Department of Psychiatry, University of Hong Kong, Pokfulam Road, Hong Kong 2
|
|
|
- April Rose
- 6 years ago
- Views:
Transcription
1 Evidence-Based Complementary and Alternative Medicine Volume 2012, Article ID , 16 pages doi: Review Article Prescription of Chinese Herbal Medicine and Selection of Acupoints in Pattern-Based Traditional Chinese Medicine Treatment for Insomnia: A Systematic Review Wing-Fai Yeung, 1 Ka-Fai Chung, 1 Maggie Man-Ki Poon, 1 Fiona Yan-Yee Ho, 1 Shi-Ping Zhang, 2 Zhang-Jin Zhang, 3 Eric Tat-Chi Ziea, 4 and Vivian Wong Taam 4 1 Department of Psychiatry, University of Hong Kong, Pokfulam Road, Hong Kong 2 School of Chinese Medicine, Hong Kong Baptist University, Hong Kong 3 School of Chinese Medicine, University of Hong Kong, Hong Kong 4 Chinese Medicine Section, Hospital Authority, Hong Kong Correspondence should be addressed to Ka-Fai Chung, kfchung@hkucc.hku.hk Received 13 July 2012; Revised 13 October 2012; Accepted 20 October 2012 Academic Editor: Jianping Liu Copyright 2012 Wing-Fai Yeung et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Traditional Chinese medicine (TCM) treatments are often prescribed based on individuals pattern diagnoses. A systematic review of Chinese and English literatures on TCM pattern differentiation, treatment principle, and pattern-based treatment for insomnia has therefore been conducted. A total of 227 studies, subjects, and 87 TCM patterns were analyzed. There was a limited consistency in pattern-based TCM treatment of insomnia across practitioners. Except for Gui Pi Tang, An Shen Ding Zhi Wan, and Wen Dan Tang which were used more commonly for deficiency of both the heart and spleen, internal disturbance of phlegmheat, and qi deficiency of the heart and gallbladder, respectively, the selection of herbal formula for other patterns and patternbased prescription of individual herbs and acupoints were not consistent. Suanzaoren (Semen Z. spinosae), Fuling (Poria), Yejiaoteng (Caulis P. multiflori), Gancao (Radix Glycyrrhizae), Baishao (Radix P. alba), Shenmen (HT7), Yintang (EX-HN3), Sanyinjiao (SP6), Baihui (GV20), Anmian (EX-HN22), and Sishencong (EX-HN1) were commonly used, but nonspecifically for many patterns. Treatment principles underlying herb and acupoint selection were seldom reported. Although many studies were reviewed, the study quality and diagnostic process were inadequate. More high quality studies are needed to examine the additional benefits of pattern differentiation and pattern-based TCM treatment. 1. Introduction Insomnia is a frequent clinical complaint. Nearly one-third of the general population worldwide presents with insomnia symptoms, and the prevalence of insomnia symptoms accompanied by daytime consequences is approximately 9 15% [1]. Insomnia is a risk factor of a number of negative health consequences, including major depression, suicide, anxiety disorders, and alcohol and substance abuse or dependence [2]. Effective pharmacological treatments for insomnia are available. However, their uses are limited due to concerns about long-term efficacy and potential for dependence, abuse, and adverse effects [3]. Although psychological and behavioral therapies have empirical evidence for insomnia [4], they have remained underused because of the time-intensive nature and treatment nonadherence. Since the currently available treatments have their limitation, complementary and alternative medicine has been sought to treat insomnia. According to a national survey, over 1.6 million adults in the United States used complementary and alternative medicine to treat insomnia in the year 2002 [5]. Traditional Chinese medicine (TCM), a form of complementary and alternative medicine, is one of the oldest medical systems in the world. The use of TCM for insomnia can be traced more than 2000 years ago in Chinese medical texts [6, 7]. In clinical practice, TCM treatments are individualized according to the TCM pattern diagnosis. TCM pattern, in terms of TCM theory, is defined as a diagnostic conclusion
2 2 Evidence-Based Complementary and Alternative Medicine of the pathological changes of a disease state based on an individual s symptoms and signs, including pulse form and tongue appearance [8]. The patterns of bodily disharmony can be described in terms of eight major parameters: yin and yang, external and internal, hot and cold, andexcess and deficiency. Additional systems, such as qi, blood and bodyfluid differentiation, and zang fu (organ) differentiation are also used [9]. For a given disease there may be different presentations of various symptoms and signs; hence, many TCM pattern diagnoses are possible and this forms the rationale that different TCM treatments can be given for the same disease. On the other hand, different diseases may be treated with the same TCM treatment if they share the same pattern. The TCM patterns used today and the selection of herbal formulas and acupoints for specific TCM patterns are developed based on clinical experience, ancient medical texts, and some recently published TCM textbooks. It has to be acknowledged that most TCM concepts and therapies have not yet been proven by scientific method. Although it is believed that pattern-based TCM treatment will provide better efficacy, previous studies regarding the additional benefit of TCM pattern differentiation are scarce. One randomized controlled trial (RCT) found that the therapeutic effect of Chinese herbal treatment according to TCM pattern was more sustainable than the standard formula in treating irritable bowel syndrome [10]. It has also been reported in rheumatoid arthritic patients that TCM pattern diagnoses can guide the use of Western medicine [11]. However, other RCTs found that the efficacy of pattern-based individualized acupuncture was not superior to standardized acupuncture for chronic shoulder pain [12], chronic back pain [13], and hypertension [14]. A previous survey in a Chinese medicine clinic in Taiwan has summarized the commonly prescribed single Chinese herbs and herbal formulas for insomnia [15]. Another study has reviewed the randomized controlled trials of acupuncture for insomnia and determined the most frequently used acupoints [16]. To the best of our knowledge, there has been no systematic review on the TCM patterns for insomnia. Information regarding pattern-based TCM treatments for insomnia is also lacking. Given the high prevalence of insomnia in the general population and its frequent presentation to TCM practitioners, it is important to review the current application of syndrome differentiation in TCM treatments for insomnia. The objectives of this paper were (1) to summarize the commonly diagnosed TCM patterns in patients with insomnia and (2) to find out the current practice of pattern-based TCM treatments for insomnia. 2. Method The present study was part of our systematic review on TCM treatments for insomnia. Chinese herbal medicine, traditional needle acupuncture, and variants of acupuncture, including acupressure, moxibustion, transcutaneous electrical nerve stimulation, auricular acupressure, and reflexology were reviewed [17]. We searched the MEDLINE, EMBASE, Cochrane Central Register of Controlled Trials, Cumulative Index to Nursing and Allied Health Literature, and Allied and Complementary Medicine from inception to May 2010 using the grouped terms (insomnia or wakeful or sleepless or sleep ) and ((acupuncture or acupoints or acupressure or meridian or transcutaneous electrical nerve stimulation or TENS or moxibustion or tuina) or (herb or herbal medicine or traditional Chinese medicine or TCM)). The search also included China Academic Journals Full- Text Database, China Proceedings of Conference Full-Text Database, Chinese Biomedical Literature Database, China Doctor Dissertations Full-Text Database, China Master Theses Full-Text Database, Chinese Science and Technology Documents Database, Chinese Dissertation Document Bibliography Database, Chinese Academic Papers Conference Database, Digital Periodical, and Taiwan Electronic Periodical Services. The reference lists of the retrieved papers were further searched for relevant articles Selection Criteria. Studies included in this paper were case series or clinical trials that described TCM patterns of subjects who received TCM treatment for their chief complaint of insomnia. In order to obtain a full coverage of the topic, we had not set any specification for sampling procedure, treatment method, outcome measure, and study quality. In addition, to derive a general picture of TCM pattern utilization, studies were excluded if they (1) had less than 30 subjects; (2) examined male or female only; (3) focusedonsubjectsagedbelow18orabove70years;(4) focused on a specific medical and psychiatric condition, a particular life transition period, or a specific TCM pattern; (5) had no statistical information regarding the frequency of individual TCM pattern; or (6) were duplicated publications. A sample size of 30 is considered as the minimum to examine the TCM pattern diagnosis in individuals with insomnia Data Extraction Process. Two authors (W. Yeung and M. Poon) searched the databases and selected the relevant publications independently. If there were any disagreements about the eligibility of a study, the two authors would check the study against the inclusion and exclusion criteria, discuss its eligibility, and come to a further decision. One author (M. Poon) extracted the data and the other (W. Yeung) checked the extracted data. For each study, the following variables were extracted: study design, sample size, mode of recruitment, sampling and diagnostic procedure, inclusion and exclusion criteria, and participants characteristics including age, gender, and duration of insomnia. TCM patterns, treatment principles, treatment regimen, and outcome of TCM treatments were obtained. In a majority of the reviewed studies, effective rate was the only outcome measure. The definition of effective rate was not standardized, but it was most often defined as the proportion of subjects who had at least some improvement of sleep or at least 30% reduction in the severity of insomnia by rating scales. We calculated the mean, standard deviation, and 95% confidence interval of dichotomous outcome measure. All Chinese to English translations were deduced primarily from the World Health
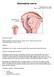
3 Evidence-Based Complementary and Alternative Medicine 3 Organization (WHO) International Standard Terminologies on Traditional Medicine in the Western Pacific Region [8], and additionally from Traditional Chinese Internal Medicine [18], a commonly used English-language TCM textbook in China Quality Assessment. For RCTs of Chinese herbal medicine, methodological quality will be assessed using Jadad scale. The Jadad scale evaluates a study in terms of the description of randomization, blinding, and dropouts. Points are awarded if the study is described as randomized, 1 point; has appropriate randomization method, 1 point; is described as double-blind, 1 point; uses appropriate blinding method, 1 point; has description of withdrawals and dropouts, 1 point. For RCTs involving acupuncture, a modified Jadad scale will be used. The modified Jadad scale takes into consideration the difficulty in blinding the acupuncturist to the treatment process. Points are awarded if the study is described as randomized, 1 point; has appropriate randomization method, 1 point; subjects blinded to intervention, 1 point; evaluator blinded to intervention, 1 point; has description of withdrawals and dropouts, 1 point [19, 20]. Both the Jadad scale and modified Jadad scale scores range from 1 to 5; RCTs with a score from 3 to 5 are regarded as better quality trials Statistical Analysis. We used SPSS version 16.0 for statistical analysis. Effective rate wassummarized using mean (SD) and 95% confidence intervals (CIs). 3. Results The search yielded potential titles for review, of which 4924 were duplicate records and 6249 were excluded for reasons of irrelevance. The full text of 2872 articles was retrieved for detailed assessment, of which 2645 were excluded for various reasons (Figure 1). Of the 227 studies which fulfilled the inclusion and exclusion criteria, 89 were on Chinese herbal medicine, 64 on acupuncture, 40 on a combination of two acupuncture treatments, 24 on a combination of Chinese herbal medicine and acupuncture, and 10 on other TCM treatments. Sample size of the 227 studies ranged from 30 to 400. TCM diagnosis was available in subjects. A total of 87 different TCM diagnoses were examined in the 227 studies. The most common pattern was deficiency of both the heart and spleen, which was diagnosed in 4056 subjects or 22.6% of the subjects; it was followed by hyperactivity of fire due to yin deficiency (N = 2926, 16.3%), liver-qi stagnation transforming into fire (N = 1817, 10.1%), heart-kidney noninteraction (N = 1157, 6.5%), internal disturbance of phlegm heat (N = 904, 5.0%), qi deficiency of the heart and gallbladder (N = 838, 4.7%), liver fireflamingupward(n = 456, 2.5%), heart deficiency with timidity (N = 356, 2.0%), disharmony between spleen and stomach (N = 325, 1.8%), and stomach disharmony (N = 162, 0.9%). The top 10 TCM patterns accounted for 72.5% of the subjects (Table 1). The criteria used for diagnosis of TCM pattern varied between studies. Twenty-one of the 227 studies (9.3%) were based on TCM textbooks, 17 (7.5%) studies used the Clinical Research Guidelines of New Chinese Herbal Medicine [21], 16 (7.0%) used the Criteria of Diagnosis and Therapeutic Effect of Diseases and Syndromes in TCM [22], 6 (2.6%) used some self-defined criteria, 3 (1.3%) adopted the criteria used by other TCM experts, and 1 used a combination of the Criteria of Diagnosis and Therapeutic Effect of Diseases and Syndromes in TCM and a textbook. One hundred and sixtythree studies (71.8%) did not report the diagnostic criteria used TCM Pattern and Chinese Herbal Medicine. Eightynine of the 227 included studies examined Chinese herbal medicine for insomnia: 54 of the 89 studies (60.7%) were case series, 8 (9.0%) were controlled studies, and 27 (30.3%) were RCTs. Of the 27 RCTs, 15 (55.6%) compared Chinese herbal medicine with Western medication, 9 (33.3%) with another Chinese herbal medicine, and 3 (11.1%) with Western medication and another Chinese herbal medicine. Twenty-six (96.3%) of the 27 RCTs were described as randomized but the randomization method, blinding, and dropouts were not presented; hence, these 26 RCTs had a Jadad score of 1. Only 1 (3.7%) of the 27 RCTs had appropriate randomization and double-blind design and obtained a Jadad score of 3. Gui Pi Tang or its modification was the most frequently used Chinese herbal formula for the treatment of insomnia in patients diagnosed with deficiency of both the heart and spleen (Table 2); for hyperactivity of fire due to yin deficiency, Huang Lian E Jiao Tang was the most frequently used formula. Modified Long Dan Xie Gan Tang and Dan Zhi Xiao Yao San were the most often used herbal formula for liver-qi stagnation transforming into fire. Forinternal disturbance of phlegm heat, the most frequently used formula was modified to Wen Dan Tang; lastly, for qi deficiency of the heart and gallbladder, modified An Shen Ding Zhi Wan was the most frequently used. There was a great variation in Chinese herbal treatment among patients diagnosed with heartkidney noninteraction and heart deficiency with timidity,with no single formula being studied twice. Studies on liver fire flaming upward, disharmony between spleen and stomach, and stomach disharmony were so limited that reliable information was not possible (Table 2). The TCM treatment principles and ingredients of the Chinese herbal formulas for treating insomnia are presented in Table 2. Due to a wide variation in the composition of herbal formulas, we only listed those individual herbs that were used in at least 20% of the studies on the TCM pattern. Suanzaoren (Semen Z. spinosae), Danggui (Radix A. sinensis), Yuanzhi (Radix Polygalae), Dangshen (Radix Condonopsis), Huangqi (Radix Astragali), Fuling (Poria), Baizhu (Rhizoma A. macrocephalae), Yejiaoteng (Caulis P. multiflori), Fushen (Poria cum Radix Pini), Muxiang (Radix Aucklandiae), Longyanrou (Arillus longan), Honey-toasted Gancao (Radix Glycyrrhizae), Gancao (Radix Glycyrrhizae), Baishao (Radix P. alba), Dazao (Fructus Jujibae), Wuweizi (Fructus S. Chinensis), Hehuanpi (Cortex Albiziae), Baiziren (Semen Platycladi), and Shengjiang (Rhizoma Zingiberis) were common individual herbs for the treatment of insomnia
4 4 Evidence-Based Complementary and Alternative Medicine records identified through database searching 149 records identified through other sources Identical citations: records after duplicates removed Irrelevant papers: full-text articles assessed for eligibility 227 studies examined TCM interventions for insomnia with TCM pattern diagnosis Chinese herbal medicine (n = 89) Acupuncture (n = 64) Acupuncture and its variants based on meridian acupoints, n = 57 Auricular acupressure, n = 7 Combined and other TCM treatments (n = 74) Chinese herbal medicine plus acupuncture, n = 24 Combination treatment of 2 different forms of acupuncture, n = 40 Other TCM treatments, n = 10 Excluded (n = 2645) Not a case-series study or clinical trial: 643 Not primarily on insomnia: 46 Without TCM patterns: 919 Without statistical information regarding TCM patterns : 603 Specific medical and psychiatric condition: 49 Particular development or life transition period: 4 Specific TCM pattern: 237 Aged below 18 or above 70: 15 Specific gender: 2 Cases <30: 61 Duplicate publication: 46 Non-English, non- Chinese languages: 12 Failure to retrieve: 8 Figure 1: Study selection flowchart. TCM pattern Table 1: The 10 most common TCM patterns diagnosed in patients with insomnia. Chinese name Number of subjects diagnosed with the TCM pattern (%) (total N = 17916) Number of studies that examined the TCM pattern (%) (total N = 227) Deficiency of both the heart and spleen 心脾兩虛 4056 (22.6) 180 (79.3) Hyperactivity of fire due to yin deficiency 陰虛火旺 2926 (16.3) 132 (58.1) Liver-qi stagnation transforming into fire 肝鬱化火 1817 (10.1) 91 (40.0) Heart-kidney noninteraction 心腎不交 1157 (6.5) 60 (26.4) Internal disturbance of phlegm heat 痰熱內擾 904 (5.0) 78 (34.4) Qi deficiency of the heart and gallbladder 心膽氣虛 838 (4.7) 63 (27.8) Liver fire flaming upward 肝火上擾 456 (2.5) 25 (11.0) Heart deficiency with timidity 心虛膽怯 356 (2.0) 31 (13.7) Disharmony between spleen and stomach 脾胃不和 325 (1.8) 19 (8.4) Stomach disharmony 胃腑不和 162 (0.9) 17 (7.5) in patients with deficiency of both the heart and spleen, and the most frequently used TCM treatment principle was to nourish heart and spleen. For hyperactivity of fire due to yin deficiency, Suanzaoren (Semen Z. spinosae), Shengdihuang (Radix Rehmanniae), Yejiaoteng (Caulis P. multiflori), Ejiao (Colla C. asini), Huanglian (Rhizoma Coptidis), Gancao (Radix Glycyrrhizae), Baishao (Radix P. alba), Hehuanpi (Cortex Albizziae), Fuling (Poria), Zhimu (Rhizoma Anemarrhenae), Wuweizi (Fructus S. Chinensis), Fushen (Poria cum Radix Pini), Yuanzhi (Radix Polygalae), and Huangbo (Cortex Phellodendri) were commonly used individual herbs for insomnia and the most frequently used TCM treatment principle was to nourish yin and suppress fire. For liver-qi stagnation transforming into fire, Chaihu (Radix Bupleuri), Zhizi (Fructus Gardeniae), Gancao (Radix Glycyrrhizae), Danggui (Radix A. sinensis), Suanzaoren (Semen Z. spinosae), Baishao (Radix P. alba), Yejiaoteng (Caulis P. multiflori), Longdancao (Radix Gentianae), Yujin (Radix Curcumae), Fuling (Poria), Shengdihuang (Radix Rehmanniae), Hehuanpi (Cortex Albizziae),
5 Evidence-Based Complementary and Alternative Medicine 5 Table 2: The commonly used Chinese herbal medicine for insomnia in subjects diagnosed with different TCM patterns a. Number of studies that examined the TCM pattern Commonly used Chinese herbal formula (N, % of studies that examined the TCM pattern) Number of studies that provided TCM treatment principle Most commonly used treatment principle (N, % of studies that provided TCM treatment principle) Deficiency of both the heart and spleen ( 心脾兩虛 ) Hyperactivity of fire due to yin deficiency ( 陰虛火旺 ) Liver-qi stagnation transforming into fire ( 肝鬱化火 ) Heart-kidney noninteraction ( 心腎不交 ) Internal disturbance of phlegm heat ( 痰熱內擾 ) Qi deficiency of the heart and gallbladder ( 心膽氣虛 ) Heart deficiency with timidity ( 心虛膽怯 ) N = 64 N = 53 N = 43 N = 13 N = 34 N = 20 N = 15 Modified Gui Pi Tang (19, 29.7%) Huang Lian E Jiao Tang (5, 9.4%) Modified Long Dan Xie Gan Tang (6, 14.0%); Dan ZhiXiaoYaoSan (6, 14.0%) No formula was most frequently used Modified Wen Dan Tang (10, 29.4%) Modified An Shen Ding Zhi Wan (7, 35.0%) No formula was most frequently used N = 11 N = 9 N = 8 N = 1 N = 6 N = 5 N = 1 Nourish heart and spleen (5, 45.5%) Nourish yin and suppress fire (5, 55.6%) Soothe liver and purge fire (4, 50.0%) Nourish yin, clear fire, and coordinate heart and kidney (1, 100.0%) Clear heat and resolve phlegm (5, 83.3%) Tonify qi and settle fright (5, 100.0%) Tonify qi and settle fright (1, 100.0%) Number of studies that provided the composition of herbal formula N = 54 N = 43 N = 39 N = 11 N = 29 N = 16 N = 13 Composition of herbal formula (% of studies that provided the formula s composition) b Suanzaoren (Semen Z. spinosae) 75.9% 58.1% 48.7% 45.5% 58.6% 68.8% 69.2% Fuling (Poria) 40.7% 34.9% 33.3% 27.3% 75.9% 62.5% 23.1% Yejiaoteng (Caulis P. multiflori) 33.3% 46.5% 41.0% 41.4% 37.5% 61.5% Gancao (Radix Glycyrrhizae) 27.8% 39.5% 51.3% 44.8% 37.5% 30.8% Baishao (Radix P. alba) 24.1% 39.5% 46.2% 27.3% 20.7% 23.1% Fushen (Poria cum Radix Pini) 33.3% 25.6% 23.1% 50.0% 38.5% Hehuanpi (Cortex Albizziae) 22.2% 34.9% 30.8% 27.6% 46.2% Yuanzhi (Radix Polygalae) 53.7% 23.3% 41.4% 62.5% 38.5% Wuweizi (Fructus S. Chinensis) 24.1% 27.9% 27.3% 38.5% Baiziren (Semen Platycladi) 20.4% 27.3% 23.1% Shengdihuang (Radix 48.8% 30.8% 27.3% Rehmanniae) Danggui (Radix A. sinensis) 63.0% 51.3% Dangshen (Radix Codonopsis) 51.9% 43.8% Baizhu (Rhizoma A. acrocephalae) 38.9% 20.5% Honey-toasted Gancao (Radix Glycyrrhizae) 29.6% 25.0% Dazao (Fructus Jujibae) 24.1% 27.3% Huanglian (Rhizoma Coptidis) 41.9% 51.7% Zhimu (Rhizoma Anemarrhenae) 30.2% 31.3%
6 6 Evidence-Based Complementary and Alternative Medicine Deficiency of both the heart and spleen ( 心脾兩虛 ) Hyperactivity of fire due to yin deficiency ( 陰虛火旺 ) Table 2: Continued. Liver-qi stagnation transforming into fire ( 肝鬱化火 ) Heart-kidney noninteraction ( 心腎不交 ) Internal disturbance of phlegm heat ( 痰熱內擾 ) Qi deficiency of the heart and gallbladder ( 心膽氣虛 ) Heart deficiency with timidity ( 心虛膽怯 ) Chaihu (Radix Bupleuri) 64.1% 23.1% Zhizi (Fructus Gardeniae) 53.8% 27.6% Zexie (Rhizoma Alismatis) 23.1% 27.3% Zhenzhumu (Concha Margaritifera) Shichangpu (Rhizoma A. Tatarinowii) 23.1% 46.2% 56.3% 46.2% Longchi(DensDraconis) 50.0% 30.8% Huangqi (Radix Astragali) 50.0% Ginger(RhizomaZingiberis) 20.4% Longyanrou(ArillusLongan) 31.5% Muxiang (Radix Aucklandiae) 31.5% Huangbo(CortexPhellodendri) 20.9% Ejiao (Colla C asini) 41.9% Longdancao(RadixGentianae) 35.9% Yujin(RadixCurcumae) 33.3% Danpi(CortexMoutan) 23.1% Huangqin(RadixScutellariae) 28.2% Shudihuang (Radix Rehmanniae Praeparata) Dannanxing (Rhizome Arisaematis) Chenpi (Pericarpium C. Reticulatae) Zhuru (Caulis Bambusae in Taeniam) 27.3% 27.6% 44.8% 58.6% Zhishi(FructusA.immaturus) 41.4% Lime-water processed banxia (Rhizoma Pinelliae Preparatum) 44.8% Renshen(RadixGinseng) 25.0% Hupo(Succinum) 37.5% Chuanxiong (Rhizoma Chuanxiong) 25.0% Longgu(FossiliaOssisMastodi) 23.1% a Only those TCM patterns with more than 5 studies are presented. b Individual Chinese herbs used in at least 50% of the studies on a particular TCM pattern are bolded.
7 Evidence-Based Complementary and Alternative Medicine 7 Huangqin (Radix Scutellariae), Fushen (Poria cum Radix Pini), Zexie (Rhizoma Alismatis), Zhenzhumu (Concha Margaritifera), Danpi (Cortex Moutan), and Baizhu (Rhizoma A. macrocephalae) were more often used and the most frequently used TCM treatment principle was to soothe liver and purge fire. There was no single herb being used in more than 50% of the studies on heart-kidney noninteraction, indicating that the selection of Chinese herbs varied greatly among practitioners. Suanzaoren (Semen Z. spinosae), Fuling (Poria), Yejiaoteng (Caulis P. multiflori), Gancao (Radix Glycyrrhizae), and Baishao (Radix P. alba) were the most commonly used individual herbs, but they were also the most nonspecific and were used in most of the TCM patterns. The effective rate of pattern-based Chinese herbal medicine treatment for insomnia was provided in 38 of the 89 studies on Chinese herbal medicine (Table 3). Based on the findings from RCTs, the mean effective rates were similar across TCM patterns, with the highest mean effective rate of 95.0% for liver-qi stagnation transforming into fire and the lowest at 79.4% for heart deficiency with timidity. When the case series were examined, the mean effective rates in liverqi stagnation transforming into fire and heart deficiency with timidity were very similar (79.1% and 77.8%, resp.) TCM Pattern and Acupuncture-Related Treatments. Fifty-seven of the 227 reviewed studies examined acupuncture-related treatments, including traditional needle acupuncture (n = 35), acupressure (n = 12), moxibustion (n = 3), acupoint injection (n = 3), acupoint plaster (n = 3), and acupoint embedment (n = 1). Forty-one (71.9%) of the 57 studies were case series, 4 (7.0%) were controlled studies, and 12 (21.1%) were RCTs. Of the 12 RCTs, 6 (50.0%) compared acupuncture with Western medication, 3 (25.0%) with another acupuncture treatment, 1 (8.3%) with Chinese herbal medicine, 1 (8.3%) with sleep hygiene education, and 1 (8.3%) with sham acupuncture and another acupuncture treatment. Ten (83.3%) of the 12 RCTs were described as randomized but the randomization method, blinding, and dropouts were not presented; hence, these 10 studies had a modified Jadad score of 1. One RCT (8.3%) was described as randomized and included the dropouts; hence, a score of 2 was given. Another RCT (8.3%) described the randomization method, blinding, and dropouts but not evaluator blind; hence, a score of 4 was given. Table 4 presents the acupoints that were commonly used for treating insomnia. There were only 7 studies on auricular acupressure; hence, the use of auricular points in TCM pattern-based treatment of insomnia was not presented. The treatment principles were also not presented because the number of studies with the data was too few, ranging from 0 to 3 in each TCM pattern. The commonly used acupoints in patients with deficiency of both the heart and spleen were Xinshu (BL15), Shenmen (HT7), Sanyinjiao (SP6), Pishu (BL20), Zusanli (ST36), Neiguan (PC6), Baihui (GV20), Yintang (EX-HN3), Anmian (EX-HN22), Sishencong (EX-HN1), Fengchi (GB20), and Zhongwan (CV12). For hyperactivity of fire due to yin deficiency, Shenmen (HT7), Sanyinjiao (SP6), Shenshu (BL23), Taixi (Kl13), Xinshu (BL15), Baihui (GV20), Neiguan (PC6), Zhongwan (CV12), Sishencong (EX-HN1), Qihai (CV6), Yintang (EX- HN3), Anmian (EX-HN22), Fengchi (GB20), Zhaohai (Kl6), and Guanyuan (CV4) were commonly used acupoints. Sanyinjiao (SP6), Taichong (LR3), Shenmen (HT7), Ganshu (BL18), Zhongwan (CV12), Neiguan (PC6), Qihai (CV6), Fengchi (GB20), Guanyuan (CV4), Baihui (GV20), Xiawan (CV10), Shenshu (BL23), and Yintang (EX-HN3) were commonly used acupoints in patients with liver-qi stagnation transforming into fire. The selection of acupoints in other TCM patterns is shown in Table 4. There was no acupoint being used in more than 50% of the studies on liver-qi stagnation transforming into fire and heart-kidney noninteraction, indicating that the selection of acupoints for these 2 TCM patterns varied greatly. Shenmen (HT7), Yintang (EX-HN3), Sanyinjiao (SP6), Baihui (GV20), Anmian (EX-HN22), and Sishencong (EX-HN1) were the most common acupoints for the treatment of insomnia. The effective rate of pattern-based acupuncture-related treatments for insomnia was provided in 24 of the 64 studies on acupuncture-related treatments (Table 3). As there were few RCTs available for comparison, based on the case series findings, the mean effective rates of acupuncture for the different TCM patterns were similar, with the highest mean effective rate of 98.1% for disharmony between spleen and stomach and the lowest at 75.0% for qi deficiency of the heart and gallbladder TCM Pattern and Combined TCM Treatments Chinese Herbal Medicine Plus Acupuncture-Related Therapies. Twenty-four studies examined Chinese herbal medicine plus acupuncture-related treatments for insomnia. Thirteen (54.2%) of the 24 studies were case series, 1 (4.2%) was a controlled study, and 10 (41.7%) were RCTs. Of the 10 RCTs, 5 (50.0%) used Chinese herbal medicine for comparison, 3 (30.0%) used Western medication, and 2 (20.0%) compared with usual care. All 10 RCTs had a modified Jadad score of 1 as they were only described as randomized, but the randomization method, blinding, and dropouts were not presented. We only presented the results of Chinese herbal medicine plus traditional needle acupuncture in deficiency of both the heart and spleen, hyperactivity of fire due to yin deficiency, and liver-qi stagnation transforming into fire, because studies on other TCM patterns and other forms of acupuncture were too few to give reliable information (Table 5). For deficiency of both the heart and spleen, the commonly used herbal ingredients for insomnia were Suanzaoren (Semen Z. spinosae), Baizhu (Rhizoma A. macrocephalae), Danggui (Radix A. sinensis), Huangqi (Radix Astragali), Yuanzhi (Radix Polygalae), Muxiang (Radix Aucklandiae), Fuling (Poria), Longyanrou (Arillus Longan), Hehuanhua (Flos Albiziae), Dazao (Fructus Jujibae), Gancao (Radix Glycyrrhizae), Yejiaoteng (Caulis P. multiflori), Wuweizi (Fructus S. Chinensis), Renshen (Radix Ginseng), Fushen (Poria cum Radix Pini), Honey-toasted Gancao (Radix
8 8 Evidence-Based Complementary and Alternative Medicine Table 3: The mean effective rate of pattern-based TCM treatments for insomnia. TCM pattern Chinese name Chinese herbal medicine Deficiency of both the heart and spleen Hyperactivity of fire due to yin deficiency Liver-qi stagnation transforming into fire 心脾兩虛 9 陰虛火旺 10 肝鬱化火 6 Heart-kidney noninteraction 心腎不交 1 Internal disturbance of phlegm heat Qi deficiency of the heart and gallbladder 痰熱內擾 5 Randomized controlled trials Controlled trials Case series No. of studies No. of studies No. of studies Mean effective rate in % (range, SD, 95% CI) 88.9 ( , 11.4, ) 86.1 ( , 9.8, ) 95.0 ( , 4.7, ) ( , 20.7, ) 心膽氣虛 Mean effectiveratein % (range, SD, 95% CI) 97.6 ( , 4.1, ) 79.2 ( , 25.3, ) 96.7 ( , 4.7, ) 0 4 Liver fire flaming upward 肝火上擾 Heart deficiency with timidity 心虛膽怯 5 Disharmony between spleen and stomach Stomach disharmony 胃腑不和 1 Acupuncture Deficiency of both the heart and spleen Hyperactivity of fire due to yin deficiency Liver-qi stagnation transforming into fire 79.4 ( , 22.0, ) 脾胃不和 心脾兩虛 4 陰虛火旺 4 肝鬱化火 1 Heart-kidney noninteraction 心腎不交 ( , 3.9, ) 81.9 ( , 21.8, ) Mean effective ratein % (range, SD, 95% CI) 86.5 ( , 12.1, ) 88.3 ( , 10.6, ) 79.1 ( , 28.6, ) 86.9 ( , 2.1, ) 86.3 ( , 18.0, ) 75.3 ( , 30.0, ) ( , 17.1, ) 87.7 ( , 10.4, ) 97.6 ( , 1.0, ) ( , 8.7, ) 88.8 ( , 18.3, ) 81.5 ( , 19.8, ) 96.3 ( , 5.6, )
9 Evidence-Based Complementary and Alternative Medicine 9 TCM pattern Chinese name Internal disturbance of phlegm heat Qi deficiency of the heart and gallbladder 痰熱內擾 2 Liver fire flaming upward 肝火上擾 2 Heart deficiency with timidity 心虛膽怯 1 Disharmony between spleen and stomach Stomach disharmony 胃腑不和 2 a Effective rate was the same in the 2 studies. Table 3: Continued. Randomized controlled trials Controlled trials Case series No. of studies No. of studies No. of studies Mean effective rate in % (range, SD, 95% CI) 94.5 ( , 7.8, ) 心膽氣虛 a Mean effectiveratein % (range, SD, 95% CI) ( , 3.3, ) 脾胃不和 a Mean effective ratein % (range, SD, 95% CI) 95.0 ( , 4.7, ) 75.0 ( , 50.0, ) 87.9 ( , 21.0, ) 90.1 ( , 14.1, ) 98.1 ( , 3.2, ) 90.0 ( , 14.1, )
10 10 Evidence-Based Complementary and Alternative Medicine Table 4: The commonly used acupoints for insomnia in subjects diagnosed with different TCM patterns a. Deficiency of both the heart and spleen ( 心脾兩虛 ) Hyperactivity of fire due to yin deficiency ( 陰虛火旺 ) Liver-qi stagnation transforming into fire ( 肝鬱化火 ) Heart-kidney noninteraction ( 心腎不交 ) Internal disturbance of phlegm heat ( 痰熱內擾 ) Qi deficiency of the heart and gallbladder ( 心膽氣虛 ) Liver fire flaming upward ( 肝火上擾 ) Heart deficiency with timidity ( 心虛膽怯 ) Disharmony between spleen and stomach ( 脾胃不和 ) No. of studies N = 47 N = 33 N = 15 N = 21 N = 14 N = 17 N = 9 N = 6 N = 10 Acupoints b Shenmen (HT7) 55.3% 54.5% 40.0% 47.6% 64.3% 47.1% 88.9% 50.0% 40.0% Yintang (EX-HN3) 29.8% 24.2% 20.0% 23.8% 35.7% 23.5% 33.3% 33.3% 30.0% Sanyinjiao (SP6) 53.2% 42.4% 46.7% 42.9% 42.9% 29.4% 44.4% 33.3% 50.0% Baihui (GV20) 34.0% 33.3% 20.0% 35.7% 35.3% 44.4% 33.3% Anmian (EX-HN22) 25.5% 24.2% 23.8% 23.5% 55.6% 33.3% 20.0% Sishencong (EX-HN1) 23.4% 24.2% 28.6% 21.4% 33.3% 33.3% 30.0% Xinshu (BL15) 72.3% 39.4% 42.9% 42.9% 35.3% 83.3% Neiguan (PC6) 34.0% 30.3% 33.3% 57.1% 33.3% 20.0% Zhongwan (CV12) 21.3% 27.3% 33.3% 57.1% 23.5% 20.0% Zusanli (ST36) 44.7% 50.0% 23.5% 22.2% 33.3% 30.0% Fengchi (GB20) 23.4% 24.2% 26.7% 50.0% 44.4% 33.3% Qihai (CV6) 24.2% 33.3% 42.9% 23.5% 20.0% Shenshu (BL23) 45.5% 20.0% 38.1% 21.4% Guanyuan (CV4) 21.2% 26.7% 42.9% Ganshu (BL18) 40.0% 21.4% 33.3% Pishu (BL20) 51.1% 28.6% Danshu (BL19) 35.3% 83.3% Weishu (BL21) 21.4% 30.0% Taixi (Kl13) 42.4% 42.9% Zhaohai (KI6) 21.2% 11.1% Xiawan (CV10) 20.0% 21.4% Shenmai (BL62) 21.4% 11.1% Cuanzhu (BL2) 21.4% 33.3% Taichong (LR3) 40.0% 100.0% Fenglong (ST40) 57.1% Qingming (BL1) 21.4% Xingjian (LR2) 66.7% Hegu (Ll4) 22.2% Xuehai (SP10) 22.2% Yanglingquan (GB34) 33.3% Yuyao (EX-HN4) 33.3% Sibai (ST2) 33.3% Daling(PC7) 33.3% Jianjing (GB21) 33.3% Tianshu (ST25) 20.0% a Studies on stomach disharmony are too few to give reliable information. b Acupoints that were used in at least 50% of the studies on a particular TCM pattern are bolded.
11 Evidence-Based Complementary and Alternative Medicine 11 Glycyrrhizae), Chuanxiong (Rhizoma Chuanxiong), Ginger (Rhizoma Z. recens), Baiziren (Semen Platycladi), Dangshen (Radix Codonopsis), Chaihu (Radix Bupleuri) in combination with acupuncture at Shenmen (HT7), Sanyinjiao (SP6), Xinshu (BL15), Pishu (BL20), Neiguan (PC6), Zusanli (ST36), Sishencong (EX-HN1), and Baihui (GV20). The selection of herbs and acupoints combination and TCM treatment principles in other TCM patterns is shown in Table 5. Danggui (Radix A. sinensis), Chaihu (Radix Bupleuri), and Gancao (Radix Glycyrrhizae) and Shenmen (HT7), Sanyinjiao (SP6), Neiguan (PC6), Zusanli (ST36), Sishencong (EX-HN1), and Baihui (GV20) were the common Chinese herbs and acupoints, respectively, in the combined Chinese herbal medicine and traditional needle acupuncture treatment for insomnia in deficiency of both the heart and spleen, hyperactivity of fire due to yin deficiency, and liver-qi stagnation transforming into fire Combination of Acupuncture Treatments. Forty studies examined the combination of 2 different acupuncture modalities for the treatment of insomnia. The TCM treatment principles were not presented due to the small number of studies with relevant information. Twenty-nine (72.5%) of the 40 studies were case series, 1 (2.5%) was a controlled study, and 10 (25.0%) were RCTs. Of the 10 RCTs, 5 (50.0%) used another acupuncture treatment for comparison, 4 (40.0%) used Western medication, and 1 (10.0%) used Chinese herbal medicine. Nine (90.0%) of the RCTs had a modified Jadad score of 1, and the other RCT (10.0%) presented the appropriate randomization method; hence, a score of 2 was given. Only the studies that examined traditional needle acupuncture plus auricular acupressure are presented, because studies on other combinations are too few to give reliable information (Table 6). For deficiency of both the heart and spleen, the commonly used acupoints were Baihui (GV20), Sanyinjiao (SP6), Shenmen (HT7), Sishencong (EX-HN1), Neiguan (PC6), Xinshu (BL15), Zusanli (ST36), Pishu (BL20), Anmian (EX-HN22), Fengchi (GB20); while the commonly used auricular points were shenmen, subcortex, heart, spleen, sympathesis, kidney, brain, endocrine, neurasthenia point, stomach, liver, and occiput. The selection of acupoints and auricular points for other TCM patterns is shown in Table 6. Sanyinjiao (SP6), Baihui (GV20), Shenmen (HT7), Sishencong (EX-HN1), and Neiguan (PC6) and shenmen, subcortex, heart, kidney, sympathesis, spleen, and liver were the commonly used acupoints and auricular points, respectively, in the combined traditional needle acupuncture and auricular acupressure for insomnia. 4. Discussion This study is the first systematic review of English and Chinese literature, involving 227 studies and subjects on the classification and treatment of insomnia using the TCM diagnostic system. We found that the TCM pattern diagnoses for insomnia were diverse, with a total of 87 different TCM patterns identified. Deficiency of both the heart and spleen was the most commonly used TCM pattern in subjects with insomnia, followed by hyperactivityoffiredueto yin deficiency, liver-qi stagnation transforming into fire, heartkidney noninteraction, internal disturbance of phlegm-heat, qi deficiency of the heart and gallbladder, liver fire flaming upward, stomach disharmony, heart deficiency with timidity, and disharmony between spleen and stomach. Pattern-based TCM treatment was more common in deficiency of both the heart and spleen, internal disturbance of phlegm heat, andqi deficiency of the heart and gallbladder, but limited to the use of Chinese herbal medicine formula. Gui Pi Tang was the most frequently used herbal formula in Deficiency of both the heart and spleen; forinternal disturbance of phlegm heat and qi deficiency of the heart and gallbladder, it was Wen Dan Tang andanshendingzhiwan,respectively.forothertcm patterns, no single formula could be regarded as commonly used across TCM practitioners. We could not identify certain combinations of herbal agents or acupoints being used for particular TCM patterns. Suanzaoren (Semen Z. spinosae), Fuling (Poria), Yejiaoteng (Caulis P. multiflori), Gancao (Radix Glycyrrhizae), and Baishao (Radix P. alba) and Shenmen (HT7), Yintang (EX- HN3), Sanyinjiao (SP6), Baihui (GV20), Anmian (EX- HN22), and Sishencong (EX-HN1) were the commonly used Chinese herbs and acupoints, respectively, and they were being used nonspecifically for treating insomnia in many different TCM patterns. Treatment principles underlying the selection of herbal combinations were seldomy reported and it was more obvious with pattern-based acupuncture studies. One explanation for the variability in pattern-based TCM treatment may be the variability in treatment principle. It is important that treatment principles should be included in future pattern-based TCM treatment studies. Further research on the link between TCM pattern, treatment principle, and treatment is warranted. The effective rates of TCM treatments were quite similar across different TCM patterns. However, the effective rate summarized in this paper was based on case-series and clinical trials with inadequate study quality. Further studies with better methodological design should be performed to compare the efficacy of TCM treatment in different TCM patterns. The present paper found that some Chinese herbs, such as Suanzaoren (Semen Z. spinosae), Fuling (Poria), Yejiaoteng (Caulis P. multiflori), Gancao (Radix Glycyrrhizae), and Baishao (Radix P. alba) were frequently used to treat insomnia regardless of the TCM pattern. In TCM theory, a standard Chinese herbal formula is consisted of Sovereign, Minister, Assistant, and Courier herbs. The Sovereign is used for treating the principal diseases; the Minister has synergistic effects with Sovereign herbs and helps to alleviate other accompanying symptoms; the Assistant is for enhancing the therapeutic effects and modulating the adverse effects of Sovereign and Minister herbs; while the Courier is used for harmonizing the actions of the others [23]. Suanzaoren (Semen Z. spinosae) and Yejiaoteng (Caulis P. multiflori) are classified as Anshen (mind tranquilizing) herbs and can act as Sovereign or Minister herbs in the treatment of insomnia. Fuling (Poria),
12 12 Evidence-Based Complementary and Alternative Medicine Table 5: The commonly used Chinese herbal medicine and acupoints in the combined Chinese herbal medicine and traditional needle acupuncture treatment for insomnia in subjects diagnosed with different TCM patterns a. Deficiency of both the heart and spleen ( 心脾兩虛 ) Hyperactivity of fire due to yin deficiency ( 陰虛火旺 ) Liver-qi stagnation transforming into fire ( 肝鬱化火 ) No. of studies that examined the TCM pattern N = 12 N = 6 N = 7 No. of studies that provided TCM treatment principle N = 5 N = 4 N = 3 Most frequently used TCM treatment principle (N, % of studies that provided TCM treatment principle) Nourish heart and spleen (3, 60.0%) Nourish yin and suppress fire (4, 100.0%) Soothe liver and purge fire (2, 66.7%) Individual Chinese herbs b Danggui (Radix A. sinensis) 75.0% 33.3% 71.4% Chaihu (Radix Bupleuri) 25.0% 33.3% 85.7% Gancao (Radix Glycyrrhizae) 41.7% 33.3% 42.9% Suanzaoren (Semen Z. spinosae) 100.0% 83.3% Huangqin (Radix Scutellariae) 66.7% 85.7% Baishao (Radix P. alba) 66.7% 28.6% Fushen (Poria cum Radix Pini) 33.3% 28.6% Shengdihuang (Radix Rehmanniae) 33.3% 57.1% Yejiaoteng (Caulis P. multiflori) 41.7% 50.0% Fuling (Poria) 50.0% 33.3% Hehuanhua (Flos Albiziae) 50.0% 33.3% Honey-toasted Gancao (Radix Glycyrrhizae) 33.3% 33.3% Baizhu (Rhizoma A. macrocephalae) 83.3% Huangqi (Radix Astragali) 75.0% Yuanzhi (Radix Polygalae) 66.7% Muxiang (Radix Aucklandiae) 58.3% Longyanrou (Arillus Longan) 50.0% Dazao (Fructus Jujibae) 41.7% Renshen (Radix Ginseng) 33.3% Wuweizi (Fructus S. Chinensis) 33.3% Baiziren (Semen Platycladi) 25.0% Chuanxiong (Rhizoma Chuanxiong ) 25.0% Dangshen (Radix Codonopsis) 25.0% Ginger (Rhizoma Z. recens) 25.0% Huanglian (Rhizoma Coptidis) 83.3% Egg yolk (Vitellus Galli) 50.0% Ejiao (Colla C. asini) 50.0% Zhizi (Fructus Gardeniae) 100.0% Cheqianzi (Semen Plantaginis) 71.4% Longgu (Fossilia Ossis Mastodi) 71.4% Muli (Concha Ostreae) 71.4% Longdancao (Radix Gentianae) 57.1% Mutong (Caulis C. armandii) 57.1% Zexie (Rhizoma Alismatis) 57.1% Hehuanpi (Cortex Albizziae) 42.9% Yujin (Radix Curcumae) 42.9% Danpi (Cortex Moutan) 28.6%
13 Evidence-Based Complementary and Alternative Medicine 13 Acupoints b Table 5: Continued. Deficiency of both the heart and spleen ( 心脾兩虛 ) Hyperactivity of fire due to yin deficiency ( 陰虛火旺 ) Liver-qi stagnation transforming into fire ( 肝鬱化火 ) Shenmen (HT7) 100.0% 100.0% 100.0% Sanyinjiao (SP6) 83.3% 50.0% 71.4% Neiguan (PC6) 58.3% 50.0% 57.1% Sishencong (EX-HN1) 41.7% 33.3% 71.4% Baihui (GV20) 33.3% 50.0% 42.9% Zusanli (ST36) 58.3% 33.3% 28.6% Taichong (LR3) 66.7% 71.4% Hegu (Ll4) 33.3% 57.1% Xinshu (BL15) 75.0% Pishu (BL20) 66.7% Taixi (Kl13) 66.7% Daling (PC7) 50.0% Shenshu (BL23) 33.3% Taiyuan (LU9) 33.3% Zhaohai (Kl6) 33.3% Anmian (EX-HN22) 28.6% Fengchi (GB20) 28.6% Ganshu (BL18) 28.6% Houxi (SI3) 28.6% Shenmai (BL62) 28.6% a Other TCM patterns are not listed because studies are too few to give reliable information. b Individual Chinese herbs and acupoints used in at least 50% of the studies on a particular TCM pattern are bolded. Gancao (Radix Glycyrrhizae), and Baishao (Radix P. alba) have no specific tranquilizing effect in TCM and can be regarded as Assistant or Courier herbs in the herbal formulae commonly used for insomnia. The pharmacological basis for the different roles of the herbal agents in the treatment of insomnia remains to be determined. We also observed that a few herbs were specifically used for particular TCM patterns; for instance, Huangbo (Cortex Phellodendri), an Qingre (clear heat) agent, was exclusively used in hyperactivity of fire due to yin deficiency; Zhuru (Caulis Bambusae in Taeniam) and Dannanxing (Rhizome Arisaematis), which are classified as Huatan (resolve phlegm) herbs, were only used in internal disturbance of phlegm heat. As these herbs have no anxiolytic or sedative properties, we believe that the primary function of these herbs is not to directly treat insomnia but to alleviate the underlying causes of body imbalance. For acupuncture-related therapies, we identified some acupoints, including Shenmen (HT7), Yintang (EX-HN3), Sanyinjiao (SP6), Baihui (GV20), Anmian (EX-HN22), and Sishencong (EX-HN1), which were generally used for insomnia regardless of the TCM pattern. All these commonly used acupoints are historically used for treating insomnia [24]. Similar to Chinese herbal medicine, we observed that a few acupoints were specifically used for particular TCM patterns; for example, Fenglong (ST40), based on the TCM theory, is used to remove phlegm and was exclusively used in internal disturbance of phlegm heat; Xingjian (LR2), which has the function of draining liver fire, was only used in liver fire flaming upward. We are unsure whether the few herbal agents and acupoints are essential for the treatment of insomnia in the particular TCM patterns. Further studies are needed to clarify the value of individual herbs and specific acupoints in pattern-based TCM treatments for insomnia. When traditional needle acupuncture treatment was combined with Chinese herbal medicine, Shenmen (HT7) was the most commonly used acupoint for the treatment of insomnia, but when traditional needle acupuncture was combined with auricular acupressure, Baihui (GV20) was more often used. Since there is an auricular point also called Shenmen which has a similar function to acupoint Shenmen (HT7) on the wrist, this may explain why Shenmen (HT7) was less frequently used when combined with auricular acupressure. Our finding suggested that the acupoint selection in traditional needle acupuncture might vary when it was combined with different TCM treatments. The key shortcoming of incorporating TCM pattern diagnosis is that there is no standardization in terminology, and the diagnostic process is highly subjective. Considerable variability in TCM diagnosis has been found across practitioners in previous studies of menopausal
14 14 Evidence-Based Complementary and Alternative Medicine Table 6: The most commonly used acupoints and auricular points in the combined traditional needle acupuncture and auricular acupressure treatment for insomnia in subjects diagnosed with different TCM patterns a. Deficiency of both the heart and spleen ( 心脾兩虛 ) Hyperactivity of fire due to yin deficiency ( 陰虛火旺 ) Liver-qi stagnation transforming into fire ( 肝鬱化火 ) Heart-kidney noninteraction ( 心腎不交 ) Qi deficiency of the heart and gallbladder ( 心膽氣虛 ) No. of studies that examined the TCM pattern N = 15 N = 8 N = 6 N = 8 N = 6 Acupoints b Sanyinjiao (SP6) 66.7% 50.0% 83.3% 62.5% 66.7% Baihui (GV20) 66.7% 75.0% 83.3% 62.5% 50.0% Shenmen (HT7) 66.7% 62.5% 33.3% 75.0% 66.7% Sishencong (EX-HN1) 53.3% 62.5% 66.7% 25.0% 50.0% Neiguan (PC6) 46.7% 37.5% 50.0% 50.0% 33.3% Anmian (EX-HN22) 33.3% 37.5% 37.5% 33.3% Zusanli (ST36) 40.0% 25.0% 33.3% Taixi (Kl13) 75.0% 62.5% 33.3% Taichong (LR3) 25.0% 83.3% Xinshu (BL15) 46.7% 75.0% Fengchi (GB20) 20.0% 25.0% Shenshu (BL23) 25.0% 50.0% Pishu (BL20) 40.0% Benshen (GB13) 25.0% Shenting (GV24) 25.0% Yintang (EX-HN3) 37.5% Ganshu (BL18) 33.3% Dazhui (GVl4) 25.0% Shenmai (BL62) 25.0% Zhaohai (Kl6) 25.0% Danshu(BLl9) 33.3% Auricular points b Shenmen 100.0% 100.0% 100.0% 100.0% 100.0% Subcortex 80.0% 100.0% 83.3% 50.0% 100.0% Heart 73.3% 62.5% 50.0% 62.5% 83.3% Kidney 46.7% 50.0% 33.3% 75.0% 66.7% Sympathesis 46.7% 62.5% 66.7% 25.0% 50.0% Spleen 66.7% 25.0% 33.3% 37.5% 50.0% Liver 26.7% 37.5% 66.7% 25.0% 66.7% Endocrine 26.7% 62.5% 50.0% 50.0% Brain 40.0% 25.0% 50.0% 33.3% Occiput 20.0% 25.0% 33.3% 25.0% Neurasthenia point 26.7% 37.5% 33.3% Stomach 26.7% Gallbladder 33.3% a Other TCM patterns are not listed because studies are too few to give reliable information. b Acupoints and auricular points used in at least 50% of the studies on a particular TCM pattern are bolded. syndrome, irritable bowel syndrome, rheumatoid arthritis, and low-back pain [25 28]. To further examine patternbased TCM therapies, a standardized and reliable TCM pattern differentiation procedure should be explored. We have recently developed a standardized symptom checklist for TCM pattern differentiation in patients with insomnia [29]. The diagnostic tool, consisting of 13 sleep-related, 61 nonsleep-related, 11 tongue, and 7 pulse items, can be further validated for TCM diagnostic purpose. In addition, more than two-third of the reviewed studies did not report
15 Evidence-Based Complementary and Alternative Medicine 15 the criteria used for pattern diagnosis. This variability in the sets of rules for diagnosis is also a major reason for the disagreement between practitioners. There are strengths as well as methodologic limitations of the study. Our data was generated from a systematic review of more than 200 articles involving almost subjects, which provided less biased results than those derived from TCM experts. The breadth of this paper would inevitably result in some uncertainties regarding the quality of data and accuracy of the TCM diagnosis. We included studies of different design, ranging from case series to RCTs; therefore, the comparison of efficacy of TCM treatments across TCM patterns should be treated with caution. In addition, most of the reviewed studies did not mention the TCM diagnostic procedure and diagnostic criteria used; hence, the quality of the diagnostic process was uncertain. Although a large number of studies were reviewed, information regarding the use of individual Chinese herbs and acupoints in some TCM patterns was still limited. Despite the limitations, the present study, for the first time, systematically and comprehensively summarized important data on pattern-based TCM treatments for insomnia. Since TCM pattern differentiation is an essential component of TCM treatment, our data should be useful for both clinical practice and research of TCM. More high quality studies incorporating TCM pattern differentiation and treatment principle are needed to examine the efficacy of TCM treatments and the additional benefit of pattern differentiation. Conflict of Interests No competing financial interests exist. Acknowledgment The present study was supported by the Hospital Authority of Hong Kong. References [1] M. M. Ohayon, Epidemiology of insomnia: what we know and what we still need to learn, Sleep Medicine Reviews, vol. 6, no. 2, pp , [2] D. J. Taylor, K. L. Lichstein, and H. H. Durrence, Insomnia as a health risk factor, Behavioral Sleep Medicine, vol. 1, no. 4, pp , [3] National Institutes of Health, National Institutes of Health State of the Science Conference statement on manifestations and management of chronic insomnia in adults, June 13 15, 2005, Sleep, vol. 28, no. 9, pp , [4] C. M. Morin, R. R. Bootzin, D. J. Buysse, J. D. Edinger, C. A. Espie, and K. L. Lichstein, Psychological and behavioral treatment of insomnia: update of the recent evidence ( ), Sleep, vol. 29, no. 11, pp , [5] N. J. Pearson, L. L. Johnson, and R. L. Nahin, Insomnia, trouble sleeping, and complementary and alternative medicine: analysis of the 2002 National Health Interview Survey data, Archives of Internal Medicine, vol. 166, no. 16, pp , [6] D. H. Tian, Spiritual Axis, People s Health Publishing House, Beijing, China, [7] B. Wang, The Yellow Emperor s Classic of Internal Medicine Simple Questions, People s Health Publishing House, Beijing, China, [8] World Health Organization, WHO International Standard Terminologies on Traditional Medicine in the Western Pacific Region, World Health Organization, Western Pacific Region, [9] W. Yang, F. Meng, and Y. Jiang, Diagnostics of Traditional Chinese Medicine, Academy Press, Beijing, China, [10] A. Bensoussan, N. J. Talley, M. Hing, R. Menzies, A. Guo, and M. Ngu, Treatment of irritable bowel syndrome with Chinese herbal medicine: a randomized controlled trial, Journal of the American Medical Association, vol. 280, no. 18, pp , [11] Q. L. Zha, Y. T. He, and J. P. Yu, Correlations between diagnostic information and therapeutic efficacy in rheumatoid arthritis analyzed with decision tree model, Chinese Journal of Integrated Traditional and Western Medicine, vol. 26, no. 10, pp , [12] A. T. Lathia, S. M. Jung, and L. X. Chen, Efficacy of acupuncture as a treatment for chronic shoulder pain, The Journal of Alternative and Complement Medicine, vol. 15, no. 6, pp , [13] D. C. Cherkin, K. J. Sherman, A. L. Avins et al., A randomized trial comparing acupuncture, simulated acupuncture, and usual care for chronic low back pain, Archives of Internal Medicine, vol. 169, no. 9, pp , [14] E. A. Macklin, P. M. Wayne, L. A. Kalish et al., Stop Hypertension with the Acupuncture Research Program (SHARP): results of a randomized, controlled clinical trial, Hypertension, vol. 48, no. 5, pp , [15] L. C. Chen, I. C. Chen, B. R. Wang, and C. H. Shao, Druguse pattern of Chinese herbal medicines in insomnia: a 4- year survey in Taiwan, Journal of Clinical Pharmacy and Therapeutics, vol. 34, no. 5, pp , [16] W. F. Yeung, K. F. Chung, Y. K. Leung, S. P. Zhang, and A. C. K. Law, Traditional needle acupuncture treatment for insomnia: a systematic review of randomized controlled trials, Sleep Medicine, vol. 10, no. 7, pp , [17] W. F. Yeung, K. F. Chung, M. K. Poon et al., Chinese herbal medicine for insomnia: a systematic review of randomized controlled trials, Sleep Medicine Reviews, vol. 16, no. 6, pp , [18] B. Peng and J. Xie, Traditional Chinese Internal Medicine, People s Medical Publishing House, Beijing, China, 2nd edition, [19] A. R. Jadad, R. A. Moore, D. Carroll et al., Assessing the quality of reports of randomized clinical trials: is blinding necessary? Controlled Clinical Trials, vol. 17, no. 1, pp. 1 12, [20] A. R. White and E. Ernst, A systematic review of randomized controlled trials of acupuncture for neck pain, Rheumatology, vol. 38, no. 2, pp , [21] Ministry of Health of the People s Republic of China, Clinical Research Guidelines of New Chinese Herbal Medicine, Ministry of Health of China, Beijing, China, [22] State Administration of Traditional Chinese Medicine of the People s Republic of China, Criteria of Diagnosis and Therapeutic Effect of Diseases and Syndromes in Traditional Chinese Medicine, Nanjing University, Nanjing, China, [23] K. Chan, Progress in traditional Chinese medicine, Trends in Pharmacological Sciences, vol. 16, no. 6, pp , 1995.
16 16 Evidence-Based Complementary and Alternative Medicine [24] A. Ellis, N. Wiseman, and K. Boss, Fundamentals of Chinese Acupuncture, Paradigm Publications, Brookline, Mass, USA, [25] J. J. Y. Sung, W. K. Leung, J. Y. L. Ching et al., Agreements among traditional Chinese medicine practitioners in the diagnosis and treatment of irritable bowel syndrome, Alimentary Pharmacology and Therapeutics, vol. 20, no. 10, pp , [26] C. J. Hogeboom, K. J. Sherman, and D. C. Cherkin, Variation in diagnosis and treatment of chronic low back pain by traditional Chinese medicine acupuncturists, Complementary Therapies in Medicine, vol. 9, no. 3, pp , [27]B.Zell,J.Hirata,A.Marcus,B.Ettinger,A.Pressman,and K. M. Ettinger, Diagnosis of symptomatic postmenopausal women by traditional Chinese medicine practitioners, Menopause, vol. 7, no. 2, pp , [28] G. G. Zhang, B. Bausell, L. Lao, W. L. Lee, B. Handwerger, and B. Berman, The variability of TCM pattern diagnosis and herbal prescription on rheumatoid arthritis patients, Alternative Therapies in Health and Medicine, vol.10,no.1, pp , [29] M.K. Poon, K.F. Chung, W.F. Yeung, H.K. Yau, and S.P. Zhang, Classification of insomnia using the traditional Chinese medicine system: a systematic review, Evidence-Based Complementary and Alternative Medicine, vol. 2012, Article ID , 9 pages, 2012.
17 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Journal of Diabetes Research International Journal of Journal of Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Journal of Obesity Journal of Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Journal of Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Post-Stroke Depression Relief With Acupuncture
 Post-Stroke Depression Relief With Acupuncture Published by HealthCMi on August 2017 Acupuncture is more effective than the antidepressant paroxetine for the treatment of depression following a stroke.
Post-Stroke Depression Relief With Acupuncture Published by HealthCMi on August 2017 Acupuncture is more effective than the antidepressant paroxetine for the treatment of depression following a stroke.
Acupuncture and Herbs Eliminate Meniere s Disease
 Acupuncture and Herbs Eliminate Meniere s Disease Published by HealthCMi on June 2018 Acupuncture has been proven clinically effective for the treatment of Meniere s disease, a disorder characterized by
Acupuncture and Herbs Eliminate Meniere s Disease Published by HealthCMi on June 2018 Acupuncture has been proven clinically effective for the treatment of Meniere s disease, a disorder characterized by
Chronic Fatigue Recovery With Acupuncture
 Chronic Fatigue Recovery With Acupuncture Published by HealthCMi on August 2017 Shenzhen Hospital of Chinese Medicine researchers determined that acupuncture is safe and effective for the alleviation of
Chronic Fatigue Recovery With Acupuncture Published by HealthCMi on August 2017 Shenzhen Hospital of Chinese Medicine researchers determined that acupuncture is safe and effective for the alleviation of
Acupuncture Heals Erectile Dysfunction Finding
 Acupuncture Heals Erectile Dysfunction Finding Published by HealthCMI on 02 May 2018. erectile dysfunction. Acupuncture and herbs are effective for the treatment of erectile dysfunction. In research conducted
Acupuncture Heals Erectile Dysfunction Finding Published by HealthCMI on 02 May 2018. erectile dysfunction. Acupuncture and herbs are effective for the treatment of erectile dysfunction. In research conducted
Acupuncture Premature Ovarian Failure Finding
 Acupuncture Premature Ovarian Failure Finding Published by HealthCMi on October 2017 Controlled studies find acupuncture effective for the treatment of premature ovarian failure (primary ovarian insufficiency).
Acupuncture Premature Ovarian Failure Finding Published by HealthCMi on October 2017 Controlled studies find acupuncture effective for the treatment of premature ovarian failure (primary ovarian insufficiency).
Acupuncture Today, July, 2010.
 The Herbalist Corner Acupuncture Today, July, 2010. BROADENING STRATEGIES IN THE TREATMENT OF INSOMNIA Jake Paul Fratkin, OMD, L.Ac. Successful treatment of insomnia can be an elusive goal, especially
The Herbalist Corner Acupuncture Today, July, 2010. BROADENING STRATEGIES IN THE TREATMENT OF INSOMNIA Jake Paul Fratkin, OMD, L.Ac. Successful treatment of insomnia can be an elusive goal, especially
Acupuncture and Drugs Found Equally Effective For Mild Depression
 Acupuncture and Drugs Found Equally Effective For Mild Depression Published by HealthCMi on 25 May 2018 Guangdong Province Traditional Chinese Medicine Hospital researchers find acupuncture with moxibustion
Acupuncture and Drugs Found Equally Effective For Mild Depression Published by HealthCMi on 25 May 2018 Guangdong Province Traditional Chinese Medicine Hospital researchers find acupuncture with moxibustion
Acupuncture And Herbs Proven Effective For PID Treatment
 Acupuncture And Herbs Proven Effective For PID Treatment Published by HealthCMi on 29 May 2018 Researchers find acupuncture combined with herbal medicine effective for the treatment of chronic pelvic inflammatory
Acupuncture And Herbs Proven Effective For PID Treatment Published by HealthCMi on 29 May 2018 Researchers find acupuncture combined with herbal medicine effective for the treatment of chronic pelvic inflammatory
TOWARDS A SPIRIT AT PEACE Understanding the treatment of shen disorders with chinese medicine
 TOWARDS A SPIRIT AT PEACE Understanding the treatment of shen disorders with chinese medicine TCM 11 1/6 PART 5 Acupuncture Treatment Protocols Acupuncture for Shen Disorders The effective points described
TOWARDS A SPIRIT AT PEACE Understanding the treatment of shen disorders with chinese medicine TCM 11 1/6 PART 5 Acupuncture Treatment Protocols Acupuncture for Shen Disorders The effective points described
Acupuncture Outmatches Drug For IBS
 Acupuncture Outmatches Drug For IBS Published by HealthCMi on December 2017 Acupuncture and Chinese herbal medicine are found effective for the alleviation of IBS (irritable bowel syndrome). Two independent
Acupuncture Outmatches Drug For IBS Published by HealthCMi on December 2017 Acupuncture and Chinese herbal medicine are found effective for the alleviation of IBS (irritable bowel syndrome). Two independent
The Herbalist s Corner
 Acupuncture Today, July 2008 The Herbalist s Corner Jake Paul Fratkin, OMD. L.Ac. MANAGING A PATIENT WITH MULTIPLE COMPLAINTS A situation common to American herbalist/acupuncturists is the arrival of a
Acupuncture Today, July 2008 The Herbalist s Corner Jake Paul Fratkin, OMD. L.Ac. MANAGING A PATIENT WITH MULTIPLE COMPLAINTS A situation common to American herbalist/acupuncturists is the arrival of a
Acupuncture Found Effective For IBS-D
 Acupuncture Found Effective For IBS-D Published by HealthCMI on 26 February 2018. Investigators find acupuncture effective for the treatment of IBS (irritable bowel syndrome). In a controlled study, Yiwu
Acupuncture Found Effective For IBS-D Published by HealthCMI on 26 February 2018. Investigators find acupuncture effective for the treatment of IBS (irritable bowel syndrome). In a controlled study, Yiwu
Hypertension Regulated By Acupuncture Finding
 Hypertension Regulated By Acupuncture Finding Published by HealthCMi on November 2017 Heilongjiang Woniutuzhen Hospital researchers find acupuncture effective for the treatment of essential hypertension.
Hypertension Regulated By Acupuncture Finding Published by HealthCMi on November 2017 Heilongjiang Woniutuzhen Hospital researchers find acupuncture effective for the treatment of essential hypertension.
Evidence-based Traditional Chinese Medicine Therapies for Dysmenorrhea
 Evidence-based Traditional Chinese Medicine Therapies for Dysmenorrhea Ju-Tzu Li M.D. (Taiwan), MSAOM Dysmenorrhea, painful menstruation, is a common women s disorder. This is also one of the common causes
Evidence-based Traditional Chinese Medicine Therapies for Dysmenorrhea Ju-Tzu Li M.D. (Taiwan), MSAOM Dysmenorrhea, painful menstruation, is a common women s disorder. This is also one of the common causes
TOWARDS A SPIRIT AT PEACE Understanding the treatment of shen disorders with chinese medicine
 TOWARDS A SPIRIT AT PEACE Understanding the treatment of shen disorders with chinese medicine TCM 10 1/7 PART 4 Acupuncture Points Acupuncture Points for Treatment of Shen Disorders Practitioners of acupuncture
TOWARDS A SPIRIT AT PEACE Understanding the treatment of shen disorders with chinese medicine TCM 10 1/7 PART 4 Acupuncture Points Acupuncture Points for Treatment of Shen Disorders Practitioners of acupuncture
Chapter 8 Depression. Etiology and Pathology
 Chapter 8 Depression Depression is a condition brought about by pent-up passions and impeded Qi movement. In addition to the pent-up emotions, it manifests mainly as emotional lability, chest fullness
Chapter 8 Depression Depression is a condition brought about by pent-up passions and impeded Qi movement. In addition to the pent-up emotions, it manifests mainly as emotional lability, chest fullness
Thirty-two Cases of Vascular Headache Treated by Acupuncture Combined with Chinese Herbal Decoction
 Journal of Traditional Chinese Medicine, December 2009, Vol. 29, No. 4 253 Thirty-two Cases of Vascular Headache Treated by Acupuncture Combined with Chinese Herbal Decoction HE Qing-yong 1, LIANG Jun
Journal of Traditional Chinese Medicine, December 2009, Vol. 29, No. 4 253 Thirty-two Cases of Vascular Headache Treated by Acupuncture Combined with Chinese Herbal Decoction HE Qing-yong 1, LIANG Jun
Professor Huang Huang
 Clinical Application of Jing Fang (Classical Formulas) A seminar with Professor Huang Huang Nanjing University of Chinese Medicine February 2014 Sydney Melbourne Proudly brought to you by CHINA BOOKS EDUCATION
Clinical Application of Jing Fang (Classical Formulas) A seminar with Professor Huang Huang Nanjing University of Chinese Medicine February 2014 Sydney Melbourne Proudly brought to you by CHINA BOOKS EDUCATION
ACUPUNCTURE TREATMENT FOR INSOMNIA: A LITERATURE REVIEW JOTIKA HUY TRUONG
 SOUTH BAYLO UNIVERSITY ACUPUNCTURE TREATMENT FOR INSOMNIA: A LITERATURE REVIEW by JOTIKA HUY TRUONG A RESEARCH PROJECT SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE Doctor of Acupuncture
SOUTH BAYLO UNIVERSITY ACUPUNCTURE TREATMENT FOR INSOMNIA: A LITERATURE REVIEW by JOTIKA HUY TRUONG A RESEARCH PROJECT SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE Doctor of Acupuncture
Acupuncture Found Effective for Chronic Fatigue Syndrome
 Acupuncture Found Effective for Chronic Fatigue Syndrome Published by HealthCMi on 07 June 2018 Acupuncture is effective for the treatment of chronic fatigue syndrome (CFS). Researchers at the Beijing
Acupuncture Found Effective for Chronic Fatigue Syndrome Published by HealthCMi on 07 June 2018 Acupuncture is effective for the treatment of chronic fatigue syndrome (CFS). Researchers at the Beijing
POST GRADUATE DIPLOMA IN ACUPUNCTURE (PGDACP) PGDACP-03 : TREATMENT OF COMMON DISEASES/ EAR & SCALP ACUPUNCTURE
 No. of Printed Pages : 11 PGDACP - 03 POST GRADUATE DIPLOMA IN ACUPUNCTURE (PGDACP) 00732 Term-End Examination December, 2010 PGDACP-03 : TREATMENT OF COMMON DISEASES/ EAR & SCALP ACUPUNCTURE Time : 2
No. of Printed Pages : 11 PGDACP - 03 POST GRADUATE DIPLOMA IN ACUPUNCTURE (PGDACP) 00732 Term-End Examination December, 2010 PGDACP-03 : TREATMENT OF COMMON DISEASES/ EAR & SCALP ACUPUNCTURE Time : 2
Clinical treatment of depressive patients with Anshendingzhi decoction
 Online Submissions: http://www.journaltcm.com J Tradit Chin Med 2014 December 15; 34(6): 652-656 info@journaltcm.com ISSN 0255-2922 2014 JTCM. All rights reserved. CLINICAL STUDY TOPIC Clinical treatment
Online Submissions: http://www.journaltcm.com J Tradit Chin Med 2014 December 15; 34(6): 652-656 info@journaltcm.com ISSN 0255-2922 2014 JTCM. All rights reserved. CLINICAL STUDY TOPIC Clinical treatment
Our ongoing interest in spirit
 Soothing the Troubled Spirit with Blue Poppy Originals Formulas with Honora Lee Wolfe Our ongoing interest in spirit Western practitioners of Chinese medicine have always had more interest in diseases
Soothing the Troubled Spirit with Blue Poppy Originals Formulas with Honora Lee Wolfe Our ongoing interest in spirit Western practitioners of Chinese medicine have always had more interest in diseases
Damage to liver function
 Damage to liver function All types of radiotherapy and chemotherapy can damage the liver function. The hepatic cells can become inflamed, although the mechanism is not the same as in viral hepatitis. Radiation
Damage to liver function All types of radiotherapy and chemotherapy can damage the liver function. The hepatic cells can become inflamed, although the mechanism is not the same as in viral hepatitis. Radiation
In Western medicine, there are three stages to a miscarriage or spontaneous
 7 Prevention of Miscarriage In Western medicine, there are three stages to a miscarriage or spontaneous abortion: 1) threatened miscarriage, 2) incomplete miscarriage, and 3) complete miscarriage. The
7 Prevention of Miscarriage In Western medicine, there are three stages to a miscarriage or spontaneous abortion: 1) threatened miscarriage, 2) incomplete miscarriage, and 3) complete miscarriage. The
ACUPUNCTURE AND TOUCH PROTOCOL
 ACUPUNCTURE AND TOUCH PROTOCOL The Role of Acupuncture Treatment with the Management of Threatened Miscarriage: An exploratory study Acupuncture treatment This involves receiving an acupuncture treatment
ACUPUNCTURE AND TOUCH PROTOCOL The Role of Acupuncture Treatment with the Management of Threatened Miscarriage: An exploratory study Acupuncture treatment This involves receiving an acupuncture treatment
Commentary on Formula Design in the Fuxing jue Chapter on Heart Organ Disease Patterns
 Commentary on Formula Design in the Fuxing jue Chapter on Heart Organ Disease Patterns by michael dell orfano [1 st ] Minor Purge the Heart Decoction Analysis Longdancao is the emperor herb in this formula,
Commentary on Formula Design in the Fuxing jue Chapter on Heart Organ Disease Patterns by michael dell orfano [1 st ] Minor Purge the Heart Decoction Analysis Longdancao is the emperor herb in this formula,
ANXIETY 1. ANXIETY IN WESTERN MEDICINE. The anxiety disorders discussed in Western medicine are:
 ANXIETY Anxiety is a normal reaction to stress. It helps one deal with a tense situation in the office, study harder for an exam, keep focussed on an important speech. In general, it helps one cope. But
ANXIETY Anxiety is a normal reaction to stress. It helps one deal with a tense situation in the office, study harder for an exam, keep focussed on an important speech. In general, it helps one cope. But
TOPICS IN GYNAECOLOGY PART ONE MENOPAUSE
 TOPICS IN GYNAECOLOGY PART ONE MENOPAUSE JANE LYTTLETON INTRODUCTION This series of articles addresses the health problems particular to women in their forties, fifties and onwards, i.e. the sorts of things
TOPICS IN GYNAECOLOGY PART ONE MENOPAUSE JANE LYTTLETON INTRODUCTION This series of articles addresses the health problems particular to women in their forties, fifties and onwards, i.e. the sorts of things
Journal of Traditional Chinese Medicine, June 2010, Vol. 30, No. 2
 132 Experts Experience LIU De-xi s Experience in the TCM Differential Treatment of Liver for Male Climacteric Syndrome WU Pei-tian Sanya Municipal Hospital of Traditional Chinese Medicine, Sanya, Hainan
132 Experts Experience LIU De-xi s Experience in the TCM Differential Treatment of Liver for Male Climacteric Syndrome WU Pei-tian Sanya Municipal Hospital of Traditional Chinese Medicine, Sanya, Hainan
Appendix 2. Detailed information about herbal prescriptions used in the included trials
 Appendix 2. Detailed information about herbal prescriptions used in the included trials First author (Year) Herbal Medicinal Preparation Name Chen Tongqiao (2013) 22 huoxue Guo Biyan (2004) 23 Qingdu Granule
Appendix 2. Detailed information about herbal prescriptions used in the included trials First author (Year) Herbal Medicinal Preparation Name Chen Tongqiao (2013) 22 huoxue Guo Biyan (2004) 23 Qingdu Granule
Contents. Basic Theory of Acupuncture. (Page 1) Acupuncture Points. (Page 31) Side Effects of Acupuncture. (Page 51)
 VII Contents Basic Theory of Acupuncture (Page 1) Scientific Aspects of Acupuncture..................... 2 Indication and Direction of Action of Acupuncture.................................... 12 Relative
VII Contents Basic Theory of Acupuncture (Page 1) Scientific Aspects of Acupuncture..................... 2 Indication and Direction of Action of Acupuncture.................................... 12 Relative
Liu Jing and Liu Jing Diagnosis System in Classical TCM Discussions of Six Divisions or Six Confirmations Diagnosis System in Classical TCM Texts
 Liu Jing and Liu Jing Diagnosis System in Classical TCM Discussions of Six Divisions or Six Confirmations Diagnosis System in Classical TCM Texts Liu Jing Bian Zheng system had developed about 1800 years
Liu Jing and Liu Jing Diagnosis System in Classical TCM Discussions of Six Divisions or Six Confirmations Diagnosis System in Classical TCM Texts Liu Jing Bian Zheng system had developed about 1800 years
EXPLAINING 4 Imbalances and 5 Organs
 4 IMBALANCES AND 5 ORGANS A New System for Diagnosis and Treatment EXPLAINING 4 Imbalances and 5 Organs Jeremy Ross www.jeremyross.com DIFFERENTIAL QUESTIONS A New System for Diagnosis 90 Organ syndromes
4 IMBALANCES AND 5 ORGANS A New System for Diagnosis and Treatment EXPLAINING 4 Imbalances and 5 Organs Jeremy Ross www.jeremyross.com DIFFERENTIAL QUESTIONS A New System for Diagnosis 90 Organ syndromes
Acupuncture Headache Relief Discovered
 Acupuncture Headache Relief Discovered Published by HealthCMi on November 2017 Acupuncture enhances positive patient outcome rates for patients suffering from headaches. In separate and independent investigations,
Acupuncture Headache Relief Discovered Published by HealthCMi on November 2017 Acupuncture enhances positive patient outcome rates for patients suffering from headaches. In separate and independent investigations,
Guide to Complete PLAR (Prior Learning Assessment)
 Guide to Complete PLAR (Prior Learning Assessment) Table of Contents Introduction... 2 Routes through the PLAR process... 3 Payment and Confirmation... 3 Case Study Assessment (Primary Route)... 4 Sample
Guide to Complete PLAR (Prior Learning Assessment) Table of Contents Introduction... 2 Routes through the PLAR process... 3 Payment and Confirmation... 3 Case Study Assessment (Primary Route)... 4 Sample
Theoretical Approaches
 Journal of Traditional Chinese Medicine, June 2010, Vol. 30, No. 2 83 Theoretical Approaches Treatment of Depression Based on Differentiation of the Shaoyang Channels ZHANG Huai-liang The First Affiliated
Journal of Traditional Chinese Medicine, June 2010, Vol. 30, No. 2 83 Theoretical Approaches Treatment of Depression Based on Differentiation of the Shaoyang Channels ZHANG Huai-liang The First Affiliated
The progressing research of traditional Chinese medicine treatment of. insomnia. Liu Jing1 a
 4th International Conference on Education, Management and Computing Technology (ICEMCT 2017) The progressing research of traditional Chinese medicine treatment of insomnia Liu Jing1 a 1 Shandong University
4th International Conference on Education, Management and Computing Technology (ICEMCT 2017) The progressing research of traditional Chinese medicine treatment of insomnia Liu Jing1 a 1 Shandong University
Poon, MMK; Chung, KF; Yeung, WF; Yau, VHK; Zhang, SP
 Title Classification of insomnia using the traditional chinese medicine system: A systematic review Author(s) Poon, MMK; Chung, KF; Yeung, WF; Yau, VHK; Zhang, SP Citation Evidence-Based Complementary
Title Classification of insomnia using the traditional chinese medicine system: A systematic review Author(s) Poon, MMK; Chung, KF; Yeung, WF; Yau, VHK; Zhang, SP Citation Evidence-Based Complementary
A systematic review on use of Chinese medicine and acupuncture for treatment of obesityobr_
 obesity reviews doi: 10.1111/j.1467-789X.2011.00979.x Obesity Treatment A systematic review on use of Chinese medicine and acupuncture for treatment of obesityobr_979 409..430 Y. Sui 1 *, H. L. Zhao 1
obesity reviews doi: 10.1111/j.1467-789X.2011.00979.x Obesity Treatment A systematic review on use of Chinese medicine and acupuncture for treatment of obesityobr_979 409..430 Y. Sui 1 *, H. L. Zhao 1
INTRODUCTION TO HERBAL MEDICINE
 COURSE DESCRIPTION This course provides students with an overview of the ideas and concepts they will encounter in their study of Chinese Herbology throughout the Masters program, as well as the basic
COURSE DESCRIPTION This course provides students with an overview of the ideas and concepts they will encounter in their study of Chinese Herbology throughout the Masters program, as well as the basic
Endometrial cancer. Endometrial/uterine adenocarcinoma; Uterine cancer; Adenocarcinoma of the endometrium/uterus; Cancer - uterine
 Endometrial cancer TCM Anti-Cancer Centre Zhao Cheng R.TCMP, R.Ac., Ph.D. Alternative names Endometrial/uterine adenocarcinoma; Uterine cancer; Adenocarcinoma of the endometrium/uterus; Cancer - uterine
Endometrial cancer TCM Anti-Cancer Centre Zhao Cheng R.TCMP, R.Ac., Ph.D. Alternative names Endometrial/uterine adenocarcinoma; Uterine cancer; Adenocarcinoma of the endometrium/uterus; Cancer - uterine
3 Clouded Vision (Mu Hun)
 The Treatment of Disease in TCM Vol. 2: Diseases of the Eyes, Ears, Nose & Throat Author: Sionneau, Philippe & Lü, Gang www.bluepoppy.com www.sionneau.com 3 Clouded Vision (Mu Hun) This refers to dimness
The Treatment of Disease in TCM Vol. 2: Diseases of the Eyes, Ears, Nose & Throat Author: Sionneau, Philippe & Lü, Gang www.bluepoppy.com www.sionneau.com 3 Clouded Vision (Mu Hun) This refers to dimness
Acupuncture Soothes Essential Tremor
 Acupuncture Soothes Essential Tremor Published by HealthCMI on 11 February 2018. Heilongjiang University of Chinese Medicine researchers find two types of acupuncture effective for the treatment of essential
Acupuncture Soothes Essential Tremor Published by HealthCMI on 11 February 2018. Heilongjiang University of Chinese Medicine researchers find two types of acupuncture effective for the treatment of essential
Chinese Medicine in the omics era
 Chinese Medicine in the omics era Prof. Giovanna Franconi Systems Medicine Department Tor Vergata University, Rome, Italy giovanna.franconi@uniroma2.it Western Medicine crisis: Exponential increase of
Chinese Medicine in the omics era Prof. Giovanna Franconi Systems Medicine Department Tor Vergata University, Rome, Italy giovanna.franconi@uniroma2.it Western Medicine crisis: Exponential increase of
The Qi-regulating Massotherapy for Treatment of Tonic Headache in 150 Cases
 Journal of Traditional Chinese Medicine, March 2009, Vol. 29, No. 1 13 The Qi-regulating Massotherapy for Treatment of Tonic Headache in 150 Cases TAN Tao, WANG Jin-gui, SUN Qing & SHI Yu-sheng Department
Journal of Traditional Chinese Medicine, March 2009, Vol. 29, No. 1 13 The Qi-regulating Massotherapy for Treatment of Tonic Headache in 150 Cases TAN Tao, WANG Jin-gui, SUN Qing & SHI Yu-sheng Department
POLYCYSTIC OVARY SYNDROME WESTERN PERSPECTIVE
 POLYCYSTIC OVARY SYNDROME WESTERN PERSPECTIVE DESCRIPTION Originally described by Stein and Leventhal, Polycystic ovary syndrome (PCOS) is one of the most common endocrinopathies in women of reproductive
POLYCYSTIC OVARY SYNDROME WESTERN PERSPECTIVE DESCRIPTION Originally described by Stein and Leventhal, Polycystic ovary syndrome (PCOS) is one of the most common endocrinopathies in women of reproductive
A LITERATURE REVIEW OF THE EFFECTIVENESS OF ACUPUNCTURE ON INSOMNIA
 SOUTH BAYLO UNIVERSITY A LITERATURE REVIEW OF THE EFFECTIVENESS OF ACUPUNCTURE ON INSOMNIA by FAKHTEH KHALAJHEDAYATI A RESEARCH PROJECT SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE
SOUTH BAYLO UNIVERSITY A LITERATURE REVIEW OF THE EFFECTIVENESS OF ACUPUNCTURE ON INSOMNIA by FAKHTEH KHALAJHEDAYATI A RESEARCH PROJECT SUBMITTED IN PARTIAL FULFILLMENT OF THE REQUIREMENTS FOR THE DEGREE
GYNECOLOGY & TCM. On line course provided by. Taught by Clara Cohen
 GYNECOLOGY & TCM On line course provided by Taught by Clara Cohen 1 GYNECOLOGY & TCM INTRODUCTION WOMEN S PHYSIOLOGY MENSTRUATION CONCEPTION PREGNANCY MENOPAUSE CAUSES OF IMBALANCE PREVENTION 2 Physiology
GYNECOLOGY & TCM On line course provided by Taught by Clara Cohen 1 GYNECOLOGY & TCM INTRODUCTION WOMEN S PHYSIOLOGY MENSTRUATION CONCEPTION PREGNANCY MENOPAUSE CAUSES OF IMBALANCE PREVENTION 2 Physiology
POST GRADUATE DIPLOMA IN ACUPUNCTURE Term-End Examination June, 2015
 No. of Printed Pages : 16 PGDACP-03 POST GRADUATE DIPLOMA IN ACUPUNCTURE Term-End Examination 0 June, 2015 PGDACP-03: TREATMENT OF COMMON DISEASES/ EAR & SCALP ACUPUNCTURE Time : 2 hours Maximum Marks
No. of Printed Pages : 16 PGDACP-03 POST GRADUATE DIPLOMA IN ACUPUNCTURE Term-End Examination 0 June, 2015 PGDACP-03: TREATMENT OF COMMON DISEASES/ EAR & SCALP ACUPUNCTURE Time : 2 hours Maximum Marks
Literature-based analysis on relationship of symptoms, drugs and therapies in treatment of intestinal diseases
 Online Submissions: http://www.journaltcm.com J Tradit Chin Med 0 February ; (): 6- info@journaltcm.com ISSN 05-9 0 JTCM. All rights reserved. LITERATURE STUDY TOPIC Literature-based analysis on relationship
Online Submissions: http://www.journaltcm.com J Tradit Chin Med 0 February ; (): 6- info@journaltcm.com ISSN 05-9 0 JTCM. All rights reserved. LITERATURE STUDY TOPIC Literature-based analysis on relationship
CMAC212. Session 8. Special Point Categories. Focusing on Lung, Spleen & Stomach. Chinese Medicine Department.
 CMAC212 Session 8 Special Point Categories Focusing on Lung, Spleen & Stomach Chinese Medicine Department www.endeavour.edu.au Session 8 Today we shall: o Explore points on the Lung channel o Explore points
CMAC212 Session 8 Special Point Categories Focusing on Lung, Spleen & Stomach Chinese Medicine Department www.endeavour.edu.au Session 8 Today we shall: o Explore points on the Lung channel o Explore points
Course: Formulas 1 Date: December 2, 2009 Class #: 10. Function in Formula. Disperse stagnation
 Course: Formulas 1 Date: December 2, 2009 Class #: 10 Xi Jiao Di Huang Tang : o Clear Heat toxins o o Disperse stagnation : o Heat in the blood Xi jiao Sheng di Shao yao Mu dan pi Clear Heart heat Nourish
Course: Formulas 1 Date: December 2, 2009 Class #: 10 Xi Jiao Di Huang Tang : o Clear Heat toxins o o Disperse stagnation : o Heat in the blood Xi jiao Sheng di Shao yao Mu dan pi Clear Heart heat Nourish
EMPEROR'S COLLEGE MTOM COURSE SYLLABUS HERB FORMULAE II
 COURSE DESCRIPTION The second of three courses in the Herb Formulae series. Categories covered in Formulae II include the Tonify Qi and Blood, Regulate Qi, Invigorate the Blood, Stop Bleeding, Stabilize
COURSE DESCRIPTION The second of three courses in the Herb Formulae series. Categories covered in Formulae II include the Tonify Qi and Blood, Regulate Qi, Invigorate the Blood, Stop Bleeding, Stabilize
N allocated to acupuncture: 53 Style of acupuncture: Not reported Point selection: Not reported
 Table B. Full details of the characteristics of the included trials, including all information about methods, patients, interventions, and outcomes collected* [posted as supplied by author] Study Benson
Table B. Full details of the characteristics of the included trials, including all information about methods, patients, interventions, and outcomes collected* [posted as supplied by author] Study Benson
4-1 Dyspnea (Chuan, 喘 )
 4-1 Dyspnea (Chuan, 喘 ) Concept Breathing with difficulty (open wide mouth, raise shoulders) Etiology and pathogenesis Climatic factors Phlegm fluid Emotion Chronic diseases Exertion Over sex Diagnosis
4-1 Dyspnea (Chuan, 喘 ) Concept Breathing with difficulty (open wide mouth, raise shoulders) Etiology and pathogenesis Climatic factors Phlegm fluid Emotion Chronic diseases Exertion Over sex Diagnosis
Functions and applications of Long Yan Rou and Suan Zao Ren By Alexandre Djukanovic
 Functions and applications of Long Yan Rou and Suan Zao Ren By Alexandre Djukanovic 龍眼肉 lóng yăn ròu, "dragon eye flesh 酸棗仁 suān zăo rén, "sour date seed" 1. Summary In this paper the functions and uses
Functions and applications of Long Yan Rou and Suan Zao Ren By Alexandre Djukanovic 龍眼肉 lóng yăn ròu, "dragon eye flesh 酸棗仁 suān zăo rén, "sour date seed" 1. Summary In this paper the functions and uses
PROSPERO International prospective register of systematic reviews
 PROSPERO International prospective register of systematic reviews Review title and timescale 1 Review title Give the working title of the review. This must be in English. Ideally it should state succinctly
PROSPERO International prospective register of systematic reviews Review title and timescale 1 Review title Give the working title of the review. This must be in English. Ideally it should state succinctly
EMPEROR'S COLLEGE MTOM COURSE SYLLABUS HERB FORMULAE I
 COURSE DESCRIPTION The first of three courses in the Herb Formulae series. These courses can be taken in any order. The Herb Formulae series analyzes the functions, ingredients, and properties of approximately
COURSE DESCRIPTION The first of three courses in the Herb Formulae series. These courses can be taken in any order. The Herb Formulae series analyzes the functions, ingredients, and properties of approximately
A Channel Based Approach
 A Channel Based Approach Meridian Circuits A meridian circuit is composed of meridians that are interconnected according to either their Chinese names, the internal-external relationships, or the horary
A Channel Based Approach Meridian Circuits A meridian circuit is composed of meridians that are interconnected according to either their Chinese names, the internal-external relationships, or the horary
Research Article Acupoints Stimulation for Anxiety and Depression in Cancer Patients: A Quantitative Synthesis of Randomized Controlled Trials
 Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 5645632, 15 pages http://dx.doi.org/10.1155/2016/5645632 Research Article Acupoints Stimulation for Anxiety and Depression
Evidence-Based Complementary and Alternative Medicine Volume 2016, Article ID 5645632, 15 pages http://dx.doi.org/10.1155/2016/5645632 Research Article Acupoints Stimulation for Anxiety and Depression
Acupuncture Treatment of Insomnia by Regulating the Defensive-qi and Strengthening the Brain and the Spinal Cord
 222 Journal of Traditional Chinese Medicine, September 2010, Vol. 30, No. 3 Acupuncture Treatment of Insomnia by Regulating the Defensive-qi and Strengthening the Brain and the Spinal Cord GAO Xi-yan 高希言,
222 Journal of Traditional Chinese Medicine, September 2010, Vol. 30, No. 3 Acupuncture Treatment of Insomnia by Regulating the Defensive-qi and Strengthening the Brain and the Spinal Cord GAO Xi-yan 高希言,
TWO CASES OF HYPERTHYROIDISM
 The Herbalist s Corner Jake Paul Fratkin, OMD, L.Ac. Acupuncture Today, January, 2008 TWO CASES OF HYPERTHYROIDISM Hyperthyroidism is not often seen in the clinic, but Chinese herbal medicine can be very
The Herbalist s Corner Jake Paul Fratkin, OMD, L.Ac. Acupuncture Today, January, 2008 TWO CASES OF HYPERTHYROIDISM Hyperthyroidism is not often seen in the clinic, but Chinese herbal medicine can be very
Colon cancer. Stages of cancer. TCM Anti-Cancer Centre Zhao Cheng R.TCMP, R.Ac., Ph.D.
 Colon cancer TCM Anti-Cancer Centre Zhao Cheng R.TCMP, R.Ac., Ph.D. Stages of cancer The staging of a carcinoma has to do with the size of the tumor, and the degree to which it has penetrated. When the
Colon cancer TCM Anti-Cancer Centre Zhao Cheng R.TCMP, R.Ac., Ph.D. Stages of cancer The staging of a carcinoma has to do with the size of the tumor, and the degree to which it has penetrated. When the
How Acupuncture and Oriental Medicine Can Help You Build a Resilient Body ALYSSA JOHNSON, L. AC, MA. OM
 How Acupuncture and Oriental Medicine Can Help You Build a Resilient Body ALYSSA JOHNSON, L. AC, MA. OM What is Oriental Medicine? or Traditional Chinese Medicine Oriental Medicine (OM) =Traditional Chinese
How Acupuncture and Oriental Medicine Can Help You Build a Resilient Body ALYSSA JOHNSON, L. AC, MA. OM What is Oriental Medicine? or Traditional Chinese Medicine Oriental Medicine (OM) =Traditional Chinese
Tonification and Dispersion Points for Each Pattern of Imbalance
 Tonification and Dispersion Points for Each Pattern of Imbalance The principles and usages for a number of different point selection methods were mentioned above. Next, the tonification and dispersion
Tonification and Dispersion Points for Each Pattern of Imbalance The principles and usages for a number of different point selection methods were mentioned above. Next, the tonification and dispersion
Principles of Differentiation and Prescription for Vitiligo in Traditional Chinese Medicine Based on a Literature Investigation
 Received: May 13, 2015 Accepted after revision: October 19, 2015 Published online: December 3, 2015 2015 The Author(s) Published by S. Karger AG, Basel 2296 7362/15/0024 0149$39.50/0 This article is licensed
Received: May 13, 2015 Accepted after revision: October 19, 2015 Published online: December 3, 2015 2015 The Author(s) Published by S. Karger AG, Basel 2296 7362/15/0024 0149$39.50/0 This article is licensed
 PROGRAMME CODE-UAC03 ASSOCIATE DEGREE IN ACUPUNCTURE - SYLLABUS FIRST YEAR CODE SUBJECT CREDITS UAC03-1 CLINICAL ACUPUNCTURE 8 CREDITS UAC03-2 TRADITIONAL ACUPUNCTURE 8 CREDITS UAC03-3 PRACTICAL-I 8 CREDITS
PROGRAMME CODE-UAC03 ASSOCIATE DEGREE IN ACUPUNCTURE - SYLLABUS FIRST YEAR CODE SUBJECT CREDITS UAC03-1 CLINICAL ACUPUNCTURE 8 CREDITS UAC03-2 TRADITIONAL ACUPUNCTURE 8 CREDITS UAC03-3 PRACTICAL-I 8 CREDITS
Root & Branch Bulk Formula List
 An asterisk * indicates the inclusion of 1 or more granule versions of an herb because of limited availability on the American herbal market. These products are usually animal in nature like E Jiao, Shui
An asterisk * indicates the inclusion of 1 or more granule versions of an herb because of limited availability on the American herbal market. These products are usually animal in nature like E Jiao, Shui
Review Article Effect of Acupuncture on Heart Rate Variability: A Systematic Review
 Evidence-Based Complementary and Alternative Medicine Volume, Article ID 819871, 19 pages http://dx.doi.org/10.15//819871 Review Article Effect of Acupuncture on Heart Rate Variability: A Systematic Review
Evidence-Based Complementary and Alternative Medicine Volume, Article ID 819871, 19 pages http://dx.doi.org/10.15//819871 Review Article Effect of Acupuncture on Heart Rate Variability: A Systematic Review
Good Practice in Traditional Chinese Medicine Research in the Post-genomic Era GP-TCM D5.7
 Good Practice in Traditional Chinese Medicine Research in the Post-genomic Era GP-TCM 223154 D5.7 Elaboration of a priority list of CMH for future research in CMH in animal models GP-TCM / WP5 / D5.7 Page
Good Practice in Traditional Chinese Medicine Research in the Post-genomic Era GP-TCM 223154 D5.7 Elaboration of a priority list of CMH for future research in CMH in animal models GP-TCM / WP5 / D5.7 Page
Course: Formulas 1 Date: September 30, 2009 Class #: 2 Prof: Dr. Ma
 Course: Formulas 1 Date: September 30, 2009 Class #: 2 Prof: Dr. Ma WEEK TWO: Class 2 Goals: Students will learn traditional treatment methods - sweating, vomiting, draining downward, harmonizing, warming,
Course: Formulas 1 Date: September 30, 2009 Class #: 2 Prof: Dr. Ma WEEK TWO: Class 2 Goals: Students will learn traditional treatment methods - sweating, vomiting, draining downward, harmonizing, warming,
HISTORICAL BASIS OF CHINESE MEDICINE. Linda Boggie, DVM Okkenbroek, The Netherlands
 HISTORICAL BASIS OF CHINESE MEDICINE Linda Boggie, DVM Okkenbroek, The Netherlands Chinese Medical Theory Based on observation of phenomena and integrated with Chinese philosophy Chinese philosophy has
HISTORICAL BASIS OF CHINESE MEDICINE Linda Boggie, DVM Okkenbroek, The Netherlands Chinese Medical Theory Based on observation of phenomena and integrated with Chinese philosophy Chinese philosophy has
A Trend Analysis of Case Reports and Case Series on Hwa-byung in Korea
 J Korean Med. 2015;36(4):129-144 pissn 1010-0695 eissn 2288-3339 Case Report A Trend Analysis of Case Reports and Case Series on Hwa-byung in Korea Soo-Hyun Sung 1, Jong-Hyun Park 2, Young-Joon Lee 3,
J Korean Med. 2015;36(4):129-144 pissn 1010-0695 eissn 2288-3339 Case Report A Trend Analysis of Case Reports and Case Series on Hwa-byung in Korea Soo-Hyun Sung 1, Jong-Hyun Park 2, Young-Joon Lee 3,
Introduction to Acupuncture
 Introduction to Acupuncture The TCM paradigm Objective- To explain the following: Definition of Acupuncture Overview of Traditional Chinese Medicine (TCM) Meridian Theory The Eight Principles Pathogenic
Introduction to Acupuncture The TCM paradigm Objective- To explain the following: Definition of Acupuncture Overview of Traditional Chinese Medicine (TCM) Meridian Theory The Eight Principles Pathogenic
In the October, 2009 issue of ACUPUNCTURE TODAY, I wrote on how to use pulse
 The Herbalist s Corner Acupuncture Today, April, 2010 TREATING COMPLEX MULTI-LAYERED CASES Part 2: Treatment Jake Paul Fratkin, OMD, L.Ac. In the October, 2009 issue of ACUPUNCTURE TODAY, I wrote on how
The Herbalist s Corner Acupuncture Today, April, 2010 TREATING COMPLEX MULTI-LAYERED CASES Part 2: Treatment Jake Paul Fratkin, OMD, L.Ac. In the October, 2009 issue of ACUPUNCTURE TODAY, I wrote on how
CMHB221 Chinese Herbal Formulae
 CMHB221 Chinese Herbal Formulae Session Four Tonifying Chinese herbal formulae: Xue; Qi and Xue: o o o o o English name; Pin yin name and Chinese name Composition; dosage and administration Functions and
CMHB221 Chinese Herbal Formulae Session Four Tonifying Chinese herbal formulae: Xue; Qi and Xue: o o o o o English name; Pin yin name and Chinese name Composition; dosage and administration Functions and
Section 3. Blood-Tonifying Herbs. Dang Gui (Radicis Angelicae Sinensis) Chapter 17 Section 3 Blood-Tonifying Herbs
 Section 3 Blood-Tonifying Herbs Pinyin Name: Dang Gui Literal Name: state of return, ought to return Alternate Chinese Names: Xi Gui, Gan Gui, Quan Dang Gui, Qin Dang Gui, Yun Dang Gui, Chuan Dang Gui
Section 3 Blood-Tonifying Herbs Pinyin Name: Dang Gui Literal Name: state of return, ought to return Alternate Chinese Names: Xi Gui, Gan Gui, Quan Dang Gui, Qin Dang Gui, Yun Dang Gui, Chuan Dang Gui
CMAC311. Session 4. Chinese Medicine Department MENSTRUATION DISORDERS. Pre-menstrual Syndrome (PMS) Dysmenorrhea (painful periods)
 CMAC311 Session 4 MENSTRUATION DISORDERS Pre-menstrual Syndrome (PMS) Dysmenorrhea (painful periods) Chinese Medicine Department www.endeavour.edu.au Session Contents o Explain the aetiology factors &
CMAC311 Session 4 MENSTRUATION DISORDERS Pre-menstrual Syndrome (PMS) Dysmenorrhea (painful periods) Chinese Medicine Department www.endeavour.edu.au Session Contents o Explain the aetiology factors &
Effects of Chai Hu (Radix Burpleuri) Containing Formulation on Plasma β-endorphin, Epinephrine and Dopamine in Patients
 The American Journal of Chinese Medicine, Vol. 33, No. 5, 737 745 2005 World Scientific Publishing Company Institute for Advanced Research in Asian Science and Medicine Effects of Chai Hu (Radix Burpleuri)
The American Journal of Chinese Medicine, Vol. 33, No. 5, 737 745 2005 World Scientific Publishing Company Institute for Advanced Research in Asian Science and Medicine Effects of Chai Hu (Radix Burpleuri)
In this chapter, I present the general treatment principles used in Chinese andrology
 Book 1 Chapter 7 General Treatment Principles in Chinese Andrology In this chapter, I present the general treatment principles used in Chinese andrology and correlate them with common Chinese medicinal
Book 1 Chapter 7 General Treatment Principles in Chinese Andrology In this chapter, I present the general treatment principles used in Chinese andrology and correlate them with common Chinese medicinal
PERIOPERATIVE ACUPUNCTURE IN PEDIATRIC ANESTHESIA
 PERIOPERATIVE ACUPUNCTURE IN PEDIATRIC ANESTHESIA Shu-Ming Wang.,MD. Woodland Anesthesiology Associates, PC Trinity Health of New England Professor Department of Anesthesiology University of Connecticut
PERIOPERATIVE ACUPUNCTURE IN PEDIATRIC ANESTHESIA Shu-Ming Wang.,MD. Woodland Anesthesiology Associates, PC Trinity Health of New England Professor Department of Anesthesiology University of Connecticut
Course: Acupuncture Treatment of Disease 1 Date: Oct 8, 2008 Doc: Test 1 Review
 Course: Acupuncture Treatment of Dise 1 Date: Oct 8, 2008 Doc: Test 1 Review This test consists of 1. 40 questions. 6 case studies in it. Must be able to analyze, just like the case studies he gave in
Course: Acupuncture Treatment of Dise 1 Date: Oct 8, 2008 Doc: Test 1 Review This test consists of 1. 40 questions. 6 case studies in it. Must be able to analyze, just like the case studies he gave in
Research Article The Traditional Chinese Medicine Prescription Pattern of Endometriosis Patients in Taiwan: A Population-Based Study
 Hindawi Publishing Corporation Evidence-Based Complementary and Alternative Medicine Volume 2012, Article ID 591391, 9 pages doi:10.1155/2012/591391 Research Article The Traditional Chinese Medicine Prescription
Hindawi Publishing Corporation Evidence-Based Complementary and Alternative Medicine Volume 2012, Article ID 591391, 9 pages doi:10.1155/2012/591391 Research Article The Traditional Chinese Medicine Prescription
Acupuncture and moxibustion for lateral elbow pain: a systematic review of randomized controlled trials
 Gadau et al. BMC Complementary and Alternative Medicine 2014, 14:136 RESEARCH ARTICLE Open Access Acupuncture and moxibustion for lateral elbow pain: a systematic review of randomized controlled trials
Gadau et al. BMC Complementary and Alternative Medicine 2014, 14:136 RESEARCH ARTICLE Open Access Acupuncture and moxibustion for lateral elbow pain: a systematic review of randomized controlled trials
Dang Gui Si Ni Tang Tangkuei Decoction for Frigid Extremities
 Dang Gui Si Ni Tang Tangkuei Decoction for Frigid Extremities D F E G ctions: Warms the channels, disperses cold, nourishes the xue, and unblocks the xue vessels. hief Deputy (a) Dang Gui (b) Gui Zhi (c)
Dang Gui Si Ni Tang Tangkuei Decoction for Frigid Extremities D F E G ctions: Warms the channels, disperses cold, nourishes the xue, and unblocks the xue vessels. hief Deputy (a) Dang Gui (b) Gui Zhi (c)
New and Improved 8 Principles in Clinical Practice: 3 Most Important Dichotomies. Bruce Ferguson, DVM, MS Holistic Veterinary Care
 New and Improved 8 Principles in Clinical Practice: 3 Most Important Dichotomies Bruce Ferguson, DVM, MS Holistic Veterinary Care www.naturalvet.org Introduction It is said that Chinese Medicine (TCVM)
New and Improved 8 Principles in Clinical Practice: 3 Most Important Dichotomies Bruce Ferguson, DVM, MS Holistic Veterinary Care www.naturalvet.org Introduction It is said that Chinese Medicine (TCVM)
CMHB221 Chinese Herbal Formulae
 CMHB221 Chinese Herbal Formulae Session Three Tonifying Chinese herbal formulae: Qi: o o o o o English name; Pin yin name and Chinese name Composition; dosage and administration Functions and indications
CMHB221 Chinese Herbal Formulae Session Three Tonifying Chinese herbal formulae: Qi: o o o o o English name; Pin yin name and Chinese name Composition; dosage and administration Functions and indications
Pin-Yi Lin, 1 Yueh-Ting Tsai, 1 Jung-Nien Lai, 1,2 Chia-Hao Yeh, 3 and Ruei-Chi Fang Introduction
 Hindawi Publishing Corporation Evidence-Based Complementary and Alternative Medicine Volume 2014, Article ID 460386, 11 pages http://dx.doi.org/10.1155/2014/460386 Research Article Bian Zheng Lun Zhi as
Hindawi Publishing Corporation Evidence-Based Complementary and Alternative Medicine Volume 2014, Article ID 460386, 11 pages http://dx.doi.org/10.1155/2014/460386 Research Article Bian Zheng Lun Zhi as
Acupuncture Beats Ibuprofen For Knee Arthritis
 Acupuncture Beats Ibuprofen For Knee Arthritis Published by HealthCMI on 1 March 2018. Researchers find acupuncture combined with tuina massage more effective for the treatment of knee osteoarthritis than
Acupuncture Beats Ibuprofen For Knee Arthritis Published by HealthCMI on 1 March 2018. Researchers find acupuncture combined with tuina massage more effective for the treatment of knee osteoarthritis than
copyright 2017 by AJTCVM All Rights Reserved Herbal Formula Spotlight
 copyright 2017 by AJTCVM All Rights Reserved Herbal Formula Spotlight Tao Hong Si Wu Tang (Four-Substance Decoction with Safflower and Peach Pit) Tao Hong Si Wu Tang (Four-Substance Decoction with Safflower
copyright 2017 by AJTCVM All Rights Reserved Herbal Formula Spotlight Tao Hong Si Wu Tang (Four-Substance Decoction with Safflower and Peach Pit) Tao Hong Si Wu Tang (Four-Substance Decoction with Safflower
CLINICAL ACUPUNCTURE TRIAL ON INSOMNIA PATIENTS---A TAIWAN EXPERIENCE
 J Chin Med 20(1,2): 35-45, 2009 35 CLINICAL ACUPUNCTURE TRIAL ON INSOMNIA PATIENTS---A TAIWAN EXPERIENCE Yu-Yang Chiang 1, Heng-Yi Hsu 1, Chiung-Hui Hsieh 1, Tsai-Yu Lin 1, Lu-Chun Tsai 2, Pei-Ching Chen
J Chin Med 20(1,2): 35-45, 2009 35 CLINICAL ACUPUNCTURE TRIAL ON INSOMNIA PATIENTS---A TAIWAN EXPERIENCE Yu-Yang Chiang 1, Heng-Yi Hsu 1, Chiung-Hui Hsieh 1, Tsai-Yu Lin 1, Lu-Chun Tsai 2, Pei-Ching Chen
Medicated diet. Tonify the Qi
 Medicated diet Tonify the Qi 1. Ren shen ginseng root Properties: sweet, slightly bitter, slightly warm Channels entered: LU, SP a. Strongly tonifies the basal qi, Tonifies the lung and spleen qi. a. Benefits
Medicated diet Tonify the Qi 1. Ren shen ginseng root Properties: sweet, slightly bitter, slightly warm Channels entered: LU, SP a. Strongly tonifies the basal qi, Tonifies the lung and spleen qi. a. Benefits
Bussell J. Acupuncture and anxiety 2013: The year in (literature) review. OA Alternative Medicine 2014 Feb 22;2(1):3.
 Bussell J. Acupuncture and anxiety 2013: The year in (literature) review. OA Alternative Medicine 2014 Feb 22;2(1):3. Licensee OA Publishing London 2014. Creative Commons Attribution License (CC-BY) Competing
Bussell J. Acupuncture and anxiety 2013: The year in (literature) review. OA Alternative Medicine 2014 Feb 22;2(1):3. Licensee OA Publishing London 2014. Creative Commons Attribution License (CC-BY) Competing
by Subhuti Dharmananda, Ph.D., Director, Institute for Traditional Medicine, Portland, Oregon
 AN INTRODUCTION TO ACUPUNCTURE AND HOW IT WORKS by Subhuti Dharmananda, Ph.D., Director, Institute for Traditional Medicine, Portland, Oregon There are two very different ways of looking at acupuncture:
AN INTRODUCTION TO ACUPUNCTURE AND HOW IT WORKS by Subhuti Dharmananda, Ph.D., Director, Institute for Traditional Medicine, Portland, Oregon There are two very different ways of looking at acupuncture:
Acupuncture to relieve unilateral numbness and tingling in the upper extremities: A case report
 Acupuncture to relieve unilateral numbness and tingling in the upper extremities: A case report KEYWORDS: acupuncture, tingling, numbness, increase, blood flow. Student/Author: Sophia Mitsiki-Murray Student
Acupuncture to relieve unilateral numbness and tingling in the upper extremities: A case report KEYWORDS: acupuncture, tingling, numbness, increase, blood flow. Student/Author: Sophia Mitsiki-Murray Student
The Foundations of Oriental Medicine Abbreviated Content Outline
 The Foundations of Oriental Medicine Abbreviated Content Outline (Effective as of February 1, 2014) Note to Candidate: This document serves as a guide to assist in examination preparation for candidates
The Foundations of Oriental Medicine Abbreviated Content Outline (Effective as of February 1, 2014) Note to Candidate: This document serves as a guide to assist in examination preparation for candidates
Acupuncture for persistent insomnia associated with major depressive disorder: a randomised controlled trial
 Title Acupuncture for persistent insomnia associated with major depressive disorder: a randomised controlled trial Author(s) Chung, KF; Yeung, WF; Zhang, SP; Zhang, Z; Wong, MT; Lee, WK; Chan, KW Citation
Title Acupuncture for persistent insomnia associated with major depressive disorder: a randomised controlled trial Author(s) Chung, KF; Yeung, WF; Zhang, SP; Zhang, Z; Wong, MT; Lee, WK; Chan, KW Citation
Chinese herb formulae for treatment of erectile dysfunction: a systematic review of randomised controlled clinical trials
 REVIEW ARTICLE Chinese herb formulae for treatment of erectile dysfunction: a systematic review of randomised controlled clinical trials G. Xiong 1,B.Li 2,K.Wang 1 &H.Li 1 1 Department of Urology, West
REVIEW ARTICLE Chinese herb formulae for treatment of erectile dysfunction: a systematic review of randomised controlled clinical trials G. Xiong 1,B.Li 2,K.Wang 1 &H.Li 1 1 Department of Urology, West
Mohammad Ali Heidarnia MD, MPH Specialist n Community Medicine Acupuncturist
 Mohammad Ali Heidarnia MD, MPH Specialist n Community Medicine Acupuncturist Principles of Medical Ethics AUTONOMY NON-MALEFICENCE BENEFICENCE JUSTICE 2 Definition of Adverse Event An adverse event is
Mohammad Ali Heidarnia MD, MPH Specialist n Community Medicine Acupuncturist Principles of Medical Ethics AUTONOMY NON-MALEFICENCE BENEFICENCE JUSTICE 2 Definition of Adverse Event An adverse event is
