Anaphylaxis: clinical features, management and avoidance
|
|
|
- Chastity Wood
- 6 years ago
- Views:
Transcription
1 Anaphylaxis: clinical features, management and avoidance James Bateman MRCP and Robin Ferner MSc, MD, FRCP VM Our series on serious ADRs focusses on rare but potentially fatal drug reactions and how to recognise and avoid them. This article describes the features, causes and management of anaphylaxis and how to avoid a recurrence. Figure 1. Intramuscular injection is the most effective way to give adrenaline, and those at considerable risk of anaphylaxis should carry an adrenaline pen Anaphylaxis is an important and potentially fatal immunologically-mediated reaction that presents as a medical emergency. Drugs, of course, are an important cause. Accurate clinical diagnosis and prompt treatment with the correct therapy saves lives. Death is usually a result of circulatory collapse and bronchospasm. All practitioners should understand the causes of anaphylaxis, know how to diagnose it and be able to administer effective treatment. In general all patients with suspected anaphylaxis should be referred to hospital for further clinical assessment and monitoring. Incidence Anaphylaxis is a severe allergic reaction of abrupt onset. It occurs when an antigen binds to immunoglobulin E (IgE) attached to mast cells, releasing inflammatory mediators. The true incidence of anaphylaxis is not known because events are rare, data are collected retrospectively and case definitions vary. In the UK, about four persons per per year are treated in hospital for anaphylaxis, and it is the reason for between 1 in 2300 to 1 in 5800 attendances to casualty departments. The risk of a fatal anaphylactic reaction to a prescribed penicillin is estimated as 2 per in the general population. 1 A recent study suggested that 1-15 per cent of the USA population were potentially at risk from an anaphylactic reaction, reflecting the great uncertainty in the estimates. 2 The rate of fatal and serious anaphylactic reactions to food allergens has probably increased over the past two decades. Pathophysiology Allergens cause anaphylaxis via their binding to specific IgE receptors attached to mast cells. The antigen-antibody complex then activates an immunological cascade, in which mast cells and basophils release mediators including histamine, cyclo-oxygenase products such as thromboxane A 2, leukotrienes and mast cell tryptase that in turn activate other vasoactive mediators such as bradykinin. The mediators increase smooth muscle tone in bronchi, 12 Prescriber 19 May
2 blood vessels and gut, and increase capillary permeability so that fluid leaks from the circulating blood volume, causing both hypotension and oedema and making airways obstruction worse. 3 Anaphylactoid reactions cause a clinically indistinguishable syndrome as a result of mast cell degranulation without the involvement of IgE. Triggers in such reactions act on the mast cells and mediator release is directly related to drug concentration. Consequently, such reactions are more readily terminated, tend to be more rare and are less serious. Angioedema is a more localised response but may be lifethreatening if it involves the upper airway. Some attacks may be triggered by medication. Clinical features The history often gives clues to the diagnosis of anaphylaxis, eg the recent intravenous administration of a drug or the introduction of a new treatment. Parenteral medications are more likely to result in severe anaphylactic reactions of rapid onset. A drug is unlikely to have caused anaphylaxis if the onset of symptoms is delayed for more than half an hour after intravenous administration of the putative allergen, although longer delays are possible after oral administration. A previous history of anaphylaxis to an allergen places the individual at high risk of further attacks if given the same allergen or a cross-reaction allergen of chemical structure, eg cephalosporins in a patient know to be allergic to penicillin. Patients with atopy are at higher risk, and patients with pre-existing asthma more likely to come to harm. System general pulmonary cardiovascular dermatological GI Clinical features collapse, shock, anxiety, restlessness, rhinitis, flushing, pallor respiratory distress, wheeze, stridor, airways oedema hypotension, collapse, loss of consciousness, tachycardia erythema, urticaria, oedema, pruritus abdominal cramp, vomiting, diarrhoea Table 1. Clinical features of anaphylaxis (key features in italics) Table 1 lists the signs and symptoms of anaphylaxis. Respiratory distress (due to bronchospasm and laryngeal or airways oedema) and hypotension (from loss of intravascular fluid) are two of the cardinal features of severe anaphylaxis. Urticaria or generalised erythema is also common. Anxiety disorder, asthma and vasovagal syncope can all be confused with anaphylaxis in the clinical context. Causes Adverse drug reactions comprise one-third of all cases of anaphylaxis. Reactions to foodstuffs, insect bites and hymenoptera stings are responsible for the other two-thirds. The most commonly used group of drugs to cause anaphylaxis are the penicillin derivatives. Other causes include other antibiotics, blood and immunological products, drugs used in anaesthesia and radiocontrast media. The common drugs causing anaphylaxis are shown in Table 2. Commonly used drugs that result in anaphylactoid reactions include NSAIDs, codeine phosphate and N-acetylcysteine. Management of anaphylaxis The cornerstone of management of anaphylaxis is the administration of adrenaline by intramuscular injection. The Resuscitation Council (UK) has issued guidelines for the management of anaphylaxis both in and outside of the hospital. 4 They are based on expert opinion and experience rather than randomised controlled clinical trials. Outside hospital, the presence of hypotension, cardiovascular collapse or respiratory distress should prompt basic life support measures and a call for an ambulance. Where relevant, further exposure to the allergen should be avoided. Adrenaline should be administered, either in or outside hospital, and oxygen should be given. Antihistamines, hydrocortisone, fluid replacement and nebulised salbutamol also play a role in management. Adrenaline Adrenaline has alpha- and betaagonist activity, increasing peripheral vascular tone, myocardial contractility and heart rate, and relaxing bronchial smooth muscle. There are several available preparations of adrenaline, of different concentrations and suitable for different routes of administration. This can lead to medication errors by emergency medical and paramedical staff. Intramuscular administration The safest effective way to give adrenaline is by intramuscular injection. The correct initial dose Prescriber 19 May
3 Antibiotics Contrast media Immunosuppressants Parenteral Miscellaneous penicillins iodine-based ciclosporin blood products NSAIDs* cephalosporins contrast media methotrexate immunoglobulin aspirin* tetracyclines vaccinations opiates* macrolides insulin local anaesthetics quinolones neuromuscular- hyposensitising blocking drugs (allergen) preparations heparin horse sera (eg snake antivenom) Table 2. Common groups of drugs causing anaphylaxis (*may be anaphylactoid) in an adult is 500µg, administered as a dose of 0.5ml im of a 1mg per ml (1:1000) preparation. Repeated doses of adrenaline can be given at two- to five-minute intervals until symptoms improve. The doses recommended by the Resuscitation Council (UK) in conjunction with the BNF are shown in Table 3. The available evidence suggests that the early administration of adrenaline increases survival in severe anaphylaxis. This means that adrenaline treatment should be given as soon as the clinical diagnosis is apparent, even though Age Adult Adult but taking TCA or MAOI Over 12 years Over 12 years but small or prepubertal From 6-12 years From 6 months- 6 years Less than 6 months adrenaline has potential adverse effects. Intravenous administration In life-threatening circumstances such as circulatory collapse, intravenous adrenaline administration may be warranted (in conjunction with intravenous access, suitable monitoring equipment and medical personnel experienced in its use). It should not normally be used, however, because intravenous adrenaline administration commonly causes serious ventricular arrhythmias, requires preexisting venous access and is prone to medication errors. 500µg im (0.5ml 1mg per ml solution) 250µg im (0.25ml 1mg per ml solution) up to 500µg im (0.5ml 1mg per ml solution) 250µg im (0.25ml 1mg per ml solution) 250µg im (0.25ml 1mg per ml solution) 120µg im (0.12ml 1mg per ml solution) 50µg im (0.05ml 1mg per ml solution; absolute accuracy not essential) Table 3. Intramuscular adrenaline doses in anaphylaxis Intramuscular adrenaline dose (strength always 1mg per ml) The intravenous dose is only one-tenth the intramuscular dose, and the concentration of solutions of adrenaline for intravenous administration is correspondingly 100µg per ml. Adrenaline is poorly and unreliably absorbed after subcutaneous administration, which is therefore inappropriate. Serious adverse reactions, including ventricular arrhythmia, are generally the result of administration of toxic doses, and especially of dosing errors if adrenaline has been given intravenously. This is a further reason for preferring the intramuscular route. 5 Other drugs can affect the actions of adrenaline. Patients taking beta-blockers, eg atenolol, may require larger doses of adrenaline because of competitive antagonism. Such patients may also be at increased risk of severe anaphylaxis in the first place. ACE inhibitors that inhibit the breakdown of bradykinin, an important mediator of anaphylaxis and angioedema, can also increase the risk of severe anaphylaxis. Adrenaline can precipitate arrhythmia in patients taking TCAs and provoke hypertensive crises in those taking MAOIs. The Resuscitation Council (UK) suggests that the dose of adrenaline should be halved in these patients. 14 Prescriber 19 May
4 Summary points anaphylaxis is a rare but potentially fatal immune-mediated reaction the diagnosis of anaphylaxis is made on the history and physical signs once anaphylaxis is identified, prompt treatment is vital intramuscular adrenaline is the emergency treatment of choice oxygen, chlorphenamine, and hydrocortisone are also valuable elevated activity of serum mast cell tryptase can support the diagnosis observe patients for at least 8 hours after severe anaphylaxis measures to prevent or treat recurrence should be put in place at the time of discharge Additional treatments Chlorphenamine, a histamine H 1 - antagonist, is the antihistamine of choice and can be given intravenously, acting within about 10 minutes of injection. It counteracts histamine-mediated vasodilatation, reduces the itching associated with urticaria and may reduce histamine-mediated bronchoconstriction. It is sedative, but this is not significant in this context. Hydrocortisone injection may hasten recovery by inhibiting leukotriene synthesis. It may take several hours to act, but can be of help in so-called biphasic anaphylactic reactions. Intravenous fluids should be considered in any patient with hypotension. In patients with predominant bronchoconstriction, nebulised salbutamol may also be helpful. Anaphylactoid reactions are common in some circumstances. For example, they occur during use of acetylcysteine (Parvolex) in paracetamol poisoning, and in codeine overdose. True anaphylactic reactions are almost unknown in these circumstances, where the use of chlorphenamine and salbutamol is normally all that is required. Subsequent management If there is doubt about the diagnosis, it can be supported by Prescriber 19 May
5 measurement of serum mast cell tryptase levels one and five hours following the event. Enzyme activity is high after mast cell degranulation, and so the test cannot distinguish anaphylaxis from an anaphylactoid reaction. Patients should be observed following resuscitation to ensure that all the clinical features resolve. In rare cases, features recur as late as eight hours after the initial event, so patients should be observed for at least that time. At discharge following a severe reaction, patients should be counselled about the suspected aetiology of the reaction and given information on avoidance. Staff should endorse the medical records and inform the GP of any suspected drug allergy. Preloaded auto-injector adrenaline syringes are appropriate for patients with severe anaphylactic reactions induced by environmental allergens such as food or insect stings, but not usually for patients with drug-induced anaphylaxis. Patients may wish to wear 16 Prescriber 19 May
6 identification, such as a Medic- Alert bracelet. Avoiding anaphylaxis A history of allergy to a drug is a relative contraindication to repeat administration. However, drug allergy reported by a patient may not represent a true IgE-mediated hypersensitivity reaction. For example, features such as diarrhoea and headache would not constitute an allergy, and the rash associated with ampicillin used in glandular fever does not herald anaphylaxis on re-exposure. Occasionally, records may show that patients state they are allergic to drugs that they have been reexposed to with no adverse effects. This sometimes happens with penicillins, and the likely explanation in this case is that impurities were present in early pharmaceutical preparations, which are no longer present due to more modern manufacturing processes. The most common drug allergy is to penicillin compounds. Prescriber 19 May
7 Penicillin therapy is often limited by unsubstantiated reporting of penicillin hypersensitivity. Skinprick testing has been used in an attempt to determine the response to penicillin. 6 Research estimates that only per cent of patients react to such testing. It is estimated that 98 per cent of patients with a negative skin prick test can safely take a penicillin derivative, although it does not exclude the risk of anaphylaxis. As such it should only be carried out in hospital by experienced staff, and with full resuscitation facilities available. People allergic to penicillins are at increased risk of reaction to cephalosporin antibiotics, which are of similar chemical structure. The practitioner may choose to avoid the cephalosporin group of drugs in patients thought to be allergic to penicillins. Alternatively, skin-prick testing can be carried out using penicillin in patients with a history of penicillin allergy. If the testing is negative, it is likely that the patient can receive the cephalosporin safely. Although the risk of an allergic response to cephalosporins in patients with true penicillin allergy is fairly low (approximately 2 per cent), it is probably best to avoid cephalosporins in any patient where there is a good history of moderate or severe reactions to penicillin. 7 Because anaphylaxis is a rare but dangerous and potentially recurrent condition, patients who have suffered a moderate or severe episode should ideally be referred for specialist evaluation and advice. Conclusion Anaphylaxis is rare and can often be avoided by taking a careful medical history including any previous drug allergies. Clinical symptoms and signs can evolve over a short period. Prompt recognition of the features of anaphylaxis will help in early identification. In the community setting adrenaline administration should be via the intramuscular route. All patients with suspected anaphylaxis should be urgently sent to hospital for assessment. Given the unpredictability of this potentially fatal adverse drug reaction, anyone who may prescribe or give drugs should know how to recognise and treat this life-threatening adverse effect. References 1. Peng MM, Jick H. A populationbased study of the incidence, cause, and severity of anaphylaxis in the United Kingdom. Arch Int Med 2004; 164: Neugut AI, Ghatak AT, Miller RL. Anaphylaxis in the United States: an investigation into its epidemiology. Arch Intern Med 2001;161: Ewan PW. Anaphylaxis. BMJ 1998; 316: Resuscitation Council UK. Emergency medical treatment of anaphylactic reactions for first medical responders and for community nurses (Revised January 2002). org.uk. 5. McLean-Tooke AP, Bethune CA, Fay AC, et al. Adrenaline in the treatment of anaphylaxis: what is the evidence? BMJ 2003;327: Salkind AR, Cuddy PG, Foxworth JW. The rational clinical examination. Is this patient allergic to penicillin? An evidence-based analysis of the likelihood of penicillin allergy. JAMA 2001;285: Kelkar PS, Li JT. Cephalosporin allergy. N Eng J Med 2001;345: Dr Bateman is specialist registrar in rheumatology, Mid Staffordshire NHS Trust, and Dr Ferner is consultant physician at City Hospital, Birmingham, and director of the West Midlands Centre for Adverse Drug Reaction Reporting 18 Prescriber 19 May
Management of an immediate adverse event following immunisation
 Management of an immediate adverse event following immunisation The vaccinated person should remain under observation for a short interval to ensure that they do not experience an immediate adverse event.
Management of an immediate adverse event following immunisation The vaccinated person should remain under observation for a short interval to ensure that they do not experience an immediate adverse event.
Anaphylaxis: Treatment in the Community
 : Treatment in the Community is likely if a patient who, within minutes of exposure to a trigger (allergen), develops a sudden illness with rapidly progressing skin changes and life-threatening airway
: Treatment in the Community is likely if a patient who, within minutes of exposure to a trigger (allergen), develops a sudden illness with rapidly progressing skin changes and life-threatening airway
Urticaria Moderate Allergic Reaction Mild signs/symptoms with any of following: Dyspnea, possibly with wheezes Angioneurotic edema Systemic, not local
 Allergic Reactions & Anaphylaxis Incidence In USA - 400 to 800 deaths/year Parenterally administered penicillin accounts for 100 to 500 deaths per year Hymenoptera stings account for 40 to 100 deaths per
Allergic Reactions & Anaphylaxis Incidence In USA - 400 to 800 deaths/year Parenterally administered penicillin accounts for 100 to 500 deaths per year Hymenoptera stings account for 40 to 100 deaths per
Policy for the Treatment of Anaphylaxis in Adults and Children
 Policy for the Treatment of Anaphylaxis in Adults and Children June 2008 Policy Title: Policy for the Treatment of Anaphylaxis in Adults or Children Policy Reference Number: PrimCare08/17 Implementation
Policy for the Treatment of Anaphylaxis in Adults and Children June 2008 Policy Title: Policy for the Treatment of Anaphylaxis in Adults or Children Policy Reference Number: PrimCare08/17 Implementation
Sign up to receive ATOTW weekly -
 ANAPHYLAXIS ANAESTHESIA TUTORIAL OF THE WEEK 38 1 th DECEMBER 2006 Dr. Sara Rees Cardiff, UK Case History You are anaesthetising a fit and well 40 year old woman for total abdominal hysterectomy for menorrhagia.
ANAPHYLAXIS ANAESTHESIA TUTORIAL OF THE WEEK 38 1 th DECEMBER 2006 Dr. Sara Rees Cardiff, UK Case History You are anaesthetising a fit and well 40 year old woman for total abdominal hysterectomy for menorrhagia.
VACCINE-RELATED ALLERGIC REACTIONS
 VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis Public Health Immunization Program June 2018 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever,
VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis Public Health Immunization Program June 2018 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever,
VACCINE-RELATED ALLERGIC REACTIONS
 VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
VACCINE-RELATED ALLERGIC REACTIONS Management of Anaphylaxis IERHA Immunization Program September 2016 VACCINE-RELATED ADVERSE EVENTS Local reactions pain, edema, erythema Systemic reactions fever, lymphadenopathy
Anaphylaxis: treatment in the community
 : treatment in the community Item Type Guideline Authors Health Service Executive Citation Health Service Executive. : treatment in the community. Dublin: Health Service Executive;. 5p. Publisher Health
: treatment in the community Item Type Guideline Authors Health Service Executive Citation Health Service Executive. : treatment in the community. Dublin: Health Service Executive;. 5p. Publisher Health
ANAPHYLAXIS EMET 2015
 ANAPHYLAXIS EMET 2015 ANA = AGAINST PHYLAX = PROTECTION No standardised definition (they re working on it) All include the similar concept of: A serious, generalised or systemic, allergic or hypersensitivity
ANAPHYLAXIS EMET 2015 ANA = AGAINST PHYLAX = PROTECTION No standardised definition (they re working on it) All include the similar concept of: A serious, generalised or systemic, allergic or hypersensitivity
Anaphylaxis 5/31/2015
 1 Definition of anaphylaxis Anaphylaxis Jon Kyle Andersen Anaphylaxis is a severe, life-threatening, generalised or systemic hypersensitivity reaction. It is characterised by rapidly developing, life-threatening
1 Definition of anaphylaxis Anaphylaxis Jon Kyle Andersen Anaphylaxis is a severe, life-threatening, generalised or systemic hypersensitivity reaction. It is characterised by rapidly developing, life-threatening
PROCEDURE FOR MANAGING AN ANAPHYLACTIC EMERGENCY
 MULTIDISCIPLINARY PROCEDURE PROCEDURE FOR MANAGING AN ANAPHYLACTIC EMERGENCY First Issued June 2011 Issue Version Four Purpose of Issue/Description of Change Planned Review Date To promote safe and consistent
MULTIDISCIPLINARY PROCEDURE PROCEDURE FOR MANAGING AN ANAPHYLACTIC EMERGENCY First Issued June 2011 Issue Version Four Purpose of Issue/Description of Change Planned Review Date To promote safe and consistent
Anaphylaxis: clinical features and GP s role in management
 n PRESCRIBING IN PRACTICE Anaphylaxis: clinical features and GP s role in management Priya Sellaturay BSc, MRCP, Krzysztof Rutkowski MD, MRCP and Shuaib Nasser MA, MD, FRCP SPL Anaphylaxis can be fatal
n PRESCRIBING IN PRACTICE Anaphylaxis: clinical features and GP s role in management Priya Sellaturay BSc, MRCP, Krzysztof Rutkowski MD, MRCP and Shuaib Nasser MA, MD, FRCP SPL Anaphylaxis can be fatal
Anaphylaxis/Latex Allergy
 Children s Acute Transport Service CATS Clinical Guideline Anaphylaxis/Latex Allergy Document Control Information Author D Lutman Author Position Consultant Document Owner E Polke Document Owner Position
Children s Acute Transport Service CATS Clinical Guideline Anaphylaxis/Latex Allergy Document Control Information Author D Lutman Author Position Consultant Document Owner E Polke Document Owner Position
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2
 CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
Anaphylaxis ASCIA Education Resources Information for health professionals
 Anaphylaxis ASCIA Education Resources Information for health professionals Anaphylaxis is a rapidly evolving, generalised multi-system allergic reaction characterized by one or more symptoms or signs of
Anaphylaxis ASCIA Education Resources Information for health professionals Anaphylaxis is a rapidly evolving, generalised multi-system allergic reaction characterized by one or more symptoms or signs of
Antiallergics and drugs used in anaphylaxis
 Antiallergics and drugs used in anaphylaxis Antiallergics and drugs used in anaphylaxis The H 1 -receptor antagonists are generally referred to as antihistamines. They inhibit the wheal, pruritus, sneezing
Antiallergics and drugs used in anaphylaxis Antiallergics and drugs used in anaphylaxis The H 1 -receptor antagonists are generally referred to as antihistamines. They inhibit the wheal, pruritus, sneezing
Adverse drug reactions. Dr. Mark Haworth MBChB DA MRCA
 Adverse drug reactions Dr. Mark Haworth MBChB DA MRCA Types of drug reaction The appearance of known side effects to a drug e.g. respiratory depression following the administration of opioid analgesics
Adverse drug reactions Dr. Mark Haworth MBChB DA MRCA Types of drug reaction The appearance of known side effects to a drug e.g. respiratory depression following the administration of opioid analgesics
Allergic Emergencies and Anaphylaxis. George Porfiris MD, CCFP(EM),FCFP TEGH
 Allergic Emergencies and Anaphylaxis George Porfiris MD, CCFP(EM),FCFP TEGH Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Allergic Emergencies and Anaphylaxis George Porfiris MD, CCFP(EM),FCFP TEGH Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
learning zone Recognition and management of patients with anaphylaxis CONTINUING PROFESSIONAL DEVELOPMENT Summary Authors Keywords
 learning zone CONTINUING PROFESSIONAL DEVELOPMENT Page 58 Anaphylaxis multiple choice questionnaire Page 59 Read Samantha Nichols practice profile on chronic diarrhoea Page 60 Guidelines on how to write
learning zone CONTINUING PROFESSIONAL DEVELOPMENT Page 58 Anaphylaxis multiple choice questionnaire Page 59 Read Samantha Nichols practice profile on chronic diarrhoea Page 60 Guidelines on how to write
EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT. Michael J. Calice MD, FACEP St. Mary Mercy Hospital
 EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT Michael J. Calice MD, FACEP St. Mary Mercy Hospital Case #1 NR is an 8 yo male c/o hot mouth and stomach ache after eating jelly
EPIPEN INSERVICE Emergency Administration of Epinephrine for the Basic EMT Michael J. Calice MD, FACEP St. Mary Mercy Hospital Case #1 NR is an 8 yo male c/o hot mouth and stomach ache after eating jelly
Student Health Center
 Referring Allergist Agreement Your patient is requesting that the University of Mary Washington Student Health Center (UMWSHC) administer allergy extracts provided by your office. Consistent with our policies
Referring Allergist Agreement Your patient is requesting that the University of Mary Washington Student Health Center (UMWSHC) administer allergy extracts provided by your office. Consistent with our policies
Who Should Be Premediciated for Contrast-Enhanced Exams?
 Who Should Be Premediciated for Contrast-Enhanced Exams? Jeffrey C. Weinreb, MD,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Types of Intravenous Contrast Media Iodinated Contrast Agents
Who Should Be Premediciated for Contrast-Enhanced Exams? Jeffrey C. Weinreb, MD,FACR Yale University School of Medicine jeffrey.weinreb@yale.edu Types of Intravenous Contrast Media Iodinated Contrast Agents
Anaphylaxis. Perceive the differences between anaphylactic shock and other types of shock. Recognize its nature, causes & characteristics.
 Anaphylaxis Red : important Black : in male / female slides Pink : in female s slides only Blue : in male s slides only Females doctor notes Grey: Males doctor notes OBJECTIVES: By the end of this lecture,
Anaphylaxis Red : important Black : in male / female slides Pink : in female s slides only Blue : in male s slides only Females doctor notes Grey: Males doctor notes OBJECTIVES: By the end of this lecture,
Emergency Treatment of Anaphylaxis Policy and Guidelines
 Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document supersedes: PAT/EC 3 v.6 Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document should be used
Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document supersedes: PAT/EC 3 v.6 Emergency Treatment of Anaphylaxis Policy and Guidelines This procedural document should be used
Food allergy in children. nice bulletin. NICE Bulletin Food Allergy in Chlidren.indd 1
 nice bulletin Food allergy in children NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin Food Allergy in Chlidren.indd 1 23/01/2012 11:04
nice bulletin Food allergy in children NICE provided the content for this booklet which is independent of any company or product advertised NICE Bulletin Food Allergy in Chlidren.indd 1 23/01/2012 11:04
Chapter 65 Allergy and Immunology for the Internist. ingestion provoke an IgE antibody response and clinical symptoms in sensitive individuals.
 Chapter 65 Allergy and Immunology for the Internist 1 I. Basic Information A. Definition of Allergens: Proteins of appropriate size that after inhalation, injection (e.g. drug, venom) or ingestion provoke
Chapter 65 Allergy and Immunology for the Internist 1 I. Basic Information A. Definition of Allergens: Proteins of appropriate size that after inhalation, injection (e.g. drug, venom) or ingestion provoke
Respiratory Pharmacology
 Allergy Targets of allergies Type I Histamine Leukotrienes Prostaglandins Bradykinin Hypersensitivity reactions Asthma Characterised by Triggered by Intrinsic Extrinsic (allergic) Mediators Result Early
Allergy Targets of allergies Type I Histamine Leukotrienes Prostaglandins Bradykinin Hypersensitivity reactions Asthma Characterised by Triggered by Intrinsic Extrinsic (allergic) Mediators Result Early
Emergency treatment of anaphylaxis in adults: concise guidance
 CONCISE GUIDELINES Emergency treatment of anaphylaxis in adults: concise guidance Jasmeet Soar on behalf of the multidisciplinary Guideline Development Group* ABSTRACT Anaphylaxis is a severe, life-threatening,
CONCISE GUIDELINES Emergency treatment of anaphylaxis in adults: concise guidance Jasmeet Soar on behalf of the multidisciplinary Guideline Development Group* ABSTRACT Anaphylaxis is a severe, life-threatening,
Five things to know about anaphylaxis
 Five things to know about anaphylaxis Magdalena Berger, MD FRCPC Allergist and Clinical Immunologist New Brunswick Internal Medicine Update April 22, 2016 Disclosures None relevant to this presentation
Five things to know about anaphylaxis Magdalena Berger, MD FRCPC Allergist and Clinical Immunologist New Brunswick Internal Medicine Update April 22, 2016 Disclosures None relevant to this presentation
Chapter 8. Learning Objectives. Learning Objectives 9/11/2012. Anaphylaxis. List symptoms of anaphylactic shock
 Chapter 8 Anaphylaxis Learning Objectives List symptoms of anaphylactic shock Discuss role of immune system in fighting antigens Define allergic response Learning Objectives Describe body s response to
Chapter 8 Anaphylaxis Learning Objectives List symptoms of anaphylactic shock Discuss role of immune system in fighting antigens Define allergic response Learning Objectives Describe body s response to
The Diagnosis and Management of Anaphylaxis
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/focus-on-allergy/the-diagnosis-and-management-of-anaphylaxis/3919/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/focus-on-allergy/the-diagnosis-and-management-of-anaphylaxis/3919/
02/06/2013. Goal of program. A few definitions. Objectives of the training. Legal context. Legal context in schools
 2 Goal of program Administering epinephrine for acute anaphylactic type allergic reactions Reduce the morbidity and mortality associated with acute anaphylactic type allergic reactions. Training for first
2 Goal of program Administering epinephrine for acute anaphylactic type allergic reactions Reduce the morbidity and mortality associated with acute anaphylactic type allergic reactions. Training for first
Following up patients after treatment for anaphylaxis
 Following up patients after treatment for anaphylaxis Unsworth D J. Following up patients after treatment for anaphylaxis. Practitioner 2012;256 (1749):21-24 Dr David J Unsworth PhD FRCP FRCPath Consultant
Following up patients after treatment for anaphylaxis Unsworth D J. Following up patients after treatment for anaphylaxis. Practitioner 2012;256 (1749):21-24 Dr David J Unsworth PhD FRCP FRCPath Consultant
Anaphylaxis: The Atypical Varieties
 Anaphylaxis: The Atypical Varieties John Johnson, D.O., PGY-4 Allergy/Immunology Fellow University Hospitals of Cleveland Case Western Reserve University School of Medicine Disclosures: None What is Anaphylaxis?
Anaphylaxis: The Atypical Varieties John Johnson, D.O., PGY-4 Allergy/Immunology Fellow University Hospitals of Cleveland Case Western Reserve University School of Medicine Disclosures: None What is Anaphylaxis?
Allergy Medications. Antihistamines. are very safe. Although usually taken as tablets, they may be prescribed as a liquid or syrup for young children
 The treatments prescribed for allergy control the symptoms and reactions; they do not cure the condition. However, using treatments as prescribed can show a huge change in a patient s health, mood and
The treatments prescribed for allergy control the symptoms and reactions; they do not cure the condition. However, using treatments as prescribed can show a huge change in a patient s health, mood and
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
REFERRAL GUIDELINES - SUMMARY
 Clinical Immunology & Allergy Unit LEEDS TEACHING HOSPITALS NHS TRUST REFERRAL GUIDELINES - SUMMARY THESE GUIDELINES ARE DESIGNED TO ENSURE THAT PATIENTS REQUIRING SECONDARY CARE ARE SEEN EFFICIENTLY AND
Clinical Immunology & Allergy Unit LEEDS TEACHING HOSPITALS NHS TRUST REFERRAL GUIDELINES - SUMMARY THESE GUIDELINES ARE DESIGNED TO ENSURE THAT PATIENTS REQUIRING SECONDARY CARE ARE SEEN EFFICIENTLY AND
MANAGING COMMON PRESENTATIONS OF ALLERGY IN PRIMARY CARE. Helen Bourne Consultant Immunologist
 MANAGING COMMON PRESENTATIONS OF ALLERGY IN PRIMARY CARE Helen Bourne Consultant Immunologist AIMS Presentation of Allergic Disease in Adults Rhinitis/ Rhinoconjuctivitis Urticaria and Angioedema Food
MANAGING COMMON PRESENTATIONS OF ALLERGY IN PRIMARY CARE Helen Bourne Consultant Immunologist AIMS Presentation of Allergic Disease in Adults Rhinitis/ Rhinoconjuctivitis Urticaria and Angioedema Food
Administering epinephrine for acute anaphylactic type allergic reactions
 Administering epinephrine for acute anaphylactic type allergic reactions Training for first aiders People known to be allergic (1.5 hours) MAJ 2012-3 2 Objectives of the training Understand the legal context
Administering epinephrine for acute anaphylactic type allergic reactions Training for first aiders People known to be allergic (1.5 hours) MAJ 2012-3 2 Objectives of the training Understand the legal context
About the immune system
 The immune system and anaphylaxis edward.purssell@kcl.ac.uk About the immune system The immune system Protects the body from infectious organisms, foreign bodies and malignancies Surface barriers Innate
The immune system and anaphylaxis edward.purssell@kcl.ac.uk About the immune system The immune system Protects the body from infectious organisms, foreign bodies and malignancies Surface barriers Innate
Product Information BROWN SNAKE ANTIVENOM AUST R 74897
 Product Information APPROVED NAME BROWN SNAKE ANTIVENOM AUST R 74897 DESCRIPTION BROWN SNAKE ANTIVENOM is prepared from the plasma of horses immunised with the venom of the brown snake (Pseudonaja textilis).
Product Information APPROVED NAME BROWN SNAKE ANTIVENOM AUST R 74897 DESCRIPTION BROWN SNAKE ANTIVENOM is prepared from the plasma of horses immunised with the venom of the brown snake (Pseudonaja textilis).
SAN JOAQUIN COUNTY EMERGENCY MEDICAL SERVICES AGENCY. Administration of Epinephrine Auto-Injector Training
 SAN JOAQUIN COUNTY EMERGENCY MEDICAL SERVICES AGENCY Administration of Epinephrine Auto-Injector Training Disclaimer: Authorization - EMT Optional Skills Only authorized Emergency Medical Technicians (EMT)
SAN JOAQUIN COUNTY EMERGENCY MEDICAL SERVICES AGENCY Administration of Epinephrine Auto-Injector Training Disclaimer: Authorization - EMT Optional Skills Only authorized Emergency Medical Technicians (EMT)
Food-allergy-FINAL.mp3. Duration: 0:07:39 START AUDIO
 BMJ LEARNING VIDEO TRANSCRIPT File: Duration: 0:07:39 Food-allergy-FINAL.mp3 START AUDIO Adam Fox: Food allergy is an inappropriate immune response to food. Our immune systems should ignore food completely,
BMJ LEARNING VIDEO TRANSCRIPT File: Duration: 0:07:39 Food-allergy-FINAL.mp3 START AUDIO Adam Fox: Food allergy is an inappropriate immune response to food. Our immune systems should ignore food completely,
Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen
 Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen Anaphylaxis Fatalities Estimated 500 1000 deaths annually
Myth: Prior Episodes Predict Future Reactions REALITY: No predictable pattern Severity depends on: Sensitivity of the individual Dose of the allergen Anaphylaxis Fatalities Estimated 500 1000 deaths annually
Diagnosis and management of suspected drug allergies
 Diagnosis and management of suspected drug allergies SPL Sophie Farooque MRCP Allergic reactions can be caused by commonly prescribed drugs and can lead to fatal anaphylaxis. Here, the author describes
Diagnosis and management of suspected drug allergies SPL Sophie Farooque MRCP Allergic reactions can be caused by commonly prescribed drugs and can lead to fatal anaphylaxis. Here, the author describes
Anaphylaxis Angioedema Transplantation & graft rejection
 Anaphylaxis Angioedema Transplantation & graft rejection 1 Learning objectives 1.Anaphylaxis: definition, causes, C/P, Ix, Rx 2.Angioedema: definition, causes, C/P, IX,RX 3.Transplantation & graft rejection:
Anaphylaxis Angioedema Transplantation & graft rejection 1 Learning objectives 1.Anaphylaxis: definition, causes, C/P, Ix, Rx 2.Angioedema: definition, causes, C/P, IX,RX 3.Transplantation & graft rejection:
Anaphylaxis. Emergencies for the general physician. Shuaib Nasser Consultant in Allergy and Asthma Cambridge University Hospitals NHS Foundation Trust
 Anaphylaxis Emergencies for the general physician Shuaib Nasser Consultant in Allergy and Asthma Cambridge University Hospitals NHS Foundation Trust Definition- Anaphylaxis A potentially life-threatening
Anaphylaxis Emergencies for the general physician Shuaib Nasser Consultant in Allergy and Asthma Cambridge University Hospitals NHS Foundation Trust Definition- Anaphylaxis A potentially life-threatening
The administration of epinephrine for severe anaphylactic type allergic reactions. Training for Quebec first aiders 2012-MAJ-3
 The administration of epinephrine for severe anaphylactic type allergic reactions Training for Quebec first aiders 2012-MAJ-3 2 Objectives Understand the causes and mechanisms of anaphylaxis Know the symptoms
The administration of epinephrine for severe anaphylactic type allergic reactions Training for Quebec first aiders 2012-MAJ-3 2 Objectives Understand the causes and mechanisms of anaphylaxis Know the symptoms
TREATMENT OF ANAPHYLACTIC REACTION WITH EPINEPHRINE
 TREATMENT OF ANAPHYLACTIC REACTION WITH EPINEPHRINE FILE: JGCDC Background: The Bibb County School System recognizes the growing concern with severe life-threatening allergic reactions to food items, latex,
TREATMENT OF ANAPHYLACTIC REACTION WITH EPINEPHRINE FILE: JGCDC Background: The Bibb County School System recognizes the growing concern with severe life-threatening allergic reactions to food items, latex,
ANAPHYLAXIS Following Vaccination. A Severe Adverse Event. Developed for the Grampians Infection Control Group (GRICG) Version 2.
 ANAPHYLAXIS Following Vaccination A Severe Adverse Event Developed for the Grampians Infection Control Group () Version 2.0:2014 Adverse Event Following Immunisation Adverse event following immunisation
ANAPHYLAXIS Following Vaccination A Severe Adverse Event Developed for the Grampians Infection Control Group () Version 2.0:2014 Adverse Event Following Immunisation Adverse event following immunisation
Allergy Immunotherapy in the Primary Care Setting
 Allergy Immunotherapy in the Primary Care Setting New York State College Health Association 2008 COMBINED ANNUAL MEETING October 2008 Mary Madsen RN BC University of Rochester Issues in Primary Care Practice
Allergy Immunotherapy in the Primary Care Setting New York State College Health Association 2008 COMBINED ANNUAL MEETING October 2008 Mary Madsen RN BC University of Rochester Issues in Primary Care Practice
Recognition & Management of Anaphylaxis in the Community. S. Shahzad Mustafa, MD, FAAAAI
 Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures None Outline Define anaphylaxis Pathophysiology Common causes Recognition and Management Definition Acute,
Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures None Outline Define anaphylaxis Pathophysiology Common causes Recognition and Management Definition Acute,
ASDIN 10th Annual Scientific Meeting Final. COI Disclosure Statement. Intravenous Contrast Media: Basics
 COI Disclosure Statement There are no financial relationships or conflicts of interest to disclose with this presentation Melissa Hicks, BA, RT(R)(VI) Vascular Interventional Technologist University of
COI Disclosure Statement There are no financial relationships or conflicts of interest to disclose with this presentation Melissa Hicks, BA, RT(R)(VI) Vascular Interventional Technologist University of
Course Objectives: Upon completion of this presentation, the attendee will be able to:
 Course Objectives: Upon completion of this presentation, the attendee will be able to: Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP 1. Identify the newest diagnostic criteria
Course Objectives: Upon completion of this presentation, the attendee will be able to: Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP 1. Identify the newest diagnostic criteria
: ALLERGIC REACTION
 6208.05: ALLERGIC REACTION INTRODUCTION Allergic (hypersensitivity) reactions are most often secondary to an exaggerated immune system response to a harmless foreign antigen (e.g. insect bite or sting,
6208.05: ALLERGIC REACTION INTRODUCTION Allergic (hypersensitivity) reactions are most often secondary to an exaggerated immune system response to a harmless foreign antigen (e.g. insect bite or sting,
Terms What is Anaphylaxis? Causes Signs & Symptoms Management Education Pictures Citations. Anaphylaxis; LBodak
 Leslie Bodak, EMT-P Terms What is Anaphylaxis? Causes Signs & Symptoms Management Education Pictures Citations Allergic Reaction: an abnormal immune response the body develops when a person has been previously
Leslie Bodak, EMT-P Terms What is Anaphylaxis? Causes Signs & Symptoms Management Education Pictures Citations Allergic Reaction: an abnormal immune response the body develops when a person has been previously
IMMUNOLOGY. Referral Guidelines NATIONAL REFERRAL GUIDELINES : IMMUNOLOGY. As above Specialist assessment is essential.
 PAGE 1 IMMUNOLOGY National PRIMARY IMMUNODEFICIENCY Primary immunodeficiency should be suspected in any patient with recurrent or persistent infection or unusual infection. Recurrent sinopulmonary infections
PAGE 1 IMMUNOLOGY National PRIMARY IMMUNODEFICIENCY Primary immunodeficiency should be suspected in any patient with recurrent or persistent infection or unusual infection. Recurrent sinopulmonary infections
Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP. Course Objectives:
 Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP Course Objectives: Upon completion of this presentation, the attendee will be able to: 1. Identify the newest diagnostic criteria
Kevin Letz DNP, MBA, MSN, RN, CNE, CEN, FNP-C, PNP-BC, ANP-BC, FAPPex, FAANP Course Objectives: Upon completion of this presentation, the attendee will be able to: 1. Identify the newest diagnostic criteria
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Core Safety Profile. Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg. Date of FAR:
 Core Safety Profile Active substance: Bisoprolol Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg P - RMS: FI/H/PSUR/0002/002 Date of FAR: 13.12.2011
Core Safety Profile Active substance: Bisoprolol Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg P - RMS: FI/H/PSUR/0002/002 Date of FAR: 13.12.2011
Emergency Department Guideline. Anaphylaxis
 Emergency Department Guideline Inclusion criteria: 1. Acute onset of an illness (minutes to hours) with a AND (b OR c): a. Skin and/or mucosa (pruritus, flushing, hives, angioedema) b. Respiratory compromise
Emergency Department Guideline Inclusion criteria: 1. Acute onset of an illness (minutes to hours) with a AND (b OR c): a. Skin and/or mucosa (pruritus, flushing, hives, angioedema) b. Respiratory compromise
Anaphylaxis. Choosing Wisely with Academic Detailing Conference October 21, 2017
 Anaphylaxis Choosing Wisely with Academic Detailing Conference October 21, 2017 Disclosure Natasha Rodney-Cail, Pharmacist, Drug Evaluation Unit DEU funded by the Drug Evaluation Alliance of Nova Scotia
Anaphylaxis Choosing Wisely with Academic Detailing Conference October 21, 2017 Disclosure Natasha Rodney-Cail, Pharmacist, Drug Evaluation Unit DEU funded by the Drug Evaluation Alliance of Nova Scotia
Learning Objectives. Introduction. Allergic Reactions 9/18/2012. Allergies - common problem. Antibody-antigen reaction gone haywire
 Chapter 14 Allergies Learning Objectives Describe mechanisms of allergic response, implication for airway management Recognize patient experiencing allergic reaction Describe emergency medical care of
Chapter 14 Allergies Learning Objectives Describe mechanisms of allergic response, implication for airway management Recognize patient experiencing allergic reaction Describe emergency medical care of
FOOD ALLERGY. Dr Colin J Lumsden. Senior Lecturer and Honorary Consultant Paediatrician. Royal Preston Hospital
 FOOD ALLERGY Dr Colin J Lumsden Senior Lecturer and Honorary Consultant Paediatrician Royal Preston Hospital LEARNING OUTCOMES Pathophysiology Presentation Diagnosis Investigation Management Milk Allergy
FOOD ALLERGY Dr Colin J Lumsden Senior Lecturer and Honorary Consultant Paediatrician Royal Preston Hospital LEARNING OUTCOMES Pathophysiology Presentation Diagnosis Investigation Management Milk Allergy
Path2220 INTRODUCTION TO HUMAN DISEASE ALLERGY. Dr. Erika Bosio
 Path2220 INTRODUCTION TO HUMAN DISEASE ALLERGY Dr. Erika Bosio Research Fellow Centre for Clinical Research in Emergency Medicine, Harry Perkins Institute of Medical Research University of Western Australia
Path2220 INTRODUCTION TO HUMAN DISEASE ALLERGY Dr. Erika Bosio Research Fellow Centre for Clinical Research in Emergency Medicine, Harry Perkins Institute of Medical Research University of Western Australia
7/25/2016. Use of Epinephrine in the Community. Knowledge Amongst Paramedics. Knowledge Amongst Paramedics survey of 3479 paramedics
 Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures Speaker s bureau Genentech, Teva Consultant Genentech, Teva Outline Knowledge gap Definition Pathophysiology
Recognition & Management of Anaphylaxis in the Community S. Shahzad Mustafa, MD, FAAAAI Disclosures Speaker s bureau Genentech, Teva Consultant Genentech, Teva Outline Knowledge gap Definition Pathophysiology
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host.
 Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Hypersensitivity is the term used when an immune response results in exaggerated or inappropriate reactions harmful to the host. Hypersensitivity vs. allergy Hypersensitivity reactions require a pre-sensitized
Allergic Reactions and Envenomations. Chapter 16
 Allergic Reactions and Envenomations Chapter 16 Allergic Reactions Allergic reaction Exaggerated immune response to any substance Histamines and leukotrienes Chemicals released by the immune system Anaphylaxis
Allergic Reactions and Envenomations Chapter 16 Allergic Reactions Allergic reaction Exaggerated immune response to any substance Histamines and leukotrienes Chemicals released by the immune system Anaphylaxis
Immunocompetence The immune system responds appropriately to a foreign stimulus
 Functions of the immune system Protect the body s internal environment against invading organisms Maintain homeostasis by removing damaged cells from the circulation Serve as a surveillance network for
Functions of the immune system Protect the body s internal environment against invading organisms Maintain homeostasis by removing damaged cells from the circulation Serve as a surveillance network for
Diagnosing and managing peanut allergy in children
 Diagnosing and managing peanut allergy in children Tibbott R, Clark A, Diagnosing and managing peanut allergy in children. Practitioner 2014;258 (1772):21-24 Dr Rebecca Tibbott MBBS BSc MRCPCH Academic
Diagnosing and managing peanut allergy in children Tibbott R, Clark A, Diagnosing and managing peanut allergy in children. Practitioner 2014;258 (1772):21-24 Dr Rebecca Tibbott MBBS BSc MRCPCH Academic
Immunology. Lecture- 8
 Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
Immunology Lecture- 8 Immunological Disorders Immunodeficiency Autoimmune Disease Hypersensitivities Immunodeficiency 1. Immunodeficiency --> abnormal production or function of immune cells, phagocytes,
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 22.1 Define key terms introduced in this chapter. Slides 10, 14, 19, 37, 39 22.2 Differentiate between the signs and symptoms of an allergic reaction
Introduction to Emergency Medical Care 1 OBJECTIVES 22.1 Define key terms introduced in this chapter. Slides 10, 14, 19, 37, 39 22.2 Differentiate between the signs and symptoms of an allergic reaction
PM-03 PED ALLERGY/ANAPHYLAXIS. Protocol SECTION: PM-03 PROTOCOL TITLE: PED ALLERGY/ANAPHYLAXIS REVISED: 01MAY2018
 SECTION: PROTOCOL TITLE: REVISED: 01MAY2018 BLS SPECIFIC CARE: See General Pediatric Care Protocol PM-1 - Determine patient s color category on length based resuscitation tape (Broselow Tape) Epi Pen Protocol
SECTION: PROTOCOL TITLE: REVISED: 01MAY2018 BLS SPECIFIC CARE: See General Pediatric Care Protocol PM-1 - Determine patient s color category on length based resuscitation tape (Broselow Tape) Epi Pen Protocol
Case Report. Mechanisms of Anaphylaxis. Case Report. Case Report 37 y/o WF Is this anaphylaxis? What would you do at this point?
 Mechanisms of Anaphylaxis Richard F. Lockey, M.D. Division of Allergy and Immunology Department of Internal Medicine University of South Florida Morsani College of Medicine and James A. Haley Veterans
Mechanisms of Anaphylaxis Richard F. Lockey, M.D. Division of Allergy and Immunology Department of Internal Medicine University of South Florida Morsani College of Medicine and James A. Haley Veterans
Anaphylaxis Guidelines
 Anaphylaxis Guidelines 2015 FAMILY NURSING & HOME CARE RATIFICATION FORM Type i.e. Strategy, Policy, Education Package etc. Name Guideline Anaphylaxis Guidelines Category i.e. organisational, clinical,
Anaphylaxis Guidelines 2015 FAMILY NURSING & HOME CARE RATIFICATION FORM Type i.e. Strategy, Policy, Education Package etc. Name Guideline Anaphylaxis Guidelines Category i.e. organisational, clinical,
LIFE THREATENING ALLERGIES POLICY
 LIFE THREATENING ALLERGIES POLICY What is Anaphylaxis? Anaphylaxis is a severe systemic allergic reaction at the extreme end of the allergic spectrum. The whole body is affected usually within minutes
LIFE THREATENING ALLERGIES POLICY What is Anaphylaxis? Anaphylaxis is a severe systemic allergic reaction at the extreme end of the allergic spectrum. The whole body is affected usually within minutes
ANAPHYLAXIS POLICY & PROCEDURES
 PHOENIX P-12 COMMUNITY COLLEGE ANAPHYLAXIS POLICY & PROCEDURES Policy Statement Anaphylaxis is a severe, rapidly progressive allergic reaction that involves various areas of the body simultaneously and
PHOENIX P-12 COMMUNITY COLLEGE ANAPHYLAXIS POLICY & PROCEDURES Policy Statement Anaphylaxis is a severe, rapidly progressive allergic reaction that involves various areas of the body simultaneously and
Allergic Reactions and Anaphylaxis. William Mapes, NRP, I/C Chief, Brandon Area Rescue Squad Brandon, VT
 Allergic Reactions and Anaphylaxis William Mapes, NRP, I/C Chief, Brandon Area Rescue Squad Brandon, VT Allergy to Anaphylaxis Defined as a histamine-mediated spectrum of physiologic events that include:
Allergic Reactions and Anaphylaxis William Mapes, NRP, I/C Chief, Brandon Area Rescue Squad Brandon, VT Allergy to Anaphylaxis Defined as a histamine-mediated spectrum of physiologic events that include:
ANAPHYLAXIS. Following Vaccination of Adults. A Severe Adverse Event
 ANAPHYLAXIS Following Vaccination of Adults A Severe Adverse Event Developed for the Grampians Infection Control Group () Version 3.0:2018 Target audience This information package is for nurse immunisers
ANAPHYLAXIS Following Vaccination of Adults A Severe Adverse Event Developed for the Grampians Infection Control Group () Version 3.0:2018 Target audience This information package is for nurse immunisers
Local Omalizumab Treatment Protocol (For children 6 to <12 years of age)
 Local Omalizumab Treatment Protocol (For children 6 to
Local Omalizumab Treatment Protocol (For children 6 to
West Houston Allergy & Asthma, P.A.
 Consent to Receive Immunotherapy (ALLERGY SHOTS) Procedure Allergy injections are usually started at a very low dose. This dose is gradually increased on a regular (usually 1-2 times per week) basis until
Consent to Receive Immunotherapy (ALLERGY SHOTS) Procedure Allergy injections are usually started at a very low dose. This dose is gradually increased on a regular (usually 1-2 times per week) basis until
Medical Documentation/Records. ADVERSE DRUG REACTIONS (ADRs) AND ALLERGIES TO MEDICATIONS
 FLORIDA STATE HOSPITAL OPERATING PROCEDURE NO. 151-24 STATE OF FLORIDA DEPARTMENT OF CHILDREN AND FAMILIES CHATTAHOOCHEE, April 26, 2017 Medical Documentation/Records ADVERSE DRUG REACTIONS (ADRs) AND
FLORIDA STATE HOSPITAL OPERATING PROCEDURE NO. 151-24 STATE OF FLORIDA DEPARTMENT OF CHILDREN AND FAMILIES CHATTAHOOCHEE, April 26, 2017 Medical Documentation/Records ADVERSE DRUG REACTIONS (ADRs) AND
Supplementary Online Content
 Supplementary Online Content Shenoy E, Macy E, Rowe TA, Blumenthal KG. Evaluation and management of penicillin allergy. JAMA. doi:10.1001/jama.2018.19283 Table 1. Hypersensitivity reaction types Table
Supplementary Online Content Shenoy E, Macy E, Rowe TA, Blumenthal KG. Evaluation and management of penicillin allergy. JAMA. doi:10.1001/jama.2018.19283 Table 1. Hypersensitivity reaction types Table
Medical Emergencies and Current Management in Dentistry. Prof. Mark Greenwood Newcastle University
 Medical Emergencies and Current Management in Dentistry Prof. Mark Greenwood Newcastle University Lancaster 1.02.12 PREVENTION! Attitude and environment Usually a clue in the history PREVENTION! Attitude
Medical Emergencies and Current Management in Dentistry Prof. Mark Greenwood Newcastle University Lancaster 1.02.12 PREVENTION! Attitude and environment Usually a clue in the history PREVENTION! Attitude
Management of ANAPHYLAXIS in the School Setting. Updated September 2010
 Management of ANAPHYLAXIS in the School Setting Updated September 2010 What is an Allergy? Allergies occur when the immune system becomes unusually sensitive and over reacts to common substance that are
Management of ANAPHYLAXIS in the School Setting Updated September 2010 What is an Allergy? Allergies occur when the immune system becomes unusually sensitive and over reacts to common substance that are
Systemic Allergic & Immunoglobulin Disorders
 Systemic Allergic & Immunoglobulin Disorders Bryan L. Martin, DO, MMAS, FACAAI, FAAAAI, FACP, FACOI Emeritus Professor of Medicine and Pediatrics President, American College of Allergy, Asthma & Immunology
Systemic Allergic & Immunoglobulin Disorders Bryan L. Martin, DO, MMAS, FACAAI, FAAAAI, FACP, FACOI Emeritus Professor of Medicine and Pediatrics President, American College of Allergy, Asthma & Immunology
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Allergy Management Policy
 Allergy Management Policy Food Allergy People with allergies have over-reactive immune systems that target otherwise harmless elements of our diet and environment. During an allergic reaction to food,
Allergy Management Policy Food Allergy People with allergies have over-reactive immune systems that target otherwise harmless elements of our diet and environment. During an allergic reaction to food,
Hypersensitivity diseases
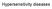 Hypersensitivity diseases Downloaded from: StudentConsult (on 18 July 2006 11:40 AM) 2005 Elsevier Type-I Hypersensitivity Basic terms Type-I = Early= IgE-mediated = Atopic = Anaphylactic type of hypersensitivity
Hypersensitivity diseases Downloaded from: StudentConsult (on 18 July 2006 11:40 AM) 2005 Elsevier Type-I Hypersensitivity Basic terms Type-I = Early= IgE-mediated = Atopic = Anaphylactic type of hypersensitivity
Epinephrine Intramuscular (IM) Injection Administration EMT Optional Scope Highlights
 Epinephrine Intramuscular (IM) Injection Administration EMT Optional Scope Highlights Nor-Cal EMS February 2018 version 1 Special Thank You To Seattle / King County EMS NY State Department of Health, Check
Epinephrine Intramuscular (IM) Injection Administration EMT Optional Scope Highlights Nor-Cal EMS February 2018 version 1 Special Thank You To Seattle / King County EMS NY State Department of Health, Check
Idiopathic Anaphylaxis. Paul A. Greenberger, MD, FAAAAI 2/28/2014 Course # 1605
 Idiopathic Anaphylaxis Paul A. Greenberger, MD, FAAAAI 2/28/2014 Course # 1605 Objectives Review definition and classification of idiopathic anaphylaxis Consider the differential diagnosis Critique lab
Idiopathic Anaphylaxis Paul A. Greenberger, MD, FAAAAI 2/28/2014 Course # 1605 Objectives Review definition and classification of idiopathic anaphylaxis Consider the differential diagnosis Critique lab
Sierra Sacramento Valley EMS Agency
 Sierra Sacramento Valley EMS Agency BLS AUTO-INJECTOR EPINEPHRINE ADMINISTRATION OPTIONAL SKILL (UPDATED 08/2017) In order for PSFA, EMR or EMT personnel to administer auto-injector epinephrine, they must:
Sierra Sacramento Valley EMS Agency BLS AUTO-INJECTOR EPINEPHRINE ADMINISTRATION OPTIONAL SKILL (UPDATED 08/2017) In order for PSFA, EMR or EMT personnel to administer auto-injector epinephrine, they must:
Core Safety Profile. Pharmaceutical form(s)/strength: Sterile eye drops 1%, 2% Date of FAR:
 Core Safety Profile Active substance: Carteolol Pharmaceutical form(s)/strength: Sterile eye drops 1%, 2% P - RMS: SK/H/PSUR/0002/002 Date of FAR: 16.03.2012 4.1 THERAPEUTIC INDICATIONS Ocular hypertension
Core Safety Profile Active substance: Carteolol Pharmaceutical form(s)/strength: Sterile eye drops 1%, 2% P - RMS: SK/H/PSUR/0002/002 Date of FAR: 16.03.2012 4.1 THERAPEUTIC INDICATIONS Ocular hypertension
Community presentations of anaphylaxis in Tasmania: Who is administering the adrenaline?
 Volume 13 Issue 1 Article 2 Community presentations of anaphylaxis in Tasmania: Who is administering the adrenaline? Dale Edwards University of Tasmania, Hobart Melanie Blackhall University of Tasmania,
Volume 13 Issue 1 Article 2 Community presentations of anaphylaxis in Tasmania: Who is administering the adrenaline? Dale Edwards University of Tasmania, Hobart Melanie Blackhall University of Tasmania,
Systemic Anti-Cancer Treatment (SACT) Hypersensitivity Guideline
 This is an official Northern Trust policy and should not be edited in any way Systemic Anti-Cancer Treatment (SACT) Hypersensitivity Guideline Reference Number: NHSCT/12/518 Target audience: This document
This is an official Northern Trust policy and should not be edited in any way Systemic Anti-Cancer Treatment (SACT) Hypersensitivity Guideline Reference Number: NHSCT/12/518 Target audience: This document
Scope of Practice Allergy Skin Testing in Australia In relation to revised Medicare Benefits Schedule item numbers effective 1 November 2018
 Scope of Practice Allergy Skin Testing in Australia In relation to revised Medicare Benefits Schedule item numbers effective 1 November 2018 A. Introduction The Australasian Society of Clinical Immunology
Scope of Practice Allergy Skin Testing in Australia In relation to revised Medicare Benefits Schedule item numbers effective 1 November 2018 A. Introduction The Australasian Society of Clinical Immunology
Chapter 20 - Immunologic Emergencies
 1 2 3 4 5 6 7 8 9 10 National EMS Education Standard Competencies (1 of 2) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an
1 2 3 4 5 6 7 8 9 10 National EMS Education Standard Competencies (1 of 2) Medicine Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Anaphylaxis in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Anaphylaxis in Children. These podcasts are designed to give medical students an overview of key topics in pediatrics.
GUIDELINES FOR THE USE OF NALOXONE INJECTION FEBRUARY 2018
 GUIDELINES FOR THE USE OF NALOXONE INJECTION FEBRUARY 2018 Guidelines for the use of naloxone injection in acute services Policy title Policy reference PHA58 Policy category Clinical Relevant to All medical,
GUIDELINES FOR THE USE OF NALOXONE INJECTION FEBRUARY 2018 Guidelines for the use of naloxone injection in acute services Policy title Policy reference PHA58 Policy category Clinical Relevant to All medical,
Package leaflet: Information for the user
 Package leaflet: Information for the user Emerade 150 micrograms solution for injection in pre-filled pen Emerade 300 micrograms solution for injection in pre-filled pen Emerade 500 micrograms solution
Package leaflet: Information for the user Emerade 150 micrograms solution for injection in pre-filled pen Emerade 300 micrograms solution for injection in pre-filled pen Emerade 500 micrograms solution
