a second-line injectable, XDR=extensively drug-resistant. WHO regions: AFR=African, AMR=Americas, EMR=Eastern Mediterranean, EUR=European, SEA=South-East Asia, WPR=Western Pacific. Brackets denote interquartile range. Numbers to three significant figures. Total Estimates of incident tuberculosis in children by drug resistance type Estimates of incident MDR-tuberculosis in children by drug resistance type DS HMR RMR MDR MDR# FQR SLR XDR AFR 338,000 [218, ,000] 309,000 [200, ,000] 16,800 [10,800-25,700] 2,890 [1,860-4,460] 8,230 [5,190-12,800] 6,560 [4,120-10,200] 577 [ ] 713 [436-1,150] 245 [ ] AMR 25,000 [16,100-38,500] 23,100 [14,900-35,700] 1,170 [743-1,810] 113 [69-191] 525 [ ] 287 [ ] 57 [35-95] 109 [66-179] 51 [31-86] EMR 75,700 [49, ,000] 64,100 [42,200-96,700] 6,640 [4,280-10,100] 1,290 [811-2,040] 3,340 [2,120-5,160] 2,140 [1,360-3,320] 635 [397-1,000] 303 [ ] 185 [ ] EUR 13,500 [8,690-21,000] 9,590 [6,180-14,900] 1,610 [1,030-2,510] 179 [ ] 2,120 [1,320-3,310] 981 [603-1,540] 374 [ ] 480 [ ] 168 [ ] SEA 294,000 [190, ,000] 264,000 [171, ,000] 21,200 [13,700-33,000] 1,820 [1,180-2,840] 6,370 [4,100-9,910] 3,780 [2,400-5,870] 1,080 [678-1,730] 1,070 [520-2,020] 199 [ ] WPR 91,800 [60, ,000] 77,600 [51, ,000] 9,670 [6,320-14,700] 1,080 [705-1,690] 3,540 [2,320-5,400] 1,960 [1,280-3,020] 877 [573-1,350] 437 [ ] 244 [ ] GLOBAL 847,000 [558,000-1,280,000] 756,000 [499,000-1,140,000] 58,300 [38,300-87,800] 7,630 [5,010-11,500] 24,800 [16,100-37,400] 16,200 [10,500-24,500] 3,810 [2,500-5,840] 3,390 [2,140-5,290] 1,160 [757-1,770]
12 Table 2: Estimates of the numbers of children infected with Mycobacterium tuberculosis by drug resistance type and WHO region, DS=drug-susceptible, HMR=isoniazid mono-resistant, RMR=rifampicin mono-resistant, MDR=multidrug-resistant; MDR#=MDR only, FQR=MDR# + resistant to a fluoroquinolone, SLR=MDR# + resistant to a second-line injectable, XDR=extensively drug-resistant. WHO regions: AFR=African, AMR=Americas, EMR=Eastern Mediterranean, EUR=European, SEA=South-East Asia, WPR=Western Pacific. Brackets denote interquartile range. Numbers to three significant figures. Total Estimates of children infected with M. tuberculosis by drug resistance type Estimates of children infected with MDR M. tuberculosis by drug resistance type DS HMR RMR MDR MDR# FQR SLR XDR AFR 20,900,000 [16,400,000-27,000,000] 19,200,000 [15,000,000-24,700,000] 1,040,000 [797,000-1,360,000] 180,000 [137, ,000] 489,000 [373, ,000] 385,000 [291, ,000] 35,800 [24,500-52,700] 45,000 [31,600-65,100] 15,800 [11,200-22,100] AMR 2,110,000 [1,590,000-2,780,000] 1,950,000 [1,470,000-2,580,000] 97,600 [73, ,000] 9,560 [6,760-14,200] 44,500 [33,000-60,900] 24,300 [17,400-34,500] 4,920 [3,360-7,180] 9,340 [6,300-13,800] 4,480 [3,030-6,720] EMR 6,500,000 [4,960,000-8,350,000] 5,490,000 [4,190,000-7,050,000] 583,000 [437, ,000] 106,000 [75, ,000] 288,000 [212, ,000] 188,000 [137, ,000] 52,900 [39,000-71,600] 26,300 [17,800-39,700] 15,400 [10,500-22,800] EUR 1,400,000 [1,040,000-1,880,000] 992,000 [746,000-1,330,000] 166,000 [123, ,000] 17,800 [13,200-24,200] 219,000 [160, ,000] 100,000 [72, ,000] 38,300 [25,100-61,300] 50,400 [33,700-76,600] 17,300 [12,500-24,100] SEA 27,000,000 [20,500,000-35,300,000] 24,300,000 [18,400,000-31,700,000] 1,950,000 [1,470,000-2,570,000] 162,000 [122, ,000] 586,000 [442, ,000] 339,000 [251, ,000] 102,000 [74, ,000] 105,000 [56, ,000] 18,300 [12,900-26,100] WPR 8,600,000 [6,670,000-11,100,000] 7,250,000 [5,630,000-9,370,000] 901,000 [696,000-1,170,000] 103,000 [79, ,000] 344,000 [264, ,000] 185,000 [142, ,000] 89,300 [67, ,000] 43,800 [33,500-57,100] 24,700 [18,600-32,300] GLOBAL 67,000,000 [52,300,000-85,700,000] 59,600,000 [46,500,000-76,200,000] 4,810,000 [3,750,000-6,160,000] 594,000 [463, ,000] 2,000,000 [1,560,000-2,580,000] 1,250,000 [968,000-1,610,000] 339,000 [262, ,000] 301,000 [221, ,000] 101,000 [78, ,000]
13 Discussion Our modelling analysis suggests large numbers of children develop tuberculosis disease each year with a global incidence estimate of nearly 847,000. We also estimate a large burden of children with DR-tuberculosis each year: in the region of 58,000 with HMR-tuberculosis, 25,000 with MDR-tuberculosis, and 1,200 with XDR-tuberculosis. A much larger number of children will be infected with M. tuberculosis; our estimate is that there are currently nearly 67 million children globally infected. Of these there are a significant number with drugresistant infections: approaching 5 million with HMR, 2 million with MDR, and 100,000 with XDR. While the WHO Africa and South-East Asia regions dominate the overall contribution to tuberculosis in children, EMR, EUR and WPR are substantial contributors to the burden of DR disease due to their much higher proportions of drug resistance. The estimated burden of DR-tuberculosis disease cases highlights a vast gap between incidence and treatment. Currently few children globally are treated for DR-tuberculosis. A recent individual patient systematic review and meta-analysis of children treated at any time in the past for MDR-tuberculosis was only able to identify 1,000 children. 21 As we estimate 25,000 children develop MDR-tuberculosis each year, clearly many children not being diagnosed and started on treatment, especially considering that rifampicin mono-resistance is clinically managed in the same way as MDR-tuberculosis. If more children are to be treated, the implications for diagnostics, funding, training, and an adequate supply of child-friendly drugs are profound. With the roll out of Xpert MTB/RIF, the significant risk of HMR in some regions may be overlooked and result in suboptimal treatment. If only Xpert MTB/RIF is used, HMR source cases may be diagnosed but considered susceptible to both rifampicin and isoniazid, and child contacts (who are likely infected with a HMR strain) given IPT. Although IPT will be effective for RMR-tuberculosis, it is unlikely that this will be diagnosed if only Xpert MTB/RIF is used; a positive rpob gene mutation result usually results in the case being managed as MDR-tuberculosis. The child is unlikely to be given isoniazid, although this would be effective. In areas with high rates of HMR, where Xpert MTB/RIF is used alone, consideration could be given to using three months of both isoniazid and rifampicin as preventive therapy, so that if the source case has undiagnosed HMR-tuberculosis, the child will still benefit from rifampicin. It is also vital that Xpert MTB/RIF testing is followed up with testing for isoniazid susceptibility. If a child is exposed to an MDR-tuberculosis case, it is unlikely that either rifampicin or isoniazid would be effective as preventive therapy. An evolving body of evidence suggests fluoroquinolone-based regimens may be effective and three clinical trials are underway to investigate alternative treatments. 22 The high rates of drug resistance in some regions will also have implications for the choice of drugs in the treatment of children with confirmed disease prior to the full DST becoming available (or where a full DST is unavailable) and also for children with clinically-diagnosed disease without a full DST profile from the source case. We can compare our estimates of paediatric MDR-tuberculosis and isoniazid-resistant tuberculosis with those of Jenkins et al. 3 and Yuen et al., 16 respectively. Our estimates of the incidence of MDR-tuberculosis are somewhat lower than the 32,000 estimate of Jenkins et al. 3 for Our global paediatric tuberculosis incidence estimate is approximately 20% smaller than that of Jenkins et al. 3, but differences are heterogeneous by location: the
14 difference in MDR-tuberculosis incidence estimates is largely accounted for by our substantially smaller estimates for underlying paediatric tuberculosis incidence in China, India and Russia, without considering any differences in drug-resistance proportions. These countries account for a difference of over 7,000 paediatric MDR cases assuming the same proportion of MDR resistance (data not shown). To compare with the existing estimate of isoniazid resistance of 120,000 in Yuen et al. 16 (which uses the underlying burden estimates from Jenkins et al. 3 ), we need to aggregate our HMR and MDR categories (giving a global estimate in the region of 84,000 for all isoniazid resistance). Thus our estimate for isoniazid resistance is lower than that of Yuen et al. 16 and as with MDR, the difference is largest in the WHO EUR, SEA and WPR regions and almost entirely accounted for by differences in underlying burden (data not shown), notably in China, India and Russia. It is a limitation of our approach that we have aggregated over subnational data in India and Russia; nationallyrepresentative surveys of drug-resistance in India and China are on-going. Our global estimate of 2.9% MDR in incident childhood tuberculosis is slightly lower than the WHO global estimate of 3.3% in all treatment naïve cases, largely reflecting lower MDR proportions in regions with higher proportions of tuberculosis incidence among children. Our analysis has several limitations, associated both with the mathematical model quantifying the burden of infection and disease, and with the analysis of patterns of drug resistance. The burden model inherits any limitations associated with WHO s estimates of tuberculosis prevalence, and has recognised uncertainties in its treatment of HIV as a risk factor for disease progression, BCG vaccination as a source of protection, and ignores potential host or pathogen variation as sources of variation in progression rates. 2 However, our burden model produces estimates that are comparable with an independent approach based on notification data, 3 and has strengths in generating estimates of latent infection and age-disaggregated incidence. Our main focus was on TB disease in the year 2014, but in the absence of clear trends, we used aggregated drug-resistance data over a decade to inform proportions with each type. This may average over trends that exist in reality but for which these data do not have the power to detect. In estimating the burden of M. tuberculosis infection, we also assumed that the annual risk of infection has remained constant during years The global tuberculosis prevalence per capita (country mean, weighted by current child population) was nearly 60% higher in 1999 than in 2014: the higher annual risks of infection in the past could imply today s burden of latent M. tuberculosis infection is up to 30% larger than an estimate based on current infection risks. Some of the limitations may apply particularly to the inclusion of drug resistance: we have assumed that drug-resistance type is not correlated with exposure, infectiousness or likelihood of progression. We have assumed that the proportion of first-line drug resistance types in treatment-naïve patients reflects that in children and have not included any uncertainty in this relation. However, this assumption is supported for isoniazid resistance and MDR by systematic review. 3,16 For second-line drug resistance, we have assumed that the proportions of different drug resistance in all patients reflects that in children, which may over-estimate levels of second-line drug resistance in children by including data from previously treated patients. Patients with MDR-tuberculosis with additional second-line resistance (including XDR-tuberculosis) may be epidemiologically and socially different to other groups with drug-resistant tuberculosis. They may be more likely to have been hospitalised or imprisoned and clustering may mean that the probability of a child being
15 exposed to a case is less than for other forms of disease. Although, they are more likely to have been retreated, it is reassuring that analysis of surveillance data has failed to find a difference between first-line resistance proportions in children and adults of any treatment status. 17 Finally, we have only evaluated the drug resistance categories determined by the drugs defining MDR- and XDR-tuberculosis. Resistance to other drugs has not been estimated due to shortage of data, partly resulting from technical difficulties in DST (e.g. cycloserine and clofazimine) and partly due to lack of good quality diagnostics in much of the world (e.g. pyrazinamide). As a result we expect that global needs in terms of effective regimens will be higher than that implied by the burden estimates that we report. A strength of our work is our treatment of uncertainty. Our analysis of drug-resistance patterns is an improvement over previous work in this respect, since it captures the uncertainty implicit in the numbers of cases determining proportions, and could be applied to determining the burden of drug-resistant tuberculosis in all age groups. While a geographically-structured hierarchical model may have allowed use of country-level variables in imputing missing drug resistance patterns, our regional resampling approach does capture regional patterns and variance from resampling, and is relatively simple and transparent. This approach could be built upon to analyse differences between countries and between regions, and to identify drivers of drug resistance patterns. As more data become available, it may be possible validate the model and also use it to make predictions into the future. Quantifying the levels of disease incidence and infection prevalence with particular drugresistance phenotypes can also feed into market size calculations for second-line drugs, and for new drugs. Finally, this framework would allow investigation of different options for empirical studies and their location to improve the precision of these estimates. Comparison with other burden estimates of DR-tuberculosis, where there is overlap, highlights the importance of better quantifying the underlying burden of childhood tuberculosis in key settings such as China, India and Russia. Conclusion Far more DR-tuberculosis occurs in children than is diagnosed, and there is a large pool of DR-tuberculosis infection. This could have implications for approaches to empiric treatment and preventive therapy in some regions. Acknowledgements We would like to thank Helen Jenkins for sharing country-level burden estimates for comparison, and Anna Dean, Dennis Falzon, Matteo Zignol and Philippe Glaziou for comments on the manuscript. Charalambos Sismanidis is a staff member of the World Health Organization. The author alone is responsible for the views expressed in this publication and they do not necessarily represent the decisions or policies of the World Health Organization.
16 This work was funded from the STEP-TB grant from UNITAID to TB Alliance. Contributions PJD and JAS conceived and designed the study, and wrote a first draft of the article. CS advised on interpretation of data, critiqued the method and contributed to writing the article. PJD performed all data analysis and modelling. Conflicts of interest We declare that we have no conflicts of interest.
17 References 1. Seddon JA, Jenkins HE, Liu L, Cohen T, Black RE, Becerra MC, et al. Counting Children with Tuberculosis: Why Numbers Matter. The international journal of tuberculosis and lung disease: the official journal of the International Union against Tuberculosis and Lung Disease. 2015;19(0 1):9. 2. Dodd PJ, Gardiner E, Coghlan R, Seddon JA. Burden of childhood tuberculosis in 22 high-burden countries: a mathematical modelling study. Lancet Glob Health Aug;2(8):e Jenkins HE, Tolman AW, Yuen CM, Parr JB, Keshavjee S, Pérez-Vélez CM, et al. Incidence of multidrug-resistant tuberculosis disease in children: systematic review and global estimates. The Lancet. 2014;383(9928): World Health Organisation. Global tuberculosis control Geneva: World Health Organization; Marais BJ, Gie RP, Schaaf HS, Hesseling AC, Obihara CC, Nelson LJ, et al. The clinical epidemiology of childhood pulmonary tuberculosis: a critical review of literature from the pre-chemotherapy era. Int J Tuberc Lung Dis Mar;8(3): Marais BJ, Gie RP, Schaaf HS, Hesseling AC, Obihara CC, Starke JJ, et al. The natural history of childhood intra-thoracic tuberculosis: a critical review of literature from the pre-chemotherapy era. Int J Tuberc Lung Dis Apr;8(4): World Health Organization. Guidance for national tuberculosis programmes on the management of tuberculosis in children [Internet]. Geneva: World Health Organization; 2014 [cited 2016 Jan 29]. Available from: 8. Smieja MJ, Marchetti CA, Cook DJ, Smaill FM. Isoniazid for preventing tuberculosis in non-hiv infected persons. Cochrane Database Syst Rev. 2000;(2):CD Zar HJ, Cotton MF, Strauss S, Karpakis J, Hussey G, Schaaf HS, et al. Effect of isoniazid prophylaxis on mortality and incidence of tuberculosis in children with HIV: randomised controlled trial. BMJ Jan 18;334(7585): Jenkins HE, Yuen CM, Rodriguez CA, Nathavitharana RR, McLaughlin M, Donald P, et al. Mortality among children diagnosed with tuberculosis: Systematic review and metaanalysis. Submitted. 2016; 11. Moore BK, Anyalechi E, van der Walt M, Smith S, Erasmus L, Lancaster J, et al. Epidemiology of drug-resistant tuberculosis among children and adolescents in South Africa, Int J Tuberc Lung Dis Jun;19(6): Dye C, Glaziou P, Floyd K, Raviglione M. Prospects for tuberculosis elimination. Annual review of public health. 2013;34:
18 13. Seddon JA, Fred D, Amanullah F, Schaaf HS, Starke JR, Keshavjee S, et al. Postexposure management of multidrug-resistant tuberculosis contacts: evidence-based recommendations. Policy Brief No. 1. Dubai, United Arab Emirates: Harvard Medical School Center for Global Health Delivery Dubai.; Schaaf HS, Gie RP, Kennedy M, Beyers N, Hesseling PB, Donald PR. Evaluation of young children in contact with adult multidrug-resistant pulmonary tuberculosis: a 30- month follow-up. Pediatrics. 2002;109(5): Schaaf HS, Van Rie A, Gie RP, Beyers N, Victor TC, van Helden PD, et al. Transmission of multidrug-resistant tuberculosis. The Pediatric infectious disease journal. 2000;19(8): Yuen CM, Jenkins HE, Rodriguez CA, Keshavjee S, Becerra MC. Global and Regional Burden of Isoniazid-Resistant Tuberculosis. Pediatrics May 1;peds Zignol M, Sismanidis C, Falzon D, Glaziou P, Dara M, Floyd K. Multidrug-resistant tuberculosis in children: evidence from global surveillance. European Respiratory Journal. 2013;42(3): World Health Organization. Guidelines for surveillance of drug resistance in tuberculosis [Internet]. 5th edition. Geneva: World Health Organization; 2015 [cited 2016 Jan 29]. Available from: Glaziou P, Sismanidis, Charalambos, Pretorius C, Timimi, H, Floyd K. Global TB Report 2015: Technical appendix on methods used to estimate the global burden of disease caused by TB. Geneva: WHO; Gastner MT, Newman MEJ. Diffusion-based method for producing density-equalizing maps. PNAS May 18;101(20): Harausz E, Garcia-Prats A, Schaaf HS, Hesseling AC, Furin JJ, Menzies R, et al. Global treatment outcomes in children with paediatric MDR-TB: systematic review and metaanalysis. In Cape Town, South Africa; Available from: capetown.worldlunghealth.org/abstract_book_2015-web.pdf 22. Harvard Medical School Center for Global Health Delivery Dubai. Global consultation on best practices in the delivery of preventive therapy for household contacts of patients with drug-resistant tuberculosis. Proceedings of the Harvard Medical School Center for Global Health Delivery Dubai. 2015;1(1).
19 Figure 1 All TB Resistant to second line MDR TB injectables DS SLR RMR MDR# XDR HMR FQR Rifampicin resistant TB Resistant to Isoniazid resistant TB fluoroquinolones
20 Figure 2a 100 Proportion of incident tuberculosis in children (%) DR type DS HMR RMR MDR 0 AFR AMR EMR EUR SEA WPR GLOBAL WHO region
21 Figure 2b 100 Proportion of incident MDR tuberculosis in children (%) MDR type MDR# FQR SLR XDR 0 AFR AMR EMR EUR SEA WPR GLOBAL WHO region
22 Figure 3 MDR (%)
23 Appendix Click here to download Necessary additional data: DR_burden_appendixR1.pdf The global burden of drug-resistant tuberculosis in children: a mathematical model (Supplementary Information) P.J. Dodd 1, C. Sismanidis 2, and J.A. Seddon 3 1. School of Health and Related Research, University of Sheffield, Sheffield, UK 2. Global TB Programme, World Health Organization, Geneva, Switzerland 3. Department of Paediatric Infectious Diseases, Imperial College London, London, UK Underlying mathematical model of tuberculosis burden in children... 3 Summary of methods... 3 Figure 1: Overview of modelling logic. Diamonds represent data sources, squares represent numbers estimated at each stage, and stadiums represent modelling stages Description of data used... 3 Country linking and exclusions... 4 Figure 2: The 180 countries included in our analysis (color by estimated per-capita tuberculosis incidence)... 5 Summary of differences from previous work... 5 Analysis of drug-resistance patterns... 6 Data availability by region... 6 Figure 3: Countries with data on resistance to first-line anti-tuberculosis drugs in new cases... 6 Figure 4: Countries with data resistance to second-line anti-tuberculosis drugs Nearest neighbor construction & interpretation of survey data... 7 Figure 5: Ranked implied design effects in survey data on MDR in new cases based on reported confidence intervals and sample size. Red line at Figure 6: The network of 5 nearest-neighbors used for imputing drug resistance patterns for countries without data WHO regions used... 8 Figure 7: Map of standard WHO regions... 8 Figure 8: Map of WHO epidemiological regions used for resampling scheme Missing data... 9 Source of data for country estimates Figure 9: Source of data for each country used in first-line drug-resistance estimates Figure 10: Source of data for each country used in second-line drug-resistance estimates Supplementary results Tables Table 1: Percentage of incident tuberculosis in children by resistance type in IQR in brackets Table 2: Estimates of incident tuberculosis in children under 5 by drug resistance type and WHO region, Maps of incidence and infection burden Figure 11: Percentage of tuberculosis disease in children by first-line resistance types,
24 Figure 12: Percentage of MDR tuberculosis disease in children by second-line resistance type, Figure 13: Tuberculosis incidence in children by first-line resistance type, Figure 14: Tuberculosis incidence in children by second-line resistance type, Figure 15: LTBI in children by first-line resistance type, Figure 16: LTBI in children by second-line resistance type,
25 Underlying mathematical model of tuberculosis burden in children A mechanistic mathematical model that uses estimates of adult tuberculosis prevalence to model the process of infection and progression to disease in different age-groups was used to generate estimates of latent infection and tuberculosis incidence in 180 countries in The model has been previously published and subsequently extended from the 22 high tuberculosis burden countries to a global model covering 180 countries. The model has a number of uncertain data and natural history inputs, and the uncertainty inherent in these quantities is represented by generating a sample of 10,000 outputs running the model across a Latin hypercube sample from the distributions characterizing these input values. A summary is provided below. Summary of methods y v c c s c y s sk x s c c c y ss s s c c c y c s c s Figure 1: Overview of modelling logic. Diamonds represent data sources, squares represent numbers estimated at each stage, and stadiums represent modelling stages. Description of data used We obtained data on country demography for 2013 from UN ESA, Population Division. Where necessary, 5-year age categories were disaggregated under the assumption of uniformly distributed ages. These data were used to generate the number of children at risk in each country by age. 3
26 WHO estimates of adult tuberculosis prevalence were obtained from for 2014, together with 95% uncertainty bounds. Uncertainty in per-capita prevalence was represented by gamma distributions, parameterised by taking the quoted ranges defined by the upper and lower bounds as 1.96 x the standard deviation, and the quoted point estimate as the mean. WHO notification data from 2010 were used to estimate the proportion of incident tuberculosis that is smear positive for the community ARI estimate. The same estimate was used for all countries to avoid bias resulting from different case detection infrastructures etc. BCG vaccination coverage estimates were obtained for 2014 from WHO. The BCG vaccination coverages were used to determine the fraction of children whose risks of progression from infection to disease were moderated by BCG. HIV prevalence estimates in those aged under 15 were available for 82 countries from UNAIDS, together with 95% uncertainty bounds. Countries for which there were not estimates reported from this source were assumed to have negligible HIV prevalence in those under 15 years of age. Uncertainty in the prevalences was represented by gamma distributions, parameterised by taking the quoted ranges defined by the upper and lower bounds were taken as 1.96 x the standard deviation, and the quoted point estimate as the mean. This HIV prevalence was assumed to be uniform by age in those under 15. Degree of immunosuppression or ART was not considered. Country linking and exclusions The WHO tuberculosis estimate and notification data were linked with the demographic, HIV, and BCG sets by 3 letter ISO code where possible, and by hand otherwise. Various countries were excluded where it was not possible to link them across the data. The WHO version of country names was used. 4
27 TB incidence in 2014 per 100,000 per year 0 to to to to to to 750 Figure 2: The 180 countries included in our analysis (color by estimated per-capita tuberculosis incidence) Summary of differences from previous work The largest difference is the set of countries to which the method is applied. Here, we apply the model to a set of 180 countries and use tuberculosis data from 2014; whereas in our previously published report (see reference in main article), we considered only the 22 highest burden tuberculosis countries (HBCs), using data largely from We only consider the community model of infection in this work, as data to inform the household method were not available for a large enough number of countries. We also shifted from using the latitude of a country s capital to the latitude of a country s centroid in the model variant with latitude variation in BCG efficacy. 5
28 Analysis of drug-resistance patterns Data availability by region first line resistance data FALSE TRUE Figure 3: Countries with data on resistance to first-line anti-tuberculosis drugs in new cases second line resistance data FALSE TRUE Figure 4: Countries with data resistance to second-line anti-tuberculosis drugs. 6
29 7 Nearest neighbor construction & interpretation of survey data Figure 5: Ranked implied design effects in survey data on MDR in new cases based on reported confidence intervals and sample size. Red line at 1. Figure 6: The network of 5 nearest-neighbors used for imputing drug resistance patterns for countries without data Sorted survey Estimated design effect
30 WHO regions used The three key differences between the two sets of regions are (i) the split between Central and Eastern Europe based on well-studied and known differences in MDR-TB epidemiology, (ii) the separate region of high-income countries across the world who are expected to have stronger health systems that are closer to universal health coverage (considered proxy for lower levels of acquired drug resistance), and (iii) the split of the African region into high and low HIV prevalence (HIV being a key determinant of TB burden). The nine epidemiological regions are African countries with high HIV prevalence, African countries with low HIV prevalence, Central Europe, Eastern Europe, high-income countries, Latin America, the Eastern Mediterranean Region (excluding high-income countries), the South-East Asia Region (excluding high-income countries) and the Western Pacific Region (excluding highincome countries). WHO regions AFR AMR EMR EUR SEA WPR Figure 7: Map of standard WHO regions 8
31 epi regions AFRhigh AFRlow CEUR EEUR EME EMR LAC Not included SEAR WPR Figure 8: Map of WHO epidemiological regions used for resampling scheme. Missing data With complete data on the counts of susceptible, HMR, RMR, and MDR tuberculosis we assumed a # (i.e. flat) prior on the proportions. Since this is conjugate to the multinomial distribution, the posterior was therefore #. When, additionally (and e.g.) data was available on the total count, and the number MDR ( all missing due to incomplete DST), we sampled from the posterior summing over all possible unobserved missing counts compatible with the total. In effect, this amounts to a draw from a mixture of Dirichlet distributions. In combination # Gibbs sampling was used to sample from these distributions using every 30 th draw in a chain of 30,000 iterations (after a burn-in of 1,000 iterations). Other combinations of missing drug resistance counts described in the article were handled analogously. 9
32 Source of data for country estimates Data sources for 1st line DR estimates neighbour regional self Not included Figure 9: Source of data for each country used in first-line drug-resistance estimates Data sources for 2nd line DR estimates neighbour regional self Not included Figure 10: Source of data for each country used in second-line drug-resistance estimates 10
33 Supplementary results Tables Table 1: Percentage of incident tuberculosis in children by resistance type in IQR in brackets. # %& %()& +%,( )&./ )0%0 1& ) /2) # %& %()& 345 +%,( )&./ )0%0 1& ) /2) S INH RIF MDR MDR# FQR SLR XDR AFR 91.6 [ ] 4.9 [ ] 0.9 [ ] 2.5 [ ] 80.5 [ ] 7.2 [ ] 8.8 [ ] 3.0 [ ] AMR 92.9 [ ] 4.7 [ ] 0.4 [ ] 2.0 [ ] 56.7 [ ] 11.1 [ ] 20.9 [ ] 9.9 [ ] EMR 85.1 [ ] 8.7 [ ] 1.7 [ ] 4.3 [ ] 65.2 [ ] 19.2 [ ] 9.1 [ ] 5.6 [ ] EUR 70.9 [ ] 11.9 [ ] 1.3 [ ] 15.8 [ ] 48.0 [ ] 17.4 [ ] 23.1 [ ] 8.0 [ ] SEA 89.9 [ ] 7.3 [ ] 0.6 [ ] 2.2 [ ] 60.9 [ ] 17.1 [ ] 18.8 [ ] 3.1 [ ] WPR 84.4 [ ] 10.5 [ ] 1.2 [ ] 3.9 [ ] 55.3 [ ] 25.0 [ ] 12.4 [ ] 7.0 [ ] GLOBAL 89.3 [ ] 6.9 [ ] 0.9 [ ] 2.9 [ ] 65.9 [ ] 15.4 [ ] 13.8 [ ] 4.7 [ ]
34 Table 2: Estimates of incident tuberculosis in children under 5 by drug resistance type and WHO region, Total Estimates of incident tuberculosis in children <5 by drug resistance type Estimates of incident MDR-tuberculosis in children <5 by drug resistance type DS HMR RMR MDR MDR# FQR SLR XDR AFR 181,000 [113, ,000] 166,000 [104, ,000] 9,030 [5,600-13,900] 1,560 [968-2,390] 4,380 [2,720-6,790] 3,500 [2,150-5,430] 304 [ ] 376 [ ] 130 [78-210] AMR 12,100 [7,750-18,600] 11,200 [7,210-17,300] 564 [ ] 56 [33-92] 253 [ ] 139 [84-219] 28 [16-46] 53 [31-87] 25 [15-41] EMR 38,400 [24,300-58,000] 32,700 [20,700-49,200] 3,320 [2,110-5,110] 666 [399-1,070] 1,680 [1,050-2,610] 1,080 [671-1,660] 322 [ ] 152 [89-257] 95 [55-159] EUR 6,770 [4,170-10,700] 4,790 [2,970-7,510] 815 [499-1,300] 92 [56-146] 1,070 [652-1,730] 496 [ ] 188 [ ] 245 [ ] 86 [52-139] SEA 143,000 [90, ,000] 128,000 [81, ,000] 10,300 [6,500-15,800] 883 [559-1,360] 3,080 [1,940-4,710] 1,810 [1,140-2,780] 521 [ ] 508 [ ] 96 [58-155] WPR 45,900 [29,300-69,400] 38,800 [24,700-58,500] 4,840 [3,080-7,260] 548 [ ] 1,790 [1,140-2,720] 990 [629-1,500] 445 [ ] 221 [ ] 124 [77-189] GLOBAL 435,000 [278, ,000] 389,000 [248, ,000] 29,500 [18,800-44,300] 3,920 [2,510-5,960] 12,700 [8,020-19,000] 8,330 [5,270-12,500] 1,940 [1,210-2,910] 1,720 [1,050-2,680] 596 [ ] 12
Epidemiology of drug-resistant tuberculosis among children and adolescents in South Africa
 Epidemiology of drug-resistant tuberculosis among children and adolescents in South Africa 2005 2010 BK Moore 1, E Anyalechi 1, M van der Walt 2, S Smith 1, L Erasmus 3, J Lancaster 2, S Morris 1, N Ndjeka
Epidemiology of drug-resistant tuberculosis among children and adolescents in South Africa 2005 2010 BK Moore 1, E Anyalechi 1, M van der Walt 2, S Smith 1, L Erasmus 3, J Lancaster 2, S Morris 1, N Ndjeka
Latest developments in WHO estimates of TB disease burden
 Latest developments in WHO estimates of TB disease burden WHO Global Task Force on TB Impact Measurement meeting Glion, 1-4 May 2018 Philippe Glaziou, Katherine Floyd 1 Contents Introduction 3 1. Recommendations
Latest developments in WHO estimates of TB disease burden WHO Global Task Force on TB Impact Measurement meeting Glion, 1-4 May 2018 Philippe Glaziou, Katherine Floyd 1 Contents Introduction 3 1. Recommendations
Epidemiology and diagnosis of MDR-TB in children H Simon Schaaf
 Epidemiology and diagnosis of MDR-TB in children H Simon Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health, Stellenbosch University, and Tygerberg Children s Hospital (TCH) Definitions
Epidemiology and diagnosis of MDR-TB in children H Simon Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health, Stellenbosch University, and Tygerberg Children s Hospital (TCH) Definitions
MDR-TB preventive treatment considerations. HS Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health Stellenbosch University
 MDR-TB preventive treatment considerations HS Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health Stellenbosch University Conflict of interest disclosure X I have no Conflict of Interest
MDR-TB preventive treatment considerations HS Schaaf Desmond Tutu TB Centre Department of Paediatrics and Child Health Stellenbosch University Conflict of interest disclosure X I have no Conflict of Interest
The epidemiology of tuberculosis
 The epidemiology of tuberculosis Tuberculosis Workshop Shanghai, 12-22 May 28 Philippe Glaziou World Health Organization Outline Epidemiology refresher Estimates of tuberculosis disease burden Notifications
The epidemiology of tuberculosis Tuberculosis Workshop Shanghai, 12-22 May 28 Philippe Glaziou World Health Organization Outline Epidemiology refresher Estimates of tuberculosis disease burden Notifications
WHAT'S IN A NUMBER? TWO RECENT REPORTS ESTIMATING CHILDHOOD TB CASES.
 WHAT'S IN A NUMBER? TWO RECENT REPORTS ESTIMATING CHILDHOOD TB CASES. Helen Jenkins, Peter Dodd, Andrea Cruz Instructor, Brigham and Women's Hospital, Boston, USA Research Associate, University of Sheffield,
WHAT'S IN A NUMBER? TWO RECENT REPORTS ESTIMATING CHILDHOOD TB CASES. Helen Jenkins, Peter Dodd, Andrea Cruz Instructor, Brigham and Women's Hospital, Boston, USA Research Associate, University of Sheffield,
What is new in WHO-guidelines relevant for childhood TB?
 Photo: Riccardo Venturi What is new in WHO-guidelines relevant for childhood TB? Dr Malgosia Grzemska Coordinator, Technical Support, Stop TB Department World Health Organization, Geneva, Switzerland 12th
Photo: Riccardo Venturi What is new in WHO-guidelines relevant for childhood TB? Dr Malgosia Grzemska Coordinator, Technical Support, Stop TB Department World Health Organization, Geneva, Switzerland 12th
Multidrug-resistant tuberculosis in children
 Multidrug-resistant tuberculosis in children James Seddon Clinical Lecturer Imperial College London UCL-TB and LSHTM TB Centre World TB Day 2015 24th March 2015 Outline Burden Recent studies Preventive
Multidrug-resistant tuberculosis in children James Seddon Clinical Lecturer Imperial College London UCL-TB and LSHTM TB Centre World TB Day 2015 24th March 2015 Outline Burden Recent studies Preventive
Recognizing MDR-TB in Children. Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention February 2016
 Recognizing MDR-TB in Children Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention 17-18 February 2016 Objectives Review the definitions and categorization of drugresistant tuberculosis Understand the
Recognizing MDR-TB in Children Ma. Cecilia G. Ama, MD 23 rd PIDSP Annual Convention 17-18 February 2016 Objectives Review the definitions and categorization of drugresistant tuberculosis Understand the
Principle of Tuberculosis Control. CHIANG Chen-Yuan MD, MPH, DrPhilos
 Principle of Tuberculosis Control CHIANG Chen-Yuan MD, MPH, DrPhilos Estimated global tuberculosis burden 2015 an estimated 10.4 million incident cases of TB (range, 8.7 million 12.2 million) 142 cases
Principle of Tuberculosis Control CHIANG Chen-Yuan MD, MPH, DrPhilos Estimated global tuberculosis burden 2015 an estimated 10.4 million incident cases of TB (range, 8.7 million 12.2 million) 142 cases
511,000 (57% new cases) ~50,000 ~30,000
 Latest global TB estimates - 2007 (Updated Mar 2009) All forms of TB Greatest number of cases in Asia; greatest rates per capita in Africa Multidrug-resistant TB (MDR-TB) Estimated number of cases 9.27
Latest global TB estimates - 2007 (Updated Mar 2009) All forms of TB Greatest number of cases in Asia; greatest rates per capita in Africa Multidrug-resistant TB (MDR-TB) Estimated number of cases 9.27
Global epidemiology of drug-resistant tuberculosis. Factors contributing to the epidemic of MDR/XDR-TB. CHIANG Chen-Yuan MD, MPH, DrPhilos
 Global epidemiology of drug-resistant tuberculosis Factors contributing to the epidemic of MDR/XDR-TB CHIANG Chen-Yuan MD, MPH, DrPhilos By the end of this presentation, participants would be able to describe
Global epidemiology of drug-resistant tuberculosis Factors contributing to the epidemic of MDR/XDR-TB CHIANG Chen-Yuan MD, MPH, DrPhilos By the end of this presentation, participants would be able to describe
Paediatric TB: disease burden estimation and the opportunities it creates to strengthening surveillance
 Paediatric TB: disease burden estimation and the opportunities it creates to strengthening surveillance Workshop 04 44 th Union World Conference on Lung Health Paris, 31 October, 2013 GLOBAL TB PROGRAMME
Paediatric TB: disease burden estimation and the opportunities it creates to strengthening surveillance Workshop 04 44 th Union World Conference on Lung Health Paris, 31 October, 2013 GLOBAL TB PROGRAMME
What can be done against XDR-TB?
 What can be done against XDR-TB? Dr Matteo Zignol Stop TB Dep. World Health Organization Geneva 16 th Swiss Symposium on tuberculosis Münchenwiler, 22 March 2007 XDR-TB Extensive Drug Resistance XDR =
What can be done against XDR-TB? Dr Matteo Zignol Stop TB Dep. World Health Organization Geneva 16 th Swiss Symposium on tuberculosis Münchenwiler, 22 March 2007 XDR-TB Extensive Drug Resistance XDR =
BACKGROUND DOCUMENT 8c. Estimating the incidence of childhood tuberculosis and multidrug-resistant tuberculosis. Prepared by: Helen Jenkins, Ted Cohen
 BACKGROUND DOCUMENT 8c Estimating the incidence of childhood tuberculosis and multidrug-resistant tuberculosis Prepared by: Helen Jenkins, Ted Cohen Questions for discussion 1. Given that our method attempts
BACKGROUND DOCUMENT 8c Estimating the incidence of childhood tuberculosis and multidrug-resistant tuberculosis Prepared by: Helen Jenkins, Ted Cohen Questions for discussion 1. Given that our method attempts
Childhood TB and new TB drugs in the WHO European Region
 Andrei Dadu Carl Cordonnier Maxim Dondiuk Childhood TB and new TB drugs in the WHO European Region Kigali, Rwanda, 09/10/ 2017 Dr Martin van den Boom, MD, MSc PH, WHO Regional Office for Europe, Joint
Andrei Dadu Carl Cordonnier Maxim Dondiuk Childhood TB and new TB drugs in the WHO European Region Kigali, Rwanda, 09/10/ 2017 Dr Martin van den Boom, MD, MSc PH, WHO Regional Office for Europe, Joint
Estimates of TB incidence, prevalence and mortality. Philippe Glaziou Cairo, October 2009
 Estimates of TB incidence, prevalence and mortality Philippe Glaziou Cairo, October 2009 Outline Main sources of information Incidence From incidence to prevalence From incidence to mortality TB/HIV MDR-TB
Estimates of TB incidence, prevalence and mortality Philippe Glaziou Cairo, October 2009 Outline Main sources of information Incidence From incidence to prevalence From incidence to mortality TB/HIV MDR-TB
Annual surveillance report 2016
 Annual surveillance report 216 Acknowledgements The Public Health Agency Northern Ireland gratefully acknowledges all those who contributed to this report, including; physicians, nurses, microbiologists,
Annual surveillance report 216 Acknowledgements The Public Health Agency Northern Ireland gratefully acknowledges all those who contributed to this report, including; physicians, nurses, microbiologists,
Annual surveillance report 2015
 Annual surveillance report 215 Acknowledgements The Public Health Agency Northern Ireland gratefully acknowledges all those who contributed to this report, including; physicians, nurses, microbiologists,
Annual surveillance report 215 Acknowledgements The Public Health Agency Northern Ireland gratefully acknowledges all those who contributed to this report, including; physicians, nurses, microbiologists,
Children as Sentinels for Transmission and Policy Response Mercedes Becerra, ScD
 Children as Sentinels for Transmission and Policy Response Mercedes Becerra, ScD Associate Professor, Harvard Medical School, Boston, MA, USA TB Specialist, Partners In Health, Boston, MA, USA Overview
Children as Sentinels for Transmission and Policy Response Mercedes Becerra, ScD Associate Professor, Harvard Medical School, Boston, MA, USA TB Specialist, Partners In Health, Boston, MA, USA Overview
Management of Multidrug- Resistant TB in Children. Jennifer Furin, MD., PhD. Sentinel Project, Director of Capacity Building
 Management of Multidrug- Resistant TB in Children Jennifer Furin, MD., PhD. Sentinel Project, Director of Capacity Building Objectives To review data on best practices for diagnosis, treatment and prevention
Management of Multidrug- Resistant TB in Children Jennifer Furin, MD., PhD. Sentinel Project, Director of Capacity Building Objectives To review data on best practices for diagnosis, treatment and prevention
TUBERCULOSIS CONTROL IN THE WHO WESTERN PACIFIC REGION In the WHO Western Pacific Region 2002 Report
 TUBERCULOSIS CONTROL IN THE WHO WESTERN PACIFIC REGION 2000 Tuberculosis Control In the WHO Western Pacific Region 2002 Report World Health Organization Office for the Western Pacific Region iii TUBERCULOSIS
TUBERCULOSIS CONTROL IN THE WHO WESTERN PACIFIC REGION 2000 Tuberculosis Control In the WHO Western Pacific Region 2002 Report World Health Organization Office for the Western Pacific Region iii TUBERCULOSIS
Tuberculosis in children: gaps and opportunities
 Tuberculosis in children: gaps and opportunities Mark Nicol Division of Medical Microbiology and Institute for Infectious Diseases and Molecular Medicine, University of Cape Town and National Health Laboratory
Tuberculosis in children: gaps and opportunities Mark Nicol Division of Medical Microbiology and Institute for Infectious Diseases and Molecular Medicine, University of Cape Town and National Health Laboratory
TB epidemic and progress towards the Millennium Development Goals
 Open Forum 4: Key issues in TB Drug Development, August 18, 2010, Addis Ababa, Ethiopia TB epidemic and progress towards the Millennium Development Goals Haileyesus Getahun Stop TB Department, WHO Geneva,
Open Forum 4: Key issues in TB Drug Development, August 18, 2010, Addis Ababa, Ethiopia TB epidemic and progress towards the Millennium Development Goals Haileyesus Getahun Stop TB Department, WHO Geneva,
Multidrug-Resistant TB
 Multidrug-Resistant TB Diagnosis Treatment Linking Diagnosis and Treatment Charles L. Daley, M.D. National Jewish Health University of Colorado Denver Disclosures Chair, Data Monitoring Committee for delamanid
Multidrug-Resistant TB Diagnosis Treatment Linking Diagnosis and Treatment Charles L. Daley, M.D. National Jewish Health University of Colorado Denver Disclosures Chair, Data Monitoring Committee for delamanid
Mathematical modelling approach to estimating TB burden in children Pete Dodd (University of Sheffield) & James Seddon (Imperial College London)
 Mathematical modelling approach to estimating TB burden in children Pete Dodd (University of Sheffield) & (Imperial College London) Wednesday, 1 April 215 Health Economics & Decision Science School of
Mathematical modelling approach to estimating TB burden in children Pete Dodd (University of Sheffield) & (Imperial College London) Wednesday, 1 April 215 Health Economics & Decision Science School of
Title: Meta-analysis of Individual patient Data (IPD) of Patients with INH (mono or poly-drug) Resistant Tuberculosis.
 Title: Meta-analysis of Individual patient Data (IPD) of Patients with INH (mono or poly-drug) Resistant Tuberculosis. Principal Investigator: Dick Menzies, MD Evidence base for treatment of INH resistant
Title: Meta-analysis of Individual patient Data (IPD) of Patients with INH (mono or poly-drug) Resistant Tuberculosis. Principal Investigator: Dick Menzies, MD Evidence base for treatment of INH resistant
Drug Resistant Tuberculosis Biology, Epidemiology and Control Dr. Christopher Dye
 Director of Health Information World Health Organization Geneva 1 1. Why TB patients are treated with drugs 2 Natural history and control of TB Fast 5/1 Slow 5/1 Uninfected Latent Active 1 1 infection/case
Director of Health Information World Health Organization Geneva 1 1. Why TB patients are treated with drugs 2 Natural history and control of TB Fast 5/1 Slow 5/1 Uninfected Latent Active 1 1 infection/case
The United Nations flag outside the Secretariat building of the United Nations, New York City, United States of America
 The United Nations flag outside the Secretariat building of the United Nations, New York City, United States of America Mike Segar / Reuters Executive Summary Context On 26 September 2018, the United Nations
The United Nations flag outside the Secretariat building of the United Nations, New York City, United States of America Mike Segar / Reuters Executive Summary Context On 26 September 2018, the United Nations
TB: A Supplement to GP CLINICS
 TB: A Supplement to GP CLINICS Chapter 10: Childhood Tuberculosis: Q&A For Primary Care Physicians Author: Madhukar Pai, MD, PhD Author and Series Editor What is Childhood TB and who is at risk? India
TB: A Supplement to GP CLINICS Chapter 10: Childhood Tuberculosis: Q&A For Primary Care Physicians Author: Madhukar Pai, MD, PhD Author and Series Editor What is Childhood TB and who is at risk? India
Global Perspective on Transmission: Value in Genotype Mapping of Disease Transmission Dynamics
 Global Perspective on Transmission: Value in Genotype Mapping of Disease Transmission Dynamics Neel R. Gandhi, MD Emory Rollins School of Public Health January 17, 2013 Medical Research Council BMJ 1948
Global Perspective on Transmission: Value in Genotype Mapping of Disease Transmission Dynamics Neel R. Gandhi, MD Emory Rollins School of Public Health January 17, 2013 Medical Research Council BMJ 1948
Selected vaccine introduction status into routine immunization
 Selected introduction status into routine infant immunization worldwide, 2003 This report summarizes the current status of national immunization schedules in 2003, as reported by Member States in the /UNICEF
Selected introduction status into routine infant immunization worldwide, 2003 This report summarizes the current status of national immunization schedules in 2003, as reported by Member States in the /UNICEF
Implementation and scale-up of the Xpert MTB/RIF system for rapid diagnosis of TB and MDR-TB. Global Consultation
 Implementation and scale-up of the Xpert MTB/RIF system for rapid diagnosis of TB and MDR-TB Global Consultation Geneva, 30 November 2010 Mario C. Raviglione, M.D. Director, Stop TB Department WHO, Geneva,
Implementation and scale-up of the Xpert MTB/RIF system for rapid diagnosis of TB and MDR-TB Global Consultation Geneva, 30 November 2010 Mario C. Raviglione, M.D. Director, Stop TB Department WHO, Geneva,
CMH Working Paper Series
 CMH Working Paper Series Paper No. WG5 : 8 Title Interventions to reduce tuberculosis mortality and transmission in low and middle-income countries: effectiveness, cost-effectiveness, and constraints to
CMH Working Paper Series Paper No. WG5 : 8 Title Interventions to reduce tuberculosis mortality and transmission in low and middle-income countries: effectiveness, cost-effectiveness, and constraints to
MDR, XDR and Untreatable Tuberculosis and Laboratory Perspectives. Martie van der Walt TUBERCULOSIS EPIDEMIOLOGY & INTERVENTION RESEARCH UNIT
 TUBERCULOSIS EPIDEMIOLOGY & INTERVENTION RESEARCH UNIT MDR, XDR and Untreatable Tuberculosis and Laboratory Perspectives Martie van der Walt IOM Meeting 15-17 January 2013 introduction 1 min 150 words
TUBERCULOSIS EPIDEMIOLOGY & INTERVENTION RESEARCH UNIT MDR, XDR and Untreatable Tuberculosis and Laboratory Perspectives Martie van der Walt IOM Meeting 15-17 January 2013 introduction 1 min 150 words
Burden of disease from the joint effects of household and ambient Air pollution for 2016
 Burden of disease from the joint effects of household and ambient Air pollution for 2016 v2 May 2018 Summary of results Globally, 7 million deaths were attributable to the joint effects of household (HAP)
Burden of disease from the joint effects of household and ambient Air pollution for 2016 v2 May 2018 Summary of results Globally, 7 million deaths were attributable to the joint effects of household (HAP)
2010 global TB trends, goals How DOTS happens at country level - an exercise New strategies to address impediments Local challenges
 Outline of what it will take Tuberculosis Elimination 25: Global and Local Challenges Anne Fanning, MD November 9, 211 21 global TB trends, goals How DOTS happens at country level - an exercise New strategies
Outline of what it will take Tuberculosis Elimination 25: Global and Local Challenges Anne Fanning, MD November 9, 211 21 global TB trends, goals How DOTS happens at country level - an exercise New strategies
Multidrug-/ rifampicinresistant. (MDR/RR-TB): Update 2017
 Multidrug-/ rifampicinresistant TB (MDR/RR-TB): Update 2017 The global TB situation (1) Estimated incidence, 2016 Estimated number of deaths, 2016 All forms of TB HIV-associated TB Multidrug- / rifampicin-resistant
Multidrug-/ rifampicinresistant TB (MDR/RR-TB): Update 2017 The global TB situation (1) Estimated incidence, 2016 Estimated number of deaths, 2016 All forms of TB HIV-associated TB Multidrug- / rifampicin-resistant
Definitions and reporting framework for tuberculosis 2013 revision. Dennis Falzon Global Forum of Xpert MTB/RIF Implementers Annecy 17 April 2013
 Definitions and reporting framework for tuberculosis 2013 revision Dennis Falzon Global Forum of Xpert MTB/RIF Implementers Annecy 17 April 2013 2-year revision process WHO/HTM/TB/2013.2 2 www.who.int/iris/bitstream/10665/79199/1/9789241505345_eng.pdf
Definitions and reporting framework for tuberculosis 2013 revision Dennis Falzon Global Forum of Xpert MTB/RIF Implementers Annecy 17 April 2013 2-year revision process WHO/HTM/TB/2013.2 2 www.who.int/iris/bitstream/10665/79199/1/9789241505345_eng.pdf
TB surveillance. Philippe Glaziou Dubrovnik, May 2009
 TB surveillance Philippe Glaziou Dubrovnik, May 2009 What are the global TB targets? Outcome targets (World Health Assembly, STB Partnership) Case detection ratio > 70% Treatment success > 85% 2015 Impact
TB surveillance Philippe Glaziou Dubrovnik, May 2009 What are the global TB targets? Outcome targets (World Health Assembly, STB Partnership) Case detection ratio > 70% Treatment success > 85% 2015 Impact
C R E A E. Consortium to Respond Effectively to the AIDS-TB Epidemic. An International Research Partnership
 C R E A E Consortium to Respond Effectively to the AIDS-TB Epidemic An International Research Partnership Supported by the Bill and Melinda Gates Foundation http://www.tbhiv-create.org Overview What is
C R E A E Consortium to Respond Effectively to the AIDS-TB Epidemic An International Research Partnership Supported by the Bill and Melinda Gates Foundation http://www.tbhiv-create.org Overview What is
MULTIDRUG- RESISTANT TUBERCULOSIS. Dean Tsukayama Hennepin County Medical Center Hennepin County Public Health Clinic
 MULTIDRUG- RESISTANT TUBERCULOSIS Dean Tsukayama Hennepin County Medical Center Hennepin County Public Health Clinic I have no relevant financial relationships. Discussion includes off label use of: amikacin
MULTIDRUG- RESISTANT TUBERCULOSIS Dean Tsukayama Hennepin County Medical Center Hennepin County Public Health Clinic I have no relevant financial relationships. Discussion includes off label use of: amikacin
EPIDEMIOLOGY OF TUBERCULOSIS AND the IMPACT ON CHILDREN
 EPIDEMIOLOGY OF TUBERCULOSIS AND the IMPACT ON CHILDREN Anneke C. Hesseling Professor in Paediatrics and Child Health Director: Desmond Tutu TB center Stellenbosch University 11 September 11 th International
EPIDEMIOLOGY OF TUBERCULOSIS AND the IMPACT ON CHILDREN Anneke C. Hesseling Professor in Paediatrics and Child Health Director: Desmond Tutu TB center Stellenbosch University 11 September 11 th International
Diagnosis of drug resistant TB
 Diagnosis of drug resistant TB Megan Murray, MD, ScD Harvard School of Public Health Brigham and Women s Hospital Harvard Medical School Broad Institute Global burden of TB 9 million new cases year 2 million
Diagnosis of drug resistant TB Megan Murray, MD, ScD Harvard School of Public Health Brigham and Women s Hospital Harvard Medical School Broad Institute Global burden of TB 9 million new cases year 2 million
TB disease burden estimation in children: an overview of progress
 TB disease burden estimation in children: an overview of progress Childhood TB subgroup: annual meeting Barcelona, 27 October 2014 Babis Sismanidis sismanidisc@who.int GLOBAL TB PROGRAMME Acknowledgements
TB disease burden estimation in children: an overview of progress Childhood TB subgroup: annual meeting Barcelona, 27 October 2014 Babis Sismanidis sismanidisc@who.int GLOBAL TB PROGRAMME Acknowledgements
Pediatric TB research Barriers and progress
 Pediatric TB research Barriers and progress Ben Marais www.sydney.edu.au/mbi www.tbcre.org.au Global Burden of TB - 2012 Estimated Incidence Estimated number of deaths All forms of TB 8.6 million (8.3
Pediatric TB research Barriers and progress Ben Marais www.sydney.edu.au/mbi www.tbcre.org.au Global Burden of TB - 2012 Estimated Incidence Estimated number of deaths All forms of TB 8.6 million (8.3
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Günther G, Lange C, Alexandru S, et al. Treatment outcomes
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Günther G, Lange C, Alexandru S, et al. Treatment outcomes
Latent tuberculosis infection
 Latent tuberculosis infection Updated and consolidated guidelines for programmatic management ANNEX 3 Values and preferences for the management of latent tuberculosis infection: survey of populations affected
Latent tuberculosis infection Updated and consolidated guidelines for programmatic management ANNEX 3 Values and preferences for the management of latent tuberculosis infection: survey of populations affected
Online Annexes (5-8)
 2016 Online Annexes (5-8) to WHO Policy guidance: The use of molecular line probe assay for the detection of resistance to second-line anti-tuberculosis drugs 1 Contents: Annex 5: GRADE summary of findings
2016 Online Annexes (5-8) to WHO Policy guidance: The use of molecular line probe assay for the detection of resistance to second-line anti-tuberculosis drugs 1 Contents: Annex 5: GRADE summary of findings
TB in the SEA Region. Review Plans and Progress. Dr Md Khurshid Alam Hyder Medical Officer TB SEARO/WHO
 TB in the SEA Region Review Plans and Progress Dr Md Khurshid Alam Hyder Medical Officer TB SEARO/WHO The SEA Region: 25% of the world s people, but >33% of TB patients Eastern M editerranean Region 5%
TB in the SEA Region Review Plans and Progress Dr Md Khurshid Alam Hyder Medical Officer TB SEARO/WHO The SEA Region: 25% of the world s people, but >33% of TB patients Eastern M editerranean Region 5%
Assessing the programmatic management of drug-resistant TB
 Assessing the programmatic management of drug-resistant TB a. Review the programmatic management of drug-resistant TB patients with the TB manager. i. What is the size of MDR-TB problem locally? How many
Assessing the programmatic management of drug-resistant TB a. Review the programmatic management of drug-resistant TB patients with the TB manager. i. What is the size of MDR-TB problem locally? How many
: uptake and impact of Xpert MTB/RIF
 Photo: Riccardo Venturi 21-215: uptake and impact of Xpert MTB/RIF Wayne van Gemert WHO Global TB Programme, Geneva Joint Partners Forum for Strengthening and Aligning TB Diagnosis and Treatment 27-3 April
Photo: Riccardo Venturi 21-215: uptake and impact of Xpert MTB/RIF Wayne van Gemert WHO Global TB Programme, Geneva Joint Partners Forum for Strengthening and Aligning TB Diagnosis and Treatment 27-3 April
Online Annexes (5-8)
 Online Annexes (5-8) to WHO Policy guidance: The use of molecular line probe assay for the detection of resistance to second-line anti-tuberculosis drugs THE END TB STRATEGY Online Annexes (5-8) to WHO
Online Annexes (5-8) to WHO Policy guidance: The use of molecular line probe assay for the detection of resistance to second-line anti-tuberculosis drugs THE END TB STRATEGY Online Annexes (5-8) to WHO
Childhood Tuberculosis: Progress Requires Advocacy Strategy Now
 ERJ Express. Published on February 23, 2012 as doi: 10.1183/09031936.00187711 Childhood Tuberculosis: Progress Requires Advocacy Strategy Now Andreas Sandgren 1, Luis E Cuevas 2,*, Masoud Dara 3, Robert
ERJ Express. Published on February 23, 2012 as doi: 10.1183/09031936.00187711 Childhood Tuberculosis: Progress Requires Advocacy Strategy Now Andreas Sandgren 1, Luis E Cuevas 2,*, Masoud Dara 3, Robert
TB & HIV CO-INFECTION IN CHILDREN. Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012
 TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
TB & HIV CO-INFECTION IN CHILDREN Reené Naidoo Paediatric Infectious Diseases Broadreach Healthcare 19 April 2012 Introduction TB & HIV are two of the leading causes of morbidity & mortality in children
The emerging threat of multidrug resistant TB: Global and local challenges and solutions
 Summary of IOM-ASSAf Workshop on: The emerging threat of multidrug resistant TB: Global and local challenges and solutions Salim S. Abdool Karim Pretoria - March, 2010 Why this workshop? Why is it on MDR
Summary of IOM-ASSAf Workshop on: The emerging threat of multidrug resistant TB: Global and local challenges and solutions Salim S. Abdool Karim Pretoria - March, 2010 Why this workshop? Why is it on MDR
Tuberculosis in Wales Annual Report 2015
 Tuberculosis in Wales Annual Report 2015 Author: Communicable Disease Surveillance Centre Date: 10/03/2016 Version: 1 Status: Final Intended Audience: Health Purpose and Summary of Document: This annual
Tuberculosis in Wales Annual Report 2015 Author: Communicable Disease Surveillance Centre Date: 10/03/2016 Version: 1 Status: Final Intended Audience: Health Purpose and Summary of Document: This annual
WHO Global Task Force on TB Impact Measurement An overview
 WHO Global Task Force on TB Impact Measurement An overview Katherine Floyd (WHO/GTB/TME) 3 rd meeting of the TB estimates subgroup Glion-sur-Montreux, 31March 2 April 2015 GLOBAL TB PROGRAMME 1. Broad
WHO Global Task Force on TB Impact Measurement An overview Katherine Floyd (WHO/GTB/TME) 3 rd meeting of the TB estimates subgroup Glion-sur-Montreux, 31March 2 April 2015 GLOBAL TB PROGRAMME 1. Broad
Controlling TB in the era of HIV
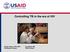 Controlling TB in the era of HIV Christy Hanson, PhD, MPH TB Research Advisor Amy Bloom, MD TB/HIV Advisor TB Incidence rates highest in Africa Estimated new TB cases (all forms) per 100 000 population
Controlling TB in the era of HIV Christy Hanson, PhD, MPH TB Research Advisor Amy Bloom, MD TB/HIV Advisor TB Incidence rates highest in Africa Estimated new TB cases (all forms) per 100 000 population
Costing of the Sierra Leone National Strategic Plan for TB
 Costing of the Sierra Leone National Strategic Plan for TB 2016-2020 Introduction The Government of Sierra Leone established the National Leprosy Control Programme in 1973 with support from the German
Costing of the Sierra Leone National Strategic Plan for TB 2016-2020 Introduction The Government of Sierra Leone established the National Leprosy Control Programme in 1973 with support from the German
Finding the missing TB cases
 Finding the missing TB cases Optimizing strategies to enhance case detection in high HIV burden settings Dr Malgosia Grzemska Global TB Programme, WHO/HQ, Geneva SWITZERLAND Child and Adolescent TB Working
Finding the missing TB cases Optimizing strategies to enhance case detection in high HIV burden settings Dr Malgosia Grzemska Global TB Programme, WHO/HQ, Geneva SWITZERLAND Child and Adolescent TB Working
The WHO Global Project on anti-tb drug resistance surveillance: background, objectives, achievements, challenges, next steps
 The WHO Global Project on anti-tb drug resistance surveillance: background, objectives, achievements, challenges, next steps Matteo Zignol STOP TB Department World Health Organization TB surveillance and
The WHO Global Project on anti-tb drug resistance surveillance: background, objectives, achievements, challenges, next steps Matteo Zignol STOP TB Department World Health Organization TB surveillance and
Change the Game. An agenda for action on childhood tuberculosis
 Change the Game An agenda for action on childhood tuberculosis Four-year-old Nyajime Guet was suffering from severe acute malnutrition (SAM) when she was admitted to a UNICEF-supported clinic a in Juba,
Change the Game An agenda for action on childhood tuberculosis Four-year-old Nyajime Guet was suffering from severe acute malnutrition (SAM) when she was admitted to a UNICEF-supported clinic a in Juba,
Isoniazid Preventive Therapy (IPT)
 Isoniazid Preventive Therapy (IPT) Josefina Cadorna-Carlos, M.D. Professor of Pediatrics U E R M M M C Objectives 1. Define IPT. 2. Discuss the indications for IPT. 3. Present RCT s for IPT (6H vs 9H).
Isoniazid Preventive Therapy (IPT) Josefina Cadorna-Carlos, M.D. Professor of Pediatrics U E R M M M C Objectives 1. Define IPT. 2. Discuss the indications for IPT. 3. Present RCT s for IPT (6H vs 9H).
Latent tuberculosis infection
 EXECUTIVE SUMMARY Latent tuberculosis infection Updated and consolidated guidelines for programmatic management Executive summary Latent tuberculosis infection (LTBI) is defined as a state of persistent
EXECUTIVE SUMMARY Latent tuberculosis infection Updated and consolidated guidelines for programmatic management Executive summary Latent tuberculosis infection (LTBI) is defined as a state of persistent
Global TB control: Current status with particular attention to TB among women and children
 Global TB control: Current status with particular attention to TB among women and children Katherine Floyd Stop TB Department World Health Organization 42 nd Union World Conference on Lung Health Stop
Global TB control: Current status with particular attention to TB among women and children Katherine Floyd Stop TB Department World Health Organization 42 nd Union World Conference on Lung Health Stop
TB/HIV in the WHO European Region Overview, Priorities & Response
 TB/HIV in the WHO European Region Overview, Priorities & Response 16 th Core Group Meeting TB/HIV Working Group Stop TB Partnership Almaty, Kazakhstan May 2010 Martin Donoghoe Andrei Dadu, Smiljka de Lussigny
TB/HIV in the WHO European Region Overview, Priorities & Response 16 th Core Group Meeting TB/HIV Working Group Stop TB Partnership Almaty, Kazakhstan May 2010 Martin Donoghoe Andrei Dadu, Smiljka de Lussigny
Stop TB Working Group on DOTS-Plus for MDR-TB Strategic Plan
 Stop TB Working Group on DOTS-Plus for MDR-TB Strategic Plan 2006-2015 Background Current threat and status of the global epidemic of multidrug resistant tuberculosis (MDR-TB) Along with HIV/AIDS, MDR-TB
Stop TB Working Group on DOTS-Plus for MDR-TB Strategic Plan 2006-2015 Background Current threat and status of the global epidemic of multidrug resistant tuberculosis (MDR-TB) Along with HIV/AIDS, MDR-TB
Global MDR-TB Update GIDC. Paul Nunn, MA, FRCP(UK) Director, Global Infectious Disease Consulting London, UK
 Global MDR-TB Update Paul Nunn, MA, FRCP(UK) Director, Global Infectious Disease Consulting London, UK Acknowledgements Matteo Zignol Mario Raviglione All the WHO staff in drug resistance surveillance
Global MDR-TB Update Paul Nunn, MA, FRCP(UK) Director, Global Infectious Disease Consulting London, UK Acknowledgements Matteo Zignol Mario Raviglione All the WHO staff in drug resistance surveillance
Epidemiology of measles in infants younger than 6 months: analysis of surveillance data
 Epidemiology of measles in infants younger than 6 months: analysis of surveillance data 2011-2016 An analysis of the epidemiology of measles in infants younger than 6 months was conducted by the U.S. CDC
Epidemiology of measles in infants younger than 6 months: analysis of surveillance data 2011-2016 An analysis of the epidemiology of measles in infants younger than 6 months was conducted by the U.S. CDC
Tuberculosis and BCG
 Tuberculosis and BCG Steve Graham Centre for International Child Health University of Melbourne Department of Paediatrics Royal Children s Hospital Melbourne Child Lung Health International Union Against
Tuberculosis and BCG Steve Graham Centre for International Child Health University of Melbourne Department of Paediatrics Royal Children s Hospital Melbourne Child Lung Health International Union Against
M ultidrug resistant (MDR) tuberculosis (TB) has
 1106 ORIGINAL ARTICLE Culture confirmed multidrug resistant tuberculosis: diagnostic delay, clinical features, and outcome H S Schaaf, K Shean, P R Donald... See end of article for authors affiliations...
1106 ORIGINAL ARTICLE Culture confirmed multidrug resistant tuberculosis: diagnostic delay, clinical features, and outcome H S Schaaf, K Shean, P R Donald... See end of article for authors affiliations...
Guidelines for TB contact tracing in Pacific Island countries and territories
 Guidelines for TB contact tracing in Pacific Island countries and territories Background Tuberculosis (TB) continues to be a public health issue of major significance around the world. The World Health
Guidelines for TB contact tracing in Pacific Island countries and territories Background Tuberculosis (TB) continues to be a public health issue of major significance around the world. The World Health
Multidrug- and extensively drug-resistant tuberculosis: a persistent problem in the European Union European Union and European Economic Area
 Rapid communications Multidrug- and extensively drug-resistant tuberculosis: a persistent problem in the European Union European Union and European Economic Area C Ködmön (csaba.kodmon@ecdc.europa.eu)
Rapid communications Multidrug- and extensively drug-resistant tuberculosis: a persistent problem in the European Union European Union and European Economic Area C Ködmön (csaba.kodmon@ecdc.europa.eu)
Global TB Report 2015: Technical appendix on methods used to estimate the global burden of disease caused by TB
 Global TB Report 2015: Technical appendix on methods used to estimate the global burden of disease caused by TB Glaziou P a, Sismanidis C a, Pretorius C b, Timimi H a and Floyd K a a Global TB Programme,
Global TB Report 2015: Technical appendix on methods used to estimate the global burden of disease caused by TB Glaziou P a, Sismanidis C a, Pretorius C b, Timimi H a and Floyd K a a Global TB Programme,
Transmissibility, virulence and fitness of resistant strains of M. tuberculosis. CHIANG Chen-Yuan MD, MPH, DrPhilos
 Transmissibility, virulence and fitness of resistant strains of M. tuberculosis CHIANG Chen-Yuan MD, MPH, DrPhilos Transmissibility, Virulence and Fitness of resistant strains of M. tuberculosis For infectious
Transmissibility, virulence and fitness of resistant strains of M. tuberculosis CHIANG Chen-Yuan MD, MPH, DrPhilos Transmissibility, Virulence and Fitness of resistant strains of M. tuberculosis For infectious
Drug-resistant Tuberculosis
 page 1/6 Scientific Facts on Drug-resistant Tuberculosis Source document: WHO (2008) Summary & Details: GreenFacts Context - Tuberculosis (TB) is an infectious disease that affects a growing number of
page 1/6 Scientific Facts on Drug-resistant Tuberculosis Source document: WHO (2008) Summary & Details: GreenFacts Context - Tuberculosis (TB) is an infectious disease that affects a growing number of
Guidance on Matching Funds: Tuberculosis Finding the Missing People with TB
 February 2017 Guidance on Matching Funds: Tuberculosis Finding the Missing People with TB 1. Background TB is the leading cause of death by infectious disease, killing 1.8 million people in 2015. Each
February 2017 Guidance on Matching Funds: Tuberculosis Finding the Missing People with TB 1. Background TB is the leading cause of death by infectious disease, killing 1.8 million people in 2015. Each
Why can t we eliminate tuberculosis?
 Why can t we eliminate tuberculosis? Neil W. Schluger, M.D. Professor of Medicine, Epidemiology and Environmental Health Sciences Columbia University Chief Scientific Officer World Lung Foundation Current
Why can t we eliminate tuberculosis? Neil W. Schluger, M.D. Professor of Medicine, Epidemiology and Environmental Health Sciences Columbia University Chief Scientific Officer World Lung Foundation Current
Background paper number 5
 Background paper number 5 Assessing the quality and coverage of surveillance data in the UK: how is it done and how can HPA help to develop the Task Force framework for assessment of surveillance data,
Background paper number 5 Assessing the quality and coverage of surveillance data in the UK: how is it done and how can HPA help to develop the Task Force framework for assessment of surveillance data,
Programmatic management of LTBI : a two pronged approach for ending the TB epidemic. Haileyesus Getahun Global TB Programme WHO/HQ
 Programmatic management of LTBI : a two pronged approach for ending the TB epidemic Haileyesus Getahun Global TB Programme WHO/HQ What is latent TB infection? A state of persistent immune response to stimulation
Programmatic management of LTBI : a two pronged approach for ending the TB epidemic Haileyesus Getahun Global TB Programme WHO/HQ What is latent TB infection? A state of persistent immune response to stimulation
1. TIME. TIME comprises two models:
 1. TIME TIME comprises two models: TIME Estimates: This module is used for producing estimated and projected values for key TB indicators. These TB indicators include: TB incidence (particularly its split
1. TIME TIME comprises two models: TIME Estimates: This module is used for producing estimated and projected values for key TB indicators. These TB indicators include: TB incidence (particularly its split
Latent TB Infection in the WHO European Region and recommendations on LTBI s M&E framework
 Latent TB Infection in the WHO European Region and recommendations on LTBI s M&E framework 18 th Wolfheze workshops / 15 th NTP managers meeting, 31 May 02 June 2017 Dr Andrei DADU Technical officer, Joint
Latent TB Infection in the WHO European Region and recommendations on LTBI s M&E framework 18 th Wolfheze workshops / 15 th NTP managers meeting, 31 May 02 June 2017 Dr Andrei DADU Technical officer, Joint
INTENSIFIED TB CASE FINDING
 INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
INTENSIFIED TB CASE FINDING My friends call me Intensified Case Finding (ICF) I undertake regularly screening all people with, or at high risk of HIV, for symptoms of TB in health care facilities, communities
HIV and Tuberculosis in Eastern Europe
 HIV and Tuberculosis in Eastern Europe Daria N. Podlekareva Meeting Standard of Care for HIV and Coinfections in Europe Rome, November 25-16 2014 TB notification rates (per 100.000) European region 2012
HIV and Tuberculosis in Eastern Europe Daria N. Podlekareva Meeting Standard of Care for HIV and Coinfections in Europe Rome, November 25-16 2014 TB notification rates (per 100.000) European region 2012
Tuberculosis in Wales Annual Report 2013
 Tuberculosis in Wales Annual Report 2013 Author: Communicable Disease Surveillance Centre Date: 16/12/13 Version: 1 Status: Final Intended Audience: Health Purpose and Summary of Document: This report
Tuberculosis in Wales Annual Report 2013 Author: Communicable Disease Surveillance Centre Date: 16/12/13 Version: 1 Status: Final Intended Audience: Health Purpose and Summary of Document: This report
The WHO END-TB Strategy
 ENDING TB and MDR-TB The WHO END-TB Strategy Dr Mario RAVIGLIONE Director Joint GDI/GLI Partners Forum WHO Geneva, 27 April 2015 This talk will deal with TB Burden Progress, Challenges Way Forward Who
ENDING TB and MDR-TB The WHO END-TB Strategy Dr Mario RAVIGLIONE Director Joint GDI/GLI Partners Forum WHO Geneva, 27 April 2015 This talk will deal with TB Burden Progress, Challenges Way Forward Who
The treatment of patients with initial isoniazid resistance
 The treatment of patients with initial isoniazid resistance 2011 INTERTB Meeting, St George s, London Patrick Phillips, MRC Clinical Trials Unit DA Mitchison, AJ Nunn. 21 st October 2011 Outline Background
The treatment of patients with initial isoniazid resistance 2011 INTERTB Meeting, St George s, London Patrick Phillips, MRC Clinical Trials Unit DA Mitchison, AJ Nunn. 21 st October 2011 Outline Background
Kenya Perspectives. Post-2015 Development Agenda. Tuberculosis
 Kenya Perspectives Post-2015 Development Agenda Tuberculosis SPEAKERS Anna Vassall Anna Vassall is Senior Lecturer in Health Economics at the London School of Hygiene and Tropical Medicine. She is a health
Kenya Perspectives Post-2015 Development Agenda Tuberculosis SPEAKERS Anna Vassall Anna Vassall is Senior Lecturer in Health Economics at the London School of Hygiene and Tropical Medicine. She is a health
GOAL 2: ACHIEVE RUBELLA AND CRS ELIMINATION. (indicator G2.2) Highlights
 GOAL 2: ACHIEVE RUBELLA AND CRS ELIMINATION (indicator G2.2) Highlights As of December 2014, 140 Member States had introduced rubella vaccines; coverage, however, varies from 12% to 94% depending on region.
GOAL 2: ACHIEVE RUBELLA AND CRS ELIMINATION (indicator G2.2) Highlights As of December 2014, 140 Member States had introduced rubella vaccines; coverage, however, varies from 12% to 94% depending on region.
Predicting outcomes and drug resistance with standardised treatment of active tuberculosis
 Eur Respir J 21; 36: 87 877 DOI: 1.1183/931936.15179 CopyrightßERS 21 Predicting outcomes and drug resistance with standardised treatment of active tuberculosis O. Oxlade*,#, K. Schwartzman*,#, M. Pai*,#,
Eur Respir J 21; 36: 87 877 DOI: 1.1183/931936.15179 CopyrightßERS 21 Predicting outcomes and drug resistance with standardised treatment of active tuberculosis O. Oxlade*,#, K. Schwartzman*,#, M. Pai*,#,
NIH Public Access Author Manuscript Int J Tuberc Lung Dis. Author manuscript; available in PMC 2013 August 06.
 NIH Public Access Author Manuscript Published in final edited form as: Int J Tuberc Lung Dis. 2013 May ; 17(5): 624 629. doi:10.5588/ijtld.12.0792. Outcomes of children treated for tuberculosis with second-line
NIH Public Access Author Manuscript Published in final edited form as: Int J Tuberc Lung Dis. 2013 May ; 17(5): 624 629. doi:10.5588/ijtld.12.0792. Outcomes of children treated for tuberculosis with second-line
ANALYSIS AND USE OF HEALTH FACILITY DATA. Guidance for tuberculosis programme managers
 ANALYSIS AND USE OF HEALTH FACILITY DATA Guidance for tuberculosis programme managers WORKING DOCUMENT SEPTEMBER 2018 World Health Organization 2018 All rights reserved. This is a working document and
ANALYSIS AND USE OF HEALTH FACILITY DATA Guidance for tuberculosis programme managers WORKING DOCUMENT SEPTEMBER 2018 World Health Organization 2018 All rights reserved. This is a working document and
Tuberculosis in Wales Annual Report 2014
 Tuberculosis in Wales Annual Report 2014 Author: Communicable Disease Surveillance Centre Date: 20/03/2015 Version: 1 Status: Final Intended Audience: Health Purpose and Summary of Document: This report
Tuberculosis in Wales Annual Report 2014 Author: Communicable Disease Surveillance Centre Date: 20/03/2015 Version: 1 Status: Final Intended Audience: Health Purpose and Summary of Document: This report
ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM
 ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM The form and content of the explanatory note is to: Inform those responsible for completing the DMR 164 Reporting Form - as to
ANNEXURE A: EXPLANATORY NOTES ON THE DMR 164 REPORTING ON HIV AND TB FORM The form and content of the explanatory note is to: Inform those responsible for completing the DMR 164 Reporting Form - as to
REVIEW OF TUBERCULOSIS EPIDEMIOLOGY
 Part I REVIEW OF TUBERCULOSIS EPIDEMIOLOGY 1. 2. 3. Estimated Tuberculosis Burden 7 Tuberculosis Case Notification 10 Prevalence and Tuberculin Surveys 22 PART 1 5 TABLE 1: Latest notification of tuberculosis
Part I REVIEW OF TUBERCULOSIS EPIDEMIOLOGY 1. 2. 3. Estimated Tuberculosis Burden 7 Tuberculosis Case Notification 10 Prevalence and Tuberculin Surveys 22 PART 1 5 TABLE 1: Latest notification of tuberculosis
DRUG RESISTANCE IN TUBERCULOSIS CONTROL. A GLOBAL AND INDIAN SITUATION
 JOURNAL OF PREVENTIVE MEDICINE 2008; 16(3-4): 3-9 Inviting Editorial DRUG RESISTANCE IN TUBERCULOSIS CONTROL. A GLOBAL AND INDIAN SITUATION Harshad Thakur Centre for Health Policy, Planning and Management,
JOURNAL OF PREVENTIVE MEDICINE 2008; 16(3-4): 3-9 Inviting Editorial DRUG RESISTANCE IN TUBERCULOSIS CONTROL. A GLOBAL AND INDIAN SITUATION Harshad Thakur Centre for Health Policy, Planning and Management,
Online Annexes (2-4)
 Online Annexes (2-4) to WHO Policy update: The use of molecular line probe assays for the detection of resistance to isoniazid and rifampicin THE END TB STRATEGY Online Annexes (2-4) to WHO Policy update:
Online Annexes (2-4) to WHO Policy update: The use of molecular line probe assays for the detection of resistance to isoniazid and rifampicin THE END TB STRATEGY Online Annexes (2-4) to WHO Policy update:
Chapter 1 Overview of Tuberculosis Epidemiology in the United States
 Chapter 1 Overview of Tuberculosis Epidemiology in the United States Table of Contents Chapter Objectives.... 1 Progress Toward TB Elimination in the United States... 3 TB Disease Trends in the United
Chapter 1 Overview of Tuberculosis Epidemiology in the United States Table of Contents Chapter Objectives.... 1 Progress Toward TB Elimination in the United States... 3 TB Disease Trends in the United
Population Health Impact and Cost-Effectiveness of Tuberculosis Diagnosis with Xpert MTB/RIF: A Dynamic Simulation and Economic Evaluation
 Population Health Impact and Cost-Effectiveness of Tuberculosis Diagnosis with Xpert MTB/RIF: A Dynamic Simulation and Economic Evaluation The Harvard community has made this article openly available.
Population Health Impact and Cost-Effectiveness of Tuberculosis Diagnosis with Xpert MTB/RIF: A Dynamic Simulation and Economic Evaluation The Harvard community has made this article openly available.
