determine need but regimen does not change based on risk factor ED medicine attending meets
|
|
|
- Arabella French
- 5 years ago
- Views:
Transcription
1 HIV PEP Guidelines after Sexual Assault Harborview Medical Center January 2015 Initial risk assessment and discussion with patient about risk and PEP is by clinician who does exam (SANE, Ob-Gyn resident, pediatrics resident.) ED Medicine attending meets with all patients in Low to moderate risk category, and with any patient in other risk categories who wishes to talk about or consider HIV PEP. Follow-up: All patients who start PEP will have follow-up through Madison Clinic. Leave voice message with Madison Clinic PCC ( ) who will arrange appointment. Medication: Patient needs 5 days of medication in hand when leaving ED. Dispense from Pyxis. Risk factors of assailant Risk factors of contact Time since contact HIV PEP Regimen Lowest risk HIV PEP not indicated Ongoing unprotected sexual contact (e.g. intimate partner) No semen to mucosal or wound contact PEP not indicated Very low risk Option of PEP should be discussed with patient by medical provider (SANE). PEP may be prescribed if patient wishes after full discussion of risks/benefits Assailant is: Man who has sex with women OR Unknown risk factors Note: man who has been recently incarcerated has same risk as general male population (<1%) Semen to mucosal contact, one assailant Low to moderate risk Recommendation for PEP should be discussed with patient, with full discussion of risks and benefits Assailant is: Man known or suspected HIV positive (most important factor) Man who has sex with men (HIV prevalence 12-15%) Known IV drug use (HIV prevalence ~2%) (prevalence in King County) Semen to mucosal contact, 2 or more assailants Victim is man assaulted by man Victim has grossly visible vaginal or anal tears Exposure semen to rectum Exposure blood to mucosa Exposure blood to open wound PEP must be initiated within 72 hours of exposure Risk factor is used to help determine need but regimen does not change based on risk factor Updated Regimen: for any patient requesting HIV PEP Truvada 1 tab po daily plus Raltegravir 400mg BID First 5 days of 28 day course is given in ED Patient Ed Discussion with patient Use Information about HIV for Patients attached Use condoms for consensual relations for 6 months Advise ED medicine attending meets HIV serology may patient to discuss PEP if patient be obtained at f/u is interested medical, 6 wks, 3 Advise: HIV serology should be and 6 months obtained at 6 wks, 3 and 6 mo If using Antibody/Antigen testing, testing done at 6 weeks and 16 weeks Full course is 28 days Reevaluate at Madison Clinic follow-up ED Medicine Attending meets all patients in this risk category to discuss HIV PEP HIV PEP after sexual assault update March
2 If patient is appropriate candidate for medication, discuss: 28 days medication course needed. 5 days of medication will be provided in ED. Must come to Madison Clinic appointment within 4 days for evaluation of medication and decision to complete course (see below for how to arrange appt) Costs: Crime Victims Compensation may cover cost medication, but only if patient applies for CVC (to qualify pt must cooperate with law enforcement, assault must have occurred in Washington state.). Patient may qualify for charity care, or insurance may cover costs. Med should be obtained at HMC unless pt has insurance. Baseline labs if patient starts PEP Pregnancy test if positive, Truvada, and Raltegravir are safe in pregnancy. Weigh the risks and benefits Urine NAAT for chlamydia and gonorrhea HIV antibody/antigen CBC platelets Creatinine Liver function panel (Hepatic panel A) RPR Medications Prescribe usual post-exposure medications: Azithromycin 1 gm, Cefixime 400 mg (Ceftriaxone 250 mg IM for MSM patients) and Hepatitis B vaccine if not previously fully immunized. Levonorgestrel emergency contraception as indicated. Standard regimen: Truvada 1 tablet daily (tenofovir 300 mg + emtricitabine 200 mg) + Raltegravir (brand name Isentress) 400 mg BID Generally well-tolerated May cause nausea, vomiting, diarrhea, flatulence, headache, renal impairment Rare but serious lactic acidosis and hepatic steatosis Safe in pregnancy (Category B). There are potential significant interactions with rifampin May cause diarrhea, nausea, vomiting Discuss before administering to patients with o Hx of liver problems o Hx of rhabdomyolysis or myopathy o Increased creatinine kinase o Hx of PKU (Raltegravir chewables contain phenylalanine) Consult with infectious disease specialist to choose alternate meds if source patient is taking antiretroviral. May call HIV MedCon (attending provider) if any questions regarding treatment Providing initial doses Provide initial 5-day supply from HMC Pharmacy. Follow-up For sexual assault patients only HIV PEP after sexual assault update March
3 TC to Madison clinic to inform of pt s name and need for follow up visit (confirm correct contact number of patient to leave on Madison clinic voice mail) Medical follow-up will be at Madison (initially in 2-4 days, and 6 weeks) All patients will get social work outreach call from HCSATS Counseling follow-up will be at HCSATS (if patient wishes) Resources on drug interactions: Harborview Madison Clinic Pharmacy ( ) and This guideline was developed and approved by: Amy Baernstein MD Attending physician Emergency Department Harborview Medical Center. Associate Professor, Medicine/General Internal Medicine University of Washington. Shireesha Dhanireddy MD Attending physician Madison Clinic Harborview Medical Center Associate Professor, Allergy & Infectious Diseases, University of Washington. Robert Harrington MD Professor Allergy and Infectious Disease University of Washington, Madison Clinic Harborview Medical Center Naomi Sugar MD Medical Director, Harborview Center for Sexual Assault and Traumatic Stress. Clinical Professor Pediatrics, University of Washington. HIV PEP after sexual assault update March
4 Risk of Transmision Do not over-prescribe HIV PEP Do not prescribe PEP if blood contacted only intact skin. Do not prescribe PEP for exposures to: Saliva (unless visibly bloody) Sweat Tears Vomit Feces Urine Nasal secretions Information for Providers even if these contacted mucous membrane or non-intact skin. Do not prescribe PEP for bites, unless source person s mouth was bloody AND exposed person s skin was visibly broken. Estimated per-act for acquisition of HIV from HIV + source, by exposure route 1 Action Predicted conversions per 10,000 acts Blood transfusion 9000 Needle sharing 67 (0.67 per 100 exposures with HIV+ source) Receptive anal intercourse 50 Needle stick 30 Receptive penile- vaginal intercourse 10 (0.1 per 100 exposures with HIV + source) Blood to mucous membranes 9 Insertive anal intercourse 6.5 Insertive penile vaginal intercourse 5 Receptive oral intercourse 1 (.01 per 100 exposures with HIV+ source) Man receiving oral sex 0.5 Risk that source patient is HIV+ (for King County) General population: < 1% Incarcerated men ~ 1% Injection drug users 2% Men who have sex with men: 12-15% Man who has sex with men and and injection drug use: 22% References 1. CDC Antiretroviral Postexposure Prophylaxis after sexual, injection-drug use, or other nonoccupational exposure to HIV in the United States. MMWR Reports and recommendations 2005; 54 (No. RR-2). 2. CDC Updated U.S. Public Health Service Guidelines for the Management of Occupational Exposures 3. to HIV and Recommendations for Postexposure Prophylaxis 2005 ; Vol. 54 (No. RR-9) 4. Garcia MT, Figueriredo RM, Moretti ML, Resende MR, Bedoni AJ, Papaiordanou. Postexposure prophylaxis after sexual assaults: a prospective cohort study. Sex Transm Dis Apr; 32(4): Wiebe ER, Comay SE, McGregor M, Ducceschi S. Offering HIV prophylaxis to people who have been sexually assaulted: 16 months' experience in a sexual assault service. CMAJ Mar 7;162(5): HIV PEP after sexual assault update March
5 Case Examples 1. Woman assaulted by male acquaintance, risk factors of male unknown. Penile-vaginal and penile-oral contact, no condom, no visible genital anal injuries. Assessment: Very low risk Action: Option of PEP should be discussed with patient Who: By medical provider (SANE), ED medicine attending if patient wishes medication. Treatment: PEP may be prescribed if patient wishes after full discussion of risks/ Basic regimen. 2. Woman assaulted by male acquaintance, risk factors of male unknown. Penile-vaginal, penile-oral, and penile-anal contact, no condom, no visible genital anal injuries. Assessment: Low to moderate risk. Treatment: Basic regimen is appropriate, depending on clinician judgment and patient preference. 3. Woman assaulted by male acquaintance, Man thought to be an IV drug user, unknown other risk factors. Penile vaginal contact only Assessment: Low to moderate risk Treatment: Basic regimen OR expanded regimen may be appropriate, depending on clinician judgment and patient preference. 4. Woman assaulted by 2 males 4 days prior to exam Assessment: outside of time frame for HIV PEP Action: Discuss with patient Who: Initial discussion by primary examiner, ED Medicine attending should meet with patient to discuss if further questions Treatment: No HIV PEP medication. Recommend baseline, 6 weeks 3 months and 6 month HIV serology. Baseline serology can be done at HCSATS follow-up. 4. Woman assaulted by male 24 hours ago. Penile-oral and penile-vaginal contact, condom used. Visible posterior fourchette tear. Assessment: Low to moderate risk Treatment: Basic regimen appropriate, 5. Male assaulted by male stranger. Unknown other risk factors. Penile-oral contact only. No mouth lesions. Assessment: Low to moderate risk (although contact is very low risk, but assailant is likely MSM, risk of HIV in assailant is higher than average) Treatment: Basic regimen OR expanded regimen may be appropriate, depending on clinician judgment and patient preference. 5. Male assaulted by male stranger. Risk factors unknown. Penile-oral and penile-anal contact. Assessment: Low to moderate risk. HIV PEP after sexual assault update March
6 Treatment: Basic regimen OR expanded regimen may be appropriate, depending on clinician judgment and patient preference. INFORMATION ABOUT HIV FOR PATIENTS HIV (human immunodeficiency virus) is the virus which can cause AIDS. Getting HIV is often a fear that people have after a sexual assault. For most individuals the risk of getting HIV from a sexual assault in Washington State is extremely low. For women the risk is less than 1 in An assailant must be infected with HIV in order to transmit it. If the assailant were HIV-infected, it is estimated that there is a less than 3% chance of transmitting it during sexual assault. In the Pacific Northwest, the rate of HIV infection in the male population is about 1 to 2 %. Most men who have HIV are homosexually active. The rate of HIV infection in injection drug users is approximately 2%. Medicines are available which can decrease the risk of acquiring HIV. The medicines must be started within 72 hours of the exposure and taken for 28 days month in order to be effective. These medications can cause mild gastrointestinal symptoms (nausea, diarrhea, fatigue, and muscle aches) and are not recommended in very low risk situations. For men who have been sexually assaulted by men there is a higher, although still small chance of getting HIV. About 1 in 7 gay men in Seattle are HIV+, but the risk of HIV transmission, even without condoms is around 1%. Under these circumstances, the risks and benefits of preventive medicine should be discussed with a health care provider. The risk of HIV infection is quite low. But this was not a risk that you chose to take. If you wish, you can get blood testing for HIV at your follow-up appointment. A repeat test is needed 6 weeks and 3 months later in order to know for certain that you have not been infected, and a final test can be done 6 months after the assault. During this time, it is important to use condoms for all voluntary sexual relations. HIV PEP after sexual assault update March
TO DECREASE THE CHANCE OF GETTING
 POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
POST ASSAULT MEDICATIONS Terri Stewart RN Naomi Sugar MD TO DECREASE THE CHANCE OF GETTING Pregnant STDs Chlamydia Gonorrhea Trichomonas Hep B HIV EMERGENCY CONTRACEPTION Plan B Levonorgestrel PLAN B Plan
FAMILY HIV CENTER NJ CARES SANE
 HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
HIV, Hepatitis B & C Postexposure Prophylaxis for Sexual Assault Victims Update for Case Managers Susan Burrows-Clark, RN, MSN, CNS, C. 10/17/11 Antiretroviral Postexposure Prophylaxis After Sexual, Injection-Drug
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft:
 Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
Guidelines for Implementing Pre-Exposure Prophylaxis For The Prevention of HIV in Youth Peter Havens, MD MS Draft: 10-2-2015 Clinical studies demonstrate that when a person without HIV infection takes
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: NON- OCCUPATIONAL EXPOSURE TO BLOOD-BORNE PATHOGENS (HIV, Hepatitis B, AND Hepatitis C)
 General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
General Definition: Blood-borne pathogens are infectious agents that can be transmitted through contact with blood or certain other body fluids. The primary pathogens are HIV, Hepatitis B, and C. Before
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
An International Antiviral Society-USA
 Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
Doug Campos-Outcalt, MD, MPA University of Arizona, Phoenix dougco@email.arizona. edu A look at new guidelines for HIV treatment and prevention Start antiretroviral therapy as soon as possible after HIV
Post-Sexual Exposure Prophylaxis (npep)
 Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Projeto Praça Onze Universidade Federal do Rio de Janeiro Post-Sexual Exposure Prophylaxis (npep) Mauro Schechter Principal Investigator, Projeto Praça Onze Professor of Infectious Diseases Universidade
Non-Occupational Post-Exposure HIV Prophylaxis npep
 Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
Non-Occupational Post-Exposure HIV Prophylaxis npep Peter Meacher MD (Chief Medical Officer) Anthony Vavasis MD (Director of Medicine) Callen-Lorde Community Health Center Objectives - at the end of the
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
PREVENTION OF HIV IN THE TIMES OF PREP. Daniela Chiriboga, MD Florida Department of Health in Polk County
 PREVENTION OF HIV IN THE TIMES OF PREP Daniela Chiriboga, MD Florida Department of Health in Polk County MAKING THE CASE FOR PREVENTION The Epidemic in Florida Population in 2014: 19.6 million (3 rd in
PREVENTION OF HIV IN THE TIMES OF PREP Daniela Chiriboga, MD Florida Department of Health in Polk County MAKING THE CASE FOR PREVENTION The Epidemic in Florida Population in 2014: 19.6 million (3 rd in
Blood-Borne Pathogens and Post-Exposure Prophylaxis
 Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Blood-Borne Pathogens and Post-Exposure Prophylaxis Christopher Behrens MD Northwest Association of Occupational and Environmental Medicine October 2017 with thanks to Shireesha Dhanireddy MD Disclosures
Chapter 67 Sexual Assault Episode Overview. Rosen s in Perspective. Crack Cast Show Notes Sexual Assault March
 Chapter 67 Sexual Assault Episode Overview 1) What precautions should be taken prior to engaging in potential sexual abuse cases? 2) What information can be useful in determining the location and likelihood
Chapter 67 Sexual Assault Episode Overview 1) What precautions should be taken prior to engaging in potential sexual abuse cases? 2) What information can be useful in determining the location and likelihood
MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE
 Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
Sandyford Protocols MANAGEMENT OF SEXUAL EXPOSURE TO HIV: PEPSE www.hiv-druginteractions.org If you require information on occupational exposure to blood borne viruses, including HIV, please refer to the
PrEP and npep for HIV Prevention. Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine
 PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
PrEP and npep for HIV Prevention Harry Rosado-Santos MD, FACP Associate Professor UU School of Medicine Case Study A 26 y/o M presents for routine asymptomatic screening for sexually transmitted infections
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Non-occupational HIV Post Exposure Prophylaxis (npep)
 Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
Mountain West AIDS Education and Training Center Non-occupational HIV Post Exposure Prophylaxis (npep) Robert Harrington, M.D. This presentation is intended for educational use only, and does not in any
Postexposure prophylaxis (PEP)
 Postexposure Prophylaxis Against Human Immunodeficiency Virus MICHAEL A. TOLLE, MD, MPH, and HEIDI L. SCHWARZWALD, MD, MPH, Baylor College of Medicine, Houston, Texas Family physicians often encounter
Postexposure Prophylaxis Against Human Immunodeficiency Virus MICHAEL A. TOLLE, MD, MPH, and HEIDI L. SCHWARZWALD, MD, MPH, Baylor College of Medicine, Houston, Texas Family physicians often encounter
CCC Guidance for Pediatric HIV PEP Outside of the Perinatal Period
 CCC Guidance for Pediatric HIV PEP Outside of the Perinatal Period There are currently no published guidelines for post-exposure prophylaxis from the CDC/PHS specific to the pediatric population. This
CCC Guidance for Pediatric HIV PEP Outside of the Perinatal Period There are currently no published guidelines for post-exposure prophylaxis from the CDC/PHS specific to the pediatric population. This
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
SFAF CLINICAL PROTOCOLS
 SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
SFAF CLINICAL PROTOCOLS Page 1 of Supersedes Date: December 31, 2016 Original Date: August 20, 2014 Version: 03 Policy Section: Patient Care Non-Occupational Post Exposure Prophylaxis Program Back ground:
CARE PRESENTATION. Diana Arriola, M.D. House Officer I
 CARE PRESENTATION Diana Arriola, M.D. House Officer I CASE PRESENTATION 12 y/o F presents to ED 2 days following sexual assault by 2 male individuals (16y/o and 19 y/o) both involving penile-vaginal and
CARE PRESENTATION Diana Arriola, M.D. House Officer I CASE PRESENTATION 12 y/o F presents to ED 2 days following sexual assault by 2 male individuals (16y/o and 19 y/o) both involving penile-vaginal and
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
PrEP for HIV Prevention. Adult Clinical Guideline from the New York State Department of Health AIDS Institute
 PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
PrEP for HIV Prevention Adult Clinical Guideline from the New York State Department of Health AIDS Institute www.hivguidelines.org Purpose of the PrEP Guideline Raise awareness of PrEP among healthcare
Important Safety Information About Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP)
 Important Safety Information About Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) For Healthcare Providers About Emtricitabine/Tenofovir Disoproxil
Important Safety Information About Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) For Healthcare Providers About Emtricitabine/Tenofovir Disoproxil
Cleveland Prevention Update. Zach Reau HIV Prevention Program Manager Ohio Department of Health
 Cleveland Prevention Update Zach Reau HIV Prevention Program Manager Ohio Department of Health May 21-22, 2018 ODH HIV PREVENTION PROGRAM 2018-2019 Overview Client Services Team Client Services Administrator-
Cleveland Prevention Update Zach Reau HIV Prevention Program Manager Ohio Department of Health May 21-22, 2018 ODH HIV PREVENTION PROGRAM 2018-2019 Overview Client Services Team Client Services Administrator-
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Blood/Body Fluid Exposure Option
 Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Introduction: Transmission of bloodborne pathogens [e.g., Hepatitis B virus (HBV), Hepatitis C virus (HBC), Human Immunodeficiency Virus (HIV)] from patients to healthcare workers (HCW) is an important
Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
 PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
PROPHYLAXISFOLLOWINGHIV, HEPB ANDC EXPOSURES: WHAT SNEW Antonio E. Urbina, M.D. Associate Medical Director Center for Comprehensive Care, West 17 th Street Clinic St. Luke s Roosevelt Hospital DISCLOSURES
Disclosure. Learning Objectives. Epidemiology. Transmission. Risk of Transmission PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION 50,000.
 Disclosure PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION I have no financial interest in and/or affiliation with any external organizations in relation to this CE program. DaleMarie Vaughan, PharmD
Disclosure PRE-EXPOSURE PROPHYLAXIS (PREP) FOR HIV PREVENTION I have no financial interest in and/or affiliation with any external organizations in relation to this CE program. DaleMarie Vaughan, PharmD
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
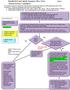 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
POST-EXPOSURE PROPHYLAXIS, PRE-EXPOSURE PROPHYLAXIS, & TREATMENT OF HIV
 POST-EXPOSURE PROPHYLAXIS, PRE-EXPOSURE PROPHYLAXIS, & TREATMENT OF HIV DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none
POST-EXPOSURE PROPHYLAXIS, PRE-EXPOSURE PROPHYLAXIS, & TREATMENT OF HIV DISCLOSURE Relevant relationships with commercial entities none Potential for conflicts of interest within this presentation none
HIV Prevention Pearls
 HIV Prevention Pearls Meghan Rothenberger, MD Assistant Professor Division of Infectious Diseases University of Minnesota Director, Youth and AIDS Projects October 27, 2017 Disclosure Information I have
HIV Prevention Pearls Meghan Rothenberger, MD Assistant Professor Division of Infectious Diseases University of Minnesota Director, Youth and AIDS Projects October 27, 2017 Disclosure Information I have
Important Safety Information About TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication. For Healthcare Providers
 Important Safety Information About TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication For Healthcare Providers About TRUVADA for a PrEP Indication INDICATION AND PRESCRIBING CONSIDERATIONS TRUVADA,
Important Safety Information About TRUVADA for a Pre-exposure Prophylaxis (PrEP) Indication For Healthcare Providers About TRUVADA for a PrEP Indication INDICATION AND PRESCRIBING CONSIDERATIONS TRUVADA,
PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER
 PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER THE NEED FOR CONTINUED HIV PREVENTION Estimated new HIV infections in the US for the most
PREP IN PRIMARY CARE TRACY SALAMEH RN, BSN, ACRN HIV CLINICAL SPECIALIST DAKOTA AIDS EDUCATION AND TRAINING CENTER THE NEED FOR CONTINUED HIV PREVENTION Estimated new HIV infections in the US for the most
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
For People Who Have Been Sexually Assaulted... What You Need To Know about STDs and Emergency Contraception
 For People Who Have Been Sexually Assaulted... What You Need To Know about STDs and Emergency Contraception FOR PEOPLE WHO HAVE BEEN SEXUALLY ASSAULTED What You Need to Know about STDs and Emergency Contraception
For People Who Have Been Sexually Assaulted... What You Need To Know about STDs and Emergency Contraception FOR PEOPLE WHO HAVE BEEN SEXUALLY ASSAULTED What You Need to Know about STDs and Emergency Contraception
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
M F. Interpreter Name
 PATIENT INFORMATION D L V Name Gender M F Age Time Date HMC# Street Address Apt. Phone City State Zip OK to call with msg? Yes No Police Report Made Yes No Accompanied by Contact Person Relationship Relationship
PATIENT INFORMATION D L V Name Gender M F Age Time Date HMC# Street Address Apt. Phone City State Zip OK to call with msg? Yes No Police Report Made Yes No Accompanied by Contact Person Relationship Relationship
People who experience gender based violence are more at risk of HIV.
 Know the HIV risk People who experience gender based violence are more at risk of HIV. HIV Human Immunodeficiency Virus is the virus that causes AIDS by interfering with the body s ability to fight off
Know the HIV risk People who experience gender based violence are more at risk of HIV. HIV Human Immunodeficiency Virus is the virus that causes AIDS by interfering with the body s ability to fight off
Study finds PEP not 100% effective in preventing HIV infection
 From TreatmentUpdate 152 Study finds PEP not 100% effective in preventing HIV infection Some doctors and nurses who care for PHAs may sustain needle-stick injuries. This raises the possibility that they
From TreatmentUpdate 152 Study finds PEP not 100% effective in preventing HIV infection Some doctors and nurses who care for PHAs may sustain needle-stick injuries. This raises the possibility that they
Prophylaxis: Partnering to Improve. Presented by MATEC Malinda Boehler, MSW, LCSW April Grudi, MPH, CHES Pamela Terrill, MS, ARNP, SANE-A
 HIV/STI Screening & Post Exposure Prophylaxis: Partnering to Improve Care Presented by MATEC Malinda Boehler, MSW, LCSW April Grudi, MPH, CHES Pamela Terrill, MS, ARNP, SANE-A Disclosures Malinda Boehler,
HIV/STI Screening & Post Exposure Prophylaxis: Partnering to Improve Care Presented by MATEC Malinda Boehler, MSW, LCSW April Grudi, MPH, CHES Pamela Terrill, MS, ARNP, SANE-A Disclosures Malinda Boehler,
Billing and Coding for HIV Services
 Billing and Coding for HIV Services Financial Disclosure This speaker does not have any financial relationships with commercial entities to disclose. This speaker will not discuss any off-label use or
Billing and Coding for HIV Services Financial Disclosure This speaker does not have any financial relationships with commercial entities to disclose. This speaker will not discuss any off-label use or
NON-OCCUPATIONAL POST EXPOSURE PROPHYLAXIS IN HIV PREVENTION. Jason E. Vercher, PA-C, AAHIVM
 NON-OCCUPATIONAL POST EXPOSURE PROPHYLAXIS IN HIV PREVENTION Jason E. Vercher, PA-C, AAHIVM Disclosures No disclosures to report Learning Objectives q Identify Individuals who would benefit from non-occupational
NON-OCCUPATIONAL POST EXPOSURE PROPHYLAXIS IN HIV PREVENTION Jason E. Vercher, PA-C, AAHIVM Disclosures No disclosures to report Learning Objectives q Identify Individuals who would benefit from non-occupational
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Post Exposure Prophylaxis for HIV following Sexual Exposure (PEPSE) Assessment Proforma PART A: FOR COMPLETION AT INITIAL PRESENTATION
 Addressograph or Name D.O.B Address Clinic no DOB Post Exposure Prophylaxis for HIV following Sexual Exposure (PEPSE) Assessment Proforma PART A: FOR COMPLETION AT INITIAL PRESENTATION The use of PEP following
Addressograph or Name D.O.B Address Clinic no DOB Post Exposure Prophylaxis for HIV following Sexual Exposure (PEPSE) Assessment Proforma PART A: FOR COMPLETION AT INITIAL PRESENTATION The use of PEP following
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
ALASKA NATIVE MEDICAL CENTER SEXUALLY TRANSMITTED DISEASE SCREENING AND TREATMENT GUIDELINES
 ALASKA NATIVE MEDICAL CENTER SEXUALLY TRANSMITTED DISEASE SCREENING AND TREATMENT GUIDELINES A. Screening Page Chlamydia and Gonorrhea 1 HIV 1 Syphilis 1 Genital Herpes 2 Hepatitis A 2 Hepatitis B 2 Hepatitis
ALASKA NATIVE MEDICAL CENTER SEXUALLY TRANSMITTED DISEASE SCREENING AND TREATMENT GUIDELINES A. Screening Page Chlamydia and Gonorrhea 1 HIV 1 Syphilis 1 Genital Herpes 2 Hepatitis A 2 Hepatitis B 2 Hepatitis
South African Guidelines for the Safe Use of. Dr. Oscar Radebe
 South African Guidelines for the Safe Use of PrEP in MSM Dr. Oscar Radebe Background Globally MSM(men who have sex with men) have been disproportionately at high risk of HIV transmission. Biological &
South African Guidelines for the Safe Use of PrEP in MSM Dr. Oscar Radebe Background Globally MSM(men who have sex with men) have been disproportionately at high risk of HIV transmission. Biological &
Answers to those burning questions -
 Answers to those burning questions - Ann Avery MD Infectious Diseases Physician-MetroHealth Medical Center Assistant Professor- Case Western Reserve University SOM Medical Director -Cleveland Department
Answers to those burning questions - Ann Avery MD Infectious Diseases Physician-MetroHealth Medical Center Assistant Professor- Case Western Reserve University SOM Medical Director -Cleveland Department
Summary of Management for Sexual Assault:> 12 years Sexual Assault Procedures and Measures to Aid Victims
 Summary of Management for Sexual Assault:> 12 years Sexual Assault Procedures and Measures to Aid Victims SANE Criteria Age >12 Assault < 120 hours Medically cleared Able to consent ED, Menino ICU only
Summary of Management for Sexual Assault:> 12 years Sexual Assault Procedures and Measures to Aid Victims SANE Criteria Age >12 Assault < 120 hours Medically cleared Able to consent ED, Menino ICU only
Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically -
 ASK SCREEN Test for HIV and STI Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically - Routinely obtain a thorough sexual history from all
ASK SCREEN Test for HIV and STI Practice Steps for Implementation of Guidelines Recommendations The guideline recommendations are shown schematically - Routinely obtain a thorough sexual history from all
For further information, please contact BC Women s Sexual Assault Service at Thank-you.
 The following guideline has been developed for use within BC Women s Hospital and Health Centre. There are support systems at BC Women s Hospital and Health Centre that may not exist in other clinical
The following guideline has been developed for use within BC Women s Hospital and Health Centre. There are support systems at BC Women s Hospital and Health Centre that may not exist in other clinical
Trends in Sexually Transmitted Infections (STIs) C. Junda Woo, MD, MPH, Medical Director San Antonio Metropolitan Health District June 3, 2017
 Trends in Sexually Transmitted Infections (STIs) C. Junda Woo, MD, MPH, Medical Director San Antonio Metropolitan Health District June 3, 2017 1 Speaker Disclosure Dr. Woo has disclosed that she has no
Trends in Sexually Transmitted Infections (STIs) C. Junda Woo, MD, MPH, Medical Director San Antonio Metropolitan Health District June 3, 2017 1 Speaker Disclosure Dr. Woo has disclosed that she has no
Pre-Exposure Prophylaxis (PrEP) for HIV Infection
 Pre-Exposure Prophylaxis (PrEP) for HIV Infection Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health University of California Los Angeles Attending Physician UCLA Center AIDS Research
Pre-Exposure Prophylaxis (PrEP) for HIV Infection Jeffrey D. Klausner, MD, MPH Professor of Medicine and Public Health University of California Los Angeles Attending Physician UCLA Center AIDS Research
PrEP in the Real World: Clinical Case Studies
 PrEP in the Real World: Clinical Case Studies Kevin L. Ard, MD, MPH April 30, 2015 Massachusetts General Hospital, National LGBT Health Education Center Continuing Medical Education Disclosure Program
PrEP in the Real World: Clinical Case Studies Kevin L. Ard, MD, MPH April 30, 2015 Massachusetts General Hospital, National LGBT Health Education Center Continuing Medical Education Disclosure Program
Case Studies in PrEP Management. Kevin L. Ard, MD, MPH Massachusetts General Hospital, National LGBT Health Education Center April 15, 2016
 Case Studies in PrEP Management Kevin L. Ard, MD, MPH Massachusetts General Hospital, National LGBT Health Education Center April 15, 2016 Continuing Medical Education Disclosure Program Faculty: Kevin
Case Studies in PrEP Management Kevin L. Ard, MD, MPH Massachusetts General Hospital, National LGBT Health Education Center April 15, 2016 Continuing Medical Education Disclosure Program Faculty: Kevin
For. Correctional. Officers. Your. Health Risks. in Correctional Settings. Facts. About HIV
 For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
For Correctional Officers Your Health Risks in Correctional Settings Facts About HIV Working in close quarters with inmates in a correctional facility puts correctional officers (COs) at increased risk
PrEP 201: Beyond the Basics
 NORTHWEST AIDS EDUCATION AND TRAINING CENTER PrEP 201: Beyond the Basics Joanne Stekler, MD MPH Associate Professor of Medicine University of Washington February 19, 2015 Disclosures and Disclaimers I
NORTHWEST AIDS EDUCATION AND TRAINING CENTER PrEP 201: Beyond the Basics Joanne Stekler, MD MPH Associate Professor of Medicine University of Washington February 19, 2015 Disclosures and Disclaimers I
I M ENDING HIV PATIENT INFORMATION. endinghiv.org.au/prep
 I M ENDING HIV PrEP PATIENT INFORMATION endinghiv.org.au/prep THIS BOOKLET PROVIDES YOU WITH INFORMATION ABOUT Pre-Exposure Prophylaxis (PrEP) for HIV. CONTENTS 06 Who will benefit from PrEP? 04 What is
I M ENDING HIV PrEP PATIENT INFORMATION endinghiv.org.au/prep THIS BOOKLET PROVIDES YOU WITH INFORMATION ABOUT Pre-Exposure Prophylaxis (PrEP) for HIV. CONTENTS 06 Who will benefit from PrEP? 04 What is
HIV Pre-Exposure Prophylaxis (HIV PrEP) in Scotland. An update for registered practitioners September 2017
 HIV Pre-Exposure Prophylaxis (HIV PrEP) in Scotland An update for registered practitioners September 2017 Key Messages HIV is a major public health challenge for Scotland with an annual average of 359
HIV Pre-Exposure Prophylaxis (HIV PrEP) in Scotland An update for registered practitioners September 2017 Key Messages HIV is a major public health challenge for Scotland with an annual average of 359
Ready, set, PrEP! Renee-Claude Mercier PharmD, PhC, BCPS-AQ ID, FCCP Professor of Pharmacy and Medicine University of New Mexico
 Ready, set, PrEP! Renee-Claude Mercier PharmD, PhC, BCPS-AQ ID, FCCP Professor of Pharmacy and Medicine University of New Mexico Objectives At the end of the talk the audience should be able to: Understand
Ready, set, PrEP! Renee-Claude Mercier PharmD, PhC, BCPS-AQ ID, FCCP Professor of Pharmacy and Medicine University of New Mexico Objectives At the end of the talk the audience should be able to: Understand
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
Modernization of North Carolina s HIV control measures
 Modernization of North Carolina s HIV control measures North Carolina Division of Public Health Victoria Mobley, MD MPH Evelyn Foust, MPH CPM Agenda Introduction Summary of scientific evidence used to
Modernization of North Carolina s HIV control measures North Carolina Division of Public Health Victoria Mobley, MD MPH Evelyn Foust, MPH CPM Agenda Introduction Summary of scientific evidence used to
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital
 HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
HIV prophylaxis for health care providers. Dr. A. K. M. Humayon Kabir Assistant Professor Department of Medicine Dhaka Medical College Hospital HIV continues to be a major global public health issue, Approximately
EQuIP 5 - This version June 2011 Revision Due June 2014
 Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
Preamble Rockingham Peel Group Non-Occupational Post-Exposure Prophylaxis (NPEP) To Prevent HIV in Western Australia Protocol The purpose of this protocol is to clarify the appropriate use and methods
CHAMP Program Child and Adolescent Sexual Offence Post-Assault Testing and Treatment Guide
 CHAMP Program Child and Adolescent Sexual Offence Post-Assault Testing and Treatment Guide Every child and adolescent suspected of sexual assault or abuse should have a complete physical examination. Even
CHAMP Program Child and Adolescent Sexual Offence Post-Assault Testing and Treatment Guide Every child and adolescent suspected of sexual assault or abuse should have a complete physical examination. Even
If you are a man that ONLY has sex with women this may not be the brochure for you.
 If you are a man that ONLY has sex with women this may not be the brochure for you. To find resources that best meet your needs check out the following website: http://www.cdc.gov/men Whether you are gay,
If you are a man that ONLY has sex with women this may not be the brochure for you. To find resources that best meet your needs check out the following website: http://www.cdc.gov/men Whether you are gay,
Nursing Interventions
 Chapter 16 H I Human Immunodeficiency V Virus A Acquired I Immuno D Deficiency S Syndrome Slide 1 Nursing Interventions Duty to treat Health care professionals may not pick and choose their patients Rehabilitation
Chapter 16 H I Human Immunodeficiency V Virus A Acquired I Immuno D Deficiency S Syndrome Slide 1 Nursing Interventions Duty to treat Health care professionals may not pick and choose their patients Rehabilitation
HIV Basics for the Family Practitioner Olha Smolynets, DO
 HIV BASICS FOR FAMILY PRACTITIONER, MS DISCLOSURES Dr. Smolynets has provided no disclosures. OBJECTIVES Indications for HIV screening Prevention counseling Prophylaxis: PrEP, PEP and npep Diagnosis Basic
HIV BASICS FOR FAMILY PRACTITIONER, MS DISCLOSURES Dr. Smolynets has provided no disclosures. OBJECTIVES Indications for HIV screening Prevention counseling Prophylaxis: PrEP, PEP and npep Diagnosis Basic
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Contamination Incidents Frequently Asked Questions
 Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
Contamination Incidents Frequently Asked Questions WWR- 004 Index 1. What is a contamination injury? 2. What should I do immediately if I have sustained a contamination injury? 3. What should I do immediately
HIV PrEP in Ireland. Information booklet for people who are accessing PrEP themselves or are considering accessing PrEP
 HIV PrEP in Ireland Information booklet for people who are accessing PrEP themselves or are considering accessing PrEP The HSE Sexual Health and Crisis Pregnancy Programme (SHCPP) and the HIV PrEP working
HIV PrEP in Ireland Information booklet for people who are accessing PrEP themselves or are considering accessing PrEP The HSE Sexual Health and Crisis Pregnancy Programme (SHCPP) and the HIV PrEP working
HIV and PEP. LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED
 HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
HIV and PEP LTC Rose Ressner WRNMMC ID staff Oct 2014 UNCLASSIFIED Disclaimer The views expressed in this presentation are those of the speaker and do not reflect the official policy of the Department
Post-exposure prophylaxis (PEP)
 Post-exposure prophylaxis (PEP) Summary Post-exposure prophylaxis, or PEP, is a way to help prevent the transmission of HIV in an HIV-negative person who may have been recently exposed to HIV. It involves
Post-exposure prophylaxis (PEP) Summary Post-exposure prophylaxis, or PEP, is a way to help prevent the transmission of HIV in an HIV-negative person who may have been recently exposed to HIV. It involves
Primary Care of LGBT Patients
 Primary Care of LGBT Patients Basics Primary care of LGBT patients is primary care of a population with unique barriers to care Like any patient population there are population specific disease risks concerns
Primary Care of LGBT Patients Basics Primary care of LGBT patients is primary care of a population with unique barriers to care Like any patient population there are population specific disease risks concerns
HIV Update Objectives. Epidemiology. Epidemiology, Transmission and Natural History. Transmission Risk by Exposure. Transmission 9/29/2014
 Objectives HIV Update 2014 Jay Sizemore, MD, MPH Medical Director Chattanooga CARES Assistant Professor UTCOM Chattanooga 2October 2014 Review HIV epidemiology and screening/testing guidelines Discuss
Objectives HIV Update 2014 Jay Sizemore, MD, MPH Medical Director Chattanooga CARES Assistant Professor UTCOM Chattanooga 2October 2014 Review HIV epidemiology and screening/testing guidelines Discuss
NEW CANADIAN. GUIDELINES: Public health and community perspectives. Camille Arkell, Moderator Dr. Darrell Tan, Gilles Charette, Dr.
 NEW CANADIAN HIV PrEP/nPEP GUIDELINES: Public health and community perspectives PRESENTED BY Camille Arkell, Moderator Dr. Darrell Tan, Gilles Charette, Dr. Joss Reimer May 16, 2018 Webinar Agenda (1 hour)
NEW CANADIAN HIV PrEP/nPEP GUIDELINES: Public health and community perspectives PRESENTED BY Camille Arkell, Moderator Dr. Darrell Tan, Gilles Charette, Dr. Joss Reimer May 16, 2018 Webinar Agenda (1 hour)
HIV. The Role of Pre-Exposure Prophylaxis (PrEP) for the Prevention of HIV. Brief History of HIV AIDS. Global HIV Infection.
 The Role of Pre-Exposure Prophylaxis (PrEP) for the Prevention of HIV HIV Sarah Kemink, PharmD, AAHIVP WMSHP Spring Seminar 5/05/2015 AIDS CD4 less than 200 +/- AIDS-defining illness Most common: Candidiasis
The Role of Pre-Exposure Prophylaxis (PrEP) for the Prevention of HIV HIV Sarah Kemink, PharmD, AAHIVP WMSHP Spring Seminar 5/05/2015 AIDS CD4 less than 200 +/- AIDS-defining illness Most common: Candidiasis
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Management
 01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
01.02 Blood Borne Pathogens (BBP) Occupational Post Exposure Purpose Audience Policy Definitions Establish protocol for management of occupational exposures to blood or potentially infectious materials.
WVU Occupational Medicine Program for evaluation and treatment of persons exposed to Lentivirus Vectors
 Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Extragenital Gonorrhea and Chlamydia among MSM
 Extragenital Gonorrhea and Chlamydia among MSM Laura Quilter, MD Infectious Disease and STD PTC Fellow University of Washington Division of Allergy and Infectious Diseases 3/28/2016 uwptc@uw.edu uwptc.org
Extragenital Gonorrhea and Chlamydia among MSM Laura Quilter, MD Infectious Disease and STD PTC Fellow University of Washington Division of Allergy and Infectious Diseases 3/28/2016 uwptc@uw.edu uwptc.org
Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) Training Guide for Healthcare Providers
 Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) Training Guide for Healthcare Providers About emtricitabine/tenofovir disoproxil fumarate for HIV-1 PrEP
Emtricitabine/Tenofovir Disoproxil Fumarate 200 mg/300 mg for HIV-1 Pre-exposure Prophylaxis (PrEP) Training Guide for Healthcare Providers About emtricitabine/tenofovir disoproxil fumarate for HIV-1 PrEP
Clinical management of non-occupational and occupational exposure to blood borne pathogens. - A Pocket Reference -
 Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
Pocket P.E.P. Clinical management of non-occupational and occupational eposure to blood borne pathogens Development Team: Deborah Yoong, PharmD 1 1, 2, 3 Kevin Gough, MD, MEd 1 Positive Care Clinic, Toronto,
STI s. (Sexually Transmitted Infections)
 STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
PrEP in Scotland. PrEP. in Scotland. PrEP. PrEP. PrEP. PrEP is a combination pill that prevents HIV.
 PrEP in Scotland PrEP PrEP PrEP PrEP is a combination pill that prevents HIV. 1 Contents Introduction 3 What is PrEP 3 Who should take PrEP 4 Getting PrEP in Scotland 5 Side effects and interactions with
PrEP in Scotland PrEP PrEP PrEP PrEP is a combination pill that prevents HIV. 1 Contents Introduction 3 What is PrEP 3 Who should take PrEP 4 Getting PrEP in Scotland 5 Side effects and interactions with
Victorian guidelines for post-exposure prophylaxis following non-occupational exposure to HIV
 Victorian guidelines for post-exposure prophylaxis following non-occupational exposure to HIV Victorian NPEP Guidelines 2016 Victorian NPEP Service Alfred Hospital Written by Dr Anna Pierce Endorsed by
Victorian guidelines for post-exposure prophylaxis following non-occupational exposure to HIV Victorian NPEP Guidelines 2016 Victorian NPEP Service Alfred Hospital Written by Dr Anna Pierce Endorsed by
Module 1: HIV epidemiology, transmission and prevention
 Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Session 2 Module goals Module 1 Participants will be able to: -offer an insight into the epidemiological situation in the country and worldwide -present the HIV transmission modes and the broad approaches
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Answering basic questions about HIV
 Answering basic questions about HIV Sixth Edition This booklet is for you if you have basic questions about HIV such as what it is, how it is transmitted and how it affects the body. If you have HIV and
Answering basic questions about HIV Sixth Edition This booklet is for you if you have basic questions about HIV such as what it is, how it is transmitted and how it affects the body. If you have HIV and
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Fast-Track Your PrEP Knowledge. Jonathan Fritz PrEP Coordinator MDHHS Division of HIV and STD Programs
 Fast-Track Your PrEP Knowledge Jonathan Fritz PrEP Coordinator MDHHS Division of HIV and STD Programs Session objectives Increase knowledge of the basics of PrEP and clinical procedures Identify financial
Fast-Track Your PrEP Knowledge Jonathan Fritz PrEP Coordinator MDHHS Division of HIV and STD Programs Session objectives Increase knowledge of the basics of PrEP and clinical procedures Identify financial
Training for Employees of Taylor Special Care Services, Inc.
 Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
Training for Employees of Taylor Special Care Services, Inc. TSCS Taylor Special Care Services housing staffing counseling on-going support Simon Pop, MBA Chief Operating Officer 2015 2016 Guidelines:
HIV PREVENTION WITH PRE-EXPOSURE PROPHYLAXIS: A PRIMER FOR PHARMACISTS. Speaker: Susan MK Lee, PharmD, BCPS, CDE
 Clinical Education Initiative Support@ceitraining.org HIV PREVENTION WITH PRE-EXPOSURE PROPHYLAXIS: A PRIMER FOR PHARMACISTS Speaker: Susan MK Lee, PharmD, BCPS, CDE 12/13/2016 HIV Prevention with Pre-Exposure
Clinical Education Initiative Support@ceitraining.org HIV PREVENTION WITH PRE-EXPOSURE PROPHYLAXIS: A PRIMER FOR PHARMACISTS Speaker: Susan MK Lee, PharmD, BCPS, CDE 12/13/2016 HIV Prevention with Pre-Exposure
Getting Prepped for PrEP. Ken Ho, MD, MPH World AIDS Day
 Getting Prepped for PrEP Ken Ho, MD, MPH World AIDS Day Objectives HIV epidemiology What is PrEP? Does it Work? Who gets PrEP? How do I prescribe PrEP What to do at the first visit? What to do at follow
Getting Prepped for PrEP Ken Ho, MD, MPH World AIDS Day Objectives HIV epidemiology What is PrEP? Does it Work? Who gets PrEP? How do I prescribe PrEP What to do at the first visit? What to do at follow
STI Indicators by STI
 STI Indicators by STI Table of Contents pg. 2 Sexual History pg. 3-4 Syphilis pg. 5-6 Gonorrhea pg. 7-9 Chlamydia pg. 10 HIV/PrEP 1 Sexual History Comprehensive Sexual History Elements Percentage of patients
STI Indicators by STI Table of Contents pg. 2 Sexual History pg. 3-4 Syphilis pg. 5-6 Gonorrhea pg. 7-9 Chlamydia pg. 10 HIV/PrEP 1 Sexual History Comprehensive Sexual History Elements Percentage of patients
Pre-exposure prophylaxis (PrEP)
 FACTSHEET Pre-exposure prophylaxis (PrEP) Summary Pre-exposure prophylaxis, or PrEP, is a way for an HIV-negative person who is at risk of HIV infection to reduce their risk of becoming infected with HIV.
FACTSHEET Pre-exposure prophylaxis (PrEP) Summary Pre-exposure prophylaxis, or PrEP, is a way for an HIV-negative person who is at risk of HIV infection to reduce their risk of becoming infected with HIV.
Update on Sexually Transmitted Infections Jeanne Marrazzo, MD, MPH
 Update on Sexually Transmitted Infections Jeanne Marrazzo, MD, MPH Division of Infectious Diseases University of Alabama at Birmingham School of Medicine Birmingham, Alabama Outline Syphilis in all its
Update on Sexually Transmitted Infections Jeanne Marrazzo, MD, MPH Division of Infectious Diseases University of Alabama at Birmingham School of Medicine Birmingham, Alabama Outline Syphilis in all its
Overview: A-Z Sexual Assault
 Definitions of Sexual Assault Overview: A-Z Sexual Assault Cheryl Ann Graf ARNP, MSN, MBA Rape = forced sexual penetration (vaginal, oral, anal, digital, object) Attempted rape = uncompleted attempt at
Definitions of Sexual Assault Overview: A-Z Sexual Assault Cheryl Ann Graf ARNP, MSN, MBA Rape = forced sexual penetration (vaginal, oral, anal, digital, object) Attempted rape = uncompleted attempt at
