keywords Malaria, Plasmodium falciparum, artemisinin-based combination therapy, drug resistance, Somalia
|
|
|
- Logan Carter
- 5 years ago
- Views:
Transcription
1 Tropical Medicine and International Health doi: /tmi volume 20 no 4 pp april 2015 Treatment of uncomplicated malaria with artesunate plus sulfadoxine pyrimethamine is failing in Somalia: evidence from therapeutic efficacy studies and Pfdhfr and Pfdhps mutant alleles Marian Warsame 1, Abdillahi Mohamed Hassan 2, Amy Barrette 1, Ali Mohamed Jibril 3, Husein Haji Elmi 4, Abdulkadir Mohamed Arale 5, Hanan El Mohammady 6, Rania A. Nada 6, Jamal Ghilan Hefzullah Amran 7, Abdikarim Muse 8, Fahmi Essa Yusuf 8 and Abdiqani Sheikh Omar 5 1 Global Malaria Programme, World Health Organization, Geneva, Switzerland 2 World Health Organization, WHO Office, Mogadishu, Somalia 3 INTERSOS, Jowhar Hospital, Middle Shabele, Somalia 4 Muslim Aid UK, Jamame, Lower Juba Region, Somalia 5 Ministry of Health and Human Service, Mogadishu, Somalia 6 US Naval Medical Research Unit-3, Cairo, Egypt 7 World Health Organization, WHO Somalia, Warwick Centre UN Avenue, Nairobi, Kenya 8 World Health Organization, WHO Office, Hargeisa, Somalia Abstract objective Artesunate plus sulfadoxine pyrimethamine (AS + SP) has been Somalia s national treatment policy since Routine monitoring of first-line malaria treatment is needed to ensure appropriate national malaria treatment policy and early detection of drug resistance. For this purpose, we conducted therapeutic efficacy studies of AS + SP for the treatment of uncomplicated malaria in Somalia in methods Studies were conducted in three sentinel sites. Eligible patients were evaluated for clinical and parasitological outcomes according to the WHO standard protocol. Molecular surveillance was conducted on resistance conferring mutations in the P.falciparum dihydrofolate reductase (dfhr) and dihydropteroate synthase (dhps) genes. results The proportion of PCR-corrected treatment failures was high in Jamame (22%, 95% CI: %) and low (<5%) in Janale and Jowhar. All patients cleared parasites by day 3. Molecular markers associated with SP resistance were detected in all three sites. Treatment failure was associated with the presence of the double mutant dhps A437G/K540E (OR = 22.4, 95% CI: ), quadruple mutant dhfr N51I/S108N+dhps A437G/K540E (OR = 5.5, 95% CI: ), quintuple mutant dhfr N51I/C59R/S108N+dhps A437G/K540E (OR = 3.5, 95% CI: ) and younger age (OR=0.86, 95% CI: ). conclusions The high treatment failure rate observed in Jamame, together with the presence of molecular mutations associated with SP resistance, indicates P. falciparum resistance to SP. In Jowhar, high treatment failure rates were absent despite the presence of molecular mutations; signs of resistance in vivo may have been masked by the stronger immunity of the older study population. The study underscores the need to update Somalia s national malaria treatment policy. keywords Malaria, Plasmodium falciparum, artemisinin-based combination therapy, drug resistance, Somalia Introduction Malaria remains an important public health problem in Somalia [1]. Transmission is moderate along the Juba and Shabele rivers, while the remaining areas of the country are characterised by low transmission, with occasional epidemics [2, 3]. Artesunate plus sulfadoxine pyrimethamine (AS + SP) is the current national treatment policy and one of five artemisinin-based combination therapies (ACTs) recommended by WHO [4, 5]. Therapeutic efficacy studies John Wiley & Sons Ltd
2 of AS + SP were conducted in Somalia between 2003 and 2006; high treatment efficacy (95 100%) was observed in each of the country s three sentinel sites [3]. These studies led to the adoption and implementation of AS + SP as Somalia s first-line treatment for uncomplicated falciparum malaria in The ACT is the recommended firstline treatment for uncomplicated P.falciparum malaria in most endemic countries located in the Middle East and in Central Asia [4]. Sulfadoxine pyrimethamine (SP) is the recommended medicine for intermittent preventive treatment in pregnancy (IPTp) in areas of moderate to high malaria transmission in Sub-Saharan Africa [6] including Somalia. In Somalia, SP is available in private drug stores and is frequently used as a monotherapy (M. Warsame, personal communication). Routine monitoring of the therapeutic efficacy of ACTs is needed for the early detection of drug resistance, which can emerge to the artemisinin and the partner drug independently, due to their different modes of action. Resistance to artemisinin is suspected when 10% of patients fail to clear parasites by day 3 after treatment with an ACT [7]. WHO recommends a change in national malaria treatment policy if the total treatment failure rate is 10%, as assessed through in vivo monitoring of therapeutic efficacy [4, 5]. Resistance to sulfadoxine pyrimethamine is mediated through point mutations that accumulate at several sites in the dihydrofolate reductase (dhfr) and dihydropteroate synthase (dhps) genes of P. falciparum [8]. Detection of these mutations has been an effective tool for monitoring SP resistance [9]. Mutations associated with SP resistance have been identified in codons 16, 51, 59, 108, 140 and 164 in the dhfr gene, and codons 436, 437, 540, 581 and 613 in the dhps gene [10]. The occurrence of the dhfr triple mutant (N51I/C59R/S108N) in combination with the dhps double mutant (A437G/K540E), called a quintuple mutant, has been associated with SP treatment failure [8, 11 13]. Other findings have suggested that the dhfr triple mutant (N51I/C59R/S108N) alone is a useful predictor of treatment failure [14, 15]. This study investigated the therapeutic efficacy of AS + SP and the presence of SP resistance conferring molecular markers in three surveillance sites in Somalia in This study is the first to examine molecular markers for SP resistance (dhfr and dhps) in Somalia. The findings have important implications for Somalia s current national malaria treatment policy. Methods Study sites The studies were conducted during the peak malaria transmission period in Somalia s three sentinel sites. The sites are situated along the belt of Juba and Shabele rivers: Jamame in the Lower Juba region, Janale in the Lower Shabele region and Jowhar in the Middle Shabele region. Mobile clinics were set up for patients living in rural communities within 10 km of each site. Studies were conducted in 2011, between July and September in Jamame and Jowhar, and from September to October in Janale. Patients Patients were eligible for inclusion if they were 6 months of age or above, had fever or history of fever in the previous 24 hours ( 37.5 C) and P. falciparum mono-infection with parasite density of asexual parasites/ll. Patients were excluded if they had one or more signs of severe or complicated malaria, mixed infection or infection with another species, or a febrile illness other than malaria. Female minors and unmarried women were also excluded, due to social and cultural norms related to requesting a pregnancy test from this population. Study procedures The study was an open-label, one-arm prospective evaluation of the therapeutic efficacy of AS + SP for the treatment of uncomplicated malaria. Methods were based on the standardised WHO protocol for monitoring antimalarial drug efficacy [16]. Clinical examination, including axillary temperature, was performed at enrolment (day 0) and on days 1, 2, 3, 7, 14, 21 and 28. Blood smear for determining parasite counts was taken on the same days except for day 1. Patients were also asked to report to the clinic at any time if new or recurrent symptoms occurred. Blood was obtained through finger prick for blood smears and stained with 2.5% Giemsa for 30 min. Parasite densities were determined on Giemsa-stained thick films and recorded as the number of asexual parasites per 200 white blood cells (or per 500, if the count was <10 parasites/200 white blood cells), assuming a white blood cell count of 8000 ll. A smear was declared negative if no parasites were seen after 1000 white blood cells were counted. For Plasmodium species detection, thin blood smears were taken on day 0. For quality assurance, all blood smears were re-read by a second microscopist. Blood smears with non-concordant results (difference in species or in parasite density of >50%) were re-read by a third microscopist, and the average parasite density of the two most concordant counts was used. Prior to enrolment, individual informed consent was obtained for all study patients. Consent was requested 2015 John Wiley & Sons Ltd 511
3 from parent/guardians of children aged less than 17 years. Permission to conduct the studies was obtained from the Ministry of Health of the Transitional Government of Somalia. The study team also sought permission from the community leaders and held public meetings in each study community to inform about the study objectives and procedures. The study information was read to each parent/guardian or patient at the time of individual patient recruitment by the study clinician, in the presence of the accompanying relative/friend. In cases where there was no accompanying relative/friend, a community representative was present. The required sample size was estimated based on an expected treatment failure rate of 5%. With a confidence level of 95% and precision of 5%, the target sample size was 73 patients per site. An additional 20% was added to ensure the sample size would be achieved after exclusion of patients due to loss to follow up and withdrawal. Treatment regimen All patients received the standard therapeutic dose of artesunate (4 mg/kg on days 0, 1 and 2), co-administered with SP (single dose of 25 mg sulfadoxine/1.25 mg pyrimethamine per kg with first artesunate dose). Study medicine was provided by WHO. All tablets were divided into quarters and given under direct supervision. If a patient vomited within 30 min of treatment, a full dose was readministered. All patients who failed treatment were treated with artemether plus lumefantrine. Drug tolerability and safety were assessed clinically. Adverse events and severe adverse events were monitored at enrolment and at each follow-up visit. An adverse event was defined as any untoward medical occurrence irrespective of its suspected relationship to the study medications. Severe adverse events were defined as any untoward medical occurrence requiring hospitalisation or resulting in death. Treatment outcomes Treatment outcomes were based on parasitological and clinical outcomes according to the methods recommended by WHO [16]. Therapeutic response was classified as either: early treatment failure (ETF), late clinical failure (LCF), late parasitological failure (LPF) or adequate clinical and parasitological response (ACPR). The proportion of cases positive on day 3 was also recorded. Polymerase chain reaction (PCR) analysis was conducted to distinguish between recrudescence and reinfection. Parasite DNA was extracted from blood spots on day 0 and on the day of reappearance of asexual parasitemia. Spots were tested using nested PCR targeting polymorphic variant genes msp1, msp2 (merozoite surface proteins) and glurp (glutamate-rich protein) according to WHO recommended methods [17]. Molecular markers of sulfadoxine pyrimethamine resistance Mutations conferring resistance to sulphadoxine pyrimethamine were detected by analysing extracted DNA from all day 0 samples, to determine the mutations in the dihydrofolate reductase (dhfr) and dihydropteroate synthetase (dhps) genes. Briefly, both dhfr and dhps genes were amplified using nested PCR, as described elsewhere [18]. Subsequently, positive PCR products were subjected to DNA sequencing using BigDye terminator chemistry (Applied Biosystems, Foster City, CA) on a 3130xl Genetic Analyzer (Applied Biosystems, Foster City, CA). DNA sequences were assembled and mutations were verified by inspection of both forward and reverse strands using BioEdit version [19]. DNA sequencing analysis of the dhfr fragment was carried out to detect mutations at codons 16, 51, 59, 108 and 164, whereas dhps fragment was evaluated at codons 436, 437, 540, 581 and 613. Statistical analysis Data were double-entered and validated using a programme developed by WHO ( malaria/publications/atoz/ /en/). Statistical analysis was performed using Stata/IC 11.0 (Stata Corporation, College Station, TX, USA). Patient characteristics at baseline were compared across the three sites. Patients who were subsequently lost to follow up, had reinfections, or unknown PCR, were excluded from the per-protocol analysis of treatment outcomes, but included in the Kaplan Meier analysis until the day of withdrawal from the study. Differences in categorical data were compared using the chi-square test or the Fisher s exact test where cell counts were 5. Comparisons of mean age between groups were computed using the t-test. Exact confidence intervals were calculated for proportions. Logistic regression was used to estimate the association between treatment failure and the presence of dhfr/dhps mutations and patient age. Results A total of 283 patients were enrolled in the three sites, of which 89 were in Jamame, 92 in Janale and 102 in Jowhar. Patient characteristics on admission are summarised for each site in Table 1. Patient age ranged from John Wiley & Sons Ltd
4 6 months to 60 years. The study population in Jamame was younger than the other two sites, with a greater proportion of patients under 5 years of age (n = 32, 36%, 95% CI: ) than in Janale (n = 16, 17.4%, 95% CI: %, v 2 = 8.0, P = 0.005) and Jowhar (n = 12, 11.8%, 95% CI: %, v 2 = 15.7, P < 0.001). Jamame also had fewer older patients than the other two sites, with only 1 patient over 15 years of age (1.1%, 95% CI: 0 6.1%), compared to 17 patients in Janale (18.5%, 95% CI: %, P < 0.001) and 27 patients in Jowhar (26.5%, 95% CI: %, P < 0.001). No other differences in admission characteristics were observed between the three sites. Of the 283 patients, 14 were censored from the analysis of PCR-corrected treatment outcomes: 5 patients were lost to follow up (1 in Jamame on day 14 and 4 in Jowhar on day 7), 6 patients were excluded due to reinfections (2 on day 21 and 3 on day 28 in Jamame, 1 in Jowhar on day 21), and 3 were excluded due to unknown PCR results (2 in Jamame and 1 in Janale). As shown in Table 2, all patients cleared parasitaemia before day 3. The percentage of PCR-corrected treatment failures was higher in Jamame (n = 18, 22.2%, 95% CI: ) than in Janale (n = 4, 4.4%, 95% CI: %, P < 0.001) and Jowhar (n = 1, 1%, 95% CI: 0 5.6%, P < 0.001). Overall, patients with treatment Table 1 Patient characteristics at baseline Jamame (n = 89) Janale (n = 92) Jowhar (n = 102) Number of 55/34 46/46 68/34 male/female patients Age at baseline n (%) (95% CI) n (%) (95% CI) n (%) (95% CI) <5 years 32 (36.0) ( )* 16 (17.4) ( ) 12 (11.8) ( ) 5 15 years 56 (62.9) ( ) 59 (64.1) ( ) 63 (61.8) ( ) >15 years 1 (1.1) (0 6.1)* 17 (18.5) ( ) 27 (26.5) ( ) Temperature C mean (SD) a mean (SD) a mean (SD) a 38.2 (0.7) 38.1 (0.4) 37.7 (0.8) Parasitemia ll mean b (95% CI) mean b (95% CI) mean b (95% CI) ( ) ( ) ( ) a standard deviation, b geometric mean. *Statistically significant difference between Jamame and both of the other two sites (P < 0.05). Table 2 Clinical and parasitological outcomes Jamame (n = 89) Janale (n = 92) Jowhar (n = 102) Outcomes n (%) 95% CI n (%) 95% CI n (%) 95% CI Parasitemia, D3 0 (0) (0 4.0) 0 (0) (0 4.0) 0 (0) (0 4.0) PCR-uncorrected, D28 Lost to follow up/excluded 1 (1.1) (0 6.1) 0 (0) (0 0.4) 4 (3.9) ( ) ACPR 63 (71.6) ( )* 87 (94.6) ( ) 96 (98.0) ( ) Treatment failure 25 (28.4) ( )* 5 (5.4) ( ) 2 (2.0) ( ) LCF 7 (8.0) ( ) 5 (5.4) ( ) 2 (2.0) ( ) LPF 18 (20.5) ( )* 0 (0) (0 0.4) 0 (0) ( ) PCR-corrected, D28 Lost to follow up/excluded 8 (9.0) ( ) 1 (1.1) ( ) 5 (4.9) ( ) ACPR 63 (77.8) ( )* 87 (95.6) ( ) 96 (99) ( ) Treatment failure 18 (22.2) ( )* 4 (4.4) ( ) 1 (1.0) (0 5.6) LCF 4 (4.9) ( ) 4 (4.4) ( ) 1 (1.0) (0 5.6) LPF 14 (17.3) ( )* 0 (0) (0 4.0) 0 (0) (0 3.7) Kaplan Meier 18 (20.7) ( )* 4 (4.4) ( ) 1 (1.0) ( ) LCF, late clinical failure; LPF, late parasitological failure; ACPR, adequate clinical and parasitological response. *Statistically significant difference between Jamame and the other two sites (P < 0.05) John Wiley & Sons Ltd 513
5 Percentage of patients S108N dhfr N51I/S108N Jamame C59R/S108N Janale N51I/C59R/S108N wild type Jowhar dhps S436A A437G A437G/K540E Figure 1 Distribution of the prevalence of dfhr and dhps mutations, at sentinel sites at enrolment. failure were younger in age (n = 23, mean = 5.7 years, 95% CI: %) than those with treatment success (n = 246, mean = 11.1 years, 95% CI: ), (t = 2.47, P = 0.01). All therapeutic regimens of the study drug were well-tolerated and safe. No adverse events or deaths occurred. The prevalence of dhfr and dhps resistance conferring mutations is shown for each site in Figure 1. The presence of molecular markers could not be determined for 14 of the 283 patients who had missing values for both dhfr and dhps (1 from Jamame and 13 from Janale), and 2 additional patients who had missing values for dhps only (both from Jamame). All study patients carried the dhfr S108N mutation; however, only 5 patients, all from Janale, carried this as a single mutation. Double dhfr mutations (N51I/S108N or C59R/S108N) were observed among 60 (68.2%) patients in Jamame, 52 (65.8%) patients in Janale, and 52 (51%) patients in Jowhar. Between the two possible double mutations, the dhfr N51I/S108N combination pre-dominated in each site. The triple dhfr mutation (N51I/C59R/S108N) was observed among 28 (31.8%) patients in Jamame, 22 (27.9%) patients in Janale and 50 (49%) patients in Jowhar. No patients were observed to carry mutations at dhfr codons 16 or 164. Overall, dhps mutations were less prevalent (Figure 1). The dhps wild type was found among 33 (38.4%) patients in Jamame, 70 (88.6%) patients in Janale and 58 (56.9%) patients in Jowhar. The proportion of dhps sensitive patients in Janale was significantly higher than the other two sites (v 2 = 37.6, P < 0.001). Single mutations at S436A and A437G were found among 7 patients. The double dhps A437G/K540E mutation was found among 51 (59.3%) patients in Jamame, 6 (7.6%) patients in Janale and 42 (41.2%) patients in Jowhar. All 99 patients with the dhps double mutant A437G/K540E also had either a quadruple or quintuple mutation (discussed below). No mutations were observed at dhps codons 581 or 613. The distribution of dhps and dhfr mutations occurring in combination is shown for each site in Figure 2. The majority of patients in Jamame (n = 51, 59.3%) carried a quadruple or quintuple mutation, significantly more than the 6 patients in Janale (7.6%, v 2 = 48.7, P < 0.001), or the 42 patients in Jowhar (41.2%, v 2 = 6.1, P < 0.05). Only 5 of the 28 patients in Jamame who carried the dhfr N51I/C59R/S108N triple mutant were found to carry the dhps wild type. In Janale, most patients carried either the dhfr N51I/S108N or C59R/S108N double mutant and the dhps wild type, observed in 47 (59.5%) patients, or the dhfr N51I/C59R/S108N triple mutant and dhps wild type, observed in 18 (22.8%) patients. Jowhar had a more even distribution of mutations, with the dhfr double mutant (N51I/S108N) and dhps wild type found among 23 (22.5%) patients, the dhfr triple mutant (N51I/C59R/S108N) and dhps wild type among 34 (33.3%) patients, the quadruple mutant (dhfr N51I, S108N + dhps A437G, K540E) among 23 (22.6%) patients, and the quintuple mutant (dhfr N51I/C59R/ S108N + dhps A437G/K540E) among 16 (15.7%) patients. Further analysis revealed an association between treatment failure, multiple mutations and age. The odds of treatment failure were increased among patients who Percentage of patients Jamame (n = 86) Janale (n = 79) Quintuple Quadruple Triple Double Single Other Treatment failure 10% treatment failure Jowhar threshold for policy (n = 102) change Figure 2 Frequency distribution of patients with dfhr/dhps mutations at sentinel sites at enrolment and treatment failure rates at day 28. quintuple: dhfr N51I/C59R/S108N + dhps A437G/K540E; quadruple: dhfr N51I/S108N + dhps A437G/ K540E, or dhfr C59R/S108N + dhps A437G/K540E; triple: dhfr N51I/C59R/S108N + dhps wild type; double: dhfr N51I/ S108N + dhps wild type, or dhfr C59R/S108N + dhps wild type; single: dhfr S108N + dhps wild type; other: dhfr N51I/ S108N + dhps S436A, or dhfr C59R/S108N + dhps S436A, or dhfr C59R/S108N + dhps A437G John Wiley & Sons Ltd
6 carried the double mutant dhps A437G/K540E (n = 21, OR = 22.4, 95% CI: ), the quadruple mutant dhfr N51I/S108N + dhps A437G/K540E (n = 11, OR = 5.5, 95% CI: ), and the quintuple mutant (n = 8, OR = 3.5 (95% CI: ). Patients who carried either the quadruple or quintuple mutation and experienced treatment failure (n = 21) also had a lower mean age (5.6 years, 95% CI: ) than the patients with quadruple or quintuple mutations who recovered following treatment (n = 74, 9.9 years, 95% CI: years), t = 2.7, P < Overall, treatment failure was associated with younger age (OR = 0.86, 95% CI: ). Discussion In this study, the PCR-corrected treatment failure rate in one of the three study sites, Jamame (22.2%), surpassed the threshold of 10% which is recommended by WHO for reviewing and updating treatment policy [4, 5]. The high proportion of treatment failures and the high prevalence of molecular mutations associated with SP resistance provide clear evidence of the presence of resistance to the partner drug in Jamame. Artemisinins tend to kill the mass of parasites, after which the partner drug eliminates the remaining parasites. Given that all patients in this study cleared parasites by microscopy on day 3, the artemisinin component of the combination is still effective in all three sites [4]. It is worth noting that patients who had recrudescence likely had submicroscopic levels of parasitemia on day 3. Therefore, SP failed to clear the residual parasites. The odds of treatment failure were higher among younger patients and patients with quadruple and quintuple mutations. The high treatment failure rate in Jamame was expected, given the high prevalence of multiple mutations. Studies previously conducted in Kenya, Malawi and Uganda found an association between quintuple mutations and treatment failure [11, 20, 21]. Apart from the higher prevalence of drug resistance associated mutations, the lower age of the patients in Jamame may have contributed to the higher failure rate. Younger patients have less background immunity and children under five may have lower pyrimethamine and sulfadoxine levels than older children and adults [22]. However, in this study, we did not measure drug blood levels. In Jowhar, the treatment failure rate remained low (1%) despite a substantial number of patients carrying quadruple or quintuple mutations (41%). This inconsistency may be explained by the fact that patients in Jowhar were older than those in Jamame. Study patients in Jowhar are likely to have acquired a higher degree of immunity, which may have been responsible for clearing SP resistant parasites during treatment, effectively masking the presence of resistance. Similar findings have been reported elsewhere [21, 23, 24]. It is likely that in all sites, the prevalence of mutations will increase with sustained drug pressure. Unofficial use of SP as a monotherapy in Somalia is likely to further accelerate the proliferation of dhfr and dhps mutations [25]. Dhfr triple mutations (N51I/C59R/S108N) were observed in all three sites, indicating the presence of resistance to pyrimethamine. Previous studies have shown that the emergence of the triple dhfr (N51I/C59R/S108N) mutation precedes that of double dhps (A437G/K540E) mutant [8, 26, 27]. It is interesting to note that in this study, all patients who carried the dhps double mutant (A437G/K540E) also carried either the quadruple or quintuple mutation. The high prevalence of molecular markers associated with SP resistance detected in this study raises concerns about the life span of SP for IPTp. One study from Tanzania has shown that IPTp with SP fails to provide benefit in areas where SP resistance is widespread [28]. However, other evidence suggests that in sub-saharan Africa, in spite of the increased frequency of quintuple mutant dhfr/dhps haplotypes, IPTp-SP remains beneficial during pregnancy in preventing peripheral parasitemia, maternal anaemia, clinical malaria during pregnancy and is associated with reduced neonatal mortality [29 33]. Vigilant monitoring of the efficacy of SP for the prevention of malaria in pregnancy is encouraged. The high prevalence of treatment failures in Jamame, and the presence of dhfr and dhps mutations associated with SP resistance in all three sites, indicates the need to revise the current treatment policy of Somalia from AS + SP to a more effective ACT. With the failure of the partner drug SP, continued use of AS + SP as the first-line treatment in Somalia endangers patients lives. Furthermore, treatment effectively becomes a 3-day course of artesunate alone, which is insufficient to kill all parasites. Consequently, this will put the parasites under artesunate drug pressure, which facilitates the development of artemisinin resistance. Sustained use of an ACT with a failing partner drug will eventually compromise the artemisinin component. Routine monitoring of ACTs should be conducted in all malaria endemic countries for the early detection of P. falciparum resistance. Acknowledgements We would like to express our gratitude to all of the study patients, and to the parents and guardians of the children who participated. We thank the staff of the sentinel sites, 2015 John Wiley & Sons Ltd 515
7 especially Kaltumo Abdullahi Ali, Mohamed Mohamoud Jimale, Hussein Hirey Kulane, Mulki Nor Warsame and Aden Isak Ali in Janale; Ahmed Hassan Gomey, Ali Haji Mohamed, Liban Omar Afrah and Ibrahim Muse Mahaad in Jowhar; and Abdi Omar Abdi, Omar Ali Sharif and Ahmed Abdulkadir Mohamed and Ali Abdi Isak in Jamame. We are also grateful to Dr Pascal Ringwald for his collaboration. We thank the technical staff, especially Irene Kamal, Ismail Raafat and Mireille Kamel for their hard work. Financial support for the studies was provided by the Bill and Melinda Gates Foundation. References 1. WHO. World Malaria Report World Health Organization: Geneva, Noor AM, Clements AC, Gething PW et al. Spatial prediction of Plasmodium falciparum prevalence in Somalia. Malaria J 2008: 7: Warsame M, Atta H, Klena JD et al. Efficacy of monotherapies and artesunate-based combination therapies in children with uncomplicated malaria in Somalia. Acta Trop 2009: 109: WHO. Global Report on Antimalarial Efficacy and Drug Resistance: World Health Organization: Geneva, WHO. Guidelines for the Treatment of Malaria (2nd edn), World Health Organization: Geneva, WHO. Updated WHO Policy Recommendation: Intermittent Preventive Treatment of Malaria in Pregnancy Using Sulfadoxine-Pyrimethamine (IPTp-SP). World Health Organization: Geneva, WHO. Status Report on Artemisinin Resistance. World Health Organization: Geneva, [01 January 2015] 8. Roper C, Pearce R, Bredenkamp B et al. Antifolate antimalarial resistance in southeast Africa: a population-based analysis. Lancet 2003: 361: Plowe CV. Antimalarial drug resistance in Africa: strategies for monitoring and deterrence. Curr Top Microbiol Immunol 2005: 295: Wernsdorfer WH, Noedl H. Molecular markers for drug resistance in malaria: use in treatment, diagnosis and epidemiology. Curr Opin Infect Dis 2003: 16: Kublin JG, Dzinjalamala FK, Kamwendo DD et al. Molecular markers for failure of sulfadoxine-pyrimethamine and chlorproguanil-dapsone treatment of Plasmodium falciparum malaria. J Infect Dis 2002: 185: Mombo-Ngoma G, Oyakhirome S, Ord R et al. High prevalence of dhfr triple mutant and correlation with high rates of sulphadoxine-pyrimethamine treatment failures in vivo in Gabonese children. Malaria J 2011: 10: Mugittu K, Ndejembi M, Malisa A et al. Therapeutic efficacy of sulfadoxine-pyrimethamine and prevalence of resistance markers in Tanzania prior to revision of malaria treatment policy: Plasmodium falciparum dihydrofolate reductase and dihydropteroate synthase mutations in monitoring in vivo resistance. Am J Trop Med Hyg 2004: 71: Basco LK, Tahar R, Keundjian A, Ringwald P. Sequence variations in the genes encoding dihydropteroate synthase and dihydrofolate reductase and clinical response to sulfadoxine-pyrimethamine in patients with acute uncomplicated falciparum malaria. J Infect Dis 2000: 182: Nzila AM, Nduati E, Mberu EK et al. Molecular evidence of greater selective pressure for drug resistance exerted by the long-acting antifolate Pyrimethamine/Sulfadoxine compared with the shorter-acting chlorproguanil/dapsone on Kenyan Plasmodium falciparum. J Infect Dis 2000: 181: WHO. Methods for Surveillance of Antimalarial Drug Efficacy. World Health Organization: Geneva, WHO. Methods and Techniques for Clinical Trials on Antimalarial Drug Efficacy: Genotyping to Identify Parasite Populations. World Health Organization: Geneva, Reeder JC, Rieckmann KH, Genton B, Lorry K, Wines B, Cowman AF. Point mutations in the dihydrofolate reductase and dihydropteroate synthetase genes and in vitro susceptibility to pyrimethamine and cycloguanil of Plasmodium falciparum isolates from Papua New Guinea. Am J Trop Med Hyg 1996: 55: Hall TA. BioEdit: a user-friendly biological sequence alignment editor and analysis program for Windows 95/98/NT. Nucleic Acids Symp Ser 1999: 41: Omar SA, Adagu IS, Warhurst DC. Can pretreatment screening for dhps and dhfr point mutations in Plasmodium falciparum infections be used to predict sulfadoxine-pyrimethamine treatment failure? Trans R Soc Trop Med Hyg 2001: 95: Staedke SG, Sendagire H, Lamola S, Kamya MR, Dorsey G, Rosenthal PJ. Relationship between age, molecular markers, and response to sulphadoxine-pyrimethamine treatment in Kampala, Uganda. Tropical Med Int Health 2004: 9: Barnes KI, Watkins WM, White NJ. Antimalarial dosing regimens and drug resistance. Trends Parasitol 2008: 24: Djimde AA, Doumbo OK, Traore O et al. Clearance of drug-resistant parasites as a model for protective immunity in Plasmodium falciparum malaria. Am J Trop Med Hyg 2003: 69: Happi CT, Gbotosho GO, Folarin OA et al. Polymorphisms in Plasmodium falciparum dhfr and dhps genes and age related in vivo sulfadoxine-pyrimethamine resistance in malaria-infected patients from Nigeria. Acta Trop 2005: 95: Raman J, Mauff K, Muianga P, Mussa A, Maharaj R, Barnes KI. Five years of antimalarial resistance marker surveillance in Gaza Province, Mozambique, following artemisinin-based combination therapy roll out. PLoS ONE 2011: 6: e John Wiley & Sons Ltd
8 26. Allen EN, Little F, Camba T et al. Efficacy of sulphadoxinepyrimethamine with or without artesunate for the treatment of uncomplicated Plasmodium falciparum malaria in southern Mozambique: a randomized controlled trial. Malaria J 2009: 8: Roper C, Pearce R, Nair S, Sharp B, Nosten F, Anderson T. Intercontinental spread of pyrimethamine-resistant malaria. Science 2004: 305: Harrington WE, Mutabingwa TK, Kabyemela E, Fried M, Duffy PE. Intermittent treatment to prevent pregnancy malaria does not confer benefit in an area of widespread drug resistance. Clin Infect Dis 2011: 53: Kapito-Tembo A, Meshnick SR, van Hensbroek MB, Phiri K, Fitzgerald M, Mwapasa V. Marked reduction in prevalence of malaria parasitemia and anemia in HIV-infected pregnant women taking cotrimoxazole with or without sulfadoxine-pyrimethamine intermittent preventive therapy during pregnancy in Malawi. J Infect Dis 2011: 203: Menendez C, Bardaji A, Sigauque B et al. A randomized placebo-controlled trial of intermittent preventive treatment in pregnant women in the context of insecticide treated nets delivered through the antenatal clinic. PLoS ONE 2008: 3: e Menendez C, Bardaji A, Sigauque B et al. Malaria prevention with IPTp during pregnancy reduces neonatal mortality. PLoS ONE 2010: 5: e Mockenhaupt FP, Bedu-Addo G, Eggelte TA et al. Rapid increase in the prevalence of sulfadoxine-pyrimethamine resistance among Plasmodium falciparum isolated from pregnant women in Ghana. J Infect Dis 2008: 198: Wilson NO, Ceesay FK, Obed SA et al. Intermittent preventive treatment with sulfadoxine-pyrimethamine against malaria and anemia in pregnant women. Am J Trop Med Hyg 2011: 85: Corresponding Author Marian Warsame, Global Malaria Programme, World Health Organization 20 Avenue Appia, 1211 Geneva 27, Switzerland. warsamem@who.int 2015 John Wiley & Sons Ltd 517
REPORT OF THE TECHNICAL CONSULTATION BACKGROUND
 Defining and validating a measure of parasite resistance to sulfadoxinepyrimethamine (SP) that would be indicative of the protective efficacy of SP for intermittent preventive treatment in infancy (SP-IPTi)
Defining and validating a measure of parasite resistance to sulfadoxinepyrimethamine (SP) that would be indicative of the protective efficacy of SP for intermittent preventive treatment in infancy (SP-IPTi)
A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation
 JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 4, 2012 A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation by Akintunde
JOURNAL OF TROPICAL PEDIATRICS, VOL. 58, NO. 4, 2012 A Simple Dose Regimen of Artesunate and Amodiaquine Based on Arm Span- or Age Range for Childhood Falciparum Malaria: A Preliminary Evaluation by Akintunde
Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
 Tropical Medicine and International Health doi:10.1111/j.1365-3156.2007.01977.x volume 13 no 1 pp 83 90 january 2008 Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
Tropical Medicine and International Health doi:10.1111/j.1365-3156.2007.01977.x volume 13 no 1 pp 83 90 january 2008 Risk associated with asymptomatic parasitaemia occurring post-antimalarial treatment
Downloaded from:
 Myrick, A; Leemann, E; Dokomajilar, C; Hopkins, H; Dorsey, G; Kamya, MR; Rosenthal, PJ (2006) Short report: Dynamics of Plasmodium falciparum malaria after sub-optimal therapy in Uganda. The American journal
Myrick, A; Leemann, E; Dokomajilar, C; Hopkins, H; Dorsey, G; Kamya, MR; Rosenthal, PJ (2006) Short report: Dynamics of Plasmodium falciparum malaria after sub-optimal therapy in Uganda. The American journal
Clinical Analysis Report For Study Sample Study
 Clinical Analysis Report For Study Sample Study Automated report generated by WWARN May 9, 2014 Falciparum class org.wwarn.csr.clinicalstudyreport Version 1.020140508-1558 1 Contents 1 Executive Summary
Clinical Analysis Report For Study Sample Study Automated report generated by WWARN May 9, 2014 Falciparum class org.wwarn.csr.clinicalstudyreport Version 1.020140508-1558 1 Contents 1 Executive Summary
Antimalarial drug resistance
 Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
Antimalarial drug resistance Md Mushfiqur Rahman*, Leonard Ortega**, R M Rastogi* and Krongthong Thimasarn* Abstract Antimalarial drug resistance is of great concern in the WHO South-East Asia (SEA) Region.
MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH MONITORING THE THERAPEUTIC EFFICACY OF ANTIMALARIALS AGAINST UNCOMPLICATED FALCIPARUM MALARIA IN THAILAND C Rojanawatsirivej 1, S Vijaykadga 1, I Amklad 1, P Wilairatna
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Fernandes S, Sicuri E, Kayentao K, et al. Cost-effectiveness
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Fernandes S, Sicuri E, Kayentao K, et al. Cost-effectiveness
Summary. keywords malaria, drug resistance, drug policy, genotypes, antimalarial drugs, Congo
 Tropical Medicine and International Health doi:10.1111/j.1365-3156.2005.01490.x volume 10 no 10 pp 1030 1037 october 2005 Epidemiology of drug-resistant malaria in Republic of Congo: using molecular evidence
Tropical Medicine and International Health doi:10.1111/j.1365-3156.2005.01490.x volume 10 no 10 pp 1030 1037 october 2005 Epidemiology of drug-resistant malaria in Republic of Congo: using molecular evidence
Evolution of Resistance to Sulfadoxine-Pyrimethamine in Plasmodium falciparum
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, June 2004, p. 2116 2123 Vol., No. 6 0066-04/04/$08.00 0 DOI: 10.1128/AAC..6.2116 2123.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, June 2004, p. 2116 2123 Vol., No. 6 0066-04/04/$08.00 0 DOI: 10.1128/AAC..6.2116 2123.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved.
CONCISE COMMUNICATION
 624 CONCISE COMMUNICATION Sequence Variations in the Genes Encoding Dihydropteroate Synthase and Dihydrofolate Reductase and Clinical Response to Sulfadoxine- Pyrimethamine in Patients with Acute Uncomplicated
624 CONCISE COMMUNICATION Sequence Variations in the Genes Encoding Dihydropteroate Synthase and Dihydrofolate Reductase and Clinical Response to Sulfadoxine- Pyrimethamine in Patients with Acute Uncomplicated
INTERMITTENT PREVENTIVE TREATMENT OF MALARIA IN PREGNANCY WITH SULPHADOXINE/PYRIMETHAMINE
 INTERMITTENT PREVENTIVE TREATMENT OF MALARIA IN PREGNANCY WITH SULPHADOXINE/PYRIMETHAMINE WHO EVIDENCE REVIEW GROUP WHO, Geneva, July 9 th 11 th 2012 MPAC MEETING September 11 th - 13 th 2012 CURRENT WHO
INTERMITTENT PREVENTIVE TREATMENT OF MALARIA IN PREGNANCY WITH SULPHADOXINE/PYRIMETHAMINE WHO EVIDENCE REVIEW GROUP WHO, Geneva, July 9 th 11 th 2012 MPAC MEETING September 11 th - 13 th 2012 CURRENT WHO
METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN
 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN 978 92 4 159753 1 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY WHO Library Cataloguing-in-Publication
METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY ISBN 978 92 4 159753 1 METHODS FOR SURVEILLANCE OF ANTIMALARIAL DRUG EFFICACY WHO Library Cataloguing-in-Publication
History, Dynamics, and Public Health Importance of Malaria Parasite Resistance
 CLINICAL MICROBIOLOGY REVIEWS, Jan. 2004, p. 235 254 Vol. 17, No. 1 0893-8512/04/$08.00 0 DOI: 10.1128/CMR.17.1.235 254.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved. History,
CLINICAL MICROBIOLOGY REVIEWS, Jan. 2004, p. 235 254 Vol. 17, No. 1 0893-8512/04/$08.00 0 DOI: 10.1128/CMR.17.1.235 254.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved. History,
Sponsor / Company: Sanofi Drug substance(s): artesunate plus amodiaquine Title of the study:
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Thesis: Community-based studies on the epidemiology, treatment and prevention of malaria in an area of intense malaria transmission in western Kenya
 Summary and discussion Thesis: Community-based studies on the epidemiology, treatment and prevention of malaria in an area of intense malaria transmission in western Kenya Anja Terlouw 16 October 2003
Summary and discussion Thesis: Community-based studies on the epidemiology, treatment and prevention of malaria in an area of intense malaria transmission in western Kenya Anja Terlouw 16 October 2003
Molecular identification of sulfadoxine pyrimethamine resistance in malaria infected women who received intermittent preventive treatment in the
 https://doi.org/10.1186/s12936-017-2160-x Malaria Journal RESEARCH Open Access Molecular identification of sulfadoxine pyrimethamine resistance in malaria infected women who received intermittent preventive
https://doi.org/10.1186/s12936-017-2160-x Malaria Journal RESEARCH Open Access Molecular identification of sulfadoxine pyrimethamine resistance in malaria infected women who received intermittent preventive
Sixth intercountry meeting of national malaria control programme managers from HANMAT and PIAM-Net countries
 Report on the Sixth intercountry meeting of national malaria control programme managers from HANMAT and PIAM-Net countries Cairo, Egypt 13 14 August 2014 Report on the Sixth intercountry meeting of national
Report on the Sixth intercountry meeting of national malaria control programme managers from HANMAT and PIAM-Net countries Cairo, Egypt 13 14 August 2014 Report on the Sixth intercountry meeting of national
MALARIA IS ONE OF THE
 ORIGINAL CONTRIBUTION Combination Therapy for Uncomplicated Falciparum Malaria in Ugandan Children A Randomized Trial Grant Dorsey, MD, PhD Sarah Staedke, MD Tamara D. Clark, MPH Denise Njama-Meya, MB
ORIGINAL CONTRIBUTION Combination Therapy for Uncomplicated Falciparum Malaria in Ugandan Children A Randomized Trial Grant Dorsey, MD, PhD Sarah Staedke, MD Tamara D. Clark, MPH Denise Njama-Meya, MB
38 Current Concepts in
 38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
38 Current Concepts in Management of Falciparum Malaria Abstract: Artemisinin based Combination Therapy (ACT) is the preferred agent to treat drug resistance uncomplicated Plasmodium Falciparum (PF) Malaria.
DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER Chaiporn Rojanawatsirivet 1, Kanungnit Congpuong 1, Saowanit Vijaykadga
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH DECLINING MEFLOQUINE SENSITIVITY OF PLASMODIUM FALCIPARUM ALONG THE THAI-MYANMAR BORDER Chaiporn Rojanawatsirivet 1, Kanungnit Congpuong 1, Saowanit Vijaykadga
Is there Artemisinin Resistance in Western Cambodia?
 Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
Is there Artemisinin Resistance in Western Cambodia? Preliminary results, February 2008 Arjen Dondorp on behalf of the Task Force on Antimalarial Drug Resistance in Cambodia S769N PfATPase6 mutation Artemether
Summary. keywords in vivo efficacy, sulphadoxine pyrimethamine, chloroquine, amodiaquine, combination therapy, falciparum malaria, Uganda
 Tropical Medicine and International Health volume 9 no 2 pp 222 229 february 2004 Efficacy of sulphadoxine pyrimethamine alone or combined with amodiaquine or chloroquine for the treatment of uncomplicated
Tropical Medicine and International Health volume 9 no 2 pp 222 229 february 2004 Efficacy of sulphadoxine pyrimethamine alone or combined with amodiaquine or chloroquine for the treatment of uncomplicated
Statistical Analysis Plan (SAP)
 Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
Statistical Analysis Plan (SAP) Comparison of artemether-lumefantrine and chloroquine with and without primaquine for the treatment of Plasmodium vivax in Ethiopia: a randomized controlled trial Contents
Addressing Malaria in Pregnancy: A Comprehensive Approach to Maternal and Newborn Health Outcomes
 Addressing Malaria in Pregnancy: A Comprehensive Approach to Maternal and Newborn Health Outcomes Malaria is a major public health crisis, especially in sub-saharan Africa, where 90% of all malaria-related
Addressing Malaria in Pregnancy: A Comprehensive Approach to Maternal and Newborn Health Outcomes Malaria is a major public health crisis, especially in sub-saharan Africa, where 90% of all malaria-related
Clinical manifestations of new versus recrudescent malaria infections following anti-malarial drug treatment
 Shaukat et al. Malaria Journal 2012, 11:207 RESEARCH Open Access Clinical manifestations of new versus recrudescent malaria infections following anti-malarial drug treatment Ayesha M Shaukat 1, Elizabeth
Shaukat et al. Malaria Journal 2012, 11:207 RESEARCH Open Access Clinical manifestations of new versus recrudescent malaria infections following anti-malarial drug treatment Ayesha M Shaukat 1, Elizabeth
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia)
 PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
PARASITOLOGY CASE HISTORY #14 (BLOOD PARASITES) (Lynne S. Garcia) A 37-year-old woman, who had traveled to New Guinea for several weeks, presented to the medical clinic with fever, chills, and rigors within
Malaria. Edwin J. Asturias, MD
 Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
Malaria Edwin J. Asturias, MD Associate Professor of Pediatrics and Epidemiology Director for Latin America Center for Global Health, Colorado School of Public Health Global Health and Disasters Course
HIV and Malaria Interactions
 HIV and Malaria Interactions Dr. Moses R. Kamya Chair and Professor of Medicine Makerere University College of Health Sciences Kampala, Uganda INTEREST, Mombasa, Kenya 8 th -11 th May 2012 1 Outline Brief
HIV and Malaria Interactions Dr. Moses R. Kamya Chair and Professor of Medicine Makerere University College of Health Sciences Kampala, Uganda INTEREST, Mombasa, Kenya 8 th -11 th May 2012 1 Outline Brief
Clinical Study Therapeutic Efficacy of Artemether-Lumefantrine for the Treatment of Uncomplicated Plasmodium falciparum Malaria in Northern Ethiopia
 Malaria Research and Treatment Volume 2012, Article ID 548710, 6 pages doi:10.1155/2012/548710 Clinical Study Therapeutic Efficacy of Artemether-Lumefantrine for the Treatment of Uncomplicated Plasmodium
Malaria Research and Treatment Volume 2012, Article ID 548710, 6 pages doi:10.1155/2012/548710 Clinical Study Therapeutic Efficacy of Artemether-Lumefantrine for the Treatment of Uncomplicated Plasmodium
Malaria and HIV infection
 Malaria and HIV infection Philip Rosenthal Dept. of Medicine UCSF The co-epidemics of malaria and HIV infection Malaria 300-500 million episodes each year (~90% in Africa) Over 1 million deaths each year
Malaria and HIV infection Philip Rosenthal Dept. of Medicine UCSF The co-epidemics of malaria and HIV infection Malaria 300-500 million episodes each year (~90% in Africa) Over 1 million deaths each year
Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries
 Summary report on the Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries WHO-EM/MAL/384/E Islamabad, Pakistan 12 14 December 2016 Summary report on the
Summary report on the Eighth intercountry meeting of national malaria programme managers from HANMAT and PIAM-Net countries WHO-EM/MAL/384/E Islamabad, Pakistan 12 14 December 2016 Summary report on the
Interpretation of the World Malaria Report Country Profile
 Interpretation of the World Malaria Report Country Profile Acknowledgements This presentation was developed to help explain the components of the World Malaria Report Country Profile. The 2017 World Malaria
Interpretation of the World Malaria Report Country Profile Acknowledgements This presentation was developed to help explain the components of the World Malaria Report Country Profile. The 2017 World Malaria
Authors Depoortere, E; Guthmann, J P; Pressé, J; Sipilanyambe, N; Nkandu, E; Balkan, S; de Pécoulas, P E; Legros, D /j
 MSF Field Research Efficacy and effectiveness of the combination of sulfadoxine/pyrimethamine and a 3-day course of artesunate for the treatment of uncomplicated falciparum malaria in a refugee settlement
MSF Field Research Efficacy and effectiveness of the combination of sulfadoxine/pyrimethamine and a 3-day course of artesunate for the treatment of uncomplicated falciparum malaria in a refugee settlement
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1
 Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Antimalarials in the WHO Essential Drugs List for Children Reviewer No.1 Part I: Evaluation of the current list Proposed grouping from the March 2007 meeting 6.5.3 Antimalarial medicines 6.5.3.1 For curative
Summary World Malaria Report 2010
 Summary The summarizes information received from 106 malaria-endemic countries and other partners and updates the analyses presented in the 2009 Report. It highlights continued progress made towards meeting
Summary The summarizes information received from 106 malaria-endemic countries and other partners and updates the analyses presented in the 2009 Report. It highlights continued progress made towards meeting
Fang Huang 1, Linhua Tang 1*, Henglin Yang 2, Shuisen Zhou 1, Xiaodong Sun 2 and Hui Liu 2
 Huang et al. Malaria Journal 2012, 11:278 RESEARCH Open Access Therapeutic efficacy of artesunate in the treatment of uncomplicated Plasmodium falciparum malaria and anti-malarial, drug-resistance marker
Huang et al. Malaria Journal 2012, 11:278 RESEARCH Open Access Therapeutic efficacy of artesunate in the treatment of uncomplicated Plasmodium falciparum malaria and anti-malarial, drug-resistance marker
Combination Anti-malarial Therapy and WHO Recommendations
 Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Prakaykaew Charunwatthana 2, and Sasithon Pukrittayakamee 1,2 1 Associate Fellow of the Royal Institute, Academy of Science 2 Department of Clinical Tropical Medicine, Faculty of Tropical Medicine, Mahidol
Minutes of the Technical Expert Group (TEG) on Drug Efficacy and Response
 Malaria Policy Advisory Committee Meeting 16 17 March 2016, Geneva, Switzerland Background document for Session 3 Minutes of the Technical Expert Group (TEG) on Drug Efficacy and Response Crowne Plaza
Malaria Policy Advisory Committee Meeting 16 17 March 2016, Geneva, Switzerland Background document for Session 3 Minutes of the Technical Expert Group (TEG) on Drug Efficacy and Response Crowne Plaza
Akintunde Sowunmi 1,2,5*, Kazeem Akano 1, Adejumoke I. Ayede 3, Godwin Ntadom 4, Temitope Aderoyeje 5, Elsie O. Adewoye 6 and Bayo Fatunmbi 7
 Sowunmi et al. BMC Infectious Diseases (2016) 16:240 DOI 10.1186/s12879-016-1565-4 RESEARCH ARTICLE Clinical illness and outcomes in Nigerian children with late-appearing anaemia after artemisinin-based
Sowunmi et al. BMC Infectious Diseases (2016) 16:240 DOI 10.1186/s12879-016-1565-4 RESEARCH ARTICLE Clinical illness and outcomes in Nigerian children with late-appearing anaemia after artemisinin-based
Downloaded from:
 Dunyo, S; Ord, R; Hallett, R; Jawara, M; Walraven, G; Mesa, E; Coleman, R; Sowe, M; Alexander, N; Targett, GA; Pinder, M; Sutherland, CJ (2006) Randomised Trial of Chloroquine/Sulphadoxine-Pyrimethamine
Dunyo, S; Ord, R; Hallett, R; Jawara, M; Walraven, G; Mesa, E; Coleman, R; Sowe, M; Alexander, N; Targett, GA; Pinder, M; Sutherland, CJ (2006) Randomised Trial of Chloroquine/Sulphadoxine-Pyrimethamine
Domain Dedication waiver
 NAOSITE: Nagasaki University's Ac Title Author(s) Two novel mutations of pfdhps K540T pyrimethamine-resistant response in Banjar district, South Kalimantan P Basuki, Sukmawati; Fitriah; Riyanto Uemura,
NAOSITE: Nagasaki University's Ac Title Author(s) Two novel mutations of pfdhps K540T pyrimethamine-resistant response in Banjar district, South Kalimantan P Basuki, Sukmawati; Fitriah; Riyanto Uemura,
Implementing the Abuja Declaration and Plan of Action: the journey so far
 Implementing the Abuja Declaration and Plan of Action: the journey so far The Abuja Declaration African leaders who met on 25 April 2000 in Abuja, Nigeria, laid out the foundation for a sustained battle
Implementing the Abuja Declaration and Plan of Action: the journey so far The Abuja Declaration African leaders who met on 25 April 2000 in Abuja, Nigeria, laid out the foundation for a sustained battle
Early rising asexual parasitaemia in Nigerian children following a first dose of artemisinin-based combination treatments of falciparum malaria
 Sowunmi et al. BMC Infectious Diseases (2017) 17:110 DOI 10.1186/s12879-016-2173-z RESEARCH ARTICLE Early rising asexual parasitaemia in Nigerian children following a first dose of artemisinin-based combination
Sowunmi et al. BMC Infectious Diseases (2017) 17:110 DOI 10.1186/s12879-016-2173-z RESEARCH ARTICLE Early rising asexual parasitaemia in Nigerian children following a first dose of artemisinin-based combination
Output... Links... Efficacy of artesunate pl...
 Efficacy of artesunate plus pyrimethamine-sulphadoxine for uncomplicated malaria in Gambian children: a double-blind, randomised, controlled trial [Articles] von Seidlein, Lorenz; Milligan, Paul; Pinder,
Efficacy of artesunate plus pyrimethamine-sulphadoxine for uncomplicated malaria in Gambian children: a double-blind, randomised, controlled trial [Articles] von Seidlein, Lorenz; Milligan, Paul; Pinder,
Comparison of light microscopy and nested PCR assay in detecting of malaria mixed species infections in an endemic area of Iran
 Comparison of light microscopy and nested PCR assay in detecting of malaria mixed species infections in an endemic area of Iran Aliehsan Heidari, Manizheh Nourian, Hossein Keshavarz Associate Prof. Dept.
Comparison of light microscopy and nested PCR assay in detecting of malaria mixed species infections in an endemic area of Iran Aliehsan Heidari, Manizheh Nourian, Hossein Keshavarz Associate Prof. Dept.
Downloaded from:
 Bukirwa, H; Yeka, A; Kamya, MR; Talisuna, A; Banek, K; Bakyaita, N; Rwakimari, JB; Rosenthal, PJ; Wabwire-Mangen, F; Dorsey, G; Staedke, SG (2006) Artemisinin combination therapies for treatment of uncomplicated
Bukirwa, H; Yeka, A; Kamya, MR; Talisuna, A; Banek, K; Bakyaita, N; Rwakimari, JB; Rosenthal, PJ; Wabwire-Mangen, F; Dorsey, G; Staedke, SG (2006) Artemisinin combination therapies for treatment of uncomplicated
OF ANTIMALARIAL DRUGS
 THE USE OF ANTIMALARIAL DRUGS THE USE OF ANTIMALARIAL DRUGS Report of an Informal Consultation World Health Organization, Geneva WHO, 2001 Technical Review: A. Bosman, C. Delacollette, P. Olumese, R. G.
THE USE OF ANTIMALARIAL DRUGS THE USE OF ANTIMALARIAL DRUGS Report of an Informal Consultation World Health Organization, Geneva WHO, 2001 Technical Review: A. Bosman, C. Delacollette, P. Olumese, R. G.
Malaria Updates. Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine
 Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
Malaria Updates Fe Esperanza Espino Department of Parasitology Research Institute for Tropical Medicine Outline General epidemiology of malaria in the Philippines P falciparum Updates in treatment Recognizing
Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies
 DOI 10.1186/s12936-017-1775-2 Malaria Journal RESEARCH Open Access Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies Moe Kyaw Myint
DOI 10.1186/s12936-017-1775-2 Malaria Journal RESEARCH Open Access Therapeutic efficacy and artemisinin resistance in northern Myanmar: evidence from in vivo and molecular marker studies Moe Kyaw Myint
Checchi, F; Piola, P; Kosack, C; Ardizzoni, E; Klarkowski, D; Kwezi, E; Priotto, G; Balkan, S; Bakyaita, N; Brockman, A; Guthmann, J P
 MSF Field Research Antimalarial efficacy of sulfadoxine-pyrimethamine, amodiaquine and a combination of chloroquine plus sulfadoxinepyrimethamine in Bundi Bugyo, western Uganda. Authors Citation DOI Publisher
MSF Field Research Antimalarial efficacy of sulfadoxine-pyrimethamine, amodiaquine and a combination of chloroquine plus sulfadoxinepyrimethamine in Bundi Bugyo, western Uganda. Authors Citation DOI Publisher
ISSN X (Print) Original Research Article. DOI: /sjams India
 DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
DOI: 10.21276/sjams.2016.4.6.22 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(6B):1981-198 5 Scholars Academic and Scientific Publisher (An International Publisher
A systematic approach to the development of a rational malaria treatment policy in Zambia
 Tropical Medicine and International Health volume 3 no 7 pp 535 542 july 1998 A systematic approach to the development of a rational malaria treatment policy in Zambia Lawrence M. Barat 1, Benson Himonga
Tropical Medicine and International Health volume 3 no 7 pp 535 542 july 1998 A systematic approach to the development of a rational malaria treatment policy in Zambia Lawrence M. Barat 1, Benson Himonga
The contribution of clinical pharmacology to antimalarial drug discovery and development
 Blackwell Science, LtdOxford, UKBCPBritish Journal of Clinical Pharmacology0306-5251Blackwell Publishing 2003? 200355?464468Original ArticleMalaria chemotherapyp. Winstanley The contribution of clinical
Blackwell Science, LtdOxford, UKBCPBritish Journal of Clinical Pharmacology0306-5251Blackwell Publishing 2003? 200355?464468Original ArticleMalaria chemotherapyp. Winstanley The contribution of clinical
Low Efficacy of Vocamine (MMH8, Pediatric Formulation) in the Treatment of Uncomplicated Plasmodium falciparum Malaria
 8 The Open Tropical Medicine Journal, 2009, 2, 8-12 Low Efficacy of Vocamine (MMH8, Pediatric Formulation) in the Treatment of Uncomplicated Plasmodium falciparum Malaria Open Access Didier Ménard 1,*,
8 The Open Tropical Medicine Journal, 2009, 2, 8-12 Low Efficacy of Vocamine (MMH8, Pediatric Formulation) in the Treatment of Uncomplicated Plasmodium falciparum Malaria Open Access Didier Ménard 1,*,
Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative
 Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative I. Background For many years, the border area between Cambodia and Thailand has been the source
Progress on the Containment of Artemisinin Tolerant Malaria Parasites in South-East Asia (ARCE) Initiative I. Background For many years, the border area between Cambodia and Thailand has been the source
drug efficacy and drug resistance:
 Global report on antimalarial drug efficacy and drug resistance: 2000 2010 WHO Library Cataloguing-in-Publication Data Global report on antimalarial drug efficacy and drug resistance: 2000-2010. 1.Malaria
Global report on antimalarial drug efficacy and drug resistance: 2000 2010 WHO Library Cataloguing-in-Publication Data Global report on antimalarial drug efficacy and drug resistance: 2000-2010. 1.Malaria
DETERMINANTS OF PARASITE CLEARANCE TIME AND RECRUDESCENCE IN PATIENTS TREATED FOR UNCOMPLICATED PLASMODIUM FALCIPARUM MALARIA IN SUB-SAHARAN AFRICA
 DETERMINANTS OF PARASITE CLEARANCE TIME AND RECRUDESCENCE IN PATIENTS TREATED FOR UNCOMPLICATED PLASMODIUM FALCIPARUM MALARIA IN SUB-SAHARAN AFRICA Mary A. Woessner A dissertation submitted to the faculty
DETERMINANTS OF PARASITE CLEARANCE TIME AND RECRUDESCENCE IN PATIENTS TREATED FOR UNCOMPLICATED PLASMODIUM FALCIPARUM MALARIA IN SUB-SAHARAN AFRICA Mary A. Woessner A dissertation submitted to the faculty
Study No.: Title: Rationale: Phase: Study Period: Study Design: Centers: Indication: Treatment: Objective: Primary Outcome/Efficacy Variable:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
Manuscripts for the WHO Evidence Review Group for malaria in pregnancy (MiP-ERG), July 2015
 Malaria Policy Advisory Committee Meeting 5 7 March 2015, Geneva, Switzerland Background document for Session 4 Manuscripts for the WHO Evidence Review Group for malaria in pregnancy (MiP-ERG), July 2015
Malaria Policy Advisory Committee Meeting 5 7 March 2015, Geneva, Switzerland Background document for Session 4 Manuscripts for the WHO Evidence Review Group for malaria in pregnancy (MiP-ERG), July 2015
Sponsor / Company: Sanofi Drug substance(s): SSR103371
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Clinical Study Clinical Efficacy of Artemether-Lumefantrine in Congolese Children with Acute Uncomplicated Falciparum Malaria in Brazzaville
 Malaria Research and Treatment Volume 2012, Article ID 749479, 5 pages doi:10.1155/2012/749479 Clinical Study Clinical Efficacy of Artemether-Lumefantrine in Congolese Children with Acute Uncomplicated
Malaria Research and Treatment Volume 2012, Article ID 749479, 5 pages doi:10.1155/2012/749479 Clinical Study Clinical Efficacy of Artemether-Lumefantrine in Congolese Children with Acute Uncomplicated
In several African countries in sub-saharan Africa, malaria is the leading cause of death in children under five.
 TECHNICAL SEMINAR - MALARIA SLIDE 1 Technical Seminar - Malaria Malaria is an extremely important cause of mortality in different parts of world. In this technical seminar, I ll discuss the rationale for
TECHNICAL SEMINAR - MALARIA SLIDE 1 Technical Seminar - Malaria Malaria is an extremely important cause of mortality in different parts of world. In this technical seminar, I ll discuss the rationale for
Coulibaly et al. Malaria Journal 2014, 13:41
 Coulibaly et al. Malaria Journal 2014, 13:41 RESEARCH Open Access Parasite clearance following treatment with sulphadoxine-pyrimethamine for intermittent preventive treatment in Burkina-Faso and Mali:
Coulibaly et al. Malaria Journal 2014, 13:41 RESEARCH Open Access Parasite clearance following treatment with sulphadoxine-pyrimethamine for intermittent preventive treatment in Burkina-Faso and Mali:
Genetic Diversity of Plasmodium falciparum Strains in Children under Five Years of Age in Southeastern Tanzania
 10 The Open Tropical Medicine Journal, 2010,, 10-14 Open Access Genetic Diversity of Plasmodium falciparum Strains in Children under Five Years of Age in Southeastern Tanzania Deborah Sumari *,1, Ken M.
10 The Open Tropical Medicine Journal, 2010,, 10-14 Open Access Genetic Diversity of Plasmodium falciparum Strains in Children under Five Years of Age in Southeastern Tanzania Deborah Sumari *,1, Ken M.
MAJOR ARTICLE. malaria; artemether/lumefantrine; vivax; effectiveness.
 MAJOR ARTICLE Effectiveness of Artemether/Lumefantrine for the Treatment of Uncomplicated Plasmodium vivax and P. falciparum Malaria in Young Children in Papua New Guinea Nicolas Senn, 1,2,3,4 Patricia
MAJOR ARTICLE Effectiveness of Artemether/Lumefantrine for the Treatment of Uncomplicated Plasmodium vivax and P. falciparum Malaria in Young Children in Papua New Guinea Nicolas Senn, 1,2,3,4 Patricia
Effect of HIV-1 Infection on Antimalarial Treatment Outcomes in Uganda: A Population-Based Study
 MAJOR ARTICLE Effect of HIV-1 Infection on Antimalarial Treatment Outcomes in Uganda: A Population-Based Study Moses R. Kamya, 1 Anne F. Gasasira, 1 Adoke Yeka, 2 Nathan Bakyaita, 2 Samuel L. Nsobya, 1
MAJOR ARTICLE Effect of HIV-1 Infection on Antimalarial Treatment Outcomes in Uganda: A Population-Based Study Moses R. Kamya, 1 Anne F. Gasasira, 1 Adoke Yeka, 2 Nathan Bakyaita, 2 Samuel L. Nsobya, 1
Molecular surveillance of drug-resistance associated mutations of Plasmodium falciparum in south-west Tanzania
 Malaria Journal This Provisional PDF corresponds to the article as it appeared upon acceptance. Copyedited and fully formatted PDF and full text (HTML) versions will be made available soon. Molecular surveillance
Malaria Journal This Provisional PDF corresponds to the article as it appeared upon acceptance. Copyedited and fully formatted PDF and full text (HTML) versions will be made available soon. Molecular surveillance
Rectal artesunate for pre-referral treatment of severe malaria
 Global Malaria Programme Rectal artesunate for pre-referral treatment of severe malaria october 2017 information note Background Severe malaria is a medical emergency: mortality from untreated severe malaria
Global Malaria Programme Rectal artesunate for pre-referral treatment of severe malaria october 2017 information note Background Severe malaria is a medical emergency: mortality from untreated severe malaria
Outcome of Presumptive Ukwaja K. et al 179
 Outcome of Presumptive Ukwaja K. et al 179 ORIGINAL ARTICLE OUTCOME OF PRESUMPTIVE VERSUS RAPID DIAGNOSTIC TESTS-BASED MANAGEMENT OF CHILDHOOD MALARIA PNEUMONIA OVERLAP IN URBAN NIGERIA: A PILOT QUASI-
Outcome of Presumptive Ukwaja K. et al 179 ORIGINAL ARTICLE OUTCOME OF PRESUMPTIVE VERSUS RAPID DIAGNOSTIC TESTS-BASED MANAGEMENT OF CHILDHOOD MALARIA PNEUMONIA OVERLAP IN URBAN NIGERIA: A PILOT QUASI-
APPLICATION FOR REVISION AND INCLUSION OF MALARIA MEDICINES IN WHO MODEL LIST OF ESSENTIAL MEDICINES
 APPLICATION FOR REVISION AND INCLUSION OF MALARIA MEDICINES IN WHO MODEL LIST OF ESSENTIAL MEDICINES The objective of this application is to assure compatibility between the WHO Model list of essential
APPLICATION FOR REVISION AND INCLUSION OF MALARIA MEDICINES IN WHO MODEL LIST OF ESSENTIAL MEDICINES The objective of this application is to assure compatibility between the WHO Model list of essential
Ending Malaria in Nigeria: The WHO Agenda
 Nigeria Institute of Medical Research 2016 World Malaria Day Lecture 27 April, 2016 Ending Malaria in Nigeria: The WHO Agenda Dr Tolu Arowolo Malaria Containment Programme, WHO, Nigeria arowolot@who.int
Nigeria Institute of Medical Research 2016 World Malaria Day Lecture 27 April, 2016 Ending Malaria in Nigeria: The WHO Agenda Dr Tolu Arowolo Malaria Containment Programme, WHO, Nigeria arowolot@who.int
Prevalence of polymorphisms in antifolate drug resistant molecular marker. genes, pvdhfr and pvdhps in clinical isolates from Kolkata, India
 AAC Accepts, published online ahead of print on 21 October 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.01171-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 1 2 Prevalence
AAC Accepts, published online ahead of print on 21 October 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.01171-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 1 2 Prevalence
Original Article. Ayan Basu 1, Santanu Saha 2, Subhasish Kamal Guha 3. Introduction. Abstract
 32 Journal of The Association of Physicians of India Vol. 63 May 2015 Original Article Comparative Study of Effectiveness and Resistance Profile of Chloroquine and Sulfadoxine-Pyrimethamine in Uncomplicated
32 Journal of The Association of Physicians of India Vol. 63 May 2015 Original Article Comparative Study of Effectiveness and Resistance Profile of Chloroquine and Sulfadoxine-Pyrimethamine in Uncomplicated
Issue 8: January December 2016 National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana
 Issue 8: January December National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights 1 Malaria Burden 2 Key Activities Undertaken in 2 Malaria
Issue 8: January December National Malaria Control Programme (NMCP) Box KB 493 Korle - Bu Accra Ghana Contents Page Editorial and Report Highlights 1 Malaria Burden 2 Key Activities Undertaken in 2 Malaria
POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region
 POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region Background Malaria is a substantial public health threat in the Americas. In 2010, the Americas had approximately
POLICY BRIEF Review of Antimalarial Medicines Available to Treat P. falciparum in the Amazon Region Background Malaria is a substantial public health threat in the Americas. In 2010, the Americas had approximately
High level Plasmodium falciparum sulfadoxine pyrimethamine resistance with the concomitant occurrence of septuple haplotype in Tanzania
 DOI 10.1186/s12936-015-0977-8 RESEARCH Open Access High level Plasmodium falciparum sulfadoxine pyrimethamine resistance with the concomitant occurrence of septuple haplotype in Tanzania Vito Baraka 1,2*,
DOI 10.1186/s12936-015-0977-8 RESEARCH Open Access High level Plasmodium falciparum sulfadoxine pyrimethamine resistance with the concomitant occurrence of septuple haplotype in Tanzania Vito Baraka 1,2*,
Repellent Soap. The Jojoo Mosquito. Africa s innovative solution to Malaria prevention. Sapphire Trading Company Ltd
 The Jojoo Mosquito Repellent Soap Africa s innovative solution to Malaria prevention Sapphire Trading Company Ltd P.O.Box: 45938-00100 Nairobi, Kenya. Tel: +254 735 397 267 +254 733 540 868 +254 700 550
The Jojoo Mosquito Repellent Soap Africa s innovative solution to Malaria prevention Sapphire Trading Company Ltd P.O.Box: 45938-00100 Nairobi, Kenya. Tel: +254 735 397 267 +254 733 540 868 +254 700 550
A Head-to-Head Comparison of Four Artemisinin-Based Combinations for Treating Uncomplicated Malaria in African Children: A Randomized Trial
 A Head-to-Head Comparison of Four Artemisinin-Based Combinations for Treating Uncomplicated Malaria in African Children: A Randomized Trial The Four Artemisinin-Based Combinations (4ABC) Study Group* "
A Head-to-Head Comparison of Four Artemisinin-Based Combinations for Treating Uncomplicated Malaria in African Children: A Randomized Trial The Four Artemisinin-Based Combinations (4ABC) Study Group* "
Chloroquine/sulphadoxinepyrimethamine. Children with Malaria: Transmission to Mosquitoes of Multidrug-Resistant Plasmodium falciparum
 Chloroquine/Sulphadoxine-Pyrimethamine for Gambian Children with Malaria: Transmission to Mosquitoes of Multidrug-Resistant Plasmodium falciparum Rachel L. Hallett 1, Samuel Dunyo 2, Rosalynn Ord 1, Musa
Chloroquine/Sulphadoxine-Pyrimethamine for Gambian Children with Malaria: Transmission to Mosquitoes of Multidrug-Resistant Plasmodium falciparum Rachel L. Hallett 1, Samuel Dunyo 2, Rosalynn Ord 1, Musa
Disclosure Information
 Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Malaria Medications Charlie Mosler, RPh, PharmD, CGP, FASCP Assistant Professor of Pharmacy Practice The University of Findlay College of Pharmacy Findlay, OH mosler@findlay.edu Disclosure Information
Kustantajan versio View/Open
 This document has been downloaded from Tampub The Institutional Repository of University of Tampere Kustantajan versio 150.6Kb View/Open Author(s): Luntamo, Mari; Rantala, Anne-Maria; Meshnick, Steven
This document has been downloaded from Tampub The Institutional Repository of University of Tampere Kustantajan versio 150.6Kb View/Open Author(s): Luntamo, Mari; Rantala, Anne-Maria; Meshnick, Steven
Downloaded from:
 Kapisi, J; Bigira, V; Clark, T; Kinara, S; Mwangwa, F; Achan, J; Kamya, M; Soremekun, S; Dorsey, G (2015) Efficacy and safety of artemether-lumefantrine for the treatment of uncomplicated malaria in the
Kapisi, J; Bigira, V; Clark, T; Kinara, S; Mwangwa, F; Achan, J; Kamya, M; Soremekun, S; Dorsey, G (2015) Efficacy and safety of artemether-lumefantrine for the treatment of uncomplicated malaria in the
Roger CK Tine *, Babacar Faye, Khadime Sylla, Jean L Ndiaye, Magatte Ndiaye, Doudou Sow, Aminata C Lo, Annie Abiola, Mamadou C Ba and Oumar Gaye
 Tine et al. Malaria Journal 2012, 11:416 RESEARCH Open Access Efficacy and tolerability of a new formulation of artesunate-mefloquine for the treatment of uncomplicated malaria in adult in Senegal: open
Tine et al. Malaria Journal 2012, 11:416 RESEARCH Open Access Efficacy and tolerability of a new formulation of artesunate-mefloquine for the treatment of uncomplicated malaria in adult in Senegal: open
Directorate of National Vector Borne Disease Control Programme
 NATIONAL DRUG POLICY ON MALARIA (2008) Directorate of National Vector Borne Disease Control Programme (Directorate General of Health Services) Ministry of Health and Family Welfare 22-Shamnath Marg,, Delhi-110054..
NATIONAL DRUG POLICY ON MALARIA (2008) Directorate of National Vector Borne Disease Control Programme (Directorate General of Health Services) Ministry of Health and Family Welfare 22-Shamnath Marg,, Delhi-110054..
A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis
 A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis and its Chinese Partners Hans Rietveld, Director, Global Access and Marketing, Malaria Initiative, Novartis Pharma AG Workshop on Access
A New Class of Malaria Drugs: The Coartem Breakthrough from Novartis and its Chinese Partners Hans Rietveld, Director, Global Access and Marketing, Malaria Initiative, Novartis Pharma AG Workshop on Access
14th Stakeholders Meeting
 14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 David Hughes, Novartis 12th October 2017 Defeating Malaria
14th Stakeholders Meeting Steady progress towards malaria elimination: Interventions for today and tomorrow Denpasar, Bali 11 12 October 2017 David Hughes, Novartis 12th October 2017 Defeating Malaria
IHI Biomedical Sciences Group. Joseph Mugasa, PhD, PD. Stakeholders Meeting
 IHI Biomedical Sciences Group Joseph Mugasa, PhD, PD Stakeholders Meeting Jan 2013 Overview Biomedical group carries out a range of laboratory studies with the aim of understanding the pathogenesis, diagnosis
IHI Biomedical Sciences Group Joseph Mugasa, PhD, PD Stakeholders Meeting Jan 2013 Overview Biomedical group carries out a range of laboratory studies with the aim of understanding the pathogenesis, diagnosis
HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA
 HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA Pages with reference to book, From 8 To 10 Mushtaq A. Khan, Gui Nayyer Rehman, S.A. Qazi ( Children Hospital, Pakistan Institute
HALOFANTRINE HYDROCHLORIDE - EFFICACY AND SAFETY IN CHILDREN WITH ACUTE MALARIA Pages with reference to book, From 8 To 10 Mushtaq A. Khan, Gui Nayyer Rehman, S.A. Qazi ( Children Hospital, Pakistan Institute
Atovaquone Proguanil (Malarone): an Effective Treatment for Uncomplicated Plasmodium falciparum Malaria in Travelers from Denmark
 Atovaquone Proguanil (Malarone): an Effective Treatment for Uncomplicated Plasmodium falciparum Malaria in Travelers from Denmark Sören Thybo, Ida Gjorup,Anita M. Ronn, Dan Meyrowitsch, and Ib C. Bygberg
Atovaquone Proguanil (Malarone): an Effective Treatment for Uncomplicated Plasmodium falciparum Malaria in Travelers from Denmark Sören Thybo, Ida Gjorup,Anita M. Ronn, Dan Meyrowitsch, and Ib C. Bygberg
Downloaded from:
 Abreha, T; Alemayehu, B; Assefa, A; Awab, GR; Baird, JK; Bezabih, B; Cheah, PY; Day, NP; Devine, A; Dorda, M; Dondorp, AM; Girma, S; Hien, TT; Jima, D; Kassa, M; Kebende, A; Khu, NH; Leslie, T; Ley, B;
Abreha, T; Alemayehu, B; Assefa, A; Awab, GR; Baird, JK; Bezabih, B; Cheah, PY; Day, NP; Devine, A; Dorda, M; Dondorp, AM; Girma, S; Hien, TT; Jima, D; Kassa, M; Kebende, A; Khu, NH; Leslie, T; Ley, B;
WHO Consultation on universal access to core malaria interventions in high burden countries: main conclusions and recommendations
 WHO Consultation on universal access to core malaria interventions in high burden countries: main conclusions and recommendations 12-15 February 2018 Salle XI, ILO Building, Geneva, Switzerland Country
WHO Consultation on universal access to core malaria interventions in high burden countries: main conclusions and recommendations 12-15 February 2018 Salle XI, ILO Building, Geneva, Switzerland Country
IN VIVO EFFICACY AND SAFETY OF QUININE-DOXYCYCLINE COMBINATION IN ACUTE PLASMODIUM FALCIPARUM MALARIA
 Original Article IN VIVO EFFICACY AND SAFETY OF QUININE-DOXYCYCLINE COMBINATION IN ACUTE PLASMODIUM FALCIPARUM MALARIA Abdul Rasheed 1, Shahzad Saeed 2 ABSTRACT Objective: To find out the in vivo efficacy
Original Article IN VIVO EFFICACY AND SAFETY OF QUININE-DOXYCYCLINE COMBINATION IN ACUTE PLASMODIUM FALCIPARUM MALARIA Abdul Rasheed 1, Shahzad Saeed 2 ABSTRACT Objective: To find out the in vivo efficacy
THE EFFECTS OF HAEMOGLOBINOPATHIES AND G6PD DEFICIENCY ON MALARIA AMONG CHILDREN OF THE KINTAMPO NORTH MUNICIPALITY OF GHANA
 THE EFFECTS OF HAEMOGLOBINOPATHIES AND G6PD DEFICIENCY ON MALARIA AMONG CHILDREN OF THE KINTAMPO NORTH MUNICIPALITY OF GHANA Presenter: Amoako Nicholas 1 Supervisors: Dr. Kwaku Poku Asante 1, Dr. Bimi
THE EFFECTS OF HAEMOGLOBINOPATHIES AND G6PD DEFICIENCY ON MALARIA AMONG CHILDREN OF THE KINTAMPO NORTH MUNICIPALITY OF GHANA Presenter: Amoako Nicholas 1 Supervisors: Dr. Kwaku Poku Asante 1, Dr. Bimi
Box 1. Recommendations unchanged from the first edition of the Guidelines (2006)
 Executive summary Executive Summary Malaria case management remains a vital component of the malaria control strategies. This entails early diagnosis and prompt treatment with effective antimalarial medicines.
Executive summary Executive Summary Malaria case management remains a vital component of the malaria control strategies. This entails early diagnosis and prompt treatment with effective antimalarial medicines.
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS
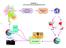 APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
APPENDIX 1 DATA COLLECTION AND DISSEMINATION STEPS 97 Country/ area APPENDIX 2a DRUG REGIMENS SEA REGION, 2001 (dosage for adults) : P. falciparum Lab confirmed Treatment failure Severe malaria Pregnancy
Artesunate combinations for treatment of malaria: meta-analysis
 Articles Artesunate combinations for treatment of malaria: meta-analysis International Artemisinin Study Group* Summary Background Addition of artemisinin derivatives to existing drug regimens for malaria
Articles Artesunate combinations for treatment of malaria: meta-analysis International Artemisinin Study Group* Summary Background Addition of artemisinin derivatives to existing drug regimens for malaria
WHO Malaria Surveillance Reference Manual. Dr Abdisalan M Noor, Team Leader, Surveillance, Monitoring and Evaluation Webinar, 29 May 2018
 WHO Malaria Surveillance Reference Manual Dr Abdisalan M Noor, Team Leader, Surveillance, Monitoring and Evaluation Webinar, 29 May 2018 Pillar 3 of the GTS Previous documents and the elimination framework
WHO Malaria Surveillance Reference Manual Dr Abdisalan M Noor, Team Leader, Surveillance, Monitoring and Evaluation Webinar, 29 May 2018 Pillar 3 of the GTS Previous documents and the elimination framework
Phenotyping Plasmodium vivax in Indonesia using Standard Chloroquine Therapy. Puji Budi Setia Asih. Eijkman Institute for Molecular Biology
 Phenotyping Plasmodium vivax in Indonesia using Standard Chloroquine Therapy Puji Budi Setia Asih Eijkman Institute for Molecular Biology Background Plasmodium vivax threatens 2.6 billion people with a
Phenotyping Plasmodium vivax in Indonesia using Standard Chloroquine Therapy Puji Budi Setia Asih Eijkman Institute for Molecular Biology Background Plasmodium vivax threatens 2.6 billion people with a
Am. J. Trop. Med. Hyg., 60(2), 1999, pp Copyright 1999 by The American Society of Tropical Medicine and Hygiene
 Am. J. Trop. Med. Hyg., 60(2), 1999, pp. 238 243 Copyright 1999 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED, DOUBLE-BLIND, COMPARATIVE TRIAL OF A NEW ORAL COMBINATION OF ARTEMETHER
Am. J. Trop. Med. Hyg., 60(2), 1999, pp. 238 243 Copyright 1999 by The American Society of Tropical Medicine and Hygiene A RANDOMIZED, DOUBLE-BLIND, COMPARATIVE TRIAL OF A NEW ORAL COMBINATION OF ARTEMETHER
