Eosinophilic gastroenteritis (EG) is a rare condition
|
|
|
- Brandon Bond
- 6 years ago
- Views:
Transcription
1 C a s e R e p o r t Simultaneous Mucosal and Subserosal Eosinophilic Gastroenteritis: A Rare and Severe Presentation Rhyl Ann F. Faeldonea-Seruelo, MD Michael Altman, MD Marylee M. Kott, MD Kathryn Peterson, MD Douglas G. Adler, MD Eosinophilic gastroenteritis (EG) is a rare condition of undetermined cause that is characterized by peripheral eosinophilia, infiltration of the gastrointestinal tract by eosinophils, and gastrointestinal symptomatology. 1,2 In EG, eosinophilic infiltration of the gastrointestinal tract is frequently confined to specific layers of the gut wall. This article reports a severe case of EG that involved multiple layers of the gastrointestinal tract (both mucosal and subserosal) as well as several organs, making this particular presentation unusual. This article also reviews the clinical features, diagnosis, and management of EG. CASE PRESENTATION Initial Presentation and History A 20-year-old Hispanic man in apparent good health presented to the emergency department with a 6-week history of a burning sensation in the upper abdomen, nausea, and loose nonbloody stools. He denied vomiting, fever, joint pains, gastrointestinal bleeding, weight loss, or other symptoms. Two weeks prior to presentation, the patient began to notice gradual swelling of his abdomen. The only history of travel outside the United States occurred 2 months previously when he traveled to Mexico. Past medical history revealed no previous hospitalizations or history of asthma, allergic rhinitis, atopic dermatitis, food allergy, or similar symptoms in the past. Physical Examination Initial physical examination revealed a well-appearing young man who appeared comfortable but voiced concern about his abdominal distention. The patient was afebrile, with nonicteric conjunctivae, no lymphadenopathy, and a normal cardiopulmonary examination. His abdomen was moderately distended, with moderate ascites confirmed by a positive fluid wave. He had no peritoneal signs and no focal areas of tenderness to deep palpation. Extremity examination revealed no edema or any joint tenderness or swelling. The remainder of the physical examination was unremarkable. Laboratory and Imaging Studies The patient s complete blood count revealed an elevated white blood cell (WBC) count of 21,000/mL (normal, ,000/mL) with marked eosinophilia of 66% and an absolute eosinophil count of 14,000/ ml (normal, 0% 1% and < 350/mL, respectively). Peripheral blood smear revealed marked mature eosinophilia, and liver function tests revealed decreased total protein (5.8 g/dl [normal, g/dl]) and decreased albumin (3.1 g/dl [normal, g/dl]). Diagnostic paracentesis was performed, and the patient was administered empiric intravenous ceftriaxone due to concern for possible spontaneous bacterial peritonitis. Fluid obtained from the paracentesis was yellow in color with a WBC count of 31,200/mL, a red blood cell count of 6750/mL, markedly elevated eosinophils (93%), and decreased polymorphonuclear neutrophils (2%), lymphocytes (3%), and histiocytes (2%). Analysis of the paracentesis fluid revealed a lactate dehydrogenase level of 171 U/L, protein level of Dr. Faeldonea-Seruelo is a resident, and Dr. Altman is an assistant professor; both are at the Department of Family Medicine, University of Texas-Houston Medical School, Houston, TX. Dr. Kott is an assistant professor, Department of Pathology, University of Texas-Houston Medical School. Dr. Peterson and Dr. Adler are assistant professors, Division of Gastroenterology and Hepatology, University of Utah School of Medicine, Salt Lake City, UT. Hospital Physician September
2 Figure 2. Endoscopic appearance of the stomach. Note diffuse, raised erythematous patches of mucosa predominantly seen in the gastric antrum without frank ulceration or mucosal breaks. Figure 1. Computed tomography scan of abdomen demonstrating diffuse thickening of the entire small bowel and ascites. 4.3 g/dl, and glucose level of 70 mg/dl. The fluid was negative for malignant cells or acid-fast bacilli. Once spontaneous bacterial peritonitis was ruled out, ceftriaxone was discontinued and the patient was managed conservatively with medications as needed for nausea. Computed tomography (CT) imaging of his abdomen was performed with and without intravenous contrast and demonstrated a moderate amount of ascites and diffuse concentric bowel wall thickening involving the entire small bowel, with the large bowel largely unaffected (Figure 1). No obstruction was seen on the CT scan, and the other intra-abdominal organs were felt to be unremarkable in appearance. Consultation and Diagnosis Gastroenterology was consulted given the CT findings. The patient then underwent esophagogastroduodenoscopy (EGD) and colonoscopy, both with multiple biopsies. EGD revealed a normal esophagus and proximal stomach as well as raised erythematous patches of mucosa predominantly in the distal gastric antrum and the proximal duodenum without frank ulceration or mucosal breaks (Figure 2). The colonoscopy revealed a diffusely inflamed and erythematous terminal ileum, a patulous, inflamed ileocecal valve, and right-sided colonic mucosal erythematous patches similar to that seen in the stomach and duodenum (Figure 3). Esophageal biopsy results were unremarkable. Evaluation of gastric, small bowel, and large bowel biopsy specimens revealed diffuse infiltration of eosinophils and multifocal chronic inflammatory infiltrates in the antrum, duodenal bulb, terminal ileum, and colon (Figure 4). Biopsy specimens were negative for fungi or parasites. Four stool cultures were completed over 3 days and were negative for ova or parasites. Given the history, physical examination, laboratory, imaging, endoscopy, and pathologic findings, the patient was diagnosed with severe EG. Management Oral prednisone 40 mg daily for 2 weeks was initiated, to be followed by a rapid taper over 2 weeks. The patient s nausea resolved once he was placed on nothingby-mouth status and prednisone was instituted. Diet was slowly reintroduced over several days from clear fluids through regular food without recurrence of nausea. The patient felt less fatigued over several days and was discharged on hospital day 6 with instructions to followup at the family medicine clinic. Despite his initial improvement, his abdominal distension did not change during his hospitalization. The patient was seen at the family medicine clinic 4 weeks after discharge, coincident with the completion of his steroid taper. He reported complete resolution of his abdominal distention and abdominal burning. Likewise, his stools were normal in caliber and consistency and he remained free of nausea. His physical examination was normal, showing neither evidence of ascites nor abdominal tenderness. Complete blood count with differential obtained at this time showed 6400 WBCs/mL, with 53% neutrophils, 32% lymphocytes, 8% monocytes, 32 Hospital Physician September
3 Figure 3. Endoscopic appearance of the cecum. Note inflamed, patulous ileocecal valve in foreground and patchy erythema on cecal mucosa (arrow). 1% basophils, and 6% eosinophils (absolute eosinophil count, 384/mL). Total protein was 6.7 g/dl with serum albumin of 4.2 g/dl. Repeat CT of the abdomen with and without contrast showed resolution of the ascites, although the patient did have some residual small bowel wall thickening. He has done well for 1 year thereafter and has remained asymptomatic. EOSINOPHILIC GASTROENTERITIS Clinical Features and Diagnosis EG is a rare condition of unknown etiology characterized by peripheral eosinophilia, eosinophilic infiltration of the gastrointestinal tract, and gastrointestinal symptomatology. 1,2 It is generally classified according to the layers of the gastrointestinal tract that are involved. EG was subdivided into predominant mucosal layer disease, predominant muscle layer disease, and predominant subserosal disease by Klein and colleagues in The frequency of involvement of each layer varies, but retrospective studies show that mucosal EG is most common (25% 60%), followed by muscular layer EG (13% 37%) and subserosal EG (13% 40%). 4 6 EG can have a varying clinical presentation depending on the layer that is involved. 7 Mucosal involvement may result in abdominal pain, nausea, vomiting, diarrhea, weight loss, anemia, protein-losing enteropathy, and intestinal perforation. Patients with muscular layer disease generally have obstructive symptoms. Subserosal eosinophilic infiltration may result in the development of eosinophilic ascites. 1 The case patient had features of both mucosal and subserosal EG, which is highly unusual. Figure 4. Specimen from the terminal ileum showing moderate to severe eosinophilic infiltrate in the lamina propria consistent with eosinophilic gastroenteritis (hematoxylin and eosin, 400x). Common presenting symptoms of EG include episodic abdominal pain (77% 100%), diarrhea (42% 62.5%), vomiting (33% 62.5%), and nausea (50% 67%). 4,5,8,9 The stomach was the most common site of involvement (43%), although 36% of patients were found to have 2 or more sites of disease at the time of presentation. 8 Ultrasound and CT scans may reveal the characteristic thickening of the intestinal wall. 4,10,11 The most common CT finding is nodular and irregular fold thickening in the distal stomach and proximal small bowel; it is this characteristic involvement of only the gastric antrum and proximal small bowel that suggests the diagnosis of EG. 10 The gold standard for diagnosis, usually demonstrated on endoscopic biopsies, is prominent tissue eosinophilia consisting of more than 20 eosinophils per high-power field on microscopic examination. 1,2,7,12 The diagnosis can sometimes be obscured by the patchy nature of the disease. In some cases, full-thickness biopsies are required to arrive at a definitive diagnosis. 2 In the case patient, the presenting symptoms were abdominal distention as well as upper abdominal pain, nausea, vomiting, and diarrhea. The biopsies from his EGD and colonoscopy revealed marked eosinophilia, which was also found in his ascitic fluid. CT imaging showed extensive small bowel involvement, with bowel wall thickening from the level of the antrum to the cecum and the large bowel seemingly spared, although colonoscopy ultimately demonstrated mucosal changes in the proximal colon. As mentioned, the case patient demonstrated symptoms of both subserosal and mucosal involvement, which is an unusual and rare presentation. 1,13 There have been several case reports of EG presenting with eosinophilic ascites and peripheral Hospital Physician September
4 eosinophilia. Full-thickness biopsies from the gastrointestinal tract of these patients revealed intense eosinophilic infiltration involving both muscular and serosal layers and extending from the stomach to the ileum. 14 Patients with uncomplicated ascites should undergo a paracentesis for diagnosis. Paracentesis often reveals exudative fluid rich in eosinophils, as was seen in the case patient. 15,16 In EG, eosinophilic intestinal inflammation also occurs secondarily in the gastrointestinal tract in inflammatory bowel disease, autoimmune diseases, reactions to medications, infections, and hypereosinophilia syndrome (HES) and after solid organ transplantation. 17 EG may be confused with irritable bowel syndrome or dyspepsia and, rarely, mimics pancreatitis or appendicitis. 7 The differential diagnosis for patients with presenting complaints similar to the case patient s would include parasitic infections (which could also elevate the peripheral blood eosinophil count) as well and inflammatory bowel disease (which could produce both small and large bowel wall thickening on CT scan). Crohn s disease could produce small and large bowel wall changes, while ulcerative colitis would produce predominately large bowel findings on imaging studies. Ascites would be uncommon with either Crohn s disease or ulcerative colitis. Idiopathic HES is a condition of sustained hypereosinophilia that affects multiple organs including the lung, skin, blood vessels, and nervous system. HES can produce gastrointestinal symptoms through thrombosis and should be considered in patients with abdominal pain and hypereosinophilia. Lastly, a variety of medications and malignancies can produce eosinophilia and abdominal pain as side effects. Treatment Most patients will improve with administration of oral steroids regardless of the intestinal layer involved. 4,5,8,14 16,18,19 Short courses of corticosteroids are the mainstay of treatment, although some patients with relapsing disease require long-term low-dose steroids. 5 Up to 90% of patients with EG reported rapid clinical improvement with institution of steroid therapy. 8 Patients with mild and sporadic symptoms can be managed with reassurance and expectant observation. 1,12 Patients with disabling symptoms can be effectively treated with corticosteroids after other systemic disorders associated with peripheral eosinophilia have been excluded. 1 Data on steroid-sparing treatment regimens for EG are limited but encouraging. Sodium cromoglycate, a mast cell stabilizing agent, has been used in case reports to treat EG with good results. 20,21 Specific food allergies have been implicated in some patients (eg, milk, fish) and can be treated with modified or simplified diets. 22 Reports of favorable responses to leukotriene inhibitors in patients with EG have been published. 23 Promising new drugs for EG also include suplaplast tosilate, a selective Th2 cytokine inhibitor with inhibitory effects on allergy-induced eosinophilic infiltration and IgE production. 7 Questions regarding the natural history of EG; optimal duration of therapy; safer steroid-sparing long-term therapeutic agents; and the means of reliable and noninvasive follow-up require further investigation. 17 CONCLUSION This article presents the case of a young man who developed symptoms of both mucosal and serosal EG with striking laboratory, imaging, and pathologic features. His extensive small bowel involvement was quite impressive, and is unusual. EG should be suspected in a patient with abdominal pain and nausea presenting with ascites and peripheral eosinophilia. This case underscores the well-documented dramatic response of even severe EG to systemic steroid therapy with the complete resolution of the patient s ascites and serum eosinophilia, emphasizing the need for accurate diagnosis. HP Corresponding author: Douglas G. Adler MD, University of Utah Gastroenterology Division, 30 North 1900 East, SOM 4R118, Salt Lake City, UT 84132; douglas.adler@hsc.utah.edu. REFERENCES 1. Lee M, Hodges WG, Huggins TL, Lee EL. Eosinophilic gastroenteritis. South Med J 1996;89: Khan S, Orenstein SR. Eosinophilic gastroenteritis: epidemiology, diagnosis and management. Paediatr Drugs 2002;4: Klein NC, Hargrove RL, Sleisinger MH, Jeffries GH. Eosinophilic gastroenteritis. Medicine (Baltimore) 1970;49: Lee CM, Changchien CS, Chen PC, et al. Eosinophilic gastroenteritis: 10 years experience. Am J Gastroenterol 1993;88: Chen MJ, Chu CH, Lin SC, et al. Eosinophilic gastroenteritis: clinical experience with 15 patients. World J Gastroenterol 2003;9: Talley NJ, Shorter RG, Phillips SF, Zinsmeister AR. Eosinophilic gastroenteritis: a clinicopathological study of patients with disease of the mucosa, muscle layer, and subserosal tissues. Gut 1990;31: Daneshjoo R, J Talley N. Eosinophilic gastroenteritis. Curr Gastroenterol Rep 2002;4: Naylor AR. Eosinophilic gastroenteritis. Scott Med J 1990;35: Kalantar SJ, Marks R, Lambert JR, et al. Dyspepsia due to 34 Hospital Physician September
5 eosinophilic gastroenteritis. Dig Dis Sci 1997;42: Horton KM, Corl FM, Fishman EK. CT of nonneoplastic diseases of the small bowel: spectrum of disease. J Comput Assist Tomogr 1999;23: Marco-Domenech SF, Gil-Sanchez S, Jornet-Fayos J, et al. Eosinophilic gastroenteritis: percutaneous biopsy under ultrasound guidance. Abdom Imaging 1998;23: Baig MA, Qadir A, Rasheed J. A review of eosinophilic gastroenteritis. J Natl Med Assoc 2006;98: Sanchez-Fayos MP, Miranda R, Renedo L, et al. [Eosinophilia and ascites as an expression of a subserous form of eosinophilic gastroenteritis.] [Article in Spanish.] Rev Clin Esp 1992;191: Santos J, Junquera F, de Torres I, et al. Eosinophilic gastroenteritis presenting as ascites and splenomegaly. Eur J Gastroenterol Hepatol 1995;7: Tai YG, Liu JD, Lin KY, et al. Eosinophilic gastroenteritis with eosinophilic ascites: report of a case. J Formos Med Assoc 1990;89: Wachter B, Jager-Arand E, Engers R, et al. [Eosinophilic gastroenteritis with serosa involvement. A rare differential diagnosis of ascites.] [Article in German.] Z Gastroenterol 1992;30: Khan S. Eosinophilic gastroenteritis. Best Pract Res Clin Gastroenterol 2005;19: Harmon WA, Helman CA. Eosinophilic gastroenteritis and ascites. J Clin Gastroenterol 1981;3: McNabb PC, Fleming CR, Higgins JA, Davis GL. Transmural eosinophilic gastroenteritis with ascites. Mayo Clin Proc 1979;54: Perez-Millan A, Martin-Lorente JL, Lopez-Morante A, et al. Subserosal eosinophilic gastroenteritis treated efficaciously with sodium cromoglycate. Dig Dis Sci 1997;42: Di Gioacchino M, Pizzicannella G, Fini N, et al. Sodium cromoglycate in the treatment of eosinophilic gastroenteritis. Allergy 1990;45: Park HS, Kim HS, Jang HJ. Eosinophilic gastroenteritis associated with food allergy and bronchial asthma. J Korean Med Sci 1995;10: Schwartz DA, Pardi DS, Murray JA. Use of montelukast as steroid-sparing agent for recurrent eosinophilic gastroenteritis. Dig Dis Sci 2001;46: Copyright 2007 by Turner White Communications Inc., Wayne, PA. All rights reserved. Hospital Physician September
Case Report Eosinophilic Gastrointestinal Disorder in Coeliac Disease: ACaseReportandReview
 Case Reports in Gastrointestinal Medicine Volume 2012, Article ID 124275, 4 pages doi:10.1155/2012/124275 Case Report Eosinophilic Gastrointestinal Disorder in Coeliac Disease: ACaseReportandReview Dennis
Case Reports in Gastrointestinal Medicine Volume 2012, Article ID 124275, 4 pages doi:10.1155/2012/124275 Case Report Eosinophilic Gastrointestinal Disorder in Coeliac Disease: ACaseReportandReview Dennis
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK. Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center
 ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
ABDOMINAL PAIN AND DIARRHEA - IT S NOT (ALWAYS) WHAT YOU THINK Yakov Wainer, MD Gastroenterology and Hepatology Meir Medical Center 1 ST ADMISSION - 2015 38 y/o female Abdominal pain, diarrhea - intermittent
Eosinophilic gastroenteritis (EG) is a rare disease
 Case Report 354 A Rare Case of Spontaneous Resolution of Eosinophilic Ascites in A Patient with Primary Eosinophilic Gastroenteritis Wei-Hsuan Liao, MD; Kuo-Liang Wei, MD; Po-Yen-Lin 1, MD; Cheng-Shyong
Case Report 354 A Rare Case of Spontaneous Resolution of Eosinophilic Ascites in A Patient with Primary Eosinophilic Gastroenteritis Wei-Hsuan Liao, MD; Kuo-Liang Wei, MD; Po-Yen-Lin 1, MD; Cheng-Shyong
Eosinophilic Esophagitis (EoE)
 Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Grand Round Presentation Dipendra Parajuli
 Grand Round Presentation Dipendra Parajuli 2-19-04 Case Report: -A 51 y/o causasian male was referred to a gastroenterology office by his primary care provider for the evaluation of new onset ascites.
Grand Round Presentation Dipendra Parajuli 2-19-04 Case Report: -A 51 y/o causasian male was referred to a gastroenterology office by his primary care provider for the evaluation of new onset ascites.
ORIGINAL ARTICLES ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:950 956 ORIGINAL ARTICLES ALIMENTARY TRACT Natural History of Eosinophilic Gastroenteritis GUILLAUME PINETON DE CHAMBRUN,*,,, FLORENT GONZALEZ,*,, JEAN YVES
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:950 956 ORIGINAL ARTICLES ALIMENTARY TRACT Natural History of Eosinophilic Gastroenteritis GUILLAUME PINETON DE CHAMBRUN,*,,, FLORENT GONZALEZ,*,, JEAN YVES
Esophageal Eosinophilia and Eosinophilic Esophagitis. Bible Class 09. Mai 2018
 Esophageal Eosinophilia and Eosinophilic Esophagitis Bible Class 09. Mai 2018 61 yo male No upper-gi symptoms Gastroscopy vor bariatric Operation Lesion: Papilloma Histology of the surrounding mucosa:
Esophageal Eosinophilia and Eosinophilic Esophagitis Bible Class 09. Mai 2018 61 yo male No upper-gi symptoms Gastroscopy vor bariatric Operation Lesion: Papilloma Histology of the surrounding mucosa:
12 Blueprints Q&A Step 2 Surgery
 12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
12 Blueprints Q&A Step 2 Surgery 34. A 40-year-old female has been referred to you for a recent ER and hospital admission, from which she was given a diagnosis of acute diverticulitis. Treatment at that
Eosinophilic Gastroenteritis: Review of a Rare and Treatable Disease of the Gastrointestinal Tract
 Published online: July 16, 2013 1662 0631/13/0072 0293$38.00/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license),
Published online: July 16, 2013 1662 0631/13/0072 0293$38.00/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license),
A Case of Steroid Dependent Eosinophilic Gastroenteritis Presenting as a Huge Gastric Ulcer
 The Korean Journal of Helicobacter and Upper Gastrointestinal Research Vol. 12, No. 2, 103-107, June 2012 http://dx.doi.org/10.7704/kjhugr.2012.12.2.103 A Case of Steroid Dependent Eosinophilic Gastroenteritis
The Korean Journal of Helicobacter and Upper Gastrointestinal Research Vol. 12, No. 2, 103-107, June 2012 http://dx.doi.org/10.7704/kjhugr.2012.12.2.103 A Case of Steroid Dependent Eosinophilic Gastroenteritis
Treatment of Inflammatory Bowel Disease. Michael Weiss MD, FACG
 Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
Treatment of Inflammatory Bowel Disease Michael Weiss MD, FACG What is IBD? IBD is an immune-mediated chronic intestinal disorder, characterized by chronic or relapsing inflammation within the GI tract.
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Abstracting Hematopoietic Neoplasms
 CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
Eosinophilic esophagitis. Kathleen Boynton MD University of Utah Gastroenterology Division
 Eosinophilic esophagitis Kathleen Boynton MD University of Utah Gastroenterology Division Financial disclosures: Janssen Genetech UCB All for research support Learning Objectives To identify the clinical
Eosinophilic esophagitis Kathleen Boynton MD University of Utah Gastroenterology Division Financial disclosures: Janssen Genetech UCB All for research support Learning Objectives To identify the clinical
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 4 Isolated Jejunal Crohn s Disease, A Diagnostic Dilemma Elise Biesboer BS Lacey Stelle MD Michelle M. Olson MD, MACM Paul Tender MD University
World Journal of Colorectal Surgery Volume 6, Issue 5 2016 Article 4 Isolated Jejunal Crohn s Disease, A Diagnostic Dilemma Elise Biesboer BS Lacey Stelle MD Michelle M. Olson MD, MACM Paul Tender MD University
Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased
 1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
1 2 3 4 5 6 7 Chapter 32 Gastroenterology General Pathophysiology General Risk Factors for GI emergencies: Excessive Consumption Excessive Smoking Increased Ingestion of Caustic Substances Poor Bowel Habits
Citywide Infectious Disease Conference. March 27 th, 2018
 Citywide Infectious Disease Conference March 27 th, 2018 Citywide Show and Tell Case 1 Summary 60 s year old Puerto Rican born man SCC of Esophagus, treated with radiation and chemotherapy and then esophageal
Citywide Infectious Disease Conference March 27 th, 2018 Citywide Show and Tell Case 1 Summary 60 s year old Puerto Rican born man SCC of Esophagus, treated with radiation and chemotherapy and then esophageal
Case Report Eosinophilic Ascites and Duodenal Obstruction in a Patient with Liver Cirrhosis
 Case Reports in Gastrointestinal Medicine, Article ID 928496, 4 pages http://dx.doi.org/10.1155/2014/928496 Case Report Eosinophilic Ascites and Duodenal Obstruction in a Patient with Liver Cirrhosis Nasrollah
Case Reports in Gastrointestinal Medicine, Article ID 928496, 4 pages http://dx.doi.org/10.1155/2014/928496 Case Report Eosinophilic Ascites and Duodenal Obstruction in a Patient with Liver Cirrhosis Nasrollah
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה
 ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentaion: S.A is 38 years old. Referred for rectal bleeding investigation. Describes several occasions of bleeding and abdominal pain.
ד"ר דוד ירדני המכון לגסטרואנטרולוגיה ומחלות כבד מרכז רפואי סורוקה Presentaion: S.A is 38 years old. Referred for rectal bleeding investigation. Describes several occasions of bleeding and abdominal pain.
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Kids Like to Break the Rules: Gastrointestinal Pathology in Children
 Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Kids Like to Break the Rules: Gastrointestinal Pathology in Children Jeffrey Goldsmith MD Director of Surgical Pathology, Beth Israel Deaconess Medical Center; Consultant in Gastrointestinal Pathology,
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 Final Pathology:
 Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Learning Objectives. Disclaimer 9/8/2015. Jean Marie Osborne MS, RN, ANP-C
 Jean Marie Osborne MS, RN, ANP-C Learning Objectives 1. Understand the pathophysiologic process of EoE. 2. Dietary indiscretions 3. Management None to report Disclaimer 1 History EoE as an allergic disease
Jean Marie Osborne MS, RN, ANP-C Learning Objectives 1. Understand the pathophysiologic process of EoE. 2. Dietary indiscretions 3. Management None to report Disclaimer 1 History EoE as an allergic disease
Disclosure. Learning Objectives 4/25/2014. I have no disclosures
 Alka Goyal MD Division of Pediatric Gastroenterology Hepatology and Nutrition Children s Hospital of Pittsburgh of UPMC Disclosure I have no disclosures Learning Objectives Diagnosis of Eosinophilic Esophagitis
Alka Goyal MD Division of Pediatric Gastroenterology Hepatology and Nutrition Children s Hospital of Pittsburgh of UPMC Disclosure I have no disclosures Learning Objectives Diagnosis of Eosinophilic Esophagitis
Eosinophilic Gastroenteritis Complicated with Helicobacter pylori Infection Unresponsive to Eradication Therapy
 CSE REPORT Eosinophilic Gastroenteritis Complicated with Helicobacter pylori Infection Unresponsive to Eradication Therapy kira Nakamura 1, Yugo Iwaya 2, Mai Iwaya 3, Takuma Okamura 1, Satoshi Kobayashi
CSE REPORT Eosinophilic Gastroenteritis Complicated with Helicobacter pylori Infection Unresponsive to Eradication Therapy kira Nakamura 1, Yugo Iwaya 2, Mai Iwaya 3, Takuma Okamura 1, Satoshi Kobayashi
Gastrointestinal Tract. Anatomy of GI Tract. Anatomy of GI Tract. (Effective February 2007) (1%-5%)
 Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
Gastrointestinal Tract (Effective February 2007) (1%-5%) Anatomy of GI Tract Esophagus bulls-eye or target EG junction seen on sagittal scan posterior to left lobe of liver and anterior to aorta Anatomy
IBD 101. Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition
 IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
IBD 101 Ronen Stein, MD Assistant Professor of Clinical Pediatrics Division of Gastroenterology, Hepatology, and Nutrition Objectives Identify factors involved in the development of inflammatory bowel
Eosinophilic Esophagitis. Kristine J. Krueger M.D. June 2014
 Eosinophilic Esophagitis Kristine J. Krueger M.D. June 2014 A Most Interesting Patient 36 year old self employed tree surgeon with long standing history of intermittent dysphagia and atypical GERD, NOT
Eosinophilic Esophagitis Kristine J. Krueger M.D. June 2014 A Most Interesting Patient 36 year old self employed tree surgeon with long standing history of intermittent dysphagia and atypical GERD, NOT
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding
 Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Allergic Colitis Clinical and Endoscopic Aspects of Infants. with Rectal Bleeding Allergic Colitis is an inflammatory disorder of the colon which occurs mainly in preschool children. It is caused by an
Perforation of a Duodenal Diverticulum. Elective Student S. C.
 Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Perforation of a Duodenal Diverticulum 2008 4 Elective Student S. C. Case History An elderly male presented to the Emergency Department with abdominal pain. Chief Complaint: Worsening, diffuse abdominal
Ulcerative Colitis. ulcerative colitis usually only affects the colon.
 Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
Ulcerative Colitis Introduction Ulcerative colitis is an inflammatory bowel disease. It is one of the 2 most common inflammatory bowel diseases. The other one is Crohn s disease. Ulcerative colitis and
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Digestion: Small and Large Intestines Pathology
 Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Digestion: Small and Large Intestines Pathology Dr. Ritamarie Loscalzo Medical Disclaimer: The information in this presentation is not intended to replace a one onone relationship with a qualified health
Surgical Management of IBD. Val Jefford Grand Rounds October 14, 2003
 Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
Surgical Management of IBD Val Jefford Grand Rounds October 14, 2003 Introduction Important Features Clinical Presentation Evaluation Medical Treatment Surgical Treatment Cases Overview Introduction Two
ACG Clinical Guideline: Evidenced Based Approach to the Diagnosis and Management of Esophageal Eosinophilia and Eosinophilic Esophagitis (EoE)
 ACG Clinical Guideline: Evidenced Based Approach to the Diagnosis and Management of Esophageal Eosinophilia and Eosinophilic Esophagitis (EoE) Evan S. Dellon, MD, MPH, 1,6 Nirmala Gonsalves, MD, 2,6 Ikuo
ACG Clinical Guideline: Evidenced Based Approach to the Diagnosis and Management of Esophageal Eosinophilia and Eosinophilic Esophagitis (EoE) Evan S. Dellon, MD, MPH, 1,6 Nirmala Gonsalves, MD, 2,6 Ikuo
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint
 GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
GASTROENTEROLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Gastroenterology MOC exam blueprint Based on feedback from physicians that MOC assessments
Allergic disorders of the gastrointestinal tract
 Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Allergic disorders of the gastrointestinal tract Christopher Justinich, MD Introduction The patient with presumed food hypersensitivity continues to present a challenge for the clinician. In certain instances,
Capsule Endoscopy: Is it Really Helpful in the Diagnosis of Small Bowel Diseases? Kashif Malik, Muhammad Joher Amin, Syed Waqar Hassan Shah
 Original Article Capsule Endoscopy: Is it Really Helpful in the Diagnosis of Small Bowel Diseases? Kashif Malik, Muhammad Joher Amin, Syed Waqar Hassan Shah ABSTRACT Objective: To determine the diagnostic
Original Article Capsule Endoscopy: Is it Really Helpful in the Diagnosis of Small Bowel Diseases? Kashif Malik, Muhammad Joher Amin, Syed Waqar Hassan Shah ABSTRACT Objective: To determine the diagnostic
Eosinophilic enteritis: A case report
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Eosinophilic enteritis: A case report Ilavarasi Lakshmanan, Ratnakar Kini, Pugazhendhi Thangavelu, Mohammed Ali ABSTRACT Introduction: Eosinophils
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Eosinophilic enteritis: A case report Ilavarasi Lakshmanan, Ratnakar Kini, Pugazhendhi Thangavelu, Mohammed Ali ABSTRACT Introduction: Eosinophils
Deep Enteroscopy Methods to Diagnose Small Bowel IBD
 Deep Enteroscopy Methods to Diagnose Small Bowel IBD Name: Institution: Peter Draganov University of Florida, Gainesville, FL Overview Types of enteroscopy Enteroscopy equipment Enetoscopy do and don'ts
Deep Enteroscopy Methods to Diagnose Small Bowel IBD Name: Institution: Peter Draganov University of Florida, Gainesville, FL Overview Types of enteroscopy Enteroscopy equipment Enetoscopy do and don'ts
GASTROENTEROLOGY ESSENTIALS
 GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
GASTROENTEROLOGY ESSENTIALS Practical Gastroenterology 8/25/2018 Jahnavi Koppala, MBBS Abdullah Abdussalam, MD A 48-year-old male was evaluated for noncardiac chest pain. Treatment with PPI twice daily
Case Report Collagenous Colitis Associated with Protein Losing Enteropathy in a Toddler
 Case Reports in Gastrointestinal Medicine, Article ID 209624, 4 pages http://dx.doi.org/10.1155/2014/209624 Case Report Collagenous Colitis Associated with Protein Losing Enteropathy in a Toddler Osama
Case Reports in Gastrointestinal Medicine, Article ID 209624, 4 pages http://dx.doi.org/10.1155/2014/209624 Case Report Collagenous Colitis Associated with Protein Losing Enteropathy in a Toddler Osama
Eosinophilic gastrointestinal disorders (EGIDs) are
 G&H CLINICAL CASE STUDIES Esophageal Obstruction as a Result of Isolated Eosinophilic Gastroenteritis Petros C. Benias, MD Ayaz Matin, MD Gil Ignacio Ascunce, MD David L. Carr-Locke, MD Division of Digestive
G&H CLINICAL CASE STUDIES Esophageal Obstruction as a Result of Isolated Eosinophilic Gastroenteritis Petros C. Benias, MD Ayaz Matin, MD Gil Ignacio Ascunce, MD David L. Carr-Locke, MD Division of Digestive
Case History B Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment
 Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Case History B-1325945 Female patient 1970 Clinical History : crampy abdominal pain and episodes of bloody diarrhea Surgical treatment Case History B-1325945 Pathology Submucosa & Muscularis Endometriosis
Intestinal tuberculosis and tuberculous peritonitis
 Intestinal tuberculosis and tuberculous peritonitis GAO Hong Department of Gastroenterology, Zhongshan Hospital Fudan University Objectives 1. To master the clinical manifestations, complications, diagnosis
Intestinal tuberculosis and tuberculous peritonitis GAO Hong Department of Gastroenterology, Zhongshan Hospital Fudan University Objectives 1. To master the clinical manifestations, complications, diagnosis
HCPCS Codes (Alphanumeric, CPT AMA) ICD-9-CM Codes Covered by Medicare Program
 HCPCS s (Alphanumeric, CPT AMA) 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal neoplasm screening ICD-9-CM
HCPCS s (Alphanumeric, CPT AMA) 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal neoplasm screening ICD-9-CM
Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego
 Severe and Emergency Presentations of Celiac Disease Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Case Presentation (1) 63 year old male transferred
Severe and Emergency Presentations of Celiac Disease Sheila E. Crowe, MD, FRCPC, FACP, FACG, AGAF Department of Medicine University of California, San Diego Case Presentation (1) 63 year old male transferred
Rings in the esophagus are not always eosinophilic esophagitis: Case series of ring forming lymphocytic esophagitis and review of the literature
 Rings in the esophagus are not always eosinophilic esophagitis: Case series of ring forming lymphocytic esophagitis and review of the literature Authors Julia L. Pleet 1,SofiaTaboada 2, Arvind Rishi 2,
Rings in the esophagus are not always eosinophilic esophagitis: Case series of ring forming lymphocytic esophagitis and review of the literature Authors Julia L. Pleet 1,SofiaTaboada 2, Arvind Rishi 2,
A Case of Eosinophilic Gastrointestinal Disorders Presenting with Chronic Diarrhea and Abdominal Pain
 Korean J Fam Med. 2011;32:257-262 doi:10.4082/kjfm.2011.32.4.257 A Case of Eosinophilic Gastrointestinal Disorders Presenting with Chronic Diarrhea and Abdominal Pain Case Report Dong-Ryul Lee* Department
Korean J Fam Med. 2011;32:257-262 doi:10.4082/kjfm.2011.32.4.257 A Case of Eosinophilic Gastrointestinal Disorders Presenting with Chronic Diarrhea and Abdominal Pain Case Report Dong-Ryul Lee* Department
HDF Case Whipple s disease
 HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
HDF Case 952556 Whipple s disease 63 yo female complaining of a diarrhea for 2 months, weigth loss (12 Kg in 3 months), and joint pains. Duodenal biopsy performed. Scanning view, enlarged intestinal villi,
NCD for Fecal Occult Blood Test
 NCD for Fecal Occult Blood Test Applicable CPT Code(s): 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal
NCD for Fecal Occult Blood Test Applicable CPT Code(s): 82272 Blood, occult, by peroxidase activity (e.g., guaiac), qualitative, feces, 1-3 simultaneous determinations, performed for other than colorectal
But.. Capsule Endoscopy. Guidelines (OMED ECCO) Why is Enteroscopy so Important? 4/19/2017
 Dr. Elizabeth Odstrcil Digestive Health Associates of Texas April 22, 2017 But.. Capsules fail to reach the cecum in as many as 25% of patients Patients with known CD have a risk of capsule retention of
Dr. Elizabeth Odstrcil Digestive Health Associates of Texas April 22, 2017 But.. Capsules fail to reach the cecum in as many as 25% of patients Patients with known CD have a risk of capsule retention of
METASTASES FROM GASTRIC CARCINOMA TO COLON LESIONS: A CASE REPORT IN THE FORM OF MULTIPLE FLAT ELEVATED CASE PRESENTATION
 H.C. Lee, M.T. Yang, K.Y. Lin, et al METASTASES FROM GASTRIC CARCINOMA TO COLON IN THE FORM OF MULTIPLE FLAT ELEVATED LESIONS: A CASE REPORT Hsi-Chang Lee, Min-Ta Yang, 1 Kuang-Yang Lin, 1 Hsing-Yang Tu,
H.C. Lee, M.T. Yang, K.Y. Lin, et al METASTASES FROM GASTRIC CARCINOMA TO COLON IN THE FORM OF MULTIPLE FLAT ELEVATED LESIONS: A CASE REPORT Hsi-Chang Lee, Min-Ta Yang, 1 Kuang-Yang Lin, 1 Hsing-Yang Tu,
A Case of Pneumatosis Cystoides Intestinalis Mimicking Intestinal Perforation
 Showa Univ J Med Sci 26 2, 169 173, June 2014 Case Report A Case of Pneumatosis Cystoides Intestinalis Mimicking Intestinal Perforation Takahiro UMEMOTO 1, Yoshikuni HARADA 1, Makiko SAKATA 1, Gaku KIGAWA
Showa Univ J Med Sci 26 2, 169 173, June 2014 Case Report A Case of Pneumatosis Cystoides Intestinalis Mimicking Intestinal Perforation Takahiro UMEMOTO 1, Yoshikuni HARADA 1, Makiko SAKATA 1, Gaku KIGAWA
Implementation of disease and safety predictors during disease management in UC
 Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
Implementation of disease and safety predictors during disease management in UC DR ARIELLA SHITRIT DIGESTIVE DISEASES INSTITUTE SHAARE ZEDEK MEDICAL CENTER JERUSALEM Case presentation A 52 year old male
The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems.
 GASTROINTESTINAL AND HEPATOBILIARY SYSTEMS The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems. GASTROINTESTINAL SYSTEM AND HEPATOBILIARY SYSTEM We will examine
GASTROINTESTINAL AND HEPATOBILIARY SYSTEMS The focus of this week s lab will be pathology of the gastrointestinal and hepatobiliary systems. GASTROINTESTINAL SYSTEM AND HEPATOBILIARY SYSTEM We will examine
The London Gastroenterology Partnership CROHN S DISEASE
 CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
Accepted Article. Granulomatous appendicitis as an uncommon cause of abdominal pain. Description of a case
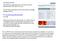 Accepted Article Granulomatous appendicitis as an uncommon cause of abdominal pain. Description of a case Carmen Salvia López Ramos, Ana Fuentes Coronel, Santiago Rodríguez Gómez DOI: 10.17235/reed.2015.3763/2015
Accepted Article Granulomatous appendicitis as an uncommon cause of abdominal pain. Description of a case Carmen Salvia López Ramos, Ana Fuentes Coronel, Santiago Rodríguez Gómez DOI: 10.17235/reed.2015.3763/2015
Eosinophilic ascites - a rare presentation of eosinophilic gastroenteritis with spontaneous remission and relapse in an adolescent
 International Journal of Gastroenterology, Hepatology, Transplant & Nutrition Case Report Eosinophilic ascites - a rare presentation of eosinophilic gastroenteritis with spontaneous remission and relapse
International Journal of Gastroenterology, Hepatology, Transplant & Nutrition Case Report Eosinophilic ascites - a rare presentation of eosinophilic gastroenteritis with spontaneous remission and relapse
MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS
 MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS Wai K. Leung Li Shu Fan Medical Foundation Professor in Gastroenterology Associate Dean (Human Capital), LKS Faculty of Medicine, University
MANAGEMENT OF IMMUNOTHERAPY RELATED GI AND HEPATIC ADVERSE EVENTS Wai K. Leung Li Shu Fan Medical Foundation Professor in Gastroenterology Associate Dean (Human Capital), LKS Faculty of Medicine, University
Objectives. Disclosures. Eosinophilic Esophagitis and Nutritional Consequences. Food Allergy In Schools
 Eosinophilic Esophagitis and Nutritional Consequences Douglas T. Johnston, DO, FACAAI, FAAAAI Assistant Professor of Internal Medicine / Allergy & Immunology Edward Via College of Osteopathic Medicine
Eosinophilic Esophagitis and Nutritional Consequences Douglas T. Johnston, DO, FACAAI, FAAAAI Assistant Professor of Internal Medicine / Allergy & Immunology Edward Via College of Osteopathic Medicine
LIVER CIRRHOSIS. The liver extracts nutrients from the blood and processes them for later use.
 LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
LIVER CIRRHOSIS William Sanchez, M.D. & Jayant A. Talwalkar, M.D., M.P.H. Advanced Liver Disease Study Group Miles and Shirley Fiterman Center for Digestive Diseases Mayo College of Medicine Rochester,
Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic
 Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic Hepatocellular Carcinoma Chih-Hao Shen, MD 3, Jung-Chung Lin, MD, PhD 2, Hsuan-Hwai Lin, MD 1, You-Chen Chao, MD 1, and Tsai-Yuan
Early Klebsiella pneumoniae Liver Abscesses associated with Pylephlebitis Mimic Hepatocellular Carcinoma Chih-Hao Shen, MD 3, Jung-Chung Lin, MD, PhD 2, Hsuan-Hwai Lin, MD 1, You-Chen Chao, MD 1, and Tsai-Yuan
A rare cause of abdominal pain and gastrointestinal bleeding: Colonic lipoma causing intussusception
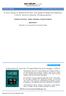 www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS A rare cause of abdominal pain and gastrointestinal bleeding: Colonic lipoma causing intussusception Daniela Ferreira, Marta Salgado, Isabel
www.edoriumjournals.com CLINICAL IMAGES PEER REVIEWED OPEN ACCESS A rare cause of abdominal pain and gastrointestinal bleeding: Colonic lipoma causing intussusception Daniela Ferreira, Marta Salgado, Isabel
Imaging techniques in the diagnosis, staging and follow up of GI cancers. Moderators: Banke Agarwal, MD and Paul Schultz, MD
 Imaging techniques in the diagnosis, staging and follow up of GI cancers Moderators: Banke Agarwal, MD and Paul Schultz, MD Panelists Axel Grothey, MD Professor of Oncology Division of Medical Oncology
Imaging techniques in the diagnosis, staging and follow up of GI cancers Moderators: Banke Agarwal, MD and Paul Schultz, MD Panelists Axel Grothey, MD Professor of Oncology Division of Medical Oncology
Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori
 Gut and Liver, Vol. 6, No. 2, April 2012, pp. 270-274 CASE REPORT Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori Soo-Kyung Park, Hwoon-Yong Jung, Do Hoon Kim,
Gut and Liver, Vol. 6, No. 2, April 2012, pp. 270-274 CASE REPORT Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori Soo-Kyung Park, Hwoon-Yong Jung, Do Hoon Kim,
Interesting Pediatric ultrasound cases. Presented by: Falguni Patel (RDMS, RVT)
 Interesting Pediatric ultrasound cases Presented by: Falguni Patel (RDMS, RVT) Role of ultrasound to rule out Appendicitis Overview: Ultrasound is relatively inexpensive, safe and quick solution to rule
Interesting Pediatric ultrasound cases Presented by: Falguni Patel (RDMS, RVT) Role of ultrasound to rule out Appendicitis Overview: Ultrasound is relatively inexpensive, safe and quick solution to rule
What s Your Diagnosis?
 Claire Legallet What s Your Diagnosis? Signalment: Species: Canine Breed: Catahoula Sex: Female Intact Age at presentation: 6 months Presenting Complaint: Chronic intermittent bloody diarrhea and vomiting
Claire Legallet What s Your Diagnosis? Signalment: Species: Canine Breed: Catahoula Sex: Female Intact Age at presentation: 6 months Presenting Complaint: Chronic intermittent bloody diarrhea and vomiting
Title: unusual case report of inflammatory. fibrous polyps in the upper gastrointestinal tract. Authors: Baifang Wang, Guoqing Xiang, Jia Zhu
 Title: An unusual case report of inflammatory fibrous polyps in the upper gastrointestinal tract Authors: Baifang Wang, Guoqing Xiang, Jia Zhu DOI: 10.17235/reed.2018.5734/2018 Link: PubMed (Epub ahead
Title: An unusual case report of inflammatory fibrous polyps in the upper gastrointestinal tract Authors: Baifang Wang, Guoqing Xiang, Jia Zhu DOI: 10.17235/reed.2018.5734/2018 Link: PubMed (Epub ahead
Recurrent Intestinal Obstruction in a Patient with Selective IgA Deficiency
 Case Report Recurrent Intestinal Obstruction in a Patient with Selective IgA Deficiency Chee-Kin Hui 1,2 Submitted: 27 May 2015 Accepted: 27 Mar 2016 Online: 7 Dec 2016 1 Centre for Alimentary Studies,
Case Report Recurrent Intestinal Obstruction in a Patient with Selective IgA Deficiency Chee-Kin Hui 1,2 Submitted: 27 May 2015 Accepted: 27 Mar 2016 Online: 7 Dec 2016 1 Centre for Alimentary Studies,
Case Discussion. Nutrition in IBD. Rémy Meier MD. Ulcerative colitis. Crohn s disease
 26.08.2017 Case Discussion Nutrition in IBD Crohn s disease Ulcerative colitis Rémy Meier MD Case Presentation 30 years old female, with diarrhea for 3 months Shool frequency 3-4 loose stools/day with
26.08.2017 Case Discussion Nutrition in IBD Crohn s disease Ulcerative colitis Rémy Meier MD Case Presentation 30 years old female, with diarrhea for 3 months Shool frequency 3-4 loose stools/day with
Eosinophilic oesophagitis
 Eosinophilic oesophagitis Food Allergy (Allergic food hypersensitivity) Mike Levin Paediatric Allergy Red Cross Hospital UCT IgE mediated Mixed Non IgE mediated Disease Mechanisms in EGID Rothenberg, JACI,
Eosinophilic oesophagitis Food Allergy (Allergic food hypersensitivity) Mike Levin Paediatric Allergy Red Cross Hospital UCT IgE mediated Mixed Non IgE mediated Disease Mechanisms in EGID Rothenberg, JACI,
WHAT IS ULCERATIVE COLITIS?
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Ulcerative Colitis WHAT IS ULCERATIVE COLITIS? Ulcerative colitis is
Lymphoplasmacytic-Plasmacytic Gastroenteritis
 Lymphoplasmacytic-Plasmacytic Gastroenteritis (Inflammation of the Stomach and Intestines, Characterized by the Presence of Lymphocytes and Plasmacytes [Types of White Blood Cell]) Basics OVERVIEW An inflammatory
Lymphoplasmacytic-Plasmacytic Gastroenteritis (Inflammation of the Stomach and Intestines, Characterized by the Presence of Lymphocytes and Plasmacytes [Types of White Blood Cell]) Basics OVERVIEW An inflammatory
Patho Basic Chronic Inflammatory Bowel Diseases. Jürg Vosbeck Pathology
 Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Patho Basic Chronic Inflammatory Bowel Diseases Jürg Vosbeck Pathology General Group of chronic relapsing diseases with chronic bloody or watery diarrhea Usually ulcerative colitis (UC) or Crohn s disease
Gastroenterology Tutorial
 Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis?
 CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
CASE REPORT IgG4-Negative Autoimmune Pancreatitis with Sclerosing Cholangitis and Colitis: Possible Association with Primary Sclerosing Cholangitis? Keita Saeki 1, Shigenari Hozawa 1, Naoteru Miyata 1,
General Data. 王 X 村 78 y/o 男性
 General Data 王 X 村 78 y/o 男性 Chief Complaint Vomiting twice this early morning Fever up to 38.9ºC was noted Present Illness (1) Old CVA with left side weakness for more than 10 years and with bed ridden
General Data 王 X 村 78 y/o 男性 Chief Complaint Vomiting twice this early morning Fever up to 38.9ºC was noted Present Illness (1) Old CVA with left side weakness for more than 10 years and with bed ridden
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 09/17/2011 Radiology Quiz of the Week # 38 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN
 UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
UNDERSTANDING X-RAYS: ABDOMINAL IMAGING THE ABDOMEN Radiology Enterprises radiologyenterprises@gmail.com www.radiologyenterprises.com STOMACH AND SMALL BOWEL STOMACH AND SMALL BOWEL Swallowed air is a
Terumitsu; Nagayasu, Takeshi
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
CHRONIC DIARRHEA DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE THAN 4 WEEKS
 DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
DR. PHILIP K. BLUSTEIN M.D. F.R.C.P.(C) 415 14 TH ST. NW. CALGARY AB T2N2A1 PHONE (403) 270-9555 FAX (403) 270-7479 CHRONIC DIARRHEA DEFINITION: *LOOSE, WATERY STOOLS *MORE THAN 3 TIMES A DAY *FOR MORE
Bleeding in the Digestive Tract
 Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Bleeding in the Digestive Tract National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH U.S. Department of Health
Eosinophilic Esophagitis in Children and Adults
 Journal of Pediatric Gastroenterology and Nutrition 37:S23 S28 November/December 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Eosinophilic Esophagitis in Children and Adults Chris A. Liacouras
Journal of Pediatric Gastroenterology and Nutrition 37:S23 S28 November/December 2003 Lippincott Williams & Wilkins, Inc., Philadelphia Eosinophilic Esophagitis in Children and Adults Chris A. Liacouras
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Ultrasound of: Appendicitis Intussusception Pyloric Stenosis
 Ultrasound of: Appendicitis Intussusception Pyloric Stenosis Andrew Phelps MD Assistant Professor Pediatric Radiology UCSF Benioff Children s Hospital No Disclosures Take Home Message Appendicitis occurs
Ultrasound of: Appendicitis Intussusception Pyloric Stenosis Andrew Phelps MD Assistant Professor Pediatric Radiology UCSF Benioff Children s Hospital No Disclosures Take Home Message Appendicitis occurs
Gastroenterology Fellowship Program
 Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
Gastroenterology Fellowship Program Outpatient Clinical Rotations I. Overview A. Three Year Continuity Clinic Experience All gastroenterology fellows will be required to have a ½ day continuity clinic
SARCINA VENTICULARI IS A POSSIBLE CAUSATIVE MICROORGANISM OTHER THAN H.PYLORI IN GASTRIC OUTLET OBSTRUCTION PATHOGENESIS
 SARCINA VENTICULARI IS A POSSIBLE CAUSATIVE MICROORGANISM OTHER THAN H.PYLORI IN GASTRIC OUTLET OBSTRUCTION PATHOGENESIS 55 years old male, Farm worker, married, from Ibb Heavy Smoker, Khat chewer non-alcohol
SARCINA VENTICULARI IS A POSSIBLE CAUSATIVE MICROORGANISM OTHER THAN H.PYLORI IN GASTRIC OUTLET OBSTRUCTION PATHOGENESIS 55 years old male, Farm worker, married, from Ibb Heavy Smoker, Khat chewer non-alcohol
At the outset, we want to clear up some terminology issues. IBS is COPYRIGHTED MATERIAL. What Is IBS?
 1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
What is ulcerative colitis?
 What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
What is ulcerative colitis? Ulcerative colitis is a disease that causes inflammation and sores, called ulcers, in the lining of the rectum and colon. Ulcers form where inflammation has killed the cells
What is Crohn's disease?
 What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
What is Crohn's disease? Crohn's disease is a chronic inflammatory disorder that causes inflammation of the digestive tract. It can affect any area of the GI tract, from the mouth to the anus, but it most
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Report An Uncommon Cause of a Small-Bowel Obstruction
 Hindawi Case Reports in Gastrointestinal Medicine Volume 2017, Article ID 1628215, 4 pages https://doi.org/10.1155/2017/1628215 Case Report An Uncommon Cause of a Small-Bowel Obstruction Ali Zakaria, Bayan
Hindawi Case Reports in Gastrointestinal Medicine Volume 2017, Article ID 1628215, 4 pages https://doi.org/10.1155/2017/1628215 Case Report An Uncommon Cause of a Small-Bowel Obstruction Ali Zakaria, Bayan
Chronic Diarrhea in Dogs
 Chronic Diarrhea in Dogs Basics OVERVIEW A change in the frequency, consistency, and volume of bowel movement (feces) for more than 3 weeks Can be either small bowel (small intestine) diarrhea, large bowel
Chronic Diarrhea in Dogs Basics OVERVIEW A change in the frequency, consistency, and volume of bowel movement (feces) for more than 3 weeks Can be either small bowel (small intestine) diarrhea, large bowel
Small Bowel and Colon Surgery
 Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
Small Bowel and Colon Surgery Why Do I Need a Small Bowel Resection? A variety of conditions can damage your small bowel. In severe cases, your doctor may recommend removing part of your small bowel. Conditions
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND. Fabrizio Parente
 NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
NON INVASIVE MONITORING OF MUCOSAL HEALING IN IBD. THE ROLE OF BOWEL ULTRASOUND Fabrizio Parente Gastrointestinal Unit, A.Manzoni Hospital, Lecco & L.Sacco School of Medicine,University of Milan - Italy
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID
 ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
Last Revised: September 15 Last Reviewed: September EOSINOPHILIC ESOPHAGITIS (EOE)/PPI-RESPONSIVE ESOPHAGEAL EOSINOPHILIA (PPI-REE)
 7.0 GASTROENTEROLOGY Last Revised: September 5 Last Reviewed: September 5 7. EOSINOPHILIC ESOPHAGITIS (EOE)/PPI-RESPONSIVE ESOPHAGEAL EOSINOPHILIA (PPI-REE) Significant changes: ) Addition of PPI-REE as
7.0 GASTROENTEROLOGY Last Revised: September 5 Last Reviewed: September 5 7. EOSINOPHILIC ESOPHAGITIS (EOE)/PPI-RESPONSIVE ESOPHAGEAL EOSINOPHILIA (PPI-REE) Significant changes: ) Addition of PPI-REE as
